Introduction to Wound Assessment & Management. Clinical Skills
|
|
|
- Grace Booker
- 5 years ago
- Views:
Transcription
1 Clinical Skills Introduction to Wound Assessment and Management Sian Williams (Clinical Skills Tutor/Manager)
2 Aims & Outcomes Aims & Outcomes The aim of this module is to facilitate student learning regarding the management of acute wounds. It has been produced using guidance from the National Institute for Clinical Excellence (NICE), Clinical Knowledge Guidance, and photography from local sources. The learning outcomes for this module are for the student to be able to: Describe the principles of wound healing. Assess a wound or laceration and recognise an infected wound. Describe how to manage a wound according to the level of risk of infection. Define the management of infected wounds. Evaluate own knowledge of acute wound care and formulate an action plan to compensate for any deficits.
3 Introduction Introduction Most health care professionals will be asked at some time for advice on the management of minor wounds and lacerations. This module has been designed to help you understand the concept of wound healing and how to manage wounds to create the optimum conditions for wound healing to occur. Trauma wounds are defined as wounds caused by injury. They range from extensive loss of tissue to simple abrasions. Minor traumatic wounds are often encountered in Primary Care. Wound healing is an intricate process in which the skin (or other organ ) heals itself after injury. In normal skin, the epidermis and dermis exists in a state of equilibrium, forming a protective barrier against the external environment. Once the protective barrier is broken, the process of wound healing is immediately set in motion. The classic model of wound healing can be divided into four sequential, yet linking phases: Haemostasis Inflammatory Proliferative Remodeling
4 Phases of wound healing Phases of wound healing -Haemostasis Immediately following cutaneous injury, blood elements and vasoactive amines extravasate from locally damaged blood vessels within the dermis. Vascular permeability is temporarily increased to allow neutrophils [polymorphonuclear neutrophils (PMNs)], platelets and plasma proteins to infiltrate the wound. Vasoconstriction follows, in response to factors released by these cells. Coagulation then occurs as platelets aggregate with fibrin, which is deposited in the wound following its conversion from fibrinogen. Platelet Erythrocyte Neutrophil
5 Phases of wound healing Phases of wound healing - Inflammation Platelets release several factors, including platelet-derived growth factor (PDGF) and transforming growth factor β (TGF-β), which attract PMNs to the wound, signalling the beginning of inflammation. Neutrophil Fibrin thread Macrophage Platelet Erythrocyte
6 Phases of wound healing Phases of wound healing - Proliferation After 48 h, macrophages replace PMNs as the principal inflammatory cell. Macrophage Fibrin thread Platelet Together, PMNs and macrophages remove debris from the wound, release growth factors, and begin to reorganise the extracellular matrix. The proliferation phase begins at about 72 h as fibroblasts, recruited to the wound by growth factors released by inflammatory cells, begin to synthesise collagen. Neutrophil Erythrocyte
7 Phases of wound healing Phases of wound healing - Remodelling Although the rate of collagen synthesis slows down after about three weeks, collagen crosslinking and reorganisation occur for months after injury in the remodelling phase of repair.
8 Wound Assessment Wound Assessment Initial Management While the temptation may be to focus solely on the injury itself, it is very important to assess the the whole person. Begin with a primary survey - that is, airway, breathing, circulatory volume and level of consciousness. If this survey is overlooked, a potentially life-threatening injury may be missed. A patient with a bleeding laceration should have gentle pressure applied with a sterile dressing to control the haemorrhage, and the affected area should be elevated. If the patient feels or looks faint they should be asked to lie down. Analgesia should be given as appropriate. Avoid anti inflammatory medication as it may interfere with the bodies natural responses to injury. The removal of a large foreign body, such as a knife, should only be undertaken in theatre. This reduces the risk of uncontrolled bleeding and allows any serious underlying damage to be treated immediately.
9 Wound Assessment Wound Assessment History-taking Once the patient has been stabilised, a more detailed history should be taken. A patient in A&E may be triaged by a Health care Professional (HCP) who will take a history. Details should include: How did the injury occur? The mechanism of the injury is vital to the assessment and care of the patient, as it provides clues to the type and amount of tissue damage. Where was the wound sustained? This is important as wounds sustained in an unclean environment are at a very high risk of contamination with bacteria, fungi and spores - for example, Clostridium tetani. When did the wound occur? Research indicates that the greater the time between wounding and good wound care, the greater the chance of infection Why did the wound occur? The reason why the wound occurred should be established, as it may be an outward manifestation of abuse or underlying medical disorder. Wound assessment charts are commonly used when assessing wounds. Check local policy.
10 Wound Assessment-When intervention is required Wound Assessment-When intervention is required Wound assessment should note the environment where the injury occurred, and include a holistic assessment of the individual. You should consult with senior colleagues if any of the following present. Vascular damage arterial bleeding from wound, loss of pulse, or poor perfusion distal to the injury. Nerve damage loss of light touch or motor function distal to the injury. Tendon injury, including injury to the sheath. Facial lacerations for which a good cosmetic repair is important, particularly lacerations crossing the margins of lips, nose, or ears. Lacerations of palm of hand with any signs of infection. Lacerations associated with marked cellulitis over a joint. Possible foreign body remaining in the wound after cleaning, including all injuries caused by glass. Complex, widely gaping, or extensively devitalized lacerations. Burns
11 Types of Wound Types of Acute Wound The next 6 slides show in graphic detail the type of acute wounds that are presented in A&E Departments every day. I will briefly describe the background to the accident
12 Types of Wound Types of Acute Wound - Avulsion Made by strong shearing forces and friction that can result in significant tearing and destruction of tissues...patient amputated the end of the finger whilst working with a crane..
13 Types of Wound Types of Acute Wound - Laceration Made by an object that tears tissues, producing jagged, irregular edges, such as glass, jagged wire, or a blunt knife...separating frozen burgers with knife. Knife slipped..
14 Types of Wound Types of Acute Wound - Contusion Made by blunt force causing tissue damage with bruising and swelling, typically not breaking the skin...fell down the stairs causing a contusion and laceration..
15 Types of Wound Types of Acute Wound Puncture Wound Made by a pointed instrument, such as an ice pick, bullet, or nail...using a power drill, accidentally drilled finger..
16 Types of Wound Types of Acute Wound Burn Caused by thermal, chemical, or electrical injury to the skin...a security tag exploded on hand causing burn..
17 Types of Wound Types of Acute Wound Abrasion Injury where a superficial layer of tissue is removed...fell off bike on to tarmac path..
18 Types of Wound Types of Acute Wound Made by strong shearing forces and friction that can result in significant tearing and destruction of tissues - e.g., degloving injury. Made by an object that tears tissues, producing jagged, irregular edges, such as glass, jagged wire, or a blunt knife. Made by blunt force causing tissue damage with bruising and swelling, typically not breaking the skin. Made by a clean cut of a sharp instrument, such as a surgical incision with a scalpel. Avulsion wounds Lacerated wounds Contused wounds Incised wounds Caused by thermal, chemical, or electrical injury to the skin. Made by a pointed instrument, such as an ice pick, bullet, or nail. Injury where a superficial layer of tissue is removed. Burn wounds Puncture wounds Abrasions
19 Wound Assessment Wound Management It is important the wound is managed according to the level of risk of infection. There are 3 broad categories: Low Risk A wound that is assessed not to be infected or at high risk of infection. High Risk A wound that has been assessed as not being infected, but is at high risk of infection. Infected A dirty-infected wound is one that retains devitalised tissue or involves preoperativelyexisting infection or perforated viscera. Skip
20 Low Risk Lacerations Low Risk Lacerations As a reminder: A Low Risk laceration may be defined as: A wound that is assessed not to be infected or at high risk of infection. Example of a Low risk wound. Clean, shallow and fairly straight. The wound will not be contaminated with soil, faeces, bodily fluids, or pus. It may present as a sharp neat, usually shallow cut, typically made in a straight, single slash. Classically these are caused by knives but can be due to falling through glass, accidents with sheet metal, in fact anything with a sharp, cutting edge. If these edges can be approximated easily, blood loss can be minimised and the risk of infection is minimal. Indiscriminate use of prophylactic antimicrobials in low risk wounds is not warranted (8).
21 Low Risk Lacerations - Cleaning the wound 1. Low Risk Lacerations-Cleaning the wound Disinfect the skin around the wound with an antiseptic if necessary, but avoid getting antiseptic into the wound. A device that may be used for low pressure irrigation of a wound Keep hair out of the wound. Cut hair along the wound edge and flatten it away from the wound with ointment. Debride devitalized tissue and pick out as much foreign material as possible if there may be glass in the wound, refer for radiography. Irrigate the wound with normal saline, drinking-quality water, or cooled boiled water. Low-pressure irrigation using a syringe is sufficient for lacerations that are not visibly contaminated.
22 Low Risk Lacerations - Closing the wound 2. Low Risk Lacerations-Closing the wound Sutures are the preferred method of closing lacerations that are longer than 5 cm long, or those 5 cm or shorter when: Deep dermal sutures are required, to allow low-tension apposition of the wound edges. The wound is subject to excessive flexing, tension, or wetting. Local anaesthetic is required before suturing. See the e-module on Suturing for more guidance.
23 Low Risk Lacerations - Closing the wound 2. Low Risk Lacerations-Closing the wound Tissue adhesives and adhesive strips are equally preferred to sutures to close wounds 5 cm or shorter when: There are no risk factors for infection and The wound edges are easily apposed without leaving any dead space and The wound is not subject to excessive flexing, tension, or wetting.
24 Low Risk Lacerations - Closing the wound 2. Low Risk Lacerations-Closing the wound Adhesive strips are preferred to tissue adhesives to close wounds 5 cm or shorter when: The laceration is a pretibial flap or There are any risk factors for infection and The wound edges are easily apposed without leaving any dead space and The wound is not subject to excessive flexing, tension, or wetting.
25 Low Risk Lacerations - Dressing the wound 3. Low Risk Lacerations-Dressing the wound Apply a dressing after closing the laceration: For lacerations with minimal exudate, dress with a clear vapour-permeable dressing(a). For lacerations with modest exudate, dress with a low-adherence, absorbent, perforated dressing with an adhesive border(b). For more information about aeseptic technique and dressing a wound, watch this tutorial provided by Queen Mary's University: a b
26 Low Risk Lacerations - Follow-up points 4. Low Risk Lacerations - Follow-up points If symptoms and signs of infection develop after closure of the laceration: Remove sutures or adhesive strips and incise if it is not draining. Incise through tissue adhesive (e.g..) to allow drainage. Take swabs from any discharge for microbiological investigation, and start empirical antibiotics while awaiting results. Remove sutures after: 3 5 days on the head days over joints days at other sites. Remove adhesive strips after: 3 5 days on the head days at other sites. Tissue adhesive does not need to be removed; it will slough off naturally after 7 10 days. Removal of dressings: Keep the laceration dressed until sutures or adhesive strips are due to be removed. Low adherence absorbent dressings should be replaced if exudate has caused significant wetting of the dressing.
27 High Risk Lacerations High Risk Lacerations As a reminder: A High Risk laceration may be defined as: a wound that has been assessed as not being infected, but is at high risk of infection. The wound may be contaminated with soil, faeces, bodily fluids, or pus. People may have additional risk factors. These include: Diabetes. Oral steroid therapy and other causes of immunosuppression. Age older than 65 years. Foreign body present before cleaning of wound. Stellate shape or jagged wound margins. Visible contamination with substances other than soil, faeces, saliva, or pus. Presentation longer than 6 hours after injury. Wounds longer than 5 cm. A lizard bite High risk
28 High Risk Lacerations - Cleaning the wound 1. High Risk Lacerations - Cleaning the wound Disinfect the skin around the wound with an antiseptic, but avoid getting antiseptic into the wound. Keep hair out of the wound. Cut hair along the wound edge and flatten it away from the wound with ointment. Debride devitalized tissue and pick out as much foreign material as possible if there may be glass in the wound, refer for radiography. Irrigate the wound with normal saline, drinking-quality water, or cooled boiled water. High-pressure irrigation should be used to remove visible debris from the wound, using a syringe and a green needle. High pressure irrigation
29 High Risk Lacerations - Closing the wound 2. High Risk Lacerations - Dressing the wound Important: Wounds that are of High Risk of Infection are dressed but not closed. a Prevent apposition of the wound edges by packing with a non-adherent dressing. Cover all lacerations at high risk of infection with a non-adherent, absorbent dressing: For lacerations with small quantities of exudate, dress with a non-adherent or topical iodine dressing (a). For lacerations with more exudate, cover with a non-adherent or hydrofibre dressing (b) (good for cavities), or a foam dressing. Arrange review 3 5 days after initial presentation. b
30 High Risk Lacerations- Antibiotic Therapy and Tetanus 3. High Risk Lacerations- Antibiotic Therapy and Tetanus Treat lacerations that may be contaminated with soil, faeces, saliva, or purulent exudates with co-amoxiclav. If the person is allergic to penicillin, treat with erythromycin combined with metronidazole. Treat lacerations that are not obviously contaminated with flucloxacillin. Use erythromycin if the person is allergic to penicillin. Refer people with a tetanus-prone wound which is at high risk of contamination with human tetanus immunoglobulin, regardless of tetanus immunization status. Check the person's tetanus immunization status and administer an opportunistic booster dose of tetanus vaccine if they are not up to date. A fully immunized person will have had a primary course of three vaccines followed by two boosters spaced 10 years apart. For further information on contraindications, cautions, drug interactions, and adverse effects, see the electronic Medicines Compendium (emc) ( or the British National Formulary (BNF) ( Also refer to local policy when prescribing anti-biotic therapy.
31 High Risk Lacerations - Closing the wound following the 3 day review 4. High Risk Lacerations-Closing the wound following the 3 day review. Review and close the laceration 3 5 days after presentation if there are no signs of infection. If infection is present, see Managing an infected laceration. Tissue adhesives are not recommended for delayed closure of lacerations at high risk of infection because they are not easily removed to allow drainage. Skin closure strips are recommended because they are easily removed if infection develops and have been shown to be an effective method of closing simple lacerations in children compared with tissue adhesives. Review and close the laceration 3 5 days after presentation if there are no signs of infection. (see Low Risk Lacerations - Closing the wound) Apply a dressing after closing the laceration. (see Low Risk Lacerations - Dressing the wound)
32 High Risk Lacerations - Follow-up points 5. High Risk Lacerations-Follow-up points If symptoms and signs of infection develop after closure of the laceration: Remove sutures or adhesive strips and incise if it is not draining. Take swabs from any discharge for microbiological investigation, and start empirical antibiotics while awaiting results. Remove sutures after: 3 5 days on the head days over joints days at other sites. Remove adhesive strips after: 3 5 days on the head days at other sites. Removal of dressings: Keep the laceration dressed until sutures or adhesive strips are due to be removed. Low adherence absorbent dressings should be replaced if exudate has caused significant wetting of the dressing.
33 Infected Lacerations Infected Lacerations As a reminder: A Infected laceration may be defined as: one that retains devitalised tissue or involves preoperatively-existing infection or perforated viscera. An infected laceration may present with: Erythema spreading from the laceration Heat at site Cellulitis General malaise Fever Discharge (serous exudate with pus, seropurulent or haemopurulent Abnormal smell Friable granulation tissue Pain and tenderness at the site Delayed healing (compared with expected rate for site and condition) An infected wound (dog bite)
34 Infected Lacerations - Cleaning the wound 1. Infected Lacerations - Cleaning the wound Before cleaning the laceration, take swabs for microbiological investigation from deep within the infected wound. Disinfect around the wound area with antiseptic, but avoid getting antiseptic into the wound. Keep hair out of the wound. Anaesthetize the laceration before cleaning if debridement or exploration of the wound for foreign bodies is necessary and is likely to be painful. Debride devitalized tissue and pick out as much foreign material as possible if there may be glass in the wound, refer for radiography. Irrigate the wound with normal saline, drinking-quality water, or cooled boiled water.
35 Infected Lacerations - Dressing the wound 2. Infected Lacerations-Dressing the wound Important: Wounds that are infected are dressed but not closed. Prevent apposition of the wound edges by packing with a non-adherent dressing. Cover all lacerations at high risk of infection with a non-adherent, absorbent dressing: For lacerations with small quantities of exudate, dress with a non-adherent or topical iodine dressing. For lacerations with more exudate, cover with a hydrofibre (good for a cavity) dressing or a foam dressing. Consider topical anti-microbials. Arrange review 3 5 days after initial presentation. Infected dog bite an appropriate dressing.
36 Infected Lacerations - Antibiotic Therapy and Tetanus 3. Infected Lacerations- Antibiotic Therapy and Tetanus Take a detailed history and ascertain whether the wound was originally contaminated with high-risk material (soil, faeces, bodily fluids, or purulent exudates): Treat contaminated lacerations with eg co-amoxiclav. If the person is allergic to penicillin, treat with erythromycin combined with metronidazole. Metronidazole provides additional coverage for anaerobes that are not susceptible to erythromycin. It is licensed for various deep soft-tissue infections in which anaerobes are likely to proliferate. If the wound has not improved and bacteria culture indicates resistance to the firstchoice antibiotic, change to a suitable antibiotic guided by the results of sensitivity testing. Check your local policy regarding anti-biotic therapy.
37 Infected Lacerations - Antibiotic Therapy and Tetanus 3. Infected Lacerations-Antibiotic Therapy and Tetanus Refer urgently if the person has signs or symptoms of tetanus (generalized rigidity and spasm of skeletal muscles, including lockjaw) and has had a laceration in the previous days or weeks. Refer people with a tetanus-prone wound which is at high risk of contamination to hospital for treatment with human tetanus immunoglobulin, regardless of tetanus immunization status. Check the person's tetanus immunization status and administer a booster dose of tetanus vaccine if needed (a fully immunized person will have had a primary course of three vaccines followed by two boosters spaced 10 years apart) For further information on contraindications, cautions, drug interactions, and adverse effects, see the electronic Medicines Compendium (emc) ( or the British National Formulary (BNF) (
38 Previously Infected Lacerations - Closing the wound 4. Previously Infected Lacerations-Closing the wound Review 3 5 days after presentation: Close the laceration if there are no signs of infection. If signs of infection persist, review the swab results, change the antibiotics if indicated, and arrange further review. Review and close the laceration 3 5 days after presentation if there are no signs of infection. (see Low Risk Lacerations - Closing the wound) Apply a dressing after closing the laceration. (see Low Risk Lacerations - Dressing the wound)
39 Infected Lacerations - Follow-up points 4. Infected Lacerations-Follow-up points If symptoms and signs of infection develop after closure of the laceration: Remove sutures or adhesive strips and incise if it is not draining. Take swabs from any discharge for microbiological investigation, and start empirical antibiotics while awaiting results. Remove sutures after: 3 5 days on the head days over joints days at other sites. Remove adhesive strips after: 3 5 days on the head days at other sites. Removal of dressings: Keep the laceration dressed until sutures or adhesive strips are due to be removed. Low adherence absorbent dressings should be replaced if exudate has caused significant wetting of the dressing.
40 Low Risk High Risk Infected Introduction to Wound Assessment & Management Advice to Patients Advice to Patients Seek medical attention if infection develops. Look out for increasing pain, redness, or swelling spreading from the laceration. Report fever or general malaise. Take simple analgesia, such as paracetamol or ibuprofen, if the wound is painful. Keep the wound dry. Waterproof dressings, such as vapour-permeable dressings, allow light wetting (as from showering) without the dressing separating or the wound becoming wet. Seek medical attention if infection develops. Look out for increasing pain, redness, or swelling spreading from the laceration. Report fever or general malaise. Take simple analgesia, such as paracetamol or ibuprofen, if the wound is painful. Keep the wound dry. Waterproof dressings, such as vapour-permeable dressings, allow light wetting (as from showering) without the dressing separating or the wound becoming wet. Seek medical attention if the infection develops further. Look out for increasing pain, redness, or swelling spreading from the laceration. Report unresolved fever or general malaise. Take simple analgesia, such as paracetamol or ibuprofen, if the wound is painful. Keep the wound dry. Waterproof dressings, such as vapour-permeable dressings, allow light wetting (as from showering) without the dressing separating or the wound becoming wet.
41 Important note: Child Maltreatment Child Maltreatment Although rare, suspect child maltreatment if: A child has lacerations, abrasions, burns or scars and the explanation is unsuitable. Examples include wounds On a child who is not independently mobile. That are multiple. With a symmetrical distribution. On areas usually protected by clothing (such as the back, chest, abdomen, axilla, genital area). On the eyes, ears, or sides of face. On the neck, ankles, or wrists that look like ligature marks (4). See your local policy on reporting concerns regarding child protection immediately.
42 References References 1. NHS Clinical Knowledge Guidance Rainey, J (2002). Wound Care: A Handbook for Community Nurses. Philadelphia, Philadelphia Whurr Publishing. 3. NICE (2009) When to suspect child maltreatment (NICE guideline). National Institute for Health and Clinical Excellence. 4. Edlich, R.F. and Reddy, V.R. (2001) 5th Annual David R. Boyd, MD Lecture: revolutionary advances in wound repair in emergency medicine during the last three decades. A view toward the new millennium. Journal of Emergency Medicine 20(2), Marion, K., Osmond, M.H., Hartling, L. et al. (2001) Tissue adhesives for traumatic lacerations in children and adults (Cochrane Review). The Cochrane Library. Issue 1. John Wiley & Sons, Ltd
43 References References 6. Cutting KF, Harding KG (1994). Criteria for identifying wound infection. Journal of Wound Care. 3, 4, Dearden C (2001). Traumatic wounds: nursing assessment and management. Nursing Times. 97, 24, p Cassel, O. C., and Ion, L. Are antibiotics necessary in the surgical management of upper limb lacerations?' British Journal of Plastic Surgery 50(7) 523-9, 199.7
Basic Wound Care. Practical Skills Teaching. Year 3 Medical Students MB BCh
 Basic Wound Care Practical Skills Teaching Year 3 Medical Students MB BCh 2012-2013 Contents Introduction to workshop... 3 Overall Session Aim... 4 Intended Learning Objectives... 4 Workshop Structure
Basic Wound Care Practical Skills Teaching Year 3 Medical Students MB BCh 2012-2013 Contents Introduction to workshop... 3 Overall Session Aim... 4 Intended Learning Objectives... 4 Workshop Structure
WOUNDS. Emergency Procedures in PT
 WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
Skin Integrity and Wound Care
 Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
INJURIES AND THEIR MANAGEMENT
 INJURIES AND THEIR MANAGEMENT INJURIES AND THEIR MANAGEMENT An injury is damage to the body caused by external forces, which may be physical or chemical. 1) Incisions 2) Types of wounds and their closure
INJURIES AND THEIR MANAGEMENT INJURIES AND THEIR MANAGEMENT An injury is damage to the body caused by external forces, which may be physical or chemical. 1) Incisions 2) Types of wounds and their closure
Principle Management of Wound and Fracture in Emergency Department
 Principle Management of Wound and Fracture in Emergency Department Presented in Clinical Update Seminar January 15 th 2011 dr. Tedjo Rukmoyo, SpOT (K) Spine Initial Management ATLS Procedure A : airway
Principle Management of Wound and Fracture in Emergency Department Presented in Clinical Update Seminar January 15 th 2011 dr. Tedjo Rukmoyo, SpOT (K) Spine Initial Management ATLS Procedure A : airway
LRI Emergency Department
 LRI Emergency Department Guideline for the management of: Finger Tip Injuries in Children In the Paediatric Emergency Department (UHL Category C Guidance) Staff relevant to: ED Medical and Nursing staff
LRI Emergency Department Guideline for the management of: Finger Tip Injuries in Children In the Paediatric Emergency Department (UHL Category C Guidance) Staff relevant to: ED Medical and Nursing staff
Wound Management for Nurses/Technicians What do we need to know?
 Wound Management for Nurses/Technicians What do we need to know? Laura Owen European Specialist in Small Animal Surgery Lecturer in Small Animal Surgery, University of Cambridge The Acute Open Wound PPE
Wound Management for Nurses/Technicians What do we need to know? Laura Owen European Specialist in Small Animal Surgery Lecturer in Small Animal Surgery, University of Cambridge The Acute Open Wound PPE
FIRST AID & EMERGENCIES
 FIRST AID & EMERGENCIES Kelly Pederson, RN Chris DeLapp, CCH Education Manager Safety & Emergencies What is First Aid? Scene Survey Victim Assessment Bleeding Control Shock Burns Choking Basic First Aid
FIRST AID & EMERGENCIES Kelly Pederson, RN Chris DeLapp, CCH Education Manager Safety & Emergencies What is First Aid? Scene Survey Victim Assessment Bleeding Control Shock Burns Choking Basic First Aid
Chapter 14 8/23/2016. Surgical Wound Care. Wound Classifications. Wound Healing. Classified According to. Phases
 Chapter 14 Surgical Wound Care All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Wound Classifications Classified According to Cause Incision
Chapter 14 Surgical Wound Care All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Wound Classifications Classified According to Cause Incision
PRODIGY Quick Reference Guide
 PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
SKIN INTEGRITY & WOUND CARE
 SKIN INTEGRITY & WOUND CARE Chapter 34 1 skin integrity: intact skin refers to the presence of normal skin layer uninterrupted by wound 2 WOUNDS DISRUPTION IN THE INTEGRITY OF BODY TISSUE CLASSIFIED AS:
SKIN INTEGRITY & WOUND CARE Chapter 34 1 skin integrity: intact skin refers to the presence of normal skin layer uninterrupted by wound 2 WOUNDS DISRUPTION IN THE INTEGRITY OF BODY TISSUE CLASSIFIED AS:
Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types. Summary
 Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Surgical Wounds & Incisions
 Surgical Wounds & Incisions A Comprehensive Review Assessment & Management Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist www.woundcarenurses.org 1
Surgical Wounds & Incisions A Comprehensive Review Assessment & Management Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist www.woundcarenurses.org 1
SAMPLE. HLTEN406A Undertake basic wound care. Learner resource. HLT07 Health Training Package. Version 2
 HLT07 Health Training Package HLTEN406A Undertake basic wound care Learner resource Version 2 Training and Education Support Industry Skills Unit Meadowbank Acknowledgments The TAFE NSW Training and Education
HLT07 Health Training Package HLTEN406A Undertake basic wound care Learner resource Version 2 Training and Education Support Industry Skills Unit Meadowbank Acknowledgments The TAFE NSW Training and Education
Burns and Scalds. Treatment and Management. Accident and Emergency Department. Royal Surrey County Hospital. Patient information leaflet
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Burns and Scalds Treatment and Management Accident and Emergency Department A Burn is an injury caused to the skin by thermal
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Burns and Scalds Treatment and Management Accident and Emergency Department A Burn is an injury caused to the skin by thermal
Assessment & Management of Wounds in primary practice.
 Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
Skin Anatomy and Physiology
 Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
Open Fractures. Ria Dindial. Photo courtesy pic2fly.com
 Open Fractures Ria Dindial Photo courtesy pic2fly.com CLINICAL PEARL TYPE WOUND DESCRIPTION OTHER CRITERIA I < 1cm (puncture wounds) - II 1-10 cm - IIIA >10 cm, coverage available Segmental fractures,
Open Fractures Ria Dindial Photo courtesy pic2fly.com CLINICAL PEARL TYPE WOUND DESCRIPTION OTHER CRITERIA I < 1cm (puncture wounds) - II 1-10 cm - IIIA >10 cm, coverage available Segmental fractures,
Subtle Signs of Child Abuse Child s Protection Office MOH Presented by Dr.Fatoumah Alabdulrazzaq M.D,FRCPC,FAAP,PEM(C)
 Subtle Signs of Child Abuse Child s Protection Office MOH Presented by Dr.Fatoumah Alabdulrazzaq M.D,FRCPC,FAAP,PEM(C) Cutaneous Injuries Bruise : injury to soft tissues in which skin is not broken, characterized
Subtle Signs of Child Abuse Child s Protection Office MOH Presented by Dr.Fatoumah Alabdulrazzaq M.D,FRCPC,FAAP,PEM(C) Cutaneous Injuries Bruise : injury to soft tissues in which skin is not broken, characterized
Property Latmedical, LLC.
 Dr. Goed provides a complete and innovate product portfolio solution to the growing healthcare need within the field of non-invasive orthopedics, sports medicine, bandaging, wound care and compression
Dr. Goed provides a complete and innovate product portfolio solution to the growing healthcare need within the field of non-invasive orthopedics, sports medicine, bandaging, wound care and compression
NovoSorb BTM. A unique synthetic biodegradable wound scaffold. Regenerating tissue. Changing lives.
 NovoSorb BTM A unique synthetic biodegradable wound scaffold Regenerating tissue. Changing lives. Overview NovoSorb BTM is a unique synthetic biodegradable wound scaffold that delivers good cosmetic and
NovoSorb BTM A unique synthetic biodegradable wound scaffold Regenerating tissue. Changing lives. Overview NovoSorb BTM is a unique synthetic biodegradable wound scaffold that delivers good cosmetic and
Wound Care in the Community. Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts
 Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
Chapter 4 Inflammation and Infection
 Chapter 4 Inflammation and Infection Defense Mechanisms Three lines of defense protect the body against foreign invasion: Physical or surface barriers Inflammation Immune response Inflammation Non-specific
Chapter 4 Inflammation and Infection Defense Mechanisms Three lines of defense protect the body against foreign invasion: Physical or surface barriers Inflammation Immune response Inflammation Non-specific
You Are the Emergency Medical Responder
 Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Wound Care Discharge Instructions
 Wound Care Discharge Instructions Wound Care Discharge Instructions DESCRIPTION Caring for your wound is important to promote healing, avoid infection, and minimize scarring. Wounds heal more quickly when
Wound Care Discharge Instructions Wound Care Discharge Instructions DESCRIPTION Caring for your wound is important to promote healing, avoid infection, and minimize scarring. Wounds heal more quickly when
WHY WOUNDS FAIL TO HEAL SIMPLIFIED
 WHY WOUNDS FAIL TO HEAL SIMPLIFIED 10 Some of the common signs of failure to heal with possible causes and some interventions WHY WOUNDS FAIL TO HEAL There must be adequate supplies of nutrients and oxygen
WHY WOUNDS FAIL TO HEAL SIMPLIFIED 10 Some of the common signs of failure to heal with possible causes and some interventions WHY WOUNDS FAIL TO HEAL There must be adequate supplies of nutrients and oxygen
Hemostasis Inflammatory Phase Proliferative/rebuilding Phase Maturation Phase
 The presenters are staff members of the CHI Health St. Elizabeth Burn and Wound Center. Many of the products discussed are used in our current practice but we have no conflict of interest to disclose.
The presenters are staff members of the CHI Health St. Elizabeth Burn and Wound Center. Many of the products discussed are used in our current practice but we have no conflict of interest to disclose.
First Responders to Orthopaedic Emergencies
 First Responders to Orthopaedic Emergencies Tom McPartland MD FABOS, FAAP Assistant Clinical Professor Rutgers-RWJMS October 17,2018 Goals Review Epidemiology of School Injuries Review Definitions of Different
First Responders to Orthopaedic Emergencies Tom McPartland MD FABOS, FAAP Assistant Clinical Professor Rutgers-RWJMS October 17,2018 Goals Review Epidemiology of School Injuries Review Definitions of Different
QI. Read the following questions and choose the most correct answer (20 Marks):
 Question One: QI. Read the following questions and choose the most correct answer (20 Marks): 1- Some people are very allergic to some drugs like penicillin. This condition is called: a) Septic shock.
Question One: QI. Read the following questions and choose the most correct answer (20 Marks): 1- Some people are very allergic to some drugs like penicillin. This condition is called: a) Septic shock.
INTRODUCTION TO WOUND DRESSINGS
 WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
Procedures/Risks:central venous catheter
 Procedures/Risks:central venous catheter Central Venous Catheter Placement Procedure: Placement of the central venous catheter will take place in the Interventional Radiology Department (IRD) at The Ohio
Procedures/Risks:central venous catheter Central Venous Catheter Placement Procedure: Placement of the central venous catheter will take place in the Interventional Radiology Department (IRD) at The Ohio
I ve a drawer full of dressings i don t know how to use!
 I ve a drawer full of dressings i don t know how to use! Introduction: Originating from battlefield medicine much of what we use today is an evolution of material science combined with our understanding
I ve a drawer full of dressings i don t know how to use! Introduction: Originating from battlefield medicine much of what we use today is an evolution of material science combined with our understanding
3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing Description 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing is used
 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing Description 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing is used to cover and protect catheter sites and to secure devices
3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing Description 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing is used to cover and protect catheter sites and to secure devices
Introduction. Follow standard infection control precautions
 Patient Handbook 1 TABLE OF CONTENTS 1. Introduction. 2 2. Indications for Use. 3 3. Contraindications... 3 4. Warnings 4 5. Precautions.. 6 6. Patient Information Guide. 6 7. Key Pad Features.. 7 8. Battery
Patient Handbook 1 TABLE OF CONTENTS 1. Introduction. 2 2. Indications for Use. 3 3. Contraindications... 3 4. Warnings 4 5. Precautions.. 6 6. Patient Information Guide. 6 7. Key Pad Features.. 7 8. Battery
Kettering Breast Service. Advice and Arm Exercises Following Breast Surgery. Information
 Kettering Breast Service Advice and Arm Exercises Following Breast Surgery Information Exercises following breast surgery are an important part of post-operative care. The gentle exercises contained in
Kettering Breast Service Advice and Arm Exercises Following Breast Surgery Information Exercises following breast surgery are an important part of post-operative care. The gentle exercises contained in
New approach to the wounds by moist wound healing in Japan. Yoshihiko Mochizuki Japan
 New approach to the wounds by moist wound healing in Japan. Yoshihiko Mochizuki M.D. @Tokyo Japan What is the meaning of wound healing? I think there are two types of wound healing. 1. True healing moist
New approach to the wounds by moist wound healing in Japan. Yoshihiko Mochizuki M.D. @Tokyo Japan What is the meaning of wound healing? I think there are two types of wound healing. 1. True healing moist
Chapter 28. Wound Care. Copyright 2019 by Elsevier, Inc. All rights reserved.
 Chapter 28 Wound Care Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 28.1 Define the key terms and key abbreviations in this chapter. Describe skin tears, circulatory ulcers, and diabetic
Chapter 28 Wound Care Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 28.1 Define the key terms and key abbreviations in this chapter. Describe skin tears, circulatory ulcers, and diabetic
Venous. Arterial. Neuropathic (e.g. diabetic foot ulcer) Describe Wound Types & Stages of. Pressure Ulcers. Identify Phases of Healing & Wound Care
 A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
Patient Care Information
 Patient Care Information A Guide to Healing Diabetic Foot Ulcers Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1 Dermal Regeneration Matrix Overview Diabetic foot ulcers are
Patient Care Information A Guide to Healing Diabetic Foot Ulcers Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1 Dermal Regeneration Matrix Overview Diabetic foot ulcers are
M A H O M E W O R K # 2 P a g e Outpatient surgery is generally limited to procedures requiring less than 60
 M A 2 0 5 H O M E W O R K # 2 P a g e 1 NAME: DATE: CHAPTER 42 Assisting with Minor Surgery True/False: 1. Outpatient surgery is generally limited to procedures requiring less than 60 minutes to perform.
M A 2 0 5 H O M E W O R K # 2 P a g e 1 NAME: DATE: CHAPTER 42 Assisting with Minor Surgery True/False: 1. Outpatient surgery is generally limited to procedures requiring less than 60 minutes to perform.
Wound Repair. Epidemiology. History. Location of Injuries Face/Scalp Extremities. Legal Risk Missed FB and Fx Infection
 Wound Repair Edwin W. Schaefer, DNP, R.N. - FNP Emergency Nurse Practitioner Epidemiology Location of Injuries Face/Scalp Extremities Legal Risk Missed FB and Fx Infection History Mechanism of Injury Associated
Wound Repair Edwin W. Schaefer, DNP, R.N. - FNP Emergency Nurse Practitioner Epidemiology Location of Injuries Face/Scalp Extremities Legal Risk Missed FB and Fx Infection History Mechanism of Injury Associated
FOOT AND ANKLE ARTHROSCOPY
 FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
Chapter 24 Soft Tissue Injuries Presentation Notes
 Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
V.A.C. Therapy Safety Information
 Bringing Safety Home V.A.C. Therapy Safety Information Bleeding Precautions Dressing Change Frequency Foam Removal Important Information 2 Prior to use of V.A.C. Therapy System it is important for the
Bringing Safety Home V.A.C. Therapy Safety Information Bleeding Precautions Dressing Change Frequency Foam Removal Important Information 2 Prior to use of V.A.C. Therapy System it is important for the
Review. A. abrasion B. contusion C. hematoma D. avulsion
 Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
INFORMATION REGARDING YOUR NASAL SURGERY
 INFORMATION REGARDING YOUR NASAL SURGERY This document contains information about the following aspects of nasal surgery: Pre-op information: How to prepare for surgery. Procedure: Wat is done during surgery.
INFORMATION REGARDING YOUR NASAL SURGERY This document contains information about the following aspects of nasal surgery: Pre-op information: How to prepare for surgery. Procedure: Wat is done during surgery.
Decision-Making in the Acute Management of Blunt and Penetrating Wounds Mary Somerville, DVM, DACVS
 Decision-Making in the Acute Management of Blunt and Penetrating Wounds Mary Somerville, DVM, DACVS Providing the best quality care and service for the patient, the client, and the referring veterinarian.
Decision-Making in the Acute Management of Blunt and Penetrating Wounds Mary Somerville, DVM, DACVS Providing the best quality care and service for the patient, the client, and the referring veterinarian.
Methicillin-Resistant Staphylococcus aureus (MRSA) in schools and among athletes
 Methicillin-Resistant Staphylococcus aureus (MRSA) in schools and among athletes Frequently asked questions What is Staphylococcus aureus?...2 What is Methicillin Resistant Staphylococcus aureus (MRSA)?...2
Methicillin-Resistant Staphylococcus aureus (MRSA) in schools and among athletes Frequently asked questions What is Staphylococcus aureus?...2 What is Methicillin Resistant Staphylococcus aureus (MRSA)?...2
COURSE DESCRIPTION. Page 1 of 18. Rev 3.0 February 2016
 COURSE DESCRIPTION Proper CPT wound repair coding is often a challenging process. The coder must first understand the various classifications of wound repair coding as well as the CPT manual s guidelines
COURSE DESCRIPTION Proper CPT wound repair coding is often a challenging process. The coder must first understand the various classifications of wound repair coding as well as the CPT manual s guidelines
Burn Wound Assessment and Infections
 Burn Wound Assessment and Infections Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Family Health:
Burn Wound Assessment and Infections Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Family Health:
Lecture 1 Surgical preparation
 Lecture 1 Surgical preparation 1. Standard instrument set 2. Preparation for surgery 3. Suture Patterns 1. Standard instrument set female set Preparation of instrument pack Video: Female set preparation
Lecture 1 Surgical preparation 1. Standard instrument set 2. Preparation for surgery 3. Suture Patterns 1. Standard instrument set female set Preparation of instrument pack Video: Female set preparation
Abscess. A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body.
 Abscess A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body. Ethyology Bacteria causing cutaneous abscesses are typically indigenous
Abscess A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body. Ethyology Bacteria causing cutaneous abscesses are typically indigenous
Determining Wound Diagnosis and Documentation Tips Job Aid
 Determining Wound Diagnosis and Job Aid 1 Coding Is this a traumatic injury from an accident? 800 Codes - Injury Section of the Coding Manual Code by specific site of injury. Only use for accidents or
Determining Wound Diagnosis and Job Aid 1 Coding Is this a traumatic injury from an accident? 800 Codes - Injury Section of the Coding Manual Code by specific site of injury. Only use for accidents or
Wound culture. (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center
 Wound culture (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center Infection is a major impairment in delayed and nonhealing chronic wounds. Cultures of chronic wounds are not routinely performed
Wound culture (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center Infection is a major impairment in delayed and nonhealing chronic wounds. Cultures of chronic wounds are not routinely performed
Appropriate Dressing Selection For Treating Wounds
 Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Wound Management in Urgent Care
 Wound Management in Urgent Care Brittany Busse Wound Management in Urgent Care Brittany Busse, MD Med 7 Urgent Care Folsom, CA, USA ISBN 978-3-319-27426-3 DOI 10.1007/978-3-319-27428-7 ISBN 978-3-319-27428-7
Wound Management in Urgent Care Brittany Busse Wound Management in Urgent Care Brittany Busse, MD Med 7 Urgent Care Folsom, CA, USA ISBN 978-3-319-27426-3 DOI 10.1007/978-3-319-27428-7 ISBN 978-3-319-27428-7
Advazorb. Hydrophilic foam dressing range
 Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Advanced Wound Care. Cut Shape Innovate
 Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
Dynamic hip screw (sliding hip screw)
 Dynamic hip screw (sliding hip screw) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a dynamic hip screw, sometimes also known as a sliding hip
Dynamic hip screw (sliding hip screw) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a dynamic hip screw, sometimes also known as a sliding hip
Exploring best practice in the management of skin tears in older people
 Exploring best practice in the management of skin tears in older people An overview of the definition, prevention and management of skin tears Abstract Battersby, L. (2009) Best practice in the management
Exploring best practice in the management of skin tears in older people An overview of the definition, prevention and management of skin tears Abstract Battersby, L. (2009) Best practice in the management
How Wounds Heal: A Guide for the Wound-care Novice
 C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
Wound Healing Basic Concept
 Department of Orthopaedic & Traumatology The Chinese University of Hong Kong Wound Healing Basic Concept Dr TSE Lung Fung ( 謝龍峰醫生 ) MBChB(CUHK),FRCS(Edin),FRCSEd(Orth),FHKCOS,FHKAM(Ortho) Tissue Damage
Department of Orthopaedic & Traumatology The Chinese University of Hong Kong Wound Healing Basic Concept Dr TSE Lung Fung ( 謝龍峰醫生 ) MBChB(CUHK),FRCS(Edin),FRCSEd(Orth),FHKCOS,FHKAM(Ortho) Tissue Damage
UNIT 4: DISASTER MEDICAL OPERATIONS
 UNIT 4: DISASTER MEDICAL OPERATIONS PART 2 Patient Evaluation: How to perform a head-to-toe assessment to identify and treat injuries. Basic Treatment How to: Treat burns Dress and bandage wounds Treat
UNIT 4: DISASTER MEDICAL OPERATIONS PART 2 Patient Evaluation: How to perform a head-to-toe assessment to identify and treat injuries. Basic Treatment How to: Treat burns Dress and bandage wounds Treat
DRESSING SELECTION SIMPLIFIED
 10 DRESSING SELECTION SIMPLIFIED It must be recognised that no one dressing provides the optimum environment for the healing of all wounds (Mahoney, 2015) DRESSING SELECTION SIMPLIFIED Selecting the correct
10 DRESSING SELECTION SIMPLIFIED It must be recognised that no one dressing provides the optimum environment for the healing of all wounds (Mahoney, 2015) DRESSING SELECTION SIMPLIFIED Selecting the correct
We look forward to serving you.
 ADVANCED CARE GEMCORE360 offers healthcare professionals a simple, clear and cost-effective wound care range while ensuring excellent clinical outcomes for their patients. 1 At GEMCO Medical, we strive
ADVANCED CARE GEMCORE360 offers healthcare professionals a simple, clear and cost-effective wound care range while ensuring excellent clinical outcomes for their patients. 1 At GEMCO Medical, we strive
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 5 Basic Surgical Procedures Key Points 2 5.1 Wound Management Many important procedures can be performed under local anesthesia and do not require a surgical specialist
Surgical Care at the District Hospital 1 5 Basic Surgical Procedures Key Points 2 5.1 Wound Management Many important procedures can be performed under local anesthesia and do not require a surgical specialist
Resources to Guide the Management of Suspected Infection in Chronic Wounds
 Resources to Guide the Management of Suspected Infection in Chronic Wounds Health Improvement Scotland published their 13th Health Technology Assessment (HTA 13) in December 2015 entitled, Antimicrobial
Resources to Guide the Management of Suspected Infection in Chronic Wounds Health Improvement Scotland published their 13th Health Technology Assessment (HTA 13) in December 2015 entitled, Antimicrobial
Application Guide for Full-Thickness Wounds
 Application Guide for Full-Thickness Wounds PriMatrix Dermal Repair Scaffold PriMatrix Ag Antimicrobial Dermal Repair Scaffold Application Guide for Full Thickness Wounds PriMatrix is a unique dermal repair
Application Guide for Full-Thickness Wounds PriMatrix Dermal Repair Scaffold PriMatrix Ag Antimicrobial Dermal Repair Scaffold Application Guide for Full Thickness Wounds PriMatrix is a unique dermal repair
Topic Page: Wound healing SKIN ANATOMY.
 Topic Page: Wound healing Definition: wound healing from Dictionary of Medical Terms the replacement of dead tissue with new tissue Summary Article: Overview of Wound Healing: Anatomy and Physiology from
Topic Page: Wound healing Definition: wound healing from Dictionary of Medical Terms the replacement of dead tissue with new tissue Summary Article: Overview of Wound Healing: Anatomy and Physiology from
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department
 Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department Functions Definition A burn is a type of injury to the skin caused by heat, electricity, chemicals, light, radiation or
Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department Functions Definition A burn is a type of injury to the skin caused by heat, electricity, chemicals, light, radiation or
Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System
 1 Chapter 20 Soft-Tissue Injury 2 Introduction to Soft-Tissue Injury Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System 3 Epidemiology Most
1 Chapter 20 Soft-Tissue Injury 2 Introduction to Soft-Tissue Injury Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System 3 Epidemiology Most
( PLUM BOROUGH SCHOOL DISTRICT
 No. 209.1 ( PLUM BOROUGH SCHOOL DISTRICT SECTION: PUPILS TITLE: FIRST AID STANDING ORDERS ADOPTED: March 27,1990 REVISED: February 27, 2001 209.1. FIRST AID STANDING ORDERS 1. Guidelines When a student
No. 209.1 ( PLUM BOROUGH SCHOOL DISTRICT SECTION: PUPILS TITLE: FIRST AID STANDING ORDERS ADOPTED: March 27,1990 REVISED: February 27, 2001 209.1. FIRST AID STANDING ORDERS 1. Guidelines When a student
Disaster Medical Operations Part 2. CERT Basic Training Unit 4
 Disaster Medical Operations Part 2 Unit 4 Unit 3 Review 3 Killers Airway obstruction Excessive bleeding Shock 4-1 CERT Sizeup 1. Gather Facts 2. Assess Damage 3. Consider Probabilities 4. Assess Your Situation
Disaster Medical Operations Part 2 Unit 4 Unit 3 Review 3 Killers Airway obstruction Excessive bleeding Shock 4-1 CERT Sizeup 1. Gather Facts 2. Assess Damage 3. Consider Probabilities 4. Assess Your Situation
After this presentation and discussion, the participants should be able to:
 Tissue Repair Robert F. Diegelmann, Ph.D. OBJECTIVES After this presentation and discussion, the participants should be able to: 1. Define the biochemical responses to tissue injury 2. Describe the mechanisms
Tissue Repair Robert F. Diegelmann, Ph.D. OBJECTIVES After this presentation and discussion, the participants should be able to: 1. Define the biochemical responses to tissue injury 2. Describe the mechanisms
Dr. Nuelle Total/Partial Hip Replacement: Discharge Care Instructions
 Dr. Nuelle Total/Partial Hip Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your hip replacement surgery. We hope that you had a good stay with us. These
Dr. Nuelle Total/Partial Hip Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your hip replacement surgery. We hope that you had a good stay with us. These
Skin lesions & Abrasions
 Skin lesions & Abrasions What Are Skin Lesions? A skin lesion is a part of the skin that has an abnormal growth or appearance compared to the skin around it Types of Skin Lesions Two types of skin lesions
Skin lesions & Abrasions What Are Skin Lesions? A skin lesion is a part of the skin that has an abnormal growth or appearance compared to the skin around it Types of Skin Lesions Two types of skin lesions
Types of Wisdom Teeth Positions
 The Wise Guide to Wisdom Teeth Extraction H. Ryan Kazemi, DMD 11 Types of Wisdom Teeth Positions Erupted: The tooth has completely emerged through the gum tissue and is visible. This occurs when there
The Wise Guide to Wisdom Teeth Extraction H. Ryan Kazemi, DMD 11 Types of Wisdom Teeth Positions Erupted: The tooth has completely emerged through the gum tissue and is visible. This occurs when there
Categorisation of Wound Care and Associated Products
 Categorisation of Wound Care and Associated Products Version 9 March 2018 Surgical Dressing Manufacturers Association 2018 TAPES AND TRADITIONAL DRESSINGS Wound Dressings Swabs Taping Traditional Wound
Categorisation of Wound Care and Associated Products Version 9 March 2018 Surgical Dressing Manufacturers Association 2018 TAPES AND TRADITIONAL DRESSINGS Wound Dressings Swabs Taping Traditional Wound
Hemiarthroplasty (half hip replacement)
 Hemiarthroplasty (half hip replacement) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a half hip replacement. It gives information about the
Hemiarthroplasty (half hip replacement) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a half hip replacement. It gives information about the
Disclosures for Tarik Alam. Wound Bed Preparation. Wound Prognosis. Session Objectives. Debridement 4/26/2015
 Disclosures for Tarik Alam Challenges in Managing Bioburden and Devitalized Tissue Tarik Alam RN, BScN, ET, MClSc(WH) Enterostomal Therapy Nurse tarikalam@hotmail.com Clinical Affairs Manager for Hollister
Disclosures for Tarik Alam Challenges in Managing Bioburden and Devitalized Tissue Tarik Alam RN, BScN, ET, MClSc(WH) Enterostomal Therapy Nurse tarikalam@hotmail.com Clinical Affairs Manager for Hollister
YOUR PATH TO RECOVERY AFTER SHOULDER REPLACEMENT
 YOUR PATH TO RECOVERY AFTER SHOULDER REPLACEMENT Revised 11/2015 Day of Surgery: # 0 After Surgery Day: # 1 Precautions DO NOT actively move your shoulder, lift, carry, reach, bear weight, or reach behind
YOUR PATH TO RECOVERY AFTER SHOULDER REPLACEMENT Revised 11/2015 Day of Surgery: # 0 After Surgery Day: # 1 Precautions DO NOT actively move your shoulder, lift, carry, reach, bear weight, or reach behind
Wound Dressing. Choosing the Right Dressing
 Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
patient group direction
 REVAXIS v01 1/12 REVAXIS (DIPHTHERIA, TETANUS AND POLIOMYELITIS (INACTIVATED) VACCINE (ADSORBED, REDUCED ANTIGEN(S) CONTENT)) PGD Details Version 1.0 Legal category Staff grades Approved by POM Paramedic
REVAXIS v01 1/12 REVAXIS (DIPHTHERIA, TETANUS AND POLIOMYELITIS (INACTIVATED) VACCINE (ADSORBED, REDUCED ANTIGEN(S) CONTENT)) PGD Details Version 1.0 Legal category Staff grades Approved by POM Paramedic
The Triangle of Wound Assessment
 The Triangle of Wound Assessment A simple and holistic framework for wound management CPWSC_TOWA_Brochure_210x210_2018.indd 1 10/01/2018 15.13 ? We asked healthcare professionals around the world about
The Triangle of Wound Assessment A simple and holistic framework for wound management CPWSC_TOWA_Brochure_210x210_2018.indd 1 10/01/2018 15.13 ? We asked healthcare professionals around the world about
DEBRIDEMENT. Professor Donald G. MacLellan Executive Director Health Education & Management Innovations
 DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
Practice review. Exploring best practice in the management of skin tears in older people
 Keywords Tissue Viability Skin tears Older people Exploring best practice in the management of skin tears in older people An overview of the definition, prevention and management of skin tear Author Lisa
Keywords Tissue Viability Skin tears Older people Exploring best practice in the management of skin tears in older people An overview of the definition, prevention and management of skin tear Author Lisa
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet February 2018 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used
Epidural Continuous Infusion Patient information Leaflet February 2018 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used
FM 3.0.MH.1 Medical Handbook
 FM 3.0.MH.1 Medical Handbook DISTRIBUTION RESTRICITON: Distribution authorized to 3 rd Battalion, 75th Ranger Regiment Senior Leadership and Instructors to protect operational information that is of use.
FM 3.0.MH.1 Medical Handbook DISTRIBUTION RESTRICITON: Distribution authorized to 3 rd Battalion, 75th Ranger Regiment Senior Leadership and Instructors to protect operational information that is of use.
Foam dressings have frequently
 The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
BLS, ILS, ALS OTEP BURNS BURN INTRODUCTION TYPES OF BURNS
 BURNS BLS, ILS, ALS OTEP While we do understand this presentation is an instructional tool for all levels of certification, taking this into consideration everyone taking this class must remember that
BURNS BLS, ILS, ALS OTEP While we do understand this presentation is an instructional tool for all levels of certification, taking this into consideration everyone taking this class must remember that
CASE 1: TYPE-II DIABETIC FOOT ULCER
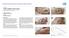 CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
Management of Penetrating Wrist Injuries in the Emergency Department
 Management of Penetrating Wrist Injuries in the Emergency Department Ioannis E. Bitzos, MD, and Mark S. Granick, MD Division of Plastic Surgery, New Jersey Medical School, University of Medicine and Dentistry
Management of Penetrating Wrist Injuries in the Emergency Department Ioannis E. Bitzos, MD, and Mark S. Granick, MD Division of Plastic Surgery, New Jersey Medical School, University of Medicine and Dentistry
Shoulder Instability
 Shoulder Instability The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The
Shoulder Instability The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The
Integra. PriMatrix Dermal Repair Scaffold PATIENT INFORMATION. Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1
 Integra PriMatrix Dermal Repair Scaffold PATIENT INFORMATION Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1 Your Path to Recovery Your health care provider has chosen to use
Integra PriMatrix Dermal Repair Scaffold PATIENT INFORMATION Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1 Your Path to Recovery Your health care provider has chosen to use
Orthopedic Nursing, Part 2. External Fixation. Nursing Best Practice Guidelines
 Orthopedic Nursing, Part 2 External Fixation Nursing Best Practice Guidelines Reasons for External Fixation Device Placement.. a technique of fracture immobilization a series of transfixing pins are inserted
Orthopedic Nursing, Part 2 External Fixation Nursing Best Practice Guidelines Reasons for External Fixation Device Placement.. a technique of fracture immobilization a series of transfixing pins are inserted
FINGERTIP INJURIES ARE THEY REALLY THAT SIMPLE? SANJAY K SHARMA, MD, FACS INSTITUTE OF RECONSTRUCTIVE PLASTIC SURGERY
 FINGERTIP INJURIES ARE THEY REALLY THAT SIMPLE? SANJAY K SHARMA, MD, FACS INSTITUTE OF RECONSTRUCTIVE PLASTIC SURGERY Austin Trauma and Critical Care Conference 2018 May 31-June 1, 2018 Outline 1. Scope
FINGERTIP INJURIES ARE THEY REALLY THAT SIMPLE? SANJAY K SHARMA, MD, FACS INSTITUTE OF RECONSTRUCTIVE PLASTIC SURGERY Austin Trauma and Critical Care Conference 2018 May 31-June 1, 2018 Outline 1. Scope
Bandaging & Plaster Techniques
 Bandaging & Plaster Techniques Dr. Ashish Gohiya MS, FIAS, FIOS (UK) Associate Professor Abrasion Contusion Lacerated W Incised W Degloving Crush DRESSING BANDAGE DRESSINGS PURPOSE OF DRESSINGS -Control
Bandaging & Plaster Techniques Dr. Ashish Gohiya MS, FIAS, FIOS (UK) Associate Professor Abrasion Contusion Lacerated W Incised W Degloving Crush DRESSING BANDAGE DRESSINGS PURPOSE OF DRESSINGS -Control
Transfemoral Amputation
 Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
