The Canadian multicentre study of deep brain stimulation for cervical dystonia
|
|
|
- Randolf Russell
- 6 years ago
- Views:
Transcription
1 doi: /brain/awm229 The Canadian multicentre study of deep brain stimulation for cervical dystonia Brain (2007), 130, 2879^2886 Zelma H. T. Kiss, 1 Kristina Doig-Beyaert, 1 Michael Eliasziw, 1,2 Joseph Tsui, 4 Angela Haffenden 1,3 and Oksana Suchowersky 1 on behalf of the Functional and Stereotactic Section of the Canadian Neurosurgical Society and the Canadian Movement Disorders Group 1 Department of Clinical Neuroscience, 2 Department of Community Health Sciences, University of Calgary, 3 Department of Psychology, Calgary Health Region, Calgary and 4 Department of Medicine,University of British Columbia, Vancouver, Canada Correspondence to: Dr Zelma H. T. Kiss, Room 182A, Heritage Medical Research Building, 3330 Hospital Drive NW, Calgary, Alberta, Canada T2N 4N1 zkiss@ucalgary.ca Deep brain stimulation (DBS) of the globus pallidus pars interna (GPi) is an effective treatment for generalized dystonia. Its role in the management of other types of dystonia is uncertain.therefore we performed a prospective, single-blind, multicentre study assessing the efficacy and safety of bilateral GPi-DBS in 10 patients with severe, chronic, medication-resistant cervical dystonia. Two blinded neurologists assessed patients before surgery and at 6 and 12 months post-operatively using the Toronto Western Spasmodic Torticollis Rating Scale (TWSTRS). The primary outcome measure was the severity subscore (range 0^30, higher scores indicating greater impairment). Secondary outcomes included disability (0 to 30), pain (0 to 40) subscores and total scores of thetwstrs, Short Form-36 and Beck depression inventory. Swallowing and neuropsychological assessment were also performed at baseline and 12 months. One-way repeated measures analysis of variance was used to analyse the data. The TWSTRS severity score improved from a mean (SD) of 14.7 (4.2) before surgery to 8.4 (4.4) at 12 months post-operatively (P = 0.003). The disability and pain scores improved from 14.9 (3.8) and 26.6 (3.6) before surgery, to 5.4 (7.0) and 9.2 (13.1) at 12 months, respectively (both P _ 0.001). General health and physical functioning as well as depression scores improved significantly. Complications were mild and reversible in four patients. Some changes in neuropsychological tests were observed, although these did not impact daily life or employment. Our results support the efficacy and safety of GPi-DBS for the treatment of patients with severe and prolonged cervical dystonia who have failed medical management. Keywords: dystonia; torticollis; deep brain stimulation; clinical trial; globus pallidus; high-frequency stimulation Abbreviations: BDI = Beck depression inventory; DBS = deep brain stimulation; MRI = magnetic resonance imaging Received May 4, Revised August 9, 2007.AcceptedAugust24,2007. Advance Access publication September 28, 2007 Introduction Deep brain stimulation (DBS), a reversible and safe surgery used to treat to movement disorders since the 1990s, has recently been reported to improve generalized dystonia (Coubes et al., 2000; Tronnier and Fogel, 2000; Vidailhet et al., 2005). Stimulation of the globus pallidus pars interna (GPi) for cervical dystonia was first reported in 1999 (Krauss et al., 1999) and was followed by several case reports and small series (Kulisevsky et al., 2000; Krauss et al., 2002). However case series often combined multiple different dystonia types (Bereznai et al., 2002; Krauss et al., 2002; Yianni et al., 2003; Eltahawy et al., 2004a, b; Bittar et al., 2005), and the ability to draw conclusions was limited by variations in selection criteria, use of validated clinical scoring methods, unblinded outcome measures (Hung et al., 2007), the same patients reported more than once, and short duration of follow-up (Krauss et al., 1999; Islekel et al., 1999). Therefore, we conducted a prospective, multicentre pilot study to determine the effect of bilateral pallidal DBS on severity, disability, pain and quality of life in patients with cervical dystonia, using standardized and blinded measures. Materials and methods Each site obtained institutional ethics committee review for this study and each patient provided informed consent. This pilot project was registered with NIH ClinicalTrials.gov (NCT ). ß The Author (2007). Published by Oxford University Press on behalf ofthe Guarantors of Brain. Allrights reserved. For Permissions, please journals.permissions@oxfordjournals.org
2 2880 Brain (2007), 130, 2879^2886 Z. H. T. Kiss et al. Patients Ten patients were consecutively recruited at five academic centres in Canada. Inclusion criteria were clinically diagnosed cervical dystonia for at least 5 years; initial response and subsequent failure of botulinum toxin A and/or B injections; no secondary cause; a normal neurological examination except for dystonia; normal findings on magnetic resonance imaging (MRI) of the brain; the absence of psychiatric disturbances; normal cognitive function, as reflected by neuropsychology assessments. Patients with generalized dystonia were excluded. Study design and outcome measures The primary outcome measure was the severity subscale of the Toronto Western Spasmodic Torticollis Rating Scale (TWSTRS), as assessed by two blinded neurologists. The TWSTRS is a validated and widely utilized scale (Consky and Lang, 1994; Comella et al.,1997) consisting of three sections: severity (range 0 30), disability (range 0 30) and pain (range 0 40), with higher scores indicating greater impairment. Severity was judged on the basis of standardized videotapes and disability and pain assessed by means of patient questionnaires. Secondary outcomes included the TWSTRS subscores for pain and disability, the Beck depression inventory (BDI) (Beck, 1997), ShortForm-36 (SF-36) to measure quality of life (Ware and Sherbourne, 1992), global assessment of change and adverse events. The TWSTRS and other assessments were performed at baseline (at least 3 months after the last botulinum toxin injection, if patients were still receiving it), 6 months and 12 months postoperatively. Follow-up was measured as time from implantation of pulse generator. At the completion of the study all 30 videotapes were randomized and scored by two neurologists blinded to patient name and time of assessment. Severity scores were then averaged. Additional visits occurred at 3 months after surgery to determine early adverse events. Swallowing studies and neuropsychological assessments were performed pre-operatively and at 12 months follow-up. Neuropsychological assessments were performed as per routine in each centre; neither the tests nor the normative data were standardized across centres. Surgery All centres had significant experience in GPi brain mapping and DBS surgery. The initial implantation target was 2 mm anterior to, mm lateral to and 2 6 mm below the midcommissural point; the final implantation site was further refined by a combination of direct visualization on MRI, microelectrode recordings, and intraoperative stimulation (as per local practice). Firing rates of GPi neurons were slightly lower than those reported for Parkinson s patients (Tang et al., 2007). However, the overall pattern of recordings passing from anterodorsal to posteroventral (very low frequency firing cells in the putamen, mid frequency firing in the globus pallidus pars externa and the highest firing rates in the GPi), similar to that seen in Parkinson s disease patients, was maintained (Kiss et al., 2004a). DBS leads were implanted bilaterally in one or two sessions with the patient under local anaesthesia with or without sedation. In three centres (N =6 patients) microelectrode recordings were used to perform the brain mapping (Lozano et al., 1996), whereas in two centres (N = 4 patients) macrostimulation alone was utilized (Laitinen et al., 1992). Macrostimulation was performed to map the posteroventral GPi, as previously described for pallidotomy (Honey and Nugent, 2000). After brain mapping the quadripolar DBS electrode (3387, Medtronic, Minneapolis, USA) was implanted and either immediately or several days later, connected to a neurostimulator (Kinetra, Medtronic, USA) implanted in the subclavicular region under general anaesthesia. All patients underwent post-operative MRI to confirm correct electrode placement and to assess for surgical complications. MRIs were not standardized with respect to imaging sequences, but performed as per routine at each centre. Images were checked by two neurosurgeons from another centre, blind to patient outcome and centre. Each neurosurgeon independently decided whether each electrode was adequately positioned in the posteroventral GPi, or whether an electrode was too medial/lateral, dorsal/ventral or anterior/posterior. Programming was performed as was customary in each centre: by nurse specialists in four hospitals and a neurosurgical fellow in the fifth centre. Initially programming was performed as recommended by previously published work (Kumar, 2002); however, after the lead centres initial experience (Kiss et al., 2004b), we recommended not waiting more than 1 week before altering programming parameters, in case of insufficient improvement. Programming commenced using monopolar stimulation trying each pole in sequence, with a pulse width of 210 ms and frequency 180 Hz, with subsequent changes in voltage, frequency, pulse width and polarity to optimize clinical benefit. If monopolar stimulation produced adverse effects, bipolar stimulation was subsequently tested. Statistical analysis Data are shown as mean SD. Percent change was calculated using the formula (pre-op score 12 month post-op score)/preop score. One-way repeated measures analysis of variance was used to compare 6-month and 12-month outcome scores to baseline pre-operative scores. Post hoc comparisons were performed using Dunnett s test. All tests were two-tailed and results with P values were considered to be statistically significant. Results Table 1 summarizes the clinical characteristics of the patients. The median age of the patients at surgery was 57.5 years (range 47 64). The median age at the onset of dystonia was 43 years (range 19 51), such that the median duration of the disease was 16.5 years (range 5 28). Five patients had prominent associated tremor, three had minimal tremor and two had no tremor at all. A mild head injury was reported as initiating the dystonia in one patient. Another patient had some writer s cramp, which was mild and had not required treatment. Three patients had previous surgery, which was ineffective. These patients represented those who had the most severe symptoms and were most willing to try new procedures, despite having failed previous surgery. The primary outcome measure, TWSTRS severity score (Fig. 1) improved from a mean (SD) of 14.7 (4.2) before surgery to 10.6 (4.8) at 6 months and 8.4 (4.4) at 12 months post-operatively (P = 0.003). In comparison to
3 DBS for cervical dystonia Brain (2007), 130, 2879^ Table 1 Clinical features of patients and therapies applied No. Sex Age (years) Age at onset (years) Duration of disease (years) Precipitating/ exacerbating factors Other therapies attempted pre-op a Medications Pre-op (daily dose) Medications At 12 months post-op (daily dose) 1 M None Microvascular decompression at XI nerve Lorazepam 12 mg Valproic acid 150 mg Propranolol 240 mg Valproic acid 75 mg/day Propranolol 120 mg 2 M None Ibuprofen occasionally 3 F Mild concussion Clonazepam 4 mg Clonazepam 2 mg 4 M None Peripheral denervation cervical muscles trihexyphenidyl 4 mg Acetaminophen 2.6^3.25 g Codeine 240 ^300 mg Clonazepam 4 ^5 mg Trihexyphenidyl 6 mg Codeine 45 mg Ibuprofen 600 mg Clonazepam 1.5mg 5 M Vertigo, changein Intradural Trihexyphenidyl 4 mg Trihexyphenidyl 4 mg head position rhizotomy C1-3 6 F None Clonazepam 0.5^5 mg Clonazepam 0.5^5 mg 7 F None Occasional methocarbamol 400mg Acetaminophen 325 mg Lorazepam 1mg Baclofen 30 mg Venlafaxine 150 mg 8 F None 9 F Stress, fatigue 10 M None Cyclobenzaprine 10 mg Naproxen 250 mg a All patients had tried and failed Botulinum toxin A (and/or B) injection therapy. No patient received injection therapy after surgery. Only pain, mood or movement disorder relevant medications are listed; some patients were also taking drugs for osteoporosis, hypertension and other medical conditions. and 9.2 (13.1) at 12 months post-op, respectively (P and P50.001, respectively). Beck depression scores improved from 14.2 (7.2) at baseline to 6.0 (3.5) at 12 months (P50.001, Fig. 3A). Quality of life as measured by SF-36 improved from 90.9 (11.3) at baseline to (18.0) at 12 months (P = 0.003) (Fig. 3B). All patients, treating neurologists and neurosurgeons scored the global assessment of outcome as good or very good improvement at the 12-month time point, except in one case. Patient 7 was discovered to be suffering from significant depression after surgery (despite scoring within acceptable range on the Beck depression inventory). After the depression was treated, she allowed the stimulator to be turned on, but nonetheless, her responses to stimulation were unusual and with blinded severity measurements, her dystonia worsened. Fig. 1 Primary outcome measure, thetoronto Western Spasmodic Torticollis Rating Scale (TWSTRS) change over time. Each patient is illustrated as an individual symbol and line indicating their outcomes. The mean (SD) scores for the whole group are shown as bar graphs. Severity is significantly better at both 6 and 12 months post-operatively in comparison to baseline scores (P =0.003, RM-ANOVA). baseline, both 6 and 12 month severity scores were significantly reduced. Figure 2 shows similar results for the secondary outcomes. The TWSTRS disability and pain scores improved from 14.9 (3.8) and 26.6 (3.6) before surgery, to 5.4 (7.0) Stimulation variables This study did not dictate specific stimulation parameters to utilize at each centre. We suggested that each programmer follow published recommendations based on experience with generalized dystonia (Kumar, 2002), but starting with a pulse width of 210 ms. After our initial experience (Kiss et al., 2004b), centres were instructed to wait no more than 1 week between programming sessions to determine the effects of stimulation. DBS frequency at 12 months was 170 (20) Hz, pulse width was 204 (49) ms and amplitude was 3.3 (0.7) V. Table 2 (Supplementary Material) reports the electrode poles utilized for each patient.
4 2882 Brain (2007), 130, 2879^2886 Z. H. T. Kiss et al. Fig. 2 Secondary outcomes from the TWSTRS: disability (A) and pain (B) subscores. Individual patient results are shown as symbols and lines, and the group mean (SD) is shown as bar graphs. Significant reduction in patient-reported outcomes occurred at 6 and 12 months after DBS surgery (P50.001, RM-ANOVA). Fig. 3 Beck depression (A) and quality of life (SF-36, B) scores pre-operatively and at 6 and 12 months post-operatively, showing significant improvements over time (A: P50.001, B: P =0.003, RM-ANOVA). Each patient score is illustrated as a distinct symbol and line, and the group mean (SD) as the bar graphs. In case 2, described in our preliminary report (Kiss et al., 2004b), DBS programming initially produced no benefit for the first 3 months. At the 3-month post-surgery follow-up appointment, both the patient and programming nurse had concluded that DBS was not effective. Monopolar stimulation had been applied to the most dorsal electrode poles (3/7) bilaterally. At this delayed time point, stimulation was altered such that bipolar stimulation using the most ventral poles (poles 0/4, at 180 Hz, 180 ms pulse width) allowed an amplitude of 3.0 V to be reached without side effects. It resulted in an immediate improvement in subjective tightness of the neck and shoulder, followed by a gradual visible straightening of the head over the ensuing few days. One week after these settings were initiated, the patient displayed little residual torticollis (videos available from Kiss et al., 2004b). The time course of benefit for the other patients ranged from immediate improvement (as described earlier) to a requirement for several weeks (1 8 weeks) or even 6 months (one patient) of stimulation. Medical treatment Pre-operatively, eight patients were taking medication for their cervical dystonia, either for pain or the movement disorder itself (Table 1). All had initially responded but secondarily failed botulinum toxin A and/or B. After DBS surgery, no patient received further injections and most patients were able to reduce their pain or muscle relaxant drugs.
5 DBS for cervical dystonia Brain (2007), 130, 2879^ second side DBS implant was delayed by 1 month. A small chronic subdural fluid collection was seen at the second side surgery and drained during that procedure. This same patient had a very subtle hemiparesis (seen only on gait) that was present at 6-month follow-up, but resolved completely by 12 months. Two patients had mild difficulties with swallowing and two others had mild improvements on swallowing tests. There were some changes seen on neuropyschological testing as detailed in Supplementary Table 2. Significant declines (as defined by >2 SD) were seen in two patients. In one patient this degree of decline was limited to phonemic fluency, and in the other patient it was limited to verbal memory. However, these changes along with the other smaller changes seen were not significant enough to impact daily life or working ability. Fig. 4 T1-weighted MR images of DBS electrode placement in patient 1 (who had 80% improvement) in (A) axial and(b) coronal views, showing most ventral electrode pole in posteroventral GPi. Scale bar indicates 5 cm. T2-weighted axial MRI from patient 7 (C) also shows well-placed electrodes extending from (i) the most ventral pole, just above the optic tract to (ii) the most dorsal at the external pallidus/putaminal border, yet this patient fared worse after surgery (change in severity score 33%). MR imaging All patients underwent MR imaging post-operatively to confirm correct electrode placement and detect complications. Images were reviewed by the lead site neurosurgeon and another neurosurgeon blinded to patient outcome and centre. The only post-operative imaging complication was a small subdural fluid collection in a patient who remained asymptomatic (Supplementary Table 2). There was no obvious relationship between successful outcome and electrode placement. The only patient who deteriorated after surgery, had well-placed electrodes into both posteroventral GPi (Fig. 4). Adverse events Four adverse events occurred in four patients in the postoperative period; all resolved rapidly without permanent morbidity (Supplementary Table 2). One patient had dysphagia for the first few weeks post-operatively. This subsided with a decrease in stimulation amplitude, although was detected on the modified barium swallow at 1 year. Another patient had dysarthria that also resolved with a change in stimulation parameters. One patient had a transient facial weakness immediately post-operatively that resolved before the 3-month visit. Another patient developed shingles in the left ophthalmic division of the trigeminal nerve, after her first side surgery; therefore her Discussion Bilateral pallidal DBS in patients with primary cervical dystonia, led to a significant and sustained improvement in head and neck postures over a 1-year period. The mean improvement in dystonia severity was 43% compared with pre-operative scores. When combined with patient reported pain and disability scores, the total TWSTRS improved by 59%. There were significant improvements in quality of life (24%) and depression scores (58%), minor effects on swallowing and cognitive tests. Medications were reduced after surgery and no further botulinum toxin injections performed. Our results, obtained from a prospective trial of patients meeting strict inclusion criteria, confirm results obtained in individual patients (Islekel et al., 1999) and small single site series (Krauss et al., 1999, 2002; Bereznai et al., 2002;Yianni et al., 2003; Eltahawy et al., 2004b; Bittar et al., 2005; Hung et al., 2007). In these previous published series, severity subscores improved by 48 (Krauss et al., 1999) to 63% (Krauss et al., 2002) and only one report failed to identify motor improvement (Kulisevsky et al., 2000). The largest case series in which 10 patients with isolated cervical dystonia were operated at a single centre, found 55% improvement in severity scores; however, these were obtained in a non-blinded fashion (Hung et al., 2007). It is not surprising that our results obtained from multiple centres, using blinded severity measurements are not quite as good as those reported from open-label series. Instead our results are very similar to those reported by Kupsch et al. (2006) in which patients with generalized and segmental dystonia were randomized to active or sham neurostimulation. These authors found a 39% improvement in the motor score using the Burke Fahn Marsden Dystonia Rating Scale, as measured by two blinded neurologists at 3 months follow-up. While it is impossible to directly compare our studies, because the European trial did not report the number of patients with isolated cervical dystonia, different scales were utilized, and it involved a
6 2884 Brain (2007), 130, 2879^2886 Z. H. T. Kiss et al. shorter follow-up, it is nonetheless encouraging that similar improvements in motor scores were obtained in both the trials. There are several strengths to our study including its prospective multicentre design, the use of standardized videos and a validated scale for severity assessment by two neurologists unaware of the patients pre-operative or post-operative status. In addition, we did not dictate surgical technique or minimum severity of dystonia for study inclusion. Despite the original design as a small feasibility study, we achieved statistical significance for all outcomes. While it would have been ideal to perform a doubleblind study (Kupsch et al., 2006), we have been unable to blind our cervical dystonia patients involved in a comparative study on the effects of unilateral versus bilateral stimulation. Our patients know immediately which side is on or off because they experience a sensation of tingling, muscle relaxation or tightening. Only in patient 2, in whom stimulation was applied too dorsal in the globus pallidus initially, was a blinded N of one study inadvertently performed. Both the nurse and patient thought optimal stimulation was being applied. Instead the electrode poles activated were likely in the external segment of the globus pallidus. When the cathodal active electrode was switched to one in the posteroventral GPi, rapid clinical benefit was obtained. Results of DBS for cervical dystonia are better than those obtained from other contemporary surgical interventions. The only procedure still in use is the selective peripheral denervation and myectomy of neck muscles (Albanese et al., 2006). This operation produces improvements of 20 30% (Ford et al., 1999; Munchau et al., 2001). While a denervating procedure may be more economical than bilateral DBS implants, it requires specialized expertise, extensive post-operative physiotherapy (Bertrand and Lenz, 1995) and may require re-operation for re-innervation of target muscles (Albanese et al., 2006). We could not identify factors that would predict degree of improvement in cervical dystonia. Matching that reported in an open-label series (Hung et al., 2007), 6 of the 10 patients had approximately 50% or better improvement in cervical dystonia severity as measured by TWSTRS (median 63% improvement). Three patients had 530% improvement (median 23% improvement) and one patient fared worse after surgery (by 33%). This individual may have deteriorated due to depression, although worsening of dystonia was also observed in the European randomized controlled trial (Kupsch et al., 2006). To determine potential reasons why this patient and the other three improved less than the others, we examined specific factors thought to influence outcome, such as DBS electrode placement, surgical technique, experience and type of dystonia. The patient whose dystonia severity was worse at 12 months follow-up had correct DBS placement on MR imaging (Fig. 4C) as judged by two neurosurgeons unaware of clinical outcome. In one case with 23% improvement, the DBS electrodes may have been too medial (patient 4). In the other two patients, DBS electrodes were judged adequately positioned. The absence of an obvious relationship between electrode positioning and degree of improvement has been observed by others (Hung et al., 2007). The four patients with 530% improvement in TWSTRS severity scores had surgery in four different centres, two of which used microelectrode brain mapping and two centres that did not. Similar to other reports (Hung et al., 2007), clinical features of the cervical dystonia such as the presence of tremor or tonic/phasic components were not predictive of outcome. Therefore while there was some variability in the magnitude of response to therapy, 90% of the patients improved and 60% improved by 50% or greater on motor scores. These objective scores do not take into account functional improvements which were better assessed by the total TWSTRS scores. Interestingly, despite 530% motor improvement in 4 patients, they all reported improvements in pain, disability and quality of life. Generally, patientreported secondary outcome measures were consistent with the decreases in the severity of dystonia. Adverse events were similar to that reported by other groups, although we had fewer hardware-related problems and more declines identified on neuropsychological testing. Complications were those inherent to DBS surgery, including self-limited mild weakness and stimulationinduced swallowing/speech disturbance. There were no hardware-related complications, despite cervical dystonia being a known risk factor for lead fracture (Yianni et al., 2004). This was likely because we devised specific methods to reduce this complication (Kiss et al., 2004b). Other larger trials such as the one published by the European DBS for Dystonia Study group reported four infections, and two hardware problems in 40 patients (Kupsch et al., 2006). One delayed infection requiring electrode removal occurred in a series of 10 patients with cervical dystonia alone (Hung et al., 2007). Because our sample size was small and follow-up was only 1 year, we may have underestimated the surgical risks of GPi-DBS in this study. Our trial did identify changes in neuropsychological assessments in four patients Supplementary Material Table 2. These involved mainly subtle changes (1 SD or less) in memory and verbal skills. However significant declines (>2 SD) were seen in one patient in phonemic verbal fluency, and in another patient on tests of verbal memory. While this testing was performed on all patients as part of their routine care, it was not standardized. In fact, three of the four patients who showed changes and the only two with significant declines were from one centre. Although the neuropsychological data are notable, the changes were not global, and most importantly, all of these patients returned to their previous work and lifestyle. Therefore the clinical relevance of these changes is uncertain. While this finding requires further investigation
7 DBS for cervical dystonia Brain (2007), 130, 2879^ with uniform tests and normative data across centres, the changes are likely limited to specific cognitive domains. Two other studies examined neuropsychological outcomes in dystonia patients subjected to GPi-DBS. Hälbig et al. (2005) found similar changes: while there were no changes in the overall scores, individual patients improved and declined on certain tests. Vidailhet et al. (2007) reported improvements in neuropsychological scores in 22 young patients (median age 30 years) with generalized dystonia. The European DBS for Dystonia Study group trial did not perform neuropsychology as part of its protocol, and the other case series only performed the testing in selected patients (Hung et al., 2007). Conclusion This pilot, prospective, single blind study demonstrated that bilateral stimulation of the posterior ventral internal pallidus resulted in a sustained decrease in the severity of cervical dystonia, including improvements in pain, disability and quality of life in adults with cervical dystonia. Acknowledgements Funding for this study was obtained from the Canadian Institutes of Health Research (CIHR Dyskinesia and Torticollis Fund) and the Calgary Health Region. Implantable devices were provided by Medtronic Canada, however, they had no involvement in study design or data analysis. We thank Dr Scott Kraft for assisting with videotapes and programming protocols and Dr Sam Wiebe for suggestions on earlier versions of the manuscript. References Albanese A, Barnes MP, Bhatia KP, Fernandez-Alvarez E, Filippini G, Gasser T, et al. A systematic review on the diagnosis and treatment of primary (idiopathic) dystonia and dystonia plus syndromes: report of an EFNS/MDS-ES Task Force. Eur J Neurol 2006; 13: Beck AT. Beck depression inventory. San Antonio, Texas, USA: Psychological Corporation; Bereznai B, Steude U, Seelos K, Botzel K. Chronic high-frequency globus pallidus internus stimulation in different types of dystonia: a clinical, video, and MRI report of six patients presenting with segmental, cervical, and generalized dystonia. Mov Disord 2002; 17: Bertrand C, Lenz FA. Surgical treatment of dystonias. In: Tsui JKC, Calne DB, editors. Handbook of Dystonia. New York: Marcel Dekker, 1995; pp Bittar RG, Yianni J, Wang S, Liu X, Nandi D, Joint C, et al. Deep brain stimulation for generalised dystonia and spasmodic torticollis. J Clin Neurosci 2005; 12: Comella CL, Stebbins GT, Goetz CG, Chmura TA, Bressman SB, Lang AE. Teaching tape for the motor section of the Toronto Western Spasmodic Torticollis Scale. Mov Disord 1997; 12: Consky ES, Lang AE. Clinical assessments of patients with cervical dystonia. In: Jankovic J, Hallett M, editors. Therapy with botulinum toxin. New York: Marcel Dekker, 1994; pp Coubes P, Roubertie A, Vayssiere N, Hemm S, Echenne B. Treatment of DYT1-generalised dystonia by stimulation of the internal globus pallidus. Lancet 2000; 355: Eltahawy HA, Saint-Cyr JA, Giladi N, Lang AE, Lozano AM. Primary dystonia is more responsive than secondary dystonia to pallidal interventions: outcome after pallidotomy or pallidal deep brain stimulation. Neurosurgery 2004a; 54: Eltahawy HA, Saint-Cyr JA, Lang AE, Lozano AM. Pallidal deep brain stimulation in cervical dystonia: clinical outcome in four cases. Can J Neurol Sci 2004b; 31: Ford B, Louis ED, Greene P, Fahn S. Outcome of selective ramisectomy for botulinum toxin resistant torticollis. J Neurol Neurosurg Psychiatry 1999; 65: Halbig TD, Gruber D, Kopp UA, Schneider GH, Trottenberg T, Kupsch A. Pallidal stimulation in dystonia: effects on cognition, mood, and quality of life. J Neurol Neurosurg Psychiatry 2005; 76: Honey CR, Nugent RA. A prospective randomized comparison of CT and MRI pre-operative localization for pallidotomy. Can J Neurol Sci 2000; 27: Hung SW, Hamani C, Lozano AM, Poon YY, Piboolnurak P, Miyasaki JM, et al. Long-term outcome of bilateral pallidal deep brain stimulation for primary cervical dystonia. Neurology 2007; 68: Islekel S, Zileli M, Zileli B. Unilateral pallidal stimulation in cervical dystonia. Stereotact Funct Neurosurg 1999; 72: Kiss ZHT, Anderson TR, Iremonger KJ, Lavrentieva E, Hu B. Globus pallidus firing rates and patterns in humans with cervical dystonia. International Basal Ganglia Society Meeting, Crieff, Scotland; 2004a (abstract). Kiss ZHT, Doig K, Eliasziw M, Ranawaya R, Suchowersky O. The Canadian multicentre trial of pallidal deep brain stimulation for cervical dystonia: preliminary results in three patients. Neurosurg Focus 2004b; 17: E5 32 E5 38. Krauss JK, Loher TJ, Pohle T, Weber S, Taub E, Barlocher CB, et al. Pallidal deep brain stimulation in patients with cervical dystonia and severe cervical dyskinesias with cervical myelopathy. J Neurol Neurosurg Psychiatry 2002; 72: Krauss JK, Pohle T, Weber S, Ozdoba C, Burgunder JM. Bilateral stimulation of globus pallidus internus for treatment of cervical dystonia. Lancet 1999; 354: Kulisevsky J, Lleo A, Gironell A, Molet J, Pascual-Sedano B, Pares P. Bilateral pallidal stimulation for cervical dystonia: dissociated pain and motor improvement. Neurology 2000; 55: Kumar R. Methods for programming and patient management with deep brain stimulation of the globus pallidus for the treatment of advanced Parkinson s disease and dystonia. Mov Disord 2002; 17: S Kupsch A, Benecke R, Muller J, Trottenberg T, Schneider GH, Poewe W, et al. Pallidal deep-brain stimulation in primary generalized or segmental dystonia. N Engl J Med 2006; 355: Laitinen LV, Bergenheim AT, Hariz MI. Leksell s posteroventral pallidotomy in the treatment of Parkinson s disease. J Neurosurg 1992; 76: Lozano AM, Hutchison WD, Kiss ZHT, Tasker RR, Davis KD, Dostrovsky JO. Methods for microelectrode-guided posteroventral pallidotomy. J Neurosurg 1996; 84: Munchau A, Palmer JD, Dressler D, O Sullivan JD, Tsang KL, Jahanshahi M, et al. Prospective study of selective peripheral denervation for botulinum-toxin resistant patients with cervical dystonia. Brain 2001; 124: Tang JK, Moro E, Mahant N, Hutchison WD, Lang AE, Lozano AM, et al. Neuronal firing rates and patterns in the globus pallidus internus of patients with cervical dystonia differ from those with Parkinson s disease. J Neurophysiol 2007; 98: Tronnier VM, Fogel W. Pallidal stimulation for generalized dystonia. Report of three cases. J Neurosurg 2000; 92: Vidailhet M, Vercueil L, Houeto JL, Krystkowiak P, Benabid AL, Cornu P, et al. Bilateral deep-brain stimulation of the globus pallidus in primary generalized dystonia. N Engl J Med 2005; 352: Vidailhet M, Vercueil L, Houeto JL, Krystkowiak P, Lagrange C, Yelnik J, et al. Bilateral, pallidal, deep-brain stimulation in primary generalised dystonia: a prospective 3 year follow-up study. Lancet Neurol 2007; 6: Ware JE, Jr, Sherbourne CD. The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med Care 1992; 30:
8 2886 Brain (2007), 130, 2879^2886 Z. H. T. Kiss et al. Yianni J, Bain PG, Giladi N, Auca M, Gregory R, Joint C, et al. Globus pallidus internus deep brain stimulation for dystonic conditions: a prospective audit. Mov Disord 2003; 18: Yianni J, Nandi D, Shad A, Bain P, Gregory R, Aziz T. Increased risk of lead fracture and migration in dystonia compared with other movement disorders following deep brain stimulation. J Clin Neurosci 2004; 11: Appendix Members of the Canadian Study Group were as follows: Neurologists: Vancouver: Joseph Tsui; Edmonton: Wayne Martin; Calgary: Scott Kraft, Ranjiit Ranawaya, Oksana Suchowersky; Winnipeg: Douglas Hobson; London: Mandar Jog. Neurosurgeons: Vancouver: Christopher Honey; Edmonton: Matt Wheatley, John McKean; Calgary: Zelma Kiss; Winnipeg: Jerry Krcek; London: Andrew Parrent. Programming: Vancouver: Rodrigo Mercado; Edmonton: Bernadette Martin; Calgary: Kristina Doig-Beyaert; Winnipeg: Renée Krcek; London: Linda Hall. Intraoperative neurophysiology assessments: Calgary: Trent Anderson, Karl Iremonger, Elena Lavrentieva; Winnipeg: Marshall Wilkinson; London: Frank Behari. Neuropsychological evaluation: Vancouver: Marci Sinden, Nicholas Bogod; Edmonton: N. Fisher; Calgary: Angela Haffenden, Stuart Longman; Winnipeg: Andrea Kilgour, John Arnett; London: Gloria Grace. Swallowing evaluation: Vancouver: Caroline Chow, Barbara Henn-Pander; Edmonton: Caitlin Ryan; Calgary: Chelsea Reidel; Winnipeg: Shelley Irvine-Day; London: Angle South. Biostatistician: Michael Eliasziw
The Canadian multicentre study of deep brain stimulation for cervical dystonia
 Brain Advance Access published September 28, 2007 doi:10.1093/brain/awm229 Brain (2007) Page 1 of 8 The Canadian multicentre study of deep brain stimulation for cervical dystonia Zelma H. T. Kiss, 1 Kristina
Brain Advance Access published September 28, 2007 doi:10.1093/brain/awm229 Brain (2007) Page 1 of 8 The Canadian multicentre study of deep brain stimulation for cervical dystonia Zelma H. T. Kiss, 1 Kristina
Outcome predictors of pallidal stimulation in patients with primary dystonia: the role of disease duration
 doi:10.1093/brain/awn120 Brain (2008), 131,1895^1902 Outcome predictors of pallidal stimulation in patients with primary dystonia: the role of disease duration Ioannis U. Isaias, 1 Ron L. Alterman 2 and
doi:10.1093/brain/awn120 Brain (2008), 131,1895^1902 Outcome predictors of pallidal stimulation in patients with primary dystonia: the role of disease duration Ioannis U. Isaias, 1 Ron L. Alterman 2 and
doi: /brain/awt009 Brain 2013: 136; Bilateral pallidal stimulation in cervical dystonia: blinded evidence of benefit beyond 5 years
 doi:10.1093/brain/awt009 Brain 2013: 136; 761 769 761 BRAIN A JOURNAL OF NEUROLOGY Bilateral pallidal stimulation in cervical dystonia: blinded evidence of benefit beyond 5 years Richard A. Walsh, 1,2
doi:10.1093/brain/awt009 Brain 2013: 136; 761 769 761 BRAIN A JOURNAL OF NEUROLOGY Bilateral pallidal stimulation in cervical dystonia: blinded evidence of benefit beyond 5 years Richard A. Walsh, 1,2
Deep brain stimulation of globus pallidus internus for DYT1 positive primary generalized dystonia
 Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Deep brain stimulation of globus pallidus internus for DYT1 positive primary generalized dystonia
Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Deep brain stimulation of globus pallidus internus for DYT1 positive primary generalized dystonia
Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech?
 Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech? Jana Zalmanowitz M.Cl.Sc (SLP) Candidate University of Western Ontario: School of Communication Sciences
Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech? Jana Zalmanowitz M.Cl.Sc (SLP) Candidate University of Western Ontario: School of Communication Sciences
Pallidal Deep Brain Stimulation
 Pallidal Deep Brain Stimulation Treatment for Dystonia Dystonia Dystonia is a neurological disorder characterized by involuntary muscle contractions resulting in abnormal postures. These movements may
Pallidal Deep Brain Stimulation Treatment for Dystonia Dystonia Dystonia is a neurological disorder characterized by involuntary muscle contractions resulting in abnormal postures. These movements may
Treatment of Dystonia with Deep Brain Stimulation
 Neurotherapeutics: The Journal of the American Society for Experimental NeuroTherapeutics Treatment of Dystonia with Deep Brain Stimulation Jill L. Ostrem* and Philip A. Starr *Department of Neurology,
Neurotherapeutics: The Journal of the American Society for Experimental NeuroTherapeutics Treatment of Dystonia with Deep Brain Stimulation Jill L. Ostrem* and Philip A. Starr *Department of Neurology,
Changes in Cortical and Pallidal Oscillatory Activity during the Execution of a Sensory Trick in Patients with Cervical Dystonia
 Changes in Cortical and Pallidal Oscillatory Activity during the Execution of a Sensory Trick in Patients with Cervical Dystonia Joyce KH Tang 1 Neil Mahant 2 Danny Cunic 2 Robert Chen 2 Elena Moro 2 Anthony
Changes in Cortical and Pallidal Oscillatory Activity during the Execution of a Sensory Trick in Patients with Cervical Dystonia Joyce KH Tang 1 Neil Mahant 2 Danny Cunic 2 Robert Chen 2 Elena Moro 2 Anthony
P rimary generalised dystonia (PGD) is a movement disorder
 1314 PAPER Effect of electrode contact location on clinical efficacy of pallidal deep brain stimulation in primary generalised dystonia S Tisch, L Zrinzo, P Limousin, K P Bhatia, N Quinn, K Ashkan, M Hariz...
1314 PAPER Effect of electrode contact location on clinical efficacy of pallidal deep brain stimulation in primary generalised dystonia S Tisch, L Zrinzo, P Limousin, K P Bhatia, N Quinn, K Ashkan, M Hariz...
Review Article Dystonia and the Role of Deep Brain Stimulation
 International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 193718, 5 pages doi:10.5402/2011/193718 Review Article Dystonia and the Role of Deep Brain Stimulation Thomas L. Ellis Wake
International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 193718, 5 pages doi:10.5402/2011/193718 Review Article Dystonia and the Role of Deep Brain Stimulation Thomas L. Ellis Wake
Deep Brain Stimulation: Patient selection
 Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
Bilateral, pallidal, deep-brain stimulation in primary generalised dystonia: a prospective 3 year follow-up study
 Bilateral, pallidal, deep-brain stimulation in primary generalised dystonia: a prospective 3 year follow-up study Marie Vidailhet, Laurent Vercueil, Jean-Luc Houeto, Pierre Krystkowiak, Christelle Lagrange,
Bilateral, pallidal, deep-brain stimulation in primary generalised dystonia: a prospective 3 year follow-up study Marie Vidailhet, Laurent Vercueil, Jean-Luc Houeto, Pierre Krystkowiak, Christelle Lagrange,
ORIGINAL CONTRIBUTION. Acute Deep-Brain Stimulation of the Internal and External Globus Pallidus in Primary Dystonia
 ORIGINAL CONTRIBUTION Acute Deep-Brain Stimulation of the Internal and External Globus Pallidus in Primary Dystonia Functional Mapping of the Pallidum Jean-Luc Houeto, MD, PhD; Jérôme Yelnik, MD, PhD;
ORIGINAL CONTRIBUTION Acute Deep-Brain Stimulation of the Internal and External Globus Pallidus in Primary Dystonia Functional Mapping of the Pallidum Jean-Luc Houeto, MD, PhD; Jérôme Yelnik, MD, PhD;
Bilateral Deep-Brain Stimulation of the Globus Pallidus in Primary Generalized Dystonia
 original article Bilateral Deep-Brain Stimulation of the Globus Pallidus in Primary Generalized Dystonia Marie Vidailhet, M.D., Ph.D., Laurent Vercueil, M.D., Jean-Luc Houeto, M.D., Ph.D., Pierre Krystkowiak,
original article Bilateral Deep-Brain Stimulation of the Globus Pallidus in Primary Generalized Dystonia Marie Vidailhet, M.D., Ph.D., Laurent Vercueil, M.D., Jean-Luc Houeto, M.D., Ph.D., Pierre Krystkowiak,
ORIGINAL CONTRIBUTION. Subthalamic Stimulation in Parkinson Disease
 Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
Pallidal Deep-Brain Stimulation in Primary Generalized or Segmental Dystonia
 The new england journal of medicine original article Pallidal Deep-Brain Stimulation in Primary Generalized or Segmental Dystonia Andreas Kupsch, M.D., Reiner Benecke, M.D., Jörg Müller, M.D., Thomas Trottenberg,
The new england journal of medicine original article Pallidal Deep-Brain Stimulation in Primary Generalized or Segmental Dystonia Andreas Kupsch, M.D., Reiner Benecke, M.D., Jörg Müller, M.D., Thomas Trottenberg,
Surgical Treatment of Movement Disorders. Surgical Treatment of Movement Disorders. New Techniques: Procedure is safer and better
 Surgical Treatment of Movement Stephen Grill, MD, PHD Johns Hopkins University and Parkinson s and Movement Center of Maryland Surgical Treatment of Movement Historical Aspects Preoperative Issues Surgical
Surgical Treatment of Movement Stephen Grill, MD, PHD Johns Hopkins University and Parkinson s and Movement Center of Maryland Surgical Treatment of Movement Historical Aspects Preoperative Issues Surgical
Subthalamic nucleus deep brain stimulation for severe idiopathic dystonia: impact on severity, neuropsychological status, and quality of life
 J Neurosurg 107:29 36, 2007 Subthalamic nucleus deep brain stimulation for severe idiopathic dystonia: impact on severity, neuropsychological status, and quality of life GALIT KLEINER-FISMAN, M.D., 1 GRACE
J Neurosurg 107:29 36, 2007 Subthalamic nucleus deep brain stimulation for severe idiopathic dystonia: impact on severity, neuropsychological status, and quality of life GALIT KLEINER-FISMAN, M.D., 1 GRACE
Deep brain stimulation in the treatment of dyskinesia and dystonia
 Neurosurg Focus 17 (1):E2, 2004, Click here to return to Table of Contents Deep brain stimulation in the treatment of dyskinesia and dystonia HIROKI TODA, M.D., PH.D., CLEMENT HAMANI, M.D., PH.D., AND
Neurosurg Focus 17 (1):E2, 2004, Click here to return to Table of Contents Deep brain stimulation in the treatment of dyskinesia and dystonia HIROKI TODA, M.D., PH.D., CLEMENT HAMANI, M.D., PH.D., AND
Surgical Treatment for Movement Disorders
 Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Palladotomy and Pallidal Deep Brain Stimulation
 Palladotomy and Pallidal Deep Brain Stimulation Parkinson s disease Parkinson s Disease is a common neurodegenerative disorder that affects about 1:100 individuals over the age of 60. In a small percentage
Palladotomy and Pallidal Deep Brain Stimulation Parkinson s disease Parkinson s Disease is a common neurodegenerative disorder that affects about 1:100 individuals over the age of 60. In a small percentage
Parkinson's Disease Center and Movement Disorders Clinic
 Parkinson's Disease Center and Movement Disorders Clinic 7200 Cambridge Street, 9th Floor, Suite 9A Houston, Texas 77030 713-798-2273 phone www.jankovic.org Dystonia Diagnosis Dystonia is a neurologic
Parkinson's Disease Center and Movement Disorders Clinic 7200 Cambridge Street, 9th Floor, Suite 9A Houston, Texas 77030 713-798-2273 phone www.jankovic.org Dystonia Diagnosis Dystonia is a neurologic
Journal of Anesthesia & Pain Medicine
 Case Report To spasm, or Not to Spasm, That is the Question Journal of Anesthesia & Pain Medicine John C McDonald BA 1 and Terence K Gray DO 1,2* 1 Mercy Pain Center, Mercy Hospital, Portland, Maine, USA
Case Report To spasm, or Not to Spasm, That is the Question Journal of Anesthesia & Pain Medicine John C McDonald BA 1 and Terence K Gray DO 1,2* 1 Mercy Pain Center, Mercy Hospital, Portland, Maine, USA
Deep Brain Stimulation: Indications and Ethical Applications
 Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
DBS Programming. Paul S Fishman MD, PhD University of Maryland School of Medicine PFNCA 3/24/18
 DBS Programming Paul S Fishman MD, PhD University of Maryland School of Medicine PFNCA 3/24/18 Disclosure The University of Maryland has received research funding form InSightec and the Focused Ultrasound
DBS Programming Paul S Fishman MD, PhD University of Maryland School of Medicine PFNCA 3/24/18 Disclosure The University of Maryland has received research funding form InSightec and the Focused Ultrasound
10/13/2017. Disclosures. Deep Brain Stimulation in the Treatment of Movement Disorders. Deep Brain Stimulation: Objectives.
 Deep Brain Stimulation in the Treatment of Movement Disorders Disclosures None Eleanor K Orehek, M.D. Movement Disorders Specialist Noran Neurological Clinic 1 2 Objectives To provide an overview of deep
Deep Brain Stimulation in the Treatment of Movement Disorders Disclosures None Eleanor K Orehek, M.D. Movement Disorders Specialist Noran Neurological Clinic 1 2 Objectives To provide an overview of deep
Understand the New 2019 Neurostimulator Analysis-Programming CPT Coding Structure and Associated Relative Value Units
 Understand the New 2019 Neurostimulator Analysis-Programming CPT Coding Structure and Associated Relative Units The American Academy of Neurology (AAN) presents the following case studies to help you understand
Understand the New 2019 Neurostimulator Analysis-Programming CPT Coding Structure and Associated Relative Units The American Academy of Neurology (AAN) presents the following case studies to help you understand
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor
 Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
Troubleshooting algorithms for common DBS related problems in tremor and dystonia
 Troubleshooting algorithms for common DBS related problems in tremor and dystonia Elena Moro, MD, PhD, FEAN, FAAN Movement Disorder Center, CHU Grenoble, Grenoble Alpes University, INSERM U1216, Grenoble,
Troubleshooting algorithms for common DBS related problems in tremor and dystonia Elena Moro, MD, PhD, FEAN, FAAN Movement Disorder Center, CHU Grenoble, Grenoble Alpes University, INSERM U1216, Grenoble,
Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology
 Deep Brain Stimulation for Movement Disorders Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology History of DBS 1 History of DBS 1987
Deep Brain Stimulation for Movement Disorders Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology History of DBS 1 History of DBS 1987
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS)
 Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici
 DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici TECNICHE DI NEUROMODULAZIONE Invasiva: odeep Brain Stimulation Non Invasiva: o Transcranial Magnetic Stimulation (TMS) o Transcranial
DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici TECNICHE DI NEUROMODULAZIONE Invasiva: odeep Brain Stimulation Non Invasiva: o Transcranial Magnetic Stimulation (TMS) o Transcranial
Deep brain stimulation in movement disorders: stereotactic coregistration of two-dimensional electrical field modeling and magnetic resonance imaging
 J Neurosurg 103:949 955, 2005 Deep brain stimulation in movement disorders: stereotactic coregistration of two-dimensional electrical field modeling and magnetic resonance imaging SIMONE HEMM, PH.D, GÉRARD
J Neurosurg 103:949 955, 2005 Deep brain stimulation in movement disorders: stereotactic coregistration of two-dimensional electrical field modeling and magnetic resonance imaging SIMONE HEMM, PH.D, GÉRARD
See Policy CPT/HCPCS CODE section below for any prior authorization requirements
 Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Outcome of selective ramisectomy for botulinum toxin resistant torticollis
 472 Center for Dystonia, Neurological Institute, Columbia-Presbyterian Medical Center B Ford E D Louis P Greene S Fahn Sergievsky Center, Columbia University, New York, USA E D Louis Correspondence to:
472 Center for Dystonia, Neurological Institute, Columbia-Presbyterian Medical Center B Ford E D Louis P Greene S Fahn Sergievsky Center, Columbia University, New York, USA E D Louis Correspondence to:
Deep Brain Stimulation Surgery for Parkinson s Disease
 Deep Brain Stimulation Surgery for Parkinson s Disease Demystifying Medicine 24 January 2012 Kareem A. Zaghloul, MD, PhD Staff Physician, Surgical Neurology Branch NINDS Surgery for Parkinson s Disease
Deep Brain Stimulation Surgery for Parkinson s Disease Demystifying Medicine 24 January 2012 Kareem A. Zaghloul, MD, PhD Staff Physician, Surgical Neurology Branch NINDS Surgery for Parkinson s Disease
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Common Misdiagnosis of a Common Neurological Disorder How Are We Misdiagnosing Essential Tremor? Samay Jain, MD; Steven E. Lo, MD; Elan D. Louis, MD, MS Background: As a common neurological
ORIGINAL CONTRIBUTION Common Misdiagnosis of a Common Neurological Disorder How Are We Misdiagnosing Essential Tremor? Samay Jain, MD; Steven E. Lo, MD; Elan D. Louis, MD, MS Background: As a common neurological
Parkinson disease: Parkinson Disease
 Surgical Surgical treatment treatment for for Parkinson disease: Parkinson Disease the Present and the Future the Present and the Future Olga Klepitskaya, MD Associate Professor of Neurology Co-Director,
Surgical Surgical treatment treatment for for Parkinson disease: Parkinson Disease the Present and the Future the Present and the Future Olga Klepitskaya, MD Associate Professor of Neurology Co-Director,
Surgery for Parkinson s disease improves disability but not impairment components of the UPDRS-II
 Parkinsonism and Related Disorders 13 (2007) 399 405 www.elsevier.com/locate/parkreldis Surgery for Parkinson s disease improves disability but not impairment components of the UPDRS-II A. Haffenden, U.
Parkinsonism and Related Disorders 13 (2007) 399 405 www.elsevier.com/locate/parkreldis Surgery for Parkinson s disease improves disability but not impairment components of the UPDRS-II A. Haffenden, U.
DEEP BRAIN STIMULATION
 DEEP BRAIN STIMULATION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
DEEP BRAIN STIMULATION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Citation for published version (APA): Contarino, M. F. (2013). Improving surgical treatment for movement disorders
 UvA-DARE (Digital Academic Repository) Improving surgical treatment for movement disorders Contarino, M.F. Link to publication Citation for published version (APA): Contarino, M. F. (2013). Improving surgical
UvA-DARE (Digital Academic Repository) Improving surgical treatment for movement disorders Contarino, M.F. Link to publication Citation for published version (APA): Contarino, M. F. (2013). Improving surgical
SUPPLEMENTAL DIGITAL CONTENT
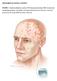 SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
Deep Brain Stimulation and Movement Disorders
 Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Dystonia is characterized by sustained muscle
 This article has been updated from its originally published version to replace Figure 2 and update the legend. See the corresponding erratum notice, DOI: 10.3171/10.3171/ 2013.11.JNS13844a, for full details.
This article has been updated from its originally published version to replace Figure 2 and update the legend. See the corresponding erratum notice, DOI: 10.3171/10.3171/ 2013.11.JNS13844a, for full details.
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD
 PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
The phenomenology and treatment of idiopathic adult-onset truncal dystonia: a retrospective review
 Ehrlich and Frucht Journal of Clinical Movement Disorders (2016) 3:15 DOI 10.1186/s40734-016-0044-9 RESEARCH ARTICLE Open Access The phenomenology and treatment of idiopathic adult-onset truncal dystonia:
Ehrlich and Frucht Journal of Clinical Movement Disorders (2016) 3:15 DOI 10.1186/s40734-016-0044-9 RESEARCH ARTICLE Open Access The phenomenology and treatment of idiopathic adult-onset truncal dystonia:
Deep brain stimulation for dystonia
 Hu and Stead Translational Neurodegeneration 2014, 3:2 Translational Neurodegeneration REVIEW Deep brain stimulation for dystonia Wei Hu * and Matt Stead * Open Access Abstract Deep brain stimulation (DBS)
Hu and Stead Translational Neurodegeneration 2014, 3:2 Translational Neurodegeneration REVIEW Deep brain stimulation for dystonia Wei Hu * and Matt Stead * Open Access Abstract Deep brain stimulation (DBS)
Ablative procedures for the treatment of Parkinson s disease
 Ablative procedures for the treatment of Parkinson s disease Zeiad Y. Fayed MD Neurosurgery department Ain Shams University 1 2 Pallidotomy Pallidotomy Indications: Non tremor dominant PD Levodopa induced
Ablative procedures for the treatment of Parkinson s disease Zeiad Y. Fayed MD Neurosurgery department Ain Shams University 1 2 Pallidotomy Pallidotomy Indications: Non tremor dominant PD Levodopa induced
I n 1991 Benabid et al introduced deep brain stimulation
 PAPER Multicentre European study of thalamic stimulation in essential tremor: a six year follow up O Sydow, S Thobois, F Alesch, J D Speelman, study collaborators... See Editorial Commentary, pp1361 2
PAPER Multicentre European study of thalamic stimulation in essential tremor: a six year follow up O Sydow, S Thobois, F Alesch, J D Speelman, study collaborators... See Editorial Commentary, pp1361 2
Outcomes after stereotactically guided pallidotomy for advanced Parkinson s disease
 J Neurosurg 90:197 202, 1999 Outcomes after stereotactically guided pallidotomy for advanced Parkinson s disease DOUGLAS KONDZIOLKA, M.D., F.R.C.S.(C), EUGENE BONAROTI, M.D., SUSAN BASER, M.D., FRAN BRANDT,
J Neurosurg 90:197 202, 1999 Outcomes after stereotactically guided pallidotomy for advanced Parkinson s disease DOUGLAS KONDZIOLKA, M.D., F.R.C.S.(C), EUGENE BONAROTI, M.D., SUSAN BASER, M.D., FRAN BRANDT,
F unctional stereotactic surgery is now well established for
 PAPER Effect of chronic pallidal deep brain on off period dystonia and sensory symptoms in advanced Parkinson s disease T J Loher, J-M Burgunder, S Weber, R Sommerhalder, J K Krauss... See end of article
PAPER Effect of chronic pallidal deep brain on off period dystonia and sensory symptoms in advanced Parkinson s disease T J Loher, J-M Burgunder, S Weber, R Sommerhalder, J K Krauss... See end of article
Deep brain stimulation for camptocormia in dystonia and Parkinson s disease
 J Neurol (2011) 258:96 103 DOI 10.1007/s00415-010-5695-0 ORIGINAL COMMUNICATION Deep brain stimulation for camptocormia in dystonia and Parkinson s disease Hans-Holger Capelle Christoph Schrader Christian
J Neurol (2011) 258:96 103 DOI 10.1007/s00415-010-5695-0 ORIGINAL COMMUNICATION Deep brain stimulation for camptocormia in dystonia and Parkinson s disease Hans-Holger Capelle Christoph Schrader Christian
Pallidal stimulation for acquired dystonia due to cerebral palsy: beyond 5 years
 ORIGINAL ARTICLE Pallidal stimulation for acquired dystonia due to cerebral palsy: beyond 5 years L. M. Romito a,b, *, G. Zorzi a, *, C. E. Marras c, A. Franzini a, N. Nardocci a and A. Albanese a,b a
ORIGINAL ARTICLE Pallidal stimulation for acquired dystonia due to cerebral palsy: beyond 5 years L. M. Romito a,b, *, G. Zorzi a, *, C. E. Marras c, A. Franzini a, N. Nardocci a and A. Albanese a,b a
Survey of practices employed by neurologists for the definition and management of secondary nonresponse to botulinum toxin in cervical dystonia
 Survey of practices employed by neurologists for the definition and management of secondary nonresponse to botulinum toxin in cervical dystonia Joaquim J. Ferreira, MD, PhD a Roongroj Bhidayasiri, MD b,c
Survey of practices employed by neurologists for the definition and management of secondary nonresponse to botulinum toxin in cervical dystonia Joaquim J. Ferreira, MD, PhD a Roongroj Bhidayasiri, MD b,c
No Financial Disclosures
 Deep Brain Stimulation: A Physician and Patient Perspective Jessica McClure Warren Marks, MD Cook Children s Medical Center Cook Children s Health Foundation Endowed Chair in Neurosciences Department of
Deep Brain Stimulation: A Physician and Patient Perspective Jessica McClure Warren Marks, MD Cook Children s Medical Center Cook Children s Health Foundation Endowed Chair in Neurosciences Department of
Deep Brain Stimulation
 Deep Brain Stimulation Policy Number: 7.01.63 Last Review: 8/2017 Origination: 8/2001 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for deep brain
Deep Brain Stimulation Policy Number: 7.01.63 Last Review: 8/2017 Origination: 8/2001 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for deep brain
Deep brain stimulation: What can patients expect from it?
 MEDICAL GRAND ROUNDS ANDRE MACHADO, MD, PhD* Director, Center for Neurological Restoration, Neurological Institute, Cleveland Clinic HUBERT H. FERNANDEZ, MD Section Head, Movement Disorders, Center for
MEDICAL GRAND ROUNDS ANDRE MACHADO, MD, PhD* Director, Center for Neurological Restoration, Neurological Institute, Cleveland Clinic HUBERT H. FERNANDEZ, MD Section Head, Movement Disorders, Center for
ORIGINAL CONTRIBUTION. Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement
 ORIGINAL CONTRIBUTION Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement Effects of Reimplantation Mathieu Anheim, MD; Alina Batir, MD; Valérie Fraix, MD;
ORIGINAL CONTRIBUTION Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement Effects of Reimplantation Mathieu Anheim, MD; Alina Batir, MD; Valérie Fraix, MD;
Dystonia: Title. A real pain in the neck. in All the Wrong Places
 Focus on CME at the University of Western Ontario Dystonia: Title in All the Wrong Places A real pain in the neck By Mandar Jog, MD, FRCPC and; Mary Jenkins, MD, FRCPC What is dystonia? Dystonia is a neurologic
Focus on CME at the University of Western Ontario Dystonia: Title in All the Wrong Places A real pain in the neck By Mandar Jog, MD, FRCPC and; Mary Jenkins, MD, FRCPC What is dystonia? Dystonia is a neurologic
The webinar will begin momentarily. Tractography-based Targeting for Functional Neurosurgery
 Welcome The webinar will begin momentarily. Tractography-based Targeting for Functional Neurosurgery Vibhor Krishna, MD, SM Assistant Professor, Center for Neuromoduation, Dept. of Neurosurgery and Dept.
Welcome The webinar will begin momentarily. Tractography-based Targeting for Functional Neurosurgery Vibhor Krishna, MD, SM Assistant Professor, Center for Neuromoduation, Dept. of Neurosurgery and Dept.
Patient selection for surgery: Hyperkinetic movement disorders
 Patient selection for surgery: Hyperkinetic movement disorders Alfons Schnitzler, MD, PhD Dept. of Neurology, Movement Disorder and Neuromodulation, Heinrich-Heine-University Düsseldorf, Germany Hyperkinetic
Patient selection for surgery: Hyperkinetic movement disorders Alfons Schnitzler, MD, PhD Dept. of Neurology, Movement Disorder and Neuromodulation, Heinrich-Heine-University Düsseldorf, Germany Hyperkinetic
Deep brain stimulation (DBS) has been
 TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES Do Stable Patients With a Premorbid Depression History Have a Worse Outcome After Deep Brain Stimulation for Parkinson Disease? Michael
TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES Do Stable Patients With a Premorbid Depression History Have a Worse Outcome After Deep Brain Stimulation for Parkinson Disease? Michael
Supplementary Information for Decreased activity of single subthalamic nucleus neurons in Parkinson patients responding to placebo
 Supplementary Information for Decreased activity of single subthalamic nucleus neurons in Parkinson patients responding to placebo Fabrizio Benedetti, 1,2 Luana Colloca, 1,2 Elena Torre, 1 Michele Lanotte,
Supplementary Information for Decreased activity of single subthalamic nucleus neurons in Parkinson patients responding to placebo Fabrizio Benedetti, 1,2 Luana Colloca, 1,2 Elena Torre, 1 Michele Lanotte,
Surgical Treatment: Patient Edition
 Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
E ssential tremor is a commonly diagnosed movement
 684 PAPER Bilateral thalamic deep brain stimulation: midline tremor control J D Putzke, R J Uitti, A A Obwegeser, Z K Wszolek, R E Wharen... See end of article for authors affiliations... Correspondence
684 PAPER Bilateral thalamic deep brain stimulation: midline tremor control J D Putzke, R J Uitti, A A Obwegeser, Z K Wszolek, R E Wharen... See end of article for authors affiliations... Correspondence
Factors affecting the health-related quality of life of patients with cervical dystonia and the impact of botulinum toxin type A injections
 Factors affecting the health-related quality of life of patients with cervical dystonia and the impact of botulinum toxin type A injections Jaroslaw Slawek a Andrzej Friedman b Anna Potulska b Pierre Krystkowiak
Factors affecting the health-related quality of life of patients with cervical dystonia and the impact of botulinum toxin type A injections Jaroslaw Slawek a Andrzej Friedman b Anna Potulska b Pierre Krystkowiak
Imaging alone versus microelectrode recording guided targeting of the STN in patients with Parkinson s disease
 CLINICAL ARTICLE Imaging alone versus microelectrode recording guided targeting of the STN in patients with Parkinson s disease Christopher S. Lozano, BSc, 1 Manish Ranjan, MBBS, 1 Alexandre Boutet, MD,
CLINICAL ARTICLE Imaging alone versus microelectrode recording guided targeting of the STN in patients with Parkinson s disease Christopher S. Lozano, BSc, 1 Manish Ranjan, MBBS, 1 Alexandre Boutet, MD,
Quantitative Assessment of Botulinum Toxin Treatment in 43 Patients with Head Tremor
 ~~~~~ ~ ~ Movement Disorder& Vol. 12, NO. 5, 1997, pp 122-126 0 1997 Movemcnt Disorder Society Quantitative Assessment of Botulinum Toxin Treatment in 43 Patients with Head Tremor "tjorg Wissel, "Florian
~~~~~ ~ ~ Movement Disorder& Vol. 12, NO. 5, 1997, pp 122-126 0 1997 Movemcnt Disorder Society Quantitative Assessment of Botulinum Toxin Treatment in 43 Patients with Head Tremor "tjorg Wissel, "Florian
THE MEDICAL AND SURGICAL TREATMENT OF DYSTONIA
 THE MEDICAL AND SURGICAL TREATMENT OF DYSTONIA Samuel Frank, MD Beth Israel Deaconess Medical Center Boston, MA Dystonia may present as an isolated disorder or as part of another disease process. The clinical
THE MEDICAL AND SURGICAL TREATMENT OF DYSTONIA Samuel Frank, MD Beth Israel Deaconess Medical Center Boston, MA Dystonia may present as an isolated disorder or as part of another disease process. The clinical
National Institute for Health and Clinical Excellence
 National Institute for Health and Clinical Excellence 319 Deep brain stimulation for tremor and dystonia (excluding Parkinson s disease) nts table IPAC date: 16 June 2006 Consultee name nts The Dystonia
National Institute for Health and Clinical Excellence 319 Deep brain stimulation for tremor and dystonia (excluding Parkinson s disease) nts table IPAC date: 16 June 2006 Consultee name nts The Dystonia
Evidence compendium. Research study summaries supporting the use of Medtronic deep brain stimulation (DBS) for Parkinson s disease
 Evidence compendium Research study summaries supporting the use of Medtronic deep brain stimulation (DBS) for Parkinson s disease CONTENTS Introduction... 4 Index of study summaries... 6 Parkinson s disease
Evidence compendium Research study summaries supporting the use of Medtronic deep brain stimulation (DBS) for Parkinson s disease CONTENTS Introduction... 4 Index of study summaries... 6 Parkinson s disease
Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease
 CLINICAL ARTICLE Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease Leonardo A. Frizon, MD, 1,2 Sean J. Nagel, MD, 1 Francis J. May, MS, 1 Jianning Shao,
CLINICAL ARTICLE Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease Leonardo A. Frizon, MD, 1,2 Sean J. Nagel, MD, 1 Francis J. May, MS, 1 Jianning Shao,
Which patients with dystonia benefit from deep brain stimulation? A metaregression of individual patient outcomes
 1 Lysholm Department of Neuroradiology, National Hospital for Neurology & Neurosurgery, London, UK 2 Unit of Functional Neurosurgery, Sobell Department of Motor Neuroscience, UCL Institute of Neurology,
1 Lysholm Department of Neuroradiology, National Hospital for Neurology & Neurosurgery, London, UK 2 Unit of Functional Neurosurgery, Sobell Department of Motor Neuroscience, UCL Institute of Neurology,
Deep Brain Stimulation: Surgical Process
 Deep Brain Stimulation: Surgical Process Kia Shahlaie, MD, PhD Assistant Professor Bronte Endowed Chair in Epilepsy Research Director of Functional Neurosurgery Minimally Invasive Neurosurgery Department
Deep Brain Stimulation: Surgical Process Kia Shahlaie, MD, PhD Assistant Professor Bronte Endowed Chair in Epilepsy Research Director of Functional Neurosurgery Minimally Invasive Neurosurgery Department
Parkinson s Disease Webcast January 31, 2008 Jill Ostrem, M.D. What is Parkinson s Disease?
 Parkinson s Disease Webcast January 31, 2008 Jill Ostrem, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or Patient
Parkinson s Disease Webcast January 31, 2008 Jill Ostrem, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or Patient
DEEP BRAIN STIMULATION (DBS) is a standard treatment
 1320 ORIGINAL ARTICLE Fast-Track Programming and Rehabilitation Model: A Novel Approach to Postoperative Deep Brain Stimulation Patient Care David B. Cohen, MD, Michael Y. Oh, MD, Susan M. Baser, MD, Cindy
1320 ORIGINAL ARTICLE Fast-Track Programming and Rehabilitation Model: A Novel Approach to Postoperative Deep Brain Stimulation Patient Care David B. Cohen, MD, Michael Y. Oh, MD, Susan M. Baser, MD, Cindy
Cerebral Magnetic Resonance Imaging Feasibility in Patients with Implanted Neurostimulation System for Deep Brain Stimulation
 The Open Magnetic Resonance Journal, 2008, 1, 1-8 1 Cerebral Magnetic Resonance Imaging Feasibility in Patients with Implanted Neurostimulation System for Deep Brain Stimulation X.A. Vasques 1-5, C. Tancu
The Open Magnetic Resonance Journal, 2008, 1, 1-8 1 Cerebral Magnetic Resonance Imaging Feasibility in Patients with Implanted Neurostimulation System for Deep Brain Stimulation X.A. Vasques 1-5, C. Tancu
Name of Policy: Deep Brain Stimulation
 Name of Policy: Deep Brain Stimulation Policy #: 347 Latest Review Date: June 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable under Blue Cross and
Name of Policy: Deep Brain Stimulation Policy #: 347 Latest Review Date: June 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable under Blue Cross and
Beta and Tremor-Related Oscillations in the Motor Thalamus of Essential Tremor Patients
 IETF - WD Hutchison Feb 214 requesting $25, Beta and Tremor-Related Oscillations in the Motor Thalamus of Essential Tremor Patients 1. Specific aims of proposal The proposed study will examine beta oscillations
IETF - WD Hutchison Feb 214 requesting $25, Beta and Tremor-Related Oscillations in the Motor Thalamus of Essential Tremor Patients 1. Specific aims of proposal The proposed study will examine beta oscillations
Pallidal neurostimulation in patients with medication-refractory cervical dystonia: a randomised, sham-controlled trial
 Pallidal neurostimulation in patients with medication-refractory cervical dystonia: a randomised, sham-controlled trial Jens Volkmann, Joerg Mueller, Günther Deuschl, Andrea A Kühn, Joachim K Krauss, Werner
Pallidal neurostimulation in patients with medication-refractory cervical dystonia: a randomised, sham-controlled trial Jens Volkmann, Joerg Mueller, Günther Deuschl, Andrea A Kühn, Joachim K Krauss, Werner
Deep Brain Stimulation. Is It Right for You?
 Deep Brain Stimulation Is It Right for You? Northwestern Medicine Deep Brain Stimulation What is DBS? Northwestern Medicine Central DuPage Hospital is a regional destination for the treatment of movement
Deep Brain Stimulation Is It Right for You? Northwestern Medicine Deep Brain Stimulation What is DBS? Northwestern Medicine Central DuPage Hospital is a regional destination for the treatment of movement
Selective peripheral denervation for spasmodic torticollis: 13-year experience with 155 patients
 J Neurosurg (Spine 2) 97:207 212, 2002 Selective peripheral denervation for spasmodic torticollis: 13-year experience with 155 patients VEIT BRAUN, M.D., AND HANS-PETER RICHTER, M.D. Department of Neurosurgery,
J Neurosurg (Spine 2) 97:207 212, 2002 Selective peripheral denervation for spasmodic torticollis: 13-year experience with 155 patients VEIT BRAUN, M.D., AND HANS-PETER RICHTER, M.D. Department of Neurosurgery,
EMERGING TREATMENTS FOR PARKINSON S DISEASE
 EMERGING TREATMENTS FOR PARKINSON S DISEASE Katerina Markopoulou, MD, PhD Director Neurodegenerative Diseases Program Department of Neurology NorthShore University HealthSystem Clinical Assistant Professor
EMERGING TREATMENTS FOR PARKINSON S DISEASE Katerina Markopoulou, MD, PhD Director Neurodegenerative Diseases Program Department of Neurology NorthShore University HealthSystem Clinical Assistant Professor
The oscillatory activity in the Parkinsonian subthalamic nucleus investigated using the macro-electrodes for deep brain stimulation
 Clinical Neurophysiology 113 (2002) 1 6 www.elsevier.com/locate/clinph The oscillatory activity in the Parkinsonian subthalamic nucleus investigated using the macro-electrodes for deep brain stimulation
Clinical Neurophysiology 113 (2002) 1 6 www.elsevier.com/locate/clinph The oscillatory activity in the Parkinsonian subthalamic nucleus investigated using the macro-electrodes for deep brain stimulation
Deep-brain stimulation of the subthalamic nucleus or the pars interna of the globus pallidus in Parkinson's disease
 Article Deep-brain stimulation of the subthalamic nucleus or the pars interna of the globus pallidus in Parkinson's disease Deep-Brain Stimulation for Parkinson's Disease Study Group KRACK, Paul (Collab.)
Article Deep-brain stimulation of the subthalamic nucleus or the pars interna of the globus pallidus in Parkinson's disease Deep-Brain Stimulation for Parkinson's Disease Study Group KRACK, Paul (Collab.)
POSTOPERATIVE PATIENT MANAGEMENT
 POSTOPERATIVE PATIENT MANAGEMENT INTRODUCTION Deep brain stimulation of the internal globus pallidus (GPi) or the subthalamic nucleus (STN) effectively reduces parkinsonian motor symptoms and alleviates
POSTOPERATIVE PATIENT MANAGEMENT INTRODUCTION Deep brain stimulation of the internal globus pallidus (GPi) or the subthalamic nucleus (STN) effectively reduces parkinsonian motor symptoms and alleviates
Measuring symptom change in patients with Parkinson s disease
 Age and Ageing 2000; 29: 41 45 2000, British Geriatrics Society Measuring symptom change in patients with Parkinson s disease JOHN E. HARRISON, SARAH PRESTON 1,STAVIA B. BLUNT 1 CeNeS Ltd, Compass House,
Age and Ageing 2000; 29: 41 45 2000, British Geriatrics Society Measuring symptom change in patients with Parkinson s disease JOHN E. HARRISON, SARAH PRESTON 1,STAVIA B. BLUNT 1 CeNeS Ltd, Compass House,
Hemifacial spasm. Parkinson's Disease Center and Movement Disorders Clinic
 Parkinson's Disease Center and Movement Disorders Clinic 7200 Cambridge Street, 9th Floor, Suite 9A Houston, Texas 77030 713-798-2273 phone www.jankovic.org Hemifacial spasm Diagnosis Hemifacial spasm
Parkinson's Disease Center and Movement Disorders Clinic 7200 Cambridge Street, 9th Floor, Suite 9A Houston, Texas 77030 713-798-2273 phone www.jankovic.org Hemifacial spasm Diagnosis Hemifacial spasm
symptoms of Parkinson s disease EXCEPT.
 M. Angele Theard, M.D Asst. Professor, Washington University, St. Louis, MO Quiz team; Shobana Rajan, M.D; Suneeta Gollapudy, MD; Verghese Cherian, M.D, M. Angele Theard, MD This quiz is being published
M. Angele Theard, M.D Asst. Professor, Washington University, St. Louis, MO Quiz team; Shobana Rajan, M.D; Suneeta Gollapudy, MD; Verghese Cherian, M.D, M. Angele Theard, MD This quiz is being published
UNILATERAL STEREOTACTIC POSTEROVENTRAL GLOBUS PALLIDUS INTERNUS PALLIDOTOMY FOR PARKINSON S DISEASE: SURGICAL TECHNIQUES AND 2-YEAR FOLLOW-UP
 Pallidotomy for Parkinson s disease UILATERAL STEREOTACTIC POSTEROVETRAL GLOBUS PALLIDUS ITERUS PALLIDOTOMY FOR PARKISO S DISEASE: SURGICAL TECHIQUES AD 2-YEAR FOLLOW-UP Chun-Po Yen, Shiao-Jing Wu, Yu-Feng
Pallidotomy for Parkinson s disease UILATERAL STEREOTACTIC POSTEROVETRAL GLOBUS PALLIDUS ITERUS PALLIDOTOMY FOR PARKISO S DISEASE: SURGICAL TECHIQUES AD 2-YEAR FOLLOW-UP Chun-Po Yen, Shiao-Jing Wu, Yu-Feng
SCIENTIFIC PROGRAMME. WEDNESDAY, May 8 th 2019
 SCIENTIFIC PROGRAMME WEDNESDAY, May 8 th 2019 2 nd International Conference on Sports Dystonia K. Alter, C. Ioannou 16:30-18:00 16:30 C. Ioannou Reinvestment and Motor Disorders in Athletes and Musicians
SCIENTIFIC PROGRAMME WEDNESDAY, May 8 th 2019 2 nd International Conference on Sports Dystonia K. Alter, C. Ioannou 16:30-18:00 16:30 C. Ioannou Reinvestment and Motor Disorders in Athletes and Musicians
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Functional Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Functional Neurosurgery Functional
Introduction to Neurosurgical Subspecialties: Functional Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Functional Neurosurgery Functional
Deep Brain Stimulation
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
THE EFFECTS OF SUBTHALAMIC NUCLEUS DEEP BRAIN STIMULATION ON VOCAL TRACT DYNAMICS IN PARKINSON S DISEASE
 11 th Bienniel Speech Motor Control Conference, Colonial Williamsburg, Virginia, 2002. THE EFFECTS OF SUBTHALAMIC NUCLEUS DEEP BRAIN STIMULATION ON VOCAL TRACT DYNAMICS IN PARKINSON S DISEASE Steven Barlow,
11 th Bienniel Speech Motor Control Conference, Colonial Williamsburg, Virginia, 2002. THE EFFECTS OF SUBTHALAMIC NUCLEUS DEEP BRAIN STIMULATION ON VOCAL TRACT DYNAMICS IN PARKINSON S DISEASE Steven Barlow,
High-Field in vivo Visualization of the Human Globus Pallidus Using 7T MRI
 Niederer 1 High-Field in vivo Visualization of the Human Globus Pallidus Using 7T MRI Abstract In the past several decades the introduction of high-resolution, three-dimensional modeling techniques have
Niederer 1 High-Field in vivo Visualization of the Human Globus Pallidus Using 7T MRI Abstract In the past several decades the introduction of high-resolution, three-dimensional modeling techniques have
Patient selection for surgery: Parkinson s disease
 Patient selection for surgery: Parkinson s disease Dr. María C. Rodríguez-Oroz Neurology and Neuroscience. University Hospital Donostia, Research Institute BioDonostia, Ikerbasque Senior Researcher San
Patient selection for surgery: Parkinson s disease Dr. María C. Rodríguez-Oroz Neurology and Neuroscience. University Hospital Donostia, Research Institute BioDonostia, Ikerbasque Senior Researcher San
Globus pallidus internus stimulation in primary generalized dystonia: a H 2 15 O PET study
 DOI: 10.1093/brain/awh213 Brain (2004), 127, 1899 1908 Globus pallidus internus stimulation in primary generalized dystonia: a H 2 15 O PET study Olivier Detante, 1,3 Laurent Vercueil, 1 Stéphane Thobois,
DOI: 10.1093/brain/awh213 Brain (2004), 127, 1899 1908 Globus pallidus internus stimulation in primary generalized dystonia: a H 2 15 O PET study Olivier Detante, 1,3 Laurent Vercueil, 1 Stéphane Thobois,
What contributes to quality of life in patients with Parkinson s disease?
 308 Department of Neurology, Institute of Neurology, Queen Square, London WC1N 3BG, UK A Schrag M Jahanshahi N Quinn Correspondence to: Professor NP Quinn n.quinn@ion.ucl.ac.uk Received 2 Sepyember 1999
308 Department of Neurology, Institute of Neurology, Queen Square, London WC1N 3BG, UK A Schrag M Jahanshahi N Quinn Correspondence to: Professor NP Quinn n.quinn@ion.ucl.ac.uk Received 2 Sepyember 1999
Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association.
 Deep Brain Stimulation Page 1 of 31 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association. Title: Deep Brain Stimulation Professional Institutional Original Effective Date:
Deep Brain Stimulation Page 1 of 31 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association. Title: Deep Brain Stimulation Professional Institutional Original Effective Date:
