Temporomandibular disorders and psychosocial status in osteogenesis imperfecta - a cross-sectional study
|
|
|
- Clementine Greer
- 5 years ago
- Views:
Transcription
1 Bendixen et al. BMC Oral Health (2018) 18:35 RESEARCH ARTICLE Open Access Temporomandibular disorders and psychosocial status in osteogenesis imperfecta - a cross-sectional study K. H. Bendixen 1*, H. Gjørup 2, L. Baad-Hansen 1, J. Dahl Hald 3, T. Harsløf 3, M. H. Schmidt 4, B. L. Langdahl 3 and D. Haubek 5 Abstract Background: Osteogenesis Imperfecta (OI) is characterized by a number of deviations in the orofacial region. The aims of the present study were to investigate the occurrence of temporomandibular disorders, to evaluate the psychosocial status, and to assess the dental occlusion in a population of adult OI patients. Methods: Participants (n = 75) were classified with mild OI, type I (n = 56), or moderate-severe OI, type III and IV (n = 19). OI patients were examined according to the Research Diagnostic Criteria for Temporomandibular Disorders (axis I and II). Results: Temporomandibular disorders and functional limitations in the orofacial region were rare and did not differ between patients with mild and moderate-severe OI (P > 0.050). No significant differences between Graded Chronic Pain Scale grades 0, 1, and 2 were found in mild OI vs. moderate-severe OI (P > 0.160). Few patients (16%) had signs of depression, but close to half (48%) had signs of somatization. Patients with moderate-severe OI had a lower mean number of teeth compared to patients with mild OI (P < 0.050). In general, malocclusions were prevalent, and mandibular overjet and posterior cross-bite were found more often in moderate-severe OI compared with mild (P < 0.050). Conclusions: Patients with moderate-severe OI had more malocclusions than patients with mild OI. The psychosocial status of OI patients was remarkably healthy considering the severity of this disabling systemic disorder. The bodily pain complaints frequently reported in OI patients were not largely reflected in the orofacial area as painful temporomandibular disorders. Keywords: Rare diseases, Heritable connective tissue disorders, Bone fractures, Dental anomalies, Pain, Jaw function Background Osteogenesis imperfecta (OI) is a rare, heritable connective tissue disorder, characterized by fragile bones, which results in an increased risk of fractures from low energy trauma [1]. Growth retardation, blue sclerae, hearing loss, and disturbances in the dental development also occur. OI is caused by defective collagen type 1 synthesis, which constitutes an essential part of the connective tissue. The prevalence of OI is estimated to be 11 per [2]. The most frequently used * Correspondence: karina.bendixen@dent.au.dk 1 Section of Orofacial Pain and Jaw Function, Department of Dentistry and Oral Health, Aarhus University, 8000 Aarhus, DK, Denmark Full list of author information is available at the end of the article classification comprises four clinical subtypes (I-IV): OI type I (mild and no bone deformities), OI type II (severe bone deformities and perinatal death), OI type III (manifest growth retardation and severely progressing bone deformities), and OI type IV (mild growth retardation and moderate bone deformities) [3]. The classical dental aberration of OI is dentinogenesis imperfecta (DI). The clinical characteristics of DI are grayish or brownish discoloration of the dentition, obliteration of the dental cavum, shortness of the roots, and cervical constriction [4, 5]. The prevalence of DI in OI populations is 19 42% [6, 7]. Furthermore, Class III malocclusion with mandibular overjet is prevalent in OI patients, especially OI The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Bendixen et al. BMC Oral Health (2018) 18:35 Page 2 of 8 type III [8, 9]. Pain in relation to the skeleton and certain physical disabilities are frequent in OI patients [10 13]. Temporomandibular Disorders (TMD) consist of a heterogeneous collection of conditions characterized by pain and/or functional limitations in the masticatory muscles, the temporomandibular joints, and associated tissues [14 17]. The TMD major subtypes according to the Research Diagnostic Criteria for Temporomandibular Disorders (RDC/TMD) are myofascial pain, disc displacements, joint pain, and degenerative and inflammatory joint disease [14]. The estimated prevalence of TMD in the general population is 5 12% [15, 18]. TMD is considered to be the most common orofacial pain condition of non-dental origin, and are the second most frequently occurring musculoskeletal condition, resulting in pain and functional impairment [19]. Female/male ratio is approximately 2:1 [15]. The majority of TMD patients suffer from myofascial pain [20, 21]. By means of the RDC/TMD, both the axis I, the physical diagnoses and the axis II, the psychosocial status can be evaluated [22]. According to our knowledge, studies on pain and functional limitations related to temporomandibular disorders in OI patients are absent. Taken the disabling impacts of some OI types in account, we hypothesize that these circumstances are also reflected in the orofacial area. The aims of the present study were: i) to report on the occurrence of temporomandibular disorders (axis I), ii) to assess jaw function, iii) to evaluate the psychosocial status (axis II), and iiii) to assess the dental occlusion in adult OI patients. Methods Study population The present study was conducted as a part of a crosssectional study investigating adult Danish patients with OI [23]. The patients were identified by search in medical files of the university hospitals in Denmark, by contact to doctors at regional hospitals, and by contact to the Danish Osteogenesis Imperfecta Society. Ninety-one individuals gave their consent to participate in the main study, and the OI diagnosis was confirmed in 85 of these individuals. The 85 participants were classified into OI types I, III, and IV [3] and asked to participate in the study investigating orofacial health. A total of 75 patients accepted the invitation (OI type I: n = 56, type III: n =7, and type IV: n = 12). The ten persons who declined to participate were OI type I: n = 4, type III: n = 4, and type IV: n = 2. The RDC/TMD examinations were carried out at the Department of Dentistry and Oral Health, Health, Aarhus University, Denmark in the years 2011 to Thus, a total of 75 OI patients (53.3% females and 46.7% males, the mean age 45.5 yrs., SD = 14.7, range: 20 to 77) were enrolled in the present study and subsequently grouped into mild OI (OI type I) and moderate-severe OI (OI type III and IV). Study design The study was conducted in accordance with the guidelines of the Helsinki Declaration and approved by the Central Denmark Region Committees on Biomedical Research Ethics (M ). The study conforms to STROBE Guidelines. The temporomandibular function of the OI patients was assessed in accordance with the guidelines of the RDC/TMD, in relation to both axis I and II [14]. One of three involved examiners (MHS, HG, and RF) performed the RDC/TMD clinical examination. An experienced user of the RDC/TMD clinical examination method (LBH) trained the three examiners. All 75 patients underwent the RDC/TMD examination (axis I) and filled out the RDC/TMD History Questionnaire (axis II) for the assessment of the psychosocial status [14, 22]. The presence of temporomandibular disorders was assessed in relation to OI subtypes and categorized in Group I: Muscle Disorders (Myofascial pain (Ia), Myofascial pain with limited opening (Ib), and No Group (Idx) (which is no group I diagnosis)); Group II: Disc Displacements (Disc displacement with reduction (IIa), Disc displacement without reduction with limited opening (IIb), Disc displacement without reduction without limited opening (IIc), and No Group II Diagnosis), and Group III: Other joint conditions (Arthralgia (IIIa), Osteoarthritis (IIIb), Osteoarthrosis (IIIc), and No Group III Diagnosis). Psychosocial status were assessed by means of the Graded Chronic Pain Scale (GCPS) [24] to rate the level of the severity of chronic pain and by the use of the Symptom Checklist 90-R (SCL-90-R) for the evaluation of depression (DEP) and somatization (i.e., non-specific physical symptoms, pain items included) (SOM) levels [25]. The GCPS, which is a valid instrument based on selfreporting, consists of six items assessed on a 10-point scales. It categorizes patients according to severity in five levels of chronic pain grades: 0 = No disability, 1 = Low disability and low pain intensity, 2 = Low disability and high pain intensity, 3 = High disability and moderately limiting, and 4 = High disability and severely limiting [24, 26]. DEP and SOM levels were assessed by the use of a 20-item instrument. Both the DEP and the SOM scores were calculated and categorized according to severity. DEP: < = normal, = indication of moderate depression, and > = the presence of severe depressive symptoms. SOM: < 0.5 = normal, = indication of moderate somatization, and > 1.0 = the presence of severe somatization symptoms [25, 26]. The dental occlusion was evaluated on the digital study models and from the clinical photos and
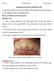
3 Bendixen et al. BMC Oral Health (2018) 18:35 Page 3 of 8 performed by an experienced orthodontist (HG) (Fig. 1). The evaluation of occlusion included any fixed dental prosthesis, but not removable dentures. The horizontal overjet (HO) was evaluated as normal (0 mm < HO < 6 mm), reduced (HO 0 mm), or increased (HO 6 mm) according to a modification of methods by Bjørk and coworkers [27]. Reduced HO was characterized as mandibular overbite (MOB). The anterior occlusion was characterized as open (frontal open bite), if the upper incisors did not occlude with the lower dentition. Non-occlusion posteriorly was defined as the absence of occlusion between premolars and molars in the same side. The non-occlusion had to be present either in one or in both sides. Non-occlusion, because of missing teeth, was included. Posterior cross-bite was defined as the presence of cross-bite on at least two teeth (premolars or molars) in the same side. The posterior cross-bite had to be present either in one or in both sides. If both premolars and molars of the same side were absent in the same jaw, registration of that side was omitted. Statistical analyses Descriptive statistics were used to summarize all data. The frequencies of the temporomandibular disorders diagnoses, the GCPS, DEP, and SOM scores are presented in %. All differences, including the number of teeth and the presence of malocclusion according to OI type (mild or moderate-severe), were evaluated by Students t-test or Fisher s Exact Test. Prior to analyses data were tested for normality by the use of QQ-plots. Data are presented as mean ± standard deviation (SD). Values of P < were considered statistically significant. Results Temporomandibular disorders (axis I) The Group I disorders, Myofascial pain (Ia) and Myofascial pain with limited opening (Ib), were rare in the mild as well as in the moderate-severe OI type as reported in Table 1, and no differences between the groups were found (P > 0.999). The proportion of the Group II disorder Disc displacement with reduction (IIa) did not differ between the groups (P = 0.273) (Table 1). The two remaining Group II disorders Disc displacement without reduction with limited opening (IIb) or Disc displacement without reduction without limited opening (IIc) were not present in the study population (Table 1). The Group III disorders, including Arthralgia (IIIa), Osteoarthritis (IIIb), and Osteoarthrosis (IIIc), were rare, and there were no differences between the groups (P > 0.566) (Table 1). Group II and III diagnoses were recorded if present in one or in both joints. In total, 7 patients, all of whom were mild OI type, had more than one TMD diagnosis. Functional status The mean value of the maximum unassisted opening capacity was 50.6 mm ± 8.1 mm in the mild OI type, ranging from 32 mm to 70 mm, and 46.1 mm ± 7.9 mm in moderate-severe OI, ranging from 35 mm to 58 mm (P = 0.055) (Table 2). Reduced jaw opening capacity (< 40 mm including vertical overlap) was seen in 8.9% of the patients with mild OI and in 25.0% of patients with moderate-severe OI (P = 0.037) (Table 2). Functional limitations (Question 19) were detected to a minor extent, apart from chewing (6.7% in mild and 16.7% in moderate-severe OI) (P = 0.340) and eating hard foods (21.7% in mild and 44.4% in moderate-severe OI type) (P = 0.119) (Table 2). All other potential limitations were present below 9%, and no differences between groups were found (P > 0.493). Psychosocial status (axis II) Scores from the GCPS revealed Grade 0, which is no TMD pain in the prior six months, in 44 of the 56 patients (78.6%) with mild OI, and in 18 of the 19 (94.8%) with moderate-severe OI (Table 3). There was no significant difference between the groups (P = 0.161). Grade 1 (low disability and low pain intensity) was found in 10 of the 56 (17.9%) patients with mild OI and in one of the 19 (5.6%) patients with moderate-severe OI, but the difference between the groups was not significant (P = 0.272). Grade 2 (low disability and high pain intensity) was present in two patients (3.6%) with mild OI, but not Fig. 1 Patient Case - OI Type IV. a Lateral Cephalogram. b Clinical Photo Frontal Aspect in Maximum Occlusion. c Digital Study Models Obtained by O3DM (Ortolab, Częstochowa, Poland)
4 Bendixen et al. BMC Oral Health (2018) 18:35 Page 4 of 8 Table 1 Temporomandibular Disorders Prevalence According to the Research Diagnostic Criteria for Temporomandibular Disorders (RDC/TMD) Related to Osteogenesis Imperfacta (OI) Subtypes OI TYPE Mild (n = 56) Moderate-severe (n = 19) Group I 1 Myofascial pain (Ia) 3 (5.4%) 1 (5.3%) 2 Myofascial pain with limited opening (Ib) 2 (3.6%) 0 0 No group (Idx) 51 (91.1%) 18 (94.7%) Group II 1 Disc displacement with reduction (IIa) 10 (18.2%) 1 (5.6%) 2 Disc displacement without reduction with limited opening (IIb) Disc displacement without reduction without limited opening (IIc) No group II Diagnosis 45 (81.8%) 17 (94.4%) Group III 1 Arthralgia (IIIa) 3 (5.7%) 0 2 Osteoarthritis (IIIb) 2 (3.8%) 0 3 Osteoarthrosis (IIIc) 4 (7.5%) 2 (11.1%) 0 No group III Diagnosis 44 (83.0%) 16 (88.9%) Mild: OI type 1. Moderate-severe: OI type 3 and 4. Group I: Muscle Conditions. Group II: Disc Displacements. Group III: Other Joint Conditions. Group II and III diagnoses: Either present in one or both joints. Missing data: Group I: None. Group II: One mild type and one moderate-severe type. Group III: Three mild types and one moderate-severe type present in any of the patients with moderate-severe OI. There was no difference between the groups (P > 0.999). Grade 3 (high disability and moderately limiting) and grade 4 (high disability and severely limiting) were not found in any OI patients (Table 3). DEP scores were obtained from 78.6% of the patients with mild OI and from 73.7% of the patients with moderate-severe OI as reported in Table 3. Data from 12 patients with mild OI and 5 with moderate-severe OI were missing, i.e., if the questionnaire was not correctly Table 2 Prevalence of Jaw Function and Limitations Related to Osteogenesis Imperfecta (OI) Subtypes OI TYPE Mild (n = 56) Moderate-severe (n = 19) Function Maximum unassisted opening (mm) (mean ± SD) 50.6 ± ± 7.9 a Reduced jaw opening capacity (%) * Limitations (%) Chewing 6.7 b 16.7 a Drinking 0.0 b 0.0 a Exercising 0.0 b 0.0 a Eating hard foods 21.7 b 44.4 a Eating soft foods 0.0 b 0.0 a Smiling/laughing 4.4 b 5.5 a Sexual activity 2.2 b 5.5 a Cleaning teeth or face 6.7 b 0.0 a Yawning 8.9 b 5.5 a Swallowing 2.2 b 0.0 a Talking 0.0 b 0.0 a Having the usual facial appearance 0.0 b 0.0 a Mild: OI type 1. Moderate-severe: OI type 3 and 4 Missing data: a n =1 3; b n =10 12 * P = 0.037, Fischer s Exact Test
5 Bendixen et al. BMC Oral Health (2018) 18:35 Page 5 of 8 Table 3 Psycosocial Status - Prevalence of RDC/TMD Axis II Findings According to OI Type OI TYPE Mild (n = 56) Moderate-severe (n = 19) Chronic Pain Grade Classification Grade 0 44 (78.6%) 18 (94.8%) Grade 1 10 (17.9%) 1 (5.6%) Grade 2 2 (3.6%) 0 Grade Grade Depression Normal 37 (84.1%) 12 (85.8%) Moderate 3 (6.8%) 2 (14.3%) Severe 4 (9.1%) 0 Somatization Normal 26 (53.1%) 9 (50.0%) Moderate 16 (32.7%) 4 (22.2%) Severe 7 (14.3%) 5 (27.8%) Grade 0: No TMD pain in the prior 6 months. Grade 1: Low disability - Low Intensity = CPI < 50, and less than 3 DP. Grade 2: Low Disability - High Intensity = CPI 50, and less than 3 DP. Grade 3: High Disability - Moderately Limiting = 3 to 4 DP, regardless of CPI. Grade 4: High Disability - Severely Limiting = 5 to 6 DP, regardless of CPI. CPI: Characteristic Pain Intensity. DP: Disability Points Depression: Missing data: Mild OI: n = 12; moderate-severe OI: n = 5. Normal: < 0.535; Moderate: ; Severe: < Somatization: Missing data mild OI: n = 7; moderate-severe OI: n = 1. Normal: < 0.5; Moderate: ; Severe: > 1.0 filled out. No significant differences between groups in any of the DEP score levels were found (P = 0.564). Likewise, SOM scores were obtained from 87.5% of the patients with mild OI and from 94.7% of the patients with moderate-severe OI as reported in Table 3. Data from seven patients with mild OI type and one patient with moderate-severe OI were missing. No significant differences between groups in any of the SOM score levels were found (P = 0.282). Occlusion Registration of the occlusion was omitted in six out of 75 patients because of missing teeth or missing data. Three patients (OI type I) had a full denture in the edentulous upper jaw. Two patients (one OI type I and one OI type III) had extensive loss of teeth in both the upper and lower jaw. In addition, neither clinical photos nor study cast were obtained in one patient (OI type III). The mean number of teeth was significantly reduced in patients with moderate-severe OI compared to patients with mild OI (P < 0.050) (Table 4). However, the three patients with full denture in the upper jaw and one patient with unspecified tooth loos all had mild OI, and the range of tooth number was greatest in the group with mild OI (Table 4). Malocclusion, in terms of mandibular overjet and posterior cross-bite, was a dominant finding in the group with moderate-severe OI compared to the mildly affected OI group (P < 0.050) (Table 4). Frontal open bite and non-occlusion posteriorly were prevalent in both mild and moderate-severe OI. Discussion The main findings in the present study were that fewer OI patients than expected, independently of the disorder Table 4 Dental Occlusion and Mean Number of Teeth in 69 OI Patients According to OI Type OI TYPE Mild (n = 52) Moderate-severe (n = 17) Mean number of natural teeth * Min.-max. Number of natural teeth % CI Mandibular overjet 2 (4%) 11(64%) ** Increased maxillary overjet ( 6 mm) 1 (2%) 0 Deep bite ( 5 mm) 2 (4%) 0 Frontal open bite 5 (10%) 5 (29%) Non-occlusion posterior (in one or in both sides) 4 (8%) 3 (18%) Posterior cross bite (in one or in both sides) a 7 (15%) 15 (88%) * * P < 0.050, Students t-test. ** P < 0.050, Fischer s Exact Test a Mild OI: n = 48; moderate-severe OI: n =17
6 Bendixen et al. BMC Oral Health (2018) 18:35 Page 6 of 8 severity, suffered from temporomandibular disorders, had jaw functional limitations, and/or were psychosocially affected. To our knowledge, it is the first time TMD prevalence and jaw function have been investigated in an OI population. The total number of adult patients with OI in Denmark is estimated to be approximately 500. A major strength of the present study is the relatively large number of patients included, but it is however a weakness due to the risk of selection bias that not all Danish OI patients were enrolled. The ten persons who declined to participate in the investigation of orofacial health declined for logistic and time reasons. To avoid too small study groups, the moderate and the severe OI types were merged prior to data analysis. This grouping is supported by the fact that OI type I is characterized by quantitative deviations in type 1 collagen, whereas type III and IV are characterized by qualitative deviations in type 1 collagen [23, 28, 29]. Too disproportional group sizes could possibly contribute to the lack of significant differences of the conditions studied. The study is cross-sectional, and all OI types were included. Usually, mild disorder cases are difficult to enroll and often only patients who suffer from the severe types of a disorder are willing to participate in clinical studies. It is a strength in the present study that the whole spectrum of OI patients was enrolled. The missing control group is an obvious limitation of the study, but the knowledge on TMD prevalence and jaw functional limitations, which are available in the literature [15, 21, 30], can serve as a source for comparison. In general, the participating OI patients were positive to the project and contributive to the data collection process. Nevertheless, a study limitation was that a complete data set was not obtained for all participants, resulting in some missing data. For example, some questions in the RDC/TMD History Questionnaire were left unanswered by the patients. Although professionals were present and ready to assist with the questionnaires and help during examination procedures, health limitations and the voluntary aspect of filling out questionnaires had to be respected. Due to the quite personal character of some questions, it was expected that some participants would leave some questions unanswered resulting in some missing data. A surprising finding of the study was that temporomandibular pain disorders, i.e., myofascial pain without and with limited opening, arthralgia, and osteoarthritis in the OI population were rare and only found in nine out of 75 (12.0%) OI patients. This proportion is very similar to the one in the general population [15, 21]. In contrast to the painful temporomandibular disorders, physical disabilities and skeletal pain are generally very frequent in all OI types [12]. The overall body expression in many OI patients is considerably different compared to healthy subjects, which can provide an expectation of similar alterations orofacially. The pain and disabilities are apparently mainly due to the common fractures related to OI. Fractures in the orofacial area are uncommon, and this might explain the differences in the occurrence of pain. Limited information is available concerning fractures in the orofacial area; however, fractures of facial bones are expected to be rare compared with load-bearing long bones [31, 32]. Of the disc displacement diagnoses, disc displacement with reduction was the only diagnosis found in this OI population (11 (14.7%) OI patients). Osteoarthrosis was found in six (8.0%) patients. Disc displacement and osteoarthrosis are the most common non-painful TMD disorders. The prevalence of these disorders in the present OI population is similar to the general population [21]. The mean jaw opening capacity was normal in both mild and moderate-severe OI patients, however, significantly more moderate-severe OI patients with reduced jaw opening capacity were found compared to mild OI patients. The functional limitations reported were generally minor, apart from limitations related to chewing hard foods, which, however, did not differ significantly between the mild and the moderate-severe OI patients. It is likely that these findings are related to dental factors as the severe OI patients are characterized by more malocclusions compared to the mild OI patients in which the occlusion are less remarkable. Findings of frontal open bite and non-occlusion posteriorly are prevalent in both mild and moderate-severe OI types (Table 4). Psychosocial status assessment by the use of the GCPS revealed that 62 out of 75 (82.7%) OI patients did not have TMD pain in the prior six months. The remaining scored grade 1 or 2. Grade 1 and 2 with low disability and low/high pain intensity are considered to be reversible conditions. Interestingly, despite their OI condition, no patients demonstrated the grades 3 or 4, high disability and moderately/severely limiting, levels considered to be irreversible. Fifty-eight out of 75 (77.3%) OI patients answered the RDC/TMD questions for depression symptoms assessment of which 47 (62.7%) demonstrated no signs of such symptoms. Indications of moderate degree of depressive symptoms were revealed in five (6.7%) OI patients and severe in four (5.3%) patients of which the latter were patients with mild OI. It is a limitation of the present study that about 1/5 of the patients did not fill out the questionnaires correctly leading to missing data. A risk of underestimation of the true level of signs of depression due to the missing answers exists and taken the severity of the disorder into account, a high level of depressive symptoms could have been expected. On the other hand, the findings correspond very well with previous findings describing that OI patients are
7 Bendixen et al. BMC Oral Health (2018) 18:35 Page 7 of 8 remarkably resilient and able to adapt to difficult life circumstances [33]. Moderate and severe levels of non-specific physical symptoms (somatization), including pain symptoms, were found in 32 (47.8%) of the OI patients. This finding may be due to OI inherent physical symptoms. Yet, half of the patients in both groups had no signs of somatization, which again supports the perception of the resilient nature of OI patients. Conclusions Patients with moderate-severe OI had significantly more malocclusions and lower mean number of natural teeth than patients with mild OI. The psychosocial status of OI patients was remarkably good considering the severity of this disabling systemic disorder. The bodily pain complaints frequently reported to occur in patients with OI are not largely reflected in the orofacial area as painful temporomandibular disorders. Abbreviations DEP: Depression; DI: Dentinogenesis imperfecta; GCPS: Graded chronic pain scale; HO: Horizontal overjet; MOB: Mandibular overbite; OI: Osteogenesis imperfecta; RDC/TMD: Research diagnostic criteria for temporomandibular disorders; SCL-90-R: Symptom checklist 90-R; SOM: Somatization; TMD: Temporomandibular disorders Acknowledgements We wish to thank dental hygienist Rikke Frandsen for doing some of the RDC/TMD clinical examinations and for her help in efficient assistance during the study. This work was supported by Central Region of Denmark; Osteoporoseforeningen, Denmark; The Danish Association for Public Dentists (TNL/DOFT/ATO), and Care4BrittleBones. Funding Central Region of Denmark; Osteoporoseforeningen, Denmark; The Danish Association for Public Dentists (TNL/DOFT/ATO), and Care4BrittleBones. The role of the funding agencies was financial support, and they were not involved in the design of the study or collection, analysis, and interpretation of data or in writing the manuscript. Availability of data and materials The data that support the findings of this study are available from Jannie Dahl Hald (co-author), but restrictions apply to the availability of these data, which were used under license for the current study, and so are not publicly available. Data are, however, available from the authors upon reasonable request and with permission of Jannie Dahl Hald. Authors contributions KHB contributed to data analysis and interpretation, drafted, and critically revised the manuscript; HG contributed to conception, design, clinical examinations and data acquisition, data analysis and interpretation, and critically revised the manuscript; LBH contributed to clinical examinations and data acquisition, data analysis and interpretation, and critically revised the manuscript; JDH contributed to conception of the study, recruited the participants, contributed to interpretation of the data, and critically revised the manuscript; TH contributed to conception of the study, interpretation of the data, and critically revised the manuscript; MHS contributed to clinical examinations and data acquisition and critically revised the manuscript; BLL contributed to conception of the study, interpretation of the data, and critically revised the manuscript; DH contributed to conception, design, data acquisition, analysis, and interpretation, and critically revised the manuscript. All authors gave final approval and agree to be accountable for all aspects of the work. Authors information Not applicable. Ethics approval and consent to participate The study was conducted in accordance with the guidelines of the Helsinki Declaration and approved by the Central Denmark Region Committees on Biomedical Research Ethics (M ). The study conforms to STROBE Guidelines. All patients gave their written consent to participate in the study prior to inclusion. Consent for publication Not applicable. Competing interests The authors declare that they have no competing interests. Publisher s Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. Author details 1 Section of Orofacial Pain and Jaw Function, Department of Dentistry and Oral Health, Aarhus University, 8000 Aarhus, DK, Denmark. 2 Center for Oral Health in Rare Diseases, Department of Maxillofacial Surgery, Aarhus University Hospital, Aarhus, Denmark. 3 Department of Endocrinology and Internal Medicine, Aarhus University Hospital, Aarhus, Denmark. 4 Aarhus Municipality, Aarhus, Denmark. 5 Section for Pediatric Dentistry, Department of Dentistry and Oral Health, Aarhus University, Aarhus, Denmark. Received: 3 August 2017 Accepted: 1 March 2018 References 1. Glorieux FH. Osteogenesis imperfecta. Best Pract Res Clin Rheumatol. 2008; 22: Andersen PE Jr, Hauge M. Osteogenesis imperfecta: a genetic, radiological, and epidemiological study. Clin Genet. 1989;36: Sillence DO, Senn A, Danks DM. Genetic heterogeneity in osteogenesis imperfecta. J Med Genet. 1979;16: Shields ED, Bixler D, el-kafrawy AM. A proposed classification for heritable human dentine defects with a description of a new entity. Arch Oral Biol. 1973;18: Barron MJ, McDonnell ST, Mackie I, Dixon MJ. Hereditary dentine disorders: dentinogenesis imperfecta and dentine dysplasia. Orphanet J Rare Dis. 2008;3: Malmgren B, Norgren S. Dental aberrations in children and adolescents with osteogenesis imperfecta. Acta Odontol Scand. 2002;60: Saeves R, Lande Wekre L, Ambjornsen E, Axelsson S, Nordgarden H, Storhaug K. Oral findings in adults with osteogenesis imperfecta. Spec Care Dentist. 2009;29: Stenvik A, Larheim TA, Storhaug K. Incisor and jaw relationship in 27 persons with osteogenesis imperfecta. Scand J Dent Res. 1985;93: Jensen BL, Lund AM. Osteogenesis imperfecta: clinical, cephalometric, and biochemical investigations of OI types I, III, and IV. J Craniofac Genet Dev Biol. 1997;17: Rauch F, Glorieux FH. Osteogenesis imperfecta. Lancet. 2004;363: Wekre LL, Froslie KF, Haugen L, Falch JA. A population-based study of demographical variables and ability to perform activities of daily living in adults with osteogenesis imperfecta. Disabil Rehabil. 2010;32: Balkefors V, Mattsson E, Pernow Y, Sääf M. Functioning and quality of life in adults with mild-to-moderate osteogenesis imperfecta. Physiother Res Int. 2013;18: Bishop NJ, Walsh JS. Osteogenesis imperfecta in adults. J Clin Invest. 2014; 124: Dworkin SF, LeResche L. Research diagnostic criteria for temporomandibular disorders: review, criteria, examinations and specifications, critique. J Craniomandib Disord. 1992;6: LeResche L. Epidemiology of temporomandibular disorders: implications for the investigation of etiologic factors. Crit Rev Oral Biol Med. 1997;8: Fernández-de-las-Penas C, Svensson P. Myofascial temporomandibular disorder. Curr Rheumatol Rev. 2016;12:40 54.
8 Bendixen et al. BMC Oral Health (2018) 18:35 Page 8 of Slade GD, Ohrbach R, Greenspan JD, Fillingim RB, Bair E, Sanders AE, Dubner R, Diatchenko L, Meloto CB, Smith S, Maixner W. Painful temporomandibular disorder: decade of discovery from OPPERA studies. J Dent Res. 2016;95: Okeson JP, de Kanter RJ. Temporomandibular disorders in the medical practice. J Fam Pract. 1996;43: National Institute of Dental and Craniofacial Research [February, 2018]; Facial pain Lobbezoo F, Drangsholt M, Peck C, Sato H, Kopp S, Svensson P. Topical review: new insights into the pathology and diagnosis of disorders of the temporomandibular joint. J Orofac Pain. 2004;18: Manfredini D, Arveda N, Guarda-Nardini L, Segù M, Collesano V. Distribution of diagnoses in a population of patients with temporomandibular disorders. Oral Surg Oral Med Oral Pathol Oral Radiol. 2012;114:e Dworkin SF, Sherman J, Mancl L, Ohrbach R, LeResche L, Truelove E. Reliability, validity, and clinical utility of the research diagnostic criteria for temporomandibular disorders Axis II scales: depression, non-specific physical symptoms, and graded chronic pain. J Orofac Pain. 2002;16: Hald JD, Folkestad L, Harsløf T, Lund AM, Duno M, Jensen JB, Neghabat S, Brixen K, Langdahl B. Skeletal phenotypes in adult patients with osteogenesis imperfecta-correlations with COL1A1/COL1A2 genotype and collagen structure. Osteoporos Int. 2016;27: Von Korff M, Ormel J, Keefe FJ, Dworkin SF. Grading the severity of chronic pain. Pain. 1992;50: Derogatis LR. SCL-90-R: administration, scoring & procedures manual-ii for the R (evised) version and other instruments of the psychopathology rating scale series. 2nd ed. Towson: Clinic Psychometric Research; Manfredini D, Winocur E, Ahlberg J, Guarda-Nardini L, Lobbezoo F. Psychosocial impairment in temporomandibular disorders patients. RDC/ TMD axis II findings from a multicentre study. J Dent. 2010;38: Bjoerk A, Krebs A, Solow B. A method for epidemiological registration of malocclusion. Acta Odontol Scand. 1964;22: Genovese C, Rowe D. Analysis of cytoplasmic and nuclear messenger RNA in fibroblasts from patients with type I osteogenesis imperfecta. Methods Enzymol. 1987;145: Korkko J, Ala-Kokko L, De Paepe A, Nuytinck L, Earley J, Prockop DJ. Analysis of the COL1A1 and COL1A2 genes by PCR amplification and scanning by conformation-sensitive gel electrophoresis identifies only COL1A1 mutations in 15 patients with osteogenesis imperfecta type I: identification of common sequences of null-allele mutations. Am J Hum Genet. 1998;62: Manfredini D, Guarda-Nardini L, Winocur E, Piccotti F, Ahlberg J, Lobbezoo F. Research diagnostic criteria for temporomandibular disorders: a systematic review of axis I epidemiologic findings. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2011;112: Ram H, Shadab M, Vardaan A, Aga P. Fracture of mandible during yawning in a patient with osteogenesis imperfecta. BMJ Case Rep. 2014; Folkestad L, Hald JD, Ersbøll AK, Gram J, Hermann AP, Langdahl B, Abrahamsen B, Brixen K. Fracture rates and fracture sites in patients with osteogenesis imperfecta: a Nationwide register-based cohort study. J Bone Miner Res. 2017;32: Ablon J. Personality and stereotype in osteogenesis imperfecta: behavioral phenotype or response to life s hard challenges? Am J Med Genet A. 2003; 122A: Submit your next manuscript to BioMed Central and we will help you at every step: We accept pre-submission inquiries Our selector tool helps you to find the most relevant journal We provide round the clock customer support Convenient online submission Thorough peer review Inclusion in PubMed and all major indexing services Maximum visibility for your research Submit your manuscript at
Prevalence of Temporomandibular Disorder Diagnoses and Psychologic Status in Croatian patients
 Prevalence of Temporomandibular Disorder Diagnoses and Psychologic Status in Croatian patients Robert ΔeliÊ 1 Samuel Dworkin 2 Vjekoslav Jerolimov 1 Mirela Maver -BiπÊanin 3 Milica Julia Bago 4 1 Department
Prevalence of Temporomandibular Disorder Diagnoses and Psychologic Status in Croatian patients Robert ΔeliÊ 1 Samuel Dworkin 2 Vjekoslav Jerolimov 1 Mirela Maver -BiπÊanin 3 Milica Julia Bago 4 1 Department
Distribution of depression, somatization and pain-related impairment in patients with chronic temporomandibular disorders
 Original Article http://dx.doi.org/10.1590/1678-7757-2018-0210 Distribution of depression, somatization and pain-related impairment in patients with chronic temporomandibular disorders Abstract Giancarlo
Original Article http://dx.doi.org/10.1590/1678-7757-2018-0210 Distribution of depression, somatization and pain-related impairment in patients with chronic temporomandibular disorders Abstract Giancarlo
Age peaks of different RDC/TMD diagnoses in a patient population
 journal of dentistry 38 (2010) 392 399 available at www.sciencedirect.com journal homepage: www.intl.elsevierhealth.com/journals/jden Age peaks of different RDC/TMD diagnoses in a patient population Daniele
journal of dentistry 38 (2010) 392 399 available at www.sciencedirect.com journal homepage: www.intl.elsevierhealth.com/journals/jden Age peaks of different RDC/TMD diagnoses in a patient population Daniele
Osteogenesis imperfecta Report from observation charts
 Orofacial function of persons having Osteogenesis imperfecta Report from observation charts The survey comprises 23 observation charts. Estimated occurrence: 5:100 000 live births. Etiology: The protein
Orofacial function of persons having Osteogenesis imperfecta Report from observation charts The survey comprises 23 observation charts. Estimated occurrence: 5:100 000 live births. Etiology: The protein
Natural course of temporomandibular disorders with low pain-related impairment: a 2-to-3-year follow-up study
 J o u r n a l o f Oral Rehabilitation Journal of Oral Rehabilitation 2013 Natural course of temporomandibular disorders with low pain-related impairment: a 2-to-3-year follow-up study D. MANFREDINI, L.
J o u r n a l o f Oral Rehabilitation Journal of Oral Rehabilitation 2013 Natural course of temporomandibular disorders with low pain-related impairment: a 2-to-3-year follow-up study D. MANFREDINI, L.
Chapter 2 Etiology and Epidemiology Daniele Manfredini and Luca Guarda-Nardini
 Chapter 2 Etiology and Epidemiology Daniele Manfredini and Luca Guarda-Nardini In the present chapter, which is dedicated to the provision of examples of the different strategies to investigate for the
Chapter 2 Etiology and Epidemiology Daniele Manfredini and Luca Guarda-Nardini In the present chapter, which is dedicated to the provision of examples of the different strategies to investigate for the
Definition and History of Orthodontics
 In the name of GOD Definition and History of Orthodontics Presented by: Dr Somayeh Heidari Orthodontist Reference: Contemporary Orthodontics Chapter 1 William R. Proffit, Henry W. Fields, David M.Sarver.
In the name of GOD Definition and History of Orthodontics Presented by: Dr Somayeh Heidari Orthodontist Reference: Contemporary Orthodontics Chapter 1 William R. Proffit, Henry W. Fields, David M.Sarver.
Dental Services Referral Form- Orthodontic Clinic
 Dental Services Referral Form- Orthodontic Clinic Date / / Title: Surname Given name Date of birth: Street address Suburb Postcode Name of Residential Facility (if applicable) Room: Phone - Home: Mobile:
Dental Services Referral Form- Orthodontic Clinic Date / / Title: Surname Given name Date of birth: Street address Suburb Postcode Name of Residential Facility (if applicable) Room: Phone - Home: Mobile:
Osseous changes and condyle position in TMJ tomograms: impact of RDC/TMD clinical diagnoses on agreement between expected and actual findings
 Osseous changes and condyle position in TMJ tomograms: impact of RDC/TMD clinical diagnoses on agreement between expected and actual findings Mie Wiese, DDS, a Ann Wenzel, DrOdont, PhD, DDS, b Hanne Hintze,
Osseous changes and condyle position in TMJ tomograms: impact of RDC/TMD clinical diagnoses on agreement between expected and actual findings Mie Wiese, DDS, a Ann Wenzel, DrOdont, PhD, DDS, b Hanne Hintze,
Volume 22 No. 14 September Dentists, Federally Qualified Health Centers and Health Maintenance Organizations For Action
 State of New Jersey Department of Human Services Division of Medical Assistance & Health Services Volume 22 No. 14 September 2012 TO: Dentists, Federally Qualified Health Centers and Health Maintenance
State of New Jersey Department of Human Services Division of Medical Assistance & Health Services Volume 22 No. 14 September 2012 TO: Dentists, Federally Qualified Health Centers and Health Maintenance
Osteogenesis imperfecta, also known as brittle
 ORIGINAL ARTICLE Evaluation of the severity of malocclusions in children affected by osteogenesis imperfecta with the peer assessment rating and discrepancy indexes Jean Rizkallah, a Stephane Schwartz,
ORIGINAL ARTICLE Evaluation of the severity of malocclusions in children affected by osteogenesis imperfecta with the peer assessment rating and discrepancy indexes Jean Rizkallah, a Stephane Schwartz,
Archived SECTION 14 - SPECIAL DOCUMENTATION REQUIREMENTS
 SECTION 14 - SPECIAL DOCUMENTATION REQUIREMENTS 14.1 CERTIFICATE OF MEDICAL NECESSITY...2 14.2 OPERATIVE REPORT...2 14.2.A PROCEDURES REQUIRING A REPORT...2 14.3 PRIOR AUTHORIZATION REQUEST...2 14.3.A
SECTION 14 - SPECIAL DOCUMENTATION REQUIREMENTS 14.1 CERTIFICATE OF MEDICAL NECESSITY...2 14.2 OPERATIVE REPORT...2 14.2.A PROCEDURES REQUIRING A REPORT...2 14.3 PRIOR AUTHORIZATION REQUEST...2 14.3.A
Age-related associations between psychological characteristics and pain intensity among Japanese patients with temporomandibular disorder
 221 Journal of Oral Science, Vol. 56, No. 3, 221-225, 2014 Original Age-related associations between psychological characteristics and pain intensity among Japanese patients with temporomandibular disorder
221 Journal of Oral Science, Vol. 56, No. 3, 221-225, 2014 Original Age-related associations between psychological characteristics and pain intensity among Japanese patients with temporomandibular disorder
Prevalence of Temporomandibular Disorders in Pregnancy
 Prevalence of Temporomandibular Disorders in Pregnancy Özlem Solak 1, Nurten Turhan-Haktanır 2, Gülengül Köken 3, Hasan Toktas 1, Özkan Güler 4, Vural Kavuncu 1, Yavuz Demir 2 1 of Physical Medicine and
Prevalence of Temporomandibular Disorders in Pregnancy Özlem Solak 1, Nurten Turhan-Haktanır 2, Gülengül Köken 3, Hasan Toktas 1, Özkan Güler 4, Vural Kavuncu 1, Yavuz Demir 2 1 of Physical Medicine and
PREVALENCE OF DISK DISPLACEMENT DISORDERS OF TMJ AMONG DENTAL STUDENTS
 International Journal of Research in Social Sciences Vol. 7 Issue 7, July 2017, ISSN: 2249-2496 Impact Factor: 7.081 Journal Homepage: Double-Blind Peer Reviewed Refereed Open Access International Journal
International Journal of Research in Social Sciences Vol. 7 Issue 7, July 2017, ISSN: 2249-2496 Impact Factor: 7.081 Journal Homepage: Double-Blind Peer Reviewed Refereed Open Access International Journal
Introduction. Facial findings. Intraoral findings. Frontal and lateral cephalometric photographs
 Journal of Dental and Oral Health Scient Open Access Exploring the World of Science ISSN: 2369-4475 Case Report A Case of Orthodontic Treatment for a Patient with Occlusal Abnormality This article was
Journal of Dental and Oral Health Scient Open Access Exploring the World of Science ISSN: 2369-4475 Case Report A Case of Orthodontic Treatment for a Patient with Occlusal Abnormality This article was
MEDICAL ASSISTANCE BULLETIN COMMONWEALTH OF PENNSYLVANIA DEPARTMENT OF PUBLIC WELFARE
 MEDICAL ASSISTANCE BULLETIN COMMONWEALTH OF PENNSYLVANIA DEPARTMENT OF PUBLIC WELFARE ISSUE DATE EFFECTIVE DATE NUMBER October 21,1996 October 28,1996 03-96-06 SUBJECT BY Information on New Procedures
MEDICAL ASSISTANCE BULLETIN COMMONWEALTH OF PENNSYLVANIA DEPARTMENT OF PUBLIC WELFARE ISSUE DATE EFFECTIVE DATE NUMBER October 21,1996 October 28,1996 03-96-06 SUBJECT BY Information on New Procedures
ORTHOGNATHIC SURGERY
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: orthodontics_for_pediatric_patients 2/2014 10/2017 10/2018 10/2017 Description of Procedure or Service Children
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: orthodontics_for_pediatric_patients 2/2014 10/2017 10/2018 10/2017 Description of Procedure or Service Children
The following standards and procedures apply to the provision of orthodontic services for children in the Medicaid/NJ FamilyCare (NJFC) programs.
 B.4.2.11 Orthodontic Services The following standards and procedures apply to the provision of orthodontic services for children in the Medicaid/NJ FamilyCare (NJFC) programs. Orthodontic Consultation
B.4.2.11 Orthodontic Services The following standards and procedures apply to the provision of orthodontic services for children in the Medicaid/NJ FamilyCare (NJFC) programs. Orthodontic Consultation
Attachment G. Orthodontic Criteria Index Form Comprehensive D8080. ABBREVIATIONS CRITERIA for Permanent Dentition YES NO
 First Review IL HFS Dental Program Models Second Review Ortho cad Attachment G Orthodontic Criteria Index Form Comprehensive D8080 Ceph Film X-Rays Photos Narrative Patient Name: DOB: ABBREVIATIONS CRITERIA
First Review IL HFS Dental Program Models Second Review Ortho cad Attachment G Orthodontic Criteria Index Form Comprehensive D8080 Ceph Film X-Rays Photos Narrative Patient Name: DOB: ABBREVIATIONS CRITERIA
Case Report Typical Radiographic Findings of Dentin Dysplasia Type 1b with Dental Fluorosis
 Case Reports in Dentistry Volume 2013, Article ID 902861, 4 pages http://dx.doi.org/10.1155/2013/902861 Case Report Typical Radiographic Findings of Dentin Dysplasia Type 1b with Dental Fluorosis S. Venkata
Case Reports in Dentistry Volume 2013, Article ID 902861, 4 pages http://dx.doi.org/10.1155/2013/902861 Case Report Typical Radiographic Findings of Dentin Dysplasia Type 1b with Dental Fluorosis S. Venkata
Title: Shortened Dental Arch and Restorative Therapies: Evidence for Functional Dentition
 Title: Shortened Dental Arch and Restorative Therapies: Evidence for Functional Dentition Date: 15 May 2008 Context and policy issues: For patients who lose teeth due to various reasons, a fundamental
Title: Shortened Dental Arch and Restorative Therapies: Evidence for Functional Dentition Date: 15 May 2008 Context and policy issues: For patients who lose teeth due to various reasons, a fundamental
Clinical UM Guideline
 Clinical UM Guideline Subject: Non-Medically Necessary Orthodontia Care Guideline #: #08-002 Current Publish Date: 10/16/2017 Status: Reviewed Last Review Date: 10/11/2017 Description This document addresses
Clinical UM Guideline Subject: Non-Medically Necessary Orthodontia Care Guideline #: #08-002 Current Publish Date: 10/16/2017 Status: Reviewed Last Review Date: 10/11/2017 Description This document addresses
Concepts of occlusion Balanced occlusion. Monoplane occlusion. Lingualized occlusion. Figure (10-1)
 Any contact between teeth of opposing dental arches; usually, referring to contact between the occlusal surface. The static relationship between the incising or masticatory surfaces of the maxillary or
Any contact between teeth of opposing dental arches; usually, referring to contact between the occlusal surface. The static relationship between the incising or masticatory surfaces of the maxillary or
Surface Electromyography Findings in Unilateral Myofascial Pain Patients: Comparison of Painful vs Non Painful Sides
 bs_bs_banner Pain Medicine 2013; 14: 1848 1853 Wiley Periodicals, Inc. Surface Electromyography Findings in Unilateral Myofascial Pain Patients: Comparison of Painful vs Non Painful Sides Daniele Manfredini,
bs_bs_banner Pain Medicine 2013; 14: 1848 1853 Wiley Periodicals, Inc. Surface Electromyography Findings in Unilateral Myofascial Pain Patients: Comparison of Painful vs Non Painful Sides Daniele Manfredini,
Fracture of mandible during yawning in a patient with osteogenesis imperfecta
 1 Department of Oral and Maxillofacial Surgery, King George s Medical University, Lucknow, Uttar Pradesh, India 2 King George s Medical University, Lucknow, Uttar Pradesh, India 3 Department of Medicine,
1 Department of Oral and Maxillofacial Surgery, King George s Medical University, Lucknow, Uttar Pradesh, India 2 King George s Medical University, Lucknow, Uttar Pradesh, India 3 Department of Medicine,
Ankylosed primary teeth with no permanent successors: What do you do? -- Part 1
 Ankylosed primary teeth with no permanent successors: What do you do? -- Part 1 March 3, 2015 By David M. Sarver, DMD, MS The clinical problem You have a seven-year-old patient who comes to your office
Ankylosed primary teeth with no permanent successors: What do you do? -- Part 1 March 3, 2015 By David M. Sarver, DMD, MS The clinical problem You have a seven-year-old patient who comes to your office
Evaluation for Severe Physically Handicapping Malocclusion. August 23, 2012
 Evaluation for Severe Physically Handicapping Malocclusion August 23, 2012 Presenters: Office of Health Insurance Programs Division of OHIP Operations Lee Perry, DDS, MBA, Medicaid Dental Director Gulam
Evaluation for Severe Physically Handicapping Malocclusion August 23, 2012 Presenters: Office of Health Insurance Programs Division of OHIP Operations Lee Perry, DDS, MBA, Medicaid Dental Director Gulam
Outline. Limiting your risk when treating patients with TMD. Temporomandibular Disorders 20/01/2014. TMD diagnosis. Condylar position and TMD risk
 Outline American Association of Orthodontists Limiting your risk when treating patients with TMD Ambra Michelotti michelot@unina.it TMD diagnosis Condylar position and TMD risk Occlusal interference and
Outline American Association of Orthodontists Limiting your risk when treating patients with TMD Ambra Michelotti michelot@unina.it TMD diagnosis Condylar position and TMD risk Occlusal interference and
Osteogenesis imperfecta (OI) is a heterogeneous
 Case Report 138 Dentinogenesis Imperfecta Associated with Osteogenesis Imperfecta: Report of Two Cases Chia-Ling Tsai, BDS, MS; Yng-Tzer Lin, BDS, MS; Yai-Tin Lin, BDS Osteogenesis imperfecta (OI) is a
Case Report 138 Dentinogenesis Imperfecta Associated with Osteogenesis Imperfecta: Report of Two Cases Chia-Ling Tsai, BDS, MS; Yng-Tzer Lin, BDS, MS; Yai-Tin Lin, BDS Osteogenesis imperfecta (OI) is a
Significant improvement with limited orthodontics anterior crossbite in an adult patient
 VARIA Significant improvement with limited orthodontics anterior crossbite in an adult patient Arzu Ari-Demirkaya Istanbul, Turkey Summary Objectives. Orthodontic treatment is known to last as long as
VARIA Significant improvement with limited orthodontics anterior crossbite in an adult patient Arzu Ari-Demirkaya Istanbul, Turkey Summary Objectives. Orthodontic treatment is known to last as long as
Lars Jacobsson 1,2,3* and Jan Lexell 1,3,4
 Jacobsson and Lexell Health and Quality of Life Outcomes (2016) 14:10 DOI 10.1186/s12955-016-0405-y SHORT REPORT Open Access Life satisfaction after traumatic brain injury: comparison of ratings with the
Jacobsson and Lexell Health and Quality of Life Outcomes (2016) 14:10 DOI 10.1186/s12955-016-0405-y SHORT REPORT Open Access Life satisfaction after traumatic brain injury: comparison of ratings with the
Dental Anatomy and Occlusion
 CHAPTER 53 Dental Anatomy and Occlusion Ma Lou C. Sabino DDS, and Emily G. Smythe, DDS What numerical system is used most commonly in the United States for designating the adult dentition? Pediatric dentition?
CHAPTER 53 Dental Anatomy and Occlusion Ma Lou C. Sabino DDS, and Emily G. Smythe, DDS What numerical system is used most commonly in the United States for designating the adult dentition? Pediatric dentition?
Orofacial function of persons having. Report from questionnaires. Turner syndrome
 Orofacial function of persons having Turner syndrome Report from questionnaires The survey comprises questionnaires. Estimated occurrence: : girls born. Etiology: Girls with Turner syndrome are either
Orofacial function of persons having Turner syndrome Report from questionnaires The survey comprises questionnaires. Estimated occurrence: : girls born. Etiology: Girls with Turner syndrome are either
Citation for published version (APA): Koutris, M. (2013). Masticatory muscle pain: Causes, consequences, and diagnosis
 UvA-DARE (Digital Academic Repository) Masticatory muscle pain: Causes, consequences, and diagnosis Koutris, M. Link to publication Citation for published version (APA): Koutris, M. (2013). Masticatory
UvA-DARE (Digital Academic Repository) Masticatory muscle pain: Causes, consequences, and diagnosis Koutris, M. Link to publication Citation for published version (APA): Koutris, M. (2013). Masticatory
Temporomandibular disorders and the need for stomatognathic treatment in orthodontically treated and untreated girls
 European Journal of Orthodontics 22 (2000) 283 292 2000 European Orthodontic Society Temporomandibular disorders and the need for stomatognathic treatment in orthodontically treated and untreated girls
European Journal of Orthodontics 22 (2000) 283 292 2000 European Orthodontic Society Temporomandibular disorders and the need for stomatognathic treatment in orthodontically treated and untreated girls
MDJ Stabilization Splint (Night Guard, Mouth Guard) Vol.:6 No.:2 2009
 MDJ Stabilization Splint (Night Guard, Mouth Guard) Comparative Research Dr. Kais George Zia B.D.S, M.Sc, Ph.D. Abstract This research compares between the effect of flexible and hard stabilization splint
MDJ Stabilization Splint (Night Guard, Mouth Guard) Comparative Research Dr. Kais George Zia B.D.S, M.Sc, Ph.D. Abstract This research compares between the effect of flexible and hard stabilization splint
Comparison of three different options for immediate treatment of painful temporomandibular disorders: a randomized, controlled pilot trial
 ACTA ODONTOLOGICA SCANDINAVICA, 2016 VOL. 74, NO. 6, 480 486 http://dx.doi.org/10.1080/00016357.2016.1204558 ORIGINAL ARTICLE Comparison of three different options for immediate treatment of painful temporomandibular
ACTA ODONTOLOGICA SCANDINAVICA, 2016 VOL. 74, NO. 6, 480 486 http://dx.doi.org/10.1080/00016357.2016.1204558 ORIGINAL ARTICLE Comparison of three different options for immediate treatment of painful temporomandibular
Angle Class II, division 2 malocclusion with deep overbite
 BBO Case Report Angle Class II, division 2 malocclusion with deep overbite Arno Locks 1 Angle Class II, division 2, malocclusion is characterized by a Class II molar relation associated with retroclined
BBO Case Report Angle Class II, division 2 malocclusion with deep overbite Arno Locks 1 Angle Class II, division 2, malocclusion is characterized by a Class II molar relation associated with retroclined
Int J Clin Exp Med 2017;10(11): /ISSN: /IJCEM
 Int J Clin Exp Med 2017;10(11):15323-15328 www.ijcem.com /ISSN:1940-5901/IJCEM0033200 Original Article Assessment of oral parafunctional behaviors and electromyographic activities of the masticatory muscles
Int J Clin Exp Med 2017;10(11):15323-15328 www.ijcem.com /ISSN:1940-5901/IJCEM0033200 Original Article Assessment of oral parafunctional behaviors and electromyographic activities of the masticatory muscles
Arrangement of the artificial teeth:
 Lecture Prosthodontic Dr. Osama Arrangement of the artificial teeth: It s the placement of the teeth on a denture with definite objective in mind or it s the setting of teeth on temporary bases. Rules
Lecture Prosthodontic Dr. Osama Arrangement of the artificial teeth: It s the placement of the teeth on a denture with definite objective in mind or it s the setting of teeth on temporary bases. Rules
Class II Correction using Combined Twin Block and Fixed Orthodontic Appliances: A Case Report
 Case Report Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/506 Class II Correction using Combined Twin Block and Fixed Orthodontic Appliances: A Case Report Ahmed Alassiry Assistant
Case Report Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/506 Class II Correction using Combined Twin Block and Fixed Orthodontic Appliances: A Case Report Ahmed Alassiry Assistant
When first published in 1992, the Research Diagnostic
 The Research Diagnostic Criteria for Temporomandibular Disorders. IV: Evaluation of Psychometric Properties of the Axis II Measures Richard Ohrbach, DDS, PhD Associate Professor Department of Oral Diagnostic
The Research Diagnostic Criteria for Temporomandibular Disorders. IV: Evaluation of Psychometric Properties of the Axis II Measures Richard Ohrbach, DDS, PhD Associate Professor Department of Oral Diagnostic
ORTHODONTIC INITIAL ASSESSMENT FORM (OIAF) w/ INSTRUCTIONS
 Use the accompanying Tip Sheet and How to Score the Orthodontic Initial Assessment Form for guidance in completion of the assessment form. You will need this score sheet and a disposable ruler (or a Boley
Use the accompanying Tip Sheet and How to Score the Orthodontic Initial Assessment Form for guidance in completion of the assessment form. You will need this score sheet and a disposable ruler (or a Boley
Hereditary Opalescent Dentin: A Report of Two Cases
 Hereditary Opalescent Dentin: A Report of Two Cases Siddharth Gupta, BDS, MDS; Rahul R. Bhowate, BDS, MDS; Ashok Bhati, BDS, MDS Abstract Aim: The aim of this case report is to present the clinical and
Hereditary Opalescent Dentin: A Report of Two Cases Siddharth Gupta, BDS, MDS; Rahul R. Bhowate, BDS, MDS; Ashok Bhati, BDS, MDS Abstract Aim: The aim of this case report is to present the clinical and
Lingual correction of a complex Class III malocclusion: Esthetic treatment without sacrificing quality results.
 SM 3M Health Care Academy Lingual correction of a complex Class III malocclusion: Esthetic treatment without sacrificing quality results. Christopher S. Riolo, DDS, M.S, Ph.D. Dr. Riolo received his DDS
SM 3M Health Care Academy Lingual correction of a complex Class III malocclusion: Esthetic treatment without sacrificing quality results. Christopher S. Riolo, DDS, M.S, Ph.D. Dr. Riolo received his DDS
Differences in clinical variables and risk factors between patients with osteoarthritis and osteoarthrosis of the temporomandibular joint (TMJ)
 Journal section: Oral Medicine and Pathology Publication Types: Research doi:10.4317/jced.3.e303 Differences in clinical variables and risk factors between patients with osteoarthritis and osteoarthrosis
Journal section: Oral Medicine and Pathology Publication Types: Research doi:10.4317/jced.3.e303 Differences in clinical variables and risk factors between patients with osteoarthritis and osteoarthrosis
Incidence of temporomandibular joint clicking in adolescents with and without unilateral posterior cross-bite: a 10-year follow-up study
 J o u r n a l o f Oral Rehabilitation Journal of Oral Rehabilitation 2016 43; 16 22 Incidence of temporomandibular joint clicking in adolescents with and without unilateral posterior cross-bite: a 10-year
J o u r n a l o f Oral Rehabilitation Journal of Oral Rehabilitation 2016 43; 16 22 Incidence of temporomandibular joint clicking in adolescents with and without unilateral posterior cross-bite: a 10-year
Unusual root canal anatomy in a maxillary second molar
 www.edoriumjournals.com CLINICAL IMAGES PEER REVIEWED OPEN ACCESS Unusual root canal anatomy in a maxillary second molar Toshiko Inoue, Makoto Saito, Fumio Nishimura, Takashi Miyazaki ABSTRACT Abstract
www.edoriumjournals.com CLINICAL IMAGES PEER REVIEWED OPEN ACCESS Unusual root canal anatomy in a maxillary second molar Toshiko Inoue, Makoto Saito, Fumio Nishimura, Takashi Miyazaki ABSTRACT Abstract
EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: Dr. Stefan Blasius Year: 2010 WBLO 01 EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: Dr. Stefan Blasius Year: 2010 WBLO 01 RÉSUMÉ
EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: Dr. Stefan Blasius Year: 2010 WBLO 01 EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: Dr. Stefan Blasius Year: 2010 WBLO 01 RÉSUMÉ
TMD Management in 2010: Science or Smoke and Mirrors
 California Dental Association Annual Meeting 2010 TMD Management in 2010: Science or Smoke and Mirrors Clinical Professor, Advanced Education in Prosthodontics University of Southern California School
California Dental Association Annual Meeting 2010 TMD Management in 2010: Science or Smoke and Mirrors Clinical Professor, Advanced Education in Prosthodontics University of Southern California School
Dr Robert Drummond. BChD, DipOdont Ortho, MChD(Ortho), FDC(SA) Ortho. Canad Inn Polo Park Winnipeg 2015
 Dr Robert Drummond BChD, DipOdont Ortho, MChD(Ortho), FDC(SA) Ortho Canad Inn Polo Park Winnipeg 2015 Severely compromised FPM with poor prognosis Children often present with a developing dentition affected
Dr Robert Drummond BChD, DipOdont Ortho, MChD(Ortho), FDC(SA) Ortho Canad Inn Polo Park Winnipeg 2015 Severely compromised FPM with poor prognosis Children often present with a developing dentition affected
RESEARCH DIAGNOSTIC CRITERIA FOR TEMPOROMANDIBULAR DISORDERS
 DEPARTMENT OF ORAL MEDICINE OROFACIAL PAIN RESEARCH GROUP RESEARCH DIAGNOSTIC CRITERIA FOR TEMPOROMANDIBULAR DISORDERS AXIS I: CLINICAL PHYSICAL EXAMINATION FORMS AND SPECIFICATIONS INSTRUCTIONS FOR SCORING
DEPARTMENT OF ORAL MEDICINE OROFACIAL PAIN RESEARCH GROUP RESEARCH DIAGNOSTIC CRITERIA FOR TEMPOROMANDIBULAR DISORDERS AXIS I: CLINICAL PHYSICAL EXAMINATION FORMS AND SPECIFICATIONS INSTRUCTIONS FOR SCORING
ORTHODONTICS Treatment of malocclusion Assist.Lec.Kasem A.Abeas University of Babylon Faculty of Dentistry 5 th stage
 Lec: Treatment of class I malocclusion Class I occlusion can be defined by Angles, classification as the mesiobuccal cusp of the upper 1 st permanent molar occlude with the developmental groove of the
Lec: Treatment of class I malocclusion Class I occlusion can be defined by Angles, classification as the mesiobuccal cusp of the upper 1 st permanent molar occlude with the developmental groove of the
Ortho-surgical Management of Severe Vertical Dysplasia: A Case Report
 Case Report Ortho-surgical Management of Severe Vertical Dysplasia: A Case Report 1 Vinni Arora, 2 Rekha Sharma, 3 Sachin Parashar 1 Senior Resident, 2 Professor and Head of Department, 3 Former Resident
Case Report Ortho-surgical Management of Severe Vertical Dysplasia: A Case Report 1 Vinni Arora, 2 Rekha Sharma, 3 Sachin Parashar 1 Senior Resident, 2 Professor and Head of Department, 3 Former Resident
Benefit Changes for Texas Health Steps Orthodontic Dental Services Effective January 1, 2012
 Benefit Changes for Texas Health Steps Orthodontic Dental Services Effective January 1, 2012 Information posted November 14, 2011 Effective for dates of service on or after January 1, 2012, the following
Benefit Changes for Texas Health Steps Orthodontic Dental Services Effective January 1, 2012 Information posted November 14, 2011 Effective for dates of service on or after January 1, 2012, the following
APPENDIX A. MEDICAID ORTHODONTIC INITIAL ASSESSMENT FORM (IAF) You will need this scoresheet and a disposable ruler (or a Boley Gauge)
 APPENDIX A MEDICAID ORTHODONTIC INITIAL ASSESSMENT FORM (IAF) You will need this scoresheet and a disposable ruler (or a Boley Gauge) Name: _ I. D. Number: Conditions: 1. Cleft palate deformities 2. Deep
APPENDIX A MEDICAID ORTHODONTIC INITIAL ASSESSMENT FORM (IAF) You will need this scoresheet and a disposable ruler (or a Boley Gauge) Name: _ I. D. Number: Conditions: 1. Cleft palate deformities 2. Deep
22q11 deletion syndrome Report from observation charts
 Orofacial function of persons having 22q11 deletion syndrome Report from observation charts The survey comprises 147 observation charts. Synonyms: CATCH 22, Di George syndrome, Velocardiofacial syndrome
Orofacial function of persons having 22q11 deletion syndrome Report from observation charts The survey comprises 147 observation charts. Synonyms: CATCH 22, Di George syndrome, Velocardiofacial syndrome
Correlation between clinical diagnosis based on RDC/TMD and MRI findings of TMJ internal derangement
 Int. J. Oral Maxillofac. Surg. 2012; 41: 103 108 doi:10.1016/j.ijom.2011.09.010, available online at http://www.sciencedirect.com Clinical paper TMJ disorders Correlation between clinical diagnosis based
Int. J. Oral Maxillofac. Surg. 2012; 41: 103 108 doi:10.1016/j.ijom.2011.09.010, available online at http://www.sciencedirect.com Clinical paper TMJ disorders Correlation between clinical diagnosis based
Sample Case #1. Disclaimer
 ABO Sample Cases Disclaimer Sample Case #1 The following sample questions and answers were composed and vetted by a panel of experts in orthodontics and are intended to provide an example of the types
ABO Sample Cases Disclaimer Sample Case #1 The following sample questions and answers were composed and vetted by a panel of experts in orthodontics and are intended to provide an example of the types
Characteristics of middle-aged and older patients with temporomandibular disorders and burning mouth syndrome
 355 Journal of Oral Science, Vol. 57, No. 4, 355-360, 2015 Original Characteristics of middle-aged and older patients with temporomandibular disorders and burning mouth syndrome Mika Honda 1), Takashi
355 Journal of Oral Science, Vol. 57, No. 4, 355-360, 2015 Original Characteristics of middle-aged and older patients with temporomandibular disorders and burning mouth syndrome Mika Honda 1), Takashi
Orthodontics. Anomalies
 Orthodontics Anomalies Anomalies of Teeth Groups of teeth Jaws Intermaxilary relations Anomalies of tooth number Hypodontics (hypodontia) the tooth (or teeth) are missing Third molars (if third molars
Orthodontics Anomalies Anomalies of Teeth Groups of teeth Jaws Intermaxilary relations Anomalies of tooth number Hypodontics (hypodontia) the tooth (or teeth) are missing Third molars (if third molars
UNLV School of Dental Medicine Advanced Education in Orthodontics and Dentofacial Orthopedics Course Descriptions, updated Dec.
 UNLV School of Dental Medicine Advanced Education in and Dentofacial Orthopedics Course Descriptions, updated Dec. 2012 Year 1 Summer Courses Intro to 8001 8011 8201 Cephlometrics Year 1 Fall Courses 1.
UNLV School of Dental Medicine Advanced Education in and Dentofacial Orthopedics Course Descriptions, updated Dec. 2012 Year 1 Summer Courses Intro to 8001 8011 8201 Cephlometrics Year 1 Fall Courses 1.
Phonophoresis in temporomandibular joint disorders: A clinical trial
 Journal of Advanced Clinical & Research Insights (2015), 2, 259 264 ORIGINAL ARTICLE Phonophoresis in temporomandibular joint disorders: A clinical trial K. R. Vijayalakshmi, Mubeen Khan, Preeti Rajguru
Journal of Advanced Clinical & Research Insights (2015), 2, 259 264 ORIGINAL ARTICLE Phonophoresis in temporomandibular joint disorders: A clinical trial K. R. Vijayalakshmi, Mubeen Khan, Preeti Rajguru
Validation of the chinese version of the oral health impact profile for TMDs (OHIP- TMDs-C)
 Journal section: Oral Medicine and Pathology Publication Types: Research doi:10.4317/medoral.20243 http://dx.doi.org/doi:10.4317/medoral.20243 Validation of the chinese version of the oral health impact
Journal section: Oral Medicine and Pathology Publication Types: Research doi:10.4317/medoral.20243 http://dx.doi.org/doi:10.4317/medoral.20243 Validation of the chinese version of the oral health impact
Mandibular incisor extraction: indications and long-term evaluation
 European Journal of Orthodontics 18 (1996) 485-489 O 1996 European Orthodontic Society Mandibular incisor extraction: indications and long-term evaluation Jose-Antonio Canut University of Valencia, Spain
European Journal of Orthodontics 18 (1996) 485-489 O 1996 European Orthodontic Society Mandibular incisor extraction: indications and long-term evaluation Jose-Antonio Canut University of Valencia, Spain
Preventive Orthodontics
 Semmelweis University Faculty of Dentistry Department in Community Dentistry director: Dr. Kivovics Péter assoc.prof. http://semmelweis-egyetem.hu/fszoi/ https://www.facebook.com/fszoi Preventive Orthodontics
Semmelweis University Faculty of Dentistry Department in Community Dentistry director: Dr. Kivovics Péter assoc.prof. http://semmelweis-egyetem.hu/fszoi/ https://www.facebook.com/fszoi Preventive Orthodontics
Correlation Between Naso Labial Angle and Effective Maxillary and Mandibular Lengths in Untreated Class II Patients
 9 International Journal of Interdisciplinary and Multidisciplinary Studies,2014,Vol 1,No.3,9-14. Available online at httt://www.ijims.com ISSN: 2348 0343 Correlation Between Naso Labial Angle and Effective
9 International Journal of Interdisciplinary and Multidisciplinary Studies,2014,Vol 1,No.3,9-14. Available online at httt://www.ijims.com ISSN: 2348 0343 Correlation Between Naso Labial Angle and Effective
Influence of Kinesio tape application on masticatory muscles activity evaluated using surface electromyography a pilot study
 Influence of Kinesio tape application on masticatory muscles activity evaluated using surface electromyography a pilot study Michał Ginszt 1, Marcin Berger 2, Magdalena Bakalczuk 2, Piotr Gawda 3, Jacek
Influence of Kinesio tape application on masticatory muscles activity evaluated using surface electromyography a pilot study Michał Ginszt 1, Marcin Berger 2, Magdalena Bakalczuk 2, Piotr Gawda 3, Jacek
Jefferson Cephalometric Analysis--Face and Health Focused
 Jefferson Cephalometric Analysis--Face and Health Focused Google: Jefferson Ceph Analysis Video Instruction for video instruction. Note: video instruction teaches how to find Center O. Center O is now
Jefferson Cephalometric Analysis--Face and Health Focused Google: Jefferson Ceph Analysis Video Instruction for video instruction. Note: video instruction teaches how to find Center O. Center O is now
Evaluation of maxillary protrusion malocclusion treatment effects with prosth-orthodontic method in old adults
 Evaluation of maxillary protrusion malocclusion treatment effects with prosth-orthodontic method in old adults Peicheng Xu, DDS, MSD, a and Honghu Liu, DDS, PhD b a Shanghai Xuhui Dental Hospital and b
Evaluation of maxillary protrusion malocclusion treatment effects with prosth-orthodontic method in old adults Peicheng Xu, DDS, MSD, a and Honghu Liu, DDS, PhD b a Shanghai Xuhui Dental Hospital and b
4 Smallest detectable difference of maximal mouth opening in patients with painfully restricted temporomandibular joint function.
 4 Smallest detectable difference of maximal mouth opening in patients with painfully restricted temporomandibular joint function. Kropmans ThJB, Dijkstra PU, Stegenga B, Stewart R, de Bont LGM European
4 Smallest detectable difference of maximal mouth opening in patients with painfully restricted temporomandibular joint function. Kropmans ThJB, Dijkstra PU, Stegenga B, Stewart R, de Bont LGM European
Use of Angular Measurements in Cephalometric Analyses
 Use of Angular Measurements in Cephalometric Analyses GEOFFREY F. WALKER and CHARLES J. KOWALSKI School of Dentistry, University of Michigan, Ann Arbor, Michigan 48104, USA Most cephalometric analyses
Use of Angular Measurements in Cephalometric Analyses GEOFFREY F. WALKER and CHARLES J. KOWALSKI School of Dentistry, University of Michigan, Ann Arbor, Michigan 48104, USA Most cephalometric analyses
Changes of the Transverse Dental Arch Dimension, Overjet and Overbite after Rapid Maxillary Expansion (RME)
 Dental Journal Changes of the Transverse Dental Arch Dimension, Overjet and Overbite after Rapid Maxillary Expansion (RME) Department of Advanced General Dentistry Faculty of Dentistry, Mahidol University.
Dental Journal Changes of the Transverse Dental Arch Dimension, Overjet and Overbite after Rapid Maxillary Expansion (RME) Department of Advanced General Dentistry Faculty of Dentistry, Mahidol University.
Prevalence and Pattern of Congenital Missing Teeth in a Group of Iranian Adolescents
 Prevalence and Pattern of Congenital Missing Teeth in a Group of Iranian Adolescents Ajami B. a, Shabzendedar M. a*, Afzal Agaee M. b, Mehrjerdian M. c a Dept. of Pediatric Dentistry, Faculty of Dentistry,
Prevalence and Pattern of Congenital Missing Teeth in a Group of Iranian Adolescents Ajami B. a, Shabzendedar M. a*, Afzal Agaee M. b, Mehrjerdian M. c a Dept. of Pediatric Dentistry, Faculty of Dentistry,
Williams syndrome Report from observation charts
 Orofacial function of persons having Williams syndrome Report from observation charts The survey comprises 88 observation charts. Synonyms: William-Beuren syndrome. Estimated occurrence: 5-10:100 000 live
Orofacial function of persons having Williams syndrome Report from observation charts The survey comprises 88 observation charts. Synonyms: William-Beuren syndrome. Estimated occurrence: 5-10:100 000 live
Fellowship. Digital Case Documentation Format for Fellowship Case Presentation. OCCLUSION CONNECTIONS Dot Dentistry
 Digital Case Documentation Format for Case Presentation TMD Candidate s Name: CLAYTON A. CHAN, D.D.S. Case No.: 1 Our Disciplines ORTHOPEDIC Patient s Initials: CL (EXAMPLE CASE) RESTORATIVE OCCLUSION
Digital Case Documentation Format for Case Presentation TMD Candidate s Name: CLAYTON A. CHAN, D.D.S. Case No.: 1 Our Disciplines ORTHOPEDIC Patient s Initials: CL (EXAMPLE CASE) RESTORATIVE OCCLUSION
Torsion bottle, a very simple, reliable, and cheap tool for a basic scoliosis screening
 Romano and Mastrantonio Scoliosis and Spinal Disorders (2018) 13:4 DOI 10.1186/s13013-018-0150-6 RESEARCH Open Access Torsion bottle, a very simple, reliable, and cheap tool for a basic scoliosis screening
Romano and Mastrantonio Scoliosis and Spinal Disorders (2018) 13:4 DOI 10.1186/s13013-018-0150-6 RESEARCH Open Access Torsion bottle, a very simple, reliable, and cheap tool for a basic scoliosis screening
Research diagnostic criteria for temporomandibular disorders: a systematic review of axis I epidemiologic findings
 Research diagnostic criteria for temporomandibular disorders: a systematic review of axis I epidemiologic findings Daniele Manfredini, DDS, a Luca Guarda-Nardini, MD, DDS, a Ephraim Winocur, DMD, b Fabio
Research diagnostic criteria for temporomandibular disorders: a systematic review of axis I epidemiologic findings Daniele Manfredini, DDS, a Luca Guarda-Nardini, MD, DDS, a Ephraim Winocur, DMD, b Fabio
The America Association of Oral and Maxillofacial Surgeons classify occlusion/malocclusion in to the following three categories:
 Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
Invisalign technique in the treatment of adults with pre-restorative concerns
 Mampieri and Giancotti Progress in Orthodontics 2013, 14:40 REVIEW Open Access Invisalign technique in the treatment of adults with pre-restorative concerns Gianluca Mampieri * and Aldo Giancotti Abstract
Mampieri and Giancotti Progress in Orthodontics 2013, 14:40 REVIEW Open Access Invisalign technique in the treatment of adults with pre-restorative concerns Gianluca Mampieri * and Aldo Giancotti Abstract
Temporomandibular Joint Clicking Noises Caused by a Multilocular Bone Cyst: A Case Report
 Temporomandibular Joint Clicking Noises Caused by a Multilocular Bone Cyst: A Case Report Abstract When diagnosing patients with temporomandibular disorder (TMD) symptoms, the possibility of unusual causes
Temporomandibular Joint Clicking Noises Caused by a Multilocular Bone Cyst: A Case Report Abstract When diagnosing patients with temporomandibular disorder (TMD) symptoms, the possibility of unusual causes
Correction of Crowding using Conservative Treatment Approach
 Case Report Correction of Crowding using Conservative Treatment Approach Dr Tapan Shah, 1 Dr Tarulatha Shyagali, 2 Dr Kalyani Trivedi 3 1 Senior Lecturer, 2 Professor, Department of Orthodontics, Darshan
Case Report Correction of Crowding using Conservative Treatment Approach Dr Tapan Shah, 1 Dr Tarulatha Shyagali, 2 Dr Kalyani Trivedi 3 1 Senior Lecturer, 2 Professor, Department of Orthodontics, Darshan
Temporomandibular Joint Disorders
 Temporomandibular Joint Disorders Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can cause headaches, ear pain,
Temporomandibular Joint Disorders Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can cause headaches, ear pain,
Prevalence amongst adolescents in Bergen, Western Norway of temporomandibular disorders according to the DC/TMD criteria and examination protocol
 Prevalence amongst adolescents in Bergen, Western Norway of temporomandibular disorders according to the DC/TMD criteria and examination protocol Graue Anne Marit¹, Jokstad Asbjørn², Assmus Jörg³, Skeie
Prevalence amongst adolescents in Bergen, Western Norway of temporomandibular disorders according to the DC/TMD criteria and examination protocol Graue Anne Marit¹, Jokstad Asbjørn², Assmus Jörg³, Skeie
An Anterior Tooth Size Comparison in Unilateral and Bilateral Congenitally Absent Maxillary Lateral Incisors
 An Anterior Tooth Size Comparison in Unilateral and Bilateral Congenitally Absent Maxillary Lateral Incisors Abstract The purpose of this study is to compare the anterior tooth size width in patients with
An Anterior Tooth Size Comparison in Unilateral and Bilateral Congenitally Absent Maxillary Lateral Incisors Abstract The purpose of this study is to compare the anterior tooth size width in patients with
Fellowship Awards Application
 Discipline. Dedication. Competency. Skilled OC (To be Typed or printed) Fellowship Awards Application Prerequisite: OC Alumni Status, Completed OC Levels 1-4 Curriculum Who can apply for OC Fellowship?
Discipline. Dedication. Competency. Skilled OC (To be Typed or printed) Fellowship Awards Application Prerequisite: OC Alumni Status, Completed OC Levels 1-4 Curriculum Who can apply for OC Fellowship?
Case Report: Long-Term Outcome of Class II Division 1 Malocclusion Treated with Rapid Palatal Expansion and Cervical Traction
 Case Report Case Report: Long-Term Outcome of Class II Division 1 Malocclusion Treated with Rapid Palatal Expansion and Cervical Traction Roberto M. A. Lima, DDS a ; Anna Leticia Lima, DDS b Abstract:
Case Report Case Report: Long-Term Outcome of Class II Division 1 Malocclusion Treated with Rapid Palatal Expansion and Cervical Traction Roberto M. A. Lima, DDS a ; Anna Leticia Lima, DDS b Abstract:
Initial Doctor Questionnaire
 Initial Doctor Questionnaire DO NOT enter the patient in this study: if your patient does not have a TMD pain diagnosis if your patient does not need treatment at this time if you are not going to treat
Initial Doctor Questionnaire DO NOT enter the patient in this study: if your patient does not have a TMD pain diagnosis if your patient does not need treatment at this time if you are not going to treat
Screening orthodontic patients for temporomandibular disorders
 Clin Dent Rev (2017) 1:8 https://doi.org/10.1007/s41894-017-0007-z DIAGNOSIS Screening orthodontic patients for temporomandibular disorders Gary Klasser 1 Charles Greene 2 Received: 5 April 2017 / Accepted:
Clin Dent Rev (2017) 1:8 https://doi.org/10.1007/s41894-017-0007-z DIAGNOSIS Screening orthodontic patients for temporomandibular disorders Gary Klasser 1 Charles Greene 2 Received: 5 April 2017 / Accepted:
pc oral surgery international
 pc oral surgery international Evidence-based TMJ Surgery 2013 Professor Paul Coulthard BDS FGDP(UK) MDS FDSRCS FDSRCS(OS) PhD evidence-based practice? - the integration of best research evidence with clinical
pc oral surgery international Evidence-based TMJ Surgery 2013 Professor Paul Coulthard BDS FGDP(UK) MDS FDSRCS FDSRCS(OS) PhD evidence-based practice? - the integration of best research evidence with clinical
The Research Diagnostic Criteria for Temporomandibular Disorders. V: Methods Used to Establish and Validate Revised Axis I Diagnostic Algorithms
 The Research Diagnostic Criteria for Temporomandibular Disorders. V: Methods Used to Establish and Validate Revised Axis I Diagnostic Algorithms Eric L. Schiffman, DDS, MS Associate Professor Department
The Research Diagnostic Criteria for Temporomandibular Disorders. V: Methods Used to Establish and Validate Revised Axis I Diagnostic Algorithms Eric L. Schiffman, DDS, MS Associate Professor Department
Up Date on TMD WHAT IS TMD? Temporomandibular Disorders (TMD)*: Donald Nixdorf DDS, MS
 Up Date on TMD Donald Nixdorf DDS, MS Associate Professor Division of TMD and Orofacial Pain WHAT IS TMD? Temporomandibular Disorders (TMD)*: MUSCLE and JOINT DISORDERS * Temporomandibular Muscle and Joint
Up Date on TMD Donald Nixdorf DDS, MS Associate Professor Division of TMD and Orofacial Pain WHAT IS TMD? Temporomandibular Disorders (TMD)*: MUSCLE and JOINT DISORDERS * Temporomandibular Muscle and Joint
TEMPORO-MANDIBULAR JOINT DISORDERS
 Disclaimer This movie is an educational resource only and should not be used to manage your dental health. All decisions about the management of TMJ Disorders must be made in conjunction with your Dental
Disclaimer This movie is an educational resource only and should not be used to manage your dental health. All decisions about the management of TMJ Disorders must be made in conjunction with your Dental
U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health
 T M J D I S O R D E R S U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health CONTENTS 2 4 6 7 8 9 14 WHAT IS THE TEMPOROMANDIBULAR JOINT? WHAT ARE TMJ DISORDERS? WHAT CAUSES TMJ DISORDERS?
T M J D I S O R D E R S U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health CONTENTS 2 4 6 7 8 9 14 WHAT IS THE TEMPOROMANDIBULAR JOINT? WHAT ARE TMJ DISORDERS? WHAT CAUSES TMJ DISORDERS?
Ibelieve the time has come for the general dentists to
 EARLY ORTHODONTIC TREATMENT Brock Rondeau, D.D.S. I.B.O., D.A.B.C.P., D-A.C.S.D.D., D.A.B.D.S.M., D.A.B.C.D.S.M. Ibelieve the time has come for the general dentists to get serious and educated in an effort
EARLY ORTHODONTIC TREATMENT Brock Rondeau, D.D.S. I.B.O., D.A.B.C.P., D-A.C.S.D.D., D.A.B.D.S.M., D.A.B.C.D.S.M. Ibelieve the time has come for the general dentists to get serious and educated in an effort
Peninsula Dental Social Enterprise (PDSE)
 Peninsula Dental Social Enterprise (PDSE) Orthodontic Checklist for Clinics Version 3.0 Date approved: November 2017 Approved by: The Board Review due: November 2018 Policy will be updated as required
Peninsula Dental Social Enterprise (PDSE) Orthodontic Checklist for Clinics Version 3.0 Date approved: November 2017 Approved by: The Board Review due: November 2018 Policy will be updated as required
ABSTRACT. are of greater importance than others, the most important of
 10.5005/jp-journals-10015-1237 Ranjit ORIGINAL Kamble RESEARCH et al Assessment of Positional Variation of Maxillary Permanent First Molar with respect to the Infrazygomatic Crest (Key Ridge) in Skeletal
10.5005/jp-journals-10015-1237 Ranjit ORIGINAL Kamble RESEARCH et al Assessment of Positional Variation of Maxillary Permanent First Molar with respect to the Infrazygomatic Crest (Key Ridge) in Skeletal
Dental Research Journal
 Dental Research Journal Case Report Dentinogenesis imperfecta associated with osteogenesis imperfecta Mina Biria 1, Fatemeh Mashhadi Abbas 2, Sedighe Mozaffar 3, Rahil Ahmadi 3 1 Departments of Pediatric,
Dental Research Journal Case Report Dentinogenesis imperfecta associated with osteogenesis imperfecta Mina Biria 1, Fatemeh Mashhadi Abbas 2, Sedighe Mozaffar 3, Rahil Ahmadi 3 1 Departments of Pediatric,
