Medical Nucleus Medical Art, Inc. Medical Nucleus Medical Art, Inc.
|
|
|
- Steven Evans
- 5 years ago
- Views:
Transcription
1 M Description The spine consists of five separate divisions: cervical (seven vertebrae), thoracic (12 vertebrae), lumbar (five vertebrae), the sacrum, and the coccyx. Each vertebra, interlocks with the segment above and below it through the superior and inferior articular processes. Between each vertebra is an intervertebral disc that provides cushioning for the spine. The lamina and pedicle, along with the vertebral body, provide the borders that create the spinal canal, which the spinal cord runs through to transmit nerve signals. There are several different scenarios or conditions that may produce symptoms that would lead your physician to further investigate, and possibly recommend this surgery. Medical Nucleus Medical Art, Inc. Stenosis causing Radicular Pain Spinal stenosis is the narrowing of the articular spaces within the spine; this may impinge on the nerves or the spinal cord. This is a degenerative process and may eventually lead to further changes on the spine over time. Radicular symptoms are pain, numbness, weakness, tingling, etc., that radiate along a specific nerve root (or dermatome) to other parts of the body outside of the spine. Surgical correction of this problem may include a minimally invasive decompression (shaving bone away to create more space around the nerve), often referred to as a laminectomy (removing part or all of the lamina in order to provide more space and relieve impingement). In some cases, movement of one vertebrae slipping against another (spondylolisthesis), may require a vertebral fusion. This may be performed open vs. minimally invasive. Disc Herniation Herniation of the intervertebral disc may be due to an acute traumatic incident. However, it is usually due to a degenerative process that creates a tear in the outer part of the disc called the annulus, causing it to impinge upon nerves, or the spinal cord itself. As the herniation becomes more of a chronic process, it causes increased narrowing, also known as stenosis. This in turn, may create instability in the vertebrae, causing them to slide against each other (spondylolisthesis). This movement can be very painful and if severe enough, requires surgical fusion to stabilize the area and relieve symptoms. Medical Illustration@2016 Nucleus Medical Art, Inc. Surgical correction of a disc herniation requires a minimally invasive discectomy, or removal of the disc. Many times this is done in combination with a decompression/laminectomy in order to obtain the best results.
2 Nature of Procedure Anterior lumbar interbody fusion is a procedure which enables the surgeon to fuse two vertebrae together, by removing the disc and placing bone between the vertebral bodies, in place of the disc, through an anterior approach. An anterior approach consists of an incision on the abdomen, mobilizing the abdominal muscles without cutting across the muscle fibers, gently going around the abdominal contents to the side and getting access to the font of the spine. A vascular surgeon is often used to help with the surgical approach exposure of the spine. During the process of fusion, which may take from 6 months to a year, the bone will try to grow from one vertebra to the other, effectively making one solid vertebra out of two. This bone can come from a donor, or it can come from the patient and may be placed in a cage. A plate and screws may be used. This plate is designed to immobilize the spine, and create a more stable environment for the bone to grow across from one vertebra to the other. Possible Complications and Instructions Surgery is undertaken to improve your condition. With all procedures, there are anticipated benefits and inherent risks. While your surgeon and team will do everything possible to minimize those risks, it is important for you to be aware of the more common risks. Many of these risks are altered by preexisting patient conditions such as diabetes, obesity, smoking, vascular disease, etc. You may have undergone preoperative medical evaluation to limit the effect of these conditions. The potential risks include, but are not limited to complications associated with having anesthesia (for example, reaction to medications, and difficulty with your airway). Your anesthesia provider will be able to give you further information regarding this matter. The more common complications following any surgical procedure are urinary tract infections, atelectasis (collapsed airspaces in the lungs), pneumonia and wound infection or bleeding. Such complications may require surgical interventions. Less frequent, but more serious complications include thrombosis or blood clots in the blood vessels of the arms, legs, or pelvis. They may lead to pulmonary embolus (clot to the lungs). Other such complications include blood loss, which may require transfusion of blood products, heart attack, stroke, or even death. The risks of the surgery may include damage or irritation to the nerves that may be temporary or permanent. This may cause numbness, weakness, or pain in the involved arm or leg. There is also a possibility of paralysis, loss of bowel or bladder function, sexual dysfunction, deep infections requiring chronic antibiotic therapy, meningitis, stroke, blindness, chronic pain and additional surgery. You should be aware that surgery has no assurances and individual results are variable. Your participation with the post-operative instructions and your current health does influence the outcome of surgery. Certainly, your surgical team will try their best to get the most optimal result for you. Some of the risks more specific to your surgical plan include: In this type of surgery, the approach utilized is through the abdomen to reach the front of the spine, also known as an anterior approach. Some of the organs in the abdominal cavity will be pushed to the side. There is a very low risk of injury to such organs. Similarly, there are large blood vessels in the front of the spine (which are responsible for the blood flow in the legs and pelvis). Often, it is required to move these vessels out of the way for safe access to the spine. This may lead to temporary swelling or discoloration of the genitalia or legs. It is for this reason that often a vascular surgeon will be utilized to perform the anterior approach.
3 The ureter is a tube which takes the urine from the kidneys to the bladder. Often the ureter is encountered along the way and is moved to the side as well. Additionally, in the path of reaching the front of the spine, there are small nerves. Injury to these nerves may cause a leg to have altered temperature perception, which is rare. There are also nerves which control ejaculation during sex in a male. If these nerves are affected during the surgery, the sexual functions of erection and orgasm are typically not affected but the male patient will not be able to ejaculate during sex. The ejaculate will shoot into the bladder causing infertility issues. Bone graft is used to accomplish a fusion. This bone can come from a donor, or it can come from the patient. Donor bone goes through a rigorous process of screening and sterilization and risk of disease transmission is extremely low. If your bone is being used, you can expect to have some numbness and pain over the area where the bone will be harvested. Pain from the donor site is expected, but usually subsides with time. Bone morphogenic protein is a protein, which is sometimes used to help the donor bone in the fusion process. While this protein has been extensively tested, there has been some controversy around its use. Other potential side effects can occur, which you should discuss with your surgeon if you are receiving bone morphogenic protein. There is a very low risk of developing a hernia at the site of the surgery. Feel free to contact our office if you feel you are experiencing any of these complications. Preparing for surgery Medical Evaluation In preparing for your spine surgery, we may ask you to have a complete physical examination done by your primary care doctor before your surgical procedure. This is necessary to assess your health and identify any conditions that can interfere with your surgery or recovery. We may need additional clearances if you also receive medical care from a specialist like a cardiologist or urologist. Tests Several tests may be needed to help plan your surgery: blood and urine samples may be tested. An electrocardiogram (EKG) and chest x-rays (radiographs) may be obtained. Medications Tell your orthopedic surgeon about the medications you are taking. Your orthopedist or your primary care doctor will advise you which medications you should stop or can continue taking before surgery. Weight Loss If you are overweight, your doctor may ask you to lose some weight before surgery to minimize the stress on your joint and possibly decrease the risks of surgery. Dental Evaluation Although infections after spine surgery are not common, an infection can occur if bacteria enter your bloodstream. Because bacteria can enter the bloodstream during dental procedures, you should consider getting treatment for significant dental diseases (including tooth extractions and periodontal work) before your spine surgery. Routine cleaning of your teeth should be delayed for several weeks after surgery. Urinary Evaluation Individuals with a history of recent or frequent urinary infections and older men with prostate disease should consider a urological evaluation before surgery.
4 Social Planning You will need some help with tasks such as cooking, shopping, bathing and laundry in the weeks following your surgery. Please arrange for a support team to help you with these tasks. What to expect at surgery You will arrive at the surgery registration area where the registration clerk will check you in. All of your insurance information will be verified and you will be escorted to the pre-operative area. You will change into a hospital gown and support stockings. All of your personal items will be marked and placed in a bag for safekeeping. They will be returned to you after surgery. Your nurse will usually check your blood pressure, heart rate, temperature, respiratory rate and oxygen level. You will also have a chance to empty your bladder before surgery. Your surgical site will be cleaned and an IV (intravenous) line will be placed to administer fluids. This line provides fluids to your body and allows access to administer medications during and after surgery. You may find that you are asked to repeat information several times or be asked the same questions throughout your stay. This is for your safety. Every team member is dedicated to making your safety of primary importance. Pre-Operative Your anesthesiologist will meet with you in the pre-operative area. He or she will discuss with you the available types of anesthesia and answer any questions you may have. Your surgeon will greet you and mark the area of your operative site. Once you have been prepared in the pre-operative area, you will be brought back to the operating room. Operating Room You will meet many people in the operating suite, all of whom play an important part in your surgery. You will be assisted by your team onto the operating table and made comfortable. Your team will help to position you and prepare your surgical site. The anesthesiologist begins by giving the medications and you will fall asleep. There will be a designated area for your family and friends to wait while you are having surgery. A member of our healthcare team will be available to keep your family and friends updated about your progress. Your surgeon will also talk with them when completing your surgery. After your surgery has been completed, you will be transported to the post-anesthesia care unit (PACU). Post Anesthesia Care Unit: PACU Here, the nursing personnel will place you on monitors to follow your blood pressure, heart rate, oxygen levels, alertness and will check your pain level. The PACU is an important transitional place before you go to your hospital room. Making sure you are comfortable and all of your vitals are stable is the PACU s main purpose. Pain medications will be administered as needed through your IV line. You may experience some nausea and medications are available to assist with your nausea. Warm blankets are also available to ensure your comfort. Your family and friends will be notified of your progress. Once you are stable and your PACU team feels you are ready, you will be taken to your hospital room. Your family will be notified and may join you in your room.
5 Pain Management After surgery, it is normal to have pain or discomfort. Inform your nurse if you are uncomfortable and they can administer the appropriate medications. Your nursing team will also provide you with ice packs and instruct you on the amount of time you can ice the area. You may be asked to rate your pain on a scale of 1 to 10, with 10 being the worst pain. If your pain is not being relieved with the ordered medications, your surgeon will be notified. The goal is to control your pain so that you can begin therapy immediately after surgery and start the road to recovery. If you are not nauseated after surgery, you will be able to start oral pain medications immediately. Otherwise, you may receive intravenous medications. By post-operative day one, it is preferred to manage your pain with oral pain medications. Your oral pain medications will give you longer lasting pain relief and allows you to feel less groggy and actively participate in therapy. Therapy Therapy is an important part of your hospital stay and vital to your overall success after surgery. The therapy team will work with you during your stay. They will assist you with general mobility, improving your strength and overall condition. If surgery is uncomplicated, you are encouraged to begin walking as soon as possible. Care After Surgery When you are stable and your pain controlled, you can be discharged home. Certain patients may discharged to rehab center to recover further before they eventually go home. After surgery, there will be pain at the incision site, which will improve over time. You may be placed in a brace after surgery. Follow up after surgery with your surgeon is required, and x-rays will be performed from time to time. You may shower on the third day after surgery as long as the wound is not draining. You should keep the incision clean and dry. Diet The bowel function may take some time to wake up and resume its normal function. This may cause some distension of the abdomen and nausea. It is for this reason that after surgery your diet may be held and later started with liquids only, and only advanced over time, to try to minimize such events. Some loss of appetite following surgery is common. Make sure you are eating a balanced diet rich in protein to promote muscle healing and strength. It may help to eat smaller meals more frequently and drink plenty of liquids. If you cannot manage solid foods, try a nutritional meal replacement drink. If you are still experiencing problems with your appetite after one week, call your surgeon. Some surgeries may require an altered diet for a short period of time after. Your healthcare team will assess your needs and provide education regarding specific recommendations. Physical Therapy and Activity You will be encouraged to walk often, being careful not do any excessive bending, lifting, or twisting. For specific instructions, speak to your surgeon.
6 Ice Ice therapy may continue to provide comfort, decrease swelling and help with pain control for up to two weeks following surgery. Be sure to place a towel between the skin and the ice bag. Ice the area for 20 minutes or less to prevent frostbite. Blood Clot Prevention After an orthopedic surgery, patients are at an increased risk for developing blood clots or deep venous thrombosis (DVT). Upon discharge, you will be given a specific regimen that may include aspirin or prescription blood thinners. It is important to follow the instructions exactly and attend all scheduled follow up appointments. You should wear the compression stockings (TED hose) for 3 weeks, or as directed. Staying active as reasonably possible will also decrease your chances of forming a blood clot and improves your overall health as well. Let pain be your guide when deciding on what activities you can participate in. Symptoms of deep venous thrombosis or pulmonary embolism may include swelling or tenderness in the calves, legs or arms, shortness of breath, increased heart rate or palpitations, or chest pain. If you experience any of these symptoms, notify your surgeon and go to an emergency room. Wound Care You have a surgical wound that requires daily attention and monitoring. Your healthcare team will instruct you about how to care for your wound before you leave the hospital. Please keep your incision clean and dry at all times. Do not immerse your incision in water. This includes pools, hot tubs, lakes, and bath water. You may shower on the third day after surgery, as long as your wound is not draining. Do not apply any lotions, creams or ointments unless prescribed by your surgeon. Your healed wound is new skin and should be protected from the sun with sun block especially in the year following surgery. Monitor your incision daily for any signs of infection. Some swelling and redness is normal but if there is an increase or if you develop any of the symptoms below notify your surgeon. Symptoms of a wound infection may include redness, drainage, swelling, warmth at/around the incision site or if you experience chills, shaking, an increase in pain or a fever over 101 orally. If you experience any of these symptoms, notify your surgeon immediately. A follow-up appointment will have already been scheduled for you days following surgery for an incision check and removal of any sutures. Preventing Infection Following your surgery, antibiotics should be taken before any dental or invasive procedure (i.e. dental cleaning, oral surgery, bladder scopes, urinary catheterizations, colonoscopy, etc.). Your surgeon will give you exact instructions after surgery. Please feel free to contact our office with any questions. Symptoms of possible infection are persistent fever (higher than 101 orally), shaking, chills, increased redness/tenderness/pain at surgical site. Medications Resuming your home medications will be determined by your physician. Please follow up with your primary care physician to ensure you are back on your prior medication regimen.
7 Pain Medications After an orthopedic surgery, most patients will require prescription pain medications, including narcotics, to treat their post-operative pain. Narcotic pain medications are controlled substances and need to be monitored closely. With chronic use, they pose a risk for addiction. Patients should treat their pain only as needed with these medications and wean off narcotics in the first few weeks following surgery. These medications can cause side effects, which may include nausea, lightheadedness, confusion, sedation, urinary retention and constipation. To avoid constipation increase your water intake, eat well-balanced meals that include fruits and vegetables and incorporate an over-the-counter stool softener such as Docusate or Senna. If you require a refill of your narcotic pain medication, please notify your surgeon early. Federal law prohibits filling most narcotics by phone; a written prescription is needed. Narcotic pain medications cannot be renewed after hours or on the weekends. If you have questions about your prescriptions, pain or find that your pain is not relieved by your medication, please notify your surgeon. Questions The CORE Institute is dedicated to your outcome. If any questions or concerns arise, please call The CORE Institute at
Medical Nucleus Medical Art, Inc.
 Description The spine consists of five separate divisions: cervical (seven vertebrae), thoracic (12 vertebrae), lumbar (five vertebrae), the sacrum, and the coccyx. Each vertebra interlocks with the segment
Description The spine consists of five separate divisions: cervical (seven vertebrae), thoracic (12 vertebrae), lumbar (five vertebrae), the sacrum, and the coccyx. Each vertebra interlocks with the segment
While complications from surgery are uncommon some can be serious and may include:
 PROCEDURE A Cervical Laminectomy is usually performed for spinal cord compression from cervical arthritis, nerve root compression from a cervical disc protrusion, or for an arthritic spur. These are painful
PROCEDURE A Cervical Laminectomy is usually performed for spinal cord compression from cervical arthritis, nerve root compression from a cervical disc protrusion, or for an arthritic spur. These are painful
The time required for surgery will vary depending upon the procedure recommended. The surgery may last 3 8 hours.
 PROCEDURE Your surgeon has recommended the removal of a spine tumor. Lesions of the spine may occur in the neck region (cervical), mid-back region (thoracic), or low-back region (lumbar-sacral). There
PROCEDURE Your surgeon has recommended the removal of a spine tumor. Lesions of the spine may occur in the neck region (cervical), mid-back region (thoracic), or low-back region (lumbar-sacral). There
ANTERIOR CERVICAL DISCECTOMY AND FUSION
 PROCEDURE An Anterior Cervical Discectomy is the surgical removal of a disc. The procedure is used when a disc protrusion or arthritic bone spur is placing pressure on a nerve and causing arm or neck pain.
PROCEDURE An Anterior Cervical Discectomy is the surgical removal of a disc. The procedure is used when a disc protrusion or arthritic bone spur is placing pressure on a nerve and causing arm or neck pain.
Thank you for choosing Saint Joseph s Hospital Health Center for your spine surgery. Updated Jan 2017
 Thank you for choosing Saint Joseph s Hospital Health Center for your spine surgery Updated Jan 2017 This class is designed to give you some basic, important information about spine surgery We will cover
Thank you for choosing Saint Joseph s Hospital Health Center for your spine surgery Updated Jan 2017 This class is designed to give you some basic, important information about spine surgery We will cover
If you have a condition that compresses your nerves, causing debilitating back pain or numbness along the back of your leg.
 Below, we have provided some basic information for your benefit. Please use this information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk
Below, we have provided some basic information for your benefit. Please use this information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk
POSTERIOR CERVICAL LAMINECTOMY AND FUSION
 PROCEDURE A Posterior Cervical Laminectomy and Fusion surgical procedure is usually performed to treat spinal cord compression resulting from cervical canal narrowing. At times, it is also recommended
PROCEDURE A Posterior Cervical Laminectomy and Fusion surgical procedure is usually performed to treat spinal cord compression resulting from cervical canal narrowing. At times, it is also recommended
POSTERIOR CERVICAL FUSION
 AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
ANTERIOR LUMBAR INTERBODY FUSION (ALIF)
 PROCEDURE An Anterior Lumbar Interbody Fusion (ALIF) is a surgical procedure performed when there is disabling pain from a degenerated disc or nerve root compression. During the operation, your surgeon
PROCEDURE An Anterior Lumbar Interbody Fusion (ALIF) is a surgical procedure performed when there is disabling pain from a degenerated disc or nerve root compression. During the operation, your surgeon
ADULT SPINAL DEFORMITY SURGERY
 PROCEDURE Spinal deformity correction surgery involves many techniques to correct the scoliosis, kyphosis, or other deformities of your spine to a more normal alignment. During the procedure, your surgeon
PROCEDURE Spinal deformity correction surgery involves many techniques to correct the scoliosis, kyphosis, or other deformities of your spine to a more normal alignment. During the procedure, your surgeon
POSTERIOR LATERAL FUSION LUMBAR
 PROCEDURE A Posterior Lateral Fusion (PLF) is spine surgery performed to treat disabling back pain, leg pain, leg weakness or numbness, or spinal instability. During this procedure, your surgeon will remove
PROCEDURE A Posterior Lateral Fusion (PLF) is spine surgery performed to treat disabling back pain, leg pain, leg weakness or numbness, or spinal instability. During this procedure, your surgeon will remove
Discharge Instructions What to Expect After Cervical Fusion
 Discharge Instructions What to Expect After Cervical Fusion Incision Care You may shower 72 hours after you have been discharged from the hospital unless otherwise stated by Dr. Valente. Please do not
Discharge Instructions What to Expect After Cervical Fusion Incision Care You may shower 72 hours after you have been discharged from the hospital unless otherwise stated by Dr. Valente. Please do not
GEORGETOWN ORTHOPAEDIC SPINE SURGERY POSTERIOR CERVICAL SURGERY (LAMINOPLASTY, LAMINECTOMY WITH FUSION)
 POSTERIOR CERVICAL SURGERY (LAMINOPLASTY, LAMINECTOMY WITH FUSION) PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS
POSTERIOR CERVICAL SURGERY (LAMINOPLASTY, LAMINECTOMY WITH FUSION) PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GEORGETOWN ORTHOPAEDIC SPINE SURGERY. Lumbar Decompression
 Lumbar Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS FOR 7-10 DAYS BEFORE SURGERY. These medications
Lumbar Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS FOR 7-10 DAYS BEFORE SURGERY. These medications
Posterior Lumbar Spinal Fusion
 Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
ANTERIOR CERVICAL DECOMPRESSION AND FUSION
 NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, etc) OR ASPIRIN PRODUCTS FOR 7-10 DAYS BEFORE SURGERY. These medications can increase bleeding
NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, etc) OR ASPIRIN PRODUCTS FOR 7-10 DAYS BEFORE SURGERY. These medications can increase bleeding
Dhruv B. Pateder, MD, FAAOS
 Dhruv B. Pateder, MD, FAAOS TOWN CENTER ORTHOPEDIC ASSOCIATES SPINE SURGERY POST-OPERATIVE DISCHARGE INSTRUCTIONS: CERVICAL (NECK) FUSION SPINE SURGERY 1.ANTERIOR DECOMPRESSION AND FUSION WITH INSTRUMENTATION
Dhruv B. Pateder, MD, FAAOS TOWN CENTER ORTHOPEDIC ASSOCIATES SPINE SURGERY POST-OPERATIVE DISCHARGE INSTRUCTIONS: CERVICAL (NECK) FUSION SPINE SURGERY 1.ANTERIOR DECOMPRESSION AND FUSION WITH INSTRUMENTATION
Discharge Instructions: What to Expect After Lumbar Fusion
 Discharge Instructions: What to Expect After Lumbar Fusion Incision Care You may shower 72 hours after you have been discharged from the hospital unless otherwise stated by Dr. Valente. Please do not take
Discharge Instructions: What to Expect After Lumbar Fusion Incision Care You may shower 72 hours after you have been discharged from the hospital unless otherwise stated by Dr. Valente. Please do not take
Cervical Spine Discharge Instructions
 Pain After surgery you may experience pain in the region of the incision. Some neck and arm pain as well as tingling or numbness may also be present. Initially it may be of greater intensity than pre-operatively,
Pain After surgery you may experience pain in the region of the incision. Some neck and arm pain as well as tingling or numbness may also be present. Initially it may be of greater intensity than pre-operatively,
Home Care Instructions. Cervical Laminoplasty
 Home Care Instructions Cervical Laminoplasty You are recovering from a posterior cervical decompression in which your surgeon removed the pressure on your spinal nerves in an attempt to reduce pain and/or
Home Care Instructions Cervical Laminoplasty You are recovering from a posterior cervical decompression in which your surgeon removed the pressure on your spinal nerves in an attempt to reduce pain and/or
Anterior Cervical Discectomy and Fusion Surgery
 Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
Minimally Invasive Discectomy/ Decompression
 Minimally Invasive Discectomy/ Decompression What Is A Minimally Invasive Lumbar Discectomy? A lumbar discectomy is a surgical procedure that involves relieving the pressure placed on nerve roots and/or
Minimally Invasive Discectomy/ Decompression What Is A Minimally Invasive Lumbar Discectomy? A lumbar discectomy is a surgical procedure that involves relieving the pressure placed on nerve roots and/or
Patient Education GANZ PERIACETABULAR OSTEOTOMY
 GANZ PERIACETABULAR OSTEOTOMY Thank you for the opportunity of allowing us to take care of you. We understand that there are many questions regarding your hip surgery for you and your parents. This information
GANZ PERIACETABULAR OSTEOTOMY Thank you for the opportunity of allowing us to take care of you. We understand that there are many questions regarding your hip surgery for you and your parents. This information
Posterior Cervical Decompression
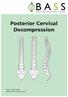 Posterior Cervical Decompression Issue 5: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a narrowing of your
Posterior Cervical Decompression Issue 5: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a narrowing of your
Patient Information. Spinal Fusion Using the ST360 or Silhouette Pedicle Screw System
 Patient Information Spinal Fusion Using the ST360 or Silhouette Pedicle Screw System Spinal Fusion Using the ST360 or Silhouette Pedicle Screw System Your doctor has recommended spinal fusion surgery using
Patient Information Spinal Fusion Using the ST360 or Silhouette Pedicle Screw System Spinal Fusion Using the ST360 or Silhouette Pedicle Screw System Your doctor has recommended spinal fusion surgery using
GUIDELINES FOR PATIENTS HAVING CERVICAL DISCECTOMY AND FUSION SURGERY
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING CERVICAL DISCECTOMY AND FUSION SURGERY Please
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING CERVICAL DISCECTOMY AND FUSION SURGERY Please
Anterior Cervical Discectomy and Fusion (ACDF)
 Anterior Cervical Discectomy and Fusion (ACDF) What Is an ACDF? Anterior Cervical Discectomy and Fusion (ACDF) is a surgical procedure that involves decompressing spinal cord and nerves in the cervical
Anterior Cervical Discectomy and Fusion (ACDF) What Is an ACDF? Anterior Cervical Discectomy and Fusion (ACDF) is a surgical procedure that involves decompressing spinal cord and nerves in the cervical
Dr. Nuelle Knee Replacement: Discharge Care Instructions
 Dr. Nuelle Knee Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your knee replacement surgery. We hope that you had a good stay with us. These discharge
Dr. Nuelle Knee Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your knee replacement surgery. We hope that you had a good stay with us. These discharge
Patient Information ACDF. Anterior Cervical Discectomy and Fusion
 Patient Information ACDF Anterior Cervical Discectomy and Fusion Table of Contents Anatomy of the Spine...2-3 General Conditions of the Cervical Spine...4 5 What is an ACDF?...6 How is an ACDF performed?...7
Patient Information ACDF Anterior Cervical Discectomy and Fusion Table of Contents Anatomy of the Spine...2-3 General Conditions of the Cervical Spine...4 5 What is an ACDF?...6 How is an ACDF performed?...7
LUMBAR MICROSURGERY. Low Back Surgery to Reduce Your Pain
 LUMBAR MICROSURGERY Low Back Surgery to Reduce Your Pain Planning for Low Back Surgery Having a low back (lumbar) problem can be frustrating. You may have pain when you sit, stand, or walk. Even a simple
LUMBAR MICROSURGERY Low Back Surgery to Reduce Your Pain Planning for Low Back Surgery Having a low back (lumbar) problem can be frustrating. You may have pain when you sit, stand, or walk. Even a simple
Ileal Conduit Diversion Surgery
 Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
TRANSURETHRAL RESECTION OF THE PROSTATE
 TRANSURETHRAL RESECTION OF THE PROSTATE A discussion of the operation and the pre and post operative care You and your doctor have considered the possibility that you have a transurethral resection of
TRANSURETHRAL RESECTION OF THE PROSTATE A discussion of the operation and the pre and post operative care You and your doctor have considered the possibility that you have a transurethral resection of
Anterior Cervical Discectomy and Fusion for Cervical Radiculopathy or Cervical Myelopathy (ACDF)
 Anterior Cervical Discectomy and Fusion for Cervical Radiculopathy or Cervical Myelopathy (ACDF) About your condition The pressure from your bulging disc(s) might be causing your pain, numbness or weakness.
Anterior Cervical Discectomy and Fusion for Cervical Radiculopathy or Cervical Myelopathy (ACDF) About your condition The pressure from your bulging disc(s) might be causing your pain, numbness or weakness.
PRE- AND POST-SURGERY INSTRUCTIONS FOR SPINE PATIENTS
 PRE- AND POST-SURGERY INSTRUCTIONS FOR SPINE PATIENTS Medications: Narcotics: The orthopaedic office does not prescribe narcotics for pain prior to operations, with some exceptions. If you have pain that
PRE- AND POST-SURGERY INSTRUCTIONS FOR SPINE PATIENTS Medications: Narcotics: The orthopaedic office does not prescribe narcotics for pain prior to operations, with some exceptions. If you have pain that
Patient Education Total Knee Arthroplasty
 Explanation of Diagnosis and Procedure The knee is the largest joint in the body. Normal knee function is required to perform most everyday activities. The knee is made up of the lower end of the thighbone
Explanation of Diagnosis and Procedure The knee is the largest joint in the body. Normal knee function is required to perform most everyday activities. The knee is made up of the lower end of the thighbone
Simple removal of the kidney (simple nephrectomy): procedure-specific information
 PATIENT INFORMATION Simple removal of the kidney (simple nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
PATIENT INFORMATION Simple removal of the kidney (simple nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
Procedure Specific Information Sheet Open Radical Prostatectomy
 Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
ANTERIOR CERVICAL DISCECTOMY AND FUSION (ACDF) SURGERY INFORMATION
 ANTERIOR CERVICAL DISCECTOMY AND FUSION (ACDF) SURGERY INFORMATION WHAT IS ANTERIOR CERVICAL DISCECTOMY AND FUSION (ACDF) SURGERY? Anterior Cervical Discectomy and Fusion (ACDF) is a surgical procedure
ANTERIOR CERVICAL DISCECTOMY AND FUSION (ACDF) SURGERY INFORMATION WHAT IS ANTERIOR CERVICAL DISCECTOMY AND FUSION (ACDF) SURGERY? Anterior Cervical Discectomy and Fusion (ACDF) is a surgical procedure
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Table of Contents. What is Spinal Fusion? Pre-Register for Surgery How Do I Prepare for Surgery?... 3
 www.cpmc.org/learning Spinal Fusion Table of Contents What is Spinal Fusion?... 2 Pre-Register for Surgery... 2 How Do I Prepare for Surgery?... 3 What Can I Expect During My Hospital Stay?... 3 If You
www.cpmc.org/learning Spinal Fusion Table of Contents What is Spinal Fusion?... 2 Pre-Register for Surgery... 2 How Do I Prepare for Surgery?... 3 What Can I Expect During My Hospital Stay?... 3 If You
At Home After Surgery
 Now that your surgery is done, your focus should be on healing. If you follow the recommendations listed in this section, you will help ensure that your new hip will last for the rest of your life. patients.d-h.org/ortho/hips
Now that your surgery is done, your focus should be on healing. If you follow the recommendations listed in this section, you will help ensure that your new hip will last for the rest of your life. patients.d-h.org/ortho/hips
Radical Cystectomy A Patient s Guide
 Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
Jason Barry, M.D. Knee Arthroscopy with Anterior Cruciate Ligament (ACL) Reconstruction
 Jason Barry, M.D. Knee Arthroscopy with Anterior Cruciate Ligament (ACL) Reconstruction Arthroscopy (scope) is a minimally invasive surgical procedure orthopedic surgeons use to visualize, diagnose and
Jason Barry, M.D. Knee Arthroscopy with Anterior Cruciate Ligament (ACL) Reconstruction Arthroscopy (scope) is a minimally invasive surgical procedure orthopedic surgeons use to visualize, diagnose and
PREMIER SPINE CARE. Adrian P. Jackson, MD (Cervical Spine Specialist) Anterior Cervical Discectomy and Fusion (ACDF)
 PREMIER SPINE CARE Adrian P. Jackson, MD (Cervical Spine Specialist) Anterior Cervical Discectomy and Fusion (ACDF) After your physical examination and a review of your films, you have been recommended
PREMIER SPINE CARE Adrian P. Jackson, MD (Cervical Spine Specialist) Anterior Cervical Discectomy and Fusion (ACDF) After your physical examination and a review of your films, you have been recommended
Review date: February Lumbar Discectomy
 Review date: February 2019 Lumbar Discectomy Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as having a lumbar disc protrusion, resulting in nerve root
Review date: February 2019 Lumbar Discectomy Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as having a lumbar disc protrusion, resulting in nerve root
Dr. Nuelle Fracture Surgery Discharge Care Instructions
 Dr. Nuelle Fracture Surgery Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your injury. We hope that you had a good stay with us. These discharge instructions are
Dr. Nuelle Fracture Surgery Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your injury. We hope that you had a good stay with us. These discharge instructions are
Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients
 Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients i What is a retroperitoneal lymph node dissection (RPLND)? You have probably already undergone surgery and treatment
Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients i What is a retroperitoneal lymph node dissection (RPLND)? You have probably already undergone surgery and treatment
TOTAL HIP ARTHROPLASTY (Total Hip Replacement)
 (Total Hip Replacement) The Hip Joint The hip is a ball and socket joint. The joint is formed by the head of the femur (thighbone) and the acetabulum (pelvis). The bones are coated in cartilage, which
(Total Hip Replacement) The Hip Joint The hip is a ball and socket joint. The joint is formed by the head of the femur (thighbone) and the acetabulum (pelvis). The bones are coated in cartilage, which
TransUrethral Resection for a Bladder Tumour ~ TURBT Women ~
 TransUrethral Resection for a Bladder Tumour ~ TURBT Women ~ To learn about TransUrethral Resection of a Bladder Tumour, you will need to know what these words mean: The bladder stores urine that is made
TransUrethral Resection for a Bladder Tumour ~ TURBT Women ~ To learn about TransUrethral Resection of a Bladder Tumour, you will need to know what these words mean: The bladder stores urine that is made
YOUR OPERATION EXPLAINED
 RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
PATIENT: DOB: TODAY S DATE:
 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand this material. I also understand that if certain sections are not
1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand this material. I also understand that if certain sections are not
LAPAROSCOPIC PYELOPLASTY INFORMATION LEAFLET
 LAPAROSCOPIC PYELOPLASTY INFORMATION LEAFLET Laparoscopic Pyeloplasty Page 1 of 8 LAPAROSCOPIC PYELOPLASTY This leaflet has been written to answers questions that you may have about your operation. If
LAPAROSCOPIC PYELOPLASTY INFORMATION LEAFLET Laparoscopic Pyeloplasty Page 1 of 8 LAPAROSCOPIC PYELOPLASTY This leaflet has been written to answers questions that you may have about your operation. If
ACDF. Anterior Cervical Discectomy and Fusion. An introduction to
 An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
Partial Removal of the Kidney
 Who can I contact if I have a problem when I get home? If you experience any problems related to your surgery or admission once you have been discharged home. Please feel free to contact Ward 4A, 4B or
Who can I contact if I have a problem when I get home? If you experience any problems related to your surgery or admission once you have been discharged home. Please feel free to contact Ward 4A, 4B or
RADICAL PROSTATECTOMY
 Tennyson Centre Suite 19 520 South Road Kurralta Park SA 5037 P 08 8292 2399 F 08 8292 2388 admin@urologicalsolutions.com.au www.urologicalsolutions.com.au Darwin Private Hospital Suite 5 Rocklands Drive
Tennyson Centre Suite 19 520 South Road Kurralta Park SA 5037 P 08 8292 2399 F 08 8292 2388 admin@urologicalsolutions.com.au www.urologicalsolutions.com.au Darwin Private Hospital Suite 5 Rocklands Drive
Transplant Surgery. Patient Education Guide to Your Kidney/Pancreas Transplant Page 9-1. For a kidney/pancreas transplant. Before Your Surgery
 Patient Education Page 9-1 Transplant Surgery For a kidney/pancreas transplant By the time you have your transplant surgery, you may have been waiting for some time. Reading this chapter before surgery
Patient Education Page 9-1 Transplant Surgery For a kidney/pancreas transplant By the time you have your transplant surgery, you may have been waiting for some time. Reading this chapter before surgery
Robotic-Assisted Laparoscopic Pyeloplasty
 Robotic-Assisted Laparoscopic Pyeloplasty What is a? Robotic-assisted pyeloplasty is a procedure to remove a blockage in the urinary tract that occurs where the kidney meets the ureter the Ureteropelvic
Robotic-Assisted Laparoscopic Pyeloplasty What is a? Robotic-assisted pyeloplasty is a procedure to remove a blockage in the urinary tract that occurs where the kidney meets the ureter the Ureteropelvic
North American Spine Society Public Education Series
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Dr. Anant Kumar, M.D. Post-Operative Instructions after Cervical Spine Surgery
 Dr. Anant Kumar, M.D. Post-Operative Instructions after Cervical Spine Surgery We want to make this experience as pleasant as possible for you and your family. If you have any questions before or after
Dr. Anant Kumar, M.D. Post-Operative Instructions after Cervical Spine Surgery We want to make this experience as pleasant as possible for you and your family. If you have any questions before or after
Cervical Artificial Disc Replacement Preoperative, Postoperative and Home Recovery Guide
 1 Cervical Artificial Disc Replacement Preoperative, Postoperative and Home Recovery Guide Introduction The purpose of this guide is to provide you and your family with information regarding your medical
1 Cervical Artificial Disc Replacement Preoperative, Postoperative and Home Recovery Guide Introduction The purpose of this guide is to provide you and your family with information regarding your medical
PATIENT INFORMATION BROCHURE
 PATIENT INFORMATION BROCHURE PATIENT INFORMATION BROCHURE This brochure is designed to help you make an informed decision about your surgery. Please read this entire document carefully. Keep this document
PATIENT INFORMATION BROCHURE PATIENT INFORMATION BROCHURE This brochure is designed to help you make an informed decision about your surgery. Please read this entire document carefully. Keep this document
Posterior. Lumbar Fusion. Disclaimer. Integrated web marketing. Multimedia Health Education
 Posterior Lumbar Fusion Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Posterior Lumbar Fusion Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Robot Assisted Total Laparoscopic Hysterectomy
 Robot Assisted Total Laparoscopic Hysterectomy What is a robot assisted total laparoscopic hysterectomy? It is the removal of the uterus, including the cervix, through four small (1/2-1 ) abdominal incisions
Robot Assisted Total Laparoscopic Hysterectomy What is a robot assisted total laparoscopic hysterectomy? It is the removal of the uterus, including the cervix, through four small (1/2-1 ) abdominal incisions
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
What You Need to Know about a Kidney Transplant
 Page 1 of 5 What You Need to Know about a Kidney Transplant This information will help you understand the risks, benefits and possible complications involved in a kidney transplant. Please read it carefully.
Page 1 of 5 What You Need to Know about a Kidney Transplant This information will help you understand the risks, benefits and possible complications involved in a kidney transplant. Please read it carefully.
MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION AN INTRODUCTION TO
 AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
Further information You can get more information and share your experience at
 GS11 Open Inguinal Hernia Repair (female) Further information You can get more information and share your experience at www.aboutmyhealth.org You can get information locally from: Hospital switchboard,
GS11 Open Inguinal Hernia Repair (female) Further information You can get more information and share your experience at www.aboutmyhealth.org You can get information locally from: Hospital switchboard,
Femoral shaft fracture surgery (femoral nailing)
 Femoral shaft fracture surgery (femoral nailing) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that
Femoral shaft fracture surgery (femoral nailing) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that
Patient Information Brochure
 Patient Information Brochure Patient Information Brochure This brochure is designed to help you make an informed decision about your surgery. Please read this entire document carefully. Keep this document
Patient Information Brochure Patient Information Brochure This brochure is designed to help you make an informed decision about your surgery. Please read this entire document carefully. Keep this document
ACL RECONSTRUCTION. Date of Surgery. Please bring this booklet the day of your surgery. QHC#65
 ACL RECONSTRUCTION Date of Surgery Please bring this booklet the day of your surgery. QHC#65 The ACL (Anterior Cruciate Ligament) is the major stabilizing ligament of the knee. The ACL is located in the
ACL RECONSTRUCTION Date of Surgery Please bring this booklet the day of your surgery. QHC#65 The ACL (Anterior Cruciate Ligament) is the major stabilizing ligament of the knee. The ACL is located in the
Knee Replacement Recovery Guide
 Knee Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Range of Motion... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering... 3 Bruising...
Knee Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Range of Motion... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering... 3 Bruising...
 Introduction Posterior cervical fusion is done through the back posterior of the neck. The surgery joins two or more neck vertebrae into one solid section of bone. The medical term for fusion is arthrodesis.
Introduction Posterior cervical fusion is done through the back posterior of the neck. The surgery joins two or more neck vertebrae into one solid section of bone. The medical term for fusion is arthrodesis.
Lumbar Decompression and Stabilisation for Spondylitic Spondylolisthesis
 Lumbar Decompression and Stabilisation for Spondylitic Spondylolisthesis Issue 6: March 2016 Review date: February 2019 Following your recent investigations and consultation with your spinal surgeon, it
Lumbar Decompression and Stabilisation for Spondylitic Spondylolisthesis Issue 6: March 2016 Review date: February 2019 Following your recent investigations and consultation with your spinal surgeon, it
A Patient's Guide to Cervical Laminectomy
 Introduction A laminectomy is a surgical procedure to relieve pressure on the spinal cord due to spinal stenosis. In spinal stenosis, bone spurs press against the spinal cord, leading to a condition called
Introduction A laminectomy is a surgical procedure to relieve pressure on the spinal cord due to spinal stenosis. In spinal stenosis, bone spurs press against the spinal cord, leading to a condition called
POSTERIOR LUMBAR FUSION SURGERY INFORMATION
 POSTERIOR LUMBAR FUSION SURGERY INFORMATION WHAT IS LUMBAR FUSION SURGERY? Spinal fusion is a surgical procedure that joins or fuses 2 or more vertebrae (bones) so that movement no longer occurs between
POSTERIOR LUMBAR FUSION SURGERY INFORMATION WHAT IS LUMBAR FUSION SURGERY? Spinal fusion is a surgical procedure that joins or fuses 2 or more vertebrae (bones) so that movement no longer occurs between
Gynaecology Department Patient Information Leaflet
 Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Patient Information for Consent
 Patient Information for Consent OS12 Femoral Shaft Fracture Surgery (Femoral Nailing) Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your
Patient Information for Consent OS12 Femoral Shaft Fracture Surgery (Femoral Nailing) Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your
LUMBAR DECOMPRESSION / DISCECTOMY SURGERY INFORMATION
 LUMBAR DECOMPRESSION / DISCECTOMY SURGERY INFORMATION WHAT IS LUMBAR DECOMPRESSION / DISCECTOMY SURGERY? During lumbar decompression/ discectomy back surgery, a small portion of the bone over the nerve
LUMBAR DECOMPRESSION / DISCECTOMY SURGERY INFORMATION WHAT IS LUMBAR DECOMPRESSION / DISCECTOMY SURGERY? During lumbar decompression/ discectomy back surgery, a small portion of the bone over the nerve
Transforaminal Lumbar Interbody Fusion
 Transforaminal Lumbar Interbody Fusion Issue 6: March 2016 Review date: February 2019 Following your discography investigation and consultation with your spinal surgeon, the possibility of undergoing lumbar
Transforaminal Lumbar Interbody Fusion Issue 6: March 2016 Review date: February 2019 Following your discography investigation and consultation with your spinal surgeon, the possibility of undergoing lumbar
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Author: Vancouver Island Neurosurgical Foundation. Reviewed: July 28/2016
 My Anterior Cervical Spine Surgery The Surgery Team has prepared this insert containing discharge information to help you and your family after surgery. It has information about what you can do after your
My Anterior Cervical Spine Surgery The Surgery Team has prepared this insert containing discharge information to help you and your family after surgery. It has information about what you can do after your
Cervical laminectomy for spinal cord compression. Information for patients Neurosurgery
 Cervical laminectomy for spinal cord compression Information for patients Neurosurgery What is a compression of the spinal cord and how has it been caused? The bones in our back are called vertebras and
Cervical laminectomy for spinal cord compression Information for patients Neurosurgery What is a compression of the spinal cord and how has it been caused? The bones in our back are called vertebras and
Surgery to the jaw joint (TMJ surgery) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Surgery to the jaw joint (TMJ surgery) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained
Surgery to the jaw joint (TMJ surgery) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained
North American Spine Society Public Education Series
 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Open Radical Removal of the Kidney
 Who can I contact if I have a problem when I get home? If you experience any problems related to your surgery or admission once you have been discharged home. Please feel free to contact 4A, 4B or 4C ward
Who can I contact if I have a problem when I get home? If you experience any problems related to your surgery or admission once you have been discharged home. Please feel free to contact 4A, 4B or 4C ward
All About? What is Sciatica. Disclaimer. Integrated web marketing. Multimedia Health Education
 What is Sciatica All About? Disclaimer This movie is an educational resource only and should not be used to manage sciatica. All decisions about the management of sciatica must be made in conjunction with
What is Sciatica All About? Disclaimer This movie is an educational resource only and should not be used to manage sciatica. All decisions about the management of sciatica must be made in conjunction with
Fracture Surgery. Post-Operative Care. And. Rehabilitation Protocol
 PATIENT NAME: Fracture Surgery Post-Operative Care And Rehabilitation Protocol After Surgery Care and Information Many questions arise during the first week after surgery. There are many new sensations
PATIENT NAME: Fracture Surgery Post-Operative Care And Rehabilitation Protocol After Surgery Care and Information Many questions arise during the first week after surgery. There are many new sensations
Open Incisional Hernia Repair
 www.mogodaysurgery.com.au Mr. Sanjay Singh MBBS, MS, FRACS, FRCS (UK) Consultant Surgeon 2-4 Charles Street MOGO NSW 2536 Tel: 02 4474 3774 Fax: 02 4474 3775 Write questions or notes here: Open Incisional
www.mogodaysurgery.com.au Mr. Sanjay Singh MBBS, MS, FRACS, FRCS (UK) Consultant Surgeon 2-4 Charles Street MOGO NSW 2536 Tel: 02 4474 3774 Fax: 02 4474 3775 Write questions or notes here: Open Incisional
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis This article is also available in Spanish: Estenosis de la columna lumbar (topic.cfm?topic=a00701). A common cause of low back and leg pain is lumbar spinal stenosis. As we age,
Lumbar Spinal Stenosis This article is also available in Spanish: Estenosis de la columna lumbar (topic.cfm?topic=a00701). A common cause of low back and leg pain is lumbar spinal stenosis. As we age,
Robot Assisted Laparoscopic Radical Prostatectomy
 Robot Assisted Laparoscopic Radical Prostatectomy Robot Assisted Laparoscopic Radical Prostatectomy is an alternative to Open Radical Prostatectomy. It will be performed by your Consultant Urologist at
Robot Assisted Laparoscopic Radical Prostatectomy Robot Assisted Laparoscopic Radical Prostatectomy is an alternative to Open Radical Prostatectomy. It will be performed by your Consultant Urologist at
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
LAPAROSCOPIC HERNIA REPAIR
 LAPAROSCOPIC HERNIA REPAIR Treating Your Hernia with Laparoscopy When You Have a Hernia Anyone can have a hernia. This is a weakness or tear in the wall of the abdomen. It often results from years of wear
LAPAROSCOPIC HERNIA REPAIR Treating Your Hernia with Laparoscopy When You Have a Hernia Anyone can have a hernia. This is a weakness or tear in the wall of the abdomen. It often results from years of wear
Aortic valve replacement. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Aortic replacement Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information in
Aortic replacement Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information in
Lumbar Nerve Root Decompression for Foraminal Stenosis
 Lumbar Nerve Root Decompression for Foraminal Stenosis Issue 5: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as
Lumbar Nerve Root Decompression for Foraminal Stenosis Issue 5: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as
Total ankle replacement. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Total ankle replacement Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Total ankle replacement Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Dr. Roy Davidovitch Next Day Discharge Total Hip Replacement Recovery Guide
 Dr. Roy Davidovitch Next Day Discharge Total Hip Replacement Recovery Guide PREOPERATIVE INSTRUCTIONS Your Preadmission Testing Visit About 2 weeks prior to your surgical date, you will be required to
Dr. Roy Davidovitch Next Day Discharge Total Hip Replacement Recovery Guide PREOPERATIVE INSTRUCTIONS Your Preadmission Testing Visit About 2 weeks prior to your surgical date, you will be required to
POST OP INSTRUCTIONS CERVICAL
 POST OP INSTRUCTIONS CERVICAL Post-Op Pain It is not unusual to experience the following symptoms in the first few weeks after surgery: 1. Pain in and around the incision(s) 2. Some persistent neck or
POST OP INSTRUCTIONS CERVICAL Post-Op Pain It is not unusual to experience the following symptoms in the first few weeks after surgery: 1. Pain in and around the incision(s) 2. Some persistent neck or
Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery
 Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery 221 Madison Ave Morristown, New Jersey 07960 (973) 538 4444 Fax (973) 538 0420 Patient
Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery 221 Madison Ave Morristown, New Jersey 07960 (973) 538 4444 Fax (973) 538 0420 Patient
