Urology Residency Training - URO-2 (PGY 3) Rotations: Overton Brooks VA Medical Center 6 months and LSU University Hospital 6 months
|
|
|
- Ella Wade
- 5 years ago
- Views:
Transcription
1 COMPETENCY-BASED GOALS AND OBJECTIVES FOR UROLOGY RESIDENT EDUCATION [Adapted (with modifications) from: Objectives For Urology Residency Education 5 th Ed. 2001, SUU And ACGME s Outcomes Project]] Urology Residency Training - URO-2 (PGY 3) Rotations: Overton Brooks VA Medical Center 6 months and LSU University Hospital 6 months NOTE: Goals and objectives from the preceding years (PGY 1&2) should be refined, reinforced, and further developed. In addition, this year of education and training should focus on the following specific goals and objectives: I. Observe through interactions with fellow residents and supervising, attending physicians the daily practice of Urology, and continue to develop experiences and knowledge in the six (6) clinical competencies assigned last year. A. Participate in the preoperative evaluation and postoperative follow up of patients in the outpatient clinic setting. 1. Describe the essentials of office urology and be able to apply them in accordance within the framework of a hospital-based office setting. 2. Contrast the scope of care deliverable in a typical private office setting compared to that provided in the university- or hospital-based urology clinic with specific reference to: a. Office consultations b. Diagnostic procedures practical in the private vs. hospital-based office setting. c. Therapeutic modalities practical in the private vs. hospital-based office setting. d. Recognition of common urologic conditions seen in a typical private vs. hospital-based office setting. e. Sexual and fertility counseling. B. Participate in the inpatient care of hospitalized patients on the Urology Service. 1. Perform history and physical examinations on these inpatients and compare and discuss findings with fellow residents and attending physicians. 2. Make daily rounds on hospitalized patients, write progress notes, and discuss patients status with chief resident and supervising attending physicians. 3. Demonstrate a willingness and ability to function as a member of a team. a. Demonstrate mutual respect and cooperation among medical and paramedical personnel. b. Obtain and provide consultative services whenever appropriate. c. Demonstrate empathy, understanding, compassion, integrity, and honesty in the interactions with patients, family members, attending physicians, colleagues, and other medical and paramedical personnel. C. Participate as Assistant Surgeon or Surgeon (under the supervision of attending surgeon) in the operative management of urologic patients. D. Communicate daily with chief resident and attending faculty in selecting the cases from the operative schedule for participation in order to obtain maximal educational benefit from the variety of cases which may be available. II. Demonstrate expanded clinical experiences and increasing knowledge and competence in the following situations or in the performance of the following procedures: A. Demonstrate competence in performing the following outpatient clinic procedures: 1. Rigid and flexible cystourethroscopy; 2. Retrograde pyelography, retrograde and antegrade techniques to bypass ureteral obstruction and JJ stent placement; 3. Cold cup bladder biopsy; 4. Fulguration of minor bleeding (e.g., from cold cup biopsy sites) utilizing electrocautery under local anesthesia;
2 5. Retrograde urethrography and urethral dilation with sounds and balloons; 6. Local instillation therapy (e.g., BCG, DMSO, chemotherapy) including indications, complications, and management; 7. Oral and parenteral medication administration for active infection and / or prophylaxis; 8. Urethral and suprapubic catheter care; 9. Stomal care; 10. Wound care; 11. Vasectomy; 12. Neonatal circumcision; 13. Urodynamic evaluation, including CMG, flowmetry, VCUG, pressure / flow study, Valsalva Leak Point Pressure determination, and pelvic floor EMG measurement; a. Recognize the urodynamic patterns of: Detrusor Overactivity, Hypotonicity, Hyperreflexia, Autonomic Dysreflexia, Cystoparesis, Intrinsic Urethral Sphincter Deficiency, Stress Incontinence, Urge Incontinence, Mixed Incontinence, Detrusor External-Sphincter Dyssynergia (DESD), Functional Bladder Neck Obstruction, and Outlet Obstruction (from Prostate or USD); b. Discuss management options for the above voiding dysfunctions; c. Describe the indications for and technique to perform and interpret a Whitaker Perfusion Pressure Test; d. Describe the indications for and technique to perform and interpret a Bethanechol Supersensitivity (Lapides) Test; 14. Percutaneous suprapubic catheter placement; 15. Percutaneous nephrostomy tube placement; 16. Urologic applications of ultrasound, including: a. BladderScan PVR measurement and U/S evaluation of the bladder; b. Renal U/S and guidance for needle biopsy or access to collecting system of kidney; c. Small organ U/S, including penis, scrotum, testes, spermatic cord, and inguinal canals; d. Transrectal U/S (TRUS) for diagnosis of disorders of the Prostate, Seminal Vesicles, and Ejaculatory Duct; e. Digitally and TRUS-guided prostate needle biopsies; f. Color flow Doppler assessment of testicular blood flow in evaluating the acute scrotum; 17. Sclerotherapy for hydrocele; B. Demonstrate expanded knowledge of the causes and management of the following specific conditions: 1. Male Infertility a. Demonstrate an understanding of the hypothalamic-pituitary-gonadal axis, its endocrine control of testicular function, and abnormalities of hormone production which affect fertility; b. Describe the processes of spermatogenesis, sperm maturation, and sperm transport and storage; c. Demonstrate an understanding of the normal and abnormal anatomy and physiology of the male reproductive tract; d. Describe a rational, systematic approach to the clinical and laboratory evaluation of the infertile male; e. Select methodology for the clinical management (surgical and / or medical) of the infertile male and describe the anatomic and / or physiological basis for selection of specific treatment plans for the following conditions: (1) Endocrinopathies such as Kallman s Syndrome (hypogonadotrophic hypogonadism), primary testicular failure (hypergonadotrophic hypogonadism), and congenital adrenal hyperplasia; (2) Sperm maturation abnormalities, such as maturation arrest; 2
3 (3) Sperm transport abnormalities, such as absent vas, epididymal obstruction, or ejaculatory duct obstruction; (4) Ejaculatory dysfunction, such as absence of ejaculation or retrograde ejaculation; (5) Varicocele and oligospermia with stress pattern ; (6) Kleinfelter s Syndrome; f. Discuss ancillary methods of interdisciplinary management of male infertility including: (1) Artificial insemination (husband or donor) (2) Sperm processing and preservation techniques (3) Intrauterine insemination (4) In vitro fertilization (5) Gamete intra-fallopian transfer (6) Intracytoplasmic Injection of Sperm (ICSI) (7) Adoption 2. Urolithiasis a. Demonstrate a depth of knowledge of the etiology, pathophysiology, diagnosis, treatment and prevention of urolithiasis; b. Demonstrate an understanding of epidemiologic factors affecting stone formation, including: (1) Geographic differences in stone formation risks; (2) Incidence in relation to race, sex, age, and ethnic & climatic factors; (3) Effects of diet and fluid intake on occurrence; c. Describe the crystalline architecture of urinary calculi and discuss the theoretical factors affecting crystallization; (1) Crystallizable elements in urine; (2) Nucleation, growth, and aggregation of crystals; (3) Effects of ph on crystallization; (4) Other factors affecting crystallization, e.g., Citrate, Magnesium, Phosphate, and mucoprotein levels; (5) Concepts of stone size & shape and their effects on spontaneous passage rates; d. Demonstrate a knowledge of the effects of obstruction of the urinary tract from stones; (1) Describe changes in renal blood flow following acute ureteral obstruction; (2) Describe the changes in urine flow and intrarenal pressure with acute obstruction; (3) Describe the alteration in the above factors with chronic obstruction; e. Present a working classification of the types of metabolic stone disease and discuss their individual management; f. Demonstrate the ability to elicit a problem-directed history compatible with stone disease, including references to: (1) Pain patterns as an aid to localization; (2) Family history and personal (occupational) history; (3) Immobilization syndrome; (4) Diet and medications; (5) Fluid intake; (6) Previous stones and their management; g. Demonstrate an understanding of the information to be gained from urinalysis by discussing: (1) Appearance of typical crystals under the microscope; (2) Relationship of ph and specific gravity; (3) Possible significance of presence of bacteria; (4) 24-hour urinary excretion of creatinine, calcium, citrate, magnesium, phosphate, oxalate, and uric acid; 3
4 h. Select and evaluate results of specific blood tests to order, when evaluating patients with urolithiasis. i. Describe the value of crystallographic and chemical stone analysis. j. Demonstrate the ability and discuss limitations of various radiologic tests in diagnosing and differentiating by radiologic appearance alone the different types of urolithiasis: (1) Uric acid (2) Cystine (3) Milk of Calcium (4) Calcium oxalate (monohydrate and dihydrate forms) (5) Calcium phosphate (Apatite) (6) Infection stones (Struvite) k. Demonstrate the ability to select in a timely manner the appropriate therapy for a given patient and be able to defend the choice with reference to risks, benefits, and cost. (1) Dietary restriction and adjustment in fluid intake (2) Medications (a) Phosphates (b) Magnesium (c) Diuretics and sodium restriction (d) Citrate augmentation by medication or lemonade (e) Allopurinol and urine alkalinization (f) Chelating agents for cystine stones (e.g., penicillamine / cupramine or mucomyst ) (3) Genetic counseling when inheritable forms of stone disease are discovered (e.g., RTA) (4) Percutaneous nephrostolithotomy techniques (a) Access site selection (b) Techniques for tract dilation (e.g., high-pressure balloons vs. Amplatz dilators) (c) Techniques for stone fragmentation (e.g., EHL, U/S, Laser, or Pneumatic impactors) (d) Techniques for chemolysis (e) Relook nephrostolithotomy (5) Transurethral and ureteroscopic techniques discuss equipment, techniques, risks and benefits. (a) Describe the techniques for ureteral dilation (b) Describe the range of available endoscopes and discuss limitations and applications. (c) Be familiar with the working instruments for each of the above scopes and their usage. (d) Be familiar with the complications of ureteroscopic manipulation and their management. (6) Open surgical techniques discuss risks and benefits and describe individual techniques (a) Pyelolithotomy and Gil-Vernet Extended Pyelolithotomy (b) Coagulum pyelolithotomy (c) Nephrotomy with extraction (d) Anatrophic nephrolithotomy (e) Partial Nephrectomy (f) Simple Nephrectomy (7) Extracorporeal Shock Wave Lithotripsy (ESWL) (a) List the types of machines available sources of energy, methods of coupling, imaging / targeting systems, comparative costs, and relative advantages / disadvantages. 4
5 (b) List relative and absolute contraindications to ESWL management of certain stones. (c) Demonstrate ability to successfully image, target, and treat a patient on the ESWL unit. (d) Demonstrate a working knowledge of the control panel and optimal instrument settings for ESWL. (e) Demonstrate knowledge of safety limits for energy level and total # of shocks to be delivered per treatment episode for ureteral or renal stones. (f) Discuss the alterations in technique for pediatric or obese patients. (g) Discuss the physics of shockwave generation and mechanism of stone fragmentation. (h) Describe appearance of successfully treated stone. (i) Discuss pain management during lithotripsy. (j) Discuss post-eswl management. 3. Female Urology A. Demonstrate the ability to evaluate, diagnose and treat a wide variety of lower urinary tract and vaginal conditions occurring in the female including: 1. Genuine stress urinary incontinence 2. Urge incontinence 3. Intrinsic sphincter deficiency 4. Vesicovaginal fistula 5. Neuropathic dysfunctions of the lower urinary tracts 6. Interstitial cystitis 7. Vaginal, uterine, and rectal prolapse 8. Endometriosis and its effects on the urinary tract 9. Vaginitis and female urethral syndrome 10. Urinary tract infection 11. Urinary obstruction anatomic and functional 12. Urethral prolapse 13. Urethral diverticulum 14. Urethral caruncle B. Demonstrate the ability to choose, perform and/or recommend appropriate therapies from the list below, for the above conditions. 1. Kegel pelvic floor exercises 2. Pharmacological and hormonal therapy when indicated 3. Anterior colporrhaphy (Kelly plication) / posterior colporrhaphy 4. MMK / Burch urethropexy 5. Transvaginal needle suspensions 6. Pubovaginal sling procedures 7. Urethrolysis (take-down of obstructing urethral suspension operations) 8. Periurethral injection therapy 9. Artificial Urinary Sphincter Implantation 10. Sacral nerve stimulation 11. Bladder augmentation (enterocystoplasty) 12. Self Intermittent Catheterization 13. Vesicostomy and catheterizable stomas (Mitrofanoff Procedure) 14. Supravesical diversion, including conduits, continent reservoirs, and neobladders 15. Transvaginal and transabdominal techniques for vesicovaginal fistula repairs 4. Obstructive uropathy A. List and discuss the causes of obstructive uropathy (congenital, iatrogenic, and acquired) and discuss their pathophysiology; 5
6 B. Recognize the clinical signs and symptoms C. Select appropriate diagnostic tests to define the cause be able to defend the choice of studies and state the advantages, hazards, and complications of the studies selected. D. Presented with an example of an obstructed condition, discuss a solution for a patient with obstructive uropathy. 1). Demonstrate an understanding of the natural history of the lesion and how the outcome can be most favorably altered. 2) Discuss the available diagnostic and therapeutic modalities with consideration given to the advantages, hazards, and complications of each treatment indicated below: a. Surgical repair or correction of obstruction b. Minimally invasive surgical alternative (e.g., endourological management) c. Temporary and permanent diversion with or without tubes or catheters. d. Pharmacological management 3) Discuss the acute and chronic effects of urinary obstruction upon the structure and function of the various portions of the urinary tract and comment on the relationship of the degree and duration of obstruction to function and restoration of function. 5. Diagnosis and endoscopic management of bladder cancer. A. Demonstrate the ability to diagnose a patient with cancer of the bladder and list the various types of bladder abnormality. 1) TCC and CIS 2) Adenocarcinoma 3) Squamous Cell Ca 4) Cystitis cystica and glandularis 5) Squamous metaplasia 6) Malakoplakia 7) Sarcoma B. Discuss epidemiological aspects of bladder cancer and list some common risk factors. 1) Family history 2) Cigarette smoking direct and secondary smoke inhalation 3) Chemical carcinogen exposure e.g., alanine dyes or tryptophan or its metabolites 4) Chemotherapy e.g., cytoxan (cyclophosphamide) 5) Chronic inflammation e.g., stones, infection, schistosomiasis C. Identify and differentiate the various forms of bladder cancer and distinguish them from other entities that may mimic bladder cancer. D. Describe the TNM classification for staging of bladder cancer. E. Demonstrate the ability to elicit a history of the possible presence of bladder cancer. F. Demonstrate the ability to recognize by endoscopy (or 35 mm slides) of typical bladder cancer. G. Describe staging techniques physical exam, radiologic and pathologic H. Discuss the endoscopic management of clinically superficial TCC I. Discuss the endoscopic management of clinically locally invasive TCC J. Discuss the management of metastatic TCC K. Discuss the roles of topical chemotherapy and immunotherapy in management of TCC. L. Discuss the concepts of induction and maintenance and describe a typical regimen for BCG treatments in a patient who has recently been diagnosed as having recurrent superficial (Ta or T1), grade 2 TCC. M. Discuss the rationale and changing trends in standard of care for the use of various forms of radiation therapy alone or in conjunction with surgery and/or chemotherapy. N. Discuss various types of supravesical urinary diversion and considerations of their suitability in the context of particular disease stage and patient condition and motivation. 6
7 O. Discuss the rationale for use of systemic chemotherapy in the treatment of regional and metastatic TCC and list some of the more active agents. 6. Diagnosis and management of benign prostatic hyperplasia (BPH). A. Discuss the incidence / prevalence of BPH B. Discuss its pathophysiology with reference to the following: 1) Androgen dependence and the role of DHT and 5 alpha reductase enzyme explain mechanism of action of finasteride 2) Stromal and epithelial cell interaction and proliferation 3) Alpha adrenergic mediated smooth muscle tone in the prostate and bladder neck explain mechanism of action of alpha 1 blockers (Cardura and Hytrin) and the newer super selective alpha-1-c blockers (tamsulosin or Flomax). C. Demonstrate competency in assessing a patient s lower urinary tract symptoms (LUTS) and determining their AUA Symptom Score and their symptoms effect on quality of life ( bothersomeness score). D. List the specific indications for upper tract imaging and/or endoscopy in the evaluation of a man with moderate LUTS compatible with BPH. E. Describe the possible usefulness of uroflow studies, pressure/flow studies, CMG, PVR determinations, serum creatinine determinations, and urinalysis in evaluating BPH. F. Discuss the appropriateness of surgical intervention in men with serious complications of BPH, including urinary retention, intractable hematuria, bladder stones, and renal failure secondary to BPH. G. Discuss various treatment options and their relative risks, benefits, costs, and side effects. H. Discuss indications and demonstrate technical ability in preoperative, operative, and postoperative management of open subtotal prostatectomy for BPH. I. Discuss indications and demonstrate technical ability in performance of endoscopic management of BPH. 1) Demonstrate competence in the procedures: TURP and TUIP - discuss their relative indications and results. 2) Demonstrate knowledge of and ability to manage intraoperative and postoperative complications of TURP. 3) Be able to discuss the principles of electrocautery and its risks and benefits: J. Discuss the rationale, indications, relative effectiveness, and complications of the newer minimally invasive therapies for BPH, including laser prostatectomy (or ablation) [using contact, noncontact, or interstitial laser applications], balloon dilation, hyperthermia, thermal coagulation therapies, stents, and intraprostatic injection of absolute alcohol. K. Discuss the appropriate follow up of patients undergoing watchful waiting, as well as those on medical therapy and those having received one or more of the minimally invasive surgical alternatives. 7. Demonstrate an understanding of the neurology and muscle physiology of the bladder and urethral and their relationship to male continence and incontinence. A. List the types of male urinary incontinence including: overflow, urge, total, stress, functional, and enuretic. B. Discuss the history in differentiating the various etiologies including: congenital anomalies, neuropathic bladder dysfunction related to disease or injury to the CNS or peripheral nerves, trauma to sphincter, iatrogenic (including post-surgical), neoplasm, stricture, radiation induced, and psychogenic. 8. Describe the anatomic and physiological causes and effects of renal vascular hypertension. A. Provide a differential diagnosis and discuss management of the various types. B. Select and interpret appropriate diagnostic studies and discuss treatment recommendations and results. 1) Medical antihypertensive management 7
8 2) Percutaneous transluminal angioplasty (PTA) 3) Surgery including: bypass operations / revascularization / nephrectomy (or partial nephrectomy), endarterectomy, aneurysmectomy, and autotransplantation 9. Identify the signs and symptoms of urogenital trauma, clinically select the appropriate diagnostic studies, interpret them correctly, and then manage cases of trauma to the upper and lower urinary tract. 10. Discuss management of blunt and penetrating injuries to the kidney, ureter, bladder, urethra, and external genitalia. Discuss the results and complications of each course of treatment selected. 11. Demonstrate knowledge of cell and molecular biology pertaining to urologic diseases. A. Describe the mechanism of DNA storage, RNA transcription, and mrna transcription and translation. B. Identify the critical steps involved in the selective expression of eukaryotic cells. C. Demonstrate an awareness of the molecules involved in hormone action and cellular signal transduction, e.g., growth factors that mediate cellular function and reproduction. D. Discuss and provide examples of specific molecular defects associated with GU tumors and certain benign urological diseases. E. Identify specific molecular defects associated with various GU malignancies and discuss processes of gene amplification, gene deletion, gene rearrangement, and integrated viral gene activity. F. Discuss and provide specific examples of the classes of gene products associated with oncogenesis of the GU tract, including oncogenes, tumor suppressor genes, and cell death (apoptosis) suppressor and initiator genes. G. Discuss the molecular defects associated with benign GU diseases, e.g., papillomatosis and renal cystic disease. 12. Through supervised daily medical practice and through participation in clinical competencybased evaluation exercises, you should continue to acquire the necessary skills to achieve competence in the six (6) medical competencies: Patient Care, Medical Knowledge, Interpersonal and Communication Skills, Professionalism, Practice-Based Learning and Improvement, and Systems-Based Practice. I have reviewed with the resident his / her progress toward accomplishment of the stated goals and objectives for the current level of training and have provided individual feedback evaluation. Signed: Date: Program Director Note to Resident: At the end of each training year you will also be asked to self-evaluate your personal attainment of each educational goal and objective. You will indicate your perception of accomplishment of each stated goal and objective by marking in the margin alongside each the following coded response: + indicates satisfactory accomplishment of this particular goal or objective. indicates exposure to, but incomplete acquisition of, knowledge or experience.** - indicates perceived deficiency in knowledge or clinical experience in this area.** ** You are expected to carry these goals & objectives over to subsequent years. I have reviewed with the Program Director my understanding of educational goals and objectives expected during this year/level of training (prior to beginning this year), and have received individual feedback regarding my degree of accomplishment of the stated goals and objectives 8
9 including acquisition of competency in the six designated competencies (at the completion of this year). Signed: Date: Urology Resident 9
Goals & Objectives by Year in Training: U-1
 Goals & Objectives by Year in Training: U-1 U-1 (PGY-2, 3) Resident Responsibilities, Goals and Objectives In addition to the goals listed for PGY-1, the U-1 resident will add to his/her knowledge base
Goals & Objectives by Year in Training: U-1 U-1 (PGY-2, 3) Resident Responsibilities, Goals and Objectives In addition to the goals listed for PGY-1, the U-1 resident will add to his/her knowledge base
GENERAL GOALS & OBJECTIVES U-1. U-1 (PGY-2, 3) GENERAL GOALS and OBJECTIVES
 GENERAL GOALS & OBJECTIVES U-1 U-1 (PGY-2, 3) GENERAL GOALS and OBJECTIVES In addition to the goals listed for PGY-1, the U-1 resident will add to his/her knowledge base by participating actively in conferences,
GENERAL GOALS & OBJECTIVES U-1 U-1 (PGY-2, 3) GENERAL GOALS and OBJECTIVES In addition to the goals listed for PGY-1, the U-1 resident will add to his/her knowledge base by participating actively in conferences,
Hong Kong College of Surgical Nursing
 Hong Kong College of Surgical Nursing Higher Surgical Nursing Training: Part B Specialty - Urological Nursing Curriculum TABLE OF CONTENTS No. Contents Page. Introduction. Aims. Learning Objectives 4.
Hong Kong College of Surgical Nursing Higher Surgical Nursing Training: Part B Specialty - Urological Nursing Curriculum TABLE OF CONTENTS No. Contents Page. Introduction. Aims. Learning Objectives 4.
LOGBOOK EBU ORAL EXAM 2015
 LOGBOOK EBU ORAL EXAM 2015 Surname First Name Date of Birth (daymonthyear) MEDICAL DEGREE (MD) UROLOGIST TRAINING: - Training in urology - Training in surgery (as part of the urology training) - Other
LOGBOOK EBU ORAL EXAM 2015 Surname First Name Date of Birth (daymonthyear) MEDICAL DEGREE (MD) UROLOGIST TRAINING: - Training in urology - Training in surgery (as part of the urology training) - Other
Morbidity Audit and Logbook Tool SNOMED Board Reporting Terms for SET and IMG Urology ENDOSCOPIC LOWER URINARY TRACT
 ENDOSCOPIC LOWER URINARY TRACT Cystolitholapaxy Cystoscopic removal of foreign body from bladder Cystoscopic removal of ureteric stent Cystoscopy and cystodiathermy Cystoscopy and transurethral biopsy
ENDOSCOPIC LOWER URINARY TRACT Cystolitholapaxy Cystoscopic removal of foreign body from bladder Cystoscopic removal of ureteric stent Cystoscopy and cystodiathermy Cystoscopy and transurethral biopsy
Urolithiasis. Ali Kasraeian, MD, FACS Kasraeian Urology Advanced Laparoscopic, Robotic & Minimally Invasive Urologic Surgery
 Urolithiasis Ali Kasraeian, MD, FACS Kasraeian Urology Advanced Laparoscopic, Robotic & Minimally Invasive Urologic Surgery Urolithiasis: Why should we care? Affects 5% of US men and women Men twice as
Urolithiasis Ali Kasraeian, MD, FACS Kasraeian Urology Advanced Laparoscopic, Robotic & Minimally Invasive Urologic Surgery Urolithiasis: Why should we care? Affects 5% of US men and women Men twice as
The number following the procedure code is the TRICARE payment group. KIDNEY
 TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
What You Need to Know
 UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablative therapies, transurethral needle ablation, Adverse events, sexual side effects of BPH Aging, and incidence of BPH associated with
Index Note: Page numbers of article titles are in boldface type. A Ablative therapies, transurethral needle ablation, Adverse events, sexual side effects of BPH Aging, and incidence of BPH associated with
4 th Year Urology Core Objectives Keith Rourke (Revised June 1, 2007)
 4 th Year Urology Core Objectives Keith Rourke (Revised June 1, 2007) I. Genitourinary Trauma: 1. Goal: The student will be able to demonstrate a basic clinical approach to the management & diagnosis of
4 th Year Urology Core Objectives Keith Rourke (Revised June 1, 2007) I. Genitourinary Trauma: 1. Goal: The student will be able to demonstrate a basic clinical approach to the management & diagnosis of
UNM SRMC UROLOGY CLINICAL PRIVILEGES.
 o o o Initial privileges (initial appointment) Renewal of privileges (reappointment) Expansion of privileges (modification) INSTRUCTIONS All new applicants must meet the following requirements as approved
o o o Initial privileges (initial appointment) Renewal of privileges (reappointment) Expansion of privileges (modification) INSTRUCTIONS All new applicants must meet the following requirements as approved
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
RATIONALE: The organs making up the urinary system consist of the kidneys, bladder, urethra, and ureters.
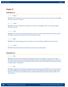 Chapter 12 Section Review 12.1 1. A. Kidneys RATIONALE: The renal pelvis receives urine from the kidney, travels through the ureters on the way to the bladder, but urine is formed in the kidney. 2. C.
Chapter 12 Section Review 12.1 1. A. Kidneys RATIONALE: The renal pelvis receives urine from the kidney, travels through the ureters on the way to the bladder, but urine is formed in the kidney. 2. C.
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH
 MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
Indiana Regional Medical Center Procedures to Labs/Tests June 1, 2011
 Indiana Regional Medical Center Procedures to Labs/Tests June 1, 2011 Urologic AMPUTATION OF PENIS Table 1 BIOPSY BLADDER Table 1 BIOPSY PENILE Table 1 BIOPSY URETERAL LESION Table 1 BLADDER DIVERTICULECTOMY
Indiana Regional Medical Center Procedures to Labs/Tests June 1, 2011 Urologic AMPUTATION OF PENIS Table 1 BIOPSY BLADDER Table 1 BIOPSY PENILE Table 1 BIOPSY URETERAL LESION Table 1 BLADDER DIVERTICULECTOMY
Benign Prostatic Hyperplasia (BPH):
 Benign Prostatic Hyperplasia (BPH): Evidence Based Guidelines for Primary Care Providers Jeanne Martin, DNP, ANP-BC Objectives 1. Understand the pathophysiology and prevalence of BPH 2. Select the appropriate
Benign Prostatic Hyperplasia (BPH): Evidence Based Guidelines for Primary Care Providers Jeanne Martin, DNP, ANP-BC Objectives 1. Understand the pathophysiology and prevalence of BPH 2. Select the appropriate
RESIDENT GOALS AND OBJECTIVES BY ROTATION U-1 U-1 (PGY-2,3) GOALS AND OBJECTIVES BY ROTATION
 RESIDENT GOALS AND OBJECTIVES BY ROTATION U-1 U-1 (PGY-2,3) GOALS AND OBJECTIVES BY ROTATION The following G&O s are representative of the unique experience gained at the individual institutions and represent
RESIDENT GOALS AND OBJECTIVES BY ROTATION U-1 U-1 (PGY-2,3) GOALS AND OBJECTIVES BY ROTATION The following G&O s are representative of the unique experience gained at the individual institutions and represent
At the end of the observership, the observer should be able to understand:
 PROGRAM A This program designed to refine the observer s skills in a urology subspecialty. The observers will be immersed, for 2 to 4 weeks, into the urology subspecialty of their choice. SPECIFIC ACADEMIC
PROGRAM A This program designed to refine the observer s skills in a urology subspecialty. The observers will be immersed, for 2 to 4 weeks, into the urology subspecialty of their choice. SPECIFIC ACADEMIC
Overview. Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia. Iain McAuley September 15, 2014
 Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia Iain McAuley September 15, 2014 Overview Review of the most recent guidelines for ED and BPH ED Guidelines CUA 2006 AUA 2011
Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia Iain McAuley September 15, 2014 Overview Review of the most recent guidelines for ED and BPH ED Guidelines CUA 2006 AUA 2011
UROLOGY TOPICS FOR SENIOR CLERKSHIP HEMATURIA
 UROLOGY TOPICS FOR SENIOR CLERKSHIP HEMATURIA Blood in urine is an important presenting symptom for many diseases of the urinary tract as well as for systemic disorders. Degree of hematuria has poor correlation
UROLOGY TOPICS FOR SENIOR CLERKSHIP HEMATURIA Blood in urine is an important presenting symptom for many diseases of the urinary tract as well as for systemic disorders. Degree of hematuria has poor correlation
Percutaneous nephrolithotomy (PCNL) (including cyctoscopy and retrograde catheterisation)
 UROLOGY PROCEDURE A ( RM 4401 - RM 4800 ) 1 Brachytherapy of prostate Radical prostatectomy, reconstruction of urinary bladder neck including bilateral 2 pelvic lymphadenectomy (Laparoscopic/Robotic) 3
UROLOGY PROCEDURE A ( RM 4401 - RM 4800 ) 1 Brachytherapy of prostate Radical prostatectomy, reconstruction of urinary bladder neck including bilateral 2 pelvic lymphadenectomy (Laparoscopic/Robotic) 3
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
SECTION R: UROLOGICAL SURGERY. Class Anae. Visits
 Visits Fee Class Anae 5R Initial Assessment $111.00 -- of a specific condition includes: pertinent family history, patient history, history of presenting complaint, functional enquiry, examination of affected
Visits Fee Class Anae 5R Initial Assessment $111.00 -- of a specific condition includes: pertinent family history, patient history, history of presenting complaint, functional enquiry, examination of affected
Loma Linda University Children s Hospital Loma Linda, CA UROLOGY PRIVILEGE FORM
 Name: Page 1 of 6 REQUEST CATEGORY MEMBERSHIP CATEGORY Provisional (Bylaws 4.3) Administrative (Bylaws 4.7) Affiliate (Bylaws(4.9) Active (Bylaws 4.2) Courtesy (Bylaws 4.4) Consulting (Bylaws 4.5) All
Name: Page 1 of 6 REQUEST CATEGORY MEMBERSHIP CATEGORY Provisional (Bylaws 4.3) Administrative (Bylaws 4.7) Affiliate (Bylaws(4.9) Active (Bylaws 4.2) Courtesy (Bylaws 4.4) Consulting (Bylaws 4.5) All
LIST OF CLINICAL PRIVILEGES UROLOGY
 AUTHORITY: Title 10, U.S.C. Chapter 55, Sections 1094 and 1102. PRINCIPAL PURPOSE: To define the scope and limits of practice for individual providers. Privileges are based on evaluation of the individual
AUTHORITY: Title 10, U.S.C. Chapter 55, Sections 1094 and 1102. PRINCIPAL PURPOSE: To define the scope and limits of practice for individual providers. Privileges are based on evaluation of the individual
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Benign Prostatic Hyperplasia (BPH)
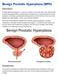 Benign Prostatic Hyperplasia (BPH) Definition Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate gland enlargement can cause bothersome
Benign Prostatic Hyperplasia (BPH) Definition Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate gland enlargement can cause bothersome
Clinical Curriculum: Urogynecology
 Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
PRIVILEGE APPLICATION FORM - [Mercy Medical Center]
![PRIVILEGE APPLICATION FORM - [Mercy Medical Center] PRIVILEGE APPLICATION FORM - [Mercy Medical Center]](/thumbs/78/77615248.jpg) Current Privilege Status Key Practitioner's Current Privilege status is signified in ( ) preceding each privilege. G = W = Withdrawn T = Temporary P = With Proctor A = Assist with C = With Consult E =
Current Privilege Status Key Practitioner's Current Privilege status is signified in ( ) preceding each privilege. G = W = Withdrawn T = Temporary P = With Proctor A = Assist with C = With Consult E =
SERVICE: Urology - Sinai, PGY 1
 SERVICE: Urology - Sinai, PGY 1 General description: The Sinai surgical residents will rotate in the Department of Urology at Sinai Hospital during their intern year. The duration of this rotation is 6
SERVICE: Urology - Sinai, PGY 1 General description: The Sinai surgical residents will rotate in the Department of Urology at Sinai Hospital during their intern year. The duration of this rotation is 6
Female Pelvic Medicine & Reconstructive Surgery
 Female Pelvic Medicine & Reconstructive Surgery APPLICATION FOR NEW FELLOWSHIP Name of Institution: McGill University Location: Royal Victoria Hospital (Glen Site), St Mary s Hospital Centre Type of Fellowship:
Female Pelvic Medicine & Reconstructive Surgery APPLICATION FOR NEW FELLOWSHIP Name of Institution: McGill University Location: Royal Victoria Hospital (Glen Site), St Mary s Hospital Centre Type of Fellowship:
An Undergraduate Syllabus for Urology. Produced on behalf of the British Association of Urological Surgeons. March 2012
 An Undergraduate Syllabus for Urology Produced on behalf of the British Association of Urological Surgeons March 2012 Authors H Hashim, P Jones, KJ O Flynn, I Pearce, J Royle, M Shaw, AM Sinclair Correspondence
An Undergraduate Syllabus for Urology Produced on behalf of the British Association of Urological Surgeons March 2012 Authors H Hashim, P Jones, KJ O Flynn, I Pearce, J Royle, M Shaw, AM Sinclair Correspondence
Original Policy Date
 MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
The 6-month course of the program is mainly dedicated to clinical experience (research time is also provided).
 Oncology Fellowship The oncology fellowship training course at Yonsei University Health System (Severance Hospital), comprising a 6-month and 1-year format, provides good quality and wide experience in
Oncology Fellowship The oncology fellowship training course at Yonsei University Health System (Severance Hospital), comprising a 6-month and 1-year format, provides good quality and wide experience in
Mini-Invasive Treatment in Urological Diseases Dott. Alberto Saita Responsabile Endourologia Istituto Clinico Humanitas - Rozzano
 Dipartimento di Urologia Direttore Prof. Giorgio Guazzoni Mini-Invasive Treatment in Urological Diseases Dott. Alberto Saita Responsabile Endourologia Istituto Clinico Humanitas - Rozzano alberto.saita@humanitas.it
Dipartimento di Urologia Direttore Prof. Giorgio Guazzoni Mini-Invasive Treatment in Urological Diseases Dott. Alberto Saita Responsabile Endourologia Istituto Clinico Humanitas - Rozzano alberto.saita@humanitas.it
Management of Voiding Dysfunction after Prostate Radiotherapy
 Management of Voiding Dysfunction after Prostate Radiotherapy Up to Date Symposium on Uro-Oncology December 7, 2012 Belo Horizonte, Brazil Jaspreet S. Sandhu, MD Department of Surgery/Urology Memorial
Management of Voiding Dysfunction after Prostate Radiotherapy Up to Date Symposium on Uro-Oncology December 7, 2012 Belo Horizonte, Brazil Jaspreet S. Sandhu, MD Department of Surgery/Urology Memorial
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation, of prostate, holmium laser, 485 495 African prune tree (Pygeum africanum), 454 455 Alfuzosin, 445 446 Alpha-adrenergic agonists,
Index Note: Page numbers of article titles are in boldface type. A Ablation, of prostate, holmium laser, 485 495 African prune tree (Pygeum africanum), 454 455 Alfuzosin, 445 446 Alpha-adrenergic agonists,
The Correction of Common Coding Problems in Urology
 2012 AAPC National Conference Las Vegas, Nevada April 1-4, 2012 Michael A. Ferragamo MD, FACS Clinical Assistant Professor of Urology State University of New York Stony Brook, Long Island, New York Editor:
2012 AAPC National Conference Las Vegas, Nevada April 1-4, 2012 Michael A. Ferragamo MD, FACS Clinical Assistant Professor of Urology State University of New York Stony Brook, Long Island, New York Editor:
HEALTHMAN UROLOGY COSTING GUIDE 2013
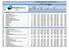 HEALTHMAN UROLOGY COSTING GUIDE COMPARATIVE TARIFFS: Scheme Rates Base Rates Practice Cost Tariff (VAT Incl.) Discovery (VAT incl.) Consultations: Units R R R R R R R R R R See the Notes below for All
HEALTHMAN UROLOGY COSTING GUIDE COMPARATIVE TARIFFS: Scheme Rates Base Rates Practice Cost Tariff (VAT Incl.) Discovery (VAT incl.) Consultations: Units R R R R R R R R R R See the Notes below for All
Policy for Prostatism/Lower Urinary Tract Symptoms in men
 NHS Halton Clinical Commissioning Group NHS Liverpool Clinical Commissioning Group NHS St Helens Clinical Commissioning Group NHS South Sefton Clinical Commissioning Group NHS Southport and Formby Clinical
NHS Halton Clinical Commissioning Group NHS Liverpool Clinical Commissioning Group NHS St Helens Clinical Commissioning Group NHS South Sefton Clinical Commissioning Group NHS Southport and Formby Clinical
MODULE 3: BENIGN PROSTATIC HYPERTROPHY
 MODULE 3: BENIGN PROSTATIC HYPERTROPHY KEYWORDS: Prostatic hypertrophy, prostatic hyperplasia, PSA, voiding dysfunction, lower urinary tract symptoms (LUTS) At the end of this clerkship, the medical student
MODULE 3: BENIGN PROSTATIC HYPERTROPHY KEYWORDS: Prostatic hypertrophy, prostatic hyperplasia, PSA, voiding dysfunction, lower urinary tract symptoms (LUTS) At the end of this clerkship, the medical student
URINARY INCONTINENCE. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
Urinary Adverse Events after Radiation Therapy for Prostate Cancer
 Urinary Adverse Events after Radiation Therapy for Prostate Cancer Sexual Medicine Society of North America Scottsdale, Arizona 2016 Jaspreet S. Sandhu, MD Department of Surgery/Urology Memorial Sloan
Urinary Adverse Events after Radiation Therapy for Prostate Cancer Sexual Medicine Society of North America Scottsdale, Arizona 2016 Jaspreet S. Sandhu, MD Department of Surgery/Urology Memorial Sloan
Module Title: GENITO-URINARY TRACT Date: May 2013 Module Rationale and Competencies
 Module Title: Date: May 2013 Module Rationale and Competencies A paediatric surgeon is required to have a thorough understanding of normal anatomy and physiology, pathophysiology, investigations, differential
Module Title: Date: May 2013 Module Rationale and Competencies A paediatric surgeon is required to have a thorough understanding of normal anatomy and physiology, pathophysiology, investigations, differential
The 82 nd UWI/BAMP CME Conference November 18, Jeetu Nebhnani MBBS D.M. Urology Consultant Urologist
 The 82 nd UWI/BAMP CME Conference November 18, 2017 Jeetu Nebhnani MBBS D.M. Urology Consultant Urologist Disclosures Outline Index case Introduction Etiology Risk factors Acute stone event Conservative
The 82 nd UWI/BAMP CME Conference November 18, 2017 Jeetu Nebhnani MBBS D.M. Urology Consultant Urologist Disclosures Outline Index case Introduction Etiology Risk factors Acute stone event Conservative
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
The Enlarged Prostate Symptoms, Diagnosis and Treatment
 The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
Regions Hospital Delineation of Privileges Urology
 Regions Hospital Delineation of s Urology Applicant s Name: Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic formal training
Regions Hospital Delineation of s Urology Applicant s Name: Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic formal training
Ralph & Berryl Goldman Fellowship in Neuro urology, voiding dysfunction and bladder reconstruction
 Ralph & Berryl Goldman Fellowship in Neuro urology, voiding dysfunction and bladder reconstruction Length of fellowship: A 1 year Fellowship: This fellowship has been designed for Urology or Gynecology
Ralph & Berryl Goldman Fellowship in Neuro urology, voiding dysfunction and bladder reconstruction Length of fellowship: A 1 year Fellowship: This fellowship has been designed for Urology or Gynecology
Lec-8 جراحة بولية د.نعمان
 4th stage Lec-8 جراحة بولية د.نعمان 11/10/2015 بسم هللا الرحمن الرحيم Ureteric, Vesical, & urethral stones Ureteric Calculus Epidemiology like renal stones Etiology like renal stones Risk factors like
4th stage Lec-8 جراحة بولية د.نعمان 11/10/2015 بسم هللا الرحمن الرحيم Ureteric, Vesical, & urethral stones Ureteric Calculus Epidemiology like renal stones Etiology like renal stones Risk factors like
EAU GUIDELINES POCKET EDITION 3
 EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
University of Alberta Reconstructive Urology Fellowship
 FACULTY OF MEDICINE AND DENTISTRY DEPARTMENT OF SURGERY DIVISION OF UROLOGY Keith Rourke, MD, FRCSC Reconstructive Urology Professor Chair of Academic Urology Reconstructive Urology Fellowship Director
FACULTY OF MEDICINE AND DENTISTRY DEPARTMENT OF SURGERY DIVISION OF UROLOGY Keith Rourke, MD, FRCSC Reconstructive Urology Professor Chair of Academic Urology Reconstructive Urology Fellowship Director
Incontinence. When I was given this topic in urology to discuss with you today I
 Incontinence When I was given this topic in urology to discuss with you today I was slightly disappointed. I personally see mostly men for problems such as stones, benign prostatic hyperplasia, prostate
Incontinence When I was given this topic in urology to discuss with you today I was slightly disappointed. I personally see mostly men for problems such as stones, benign prostatic hyperplasia, prostate
HMM 4401 Genito-urinary tract diseases
 HMM 4401 Genito-urinary tract diseases Urine production Core elements: Glomerulus, proximal and distal convoluted tube, loop of Henle, collecting tubules, ureters, bladder, sphincter, uretra, and out
HMM 4401 Genito-urinary tract diseases Urine production Core elements: Glomerulus, proximal and distal convoluted tube, loop of Henle, collecting tubules, ureters, bladder, sphincter, uretra, and out
WJ UROGENITAL SYSTEM. UROLOGY
 WJ UROGENITAL SYSTEM. UROLOGY 1 Societies 11 History Include all aspects 13 Dictionaries. Encyclopaedias. Bibliographies Use for general works only. Classify with specific aspect where possible 15 Classification.
WJ UROGENITAL SYSTEM. UROLOGY 1 Societies 11 History Include all aspects 13 Dictionaries. Encyclopaedias. Bibliographies Use for general works only. Classify with specific aspect where possible 15 Classification.
M E M O R A N D U M. RE: Resident Surgical Index Case List Redefined For 2009: Recommended Minimum Numbers and Core Domains Emphasized
 M E M O R A N D U M TO: FROM: Urology Program Directors Louise King Executive Director, Residency Review Committee for Urology 312.755.5498 lking@acgme.org Members, Review Committee for Urology DATE: February
M E M O R A N D U M TO: FROM: Urology Program Directors Louise King Executive Director, Residency Review Committee for Urology 312.755.5498 lking@acgme.org Members, Review Committee for Urology DATE: February
Atlas of Urologic Surgery
 Atlas of Urologic Surgery Hinman, F ISBN-13: 9781416042105 Table of Contents Section I: Surgical Basics Chapter 1 Surgical Basics Section II: The Urologist at Work Chapter 2 Basic Surgical Techniques Chapter
Atlas of Urologic Surgery Hinman, F ISBN-13: 9781416042105 Table of Contents Section I: Surgical Basics Chapter 1 Surgical Basics Section II: The Urologist at Work Chapter 2 Basic Surgical Techniques Chapter
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Alcohol abusers Allergy(ies) Anesthesia/anesthetics, 497 519. See also Office-based anesthesia (OBA) for sperm retrieval for infertility,
Index Note: Page numbers of article titles are in boldface type. A Alcohol abusers Allergy(ies) Anesthesia/anesthetics, 497 519. See also Office-based anesthesia (OBA) for sperm retrieval for infertility,
What is Benign Prostatic Hyperplasia (BPH)?
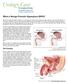 What is Benign Prostatic Hyperplasia (BPH)? Benign prostatic hyperplasia (BPH) is an enlarged prostate. The prostate goes through two main growth periods as a man ages. The first occurs early in puberty,
What is Benign Prostatic Hyperplasia (BPH)? Benign prostatic hyperplasia (BPH) is an enlarged prostate. The prostate goes through two main growth periods as a man ages. The first occurs early in puberty,
2017 Coding and Reimbursement Survival Guide
 2017 Coding and Reimbursement Survival Guide Chapter 20: Urology CPT Changes: Key Into Guideline Updates for Successful Procedure Coding in 2017 Plus: New coding tips also will help keep you on track.
2017 Coding and Reimbursement Survival Guide Chapter 20: Urology CPT Changes: Key Into Guideline Updates for Successful Procedure Coding in 2017 Plus: New coding tips also will help keep you on track.
Hydronephrosis. What is hydronephrosis?
 What is hydronephrosis? Hydronephrosis Hydronephrosis describes the situation where the urine collecting system of the kidney is dilated. This may be a normal variant or it may be due to an underlying
What is hydronephrosis? Hydronephrosis Hydronephrosis describes the situation where the urine collecting system of the kidney is dilated. This may be a normal variant or it may be due to an underlying
All about the Prostate
 MEN S HEALTH Dr Nick Pendleton January 16 th 2018 All about the Prostate 1 What does it do? Functions of the Prostate 1. Secretes Prostatic Fluid slightly alkaline fluid, 30% of volume of seminal fluid,
MEN S HEALTH Dr Nick Pendleton January 16 th 2018 All about the Prostate 1 What does it do? Functions of the Prostate 1. Secretes Prostatic Fluid slightly alkaline fluid, 30% of volume of seminal fluid,
Urologist. From Wikipedia, the free encyclopedia. Occupation. Occupation type Activity sectors
 1 of 6 1/5/2017 2:03 PM From Wikipedia, the free encyclopedia Urology (from Greek οὖρον ouron "urine" and -λογία -logia "study of"), also known as genitourinary surgery, is the branch of medicine that
1 of 6 1/5/2017 2:03 PM From Wikipedia, the free encyclopedia Urology (from Greek οὖρον ouron "urine" and -λογία -logia "study of"), also known as genitourinary surgery, is the branch of medicine that
Introduction/Learning Objectives. Incontinence: Natural History. Course Outline 10/14/2016. Urinary Incontinence: Conservative Measures
 Management of Urinary Complications after Prostatectomy Course Faculty: Introduction/Learning Objectives Jaspreet S. Sandhu, MD Associate Attending Urologist Department of Surgery/Urology Memorial Sloan
Management of Urinary Complications after Prostatectomy Course Faculty: Introduction/Learning Objectives Jaspreet S. Sandhu, MD Associate Attending Urologist Department of Surgery/Urology Memorial Sloan
Voiding Dysfunction Block lecture, 5 th year student. Choosak Pripatnanont, Department of Surgery, PSU.
 Voiding Dysfunction 2009 Block lecture, 5 th year student. Choosak Pripatnanont, Department of Surgery, PSU. Objectives Understand and explain physiologic function and dysfunction of lower urinary tract.
Voiding Dysfunction 2009 Block lecture, 5 th year student. Choosak Pripatnanont, Department of Surgery, PSU. Objectives Understand and explain physiologic function and dysfunction of lower urinary tract.
RESIDENCY TRAINING PROGRAMME IN UROLOGY CERTIFICATION APPLICATION FORM PARTICIPATING INSTITUTE(S)
 Date application Name primary institute RESIDENCY TRAINING PROGRAMME IN UROLOGY CERTIFICATION APPLICATION FORM Name affiliated institute(s) Name Programme Director PARTICIPATING INSTITUTE(S) This form
Date application Name primary institute RESIDENCY TRAINING PROGRAMME IN UROLOGY CERTIFICATION APPLICATION FORM Name affiliated institute(s) Name Programme Director PARTICIPATING INSTITUTE(S) This form
Loss of Bladder Control
 BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
Rezūm procedure for the Prostate
 Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
University of Alberta Reconstructive Urology Fellowship
 University of Alberta Reconstructive Urology Fellowship 1. Overview 2. Eligibility Requirements 3. Funding 4. Clinical Expectations 5. Academic Expectations 6. Objectives of Training 7. Teaching Methods
University of Alberta Reconstructive Urology Fellowship 1. Overview 2. Eligibility Requirements 3. Funding 4. Clinical Expectations 5. Academic Expectations 6. Objectives of Training 7. Teaching Methods
Victoria Sharp, MD, MBA, FAAFP. Clinical Professor of Urology and Family Medicine
 Victoria Sharp, MD, MBA, FAAFP Clinical Professor of Urology and Family Medicine Victoria Sharp, MD, MBA, FAAFP Market Chief Medial Officer AmeriHealth Caritas Family of Companies Office phone: (515) 330-3740
Victoria Sharp, MD, MBA, FAAFP Clinical Professor of Urology and Family Medicine Victoria Sharp, MD, MBA, FAAFP Market Chief Medial Officer AmeriHealth Caritas Family of Companies Office phone: (515) 330-3740
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics. Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital
 Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Urogynecology ICD-9 to ICD-10 Crosswalks
 1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
Shlomi Albert, M.D., Inc Warner Avenue, Suite 423 Fountain Valley, Ca Tel (714) Fax (714) Kidney Stone Disease in Adults
 Shlomi Albert, M.D., Inc. 11160 Warner Avenue, Suite 423 Fountain Valley, Ca 92708 Tel (714)549-3333 Fax (714)549-3334 Kidney Stone Disease in Adults Overview Kidney stones are one of the most painful
Shlomi Albert, M.D., Inc. 11160 Warner Avenue, Suite 423 Fountain Valley, Ca 92708 Tel (714)549-3333 Fax (714)549-3334 Kidney Stone Disease in Adults Overview Kidney stones are one of the most painful
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
SURGICAL PROCEDURES OPERATIONS ON THE UROGENITAL SYSTEM
 KIDNEYS AND PERINEPHRUM 1. No additional claim should be made for nephroscopy when done at the time of pyelolithotomy or nephrolithotomy. 2. In a routine surgical approach to the kidney and related procedures,
KIDNEYS AND PERINEPHRUM 1. No additional claim should be made for nephroscopy when done at the time of pyelolithotomy or nephrolithotomy. 2. In a routine surgical approach to the kidney and related procedures,
Prostate Health PHARMACIST VIEW
 Prostate Health PHARMACIST VIEW Prostate Definition Prostate is a gland made of fibromuscular tissue. It is about 4 cm and surrounds the neck of the bladder and the urethra. It produces seminal fluid.
Prostate Health PHARMACIST VIEW Prostate Definition Prostate is a gland made of fibromuscular tissue. It is about 4 cm and surrounds the neck of the bladder and the urethra. It produces seminal fluid.
January Dear Medical Director:
 January 2010 Dear Medical Director: It is the position of the American Urological Association (AUA) that urologists are appropriately trained in the performance of sonographic procedures. In spite of this,
January 2010 Dear Medical Director: It is the position of the American Urological Association (AUA) that urologists are appropriately trained in the performance of sonographic procedures. In spite of this,
Definition Prostate cancer
 Prostate cancer 61 Definition Prostate cancer is a malignant neoplasm that arises from the prostate gland and the most common form of cancer in men. localized prostate cancer is curable by surgery or radiation
Prostate cancer 61 Definition Prostate cancer is a malignant neoplasm that arises from the prostate gland and the most common form of cancer in men. localized prostate cancer is curable by surgery or radiation
Urological Procedure Coding
 Urological Procedure Coding AAPC Annual Conference April 6, 2011 Long Beach, California Objectives Understand anatomy and CPT procedural terminology related to urological procedures Recognize and code
Urological Procedure Coding AAPC Annual Conference April 6, 2011 Long Beach, California Objectives Understand anatomy and CPT procedural terminology related to urological procedures Recognize and code
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Limited text update March 2015) B. Blok (Co-chair), J. Pannek (Co-chair), D. Castro Diaz, G. del Popolo, J. Groen, T. Gross (Guidelines ssociate), R. Hamid, G. Karsenty, T.M.
GUIDELINES ON NEURO-UROLOGY (Limited text update March 2015) B. Blok (Co-chair), J. Pannek (Co-chair), D. Castro Diaz, G. del Popolo, J. Groen, T. Gross (Guidelines ssociate), R. Hamid, G. Karsenty, T.M.
Specific Basic Standards for Osteopathic Fellowship Training in Nephrology
 Specific Basic Standards for Osteopathic Fellowship Training in Nephrology American Osteopathic Association and American College of Osteopathic Internists BOT Rev. 2/2011 These specific basic standards
Specific Basic Standards for Osteopathic Fellowship Training in Nephrology American Osteopathic Association and American College of Osteopathic Internists BOT Rev. 2/2011 These specific basic standards
We welcome comments and corrections which will be used to improve the system annually.
 ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
NON-Neurogenic Chronic Urinary Retention AUA White Paper
 NON-Neurogenic Chronic Urinary Retention AUA White Paper Great Lakes SUNA Inside Urology March 16, 2018 Michelle J. Lajiness FNP-BC Nurse Practitioner DMC Urology Incidence Really unknown Lack consensus
NON-Neurogenic Chronic Urinary Retention AUA White Paper Great Lakes SUNA Inside Urology March 16, 2018 Michelle J. Lajiness FNP-BC Nurse Practitioner DMC Urology Incidence Really unknown Lack consensus
Urinary System Part of the Excretory System
 Urinary System Part of the Excretory System Bellwork **only write the term and underlined definition INCONTINENCE involuntary urination, often seem in older persons, or due to illness and disease ENURESIS
Urinary System Part of the Excretory System Bellwork **only write the term and underlined definition INCONTINENCE involuntary urination, often seem in older persons, or due to illness and disease ENURESIS
AQUA Registry 2019 Non-QPP Measure Specifications. Denominator Exceptions. IPSS<8 None None Yes Patient Reported Outcome (PRO)
 AQUA12 Benign Prostate Hyperplasia: IPSS improvement after diagnosis with NEW diagnosis of clinically significant BPH who had IPSS (international prostate symptoms score) or AUASS (American urological
AQUA12 Benign Prostate Hyperplasia: IPSS improvement after diagnosis with NEW diagnosis of clinically significant BPH who had IPSS (international prostate symptoms score) or AUASS (American urological
Imaging Ejaculatory Disorders and Hematospermia
 ATHENS 4-6 October 2018 European Society of Urogenital Radiology Imaging Ejaculatory Disorders and Hematospermia Parvati Ramchandani, MD Professor, Radiology and Surgery University of Pennsylvania Medical
ATHENS 4-6 October 2018 European Society of Urogenital Radiology Imaging Ejaculatory Disorders and Hematospermia Parvati Ramchandani, MD Professor, Radiology and Surgery University of Pennsylvania Medical
Canadian Undergraduate Urology Curriculum (CanUUC): Prostate Diseases
 Canadian Undergraduate Urology Curriculum (CanUUC): Prostate Diseases LUTS/Benign Prostate Hyperplasia Objectives 1. List the lower urinary tract symptoms (LUTS) found in men with BPH. 2. List the differential
Canadian Undergraduate Urology Curriculum (CanUUC): Prostate Diseases LUTS/Benign Prostate Hyperplasia Objectives 1. List the lower urinary tract symptoms (LUTS) found in men with BPH. 2. List the differential
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA. A Minimally Invasive Innovative Treatment
 PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
Subspecialty Procedural Volume Guidelines
 Subspecialty Review Committee for Obstetrics and Gynecology In response to requests from program directors, and in an effort to be transparent, the Review Committee for Obstetrics and Gynecology has elected
Subspecialty Review Committee for Obstetrics and Gynecology In response to requests from program directors, and in an effort to be transparent, the Review Committee for Obstetrics and Gynecology has elected
When to worry, when to test?
 Focus on CME at the University of Calgary Prostate Cancer: When to worry, when to test? Bryan J. Donnelly, MSc, MCh, FRCSI, FRCSC Presented at a Canadian College of Family Practitioner s conference (October
Focus on CME at the University of Calgary Prostate Cancer: When to worry, when to test? Bryan J. Donnelly, MSc, MCh, FRCSI, FRCSC Presented at a Canadian College of Family Practitioner s conference (October
Management of Voiding Problems in Older Men. Dr. John Fenn Consultant, QEH 10 th October, 2005
 Management of Voiding Problems in Older Men Dr. John Fenn Consultant, QEH 10 th October, 2005 Voiding Problems Poor stream Hesitancy Straining Incomplete emptying Intermittent micturition Terminal dribbling
Management of Voiding Problems in Older Men Dr. John Fenn Consultant, QEH 10 th October, 2005 Voiding Problems Poor stream Hesitancy Straining Incomplete emptying Intermittent micturition Terminal dribbling
Managing urinary morbidity after brachytherapy. Kieran O Flynn Department of Urology, Salford Royal Foundation Trust, Manchester
 Managing urinary morbidity after brachytherapy Kieran O Flynn Department of Urology, Salford Royal Foundation Trust, Manchester Themes Can we predict urinary morbidity? Prevention of urinary morbidity
Managing urinary morbidity after brachytherapy Kieran O Flynn Department of Urology, Salford Royal Foundation Trust, Manchester Themes Can we predict urinary morbidity? Prevention of urinary morbidity
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
KIDNEY STONES. When to call for help Call these rooms if any of the following occur:
 KIDNEY STONES Background Kidney stones that move into the ureter (the narrow tube that drains each kidney) often cause a lot of pain. If the stones measure 5mm or less in diameter then most will eventually
KIDNEY STONES Background Kidney stones that move into the ureter (the narrow tube that drains each kidney) often cause a lot of pain. If the stones measure 5mm or less in diameter then most will eventually
Associated Terms: Bladder Stones, Ureteral Stones, Kidney Stones, Cystotomy, Urolithiasis, Cystic Calculi
 Associated Terms: Bladder Stones, Ureteral Stones, Kidney Stones, Cystotomy, Urolithiasis, Cystic Calculi The term "ACVS Diplomate" refers to a veterinarian who has been board certified in veterinary surgery.
Associated Terms: Bladder Stones, Ureteral Stones, Kidney Stones, Cystotomy, Urolithiasis, Cystic Calculi The term "ACVS Diplomate" refers to a veterinarian who has been board certified in veterinary surgery.
