NEONATAL SKIN AND WOUND CARE
|
|
|
- Christine Lyons
- 5 years ago
- Views:
Transcription
1 NEONATAL SKIN AND WOUND CARE
2 Objectives Review the different categories of wounds seen in neonates and children. Understand the physiologic and structural differences between neonatal skin and adult skin. Review the risk factors associated with pressure ulcers in neonates. Review the different categories of pressure ulcers and how they present in neonates. Discuss wound care dressings that are safe and effective in neonates. Review the management of IV infiltrates in neonates. Purpose To reduce swelling. To minimise pain and discomfort. To prevent further damage to vulnerable tissue. To reduce incidence and severity of scarring. To provide protection and allow fluid to escape from tissues. To ensure comprehensive assessment and documentation. To provide a record for infants notes. Neonatal Wound Types Pressure Injuries Contact irritation Extravasation Wounds Surgical Wounds Trauma/Shear Injuries/Miscellaneous Infections Burns
3 Wound Healing Principles Adequate Debridement Proper moisture balance Control of infection and inflammation Appropriate choice of dressing Unique features of Neonatal Skin Skin does not mature until 32 weeks gestation or about days post birth for those born at less than 32 weeks. Skin integrity of premature infants is weak and far from complete. Stratum corneum is the outermost section of the epidermis. Composed of nonviable skin cells packed on top of each other to create a protective barrier. Key function of Stratum corneum is to control transepidermal water loss (TEWL) and to prevent absorption of toxic substances. Stratum Corneum In full term infants and adults the Stratum corneum is layers thick Premature neonates <30 weeks have less than 2-3 layers week preterm infants have virtually no stratum corneum
4 Basement Membrane In premature infants, the connection at the dermal-epidermal junction is weak due to fewer hemidesmosomes and anchoring fibrils. They are also spaced further apart. Trauma to the epidermis can therefore arise when removing adhesive dressing in which the bond between adhesive dressing is stronger than the bond between dermis and epidermis. This factor, therefore, places the premature infant at greater risk for blistering or thermal insults. Dermis The dermis of premature infants has less collagen and fewer elastin fibres. This increases the risk for oedema. Oedema can in turn raise the risk for pressure ulcers and other ischaemic injury due to reduced blood flow.
5 Epidermal stripping Definition Skin (Epidermal) stripping Removal of one or more layers of the Stratum corneum occuring following removal of adhesive tape or dressing. Lesions are frequently shallow and irregular in shape and the skin may appear shiny. Open lesions may be accompanied by erythema and blister formation. Action All staff must keep their fingernails short and ensure that all stoned rings are removed as, in some cases, handling alone may cause epidermal stripping. Minimal use of adhesive tape. Do not use tape on the skin when securing umbilical lines. A layer of hydrocolloid (Duoderm) should be used under tape as appropriate e.g. for nasogastric tube fixation. Careful removal of tapes and adhesive dressings following manufacturer s instructions e.g. Remove film dressing by stretching the dressing parallel to the patient s skin while stabilising the skin and IV catheter with the other hand. Use of adhesive removers if needed. ( Appeel wipes)
6 Neonatal pressure injuries Definition A pressure ulcer is localized injury to the skin and/or underlying tissue usually over a bony prominence, as a result of pressure, or pressure in combination with shear. A number of contributing or confounding factors are also associated with pressure ulcers moisture, nutrition, tissue perfusion, mobility and activity. Stage I: Non-blanching erythema Intact skin with non-blanching redness of a localized area usually over a bony prominence. Darkly pigmented skin may not have visible blanching; its colour may differ from the surrounding area. The area may be painful, firm, soft, warmer or cooler as compared to adjacent tissue.
7 Stage II: Partial thickness skin loss Partial thickness loss of dermis presenting as a shallow open ulcer with a red pink wound bed, without slough. May also present as an intact or open/ruptured and serum-filled. Presents as a shiny or dry shallow ulcer without slough or bruising. Bruising indicates deep tissue injury. This category should not be used to describe skin tears, tape burns, incontinence associated dermatitis, maceration or excoriation. Stage III: Full thickness skin loss Full thickness tissue loss. Subcutaneous fat may be visible but bone, tendon or muscles are not exposed. Slough may be present but does not obscure the depth of tissue loss. May include undermining and tunnelling. Bone/tendon is not visible or directly affected.
8 Stage IV: Full thickness tissue loss Full thickness tissue loss with exposed bone, tendon or muscle. Slough or eschar may be present. Often includes undermining and tunnelling. Category/Stage IV ulcers can extend into muscle and/or supporting structures e.g., fascia, tendon or joint capsule making osteomyelitis likely to occur. Unstageable: Full thickness skin or tissue loss depth unknown Full thickness tissue loss in which actual depth of the ulcer is completely obscured by slough (yellow, tan, green or brown) and/or eschar (tan, brown or black) in the wound bed. Until enough slough and/or eschar are removed to expose the base of the wound, the true depth cannot be determined but it will be either a Category/Stage III or IV.
9 Suspected Deep Tissue Injury depth unknown Purple or maroon localized area of discoloured intact skin or blood-filled blister due to damage of underlying soft tissue from pressure and/or shear. The area may be preceded by tissue that is painful, firm, mushy, boggy, warmer or cooler as compared to adjacent tissue. Deep tissue injury may be difficult to detect in individuals with dark skin tones. Evolution may include a thin blister over a dark wound bed. The wound may further evolve and become covered by thin eschar. Evolution may be rapid exposing additional layers of tissue even with optimal treatment. Risk factors for Neonatal Pressure Ulcers Identifying babies at risk for pressure ulcers is the key to their prevention Among neonates and children, 50% of pressure ulcers are equipment and device related (nasal prongs, CPAP masks, tubing, lines, tracheostomy devices, O2 monitors and bedding) Acutely ill and immobilised neonates are at high risk for pressure injuries. Such patients are often nutritionally challenged which directly affects skin integrity. Extremely premature infants less than 28 weeks are at greatest risk for pressure ulcers.
10 Risk Factors Bedding Devices Oedema
11 Action Timing of re-siting of probes will depend on the assessment of the individual infant s skin condition and will be documented on the infant s chart but saturation probes must be resited at least 4 hourly ( as per MHRA advice) Change infant position as tolerated to alleviate pressure and reduce risk for pressure injuries. Use Duoderm under CPAP nasal prongs and mask on or apply to nasal septum and nasal bridge. Relieve pressure by alternating mask and prongs, as tolerated. Ensure that small plastic covers and caps from medical devices e.g. the ends of administration sets or IV cannulae, are discarded rather than left in the infant s bed. These can cause pressure damage if the infant inadvertently lies on them for a period of time.
12 Extravasation Wound Care Definition Extravasation is the accidental leakage of certain medicines into the body from an IV drip in the vein. Some medicines, such as TPN, blood products, calcium and sodium bicarbonate can be dangerous when they escape from the drip or the vein. The symptoms can vary from blisters to severe tissue injury or even cause the cells or tissue to die. In severe cases, extravasation injuries can require surgical reconstruction or can lead to amputation. What causes extravasation injuries? Extravasation injuries are caused when certain medicines accidentally come into contact with tissue when being administered through an IV drip or needle. Some medicines will only cause slight damage and are called irritants. Medicines that cause more serious damage are called vesicants. The medicine can come into contact with the surrounding tissue by leakage or direct exposure. The device that administers the medicine may not be secured properly, may be the incorrect size or may be placed on an area that moves a lot so can become loose or dislodged. A needle may puncture the vein and the medicine goes into the surrounding tissue, or the same vein may be used multiple times, which weakens it. Also, young patients have small veins can easily be damaged by the cannula itself. What are the signs and symptoms of extravasation injuries? Symptoms of an extravasation injury can include: Coolness or blanching at the medicine insertion site. Swelling - Infusion rates are often very low in neonates e.g. 0.1ml/hr so you may not observe any swelling prior to an extravasation injury. Tenderness/discomfort. Taut or stretched skin. Leakage of fluid at the insertion site. Inability to obtain blood return (not always present). Change in quality and flow of the infusion or injection. Numbness, tingling or a pins and needles feeling. Burning, stinging pain Redness may occur followed by blistering, tissue necrosis and ulceration. In severe cases of central line extravasation the infusate can enter the pleural or pericardial space and cause sudden unexpected collapse.
13 How extravasation injuries are normally diagnosed? Sometimes, other conditions will need to be ruled out. Some symptoms can resemble other conditions, such as vessel irritation or hypersensitivity. However, as extravasation injuries can be very serious, a nurse or doctor will always be extra cautious and treat the child as though it is an extravasation injury. How are extravasation injuries treated? Extravasation injuries are considered to be medical emergencies. Early detection of the condition is best to avoid complications. Immediate treatment will be to stop the flow of medicine. The cannula (the flexible tube) may be left in place in case the doctor needs to administer any treatment or antidote. The affected site will be elevated and monitored for any changes or gently washed out with Hyaluronidase/Saline and a dressing applied. What happens next? The injury will be observed and elevated until it regains a normal appearance. Sometimes, surgical reconstruction by a plastic surgeon is necessary. To reduce the risk of extravasations Use splints if necessary to support cannula site to reduce the risk of extravasation injury Intravenous cannulae and peripheral longlines should be secured with a sterile clearfilm dressing to ensure cannulation site is clearly visible. A small piece of
14 gauze can be applied to support cannulae (UAC and UVC should be secured according to guidelines) A central line should ideally be sited for the administration of Total Parental Nutrition and infusions that contain glucose in concentrations greater than 12.5% and certain drugs Positioning of limb to aid visibility of site of infusion. This may involve nursing infant in an incubator if temperature cannot be maintained with the limb exposed. At least hourly assessment of the infusion site. Regular visual assessment of lines, ensuring the dressing is secure. Use infusion devices with continuous in line pressure monitoring Check the pressure limit alarm on the pump is set correctly when taking over infant s care. Significant extravasation: (STAGE 3-4) When an extravasation injury has occurred treatment should be initiated without delay. Immediately stop the infusion/injection Elevate the limb Notify the neonatal doctor An extravasation of fluid into the pleural cavity or pericardial space is an emergency and requires immediate assessment and possibly intervention by a senior member of the medical team. If necessary, aspirate as much of the residual drug as possible to minimise the injury caused by the residue of the drug DO NOT FLUSH THE CANNULA Complete a DATIX form Take a photograph of the site. (Parental consent MUST be obtained before the pictures are attached to the patients records. If consent is refused, then pictures must be deleted. Use Hyaluronidase as soon as possible
15 Hyaluronidase for extravasation injuries Equipment 1% Lignocaine (no adrenaline) 1 vial Hyaluronidase (1500units). Dilute with 1ml of water for injection (as per neonatal formulary) then add to 9mls of 0.9% sodium chloride to give a solution of 150IU/ml 0.9% Sodium Chloride ampoules 2ml or 5ml syringe 10ml/20ml syringes Pink blunt ended needles Absorbent sheets or towel to prevent large volumes of liquid from making the infant cold during the procedure Method Use aseptic technique, Appendix 1 Give sucrose, as appropriate Infiltrate 1% Lignocaine in and around the extravasation site (0.3ml/kg maximum ) Wait 3-5 minutes after infiltrating the anaesthetic agent Using a Pink blunt ended needle, infiltrate Hyaluronidase in 0.25 ml aliquots into the subcutaneous tissue (1 vial is diluted with 1ml of water for injection, as stated above) in separate sites around the extravasation aiming toward the centre of the site. Wait 3-15 minutes after administrating the Hyaluronidase. Flush 0.9% sodium chloride through the subcutaneous space in 5ml aliquots. The saline is irrigated through 4-5 of the exit wound sites, exiting as a shower through the remainder - *The amount of fluid used depends on the size of the baby and extent of the wound Gentle massage of the limb can be performed to express fluid through the injection site
16 Apply the dressing and place the limb in a comfortable neutral position. Dressing Plan - Hydrogel Clear Film Change after 24 hours The site must be reviewed on a regular basis Post procedural photographs are recommended If necessary, the patient will be followed up by the plastic surgery service in conjunction with the neonatal service (community and outpatient follow up)
17 Glycerine Trinitrate (GTN) treatment Rationale for use: For use in poor perfusion of extremities, for example dusky toes or fingers Can be used after extravasation with certain agents such as, Dopamine, Dobutamine and Adrenaline, following review and assessment by Consultant. Current indication for use: Ischaemia secondary to arterial cannulation Side effects Systemic vasodilatation and a rise in methaemoglobin level. If used for prolonged periods, measure MetHb levels Hypotension Action to be taken: Inform doctors of the problem and refer to vascular emergency guideline Take photographs if necessary (Gain consent from parents) Follow prescription as stated by doctors Discuss need for analgesia in response to pain score Blood pressure should be monitored closely Close observation of affected limbs/ fingers/toes An online referral may need to be completed for plastic review
18 Dosage and duration Transdermal patch Apply a 1/8 th of a patch (delivers 5mg/day) to the affected area for 24 hours or less Review and reassess on a regular basis. REMEMBER: Document all findings and actions with timings very carefully in the notes. Take photos (parental consent needed) where possible.
19 Wound beds and dressings EPITHELIALISING WOUNDS Characterised by Wound bed pink in appearance tissue very fragile and needs to be kept moist. To protect new tissue growth. Management aims LEVEL OF EXUDATE PRIMARY DRESSINGS LOW Silflex MEDIUM N/A HIGH N/A
20 GRANULATING WOUNDS Characterised by Wound has granular appearance, looks red and bleeds easily. Management aims To maintain a warm moist environment to promote angiogenesis and therefore promote healing LEVEL OF EXUDATE PRIMARY DRESSINGS LOW Silflex Jelonet MEDIUM Silflex Jelonet HIGH Jelonet
21 SLOUGHY WOUNDS Characterised by Formation of viscous predominately yellow soft necrotic tissue. To debride wound bed of sloughy tissue. Management aims LEVEL OF EXUDATE PRIMARY DRESSINGS LOW MEDIUM HIGH Activon tulle Hydrogel Duoderm Activon tulle Aquacel Hydrogel Activon tulle Aquacel Cutimed Sorbact
22 NECROTIC WOUNDS Characterised by Presence of dead devitalised tissues black / brown in colouration. Management aims To rehydrate eschar. This should only be done once a member of the wound care team had reviewed patient. LEVEL OF EXUDATE PRIMARY DRESSINGS LOW MEDIUM Activon tulle Hydrogel Duoderm Activon tulle HIGH Aquacel
23 INFECTED WOUNDS Characterised by Localised heat and increase in exudate, malodour and deterioration in wound bed, colouration yellow/ green. Management aims To identify infection, reduce level of bacteria, control odour and exudate. Wound swab to be taken, Doctors to review and wound care team referral to be made. LEVEL OF EXUDATE PRIMARY DRESSINGS LOW Activon tulle MEDIUM HIGH Cutimed Sorbact Activon tulle Sorbsan Cutimed Sorbact Sorbsan
24 Silflex Non adherent primary dressing. Type of dressing Suitable for Use on lightly exudating wounds. Wounds with fragile surrounding edges. Ideal for traumatic surgical & chronic. Minimise Trauma to wound and infant Minimise pain felt by infant Benefits Allows exudate to pass through the secondary dressing without the need to be changed, therefore reducing trauma to the wound bed Change frequency Can remain in place for up to 14 days - Secondary dressing will need to be changed regularly.
25 Activon tulle Honey dressing Type of dressing Suitable for Use on low to moderate exudating wounds. Benefits Draws exudate out into secondary dressing. Antibacterial properties Change frequency Can be left on for 72 hours.
26 Cavilon Barrier Stick Barrier film preparation Type of dressing Suitable for Protects peri-wound skin Protection from body fluids/ adhesives Transparent Non-sting Benefits Acts as a barrier to protect healthy skin Change frequency Protects for up to 72 hours (therefore no need to re-apply with each change)
27 Duoderm Hydrocolloid dressing Type of dressing Suitable for For use on non-lightly exudating wounds Can be used as a skin protector Benefits Provides bacterial and viral barrier Atraumatic on removal Reduces risk of skin breakdown Change frequency Change as dictated by the amount of exudate. Maximum wear time is 7 days.
28 Sorbsan Calcium Alginate dressing. Type of dressing Suitable for Absorbs moderate high amounts of exudate Suitable for flat shallow or cavity wounds Benefits Encourages bacteria into the secondary dressing Conforms to shape of the wound Can be left in place for 72 hours Change frequency
29 Hydrogel Hydrogel Type of dressing Suitable for For use of dry light exudating wounds Rehydrates necrosis and slough Benefits Can be left in place for 72 hours Change frequency
30 Aquacel Extra Type of dressing Hydrocolloid Fibrous Dressing (Hydrofibre) Suitable for Absorbs moderate - heavy amounts of exudate Will require secondary dressing Benefits Re-hydrates & debrides necrotic tissue or dry slough Reduces maceration to surrounding skin Provides a bacterial barrier Use with 0.9% sodium chloride when applied to necrotic areas to hydrate and debride necrosis Change frequency Change as dictated by the amount of exudate. Maximum wear time is 7 days. Removal Aquacel maintains its integrity when gelled, allowing one-piece removal. If adherence occurs, assist removal by gently irrigating with warmed sodium chloride 0.9% solution.
31 Appeel Silicone Adhesive remover Type of dressing Suitable for Use to remove adhesive wound dressings Non Sting Completely removes adhesive Leaves no residue on skin Reduces trauma to fragile skin Benefits Can be used as often as required Change frequency
32 Kaltostat Type of dressing Sterile non-woven calcium-sodium alginate fibre Suitable for Moderate to heavily exuding wounds and the local management of bleeding minor wounds. Benefits On contact with a bleeding wound, promotes haemostasis Change frequency Change as dictated by the amount of exudate. Maximum wear time is 7 days. Removal Kaltostat maintains its integrity when gelled, allowing one-piece removal. If adherence occurs, assist removal by gently irrigating with warmed 0.9% sodium chloride solution.
33 Cutimed Sorbact Type of dressing Sorbact Technology-coated antimicrobial dressings Unlike dressings which depend on antimicrobials or antiseptics to remove bacteria from contaminated and infected wounds, Cutimed Sorbact is the first range of wound dressings to work without a chemically active agent. By the physical principle of hydrophobic interaction, within 30 seconds, bacteria and fungi become physically and irreversibly bound to the dressings' specially coated surface of Sorbact Technology. Therefore with every dressing change, the bound bacteria and fungi are simply removed from the wound bed. Suitable for Cutimed Sorbact can be used safely on all types of colonised or infected wounds regardless of their aetiology: Chronic wounds such as venous, pressure or diabetic foot ulcers Post-operative or dehisced surgical wounds Traumatic wounds Wounds after excision of abscesses Benefits The use of Cutimed Sorbact dressings are also not linked to contraindications and side effects that are associated with the use of other antimicrobial dressings
34 Reducing the bacterial bioburden in a wound improves the conditions for wound healing to take place. By removing bacteria with each dressing change, Cutimed Sorbact reduces not only their number but also the level of harmful toxins, improving conditions for wound healing to take place. None of the drawbacks of conventional antimicrobial dressings. There is no cytotoxicity, no disturbance in wound inspection and no contra-indications - the dressing can be used safely during pregnancy, breastfeeding and on children. Safe to use for pro-longed periods of time as no chemicals are donated into the wound Change frequency Cutimed Sorbact is to be applied as a single layer only. Change as dictated by the amount of exudate. Maximum wear time is 7 days - Secondary dressing will need to be changed regularly.
35 Jelonet Type of dressing Jelonet consists of a leno-weave fabric, of cotton or cotton and viscose, which has been impregnated with white soft paraffin. Suitable for Minor Burns and scalds Donor sites Graft sites Trauma Allows the wound to drain freely Soothes Protects Easy removal Benefits Change frequency Change dressing daily or more often according to the condition of the wound. A double layer of Jelonet will prevent the dressing from sticking to the wound bed.
36
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
Pressure Ulcer Staging and Documentation. Carolyn Watts MSN, RN, CWON Vanderbilt Medical Center
 Pressure Ulcer Staging and Documentation Carolyn Watts MSN, RN, CWON Vanderbilt Medical Center Overview of the Pressure Ulcer Problem Scope Over 1 million cases each year, 1 in 4 patients Cost In acute
Pressure Ulcer Staging and Documentation Carolyn Watts MSN, RN, CWON Vanderbilt Medical Center Overview of the Pressure Ulcer Problem Scope Over 1 million cases each year, 1 in 4 patients Cost In acute
Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell
 Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell Objectives Identify the stages of pressure ulcer according to the depth of tissue destruction. Discuss the differences
Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell Objectives Identify the stages of pressure ulcer according to the depth of tissue destruction. Discuss the differences
Risk factors and drugs/infusion commonly associated with tissue damage include: Extreme Prematurity Dextrose greater than 12.
 Neonatal Intensive Care Unit Clinical Guideline Extravasation injuries Extravasation is defined as the inadvertent leakage of infused fluid into the surrounding tissue. The resultant damage to tissue can
Neonatal Intensive Care Unit Clinical Guideline Extravasation injuries Extravasation is defined as the inadvertent leakage of infused fluid into the surrounding tissue. The resultant damage to tissue can
Pressure Ulcer Staging. Staging of Wounds are based on the deepest level of tissue damage
 Pressure Ulcer Staging Staging of Wounds are based on the deepest level of tissue damage Pressure Ulcer Staging New Pressure Ulcer Staging Stage I Stage II Stage III Stage IV Unstageable Suspected Deep
Pressure Ulcer Staging Staging of Wounds are based on the deepest level of tissue damage Pressure Ulcer Staging New Pressure Ulcer Staging Stage I Stage II Stage III Stage IV Unstageable Suspected Deep
Appropriate Dressing Selection For Treating Wounds
 Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Extravasation injuries. Amendments Date Page(s) Comments Approved by 03/16 ALL Completely updated guideline
 Note: Guidance comments are written in italics Extravasation injuries Amendments Date Page(s) Comments Approved by 03/16 ALL Completely updated guideline Compiled by: In Consultation with: Ratified by:
Note: Guidance comments are written in italics Extravasation injuries Amendments Date Page(s) Comments Approved by 03/16 ALL Completely updated guideline Compiled by: In Consultation with: Ratified by:
Tissue Viability Service Wound Management Primary Care Formulary 2017
 Tissue Viability Service Wound Management Primary Care Formulary 2017 WMPF/TVS: March 2017 Review date: March 2019 Product Group Current Product Sizes Price per Item Hydrogel 1st Activheal Hydrogel 2nd
Tissue Viability Service Wound Management Primary Care Formulary 2017 WMPF/TVS: March 2017 Review date: March 2019 Product Group Current Product Sizes Price per Item Hydrogel 1st Activheal Hydrogel 2nd
Advanced Clinical Solutions. Pressure Ulcer. Carilex Medical Group 1
 Advanced Clinical Solutions Pressure Ulcer Carilex Medical Group 1 Advanced Clinical Solutions Contents About Pressure Ulcer! 2 Stages of Pressure Ulcer! 5 Reference! 7 Carilex Medical Group 1 About Pressure
Advanced Clinical Solutions Pressure Ulcer Carilex Medical Group 1 Advanced Clinical Solutions Contents About Pressure Ulcer! 2 Stages of Pressure Ulcer! 5 Reference! 7 Carilex Medical Group 1 About Pressure
Tissue Viability Service Wound Management Primary Care Formulary 2017
 Tissue Viability Service Wound Management Primary Care Formulary 2017 WMPF/TVS: March 2017 Review date: March 2019 Product Group Current Product Sizes Price per Item Hydrogel 1st Activheal Hydrogel 2nd
Tissue Viability Service Wound Management Primary Care Formulary 2017 WMPF/TVS: March 2017 Review date: March 2019 Product Group Current Product Sizes Price per Item Hydrogel 1st Activheal Hydrogel 2nd
Wound Jeopardy: Name That Wound Session 142 Saturday, September 10 th 2011
 Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
The Importance of Skin Examination. following Spinal Cord Injury
 The Importance of Skin Examination following Spinal Cord Injury An individual who sustains a spinal cord injury (SCI) has a lifetime of increased susceptibility to skin problems, including pressure ulcers
The Importance of Skin Examination following Spinal Cord Injury An individual who sustains a spinal cord injury (SCI) has a lifetime of increased susceptibility to skin problems, including pressure ulcers
Pressure Ulcer. Patient information leaflet. Category I. Category II. Category III. Category IV. Unstageable. Deep Tissue Injury
 Pressure Ulcers Patient information leaflet Pressure Ulcer Category I Category II Category III Category IV Unstageable Deep Tissue Injury Introduction This leaflet is about pressure ulcers and includes
Pressure Ulcers Patient information leaflet Pressure Ulcer Category I Category II Category III Category IV Unstageable Deep Tissue Injury Introduction This leaflet is about pressure ulcers and includes
DRESSING SELECTION SIMPLIFIED
 10 DRESSING SELECTION SIMPLIFIED It must be recognised that no one dressing provides the optimum environment for the healing of all wounds (Mahoney, 2015) DRESSING SELECTION SIMPLIFIED Selecting the correct
10 DRESSING SELECTION SIMPLIFIED It must be recognised that no one dressing provides the optimum environment for the healing of all wounds (Mahoney, 2015) DRESSING SELECTION SIMPLIFIED Selecting the correct
GP Practice Woundcare Formulary
 Agreed jointly by Ipswich and East Suffolk and West Suffolk Clinical Commissioning Groups GP Practice Woundcare Formulary Version 28 October 2017 Formulary items should be prescribed wherever possible.
Agreed jointly by Ipswich and East Suffolk and West Suffolk Clinical Commissioning Groups GP Practice Woundcare Formulary Version 28 October 2017 Formulary items should be prescribed wherever possible.
Welcome to NuMed! Our Commitment: Quality Products, Cost Savings, Exceptional Service
 It s a New Day in Wound Care Welcome to NuMed! Our Commitment: Quality Products, Cost Savings, Exceptional Service NuMed Industries is a manufacturing company that specializes in Advanced Wound Care products.
It s a New Day in Wound Care Welcome to NuMed! Our Commitment: Quality Products, Cost Savings, Exceptional Service NuMed Industries is a manufacturing company that specializes in Advanced Wound Care products.
PRESSURE ULCERS SIMPLIFIED
 10 PRESSURE ULCERS SIMPLIFIED This leaflet is intended to give you information and answers to some question you may have around pressure ulcers PRESSURE ULCERS SIMPLIFIED Pressure ulcer development has
10 PRESSURE ULCERS SIMPLIFIED This leaflet is intended to give you information and answers to some question you may have around pressure ulcers PRESSURE ULCERS SIMPLIFIED Pressure ulcer development has
If both a standardized, validated screening tool and an evaluation of clinical factors are utilized, select Response 2.
 (M1300) Pressure Ulcer Assessment: Was this patient assessed for Risk of Developing Pressure Ulcers? 0 - No assessment conducted [Go to M1306 ] 1 - Yes, based on an evaluation of clinical factors (for
(M1300) Pressure Ulcer Assessment: Was this patient assessed for Risk of Developing Pressure Ulcers? 0 - No assessment conducted [Go to M1306 ] 1 - Yes, based on an evaluation of clinical factors (for
DRESSING SELECTION. Rebecca Aburn MN NP Candidate
 DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
Negative Pressure Wound Therapy
 Origination: 6/29/04 Revised: 8/24/16 Annual Review: 11/10/16 Purpose: To provide Negative Pressure Wound Therapy (wound care treatment) guidelines for the Medical Department staff to reference when making
Origination: 6/29/04 Revised: 8/24/16 Annual Review: 11/10/16 Purpose: To provide Negative Pressure Wound Therapy (wound care treatment) guidelines for the Medical Department staff to reference when making
Objectives. Major Changes to Section M. MDS 3.0 Section M Pressure Ulcers. Risk assessment Introduction of NPUAP guidelines
 MDS 3.0 Section M Pressure Ulcers Moderator: Barbara Baylis Sr. VP of Clinical and Residential Services, Kindred Healthcare Presenter: Glenda Mack, Sr. Director of Clinical Operations, Peoplefirst Rehabilitation
MDS 3.0 Section M Pressure Ulcers Moderator: Barbara Baylis Sr. VP of Clinical and Residential Services, Kindred Healthcare Presenter: Glenda Mack, Sr. Director of Clinical Operations, Peoplefirst Rehabilitation
Pressure Injury Staging Update 2016
 Pressure Injury Staging Update 2016 A Review of the New Changes for Pressure Injury Documentation and Staging Jeanne Terefenko, BSN, RN, CWOCN Ext. 5855 Pressure Ulcer Staging Updates: In April, 2016,
Pressure Injury Staging Update 2016 A Review of the New Changes for Pressure Injury Documentation and Staging Jeanne Terefenko, BSN, RN, CWOCN Ext. 5855 Pressure Ulcer Staging Updates: In April, 2016,
Assisted Living Resident Assessment (To be used when yes is indicated for skin issues under Section 5 of Assisted Living Resident Assessment)
 Skin Assessment Current open skin areas: Yes No Current pressure ulcer: Yes No A. Stage 1 Ulcers Report based on highest stage of existing ulcers at its worst; do not reverse stage. Number of existing
Skin Assessment Current open skin areas: Yes No Current pressure ulcer: Yes No A. Stage 1 Ulcers Report based on highest stage of existing ulcers at its worst; do not reverse stage. Number of existing
Recognizing Pressure Injury
 Recognizing Pressure Injury Karen Zulkowski, DNS, RN Hawaii Recorded on March 8, 2017 1 A Little About Myself Executive editor of the Journal of the World Council of Enterostomal Therapists (JWCET) and
Recognizing Pressure Injury Karen Zulkowski, DNS, RN Hawaii Recorded on March 8, 2017 1 A Little About Myself Executive editor of the Journal of the World Council of Enterostomal Therapists (JWCET) and
Lower Extremity Wound Evaluation and Treatment
 Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
2. Advanced wound therapies... 4 (i) Maggots... 4 (ii) Negative Pressure Wound Therapy (NPWT)... 4
 Contents: Wound management Medicines Formulary 1. Interactive dressings... 2 (i) Hydrocolloid dressings... 2 (ii) Hydrogel dressings... 2 (iii) Alginate dressings... 2 (iv) Fibrous absorbent dressings...
Contents: Wound management Medicines Formulary 1. Interactive dressings... 2 (i) Hydrocolloid dressings... 2 (ii) Hydrogel dressings... 2 (iii) Alginate dressings... 2 (iv) Fibrous absorbent dressings...
Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types. Summary
 Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Guidelines for the Treatment of Pressure Ulcers (Adapted from EPUAP & NPUAP 2009)
 Guidelines for the Treatment of Pressure Ulcers (Adapted from EPUAP & NPUAP 2009) This guidance should be read in conjunction with your local dressing formulary and anti-biotic prescribing guidelines.
Guidelines for the Treatment of Pressure Ulcers (Adapted from EPUAP & NPUAP 2009) This guidance should be read in conjunction with your local dressing formulary and anti-biotic prescribing guidelines.
Pressure Injury Definition and Stages
 Program Objective Pressure Injury Definition and Stages Identify the changes to the 2016 NPUAP staging system Changes to the Staging System in 2016 2 Anatomy of the Skin Anatomy of the Skin Largest organ
Program Objective Pressure Injury Definition and Stages Identify the changes to the 2016 NPUAP staging system Changes to the Staging System in 2016 2 Anatomy of the Skin Anatomy of the Skin Largest organ
Bed Sores No More! Pressure Injuries Risk Factors and Updated Staging Methodology. Nicolle Samuels, MSPT, CLT-LANA, CWS, CKTP
 Bed Sores No More! Pressure Injuries Risk Factors and Updated Staging Methodology Nicolle Samuels, MSPT, CLT-LANA, CWS, CKTP Objectives Understand updated definitions as well as staging and classification
Bed Sores No More! Pressure Injuries Risk Factors and Updated Staging Methodology Nicolle Samuels, MSPT, CLT-LANA, CWS, CKTP Objectives Understand updated definitions as well as staging and classification
(Words Pressure Wound Video Series and Part II appear on screen with the SCIRE logo at the top right corner.)
 (Words Pressure Wound Video Series and Part II appear on screen with the SCIRE logo at the top right corner.) (Fades to next slide titled Pressure Ulcer Staging. *Video contains Graphic Imagery is noted
(Words Pressure Wound Video Series and Part II appear on screen with the SCIRE logo at the top right corner.) (Fades to next slide titled Pressure Ulcer Staging. *Video contains Graphic Imagery is noted
ASHFORD & ST PETER S HOSPITALS NHS TRUST Neonatal Unit. Neonatal Skin and Wound Care Guideline
 ASHFORD & ST PETER S HOSPITALS NHS TRUST Neonatal Unit Neonatal Skin and Wound Care Guideline Contents Preventative measures 2 Initiating wound care 3 Wound classification and management 4 Recommended
ASHFORD & ST PETER S HOSPITALS NHS TRUST Neonatal Unit Neonatal Skin and Wound Care Guideline Contents Preventative measures 2 Initiating wound care 3 Wound classification and management 4 Recommended
Anseong Factory : 70-17, Wonam-ro, Wongok-myeon, Anseong-si, Gyeonggi-do , REPUBLIC OF KOREA
 Care for tomorrow The Solution for Management HQ & Factory : 7, Hyeongjero4Beon-gil, Namsa-myeon, Cheoin-gu, Yong-in-si, Gyeonggi-do 449-884, REPUBLIC OF KOREA TEL: +8-3-33-33 / FAX: +8-3-33-34 Anseong
Care for tomorrow The Solution for Management HQ & Factory : 7, Hyeongjero4Beon-gil, Namsa-myeon, Cheoin-gu, Yong-in-si, Gyeonggi-do 449-884, REPUBLIC OF KOREA TEL: +8-3-33-33 / FAX: +8-3-33-34 Anseong
THERAPIES. HAND IN HAND. Need safe and efficient infection prevention and management? 1 The Cutimed. Closing wounds. Together.
 Closing wounds. Together. Need safe and efficient infection prevention and management? 1 The Cutimed Sorbact range. A responsible choice. THERAPIES. HAND IN HAND. www.bsnmedical.co.uk TOGETHER WE CAN MAKE
Closing wounds. Together. Need safe and efficient infection prevention and management? 1 The Cutimed Sorbact range. A responsible choice. THERAPIES. HAND IN HAND. www.bsnmedical.co.uk TOGETHER WE CAN MAKE
Wound Care Program for Nursing Assistants-
 Wound Care Program for Nursing Assistants- Wound Cleansing,Types & Presentation Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion
Wound Care Program for Nursing Assistants- Wound Cleansing,Types & Presentation Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion
Wound Care per HHVNA Wound Product Formulary
 Venous Ulcers ABI of 0.9-1.2 = normal blood flow An ABI MUST be obtained prior to inititiation of compression therapy. Compression is the Gold Standard of care to promote wound of venous ulcers. Elevation
Venous Ulcers ABI of 0.9-1.2 = normal blood flow An ABI MUST be obtained prior to inititiation of compression therapy. Compression is the Gold Standard of care to promote wound of venous ulcers. Elevation
Advazorb. Hydrophilic foam dressing range
 Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
SDMA Categorisation of Wound Care and Associated Products
 Version 7 - February 2015 TAPES AND TRADITIONAL DRESSINGS Traditional Wound Dressings Wound Dressings Packs Swabs Swabs Swab Products Adhesive Tapes Taping Sheets Absorbent Wadding Absorbent Dressings
Version 7 - February 2015 TAPES AND TRADITIONAL DRESSINGS Traditional Wound Dressings Wound Dressings Packs Swabs Swabs Swab Products Adhesive Tapes Taping Sheets Absorbent Wadding Absorbent Dressings
WHY WOUNDS FAIL TO HEAL SIMPLIFIED
 WHY WOUNDS FAIL TO HEAL SIMPLIFIED 10 Some of the common signs of failure to heal with possible causes and some interventions WHY WOUNDS FAIL TO HEAL There must be adequate supplies of nutrients and oxygen
WHY WOUNDS FAIL TO HEAL SIMPLIFIED 10 Some of the common signs of failure to heal with possible causes and some interventions WHY WOUNDS FAIL TO HEAL There must be adequate supplies of nutrients and oxygen
E-learning module: Stages of pressure injuries. Disclaimer
 E-learning module: Stages of pressure injuries 1 Disclaimer Classification of pressure injuries The International Pressure Injury Category System (2009) was developed by:! the National Pressure Ulcer Advisory
E-learning module: Stages of pressure injuries 1 Disclaimer Classification of pressure injuries The International Pressure Injury Category System (2009) was developed by:! the National Pressure Ulcer Advisory
We look forward to serving you.
 ADVANCED CARE GEMCORE360 offers healthcare professionals a simple, clear and cost-effective wound care range while ensuring excellent clinical outcomes for their patients. 1 At GEMCO Medical, we strive
ADVANCED CARE GEMCORE360 offers healthcare professionals a simple, clear and cost-effective wound care range while ensuring excellent clinical outcomes for their patients. 1 At GEMCO Medical, we strive
Assessment & Management of Wounds in primary practice.
 Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
INTRODUCTION TO WOUND DRESSINGS
 WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
Yorkshire & Humber Neonatal ODN (South) Clinical Guideline
 Yorkshire & Humber Neonatal ODN (South) Clinical Guideline Title: Extravasation Injuries in Neonates Author: Dr Pauline Adiotomre, Lynn Elliot Date Written: March 2005, Reviewed July 2018 by Dr Pauline
Yorkshire & Humber Neonatal ODN (South) Clinical Guideline Title: Extravasation Injuries in Neonates Author: Dr Pauline Adiotomre, Lynn Elliot Date Written: March 2005, Reviewed July 2018 by Dr Pauline
Categorisation of Wound Care and Associated Products
 Categorisation of Wound Care and Associated Products Version 9 March 2018 Surgical Dressing Manufacturers Association 2018 TAPES AND TRADITIONAL DRESSINGS Wound Dressings Swabs Taping Traditional Wound
Categorisation of Wound Care and Associated Products Version 9 March 2018 Surgical Dressing Manufacturers Association 2018 TAPES AND TRADITIONAL DRESSINGS Wound Dressings Swabs Taping Traditional Wound
Pressure Ulcers ecourse
 Pressure Ulcers ecourse Knowledge Checkup Module 2 Handout College of Licensed Practical Nurses of Alberta (Canada) CLPNA.com and StudywithCLPNA.com CLPNA Pressure Ulcers ecourse Knowledge Checkup Module
Pressure Ulcers ecourse Knowledge Checkup Module 2 Handout College of Licensed Practical Nurses of Alberta (Canada) CLPNA.com and StudywithCLPNA.com CLPNA Pressure Ulcers ecourse Knowledge Checkup Module
SOMERSET COMMUNITY HEALTH WOUND FORMULARY. 12 January 2011
 SOMERSET COMMUNITY HEALTH WOUND FORMULARY 12 January 2011 INTRODUCTION The purpose of this is to aid clinical staff in selecting the most appropriate dressing for wounds healing by secondary intention.
SOMERSET COMMUNITY HEALTH WOUND FORMULARY 12 January 2011 INTRODUCTION The purpose of this is to aid clinical staff in selecting the most appropriate dressing for wounds healing by secondary intention.
Skin Integrity and Wound Care
 Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Basic Dressing Categories
 Category of Dressing Examples Advantages/Indications Disadvantages/Contraindications Hydrofiber Aquacel AG - ConvaTec Aquacel - Convatec Excellent for absorbing excess exudate These dressings form a gel
Category of Dressing Examples Advantages/Indications Disadvantages/Contraindications Hydrofiber Aquacel AG - ConvaTec Aquacel - Convatec Excellent for absorbing excess exudate These dressings form a gel
Stop The Pressure: Patient Safety and Tissue Viability
 Portsmouth Hospitals NHS Trust Stop The Pressure: Patient Safety and Tissue Viability Alison Cole Claire Brett Karen Oakley Presentation Focus Etiology and cause of a pressure ulcer The impact of pressure
Portsmouth Hospitals NHS Trust Stop The Pressure: Patient Safety and Tissue Viability Alison Cole Claire Brett Karen Oakley Presentation Focus Etiology and cause of a pressure ulcer The impact of pressure
ד"ר בוריס פונצ' קי PRESSURE ULCERS
 ד"ר בוריס פונצ' קי 25.12.2013 PRESSURE ULCERS International EPUAP-NPUAP Pressure Ulcer Definition: (European Pressure Ulcer Advisory Panel and National Pressure Ulcer Advisory Panel, 2010).. is localized
ד"ר בוריס פונצ' קי 25.12.2013 PRESSURE ULCERS International EPUAP-NPUAP Pressure Ulcer Definition: (European Pressure Ulcer Advisory Panel and National Pressure Ulcer Advisory Panel, 2010).. is localized
Durable Medical Equipment Providers
 August 2009 Provider Bulletin Number 974 Durable Medical Equipment Providers Vacuum Assisted Wound Closure Therapy Negative pressure wound therapy (NPWT) must be requested and supplied by an enrolled durable
August 2009 Provider Bulletin Number 974 Durable Medical Equipment Providers Vacuum Assisted Wound Closure Therapy Negative pressure wound therapy (NPWT) must be requested and supplied by an enrolled durable
SECTION M: SKIN CONDITIONS. M0210: Unhealed Pressure Ulcer(s) Item Rationale
 SECTION M: SKIN CONDITIONS Intent: The items in this section of the April 1, 2014 release of the LTCH CARE Data Set Version 2.01 document the presence, appearance, and change of pressure ulcers. If warranted
SECTION M: SKIN CONDITIONS Intent: The items in this section of the April 1, 2014 release of the LTCH CARE Data Set Version 2.01 document the presence, appearance, and change of pressure ulcers. If warranted
Treat the whole patient, not just the hole in the patient! 3/21/2017 CAN YOU CONNECT THE DOTS?? PHILOSOPHY OBJECTIVES
 CAN YOU CONNECT THE DOTS?? Boone Hospital Wound Healing Center Kimberly Jamison, MD, FACP, FAPWCA, PCWC Kim Mitchell, RN, BSN OBJECTIVES Describe the basic concepts of chronic wound care to ensure an optimal
CAN YOU CONNECT THE DOTS?? Boone Hospital Wound Healing Center Kimberly Jamison, MD, FACP, FAPWCA, PCWC Kim Mitchell, RN, BSN OBJECTIVES Describe the basic concepts of chronic wound care to ensure an optimal
2 Pressure Ulcer or Pressure Injury? (Do you have skin in the game?)
 Pressure Ulcer or Pressure Injury? (Do you have skin in the game?) Ann Rambusch, MSN, HCS D, HCS O, RN June 28, 2016 1 Pressure Ulcer or Pressure Injury? (Do you have skin in the game?) Understanding NPUAP
Pressure Ulcer or Pressure Injury? (Do you have skin in the game?) Ann Rambusch, MSN, HCS D, HCS O, RN June 28, 2016 1 Pressure Ulcer or Pressure Injury? (Do you have skin in the game?) Understanding NPUAP
Ann Leland, APRN, CNP, DNP Instructor, college of surgery
 Ann Leland, APRN, CNP, DNP Instructor, college of surgery leland.ann@mayo.edu 2015 MFMER 3543652-1 Pressure ulcers Mayo School of Continuous Professional Development 2nd Annual Inpatient Medicine for NPs
Ann Leland, APRN, CNP, DNP Instructor, college of surgery leland.ann@mayo.edu 2015 MFMER 3543652-1 Pressure ulcers Mayo School of Continuous Professional Development 2nd Annual Inpatient Medicine for NPs
OASIS NP August 2011: Special Training. OASIS-C Integument Assessment. Rhonda Will, RN, BS, COS-C, HCS-D Assistant Director OASIS Competency Institute
 OASIS NP August 211: Special Training OASIS-C Integument Assessment Rhonda Will, RN, BS, COS-C, HCS-D Assistant Director OASIS Competency Institute 243 King Street, Suite 246 Northampton, MA 16 413-584-53
OASIS NP August 211: Special Training OASIS-C Integument Assessment Rhonda Will, RN, BS, COS-C, HCS-D Assistant Director OASIS Competency Institute 243 King Street, Suite 246 Northampton, MA 16 413-584-53
Pressure Ulcer Prevention Guidelines
 EUROPEAN PRESSURE ULCER ADVISORY PANEL Pressure Ulcer Prevention Guidelines INTRODUCTION Pressure damage is common in many healthcare settings across Europe, affecting all age groups, and is costly both
EUROPEAN PRESSURE ULCER ADVISORY PANEL Pressure Ulcer Prevention Guidelines INTRODUCTION Pressure damage is common in many healthcare settings across Europe, affecting all age groups, and is costly both
New Strategies to Improve Assessment, Documentation and Prevention of Pressure Injuries
 New Strategies to Improve Assessment, Documentation and Prevention of Pressure Injuries Janet Cuddigan, PhD, RN, CWCN, FAAN Professor, UNMC College of Nursing Omaha, NE Focus of this Presentation New developments
New Strategies to Improve Assessment, Documentation and Prevention of Pressure Injuries Janet Cuddigan, PhD, RN, CWCN, FAAN Professor, UNMC College of Nursing Omaha, NE Focus of this Presentation New developments
Wound Care in the Community. Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts
 Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
Vacuumed Assisted Closure
 Vacuumed Assisted Closure Louise Morris Lead Nurse in Tissue Viability Jackie Stephen-Haynes Consultant Nurse and senior Lecturer in Tissue Viability 2009 Aims and Objectives To develop an awareness of
Vacuumed Assisted Closure Louise Morris Lead Nurse in Tissue Viability Jackie Stephen-Haynes Consultant Nurse and senior Lecturer in Tissue Viability 2009 Aims and Objectives To develop an awareness of
Galen ( A.D) Advanced Wound Dressing
 Galen (120-201A.D) Advanced Wound Dressing Wounds heal optimally in a moist environment นพ.เก งกาจ ว น ยโกศล Wound assessment Ideal wound dressing Type of wound Clinical appearance Wound location Measurement
Galen (120-201A.D) Advanced Wound Dressing Wounds heal optimally in a moist environment นพ.เก งกาจ ว น ยโกศล Wound assessment Ideal wound dressing Type of wound Clinical appearance Wound location Measurement
Wound Dressing. Choosing the Right Dressing
 Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
Teaming Together to Understand Pressure Injuries / (Ulcers): NPUAP Terminology and Staging Clarification
 Teaming Together to Understand Pressure Injuries / (Ulcers): NPUAP Terminology and Staging Clarification We encourage you to share this information with your staff and colleagues by facilitating clinician
Teaming Together to Understand Pressure Injuries / (Ulcers): NPUAP Terminology and Staging Clarification We encourage you to share this information with your staff and colleagues by facilitating clinician
PRODIGY Quick Reference Guide
 PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
WOUND CARE. By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare
 WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
TIME CONCEPT AND LOCAL WOUND MANAGEMENT
 TIME CONCEPT AND LOCAL WOUND MANAGEMENT B. BRAUN WOUND CARE INTRODUCTION: TIME is a global care framework used to implement appropriate care plans and promote wound healing Tissue Management Inflammation
TIME CONCEPT AND LOCAL WOUND MANAGEMENT B. BRAUN WOUND CARE INTRODUCTION: TIME is a global care framework used to implement appropriate care plans and promote wound healing Tissue Management Inflammation
Pathway to excellence. A comprehensive clinical education platform from Smith & Nephew
 Pathway to excellence A comprehensive clinical education platform from Smith & Nephew Pathway to Excellence Support Each year, we train more than 150,000 healthcare professional around the globe. In addition
Pathway to excellence A comprehensive clinical education platform from Smith & Nephew Pathway to Excellence Support Each year, we train more than 150,000 healthcare professional around the globe. In addition
Foam dressings have frequently
 The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
Wound Assessment & Treatment
 Wound Assessment & Treatment Cathy Lyle Advanced Practice Nurse Providence Care, SMOL site LTC Physicians CME June 2011 Outline l Is it healing? l Will it heal? l What colour is it? l How wet is it? l
Wound Assessment & Treatment Cathy Lyle Advanced Practice Nurse Providence Care, SMOL site LTC Physicians CME June 2011 Outline l Is it healing? l Will it heal? l What colour is it? l How wet is it? l
Table of Contents. Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings
 Table of Contents Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings Dialysis Port Care Know What Type of Vascular Access You Have. Fistula: An artery in your forearm
Table of Contents Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings Dialysis Port Care Know What Type of Vascular Access You Have. Fistula: An artery in your forearm
Successful IV Starts Revised February 2014
 Successful IV Starts Revised February 2014 Why Intravenous Therapy? Used for access to the body s circulation Indications: Administer fluids, blood, medications, and nutrition Obtain laboratory specimens
Successful IV Starts Revised February 2014 Why Intravenous Therapy? Used for access to the body s circulation Indications: Administer fluids, blood, medications, and nutrition Obtain laboratory specimens
A GUIDE TO THE TREATMENT OF PRESSURE ULCERS FROM GRADE 1 GRADE 4
 A GUIDE TO THE TREATMENT OF PRESSURE ULCERS FROM GRADE 1 GRADE 4 Gill Wicks, Nurse Consultant, Tissue Viability for Wiltshire Primary Care Trust and Lecturer at University of West England Pressure ulcers
A GUIDE TO THE TREATMENT OF PRESSURE ULCERS FROM GRADE 1 GRADE 4 Gill Wicks, Nurse Consultant, Tissue Viability for Wiltshire Primary Care Trust and Lecturer at University of West England Pressure ulcers
Northern Ireland Wound Care Formulary
 Northern Ireland Wound Care Formulary 2nd Edition April 2011 Wound Care Formulary 2 Wounds cause pain and discomfort to many people in Northern Ireland. Management of wounds requires considerable resources
Northern Ireland Wound Care Formulary 2nd Edition April 2011 Wound Care Formulary 2 Wounds cause pain and discomfort to many people in Northern Ireland. Management of wounds requires considerable resources
Essity Internal. Taking the fear out of wound infection: conquering everyday issues
 Taking the fear out of wound infection: conquering everyday issues Learning objectives 1. Identifying the cost which wound infection can have on both the patient and healthcare organisations 2. Understanding
Taking the fear out of wound infection: conquering everyday issues Learning objectives 1. Identifying the cost which wound infection can have on both the patient and healthcare organisations 2. Understanding
Excellence in OASIS-C COS-C Prep & OASIS Training
 Excellence in OASIS-C COS-C Prep & OASIS Training Webinar Series - Session 5 April 2, 2014 2:00 3:00PM EST PRESENTER: JOAN L. USHER, BS, RHIA, COS-C, ACE JLU HEALTH RECORD SYSTEMS TEL: (781) 829-9632 FAX:
Excellence in OASIS-C COS-C Prep & OASIS Training Webinar Series - Session 5 April 2, 2014 2:00 3:00PM EST PRESENTER: JOAN L. USHER, BS, RHIA, COS-C, ACE JLU HEALTH RECORD SYSTEMS TEL: (781) 829-9632 FAX:
POLYHEAL MICRO - INSTRUCTIONS FOR USE
 POLYHEAL MICRO - INSTRUCTIONS FOR USE PRODUCT DESCRIPTION PolyHeal Micro is a medical device indicated for the treatment of wounds. It is comprised of a suspension of polystyrene negatively charged microspheres
POLYHEAL MICRO - INSTRUCTIONS FOR USE PRODUCT DESCRIPTION PolyHeal Micro is a medical device indicated for the treatment of wounds. It is comprised of a suspension of polystyrene negatively charged microspheres
Central venous access devices for children with lysosomal storage disorders
 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Central venous access devices for children with lysosomal storage disorders This information explains about central
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Central venous access devices for children with lysosomal storage disorders This information explains about central
Promoting Skin Integrity in End of Life Care. Part 1. Tracey McKenzie Head of Tissue Viability Services TSDFT
 Promoting Skin Integrity in End of Life Care Part 1 Tracey McKenzie Head of Tissue Viability Services TSDFT To Understand the Extrinsic Factors of Pressure Ulcer (PU) development To understand the Intrinsic
Promoting Skin Integrity in End of Life Care Part 1 Tracey McKenzie Head of Tissue Viability Services TSDFT To Understand the Extrinsic Factors of Pressure Ulcer (PU) development To understand the Intrinsic
Consider the possibility of pressure ulcer development
 Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
C A R O L S I E M M S N, R N, B C, G N P M U S I N C L A I R S C H O O L O F N U R S I N G Q I P M O WHAT S IN A NAME?
 M D S A N D P R E S S U R E U L C E R S C A R O L S I E M M S N, R N, B C, G N P M U S I N C L A I R S C H O O L O F N U R S I N G Q I P M O WHAT S IN A NAME? 1777: decubitus is the oldest term used 1942
M D S A N D P R E S S U R E U L C E R S C A R O L S I E M M S N, R N, B C, G N P M U S I N C L A I R S C H O O L O F N U R S I N G Q I P M O WHAT S IN A NAME? 1777: decubitus is the oldest term used 1942
The Triangle of Wound Assessment
 The Triangle of Wound Assessment A simple and holistic framework for wound management CPWSC_TOWA_Brochure_210x210_2018.indd 1 10/01/2018 15.13 ? We asked healthcare professionals around the world about
The Triangle of Wound Assessment A simple and holistic framework for wound management CPWSC_TOWA_Brochure_210x210_2018.indd 1 10/01/2018 15.13 ? We asked healthcare professionals around the world about
BIOSORB GELLING FIBRE DRESSING. Key facts: In vitro evidence
 BIOSORB GELLING FIBRE DRESSING Key facts: In vitro evidence BIOSORB Gelling Fibre Dressing WHAT IS IT? BIOSORB Gelling Fibre Dressing is a soft, conformable non-woven dressing made from sodium carboxymethyl
BIOSORB GELLING FIBRE DRESSING Key facts: In vitro evidence BIOSORB Gelling Fibre Dressing WHAT IS IT? BIOSORB Gelling Fibre Dressing is a soft, conformable non-woven dressing made from sodium carboxymethyl
Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL. of the infection risk in chronic wound
 Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL of the infection risk in chronic wound Introduction The impact of infection on patients is well
Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL of the infection risk in chronic wound Introduction The impact of infection on patients is well
Spinal Cord Injury Info Sheet An information series produced by the Spinal Cord Program at GF Strong Rehab Centre.
 Spinal Cord Injury Info Sheet An information series produced by the Spinal Cord Program at GF Strong Rehab Centre. What does skin do? 1. It protects you. 2. It provides sensory information. 3. It helps
Spinal Cord Injury Info Sheet An information series produced by the Spinal Cord Program at GF Strong Rehab Centre. What does skin do? 1. It protects you. 2. It provides sensory information. 3. It helps
Cuticell Contact. Silicone Wound Contact Layer. Highly Flexible Atraumatic Single-sided adherence
 Cuticell Contact Silicone Wound Contact Layer Highly Flexible Atraumatic Single-sided adherence Cuticell Contact impressively wound calming Cuticell Contact is a silicone wound contact layer that has a
Cuticell Contact Silicone Wound Contact Layer Highly Flexible Atraumatic Single-sided adherence Cuticell Contact impressively wound calming Cuticell Contact is a silicone wound contact layer that has a
ASSESSMENT AND CARE Monitor for the following and remove catheter if there is: redness, pain, swelling, firm tissue, exudates, bleeding or leakage.
 POLICY An Indwelling subcutaneous catheter may be inserted when an infant requires regular subcutaneous injections (At least one subcutaneous injection per day). SUPPORTIVE DATA In the NICU medications
POLICY An Indwelling subcutaneous catheter may be inserted when an infant requires regular subcutaneous injections (At least one subcutaneous injection per day). SUPPORTIVE DATA In the NICU medications
DMEPOS: hospital beds, bed accessories, and pressurereducing
 ACTION: Final DATE: 07/02/2018 10:03 AM 5160-10-18 DMEPOS: hospital beds, bed accessories, and pressurereducing support surfaces. (A) Definitions and explanations. (1) "Group 1," "group 2," and "group
ACTION: Final DATE: 07/02/2018 10:03 AM 5160-10-18 DMEPOS: hospital beds, bed accessories, and pressurereducing support surfaces. (A) Definitions and explanations. (1) "Group 1," "group 2," and "group
Choosing an appropriate dressing for chronic wounds Denise Bell BSc, RGN and Dot Hyam RGN, DipHE
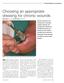 Choosing an appropriate dressing for chronic wounds Denise Bell BSc, RGN and Dot Hyam RGN, DipHE Chronic wounds are nonhealing with a sometimes complex aetiology, and dressing such wounds can be difficult
Choosing an appropriate dressing for chronic wounds Denise Bell BSc, RGN and Dot Hyam RGN, DipHE Chronic wounds are nonhealing with a sometimes complex aetiology, and dressing such wounds can be difficult
Beyond the Basics ImprovingYour Wound Care Knowledge. Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN
 Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
January Adult Burn Injured patients
 Guideline Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version goes out of date): Explicit definition
Guideline Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version goes out of date): Explicit definition
Managing Wounds. Esther White Tissue Viability Nurse
 Managing Wounds Esther White Tissue Viability Nurse First things first.. Assess, measure and photograph Know what you re dealing with, look at anatomical position and the bigger picture to look for extra
Managing Wounds Esther White Tissue Viability Nurse First things first.. Assess, measure and photograph Know what you re dealing with, look at anatomical position and the bigger picture to look for extra
3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing Description 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing is used
 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing Description 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing is used to cover and protect catheter sites and to secure devices
3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing Description 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing is used to cover and protect catheter sites and to secure devices
SOUTHERN HEALTH & SOCIAL CARE TRUST. Children & Young People s Directorate Procedure/Guidelines/Protocol Checklist & Version Control Sheet
 Children & Young People s Directorate Procedure/Guidelines/Protocol Checklist & Version Control Sheet 1 Name of Procedure/Guidelines/ Protocol: PROCEDURE FOR PERIPHERAL ARTERIAL CANNULATION 2 Purpose of
Children & Young People s Directorate Procedure/Guidelines/Protocol Checklist & Version Control Sheet 1 Name of Procedure/Guidelines/ Protocol: PROCEDURE FOR PERIPHERAL ARTERIAL CANNULATION 2 Purpose of
The Power of a Hydroconductive Wound Dressing with LevaFiber Technology
 The Power of a Hydroconductive Wound Dressing with LevaFiber Technology The first step in healing a chronic wound is to detoxify it by removing slough, necrotic tissue, exudate and bacteria, while keeping
The Power of a Hydroconductive Wound Dressing with LevaFiber Technology The first step in healing a chronic wound is to detoxify it by removing slough, necrotic tissue, exudate and bacteria, while keeping
The Proven Multifunctional Dressing
 The Proven Multifunctional Dressing belongs to an innovative class of multifunctional wound care dressings. dressings effectively cleanse, fill, absorb and moisten wounds throughout the healing continuum.
The Proven Multifunctional Dressing belongs to an innovative class of multifunctional wound care dressings. dressings effectively cleanse, fill, absorb and moisten wounds throughout the healing continuum.
Making the Most of your Dressing Products Catherine Hammond CNS/CNE
 Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
Palliative Care. EPUAP/NPUAP Publish New Pressure Ulcer Guidelines for. Treatment. Improving Quality of Care Based on CMS Guidelines 39
 Treatment EPUAP/NPUAP Publish New Pressure Ulcer Guidelines for Palliative Care Dealing with the end of a loved one s life is difficult enough, but when wound and skin care issues are involved, the decisions
Treatment EPUAP/NPUAP Publish New Pressure Ulcer Guidelines for Palliative Care Dealing with the end of a loved one s life is difficult enough, but when wound and skin care issues are involved, the decisions
Application Guide for Full-Thickness Wounds
 Application Guide for Full-Thickness Wounds PriMatrix Dermal Repair Scaffold PriMatrix Ag Antimicrobial Dermal Repair Scaffold Application Guide for Full Thickness Wounds PriMatrix is a unique dermal repair
Application Guide for Full-Thickness Wounds PriMatrix Dermal Repair Scaffold PriMatrix Ag Antimicrobial Dermal Repair Scaffold Application Guide for Full Thickness Wounds PriMatrix is a unique dermal repair
