Cervical Medial Branch Blocks for Chronic Cervical Facet Joint Pain
|
|
|
- Gerard Collins
- 5 years ago
- Views:
Transcription
1 Cervical Medial Branch Blocks for Chronic Cervical Facet Joint Pain A Randomized, Double-Blind, Controlled Trial With One-Year Follow-up Laxmaiah Manchikanti, MD,* Vijay Singh, MD, Frank J. E. Falco, MD, Kimberly M. Cash, RT,* and Bert Fellows, MA* SPINE Volume 33, Number 17, pp , Lippincott Williams & Wilkins Study Design. A double-blind, randomized, controlled trial. Objective. To determine the clinical effectiveness of therapeutic local anesthetic cervical medial branch blocks with or without steroid in managing chronic neck pain of facet joint origin. Summary of Background Data. The prevalence of persistent neck pain, secondary to involvement of cervical facet or zygapophysial joints, has been described in controlled studies as varying from 39% to 67%. Intra-articular injections, medial branch nerve blocks, and neurolysis of medial branch nerves have been described in managing chronic neck pain of facet joint origin. Methods. A total of 120 patients were included, with 60 patients in each of the local anesthetic and steroid groups. All the patients met the diagnostic criteria of cervical facet joint pain by means of comparative, controlled diagnostic blocks, and the inclusion criteria. Group I consisted of medial branch blocks with bupivacaine. Group II consisted of cervical medial branch blocks with bupivacaine and steroid. Numerical pain scores, Neck Disability Index, opioid intake, and work status were evaluated at baseline, 3 months, 6 months, and 12 months. Results. Significant pain relief ( 50%) and functional status improvement was observed at 3 months, 6 months, and 12 months in over 83% of patients. The average number of treatments for 1 year was in the nonsteroid group and in the steroid group. Duration of average pain relief with each procedure was weeks in the nonsteroid group, and it was weeks in the steroid group. Significant relief and functional improvement was reported for 46 to 48 weeks in a year. Conclusion. Therapeutic cervical medial branch nerve blocks, with or without steroids, may provide effective management for chronic neck pain of facet joint origin. Key words: chronic neck pain, cervical facet or zygapophysial joint pain, medial branch blocks, comparative controlled local anesthetic blocks, therapeutic cervical facet joint nerve blocks. Spine 2008;33: From the *Pain Management Center of Paducah, Paducah, KY; Pain Diagnostic Associates, Niagara, WI; and Mid Atlantic Spine and Pain Specialists of Newark, DE. Acknowledgment date: November 20, First revision date: February 14, Acceptance date: March 4, The device(s)/drug(s) is/are FDA-approved or approved by corresponding national agency for this indication. No funds were received in support of this work. No benefits in any form have been or will be received from a commercial party related directly or indirectly to the subject of this manuscript. Address correspondence and reprint requests to Laxmaiah Manchikanti, MD, 2831 Lone Oak Road, Paducah, KY 42003; drlm@ thepainmd.com Chronic neck pain is seen in up to 60% of patients 5 years or longer after the initial episode. 1 5 The study of the prevalence of neck pain and the impact on general health showed 14% of patients reporting grade 2 to 4 neck pain defined as high pain intensity with disability. Thus, chronic, function-limiting neck pain is not only common but is also associated with significant economic, social, and health impact. 1,5,6 Bogduk and McGuirk 7 and the Quebec Task Force 8 found either no or scant literature to substantiate the use of commonly practiced treatments in managing chronic neck pain. Based on responses to controlled diagnostic blocks in accordance with the criteria established by the International Association for the Study of Pain (IASP), 9 facet or zygapophysial joints have been implicated as the source of chronic pain in 39% to 67% of patients with chronic neck pain of heterogeneous origin Cervical facet joints have been shown to have an abundant nerve supply with nociceptors and mechanoreceptors, and to be a source of pain in the neck and referred pain in the head and upper extremities. 16 Further, cervical facet joints meet the first 3 of the 4 criteria proposed by Bogduk 17 establishing that for a painful structure must have (1) a nerve supply, (2) capable of causing pain similar to that seen clinically, ideally in normal volunteers, (3) have been shown to be a source of pain in patients using diagnostic techniques of known reliability and validity, and (4) susceptible to diseases or injuries that are known to be painful. Despite a preponderance of evidence supporting the existence of cervical facet joint pain, the essence of controlled diagnostic blocks and diagnosis by that means has been recently questioned. 20 Multiple therapeutic techniques have been described in managing chronic neck pain of facet joint origin including intraarticular injections, medial branch blocks, and radiofrequency neurotomy with variable evidence Systematic reviews 21,22 have provided limited evidence for cervical intra-articular injections, 26 moderate evidence for cervical medial branch blocks, 27,28 strong evidence for radiofrequency neurotomy using a technique described by Bogduk 29,30 and moderate evidence using traditional technique. 21 Thus, an alternative to percutaneous radiofrequency neurotomy, therapeutic cervical medial branch blocks have been described. 27,28 Radiofrequency neurotomy provides temporary or long-term relief of pain by denaturing the nerves that innervate the painful joint. 29,30 In contrast with cervical medial branch 1813
2 1814 Spine Volume 33 Number blocks the exact phenomenon of therapeutic effect is not known. However, both techniques may be repeated to reinstate the relief. This report consists of the 1-year results of the randomized, double-blind, controlled study in patients with a confirmed diagnosis of cervical facet joint pain by means of comparative, controlled, local anesthetic blocks based on criteria of IASP. 9,27 Materials and Methods The study was conducted at an interventional pain management practice, a specialty referral center, in a private practice setting in the United States. The study protocol was approved by the Institutional Review Board and the study has been registered with clinical trial registry as NCT Participants Patients were assigned to 1 of 2 groups with group I constituting a nonsteroid group, and group II encompassing a steroid group. Both groups were also divided into 2 categories each with the addition of Sarapin. Consequently, group I, category A patients received medial branch blocks with injections of bupivacaine 0.25%, whereas group I, category B patients received a mixture with Sarapin, group II, category A patients also received Sarapin. All mixtures consisted of clear solutions. Sarapin and bupivacaine were mixed in equal volumes, and 0.15 mg of nonparticulate betamethasone was added per ml of solution. Inclusion and Exclusion Criteria Only patients with nonspecific neck pain with a duration of at least 6 months were included. Patients suspected of disc-related pain with radicular symptoms were excluded based on radiologic testing and symptomatology involving predominately the upper extremity, and by neurologic examination including reflex suppression and focal neurologic deficits. In addition, all patients included for the diagnosis of cervical facet joint pain had failed conservative management, including physical therapy, chiropractic manipulation, exercises, drug therapy, and bed rest. Inclusion criteria for this study included diagnosis of facet joint pain by means of comparative local anesthetic blocks; patients who were 18 years of age; patients with a history of chronic, function-limiting neck pain of at least 6 months duration; patients who were able to provide voluntary, written informed consent to participate in this evaluation; patients willing to return for follow-ups; and patients without radicular pain and patients without a history of recent surgical procedures within the last 3 months. Negative responses to controlled comparative local anesthetic blocks, uncontrolled major depression or psychiatric disorders, heavy opioid usage, acute or uncontrolled medical illness, chronic severe conditions that could interfere with the interpretations of the outcome assessments, women who were pregnant or lactating, patients unable to be positioned in a prone position, and patients with histories of adverse reactions to local anesthetic, Sarapin, or steroids were considered as exclusion criteria. Interventions Institutional Review Board approved informed consent and protocol were provided to all the patients, which described details of the trial including side effects and the mechanism of withdrawal from the study. Cervical Medial Branch Blocks In the diagnostic phase, facet or zygapophysial joint pain was investigated in all patients starting with diagnostic blocks using 0.5 ml of 1% lidocaine, as per the criteria established by the IASP. 9 Patients with lidocaine-positive results were further studied using 0.5 ml of 0.25% bupivacaine on a separate occasion, usually 3 to 4 weeks after the first injection. The blocks were performed with intermittent fluoroscopic visualization using a 22-gauge, 2-inch spinal needle at each of the indicated medial branches. Intravenous access was established and light sedation with midazolam was offered to all patients in the diagnostic phase. To be considered positive, pain relief from block had to last at least 2 hours when lidocaine was used, and at least 3 hours, or greater than the duration of relief with lidocaine, when bupivacaine was used, and the intensity of relief should have been 80% or more. Any other response was considered as a negative outcome. However, the diagnostic phase was not part of this study. In the therapeutic phase, all medial branches were performed under fluoroscopy in an ambulatory surgery center with a 22-gauge, 2-inch spinal needle with the injection of a 0.5 to 1 ml mixture as assigned by grouping at each level. Medial branch blocks were repeated based on the response to prior interventions with improvement in physical and functional status and only when increased levels of pain were reported and it was greater than the 50% level or relief had deteriorated to below 50%. Cointerventions No specific cointerventions, such as physical therapy, occupational therapy, or bracing, were provided. However, the same cointerventions as needed with opioid and nonopioid analgesics, adjuvant analgesics, and previously directed exercise programs before enrollment were continued in all patients. In addition, adjustments in medical therapy were carried out based on response, and physical and functional needs. Additional Interventions All the patients underwent assigned treatments. Protocol allowed additional interventions if indicated. Medial branch blocks were provided based on their responses, either after unblinding or without unblinding. Protocol allowed the assigned treatments except in patients who were unblinded receiving either the assigned treatment or another treatment based on their responses. The patients who were nonresponsive and in situations where medial branch blocks were stopped and other treatments were provided, these patients were considered to be withdrawn from the study, and no subsequent data were collected. Objective To determine the clinical effectiveness of therapeutic local anesthetic cervical medial branch blocks with or without steroid in managing chronic neck pain of facet joint origin. Outcomes Outcomes measures included NRS pain scale, Neck Disability Index, work status, and opioid intake assessed at baseline, 3 months, 6 months, and 12 months post-treatment. At least 50% pain relief with at least 40% improvement in Neck Disability Index was considered as significant improvement. The Neck Disability Index has been shown to be valid
3 Cervical Medial Branch Blocks Manchikanti et al 1815 and reliable in patients with mechanical neck pain. 31,32 Thresholds for the minimum clinically important difference for the Neck Disability Index varied from a 10% to 19% change. Patients unemployed or employed on a part-time basis with limited or no employment due to pain were classified as employable. Patients who chose not to work, were retired, or were homemakers (not working, but not due to pain) were considered as not employable. Sample Size A sample size of 60 patients was chosen for each group. The estimated sample size was based on previous studies of cervical 29 and lumbar medial branch neurotomies, 33 which included less than 20 patients in each group, and other literature of interventional techniques identifying as 50 patients as acceptable. 34 Randomization From a total of 120 patients, 60 patients were randomly assigned into each group, and 30 patients into each category for Sarapin. Sequence Generation Randomization was performed by computer-generated random allocations sequence in blocks of 20 patients. Allocation Concealment The operating room nurse assisting with the procedure, randomized the patients and prepared the drugs appropriately. Implementation Participants were invited to enroll in the study if they met inclusion criteria. One of the 3 nurses assigned as coordinators of the study enrolled the participants and assigned participants to their respective groups. Blinding The random allocation was not revealed to personnel in the recovery room or to the physician performing the procedure. Patients were unblinded if they requested to be unblinded or after completing 24 months of the study. Patients were also given an opportunity to discontinue or withdraw from the study for lack of pain relief, for lack of interest, or for any other reason. Further, patients were considered to be withdrawn if follow-up was lost. For this evaluation and 1-year follow-up report, all the patients completing the evaluation of 24 months (thus unblinded), and the remaining patients were included with data being obtained by the statistician without unblinding. Thus, the randomization and double-blind nature of the study were preserved. Statistical Methods Statistical analysis included 2 statistic, Fisher exact test, paired t test, Wilcoxon signed ranks test, Mann-Whitney test, and one-way analysis of variance were used. 2 statistic was used to test the differences in proportions. Fisher exact test was used wherever the expected value was less than 5, a paired t test was used to compare the pre- and posttreatment results of average pain scores and the Neck Disability Index measurements at baseline versus 3 months, 6 months, and 12 months. For comparison of mean scores between groups, t test was performed. One-way analysis of variance was used for comparison of means among groups. Initially, categories with or without Sarapin in each group were analyzed by comparing them to each other. Subsequently, if there were no differences, local anesthetic and steroid groups were compared. Intent-to-Treat-Analysis An intent-to-treat-analysis was used on all patients using the last follow-up data. Initial data were used in the patients who dropped out of the study without further follow-up. Results Participant Flow Figure 1 illustrates the participant flow. Recruitment The recruitment period lasted from November 2003 to July Baseline Data Demographic characteristics are illustrated in Table 1. There were no significant differences noted among the groups. The number of joints involved was as follows: 2 joints were involved in 48% of the patients, 3 joints were involved in 52% of the patients, and 4 joints were involved in 2% of the patients. Bilateral involvement was seen in 73% of the patients. Analysis of Data Data were analyzed for both categories in each group to evaluate the influence of Sarapin. There were no significant differences. Thus, descriptions are provided for 2 groups with local anesthetic with or without steroid. Numbers Analyzed Figure 1 illustrates the details of analysis. All 120 patients were used in the analysis. Six patients were lost to follow-up in group I with 1 patient lost to follow-up after the baseline assessment, 4 patients lost to follow-up after 3 months, and 1 patient lost to follow-up after 6 months. In group II, 3 patients were lost to follow-up. One patient was lost to follow-up after 3 months, whereas, 2 patients were lost to follow-up after 6 months. Intent-to-treat analysis was performed because of nonavailable data on 13 occasions in group I and on 12 occasions for group II, with a total data collection of 120 patients at baseline, 3 months, 6 months, and 12 months. Outcomes Pain Relief Numerical pain scale scores reported at baseline, 3 months, 6 months, and 12 months are illustrated in Table 2 and Figure 2. There were significant changes in pain scores from baseline, at 3 months, 6 months, and 12 months in all the groups, with no differences among groups I and II. Table 3 illustrates therapeutic procedural characteristics with average pain relief over a period of 1 year. Table 4 shows therapeutic procedural characteristics with an average total pain relief over a period of 52 weeks.
4 1816 Spine Volume 33 Number Eligible Patients Assessed 144 Patients Excluded Patients Not Meeting Inclusion Criteria=16 Patients Refusing to Participate = 8 Patients randomized 120 GROUP I GROUP II Medial branch blocks with bupivacaine (IA) and medial branch blocks with bupivacaine and Sarapin (IB) Medial branch blocks with bupivacaine and steroid (IIA) and medial branch blocks with bupivacaine, Sarapin, and steroid (IIB) Patients lost to follow-up=6 1 patient after baseline 4 patients after 3 months 1 patient after 6 months Patients lost to follow-up=3 1 patient after 3 months 2 patients after 6 months Patients included in analysis = 60 Patients included in analysis = 60 Patients unblinded prematurely= 0 Patients unblinded prematurely = 0 Intent to treat analysis was performed on 1 occasion at 3 months, 4 occasions at 6 months, and 8 occasions at 12 months for missing data Figure 1. Schematic presentation of patient flow at 1-year follow-up. Functional Assessment Table 5 and Figure 3 illustrates functional assessment characteristics evaluated by Neck Disability Index. At Table 1. Demographic Characteristics Group I (Bupivacaine Group II (Bupivacaine Gender Male 32% (19) 20% (12) Female 68% (41) 80% (48) Age Mean SD Height (in.) Mean SD Weight (lbs) Mean SD Duration of pain (mo) Mean SD Mode of onset of pain Gradual 57% (34) 57% (34) Sudden 11% (7) 11% (7) WC/MVA 32% (19) 32% (19) WC indicates workers compensation; MVA, motor vehicle injury. Intent to treat analysis was performed on 1 occasion at 3 months, 5 occasions at 6 months, and 6 occasions at 12 months for missing data least 40% improvement was seen in 85% of patients in both groups and 50% improvement was seen in 63% in group I and 68% in group II. Employment Characteristics Table 6 illustrates the summary of employment characteristics in both groups. Among the patients eligible for employment, total employed changed from 10 at baseline to 22 at the end of 12 months in group I, whereas it Table 2. Pain Relief Characteristics Nonsteroid Groups Group I (Bupivacaine Steroid Groups Group II (Bupivacaine Average pain scores (mean SD) Baseline mo 3.8* * mo 3.6* * mo 3.7* * 0.9 *Significant difference with baseline values.
5 Cervical Medial Branch Blocks Manchikanti et al 1817 Figure 2. Pain relief characteristics with average pain scores. changed from 11 to 18 in group II, a nonsignificant increase of 120% in group I and 61% in group II. Adverse Events There were no adverse events reported during this study. Discussion The 1-year follow-up data of this randomized, doubleblind trial in patients undergoing therapeutic cervical medial branch nerve blocks showed significant improvement with decreased pain and improved functional status. Over 83% of the patients noted significant pain relief ( 50%) of varying duration and at least 40% improvement in the Neck Disability Index. The average pain relief per procedure ranged from 14 to 16 weeks and patients experienced 46 to 48 weeks of significant pain relief during a 1 year period. Although there was no change in opioid intake, employment status showed statistically insignificant but clinically important improvement. The results of the current study in treating patients with chronic neck pain with therapeutic facet joint nerve blocks were superior to a prior evaluation of clinical effectiveness of therapeutic cervical medial branch blocks in a prospective evaluation. 28 The lack of a placebo group is a shortcoming of this study. However, issues of ethics, feasibility, and cost pose challenges to the inclusion of a placebo group in the United States. Further, in modern evaluations, pragmatic Table 3. Therapeutic Procedural Characteristics Over a Period of One Year With Average Relief per Procedure in Weeks No. Procedures Group I (Bupivacaine Group II (Bupivacaine One (3) 52 (2) Two (7) (9) Three (14) (14) Four (27) (31) Five 10 0 (9) (4) Average relief per procedure (wk) (60) (60) studies are considered more appropriate, rather than explanatory trials. 35 Explanatory trials measure efficacy, whereas pragmatic trials, also known as practical clinical trials, measure effectiveness. 36 Practical clinical trials are best designed to provide the results of the benefit of treatments produced in routine clinical practice and also address questions about the risks, benefits, and costs of an intervention as they occur in routine clinical practice better than an explanatory trial. 36 Consequently, without a placebo group, in pragmatic approaches, the treatment response is the combination of the treatment effect and placebo effect, as this will best reflect the likely clinical response in actual practice. This study also resolves the issue of the addition of Sarapin and steroid. In the past, conflicting results demonstrated the effect of Sarapin and steroid. 37,38 However, the present study showed no significant differences not only with the addition of Sarapin, but also with the addition of steroid. The equal effectiveness of local anesthetic with or without steroid for cervical medial branch blocks provides information that there is no significant role for steroids in cervical medial branch blocks. Most studies describe that epidural corticosteroids provide a certain level of efficacy by their anti-inflammatory, immunosuppressive, antiedema effects, and inhibition of neurotransmission within the C-fibers Although local anesthetics are well known to provide short-term symp- Table 4. Therapeutic Procedural Characteristics With Average Total Relief in Weeks Over a Period of One Year No. Procedures Non-Steroid Groups Group I (Bupivacaine Steroid Groups Group II (Bupivacaine One (3) 52 (2) Two (7) (9) Three (14) (14) Four (27) (31) Five 52 0 (9) (4) Total (For 1 yr) (60) (60)
6 1818 Spine Volume 33 Number Table 5. Functional Assessment Evaluated by Neck Disability Index Group I (Bupivacaine Group II (Bupivacaine Neck disability scores (Mean SD) Baseline mo 12.0* * mo 12.0* * mo 11.7* * 4.6 *Indicates significant difference with baseline values. tomatic relief, the mechanism of the relief of local anesthetics on a long-term basis remains an enigma. Pasqualucci et al 43 postulated the effectiveness obtained from local anesthetics may be explained by the direct effects of the local anesthetic on various mechanisms in chronic pain. The pathophysiologic mechanisms that formed the basis for chronic pain include the presence of noxious peripheral stimulation, and excess nociception resulting in the sensitization of the pain pathways at several neuronal levels. 44,45 Further, excess release of neurotransmitters is considered responsible for complex central responses such as secondary hyperalgesia, or windup. 43 Consequently, these responses result in an increase in nociceptive sensitization of the nervous system, 46,47 and phenotypic changes considered part of neuronal plasticity, 46,48 similar to neuropathic pain. 46,47,49 Although corticosteroids are not effective in neuropathic pain, local anesthetics have been shown to be effective in the treatment of neuropathic pain 50 including the prevention of onset and the treatment of phantom-limb syndrome. 45,51,52 Thus, it is postulated that local anesthetics provide relief by suppression of nociceptive discharge, 53 the block of the axonal transport, 54,55 the block of the sympathetic reflex arc, 40,56 the block of sensitization, 44,45 and anti-inflammatory effects. 57 Local anesthetics also block the axonal transport of nerve fibers with lower concentrations compared with those which Table 6. Employment Characteristics Employment Status Group I (Bupivacaine Group II (Bupivacaine Baseline 12 mo Baseline 12 mo Employed part-time Employed full-time Total employed Unemployed due to pain Unemployed-student Total unemployed Housewife Disabled Over 65 yr of age Total not working Total are necessary for a block of nerve conduction. 54,55 A host of previous studies have also shown prolonged relief after local anesthetic nerve block or epidural injections. 37,38,53,58 60 In 1941, Wertheim and Rovenstine 58 reported that the analgesic effect of a 2% procaine injection may continue for 4 to 6 weeks. Arner et al 53 in 1990 reported conduction block outlasting the expected duration of local anesthetics with a period of complete pain relief from 12 to 48 hours and further relief lasting 4 to 6 days. In addition, pain relief beyond the expected duration of local anesthesia after a series of blocks and sometimes even after a single block has been reported over the years in various textbooks and also in anecdotal reports Although these results describe patients in a private practice interventional pain management setting in a practical and pragmatic clinical trial, the results are not applicable in the general population unless the same methodology is used with the diagnosis and therapy. Further, generalizability of the findings of this study may only be feasible in studies using larger populations in multiple settings. Overall, evidence in this report demonstrates cervical facet joint pain diagnosed by controlled, comparative Figure 3. Functional assessment evaluated by neck disability index.
7 Cervical Medial Branch Blocks Manchikanti et al 1819 local anesthetic blocks with the criteria of 80% pain relief, which is sustained after prior painful movements for appropriate duration of action of local anesthetic, may be treated with cervical medial branch blocks with or without steroid providing approximately 14 to 16 weeks of relief and requiring 3 to 4 episodes of treatment per year. Key Points Involvement of facet joints in chronic neck pain has been reported in 39% to 67% of patients based on response to controlled diagnostic blocks in accordance with the criteria established by the International Association for the Study of Pain. This study of 120 patients receiving therapeutic cervical medial branch blocks with bupivacaine or bupivacaine and steroid provided significant relief to patients with chronic neck pain. Patients in both groups experienced relief lasting approximately 14 to 16 weeks with a single block and the number of blocks required per year was approximately 3 to 4. Significant pain relief and functional improvement was maintained approximately 46 to 48 weeks out of 52 weeks. There were no significant differences noted between the use of local anesthetic or local anesthetic with steroid with therapeutic cervical medial branch blocks. References 1. Enthoven P, Skargren E, Oberg B. Clinical course in patients seeking primary care for back or neck pain: a prospective 5-year follow-up of outcome and health care consumption with subgroup analysis. Spine 2004;29: Brattberg G. Do pain problems in young school children persist into early adulthood? A 13-year follow-up. Eur J Pain 2004;8: Hoving JL, de Vet HC, Twisk JW, et al. Prognostic factors for neck pain in general practice. Pain 2004;110: Cote P, Cassidy JD, Carroll LJ, et al. The annual incidence and course of neck pain in the general population: A population-based cohort study. Pain 2004; 112: Cote P, Cassidy JD, Carroll L. The Saskatchewan Health and Back Pain Survey: the prevalence of neck pain and related disability. Spine 1998;23: Reyes-Gibby CC, Aday L, Cleeland C. Impact of pain on self-rated health in the community-dwelling older adults. Pain 2002;95: Bogduk N, McGuirk B. Management of Acute and Chronic Neck Pain. An Evidence-Based Approach. Amsterdam: Elsevier; Spitzer WO, LeBlanc FE, Dupuis M. Scientific approach to the assessment and management of activity-related spinal disorders: a monograph for clinicians. Report of Quebec Task Force on Spinal Disorders. Spine 1987;12:S1 S Merskey H, Bogduk N. Classification of Chronic Pain: Descriptions of Chronic Pain Syndromes and Definitions of Pain Terms. 2nd ed. Seattle, WA: IASP Press; Manchikanti L, Boswell MV, Singh V, et al. Prevalence of facet joint pain in chronic spinal pain of cervical, thoracic, and lumbar regions. BMC Musculoskelet Disord 2004;5: Manchikanti L, Singh V, Rivera JJ, et al. Prevalence of cervical facet joint pain in chronic neck pain. Pain Physician 2002;5: Manchikanti L, Singh V, Pampati V, et al. Is there correlation of facet joint pain in lumbar and cervical spine? Pain Physician 2002;5: Manchukonda R, Manchikanti KN, Cash KA, et al. Facet joint pain in chronic spinal pain: an evaluation of prevalence and false-positive rate of diagnostic blocks. J Spinal Disord Tech 2007;20: Barnsley L, Lord SM, Wallis BJ, et al. The prevalence of chronic cervical zygapophysial joint pain after whiplash. Spine 1995;20: Lord SM, Barnsley L, Wallis BJ, et al. Chronic cervical zygapophysial joint pain with whiplash: a placebo-controlled prevalence study. Spine 1996;21: Bogduk N. International spinal injection society guidelines for the performance of spinal injection procedures. Part 1. Zygapophysial joint blocks. Clin J Pain 1997;13: Bogduk N. Low back pain. In: Clinical Anatomy of Lumbar Spine and Sacrum. 4th ed. New York, NY: Churchill Livingstone; 2005: Boswell MV, Singh V, Staats PS, et al. Accuracy of precision diagnostic blocks in the diagnosis of chronic spinal pain of facet or zygapophysial joint origin. Pain Physician 2003;6: Seghal N, Dunbar EE, Shah RV, et al. Systematic review of diagnostic utility of facet (zygapophysial) joint injections in chronic spinal pain: an update. Pain Physician 2007;10: Carragee EJ, Haldeman S, Hurwitz E. The pyrite standard: the Midas touch in the diagnosis of axial pain syndrome. Spine J 2007;7: Boswell MV, Trescot AM, Datta S, et al. Interventional techniques: evidencebased practice guidelines in the management of chronic spinal pain. Pain Physician 2007;10: Boswell MV, Colson JD, Spillane WF. Therapeutic facet joint interventions in chronic spinal pain: a systematic review of effectiveness and complications. Pain Physician 2005;8: Manchikanti L, Singh V, Vilims BD, et al. Medial branch neurotomy in management of chronic spinal pain: systematic review of the evidence. Pain Physician 2002;5: Geurts JW, van Wijk RM, Stolker RJ, et al. Efficacy of radiofrequency procedures for the treatment of spinal pain: a systematic review of randomized clinical trials. Reg Anesth Pain Med 2001;26: Niemistö L, Kalso E, Malmivaara A, et al. Radiofrequency denervation for neck and back pain: a systematic review within the framework of the Cochrane Collaboration Back Review Group. Spine 2003;28: Barnsley L, Lord SM, Wallis BJ, et al. Lack of effect of intra-articular corticosteroids for chronic pain in the cervical zygapophyseal joints. N Engl J Med 1994;330: Manchikanti L, Damron KS, Cash KA, et al. Therapeutic medial branch blocks in managing chronic neck pain: a preliminary report of a randomized, double-blind, controlled trial: clinical Trial NCT Pain Physician 2006;9: Manchikanti L, Manchikanti KN, Damron KS, et al. Effectiveness of cervical medial branch blocks in chronic neck pain: a prospective outcome study. Pain Physician 2004;7: Lord SM, Barnsley L, Wallis BJ, et al. Percutaneous radiofrequency neurotomy for chronic cervical zygapophysial joint pain. N Engl J Med 1996;335: Barnsley L. Percutaneous radiofrequency neurotomy for chronic neck pain: outcomes in a series of consecutive patients. Pain Med 2005;6: Pietrobon R, Coeytaux RR, Carey TS, et al. Standard scales for measurement of functional outcome for cervical pain or dysfunction: a systematic review. Spine 2002;27: Cleland JA, Childs JD, Whitman JM. Psychometric properties of the neck disability index and numeric pain rating scale in patients with mechanical neck pain. Arch Phys Med Rehabil 2008;89: van Kleef M, Barendse GA, Kessels A, et al. Randomized trial of radiofrequency lumbar facet denervation for chronic low back pain. Spine 1999;24: Koes BW, Scholten RJ, Mens JM, et al. Efficacy of epidural steroid injections for low-back pain and sciatica: a systematic review of randomized clinical trials. Pain 1995;63: Tunis SR, Stryer DB, Clancy CM. Practical Clinical Trials. Increasing the value of clinical research for decision making in clinical and health policy. JAMA 2003;290: Roland M, Torgerson DJ. What are pragmatic trials? BMJ 1998;316: Manchikanti L, Pampati V, Fellows B, et al. The diagnostic validity and therapeutic value of lumbar facet joint nerve blocks with or without adjuvant agents. Curr Rev Pain 2000;4: Manchikanti KN, Pampati V, Damron KS, et al. A double-blind, controlled evaluation of the value of Sarapin in neural blockade. Pain Physician 2004; 7: Grenier B, Castagnera L, Maurette P, et al. Chronic cervico-brachial neuralgia treated by cervical epidural injection of corticosteroids. Long-term results. Ann Fr Anesth Reanim 1995;14: Hayashi N, Weinstein JN, Meller ST, et al. The effect of epidural injection of
8 1820 Spine Volume 33 Number betamethasone or bupivacaine in a rat model of lumbar radiculopathy. Spine 1998;23: Lee HM, Weinstein JN, Meller ST, et al. The role of steroids and their effects on phospholipase A2. An animal model of radiculopathy. Spine 1998;23: Johansson A, Hao J, Sjolund B. Local corticosteroid application blocks transmission in normal nociceptive C-fibres. Acta Anaesthesiol Scand 1990; 34: Pasqualucci A, Varrassi G, Braschi A, et al. Epidural local anesthetic plus corticosteroid for the treatment of cervical brachial radicular pain: single injection versus continuous infusion. Clin J Pain 2007;23: Katz WA, Rothenberg R. The nature of pain: pathophysiology. J Clin Rheumatol 2005;11(2 Suppl):S11 S Melzack R, Coderre TJ, Katz J, et al. Central neuroplasticity and pathological pain. Ann N Y Acad Sci 2001;933: Kawakami M, Weinstein JN, Chatani K, et al. Experimental lumbar radiculopathy. Behavioral and histologic changes in a model of radicular pain after spinal nerve root irritation with chromic gut ligatures in the rat. Spine 1994;19: Decosterd I, Woolf CJ. Spared nerve injury: an animal model of persistent peripheral neuropathic pain. Pain 2000;87: Pennypacker KR, Hong JS, McMillian MK. Implications of prolonged expression of Fos-related antigens. Trends Pharmacol Sci 1995;16: Ji RR, Woolf CJ. Neuronal plasticity and signal transduction in nociceptive neurons: implications for the initiation and maintenance of pathological pain. Neurobiol Dis 2001;8: Mao J, Chen LL. Systemic lidocaine for neuropathic pain relief. Pain 2000; 87: Pasqualucci A. Experimental and clinical studies about the preemptive analgesia with local anesthetics. Possible reasons of the failure. Minerva Anestesiol 1998;64: Ferrante FM, Paggioli J, Cherukuri S, et al. The analgesic response to intravenous lidocaine in the treatment of neuropathic pain. Anesth Analg 1996; 82: Arner S, Lindblom U, Meyerson BA, et al. Prolonged relief of neuralgia after regional anesthetic block. A call for further experimental and systematic clinical studies. Pain 1990;43: Lavoie PA, Khazen T, Filion PR. Mechanisms of the inhibition of fast axonal transport by local anesthetics. Neuropharmacology 1989;28: Bisby MA. Inhibition of axonal transport in nerves chronically treated with local anesthetics. Exp Neurol 1975;47: Benzon HT. Epidural steroid injections for low back pain and lumbosacral radiculopathy. Pain 1986;24: Cassuto J, Sinclair R, Bonderovic M. Anti-inflammatory properties of local anesthetics and their present and potential clinical implications. Acta Anaesthesiol Scand 2006;50: Wertheim HM, Rovenstine EA. Suprascapular nerve block. Anesthesiology 1941;2: Riew KD, Park JB, Cho YS, et al. Nerve root blocks in the treatment of lumbar radicular pain. A minimum five-year follow-up. J Bone Joint Surg Am 2006;88: Riew KD, Yin Y, Gilula L, et al. The effect of nerve-root injections on the need for operative treatment of lumbar radicular pain. A prospective, randomized, controlled, double-blind study. J Bone Joint Surg Am 2000;82-A: Abram SE, Likavec MJ. Pain syndromes and rationale for management. Neurogenic pain. In: Raj P, ed. Practical Management of Pain. Chicago, IL: Year Book Medical Publishers; 1986: Bonica JJ. The Management of Pain. Philadelphia, PA: Lea and Febiger; Bonica JJ. Current role of nerve blocks in diagnosis and therapy of pain. In: Bonica JJ, ed. Advances in Neurology, Vol. 4. New York, NY: Raven Press; 1974: Livingston WK. Pain Mechanisms. New York, NY: Macmillan; Raj PP. Prognostic and therapeutic local anaesthetic blockade. In: Cousins MJ, Bridenbaugh PO, eds. Neural Blockade. Philadelphia, PA: Lippincott; 1988: Kibler RF, Nathan PW. Relief of pain and paraesthesiae by nerve block distal to a lesion. J Neurol Neurosurg Psychiatr 1960;23: Xavier AV, McDanal J, Kissin I. Relief of sciatic radicular pain by sciatic nerve block. Anesth Analg 1988;67:
Randomized Trial. Pain Physician 2008; 11: ISSN
 Pain Physician 2008; 11:491-504 ISSN 1533-3159 Randomized Trial Effectiveness of Thoracic Medial Branch Blocks in Managing Chronic Pain: A Preliminary Report of a Randomized, Double-Blind Controlled Trial;
Pain Physician 2008; 11:491-504 ISSN 1533-3159 Randomized Trial Effectiveness of Thoracic Medial Branch Blocks in Managing Chronic Pain: A Preliminary Report of a Randomized, Double-Blind Controlled Trial;
Outcome Measures: Numeric Rating Scale (NRS) pain scale, the Oswestry Disability Index 2.0 (ODI), employment status, and opioid intake.
 Pain Physician 2007; 10:425-440 ISSN 1533-3159 Randomized Trial Evaluation of Lumbar Facet Joint Nerve Blocks in the Management of Chronic Low Back Pain: Preliminary Report of A Randomized, Double-Blind
Pain Physician 2007; 10:425-440 ISSN 1533-3159 Randomized Trial Evaluation of Lumbar Facet Joint Nerve Blocks in the Management of Chronic Low Back Pain: Preliminary Report of A Randomized, Double-Blind
Systematic Review of Diagnostic Utility and Therapeutic Effectiveness of Thoracic Facet Joint Interventions
 Pain Physician 2008; 11:611-629 ISSN 1533-3159 Systematic Review Systematic Review of Diagnostic Utility and Therapeutic Effectiveness of Thoracic Facet Joint Interventions Sairam Atluri, MD 1, Sukdeb
Pain Physician 2008; 11:611-629 ISSN 1533-3159 Systematic Review Systematic Review of Diagnostic Utility and Therapeutic Effectiveness of Thoracic Facet Joint Interventions Sairam Atluri, MD 1, Sukdeb
Re: Treatment Modalities for Facetogenic Pain, Policy #141
 March 30, 2017 Blue Cross and Blue Shield of Alabama Attn: Health Management - Medical Policy P.O. Box 995 Birmingham, AL 35298-0001 Fax: 205-220-0878 Re: Treatment Modalities for Facetogenic Pain, Policy
March 30, 2017 Blue Cross and Blue Shield of Alabama Attn: Health Management - Medical Policy P.O. Box 995 Birmingham, AL 35298-0001 Fax: 205-220-0878 Re: Treatment Modalities for Facetogenic Pain, Policy
A Randomized, Prospective, Double-Blind, Placebo-Controlled Evaluation of the Effect of Sedation on Diagnostic Validity of Cervical Facet Joint Pain
 Manchikanti et al Effect of Sedation on Diagnostic Validity of Cervical Facet Joint Pain 301 Pain Physician. 2004;7:301-309, ISSN 1533-3159 A Randomized Evaluation A Randomized, Prospective, Double-Blind,
Manchikanti et al Effect of Sedation on Diagnostic Validity of Cervical Facet Joint Pain 301 Pain Physician. 2004;7:301-309, ISSN 1533-3159 A Randomized Evaluation A Randomized, Prospective, Double-Blind,
5/31/2013. Disclosures. Lumbar Facet Joint Pain: Evidence. I have nothing to disclose
 Disclosures : Evidence I have nothing to disclose David J. Lee, MD Professor Pain Management Center Department of Anesthesia Facet Joint Pain Prevalence Spinal pain 54-80% lifetime 80-90% resolve in 6
Disclosures : Evidence I have nothing to disclose David J. Lee, MD Professor Pain Management Center Department of Anesthesia Facet Joint Pain Prevalence Spinal pain 54-80% lifetime 80-90% resolve in 6
Original Contribution
 Original Contribution 354 Pain Physician, Volume 5, Number 4, pp 354-359 2002, American Society of Interventional Pain Physicians ISSN 1533-3159 Evaluation of the Prevalence of Facet Joint Pain in Chronic
Original Contribution 354 Pain Physician, Volume 5, Number 4, pp 354-359 2002, American Society of Interventional Pain Physicians ISSN 1533-3159 Evaluation of the Prevalence of Facet Joint Pain in Chronic
CLINICAL GUIDELINES. CMM-201 ~ Facet Joint Injections. Version 19.0 Effective August 11, 2017
 CLINICAL GUIDELINES CMM-201 ~ Facet Joint Injections Version 19.0 Effective August 11, 2017 evicore healthcare Clinical Decision Support Tool Diagnostic Strategies:This tool addresses common symptoms and
CLINICAL GUIDELINES CMM-201 ~ Facet Joint Injections Version 19.0 Effective August 11, 2017 evicore healthcare Clinical Decision Support Tool Diagnostic Strategies:This tool addresses common symptoms and
FACET JOINT INJECTIONS Version 18.0; Effective
 evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
Cigna Medical Coverage Policies Musculoskeletal Facet Joint Injections/Medial Branch Blocks
 Cigna Medical Coverage Policies Musculoskeletal January 15, 2018 Instructions for use The following coverage policy applies to health benefit plans administered by Cigna. Coverage policies are intended
Cigna Medical Coverage Policies Musculoskeletal January 15, 2018 Instructions for use The following coverage policy applies to health benefit plans administered by Cigna. Coverage policies are intended
INTERVENTIONAL TREATMENT FOR PAIN OF SPINAL ORIGIN
 INTERVENTIONAL TREATMENT FOR PAIN OF SPINAL ORIGIN Dr John MacVicar, Medical Director Southern Rehab, Christchurch, NZ AOCPRM Nov 23 rd 2018 INTERVENTIONAL TREATMENT FOR PAIN OF SPINAL ORIGIN An evidence-based
INTERVENTIONAL TREATMENT FOR PAIN OF SPINAL ORIGIN Dr John MacVicar, Medical Director Southern Rehab, Christchurch, NZ AOCPRM Nov 23 rd 2018 INTERVENTIONAL TREATMENT FOR PAIN OF SPINAL ORIGIN An evidence-based
Guideline Number: NIA_CG_301 Last Revised Date: March 2018 Responsible Department: Clinical Operations
 Magellan Healthcare Clinical guidelines PARAVERTEBRAL FACET JOINT INJECTIONS OR BLOCKS (no U/S) CPT Codes: Cervical Thoracic Region: 64490 (+ 64491, +64492) Lumbar Sacral Region: 64493 (+64494, +64495)
Magellan Healthcare Clinical guidelines PARAVERTEBRAL FACET JOINT INJECTIONS OR BLOCKS (no U/S) CPT Codes: Cervical Thoracic Region: 64490 (+ 64491, +64492) Lumbar Sacral Region: 64493 (+64494, +64495)
CLINICAL GUIDELINES. CMM-201: Facet Joint Injections/Medial Branch Blocks. Version Effective October 22, 2018
 CLINICAL GUIDELINES CMM-201: Facet Joint Injections/Medial Branch Blocks Version 20.0.2018 Effective October 22, 2018 Clinical guidelines for medical necessity review of speech therapy services. CMM-201:
CLINICAL GUIDELINES CMM-201: Facet Joint Injections/Medial Branch Blocks Version 20.0.2018 Effective October 22, 2018 Clinical guidelines for medical necessity review of speech therapy services. CMM-201:
Randomized Trial. Pain Physician 2010; 13: ISSN
 Pain Physician 2010; 13:437-450 ISSN 1533-3159 Randomized Trial Comparative Outcomes of a 2-Year Follow-Up of Cervical Medial Branch Blocks in Management of Chronic Neck Pain: A Randomized, Double-Blind
Pain Physician 2010; 13:437-450 ISSN 1533-3159 Randomized Trial Comparative Outcomes of a 2-Year Follow-Up of Cervical Medial Branch Blocks in Management of Chronic Neck Pain: A Randomized, Double-Blind
Re: Occipital Neuralgia and Headache Treatment, Policy Number: 2018T0080Y
 May 10, 2018 United Healthcare Medical Policy Department 9500 Bren Road East Minnetonka, MN 55343 via Email: mpq@uhc.com Re: Occipital Neuralgia and Headache Treatment, Policy Number: 2018T0080Y To Whom
May 10, 2018 United Healthcare Medical Policy Department 9500 Bren Road East Minnetonka, MN 55343 via Email: mpq@uhc.com Re: Occipital Neuralgia and Headache Treatment, Policy Number: 2018T0080Y To Whom
Dr Ian Wallbridge. Musculoskeletal Specialist Rotorua. 11:30-12:00 Managing Intractable Spinal pain
 Dr Ian Wallbridge Musculoskeletal Specialist Rotorua 11:30-12:00 Managing Intractable Spinal pain 2 years of pain 2 years of pain 2 years of pain Intractable spinal pain KEY POINT #1 2 types: SOMATIC
Dr Ian Wallbridge Musculoskeletal Specialist Rotorua 11:30-12:00 Managing Intractable Spinal pain 2 years of pain 2 years of pain 2 years of pain Intractable spinal pain KEY POINT #1 2 types: SOMATIC
Management of lumbar zygapophysial (facet) joint pain
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v7.i5.315 World J Orthop 2016 May 18; 7(5): 315-337 ISSN 2218-5836 (online) 2016 Baishideng
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v7.i5.315 World J Orthop 2016 May 18; 7(5): 315-337 ISSN 2218-5836 (online) 2016 Baishideng
Cigna Medical Coverage Policies Musculoskeletal Facet Joint Injections/Medial Branch Blocks
 Cigna Medical Coverage Policies Musculoskeletal January 15, 2019 Instructions for use The following coverage policy applies to health benefit plans administered by Cigna. Coverage policies are intended
Cigna Medical Coverage Policies Musculoskeletal January 15, 2019 Instructions for use The following coverage policy applies to health benefit plans administered by Cigna. Coverage policies are intended
Dr Jim Borowczyk. Dr John Robinson. Dr Peter McKenzie. Dr John MacVicar
 Dr Jim Borowczyk Musculoskeletal Physician Christchurch Dr Peter McKenzie Musculoskeletal Physician Nelson Dr John Robinson General Practitioner Otumoetai Doctors Tauranga Dr John MacVicar Medical Director
Dr Jim Borowczyk Musculoskeletal Physician Christchurch Dr Peter McKenzie Musculoskeletal Physician Nelson Dr John Robinson General Practitioner Otumoetai Doctors Tauranga Dr John MacVicar Medical Director
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Facet Joint Denervation Page 1 of 20 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Facet Joint Denervation Professional Institutional Original Effective Date:
Facet Joint Denervation Page 1 of 20 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Facet Joint Denervation Professional Institutional Original Effective Date:
An Update of Evaluation of Therapeutic Thoracic Facet Joint Interventions
 Pain Physician 2012; 15:E463-E481 ISSN 2150-1149 Systematic Review An Update of Evaluation of Therapeutic Thoracic Facet Joint Interventions Kavita N. Manchikanti, MD 1, Sairam Atluri, MD 2, Vijay Singh,
Pain Physician 2012; 15:E463-E481 ISSN 2150-1149 Systematic Review An Update of Evaluation of Therapeutic Thoracic Facet Joint Interventions Kavita N. Manchikanti, MD 1, Sairam Atluri, MD 2, Vijay Singh,
A Best-Evidence Systematic Appraisal of the Diagnostic Accuracy and Utility of Facet (Zygapophysial) Joint Injections in Chronic Spinal Pain
 Pain Physician 2015; 18:E497-E533 ISSN 2150-1149 Systematic Review From: 1 Department of Anesthesiology and Perioperative Medicine, University of Louisville, Louisville, KY; 2 Pain Management Center of
Pain Physician 2015; 18:E497-E533 ISSN 2150-1149 Systematic Review From: 1 Department of Anesthesiology and Perioperative Medicine, University of Louisville, Louisville, KY; 2 Pain Management Center of
FEP Medical Policy Manual
 FEP Medical Policy Manual Effective Date: April 15, 2018 Related Policies: 6.01.23 Diagnosis and Treatment of Sacroiliac Joint Pain 7.01.120 Facet Arthroplasty Facet Joint Denervation Description Percutaneous
FEP Medical Policy Manual Effective Date: April 15, 2018 Related Policies: 6.01.23 Diagnosis and Treatment of Sacroiliac Joint Pain 7.01.120 Facet Arthroplasty Facet Joint Denervation Description Percutaneous
Systematic Review of Diagnostic Utility and Therapeutic Effectiveness of Cervical Facet Joint Interventions
 Pain Physician 2009; 12:323-344 ISSN 1533-3159 Systematic Review Systematic Review of Diagnostic Utility and Therapeutic Effectiveness of Cervical Facet Joint Interventions Frank J.E. Falco, MD 1, Stephanie
Pain Physician 2009; 12:323-344 ISSN 1533-3159 Systematic Review Systematic Review of Diagnostic Utility and Therapeutic Effectiveness of Cervical Facet Joint Interventions Frank J.E. Falco, MD 1, Stephanie
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Facet Joint Denervation Page 1 of 22 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Facet Joint Denervation Professional Institutional Original Effective Date:
Facet Joint Denervation Page 1 of 22 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Facet Joint Denervation Professional Institutional Original Effective Date:
Cigna Medical Coverage Policies Musculoskeletal Radiofrequency Joint Ablation/Denervation
 Cigna Medical Coverage Policies Musculoskeletal Radiofrequency Joint Ablation/Denervation Effective January 1, 2016 Instructions for use The following coverage policy applies to health benefit plans administered
Cigna Medical Coverage Policies Musculoskeletal Radiofrequency Joint Ablation/Denervation Effective January 1, 2016 Instructions for use The following coverage policy applies to health benefit plans administered
To: Manuel Suarez, M.D. Medical Director Neighborhood Health Plan Management Department 5757 Plaza Dr. Cyprus, CA Mailstop: CA
 To: Manuel Suarez, M.D. Medical Director Neighborhood Health Plan Management Department 5757 Plaza Dr. Cyprus, CA 30630 Mailstop: CA124-01290 Subject: Denial of Cervical Spinal Injection Procedures Dear
To: Manuel Suarez, M.D. Medical Director Neighborhood Health Plan Management Department 5757 Plaza Dr. Cyprus, CA 30630 Mailstop: CA124-01290 Subject: Denial of Cervical Spinal Injection Procedures Dear
Radiofrequency Denervation for Neck and Back Pain: A Systematic Review Within the Framework of the Cochrane Collaboration Back Review Group
 Radiofrequency Denervation for Neck and Back Pain: A Systematic Review Within the Framework of the Cochrane Collaboration Back Review Group 1 Spine August 15, 2003; 28(16):1877-1888 Leena Niemistö, MD;
Radiofrequency Denervation for Neck and Back Pain: A Systematic Review Within the Framework of the Cochrane Collaboration Back Review Group 1 Spine August 15, 2003; 28(16):1877-1888 Leena Niemistö, MD;
Laxmaiah Manchikanti, MD, Kimberly A. Cash, RT, Vidyasagar Pampati, MSc, Bradley W. Wargo, DO, and Yogesh Malla, MD
 Pain Physician 2010; 13:E265-E278 ISSN 2150-1149 Randomized Trial Cervical Epidural Injections in Chronic Discogenic Neck Pain Without Disc Herniation or Radiculitis: Preliminary Results of a Randomized,
Pain Physician 2010; 13:E265-E278 ISSN 2150-1149 Randomized Trial Cervical Epidural Injections in Chronic Discogenic Neck Pain Without Disc Herniation or Radiculitis: Preliminary Results of a Randomized,
MEDICAL POLICY SUBJECT: RADIOFREQUENCY FACET DENERVATION
 MEDICAL POLICY PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
MEDICAL POLICY PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
Randomized Trial. Pain Physician 2008; 11: ISSN
 Pain Physician 2008; 11:801-815 ISSN 1533-3159 Randomized Trial Preliminary Results of a Randomized, Equivalence Trial of Fluoroscopic Caudal Epidural Injections in Managing Chronic Low Back Pain: Part
Pain Physician 2008; 11:801-815 ISSN 1533-3159 Randomized Trial Preliminary Results of a Randomized, Equivalence Trial of Fluoroscopic Caudal Epidural Injections in Managing Chronic Low Back Pain: Part
NEUROABLATION FOR TREATMENT OF CHRONIC PAIN
 NEUROABLATION FOR TREATMENT OF CHRONIC PAIN Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical
NEUROABLATION FOR TREATMENT OF CHRONIC PAIN Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical
Facet Joint Denervation. Populations Interventions Comparators Outcomes Individuals: With suspected facet joint pain
 Protocol Facet Joint Denervation (701116) Medical Benefit Effective Date: 01/01/16 Next Review Date: 11/18 Preauthorization Yes Review Dates: 09/09, 09/10, 07/11, 07/12, 05/13, 05/14, 01/15, 11/15, 11/16,
Protocol Facet Joint Denervation (701116) Medical Benefit Effective Date: 01/01/16 Next Review Date: 11/18 Preauthorization Yes Review Dates: 09/09, 09/10, 07/11, 07/12, 05/13, 05/14, 01/15, 11/15, 11/16,
MEDICAL POLICY SUBJECT: RADIOFREQUENCY JOINT ABLATION / DENERVATION
 MEDICAL POLICY SUBJECT: RADIOFREQUENCY JOINT PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including
MEDICAL POLICY SUBJECT: RADIOFREQUENCY JOINT PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including
Facet Joint Denervation. Description
 Section: Surgery Effective Date: April 15, 2015 Subject: Facet Joint Denervation Page: 1 of 14 Last Review Status/Date: March 2015 Facet Joint Denervation Description Facet joint denervation is performed
Section: Surgery Effective Date: April 15, 2015 Subject: Facet Joint Denervation Page: 1 of 14 Last Review Status/Date: March 2015 Facet Joint Denervation Description Facet joint denervation is performed
Vijay Singh, M.D Roosevelt Rd., Niagara, WI 54151
 Publications and Book Chapters Vijay Singh, M.D. 1601 Roosevelt Rd., Niagara, WI 54151 PUBLICATIONS Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 July 2012 July 2012 May-Jun 2012 May-Jun
Publications and Book Chapters Vijay Singh, M.D. 1601 Roosevelt Rd., Niagara, WI 54151 PUBLICATIONS Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 July 2012 July 2012 May-Jun 2012 May-Jun
d EFFECTIVE DATE: POLICY LAST UPDATED:
 Medical Coverage Policy Epidural Injections for Pain Management d EFFECTIVE DATE: 04 01 2018 POLICY LAST UPDATED: 03 20 2018 OVERVIEW Epidural injections are generally performed to treat pain arising from
Medical Coverage Policy Epidural Injections for Pain Management d EFFECTIVE DATE: 04 01 2018 POLICY LAST UPDATED: 03 20 2018 OVERVIEW Epidural injections are generally performed to treat pain arising from
Facet Joint Denervation. Description
 Section: Surgery Effective Date: April 15, 2014 Subject: Facet Joint Denervation Page: 1 of 16 Last Review Status/Date: March 2014 Facet Joint Denervation Description Facet joint denervation is performed
Section: Surgery Effective Date: April 15, 2014 Subject: Facet Joint Denervation Page: 1 of 16 Last Review Status/Date: March 2014 Facet Joint Denervation Description Facet joint denervation is performed
Facet Joint Injections and Facet Joint Nerve Blocks Effective Date December 15, 2014 Original Policy Date March 16, 1988
 BSC6.03 Section 7.0 Surgery Subsection 7.01 Surgery Facet Joint Injections and Facet Joint Nerve Blocks Effective Date December 15, 2014 Original Policy Date March 16, 1988 Next Review Date December 2015
BSC6.03 Section 7.0 Surgery Subsection 7.01 Surgery Facet Joint Injections and Facet Joint Nerve Blocks Effective Date December 15, 2014 Original Policy Date March 16, 1988 Next Review Date December 2015
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: facet_joint_denervation 6/2009 4/2017 4/2018 4/2017 Description of Procedure or Service Facet joint denervation
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: facet_joint_denervation 6/2009 4/2017 4/2018 4/2017 Description of Procedure or Service Facet joint denervation
Accuracy of Precision Diagnostic Blocks in the Diagnosis of Chronic Spinal Pain of Facet or Zygapophysial Joint Origin:
 Boswell et al Diagnostic Facet Joint Blocks 449 Pain Physician. 2003;6:449-456, ISSN 1533-3159 A Systematic Review Accuracy of Precision Diagnostic Blocks in the Diagnosis of Chronic Spinal Pain of Facet
Boswell et al Diagnostic Facet Joint Blocks 449 Pain Physician. 2003;6:449-456, ISSN 1533-3159 A Systematic Review Accuracy of Precision Diagnostic Blocks in the Diagnosis of Chronic Spinal Pain of Facet
Facet Joint Denervation
 Facet Joint Denervation Policy Number: 7.01.116 Last Review: 5/2014 Origination: 5/2011 Next Review: 5/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for radiofrequency
Facet Joint Denervation Policy Number: 7.01.116 Last Review: 5/2014 Origination: 5/2011 Next Review: 5/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for radiofrequency
An Updated Review of the Diagnostic Utility of Cervical Facet Joint Injections
 Pain Physician 2012; 15:E807-E838 ISSN 2150-1149 Systematic Review An Updated Review of the Diagnostic Utility of Cervical Facet Joint Injections Frank J.E. Falco, MD 1, Sukdeb Datta, MD 2, Laxmaiah Manchikanti,
Pain Physician 2012; 15:E807-E838 ISSN 2150-1149 Systematic Review An Updated Review of the Diagnostic Utility of Cervical Facet Joint Injections Frank J.E. Falco, MD 1, Sukdeb Datta, MD 2, Laxmaiah Manchikanti,
Laxmaiah Manchikanti, MD, Kimberly A. Cash, RT, Vidyasagar Pampati, MSc, Bradley W. Wargo, DO, and Yogesh Malla, MD
 Pain Physician 2010; 13:223-236 ISSN 1533-3159 Randomized Trial The Effectiveness of Fluoroscopic Cervical Interlaminar Epidural Injections in Managing Chronic Cervical Disc Herniation and Radiculitis:
Pain Physician 2010; 13:223-236 ISSN 1533-3159 Randomized Trial The Effectiveness of Fluoroscopic Cervical Interlaminar Epidural Injections in Managing Chronic Cervical Disc Herniation and Radiculitis:
Original Policy Date
 MP 7.01.96 Facet Joint Denervation Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy Index
MP 7.01.96 Facet Joint Denervation Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy Index
Influence of Psychological Variables on the Diagnosis of Facet Joint Involvement in Chronic Spinal Pain
 Pain Physician 2008; 11:145-160 ISSN 1533-3159 Retrospective Evaluation Influence of Psychological Variables on the Diagnosis of Facet Joint Involvement in Chronic Spinal Pain Laxmaiah Manchikanti, MD,
Pain Physician 2008; 11:145-160 ISSN 1533-3159 Retrospective Evaluation Influence of Psychological Variables on the Diagnosis of Facet Joint Involvement in Chronic Spinal Pain Laxmaiah Manchikanti, MD,
CMM-201~Facet Joint Injections- Medical Branch Blocks
 MedSolutions, Inc. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Requests for patients with atypical symptoms or clinical presentations
MedSolutions, Inc. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Requests for patients with atypical symptoms or clinical presentations
Outcome of Caudal Epidural Steroid. Injection in Chronic Low Back Pain. {Original Article (Orthopedic) Gulzar Saeed Ahmed
 Outcome of Caudal Epidural Steroid Injection in Chronic Low Back Pain {Original Article (Orthopedic) Gulzar Saeed Ahmed Assoc. Prof. of Orthopedic Surgery and traumatology, Liaquat University of Medical
Outcome of Caudal Epidural Steroid Injection in Chronic Low Back Pain {Original Article (Orthopedic) Gulzar Saeed Ahmed Assoc. Prof. of Orthopedic Surgery and traumatology, Liaquat University of Medical
Comparison of effectiveness for fluoroscopic cervical interlaminar epidural injections with or without steroid in cervical post-surgery syndrome
 Original Article Korean J Pain 2018 October; Vol. 31, No. 4: 277-288 pissn 2005-9159 eissn 2093-0569 https://doi.org/10.3344/kjp.2018.31.4.277 Comparison of effectiveness for fluoroscopic cervical interlaminar
Original Article Korean J Pain 2018 October; Vol. 31, No. 4: 277-288 pissn 2005-9159 eissn 2093-0569 https://doi.org/10.3344/kjp.2018.31.4.277 Comparison of effectiveness for fluoroscopic cervical interlaminar
CLINICAL GUIDELINES. CMM-207: Epidural Adhesiolysis. Version Effective February 15, 2019
 CLINICAL GUIDELINES CMM-207: Version 1.0.2019 Effective February 15, 2019 Clinical guidelines for medical necessity review of speech therapy services. CMM-207: CMM-207.1: Definition 3 CMM-207.2: General
CLINICAL GUIDELINES CMM-207: Version 1.0.2019 Effective February 15, 2019 Clinical guidelines for medical necessity review of speech therapy services. CMM-207: CMM-207.1: Definition 3 CMM-207.2: General
See Policy CPT/HCPCS CODE section below for any prior authorization requirements
 Effective Date: 7/1/2018 Section: MED Policy No: 123 Medical Officer 7/1/18 Date Technology Assessment Committee Approved Date: 10/10; 12/15 Medical Policy Committee Approved Date: 8/94; 7/96; 8/97; 4/98;
Effective Date: 7/1/2018 Section: MED Policy No: 123 Medical Officer 7/1/18 Date Technology Assessment Committee Approved Date: 10/10; 12/15 Medical Policy Committee Approved Date: 8/94; 7/96; 8/97; 4/98;
National Imaging Associates, Inc. Clinical guidelines FACET JOINT INJECTIONS, MEDIAL BRANCH BLOCKS, AND FACET JOINT RADIOFREQUENCY NEUROTOMY
 National Imaging Associates, Inc. Clinical guidelines FACET JOINT INJECTIONS, MEDIAL BRANCH BLOCKS, AND FACET JOINT RADIOFREQUENCY NEUROTOMY CPT Codes: Refer to pages 5 and 6 LCD ID Number: L35936 J K
National Imaging Associates, Inc. Clinical guidelines FACET JOINT INJECTIONS, MEDIAL BRANCH BLOCKS, AND FACET JOINT RADIOFREQUENCY NEUROTOMY CPT Codes: Refer to pages 5 and 6 LCD ID Number: L35936 J K
Comprasion of Effectiveness of CT vs C-arm Guided Percutaneous Radiofrequency Lumbar Facet Rhizotomy
 Original Article Korean J Pain 2010 June; Vol. 23, No. 2: 137-141 pissn 2005-9159 eissn 2093-0569 DOI:10.3344/kjp.2010.23.2.137 Comprasion of Effectiveness of CT vs C-arm Guided Percutaneous Radiofrequency
Original Article Korean J Pain 2010 June; Vol. 23, No. 2: 137-141 pissn 2005-9159 eissn 2093-0569 DOI:10.3344/kjp.2010.23.2.137 Comprasion of Effectiveness of CT vs C-arm Guided Percutaneous Radiofrequency
Follow this and additional works at: Part of the Musculoskeletal Diseases Commons
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2016 Do Epidural Injections With Local Anesthetic
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2016 Do Epidural Injections With Local Anesthetic
Clinical Policy: Selective Nerve Root Blocks and Transforaminal Epidural Steroid Injections
 Clinical Policy: Selective Nerve Root Blocks and Transforaminal Epidural Steroid Injections Reference Number: PA.CP.MP.165 Effective Date: 09/18 Last Review Date: 09/18 Coding Implications Revision Log
Clinical Policy: Selective Nerve Root Blocks and Transforaminal Epidural Steroid Injections Reference Number: PA.CP.MP.165 Effective Date: 09/18 Last Review Date: 09/18 Coding Implications Revision Log
MEDICAL POLICY MEDICAL POLICY DETAILS POLICY STATEMENT. Page: 1 of 5
 Page: 1 of 5 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title RADIOFREQUENCY JOINT ABLATION/DENERVATION Policy Number 7.01.42 Category Technology Assessment Effective Date 10/18/01 Revised Date
Page: 1 of 5 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title RADIOFREQUENCY JOINT ABLATION/DENERVATION Policy Number 7.01.42 Category Technology Assessment Effective Date 10/18/01 Revised Date
PERCUTANEOUS FACET JOINT DENERVATION
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-95 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-95 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
MEDICAL HISTORY CHIRO PHYSICAL
 Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
Is Dexamethasone Epidural Injection Effective in Relieving Radicular Pain in an Adult Population?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 Is Dexamethasone Epidural Injection Effective
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 Is Dexamethasone Epidural Injection Effective
The Benefit of Therapeutic Medial Branch Blocks after Cervical Operations
 Pain Physician 2010; 13:527-534 ISSN 1533-3159 Retrospective Study The Benefit of Therapeutic Medial Branch Blocks after Cervical Operations Stephan Klessinger, MD From: Nova Clinic, Biberach, Germany
Pain Physician 2010; 13:527-534 ISSN 1533-3159 Retrospective Study The Benefit of Therapeutic Medial Branch Blocks after Cervical Operations Stephan Klessinger, MD From: Nova Clinic, Biberach, Germany
Variation In The Method Of Caudal Epidural Injection- A Regional Survey
 ISPUB.COM The Internet Journal of Spine Surgery Volume 5 Number 2 Variation In The Method Of Caudal Epidural Injection- A Regional Survey S Haque., J Gaskin., A Uguwoke, S Karmani Citation S Haque., J
ISPUB.COM The Internet Journal of Spine Surgery Volume 5 Number 2 Variation In The Method Of Caudal Epidural Injection- A Regional Survey S Haque., J Gaskin., A Uguwoke, S Karmani Citation S Haque., J
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN
 UnitedHealthcare Commercial Medical Policy EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: PAI001 Effective Date: May 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT
UnitedHealthcare Commercial Medical Policy EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: PAI001 Effective Date: May 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT
Clinical Policy Title: Radiofrequency ablation treatment for spine pain
 Clinical Policy Title: Radiofrequency ablation treatment for spine pain Clinical Policy Number: 03.02.02 Effective Date: June 1, 2013 Initial Review Date: March 21, 2013 Most Recent Review Date: March
Clinical Policy Title: Radiofrequency ablation treatment for spine pain Clinical Policy Number: 03.02.02 Effective Date: June 1, 2013 Initial Review Date: March 21, 2013 Most Recent Review Date: March
Accuracy of Diagnostic Lumbar Facet Joint Nerve Blocks: A 2-Year Follow-Up of 152 Patients Diagnosed with Controlled Diagnostic Blocks
 Pain Physician 2009; 12:855-866 ISSN 1533-3159 Original Contribution Accuracy of Diagnostic Lumbar Facet Joint Nerve Blocks: A 2-Year Follow-Up of 152 Patients Diagnosed with Controlled Diagnostic Blocks
Pain Physician 2009; 12:855-866 ISSN 1533-3159 Original Contribution Accuracy of Diagnostic Lumbar Facet Joint Nerve Blocks: A 2-Year Follow-Up of 152 Patients Diagnosed with Controlled Diagnostic Blocks
Clinical Policy: Caudal or Interlaminar Epidural Steroid Injections
 Clinical Policy: Reference Number: PA.CP.MP.164 Effective Date: 09/18 Last Review Date: 09/18 Coding Implications Revision Log Description Epidural steroid injections have been used for pain control in
Clinical Policy: Reference Number: PA.CP.MP.164 Effective Date: 09/18 Last Review Date: 09/18 Coding Implications Revision Log Description Epidural steroid injections have been used for pain control in
MEDICAL POLICY EFFECTIVE DATE: 08/15/13 REVISED DATE: 07/17/14 SUBJECT: SPINAL INJECTIONS (EPIDURAL AND FACET INJECTIONS) FOR PAIN MANAGEMENT
 MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
Radiofrequency Treatment of Facet-related Pain: Evidence and Controversies
 Curr Pain Headache Rep (2012) 16:19 25 DOI 10.1007/s11916-011-0237-8 ANESTHETIC TECHNIQUES IN PAIN MANAGEMENT (GJ BRENNER, SECTION EDITOR) Radiofrequency Treatment of Facet-related Pain: Evidence and Controversies
Curr Pain Headache Rep (2012) 16:19 25 DOI 10.1007/s11916-011-0237-8 ANESTHETIC TECHNIQUES IN PAIN MANAGEMENT (GJ BRENNER, SECTION EDITOR) Radiofrequency Treatment of Facet-related Pain: Evidence and Controversies
MEDICAL POLICY STATEMENT INDIANA MEDICAID Original Issue Date Next Annual Review Effective Date 11/01/ /01/ /17/2017
 MEDICAL POLICY STATEMENT INDIANA MEDICAID Original Issue Date Next Annual Review Effective Date 11/01/2017 11/01/2018 12/17/2017 Policy Name Policy Number Policy Type MEDICAL Administrative Pharmacy Reimbursement
MEDICAL POLICY STATEMENT INDIANA MEDICAID Original Issue Date Next Annual Review Effective Date 11/01/2017 11/01/2018 12/17/2017 Policy Name Policy Number Policy Type MEDICAL Administrative Pharmacy Reimbursement
INTERVENTIONAL PAIN MEDICINE PAST, PRESENT, FUTURE. No conflicts of interest. The truth does not pay
 INTERVENTIONAL PAIN MEDICINE PAST, PRESENT, FUTURE Professor Nikolai Bogduk Emeritus Professor of Pain Medicine University of Newcastle Australia No conflicts of interest The truth does not pay 1970 1980
INTERVENTIONAL PAIN MEDICINE PAST, PRESENT, FUTURE Professor Nikolai Bogduk Emeritus Professor of Pain Medicine University of Newcastle Australia No conflicts of interest The truth does not pay 1970 1980
Clinical Policy Title: Radiofrequency ablation treatment for spine pain
 Clinical Policy Title: Radiofrequency ablation treatment for spine pain Clinical Policy Number: 03.02.02 Effective Date: June 1, 2013 Initial Review Date: March 21, 2013 Most Recent Review Date: March
Clinical Policy Title: Radiofrequency ablation treatment for spine pain Clinical Policy Number: 03.02.02 Effective Date: June 1, 2013 Initial Review Date: March 21, 2013 Most Recent Review Date: March
Nonsurgical Interventional Treatments for Spinal Pain Management
 Nonsurgical Interventional Treatments for Spinal Pain Management I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain
Nonsurgical Interventional Treatments for Spinal Pain Management I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain
Phillip Weidner, DO, DABA, BCPM May 20th, 2014
 Phillip Weidner, DO, DABA, BCPM May 20th, 2014 Introduction Comprehensive Pain Management Center Interventional therapies Epidural steroid injections Sacroiliac interventions Facet joint disease Who to
Phillip Weidner, DO, DABA, BCPM May 20th, 2014 Introduction Comprehensive Pain Management Center Interventional therapies Epidural steroid injections Sacroiliac interventions Facet joint disease Who to
Ultrasound-guided Pulsed Radiofrequency of the Third Occipital Nerve
 Case Report Korean J Pain 2013 April; Vol. 26, No. 2: 186-190 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.2.186 Ultrasound-guided Pulsed Radiofrequency of the Third Occipital
Case Report Korean J Pain 2013 April; Vol. 26, No. 2: 186-190 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.2.186 Ultrasound-guided Pulsed Radiofrequency of the Third Occipital
Clinical Policy Title: Radiofrequency ablation treatment for spine pain
 Clinical Policy Title: Radiofrequency ablation treatment for spine pain Clinical Policy Number: 03.02.02 Effective Date: June 1, 2013 Initial Review Date: March 21, 2013 Most Recent Review Date: February
Clinical Policy Title: Radiofrequency ablation treatment for spine pain Clinical Policy Number: 03.02.02 Effective Date: June 1, 2013 Initial Review Date: March 21, 2013 Most Recent Review Date: February
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): February 28, 2012 Most Recent Review Date (Revised): January 28, 2014 Effective Date: April 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS
Original Issue Date (Created): February 28, 2012 Most Recent Review Date (Revised): January 28, 2014 Effective Date: April 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS
Spinal and Trigger Point Injections
 Spinal and Trigger Point Injections I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain when determined to be medically
Spinal and Trigger Point Injections I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain when determined to be medically
Quick Response code. Original Article. Access this Article online INTRODUCTION
 Original Article EFFECT OF MAITLAND VS MULLIGAN MOBILISATION TECHNIQUE ON UPPER THORACIC SPINE IN PATIENTS WITH NON-SPECIFIC NECK PAIN - A COMPARATIVE STUDY Kaur Inderpreet *1, Arunmozhi R 2, Arfath Umer
Original Article EFFECT OF MAITLAND VS MULLIGAN MOBILISATION TECHNIQUE ON UPPER THORACIC SPINE IN PATIENTS WITH NON-SPECIFIC NECK PAIN - A COMPARATIVE STUDY Kaur Inderpreet *1, Arunmozhi R 2, Arfath Umer
Re: Adoption of ACOEM Guidelines on Cervical and Thoracic Spine Disorders
 February 23, 2018 Division of Workers Compensation State of California PO Box 420603 San Francisco, CA 94142 via Email to: DWCforums@dir.ca.gov Re: Adoption of ACOEM Guidelines on Cervical and Thoracic
February 23, 2018 Division of Workers Compensation State of California PO Box 420603 San Francisco, CA 94142 via Email to: DWCforums@dir.ca.gov Re: Adoption of ACOEM Guidelines on Cervical and Thoracic
Clinical Policy Title: Spine pain facet joint injections
 Clinical Policy Title: Spine pain facet joint injections Clinical Policy Number: 03.02.07 Effective Date: April 1, 2016 Initial Review Date: June 16, 2013 Most Recent Review Date: January 11, 2018 Next
Clinical Policy Title: Spine pain facet joint injections Clinical Policy Number: 03.02.07 Effective Date: April 1, 2016 Initial Review Date: June 16, 2013 Most Recent Review Date: January 11, 2018 Next
Diagnostic cervical and lumbar medial branch blocks
 Considered Judgement Form This form is a checklist of issues that may be considered by the Purchasing Guidance Advisory Group when making purchasing recommendations Meeting date: 2 November 2015 Topic:
Considered Judgement Form This form is a checklist of issues that may be considered by the Purchasing Guidance Advisory Group when making purchasing recommendations Meeting date: 2 November 2015 Topic:
Medical Policy Facet Joint Denervation. Effective Date February 15, Subsection. 7.0 Surgery. Next Review Date December 2015
 7.01.116 Facet Joint Denervation Section 7.0 Surgery Subsection Effective Date February 15, 2015 Original Policy Date February 14, 2001 Next Review Date December 2015 Description Percutaneous radiofrequency
7.01.116 Facet Joint Denervation Section 7.0 Surgery Subsection Effective Date February 15, 2015 Original Policy Date February 14, 2001 Next Review Date December 2015 Description Percutaneous radiofrequency
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN
 EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN UnitedHealthcare Oxford Clinical Policy Policy Number: PAIN 019.21 T2 Effective Date: October 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE...
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN UnitedHealthcare Oxford Clinical Policy Policy Number: PAIN 019.21 T2 Effective Date: October 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE...
MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND FACET INJECTIONS) FOR PAIN MANAGEMENT
 MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 10 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product
MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 10 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product
PERCUTANEOUS RADIO-FREQUENCY NEUROTOMY FOR CHRONIC CERVICAL ZYGAPOPHYSEAL-JOINT PAIN
 PERCUTANEOUS RADIO-FREQUENCY NEUROTOMY FOR CHRONIC CERVICAL ZYGAPOPHYSEAL-JOINT PAIN PERCUTANEOUS RADIO-FREQUENCY NEUROTOMY FOR CHRONIC CERVICAL ZYGAPOPHYSEAL-JOINT PAIN SUSAN M. LORD, B.MED., PH.D., LESLIE
PERCUTANEOUS RADIO-FREQUENCY NEUROTOMY FOR CHRONIC CERVICAL ZYGAPOPHYSEAL-JOINT PAIN PERCUTANEOUS RADIO-FREQUENCY NEUROTOMY FOR CHRONIC CERVICAL ZYGAPOPHYSEAL-JOINT PAIN SUSAN M. LORD, B.MED., PH.D., LESLIE
Evidence based Practice Changes Spinal Injections
 Evidence based Practice Changes Spinal Injections Kathryn Mueller, MD, MPH, FACOEM Professor, School of Public Health & Department of Physiatry - University of Colorado President - American College of
Evidence based Practice Changes Spinal Injections Kathryn Mueller, MD, MPH, FACOEM Professor, School of Public Health & Department of Physiatry - University of Colorado President - American College of
Behnam Hosseini, Mohammad Hossein Ataei, Sirous Momenzadeh, Reza Jalili Khoshnood, Davood Ommi
 Original Article The comparison between steroid and hypertonic saline 10% with steroid in transforaminal epidural injection in patients with unilateral foraminal stenosis Behnam Hosseini, Mohammad Hossein
Original Article The comparison between steroid and hypertonic saline 10% with steroid in transforaminal epidural injection in patients with unilateral foraminal stenosis Behnam Hosseini, Mohammad Hossein
Lysis of Epidural Adhesions
 Medical Policy Manual Surgery, Policy No. 94 Lysis of Epidural Adhesions Next Review: September 2019 Last Review: October 2018 Effective: November 1, 2018 IMPORTANT REMINDER Medical Policies are developed
Medical Policy Manual Surgery, Policy No. 94 Lysis of Epidural Adhesions Next Review: September 2019 Last Review: October 2018 Effective: November 1, 2018 IMPORTANT REMINDER Medical Policies are developed
Interventional Pain. Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care
 Interventional Pain Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care IASP Definition of Pain Pain is an unpleasant sensory or emotional experience associated
Interventional Pain Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care IASP Definition of Pain Pain is an unpleasant sensory or emotional experience associated
Medical Affairs Policy
 Medical Affairs Policy Service: Back Pain Procedures-Epidural Injection (Caudal Epidural, Selective Nerve Root Block, Interlaminar, Transforaminal, Translaminar Epidural Injection) PUM 250-0015-1706 Medical
Medical Affairs Policy Service: Back Pain Procedures-Epidural Injection (Caudal Epidural, Selective Nerve Root Block, Interlaminar, Transforaminal, Translaminar Epidural Injection) PUM 250-0015-1706 Medical
Nerve root blocks in the treatment of lumbar radicular pain: A minimum five-year follow-up
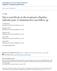 Washington University School of Medicine Digital Commons@Becker Open Access Publications 8-1-2006 Nerve root blocks in the treatment of lumbar radicular pain: A minimum five-year follow-up K. Daniel Riew
Washington University School of Medicine Digital Commons@Becker Open Access Publications 8-1-2006 Nerve root blocks in the treatment of lumbar radicular pain: A minimum five-year follow-up K. Daniel Riew
Percutaneous Discectomy
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
MEDICAL POLICY EFFECTIVE DATE: 08/15/13 REVISED DATE: 07/17/14, 06/18/15, 05/25/16, 05/18/17
 MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 10 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product,
MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 10 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product,
Key words: Rhizotomy, radiofrequency neurotomy, 2 needles, facet joint pain, low back pain, cadaveric tissue. Pain Physician 2010; 13:43-49
 Pain Physician 2010; 13:43-49 ISSN 1533-3159 Cadaveric Study The Efficacy of Two Electrodes Radiofrequency Technique: Comparison Study Using a Cadaveric Interspinous Ligament and Temperature Measurement
Pain Physician 2010; 13:43-49 ISSN 1533-3159 Cadaveric Study The Efficacy of Two Electrodes Radiofrequency Technique: Comparison Study Using a Cadaveric Interspinous Ligament and Temperature Measurement
2/5/2019. Facet Joint Pain. Biomechanics
 Facet Arthropathy as a Pain Source Evaluation and Management Shelby Spine Jan 31 st Feb 2 nd, 2019 Kushagra Verma MD, MS Adult and Pediatric Scoliosis And Spine Deformity Beach Orthopaedics Specialty Institute
Facet Arthropathy as a Pain Source Evaluation and Management Shelby Spine Jan 31 st Feb 2 nd, 2019 Kushagra Verma MD, MS Adult and Pediatric Scoliosis And Spine Deformity Beach Orthopaedics Specialty Institute
Discussion Points 10/17/16. Spine Pain is Ubiquitous. Interventional Pain Management
 Interventional Pain Management Blake Christensen, D.O. Fellowship Trained Interventional Pain Management Board Eligible in Anesthesiology and Interventional Pain Management Oklahoma Interventional Pain
Interventional Pain Management Blake Christensen, D.O. Fellowship Trained Interventional Pain Management Board Eligible in Anesthesiology and Interventional Pain Management Oklahoma Interventional Pain
Laxmaiah Manchikanti, MD, Sneha Pampati, and Kimberly A. Cash, RT
 Pain Physician 2010; 13:133-143 ISSN 1533-3159 Diagnostic Accuracy Study Making Sense of the Accuracy of Diagnostic Lumbar Facet Joint Nerve Blocks: An Assessment of the Implications of 50% Relief, 80%
Pain Physician 2010; 13:133-143 ISSN 1533-3159 Diagnostic Accuracy Study Making Sense of the Accuracy of Diagnostic Lumbar Facet Joint Nerve Blocks: An Assessment of the Implications of 50% Relief, 80%
Medical Affairs Policy
 Medical Affairs Policy Service: Back and Nerve Pain Procedures - Radiofrequency Ablation, Facet and Other Injections PUM 250-0035-1706 Cryoablation Medial Branch Neuroablation Radiofrequency Neuroablation
Medical Affairs Policy Service: Back and Nerve Pain Procedures - Radiofrequency Ablation, Facet and Other Injections PUM 250-0035-1706 Cryoablation Medial Branch Neuroablation Radiofrequency Neuroablation
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN
 EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Protocol: PAI001 Effective Date: April 1, 2018 Table of Contents Page COMMERCIAL & MEDICAID COVERAGE RATIONALE... 1 MEDICARE COVERAGE RATIONALE...
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Protocol: PAI001 Effective Date: April 1, 2018 Table of Contents Page COMMERCIAL & MEDICAID COVERAGE RATIONALE... 1 MEDICARE COVERAGE RATIONALE...
DRAFT as posted for public comment 11/8/2016 to 8 a.m. 12/9/2016. HERC Coverage Guidance
 HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: LOW BACK PAIN - CORTICOSTEROID INJECTIONS HERC Coverage Guidance Corticosteroid injections (including epidural, facet joint, medial branch, and
HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: LOW BACK PAIN - CORTICOSTEROID INJECTIONS HERC Coverage Guidance Corticosteroid injections (including epidural, facet joint, medial branch, and
