Posterior Lumbar Discectomy
|
|
|
- Veronica Edwards
- 6 years ago
- Views:
Transcription
1 1 2 Posterior Lumbar Discectomy Overview Posterior lumbar discectomy is a surgery to remove a herniated or degenerative disc in the lower spine. The incision is made posterior, through the back muscles, to reach and remove the disc pressing on the nerve. Discectomy surgery may be recommended if physical therapy or medications fail to relieve leg or back pain caused by pinched spinal nerves. It may also be needed if you have signs of nerve damage, such as weakness or loss of feeling in your legs. The surgery can be performed in an open or minimally invasive technique. What is posterior lumbar discectomy? Discectomy literally means "cutting out the disc." A discectomy can be performed anywhere along the spine from the neck (cervical) to the low back (lumbar). The surgeon reaches the damaged disc from the back (posterior) of the spine through the muscles and bone. The surgeon accesses the disc by removing a portion of the lamina. The lamina is the bone that forms the backside of the spinal canal and makes a roof over the spinal cord. Next, the spinal nerve is retracted to one side. Depending on your particular case, one disc (single-level) or more (multi-level) may be removed. A variety of surgical tools and techniques can be used to perform a discectomy. An open technique uses a large skin incision and muscle retraction so that the surgeon can directly view the area. A minimally invasive technique, called a microendoscopic discectomy, uses a small skin incision. A series of progressively larger tubes, called dilators, are used to tunnel through the muscles. Special instruments help the surgeon see and operate in a smaller space. A minimally invasive incision causes less disruption of the back muscles and may decrease recovery time. Your surgeon will recommend the technique most appropriate for your specific case. A fusion may be done at the same time as discectomy to help stabilize the spine for patients who are athletes, perform heavy labor, or have spinal instability. Fusion uses a combination of bone graft and hardware (screws/plates) to connect two vertebrae together. During the healing process, the two vertebrae fuse into one piece of bone. Fusion is rarely needed for a herniated lumbar disc [1]. Figure 1. (top view of vertebra) A herniated disc occurs when the gel-filled nucleus material escapes through a tear in the disc annulus and compresses the spinal nerve causing pain and swelling. Who is a candidate? You may be a candidate for discectomy if you have: diagnostic tests (MRI, CT, myelogram) that show a herniated disc significant pain, weakness, or numbness in your leg or foot leg pain (sciatica) worse than back pain symptoms that have not improved with physical therapy or medication leg weakness, loss of feeling in the genital area, and loss of bladder or bowel control (cauda equina syndrome) Posterior lumbar discectomy may be helpful in treating leg pain (sciatica) caused by: Bulging or herniated disc: The gel-like material within the disc can bulge or rupture through a weak area in the surrounding wall (annulus). Irritation and swelling occurs when this material squeezes out and painfully presses on a nerve (Fig. 1). Degenerative disc disease: As discs naturally wear out, bone spurs form and the facet joints inflame. The discs dry out and shrink, losing their flexibility and cushioning properties. The disc spaces get smaller. These changes lead to stenosis or disc herniation. >1
2 4 3 The surgical decision Most herniated discs heal after a few months of nonsurgical treatment. Your doctor may recommend treatment options, but only you can decide whether surgery is right for you. Be sure to consider all the risks and benefits before making your decision. Only 10% of people with herniated disc problems have enough pain after 6 weeks of nonsurgical treatment to consider surgery. Who performs the procedure? A neurosurgeon or an orthopedic surgeon can perform spine surgery. Many spine surgeons have specialized training in complex spine surgery. Ask your surgeon about their training, especially if your case is complex or you ve had more than one spinal surgery. What happens before surgery? You may be scheduled for presurgical tests (e.g., blood test, electrocardiogram, chest X-ray) several days before surgery. In the doctor s office, you will sign consent and other forms so that the surgeon knows your medical history (allergies, medicines/vitamins, bleeding history, anesthesia reactions, previous surgeries). Discuss all medications (prescription, over-the-counter, and herbal supplements) you are taking with your health care provider. Some medications need to be continued or stopped the day of surgery. Stop taking all non-steroidal anti-inflammatory medicines (Naprosyn, Advil, Motrin, Nuprin, Aleve, etc.) and blood thinners (Coumadin, Plavix, etc.) 1 to 2 weeks before surgery as directed by the doctor. Additionally, stop smoking, chewing tobacco, and drinking alcohol 1 week before and 2 weeks after surgery because these activities can cause bleeding problems. No food or drink is permitted past midnight the night before surgery. Figure 2. For an open discectomy, a 1- to 2-inch skin incision (black line) is made down the middle of your back. Muscles overlying the vertebrae are retracted to one side. For a minimally invasive discectomy, a small stab entry (green line) is made in the skin near the midline. Morning of surgery Shower using antibacterial soap. Dress in freshly washed, loose-fitting clothing. Wear flat-heeled shoes with closed backs. If you have instructions to take regular medication the morning of surgery, do so with small sips of water. Remove make-up, hairpins, contacts, body piercings, nail polish, etc. Leave all valuables and jewelry at home (including wedding bands). Bring a list of medications (prescriptions, overthe-counter, and herbal supplements) with dosages and the times of day usually taken. Bring a list of allergies to medication or foods. Arrive at the hospital 2 hours before (surgery center 1 hour before) your scheduled surgery time to complete the necessary paperwork and preprocedure work-ups. An anesthesiologist will talk with you and explain the effects of anesthesia and its risks. An intravenous (IV) line will be placed in your arm. What happens during surgery? There are five steps of the procedure. The operation generally lasts 1 to 2 hours. Step 1: prepare the patient You will lie on your back on the operative table and be given anesthesia. Once asleep, you are rolled onto your stomach with your chest and sides supported by pillows. The area where the incision will be made is cleansed and prepped. Figure 3. For a minimally invasive discectomy, a small stab entry is made in the skin. Muscles are then dilated gradually with increasingly larger tubular retractors to gain access to the spine. >2
3 6 5 Step 2: make an incision With the aid of a fluoroscope (a special X-ray), the surgeon passes a thin needle through the skin down to the bone to locate the affected vertebra and disc. In an open discectomy, a skin incision is made down the middle of your back over the affected vertebrae (Fig. 2). The length of the incision depends on how many discectomies will be performed. A single-level incision is about 1 to 2 inches long. The back muscles are retracted on one side to expose the bony vertebra. An X-ray is taken to verify the correct vertebra. In a minimally invasive discectomy, a small incision (less than 1 inch) is made to one side of your back (Fig. 3). Next, a series of progressively larger dilators are passed, one around the other, to gradually separate the muscles and create a tunnel to the bony vertebra. Figure 4. A laminotomy makes a small window by removing bone of the lamina above and below. The nerve root and spinal cord can be gently reflected to expose the herniated disc. Step 3: make a laminotomy Next, a small opening of the lamina, above and below the spinal nerve, is made with a drill or bonebiting tools (Fig. 4). A laminotomy can be done on one (unilateral) or both (bilateral) sides, or on multiple vertebrae levels. Step 4: remove the disc fragments With the lamina removed, the surgeon gently retracts the protective sac of the nerve root. The surgeon looks through a surgical microscope to find the herniated disc. Only the ruptured portion of the disc is removed to decompress the spinal nerve root. The entire disc is not removed (Fig. 5). Bone spurs or a synovial cyst that may press on the nerve root are also removed. For a single-level lumbar discectomy, fusion is rarely performed. However, other conditions, such as recurrent disc herniation or spinal instability, may be treated with a fusion. Step 5: close the incision The retractor holding the muscles is removed. The muscle and skin incisions are sewn together with sutures or staples. Steri-Strips are placed across the incision. What happens after surgery? You will awaken in the postoperative recovery area, called the PACU. Blood pressure, heart rate, and respiration will be monitored. Any pain will be addressed. Once awake, you will be moved to a regular room where you ll increase your activity level (sitting in a chair, walking). Most patients can go home the same day. Other patients can be released from the hospital in 1 to 2 days. Figure 5. The herniated disc material compressing the nerve root is removed. Discharge instructions Discomfort 1. After surgery, pain is managed with narcotic medication. Because narcotic pain pills are addictive, they are used for a limited period (2 to 4 weeks). As their regular use can cause constipation, drink lots of water and eat high fiber foods. Laxatives (e.g., Dulcolax, Senokot, Milk of Magnesia) can be bought without a prescription. Thereafter, pain is managed with acetaminophen (e.g., Tylenol). Restrictions 2. If you had a fusion, do not use non-steroidal anti-inflammatory drugs (NSAIDs) (e.g., aspirin; ibuprofen, Advil, Motrin, Nuprin; naproxen sodium, Aleve) for 6 months after surgery. NSAIDs may cause bleeding and >3
4 interfere with bone healing. 3. Do not drive for 2 to 4 weeks after surgery or until discussed with your surgeon. 4. Avoid sitting for long periods of time. 5. Do not lift anything heavier than 10 pounds (e.g., gallon of milk). Do not bend or twist at the waist. 6. Housework and yard-work are not permitted until the first follow-up office visit. This includes gardening, mowing, vacuuming, ironing, and loading/unloading the dishwasher, washer, or dryer. 7. Postpone sexual activity until your follow-up appointment unless your surgeon specifies otherwise. 8. Do not smoke. Smoking delays healing by increasing the risk of complications (e.g., infection) and inhibits the bones' ability to fuse. Activity 9. You may need help with daily activities (e.g., dressing, bathing) for the first few days. Fatigue is common. Let pain be your guide. 10. Gradually return to your normal activities. Walking is encouraged; start with a short distance and gradually increase to 1 to 2 miles daily. A physical therapy program may be recommended. Bathing/Incision Care 11. You may shower 1 to 4 days after surgery. Follow your surgeon s specific instructions. No tub baths, hot tubs, or swimming pools until your health care provider says it s safe to do so. 12. Staples or stitches, which remain in place when you go home, will need to be removed. Ask your surgeon or call the office to find out when. When to Call Your Doctor 13. If your temperature exceeds 101 F, or if the incision begins to separate or show signs of infection, such as redness, swelling, pain, or drainage. Recovery and prevention Schedule a follow-up appointment with your surgeon for 2 weeks after surgery. Physical therapy may be necessary for some people. The recovery time varies from 1 to 4 weeks depending on the underlying disease treated and your general health. You may feel pain at the site of the incision. The original pain may not be completely relieved immediately after surgery. Aim to keep a positive attitude and diligently perform your physical therapy exercises if prescribed. Most people can return to work in 2 to 4 weeks or less with jobs that are not physically challenging. Others may need to wait at least 8 to 12 weeks to return to work for jobs that require heavy lifting or operating heavy machinery. Recurrences of back pain are common. The key to avoiding recurrence is prevention: Proper lifting techniques Good posture during sitting, standing, moving, and sleeping Appropriate exercise program An ergonomic work area Healthy weight and lean body mass A positive attitude and relaxation techniques (e.g., stress management) No smoking What are the results? Good results are achieved in 80 to 90% of patients treated with lumbar discectomy [2,3]. In a study that compared surgery and nonsurgical treatment for herniated discs, the outcomes were [2]: People with leg pain (sciatica) benefit more from surgery than those with back pain. People with less severe or improving pain do well with nonsurgical treatment. People with moderate to severe pain who had surgery notice a greater improvement than those who did not have surgery. Similarly, minimally invasive discectomy techniques have been shown to be comparable in outcomes with open discectomy [4]. While the benefits of minimally invasive approaches include shorter operative time, less blood loss and muscle trauma, and faster recovery, these newer techniques are not appropriate for all patients. Ask your surgeon if minimally invasive microendoscopic discectomy is appropriate for you. Discectomy may provide faster pain relief than nonsurgical treatment. However, it is unclear whether surgery makes a difference in what treatment may be needed later on. About 5 to 15% of patients will have a recurrent disc herniation, either at the same side or the opposite side. What are the risks? No surgery is without risks. General complications of any surgery include bleeding, infection, blood clots, and reactions to anesthesia. If spinal fusion is done at the same time as a discectomy, there is a greater risk of complications. Specific complications related to a discectomy may include: Deep vein thrombosis (DVT) is a potentially serious condition caused when blood clots form inside the leg veins. If the clots break free and travel to the lungs, lung collapse or even death is a risk. However, there are several ways to treat or prevent DVT. Get up and out of bed as soon as possible so your blood is moving and less likely to clot. Support hose and pulsatile stockings can keep the blood from pooling in the veins. Drugs, such as aspirin, Heparin, or Coumadin, may also be used. > 4
5 Lung problems. Lungs need to be working their best after surgery to provide tissues with enough oxygen to heal. If the lungs have collapsed areas, mucus and bacteria build up can lead to pneumonia. Your nurse will encourage you to breath deeply and cough often. Nerve damage or persistent pain. Any operation on the spine comes with the risk of damaging the nerves or spinal cord. Damage can cause numbness or even paralysis. However, the most common cause of persistent pain is nerve damage from the disc herniation itself. Some disc herniations may permanently damage a nerve making it unresponsive to decompressive surgery (Fig. 6). In these cases, spinal cord stimulation or other treatments may provide relief. Be sure to go into surgery with realistic expectations about your pain. Discuss your expectations with your doctor. Sources & Links If you have more questions, please contact Mayfield Brain & Spine at or Sources 1) Resnick DK, et al. Guidelines for the performance of fusion procedures for degenerative disease of the lumbar spine. Part 8: lumbar fusion for disc herniation and radiculopathy. J Neurosurg Spine 2:673-78, ) Atlas SJ, et al. Long-term outcomes of surgical and nonsurgical management of sciatica secondary to a lumbar disc herniation: 10-year results from the Maine Lumbar Spine Study. Spine, 30(8): , ) Weinstien JN, et al. Surgical vs nonoperative treatment for lumbar disk herniation: the Spine Patient Outcomes Research Trial (SPORT): a randomized trial. JAMA 296: , ) Ryang YM, et al. Standard open microdiscectomy versus minimal access trocar microdiscectomy: results of a prospective randomized study. Neurosurgery 62:174-81, Links nerve healed nerve damaged Figure 6. Several months after surgery, the disc wall and nerve root should repair and heal (left). However, sometimes the nerve is unable to repair itself fully (right) and some symptoms may persist despite removing the pressure off the nerve. This situation may be similar to moving furniture off the carpet. Once the heavy couch is moved, the carpet fibers re-expand and look like new; other times the imprint is there forever. Glossary annulus (annulus fibrosis): tough fibrous outer wall of an intervertebral disc. discectomy: a type of surgery in which herniated disc material is removed so that it no longer irritates and compresses the nerve root. fusion: to join together two separate bones into one to provide stability. herniated disc: a condition in which disc material protrudes through the disc wall and irritates surrounding nerves causing pain. lamina: flat plates of bone originating from the pedicles of the vertebral body that form the posterior outer wall of the spinal canal and protect the spinal cord. Sometimes called the vertebral arch. spinal instability: abnormal movement between two vertebrae that can cause pain or damage the spinal cord and nerves. vertebra (plural vertebrae): one of 33 bones that form the spinal column, they are divided into 7 cervical, 12 thoracic, 5 lumbar, 5 sacral, and 4 coccygeal. Only the top 24 bones are moveable. updated > reviewed by > Robert Bohinski, MD, Mayfield Clinic Mayfield Certified Health Info materials are written and developed by the Mayfield Clinic. We comply with the HONcode standard for trustworthy health information. This information is not intended to replace the medical advice of your health care provider. Mayfield Clinic > 5
Spinal Decompression: Laminectomy & Laminotomy
 Spinal Decompression: Laminectomy & Laminotomy Overview Decompression surgery (laminectomy) removes the bony roof covering the spinal cord and nerves to create more space for them to move freely. Narrowing
Spinal Decompression: Laminectomy & Laminotomy Overview Decompression surgery (laminectomy) removes the bony roof covering the spinal cord and nerves to create more space for them to move freely. Narrowing
Spinal Fusion: Axial Lumbar Interbody Fusion (AxiaLIF)
 1 2 Spinal Fusion: Axial Lumbar Interbody Fusion (AxiaLIF) Overview AxiaLIF is a minimally invasive spinal fusion to treat disc problems in the low back. Fusion stabilizes the spine to stop the painful
1 2 Spinal Fusion: Axial Lumbar Interbody Fusion (AxiaLIF) Overview AxiaLIF is a minimally invasive spinal fusion to treat disc problems in the low back. Fusion stabilizes the spine to stop the painful
Anterior Cervical Discectomy & Fusion
 1 2 Anterior Cervical Discectomy & Fusion Overview Anterior cervical discectomy and fusion (ACDF) is a surgery to remove a herniated or degenerative disc in the neck area of the spine. The incision is
1 2 Anterior Cervical Discectomy & Fusion Overview Anterior cervical discectomy and fusion (ACDF) is a surgery to remove a herniated or degenerative disc in the neck area of the spine. The incision is
Anterior Cervical Discectomy & Fusion
 Anterior Cervical Discectomy & Fusion Overview Anterior cervical discectomy and fusion (ACDF) is a surgery to remove a herniated or degenerative disc in the neck. An incision is made in the throat area
Anterior Cervical Discectomy & Fusion Overview Anterior cervical discectomy and fusion (ACDF) is a surgery to remove a herniated or degenerative disc in the neck. An incision is made in the throat area
GUIDELINES FOR PATIENTS HAVING CERVICAL DISCECTOMY AND FUSION SURGERY
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING CERVICAL DISCECTOMY AND FUSION SURGERY Please
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING CERVICAL DISCECTOMY AND FUSION SURGERY Please
Minimally Invasive Discectomy/ Decompression
 Minimally Invasive Discectomy/ Decompression What Is A Minimally Invasive Lumbar Discectomy? A lumbar discectomy is a surgical procedure that involves relieving the pressure placed on nerve roots and/or
Minimally Invasive Discectomy/ Decompression What Is A Minimally Invasive Lumbar Discectomy? A lumbar discectomy is a surgical procedure that involves relieving the pressure placed on nerve roots and/or
POSTERIOR LATERAL FUSION LUMBAR
 PROCEDURE A Posterior Lateral Fusion (PLF) is spine surgery performed to treat disabling back pain, leg pain, leg weakness or numbness, or spinal instability. During this procedure, your surgeon will remove
PROCEDURE A Posterior Lateral Fusion (PLF) is spine surgery performed to treat disabling back pain, leg pain, leg weakness or numbness, or spinal instability. During this procedure, your surgeon will remove
North American Spine Society Public Education Series
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
The time required for surgery will vary depending upon the procedure recommended. The surgery may last 3 8 hours.
 PROCEDURE Your surgeon has recommended the removal of a spine tumor. Lesions of the spine may occur in the neck region (cervical), mid-back region (thoracic), or low-back region (lumbar-sacral). There
PROCEDURE Your surgeon has recommended the removal of a spine tumor. Lesions of the spine may occur in the neck region (cervical), mid-back region (thoracic), or low-back region (lumbar-sacral). There
Review date: February Lumbar Discectomy
 Review date: February 2019 Lumbar Discectomy Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as having a lumbar disc protrusion, resulting in nerve root
Review date: February 2019 Lumbar Discectomy Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as having a lumbar disc protrusion, resulting in nerve root
While complications from surgery are uncommon some can be serious and may include:
 PROCEDURE A Cervical Laminectomy is usually performed for spinal cord compression from cervical arthritis, nerve root compression from a cervical disc protrusion, or for an arthritic spur. These are painful
PROCEDURE A Cervical Laminectomy is usually performed for spinal cord compression from cervical arthritis, nerve root compression from a cervical disc protrusion, or for an arthritic spur. These are painful
LUMBAR MICROSURGERY. Low Back Surgery to Reduce Your Pain
 LUMBAR MICROSURGERY Low Back Surgery to Reduce Your Pain Planning for Low Back Surgery Having a low back (lumbar) problem can be frustrating. You may have pain when you sit, stand, or walk. Even a simple
LUMBAR MICROSURGERY Low Back Surgery to Reduce Your Pain Planning for Low Back Surgery Having a low back (lumbar) problem can be frustrating. You may have pain when you sit, stand, or walk. Even a simple
POSTERIOR CERVICAL LAMINECTOMY AND FUSION
 PROCEDURE A Posterior Cervical Laminectomy and Fusion surgical procedure is usually performed to treat spinal cord compression resulting from cervical canal narrowing. At times, it is also recommended
PROCEDURE A Posterior Cervical Laminectomy and Fusion surgical procedure is usually performed to treat spinal cord compression resulting from cervical canal narrowing. At times, it is also recommended
Table of Contents. What is Spinal Fusion? Pre-Register for Surgery How Do I Prepare for Surgery?... 3
 www.cpmc.org/learning Spinal Fusion Table of Contents What is Spinal Fusion?... 2 Pre-Register for Surgery... 2 How Do I Prepare for Surgery?... 3 What Can I Expect During My Hospital Stay?... 3 If You
www.cpmc.org/learning Spinal Fusion Table of Contents What is Spinal Fusion?... 2 Pre-Register for Surgery... 2 How Do I Prepare for Surgery?... 3 What Can I Expect During My Hospital Stay?... 3 If You
ANTERIOR CERVICAL DISCECTOMY AND FUSION
 PROCEDURE An Anterior Cervical Discectomy is the surgical removal of a disc. The procedure is used when a disc protrusion or arthritic bone spur is placing pressure on a nerve and causing arm or neck pain.
PROCEDURE An Anterior Cervical Discectomy is the surgical removal of a disc. The procedure is used when a disc protrusion or arthritic bone spur is placing pressure on a nerve and causing arm or neck pain.
A Patient s Guide to Cervical Foraminotomy
 A Patient s Guide to Cervical Foraminotomy 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Cervical Foraminotomy 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled from a variety
ANTERIOR LUMBAR INTERBODY FUSION (ALIF)
 PROCEDURE An Anterior Lumbar Interbody Fusion (ALIF) is a surgical procedure performed when there is disabling pain from a degenerated disc or nerve root compression. During the operation, your surgeon
PROCEDURE An Anterior Lumbar Interbody Fusion (ALIF) is a surgical procedure performed when there is disabling pain from a degenerated disc or nerve root compression. During the operation, your surgeon
ANTERIOR CERVICAL DECOMPRESSION AND FUSION
 NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, etc) OR ASPIRIN PRODUCTS FOR 7-10 DAYS BEFORE SURGERY. These medications can increase bleeding
NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, etc) OR ASPIRIN PRODUCTS FOR 7-10 DAYS BEFORE SURGERY. These medications can increase bleeding
GEORGETOWN ORTHOPAEDIC SPINE SURGERY POSTERIOR CERVICAL SURGERY (LAMINOPLASTY, LAMINECTOMY WITH FUSION)
 POSTERIOR CERVICAL SURGERY (LAMINOPLASTY, LAMINECTOMY WITH FUSION) PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS
POSTERIOR CERVICAL SURGERY (LAMINOPLASTY, LAMINECTOMY WITH FUSION) PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS
Dr. Anant Kumar, M.D. Post-Operative Instructions after Cervical Spine Surgery
 Dr. Anant Kumar, M.D. Post-Operative Instructions after Cervical Spine Surgery We want to make this experience as pleasant as possible for you and your family. If you have any questions before or after
Dr. Anant Kumar, M.D. Post-Operative Instructions after Cervical Spine Surgery We want to make this experience as pleasant as possible for you and your family. If you have any questions before or after
A Patient's Guide to Cervical Laminectomy
 Introduction A laminectomy is a surgical procedure to relieve pressure on the spinal cord due to spinal stenosis. In spinal stenosis, bone spurs press against the spinal cord, leading to a condition called
Introduction A laminectomy is a surgical procedure to relieve pressure on the spinal cord due to spinal stenosis. In spinal stenosis, bone spurs press against the spinal cord, leading to a condition called
ADULT SPINAL DEFORMITY SURGERY
 PROCEDURE Spinal deformity correction surgery involves many techniques to correct the scoliosis, kyphosis, or other deformities of your spine to a more normal alignment. During the procedure, your surgeon
PROCEDURE Spinal deformity correction surgery involves many techniques to correct the scoliosis, kyphosis, or other deformities of your spine to a more normal alignment. During the procedure, your surgeon
Preparing for Lumbar Spinal Fusion
 1 Preparing for Lumbar Spinal Fusion Overview A. Normal spine Spinal fusion is a surgery that permanently joins together one or more bony vertebrae of the spine. Fusing bones together can prevent painful
1 Preparing for Lumbar Spinal Fusion Overview A. Normal spine Spinal fusion is a surgery that permanently joins together one or more bony vertebrae of the spine. Fusing bones together can prevent painful
Lumbar Nerve Root Decompression for Foraminal Stenosis
 Lumbar Nerve Root Decompression for Foraminal Stenosis Issue 5: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as
Lumbar Nerve Root Decompression for Foraminal Stenosis Issue 5: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Anterior Cervical Discectomy and Fusion Surgery
 Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
Dhruv B. Pateder, MD, FAAOS
 Dhruv B. Pateder, MD, FAAOS TOWN CENTER ORTHOPEDIC ASSOCIATES SPINE SURGERY POST-OPERATIVE DISCHARGE INSTRUCTIONS: CERVICAL (NECK) FUSION SPINE SURGERY 1.ANTERIOR DECOMPRESSION AND FUSION WITH INSTRUMENTATION
Dhruv B. Pateder, MD, FAAOS TOWN CENTER ORTHOPEDIC ASSOCIATES SPINE SURGERY POST-OPERATIVE DISCHARGE INSTRUCTIONS: CERVICAL (NECK) FUSION SPINE SURGERY 1.ANTERIOR DECOMPRESSION AND FUSION WITH INSTRUMENTATION
GEORGETOWN ORTHOPAEDIC SPINE SURGERY. Lumbar Decompression
 Lumbar Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS FOR 7-10 DAYS BEFORE SURGERY. These medications
Lumbar Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS FOR 7-10 DAYS BEFORE SURGERY. These medications
Spinal Cord Stimulation
 1 2 Spinal Cord Stimulation Overview Spinal cord stimulation uses low voltage stimulation to the spine to block the feeling of pain. A small device implanted in the body transmits an electrical current
1 2 Spinal Cord Stimulation Overview Spinal cord stimulation uses low voltage stimulation to the spine to block the feeling of pain. A small device implanted in the body transmits an electrical current
A Patient s Guide to Lumbar Discectomy. PHYSIO.coza
 A Patient s Guide to Lumbar Discectomy SANDTON MEDICLINIC 011 706 7495 FAIRWAYS LIFE HOSPITAL 011 875 1827 ST STITHIANS 082 378 9642 JEPPE BOYS HIGH SCHOOL 084 816 5457 JOHANNESBURG, SANDTON@PHYSIO.CO.ZA
A Patient s Guide to Lumbar Discectomy SANDTON MEDICLINIC 011 706 7495 FAIRWAYS LIFE HOSPITAL 011 875 1827 ST STITHIANS 082 378 9642 JEPPE BOYS HIGH SCHOOL 084 816 5457 JOHANNESBURG, SANDTON@PHYSIO.CO.ZA
Spinal Fusion: Anterior Lumbar Interbody Fusion (ALIF)
 Spinal Fusion: Anterior Lumbar Interbody Fusion (ALIF) Overview Anterior lumbar interbody fusion is a surgery to treat disc problems in the low back. Fusion locks together two or more bones to stop painful
Spinal Fusion: Anterior Lumbar Interbody Fusion (ALIF) Overview Anterior lumbar interbody fusion is a surgery to treat disc problems in the low back. Fusion locks together two or more bones to stop painful
The main causes of cervical radiculopathy include degeneration, disc herniation, and spinal instability.
 SpineFAQs Cervical Radiculopathy Neck pain has many causes. Mechanical neck pain comes from injury or inflammation in the soft tissues of the neck. This is much different and less concerning than symptoms
SpineFAQs Cervical Radiculopathy Neck pain has many causes. Mechanical neck pain comes from injury or inflammation in the soft tissues of the neck. This is much different and less concerning than symptoms
Anterior Cervical Discectomy and Fusion (ACDF)
 Anterior Cervical Discectomy and Fusion (ACDF) What Is an ACDF? Anterior Cervical Discectomy and Fusion (ACDF) is a surgical procedure that involves decompressing spinal cord and nerves in the cervical
Anterior Cervical Discectomy and Fusion (ACDF) What Is an ACDF? Anterior Cervical Discectomy and Fusion (ACDF) is a surgical procedure that involves decompressing spinal cord and nerves in the cervical
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
North American Spine Society Public Education Series
 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
 The spine is made of a column of bones. Each bone, or vertebra, is formed by a round block of bone, called a vertebral body. A bony ring attaches to the back of the vertebral body. When the vertebra bones
The spine is made of a column of bones. Each bone, or vertebra, is formed by a round block of bone, called a vertebral body. A bony ring attaches to the back of the vertebral body. When the vertebra bones
Spine Conditions and Treatments. Your Guide to Common
 Your Guide to Common Spine Conditions and Treatments The spine is made up of your neck and backbone. It allows your body to bend and move freely. As you get older, it is normal to have aches and pains.
Your Guide to Common Spine Conditions and Treatments The spine is made up of your neck and backbone. It allows your body to bend and move freely. As you get older, it is normal to have aches and pains.
 Introduction Posterior cervical fusion is done through the back posterior of the neck. The surgery joins two or more neck vertebrae into one solid section of bone. The medical term for fusion is arthrodesis.
Introduction Posterior cervical fusion is done through the back posterior of the neck. The surgery joins two or more neck vertebrae into one solid section of bone. The medical term for fusion is arthrodesis.
Spinal Cord Stimulation
 Spinal Cord Stimulation Overview Spinal cord stimulation is a therapy that masks pain signals before they reach the brain. A small device, similar to a pacemaker, is implanted in the body to deliver electrical
Spinal Cord Stimulation Overview Spinal cord stimulation is a therapy that masks pain signals before they reach the brain. A small device, similar to a pacemaker, is implanted in the body to deliver electrical
POSTERIOR CERVICAL FUSION
 AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
A Healthy Lumbar Spine...2. Lumbar Discectomy...3. Understanding Discectomy Surgery...4. Lumbar Decompression...5
 Table of Contents A Healthy Lumbar Spine...2 Lumbar Discectomy...3 Understanding Discectomy Surgery...4 Lumbar Decompression...5 Understanding Decompression Surgery....6 Preparing for Surgery....7 After
Table of Contents A Healthy Lumbar Spine...2 Lumbar Discectomy...3 Understanding Discectomy Surgery...4 Lumbar Decompression...5 Understanding Decompression Surgery....6 Preparing for Surgery....7 After
Neurosurgery: Neck Surgery
 Patient & Family Guide 2015 Neurosurgery: Neck Surgery www.nshealth.ca Neurosurgery: Neck Surgery Types of surgery Discectomy is the removal of part of the disc which is pressing on a nerve. The pressure
Patient & Family Guide 2015 Neurosurgery: Neck Surgery www.nshealth.ca Neurosurgery: Neck Surgery Types of surgery Discectomy is the removal of part of the disc which is pressing on a nerve. The pressure
Cervical Spine Discharge Instructions
 Pain After surgery you may experience pain in the region of the incision. Some neck and arm pain as well as tingling or numbness may also be present. Initially it may be of greater intensity than pre-operatively,
Pain After surgery you may experience pain in the region of the incision. Some neck and arm pain as well as tingling or numbness may also be present. Initially it may be of greater intensity than pre-operatively,
Table of Contents: What is a laparoscopic nissen fundoplication?...3. Where will surgery be performed?...3
 Table of Contents: What is a laparoscopic nissen fundoplication?...3 Planning and preparing for the surgery...3-4 Where will surgery be performed?...3 What to expect during surgery and your hospital stay.
Table of Contents: What is a laparoscopic nissen fundoplication?...3 Planning and preparing for the surgery...3-4 Where will surgery be performed?...3 What to expect during surgery and your hospital stay.
Herniated Disk in the Lower Back
 Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
If you have a condition that compresses your nerves, causing debilitating back pain or numbness along the back of your leg.
 Below, we have provided some basic information for your benefit. Please use this information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk
Below, we have provided some basic information for your benefit. Please use this information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS North American Spine Society Public Education Series WHAT IS LUMBAR SPINAL STENOSIS? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
LUMBAR SPINAL STENOSIS North American Spine Society Public Education Series WHAT IS LUMBAR SPINAL STENOSIS? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
PRE- AND POST-SURGERY INSTRUCTIONS FOR SPINE PATIENTS
 PRE- AND POST-SURGERY INSTRUCTIONS FOR SPINE PATIENTS Medications: Narcotics: The orthopaedic office does not prescribe narcotics for pain prior to operations, with some exceptions. If you have pain that
PRE- AND POST-SURGERY INSTRUCTIONS FOR SPINE PATIENTS Medications: Narcotics: The orthopaedic office does not prescribe narcotics for pain prior to operations, with some exceptions. If you have pain that
SpineFAQs. Neck Pain Diagnosis and Treatment
 SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
Spine Surgery Discharge Instructions
 Spine Surgery Discharge Instructions Your sutures or staples need to stay in place for at least 10 days after surgery. To have them removed you can: Call your surgeon s office (the number is on your discharge
Spine Surgery Discharge Instructions Your sutures or staples need to stay in place for at least 10 days after surgery. To have them removed you can: Call your surgeon s office (the number is on your discharge
Thank you for choosing Saint Joseph s Hospital Health Center for your spine surgery. Updated Jan 2017
 Thank you for choosing Saint Joseph s Hospital Health Center for your spine surgery Updated Jan 2017 This class is designed to give you some basic, important information about spine surgery We will cover
Thank you for choosing Saint Joseph s Hospital Health Center for your spine surgery Updated Jan 2017 This class is designed to give you some basic, important information about spine surgery We will cover
A Patient s Guide to Cervical Radiculopathy
 A Patient s Guide to Cervical Radiculopathy 950 Breckinridge Lane Suite 220 Louisville, KY 40223 Phone: 502.708.2940 DISCLAIMER: The information in this booklet is compiled from a variety of sources. It
A Patient s Guide to Cervical Radiculopathy 950 Breckinridge Lane Suite 220 Louisville, KY 40223 Phone: 502.708.2940 DISCLAIMER: The information in this booklet is compiled from a variety of sources. It
Patient Information. Spinal Fusion Using the ST360 or Silhouette Pedicle Screw System
 Patient Information Spinal Fusion Using the ST360 or Silhouette Pedicle Screw System Spinal Fusion Using the ST360 or Silhouette Pedicle Screw System Your doctor has recommended spinal fusion surgery using
Patient Information Spinal Fusion Using the ST360 or Silhouette Pedicle Screw System Spinal Fusion Using the ST360 or Silhouette Pedicle Screw System Your doctor has recommended spinal fusion surgery using
Nucleoplasty What is Nucleoplasty? Why do I need a Nucleoplasty? What is the typical procedure? not Is this procedure effective?
 Nucleoplasty What is Nucleoplasty? Nucleoplasty is a minimally invasive procedure for percutaneous disc decompression that uses radiofrequency based technology to ablate and coagulate soft tissue to decompress
Nucleoplasty What is Nucleoplasty? Nucleoplasty is a minimally invasive procedure for percutaneous disc decompression that uses radiofrequency based technology to ablate and coagulate soft tissue to decompress
Caring for Myself after Extreme Lateral Lumbar Spinal Fusion
 Caring for Myself after Extreme Lateral Lumbar Spinal Fusion What is Extreme Lateral Lumbar Spinal Fusion? Extreme Lateral Lumbar Spinal Fusion is the placement of a cage in the disc space and possibly
Caring for Myself after Extreme Lateral Lumbar Spinal Fusion What is Extreme Lateral Lumbar Spinal Fusion? Extreme Lateral Lumbar Spinal Fusion is the placement of a cage in the disc space and possibly
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis This article is also available in Spanish: Estenosis de la columna lumbar (topic.cfm?topic=a00701). A common cause of low back and leg pain is lumbar spinal stenosis. As we age,
Lumbar Spinal Stenosis This article is also available in Spanish: Estenosis de la columna lumbar (topic.cfm?topic=a00701). A common cause of low back and leg pain is lumbar spinal stenosis. As we age,
Taking Care of Your Back
 Taking Care of Your Back Most people will feel back pain at some point in their lives, but not all back pain is the same for everyone. The good news is, most low back pain improves without any treatment
Taking Care of Your Back Most people will feel back pain at some point in their lives, but not all back pain is the same for everyone. The good news is, most low back pain improves without any treatment
Lumbar Epidural Injections. Treatment to Reduce Pain
 Lumbar Epidural Injections Treatment to Reduce Pain What Is a Lumbar Epidural Injection? Your doctor may have suggested you have a lumbar epidural injection. This procedure can help relieve low back and
Lumbar Epidural Injections Treatment to Reduce Pain What Is a Lumbar Epidural Injection? Your doctor may have suggested you have a lumbar epidural injection. This procedure can help relieve low back and
Lumbar Decompression Surgery Guide
 Kevin O Neill, MD 8450 Northwest Blvd. Indianapolis, IN 46278 317.802.2429 Lumbar Decompression Surgery Guide Table of Contents The Lumbar Spine...1 Lumbar Surgery...2 Before Surgery...3 Medications...4
Kevin O Neill, MD 8450 Northwest Blvd. Indianapolis, IN 46278 317.802.2429 Lumbar Decompression Surgery Guide Table of Contents The Lumbar Spine...1 Lumbar Surgery...2 Before Surgery...3 Medications...4
ACDF. Anterior Cervical Discectomy and Fusion. An introduction to
 An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
HERNIATED DISCS AN INTRODUCTION TO
 AN INTRODUCTION TO HERNIATED S This booklet provides general information on herniated discs. It is not meant to replace any personal conversations that you might wish to have with your physician or other
AN INTRODUCTION TO HERNIATED S This booklet provides general information on herniated discs. It is not meant to replace any personal conversations that you might wish to have with your physician or other
Patient s guide to surgery
 Patient s guide to surgery Surgery date: Time for arrival will be given a day before surgery Please make a pre-operative appointment at the hospital. Remember to take the preoperative paperwork with you
Patient s guide to surgery Surgery date: Time for arrival will be given a day before surgery Please make a pre-operative appointment at the hospital. Remember to take the preoperative paperwork with you
Posterior Lumbar Spinal Fusion
 Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
Adult Isthmic Spondylolisthesis
 Adult Isthmic Spondylolisthesis North American Spine Society Public Education Series What Is Adult Isthmic Spondylolisthesis? The spine is made up of a series of connected bones called vertebrae. In about
Adult Isthmic Spondylolisthesis North American Spine Society Public Education Series What Is Adult Isthmic Spondylolisthesis? The spine is made up of a series of connected bones called vertebrae. In about
BACK PAIN. Disclaimer. Integrated web marketing. Multimedia Health Education
 BACK PAIN Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or a licensed healthcare
BACK PAIN Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or a licensed healthcare
Patient Guide to Neck Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Posterior Cervical Fusion procedures. Patient Guide to Neck Surgery Posterior Cervical Fusion NexPosure NexPosure MIS Access provides
The following is a sampling of products offered by Zimmer Spine for use in Posterior Cervical Fusion procedures. Patient Guide to Neck Surgery Posterior Cervical Fusion NexPosure NexPosure MIS Access provides
Lumbar Discectomy. Long Island Spine Specialists, P.C. 763 Larkfield Road 2nd Floor Commack, NY Phone: (631) Fax: (631)
 A Patient s Guide to Lumbar Discectomy 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is compiled from a variety of
A Patient s Guide to Lumbar Discectomy 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is compiled from a variety of
Cervical Artificial Disc Replacement Preoperative, Postoperative and Home Recovery Guide
 1 Cervical Artificial Disc Replacement Preoperative, Postoperative and Home Recovery Guide Introduction The purpose of this guide is to provide you and your family with information regarding your medical
1 Cervical Artificial Disc Replacement Preoperative, Postoperative and Home Recovery Guide Introduction The purpose of this guide is to provide you and your family with information regarding your medical
Cervical Corpectomy (Vertebral Body Replacement) and Spinal Fusion
 Cervical Corpectomy (Vertebral Body Replacement) and Spinal Fusion Cervical Corpectomy is intended for the surgical correction and stabilization of the spine where vertebral bone removal is necessary.
Cervical Corpectomy (Vertebral Body Replacement) and Spinal Fusion Cervical Corpectomy is intended for the surgical correction and stabilization of the spine where vertebral bone removal is necessary.
Overview Anatomy of the spinal canal What is spinal stenosis? > 1
 1 Spinal Stenosis Overview Spinal stenosis is the narrowing of the bony space (canals) through which the nerves and spinal cord pass. Arthritis can cause the facet joints and ligaments to enlarge and thicken
1 Spinal Stenosis Overview Spinal stenosis is the narrowing of the bony space (canals) through which the nerves and spinal cord pass. Arthritis can cause the facet joints and ligaments to enlarge and thicken
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
Shoulder Instability Latarjet Procedure
 Explanation of Procedure and/or Diagnosis Anatomy The shoulder is a ball and socket joint and is the most mobile joint of the body. Its plays a major role in positioning your arm and hand in space. Because
Explanation of Procedure and/or Diagnosis Anatomy The shoulder is a ball and socket joint and is the most mobile joint of the body. Its plays a major role in positioning your arm and hand in space. Because
Discharge Instructions: What to Expect After Lumbar Fusion
 Discharge Instructions: What to Expect After Lumbar Fusion Incision Care You may shower 72 hours after you have been discharged from the hospital unless otherwise stated by Dr. Valente. Please do not take
Discharge Instructions: What to Expect After Lumbar Fusion Incision Care You may shower 72 hours after you have been discharged from the hospital unless otherwise stated by Dr. Valente. Please do not take
Home Care Instructions. Cervical Laminoplasty
 Home Care Instructions Cervical Laminoplasty You are recovering from a posterior cervical decompression in which your surgeon removed the pressure on your spinal nerves in an attempt to reduce pain and/or
Home Care Instructions Cervical Laminoplasty You are recovering from a posterior cervical decompression in which your surgeon removed the pressure on your spinal nerves in an attempt to reduce pain and/or
Facet Joint Syndrome / Arthritis
 Facet Joint Syndrome / Arthritis Overview Facet joint syndrome is an arthritis-like condition of the spine that can be a significant source of back and neck pain. It is caused by degenerative changes to
Facet Joint Syndrome / Arthritis Overview Facet joint syndrome is an arthritis-like condition of the spine that can be a significant source of back and neck pain. It is caused by degenerative changes to
Dr. Nuelle Total/Partial Hip Replacement: Discharge Care Instructions
 Dr. Nuelle Total/Partial Hip Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your hip replacement surgery. We hope that you had a good stay with us. These
Dr. Nuelle Total/Partial Hip Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your hip replacement surgery. We hope that you had a good stay with us. These
Spine Surgery. Lumbar Spinal Surgery
 Spine Surgery Lumbar Spinal Surgery Lumbar spinal surgery_print.indd 1 5/10/2016 11:17:59 AM Lower back problems If you have a lower back problem, you re not alone. Lower back problems are very common.
Spine Surgery Lumbar Spinal Surgery Lumbar spinal surgery_print.indd 1 5/10/2016 11:17:59 AM Lower back problems If you have a lower back problem, you re not alone. Lower back problems are very common.
PARADIGM SPINE. Patient Information. Treatment of a Narrow Lumbar Spinal Canal
 PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
A Patient s Guide to Cervical Radiculopathy
 A Patient s Guide to Cervical Radiculopathy 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Cervical Radiculopathy 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is compiled from a variety
Jason Barry, M.D. Knee Arthroscopy with Anterior Cruciate Ligament (ACL) Reconstruction
 Jason Barry, M.D. Knee Arthroscopy with Anterior Cruciate Ligament (ACL) Reconstruction Arthroscopy (scope) is a minimally invasive surgical procedure orthopedic surgeons use to visualize, diagnose and
Jason Barry, M.D. Knee Arthroscopy with Anterior Cruciate Ligament (ACL) Reconstruction Arthroscopy (scope) is a minimally invasive surgical procedure orthopedic surgeons use to visualize, diagnose and
MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION AN INTRODUCTION TO
 AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
POST-OPERATIVE INSTRUCTIONS
 POST-OPERATIVE INSTRUCTIONS Arthroscopic Subacromial Decompression with or without Distal Clavicle Excision (removal of bone spur) Dr. Sostak visit www.healthy-txt.com/drsostak for more detailed instructions
POST-OPERATIVE INSTRUCTIONS Arthroscopic Subacromial Decompression with or without Distal Clavicle Excision (removal of bone spur) Dr. Sostak visit www.healthy-txt.com/drsostak for more detailed instructions
Caring for myself after Laparoscopic Appendectomy
 Caring for myself after Laparoscopic Appendectomy What is Laparoscopy Appendectomy? Laparoscopy appendectomy is a surgery to treat appendicitis infection of the appendix. During laparoscopic surgery, surgeons
Caring for myself after Laparoscopic Appendectomy What is Laparoscopy Appendectomy? Laparoscopy appendectomy is a surgery to treat appendicitis infection of the appendix. During laparoscopic surgery, surgeons
Discharge Instructions What to Expect After Cervical Fusion
 Discharge Instructions What to Expect After Cervical Fusion Incision Care You may shower 72 hours after you have been discharged from the hospital unless otherwise stated by Dr. Valente. Please do not
Discharge Instructions What to Expect After Cervical Fusion Incision Care You may shower 72 hours after you have been discharged from the hospital unless otherwise stated by Dr. Valente. Please do not
A Patient s Guide to Pain Management: Radiofrequency Ablation
 A Patient s Guide to Pain Management: Radiofrequency Ablation 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Pain Management: Radiofrequency Ablation 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled
the back book Your Guide to a Healthy Back
 the back book Your Guide to a Healthy Back anatomy Your spine s job is to: Support your upper body and neck Increase flexibility of your spine Protect your spinal cord There are 6 primary components of
the back book Your Guide to a Healthy Back anatomy Your spine s job is to: Support your upper body and neck Increase flexibility of your spine Protect your spinal cord There are 6 primary components of
Dr. Nuelle Knee Replacement: Discharge Care Instructions
 Dr. Nuelle Knee Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your knee replacement surgery. We hope that you had a good stay with us. These discharge
Dr. Nuelle Knee Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your knee replacement surgery. We hope that you had a good stay with us. These discharge
Laparoscopy. What is Laparoscopy? Why is this surgery used? How do I prepare for surgery?
 What is? Laparoscopic surgery is where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the belly button. To help with the surgery,
What is? Laparoscopic surgery is where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the belly button. To help with the surgery,
UW MEDICINE PATIENT EDUCATION. What to expect and how to prepare DRAFT. What are liposuction and fat grafting? How do I prepare?
 UW MEDICINE PATIENT EDUCATION Liposuction and Fat Grafting for Breast Reconstruction What to expect and how to prepare This handout explains liposuction and fat grafting when used in breast reconstruction.
UW MEDICINE PATIENT EDUCATION Liposuction and Fat Grafting for Breast Reconstruction What to expect and how to prepare This handout explains liposuction and fat grafting when used in breast reconstruction.
ACL Reconstruction. Role of the Anterior Cruciate Ligament. Treatment of ACL tears. ACL Reconstruction
 Role of the Anterior Cruciate Ligament The ACL stabilizes the knee when jumping, pivoting, or cutting. It prevents the shinbone (tibia) from sliding forward on the thigh bone (femur). ACL tears often occur
Role of the Anterior Cruciate Ligament The ACL stabilizes the knee when jumping, pivoting, or cutting. It prevents the shinbone (tibia) from sliding forward on the thigh bone (femur). ACL tears often occur
LUMBAR DECOMPRESSION / DISCECTOMY SURGERY INFORMATION
 LUMBAR DECOMPRESSION / DISCECTOMY SURGERY INFORMATION WHAT IS LUMBAR DECOMPRESSION / DISCECTOMY SURGERY? During lumbar decompression/ discectomy back surgery, a small portion of the bone over the nerve
LUMBAR DECOMPRESSION / DISCECTOMY SURGERY INFORMATION WHAT IS LUMBAR DECOMPRESSION / DISCECTOMY SURGERY? During lumbar decompression/ discectomy back surgery, a small portion of the bone over the nerve
Anatomy of the Spine. Figure 1. (left) The spine has three natural curves that form an S-shape; strong muscles keep our spine in alignment.
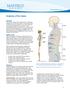 1 2 Anatomy of the Spine Overview The spine is made of 33 individual bony vertebrae stacked one on top of the other. This spinal column provides the main support for your body, allowing you to stand upright,
1 2 Anatomy of the Spine Overview The spine is made of 33 individual bony vertebrae stacked one on top of the other. This spinal column provides the main support for your body, allowing you to stand upright,
A Patient s Guide to Pain Management: Spinal Cord Stimulators
 A Patient s Guide to Pain Management: Spinal Cord Stimulators 950 Breckinridge Lane Suite 220 Louisville, KY 40223 Phone: 502.708.2940 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Pain Management: Spinal Cord Stimulators 950 Breckinridge Lane Suite 220 Louisville, KY 40223 Phone: 502.708.2940 DISCLAIMER: The information in this booklet is compiled from a variety
