Proximal Gastric Vagotomy Without Drainage for Treatment of Perforated Duodenal Ulcer
|
|
|
- Felix Rich
- 6 years ago
- Views:
Transcription
1 GASTROENTEROLOGY 1982; Proximal Gastric Vagotomy Without Drainage for Treatment of Perforated Duodenal Ulcer PAUL H. JORDAN, Jr. Surgical Services of the Cora and Webb Mading Department of Surgery, Baylor College of Medicine, and the Veterans Administration Medical Center, Houston, Texas One hundred and nine patients with perforated duodenal ulcer were treated by operation between 1973 and The operations performed included simple closure in 37 patients, vagotomy and drainage or gastric resection in 12 patients, and proximal gastric vagotomy without drainage and with omental patch of the perforation in 60 patients. Patients who were treated by proximal gastric vagotomy have been observed for 1-8 yr and form the basis of this study. There was no operative mortality. One patient with a postoperative infection required secondary drainage and a second patient with intestinal obstruction required lysis of adhesions. There were no other important complications. Persistent mild dumping occurred in 1 patient. Diarrhea was not a complication for any patient. One patient developed a recurrent ulcer and underwent truncal vagotomy and pyloroplasty. All patients except the patient with a recurrent ulcer had a Visick grading of lor II. Proximal gastric vagotomy, omental patch of the ulcer, and no drainage procedure is the ideal operation for patients who are candidates for definitive treatment of a perforated duodenal ulcer. In 1976 (1) we reported excellent, early results of proximal gastric vagotomy (PGV) and omental patch for treatment of perforated duodenal ulcers. In our opinion, this procedure was ideal to protect patients with a perforated ulcer against further ulcer complications. This report extends the previous study by presenting the 1-8 yr follow-up study results of this method performed upon 60 patients with a perforated duodenal ulcer. It was emphasized in the previous report that the opinion regarding the relative Received September 30, Accepted January 25, Address request for reprints to: Paul H. Jordan, [r., M.D., 1200 Moursund, Houston, Texas by the American Gastroenterological Association /82/ $02.50 merits of definitive surgery or simple closure of a perforated ulcer did not rest entirely on the operative risk of the two methods of therapy. If poor risk patients, either because of their specific medical problems or because of complications of peritonitis, are relegated to simple closure, the remaining patients can undergo either definitive surgery or simple closure with virtually no mortality. The problem is the identification of patients who should undergo definitive surgery in order to avoid further ulcer complications. The major concern regarding the use of definitive surgery rather than simple closure is the possibility that as a consequence of a definitive operation, gastric symptoms might unnecessarily be inflicted upon a patient who would not have had further ulcer-related symptoms after simple closure. Two-thirds to three-fourths of the patients with perforated duodenal ulcer will have further significant ulcer symptoms after simple closure. Yet, a certain number of patients who because of their age, sex, and chronic history might be expected to have further ulcer symptoms do not. In other patients the need for a definitive operation is not recognized because they fail to reveal their chronic peptic ulcer history until after recovery from operation. These patients fail to give an accurate history because the pain of perforation is so great that their previous symptoms fade into insignificance by comparison. Failure to perform definitive operation in these patients partially accounts for subsequent peptic ulcer symptoms after simple closure in 14%-25% of patients thought to have an acute ulcer (2-5). It is difficult to recommend truncal vagotomy and antrectomy or pyloroplasty for all patients with perforated duodenal ulcer because these procedures, associated with identifiable postoperative sequelae, are unnecessary in approximately 15%-20% of patients with chronic ulcers and 75% of patients with acute ulcers. The specific patients who are at risk of
2 180 JORDAN GASTROENTEROLOGY Vol. 83, No.1, Part 2 having an unnecessary definitive operation cannot be identified at time of operation. Our objectives for the ideal definitive operation for perforated duodenal ulcer patients are a negligible mortality rate, no postoperative gastric sequelae, and good protection against recurrent ulcers. During the past 8 yr, PGV without drainage and with omental patch of the perforation was performed in 60 patients with perforated duodenal ulcer in whom it was considered safe and technically possible to perform a definitive procedure. In our opinion PGV provides excellent definitive treatment of a perforated duodenal ulcer without the fear that patients might have incapacitating gastric symptoms develop as the result of an operation that they might not have needed. Patients and Methods Between August 1973 and November 1980, 109 patients were operated upon for perforated duodenal ulcer. Treatment consisted of simple closure of the ulcer using an omental patch in 37 patients, PGV without drainage and closure of the ulcer with an omental patch in 60 patients, and other definitive methods including vagotomy, antrectomy, and Billroth I or II in 6 patients, vagotomy and drainage in 4 patients, and antrectomy and Billroth II in 2 patients. No patient during this period was treated knowingly by a nonoperative approach. This paper is based primarily upon the 60 patients who were observed 1-8 yr after treatment of their perforated duodenal ulcer by PGV. Their mean age was 47 yr (range, yr). The mean time from perforation to operation was 9 h (range, 4-24 h). The length of ulcer history of the patient before perforation was no history in 3 patients, less than 3 mo in 5 patients, 3-12 mo in 4 patients, more than 1 yr in 48 patients, and more than 5 yr in 33 patients. The length of ulcer history was ascertained after operation in many patients because they denied having ulcer symptoms preoperatively. Ten patients who had definitive surgery other than PGV and a few of the patients in whom simple closure was performed would have been candidates for PGV had the author been available to supervise the operations. Two patients underwent definitive operations other than PGV because of a second duodenal ulcer that was bleeding. Three patients had a simple closure rather than PGV because the inflammatory response obscured the nerves of Latarjet so that they could not be identified satisfactorily. Ancillary procedures at the time of PGV included an antireflux procedure in 2 patients and appendectomy in 3 patients. Splenectomy was required as a consequence of splenic injury in 3 patients. The ulcers were not closed until after the vagotomy in order to prevent dislodgement of the omental patch from the ulcer during the manipulation required by the vagotomy. When the adequacy of the pyloric lumen was questioned, a 40F dilator was passed through the mouth and into the stomach. Passage of the dilator through the pylo- rus and into the duodenum without the application of force insured against postoperative obstruction. The abdomens were liberally irrigated with saline and antibiotics begun preoperatively were continued for an appropriate period postoperatively. After operation, efforts were made to interview patients at 6 and 12 mo and every 12 mo thereafter. All patients were not, however, studied at each time interval. The patients who were treated for perforation were more recalcitrant and less cooperative to undergo postoperative studies than those who had undergone elective operations. Many of the follow-up evaluations were done by telephone. Basal acid output (BAO) and maximal acid output (MAO) in response to histolog were tested at these time intervals if the patients permitted. The clinical results were graded at each time period according to the Visick classification. Results The results of treatment of those patients undergoing simple closure are seen in Table 1. Factors contributing to the 20 deaths in the 37 patients who underwent simple closure included head and neck and pulmonary cancer in 6 patients, chronic obstructive pulmonary disease treated with steroids in 5, over the age of 70 yr and emaciation in 3, severe cardiac pathologic features in 4, renal failure and on dialysis in 2, surgery delayed by 2 wk in 2, ischemic colitis in 1, and reoperation required for bleeding from a second ulcer in 1 patient. The results of definitive therapy by means other than PGV involved too few patients to make an analysis meaningful. There was no operative mortality in this group. One patient who underwent antrecto my and Billroth II anastomosis without vagotomy had a recurrent ulcer develop. During the period of this study, simple closure with an omental patch combined with PGV without drainage was used in 55% of the patients with a perforated duodenal ulcer. On the basis of our experience, it is estimated that 75% of the patients with a perforated ulcer would be considered candidates for PGV. This estimate is the same as the actual percentage of patients being treated in this way by Johnston (6). The operative mortality was zero. Of 5 Table 1. Thirty-seven Patients Treated by Simple Closure Group Postoperative deaths Late deaths Asymptomatic Reoperated for ulcer Remain symptomatic No. of patients
3 July 1982 PGV AND PERFORATED DUODENAL ULCER 181 Table 2. Results of the Last Gastric Analysis Performed on Each Patient Treated by Proximal Gastric Vagotomy Time BAO (rneq/h) MAO (meq /h) postoperative (yr) n > > patients who had late deaths, 3 were due to squamous cell carcinoma, 1 to chronic pulmonary disease, and 1 to unknown causes. There were 2 postoperative complications. One was a right subhepatic abscess that was drained extraperitoneally. The other complication was intestinal obstruction that required lysis of adhesions. All patients were observed for at least 1 yr except for 2 patients with carcinoma of the lung who died between 2 and 6 mo after operation. Eighty-two percent of the patients were observed 2 yr or longer. Dumping was reported at some time during the follow-up period by 6 patients. It was persistent in only 1 patient (2%). Dumping was mild and was readily controlled by minor diet modifications consisting of either avoidance of overeating or the elimination or reduction of liquids with meals. Intolerance of sugar was no problem. These restrictions were usually unconsciously invoked by the patients and may account for the low rate of persistent dumping. Intolerance to milk was persistent in 1 patient which was less frequent than occurred after elective PGV. Diarrhea was reported during the study by only 3 patients (5%) and in no patient was it persistent and in no patient did it ever cause a problem. Dysphagia was reported in the early postoperative period in 10 patients but it was not persistent in any patient. Reflux was noted late in the follow-up period by 3 patients but has not been a persistent problem for any patient. The weight of each patient at the time of their last follow-up examination when compared with their preoperative weight was unchanged in 32 patients, increased more than 5 lb in 13 patients, and decreased more than 5 lb in 15 patients. Three of the 15 patients who lost weight died of cancer. The results of the last gastric analysis performed on the patients are summarized in Table 2. We have postoperative studies on 52 patients. No studies were performed on 8 patients and many patients did not permit repeat studies on subsequent visits. The BAO was :52 meqlh in 71% and the MAO was <10 meqlh in 54% of the patients who were studied. Twenty-seven patients had repeat gastric studies that spanned a 2-yr period. The BAO remained the same over this period in 24 patients and increased in 3 patients. The MAO remained the same or decreased in 22 patients and increased in 5 patients. Five patients complained of symptoms at some time after operation that were of concern because of the possibility that they might represent recurrent peptic ulcer disease. One patient did have a recurrent ulcer 2 yr after operation (2% rate of recurrence). After 1 yr of medical treatment he underwent truncal vagotomy and pyloroplasty. For 6 mo after the second operation this patient complained of dumping, diarrhea, and intolerance to milk and sugar. He had experienced none of these symptoms following PGV. After 1 yr all of these symptoms except diarrhea subsided. Of the 4 remaining patients with worrisome symptoms, 1 patient had pancreatitis, 1 had esophageal reflux, and 2 patients had symptoms of unknown causes that completely subsided. Recurrent ulcer was never documented by endoscopy in these patients. The clinical results according to the Visick grading system are tabulated in Table 3. A grade is given to each patient for each follow-up period. A total of 49 patients were observed for 2 yr or longer. The clinical results achieved by these patients at their last follow-up visit were Visick I in42 patients, Visick II in 6 patients, and Visick IV in the1 patient who had a recurrent ulcer develop. Discussion There are basically three methods of treating a patient with perforated duodenal ulcer. They are: (a) nonoperative, which relies primarily on nasogastric suction, antibiotics, and supportive treatment, (b) simple closure of the perforation and cleansing of the abdominal cavity, and (c) definitive surgery. The mortality of the patients who underwent sim-
4 182 JORDAN GASTROENTEROLOGY Vol. 83, No.1, Part 2 Table 3. The Visick Gradings at Each Follow-up Period after Proximal Gastric Vagotomy Time postoperative (yr) n II III IV patients followed ~2 yr ple closure was 41 %. This is higher than 21% and 29% reported in other series in which the poor risk patient constituted the majority of patients who underwent simple closure (7,8). Even if all our patients upon whom a definitive operation was performed had undergone simple closure, the mortality rate for simple closure would not have been better than 14%. This is higher than the 5%-7% reported by those who perform simple closure as their principal operative procedure. These observations emphasize that certain patients who were too ill to survive even simple closure might have been better treated by the nonoperative methods outlined by Berne and Rosoff (9) and Donovan (8). We were much more perceptive in selecting patients who could successfully withstand definitive surgery than we were those who could withstand simple closure. There were no deaths in the 72 patients who were treated by the various definitive methods used. If simple closure and definitive surgery were performed upon patients of equal risk, one might conclude that the operative mortality after definitive operation would be greater than the mortality of simple closure because the operation is longer and more traumatic. But just how much greater the risk, is difficult to say. The patients who undergo simple closure have been exposed to the same trauma of perforation, anesthesia, and laparotomy as those patients who undergo definitive operation. In addition, death from a complication of d~odenal ulcer that would have been prevented if definitive therapy rather than simple closure had been performed originally should be attributed to simple closure. For example, 1 patient in our study (3%) died after simple closure because of a bleeding ulcer. If this factor were considered in the mortality analysis, definitive treatment would almost certainly be as safe if not more so than simple closure in most reports. No matter how patients with perforated duodenal ulcer are categorized, if simple closure were performed upon all patients there would be many in each category who would ultimately need additional surgery. It is equally evident that a definitive operation performed upon on all patients capable of undergoing operation successfully would result in some patients having such an operation unnecessarily. Based on duration of the history or the pathological findings at operation, there were in our study approximately 8 patients who might not have needed a definitive operation, but we are not sure. It is recognized that a good gastric surgeon exercising good surgical judgment can perform definitive surgery in carefully selected patients at the time of perforation with a mortality of 0%-2.2% (7,10). Our original reservations about performing definitive surgery were based upon the possibility that gastric sequelae might occur after truncal vagotomy combined with antrectomy or a drainage procedure in patients who would not have subsequently required a definitive operation. A previous prospective, randomized study (11) demonstrated that PGV can be performed with no mortality and without postoperative gastric sequelae for the elective treatment of duodenal ulcer. The present study demonstrates that PGV can be safely applied also in patients with perforated duodenal ulcer without morbidity and mortality. Our total experience consists of PGV in 63 patients with perforated duodenal ulcer. The mortality remains zero. Of the 60 patients who have been observed 1 yr or longer, the morbidity is inconsequential and the recurrence rate is 1. 7%. Although this patient is considered a failure, the consequences of the ulcer in this patient are no different than if a persistent ulcer after simple closure had developed. Our results confirm those of others (12,13) who suggest that PGV is an excellent choice for the treatment of perforated duodenal ulcer in patients who by virtue of their age, fitness, and status of the peritoneal cavity are candidates for definitive surgery. It inflicts virtually none of the morbidity that occurs with other forms of definitive treatment upon patients who might not have needed a definitive operation. At the same time it provides definitive therapy for the larger number of patients who would have subsequently required a second operation for continued ulcer disease if simple closure alone were performed. References 1. Jordan PH Ir. Korompai FL. Evolvement of a new treatment for perforated duodenal ulcer. Surg. Gynecol Obstet 1976 ; 142 :391-5.
5 July 1982 PGV AND PERFORATED DUODENAL ULCER Steiger E, Cooperman AM. Considerations in the nianagement of perforated peptic ulcers. Surg Clin N Am 1976;56: Drury JK, MacKay AI. Hutchinson JSF, Joffe SN. Natural history of perforated duodenal ulcers treated by suture closure. Lancet 1978;2: Kay PH, Moore KTH, Clark RG. The treatment of perforated duodenal ulcer. Br J Surg 1978;65: Kirkpatrick JR, Bowman DL. A logical solution to the perforated ulcer controversy. Surg Gynecol Obstet 1980;150: Johnston D. Treatment of peptic ulcer and its complications. In: Taylor S, ed. Recent advances in surgery, No. 10, Chap. 16. London: Churchill-Livingstone, 1980: Jordan GL [r, DeBakey ME, Duncan JM Jr. Surgical management of perforated peptic ulcer. Ann Surg 1974;179: Donovan AI. Vinson TL, Maulsby GO, Gewin JR. Selective treatment of duodenal ulcer with perforation. Ann Surg 1979;189: Berne C], Rosoff L Sr. Acute perforation of peptic ulcer. In: Nyhus LM, Waste II C, eds. Surgery of the stomach and duodenum. 3rd ed. Boston: Little, Brown & Co., 1977: Lowdon AGR. The treatment of acute perforated peptic ulcer by primary partial gastrectomy. Lancet 1952;1: Jordan PH Jr. An interim report on parietal cell vagotomy versus selective vagotomy and antrectomy for treatment of duodenal ulcer. Ann Surg 1979;189: Johnston D, Lyndon PI. Smith RB, Humphrey CS. Highly selective vagotomy without a drainage procedure in the treatment of hemorrhage, perforation and pyloric stenosis due to peptic ulcer. Br J Surg 1973;60: Sawyers JL, Herrington JL. Perforated duodenal ulcer managed by proximal gastric vagotomy and suture plication. Ann Surg 1977;185:
Perforated duodenal ulcer: which operation?
 The Ulster Medical Journal, Volume 56, No. 2, pp. 130-134, October 1987. Perforated duodenal ulcer: which operation? P J Gill, C F J Russell Accepted 7 September 1987. SUMMARY Between January 1968 and
The Ulster Medical Journal, Volume 56, No. 2, pp. 130-134, October 1987. Perforated duodenal ulcer: which operation? P J Gill, C F J Russell Accepted 7 September 1987. SUMMARY Between January 1968 and
OPERATIVE TREATMENT OF ULCER DISEASE
 Página 1 de 8 Copyright 2001 Lippincott Williams & Wilkins Greenfield, Lazar J., Mulholland, Michael W., Oldham, Keith T., Zelenock, Gerald B., Lillemoe, Keith D. Surgery: Scientific Principles & Practice,
Página 1 de 8 Copyright 2001 Lippincott Williams & Wilkins Greenfield, Lazar J., Mulholland, Michael W., Oldham, Keith T., Zelenock, Gerald B., Lillemoe, Keith D. Surgery: Scientific Principles & Practice,
Perforated duodenal ulcer in Reading from 1950 to 1959
 Gut, 1969, 1, 454-459 Perforated duodenal ulcer in Reading from 195 to 1959 PAUL CASSELL From the Royal Berkshire Hospital, Reading During the last 15 years there has been an evolution in the management
Gut, 1969, 1, 454-459 Perforated duodenal ulcer in Reading from 195 to 1959 PAUL CASSELL From the Royal Berkshire Hospital, Reading During the last 15 years there has been an evolution in the management
Surgery for Complications of Peptic Ulcer Disease (Definitive Treatment)
 Surgery for Complications of Peptic Ulcer Disease (Definitive Treatment) Amid Keshavarzi, MD UCHSC Grand Round 3/20/2006 Department of Surgery Introduction Epidemiology Pathophysiology Clinical manifestation
Surgery for Complications of Peptic Ulcer Disease (Definitive Treatment) Amid Keshavarzi, MD UCHSC Grand Round 3/20/2006 Department of Surgery Introduction Epidemiology Pathophysiology Clinical manifestation
The late prognosis of perforated duodenal ulcer
 Gut, 1962, 3, 6 The late prognosis of perforated duodenal ulcer A. C. B. DEAN,1 C. G. CLARK, AND A. H. SINCLAIR-GIEBEN From Aberdeen Royal Infirmary and the Department of Mental Health, niversity of Aberdeen
Gut, 1962, 3, 6 The late prognosis of perforated duodenal ulcer A. C. B. DEAN,1 C. G. CLARK, AND A. H. SINCLAIR-GIEBEN From Aberdeen Royal Infirmary and the Department of Mental Health, niversity of Aberdeen
Perforated peptic ulcers. Dr V. Roudnitsky KCH
 Perforated peptic ulcers Dr V. Roudnitsky KCH Peptic ulcer disease Peptic ulcers are focal defects in the gastric or duodenal mucosa that extend into the submucosa or deeper Caused by an imbalance between
Perforated peptic ulcers Dr V. Roudnitsky KCH Peptic ulcer disease Peptic ulcers are focal defects in the gastric or duodenal mucosa that extend into the submucosa or deeper Caused by an imbalance between
STOMACH and DUODENUM DISEASE
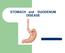 STOMACH and DUODENUM DISEASE STOMACH ANATOMY In the living and upright posture, the stomach is a j-shaped. It has two surfaces, two curvatures and two openings. Esophagus Fundus cardia Pylorus B o d y
STOMACH and DUODENUM DISEASE STOMACH ANATOMY In the living and upright posture, the stomach is a j-shaped. It has two surfaces, two curvatures and two openings. Esophagus Fundus cardia Pylorus B o d y
Non Operative Management of Perforated Duodenal Ulcers. Rabih Nemr M.D. Kings County Hospital Sept 2006
 Non Operative Management of Perforated Duodenal Ulcers Rabih Nemr M.D. Kings County Hospital Sept 2006 Case presentation 40 year old male presenting with abdominal pain: Epigastric Worsening over the last
Non Operative Management of Perforated Duodenal Ulcers Rabih Nemr M.D. Kings County Hospital Sept 2006 Case presentation 40 year old male presenting with abdominal pain: Epigastric Worsening over the last
Retrospective study analyzing the data on non-traumatic abdominal emergency surgeries done tertiary care hospital, Chennai
 Original Research Article Retrospective study analyzing the data on non-traumatic abdominal emergency surgeries done tertiary care hospital, Chennai S. Vijayalakshmi 1, Sriramchristopher M 2* 1 Associate
Original Research Article Retrospective study analyzing the data on non-traumatic abdominal emergency surgeries done tertiary care hospital, Chennai S. Vijayalakshmi 1, Sriramchristopher M 2* 1 Associate
Stomach. R.B. Kolachalam, MD
 Stomach R.B. Kolachalam, MD Relevent Anatomy 1.four regions: Cardia, Fundus, Body, and the Pylorus 2. fixed in two locations- at the GEJ and the duodenum Gastric Anatomy body of the stomach: site of mechanical
Stomach R.B. Kolachalam, MD Relevent Anatomy 1.four regions: Cardia, Fundus, Body, and the Pylorus 2. fixed in two locations- at the GEJ and the duodenum Gastric Anatomy body of the stomach: site of mechanical
Emergency Operations for Bleeding Duodenal Ulcer:A simple option to consider Case Report Abstract Key words Case Report
 Vtáx exñéüà :A simple option to consider: Case Report Gamal E H A El Shallaly, Eltayeb A Ali, Suzan Salih Abstract We report a 46 years-old man who had severe bleeding from a posterior duodenal ulcer (DU)
Vtáx exñéüà :A simple option to consider: Case Report Gamal E H A El Shallaly, Eltayeb A Ali, Suzan Salih Abstract We report a 46 years-old man who had severe bleeding from a posterior duodenal ulcer (DU)
Removal of a lap band and revision to an alternative bariatric procedure in one procedure.
 How to Discuss the Case with Insurance Plan Medical Director, Letter of Medical Necessity, and Increasing the Chance of Letters of Medical Necessity are a well-known requirement when requesting authorization
How to Discuss the Case with Insurance Plan Medical Director, Letter of Medical Necessity, and Increasing the Chance of Letters of Medical Necessity are a well-known requirement when requesting authorization
-Ist hour and 2nd hour.
 Vol. 12, No. 5. October. 1971. SINGAPORE MEDICAL JOURNAL 291 ASSESSMENT OF VAGOTOMY BY THE INSULIN TEST By W. P. Fung SYNOPSIS The insulin test for vagal innervation was done in 21 patients, who had vagotomy
Vol. 12, No. 5. October. 1971. SINGAPORE MEDICAL JOURNAL 291 ASSESSMENT OF VAGOTOMY BY THE INSULIN TEST By W. P. Fung SYNOPSIS The insulin test for vagal innervation was done in 21 patients, who had vagotomy
The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control
 ORIGINAL ARTICLES The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control Mark B. Orringer, M.D., and Jay S. Orringer, M.D. ABSTRACT This report summarizes the clinical experience with
ORIGINAL ARTICLES The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control Mark B. Orringer, M.D., and Jay S. Orringer, M.D. ABSTRACT This report summarizes the clinical experience with
Perforated peptic ulcer
 Perforated peptic ulcer - Despite the widespread use of gastric anti-secretory agents and eradication therapy, the incidence of perforated peptic ulcer has changed little, age limits increase NSAIDs elderly
Perforated peptic ulcer - Despite the widespread use of gastric anti-secretory agents and eradication therapy, the incidence of perforated peptic ulcer has changed little, age limits increase NSAIDs elderly
Symptomatic significance of gastric mucosal changes
 Gut, 1977, 18, 295-300 Symptomatic significance of gastric mucosal changes after surgery for peptic ulcer A. M. HOARE, E. L. JONES, J. ALEXANDER-WILLIAMS, AND C. F. HAWKINS From the Queen Elizabeth Hospital,
Gut, 1977, 18, 295-300 Symptomatic significance of gastric mucosal changes after surgery for peptic ulcer A. M. HOARE, E. L. JONES, J. ALEXANDER-WILLIAMS, AND C. F. HAWKINS From the Queen Elizabeth Hospital,
WHEN To Initiate Parenteral Nutrition A Frequent Question With New Answers
 WHEN To Initiate Parenteral Nutrition A Frequent Question With New Answers Ainsley Malone, MS, RD, LD, CNSC, FAND, FASPEN Dubai International Nutrition Conference 2018 Disclosures No commercial relationship
WHEN To Initiate Parenteral Nutrition A Frequent Question With New Answers Ainsley Malone, MS, RD, LD, CNSC, FAND, FASPEN Dubai International Nutrition Conference 2018 Disclosures No commercial relationship
Chapter 14: Training in Radiology. DDSEP Chapter 1: Question 12
 DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
An alternative plan for the treatment of a perforated duodenal ulcer is proposed. We
 Perforated Duodenal Ulcer An Alternative Therapeutic Plan SPECIAL ARTICLE Arthur J. Donovan, MD; Thomas V. Berne, MD; John A. Donovan, MD An alternative plan for the treatment of a perforated duodenal
Perforated Duodenal Ulcer An Alternative Therapeutic Plan SPECIAL ARTICLE Arthur J. Donovan, MD; Thomas V. Berne, MD; John A. Donovan, MD An alternative plan for the treatment of a perforated duodenal
Chapter 14 GASTROINTESTINAL IMPAIRMENT
 Chapter 14 GASTROINTESTINAL IMPAIRMENT Introduction This chapter provides criteria for assessing permanent impairment from entitled conditions of the gastrointestinal tract and the accessory organs of
Chapter 14 GASTROINTESTINAL IMPAIRMENT Introduction This chapter provides criteria for assessing permanent impairment from entitled conditions of the gastrointestinal tract and the accessory organs of
SARCINA VENTICULARI IS A POSSIBLE CAUSATIVE MICROORGANISM OTHER THAN H.PYLORI IN GASTRIC OUTLET OBSTRUCTION PATHOGENESIS
 SARCINA VENTICULARI IS A POSSIBLE CAUSATIVE MICROORGANISM OTHER THAN H.PYLORI IN GASTRIC OUTLET OBSTRUCTION PATHOGENESIS 55 years old male, Farm worker, married, from Ibb Heavy Smoker, Khat chewer non-alcohol
SARCINA VENTICULARI IS A POSSIBLE CAUSATIVE MICROORGANISM OTHER THAN H.PYLORI IN GASTRIC OUTLET OBSTRUCTION PATHOGENESIS 55 years old male, Farm worker, married, from Ibb Heavy Smoker, Khat chewer non-alcohol
The clinical significance of radiological changes in duodenal ulcer patients
 Ital J Gastroanter ol 1986; 18: CLINICAL REPORT 8-92 The clinical significance of radiological changes in duodenal ulcer patients RJ EARLAM, RS MURRAY, JC SWANN, EGW SLATER and SJW EVANS 1 The London Hospital,
Ital J Gastroanter ol 1986; 18: CLINICAL REPORT 8-92 The clinical significance of radiological changes in duodenal ulcer patients RJ EARLAM, RS MURRAY, JC SWANN, EGW SLATER and SJW EVANS 1 The London Hospital,
GRANULOMATOUS COLITIS: SIGNIFICANCE OF INVOLVEMENT OF THE TERMINAL ILEUM
 GASTROENTEROLOGY 64: 1071-1076, 1973 Copyright 1973 by The Williams & Wilkins Co. Vol. 64, No.6 Printed in U.S.A. GRANULOMATOUS COLITIS: SIGNIFICANCE OF INVOLVEMENT OF THE TERMINAL ILEUM JAMES A. NELSON,
GASTROENTEROLOGY 64: 1071-1076, 1973 Copyright 1973 by The Williams & Wilkins Co. Vol. 64, No.6 Printed in U.S.A. GRANULOMATOUS COLITIS: SIGNIFICANCE OF INVOLVEMENT OF THE TERMINAL ILEUM JAMES A. NELSON,
Postgastrectomy Syndromes
 Postgastrectomy Syndromes Postgastrectomy syndromes are iatrogenic conditions that may arise from partial gastrectomies, independent of whether the gastric surgery was initially performed for peptic ulcer
Postgastrectomy Syndromes Postgastrectomy syndromes are iatrogenic conditions that may arise from partial gastrectomies, independent of whether the gastric surgery was initially performed for peptic ulcer
Key words: gastric cancer, postoperative complication, total gastrectomy
 Key words: gastric cancer, postoperative complication, total gastrectomy 115 (115) Fig. 1 Technique of esophagojejunostomy (Quotation from Shimotsuma M and Nakamura R')). A, Technique for hand suture for
Key words: gastric cancer, postoperative complication, total gastrectomy 115 (115) Fig. 1 Technique of esophagojejunostomy (Quotation from Shimotsuma M and Nakamura R')). A, Technique for hand suture for
Audit of mortality in upper gastrointestinal bleeding
 Postgraduate Medical Journal (1989) 65, 913-917 Medical Audit Audit of mortality in upper gastrointestinal bleeding B.D. Katschinski', R.F.A. Logan2, J. Davies3 and M.J.S. Langman4 'Division of Gastroenterology,
Postgraduate Medical Journal (1989) 65, 913-917 Medical Audit Audit of mortality in upper gastrointestinal bleeding B.D. Katschinski', R.F.A. Logan2, J. Davies3 and M.J.S. Langman4 'Division of Gastroenterology,
Combined Collis-Nissen Reconstruction. of the esophagogastric junction at. Mark B. Orringer, M.D., and Herbert Sloan, M.D.
 Combined Collis-Nissen Reconstruction of the Esophagogastric Junction Mark B. Orringer, M.D., and Herbert Sloan, M.D. ABSTRACT Recent reports have indicated that combined Collis-Belsey reconstruction of
Combined Collis-Nissen Reconstruction of the Esophagogastric Junction Mark B. Orringer, M.D., and Herbert Sloan, M.D. ABSTRACT Recent reports have indicated that combined Collis-Belsey reconstruction of
Bariatric Surgery Risk Education Packet Walter J. Chlysta MD, FACS
 Date: Patient Name: Height: Weight: Ideal Body Weight: Excess Weight: Realistic Gastric Bypass Weight Goal (77 % Excess weight loss): Realistic Sleeve Gastrectomy Weight Goal (70 % Excess weight loss):
Date: Patient Name: Height: Weight: Ideal Body Weight: Excess Weight: Realistic Gastric Bypass Weight Goal (77 % Excess weight loss): Realistic Sleeve Gastrectomy Weight Goal (70 % Excess weight loss):
Management of acute abdomen: Study of 110 cases
 Original Research Article Management of acute abdomen: Study of 110 cases Samir Ray 1, Manthan Patel 2, Hiren Parmar 3* 1 Associate Professor, Department of Surgery, GMERS Medical College, Gotri, Vadodara,
Original Research Article Management of acute abdomen: Study of 110 cases Samir Ray 1, Manthan Patel 2, Hiren Parmar 3* 1 Associate Professor, Department of Surgery, GMERS Medical College, Gotri, Vadodara,
duodenal ulcer by vagotomy and gastric drainage operation
 Gut, 1961, 2,158 A clinical appraisal of the treatment of chronic duodenal ulcer by vagotomy and gastric drainage operation W. GERALD AUSTEN' AND HAROLD C. EDWARDS From King's College Hospital, London
Gut, 1961, 2,158 A clinical appraisal of the treatment of chronic duodenal ulcer by vagotomy and gastric drainage operation W. GERALD AUSTEN' AND HAROLD C. EDWARDS From King's College Hospital, London
Reoperation Bariatric Surgery:
 Reoperative Bariatric Surgery, Achieving Insurance Authorization Achieving insurance authorization for reoperative bariatric procedures is not difficult provided that prior insurance company authorization
Reoperative Bariatric Surgery, Achieving Insurance Authorization Achieving insurance authorization for reoperative bariatric procedures is not difficult provided that prior insurance company authorization
Peptic ulcer disease. Nomin-Erdene. D SOM-531
 Peptic ulcer disease Nomin-Erdene. D SOM-531 Learning objectives Stomach gross anatomy PUD Epidemiology Pathogenesis Clinical manifestation Diagnosing Treatment Complicated ulcer disease Surgical procedures
Peptic ulcer disease Nomin-Erdene. D SOM-531 Learning objectives Stomach gross anatomy PUD Epidemiology Pathogenesis Clinical manifestation Diagnosing Treatment Complicated ulcer disease Surgical procedures
Gastrointestinal Complications of Hepatic Transplantation
 Gastrointestinal Complications of Hepatic Transplantation L. J. Koep, T. E. Starzl, and R. Weil III I N THE largest series of orthotopic liver transplants, now numbering 150 patients, the largest number
Gastrointestinal Complications of Hepatic Transplantation L. J. Koep, T. E. Starzl, and R. Weil III I N THE largest series of orthotopic liver transplants, now numbering 150 patients, the largest number
is time consuming and expensive. An intra-operative assessment is not going to be helpful if there is no more tissue that can be taken to improve the
 My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery
 SCIENTIFIC PAPER Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery Steven J. Binenbaum, MD, Michael A. Goldfarb, MD ABSTRACT Background: Inadvertent enterotomy (IE) in laparoscopic abdominal
SCIENTIFIC PAPER Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery Steven J. Binenbaum, MD, Michael A. Goldfarb, MD ABSTRACT Background: Inadvertent enterotomy (IE) in laparoscopic abdominal
Reflux after cardiomyotomy
 Gut, 1965, 6, 80 FRANK ELLIS AND F. L. COLE From the Departments of Surgery and Radiology, Guy's Hospital, London EDITORIAL SYNOPSIS A series of 56 patients with achalasia of the cardia included 16 with
Gut, 1965, 6, 80 FRANK ELLIS AND F. L. COLE From the Departments of Surgery and Radiology, Guy's Hospital, London EDITORIAL SYNOPSIS A series of 56 patients with achalasia of the cardia included 16 with
Vagotomy for gastric ulcer
 Gut, 1970, 11, 540-545 Progress report Vagotomy for gastric ulcer In all aspects of the surgical treatment of peptic ulcer the trend, in the past decade, has been to substitute vagotomy and a drainage
Gut, 1970, 11, 540-545 Progress report Vagotomy for gastric ulcer In all aspects of the surgical treatment of peptic ulcer the trend, in the past decade, has been to substitute vagotomy and a drainage
SURGICAL MANAGEMENT OF PEPTIC ULCER DISEASE IN PROTON PUMP INHIBITOR ERA
 ORIGINAL ARTICLE ABSTRACT SURGICAL MANAGEMENT OF PEPTIC ULCER DISEASE IN PROTON PUMP INHIBITOR ERA M.A.NASIR MALIK, OMER SALAHUDDIN, MOBASHER AHMAD, MUHAMMAD AZHAR, OMER DILAWAR, AYESHA SALAHUDDIN Objective
ORIGINAL ARTICLE ABSTRACT SURGICAL MANAGEMENT OF PEPTIC ULCER DISEASE IN PROTON PUMP INHIBITOR ERA M.A.NASIR MALIK, OMER SALAHUDDIN, MOBASHER AHMAD, MUHAMMAD AZHAR, OMER DILAWAR, AYESHA SALAHUDDIN Objective
Two Cases of Laparoscopic Adhesiolysis for Chronic Abdominal Pain without Intestinal Obstruction after Total Gastrectomy
 J Gastric Cancer 2012;12(4):249-253 http://dx.doi.org/10.5230/jgc.2012.12.4.249 Case Report Two Cases of Laparoscopic Adhesiolysis for Chronic Abdominal Pain without Intestinal Obstruction after Total
J Gastric Cancer 2012;12(4):249-253 http://dx.doi.org/10.5230/jgc.2012.12.4.249 Case Report Two Cases of Laparoscopic Adhesiolysis for Chronic Abdominal Pain without Intestinal Obstruction after Total
DATA REPORT. August 2014
 AUDIT DATA REPORT August 2014 Prepared for the Australian and New Zealand Gastric and Oesophageal Surgical Association by the Royal Australasian College of Surgeons 199 Ward St, North Adelaide, SA 5006
AUDIT DATA REPORT August 2014 Prepared for the Australian and New Zealand Gastric and Oesophageal Surgical Association by the Royal Australasian College of Surgeons 199 Ward St, North Adelaide, SA 5006
Difficult Abdominal Closure. Mark A. Carlson, MD
 Difficult Abdominal Closure Mark A. Carlson, MD Illustrative case 14 yo boy with delayed diagnosis of appendicitis POD9 Appendectomy 2 wk after onset of symptoms POD4: return to OR for midline laparotomy
Difficult Abdominal Closure Mark A. Carlson, MD Illustrative case 14 yo boy with delayed diagnosis of appendicitis POD9 Appendectomy 2 wk after onset of symptoms POD4: return to OR for midline laparotomy
By incision of the pyloric muscle and plastic reconstruction
 Pyloroplasty Jon Arne Söreide, MD, PhD, FACS and Kjetil Söreide, MD By incision of the pyloric muscle and plastic reconstruction of the pyloric channel, pyloroplasty facilitates gastric emptying when the
Pyloroplasty Jon Arne Söreide, MD, PhD, FACS and Kjetil Söreide, MD By incision of the pyloric muscle and plastic reconstruction of the pyloric channel, pyloroplasty facilitates gastric emptying when the
Clinical Case Presentation. Jared B. Smith, M.D. Surgical Grand Rounds, August 21, 2006
 Clinical Case Presentation Jared B. Smith, M.D. Surgical Grand Rounds, August 21, 2006 Clinical History CC: Can t swallow anything HPI: 50 y.o. male from western Colorado, greater than 2 years of emesis
Clinical Case Presentation Jared B. Smith, M.D. Surgical Grand Rounds, August 21, 2006 Clinical History CC: Can t swallow anything HPI: 50 y.o. male from western Colorado, greater than 2 years of emesis
Peptic ulcer disease Disorders of the esophagus
 Peptic ulcer disease Disorders of the esophagus Peptic ulcer disease Burning epigastric pain Exacerbated by fasting Improved with meals Ulcer: disruption of mucosal integrity >5 mm in size, with depth
Peptic ulcer disease Disorders of the esophagus Peptic ulcer disease Burning epigastric pain Exacerbated by fasting Improved with meals Ulcer: disruption of mucosal integrity >5 mm in size, with depth
Here are some types of gastric bypass surgery:
 Gastric Bypass- Definition By Mayo Clinic staff Weight-loss (bariatric) surgeries change your digestive system, often limiting the amount of food you can eat. These surgeries help you lose weight and can
Gastric Bypass- Definition By Mayo Clinic staff Weight-loss (bariatric) surgeries change your digestive system, often limiting the amount of food you can eat. These surgeries help you lose weight and can
Perforated Peptic Ulcer Disease at Kenyatta National Hospital, Nairobi.
 Perforated Peptic Ulcer Disease at Kenyatta National Hospital, Nairobi. N.A. Nasio 1, H. Saidi 1,2 1 Department of Surgery, 2 Department of Human Anatomy, University of Nairobi Correspondence to: Nasio
Perforated Peptic Ulcer Disease at Kenyatta National Hospital, Nairobi. N.A. Nasio 1, H. Saidi 1,2 1 Department of Surgery, 2 Department of Human Anatomy, University of Nairobi Correspondence to: Nasio
Clinical, Diagnostic, and Operative Correlation of Acute Abdomen
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/163 Clinical, Diagnostic, and Operative Correlation of Acute Abdomen Madipeddi Venkanna 1, Doolam Srinivas 2, Budida
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/163 Clinical, Diagnostic, and Operative Correlation of Acute Abdomen Madipeddi Venkanna 1, Doolam Srinivas 2, Budida
Penetrating Abdominal Stab Wounds. Laparotomy or Selective Surgical Abstention: Practice About 28 Cases at University Hospital of Treichville
 Cronicon OPEN ACCESS EC GASTROENTEROLOGY AND DIGESTIVE SYSTEM Research Article Penetrating Abdominal Stab Wounds. Laparotomy or Selective Surgical Abstention: Practice About 28 Cases at University Laurent
Cronicon OPEN ACCESS EC GASTROENTEROLOGY AND DIGESTIVE SYSTEM Research Article Penetrating Abdominal Stab Wounds. Laparotomy or Selective Surgical Abstention: Practice About 28 Cases at University Laurent
Laparoscopic Gastric Bypass Information
 1441 Constitution Boulevard, Salinas, CA 93906 (831) 783-2556 www.natividad.com/weight-loss (Roux-en-Y Gastric Bypass) What is gastric bypass surgery? Gastric bypass surgery, a type of bariatric surgery
1441 Constitution Boulevard, Salinas, CA 93906 (831) 783-2556 www.natividad.com/weight-loss (Roux-en-Y Gastric Bypass) What is gastric bypass surgery? Gastric bypass surgery, a type of bariatric surgery
Selective Nonoperative Management of Contained Intrathoracic Esophageal Disruptions
 Selective Nonoperative Management of Contained Intrathoracic Esophageal Disruptions John L. Cameron, M.D., Richard F. Kieffer, M.D., Thomas R. Hendrix, M.D., Denis G. Mehigan, M.., and R. Robinson aker,
Selective Nonoperative Management of Contained Intrathoracic Esophageal Disruptions John L. Cameron, M.D., Richard F. Kieffer, M.D., Thomas R. Hendrix, M.D., Denis G. Mehigan, M.., and R. Robinson aker,
Postgastrectomy and Postvagotomy Syndromes
 H. D. Becker W.F. Caspary Postgastrectomy and Postvagotomy Syndromes With 84 Figures (Mainly in Two Colors) Springer-Verlag Berlin Heidelberg New York 1980 Professor Dr. med. H. D. Becker KlInik und PolIklImk
H. D. Becker W.F. Caspary Postgastrectomy and Postvagotomy Syndromes With 84 Figures (Mainly in Two Colors) Springer-Verlag Berlin Heidelberg New York 1980 Professor Dr. med. H. D. Becker KlInik und PolIklImk
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL. September 17, Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous
 Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Emergency Surgery Board Department of General Surgery Rambam Health Care Campus
 Emergency Surgery Board Department of General Surgery Rambam Health Care Campus Surgical Complications of Peptic Ulcer Disease Case Presentation and Review of the Literature Case Presentation 40y male
Emergency Surgery Board Department of General Surgery Rambam Health Care Campus Surgical Complications of Peptic Ulcer Disease Case Presentation and Review of the Literature Case Presentation 40y male
OPEN ACCESS TEXTBOOK OF GENERAL SURGERY
 OPEN ACCESS TEXTBOOK OF GENERAL SURGERY PEPTIC ULCER DISEASE PC Bornman RS Du Toit EPIDEMIOLOGY AND PATHOGENESIS The prevalence of duodenal ulcer disease has a variable geographical distribution and differs
OPEN ACCESS TEXTBOOK OF GENERAL SURGERY PEPTIC ULCER DISEASE PC Bornman RS Du Toit EPIDEMIOLOGY AND PATHOGENESIS The prevalence of duodenal ulcer disease has a variable geographical distribution and differs
CLINICAL STUDY OF ABDOMINAL HOLLOW VISCERAL PERFORATION-NON TRAUMATIC Vinod Kumar B 1, A. S. Mathew 2
 CLINICAL STUDY OF ABDOMINAL HOLLOW VISCERAL PERFORATION-NON TRAUMATIC Vinod Kumar B 1, A. S. Mathew 2 HOW TO CITE THIS ARTICLE: Vinod Kumar B, A. S. Mathew. Clinical Study of Abdominal Hollow Visceral
CLINICAL STUDY OF ABDOMINAL HOLLOW VISCERAL PERFORATION-NON TRAUMATIC Vinod Kumar B 1, A. S. Mathew 2 HOW TO CITE THIS ARTICLE: Vinod Kumar B, A. S. Mathew. Clinical Study of Abdominal Hollow Visceral
Factors relevant to the prognosis of chronic
 Gut, 1975, 16, 714-718 Factors relevant to the prognosis of chronic gastric ulcer D. W. PIPER, MARGARET GREIG, G. A. E. COUPLAND, ELIZABETH HOBBIN, AND JANE SHINNERS From the Departments of Medicine and
Gut, 1975, 16, 714-718 Factors relevant to the prognosis of chronic gastric ulcer D. W. PIPER, MARGARET GREIG, G. A. E. COUPLAND, ELIZABETH HOBBIN, AND JANE SHINNERS From the Departments of Medicine and
Gastric emptying following vagotomy and antrectomy and proximal gastric vagotomy
 Gut, 1975, 16, 509-513 Gastric emptying following vagotomy and antrectomy and proximal gastric vagotomy H. KALBASI, F. R. HUDSON, A. HERRING, S. MOSS, H. I. GLASS, AND J. SPENCER From the Departments of
Gut, 1975, 16, 509-513 Gastric emptying following vagotomy and antrectomy and proximal gastric vagotomy H. KALBASI, F. R. HUDSON, A. HERRING, S. MOSS, H. I. GLASS, AND J. SPENCER From the Departments of
GASTRIC HETEROTOPIA IN THE ILEUM WITH ULCERATION AND CHRONIC BLEEDING
 GASTROENTEROLOGY 66: 113-117, 1974 Copyright 1974 by The Williams & Wilkins Co. Vol. 66, No.1 Printed in U.S.A. CASE REPORTS GASTRIC HETEROTOPIA IN THE ILEUM WITH ULCERATION AND CHRONIC BLEEDING KARIM
GASTROENTEROLOGY 66: 113-117, 1974 Copyright 1974 by The Williams & Wilkins Co. Vol. 66, No.1 Printed in U.S.A. CASE REPORTS GASTRIC HETEROTOPIA IN THE ILEUM WITH ULCERATION AND CHRONIC BLEEDING KARIM
Safety of Repair for Severe Duodenal Injuries
 World J Surg (2008) 32:7 12 DOI 10.1007/s00268-007-9255-4 Safety of Repair for Severe Duodenal Injuries George C. Velmahos Æ Constantinos Constantinou Æ George Kasotakis Published online: 22 October 2007
World J Surg (2008) 32:7 12 DOI 10.1007/s00268-007-9255-4 Safety of Repair for Severe Duodenal Injuries George C. Velmahos Æ Constantinos Constantinou Æ George Kasotakis Published online: 22 October 2007
Peptic ulcer perforation in young Indians the causation and the trend
 International Surgery Journal Sabhnani G et al. Int Surg J. 2018 Jan;5(1):200-204 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20175895
International Surgery Journal Sabhnani G et al. Int Surg J. 2018 Jan;5(1):200-204 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20175895
Emergency abdominal surgery in the aged
 Br. J. Surg. Vol. 63 (1976) 956-960 Emergency abdominal surgery in the aged RICHARD BLAKE AND JOHN LYNN* SUMMARY The results of 375 emergency abdominal operations in elderly patients over the age of 75
Br. J. Surg. Vol. 63 (1976) 956-960 Emergency abdominal surgery in the aged RICHARD BLAKE AND JOHN LYNN* SUMMARY The results of 375 emergency abdominal operations in elderly patients over the age of 75
Acute Care Surgery: Diverticulitis
 Acute Care Surgery: Diverticulitis Madhulika G. Varma, MD Associate Professor and Chief Section of Colorectal Surgery University of California, San Francisco Modern Treatment of Diverticular Disease Increasing
Acute Care Surgery: Diverticulitis Madhulika G. Varma, MD Associate Professor and Chief Section of Colorectal Surgery University of California, San Francisco Modern Treatment of Diverticular Disease Increasing
Ileo-rectal anastomosis for Crohn's disease of
 Ileo-rectal anastomosis for Crohn's disease of the colon W. N. W. BAKER From the Research Department, St Mark's Hospital, London Gut, 1971, 12, 427-431 SUMMARY Twenty-six cases of Crohn's disease of the
Ileo-rectal anastomosis for Crohn's disease of the colon W. N. W. BAKER From the Research Department, St Mark's Hospital, London Gut, 1971, 12, 427-431 SUMMARY Twenty-six cases of Crohn's disease of the
PROGRESS IN GASTROENTEROLOGY
 GASTROENTEROLOGY 68:1615-1628, 1975 Copyright 1975 by The Williams & Wilkins Co. Vol.68, No.6 Printed in U.SA. PROGRESS IN GASTROENTEROLOGY VAGOTOMY IN THE ELECTIVE TREATMENT OF DUODENAL ULCER THEODORE
GASTROENTEROLOGY 68:1615-1628, 1975 Copyright 1975 by The Williams & Wilkins Co. Vol.68, No.6 Printed in U.SA. PROGRESS IN GASTROENTEROLOGY VAGOTOMY IN THE ELECTIVE TREATMENT OF DUODENAL ULCER THEODORE
DIGESTIVE SYSTEM SURGICAL PROCEDURES December 22, 2015 (effective March 1, 2016) INTESTINES (EXCEPT RECTUM) Asst Surg Anae
 December 22, 2015 (effective March 1, 201) INTESTINES (EXCEPT RECTUM) Z513 Hydrostatic - Pneumatic dilatation of colon stricture(s) through colonoscope... 10.50 Z50 Fulguration of first polyp through colonoscope...
December 22, 2015 (effective March 1, 201) INTESTINES (EXCEPT RECTUM) Z513 Hydrostatic - Pneumatic dilatation of colon stricture(s) through colonoscope... 10.50 Z50 Fulguration of first polyp through colonoscope...
Postoperative Ultrasound Evaluation of Gastric Distension; A Pilot study
 Postoperative Ultrasound Evaluation of Gastric Distension; A Pilot study M Jaronczyk MD, W Boyan Jr. MD, M Goldfarb MD. FACS. MMC Dept of Surgery Nausea and vomiting are common complaints of postoperative
Postoperative Ultrasound Evaluation of Gastric Distension; A Pilot study M Jaronczyk MD, W Boyan Jr. MD, M Goldfarb MD. FACS. MMC Dept of Surgery Nausea and vomiting are common complaints of postoperative
Clinical Study Adhesive Intestinal Obstruction in Infants and Children: The Place of Conservative Treatment
 International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 645104, 4 pages doi:10.5402/2011/645104 Clinical Study Adhesive Intestinal Obstruction in Infants and Children: The Place of
International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 645104, 4 pages doi:10.5402/2011/645104 Clinical Study Adhesive Intestinal Obstruction in Infants and Children: The Place of
Introduction. Roxanne L. Massoumi 1 Colleen M. Trevino
 World J Surg (2017) 41:935 939 DOI 10.1007/s00268-016-3816-3 ORIGINAL SCIENTIFIC REPORT Postoperative Complications of Laparoscopic Cholecystectomy for Acute Cholecystitis: A Comparison to the ACS-NSQIP
World J Surg (2017) 41:935 939 DOI 10.1007/s00268-016-3816-3 ORIGINAL SCIENTIFIC REPORT Postoperative Complications of Laparoscopic Cholecystectomy for Acute Cholecystitis: A Comparison to the ACS-NSQIP
Spleen indications of splenectomy complications OPSI
 Intestinal obstruction Differences between adynamic ileus and mechanical obstruction Aetiology Pathophysiology (Cluster contractions- bowel proximal to the obstruction dilate- wall of obstructed gut is
Intestinal obstruction Differences between adynamic ileus and mechanical obstruction Aetiology Pathophysiology (Cluster contractions- bowel proximal to the obstruction dilate- wall of obstructed gut is
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
PARTIAL GASTRECTOMY FOR PEPTIC ULCER
 Gut, 1960, 1, 149. PARTIAL GASTRECTOMY FOR PEPTIC ULCER BY VICTOR S. BROOKES, J. A. H. WATERHOUSE, and P. A. THORN From the University of Birmingham, the United Birmingham Hospitals, and Wolverhampton
Gut, 1960, 1, 149. PARTIAL GASTRECTOMY FOR PEPTIC ULCER BY VICTOR S. BROOKES, J. A. H. WATERHOUSE, and P. A. THORN From the University of Birmingham, the United Birmingham Hospitals, and Wolverhampton
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES
 JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
Index. Note: Page numbers of article title are in boldface type.
 Index Note: Page numbers of article title are in boldface type. A Abscess(es) in Crohn s disease, 168 169 IPAA and, 110 114 as unexpected finding in colorectal surgery, 46 Adhesion(s) trocars-related laparoscopy
Index Note: Page numbers of article title are in boldface type. A Abscess(es) in Crohn s disease, 168 169 IPAA and, 110 114 as unexpected finding in colorectal surgery, 46 Adhesion(s) trocars-related laparoscopy
Role Of Laparoscopy In Diagnosis And Management Of Acute Abdomen In South Indian Population
 ISPUB.COM The Internet Journal of Surgery Volume 30 Number 4 Role Of Laparoscopy In Diagnosis And Management Of Acute Abdomen In South Indian Population P B Babannavar, P Thejeswi, Ravishankar, S P Rao,
ISPUB.COM The Internet Journal of Surgery Volume 30 Number 4 Role Of Laparoscopy In Diagnosis And Management Of Acute Abdomen In South Indian Population P B Babannavar, P Thejeswi, Ravishankar, S P Rao,
Gastric bypass vs. Sleeve gastrectomy
 Gastric bypass vs. Sleeve gastrectomy SLEEVEPASS-study Sleeve gastrectomy Paulina Salminen, M.D., PhD Turku University Hospital Department of Surgery Stockholms Obesitasdagar 19.4.2012 Swedish Obese Subjects
Gastric bypass vs. Sleeve gastrectomy SLEEVEPASS-study Sleeve gastrectomy Paulina Salminen, M.D., PhD Turku University Hospital Department of Surgery Stockholms Obesitasdagar 19.4.2012 Swedish Obese Subjects
Takayuki; Eguchi, Susumu; Kanematsu. Citation Pediatric surgery international, 27
 NAOSITE: Nagasaki University's Ac Title Author(s) Endoscopic balloon dilatation for c jejunum in an infant. Mochizuki, Kyoko; Obatake, Masayuki Takayuki; Eguchi, Susumu; Kanematsu Citation Pediatric surgery
NAOSITE: Nagasaki University's Ac Title Author(s) Endoscopic balloon dilatation for c jejunum in an infant. Mochizuki, Kyoko; Obatake, Masayuki Takayuki; Eguchi, Susumu; Kanematsu Citation Pediatric surgery
Surgical Apgar Score Predicts Post- Laparatomy Complications
 ORIGINAL ARTICLE Surgical Apgar Score Predicts Post- Laparatomy Complications Dullo M 1, Ogendo SWO 2, Nyaim EO 2 1 Kitui District Hospital 2 School of Medicine, University of Nairobi Correspondence to:
ORIGINAL ARTICLE Surgical Apgar Score Predicts Post- Laparatomy Complications Dullo M 1, Ogendo SWO 2, Nyaim EO 2 1 Kitui District Hospital 2 School of Medicine, University of Nairobi Correspondence to:
Last Revised: September 15 Last Reviewed: September EOSINOPHILIC ESOPHAGITIS (EOE)/PPI-RESPONSIVE ESOPHAGEAL EOSINOPHILIA (PPI-REE)
 7.0 GASTROENTEROLOGY Last Revised: September 5 Last Reviewed: September 5 7. EOSINOPHILIC ESOPHAGITIS (EOE)/PPI-RESPONSIVE ESOPHAGEAL EOSINOPHILIA (PPI-REE) Significant changes: ) Addition of PPI-REE as
7.0 GASTROENTEROLOGY Last Revised: September 5 Last Reviewed: September 5 7. EOSINOPHILIC ESOPHAGITIS (EOE)/PPI-RESPONSIVE ESOPHAGEAL EOSINOPHILIA (PPI-REE) Significant changes: ) Addition of PPI-REE as
Complication of Percutaneous Endoscopic Gastrostomy
 Complication of Percutaneous Endoscopic Gastrostomy Tube Ogori N. Kalu MD Morbidity & Mortality Conference General Surgery Service Kings County Hospital Center ACGME Core Competencies 1. Medical knowledge
Complication of Percutaneous Endoscopic Gastrostomy Tube Ogori N. Kalu MD Morbidity & Mortality Conference General Surgery Service Kings County Hospital Center ACGME Core Competencies 1. Medical knowledge
Acute Upper Gastrointestinal Hemorrhage Surgical Perspective. Dr.J.H.Barnard Dept. of Surgery PAH
 Acute Upper Gastrointestinal Hemorrhage Surgical Perspective Dr.J.H.Barnard Dept. of Surgery PAH Introduction: AGH is a leading cause of admissions into ICU. Overall mortality 5-12%, but increases to 40%
Acute Upper Gastrointestinal Hemorrhage Surgical Perspective Dr.J.H.Barnard Dept. of Surgery PAH Introduction: AGH is a leading cause of admissions into ICU. Overall mortality 5-12%, but increases to 40%
C.Y. Lin, B.Y. Lin, and P.L. Kang Aortic aneurysm Figure 1. Preoperative computerized tomography shows a 6.8 cm infrarenal abdominal aortic aneurysm.
 DUODENAL OBSTRUCTION AFTER ELECTIVE ABDOMINAL AORTIC ANEURYSM REPAIR: A CASE REPORT Chun-Yao Lin, Bor-Yen Lin, and Pei-Luen Kang Division of Cardiology, Department of Surgery, Kaohsiung Veterans General
DUODENAL OBSTRUCTION AFTER ELECTIVE ABDOMINAL AORTIC ANEURYSM REPAIR: A CASE REPORT Chun-Yao Lin, Bor-Yen Lin, and Pei-Luen Kang Division of Cardiology, Department of Surgery, Kaohsiung Veterans General
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY 2013/12/21
 THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
Helicobacter Pylori Testing HELICOBACTER PYLORI TESTING HS-131. Policy Number: HS-131. Original Effective Date: 9/17/2009
 Easy Choice Health Plan, Inc. Harmony Health Plan of Illinois, Inc. Missouri Care, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance of Arizona, Inc. WellCare Health Insurance of Illinois,
Easy Choice Health Plan, Inc. Harmony Health Plan of Illinois, Inc. Missouri Care, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance of Arizona, Inc. WellCare Health Insurance of Illinois,
SETTING Fudan University Shanghai Cancer Center. RESPONSIBLE PARTY Haiquan Chen MD.
 OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
SECONDARIES: A PRELIMINARY REPORT
 HPB Surgery, 1990, Vol. 2, pp. 69-72 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORTS
HPB Surgery, 1990, Vol. 2, pp. 69-72 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORTS
Surgery and Crohn s. Crohn s Disease 70 % Why Operate? Complications of Disease. The Gastrointestinal Tract. Surgery for Inflammatory Bowel Disease
 The Gastrointestinal Tract Surgery for Inflammatory Bowel Disease Jonathan Chun, MD The regon Clinic Gastrointestinal and Minimally Invasive Surgery Crohn s Disease Can affect anywhere in the GI tract,
The Gastrointestinal Tract Surgery for Inflammatory Bowel Disease Jonathan Chun, MD The regon Clinic Gastrointestinal and Minimally Invasive Surgery Crohn s Disease Can affect anywhere in the GI tract,
RECONSTRUCTION OF THE CARDIA AND FUNDUS OF THE STOMACH
 Thorax (1956), 11, 275. RECONSTRUCTION OF THE CARDIA AND FUNDUS OF THE STOMACH BY From tile United Leeds Hospitals (RECEIVED FOR PUBLICATION SEPTEMBER 15, 1956) This is a preliminary report describing
Thorax (1956), 11, 275. RECONSTRUCTION OF THE CARDIA AND FUNDUS OF THE STOMACH BY From tile United Leeds Hospitals (RECEIVED FOR PUBLICATION SEPTEMBER 15, 1956) This is a preliminary report describing
International Journal of Medical Science and Health Research
 A Retrospective Study of Clinicopathological Profiles of Proximal Gastrectomy Vs Distal Gastrectomy in Carcinoma Stomach and Its Incidence in our Population Dr Magesh kumar J 1, Dr V Naveen Kumar 2, Dr
A Retrospective Study of Clinicopathological Profiles of Proximal Gastrectomy Vs Distal Gastrectomy in Carcinoma Stomach and Its Incidence in our Population Dr Magesh kumar J 1, Dr V Naveen Kumar 2, Dr
Laparoscopic or Endoscopic Gastrostomy in Children: Comparison of Two Methods. H. STEYAERT, L. CARFAGNA, M.A. LEMBO, E. TREVINO, and J.S.
 Pediatric Endosurgery & Innovative Techniques Volume 7, Number 2, 2003 Mary Ann Liebert, Inc. Laparoscopic or Endoscopic Gastrostomy in Children: Comparison of Two Methods H. STEYAERT, L. CARFAGNA, M.A.
Pediatric Endosurgery & Innovative Techniques Volume 7, Number 2, 2003 Mary Ann Liebert, Inc. Laparoscopic or Endoscopic Gastrostomy in Children: Comparison of Two Methods H. STEYAERT, L. CARFAGNA, M.A.
Penetrating abdominal trauma clinical view. Ari Leppäniemi, MD Department of Abdominal Surgery Meilahti hospital University of Helsinki Finland
 Penetrating abdominal trauma clinical view Ari Leppäniemi, MD Department of Abdominal Surgery Meilahti hospital University of Helsinki Finland Meilahti hospital - one of Helsinki University hospitals -
Penetrating abdominal trauma clinical view Ari Leppäniemi, MD Department of Abdominal Surgery Meilahti hospital University of Helsinki Finland Meilahti hospital - one of Helsinki University hospitals -
Key words: duodenal ulcer, perforation, retroperitoneal abscess
 Key words:, perforation, retroperitoneal abscess Fig. 1 Plain abdominal X-ray film in the standing position on admission shows abnormal gas with niveau (arrow) on the medial side of the gas in the 2nd
Key words:, perforation, retroperitoneal abscess Fig. 1 Plain abdominal X-ray film in the standing position on admission shows abnormal gas with niveau (arrow) on the medial side of the gas in the 2nd
INVESTIGATIONS OF GASTROINTESTINAL DISEAS
 INVESTIGATIONS OF GASTROINTESTINAL DISEAS Lecture 1 and 2 دز اسماعيل داود فرع الطب كلية طب الموصل Radiological tests of structure (imaging) Plain X-ray: May shows soft tissue outlines like liver, spleen,
INVESTIGATIONS OF GASTROINTESTINAL DISEAS Lecture 1 and 2 دز اسماعيل داود فرع الطب كلية طب الموصل Radiological tests of structure (imaging) Plain X-ray: May shows soft tissue outlines like liver, spleen,
AN ARGUMENT FOR SURGERY FOR GASTRINOMA. Lauren Wilson R1 General Surgery
 AN ARGUMENT FOR SURGERY FOR GASTRINOMA Lauren Wilson R1 General Surgery WHAT IS A GASTRINOMA? Gastrin secreting cells derived from multipotential stem cells of endodermal origin or enteroendocrine cells
AN ARGUMENT FOR SURGERY FOR GASTRINOMA Lauren Wilson R1 General Surgery WHAT IS A GASTRINOMA? Gastrin secreting cells derived from multipotential stem cells of endodermal origin or enteroendocrine cells
FACTORS AFFECTING MORBIDITY AND MORTALITY IN PERFORATED DUODENAL ULCER
 Basrah Journal Original Article Of Surgery FACTORS AFFECTING MORBIDITY AND MORTALITY IN PERFORATED DUODENAL ULCER kassim Trayem Hayef* & Adnan Yassin Abdul-Wahab @ *MBChB, Al-Sader Teaching Hospital, Basrah.
Basrah Journal Original Article Of Surgery FACTORS AFFECTING MORBIDITY AND MORTALITY IN PERFORATED DUODENAL ULCER kassim Trayem Hayef* & Adnan Yassin Abdul-Wahab @ *MBChB, Al-Sader Teaching Hospital, Basrah.
Colon Patch Esophagoplasty: A Clinical Study For Chemical Burn Esophageal Stricture
 ISPUB.COM The Internet Journal of Surgery Volume 5 Number 1 Colon Patch Esophagoplasty: A Clinical Study For Chemical Burn Esophageal Stricture M Hourang, V Mehrabi Citation M Hourang, V Mehrabi. Colon
ISPUB.COM The Internet Journal of Surgery Volume 5 Number 1 Colon Patch Esophagoplasty: A Clinical Study For Chemical Burn Esophageal Stricture M Hourang, V Mehrabi Citation M Hourang, V Mehrabi. Colon
Outcome after emergency surgery in patients with a free perforation caused by gastric cancer
 experimental and therapeutic medicine 1: 199-203, 2010 199 Outcome after emergency surgery in patients with a free perforation caused by gastric cancer Hironori Tsujimoto 1, Shuichi Hiraki 1, Naoko Sakamoto
experimental and therapeutic medicine 1: 199-203, 2010 199 Outcome after emergency surgery in patients with a free perforation caused by gastric cancer Hironori Tsujimoto 1, Shuichi Hiraki 1, Naoko Sakamoto
QUESTIONS IN SURGERY General Surgery (3rd year) Surgery nr.1 (4th year)
 QUESTIONS IN SURGERY General Surgery (3 rd year) 1. Bleeding: definition, classification. Physiological mechanisms of compensation and pathological mechanisms of decompensation in case of hemorrhage. Physiologic
QUESTIONS IN SURGERY General Surgery (3 rd year) 1. Bleeding: definition, classification. Physiological mechanisms of compensation and pathological mechanisms of decompensation in case of hemorrhage. Physiologic
E n t e r o c u t a n e o u s F i s t u l a : Outcome in a Tertiary Center in Nigeria
 E n t e r o c u t a n e o u s F i s t u l a : Aetiology and Management Outcome in a Tertiary Center in Nigeria 2 2 Okoli C, Oparocha D, Onyemkpa J ABSTRACT Background: Enterocutaneous fistula is a major
E n t e r o c u t a n e o u s F i s t u l a : Aetiology and Management Outcome in a Tertiary Center in Nigeria 2 2 Okoli C, Oparocha D, Onyemkpa J ABSTRACT Background: Enterocutaneous fistula is a major
