Perioperative care for lumbar microdiscectomy: a survey of Australasian neurosurgeons
|
|
|
- Melina Anne Poole
- 5 years ago
- Views:
Transcription
1 Original Study Perioperative care for lumbar microdiscectomy: a survey of Australasian neurosurgeons Christopher D. Daly 1,2,3, Kai Zheong Lim 1,2, Peter Ghosh 3,4, Tony Goldschlager 1,2,3 1 Department of Neurosurgery, Monash Medical Centre, Clayton, Victoria, Australia; 2 Department of Surgery, Monash University, Clayton, Victoria, Australia; 3 The Ritchie Centre, Hudson Institute of Medical Research, Monash University, Clayton, Victoria, Australia; 4 Proteobioactives Pty. Ltd., Brookvale, New South Wales, Australia Contributions: (I) Conception and design: CD Daly, KZ Lim, T Goldschlager; (II) Administrative support: None; (III) Provision of study materials or patients: None; (IV) Collection and assembly of data: CD Daly; (V) Data analysis and interpretation: All authors; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Dr. Christopher D. Daly, MBBS, MPhil. Department of Neurosurgery, Monash Medical Centre, 246 Clayton Rd., Clayton, Victoria 3168, Australia. christopher.daly@monash.edu. Background: Lumbar microdiscectomy is the most commonly performed spine surgery procedure. Over time it has evolved to a minimally invasive procedure. Traditionally patients were advised to restrict activity following lumbar spine surgery. However, post-operative instructions are heterogeneous. The purpose of this report is to assess, by survey, the perioperative care practices of Australasian neurosurgeons in the minimally invasive era. Methods: A survey was conducted by invitation sent to all full members of the Neurosurgical Society of Australasia (NSA). This consisted of 11 multi-choice questions relating to operative indications, technique, and post-operative instructions for lumbar microdiscectomy answered by an electronically distributed anonymized online survey. Results: The survey was sent to all Australasian Neurosurgeons. In total, 68 complete responses were received (28.9%). Most surgeons reported they would consider a period of either 4 to 8 weeks (42.7%) or 8 to 12 weeks (32.4%) as the minimum duration of radicular pain adequate to offer surgery. Unilateral muscle dissection with unilateral discectomy was practiced by 76.5%. Operative microscopy was the most commonly employed method of magnification (76.5%). The majority (55.9%) always refer patients to undergo inpatient physiotherapy. Sitting restrictions were advised by 38.3%. Lifting restrictions were advised by 83.8%. Conclusions: Australasian neurosurgical lumbar microdiscectomy perioperative care practices are generally consistent with international practices and demonstrate a similar degree of heterogeneity. Recommendation of post-operative activity restrictions by Australasian neurosurgeons is still common. This suggests a role for the investigation of the necessity of such restrictions in the era of minimally invasive spine surgery. Keywords: Spine; discectomy; perioperative care; neurosurgery; surveys and questionnaires Submitted Jul 29, Accepted for publication Jan 17, doi: /jss View this article at:
2 2 Daly et al. Lumbar discectomy perioperative care Introduction Lumbar microdiscectomy is the most commonly performed spine surgery procedure with over 300,000 operations performed annually in the United States alone (1). The first lumbar discectomy for a patient with a preoperative diagnosis of ruptured intervertebral disk is credited to Mixter and Barr in 1932 and was performed via a multi-level lumbar laminectomy (2). Since the initial description of the lumbar discectomy procedure the operation has progressed towards its current minimally invasive form. In tandem with the reduction in invasiveness, some surgeons have reduced the restrictions imposed in post-operative care instructions (3). However, significant heterogeneity in surgical technique and perioperative care still exists around the world (4-7) and there is a paucity of literature about the current state of play in Australia. Understanding current practices would be helpful to patients together with care providers, including referring practitioners, nursing staff, physiotherapists and perhaps other surgeons. The purpose of this survey is to determine current lumbar microdiscectomy perioperative practices amongst Australasian neurosurgeons. Methods A survey of Australasian Neurosurgeons was conducted by invitation sent to all full members of the Neurosurgical Society of Australasia (NSA). All invitees received a further two reminders. The survey consisted of 11 multi-choice questions conducted by an anonymized online survey. Statistical analysis was performed with Prism 7.0 (GraphPad Software Inc., La Jolla, CA, USA) and SPSS Statistics Version 24 (IBM Corp., Amonk, NY, USA). Pearson chi-squared statistic was used to assess the statistical significance of relationships between surgeon seniority and response to variables. Ethics approval was provided by Monash Human Research Ethics Committee. Results The survey was sent to 235 Australasian Neurosurgeons (NSA Members). Seventy-one responses were received of which 68 were complete (28.9% complete response rate). Only complete responses were included in the attached report. The questions and results of the survey are detailed below in Table 1. Surgical procedure The majority of surgeons (97.1%) performed a unilateral approach; 76.5% of surgeons used a microdiscectomy retractor and 20.6% used a tubular retractor system to perform a unilateral muscle dissection with unilateral discectomy. Only 2.9% of respondents performed bilateral muscle dissection with unilateral discectomy. Magnification The operative microscope was the most commonly employed method of magnification, practiced by 76.5% of surgeons. The operative microscope was used by surgeons performing the unilateral muscle dissection technique with a microdiscectomy retractor (58.8%) and those utilizing a tubular retractor system (17.6%). Loupes were used by 20.6% of surgeons 16.2% using the unilateral approach with microdiscectomy retractor, 2.9% using the tubular retractor system and 1.5% using the bilateral muscle dissection approach. Only 2.9% of surgeons elected to use no magnification and these were evenly split between the bilateral and unilateral muscle dissection approach. Operative indications In the absence of cauda equina syndrome or severe neurological deficit most surgeons reported that they would consider a period of either 4 to 8 weeks (42.7%) or 8 to 12 weeks (32.4%) of radicular pain the minimum duration of symptoms before offering surgery. Of the remaining surgeons 4.4% considered less than 2 weeks appropriate, 11.8% reported 2 to 4 weeks and 8.7% deemed more than 12 weeks an acceptable period of radicular pain after which surgery could be offered. Post-operative management The majority of surgeons (57.4%) mobilized patients upon returning to the ward on the day of surgery. Slightly less than one third of surgeons (32.4%) mobilized patients a few hours after surgery with the remainder (10.2%) mobilizing patients on day 1 following operation. Post-operative physiotherapy Most surgeons (55.9%) always referred patients to inpatient physiotherapy. Only 13.2% of surgeons stated they never
3 Journal of Spine Surgery, Vol 4, No 1 March Table 1 Survey questions and results Question Response Percentage (%) 1. Which surgical technique do you perform as a standard procedure for lumbar discectomy? Bilateral muscle dissection with bilateral discectomy 0 Bilateral muscle dissection with unilateral discectomy 2.9 Unilateral muscle dissection with unilateral discectomy 76.5 Unilateral muscle dissection with unilateral discectomy via tubular system Do you use magnification when performing lumbar discectomy operations and if so what kind? No magnification 2.9 Loupes In the absence of cauda equina syndrome or severe neurological deficit, what is the minimum duration of radicular pain a patient must report for you to offer lumbar discectomy surgery? Microscope 76.5 <2 weeks weeks weeks weeks 32.4 >12 weeks In the absence of CSF leak when do you allow your lumbar discectomy patients to mobilize following their operation? Day 0, upon returning to the ward 57.4 Day 0, after a few hours 32.4 Day Day Do you prescribe inpatient post-operative physiotherapy during admission following lumbar discectomy? Never 13.2 Rarely 8.8 Sometime 8.8 Often 13.3 Always Do you prescribe postoperative outpatient physiotherapy after discharge following lumbar discectomy? Never 23.5 Rarely 17.7 Sometime 35.2 Often 7.4 Always Do you advise sitting restrictions in the post-operative period following lumbar discectomy? No sitting restrictions 22.0 As comfort allows 39.7 <30 min per hour 20.6 <15 min per hour 10.3 Avoid sitting entirely if possible 7.4 Table 1 (continued)
4 4 Daly et al. Lumbar discectomy perioperative care Table 1 (continued) Question Response Percentage (%) 8. How long after lumbar discectomy do you advise patients to restrict sitting time? I don t advise sitting restrictions 30.9 Until comfortable 25.0 <1 week weeks weeks weeks 11.8 >8 weeks 0 9. Do you advise lifting restrictions in the post-operative period? I don t advise lifting restrictions 16.2 <40 kg 0 <20 kg 1.5 <10 kg 39.6 <5 kg How long after microdiscectomy do you advise patients to restrict lifting? No lifting restrictions 7.4 Until comfortable 13.2 <1 week weeks weeks 52.9 >8 weeks How many years have you been practicing as a Consultant Neurosurgeon? 0 5 years years years years 13.2 >20 years 36.8 The table lists all survey questions, responses and the percentage of surgeons who selected each response. CSF, cerebrospinal fluid. referred patients to undergo inpatient physiotherapy. Outpatient physiotherapy referral practices were more varied, with 23.5% of surgeons indicating that they never referred patients for outpatient physiotherapy and 16.2% always referring patients for outpatient physiotherapy. The remaining surgeons fell between these extremes. Table 1 and Figure 1. When sitting restrictions were recommended the duration varied between avoiding sitting until comfortable (25.0%) and 4 to 8 weeks (11.8%). Sitting restrictions of 2 to 4 weeks were advised by 17.7% of surgeons. Restrictions of 1 week or less were rarely recommended (1.4%). Sitting restrictions Just over one third of surgeons (38.3%) recommended the application of sitting restrictions whilst the remainder (61.7%) recommended no restrictions beyond that afforded by comfort. The breakdown of this advice can be seen in Lifting restrictions Lifting restrictions were advised by the majority of surgeons (83.8%). Lifting restrictions of <5 kg (42.7%) and <10 kg (39.6%) were most frequently offered. No lifting restrictions were recommended by 16.2% of surgeons
5 Journal of Spine Surgery, Vol 4, No 1 March Figure 1 Sitting restrictions. Percentage of surgeons. No sitting restrictions As comfort allows <30 min per hr <15 min per hr Avoid sitting entirely Don t advise lifting restrictions <20 kg <10 kg <5 kg Figure 2 Lifting restrictions. Percentage of surgeons. (Figure 2). One surgeon contacted the authors directly to stress the importance of the avoidance of spinal flexion rather than lifting per se. A majority of surgeons advised patients to follow lifting restrictions for a period of 4 to 8 weeks (52.9%). The next most common period was 2 to 4 weeks (19.1%). The application of restrictions until comfortable was advised by 13.2% of surgeons and no period of lifting restrictions advised by 7.4%. A minority of surgeons advised extension of lifting restrictions beyond 8 weeks (5.9%) or for less than 1 week (1.5%). Seniority and relationship to advising restrictions There was a representative range of surgeon experience in this study, with surgeons of less than 5 years (25.0% of respondents) to more than 20 years of experience (36.8% of respondents) contributing to the survey. Surgeons 5 years or less post fellowship were more likely to use the operative microscope (94.1%) than those 6 or more years post fellowship (69.2%). The only surgeons who did not use intraoperative magnification had more than 20 years experience post fellowship. No relationship between surgical seniority and any other variable achieved statistical significance. Discussion This is the first survey of Australasian neurosurgeons detailing the peri-operative management of patients undergoing lumbar discectomy. Australasian practice is generally consistent with international practice and demonstrates a similar degree of heterogeneity (4-7). A limitation of this study is the 28.9% complete response rate. A trend towards declining responses to clinician surveys has been noted previously (8,9). Reasons cited for this trend include clinicians being swamped by questionnaires (10), a lack of incentive for involvement (10) and many clinicians having a policy of non-response (9). Furthermore Australasian clinicians have been noted to be amongst the worst survey responders (8). The response rate is comparable to the 36% rate in a survey of members of the International Society for the Study of the Lumbar Spine regarding post-operative activity restrictions (11). The distribution of surgeon seniority in this survey approximates that of the neurosurgical workforce as described in the 2016 Royal Australasian College of Surgeons Activities Report suggesting that responders are representative in this regard (12). The potential for non-responder bias must, however, be recognized. Unilateral muscle dissection with unilateral discectomy is the approach taken by the majority of Australasian neurosurgeons and is consistent with the reported practices of Dutch spine surgeons (4). The nature of the operative approach preferred by British, Canadian and Italian surgeons was not reported. Concurrent with the trend towards reduced soft tissue dissection in lumbar discectomy increased use of operative magnification has also been practiced (13). The operating microscope was introduced to lumbar discectomy surgery by Yasargil in 1967 and reported as part of a series of patients in 1977 (14). Its use was subsequently popularized by the pioneering orthopedic spine surgeon John McCulloch (13,15) and is the practice of over three quarters of Australasian neurosurgeons surveyed. Canadian neurosurgeons reported a similar practice with 70% using the microscope (5). Similarly, 82.5% of neurosurgeons from Lombardy reported using either loupes or the operative microscope (the two were not distinguished in the Italian survey) while 17.5% reported no use of magnification,
6 6 Daly et al. Lumbar discectomy perioperative care much higher than the 3% in our survey. The figures for Dutch and British surgeons were not reported. Variation among spine surgeons regarding timing of surgery in patients with radicular pain has been noted in previous studies (4). The majority of Australasian neurosurgeons surveyed consider a period of 4 to 8 weeks (42.65%) or 8 to 12 weeks (32.35%) the minimum period of radicular pain a patient must report prior to being offered lumbar discectomy surgery in the absence of cauda equina syndrome. These figures are very similar to those reported by Dutch spine surgeons 34% of surgeons indicated they would offer surgery to patients with 4 to 8 weeks of symptoms and a further 42% would offer surgery at 8 to 12 weeks (4). Timing of surgery for lumbar disk herniation associated sciatica is a long-standing controversy amongst spine surgeons. Surgical practice has swung from periods of early surgical intervention for acute radicular pain (16) to the current approach favored by most surgeons of performing a trial of conservative management lasting a number of weeks. The evidence from randomized controlled trials suggests early surgical intervention may offer symptomatic benefit. On as-treated analysis, the Spine Patient Outcomes Research Trial (SPORT) (17,18), demonstrated statistically significant benefits to surgery at all time-points from 3 months to 4 years (17,18). Similarly, the Sciatica Trial, comparing early (6 to 14 weeks) surgery for sciatica with 6 months of conservative management and surgery thereafter if required, demonstrated faster pain relief and perceived recovery in those who received early surgery (19). Just over half of Australian neurosurgeons always prescribe post-operative inpatient physiotherapy with less, only 1 in 6, always prescribing outpatient physiotherapy. International practice regarding physiotherapy referral varied significantly: 85.7% of Dutch surgeons prescribed inpatient physiotherapy while only 6% of Italian neurosurgeons did the same. This reflects the lack of clarity regarding the role of post-operative physiotherapy following lumbar microdiscectomy. A recent Cochrane review of post-operative rehabilitation programs following lumbar microdiscectomy indicated that there is, at best, low level evidence that physiotherapy programs started 4 to 6 weeks post-surgery led to better function than no treatment (20). Post-operative activity restrictions are commonly imposed following lumbar discectomy. This can be observed in our survey and a survey of international surgeons specifically addressing lifting restrictions following spine surgery (11). Our survey results reflect the persistence of this practice with approximately 40% of Australasian neurosurgeons recommending specific sitting restrictions. A survey of British spine surgeons indicated that 31% request their patients do not sit for between 2 days to 6 weeks following a spine surgical procedure (6). The British survey does not provide further detail on sitting restrictions and data for post-operative sitting restrictions were not available for Dutch, Italian or Canadian spine surgeons. Lifting restrictions were more common, with specific lifting restrictions advised by the majority of Australasian neurosurgeons (83.2%). Approximately half of Australasian neurosurgeons advised the application of such restrictions for a period of 4 to 8 weeks. The recommendation for lifting restrictions is relatively consistent with the practice among British spine surgeons and surgeons of the International Society for the Study of Lumbar Spine Surgery, 85% (6) and 96.3% (11) of whom respectively advised lifting restrictions (6). The variety of lifting restrictions demonstrated in this survey are consistent with earlier reports of European spine surgeon recommendations in which the authors noted a lack of consistency (11). The underlying rationale for sitting and lifting restrictions is that following surgery the spine is weaker due to disruption of the functional spinal motion unit and thus potentially more prone to injury (11). However, there appears to be little evidence to support this theory, empirically or biomechanically, or the imposition of such restrictions (11,21). The purpose of such restrictions in the era of microdiscectomy has been questioned in the literature since at least the mid-1990s (3,22). Carragee et al. reported a prospective study of 152 patients who did not observe activity restrictions following lumbar microdiscectomy. This cohort achieved similar outcomes, with the exception of achieving earlier return to work, compared to literature reported outcomes for the standard practice of postoperative restrictions. Bono et al. (23) recently reported the first randomized controlled trial comparing postoperative activity restriction protocols following lumbar microdiscectomy. No significant differences in outcomes or disk herniation recurrence rates were observed with activity restriction protocols of 2 or 6 weeks. The study was, however, underpowered to detect a significant difference in reherniation rates. We are currently performing the first randomized controlled trial comparing a patient group observing no post-operative activity restrictions with a control group observing a one month period of activity restrictions (24). Additionally, our study will track patient adherence to activity restrictions following spine surgery
7 Journal of Spine Surgery, Vol 4, No 1 March through use of a wearable activity monitory, an innovation of importance given the difficulty of verifying patient adherence to activity restrictions through self-report. Conclusions In conclusion, the surgical techniques and magnification preference of Australian neurosurgeons are generally consistent with their international colleagues. Sitting and lifting restrictions are still frequently advised by Australasian neurosurgeons. This survey demonstrates the heterogeneity in peri-operative practices of Australasian neurosurgeons and suggests the potential for investigation of the role of post-operative activity restrictions following lumbar microdiscectomy given the prevalence and variety of these practices in the era of minimally invasive spine surgery. Acknowledgements Dr. CD Daly is the recipient of the Foundation for Surgery Richard Jepson Research Scholarship. The authors thank the Neurosurgical Society of Australasia and its members for their participation and contribution to this report. Footnote Conflicts of Interest: The authors have no conflicts of interest to declare. Ethical Statement: Ethics approval was provided by Monash Human Research Ethics Committee (No L). References 1. Parker SL, Xu R, McGirt MJ, et al. Long-term back pain after a single-level diskectomy for radiculopathy: incidence and health care cost analysis. J Neurosurg Spine 2010;12: Mixter WJ, Barr JS. Rupture of the intervertebral disk with involvement of the spinal canal. N Engl J Med 1934;211: Carragee EJ, Helms E, O'Sullivan GS. Are postoperative activity restrictions necessary after posterior lumbar diskectomy? A prospective study of outcomes in 50 consecutive cases. Spine (Phila Pa 1976) 1996;21: Arts MP, Peul WC, Koes BW, et al. Management of sciatica due to lumbar disk herniation in the Netherlands: a survey among spine surgeons. J Neurosurg Spine 2008;9: Cenic A, Kachur E. Lumbar diskectomy: a national survey of neurosurgeons and literature review. Can J Neurol Sci 2009;36: McGregor AH, Dicken B, Jamrozik K. National audit of post-operative management in spinal surgery. BMC Musculoskelet Disord 2006;7: Zoia C, Bongetta D, Poli JC, et al. Intraregional differences of perioperative management strategy for lumbar disk herniation: is the Devil really in the details? Int J Spine Surg 2017;11:1. 8. Cook JV, Dickinson HO, Eccles MP. Response rates in postal surveys of healthcare professionals between 1996 and 2005: An observational study. BMC Health Serv Res 2009;9: Wiebe ER, Kaczorowski J, MacKay J. Why are response rates in clinician surveys declining? Can Fam Physician 2012;58:e McAvoy BR, Kaner EF. General practice postal surveys: a questionnaire too far? BMJ 1996;313:732-3; discussion Magnusson ML, Pope MH, Wilder DG, et al. Is there a rational basis for post-surgical lifting restrictions? 1. Current understanding. Eur Spine J 1999;8: RACS. Royal Australasian College of Surgeons 2016 Annual Activities Report. 2017: Truumees E. A history of lumbar disk herniation from Hippocrates to the 1990s. Clin Orthop Relat Res 2015;473: Yasargil MG. Microsurgical Operation of Herniated Lumbar Disk. In: Wüllenweber R, Brock M, Hamer J, et al. editors. Lumbar Disk Adult Hydrocephalus. Berlin: Springer, 1977: McCulloch JA. Focus issue on lumbar disk herniation: macro- and microdiskectomy. Spine (Phila Pa 1976) 1996;21:45S-56S. 16. Postacchini F, Postacchini R. Operative management of lumbar disc herniation: the evolution of knowledge and surgical techniques in the last century. Acta Neurochir Suppl 2011;108: Weinstein JN, Tosteson TD, Lurie JD, et al. Surgical vs nonoperative treatment for lumbar disk herniation: the Spine Patient Outcomes Research Trial (SPORT): a randomized trial. JAMA 2006;296: Weinstein JN, Lurie JD, Tosteson TD, et al. Surgical versus nonoperative treatment for lumbar disc herniation: four-year results for the Spine Patient Outcomes Research Trial (SPORT). Spine (Phila Pa 1976) 2008;33:
8 8 Daly et al. Lumbar discectomy perioperative care 19. Peul WC, van Houwelingen HC, van den Hout WB, et al. Surgery versus prolonged conservative treatment for sciatica. N Engl J Med 2007;356: Oosterhuis T, Costa LO, Maher CG, et al. Rehabilitation after lumbar disk surgery. Cochrane Database Syst Rev 2014;(3):CD Pope MH, Magnusson ML, Wilder DG, et al. Is there a rational basis for post-surgical lifting restrictions? 2. Possible scientific approach. Eur Spine J 1999;8: Carragee EJ, Han MY, Yang B, et al. Activity restrictions after posterior lumbar diskectomy. A prospective study of outcomes in 152 cases with no postoperative restrictions. Spine (Phila Pa 1976) 1999;24: Bono CM, Leonard DA, Cha TD, et al. The effect of short (2-weeks) versus long (6-weeks) post-operative restrictions following lumbar diskectomy: a prospective randomized control trial. Eur Spine J 2017;26: Daly CD, Lim KZ, Lewis J, et al. Lumbar microdiscectomy and post-operative activity restrictions: a protocol for a single blinded randomised controlled trial. BMC Musculoskelet Disord 2017;18:312. Cite this article as: Daly CD, Lim KZ, Ghosh P, Goldschlager T. Perioperative care for lumbar microdiscectomy: a survey of Australasian neurosurgeons.. doi: /jss
Lumbar microdiscectomy and post-operative activity restrictions: a protocol for a single blinded randomised controlled trial
 Daly et al. BMC Musculoskeletal Disorders (2017) 18:312 DOI 10.1186/s12891-017-1681-3 STUDY PROTOCOL Open Access Lumbar microdiscectomy and post-operative activity restrictions: a protocol for a single
Daly et al. BMC Musculoskeletal Disorders (2017) 18:312 DOI 10.1186/s12891-017-1681-3 STUDY PROTOCOL Open Access Lumbar microdiscectomy and post-operative activity restrictions: a protocol for a single
Lumbar disc herniation
 Lumbar disc herniation Thomas Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Symptoms and Signs Radicular Pain in the distribution of the involved nerve Neurological deficit motor,
Lumbar disc herniation Thomas Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Symptoms and Signs Radicular Pain in the distribution of the involved nerve Neurological deficit motor,
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/29800 holds various files of this Leiden University dissertation. Author: Moojen, Wouter Anton Title: Introducing new implants and imaging techniques for
Cover Page The handle http://hdl.handle.net/1887/29800 holds various files of this Leiden University dissertation. Author: Moojen, Wouter Anton Title: Introducing new implants and imaging techniques for
Clinical Policy: Disc Decompression Procedures Reference Number: CP.MP.114
 Clinical Policy: Reference Number: CP.MP.114 Effective Date: 07/16 Last Review Date: 07/16 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.114 Effective Date: 07/16 Last Review Date: 07/16 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
THRESHOLD POLICY T17 SPINAL SURGERY FOR ACUTE LUMBAR CONDITIONS
 THRESHOLD POLICY T17 SPINAL SURGERY FOR ACUTE LUMBAR CONDITIONS Policy author: Ipswich and East Suffolk and West Suffolk CCGs with support from Public Health Suffolk Policy start date: September 2014 Subsequent
THRESHOLD POLICY T17 SPINAL SURGERY FOR ACUTE LUMBAR CONDITIONS Policy author: Ipswich and East Suffolk and West Suffolk CCGs with support from Public Health Suffolk Policy start date: September 2014 Subsequent
Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS NASS COVERAGE POLICY RECOMMENDATIONS TASKFORCE
 NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
Better Outcomes for Older People with Spinal Trouble (BOOST) Research Programme
 Better Outcomes for Older People with Spinal Trouble (BOOST) Research Programme Background Low back pain (LBP) is now recognised as the leading disabling condition in the world. LBP is a highly variable
Better Outcomes for Older People with Spinal Trouble (BOOST) Research Programme Background Low back pain (LBP) is now recognised as the leading disabling condition in the world. LBP is a highly variable
Standard Disscectomy versus Microdiscectomy: Short Term and Long Term Outcome Comparison in Treatment of Lateral Lumbar Disc Hernaiation
 Iraqi JMS Published by Al-Nahrain College of Medicine P-ISSN 1681-6579 E-ISSN 2224-4719 Email: iraqijms@colmed-alnahrain.edu.iq http://www.colmed-alnahrain.edu.iq http://www.iraqijms.net Standard Disscectomy
Iraqi JMS Published by Al-Nahrain College of Medicine P-ISSN 1681-6579 E-ISSN 2224-4719 Email: iraqijms@colmed-alnahrain.edu.iq http://www.colmed-alnahrain.edu.iq http://www.iraqijms.net Standard Disscectomy
Clinical Policy: Disc Decompression Procedures Reference Number: CP.MP.114
 Clinical Policy: Reference Number: CP.MP.114 Effective Date: 07/16 Last Review Date: 07/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.114 Effective Date: 07/16 Last Review Date: 07/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life
 Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
NUHS Evidence Based Practice I Journal Club. Date:
 Topic NUHS Evidence Based Practice I Journal Club Team Members: Date: Featured Research Article: Vancouver format example: Weinstein JN, Tosteson TD, Lurie JD, Tosteson AN, Hanscom B, Skinner JS, Abdu
Topic NUHS Evidence Based Practice I Journal Club Team Members: Date: Featured Research Article: Vancouver format example: Weinstein JN, Tosteson TD, Lurie JD, Tosteson AN, Hanscom B, Skinner JS, Abdu
Surgery has long been an accepted treatment for. Patient-specific factors affecting hospital costs in lumbar spine surgery
 clinical article J Neurosurg Spine 24:1 6, 2016 Patient-specific factors affecting hospital costs in lumbar spine surgery Ross C. Puffer, MD, Ryan Planchard, BE, Grant W. Mallory, MD, and Michelle J. Clarke,
clinical article J Neurosurg Spine 24:1 6, 2016 Patient-specific factors affecting hospital costs in lumbar spine surgery Ross C. Puffer, MD, Ryan Planchard, BE, Grant W. Mallory, MD, and Michelle J. Clarke,
Lumbar disc reherniation after transforaminal lumbar endoscopic discectomy
 Original Article Page 1 of 5 Lumbar disc reherniation after transforaminal lumbar endoscopic discectomy Thomas A. Kosztowski, David Choi, Jared Fridley, Michael Galgano, Ziya Gokaslan, Adetokunbo Oyelese,
Original Article Page 1 of 5 Lumbar disc reherniation after transforaminal lumbar endoscopic discectomy Thomas A. Kosztowski, David Choi, Jared Fridley, Michael Galgano, Ziya Gokaslan, Adetokunbo Oyelese,
Patient Selection and Lumbar Operative Interventions
 Patient Selection and Lumbar Operative Interventions John C France MD Professor of Orthopaedic & Neurosurgery West Virginia University Low back pain is a symptom not a diagnosis Epidemiology of LBP General
Patient Selection and Lumbar Operative Interventions John C France MD Professor of Orthopaedic & Neurosurgery West Virginia University Low back pain is a symptom not a diagnosis Epidemiology of LBP General
Physician Reference Manual
 Nucleotome Physician Reference Manual Automated Percutaneous Lumbar Discectomy 900487-001-00, Page 1 Nucleotome Automated Percutaneous Lumbar Discectomy (APLD) Table of Contents Section 1 I. Description
Nucleotome Physician Reference Manual Automated Percutaneous Lumbar Discectomy 900487-001-00, Page 1 Nucleotome Automated Percutaneous Lumbar Discectomy (APLD) Table of Contents Section 1 I. Description
of thoracolumbar burst fractures
 Clin Orthop Relat Res (2016) 474:619 624 / DOI 10.1007/s11999-015-4305-y Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons Published online: 23 April
Clin Orthop Relat Res (2016) 474:619 624 / DOI 10.1007/s11999-015-4305-y Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons Published online: 23 April
Placename CCG. Policies for the Commissioning of Healthcare. Policy for Managing Back Pain- Spinal Injections
 Placename CCG Policies for the Commissioning of Healthcare Policy for Managing Back Pain- Spinal Injections 1 Introduction 1.1 This document is part of a suite of policies that the CCG uses to drive its
Placename CCG Policies for the Commissioning of Healthcare Policy for Managing Back Pain- Spinal Injections 1 Introduction 1.1 This document is part of a suite of policies that the CCG uses to drive its
Lumbar Discectomy and Decompression INFORMATION FOR PATIENTS UNDERGOING SURGERY
 Lumbar Discectomy and Decompression INFORMATION FOR PATIENTS UNDERGOING SURGERY Informed consent is the process of the surgical team providing information to the patient and their carers to enable them
Lumbar Discectomy and Decompression INFORMATION FOR PATIENTS UNDERGOING SURGERY Informed consent is the process of the surgical team providing information to the patient and their carers to enable them
SPORT Lumbar Intervertebral Disk Herniation and Back Pain
 SPORT Lumbar Intervertebral Disk Herniation and Back Pain Does Treatment, Location, or Morphology Matter? Adam M. Pearson, MD, MS,* Emily A. Blood, MS,* John W. Frymoyer, MD,* Harry Herkowitz, MD, William
SPORT Lumbar Intervertebral Disk Herniation and Back Pain Does Treatment, Location, or Morphology Matter? Adam M. Pearson, MD, MS,* Emily A. Blood, MS,* John W. Frymoyer, MD,* Harry Herkowitz, MD, William
Populations Interventions Comparators Outcomes Individuals: With lumbar spinal stenosis
 Image-Guided Minimally Invasive Decompression for Spinal (701126) (Formerly Image-Guided Minimally Invasive Lumbar Decompression for Spinal ) Medical Benefit Effective Date: 10/01/17 Next Review Date:
Image-Guided Minimally Invasive Decompression for Spinal (701126) (Formerly Image-Guided Minimally Invasive Lumbar Decompression for Spinal ) Medical Benefit Effective Date: 10/01/17 Next Review Date:
A Canadian perspective on anterior cervical discectomies: practice patterns and preferences
 Original Study A Canadian perspective on anterior cervical discectomies: practice patterns and preferences Reena K. Baweja 1, Michael Bennardo 1, Forough Farrokhyar 2, Amanda Martyniuk 1, Kesava Reddy
Original Study A Canadian perspective on anterior cervical discectomies: practice patterns and preferences Reena K. Baweja 1, Michael Bennardo 1, Forough Farrokhyar 2, Amanda Martyniuk 1, Kesava Reddy
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Segmental stability following minimally invasive decompressive surgery with tubular retractor for lumbar spinal stenosis
 Segmental stability following minimally invasive decompressive surgery with tubular retractor for lumbar spinal stenosis Department of Spinal surgery, Research Institute for Brain and Blood Vessels-Akita
Segmental stability following minimally invasive decompressive surgery with tubular retractor for lumbar spinal stenosis Department of Spinal surgery, Research Institute for Brain and Blood Vessels-Akita
Original Article Discectomy for Herniated Lumbar Disc in Resource Limited Settings: Loupe or Microscope?
 Egyptian Journal of Neurosurgery Volume 30 / No. 4 / October - December 2015 299-306 Original Article Discectomy for Herniated Lumbar Disc in Resource Limited Settings: Loupe or Microscope? Salah M Hamada
Egyptian Journal of Neurosurgery Volume 30 / No. 4 / October - December 2015 299-306 Original Article Discectomy for Herniated Lumbar Disc in Resource Limited Settings: Loupe or Microscope? Salah M Hamada
CAN WE PREDICT SURGERY FOR SCIATICA?
 7 CAN WE PREDICT SURGERY FOR SCIATICA? Improving prediction of inevitable surgery during non-surgical treatment of sciatica. Wilco C. Peul Ronald Brand Raph T.W.M. Thomeer Bart W. Koes Submitted for publication
7 CAN WE PREDICT SURGERY FOR SCIATICA? Improving prediction of inevitable surgery during non-surgical treatment of sciatica. Wilco C. Peul Ronald Brand Raph T.W.M. Thomeer Bart W. Koes Submitted for publication
ASJ. Asian Spine Journal. Introduction
 Asian Spine Journal Asian Spine Clinical Journal Study Asian Prolonged Spine J 2017;11(4):531-537 physiotherapy versus https://doi.org/10.4184/asj.2017.11.4.531 early surgical intervention Prolonged Physiotherapy
Asian Spine Journal Asian Spine Clinical Journal Study Asian Prolonged Spine J 2017;11(4):531-537 physiotherapy versus https://doi.org/10.4184/asj.2017.11.4.531 early surgical intervention Prolonged Physiotherapy
Responses to Key Questions for Washington State Health Care Authority Health Technology Assessment of Surgery for Symptomatic Lumbar Radiculopathy
 The American Academy of Orthopaedic Surgeons (AAOS), American Association of Neurological Surgeons (AANS), AANS/CNS Section on Disorders of the Spine and Peripheral Nerves (DSPN), Congress of Neurological
The American Academy of Orthopaedic Surgeons (AAOS), American Association of Neurological Surgeons (AANS), AANS/CNS Section on Disorders of the Spine and Peripheral Nerves (DSPN), Congress of Neurological
Waveflex elastic fixation and discectomy annulus in repair and reconstruction of spinal stability in patients with lumbar disc herniation
 19 44 20151022 Chinese Journal of Tissue Engineering Research October 22, 2015 Vol.19, No.44 Waveflex ( 221009) 1 Waveflex 2 3 Waveflex Waveflex (XZB201311) Waveflex Waveflex 38 18 Waveflex 20 (JOA)Oswestry
19 44 20151022 Chinese Journal of Tissue Engineering Research October 22, 2015 Vol.19, No.44 Waveflex ( 221009) 1 Waveflex 2 3 Waveflex Waveflex (XZB201311) Waveflex Waveflex 38 18 Waveflex 20 (JOA)Oswestry
Post Operative Care Following Spinal Surgery For A Cervical Herniated Disc
 Post Operative Care Following Spinal Surgery For A Cervical Herniated Disc The patient services department (PSD) supports LSI patients post surgery. Herniated Disc searching for the most effective solution
Post Operative Care Following Spinal Surgery For A Cervical Herniated Disc The patient services department (PSD) supports LSI patients post surgery. Herniated Disc searching for the most effective solution
Christopher I. Shaffrey, MD
 CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
BARRICAID PROSTHESIS for Partial Anulus Replacement. Optimizing discectomy outcomes in high-risk patients. Prevent Reherniation. Preserve Disc.
 BARRICAID PROSTHESIS for Partial Anulus Replacement Optimizing discectomy outcomes in high-risk patients Prevent Reherniation. Preserve Disc. Today s standard discectomy is performed in such manner that
BARRICAID PROSTHESIS for Partial Anulus Replacement Optimizing discectomy outcomes in high-risk patients Prevent Reherniation. Preserve Disc. Today s standard discectomy is performed in such manner that
Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Anthem Blue Cross and Blue Shield Central Region Clinical Claim Edit
 Subject: Laminotomy (Hemilaminectomy) with Decompression of Nerve Root(s), Including Partial Facetectomy, Foraminotomy and/or Excision of Herniated Intervertebral Disc, Reexploration, Single Interspace-Lumbar
Subject: Laminotomy (Hemilaminectomy) with Decompression of Nerve Root(s), Including Partial Facetectomy, Foraminotomy and/or Excision of Herniated Intervertebral Disc, Reexploration, Single Interspace-Lumbar
Citation for the published paper: Spine J Jun 1;15(6): doi: /j.spinee Epub 2015 Feb 17.
 This is an author produced version of a paper published in Spine Journal. This paper has been peer-reviewed but does not include the final publisher proof-corrections or journal pagination. Citation for
This is an author produced version of a paper published in Spine Journal. This paper has been peer-reviewed but does not include the final publisher proof-corrections or journal pagination. Citation for
Characteristics and Neurological Manifestations of Patients with Operated Lumbar Disc Herniation
 Original article ISSN: 2203-1413 Vol.2 No.1 Characteristics and Neurological Manifestations of Patients with Operated Lumbar Disc Herniation Amir Mohammad Bazzazi 1, Amir Abbas Ghasemi 1*, Roghayeh Mirsoltani
Original article ISSN: 2203-1413 Vol.2 No.1 Characteristics and Neurological Manifestations of Patients with Operated Lumbar Disc Herniation Amir Mohammad Bazzazi 1, Amir Abbas Ghasemi 1*, Roghayeh Mirsoltani
Populations Interventions Comparators Outcomes Individuals: With lumbar spinal stenosis
 Image-Guided Minimally Invasive Decompression for Spinal (701126) Medical Benefit Effective Date: 10/01/18 Next Review Date: 07/19 Preauthorization No Review Dates: 09/10, 07/11, 07/12, 07/13, 07/14, 07/15,
Image-Guided Minimally Invasive Decompression for Spinal (701126) Medical Benefit Effective Date: 10/01/18 Next Review Date: 07/19 Preauthorization No Review Dates: 09/10, 07/11, 07/12, 07/13, 07/14, 07/15,
Functional Outcome of Patients with Lumbar Intervertebral Disc Herniation after Minimally Invasive Microdiscectomy
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. II (July. 2017), PP 35-39 www.iosrjournals.org Functional Outcome of Patients with Lumbar
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. II (July. 2017), PP 35-39 www.iosrjournals.org Functional Outcome of Patients with Lumbar
Microdiscectomy for the Treatment of Lumbar Disc Herniation: An Evaluation of Reoperations and Long-Term Outcomes
 Original Research 77 Microdiscectomy for the Treatment of Lumbar Disc Herniation: An Evaluation of Reoperations and Long-Term Outcomes Alexander Aichmair 1 Jerry Y. Du 1 Jennifer Shue 1 Gisberto Evangelisti
Original Research 77 Microdiscectomy for the Treatment of Lumbar Disc Herniation: An Evaluation of Reoperations and Long-Term Outcomes Alexander Aichmair 1 Jerry Y. Du 1 Jennifer Shue 1 Gisberto Evangelisti
REVIEW OF LITERATURE BMJ 2007; 334(7607): Diagnosis and treatment of sciatica. Bart W. Koes Maurits W. van Tulder Wilco C.
 2 REVIEW OF LITERATURE Diagnosis and treatment of sciatica Bart W. Koes Maurits W. van Tulder Wilco C. Peul BMJ 2007; 334(7607):1313-1317 22 CHAPTER 2 DIAGNOSIS AND TREATMENT OF SCIATICA 23 INTRODUCTION
2 REVIEW OF LITERATURE Diagnosis and treatment of sciatica Bart W. Koes Maurits W. van Tulder Wilco C. Peul BMJ 2007; 334(7607):1313-1317 22 CHAPTER 2 DIAGNOSIS AND TREATMENT OF SCIATICA 23 INTRODUCTION
Lumbar microdiscectomy for sciatica in adolescents: a multicentre observational registry-based study
 Acta Neurochir (2017) 159:509 516 DOI 10.1007/s00701-017-3077-4 ORIGINAL ARTICLE - SPINE Lumbar microdiscectomy for sciatica in adolescents: a multicentre observational registry-based study Sasha Gulati
Acta Neurochir (2017) 159:509 516 DOI 10.1007/s00701-017-3077-4 ORIGINAL ARTICLE - SPINE Lumbar microdiscectomy for sciatica in adolescents: a multicentre observational registry-based study Sasha Gulati
Pasquale Donnarumma 1, Roberto Tarantino 1, Lorenzo Nigro 1, Marika Rullo 2, Domenico Messina 3, Daniele Diacinti 4, Roberto Delfini 1.
 Original Study Decompression versus decompression and fusion for degenerative lumbar stenosis: analysis of the factors influencing the outcome of back pain and disability Pasquale Donnarumma 1, Roberto
Original Study Decompression versus decompression and fusion for degenerative lumbar stenosis: analysis of the factors influencing the outcome of back pain and disability Pasquale Donnarumma 1, Roberto
5 Steps to a More Prosperous ASC June 12, Greg Poulter, MD, Vail Summit Orthopaedics
 Greg Poulter, MD, Vail Summit Orthopaedics 1 Complex Spine Surgery Complex Spine Surgery Capital intensive Challenging setup Technically difficult Minimally invasive Little pain May be outpatient 2 Concerns
Greg Poulter, MD, Vail Summit Orthopaedics 1 Complex Spine Surgery Complex Spine Surgery Capital intensive Challenging setup Technically difficult Minimally invasive Little pain May be outpatient 2 Concerns
Medical Policy Original Effective Date: Revised Date: Page 1 of 11
 Page 1 of 11 Content Disclaimer Description Coverage Determination Clinical Indications Lumbar Spine Surgery Lumbar Spine Surgery Description Indication Coding Lumbar Spinal Fusion (single level)surgery
Page 1 of 11 Content Disclaimer Description Coverage Determination Clinical Indications Lumbar Spine Surgery Lumbar Spine Surgery Description Indication Coding Lumbar Spinal Fusion (single level)surgery
Innovative Techniques in Minimally Invasive Cervical Spine Surgery. Bruce McCormack, MD San Francisco California
 Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion
 Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion Andrei Stefan Iencean ROMANIA DOI:
Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion Andrei Stefan Iencean ROMANIA DOI:
Herniated Disk in the Lower Back
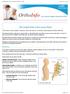 Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
Is unilateral pedicle screw fixation superior than bilateral pedicle screw fixation for lumbar degenerative diseases: a meta-analysis
 Lu et al. Journal of Orthopaedic Surgery and Research (2018) 13:296 https://doi.org/10.1186/s13018-018-1004-x SYSTEMATIC REVIEW Open Access Is unilateral pedicle screw fixation superior than bilateral
Lu et al. Journal of Orthopaedic Surgery and Research (2018) 13:296 https://doi.org/10.1186/s13018-018-1004-x SYSTEMATIC REVIEW Open Access Is unilateral pedicle screw fixation superior than bilateral
MEDICAL POLICY. Proprietary Information of YourCare Health Plan
 MEDICAL POLICY SUBJECT: INTERVERTEBRAL DISC DECOMPRESSION: PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
MEDICAL POLICY SUBJECT: INTERVERTEBRAL DISC DECOMPRESSION: PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
A COMPARATIVE STUDY OF THE
 A COMPARATIVE STUDY OF THE OUTCOMES OF PRIMARY AND REVISION DISCECTOMY SURGERY MS Patel, J Braybrooke, M Newey, P Sell BACKGROUND Following primary discectomy, a recurrent lumbar disc herniation at the
A COMPARATIVE STUDY OF THE OUTCOMES OF PRIMARY AND REVISION DISCECTOMY SURGERY MS Patel, J Braybrooke, M Newey, P Sell BACKGROUND Following primary discectomy, a recurrent lumbar disc herniation at the
GENDER & SCIATICA. Accepted for publication by Pain (in press 2008)
 8 GENDER & SCIATICA Influence of gender and other prognostic factors on outcome of sciatica; a post-hoc analysis of a randomized trial Wilco C. Peul Ronald Brand Raph T.W.M. Thomeer Bart W. Koes Accepted
8 GENDER & SCIATICA Influence of gender and other prognostic factors on outcome of sciatica; a post-hoc analysis of a randomized trial Wilco C. Peul Ronald Brand Raph T.W.M. Thomeer Bart W. Koes Accepted
Worldwide, many patients are affected
 TOPIC RESEARCH HUMAN CLINICAL TRIALS RESEARCH HUMAN CLINICAL TRIALS Tubular Diskectomy vs Conventional Microdiskectomy for the Treatment of Lumbar Disk Herniation: 2-Year Results of a Double-Blind Randomized
TOPIC RESEARCH HUMAN CLINICAL TRIALS RESEARCH HUMAN CLINICAL TRIALS Tubular Diskectomy vs Conventional Microdiskectomy for the Treatment of Lumbar Disk Herniation: 2-Year Results of a Double-Blind Randomized
Techniques and Applications of Endoscopic Spine Surgery. Part II: Safety and. Effectiveness of Endoscopic Spine Surgery in Treating Spinal Conditions
 Techniques and Applications of Endoscopic Spine Surgery. Part II: Safety and Effectiveness of Endoscopic Spine Surgery in Treating Spinal Conditions Kai-Xuan Liu, MD, PhD Atlantic Spine Center West Orange,
Techniques and Applications of Endoscopic Spine Surgery. Part II: Safety and Effectiveness of Endoscopic Spine Surgery in Treating Spinal Conditions Kai-Xuan Liu, MD, PhD Atlantic Spine Center West Orange,
Safety, Outcomes, and Cost Effectiveness of Outpatient Cervical ArthroplastieS
 Safety, Outcomes, and Cost Effectiveness of Outpatient Cervical ArthroplastieS Richard Wohns, M.D., J.D., MBA NeoSpine Puget Sound Region, WA NeoSpine Microsurgical Spine Center First outpatient ACDF in
Safety, Outcomes, and Cost Effectiveness of Outpatient Cervical ArthroplastieS Richard Wohns, M.D., J.D., MBA NeoSpine Puget Sound Region, WA NeoSpine Microsurgical Spine Center First outpatient ACDF in
This procedure lacks scientific evidence of effectiveness, and is not covered.
 ARBenefits Approval: 09-21-2011 Effective Date: 01-01-2012 Revision Date: Code(s): 0275T Medical Policy Title: Minimally Invasive, Image-Guided Lumbar Decompression for Spinal Stenosis Document: ARB0186
ARBenefits Approval: 09-21-2011 Effective Date: 01-01-2012 Revision Date: Code(s): 0275T Medical Policy Title: Minimally Invasive, Image-Guided Lumbar Decompression for Spinal Stenosis Document: ARB0186
QF-78. S. Tanaka 1, T.Yokoyama 1, K.Takeuchi 1, K.Wada 2, T. Tanaka 2, S.Abrakawa 2, G.Kumagai 2, T.Asari 2, A.Ono 2, Y.
 QF-78 Patient-oriented outcomes after musclepreserving interlaminar decompression for patients with lumbar spinal canal stenosis: Multi-center study to identify risk factors for poor outcomes S. Tanaka
QF-78 Patient-oriented outcomes after musclepreserving interlaminar decompression for patients with lumbar spinal canal stenosis: Multi-center study to identify risk factors for poor outcomes S. Tanaka
Lumbar Disc Prolapse. Dr. Ahmed Salah Eldin Hassan. Professor of Neurosurgery & Consultant spinal surgeon
 Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Research Article. Abstract
 Research Article Prolonged Preoperative Weakness Affects Recovery of Motor Function After Anterior Cervical Diskectomy and Fusion Tyler Kreitz, MD Ronald Huang, MD David Beck, MD Andrew G. Park, MD Alan
Research Article Prolonged Preoperative Weakness Affects Recovery of Motor Function After Anterior Cervical Diskectomy and Fusion Tyler Kreitz, MD Ronald Huang, MD David Beck, MD Andrew G. Park, MD Alan
Central Cord Syndrome: Does early surgical intervention improve neurological outcome
 Central Cord Syndrome: Does early surgical intervention improve neurological outcome Ciara Stevenson, Jonathan Warnock, Suzanne Maguire, Niall Eames Department of Trauma and Orthopaedic Surgery, Royal
Central Cord Syndrome: Does early surgical intervention improve neurological outcome Ciara Stevenson, Jonathan Warnock, Suzanne Maguire, Niall Eames Department of Trauma and Orthopaedic Surgery, Royal
Lumbar discectomy is the most common spinal procedure. FOCUS Neurosurg Focus 44 (5):E12, 2018
 NEUROSURGICAL FOCUS Neurosurg Focus 44 (5):E12, 2018 Propensity-matched comparison of outcomes and cost after macroscopic and microscopic lumbar discectomy using a national longitudinal database *Arjun
NEUROSURGICAL FOCUS Neurosurg Focus 44 (5):E12, 2018 Propensity-matched comparison of outcomes and cost after macroscopic and microscopic lumbar discectomy using a national longitudinal database *Arjun
Discectomy. Policy Number: Last Review: 12/2018 Origination: 12/2014 Next Review: 12/2019
 Discectomy Policy Number: 7.01.146 Last Review: 12/2018 Origination: 12/2014 Next Review: 12/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Discectomy when it
Discectomy Policy Number: 7.01.146 Last Review: 12/2018 Origination: 12/2014 Next Review: 12/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Discectomy when it
Syddansk Universitet. Published in: Danish Medical Journal. Publication date: Document version Publisher's PDF, also known as Version of record
 Syddansk Universitet Patient are satisfied one year after decompression surgery for lumbar spinal stenosis Tendal Paulsen, Rune; Bouknaitir, Jamal Bech; Fruensgaard, Søren; Carreon, Leah Y; Andersen, Mikkel
Syddansk Universitet Patient are satisfied one year after decompression surgery for lumbar spinal stenosis Tendal Paulsen, Rune; Bouknaitir, Jamal Bech; Fruensgaard, Søren; Carreon, Leah Y; Andersen, Mikkel
Posterior decompression via total laminectomy and
 CASE REPORT J Neurosurg Spine 27:352 356, 2017 Anterior lumbar discectomy and fusion for acute cauda equina syndrome caused by recurrent disc prolapse: report of 3 cases Kimberly-Anne Tan, MBBS, 1,2 Mathew
CASE REPORT J Neurosurg Spine 27:352 356, 2017 Anterior lumbar discectomy and fusion for acute cauda equina syndrome caused by recurrent disc prolapse: report of 3 cases Kimberly-Anne Tan, MBBS, 1,2 Mathew
Effects of Viewing an Evidence-Based Video Decision Aid on Patients Treatment Preferences for Spine Surgery. ACCEPTED
 Spine Publish Ahead of Print DOI: 10.1097/BRS.0b013e3182055c1e Effects of Viewing an Evidence-Based Video Decision Aid on Patients Treatment Preferences for Spine Surgery. Jon D. Lurie, MD, MS; Kevin F.
Spine Publish Ahead of Print DOI: 10.1097/BRS.0b013e3182055c1e Effects of Viewing an Evidence-Based Video Decision Aid on Patients Treatment Preferences for Spine Surgery. Jon D. Lurie, MD, MS; Kevin F.
Byung-Joon Shin. Soonchunhyang University College of Medicine, Seoul, Korea
 Asian Spine Journal Asian Spine Review Journal Article Asian Spine J 2014;8(2):211-215 http://dx.doi.org/10.4184/asj.2014.8.2.211 Recurrent disc 211 Risk Factors for Recurrent Lumbar Disc Herniations Byung-Joon
Asian Spine Journal Asian Spine Review Journal Article Asian Spine J 2014;8(2):211-215 http://dx.doi.org/10.4184/asj.2014.8.2.211 Recurrent disc 211 Risk Factors for Recurrent Lumbar Disc Herniations Byung-Joon
Torres del Paine, Patagonia
 Torres del Paine, Patagonia Chapter 7 Two-year results of the trial Tubular discectomy versus conventional microdiscectomy for the treatment of lumbar disc herniation: two-year results of a double-blind
Torres del Paine, Patagonia Chapter 7 Two-year results of the trial Tubular discectomy versus conventional microdiscectomy for the treatment of lumbar disc herniation: two-year results of a double-blind
Review date: February Lumbar Discectomy
 Review date: February 2019 Lumbar Discectomy Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as having a lumbar disc protrusion, resulting in nerve root
Review date: February 2019 Lumbar Discectomy Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as having a lumbar disc protrusion, resulting in nerve root
Automated Percutaneous and Endoscopic Discectomy. Original Policy Date
 MP 7.01.13 Automated Percutaneous and Endoscopic Discectomy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return
MP 7.01.13 Automated Percutaneous and Endoscopic Discectomy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return
How I do it: percutaneous transforaminal endoscopic discectomy for lumbar disk herniation
 Acta Neurochirurgica (2018) 160:2473 2477 https://doi.org/10.1007/s00701-018-3723-5 HOW I DO IT - SPINE DEGENERATIVE How I do it: percutaneous transforaminal endoscopic discectomy for lumbar disk herniation
Acta Neurochirurgica (2018) 160:2473 2477 https://doi.org/10.1007/s00701-018-3723-5 HOW I DO IT - SPINE DEGENERATIVE How I do it: percutaneous transforaminal endoscopic discectomy for lumbar disk herniation
LUMBAR MICRODISCECTOMY: TECHNIQUE, ADVANTAGES AND OUTCOMES. SURABAYA EXPERIENCE ON 83 PATIENTS
 Lumbar Microdiscectomy: Technique, Advantages and Outcomes. Surabaya Experience on 83 Patients (Abdul Hafid Bajamal) LUMBAR MICRODISCECTOMY: TECHNIQUE, ADVANTAGES AND OUTCOMES. SURABAYA EXPERIENCE ON 83
Lumbar Microdiscectomy: Technique, Advantages and Outcomes. Surabaya Experience on 83 Patients (Abdul Hafid Bajamal) LUMBAR MICRODISCECTOMY: TECHNIQUE, ADVANTAGES AND OUTCOMES. SURABAYA EXPERIENCE ON 83
The SPORT Study: What Have We Learned About Non- Operative Care? SPORT Study. In All Matters of Opinion, Our Adversaries are Insane
 The SPORT Study: What Have We Learned About Non- Operative Care? Joel S. Saal, M.D. SOAR, Physiatry Medical Group Redwood City, California In All Matters of Opinion, Our Adversaries are Insane Mark Twain
The SPORT Study: What Have We Learned About Non- Operative Care? Joel S. Saal, M.D. SOAR, Physiatry Medical Group Redwood City, California In All Matters of Opinion, Our Adversaries are Insane Mark Twain
Artificial Disc Replacement, Cervical
 Artificial Disc Replacement, Cervical Policy Number: Original Effective Date: MM.06.001 02/01/2010 Line(s) of Business: Current Effective Date: HMO; PPO 11/01/2011 Section: Surgery Place(s) of Service:
Artificial Disc Replacement, Cervical Policy Number: Original Effective Date: MM.06.001 02/01/2010 Line(s) of Business: Current Effective Date: HMO; PPO 11/01/2011 Section: Surgery Place(s) of Service:
Original Article First 30 Days Outcome of Conventional Discectomy for De Novo Lumbar Disc Herniation
 Egyptian Journal of Neurosurgery Volume 30 / No. 3 / July - September 2015 227-232 Original Article First 30 Days Outcome of Conventional Discectomy for De Novo Lumbar Disc Herniation 1 Mohamed Nosseir
Egyptian Journal of Neurosurgery Volume 30 / No. 3 / July - September 2015 227-232 Original Article First 30 Days Outcome of Conventional Discectomy for De Novo Lumbar Disc Herniation 1 Mohamed Nosseir
MOTORIZED SPINAL TRACTION
 MOTORIZED SPINAL TRACTION UnitedHealthcare Commercial Medical Policy Policy Number: PAI010 Effective Date: January 1, 2019 Table of Contents Page COVERAGE RATIONALE... 1 APPLICABLE CODES... 1 DESCRIPTION
MOTORIZED SPINAL TRACTION UnitedHealthcare Commercial Medical Policy Policy Number: PAI010 Effective Date: January 1, 2019 Table of Contents Page COVERAGE RATIONALE... 1 APPLICABLE CODES... 1 DESCRIPTION
ifuse implant system for treating chronic sacroiliac joint pain
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE ifuse implant system for treating chronic sacroiliac joint pain 1 Technology 1.1 Description of the technology The ifuse
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE ifuse implant system for treating chronic sacroiliac joint pain 1 Technology 1.1 Description of the technology The ifuse
Incomplete cauda equina syndrome in adult monozygotic twins
 Incomplete cauda equina syndrome in adult monozygotic twins J. Mohar, R. Kramar, N. Hero, R. J. Cirman Department of Spine Surgery and Paediatric Orthopaedics, Orthopaedic Hospital Valdoltra, Ankaran,
Incomplete cauda equina syndrome in adult monozygotic twins J. Mohar, R. Kramar, N. Hero, R. J. Cirman Department of Spine Surgery and Paediatric Orthopaedics, Orthopaedic Hospital Valdoltra, Ankaran,
STUDY OF FUNCTIONAL OUTCOME OF DISCECTOMY FOR LUMBAR DISC PROLAPSE
 STUDY OF FUNCTIONAL OUTCOME OF DISCECTOMY FOR LUMBAR DISC PROLAPSE P. Ashok Kumar 1, Ch. V. Murali Krishna 2, K. Srinivasa Rao 3, P. Rambabu 4, K. Vamsi Krishna 5, V. Krishna Swamy 6, Jameer Shaik 7, K.
STUDY OF FUNCTIONAL OUTCOME OF DISCECTOMY FOR LUMBAR DISC PROLAPSE P. Ashok Kumar 1, Ch. V. Murali Krishna 2, K. Srinivasa Rao 3, P. Rambabu 4, K. Vamsi Krishna 5, V. Krishna Swamy 6, Jameer Shaik 7, K.
Foundation Trust, Manchester, UK b Department of Neuroanaesthesia, Greater Manchester Neurosciences Centre, Salford Royal
 This article was downloaded by: [Kanna Gnanalingham] On: 07 September 2015, At: 00:20 Publisher: Taylor & Francis Informa Ltd Registered in England and Wales Registered Number: 1072954 Registered office:
This article was downloaded by: [Kanna Gnanalingham] On: 07 September 2015, At: 00:20 Publisher: Taylor & Francis Informa Ltd Registered in England and Wales Registered Number: 1072954 Registered office:
Darshan Vora 1, Matthew Kinnard 1, David Falk 1, Michael Hoy 1, Sachin Gupta 1, Christine Piper 1, Warren Yu 1, Faisal Siddiqui 2, Joseph O Brien 3
 Original Study A comparison of narcotic usage and length of post-operative hospital stay in open versus minimally invasive lumbar interbody fusion with percutaneous pedicle screws Darshan Vora 1, Matthew
Original Study A comparison of narcotic usage and length of post-operative hospital stay in open versus minimally invasive lumbar interbody fusion with percutaneous pedicle screws Darshan Vora 1, Matthew
Straight Leg Raising Test a snapshot summary of evidence (May 2013) Key messages
 Straight Leg Raising Test a snapshot summary of evidence (May 2013) Key messages The passive straight leg raising test (PSLR) is commonly used as an aid to the diagnosis of Lower Back Pain and is considered
Straight Leg Raising Test a snapshot summary of evidence (May 2013) Key messages The passive straight leg raising test (PSLR) is commonly used as an aid to the diagnosis of Lower Back Pain and is considered
Artificial Disc Replacement, Cervical
 Artificial Disc Replacement, Cervical Policy Number: Original Effective Date: MM.06.001 02/01/2010 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 01/01/2014 Section: Surgery Place(s) of Service:
Artificial Disc Replacement, Cervical Policy Number: Original Effective Date: MM.06.001 02/01/2010 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 01/01/2014 Section: Surgery Place(s) of Service:
Minimally Invasive Discectomy/ Decompression
 Minimally Invasive Discectomy/ Decompression What Is A Minimally Invasive Lumbar Discectomy? A lumbar discectomy is a surgical procedure that involves relieving the pressure placed on nerve roots and/or
Minimally Invasive Discectomy/ Decompression What Is A Minimally Invasive Lumbar Discectomy? A lumbar discectomy is a surgical procedure that involves relieving the pressure placed on nerve roots and/or
Percutaneous Laser Disc Decompression
 Percutaneous Laser Disc Decompression , MD Assistant Clinical Professor of Medicine, Columbia University College of Physicians & Surgeons, New York, New York; and Director of Laser Spine Center, New York,
Percutaneous Laser Disc Decompression , MD Assistant Clinical Professor of Medicine, Columbia University College of Physicians & Surgeons, New York, New York; and Director of Laser Spine Center, New York,
Cox Technic Case Report #169 published at (sent 5/9/17) 1
 Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Fusion and repeat discectomy following single level open lumbar discectomies. Survival analysis
 Fusion and repeat discectomy following single level open lumbar discectomies. Survival analysis Dr John Mortimer Mr Chris Hoffman CCDHB and TBI Health group Sciatica = Leg Dominant Pain Patients referred
Fusion and repeat discectomy following single level open lumbar discectomies. Survival analysis Dr John Mortimer Mr Chris Hoffman CCDHB and TBI Health group Sciatica = Leg Dominant Pain Patients referred
DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL
 SPINAL CHAPTER, NESON DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL INTRODUCTION DEGENERATIVE SPINAL DISEASE Gradual loss of normal structure and function of spine with time Also
SPINAL CHAPTER, NESON DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL INTRODUCTION DEGENERATIVE SPINAL DISEASE Gradual loss of normal structure and function of spine with time Also
Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion. Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD
 ORIGINAL ARTICLE Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD Study Design: A prospective study assessing
ORIGINAL ARTICLE Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD Study Design: A prospective study assessing
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of percutaneous endoscopic laser lumbar discectomy Symptomatic lumbar disc prolapse
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of percutaneous endoscopic laser lumbar discectomy Symptomatic lumbar disc prolapse
Reading** *Journal 吳孟玲. Presenter:Int. Outcome Evaluation of Surgical and Nonsurgical Management of Lumbar Disc Protrusion Causing Radiculopathy
 *Journal Reading** Outcome Evaluation of Surgical and Nonsurgical Management of Lumbar Disc Protrusion Causing Radiculopathy 2007-06-26 Presenter:Int. 吳孟玲 Background lumbar disc protrusion causing radiculopathy
*Journal Reading** Outcome Evaluation of Surgical and Nonsurgical Management of Lumbar Disc Protrusion Causing Radiculopathy 2007-06-26 Presenter:Int. 吳孟玲 Background lumbar disc protrusion causing radiculopathy
Evidence based management of low back pain surprising findings from historical research
 Evidence based management of low back pain surprising findings from historical research Dr Paul R. Mason Sport and Exercise Medicine Physician FACSEP MBBS (Honors) University of Sydney Bachelor of Physiotherapy
Evidence based management of low back pain surprising findings from historical research Dr Paul R. Mason Sport and Exercise Medicine Physician FACSEP MBBS (Honors) University of Sydney Bachelor of Physiotherapy
The Value of Adding Chiropractic Care to Worksite Health Clinics
 4 th National Association of Worksite Health Centers Annual Forum September 8, 2016, Milwaukee, Wisconsin Curt A. Krause, DC, MS Cerner Healthe Clinic LinkedIn Profile: http://t.co/l0twuh2s9r Slide 1:
4 th National Association of Worksite Health Centers Annual Forum September 8, 2016, Milwaukee, Wisconsin Curt A. Krause, DC, MS Cerner Healthe Clinic LinkedIn Profile: http://t.co/l0twuh2s9r Slide 1:
Disclosure. Thoracolumbar Tumors. Intraspinal Tumor Removal Options 6/4/2011. Minimally Invasive Approaches for Spinal Tumors
 Minimally Invasive Approaches for Spinal Tumors Praveen V. Mummaneni, M.D. Disclosure Medtronic (Consultant, Grants) DePuy (Consultant, Other Financial Support) Associate Professor Dept. of Neurosurgery
Minimally Invasive Approaches for Spinal Tumors Praveen V. Mummaneni, M.D. Disclosure Medtronic (Consultant, Grants) DePuy (Consultant, Other Financial Support) Associate Professor Dept. of Neurosurgery
NICE guidelines development Low back pain and sciatica: Management of non-specific low back pain and sciatica
 NICE guidelines development Low back pain and sciatica: Management of non-specific low back pain and sciatica Steven Vogel Vice Principal (Research), The British School of Osteopathy Editor-in-Chief, The
NICE guidelines development Low back pain and sciatica: Management of non-specific low back pain and sciatica Steven Vogel Vice Principal (Research), The British School of Osteopathy Editor-in-Chief, The
Disc herniation caused by a viscoelastic nucleus after total lumbar disc replacement a case report
 Case Report Disc herniation caused by a viscoelastic nucleus after total lumbar disc replacement a case report Lukas Grassner 1,2,3,4, Andreas Grillhösl 5, Michael Bierschneider 1, Martin Strowitzki 1
Case Report Disc herniation caused by a viscoelastic nucleus after total lumbar disc replacement a case report Lukas Grassner 1,2,3,4, Andreas Grillhösl 5, Michael Bierschneider 1, Martin Strowitzki 1
Int J Clin Exp Med 2016;9(2): /ISSN: /IJCEM Sheng Huang, Jiaquan Luo, Liangping Li, Shuai Huang
 Int J Clin Exp Med 2016;9(2):888-898 www.ijcem.com /ISSN:1940-5901/IJCEM0017704 Original Article The efficacy and safety of microendoscopic discectomy compared with conventional microsurgical discectomy:
Int J Clin Exp Med 2016;9(2):888-898 www.ijcem.com /ISSN:1940-5901/IJCEM0017704 Original Article The efficacy and safety of microendoscopic discectomy compared with conventional microsurgical discectomy:
Magnetic Resonance Imaging Interpretation in Patients With Symptomatic Lumbar Spine Disc Herniations
 Magnetic Resonance Imaging Interpretation in Patients With Symptomatic Lumbar Spine Disc Herniations Comparison of Clinician and Radiologist Readings Jon D. Lurie, MD, MS,* David M. Doman, MD, Kevin F.
Magnetic Resonance Imaging Interpretation in Patients With Symptomatic Lumbar Spine Disc Herniations Comparison of Clinician and Radiologist Readings Jon D. Lurie, MD, MS,* David M. Doman, MD, Kevin F.
Musculoskeletal Health
 CLINICAL PATHWAY Musculoskeletal Health Lumbar Disc Herniation and Radiculopathy Pathway Lumbar Disc Herniation and Radiculopathy Pathway Table of Contents (tap to jump to page) INTRODUCTION 1 Scope of
CLINICAL PATHWAY Musculoskeletal Health Lumbar Disc Herniation and Radiculopathy Pathway Lumbar Disc Herniation and Radiculopathy Pathway Table of Contents (tap to jump to page) INTRODUCTION 1 Scope of
Neurological Surgery, P.C. Brings Progressive Spine Surgery to Long Island. Long Island
 Long Island A BUSINESS & PRACTICE MANAGEMENT MAGAZINE ABOUT PHYSICIANS FROM PHYSICIANS FOR PHYSICIANS Neurological Surgery, P.C. Brings Progressive Spine Surgery to Long Island Neurological Surgery, P.C.
Long Island A BUSINESS & PRACTICE MANAGEMENT MAGAZINE ABOUT PHYSICIANS FROM PHYSICIANS FOR PHYSICIANS Neurological Surgery, P.C. Brings Progressive Spine Surgery to Long Island Neurological Surgery, P.C.
Lumbar Disc Prolapse: Management and Outcome Analysis of 96 Surgically treated Patients
 Lumbar Disc Prolapse: Management and Outcome Analysis of 96 Surgically treated Patients A. Akbar ( Department of Neurosurgery, Chandka Medical College, Larkana. ) A. Mahar ( Department of Orthopedic Surgery,
Lumbar Disc Prolapse: Management and Outcome Analysis of 96 Surgically treated Patients A. Akbar ( Department of Neurosurgery, Chandka Medical College, Larkana. ) A. Mahar ( Department of Orthopedic Surgery,
Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment
 Tohoku J. Exp. Med., 2006, 209, 1-6 Cauda Equina Tumors 1 Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment YOICHI SHIMADA, NAOHISA MIYAKOSHI, 1 YUJI KASUKAWA, 1 MICHIO HONGO, 1 SHIGERU
Tohoku J. Exp. Med., 2006, 209, 1-6 Cauda Equina Tumors 1 Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment YOICHI SHIMADA, NAOHISA MIYAKOSHI, 1 YUJI KASUKAWA, 1 MICHIO HONGO, 1 SHIGERU
