Arterial Leg Ulcer Clinical Pathway
|
|
|
- Chad Price
- 6 years ago
- Views:
Transcription
1 Waterloo Wellington Integrated Wound Care Program Evidence-Based Wound Care Arterial Leg Ulcer Clinical Pathway 0-7 Days Expected Outcomes Notes Patient admitted to service/facility Most Responsible Physician(MRP)/Nurse Practitioner (NP) identified/informed Medical/surgical history and co-morbidity management considered within care plan Current ongoing adjunctive therapies integrated into care plan Refer patient to Care Connects if no responsible practioner currently involved with patient Determine if MRP/NP is part of family health team (FHT) or community health centre (CHC) and consider additional supports available Risk factors include: Chronic renal disease Smoking Congestive heart failure Diabetes mellitus Impaired liver function Hyperlipidemia Use of systemic steroids, Hypertension immunosuppressives and chemotherapy Poor nutrition >70 years of age Low hemoglobin Age years with history of diabetes Obesity or smoking Decreased thyroid function < 50 years with diabetes and one other Coronary artery disease atherosclerotic factor Psoriasis History of vascular surgery or deep vein History of cerebral vascular accident thrombosis (CVA) Bleeding disorders Autoimmune diseases Family history of arterial disease Medication reconciliation and their impact on wound healing reviewed Recent blood work and other diagnostic test results reviewed and implictions for wound healing considered Physical examination performed Prescription, non-prescription, naturopathic and illicit drug use (including e-cigarettes, inhaled substances and nicotine replacement therapy) Medications that can affect healing include: chemotherapy, anticoagulants, antiplatelets, corticosteroids, vasoconstrictors, antihypertensives, diuretics and immunosepressive drugs Other medications used to treat acute episodic illnesses may affect healing (eg. antibiotics, colchicine, anti-rheumatoid arthritics) Vitamin and mineral supplementation Determine bloodwork and other diagnostic tests required Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
2 Bilateral lower leg assessment completed Signs and symptoms of Peripheral Arterial Disease could include: Pain with elevation of lower limbs, rest pain, nocturnal pain and pain on walking (caused by intermittent claudication) Dependent rubor in lower legs and feet Pallor in feet on elevation Dry, shiny skin on lower legs Edema subsequent to leg being dependent Thick or flaking toe nails Hairless lower legs and feet Weak or absent pulses Intense hyperesthesia (sensitive to light touch) Limb muscle may appear wasted from ischemic atrophy Delayed capillary refill Distal gangrene Erectile dysfunction in men Non-healing wound ABPI 0.5 to 0.8 TBPI 0.64 to 0.7 Suggest Transcutaneous Oxygen Pressure(TcPo 2 ), Laser Doppler Flowmetry, Doppler Arterial Waveforms or Segmental Doppler Pressure studies ABPI <0.5 TBPI <0.64 Urgent vascular surgical consult needed ABPI/TPBI completed within last 3 mths and results documented If unable to obtain ABPI/TPBI, referral to vascular surgeon is recommended Assess pulses (popliteal behind knee, dorsalis pedis top of foot, posterior tibial medial ankle) Measurement of edema Assess capillary refill (normal less than 3 seconds) Leg measurements (foot, ankle, calf, thigh) Ankle range of motion (ROM) Foot deformities Ankle flare Skin temperature (compare both legs) Skin colour (dependent and on elevation) Presence of pain Nail changes Presence of hair on lower leg, feet and toes Presence of varicosities (varicose veins) Dermatological changes due to impaired blood flow Repeat ABPI/TPBI assessment every 3 months if healing is not progressing Acute arterial occlusion is a life and limb-threatening situation which requires immediate emergency intervention Signs and symptoms that may become severe may be associated with the following: Pale or blue skin Skin cold to the touch Sudden decrease in mobility No pulse where one was present prior to this Sudden and severe pain Wound Assessment completed Complete: Bates-Jensen Wound Assessment Tool (BWAT) OR 4 P s of Arterial Ulcers Leg Ulcer Measurement Tool (LUMT) Pale wound base Determine wound etiology Punched-out appearance Arterial ulcers are typically pale at base of wound, have punched out appearance, are more painful than expected and have low to no exudate Painful Results of LLA and ABPI/TPBI Parched (low to no exudate) Document percentage of healing since last visit Assessment for infection (NERDS and STONEES) Obtain photos following best practice as per framework for individual organization policies and procedures. Suggest following publication as guideline: Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
3 Compression therapy history documented and considered in plan Compression is typically contraindicated in the presence of peripheral arterial disease. In some circumstances light compression may be beneficial, but only if arterial supply is sufficient. Sufficient arterial supply should be objectively evidenced by diagnostic tests. In such cases, compression should be ordered by an advanced wound care physician or nurse practitioner only! Pain management initiated Arterial pain is typically described as: Pain with elevation of lower limbs, rest pain, nocturnal pain and pain on walking (caused by intermittent claudication) History of: Previous compression garments Age of compression garments Adherence Application and removal of compression in past Finances Reason compression treatment plan has changed if applicable Complete: Brief Pain Inventory Short Form (BPI-SF) Obtain physician/nurse practitioner orders for analgesics (opioids and non-opioids) Patient s nutritional status optimized Review blood work results Calculate Body Mass Index (BMI) Determine recent weight loss/gain Complete Mini Nutritional Assessment (MNA) If screening section results < 11 = complete assessment section If Assessment section results< 24 = Registered Dietician referral required Wound etiology and appropriate pathway established Patient and caregiver concerns and goals integrated into the care plan and shared with care team Wound treatment plan determined in accordance to treatment goal (healable, maintenance or non-healable) Caution: USE DRY WOUND HEALING 1. Keep eschar dry 2. No occlusive dressings 3. Do NOT debride 4. Avoid tourniquet effect when securing dressings 5. If eschar becomes wet/boggy URGENT referral to advanced wound care specialist is recommended Complete: Cardiff Wound Impact Questionnaire OR World Health Organization Quality of Life (WHOQOL) form Arrange for physician/nurse practitioner orders as required to begin plan of care including agreeance to professional referral recommendations Identify any potential barriers to wound treatment plan Utilize toolkit to determine wound cleansing, debridement and dressing selection (South West Region Wound Care Program: Wound Cleansing Table and Dressing Selection and Cleansing enablers and CAWC Product Picker chart) Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
4 Patient counselled on the benefit of activity rest and head elevation in moderation (balancing need for pressure relief) for comfort measures and wound healing Recent changes in overall activity level Daily routine Personal assistance available to perform activities of daily living Ankle range of motion allowing for calf muscle pump to function Determine where patient sleeps at night Patient/caregiver educational plan initiated Emergency signs and symptoms of Peripheral Arterial Disease that require immediate medical attention (refer to lower leg assessment section) Compression is typically contraindicated in the presence of peripheral arterial disease. In some circumstances light compression may be beneficial. In such cases, compression should be ordered by an advanced wound care physician or nurse practitioner only! See algorithm in guidelines. Risks of compression Smoking cessation including e-cigarettes and nicotene replacement Appropriate footwear as discussed with foot care specialist (encourage use of white socks) Skin care Nail care (suggest use of foot care specialist) Wound self care Pain management Encourage patient to sleep in bed with no lower limb elevation (most arterial pain increases when feet elevated above heart level) Mobility and dexterity aids currently being used Safety of transfers Recommendations for exercise Consider Occupational Therapist referral for comfort measures Diagnostic testing Dietary Rest/Activity Prevention of injury avoid extremes (hot/cold, loose/tight) When to call primary care giver (eg. signs and symptoms of infection, deep vein thrombosis, cellulitis, impaired blood flow, difficulties with compression) Self lower-leg assessment Community support groups (i.e. walking groups) Other Ability to self-manage optimized Barriers to participate (transportation, socioeconomic, social environment, other co-morbidities) Cognitive ability Review importance and potential barriers to smoking cessation at every visit Hygeine Waterloo Wellington Integrated Wound Care Program Arterial Pathway May Foot inspection (including bottom of foot and between toes) Enviroment Wound care Compression application and removal if prescribed Coping strategies implemented into plan of care Patient s concerns and fears Signs of anxiety or other mental health issues (eg. delusions, hallucinations, paranoid behaviour) Depression screen using Geriatric Depression Scale assessment form GDS15 Suicide assessment if applicable ETOH and illicit /recreational drug use
5 Family and caregiver support identified and incorporated into plan Family/caregiver actively able to participate in treatment plan of care Social supports/community resources currently utilized is integrated Family support into plan of care Funding Community resources Caregiver conflicts Long or short term placement Assistance provided for financial concerns patient is experiencing Determine: Private insurance availability Eligibility for Assistive Devices Program (ADP [lymphedema only], ODSP, High-needs fund, Veterans Affairs Canada or Aborignal Services) Professional referrals are initiated Primary Care Physician Pharmacist Advanced Wound Specialist Occupational Therapist Nurse Practitioner Physiotherapy Infectious Disease Specialist Chiropodist Vascular Surgeon Certified Pedorothist Dermatologist Certified Orthotist Plastic surgeon Certified Prosthetist Internist/Endocrinologist Podiatrist Mental Health Specialist Lymphatic Massage Psychologists Compression Stocking Fitter Social work Other: Registered Dietitian Physician/nurse practitioner orders received as required to change plan of care including agreeance to professional referral recommendations Appropriate documents shared Identify need to reassess ABPI/TPBI in 6 months Acute care Lower leg assessment Complex Continuing Care/Rehab Recent vascular study results (eg. ABPI, TPBI, Transcutaneous Oxygen Pressure(TcPo 2 ), Laser Doppler Flowmetry, Doppler Arterial Waveforms or Segmental Doppler Pressure studies) Long-term care Community care Primary care physician/nurse Practioner Professionals referred to Relevant consultation notes Other Diagnostic results Current treatment plan If wound closed or eschar is stable send discharge summary outlining outstanding issues and teaching completed to: Referral source and most responsible physician (MRP)/nurse Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
6 practitioner (NP) 8-21 Days Expected Outcomes Notes Most Responsible Physician(MRP)/Nurse Practitioner (NP) identified/informed Assessment of wound performed and percentage of healing documented 4 P s of Arterial Ulcers Pale wound base Punched-out appearance Painful Parched (low to no exudate) Wound treatment/compression plan is being followed Communication with primary care physician and/or Nurse Practioner to update on any significant changes in patient s condition. Refer patient to Care Connects if no responsible practioner currently involved with patient Determine if MRP/NP is part of family health team (FHT) or community health centre (CHC) and consider additional supports available Complete: Bates-Jensen Wound Assessment Tool (BWAT) OR Leg Ulcer Measurement Tool (LUMT) Determine wound etiology Arterial ulcers are typically pale at base of wound, have punched out appearance, are more painful than expected and have low to no exudate Results of LLA and ABPI/TPBI Document percentage of healing since admission Assessment for infection (NERDS and STONEES) Potential need for wound care specialist considered if wound healing is not progressing and infection is absent Obtain photos following best practice as per framework for individual organization policies and procedures. Suggest following publication as guideline: Review: Adherence to plan Real or potential barriers to wound treatment plan Caution: USE DRY WOUND HEALING 1. Keep eschar dry 2. No occlusive dressings 3. Do NOT debride 4. Avoid tourniquet effect when securing dressings 5. If eschar becomes wet/boggy URGENT referral to algorithm in guidelines. Waterloo Wellington advanced wound Integrated care specialist Wound Care is recommended Program Arterial Pathway May Compression is typically contraindicated in the presence of peripheral arterial disease. In some circumstances light compression may be beneficial. In such cases, compression should be ordered by an advanced wound care physician or nurse practitioner only! See
7 Pain management reviewed Arterial pain is typically described as: Pain with elevation of lower limbs, rest pain, nocturnal pain and pain on walking (caused by intermittent claudication) Medical/surgical history and co-morbidity management considered within care plan Medication reconciliation and their impact on wound healing reviewed Review for changes Brief Pain Inventory Short Form (BPI-SF) Obtain physician/nurse practitioner orders for analgesics required (opioids and nonopioids) Review for changes Review for changes: Prescription, non-prescription, naturopathic and illicit drug use Recent blood work and other diagnostic test results reviewed and implictions for wound healing considered Determine bloodwork and other diagnostic tests required Bilateral lower leg assessment completed Signs and symptoms of Peripheral Arterial Disease could include: Pain with elevation of lower limbs, rest pain, nocturnal pain and pain on walking (caused by intermittent claudication) Dependent rubor in lower legs and feet Pallor in feet on elevation Dry, shiny skin on lower legs Edema subsequent to leg being dependent Thick or flaking toe nails Hairless lower legs and feet Weak or absent pulses Intense hyperesthesia (sensitive to light touch) Limb muscle may appear wasted from ischemic atrophy Delayed capillary refill Distal gangrene Erectile dysfunction in men Non-healing wound ABPI/TPBI completed within last 3 mths and results documented If unable to obtain ABPI/TPBI, referral to vascular surgeon is recommended Assess pulses (popliteal behind knee, dorsalis pedis top of foot, posterior tibial medial ankle) Measurement of edema Assess capillary refill (normal less than 3 seconds) Leg measurements (foot, ankle, calf, thigh) Ankle range of motion (ROM) Foot deformities Ankle flare Skin temperature (compare both legs) Skin colour (dependent and on elevation) Presence of pain Nail changes Presence of hair on lower leg, feet and toes Presence of varicosities (varicose veins) Dermatological changes due to impaired blood flow Repeat ABPI/TPBI assessment every 3 months if healing is not progressing ABPI 0.5 to 0.8 TBPI 0.64 to 0.7 Suggest Transcutaneous Oxygen Pressure(TcPo 2 ), Laser Doppler Acute arterial occlusion is a life and limb-threatening situation which requires Flowmetry, Doppler Arterial Waveforms immediate emergency intervention or Segmental Doppler Pressure studies Signs and symptoms that may become severe may be associated with the following: Waterloo be Wellington performed Integrated Wound Care Program Arterial Pathway May Pale or blue skin 7 ABPI <0.5 TBPI <0.64 Skin cold to the touch Urgent vascular surgical consult needed Sudden decrease in mobility
8 Patient s nutritional status optimized Review: Recent blood work results Significant weight changes Adherence to diet plan Identify barriers to good nutrition Patient and caregiver concerns and goals integrated into the care Review for changes: plan and shared with care team Cardiff Wound Impact Questionnaire OR World Health Organization Quality of Life (WHOQOL) form Patient counselled on the benefit of activity rest and head elevation Review for changes: Encourage patient to sleep in bed with in moderation (balancing need for pressure relief) for comfort Recent changes in overall activity level no lower limb elevation (most arterial measures and wound healing Daily routine pain increases when feet elevated Personal assistance available to above heart level) perform activities of daily living Mobility and dexterity aids currently Ankle range of motion allowing for calf being used muscle pump to function Safety of transfers Determine where patient sleeps at Recommendations for exercise night Consider Occupational Therapist referral for comfort measures Patient/caregiver educational needs reviewed using teach-back Emergency signs and symptoms of Diagnostic testing method Peripheral Arterial Disease that require Dietary immediate medical attention (refer to Rest/Activity lower leg assessment section) Prevention of injury avoid extremes Risks of compression (hot/cold, loose/tight) Smoking cessation including e- cigarettes and nicotene replacement When to call primary care giver (eg. signs and symptoms of infection, deep Appropriate footwear as discussed with foot care specialist (encourage use of white socks) vein thrombosis, cellulitis, impaired blood flow, difficulties with compression) Skin care Self lower-leg assessment Nail care (suggest use of foot care specialist) Community support groups (i.e. walking groups) Wound self care Other Pain management Ability to self-manage optimized Review for changes: Hygeine Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
9 Coping strategies implemented into plan of care Family and caregiver support identified and incorporated into plan of care Adherence to plan Foot inspection (including bottom of Barriers to participate (transportation, foot and between toes) socioeconomic, social environment, Enviroment other co-morbidities) Wound care Cognitive ability Compression application and removal if Review importance and potential barriers to smoking cessation at every visit prescribed Review for changes Patient s concerns and fears Signs of anxiety or other mental health issues (eg. delusions, hallucinations, paranoid behaviour) Depression screen using Geriatric Depression Scale assessment form GDS15 Suicide assessment if applicable ETOH and illicit /recreational drug use Review: Availability of assistance required Social supports/community resources currently utilized is integrated Family support into plan of care Funding Community resources Caregiver conflicts Long or short term placement Assistance provided for financial concerns patient is experiencing Review: Private insurance availability Eligibility for Assistive Devices Program (ADP [lymphedema only], ODSP, High-needs fund, Veterans Affairs Canada or Aborignal Services) Professional referral status reviewed Primary Care Physician Pharmacist Advanced Wound Specialist Occupational Therapist Nurse Practitioner Physiotherapy Infectious Disease Specialist Chiropodist Vascular Surgeon Certified Pedorothist Dermatologist Certified Orthotist Plastic surgeon Certified Prosthetist Internist/Endocrinologist Podiatrist Mental Health Specialist Lymphatic Massage Psychologists Compression Stocking Fitter Social work Other: Registered Dietitian Physician/nurse practitioner orders received as required to change plan of care including agreeance to professional referral Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
10 recommendations Appropriate documents shared Identify need to reassess ABPI/TPBI in 6 months Lower leg assessment Recent vascular study results (eg. ABPI, TPBI, Transcutaneous Oxygen Pressure(TcPo 2 ), Laser Doppler Flowmetry, Doppler Arterial Waveforms or Segmental Doppler Pressure studies) Relevant consultation notes Diagnostic results Current treatment plan Acute care Complex Continuing Care/Rehab Long-term care Community care Primary care physician/nurse Practioner Professionals referred to Other If wound closed or eschar is stable send discharge summary outlining outstanding issues and teaching completed to: Referral source and most responsible physician (MRP)/nurse practitioner (NP) Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
11 21-28 Days Expected Outcomes Notes Most Responsible Physician(MRP)/Nurse Practitioner (NP) identified/informed Communication with primary care physician and/or Nurse Practioner to update on any significant changes in patient s condition. Refer patient to Care Connects if no responsible practioner currently involved with patient Determine if MRP/NP is part of family health team (FHT) or community health centre (CHC) and consider additional supports available Assessment of wound performed and percentage of healing documented 4 P s of Arterial Ulcers Pale wound base Punched-out appearance Painful Parched (low to no exudate) Arterial ulcers do not follow trajectory healing rate of venous ulcers (30% week 4 & healed at 12 weeks). Further intervention should be considered if conservative treatment does not improve healing in 4-6 weeks Wound treatment/compression plan is being followed Caution: USE DRY WOUND HEALING 1. Keep eschar dry 2. No occlusive dressings 3. Do NOT debride 4. Avoid tourniquet effect when securing dressings 5. If eschar becomes wet/boggy URGENT referral to advanced wound care specialist is recommended Complete: Bates-Jensen Wound Assessment Tool (BWAT) OR Leg Ulcer Measurement Tool (LUMT) Determine wound etiology Arterial ulcers are typically pale at base of wound, have punched out appearance, are more painful than expected and have low to no exudate Results of LLA and ABPI/TPBI Document percentage of healing since admission Assessment for infection (NERDS and STONEES) Potential need for wound care specialist considered if wound healing is not progressing and infection is absent Obtain photos following best practice as per framework for individual organization policies and procedures. Suggest following publication as guideline: Review: Adherence to plan Real or potential barriers to wound treatment plan Compression is typically contraindicated in the presence of peripheral arterial disease. In some circumstances light compression may be beneficial. In such cases, compression should be ordered by an advanced wound care physician or nurse practitioner only! See algorithm in guidelines. Pain management reviewed Review for changes Brief Pain Inventory Short Form (BPI-SF) Arterial pain is typically described as: Obtain physician/nurse practitioner orders for analgesics required (opioids and non-opioids) Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
12 Pain with elevation of lower limbs, rest pain, nocturnal pain and pain on walking (caused by intermittent claudication) Medical/surgical history and co-morbidity management considered within care plan Medication reconciliation and their impact on wound healing reviewed Review for changes Review for changes: Prescription, non-prescription, naturopathic and illicit drug use Recent blood work and other diagnostic test results reviewed and implictions for wound healing considered Bilateral lower leg assessment completed Signs and symptoms of Peripheral Arterial Disease could include: Pain with elevation of lower limbs, rest pain, nocturnal pain and pain on walking (caused by intermittent claudication) Dependent rubor in lower legs and feet Pallor in feet on elevation Dry, shiny skin on lower legs Edema subsequent to leg being dependent Thick or flaking toe nails Hairless lower legs and feet Weak or absent pulses Intense hyperesthesia (sensitive to light touch) Limb muscle may appear wasted from ischemic atrophy Delayed capillary refill Distal gangrene Erectile dysfunction in men Non-healing wound Determine bloodwork and other diagnostic tests required ABPI/TPBI completed within last 3 mths and results documented If unable to obtain ABPI/TPBI, referral to vascular surgeon is recommended Assess pulses (popliteal behind knee, dorsalis pedis top of foot, posterior tibial medial ankle) Measurement of edema Assess capillary refill (normal less than 3 seconds) Leg measurements (foot, ankle, calf, thigh) Ankle range of motion (ROM) Foot deformities Ankle flare Skin temperature (compare both legs) Skin colour (dependent and on elevation) Presence of pain Nail changes Presence of hair on lower leg, feet and toes Presence of varicosities (varicose veins) Dermatological changes due to impaired blood flow Repeat ABPI/TPBI assessment every 3 months if healing is not progressing ABPI 0.5 to 0.8 TBPI 0.64 to 0.7 Suggest Transcutaneous Oxygen Pressure(TcPo 2 ), Laser Doppler Flowmetry, Doppler Arterial Waveforms or Segmental Doppler Pressure studies ABPI <0.5 TBPI <0.64 Urgent vascular surgical consult needed Acute arterial occlusion is a life and limb-threatening situation which requires immediate emergency intervention Signs and symptoms that may become severe may be associated with the following: Pale or blue skin Skin cold to the touch Sudden decrease in mobility No pulse where one was present prior to this Sudden and severe pain Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
13 Patient s nutritional status optimized Patient and caregiver concerns and goals integrated into the care plan and shared with care team Patient counselled on the benefit of activity rest and head elevation in moderation (balancing need for pressure relief) for comfort measures and wound healing Patient/caregiver educational needs reviewed using teach-back method Ability to self-manage optimized Review: Recent blood work results Significant weight changes Adherence to diet plan Identify barriers to good nutrition Review for changes: Cardiff Wound Impact Questionnaire OR World Health Organization Quality of Life (WHOQOL) form Review for changes: Encourage patient to sleep in bed with Recent changes in overall activity level no lower limb elevation (most arterial Daily routine pain increases when feet elevated Personal assistance available to perform above heart level) activities of daily living Mobility and dexterity aids currently Ankle range of motion allowing for calf being used muscle pump to function Safety of transfers Determine where patient sleeps at night Recommendations for exercise Consider Occupational Therapist referral for comfort measures Emergency signs and symptoms of Pain management Peripheral Arterial Disease that require Diagnostic testing immediate medical attention (refer to Dietary lower leg assessment section) Rest/Activity Risks of compression Prevention of injury avoid extremes Smoking cessation including e-cigarettes (hot/cold, loose/tight) and nicotene replacement When to call primary care giver (eg. Appropriate footwear as discussed with signs and symptoms of infection, deep foot care specialist (encourage use of vein thrombosis, cellulitis, impaired white socks) blood flow, difficulties with Skin care compression) Nail care (suggest use of foot care Self lower-leg assessment specialist) Community support groups (i.e. walking Wound self care groups) Other Review for changes: Adherence to plan Barriers to participate (transportation, socioeconomic, social environment, other comorbidities) Cognitive ability Review importance and potential barriers to smoking cessation at every visit Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
14 Coping strategies implemented into plan of care Family and caregiver support identified and incorporated into plan of care Hygeine Foot inspection (including bottom of foot and between toes) Enviroment Wound care Compression application and removal if prescribed Review for changes Patient s concerns and fears Signs of anxiety or other mental health issues (eg. delusions, hallucinations, paranoid behaviour) Depression screen using Geriatric Depression Scale assessment form GDS15 Suicide assessment if applicable ETOH and illicit /recreational drug use Review: Availability of assistance required Social supports/community resources currently utilized is Family support integrated into plan of care Funding Community resources Caregiver conflicts Long or short term placement Assistance provided for financial concerns patient is experiencing Review: Private insurance availability Eligibility for Assistive Devices Program (ADP [lymphedema only], ODSP, High-needs fund, Veterans Affairs Canada or Aborignal Services) Professional referral status reviewed Primary Care Physician Pharmacist Advanced Wound Specialist Occupational Therapist Nurse Practitioner Physiotherapy Infectious Disease Specialist Chiropodist Vascular Surgeon Certified Pedorothist Dermatologist Certified Orthotist Plastic surgeon Certified Prosthetist Internist/Endocrinologist Podiatrist Mental Health Specialist Lymphatic Massage Psychologists Compression Stocking Fitter Social work Other: Registered Dietitian Physician/nurse practitioner orders received as required to change plan of care including agreeance to professional referral recommendations Appropriate documents shared Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
15 Identify need to reassess ABPI/TPBI in 6 months Lower leg assessment Recent vascular study results (eg. ABPI, TPBI, Transcutaneous Oxygen Pressure(TcPo 2 ), Laser Doppler Flowmetry, Doppler Arterial Waveforms or Segmental Doppler Pressure studies) Relevant consultation notes Diagnostic results Current treatment plan Acute care Complex Continuing Care/Rehab Long-term care Community care Primary care physician/nurse Practioner Professionals referred to Other If wound closed or eschar is stable send discharge summary outlining outstanding issues and teaching completed to: Referral source and most responsible physician (MRP)/nurse practitioner (NP) Collaborative team/patient conference arranged to discuss barriers to healing and care plan if progression to healing is stalled Arrange a Collaborative team/patient meeting to discuss barriers to healing and care plan Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
16 77-84 Days Expected Outcomes Notes Most Responsible Physician(MRP)/Nurse Practitioner (NP) identified/informed Assessment of wound performed and percentage of healing documented Wound treatment/compression plan is being followed Pain management reviewed 4 P s of Arterial Ulcers Pale wound base Punched-out appearance Painful Parched (low to no exudate) Arterial ulcers do not follow trajectory healing rate of venous ulcers (30% week 4 & healed at 12 weeks). Further intervention should be considered if conservative treatment does not improve healing in 4-6 weeks Caution: USE DRY WOUND HEALING 1. Keep eschar dry 2. No occlusive dressings 3. Do NOT debride 4. Avoid tourniquet effect when securing dressings 5. If eschar becomes wet/boggy URGENT referral to advanced wound care specialist is recommended Arterial pain is typically described as: Pain with elevation of lower limbs, rest pain, nocturnal pain and pain on walking (caused by intermittent claudication) Medical/surgical history and co-morbidity management considered within care plan Communication with primary care physician and/or Nurse Practioner to update on any significant changes in patient s condition. Refer patient to Care Connects if no responsible practioner currently involved with patient Determine if MRP/NP is part of family health team (FHT) or community health centre (CHC) and consider additional supports available Complete: Bates-Jensen Wound Assessment Tool (BWAT) OR Leg Ulcer Measurement Tool (LUMT) Determine wound etiology Arterial ulcers are typically pale at base of wound, have punched out appearance, are more painful than expected and have low to no exudate Results of LLA and ABPI/TPBI Document percentage of healing since admission Assessment for infection (NERDS and STONEES) Potential need for wound care specialist considered if wound healing is not progressing and infection is absent Obtain photos following best practice as per framework for individual organization policies and procedures. Suggest following publication as guideline: Adherence to plan Real or potential barriers to wound treatment plan Compression is typically contraindicated in the presence of peripheral arterial disease. In some circumstances light compression may be beneficial. In such cases, compression should be ordered by an advanced wound care physician or nurse practitioner only! See algorithm in guidelines. Brief Pain Inventory Short Form (BPI-SF) Obtain physician/nurse practitioner orders for analgesics required (opioids and non-opioids) Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
17 Medication reconciliation and their impact on wound healing reviewed Prescription, non-prescription, naturopathic and illicit drug use Recent blood work and other diagnostic test results reviewed and implictions for wound healing considered Bilateral lower leg assessment completed Signs and symptoms of Peripheral Arterial Disease could include: Pain with elevation of lower limbs, rest pain, nocturnal pain and pain on walking (caused by intermittent claudication) Dependent rubor in lower legs and feet Pallor in feet on elevation Dry, shiny skin on lower legs Edema subsequent to leg being dependent Thick or flaking toe nails Hairless lower legs and feet Weak or absent pulses Intense hyperesthesia (sensitive to light touch) Limb muscle may appear wasted from ischemic atrophy Delayed capillary refill Distal gangrene Erectile dysfunction in men Non-healing wound Determine bloodwork and other diagnostic tests required ABPI/TPBI completed within last 3 mths and results documented If unable to obtain ABPI/TPBI, referral to vascular surgeon is recommended Assess pulses (popliteal behind knee, dorsalis pedis top of foot, posterior tibial medial ankle) Measurement of edema Assess capillary refill (normal less than 3 seconds) Leg measurements (foot, ankle, calf, thigh) Ankle range of motion (ROM) Foot deformities Ankle flare Skin temperature (compare both legs) Skin colour (dependent and on elevation) Presence of pain Nail changes Presence of hair on lower leg, feet and toes Presence of varicosities (varicose veins) Dermatological changes due to impaired blood flow Repeat ABPI/TPBI assessment every 3 months if healing is not progressing ABPI 0.5 to 0.8 TBPI 0.64 to 0.7 Suggest Transcutaneous Oxygen Pressure(TcPo 2 ), Laser Doppler Flowmetry, Doppler Arterial Waveforms or Segmental Doppler Pressure studies ABPI <0.5 TBPI <0.64 Urgent vascular surgical consult needed Acute arterial occlusion is a life and limb-threatening situation which requires immediate emergency intervention Signs and symptoms that may become severe may be associated with the following: Pale or blue skin Skin cold to the touch Sudden decrease in mobility No pulse where one was present prior to this Sudden and severe pain Patient s nutritional status optimized Recent blood work results Significant weight changes Adherence to diet plan Identify barriers to good nutrition Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
18 Patient and caregiver concerns and goals integrated into the care plan and shared with care team Patient counselled on the benefit of activity rest and head elevation in moderation (balancing need for pressure relief) for comfort measures and wound healing Patient/caregiver educational needs reviewed using teach-back method Cardiff Wound Impact Questionnaire OR World Health Organization Quality of Life (WHOQOL) form Encourage patient to sleep in bed with Recent changes in overall activity level no lower limb elevation (most arterial Daily routine pain increases when feet elevated Personal assistance available to perform above heart level) activities of daily living Mobility and dexterity aids currently Ankle range of motion allowing for calf being used muscle pump to function Safety of transfers Determine where patient sleeps at night Recommendations for exercise Consider Occupational Therapist referral for comfort measures Emergency signs and symptoms of Pain management Peripheral Arterial Disease that require Diagnostic testing immediate medical attention (refer to Dietary lower leg assessment section) Rest/Activity Risks of compression Prevention of injury avoid extremes Smoking cessation including e-cigarettes (hot/cold, loose/tight) and nicotene replacement When to call primary care giver (eg. Appropriate footwear as discussed with signs and symptoms of infection, deep foot care specialist (encourage use of vein thrombosis, cellulitis, impaired white socks) blood flow, difficulties with Skin care compression) Nail care (suggest use of foot care Self lower-leg assessment specialist) Community support groups (i.e. walking Wound self care groups) Other Ability to self-manage optimized Hygeine Adherence to plan Foot inspection (including bottom of Barriers to participate (transportation, foot and between toes) socioeconomic, social environment, Enviroment other co-morbidities) Wound care Cognitive ability Compression application and removal if Review importance and potential prescribed barriers to smoking cessation at every visit Coping strategies implemented into plan of care Patient s concerns and fears Signs of anxiety or other mental health issues (eg. delusions, hallucinations, paranoid Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
19 Family and caregiver support identified and incorporated into plan of care behaviour) Depression screen using Geriatric Depression Scale assessment form GDS15 Suicide assessment if applicable ETOH and illicit /recreational drug use Availability of assistance required Social supports/community resources currently utilized is integrated into plan of care Family support Funding Community resources Caregiver conflicts Long or short term placement Assistance provided for financial concerns patient is experiencing Private insurance availability Eligibility for Assistive Devices Program (ADP [lymphedema only], ODSP, High-needs fund, Veterans Affairs Canada or Aborignal Services) Professional referral status reviewed Primary Care Physician Pharmacist Advanced Wound Specialist Occupational Therapist Nurse Practitioner Physiotherapy Infectious Disease Specialist Chiropodist Vascular Surgeon Certified Pedorothist Dermatologist Certified Orthotist Plastic surgeon Certified Prosthetist Internist/Endocrinologist Podiatrist Mental Health Specialist Lymphatic Massage Psychologists Compression Stocking Fitter Social work Other: Registered Dietitian Physician/nurse practitioner orders received as required to change plan of care including agreeance to professional referral recommendations Appropriate documents shared Identify need to reassess ABPI/TPBI in 6 months Lower leg assessment Recent vascular study results (eg. ABPI, TPBI, Transcutaneous Oxygen Pressure(TcPo 2 ), Laser Doppler Flowmetry, Doppler Arterial Waveforms or Segmental Doppler Pressure studies) Relevant consultation notes Acute care Complex Continuing Care/Rehab Long-term care Community care Primary care physician/nurse Practioner Professionals referred to Other Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
20 Diagnostic results Current treatment plan If wound closed or eschar is stable send discharge summary outlining outstanding issues and teaching completed to: Referral source and most responsible physician (MRP)/nurse practitioner (NP) Collaborative team/patient conference arranged to discuss barriers to healing and care plan if progression to healing is stalled Arrange a Collaborative team/patient meeting to discuss barriers to healing and care plan Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
21 91-98 Days Expected Outcomes Notes Most Responsible Physician(MRP)/Nurse Practitioner (NP) identified/informed Assessment of wound performed and percentage of healing documented 4 P s of Arterial Ulcers Pale wound base Punched-out appearance Painful Parched (low to no exudate) Arterial ulcers do not follow trajectory healing rate of venous ulcers (30% week 4 & healed at 12 weeks). Further intervention should be considered if conservative treatment does not improve healing in 4-6 weeks Wound treatment/compression plan is being followed Caution: USE DRY WOUND HEALING 1. Keep eschar dry 2. No occlusive dressings 3. Do NOT debride 4. Avoid tourniquet effect when securing dressings 5. If eschar becomes wet/boggy URGENT referral to advanced wound care specialist is recommended Pain management reviewed Arterial pain is typically described as: Pain with elevation of lower limbs, rest pain, nocturnal pain and pain on walking (caused by intermittent claudication) Medical/surgical history and co-morbidity management considered within care plan Medication reconciliation and their impact on wound healing Communication with primary care physician and/or Nurse Practioner to update on any significant changes in patient s condition. Refer patient to Care Connects if no responsible practioner currently involved with patient Determine if MRP/NP is part of family health team (FHT) or community health centre (CHC) and consider additional supports available Complete: Bates-Jensen Wound Assessment Tool (BWAT) OR Leg Ulcer Measurement Tool (LUMT) Determine wound etiology Arterial ulcers are typically pale at base of wound, have punched out appearance, are more painful than expected and have low to no exudate Results of LLA and ABPI/TPBI Document percentage of healing since admission Assessment for infection (NERDS and STONEES) Potential need for wound care specialist considered if wound healing is not progressing and infection is absent Obtain photos following best practice as per framework for individual organization policies and procedures. Suggest following publication as guideline: Adherence to plan Real or potential barriers to wound treatment plan Compression is typically contraindicated in the presence of peripheral arterial disease. In some circumstances light compression may be beneficial. In such cases, compression should be ordered by an advanced wound care physician or nurse practitioner only! See algorithm in guidelines. Brief Pain Inventory Short Form (BPI-SF) Obtain physician/nurse practitioner orders for analgesics required (opioids and non-opioids) Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
22 reviewed Prescription, non-prescription, naturopathic and illicit drug use Recent blood work and other diagnostic test results reviewed and implictions for wound healing considered Determine bloodwork and other diagnostic tests required Bilateral lower leg assessment completed Signs and symptoms of Peripheral Arterial Disease could include: Pain with elevation of lower limbs, rest pain, nocturnal pain and pain on walking (caused by intermittent claudication) Dependent rubor in lower legs and feet Pallor in feet on elevation Dry, shiny skin on lower legs Edema subsequent to leg being dependent Thick or flaking toe nails Hairless lower legs and feet Weak or absent pulses Intense hyperesthesia (sensitive to light touch) Limb muscle may appear wasted from ischemic atrophy Delayed capillary refill Distal gangrene Erectile dysfunction in men Non-healing wound ABPI 0.5 to 0.8 TBPI 0.64 to 0.7 Suggest Transcutaneous Oxygen Pressure(TcPo 2 ), Laser Doppler Flowmetry, Doppler Arterial Waveforms or Segmental Doppler Pressure studies ABPI <0.5 TBPI <0.64 Urgent vascular surgical consult needed ABPI/TPBI completed within last 3 mths and results documented If unable to obtain ABPI/TPBI, referral to vascular surgeon is recommended Assess pulses (popliteal behind knee, dorsalis pedis top of foot, posterior tibial medial ankle) Measurement of edema Assess capillary refill (normal less than 3 seconds) Leg measurements (foot, ankle, calf, thigh) Ankle range of motion (ROM) Foot deformities Ankle flare Skin temperature (compare both legs) Skin colour (dependent and on elevation) Presence of pain Nail changes Presence of hair on lower leg, feet and toes Presence of varicosities (varicose veins) Dermatological changes due to impaired blood flow Repeat ABPI/TPBI assessment every 3 months if healing is not progressing Acute arterial occlusion is a life and limb-threatening situation which requires immediate emergency intervention Signs and symptoms that may become severe may be associated with the following: Pale or blue skin Skin cold to the touch Sudden decrease in mobility No pulse where one was present prior to this Sudden and severe pain Patient s nutritional status optimized Recent blood work results Significant weight changes Adherence to diet plan Identify barriers to good nutrition Patient and caregiver concerns and goals integrated into the care plan and shared with care team Cardiff Wound Impact Questionnaire Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
23 Patient counselled on the benefit of activity rest and head elevation in moderation (balancing need for pressure relief) for comfort measures and wound healing Patient/caregiver educational needs reviewed using teach-back method OR World Health Organization Quality of Life (WHOQOL) form Encourage patient to sleep in bed with Recent changes in overall activity level no lower limb elevation (most arterial Daily routine pain increases when feet elevated Personal assistance available to perform above heart level) activities of daily living Mobility and dexterity aids currently Ankle range of motion allowing for calf being used muscle pump to function Safety of transfers Determine where patient sleeps at night Recommendations for exercise Consider Occupational Therapist referral for comfort measures Emergency signs and symptoms of Pain management Peripheral Arterial Disease that require Diagnostic testing immediate medical attention (refer to Dietary lower leg assessment section) Rest/Activity Risks of compression Prevention of injury avoid extremes Smoking cessation including e-cigarettes (hot/cold, loose/tight) and nicotene replacement When to call primary care giver (eg. Appropriate footwear as discussed with signs and symptoms of infection, deep foot care specialist (encourage use of vein thrombosis, cellulitis, impaired white socks) blood flow, difficulties with Skin care compression) Nail care (suggest use of foot care Self lower-leg assessment specialist) Community support groups (i.e. walking Wound self care groups) Other Ability to self-manage optimized Hygeine Adherence to plan Foot inspection (including bottom of Barriers to participate (transportation, foot and between toes) socioeconomic, social environment, Enviroment other co-morbidities) Wound care Cognitive ability Compression application and removal if Review importance and potential prescribed barriers to smoking cessation at every visit Coping strategies implemented into plan of care Patient s concerns and fears Signs of anxiety or other mental health issues (eg. delusions, hallucinations, paranoid behaviour) Depression screen using Geriatric Depression Scale assessment form GDS15 Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
24 Suicide assessment if applicable ETOH and illicit /recreational drug use Family and caregiver support identified and incorporated into plan of care Availability of assistance required Social supports/community resources currently utilized is integrated into plan of care Family support Funding Community resources Caregiver conflicts Long or short term placement Assistance provided for financial concerns patient is experiencing Private insurance availability Eligibility for Assistive Devices Program (ADP [lymphedema only], ODSP, High-needs fund, Veterans Affairs Canada or Aborignal Services) Professional referral status reviewed Primary Care Physician Pharmacist Advanced Wound Specialist Occupational Therapist Nurse Practitioner Physiotherapy Infectious Disease Specialist Chiropodist Vascular Surgeon Certified Pedorothist Dermatologist Certified Orthotist Plastic surgeon Certified Prosthetist Internist/Endocrinologist Podiatrist Mental Health Specialist Lymphatic Massage Psychologists Compression Stocking Fitter Social work Other: Registered Dietitian Physician/nurse practitioner orders received as required to change plan of care including agreeance to professional referral recommendations Appropriate documents shared Identify need to reassess ABPI/TPBI in 6 months Lower leg assessment Recent vascular study results (eg. ABPI, TPBI, Transcutaneous Oxygen Pressure(TcPo 2 ), Laser Doppler Flowmetry, Doppler Arterial Waveforms or Segmental Doppler Pressure studies) Relevant consultation notes Diagnostic results Current treatment plan Acute care Complex Continuing Care/Rehab Long-term care Community care Primary care physician/nurse Practioner Professionals referred to Other Waterloo Wellington Integrated Wound Care Program Arterial Pathway May
Arterial Leg Ulcer Clinical Pathway
 Waterloo Wellington Integrated Wound Care Program Evidence-Based Wound Care Arterial Leg Ulcer Clinical Pathway 0-7 Days Expected Outcomes Notes Most Responsible Physician(MRP)/Nurse Practitioner (NP)
Waterloo Wellington Integrated Wound Care Program Evidence-Based Wound Care Arterial Leg Ulcer Clinical Pathway 0-7 Days Expected Outcomes Notes Most Responsible Physician(MRP)/Nurse Practitioner (NP)
Diabetic Foot Ulcer Clinical Pathway
 Page 1 of 10 Waterloo Wellington Integrated Wound Care Program Evidence-Based Wound Care Diabetic Foot Ulcer Clinical Pathway 0-7 Days Expected Outcomes Notes Most Responsible Physician(MRP)/Nurse Practitioner
Page 1 of 10 Waterloo Wellington Integrated Wound Care Program Evidence-Based Wound Care Diabetic Foot Ulcer Clinical Pathway 0-7 Days Expected Outcomes Notes Most Responsible Physician(MRP)/Nurse Practitioner
Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline
 Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline Description Domain I: Assessment and Care Planning 010000 40 Task 1: Obtain focused
Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline Description Domain I: Assessment and Care Planning 010000 40 Task 1: Obtain focused
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
All WALES LYMPHOEDEMA GUIDANCE:
 All WALES LYMPHOEDEMA GUIDANCE: Lymphoedema Vascular Assessment Policy (Toe Brachial Pressure Index / TBPI) April 2013 Created by the All Wales Lymphoedema Service Leads 1 Background The presence of peripheral
All WALES LYMPHOEDEMA GUIDANCE: Lymphoedema Vascular Assessment Policy (Toe Brachial Pressure Index / TBPI) April 2013 Created by the All Wales Lymphoedema Service Leads 1 Background The presence of peripheral
Appendix D: Leg Ulcer Assessment Form
 Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Address: Left Leg. other: Nails: thick yellow brittle fungus abnormal thick yellow brittle fungus abnormal
 South West Regional Wound Care Toolkit: Interdisciplinary Lower Leg Assessment Form Instructions for use: Competent/ Proficient/ Expert level HCP to complete if lower leg ulcer present or risk of ulcer
South West Regional Wound Care Toolkit: Interdisciplinary Lower Leg Assessment Form Instructions for use: Competent/ Proficient/ Expert level HCP to complete if lower leg ulcer present or risk of ulcer
Leg ulcer assessment and management
 Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Diabetic Foot Ulcers. Care for Patients in All Settings
 Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Peripheral Vascular Examination. Dr. Gary Mumaugh Western Physical Assessment
 Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
Venous Insufficiency Ulcers. Patient Assessment: Superficial varicosities. Evidence of healed ulcers. Dermatitis. Normal ABI.
 Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
Wound Assessment Report
 Wound Assessment Report Single Assessment, Single Wound Mary Taylor Assessment Patient ID MT4367147 Date of Birth 1939-4-18 Left Foot, Sole: Wound A Image taken 16-45-43 Area 1.7cm2 Perimeter 48mm Maximum
Wound Assessment Report Single Assessment, Single Wound Mary Taylor Assessment Patient ID MT4367147 Date of Birth 1939-4-18 Left Foot, Sole: Wound A Image taken 16-45-43 Area 1.7cm2 Perimeter 48mm Maximum
Leg Ulcer Case Study
 Leg Ulcer Case Study Wound Healing Community Outreach Service Mrs Ivy Hurtzalot, a 71-year-old lady, presents to her general practitioner with an ulcer on her right medial malleolus. Ivy reveals that the
Leg Ulcer Case Study Wound Healing Community Outreach Service Mrs Ivy Hurtzalot, a 71-year-old lady, presents to her general practitioner with an ulcer on her right medial malleolus. Ivy reveals that the
Person s Name: ID Number: Date:
 South West Regional Wound Care Program Person s Name: ID Number: Interdisciplinary Diabetic/Neuropathic Foot Assessment Form MEDICAL HISTORY: Question Year diabetes diagnosed: Characteristics of onset
South West Regional Wound Care Program Person s Name: ID Number: Interdisciplinary Diabetic/Neuropathic Foot Assessment Form MEDICAL HISTORY: Question Year diabetes diagnosed: Characteristics of onset
Lower Leg Ulceration. Wendy McInnes Vascular Nurse Practitioner; Northern Adelaide Local Health Network;
 Lower Leg Ulceration Wendy McInnes Vascular Nurse Practitioner; Northern Adelaide Local Health Network; wendy.mcinnes@sa.gov.au 0447 051 036 1 Lower Leg Ulceration A manifestation of underlying pathology/disease
Lower Leg Ulceration Wendy McInnes Vascular Nurse Practitioner; Northern Adelaide Local Health Network; wendy.mcinnes@sa.gov.au 0447 051 036 1 Lower Leg Ulceration A manifestation of underlying pathology/disease
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care
 The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
Peripheral Arterial Disease Extremity
 Peripheral Arterial Disease Lower Extremity 05 Contributor Dr Steven Chong Advisors Dr Ashish Anil Dr Tay Jam Chin Introduction Risk Factors Clinical Presentation Classification History PHYSICAL examination
Peripheral Arterial Disease Lower Extremity 05 Contributor Dr Steven Chong Advisors Dr Ashish Anil Dr Tay Jam Chin Introduction Risk Factors Clinical Presentation Classification History PHYSICAL examination
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT
 VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
Will it heal? How to assess the probability of wound healing
 Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS
 VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
Steven Hadesman, MD Chief Medical Officer, MeridianRx Internal Medicine Physician, St. John Hospital
 Steven Hadesman, MD Chief Medical Officer, MeridianRx Internal Medicine Physician, St. John Hospital Deep Venous Thrombosis Varicose Veins Venous insufficiency Phlebitis Lymphedema Elephantiasis nostras
Steven Hadesman, MD Chief Medical Officer, MeridianRx Internal Medicine Physician, St. John Hospital Deep Venous Thrombosis Varicose Veins Venous insufficiency Phlebitis Lymphedema Elephantiasis nostras
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists
 EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
Reality TV Managing patients in the real world. Wounds UK Harrogate 2009
 Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
How to manage leg ulcers in the elderly
 How to manage leg ulcers in the elderly David Riding Clinical Research Fellow / Specialty Registrar in Vascular Surgery University of Manchester / MFT British Geriatric Society Trainees Meeting 2018 Objectives
How to manage leg ulcers in the elderly David Riding Clinical Research Fellow / Specialty Registrar in Vascular Surgery University of Manchester / MFT British Geriatric Society Trainees Meeting 2018 Objectives
Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2)
 Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2) Definition Vascular surgery is the specialty concerned with the diagnosis and management of congenital and acquired diseases of the
Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2) Definition Vascular surgery is the specialty concerned with the diagnosis and management of congenital and acquired diseases of the
PDP SELF-TEST QUESTIONNAIRE
 Number 5 CORE TUTORIALS IN DERMATOLOGY FOR PRIMARY CARE PDP SELF-TEST QUESTIONNAIRE METEOR CRATER, ARIZONA, USA LEG ULCERS Ulcer Full thickness loss of epidermis and some dermis, which will heal with scarring
Number 5 CORE TUTORIALS IN DERMATOLOGY FOR PRIMARY CARE PDP SELF-TEST QUESTIONNAIRE METEOR CRATER, ARIZONA, USA LEG ULCERS Ulcer Full thickness loss of epidermis and some dermis, which will heal with scarring
Improving customer care in compression hosiery
 Improving customer care in compression hosiery Introduction Within the modern NHS, the Pharmacy Team provides the front line service that most patients have contact with. Compression hosiery has a key
Improving customer care in compression hosiery Introduction Within the modern NHS, the Pharmacy Team provides the front line service that most patients have contact with. Compression hosiery has a key
Clinical Examination of VASCULAR PATIENTS. Stephanie Hirst & Alexander Sunde
 Clinical Examination of VASCULAR PATIENTS Stephanie Hirst & Alexander Sunde Goals of Medical History To record the patient s symptoms at time of presentation. To organize the events which have lead to
Clinical Examination of VASCULAR PATIENTS Stephanie Hirst & Alexander Sunde Goals of Medical History To record the patient s symptoms at time of presentation. To organize the events which have lead to
The Peripheral Vascular System
 The Peripheral Vascular System Anatomy and Physiology Arteries Arteries contain 3 concentric layers of tissue: - the intima - the media - the adventitia The intima The endothelium of the intima has metabolic
The Peripheral Vascular System Anatomy and Physiology Arteries Arteries contain 3 concentric layers of tissue: - the intima - the media - the adventitia The intima The endothelium of the intima has metabolic
Model of Care for the Diabetic Foot
 Model of Care for the Diabetic Foot National Clinical Programme for Diabetes Clinical Strategy and Programme Division 2018 Revision number Document drafted by National Clinical Programme for Diabetes Working
Model of Care for the Diabetic Foot National Clinical Programme for Diabetes Clinical Strategy and Programme Division 2018 Revision number Document drafted by National Clinical Programme for Diabetes Working
End Diastolic Pneumatic Compression Boot as a Treatment of Peripheral Vascular Disease or Lymphedema. Original Policy Date
 MP 2.02.12 End Diastolic Pneumatic Compression Boot as a Treatment of Peripheral Vascular Disease or Lymphedema Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
MP 2.02.12 End Diastolic Pneumatic Compression Boot as a Treatment of Peripheral Vascular Disease or Lymphedema Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS
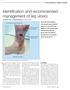 Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS thickened skin, lipodermatosclerosis skin stained haemosiderin shallow ulcer irregular shape Our
Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS thickened skin, lipodermatosclerosis skin stained haemosiderin shallow ulcer irregular shape Our
Diabetes Foot Screening and Risk Stratification Tool
 Diabetes Foot Screening and Risk Stratification Tool Welcome to the Diabetes Foot Screening and Risk Stratification Tool This tool is based on the work of the Scottish Foot Action Group (SFAG). It has
Diabetes Foot Screening and Risk Stratification Tool Welcome to the Diabetes Foot Screening and Risk Stratification Tool This tool is based on the work of the Scottish Foot Action Group (SFAG). It has
Diabetes Foot and Skin Care. Diabetes and the feet. Foot problems: Major cause of morbidity and mortality
 Session # 11 Diabetes Foot and Skin Care Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE Diabetes and the feet Diabetes affects circulation and immunity. Over time, the sensory nerves in the
Session # 11 Diabetes Foot and Skin Care Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE Diabetes and the feet Diabetes affects circulation and immunity. Over time, the sensory nerves in the
Case study: A targeted approach to healing complex wounds using the geko device.
 Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
PRODIGY Quick Reference Guide
 PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
Arterial & Venous Ulcers. A Comprehensive Review Assessment & Management
 Arterial & Venous Ulcers A Comprehensive Review Assessment & Management 1 Objectives Understand Arterial & Venous disease Understand the etiology of lower extremities ulcers Understand assessment of lower
Arterial & Venous Ulcers A Comprehensive Review Assessment & Management 1 Objectives Understand Arterial & Venous disease Understand the etiology of lower extremities ulcers Understand assessment of lower
GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND
 GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND AIM To provide evidence based principles for the measurement of Ankle Brachial Pressure Index (ABPI) using a BACKGROUND/EVIDENCE
GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND AIM To provide evidence based principles for the measurement of Ankle Brachial Pressure Index (ABPI) using a BACKGROUND/EVIDENCE
Rapid Foot Screening
 GP Symposium 2015 Workshop Rapid Foot Screening Ms Chelsea Law, Principal Podiatrist Mr Henry Lee, Podiatrist Ms Ng Jia Lin, Podiatrist Ms Polly Lim, Podiatrist Ms Wong Wan Mun, Podiatrist Mr Yeo Boon
GP Symposium 2015 Workshop Rapid Foot Screening Ms Chelsea Law, Principal Podiatrist Mr Henry Lee, Podiatrist Ms Ng Jia Lin, Podiatrist Ms Polly Lim, Podiatrist Ms Wong Wan Mun, Podiatrist Mr Yeo Boon
Northumbria Healthcare NHS Foundation Trust. Preparing For Foot and Ankle Surgery. Issued by the Orthopaedic Department
 Northumbria Healthcare NHS Foundation Trust Preparing For Foot and Ankle Surgery Issued by the Orthopaedic Department This leaflet gives you information about what is involved in foot and ankle surgery.
Northumbria Healthcare NHS Foundation Trust Preparing For Foot and Ankle Surgery Issued by the Orthopaedic Department This leaflet gives you information about what is involved in foot and ankle surgery.
ARTERIAL BYPASS GRAFTS IN THE LEG
 The Christchurch Department of Vascular Surgery is actively involved in research projects aimed at improving treatment for patients with arterial disease. Marilyn Ollett Department of Surgery Christchurch
The Christchurch Department of Vascular Surgery is actively involved in research projects aimed at improving treatment for patients with arterial disease. Marilyn Ollett Department of Surgery Christchurch
Skin Tear Management Guide South West Regional Wound Care Program Last Updated April 10,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Arterial Studies And The Diabetic Foot Patient
 Arterial Studies And The Patient George L. Berdejo, BA, RVT, FSVU gberdejo@wphospital.org Disclosures I have nothing to disclose! Diabetes mellitus continues to grow in global prevalence and to consume
Arterial Studies And The Patient George L. Berdejo, BA, RVT, FSVU gberdejo@wphospital.org Disclosures I have nothing to disclose! Diabetes mellitus continues to grow in global prevalence and to consume
A retrospective chart review will be done at the start and end of the study (anticipated 1 year duration) measuring rates of the following:
 Project name: Renal Foot Care Program Supervisor: Shaoyee Yao Background: Hemodialysis patients have significant co-morbidities including diabetes, peripheral vascular disease, neuropathy and lower limb
Project name: Renal Foot Care Program Supervisor: Shaoyee Yao Background: Hemodialysis patients have significant co-morbidities including diabetes, peripheral vascular disease, neuropathy and lower limb
End-Diastolic Pneumatic Compression Boot as a Treatment of Peripheral Vascular Disease or Lymphedema
 End-Diastolic Pneumatic Compression Boot as a Treatment of Peripheral Vascular Disease or Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary,
End-Diastolic Pneumatic Compression Boot as a Treatment of Peripheral Vascular Disease or Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary,
Alberta Health. Alberta Aids to Daily Living Compression Stockings and Lymphedema Sleeves Ready Made Benefits Policy & Procedures Manual
 Alberta Health Alberta Aids to Daily Living Compression Stockings and Lymphedema Sleeves Ready Made Benefits Policy & Procedures Manual March 7, 2016 Revision History Description Date N-03, N 05 and N-07:
Alberta Health Alberta Aids to Daily Living Compression Stockings and Lymphedema Sleeves Ready Made Benefits Policy & Procedures Manual March 7, 2016 Revision History Description Date N-03, N 05 and N-07:
Limb Salvage in Diabetic Ischemic Foot. Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017
 Limb Salvage in Diabetic Ischemic Foot Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017 Case Male 67 years old Underlying DM, HTN, TVD Present with gangrene
Limb Salvage in Diabetic Ischemic Foot Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017 Case Male 67 years old Underlying DM, HTN, TVD Present with gangrene
Independent evaluation of BEMER physical vascular regulation therapy
 of BEMER Liezl Naudé Advanced nurse specialist: wound management Advanced lower limb and wound management centre, Pretoria Heart 4 the Wounded 5-7 July Pretoria Introduction Lower limb wounds have always
of BEMER Liezl Naudé Advanced nurse specialist: wound management Advanced lower limb and wound management centre, Pretoria Heart 4 the Wounded 5-7 July Pretoria Introduction Lower limb wounds have always
AWMA MODULE ACCREDITATION. Module Five: The High Risk Foot (Including the Diabetic Foot)
 AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
How to prevent blood clots whilst in hospital and after your return home
 How to prevent blood clots whilst in hospital and after your return home Patient information WHAT What IS is DEEP deep VEIN vein THROMBOSIS? thrombosis? Deep Vein Thrombosis DVT is a blood clot within
How to prevent blood clots whilst in hospital and after your return home Patient information WHAT What IS is DEEP deep VEIN vein THROMBOSIS? thrombosis? Deep Vein Thrombosis DVT is a blood clot within
Diabetes Foot Care Clinical Pathway Healthcare Provider s Guide
 Diabetes Foot Care Clinical Pathway Healthcare Provider s Guide Diabetes, Obesity & Nutrition Strategic Clinical Network Version 1.0 Acknowledgement This healthcare provider s guide has been adapted from
Diabetes Foot Care Clinical Pathway Healthcare Provider s Guide Diabetes, Obesity & Nutrition Strategic Clinical Network Version 1.0 Acknowledgement This healthcare provider s guide has been adapted from
9 Day Certified Lymphedema & Wound Therapist (62.5 CE hrs On-line + 9 Days Live Training (8am 8pm *daily times vary; 153 CE hrs Total!
 1 9 Day Certified Lymphedema & Wound Therapist (62.5 CE hrs On-line + 9 Days Live Training (8am 8pm *daily times vary; 153 CE hrs Total!) On-Line COURSE OUTLINE/Overview of Topics (62.5hrs): Lymphatics
1 9 Day Certified Lymphedema & Wound Therapist (62.5 CE hrs On-line + 9 Days Live Training (8am 8pm *daily times vary; 153 CE hrs Total!) On-Line COURSE OUTLINE/Overview of Topics (62.5hrs): Lymphatics
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated April 7,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC
 High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC A new paradigm? Foot ulceration 101 Assessing Perfusion a new challenge Pressure
High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC A new paradigm? Foot ulceration 101 Assessing Perfusion a new challenge Pressure
Foot and Ankle Surgery
 Information about Foot and Ankle Surgery Statement of Use The information in this leaflet is intended solely for the person to whom it was given by the health care team and is provided as a general information
Information about Foot and Ankle Surgery Statement of Use The information in this leaflet is intended solely for the person to whom it was given by the health care team and is provided as a general information
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
Practical Point in Diabetic Foot Care 3-4 July 2017
 Diabetic Foot Ulcer : Role of Vascular Surgeon Practical Point in Diabetic Foot Care 3-4 July 2017 Supapong Arworn, MD Division of Vascular and Endovascular Surgery Department of Surgery, Chiang Mai University
Diabetic Foot Ulcer : Role of Vascular Surgeon Practical Point in Diabetic Foot Care 3-4 July 2017 Supapong Arworn, MD Division of Vascular and Endovascular Surgery Department of Surgery, Chiang Mai University
Complex Limb Injury. Exceptional healthcare, personally delivered
 Complex Limb Injury Exceptional healthcare, personally delivered Complex Limb Injuries Introduction This information booklet aims to help you to understand the nature, treatment and outcome of your limb
Complex Limb Injury Exceptional healthcare, personally delivered Complex Limb Injuries Introduction This information booklet aims to help you to understand the nature, treatment and outcome of your limb
KNEE ARTHROSCOPY SURGERY
 KNEE ARTHROSCOPY SURGERY SUMMARY OF PROCEDURE Arthroscopy involves looking at the inside of the knee joint with a small telescope and camera (arthroscope). The image is projected onto a television monitor
KNEE ARTHROSCOPY SURGERY SUMMARY OF PROCEDURE Arthroscopy involves looking at the inside of the knee joint with a small telescope and camera (arthroscope). The image is projected onto a television monitor
British Columbia Provincial Nursing Skin and Wound Committee
 Developed by the BC Provincial Nursing Skin and Wound Care Committee in collaboration with Wound Clinicians from: / Education Module Ankle Brachial Index(ABI) Procedure in Adults for Handheld Doppler &
Developed by the BC Provincial Nursing Skin and Wound Care Committee in collaboration with Wound Clinicians from: / Education Module Ankle Brachial Index(ABI) Procedure in Adults for Handheld Doppler &
Introduction. Risk factors of PVD 5/8/2017
 PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
National Clinical Conference 2018 Baltimore, MD
 National Clinical Conference 2018 Baltimore, MD No relevant financial relationships to disclose Wound Care Referral The patient has been maximized from a vascular standpoint. She has no other options.
National Clinical Conference 2018 Baltimore, MD No relevant financial relationships to disclose Wound Care Referral The patient has been maximized from a vascular standpoint. She has no other options.
How is 1st MTP joint fusion carried out? Patient Information: Big Toe Fusion Metatarsophalangeal (MTP)
 Patient Information: Big Toe Fusion Metatarsophalangeal (MTP) How is 1st MTP joint fusion carried out? You will be asked to wash your feet thoroughly on the day of operation and keep them clean, as this
Patient Information: Big Toe Fusion Metatarsophalangeal (MTP) How is 1st MTP joint fusion carried out? You will be asked to wash your feet thoroughly on the day of operation and keep them clean, as this
THE DIABETIC FOOT. Nicola Kilburn Diabetes Specialist Podiatrist
 THE DIABETIC FOOT Nicola Kilburn Diabetes Specialist Podiatrist Diabetic foot disease is associated with significant morbidity and mortality. Foot screening is effective in identifying an individuals risk
THE DIABETIC FOOT Nicola Kilburn Diabetes Specialist Podiatrist Diabetic foot disease is associated with significant morbidity and mortality. Foot screening is effective in identifying an individuals risk
VeinOPlus Vascular Peripheral Vascular & Wound Therapy Device
 VeinOPlus Vascular Peripheral Vascular & Wound Therapy Device Calf Muscle Pump Dysfunction Therapy Increases blood flow, accelerates wound healing, and improves CVD and PAD symptoms Tomorrow s Technology
VeinOPlus Vascular Peripheral Vascular & Wound Therapy Device Calf Muscle Pump Dysfunction Therapy Increases blood flow, accelerates wound healing, and improves CVD and PAD symptoms Tomorrow s Technology
Role of ABI in Detecting and Quantifying Peripheral Arterial Disease
 Role of ABI in Detecting and Quantifying Peripheral Arterial Disease Difference in AAA size between US and Surgeon 2 1 0-1 -2-3 0 1 2 3 4 5 6 7 Mean AAA size between US and Surgeon Kathleen G. Raman MD,
Role of ABI in Detecting and Quantifying Peripheral Arterial Disease Difference in AAA size between US and Surgeon 2 1 0-1 -2-3 0 1 2 3 4 5 6 7 Mean AAA size between US and Surgeon Kathleen G. Raman MD,
Prevention and Management of Leg Ulcers
 EWMA Educational Development Programme Curriculum Development Project Education Module: Prevention and Management of Leg Ulcers Latest revision: October 2015 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME
EWMA Educational Development Programme Curriculum Development Project Education Module: Prevention and Management of Leg Ulcers Latest revision: October 2015 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME
Pressure Injury Assessment Guide South West Regional Wound Care Program Last Updated October 31,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Promoting best practice in leg ulcer management
 Promoting best practice in leg ulcer management Sylvie Hampton MA BSc (Hons) DpSN RGN Independent Tissue Viability Consultant Nurse Leg Ulcers - What are the causes? Chronic leg ulcers are defined as those
Promoting best practice in leg ulcer management Sylvie Hampton MA BSc (Hons) DpSN RGN Independent Tissue Viability Consultant Nurse Leg Ulcers - What are the causes? Chronic leg ulcers are defined as those
Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship
 Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship CLINICAL PROBLEMS IN VASCULAR SURGERY 1. ABDOMINAL AORTIC ANEURYSM A 70 year old man presents in the emergency department with
Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship CLINICAL PROBLEMS IN VASCULAR SURGERY 1. ABDOMINAL AORTIC ANEURYSM A 70 year old man presents in the emergency department with
Foot and ankle fractures
 Foot and ankle fractures Some fractures can be managed without surgery, but others require surgery to achieve the best possible outcome. Fractures and injuries to joints have a high risk of developing
Foot and ankle fractures Some fractures can be managed without surgery, but others require surgery to achieve the best possible outcome. Fractures and injuries to joints have a high risk of developing
Non- invasive vascular testing. Pros and Cons of ABIs and Alternative Physiologic Assessments
 Non- invasive vascular testing Pros and Cons of ABIs and Alternative Physiologic Assessments Non- Invasive Physiologic Arterial Studies Segmental Systolic Pressure Measurements ABIs, TBIs, and full segmentals
Non- invasive vascular testing Pros and Cons of ABIs and Alternative Physiologic Assessments Non- Invasive Physiologic Arterial Studies Segmental Systolic Pressure Measurements ABIs, TBIs, and full segmentals
DIABETIC FOOT BOOK THE. A guide to keeping it simple and preventing complications. Practice genii. the Diabetic Foot Book
 DIABETIC THE FOOT BOOK A guide to keeping it simple and preventing complications Understanding how diabetes can affect foot health and the measures that are taken to prevent diabetic foot complications
DIABETIC THE FOOT BOOK A guide to keeping it simple and preventing complications Understanding how diabetes can affect foot health and the measures that are taken to prevent diabetic foot complications
Due to Perimed s commitment to continuous improvement of our products, all specifications are subject to change without notice.
 A summary Disclaimer The information contained in this document is intended to provide general information only. It is not intended to be, nor does it constitute, medical advice. Under no circumstances
A summary Disclaimer The information contained in this document is intended to provide general information only. It is not intended to be, nor does it constitute, medical advice. Under no circumstances
Our Vision NADA BoD Strategic Planning Session -
 Who we are NADA is a not-for-profit members-led organization established in 1995 as a result of the rising rates of diabetes among First Nations, Inuit and Métis Peoples in Canada Our Vision - 2016 NADA
Who we are NADA is a not-for-profit members-led organization established in 1995 as a result of the rising rates of diabetes among First Nations, Inuit and Métis Peoples in Canada Our Vision - 2016 NADA
Treating your leg ulcer
 Page 1 of 7 Treating your leg ulcer Introduction The information in this leaflet will answer many questions you may have about your leg ulcer. If you have any further questions about your condition or
Page 1 of 7 Treating your leg ulcer Introduction The information in this leaflet will answer many questions you may have about your leg ulcer. If you have any further questions about your condition or
Case study: Young athlete suffering from PTS recovers from traumatic foot ulcer, following use of the geko TM device.
 Case study: Young athlete suffering from PTS recovers from traumatic foot ulcer, following use of the geko TM device.... Subject 34-year-old male, ex professional rugby player. Wound Type Lower left leg
Case study: Young athlete suffering from PTS recovers from traumatic foot ulcer, following use of the geko TM device.... Subject 34-year-old male, ex professional rugby player. Wound Type Lower left leg
TURNINGPOINT CLINICAL POLICY
 1 P a g e NOTE: For services provided on December 3, 2018 and after, Horizon Blue Cross Blue Shield of New Jersey ( Horizon BCBSNJ ) has contracted with TurningPoint Healthcare Solutions, LLC to conduct
1 P a g e NOTE: For services provided on December 3, 2018 and after, Horizon Blue Cross Blue Shield of New Jersey ( Horizon BCBSNJ ) has contracted with TurningPoint Healthcare Solutions, LLC to conduct
Medical Policy Original Effective Date: 01/23/2019
 Page 1 of 12 Disclaimer Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans or the plan may have broader or more limited benefits
Page 1 of 12 Disclaimer Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans or the plan may have broader or more limited benefits
Obesity and Lymphoedema : a clinical dilemma
 Obesity and Lymphoedema : a clinical dilemma Professor Christine Moffatt CBE Professor of Clinical Nursing Research & Nurse consultant Royal Derby Hospital Foundation Trust Lymphoedema Service Chair ILF
Obesity and Lymphoedema : a clinical dilemma Professor Christine Moffatt CBE Professor of Clinical Nursing Research & Nurse consultant Royal Derby Hospital Foundation Trust Lymphoedema Service Chair ILF
Looking after your diabetic foot ulcer
 Looking after your diabetic foot ulcer diabetes information and advice leaflet Emergency Action Plan FOOT ATTACK? If your foot is red, swollen or if you have breaks in the skin PHONE 07786250788 IMMEDIATELY.
Looking after your diabetic foot ulcer diabetes information and advice leaflet Emergency Action Plan FOOT ATTACK? If your foot is red, swollen or if you have breaks in the skin PHONE 07786250788 IMMEDIATELY.
Wound Healing Community Outreach Service
 Wound Healing Community Outreach Service Wound Management Education Plan January 2011 December 2011 Author: Michelle Gibb Nurse Practitioner Wound Management Wound Healing Community Outreach Service Institute
Wound Healing Community Outreach Service Wound Management Education Plan January 2011 December 2011 Author: Michelle Gibb Nurse Practitioner Wound Management Wound Healing Community Outreach Service Institute
Dr. Sibbald is: Company/ Agency Lecturers. Objectives Participants will:
 Dr. R. Gary Sibbald MD, FRCPC (Med, Derm), MACP, FAAD, M.Ed. Professor Of Medicine / Public Health U. Of Toronto Director Of The International Interprofessional Wound Care Course President Of The World
Dr. R. Gary Sibbald MD, FRCPC (Med, Derm), MACP, FAAD, M.Ed. Professor Of Medicine / Public Health U. Of Toronto Director Of The International Interprofessional Wound Care Course President Of The World
Diabetes - Foot Care
 Diabetes - Foot Care Introduction People with diabetes are more likely than others to have problems with their feet. These problems can lead to dangerous infections of the foot. Recognizing and treating
Diabetes - Foot Care Introduction People with diabetes are more likely than others to have problems with their feet. These problems can lead to dangerous infections of the foot. Recognizing and treating
Bunion (hallux valgus deformity) surgery
 Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
National Vascular Registry
 National Vascular Registry Bypass Patient Details Patient Consent* 2 Not Required If patient not consented: Date consent recorded / / (DD/MM/YYYY) Do not record NHS number, NHS number* name(s) or postcode.
National Vascular Registry Bypass Patient Details Patient Consent* 2 Not Required If patient not consented: Date consent recorded / / (DD/MM/YYYY) Do not record NHS number, NHS number* name(s) or postcode.
Lower Extremity Venous Disease (LEVD)
 Lower Extremity Venous Disease (LEVD) Lower Extremity Venous Disease (LEVD) Wounds Etiology Lower extremity venous leg ulcers are caused by chronic venous hypertension. Failure of valves in the veins or
Lower Extremity Venous Disease (LEVD) Lower Extremity Venous Disease (LEVD) Wounds Etiology Lower extremity venous leg ulcers are caused by chronic venous hypertension. Failure of valves in the veins or
Your Orthotics service is changing
 Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
Social History. Retired internist 2 scotches a day 50 pack-year history, stopped in 2005
 April 17, 2008 HPI 78 year old internist complains of 10 days of tingling and discomfort in left toes Unable to walk or sleep due to severe pain Pain worse with movement Redness in left toes Bilateral
April 17, 2008 HPI 78 year old internist complains of 10 days of tingling and discomfort in left toes Unable to walk or sleep due to severe pain Pain worse with movement Redness in left toes Bilateral
Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme
 Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme 48 BPJ Issue 39 What are the goals? The PHO Performance Programme
Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme 48 BPJ Issue 39 What are the goals? The PHO Performance Programme
Organization of Wound Care Nurses
 Organization of Wound Care Nurses www.woundcarenurses.org Lower extremity arterial disease refers to disorders affecting the leg arteries Also known as PVD, PAOD, and PAD Cardiovascular Disease (CVD) is
Organization of Wound Care Nurses www.woundcarenurses.org Lower extremity arterial disease refers to disorders affecting the leg arteries Also known as PVD, PAOD, and PAD Cardiovascular Disease (CVD) is
Definitions and criteria
 Several disciplines are involved in the management of diabetic foot disease and having a common vocabulary is essential for clear communication. Thus, based on a review of the literature, the IWGDF has
Several disciplines are involved in the management of diabetic foot disease and having a common vocabulary is essential for clear communication. Thus, based on a review of the literature, the IWGDF has
Your Orthotics service is changing
 Your Orthotics service is changing Important information for service users on changes effective from July 2015 Why is the service changing? As demand for the Orthotics service increases, Livewell Southwest
Your Orthotics service is changing Important information for service users on changes effective from July 2015 Why is the service changing? As demand for the Orthotics service increases, Livewell Southwest
The Diabetic Foot Latest Statistics
 The Diabetic Foot Latest Statistics There are 2.6 million people with diagnosed diabetes in the UK. There are predicted to be 500,000 who have the condition but are unaware of it. There are 11,859 in TH
The Diabetic Foot Latest Statistics There are 2.6 million people with diagnosed diabetes in the UK. There are predicted to be 500,000 who have the condition but are unaware of it. There are 11,859 in TH
Administer 60 Second Foot Screen Tool*
 Basic Foot Care Screen and Self Care Education Toolkit - Central West Diabetes egional Coordination Centre 2012 Foot Care Screening Flow Map Administer 60 Second Foot Screen Tool* Client Education Throughout
Basic Foot Care Screen and Self Care Education Toolkit - Central West Diabetes egional Coordination Centre 2012 Foot Care Screening Flow Map Administer 60 Second Foot Screen Tool* Client Education Throughout
People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy.
 Form: D-5821 Treat Your Feet: Foot care for people with diabetes People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy. Diabetes raises
Form: D-5821 Treat Your Feet: Foot care for people with diabetes People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy. Diabetes raises
10/9/2015. Differential Assessment of Lower Extremity Wounds. Disclosure Statement. Program Objectives
 3M 2015. All Rights Reserved 3M 2015. All Rights Reserved 2 3M 2015. All Rights Reserved 3 Differential Assessment of Lower Extremity Wounds Presented by: Lynn Peterson RN, BSN, CWOCN 3M Health Care November
3M 2015. All Rights Reserved 3M 2015. All Rights Reserved 2 3M 2015. All Rights Reserved 3 Differential Assessment of Lower Extremity Wounds Presented by: Lynn Peterson RN, BSN, CWOCN 3M Health Care November
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) GUIDELINES FOR THE USE OF COMPRESSION HOSIERY
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) GUIDELINES FOR THE USE OF COMPRESSION HOSIERY Do not include made to measure on the prescription; the community pharmacy/dispensing practice will endorse
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) GUIDELINES FOR THE USE OF COMPRESSION HOSIERY Do not include made to measure on the prescription; the community pharmacy/dispensing practice will endorse
Sores That Will Not Heal
 Sores That Will Not Heal Introduction Some sores have trouble healing on their own. Sores that will not heal are a common problem. Open sores that will not heal are also known as wounds or skin ulcers.
Sores That Will Not Heal Introduction Some sores have trouble healing on their own. Sores that will not heal are a common problem. Open sores that will not heal are also known as wounds or skin ulcers.
Nanogen Aktiv. Naz Wahab MD, FAAFP, FAPWCA Nexderma
 Nanogen Aktiv Naz Wahab MD, FAAFP, FAPWCA Nexderma Patient BM 75 y.o female with a history of Type 2 Diabetes, HTN, Hypercholesterolemia, Renal insufficiency, Chronic back Pain, who had undergone a L3-L4
Nanogen Aktiv Naz Wahab MD, FAAFP, FAPWCA Nexderma Patient BM 75 y.o female with a history of Type 2 Diabetes, HTN, Hypercholesterolemia, Renal insufficiency, Chronic back Pain, who had undergone a L3-L4
