Spinal stimulation of the upper lumbar spinal cord modulates urethral sphincter activity in rats after spinal cord injury
|
|
|
- Norman Augustine Hood
- 6 years ago
- Views:
Transcription
1 Am J Physiol Renal Physiol 308: F1032 F1040, First published February 18, 2015; doi: /ajprenal Spinal stimulation of the upper lumbar spinal cord modulates urethral sphincter activity in rats after spinal cord injury Edsel M. Abud, 1 Ronaldo M. Ichiyama, 7 Leif A. Havton, 2,3,4,5,6 and Huiyi H. Chang 2,6 1 Department of Neurobiology and Behavior, University of California, Irvine, California; 2 Department of Anesthesiology and Perioperative Care, University of California, Irvine, California; 3 Department of Anatomy and Neurobiology, University of California, Irvine, California; 4 Department of Neurology, University of California, Irvine, California; 5 Reeve-Irvine Research Center, University of California, Irvine, California; 6 Department of Neurology, University of California, Los Angeles, California; and 7 School of Biomedical Sciences, University of Leeds, Leeds, United Kingdom Submitted 14 October 2014; accepted in final form 11 February 2015 Abud EM, Ichiyama RM, Havton LA, Chang HH. Spinal stimulation of the upper lumbar spinal cord modulates urethral sphincter activity in rats after spinal cord injury. Am J Physiol Renal Physiol 308: F1032 F1040, First published February 18, 2015; doi: /ajprenal After spinal cord injury (SCI), the neurogenic bladder is observed to develop asynchronous bladder and external urethral sphincter (EUS) contractions in a condition known as detrusor-sphincter dyssnergia (DSD). Activation of the EUS spinal controlling center located at the upper lumbar spinal cord may contribute to reduce EUS dyssynergic contractions and decrease urethral resistance during voiding. However, this mechanism has not been well studied. This study aimed at evaluating the effects of epidural stimulation (EpS) over the spinal EUS controlling center (L3) in combination with a serotonergic receptor agonist on EUS relaxation in naive rats and chronic (6 8 wk) T8 SCI rats. Cystometrogram and EUS electromyography (EMG) were obtained before and after the intravenous administration of 5HT-1A receptor agonist and antagonist. The latency, duration, frequency, amplitude, and area under curve of EpS-evoked EUS EMG responses were analyzed. EpS on L3 evoked an inhibition of EUS tonic contraction and an excitation of EUS intermittent bursting/relaxation correlating with urine expulsion in intact rats. Combined with a 5HT-1A receptor agonist, EpS on L3 evoked a similar effect in chronic T8 SCI rats to reduce urethral contraction (resistance). This study examined the effect of facilitating the EUS spinal controlling center to switch between urine storage and voiding phases by using EpS and a serotonergic receptor agonist. This novel approach of applying EpS on the EUS controlling center modulates EUS contraction and relaxation as well as reduces urethral resistance during voiding in chronic SCI rats with DSD. electromyography; epidural stimulation; serotonergic receptors; urethral resistance SPINAL CORD INJURY (SCI) has a profound effect on the health of a patient s life. Researchers have noted that patients with SCI placed bowel/bladder, sexual function, and mobility as top priorities when assessing quality of life (25). Disorganized voiding reflexes, or detrusor-sphincter dyssynergia (DSD), develop in the majority of SCI patients. During voiding, the external urethral sphincter (EUS) dyssynergically contracts instead of relaxing completely, causing urine flow to be interrupted and the bladder pressure to rise (3). Commonly, DSD leads to urinary tract infections and long-term severe renal damages (30). The urgency and timeliness to better understand Address for reprint requests and other correspondence: H. H. Chang, Dept. of Urology, Univ. of Southern California, 2011 Zonal Ave., HMR-602, Los Angeles, CA ( HuiyiHarriet.Chang@med.usc.edu). and modulate the changes occurring in the spinal circuits controlling lower urinary tract (LUT) function after SCI are evident. The urinary bladder and EUS in rats receive their efferent innervation from parasympathetic neurons and EUS motoneurons located at the caudal lumbosacral levels (L6-S1) of the spinal cord. It is generally believed that these neurons are controlled by input from the pontine micturition center that is primarily responsible for coordinating the activity of the urinary bladder and urethral outlet during micturition (11). However, studies by Chang et al. (5) suggested that the EUS bursting pattern generator is located in the L3-4 spinal segments in female rats and is also important for generating the alternating relaxations and contractions of the EUS, an essential feature for efficient voiding in rodents. Thus the voiding phase in rodents is controlled by the upper lumbar levels (L3-4) instead of the motoneurons of the L6-S1 spinal segments in rats. A recent study reported that epidural stimulation (EpS) between L3 and L6 improves bladder function after severe SCI when combined with long-term locomotor training and serotonergic receptor agonists (15). The combinatorial treatment decreased nonvoiding contractions, leak point pressure, and urethral outlet resistance. Therefore, the present study, using a rat SCI model, was designed to evaluate the modulation of EUS tonic/bursting activity by using EpS over the upper lumbar spinal cord and to understand the switch between storage and voiding phases in the chronically injured spinal cord. Furthermore, serotonergic 5HT-1A mechanisms play an important role on the modulation of LUT function, especially on EUS relaxation in rats, in part by prolonging the silent period within the bursting activity during voiding (6, 10, 12 13). While EpS elicits the inhibition of EUS tonic activity and further evokes bursting responses, a concurrent administration of a 5HT-1A receptor agonist may provide a synergistic effect. The present study was carried out as a combination of EpS on L3 spinal cord segment and serotonergic administration to investigate the mechanisms of EUS relaxation during voiding in rats with DSD. METHODS All animal use and procedures were performed in accordance with the guidelines established by the National Institutes of Health Guide for Care and Use of Laboratory Animals and approved by the Institutional Animal Care and Use Committee of the University of California, Irvine. A total of 21 animals were used in the present study and included control (n 9) and SCI (n 12) groups. F X/15 Copyright 2015 the American Physiological Society
2 F1033 Spinal cord transection. Twelve adult female rats (Sprague-Dawley, weighing g) underwent a complete spinal cord transection at spinal level T8 under gas anesthesia (isoflurane, 2 5%). The spinal cord transection was verified by visual inspection under the microscope. Cut ends were exposed and separated by Gelfoam (5). An analgesic (buprenorphine; 0.05 mg/kg) was given subcutaneously every 12 h for 48 h to relieve any postoperative pain. An antibiotic (Baytril; 5 mg/kg, sc) was given daily for 7 days to prevent urinary infections. Postoperatively, the bladder was manually expressed twice a day for 3 wk and then once a day until the end point (6 8 wk). At the end point, the animals underwent surgical preparation for EpS and urodynamic recordings. Preparation for EpS and urodynamic recordings. Both control (n 9) and SCI (n 12) groups were given urethane (1.2 g/kg sc) 1 h before the surgical preparation. Each animal was placed on a water-circulating heating pad. An established method was used to place the EpS wires (16). In brief, a laminectomy was performed at a thoracic level of T12-L2. For EpS over L3 (L3-EpS), the spinal segments of L2-3 were exposed for placements of epidural stimulating electrodes. Two Teflon-coated stainless steel wires (AS632; Cooner Wire) were placed over the midline at dorsal surface of the spinal cord. The stimulation electrodes were made by removing a small portion ( 1-mm notch) of the Teflon coating to expose the stainless steel wire on the surface facing the spinal cord and then suturing them to the dura of L2 and L3 as the anode and cathode between 2 and 4 mm, respectively, to provide the bipolar/biphasic stimulation by an isolated unit and an electrical stimulator (SIU5 and S88; GRASS Technologies). The dura remained intact. In some animals, the EpS was tested over L6 (L6-EpS). The EpS wires were placed over the midline at dorsal surface of the spinal segments and sutured to the dura of L6-S1 as the anode and cathode, respectively, to provide the bipolar/biphasic stimulation. A bladder catheter and EUS EMG wires were placed using established methods (5, 6). Briefly, a midline lower abdominal incision was made to expose the bladder. A flared tip of a PE-50 catheter (Instech Laboratories) was inserted into the top of bladder dome and secured by a surgical thread. The bladder catheter was then connected to an infusion pump (KD Scientific) and a pressure sensor (Biopac Systems) via a three-way stopcock. Two 50- m PFA-insulated platinum-iridium wire electrodes (A-M Systems) were inserted into EUS bilaterally using a 27-gauge needle. Wire electrodes were then connected to the amplifier (Biopac Systems). The infusion rate of saline was set at 0.12 ml/min. EpS was applied at 1- to 1.5-fold of the threshold intensity (1 5 V) at Hz and a 0.1- to 0.3-ms pulse width for s. The threshold intensity was set at the appearance of EUS bursting responses because EUS bursting has been an important index for voiding in rodents. The stimulation intensity was adjusted to avoid hindlimb movements and reduce the interference from the muscle twitching. The elicited EUS responses were collected before and after drug administration. 8-Hydroxy-2-(di-npropylamino)-tetralin (8-OH-DPAT, a 5HT-1A receptor agonist; 0.5 mg/kg; Sigma-Aldrich, St Louis, MO) was administrated intravenously (iv). N-{2-[4-(2-methoxyphenyl)-1-piperazinyl] ethyl}-n-(2- pyridinyl) cyclohexanecarboxamide trihydrochloride (WAY100635, a 5HT-1A receptor antagonist; 0.3 mg/kg; Sigma-Aldrich) was given iv to evaluate the effect of 8-OH-DPAT on EUS activity. Both of 8-OH-DPAT and WAY were dissolved in 0.9% of normal saline at the final dose of 1 mg/ml, aliquot in 1-m tube, and then stored in the 20 C freezer. These tubes were used within 2 wk since they were made. Outcome measurements. During continuous bladder infusion, three voiding contractions were evaluated 60 min after infusion. Outcome measures from cystometrogram and EUS electromyography (EMG) activity included the maximum intravesical pressure, resting pressure, and contraction duration as well as the maximum amplitude and area under curve (AUC). The latency of the first void (LFV) was measured as the latency from the start of empty bladder filling to the onset of the first void. The bladder capacity was calculated as the volume (ml) of [LFV (min) infusion rate (0.12 ml/min)]. The latency to EUS bursting, duration of inhibited EUS tonic activity, duration of evoked bursting activity, and maximum amplitude, AUC, and firing frequency of evoked EUS bursting were measured for three responses and then averaged in each animal before and after drug administration. Statistical analysis. Data without drugs were analyzed by t-test to examine the differences between two groups using Prism 4.0 (GraphPad Software). Repeated t-test was applied to compare the drug effect of different doses. Quantitative data are expressed as means SE. We regarded P 0.05 to indicate a statistically significant difference between groups. Fig. 1. Continuous bladder infusion in an intact rat. A: regular voiding contractions responding to the saline infusion of the bladder are shown. B: faster time tracing shows external urethral sphincter (EUS) bursting during voiding. To summarize, the rat exhibits EUS tonic activity during storage phase and switches to bursting when voiding. The infusion rate was 0.12 ml/min.
3 F1034 RESULTS Fig. 2. Representative examples acquired at different ranges of frequencies (A) at a 0.2-ms pulse width and pulse widths (B) at 40 Hz in a naive rat. The intensity was 5 V, 1.5-fold of threshold without lower extremities movement. Note the bursting reflex was used as an indicator of voiding reflex because bursting only appeared during voiding in rodents. Therefore, the suggestive optimal stimulation was a 40-Hz, 0.2-ms pulse width at 1- to 2-fold over threshold intensity. Identification of EpS-evoked EUS reflexes. In control rats (n 9) EUS EMG recordings demonstrated a low amplitude tonic activity during bladder filling. This tonic activity increased gradually as the infused volume approached the voiding threshold. During bladder contractions, EUS EMG patterns markedly changed, consisting of increased tonic and bursting activity (Fig. 1). The bladder was partially distended to examine the increase of EUS tonic activity before onset of EpS. After EUS activity was measured, EpS parameters were optimized to prevent unwanted hind limb movement by utilizing lower intensity (voltages). A range of frequencies (10 40 Hz) and pulse widths ( ms) was examined (Fig. 2). The optimal parameters of EpS were determined as 40 Hz and 0.2-ms pulse width because such EpS evoked not only inhibition of EUS tonic activity but also EUS bursting. Each stimulation episode occurred for s with a resting time of 4 5 min. EUS EMG responses to EpS were not observed if the waiting time was 4 min under these stimulating parameters. L6-EpS evoked continuous EUS tonic contraction (Fig. 3A) until EpS stopped. L3-EpS elicited several EUS responses including an initial increase of EUS activity, followed by inhibition of EUS activity and onset of evoked EUS bursting (Fig. 3B) in control rats. When the bladder was empty with modest EUS tonic activity, L3-EpS-evoked EUS bursting was shown but not the inhibition of EUS tonic activity. When the bladder was filled (62 6% of the bladder capacity based on LFV of each animal, n 9), both EUS bursting and inhibition of EUS tonic activity were evoked by L3-EpS. L3-EpS-evoked EUS burst-
4 F1035 ing was compared when the bladder was empty or distended in control rats. There were no significant EUS bursting changes of latency, duration, frequency, AUC, and maximum amplitude (Table 1). These evoked EUS responses were eliminated after an acute bilateral pudendal nerve transection or T8 spinal transection (Fig. 4). A bilateral pelvic nerve transection did not affect these L3-EpS-evoked EUS responses. After administration of 8-OH-DPAT, a 5HT-1A agonist, the maximum amplitude and AUC of evoked EUS bursting were significantly increased in control rats (Table 2). WAY100635, a 5HT-1A antagonist, reversed the effect of 8-OH-DPAT and decreased the frequency and AUC of EUS bursting. The inhibition of EUS activity was significantly prolonged by WAY compared with the condition without drug (Table 2). Examinations of EpS-evoked EUS reflexes after spinal cord injury. In rats with a chronic SCI (n 12), only large amplitude EUS tonic activity (contraction) was produced during voiding (Fig. 5A). The bladder was partially distended by infusing saline, 60% of bladder capacity based on LFV of each animal (n 12). L6-EpS evoked continuous EUS tonic contraction that persisted even after EpS was stopped (Fig. 5C). L3-EpS elicited inhibition of EUS activity (relaxation) in all Fig. 3. Representative examples of EUS bursting reflex elicited by epidural stimulation (EpS) on L6 (A) or L3 (B) spinal segment in 3 intact rats. Note EpS suppressed EUS tonic activity, and elicited EUS bursting reflex. In animals 1 and 3, the duration of suppressed tonic activity was longer and continued after EpS has been stopped. It may indicate that EpS was given close to EUS bursting pattern generator compared with the EpS location at animal 2. Dotted boxes indicate the duration of inhibited EUS tonic activity evoked by EpS. The solid bar above the tracings indicated the duration of EpS (4 6 V, 0.2-ms pulse width at 40 Hz). SCI rats but only elicited EUS bursting in 4 out of 12 SCI rats. The latency of L3-EpS-evoked EUS responses was significantly delayed compared with controls (Fig. 6). The duration of EUS bursting did not significantly differ between SCI and control groups. The firing frequency, maximum amplitude, and AUC were significantly decreased in SCI rats (Fig. 6). SCI rats had prolonged inhibition of EUS tonic activity during L3-EpS compared with controls. L3-EpS-evoked EUS responses, including inhibition of tonic activity and intermittent relaxation/ bursting, were present when the bladder was empty or distended. After administration of 8-OH-DPAT, EUS bursting during voiding was unmasked in the SCI group (Fig. 5B). All SCI rats showed EUS bursting evoked by L3-EpS. 8-OH-DPAT significantly shortened the latency of evoked EUS responses as well as enhanced the maximum amplitude, frequency, and AUC of evoked EUS bursting in all SCI rats (Fig. 5E and Table 3). WAY reversed the effect of 8-OH-DPAT, and only 3 out of 12 SCI rats showed L3-EpS-evoked EUS responses. WAY significantly decreased the duration of EUS bursting and the inhibition of EUS activity compared with the condition without drug (Table 3). Table 1. Measurements of L3-EpS-evoked EUS bursting responses when the bladder was empty or distended in the control rats Latency, s Duration, s Frequency, Hz Amplitude, mv AUC, mv/s Empty bladder (n 9) Distended bladder (n 9) EpS, epidural stimulation; EUS, external urethral sphincter; AUC, area under curve.
5 F1036 Fig. 4. Verification of the pathway of evoked EUS responses in intact rats (A) when EpS was applied over L3. The animal received bilateral pelvic nerve transection (B), and it did not affect evoked EUS responses. Then, the same animal underwent bilateral pudendal nerve transection (C). The evoked EUS responses were eliminated. In other words, the evoked EUS responses are suggested to be conducted by pudendal nerve. In another rat, an acute T8 transection (D) alone showed that the evoked EUS responses were eliminated when the pathway to the pontine micturition center was blocked acutely. DISCUSSION The present study investigated the effects of spinal electrical stimulation over the dura matter at the dorsal surface of the L3 spinal cord segment in attempts to modulate EUS relaxation during voiding. L3-EpS evoked an inhibition of EUS tonic activity and activation of EUS bursting in control animals. L3-EpS inhibited EUS tonic activity in spinal cord transected rats, and L3-EpS in combination with a serotonergic receptor agonist (8-OH-DPAT) inhibited EUS tonic activity and unmasked EUS bursting. These results indicated that L3-EpS combined 8-OH-DPAT over the EUS spinal pattern generator promotes voiding and offers a potential new strategy for EUS relaxation during voiding to ameliorate DSD after SCI. EpS of the L3 segment evokes spinal EUS reflexes in the present study and indicates possible linkage between the L3 and L6-S1 segments for LUT function, especially EUS activation. Previous histological and electrophysiological studies have shown possible connections between the L3-4 and L6-S1 spinal segments that might mediate the EUS bursting. In male rats, bursting activity was identified in the periurethral striated muscles (bulbocavernosus and ischiocavernous muscles) involved in ejaculation (20). The ejaculation reflex is mediated by a spinal pattern generator located in the L3-4 spinal segments (29). Because pseudorabies virus (PRV) tracing studies also revealed PRV-labeled neurons in this same region following injection of PRV into EUS of female rats (19), these L3-4 spinal neurons may also be responsible for the generation of EUS bursting activity during voiding (5). Other studies showed that electrical stimulation of the pudendal nerve, which contains afferents innervating the EUS, increased c-fos expression in the L3-4 spinal segments (31). In addition, electrical stimulation of the pelvic nerve, which contains afferents from the bladder and urethra, increased c-fos staining in neurons located between the L2 and S1 segments (2). These reports provide support for a circuitry connecting motor pathways in the L6-S1 spinal cord with a putative pattern generator in the L3-4 spinal segments. Our data suggest that, instead of direct stimulation of Onuf s nucleus at the lumbosacral levels (L6-S1), stimulation of the upper lumbar levels containing the EUS bursting pattern generator may provide an innovative approach to modulate LUT functions. A variety of electrical stimulation treatments are currently under investigation or already clinically available for modulating voiding dysfunction. Functional electrical stimulation devices (23), peripheral nerve stimulation (26), and intraspinal stimulation (14, 22) methods are examples of electrical stimulation approaches currently in use and/or under investigation. These electrical stimulation methods (1, 14, 22, 24, 26) target the lumbosacral levels at L6-S2 to directly activate the preganglionic parasympathetic neurons and EUS motoneurons. While the majority of prior studies have focused on electrical stimulation at lumbosacral levels, the present study demonstrates a novel method of EpS over upper lumbar levels to modulate urethral sphincter activity (5). Previous investigations have demonstrated early (ER) and late (LR) responses of pelvic-eus reflexes elicited by pelvic nerve stimulation in spinally intact rats to represent EUS tonic and bursting activities, respectively (5). EpS-evoked EUS responses are similar to the ER and LR of pelvic-eus reflexes. The ER and tonic activity were eliminated when L6-S1 segments were transected indicating EUS tonic activity is mediated by a spinal pathway. The present study confirmed that tonic activity was elicited when L6-EpS was applied in naive and spinal cord injured rats. In contrast to ER and EUS tonic activity mediated by L6-S1, the LR and EUS bursting are eliminated when L3-4 spinal segments are damaged indicating EUS bursting is mediated by a supinobulbospinal reflex pathway. L3-EpS evoked the EUS bursting. However, L3-EpS provides strong stimulation to elicit EUS bursting responses, regardless of whether the bladder is empty or distended. The Table 2. Statistical analysis of evoked EUS EMG responses in naive animals before and after drugs Naive Animals Without Drug 8-OH-DPAT 8-OH-DPAT WAY n Inhibition of EUS activity, s Latency to the beginning of inhibition, s Duration of EUS bursting, s Frequency of EUS bursting, Hz Amplitude of EUS bursting, mv * AUC of EUS bursting, mv/s * Inhibition of EUS EMG activity includes the duration of EUS bursting. WAY (0.3 mg/kg iv) was given after 8-hydroxy-2-(di-n-propylamino)- tetralin (8-OH-DPAT; 0.5 mg/kg iv). * P 0.05, significant change compared with the recordings before drug administration.
6 F1037 Fig. 5. Representative examples of continuous bladder infusion in a rat with chronic spinal cord injury (SCI). The rat produced only EUS tonic activity during storage and voiding phases, representing detrusor sphincter dyssnergia (DSD) after SCI (A). No EUS relaxation was found during the high amplitude part of the tonic contractions during voiding. After administration of 8-hydroxy-2-(di-n-propylamino)-tetralin (8-OH-DPAT; 0.5 mg/kg iv), the EUS bursting was unmasked during voiding (B). Increased EUS relaxation (silent periods between each individual burst) was also demonstrated after drug administration. The bladder infusion rate was 0.12 ml/min. When EpS was applied over L6, only continuous EUS tonic firing activity was seen (C). However, EpS over L3 evoked the inhibition of EUS tonic activity (storage) but no bursting (D). The latency was shortened and the duration of suppressed EUS tonic activity (storage) was prolonged by administration of 8-OH-DPAT (0.5 mg/kg iv; E). LR of pelvic-eus reflex requires bladder distension to be evoked by indirect stimulation of the L3-4 segments via pelvic nerve stimulation. Firing frequencies (1 2 Hz) of LR of pelvic- EUS reflexes and EpS-evoked EUS bursting indicate more EUS relaxation compared with the regular EUS bursting (6 8 Hz) when the bladder is infused by saline (4, 5, 9). In the present study, when EpS was applied directly on L3, the spinal EUS bursting center, EUS tonic activity was first suppressed and then the bursting responses were evoked. When EpS was applied slightly closer to L2, EpS-evoked EUS responses showed shorter duration of suppressed tonic activity (Fig. 3B). However, when EpS was applied on L6, it only evoked continuous EUS tonic activity. These results indicated that the optimal stimulation site may be located closely to L3. The present results showed that EpS-evoked EUS responses are not affected by transecting the pelvic nerves, but they are eliminated when the bilateral pudendal nerves are cut. Therefore, all EpS-evoked EUS responses are conducted via the pudendal nerves, which innervate the EUS muscle (21). By acutely transecting the T8 spinal segment, all evoked responses
7 F1038 Fig. 6. Statistical analysis of EpS evoked EUS responses in control (n 9) and SCI (n 4) groups without drug administration. AUC, area under the curve. *P 0.05, significant changes. were eliminated. In most chronic T8 SCI rats, L3-EpS evoked the inhibition of EUS tonic activity and EUS bursting when combined with 8-OH-DPAT. Serotonergic 5HT-1A mechanisms have a long-standing history in promoting EUS activation in rodent models (5, 6, 8, 10, 12, 18, 28). 8-OH-DPAT, a 5HT-1A receptor agonist, produces a bladder contraction leading to micturition at subthreshold bladder pressures (18). In the ventral horn, 5HT-1A binding sites are very densely located in the spinal dorsolateral nucleus of the pudendal nerve (27). Studies also indicate that 5HT-1A receptors facilitate EUS bursting duration and relaxation in rats (6, 10), which is important to expulse the urine and empty the bladder. Here we showed that 8-OH-DPAT increased the amplitude and AUC of L3-EpS-evoked EUS bursting responses in intact rats. However, in the chronic SCI rats, L3-EpS only suppressed EUS tonic activity but did not elicit EUS bursting in 8 of 12 chronic SCI rats without 8-OH-DPAT. Additionally, 8-OH-DPAT further unmasked EUS bursting and shortened the latency of EUS bursting in all SCI rats. 8-OH-DPAT also increased the amplitude, AUC, and firing frequency of EUS bursting. The excitatory effect of 8-OH- DPAT on L3-EpS-evoked EUS responses is attributable to an action in the spinal cord because it occurred in chronic SCI rats. These results appear similarly to the ER of the pelvic-eus reflex facilitated by 8-OH-DPAT in intact rats as well as in chronic T8 SCI rats and the LR of pelvic-eus reflexes facilitated by 8-OH-DPAT in chronic T8 SCI rats (5). Table 3. Statistical analysis of evoked EUS EMG responses in the animals with chronic SCI before and after drugs Chronic SCI Without Drug 8-OH-DPAT 8-OH-DPAT WAY n Inhibition of EUS activity, s Latency to the beginning of inhibition, s * Duration of EUS bursting, s Frequency of EUS bursting, Hz * Amplitude of EUS bursting, mv * AUC of EUS bursting, mv/s * SCI, spinal cord injury. Inhibition of EUS EMG activity includes the duration of EUS bursting. WAY (0.3 mg/kg iv) was given after 8-OH-DPAT (0.5 mg/kg iv). * P 0.05, significant change compared with the recordings before drug administration.
8 To validate the effects of 8-OH-DPAT in EpS-induced EUS activity, a known 5HT-1A antagonist, WAY , was used. In our study, after administration of 8-OH-DPAT, WAY extensively prolonged the inhibition of EUS tonic activity in intact rats but reduced the inhibition of EUS tonic activity and EUS bursting responses in the SCI rats. Previous studies in neurologically intact rats revealed that WAY alone not only reversed the excitatory effect of 8-OH-DPAT but also suppressed reflex bladder activity (5, 17, 28) and EUS bursting induced by bladder distension (5). This indicates that EUS bursting is facilitated by an endogenous serotonergic mechanism in anesthetized rats with an intact neuraxis. Therefore, serotonergic effects of prolonged EUS relaxation on EUS bursting center located in the L3 spinal segment can be expected from these two studies when indirect activation is provided by electrical stimulation of the pelvic afferents or directly on the L3 segment. The present study examined the possibility of modulating the EUS spinal controlling center and investigated the mechanisms for switching between urine storage and voiding phases. The overall goal of this technique is to suppress the dyssynergic EUS contraction and then empty the bladder by the later EpS-evoked EUS bursting during voiding in chronic SCI rats with DSD. Although humans do not have EUS bursting during voiding, EpS on the EUS spinal controlling center may contribute to suppress dyssynergic EUS contraction while the bladder reaches voiding threshold in the SCI patients with DSD to expulse urine. ACKNOWLEDGMENTS We thank Dr. Lisa Wulund for assisting with surgery and postoperative animal care. GRANTS The present study is partially supported by the University of California through a continuation of the Roman Reed Spinal Cord Injury Research Fund of California and the Dr. Miriam and Sheldon G. Adelson Medical Research Foundation. DISCLOSURES No conflicts of interest, financial or otherwise, are declared by the author(s). AUTHOR CONTRIBUTIONS Author contributions: E.M.A. and H.H.C. conception and design of research; E.M.A., R.M.I., and H.H.C. performed experiments; E.M.A. and H.H.C. analyzed data; E.M.A. and H.H.C. drafted manuscript; E.M.A., R.M.I., L.A.H., and H.H.C. edited and revised manuscript; E.M.A., R.M.I., L.A.H., and H.H.C. approved final version of manuscript; L.A.H. and H.H.C. interpreted results of experiments; H.H.C. prepared figures. REFERENCES 1. Bamford JA, Mushahwar VK. Intraspinal microstimulation for the recovery of function following spinal cord injury. Prog Brain Res 194: , Birder LA, Roppolo JR, Iadarola MJ, de Groat WC. Electrical stimulation of visceral afferent pathways in the pelvic nerve increases c-fos in the rat lumbosacral spinal cord. Neurosci Lett 129: , Cardenas DD, Hooton TM. Urinary tract infection in persons with spinal cord injury. Arch Phys Med Rehabil 76: , Chang HY, Cheng CL, Chen JJ, de Groat WC. Roles of glutamatergic and serotonergic mechanisms in reflex control of the external urethral sphincter in urethane-anesthetized female rats. Am J Physiol Regul Integr Comp Physiol 291: R224 R234, Chang HY, Cheng CL, Chen JJ, de Groat WC. Serotonergic drugs and spinal cord transections at different segmental levels indicate that F1039 different spinal circuits are involved in tonic and bursting external urethral sphincter activity in rats. Am J Physiol Renal Physiol 292: F1044 F1053, Chang HH, Havton LA. Serotonergic 5-HT 1A receptor agonist (8-OH- DPAT) ameliorates impaired micturition reflexes in a chronic ventral root avulsion model of incomplete cauda equina/conus medullaris injury. Exp Neurol 239: , Chen KJ, Chen LW, Liao JM, Chen CH, Ho YC, Ho YC, Cheng CL, Lin JJ, Huang PC, Lin TB. Effects of a calcineurin inhibitor, tacrolimus, on glutamate-dependent potentiation in pelvic-urethral reflex in anesthetized rats. Neuroscience 138: 69 76, Chen SC, Cheng CL, Fan WJ, Chen JJ, Lai CH, Peng CW. Effect of a 5-HT1A receptor agonist (8-OH-DPAT) on external urethral sphincter activity in a rat model of pudendal nerve injury. Am J Physiol Regul Integr Comp Physiol 301: R225 R235, Cheng CL, de Groat WC. The role of capsaicin-sensitive afferent fibers in the lower urinary tract dysfunction induced by chronic spinal cord injury in rats. Exp Neurol 187: , Cheng CL, de Groat WC. Role of 5-HT1A receptors in control of lower urinary tract function in anesthetized rats. Am J Physiol Renal Physiol 298: F771 F778, de Groat WC, Yoshimura N. Mechanisms underlying the recovery of lower urinary tract function following spinal cord injury. Prog Brain Res 152: 59 84, de Groat WC. Influence of central serotonergic mechanisms on lower urinary tract function. Urology 59: 30 36, Dolber PC, Gu B, Zhang X, Fraser MO, Thor KB, Reiter JP. Activation of the external urethral sphincter central pattern generator by a 5-HT(1A) receptor agonist in rats with chronic spinal cord injury. Am J Physiol Regul Integr Comp Physiol 292: R1699 R1706, Grill WM, Bhadra N, Wang B. Bladder and urethral pressures evoked by microstimulation of the sacral spinal cord in cats. Brain Res 836: 19 30, Horst M, Heutschi J, van den Brand R, Andersson KE, Gobet R, Sulser T, Courtine G, Eberli D. Multisystem neuroprosthetic training improves bladder function after severe spinal cord injury. J Urol 189: , Ichiyama RM, Gerasimenko YP, Zhong H, Roy RR, Edgerton VR. Hindlimb stepping movements in complete spinal rats induced by epidural spinal cord stimulation. Neurosci Lett 383: , Kakizaki H, Yoshiyama M, Koyanagi T, de Groat WC. Effects of WAY100635, a selective 5-HT1A-receptor antagonist on the micturitionreflex pathway in the rat. Am J Physiol Regul Integr Comp Physiol 280: R1407 R1413, Lecci A, Giuliani S, Santicioli P, Maggi CA. Involvement of 5-hydroxytryptamine1A receptors in the modulation of micturition reflexes in the anesthetized rat. J Pharmacol Exp Ther 262: , Marson L. Identification of central nervous system neurons that innervate the bladder body, bladder base, or external urethral sphincter of female rats: a transneuronal tracing study using pseudorabies virus. J Comp Neurol 389: , McKenna KE, Chung SK, McVary KT. A model for the study of sexual function in anesthetized male and female rats. Am J Physiol Regul Integr Comp Physiol 261: R1276 R1285, Peng CW, Chen JJ, Cheng CL, Grill WM. Improved bladder emptying in urinary retention by electrical stimulation of pudendal afferents. J Neural Eng 5: , Pikov V, Bullara L, McCreery DB. Intraspinal stimulation for bladder voiding in cats before and after chronic spinal cord injury. J Neural Eng 4: , Ragnarsson KT. Functional electrical stimulation after spinal cord injury: current use, therapeutic effects and future directions. Spinal Cord 46: , Rijkhoff NJ, Wijkstra H, van Kerrebroeck PE, Debruyne FM. Urinary bladder control by electrical stimulation: review of electrical stimulation techniques in spinal cord injury. Neurourol Urodyn 16: 39 53, Simpson LA, Eng JJ, Hsieh JT, Wolfe DL; Spinal Cord Injury Rehabilitation Evidence Scire Research Team. The health and life priorities of individuals with spinal cord injury: a systematic review. J Neurotrauma 29: , 2012.
9 F Tai C, Booth AM, de Groat WC, Roppolo JR. Bladder and urethral sphincter responses evoked by microstimulation of S2 sacral spinal cord in spinal cord intact and chronic spinal cord injured cats. Exp Neurol 190: , Thor KB, Nickolaus S, Helke CJ. Autoradiographic localization of 5-hydroxytryptamine1A, 5-hydroxytryptamine1B and 5-hydroxytryptamine1C/2 binding sites in the rat spinal cord. Neuroscience 55: , Testa R, Guarneri L, Poggesi E, Angelico P, Velasco C, Ibba M, Cilia A, Motta G, Riva C, Leonardi A. Effect of several 5-hydroxytryptamine(1A) receptor ligands on the micturition reflex in rats: comparison with WAY J Pharmacol Exp Ther 290: , Truitt WA, Coolen LM. Identification of a potential ejaculation generator in the spinal cord. Science 297: , Watanabe T, Rivas DA, Chancellor MB. Urodynamics of spinal cord injury. Urol Clin North Am 23: , Wiedey J, Alexander MS, Marson L. Spinal neurons activated in response to pudendal or pelvic nerve stimulation in female rats. Brain Res 1197: , 2008.
Neural Control of Lower Urinary Tract Function. William C. de Groat University of Pittsburgh Medical School
 Neural Control of Lower Urinary Tract Function William C. de Groat University of Pittsburgh Medical School Disclosures Current funding: NIH Grants, DK093424, DK-091253, DK-094905, DK-090006. Other financial
Neural Control of Lower Urinary Tract Function William C. de Groat University of Pittsburgh Medical School Disclosures Current funding: NIH Grants, DK093424, DK-091253, DK-094905, DK-090006. Other financial
The Time-Frequency Analysis of the Pudendo-to-Pudendal Nerve and Pelvic-to-Pudendal Nerve Reflexes in Anesthetized Intact Rats
 Journal of Medical and Biological Engineering, 24(1): 17-22 17 The Time-Frequency Analysis of the Pudendo-to-Pudendal Nerve and Pelvic-to-Pudendal Nerve Reflexes in Anesthetized Intact Rats Hui-Yi Chang
Journal of Medical and Biological Engineering, 24(1): 17-22 17 The Time-Frequency Analysis of the Pudendo-to-Pudendal Nerve and Pelvic-to-Pudendal Nerve Reflexes in Anesthetized Intact Rats Hui-Yi Chang
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury. Original Policy Date
 MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
Overactive Bladder; OAB. Aδ silent C. Adenosine triphosphate; ATP SD g n Key words
 25-32 2009 SD 200-270g n 28 4 1 2 3 4 PE-50 4-5 0.25 60 C Key words acupuncture stimulation overactive bladder rat bladder irritation C C fiber Received November 17, 2008; Accepted January 9, 2009 I Overactive
25-32 2009 SD 200-270g n 28 4 1 2 3 4 PE-50 4-5 0.25 60 C Key words acupuncture stimulation overactive bladder rat bladder irritation C C fiber Received November 17, 2008; Accepted January 9, 2009 I Overactive
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Technologies and architectures" Stimulator, electrodes, system flexibility, reliability, security, etc."
 March 2011 Introduction" Basic principle (Depolarization, hyper polarization, etc.." Stimulation types (Magnetic and electrical)" Main stimulation parameters (Current, voltage, etc )" Characteristics (Muscular
March 2011 Introduction" Basic principle (Depolarization, hyper polarization, etc.." Stimulation types (Magnetic and electrical)" Main stimulation parameters (Current, voltage, etc )" Characteristics (Muscular
University of Groningen. Neuronal control of micturition Kuipers, Rutger
 University of Groningen Neuronal control of micturition Kuipers, Rutger IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
University of Groningen Neuronal control of micturition Kuipers, Rutger IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
Neural control of the lower urinary tract in health and disease
 Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
Characterization of bladder and external urethral activity in mice with or without spinal cord injury a comparison study with rats
 Am J Physiol Regul Integr Comp Physiol 31: R752 R758, 216. First published January 27, 216; doi:1.1152/ajpregu.45.215. Characterization of bladder and external urethral activity in mice with or without
Am J Physiol Regul Integr Comp Physiol 31: R752 R758, 216. First published January 27, 216; doi:1.1152/ajpregu.45.215. Characterization of bladder and external urethral activity in mice with or without
Characterization of bladder and external urethral activity in mice with or without spinal cord injury a comparison study with rats
 Am J Physiol Regul Integr Comp Physiol 31: R752 R758, 216. First published January 27, 216; doi:1.1152/ajpregu.45.215. Characterization of bladder and external urethral activity in mice with or without
Am J Physiol Regul Integr Comp Physiol 31: R752 R758, 216. First published January 27, 216; doi:1.1152/ajpregu.45.215. Characterization of bladder and external urethral activity in mice with or without
Original Article. Annals of Rehabilitation Medicine INTRODUCTION
 Original Article Ann Rehabil Med 2014;38(3):342-346 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.342 Annals of Rehabilitation Medicine Phasic Changes in Bladder Compliance
Original Article Ann Rehabil Med 2014;38(3):342-346 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.342 Annals of Rehabilitation Medicine Phasic Changes in Bladder Compliance
c-fos Expression in Bladder-Specific Spinal Neurons after Spinal Cord Injury Using Pseudorabies Virus
 Yonsei Med J 49(3):479-485, 2008 DOI 10.3349/ymj.2008.49.3.479 c-fos Expression in Bladder-Specific Spinal Neurons after Spinal Cord Injury Using Pseudorabies Virus Young Jae Im, 1 Chang Hee Hong, 1 Mei
Yonsei Med J 49(3):479-485, 2008 DOI 10.3349/ymj.2008.49.3.479 c-fos Expression in Bladder-Specific Spinal Neurons after Spinal Cord Injury Using Pseudorabies Virus Young Jae Im, 1 Chang Hee Hong, 1 Mei
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
The Praxis FES System and Bladder/Bowel Management in Patients with Spinal Cord Injury
 The Praxis FES System and Bladder/Bowel Management in Patients with Spinal Cord Injury Brian J. Benda 1, Thierry Houdayer 2, Graham Creasey 3, Randal R. Betz 1, Brian T. Smith 1 *, Therese E. Johnston
The Praxis FES System and Bladder/Bowel Management in Patients with Spinal Cord Injury Brian J. Benda 1, Thierry Houdayer 2, Graham Creasey 3, Randal R. Betz 1, Brian T. Smith 1 *, Therese E. Johnston
Urodynamic and electrophysiological investigations in neuro-urology
 Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Electrostimulation Part 3: Bladder dysfunctions
 GBM8320 Dispositifs Médicaux Intelligents Electrostimulation Part 3: Bladder dysfunctions Mohamad Sawan et al Laboratoire de neurotechnologies Polystim!!! http://www.cours.polymtl.ca/gbm8320/! mohamad.sawan@polymtl.ca!
GBM8320 Dispositifs Médicaux Intelligents Electrostimulation Part 3: Bladder dysfunctions Mohamad Sawan et al Laboratoire de neurotechnologies Polystim!!! http://www.cours.polymtl.ca/gbm8320/! mohamad.sawan@polymtl.ca!
Neural control of the lower urinary tract
 Neural control of the lower urinary tract Jalesh N. Panicker Consultant Neurologist and Honorary Senior Lecturer The National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen
Neural control of the lower urinary tract Jalesh N. Panicker Consultant Neurologist and Honorary Senior Lecturer The National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen
GBM8320 Dispositifs Médicaux Intelligents. Electrostimulation. Part 3: Bladder dysfunctions
 GBM8320 Dispositifs Médicaux Intelligents Electrostimulation Part 3: Bladder dysfunctions Mohamad Sawan et al Laboratoire de neurotechnologies Polystim!!! http://www.cours.polymtl.ca/gbm8320/! mohamad.sawan@polymtl.ca!
GBM8320 Dispositifs Médicaux Intelligents Electrostimulation Part 3: Bladder dysfunctions Mohamad Sawan et al Laboratoire de neurotechnologies Polystim!!! http://www.cours.polymtl.ca/gbm8320/! mohamad.sawan@polymtl.ca!
Quantification of effectiveness of bilateral and unilateral neuromodulation in the rat bladder rhythmic contraction model
 Su et al. BMC Urology 2013, 13:34 RESEARCH ARTICLE Open Access Quantification of effectiveness of bilateral and unilateral neuromodulation in the rat bladder rhythmic contraction model Xin Su 1*, Angela
Su et al. BMC Urology 2013, 13:34 RESEARCH ARTICLE Open Access Quantification of effectiveness of bilateral and unilateral neuromodulation in the rat bladder rhythmic contraction model Xin Su 1*, Angela
Role of Animal Models
 Division of Urology, Department of Surgery, Duke University Medical Center Institute for Medical Research, Durham Veteran s Affairs Medical Center Role of Animal Models Matthew O. Fraser, PhD 9th Annual
Division of Urology, Department of Surgery, Duke University Medical Center Institute for Medical Research, Durham Veteran s Affairs Medical Center Role of Animal Models Matthew O. Fraser, PhD 9th Annual
Dual-Channel Neuromodulation of Pudendal Nerve with Closed-Loop Control Strategy to Improve Bladder Functions
 82 Journal of Medical and Biological Engineering, 34(1): 82-89 Dual-Channel Neuromodulation of Pudendal Nerve with Closed-Loop Control Strategy to Improve Bladder Functions Yin-Tsong Lin 1, Chien-Hung
82 Journal of Medical and Biological Engineering, 34(1): 82-89 Dual-Channel Neuromodulation of Pudendal Nerve with Closed-Loop Control Strategy to Improve Bladder Functions Yin-Tsong Lin 1, Chien-Hung
Regulation of the Urinary Bladder Chapter 26
 Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
TITLE: An Implantable Neuroprosthetic Device to Normalize Bladder Function after SCI
 AWARD NUMBER: W81XWH-11-1-819 TITLE: An Implantable Neuroprosthetic Device to Normalize Bladder Function after SCI PRINCIPAL INVESTIGATOR: Changfeng Tai, PhD CONTRACTING ORGANIZATION: University of Pittsburgh
AWARD NUMBER: W81XWH-11-1-819 TITLE: An Implantable Neuroprosthetic Device to Normalize Bladder Function after SCI PRINCIPAL INVESTIGATOR: Changfeng Tai, PhD CONTRACTING ORGANIZATION: University of Pittsburgh
Contribution of the External Urethral Sphincter to Urinary Void Size in Unanesthetized Unrestrained Rats
 Neurourology and Urodynamics 35:696 702 (2016) Contribution of the External Urethral Sphincter to Urinary Void Size in Unanesthetized Unrestrained Rats Brandon K. LaPallo, 1 Jonathan R. Wolpaw, 1,2 * Xiang
Neurourology and Urodynamics 35:696 702 (2016) Contribution of the External Urethral Sphincter to Urinary Void Size in Unanesthetized Unrestrained Rats Brandon K. LaPallo, 1 Jonathan R. Wolpaw, 1,2 * Xiang
Normal micturition involves complex
 NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
Spinal transection alters external urethral sphincter activity during spontaneous voiding in freely moving rats
 Page 1 of 60 Mary Ann Liebert, Inc. DOI: 10.1089/neu.2016.4844 1 Spinal transection alters external urethral sphincter activity during spontaneous voiding in freely moving rats Brandon K. LaPallo 1, Ph.D.,
Page 1 of 60 Mary Ann Liebert, Inc. DOI: 10.1089/neu.2016.4844 1 Spinal transection alters external urethral sphincter activity during spontaneous voiding in freely moving rats Brandon K. LaPallo 1, Ph.D.,
The Journal of Physiology Neuroscience
 J Physiol 590.19 (2012) pp 4945 4955 4945 The Journal of Physiology Neuroscience Inhibition of micturition reflex by activation of somatic afferents in posterior femoral cutaneous nerve Changfeng Tai 1,BingShen
J Physiol 590.19 (2012) pp 4945 4955 4945 The Journal of Physiology Neuroscience Inhibition of micturition reflex by activation of somatic afferents in posterior femoral cutaneous nerve Changfeng Tai 1,BingShen
The Journal of Physiology
 J Physiol 595.6 (27) pp 5687 5698 5687 Sensory feedback from the urethra evokes state-dependent lower urinary tract reflexes in rat Zachary C. Danziger and Warren M. Grill 2,3 Department of Biomedical
J Physiol 595.6 (27) pp 5687 5698 5687 Sensory feedback from the urethra evokes state-dependent lower urinary tract reflexes in rat Zachary C. Danziger and Warren M. Grill 2,3 Department of Biomedical
Spinal Cord Injury. R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH
 Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
ATLAS OF URODYNAMICS. Bladder. Pure. Pves. Pabd. Pdet EMG. Bladder. volume. Cough Strain IDC. Filling. Pure. Pves. Pabd. Pdet EMG
 2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
New Neurostimulation and Blockade Strategy to. Enhance Bladder Voiding in Paraplegics
 Contemporary Engineering Sciences, Vol. 3, 2010, no. 7, 321-337 New Neurostimulation and Blockade Strategy to Enhance Bladder Voiding in Paraplegics Fayçal Mounaïm 1, Ehab Elzayat 2, Mohamad Sawan 1, Jacques
Contemporary Engineering Sciences, Vol. 3, 2010, no. 7, 321-337 New Neurostimulation and Blockade Strategy to Enhance Bladder Voiding in Paraplegics Fayçal Mounaïm 1, Ehab Elzayat 2, Mohamad Sawan 1, Jacques
The lower urinary tract is composed of the bladder and the urethra the 2
 URINARY INCONTINENCE IN WOMEN Neurophysiology of Stress Urinary Incontinence Michael B. Chancellor, MD, Naoki Yoshimura, MD, PhD Department of Urology, University of Pittsburgh School of Medicine, Pittsburgh,
URINARY INCONTINENCE IN WOMEN Neurophysiology of Stress Urinary Incontinence Michael B. Chancellor, MD, Naoki Yoshimura, MD, PhD Department of Urology, University of Pittsburgh School of Medicine, Pittsburgh,
Urodynamics in Neurological Lower Urinary Tract Dysfunction. Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne
 Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Minimal invasive electrode implantation for conditional stimulation of the dorsal genital nerve in neurogenic detrusor overactivity
 (2011) 49, 566 572 & 2011 International Society All rights reserved 1362-4393/11 $32.00 www.nature.com/sc ORIGINAL ARTICLE Minimal invasive electrode implantation for conditional stimulation of the dorsal
(2011) 49, 566 572 & 2011 International Society All rights reserved 1362-4393/11 $32.00 www.nature.com/sc ORIGINAL ARTICLE Minimal invasive electrode implantation for conditional stimulation of the dorsal
Impact of Bioelectronic Medicine on the Neural Regulation of Pelvic Visceral Function
 Impact of Bioelectronic Medicine on the Neural Regulation of Pelvic Visceral Function William C de Groat 1 and Changfeng Tai 1,2 Departments of 1 Pharmacology and Chemical Biology and 2 Urology, University
Impact of Bioelectronic Medicine on the Neural Regulation of Pelvic Visceral Function William C de Groat 1 and Changfeng Tai 1,2 Departments of 1 Pharmacology and Chemical Biology and 2 Urology, University
TITLE: Use of GDNF-Releasing Nanofiber Nerve Guide Conduits for the Repair of Conus Medullaris/Cauda Equina Injury in the Non-Human Primate
 AD Award Number: W81XWH-10-1-0907 TITLE: Use of GDNF-Releasing Nanofiber Nerve Guide Conduits for the Repair of Conus Medullaris/Cauda Equina Injury in the Non-Human Primate PRINCIPAL INVESTIGATOR: Kari
AD Award Number: W81XWH-10-1-0907 TITLE: Use of GDNF-Releasing Nanofiber Nerve Guide Conduits for the Repair of Conus Medullaris/Cauda Equina Injury in the Non-Human Primate PRINCIPAL INVESTIGATOR: Kari
Multiple Pudendal Sensory Pathways Reflexly Modulate Bladder and Urethral Activity in Patients With Spinal Cord Injury
 Multiple Pudendal Sensory Pathways Reflexly Modulate Bladder and Urethral Activity in Patients With Spinal Cord Injury Paul B. Yoo,*, Eric E. Horvath, Cindy L. Amundsen, George D. Webster and Warren M.
Multiple Pudendal Sensory Pathways Reflexly Modulate Bladder and Urethral Activity in Patients With Spinal Cord Injury Paul B. Yoo,*, Eric E. Horvath, Cindy L. Amundsen, George D. Webster and Warren M.
Safety and Pain-relief Efficacy of Urethral Catheter with Local-anesthetic Injection Port
 Shinshu Med J, 65⑹:355~359, 2017 Safety and Pain-relief Efficacy of Urethral Catheter with Local-anesthetic Injection Port Teppei Yamamoto *, Masashi Shiozaki, Yuji Shimojima, Tomomi Haba Tomohiko Oguchi,
Shinshu Med J, 65⑹:355~359, 2017 Safety and Pain-relief Efficacy of Urethral Catheter with Local-anesthetic Injection Port Teppei Yamamoto *, Masashi Shiozaki, Yuji Shimojima, Tomomi Haba Tomohiko Oguchi,
Physiologic Anatomy and Nervous Connections of the Bladder
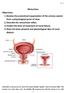 Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Chapter 23. Micturition and Renal Insufficiency
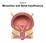 Chapter 23 Micturition and Renal Insufficiency Voiding Urine Between acts of urination, the bladder is filling. detrusor muscle relaxes urethral sphincters are tightly closed accomplished by sympathetic
Chapter 23 Micturition and Renal Insufficiency Voiding Urine Between acts of urination, the bladder is filling. detrusor muscle relaxes urethral sphincters are tightly closed accomplished by sympathetic
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests. Amelyn R.
 Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
University of Groningen. Neuronal control of micturition Kuipers, Rutger
 University of Groningen Neuronal control of micturition Kuipers, Rutger IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
University of Groningen Neuronal control of micturition Kuipers, Rutger IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
Mechanisms of Disease: central nervous system involvement in overactive bladder syndrome
 Mechanisms of Disease: central nervous system involvement in overactive bladder syndrome Karl-Erik Andersson SUMMARY The pathophysiology of overactive bladder syndrome (OABS) and detrusor overactivity
Mechanisms of Disease: central nervous system involvement in overactive bladder syndrome Karl-Erik Andersson SUMMARY The pathophysiology of overactive bladder syndrome (OABS) and detrusor overactivity
Objectives. Key Outlines:
 Objectives! Iden8fy and describe the Func8onal Anatomy of Urinary Bladder! Describe the mechanism of filling and emptying of the urinary bladder! Cystometrogram! Appreciate neurogenic control of the mechanism
Objectives! Iden8fy and describe the Func8onal Anatomy of Urinary Bladder! Describe the mechanism of filling and emptying of the urinary bladder! Cystometrogram! Appreciate neurogenic control of the mechanism
EE 791 Lecture 10. FES April 1, EE 791 Lecture 10 1
 EE 791 Lecture 10 FES April 1, 2013 EE 791 Lecture 10 1 Normal Functional Control EE 791 Lecture 10 2 Current uses of FES Cardiovascular Exercise Breathing assist Grasping and Reaching Transfer and Standing
EE 791 Lecture 10 FES April 1, 2013 EE 791 Lecture 10 1 Normal Functional Control EE 791 Lecture 10 2 Current uses of FES Cardiovascular Exercise Breathing assist Grasping and Reaching Transfer and Standing
Rewiring of hindlimb corticospinal neurons after spinal cord injury
 Rewiring of hindlimb corticospinal neurons after spinal cord injury Arko Ghosh, Florent Haiss, Esther Sydekum, Regula Schneider, Miriam Gullo, Matthias T. Wyss, Thomas Mueggler, Christof Baltes, Markus
Rewiring of hindlimb corticospinal neurons after spinal cord injury Arko Ghosh, Florent Haiss, Esther Sydekum, Regula Schneider, Miriam Gullo, Matthias T. Wyss, Thomas Mueggler, Christof Baltes, Markus
What is on the Horizon in Drug Therapy for OAB?
 What is on the Horizon in Drug Therapy for OAB? K-E Andersson, MD, PhD Wake Forest Institute for Regenerative Medicine Wake Forest University School of Medicine Winston Salem, North Carolina Disclosures
What is on the Horizon in Drug Therapy for OAB? K-E Andersson, MD, PhD Wake Forest Institute for Regenerative Medicine Wake Forest University School of Medicine Winston Salem, North Carolina Disclosures
Signal transduction underlying the control of urinary bladder smooth muscle tone Puspitoayu, E.
 UvA-DARE (Digital Academic Repository) Signal transduction underlying the control of urinary bladder smooth muscle tone Puspitoayu, E. Link to publication Citation for published version (APA): Puspitoayu,
UvA-DARE (Digital Academic Repository) Signal transduction underlying the control of urinary bladder smooth muscle tone Puspitoayu, E. Link to publication Citation for published version (APA): Puspitoayu,
Table of Contents: Chapter 1 The organization of the spinal cord Charles Watson and Gulgun Kayalioglu
 Table of Contents: Chapter 1 The organization of the spinal cord Charles Watson and Gulgun Kayalioglu The gross anatomy of the spinal cord Spinal cord segments Spinal nerves Spinal cord gray and white
Table of Contents: Chapter 1 The organization of the spinal cord Charles Watson and Gulgun Kayalioglu The gross anatomy of the spinal cord Spinal cord segments Spinal nerves Spinal cord gray and white
Effect of sacral nerve blocks on the function of the urinary bladder in humans
 Effect of sacral nerve blocks on the function of the urinary bladder in humans GAYLAN L. ROCKSWOLD, M.D., WILLIAM E. BRADLEY, M.D., AND SHELLEY N. CHOU, M.D. Departments of Neurosurgery and Neurology,
Effect of sacral nerve blocks on the function of the urinary bladder in humans GAYLAN L. ROCKSWOLD, M.D., WILLIAM E. BRADLEY, M.D., AND SHELLEY N. CHOU, M.D. Departments of Neurosurgery and Neurology,
Perineal Electrophysiologic Tests
 Perineal disorders and emg! Perineal Electrophysiologic Tests Voiding dysfunction Stress Urinary Incontinence urgency OAB Urge Incontinence nocturia Pr. Gerard Amarenco Mixed Incontinence frequency Service
Perineal disorders and emg! Perineal Electrophysiologic Tests Voiding dysfunction Stress Urinary Incontinence urgency OAB Urge Incontinence nocturia Pr. Gerard Amarenco Mixed Incontinence frequency Service
Feed-forward and feedback regulation of bladder contractility by Barrington s nucleus in cats
 J Physiol 557.1 (2004) pp 287 305 287 Feed-forward and feedback regulation of bladder contractility by Barrington s nucleus in cats Mitsuyoshi Sasaki Department of Physiology, Tokyo Medical University,
J Physiol 557.1 (2004) pp 287 305 287 Feed-forward and feedback regulation of bladder contractility by Barrington s nucleus in cats Mitsuyoshi Sasaki Department of Physiology, Tokyo Medical University,
NEUROMODULATION FOR UROGYNAECOLOGISTS
 NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
Neuropathic bladder and spinal dysraphism
 Archives of Disease in Childhood, 1981, 56, 176-180 Neuropathic bladder and spinal dysraphism MALGORZATA BORZYSKOWSKI AND B G R NEVILLE Evelina Children's Department, Guy's Hospital, London SUMMARY The
Archives of Disease in Childhood, 1981, 56, 176-180 Neuropathic bladder and spinal dysraphism MALGORZATA BORZYSKOWSKI AND B G R NEVILLE Evelina Children's Department, Guy's Hospital, London SUMMARY The
The Spinal Cord & Spinal Nerves
 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward and downward travel
The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward and downward travel
Neuropathic Bladder. Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014
 Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Re-evaluation of differential sacral rhizotomy for neurological bladder disease
 J Neurosurg 48:773-778, 1978 Re-evaluation of differential sacral rhizotomy for neurological bladder disease GAYLAN L. ROCKSWOLD, M.D., PH.D., SHELLEY N. CHOU, M.D., PH.D., AND WILLIAM E. BRADLEY, M.D.
J Neurosurg 48:773-778, 1978 Re-evaluation of differential sacral rhizotomy for neurological bladder disease GAYLAN L. ROCKSWOLD, M.D., PH.D., SHELLEY N. CHOU, M.D., PH.D., AND WILLIAM E. BRADLEY, M.D.
Development of mathematical model for lower urinary tract dysfunctions
 Development of mathematical model for lower urinary tract dysfunctions Mohanad A.Deaf 1, Mohamed A.A.Eldosoky 1, Ahmed M. El-Garhy 2, Hesham W.Gomma 2, Ahmed S.El-Azab 3 Dept. of Biomedical Engineering,
Development of mathematical model for lower urinary tract dysfunctions Mohanad A.Deaf 1, Mohamed A.A.Eldosoky 1, Ahmed M. El-Garhy 2, Hesham W.Gomma 2, Ahmed S.El-Azab 3 Dept. of Biomedical Engineering,
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
What is the role for neurophysiology in the evaluation of patients with uro-genito-anal dysfunction?
 London, 2016 What is the role for neurophysiology in the evaluation of patients with uro-genito-anal dysfunction? David B. Vodušek Medical Faculty, University of Ljubljana, Slovenia vodusek.david.b@gmail.com
London, 2016 What is the role for neurophysiology in the evaluation of patients with uro-genito-anal dysfunction? David B. Vodušek Medical Faculty, University of Ljubljana, Slovenia vodusek.david.b@gmail.com
Sacral neuromodulation (SNM), using permanent foramen S3 electrode, Early versus late treatment of voiding dysfunction with pelvic neuromodulation
 ORIGINAL RESEARCH Early versus late treatment of voiding dysfunction with pelvic neuromodulation Magdy M. Hassouna, MD, PhD; Mohamed S. Elkelini, MD See related article on page 111 Abstract Introduction:
ORIGINAL RESEARCH Early versus late treatment of voiding dysfunction with pelvic neuromodulation Magdy M. Hassouna, MD, PhD; Mohamed S. Elkelini, MD See related article on page 111 Abstract Introduction:
PREPARED FOR: U.S. Army Medical Research and Materiel Command Fort Detrick, Maryland
 Award Number: W81XWH-12-1-0445 TITLE: An investigation into the nature of non-voiding contractions resulting from detrusor hyperreflexia in neurogenic bladders following spinal cord injury PRINCIPAL INVESTIGATOR:
Award Number: W81XWH-12-1-0445 TITLE: An investigation into the nature of non-voiding contractions resulting from detrusor hyperreflexia in neurogenic bladders following spinal cord injury PRINCIPAL INVESTIGATOR:
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER
 SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER CHARLES C. HIGGINS, M.D. W. JAMES GARDNER, M.D. WM. A. NOSIK, M.D. The treatment of "cord bladder", a disturbance of bladder function from disease
SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER CHARLES C. HIGGINS, M.D. W. JAMES GARDNER, M.D. WM. A. NOSIK, M.D. The treatment of "cord bladder", a disturbance of bladder function from disease
INJ MATERIALS AND METHODS
 Official Journal of Korean Continence Society / Korean Society of Urological Research / The Korean Children s Continence and Enuresis Society / The Korean Association of Urogenital Tract Infection and
Official Journal of Korean Continence Society / Korean Society of Urological Research / The Korean Children s Continence and Enuresis Society / The Korean Association of Urogenital Tract Infection and
MITSUHARU YOSHIYAMA, JAMES R. ROPPOLO and WILLIAM C. de GROAT
 0022-3565/97/2802-0894$03.00/0 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 280, No. 2 Copyright 1997 by The American Society for Pharmacology and Experimental Therapeutics Printed in
0022-3565/97/2802-0894$03.00/0 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 280, No. 2 Copyright 1997 by The American Society for Pharmacology and Experimental Therapeutics Printed in
Neurophysiological modeling of voiding in rats: urethral nerve response to urethral pressure and flow
 Neurophysiological modeling of voiding in rats: urethral nerve response to urethral pressure and flow Joost Le Feber, Els Van Asselt and Ron Van Mastrigt Am J Physiol Regulatory Integrative Comp Physiol
Neurophysiological modeling of voiding in rats: urethral nerve response to urethral pressure and flow Joost Le Feber, Els Van Asselt and Ron Van Mastrigt Am J Physiol Regulatory Integrative Comp Physiol
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION
 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
We have heard a great deal about "overactive" bladder recently. But what
 BLADDER DYSFUNCTION Differential Diagnosis and Treatment of Impaired Bladder Emptying Naoki Yoshimura, MD, PhD, Michael B. Chancellor, MD Department of Urology, University of Pittsburgh School of Medicine,
BLADDER DYSFUNCTION Differential Diagnosis and Treatment of Impaired Bladder Emptying Naoki Yoshimura, MD, PhD, Michael B. Chancellor, MD Department of Urology, University of Pittsburgh School of Medicine,
A Novel Cystometric Model of Pelvic Floor Dysfunction After Rabbit Pelvic Floor Noxious Electrical Stimulation
 ORIGINAL ARTICLE A Novel Cystometric Model of Pelvic Floor Dysfunction After Rabbit Pelvic Floor Noxious Electrical Stimulation Amy D. Dobberfuhl, MD,* Sara Spettel, MD, Catherine Schuler, BA, Andrew H.
ORIGINAL ARTICLE A Novel Cystometric Model of Pelvic Floor Dysfunction After Rabbit Pelvic Floor Noxious Electrical Stimulation Amy D. Dobberfuhl, MD,* Sara Spettel, MD, Catherine Schuler, BA, Andrew H.
Storage is accomplished through the following mechanisms:
 NROSCI/BIOSC 1070 and MSNBIO 2070 September 13, 2017 Examples of Coordinated Autonomic and Motor Responses and Return to the Cardiovascular System 1) Micturition Micturition, or the process of emptying
NROSCI/BIOSC 1070 and MSNBIO 2070 September 13, 2017 Examples of Coordinated Autonomic and Motor Responses and Return to the Cardiovascular System 1) Micturition Micturition, or the process of emptying
Definitions of IC: U.S. perspective. Edward Stanford MD MS FACOG FACS Western Colorado
 Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Department of Medical Education, Saint Paul s Hospital, Taoyuan, Taiwan
 Am J Physiol Renal Physiol 292: F1791 F1801, 2007. First published February 6, 2007; doi:10.1152/ajprenal.00443.2006. Spinal glutamatergic NMDA-dependent pelvic nerve-to-external urethra sphincter reflex
Am J Physiol Renal Physiol 292: F1791 F1801, 2007. First published February 6, 2007; doi:10.1152/ajprenal.00443.2006. Spinal glutamatergic NMDA-dependent pelvic nerve-to-external urethra sphincter reflex
Practical urodynamics What PA s need to know. Gary E. Lemack, MD Professor of Urology and Neurology
 Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
POSTOPERATIVE URINARY RETENTION IN ABDOMINAL SURGERY. Marta Alves Servicio de Urología
 POSTOPERATIVE URINARY RETENTION IN ABDOMINAL SURGERY Marta Alves Servicio de Urología Introduction Incidence Mechanism of micturition Risk factors Prevention Diagnosis Complications/Adverse effects associated
POSTOPERATIVE URINARY RETENTION IN ABDOMINAL SURGERY Marta Alves Servicio de Urología Introduction Incidence Mechanism of micturition Risk factors Prevention Diagnosis Complications/Adverse effects associated
Neuromodulation and the pudendal nerve
 Neuromodulation and the pudendal nerve Stefan De Wachter, MD, PhD, FEBU Professor of Urology University of Antwerpen, Belgium Chairman dept of Urology, UZA Disclosures Consultant speaker: Astellas, Medtronic,
Neuromodulation and the pudendal nerve Stefan De Wachter, MD, PhD, FEBU Professor of Urology University of Antwerpen, Belgium Chairman dept of Urology, UZA Disclosures Consultant speaker: Astellas, Medtronic,
Recommandations de prise en charge des vessies neurogènes EAU 2006
 Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
The central control of micturition and continence: implications for urology
 BJU International (1999), 83, Suppl. 2, 1 6 The central control of micturition and continence: implications for urology B.F.M. BLOK and G. HOLSTEGE Department of Anatomy and Embryology, Faculty of Medical
BJU International (1999), 83, Suppl. 2, 1 6 The central control of micturition and continence: implications for urology B.F.M. BLOK and G. HOLSTEGE Department of Anatomy and Embryology, Faculty of Medical
Human Anatomy. Spinal Cord and Spinal Nerves
 Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN
 Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Spinal Cord Protection. Chapter 13 The Spinal Cord & Spinal Nerves. External Anatomy of Spinal Cord. Structures Covering the Spinal Cord
 Spinal Cord Protection Chapter 13 The Spinal Cord & Spinal Nerves We are only going to cover Pages 420-434 and 447 Together with brain forms the CNS Functions spinal cord reflexes integration (summation
Spinal Cord Protection Chapter 13 The Spinal Cord & Spinal Nerves We are only going to cover Pages 420-434 and 447 Together with brain forms the CNS Functions spinal cord reflexes integration (summation
Oral Nitric Oxide Donors: A New Pharmacological Approach to Detrusor-Sphincter Dyssynergia in Spinal Cord Injured Patients?
 European Urology European Urology 45 (24) 516 52 Oral Nitric Oxide Donors: A New Pharmacological Approach to Detrusor-Sphincter Dyssynergia in Spinal Cord Injured Patients? André Reitz a,*, Peter A. Knapp
European Urology European Urology 45 (24) 516 52 Oral Nitric Oxide Donors: A New Pharmacological Approach to Detrusor-Sphincter Dyssynergia in Spinal Cord Injured Patients? André Reitz a,*, Peter A. Knapp
Japan. J. Pharmacol. 50, (1989) 327. Effects of Central Nervous System-Acting Drugs on Urinary Bladder Contraction in Unanesthetized Rats
 Japan. J. Pharmacol. 50, 327-332 (1989) 327 Effects of Central Nervous System-Acting Drugs on Urinary Bladder Contraction in Unanesthetized Rats Hitoshi KONTANI, Mikiko NAKAGAWA and Takeshi SAKAI Department
Japan. J. Pharmacol. 50, 327-332 (1989) 327 Effects of Central Nervous System-Acting Drugs on Urinary Bladder Contraction in Unanesthetized Rats Hitoshi KONTANI, Mikiko NAKAGAWA and Takeshi SAKAI Department
Comparison of neural targets for neuromodulation of bladder micturition reflex in the rat
 m J Physiol Renal Physiol 33: F119 F12, 212. First published ugust 8, 212; doi:.12/ajprenal.343.212. omparison of neural targets for neuromodulation of bladder micturition reflex in the rat Xin Su ( ),
m J Physiol Renal Physiol 33: F119 F12, 212. First published ugust 8, 212; doi:.12/ajprenal.343.212. omparison of neural targets for neuromodulation of bladder micturition reflex in the rat Xin Su ( ),
Annual Scientific Update in Urogynaecology- Joint RCOG/BSUG Meeting Neurogenic bladder dysfunction
 Annual Scientific Update in Urogynaecology- Joint RCOG/BSUG Meeting Neurogenic bladder dysfunction Clare J.Fowler National Hospital for Neurology and Neurosurgery & Institute of Neurology, UCL Aims Background
Annual Scientific Update in Urogynaecology- Joint RCOG/BSUG Meeting Neurogenic bladder dysfunction Clare J.Fowler National Hospital for Neurology and Neurosurgery & Institute of Neurology, UCL Aims Background
Aalborg Universitet. Published in: Journal of Urology. DOI (link to publication from Publisher): /01.ju b
 Aalborg Universitet Treatment of neurogenic detrusor overactivity in spinal cord injured patients by conditional electrical stimulation Hansen, John; Media, S.; Nøhr, M.; Biering-Sørensen, F.; Sinkjær,
Aalborg Universitet Treatment of neurogenic detrusor overactivity in spinal cord injured patients by conditional electrical stimulation Hansen, John; Media, S.; Nøhr, M.; Biering-Sørensen, F.; Sinkjær,
Facilitation of reflex swallowing from the pharynx and larynx
 167 Journal of Oral Science, Vol. 51, No. 2, 167-171, 2009 Original Facilitation of reflex swallowing from the pharynx and larynx Junichi Kitagawa 1,5), Kazuharu Nakagawa 2), Momoko Hasegawa 3), Tomoyo
167 Journal of Oral Science, Vol. 51, No. 2, 167-171, 2009 Original Facilitation of reflex swallowing from the pharynx and larynx Junichi Kitagawa 1,5), Kazuharu Nakagawa 2), Momoko Hasegawa 3), Tomoyo
nerve blocks in the diagnosis and therapy of visceral disease
 Visceral Pain nerve blocks in the diagnosis and therapy of visceral disease Guy Hans, MD, PhD Dept. of Anesthesiology, Multidisciplinary Pain Center Visceral Pain? Type of nociceptive pain (although often
Visceral Pain nerve blocks in the diagnosis and therapy of visceral disease Guy Hans, MD, PhD Dept. of Anesthesiology, Multidisciplinary Pain Center Visceral Pain? Type of nociceptive pain (although often
URINARY TRACT NERVOUS SYSTEM DISORDERS: DRUG THERAPY REVIEW
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk URINARY TRACT NERVOUS SYSTEM DISORDERS: DRUG THERAPY REVIEW Author : Ian Battersby Categories : Vets Date : August 3, 2009
Vet Times The website for the veterinary profession https://www.vettimes.co.uk URINARY TRACT NERVOUS SYSTEM DISORDERS: DRUG THERAPY REVIEW Author : Ian Battersby Categories : Vets Date : August 3, 2009
OHTAC Recommendation
 OHTAC Recommendation Sacral Nerve Stimulation for the Management of Urge Incontinence, Urgency-Frequency, Urinary Retention and Fecal Incontinence March 2, 2005 1 The Ontario Health Technology Advisory
OHTAC Recommendation Sacral Nerve Stimulation for the Management of Urge Incontinence, Urgency-Frequency, Urinary Retention and Fecal Incontinence March 2, 2005 1 The Ontario Health Technology Advisory
Urethral closure mechanisms during sneezing-induced stress in anesthetized female cats
 Am J Physiol Regul Integr Comp Physiol 293: R1357 R1367, 2007. First published July 11, 2007; doi:10.1152/ajpregu.00003.2007. Urethral closure mechanisms during sneezing-induced stress in anesthetized
Am J Physiol Regul Integr Comp Physiol 293: R1357 R1367, 2007. First published July 11, 2007; doi:10.1152/ajpregu.00003.2007. Urethral closure mechanisms during sneezing-induced stress in anesthetized
APPLICATION OF HIGH FREQUENCY ELECTRICAL BLOCK ON THE EFFERENT NERVES TO THE LOWER URINARY TRACT FOR BLADDER VOIDING.
 i APPLICATION OF HIGH FREQUENCY ELECTRICAL BLOCK ON THE EFFERENT NERVES TO THE LOWER URINARY TRACT FOR BLADDER VOIDING By Adam Sprott Boger Submitted in partial fulfillment of the requirements for the
i APPLICATION OF HIGH FREQUENCY ELECTRICAL BLOCK ON THE EFFERENT NERVES TO THE LOWER URINARY TRACT FOR BLADDER VOIDING By Adam Sprott Boger Submitted in partial fulfillment of the requirements for the
Bladder Management. A guide for patients. Key points
 Bladder Management A guide for patients Key points Urinary issues remain one of the highest causes of readmission to hospital following Spinal Cord Injury (SCI). Following SCI most patients experience
Bladder Management A guide for patients Key points Urinary issues remain one of the highest causes of readmission to hospital following Spinal Cord Injury (SCI). Following SCI most patients experience
How to manage a patient with bladder dysfunction
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Teaching Course 13 How to manage a patient with autonomic dysfunction - Level 2 How to manage a patient with
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Teaching Course 13 How to manage a patient with autonomic dysfunction - Level 2 How to manage a patient with
Role of Spinal Glutamatergic Transmission in the Ascending Limb of the Micturition Reflex Pathway in the Rat 1
 0022-3565/98/2851-0022$03.00/0 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 285, No. 1 Copyright 1998 by The American Society for Pharmacology and Experimental Therapeutics Printed in
0022-3565/98/2851-0022$03.00/0 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 285, No. 1 Copyright 1998 by The American Society for Pharmacology and Experimental Therapeutics Printed in
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
