Why Focus on Low Back Pain? Care Pathway Roles and Responsibilities. The following table describes general role and responsibilities.
|
|
|
- Jade Ross
- 6 years ago
- Views:
Transcription
1 Low Back Pain This CPM presents a model of care based on scientific evidence available at the time of publication. It is not a prescription for every physician or every patient, nor does it replace clinical judgment. All statements, protocols, and recommendations herein are viewed as transitory and iterative. Although physicians are encouraged to follow the CPM to help focus on and measure quality, deviations are a means for discovering improvements in patient care and expanding the knowledge base. If you have questions or concerns regarding this information, contact: Clinical Leaders David Arredondo, MD darredond@phs.org Dion Gallant, MD dgallant@phs.org Fauzia Malik fmalik@phs.org This CPM is part of Presbyterian s Clinical Care Model is a broad, enterprisewide body of documentation covering PHS functions, programs, and care pathways, intended to build organizational acumen, facilitate cross-system collaboration, and accelerate our implementation of clinical initiatives. Find all of PHS Care Model at March 2018 This Clinical Practice Model (CPM) is designed for patients: Over the age of 18 Presenting with low back pain Being seen in an outpatient setting (PMG Clinic or PHS Hospital) This CPM recommends an evidence-based protocol for diagnosis and treatment of low back pain. These recommendations represent the work of Presbyterian s Low Back Pain EBCD initiative. Why Focus on Low Back Pain? Low back pain (LBP) is the fifth most common reason that Americans visit their physicians (ACP, APS). It has a significant impact on the cost of care, as well as absenteeism in the workplace. Evaluation and treatment of LBP remains highly variable, often with an overreliance on imaging studies. Care Pathway Roles and Responsibilities The following table describes general role and responsibilities. Responsibility Initial diagnosis and treatment for mild, moderate, or severe low back pain Initial diagnosis and treatment for mild, moderate, or severe low back pain Evaluation and development of physical therapy treatment plan Guidance on resumption of daily and physical activities Support for lifestyle modification, stress management, depression due to chronic low back pain Consultations and administration of injections or other interventional procedures Surgical consultations and surgery Evidence/Resources American Academy of Family Physicians American College of Physicians American Pain Society Choosing Wisely Clinician Physician or Advanced Practice Clinician Physical Therapist Behavioral Health Clinician Interventional Pain Specialist Spine Surgeon jump to ALGORITHM 2018 Presbyterian Healthcare Services 1
2 Assessment, Diagnosis, and Treatment: Low Back Pain Diagnosis and Testing The recommended first step in diagnosis, regardless of care setting, is a detailed history, physical examination, and the identification of any red flags. This can assist in diagnosing the pain as one of three broad types: nonspecific low back pain, back pain potentially associated with radiculopathy or spinal stenosis, or back pain potentially associated with another specific spinal cause. Typically, 85% of patients are diagnosed with nonspecific LBP (ACP & APS). Unless red flags are present or the pain has been ongoing for more than 6 weeks, imaging is not recommended. Diagnosis Administer Oswestry Low Back Pain Disability Questionnaire Document pain scale Conduct History & Physical Exam o This allows the provider to gain detailed information about the symptoms, potential cause, disabling factors, pre-injury work and health status, psychosocial risk factors, and the identification of any red flags. The focus of this exam should be on 2018 Presbyterian Healthcare Services 2
3 identifying any red flags (and the associated potential serious pathology) as opposed to developing a specific pathoanatomical diagnosis. Document presence or absence of red flags Assess for mental health concerns (sometimes referred to as yellow flags ) o Psychosocial risk factors are correlated with higher rates of chronicity o Addressing beliefs and fears regarding low back pain early on is key in avoiding chronicity o Screening for these yellow flags may include: Somatization Distress Depressive mood Passive coping strategies Fear of pain, movement, and re-injury High scores on measures such as the Fear-Avoidance Beliefs Questionnaire (FABQ) or the Pain Catastrophizing Scale (PCS) FABQ score <14 = low risk and >16 = high risk PCS score >30 = high risk Ascertain presence of radicular pain o May involve paresthesia in the lower extremities, numbness or weakness o Commonly co-presenting with related or referred lower extremity pain, such as buttock, thigh, or leg pain Refer to Physical Therapy, behavioral health clinician, interventional pain specialist, or surgical consultation as appropriate Imaging Tests Imaging tests are not recommended for low back pain within the first 6 weeks (source). Exceptions to this are when severe underlying conditions are suspected (see red flags, below). Imaging can have adverse effects through the overexposure to radiation and nocebic/iatrogenic effects due to the misinterpretation of age-related structural findings. In cases of nonspecific low back pain, there is no correlation between imaging and rate of recovery, and the cost of treatment is frequently higher when imaging is performed prior to other treatments. Red Flags & Possible Diagnoses Possible Diagnosis Red Flags/Risk Factors Imaging/other studies recommended Cancer History of cancer Unexplained weight loss Failure to improve after 1 month Age > 50 years Vertebral Infection/Epidural Abscess Fever IV drug use Recent infection Cauda equina Urinary retention Motor deficits Fecal incontinence Saddle anesthesia Vertebral compression fracture Older age History of osteoporosis Steroid use MRI ESR Lumbosacral plain radiography MRI ESR CRP MRI Lumbosacral plain radiography 2018 Presbyterian Healthcare Services 3
4 Red Flags & Possible Diagnoses Possible Diagnosis Red Flags/Risk Factors Imaging/other studies recommended Ankylosing spondylitis Younger age Morning stiffness Improvement with exercise Alternating buttock pain Awaking due to back pain (second part of the night) Herniated disc Back and leg pain Positive straight-leg-raise test or crossed straight-leg-raise test Lumbar spinal stenosis Radiating leg pain Older age Changing symptoms on downhill treadmill Pain relieved when sitting Treatment Anterior-posterior pelvis plain radiography ESR CRP HLA-B27 If symptoms < 1 month: none If symptoms > 1 month: MRI or EMG/NCV If symptoms < 1 month: none If symptoms > 1 month: MRI or EMG/NCV Treatment of LBP may vary depending on if the symptoms are classified as mild, moderate, or severe, and if the LBP is acute, sub-acute or chronic. Acute describes pain occurring for less than 6 weeks, sub-acute for 6 to 12 weeks, and chronic for longer than 12 weeks. For scheduling purposes, back pain occurring for less than 90 days may be termed acute; chronic refers to pain occurring for more than 90 days. Mild Symptoms Pain without functional impairment/disability Core Treatment Plan First-line medication options include NSAIDs or acetaminophen See Medication Therapy for other options Heat or ice may be applied to provide short-term relief of symptoms With patient education, focus is on encouraging exercise, including walking or other aerobic activity, resumption of normal physical activities, avoiding bed rest for more than 48 hours, and ergonomics If appropriate, consider a referral to a behavioral health clinician Imaging is not recommended unless the symptoms are unresolved after 6 weeks Moderate Symptoms Pain with minimal functional impairment/disability Core Treatment Plan Mild Symptoms plan, and If a worker s compensation claim is involved, complete the necessary return to work assessment In acute cases, consider referral to Physical Therapy A short-term course of skeletal muscle relaxants (see Medication Therapy) may also be appropriate for acute LBP Severe Symptoms Pain with moderate-to-severe functional impairment/disability 2018 Presbyterian Healthcare Services 4
5 Core Treatment Plan Mild/Moderate Symptoms plan, and A short-term course of opioids may be appropriate in patients with acute LBP (see Medication Therapy) Medication Therapy Depending on the diagnosis and severity of the low back pain, various medication therapies may be used. The role of pharmacological therapy is to prevent and control symptoms and assist the patient in pursuing the lifestyle therapies and adjustments necessary. Most of the research supporting the choice of medication is based on short-term (<4 weeks) courses of treatment. NSAIDs and acetaminophen are the most commonly recommended medication options for patients suffering from low back pain. Medications Drugs 1 st Line NSAIDs Acetaminophen Notes Recommended as the first step in treating low back pain at home by Choosing Wisely Found to be a moderately effective short-term treatment for acute low back pain (ACP, APS) Acetaminophen may be slightly less effective than NSAIDs, though the results of studies are inconclusive, and the safety profile of acetaminophen is more favorable The possibility of adverse gastrointestinal or cardiovascular effects with NSAIDs should be considered 2 nd Line 3 rd Line Other Skeletal muscle relaxants Opioids Benzodiazepines Tricyclic antidepressants Limited evidence, but may be moderately effective as a short-term treatment for acute low back pain (ACP, APS) Some skeletal muscle relaxants may have adverse short-term effects, such as hepatotoxicity Baclofen is preferred, though cyclobenzaprine may be used in patients under 60 years old Carisoprodol is discouraged, given its potential for abuse. Moderately effective at treating low back pain May be appropriate for short-term use in patients complaining of severe pain Given the potential for abuse, use of opioids is not recommended as a long term solution Limited evidence, but may be moderately effective at treating low back pain in the short term in ED setting Not recommended for patients >65 years old Given the potential for abuse, use of benzodiazepines is not recommended as a long term solution Found to have a small to moderate effect on short-term pain relief (ACP, APS) At this point, only tricyclic antidepressants have been demonstrated to be effective in treating low back pain, though others have not been evaluated Antiepileptic drugs Gabapentin and topiramate may be effective for patients presenting with chronic low back pain with or without radiculopathy Physical Therapy The primary recommended treatment for acute LBP is physical therapy. Referral The PCP or the PT can refer a patient for outpatient physical therapy via Epic, which will then trigger a call to schedule an appointment from Presbyterian Customer Service Center (PCSC). There have been and continue to be efforts to simplify this process and make it more efficient, including adding acute slots into the PT schedule, which can allow patients to be seen sooner than they might otherwise be. Evaluation 1. Focus on Therapeutic Outcomes (FOTO) assessment, which includes 2018 Presbyterian Healthcare Services 5
6 a. Oswestry Low Back Pain Disability Questionnaire b. Fear-Avoidance Belief Questionnaire c. Pain Catastrophizing Scale 2. Patient vitals 3. History, which generally focuses on the following elements: a. Onset of pain b. Mechanism of injury c. Time frame of symptoms/injury d. Exacerbating and alleviating factors e. Location of symptoms f. Pain pattern g. Patient goals and expectations for outcomes h. Identification of red flags 4. Physical Exam, which typically includes various tests of measures, such as a. Range of motion b. Sensitivity c. Special tests as appropriate (e.g., straight leg raise test or slump test) Assessment Once the evaluation is completed, the PT provides their assessment of the issue and the best Plan of Care. Plan of Care The PT then develops an individualized Plan of Care, which is signed by the patient s PCP. Treatment Treatment typically takes place over the course of 7 to 9 weekly visits and may include: Manual therapy to reduce pain and disability and improve mobility Trunk coordination, strengthening and endurance exercises Centralization and directional preference exercises and procedures (McKenzie therapy) Flexion exercises (Williams flexion), per PT discretion Lower-quarter nerve mobilization procedures Recommendations for at-home stretching and exercise, as appropriate Cognitive behavioral intervention as needed to address psychosocial issues If the patient s symptoms do not improve with treatment, or if they appear to be in mental distress, the PT may decide to refer the patient back to their PCP with a recommendation to pursue treatment from a behavioral health clinician, interventional pain specialist, or surgeon. Therapeutic Lifestyle Changes Exercise/Activity Walking and other aerobic exercise should be encouraged Core strengthening exercises and flexion/extension movements can be helpful Mind-body exercises, such as yoga and pilates, can be helpful Bed rest is not recommended for >48 hours (Choosing Wisely) 2018 Presbyterian Healthcare Services 6
7 Other Non-pharmacological treatment Heat/ice may provide short-term pain relief Therapeutic massage, chiropractic work, and acupuncture may benefit some individuals Condition Progression Reoccurrence of LBP after an initial acute episode is very common, appearing in approximately 70% of patients. LBP may progress from acute to chronic if it is not resolved through treatment in either a primary care or physical therapy setting. If there is no improvement with non-invasive treatment of radicular LBP over the course of 9 to 10 weeks, or if the patient presents with several radiculopathy, it may be appropriate to refer the patient to an interventional pain specialist or to a surgical specialist. Interventional Procedures After an assessment and appropriate imaging, an interventional pain specialist may elect to use pharmacological treatment or one of several injections. The most commonly used injections are: Epidural Steroid Injection (may require a prior authorization) Facet Steroid injection Medial Branch Nerve Block Radiofrequency Discogram is less common, but also available. In some cases, these injections will provide short- or long-term relief for patients, and may be given up to 4 times per year. For patients with degenerative diseases, such as degenerative disc disease, treatment can continue for several years. Injections may also be used in conjunction with physical therapy or exercise programs. If the injections do not alleviate the symptoms, however, many providers choose to refer patients for surgical consultation. Both prior to and while undergoing pharmacological treatment of symptoms, patients may be assessed for potential misuse of opioids using either the Screener and Opioid Assessment for Patients with Pain- Revised (SOAPP -R) or the Current Opioid Misuse Measure (COMM). A pain psychologist is also available to treat those patients who struggle with psychosocial issues related to chronic pain. Surgery or Other Interventional Procedures If the patient is not able to manage their low back pain with the assistance of either physical therapy or treatment by an interventional pain specialist, a surgical consultation may be appropriate. Patient Education and Support Key aspects of patient education include helping patients Understand the generally favorable prognosis of low back pain Use active pain coping strategies for helping decrease fear and catastrophizing Rapidly resume vocational and daily activities, even if some pain persists Develop an appropriate self-care regimen that includes activities like walking and core strengthening exercise In many cases, it is also recommended to Discourage extended bed-rest (>48 hours) Avoid providing in-depth patho-anatomical explanations for the specific cause of the pain 2018 Presbyterian Healthcare Services 7
8 When dealing with chronic pain, some patients may benefit from treatment by a behavioral health clinician. Patient Education Materials In a primary care or urgent care setting, patient education materials provided by ExitCare are available on Epic. In PT, individualized patient education materials are created through Visual Health Information and Home Exercise To Go. Measurement and Reporting The key metric reported on LBP is the use of imaging studies. The percentage of patients with low back pain who receive imaging studies in less than 28 days are reported monthly via HEDIS and to CMS. Internal measures of success focus on the issues of access and improving patient outcomes, particularly with regard to physical therapy. The EBCD LBP initiative in 2014 resulted in a significant decrease in the average wait time for physical therapy services, from 40 days in January 2015 to 8 days in December There has also been a significant improvement in patients functional outcomes post-physical therapy according to pre- and post-treatment scores on the Oswestry Low Back Pain Disability Questionnaire. Clinical Definitions Access Evidence-Based Care Design (EBCD) Overuse The timely use of personal health services to achieve the best possible outcome. Key components of access: Gaining entry into the health care system. Getting access to sites of care where patients can receive needed services. Finding providers who meet the needs of individual patients and with whom patients can develop a relationship based on mutual communication and trust. A formal, evidence-driven, cross-disciplinary method for clinical workflow development, redesign, or augmentation. When a drug or treatment is given without medical justification or strong scientific evidence. Overuse includes failing to follow effective options that cost less or cause fewer side effects. For example, antibiotics are prescribed for children s ear infections 80 percent of the time, despite the finding that these infections usually resolve within three days without antibiotics. Additional References Related Care Model Topics Chronic Opioid Therapy for Chronic Pain (pending) Evidence-Based Care Design Patient-Centered Medical Home (PCMH) Policies and Procedures [PHS login required] Epidural Corticosteroid Injections for Back Pain Other Resources Chou R, Qaseem A, Snow V, Casey D, Shekelle P, Owens DK. Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society. Annals of Internal Medicine. 2007;147(7): doi: / Presbyterian Healthcare Services 8
9 Oswestry Low Back Pain Disability Questionnaire Patient Name: Date: Instructions: This questionnaire has been designed to give us information as to how your back or leg pain is affecting your ability to manage in everyday life. Please answer by checking ONE box in each section for the statement which best applies to you. We realize you may consider that two or more statements in any one section apply but please just shade out the spot that indicates the statement which most clearly describes your problem. Section 1 Pain Intensity I have no pain at the moment The pain is very mild at the moment The pain is moderate at the moment The pain is fairly severe at the moment The pain is very severe at the moment The pain is the worst imaginable at the moment Section 2 Personal care (washing, dressing, etc) I can look after myself normally without causing extra pain I can look after myself normally but it causes extra pain It is painful to look after myself and I am slow and careful I need some help but manage most of my personal care I need help every day in most aspects of self-care I do not get dressed, I wash with difficulty and stay in bed Section 3 Lifting I can lift heavy weights without extra pain I can lift heavy weights but it gives extra pain Pain prevents me from lifting heavy weights off the floor, but I can manage if they are conveniently placed eg. on a table. Pain prevents me from lifting heavy weights, but I can manage light to medium weights if they are conveniently positioned I can lift very light weights I cannot lift or carry anything at all Section 4 Walking Pain does not prevent me walking any distance Pain prevents me from walking more than 2 kilometers Pain prevents me from walking more than 1 kilometer Pain prevents me from walking more than 500 meters I can only walk using a stick or crutches I am in bed most of the time 2018 Presbyterian Healthcare Services 9
10 Section 5 Sitting I can sit in any chair as long as I like I can only sit in my favorite chair as long as I like Pain prevents me sitting more than one hour Pain prevents me from sitting more than 30 minutes Pain prevents me from sitting more than 10 minutes Pain prevents me from sitting at all Section 8 Sex Life (if applicable) My sex life is normal and causes no extra pain My sex life is normal but causes some extra pain My sex life is nearly normal but is very painful My sex life is severely restricted by pain My sex life is nearly absent because of pain Pain prevents any sex life at all Section 6 Standing I can stand as long as I want without extra pain I can stand as long as I want but it gives me extra pain Pain prevents me from standing for more than 1 hour Pain prevents me from standing for more than 3 minutes Pain prevents me from standing for more than 10 minutes Pain prevents me from standing at all Section 7 Sleeping My sleep is never disturbed by pain My sleep is occasionally disturbed by pain Because of pain I have less than 6 hours sleep Because of pain I have less than 4 hours sleep Because of pain I have less than 2 hours sleep Pain prevents me from sleeping at all Section 9 Social life My social life is normal and gives me no extra pain My social life is normal but increases the degree of pain Pain has no significant effect on my social life apart from limiting my more energetic interests eg, sport Pain has restricted my social life and I do not go out as often Pain has restricted my social life to my home I have no social life because of pain Section 10 Travelling I can travel anywhere without pain I can travel anywhere but it gives me extra pain Pain is bad but I manage journeys over two hours Pain restricts me to journeys of less than one hour Pain restricts me to short necessary journeys under 30 minutes Pain prevents me from travelling except to receive treatment 2018 Presbyterian Healthcare Services 10
11 Scoring Instructions: For each section the total possible score is 5. If the first statement is marked the section score = 0. If the last statement is marked, it=5. If all 10 sections are completed the score is calculated as follows: Example: 16 (patient score) / 50 (total possible score) x 100 = 32% If one section is missed or not applicable the score is calculated: Example: 16 (patient score) / 45 (total possible score) x 100 = 35.5% Minimum detectable change (90% confidence): 10% points (change of less than this may be attributable to error in the measurement) Interpretation of scores: 0 to 20%: minimal disability The patient can cope with most living activities. Usually no treatment is indicated apart from advice on lifting sitting and exercise %: moderate disability The patient experiences more pain and difficulty with sitting, lifting, and standing. Travel and social life are more difficult and they may be disabled from work. Personal care, sexual activity and sleeping are not grossly affected and the patient can usually be managed by conservative means %: severe disability Pain remains the main problem in this group but activities of daily living are affected. These patients require a detailed investigation %: crippled Back pain impinges on all aspects of the patient s life. Positive intervention is required %: These patients are either bed bound or exaggerating their symptoms Presbyterian Healthcare Services 11
12 Fear Avoidance Behavior Questionnaire (FABQ) Work Description: This module assesses fear-avoidance beliefs in respect to performing physical activities and work-related activities. Use to generate measures of the impact of fear-avoidance that may affect the outcomes for your patient. Originally, the fear- avoidance beliefs questionnaire (FABQ) was designed to assess fear-avoidance for patients with lumbar syndromes, but we have modified the questionnaire to be generic, i.e., no reference to the back or any other body part. This module can be used for any patient who has fear of activities or work. The FABQ-Work is also now being administered with Computer Adaptive Testing, so that all patients do not have to answer all questions. What will be reported: FOTO reports the Work Fear-Avoidance Behavior Questionnaire subscale both on an adjusted 100 point scale (first score) and on the standard scoring. The questionnaire has a score range from 0 (low fear) to 42 (high fear). High scores represent high fear. Low scores represent low levels of fear-avoidance, which is good. A useful cut point for clinical management is 35 or more for Work. When a patient has high (i.e. >35 Work FABQ), adjust treatment to manage the patient's fears of work activities to increase the probability of good functional status outcomes. Research Reference: Waddell G, Newton M, Henderson I, Somerville D, Main CJ, A Fear- Avoidance Beliefs Questionnaire (FABQ) and the role of fear-avoidance beliefs in chronic low-back pain and disability. Pain, 1993;52: Responses for all questions: Completely disagree Somewhat disagree Unsure Somewhat agree Completely disagree Questions (possible -- not all questions will be asked of all patients): This is a statement other patients have made. Please rate your level of agreement. I cannot do my normal work with my present pain. I should not do my work with my present pain. I cannot do my normal work until my pain is treated. My work is too heavy for me. I do not think I will be back to my normal work within 3 months. I have a claim for compensation for my pain. My work might harm me. My work aggravated my pain Presbyterian Healthcare Services 12
13 Pain Catastrophizing Scale Description: This assessment asks the patient to reflect on past painful experiences, and to indicate the degree to which they experienced each of 13 thoughts or feelings when experiencing pain, which enables treatment plans to be more individually tailored. What is reported: The PCS yields a total score and three subscale scores assessing rumination, magnification, and helplessness, based on patient responses on a 5-point scale with the end points (0) not at all and (4) all the time. The total score is computed by summing responses to all 13 items and range from Subscales are computed by summing the responses of the following items: Rumination: Sum of items 8, 9, 10, 11 Magnification: Sum of Items 6, 7, 13 Helplessness: Sum of items 1, 2, 3, 4, 5, 12 Reference: Sullivan, Michael JL, Ph.D, Department of Psychology, Medicine and Neurology, School of Physical & Occupational Therapy McGill University, Montreal, Quebec H3A 181. Responses: 0 = not at all 1 = to a slight degree 2 = to a moderate degree 3 = to a great degree 4 = all the time Questions: When I'm in pain... I worry all the time about whether the pain will end. I feel I can't go on. It's terrible and I think it's never going to get any better. It's awful and I feel that it overwhelms me. I feel I can't stand it anymore. I become afraid that the pain will get worse. I keep thinking of other painful events. I anxiously want the pain to go away. I can't seem to keep it out of my mind. I keep thinking about how much it hurts. I keep thinking about how badly I want the pain to stop. There's nothing I can do to reduce the intensity of the pain. I wonder whether something serious may happen Presbyterian Healthcare Services 13
Chiropractic Health Plan - Diagnosis of Low Back Pain
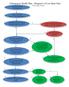 Chiropractic Health Plan - Diagnosis of Low Back Pain 1 Adult Patient with ot for major Trauma Low back pain 2 Intake Evaluation (Inset 1) Recommendation 1 3 Potentially Serious Condition Strongly Suspected
Chiropractic Health Plan - Diagnosis of Low Back Pain 1 Adult Patient with ot for major Trauma Low back pain 2 Intake Evaluation (Inset 1) Recommendation 1 3 Potentially Serious Condition Strongly Suspected
Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society
 Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society Annals of Internal Medicine October 2007 Volume 147,
Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society Annals of Internal Medicine October 2007 Volume 147,
Worker s Compensation Form
 Worker s Compensation Form Patient Name: Today s Date: Patient Address: Patient Phone Number: ( ) Cell: ( ) Patient Date of Birth Occupation: Male Female SSN: - - Name of Employer: Contact Person: Address:
Worker s Compensation Form Patient Name: Today s Date: Patient Address: Patient Phone Number: ( ) Cell: ( ) Patient Date of Birth Occupation: Male Female SSN: - - Name of Employer: Contact Person: Address:
Disclosure Statement of Financial Interest. Evidence Based Evaluation and. Learning Objectives. What is Low Back Pain?
 Disclosure Statement of Financial Interest Evidence Based Evaluation and Management of Low Back Pain June 28, 2013 St. Charles Medical Center Summer Boslaugh and Alison Little DO NOT have a financial interest/arrangement
Disclosure Statement of Financial Interest Evidence Based Evaluation and Management of Low Back Pain June 28, 2013 St. Charles Medical Center Summer Boslaugh and Alison Little DO NOT have a financial interest/arrangement
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽
 외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
Pain Intensity (mark only 1) Personal Care (washing, dressing, etc.) Lifting (mark only 1) Walking (mark only 1) Sitting (mark only 1)
 Pain Intensity Personal Care (washing, dressing, etc.) Lifting Walking Sitting Standing Sleeping Sex Life OSWESTRY v2 Patient s copy I have no pain at the moment The pain is very mild at the moment The
Pain Intensity Personal Care (washing, dressing, etc.) Lifting Walking Sitting Standing Sleeping Sex Life OSWESTRY v2 Patient s copy I have no pain at the moment The pain is very mild at the moment The
CLINICAL GUIDELINES. Primary Care Guideline Summary Lumbar Spine Thomas J. Gilbert M.D., M.P.P. 3/17/15 revision
 CLINICAL GUIDELINES Primary Care Guideline Summary Lumbar Spine Thomas J. Gilbert M.D., M.P.P. 3/17/15 revision TRIAGE At the initial visit, a focused history and physical examination is performed to assign
CLINICAL GUIDELINES Primary Care Guideline Summary Lumbar Spine Thomas J. Gilbert M.D., M.P.P. 3/17/15 revision TRIAGE At the initial visit, a focused history and physical examination is performed to assign
Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology
 Physical Therapy Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology Scott Behjani, DPT, OCS Introduction Prevalence 1-year incidence of first-episode LBP ranges from
Physical Therapy Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology Scott Behjani, DPT, OCS Introduction Prevalence 1-year incidence of first-episode LBP ranges from
LOW BACK PAIN EPIDEMIOLOGY:
 LOW BACK PAIN OBJECTIVES: Discuss epidemiology of low back pain Summarize diagnosis/ special tests Review Red Flags Discuss treatment and referral guidelines Discuss light duty guidelines EPIDEMIOLOGY:
LOW BACK PAIN OBJECTIVES: Discuss epidemiology of low back pain Summarize diagnosis/ special tests Review Red Flags Discuss treatment and referral guidelines Discuss light duty guidelines EPIDEMIOLOGY:
CHRISTIANA SPINE CENTER NEW PATIENT QUESTIONNAIRE
 CHRISTIANA SPINE CENTER NEW PATIENT QUESTIONNAIRE NAME Today s Date CHIEF COMPLAINT _ (Please use your pen to mark painful areas) Front Back Date of Birth When did the pain begin: Allergies and reaction:
CHRISTIANA SPINE CENTER NEW PATIENT QUESTIONNAIRE NAME Today s Date CHIEF COMPLAINT _ (Please use your pen to mark painful areas) Front Back Date of Birth When did the pain begin: Allergies and reaction:
Good. Poor [ ] [ ] Yes, at all [ A ] Moderate activities, such as moving a table, pushing a vacuum cleaner, bowling, or playing golf [ ] [ ]
![Good. Poor [ ] [ ] Yes, at all [ A ] Moderate activities, such as moving a table, pushing a vacuum cleaner, bowling, or playing golf [ ] [ ] Good. Poor [ ] [ ] Yes, at all [ A ] Moderate activities, such as moving a table, pushing a vacuum cleaner, bowling, or playing golf [ ] [ ]](/thumbs/96/126804246.jpg) PATIENT I.D. This survey asks for your views about your health. This information will help keep track of how you feel and how well you are able to do your usual activities. For each of the following questions,
PATIENT I.D. This survey asks for your views about your health. This information will help keep track of how you feel and how well you are able to do your usual activities. For each of the following questions,
Treatments for Common Pain Disorders. Matthew R. Kohler, MD Hudson Spine and Pain Medicine 03/01/2017
 Treatments for Common Pain Disorders Matthew R. Kohler, MD Hudson Spine and Pain Medicine 03/01/2017 Acute Disc Herniation Conservative Approach (Four to Six Weeks) Physical Therapy, exercise and gentle
Treatments for Common Pain Disorders Matthew R. Kohler, MD Hudson Spine and Pain Medicine 03/01/2017 Acute Disc Herniation Conservative Approach (Four to Six Weeks) Physical Therapy, exercise and gentle
NW Family Wellness Center SE Sunnyside Rd. Suite 210 Clackamas, OR P: F: ACCIDENT INFORMATION FORM
 ACCIDENT INFORMATION FORM Name DOB Date Date of Accident Your Insurance Information Name of Policy Holder Policy Holder s Insurance Company Insurance Company Address Claim s Adjuster Name Adjuster phone
ACCIDENT INFORMATION FORM Name DOB Date Date of Accident Your Insurance Information Name of Policy Holder Policy Holder s Insurance Company Insurance Company Address Claim s Adjuster Name Adjuster phone
NAME: DATE: SPINE CENTER NEW PATIENT QUESTIONNAIRE
 Please complete and give to the receptionist when you arrive at the office for your appointment. NAME: DATE: SPINE CENTER NEW PATIENT QUESTIONNAIRE Page 1 of 6 Primary Care Physician s Name Primary Care
Please complete and give to the receptionist when you arrive at the office for your appointment. NAME: DATE: SPINE CENTER NEW PATIENT QUESTIONNAIRE Page 1 of 6 Primary Care Physician s Name Primary Care
Back and Neck Pain Questionnaire
 www.orthonc.com Back and Neck Pain Questionnaire Please print legibly in black ink. Answer only questions applicable to your condition. Leave other spaces blank. Date you are filling out this form: PERSONAL
www.orthonc.com Back and Neck Pain Questionnaire Please print legibly in black ink. Answer only questions applicable to your condition. Leave other spaces blank. Date you are filling out this form: PERSONAL
Getting at the CORE of Low-back pain Treatment Dr. John Flannery Dr. Carlo Ammendolia
 Disclosure & Acknowledgment Getting at the CORE of Low-back pain Treatment Dr. John Flannery Dr. Carlo Ammendolia Disclosures - None Acknowledgements Dr. Andrea Furlan Dr. Julia Alleyne Dr. Hamilton Hall
Disclosure & Acknowledgment Getting at the CORE of Low-back pain Treatment Dr. John Flannery Dr. Carlo Ammendolia Disclosures - None Acknowledgements Dr. Andrea Furlan Dr. Julia Alleyne Dr. Hamilton Hall
NAME OF PATIENT: STREET ADDRESS: CITY: STATE: ZIP: SEX: Male Female AGE: BIRTHDATE: MARITAL STATUS: PATIENT EMPLOYED BY: BUSINESS ADDRESS:
 DATE: HOME PHONE: NAME OF PATIENT: (Last name) (First name) (Middle) RESPONSIBLE PARTY (if a minor): STREET ADDRESS: CITY: STATE: ZIP: SEX: Male Female AGE: BIRTHDATE: MARITAL STATUS: PATIENT EMPLOYED
DATE: HOME PHONE: NAME OF PATIENT: (Last name) (First name) (Middle) RESPONSIBLE PARTY (if a minor): STREET ADDRESS: CITY: STATE: ZIP: SEX: Male Female AGE: BIRTHDATE: MARITAL STATUS: PATIENT EMPLOYED
Hailee Gibson, CCPA Neurosurgery Physician Assistant. Windsor Neurosurgery & Spine Associates. Windsor Regional Hospital Ouellette Campus
 Hailee Gibson, CCPA Neurosurgery Physician Assistant Windsor Neurosurgery & Spine Associates Windsor Regional Hospital Ouellette Campus Disclosures I have no disclosures Learning Objectives Provide information
Hailee Gibson, CCPA Neurosurgery Physician Assistant Windsor Neurosurgery & Spine Associates Windsor Regional Hospital Ouellette Campus Disclosures I have no disclosures Learning Objectives Provide information
Regional Back Pain and Radicular Pain Pathway Frequently asked Questions and Answers
 In Partnership with Regional Back Pain and Radicular Pain Pathway Frequently asked Questions and Answers Moving BACK to health Don t let your back pain get the better of you! The Regional Back Pain and
In Partnership with Regional Back Pain and Radicular Pain Pathway Frequently asked Questions and Answers Moving BACK to health Don t let your back pain get the better of you! The Regional Back Pain and
Quality Standards. Low Back Pain Care for Adults With Acute Low Back Pain. April 2018
 Quality Standards Low Back Pain Care for Adults With Acute Low Back Pain April 2018 Draft do not cite. Report is a work in progress and could change following public consultation. Summary This quality
Quality Standards Low Back Pain Care for Adults With Acute Low Back Pain April 2018 Draft do not cite. Report is a work in progress and could change following public consultation. Summary This quality
Dr. Cheng s NECK & BACK QUESTIONNAIRE FOR NEW PATIENT (Please complete this form and bring it with you on your visit)
 Dr. Cheng s NECK & BACK QUESTIONNAIRE FOR NEW PATIENT (Please complete this form and bring it with you on your visit) Last name: First Name: Title: Mr. Mrs. Dr. Appt Date: Refer by: (Please provide name
Dr. Cheng s NECK & BACK QUESTIONNAIRE FOR NEW PATIENT (Please complete this form and bring it with you on your visit) Last name: First Name: Title: Mr. Mrs. Dr. Appt Date: Refer by: (Please provide name
MOTOR VEHICLE ACCIDENT PAIN CHART
 MOTOR VEHICLE ACCIDENT PAIN CHART Name Today s Date (D/M/Y) Area of Concern What is the WORST pain you have ever experienced? (other than the pain you are experiencing NOW!) What was the date of this painful
MOTOR VEHICLE ACCIDENT PAIN CHART Name Today s Date (D/M/Y) Area of Concern What is the WORST pain you have ever experienced? (other than the pain you are experiencing NOW!) What was the date of this painful
A Patient s Guide to Treatment Guidelines for Low Back Pain
 A Patient s Guide to Treatment Guidelines for Low Back Pain 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Treatment Guidelines for Low Back Pain 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled
Common Thoraco- Lumbar Problems in the Mature Athlete
 Common Thoraco- Lumbar Problems in the Mature Athlete Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University Objectives Review the pathophysiology of the
Common Thoraco- Lumbar Problems in the Mature Athlete Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University Objectives Review the pathophysiology of the
Acute Low Back Pain. North American Spine Society Public Education Series
 Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
The NICE revised guidelines for the management of non-specific low back pain and; Implications for Practice
 The NICE revised guidelines for the management of non-specific low back pain and; Implications for Practice David Walsh David.walsh@nottingham.ac.uk National Clinical Guideline Centre Commissioned by NICE
The NICE revised guidelines for the management of non-specific low back pain and; Implications for Practice David Walsh David.walsh@nottingham.ac.uk National Clinical Guideline Centre Commissioned by NICE
A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT
 LUMBAR SPINE CASE #3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
LUMBAR SPINE CASE #3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
Mr. LBP: Case Presentation
 CLINICAL CASES Case: Mr. LBP Mr. LBP: Case Presentation Mr. LBP is a 35-year-old male He fell down while participating in a recreational sports activity He subsequently developed low back pain Upon arrival
CLINICAL CASES Case: Mr. LBP Mr. LBP: Case Presentation Mr. LBP is a 35-year-old male He fell down while participating in a recreational sports activity He subsequently developed low back pain Upon arrival
Are you getting the best treatment for your low back pain?
 Are you getting the best treatment for your low back pain? Dr.Rahimian Orthopedic surgon Spine fellowship resident Why are we here? To update you on the best evidence for the treatments available To give
Are you getting the best treatment for your low back pain? Dr.Rahimian Orthopedic surgon Spine fellowship resident Why are we here? To update you on the best evidence for the treatments available To give
Back Pain Update. Steven Andersen, MD Providence Physiatry Clinic 2016
 Back Pain Update Steven Andersen, MD Providence Physiatry Clinic 2016 Back Pain is Very Common Lifetime prevalence 80% 12 month prevalence 40% Point prevalence 20% Centers for Disease Control and Prevention.
Back Pain Update Steven Andersen, MD Providence Physiatry Clinic 2016 Back Pain is Very Common Lifetime prevalence 80% 12 month prevalence 40% Point prevalence 20% Centers for Disease Control and Prevention.
NON-INJURY QUESTIONNAIRE
 Patient Name: Appointment Date: Appointment with: Dr. Jeffrey A. Kozak NON-INJURY QUESTIONNAIRE Why did you make an appointment to see the doctor? Evaluation Surgical Opinion Reassurance Other Specify:
Patient Name: Appointment Date: Appointment with: Dr. Jeffrey A. Kozak NON-INJURY QUESTIONNAIRE Why did you make an appointment to see the doctor? Evaluation Surgical Opinion Reassurance Other Specify:
LUMBAR SPINE CASE 3. Property of VOMPTI, LLC. For Use of Participants Only. No Use or Reproduction Without Consent 1. L4-5, 5-S1 disc, facet (somatic)
 LUMBAR SPINE CASE 3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Richmond 2018-2019 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
LUMBAR SPINE CASE 3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Richmond 2018-2019 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
R Number. Patient Intake
 Date: dd/mm/yy Patient Information Name: OHIP #: Female Male Age: Date of Birth: dd/mm/yy Phone: Address: Email: City: Postal Code: What is your current marital status? Married Common-law Single (never
Date: dd/mm/yy Patient Information Name: OHIP #: Female Male Age: Date of Birth: dd/mm/yy Phone: Address: Email: City: Postal Code: What is your current marital status? Married Common-law Single (never
Corner on Wellness Chiropractic Center Therapeutic Massage
 Corner on Wellness Chiropractic Center Therapeutic Massage Patient Name Date Address _ City State Zip Phone Email Emergency Contact Name Phone Employer Work Phone Date of Birth Social Security # Is condition
Corner on Wellness Chiropractic Center Therapeutic Massage Patient Name Date Address _ City State Zip Phone Email Emergency Contact Name Phone Employer Work Phone Date of Birth Social Security # Is condition
BOTHELL INTEGRATED HEALTH, LLC Therapeutic Massage
 BOTHELL INTEGRATED HEALTH, LLC Therapeutic Massage Patient Name Date Address City State Zip Phone (home) (cell) Emergency Contact Name Phone Employer Date of Birth Work Phone Social Security # Is condition
BOTHELL INTEGRATED HEALTH, LLC Therapeutic Massage Patient Name Date Address City State Zip Phone (home) (cell) Emergency Contact Name Phone Employer Date of Birth Work Phone Social Security # Is condition
Health Today BACK PAIN
 SEEMINGLY SIMPLE THINGS MAY ALSO BE THE SOURCE OF YOUR ACHES AND PAINS. IN FACT, YOU MAY HAVE BEEN UNKNOW- INGLY LIFTING THINGS IN A MANNER THAT CAN CAUSE SUDDEN AGONY FROM A SIMPLE MOVEMENT OR YOU COULD
SEEMINGLY SIMPLE THINGS MAY ALSO BE THE SOURCE OF YOUR ACHES AND PAINS. IN FACT, YOU MAY HAVE BEEN UNKNOW- INGLY LIFTING THINGS IN A MANNER THAT CAN CAUSE SUDDEN AGONY FROM A SIMPLE MOVEMENT OR YOU COULD
In order to receive the maximum benefit from your rehabilitation program, it is important to understand and comply with the following guidelines:
 Arrival Policy 900 2 nd Ave., Madison, MN 56256 In order to receive the maximum benefit from your rehabilitation program, it is important to understand and comply with the following guidelines: Attend
Arrival Policy 900 2 nd Ave., Madison, MN 56256 In order to receive the maximum benefit from your rehabilitation program, it is important to understand and comply with the following guidelines: Attend
LOTHIAN LUMBAR SPINE PATHWAYS
 LOTHIAN LUMBAR SPINE PATHWAYS Patient Completes STarT Back form Assess patient and screen for Red Flags. If present refer to Appendix 1 Establish if Neurogenic. If so refer to Appendix 2 Children under
LOTHIAN LUMBAR SPINE PATHWAYS Patient Completes STarT Back form Assess patient and screen for Red Flags. If present refer to Appendix 1 Establish if Neurogenic. If so refer to Appendix 2 Children under
LUMBAR Orthopedic Specialists of Louisiana Pierce D. Nunley, MD PERSONAL INFORMATION. Patient Name:
 PERSONAL INFORMATION (Please Print or Type) Patient Name: Last First MI Registration Date: / / Birthdate: / / Age: Social Security #: - - Sex: Address: Apt. # Street Telephone Numbers: ( ) Occupation:
PERSONAL INFORMATION (Please Print or Type) Patient Name: Last First MI Registration Date: / / Birthdate: / / Age: Social Security #: - - Sex: Address: Apt. # Street Telephone Numbers: ( ) Occupation:
Cox Technic Case Report #126 published at (sent December 2013 ) 1
 Cox Technic Case Report #126 published at www.coxtechnic.com (sent December 2013 ) 1 Cox Technic Decompression Spinal Manipulation Resolves Symptoms Associated with Disc Protrusion and S1 Radiculopathy,
Cox Technic Case Report #126 published at www.coxtechnic.com (sent December 2013 ) 1 Cox Technic Decompression Spinal Manipulation Resolves Symptoms Associated with Disc Protrusion and S1 Radiculopathy,
NEW PATIENT QUESTIONNAIRE Spine pt acct #
 NEW PATIENT QUESTIONNAIRE Spine pt acct # Name: Date of Visit: Male Female (please fill in the circles) Date of Birth: Height: Weight: Age Today: What studies have been done on your spine? Where/When?
NEW PATIENT QUESTIONNAIRE Spine pt acct # Name: Date of Visit: Male Female (please fill in the circles) Date of Birth: Height: Weight: Age Today: What studies have been done on your spine? Where/When?
Agenda. Oregon Health Plan Back Pain Coverage Changes
 Oregon Health Plan Back Pain Coverage Changes Effective July 1, 2016 Alison Little, MD, MPH Medical Director, Medicaid, PacificSource Community Solutions PR3755_06202016 Agenda History Evidence on treatment
Oregon Health Plan Back Pain Coverage Changes Effective July 1, 2016 Alison Little, MD, MPH Medical Director, Medicaid, PacificSource Community Solutions PR3755_06202016 Agenda History Evidence on treatment
Regional Pain Syndromes: Neck and Low Back
 Regional Pain Syndromes: Neck and Low Back Srinivas Nalamachu, MD Disclosures Consultant/Independent Contractor/Honoraria: Ferring 1 Learning Objectives Identify the most common painful conditions in the
Regional Pain Syndromes: Neck and Low Back Srinivas Nalamachu, MD Disclosures Consultant/Independent Contractor/Honoraria: Ferring 1 Learning Objectives Identify the most common painful conditions in the
Welcome to NHS Highland Pain Management Service
 Welcome to NHS Highland Pain Management Service Information from this questionnaire helps us to understand your pain problem better. It is important that you read each question carefully and answer as
Welcome to NHS Highland Pain Management Service Information from this questionnaire helps us to understand your pain problem better. It is important that you read each question carefully and answer as
KAISER PERMANENTE SPINE
 KAISER PERMANENTE SPINE The following forms are specially designed to give your doctor valuable information about the health of your spine. The same way an EKG gives us information about your heart. It
KAISER PERMANENTE SPINE The following forms are specially designed to give your doctor valuable information about the health of your spine. The same way an EKG gives us information about your heart. It
Managing back pain a new approach
 Managing back pain a new approach David Rogers Clinical Lead Functional Restoration Service Extended Scope Physiotherapist Royal Orthopaedic Hospital Setting the scene Back pain is one of the most common
Managing back pain a new approach David Rogers Clinical Lead Functional Restoration Service Extended Scope Physiotherapist Royal Orthopaedic Hospital Setting the scene Back pain is one of the most common
CERVICAL Orthopedic Specialists of Louisiana Pierce D. Nunley, MD PERSONAL INFORMATION. Patient Name:
 PERSONAL INFORMATION (Please Print or Type) Patient Name: Last First MI Registration Date: / / Birthdate: / / Age: Social Security #: - - Sex: Address: Apt. # Street Telephone Numbers: ( ) Occupation:
PERSONAL INFORMATION (Please Print or Type) Patient Name: Last First MI Registration Date: / / Birthdate: / / Age: Social Security #: - - Sex: Address: Apt. # Street Telephone Numbers: ( ) Occupation:
Epidemiology of Low back pain
 Low Back Pain Definition Pain felt in your lower back may come from the spine, muscles, nerves, or other structures in that region. It may also radiate from other areas like the mid or upper back, a inguinal
Low Back Pain Definition Pain felt in your lower back may come from the spine, muscles, nerves, or other structures in that region. It may also radiate from other areas like the mid or upper back, a inguinal
STRETCHING EXERCISES FOR PAIN REDUCTION
 PHYSICAL THERAPY RESOURCES STRETCHING EXERCISES FOR PAIN REDUCTION This material is presented for informational and educational purposes only. If you experience any pain or difficulty with these exercises,
PHYSICAL THERAPY RESOURCES STRETCHING EXERCISES FOR PAIN REDUCTION This material is presented for informational and educational purposes only. If you experience any pain or difficulty with these exercises,
PAIN HISTORY. Please describe your pain:
 Name: Date: PAIN HISTORY Please describe your pain: List surgeries/hospital admissions and dates (Skip if you have already provided this information on Medical History Questionnaire): Please list current
Name: Date: PAIN HISTORY Please describe your pain: List surgeries/hospital admissions and dates (Skip if you have already provided this information on Medical History Questionnaire): Please list current
Re-Exam Questionnaire
 Re-Exam Questionnaire Patient Name: Date: The following hi-lighted symptoms are what brought you into our office originally. DIRECTIONS: Please rate ALL hi-lighted symptoms: S = same; B = better; W = worse
Re-Exam Questionnaire Patient Name: Date: The following hi-lighted symptoms are what brought you into our office originally. DIRECTIONS: Please rate ALL hi-lighted symptoms: S = same; B = better; W = worse
Heritage Chiropractic Clinic Geoffrey A. Sandels, D.C Lenora Church Road / Snellville, Georgia / Welcome to our office!
 Heritage Chiropractic Clinic Geoffrey A. Sandels, D.C. 2407 Lenora Church Road / Snellville, Georgia 30078-6916 / 770-979-2731 Welcome to our office! Today's Date: / / Your Name: [ ] Male [ ] Female What
Heritage Chiropractic Clinic Geoffrey A. Sandels, D.C. 2407 Lenora Church Road / Snellville, Georgia 30078-6916 / 770-979-2731 Welcome to our office! Today's Date: / / Your Name: [ ] Male [ ] Female What
SPINAL PAIN. Mr. Yagnesh Vellore FRACS Neurosurgeon and Spine Surgeon
 SPINAL PAIN Mr. Yagnesh Vellore FRACS Neurosurgeon and Spine Surgeon PAIN GENERATORS IN THE SPINE Ligaments: ALL,PLL Muscle Periosteum bone Outer 1/3 annulus disc Facet joints Sacro-iliac joint sinuvertebral
SPINAL PAIN Mr. Yagnesh Vellore FRACS Neurosurgeon and Spine Surgeon PAIN GENERATORS IN THE SPINE Ligaments: ALL,PLL Muscle Periosteum bone Outer 1/3 annulus disc Facet joints Sacro-iliac joint sinuvertebral
Cervical Plating BACK PAIN
 BACK PAIN Back Pain Back pain is frequent complaint. It is the commonest cause of work-related absence in the world. Although back pain may be painful and uncomfortable, it is not usually serious. Even
BACK PAIN Back Pain Back pain is frequent complaint. It is the commonest cause of work-related absence in the world. Although back pain may be painful and uncomfortable, it is not usually serious. Even
Chad J Anderson D.C.
 Chad J Anderson D.C. New Patient Health History Form NAME: DATE: / / DOB: / / AGE: MARITAL STATUS: M / S / D / W ADDRESS: CITY: STATE: ZIP: PHONE: CELL PHONE: EMAIL: EMERGENCY CONTACT: PHONE#: RELATIONSHIP:
Chad J Anderson D.C. New Patient Health History Form NAME: DATE: / / DOB: / / AGE: MARITAL STATUS: M / S / D / W ADDRESS: CITY: STATE: ZIP: PHONE: CELL PHONE: EMAIL: EMERGENCY CONTACT: PHONE#: RELATIONSHIP:
Medical Affairs Policy
 Medical Affairs Policy Service: Back Pain Procedures-Epidural Injection (Caudal Epidural, Selective Nerve Root Block, Interlaminar, Transforaminal, Translaminar Epidural Injection) PUM 250-0015-1706 Medical
Medical Affairs Policy Service: Back Pain Procedures-Epidural Injection (Caudal Epidural, Selective Nerve Root Block, Interlaminar, Transforaminal, Translaminar Epidural Injection) PUM 250-0015-1706 Medical
The Complex/Challenging Spine Patient Steve Wisniewski, M.D. Department of PM&R
 The Complex/Challenging Spine Patient Steve Wisniewski, M.D. Department of PM&R 2011 MFMER slide-1 Disclosures None 2011 MFMER slide-2 Learning Objectives Review indications for obtaining imaging studies
The Complex/Challenging Spine Patient Steve Wisniewski, M.D. Department of PM&R 2011 MFMER slide-1 Disclosures None 2011 MFMER slide-2 Learning Objectives Review indications for obtaining imaging studies
Past Surgical History
 Name: DOB: Check All That Apply Past Medical History o Anemia o Aneurysm o Asthma o Bipolar o Bleeding Disorder o Blood Clot o Brain Tumor o Bronchitis o Cancer o Crohn s Disease/Ulcerative Colitis o Depression
Name: DOB: Check All That Apply Past Medical History o Anemia o Aneurysm o Asthma o Bipolar o Bleeding Disorder o Blood Clot o Brain Tumor o Bronchitis o Cancer o Crohn s Disease/Ulcerative Colitis o Depression
Premier Orthopedic Spine Center
 Premier Orthopedic Spine Center Atrium Medical Center Professional Buliding 200 Medical Center Dr., Ste. 375 Middletown, Ohio 45005 Neck Questionnaire Patient Date Family Physician The onset of my neck
Premier Orthopedic Spine Center Atrium Medical Center Professional Buliding 200 Medical Center Dr., Ste. 375 Middletown, Ohio 45005 Neck Questionnaire Patient Date Family Physician The onset of my neck
Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis
 Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis The program consisted of manual therapy twice per week (eg, soft tissue and neural The components of the Boot Camp Program
Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis The program consisted of manual therapy twice per week (eg, soft tissue and neural The components of the Boot Camp Program
North American Spine Society Public Education Series
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Name Date of Birth Today s Date
 SWEDISH PAIN SERVICES: Initial Visit Questionnaire Name Date of Birth Today s Date We realize that some of the questions might not address your exact situation but please answer them to your best ability.
SWEDISH PAIN SERVICES: Initial Visit Questionnaire Name Date of Birth Today s Date We realize that some of the questions might not address your exact situation but please answer them to your best ability.
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Facet Injection Please check the indication (reason)
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Facet Injection Please check the indication (reason)
Objectives. Identify and differentiate appropriate surgical cases. Good Surgical Outcomes
 ECHO February 5 th, 2015 Surgical Selection for Low Back Pain Objectives Identify and differentiate appropriate surgical cases Disclosures Medical director for UHN Rehabilitations Solution Back and Neck
ECHO February 5 th, 2015 Surgical Selection for Low Back Pain Objectives Identify and differentiate appropriate surgical cases Disclosures Medical director for UHN Rehabilitations Solution Back and Neck
Cox Technic Case Report #169 published at (sent 5/9/17) 1
 Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
The evidence for SMT in CLBP
 The evidence for SMT in CLBP Peter Tuchin BSc, GradDipChiro, DipOHS PhD FACC Associate Professor, MU (1991 - ) Past President, COCA 1 Peter Tuchin Peter Tuchin 2 WCA 2007 Peter Tuchin 3 Number of injuries
The evidence for SMT in CLBP Peter Tuchin BSc, GradDipChiro, DipOHS PhD FACC Associate Professor, MU (1991 - ) Past President, COCA 1 Peter Tuchin Peter Tuchin 2 WCA 2007 Peter Tuchin 3 Number of injuries
A Patient s Guide to Cervical Foraminotomy
 A Patient s Guide to Cervical Foraminotomy 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Cervical Foraminotomy 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled from a variety
Get back to: my life. Non-fusion treatment for lumbar spinal stenosis
 Get back to: my life Non-fusion treatment for lumbar spinal stenosis Do you have any of these symptoms? numbness, weakness or pain in the lower legs When any of these conditions occur, the spinal nerve,
Get back to: my life Non-fusion treatment for lumbar spinal stenosis Do you have any of these symptoms? numbness, weakness or pain in the lower legs When any of these conditions occur, the spinal nerve,
Spine New Patient Questionnaire Rev
 Spine New Patient Questionnaire Rev 10.13.10 Name: Male Female Temp: Height: Weight: Date of Visit: Date of Birth: Age Today: *Please note this is a multi-part questionnaire. When you are done, please
Spine New Patient Questionnaire Rev 10.13.10 Name: Male Female Temp: Height: Weight: Date of Visit: Date of Birth: Age Today: *Please note this is a multi-part questionnaire. When you are done, please
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Epidural Injection Please check the indication (reason)
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Epidural Injection Please check the indication (reason)
PATIENT CONSULTATION WORKSHEET
 PATIENT CONSULTATION WORKSHEET Today s Date: Name: Referred By: Birthdate: Address: City: State: Zip: Home Phone: Work: Ext: Cell Phone: E-Mail Address: Best way for us to keep in touch with you (check
PATIENT CONSULTATION WORKSHEET Today s Date: Name: Referred By: Birthdate: Address: City: State: Zip: Home Phone: Work: Ext: Cell Phone: E-Mail Address: Best way for us to keep in touch with you (check
Taking Care of Your Back
 Taking Care of Your Back Most people will feel back pain at some point in their lives, but not all back pain is the same for everyone. The good news is, most low back pain improves without any treatment
Taking Care of Your Back Most people will feel back pain at some point in their lives, but not all back pain is the same for everyone. The good news is, most low back pain improves without any treatment
REVIEW OF LITERATURE BMJ 2007; 334(7607): Diagnosis and treatment of sciatica. Bart W. Koes Maurits W. van Tulder Wilco C.
 2 REVIEW OF LITERATURE Diagnosis and treatment of sciatica Bart W. Koes Maurits W. van Tulder Wilco C. Peul BMJ 2007; 334(7607):1313-1317 22 CHAPTER 2 DIAGNOSIS AND TREATMENT OF SCIATICA 23 INTRODUCTION
2 REVIEW OF LITERATURE Diagnosis and treatment of sciatica Bart W. Koes Maurits W. van Tulder Wilco C. Peul BMJ 2007; 334(7607):1313-1317 22 CHAPTER 2 DIAGNOSIS AND TREATMENT OF SCIATICA 23 INTRODUCTION
What guidelines are available for sciatica and radicular pain?
 Chapter 5 What guidelines are available for sciatica and radicular pain? Paolo Marchettini Guidelines for the management of low back pain (LBP) and lumbar or cervical radiculopathy resulting from sciatica
Chapter 5 What guidelines are available for sciatica and radicular pain? Paolo Marchettini Guidelines for the management of low back pain (LBP) and lumbar or cervical radiculopathy resulting from sciatica
A Patient's Guide to Cervical Laminectomy
 Introduction A laminectomy is a surgical procedure to relieve pressure on the spinal cord due to spinal stenosis. In spinal stenosis, bone spurs press against the spinal cord, leading to a condition called
Introduction A laminectomy is a surgical procedure to relieve pressure on the spinal cord due to spinal stenosis. In spinal stenosis, bone spurs press against the spinal cord, leading to a condition called
DOCTOR DISCUSSION GUIDE
 DOCTOR DISCUSSION GUIDE BE PREPARED For the best outcome from a visit with your doctor, it s important to be prepared. The more completely and clearly you describe the pain you re experiencing, the easier
DOCTOR DISCUSSION GUIDE BE PREPARED For the best outcome from a visit with your doctor, it s important to be prepared. The more completely and clearly you describe the pain you re experiencing, the easier
WHAT IS SCIATICA? Apart from the compression of one of the nerves, there are other known causes of sciatica which include:
 WHAT IS SCIATICA? If you suffer from Sciatica, or you re close to someone who does, you already know that it is one of those conditions that can be quite overwhelming and incapacitating while causing a
WHAT IS SCIATICA? If you suffer from Sciatica, or you re close to someone who does, you already know that it is one of those conditions that can be quite overwhelming and incapacitating while causing a
An Osteopathic Approach to Low Back Pain. Ryan Seals DO Interim Chair of Family Medicine and OMM
 An Osteopathic Approach to Low Back Pain Ryan Seals DO Interim Chair of Family Medicine and OMM Objectives Review Osteopathic Philosophy and Principles Discuss how somatic dysfunction influences low back
An Osteopathic Approach to Low Back Pain Ryan Seals DO Interim Chair of Family Medicine and OMM Objectives Review Osteopathic Philosophy and Principles Discuss how somatic dysfunction influences low back
Paul Allan Regional Clinical Lead - South. Lumbar Spine. Assessment & Differential Diagnosis
 Paul Allan Regional Clinical Lead - South Lumbar Spine Assessment & Differential Diagnosis Aims Refresh lumbar spine anatomy Red flags Discuss common pathologies seen in general practice Subjective and
Paul Allan Regional Clinical Lead - South Lumbar Spine Assessment & Differential Diagnosis Aims Refresh lumbar spine anatomy Red flags Discuss common pathologies seen in general practice Subjective and
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Name: DOB: Age: Phone: Phone: Is this an injury related to a : (circle one) Other? Yes / No (Please Explain)
 Family/Primary Doctor: Emergency Contact: Name Phone: Phone: Who referred you to our office? Who else have you seen for this condition? INSTRUCTIONS: Please provide the following information, in detail.
Family/Primary Doctor: Emergency Contact: Name Phone: Phone: Who referred you to our office? Who else have you seen for this condition? INSTRUCTIONS: Please provide the following information, in detail.
PERSONAL INJURY QUESTIONNAIRE
 PERSONAL INJURY QUESTIONNAIRE Name Date of Birth Age Address City State Zip NATURE OF ACCIDENT: 1. Date of Accident Time of Day (AM / PM) 2. Please state how the accident happened in your own words: 3.
PERSONAL INJURY QUESTIONNAIRE Name Date of Birth Age Address City State Zip NATURE OF ACCIDENT: 1. Date of Accident Time of Day (AM / PM) 2. Please state how the accident happened in your own words: 3.
Herniated Disk in the Lower Back
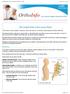 Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
Do not write in this box. Name: Appointment: Date: Appointment Time: Primary Care Provider: Phone: Fax: Referring Physician: Address:
 3901 Rainbow Boulevard Do not write in this box Appointment: Date: Appointment Time: Birth date: Age: Gender: Male Female Primary Care Provider: Phone: Fax: Referring Physician: Address: Phone: Fax: CHIEF
3901 Rainbow Boulevard Do not write in this box Appointment: Date: Appointment Time: Birth date: Age: Gender: Male Female Primary Care Provider: Phone: Fax: Referring Physician: Address: Phone: Fax: CHIEF
Thank you for choosing Saint Joseph s Hospital Health Center for your spine surgery. Updated Jan 2017
 Thank you for choosing Saint Joseph s Hospital Health Center for your spine surgery Updated Jan 2017 This class is designed to give you some basic, important information about spine surgery We will cover
Thank you for choosing Saint Joseph s Hospital Health Center for your spine surgery Updated Jan 2017 This class is designed to give you some basic, important information about spine surgery We will cover
RED FLAGS IN LOW BACK PAIN NAOEM
 RED FLAGS IN LOW BACK PAIN NAOEM Annual Scientific Conference 2016 Dianna Chamblin, MD LOW BACK PAIN : FIRST THE BAD NEWS LOW BACK PAIN: [DEPRESSING] STATS Leading cause of disability in the US as of 2010.
RED FLAGS IN LOW BACK PAIN NAOEM Annual Scientific Conference 2016 Dianna Chamblin, MD LOW BACK PAIN : FIRST THE BAD NEWS LOW BACK PAIN: [DEPRESSING] STATS Leading cause of disability in the US as of 2010.
If you have a condition that compresses your nerves, causing debilitating back pain or numbness along the back of your leg.
 Below, we have provided some basic information for your benefit. Please use this information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk
Below, we have provided some basic information for your benefit. Please use this information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk
Integrative Pain Treatment Center Programs Scope of Services
 Integrative Pain Treatment Center Programs Scope of Services The Integrative Pain Treatment Center at Marianjoy Rehabilitation Hospital, part of Northwestern Medicine, offers two specialized 21-day outpatient
Integrative Pain Treatment Center Programs Scope of Services The Integrative Pain Treatment Center at Marianjoy Rehabilitation Hospital, part of Northwestern Medicine, offers two specialized 21-day outpatient
 Introduction Posterior cervical fusion is done through the back posterior of the neck. The surgery joins two or more neck vertebrae into one solid section of bone. The medical term for fusion is arthrodesis.
Introduction Posterior cervical fusion is done through the back posterior of the neck. The surgery joins two or more neck vertebrae into one solid section of bone. The medical term for fusion is arthrodesis.
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis This article is also available in Spanish: Estenosis de la columna lumbar (topic.cfm?topic=a00701). A common cause of low back and leg pain is lumbar spinal stenosis. As we age,
Lumbar Spinal Stenosis This article is also available in Spanish: Estenosis de la columna lumbar (topic.cfm?topic=a00701). A common cause of low back and leg pain is lumbar spinal stenosis. As we age,
Patient Summary Form PSF-750 (Rev:2/18/2009) Patient Information
 atient Summary Form SF-750 (ev:2/18/2009) atient nformation Female nstructions lease complete this form within the specified timeline and fax to the specified fax number as indicated on lan Summary or
atient Summary Form SF-750 (ev:2/18/2009) atient nformation Female nstructions lease complete this form within the specified timeline and fax to the specified fax number as indicated on lan Summary or
PLEASE READ THESE IMPORTANT INSTRUCTIONS BELOW:
 Welcome to the Montana Spine and Pain Center We have you scheduled to see: Your appointment is scheduled for: Check in Time: Appointment Time: PLEASE READ THESE IMPORTANT INSTRUCTIONS BELOW: Complete this
Welcome to the Montana Spine and Pain Center We have you scheduled to see: Your appointment is scheduled for: Check in Time: Appointment Time: PLEASE READ THESE IMPORTANT INSTRUCTIONS BELOW: Complete this
PAIN MEDICINE FOR THE NON-PAIN SPECIALIST 2017
 PAIN MEDICINE FOR THE NON-PAIN SPECIALIST 2017 FEBRUARY 16-18, 2017 JW MARRIOTT DESERT SPRINGS RESORT & SPA PALM DESERT, CALIFORNIA Learn the latest treatment strategies and multidisciplinary management
PAIN MEDICINE FOR THE NON-PAIN SPECIALIST 2017 FEBRUARY 16-18, 2017 JW MARRIOTT DESERT SPRINGS RESORT & SPA PALM DESERT, CALIFORNIA Learn the latest treatment strategies and multidisciplinary management
Robert J. Brownsberger, M.D., PC New Patient Paperwork
 1 Today s Date: Robert J. Brownsberger, M.D., PC New Patient Paperwork Your Name: Date of Birth: SS#: Email: Race/Ethnicity: Primary Language: Mailing address: Home Phone: Cell Phone: Preferred Pharmacy:
1 Today s Date: Robert J. Brownsberger, M.D., PC New Patient Paperwork Your Name: Date of Birth: SS#: Email: Race/Ethnicity: Primary Language: Mailing address: Home Phone: Cell Phone: Preferred Pharmacy:
Cornerstone Health, 500 Davis Street, Suite #109, Evanston IL 60201
 Patient's Name Number Date NECK DISABILITY INDEX This questionnaire has been designed to give the doctor information as to how your neck pain has affected your ability to manage in everyday life. Please
Patient's Name Number Date NECK DISABILITY INDEX This questionnaire has been designed to give the doctor information as to how your neck pain has affected your ability to manage in everyday life. Please
Rational Approach to Treating Low Back Pain
 Rational Approach to Treating Low Back Pain Susie Jang, MD Faculty, Department of Anesthesia, Critical Care & Pain Medicine Beth Israel Deaconess Medical Center Instructor, Harvard Medical School Learning
Rational Approach to Treating Low Back Pain Susie Jang, MD Faculty, Department of Anesthesia, Critical Care & Pain Medicine Beth Israel Deaconess Medical Center Instructor, Harvard Medical School Learning
