|
|
|
- Curtis Allen
- 5 years ago
- Views:
Transcription
1 Page 1 de 6 Brief Summary GUIDELINE TITLE Neck and upper back (acute & chronic). BIBLIOGRAPHIC SOURCE(S) Work Loss Data Institute. Neck and upper back (acute & chronic). Corpus Christi (TX): Work Loss Data Institute; p. [329 references] GUIDELINE STATUS This is the current release of the guideline. This guideline updates a previous version: Work Loss Data Institute. Neck and upper back (acute & chronic). Corpus Christi (TX): Work Loss Data Institute; 2007 Jul p. The Official Disability Guidelines product line, including ODG Treatment in Workers Comp, is updated annually, as it has been since the first release in FDA WARNING/REGULATORY ALERT ** REGULATORY ALERT ** Note from the National Guideline Clearinghouse: This guideline references a drug(s) for which important revised regulatory and/or warning information has been released. August 3, OnabotulinumtoxinA (Botox/Botox Cosmetic), AbobotulinumtoxinA (Dysport) and RimabotulinumtoxinB (Myobloc): The U.S. Food and Drug Administration (FDA) notified healthcare professionals of changes to the established drug names for Botox/Botox Cosmetic, Dysport and Myobloc to reinforce individual potencies and prevent medication errors, and provided recommendations for healthcare professionals to consider, plus information for patients, family members, and caregivers. ** REGULATORY ALERT ** RECOMMENDATIONS EVIDENCE SUPPORTING THE RECOMMENDATIONS IDENTIFYING INFORMATION AND AVAILABILITY DISCLAIMER Go to the Complete Summary BRIEF SUMMARY CONTENT MAJOR RECOMMENDATIONS Identify Neurologic Findings RECOMMENDATIONS First visit: may be with Primary Care Physician MD/DO (50%), Orthopedist (35%), or Chiropractor (15%) Determine Neurologic Findings -- Initial Evaluation History Note any previous neck problems or related disabilities. Determine the onset of the injury and mechanism of injury (any direct trauma, head injury, or fall). Determine any history of trauma to the neck and any initial acute episode of pain or whiplash injury. Search for any symptoms of possible neurologic impairment, such as weakness in an upper extremity, numbness, or radicular pain radiating into upper extremities. History of work activities, hobbies, and sports Note any psychosocial problems, such as substance abuse, job dissatisfaction, conflict with supervisors, marital problems, and/or financial problems. Determine relevant medical history, history of systemic disease, or previous neck injury or disability. Note any history which produces radiating pain in the neck from structures such as the thyroid, the lymph nodes, the esophagus, the trachea, or from a Pancoast tumor in the apex of the lung. Note any history of cancer. Physical Examination
2 Page 2 de 6 Perform a comprehensive examination of the neck and upper extremities including attention to flexibility, strength, and range-of-motion of the neck. Perform a careful limited neurological examination of the neck and the upper and lower extremities to determine which diagnostic tests and therapy should be performed. This examination should include reflexes of the biceps, triceps, and brachioradialis tendons and those of the lower extremities, as well as weakness and sensory changes to pin prick by anatomical area (dermatomes) when needed. Check for long tract signs (Babinski and clonus). Evaluate for any evidence of weakness or atrophy of muscle groups of the arm. Evaluate for any signs of systemic disease. Note that any patient with an acute injury and positive neurologic findings requires a neck splint, immobilization, and referral to a spinal surgeon. Imaging Imaging modalities are often not necessary for patients with typical nontraumatic acute neck pain, but due to the risk of treating patients with undiagnosed cervical vertebral fractures, x-rays are necessary if there is any possibility of a fracture, even in patients without neurologic findings. Any patient with a minimal fracture of the cervical spine should have a computed tomography (CT) scan to evaluate the status of the neural arch. Indications for x-rays of the cervical spine include the following: A history of direct trauma, blow to the head, any significant whiplash type injury, or any significant fall. These patients should have an x-ray of the cervical spine. Patients with fractures of the cervical spine should be referred to a spinal surgeon. Whiplash with any evidence of neurologic deficit or persistent pain Chronic, slow onset of pain, especially if it is increasing or night pain A history of systemic disease such as cancer, long-term steroid therapy, or alcohol abuse Patients over 50 years of age with any question of etiology of symptoms Patients with significant stiffness of the cervical spine Lateral flexion and extension views may demonstrate instability of the spine and indicate the need for consultation even in the absence of a fracture (fingertip test), muscle atrophy (calf measurement), local areas of tenderness, visual pain analog Indications for magnetic resonance imaging (MRI) of the cervical spine include the following: Any suggestion of abnormal neurologic findings below the level of injury Progressive neurologic deficit Persistent unremitting pain with or without positive neurologic findings Previous herniated intervertebral disk within the last two years and radicular pain with positive neurologic findings Patients with significant neurologic findings and failure to respond to conservative therapy despite compliance with the therapeutic regimen Imaging procedures such as CT scans are necessary for any fracture of the cervical spine, with referral to a spinal surgeon. Additional imaging procedures, such as bone scan, myelography, etc., have special indications and are rarely needed at this stage, unless strong evidence of systemic disease exists and further evaluations thought necessary by the spinal surgeon. Other tests such as electromyography (EMG) or nerve conduction studies are not necessary in the initial evaluation of patients with new symptoms, due to the fact that these tests will not become positive until four to six weeks after the onset of symptoms. An EMG is not necessary for the diagnosis of intervertebral disk disease with radiculopathy; rather, its value lies in differentiating other types of neuritis, neuropathy, or muscle abnormalities from radicular neuropathy and for cases where the etiology of the pain is not clear. An EMG is most appropriate to perform after an evaluation by a specialist. Consider the New Classification System for Neck Pain from the Bone and Joint Decade Task Force on Neck Pain. Presumptive Diagnosis (see original guideline document for International Classification of Diseases, Ninth Revision [ICD-9] codes) Without Neurologic Findings Neck pain with no radiation of pain beyond the neck area Neck pain with radiation of pain in shoulders and upper back, but with no radicular signs Chronic neck pain or chronic neck problems or whiplash With Neurologic Findings Fracture of cervical spine Radicular pain and positive signs indicate a presumptive diagnosis of herniated intervertebral disk Neurologic signs and symptoms at the cervical level and in the lower body or lower extremities Radicular pain and positive signs indicate a presumptive diagnosis of herniated intervertebral disk and an MRI or CT scan shows positive findings of a herniated intervertebral disk that matches the clinical findings
3 Page 3 de 6 Cases Without Neurologic Findings (95% of cases) Also first visit (day 1): Prescribe decreased activity if necessary based on severity and difficulty of job, passive therapy with heat/ice (3 to 4 times/day), stretching/exercise, appropriate analgesia (i.e., acetaminophen) and/or anti-inflammatory (i.e., ibuprofen) [Benchmark cost: $14], back to work except for severe cases in 72 hours, possibly modified duty. Avoid bed rest. No x-rays unless major trauma (e.g., a fall) If muscle spasms, then prescribe muscle relaxant with limited sedative side effects [Benchmark cost: $44] Reassure patient: common problem (90% of patients recover spontaneously in 4 weeks) Official Disability Guidelines (ODG) Return-To-Work Pathways (neck sprain) Whiplash grade 0 (Quebec Task Force grades): 0 days (See ODG Capabilities & Activity Modifications for Restricted Work under "Work" in the Procedure Summary of the original guideline document) Second visit (day 3 to 10 about 1 week after first visit, or sooner, because delayed treatment is not recommended) Document progress (areas of tenderness, motor strength) If still 50% disabled then prescribe manual therapy [Benchmark cost: $250]: Refer to massage therapist, chiropractor, physical therapist, or occupational therapist (3 visits in first week), or by treating DO Probably discontinue muscle relaxant ODG Return-To-Work Pathways (neck sprain) Whiplash grade I-III, clerical/modified work: 5 days Third visit (day 10 to 17 about 1 week after second visit) Document progress Prescribe muscle-conditioning exercises At this point 66% to 75% should be back to regular work If still disabled, then first imaging study (anteroposterior [AP]/lateral 2-view x-ray of upper back) [Benchmark cost: $150] to rule out cervical spondylolysis or joint narrowing/spinal stenosis (age related, not caused by recent trauma - will not change treatment) Continue therapist, change from passive to active modality, 2 visits in next week, teach home exercises End manual therapy (physical therapy or manipulation) at 4 weeks ODG Return-To-Work Pathways (neck sprain) Whiplash grade I-III, manual work: 21 days Whiplash grade I-III, heavy manual work: 28 days Up to 3 more visits for follow up and documentation of progress Cases With Neurologic Findings (5% of cases) Also first visit (day 1) Same as non-radicular ODG Return-To-Work Pathways (cervical disc disorders) Mild cases with back pain, avoid strenuous activity: 0 days Initial conservative medical treatment, clerical/modified work: 0 to 3 days Second visit (day 3 to 10 about 1 week after first visit) Same as non-radicular Reassure, but warn of increased numbness or weakness of either arm: if so, get back to provider in one day Consider referral to musculoskeletal physician (orthopedist/physical medicine and rehabilitation (PM&R)/sports medicine) Third visit (day 10 to 17 about 1 week after second visit) Same as non-radicular About 50% can be back at modified duty If improvement, then add strengthening exercises, increased activity Fourth visit (day 21 to 28 about 1 to 2 weeks after third visit)
4 Page 4 de 6 Document, if no improvement then: First MRI (about 3% of total cases, or 30% of cases with neurologic symptoms) to confirm extruded disk with nerve root displacement [Benchmark cost: $1,600] MRI or CT not indicated without obvious clinical level of nerve root dysfunction or before 3 to 4 weeks Consider epidural steroid injection (ESI) for severe cases hoping to avoid surgery [Benchmark cost: $676] Bone scan if spondylolisthesis Second MRI only if progression of neurological symptoms (less than 1% of cases) Refer to fellowship trained Spine Surgeon: Neurosurgeon (50%), Orthopedist (50%) Before surgery, screen for psychological symptoms that could affect surgical outcome (e.g., substance abuse, child abuse, work conflicts, somatization, verbalizations, attorney involvement, smoking) If psychological factors retarding recovery are suspected, possibly refer to psychologist for testing (Minnesota Multiphasic Personality Inventory [MMPI] or, better, Waddell test) [Benchmark cost: $540] ODG Return-To-Work Pathways (cervical disc disorders) Initial conservative medical treatment, manual work: 35 days Surgery (day 28 to 35) (about 2% of total cases, or 20% of radicular cases) (See also "ODG Indications for Surgery Discectomy" in the Procedure Summary of the original guideline document.) Review options/outcomes with patient, let patient decide Simple discectomy/laminectomy, minimally invasive [Benchmark cost: $17,400] Outpatient (23 hour stay) Post-operative pain, walking exercises ODG Return-To-Work Pathways (cervical disc disorders) Cervical discectomy, clerical/modified work: 28 to 56 days Cervical discectomy, manual work: 56 days Cervical discectomy, heavy manual work: 126 days to indefinite Cervical laminectomy/decompression, clerical/modified work: 28 days Cervical laminectomy/decompression, manual work: 63 days Cervical laminectomy/decompression, heavy manual work: 105 days to indefinite Follow-up visits as required CLINICAL ALGORITHM(S) None provided EVIDENCE SUPPORTING THE RECOMMENDATIONS TYPE OF EVIDENCE SUPPORTING THE RECOMMENDATIONS During the comprehensive medical literature review, preference was given to high quality systematic reviews, meta-analyses, and clinical trials over the past ten years, plus existing nationally recognized treatment guidelines from the leading specialty societies. The heart of each Work Loss Data Institute guideline is the Procedure Summary (see the original guideline document), which provides a concise synopsis of effectiveness, if any, of each treatment method based on existing medical evidence. Each summary and subsequent recommendation is hyper-linked into the studies on which they are based, in abstract form, which have been ranked, highlighted and indexed. BIBLIOGRAPHIC SOURCE(S) IDENTIFYING INFORMATION AND AVAILABILITY Work Loss Data Institute. Neck and upper back (acute & chronic). Corpus Christi (TX): Work Loss Data Institute; p. [329 references] ADAPTATION Not applicable: The guideline was not adapted from another source. DATE RELEASED 2003 (revised 2008 May 7)
5 Page 5 de 6 GUIDELINE DEVELOPER(S) Work Loss Data Institute - Public For Profit Organization SOURCE(S) OF FUNDING Not stated GUIDELINE COMMITTEE Not stated COMPOSITION OF GROUP THAT AUTHORED THE GUIDELINE Editor-in-Chief, Philip L. Denniston, Jr. and Senior Medical Editor, Charles W. Kennedy, MD, together pilot the group of approximately 80 members. See the ODG Treatment in Workers Comp Editorial Advisory Board. FINANCIAL DISCLOSURES/CONFLICTS OF INTEREST There are no conflicts of interest among the guideline development members. GUIDELINE STATUS This is the current release of the guideline. This guideline updates a previous version: Work Loss Data Institute. Neck and upper back (acute & chronic). Corpus Christi (TX): Work Loss Data Institute; 2007 Jul p. The Official Disability Guidelines product line, including ODG Treatment in Workers Comp, is updated annually, as it has been since the first release in GUIDELINE AVAILABILITY Electronic copies: Available to subscribers from the Work Loss Data Institute Web site. Print copies: Available from the Work Loss Data Institute, 169 Saxony Road, Suite 210, Encinitas, CA 92024; Phone: , , Fax: ; AVAILABILITY OF COMPANION DOCUMENTS The following are available: Background information on the development of the Official Disability Guidelines of the Work Loss Data Institute is available from the Work Loss Data Institute Web site. Appendix A. ODG Treatment in Workers' Comp. Methodology description using the AGREE instrument. Available to subscribers from the Work Loss Data Institute Web site. PATIENT RESOURCES The following is available: Appendix C. ODG Treatment in Workers' Comp. Patient information resources Electronic copies: Available to subscribers from the Work Loss Data Institute Web site. Print copies: Available from the Work Loss Data Institute, 169 Saxony Road, Suite 210, Encinitas, CA 92024; Phone: , , Fax: ; Please note: This patient information is intended to provide health professionals with information to share with their patients to help them better understand their health and their diagnosed disorders. By providing access to this patient information, it is not the intention of NGC to provide specific medical advice for particular patients. Rather we urge patients and their representatives to review this material and then to consult with a licensed health professional for evaluation of treatment options suitable for them as well as for diagnosis and answers to their personal medical questions. This patient information has been derived and prepared from a guideline for health care professionals included on NGC by the authors or publishers of that original guideline. The patient information is not reviewed by NGC to establish whether or not it accurately reflects the original guideline's content. NGC STATUS This summary was completed by ECRI on February 2, The information was verified by the guideline developer on February 13, This NGC summary was updated by ECRI on March 28, 2005, January 13, 2006, April 12, 2006, November 13, 2006, April 2, 2007, and August 28, This NGC summary was updated by ECRI Institute on January 22, This summary was updated by ECRI Institute on May 26, 2009, following the U.S. Food and Drug Administration advisory on Botox, Botox Cosmetic (Botulinum toxin Type A), and Myobloc (Botulinum toxin Type B). This summary was updated by ECRI Institute on August 17, 2009, following the updated FDA advisory on Botox and Botox Cosmetic (Botulinum toxin Type A), and Myobloc (Botulinum toxin Type B). COPYRIGHT STATEMENT This NGC summary is based on the original guideline, which is subject to the guideline developer's copyright restrictions. DISCLAIMER
6 Page 6 de 6 NGC DISCLAIMER The National Guideline Clearinghouse (NGC) does not develop, produce, approve, or endorse the guidelines represented on this site. All guidelines summarized by NGC and hosted on our site are produced under the auspices of medical specialty societies, relevant professional associations, public or private organizations, other government agencies, health care organizations or plans, and similar entities. Guidelines represented on the NGC Web site are submitted by guideline developers, and are screened solely to determine that they meet the NGC Inclusion Criteria which may be found at NGC, AHRQ, and its contractor ECRI Institute make no warranties concerning the content or clinical efficacy or effectiveness of the clinical practice guidelines and related materials represented on this site. Moreover, the views and opinions of developers or authors of guidelines represented on this site do not necessarily state or reflect those of NGC, AHRQ, or its contractor ECRI Institute, and inclusion or hosting of guidelines in NGC may not be used for advertising or commercial endorsement purposes. Readers with questions regarding guideline content are directed to contact the guideline developer.
GET BACK TO YOUR FUTURE WITH SPECIALIZED SPINE CARE. A Guide for Patients
 GET BACK TO YOUR FUTURE WITH SPECIALIZED SPINE CARE A Guide for Patients Your Spine Deserves Special Care Your spine is at the center of a delicately balanced system that controls all of your body s movements.
GET BACK TO YOUR FUTURE WITH SPECIALIZED SPINE CARE A Guide for Patients Your Spine Deserves Special Care Your spine is at the center of a delicately balanced system that controls all of your body s movements.
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Epidural Injection Please check the indication (reason)
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Epidural Injection Please check the indication (reason)
Corporate Medical Policy
 Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Facet Injection Please check the indication (reason)
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Facet Injection Please check the indication (reason)
Complete Summary GUIDELINE TITLE. Cervical cytology screening. BIBLIOGRAPHIC SOURCE(S)
 Complete Summary GUIDELINE TITLE Cervical cytology screening. BIBLIOGRAPHIC SOURCE(S) American College of Obstetricians and Gynecologists (ACOG). Cervical cytology screening. Washington (DC): American
Complete Summary GUIDELINE TITLE Cervical cytology screening. BIBLIOGRAPHIC SOURCE(S) American College of Obstetricians and Gynecologists (ACOG). Cervical cytology screening. Washington (DC): American
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested is: Please check the indication (reason) for this procedure
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested is: Please check the indication (reason) for this procedure
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Epidural Adhesiolysis Please check the indication (reason)
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Epidural Adhesiolysis Please check the indication (reason)
HIGH LEVEL - Science
 Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
North American Spine Society Public Education Series
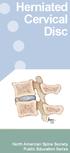 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
IEHP UM Subcommittee Approved Authorization Guidelines Referrals to Pain Management Specialists
 IEHP Policy: Based on a review of the currently available literature and community standards of practice, the IEHP UM Subcommittee will consider referrals to Pain Management Specialists medically necessary
IEHP Policy: Based on a review of the currently available literature and community standards of practice, the IEHP UM Subcommittee will consider referrals to Pain Management Specialists medically necessary
Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society
 Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society Annals of Internal Medicine October 2007 Volume 147,
Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society Annals of Internal Medicine October 2007 Volume 147,
A Patient s Guide to Cervical Radiculopathy
 A Patient s Guide to Cervical Radiculopathy 950 Breckinridge Lane Suite 220 Louisville, KY 40223 Phone: 502.708.2940 DISCLAIMER: The information in this booklet is compiled from a variety of sources. It
A Patient s Guide to Cervical Radiculopathy 950 Breckinridge Lane Suite 220 Louisville, KY 40223 Phone: 502.708.2940 DISCLAIMER: The information in this booklet is compiled from a variety of sources. It
IEHP UM Subcommittee Approved Authorization Guidelines Referrals to Pain Management Specialists
 IEHP Policy: Based on a review of the currently available literature and community standards of practice, the IEHP UM Subcommittee will consider referrals to Pain Management Specialists medically necessary
IEHP Policy: Based on a review of the currently available literature and community standards of practice, the IEHP UM Subcommittee will consider referrals to Pain Management Specialists medically necessary
 The spine is made of a column of bones. Each bone, or vertebra, is formed by a round block of bone, called a vertebral body. A bony ring attaches to the back of the vertebral body. When the vertebra bones
The spine is made of a column of bones. Each bone, or vertebra, is formed by a round block of bone, called a vertebral body. A bony ring attaches to the back of the vertebral body. When the vertebra bones
Guideline Summary NGC-3246
 NGC banner Guideline Summary NGC-3246 Guideline Title Metatarsalgia/intractable plantar keratosis/tailor's bunion. Bibliographic Source(s) Academy of Ambulatory Foot and Ankle Surgery. Metatarsalgia/intractable
NGC banner Guideline Summary NGC-3246 Guideline Title Metatarsalgia/intractable plantar keratosis/tailor's bunion. Bibliographic Source(s) Academy of Ambulatory Foot and Ankle Surgery. Metatarsalgia/intractable
What Is Back Pain? Can Back Pain Be Prevented? When Should I See a Doctor for Pain? How Is Back Pain Diagnosed?
 What Is Back Pain? Back pain can also occur with some conditions and diseases, such as: Scoliosis Spondylolisthesis Arthritis Spinal stenosis Pregnancy Kidney stones Infections Endometriosis Fibromyalgia.
What Is Back Pain? Back pain can also occur with some conditions and diseases, such as: Scoliosis Spondylolisthesis Arthritis Spinal stenosis Pregnancy Kidney stones Infections Endometriosis Fibromyalgia.
Regional Review of Musculoskeletal System: Head, Neck, and Cervical Spine Presented by Michael L. Fink, PT, DSc, SCS, OCS Pre- Chapter Case Study
 Regional Review of Musculoskeletal System: Presented by Michael L. Fink, PT, DSc, SCS, OCS (20 minutes CEU Time) Subjective A 43-year-old male, reported a sudden onset of left-sided neck and upper extremity
Regional Review of Musculoskeletal System: Presented by Michael L. Fink, PT, DSc, SCS, OCS (20 minutes CEU Time) Subjective A 43-year-old male, reported a sudden onset of left-sided neck and upper extremity
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
North American Spine Society Public Education Series
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
What Is Back Pain? Fast Facts: An Easy-to-Read Series of Publications for the Public. Who Gets Back Pain? What Are the Causes of Back Pain?
 Back pain can range from a dull, constant ache to a sudden, sharp pain that makes it hard to move. It can start quickly if you fall or lift something too heavy, or it can get worse slowly. Who Gets Back
Back pain can range from a dull, constant ache to a sudden, sharp pain that makes it hard to move. It can start quickly if you fall or lift something too heavy, or it can get worse slowly. Who Gets Back
Epidemiology of Low back pain
 Low Back Pain Definition Pain felt in your lower back may come from the spine, muscles, nerves, or other structures in that region. It may also radiate from other areas like the mid or upper back, a inguinal
Low Back Pain Definition Pain felt in your lower back may come from the spine, muscles, nerves, or other structures in that region. It may also radiate from other areas like the mid or upper back, a inguinal
** REGULATORY ALERT **
 Complete Summary GUIDELINE TITLE Fibromyalgia. BIBLIOGRAPHIC SOURCE(S) Fibromyalgia. Philadelphia (PA): Intracorp; 2004. Various p. GUIDELINE STATUS This is the current release of the guideline. All Intracorp
Complete Summary GUIDELINE TITLE Fibromyalgia. BIBLIOGRAPHIC SOURCE(S) Fibromyalgia. Philadelphia (PA): Intracorp; 2004. Various p. GUIDELINE STATUS This is the current release of the guideline. All Intracorp
Corporate Medical Policy
 Corporate Medical Policy Paraspinal Surface Electromyography (SEMG) File Name: Origination: Last CAP Review: Next CAP Review: Last Review: paraspinal_surface_electromyography_(emg) 4/2005 5/2018 5/2019
Corporate Medical Policy Paraspinal Surface Electromyography (SEMG) File Name: Origination: Last CAP Review: Next CAP Review: Last Review: paraspinal_surface_electromyography_(emg) 4/2005 5/2018 5/2019
Why choose Ottauquechee PT
 Why does your back hurt? Low back pain is one of the most common patient complaints affecting 80% of adults at some point in their lives. Generally the source of pain is in the spine and/or its supporting
Why does your back hurt? Low back pain is one of the most common patient complaints affecting 80% of adults at some point in their lives. Generally the source of pain is in the spine and/or its supporting
Guideline Summary NGC-8514
 NGC banner Guideline Summary NGC-8514 Guideline Title Head (trauma, headaches, etc., not including stress & mental disorders). Bibliographic Source(s) Work Loss Data Institute. Head (trauma, headaches,
NGC banner Guideline Summary NGC-8514 Guideline Title Head (trauma, headaches, etc., not including stress & mental disorders). Bibliographic Source(s) Work Loss Data Institute. Head (trauma, headaches,
Practice parameter: immunotherapy for Guillain-Barre syndrome: report of the Quality Standards Subcommittee of the American Academy of Neurology.
 Complete Summary GUIDELINE TITLE Practice parameter: immunotherapy for Guillain-Barre syndrome: report of the Quality Standards Subcommittee of the American Academy of Neurology. BIBLIOGRAPHIC SOURCE(S)
Complete Summary GUIDELINE TITLE Practice parameter: immunotherapy for Guillain-Barre syndrome: report of the Quality Standards Subcommittee of the American Academy of Neurology. BIBLIOGRAPHIC SOURCE(S)
A Patient s Guide to Cervical Radiculopathy
 A Patient s Guide to Cervical Radiculopathy 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Cervical Radiculopathy 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is compiled from a variety
SpineFAQs. Neck Pain Diagnosis and Treatment
 SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
Acute Low Back Pain. North American Spine Society Public Education Series
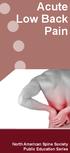 Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Complete Summary GUIDELINE TITLE
 Complete Summary GUIDELINE TITLE Practice parameter: thymectomy for autoimmune myasthenia gravis (an evidence-based review). Report of the Quality Standards Subcommittee of the American Academy of Neurology.
Complete Summary GUIDELINE TITLE Practice parameter: thymectomy for autoimmune myasthenia gravis (an evidence-based review). Report of the Quality Standards Subcommittee of the American Academy of Neurology.
The main causes of cervical radiculopathy include degeneration, disc herniation, and spinal instability.
 SpineFAQs Cervical Radiculopathy Neck pain has many causes. Mechanical neck pain comes from injury or inflammation in the soft tissues of the neck. This is much different and less concerning than symptoms
SpineFAQs Cervical Radiculopathy Neck pain has many causes. Mechanical neck pain comes from injury or inflammation in the soft tissues of the neck. This is much different and less concerning than symptoms
SPINAL PAIN. Mr. Yagnesh Vellore FRACS Neurosurgeon and Spine Surgeon
 SPINAL PAIN Mr. Yagnesh Vellore FRACS Neurosurgeon and Spine Surgeon PAIN GENERATORS IN THE SPINE Ligaments: ALL,PLL Muscle Periosteum bone Outer 1/3 annulus disc Facet joints Sacro-iliac joint sinuvertebral
SPINAL PAIN Mr. Yagnesh Vellore FRACS Neurosurgeon and Spine Surgeon PAIN GENERATORS IN THE SPINE Ligaments: ALL,PLL Muscle Periosteum bone Outer 1/3 annulus disc Facet joints Sacro-iliac joint sinuvertebral
Cox Technic Case Report #169 published at (sent 5/9/17) 1
 Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
DOCTOR DISCUSSION GUIDE
 DOCTOR DISCUSSION GUIDE BE PREPARED For the best outcome from a visit with your doctor, it s important to be prepared. The more completely and clearly you describe the pain you re experiencing, the easier
DOCTOR DISCUSSION GUIDE BE PREPARED For the best outcome from a visit with your doctor, it s important to be prepared. The more completely and clearly you describe the pain you re experiencing, the easier
Chapter 2 Diagnostic Algorithms. 4 Traumatic Neck Pain Algorithm
 Chapter 2 Diagnostic Algorithms 4 Traumatic Neck Pain Algorithm Patient presents with a traumatic onset of neck pain. In general, radiographs should be ordered with a history of recent, significant trauma.
Chapter 2 Diagnostic Algorithms 4 Traumatic Neck Pain Algorithm Patient presents with a traumatic onset of neck pain. In general, radiographs should be ordered with a history of recent, significant trauma.
Herniated Disk in the Lower Back
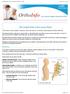 Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
Can angled sagittal MRI of neural foramen combined with neurological findings determine the affected nerve root in cervical radiculopathy?
 Can angled sagittal MRI of neural foramen combined with neurological findings determine the affected nerve root in cervical radiculopathy? Masatoshi Morimoto, MD., Akihiro Nagamachi, MD. PhD., Kosuke Sugiura,
Can angled sagittal MRI of neural foramen combined with neurological findings determine the affected nerve root in cervical radiculopathy? Masatoshi Morimoto, MD., Akihiro Nagamachi, MD. PhD., Kosuke Sugiura,
Neck Pain Guide. Understanding Causes, Treatment and Prevention
 Neck Pain Guide Understanding Causes, Treatment and Prevention Neck pain may be more than a nuisance; it could be a symptom of an underlying condition. Use this guide to help you understand common causes
Neck Pain Guide Understanding Causes, Treatment and Prevention Neck pain may be more than a nuisance; it could be a symptom of an underlying condition. Use this guide to help you understand common causes
Spine Center. at Stamford Hospital s Orthopedic Institute
 Spine Center at Stamford Hospital s Orthopedic Institute Back pain related to spinal deformity and injury or congenital conditions is a common health complaint, which can be very debilitating. At Stamford
Spine Center at Stamford Hospital s Orthopedic Institute Back pain related to spinal deformity and injury or congenital conditions is a common health complaint, which can be very debilitating. At Stamford
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
Clinical guidelines for best practice management of acute and chronic whiplash-associated disorders. Clinical resource guide
 Clinical guidelines for best practice management of acute and chronic whiplash-associated disorders Clinical resource guide TRACsa was integrated into the Motor Accident Commission (MAC) in November 2008.
Clinical guidelines for best practice management of acute and chronic whiplash-associated disorders Clinical resource guide TRACsa was integrated into the Motor Accident Commission (MAC) in November 2008.
LUMBAR SPINAL STENOSIS
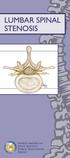 LUMBAR SPINAL STENOSIS North American Spine Society Public Education Series WHAT IS LUMBAR SPINAL STENOSIS? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
LUMBAR SPINAL STENOSIS North American Spine Society Public Education Series WHAT IS LUMBAR SPINAL STENOSIS? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
THE SPINE AMA GUIDES CHAPTER 15
 THE SPINE AMA GUIDES CHAPTER 15 Tim Mussack Marlene Phillips Bradford & Barthel, LLP AMA Analysis and Ratings Division HOUSEKEEPING ITEMS To control background noise, all attendees will be muted. Access
THE SPINE AMA GUIDES CHAPTER 15 Tim Mussack Marlene Phillips Bradford & Barthel, LLP AMA Analysis and Ratings Division HOUSEKEEPING ITEMS To control background noise, all attendees will be muted. Access
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) 6565 Fannin Street Houston, TX 77030 Phone: 713-790-3333 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) 6565 Fannin Street Houston, TX 77030 Phone: 713-790-3333 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
Postnatal corticosteroids to treat or prevent chronic lung disease in preterm infants.
 Complete Summary GUIDELINE TITLE Postnatal corticosteroids to treat or prevent chronic lung disease in preterm infants. BIBLIOGRAPHIC SOURCE(S) Postnatal corticosteroids to treat or prevent chronic lung
Complete Summary GUIDELINE TITLE Postnatal corticosteroids to treat or prevent chronic lung disease in preterm infants. BIBLIOGRAPHIC SOURCE(S) Postnatal corticosteroids to treat or prevent chronic lung
Critical Appraisal of a Clinical Practice Guideline
 Critical Appraisal of a Clinical Practice Guideline Goal: To critically evaluate a guideline, using the Users Guides (reference below). Objectives: 1. Assess the validity of a guideline 2. Understand the
Critical Appraisal of a Clinical Practice Guideline Goal: To critically evaluate a guideline, using the Users Guides (reference below). Objectives: 1. Assess the validity of a guideline 2. Understand the
Guideline Summary NGC-3241
 NGC banner Guideline Summary NGC-3241 Guideline Title Ingrown toenails. Bibliographic Source(s) Academy of Ambulatory Foot and Ankle Surgery. Ingrown toenails. Philadelphia (PA): Academy of Ambulatory
NGC banner Guideline Summary NGC-3241 Guideline Title Ingrown toenails. Bibliographic Source(s) Academy of Ambulatory Foot and Ankle Surgery. Ingrown toenails. Philadelphia (PA): Academy of Ambulatory
Adult Isthmic Spondylolisthesis
 Adult Isthmic Spondylolisthesis North American Spine Society Public Education Series What Is Adult Isthmic Spondylolisthesis? The spine is made up of a series of connected bones called vertebrae. In about
Adult Isthmic Spondylolisthesis North American Spine Society Public Education Series What Is Adult Isthmic Spondylolisthesis? The spine is made up of a series of connected bones called vertebrae. In about
MUSCULOSKELETAL PROGRAM OF CARE
 MUSCULOSKELETAL PROGRAM OF CARE AUGUST 1, 2014 Table of contents Acknowledgements... 3 MSK POC Scope... 3 The Evidence... 3 Objectives.... 4 Target Population.... 4 Assessment of Flags and Barriers to
MUSCULOSKELETAL PROGRAM OF CARE AUGUST 1, 2014 Table of contents Acknowledgements... 3 MSK POC Scope... 3 The Evidence... 3 Objectives.... 4 Target Population.... 4 Assessment of Flags and Barriers to
NAME: DATE: SPINE CENTER NEW PATIENT QUESTIONNAIRE
 Please complete and give to the receptionist when you arrive at the office for your appointment. NAME: DATE: SPINE CENTER NEW PATIENT QUESTIONNAIRE Page 1 of 6 Primary Care Physician s Name Primary Care
Please complete and give to the receptionist when you arrive at the office for your appointment. NAME: DATE: SPINE CENTER NEW PATIENT QUESTIONNAIRE Page 1 of 6 Primary Care Physician s Name Primary Care
Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis
 Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis The program consisted of manual therapy twice per week (eg, soft tissue and neural The components of the Boot Camp Program
Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis The program consisted of manual therapy twice per week (eg, soft tissue and neural The components of the Boot Camp Program
LOW BACK PAIN EPIDEMIOLOGY:
 LOW BACK PAIN OBJECTIVES: Discuss epidemiology of low back pain Summarize diagnosis/ special tests Review Red Flags Discuss treatment and referral guidelines Discuss light duty guidelines EPIDEMIOLOGY:
LOW BACK PAIN OBJECTIVES: Discuss epidemiology of low back pain Summarize diagnosis/ special tests Review Red Flags Discuss treatment and referral guidelines Discuss light duty guidelines EPIDEMIOLOGY:
Neck Pain: Help! Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto
 Neck Pain: Help! Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
Neck Pain: Help! Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
Lumbar disc herniation
 Lumbar disc herniation Thomas Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Symptoms and Signs Radicular Pain in the distribution of the involved nerve Neurological deficit motor,
Lumbar disc herniation Thomas Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Symptoms and Signs Radicular Pain in the distribution of the involved nerve Neurological deficit motor,
Spinal Fusion. North American Spine Society Public Education Series
 Spinal Fusion North American Spine Society Public Education Series What Is Spinal Fusion? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
Spinal Fusion North American Spine Society Public Education Series What Is Spinal Fusion? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
Case Studies, Impairment of the Spine in Washington State
 Case Studies, Impairment of the Spine in Washington State NAOEM at Skamania, 2015 25 Sep, 2015 Tim Gilmore, MD Several Slides from this Presentation Borrowed with permission from the Washington State Department
Case Studies, Impairment of the Spine in Washington State NAOEM at Skamania, 2015 25 Sep, 2015 Tim Gilmore, MD Several Slides from this Presentation Borrowed with permission from the Washington State Department
National Imaging Associates, Inc. Clinical guidelines
 National Imaging Associates, Inc. Clinical guidelines Original Date: September 1997 THORACIC SPINE CT Page 1 of 5 CPT Codes: 72128, 72129, 72130 Last Review Date: May 2013 Guideline Number: NIA_CG_043
National Imaging Associates, Inc. Clinical guidelines Original Date: September 1997 THORACIC SPINE CT Page 1 of 5 CPT Codes: 72128, 72129, 72130 Last Review Date: May 2013 Guideline Number: NIA_CG_043
CLINICAL GUIDELINES. Primary Care Guideline Summary Lumbar Spine Thomas J. Gilbert M.D., M.P.P. 3/17/15 revision
 CLINICAL GUIDELINES Primary Care Guideline Summary Lumbar Spine Thomas J. Gilbert M.D., M.P.P. 3/17/15 revision TRIAGE At the initial visit, a focused history and physical examination is performed to assign
CLINICAL GUIDELINES Primary Care Guideline Summary Lumbar Spine Thomas J. Gilbert M.D., M.P.P. 3/17/15 revision TRIAGE At the initial visit, a focused history and physical examination is performed to assign
d EFFECTIVE DATE: POLICY LAST UPDATED:
 Medical Coverage Policy Epidural Injections for Pain Management d EFFECTIVE DATE: 04 01 2018 POLICY LAST UPDATED: 03 20 2018 OVERVIEW Epidural injections are generally performed to treat pain arising from
Medical Coverage Policy Epidural Injections for Pain Management d EFFECTIVE DATE: 04 01 2018 POLICY LAST UPDATED: 03 20 2018 OVERVIEW Epidural injections are generally performed to treat pain arising from
Original Policy Date
 MP 6.01.39 Positional Magnetic Resonance Imaging Medical Policy Section Radiology Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
MP 6.01.39 Positional Magnetic Resonance Imaging Medical Policy Section Radiology Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
Objectives. Identify and differentiate appropriate surgical cases. Good Surgical Outcomes
 ECHO February 5 th, 2015 Surgical Selection for Low Back Pain Objectives Identify and differentiate appropriate surgical cases Disclosures Medical director for UHN Rehabilitations Solution Back and Neck
ECHO February 5 th, 2015 Surgical Selection for Low Back Pain Objectives Identify and differentiate appropriate surgical cases Disclosures Medical director for UHN Rehabilitations Solution Back and Neck
Chiropractic , The Patient Education Institute, Inc. amf10101 Last reviewed: 01/17/2018 1
 Chiropractic Introduction Chiropractic is health care that focuses on disorders of the musculoskeletal system and the nervous system, and the way these disorders affect general health. Chiropractic uses
Chiropractic Introduction Chiropractic is health care that focuses on disorders of the musculoskeletal system and the nervous system, and the way these disorders affect general health. Chiropractic uses
Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS AND PAIN
 Cox Technic Case Report #100 published at www.coxtechnic.com (sent October 2011 on 10/11/11 ) 1 Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS
Cox Technic Case Report #100 published at www.coxtechnic.com (sent October 2011 on 10/11/11 ) 1 Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS
Inova. Spine Institute
 Inova Spine Institute At Inova Spine Institute, you ll find a wide range of treatment alternatives, from physical therapy and rehabilitation to pain management. For patients who require surgery, Inova
Inova Spine Institute At Inova Spine Institute, you ll find a wide range of treatment alternatives, from physical therapy and rehabilitation to pain management. For patients who require surgery, Inova
A Patient s Guide to Pain Management: Complex Regional Pain Syndrome
 A Patient s Guide to Pain Management: Complex Regional Pain Syndrome Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER:
A Patient s Guide to Pain Management: Complex Regional Pain Syndrome Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER:
Low back pain, radiculopathy left leg icd 10 code
 Home Search Low back pain, radiculopathy left leg icd 10 code 2018 ICD - 10 code for Radiculopathy is M54.1. Lookup the complete ICD 10 Code details for M54.1.. Low back pain ; M54.6 - Pain in thoracic
Home Search Low back pain, radiculopathy left leg icd 10 code 2018 ICD - 10 code for Radiculopathy is M54.1. Lookup the complete ICD 10 Code details for M54.1.. Low back pain ; M54.6 - Pain in thoracic
A Patient s Guide to Quadrilateral Space Syndrome
 A Patient s Guide to Quadrilateral Space Syndrome Orthopedic and Sports Medicine 825 South 8th Street, #550 Minneapolis, MN 55404 Phone: 612-333-5000 Fax: 612-333-6922 DISCLAIMER: The information in this
A Patient s Guide to Quadrilateral Space Syndrome Orthopedic and Sports Medicine 825 South 8th Street, #550 Minneapolis, MN 55404 Phone: 612-333-5000 Fax: 612-333-6922 DISCLAIMER: The information in this
A Patient s Guide to Cervical Foraminotomy
 A Patient s Guide to Cervical Foraminotomy 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Cervical Foraminotomy 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled from a variety
Stand-Alone Technology. Reginald Davis, M.D., FAANS, FACS Director of Clinical Research
 Stand-Alone Technology Reginald Davis, M.D., FAANS, FACS Director of Clinical Research Disclosures Stand-Alone Devices Optio-C Stalif C Coalition Prevail ROI-C Technology Descriptions Optio-C A no profile,
Stand-Alone Technology Reginald Davis, M.D., FAANS, FACS Director of Clinical Research Disclosures Stand-Alone Devices Optio-C Stalif C Coalition Prevail ROI-C Technology Descriptions Optio-C A no profile,
Interventional Pain Management
 Origination: 5/21/08 Revised: 10/02/17 Annual Review: 11/02/17 Purpose: To provide interventional pain management clinical coordination criteria for the Medical Department staff to reference when making
Origination: 5/21/08 Revised: 10/02/17 Annual Review: 11/02/17 Purpose: To provide interventional pain management clinical coordination criteria for the Medical Department staff to reference when making
Primary care referral criteria for musculoskeletal MRI scans
 Appendix 1 Primary care referral criteria for musculoskeletal MRI scans Accepted Criteria for Direct Access MRI Body Part Symptoms Imaging indicated Lumbar Spine Low Back Pain with adverse symptoms or
Appendix 1 Primary care referral criteria for musculoskeletal MRI scans Accepted Criteria for Direct Access MRI Body Part Symptoms Imaging indicated Lumbar Spine Low Back Pain with adverse symptoms or
REVIEW OF LITERATURE BMJ 2007; 334(7607): Diagnosis and treatment of sciatica. Bart W. Koes Maurits W. van Tulder Wilco C.
 2 REVIEW OF LITERATURE Diagnosis and treatment of sciatica Bart W. Koes Maurits W. van Tulder Wilco C. Peul BMJ 2007; 334(7607):1313-1317 22 CHAPTER 2 DIAGNOSIS AND TREATMENT OF SCIATICA 23 INTRODUCTION
2 REVIEW OF LITERATURE Diagnosis and treatment of sciatica Bart W. Koes Maurits W. van Tulder Wilco C. Peul BMJ 2007; 334(7607):1313-1317 22 CHAPTER 2 DIAGNOSIS AND TREATMENT OF SCIATICA 23 INTRODUCTION
Evidence Supporting the Recommendations. Implementation of the Guideline. Benefits/Harms of Implementing the Guideline Recommendations
 1 / 6 Surgical safety checklist in obstetrics and gynaecology Guideline Developer(s) Society of Obstetricians and Gynaecologists of Canada Date Released 2013 Jan Full Text Guideline Surgical safety checklist
1 / 6 Surgical safety checklist in obstetrics and gynaecology Guideline Developer(s) Society of Obstetricians and Gynaecologists of Canada Date Released 2013 Jan Full Text Guideline Surgical safety checklist
Radiographic Assessment for Back Pain
 Radiographic Assessment for Back Pain North American Spine Society Public Education Series What Are Radiographic Assessments? Radiographic assessments for low back pain involve the use of X-rays to determine
Radiographic Assessment for Back Pain North American Spine Society Public Education Series What Are Radiographic Assessments? Radiographic assessments for low back pain involve the use of X-rays to determine
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis This article is also available in Spanish: Estenosis de la columna lumbar (topic.cfm?topic=a00701). A common cause of low back and leg pain is lumbar spinal stenosis. As we age,
Lumbar Spinal Stenosis This article is also available in Spanish: Estenosis de la columna lumbar (topic.cfm?topic=a00701). A common cause of low back and leg pain is lumbar spinal stenosis. As we age,
Table of Contents: Part 1 General principles. Section 1: Introduction. 1. Past, present and future of interventional physiatry 2.
 Table of Contents: Part 1 General principles Section 1: Introduction 1. Past, present and future of interventional physiatry 2. Epidemiology Section 2: Spinal pain 3. Inflammatory basis of spinal pain
Table of Contents: Part 1 General principles Section 1: Introduction 1. Past, present and future of interventional physiatry 2. Epidemiology Section 2: Spinal pain 3. Inflammatory basis of spinal pain
APPROPRIATE USE GUIDELINES
 APPROPRIATE USE GUIDELINES Appropriateness of Advanced Imaging Procedures (MRI, CT, Bone Scan/PET) in Patients with Neck Pain CDI QUALITY INSTITUTE: PROVIDER LED ENTITY (PLE) Updated June, 2017 Contents
APPROPRIATE USE GUIDELINES Appropriateness of Advanced Imaging Procedures (MRI, CT, Bone Scan/PET) in Patients with Neck Pain CDI QUALITY INSTITUTE: PROVIDER LED ENTITY (PLE) Updated June, 2017 Contents
Chiropractic Healthcare. What, How, & Why
 Chiropractic Healthcare What, How, & Why Table of Contents Introduction 3 Topics Why Should Anyone go to a Chiropractor? 4 What to Expect on Your First Visit 7 Chiropractic and Exercise: Better than Drugs
Chiropractic Healthcare What, How, & Why Table of Contents Introduction 3 Topics Why Should Anyone go to a Chiropractor? 4 What to Expect on Your First Visit 7 Chiropractic and Exercise: Better than Drugs
Piriformis Syndrome. Midwest Bone & Joint Institute 2350 Royal Boulevard Suite 200 Elgin, IL Phone: Fax:
 A Patient s Guide to Piriformis Syndrome 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Piriformis Syndrome 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
Spinal Stenosis Surgical
 Spinal Stenosis Surgical Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Spinal Stenosis Surgical Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Kinematic Cervical Spine Magnetic Resonance Imaging in Low-Impact Trauma Assessment
 Kinematic Cervical Spine Magnetic Resonance Imaging in Low-Impact Trauma Assessment 1 Seminars in Ultrasound, CT, and MRI June 2009; Volume 30; Number 3; pp. 168-173 Vincenzo Giuliano, MD, Antonio Pinto,
Kinematic Cervical Spine Magnetic Resonance Imaging in Low-Impact Trauma Assessment 1 Seminars in Ultrasound, CT, and MRI June 2009; Volume 30; Number 3; pp. 168-173 Vincenzo Giuliano, MD, Antonio Pinto,
Misdiagnosis in cervical spondylosis myelopathy.
 Journal of the International Society of Head and Neck Trauma (ISHANT) Case report Misdiagnosis in cervical spondylosis myelopathy. Dr. Reinel A. Junco Martin. Neurosurgeon. Assistant professor Miguel Enriquez
Journal of the International Society of Head and Neck Trauma (ISHANT) Case report Misdiagnosis in cervical spondylosis myelopathy. Dr. Reinel A. Junco Martin. Neurosurgeon. Assistant professor Miguel Enriquez
Fractures of the Thoracic and Lumbar Spine
 A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
PATIENT REGISTRATION FORM
 PATIENT REGISTRATION FORM NAME: D.O.B AGE: SEX: STREET: CITY: STATE: ZIP: SS #: ETHNICITY: RACE: LANGUAGE: PHONE # TO LEAVE A PERSONAL MESSAGE: HOME PHONE #: WORK #: CELL #: E MAIL ADDRESS: EMERGENCY CONTACT:
PATIENT REGISTRATION FORM NAME: D.O.B AGE: SEX: STREET: CITY: STATE: ZIP: SS #: ETHNICITY: RACE: LANGUAGE: PHONE # TO LEAVE A PERSONAL MESSAGE: HOME PHONE #: WORK #: CELL #: E MAIL ADDRESS: EMERGENCY CONTACT:
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Mr. LBP: Case Presentation
 CLINICAL CASES Case: Mr. LBP Mr. LBP: Case Presentation Mr. LBP is a 35-year-old male He fell down while participating in a recreational sports activity He subsequently developed low back pain Upon arrival
CLINICAL CASES Case: Mr. LBP Mr. LBP: Case Presentation Mr. LBP is a 35-year-old male He fell down while participating in a recreational sports activity He subsequently developed low back pain Upon arrival
Spinal Trauma. General Rehabilitation of Patient with Spinal Trauma. Common Spinal Injuries. Important Anatomical Structures at each Vertebral Level
 Asian Association for Dynamic Osteosynthesis Workshop on Management of Spinal Trauma 22 April 2007 (Sunday) Orthopaedic Learning Centre, PWH, Shatin, Hong Kong General Rehabilitation of Patient with Spinal
Asian Association for Dynamic Osteosynthesis Workshop on Management of Spinal Trauma 22 April 2007 (Sunday) Orthopaedic Learning Centre, PWH, Shatin, Hong Kong General Rehabilitation of Patient with Spinal
Back and Neck Injuries: Surgical Advances and Treatment
 Back and Neck Injuries: Surgical Advances and Treatment Ara Deukmedjian, MD Board Certified Neurosurgeon June 8, 2017 1 2 Spinal Joints: Anatomy Two types of Spinal Joints: Spinal (intervertebral) disc
Back and Neck Injuries: Surgical Advances and Treatment Ara Deukmedjian, MD Board Certified Neurosurgeon June 8, 2017 1 2 Spinal Joints: Anatomy Two types of Spinal Joints: Spinal (intervertebral) disc
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽
 외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
Impingement syndrome. Clinical features. Management. Rotator cuff tear diagnosed. Go to rotator cuff tear
 Impingement syndrome Clinical features Management Poor response Good response Refer to orthopaedic surgery R Review as appropriate Investigations Rotator cuff tear diagnosed Go to rotator cuff tear Consider
Impingement syndrome Clinical features Management Poor response Good response Refer to orthopaedic surgery R Review as appropriate Investigations Rotator cuff tear diagnosed Go to rotator cuff tear Consider
Cervical intervertebral disc disease Degenerative diseases F 04
 Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Medical Affairs Policy
 Medical Affairs Policy Service: Back Pain Procedures-Epidural Injection (Caudal Epidural, Selective Nerve Root Block, Interlaminar, Transforaminal, Translaminar Epidural Injection) PUM 250-0015-1706 Medical
Medical Affairs Policy Service: Back Pain Procedures-Epidural Injection (Caudal Epidural, Selective Nerve Root Block, Interlaminar, Transforaminal, Translaminar Epidural Injection) PUM 250-0015-1706 Medical
Regional Pain Syndromes: Neck and Low Back
 Regional Pain Syndromes: Neck and Low Back Srinivas Nalamachu, MD Disclosures Consultant/Independent Contractor/Honoraria: Ferring 1 Learning Objectives Identify the most common painful conditions in the
Regional Pain Syndromes: Neck and Low Back Srinivas Nalamachu, MD Disclosures Consultant/Independent Contractor/Honoraria: Ferring 1 Learning Objectives Identify the most common painful conditions in the
CERVICAL STRAIN AND SPRAIN (Whiplash)
 CERVICAL STRAIN AND SPRAIN (Whiplash) Description time and using proper technique decrease the frequency of Whiplash is an injury to the neck caused when it is forcefully whipped or forced backward or
CERVICAL STRAIN AND SPRAIN (Whiplash) Description time and using proper technique decrease the frequency of Whiplash is an injury to the neck caused when it is forcefully whipped or forced backward or
Degenerative Disease of the Spine
 Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
A Patient s Guide to Treatment Guidelines for Low Back Pain
 A Patient s Guide to Treatment Guidelines for Low Back Pain 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Treatment Guidelines for Low Back Pain 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled
