Compression Bandaging Formulary 2017
|
|
|
- Baldwin Banks
- 6 years ago
- Views:
Transcription
1 Area Drugs Therapeutics Committee Compression Bandaging Formulary 2017 Compression Bandaging Formulary 2017 Developed by the NHS Fife Wound and Skin Care Forum (WSCF) Group Approved: October 2017 Review: October 2020
2 Contents Page Foreword/Disclaimer/Acknowledgements Introduction 4 Accountability and Responsibility / Scope of Practice.4 Patient Centred Involvement in Management Plan.5 General Information for Management of Leg Ulcers 6 Categories of Bandaging.6 Choice of compression system according to ABPI results.7 BANDAGING SYSTEMS Two Layer Kit (Latex Free) Full Compression Coban 2, Urgo K Reduced Compression, Coban 2 Lite, Urgo K2 reduced. 9 Multi Layer Kit (Latex Free) Full Compression Ultra Four, Profore.. 10 Reduced Compression Ultra Four RC, Profore Lite.. 10 Short Stretch Compression Bandage Comprilan, Actico 11 Orthopaedic Wadding 12 Compression Hosiery 13 Self managed compression systems.. 14 References / Further Reading 15 Appendix 1: Leg Ulcer Assessment Chart.16 Appendix 2: Patient Information Leaflet 18
3 Disclaimer NHS Fife Compression Bandaging Formulary 2017 Detailed discussion on the aetiology and pathophysiology of Chronic Venous Insufficiency is out with the scope of this Guideline. Clinicians are directed to best practice literature to guide them on the needs of the patient and the organisation prior to choosing, prescribing and applying compression bandaging. Guideline users should also be mindful that, as with any clinical guideline, recommendations may not be appropriate for use in all circumstances. Clearly, a limitation of any guideline is that it simplifies clinical decision making processes and recommendations. Decisions to adopt any particular recommendations must be made by the practitioner in the light of available resources, local services, policies and protocols. The particular patient s circumstances and wishes, available personnel and equipment, clinical experience of the practitioner and knowledge of more recent research findings, must all be considered and decisions must be clearly documented in the patient s notes. Acknowledgements The NHS Fife Wound and Skin Care Forum would like to acknowledge the contribution of both Fife Health and Social Care Partnership and NHS Fife Acute Services Division staff in the development of these Guidelines. The WSCF also thank Greater Glasgow Health Board for allowing us to use some of the information contained within their Guidelines. Foreword This formulary has been developed by the NHS Fife Wound and Skin Care Forum (WSCF). Input was also sought from experienced Community and Practice Nurses involved with the care of patients with chronic leg ulcers. As with the introduction of the Wound Formulary, compression bandaging systems will be advocated, which aim to meet the needs of the majority of patients with Chronic Venous Insufficiency (CVI). It is anticipated that the utilisation of this Guideline will lead to the following advantages: Facilitation of best practice Standardisation of use of products Cost Effectiveness Reduction of Waste It is understood that there are occasions when products which are not on formulary are required. If this is the case then an Exception Form should be completed (available on the ADTC website: and sent to the Prescribing Support Nurse Team Fife-UHB.Fifeprescribingsupportnurse@nhs.net 3
4 Introduction Chronic venous insufficiency (CVI) is a progressive circulatory disease causing stasis, venous hypertension, oedema and ulceration in the lower limbs. Graduated or sustained compression therapy is the recommended therapeutic intervention in the treatment and prevention of CVI. Over 80 % of lower leg ulcers are caused by venous insufficiency (Vishwanath, 2014). To achieve the most effective outcome, it is recommended that following an holistic assessment, including ankle brachial pressure index (ABPI), patients are placed into the highest level of therapeutic compression that can be safely and comfortably tolerated (Table1) Accountability and Responsibility / Scope of Practice Compression bandages should only be applied by those clinicians competent to do so. For this reason, clinicians must ensure that they are up to date with evidence based, best practice and that this is demonstrated in KSF profiles. Staff developing this skill should have this identified within their individual PDP as agreed by their line manager. 4
5 Patient-Centred Involvement in Management Plan Following a comprehensive, holistic assessment, clinicians involved in the management of CVI and leg ulcers should consider the following important factors in the determination of effective treatment pathways (Table2) Table 2: Factors to consider in managing patients with compression bandages (adapted from SIGN 120) ASSESSMENT Inform the patient: A full leg ulcer assessment will be carried out, including investigation of ABPI, to confirm whether treatment with compression is appropriate. Sign 120 recommends ABPI assessment if an ulcer fails to heal 4 weeks after presentation, with conventional treatment. Routine swabbing of leg ulcers is not recommended The patient will be asked if there are any known allergies, prior to product selection and application. TREATMENT To optimise concordance, inform the patient of the following: Compression treatment with bandages or hosiery is the single most important treatment for a leg ulcer. Bandages only require weekly changes unless conditions dictate otherwise. If condition fails to progress, specialist referral (i.e. vascular or dermatology) may be indicated. Ongoing and regular holistic reassessment is required. Recent recommendations suggest 6 monthly intervals, Wounds UK (2016) DIRECT PATIENT INVOLVEMENT Discuss with the patient the importance of: Exercise - Regular ankle /calf exercises Elevation of legs at rest Exploring sleeping pattern and encourage bed rest at night Skin care maintaining skin hydration using simple emollients e.g. QV cream All holistic assessments and ongoing management of leg ulceration should be recorded within a recognised Leg Ulcer Assessment Tool (Appendix 1) 5
6 General Bandaging Considerations NHS Fife Compression Bandaging Formulary 2017 Once an assessment is carried out to determine if compression bandaging is indicated, consideration of general factors relating to bandaging should be taken to help inform best practice for choice and application. (Table 3). Table 3 General Information for Management of CVI and Leg Ulcers Any bandaging of the lower limbs should start at the base of the toes, and extend to 2cm below the popliteal space, with either a spiral or a figure of eight application as per the manufacturer s instructions. This is to aid in the effective redistribution and reduction of oedema, and minimise the risk of potential bandage trauma (i.e. a tourniquet effect.) Mixed aetiology ulcers (e.g. in patients with diabetes, Peripheral Vascular Disease, Rheumatoid Arthritis) may require specialist investigation and referral to explore the most appropriate bandage choice. Light support bandages (e.g. Clinifast) can be used to contain primary dressings, absorb exudate and support the leg where compression is contraindicated. Table 4 Categories of Bandages Category 1: Short Stretch Inelastic Systems: Can be used for the management of leg ulcers and chronic oedema. Available as single components or as kits. e.g. Comprilan Category 2: Multi layer Elastic / Inelastic Bandage Kits: 2.1 Two Layer kits: Achieve the same levels of compression as four layer; may lead to greater concordance for patients and should therefore be the preferred choice. e.g. Coban 2, Urgo K2 2.2 Four-layer Elastic Kits: Have been historically used to provide full compression and may be more convenient for certain situations. e.g Robinson Ultra Four, Profore 4 layer 2.3 Single-layer High Compression Bandage: Used with specialist advice only, if multi layer combinations will not provide optimum treatment outcomes. For use with a padding layer, e.g. Softban. Category 3: Two-layer Reduced Elastic / Inelastic Bandage Kits: Used for patients with mixed aetiology. e.g Coban Lite, Urgo K2 Lite 6
7 GUIDELINE FOR CHOICE OF COMPRESSION ACCORDING TO RESULTS OF ABPI *ABPI between 0.6 and 0.8 REDUCED COMPRESSION 2 Layer system (Coban Light, KTwo Light) Or 3 Layer system (Profore Lite) ABPI between 0.8 and 1.3 FULL COMPRESSION 2 Layer system (Coban, KTwo) Or 4 Layer system (Robinsons Ultra 4) Compression bandaging is not suitable for patients with arterial ulcers and/or arterial disease. Caution should be used when applying reduced compression on patients with an *ABPI less than 0.8, and further advice sought from Vascular Nurse Specialist or Tissue Viability (Community) ABPI less than 0.6, urgent vascular referral recommended Patients with the following features should be referred to the appropriate specialist at an early stage. Suspicion of malignancy Peripheral arterial disease (ABPI<0.8) Rheumatoid/Vasculitis Suspected contact dermatitis or dermatitis resistant to topical steroids Diabetes Atypical distribution of ulcers Non healing ulcers Severe pain Please see Leg Ulcer Referral Pathway for further guidance (Appendix 3) 7
8 Two Layer Kit Latex Free Full Compression 1 st choice - Coban 2 2 nd choice -Urgo KTwo Description Coban 2 is a two-layer compression system, for venous leg ulcers, that delivers sustained, therapeutic compression. Comprises a latex-free foam padding layer and a latex-free, cohesive, compression bandage. Once applied, the two layers bond to form a single-layer bandage. Can be worn for up to seven days. UrgoKTwo is a two-layer bandage system combining elastic and inelastic components that work together to provide sustained graduated compression for up to seven days. The first layer, KTech, is the inelastic component providing compression, absorbency and massage effect. KPress, the second layer, is an elastic, cohesive bandage that keeps the system in place and delivers additional compression to achieve therapeutic pressures and maintain resting pressures. UrgoKTwo donates an average pressure of 40mmHg at the ankle. Indications For the treatment of venous leg ulcers, venous oedema and lymphoedema. Contra-indications Arterial disease (ABPI <0.8). Diabetic microangiopathy, ischaemic phlebitis and septic thrombosis. Allergy to any of the components. Ulceration caused by infection. The systems are designed to be used as a kit and should not be used with other wadding or bandages. Ankle Circumference Drug Tariff Price Sept2017 (Each) Coban 2 (3M) One size 8.24 UrgoKTwo Latex Free (Urgo) 18-25cm (10cm) 25-32cm (10cm)
9 Two Layer Kit Latex Free Reduced Compression 1 st choice -Coban 2 Lite 2 nd choice - UrgoKTwo Reduced Description Coban 2 Lite is a two-layer compression system, for venous leg ulcers, designed to achieve sustained, therapeutic compression with reduced sub-bandage resting pressures. Comprises a latex-free foam padding layer and a latex-free, cohesive, compression bandage. Once applied, the two layers bond to form a single-layer bandage. Can be worn for up to seven days. UrgoKTwo Reduced is a two-layer bandage system combining elastic and inelastic components that work together to provide sustained graduated compression for up to seven days. The first layer, KTech Reduced, is the inelastic component providing compression, absorbency and massage effect. KPress, the second layer, is an elastic, cohesive bandage that keeps the system in place and delivers additional compression to achieve therapeutic pressures and maintain resting pressures. UrgoKTwo Reduced donates an average pressure of 20mmHg at the ankle. Indications For the management of mixed aetiology leg ulcers, lymphoedema and venous leg ulcers where patients cannot tolerate full compression or where full compression is otherwise inappropriate. Contra-indications Must not be applied to patients with an ABPI <0.6. The systems are designed to be used as a kit and should not be used with other wadding or bandages. Coban 2 Lite (3M) Ankle Circumference One size Drug Tariff Price Sept 2017 (Each) 8.24 UrgoKTwo Reduced Latex Free (Urgo) 18-25cm (10cm)
10 Mutli Layer Kit Latex Free Full Compression 1 st choice - Ultra Four 2 nd choice - Profore - Description Ultra Four is a latex-free multilayer compression bandage system. Components: Ultra Soft wadding; Ultra Lite; Ultra Plus; Ultra Fast. Profore is a latex-free multilayer compression bandaging system. Profore #1 Latex-free (10cmx3.5cm); Profore #2 Latex-free (10cmx4.5m); Profore #3 Latex-free (10cmx8.7m); Profore #4 Latex-free (10cmx2.5m); Profore + Latexfree (10cmx3m) Indications For the management of venous leg ulcers and associated conditions. Contra-indications Four layer bandage systems are not suitable for patients with arterial ulcers and arterial disease. Do not use on patients with an ABPI of <0.8. Do not use on diabetic patients with advanced small vessel disease. For details of precautions please contact supplier. Ultra Four (Robinson) Profore Latex Free (Smith and Nephew) Ankle Circumference Up to 18cm 18-25cm 18-25cm Drug Tariff Price Sept 2017 (Each) Multi Layer Kit Latex Free Reduced Compression 1 st choice - Ultra Four RC - 2 nd choice - Profore Lite - Description Ultra Four RC is a latex-free multilayer compression bandage system. Components: Ultra Soft wadding; Ultra Lite; Ultra Fast. Profore Lite is a latex-free multilayer compression bandaging system. Profore #1 Latex-free (10cmx3.5cm); Profore #2 Latex-free (10cmx4.5m); Profore #4 Latex-free (10cmx2.5m). 10
11 Indications For the management of mixed aetiology leg ulcers, lymphoedema and venous leg ulcers where patients cannot tolerate full compression or where full compression is otherwise inappropriate. Contra-indications Must not be applied to patients with an ABPI <0.6. Ankle Circumference Drug Tariff Price Sept 2017 (Each) Ultra Four RC 18-25cm 4.14 (Robinson) Profore Lite Latex Free 18+cm 6.05 (Smith and Nephew) Short Stretch Compression Comprilan (Non Cohesive, Latex Free) Actico (Cohesive, Contains Latex) Orthopaedic Wadding layer should be ordered separately (See page 11) Do not confuse with Actico 2C Multi layer bandaging kit. Description Inelastic short stretch compression bandage Indications Varicosis, chronic venous insufficiency, venous leg ulcers, thrombophlebitis, deep venous thrombosis, after venous surgery, primary and secondary lymphoedema. Contra-indications Advanced peripheral arterial occlusive disease, decompensated cardiac insufficiency, septic phlebitis; phlegmasia coerulea dolens (painful blue oedema, caused by an uncommon, severe form of deep venous thrombosis). N.B LAYER OF ORTHOPAEDIC WADDING MUST BE APPLIED UNDER SHORT STRETCH BANDAGE (See p11) Size Drug Tariff Price Sept 2017 (Each) Actico 10cm x 6m 3.41 (Activa) Comprilan 10cm x 5m 3.44 (Paul Hartman) 11
12 Orthopaedic Wadding 1 st choice: 2 nd choice: 1 st choice: 2 nd choice: NHS Fife Compression Bandaging Formulary 2017 Softban Natural/Synthetic- ADC only Lantor- ADC only UltraSoft- Prescribing only K-Soft- Prescribing only Description Softban Natural - soft, natural viscose, protective orthopaedic padding. Softban Eco- synthetic, protective orthopaedic padding. Indications Used to reduce the effects of compression bandages or orthopaedic casting materials on the skin. May also be use to reshape the leg around the calf and ankle, to ensure correct pressure are achieved when applying multilayer compression and to protect the bony prominences. Size (2.75m lengths) (Pack Size) Drug Tariff Price - Sept 2017 (Each) Natural Softban Natural (BSN) 10cm(12) ADC only 15cm(12) Synthetic Softban Eco (BSN) 7.5cm(12) ADC only 10cm(12) 15cm(12) For Prescribing only Ultra Soft (Robinsons) 10cm x 3.5m 0.39 Self Management Compression Systems With an increase in chronic leg ulceration anticipated in the coming years, related to an ageing population, the use of self management compression systems will increase. These systems should be considered when patients are keen to be more involved with their leg ulcer care, and are able to manage the application of the system. They will be particularly appropriate for younger patients and can improve the quality of life of the patient, with less involvement of nursing staff, particularly if the patient is working. Self management compression options also help in the management of skin problems associated with venous hypertension, e.g. varicose eczema and hyperkeratosis, by allowing for daily access to cleanse the skin and subsequent application of emollients or topical steroid therapy. All Wales Tissue Viability Nurses Forum (2014). 12
13 When considering use of these systems, please contact the vascular nurse specialist for further advice and support. The following systems are available on GP10:- Juxtacures, Medi UK - Farrow Wrap BSN Medical ReadyWrap - Activa Healthcare Short video guidance on how to measure and apply the compression systems, are available on the company websites. Compression Hosiery Conservative treatment of venous disease is aimed at improving the condition by means of compression and exercise therapy. Compression hosiery presses the distended veins together so that the venous valves can close again, thus preventing the blood from flowing in the wrong direction namely away from the heart. The necessary compression can be provided by using compression stockings or tights, which prevent new varicose veins from forming, and keep existing venous disease under control. Untreated venous disease will continue to progress and may become chronic. This is why it is important that patients are advised that they should wear compression stockings to prevent further deterioration, or recurrence of venous leg ulcers. Indications for use: 14-17mmHg Class 1 GP10 Provides light compression and should be used for superficial or early varicose veins and swollen ankles (e.g. during pregnancy) 18-24mmHg - Class 2 GP10 Provides medium compression and should be used in medium severity varicose veins and mild oedema. Can be used for the treatment of, and to prevent the recurrence of venous leg ulcers mmHg Class 3 GP10 Provides strong compression and should be used for severe varicose veins and gross oedema. Used for chronic venous insufficiency, and in the treatment and prevention of venous leg ulcers. (Please note above are British Standard Classifications of compression hosiery as used in the Scottish Drug Tariff. European Classifications can be found within the 2015 Wounds UK Best Practice Statement on Compression Hoisery). Contraindications Significant arterial disease Current acute inflammatory episode Acute deep vein thrombosis Patient with diabetes or rheumatoid arthritis, unless after specialist referral and under supervision, due to risk of micro vascular disease Congestive heart failure, as compression could lead to cardiac overload 13
14 Sensory disorders of the limb i.e. peripheral neuropathy Known sensitivity to the fabric Please refer to the Wounds UK Best Practice Statement Compression Hosiery (2015) for further information. Made to measure versus standard hosiery Where possible, every effort should be made to use standard size hosiery, as there can be a significant cost difference associated with made to measure stockings. In cases where the leg is an unusual shape, or the patient has gross lymphoedema, made to measure stockings may be used. Legs should be measured and hosiery prescribed according to each manufacturer s own measuring guide, as sizes vary according to manufacturer. Every effort must be made to reduce oedema before hosiery is measured. (Best Practice Statement Compression hosiery, 2015) Leg Ulcer Hosiery Kits There are patients who have difficulty applying their stockings, or are unable to tolerate compression bandaging, and this should be considered as part of their overall assessment. As long as exudate levels are low, concordance may often be improved with the use of leg ulcer hosiery kits. These kits consist of a liner stocking, which makes it easier to apply the compression stocking on top. Each kit contains one stocking and two liner stockings. There are companies who also make a leg ulcer kit with a zip in the compression stocking. Please refer to the BNF section on compression hosiery for further information. Accessories A variety of accessories are available for patients, to help them with managing their hosiery. Please refer to the BNF section on compression garments and accessories. N.B In normal circumstances two pairs of stockings should last 6 months, therefore patients should be prescribed no more than four pairs per year. 14
15 Table 4: Recommended reading to complement this formulary, and to support patient centred care: (this is for guidance only and not an exhaustive list) 1 All Wales Tissue Viability Nurses Forum (2014) All Wales guidance for the management of hyperkeratosis of the lower limb. Wounds UK, London 2 Moffat CJ, Edwards L, Collier M, et al (2008) A randomized controlled 8 week crossover clinical evaluation of the 3M Coban 2 layer Compression System versus Profore to evaluate the product performance in patients with venous leg ulcers, International Wound journal, Vol 5, Issue 2, May, pages SIGN 120 (2010) Management of chronic venous leg ulcers 4 Vishwanath V, (2014) Quality of Life: Venous Leg Ulcers. Indian Dermatol Online J. July-Sep; 5(3): Weller C, Evans S (2012) Venous leg ulcer management in general practice: Practice nurses and evidence based guidelines, Australian Family Physician, Vol. 41, No.5, May, , Wounds UK best Practice Statement (2015) Compression hosiery (2 nd edn) London: Wounds UK. Available to download from 7 Wounds UK Best Practice Statement (2016): Holistic Management of Venous Leg Ulceration. London: Wounds UK. Available to download from: 8 Young T, et al, Cleanse and compress unique combinations to treat venous leg ulceration. The clinician and patient perspective, Journal of Community Nursing Supplement, (2017), Vol 31, No. 3 15
16 APPENDIX 1 Leg Ulcer Assessment Form 16
17 17
18 LEG ULCER ASSESSMENT SHEET N Compresssion bandage patient info 18
PRODIGY Quick Reference Guide
 PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS
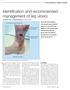 Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS thickened skin, lipodermatosclerosis skin stained haemosiderin shallow ulcer irregular shape Our
Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS thickened skin, lipodermatosclerosis skin stained haemosiderin shallow ulcer irregular shape Our
HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING
 HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING Alison Hopkins is Clinical Nurse Specialist, East London Wound Healing Centre, Tower Hamlets Primary Care Trust Compression therapy is essential
HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING Alison Hopkins is Clinical Nurse Specialist, East London Wound Healing Centre, Tower Hamlets Primary Care Trust Compression therapy is essential
Reality TV Managing patients in the real world. Wounds UK Harrogate 2009
 Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
JoyTickle, Tissue Viability Nurse Specialist, Shropshire Community Health NHS Trust
 Lower limb Ulceration Pathway: Leanne Atkin, Lecturer practitioner/vascular Nurse Specialist, School of Human and Health Sciences, University of Huddersfield and Mid Yorkshire NHS Trust, E mail: l.atkin@hud.ac.uk
Lower limb Ulceration Pathway: Leanne Atkin, Lecturer practitioner/vascular Nurse Specialist, School of Human and Health Sciences, University of Huddersfield and Mid Yorkshire NHS Trust, E mail: l.atkin@hud.ac.uk
Wound Management / Bandages - Cohesive
 Wound Management / Bandages - Cohesive 3M Coban Self-Adherent Wrap The self-adherent wrap that sticks to itself without the need for adhesives, clips or pins. Can be used to secure, compress and support
Wound Management / Bandages - Cohesive 3M Coban Self-Adherent Wrap The self-adherent wrap that sticks to itself without the need for adhesives, clips or pins. Can be used to secure, compress and support
West Gloucestershire Primary Care Trust Community Nursing Service. Leg Ulcer Audit. Gloucestershire Primary & Community Care Audit Group
 West Gloucestershire Primary Care Trust Community Nursing Service Leg Ulcer Audit 2006 Gloucestershire Primary & Community Care Audit Group Contents Page number Background 3 Audit Aims 4 Methodology 4
West Gloucestershire Primary Care Trust Community Nursing Service Leg Ulcer Audit 2006 Gloucestershire Primary & Community Care Audit Group Contents Page number Background 3 Audit Aims 4 Methodology 4
Managing venous leg ulcers and oedema using compression hosiery
 Managing venous leg ulcers and oedema using compression hosiery Tickle J (2015) Managing venous leg ulcers and oedema using compression hosiery. Nursing Standard. 30, 8, 57-63. Date of submission: July
Managing venous leg ulcers and oedema using compression hosiery Tickle J (2015) Managing venous leg ulcers and oedema using compression hosiery. Nursing Standard. 30, 8, 57-63. Date of submission: July
GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND
 GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND AIM To provide evidence based principles for the measurement of Ankle Brachial Pressure Index (ABPI) using a BACKGROUND/EVIDENCE
GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND AIM To provide evidence based principles for the measurement of Ankle Brachial Pressure Index (ABPI) using a BACKGROUND/EVIDENCE
All WALES LYMPHOEDEMA GUIDANCE:
 All WALES LYMPHOEDEMA GUIDANCE: Lymphoedema Vascular Assessment Policy (Toe Brachial Pressure Index / TBPI) April 2013 Created by the All Wales Lymphoedema Service Leads 1 Background The presence of peripheral
All WALES LYMPHOEDEMA GUIDANCE: Lymphoedema Vascular Assessment Policy (Toe Brachial Pressure Index / TBPI) April 2013 Created by the All Wales Lymphoedema Service Leads 1 Background The presence of peripheral
TREATING LOWER LIMB LYMPHOEDEMA WITH COMPRESSION BANDAGING
 TREATING LOWER LIMB LYMPHOEDEMA WITH COMPRESSION BANDAGING Debra Doherty is Senior Lecturer, Centre for Research and implementation of Clinical Practice, Thames Valley University Multilayer continues to
TREATING LOWER LIMB LYMPHOEDEMA WITH COMPRESSION BANDAGING Debra Doherty is Senior Lecturer, Centre for Research and implementation of Clinical Practice, Thames Valley University Multilayer continues to
Part III (b) Bandages
 Part III (b) Bandages 1. The term bandage used in a prescription form without qualification is to be interpreted to mean an Open-Wove Bandage, Type 1 BP 5cm x 5m. All bandages supplied are to be of the
Part III (b) Bandages 1. The term bandage used in a prescription form without qualification is to be interpreted to mean an Open-Wove Bandage, Type 1 BP 5cm x 5m. All bandages supplied are to be of the
Part III (b) Bandages. Contents:
 Part III (b) Bandages 1. The term bandage used in a prescription form without qualification is to be interpreted to mean an Open-Wove Bandage, Type 1 BP 5cm x 5m. All bandages supplied are to be of the
Part III (b) Bandages 1. The term bandage used in a prescription form without qualification is to be interpreted to mean an Open-Wove Bandage, Type 1 BP 5cm x 5m. All bandages supplied are to be of the
easy made UrgoKTwo Compression Bandage System Introduction
 PRODUCTS FOR PRACTICE UrgoKTwo Compression Bandage System made easy Volume 4 Issue 1 February 2013 www.woundsinternational.com Introduction Compression therapy has been considered the gold standard of
PRODUCTS FOR PRACTICE UrgoKTwo Compression Bandage System made easy Volume 4 Issue 1 February 2013 www.woundsinternational.com Introduction Compression therapy has been considered the gold standard of
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) GUIDELINES FOR THE USE OF COMPRESSION HOSIERY
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) GUIDELINES FOR THE USE OF COMPRESSION HOSIERY Do not include made to measure on the prescription; the community pharmacy/dispensing practice will endorse
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) GUIDELINES FOR THE USE OF COMPRESSION HOSIERY Do not include made to measure on the prescription; the community pharmacy/dispensing practice will endorse
Compression therapy can
 What are the benefits of using cohesive inelastic compression bandages in the community? Compression therapy can play a vital role in improving the quality of life for those with chronic venous insufficiency,
What are the benefits of using cohesive inelastic compression bandages in the community? Compression therapy can play a vital role in improving the quality of life for those with chronic venous insufficiency,
Venous and lymphatic disease
 Welcome to JCN s learning zone. By reading the article in each issue, you can learn all about the key principles of subjects that are vital to your role as a community nurse. Once you have read the article,
Welcome to JCN s learning zone. By reading the article in each issue, you can learn all about the key principles of subjects that are vital to your role as a community nurse. Once you have read the article,
Providing optimal sub-bandage pressure in compression therapy
 Providing optimal sub-bandage pressure in compression therapy Simon Barrett If left untreated, leg ulcers can descend into a cycle of tissue breakdown and healing, resulting in chronic venous leg ulcers,
Providing optimal sub-bandage pressure in compression therapy Simon Barrett If left untreated, leg ulcers can descend into a cycle of tissue breakdown and healing, resulting in chronic venous leg ulcers,
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Jackie Stephen-Haynes. Compression therapies- Does. Jackie Stephen-Haynes 2011
 Jackie Stephen-Haynes Compression therapies- Does compression meet the patients needs? 2011 Aims For practitioner to be able to consider compression options and the impact for the patient Leg Ulcer Definition
Jackie Stephen-Haynes Compression therapies- Does compression meet the patients needs? 2011 Aims For practitioner to be able to consider compression options and the impact for the patient Leg Ulcer Definition
Promoting best practice in leg ulcer management
 Promoting best practice in leg ulcer management Sylvie Hampton MA BSc (Hons) DpSN RGN Independent Tissue Viability Consultant Nurse Leg Ulcers - What are the causes? Chronic leg ulcers are defined as those
Promoting best practice in leg ulcer management Sylvie Hampton MA BSc (Hons) DpSN RGN Independent Tissue Viability Consultant Nurse Leg Ulcers - What are the causes? Chronic leg ulcers are defined as those
It is estimated that 730,000 patients suffer with
 The leg ulceration pathway: impact of implementation Leg ulceration continues to be a common cause of suffering for patients and the treatment of these patients continues to place a significant burden
The leg ulceration pathway: impact of implementation Leg ulceration continues to be a common cause of suffering for patients and the treatment of these patients continues to place a significant burden
4-layer compression bandaging system (includes microbe binding wound contact layer) Latex-free, 4-layer compression bandaging system
 JOBST Comprifore JOBST Comprifore at a glance: provides effective levels of sustained graduated compression provides built in safety and ease of application Insures compliance and maximum healing for cost
JOBST Comprifore JOBST Comprifore at a glance: provides effective levels of sustained graduated compression provides built in safety and ease of application Insures compliance and maximum healing for cost
The Management of Lower Limb Oedema. Catherine Hammond CNS/CNE 2018
 The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
The Juxta CURES adjustable compression system for treating venous leg ulcers
 Medtech innovation The Juxta CURES adjustable compression system for treating Published: 25 March 2015 Summary The Juxta CURES system provides adjustable compression management of and is designed to be
Medtech innovation The Juxta CURES adjustable compression system for treating Published: 25 March 2015 Summary The Juxta CURES system provides adjustable compression management of and is designed to be
In line with the professional requirements of the Nursing and Midwifery Council
 STANDARDS OF PRACTICE FOR LEG CLUB STAFF October 2010 Foreword In line with the professional requirements of the Nursing and Midwifery Council Code: Standards of conduct, performance and ethics for nurses
STANDARDS OF PRACTICE FOR LEG CLUB STAFF October 2010 Foreword In line with the professional requirements of the Nursing and Midwifery Council Code: Standards of conduct, performance and ethics for nurses
CLINICAL PROTOCOL - VENOUS LEG ULCER MANAGEMENT. SCOPE: Western Australia. Clinical Protocol for Venous Leg Ulcer Management
 CLINICAL PROTOCOL - VENOUS LEG ULCER MANAGEMENT SCOPE: Western Australia Clinical Protocol for Venous Leg Ulcer The following protocol outlines the sequence of events in the assessment and management of
CLINICAL PROTOCOL - VENOUS LEG ULCER MANAGEMENT SCOPE: Western Australia Clinical Protocol for Venous Leg Ulcer The following protocol outlines the sequence of events in the assessment and management of
Priorities Forum Statement
 Priorities Forum Statement Number 9 Subject Varicose Vein Surgery Date of decision September 2014 Date refreshed March 2017 Date of review September 2018 Relevant OPCS codes: L841-46, L848-49, L851-53,
Priorities Forum Statement Number 9 Subject Varicose Vein Surgery Date of decision September 2014 Date refreshed March 2017 Date of review September 2018 Relevant OPCS codes: L841-46, L848-49, L851-53,
Venous Insufficiency Ulcers. Patient Assessment: Superficial varicosities. Evidence of healed ulcers. Dermatitis. Normal ABI.
 Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
Improving customer care in compression hosiery
 Improving customer care in compression hosiery Introduction Within the modern NHS, the Pharmacy Team provides the front line service that most patients have contact with. Compression hosiery has a key
Improving customer care in compression hosiery Introduction Within the modern NHS, the Pharmacy Team provides the front line service that most patients have contact with. Compression hosiery has a key
The key to successful. Impact of compression therapy on chronic. venous disease
 Acute WOUNDS Impact of compression therapy on chronic venous disease Chronic venous disease is known to affect up to 50% of the adult population and it is estimated that 1% of individuals will suffer from
Acute WOUNDS Impact of compression therapy on chronic venous disease Chronic venous disease is known to affect up to 50% of the adult population and it is estimated that 1% of individuals will suffer from
Treating your leg ulcer
 Page 1 of 7 Treating your leg ulcer Introduction The information in this leaflet will answer many questions you may have about your leg ulcer. If you have any further questions about your condition or
Page 1 of 7 Treating your leg ulcer Introduction The information in this leaflet will answer many questions you may have about your leg ulcer. If you have any further questions about your condition or
NHS Greater Glasgow & Clyde Compression Therapy Formulary: Hosiery and Bandages Review date: November 2017
 NHS Greater Glasgow & Clyde Compression Therapy Formulary: Hosiery and Bandages Review date: November 2017 Primary Care and Acute Joint Formulary The emphasis of this formulary is on the use of hosiery
NHS Greater Glasgow & Clyde Compression Therapy Formulary: Hosiery and Bandages Review date: November 2017 Primary Care and Acute Joint Formulary The emphasis of this formulary is on the use of hosiery
Leg Ulcer Policy. Control Aseptic Technique Policy NSCP Wound Formulary Consent Policy Clinical photography. Safe Caring Effective Responsive Well Led
 Leg Ulcer Policy Author(s) & Designation Lead Clinician if appropriate In consultation with To be read in association with Ratified by Sarah Williams, Tissue Viability Specialist Nurse Mary Lewis, Director
Leg Ulcer Policy Author(s) & Designation Lead Clinician if appropriate In consultation with To be read in association with Ratified by Sarah Williams, Tissue Viability Specialist Nurse Mary Lewis, Director
Wounds UK. Development and evaluation of a hosiery selection algorithm in an acute and community healthcare NHS Trust
 Reprint Volume 9 Issue 4 Wounds UK Development and evaluation of a hosiery selection algorithm in an acute and community healthcare NHS Trust Authors Jackie Stephen-Haynes, Rachael Sykes RESEARCH AND
Reprint Volume 9 Issue 4 Wounds UK Development and evaluation of a hosiery selection algorithm in an acute and community healthcare NHS Trust Authors Jackie Stephen-Haynes, Rachael Sykes RESEARCH AND
Use of a velcro wrap system in the management of lower limb lymphoedema/chronic oedema. Sue Lawrance
 Use of a velcro wrap system in the management of lower limb lymphoedema/chronic oedema Sue Lawrance Abstract Lymphoedema and chronic lower limb oedema are conventionally treated with multi-layer bandaging,
Use of a velcro wrap system in the management of lower limb lymphoedema/chronic oedema Sue Lawrance Abstract Lymphoedema and chronic lower limb oedema are conventionally treated with multi-layer bandaging,
Venous leg ulcers: importance of early assessment and intervention for long-term success
 Venous leg ulcers: importance of early assessment and intervention for long-term success Introduction A venous leg ulcer (VLU) can be defined as: an open lesion between the knee and ankle joint that occurs
Venous leg ulcers: importance of early assessment and intervention for long-term success Introduction A venous leg ulcer (VLU) can be defined as: an open lesion between the knee and ankle joint that occurs
 More information about the Comfi range of woundcare solutions and helpful information and tools for healthcare professionals can be found on our website at www.comfi-range.com Synergy Health (UK) Ltd,
More information about the Comfi range of woundcare solutions and helpful information and tools for healthcare professionals can be found on our website at www.comfi-range.com Synergy Health (UK) Ltd,
PDP SELF-TEST QUESTIONNAIRE LEG ULCERS. Ulcer Full thickness loss of epidermis and some dermis, which will heal with scarring.
 Number 5 CORE TUTORIALS IN DERMATOLOGY FOR PRIMARY CARE PDP SELF-TEST QUESTIONNAIRE METEOR CRATER, ARIZONA, USA LEG ULCERS UPDATED PDP SELF-TEST QUESTIONNAIRE SEPTEMBER 2013 Ulcer Full thickness loss of
Number 5 CORE TUTORIALS IN DERMATOLOGY FOR PRIMARY CARE PDP SELF-TEST QUESTIONNAIRE METEOR CRATER, ARIZONA, USA LEG ULCERS UPDATED PDP SELF-TEST QUESTIONNAIRE SEPTEMBER 2013 Ulcer Full thickness loss of
BANDAGES: SELECTION AND APPLICATION POLICY
 BANDAGES: SELECTION AND APPLICATION POLICY DOCUMENT CONTROL: Version: 2 Ratified by: Clinical Quality Standards Group Date ratified: 4 August 2015 Name of originator/author: Clinical Nurse Specialist in
BANDAGES: SELECTION AND APPLICATION POLICY DOCUMENT CONTROL: Version: 2 Ratified by: Clinical Quality Standards Group Date ratified: 4 August 2015 Name of originator/author: Clinical Nurse Specialist in
Wound Healing Community Outreach Service
 Wound Healing Community Outreach Service Wound Management Education Plan January 2011 December 2011 Author: Michelle Gibb Nurse Practitioner Wound Management Wound Healing Community Outreach Service Institute
Wound Healing Community Outreach Service Wound Management Education Plan January 2011 December 2011 Author: Michelle Gibb Nurse Practitioner Wound Management Wound Healing Community Outreach Service Institute
Four Layer Versus Actico Cohesive Short Stretch Bandage Background
 Four Layer Versus Actico Cohesive Short Stretch Bandage Background Cochrane Systematic Review 6/2/01 "Five small studies found no difference in healing between multi-layer high compression (4-layer bandage
Four Layer Versus Actico Cohesive Short Stretch Bandage Background Cochrane Systematic Review 6/2/01 "Five small studies found no difference in healing between multi-layer high compression (4-layer bandage
Understanding compression stockings (hosiery) Leg Ulcer Management Team Patient Information Leaflet
 Understanding compression stockings (hosiery) Leg Ulcer Management Team Patient Information Leaflet Introduction Your leg ulcer clinic coordinator, nurse or health professional has recommended that you
Understanding compression stockings (hosiery) Leg Ulcer Management Team Patient Information Leaflet Introduction Your leg ulcer clinic coordinator, nurse or health professional has recommended that you
pat hways Medtech innovation briefing Published: 25 March 2015 nice.org.uk/guidance/mib25
 pat hways The Juxta CURES adjustable compression system for treating venous leg ulcers Medtech innovation briefing Published: 25 March 2015 nice.org.uk/guidance/mib25 Summary The Juxta CURES system provides
pat hways The Juxta CURES adjustable compression system for treating venous leg ulcers Medtech innovation briefing Published: 25 March 2015 nice.org.uk/guidance/mib25 Summary The Juxta CURES system provides
Clinical Guidance on the treatment of Leg Ulcers January 2013
 Clinical Guidance on the treatment of Leg Ulcers January 2013 Author(S) & Linda Davies Tissue Viability Nurse Designation: Lead Clinician (if Linda Davies appropriate): In consultation with: Linda Davies
Clinical Guidance on the treatment of Leg Ulcers January 2013 Author(S) & Linda Davies Tissue Viability Nurse Designation: Lead Clinician (if Linda Davies appropriate): In consultation with: Linda Davies
Rosidal TCS Trust our strength
 Rosidal TCS Trust our strength effective, comfortable, safe compression www.lohmann-rauscher.us Rosidal TCS provides effective compression The two components of Rosidal TCS work together to deliver effective
Rosidal TCS Trust our strength effective, comfortable, safe compression www.lohmann-rauscher.us Rosidal TCS provides effective compression The two components of Rosidal TCS work together to deliver effective
JOBST FARROWWRAP LYMPHOEDEMA MANAGEMENT MADE SIMPLE THROUGH ADJUSTABLE SHORT-STRETCH WRAP SOLUTIONS THERAPIES. HAND IN HAND.
 JOBST FARROWWRAP LYMPHOEDEMA MANAGEMENT MADE SIMPLE THROUGH ADJUSTABLE SHORT-STRETCH WRAP SOLUTIONS THERAPIES. HAND IN HAND. HOW DO YOU STRIKE THE RIGHT BALANCE BETWEEN BOTH YOUR PATIENT S MEDICAL NEEDS
JOBST FARROWWRAP LYMPHOEDEMA MANAGEMENT MADE SIMPLE THROUGH ADJUSTABLE SHORT-STRETCH WRAP SOLUTIONS THERAPIES. HAND IN HAND. HOW DO YOU STRIKE THE RIGHT BALANCE BETWEEN BOTH YOUR PATIENT S MEDICAL NEEDS
Prevention and Management of Leg Ulcers
 EWMA Educational Development Programme Curriculum Development Project Education Module: Prevention and Management of Leg Ulcers Latest revision: October 2015 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME
EWMA Educational Development Programme Curriculum Development Project Education Module: Prevention and Management of Leg Ulcers Latest revision: October 2015 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME
Between 1% and 2% of the. Juxta CURES : when is it appropriate?
 Juxta CURES : when is it appropriate? Compression therapy is the optimum treatment for venous leg ulcers (Nelson, 2011). Through case study evidence, this article challenges the view that the current gold
Juxta CURES : when is it appropriate? Compression therapy is the optimum treatment for venous leg ulcers (Nelson, 2011). Through case study evidence, this article challenges the view that the current gold
Level 2 Leg Ulcer Management Service. Service Level Agreement Background. Contents:
 Level 2 Leg Ulcer Management Service Service Level Agreement 2016-2019 Contents: 1. Background to Leg Ulcer Management Service 2. Service Details 3. Accreditation 4. Service Standards 5. Finance Details
Level 2 Leg Ulcer Management Service Service Level Agreement 2016-2019 Contents: 1. Background to Leg Ulcer Management Service 2. Service Details 3. Accreditation 4. Service Standards 5. Finance Details
VTE Prophylaxis. NEW NICE guidance. Providing venous thromboembolism (VTE) prophylaxis to all at risk hospital patients
 NEW NICE guidance NICE guidance (MTG19) supports the use of the geko device for people who have a high risk of VTE and for whom pharmacological or other mechanical methods of VTE prevention are impractical
NEW NICE guidance NICE guidance (MTG19) supports the use of the geko device for people who have a high risk of VTE and for whom pharmacological or other mechanical methods of VTE prevention are impractical
Leg Ulcer Clinic Audit
 Gloucestershire PCT Community Nursing Service Leg Ulcer Clinic Audit 2007 Contents Page number Background 3 Audit Aims 4 Methodology 4 Results 5-11 Discussion 13-15 Action Plan References 2 Background
Gloucestershire PCT Community Nursing Service Leg Ulcer Clinic Audit 2007 Contents Page number Background 3 Audit Aims 4 Methodology 4 Results 5-11 Discussion 13-15 Action Plan References 2 Background
PDP SELF-TEST QUESTIONNAIRE
 Number 5 CORE TUTORIALS IN DERMATOLOGY FOR PRIMARY CARE PDP SELF-TEST QUESTIONNAIRE METEOR CRATER, ARIZONA, USA LEG ULCERS Ulcer Full thickness loss of epidermis and some dermis, which will heal with scarring
Number 5 CORE TUTORIALS IN DERMATOLOGY FOR PRIMARY CARE PDP SELF-TEST QUESTIONNAIRE METEOR CRATER, ARIZONA, USA LEG ULCERS Ulcer Full thickness loss of epidermis and some dermis, which will heal with scarring
Wound debridement: guidelines and practice to remove barriers to healing
 Wound debridement: guidelines and practice to remove barriers to healing Learning objectives 1. The burden of wounds and the impact to the NHS 2. Understand what debridement is and why it is needed 3.
Wound debridement: guidelines and practice to remove barriers to healing Learning objectives 1. The burden of wounds and the impact to the NHS 2. Understand what debridement is and why it is needed 3.
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
VTE Prophylaxis. NICE guidance. Providing venous thromboembolism (VTE) prophylaxis to all at risk hospital patients
 NICE guidance NICE guidance (MTG19) supports the use of the geko device for people who have a high risk of VTE and for whom pharmacological or other mechanical methods of VTE prevention are impractical
NICE guidance NICE guidance (MTG19) supports the use of the geko device for people who have a high risk of VTE and for whom pharmacological or other mechanical methods of VTE prevention are impractical
made easy n Proven clinical effectiveness n Enhances calf muscle pump function
 PRODUCTS FOR PRACTICE 3M Coban 2 Compression made easy Volume 2 Issue 1 February 2011 www.woundsinternational.com Introduction The 3M TM Coban TM 2 Compression System is designed to address some of the
PRODUCTS FOR PRACTICE 3M Coban 2 Compression made easy Volume 2 Issue 1 February 2011 www.woundsinternational.com Introduction The 3M TM Coban TM 2 Compression System is designed to address some of the
Categorisation of Wound Care and Associated Products
 Categorisation of Wound Care and Associated Products Version 9 March 2018 Surgical Dressing Manufacturers Association 2018 TAPES AND TRADITIONAL DRESSINGS Wound Dressings Swabs Taping Traditional Wound
Categorisation of Wound Care and Associated Products Version 9 March 2018 Surgical Dressing Manufacturers Association 2018 TAPES AND TRADITIONAL DRESSINGS Wound Dressings Swabs Taping Traditional Wound
SDMA Categorisation of Wound Care and Associated Products
 Version 7 - February 2015 TAPES AND TRADITIONAL DRESSINGS Traditional Wound Dressings Wound Dressings Packs Swabs Swabs Swab Products Adhesive Tapes Taping Sheets Absorbent Wadding Absorbent Dressings
Version 7 - February 2015 TAPES AND TRADITIONAL DRESSINGS Traditional Wound Dressings Wound Dressings Packs Swabs Swabs Swab Products Adhesive Tapes Taping Sheets Absorbent Wadding Absorbent Dressings
Venous disease made easy. medi. I feel better.
 Venous disease made easy 2019 medi. I feel better. medi medi is one of the largest manufacturers of compression garments in the world and has built a reputation for quality and innovation over the past
Venous disease made easy 2019 medi. I feel better. medi medi is one of the largest manufacturers of compression garments in the world and has built a reputation for quality and innovation over the past
Advazorb. Hydrophilic foam dressing range
 Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Silver Dressings. Sajida Khatri PrescQIPP Primary Care Lead.
 Silver Dressings Sajida Khatri PrescQIPP Primary Care Lead www.prescqipp.info Available at: www.prescqipp.info/silverdressings 2 Introduction PrescQIPP Silver dressings bulletin published in March 2014
Silver Dressings Sajida Khatri PrescQIPP Primary Care Lead www.prescqipp.info Available at: www.prescqipp.info/silverdressings 2 Introduction PrescQIPP Silver dressings bulletin published in March 2014
Juxta CURES Compression Ulcer Recovery System
 medi UK Ltd. Plough Lane Hereford HR4 OEL United Kingdom T 01432 37 35 00 F 01432 37 35 10 enquiries@mediuk.co.uk www.mediuk.co.uk 97C28/01.2013 Juxta CURES Compression Ulcer Recovery System Patient Information
medi UK Ltd. Plough Lane Hereford HR4 OEL United Kingdom T 01432 37 35 00 F 01432 37 35 10 enquiries@mediuk.co.uk www.mediuk.co.uk 97C28/01.2013 Juxta CURES Compression Ulcer Recovery System Patient Information
Efficacy of Velcro Band Devices in Venous and. Mixed Arterio-Venous Patients
 Efficacy of Velcro Band Devices in Venous and Mixed Arterio-Venous Patients T. Noppeney Center for Vascular Diseases: Outpatient Dept. Obere Turnstrasse, Dept. for Vascular Surgery Martha-Maria Hospital
Efficacy of Velcro Band Devices in Venous and Mixed Arterio-Venous Patients T. Noppeney Center for Vascular Diseases: Outpatient Dept. Obere Turnstrasse, Dept. for Vascular Surgery Martha-Maria Hospital
Leg ulcer assessment and management
 Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Understanding compression bandages. Leg Ulcer Management Team Patient Information Leaflet
 Understanding compression bandages Leg Ulcer Management Team Patient Information Leaflet Introduction Your leg ulcer clinic coordinator, nurse or healthcare professional has recommended that you have compression
Understanding compression bandages Leg Ulcer Management Team Patient Information Leaflet Introduction Your leg ulcer clinic coordinator, nurse or healthcare professional has recommended that you have compression
Dr Paul Thibault. Phlebologist & Assistant Editor Phlebology (International Journal) Australasian College of Phlebology
 Dr Paul Thibault Phlebologist & Assistant Editor Phlebology (International Journal) Australasian College of Phlebology Prescribing Effective Compression and PTS Dr Paul Thibault Phlebologist, Newcastle,
Dr Paul Thibault Phlebologist & Assistant Editor Phlebology (International Journal) Australasian College of Phlebology Prescribing Effective Compression and PTS Dr Paul Thibault Phlebologist, Newcastle,
Herefordshire Wound Management Formulary
 Herefordshire Wound Management Formulary July 2015 Michaela Powell Tissue Viability Nurse Wye Valley NHS Trust Hereford HR1 2ER Wound Care Formulary Sub-Group Herefordshire Joint Formulary Working Group
Herefordshire Wound Management Formulary July 2015 Michaela Powell Tissue Viability Nurse Wye Valley NHS Trust Hereford HR1 2ER Wound Care Formulary Sub-Group Herefordshire Joint Formulary Working Group
Taken into account multidiscilinary aspect of Vascular Compression
 The Vascular Center : A model to improve patient care Taken into account multidiscilinary aspect of Vascular Compression F. Vin C. Gardon-Mollard Compression Therapy is an efficient treatment for the management
The Vascular Center : A model to improve patient care Taken into account multidiscilinary aspect of Vascular Compression F. Vin C. Gardon-Mollard Compression Therapy is an efficient treatment for the management
JOURNAL OF WOUND CARE. VOLUME 8. NUMBER 9. October A comparison of sub-bandage pressures produced with two multi-layer bandaging systems
 JOURNAL OF WOUND CARE VOLUME 8. NUMBER 9. October 1999 A comparison of sub-bandage pressures produced with two multi-layer bandaging systems A.D. Taylor, MSc, RGN, SCM, DN, Clinical Nurse Specialist, Salford
JOURNAL OF WOUND CARE VOLUME 8. NUMBER 9. October 1999 A comparison of sub-bandage pressures produced with two multi-layer bandaging systems A.D. Taylor, MSc, RGN, SCM, DN, Clinical Nurse Specialist, Salford
Injection sclerotherapy. Information for patients Sheffield Vascular Institute
 Injection sclerotherapy Information for patients Sheffield Vascular Institute page 2 of 8 You have been diagnosed as having varicose veins that are suitable for injection sclerotherapy. This leaflet explains
Injection sclerotherapy Information for patients Sheffield Vascular Institute page 2 of 8 You have been diagnosed as having varicose veins that are suitable for injection sclerotherapy. This leaflet explains
RESPONSE FOI Reference: OPTUM FOI SWL CCG
 , FOI Team Optum Commissioning Support Services South Kesteven District Council Offices St. Peter s Hill, Grantham, Lincolnshire NG31 6PZ 5 th October 2016 Dear Requester FREEDOM OF INFORMATION REQUEST
, FOI Team Optum Commissioning Support Services South Kesteven District Council Offices St. Peter s Hill, Grantham, Lincolnshire NG31 6PZ 5 th October 2016 Dear Requester FREEDOM OF INFORMATION REQUEST
The management of patients with lymphoedema
 Juxta-Fit compression garments in lymphoedema management Julie Mullings Julie Mullings, Tissue Viabilty Specialist Nurse, University Hospital of South Manchester - Community Services Email: Julie.mullings@uhsm.nhs.uk
Juxta-Fit compression garments in lymphoedema management Julie Mullings Julie Mullings, Tissue Viabilty Specialist Nurse, University Hospital of South Manchester - Community Services Email: Julie.mullings@uhsm.nhs.uk
Understanding how compression works: part 1
 Understanding how compression works: part 1 Georgina Ritchie, Gillian Warwick Chronic leg ulceration is an increasing burden in the UK, both financially to the health service and on a human level. This
Understanding how compression works: part 1 Georgina Ritchie, Gillian Warwick Chronic leg ulceration is an increasing burden in the UK, both financially to the health service and on a human level. This
Leg ulcers. continuing professional development
 By reading this article and writing a practice profile, you can gain a certificate of learning. You have up to a year to send in your practice profile. Guidelines on how to write and submit a profile are
By reading this article and writing a practice profile, you can gain a certificate of learning. You have up to a year to send in your practice profile. Guidelines on how to write and submit a profile are
Suspected Deep Vein Thrombosis (DVT) Pathway for Non Pregnant patients Updated November 2016, with new D-dimer reference range
 Suspected Deep Vein Thrombosis (DVT) Pathway for Non Pregnant patients Updated November 2016, with new D-dimer reference range Suspect a DVT? Complete a Two-level DVT Wells score on ICE system (see page
Suspected Deep Vein Thrombosis (DVT) Pathway for Non Pregnant patients Updated November 2016, with new D-dimer reference range Suspect a DVT? Complete a Two-level DVT Wells score on ICE system (see page
Foam dressings have frequently
 The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
Appendix D: Leg Ulcer Assessment Form
 Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Leg ulcers. Causes and management. OBJECTIVE This article outlines the assessment and management of patients with leg ulceration.
 THEME Wounds Leg ulcers Causes and management BACKGROUND A leg ulcer is not a disease but the manifestation of an underlying problem that requires a clear diagnosis. Sandra Dean RN, is nurse consultant
THEME Wounds Leg ulcers Causes and management BACKGROUND A leg ulcer is not a disease but the manifestation of an underlying problem that requires a clear diagnosis. Sandra Dean RN, is nurse consultant
Venous Leg Ulcer. A Complete Solution. Therapy Approach with Adapted Products
 Venous Leg Ulcer A Complete Solution Therapy Approach with Adapted Products A Complete Solution for Venous Leg Ulcers No two wounds are the same, yet they share one thing: every wound needs the best possible
Venous Leg Ulcer A Complete Solution Therapy Approach with Adapted Products A Complete Solution for Venous Leg Ulcers No two wounds are the same, yet they share one thing: every wound needs the best possible
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT
 VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS
 VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
Priorities Forum Statement
 Priorities Forum Statement Number 5 Subject Lymphoedema Date of decision November 2015 Date refreshed March 2017 Date of review November 2018 GUIDANCE Lymphoedema is the result of accumulation of fluid
Priorities Forum Statement Number 5 Subject Lymphoedema Date of decision November 2015 Date refreshed March 2017 Date of review November 2018 GUIDANCE Lymphoedema is the result of accumulation of fluid
Understanding our report and advice: Antimicrobial wound dressings (AWDs) for chronic wounds
 Understanding our report and advice: Antimicrobial wound dressings (AWDs) for chronic wounds Health technology assessment report 13 December 2015 Healthcare Improvement Scotland 2015 Published December
Understanding our report and advice: Antimicrobial wound dressings (AWDs) for chronic wounds Health technology assessment report 13 December 2015 Healthcare Improvement Scotland 2015 Published December
Resources to Guide the Management of Suspected Infection in Chronic Wounds
 Resources to Guide the Management of Suspected Infection in Chronic Wounds Health Improvement Scotland published their 13th Health Technology Assessment (HTA 13) in December 2015 entitled, Antimicrobial
Resources to Guide the Management of Suspected Infection in Chronic Wounds Health Improvement Scotland published their 13th Health Technology Assessment (HTA 13) in December 2015 entitled, Antimicrobial
Treatment for the management of lymphoedema is
 FarrowWrap: innovative and creative patient treatment for lymphoedema Anita Hobday, Jane Wigg Anita Hobday is Lymphoedema Consultant Practitioner, Senior Lecturer, Macmillan Lymphoedema Academy; Jane Wigg
FarrowWrap: innovative and creative patient treatment for lymphoedema Anita Hobday, Jane Wigg Anita Hobday is Lymphoedema Consultant Practitioner, Senior Lecturer, Macmillan Lymphoedema Academy; Jane Wigg
Varicose veins. Information for patients Sheffield Vascular Institute
 Varicose veins Information for patients Sheffield Vascular Institute You have been diagnosed as having varicose veins. This leaflet explains more about varicose veins and answers some of the most frequently
Varicose veins Information for patients Sheffield Vascular Institute You have been diagnosed as having varicose veins. This leaflet explains more about varicose veins and answers some of the most frequently
VENOUS LEG ULCERS (VLU)
 VENOUS LEG ULERS (VLU) REOMMENDTION S Evidence-based gradings Excellent evidence ody of evidence can be trusted to guide practice. Good evidence ody of evidence can be trusted to guide practice in most
VENOUS LEG ULERS (VLU) REOMMENDTION S Evidence-based gradings Excellent evidence ody of evidence can be trusted to guide practice. Good evidence ody of evidence can be trusted to guide practice in most
Intensive Decongestive Lymphatic Therapy for Non-Cancer Secondary Lymphoedema Criteria Based Access Protocol
 NHS Dorset Clinical Commissioning Group Intensive Decongestive Lymphatic Therapy for Non-Cancer Secondary Lymphoedema Criteria Based Access Protocol Supporting people in Dorset to lead healthier lives
NHS Dorset Clinical Commissioning Group Intensive Decongestive Lymphatic Therapy for Non-Cancer Secondary Lymphoedema Criteria Based Access Protocol Supporting people in Dorset to lead healthier lives
PROCEDURE FOR VASCULAR ASSESSMENT BY DOPPLER ULTRASOUND
 PROCEDURE FOR VASCULAR ASSESSMENT BY DOPPLER ULTRASOUND (to achieve Ankle Brachial Pressure Index) First Issued Issue Version Purpose of Issue/Description of Change Planned Review Date One To enable nurses
PROCEDURE FOR VASCULAR ASSESSMENT BY DOPPLER ULTRASOUND (to achieve Ankle Brachial Pressure Index) First Issued Issue Version Purpose of Issue/Description of Change Planned Review Date One To enable nurses
compression should be applied at the strongest class that the patient can tolerate.
 Sponsored feature A simple and effective solution to preventing recurrent venous leg ulcers When trying to prevent the recurrence of leg ulcers, many Leg ulcers It is widely accepted that good compression
Sponsored feature A simple and effective solution to preventing recurrent venous leg ulcers When trying to prevent the recurrence of leg ulcers, many Leg ulcers It is widely accepted that good compression
This article is intended as a
 Compression Hosiery and Multilayer Wraps: Proper Prescription and Usage The effect of this therapy on venous ulcers is impressive. By Steven Kravitz, DPM 123 This article is intended as a reference for
Compression Hosiery and Multilayer Wraps: Proper Prescription and Usage The effect of this therapy on venous ulcers is impressive. By Steven Kravitz, DPM 123 This article is intended as a reference for
Velcro Compression Devices
 Velcro Compression Devices Joseph A. Caprini, MD, MS, FACS, RVT, FACCWS Louis W. Biegler Chair of Surgery NorthShore University HealthSystem, Evanston, IL Clinical Professor of Surgery University of Chicago
Velcro Compression Devices Joseph A. Caprini, MD, MS, FACS, RVT, FACCWS Louis W. Biegler Chair of Surgery NorthShore University HealthSystem, Evanston, IL Clinical Professor of Surgery University of Chicago
Leg Ulcer Management Policy
 Leg Ulcer Management Policy Page1 Policy Title: Executive Summary: Leg Ulcer Management Policy This policy for the Management of Leg Ulcers is for East Cheshire Trust. The aim is that that all leg ulcers
Leg Ulcer Management Policy Page1 Policy Title: Executive Summary: Leg Ulcer Management Policy This policy for the Management of Leg Ulcers is for East Cheshire Trust. The aim is that that all leg ulcers
Leg Ulcer Management Guidelines
 CPRO28 Leg Ulcer Management Guidelines Page 1 of 46 Version: V3 Name of author: Lorraine Grothier Consultant Nurse Tissue Viability Related procedural documents Wound management guidelines Infection prevention
CPRO28 Leg Ulcer Management Guidelines Page 1 of 46 Version: V3 Name of author: Lorraine Grothier Consultant Nurse Tissue Viability Related procedural documents Wound management guidelines Infection prevention
DVT - initial management NSCCG
 Background information Information resources for patients and carers Updates to this care map Synonyms Below knee DVT and bleeding risks Patient with confirmed DVT Scan confirms superficial thrombophlebitis
Background information Information resources for patients and carers Updates to this care map Synonyms Below knee DVT and bleeding risks Patient with confirmed DVT Scan confirms superficial thrombophlebitis
Using treatment pathways to improve healing of venous leg ulceration
 Using treatment pathways to improve healing of venous leg ulceration Background: A leg ulcer prevalence audit carried out by staff working in community services within an NHS Trust identified an average
Using treatment pathways to improve healing of venous leg ulceration Background: A leg ulcer prevalence audit carried out by staff working in community services within an NHS Trust identified an average
Wound Management, & Continence Preferred Prescribing List April 2018
 Wound Management, & Continence Preferred Prescribing List April 208 Tissue Viability & Continence Service Longford Primary Care Trust Longford Road Coventry Tissue Viability Office 024 7664 677 tissue.viability@covwarkpt.nhs.uk
Wound Management, & Continence Preferred Prescribing List April 208 Tissue Viability & Continence Service Longford Primary Care Trust Longford Road Coventry Tissue Viability Office 024 7664 677 tissue.viability@covwarkpt.nhs.uk
Healthy Legs For Life! Prevention is better then cure
 Healthy Legs For Life! Prevention is better then cure Ellie Lindsay Independent Specialist Practitioner Associate Lecturer, CRICP, London Visiting Fellow, Queensland University of Technology Occurrence
Healthy Legs For Life! Prevention is better then cure Ellie Lindsay Independent Specialist Practitioner Associate Lecturer, CRICP, London Visiting Fellow, Queensland University of Technology Occurrence
Lower Limb Ulceration Policy. Version No 2.6. Review: February 2018
 Livewell Southwest Lower Limb Ulceration Policy Version No 2.6 Review: February 2018 Notice to staff using a paper copy of this guidance The policies and procedures page of Intranet holds the most recent
Livewell Southwest Lower Limb Ulceration Policy Version No 2.6 Review: February 2018 Notice to staff using a paper copy of this guidance The policies and procedures page of Intranet holds the most recent
