Abdominal Wound Dehiscence. Presenter: T Mohammed Moderator: Dr H Pienaar
|
|
|
- Clarissa Barrett
- 6 years ago
- Views:
Transcription
1 Abdominal Wound Dehiscence Presenter: T Mohammed Moderator: Dr H Pienaar
2 Introduction Wound Dehiscence is the premature "bursting" open of a wound along surgical suture. It is a surgical complication that results from poor wound healing. Risk factors in general are age, diabetes, obesity, poor knotting or grabbing of stitches, and trauma to the wound after surgery. Sometimes a pink (serosanguinous) fluid may leak out.
3 Introduction Abdominal wound dehiscence (burst abdomen, fascial dehiscence) is a severe postoperative complication, with mortality rates reported as high as 45%. The incidence as described in the literature ranges from 0.4% to 3.5%.
4 Introduction Abdominal wound dehiscence can result in evisceration, requiring immediate treatment. Prolonged hospital stay, high incidence of incision hernia, and subsequent reoperations underline the severity of this complication.
5 Introduction Despite advances in perioperative care and suture materials, incidence and mortality rates in regard to abdominal wound dehiscence have not significantly changed over the past decades. This may be attributable to increasing incidences of risk factors within patient populations outweighing the benefits of technical achievements.
6 Types of Wounds
7 Recent Literature In this study by Van Ramshorst et al (World J of Surg 2010;34:20-27) the objective was to develop a risk model to recognize high risk patients and identify independent risk factors for abdominal wound dehiscence. The study was conducted at the department of surgery, Erasmus University Medical Center, Rotterdam, Netherlands.
8 Recent Literature A total of 363 cases and 1,089 controls were analyzed. Major independent risk factors were: age, gender, chronic pulmonary disease, ascites, jaundice, anemia, emergency surgery, type of surgery, postoperative coughing, and wound infection.
9 Recent Literature In the validation population, risk scores were significantly higher (P<0.001) for patients with abdominal wound dehiscence (n = 19) compared to those without (n = 677). Resulting scores ranged from 0 to 8.5, and the risk for abdominal wound dehiscence over this range increased exponentially from 0.02% to 70.1%.
10 Risk Formula The validated risk model shows high predictive value for abdominal wound dehiscence and may help to identify patients at increased risk. The calculation of the probability of abdominal wound dehiscence for an individual surgical patient is performed in two steps.
11 Risk Formula First, the total risk score is calculated by adding the weights of the various variables shown in Table 1. In the second step, the probability of developing abdominal wound dehiscence, P, is calculated according to the logistic formula: P= e х / (1+e x )x100%;where e x represents the exponential function and x represents (1.085 x calculated total risk score).
12
13 Risk Calculation For example, the risk score for a 67-year-old man who undergoes an elective reconstruction of the abdominal aorta and is known to have a history of chronic pulmonary disease is 0.9 (score for age years) (score for male gender)? 1.3 (score for vascular surgery) (score for chronic pulmonary disease), for a total of 3.6. The probability, P, of this patient s developing abdominal wound dehiscence is: e (-8.37+(1.085x3.6)) /1+e (-8.37+(1.085x3.6)) x100%= 1.1%
14 Risk Calculation An emergency repair in a similar patient with a ruptured aneurysm and subsequent anemia results in a total score of 4.9 (i.e., subtotal of 3.6 points emergency anemia). Thus, the absolute risk rises to 4.5%.
15 Risk Score Intepretation
16 Risk factors Patients who undergo emergency surgery are generally in worse condition and nutritional state, and the chance of contamination of the surgical field is higher than in elective surgery. Moreover, the performance of the surgeon might be affected at night, which could lead to suboptimal closure of the abdomen at the end of the operation.
17 Risk factors Old age is another independent risk factor for abdominal wound dehiscence. Age has also been reported as a risk factor in other studies. The explanation for this might lie in deterioration of the tissue repair mechanism in the elderly. Especially during the first few days of the wound healing process, the immune system plays a key role.
18 Risk Factors One of the interesting risk factors found in this Rotterdam study, is gender. In previous studies, males have been reported to have a higher risk of developing abdominal wound dehiscence. This was attributed to smoking as a possible confounder and its effect on tissue repair.
19 Risk Factors Another explanation may be that men build up higher abdominal wall tension than females. An increase in intra-abdominal pressure results in higher strain on the wound edges, causing the sutures to cut through the muscles and fascia.
20 Risk Factors In the Rotterdam study, wound infection proved to be the risk factor with the highest relative weight. Its importance has been confirmed by virtually every study on this topic. Continued presence of bacteria causes influx and activation of neutrophils and increases in levels of degradative matrix metalloproteinases (MMPs).
21 Risk Factors In the absence of sufficient tissue inhibitors of MMPs, wound degradation will occur. The release of endotoxins by bacteria leads to the production of collagenase, which degrades collagen fibers. Infection thereby causes a prolongation of the inflammatory phase and negatively affects deposition of collagen and fibroblast activity.
22 Risk factors In wounds of patients with abdominal wound dehiscence, it has been observed that degradation of collagen exceeds the synthesis of collagen, which adversely affects breaking strength. Adequate tissue breaking strength is necessary, however, to provide support for the sutures that hold the wound edges together.
23 Risk Factors Low breaking strength can therefore amount to abdominal wound dehiscence, especially in the presence of increased intra-abdominal pressure and abnormal inflammatory response.
24 Risk factors Primary repair can be difficult or impossible when tissue has low breaking strength, creating the need for the use of mesh or acceptance of the high risk of recurrent abdominal wound dehiscence.
25 Risk factors Risk factors that did not have independent effects in the Rotterdam study included: 1.hypertension 2.uremia 3. corticosteroid use.
26 Risk Factors The Rotterdam study found no significant effect on the occurrence of abdominal wound dehiscence for diabetes mellitus and previous laparotomy. Malignancy, sepsis, and postoperative vomiting have been identified as risk factors by several authors, but no significant effects were found in the present study.
27 Risk factors This was surprising because it was suspected that the presence of scar tissue, microvascular changes due to hypertension and diabetes, poor tissue perfusion, and poor overall condition of the patient, associated with sepsis and malignancy, would be risk factors.
28 Risk factors Jaundice, on the other hand, was found to be an independent risk factor. The conclusion of The Rotterdam study was that wound healing is affected in jaundiced patients due to the association with low hematocrit and albumin levels and malignancy (i.e., poor nutritional status) and not to raised bilirubin levels.
29 Risk Factors Low protein and albumin levels and deficiencies of several vitamins and minerals such as vitamins A, B1, B2, B6, C and zinc, selenium and copper have been associated with poor wound repair.
30 Risk Factors Anemia is a risk factor that is related to increased perioperative stress, blood transfusions, and decreased tissue oxygenation, all of which can affect the immune system and the wound healing process.
31 American Risk Model A similar validation model of risk of dehiscence index was developed by an American group in Salt Lake City Utah in 2003 using data from the Veterans Affairs National Surgical Quality Improvement Program but lacks a formula for calculating the probability of developing dehiscence as in the Rotterdam Study.
32 American Risk Model There are several limitations to this study. Because the veterans carry more comorbidities than the general population, our results may not be generalizable to the public at large.
33 Abdominal Wall Closure For secure abdominal wall closures, the reduced tissue integrity along the border of the acute wound led to development of the concept of an optimal suture length to wound length (Suture Length-to-Wound Length) ratio for the primary closure of midline laparotomies.
34 Abdominal Wall Closure Well-done, large, prospective studies with the best follow-up found that a SL-to-WL ratio of approximately 4:1 minimized the incidence of fascial dehiscence and incisional hernia formation; this is where the surgical training dictum of 1-cm bites followed by 1 cm of progress originated.
35 Conclusion Important risk factors for abdominal wound dehiscence have been identified in the Rotterdam case-control study 2010 including: 1. age, 2. gender 3. chronic pulmonary disease, 4.ascites, jaundice, anemia, emergency surgery, type of surgery, coughing, and wound infection.
36 Conclusion 5.jaundice 6.anemia 7.emergency surgery 8.type of surgery 9.coughing 10.wound infection
37 Conclusion A number of factors for abdominal wound dehiscence have been identified but the risk of developing abdominal wound dehiscence can be reduced by preventing pneumonia and wound infection, and by applying optimal surgical technique in every patient.
38 References Abdominal wound dehiscence in adults. Van Ramshorst et al. World J of Surg 2010;34: Prognostic models of wound dehiscence. Webster et al. J Surg Research 2003, 109: The biology of acute wound failure. Dubay et al. Surg Clin North Am 2003,83:
Abdominal Wound Dehiscence in Adults: Development and Validation of a Risk Model
 World J Surg (2010) 34:20 27 DOI 10.1007/s00268-009-0277-y Abdominal Wound Dehiscence in Adults: Development and Validation of a Risk Model Gabriëlle H. van Ramshorst Jeroen Nieuwenhuizen Wim C. J. Hop
World J Surg (2010) 34:20 27 DOI 10.1007/s00268-009-0277-y Abdominal Wound Dehiscence in Adults: Development and Validation of a Risk Model Gabriëlle H. van Ramshorst Jeroen Nieuwenhuizen Wim C. J. Hop
Risk Factors for Abdominal Wound Dehiscence in Children: A Case-Control Study
 World J Surg (2009) 33:1509 1513 DOI 10.1007/s00268-009-0058-7 Risk Factors for Abdominal Wound Dehiscence in Children: A Case-Control Study Gabriëlle H. van Ramshorst Æ Nathalie E. Salu Æ Nikolaas M.
World J Surg (2009) 33:1509 1513 DOI 10.1007/s00268-009-0058-7 Risk Factors for Abdominal Wound Dehiscence in Children: A Case-Control Study Gabriëlle H. van Ramshorst Æ Nathalie E. Salu Æ Nikolaas M.
Development of a Risk Model for Abdominal Wound Dehiscence
 Surgical Science, 2016, 7, 466-474 http://www.scirp.org/journal/ss ISSN Online: 2157-9415 ISSN Print: 2157-9407 Development of a Risk Model for Abdominal Wound Dehiscence Mujahid Ahmad Mir *, Farzana Manzoor,
Surgical Science, 2016, 7, 466-474 http://www.scirp.org/journal/ss ISSN Online: 2157-9415 ISSN Print: 2157-9407 Development of a Risk Model for Abdominal Wound Dehiscence Mujahid Ahmad Mir *, Farzana Manzoor,
Medieval times in surgery Still no solution for:
 Medieval times in surgery Still no solution for: The most frequent complications of the abdominal surgeon: Adhesions Postoperative ileus Incisional hernia Anastomotic leakage Wound infection Incidence
Medieval times in surgery Still no solution for: The most frequent complications of the abdominal surgeon: Adhesions Postoperative ileus Incisional hernia Anastomotic leakage Wound infection Incidence
Difficult Abdominal Closure. Mark A. Carlson, MD
 Difficult Abdominal Closure Mark A. Carlson, MD Illustrative case 14 yo boy with delayed diagnosis of appendicitis POD9 Appendectomy 2 wk after onset of symptoms POD4: return to OR for midline laparotomy
Difficult Abdominal Closure Mark A. Carlson, MD Illustrative case 14 yo boy with delayed diagnosis of appendicitis POD9 Appendectomy 2 wk after onset of symptoms POD4: return to OR for midline laparotomy
Development of incisional herniation after midline laparotomy
 Original article Development of incisional herniation after midline laparotomy J. J. Harlaar 1, E. B. Deerenberg 1, R. S. Dwarkasing 2, A. M. Kamperman 3, G. J. Kleinrensink 4, J. Jeekel 4 andj.f.lange
Original article Development of incisional herniation after midline laparotomy J. J. Harlaar 1, E. B. Deerenberg 1, R. S. Dwarkasing 2, A. M. Kamperman 3, G. J. Kleinrensink 4, J. Jeekel 4 andj.f.lange
International Journal of Current Research and Academic Review ISSN: Volume 3 Number 1 (January-2015) pp
 International Journal of Current Research and Academic Review ISSN: 2347-3215 Volume 3 Number 1 (January-2015) pp. 348-354 www.ijcrar.com Study of Operative Procedures and their Indications in Management
International Journal of Current Research and Academic Review ISSN: 2347-3215 Volume 3 Number 1 (January-2015) pp. 348-354 www.ijcrar.com Study of Operative Procedures and their Indications in Management
A Prospective Study of Incisional Hernia with An Evaluation of Factors In Developing Post-Operative Complications
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 3 Ver. I (March. 2017), PP 25-29 www.iosrjournals.org A Prospective Study of Incisional Hernia
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 3 Ver. I (March. 2017), PP 25-29 www.iosrjournals.org A Prospective Study of Incisional Hernia
Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan
 Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Determinants of Wound Dehiscence in Abdominal Surgery in Public Sector Hospital
 Determinants of Wound Dehiscence in Abdominal Surgery in Public Sector Hospital 1 AFZAL S., 2 BASHIR M.M. 1MBBS, MCPS, Demonstrator, Department of Community Medicine, King Edward Medical University Lahore
Determinants of Wound Dehiscence in Abdominal Surgery in Public Sector Hospital 1 AFZAL S., 2 BASHIR M.M. 1MBBS, MCPS, Demonstrator, Department of Community Medicine, King Edward Medical University Lahore
Factors affecting post-operative laparotomy wound complications
 Factors affecting post-operative laparotomy wound complications Original Research Article ISSN: 2394-0026 (P) Factors affecting post-operative laparotomy wound complications Khandra Hitesh P 1*, Vyas Pratik
Factors affecting post-operative laparotomy wound complications Original Research Article ISSN: 2394-0026 (P) Factors affecting post-operative laparotomy wound complications Khandra Hitesh P 1*, Vyas Pratik
34 yo M presented in ER of KCH at 7/06/10 Painful lump lt groin + vomiting Pain started 2 hrs before presentation. PMH known left inguinal hernia PSH
 Case Presentation 34 yo M presented in ER of KCH at 7/06/10 Painful lump lt groin + vomiting Pain started 2 hrs before presentation. PMH known left inguinal hernia PSH negative NKDA Case Presentation VS:
Case Presentation 34 yo M presented in ER of KCH at 7/06/10 Painful lump lt groin + vomiting Pain started 2 hrs before presentation. PMH known left inguinal hernia PSH negative NKDA Case Presentation VS:
Colostomy & Ileostomy
 Colostomy & Ileostomy Indications, problems and preference By Waleed Omar Professor of Colorectal surgery, Mansoura University. Disclosure I have no disclosures. Presentation outline Stoma: Definition
Colostomy & Ileostomy Indications, problems and preference By Waleed Omar Professor of Colorectal surgery, Mansoura University. Disclosure I have no disclosures. Presentation outline Stoma: Definition
Prevention and Surgical management of Parastomal hernias; When to treat?
 Prevention and Surgical management of Parastomal hernias; When to treat? Sabry A. Mahmoud (MD) Prof of General & Colorectal Surgery Mansoura University It is an incisional hernia that develops at the site
Prevention and Surgical management of Parastomal hernias; When to treat? Sabry A. Mahmoud (MD) Prof of General & Colorectal Surgery Mansoura University It is an incisional hernia that develops at the site
Abdominal wound dehiscence- A look into the risk factors
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 10 Ver. I (Oct. 2015), PP 47-54 www.iosrjournals.org Abdominal wound dehiscence- A look into
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 10 Ver. I (Oct. 2015), PP 47-54 www.iosrjournals.org Abdominal wound dehiscence- A look into
Hernia. emoryhealthcare.org
 Hernia Have you noticed a bulge or pain in your abdominal wall or groin? If so you may have a hernia. You may be in the process of confirming this diagnosis with your Primary Care Physician or already
Hernia Have you noticed a bulge or pain in your abdominal wall or groin? If so you may have a hernia. You may be in the process of confirming this diagnosis with your Primary Care Physician or already
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery doi: To be assigned Early view version published: November
: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery doi: To be assigned Early view version published: November
PREVENTION OF INCISIONAL HERNIA AFTER MIDLINE LAPAROTOMY FOR ABDOMINAL AORTIC ANEURYSM TREATMENT: A RANDOMIZED CONTROLLED TRIAL
 PREVENTION OF INCISIONAL HERNIA AFTER MIDLINE LAPAROTOMY FOR ABDOMINAL AORTIC ANEURYSM TREATMENT: A RANDOMIZED CONTROLLED TRIAL F. Muysoms 1, T. Vierendeels 2, M. Huyghe 3, M. Miserez 4, M. Ruppert 5,
PREVENTION OF INCISIONAL HERNIA AFTER MIDLINE LAPAROTOMY FOR ABDOMINAL AORTIC ANEURYSM TREATMENT: A RANDOMIZED CONTROLLED TRIAL F. Muysoms 1, T. Vierendeels 2, M. Huyghe 3, M. Miserez 4, M. Ruppert 5,
Open abdomen in trauma. Ari Leppäniemi Abdominal Center Meilahti hospital University of Helsinki Finland
 Open abdomen in trauma Ari Leppäniemi Abdominal Center Meilahti hospital University of Helsinki Finland Frequency and causes of open abdomen - in 23% (344/1531) after trauma laparotomies - damage control
Open abdomen in trauma Ari Leppäniemi Abdominal Center Meilahti hospital University of Helsinki Finland Frequency and causes of open abdomen - in 23% (344/1531) after trauma laparotomies - damage control
Hernias Umbilical Hernia When to See a Surgeon? What Are Symptoms of an Umbilical Hernia? How is Repair Performed?
 Hernias Umbilical Hernia An umbilical hernia occurs when part of the intestine protrudes through the umbilical opening in the abdominal muscles. Umbilical hernias are common and typically harmless. They
Hernias Umbilical Hernia An umbilical hernia occurs when part of the intestine protrudes through the umbilical opening in the abdominal muscles. Umbilical hernias are common and typically harmless. They
Farah S, Kiyingi A, Leinkram C. The Melbourne Hernia Clinic Masada Hospital 26 Balaclava Road St Kilda East Victoria, Australia 3168.
 Medium to Long term results following open intra-abdominal repair of large incisional hernias with a new composite polypropylene and silicone mesh, without components separation. Farah S, Kiyingi A, Leinkram
Medium to Long term results following open intra-abdominal repair of large incisional hernias with a new composite polypropylene and silicone mesh, without components separation. Farah S, Kiyingi A, Leinkram
Predicting Short Term Morbidity following Revision Hip and Knee Arthroplasty
 Predicting Short Term Morbidity following Revision Hip and Knee Arthroplasty A Review of ACS-NSQIP 2006-2012 Arjun Sebastian, M.D., Stephanie Polites, M.D., Kristine Thomsen, B.S., Elizabeth Habermann,
Predicting Short Term Morbidity following Revision Hip and Knee Arthroplasty A Review of ACS-NSQIP 2006-2012 Arjun Sebastian, M.D., Stephanie Polites, M.D., Kristine Thomsen, B.S., Elizabeth Habermann,
The use of synthetic mesh in patients undergoing ventral hernia repair during colorectal resection: Risk of infection and recurrence
 Asian Journal of Surgery (2012) 35, 149e153 Available online at www.sciencedirect.com journal homepage: www.e-asianjournalsurgery.com ORIGINAL ARTICLE The use of synthetic mesh in patients undergoing ventral
Asian Journal of Surgery (2012) 35, 149e153 Available online at www.sciencedirect.com journal homepage: www.e-asianjournalsurgery.com ORIGINAL ARTICLE The use of synthetic mesh in patients undergoing ventral
Paraesophageal Hernia
 Paraesophageal Hernia Inderpal (Netu) S. Sarkaria, M.D. Vice Chairman, Clinical Affairs Director, Robotic Thoracic Surgery Co-Director, Esophageal and Lung Surgery Institute Speaker/Education: Intuitive
Paraesophageal Hernia Inderpal (Netu) S. Sarkaria, M.D. Vice Chairman, Clinical Affairs Director, Robotic Thoracic Surgery Co-Director, Esophageal and Lung Surgery Institute Speaker/Education: Intuitive
The pillars defining our quality care. We Care!
 The pillars defining our quality care We Care! 1 An umbilical hernia occurs when a tissue bulges out through an opening in time muscles on the abdomen near the navel or belly button (umbilicus). About
The pillars defining our quality care We Care! 1 An umbilical hernia occurs when a tissue bulges out through an opening in time muscles on the abdomen near the navel or belly button (umbilicus). About
After this presentation and discussion, the participants should be able to:
 Tissue Repair Robert F. Diegelmann, Ph.D. OBJECTIVES After this presentation and discussion, the participants should be able to: 1. Define the biochemical responses to tissue injury 2. Describe the mechanisms
Tissue Repair Robert F. Diegelmann, Ph.D. OBJECTIVES After this presentation and discussion, the participants should be able to: 1. Define the biochemical responses to tissue injury 2. Describe the mechanisms
REINFORCED BIOSCAFFOLDS
 REINFORCED BIOSCAFFOLDS Midline Incisional Open OviTex 1S Resorbable Clinical Case Study: Open Abdomen Incisional Herniorrhaphy in Contaminated (CDC Class IV) Operative Field Performed by Dr. Michael Sawyer,
REINFORCED BIOSCAFFOLDS Midline Incisional Open OviTex 1S Resorbable Clinical Case Study: Open Abdomen Incisional Herniorrhaphy in Contaminated (CDC Class IV) Operative Field Performed by Dr. Michael Sawyer,
Vacuum-assisted close versus conventional treatment for postlaparotomy wound dehiscence
 ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2014.87.5.260 Annals of Surgical Treatment and Research Vacuum-assisted close versus conventional treatment for postlaparotomy
ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2014.87.5.260 Annals of Surgical Treatment and Research Vacuum-assisted close versus conventional treatment for postlaparotomy
Case Report. XCM Biologic Tissue Matrix. Components separation using sandwich technique for reconstruction of abdominal wall defect.
 Case Report XCM Biologic Tissue Matrix. Components separation using sandwich technique for reconstruction of abdominal wall defect. XCM Biologic Tissue Matrix. Components separation using sandwich technique
Case Report XCM Biologic Tissue Matrix. Components separation using sandwich technique for reconstruction of abdominal wall defect. XCM Biologic Tissue Matrix. Components separation using sandwich technique
The Abdominal Compartment Syndrome
 The Abdominal Compartment Syndrome Andre R. Campbell, MD, FACS, FACP, FCCM Professor of Surgery, UCSF Endowed Chair of Surgical Education San Francisco General Hospital Outline Case presentations Review
The Abdominal Compartment Syndrome Andre R. Campbell, MD, FACS, FACP, FCCM Professor of Surgery, UCSF Endowed Chair of Surgical Education San Francisco General Hospital Outline Case presentations Review
In any operation. Indications. Anaesthesia. Position of the patient. Incision. Steps of the operation. Complications.
 In any operation Indications. Anaesthesia. Position of the patient. Incision. Steps of the operation. Complications. Abdominal operation I position for operation Supine Abdominal operation I position for
In any operation Indications. Anaesthesia. Position of the patient. Incision. Steps of the operation. Complications. Abdominal operation I position for operation Supine Abdominal operation I position for
A Case Report of a Repair of a Ruptured Incisional Hernia Using Polypropylene Mesh and Component Separation Technique A Rambhajan, T Bernard ABSTRACT
 A Case Report of a Repair of a Ruptured Incisional Hernia Using Polypropylene Mesh and Component Separation Technique A Rambhajan, T Bernard ABSTRACT Incisional hernias are a common complication of laparotomies
A Case Report of a Repair of a Ruptured Incisional Hernia Using Polypropylene Mesh and Component Separation Technique A Rambhajan, T Bernard ABSTRACT Incisional hernias are a common complication of laparotomies
COMPLICATIONS OF HERNIA REPAIR
 COMPLICATIONS OF HERNIA REPAIR Stanley Rogers, MD Associate Clinical Professor of Surgery University of Califronia, San Francisco Paré was respected as a hernia specialist, and was known to have elevated
COMPLICATIONS OF HERNIA REPAIR Stanley Rogers, MD Associate Clinical Professor of Surgery University of Califronia, San Francisco Paré was respected as a hernia specialist, and was known to have elevated
LAPAROSCOPIC HERNIA REPAIR
 LAPAROSCOPIC HERNIA REPAIR Treating Your Hernia with Laparoscopy When You Have a Hernia Anyone can have a hernia. This is a weakness or tear in the wall of the abdomen. It often results from years of wear
LAPAROSCOPIC HERNIA REPAIR Treating Your Hernia with Laparoscopy When You Have a Hernia Anyone can have a hernia. This is a weakness or tear in the wall of the abdomen. It often results from years of wear
ACTIVE INCISION MANAGEMENT: A PLAN FOR PROTECTING YOUR SURGICAL RESULTS, YOUR PATIENTS AND YOUR HOSPITAL.
 ACTIVE INCISION MANAGEMENT: A PLAN FOR PROTECTING YOUR SURGICAL RESULTS, YOUR PATIENTS AND YOUR HOSPITAL. How active hands-on involvement in managing the incision healing process helps to protect your
ACTIVE INCISION MANAGEMENT: A PLAN FOR PROTECTING YOUR SURGICAL RESULTS, YOUR PATIENTS AND YOUR HOSPITAL. How active hands-on involvement in managing the incision healing process helps to protect your
Chapter 14 8/23/2016. Surgical Wound Care. Wound Classifications. Wound Healing. Classified According to. Phases
 Chapter 14 Surgical Wound Care All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Wound Classifications Classified According to Cause Incision
Chapter 14 Surgical Wound Care All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Wound Classifications Classified According to Cause Incision
Radial Artery Pedicle Flap To Cover Exposed Mesh After Abdominal Wound Dehiscence-An Easy Solution To A Difficult Problem
 ISPUB.COM The Internet Journal of Plastic Surgery Volume 6 Number 1 Radial Artery Pedicle Flap To Cover Exposed Mesh After Abdominal Wound Dehiscence-An Easy Solution To A Difficult Problem S Tripathy,
ISPUB.COM The Internet Journal of Plastic Surgery Volume 6 Number 1 Radial Artery Pedicle Flap To Cover Exposed Mesh After Abdominal Wound Dehiscence-An Easy Solution To A Difficult Problem S Tripathy,
Keyhole Laparoscopic Hernia Repairs: What s the Benefit for Your Patients?
 InTouch ARTICLE Keyhole Laparoscopic Hernia Repairs: What s the Benefit for Your Patients? Author: Mr Steve Warren Date: Mary 2015 17 19 View Road, Highgate, London, N6 4DJ Tel. 020 8341 4182 Email. enquiries@highgatehospital.co.uk
InTouch ARTICLE Keyhole Laparoscopic Hernia Repairs: What s the Benefit for Your Patients? Author: Mr Steve Warren Date: Mary 2015 17 19 View Road, Highgate, London, N6 4DJ Tel. 020 8341 4182 Email. enquiries@highgatehospital.co.uk
Abdominal Compartment Syndrome. Jeff Johnson, MD
 Abdominal Compartment Syndrome Jeff Johnson, MD Acute Care Surgeon, Denver Health Associate Professor of Surgery, University of Colorado Denver The Abdomen A Forgotten Closed Compartment Early Animal Models
Abdominal Compartment Syndrome Jeff Johnson, MD Acute Care Surgeon, Denver Health Associate Professor of Surgery, University of Colorado Denver The Abdomen A Forgotten Closed Compartment Early Animal Models
4/30/2010. Options for abdominal wall reconstruction. Scott L. Hansen, MD
 Components Separation Scott L. Hansen, MD University of California, San Francisco Chief, Plastic and Reconstructive Surgery San Francisco General Hospital Overview Options for abdominal wall reconstruction
Components Separation Scott L. Hansen, MD University of California, San Francisco Chief, Plastic and Reconstructive Surgery San Francisco General Hospital Overview Options for abdominal wall reconstruction
Facing a Hernia Repair?
 Facing a Hernia Repair? Learn about minimally invasive da Vinci Surgery www.olarts.com The Condition: Hernia A hernia happens when part of an internal organ or tissue bulges through a hole or weak area
Facing a Hernia Repair? Learn about minimally invasive da Vinci Surgery www.olarts.com The Condition: Hernia A hernia happens when part of an internal organ or tissue bulges through a hole or weak area
COMPARISON BETWEEN SUTURING AND NON-SUTURING OF SUBCUTANEOUS TISSUE IN ELECTIVE ABDOMINAL SURGERIES
 COMPARISON BETWEEN SUTURING AND NON-SUTURING OF SUBCUTANEOUS TISSUE IN ELECTIVE ABDOMINAL SURGERIES *Amit Pal Singh Bawa, Kulwant Singh Ded and Rana Ranjit Singh Department of Surgery, Sri Guru Ramdas
COMPARISON BETWEEN SUTURING AND NON-SUTURING OF SUBCUTANEOUS TISSUE IN ELECTIVE ABDOMINAL SURGERIES *Amit Pal Singh Bawa, Kulwant Singh Ded and Rana Ranjit Singh Department of Surgery, Sri Guru Ramdas
SURGICAL TREATMENT OF INCISIONAL HERNIAS
 UNIVERSITY OF MEDICINE AND FARMACY CRAIOVA PhD School PhD Thesis Abstract SURGICAL TREATMENT OF INCISIONAL HERNIAS Scientific coordinator: PROF.UNIV.DR. DAN MOGOȘ PhD Student: SFECLAN MARIA CRISTINA CRAIOVA
UNIVERSITY OF MEDICINE AND FARMACY CRAIOVA PhD School PhD Thesis Abstract SURGICAL TREATMENT OF INCISIONAL HERNIAS Scientific coordinator: PROF.UNIV.DR. DAN MOGOȘ PhD Student: SFECLAN MARIA CRISTINA CRAIOVA
Using NSQIP as a Platform for Registries Challenges and Potential Solutions
 Using NSQIP as a Platform for Registries Challenges and Potential Solutions Mary Hawn MD, MPH FACS Professor and Chief of Gastrointestinal Surgery University of Alabama at Birmingham NSQIP Annual Meeting
Using NSQIP as a Platform for Registries Challenges and Potential Solutions Mary Hawn MD, MPH FACS Professor and Chief of Gastrointestinal Surgery University of Alabama at Birmingham NSQIP Annual Meeting
Skin Integrity and Wound Care
 Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
INCISIONAL HERNIAS. Contents What is an Incisional Hernia?... 3
 Contents What is an Incisional Hernia?................... 3 When can I return to normal activities?....... 6 YOUR GUIDE TO INCISIONAL HERNIAS An IPRS Guide to provide you with exercises and advice to ease
Contents What is an Incisional Hernia?................... 3 When can I return to normal activities?....... 6 YOUR GUIDE TO INCISIONAL HERNIAS An IPRS Guide to provide you with exercises and advice to ease
The Efficacy of NPWT on Primary Closed Incisions
 The Efficacy of NPWT on Primary Closed Incisions Pieter Zwanenburg Researcher / PhD Candidate Marja Boermeester Professor of Surgery, Academic Medical Center, Amsterdam Incisional Negative Pressure Wound
The Efficacy of NPWT on Primary Closed Incisions Pieter Zwanenburg Researcher / PhD Candidate Marja Boermeester Professor of Surgery, Academic Medical Center, Amsterdam Incisional Negative Pressure Wound
One hundred percent fascial approximation with sequential abdominal closure of the open abdomen
 The American Journal of Surgery 192 (2006) 238 242 HowIdoit One hundred percent fascial approximation with sequential abdominal closure of the open abdomen C. Clay Cothren, M.D. a,b, *, Ernest E. Moore,
The American Journal of Surgery 192 (2006) 238 242 HowIdoit One hundred percent fascial approximation with sequential abdominal closure of the open abdomen C. Clay Cothren, M.D. a,b, *, Ernest E. Moore,
ISSN X (Print) Research Article. *Corresponding author Dr. Umeshchandra D.G
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(1B):80-84 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(1B):80-84 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
The Emergency Hernia or The call you don t want at 2:00 a.m.*
 or The call you don t want at 2:00 a.m.* *Or even at 8:00 a.m. Michael G. Sarr, MD Professor of Surgery Mayo Clinic South Canada WEST CANADA EAST CANADA Clinical talk Hernias Inguinal Umbilical Incisional
or The call you don t want at 2:00 a.m.* *Or even at 8:00 a.m. Michael G. Sarr, MD Professor of Surgery Mayo Clinic South Canada WEST CANADA EAST CANADA Clinical talk Hernias Inguinal Umbilical Incisional
Present-on-Admission (POA) Coding
 1 Present-on-Admission (POA) Coding Michael Pine, MD, MBA Michael Pine and Associates, Inc 2 POA and Coding Guidelines (1) Unless otherwise specified, a POA modifier must be assigned to each principal
1 Present-on-Admission (POA) Coding Michael Pine, MD, MBA Michael Pine and Associates, Inc 2 POA and Coding Guidelines (1) Unless otherwise specified, a POA modifier must be assigned to each principal
AIDA Study:Primary Onlay Mesh Augmentation following AAA Repair Prevents Incisional Hernia a Multicenter Randomized Trial
 AIDA Study:Primary Onlay Mesh Augmentation following AAA Repair Prevents Incisional Hernia a Multicenter Randomized Trial ES Debus, H. Diener Department for Vascular Medicine, University Heart Center Hamburg
AIDA Study:Primary Onlay Mesh Augmentation following AAA Repair Prevents Incisional Hernia a Multicenter Randomized Trial ES Debus, H. Diener Department for Vascular Medicine, University Heart Center Hamburg
POLSKI 2014, 86, 2, 68 72
 POLSKI PRZEGLĄD CHIRURGICZNY 2014, 86, 2, 68 72 10.2478/pjs-2014-0012 Mesh repair of umbilical hernia without a visible abdominal scar Waldemar Kurpiewski 1, Michał Kiliańczyk 1, Rafał Szynkarczuk 1, Michał
POLSKI PRZEGLĄD CHIRURGICZNY 2014, 86, 2, 68 72 10.2478/pjs-2014-0012 Mesh repair of umbilical hernia without a visible abdominal scar Waldemar Kurpiewski 1, Michał Kiliańczyk 1, Rafał Szynkarczuk 1, Michał
PAPER. Umbilical Hernia Repair in Patients With Signs
 PAPER Umbilical Hernia Repair in Patients With Signs of Portal Hypertension Surgical Outcome and Predictors of Mortality Sung W. Cho, MB, BS, MSc; Neil Bhayani, MD; Pippa Newell, MD; Maria A. Cassera,
PAPER Umbilical Hernia Repair in Patients With Signs of Portal Hypertension Surgical Outcome and Predictors of Mortality Sung W. Cho, MB, BS, MSc; Neil Bhayani, MD; Pippa Newell, MD; Maria A. Cassera,
INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP
 INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify
INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify
Masatoku Arai 1*, Shiei Kim 1, Hiromoto Ishii 1, Jun Hagiwara 1, Shigeki Kushimoto 2 and Hiroyuki Yokota 1
 Arai et al. World Journal of Emergency Surgery (2018) 1:9 https://doi.org/10.118/s1017-018-0200-7 RESEARCH ARTICLE Open Access The long-term outcomes of early abdominal wall reconstruction by bilateral
Arai et al. World Journal of Emergency Surgery (2018) 1:9 https://doi.org/10.118/s1017-018-0200-7 RESEARCH ARTICLE Open Access The long-term outcomes of early abdominal wall reconstruction by bilateral
Surgical Wound Infection in Clean-Contaminated and Contaminated Laparotomy Wounds at Muhimbili National Hospital.
 Original Article 19 Surgical Wound Infection in Clean-Contaminated and Contaminated Laparotomy Wounds at Muhimbili National Hospital. E.V. Ussiri 1, C.A. Mkony 2, M.R. Aziz 2. 1 Specialist Surgeon, 2 Associate
Original Article 19 Surgical Wound Infection in Clean-Contaminated and Contaminated Laparotomy Wounds at Muhimbili National Hospital. E.V. Ussiri 1, C.A. Mkony 2, M.R. Aziz 2. 1 Specialist Surgeon, 2 Associate
More than 150 consecutive open umbilical hernia repairs in a major Veterans Administration Medical Center
 The American Journal of Surgery (2008) 196, 647 651 The Association of VA Surgeons More than 150 consecutive open umbilical hernia repairs in a major Veterans Administration Medical Center Buckminster
The American Journal of Surgery (2008) 196, 647 651 The Association of VA Surgeons More than 150 consecutive open umbilical hernia repairs in a major Veterans Administration Medical Center Buckminster
Surgery for Complications of Peptic Ulcer Disease (Definitive Treatment)
 Surgery for Complications of Peptic Ulcer Disease (Definitive Treatment) Amid Keshavarzi, MD UCHSC Grand Round 3/20/2006 Department of Surgery Introduction Epidemiology Pathophysiology Clinical manifestation
Surgery for Complications of Peptic Ulcer Disease (Definitive Treatment) Amid Keshavarzi, MD UCHSC Grand Round 3/20/2006 Department of Surgery Introduction Epidemiology Pathophysiology Clinical manifestation
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of reinforcement of a permanent stoma with mesh to prevent a parastomal hernia A
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of reinforcement of a permanent stoma with mesh to prevent a parastomal hernia A
Tissue repair. (3&4 of 4)
 Tissue repair (3&4 of 4) What will we discuss today: Regeneration in tissue repair Scar formation Cutaneous wound healing Pathologic aspects of repair Regeneration in tissue repair Labile tissues rapid
Tissue repair (3&4 of 4) What will we discuss today: Regeneration in tissue repair Scar formation Cutaneous wound healing Pathologic aspects of repair Regeneration in tissue repair Labile tissues rapid
Information for patients (and their families) waiting for liver transplantation
 Information for patients (and their families) waiting for liver transplantation Waiting list? What is liver transplant? Postoperative conditions? Ver.: 5/2017 1 What is a liver transplant? Liver transplantation
Information for patients (and their families) waiting for liver transplantation Waiting list? What is liver transplant? Postoperative conditions? Ver.: 5/2017 1 What is a liver transplant? Liver transplantation
A multiple logistic regression analysis of complications following microsurgical breast reconstruction
 Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
Optimizing Hernia Care (It is more than patching a hole!)
 Optimizing Hernia Care (It is more than patching a hole!) Bulent Cetindag M.D. Associate Professor of Surgery University of Iowa Carver College of Medicine Goal of Optimizing Three hundred fifty thousand
Optimizing Hernia Care (It is more than patching a hole!) Bulent Cetindag M.D. Associate Professor of Surgery University of Iowa Carver College of Medicine Goal of Optimizing Three hundred fifty thousand
Citation for published version (APA): Bartels, S. A. L. (2013). Laparoscopic colorectal surgery: beyond the short-term effects
 UvA-DARE (Digital Academic Repository) Laparoscopic colorectal surgery: beyond the short-term effects Bartels, S.A.L. Link to publication Citation for published version (APA): Bartels, S. A. L. (2013).
UvA-DARE (Digital Academic Repository) Laparoscopic colorectal surgery: beyond the short-term effects Bartels, S.A.L. Link to publication Citation for published version (APA): Bartels, S. A. L. (2013).
Causes and management of surgical wound dehiscence
 Causes and management of surgical wound dehiscence Michael S. Eisenstat, M.D. # Stanley O. Hoerr, M.D. Department of General Surgery Dehiscence of the wound after abdominal surgery is a serious complication
Causes and management of surgical wound dehiscence Michael S. Eisenstat, M.D. # Stanley O. Hoerr, M.D. Department of General Surgery Dehiscence of the wound after abdominal surgery is a serious complication
JMSCR Vol 04 Issue 04 Page April 2016
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 5.88 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i4.44 Clinical study of Incisional Hernia Authors
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 5.88 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i4.44 Clinical study of Incisional Hernia Authors
Discussion of Complex Clinical Scenarios and Variable Review ACS NSQIP Clinical Support Team
 Discussion of Complex Clinical Scenarios and Variable Review CS NSQIP Clinical Support Team SCR Open Q& Calls The CS NSQIP Clinical Team is trialing Open format Q& calls for NSQIP SCRs Participation in
Discussion of Complex Clinical Scenarios and Variable Review CS NSQIP Clinical Support Team SCR Open Q& Calls The CS NSQIP Clinical Team is trialing Open format Q& calls for NSQIP SCRs Participation in
A FAMILY HISTORY OF ABDOMINAL AORTIC ANEURYSM (AAA) DISEASE
 Important Information for You and Your Family A FAMILY HISTORY OF ABDOMINAL AORTIC ANEURYSM (AAA) DISEASE Have you been diagnosed with AAA disease? There is a 15% chance that one of your family members
Important Information for You and Your Family A FAMILY HISTORY OF ABDOMINAL AORTIC ANEURYSM (AAA) DISEASE Have you been diagnosed with AAA disease? There is a 15% chance that one of your family members
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
LAPAROSCOPIC APPENDICECTOMY
 LAPAROSCOPIC APPENDICECTOMY WHAT IS THE APPENDIX? The appendix is a small, fingerlike pouch of the intestinal tract located where the small and large join. It has no known use. It is postulated that the
LAPAROSCOPIC APPENDICECTOMY WHAT IS THE APPENDIX? The appendix is a small, fingerlike pouch of the intestinal tract located where the small and large join. It has no known use. It is postulated that the
Laparoscopic umbilical herniorrhaphy: a novel technique of hernia neck closure and outcomes in the first 19 cases
 Original Article Page 1 of 7 Laparoscopic umbilical herniorrhaphy: a novel technique of hernia neck closure and outcomes in the first 19 cases Cheyenne Vetter 1, Yagan Pillay 2 1 Department of Family Medicine,
Original Article Page 1 of 7 Laparoscopic umbilical herniorrhaphy: a novel technique of hernia neck closure and outcomes in the first 19 cases Cheyenne Vetter 1, Yagan Pillay 2 1 Department of Family Medicine,
SCOPE OF PRACTICE PGY-6 PGY-7 PGY-8
 PGY-6 Round on all plastic surgery inpatients every day. Assess progress of patients and identify real or potential problems. Review patients progress with attending physicians daily and participate in
PGY-6 Round on all plastic surgery inpatients every day. Assess progress of patients and identify real or potential problems. Review patients progress with attending physicians daily and participate in
Robotic Ventral Hernia Repair and Endoscopic Component Separation: Outcomes
 SCIENTIFIC PAPER Robotic Ventral Hernia Repair and Endoscopic Component Separation: Outcomes Rodolfo J. Oviedo, MD, FACS, Jarrod C. Robertson, MD, Apurva Sunder Desai, BS ABSTRACT Background and Objectives:
SCIENTIFIC PAPER Robotic Ventral Hernia Repair and Endoscopic Component Separation: Outcomes Rodolfo J. Oviedo, MD, FACS, Jarrod C. Robertson, MD, Apurva Sunder Desai, BS ABSTRACT Background and Objectives:
Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery
 SCIENTIFIC PAPER Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery Steven J. Binenbaum, MD, Michael A. Goldfarb, MD ABSTRACT Background: Inadvertent enterotomy (IE) in laparoscopic abdominal
SCIENTIFIC PAPER Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery Steven J. Binenbaum, MD, Michael A. Goldfarb, MD ABSTRACT Background: Inadvertent enterotomy (IE) in laparoscopic abdominal
Healing & Repair. Tissue Regeneration
 Healing & Repair Dr. Srikumar Chakravarthi Repair & Healing: Are they same? Repair :Regeneration of injured cells by cells of same type, as with regeneration of skin/oral mucosa (requires basement membrane)
Healing & Repair Dr. Srikumar Chakravarthi Repair & Healing: Are they same? Repair :Regeneration of injured cells by cells of same type, as with regeneration of skin/oral mucosa (requires basement membrane)
Further information You can get more information and share your experience at
 UG13 Elective Splenectomy Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from:......... Taunton and
UG13 Elective Splenectomy Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from:......... Taunton and
Supplementary Online Content
 Supplementary Online Content Bhangu A, Singh P, Lundy J, Bowley DM. Systemic review and meta-analysis of randomized clinical trials comparing primary vs delayed primary skin closure in contaminated and
Supplementary Online Content Bhangu A, Singh P, Lundy J, Bowley DM. Systemic review and meta-analysis of randomized clinical trials comparing primary vs delayed primary skin closure in contaminated and
INFORMED CONSENT FOR LAPAROSCOPIC ADJUSTABLE GASTRIC BAND. Please read this form carefully and ask about anything you may not understand.
 Please read this form carefully and ask about anything you may not understand. I consent to undergo laparoscopic placement of a laparoscopic Adjustable Gastric Band for the purposes of weight loss. I met
Please read this form carefully and ask about anything you may not understand. I consent to undergo laparoscopic placement of a laparoscopic Adjustable Gastric Band for the purposes of weight loss. I met
A Clinical Study on Incisional Hernia: Anatomical Repair V/S Mesh Repair
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/1 A Clinical Study on Incisional Hernia: Anatomical Repair V/S Mesh Repair Gandla Anil Kumar 1, Bejjamshetty Nagendar
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/1 A Clinical Study on Incisional Hernia: Anatomical Repair V/S Mesh Repair Gandla Anil Kumar 1, Bejjamshetty Nagendar
MBSAQIP Complex Clinical Scenarios & Variable Review
 MBSAQIP Complex Clinical Scenarios & Variable Review Disclosure The following planners, speakers, moderators, and/or panelists of the CME/CEU activity have no relevant financial relationships with commercial
MBSAQIP Complex Clinical Scenarios & Variable Review Disclosure The following planners, speakers, moderators, and/or panelists of the CME/CEU activity have no relevant financial relationships with commercial
Abdominal Wound Dehiscence in Interrupted Versus Continuous Closure of Rectus Sheath after Midline Emergency Laparotomy Incision
 ORIGINAL ARTICLE OPEN ACCESS Abdominal Wound Dehiscence in Interrupted Versus Continuous Closure of Rectus Sheath after Midline Emergency Urooj Akmal, 1 * Abdul Qaiyoume Amini, 1 Shahida Perveen Afridi
ORIGINAL ARTICLE OPEN ACCESS Abdominal Wound Dehiscence in Interrupted Versus Continuous Closure of Rectus Sheath after Midline Emergency Urooj Akmal, 1 * Abdul Qaiyoume Amini, 1 Shahida Perveen Afridi
Surgery to remove the spleen (elective splenectomy)
 Surgery to remove the spleen (elective splenectomy) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that
Surgery to remove the spleen (elective splenectomy) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that
East and Central African Journal of Surgery Volume 15 Number 2. July/August 2010.
 The Predictors, Prevalence and Outcome of Burst Abdomen in Emergency Paediatric Surgical Centre. O.D. Osifo, M.E. Ovueni. Pediatric Surgery Unit, Department of Surgery, University of Benin Teaching Hospital,
The Predictors, Prevalence and Outcome of Burst Abdomen in Emergency Paediatric Surgical Centre. O.D. Osifo, M.E. Ovueni. Pediatric Surgery Unit, Department of Surgery, University of Benin Teaching Hospital,
DGAFMS MEDICAL MEMORANDUM ON INGUINAL HERNIA AND THEIR DISPOSAL. 2. Three Primary causes can be distinguished in the etiology of Hernia.
 DGAFMS MEDICAL MEMORANDUM ON INGUINAL HERNIA AND THEIR DISPOSAL Definition :- 1. Hernia is defined as the protrusion of a viscus on part of a viscus through an abnormal opening. Etiology : 2. Three Primary
DGAFMS MEDICAL MEMORANDUM ON INGUINAL HERNIA AND THEIR DISPOSAL Definition :- 1. Hernia is defined as the protrusion of a viscus on part of a viscus through an abnormal opening. Etiology : 2. Three Primary
Damage Control in Abdominal and Pelvic Injuries
 Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
Mr John Groom The Complete Guide to Hernia
 Mr John Groom The Complete Guide to Hernia What Do They Have in Common? AA Both Subjects Controversial! Debate 1. Laparoscopic verses Open Hernia Repair Beautiful Big splash Debate 2. Use of Mesh in Hernia
Mr John Groom The Complete Guide to Hernia What Do They Have in Common? AA Both Subjects Controversial! Debate 1. Laparoscopic verses Open Hernia Repair Beautiful Big splash Debate 2. Use of Mesh in Hernia
7/2/2015. Incidence. *Mudge M et al, Br. J. Surg, 1985, 72:70-71
 Ventral Hernia Repair: Revisonal Surgery Natan Zundel MD FACS Professor of Surgery Vice-Chairman Department of Surgery FIU Herbert Wertheim College of Medicine. Miami Florida DISCLOSURE Ethicon Endosurgery
Ventral Hernia Repair: Revisonal Surgery Natan Zundel MD FACS Professor of Surgery Vice-Chairman Department of Surgery FIU Herbert Wertheim College of Medicine. Miami Florida DISCLOSURE Ethicon Endosurgery
Setting The study setting was tertiary care. The economic study was carried out in the USA.
 Laparoscopic intraperitoneal polytetrafluoroethylene (PTFE) prosthetic patch repair of ventral hernia: prospective comparison to open prefascial polypropylene mesh repair DeMaria E J, Moss J M, Sugerman
Laparoscopic intraperitoneal polytetrafluoroethylene (PTFE) prosthetic patch repair of ventral hernia: prospective comparison to open prefascial polypropylene mesh repair DeMaria E J, Moss J M, Sugerman
Incisional hernia: risk factors, clinical presentations, and pre-peritoneal polypropylene mesh repair
 International Surgery Journal Inamdar MF et al. Int Surg J. 2017 Apr;4(4):1189-1194 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20170896
International Surgery Journal Inamdar MF et al. Int Surg J. 2017 Apr;4(4):1189-1194 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20170896
Photo Diagnosis. Case 1 The upper lip of this three-year-old boy became swollen and itchy an hour after he had ingested some peanuts.
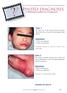 An illustrated quiz on problems seen in everyday practice Case 1 The upper lip of this three-year-old boy became swollen and itchy an hour after he had ingested some peanuts. 2. What is the treatment?
An illustrated quiz on problems seen in everyday practice Case 1 The upper lip of this three-year-old boy became swollen and itchy an hour after he had ingested some peanuts. 2. What is the treatment?
In two cases, fundamentally: - Bilateral inguinal hernia recurrent groin hernia, already treated with open surgery
 3.- What cases the hernia? It is unknown. Sometimes it is related to violent exercise or some trauma; you begin feeling discomfort and later the lump appears in the groin. It is also related to chronic
3.- What cases the hernia? It is unknown. Sometimes it is related to violent exercise or some trauma; you begin feeling discomfort and later the lump appears in the groin. It is also related to chronic
Factors Influencing Morbidity after Rectopexy for Posterior Pelvic Floor Disorders
 Factors Influencing Morbidity after Rectopexy for Posterior Pelvic Floor Disorders Ayca Fatma Gultekin 1, Jean-Benoit Hardouin 2, Guilé Romain 3, Myriam Boutami 1, Paul-Antoine Lehur 1, Guillaume Meurette
Factors Influencing Morbidity after Rectopexy for Posterior Pelvic Floor Disorders Ayca Fatma Gultekin 1, Jean-Benoit Hardouin 2, Guilé Romain 3, Myriam Boutami 1, Paul-Antoine Lehur 1, Guillaume Meurette
Bariatric Surgery Risk Education Packet Walter J. Chlysta MD, FACS
 Date: Patient Name: Height: Weight: Ideal Body Weight: Excess Weight: Realistic Gastric Bypass Weight Goal (77 % Excess weight loss): Realistic Sleeve Gastrectomy Weight Goal (70 % Excess weight loss):
Date: Patient Name: Height: Weight: Ideal Body Weight: Excess Weight: Realistic Gastric Bypass Weight Goal (77 % Excess weight loss): Realistic Sleeve Gastrectomy Weight Goal (70 % Excess weight loss):
Clinical Questions. Clinical Questions. Clinical Questions. Health-Process-Evidencebased Clinical Practice Guidelines Acute Abdomen
 Health-Process-Evidencebased Clinical Practice Guidelines Acute Abdomen 1. What is an operational concept of acute abdomen? any abdominal condition of acute onset from various causes involving the intraabdominal
Health-Process-Evidencebased Clinical Practice Guidelines Acute Abdomen 1. What is an operational concept of acute abdomen? any abdominal condition of acute onset from various causes involving the intraabdominal
-DVT and PE Reduction Strategy in AWR- Can We Win? Luciano Tastaldi, MD
 -DVT and PE Reduction Strategy in AWR- Can We Win? Luciano Tastaldi, MD Summary of the Project Objectives Present Numbers Evolution Challenges of Implementation Discuss Future Directions -Problem at CCF-
-DVT and PE Reduction Strategy in AWR- Can We Win? Luciano Tastaldi, MD Summary of the Project Objectives Present Numbers Evolution Challenges of Implementation Discuss Future Directions -Problem at CCF-
Suture antibatteriche: mito o realtà? Michele Zuolo U.O Chirurgia Generale Ospedale «Valli del Noce» Cles Direttore: Dott. M.
 Suture antibatteriche: mito o realtà? Michele Zuolo U.O Chirurgia Generale Ospedale «Valli del Noce» Cles Direttore: Dott. M. Rigamonti Background Triclosan: agente antisettico (5-cloro-2-(2,4-diclorofenossi)
Suture antibatteriche: mito o realtà? Michele Zuolo U.O Chirurgia Generale Ospedale «Valli del Noce» Cles Direttore: Dott. M. Rigamonti Background Triclosan: agente antisettico (5-cloro-2-(2,4-diclorofenossi)
Form 1: Demographics
 Form 1: Demographics Case Number: *LMRN: *DOB: / / *Gender: Male Female *Race: White Native Hawaiian/Other Pacific Islander Black or African American Asian American Indian or Alaska Native Unknown *Hispanic
Form 1: Demographics Case Number: *LMRN: *DOB: / / *Gender: Male Female *Race: White Native Hawaiian/Other Pacific Islander Black or African American Asian American Indian or Alaska Native Unknown *Hispanic
EXPLANATION OF HISTORY PRESENTATION OR REPORTING FOR A PATIENT WITH INGUINAL HERNIA INCLUDING ALGORITHM IN RESPONSE
 EXPLANATION OF HISTORY PRESENTATION OR REPORTING FOR A PATIENT WITH INGUINAL HERNIA INCLUDING ALGORITHM IN RESPONSE TO THE QUESTION; EXAMINE THIS PATIENT S GROIN? In this article the trainee will find
EXPLANATION OF HISTORY PRESENTATION OR REPORTING FOR A PATIENT WITH INGUINAL HERNIA INCLUDING ALGORITHM IN RESPONSE TO THE QUESTION; EXAMINE THIS PATIENT S GROIN? In this article the trainee will find
Open Incisional Hernia Repair
 www.mogodaysurgery.com.au Mr. Sanjay Singh MBBS, MS, FRACS, FRCS (UK) Consultant Surgeon 2-4 Charles Street MOGO NSW 2536 Tel: 02 4474 3774 Fax: 02 4474 3775 Write questions or notes here: Open Incisional
www.mogodaysurgery.com.au Mr. Sanjay Singh MBBS, MS, FRACS, FRCS (UK) Consultant Surgeon 2-4 Charles Street MOGO NSW 2536 Tel: 02 4474 3774 Fax: 02 4474 3775 Write questions or notes here: Open Incisional
