Endoscopic treatment of the Retro-trochanteric Pain Syndrome
|
|
|
- Kristin Brown
- 5 years ago
- Views:
Transcription
1 Faculty of Health Sciences Endoscopic treatment of the Retro-trochanteric Pain Syndrome A quality study with medium-term follow-up Eirik Mikkelsen Master thesis in Medicine (MED-3950) May 2018 Supervisor: MD Khaled Meknas
2 Preface The orthopaedic research group at UiT The Artic University of Norway with MD. PhD Khaled Meknas in front have had a special interest in Retro-trochanteric pain syndrome and treatment of this condition for several years. In the past ten years or so Meknas has operated patients with Retro-trochanteric pain syndrome at the University Hospital of Northern Norway with endoscopic bursectomy and microtenotomy of short rotator in the hip. The purpose of this project is to evaluate this new treatment method and if there is developed osteoarthritis or other pathology in the hip region in the operated patients. Meknas has been my supervisor and has designed this study and its objective. He has also provided the preoperative and the short-term data. Furthermore, he dedicated two days in his outpatient clinic together with the writer for the medium-term follow-up. MD Zeiad Al- Ani (radiologist) has interpreted the x-ray and MRI scans. Professor Tom Wilsgaard has offered his assistance with the statistical methods. Sincere thanks to MD Meknas for offering me this project and for excellent supervision. Thanks to all that have contributed to the project. Tromsø, Eirik Mikkelsen Stud.med I
3 List of content PREFACE... I LIST OF CONTENT... II ABSTRACT... III INTRODUCTION... 1 THE DIAGNOSIS... 2 TREATMENT... 2 OBJECTIVE... 3 ETHICS AND PROTECTION OF PRIVACY... 3 PATIENTS AND METHODS... 3 PATIENTS... 3 METHODS... 4 STATISTICS... 5 CLARIFICATION OF TERMS... 5 RESULTS... 6 DISCUSSION... 7 CONCLUSION... 9 REFERENCES TABLES ENCLOSURE SUMMARY OF QUALITY OF CENTRAL REFERENCES II
4 Abstract Introduction Retro-trochanteric pain syndrome (RTPS) is a condition characterized by pain and tenderness in the buttock region. Normally sciatica originates from pathology in the spine. In RTPS the pathology resulting in sciatica is localized in the buttock region. First line treatment for RTPS is physiotherapy. This study evaluate treatment of RTPS by endoscopic bursectomy and microtenotomy of the short rotator affecting the sciatic nerve. Patients and methods 11 patients (12 hips) operated with endoscopic bursectomy and microtenotomy of a short rotator for treatment of RTPS were included in the study. The average age of the patients (1 male and 10 female) were 57.2 years and the mean duration of symptoms were 6.7 years. All patients had failed preoperative attempts of conservative treatment such as physiotherapy, NSAIDs and local steroid injections. The short-term follow-up was 3 months and the mean medium-term follow-up was 5 years. We evaluated the level of pain (using the visual analogue scale, VAS), function and clinical examination preoperatively, at 3 months and at 5 years. We also evaluated level of satisfaction and postoperative time without symptoms. Standard radiographs of the pelvis and hips and MRI of the lumbar spine, pelvis and hips were done preoperative and at medium-term follow-up. Results Pain significantly decreased from a mean VAS of 8.3 (SD 0.99) to 2.4 (SD 1.7), p-value = at short-term and 5.1 (SD 2.6), p-value = at medium-term follow-up. The ability to sit and usage of pain medication had a significant improvement. Overall satisfaction was high. Between surgery and final follow-up five patients developed OA in the hip(s). Conclusion Endoscopic bursectomy and microtenotomy of the small rotators in the hip are a valuable treatment method for patients with RTPS, the patients had significantly reduced pain and improved function five years after operation. III
5 Introduction Retro-trochanteric pain syndrome (RTPS) is a condition characterized by pain and tenderness in the buttock region from the sacrum to the greater trochanter, often accompanied by sciatic pain radiating diffusely to the lower extremity, limping and intolerance of sitting more than min (1, 2). The syndrome is known through different terms such as piriformis syndrome, greater trochanteric pain syndrome (GTPS), internal obturator syndrome and deep gluteal syndrome among others (1, 2). We choose to use the term Retro-trochanteric pain syndrome because it is a broader term and it is recommended by Meknas et al. (1). The incidence of the syndrome is not very well mapped out, as it is an exclusion diagnosis. However, the lifetime prevalence is estimated between 10-25% in industrialized societies (3-5). The incidence in primary care setting is reported to be around 1.8 patients per 1000 per year (4). The spine surgeon Tortolani and colleges found GTPS in 62.7 % of patients they evaluated(6). The incidence is increased in women, patients with leg length discrepancies, low back pain and knee pain (1). Usually sciatic pain originates from pathology in the spine such as radiculopathy or lumbar spinal stenosis, which is not the case for RTPS. The aetiology of the syndrome is not clearly known, but many factors are reported in the literature. Anatomical variations or abnormalities in the piriformis muscle and the sciatic nerve (7) such as piriformis muscle anterior to the sciatic nerve (8), bipartite piriformis muscle (9, 10) or a split sciatic nerve that encircles the piriformis muscle may irritate the nerve and give pain (1). Carro et al. found adhesions between the sciatic nerve and the piriformis muscle and fibrous or fibrovascular bands limiting the movement of or compressing the sciatic nerve (2). The gemelli and internal obturator muscles complex and their associated bursae may cause pain (11). It is argued that trochanteric bursitis is a frequent cause of hip pain (12). Overuse, hypertrophy of the piriformis muscle or dynamic entrapment of the sciatic nerve by the piriformis may cause the piriformis syndrome, (2, 13). In two different studies; Park et al. and Yang et al. found ganglion cysts compressing the sciatic nerve causing sciatic pain (14, 15). Ischiofemoral pathology, pathology in the quadratus femoris and the hamstrings may affect the sciatic nerve and cause pain (2). Pyomyositis of the piriformis or the internal obturator is reported to cause RTPS (16, 17). It is also reported RTPS secondary to hip replacement (18). Cox et al. (11) reported that inflammation of the small external rotators and thus tendinosis of these muscle tendons may cause RTPS. Radiofrequency microtenotomy has been reported effective for treatment of lateral epicondylitis (19-21), patellar- and rotator cuff 1
6 tendinosis (22). Therefore Meknas et al.(1) suggested microtenotomy of the affected external rotator as a possible method for treatment of RTPS. The Diagnosis The syndrome is characterized by buttock and diffuse pain in the lower extremity caused by a hypertrophic or inflamed muscle, which increases the pressure from the small external rotators of the hip towards the sciatic nerve (11). Another specific symptom is disturbed or loss of sensation in the affected extremity, usually diffuse and not limited to a dermatome (1, 2). The main diagnostic sign seems to be pain or tenderness triggered by deep digital palpation over the external rotators of the hip and the sciatic nerve (23, 24). Other useful clinical tests include Freiberg s sign, Pace s sign, Lasegue s test, Trendelenburg s sign and muscle hypotrophy in the affected extremity (1, 2). Most patients with RTPS have an immediate positive response to injection of a local anaesthetic and corticosteroid in the area, which can be used both for diagnosis and therapy of the condition (25). Regarding laboratory and radiological diagnostic there is no method available to diagnose the syndrome (1, 26-29). However, standard radiographs of the pelvis and hips, and MRI of the lumbar spine and hips are useful to exclude differential diagnosis such as radiculopathy, lumbar spine stenosis, osteoarthritis (OA), femoro-acetubular impingement and gynaecological conditions that should be excluded before making the diagnosis (1, 2). Treatment A number of methods exist for the treatment of RTPS. Physical therapy is recommended as first line treatment (11, 24, 30). Other conservative methods such as non-steroidal antiinflammatory drugs (NSAIDs), muscle relaxants, ice and rest have been reported with good outcome (31, 32). Injections of anaesthetic agents with or without corticosteroids are reported with variable results (33, 34). Tendinopathies in other muscles are treated with extracorporeal shock wave therapy (ESWT) and injection of platelet-rich plasma (PRP), this may be an alternative treatment for RTPS (35-38). Several studies have been reported an immediate pain relief after tenotomy of the piriformis tendon (8, 9, 39, 40). Carro et al. (2) described an endoscopic surgical technique for piriformis tendon and fibrotic band release for patients with RTPS, they found the method useful and that it improved function and diminished pain. Meknas et al. (23, 41) described 2
7 long-term improvement after tenotomy of the internal obturator muscle in patients with a tense internal obturator tendon. Meknas et al.(1) suggested a treatment algorithm for RTPS. A procedure for treating RTPS that included endoscopic trochanteric bursectomy and microtenotomy of the short rotator affecting the sciatic nerve is described by Meknas et al. (1) The unpublished short-term data showed pain reduction and improved function. Some of these patients are also included in the current study. Objective New methods of treatment need to be evaluated. This project aims to evaluate the treatment of patients with retro-trochanteric pain syndrome operated with endoscopic bursectomy and microtenotomy of short rotators in the retro-trochanteric area. Our hypothesis is that the patients suffered from retro-trochanteric pain syndrome would have reduced pain and improved function at medium-term follow-up after endoscopic bursectomy and microtenotomy of the short rotators of the hip. Additionally, we aimed to evaluate if OA or other pathology in the hip region would develop during the follow-up period. Ethics and Protection of Privacy The Data Protection Official at the University Hospital of Northern Norway were contacted through Kristin Andersen. The Data Protection Official have evaluated the project to be regulated by 7-12 in the Personal Data Regulations and authorized by the Health Personal Act 26. According to the Data Protection Regulations 7-12 did the Data Protection Official authorize project. See enclosure 1 for the full sanction. Patients and methods Patients Eleven patients (twelve hips) one male and 10 female, mean age 57.2 (SD 10.6) years who had retro-trochanteric pain syndrome, with radiation to the lower extremity treated by endoscopic bursectomy and microtenotomy of the short rotators, were included in the study. The mean duration of symptoms was 6.7 years (SD 3.9). The demographics of the patients are presented in table I. The surgical procedure was described by Meknas et al. in 2011 (1). All patients had been through previous attempts of conservative treatment such as physical 3
8 therapy, NSAIDS and injections of local anaesthesia with corticosteroids without improvement. Patients with cancer or serious organ system failure, or poor general condition were excluded. Methods Preoperatively, at 3-month follow-up and at 5-year follow-up, all patients underwent both assessment of pain using the visual analogue scale (VAS), assessment of function and clinical examinations. Furthermore, registration of time without symptoms postoperatively, satisfaction, willingness to undergo a reoperation given the same symptoms as preoperatively and scoring by The Nonarthritic Hip Score (42) were done at the medium-term follow-up. The evaluation of function included assessment of ability to sit and walk and usage of analgesics and NSAIDs. Classification of function is presented in table II. The clinical examinations included Pace s sign, Freiberg s sign, Lasegue s test, Trendelenburg s sign, test for pain when examined with deep digital palpation over the small external rotators and the sciatic nerve, radiation of pain and evaluation of limping. Preoperatively and at final follow-up, all patients underwent standard antero-posterior radiographs of the pelvis and hips, and lateral view of the hips (bilaterally) and MRI of the lumbar spine, pelvis and hips using a Philips Intera 1.5 Tesla (Royal Philips, Electronics Amsterdam Netherlands). An independent radiologist described both the preoperative and medium-term follow-up x-rays and MRI scans. Calcaria in the area of the Greater Trochanter were graded as + /++ or -. OA in the hips were graded from 0-IV according Conventional radiograph grading of OA as following: - grade 0: normal - grade I: possible joint space narrowing and subtle osteophytes - grade II: definite joint space narrowing, defined osteophytes and some sclerosis, especially in the acetabular region - grade III: marked joint space narrowing, small osteophytes, some sclerosis and cyst formation and deformity of femoral head and acetabulum - grade IV: gross loss of joint space with above features plus large osteophytes and increased deformity of the femoral head and acetabulum Primary endpoints were registration of pain using VAS, function and satisfaction. Secondary endpoint was medium-term radiological examination and comparison with 4
9 preoperative radiological examinations. An overview of the variables used is presented in table III. Statistics The related samples Wilcoxon signed rank test was used for the longitudinal comparisons. Dichotomous variables were analysed using the McNemar test. For the Pace s sign and Pain radiation the p-value is calculated with preoperative scoring of positive tests 11/12, thus the calculated p-value for these variables is higher than the true p-value. The statistical test was done by using SPSS Statistics version 24 (International Business Machines, New York, United States). A p-value < 0.05 was considered statically significant. Clarification of terms RTPS: Retro-trochanteric pain syndrome. GTPS: Greater trochanteric pain syndrome. Freiberg s sign: Forced passive internal rotation of the extended lower limb produces pain. Pace s sign: Resisted external rotation and abduction of the thigh in sitting position produces pain. Lasegue s test: Buttock and radiating pain below the knee during passive straight leg raise (<60 ) of the extended lower limb in the supine position. Trendelenburg s sign: With the patient standing on one foot the pelvis drops on the contralateral side if the abductor musculature is weak. MRI: Magnetic resonance imaging. NSAIDs: Non-steroidal anti-inflammatory drugs. Tendinopathy: A term that is commonly used in chronic tendon disorders when the patient seeks help as a result of pain. Tendinosis: A histological confirmation of degenerative changes without inflammatory cells but with changes such as collagen fibril disorientation, rounding of tenocyte nuclei, increased ground substance and hypervascularity in the histological specimens. ESWT: Extracorporeal shock wave therapy. Microtenotomy: The Topaz electrode (Smith Nephew) with 1.0 mm tip diameter is used to perform radiofrequency (RF) applications on the tendon in a grid-like 5
10 pattern. The electrode connected to sterile isotonic saline flow system, is used for microtenotomy. A radiofrequency apparatus provided the energy delivered through the electrode. The bipolar radiofrequency -based microtenotomy is thought to induce healing by a controlled inflammatory response followed by a stimulation of an angiogenic healing in the tendon. VAS: Visual analogue scale. OA: Osteoarthritis. Calcaria: Calcareous deposition around the greater trochanter and its tendon insertions. FCF: Fracture of the collum femoris Results There was a significant decrease in pain both at 3 months and at 5 years compared to preoperative pain. Mean VAS decreased from 8.3 (SD 0.99) to 2.4 (SD 1.7) p= and 5.1 (SD 2.6) p = respectively (Table IV). The ability to walk, sit and usage of painkiller are presented in table V. Both the sitting ability and the usage of painkillers had a significant improvement at both follow-ups compared to the preoperative level. The walking ability improved significantly at the shortterm follow-up compared to before surgery, however at medium-term follow-up the improvement of walking ability was not significant. Nine of the patients was symptom free for several years postoperatively (mean 3.4 years, SD 2,5), most of the patients were satisfied with the surgery, and nine were willing to do a reoperation (if they hypothetically were to have the same symptoms as before the operation) (Table VI). All clinical examination tests preoperatively, at 3 months and 5 years are presented in Table VII. The radiological findings are presented in table VIII. Preoperatively, none of the patients had pathological changes in the lumbar spine needing surgical intervention. Two patients had unaltered herniation of intervertebral disc at 5-year follow-up. 6
11 Calcaria (+) in the area of the Greater Trochanter was found in eight hips before surgery. The corresponding was found in nine hips (one on the contralateral side) at 5-year follow-up, one had developed to ++. None of the patients had OA in the hips preoperatively. The corresponding was found in 5 patients at medium-term follow-up, two of these patients had developed bilateral OA. Of the five patients with OA, one had tendinopathy revealed by MRI examinations both preoperatively and at 5-year follow-up. The others had developed tendinopathy between the operation and the final follow-up. The MRI displayed one tendinopathy and three bursitis (of which one was at the contralateral side) preoperatively. At the final follow-up; the MRI displayed tendinopathy in the gluteus medius and / or in the small rotators in eight patients (of which two was on the contralateral side). Furthermore, the MRI casually revealed ovarian cancer in one of the patients. The cancer was successfully treated by the Gynaecologists and Oncologists at the University Hospital of Northern Norway. One patient had transient neuralgic pain anteriorly to the knee radiating to the lateral leg postoperatively which recovered after 3 months. The pain is most likely derived from irritation of the sciatic nerve during the surgery. No other complications were registered. Discussion The most important finding in this study is that pain significantly decreased. At the 3-month follow-up all the patients had less pain compered to preoperative, and at 5 years the corresponding was 9 patients. In addition, both the ability to sit, and the usage of painkillers were significantly improved at both follow-ups. These findings together show that our patients had less pain and better function after the operation. The tendency of our results is that the patients were satisfied and had good outcome of the operation both on pain and function. There was still a degree of relapse of symptoms between the short- and medium-term follow-up. The negative development seems to be driven by patient no. 1 and 5. Both patients had comorbidity that were interpreted to contribute to their bad scorings. One patients got serious relapse 6.5 years after operation and were re-operated with excellent short-term results. All things considered the operation was effective both on short- and medium-term and the overall degree of satisfaction was high. 7
12 In a recently published systematic review of surgical management of deep gluteal syndrome Kay et al.(43) found varying surgical procedures for deep gluteal syndrome. The review concluded that the results showed consistent improvement in pain and a low incidence of complications after surgery, this is in line with in this study. Among the articles included in the review there were only one randomized controlled trial (RCT). In the RCT by Meknas et al. (23), they found significant improvement of pain both short- and long-term after surgical release of the internal obturator tendon. A median VAS of 8.3 at inclusion decreased to 4.0 at the 8-year follow-up. In a retrospective study in 2017 Han et al. (44) found significant improvement of pain in 12 patients after resection of the piriformis tendon, trochanteric bursectomy and sciatic nerve neurolysis. The mean VAS score of 9.0 decreased to 3.1 at 12- month follow-up. Martin et al. (45) found decrease in pain using VAS from 6.9 to 2.4 and improved modified Harris Hip Score (MHHS) in 35 patients operated with endoscopic decompression of the sciatic nerve. Furia et al. (35) found that ESWT can be used to treat patients with GTPS that have failed other conservative treatment approaches. They found a significant decrease of pain from 8.5 to 2.7 at 12 months. Taken together; the findings in this study are in line with other studies in the literature. However, we find few articles with a long-term follow-up. There is, to our knowledge, in the literature not described a procedure involving bursectomy and microtenotomy of the affected short external rotator for treatment of RTPS In a histological and ultrastructural study, Meknas et al. (46) studied the internal obturator tendon in patients diagnosed with OA or fracture of the collum femoris (FCF) who underwent hip arthroplasty. They found significant altered pathological and ultrastructural appearance (compatible with tendinosis) in the internal obturator tendons in the patients with OA compared to the patients with FCF. To our knowledge, there are no reports in the literature that discuss whether the tendinous changes are a normal pathological process in conjunction with OA, or whether the disease actually starts in the tendon and then proceeds to the joint. Our study does not give an answer on this matter but show the same tendency that tendinopathy and OA are associated with one another. The strength of this study is medium-term follow up (mean 5 years), and that examiners independent of the surgery performed the medium-term follow-up and all radiographic assessments. 8
13 The weakness of the study is the small number of patients involved, the lack of a control group, that the study design was not an RCT and that the time between surgery and the medium-term follow-up was not constant between the patients. It is desirable that further randomized controlled studies with a greater number of patients are conducted to evaluate both this treatment method and to establish a golden standard for treatment of retro-trochanteric pain syndrome. Conclusion Endoscopic bursectomy and microtenotomy of the affected short rotator in the hip resulted in significant medium-term decrease in pain and improved function in patients with retrotrochanteric pain syndrome. Thus, the hypothesis of the present study could be verified. This lends credence to that the surgical procedure can be offered to patients suffering from RTPS resistant towards conservative treatment. 9
14 References 1. Meknas K, Johansen O, Kartus J. Retro-trochanteric sciatica-like pain: current concept. Knee Surg Sports Traumatol Arthrosc 2011; 19: Carro LP, Hernando MF, Cerezal L, et al. Deep gluteal space problems: piriformis syndrome, ischiofemoral impingement and sciatic nerve release. Muscles Ligaments Tendons J 2016; 6: Collee G, Dijkmans BA, Vandenbroucke JP, et al. Greater trochanteric pain syndrome (trochanteric bursitis) in low back pain. Scand J Rheumatol 1991; 20: Lievense A, Bierma-Zeinstra S, Schouten B, et al. Prognosis of trochanteric pain in primary care. Br J Gen Pract 2005; 55: Segal NA, Felson DT, Torner JC, et al. Greater trochanteric pain syndrome: epidemiology and associated factors. Arch Phys Med Rehabil 2007; 88: Tortolani PJ, Carbone JJ, Quartararo LG. Greater trochanteric pain syndrome in patients referred to orthopedic spine specialists. Spine J 2002; 2: Benzon HT, Katz JA, Benzon HA, et al. Piriformis syndrome: anatomic considerations, a new injection technique, and a review of the literature. Anesthesiology 2003; 98: Sayson SC, Ducey JP, Maybrey JB, et al. Sciatic entrapment neuropathy associated with an anomalous piriformis muscle. Pain 1994; 59: Chen WS. Bipartite piriformis muscle: an unusual cause of sciatic nerve entrapment. Pain 1994; 58: Kosukegawa I, Yoshimoto M, Isogai S, et al. Piriformis syndrome resulting from a rare anatomic variation. Spine (Phila Pa 1976) 2006; 31: E Cox JM, Bakkum BW. Possible generators of retrotrochanteric gluteal and thigh pain: the gemelli-obturator internus complex. J Manipulative Physiol Ther 2005; 28: Raman D, Haslock I. Trochanteric bursitis--a frequent cause of 'hip' pain in rheumatoid arthritis. Ann Rheum Dis 1982; 41: Mayrand N, Fortin J, Descarreaux M, et al. Diagnosis and management of posttraumatic piriformis syndrome: a case study. J Manipulative Physiol Ther 2006; 29: Park JH, Jeong HJ, Shin HK, et al. Piriformis ganglion: An uncommon cause of sciatica. Orthop Traumatol Surg Res 2016; 102: Yang G, Wen X, Gong Y, et al. Sciatica and claudication caused by ganglion cyst. Spine (Phila Pa 1976) 2013; 38: E Hsu WC, Hsu JY, Chen MY, et al. Obturator internus pyomyositis manifested as sciatica in a patient with subacute bacterial endocarditis: A rare case report. Medicine (Baltimore) 2016; 95: e Toda T, Koda M, Rokkaku T, et al. Sciatica caused by pyomyositis of the piriformis muscle in a pediatric patient. Orthopedics 2013; 36: e Uchio Y, Nishikawa U, Ochi M, et al. Bilateral piriformis syndrome after total hip arthroplasty. Arch Orthop Trauma Surg 1998; 117: Meknas K, Odden-Miland A, Mercer JB, et al. Radiofrequency microtenotomy: a promising method for treatment of recalcitrant lateral epicondylitis. Am J Sports Med 2008; 36: Meknas K, Al Hassoni TN, Odden-Miland A, et al. Medium-Term Results After Treatment of Recalcitrant Lateral Epicondylitis: A Prospective, Randomized Study Comparing Open Release and Radiofrequency Microtenotomy. Orthop J Sports Med 2013; 1:
15 21. Tasto JP, Cummings J, Medlock V, et al. Microtenotomy using a radiofrequency probe to treat lateral epicondylitis. Arthroscopy 2005; 21: Taverna E, Battistella F, Sansone V, et al. Radiofrequency-based plasma microtenotomy compared with arthroscopic subacromial decompression yields equivalent outcomes for rotator cuff tendinosis. Arthroscopy 2007; 23: Meknas K, Kartus J, Letto JI, et al. Surgical release of the internal obturator tendon for the treatment of retro-trochanteric pain syndrome: a prospective randomized study, with longterm follow-up. Knee Surg Sports Traumatol Arthrosc 2009; 17: Meknas K, Kartus J, Letto JI, et al. A 5-year prospective study of non-surgical treatment of retro-trochanteric pain. Knee Surg Sports Traumatol Arthrosc 2009; 17: Palamar D, Misirlioglu TO, Akgun K. Comment on "Piriformis muscle syndrome: Diagnostic criteria and treatment of a monocentric series of 250 patients" by F. Michel et al. Ann Phys Rehabil Med 2013;56: Ann Phys Rehabil Med 2015; 58: Barton PM. Piriformis syndrome: a rational approach to management. Pain 1991; 47: Jankiewicz JJ, Hennrikus WL, Houkom JA. The appearance of the piriformis muscle syndrome in computed tomography and magnetic resonance imaging. A case report and review of the literature. Clin Orthop Relat Res 1991: Lee EY, Margherita AJ, Gierada DS, et al. MRI of piriformis syndrome. AJR Am J Roentgenol 2004; 183: Papadopoulos EC, Khan SN. Piriformis syndrome and low back pain: a new classification and review of the literature. Orthop Clin North Am 2004; 35: Keskula DR, Tamburello M. Conservative management of piriformis syndrome. J Athl Train 1992; 27: Browning R, Jackson JL, O'Malley PG. Cyclobenzaprine and back pain: a metaanalysis. Arch Intern Med 2001; 161: van Tulder MW, Scholten RJ, Koes BW, et al. Nonsteroidal anti-inflammatory drugs for low back pain: a systematic review within the framework of the Cochrane Collaboration Back Review Group. Spine (Phila Pa 1976) 2000; 25: Mullin V, de Rosayro M. Caudal steroid injection for treatment of piriformis syndrome. Anesth Analg 1990; 71: Smith J, Hurdle MF, Locketz AJ, et al. Ultrasound-guided piriformis injection: technique description and verification. Arch Phys Med Rehabil 2006; 87: Furia JP, Rompe JD, Maffulli N. Low-energy extracorporeal shock wave therapy as a treatment for greater trochanteric pain syndrome. Am J Sports Med 2009; 37: Kajikawa Y, Morihara T, Sakamoto H, et al. Platelet-rich plasma enhances the initial mobilization of circulation-derived cells for tendon healing. J Cell Physiol 2008; 215: Krasny C, Enenkel M, Aigner N, et al. Ultrasound-guided needling combined with shock-wave therapy for the treatment of calcifying tendonitis of the shoulder. J Bone Joint Surg Br 2005; 87: Mishra A, Woodall J, Jr., Vieira A. Treatment of tendon and muscle using platelet-rich plasma. Clin Sports Med 2009; 28: Benson ER, Schutzer SF. Posttraumatic piriformis syndrome: diagnosis and results of operative treatment. J Bone Joint Surg Am 1999; 81: Dezawa A, Kusano S, Miki H. Arthroscopic release of the piriformis muscle under local anesthesia for piriformis syndrome. Arthroscopy 2003; 19: Meknas K, Christensen A, Johansen O. The internal obturator muscle may cause sciatic pain. Pain 2003; 104:
16 42. Christensen CP, Althausen PL, Mittleman MA, et al. The nonarthritic hip score: reliable and validated. Clin Orthop Relat Res 2003: Kay J, de Sa D, Morrison L, et al. Surgical Management of Deep Gluteal Syndrome Causing Sciatic Nerve Entrapment: A Systematic Review. Arthroscopy 2017; 33: e Han SK, Kim YS, Kim TH, et al. Surgical Treatment of Piriformis Syndrome. Clin Orthop Surg 2017; 9: Martin HD, Shears SA, Johnson JC, et al. The endoscopic treatment of sciatic nerve entrapment/deep gluteal syndrome. Arthroscopy 2011; 27: Meknas K, Johansen O, Steigen SE, et al. Could tendinosis be involved in osteoarthritis? Scand J Med Sci Sports 2012; 22:
17 Tables Table I Demography of the patients ID GENDER SIDE AGE DURATION OF SYMPTOMS (YEARS) TIME BETWEEN SURGERY AND MEDIUM-TERM FOLLOW-UP (MONTHS) 1 Female Right Female Left Female Left Female Left Male Right Female Right Female Right Female Right Female Left Female Left Female Right Left TOTAL 10 Females 1 Male 6 Right 6 Left Mean: 57.2 (SD ) Mean: 6.7 (SD 1 3.9) Mean: 62.3 (SD ) 1 SD= standard deviation Table II Classification of function Classification of walking ability Can walk without problem 1 Can walk 1 km without pain 2 Can walk 1/2 km without pain 3 Can walk only with crutches 4 Cannot walk 5 Classification of sitting ability Can sit without problem 1 Can sit 1 h without pain 2 Can sit 1/2 h without pain 3 Can only sit 10 min because of pain 4 Cannot sit at all 5 Classification of pain medication Can manage the pain without painkillers 1 Painkillers gives moderate effect on the pain 2 Painkillers have no effect on the pain 3 13
18 Table III Variables Gender Defines whether the patient is male or female Side Defines which hip that was operated Age Defines the patients age at the time of surgery Duration of symptoms Defines how long the symptoms lasted before surgery (in years) Time between surgery and medium-term Defines how long time between surgery and medium-term follow-up follow-up (in months) Time without symptoms postoperatively Defines how long time the patient was free of symptoms postoperative (in years) Satisfaction with the operation Defines how satisficed the patient was with the operation on a scale from 0-10 (0 not satisfied and 10 totally satisfied) Given the same symptoms as Defines whether or not the patient would have had a new preoperatively would you have wanted a operation given he/she had experienced the same symptoms new operation? as preoperative Nonarthritic Hip Score (0-100) at mediumterm follow-up from (0 is the lowest possible score and 100 maximum Defines the score at The Nonarthritic Hip Score on a scale score) Pain using VAS Defines the patients pain from the hip using the Visual Analogue Scale from 0-10 (0 is no pain and 10 is maximum imaginal pain) Walking ability Defines walking ability using a scale from 1-5, see table II Sitting ability Defines sitting ability using a scale from 1-5, see table II Pain medication Defines pain medication using a scale form 1-3, see table II Lasegue s test Defines whether or not Lasegue s test is positive under 60 degrees flection Freiberg s sign Defines whether or not Freiberg s sign is positive Pace s sign Defines whether or not Pace s sign is positive Trendelenburg s sign Defines whether or not Trendelenburg s sign is positive Limping Defines whether or not the patients are limping Pain radiation in the affected extremity Defines whether or not the patient experiences pain radiating down the affected lower extremity or towards the lumbar column. Radiological findings Calcaria on x-ray: Calcareous deposition around the Greater Trochanter major. Graded as + or ++ Osteoarthritis on x-ray: Osteoarthritis in the hips graded from 0-VI Tendinopathy on MRI: Whether or not there is tendinopathy revealed by MRI Bursitis on MRI: Whether or not there is bursitis revealed by MRI 14
19 Table IV VAS preoperatively, at 3-month and 5-year follow-up ID PREOPERATIVE SHORT-TERM FOLLOW-UP MEDIUM-TERM FOLLOW- UP (right side) 2 (right side) 5 (right side) 8 (left side) 3 (left side) 5 (left side) MEAN (SD 1 ) 8.3 (0.99) 2.4 (1.7) 5.1 (2.6) MEDIAN (RANGE) 8 (7-10) 3 (0-5) 5 (1-10) P-VALUES SD= Standard deviation 2 P-values versus preoperative Table V Function PREOPERATIVELY SHORT-TERM FOLLOW-UP MEDIUM-TERM FOLLOW-UP MEAN WALKING ABILITY (SD 1 ) 3,1 (0,30) 1,3 (0,47) 2,1 (1,3) MEDIAN WALKING ABILITY (RANGE) 3 (3-4) 1 (1-2) 2 (1-5) P-VALUES 2 0,002 0,056 (n.s. 3 ) MEAN SITTING ABILITY (SD 1 ) 3,3 (0,47) 1,5 (0,69) 2,2 (0,98) MEDIAN SITTING ABILITY (RANGE) 3 (3-4) 1 (1-3) 2 (1-4) P-VALUES 2 0,002 0,006 MEAN PAIN MEDICATION (SD 1 ) 2,6 (0,52) 1,5 (0,69) 1,6 (0,67) MEDIAN PAIN MEDICATION (RANGE) 3 (2-3) 1 (1-3) 2 (1-3) P-VALUES 2 0,003 0,008 1 SD= Standard deviation 2 P-values versus preoperative 3 n.s.= Not significant 15
20 Table VI Nonarthritic hip score, postoperative time without pain and satisfaction ID NONARTHRITIC HIP SCORE (0-100) AT MEDIUM-TERM FOLLOW- UP TIME WITHOUT SYMPTOMS POSTOPERATIVELY (YEARS) SATISFACTION WITH THE OPERATION (0-10) MEAN (SD 1 ) 62.4 (17.5) 3.4 (2.5) 8.2 (3.2) 1 SD= Standard deviation Table VII Clinical assessment PREOPERATIVE SHORT-TERM FOLLOW-UP MEDIUM-TERM FOLLOW-UP LASEGUE S TEST POSITIVE 11/12 2/12 1/12 P-VALUES FREIBERG S SIGN POSITIVE 10/12 1/12 3/12 P-VALUES PACE S SIGN POSITIVE 12/12 4/12 5/12 P-VALUES * 0.031* TRENDELENBURG S SIGN 11/12 3/12 2/12 P-VALUES LIMPING 9/11 1/11 3/11 P-VALUES PAIN RADIATION 12/12 2/12 6/12 P-VALUES * 0.063* (n.s. 2 ) 1 P-values versus preoperative 2 n.s.= Not significant * P-value calculated with preoperative scoring set as 11/12, thus the calculated p-value is higher than the true p- value 16
21 Table VIII Radiographic findings ID STANDARD RADIOGRAPHS MRI PREOPERATIVE MEDIUM-TERM FOLLOW-UP PREOPERATIVE 1 Calcaria (+) Calcaria (+) Tendinopathy + Bilateral OA 1, grade II at the ipsilateral side and grade III at the contralateral side MEDIUM-TERM FOLLOW-UP Tendinopathy 2 Calcaria (+) Calcaria (+) No pathology No pathology 3 Calcaria (+) Calcaria (+) + -OA 1 grade I 4 Calcaria (+) Calcaria (+) + OA 1 grade I 5 Calcaria (+) Calcaria (++) + Bilateral OA 1 grade II Bursitis No pathology Bursitis Tendinopathy + Bursitis Tendinopathy + Bursitis Bilateral tendinopathy + Bilateral bursitis 6 No pathology No pathology No pathology Contralateral tendinopathy + Contralateral bursitis 7 Calcaria (+) Bilateral calcaria (+) No pathology Bursitis 8 No pathology No pathology Contralateral bursitis No pathology 9 Calcaria (+) Calcaria (+) No pathology Tendinopathy + Bursitis 10 No pathology No pathology No pathology No pathology 11* Calcaria (+) at the left side 1 OA= Osteoarthritis *the patient is operated in both hips Calcaria (+) at the left side + OA 1 grade II at the left side No pathology Tendinopathy at the right side Bursitis at the left side 17
22 Enclosure Enclosure 1 Til Khaled Meknas Ortopedisk avdeling Deres ref.: Vår ref.: 2017/3168 Saksbehandler/dir.tlf.: Kristin Andersen/ Dato: GODKJENNING AV BEHANDLING AV PERSONOPPLYSNINGER Det vises til Meldeskjema for forskningsprosjekt, kvalitetsprosjekt og annen aktivitet som medfører behandling av personopplysninger som er melde- eller konsesjonspliktig i henhold til helseregisterloven og personopplysningsloven med forskrifter, mottatt Meldingen gjelder prosjektet/registeret: Nr Navn på prosjektet: Retrotrochantær hofte smerte Prosjektet er et kvalitetsprosjekt/studentoppgave hvor Universitetssykehuset Nord-Norge HF er behandlingsansvarlig. Formål: «Evaluering av resultat av behandling av isjias lignende smerte rundt hoften» Personvernombudet (PVO) har vurdert prosjektet, og finner at behandlingen av personopplysningene vil være regulert av 7-12 i Personopplysningsforskriften og hjemlet etter Helsepersonelloven 26. PVO forutsetter at prosjektet gjennomføres i tråd med de opplysningene som er gitt, samt i henhold til Personopplysningsloven og Helseregisterloven med forskrifter. Videre forutsettes det at data anonymiseres etter prosjektavslutning ved at kodelista slettes. PVO har på bakgrunn av og tilsendte meldeskjema med vedlegg registrert prosjektet og opprettet et eget område (mappe) på \\hn.helsenord.no\unn-avdelinger\felles.avd\forskning (o:\) med navn 0707 hvor all data i forbindelse med prosjektet skal lagres. I tillegg er det opprettet et område på \\hn.helsenord.no\unnavdelinger\felles.avd\forskning\key med navn 0707N hvor nøkkelfil skal oppbevares. Tilgang til dette området er begrenset til kun å omfatte prosjektleder og den som prosjektleder definerer. PVO vil ha tilgang til området. PVO gjør oppmerksom på at dersom registeret skal brukes til annet formål enn det som er nevnt i meldingen, må dette meldes særskilt. Postadresse: Avdeling: Kvalitets- og utviklingssenteret Telefon: UNN HF Besøksadr.: Internett: TROMSØ Fakturaadr: UNN HF, c/o Fakturamottak, Postboks 3232, 7439 Trondheim E-post: personvernombudet@unn.no 18
23 PVO skal ha melding når registeret er slettet. PVO skal også ha melding dersom registeret ikke er slettet eller ikke ferdig behandlet innen 3 år. Med hjemmel i Forskrift om behandling av personopplysninger 7-12 godkjenner PVO at behandlingen kan iverksettes. Med vennlig hilsen UNIVERSITETSSYKEHUSET NORD-NORGE HF PVO-teamet e.f. Kopi: Klinikksjef Bjørn-Yngvar Nordvåg 19
24 Summary of Quality of Central References Referanse: Kay J, de Sa D, Morrison L, et al. Surgical Management of Deep Gluteal Syndrome Causing Sciatic Nerve Entrapment: A Systematic Review. Arthroscopy 2017; 33: e1. Design: Oversiktsartikkel Dokumentasjonsnivå Formål Materiale og metode Resultater Diskusjon/kommentarer Three databases (PubMed, Ovid Sjekkliste: [MEDLINE], and Embase) were searched by 2 reviewers independently from database inception until September 7, The inclusion criteria were studies reporting on both arthroscopic and open surgery and those with Level I to IV evidence. Systematic reviews, conference abstracts, book chapters, and technical reports with no outcome data were excluded. The methodologic quality of the studies was assessed with the MINORS (Methodological Index for Non-randomized Studies) tool. To assess the causes, surgical indications, patient reported clinical outcomes, and complications in patients with deep gluteal syndrome causing sciatic nerve entrapment. Konklusjon Although most of the studies identified were case series and reports, the results consistently showed improvement in pain and a low incidence of complications, particularly for endoscopic procedures. These findings lend credence to surgical management as a viable option for buttock pain caused by deep gluteal syndrome and warrant further investigation Land Canada År data innsamling 2017 The search identified 1,539 studies, of which 28 (481 patients; mean age, 48 years) were included for assessment. Of the studies, 24 were graded as Level IV, 3 as Level III, and 1 as Level II. The most commonly identified causes were iatrogenic (30%), piriformis syndrome (26%), trauma (15%), and non-piriformis (hamstring, obturator internus) muscle pathology (14%). The decision to pursue surgical management was made based on clinical findings and diagnostic investigations alone in 50% of studies, whereas surgical release was attempted only after failed conservative management in the other 50%. Outcomes were positive, with an improvement in pain at final follow-up (mean, 23 months) reported in all 28 studies. The incidence of complications from these procedures was low: Fewer than 1% and 8% of open surgical procedures and 0% and fewer than 1% of endoscopic procedures resulted in major (deep wound infection) and minor complications, respectively. Grade: Ib Moderate to high Er formålet med artikkelen klart formulert? Yes Søkte forfatterne etter relevante studier? Yes Er det sannsynlig at alle relevante studier ble funnet? Most likely Ble kvaliteten på de inkluderte studiene tilstrekkelig vurdert? Yes Hvis resultatene er slått sammen i en metaanalyse, er dette fornuftig og forsvarlig? Not relevant Hva er resultatene? The results are presented in a descriptive manner. Decrease in pain are described as a decrease of mean from preoperative to follow-up. Hvor presise er resultatene? The results are given in mean without SD and in percentage. Kan resultatene overføres til praksis? Yes Ble alle viktige utfallsmål vurdert? Assesment of function were not done Veier fordelene opp for ulemper og kostnader? Yes Styrke Undisclosed Svakhet Limited by the quantity and quality of the studies included. Heterogeneity with respect to surgical management, adjunctive treatment and evaluated outcomes. Lack of patientreported outcomes. The surgical learning curve that exist in endoscopic release of the sciatic nerve 20
25 Referanse: Meknas K, Kartus J, Letto JI, et al. Surgical release of the internal obturator tendon for the treatment of retro-trochanteric pain syndrome: a prospective randomized study, with long-term follow-up. Knee Surg Sports Traumatol Arthrosc 2009; 17: Design: RCT Dokumentasjonsnivå Formål Materiale og metode Resultater Diskusjon/kommentarer Twelve patients with clinical signs of retro-trochanteric pain syndrome were randomized to either operative treatment or a control group. Six patients were operated on with sectioning of the tendon to the internal obturator near its insertion to the trochanter major Evaluate surgical release of the internal obturator tendon as a treatment for retrotrochanteric pain syndrome. Konklusjon Surgical release of the internal obturator muscle resulted in long-term decrease in pain in patients with retro-trochanteric pain syndrome. Land Norway År data innsamling 2009 There was no significant pain decrease in either group at 6 months. However, at 8 years, the decrease in pain was significant in the surgical group (P < 0.03) but not in the control group. Three patients in the surgical group who needed pain medication with opioids preoperatively managed without such drugs at 8 years. Two patients were working half time at the 8 year follow-up. Before the start of the study the patients had been out of work for 3 and 10 years, respectively. At inclusion 4/12 patients had minor degenerative changes at the L3-L5 level as seen on computerized tomography or magnetic resonance imaging. At 8 years, the corresponding change was found in 7/9 patients (P = 0.025). Grade: Ib Low to moderate Sjekkliste: Er formålet med studien klart formulert? Yes Ble utvalget fordelt til de ulike gruppene med randiseringsprose-dyre? Yes Ble alle deltakerne gjort rede for på slutten av studien? Yes Ble deltakere/studiepersonell blindet mht gruppetilhørighet? Not reported, judged as not blinded. Var guppene like ved starten? Yes Ble gruppene behandlet likt? Yes Ble alle deltakere gjort rede for? Yes. 1/3 dropout in the surgical group and 1/6 dropout in the controlgroup Hva er resultatene? The most important variables were controlled, and the follow-up time is long enough. The effect is decrease of mean pain. Kan resultatene overføres til praksis. Yes Ble alle utfallsmål vurdert? Yes Er fordelene verdt ulemper/kostnader? Yes Styrke: Independent examiners for long-term and radiological follow-up Svakhet: Few patients, not enough power to analyse difference between groups 21
26 Referanse: Han SK, Kim YS, Kim TH, et al. Surgical Treatment of Piriformis Syndrome. Clin Orthop Surg 2017; 9: Design: Pasientserie Dokumentasjonsnivå Formål Materiale og metode Resultater Diskusjon/kommentarer From March 2006 to February 2013, Buttock pain was more improved than we retrospectively reviewed 239 sciatica with various conservative patients who were diagnosed with PS treatments. ESWT was the most and effective conservative treatment screened them for eligibility according relieving pain. Compared with to our inclusion/exclusion criteria. All preoperatively, the patients underwent various VAS score was significantly decreased conservative treatments from a mean of 9.0 to 4.0 after the initially including activity modification, operation, and 3.1 at 12 months. medications, physical therapy, local Overall, satisfactory results were steroid injections into the piriformis obtained in 10 patients (83%) after muscle, and extracorporeal surgery. shock wave therapy for at least 3 months. We resected the piriformis muscle with/without neurolysis of the sciatic nerve in 12 patients who had intractable sciatica despite conservative treatment at least for 3 months. The average age of the patients (4 males and 8 females) was 61 years (range, 45 to 71 years). The average Styrke Undisclosed duration of symptoms before surgery Svakhet Undisclosed was 22.1 months (range, 4 to 72 months), and the mean follow-up period was 22.7 months (range, 12 to 43 months). We evaluated the degree of pain and recorded the responses using a visual analog scale (VAS) preoperatively and 3 days and 12 months postoperatively. This study analyzes the diagnostic methods and efficacy of conservative and surgical treatments for piriformis syndrome Konklusjon Piriformis syndrome is thought to be an exclusively clinical diagnosis, and if the diagnosis is performed correctly, surgery can be a good treatment option in patients with refractory sciatica despite appropriate conservative treatments Land Korea År data innsamling 2017 Grade: III Low Sjekkliste: Var studien basert på et tilfeldig utvalg fra en egnet pasientgruppe? Yes Var det sikret at utvalget ikke var selektert? Yes Var inklusjonskriteriene for utvalget klart definert? Yes Er svarprosenten høy nok? All patients were assessed Var alle pasientene i utvalget i samme stadium av sykdom? Yes Var oppfølgningen tilstrekkelig (type/omfang/tid) for å synliggjøre endepunktene? It is desirable that ability to walk and sit are assessed. It is also desirable with a longer follow-up time. Ble objektive kriterier benyttet for å vurdere/validere endepunktene? Yes Ved sammenlikninger av pasientserier, er seriene tilstrekkelig beskrevet og prognostiske faktorers fordeling beskrevet? Not relevant Var registreringen av data prospektiv? No it was retrospective 22
27 Referanse: Martin HD, Shears SA, Johnson JC, et al. The endoscopic treatment of sciatic nerve entrapment/deep gluteal syndrome. Arthroscopy 2011; 27: Design: Pasientserier Dokumentasjonsnivå Grade: III Low Formål Materiale og metode Resultater Diskusjon/kommentarer Sciatic nerve entrapment was The mean patient age was 47 years diagnosed in 35 patients (28 women (range, 20 to 66 years). The mean and 7 men). Portals for inspection of duration of symptoms was 3.7 years the posterior peritrochanteric space (range, 1 to 23 years). The mean (subgluteal space) of the hip were preoperative VAS score was 6.9 +/- used as well as an auxiliary 2.0, and the mean preoperative MHHS posterolateral portal. Patients were was / (range, 25.3 to 79.2). treated with sciatic nerve Of the patients, 21 reported decompression by resection of preoperative use of narcotics for pain; 2 fibrovascular scar bands, piriformis continued to take narcotics tendon release, obturator internus, or postoperatively (unrelated to initial quadratus femoris or by hamstring complaint). The mean time of follow-up tendon scarring. Postoperative was 12 months (range, 6 to 24 outcomes were evaluated with the months). The mean postoperative modified Harris Hip Score (MHHS), MHHS increased to 78.0 and VAS verbal analog scale (VAS) pain score, score decreased to 2.4. Eighty-three and a questionnaire related percent of patients had no specifically to sciatic hip pain. postoperative sciatic sit pain (inability to sit for >30 minutes). The purpose of this study was to investigate the historical, clinical, and radiographic presentation of deep gluteal syndrome (DGS) patients, describe the endoscopic anatomy associated with DGS, and assess the effectiveness of endoscopic surgical decompression for DGS. Konklusjon Endoscopic decompression of the sciatic nerve appears useful in improving function and diminishing hip pain in sciatic nerve entrapment/dgs. Land United States År data innsamling 2010 Sjekkliste: Var studien basert på et tilfeldig utvalg fra en egnet pasientgruppe? Yes Var det sikret at utvalget ikke var selektert? Yes Var inklusjonskriteriene for utvalget klart definert? Yes Er svarprosenten høy nok? For the Benson questionary the rate was 66%, for the other variables 100% Var alle pasientene i utvalget i samme stadium av sykdom? Yes Var oppfølgningen tilstrekkelig (type/omfang/tid) for å synliggjøre endepunktene? A little to short follow-up time Ble objektive kriterier benyttet for å vurdere/validere endepunktene? Yes Ved sammenlikninger av pasientserier, er seriene tilstrekkelig beskrevet og prognostiske faktorers fordeling beskrevet? Not relevant Var registreringen av data prospektiv? Not clear, but likely Styrke Undisclosed Svakhet Experience were a factor in preoperative evaluation and treatment. The Benson criteria data were only obtained in a subset of patients. 23
TOPAZ TM What you should know
 TOPAZ TM What you should know Not for distribution in the United States. Need to know 2 Tendon: is a tough band of fibrous connective tissue that connects muscle to bone and is capable of withstanding
TOPAZ TM What you should know Not for distribution in the United States. Need to know 2 Tendon: is a tough band of fibrous connective tissue that connects muscle to bone and is capable of withstanding
STAIRS. What s Hip: Top 5 Hip Problems in Primary Care. I have no relevant disclosures. Top 5 (or 6) Pathologies. Big 3- Questions to Ask
 I have no relevant disclosures. What s Hip: Top 5 Hip Problems in Primary Care Alan Zhang MD Assistant Professor Sports Medicine and Hip Arthroscopy UCSF Department of Orthopaedic Surgery December, 2015
I have no relevant disclosures. What s Hip: Top 5 Hip Problems in Primary Care Alan Zhang MD Assistant Professor Sports Medicine and Hip Arthroscopy UCSF Department of Orthopaedic Surgery December, 2015
Effectiveness of Endoscopic Sciatic Nerve Decompression for the Treatment of Deep Gluteal Syndrome
 ORIGINAL ARTICLE Hip Pelvis 30(1): 29-36, 2018 http://dx.doi.org/10.5371/hp.2018.30.1.29 Print ISSN 2287-3260 Online ISSN 2287-3279 Effectiveness of Endoscopic Sciatic Nerve Decompression for the Treatment
ORIGINAL ARTICLE Hip Pelvis 30(1): 29-36, 2018 http://dx.doi.org/10.5371/hp.2018.30.1.29 Print ISSN 2287-3260 Online ISSN 2287-3279 Effectiveness of Endoscopic Sciatic Nerve Decompression for the Treatment
What s Hip: Common Hip Problems and Kids and Adults
 What s Hip: Common Hip Problems and Kids and Adults Alan Zhang MD Assistant Professor Sports Medicine and Hip Arthroscopy UCSF Department of Orthopaedic Surgery I have no relevant disclosures. 2 1 Most
What s Hip: Common Hip Problems and Kids and Adults Alan Zhang MD Assistant Professor Sports Medicine and Hip Arthroscopy UCSF Department of Orthopaedic Surgery I have no relevant disclosures. 2 1 Most
Deep gluteal syndrome
 Journal of Hip Preservation Surgery Vol. 2, No. 2, pp. 99 107 doi: 10.1093/jhps/hnv029 Mini Symposium MINI SYMPOSIUM Deep gluteal syndrome Hal David Martin, 1 Manoj Reddy 1,2 and Juan Gómez-Hoyos 1,3 *
Journal of Hip Preservation Surgery Vol. 2, No. 2, pp. 99 107 doi: 10.1093/jhps/hnv029 Mini Symposium MINI SYMPOSIUM Deep gluteal syndrome Hal David Martin, 1 Manoj Reddy 1,2 and Juan Gómez-Hoyos 1,3 *
Evaluation of Posterior Hip Pain
 Evaluation of Posterior Hip Pain Anthony J. Ferretti, D.O., MHSA Hip Pain in the Adult Various etiologies: Traumatic Infectious Neurovascular Degenerative Congenital Pathologic 1 Hip Pain Complex interaction
Evaluation of Posterior Hip Pain Anthony J. Ferretti, D.O., MHSA Hip Pain in the Adult Various etiologies: Traumatic Infectious Neurovascular Degenerative Congenital Pathologic 1 Hip Pain Complex interaction
Salisbury Foundation Trust Radiology Department Referral Guidelines for Primary Care: Musculoskeletal Imaging
 Salisbury Foundation Trust Radiology Department Referral Guidelines for Primary Care: Musculoskeletal Imaging These guidelines have been issued in conjunction with the Royal College of Radiology referral
Salisbury Foundation Trust Radiology Department Referral Guidelines for Primary Care: Musculoskeletal Imaging These guidelines have been issued in conjunction with the Royal College of Radiology referral
Young Adult Hip problems. Aresh Hashemi-Nejad FRCS(Orth)
 Young Adult Hip problems Aresh Hashemi-Nejad FRCS(Orth) RNOH founded 1837 by William Little 14 year old presenting with limp Knee pain on and off 4 months Limps Aresh Hashemi-Nejad FRCS(Orth) The Royal
Young Adult Hip problems Aresh Hashemi-Nejad FRCS(Orth) RNOH founded 1837 by William Little 14 year old presenting with limp Knee pain on and off 4 months Limps Aresh Hashemi-Nejad FRCS(Orth) The Royal
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow.
 Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
Latest technology in the treatment of chronic recalcitrant tendinopathy
 Latest technology in the treatment of chronic recalcitrant tendinopathy Dr K Arjun Rao Consultant Sport & Exercise Medicine Physician FACSEP FFSEM(UK) Specialist Sportscare W.A. WA Institute of Sport School
Latest technology in the treatment of chronic recalcitrant tendinopathy Dr K Arjun Rao Consultant Sport & Exercise Medicine Physician FACSEP FFSEM(UK) Specialist Sportscare W.A. WA Institute of Sport School
DISCLOSURE. The contributing authors have no financial relationships to disclose.
 DISCLOSURE The contributing authors have no financial relationships to disclose. INTRODUCTION Greater trochanteric pain syndrome (GTPS); formerly trochanteric bursitis Common condition, wide differential
DISCLOSURE The contributing authors have no financial relationships to disclose. INTRODUCTION Greater trochanteric pain syndrome (GTPS); formerly trochanteric bursitis Common condition, wide differential
Epidural Steroid Injection
 Epidural Steroid Injection Epidural steroid injections (ESI) are performed to place anti-inflammatory medication (steroid) and local anesthetic in the epidural space to target irritated nerves and relieve
Epidural Steroid Injection Epidural steroid injections (ESI) are performed to place anti-inflammatory medication (steroid) and local anesthetic in the epidural space to target irritated nerves and relieve
Hip Arthroscopy Techniques: Deep Gluteal Space Access
 1 2 Hip Arthroscopy Techniques: Deep Gluteal Space Access 3 4 5 6 7 8 9 10 11 Carlos A. Guanche, MD Southern California Orthopedic Institute 6815 Noble Avenue Van Nuys, CA 91405 cguanche@scoi.com 12 13
1 2 Hip Arthroscopy Techniques: Deep Gluteal Space Access 3 4 5 6 7 8 9 10 11 Carlos A. Guanche, MD Southern California Orthopedic Institute 6815 Noble Avenue Van Nuys, CA 91405 cguanche@scoi.com 12 13
HIP_CASE 2_OA. Hip Forces. Function of the Hip. Property of VOMPTI, LLC. For Use of Participants Only. No Use or Reproduction Without Consent 1
 HIP_CASE 2_OA Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 Eric Magrum DPT, OCS, FAAOMPT 62 yo female AM stiffness Hip pain diffuse, variable ant>lateral>post Gradual onset Tennis
HIP_CASE 2_OA Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 Eric Magrum DPT, OCS, FAAOMPT 62 yo female AM stiffness Hip pain diffuse, variable ant>lateral>post Gradual onset Tennis
The Relationship Between Hip Physical Examination Findings and Intra-articular Pathology Seen at the Time of Hip Arthroscopy
 The Relationship Between Hip Physical Examination Findings and Intra-articular Pathology Seen at the Time of Hip Arthroscopy Craig M. Capeci, MD Mohaned Al-Humadi, MD Malachy P. McHugh, PhD Alexis Chiang-Colvin,
The Relationship Between Hip Physical Examination Findings and Intra-articular Pathology Seen at the Time of Hip Arthroscopy Craig M. Capeci, MD Mohaned Al-Humadi, MD Malachy P. McHugh, PhD Alexis Chiang-Colvin,
Piriformis Syndrome. Midwest Bone & Joint Institute 2350 Royal Boulevard Suite 200 Elgin, IL Phone: Fax:
 A Patient s Guide to Piriformis Syndrome 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Piriformis Syndrome 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
Shockwave Therapies for Musculoskeletal Problems Useful Literature
 Shockwave Therapies for Musculoskeletal Problems Useful Literature I have some 1600 references related to shockwave therapy. Those listed below are the main musculoskeletal related papers from 2005-07
Shockwave Therapies for Musculoskeletal Problems Useful Literature I have some 1600 references related to shockwave therapy. Those listed below are the main musculoskeletal related papers from 2005-07
Non Surgical Management Of Hip And Knee Osteoarthritis Toolkit. Evaluation and Diagnosis of Osteoarthritis in Primary Care
 Non Surgical Management Of Hip And Knee Osteoarthritis Toolkit Evaluation and Diagnosis of Osteoarthritis in Primary Care OA-HxPE-716.indd 1 TABLE OF CONTENTS HISTORY TAKING... 3 EVALUATION OF SUSPECTED
Non Surgical Management Of Hip And Knee Osteoarthritis Toolkit Evaluation and Diagnosis of Osteoarthritis in Primary Care OA-HxPE-716.indd 1 TABLE OF CONTENTS HISTORY TAKING... 3 EVALUATION OF SUSPECTED
October 1999, Supplement 1 Volume 15 Number 7
 October 1999, Supplement 1 Volume 15 Number 7
October 1999, Supplement 1 Volume 15 Number 7
Corporate Medical Policy
 Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis by David Borenstein, MD In a previous article on low back pain, I reviewed the anatomy of the spine and discussed three causes of low back pain: muscle strain, herniated intervertebral
Lumbar Spinal Stenosis by David Borenstein, MD In a previous article on low back pain, I reviewed the anatomy of the spine and discussed three causes of low back pain: muscle strain, herniated intervertebral
FUNCTIONAL ANATOMY AND EXAM OF THE HIP, GROIN AND THIGH
 FUNCTIONAL ANATOMY AND EXAM OF THE HIP, GROIN AND THIGH Peter G Gerbino, MD, FACSM Orthopedic Surgeon Monterey Joint Replacement and Sports Medicine Monterey, CA TPC, San Diego, 2017 The lecturer has no
FUNCTIONAL ANATOMY AND EXAM OF THE HIP, GROIN AND THIGH Peter G Gerbino, MD, FACSM Orthopedic Surgeon Monterey Joint Replacement and Sports Medicine Monterey, CA TPC, San Diego, 2017 The lecturer has no
Plantar fasciitis: p. 1/6
 Clinical trials published in the international peer-reviewed literature 1 demonstrating efficacy and safety of treatment with the EMS Swiss Dolorclast according to Evidence Based Medicine criteria 2 :
Clinical trials published in the international peer-reviewed literature 1 demonstrating efficacy and safety of treatment with the EMS Swiss Dolorclast according to Evidence Based Medicine criteria 2 :
Trochanteric Bursitis After Total Hip Arthroplasty
 The Journal of Arthroplasty Vol. 25 No. 2 2010 Trochanteric Bursitis After Total Hip Arthroplasty Incidence and Evaluation of Response to Treatment Kevin W. Farmer, MD, Lynne C. Jones, PhD, Kirstyn E.
The Journal of Arthroplasty Vol. 25 No. 2 2010 Trochanteric Bursitis After Total Hip Arthroplasty Incidence and Evaluation of Response to Treatment Kevin W. Farmer, MD, Lynne C. Jones, PhD, Kirstyn E.
Hip Region. PHTY2020: Lecture
 Region PHTY2020: Lecture 2.1 29.02.16 Functional Overview Transfer body weight form trunk to legs Allows leg to adopt numerous positions needed for standing, walking running, stairs, sitting and other
Region PHTY2020: Lecture 2.1 29.02.16 Functional Overview Transfer body weight form trunk to legs Allows leg to adopt numerous positions needed for standing, walking running, stairs, sitting and other
CLINICS IN SPORTS MEDICINE
 Clin Sports Med 25 (2006) 365 369 CLINICS IN SPORTS MEDICINE A Acetabular labrum, tears of, hip arthroscopy in, 264 Acetabular rim, trimming of, and labral repair, new method for, 293 297 Acetabulum, femoral
Clin Sports Med 25 (2006) 365 369 CLINICS IN SPORTS MEDICINE A Acetabular labrum, tears of, hip arthroscopy in, 264 Acetabular rim, trimming of, and labral repair, new method for, 293 297 Acetabulum, femoral
Anatomy Your shoulder is made up of three bones: your upper arm bone (humerus), your shoulder blade (scapula), and your collarbone (clavicle).
 Shoulder Impingement/Rotator Cuff Tendinitis One of the most common physical complaints is shoulder pain. Your shoulder is made up of several joints combined with tendons and muscles that allow a great
Shoulder Impingement/Rotator Cuff Tendinitis One of the most common physical complaints is shoulder pain. Your shoulder is made up of several joints combined with tendons and muscles that allow a great
Tendon Fenestration. Disclosures. Outline: questions. Introduction: Peritendon Steroid Injections. Jon A. Jacobson, MD. Patellar Tendon: tendinosis
 Tendon Fenestration Jon A. Jacobson, MD Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures Consultant: Bioclinica Advisory Board: GE, Philips Book
Tendon Fenestration Jon A. Jacobson, MD Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures Consultant: Bioclinica Advisory Board: GE, Philips Book
EXTRACORPOREAL SHOCK WAVE THERAPY (ESWT) FOR CHRONIC TENDINITIS AND RELATED DISORDERS
 BACKGROUND EXTRACORPOREAL SHOCK WAVE THERAPY (ESWT) FOR CHRONIC TENDINITIS AND RELATED DISORDERS REVIEW OF THE MEDICAL LITERATURE FOR EFFICACY, SAFETY, AND COST-EFFECTIVENESS Low energy ESWT is a byproduct
BACKGROUND EXTRACORPOREAL SHOCK WAVE THERAPY (ESWT) FOR CHRONIC TENDINITIS AND RELATED DISORDERS REVIEW OF THE MEDICAL LITERATURE FOR EFFICACY, SAFETY, AND COST-EFFECTIVENESS Low energy ESWT is a byproduct
Hip Joint DX 612 Orthopedics and Neurology
 Hip Joint DX 612 Orthopedics and Neurology James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Hip Anatomy Palpation Point tenderness Edema Symmetry Hip ROM Hip Contracture
Hip Joint DX 612 Orthopedics and Neurology James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Hip Anatomy Palpation Point tenderness Edema Symmetry Hip ROM Hip Contracture
Hip Anatomy. Hip Joint DX 612 Orthopedics and Neurology. Hip ROM. Palpation
 Hip Joint DX 612 Orthopedics and Neurology Hip Anatomy James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Palpation Hip ROM Point tenderness Edema Symmetry Hip Contracture
Hip Joint DX 612 Orthopedics and Neurology Hip Anatomy James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Palpation Hip ROM Point tenderness Edema Symmetry Hip Contracture
THE HIP. Cooler than cool, the pinnacle of what is "it". Beyond all trends and conventional coolness.
 THE HIP Cooler than cool, the pinnacle of what is "it". Beyond all trends and conventional coolness. Objectives Hip anatomy Causes of hip pain Hip exam Anatomy Bones Ilium Anterior Superior Iliac Spine
THE HIP Cooler than cool, the pinnacle of what is "it". Beyond all trends and conventional coolness. Objectives Hip anatomy Causes of hip pain Hip exam Anatomy Bones Ilium Anterior Superior Iliac Spine
Degenerative joint disease of the shoulder, while
 Arthroscopic Debridement of the Shoulder for Osteoarthritis David M. Weinstein, M.D., John S. Bucchieri, M.D., Roger G. Pollock, M.D., Evan L. Flatow, M.D., and Louis U. Bigliani, M.D. Summary: Twenty-five
Arthroscopic Debridement of the Shoulder for Osteoarthritis David M. Weinstein, M.D., John S. Bucchieri, M.D., Roger G. Pollock, M.D., Evan L. Flatow, M.D., and Louis U. Bigliani, M.D. Summary: Twenty-five
The University Of Jordan Faculty Of Medicine THE LOWER LIMB. Dr.Ahmed Salman Assistant Prof. of Anatomy. The University Of Jordan
 The University Of Jordan Faculty Of Medicine THE LOWER LIMB Dr.Ahmed Salman Assistant Prof. of Anatomy. The University Of Jordan Gluteal Region Cutaneous nerve supply of (Gluteal region) 1. Lateral cutaneous
The University Of Jordan Faculty Of Medicine THE LOWER LIMB Dr.Ahmed Salman Assistant Prof. of Anatomy. The University Of Jordan Gluteal Region Cutaneous nerve supply of (Gluteal region) 1. Lateral cutaneous
SPORTS MEDICINE OVERUSE MANAGEMENT PRINCIPLES FOR
 SPORTS MEDICINE OVERUSE INJURIES: DIAGNOSIS AND MANAGEMENT PRINCIPLES FOR THE FAMILY PHYSICIAN DR NG CHUNG SIEN MBBS (SPORE) MSPMED (AUSTRALIA) DFD CAW SENIOR REGISTRAR CHANGI SPORTS MEDICINE CENTRE CHANGI
SPORTS MEDICINE OVERUSE INJURIES: DIAGNOSIS AND MANAGEMENT PRINCIPLES FOR THE FAMILY PHYSICIAN DR NG CHUNG SIEN MBBS (SPORE) MSPMED (AUSTRALIA) DFD CAW SENIOR REGISTRAR CHANGI SPORTS MEDICINE CENTRE CHANGI
PARADIGM SPINE. Patient Information. Treatment of a Narrow Lumbar Spinal Canal
 PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
Jessica Jameson MD Post Falls, ID
 Jessica Jameson MD Post Falls, ID Discuss the history of interventiona l pain Discuss previous tools to manage chronic pain Discuss current novel therapies to manage chronic pain and indications HISTORY
Jessica Jameson MD Post Falls, ID Discuss the history of interventiona l pain Discuss previous tools to manage chronic pain Discuss current novel therapies to manage chronic pain and indications HISTORY
NECK AND BACK PAIN AN INTRODUCTION TO
 AN INTRODUCTION TO NECK AND BACK PAIN This booklet provides general information on neck and back pain. It is not meant to replace any personal conversations that you might wish to have with your physician
AN INTRODUCTION TO NECK AND BACK PAIN This booklet provides general information on neck and back pain. It is not meant to replace any personal conversations that you might wish to have with your physician
The Lower Limb II. Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa
 The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
ROTATOR CUFF DISORDERS/IMPINGEMENT
 ROTATOR CUFF DISORDERS/IMPINGEMENT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH
ROTATOR CUFF DISORDERS/IMPINGEMENT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH
Hospital NEO,Turku, Finland
 Hamstring syndrome from fibrous band to tendinosis Sakari Orava, Janne Sarimo, Lasse Lempainen, Jyrki Heinänen Hospital NEO,Turku, Finland 1 Hamstring muscles- ANATOMY over two big joints pelvic stabilizers
Hamstring syndrome from fibrous band to tendinosis Sakari Orava, Janne Sarimo, Lasse Lempainen, Jyrki Heinänen Hospital NEO,Turku, Finland 1 Hamstring muscles- ANATOMY over two big joints pelvic stabilizers
A Patient s Guide to Arthroscopy of the Hip
 A Patient s Guide to Arthroscopy of the Hip Introduction A hip arthroscopy is a procedure where a small video camera attached to a fiberoptic lens is inserted into the hip joint to allow a surgeon to see
A Patient s Guide to Arthroscopy of the Hip Introduction A hip arthroscopy is a procedure where a small video camera attached to a fiberoptic lens is inserted into the hip joint to allow a surgeon to see
Latest Treatments for Hip Arthritis. Michael J. Repine MD Boulder Medical Center Orthopedics You re Not Alone
 Latest Treatments for Hip Arthritis Michael J. Repine MD Boulder Medical Center Orthopedics 303-502-9404 You re Not Alone More than 43 million people have some form of arthritis. It is estimated that the
Latest Treatments for Hip Arthritis Michael J. Repine MD Boulder Medical Center Orthopedics 303-502-9404 You re Not Alone More than 43 million people have some form of arthritis. It is estimated that the
A Syndrome (Pattern) Approach to Low Back Pain. History
 A Syndrome (Pattern) Approach to Low Back Pain Hamilton Hall MD FRCSC Professor, Department of Surgery, University of Toronto Medical Director, CBI Health Group Executive Director, Canadian Spine Society
A Syndrome (Pattern) Approach to Low Back Pain Hamilton Hall MD FRCSC Professor, Department of Surgery, University of Toronto Medical Director, CBI Health Group Executive Director, Canadian Spine Society
SMF PCP Treatment & Referral Guideline Orthopedics Developed February 1, 2003 Revised: October, 2011
 SUTTER MEDICAL FOUNDATION (SMF) 2800 L Street, 7 th Floor Sacramento, CA 95816 SMF PCP Treatment & Referral Guideline Orthopedics Developed February 1, 2003 Revised: October, 2011 I. Shoulder Pain...Page
SUTTER MEDICAL FOUNDATION (SMF) 2800 L Street, 7 th Floor Sacramento, CA 95816 SMF PCP Treatment & Referral Guideline Orthopedics Developed February 1, 2003 Revised: October, 2011 I. Shoulder Pain...Page
Page 1 of 6. Appendix 1
 Page 1 Appendix 1 Rotation Objectives and Schedule 1. Introductory Month 4 weeks 2. Total Joints 4 weeks a. Diagnosis and management of hip and knee arthritis b. Indications for surgery c. Implant selection;
Page 1 Appendix 1 Rotation Objectives and Schedule 1. Introductory Month 4 weeks 2. Total Joints 4 weeks a. Diagnosis and management of hip and knee arthritis b. Indications for surgery c. Implant selection;
Piriformis Muscle: Clinical Anatomy with Computed Tomography in Korean Population
 Original Article Korean J Pain 2011 June; Vol. 24, No. 2: 87-92 pissn 2005-9159 eissn 2093-0569 DOI:10.3344/kjp.2011.24.2.87 Piriformis Muscle: Clinical Anatomy with Computed Tomography in Korean Population
Original Article Korean J Pain 2011 June; Vol. 24, No. 2: 87-92 pissn 2005-9159 eissn 2093-0569 DOI:10.3344/kjp.2011.24.2.87 Piriformis Muscle: Clinical Anatomy with Computed Tomography in Korean Population
Using proximal hamstring tendons as a landmark for ultrasound- and CT-guided injections of ischiofemoral impingement
 Radiology Case Reports Using proximal hamstring tendons as a landmark for ultrasound- and CT-guided injections of ischiofemoral impingement Yulia Volokhina, DO, and David Dang, MD Volume 8, Issue 1, 2013
Radiology Case Reports Using proximal hamstring tendons as a landmark for ultrasound- and CT-guided injections of ischiofemoral impingement Yulia Volokhina, DO, and David Dang, MD Volume 8, Issue 1, 2013
What is the clinical effectiveness of extracorporeal Shock Wave Therapy or barbotage in the management of rotator cuff calcific tendinopathy?
 Specific Question: What is the clinical effectiveness of extracorporeal Shock Wave Therapy or barbotage in the management of rotator cuff calcific tendinopathy? Clinical bottom line There is moderate evidence
Specific Question: What is the clinical effectiveness of extracorporeal Shock Wave Therapy or barbotage in the management of rotator cuff calcific tendinopathy? Clinical bottom line There is moderate evidence
Greater Trochanter: Anatomy and Pathology
 Greater Trochanter: Anatomy and Pathology Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties:
Greater Trochanter: Anatomy and Pathology Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties:
HIP FOLLOW-UP. Thank you for your attention to this matter. If you have any questions, please contact us for assistance. Thomas P.
 HIP FOLLOW-UP It is important to review the status of your hip implant(s) during an office visit at six weeks, one year, two years, and every other year postoperatively thereafter for your safety even
HIP FOLLOW-UP It is important to review the status of your hip implant(s) during an office visit at six weeks, one year, two years, and every other year postoperatively thereafter for your safety even
A Patient s Guide to Trochanteric Bursitis of the Hip
 A Patient s Guide to Trochanteric Bursitis of the Hip Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can
A Patient s Guide to Trochanteric Bursitis of the Hip Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can
Piriformis Syndrome. Long Island Spine Specialists, P.C. 763 Larkfield Road 2nd Floor Commack, NY Phone: (631) Fax: (631)
 A Patient s Guide to Piriformis Syndrome 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Piriformis Syndrome 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is compiled from a variety
Move Better, Feel Better: What Can Physical Therapy Do For You
 Back to Basics Move Better, Feel Better: What Can Physical Therapy Do For You Dr. Stephen Baxter, Dr. Dean Yamanuha Department of Physical Therapy and Rehabilitative Sciences 5/16/2017 Dr. Stephen Baxter
Back to Basics Move Better, Feel Better: What Can Physical Therapy Do For You Dr. Stephen Baxter, Dr. Dean Yamanuha Department of Physical Therapy and Rehabilitative Sciences 5/16/2017 Dr. Stephen Baxter
Ankle Arthroscopy.
 Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Common neuromusculoskeletal disorders in the workplace W. Shane Journeay, PhD, MD, MPH, FRCPC, BC-OEM
 Common neuromusculoskeletal disorders in the workplace W. Shane Journeay, PhD, MD, MPH, FRCPC, BC-OEM OEMAC Calgary September 23, 2018 OBJECTIVES 1. To name key diagnoses of neuromusculoskeletal conditions
Common neuromusculoskeletal disorders in the workplace W. Shane Journeay, PhD, MD, MPH, FRCPC, BC-OEM OEMAC Calgary September 23, 2018 OBJECTIVES 1. To name key diagnoses of neuromusculoskeletal conditions
Evaluation of the Hip
 Evaluation of the Hip Adam Lewno, DO PCSM Fellow, University of Michigan Primary Care Sports Update 2017 Disclosures Financial: None Images: I would like to acknowledge the work of the original owners
Evaluation of the Hip Adam Lewno, DO PCSM Fellow, University of Michigan Primary Care Sports Update 2017 Disclosures Financial: None Images: I would like to acknowledge the work of the original owners
Evaluating hip pathology in trochanteric pain syndrome
 August 27, 2008 By Chris Dougherty, DO [1] and John J. Dougherty, DO [2] Patients may have greater trochanteric pain syndrome for years without knowing a defining cause or seeing pain improvement. Pathology
August 27, 2008 By Chris Dougherty, DO [1] and John J. Dougherty, DO [2] Patients may have greater trochanteric pain syndrome for years without knowing a defining cause or seeing pain improvement. Pathology
Your Orthopaedic Experience: Bones, Muscles and Joints. Getting you back into motion
 Your Orthopaedic Experience: Bones, Muscles and Joints Getting you back into motion Taking on your aches and pains You want to enjoy all life has to offer. And it s when you re mobile and active, and your
Your Orthopaedic Experience: Bones, Muscles and Joints Getting you back into motion Taking on your aches and pains You want to enjoy all life has to offer. And it s when you re mobile and active, and your
Total Hip Replacement Rehabilitation: Progression and Restrictions
 Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Hailee Gibson, CCPA Neurosurgery Physician Assistant. Windsor Neurosurgery & Spine Associates. Windsor Regional Hospital Ouellette Campus
 Hailee Gibson, CCPA Neurosurgery Physician Assistant Windsor Neurosurgery & Spine Associates Windsor Regional Hospital Ouellette Campus Disclosures I have no disclosures Learning Objectives Provide information
Hailee Gibson, CCPA Neurosurgery Physician Assistant Windsor Neurosurgery & Spine Associates Windsor Regional Hospital Ouellette Campus Disclosures I have no disclosures Learning Objectives Provide information
DIRECT SUPERIOR HIP APPROACH IN TOTAL HIP ARTHROPLASTY. Anil Thomas, MD Adult Reconstruction Peachtree Orthopedics Atlanta, GA
 DIRECT SUPERIOR HIP APPROACH IN TOTAL HIP ARTHROPLASTY Anil Thomas, MD Adult Reconstruction Peachtree Orthopedics Atlanta, GA Disclosures None Direct Superior Approach History and development of the approach
DIRECT SUPERIOR HIP APPROACH IN TOTAL HIP ARTHROPLASTY Anil Thomas, MD Adult Reconstruction Peachtree Orthopedics Atlanta, GA Disclosures None Direct Superior Approach History and development of the approach
Evaluation of the Knee and Shoulder
 Evaluation of the Knee and Shoulder Karen J. Boselli, MD Northeast Regional Nurse Practitioner Conference May 2018 Knee Overview History Examination Top 5 diagnoses When to image When to refer Pain most
Evaluation of the Knee and Shoulder Karen J. Boselli, MD Northeast Regional Nurse Practitioner Conference May 2018 Knee Overview History Examination Top 5 diagnoses When to image When to refer Pain most
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A ACJ. See Acromioclavicular joint (ACJ) Acromioclavicular joint (ACJ) procedures of, 557 559 Ankle and foot procedures of, 649 671 (See also
Note: Page numbers of article titles are in boldface type. A ACJ. See Acromioclavicular joint (ACJ) Acromioclavicular joint (ACJ) procedures of, 557 559 Ankle and foot procedures of, 649 671 (See also
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽
 외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
Andrew B. Wolff, MD a Geoffrey Hogan, BA a James Capon, BS, MS a Hayden Smith, BA a Alexandra Napoli, BS a Patrick Gaspar, MD b
 Pre-operative Lumbar Plexus Block Provides Superior Post-operative Analgesia when compared with Fascia Iliaca Block or General Anesthesia alone in Hip Arthroscopy Andrew B. Wolff, MD a Geoffrey Hogan,
Pre-operative Lumbar Plexus Block Provides Superior Post-operative Analgesia when compared with Fascia Iliaca Block or General Anesthesia alone in Hip Arthroscopy Andrew B. Wolff, MD a Geoffrey Hogan,
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME
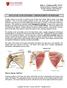 ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
The Young Adult Hip: FAI. Jason Snibbe, M.D. Snibbe Orthopedics Team Physician, University of Southern California
 The Young Adult Hip: FAI Jason Snibbe, M.D. Snibbe Orthopedics Team Physician, University of Southern California Introduction Femoroacetabular Impingment(FAI) Presentation and Exam Imaging Surgical Management
The Young Adult Hip: FAI Jason Snibbe, M.D. Snibbe Orthopedics Team Physician, University of Southern California Introduction Femoroacetabular Impingment(FAI) Presentation and Exam Imaging Surgical Management
Disorders of the Achilles tendon The ageing athlete
 Disorders of the Achilles tendon The ageing athlete John P. Negrine F.R.A.C.S. Foot and Ankle Surgeon Orthosports Sydney The Bad news Maximum heart rate decreases VO2 Max decreases Runners when compared
Disorders of the Achilles tendon The ageing athlete John P. Negrine F.R.A.C.S. Foot and Ankle Surgeon Orthosports Sydney The Bad news Maximum heart rate decreases VO2 Max decreases Runners when compared
ORTHOPEDICS BONE Recalcitrant nonunions In total hip replacement total knee surgery increased callus volume
 ORTHOPEDICS Orthopedics has to do with a variety of tissue: bone, cartilage, tendon, ligament, muscle. In this regard orthopedic and sports medicine share the same tissue targets. Orthopedics is mostly
ORTHOPEDICS Orthopedics has to do with a variety of tissue: bone, cartilage, tendon, ligament, muscle. In this regard orthopedic and sports medicine share the same tissue targets. Orthopedics is mostly
Cox Technic Case Report #126 published at (sent December 2013 ) 1
 Cox Technic Case Report #126 published at www.coxtechnic.com (sent December 2013 ) 1 Cox Technic Decompression Spinal Manipulation Resolves Symptoms Associated with Disc Protrusion and S1 Radiculopathy,
Cox Technic Case Report #126 published at www.coxtechnic.com (sent December 2013 ) 1 Cox Technic Decompression Spinal Manipulation Resolves Symptoms Associated with Disc Protrusion and S1 Radiculopathy,
The Painful Hip. Jennifer R Marks, MD
 The Painful Hip Jennifer R Marks, MD The Painful Hip A 64 yo F presents to clinic complaining of a sore hip What further questions do you have for this patient? What is on your differential diagnosis?
The Painful Hip Jennifer R Marks, MD The Painful Hip A 64 yo F presents to clinic complaining of a sore hip What further questions do you have for this patient? What is on your differential diagnosis?
Coventry Pain Clinic - Spianl Pain - Sciatica and Brachalgia
 Coventry Pain Clinic - Spianl Pain - Sciatica and Brachalgia Copyright 2002-2005 Dr. Richard S. Walker Introduction Spinal Nerve Root Pain (Radiculopathy) can arise from the problems affecting the:- C4
Coventry Pain Clinic - Spianl Pain - Sciatica and Brachalgia Copyright 2002-2005 Dr. Richard S. Walker Introduction Spinal Nerve Root Pain (Radiculopathy) can arise from the problems affecting the:- C4
In comparison to anterior and lateral knee pain, chronic. Semimembranosus Tendinopathy: One Cause of Chronic Posteromedial Knee Pain.
 [ Primary Care ] Semimembranosus Tendinopathy: One Cause of Chronic Posteromedial Knee Pain William E. Bylund, BS,* and Kevin de Weber, MD Context: Semimembranosus tendinopathy (SMT) is an uncommon cause
[ Primary Care ] Semimembranosus Tendinopathy: One Cause of Chronic Posteromedial Knee Pain William E. Bylund, BS,* and Kevin de Weber, MD Context: Semimembranosus tendinopathy (SMT) is an uncommon cause
Degenerative arthritis of Hip Bone Bangalore. Prof Sharath Rao Head, Dept. of Orthopaedics KMC Manipal
 Degenerative arthritis of Hip Prof Sharath Rao Head, Dept. of Orthopaedics KMC Manipal Hip joint Classical Synovial joint Biomechanics of hip Force coincides with trabecular pattern Hip joint Acetabulum
Degenerative arthritis of Hip Prof Sharath Rao Head, Dept. of Orthopaedics KMC Manipal Hip joint Classical Synovial joint Biomechanics of hip Force coincides with trabecular pattern Hip joint Acetabulum
Relieving Hip Pain. Austin W. Chen M.D.
 Relieving Hip Pain Austin W. Chen M.D. A little bit about me From Pittsburgh, PA Undergrad at U. of Notre Dame Medical School and Orthopaedic Surgery Residency at U. of Illinois Chicago Sports Medicine
Relieving Hip Pain Austin W. Chen M.D. A little bit about me From Pittsburgh, PA Undergrad at U. of Notre Dame Medical School and Orthopaedic Surgery Residency at U. of Illinois Chicago Sports Medicine
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT ***
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient - Certain conditions are more prevalent in particular age groups (Hip pain in children may refer to the knee from Legg-Calve-Perthes
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient - Certain conditions are more prevalent in particular age groups (Hip pain in children may refer to the knee from Legg-Calve-Perthes
Hip Cases from Clinic: Refining your history and physical
 Hip Cases from Clinic: Refining your history and physical Alan Zhang MD Assistant Professor Sports Medicine and Hip Arthroscopy UCSF Department of Orthopaedic Surgery 11/20/2017 Case #1 Healthy 21 M College
Hip Cases from Clinic: Refining your history and physical Alan Zhang MD Assistant Professor Sports Medicine and Hip Arthroscopy UCSF Department of Orthopaedic Surgery 11/20/2017 Case #1 Healthy 21 M College
Soft Tissue Rheumatism. Elinor Mody, MD Chief, Division of Rheumatology Reliant Medical Group
 Soft Tissue Rheumatism Elinor Mody, MD Chief, Division of Rheumatology Reliant Medical Group Some problems are difficult, but diagnosing and treating most causes of joint pain are not! Common areas of
Soft Tissue Rheumatism Elinor Mody, MD Chief, Division of Rheumatology Reliant Medical Group Some problems are difficult, but diagnosing and treating most causes of joint pain are not! Common areas of
Cox Technic Case Report #169 published at (sent 5/9/17) 1
 Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
405 Firemans Ave LaVale, Maryland 21502
 Dec 19, 2016 CHIEF COMPLAINT: Iris presents with a chief complaint involving her lower lumbar and sacral region, left sacroiliac region and left anterior hip and groin. ONSET OF SYMPTOMS Iris states this
Dec 19, 2016 CHIEF COMPLAINT: Iris presents with a chief complaint involving her lower lumbar and sacral region, left sacroiliac region and left anterior hip and groin. ONSET OF SYMPTOMS Iris states this
APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES
 APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES Tracy Porter, PT, DPT Des Moines University Department of Physical Therapy Objectives Review current literature related
APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES Tracy Porter, PT, DPT Des Moines University Department of Physical Therapy Objectives Review current literature related
A Structural Service Plan: Towards Better and Safer Spine Surgeries. Department of Orthopaedics & Traumatology Tuen Mun Hospital
 A Structural Service Plan: Towards Better and Safer Spine Surgeries Department of Orthopaedics & Traumatology Tuen Mun Hospital Cheung KK Wong CY Chan Andrew Tse Alfred Chow YY Department of Orthopaedics
A Structural Service Plan: Towards Better and Safer Spine Surgeries Department of Orthopaedics & Traumatology Tuen Mun Hospital Cheung KK Wong CY Chan Andrew Tse Alfred Chow YY Department of Orthopaedics
Trauma & Orthopaedic Undergraduate Syllabus
 Trauma & Orthopaedic Undergraduate Syllabus Introduction The purpose of this document is to provide a recommended syllabus for medical students in Trauma & Orthopaedics (T&0). It should help students on
Trauma & Orthopaedic Undergraduate Syllabus Introduction The purpose of this document is to provide a recommended syllabus for medical students in Trauma & Orthopaedics (T&0). It should help students on
Your Orthopaedic Experience: Bones, Muscles and Joints. Getting you back into motion. Hospitals + Health Checks + Physio + Gyms
 Your Orthopaedic Experience: Bones, Muscles and Joints. Getting you back into motion. Hospitals + Health Checks + Physio + Gyms Taking on your aches and pains. Getting you mobile your way. You want to
Your Orthopaedic Experience: Bones, Muscles and Joints. Getting you back into motion. Hospitals + Health Checks + Physio + Gyms Taking on your aches and pains. Getting you mobile your way. You want to
Impingement syndrome. Clinical features. Management. Rotator cuff tear diagnosed. Go to rotator cuff tear
 Impingement syndrome Clinical features Management Poor response Good response Refer to orthopaedic surgery R Review as appropriate Investigations Rotator cuff tear diagnosed Go to rotator cuff tear Consider
Impingement syndrome Clinical features Management Poor response Good response Refer to orthopaedic surgery R Review as appropriate Investigations Rotator cuff tear diagnosed Go to rotator cuff tear Consider
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) 6565 Fannin Street Houston, TX 77030 Phone: 713-790-3333 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) 6565 Fannin Street Houston, TX 77030 Phone: 713-790-3333 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
H.P. Teng, Y.J. Chou, L.C. Lin, and C.Y. Wong Under general or spinal anesthesia, the knee was flexed gently. In the cases of limited ROM, gentle and
 THE BENEFIT OF ARTHROSCOPY FOR SYMPTOMATIC TOTAL KNEE ARTHROPLASTY Hsiu-Peng Teng, Yi-Jiun Chou, Li-Chun Lin, and Chi-Yin Wong Department of Orthopedic Surgery, Kaohsiung Veterans General Hospital, Kaohsiung,
THE BENEFIT OF ARTHROSCOPY FOR SYMPTOMATIC TOTAL KNEE ARTHROPLASTY Hsiu-Peng Teng, Yi-Jiun Chou, Li-Chun Lin, and Chi-Yin Wong Department of Orthopedic Surgery, Kaohsiung Veterans General Hospital, Kaohsiung,
Hip Tendinopathy. Outline. Tendon Anatomy 6/6/2011. Tendinopathy Hip adductor Iliopsoas Gluteus medius / minimus Hamstring New treatments
 Hip Tendinopathy Kelly C. McInnis, DO Massachusetts General Hospital Sports Medicine Center Physical Medicine and Rehabilitation Outline Tendinopathy Hip adductor Iliopsoas Gluteus medius / minimus Hamstring
Hip Tendinopathy Kelly C. McInnis, DO Massachusetts General Hospital Sports Medicine Center Physical Medicine and Rehabilitation Outline Tendinopathy Hip adductor Iliopsoas Gluteus medius / minimus Hamstring
John J Christoforetti, MD Pittsburgh, Pennsylvania
 ARTHROSCOPIC ASSISTED PROXIMAL HAMSTRINGS REPAIR WITH HUMAN ACELLULAR DERMAL ALLOGRAFT PATCH AUGMENTATION FOR REVISION OF FAILED PROXIMAL HAMSTRINGS REPAIR: SHORT TERM CLINICAL AND MRI RESULT John J Christoforetti,
ARTHROSCOPIC ASSISTED PROXIMAL HAMSTRINGS REPAIR WITH HUMAN ACELLULAR DERMAL ALLOGRAFT PATCH AUGMENTATION FOR REVISION OF FAILED PROXIMAL HAMSTRINGS REPAIR: SHORT TERM CLINICAL AND MRI RESULT John J Christoforetti,
Leg Length Discrepancy in a Patient with Ipsilateral Total Knee and Total Hip Arthroplasty
 texas orthopaedic journal CASE REPORT Leg Length Discrepancy in a Patient with Ipsilateral Total Knee and Total Hip Arthroplasty Gaurav S. Sharma, BA; Ronald W. Lindsey, MD Department of Orthopaedic Surgery
texas orthopaedic journal CASE REPORT Leg Length Discrepancy in a Patient with Ipsilateral Total Knee and Total Hip Arthroplasty Gaurav S. Sharma, BA; Ronald W. Lindsey, MD Department of Orthopaedic Surgery
ANTERIOR TOTAL HIP ARTHOPLASTY
 ANTERIOR TOTAL HIP ARTHOPLASTY And Other Approaches Bill Rhodes PTA 236 Total Hip Arthoplasty (THA) Background THA, also know as Total Hip Replacement Regarded as the most valued development in orthopedics
ANTERIOR TOTAL HIP ARTHOPLASTY And Other Approaches Bill Rhodes PTA 236 Total Hip Arthoplasty (THA) Background THA, also know as Total Hip Replacement Regarded as the most valued development in orthopedics
Interlaminar Decompression & Stabilization. Reginald Davis, M.D., FAANS, FACS Director of Clinical Research
 Interlaminar Decompression & Stabilization Reginald Davis, M.D., FAANS, FACS Director of Clinical Research Disclosures Background Device meant to stabilize the spine without fusion following decompression
Interlaminar Decompression & Stabilization Reginald Davis, M.D., FAANS, FACS Director of Clinical Research Disclosures Background Device meant to stabilize the spine without fusion following decompression
The Lower Limb. Anatomy RHS 241 Lecture 2 Dr. Einas Al-Eisa
 The Lower Limb Anatomy RHS 241 Lecture 2 Dr. Einas Al-Eisa The bony pelvis Protective osseofibrous ring for the pelvic viscera Transfer of forces to: acetabulum & head of femur (when standing) ischial
The Lower Limb Anatomy RHS 241 Lecture 2 Dr. Einas Al-Eisa The bony pelvis Protective osseofibrous ring for the pelvic viscera Transfer of forces to: acetabulum & head of femur (when standing) ischial
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS North American Spine Society Public Education Series WHAT IS LUMBAR SPINAL STENOSIS? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
LUMBAR SPINAL STENOSIS North American Spine Society Public Education Series WHAT IS LUMBAR SPINAL STENOSIS? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Main Menu. Joint and Pelvic Girdle click here. The Power is in Your Hands
 1 Hip Joint and Pelvic Girdle click here Main Menu K.6 http://www.handsonlineeducation.com/classes//k6entry.htm[3/23/18, 2:01:12 PM] Hip Joint (acetabular femoral) Relatively stable due to : Bony architecture
1 Hip Joint and Pelvic Girdle click here Main Menu K.6 http://www.handsonlineeducation.com/classes//k6entry.htm[3/23/18, 2:01:12 PM] Hip Joint (acetabular femoral) Relatively stable due to : Bony architecture
Overview. Overview. Introduction. Introduction Anatomy History Examination Common Disorders. Introduction Anatomy History Examination Common Disorders
 Common Hip Disorders in Figure Skaters 14 th Annual Meeting of Sports Medicine and Science in Figure Skating January 25, 2009 8:15-8:45am Robert J. Dimeff, MD Medical Director of Sports Medicine Overview
Common Hip Disorders in Figure Skaters 14 th Annual Meeting of Sports Medicine and Science in Figure Skating January 25, 2009 8:15-8:45am Robert J. Dimeff, MD Medical Director of Sports Medicine Overview
Adult Isthmic Spondylolisthesis
 Adult Isthmic Spondylolisthesis North American Spine Society Public Education Series What Is Adult Isthmic Spondylolisthesis? The spine is made up of a series of connected bones called vertebrae. In about
Adult Isthmic Spondylolisthesis North American Spine Society Public Education Series What Is Adult Isthmic Spondylolisthesis? The spine is made up of a series of connected bones called vertebrae. In about
DISTINGUISHING BETWEEN ACUTE AND CHRONIC ROTATOR CUFF INJURIES IN WORKERS COMPENSATION PATIENTS
 DISTINGUISHING BETWEEN ACUTE AND CHRONIC ROTATOR CUFF INJURIES IN WORKERS COMPENSATION PATIENTS Lyndon B. Gross M.D. Ph.D. The Orthopedic Center of St. Louis SHOULDER PAIN Third most common musculoskeletal
DISTINGUISHING BETWEEN ACUTE AND CHRONIC ROTATOR CUFF INJURIES IN WORKERS COMPENSATION PATIENTS Lyndon B. Gross M.D. Ph.D. The Orthopedic Center of St. Louis SHOULDER PAIN Third most common musculoskeletal
Total Hip Arthroplasty Performed Using Conventional and Computer-Assisted, Tissue- Preserving Techniques 6
 Total Hip Arthroplasty Performed Using Conventional and Computer-Assisted, Tissue- Preserving Techniques 6 Stephen B. Murphy, MD, Timo M. Ecker, MD and Moritz Tannast, MD Introduction Less invasive techniques
Total Hip Arthroplasty Performed Using Conventional and Computer-Assisted, Tissue- Preserving Techniques 6 Stephen B. Murphy, MD, Timo M. Ecker, MD and Moritz Tannast, MD Introduction Less invasive techniques
