Management of postoperative infections after the minimally invasive pectus excavatum repair
|
|
|
- Silas Lucas
- 6 years ago
- Views:
Transcription
1 Journal of Pediatric Surgery (2005) 40, Management of postoperative infections after the minimally invasive pectus excavatum repair Casey M. Calkins, Stephen B. Shew, Ronald J. Sharp, Daniel J. Ostlie, Suzanne M. Yoder, George K. Gittes, Charles L. Snyder, Wendy Guevel, George W. Holcomb III* The Children s Mercy Hospital, University of Missouri at Kansas City School of Medicine, Kansas City, MO 66408, USA Index words: Minimally invasive pectus excavatum repair; Nuss procedure; Postoperative infection Abstract Purpose: Pectus excavatum is frequently repaired using the minimally invasive placement of a substernal bar (Nuss procedure). Infectious complications after the Nuss procedure are potentially devastating. To date, the management of postoperative infectious complications has not been well described. Methods: A retrospective review of all patients (N = 168) who underwent the Nuss procedure from January 1, 1997, to October 1, 2003, at our institution was performed. Six patients (4%) had postoperative infections, and their medical records were reviewed. Results: Of the 6 patients, 5 underwent operative drainage for wound abscesses that developed 2 to 76 weeks postoperatively. The other patient developed cellulitis 12 months postoperatively and was treated effectively with antibiotics alone. Recurrent infections were treated in 3 of 6 patients, one of whom eventually required removal of the bar resulting in a mild, residual pectus excavatum defect. One of 6 patients has had the substernal bar removed electively. The remaining 4 continue to be without clinically apparent infection at this time and are over 1 year removed from their infection. Conclusions: Although uncommon, infectious complications after the Nuss procedure require complex management strategies. Despite recurrent infection in some cases, most infectious complications occurring after the minimally invasive repair can be effectively treated without having to remove the substernal bar. D 2005 Elsevier Inc. All rights reserved. Pectus excavatum is the most common chest wall deformity in children. Since the initial description by Ravitch [1], repair of pectus excavatum has traditionally Presented at the 56th Annual Meeting of the Section on Surgery of the American Academy of Pediatrics, San Francisco, California, October 8-10, T Corresponding author. Department of Surgery, The Children s Mercy Hospital, University of Missouri at Kansas City School of Medicine, Kansas City, MO 66408, USA. Tel.: ; fax: address: gholcomb@cmh.edu (G.W. Holcomb). involved subperichondrial resection of abnormal costal cartilages with anterior displacement of the sternum to a normal position. In 1998, Nuss et al [2] reported an alternative, minimally invasive technique for repair of this anomaly. The initial description of the repair used 2 small incisions in the lateral chest wall for placement of an appropriately shaped convex metal bar that is secured inside the anterior hemicircumference of the chest. The technique has rapidly gained acceptance and is our preferred approach for the repair of pectus excavatum in children and adolescents. As with implantation of any prosthesis, /$ see front matter D 2005 Elsevier Inc. All rights reserved. doi: /j.jpedsurg
2 Management of postoperative infections after the minimally invasive pectus excavatum repair 1005 infectious complications often mandate removal of the hardware. Unfortunately, premature removal of the pectus bar may lead to recurrence of the defect. To date, no consensus exists with regard to the optimal management of infectious complications that occur after the minimally invasive placement of the pectus bar. With one of the larger single-center experiences to date, we conducted this clinical review to evaluate the incidence of pectus bar infection and explore management strategies to prevent pectus bar infection and avoid bar removal should infection occur. convex stainless steel bar (Walter Lorenz Co, Jackson, FL). The bar is bent to conform to the patient s anterior chest wall. Lateral stabilizer bars have been used routinely since September Also, since the autumn of 1999, the routine modification of a vertical subxiphoid anterior chest wall incision has been added to our repair technique. This modification involves the creation of a small subxiphoid pocket to ensure safe passage of the bar across the mediastinum. Two to 3 years after their initial MIPR procedure, patients are scheduled for removal of the bar. 1. Methods After obtaining institutional review board (IRB) approval (IRB Exempt # X), the charts of all patients who underwent the minimally invasive pectus repair (MIPR) at Children s Mercy Hospital between January 1, 1997, and October 1, 2003, (N = 168) were reviewed retrospectively. Six patients had postoperative infections and their medical records were extensively reviewed. The management of each infection was investigated, including whether or not the bar was removed to clear the infection. Patient selection for corrective repair is based on history, physical examination, and computed tomography. The deformity classification is based on assessment of computed tomography with a ratio of transverse diameter to anteroposterior diameter (distance between posterior sternum and anterior vertebral body) greater than 3.25 defining a severe deformity. The minimally invasive repair requires small (2 cm), bilateral, midaxillary transverse incisions, subcutaneous tunneling, and intrathoracic placement of a substernal 2. Results Of the 168 patients repaired during the study period, all successfully underwent MIPR. Six of the study cohort developed a postoperative infectious complication (4%). One (16%) of the 6 patients required premature removal of the substernal bar. The 6 patients and their respective outcomes are summarized in Table 1. All patients received perioperative antibiotics. Of the 6 patients, 5 developed wound abscesses that came to medical attention anywhere from 2 weeks to 19 months postoperatively. The sixth patient developed cellulitis 12 months postoperatively and was treated effectively with antibiotics alone. When obtained, positive cultures grew methicillinsensitive Staphylococcus species (aureus or epidermidis). Two of 6 patients demonstrated no evidence of nickel allergy by skin testing. Recurrent infections were treated in 3 of these 6 patients, one of which required removal of the substernal bar 1 year after the initial placement resulting in a mild, residual pectus excavatum defect. One of these 6 patients has Table 1 Summary of patients sustaining infectious complications after minimally invasive placement of pectus bar Patient age (y)/sex No. of bars placed Complication Postoperative duration to infection Treatment Outcome 14/female 1 Unilateral abscess 2 wk I&D, removal single stabilizer, IV antibiotics, postoperative antibiotic suppression 5/male 1 Unilateral abscess 18 mo I&D, removal single stabilizer, 10/male 1 Bilateral abscesses (metanchrynous) IV antibiotics 3 wk/3 mo I&D, removal bilateral stabilizer, IV antibiotics, postoperative antibiotic suppression 13/male 1 Unilateral abscess 3.5 mo I&D, wound care, IV antibiotics, postoperative antibiotic suppression 14/male 2 Bilateral abscesses 4 mo I&D, wound care, IV antibiotics, (synchronous) postoperative antibiotic suppression, removed electively Bar 1 removed 9 mo postoperatively, bar 2 removed 12 mo postoperatively 16/male 1 Unilateral cellulitis 12 mo IV antibiotics Demographics and outcomes of 6 patients who developed postoperative infection after the minimally invasive placement of a substernal bar for pectus excavatum. I&D indicates incision and drainage.
3 1006 had the substernal bar removed electively 2 years after initial placement (there was no evidence of infection present). The remaining 4 patients demonstrate no clinically apparent infection at this time. All of these 4 patients are now over 1 year removed from their infection. Patients who developed wound abscesses were admitted to the hospital. The abscess was drained and intravenous (IV) antibiotics were begun. The lateral chest wall stabilizer was removed in cases where the infection occurred within the subcutaneous pocket. The soft tissue was reapproximated over the retained bar, but the skin was left open and treated with sulfamyalon solution wet-to-dry dressing changes. No infections occurred underlying the subxiphoid incision. Initial choice of antibiotics varied; yet, either cefazolin, vancomycin, or ceftriaxone was chosen. Once the IV course was tailored to the cultured organism and completed (3 weeks to 3 months), oral antibiotic regimens were instituted and consisted of either cefadroxil or rifampin/clindamycin. Other than the individual who had isolated cellulitis and was treated successfully with 3-week IV antibiotic course, all patients received prolonged oral bsuppressive antibioticsq for 6 to 12 months in an attempt to prevent recurrent infection. The single failure of this regimen occurred in a patient who had 2 bars placed at the time of surgery for a severe pectus excavatum defect. Abscesses developed overlying both stabilizers 4 months after the placement of the bars. Local wound care and IV and oral antibiotic regimens were initially successful, but chronic wound drainage ultimately necessitated removal of the inferior bar 9 months postoperatively. The second superior bar was removed 3 months later for persistent wound drainage. 3. Discussion Since its introduction, the minimally invasive repair of pectus excavatum has become popular with patients because of perceived improved cosmetic results from a less invasive procedure and with surgeons because of reduced operating time. A 3-fold increase in patient presentation for pectus excavatum repair has been appreciated at our institution since the introduction of this new approach. The long-term outcomes and complications of this technique, however, are still being realized. In this large retrospective review, we have scrutinized our management of postoperative infectious complications. Our infection rate compares favorably with that described in other large series in which infectious complications occur in anywhere from 2% to 5% of cases [3,4]. In a review of 329 cases of the minimally invasive repair reported by Nuss et al [5], wound infection occurred in 2.6% resulting in bar infection in 3 of the 7 patients. Long-term antibiotics were successful in curing the infection in 1 patient, whereas the other 2 required bar removal at 12 and 18 months [5]. Herein, we have described 6 patients who developed an infectious complication after minimally invasive placement C.M. Calkins et al. of a substernal bar. Five of 6 developed an abscess that was treated by drainage and long-term antibiotics. Intravenous antibiotics are initially begun using a first-generation cephalosporin or vancomycin at a weight appropriate dose. These should be continued for at least 14 days and discontinued when clinical signs of infection have abated. Based on our experience, we recommend oral suppressive antibiotic therapy in patients who have been successfully treated with wound drainage and IV antibiotic therapy. The optimal duration of suppressive therapy remains unclear, yet we have maintained the last 2 individuals on oral rifampin (300 mg bid) indefinitely (until bar removal). Since the last infectious complication (August 2002), we have used additional measures in an attempt to reduce the incidence of wound infection. First, the operating surgeon and assistant use a double-gloving technique with Biogel indicator undergloves (Regent, Norcross, Ga) preceded by a strict 5-minute surgical scrub. Second, the chest is elevated off the operative table with a midline roll placed underlying the thoracic spine. Furthermore, sterile towels along the chest wall are secured with skin staples such that the sterile field is not violated when flipping the bar into position. Next, an iodine impregnated drape is placed before the start of the procedure. Before a 3-layer closure, the wounds are irrigated with antibiotic solution. Finally, perioperative antibiotics (IV cefazolin) are continued for 72 hours after the procedure. Since using these techniques, the sole infectious complication occurred in a patient who developed an abscess within a hematoma which occurred along the anterior portion of the bar after he was struck in this region by a baseball some 3 months after the procedure. In this case, the wound was opened along the right anterior chest wall overlying the subcutaneous portion of the bar lateral to the sternum. The abscess cavity was drained and local wound care used. Despite the exposed bar, the wound contracted over time and is now completely closed. We routinely use placement of lateral stabilizer bars to prevent rotational or lateral displacement of the retrosternal bar. Since we instituted this practice, we have not needed to reoperate prematurely for bar slippage [6]. Therefore, we believe that the routine use of stabilizer bars is important. Recently, Watanabe et al [7] have suggested that the use of lateral stabilizers increases the incidence of wound complications. In our cohort of patients, all patients who developed wound complications did so after placement of bilateral stabilizers. We removed the stabilizer when an abscess cavity was present overlying the hardware, yet left the bar in place and treated the wound locally and continued IV antibiotic therapy in an attempt to salvage the bar. This strategy was successful in retaining the bar in all 3 patients in whom it was used. We argue that the small risk of wound infection is outweighed by the risk of bar migration or slippage [3]. Patients who develop erythema along the substernal bar are typically treated for cellulitis, yet hypersensitivity and nickel allergy may present in a similar manner. Saitoh et al
4 Management of postoperative infections after the minimally invasive pectus excavatum repair 1007 [8] have reported nickel allergy to the substernal bar; and this entity should be considered in patients who do not respond appropriately to antibiotic therapy or have persistent erythema in the skin overlying the bar without clinical evidence of infection. We recommend a 5-minute surgical scrub, double gloving, modification of positioning and prep to ensure a sterile field, and perioperative antibiotics in an attempt to prevent infection from occurring. When a patient presents with signs and symptoms of a bar infection (fever, increasing pain along the bar, erythema along the bar, and drainage from one or more of the incision sites), hospital admission is recommended. If fluid overlying the bar or the stabilizers is suggested by physical exam findings, this is assessed by ultrasonography and drained percutaneously. Fluid is sent for Gram stain and culture, and the patient is started on parenteral antibiotics (cefazolin and clindamycin). Parenteral antibiotic therapy is then tailored to the cultured organism. Thereafter, treatment is guided based on the initial response to therapy. If clinical improvement is noted, we recommend placement of a peripherally inserted central venous catheter where the appropriate antibiotics can be administered at home. We have continued parenteral therapy in favorable cases for 3 to 6 weeks, after which oral antibiotics are continued for a prolonged duration. If the site overlying the bar breaks down or continued drainage is noted from a lateral incision, we recommend incision and drainage of the affected area. Local wound care with moist-to-dry dressing changes and administration of parenteral antibiotics continues until the wound has closed. If such therapy is unsuccessful (continued clinical deterioration or wound drainage), bar removal is unavoidable. References [1] Ravitch M. The operative treatment of pectus excavatum. Ann Surg 1949;129: [2] Nuss D, Kelly Jr RE, Croitoru DP, et al. 10-year review of a minimally invasive technique for the correction of pectus excavatum. J Pediatr Surg 1998;33: [3] Hebra A, Swoveland B, Egbert M, et al. Outcome analysis of minimally invasive repair of pectus excavatum: review of 251 cases. J Pediatr Surg 2000;35:252-7 [discussion ]. [4] Hosie S, Sitkiewicz T, Petersen C, et al. Minimally invasive repair of pectus excavatum the Nuss procedure. A European multicentre experience. Eur J Pediatr Surg 2002;12: [5] Nuss D, Croitoru DP, Kelly Jr RE, et al. Review and discussion of the complications of minimally invasive pectus excavatum repair. Eur J Pediatr Surg 2002;12: [6] Miller KA, Woods RK, Sharp RJ, et al. Minimally invasive repair of pectus excavatum: a single institution s experience. Surgery 2001;130: [discussion ]. [7] Watanabe A, Watanabe T, Obama T, et al. The use of a lateral stabilizer increases the incidence of wound trouble following the Nuss procedure. Ann Thorac Surg 2004;77: [8] Saitoh C, Yamada A, Kosaka K, et al. Allergy to pectus bar for funnel chest. Plast Reconstr Surg 2002;110: Discussion Darrell Cass, MD (Houston, TX): Is there something about the stabilizers that may predispose to infection? Were the stabilizers attached with a wire, and was the wire your source of irritation? Casey M. Calkins, MD (Kansas City, MO): That s a good question, there s been a recent report by Dr Watanabe in the JPS about whether or not the lateral stabilizers predispose to infectious complications. We put stabilizers in on both sides and secure them with an Ethibond suture. We have done so because in our early experience with technique we had a lot of problems with the bar rotation. I think the most important thing for these preventative strategies is to try to attempt to salvage or prevent infection because, since employing them, we haven t had an infectious related complication. Richard R. Ricketts, MD, FAAP (Atlanta, GA): Can you give us a little more detail about your antibiotic protocol, how long are they on IV antibiotics, how long in the hospital, how long on po antibiotics, and which ones you use? Casey M. Calkins, MD (Kansas City, MO): All the patients were initially managed with intravenous antibiotics consisting of either cefazolin or ceftriaxone. In the patients that had culture material obtained at the time of incision and drainage, all of the organisms cultured were methicillin-sensitive Staphylococcus aureus. In our institution, ceftriaxone is an adequate agent to treat that infection. So in all of these cases patients were hospitalized for either 4 to 7 days, discharged home with a PICC line in place and antibiotics continued parenterally for anywhere from 14 to 21 days. Then, oral antibiotics were continued and our current strategy is to use rifampin and that s at the behest of our infectious disease colleagues who have suggested continuing that for at least 12 months to prevent bar removal. Daniel Robie, MD, FAAP (Honolulu, HI): I think we really do need to emphasize the catastrophic nature of this complication. I have had some of these myself, not too many I hope, but I have had to remove the bars in two patients and that s very catastrophic for these patients. And so I actually talked to Dr Moriarty a couple of years ago about this very thing and I ve instituted these recommendations especially the Ioban and the adherence to strict sterile technique. Because, if these do get infected, we must assume that contamination s occurring at the operation. So there are two principles: one adopted from our orthopedic colleagues, which is absolute strict sterile technique, and then the other one is good wound closure. This can be difficult to do since all you have is the skin and subcutaneous tissues to close over these bars. Casey M. Calkins, MD (Kansas City, MO): You are absolutely correct, and we attempt to close the lateral
5 1008 wounds in two layers but to get more than two layers is difficult. Daniel Robie, MD, FAAP (Honolulu, HI): Can you comment on why you remove stabilizers but leave the bar? Casey M. Calkins, MD (Kansas City, MO): That s a good question. In the patients that had the stabilizer removed, there was a persistent area of seroma and/or purulent C.M. Calkins et al. material that we felt would be most adequately treated with removal of the stabilizer itself. We managed to salvage the bar in all of those patients but that certainly was a possibility of having to remove it should continued drainage occur and that s what happened in the one patient that wasn t treated successfully with this strategy. The stabilizers were initially removed and thereafter the bar had to be removed when that therapy was not successful.
Current Management of Pectus Deformities. George W. Holcomb, III, M.D., MBA Surgeon-in-Chief Children s Mercy Hospital Kansas City, Missouri
 Current Management of Pectus Deformities George W. Holcomb, III, M.D., MBA Surgeon-in-Chief Children s Mercy Hospital Kansas City, Missouri Pectus Deformities Pectus Excavatum Pectus Carinatum Mixed Excavatum/Carinatum
Current Management of Pectus Deformities George W. Holcomb, III, M.D., MBA Surgeon-in-Chief Children s Mercy Hospital Kansas City, Missouri Pectus Deformities Pectus Excavatum Pectus Carinatum Mixed Excavatum/Carinatum
Nuss procedure for repair of pectus excavatum after failed Ravitch procedure in adults: indications and caveats
 Original Article Nuss procedure for repair of pectus excavatum after failed Ravitch procedure in adults: indications and caveats Gregor J. Kocher 1, Nathalie Gstrein 1, Dawn E. Jaroszewski 2, Mennatallah
Original Article Nuss procedure for repair of pectus excavatum after failed Ravitch procedure in adults: indications and caveats Gregor J. Kocher 1, Nathalie Gstrein 1, Dawn E. Jaroszewski 2, Mennatallah
Short Nuss bar procedure
 Art of Operative Techniques Short Nuss bar procedure Hans Kristian Pilegaard 1,2 1 Department of Cardiothoracic and Vascular Surgery, Aarhus University Hospital, Skejby, Aarhus, Denmark; 2 Department of
Art of Operative Techniques Short Nuss bar procedure Hans Kristian Pilegaard 1,2 1 Department of Cardiothoracic and Vascular Surgery, Aarhus University Hospital, Skejby, Aarhus, Denmark; 2 Department of
The Comparison Of Measurements On Chest X-Ray For Patients With Pectus Deformity. S Gurkok, O Genc, M Dakak, A Gozubuyuk, R Gorur, K Balkanli
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 5 Number 2 The Comparison Of Measurements On Chest X-Ray For Patients With Pectus Deformity S Gurkok, O Genc, M Dakak, A Gozubuyuk,
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 5 Number 2 The Comparison Of Measurements On Chest X-Ray For Patients With Pectus Deformity S Gurkok, O Genc, M Dakak, A Gozubuyuk,
Pectus excavatum is a chest wall deformity characterized
 Minimally Invasive Repair for Pectus Excavatum in Adults Swee H. Teh, MD, Angela M. Hanna, MD, Tuan H. Pham, MD, PhD, Adriana Lee, MD, Claude Deschamps, MD, Penny Stavlo, RN, and Christopher Moir, MD Divisions
Minimally Invasive Repair for Pectus Excavatum in Adults Swee H. Teh, MD, Angela M. Hanna, MD, Tuan H. Pham, MD, PhD, Adriana Lee, MD, Claude Deschamps, MD, Penny Stavlo, RN, and Christopher Moir, MD Divisions
Pectus excavatum (PE) is one of the most common
 Analysis of the Nuss Procedure for Pectus Excavatum in Different Age Groups Do Hyung Kim, MD, Jung Joo Hwang, MD, Mi Kyeong Lee, RN, Doo Yun Lee, MD, and Hyo Chae Paik, MD Department of Thoracic and Cardiovascular
Analysis of the Nuss Procedure for Pectus Excavatum in Different Age Groups Do Hyung Kim, MD, Jung Joo Hwang, MD, Mi Kyeong Lee, RN, Doo Yun Lee, MD, and Hyo Chae Paik, MD Department of Thoracic and Cardiovascular
Moderators: Malgorzata Lutwin-Kawalec, MD, Dinesh K Choudhry, MD, FRCA. Institution: Nemours/AI DuPont Hospital for Children, Wilmington, DE
 PBLD Table # 17 A teenager with Factor V Leiden and pectus excavatum for a Nuss procedure: navigating recommendations for testing, perioperative risk of thrombosis and post-operative pain management. Moderators:
PBLD Table # 17 A teenager with Factor V Leiden and pectus excavatum for a Nuss procedure: navigating recommendations for testing, perioperative risk of thrombosis and post-operative pain management. Moderators:
Single centre experience on short bar technique for pectus excavatum
 Featured Article Single centre experience on short bar technique for pectus excavatum Hans Kristian Pilegaard 1,2 1 Department of Cardiothoracic and Vascular Surgery, Aarhus University Hospital, Aarhus,
Featured Article Single centre experience on short bar technique for pectus excavatum Hans Kristian Pilegaard 1,2 1 Department of Cardiothoracic and Vascular Surgery, Aarhus University Hospital, Aarhus,
Initial results with minimally invasive repair of pectus carinatum
 Initial results with minimally invasive repair of pectus carinatum Attila, MD Objective: Pectus carinatum is traditionally repaired by using some modification of the open Ravitch procedure, with its possible
Initial results with minimally invasive repair of pectus carinatum Attila, MD Objective: Pectus carinatum is traditionally repaired by using some modification of the open Ravitch procedure, with its possible
Optoelectronic plethysmography demonstrates abrogation of regional chest wall motion dysfunction in patients with pectus excavatum after Nuss repair
 Journal of Pediatric Surgery (2012) 47, 160 164 www.elsevier.com/locate/jpedsurg Optoelectronic plethysmography demonstrates abrogation of regional chest wall motion dysfunction in patients with pectus
Journal of Pediatric Surgery (2012) 47, 160 164 www.elsevier.com/locate/jpedsurg Optoelectronic plethysmography demonstrates abrogation of regional chest wall motion dysfunction in patients with pectus
Minimally Invasive Repair of Pectus Carinatum in Patients Unsuited to Bracing Therapy
 Korean J Thorac Cardiovasc Surg 2016;49:92-98 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) Minimally Invasive Repair of Pectus Carinatum in Patients Unsuited to Bracing Therapy Clinical Research http://dx.doi.org/10.5090/kjtcs.2016.49.2.92
Korean J Thorac Cardiovasc Surg 2016;49:92-98 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) Minimally Invasive Repair of Pectus Carinatum in Patients Unsuited to Bracing Therapy Clinical Research http://dx.doi.org/10.5090/kjtcs.2016.49.2.92
P chondrosternal depression), the most common congenital
 Pectus Excavaturn Repair Claude Deschamps, MD ectus excavatum (also known as funnel chest or P chondrosternal depression), the most common congenital chest wall deformity, involves depression or inward
Pectus Excavaturn Repair Claude Deschamps, MD ectus excavatum (also known as funnel chest or P chondrosternal depression), the most common congenital chest wall deformity, involves depression or inward
Center for Prospective Clinical Trials, The Children's Mercy Hospital, Kansas City, MO
 Journal of Pediatric Surgery (2010) 45, 236 240 www.elsevier.com/locate/jpedsurg Initial laparoscopic appendectomy versus initial nonoperative management and interval appendectomy for perforated appendicitis
Journal of Pediatric Surgery (2010) 45, 236 240 www.elsevier.com/locate/jpedsurg Initial laparoscopic appendectomy versus initial nonoperative management and interval appendectomy for perforated appendicitis
Procedure: Chest Tube Placement (Tube Thoracostomy)
 Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Pathologic abnormality of the sternoclavicular joint (SCJ)
 Surgical Management of the Infected Sternoclavicular Joint Rubie Sue Jackson, MD, Yvonne M. Carter, MD, and M. Blair Marshall, MD Pathologic abnormality of the sternoclavicular joint (SCJ) is rare. The
Surgical Management of the Infected Sternoclavicular Joint Rubie Sue Jackson, MD, Yvonne M. Carter, MD, and M. Blair Marshall, MD Pathologic abnormality of the sternoclavicular joint (SCJ) is rare. The
For the Attention of the Operating Surgeon: IMPORTANT INFORMATION ON THE MATRIXRIB FIXATION SYSTEM
 For the Attention of the Operating Surgeon: IMPORTANT INFORMATION ON THE MATRIXRIB FIXATION SYSTEM 10/16 GP2685-E-CAN DESCRIPTION The MatrixRIB Fixation System consists of locking plates, locking screws,
For the Attention of the Operating Surgeon: IMPORTANT INFORMATION ON THE MATRIXRIB FIXATION SYSTEM 10/16 GP2685-E-CAN DESCRIPTION The MatrixRIB Fixation System consists of locking plates, locking screws,
TOTAL SHOULDER REPLACEMENT The following is designed to present an overview of shoulder replacement surgery options
 SHOULDER SERVICE TOTAL SHOULDER REPLACEMENT The following is designed to present an overview of shoulder replacement surgery options SHOULDER PAIN Chronic shoulder pain can limit your activities, keep
SHOULDER SERVICE TOTAL SHOULDER REPLACEMENT The following is designed to present an overview of shoulder replacement surgery options SHOULDER PAIN Chronic shoulder pain can limit your activities, keep
Forces to be overcome in correction of pectus excavatum
 Forces to be overcome in correction of pectus excavatum Peter G. Weber, MD, Hans P. Huemmer, MD, and Bertram Reingruber, MD Objective: The Erlangen technique of funnel chest correction is carried out through
Forces to be overcome in correction of pectus excavatum Peter G. Weber, MD, Hans P. Huemmer, MD, and Bertram Reingruber, MD Objective: The Erlangen technique of funnel chest correction is carried out through
Pectus Excavatum Reconstruction With Silicone Implants. Long-Term Results and a Review of the English-Language Literature
 REVIEW ARTICLES Pectus Excavatum Reconstruction With Silicone Implants Long-Term Results and a Review of the English-Language Literature Bart Jorrit Snel, MD,* Cees A. Spronk, MD, Paul M. N. Werker, MD,
REVIEW ARTICLES Pectus Excavatum Reconstruction With Silicone Implants Long-Term Results and a Review of the English-Language Literature Bart Jorrit Snel, MD,* Cees A. Spronk, MD, Paul M. N. Werker, MD,
REINFORCED BIOSCAFFOLDS
 REINFORCED BIOSCAFFOLDS Midline Incisional Open OviTex 1S Resorbable Clinical Case Study: Open Abdomen Incisional Herniorrhaphy in Contaminated (CDC Class IV) Operative Field Performed by Dr. Michael Sawyer,
REINFORCED BIOSCAFFOLDS Midline Incisional Open OviTex 1S Resorbable Clinical Case Study: Open Abdomen Incisional Herniorrhaphy in Contaminated (CDC Class IV) Operative Field Performed by Dr. Michael Sawyer,
Procedures/Risks:central venous catheter
 Procedures/Risks:central venous catheter Central Venous Catheter Placement Procedure: Placement of the central venous catheter will take place in the Interventional Radiology Department (IRD) at The Ohio
Procedures/Risks:central venous catheter Central Venous Catheter Placement Procedure: Placement of the central venous catheter will take place in the Interventional Radiology Department (IRD) at The Ohio
Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan
 Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
MODIFICATION OF THE NUSS PROCEDURE-PREVENTION OF INJURIES OF THE HEART AND MAJOR BLOOD VESSELS
 . Bali Medical Journal (BMJ) 20, Volume 1, Number 3: 88-92 MODIFICATION OF THE NUSS PROCEDURE-PREVENTION OF INJURIES OF THE HEART AND MAJOR BLOOD VESSELS Mirko Žganjer Children s Hospital Zagreb, Department
. Bali Medical Journal (BMJ) 20, Volume 1, Number 3: 88-92 MODIFICATION OF THE NUSS PROCEDURE-PREVENTION OF INJURIES OF THE HEART AND MAJOR BLOOD VESSELS Mirko Žganjer Children s Hospital Zagreb, Department
What's new in pediatric surgery? A minimally invasive technique to correct pectus excavatum
 BUMC Proceedings 1999;12:25-28 What's new in pediatric surgery? A minimally invasive technique to correct pectus excavatum DALE COLN, MD Department of Surgery, BUMC An effective method for surgically repairing
BUMC Proceedings 1999;12:25-28 What's new in pediatric surgery? A minimally invasive technique to correct pectus excavatum DALE COLN, MD Department of Surgery, BUMC An effective method for surgically repairing
A Comparative Study for the Role of Preoperative Antibiotic Prophylaxis in Prevention of Surgical Site Infections
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 4 Ver. IV. (Apr. 2014), PP 27-31 A Comparative Study for the Role of Preoperative Antibiotic
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 4 Ver. IV. (Apr. 2014), PP 27-31 A Comparative Study for the Role of Preoperative Antibiotic
Thoracoplasty for the Management of Postpneumonectomy Empyema
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 9 Number 2 Thoracoplasty for the Management of Postpneumonectomy Empyema S Mullangi, G Diaz-Fuentes, S Khaneja Citation S Mullangi,
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 9 Number 2 Thoracoplasty for the Management of Postpneumonectomy Empyema S Mullangi, G Diaz-Fuentes, S Khaneja Citation S Mullangi,
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander.
 Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
Esophageal Perforation
 Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Nuss Ravitch modified CPT Codes repair repair modify CPT Code repair repair Nuss codes repair modified Nuss modified Ravitch procedure
 Sep 1, 2013. Nuss procedure or the Ravitch technique (original or modified), typically requiring the removal of a portion of damaged.. CPT Codes. Description: Codes Covered When Medically Necessary. 21740.
Sep 1, 2013. Nuss procedure or the Ravitch technique (original or modified), typically requiring the removal of a portion of damaged.. CPT Codes. Description: Codes Covered When Medically Necessary. 21740.
Chest Wall Tumors and Reconstruction: Lateral Chest Wall. Dr. Robert Kelly
 Chest Wall Tumors and Reconstruction: Lateral Chest Wall Dr. Robert Kelly THORACIC PROGRAMME: ADVANCES IN CHEST WALL SURGERY AND OSTEOSYNTHESIS Dr. José Ribas Milanez de Campos Assistant, Professor, Department
Chest Wall Tumors and Reconstruction: Lateral Chest Wall Dr. Robert Kelly THORACIC PROGRAMME: ADVANCES IN CHEST WALL SURGERY AND OSTEOSYNTHESIS Dr. José Ribas Milanez de Campos Assistant, Professor, Department
Table 2: Outcomes measured. Table 1: Intrapleural alteplase instillation therapy protocol
 ORIGINAL RESEARCH ARTICLE Intrapleural F brinolytic Therapy with Alteplase in Empyema Thoracis in Children conducted in the Department of Pediatric critical care and Pulmonology unit at our institution
ORIGINAL RESEARCH ARTICLE Intrapleural F brinolytic Therapy with Alteplase in Empyema Thoracis in Children conducted in the Department of Pediatric critical care and Pulmonology unit at our institution
Information for Patients
 Having a Percutaneous Drainage Information for Patients In this leaflet: Introduction 2 What is a percutaneous drainage?..... 2 Why do I need a percutaneous drainage?.....2 Are there any risks?....2 What
Having a Percutaneous Drainage Information for Patients In this leaflet: Introduction 2 What is a percutaneous drainage?..... 2 Why do I need a percutaneous drainage?.....2 Are there any risks?....2 What
Vancomycin powder to reduce surgical site infection in spine surgery
 Vancomycin powder to reduce surgical site infection in spine surgery 2014/03/25 EBM Spine Fellow 林東儀 Post-Op infection in spine surgery Wound infection: 0.7% to 11.9% Infection rates of 2.8% to 6.0% for
Vancomycin powder to reduce surgical site infection in spine surgery 2014/03/25 EBM Spine Fellow 林東儀 Post-Op infection in spine surgery Wound infection: 0.7% to 11.9% Infection rates of 2.8% to 6.0% for
Peritoneal Dialysis Catheter Placement. Peritoneal Dialysis Catheter Placement. Peritoneal Dialysis Catheter Placement
 ASDIN Advanced Techniques Pre-course Feb. 24, 2012 New Orleans, La Randall L. Rasmussen, MD Special thank you to Drs. Rajeev Narayan, San Antonio, Tx and Hemant Dhingra, Fresno Ca for lending me slides
ASDIN Advanced Techniques Pre-course Feb. 24, 2012 New Orleans, La Randall L. Rasmussen, MD Special thank you to Drs. Rajeev Narayan, San Antonio, Tx and Hemant Dhingra, Fresno Ca for lending me slides
Associate Professor of Plastic Surgery, Karol. Institute; Plastic Department, Serafimerlasarettet, Stockholm, Sweden
 A NEW METHOD OF SHAPING DEFORMED EARS By A. RAGNELL, M.D. Associate Professor of Plastic Surgery, Karol. Institute; Plastic Department, Serafimerlasarettet, Stockholm, Sweden NUMEROUS methods of shaping
A NEW METHOD OF SHAPING DEFORMED EARS By A. RAGNELL, M.D. Associate Professor of Plastic Surgery, Karol. Institute; Plastic Department, Serafimerlasarettet, Stockholm, Sweden NUMEROUS methods of shaping
Serum C-reactive protein levels correlate with clinical response in patients treated with antibiotics for wound infections after spinal surgery
 The Spine Journal 6 (2006) 311 315 Serum C-reactive protein levels correlate with clinical response in patients treated with antibiotics for wound infections after spinal surgery Mustafa H. Khan, MD a,
The Spine Journal 6 (2006) 311 315 Serum C-reactive protein levels correlate with clinical response in patients treated with antibiotics for wound infections after spinal surgery Mustafa H. Khan, MD a,
Interesting Case Series. Omental Flap for Thoracic Aortic Graft Infection
 Interesting Case Series Omental Flap for Thoracic Aortic Graft Infection Andrew A. Marano, BA, Adam M. Feintisch, MD, and Mark S. Granick, MD Division of Plastic Surgery, Department of Surgery, Rutgers
Interesting Case Series Omental Flap for Thoracic Aortic Graft Infection Andrew A. Marano, BA, Adam M. Feintisch, MD, and Mark S. Granick, MD Division of Plastic Surgery, Department of Surgery, Rutgers
Pectus excavatum is the most common congenital
 Nonprosthetic Surgical Repair of Pectus Excavatum Hiroshi Iida, MD, PhD, Yoshio Sudo, MD, PhD, Yasuyuki Yamada, MD, PhD, Yasushi Matsushita, MD, PhD, Kunihiro Eda, MD, PhD, and Yuho Inoue MD, PhD GENERAL
Nonprosthetic Surgical Repair of Pectus Excavatum Hiroshi Iida, MD, PhD, Yoshio Sudo, MD, PhD, Yasuyuki Yamada, MD, PhD, Yasushi Matsushita, MD, PhD, Kunihiro Eda, MD, PhD, and Yuho Inoue MD, PhD GENERAL
Vertical mammaplasty has been developed
 BREAST Y-Scar Vertical Mammaplasty David A. Hidalgo, M.D. New York, N.Y. Background: Vertical mammaplasty is an effective alternative to inverted-t methods. Among other benefits, it results in a significantly
BREAST Y-Scar Vertical Mammaplasty David A. Hidalgo, M.D. New York, N.Y. Background: Vertical mammaplasty is an effective alternative to inverted-t methods. Among other benefits, it results in a significantly
The posterolateral thoracotomy is still probably the
 Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Central Venous Access Devices and Infection
 Central Venous Access Devices and Infection Dr Andrew Daley Microbiology & Infectious Diseases Women s & Children s Health Melbourne Background Types of infection! Local site infection! Blood stream infection!
Central Venous Access Devices and Infection Dr Andrew Daley Microbiology & Infectious Diseases Women s & Children s Health Melbourne Background Types of infection! Local site infection! Blood stream infection!
Our Experience with Endoscopic Brow Lifts
 Aesth. Plast. Surg. 24:90 96, 2000 DOI: 10.1007/s002660010017 2000 Springer-Verlag New York Inc. Our Experience with Endoscopic Brow Lifts Ozan Sozer, M.D., and Thomas M. Biggs, M.D. İstanbul, Turkey and
Aesth. Plast. Surg. 24:90 96, 2000 DOI: 10.1007/s002660010017 2000 Springer-Verlag New York Inc. Our Experience with Endoscopic Brow Lifts Ozan Sozer, M.D., and Thomas M. Biggs, M.D. İstanbul, Turkey and
Strattice Reconstructive Tissue Matrix used in the repair of rippling
 Clinical case study Strattice Tissue Matrix Strattice Reconstructive Tissue Matrix used in the repair of rippling Steven Teitelbaum, MD* Santa Monica, CA Case summary A 48-year-old woman with a history
Clinical case study Strattice Tissue Matrix Strattice Reconstructive Tissue Matrix used in the repair of rippling Steven Teitelbaum, MD* Santa Monica, CA Case summary A 48-year-old woman with a history
Central Venous Access Devices. Stephanie Cunningham Amy Waters
 Central Venous Access Devices Stephanie Cunningham Amy Waters 5 Must Know Facts About CVAD s 1) What are CVAD s? 2) What are CVAD s used for? 3) How are these devices put in? 4) What are the complications
Central Venous Access Devices Stephanie Cunningham Amy Waters 5 Must Know Facts About CVAD s 1) What are CVAD s? 2) What are CVAD s used for? 3) How are these devices put in? 4) What are the complications
IR Central Venous Access [ ] Pre Procedure
![IR Central Venous Access [ ] Pre Procedure IR Central Venous Access [ ] Pre Procedure](/thumbs/90/104119758.jpg) IR Central Venous Access [1050200001] Pre Procedure Case Request/Scheduling Procedure Enter IR Case Request if not already completed (All hospitals except Grant Medical Center) [ ] Case Request IR Lab
IR Central Venous Access [1050200001] Pre Procedure Case Request/Scheduling Procedure Enter IR Case Request if not already completed (All hospitals except Grant Medical Center) [ ] Case Request IR Lab
One hundred percent fascial approximation with sequential abdominal closure of the open abdomen
 The American Journal of Surgery 192 (2006) 238 242 HowIdoit One hundred percent fascial approximation with sequential abdominal closure of the open abdomen C. Clay Cothren, M.D. a,b, *, Ernest E. Moore,
The American Journal of Surgery 192 (2006) 238 242 HowIdoit One hundred percent fascial approximation with sequential abdominal closure of the open abdomen C. Clay Cothren, M.D. a,b, *, Ernest E. Moore,
Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine:
 Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
HIP REPLACEMENT SURGERY
 HIP REPLACEMENT SURGERY HOW TO PREPARE FOR SURGERY AND REC0VERY Before surgery: Arrange for someone to help you around the house for a week or two after coming home from the hospital. Arrange for transportation
HIP REPLACEMENT SURGERY HOW TO PREPARE FOR SURGERY AND REC0VERY Before surgery: Arrange for someone to help you around the house for a week or two after coming home from the hospital. Arrange for transportation
INTRODUCTION MATERIALS AND METHODS
 J Korean Med Sci 2003; 18: 360-4 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences The aim of this study was to compare clinical outcomes in pectus excavatum patients undergoing a Ravitch
J Korean Med Sci 2003; 18: 360-4 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences The aim of this study was to compare clinical outcomes in pectus excavatum patients undergoing a Ravitch
BEN C. TAYLOR, MD TRAUMA FELLOW GRANT MEDICAL CENTER
 Evaluation of Primary Total Knee Arthroplasty Incision Closure with the Use of Continuous Bidirectional SCOTT STEPHENS, MD RESIDENT PHYSICIAN MOUNT CARMEL MEDICAL CENTER JOEL POLITI, MD DEPARTMENT OF ORTHOPEDIC
Evaluation of Primary Total Knee Arthroplasty Incision Closure with the Use of Continuous Bidirectional SCOTT STEPHENS, MD RESIDENT PHYSICIAN MOUNT CARMEL MEDICAL CENTER JOEL POLITI, MD DEPARTMENT OF ORTHOPEDIC
The University of Toledo Medical Center and its Medical Staff
 Name of Policy: Policy Number: Department: 3364-109-GEN-705 Infection Control Medical Staff Hospital Administration Approving Officer: Responsible Agent: Scope: Chair, Infection Control Committee Chief
Name of Policy: Policy Number: Department: 3364-109-GEN-705 Infection Control Medical Staff Hospital Administration Approving Officer: Responsible Agent: Scope: Chair, Infection Control Committee Chief
Radiological Assessment of Children with Pectus Excavatum
 51 Original Article Radiological Assessment of Children with Pectus Excavatum Arturas Kilda 1, Algidas Basevicius 2, Vidmantas Barauskas 1, Saulius Lukosevicius 2 and Donatas Ragaisis 2 1 Department of
51 Original Article Radiological Assessment of Children with Pectus Excavatum Arturas Kilda 1, Algidas Basevicius 2, Vidmantas Barauskas 1, Saulius Lukosevicius 2 and Donatas Ragaisis 2 1 Department of
NEW DEFINITION FORMAT AND DIFFICULT VARIABLE DEFINITIONS
 NEW DEFINITION FORMAT AND DIFFICULT VARIABLE DEFINITIONS Bruce L. Hall, MD, PhD, MBA, FACS Clinical Support Physician Lead Paula Farrell, RN, BSN ACS NSQIP Clinical Support Specialist Case Studies &
NEW DEFINITION FORMAT AND DIFFICULT VARIABLE DEFINITIONS Bruce L. Hall, MD, PhD, MBA, FACS Clinical Support Physician Lead Paula Farrell, RN, BSN ACS NSQIP Clinical Support Specialist Case Studies &
Osteomyelitis Samir S. Shah, MD, MSCE
 Osteomyelitis Samir S. Shah, MD, MSCE Professor, Department of Pediatrics University of Cincinnati College of Medicine Director, Division of Hospital Medicine Attending Physician in Infectious Diseases
Osteomyelitis Samir S. Shah, MD, MSCE Professor, Department of Pediatrics University of Cincinnati College of Medicine Director, Division of Hospital Medicine Attending Physician in Infectious Diseases
CASE REPORT. Mycotic Aneurysm of Ascending Aorta Due to Sarcina Lutea. G. A. Lopez, M.D., and A. R. C. Dobell, M.D.
 CASE REPORT Mycotic Aneurysm of Ascending Aorta Due to Sarcina Lutea G. A. Lopez, M.D., and A. R. C. Dobell, M.D. ABSTRACT A patient developed a mycotic aneurysm of the aortic suture line after aortic
CASE REPORT Mycotic Aneurysm of Ascending Aorta Due to Sarcina Lutea G. A. Lopez, M.D., and A. R. C. Dobell, M.D. ABSTRACT A patient developed a mycotic aneurysm of the aortic suture line after aortic
OSTEOMYELITIS. If it occurs in adults, then the axial skeleton is the usual site.
 OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
-primarily by apposition of the anterior rectus
 2 Component separation Cop HARVEY CHIM, KAREN KIM EVANS, AND SAMIR MARDINI Mater al Introduction 7 Preoperative markings 7 Intraoperative details 9 Technique modification: Component separation with preservation
2 Component separation Cop HARVEY CHIM, KAREN KIM EVANS, AND SAMIR MARDINI Mater al Introduction 7 Preoperative markings 7 Intraoperative details 9 Technique modification: Component separation with preservation
Infected cardiac-implantable electronic devices: diagnosis, and treatment
 Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
Breast Reduction Surgery Houston
 Breast Houston Reduction Surgery Breast Reduction Surgery by Houston Board Certified Plastic Surgeon Breast Reduction Surgery Houston Breast Reduction surgery is a very satisfying procedure. Heavy, large,
Breast Houston Reduction Surgery Breast Reduction Surgery by Houston Board Certified Plastic Surgeon Breast Reduction Surgery Houston Breast Reduction surgery is a very satisfying procedure. Heavy, large,
Children s Acute Transport Service
 Children s Acute Transport Service Vascular Access Document Control Information Author Ramnarayan Author Position Consultant, CATS Document Owner Polke Document Owner Position CATS Co-ordinator Document
Children s Acute Transport Service Vascular Access Document Control Information Author Ramnarayan Author Position Consultant, CATS Document Owner Polke Document Owner Position CATS Co-ordinator Document
Corporate Medical Policy
 Corporate Medical Policy Surgical Treatment of Chest Wall Deformities (Congenital or File Name: Origination: Last CAP Review: Next CAP Review: Last Review: surgical_treatment_of_chest_wall_deformities_congenital_or_acquired
Corporate Medical Policy Surgical Treatment of Chest Wall Deformities (Congenital or File Name: Origination: Last CAP Review: Next CAP Review: Last Review: surgical_treatment_of_chest_wall_deformities_congenital_or_acquired
National Healthcare Safety Network: Central Line-associated Bloodstream Case Studies Teresa C. Horan, MPH
 National Healthcare Safety Network: Central Line-associated Bloodstream Case Studies Teresa C. Horan, MPH National Center for Emerging and Zoonotic Infectious Diseases Division of Healthcare Quality Promotion
National Healthcare Safety Network: Central Line-associated Bloodstream Case Studies Teresa C. Horan, MPH National Center for Emerging and Zoonotic Infectious Diseases Division of Healthcare Quality Promotion
Emergency Approach to the Subclavian and Innominate Vessels
 Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
The Eloesser flap thoracostomy window was initially described
 Eloesser Flap Thoracostomy Window Chadrick E. Denlinger, MD Department of Surgery, Medical University of South Carolina and the Ralph H. Johnson VA Medical Center, Charleston, South Carolina. Address reprint
Eloesser Flap Thoracostomy Window Chadrick E. Denlinger, MD Department of Surgery, Medical University of South Carolina and the Ralph H. Johnson VA Medical Center, Charleston, South Carolina. Address reprint
Knee Replacement Recovery Guide
 Knee Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Range of Motion... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering... 3 Bruising...
Knee Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Range of Motion... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering... 3 Bruising...
Spinal Fusion. North American Spine Society Public Education Series
 Spinal Fusion North American Spine Society Public Education Series What Is Spinal Fusion? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
Spinal Fusion North American Spine Society Public Education Series What Is Spinal Fusion? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
Treatment for sternoclavicular joint infections: a multi-institutional study
 Original Article Treatment for sternoclavicular joint infections: a multi-institutional study Allen Murga, Hannah Copeland, Rachel Hargrove, Jason M. Wallen, Salman Zaheer Department of Thoracic and Cardiovascular
Original Article Treatment for sternoclavicular joint infections: a multi-institutional study Allen Murga, Hannah Copeland, Rachel Hargrove, Jason M. Wallen, Salman Zaheer Department of Thoracic and Cardiovascular
SURGICAL SITE INFECTIONS: SURVEILLANCE & PREVENTION
 SURGICAL SITE INFECTIONS: SURVEILLANCE & PREVENTION Facts There were an estimated 157,500 surgical site infections associated with inpatient surgeries in 2011. SSIs were the most common healthcare-associated
SURGICAL SITE INFECTIONS: SURVEILLANCE & PREVENTION Facts There were an estimated 157,500 surgical site infections associated with inpatient surgeries in 2011. SSIs were the most common healthcare-associated
Surgical site infections pose a burden on both patients
 SPINE Volume 39, Number 20, pp 1683-1687 2014, Lippincott Williams & Wilkins DEFORMITY Safety of Topical Vancomycin for Pediatric Spinal Deformity Nontoxic Serum Levels With Supratherapeutic Drain Levels
SPINE Volume 39, Number 20, pp 1683-1687 2014, Lippincott Williams & Wilkins DEFORMITY Safety of Topical Vancomycin for Pediatric Spinal Deformity Nontoxic Serum Levels With Supratherapeutic Drain Levels
Minimally invasive repair of pectus excavatum: A novel morphology-tailored, patient-specific approach
 Park et al General Thoracic Surgery Minimally invasive repair of pectus excavatum: A novel morphology-tailored, patient-specific approach Hyung Joo Park, MD, a Jin Yong Jeong, MD, a Won Min Jo, MD, a Jae
Park et al General Thoracic Surgery Minimally invasive repair of pectus excavatum: A novel morphology-tailored, patient-specific approach Hyung Joo Park, MD, a Jin Yong Jeong, MD, a Won Min Jo, MD, a Jae
Torn ACL Hamstring Graft
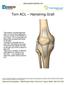 Torn ACL Hamstring Graft The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects the femur to the tibia.
Torn ACL Hamstring Graft The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects the femur to the tibia.
Hospital-wide Impact of Mandatory Infectious Disease Consultation on Staphylococcus aureus Septicemia
 Hospital-wide Impact of Mandatory Infectious Disease Consultation on Staphylococcus aureus Septicemia Amanda Guth 1 Amy Slenker MD 1,2 1 Department of Infectious Diseases, Lehigh Valley Health Network
Hospital-wide Impact of Mandatory Infectious Disease Consultation on Staphylococcus aureus Septicemia Amanda Guth 1 Amy Slenker MD 1,2 1 Department of Infectious Diseases, Lehigh Valley Health Network
Recurrent Retropharyngeal Abscess with Esophageal Perforation due to Chopstick Injury
 Recurrent Retropharyngeal Abscess with Esophageal Perforation due to Chopstick Injury Hye Kyung Chang, Jung-Tak Oh, Seung Hoon Choi, Seok Joo Han Division of Pediatric Surgery, Department of Surgery, Yonsei
Recurrent Retropharyngeal Abscess with Esophageal Perforation due to Chopstick Injury Hye Kyung Chang, Jung-Tak Oh, Seung Hoon Choi, Seok Joo Han Division of Pediatric Surgery, Department of Surgery, Yonsei
Case Study. TRAM Flap Reconstruction with an Associated Complication. Repair using DermaMatrix Acellular Dermis.
 Case Study TRAM Flap Reconstruction with an Associated Complication. Repair using DermaMatrix Acellular Dermis. TRAM Flap Reconstruction with an Associated Complication Challenge Insulin-dependent diabetes
Case Study TRAM Flap Reconstruction with an Associated Complication. Repair using DermaMatrix Acellular Dermis. TRAM Flap Reconstruction with an Associated Complication Challenge Insulin-dependent diabetes
Empyema After Pneumonectomy
 George L. Zumbro, Jr., Maj, Robert Treasure, Col, James P. Geiger, M.D., Col (Ret), and David C. Green, Col, all MC, USA ABSTRACT Ten patients who developed empyema after pneumonectomy are discussed. The
George L. Zumbro, Jr., Maj, Robert Treasure, Col, James P. Geiger, M.D., Col (Ret), and David C. Green, Col, all MC, USA ABSTRACT Ten patients who developed empyema after pneumonectomy are discussed. The
Open Retromuscular Hernia Repair: Tips and Tricks from the Masters
 Open Retromuscular Hernia Repair: Tips and Tricks from the Masters Eric M. Pauli, MD FACS FASGE Associate Professor of Surgery Director of Endoscopic Surgery Penn State Hershey Medical Center Disclosures
Open Retromuscular Hernia Repair: Tips and Tricks from the Masters Eric M. Pauli, MD FACS FASGE Associate Professor of Surgery Director of Endoscopic Surgery Penn State Hershey Medical Center Disclosures
A Standardized Protocol to Reduce Pediatric Baclofen Pump Infections: A Quality Improvement Initiative
 A Standardized Protocol to Reduce Pediatric Baclofen Pump Infections: A Quality Improvement Initiative Kathryn M. Wagner, Virendra R. Desai, Jeffrey S. Raskin, Arvind Mohan, JoWinsyl Montojo, Valentina
A Standardized Protocol to Reduce Pediatric Baclofen Pump Infections: A Quality Improvement Initiative Kathryn M. Wagner, Virendra R. Desai, Jeffrey S. Raskin, Arvind Mohan, JoWinsyl Montojo, Valentina
Arthroscopic Surgery. What is Arthroscopic Surgery?
 Arthroscopic Surgery The physicians and surgeons at Orthopaedic Asssociates of Central Texas (OACT) are leaders in caring for the joints of the body. We service patients in Williamson and surrounding Counties,
Arthroscopic Surgery The physicians and surgeons at Orthopaedic Asssociates of Central Texas (OACT) are leaders in caring for the joints of the body. We service patients in Williamson and surrounding Counties,
FOOT AND ANKLE ARTHROSCOPY
 FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
Sacral Nerve Stimulation (SNS) System Implantation
 Patient & Family Guide 2016 Sacral Nerve Stimulation (SNS) System Implantation www.nshealth.ca Sacral Nerve Stimulation (SNS) System Implantation SNS system implantation involves placing a lead ( leed,
Patient & Family Guide 2016 Sacral Nerve Stimulation (SNS) System Implantation www.nshealth.ca Sacral Nerve Stimulation (SNS) System Implantation SNS system implantation involves placing a lead ( leed,
Replacement of the mitral valve in the presence of
 Mitral Valve Replacement in Patients with Mitral Annulus Abscess Christopher M. Feindel Replacement of the mitral valve in the presence of an abscess of the mitral annulus presents a major challenge to
Mitral Valve Replacement in Patients with Mitral Annulus Abscess Christopher M. Feindel Replacement of the mitral valve in the presence of an abscess of the mitral annulus presents a major challenge to
EMERGING EVIDENCE AND BEST PRACTICES TO PREVENT SSI IN COLON PROCEDURES
 EMERGING EVIDENCE AND BEST PRACTICES TO PREVENT SSI IN COLON PROCEDURES Clifford Ko, MD, MS, MSHS, FACS, FASCRS Professor of Surgery UCLA Director, ACS NSQIP, American College of Surgeons EVIDENCE Ban
EMERGING EVIDENCE AND BEST PRACTICES TO PREVENT SSI IN COLON PROCEDURES Clifford Ko, MD, MS, MSHS, FACS, FASCRS Professor of Surgery UCLA Director, ACS NSQIP, American College of Surgeons EVIDENCE Ban
Post-LASIK infections
 Post-LASIK infections By Mohamed El-moddather Assiss. Prof. and head of department of ophthalmology AL-Azhar unizersity Assuit LASIK has become a common refractive procedure and is generally considered
Post-LASIK infections By Mohamed El-moddather Assiss. Prof. and head of department of ophthalmology AL-Azhar unizersity Assuit LASIK has become a common refractive procedure and is generally considered
THE REVERSE SHOULDER REPLACEMENT
 THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
Appendix E: Overview of Vascular
 Appendix E: Overview of Vascular 56 Peripheral Short Catheter, less than 3 inches (7.5 cm) in length; over-the-needle catheter is most common. Inserted by percutaneous venipuncture, generally into a hand
Appendix E: Overview of Vascular 56 Peripheral Short Catheter, less than 3 inches (7.5 cm) in length; over-the-needle catheter is most common. Inserted by percutaneous venipuncture, generally into a hand
MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION AN INTRODUCTION TO
 AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
Central Venous Catheter Insertion: Assisting
 Approved by: Central Venous Catheter Insertion: Assisting Gail Cameron Senior Director, Operations, Maternal, Neonatal & Child Health Programs Dr. Santiago Ensenat Medical Director, Neonatology Neonatal
Approved by: Central Venous Catheter Insertion: Assisting Gail Cameron Senior Director, Operations, Maternal, Neonatal & Child Health Programs Dr. Santiago Ensenat Medical Director, Neonatology Neonatal
An alternative approach for correction of constricted ears of moderate severity
 British Journal of Plastic Surgery (2005) 58, 389 393 An alternative approach for correction of constricted ears of moderate severity M.M. Al-Qattan* Division of Plastic Surgery, King Saud University,
British Journal of Plastic Surgery (2005) 58, 389 393 An alternative approach for correction of constricted ears of moderate severity M.M. Al-Qattan* Division of Plastic Surgery, King Saud University,
Case Study: Nadine. Conditions Treated Hip Dysplasia. Age Range During Treatment 39 years
 Case Study: Nadine Conditions Treated Hip Dysplasia Age Range During Treatment 39 years David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone
Case Study: Nadine Conditions Treated Hip Dysplasia Age Range During Treatment 39 years David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone
Pocket Management: Before, During, and After (Extended Q&A) WELCOME!
 Pocket Management: Before, During, and After (Extended Q&A) WELCOME! About LEADCONNECTION.ORG membership (1 yr. since launch) 334 Members MD 277 (83%) Allied 33 (10%) Industry/scientist 23 ( 7%) 40 countries
Pocket Management: Before, During, and After (Extended Q&A) WELCOME! About LEADCONNECTION.ORG membership (1 yr. since launch) 334 Members MD 277 (83%) Allied 33 (10%) Industry/scientist 23 ( 7%) 40 countries
Abscess cellulitis in the mouth
 Cari untuk: Cari Cari Abscess cellulitis in the mouth Cellulitis is inflammation that has spread to the surrounding soft tissues of the mouth. It is a dental emergency because, if not treated, it can cau
Cari untuk: Cari Cari Abscess cellulitis in the mouth Cellulitis is inflammation that has spread to the surrounding soft tissues of the mouth. It is a dental emergency because, if not treated, it can cau
Division of Vascular and Endovascular Surgery University of South Florida School of Medicine Tampa, Florida
 Division of Vascular and Endovascular Surgery University of South Florida School of Medicine Tampa, Florida Appearance: oearly < 3 mo. olate > 3 mo.. Extent: Szilagyi Classification: Grade I: infection
Division of Vascular and Endovascular Surgery University of South Florida School of Medicine Tampa, Florida Appearance: oearly < 3 mo. olate > 3 mo.. Extent: Szilagyi Classification: Grade I: infection
Selective Nonoperative Management of Contained Intrathoracic Esophageal Disruptions
 Selective Nonoperative Management of Contained Intrathoracic Esophageal Disruptions John L. Cameron, M.D., Richard F. Kieffer, M.D., Thomas R. Hendrix, M.D., Denis G. Mehigan, M.., and R. Robinson aker,
Selective Nonoperative Management of Contained Intrathoracic Esophageal Disruptions John L. Cameron, M.D., Richard F. Kieffer, M.D., Thomas R. Hendrix, M.D., Denis G. Mehigan, M.., and R. Robinson aker,
INSTRUCTIONS FOR USE FOR:
 INSTRUCTIONS FOR USE FOR: en English INSTRUCTIONS FOR USE GORE ENFORM PREPERITONEAL BIOMATERIAL Carefully read all instructions prior to use. Observe all instructions, warnings, and precautions noted throughout.
INSTRUCTIONS FOR USE FOR: en English INSTRUCTIONS FOR USE GORE ENFORM PREPERITONEAL BIOMATERIAL Carefully read all instructions prior to use. Observe all instructions, warnings, and precautions noted throughout.
Transabdominal pre peritoneal (TAPP) vs totally extraperitoneal (TEP) laparoscopic techniques for inguinal hernia repair
 Transabdominal pre peritoneal (TAPP) vs totally extraperitoneal (TEP) laparoscopic techniques for inguinal hernia repair An inguinal hernia (hernia of the groin) is a weakness in the wall of the abdominal
Transabdominal pre peritoneal (TAPP) vs totally extraperitoneal (TEP) laparoscopic techniques for inguinal hernia repair An inguinal hernia (hernia of the groin) is a weakness in the wall of the abdominal
2013 MCT CPC-H Quiz #8 Chapters 13 and 14
 2013 MCT CPC-H Quiz #8 Chapters 13 and 14 Name: Date: Instructor: Score: 1. A female patient presents to the outpatient clinic for excision of a 4.8 cm malignant melanoma of the left inner thigh. A 6 cm
2013 MCT CPC-H Quiz #8 Chapters 13 and 14 Name: Date: Instructor: Score: 1. A female patient presents to the outpatient clinic for excision of a 4.8 cm malignant melanoma of the left inner thigh. A 6 cm
Impact of Suture Choice on Stricture Formation Following Repair of Esophageal Atresia
 Annals of Pediatric Surgery, Vol 3, No 2, April 2007 PP 75-79 Original Article Impact of Suture Choice on Stricture Formation Following Repair of Esophageal Atresia Shawn D. St. Peter, Patricia A. Valusek,
Annals of Pediatric Surgery, Vol 3, No 2, April 2007 PP 75-79 Original Article Impact of Suture Choice on Stricture Formation Following Repair of Esophageal Atresia Shawn D. St. Peter, Patricia A. Valusek,
Case Presentation and Discussion on Posterior Neck Mass. Martin Joseph S. Cabahug
 Case Presentation and Discussion on Posterior Neck Mass Martin Joseph S. Cabahug General Data: C.A, 60 y/o male Sta. Ana, Mla Chief Complaint: Posterior Neck Mass History and Physical Exam 2 wks PTA mass,
Case Presentation and Discussion on Posterior Neck Mass Martin Joseph S. Cabahug General Data: C.A, 60 y/o male Sta. Ana, Mla Chief Complaint: Posterior Neck Mass History and Physical Exam 2 wks PTA mass,
CASE REPORT. Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur
 PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
Nuclear medicine and Prosthetic Joint Infections
 Nuclear medicine and Prosthetic Joint Infections Christophe Van de Wiele, M.D., Ph.D. Department of Nuclear Medicine, University Hospital Ghent, Belgium Orthopedic prostheses: world market 1996 Prosthetic
Nuclear medicine and Prosthetic Joint Infections Christophe Van de Wiele, M.D., Ph.D. Department of Nuclear Medicine, University Hospital Ghent, Belgium Orthopedic prostheses: world market 1996 Prosthetic
