Guideline Number: NIA_CG_304 Last Revised Date: October 2014 Responsible Department: Implementation Date: October 2014 Clinical Operations
|
|
|
- Moses Singleton
- 5 years ago
- Views:
Transcription
1 National Imaging Associates, Inc. Clinical guidelines Lumbar Spinal Fusion Surgery Lumbar Decompression Procedures Lumbar Microdiscectomy Only Procedure CPT Codes: Lumbar Fusion (Single level) = 22533, 22558, 22612, 22630, Lumbar Fusion (Multiple levels) = 22533, , 22558, , 22612, , 22630, , 22633, (+ indicates multiple level) Lumbar Decompression = 63030, , 63005, 63012, 63017, 63042, , 63047, , 63056, Lumbar Microdiscectomy = 63030, Original Date: June 1, 2013 Page 1 of 10 Last Review Date: October 2014 Guideline Number: NIA_CG_304 Last Revised Date: October 2014 Responsible Department: Implementation Date: October 2014 Clinical Operations OVERVIEW: This guideline outlines the key surgical treatments and indications for common lumbar spinal disorders and is a consensus document based upon the best available evidence. Spine surgery is a complex area of medicine and this document breaks out the treatment modalities for lumbar spine disorders into surgical categories: lumbar microdiscectomy, lumbar decompression, and lumbar fusion surgery. See the additional information section for procedures considered not medically necessary. INTRODUCTION A. Lumbar Microdiscectomy is a surgical procedure to remove part of the damaged spinal disc. The damaged spinal disc herniates into the spinal canal and irritates the nerve roots. Nerve root compression leads to symptoms like low back pain, radicular pain, numbness and tingling, muscular weakness, and paresthesia. Typical disc herniation pain is exacerbated with any movement that causes the disc to increase pressure on the nerve roots. B. Lumbar Decompression (Laminectomy, Facetectomy and Foraminotomy): Laminectomy is common decompression surgery. The American Association of Neurological Surgeons defines laminectomy as a surgery to remove the back part of vertebra, lamina, to create more space for the spinal cord and nerves. The most common indication for laminectomy is spinal stenosis. Spondylolisthesis and herniated disk are also frequent indications for laminectomy. Decompression surgery is usually performed as part of lumbar fusion surgery. C. Lumbar Fusion Surgery: Lumbar spinal fusion (arthrodesis) is a surgical procedure used to treat spinal conditions of the lumbar, e.g., degenerative disc disease, spinal stenosis, injuries/fractures of the spine, spinal instability, and spondylolisthesis. Spinal 1 Lumbar Spine Surgery Proprietary
2 fusion is a welding process that permanently fuses or joins together two or more adjacent bones in the spine, immobilizing the vertebrae and restricting motion at a painful joint. It is usually performed after other surgical procedures of the spine, such as discectomy or laminectomy. The goal of fusion is to increase spinal stability, reduce irritation of the affected nerve roots, compression on the spinal cord, disability, and pain and/or numbness. Clinical criteria for single level fusion versus multiple level fusions are outlined under the indications section. INDICATIONS FOR LUMBAR & PRE-SACRAL SURGERY: (This section of the clinical guidelines provides the clinical criteria each of the lumbar and pre-sacral spine surgery categories.) Indications for Lumbar Microdiscectomy - Surgical indications for inter-vertebral disc herniation*: o Primary radicular symptoms noted upon clinical exam that hinders daily activities; AND o Failure to improve with at least six consecutive weeks of conservative treatment; AND o Imaging studies showing evidence of inter-vertebral disc herniation *Other indications: Microdiscectomy may be used as the first line of treatment (no conservative treatment required) in the following clinical scenarios: o Progressive nerve compression resulting in an acute neurologic deficit sensory or motor due to herniated disc; OR o Cauda equina syndrome (loss of bowel or bladder control). NOTE: Percutaneous lumbar discectomy or radiofrequency disc decompression procedures are deemed investigational procedures and are not approved. Indications for Lumbar Decompression: Laminectomy, Facetectomy and Foraminotomy. These procedures allow decompression by partial or total removal of various parts of vertebral bone and ligaments. Surgical Indications for spinal canal decompression due to lumbar spinal stenosis*: o Low back pain, neurogenic claudication, and/or radicular leg pain that impairs daily activities for at least twelve (12) weeks; AND o Failure to improve with at least 6 weeks of conservative therapy; AND o Imaging findings consistent with clinical signs/symptoms; AND o Imaging studies do not show evidence of spinal instability. *Other Indications: Lumbar decompression may be used as the first line of treatment (no conservative treatment required) in the following clinical scenarios: o Progressive nerve compression resulting in an acute neurologic (sensory or motor) deficit o Cauda equina syndrome (loss of bowel or bladder control) o Spinal stenosis due to tumor, infection, or trauma Indications for Lumbar Spine Fusion: Single Level with or without decompression 2 Lumbar Spine Surgery Proprietary
3 Because of variable outcomes with fusion surgery, patients should be actively involved in the decision-making process and provided appropriate decision-support materials when considering this intervention. The following indicators must be present*: o Lumbar back pain, neurogenic claudication, and/or radicular leg pain without sensory or motor deficit that impairs daily activities for at least 6 months; AND o Failure to improve with least 6-12 weeks of conservative, non-operative therapy; AND o Imaging studies corresponding to the clinical findings; AND o At least one of the following clinical conditions: a. Spondylolisthesis [Neural Arch Defect -Spondylolytic spondylolisthesis, degenerative spondylolisthesis, and congenital unilateral neural arch hypoplasia]; OR b. Evidence of Segmental Instability -Excessive motion, as in degenerative spondylolisthesis, segmental instability, and surgically induced segmental instability; OR c. Revision surgery for failed previous operation(s) for pseudoarthorsis at the same level at least 6-12 months from prior surgery** if significant functional gains are anticipated; OR d. Revision surgery for failed previous operation(s) repeat disk herniations if significant functional gains are anticipated; OR e. Fusion for the treatment of spinal tumor, cancer, or infection; OR f. Chronic low back pain or degenerative disc disease must have failed at least 6 months of appropriate non-operative treatment (comprehensive rehabilitation) and must be evaluated on a case-by-case basis. *Other Indications: Lumbar spinal fusion may be used as the first line of treatment (no conservative treatment required) in the following clinical scenarios: o Progressive nerve compression resulting in an acute neurologic deficit sensory or motor AND one of the aforementioned clinical conditions, except chronic low back pain or degenerative disc disease. o Cauda equina syndrome (loss of bowel or bladder control) ** REPEAT LUMBAR SPINE FUSION OPERATIONS: Repeat lumbar fusion operations will be reviewed on a case-by-case basis upon submission of medical records and imaging studies that demonstrate remediable pathology. The below must also be documented and available for review of repeat fusion requests: o Rationale as to why surgery is preferred over other non-invasive or less invasive treatment procedures. o Signed documentation that the patient has participated in the decision-making process and understands the high rate of failure/complications. Instrumentation, bone formation or grafting materials, including biologics, should be used at the surgeon s discretion; however, use should be limited to FDA approved devices or biologics and indications. NOTE: Pre-sacral, axial lumbar interbody fusion (AxiaLIF) is not an approved surgical approach due to insufficient evidence. Pre-Sacral Fusion Codes: 0195T, +0196T, 22586, 0309T. Artificial lumbar disc replacement or other lumbar implants are not an approved 3 Lumbar Spine Surgery Proprietary
4 procedure due to insufficient evidence Lumbar Artificial Disc Replacement/Implant Codes: 22857, +0163T, 22862, +0164T, 22865, +0165T, 0221T, +0222T Indications for multi-level fusions with or without decompression (All multi-level fusion surgeries will be reviewed on a case-by-case basis). Because of variable outcomes with fusion surgery, patients should be actively involved in the decision-making process and provided appropriate decision-support materials when considering this intervention. The following clinical indications must be present*: o Lumbar back pain, neurogenic claudication, and/or radicular leg pain without sensory or motor deficit that impairs daily activities for at least 6 months; AND o Failure to improve with least 6-12 weeks of conservative, non-operative therapy; AND o o Imaging studies corresponding to the clinical findings; AND At least one of the following clinical conditions: a. Multiple Level Spondylolisthesis; OR b. Fusion for the treatment of spinal tumor, trauma, cancer, or infection affecting multiple levels; OR c. Intra-Operative Segmental Instability *Other Indications: Lumbar spinal fusion may be used as the first line of treatment (no conservative treatment required) in the following clinical scenarios: o Progressive nerve compression resulting in an acute neurologic deficit (sensory or motor) AND one of the aforementioned clinical conditions. Instrumentation, bone formation or grafting materials, including biologics, should be used at the surgeon s discretion; however, use should be limited to FDA approved devices or biologics and indications. This lumbar surgery guideline does not address spinal deformity surgeries or the clinical indications for spinal deformity surgery [CPT codes ]. NOTE: Pre-sacral, axial lumbar interbody fusion (AxiaLIF) is not an approved surgical approach due to insufficient evidence. Pre-Sacral Fusion Codes: 0195T, +0196T, 22586, 0309T. Artificial lumbar disc replacement or other lumbar implants are not an approved procedure due to insufficient evidence Lumbar Artificial Disc Replacement/Implant Codes: 22857, +0163T, 22862, +0164T, 22865, +0165T, 0221T, +0222T CONTRAINDICATIONS FOR SPINE SURGERY Medical contraindications to surgery, e.g., severe osteoporosis; infection of soft tissue adjacent to the spine, whether or not it has spread to the spine; severe cardiopulmonary disease; anemia; malnutrition and systemic infection Psychosocial risk factors. It is imperative to rule out non-physiologic modifiers of pain presentation or non-operative conditions mimicking radiculopathy or instability (e.g., peripheral neuropathy, piriformis syndrome, myofascial pain, sympathetically mediated pain syndromes, sacroiliac dysfunction, psychological conditions, etc.) prior to consideration of elective surgical intervention. 4 Lumbar Spine Surgery Proprietary
5 Active Tobacco use prior to fusion surgery. It is recommended that the patient refrain from smoking for at least six weeks prior to surgery and during the period of fusion healing. Morbid Obesity. Contraindication to surgery in cases where there is significant risk and concern for improper post-operative healing, post-operative complications related to morbid obesity, and/or an inability to participate in post-operative rehabilitation. ADDITIONAL INFORMATION Services Not Covered: The following procedures are considered either still under investigation or are not recommended based upon the current evidence: Percutaneous lumbar discectomy; Laser discectomy; Percutaneous Radiofrequency Disc Decompression; intradiscal electrothermal annuloplasty (IDEA) or more commonly called IDET (Intradiscal Electrothermal therapy); Nucleus Pulpous Replacement; Pre-Sacral Fusion, or Lumbar Artificial Disc Replacement. PERCUTANEOUS DISCECTOMY is an invasive operative procedure to accomplish partial removal of the disc through a needle which allows aspiration of a portion of the disc trocar under imaging control. Percutaneous discectomy is rarely indicated. It is sometimes useful in suspected septic discitis or in order to obtain diagnostic tissue. Percutaneous discectomy is not recommended for contained disc herniations or bulges with associated radiculopathy, due to lack of evidence to support long-term improvement. This includes radiofrequency disc decompression. LASER DISCECTOMY is a procedure which involves the delivery of laser energy into the center of the nucleus pulposus using a fluoroscopically guided laser fiber under local anesthesia. The energy denatures protein in the nucleus, causing a structural change which is intended to reduce intradiscal pressure. Its effectiveness has not been fully established. INTRADISCAL ELECTROTHERMAL ANNULOPLASTY (IDEA) (more commonly called IDET, or Intradiscal Electrothermal therapy) is an outpatient non-operative procedure in which a wire is guided into the identified painful disc using fluoroscopy. The wire is then heated at the nuclear-annular junction within the disc. Physicians performing this procedure must have been trained in the procedure and certified. Surgical Indications: Failure of conservative therapy including physical therapy, medication management, or therapeutic injections. Indications may include those with chronic low back pain, disc related back pain, or pain lasting for greater than 6 months. There is conflicting evidence regarding its effectiveness. NUCLEUS PULPOSUS REPLACEMENT Involves the introduction of a prosthetic implant into the intervertebral disc, replacing the nucleus pulposus while preserving the annulus fibrosus. INDICATIONS: Nucleus Pulposus Replacement is limited to investigational use in the United States at this time and is not recommended 5 Lumbar Spine Surgery Proprietary
6 LUMBAR ARTIFICIAL DISC REPLACEMENT: Involves the insertion of a prosthetic device into an intervertebral space from which a degenerated disc has been removed, sparing only the peripheral annulus. The prosthetic device is designed to distribute the mechanical load of the vertebrae in a physiologic manner and maintain range of motion. Studies do not demonstrate a long-term advantage of measured function or pain over comparison groups undergoing fusion. The longevity of this prosthetic device has not yet been determined. Lumbar Artificial Disc Replacement Codes: 22857, +0163T, 22862, +0164T, 22865, +0165T, 0221T, +0222T Conservative Therapy: (musculoskeletal) includes a combination of modalities, such as rest, ice, heat, modified activities, medical devices, (such as crutches, immobilizer, metal braces, orthotics, rigid stabilizer or splints, etc and not to include neoprene sleeves), medications, diathermy, chiropractic treatments, or physician supervised home exercise program. Part of this combination may include the physician instructing patient to rest the area or stay off the injured part. Home Exercise Program - (HEP) the following two elements are required to meet guidelines for completion of conservative therapy: o Information provided on exercise prescription/plan AND o Follow up with member with information provided regarding completion of HEP (after suitable 4-6 week period), or inability to complete HEP due to physical reasoni.e. increased pain, inability to physically perform exercises. (Patient inconvenience or noncompliance without explanation does not constitute inability to complete HEP). Claims Billing & Coding: NIA uses a combination of internally developed edits in addition to an enhanced set of industry standard editing. NIA s Claims Edit Module is a group of system edits that run multiple times per day. Edits that are part of this module include industry standard edits that apply to spine surgery services and NIA custom edits developed specifically for spine surgery. The following describes each of the edits NIA applies: Outpatient Code Editor (OCE): This edit performs all functions that require specific reference to HCPCS codes, HCPCS modifiers, and ICD-9-CM diagnosis codes. The OCE only functions on a single claim and does not have any cross claim capabilities. NIA is consistent with CMS. National Correct Coding Initiative (NCCI) editing: The edit prevents improper payment when incorrect code combinations are reported. The NCCI contains two tables of edits. The Column One/Column Two Correct Coding Edits table and the Mutually Exclusive Edits table include code pairs that should not be reported together for a number of reasons explained in the Coding Policy Manual. NIA is consistent with CMS. o Incidental edits: This edit applies if a procedure being billed is a component of another procedure that occurred on the same date of service for the same provider and tax ID and claimant. 6 Lumbar Spine Surgery Proprietary
7 o Mutually exclusive editing: This edit applies if a procedure being billed is mutually exclusive with a procedure that occurred on the same date of service for the same provider tax ID and claimant. Multiple Procedure Discounts (MPD): This edit applies a reduction to the second and any other subsequent services by the same provider, in the same setting, for the same member. We typically apply a 50% reduction. NIA follows the CMS methodology that began in January 2011 which allows for application of MPD to codes within CMS s two specific advanced imaging code families. However, NIA differs from CMS in that we apply MPD to all provider types unless health plan contracts prohibit this. Lumbar Fusion - Fusions can be performed either anteriorly, laterally, or posteriorly, or via a combined approach; although simple posterolateral fusions are indicated in the great majority of cases requiring fusion. These are the surgical approaches: Intertransverse Fusion or Posterolateral Fusion Anterior Interbody Fusion (ALIF) Lateral or Transpsoas Interbody Fusion (XLIF) Posterior or Trans-foraminal Interbody Fusion (PLIF or TLIF) Anterior/posterior Fusion (360-degree) Pre-sacral, axial lumbar interbody fusion (AxiaLIF) is still being investigated and is not recommended. Use of bone grafts including autologous or allograft which might be combined with metal or biocompatible devices to produce a rigid, bony connection between two or more adjacent vertebrae are common. Bone formation or grafting materials including biologics should be used at the surgeon s discretion; however, use of biologics should be limited to FDA approved indications in order to limit complications (especially BMP). All operative interventions must be based upon positive correlation of clinical findings, clinical course, and diagnostic tests. A comprehensive assimilation of these factors must lead to a specific diagnosis with positive identification of pathologic condition(s). It is imperative to rule out non-physiologic modifiers of pain presentation or non-operative conditions mimicking radiculopathy or instability (e.g., peripheral neuropathy, piriformis syndrome, myofascial pain, sympathetically mediated pain syndromes, sacroiliac dysfunction, psychological conditions, etc.) prior to consideration of elective surgical intervention. Operative treatment is indicated when the natural history of surgically treated lesions is better than the natural history for non-operatively treated lesions. All patients being considered for surgical intervention should first undergo a comprehensive neuro-musculoskeletal examination to identify mechanical pain generators that may respond to non-surgical techniques or may be refractory to surgical intervention. While sufficient time allowances for non-operative treatment are required to determine the natural cause and response to non-operative treatment of low back pain disorders, 7 Lumbar Spine Surgery Proprietary
8 timely decision making for operative intervention is critical to avoid de-conditioning and increased disability (exclusive of "emergent" or urgent pathology such as cauda equina syndrome or associated rapidly progressive neurologic loss). In general, if the program of non-operative treatment fails, operative treatment is indicated when: Improvement of the symptoms has plateaued or failed to occur and the residual symptoms of pain and functional disability are unacceptable at the end of 6 to 12 weeks of active treatment, or at the end of longer duration of non-operative programs for debilitated patients with complex problems; and/or Frequent recurrences of symptoms cause serious functional limitations even if a nonoperative active treatment program provides satisfactory relief of symptoms, and restoration of function on each recurrence. Lumbar spinal stenosis and associated lumbar spondylolisthesis - Spinal stenosis is narrowing of the spinal column or of the neural foramina where spinal nerves leave the spinal column, causing pressure on the spinal cord. The most common cause is degenerative changes in the lumbar spine. Neurogenic claudication is the most common symptom, referring to leg symptoms encompassing the buttock, groin and anterior thigh, as well as radiation down the posterior part of the leg to the feet. i In addition to pain, leg symptoms can include fatigue, heaviness, weakness and/or paresthesia. Some patients may also suffer from accompanying back pain. Symptoms are worse when standing or walking and are relieved by sitting. Lumbar spinal stenosis is often a disabling condition, and it is the most common reason for lumbar spinal surgery in adults over 65 years. Degenerative lumbar spondylolisthesis - is the displacement of a vertebra in the lower part of the spine; one lumbar vertebra slips forward on another with an intact neural arch and begins to press on nerves. The slippage occurs at the L4-L5 level most commonly. The most common cause, in adults, is degenerative disease although it may also result from bone diseases and fractures. Spondylolisthesis seldom occurs before the age of 50 years and it disproportionately affects women, especially black women. Degenerative spondylolisthesis is not always symptomatic. Lumbar degenerative disease without stenosis or spondylolisthesis - Spondylosis is an umbrella term describing age-related degeneration of the spine. Lumbar degenerative disease without stenosis or spondylolisthesis is characterized by disabling low back pain and spondylosis at L4-5, L5-S1, or both levels. 8 Lumbar Spine Surgery Proprietary
9 REFERENCES Atlas, S.J., Keller, R.B., Wu, Y.A., Deyo, R.A., & Singer, D.E. (2005). Long-term outcomes of surgical and nonsurgical management of lumbar spinal stenosis: 8 to 10 year results from the Maine lumbar spine study. Spine, 30(8), Retrieved from Bogduk, N., & Andersson, G. (2009). Is spinal surgery effective for back pain? F1000 Med Rep., 1, 60. doi: /M1-60. Brox, I.J., Sorensen, R., Friis, A., Nyygaard, O., Indahl, A., Keller, A., Reikeras, O. (2003). Randomized clinical trial of lumbar instrumented fusion and cognitive intervention and exercises in patients with chronic low back pain and disc degeneration. Spine, 28(17), Retrieved from Carreon, L.Y., Glassman, S.D., & Howard, J. (2008). Fusion and nonsurgical treatment for symptomatic lumbar degenerative disease: A systematic review of Oswestry Disability Index and MOS Short Form-36 outcomes. The Spine Journal, 8(5), Retrieved from Chou, R., Baisden, J., Carragee, E.J., Resnick, D.K., Shaffer, W.O., & Loeser, J.D. (2009). Surgery for low back pain: A review of the evidence for an American Pain Society Clinical Practice Guideline. Spine, 34(10), doi: /BRS.0b013e3181a105fc. Deyo, R.A., Mirza, S.K., Martin, B.I., Kreuter, W., Goodman, D.C., & Jarvik, J.G. (2010). Trends, major medical complications, and charges associated with surgery for lumbar spinal stenosis in older adults. JAMA, 303(13), doi: /jama Fardon, D.R., & Milette, P.C. (2001). Nomenclature and classification of lumbar disc pathology: Recommendations of the combined task forces of the North American Spine Society, American Society of Spine Radiology, and American Society of Neuroradiology. Spine, 26(5), E93-E113. Retrieved from re+and+classification+of+lumbar+disc+pathology%3a+recommendations+of+the+combi ned+task+forces+of+the+north+americvan+spine+society%2c+american+society+of+ Spine+Radiology%2C+and+American+Society+of+Neuroradiology.+Spine+2001%3B+26 (5)%3AE93-E113 Fritzell, P., Wessberg, P., & Nordwall, A. (2001). Swedish Lumbar Spine Study Group: Lumbar fusion versus nonsurgical treatment for chronic low back pain A multicenter randomized controlled trial from the Swedish Lumbar Spine Study Group. Spine, 26(23), Retrieved from Genevay, S., & Atlas, S.J. (2010). Lumbar spinal stenosis. Best Pract Res Clin Rheumatol, 24(2), doi: /j.berh Lumbar Spine Surgery Proprietary
10 North American Spine Society (NASS). (2009). Clinical Guidelines for Multidisciplinary Spine Care: Diagnosis and Treatment of Degenerative Lumbar Spondylolisthesis. doi: /j.spinee Peul, W.C., van Houwelingen, H.C., van den Hout, W.B., Brand R., Eekhof, J.A., Tans, J.T., Leiden-The Hague Spine Intervention Prognostic Study Group. (2007). Surgery versus prolonged conservative treatment for sciatica. N Engl J Med., 356, Retrieved from Resnick, D.K., Choudhri, T.F., Dailey, A.T., Groff, M.W., Khoo, L., Matz, P.G., Hadley, M.N. (2005). Guidelines for the performance of fusion procedures for degenerative disease of the lumbar spine. Part 7: Intractable low-back pain without stenosis or spondylolisthesis. J Neurosurg: Spine, 2, Retrieved from Tosteson, A.N.A., Tosteson,T.D., Lurie, J.D., Abdu, W., Herkowitz, H., Andersson, G., Weinstein, J.N. (2011). Comparative effectiveness evidence from the spine patient outcomes research trial: surgical versus nonoperative care for spinal stenosis, degenerative spondylolisthesis, and intervertebral disc herniation. Spine, 36(24), doi: /BRS.0b013e b. Tosteson, A.N.A., Lurie, J.D., Tosteson, T.D., Skinner, J.S., Hertowitz, H., Albert, T., Weinstein, J.N. (2008). Surgical treatment of spinal stenosis with and without degenerative spondylolisthesis: Cost-effectiveness after 2 years. Ann Intern Med, 149(2), Retrieved from Weinstein, J.N., Lurie, J.D., Tosteson, T.D., Hanscom, B., Tosteson, A.N.A., Blood E.A., Hu, S.S. (2007). Surgical versus nonsurgical treatment for lumbar degenerative spondylolisthesis. N Engl J Med., 356(22), Retrieved from 10 Lumbar Spine Surgery Proprietary
Magellan Clinical Guidelines for Medical Necessity Review
 2018-2019 Magellan Clinical Guidelines for Medical Necessity Review MUSCULOSKELETAL AND SURGERY GUIDELINES HAWAI I MEDICAL SERVICE ASSOCIATION (HMSA) Effective: July 1, 2018 2018-2019 Magellan Health,
2018-2019 Magellan Clinical Guidelines for Medical Necessity Review MUSCULOSKELETAL AND SURGERY GUIDELINES HAWAI I MEDICAL SERVICE ASSOCIATION (HMSA) Effective: July 1, 2018 2018-2019 Magellan Health,
Key Primary CPT Codes: Refer to pages: 7-9 Last Review Date: October 2016 Medical Coverage Guideline Number:
 National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
Medical Policy Original Effective Date: Revised Date: Page 1 of 11
 Page 1 of 11 Content Disclaimer Description Coverage Determination Clinical Indications Lumbar Spine Surgery Lumbar Spine Surgery Description Indication Coding Lumbar Spinal Fusion (single level)surgery
Page 1 of 11 Content Disclaimer Description Coverage Determination Clinical Indications Lumbar Spine Surgery Lumbar Spine Surgery Description Indication Coding Lumbar Spinal Fusion (single level)surgery
If you have a condition that compresses your nerves, causing debilitating back pain or numbness along the back of your leg.
 Below, we have provided some basic information for your benefit. Please use this information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk
Below, we have provided some basic information for your benefit. Please use this information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk
National Imaging Associates, Inc. Clinical guidelines
 National Imaging Associates, Inc. Clinical guidelines Original Date: September 1997 THORACIC SPINE CT Page 1 of 5 CPT Codes: 72128, 72129, 72130 Last Review Date: May 2013 Guideline Number: NIA_CG_043
National Imaging Associates, Inc. Clinical guidelines Original Date: September 1997 THORACIC SPINE CT Page 1 of 5 CPT Codes: 72128, 72129, 72130 Last Review Date: May 2013 Guideline Number: NIA_CG_043
Back Pain Policies Summary
 Back Pain Policies Summary These policies are part of the wider project, Reviewing local health policies, which is reviewing and updating more than 100 policies, of which back pain are part of. This review
Back Pain Policies Summary These policies are part of the wider project, Reviewing local health policies, which is reviewing and updating more than 100 policies, of which back pain are part of. This review
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2017 5/2018 5/2017 Description of Procedure or Service Low back pain
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2017 5/2018 5/2017 Description of Procedure or Service Low back pain
DEGENERATIVE SPONDYLOLISTHESIS
 AN INTRODUCTION TO DEGENERATIVE SPONDYLOLISTHESIS This booklet is designed to inform you about lumbar degenerative spondylolisthesis. It is not meant to replace any personal conversations that you might
AN INTRODUCTION TO DEGENERATIVE SPONDYLOLISTHESIS This booklet is designed to inform you about lumbar degenerative spondylolisthesis. It is not meant to replace any personal conversations that you might
Lumbar Spinal Fusion Corporate Medical Policy
 Lumbar Spinal Fusion Corporate Medical Policy File name: Lumbar Spinal Fusion File code: UM.SURG.15 Origination: 09/01/2016 Last Review: 09/29/2016 Next Review: 09/29/2017 Effective Date: 01/01/2017 Populations
Lumbar Spinal Fusion Corporate Medical Policy File name: Lumbar Spinal Fusion File code: UM.SURG.15 Origination: 09/01/2016 Last Review: 09/29/2016 Next Review: 09/29/2017 Effective Date: 01/01/2017 Populations
Anthem Blue Cross and Blue Shield Central Region Clinical Claim Edit
 Subject: Laminotomy (Hemilaminectomy) with Decompression of Nerve Root(s), Including Partial Facetectomy, Foraminotomy and/or Excision of Herniated Intervertebral Disc, Reexploration, Single Interspace-Lumbar
Subject: Laminotomy (Hemilaminectomy) with Decompression of Nerve Root(s), Including Partial Facetectomy, Foraminotomy and/or Excision of Herniated Intervertebral Disc, Reexploration, Single Interspace-Lumbar
Table of Contents: Part 1 General principles. Section 1: Introduction. 1. Past, present and future of interventional physiatry 2.
 Table of Contents: Part 1 General principles Section 1: Introduction 1. Past, present and future of interventional physiatry 2. Epidemiology Section 2: Spinal pain 3. Inflammatory basis of spinal pain
Table of Contents: Part 1 General principles Section 1: Introduction 1. Past, present and future of interventional physiatry 2. Epidemiology Section 2: Spinal pain 3. Inflammatory basis of spinal pain
Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS NASS COVERAGE POLICY RECOMMENDATIONS TASKFORCE
 NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
Populations Interventions Comparators Outcomes Individuals: With lumbar spinal stenosis
 Image-Guided Minimally Invasive Decompression for Spinal (701126) (Formerly Image-Guided Minimally Invasive Lumbar Decompression for Spinal ) Medical Benefit Effective Date: 10/01/17 Next Review Date:
Image-Guided Minimally Invasive Decompression for Spinal (701126) (Formerly Image-Guided Minimally Invasive Lumbar Decompression for Spinal ) Medical Benefit Effective Date: 10/01/17 Next Review Date:
University of Jordan. Professor Freih Abuhassan -
 Freih Odeh Abu Hassan F.R.C.S.(Eng.), F.R.C.S.(Tr.& Orth.). Professor of Orthopedics University of Jordan 1 A. Sacroiliitis History Trauma is very common Repetitive LS motion--lumbar rotation or axial
Freih Odeh Abu Hassan F.R.C.S.(Eng.), F.R.C.S.(Tr.& Orth.). Professor of Orthopedics University of Jordan 1 A. Sacroiliitis History Trauma is very common Repetitive LS motion--lumbar rotation or axial
FirstCarolinaCare Spinal Surgery Prior authorization Guidelines
 FirstCarolinaCare Spinal Surgery Prior authorization Guidelines Subject LUMBAR FUSION (arthrodesis) Next Review 06/2014 General Requirements for Lumbar Spinal Fusion: 1. Prior authorization is required
FirstCarolinaCare Spinal Surgery Prior authorization Guidelines Subject LUMBAR FUSION (arthrodesis) Next Review 06/2014 General Requirements for Lumbar Spinal Fusion: 1. Prior authorization is required
Cervical intervertebral disc disease Degenerative diseases F 04
 Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
You Don t Understand This Stuff???
 SPINE SURGERY You Don t Understand This Stuff??? Welcome to the club Most PCP s don t understand what we do Half of other orthopods don t get it Sometimes we can t even explain it to each other Why would
SPINE SURGERY You Don t Understand This Stuff??? Welcome to the club Most PCP s don t understand what we do Half of other orthopods don t get it Sometimes we can t even explain it to each other Why would
Corporate Medical Policy
 Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
PROCEDURES WE PERFORM
 PROCEDURES WE PERFORM Decompression, Stabilization, and More North American Spine offers a family of advanced, minimally invasive procedures that are highly effective in treating most forms of chronic
PROCEDURES WE PERFORM Decompression, Stabilization, and More North American Spine offers a family of advanced, minimally invasive procedures that are highly effective in treating most forms of chronic
ACDF. Anterior Cervical Discectomy and Fusion. An introduction to
 An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
Populations Interventions Comparators Outcomes Individuals: With lumbar spinal stenosis
 Image-Guided Minimally Invasive Decompression for Spinal (701126) Medical Benefit Effective Date: 10/01/18 Next Review Date: 07/19 Preauthorization No Review Dates: 09/10, 07/11, 07/12, 07/13, 07/14, 07/15,
Image-Guided Minimally Invasive Decompression for Spinal (701126) Medical Benefit Effective Date: 10/01/18 Next Review Date: 07/19 Preauthorization No Review Dates: 09/10, 07/11, 07/12, 07/13, 07/14, 07/15,
NIA Clinical Guidelines for Medical Necessity Review
 2018-2019 for Medical Necessity Review MUSCULOSKELETAL AND SURGERY GUIDELINES 2018-2019 Magellan Health, Inc. Proprietary Page 1 of 130 Guidelines for Clinical Review Determination Preamble NIA is committed
2018-2019 for Medical Necessity Review MUSCULOSKELETAL AND SURGERY GUIDELINES 2018-2019 Magellan Health, Inc. Proprietary Page 1 of 130 Guidelines for Clinical Review Determination Preamble NIA is committed
SpineFAQs. Lumbar Spondylolisthesis
 SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
Patient Selection and Lumbar Operative Interventions
 Patient Selection and Lumbar Operative Interventions John C France MD Professor of Orthopaedic & Neurosurgery West Virginia University Low back pain is a symptom not a diagnosis Epidemiology of LBP General
Patient Selection and Lumbar Operative Interventions John C France MD Professor of Orthopaedic & Neurosurgery West Virginia University Low back pain is a symptom not a diagnosis Epidemiology of LBP General
Common Thoraco- Lumbar Problems in the Mature Athlete
 Common Thoraco- Lumbar Problems in the Mature Athlete Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University Objectives Review the pathophysiology of the
Common Thoraco- Lumbar Problems in the Mature Athlete Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University Objectives Review the pathophysiology of the
POSTERIOR CERVICAL FUSION
 AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
SpineFAQs. Neck Pain Diagnosis and Treatment
 SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
THRESHOLD POLICY T17 SPINAL SURGERY FOR ACUTE LUMBAR CONDITIONS
 THRESHOLD POLICY T17 SPINAL SURGERY FOR ACUTE LUMBAR CONDITIONS Policy author: Ipswich and East Suffolk and West Suffolk CCGs with support from Public Health Suffolk Policy start date: September 2014 Subsequent
THRESHOLD POLICY T17 SPINAL SURGERY FOR ACUTE LUMBAR CONDITIONS Policy author: Ipswich and East Suffolk and West Suffolk CCGs with support from Public Health Suffolk Policy start date: September 2014 Subsequent
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/29800 holds various files of this Leiden University dissertation. Author: Moojen, Wouter Anton Title: Introducing new implants and imaging techniques for
Cover Page The handle http://hdl.handle.net/1887/29800 holds various files of this Leiden University dissertation. Author: Moojen, Wouter Anton Title: Introducing new implants and imaging techniques for
Anterior cervical diskectomy icd 10 procedure code
 Home Anterior cervical diskectomy icd 10 procedure code Access to discounts at hundreds of restaurants, travel destinations, retail stores, and service providers. AAPC members also have opportunities to
Home Anterior cervical diskectomy icd 10 procedure code Access to discounts at hundreds of restaurants, travel destinations, retail stores, and service providers. AAPC members also have opportunities to
Interventional Pain Management
 Origination: 5/21/08 Revised: 10/02/17 Annual Review: 11/02/17 Purpose: To provide interventional pain management clinical coordination criteria for the Medical Department staff to reference when making
Origination: 5/21/08 Revised: 10/02/17 Annual Review: 11/02/17 Purpose: To provide interventional pain management clinical coordination criteria for the Medical Department staff to reference when making
Spinal Fusion. North American Spine Society Public Education Series
 Spinal Fusion North American Spine Society Public Education Series What Is Spinal Fusion? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
Spinal Fusion North American Spine Society Public Education Series What Is Spinal Fusion? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
22110 vertebral segment; cervical vertebral segment; thoracic vertebral segment; lumbar
 The following codes are authorized by Palladian Health for applicable product lines. Visit palladianhealth.com to request authorization and to access guidelines. Palladian Musculoskeletal Program Codes
The following codes are authorized by Palladian Health for applicable product lines. Visit palladianhealth.com to request authorization and to access guidelines. Palladian Musculoskeletal Program Codes
PATIENT: DOB: TODAY S DATE:
 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand this material. I also understand that if certain sections are not
1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand this material. I also understand that if certain sections are not
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Lumbar Spinal Fusion Page 1 of 29 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Lumbar Spinal Fusion Page 1 of 29 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Anterior Cervical Discectomy and Fusion Surgery
 Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Lumbar Spinal Fusion Page 1 of 28 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Lumbar Spinal Fusion Page 1 of 28 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Guideline Number: NIA_CG_301 Last Revised Date: March 2018 Responsible Department: Clinical Operations
 Magellan Healthcare Clinical guidelines PARAVERTEBRAL FACET JOINT INJECTIONS OR BLOCKS (no U/S) CPT Codes: Cervical Thoracic Region: 64490 (+ 64491, +64492) Lumbar Sacral Region: 64493 (+64494, +64495)
Magellan Healthcare Clinical guidelines PARAVERTEBRAL FACET JOINT INJECTIONS OR BLOCKS (no U/S) CPT Codes: Cervical Thoracic Region: 64490 (+ 64491, +64492) Lumbar Sacral Region: 64493 (+64494, +64495)
Objectives. Comprehension of the common spine disorder
 Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
 The spine is made of a column of bones. Each bone, or vertebra, is formed by a round block of bone, called a vertebral body. A bony ring attaches to the back of the vertebral body. When the vertebra bones
The spine is made of a column of bones. Each bone, or vertebra, is formed by a round block of bone, called a vertebral body. A bony ring attaches to the back of the vertebral body. When the vertebra bones
Copyright 2017 Dr. David Hendrickson Discover Life Chiroprac c 5015 Tacoma Mall Blvd Ste E102 Tacoma, WA Phone #: (253)
 Copyright 2017 Dr. David Hendrickson Discover Life Chiroprac c 5015 Tacoma Mall Blvd Ste E102 Tacoma, WA 98409 Phone #: (253) 472 4400 www.discoverlifechiro.com Chiropractic and Sciatica Sciatica is a
Copyright 2017 Dr. David Hendrickson Discover Life Chiroprac c 5015 Tacoma Mall Blvd Ste E102 Tacoma, WA 98409 Phone #: (253) 472 4400 www.discoverlifechiro.com Chiropractic and Sciatica Sciatica is a
5/19/2017. Interspinous Process Fixation with the Minuteman G3. What is the Minuteman G3. How Does it Work?
 Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Spine Conditions and Treatments. Your Guide to Common
 Your Guide to Common Spine Conditions and Treatments The spine is made up of your neck and backbone. It allows your body to bend and move freely. As you get older, it is normal to have aches and pains.
Your Guide to Common Spine Conditions and Treatments The spine is made up of your neck and backbone. It allows your body to bend and move freely. As you get older, it is normal to have aches and pains.
Spinal canal stenosis Degenerative diseases F 06
 What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
Corporate Medical Policy
 Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
Related Policies None
 Medical Policy MP 7.01.541 BCBSA Ref. Policy: 7.01.141 Last Review: 06/27/2018 Effective Date: 06/27/2018 Section: Surgery Related Policies None DISCLAIMER Our medical policies are designed for informational
Medical Policy MP 7.01.541 BCBSA Ref. Policy: 7.01.141 Last Review: 06/27/2018 Effective Date: 06/27/2018 Section: Surgery Related Policies None DISCLAIMER Our medical policies are designed for informational
The main causes of cervical radiculopathy include degeneration, disc herniation, and spinal instability.
 SpineFAQs Cervical Radiculopathy Neck pain has many causes. Mechanical neck pain comes from injury or inflammation in the soft tissues of the neck. This is much different and less concerning than symptoms
SpineFAQs Cervical Radiculopathy Neck pain has many causes. Mechanical neck pain comes from injury or inflammation in the soft tissues of the neck. This is much different and less concerning than symptoms
MUSCULOSKELETAL AND SPINE SURGERY GUIDELINES DEAN HEALTH PLAN
 2017-2018 MAGELLAN 1 CLINICAL GUIDELINES FOR MEDICAL NECESSITY REVIEW MUSCULOSKELETAL AND SPINE SURGERY GUIDELINES DEAN HEALTH PLAN National Imaging Associates, Inc. is a subsidiary of Magellan Healthcare,
2017-2018 MAGELLAN 1 CLINICAL GUIDELINES FOR MEDICAL NECESSITY REVIEW MUSCULOSKELETAL AND SPINE SURGERY GUIDELINES DEAN HEALTH PLAN National Imaging Associates, Inc. is a subsidiary of Magellan Healthcare,
Virginia Spine Institute - FAQs
 Virginia Spine Institute - FAQs 1. What are common causes of back pain? Back pain is one of the most common ailments known to man. Approximately 80% of the adult population will develop a significant episode
Virginia Spine Institute - FAQs 1. What are common causes of back pain? Back pain is one of the most common ailments known to man. Approximately 80% of the adult population will develop a significant episode
Corporate Medical Policy
 Corporate Medical Policy Axial Lumbosacral Interbody Fusion File Name: Origination: Last CAP Review: Next CAP Review: Last Review: axial_lumbosacral_interbody_fusion 6/2009 10/2017 10/2018 10/2017 Description
Corporate Medical Policy Axial Lumbosacral Interbody Fusion File Name: Origination: Last CAP Review: Next CAP Review: Last Review: axial_lumbosacral_interbody_fusion 6/2009 10/2017 10/2018 10/2017 Description
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Back and Neck Injuries: Surgical Advances and Treatment
 Back and Neck Injuries: Surgical Advances and Treatment Ara Deukmedjian, MD Board Certified Neurosurgeon June 8, 2017 1 2 Spinal Joints: Anatomy Two types of Spinal Joints: Spinal (intervertebral) disc
Back and Neck Injuries: Surgical Advances and Treatment Ara Deukmedjian, MD Board Certified Neurosurgeon June 8, 2017 1 2 Spinal Joints: Anatomy Two types of Spinal Joints: Spinal (intervertebral) disc
RADICULOPATHY AN INTRODUCTION TO
 AN INTRODUCTION TO RADICULOPATHY This booklet provides general information on radiculopathy. It is not meant to replace any personal conversations that you might wish to have with your physician or other
AN INTRODUCTION TO RADICULOPATHY This booklet provides general information on radiculopathy. It is not meant to replace any personal conversations that you might wish to have with your physician or other
Degenerative Disease of the Spine
 Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Common Conditions. Visit our homepage for more info >> TABLE OF CONTENTS. Bulging/Herniated Disc... PAGE 2. Cervical (Neck) Pain...
 Common Conditions TABLE OF CONTENTS Bulging/Herniated Disc... PAGE 2 Cervical (Neck) Pain... PAGE 3 Degenerative Disc Disease... PAGE 4 Sciatica...PAGE 5 Spinal Stenosis... PAGE 6 Spondylolisthesis...
Common Conditions TABLE OF CONTENTS Bulging/Herniated Disc... PAGE 2 Cervical (Neck) Pain... PAGE 3 Degenerative Disc Disease... PAGE 4 Sciatica...PAGE 5 Spinal Stenosis... PAGE 6 Spondylolisthesis...
Clinical Policy: Disc Decompression Procedures Reference Number: CP.MP.114
 Clinical Policy: Reference Number: CP.MP.114 Effective Date: 07/16 Last Review Date: 07/16 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.114 Effective Date: 07/16 Last Review Date: 07/16 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Facet Arthroplasty. Policy Number: Last Review: 9/2018 Origination: 9/2009 Next Review: 3/2019
 Facet Arthroplasty Policy Number: 7.01.120 Last Review: 9/2018 Origination: 9/2009 Next Review: 3/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for total facet
Facet Arthroplasty Policy Number: 7.01.120 Last Review: 9/2018 Origination: 9/2009 Next Review: 3/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for total facet
2012 CPT Coding Update AANS/CNS Joint Section on Disorders of the Spine and Peripheral Nerves
 2012 CPT Coding Update AANS/CNS Joint Section on Disorders of the Spine and Peripheral Nerves Joseph S. Cheng, M.D., M.S. Associate Professor of Neurological Surgery, Orthopedic Surgery, and Rehabilitation
2012 CPT Coding Update AANS/CNS Joint Section on Disorders of the Spine and Peripheral Nerves Joseph S. Cheng, M.D., M.S. Associate Professor of Neurological Surgery, Orthopedic Surgery, and Rehabilitation
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine...2 General Conditions of the Spine...4 6 MIS-TLIF
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine...2 General Conditions of the Spine...4 6 MIS-TLIF
MEDICAL POLICY MEDICAL POLICY DETAILS POLICY STATEMENT. Page: 1 of 5
 Page: 1 of 5 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title LUMBAR DECOMPRESSION Policy Number 7.01.97 Category Technology Assessment Effective Date 06/21/18 Revised Date 12/20/18 Product Disclaimer
Page: 1 of 5 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title LUMBAR DECOMPRESSION Policy Number 7.01.97 Category Technology Assessment Effective Date 06/21/18 Revised Date 12/20/18 Product Disclaimer
Lumbar spinal canal stenosis Degenerative diseases F 08
 What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
2017 NIA Clinical Guidelines for Medical Necessity Review
 2017 for Medical Necessity Review MUSCULOSKELETAL AND SURGERY GUIDELINES 2017 Magellan Health, Inc. Proprietary Page 1 of 125 Guidelines for Clinical Review Determination Preamble NIA is committed to the
2017 for Medical Necessity Review MUSCULOSKELETAL AND SURGERY GUIDELINES 2017 Magellan Health, Inc. Proprietary Page 1 of 125 Guidelines for Clinical Review Determination Preamble NIA is committed to the
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): July 1, 2002 Most Recent Review Date (Revised): November 26, 2013 Effective Date: June 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
Original Issue Date (Created): July 1, 2002 Most Recent Review Date (Revised): November 26, 2013 Effective Date: June 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
Patient Information ACDF. Anterior Cervical Discectomy and Fusion
 Patient Information ACDF Anterior Cervical Discectomy and Fusion Table of Contents Anatomy of the Spine...2-3 General Conditions of the Cervical Spine...4 5 What is an ACDF?...6 How is an ACDF performed?...7
Patient Information ACDF Anterior Cervical Discectomy and Fusion Table of Contents Anatomy of the Spine...2-3 General Conditions of the Cervical Spine...4 5 What is an ACDF?...6 How is an ACDF performed?...7
RETROLISTHESIS. Retrolisthesis. is found mainly in the cervical spine and lumbar region but can also be often seen in the thoracic spine
 RETROLISTHESIS A retrolisthesis is a posterior displacement of one vertebral body with respect to adjacent vertebrae Typically a vertebra is to be in retrolisthesis position when it translates backward
RETROLISTHESIS A retrolisthesis is a posterior displacement of one vertebral body with respect to adjacent vertebrae Typically a vertebra is to be in retrolisthesis position when it translates backward
Lumbar Disc Prolapse. Dr. Ahmed Salah Eldin Hassan. Professor of Neurosurgery & Consultant spinal surgeon
 Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Herniated Disc Treatment Non-covered Procedures
 Herniated Disc Treatment Non-covered Procedures Date of Origin: 03/2004 Last Review Date: 03/22/2017 Effective Date: 03/22/2017 Dates Reviewed: 02/2005, 02/2006, 02/2007, 03/2008, 01/2009, 04/2009, 02/2011,
Herniated Disc Treatment Non-covered Procedures Date of Origin: 03/2004 Last Review Date: 03/22/2017 Effective Date: 03/22/2017 Dates Reviewed: 02/2005, 02/2006, 02/2007, 03/2008, 01/2009, 04/2009, 02/2011,
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis This article is also available in Spanish: Estenosis de la columna lumbar (topic.cfm?topic=a00701). A common cause of low back and leg pain is lumbar spinal stenosis. As we age,
Lumbar Spinal Stenosis This article is also available in Spanish: Estenosis de la columna lumbar (topic.cfm?topic=a00701). A common cause of low back and leg pain is lumbar spinal stenosis. As we age,
PARADIGM SPINE. Patient Information. Treatment of a Narrow Lumbar Spinal Canal
 PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
CERVICAL PROCEDURES PHYSICIAN CODING
 CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
The ABC s of LUMBAR SPINE DISEASE
 The ABC s of LUMBAR SPINE DISEASE Susan O. Smith ANP-BC University of Rochester Department of Neurological Surgery Diagnosis/Imaging/Surgery of Lumbar Spine Disorders Objectives Identify the most common
The ABC s of LUMBAR SPINE DISEASE Susan O. Smith ANP-BC University of Rochester Department of Neurological Surgery Diagnosis/Imaging/Surgery of Lumbar Spine Disorders Objectives Identify the most common
MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION AN INTRODUCTION TO
 AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
Cervical Plating BACK PAIN
 BACK PAIN Back Pain Back pain is frequent complaint. It is the commonest cause of work-related absence in the world. Although back pain may be painful and uncomfortable, it is not usually serious. Even
BACK PAIN Back Pain Back pain is frequent complaint. It is the commonest cause of work-related absence in the world. Although back pain may be painful and uncomfortable, it is not usually serious. Even
Understanding your spine and how it works can help you better understand low back pain.
 Low Back Pain Almost everyone will experience low back pain at some point in their lives. This pain can vary from mild to severe. It can be short-lived or long-lasting. However it happens, low back pain
Low Back Pain Almost everyone will experience low back pain at some point in their lives. This pain can vary from mild to severe. It can be short-lived or long-lasting. However it happens, low back pain
Epidemiology of Low back pain
 Low Back Pain Definition Pain felt in your lower back may come from the spine, muscles, nerves, or other structures in that region. It may also radiate from other areas like the mid or upper back, a inguinal
Low Back Pain Definition Pain felt in your lower back may come from the spine, muscles, nerves, or other structures in that region. It may also radiate from other areas like the mid or upper back, a inguinal
Image-Guided Minimally Invasive Lumbar Decompression (IG-MLD) for Spinal Stenosis. Original Policy Date
 MP 7.01.107 Image-Guided Minimally Invasive Lumbar Decompression (IG-MLD) for Spinal Stenosis Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed
MP 7.01.107 Image-Guided Minimally Invasive Lumbar Decompression (IG-MLD) for Spinal Stenosis Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed
Herniated Disk in the Lower Back
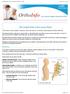 Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
Get back to: my life. Non-fusion treatment for lumbar spinal stenosis
 Get back to: my life Non-fusion treatment for lumbar spinal stenosis Do you have any of these symptoms? numbness, weakness or pain in the lower legs When any of these conditions occur, the spinal nerve,
Get back to: my life Non-fusion treatment for lumbar spinal stenosis Do you have any of these symptoms? numbness, weakness or pain in the lower legs When any of these conditions occur, the spinal nerve,
The imaging features of spondylolisthesis : what the clinician needs to know
 The imaging features of spondylolisthesis : what the clinician needs to know Poster No.: C-1018 Congress: ECR 2011 Type: Authors: Educational Exhibit D. Shah 1, C. J. Burke 1, A. C. andi 2, R. Houghton
The imaging features of spondylolisthesis : what the clinician needs to know Poster No.: C-1018 Congress: ECR 2011 Type: Authors: Educational Exhibit D. Shah 1, C. J. Burke 1, A. C. andi 2, R. Houghton
Cox Technic Case Report #169 published at (sent 5/9/17) 1
 Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Percutaneous disc decompression using nucleoplasty in patients with discogenic low back pain
 Percutaneous disc decompression using nucleoplasty in patients with discogenic low back pain Poster No.: C-2358 Congress: ECR 2012 Type: Scientific Paper Authors: P. Nikolopoulos, P. Maniatis, A. P. Giannila,
Percutaneous disc decompression using nucleoplasty in patients with discogenic low back pain Poster No.: C-2358 Congress: ECR 2012 Type: Scientific Paper Authors: P. Nikolopoulos, P. Maniatis, A. P. Giannila,
A Patient s Guide to Artificial Cervical Disc Replacement
 A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
ProDisc-L Total Disc Replacement. IDE Clinical Study.
 ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
Corporate Medical Policy Automated Percutaneous and Endoscopic Discectomy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: percutaneous_discectomy 9/1991 5/2017 5/2018 5/2017 Description of Procedure or Service Surgical management
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: percutaneous_discectomy 9/1991 5/2017 5/2018 5/2017 Description of Procedure or Service Surgical management
Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions:
 Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions: Radiating leg pain Greater leg / buttock pain than back pain Severe pain sets in when walking as
Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions: Radiating leg pain Greater leg / buttock pain than back pain Severe pain sets in when walking as
EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018
 EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018 Marc J. Levine, MD Rothman Institute Director Spine Surgery Program
EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018 Marc J. Levine, MD Rothman Institute Director Spine Surgery Program
Orthopadic cors. Topic : -Cervical spondylitis. -Development disorders(spondylolysis and Spodylolsithesis)
 Orthopadic cors Topic : -Cervical spondylitis. -Development disorders(spondylolysis and Spodylolsithesis) Cervical spondylitis. Definition : - a painful condition of the cervical spine resulting from the
Orthopadic cors Topic : -Cervical spondylitis. -Development disorders(spondylolysis and Spodylolsithesis) Cervical spondylitis. Definition : - a painful condition of the cervical spine resulting from the
Original Date: July 2008 Cervical ACDF - Anterior Decompression with Fusion Single or Multiple Levels
 National Imaging Associates, Inc. CERVICAL SPINE SURGERY: Original Date: July 2008 Cervical ACDF - Anterior Decompression with Fusion Single or Multiple Levels Page 1 of 13 Cervical Posterior Decompression
National Imaging Associates, Inc. CERVICAL SPINE SURGERY: Original Date: July 2008 Cervical ACDF - Anterior Decompression with Fusion Single or Multiple Levels Page 1 of 13 Cervical Posterior Decompression
Lumbar Fusion for Spinal Instability and Degenerative Disc Conditions, Including Sacroiliac Fusion
 Medical Coverage Policy Effective Date...01/15/2018 Next Review Date...01/15/2019 Coverage Policy Number... 0303 Lumbar Fusion for Spinal Instability and Degenerative Disc Conditions, Including Sacroiliac
Medical Coverage Policy Effective Date...01/15/2018 Next Review Date...01/15/2019 Coverage Policy Number... 0303 Lumbar Fusion for Spinal Instability and Degenerative Disc Conditions, Including Sacroiliac
All About? What is Sciatica. Disclaimer. Integrated web marketing. Multimedia Health Education
 What is Sciatica All About? Disclaimer This movie is an educational resource only and should not be used to manage sciatica. All decisions about the management of sciatica must be made in conjunction with
What is Sciatica All About? Disclaimer This movie is an educational resource only and should not be used to manage sciatica. All decisions about the management of sciatica must be made in conjunction with
Spinal Interventional Pain Management and Lumbar Spine Surgery
 Spinal Interventional Pain Management and Lumbar Spine Surgery Policy Number: Original Effective Date: MM.06.024 01/01/2014 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 08/22/2014
Spinal Interventional Pain Management and Lumbar Spine Surgery Policy Number: Original Effective Date: MM.06.024 01/01/2014 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 08/22/2014
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
Posterior. Lumbar Fusion. Disclaimer. Integrated web marketing. Multimedia Health Education
 Posterior Lumbar Fusion Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Posterior Lumbar Fusion Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
BACK PAIN. Disclaimer. Integrated web marketing. Multimedia Health Education
 BACK PAIN Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or a licensed healthcare
BACK PAIN Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or a licensed healthcare
