FACTORS CONTRIBUTING TO ANEMIA AFTER UNCOMPLICATED FALCIPARUM MALARIA
|
|
|
- Willis Burke
- 5 years ago
- Views:
Transcription
1 Am. J. Trop. Med. Hyg., 65(5), 2001, pp Copyright 2001 by The American Society of Tropical Medicine and Hygiene FACTORS CONTRIBUTING TO ANEMIA AFTER UNCOMPLICATED FALCIPARUM MALARIA RIC N. PRICE, JULIE A. SIMPSON, FRANÇOIS NOSTEN, CHRISTINE LUXEMBURGER, LILI HKIRJAROEN, FEIKO TER KUILE, TAN CHONGSUPHAJAISIDDHI, AND NICHOLAS J. WHITE Shoklo Malaria Research Unit, Mae Sod, Tak Province, Thailand; Faculty of Tropical Medicine, Mahidol University, Bangkok, Thailand; Department of Infectious Diseases and AIDS, Academic Medical Centre, University of Amsterdam, The Netherlands; Centre for Tropical Medicine, Nuffield Department of Clinical Medicine, John Radcliffe Hospital, Headington, Oxford, United Kingdom Abstract. The factors contributing to anemia in falciparum malaria were characterized in 4,007 prospectively studied patients on the western border of Thailand. Of these, 727 patients (18%) presented with anemia (haematocrit 30%), and 1% (55 of 5,253) required blood transfusion. The following were found to be independent risk factors for anemia at admission: age 5 years, a palpable spleen, a palpable liver, recrudescent infections, being female, a prolonged history of illness ( 2 days) before admission, and pure Plasmodium falciparum infections rather than mixed P. falciparum and Plasmodium vivax infections. The mean maximum fractional fall in hematocrit after antimalarial treatment was 14.1% of the baseline value (95% confidence interval [CI], ). This reduction was significantly greater in young children (aged 5 years) and in patients with a prolonged illness, high parasitemia, or delayed parasite clearance. Loss of parasitized erythrocytes accounted for 10% of overall red blood cell loss. Hematological recovery was usually complete within 6 weeks, but it was slower in patients who were anemic at admission (adjusted hazards ratio [AHR], 1.9, 95% CI, ), and those whose infections recrudesced (AHR, 1.2, 95% CI, ). Half the patients with treatment failure were anemic at 6 weeks compared with 19% of successfully treated patients (relative risk, 2.8, 95% CI, ). Patients coinfected with P. vivax (16% of the total) were 1.8 (95% CI, ) times less likely to become anemic and recovered 1.3 (95% CI, ) times faster than those with P. falciparum only. Anemia is related to drug resistance and treatment failure in uncomplicated malaria. Children aged 5 years of age were more likely than older children or adults to become anemic. Coinfection with P. vivax attenuates the anemia of falciparum malaria, presumably by modifying the severity of the infection. INTRODUCTION Malaria is a significant cause of anemia in the tropics, particularly in children. 1 The relationship between the severity and duration of anemia and the intensity of infection is complex. Anemia results from the destruction of parasitized erythrocytes, the shortened survival of unparasitized erythrocytes, and a variable degree of bone marrow dyserythropoiesis. 2 In general, the more severe the infection, the more profound the anemia. 3 The importance of drug-resistant malaria as a cause of anemia has been highlighted in recent years as chloroquine resistance has increased in Africa 4 ; the incidence of severe anemia requiring hospitalization and the need for blood transfusions have increased in parallel. 5 7 In high-transmission areas, where people are infected repeatedly, the contribution of an individual infection to anemia may be difficult to determine. The interaction between malaria and anemia has been less well studied in areas of low or unstable transmission. We report here on the relationship between anemia and falciparum malaria on the western border of Thailand, where transmission is low and multidrug resistance in Plasmodium falciparum deteriorated steadily during the past 10 years. PATIENTS AND METHODS Study site. This review is based on a series of large prospective chemotherapeutic trials aimed at optimizing antimalarial treatment regimens in an area of multidrug-resistant falciparum malaria. These studies took place between 1990 and 1995 in a Karen community, the members of which were living in 2 camps for displaced people located in an area of malarious hill forest on the western border of Thailand. 614 Studies involving 4,551 of the patients described here have been reported previously Transmission of malaria in this area is low (each person experienced approximately one bout of vivax and one bout of falciparum malaria infection every 2 years) and seasonal. 8 Nearly all falciparum malaria infections become symptomatic, and hence the treatment of every episode could be documented reliably. Between May 1990 and April 1992, a prospective malaria epidemiological study was conducted in Shoklo (one of the camps) with a population at midstudy estimated at 4,728; in total, 5,776 cases of falciparum malaria were diagnosed, and 400 (7%) of these patients were hospitalized. Thus, the overall (95% confidence interval [CI]) incidence of symptomatic falciparum malaria was 611 ( ) per 1,000 people per year. 8 This estimate incorporates both primary and recrudescent attacks. Of the 400 patients who were hospitalized, 303 patients (76%) were considered to have severe malaria, and 11 (3%) died. Thus, malaria is an important cause of morbidity and mortality in the area, and it is a major contributor to anemia, although hookworm, iron deficiency, and thalassemia also occur. Patients. All patients with uncomplicated falciparum malaria who were enrolled into therapeutic studies at the Shoklo Malaria Research Unit between 1990 and 1995 were included in the analysis. Patients of all ages were eligible to enroll in these prospective chemotherapeutic studies if they presented with slide-confirmed falciparum malaria to the Shoklo Malaria Research Unit or the outpatient clinics of Médecins Sans Frontières. Patients were recruited into prospective studies provided that they or their accompanying relatives gave fully informed consent. Pregnant women, children weighing 5 kg, and patients with concomitant disease requiring hospital ad-
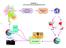
2 ANEMIA IN FALCIPARUM MALARIA 615 Mefloquine M 25 Halofantrine H 24 H 72 TABLE 1 Antimalarial treatment regimens Drug and regimen n Dose Artesunate mefloquine MA MAS1 MAS3 MAS5 MAS7 Artesunate AS5 AS7 Artemether MAM3 AM7 Quinine with or without tetracycline Q7 1, , mg/kg 24 mg/kg in 1 day 72 mg/kg over 3 days As 10 mg/kg (3 doses in 1 day) M15 As 4 mg/kg (1 dose) M25 As 4 mg/kg daily for 3 days M25 As 12 mg/kg (over 5 days) M25 As 12 mg/kg (over 7 days) M25 12 mg/kg over 5 days 12 mg/kg over 7 days Am 4 mg/kg daily for 3 days M25 12 mg/kg over 7 days 38 Q 30 mg/kg daily for 7 days Q7T7 182 Q 30 mg/kg daily for 7 days T 16 mg/kg daily As Artesunate, Am Artemether, M15 Mefloquine 15 mg/kg, M25 Mefloquine 25 mg/kg, Q Quinine, T Tetracycline. mission were all excluded. Therapeutic studies in Shoklo were carried out in 3 prospectively defined patient groups because each of these required a different treatment approach: 1) primary episodes of falciparum malaria; 2) recrudescent cases of malaria (recurrence of malaria within 63 days of a previous episode); and 3) hyperparasitemic falciparum malaria ( 4% parasitized red blood cells [RBCs]). Apart from this categorization, the inclusion and exclusion criteria were identical between studies. All studies were approved by the ethics committee of the Faculty of Tropical Medicine, Mahidol University, and the Karen Refugee Committee. Clinical and laboratory procedures and patient follow-up were similar irrespective of whether they were enrolled into a comparative drug study or monitored routinely. At admission, a full clinical examination was completed, and capillary blood was drawn for routine hematology. Hematocrit was measured from 100 L heparinized capillary blood, and packed cell volume was measured by microcentrifugation. Parasite counts were determined on Giemsa-stained thick and thin blood films. If the count on the thick film exceeded 1,000 parasites per 500 white blood cells, the thin film result (expressed as the number of erythrocytes per 1,000 RBCs) was recorded. Treatment with one of the drug regimens (Table 1) was assigned to patients in comparative randomized studies as described previously For the purposes of this analysis, they were then categorized into 4 treatment groups: mefloquine (single or split dose without artemisinin derivatives), halofantrine (high or low dose), artemisinin derivatives (artesunate or artemether with and without mefloquine), and quinine. Primaquine was not given routinely to eradicate the liver stages of Plasmodium vivax in mixed infections. Drug administration was observed in all patients. All patients were examined daily until they became asymptomatic and aparasitemic; they were then seen weekly during the follow-up period; before 1993, this was for 4 weeks, and after 1993, it was for 9 weeks. A malaria blood smear and blood for hematocrit was taken at each weekly visit, or if symptoms returned, between follow-up appointments. After recovery from the acute episode of malaria, patients with a hematocrit of 30% were prescribed a 2-week course of unsupervised ferrous sulfate and folic acid supplementation. Patients presenting with symptomatic and severe anemia (defined as hematocrit 20%) were transfused. A crosssectional malariometric survey of randomized houses in this camp was carried out in Data analysis. Data were analyzed by the statistical programs SPSS for Windows (SPSS Inc., Chicago, IL) and Epi Info 6 (CDC, Atlanta, GA). Normally distributed continuous data were compared by Student s t-test and analysis of variance. Data not conforming to a normal distribution were compared by the Mann-Whitney U test and Kruskal-Wallis analysis of variance. The association between 2 continuous variables was assessed by Spearman s rank correlation coefficient. Anemia was defined prospectively as a hematocrit 30%, and further classified as severe if the hematocrit was 20%. In patients whose infections did not recrudesce during follow-up, the fractional reduction in hematocrit attributable to malaria was defined before and after treatment as the difference between the patient s normal hematocrit on Day 42 and that on Day 0 or Day 7, respectively (see Figure 1 and Results) divided by the hematocrit on Day 42. Patients were stratified prospectively into the following age groups: young children (aged 5 years), older children (aged 5 14 years), and adults (aged 14 years). Proportions were compared by calculating by the chi-square test with Yates correction or by Fisher s exact test. Survival analysis was used to assess risk factors associated with the development of anemia during the follow-up period (for those patients not anemic at admission) and the time taken to return to a normal hematocrit (defined for each age and sex group as a hematocrit above the 25th percentile of the population hematocrit on Day 42 after antimalarial treatment) (Table 2). Cumulative incidences were calculated by the
3 616 PRICE AND OTHERS FIGURE 1. Hematological recovery after an episode of falciparum malaria (mean and 95% confidence intervals) in 4,007 patients. The malaria attributable fall in hematocrit before and after treatment was defined as the difference between the patients hematocrit on Day 42 and that on Day 0 or Day 7, respectively. product limit method and compared by the Mantel-Haenszel log rank test. When assessing independent risk factors, a Cox regression model was used. A multiple logistic regression model and a multiple linear regression model were used to determine adjusted odds ratios for risk factors for anemia at admission and adjusted regression coefficients for the variables associated with the fall in hematocrit attributable to malaria, respectively. In all multivariate analyses, independent risk factors were assessed after stratifying by the 4 treatment categories to account for potential drug effects. Any variable found to be TABLE 2 Comparison of the hematocrit values of patients at the time of complete hematological recovery* and from a survey of the general population conducted during the study period Age and sex Total 5 years 5 14 years Men Women n Survey Mean hematocrit, % (standard deviation) 36.0 (4.4) 33.8 (3.8) 36.5 (4.1) 38.7 (4.7) 35.3 (4.8) n 2, , days after acute malaria Mean hematocrit, % (standard deviation) 36.0 (3.2) 34.4 (3.1) 36.1 (2.9) 38.1 (3.5) 35.6 (2.9) 25th percentile * Derived from the predicted and actual hematocrit values on Day 42 of follow-up. associated significantly with anemia in a univariate analysis was entered into the equation and the model constructed by a forward stepwise analysis of the Wald statistic. RESULTS Between November 1990 and May 1995, 5,253 patients (2,328 female subjects and 2,925 male subjects) were enrolled into drug studies. Of these patients, 3,148 (60%) were recruited into randomized prospective studies and a further 2,105 (40%) patients presented to the clinics. Although the latter group was not part of comparative studies, they were treated in the same way and therefore included in this analysis. In total, 3,848 patients (73%) had primary infections and 1,405 (27%) had recrudescences of earlier falciparum malaria. There were 865 patients (16.5%) aged 5 years, 2,425 (46%) aged 5 14 years, and 1,963 (37%) aged 14 years old. The geometric mean parasitemia at admission was 5,347 parasites/ L (95% CI, 5,047 5,664) (Table 3). Followup was achieved in 4,294 (82%) patients to Day 28 and 2,599 (50%) to Day 42 after the start of antimalarial treatment. Hematological responses. Hematocrit data were available for 4,007 patients at admission, and the subsequent analysis in this section is confined to these patients. Of these, 3,328 patients (84%) had pure P. falciparum malaria and 634
4 ANEMIA IN FALCIPARUM MALARIA 617 TABLE 3 Admission characteristics Variable Patients with admission hematocrit, n (%) Admission hematocrit, mean (standard deviation) Anemic (hematocrit 30), n (%) Severe anemia (hematocrit 20), n (%) Total Aged 5 years Aged 5 14 years Men Women Primary infections Recrudescent infections Plasmodium falciparum only P. falciparum and Plasmodium vivax 4,007 (76) 613 (71) 1,905 (79) 786 (75) 703 (76) 3,046 (79) 961 (68) 3,328 (77) 634 (74) 34.7 (5.7) 31.1 (5.7) 34.9 (5.2) 37.4 (5.6) 34.3 (5.1) 35.3 (5.6) 33.0 (5.5) 34.7 (5.9) 35.2 (5.1) 727 (18) 235 (38) 304 (16) 63 (8) 125 (18) 476 (16) 251 (26) 630 (19) 88 (14) 40 (1.0) 20 (3.3) 16 (0.8) 1 (0.1) 3 (0.4) 25 (0.8) 15 (1.6) 35 (1.1) 4 (0.6) (16%) had mixed P. falciparum and P. vivax infection. Mixed infections occurred in 22.8% (194 of 852) of young children ( 5 years old) compared with 15.3% (659 of 4,316) in older patients (P 0.001). The mean hematocrit at admission was 34.7% (95% CI, ). Anemia (hematocrit 30%) occurred in 18% (727 of 4,007) patients. The incidence of anemia in falciparum malaria was highest in infants (56%). Admission characteristics are summarized in Table 3. The hematocrit at admission was correlated positively with age in children (r s 0.32; P 0.001) but not in adults, and overall showed a very weak positive correlation with parasitemia (r s 0.05; P 0.001). In a multivariate model, after correcting for baseline parasitemia, the following were found to be independent risk factors for anemia (defined as a hematocrit 30%) at admission: 1) children aged 5 years compared with children aged 5 14 years (adjusted odds ratio [AOR], 2.6, 95% CI, ; P 0.001); and 2) children aged 5 years compared with patients 14 years of age (AOR, 3.6, 95% CI, ; P 0.001), a palpable spleen (AOR, 2.3, 95% CI, ; P 0.001), a palpable liver (AOR, 2.0, 95% CI, ; P 0.001), recrudescent infections (AOR, 1.9, 95% CI, ; P 0.001), being female (AOR, 1.5, 95% CI, ; P 0.001), a prolonged history of illness before admission ( 2 days) (AOR, 1.5, 95% CI, ; P 0.001), and pure P. falciparum infections rather than mixed P. falciparum and P. vivax infections (AOR, 1.3, 95% CI, ; P 0.04). Hematological recovery. Overall, 55 (1%) patients required a blood transfusion. These patients were excluded from the analysis when assessing hematological profiles after admission. Since July 1993, individual patient follow-up has lasted days. In the 912 patients followed for longer than 42 days, no significant change in hematocrit was observed after Day 42, suggesting complete hematological recovery by this time (Figure 1). The Day 42 hematocrit was therefore taken as the normal value for that person. In total, only 1,372 (26%) patients had available hematocrit values on Day 42, and most of the data available came from those who received mefloquine plus 3 days of artesunate (MAS3) treatment (60%). A multivariate model was then generated with only MAS3-treated patients to predict the hematocrit value on Day 42 and thus that person s normal hematocrit, from the admission parasitemia and hematocrit values on Day 0, Day 7, and Day 28 (adjusted R ). The model was tested in 283 patients who did not receive MAS3 but who had their hematocrit measured on Day 42; we found no significant difference in the actual and predicted Day 42 hematocrit value (median difference, 0.06%, interquartile range [IQR], 2.0 to 2.0%). Data on a further 779 patients were generated by use of the model. Pooling actual and predicted Day 42 hematocrit levels demonstrated no difference in their age-stratified mean values and those obtained from a crosssectional hematocrit survey of the study population (Table 2). These observations supported the use of the Day 42 hematocrit as representing full hematological recovery from uncomplicated malaria. Malaria attributable anemia. Before treatment. Before treatment, the median fractional reduction fall in hematocrit attributable to malaria was 2.3% (IQR, 5.7 to 10.6%). This reduction was correlated weakly and negatively with both the parasitemia at admission (r 0.06, P 0.01) and age (r s 0.14, P 0.001). Children aged 5 years had a median (IQR) fractional fall in hematocrit of 7.5% ( 3.1 to 17.5%) compared with 1.4% ( 6.2 to 9.2%) in older children and 1.4% ( 6.3 to 9.2%) in adults (P 0.001). A severe reduction in hematocrit (defined as a fractional fall 25%) occurred in 13% (45 of 354) of patients aged 5 years, compared with 4% (44 of 1073) in older children and 3.2% (21 of 649) in adults (P 0.001). In a multivariate model, age 5 years, recrudescent infection, and a palpable spleen or liver were independent risk factors for a fractional reduction in hematocrit 25%, and together they explained 60% of the cases (Table 4). After treatment. The median (IQR) fractional fall in hematocrit attributable to malaria after treatment started was 8.9% ( %). The fractional fall in hematocrit was correlated positively with the admission parasite count (r s 0.25, P 0.001). Once again, the fall was greatest in the youngest age group (11.4; %) compared with 9.3 ( %) in older children and 6.6 ( %) in adults (P 0.001). Overall, 12.4% (37 of 298) of patients aged 5 years had a large fractional fall ( 25%) compared with 5.4% (50 of 930) in older children and 5.2% (31 of 595) in adults (P 0.001). In a multivariate model age, prolonged preadmission history of fever, high initial parasitemia, and delayed parasite clearance were all found to be significant independent risk factors. Together they explained 84% of cases in which the fractional fall in hematocrit exceeded 25% (Table 4). The overall mean maximal fractional reduction in hematocrit (including both pre- and posttreatment falls) resulting
5 618 PRICE AND OTHERS TABLE 4 Population attributable risk for a fractional fall in hematocrit of 25% before and after malaria treatment Risk factor Before treatment Aged 5 years Recrudescent infections Palpable spleen Palpable liver After treatment Aged 5 years High parasitemia ( 100,000 parasites/ L) Prolonged preadmission history Parasitemia not cleared in 24 hr Frequency (%) AOR (95% confidence interval)* 2.6 ( ) 1.9 ( ) 2.7 ( ) 1.8 ( ) 2.2 ( ) 2.4 ( ) 2.9 ( ) 2.7 ( ) PAR (%) P value * AOR adjusted odds ratio. AORs and 95% confidence intervals of the risk associated with the presence of the factor when compared with its absence after adjustment for the other factors in the table. AORs were calculated by logistic regression analysis. PAR population attributable risk. PAR is for a fractional drop in hematocrit from normal values of 25%. The overall PAR was calculated as 1 minus the product of 1 minus each individual PAR. Overall PAR before treatment is Overall PAR after treatment is from acute uncomplicated falciparum malaria in this series was 14.1% (95% CI, ). The effect of age on the maximal fractional drop in hematocrit proved independent of all other confounding factors (P 0.004) (Figure 2). Contribution of the loss of parasitized RBCs to anemia. From the maximal fractional fall and the Day 42 hematocrit, the mean (standard deviation [SD]) absolute loss of RBCs was calculated to be 628,000 cells/ L (440,000 cells/ L). The contribution of loss of parasitized RBCs to this figure was estimated by calculating the total number of RBCs parasitized during the infection and dividing this figure by the total number of RBCs lost. This calculation assumes that each parasitized cell was lost and that there was no reticulocyte response before the nadir of hematocrit. We have estimated previously that during the acute phase of falciparum malaria (with a parasite multiplication rate of 10-fold per cycle), 25% of the overall parasite biomass is sequestered in the microvasculature at any one time, although there is wide variability between people depending on the stage and synchronicity of each infection. 17 Taking into account these cells, the total number of malaria parasites that had occurred in the infection was calculated from the admission parasite count, assuming a previous parasite multiplication rate of 10- fold per cycle. The proportion of the total RBCs that were FIGURE 2. The age distribution of the mean maximal fractional fall in hematocrit associated with malaria.
6 ANEMIA IN FALCIPARUM MALARIA 619 FIGURE 3. Hematological recovery after a primary episode of falciparum malaria (mean and 95% confidence intervals) for patients treated successfully and patients with recrudescent infections during follow-up (n 3,021). lost as a direct result of parasitization was estimated to be 7.9% (95% CI, %). Thus, even if the majority of parasitized cells were sequestered at the time of admission, parasitization would still only account for less than one fifth of the loss in RBCs in patients with uncomplicated falciparum malaria. Hematocrit during follow-up. The mean hematocrit was lowest on Day 7 (mean, 32.8%; 95% CI, ) (Figure 1). The fractional fall in hematocrit during the first week of treatment correlated positively with hematocrit at admission (r 0.6; P 0.001), and this relationship was independent of the initial parasitemia. In those patients whose hematocrit was 30% at admission (n 3,280), the following were found by Cox regression analysis to be independent risk factors associated with the subsequent development of anemia during follow-up: 1) age 5 years compared with both children aged 5 14 years (AHR, 2.0, 95% CI, ; P 0.001), and also patients 14 years old (AHR, 2.6, 95% CI, ; P 0.001); 2) a prolonged history of illness before admission ( 2 days) (AHR, 1.7, 95% CI, ; P 0.001); 3) pure P. falciparum infections rather than mixed P. falciparum and P. vivax infections (AHR, 1.8, 95% CI, ; P 0.002); 4) a palpable liver (AHR, 1.4, 95% CI, ; P 0.05); 5) female sex (AHR, 1.3, 95% CI, ; P 0.02); 6) a high parasite count at admission ( 100,000 parasites/ L) (AHR, 1.5, 95% CI, ; P 0.008); and 7) failure to clear the peripheral parasitemia within 24 hr (AHR, 1.3, 95% CI, ; P 0.03). The time taken to return to a normal hematocrit (defined for each age and sex group as a hematocrit above the 25th percentile of the population for Day 42 hematocrit; Table 2) was significantly longer in those patients whose infections recrudesced during the follow-up period (P 0.02). By Day 42, patients who were treated successfully had a significantly higher hematocrit level compared with those whose malaria had recrudesced (36.2%, SD 3.5% versus 34.7%, SD 3.9%; P 0.001) (Figure 3). Furthermore, on this day, half (23 of 46, 50%) of patients failing their treatment were anemic (hematocrit 30%) compared with less than one fifth (235 of 1,264, 19%) of successfully treated patients (agestratified relative risk, 2.8, 95% CI, ; P 0.001). These data allow prediction of the effects of falciparum malaria on the overall hematological status of a population in an area with an attack rate of one episode of falciparum malaria per year and a treatment regimen with a 100% cure rate. In these circumstances, the overall mean drop in hematocrit per person would be very small, averaging 0.15% (95% CI, ) during the year. Three factors were found independently to delay hematological recovery: 1) anemia at admission (AHR, 1.9, 95% CI, ; P 0.001); 2) pure P. falciparum infections compared with mixed vivax and falciparum malaria (AHR, 1.3, 95% CI, ; P 0.01); and 3) recrudescence during follow-up (AHR, 1.2, 95% CI, ; P 0.03). DISCUSSION The emergence of multidrug resistance in P. falciparum on the western border of Thailand has been rapid. Patients
7 620 PRICE AND OTHERS with drug-resistant malaria responded more slowly to their antimalarial treatment, and their infections were more likely to recrudesce later. 18 These 2 factors combined to increase anemia after falciparum malaria. However, several factors have lessened the impact on the community we have studied. The infection rate with P. falciparum in the area is low (approximately one infection every 2 years, although nearly all patients become symptomatic). 8 Patients also tended to present early to malaria clinics (to which there is ready access) and begin effective antimalarial treatment before high parasite burdens developed. Elsewhere in this area, the population is more dispersed and enjoys less access to appropriate malaria treatment, and in this case, the impact of malaria on anemia would be expected to be greater. Other factors may have contributed to anemia in this series. The prevalence of hemoglobinopathies is very high in this area of the world. Nondeletional -thalassemia gene prevalences in Thailand (principally Hb Constant Spring) range 5 15%, and 0 -thalassemia genes are found in 2.5% of the population in the North. 19 Surveys in this population indicate that 6% of the population has heterozygote beta thalassemia, 2.5% has homozygous hemoglobin E, and 10% of boys or men have mild variant glucose-6-phosphate dehydrogenase (G6PD) deficiency (Weatherall D and Clegg J, unpublished data). Hookworm is also found, but egg burdens are low, and hookworm is not considered a major cause of anemia in this area (unpublished data). With the possible exception of G6PD deficiency, none of these should have contributed to the reversible reduction in hematocrit associated with malaria, although they would have contributed to the background population prevalence of anemia. The fall in hematocrit attributable to malaria in this study was greatest 1 week after presentation, with a mean reduction of 10% of the RBC mass and fall in hematocrit exceeding 25% in nearly 7% of patients. Approximately onequarter of the malaria-attributable fall in hematocrit occurred before presentation and three quarters after treatment. The hematological insult was greatest in the youngest age groups, in those with high parasite burdens, and in those presenting with a prolonged history of fever ( 2 days). As in other studies, a delay in the therapeutic response also contributed to an increased risk of malaria-associated anemia. 5 Malaria induces dyserythropoiesis, and reticulocytosis is depressed in the acute phase of the disease. 2,20 However, this cannot account for the rapidity with which anemia develops in malaria; the main causative factor is hemolysis. 2 This is conventionally attributed to loss of parasitized erythrocytes, but there is also evidence of accelerated destruction of unparasitized erythrocytes Recent studies indicate that the spleen can remove young intraerythrocytic malaria parasites and return the once-parasitized RBCs to circulation. 23 Nevertheless, even making the conservative assumption that each parasitized RBC will be destroyed at schizogony, we estimated that 90% of the RBCs lost were unparasitized in these patients with uncomplicated falciparum malaria. Although fever and the inflammatory reaction may shorten RBC survival, anemia in malaria is considerably greater than in other systemic infections. 24 Recent studies indicate that the membrane properties of unparasitized erythrocytes are altered in acute malaria, and there is reduced RBC deformability, 25 which correlates with the degree of anemia. 26 The splenic threshold for the removal of rigid or antibody-coated RBCs is lowered, and this is the most likely route of erythrocyte removal in acute falciparum malaria. 27,28 Anemia can be considered a measure of the cumulative impact of malaria on the individual patient. Protracted infections are associated with clinically significant RBC destruction, and in this study, patients with a prolonged history of fever ( 2 days) were 1.5-fold more likely to present with anemia and nearly 3 times more likely to experience a decrease in their hematocrit of 25%. The hematological burden of a heavy parasite load manifested itself mainly after treatment; indeed, patients with high parasite burdens presented with less RBC destruction before treatment compared with those with lower parasite burdens (0.3% compared with 2.7%; P 0.02). Immunity is slowly acquired with repeated malaria infection and manifests initially by reduced production of proinflammatory cytokines, as well as by a reduced response to these mediators in the face of infection (premunition). Eventually, more specific immunity supervenes, which controls and may prevent infection. Despite the low level of malaria transmission, there is evidence of acquired immunity in this community. 8 Children are more likely than adults to develop severe malaria 29 and are more likely to fail to respond to antimalarial medication. 16,30 In this study, children were also at greater risk of developing anemia, but this was still apparent after controlling for parasitemia. This suggests that children may be intrinsically more likely to develop anemia in falciparum malaria. Children with severe malaria are also more likely to develop severe anemia than adults. In this large series, children aged 5 years were 5.5 (95% CI, 3 10) times more likely to present with severe anemia (hematocrit 20%) at admission (P 0.001) and, after controlling for confounding factors, were twice as likely to experience a substantial reduction ( 25%) in their hematocrit when compared with older patients. Factors unrelated to falciparum malaria, such as previous malaria and hookworm infections (both of which were more common in children), may compound the effects of malaria and predispose the children to a greater hematological insult after infection with P. falciparum. Simultaneous coinfection with P. vivax attenuated the anemia resulting from falciparum malaria. The mean (SD) hematocrit on Day 7 was 32.5% (4.7) for pure falciparum infections compared with 33.5% (3.9) for mixed infections (P 0.001). In a recent study of the treatment of pure P. vivax infections at the same study site, the hematocrit on Day 7 after vivax malaria was found to be 35.6% (3.8). 31 In the study presented here, patients with mixed infections were 1.8 (95% CI: ) times less likely to develop anemia during follow-up, and cleared their anemia 1.3 (95% CI: ) times faster when compared with patients with pure P. falciparum infections (P 0.001). This may reflect mutual suppression of the 2 infections or earlier presentation and treatment, perhaps because of the lower pyrogenic density of P. vivax. In this community, mixed infections are also associated with a 4-fold lower risk of developing severe malaria 8 and of recrudescence after antimalarial treatment. 16 These observations further support the contention that P. vivax amelio-
8 ANEMIA IN FALCIPARUM MALARIA 621 rates falciparum malaria, 32 and they raise important questions over the value of targeting P. vivax, either with chloroquine or through the development of a vaccine, in areas where both species are prevalent. The fractional drop in hematocrit in the first week of treatment was correlated with the baseline hematocrit (r s 0.6, P 0.001), and this was independent of initial parasitemia. Hence, patients presenting with a low hematocrit are proportionally less likely to experience a drop in their hematocrit levels than those with high initial hematocrits. This suggests that RBC loss in an effectively treated uncomplicated infection is relatively fixed. Hematological recovery after an acute episode of uncomplicated falciparum malaria was complete by Day 42 of follow-up. After this time, hematocrit values did not change in those who were cured, and age-stratified values were not significantly different from those obtained from a hematological survey of the population. This period of recovery is twice that observed in healthy adults after a comparable loss of blood volume (8%). 33 This slow recovery may result from dyserythropoiesis and continued destruction of unparasitized erythrocytes after clearance of parasitemia. 21 Patients whose infections recrudesced during follow-up took significantly longer to return to a normal hematocrit, and by Day 42, these patients were nearly 3 times as likely to be anemic (P 0.001). In the majority of patients, a single episode of uncomplicated falciparum malaria, which is diagnosed and treated effectively, causes mild anemia; this resolves slowly. Drug resistance leads to an increase in anemia, and young children are particularly vulnerable because they are more likely to have recrudescent infections and have a greater decrease in hematocrit levels than older children for any given severity of infection. Acknowledgments: We thank the Karen staff members of the Shoklo Malaria Research Unit for support and technical assistance. We thank James Beeson, Daan Kuyper, Rose McGready, Stephane Proux, and Michele van Vugt for their help in conducting the hematocrit survey. This study was part of the Wellcome Trust-Mahidol University Oxford Tropical Medicine Research Programme, supported by the Wellcome Trust of Great Britain. Financial support: This study was part of the Wellcome Trust-Mahidol University Oxford Tropical Medicine Research Programme, supported by the Wellcome Trust of Great Britain. Authors addresses: Ric N. Price, Feiko ter Kuile, Christine Luxemburger, Lili Hkirjaroen, and François Nosten, Shoklo Malaria Research Unit, P.O. Box 46, Mae Sod 63110, Tak Province, Thailand. François Nosten, T. Chongsuphajaisiddhi, Julie A. Simpson, and Nicholas J. White, Faculty of Tropical Medicine, Mahidol University, Bangkok, Thailand. Feiko ter Kuile, Department of Infectious Diseases and AIDS, Academic Medical Centre, University of Amsterdam, The Netherlands. Ric N. Price, C. Luxemburger, François Nosten, and Nicholas J. White, Centre for Tropical Medicine, Nuffield Department of Clinical Medicine, John Radcliffe Hospital, Headington, Oxford, United Kingdom. Reprint requests: R. N. Price, Centre for Tropical Medicine, Nuffield Department of Clinical Medicine, John Radcliffe Hospital, Headington, Oxford, United Kingdom, Telephone: , Fax: ( ricprice@doctors.org.uk). REFERENCES 1. Hedberg K, Shaffer N, Davachi F, Hightower A, Lyamba B, Paluku KM, Nguyen Dinh P, Breman JG, Plasmodium falciparum-associated anemia in children at a large urban hospital in Zaire. Am J Trop Med Hyg 48: White NJ, Ho M, The pathophysiology of malaria. Baker JR, Muller R, eds. Advances in Parasitology. New York: Academic Press, Slutsker L, Taylor TE, Wirima JJ, Steketee RW, In-hospital morbidity and mortality due to malaria-associated severe anaemia in two areas of Malawi with different patterns of malaria infection. Trans R Soc Trop Med Hyg 88: Ekvall H, Premji Z, Bjorkman A, Chloroquine treatment for uncomplicated childhood malaria in an area with drug resistance: early treatment failure aggravates anaemia. Trans R Soc Trop Med Hyg 92: Bloland PB, Lackritz EM, Kazembe PN, Were JB, Steketee R, Campbell CC, Beyond chloroquine: implications of drug resistance for evaluating malaria therapy efficacy and treatment policy in Africa. J Infect Dis 167: Zucker JR, Lackritz EM, Ruebush TK, Hightower AW, Adungosi JE, Were JB, Campbell CC, Anaemia, blood transfusion practices, HIV and mortality among women of reproductive age in western Kenya. Trans R Soc Trop Med Hyg 88: Zucker JR, Lackritz EM, Ruebush TK, Hightower AW, Adungosi JE, Were JBO, Metchock B, Patrick E, Campbell CC, Childhood mortality during and after hospitalisation in Western Kenya: effect of malaria treatment regimens. Am J Trop Med Hyg 55: Luxemburger C, Kyaw Ley Thew, White NJ, Webster HK, Kyle DE, Maelankiri L, Chongsuphajaisiddhi T, Nosten F, The epidemiology of malaria in a Karen population on the western border of Thailand. Trans R Soc Trop Med Hyg 90: ter Kuile FO, Dolan G, Nosten F, Edstein MD, Luxemburger C, Phaipun L, Chongsuphajaisiddhi T, Webster HK, White NJ, Halofantrine versus mefloquine in the treatment of multi-drug resistant falciparum malaria. Lancet 341: Luxemburger C, ter Kuile F, Nosten F, Dolan G, Bradol JH, Phaipun L, Chongsuphajaisiddhi T, White NJ, Single day mefloquine-artesunate combination in the treatment of multi-drug resistant falciparum malaria. Trans R Soc Trop Med Hyg 88: Nosten F, Luxemburger C, ter Kuile FO, Woodrow C, Eh JP, Chongsuphajaisiddhi T, White NJ, Treatment of multidrug-resistant Plasmodium falciparum malaria with 3-day artesunate-mefloquine combination J Infect Dis 170: Luxemburger C, Nosten F, Raimond SD, Chongsuphajaisiddhi T, White NJ, Oral artesunate in the treatment of uncomplicated hyperparasitemic falciparum malaria. Am J Trop Med Hyg 53: Price RN, Nosten F, Luxemburger C, Am Kham, Brockman A, Chongsuphajaisiddhi T, White NJ, Artesunate versus artemether in combination with mefloquine for the treatment of multidrug resistant falciparum malaria. Trans R Soc Trop Med Hyg 89: Price RN, Luxemburger C, van Vugt M, Simpson J, Phaipun L, Chongsuphajaisiddhi T, Nosten F, White NJ, Treatment of uncomplicated hyperparasitaemic falciparum malaria on the Thai-Burmese border. Trans R Soc Trop Med Hyg 92: Price RN, van Vugt M, Luxemburger C, Brockman A, Phaipun L, Chongsuphajaisiddhi T, Nosten F, White NJ, Artesunate versus artemether for the treatment of recrudescent falciparum malaria. Am J Trop Med Hyg 59: Price RN, Nosten F, Luxemburger C, van Vugt M, Phaipun L, Chongsuphajaisiddhi T, White NJ, Artesunate/mefloquine treatment of multi-drug resistant falciparum malaria. Trans R Soc Trop Med Hyg 91: White NJ, Chapman D, Watt G, The effects of multiplication and synchronicity on the vascular distribution of parasites in falciparum malaria. Trans R Soc Trop Med Hyg 86: White NJ, Assessment of the pharmacodynamic properties of antimalarial drugs in vivo. Antimicrob Agents Chemother 41:
9 622 PRICE AND OTHERS 19. Hundreiser J, Sanguansermsri T, Papp T, Flatz G, Alphathalassaemia in Northern Thailand. Hum Hered 38: Phillips RE, Looareesuwan S, Warrell DA, Lee SH, Karbwang J, Warrell MJ, White NJ, Swasdichai C, Weatherall DJ, The importance of anaemia in cerebral and uncomplicated falciparum malaria: role of complications, dyserythropoiesis and iron sequestration. Q J Med 58: Looareesuwan S, Merry AH, Phillips RE, Pleehachinda R, Wattanagoon Y, Ho M, Charoenlarp P, Warrell DA, Weatherall DJ, Reduced erythrocyte survival following clearance of malarial parasitemia in Thai patients. Br J Haematol 67: Looareesuwan S, Davis TME, Pukrittayakamee S, Supanaranond W, Desakorn V, Silamut K, Krishna S, Boonamrung S, White NJ, Erythrocyte survival in severe falciparum malaria. Acta Trop 48: Angus B, Chotivanich K, Udomsangpetch R, White NJ, In vivo removal of malaria parasites from red cells without their destruction in acute falciparum malaria. Blood 90: Karle H, The pathogenesis of the anaemia of chronic disorders and the role of fever in erythrokinetics. Scand J Haematol 13: Naumann KM, Jones GL, Saul A, Smith R, Parasite-induced changes to localized erythrocyte membrane deformability in Plasmodium falciparum cultures. Immun Cell Biol 70: Dondorp AM, Angus BJ,Vreeken J, Chotivanich K, Silamut K, Ruangveerayuth R, Hardeman MR, Kager PA, White NJ, Red cell deformability as a predictor of anemia in severe falciparum malaria. Am J Trop Med Hyg 60: Looareesuwan S, Ho M, Wattanagoon Y, White NJ, Warrell DA, Bunnag D, Harinasuta T, Wyler DJ, Dynamic alteration in splenic function during acute falciparum malaria. N Engl J Med 317: Ho M, White NJ, Looareesuwan S, Wattanagoon Y, Lee SH, Walport MJ, Bunnag D, Harinasuta T, Splenic Fc receptor function in host defense and anemia in acute Plasmodium falciparum malaria. J Infect Dis 161: Luxemburger C, Ricci F, Nosten F, Raimond D, Bathet S, White NJ, The epidemiology of severe malaria in an area of low transmission in Thailand. Trans R Soc Trop Med Hyg 91: ter Kuile F, Luxemburger C, Nosten F, Phaipun L, Chongsuphajaisiddhi T, White NJ, Predictors of mefloquine treatment failure: a prospective study in 1590 patients with uncomplicated falciparum malaria. Trans R Soc Trop Med Hyg 89: Luxemburger C, van Vugt M, Jonathan S, McGready R, Looareesuwan S, White NJ, Nosten F, Treatment of vivax malaria on the western border of Thailand. Trans R Soc Trop Med Hyg 93: Maitland K, Williams TN, Newbold CI, Plasmodium vivax and P. falciparum: biological interactions and the possibility of cross-species immunity. Parasitol Today 13: Wadsworth GB, Recovery from acute haemorrhage in normal men and women. J Physiol 129:
Pharmacokinetics of Mefloquine Combined with Artesunate in Children with Acute Falciparum Malaria
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Feb. 1999, p. 341 346 Vol. 43, No. 2 0066-4804/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Pharmacokinetics of Mefloquine
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Feb. 1999, p. 341 346 Vol. 43, No. 2 0066-4804/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Pharmacokinetics of Mefloquine
Oral Artesunate Dose-Response Relationship in Acute Falciparum Malaria
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Mar. 2002, p. 778 782 Vol. 46, No. 3 0066-4804/02/$04.00 0 DOI: 10.1128/AAC.46.3.778 782.2002 Copyright 2002, American Society for Microbiology. All Rights Reserved.
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Mar. 2002, p. 778 782 Vol. 46, No. 3 0066-4804/02/$04.00 0 DOI: 10.1128/AAC.46.3.778 782.2002 Copyright 2002, American Society for Microbiology. All Rights Reserved.
Artemether-lumefantrine: a new treatment combination for multi-drug resistant falciparum malaria van Vugt, M.
 UvA-DARE (Digital Academic Repository) Artemether-lumefantrine: a new treatment combination for multi-drug resistant falciparum malaria van Vugt, M. Link to publication Citation for published version (APA):
UvA-DARE (Digital Academic Repository) Artemether-lumefantrine: a new treatment combination for multi-drug resistant falciparum malaria van Vugt, M. Link to publication Citation for published version (APA):
MONITORING THE THERAPEUTIC EFFICACY OF ANTIMALARIALS AGAINST UNCOMPLICATED FALCIPARUM MALARIA IN THAILAND
 SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH MONITORING THE THERAPEUTIC EFFICACY OF ANTIMALARIALS AGAINST UNCOMPLICATED FALCIPARUM MALARIA IN THAILAND C Rojanawatsirivej 1, S Vijaykadga 1, I Amklad 1, P Wilairatna
SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH MONITORING THE THERAPEUTIC EFFICACY OF ANTIMALARIALS AGAINST UNCOMPLICATED FALCIPARUM MALARIA IN THAILAND C Rojanawatsirivej 1, S Vijaykadga 1, I Amklad 1, P Wilairatna
Combination Anti-malarial Therapy and WHO Recommendations
 Prakaykaew Charunwatthana 2, and Sasithon Pukrittayakamee 1,2 1 Associate Fellow of the Royal Institute, Academy of Science 2 Department of Clinical Tropical Medicine, Faculty of Tropical Medicine, Mahidol
Prakaykaew Charunwatthana 2, and Sasithon Pukrittayakamee 1,2 1 Associate Fellow of the Royal Institute, Academy of Science 2 Department of Clinical Tropical Medicine, Faculty of Tropical Medicine, Mahidol
Am. J. Trop. Med. Hyg., 60(2), 1999, pp Copyright 1999 by The American Society of Tropical Medicine and Hygiene
 Am. J. Trop. Med. Hyg., 60(2), 1999, pp. 238 243 Copyright 1999 by The American Society of Tropical Medicine and Hygiene A RANDOMIZED, DOUBLE-BLIND, COMPARATIVE TRIAL OF A NEW ORAL COMBINATION OF ARTEMETHER
Am. J. Trop. Med. Hyg., 60(2), 1999, pp. 238 243 Copyright 1999 by The American Society of Tropical Medicine and Hygiene A RANDOMIZED, DOUBLE-BLIND, COMPARATIVE TRIAL OF A NEW ORAL COMBINATION OF ARTEMETHER
DOUBLE BLIND RANDOMISED CLINICAL TRIAL OF TWO DIFFERENT REGIMENS OF ORAL ARTESUNATE IN FALCIPARUM MALARIA
 DOUBLE BLIND RANDOMISED CLINICAL TRIAL OF TWO DIFFERENT REGIMENS OF ORAL ARTESUNATE IN FALCIPARUM MALARIA Danai Bunnag, Chaisin Viravan, Sornchai Looareesuwan, Juntra Karbwang and T-ranakchit Harinasuta
DOUBLE BLIND RANDOMISED CLINICAL TRIAL OF TWO DIFFERENT REGIMENS OF ORAL ARTESUNATE IN FALCIPARUM MALARIA Danai Bunnag, Chaisin Viravan, Sornchai Looareesuwan, Juntra Karbwang and T-ranakchit Harinasuta
Artemether-lumefantrine: a new treatment combination for multi-drug resistant falciparum malaria van Vugt, M.
 UvA-DARE (Digital Academic Repository) Artemether-lumefantrine: a new treatment combination for multi-drug resistant falciparum malaria van Vugt, M. Link to publication Citation for published version (APA):
UvA-DARE (Digital Academic Repository) Artemether-lumefantrine: a new treatment combination for multi-drug resistant falciparum malaria van Vugt, M. Link to publication Citation for published version (APA):
S Krudsood 1, K Chalermrut 2, C Pengruksa 2, S Srivilairit 2, U Silachamroon 3, S Treeprasertsuk 3, S Kano 4, GM Brittenham 5 and S Looareesuwan 3
 SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH COMPARATIVE CLINICAL TRIAL OF TWO-FIXED COMBINATIONS DIHYDROARTEMISININ-NAPTHOQUINE- TRIMETHOPRIM (DNP ) AND ARTEMETHER-LUMEFANTRINE (COARTEM / RIAMET ) IN THE
SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH COMPARATIVE CLINICAL TRIAL OF TWO-FIXED COMBINATIONS DIHYDROARTEMISININ-NAPTHOQUINE- TRIMETHOPRIM (DNP ) AND ARTEMETHER-LUMEFANTRINE (COARTEM / RIAMET ) IN THE
CLINICAL EXPERIENCE WITH INTRAVENOUS QUININE, INTRAMUSCULAR ARTEMETHER AND INTRAVENOUS ARTESUNATE FOR THE TREATMENT OF SEVERE MALARIA IN THAILAND
 SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH CLINICAL EXPERIENCE WITH INTRAVENOUS QUININE, INTRAMUSCULAR ARTEMETHER AND INTRAVENOUS ARTESUNATE FOR THE TREATMENT OF SEVERE MALARIA IN THAILAND Srivicha Krudsood
SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH CLINICAL EXPERIENCE WITH INTRAVENOUS QUININE, INTRAMUSCULAR ARTEMETHER AND INTRAVENOUS ARTESUNATE FOR THE TREATMENT OF SEVERE MALARIA IN THAILAND Srivicha Krudsood
Statistical Analysis Plan (SAP)
 Statistical Analysis Plan (SAP) Comparison of artemether-lumefantrine and chloroquine with and without primaquine for the treatment of Plasmodium vivax in Ethiopia: a randomized controlled trial Contents
Statistical Analysis Plan (SAP) Comparison of artemether-lumefantrine and chloroquine with and without primaquine for the treatment of Plasmodium vivax in Ethiopia: a randomized controlled trial Contents
DECLINING MEFLOQUINE SENSITIVITY OF PLASMODIUM FALCIPARUM ALONG THE THAI-MYANMAR BORDER
 SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH DECLINING MEFLOQUINE SENSITIVITY OF PLASMODIUM FALCIPARUM ALONG THE THAI-MYANMAR BORDER Chaiporn Rojanawatsirivet 1, Kanungnit Congpuong 1, Saowanit Vijaykadga
SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH DECLINING MEFLOQUINE SENSITIVITY OF PLASMODIUM FALCIPARUM ALONG THE THAI-MYANMAR BORDER Chaiporn Rojanawatsirivet 1, Kanungnit Congpuong 1, Saowanit Vijaykadga
On the pathophysiology of severe falciparum malaria with special reference to red cell deformability Dondorp, A.M.
 UvA-DARE (Digital Academic Repository) On the pathophysiology of severe falciparum malaria with special reference to red cell deformability Dondorp, A.M. Link to publication Citation for published version
UvA-DARE (Digital Academic Repository) On the pathophysiology of severe falciparum malaria with special reference to red cell deformability Dondorp, A.M. Link to publication Citation for published version
ISSN X (Print) Original Research Article. DOI: /sjams India
 DOI: 10.21276/sjams.2016.4.6.22 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2016; 4(6B):1981-198 5 Scholars Academic and Scientific Publisher (An International Publisher
DOI: 10.21276/sjams.2016.4.6.22 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2016; 4(6B):1981-198 5 Scholars Academic and Scientific Publisher (An International Publisher
EFFICACY OF PRIMAQUINE REGIMENS FOR PRIMAQUINE-RESISTANT PLASMODIUM VIVAX MALARIA IN THAILAND
 Am. J. Trop. Med. Hyg., 61(6), 1999, pp. 973 977 Copyright 1999 by The American Society of Tropical Medicine and Hygiene EFFICACY OF PRIMAQUINE REGIMENS FOR PRIMAQUINE-RESISTANT PLASMODIUM VIVAX MALARIA
Am. J. Trop. Med. Hyg., 61(6), 1999, pp. 973 977 Copyright 1999 by The American Society of Tropical Medicine and Hygiene EFFICACY OF PRIMAQUINE REGIMENS FOR PRIMAQUINE-RESISTANT PLASMODIUM VIVAX MALARIA
Artemether-lumefantrine: a new treatment combination for multi-drug resistant falciparum malaria van Vugt, M.
 UvA-DARE (Digital Academic Repository) Artemether-lumefantrine: a new treatment combination for multi-drug resistant falciparum malaria van Vugt, M. Link to publication Citation for published version (APA):
UvA-DARE (Digital Academic Repository) Artemether-lumefantrine: a new treatment combination for multi-drug resistant falciparum malaria van Vugt, M. Link to publication Citation for published version (APA):
Is there Artemisinin Resistance in Western Cambodia?
 Is there Artemisinin Resistance in Western Cambodia? Preliminary results, February 2008 Arjen Dondorp on behalf of the Task Force on Antimalarial Drug Resistance in Cambodia S769N PfATPase6 mutation Artemether
Is there Artemisinin Resistance in Western Cambodia? Preliminary results, February 2008 Arjen Dondorp on behalf of the Task Force on Antimalarial Drug Resistance in Cambodia S769N PfATPase6 mutation Artemether
NIH Public Access Author Manuscript Am J Ther. Author manuscript; available in PMC 2012 May 1.
 NIH Public Access Author Manuscript Published in final edited form as: Am J Ther. 2011 May ; 18(3): 190 197. doi:10.1097/mjt.0b013e3181d169c9. Use of area under the curve to evaluate the effects of antimalarial
NIH Public Access Author Manuscript Published in final edited form as: Am J Ther. 2011 May ; 18(3): 190 197. doi:10.1097/mjt.0b013e3181d169c9. Use of area under the curve to evaluate the effects of antimalarial
A Simple Dose Regimen of Artesunate and Amodiaquine Based on Arm Span- or Age Range for Childhood Falciparum Malaria: A Preliminary Evaluation
 JOURNAL OF TROPICAL PEDIATRICS, VOL. 58, NO. 4, 2012 A Simple Dose Regimen of Artesunate and Amodiaquine Based on Arm Span- or Age Range for Childhood Falciparum Malaria: A Preliminary Evaluation by Akintunde
JOURNAL OF TROPICAL PEDIATRICS, VOL. 58, NO. 4, 2012 A Simple Dose Regimen of Artesunate and Amodiaquine Based on Arm Span- or Age Range for Childhood Falciparum Malaria: A Preliminary Evaluation by Akintunde
ARTEMISININ FOR TREATMENT OF UNCOMPLICATED FALCIPARUM MALARIA: IS THERE A PLACE FOR MONOTHERAPY?
 Am. J. Trop. Med. Hyg., 65(6), 2001, pp. 690 695 Copyright 2001 by The American Society of Tropical Medicine and Hygiene ARTEMISININ FOR TREATMENT OF UNCOMPLICATED FALCIPARUM MALARIA: IS THERE A PLACE
Am. J. Trop. Med. Hyg., 65(6), 2001, pp. 690 695 Copyright 2001 by The American Society of Tropical Medicine and Hygiene ARTEMISININ FOR TREATMENT OF UNCOMPLICATED FALCIPARUM MALARIA: IS THERE A PLACE
Artemether-lumefantrine: a new treatment combination for multi-drug resistant falciparum malaria van Vugt, M.
 UvA-DARE (Digital Academic Repository) Artemether-lumefantrine: a new treatment combination for multi-drug resistant falciparum malaria van Vugt, M. Link to publication Citation for published version (APA):
UvA-DARE (Digital Academic Repository) Artemether-lumefantrine: a new treatment combination for multi-drug resistant falciparum malaria van Vugt, M. Link to publication Citation for published version (APA):
CONTRIBUTION OF HUMORAL IMMUNITY TO THE THERAPEUTIC RESPONSE IN FALCIPARUM MALARIA
 Am. J. Trop. Med. Hyg., 65(6), 2001, pp. 918 923 Copyright 2001 by The American Society of Tropical Medicine and Hygiene CONTRIBUTION OF HUMORAL IMMUNITY TO THE THERAPEUTIC RESPONSE IN FALCIPARUM MALARIA
Am. J. Trop. Med. Hyg., 65(6), 2001, pp. 918 923 Copyright 2001 by The American Society of Tropical Medicine and Hygiene CONTRIBUTION OF HUMORAL IMMUNITY TO THE THERAPEUTIC RESPONSE IN FALCIPARUM MALARIA
ACCEPTED. Diseases, Monash University, Commercial Road, Melbourne, Victoria 3004, Australia
 The Pediatric Infectious Disease Journal Publish Ahead of Print DOI : 10.1097/INF.0000000000000671 Plasmodium vivax malaria: challenges in diagnosis, treatment, and elimination James G Beeson 1,2, Cindy
The Pediatric Infectious Disease Journal Publish Ahead of Print DOI : 10.1097/INF.0000000000000671 Plasmodium vivax malaria: challenges in diagnosis, treatment, and elimination James G Beeson 1,2, Cindy
CLINICAL TRIAL OF HALOFANTRINE WITH MODIFIED DOSES FOR TREATMENT OF MALARIA IN THE HOSPITAL FOR TROPICAL DISEASES
 CLINICAL TRIAL OF HALOFANTRINE WITH MODIFIED DOSES FOR TREATMENT OF MALARIA IN THE HOSPITAL FOR TROPICAL DISEASES Srivicha Krudsood 1, Pratap Singhasivanon 1, Udomsak Silachamroon 2, Sombat Treeprasertsuk
CLINICAL TRIAL OF HALOFANTRINE WITH MODIFIED DOSES FOR TREATMENT OF MALARIA IN THE HOSPITAL FOR TROPICAL DISEASES Srivicha Krudsood 1, Pratap Singhasivanon 1, Udomsak Silachamroon 2, Sombat Treeprasertsuk
Downloaded from:
 Abreha, T; Alemayehu, B; Assefa, A; Awab, GR; Baird, JK; Bezabih, B; Cheah, PY; Day, NP; Devine, A; Dorda, M; Dondorp, AM; Girma, S; Hien, TT; Jima, D; Kassa, M; Kebende, A; Khu, NH; Leslie, T; Ley, B;
Abreha, T; Alemayehu, B; Assefa, A; Awab, GR; Baird, JK; Bezabih, B; Cheah, PY; Day, NP; Devine, A; Dorda, M; Dondorp, AM; Girma, S; Hien, TT; Jima, D; Kassa, M; Kebende, A; Khu, NH; Leslie, T; Ley, B;
PARASITOLOGY CASE HISTORY #14 (BLOOD PARASITES) (Lynne S. Garcia)
 PARASITOLOGY CASE HISTORY #14 (BLOOD PARASITES) (Lynne S. Garcia) A 37-year-old woman, who had traveled to New Guinea for several weeks, presented to the medical clinic with fever, chills, and rigors within
PARASITOLOGY CASE HISTORY #14 (BLOOD PARASITES) (Lynne S. Garcia) A 37-year-old woman, who had traveled to New Guinea for several weeks, presented to the medical clinic with fever, chills, and rigors within
HALOFANTRINE HYDROCHLORIDE - EFFICACY AND SAFETY IN CHILDREN WITH ACUTE MALARIA
 HALOFANTRINE HYDROCHLORIDE - EFFICACY AND SAFETY IN CHILDREN WITH ACUTE MALARIA Pages with reference to book, From 8 To 10 Mushtaq A. Khan, Gui Nayyer Rehman, S.A. Qazi ( Children Hospital, Pakistan Institute
HALOFANTRINE HYDROCHLORIDE - EFFICACY AND SAFETY IN CHILDREN WITH ACUTE MALARIA Pages with reference to book, From 8 To 10 Mushtaq A. Khan, Gui Nayyer Rehman, S.A. Qazi ( Children Hospital, Pakistan Institute
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centers: Indication: Treatment: Objective: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Malaria. Edwin J. Asturias, MD
 Malaria Edwin J. Asturias, MD Associate Professor of Pediatrics and Epidemiology Director for Latin America Center for Global Health, Colorado School of Public Health Global Health and Disasters Course
Malaria Edwin J. Asturias, MD Associate Professor of Pediatrics and Epidemiology Director for Latin America Center for Global Health, Colorado School of Public Health Global Health and Disasters Course
Hospitalization Criteria in Imported Falciparum Malaria
 306 Hospitalization Criteria in Imported Falciparum Malaria Valérie Briand, MD, MPH, * Olivier Bouchaud, MD, PhD, Jérôme Tourret, MD, Charlotte Behr, PhD, Sophie Abgrall, MD, PhD, Pascal Ralaimazava, MD,
306 Hospitalization Criteria in Imported Falciparum Malaria Valérie Briand, MD, MPH, * Olivier Bouchaud, MD, PhD, Jérôme Tourret, MD, Charlotte Behr, PhD, Sophie Abgrall, MD, PhD, Pascal Ralaimazava, MD,
INTRODUCTION. falciparum malaria (WHO, 2006). In Southeast Asia, where P. falciparum is the most drug resistant
 OPTIMUM DOSE OF ARTMISININ-PIPERAQUINE COMBINATIONS DOSE RANGING STUDIES OF NEW ARTEMISININ-PIPERAQUINE FIXED COMBINATIONS COMPARED TO STANDARD REGIMENS OF ARTEMISISNIN COMBINATION THERAPIES FOR ACUTE
OPTIMUM DOSE OF ARTMISININ-PIPERAQUINE COMBINATIONS DOSE RANGING STUDIES OF NEW ARTEMISININ-PIPERAQUINE FIXED COMBINATIONS COMPARED TO STANDARD REGIMENS OF ARTEMISISNIN COMBINATION THERAPIES FOR ACUTE
Cost of treating inpatient falciparum malaria on the Thai-Myanmar border
 Kyaw et al. Malaria Journal 2014, 13:416 RESEARCH Open Access Cost of treating inpatient falciparum malaria on the Thai-Myanmar border Shwe Sin Kyaw 1*, Tom Drake 1,2, Ronatrai Ruangveerayuth 3, Wirongrong
Kyaw et al. Malaria Journal 2014, 13:416 RESEARCH Open Access Cost of treating inpatient falciparum malaria on the Thai-Myanmar border Shwe Sin Kyaw 1*, Tom Drake 1,2, Ronatrai Ruangveerayuth 3, Wirongrong
Population Pharmacokinetic Assessment of a New Regimen of Mefloquine Used in Combination Treatment of Uncomplicated Falciparum Malaria
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, July 2006, p. 2281 2285 Vol. 50, No. 7 0066-4804/06/$08.00 0 doi:10.1128/aac.00040-06 Copyright 2006, American Society for Microbiology. All Rights Reserved. Population
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, July 2006, p. 2281 2285 Vol. 50, No. 7 0066-4804/06/$08.00 0 doi:10.1128/aac.00040-06 Copyright 2006, American Society for Microbiology. All Rights Reserved. Population
Antimalarials in the WHO Essential Drugs List for Children Reviewer No.1
 Antimalarials in the WHO Essential Drugs List for Children Reviewer No.1 Part I: Evaluation of the current list Proposed grouping from the March 2007 meeting 6.5.3 Antimalarial medicines 6.5.3.1 For curative
Antimalarials in the WHO Essential Drugs List for Children Reviewer No.1 Part I: Evaluation of the current list Proposed grouping from the March 2007 meeting 6.5.3 Antimalarial medicines 6.5.3.1 For curative
Risk associated with asymptomatic parasitaemia occurring post-antimalarial treatment
 Tropical Medicine and International Health doi:10.1111/j.1365-3156.2007.01977.x volume 13 no 1 pp 83 90 january 2008 Risk associated with asymptomatic parasitaemia occurring post-antimalarial treatment
Tropical Medicine and International Health doi:10.1111/j.1365-3156.2007.01977.x volume 13 no 1 pp 83 90 january 2008 Risk associated with asymptomatic parasitaemia occurring post-antimalarial treatment
Malaria Updates. Fe Esperanza Espino Department of Parasitology Research Institute for Tropical Medicine
 Malaria Updates Fe Esperanza Espino Department of Parasitology Research Institute for Tropical Medicine Outline General epidemiology of malaria in the Philippines P falciparum Updates in treatment Recognizing
Malaria Updates Fe Esperanza Espino Department of Parasitology Research Institute for Tropical Medicine Outline General epidemiology of malaria in the Philippines P falciparum Updates in treatment Recognizing
CLINICAL TRIALS OF MEFLOQUINE WITH TETRACYCLINE
 CLINICAL TRIALS OF MEFLOQUINE WITH TETRACYCLINE Danai Bunnag, Juntra Karbwang, Chaisin Viravan, Sunee Chitamas and Tranakchit Harinasuta Department of Clinical Tropical Medicine and Hospital for Tropical
CLINICAL TRIALS OF MEFLOQUINE WITH TETRACYCLINE Danai Bunnag, Juntra Karbwang, Chaisin Viravan, Sunee Chitamas and Tranakchit Harinasuta Department of Clinical Tropical Medicine and Hospital for Tropical
Disclosure Information
 Malaria Medications Charlie Mosler, RPh, PharmD, CGP, FASCP Assistant Professor of Pharmacy Practice The University of Findlay College of Pharmacy Findlay, OH mosler@findlay.edu Disclosure Information
Malaria Medications Charlie Mosler, RPh, PharmD, CGP, FASCP Assistant Professor of Pharmacy Practice The University of Findlay College of Pharmacy Findlay, OH mosler@findlay.edu Disclosure Information
Clinical experience of 17 cases of imported malaria at a Taiwan university hospital,
 J Microbiol Immunol Infect. 2007;40:209-215 Chung et al Original Article Clinical experience of 17 cases of imported malaria at a Taiwan university hospital, 1999-2005 Hsing-Chun Chung 1, Jann-Tay Wang
J Microbiol Immunol Infect. 2007;40:209-215 Chung et al Original Article Clinical experience of 17 cases of imported malaria at a Taiwan university hospital, 1999-2005 Hsing-Chun Chung 1, Jann-Tay Wang
Chloroquine pharmacokinetics in pregnant and nonpregnant women with vivax malaria
 Eur J Clin Pharmacol (2008) 64:987 992 DOI 10.1007/s00228-008-0500-z PHARMACOKINETICS AND DISPOSITION Chloroquine pharmacokinetics in pregnant and nonpregnant women with vivax malaria Sue Jean Lee & Rose
Eur J Clin Pharmacol (2008) 64:987 992 DOI 10.1007/s00228-008-0500-z PHARMACOKINETICS AND DISPOSITION Chloroquine pharmacokinetics in pregnant and nonpregnant women with vivax malaria Sue Jean Lee & Rose
14th Stakeholders Meeting
 14th Stakeholders Meeting Steady progress towards malaria elimination: Interventions for today and tomorrow Denpasar, Bali 11 12 October 2017 David Hughes, Novartis 12th October 2017 Defeating Malaria
14th Stakeholders Meeting Steady progress towards malaria elimination: Interventions for today and tomorrow Denpasar, Bali 11 12 October 2017 David Hughes, Novartis 12th October 2017 Defeating Malaria
APPENDIX 1 DATA COLLECTION AND DISSEMINATION STEPS
 APPENDIX 1 DATA COLLECTION AND DISSEMINATION STEPS 97 Country/ area APPENDIX 2a DRUG REGIMENS SEA REGION, 2001 (dosage for adults) : P. falciparum Lab confirmed Treatment failure Severe malaria Pregnancy
APPENDIX 1 DATA COLLECTION AND DISSEMINATION STEPS 97 Country/ area APPENDIX 2a DRUG REGIMENS SEA REGION, 2001 (dosage for adults) : P. falciparum Lab confirmed Treatment failure Severe malaria Pregnancy
38 Current Concepts in
 38 Current Concepts in Management of Falciparum Malaria Abstract: Artemisinin based Combination Therapy (ACT) is the preferred agent to treat drug resistance uncomplicated Plasmodium Falciparum (PF) Malaria.
38 Current Concepts in Management of Falciparum Malaria Abstract: Artemisinin based Combination Therapy (ACT) is the preferred agent to treat drug resistance uncomplicated Plasmodium Falciparum (PF) Malaria.
P. vivax P. falciparum coinfection and antimalarial drug resistance. Ric Price
 P. vivax P. falciparum coinfection and antimalarial drug resistance Ric Price Outline Global Burden Comparative biology of Pv and Pf Coinfections: Pv effect on Pf Relapses and the role post treatment prophylaxis
P. vivax P. falciparum coinfection and antimalarial drug resistance Ric Price Outline Global Burden Comparative biology of Pv and Pf Coinfections: Pv effect on Pf Relapses and the role post treatment prophylaxis
HIV and Malaria Interactions
 HIV and Malaria Interactions Dr. Moses R. Kamya Chair and Professor of Medicine Makerere University College of Health Sciences Kampala, Uganda INTEREST, Mombasa, Kenya 8 th -11 th May 2012 1 Outline Brief
HIV and Malaria Interactions Dr. Moses R. Kamya Chair and Professor of Medicine Makerere University College of Health Sciences Kampala, Uganda INTEREST, Mombasa, Kenya 8 th -11 th May 2012 1 Outline Brief
Antimalarial Drugs Clear Resistant Parasites from Partially Immune Hosts
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Oct. 2001, p. 2897 2901 Vol. 45, No. 10 0066-4804/01/$04.00 0 DOI: 10.1128/AAC.45.10.2897 2901.2001 Copyright 2001, American Society for Microbiology. All Rights
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Oct. 2001, p. 2897 2901 Vol. 45, No. 10 0066-4804/01/$04.00 0 DOI: 10.1128/AAC.45.10.2897 2901.2001 Copyright 2001, American Society for Microbiology. All Rights
Artemether-lumefantrine: a new treatment combination for multi-drug resistant falciparum malaria van Vugt, M.
 UvA-DARE (Digital Academic Repository) Artemether-lumefantrine: a new treatment combination for multi-drug resistant falciparum malaria van Vugt, M. Link to publication Citation for published version (APA):
UvA-DARE (Digital Academic Repository) Artemether-lumefantrine: a new treatment combination for multi-drug resistant falciparum malaria van Vugt, M. Link to publication Citation for published version (APA):
Efficacy and effectiveness of dihydroartemisinin-piperaquine versus artesunate-mefloquine in falciparum malaria: an open-label randomised comparison
 Efficacy and effectiveness of dihydroartemisinin-piperaquine versus artesunate-mefloquine in falciparum malaria: an open-label randomised comparison Frank Smithuis, Moe Kyaw Kyaw, Ohn Phe, Khin Zarli Aye,
Efficacy and effectiveness of dihydroartemisinin-piperaquine versus artesunate-mefloquine in falciparum malaria: an open-label randomised comparison Frank Smithuis, Moe Kyaw Kyaw, Ohn Phe, Khin Zarli Aye,
Akintunde Sowunmi 1,2,5*, Kazeem Akano 1, Adejumoke I. Ayede 3, Godwin Ntadom 4, Temitope Aderoyeje 5, Elsie O. Adewoye 6 and Bayo Fatunmbi 7
 Sowunmi et al. BMC Infectious Diseases (2016) 16:240 DOI 10.1186/s12879-016-1565-4 RESEARCH ARTICLE Clinical illness and outcomes in Nigerian children with late-appearing anaemia after artemisinin-based
Sowunmi et al. BMC Infectious Diseases (2016) 16:240 DOI 10.1186/s12879-016-1565-4 RESEARCH ARTICLE Clinical illness and outcomes in Nigerian children with late-appearing anaemia after artemisinin-based
doi: /s
 doi: 10.1007/s10528-008-9185-3 Lack of association of the HbE variant with protection from cerebral malaria in Thailand Izumi Naka 1, Jun Ohashi 1, Pornlada Nuchnoi 2, Hathairad Hananantachai 2, Sornchai
doi: 10.1007/s10528-008-9185-3 Lack of association of the HbE variant with protection from cerebral malaria in Thailand Izumi Naka 1, Jun Ohashi 1, Pornlada Nuchnoi 2, Hathairad Hananantachai 2, Sornchai
Downloaded from:
 Ekvall, H; Premji, Z; Bennett, S; Bjorkman, A (2001) Hemoglobin concentration in children in a malaria holoendemic area is determined by cumulated Plasmodium falciparum parasite densities. The American
Ekvall, H; Premji, Z; Bennett, S; Bjorkman, A (2001) Hemoglobin concentration in children in a malaria holoendemic area is determined by cumulated Plasmodium falciparum parasite densities. The American
EFFECT OF PRIMAQUINE STANDARD DOSE (15 MGIDAY FOR 14 DAYS) IN THE TREATMENT OF VIVAX MALARIA PATIENTS IN THAILAND
 EFFECT OF PRIMAQUINE STANDARD DOSE (15 MGIDAY FOR 14 DAYS) IN THE TREATMENT OF VIVAX MALARIA PATIENTS IN THAILAND K Buchachart', S Krudsood', P Singhasivanon', S Treeprasertsuk2, N Phophak', S Srivilairit3,
EFFECT OF PRIMAQUINE STANDARD DOSE (15 MGIDAY FOR 14 DAYS) IN THE TREATMENT OF VIVAX MALARIA PATIENTS IN THAILAND K Buchachart', S Krudsood', P Singhasivanon', S Treeprasertsuk2, N Phophak', S Srivilairit3,
The Malarias: Plasmodium falciparum Plasmodium vivax Plasmodium malariae Plasmodium ovale. Distribution of Plasmodium falciparum
 The Malarias: Plasmodium falciparum Plasmodium vivax Plasmodium malariae Plasmodium ovale Distribution of Plasmodium falciparum 1 Distribution Of Plasmodium vivax 2 Global Risk By Country-Proportionality
The Malarias: Plasmodium falciparum Plasmodium vivax Plasmodium malariae Plasmodium ovale Distribution of Plasmodium falciparum 1 Distribution Of Plasmodium vivax 2 Global Risk By Country-Proportionality
Poor response to artesunate treatment in two patients with severe malaria on the Thai Myanmar border
 https://doi.org/10.1186/s12936-018-2182-z Malaria Journal CASE REPORT Open Access Poor response to artesunate treatment in two patients with severe malaria on the Thai Myanmar border Aung Pyae Phyo 1,6*,
https://doi.org/10.1186/s12936-018-2182-z Malaria Journal CASE REPORT Open Access Poor response to artesunate treatment in two patients with severe malaria on the Thai Myanmar border Aung Pyae Phyo 1,6*,
Randomized Comparison of Artesunate and Quinine in the Treatment of Severe Falciparum Malaria
 MAJOR ARTICLE Randomized Comparison of Artesunate and Quinine in the Treatment of Severe Falciparum Malaria Paul N. Newton, 1,5 Brian J. Angus, 1,5 Wirongrong Chierakul, 1 Arjen Dondorp, 1,5 Ronatrai Ruangveerayuth,
MAJOR ARTICLE Randomized Comparison of Artesunate and Quinine in the Treatment of Severe Falciparum Malaria Paul N. Newton, 1,5 Brian J. Angus, 1,5 Wirongrong Chierakul, 1 Arjen Dondorp, 1,5 Ronatrai Ruangveerayuth,
High Postdischarge Morbidity in Ugandan Children With Severe Malarial Anemia or Cerebral Malaria
 Journal of the Pediatric Infectious Diseases Society ORIGINAL ARTICLE High Postdischarge Morbidity in Ugandan Children With Severe Malarial Anemia or Cerebral Malaria Robert O. Opoka, 1 Karen E. S. Hamre,
Journal of the Pediatric Infectious Diseases Society ORIGINAL ARTICLE High Postdischarge Morbidity in Ugandan Children With Severe Malarial Anemia or Cerebral Malaria Robert O. Opoka, 1 Karen E. S. Hamre,
Downloaded from:
 Awad, MI; Alkadru, AMY; Behrens, RH; Baraka, OZ; Eltayeb, IB (2003) Descriptive study on the efficacy and safety of artesunate suppository in combination with other antimalarials in the treatment of severe
Awad, MI; Alkadru, AMY; Behrens, RH; Baraka, OZ; Eltayeb, IB (2003) Descriptive study on the efficacy and safety of artesunate suppository in combination with other antimalarials in the treatment of severe
Activities of amodiaquine, artesunate, and artesunate-amodiaquine against asexualand -sexual stage parasites in falciparum malaria in children
 AAC Accepts, published online ahead of print on 26 February 2007 Antimicrob. Agents Chemother. doi:10.1128/aac.00077-07 Copyright 2007, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 26 February 2007 Antimicrob. Agents Chemother. doi:10.1128/aac.00077-07 Copyright 2007, American Society for Microbiology and/or the Listed Authors/Institutions.
Malaria. An Overview of Life-cycle, Morphology and Clinical Picture
 Malaria An Overview of Life-cycle, Morphology and Clinical Picture Malaria Malaria is the most important of all tropical parasitic disease,causes death and debility and is endemic throughout the tropics
Malaria An Overview of Life-cycle, Morphology and Clinical Picture Malaria Malaria is the most important of all tropical parasitic disease,causes death and debility and is endemic throughout the tropics
Quinine Pharmacokinetics and Pharmacodynamics in Children with Malaria Caused by Plasmodium falciparum
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Sept. 2005, p. 3658 3662 Vol. 49, No. 9 0066-4804/05/$08.00 0 doi:10.1128/aac.49.9.3658 3662.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved.
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Sept. 2005, p. 3658 3662 Vol. 49, No. 9 0066-4804/05/$08.00 0 doi:10.1128/aac.49.9.3658 3662.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved.
Scenario#1 Fever from Kenya. New Drugs for Malaria
 New Drugs for Malaria This talk may be politically incorrect or in bad 1 taste.viewer discretion is advised 2 Scenario#1 Fever from Kenya A 37 year old traveller returns from a one month vacation in rural
New Drugs for Malaria This talk may be politically incorrect or in bad 1 taste.viewer discretion is advised 2 Scenario#1 Fever from Kenya A 37 year old traveller returns from a one month vacation in rural
Clinical Analysis Report For Study Sample Study
 Clinical Analysis Report For Study Sample Study Automated report generated by WWARN May 9, 2014 Falciparum class org.wwarn.csr.clinicalstudyreport Version 1.020140508-1558 1 Contents 1 Executive Summary
Clinical Analysis Report For Study Sample Study Automated report generated by WWARN May 9, 2014 Falciparum class org.wwarn.csr.clinicalstudyreport Version 1.020140508-1558 1 Contents 1 Executive Summary
The Malarias: Plasmodium falciparum Plasmodium vivax Plasmodium malariae Plasmodium ovale. Watersheds of the African Continent
 The Malarias: Plasmodium falciparum Plasmodium vivax Plasmodium malariae Plasmodium ovale Global Risk By Country-Proportionality Plot P. falciparum P. vivax Distribution of Plasmodium falciparum 3 million
The Malarias: Plasmodium falciparum Plasmodium vivax Plasmodium malariae Plasmodium ovale Global Risk By Country-Proportionality Plot P. falciparum P. vivax Distribution of Plasmodium falciparum 3 million
Sponsor / Company: Sanofi Drug substance(s): artesunate plus amodiaquine Title of the study:
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
Malaria in Children. University Hospitals of Leicester NHS Trust Children's Services Medical Guidelines. Title: Malaria in children
 Management of Malaria in Children Malaria is a febrile illness caused by Plasmodium falciparum, vivax, malariae, ovale and knowlesi.delayed diagnosis can be fatal and hence a high index of suspicion is
Management of Malaria in Children Malaria is a febrile illness caused by Plasmodium falciparum, vivax, malariae, ovale and knowlesi.delayed diagnosis can be fatal and hence a high index of suspicion is
The New England Journal of Medicine
 The New England Journal of Medicine Copyright, 1996, by the Massachusetts Medical Society VOLUME 335 J ULY 11, 1996 NUMBER 2 A TRIAL OF ARTEMETHER OR QUININE IN CHILDREN WITH CEREBRAL MALARIA MICHAËL BOELE
The New England Journal of Medicine Copyright, 1996, by the Massachusetts Medical Society VOLUME 335 J ULY 11, 1996 NUMBER 2 A TRIAL OF ARTEMETHER OR QUININE IN CHILDREN WITH CEREBRAL MALARIA MICHAËL BOELE
FACTS. Approximately 2.48 million malaria cases are reported annually from South Asia. Of Which 75% cases are contributed by India alone.
 MALARIA 2 FACTS Approximately 2.48 million malaria cases are reported annually from South Asia. Of Which 75% cases are contributed by India alone. The magnitude of the problem is further enhanced by P
MALARIA 2 FACTS Approximately 2.48 million malaria cases are reported annually from South Asia. Of Which 75% cases are contributed by India alone. The magnitude of the problem is further enhanced by P
A comparison of oral artesunate and artemether antimalarial bioactivities in acute falciparum malaria
 A comparison of oral artesunate and artemether antimalarial bioactivities in acute falciparum malaria Yupin Suputtamongkol, 1 Paul N. Newton, 2,3 Brian Angus, 3 Paktiya Teja-Isavadharm, 4 Duangsuda Keeratithakul,
A comparison of oral artesunate and artemether antimalarial bioactivities in acute falciparum malaria Yupin Suputtamongkol, 1 Paul N. Newton, 2,3 Brian Angus, 3 Paktiya Teja-Isavadharm, 4 Duangsuda Keeratithakul,
Comparison of clinical profile between Plasmodium vivax and Plasmodium falciparum malaria in children in tertiary care hospital
 International Journal of Contemporary ediatrics Ravilala VK et al. Int J Contemp ediatr. 2018 Jul;5(4):1294-1299 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI:
International Journal of Contemporary ediatrics Ravilala VK et al. Int J Contemp ediatr. 2018 Jul;5(4):1294-1299 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI:
Antimalarial drug resistance
 Antimalarial drug resistance Md Mushfiqur Rahman*, Leonard Ortega**, R M Rastogi* and Krongthong Thimasarn* Abstract Antimalarial drug resistance is of great concern in the WHO South-East Asia (SEA) Region.
Antimalarial drug resistance Md Mushfiqur Rahman*, Leonard Ortega**, R M Rastogi* and Krongthong Thimasarn* Abstract Antimalarial drug resistance is of great concern in the WHO South-East Asia (SEA) Region.
Case Definitions of Clinical Malaria under Different Transmission Conditions in Kilifi District, Kenya
 MAJOR ARTICLE Case Definitions of Clinical Malaria under Different Transmission Conditions in Kilifi District, Kenya Tabitha W. Mwangi, 1 Amanda Ross, 1,2,a Robert W. Snow, 1,2 and Kevin Marsh 2 1 Kenya
MAJOR ARTICLE Case Definitions of Clinical Malaria under Different Transmission Conditions in Kilifi District, Kenya Tabitha W. Mwangi, 1 Amanda Ross, 1,2,a Robert W. Snow, 1,2 and Kevin Marsh 2 1 Kenya
Manuscripts for the WHO Evidence Review Group for malaria in pregnancy (MiP-ERG), July 2015
 Malaria Policy Advisory Committee Meeting 5 7 March 2015, Geneva, Switzerland Background document for Session 4 Manuscripts for the WHO Evidence Review Group for malaria in pregnancy (MiP-ERG), July 2015
Malaria Policy Advisory Committee Meeting 5 7 March 2015, Geneva, Switzerland Background document for Session 4 Manuscripts for the WHO Evidence Review Group for malaria in pregnancy (MiP-ERG), July 2015
Tolerability of Artemisinin based combination treatments - ACTs. Bob Taylor MD (Lond), FRCP (UK), DTM&H (Lond)
 Tolerability of Artemisinin based combination treatments - ACTs Bob Taylor MD (Lond), FRCP (UK), DTM&H (Lond) Main ACTs Artesunate + mefloquine Dihydroartemisinin + piperaquine Artemether + lumefantrine
Tolerability of Artemisinin based combination treatments - ACTs Bob Taylor MD (Lond), FRCP (UK), DTM&H (Lond) Main ACTs Artesunate + mefloquine Dihydroartemisinin + piperaquine Artemether + lumefantrine
Dose-finding and efficacy study for i.m. artemotil (beta-arteether) and comparison with i.m. artemether in acute uncomplicated P. falciparum malaria
 Dose-finding and efficacy study for i.m. artemotil (beta-arteether) and comparison with i.m. artemether in acute uncomplicated P. falciparum malaria S. Looareesuwan, 1 B. Oosterhuis, 2 B. M. Schilizzi,
Dose-finding and efficacy study for i.m. artemotil (beta-arteether) and comparison with i.m. artemether in acute uncomplicated P. falciparum malaria S. Looareesuwan, 1 B. Oosterhuis, 2 B. M. Schilizzi,
Severe Anemia in Young Children After High and Low Malaria Transmission Seasons in the Kassena- Nankana District of Northern Ghana
 University of Nebraska - Lincoln DigitalCommons@University of Nebraska - Lincoln U.S. Navy Research U.S. Department of Defense 2000 Severe Anemia in Young Children After High and Low Malaria Transmission
University of Nebraska - Lincoln DigitalCommons@University of Nebraska - Lincoln U.S. Navy Research U.S. Department of Defense 2000 Severe Anemia in Young Children After High and Low Malaria Transmission
In several African countries in sub-saharan Africa, malaria is the leading cause of death in children under five.
 TECHNICAL SEMINAR - MALARIA SLIDE 1 Technical Seminar - Malaria Malaria is an extremely important cause of mortality in different parts of world. In this technical seminar, I ll discuss the rationale for
TECHNICAL SEMINAR - MALARIA SLIDE 1 Technical Seminar - Malaria Malaria is an extremely important cause of mortality in different parts of world. In this technical seminar, I ll discuss the rationale for
Testing for G6PD deficiency for safe use of primaquine in radical cure of P. vivax and P. ovale
 Testing for G6PD deficiency for safe use of primaquine in radical cure of P. vivax and P. ovale Webinar presentation to support the dissemination of the policy brief Silvia Schwarte, WHO/GMP e-mail: schwartes@who.int
Testing for G6PD deficiency for safe use of primaquine in radical cure of P. vivax and P. ovale Webinar presentation to support the dissemination of the policy brief Silvia Schwarte, WHO/GMP e-mail: schwartes@who.int
MALARIA INFECTION AMONG THE MIGRANT POPULATION ALONG THE THAI-MYANMAR BORDER AREA
 MALARIA INFECTION AMONG THE MIGRANT POPULATION ALONG THE THAI-MYANMAR BORDER AREA Wisit Chaveepojnkamjorn and Natchaporn Pichainarong Department of Epidemiology, Faculty of Public Health, Mahidol University,
MALARIA INFECTION AMONG THE MIGRANT POPULATION ALONG THE THAI-MYANMAR BORDER AREA Wisit Chaveepojnkamjorn and Natchaporn Pichainarong Department of Epidemiology, Faculty of Public Health, Mahidol University,
Gametocyte Clearance in Uncomplicated and Severe Plasmodium falciparum Malaria after Artesunate-Mefloquine Treatment in Thailand
 Korean J Parasitol. Vol. 46, No. 2: 65-70, June 2008 DOI: 10.3347/kjp.2008.46.2.65 Gametocyte Clearance in Uncomplicated and Severe Plasmodium falciparum Malaria after Artesunate-Mefloquine Treatment in
Korean J Parasitol. Vol. 46, No. 2: 65-70, June 2008 DOI: 10.3347/kjp.2008.46.2.65 Gametocyte Clearance in Uncomplicated and Severe Plasmodium falciparum Malaria after Artesunate-Mefloquine Treatment in
A systematic approach to the development of a rational malaria treatment policy in Zambia
 Tropical Medicine and International Health volume 3 no 7 pp 535 542 july 1998 A systematic approach to the development of a rational malaria treatment policy in Zambia Lawrence M. Barat 1, Benson Himonga
Tropical Medicine and International Health volume 3 no 7 pp 535 542 july 1998 A systematic approach to the development of a rational malaria treatment policy in Zambia Lawrence M. Barat 1, Benson Himonga
Effectiveness of five artemisinin combination regimens with or without primaquine in uncomplicated falciparum malaria: an open-label randomised trial
 Effectiveness of five artemisinin combination regimens with or without primaquine in uncomplicated falciparum malaria: an open-label randomised trial Frank Smithuis, Moe Kyaw Kyaw, Ohn Phe, Thein Win,
Effectiveness of five artemisinin combination regimens with or without primaquine in uncomplicated falciparum malaria: an open-label randomised trial Frank Smithuis, Moe Kyaw Kyaw, Ohn Phe, Thein Win,
Artesunate combinations for treatment of malaria: meta-analysis
 Articles Artesunate combinations for treatment of malaria: meta-analysis International Artemisinin Study Group* Summary Background Addition of artemisinin derivatives to existing drug regimens for malaria
Articles Artesunate combinations for treatment of malaria: meta-analysis International Artemisinin Study Group* Summary Background Addition of artemisinin derivatives to existing drug regimens for malaria
Sponsor / Company: Sanofi Drug substance(s): SSR103371
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
Anaemia and malaria. Malaria Journal. Open Access REVIEW. Nicholas J. White 1,2*
 https://doi.org/10.1186/s12936-018-2509-9 Malaria Journal REVIEW Open Access Anaemia and malaria Nicholas J. White 1,2* Abstract Malaria is a major cause of anaemia in tropical areas. Malaria infection
https://doi.org/10.1186/s12936-018-2509-9 Malaria Journal REVIEW Open Access Anaemia and malaria Nicholas J. White 1,2* Abstract Malaria is a major cause of anaemia in tropical areas. Malaria infection
Evaluation of a Microcurrent Device in the Treatment of Malaria
 INTRODUCTION Malaria is one of the most widespread diseases, having a global incidence of over 0 million cases/year. In Nigeria alone over million deaths (500,000 being children below 5 years of age) per
INTRODUCTION Malaria is one of the most widespread diseases, having a global incidence of over 0 million cases/year. In Nigeria alone over million deaths (500,000 being children below 5 years of age) per
Anas Raed. - Zaid Emad. - Malik Zuhlof
 - 6 - Anas Raed - Zaid Emad - Malik Zuhlof 1 P a g e - This lecture started with the excellent presentation of chronic fatigue syndrome and the role of Vitamin B12 in its treatment by our colleague Osama
- 6 - Anas Raed - Zaid Emad - Malik Zuhlof 1 P a g e - This lecture started with the excellent presentation of chronic fatigue syndrome and the role of Vitamin B12 in its treatment by our colleague Osama
Cases of Severe Malaria and Cerebral Malaria in Apam Catholic Hospital and Manhiya District Hospital
 Cases of Severe Malaria and Cerebral Malaria in Apam Catholic Hospital and Manhiya District Hospital CL Barba, MSIV Charles Drew University of Medicine and Science Los Angeles, CA QUESTION What pediatric
Cases of Severe Malaria and Cerebral Malaria in Apam Catholic Hospital and Manhiya District Hospital CL Barba, MSIV Charles Drew University of Medicine and Science Los Angeles, CA QUESTION What pediatric
DEPARTMENT OF HEALTH AND HUMAN SERVICES CENTERS FOR DISEASE CONTROL AND PREVENTION SAFTER HEALTHIER PEOPLE TM
 MALARIA TREATMENT GUIDELINES Treatment of Malaria (Guidelines For Clinicians) If you wish to share your clinical experience, please contact us at: nciddpdmalaria@cdc.gov Treatment Table The Treatment Table
MALARIA TREATMENT GUIDELINES Treatment of Malaria (Guidelines For Clinicians) If you wish to share your clinical experience, please contact us at: nciddpdmalaria@cdc.gov Treatment Table The Treatment Table
MALARIA CONTROL FROM THE INDIVIDUAL TO THE COMMUNITY
 MALARIA CONTROL FROM THE INDIVIDUAL TO THE COMMUNITY Calvin L. Wilson MD Clinical Professor of Family Medicine and Public Health University of Colorado Anschutz OBJECTIVES 1. Understand the unique characteristics
MALARIA CONTROL FROM THE INDIVIDUAL TO THE COMMUNITY Calvin L. Wilson MD Clinical Professor of Family Medicine and Public Health University of Colorado Anschutz OBJECTIVES 1. Understand the unique characteristics
THE EFFECTS OF HAEMOGLOBINOPATHIES AND G6PD DEFICIENCY ON MALARIA AMONG CHILDREN OF THE KINTAMPO NORTH MUNICIPALITY OF GHANA
 THE EFFECTS OF HAEMOGLOBINOPATHIES AND G6PD DEFICIENCY ON MALARIA AMONG CHILDREN OF THE KINTAMPO NORTH MUNICIPALITY OF GHANA Presenter: Amoako Nicholas 1 Supervisors: Dr. Kwaku Poku Asante 1, Dr. Bimi
THE EFFECTS OF HAEMOGLOBINOPATHIES AND G6PD DEFICIENCY ON MALARIA AMONG CHILDREN OF THE KINTAMPO NORTH MUNICIPALITY OF GHANA Presenter: Amoako Nicholas 1 Supervisors: Dr. Kwaku Poku Asante 1, Dr. Bimi
CURRICULUM VITAE. Nicholas John White. Date of birth: Education: St. John's College, Southsea, Hants
 CURRICULUM VITAE Name: Nicholas John White Date of birth: 13.3.1951 Marital status: Married, 3 children Education: 1961-68 St. John's College, Southsea, Hants 1968-74 Guy's Hospital Medical School Degrees:
CURRICULUM VITAE Name: Nicholas John White Date of birth: 13.3.1951 Marital status: Married, 3 children Education: 1961-68 St. John's College, Southsea, Hants 1968-74 Guy's Hospital Medical School Degrees:
Bone marrow reticulocytes: a Plasmodium vivax affair? Alfredo Mayor a and Pietro Alano b
 Bone marrow reticulocytes: a Plasmodium vivax affair? Alfredo Mayor a and Pietro Alano b a ISGlobal, Barcelona Ctr. Int. Health Res. (CRESIB), Hospital Clínic - Universitat de Barcelona, Barcelona, Spain;
Bone marrow reticulocytes: a Plasmodium vivax affair? Alfredo Mayor a and Pietro Alano b a ISGlobal, Barcelona Ctr. Int. Health Res. (CRESIB), Hospital Clínic - Universitat de Barcelona, Barcelona, Spain;
Mefloquine antimalarial prophylaxis in pregnancy: dose finding and pharmacokinetic study
 Br. J. clin. Pharmac. (1990), 30, 79-85 Mefloquine antimalarial prophylaxis in pregnancy: dose finding and pharmacokinetic study F. NOSTEN', J. KARBWANG1, N. J. WHITE12, HONEYMOON', K. NA BANGCHANG', D.
Br. J. clin. Pharmac. (1990), 30, 79-85 Mefloquine antimalarial prophylaxis in pregnancy: dose finding and pharmacokinetic study F. NOSTEN', J. KARBWANG1, N. J. WHITE12, HONEYMOON', K. NA BANGCHANG', D.
USE OF MEFLOQUINE IN PREGNANCY
 www.uktis.org / www.toxbase.org 0844 892 0909 USE OF MEFLOQUINE IN PREGNANCY Date of issue: October 2014 Version: 2.1 This is a UKTIS monograph for use by health care professionals. For casespecific advice
www.uktis.org / www.toxbase.org 0844 892 0909 USE OF MEFLOQUINE IN PREGNANCY Date of issue: October 2014 Version: 2.1 This is a UKTIS monograph for use by health care professionals. For casespecific advice
Predictors of drug sensitive tuberculosis treatment outcomes among hospitalised
 Predictors of drug sensitive tuberculosis treatment outcomes among hospitalised patients in South Africa: a multinomial logit model Abiola O. Olaleye 1,* and Andy K. Beke 1 1 School of Health Systems and
Predictors of drug sensitive tuberculosis treatment outcomes among hospitalised patients in South Africa: a multinomial logit model Abiola O. Olaleye 1,* and Andy K. Beke 1 1 School of Health Systems and
BERTRAND LELL, LEOPOLD G. LEHMAN, J. RUPRECHT SCHMIDT-OTT, DIETER STURCHLER, JURG HANDSCHIN, AND PETER G. KREMSNER
 Am. J. Trop. ed. Hyg., 58(5), 1998, pp. 619624 Copyright 1998 by The American Society of Tropical edicine and Hygiene ALARIA CHEOTHERAPY TRIAL AT A INIAL EFFECTIVE DOSE OF EFLOQUINE/SULFADOXINE/PYRIETHAINE
Am. J. Trop. ed. Hyg., 58(5), 1998, pp. 619624 Copyright 1998 by The American Society of Tropical edicine and Hygiene ALARIA CHEOTHERAPY TRIAL AT A INIAL EFFECTIVE DOSE OF EFLOQUINE/SULFADOXINE/PYRIETHAINE
Artesunate versus quinine for treatment of severe falciparum malaria: a randomised trial
 Artesunate versus quinine for treatment of severe falciparum malaria: a randomised trial South East Asian Quinine Artesunate Malaria Trial (SEAQUAMAT) group* Summary Background In the treatment of severe
Artesunate versus quinine for treatment of severe falciparum malaria: a randomised trial South East Asian Quinine Artesunate Malaria Trial (SEAQUAMAT) group* Summary Background In the treatment of severe
GSK Medicine Study Number: Title: Rationale Phase: Study Period: Study Design: Centres: Indication: Treatment: Objectives:
 The study listed may include approved and nonapproved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and nonapproved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
