Predictors of postoperative sore throat among surgical patients at Ethiopian teaching hospitals
|
|
|
- Erika Woods
- 6 years ago
- Views:
Transcription
1 Vol. 8(1), pp. 1-11, November 2016 DOI: /JCMR Article Number: 43EF ISSN Copyright 2016 Author(s) retain the copyright of this article Journal of Clinical Medicine and Research Full Length Research Paper Predictors of postoperative sore throat among surgical patients at Ethiopian teaching hospitals Hunduma Jisha Chawaka* and Merga Haile Temesgen Anesthesia Department, College of Health Science, Jimma University, Jimma, Ethiopia. Received 6 October, 2016: Accepted 15 November, 2016 Post-operative sore throat significantly impact patients satisfaction during post-operative period. Many factors can contribute to postoperative sore throat and the incidence varies with the method of airway management. To determine the predictors and incidence of postoperative sore throat. In this facility based cross sectional study, 245 elective gynecologic and general surgical patients who had had surgery at Jimma University Teaching Hospital between February 01 and April 30, 2015 were interviewed during postoperative period between 6 and 24 h using a structured questionair. After outliers and missing value checked the data manually entered into SPSS Version 20 IBM. In addition to descriptive analysis odds ratio with 95% confidence interval was used in bivariate and multivariate logistic regression analysis to determine the effect of predictors on the postoperative sore thoat and hoarsness of voices. A total of 245 surgical patients was interviewed with a complete response rate of 228(93.1%). Their age ranges from 18 to 87years, with a majority between 31 and 40 years. From a total respondent 120 (52.6%) were females, 171(75%) American Society of Anesthesiologist class-i, 137(60.1%) cannot read and write, and 108 (47.4%) were farmer. Majority 47(20.6%) of surgery was orthopedics surgery; followed by 25(11%) breast surgery, 23(10.1%) hysterectomy and others. One hundred twenty nine (56.6%) participants had suffered postoperative sore throat and 68 of them had had hoarseness of voices. The sore throat was found to be more common with certain patient, anesthetic and surgical related factors; difficulty level of intubation, duration of ETT in trachea, being not premedicated with opioid, unexperienced anesthetists, other than ketamine anesthetic induction agent, bleeding on tip of laryngoscope/ett, perioperative hypotension and higher estimated blood loss during surgery. Significant incidence of postoperative sore throat and hoarseness of voice were seen during study period in the study area. Awareness creation on the predisposing factors and appropriate care especially during endotracheal intubation would help in reducing or avoiding the incidence of postoperative sore throat. Key words: Endotracheal intubation, elective surgery, postoperative complications, sore throat. INTRODUCTION Postoperative sore throat (POST) is one among the most common anesthesia complications during postoperative *Corresponding author. hunjisha@gmail.com. Author(s) agree that this article remain permanently open access under the terms of the Creative Commons Attribution License 4.0 International License
2 2 J. Clin. Med. Res. period. It impacts the wellbeing of patient after surgical procedures under general anesthesia. Anesthesia complication is the patient s physiologic derangement or any unwanted effect related to anesthesia management (McHardy and Chung, 1999). Safe anesthesia is multidimensional anesthetic service provision which satisfy the demand of patient care and minimizing associated complication. The important aim of good anesthetic care is to achieve a secure airway and ventilate the lung in proper physiologic manner. This can be done in a number of ways, depending on the patient characteristics and nature of the surgery intended to be performed. Safe and secure airway is achieved by endotracheal (ETT) and laryngeal mask airway (LMA), which is majorly performed by anesthetist and or anesthesiologist. The ETT is made of polyvinylchloride (PVC) and has a cuff at the distal end which is inflated after correctly placed in trachea. When intubating with the Macintosh laryngoscope, the tip of the laryngoscope has to be placed in the vallecula and lifted, which stretches these structures that may traumatize (Cirilla et al., 2015; Najafi et al., 2014). Although POST is minor problem, it has been documented that controlling POST is difficult and imposes significant impact on patient s comfort during postoperative period (Kalil et al., 2014). Wide range of POST has been documented with the incidence range from 24 to 90% and may be more in some situations (Cirilla et al., 2015; Burgard et al., 1996; Mandoe et al., 1992). This is due to multifactorial impact contributes in the occurrence and severity of POST as indicated by scholars (Cirilla et al., 2015). For instance types of airways used, technique of insertion/experience level of intubating person, duration of surgical procedure, anesthetics type, cuff pressure, method of airway management and multitude of patient feature (Mandoe et al., 1992; Soediono, 1989). Many researchers found highest incidence (14.4 to 50%) after tracheal intubation; while after laryngeal mask airway it has been reported (5.8 to 34%) and it is much less when a face mask is used for the maintenance of anesthesia (McHardy and Chung, 1999; Burgard et al., 1996). Different investigators have shown that the incidence is higher in female population because of the tight fit of the airway mucosa with airway equipment (McHardy and Chung, 1999; Cirilla et al., 2015; Jaensson et al., 2014; Ahmed et al., 2007), while some still did not find any difference among sex (Edomwonyi et al., 2006). It has been revealed that the experience of anesthetist and duration of intubation significantly affect its incidences (Cirilla et al., 2015). Another study identified that there is no difference on the rate of occurrence among gender and lubrication of ETT (Edomwonyi et al., 2006). Furthermore, method of interview affects the reporting of a sore throat, that is, whether the questions are asked directly or indirectly. Thang a et al. (2013) showed that diclofenac premedication will not prevent the occurrence of sore throat. But another study done by Shresta et al. (2010) in Nepal and Teymourian et al. (2015) in Iran showed that preoperative ketamine gargling and magnesium medication significantly reduces the incidences POST. Again it has been documented by many scholars that dexamethasone showed the promises in reducing the incidence of postoperative sore throat occurrence and severety (Zhao et al., 2014; Haider and Al-ali, 2013). Since a long time many studies have been performed to determine the incidence of postoperative sore throat and to find measures for its prevention. Most of these studies have been conducted in the developed; western countries. However, it has been documented by many researchers that there are racial differences in the occurrence of some medical events (McHardy and Chung, 1999; Ahmed et al., 2007). And limited studies have been done on predictors of postoperative sore throat in developing countries where resources and qualified man powers are limited. Therefore this study was conducted as a preliminary step to determine the magnitude of postoperative sore throat in Jimma university teaching hospital, analyze the factors contributed in its occurrence and see if it is comparable to studies done in other parts of the world. This would in turn help us to identify the preventable causes and formulate strategies for prevention of this common postoperative complication by creating awareness. MATERIALS AND METHODS Study area and setting This study conducted at Jimma University Teaching Hospital (JUTH), located 346 km away from Addis Ababa to South West of Ethiopia, from April 01 to June 30, The hospital provides a range of health care services including major surgical treatments. On average about eight major elective operations performed per day. Orthopedic surgery, hysterectomy, thyroidectomy, mastectomy, colostomy, herniorrhaphy, hemorrhoidectomy, laparotomy, prostatectomy and etc. were among the commonly performed elective surgical procedures. As an existing hospital practices informed consent was taken a day before surgery at ward where pre-anesthetic evaluation made to verify whether the scheduled patient is fit or not for surgery and anesthesia. After pre-oxygenation with 100% O 2 for 3 min, induction was given with either of (2 mg/kg ketamine, 5 mg/kg thiopental or 2 to 2.5 mg/kg propofol) and 2 mg/kg suxamethonium for intubation. Number 3 or 4 Macintosh laryngoscope blade was used. A 6.5 and 7.0 mm internal diameter cuffed polyvinyl chloride (PVC) endotracheal tube was used for the female patients, and 7.5 and 8.5 mm tube was used for the male patients. After intubation patient s lungs were manually ventilated. All patient received 100% oxygen and 1.5 to 2% halothane for maintenance throughout the surgery, and some patients get administered pethidine/tramadol intraoperatively. At the end of surgery the airway devices were removed when patients able to open their eyes to command (awake) and some of them at deep level of anesthesia. Finally the patient taken to the post anesthesia care unit (PACU) from they were shifted to the ward after adequate recovery (mostly 30 min
3 Chawaka and Temesgen 3 to 1 h later). Study design The study design is facility based cross-sectional study. Sample size Using a single population proportion formula; a maximum estimated proportion of sore throat occurrence = 50%; since there is no previous study done on this topic in this study area; with 95% CI, 5% margin of error. We found n=384 We have 3 major operation theatre which serves for both emergency and elective surgery. The number of patients gets operated per day as an elective, range from 6 to 12, on average 8 patients per day or less. So, the total of patients operated over three months of working days estimated 528 or less. Thus, the population is estimated to be < 10,000; using correction formula n=223 and with the consideration 10% of non-respondent and incomplete data collection n=246. Sampling technique For the above reason we use non-randomized convenient sampling technique; thus all patients who underwent elective surgery during study period and satisfy inclusion criteria was included until 246 patient s data were obtained. Inclusion and exclusion criteria All patients aged 18 year or above who has been diagnosed and underwent elective surgical or gynecological procedure during the study period was included. Patients who have pre-operative sore throat complaint, seriously ill (ASA class III or more), surgery done on the airway, unable to communicate or emergency surgery will be excluded. Data collection and measurement Data collectors reviewed patient s card and interviewed the patient for the presence of sore throat, hoarseness of voices and other information to be filled on a pre-designed data sheet prepared by principal investigator, developed based on previous published paper. The interview was done between 12 and 24 h post operatively; after the patient fully recovered from anesthesia and feels comfortable to be interviewed. In patients with sore throat, the responsible doctor was asked whether treatment is necessary. And the age, sex, weight, American Society of Anesthesiologists (ASA) physical status of the patients, time of intubation and extubation, type of surgical procedure, premedication given, perioperative analgesics (opioids) given, degree of postoperative pain, tube size/type/depth, level of extubation (awake/deep), laryngoscope view grade, number of intubation attempt, presence of cough during intubation and/ extubation, presence of blood on laryngoscope/ endotracheal tube (ETT) and estimated blood loss during surgery were also recorded on prepared formats. Data entry and analysis Each questionnaire and predesigned sheet was checked for completeness and coded. Data was manually entered into SPSS Version 20 IBM. Data cleaning was executed by using frequencies and cross tabulations to check accuracy, outliers, consistencies, and missing values. Accordingly, the incorrect entries were identified and re-entered. Descriptive analysis like percentage, mean, standard deviations were computed to describe the study population in respect of socio-demographic and other relevant variables. Odds ratio (OR) with 95% confidence interval (95% CI) was used in bivariate and multivariate logistic regression analysis to determine the effect of various factors on the outcome variable. In logistic regression analysis, each explanatory variable with outcome variable was assessed for its association and those variables whose p-value < 0.05 were taken as candidate variables for multiple logistic regressions for further analysis of its predictive power of sore throat. Variables with P-value less than 0.05 were reported with 95% CI. Ethical clearance A study was conducted after ethical approval letter obtained from the Jimma university ethical review committee and official permission confirmed from hospital administration. An informed consent was taken from all study participants after their volunteer participation asked. Confidentiality of the information was assured and privacy of the study population was respected and kept secret as well. Those patients who had had pain and or sore throat were reported to the concerned physician for treatment. RESULTS Pre-anesthetic characteristics of participants A total of 245 patients were enrolled in to study with a response rate of 228(93.1%). The study subjects age ranges from 18 to 87years, with a majority 113 (49.6%) between the ages of 31 and 50 years. Out of total respondents, 120 (52.6%) were females, 171(75%) ASA class I, 122(53.5%) Oromo ethnics, 146(64%) Muslim, 129 (56.6%) married, 137(60.1%) cannot read and write, and 108 (47.4%) were farmer. Three fourth (75%) of participant classified as ASA I and 25% in ASA II. About 99(43.4%) participants had information on surgeries and anesthesia complications. Eighty three (36.4%) patients had an experience of previous hospitalization. Seventy two (31.6%) patients had undergone previous surgery under local/regional anesthesia 21 (29.2%) and general anesthesia 51(70.8%), of which 49 experienced postoperative complications; 5 dry mouth, 9 head ache, 12 sore throat, 15 nausea and vomiting, and 8 combination of it. Regarding time of aforementioned surgeries, from a total of 72 patients who had experience of previous operation, 53 (73.6%) had operation within last three years and the rest before five years. Majority 64(88.9%) had only once previous operation while 8(11.1%) two times (Table 1). Orthopedics surgery was the most frequently, 47(20.6%), performed procedure and followed by 25(11%) breast surgery, 23(10.1%) hysterectomy, 23(10.1%) herniorrhaphy, 20(8.8%) prostatectomy, 20(8.8%) tissue excision, 17(7.5%) laparotomy, 13(5.7%) uretroplasty and 12(5.3%) thyrodectomy; respectively
4 4 J. Clin. Med. Res. Table 1. Pre-anaesthetic characteristics of study participants of Jima University Teaching Hospital, Variable Character N Percentage Sex Age in year ASA classification Educational status Previous history Ethnic group Others =, kullo, kafa, yem, tigre etc. Female Male > ASA I ASA II Cannot read and write Can read and write Had information about anaesthesia Had had surgery Had experienced postoperative complication Oromo Amhara Others (Figure 1). Incidence of postoperative sore throat (POST) and others complaints From a total of 228, 129 (56.6%) participant had suffered postoperative sore throat (POST) and 68 (29.8%) of them develops hoarseness of voices. The sore throat complaint was severe in 27(11.8), moderate in 43(18.9) and mild in 59(25.9) patients as they indicated on numerical scale. Majority of them noticed that the suffering started immediately while they were in PACU. About 63(27.6%) patients have three or more complaints of which 54 (23.7%) of them had two coincided complaints. In this study we found nausea and vomiting was the most frequent (68.2%) complaint of many patients and sore throat is the second (56.6%) most reported problems during postoperative period. The other postoperative complaint was; postoperative pain 46.7%, cold and thermal discomfort 44.8%, back pain 38%, dry mouth 22.2%) and others (Figures 2 and 3). Among participants who complained sore throat, 54.3% were women. Ninety three patients was premedicated with opioids and more proportion of POST complaint was seen in patients who did not pre-medicated with opioids than those who did; 98/135 vs 31/93 or (72.6% vs 33.3%), respectively. One hundred twenty four (54.4%) patients were given intra-operative analgesic medication. About 51.3%; 117/228 of intubation lasted less than 2 h and four surgeries lasted more than 4 h. Intubation was attempted more than once in 78(34.2%) patients; of which 49 patients complained sore throat. Laryngoscopic view was difficult in 47(20.6%) patients from which 31 patients develops POST (53.1%); patient intubation was done by students and the rest were done by senior who had practiced for 2 years or more. Less POST complaint was observed in patient for whom intubation was done by senior anesthetist. Ninety one (39.9%) patients coughed while tube is in; and majorly suffers sore throat. One hundred forty three (62.7%) patients were extubated during awake stages. Higher incidence of POST was noticed in these patient groups (39% vs 17.5%). Postoperative pain was controlled in 91(39.9%) participants while 32(14%) patients were suffering severe postoperative pain. In the 121 participant, blood clot was observed on tip of ETT/laryngoscope in 107(46.7%) patients. Estimated blood loss was >15% of their estimated total blood volume in 93 (40.8%) participant. Persistent hypotension for more than three minutes was recorded in 94(41.2%) cases (Table 2). Contributing factors of postoperative sore throat The bivariate analysis showed a significant association between post-operative sore throat and the following variables: Being pre-medicated with opioids, postoperative pain, duration of intubation, stage of extubation, presence of cough on ETT, presence of blood on laryngoscope tip/ ETT, anesthetist s experience, hypotension (HPT) lasting >3 min and perioperative estimated blood loss. The association was not detected when those variables entered into final model multiple
5 Chawaka and Temesgen 5 tissue excision (tisue sarcoma), 20. 9% cesarean section, 7.3% thyroidectomy, 12. 5% laparotomy (intraabdominal surgery), 17. 7% cholesystectomy, 10. 4% orthopedic surgery, % hernioraphy, 23.10% breast surgery, % laparatomy (ovarian tumor), 11. 5% hysterectomy, % prostatectomy (BPH), 20.9% urethroplasty (uretral stricture), 13.6% Figure 1. Percentsge distribution of surgical procedures performed during study period at Jima University Teaching Hospital, sore throat hoarsness of voice 5 0 Mild Moderate Severe Figure 2. Percentage distribution of severity of sore thraot and hoarsness of voices after elective surgery at Jima University Teaching Hospital, logistic regression for postoperative sore throat status, stage of extubation, presence of cough, hypotension (HPT) lasting >3 min and perioperative estimated blood loss. However, no significant associations were observed between post-operative sore throat and sex, ASA physical status, intraoperative analgesic medication, induction agent type. Multivariable linear regression was performed to determine the best linear combinations of opioid premedication, duration of intubation, presence of blood on ETT/ laryngoscope tip and anesthetists experience for predicting postoperative sore throat. (Table 3) Being premeditated with opioid and intubation with senior anesthesia has a preventive association with postoperative sore throat. That means those patients who had been premedicated with opioid had less sore throat
6 6 J. Clin. Med. Res. Figure 3. Percentage distribution of postoperative complications after elective surgery during study period at Jima University Teaching Hospital, by 0.17 time (B = 0.170, 95% CI ( ) in comparison to those who did not. Similarly in those intubation performed by a senior anaesthetist, had 0.25 time less likelihood of having postoperative sore throat (B=0.254, 95% CI ( ) when compared with those intubated by junior. The duration of intubation time positively associated with postoperative sore throat, that is, patients who has been lasted as intubated for more than 2 h would have increased the likely hood of developing sore throat on average by 8.5 times (B=8.467, 95% CI ( ) when compared to those intubation that lasted for less than 2 h. Patients in whom blood was observed on tip of laryngoscope or endotracheal tube during intubation complain sore throat 3.0 times more (B = 3.005, 95% CI ( ) than those whose blood was not observed on laryngoscope after laryngoscopy. DISCUSSION Sore throat following the use of endotracheal intubation and other airway is a common minor complication (McHardy and Chung, 1999; Cirilla et al., 2015; Hu et al., 2013). But limited studies have been done in developing countries like Ethiopia, a place where anesthesia resources are very limited. The cause of POST is not clearly known, but it is hypothesized as from inflammatory response from an injured mucosal membrane underlying the EET cuff pressure (McHardy and Chung, 1999; Kalil et al., 2014; Edomwonyi et al., 2006). An existing study results often high variable. As one might expect and know, current practice of airway management method also varied. This variety methods of airway management has varied associated problems; for inistance one study clearly showed that using glide scope vedio laryngoscope for intubation minimizes the incidence of POST compared to macintosh blade laryngoscope (Najafi et al., 2014). The study participant s age ranges from 18 to 87 years, with a majority (26.8%) between 31 and 40 years, 120 (52.6%) were females, 171(75%) ASA class I, 146(64%) Muslim, 129 (56.6%) married, 137(60.1%) cannot read and write, and 108 (47.4%) were farmer. Two studies were done in Germany to see effect of LMA on sore throat (19) and in Iraq to determine incidence of POST (Ahmed et al., 2007), which has similar sociodemographic characteristics. Multiple surgical specialties were included in this study; 47(20.6%) orthopedics surgery; 25(11%) breast surgery, 23(10.1%) hysterectomy, 23(10.1%) herniorrhaphy, 20(8.8%)
7 Chawaka and Temesgen 7 Table 2. Distribution of postoperative sore throat against different variables after elective surgery at Jima University Teaching Hospital, Variable Character Presence of sore throat No Yes n (%) n (%) Total n=228(100%) Gender Female 49(21.4) 70(30.7) 119(52.2) Male 50(21.9) 59(25.9) 109(47.8) Age (years) Physical ASA status (6.6) 24(10.5) 39(17.1) (13.6) 30(13.2) 61(26.8) (10.5) 28(12.3) 52(22.8) (9.6) 34(14.9) 56(24.6) > 65 7(3.1) 13(5.7) 20(8.8) ASA I 75(32.9) 96(42.1) 171(75) ASA II 24(10.5) 33(14.5) 57(25) Premediated with Opioid No 37(16.2) 98(43) 135(59.2) Yes 62(27.2) 31(13.6) 93(40.8) Types of drugs given as premedication Intraoperative given analgesic medication Post-operative pain controlled? Postoperative pain level Induction anesthetic agent used Laryngoscopic view grade Number of intubation attempted ETT size (internal diameter; ID in mm) ETT depth (tip of tube placement from angle of mouth; in cm) Nothing 7(3.1) 25(11) 32(14) Opioid 8(3.5) 12(5.3) 20(8.8) Diazepam 18(7.9) 29(12.7) 47(20.6) Atropine 14(6.1) 40(17.5) 54(23.2) combination (all) 47(20.6) 23(10.1) 73(32) No 48(21) 76(33.3) 124(54.4) Yes 51(22.4) 53(22.8) 104(45.6) No 42(18.4) 95(41.7) 137(60.1) Yes 57(25) 34(14.9) 91(39.9) Controlled 58(25.4) 33(14.5) 91(39.9) Mild 16(7) 42(18.4) 58(25.4) Moderate 14(6.1) 33(14.5) 47(20.6) Severe 11(4.8) 21(9.2) 32(14) other agent IVA 41(18) 83(36.4) 124(54.4) Ketamine 58(25.4) 46(20.2) 104(45.6) simple (G=I or II) 83(36.4) 98(43) 181(79.4) Difficult (G=III or IV) 16(7) 31(13.6) 47(20.6) Once 70(30.7) 80(35.1) 150(65.8) > once 29(12.7) 49(21.5) 78(34.2) (9.2) 30(13.2) 51(22.4) 7 42(18.4) 60(26.3) 102(44.7) (7.5) 14(6.1) 31(13.6) 8 18(7.9) 25(11) 43(18.9) 20 33(14.5) 52(22.8) 85(37.3) 21 29(12.7) 40(17.5) 69(30.3) 22 37(16.2) 37(16.2) 74(32.5)
8 8 J. Clin. Med. Res. Table 2. Contd. Duration of intubation 30 min 1(.4) 2(.9) 3(1.3) min 20(8.8) 11(4,8) 31(13.6) 1-2 h 61(26.8) 24(10.5) 85(37.3) 2-3 h 16(7) 71(31.1) 87(38.2) 3-4 h 1(0.4) 17(7.5) 18(7.9) > 4 h 0 4(1.8) 4(1.8) Is duration of ETT > 2 h No 81(35.5) 36(15.8) 117(51.3) Yes 18(7.9) 93(40.8) 111(48.7) Awake extubation No 45(19.7) 40(17.5) 85(37.3) Yes 54(23.7) 89(39) 143(62.7 Presence of cough No 83(36.4) 54(23.7) 137(60.1) yes (during intubation, extubation, suction) 16(17) 75(32.9) 91(39.9) Blood were observed on ETT / laryngoscope tips Qualification of Anesthetists BP drops persist for more than 3 min Estimated blood loss > 15% of EBVt? Source: Own survey data, No 74(32.5) 47(20.6) 121(53.1) Yes 25(11) 82(36) 107(46.9) student /junior 31(13.6) 98(43) 129(66.6) senior (> 2 year experience) 68(29.8) 31(13.6) 99(43.4) No 73(32) 61(26.8) 134(58.8) yes 26(11.4) 68(29.8) 94(41.2) No 68(29.8) 67(29.4) 135(59.2) Yes 31(13.6) 62(27.2) 93(40.8) Table 3. Predictors of post-operative sore throat among elective surgical patients at Jima University Teaching Hospital, Variable Character N Sex Female Male ( ) Presence of post-operative sore throat COR(95% of CI) p-value AOR(95% of CI) p-value ASA physical status Was pre-medicated with opioid? Was intra-operative analgesic medication given? Was post-operative pain controlled? Was the Laryngoscopic view difficult? That is (G=III or IV) ASA I ASA II ( ) No Yes ( )** ( )** No Yes ( ) No Yes ( )** ( ) No Yes ( ) 0.148
9 Chawaka and Temesgen 9 Table 3. Contd. Was intubation attempted more than once? Was duration of intubation lasts >2 h? Was patient extubated awake? Was patient coughed (during intubation, extubation or suctioning)? Was blood observed on ETT/laryngoscopes tip? Was the anesthetists senior (> 2 year experience)? Does hypotension (HPT) last >3 min? Does estimated blood loss > 15% TBV? No Yes ( ) No Yes ( )** ( )** No Yes ( )* ( ) No Yes ( )** ( ) No Yes ( )** ( )** No Yes ( )** ( )** No Yes ( )** ( ) No Yes ( )* ( ) Was ketamine used as induction agent? *=P 0.05; **=P 0.01; Source: Own survey data, No Yes ( )** ( ) prostatectomy, 20(8.8%) tissue excision, 17(7.5%) laparotomy, 13(5.7%) uretroplasty and 12(5.3%) thyroidectomy. Similarly many studies has evaluate the sore throat in different surgical specialties (Ahmed et al., 2007; Edomwonyi et al., 2006; Jaensson et al., 2014). This study showed 56.6% participants have complainedpostoperative sore throat from which 63% of them had hoarseness of voice. In other parts of the world it have been documented that the value varied from 20 to 50% (Ahmed et al., 2007; Edomwonyi et al., 2006), which is a bit lower than this finding. On the other side there is higher and comparable results; 64% have been reported by Mchardy and Chung (1999); and 59% in air filled ETT cuff, Navarro and Baughman (1997). This finding is higher than the result found by Jaensson et al. 40% (Jaensson et al., 2014). In another experts report it was documented 40% of participants develop POST after extubation (Orandi et al., 2013). Another systematic review paper showed a very wide range with highest 70% and lowest 30% of POST occurrences (Tanaka et al., 2009). This discrepancy might be due to sample sizes and data collection time differences. In addition to this the educational level and understanding level of the question might be different. Furthermore, sore throat was found to be more common with certain patient related, anesthetic and surgical factors, e.g. gender, difficulty level of intubation, duration of ETT in trachea, being not premedicated with opioid, anesthetists experience, induction agent, bleeding on tip of laryngoscope /ETT, perioperative hypotension and estimated blood loss during surgery. However, a bigger sample size taken from various surgical specialties and the application of more advanced statistical tests would be required to comment on the true association of sore throat with these factors. In this study women more frequently complained POST than men, (70/119 vs 59/109), but it was not statistically significant (p=0.475). Similar report were documented by Jeansson et al Orebro University Hospital (Jaensson et al., 2014) and Cirilla et al. (2015), while others still not find any difference (Jaensson, 2013). Preoperative analgesic medication was given for only 93 (40.8%) patients and we observed less incidence of POST in these patient groups. Being premedicated by opioids decreases the likely hood of postoperative sore throat by 0.17 (B=0.170, 95% CI , p=0.001) in
10 10 J. Clin. Med. Res. comparison to those who did not premedicated. Several researchers has revealed that premedication would reduce the incidences of POST; Shrestha et al (2010) in Nepal had showed preoperative ketamine gargling decreases POST incidences. Another study revealed that dexamethasone significantly lowers the incidence; 12(20%) vs 5(8.3%) (Haider and Al-ali, 2013); similar result were obtained from other study (Kalil et al., 2014). Again another study conducted, in Iran 2014 (Teymourian et al., 2015), to compare the effect of magnesium and ketamine gargling on POST showed effective reduction of complaint with superiority of magnesium. On the contrary, Tanga a et al. (2013) found no difference among diclofenac medicated and non-medicate groups. Soltani and Aghadavoudi (2002) studied to verify the effect of dexamethasone on sore throat and found significant difference with higher rate occurrence of POST (64%) in those who did not premedicated with dexamethasone. But we did not find any literature showing a reduction of POST with opioids premedication. This difference might be clients misunderstood the question with the supper imposed effect of postoperative pain from surgical site. It have been seen that bleeding during intubation or suctioning increases the occurrence of postoperative sore throat (B = 3.005, 95% CI , p=.007) in comparison to their counterparts. This is because of direct injury to the underlying tissue during laryngoscopy and suctioning with a suction catheter. This concept were explaned by one study conducted at Tabriz, Iran; which were done to compare the effect of LMA and ETT on postoperative complication (Journal, 2010). Higher incidence of POST was noticed in participants whose intubation lasted 2 h or more duration, 93/111 (83.8%) vs 36/117(30.8%). The likely hood of developing postoperative sore throat in participants whose intubation lasted more than 2 h is increased by 8.5 times (B = 8.467, 95% CI , p=0.000) when compared to those intubation lasts less than 2 h. It has been documented by many researchers that intubation duration has significant association with postoperative sore throat occurrence (Mokhtar and Choy, 2013; Ahmed et al., 2007; Edomwonyi et al., 2006). Though this study revealed relatively higher incidence of sore throat among patients with higher laryngoscopic view grade, cough while ETT is in trachea, and estimated blood loss is greater than 15% of estimated blood volume, the association and statistical significance was no found. One researcher revealed that the these factors have association with the occurrence rate of postoperative sore throat (Jaensson, 2013).We did not detect the number of intubation attempt is associated with increased frequency of POST which agreed with findings from Albany Medical Center, Albany (Cirilla II et al., 2015). One hundred twenty one (53.1%) particicpants were intubated by students and or junior anesthetists who had 2 years or less experience. Less POST complaint was observed in a patient who were intubated by senior anesthetist. Similarly, it was well documented by D.J. Cirilla II et al. (Cirilla et al., 2015), that higher incidence of POST was observed in patients who has been intubated by CRNA than those performed by experienced anesthesiologists, 26.8 Vs 52.3%, respectively. One hundred forty three (62.7%) patients were extubated during awake stages and higher incidence of POST was noticed in these patient groups (39% vs 17.5%). This might be contributed by moving the tube in and out during coughing, which traumatize the underlying mucosa of larynx. The estimated perioperative blood loss, in 93 (40.8%) participant, was more than 15% of their estimated total blood volume and persistent hypotension for more than three minutes was recorded in 94(41.2%) cases. More frequent complaint of sore throat was noticed among these patients. This might be contributed when there is hypotension the blood flow to laryngeal mucosa diminished and exacerbated by compression from tube which results in ischemia. There are a number of limitations during this study. The result will not represent other types of surgical procedure we studied on; and the predictive factors identified in this study may not necessarily be transferable to other institution. Therefore, further studies in the larger population including multiple institution are needed. The some patients were not cooperative to provide full information because of postoperative pain; however, all possible ways of time arrangement was considered in order to cooperate during pain free time for the interview. Another limitation of this study is that the assessment of symptoms of POST and PH were made over a range of time (6 to 24 h post operatively), not at a specific point of time. However, these symptoms usually emerge in the early postoperative period and, therefore, early assessment can help the providers to capture patients at risk. Also we did not used manometer to measure the endotracheal tube cuff pressure which significantly impact the result. Conclusion Significant postoperative sore throat complaint was observed during the study period. Little appreciation was given to the postoperative complications in the study area, though it is reported with a surprisingly high frequency. Nevertheless, anesthetic care justifiably has been singled out as a model for patient safety and highquality outcome. The sore throat was found to be more common with certain patient, anesthetic and surgical related factors; difficulty level of intubation, duration of ETT in trachea, being not premedicated with opioid, anesthetists experience, type of induction agent, bleeding on tip of laryngoscope/ett, perioperative hypotension and estimated blood loss during surgery. All
11 Chawaka and Temesgen 11 patients should be premedicated with analgesic medications, especially those with predictive factors, which minimizes the incidence of postoperative sore throat and optimize the patient satisfaction. Student should practice on manikin before an actual patient and not allowed for repeated attempt of laryngoscopy in case of difficulty. Laryngoscopy and sanctioning should be performed gently under close supervision of senior anesthetists The results of this study can have additional refine on the pervasive nature of minor perioperative adverse anesthetic events. Proposed measures to address the present situation include modifying the training of anesthesia providers to raise awareness on patient well-being during perioperative period. Minor adverse events need to be regularly discussed during Grand Rounds and with all patients during theirpreoperative anesthetic visit. Conflicts of interests The authors have not declared any conflict of interests. ACKNOWLEDGEMENT The authors would like to thank the hospital administration offices and participant (patients) for their co-operation in giving valuable information, sa well as the anesthesia team for their help in completing the form and nurses who helped by delivering information regarding administration of prophylactic antibiotics. REFERENCES throat after elective surgical procedures. J. Ayub. Med. Coll. Abbottabad 19(2):12-4. Edomwonyi NP, Ekwere IT, Omo E, Rupasinghe A (2006). Postoperative Throat Complications after Tracheal Intubation. Ann. Afr. Med. 5(1): Thang a P, Kamya D, Mung ayi V (2013). Effects of intravenous diclofenac on postoperative sore throat in patients undergoing laparoscopic surgery at Aga Khan University Hospital, Nairobi: a prospective, randomized, double blind controlled trial. Afr. Health Sci. 13(4): Shrestha SK, Bhattarai B, Singh J (2010). Ketamine gargling and postoperative sore throat. [Internet].; J. Nepal Med. Assoc. 49(180): Teymourian H, Mohajerani SA, Farahbod A (2005).Magnesium and Ketamine Gargle and Postoperative Sore Throat. Anesth. Pain Med. 5(3): Zhao X, Cao X, Li Q (2014). Dexamethasone for the prevention of postoperative sore throat: a systematic review and meta-analysis. J. Clin. Anesth. 27(1): Haider HS, Al-ali BT (2013). The Role of Dexamethasone in Reducing the Severity of Postoperative Sore Throat. Can J Anaesth. 12(3): Hu B, Bao R, Wang X, Liu S, Tao T, Xie Q, Yu X, Li J, Bo L, Deng X (2013). The size of endotracheal tube and sore throat after surgery: a systematic review and meta-analysis. PLoS One 8(10):e Navarro RM, Baughman VL (1997). Lidocaine in the Endotracheal Tube Cuff Reduces Postoperative Sore Throat. J. Clin. Anesth. 8180(97): Orandi A, Orandi A, Najafi A, Hajimohammadi F, Soleimani S, Zahabi S (2013).Post-intubation sore throat and menstruation cycles. Anesthesiol. Pain Med. 3(2): Tanaka Y, Nakayama T, Nishimori M, Sato Y, Furuya H (2009). Lidocaine for preventing postoperative sore throat (Review). Cochrane Database Syst. Rev. 3:3-5. Soltani H-A, Aghadavoudi O (2002). The effect of different lidocaine application methods on postoperative cough and sore throat. J. Clin. Anesth. 14(1):15-8. Journal SE (2010). Comparison of the Effects of Endotracheal Tube and Laryngeal Mask Airway on Immediate Postoperative Complications in Elective Operations. Abstract : Introduction 11(4): Mokhtar AMM, Choy CY(2013). Postoperative sore throat in children: Comparison between prosealtm LMA and classictm LMA. Middle East J. Anesthesiol. 22(1): McHardy FE, Chung F (1999). Postoperative sore throat: Cause, prevention and treatment. Anaesthesia. 54(5): Cirilla DJ, Ngo J, Vaisman V, Daly C, Ata A, Sandison M, Roberts K (2015). Does the incidence of sore throat postoperatively increase with the use of a traditional intubation blade or the GlideScope?. J. Clin. Anesth. 27(8): Najafi A, Imani F, Makarem J, Khajavi MR, Etezadi F, Habibi S, Moharari RS (2014). Postoperative Sore Throat After Laryngoscopy With Macintosh or Glide Scope Video Laryngoscope Blade in Normal Airway Patients. Anesthesiol. Pain Med. 4(1):4-7. Kalil DM, Silvestro LS, Austin PN (2014). Novel preoperative pharmacologic methods of preventing postoperative sore throat due to tracheal intubation. AANA J. 82(3): Burgard G, Möllhoff T, Prien T (1996). The effect of laryngeal mask cuff pressure on postoperative sore throat incidence. J. Clin. Anesth. 8(3): Mandoe H, Nikolajsen L, Lintrup U, Jepsen D, Molgaard J (1992). Sore throat after endotracheal intubation. Anesth. Analg. 74(6): Soediono B (1989). Factors Affecting the Incidence of Sore Throat Following General Anesthesia with Endotracheal Tube Versus Laryngeal Mask Airway. J. Chem. Inf. Model. pp. 53:160. Jaensson M (2013). Postoperative sore throat and hoarseness. Print: Örebro University, Repro 11/2013 ISSN Jaensson M, Gupta A, Nilsson U (2014). Gender differences in sore throat and hoarseness following endotracheal tube or laryngeal mask airway: a prospective study. BMC Anesthesiol.14(1):1-8. Ahmed A, Abbasi S, Ghafoor HB, Ishaq M (2007). Postoperative sore
POST-THYROIDECTOMY SORE THROAT: A COMMON PROBLEM
 Original Article POST-THYROIDECTOMY SORE THROAT: A COMMON PROBLEM Irfan Ali Kadri 1, Tariq Wahab Khanzada 2, Abdul Samad 3, Waseem Memon 4 ABSTRACT Objective: To determine the frequency of postoperative
Original Article POST-THYROIDECTOMY SORE THROAT: A COMMON PROBLEM Irfan Ali Kadri 1, Tariq Wahab Khanzada 2, Abdul Samad 3, Waseem Memon 4 ABSTRACT Objective: To determine the frequency of postoperative
Magnesium and Ketamine Gargle and Postoperative Sore Throat
 Anesth Pain Med. 2015 June; 5(3): e22367. Published online 2015 June 22. DOI: 10.5812/aapm.5(3)2015.22367 Research Article and Gargle and Postoperative Sore Throat Houman Teymourian 1,* ; Seyed Amir Mohajerani
Anesth Pain Med. 2015 June; 5(3): e22367. Published online 2015 June 22. DOI: 10.5812/aapm.5(3)2015.22367 Research Article and Gargle and Postoperative Sore Throat Houman Teymourian 1,* ; Seyed Amir Mohajerani
4/23/14 POST. Population POST POST POST POST. intervention. Comparison Outcome. Novel Preoperative Pharmacologic Methods of
 ovel Preoperative Pharmacologic Methods of David Kalil CRA, DAP Preventing Postoperative Sore Throat Sore throat and hoarseness after (GA) with tracheal intubation occurs in 30-70% of patients Usually
ovel Preoperative Pharmacologic Methods of David Kalil CRA, DAP Preventing Postoperative Sore Throat Sore throat and hoarseness after (GA) with tracheal intubation occurs in 30-70% of patients Usually
Efficacy of Ketamine Gargles in the Prevalence of Postoperative Sore Throat after Endotracheal Intubation
 Original Research Efficacy of Ketamine Gargles in the Prevalence of Postoperative Sore Throat after Endotracheal Intubation Neha P. Kamble 1,*, Manojkumar N. Gajbhare 2 1 Assistant professor, Department
Original Research Efficacy of Ketamine Gargles in the Prevalence of Postoperative Sore Throat after Endotracheal Intubation Neha P. Kamble 1,*, Manojkumar N. Gajbhare 2 1 Assistant professor, Department
ISSN X (Print) Research Article. *Corresponding author Dr. Souvik Saha
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(6B):2238-2243 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(6B):2238-2243 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Post-Intubation Airway Related Adverse Effects: A Comparison between Intra-Cuff Dexamethasone and Intra-Cuff Alkalinized Lignocaine
 Original Research Article Post-Intubation Airway Related Adverse Effects: A Comparison between Intra-Cuff Dexamethasone and Intra-Cuff Alkalinized Lignocaine Kep Kee W 1, Nadia MN 2, Melvin K 2 ( ), Muhammad
Original Research Article Post-Intubation Airway Related Adverse Effects: A Comparison between Intra-Cuff Dexamethasone and Intra-Cuff Alkalinized Lignocaine Kep Kee W 1, Nadia MN 2, Melvin K 2 ( ), Muhammad
SORE THROAT AFTER ANAESTHESIA
 Brit. J. Anaesth. (1960), 32, 219 SORE THROAT AFTER ANAESTHESIA BY C. M. CONWAY, J. S. MILLER AND F. L. H. SUGDEN Department of Anaesthesia, Charing Cross Hospital Medical School, London, W.C.2 A sore
Brit. J. Anaesth. (1960), 32, 219 SORE THROAT AFTER ANAESTHESIA BY C. M. CONWAY, J. S. MILLER AND F. L. H. SUGDEN Department of Anaesthesia, Charing Cross Hospital Medical School, London, W.C.2 A sore
Comparison of the Hemodynamic Responses with. with LMA vs Endotracheal Intubation
 Original article Comparison of the Hemodynamic Responses 10.5005/jp-journals-10045-0060 with LMA vs Endotracheal Intubation Comparison of the Hemodynamic Responses with Laryngeal Mask Airway vs Endotracheal
Original article Comparison of the Hemodynamic Responses 10.5005/jp-journals-10045-0060 with LMA vs Endotracheal Intubation Comparison of the Hemodynamic Responses with Laryngeal Mask Airway vs Endotracheal
Use of the Aintree Intubation Catheter with the Laryngeal Mask Airway and a Fiberoptic Bronchoscope in a Patient with an Unexpected Difficult Airway
 Case Report Use of the Aintree Intubation Catheter with the Laryngeal Mask Airway and a Fiberoptic Bronchoscope in a Patient with an Unexpected Difficult Airway Andrew Zura MD, D. John Doyle MD PhD FRCPC,
Case Report Use of the Aintree Intubation Catheter with the Laryngeal Mask Airway and a Fiberoptic Bronchoscope in a Patient with an Unexpected Difficult Airway Andrew Zura MD, D. John Doyle MD PhD FRCPC,
The effect of combining lidocaine with dexamethasone for attenuating postoperative sore throat, cough, and hoarseness
 Anesth Pain Med 2016; 11: 42-48 http://dx.doi.org/10.17085/apm.2016.11.1.42 Clinical Research The effect of combining lidocaine with dexamethasone for attenuating postoperative sore throat, cough, and
Anesth Pain Med 2016; 11: 42-48 http://dx.doi.org/10.17085/apm.2016.11.1.42 Clinical Research The effect of combining lidocaine with dexamethasone for attenuating postoperative sore throat, cough, and
SORE THROAT; COMPARISON OF KETAMINE NEBULISATION WITH KETAMINE GARGLES IN ATTENUATING POSTOPERATIVE SORE THROAT.
 The Professional Medical Journal DOI: 10.29309/TPMJ/18.4507 ORIGINAL PROF-4507 SORE THROAT; COMPARISON OF KETAMINE NEBULISATION WITH KETAMINE GARGLES IN ATTENUATING POSTOPERATIVE SORE THROAT. 1. MBBS,
The Professional Medical Journal DOI: 10.29309/TPMJ/18.4507 ORIGINAL PROF-4507 SORE THROAT; COMPARISON OF KETAMINE NEBULISATION WITH KETAMINE GARGLES IN ATTENUATING POSTOPERATIVE SORE THROAT. 1. MBBS,
As laparoscopic surgeries are gaining popularity, Original Article. Maharjan SK 1, Shrestha S 2 1. Introduction
 , Vol. 1, No. 1, Issue 1, Jul.-Sep., 2012 Original Article Maharjan SK 1, Shrestha S 2 1 Associate Professor, 2 Assistant Professor, Department of Anaesthesiology and Intensive Care Kathmandu Medical College,
, Vol. 1, No. 1, Issue 1, Jul.-Sep., 2012 Original Article Maharjan SK 1, Shrestha S 2 1 Associate Professor, 2 Assistant Professor, Department of Anaesthesiology and Intensive Care Kathmandu Medical College,
Dose-dependent effectiveness of ketamine nebulisation in preventing postoperative sore throat due to tracheal intubation
 Dose-dependent effectiveness of ketamine nebulisation in preventing postoperative sore throat due to tracheal intubation M Reddy *, S Fiaz 2 Professor *, Resident 2, Department of Anesthesiology Kempegowda
Dose-dependent effectiveness of ketamine nebulisation in preventing postoperative sore throat due to tracheal intubation M Reddy *, S Fiaz 2 Professor *, Resident 2, Department of Anesthesiology Kempegowda
Comparison of intracuff dexamethasone, lignocaine and normal saline on post extubation response - A prospective study
 Original Research Article Comparison of intracuff dexamethasone, lignocaine and normal saline on post extubation response - A prospective study Soumya M V 1, Sanjeev G M 2* 1 Senior Resident, 2 Associate
Original Research Article Comparison of intracuff dexamethasone, lignocaine and normal saline on post extubation response - A prospective study Soumya M V 1, Sanjeev G M 2* 1 Senior Resident, 2 Associate
Setting The setting was tertiary care. The economic study appears to have been performed in Heidelberg, Germany.
 Comparative analysis of costs of total intravenous anaesthesia with propofol and remifentanil vs. balanced anaesthesia with isoflurane and fentanyl Epple J, Kubitz J, Schmidt H, Motsch J, Bottiger B W,
Comparative analysis of costs of total intravenous anaesthesia with propofol and remifentanil vs. balanced anaesthesia with isoflurane and fentanyl Epple J, Kubitz J, Schmidt H, Motsch J, Bottiger B W,
FAILED ELECTIVE INTUBATION: PLAN A- C
 FAILED ELECTIVE INTUBATION: PLAN A- C MODULE: AIRWAY TARGET: NOVICE, BASIC LEVEL TRAINEES & ALL ANAESTHETISTS BACKGROUND: Management of the unexpectedly difficult airway is a core skill for all anaesthetists.
FAILED ELECTIVE INTUBATION: PLAN A- C MODULE: AIRWAY TARGET: NOVICE, BASIC LEVEL TRAINEES & ALL ANAESTHETISTS BACKGROUND: Management of the unexpectedly difficult airway is a core skill for all anaesthetists.
Key words: airway, complications; complications, tracheal intubation; education, untrained personnel
 British Journal of Anaesthesia, 2015, 463 9 doi: 10.1093/bja/aev234 Advance Access Publication Date: 4 August 2015 Respiration and the Airway RESPIRATION AND THE AIRWAY Tracheal intubation by trainees
British Journal of Anaesthesia, 2015, 463 9 doi: 10.1093/bja/aev234 Advance Access Publication Date: 4 August 2015 Respiration and the Airway RESPIRATION AND THE AIRWAY Tracheal intubation by trainees
MD (Anaesthesiology) Title (Plan of Thesis) (Session )
 S.No. 1. Comparative Assessment of Sequential organ failure Assessment (SOFA) score and Multiple Organ Dysfunction Score (Mode) in Outcome Prediction among ICU Patients. 2. Comparison of Backpain after
S.No. 1. Comparative Assessment of Sequential organ failure Assessment (SOFA) score and Multiple Organ Dysfunction Score (Mode) in Outcome Prediction among ICU Patients. 2. Comparison of Backpain after
Dexamethasone combined with other antiemetics for prophylaxis after laparoscopic cholecystectomy
 Original Research Article Dexamethasone combined with other antiemetics for prophylaxis after laparoscopic cholecystectomy T. Uma Maheswara Rao * Associate Professor, Department of Surgery, Konaseema Institute
Original Research Article Dexamethasone combined with other antiemetics for prophylaxis after laparoscopic cholecystectomy T. Uma Maheswara Rao * Associate Professor, Department of Surgery, Konaseema Institute
CAN T INTUBATE, CAN T VENTILATE: PLAN A- D
 CAN T INTUBATE, CAN T VENTILATE: PLAN A- D MODULE: AIRWAY TARGET: BASIC LEVEL TRAINEES & ALL ANAESTHETISTS BACKGROUND: Management of the Can t Intubate, Can t Ventilate situation is a core skill for all
CAN T INTUBATE, CAN T VENTILATE: PLAN A- D MODULE: AIRWAY TARGET: BASIC LEVEL TRAINEES & ALL ANAESTHETISTS BACKGROUND: Management of the Can t Intubate, Can t Ventilate situation is a core skill for all
HELPING REDUCE THE TRACHEAL IMPACT OF INTUBATION1. Endotracheal tubes with TaperGuard cuff technology in the operating room
 HELPING REDUCE THE TRACHEAL IMPACT OF INTUBATION1 Endotracheal tubes with TaperGuard cuff technology in the operating room SECURING AIRWAYS WITH A GENTLE TOUCH You aim to keep patients safe and comfortable
HELPING REDUCE THE TRACHEAL IMPACT OF INTUBATION1 Endotracheal tubes with TaperGuard cuff technology in the operating room SECURING AIRWAYS WITH A GENTLE TOUCH You aim to keep patients safe and comfortable
DIFFICULT AIRWAY MANAGMENT. Dr.N.SANTHOSH KUMAR MD ANESTHESIA (2 nd Yr)
 DIFFICULT AIRWAY MANAGMENT Dr.N.SANTHOSH KUMAR MD ANESTHESIA (2 nd Yr) AIRWAY MANAGEMENT AND MAINTAINING OXYGENATION ARE THE FUNDAMENTAL RESPONSIBILITIES OF ANY BASIC DOCTOR. TO MANAGE A DIFFICULT AIRWAY,
DIFFICULT AIRWAY MANAGMENT Dr.N.SANTHOSH KUMAR MD ANESTHESIA (2 nd Yr) AIRWAY MANAGEMENT AND MAINTAINING OXYGENATION ARE THE FUNDAMENTAL RESPONSIBILITIES OF ANY BASIC DOCTOR. TO MANAGE A DIFFICULT AIRWAY,
University of Zurich. Complaints of sore throat after tracheal intubation: a prospective evaluation. Zurich Open Repository and Archive
 University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2005 Complaints of sore throat after tracheal intubation: a prospective evaluation
University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2005 Complaints of sore throat after tracheal intubation: a prospective evaluation
Life Science Journal 2018;15(3)
 Comparison of Post Extubation Complications In 3 Different States of Filling Endotracheal Tube Cuff With Lidoaine 4% In Elective Surgery Patients (This is the template do not put these words about template
Comparison of Post Extubation Complications In 3 Different States of Filling Endotracheal Tube Cuff With Lidoaine 4% In Elective Surgery Patients (This is the template do not put these words about template
LMA Supreme Second Seal. Maintain the airway. Manage gastric contents. Meet NAP4 recommendations.
 LMA Supreme Second Seal Maintain the airway. Manage gastric contents. Meet NAP4 recommendations. A proven double seal The importance of the Second Seal (oesophageal seal) is significant: it can minimise
LMA Supreme Second Seal Maintain the airway. Manage gastric contents. Meet NAP4 recommendations. A proven double seal The importance of the Second Seal (oesophageal seal) is significant: it can minimise
The Mallampati Test versus the Upper Lip Bite Test in Predicting Difficult Intubation. Chance Buttars BSN, BA Bryan College of Health Sciences
 1 The Mallampati Test versus the Upper Lip Bite Test in Predicting ifficult Intubation Chance Buttars BSN, BA Bryan College of Health Sciences Keywords: Airway assessment, Mallampati test, upper lip bite
1 The Mallampati Test versus the Upper Lip Bite Test in Predicting ifficult Intubation Chance Buttars BSN, BA Bryan College of Health Sciences Keywords: Airway assessment, Mallampati test, upper lip bite
ISPUB.COM. The Video-Intubating Laryngoscope. M Weiss THE LARYNGOSCOPE INTRODUCTION TECHNICAL DESCRIPTION
 ISPUB.COM The Internet Journal of Anesthesiology Volume 3 Number 1 M Weiss Citation M Weiss.. The Internet Journal of Anesthesiology. 1998 Volume 3 Number 1. Abstract A Macintosh intubating laryngoscope
ISPUB.COM The Internet Journal of Anesthesiology Volume 3 Number 1 M Weiss Citation M Weiss.. The Internet Journal of Anesthesiology. 1998 Volume 3 Number 1. Abstract A Macintosh intubating laryngoscope
Use of the Intubating Laryngeal Mask Airway
 340 Anesthesiology 2000; 93:340 5 2000 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Use of the Intubating Laryngeal Mask Airway Are Muscle Relaxants Necessary? Janet
340 Anesthesiology 2000; 93:340 5 2000 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Use of the Intubating Laryngeal Mask Airway Are Muscle Relaxants Necessary? Janet
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Research Article. Shital S. Ahire 1 *, Shweta Mhambrey 1, Sambharana Nayak 2. Received: 22 July 2016 Accepted: 08 August 2016
 International Journal of Research in Medical Sciences Ahire SS et al. Int J Res Med Sci. 2016 Sep;4(9):3838-3844 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20162824
International Journal of Research in Medical Sciences Ahire SS et al. Int J Res Med Sci. 2016 Sep;4(9):3838-3844 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20162824
RELEVANT AREAS OF THE ANAESTHETIC CURRICULUM
 LARYNGOSPASM MODULE: CRITICAL INCIDENTS TARGET: ALL ANAESTHETISTS & INTENSIVISTS BACKGROUND: Laryngospasm is a common complication around the time of airway handling in adults and in paediatric patients.
LARYNGOSPASM MODULE: CRITICAL INCIDENTS TARGET: ALL ANAESTHETISTS & INTENSIVISTS BACKGROUND: Laryngospasm is a common complication around the time of airway handling in adults and in paediatric patients.
ASPIRATION DURING ANAESTHESIA
 ASPIRATION DURING ANAESTHESIA MODULE: CRITICAL INCIDENTS TARGET: ALL ANAESTHETISTS BACKGROUND: Passive regurgitation or vomiting can occur during the pre-, peri- or post- operative period risking aspiration
ASPIRATION DURING ANAESTHESIA MODULE: CRITICAL INCIDENTS TARGET: ALL ANAESTHETISTS BACKGROUND: Passive regurgitation or vomiting can occur during the pre-, peri- or post- operative period risking aspiration
Comparison of Ease of Insertion and Hemodynamic Response to Lma with Propofol and Thiopentone.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 12 Ver. IV (Dec. 2015), PP 22-30 www.iosrjournals.org Comparison of Ease of Insertion and Hemodynamic
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 12 Ver. IV (Dec. 2015), PP 22-30 www.iosrjournals.org Comparison of Ease of Insertion and Hemodynamic
Problem Based Learning. Problem. Based Learning
 Problem 2013 Based Learning Problem Based Learning Your teacher presents you with a problem in anesthesia, our learning becomes active in the sense that you discover and work with content that you determine
Problem 2013 Based Learning Problem Based Learning Your teacher presents you with a problem in anesthesia, our learning becomes active in the sense that you discover and work with content that you determine
Original Article Effects of pharyngeal tampon usage for postoperative nause, vomiting and sore throat in nasal surgery
 Int J Clin Exp Med 2016;9(7):14442-14447 www.ijcem.com /ISSN:1940-5901/IJCEM0027727 Original Article Effects of pharyngeal tampon usage for postoperative nause, vomiting and sore throat in nasal surgery
Int J Clin Exp Med 2016;9(7):14442-14447 www.ijcem.com /ISSN:1940-5901/IJCEM0027727 Original Article Effects of pharyngeal tampon usage for postoperative nause, vomiting and sore throat in nasal surgery
Sleep Apnea and ifficulty in Extubation. Jean Louis BOURGAIN May 15, 2016
 Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
LEVITAN S FIBREOPTIC STYLET: BEYOND BARRIERS. - Our Perspective.
 ISSN: 2250-0359 Volume 3 Issue 4 2013 LEVITAN S FIBREOPTIC STYLET: BEYOND BARRIERS - Our Perspective. Justin Ebenezer Sargunaraj * Dr.Balasubramaniam Thiagarajan * *Stanley Medical College ABSTRACT: This
ISSN: 2250-0359 Volume 3 Issue 4 2013 LEVITAN S FIBREOPTIC STYLET: BEYOND BARRIERS - Our Perspective. Justin Ebenezer Sargunaraj * Dr.Balasubramaniam Thiagarajan * *Stanley Medical College ABSTRACT: This
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Care Unit (FELLOW)
 Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
American Journal of Health Research
 American Journal of Health Research 2014; 2(4): 113-117 Published online July 30, 2014 (http://www.sciencepublishinggroup.com/j/ajhr) doi: 10.11648/j.ajhr.20140204.12 ISSN: 2330-8788 (Print); ISSN: 2330-8796
American Journal of Health Research 2014; 2(4): 113-117 Published online July 30, 2014 (http://www.sciencepublishinggroup.com/j/ajhr) doi: 10.11648/j.ajhr.20140204.12 ISSN: 2330-8788 (Print); ISSN: 2330-8796
FAILED INTUBATION DURING RSI: PLAN A, C & D
 FAILED INTUBATION DURING RSI: PLAN A, C & D MODULE: NOVICE & AIRWAY TARGET: NOVICE INITIAL ASSESSMENT OF COMPETENCY ALL ANAESTHETISTS BACKGROUND: Management of the Can t Intubate, Can t Ventilate situation
FAILED INTUBATION DURING RSI: PLAN A, C & D MODULE: NOVICE & AIRWAY TARGET: NOVICE INITIAL ASSESSMENT OF COMPETENCY ALL ANAESTHETISTS BACKGROUND: Management of the Can t Intubate, Can t Ventilate situation
Journal of Anesthesia & Clinical
 Journal of Anesthesia & Clinical Research ISSN: 2155-6148 Journal of Anesthesia & Clinical Research Balasubramanian and Menaha, J Anesth Clin Res 2017, 8:12 DOI: 10.4172/2155-6148.1000791 Research Article
Journal of Anesthesia & Clinical Research ISSN: 2155-6148 Journal of Anesthesia & Clinical Research Balasubramanian and Menaha, J Anesth Clin Res 2017, 8:12 DOI: 10.4172/2155-6148.1000791 Research Article
1. Influence of isoflurane exposure in pregnant rats on the learning and memory of offspring
 1. Influence of isoflurane exposure in pregnant rats on the learning and memory of offspring Huang W, Dong Y, Zhao G, et al. BMC Anesthesiology 2018 18:5 Concerns remain about possible effects of general
1. Influence of isoflurane exposure in pregnant rats on the learning and memory of offspring Huang W, Dong Y, Zhao G, et al. BMC Anesthesiology 2018 18:5 Concerns remain about possible effects of general
Pharyngolaryngeal Morbidity with the Laryngeal Mask Airway in Spontaneously Breathing Patients
 Anesthesiology 2001; 94:760 6 2001 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Pharyngolaryngeal Morbidity with the Laryngeal Mask Airway in Spontaneously Breathing
Anesthesiology 2001; 94:760 6 2001 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Pharyngolaryngeal Morbidity with the Laryngeal Mask Airway in Spontaneously Breathing
GENERAL ANAESTHESIA AND FAILED INTUBATION
 GENERAL ANAESTHESIA AND FAILED INTUBATION INTRODUCTION The majority of caesarean sections in the UK are performed under regional anaesthesia. However, there are situations where general anaesthesia (GA)
GENERAL ANAESTHESIA AND FAILED INTUBATION INTRODUCTION The majority of caesarean sections in the UK are performed under regional anaesthesia. However, there are situations where general anaesthesia (GA)
Anatomy and Physiology. The airways can be divided in to parts namely: The upper airway. The lower airway.
 Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
MD (Anaesthesiology) Title (Plan of Thesis) (Session )
 S.No. 1. To study the occurrence of postoperative hyponatremia in paediatric patients under 2 years of age 2. Influence of timing of intravenous fluid therapy on maternal hemodynamics in patients undergoing
S.No. 1. To study the occurrence of postoperative hyponatremia in paediatric patients under 2 years of age 2. Influence of timing of intravenous fluid therapy on maternal hemodynamics in patients undergoing
Risk Factors of Early Complications of Tracheostomy at Kenyatta National Hospital.
 Risk Factors of Early Complications of Tracheostomy at Kenyatta National Hospital. G. Karuga 1, H. Oburra 2, C. Muriithi 3. 1 Resident Ear Nose & Throat (ENT) Head & Neck Department. University of Nairobi
Risk Factors of Early Complications of Tracheostomy at Kenyatta National Hospital. G. Karuga 1, H. Oburra 2, C. Muriithi 3. 1 Resident Ear Nose & Throat (ENT) Head & Neck Department. University of Nairobi
Awake regional versus general anesthesia in preterms and ex-preterm infants for herniotomy
 Awake regional versus general anesthesia in preterms and ex-preterm infants for herniotomy Department of Anaesthesia University Children s Hospital Zurich Switzerland Epidemiology Herniotomy needed in
Awake regional versus general anesthesia in preterms and ex-preterm infants for herniotomy Department of Anaesthesia University Children s Hospital Zurich Switzerland Epidemiology Herniotomy needed in
PDF of Trial CTRI Website URL -
 Clinical Trial Details (PDF Generation Date :- Tue, 09 Oct 2018 14:20:31 GMT) CTRI Number Last Modified On 23/07/2012 Post Graduate Thesis Type of Trial Type of Study Study Design Public Title of Study
Clinical Trial Details (PDF Generation Date :- Tue, 09 Oct 2018 14:20:31 GMT) CTRI Number Last Modified On 23/07/2012 Post Graduate Thesis Type of Trial Type of Study Study Design Public Title of Study
P V Praveen Kumar 1*, P. Archana 2. Original Research Article. Abstract
 Original Research Article Comparative clinical study of attenuation of cardiovascular responses to laryngoscopy intubation diltiazem, lignocaine and combination of diltiazem and lignocaine P V Praveen
Original Research Article Comparative clinical study of attenuation of cardiovascular responses to laryngoscopy intubation diltiazem, lignocaine and combination of diltiazem and lignocaine P V Praveen
Clinical Comparison of Lightwand-guided versus Conventional Endotracheal Intubation
 Clinical Comparison of Lightwand-guided versus Conventional Endotracheal Intubation Helena Masson 1, Tyberiusz Moska 2, Anders Rehn 3, Ljubisa Janjic 4 and Jonas Åkeson 5 1 helena.masson {at} skane.se
Clinical Comparison of Lightwand-guided versus Conventional Endotracheal Intubation Helena Masson 1, Tyberiusz Moska 2, Anders Rehn 3, Ljubisa Janjic 4 and Jonas Åkeson 5 1 helena.masson {at} skane.se
Advanced Airway Management. University of Colorado Medical School Rural Track
 Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
ORIGINAL ARTICLE. Comparison of Spinal vs General Anesthesia via Laryngeal Mask Airway in Inguinal Hernia Repair
 ORIGINAL ARTICLE Comparison of Spinal vs General Anesthesia via Laryngeal Mask Airway in Inguinal Hernia Repair Richard E. Burney, MD; Mythili A. Prabhu, MD; Mary Lou V. H. Greenfield, MPH, MS; Amy Shanks,
ORIGINAL ARTICLE Comparison of Spinal vs General Anesthesia via Laryngeal Mask Airway in Inguinal Hernia Repair Richard E. Burney, MD; Mythili A. Prabhu, MD; Mary Lou V. H. Greenfield, MPH, MS; Amy Shanks,
Anaesthesia > Critical Incidents > Scenario 2 (BL) Emergency Medicine > Clinical > Scenario 3
 Anaesthesia > Critical Incidents > Scenario 2 (BL) SEIZURES MODULE: CRITICAL INCIDENTS TARGET: ANAESTHETISTS, INTENSIVISTS, EMERGENCY, ACUTE PHYSICIANS & FOUNDATION DOCTORS BACKGROUND: Management of seizures
Anaesthesia > Critical Incidents > Scenario 2 (BL) SEIZURES MODULE: CRITICAL INCIDENTS TARGET: ANAESTHETISTS, INTENSIVISTS, EMERGENCY, ACUTE PHYSICIANS & FOUNDATION DOCTORS BACKGROUND: Management of seizures
Risky Extubation. Andy Higgs. Warrington Hospitals Cheshire UK
 Andy Higgs Warrington Hospitals Cheshire UK Declaration COOKMEDICAL Extubation plan DAS guideline Airway Exchange Catheters # 11 CAEC post maxillo-facial surgery Used as intubation stylets Airway Exchange
Andy Higgs Warrington Hospitals Cheshire UK Declaration COOKMEDICAL Extubation plan DAS guideline Airway Exchange Catheters # 11 CAEC post maxillo-facial surgery Used as intubation stylets Airway Exchange
January, ; Vol2; Issue1
 January, 208 208; Vol2; Issue http://iamresearcher.online Acceptance of Medical Abortion Method and Associated Factors Among Women Attending Public and n-governmental Organization Clinics in Dire Dawa
January, 208 208; Vol2; Issue http://iamresearcher.online Acceptance of Medical Abortion Method and Associated Factors Among Women Attending Public and n-governmental Organization Clinics in Dire Dawa
Emergency Department/Trauma Adult Airway Management Protocol
 Emergency Department/Trauma Adult Airway Management Protocol Purpose: A standardized protocol for management of the airway in the setting of trauma in an academic center, with the goal of maximizing successful
Emergency Department/Trauma Adult Airway Management Protocol Purpose: A standardized protocol for management of the airway in the setting of trauma in an academic center, with the goal of maximizing successful
Joint Theater Trauma System Clinical Practice Guideline
 Page 1 of 7 Joint Theater Trauma System Clinical Practice Guideline TRAUMA AIRWAY MANAGEMENT Original Release/Approval 18 Dec 2004 Note: This CPG requires an annual review. Reviewed: May 2012 Approved:
Page 1 of 7 Joint Theater Trauma System Clinical Practice Guideline TRAUMA AIRWAY MANAGEMENT Original Release/Approval 18 Dec 2004 Note: This CPG requires an annual review. Reviewed: May 2012 Approved:
POST-ANAESTHETIC RESPIRATORY COMPLAINTS FOLLOWING ENDOTRACHEAL ANAESTHESIA IN LOWER ABDOMINAL OBSTETRIC AND GYNAECOLOGY SURGERY
 Nigerian Journal of Clinical Practice Sept 2008 Vol 11(3) :225-230 POST-ANAESTHETIC RESPIRATORY COMPLAINTS FOLLOWING ENDOTRACHEAL ANAESTHESIA IN LOWER ABDOMINAL OBSTETRIC AND GYNAECOLOGY SURGERY I.K. Kolawole,
Nigerian Journal of Clinical Practice Sept 2008 Vol 11(3) :225-230 POST-ANAESTHETIC RESPIRATORY COMPLAINTS FOLLOWING ENDOTRACHEAL ANAESTHESIA IN LOWER ABDOMINAL OBSTETRIC AND GYNAECOLOGY SURGERY I.K. Kolawole,
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Postoperative sore throat and hoarseness
 Postoperative sore throat and hoarseness To my beloved family Life is like riding a bicycle. To keep your balance you must keep moving. Albert Einstein Örebro Studies in Care Sciences 51 MARIA JAENSSON
Postoperative sore throat and hoarseness To my beloved family Life is like riding a bicycle. To keep your balance you must keep moving. Albert Einstein Örebro Studies in Care Sciences 51 MARIA JAENSSON
Z.U.M.J.Vol.19; N.5; September; 2013
 COMPARISON OF THE EFFICACY AND SAFETY OF EACH OF LEVITAN AND SHIKANI OPTICAL STYLETS EITHER USED ALONE OR WITH DIRECT LARYNGOSCOPY FOR TRACHEAL INTUBATION Islam A. Eliwa, MD, Akmal Abd Elsamad, MD, Khalid
COMPARISON OF THE EFFICACY AND SAFETY OF EACH OF LEVITAN AND SHIKANI OPTICAL STYLETS EITHER USED ALONE OR WITH DIRECT LARYNGOSCOPY FOR TRACHEAL INTUBATION Islam A. Eliwa, MD, Akmal Abd Elsamad, MD, Khalid
Dexamethasone Compared with Metoclopramide in Prevention of Postoperative Nausea and Vomiting in Orthognathic Surgery
 Article ID: WMC002013 2046-1690 Dexamethasone Compared with Metoclopramide in Prevention of Postoperative Nausea and Vomiting in Orthognathic Surgery Corresponding Author: Dr. Agreta Gashi, Anesthesiologist,
Article ID: WMC002013 2046-1690 Dexamethasone Compared with Metoclopramide in Prevention of Postoperative Nausea and Vomiting in Orthognathic Surgery Corresponding Author: Dr. Agreta Gashi, Anesthesiologist,
Tracheostomy. Information for patients and relatives
 Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
MD (Anaesthesiology) Title (Plan of Thesis) (Session )
 S.No. 1. COMPARATIVE STUDY OF CENTRAL VENOUS CANNULATION USING ULTRASOUND GUIDANCE VERSUS LANDMARK TECHNIQUE IN PAEDIATRIC CARDIAC PATIENT. 2. TO EVALUATE THE ABILITY OF SVV OBTAINED BY VIGILEO-FLO TRAC
S.No. 1. COMPARATIVE STUDY OF CENTRAL VENOUS CANNULATION USING ULTRASOUND GUIDANCE VERSUS LANDMARK TECHNIQUE IN PAEDIATRIC CARDIAC PATIENT. 2. TO EVALUATE THE ABILITY OF SVV OBTAINED BY VIGILEO-FLO TRAC
(ix) Difficult & Failed Intubation Queen Charlotte s Hospital
 (ix) Difficult & Failed Intubation Queen Charlotte s Hospital Pre-operative Assessment Clinical assessment of airway and risk of difficult intubation: (can be performed in a matter of seconds): 1. Mouth
(ix) Difficult & Failed Intubation Queen Charlotte s Hospital Pre-operative Assessment Clinical assessment of airway and risk of difficult intubation: (can be performed in a matter of seconds): 1. Mouth
Highlighted Educational/Occupational Qualifications:
 FARHAD ETEZADI Current Rank/Department: Associate Professor/Anesthesiology Tehran University of Medical Sciences Contact Information: Academic Rank: Associate Professor Department: Anesthesiology & Critical
FARHAD ETEZADI Current Rank/Department: Associate Professor/Anesthesiology Tehran University of Medical Sciences Contact Information: Academic Rank: Associate Professor Department: Anesthesiology & Critical
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Evaluation of Postoperative Complications Occurring in Patients after Desflurane or Sevoflurane in Outpatient Anaesthesia: A Comparative Study
 Original article Evaluation of Postoperative Complications Occurring in Patients after Desflurane or Sevoflurane in Outpatient Anaesthesia: A Comparative Study Shishir Ramachandra Sonkusale 1, RajulSubhash
Original article Evaluation of Postoperative Complications Occurring in Patients after Desflurane or Sevoflurane in Outpatient Anaesthesia: A Comparative Study Shishir Ramachandra Sonkusale 1, RajulSubhash
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Evaluation of Postoperative Sore Throat and Hoarseness of Voice with Three Variants of Laryngeal
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Evaluation of Postoperative Sore Throat and Hoarseness of Voice with Three Variants of Laryngeal
Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery
 Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery Martha Cordoba Amorocho, MD Iuliu Fat, MD Supplement to Cordoba Amorocho M, Fat I. Anesthetic techniques in endoscopic sinus and skull base
Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery Martha Cordoba Amorocho, MD Iuliu Fat, MD Supplement to Cordoba Amorocho M, Fat I. Anesthetic techniques in endoscopic sinus and skull base
General OR Rotations GOALS & OBJECTIVES
 General OR Rotations GOALS & OBJECTIVES Goals At the end of the CA 1 year General OR rotations, the resident should competently manage uncomplicated ambulatory, orthopedic, maxillo-facial, ENT, gynecologic,
General OR Rotations GOALS & OBJECTIVES Goals At the end of the CA 1 year General OR rotations, the resident should competently manage uncomplicated ambulatory, orthopedic, maxillo-facial, ENT, gynecologic,
Comparison of the Airtraq to the Bonfils Fibroscope for Endotracheal Intubation in a Simulated Difficult Airway
 Med. J. Cairo Univ., Vol. 77, No. 4, June: 203-207, 2009 www.medicaljournalofcairouniversity.com Comparison of the Airtraq to the Bonfils Fibroscope for Endotracheal Intubation in a Simulated Difficult
Med. J. Cairo Univ., Vol. 77, No. 4, June: 203-207, 2009 www.medicaljournalofcairouniversity.com Comparison of the Airtraq to the Bonfils Fibroscope for Endotracheal Intubation in a Simulated Difficult
The Superiority Of Mcgrath Videolaryngoscope After Failed Conventional Laryngoscopy
 ISPUB.COM The Internet Journal of Anesthesiology Volume 33 Number 1 The Superiority Of Mcgrath Videolaryngoscope After Failed Conventional Laryngoscopy S Karaman, S Arici, S Dogru, T Karaman, H Tapar,
ISPUB.COM The Internet Journal of Anesthesiology Volume 33 Number 1 The Superiority Of Mcgrath Videolaryngoscope After Failed Conventional Laryngoscopy S Karaman, S Arici, S Dogru, T Karaman, H Tapar,
HELP PROTECT YOUR PATIENTS AND PREVENT COMPLICATIONS.
 HELP PROTECT YOUR PATIENTS AND PREVENT COMPLICATIONS. Clinician-inspired tools for the operating room McGRATH MAC video laryngoscope and Shiley airway management products AIRWAY MANAGEMENT TOOLS INSPIRED
HELP PROTECT YOUR PATIENTS AND PREVENT COMPLICATIONS. Clinician-inspired tools for the operating room McGRATH MAC video laryngoscope and Shiley airway management products AIRWAY MANAGEMENT TOOLS INSPIRED
Omiros Chalkeidis*, Georgios Kotsovolis, Apostolos Kalakonas, Maria Filippidou, Christos Triantafyllou, Dimitris Vaikos, Epaminondas Koutsioumpas
 Acta Anaesthesiol Taiwan 2010;48(1):15 20 ORIGINAL ARTICLE A Comparison Between the Airtraq and Macintosh Laryngoscopes for Routine Airway Management by Experienced Anesthesiologists: A Randomized Clinical
Acta Anaesthesiol Taiwan 2010;48(1):15 20 ORIGINAL ARTICLE A Comparison Between the Airtraq and Macintosh Laryngoscopes for Routine Airway Management by Experienced Anesthesiologists: A Randomized Clinical
Impact of Endotracheal Tube Cuff Pressure on Postoperative Sore Throat: A Systematic Review and Meta-Analysis
 Impact of Endotracheal Tube Cuff Pressure on Postoperative Sore Throat: A Bao-Ji Hu 1*, Jian Xu 2*, Xiao-Hong Zhao 1*, Nan-Nan Zhang 1, Meng-Zhi Pan 1, Lu-Long Bo 3#, and Hong-Wei Duan 1# ABSTRACT Background:
Impact of Endotracheal Tube Cuff Pressure on Postoperative Sore Throat: A Bao-Ji Hu 1*, Jian Xu 2*, Xiao-Hong Zhao 1*, Nan-Nan Zhang 1, Meng-Zhi Pan 1, Lu-Long Bo 3#, and Hong-Wei Duan 1# ABSTRACT Background:
Hemodynamic response to laryngoscopy in ischemic heart disease: Macintosh blade versus GlideScope videolaryngoscope
 Original Article Hemodynamic response to laryngoscopy in ischemic heart disease: Macintosh blade versus GlideScope videolaryngoscope Eisa Bilehjani, Solmaz Fakhari ABSTRACT Objective To determine the hemodynamic
Original Article Hemodynamic response to laryngoscopy in ischemic heart disease: Macintosh blade versus GlideScope videolaryngoscope Eisa Bilehjani, Solmaz Fakhari ABSTRACT Objective To determine the hemodynamic
Anesthesia recommendations for patients suffering from Mucolipidosis II and III
 orphananesthesia Anesthesia recommendations for patients suffering from Mucolipidosis II and III Disease name: Mucolipidosis Type 2 and 3 ICD 10: E77.0 Synonyms: Mucolipidosis type 2 - I-cell disease N-acetyl-glucosamine
orphananesthesia Anesthesia recommendations for patients suffering from Mucolipidosis II and III Disease name: Mucolipidosis Type 2 and 3 ICD 10: E77.0 Synonyms: Mucolipidosis type 2 - I-cell disease N-acetyl-glucosamine
Comparison of the Berman Intubating Airway and the Williams Airway Intubator for fibreoptic orotracheal intubation in anaesthetised patients.
 Title Comparison of the Berman Intubating Airway and the Williams Airway Intubator for fibreoptic orotracheal intubation in anaesthetised patients Author(s) Greenland, KB; Ha, ID; Irwin, MG Citation Anaesthesia,
Title Comparison of the Berman Intubating Airway and the Williams Airway Intubator for fibreoptic orotracheal intubation in anaesthetised patients Author(s) Greenland, KB; Ha, ID; Irwin, MG Citation Anaesthesia,
Journal of Society of Anesthesiologists of Nepal
 SOCIETY OF ANESTHESIOLOGISTS OF NEPAL ISSN 2362-1281 A PEER REVIEWED JOURNAL Indexed in scholar NepJol, Asia Journals Online Journal TOC Index Copernicus JOURNAL OF SOCIETY OF ANESTHESIOLOGISTS OF NEPAL
SOCIETY OF ANESTHESIOLOGISTS OF NEPAL ISSN 2362-1281 A PEER REVIEWED JOURNAL Indexed in scholar NepJol, Asia Journals Online Journal TOC Index Copernicus JOURNAL OF SOCIETY OF ANESTHESIOLOGISTS OF NEPAL
The Laryngeal Mask and Other Supraglottic Airways: Application to Clinical Airway Management
 The Laryngeal Mask and Other Supraglottic Airways: Application to Clinical Airway Management D. John Doyle MD PhD FRCPC Department of General Anesthesiology Cleveland Clinic Foundation 9500 Euclid Avenue
The Laryngeal Mask and Other Supraglottic Airways: Application to Clinical Airway Management D. John Doyle MD PhD FRCPC Department of General Anesthesiology Cleveland Clinic Foundation 9500 Euclid Avenue
Do pediatric patients undergoing cardiac surgeries require larger-size cuffed endotracheal tubes? A prospective study
 Pediatric Anesthesia ISSN 1155-5645 ORIGINAL ARTICLE Do pediatric patients undergoing cardiac surgeries require larger-size cuffed endotracheal tubes? A prospective study Rasoul Azarfarin 1, Mahin Seyedhejazi
Pediatric Anesthesia ISSN 1155-5645 ORIGINAL ARTICLE Do pediatric patients undergoing cardiac surgeries require larger-size cuffed endotracheal tubes? A prospective study Rasoul Azarfarin 1, Mahin Seyedhejazi
Transient Lingual and Hypoglossal Nerve Damage After Rotator Cuff Repair. Krista Madden, MSNA. Westminster College
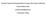 Transient Lingual and Hypoglossal Nerve Damage After Rotator Cuff Repair Krista Madden, MSNA madden.krista@gmail.com Westminster College Abstract When providing anesthesia for patients in the sitting position,
Transient Lingual and Hypoglossal Nerve Damage After Rotator Cuff Repair Krista Madden, MSNA madden.krista@gmail.com Westminster College Abstract When providing anesthesia for patients in the sitting position,
Oral Midazolam for Premedication in Children Undergoing Various Elective Surgical procedures
 Oral Midazolam for Premedication in Children Undergoing Various Elective Surgical procedures E-mail gauripanjabi@yahoo.co.in 1 st Author:. Dr Panjabi Gauri M., M.D., D.A., Senior Assistant professor. 2
Oral Midazolam for Premedication in Children Undergoing Various Elective Surgical procedures E-mail gauripanjabi@yahoo.co.in 1 st Author:. Dr Panjabi Gauri M., M.D., D.A., Senior Assistant professor. 2
Recent Advances in Airway Management HA Convention 2014
 Recent Advances in Airway Management HA Convention 2014 Dr. HK Cheng Chief of Service (Dept. of Anaesthesia & OT) Service Director (Ambulatory Surgery Centre) Tseung Kwan O Hospital Recent Advances in
Recent Advances in Airway Management HA Convention 2014 Dr. HK Cheng Chief of Service (Dept. of Anaesthesia & OT) Service Director (Ambulatory Surgery Centre) Tseung Kwan O Hospital Recent Advances in
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to
 1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
Acute And perioperative care of the burn-injured patient. Anesthesiology, V 122, No 2
 Acute And perioperative care of the burn-injured patient Anesthesiology, V 122, No 2 Reporter:R4 沈士鈞 Supervisor: 蔡欣怡醫師 Pathophysiology Initial evaluation and management Anesthetic managemen nt Pathophysiology
Acute And perioperative care of the burn-injured patient Anesthesiology, V 122, No 2 Reporter:R4 沈士鈞 Supervisor: 蔡欣怡醫師 Pathophysiology Initial evaluation and management Anesthetic managemen nt Pathophysiology
Airway Management. Key points. Rapid Sequence Intubation. Rapid Sequence Intubation Recognizing difficult airway Managing difficult airway
 Airway Management Prasha Ramanujam and Guy Shochat Department of Emergency Medicine UCSF Medical Center Key points Rapid Sequence Intubation Recognizing difficult airway Managing difficult airway Rapid
Airway Management Prasha Ramanujam and Guy Shochat Department of Emergency Medicine UCSF Medical Center Key points Rapid Sequence Intubation Recognizing difficult airway Managing difficult airway Rapid
Qing Zhu 1, Hai Wu 2, Hai-Bo Song 3, Ting Liu 1, Bei Liu 1, Chun-Lan Zheng 1, Wei Huang 1, and Han Huang 1. a standard care in contemporary anesthesia
 Journal of Anesthesia and Perioperative Medicine Original Article Effect of Intra-Cuff on Preventing Postoperative Sore Throat after Gynecological Surgery Qing Zhu, Hai Wu 2, Hai-Bo Song 3, Ting Liu, Bei
Journal of Anesthesia and Perioperative Medicine Original Article Effect of Intra-Cuff on Preventing Postoperative Sore Throat after Gynecological Surgery Qing Zhu, Hai Wu 2, Hai-Bo Song 3, Ting Liu, Bei
Succinycholine: Succinylcholine has no place in pediatric anesthesia. Wads Ames MBBS FRCA
 Succinycholine: Succinylcholine has no place in pediatric anesthesia Wads Ames MBBS FRCA Food And Drug Administration Created in 1906 Responsible for protecting and promoting public health through the
Succinycholine: Succinylcholine has no place in pediatric anesthesia Wads Ames MBBS FRCA Food And Drug Administration Created in 1906 Responsible for protecting and promoting public health through the
Nasotracheal intubation with Parker Flex-Tip versus preformed nasal endotracheal tubes for children undergoing adenotonsillectomy
 Nasotracheal intubation with Parker Flex-Tip versus preformed nasal endotracheal tubes for children undergoing adenotonsillectomy Moustafa Abdelaziz Moustafa 1 and Yasser Mohamed Ossman 2 ** Abstract:
Nasotracheal intubation with Parker Flex-Tip versus preformed nasal endotracheal tubes for children undergoing adenotonsillectomy Moustafa Abdelaziz Moustafa 1 and Yasser Mohamed Ossman 2 ** Abstract:
Airway Workshop Lecture. University of Ottawa
 Airway Workshop Lecture Department of Anesthesiology University of Ottawa Overview Ventilation Airway assessment Difficult airways Airway management equipment aids Intubation/Improving Intubation Success
Airway Workshop Lecture Department of Anesthesiology University of Ottawa Overview Ventilation Airway assessment Difficult airways Airway management equipment aids Intubation/Improving Intubation Success
Effects of Tube Depth and Infusion Rate of Continuous Humidification by Endotracheal Intubation on Humidification Effect
 Open Journal of Nursing, 2017, 7, 123-127 http://www.scirp.org/journal/ojn ISSN Online: 2162-5344 ISSN Print: 2162-5336 Effects of Tube Depth and Infusion Rate of Continuous Humidification by Endotracheal
Open Journal of Nursing, 2017, 7, 123-127 http://www.scirp.org/journal/ojn ISSN Online: 2162-5344 ISSN Print: 2162-5336 Effects of Tube Depth and Infusion Rate of Continuous Humidification by Endotracheal
Haemodynamic response to orotracheal intubation: direct laryngoscopy versus fiberoptic bronchoscopy
 Haemodynamic response to orotracheal intubation: direct laryngoscopy versus fiberoptic bronchoscopy Amir Murad Khudad* Hoshyar Najeeb Karem** ABSTRACT Background and Objectives: The cardiovascular response
Haemodynamic response to orotracheal intubation: direct laryngoscopy versus fiberoptic bronchoscopy Amir Murad Khudad* Hoshyar Najeeb Karem** ABSTRACT Background and Objectives: The cardiovascular response
Agency 71. Kansas Dental Board (Authorized by K.S.A and (Authorized by K.S.A and
 Agency 71 Kansas Dental Board Articles 71-4. CONTINUING EDUCATION REQUIREMENTS. 71-5. SEDATIVE AND GENERAL ANAESTHESIA. 71-11. MISCELLANEOUS PROVISIONS. Article 4. CONTINUING EDUCATION REQUIREMENTS 71-4-1.
Agency 71 Kansas Dental Board Articles 71-4. CONTINUING EDUCATION REQUIREMENTS. 71-5. SEDATIVE AND GENERAL ANAESTHESIA. 71-11. MISCELLANEOUS PROVISIONS. Article 4. CONTINUING EDUCATION REQUIREMENTS 71-4-1.
Exclusion Criteria 1. Operator or supervisor feels specific intra- procedural laryngoscopy device will be required.
 FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Investigating the Effect of Endotracheal Tube Cuff Pressure on Sore Throat, Hoarseness and Cough in Patients with Coronary Artery Bypass Surgery
 Investigating the Effect of Endotracheal Tube Cuff Pressure on Sore Throat, Hoarseness and Cough in Patients with Coronary Artery Bypass Surgery Ali Akbar Vaezi (1) Mohammad Hassan Mondegari Bamakan (2)
Investigating the Effect of Endotracheal Tube Cuff Pressure on Sore Throat, Hoarseness and Cough in Patients with Coronary Artery Bypass Surgery Ali Akbar Vaezi (1) Mohammad Hassan Mondegari Bamakan (2)
A comparison of endotracheal intubation and use of the laryngeal mask airway for ambulatory oral surgery patients Todd D W
 A comparison of endotracheal intubation and use of the laryngeal mask airway for ambulatory oral surgery patients Todd D W Record Status This is a critical abstract of an economic evaluation that meets
A comparison of endotracheal intubation and use of the laryngeal mask airway for ambulatory oral surgery patients Todd D W Record Status This is a critical abstract of an economic evaluation that meets
