Advanced Wound Management: Nine Myths and Realities (2008)
|
|
|
- Hilary Pearson
- 5 years ago
- Views:
Transcription
1 Advanced Wound Management: Nine Myths and Realities (2008) Marvin A. Wayne, MD, FACEP; Adam J. Singer, MD, FACEP Wherever wounds occur on the body, the goals of wound management are the same: early closure, prevention of infection, a cosmetically appealing scar, and a functional scar. All of the steps taken in managing wounds aim for these results. The history of wound closure is an interesting and somewhat bizarre one. The first written records of the treatment of wounds date from around 2,500 BC. Plants figured prominently in their treatment for more than 1,000 years. Herbs were applied in a balsam, leaves and grasses were used as bandages. Honey, butter, clay, and bark were used as medicines; urine, dung, and blood were used more for ritualistic significance. During the Middle Ages purulence was considered essential for wound healing. As a result, wounds were intentionally contaminated to produce pus. The earliest record of using sutures to close wounds comes from a mummy dating from 1100 BC. An early form of staples (developed in the early 20th century) can also be found in the ancient Hindu civilization where wounds were closed with the jaws of dead ants. The number and varieties of wounds seen by emergency physicians justify continuing interest in their care. In 2005, the most recent figures provided by the National Center for Health Statistics, of approximately 120 million emergency department visits, there were 12 million wounds, 7 million lacerations, 2.5 million abscesses, and 430, 000 burns serious enough to be treated in the ED. Lacerations occur in many parts of the body, which often influences how they are treated. Lacerations most commonly occur on the upper extremities (38%), face (27%), and trunk (13%) with eleven percent each on the lower extremities and in the head and neck area. With a long history of technique and reported results, many myths about the management of wounds still abound. This article examines some of the most common ones. Myth #1: Keeping wounds dry prevents wound infection and speeds healing Until the mid 20th century wounds were kept dry to avoid infection. Studies in pigs showed that the occlusion of partial thickness wounds doubled the rate of re-epithelization. Early studies in humans seemed to confirm that occluded wounds healed faster. Later studies have confirmed the advantages of moist wound healing. It has been shown that a moist wound healing environment helps prevent cell dehydration and death. It also promotes angiogenesis, improves phagocytosis, and growth factor elaboration. Further it improves the rate of reepithelialization, reduces pain and improves the cosmetic outcome. Those who objected to the moist healing strategy based their opinion on the concern that under occluded dressings, bacteria proliferated and would cause infection. However, most studies have not confirmed this suspicion. In fact, a meta-analysis, of over 3000 wounds covered with occlusive dressings or gauze, demonstrated that wound infection rates were significantly lower with occlusive dressings: 2.6% of those with occlusive dressings became infected versus 7.1% of those with gauze dressing, with a significant P value. Reality: Infection rates are lower and healing is faster when wounds are kept moist. 1
2 Myth #2: Using sterile technique for lacerations commonly seen in the emergency department is necessary to prevent wound infection It may seem counterintuitive that there should be a question of whether or not sterile technique will prevent wound infection. However, a study of the effect of using caps and masks on infection rates is revealing. A study of 442 lacerations, of which 239 were repaired using a cap and mask, and 203 without them, demonstrated that the incidence of infection was 2.5% in wounds treated with clinicians wearing caps and masks, and 3.9% in those treated without the presence of caps and masks with no statistically significant difference between the groups. Thus, caps and masks do not seem to prevent infection. As always, common sense should prevail. A mask should be used when the practitioner has a respiratory infection and is sneezing and coughing. Another study looked at sterile vs. non-sterile gloves as a factor in wound infections. A multicenter, single blind, randomized study looked at 816 patients randomized to laceration repair using sterile and non-sterile gloves. Most of the wounds were sutured; 25% were treated with topical antibiotics. Ninety-seven percent were followed up within one week. Of those in the sterile glove group, 6.1% developed infection vs. 4.4% in the non-sterile group. Several other similar studies have also come to the same conclusion. Reality: Using caps, masks, and sterile gloves do not appear to be necessary for the average laceration treated in the emergency department. Myth #3: Irrigation of facial and scalp lacerations is necessary to prevent wound infection While there is evidence that irrigation lowers infection rates in contaminated wounds created in animals, there is no evidence that irrigation is effective in clean, low-risk wounds in humans. Overall infection rates after traumatic laceration repair in the ED are around 3-5%, and even lower in well vascularized facial and scalp lacerations. To examine whether high pressure irrigation is necessary in facial and scalp wounds, an observational study of 1,923 wounds, of which 1,090 were irrigated and 833 were not, compared both infection rates and cosmetic outcome of low-risk wounds based on whether or not they were irrigated. (The cosmetic parameter was added because high pressure irrigation might cause wound distortion that is difficult to correct.) The groups compared were similar in terms of patient demographics and wound characteristics: length of wounds, layers of closure, and use of antibiotics. The results of this study were that infection rates were similar in those whose wounds were irrigated (0.9%) and those whose wounds were not (1.4%). In terms of cosmetic outcome, 76% of the irrigated group achieved a good result, while 82% of the non-irrigated group achieved a good result. While the difference between groups in cosmetic outcome was not statistically significant there certainly was a trend (P=0.07) favoring no irrigation. Reality: Irrigation of low-risk facial and scalp lacerations of the type generally seen in the emergency department does not lower the incidence of infection, but may result in a less optimal cosmetic result. Dirty or highly contaminated wounds still 2
3 require meticulous cleansing and irrigation. Myth # 4: Saline is more effective than tap water in preventing wound infection Somehow the idea of running tap water over a wound seems less appropriate than irrigating it with saline solution. However, saline costs more than tap water and is not readily available outside of the hospital. Is there any evidence that saline is more effective than tap water at preventing wound infections? A randomized, controlled study of 530 wounds in pediatric patients treated in the emergency department was designed to compare wound infection rates. Saline was used is 271 patients, tap water was used in 259. While the baseline characteristics in both study groups were fairly similar, there were more hand lacerations in the group randomized to tap water irrigation (which would tend to increase the rate of infections in this group!) The results were as follows: of the saline-irrigated group, 2.8% developed an infection. Of the tap-water irrigated group, 2.9% developed an infection. There was no difference whatsoever between the tap water and saline. Other studies have mimicked these results. Thus there is no evidence that saline is more effective than tap water in preventing infection, yet it is commonly used in the United States at considerable expense to healthcare institutions. In other countries in the world where saline is unaffordable, tap water is used. Assuming the tap water is not contaminated, it seems to be effective. Reality: Saline is no more effective in preventing wound infections than tap water. Myth #5: There is a direct relationship between the time interval from injury to closure and wound infection rates One of the oldest wound controversies concerns the length of the so-called golden period of the wound. This period refers to the time interval between wound injury and closure when it is still safe to close wounds without significantly increasing the risk of infection. Some have recommended that wounds older than 6-12 hours not be closed. Several studies have come up with different results based on the types of wounds and patients. One of the largest studies comes from Jamaica where many of the patients have dirty wounds and present relatively late to the ED. This study was an observational study that compared healing rates at 7 days, without infection, between wounds closed within and beyond 19 hours of injury. The results of this study are representative of other studies demonstrating that lacerations over the face, head and neck can be safely closed even after 19 hours without increasing the risk of infection. In contrast, lacerations over the lower extremities and trunk have an increased risk of infection and non-healing when closed after 19 hours from injury. Thus the golden period of the wound needs to be individualized based on patient and wound characteristics including, but not limited to, wound location. Reality: For wounds on the face, head, and neck, there is no evidence that delayed closure results in any increase in the rate of wound infection. Wounds on the truck, arms, and legs probably should not be closed after 6-12 hours. Myth #6: Mammalian bites treated with primary closure have an increased wound 3
4 infection rate. An observational study from 2000 looked at 145 patients with mammalian bites from dogs, cats, and humans (not many human bites were included) treated with primary closure, with a mean time from injury to treatment of up to 1.8 hours. Fifty seven percent were on the head and neck, and 36% were on the extremities. The infection rate in these patients with bite wounds was 5.5%, compared with infection rates for non-bite wounds of 3-7%. Essentially, the infection rate was the same. What about dog bites specifically? In 1988, 96 patients with 169 wounds were studied in a randomized clinical trial. Of these, 92 wounds were randomized to suturing and 77 were left open. Most of the wounds were short and on the hands. The average delay from wound to treatment was 2.5 hours. No systemic antibiotics were given in any of the patients. The rate of infection in both groups of patients was approximately 8%. Since the cosmetic outcome of facial lacerations is so important and overall infection rates in this area tend to be low, most facial lacerations are sutured, regardless of whether they are caused by dog, cat, or human bites. When it comes to extremities, where infection rates are higher and cosmesis less important, most small puncture wounds are closed while large wounds are loosely closed and patients are given oral antibiotics for prophylaxis. What about giving antibiotics to prevent infection in patients with dog bites? In eight randomized studies reported in the 2001 Cochrane database it was clear that antibiotics reduced infections in wounds caused by human bites, but did not reduce infections caused by dog or cat bites. However, regardless of the cause of extremity bites, these wounds benefited most from prophylactic systemic antibiotics. Reality: Lacerations on the face from any mammalian bite (especially if large) can be sutured. Regarding antibiotics, studies confirm that antibiotics reduce infections in wounds caused by human bites, and for extremity bites. Myth #7: Sutures are the best wound closure device for lacerations. While sutures have been around the longest, the question is what is the best or most appropriate method of closing wounds: sutures, staples, surgical tapes, or topical skin adhesives? All of the currently available wound closure devices have a role in wound closure, each with a set of advantages and disadvantages. Sutures are the time-honored method of closing wounds, but they are painful to insert and painful to remove for the patient. They are relatively expensive, there is a risk of a needle stick injury for the provider, they are time consuming to put in, operator dependent, and they cause greater tissue reactivity than the other wound closure devices. On the other hand, sutures provide the most meticulous closure, the greatest tensile strength, and the lowest dehiscence rate. Another major disadvantage of sutures is that most require removal. Sutures that are left in the skin beyond 7 days tend to result in the formation of ugly dots on either side of the wound. Fast absorbing sutures may be used to avoid the need for removal. In general, sutures are the most appropriate wound closure device for complex and high tension wounds and over areas where other devices may be inappropriate, such as the hair and mucous membranes. 4
5 Staples are excellent for scalp wounds. Other than washing them out, no further dressings are required. Staples are quick to apply, require little training, have low tissue reactivity, are low cost, and there is a very low risk of a needle stick. The disadvantages are that they result in a less meticulous closure, they may interfere with imaging, and they require removal, which can be painful. Surgical tape is inexpensive, has the lowest infection rates in animal models, is rapid to place, comfortable for the patient, and is the least tissue reactive of all the wound closure devices. However, the tape tends to fall off, cannot get wet, cannot be used over hair, has low tensile strength, and can cause blister formation. Surgical tapes can be used to reinforce wounds after removal of sutures or staples when the wound s bursting strength is quite low. The cyanoacrylate topical skin adhesives were first synthesized in 1949 and first used clinically in Their application is rapid, simple, painless for the patient, and relatively inexpensive. The material is a liquid monomer that polymerizes into a solid polymer upon contact with tissue anions. It is applied topically and bonds the apposed wound edges. Since the topical adhesive sloughs off spontaneously in 5-10 days as the skin renews itself, device removal is unnecessary. However, the topical adhesives are not very useful for hands and feet and for wounds directly over bending areas. Fingernail bed injuries can be closed with a topical adhesive as well as hand lacerations that are to be splinted over the next 5-10 days. The topical skin adhesives are extremely valuable for fragile skin (such as skin tears and shin lacerations). They are not particularly useful in an around mucous membranes since they tend to fall off prematurely. Extreme care should be used in lacerations around the eyes in order to prevent inadvertent runoff and matting of the eyelids. If it does get into the eye, use ophthalmic ointment to hasten sloughing of the adhesive. Reality: Sutures are not the only effective means of wound closure. Effective alternatives exist depending on wound type and location. Myth #8: Double layer suturing yields better cosmesis for facial wounds than single layer suturing Emergency physicians rarely use deep sutures. In contrast, plastic surgeons frequently use deep sutures in the face. Is there any proof that deep sutures lead to a better result in terms of infection and scar formation? Scar width is related to wound tension and correlated with the force required to close the wound. On the other hand, deep sutures increase infection rates in contaminated animal wound models. What is the evidence that deep sutures are beneficial in closing facial lacerations? A small study looking at 17 patients who were undergoing laminectomy, in whom there was closure of the upper and lower parts of the incision randomly with or without 4/0 subcuticular polyglycolic acid in addition to percutaneous nylon sutures, concluded that the width of the scar was unaffected by the presence of subcuticular sutures. A larger trial looked at time to closure and cosmesis in 60 patients with non-gaping (<10 mm width) facial lacerations randomized to a single layer of uninterrupted 6/0 polypropylene sutures or a double layer of deep dermal buried 5/0 polyglactin sutures plus simple interrupted 5/0 polypropylene sutures. The authors concluded that there was no benefit in using deep sutures in addition to the superficial single layer of percutaneous interrupted sutures. In fact, there was a time advantage in using only a single layer of sutures (six minutes) that would be expected. 5
6 Reality: In non-gaping facial lacerations there is no benefit in using double layer vs. single layer suturing. Deep dermal sutures may still be required in high tension gaping facial lacerations. Myth #9: The use of epinephrine for digital block may result in digital gangrene. Since 1888, there have been 48 cases of digital gangrene after the administration of anesthetic. In 21 of these cases epinephrine was used, however, its concentration was unknown and in many of these cases tourniquets were used making interpretation of this data difficult. In contrast there have been no reports of digital gangrene since 1948 when a commercial combination of epinephrine in lidocaine was introduced. A 1991 study randomized patients undergoing hand surgery to digital blocks with lidocaine with or without epinephrine and found no cases of gangrene. Furthermore, the addition of epinephrine reduced the need for additional injections of anesthetic and use of tourniquets, which are far more detrimental to digital blood flow than epinephrine. An ultrasonic study of digital blood flow found that injection of epinephrine resulted in a transient decrease in blood flow that completely resolved within minutes. A recent observational report of over 5000 patients undergoing digital block with lidocaine and epinephrine failed to demonstrate any cases of digital gangrene or any other complications. Reality: There is no evidence that the use of epinephrine is associated with digital gangrene. While it may have a vasoconstrictive effect, that effect may actually be desirable, and resolves within minutes. These are just some of the many myths that have purveyed our specialty concerning wound care. We all need to keep an open mind and look at the evidence behind so much that we have held to be realities. As always, clinical judgment and common sense should also be taken into consideration when determining how best to manage individual wounds. 6
7 ADDITIONAL READING 1. Singer AJ, Thode HC, Hollander JE. National trends in ED lacerations between Am J Emerg Med 2006;24: Hinman CD, Maibach H. Effect of air exposure and occlusion on experimental human skin wounds. Nature 1963;200: Hutchinson JJ. Prevalence of wound infection under occlusive dressings: a collective survey of reported research. Wound 1989;1: Perelman VS, Francis GJ, Rutledge T, Foote J, Martino F, Dranitsaris G. Sterile versus nonsterile gloves for repair of uncomplicated lacerations in the emergency department: a randomized controlled trial. Ann Emerg Med. 2004;43: Hollander JE, Richman PB, Werblud M, et al. Irrigation in facial and scalp lacerations: does it alter outcome? Ann Emerg Med 1998;31: Hollander JE, Singer AJ. Laceration management. Ann Emerg 1999;34: Singer AJ, Hollander JE, Quinn JV. Evaluation and management of traumatic lacerations. New Engl J Med 1997;337: Moscati RM, Mayrose J, Reardon RF, Janicke DM, Jehle DV. A multicenter comparison of tap water versus sterile saline for wound irrigation. Acad Emerg Med. 2007;14: Berk WA, Osbourne DD, Taylor DD. Evaluation of the golden period for wound repair: 204 cases from a third world emergency department. Ann Emerg Med 1988;17: Chen E, Hornig S, Shepherd SM, Hollander JE. Primary closure of mammalian bites. Acad Emerg Med 2000;7: Medeiros I, Saconato H. Antibiotic prophylaxis for mammalian bites. Cochrane Database of Systematic Reviews 2001, Issue 2. Art. No.: CD Singer AJ, Quinn JV, Hollander JE, Clark RE. Closure of lacerations and incisions with Octylcyanoacrylate: A multi-center randomized clinical trial. Surgery 2002;131: Singer AJ, Gulla J, Hein M, Marchini C, Chale S, Arora B. Single vs double layer closure of facial lacerations: A randomized control trial. Plast & Reconstr Surg 2005;116: Krunic AL, Wang LC, Soltani K, Weitzul S, Taylor RS. Digital anesthesia with epinephrine: an old myth revisited. J Am Acad Dermatol. 2004;51:
8 8
EVALUATION OF A LIQUID DRESSING FOR MINOR NON BLEEDING ABRASIONS AND CLASS I AND II SKIN TEARS IN THE EMERGENCY DEPARTMENT
 EVALUATION OF A LIQUID DRESSING FOR MINOR NON BLEEDING ABRASIONS AND CLASS I AND II SKIN TEARS IN THE EMERGENCY DEPARTMENT Adam J Singer, MD Department of Emergency Medicine Stony Brook University Stony
EVALUATION OF A LIQUID DRESSING FOR MINOR NON BLEEDING ABRASIONS AND CLASS I AND II SKIN TEARS IN THE EMERGENCY DEPARTMENT Adam J Singer, MD Department of Emergency Medicine Stony Brook University Stony
Chris Giaquinto, PA-C Doctors for Emergency Service Christiana Care Health System
 Chris Giaquinto, PA-C Doctors for Emergency Service Christiana Care Health System This program was sponsored by an educational grant from Ethicon. DAPA would like to thank Doctors for Emergency Service
Chris Giaquinto, PA-C Doctors for Emergency Service Christiana Care Health System This program was sponsored by an educational grant from Ethicon. DAPA would like to thank Doctors for Emergency Service
STANDARD OPERATING PROCEDURE #203 LARGE ANIMAL SURGERY
 STANDARD OPERATING PROCEDURE #203 LARGE ANIMAL SURGERY 1. PURPOSE This Standard Operating Procedure (SOP) describes procedures for general surgery of large animal species such as swine, dogs, rabbits,
STANDARD OPERATING PROCEDURE #203 LARGE ANIMAL SURGERY 1. PURPOSE This Standard Operating Procedure (SOP) describes procedures for general surgery of large animal species such as swine, dogs, rabbits,
micromend Skin Closure Device Pre-clinical Studies of Closure of Surgical Wounds in Live Pigs
 micromend Skin Closure Device Pre-clinical Studies of Closure of Surgical Wounds in Live Pigs RONALD BERENSON, M.D. and PAUL LEUNG, M.S. EXECUTIVE SUMMARY KitoTech Medical has developed a revolutionary
micromend Skin Closure Device Pre-clinical Studies of Closure of Surgical Wounds in Live Pigs RONALD BERENSON, M.D. and PAUL LEUNG, M.S. EXECUTIVE SUMMARY KitoTech Medical has developed a revolutionary
Wound Management in Urgent Care
 Wound Management in Urgent Care Brittany Busse Wound Management in Urgent Care Brittany Busse, MD Med 7 Urgent Care Folsom, CA, USA ISBN 978-3-319-27426-3 DOI 10.1007/978-3-319-27428-7 ISBN 978-3-319-27428-7
Wound Management in Urgent Care Brittany Busse Wound Management in Urgent Care Brittany Busse, MD Med 7 Urgent Care Folsom, CA, USA ISBN 978-3-319-27426-3 DOI 10.1007/978-3-319-27428-7 ISBN 978-3-319-27428-7
Adhesive strips for the closure of surgical wounds: a systematic review and meta-analysis
 Adhesive strips for the closure of surgical wounds: a systematic review and meta-analysis Presenting author: I Gkegkes, M Mavros, V Alexiou, G Peppas, M Falagas Vangelis G. Alexiou, MD, MSc General Surgery
Adhesive strips for the closure of surgical wounds: a systematic review and meta-analysis Presenting author: I Gkegkes, M Mavros, V Alexiou, G Peppas, M Falagas Vangelis G. Alexiou, MD, MSc General Surgery
Basic Laceration Repair
 videos in clinical medicine Basic Laceration Repair Todd W. Thomsen, M.D., Derek A. Barclay, M.D., and Gary S. Setnik, M.D. From the Department of Emergency Medicine, Mount Auburn Hospital, Cambridge,
videos in clinical medicine Basic Laceration Repair Todd W. Thomsen, M.D., Derek A. Barclay, M.D., and Gary S. Setnik, M.D. From the Department of Emergency Medicine, Mount Auburn Hospital, Cambridge,
Chapter 14 8/23/2016. Surgical Wound Care. Wound Classifications. Wound Healing. Classified According to. Phases
 Chapter 14 Surgical Wound Care All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Wound Classifications Classified According to Cause Incision
Chapter 14 Surgical Wound Care All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Wound Classifications Classified According to Cause Incision
STUDY. Prevention of Scar Spread on Trunk Excisions. Kevin F. Kia, MD; Molly V. Burns, MD; Travis Vandergriff, MD; Sarah Weitzul, MD
 STUDY Prevention of Scar Spread on Trunk Excisions A Rater-Blinded Randomized Controlled Trial Kevin F. Kia, MD; Molly V. Burns, MD; Travis Vandergriff, MD; Sarah Weitzul, MD Importance: Wounds that heal
STUDY Prevention of Scar Spread on Trunk Excisions A Rater-Blinded Randomized Controlled Trial Kevin F. Kia, MD; Molly V. Burns, MD; Travis Vandergriff, MD; Sarah Weitzul, MD Importance: Wounds that heal
ORIGINAL ARTICLE. A Prospective Controlled Study of Wound-Healing Characteristics. glues have been investigated
 ORIGINAL ARTICLE Efficacy of Octyl-2-Cyanoacrylate Tissue Glue in Blepharoplasty A Prospective Controlled Study of Wound-Healing Characteristics David Greene, MD; R. James Koch, MD; Richard L. Goode, MD
ORIGINAL ARTICLE Efficacy of Octyl-2-Cyanoacrylate Tissue Glue in Blepharoplasty A Prospective Controlled Study of Wound-Healing Characteristics David Greene, MD; R. James Koch, MD; Richard L. Goode, MD
DERMABOND PRINEO SKIN CLOSURE SYSTEM (22 CM)
 SKIN CLOSURE SYSTEM (22 CM) Evidence Brief: Comparative Wound Holding Strength and Tension Redistribution Introduction The is a non-invasive skin closure device that can be used to approximate the skin
SKIN CLOSURE SYSTEM (22 CM) Evidence Brief: Comparative Wound Holding Strength and Tension Redistribution Introduction The is a non-invasive skin closure device that can be used to approximate the skin
Sideline Wound Care. Erin E. Shaffer, DO, ATC
 Sideline Wound Care Erin E. Shaffer, DO, ATC 1 Objectives Know what supplies you should have on the sideline to facilitate care of athletic wounds Recognize the different stages of wound healing and be
Sideline Wound Care Erin E. Shaffer, DO, ATC 1 Objectives Know what supplies you should have on the sideline to facilitate care of athletic wounds Recognize the different stages of wound healing and be
Wound culture. (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center
 Wound culture (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center Infection is a major impairment in delayed and nonhealing chronic wounds. Cultures of chronic wounds are not routinely performed
Wound culture (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center Infection is a major impairment in delayed and nonhealing chronic wounds. Cultures of chronic wounds are not routinely performed
Is there a relationship between wound infections and laceration closure times?
 Waseem et al. International Journal of Emergency Medicine 2012, 5:32 ORIGINAL RESEARCH Open Access Is there a relationship between wound infections and laceration closure times? Muhammad Waseem 1,2*, Viraj
Waseem et al. International Journal of Emergency Medicine 2012, 5:32 ORIGINAL RESEARCH Open Access Is there a relationship between wound infections and laceration closure times? Muhammad Waseem 1,2*, Viraj
CLINICAL INVESTIGATIONS
 730 Karounis et al. d COSMETIC OUTCOMES WITH ABSORBABLE VS. NONABSORBABLE SUTURES CLINICAL INVESTIGATIONS A Randomized, Controlled Trial Comparing Long-term Cosmetic Outcomes of Traumatic Pediatric Lacerations
730 Karounis et al. d COSMETIC OUTCOMES WITH ABSORBABLE VS. NONABSORBABLE SUTURES CLINICAL INVESTIGATIONS A Randomized, Controlled Trial Comparing Long-term Cosmetic Outcomes of Traumatic Pediatric Lacerations
Section of Pediatric Surgery, Department of Surgery, CS Mott Children s Hospital, University of Michigan, Ann Arbor, MI , USA
 Journal of Pediatric Surgery (2009) 44, 1418 1422 www.elsevier.com/locate/jpedsurg A prospective, randomized comparison of skin adhesive and subcuticular suture for closure of pediatric hernia incisions:
Journal of Pediatric Surgery (2009) 44, 1418 1422 www.elsevier.com/locate/jpedsurg A prospective, randomized comparison of skin adhesive and subcuticular suture for closure of pediatric hernia incisions:
Galen ( A.D) Advanced Wound Dressing
 Galen (120-201A.D) Advanced Wound Dressing Wounds heal optimally in a moist environment นพ.เก งกาจ ว น ยโกศล Wound assessment Ideal wound dressing Type of wound Clinical appearance Wound location Measurement
Galen (120-201A.D) Advanced Wound Dressing Wounds heal optimally in a moist environment นพ.เก งกาจ ว น ยโกศล Wound assessment Ideal wound dressing Type of wound Clinical appearance Wound location Measurement
ABSTRACT. Acad. Emerg. Med. 1998; 5: ACADEMIC EMERGENCY MEDICINE FEB 1998 VOL 5/NO
 94 ACADEMIC EMERGENCY MEDICINE FEB 1998 VOL 5/NO 2 Prospective, Randomized, Controlled Trial of Tissue Adhesive (2-Octylcyanoacrylate) vs Standard Wound Closure Techniques for Laceration Repair Adam J.
94 ACADEMIC EMERGENCY MEDICINE FEB 1998 VOL 5/NO 2 Prospective, Randomized, Controlled Trial of Tissue Adhesive (2-Octylcyanoacrylate) vs Standard Wound Closure Techniques for Laceration Repair Adam J.
Wound Management for Nurses/Technicians What do we need to know?
 Wound Management for Nurses/Technicians What do we need to know? Laura Owen European Specialist in Small Animal Surgery Lecturer in Small Animal Surgery, University of Cambridge The Acute Open Wound PPE
Wound Management for Nurses/Technicians What do we need to know? Laura Owen European Specialist in Small Animal Surgery Lecturer in Small Animal Surgery, University of Cambridge The Acute Open Wound PPE
u A 14 year old female with no significant past medical history presents to the ED for evaluation of a finger laceration. While playing a card game
 Finger Lacerations u A 14 year old female with no significant past medical history presents to the ED for evaluation of a finger laceration. While playing a card game with her family, she lost her balance
Finger Lacerations u A 14 year old female with no significant past medical history presents to the ED for evaluation of a finger laceration. While playing a card game with her family, she lost her balance
Wound Care Discharge Instructions
 Wound Care Discharge Instructions Wound Care Discharge Instructions DESCRIPTION Caring for your wound is important to promote healing, avoid infection, and minimize scarring. Wounds heal more quickly when
Wound Care Discharge Instructions Wound Care Discharge Instructions DESCRIPTION Caring for your wound is important to promote healing, avoid infection, and minimize scarring. Wounds heal more quickly when
Evaluation, Repair and Treatment of Wounds. Carol O Mara, DNP, APRN, FNP-C
 Evaluation, Repair and Treatment of Wounds Carol O Mara, DNP, APRN, FNP-C Composition of skin Skin consists of four layers Epidermis Dermis Superficial fascia (SQ layer) Deep fascia Anatomy of the Skin
Evaluation, Repair and Treatment of Wounds Carol O Mara, DNP, APRN, FNP-C Composition of skin Skin consists of four layers Epidermis Dermis Superficial fascia (SQ layer) Deep fascia Anatomy of the Skin
Appropriate Dressing Selection For Treating Wounds
 Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
A Comparison of Cosmetic Outcomes of Lacerations on the Extremities and Trunk Using Absorbable Versus Nonabsorbable Sutures
 ORIGINAL CONTRIBUTION A Comparison of Cosmetic Outcomes of Lacerations on the Extremities and Trunk Using Absorbable Versus Nonabsorbable Sutures Cena Tejani, MD, Adam B. Sivitz, MD, Micheal D. Rosen,
ORIGINAL CONTRIBUTION A Comparison of Cosmetic Outcomes of Lacerations on the Extremities and Trunk Using Absorbable Versus Nonabsorbable Sutures Cena Tejani, MD, Adam B. Sivitz, MD, Micheal D. Rosen,
Surgical Gown. A disposable gown worn by medical staff during surgery. A disposable gown worn by medical staff during surgery
 Surgical Gown A disposable gown worn by medical staff during surgery Used by the surgeon during surgery; significant blood cover DOGS Surgical Gown A disposable gown worn by medical staff during surgery
Surgical Gown A disposable gown worn by medical staff during surgery Used by the surgeon during surgery; significant blood cover DOGS Surgical Gown A disposable gown worn by medical staff during surgery
Mr Zachary Moaveni Plastic Surgeon, Middlemore Hospital. Mr Adam Bialostocki Plastic Surgeon, Tauranga
 Mr Zachary Moaveni Plastic Surgeon, Middlemore Hospital Mr Adam Bialostocki Plastic Surgeon, Tauranga Mr. Adam Bialostocki Plastic Surgeon Minor Burns First Aid Remove the burning agent / wet clothes
Mr Zachary Moaveni Plastic Surgeon, Middlemore Hospital Mr Adam Bialostocki Plastic Surgeon, Tauranga Mr. Adam Bialostocki Plastic Surgeon Minor Burns First Aid Remove the burning agent / wet clothes
SKIN INTEGRITY & WOUND CARE
 SKIN INTEGRITY & WOUND CARE Chapter 34 1 skin integrity: intact skin refers to the presence of normal skin layer uninterrupted by wound 2 WOUNDS DISRUPTION IN THE INTEGRITY OF BODY TISSUE CLASSIFIED AS:
SKIN INTEGRITY & WOUND CARE Chapter 34 1 skin integrity: intact skin refers to the presence of normal skin layer uninterrupted by wound 2 WOUNDS DISRUPTION IN THE INTEGRITY OF BODY TISSUE CLASSIFIED AS:
Skin Integrity and Wound Care
 Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
FINGERTIP INJURIES ARE THEY REALLY THAT SIMPLE? SANJAY K SHARMA, MD, FACS INSTITUTE OF RECONSTRUCTIVE PLASTIC SURGERY
 FINGERTIP INJURIES ARE THEY REALLY THAT SIMPLE? SANJAY K SHARMA, MD, FACS INSTITUTE OF RECONSTRUCTIVE PLASTIC SURGERY Austin Trauma and Critical Care Conference 2018 May 31-June 1, 2018 Outline 1. Scope
FINGERTIP INJURIES ARE THEY REALLY THAT SIMPLE? SANJAY K SHARMA, MD, FACS INSTITUTE OF RECONSTRUCTIVE PLASTIC SURGERY Austin Trauma and Critical Care Conference 2018 May 31-June 1, 2018 Outline 1. Scope
소아비뇨기과관혈적수술시피부봉합제로사용된 Octyl-2-Cyanoacrylate (Dermabond TM ) 의효용성서울대학교의과대학비뇨기과학교실
 Original article J Korean Soc Pediatr Nephrol 2012;16:115-120 DOI: http://dx.doi.org/10.3339/jkspn.2012.16.2.115 ISSN 1226-5292 (print) ISSN 2234-4209 (online) 소아비뇨기과관혈적수술시피부봉합제로사용된 Octyl-2-Cyanoacrylate
Original article J Korean Soc Pediatr Nephrol 2012;16:115-120 DOI: http://dx.doi.org/10.3339/jkspn.2012.16.2.115 ISSN 1226-5292 (print) ISSN 2234-4209 (online) 소아비뇨기과관혈적수술시피부봉합제로사용된 Octyl-2-Cyanoacrylate
Topical EMLA Cream as a Pretreatment for Facial Lacerations
 Topical EMLA Cream as a Pretreatment for Facial Lacerations Original Article Sung Woo Park, Tae Suk Oh, Jong Woo Choi, Jin Sup Eom, Joon Pio Hong, Kyung S Koh, Taik Jong Lee, Eun Key Kim Department of
Topical EMLA Cream as a Pretreatment for Facial Lacerations Original Article Sung Woo Park, Tae Suk Oh, Jong Woo Choi, Jin Sup Eom, Joon Pio Hong, Kyung S Koh, Taik Jong Lee, Eun Key Kim Department of
Wound Repair. Epidemiology. History. Location of Injuries Face/Scalp Extremities. Legal Risk Missed FB and Fx Infection
 Wound Repair Edwin W. Schaefer, DNP, R.N. - FNP Emergency Nurse Practitioner Epidemiology Location of Injuries Face/Scalp Extremities Legal Risk Missed FB and Fx Infection History Mechanism of Injury Associated
Wound Repair Edwin W. Schaefer, DNP, R.N. - FNP Emergency Nurse Practitioner Epidemiology Location of Injuries Face/Scalp Extremities Legal Risk Missed FB and Fx Infection History Mechanism of Injury Associated
White Paper. Wound Closure
 White Paper Table of Contents 1. Introduction... 3 2. Primary Endpoint:... 3 3. Secondary Endpoint: Cosmetic Outcome... 4 4. Safety Endpoints... 4 5. Control Group... 5 6. Patient Recruitment and Retention...
White Paper Table of Contents 1. Introduction... 3 2. Primary Endpoint:... 3 3. Secondary Endpoint: Cosmetic Outcome... 4 4. Safety Endpoints... 4 5. Control Group... 5 6. Patient Recruitment and Retention...
V.A.C. Therapy Patient Guide. Are you suffering from a wound? Ask your doctor about V.A.C. Therapy and whether it may be right for you.
 V.A.C. Therapy Patient Guide Are you suffering from a wound? Ask your doctor about V.A.C. Therapy and whether it may be right for you. kci1.com 800.275.4524 Table of Contents Wound Healing is a Process...2
V.A.C. Therapy Patient Guide Are you suffering from a wound? Ask your doctor about V.A.C. Therapy and whether it may be right for you. kci1.com 800.275.4524 Table of Contents Wound Healing is a Process...2
Determining Wound Diagnosis and Documentation Tips Job Aid
 Determining Wound Diagnosis and Job Aid 1 Coding Is this a traumatic injury from an accident? 800 Codes - Injury Section of the Coding Manual Code by specific site of injury. Only use for accidents or
Determining Wound Diagnosis and Job Aid 1 Coding Is this a traumatic injury from an accident? 800 Codes - Injury Section of the Coding Manual Code by specific site of injury. Only use for accidents or
WOUNDS. Emergency Procedures in PT
 WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
Integra. PriMatrix Dermal Repair Scaffold PATIENT INFORMATION. Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1
 Integra PriMatrix Dermal Repair Scaffold PATIENT INFORMATION Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1 Your Path to Recovery Your health care provider has chosen to use
Integra PriMatrix Dermal Repair Scaffold PATIENT INFORMATION Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1 Your Path to Recovery Your health care provider has chosen to use
Successful IV Starts Revised February 2014
 Successful IV Starts Revised February 2014 Why Intravenous Therapy? Used for access to the body s circulation Indications: Administer fluids, blood, medications, and nutrition Obtain laboratory specimens
Successful IV Starts Revised February 2014 Why Intravenous Therapy? Used for access to the body s circulation Indications: Administer fluids, blood, medications, and nutrition Obtain laboratory specimens
Decision-Making in the Acute Management of Blunt and Penetrating Wounds Mary Somerville, DVM, DACVS
 Decision-Making in the Acute Management of Blunt and Penetrating Wounds Mary Somerville, DVM, DACVS Providing the best quality care and service for the patient, the client, and the referring veterinarian.
Decision-Making in the Acute Management of Blunt and Penetrating Wounds Mary Somerville, DVM, DACVS Providing the best quality care and service for the patient, the client, and the referring veterinarian.
Chapter 16. Cosmetic Concerns. Better Blood Supply and Circulation
 Chapter 16 FACIAL LACERATIONS KEY FIGURES: Tissue flap Suture bites: face vs. rest of body Lip anatomy Soft tissue loss The face has several unique properties that dictate the choice of treatment after
Chapter 16 FACIAL LACERATIONS KEY FIGURES: Tissue flap Suture bites: face vs. rest of body Lip anatomy Soft tissue loss The face has several unique properties that dictate the choice of treatment after
Prospective, Randomized, Blinded Study of a New Wound Closure Film Versus Cutaneous Suture for Surgical Wound Closure
 Prospective, Randomized, Blinded Study of a New Wound Closure Film Versus Cutaneous Suture for Surgical Wound Closure F ELIX K UO, MD, D ENNIS L EE, MD, y AND G ARY S. R OGERS, MD z BACKGROUND Wound closure
Prospective, Randomized, Blinded Study of a New Wound Closure Film Versus Cutaneous Suture for Surgical Wound Closure F ELIX K UO, MD, D ENNIS L EE, MD, y AND G ARY S. R OGERS, MD z BACKGROUND Wound closure
Wound Healing Basic Concept
 Department of Orthopaedic & Traumatology The Chinese University of Hong Kong Wound Healing Basic Concept Dr TSE Lung Fung ( 謝龍峰醫生 ) MBChB(CUHK),FRCS(Edin),FRCSEd(Orth),FHKCOS,FHKAM(Ortho) Tissue Damage
Department of Orthopaedic & Traumatology The Chinese University of Hong Kong Wound Healing Basic Concept Dr TSE Lung Fung ( 謝龍峰醫生 ) MBChB(CUHK),FRCS(Edin),FRCSEd(Orth),FHKCOS,FHKAM(Ortho) Tissue Damage
Lower Extremity Wound Evaluation and Treatment
 Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Application Guide for Full-Thickness Wounds
 Application Guide for Full-Thickness Wounds PriMatrix Dermal Repair Scaffold PriMatrix Ag Antimicrobial Dermal Repair Scaffold Application Guide for Full Thickness Wounds PriMatrix is a unique dermal repair
Application Guide for Full-Thickness Wounds PriMatrix Dermal Repair Scaffold PriMatrix Ag Antimicrobial Dermal Repair Scaffold Application Guide for Full Thickness Wounds PriMatrix is a unique dermal repair
Evaluation of the Use of a Silver Collagen Amorphous Gel in the Healing of Post Surgical and Dehisced Lesions
 Evaluation of the Use of a Silver Collagen Amorphous Gel in the Healing of Post Surgical and Dehisced Lesions Presented by: Kathryn Khandaker, RN, BSN, CWCN and Deanna Sue Kohl, RN, BSN, CWOCN, CFCN Introduction:
Evaluation of the Use of a Silver Collagen Amorphous Gel in the Healing of Post Surgical and Dehisced Lesions Presented by: Kathryn Khandaker, RN, BSN, CWCN and Deanna Sue Kohl, RN, BSN, CWOCN, CFCN Introduction:
NovoSorb BTM. A unique synthetic biodegradable wound scaffold. Regenerating tissue. Changing lives.
 NovoSorb BTM A unique synthetic biodegradable wound scaffold Regenerating tissue. Changing lives. Overview NovoSorb BTM is a unique synthetic biodegradable wound scaffold that delivers good cosmetic and
NovoSorb BTM A unique synthetic biodegradable wound scaffold Regenerating tissue. Changing lives. Overview NovoSorb BTM is a unique synthetic biodegradable wound scaffold that delivers good cosmetic and
Skin Anatomy and Physiology
 Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
2017 Physician Coding Survival Guide
 2017 Physician Coding Survival Guide Chapter 3: Dermatology Melanoma: Stop Melanoma Coding Errors Before They Spread If the dermatologist gets down to the fascia, would you still stick with an integumentary
2017 Physician Coding Survival Guide Chapter 3: Dermatology Melanoma: Stop Melanoma Coding Errors Before They Spread If the dermatologist gets down to the fascia, would you still stick with an integumentary
Surgery/Integumentary System ( )
 10030 The provider inserts a catheter through the skin using imaging to view the fluid. He then drains the fluid from the soft tissue in cases such as abscess, hematoma, seroma, lymphocele, or cyst. Imaging
10030 The provider inserts a catheter through the skin using imaging to view the fluid. He then drains the fluid from the soft tissue in cases such as abscess, hematoma, seroma, lymphocele, or cyst. Imaging
Patient Care Information
 Patient Care Information A Guide to Healing Diabetic Foot Ulcers Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1 Dermal Regeneration Matrix Overview Diabetic foot ulcers are
Patient Care Information A Guide to Healing Diabetic Foot Ulcers Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1 Dermal Regeneration Matrix Overview Diabetic foot ulcers are
Burns. A Comprehensive Review Assessment & Management
 Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
Prontosan. Clean. Easy Wound Healing. Wound Cleansing
 Prontosan Clean. Easy Wound Healing. Wound Cleansing CoE Infection Control Prontosan the unique combination of Betaine & Polihexanide reduces healing time removes and prevents biofilm prevents infections
Prontosan Clean. Easy Wound Healing. Wound Cleansing CoE Infection Control Prontosan the unique combination of Betaine & Polihexanide reduces healing time removes and prevents biofilm prevents infections
New approach to the wounds by moist wound healing in Japan. Yoshihiko Mochizuki Japan
 New approach to the wounds by moist wound healing in Japan. Yoshihiko Mochizuki M.D. @Tokyo Japan What is the meaning of wound healing? I think there are two types of wound healing. 1. True healing moist
New approach to the wounds by moist wound healing in Japan. Yoshihiko Mochizuki M.D. @Tokyo Japan What is the meaning of wound healing? I think there are two types of wound healing. 1. True healing moist
EACH year more than 10 million wounds are CLINICAL INVESTIGATIONS. LET versus EMLA for Pretreating Lacerations: A Randomized Trial
 ACADEMIC EMERGENCY MEDICINE March 2001, Volume 8, Number 3 223 CLINICAL INVESTIGATIONS LET versus EMLA for Pretreating Lacerations: A Randomized Trial ADAM J. SINGER, MD, MARY JO STARK, RN Abstract. Objective:
ACADEMIC EMERGENCY MEDICINE March 2001, Volume 8, Number 3 223 CLINICAL INVESTIGATIONS LET versus EMLA for Pretreating Lacerations: A Randomized Trial ADAM J. SINGER, MD, MARY JO STARK, RN Abstract. Objective:
If both a standardized, validated screening tool and an evaluation of clinical factors are utilized, select Response 2.
 (M1300) Pressure Ulcer Assessment: Was this patient assessed for Risk of Developing Pressure Ulcers? 0 - No assessment conducted [Go to M1306 ] 1 - Yes, based on an evaluation of clinical factors (for
(M1300) Pressure Ulcer Assessment: Was this patient assessed for Risk of Developing Pressure Ulcers? 0 - No assessment conducted [Go to M1306 ] 1 - Yes, based on an evaluation of clinical factors (for
Procedure: Chest Tube Placement (Tube Thoracostomy)
 Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Our Experience with Endoscopic Brow Lifts
 Aesth. Plast. Surg. 24:90 96, 2000 DOI: 10.1007/s002660010017 2000 Springer-Verlag New York Inc. Our Experience with Endoscopic Brow Lifts Ozan Sozer, M.D., and Thomas M. Biggs, M.D. İstanbul, Turkey and
Aesth. Plast. Surg. 24:90 96, 2000 DOI: 10.1007/s002660010017 2000 Springer-Verlag New York Inc. Our Experience with Endoscopic Brow Lifts Ozan Sozer, M.D., and Thomas M. Biggs, M.D. İstanbul, Turkey and
STUDY. Primary Closure vs Second-Intention Treatment of Skin Punch Biopsy Sites
 STUDY Primary Closure vs Second-Intention Treatment of Skin Punch Biopsy Sites A Randomized Trial Leslie J. Christenson, MD; P. Kim Phillips, MD; Amy L. Weaver, MS; Clark C. Otley, MD Objective: To determine
STUDY Primary Closure vs Second-Intention Treatment of Skin Punch Biopsy Sites A Randomized Trial Leslie J. Christenson, MD; P. Kim Phillips, MD; Amy L. Weaver, MS; Clark C. Otley, MD Objective: To determine
Laceration Management
 S T A T E O F T H E A R T Laceration Management From the Department of Emergency Medicine, University of Pennsylvania, Philadelphia, PA, * and the Department of Emergency Medicine, State University of
S T A T E O F T H E A R T Laceration Management From the Department of Emergency Medicine, University of Pennsylvania, Philadelphia, PA, * and the Department of Emergency Medicine, State University of
Property Latmedical, LLC.
 Dr. Goed provides a complete and innovate product portfolio solution to the growing healthcare need within the field of non-invasive orthopedics, sports medicine, bandaging, wound care and compression
Dr. Goed provides a complete and innovate product portfolio solution to the growing healthcare need within the field of non-invasive orthopedics, sports medicine, bandaging, wound care and compression
Susan G. Komen 3-Day. Medical Team Blister Protocol. Randy Pearson, MD, FAAFP, FACSM Dr. Jennifer A. Saam, DPM
 Susan G. Komen 3-Day Medical Team Blister Protocol Randy Pearson, MD, FAAFP, FACSM Dr. Jennifer A. Saam, DPM Blisters happen because of friction. Most common problem on the Komen 3-Day. Caused by friction
Susan G. Komen 3-Day Medical Team Blister Protocol Randy Pearson, MD, FAAFP, FACSM Dr. Jennifer A. Saam, DPM Blisters happen because of friction. Most common problem on the Komen 3-Day. Caused by friction
Beyond the Basics ImprovingYour Wound Care Knowledge. Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN
 Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types. Summary
 Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
How Wounds Heal: A Guide for the Wound-care Novice
 C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
TOPICAL ANAESTHETIC SOLUTIONS FOR PAIN FREE SUTURE OF LACERATIONS IN THE EMERGENCY ROOM. Dr Sylvie MARTUS, Laurence PONCIN
 Joint Meeting BELAPS, BAPA & BePPa TOPICAL ANAESTHETIC SOLUTIONS FOR PAIN FREE SUTURE OF LACERATIONS IN THE EMERGENCY ROOM Dr Sylvie MARTUS, Laurence PONCIN Dr C. GOMES, Dr M. GLASS, Dr. J. KIEFFER, Dr
Joint Meeting BELAPS, BAPA & BePPa TOPICAL ANAESTHETIC SOLUTIONS FOR PAIN FREE SUTURE OF LACERATIONS IN THE EMERGENCY ROOM Dr Sylvie MARTUS, Laurence PONCIN Dr C. GOMES, Dr M. GLASS, Dr. J. KIEFFER, Dr
Surgical Therapy. Tuesday, April 2, 13. Alessan"o Geminiani, DDS, MS
 Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
INJURIES AND THEIR MANAGEMENT
 INJURIES AND THEIR MANAGEMENT INJURIES AND THEIR MANAGEMENT An injury is damage to the body caused by external forces, which may be physical or chemical. 1) Incisions 2) Types of wounds and their closure
INJURIES AND THEIR MANAGEMENT INJURIES AND THEIR MANAGEMENT An injury is damage to the body caused by external forces, which may be physical or chemical. 1) Incisions 2) Types of wounds and their closure
First Responders to Orthopaedic Emergencies
 First Responders to Orthopaedic Emergencies Tom McPartland MD FABOS, FAAP Assistant Clinical Professor Rutgers-RWJMS October 17,2018 Goals Review Epidemiology of School Injuries Review Definitions of Different
First Responders to Orthopaedic Emergencies Tom McPartland MD FABOS, FAAP Assistant Clinical Professor Rutgers-RWJMS October 17,2018 Goals Review Epidemiology of School Injuries Review Definitions of Different
Principle Management of Wound and Fracture in Emergency Department
 Principle Management of Wound and Fracture in Emergency Department Presented in Clinical Update Seminar January 15 th 2011 dr. Tedjo Rukmoyo, SpOT (K) Spine Initial Management ATLS Procedure A : airway
Principle Management of Wound and Fracture in Emergency Department Presented in Clinical Update Seminar January 15 th 2011 dr. Tedjo Rukmoyo, SpOT (K) Spine Initial Management ATLS Procedure A : airway
Your guide to wound debridement and assessment. Michelle Greenwood. Lorraine Grothier. Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust
 Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
DISTANT FLAPS KEY FIGURES:
 Chapter 14 DISTANT FLAPS KEY FIGURES: Chest flap Cross arm flap Cross leg flap Design of groin flap Examples of groin flap Examples of free flaps A distant flap involves moving tissue (skin, fascia, muscle,
Chapter 14 DISTANT FLAPS KEY FIGURES: Chest flap Cross arm flap Cross leg flap Design of groin flap Examples of groin flap Examples of free flaps A distant flap involves moving tissue (skin, fascia, muscle,
Prof Oluwadiya KS FMCS(orthop)
 Prof Oluwadiya KS FMCS(orthop) www.oluwadiya.com Sutures are materials with which two surfaces are kept in apposition. Tensile strength is the measured level of tension that a knotted suture strand can
Prof Oluwadiya KS FMCS(orthop) www.oluwadiya.com Sutures are materials with which two surfaces are kept in apposition. Tensile strength is the measured level of tension that a knotted suture strand can
BEN C. TAYLOR, MD TRAUMA FELLOW GRANT MEDICAL CENTER
 Evaluation of Primary Total Knee Arthroplasty Incision Closure with the Use of Continuous Bidirectional SCOTT STEPHENS, MD RESIDENT PHYSICIAN MOUNT CARMEL MEDICAL CENTER JOEL POLITI, MD DEPARTMENT OF ORTHOPEDIC
Evaluation of Primary Total Knee Arthroplasty Incision Closure with the Use of Continuous Bidirectional SCOTT STEPHENS, MD RESIDENT PHYSICIAN MOUNT CARMEL MEDICAL CENTER JOEL POLITI, MD DEPARTMENT OF ORTHOPEDIC
Assessment & Management of Wounds in primary practice.
 Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
CASE 1: TYPE-II DIABETIC FOOT ULCER
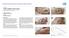 CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
COMPARATIVE MEDICINE LABORATORY ANIMAL FACILITIES STANDARD OPERATING PROCEDURE FOR RODENT SURGERY
 2.A.3 COMPARATIVE MEDICINE LABORATORY ANIMAL FACILITIES STANDARD OPERATING PROCEDURE FOR RODENT SURGERY 1.0 Purpose: Post-operative infections in rodents can and do occur. Such infections, which may not
2.A.3 COMPARATIVE MEDICINE LABORATORY ANIMAL FACILITIES STANDARD OPERATING PROCEDURE FOR RODENT SURGERY 1.0 Purpose: Post-operative infections in rodents can and do occur. Such infections, which may not
Traditional Silicone Technology
 Innovative Non-Silicone Low Trauma Adhesives versus Traditional Silicone Technology A Review and Comparison Alan Neil Medical Industry Consultant Advanced Wound Care Lohmann Corporation 2016 Chronic wound
Innovative Non-Silicone Low Trauma Adhesives versus Traditional Silicone Technology A Review and Comparison Alan Neil Medical Industry Consultant Advanced Wound Care Lohmann Corporation 2016 Chronic wound
Wound Care Program for Nursing Assistants-
 Wound Care Program for Nursing Assistants- Wound Cleansing,Types & Presentation Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion
Wound Care Program for Nursing Assistants- Wound Cleansing,Types & Presentation Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion
Patient Information Publications Warren Grant Magnuson Clinical Center National Institutes of Health
 Warren Grant Magnuson Clinical Center National Institutes of Health What is a subcutaneous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous
Warren Grant Magnuson Clinical Center National Institutes of Health What is a subcutaneous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
Chapter 11 Worksheet Code It
 Class: Date: Chapter 11 Worksheet 3 2 1 Code It True/False Indicate whether the statement is true or false. 1. Surgical destruction is considered part of the surgical procedure description. 2. Prepping
Class: Date: Chapter 11 Worksheet 3 2 1 Code It True/False Indicate whether the statement is true or false. 1. Surgical destruction is considered part of the surgical procedure description. 2. Prepping
Burns and Scalds. Treatment and Management. Accident and Emergency Department. Royal Surrey County Hospital. Patient information leaflet
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Burns and Scalds Treatment and Management Accident and Emergency Department A Burn is an injury caused to the skin by thermal
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Burns and Scalds Treatment and Management Accident and Emergency Department A Burn is an injury caused to the skin by thermal
Pa#ent Informa#on for Consent
 Pa#ent Informa#on for Consent ER_OS02 Total Knee Replacement Enhanced Recovery Expires end of November 2018 Local Informa#on For further informa0on locally you can contact the Pa0ent Advice & Liaison Service
Pa#ent Informa#on for Consent ER_OS02 Total Knee Replacement Enhanced Recovery Expires end of November 2018 Local Informa#on For further informa0on locally you can contact the Pa0ent Advice & Liaison Service
You Are the Emergency Medical Responder
 Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Clinical guideline Published: 22 October 2008 nice.org.uk/guidance/cg74
 Surgical site infections: prevention ention and treatment Clinical guideline Published: 22 October 08 nice.org.uk/guidance/cg74 NICE 18. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Surgical site infections: prevention ention and treatment Clinical guideline Published: 22 October 08 nice.org.uk/guidance/cg74 NICE 18. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Trigger Finger Release
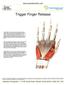 Trigger Finger Release Trigger finger, also known as stenosing tenosynovitis, occurs when one of the tendons responsible for bending a finger or the thumb develops a thickening, known as a nodule, and
Trigger Finger Release Trigger finger, also known as stenosing tenosynovitis, occurs when one of the tendons responsible for bending a finger or the thumb develops a thickening, known as a nodule, and
South West Regional Wound Care Toolkit F. PRINCIPLES OF TREATMENT BASED ON ETIOLOGY (TREAT THE CAUSE)
 F. PRINCIPLES OF TREATMENT BASED ON ETIOLOGY (TREAT THE CAUSE) F.5 SURGICAL WOUND (CLOSED AND OPEN) 5.1 Background to Etiology Closed surgical wounds are well-approximated with a palpable healing ridge
F. PRINCIPLES OF TREATMENT BASED ON ETIOLOGY (TREAT THE CAUSE) F.5 SURGICAL WOUND (CLOSED AND OPEN) 5.1 Background to Etiology Closed surgical wounds are well-approximated with a palpable healing ridge
Instructions for Use
 PRODUCTS Instructions for Use PRODUCTS Andover offers a variety of cohesive flexible bandage options. Why are CoFlex products the Best Bandage Choice? Available latex or latex-free Self-adhering - sticks
PRODUCTS Instructions for Use PRODUCTS Andover offers a variety of cohesive flexible bandage options. Why are CoFlex products the Best Bandage Choice? Available latex or latex-free Self-adhering - sticks
THE PLASTIC SURGERY CLINIC
 FACELIFT SURGERY INSTRUCTIONS FOLLOWING SURGERY WHAT TO EXPECT IMMEDIATELY AFTER SURGERY You will wake up with a helmet dressing on your head (i.e. bandages) and you may have some drains/tubes inserted
FACELIFT SURGERY INSTRUCTIONS FOLLOWING SURGERY WHAT TO EXPECT IMMEDIATELY AFTER SURGERY You will wake up with a helmet dressing on your head (i.e. bandages) and you may have some drains/tubes inserted
We look forward to serving you.
 ADVANCED CARE GEMCORE360 offers healthcare professionals a simple, clear and cost-effective wound care range while ensuring excellent clinical outcomes for their patients. 1 At GEMCO Medical, we strive
ADVANCED CARE GEMCORE360 offers healthcare professionals a simple, clear and cost-effective wound care range while ensuring excellent clinical outcomes for their patients. 1 At GEMCO Medical, we strive
ISPUB.COM. S Saad, E Shakov, V Sebastian, A Saad INTRODUCTION METHODS CASE REPORT 2 CASE REPORT 3 CASE REPORT 1
 ISPUB.COM The Internet Journal of Surgery Volume 11 Number 1 The use of Wound Vacuum-assisted Closure (V.A.C. ) system in the treatment of Recurrent or Complex Pilonidal Cyst Disease: Experience in 4 Adolescent
ISPUB.COM The Internet Journal of Surgery Volume 11 Number 1 The use of Wound Vacuum-assisted Closure (V.A.C. ) system in the treatment of Recurrent or Complex Pilonidal Cyst Disease: Experience in 4 Adolescent
Efficacy of cyanoacrylate glue in operative wound closure
 International Surgery Journal Chawada MJ et al. Int Surg J. 2016 May;3(2):792-796 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20160659
International Surgery Journal Chawada MJ et al. Int Surg J. 2016 May;3(2):792-796 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20160659
Boonlawat Homvises MD* * Department of Surgery, Faculty of Medicine, Thammasat University, Pathumthani, Thailand
 A Randomized Trial between Different Suture Materials (Polydioxanone vs. Poliglecaprone 25) and Different Suturing Techniques (Running Subcuticular Suture Alone vs. with Running Horizontal Mattress) in
A Randomized Trial between Different Suture Materials (Polydioxanone vs. Poliglecaprone 25) and Different Suturing Techniques (Running Subcuticular Suture Alone vs. with Running Horizontal Mattress) in
Understanding Debridement
 Understanding Debridement Figure 1. Wound Healing Process Wound Blood Clot Blood Blood Vessel Fat Tissue The wound in the skin exposes deep tissue layers to the air. Scab Scab Exudate Granulation Tissue
Understanding Debridement Figure 1. Wound Healing Process Wound Blood Clot Blood Blood Vessel Fat Tissue The wound in the skin exposes deep tissue layers to the air. Scab Scab Exudate Granulation Tissue
8-5cover.qxd 11/14/2006 5:09 PM Page 1 $20.00 (US)
 $20.00 (US) CASE REPORT Peer Reviewed Wound Management in a Trumpeter Swan using Honey and a Sustained Release Ionic Silver Hydrogel Christoph Mans, med vet; Janet Sunohara-Neilson, MSc; Geraldine Higginson,
$20.00 (US) CASE REPORT Peer Reviewed Wound Management in a Trumpeter Swan using Honey and a Sustained Release Ionic Silver Hydrogel Christoph Mans, med vet; Janet Sunohara-Neilson, MSc; Geraldine Higginson,
Randomized Prospective Study Comparing Conventional Subcuticular Skin Closure With Dermabond Skin Glue After Saphenous Vein Harvesting
 Randomized Prospective Study Comparing Conventional Subcuticular Skin Closure With Dermabond Skin Glue After Saphenous Vein Harvesting Bhuvaneswari Krishnamoorthy, BS,* Osman Najam, MBChB,* Ursalan A.
Randomized Prospective Study Comparing Conventional Subcuticular Skin Closure With Dermabond Skin Glue After Saphenous Vein Harvesting Bhuvaneswari Krishnamoorthy, BS,* Osman Najam, MBChB,* Ursalan A.
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
5 RIOT-CONTROL AGENTS
 Riot-Control Agents Chapter 5 RIOT-CONTROL AGENTS Summary NATO Codes: CN, CS, CR, OC, DM Signs and Symptoms: Burning and pain on exposed mucous membranes and skin, eye pain and tearing, burning in the
Riot-Control Agents Chapter 5 RIOT-CONTROL AGENTS Summary NATO Codes: CN, CS, CR, OC, DM Signs and Symptoms: Burning and pain on exposed mucous membranes and skin, eye pain and tearing, burning in the
Bandaging & Plaster Techniques
 Bandaging & Plaster Techniques Dr. Ashish Gohiya MS, FIAS, FIOS (UK) Associate Professor Abrasion Contusion Lacerated W Incised W Degloving Crush DRESSING BANDAGE DRESSINGS PURPOSE OF DRESSINGS -Control
Bandaging & Plaster Techniques Dr. Ashish Gohiya MS, FIAS, FIOS (UK) Associate Professor Abrasion Contusion Lacerated W Incised W Degloving Crush DRESSING BANDAGE DRESSINGS PURPOSE OF DRESSINGS -Control
Otoplasty. Multimedia Health Education. Disclaimer
 Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about must be made in conjunction with Your Surgeon or a licensed healthcare provider.
Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about must be made in conjunction with Your Surgeon or a licensed healthcare provider.
