Identifying Patients Most Likely to Have a Common Bile Duct Stone After a Positive Intraoperative Cholangiogram
|
|
|
- Ada Evans
- 5 years ago
- Views:
Transcription
1 Identifying Patients Most Likely to Have a Common Bile Duct Stone After a Positive Intraoperative Cholangiogram Raja Vadlamudi, MD, MPH, Jason Conway, MD, MPH, Girish Mishra, MD, MS, John Baillie, MB ChB, FRCP, John Gilliam, MD, Adolfo Fernandez, MD, and John Evans, MD, MMSc Dr Vadlamudi is a gastroenterology fellow in the Department of Medicine at SUNY Upstate Medical University in Syracuse, New York. Drs Conway, Mishra, Gilliam, Fernandez, and Evans are affiliated with the Wake Forest School of Medicine in Winston-Salem, North Carolina. Dr Conway is an assistant professor of internal medicine, director of Endoscopic Ultrasound Services and the Advanced Endoscopy Fellowship Program in the Department of Internal Medicine; Dr Mishra is an associate professor of medicine, director of Endoscopy & Clinical Services, and vice chief of the Division of Gastroenterology; Drs Gilliam and Evans are assistant professors of medicine in the Division of Gastroenterology; and Dr Fernandez is an associate professor of surgery in the Department of General Surgery. Dr Baillie is the director of medical gastroenterology at the Carteret Medical Group in Morehead City, North Carolina. Address correspondence to: Dr John Evans Division of Gastroenterology Wake Forest School of Medicine Medical Center Boulevard Winston-Salem, NC 27157; Tel: ; joevans@wakehealth.edu Keywords Common bile duct stone, intraoperative cholangiogram, endoscopic retrograde cholangiopancreatography, endoscopic ultrasound Abstract: The false-positive rates of a positive intraoperative cholangiogram (IOC) are as high as 60%. Endoscopic retrograde cholangiopancreatography (ERCP) for stone removal is required after a positive IOC. It is unclear which clinical factors identify patients most likely to have a stone after a positive IOC. This study was conducted to identify factors predictive of common bile duct (CBD) stone(s) on ERCP after a positive IOC. A retrospective review of our endoscopic database identified all ERCP and/or endoscopic ultrasound (EUS) procedures performed for a positive IOC between August 2003 and August Collected data included patient demographics; indication for cholecystectomy; IOC findings; blood tests before and after cholecystectomy, including liver function tests, complete blood count, and amylase and lipase measurements; and ERCP and/or EUS results. Patients who had a negative EUS for CBD stones and no subsequent ERCP were contacted by phone to see if they eventually required an ERCP. Univariate and multivariable analyses were performed. A total of 114 patients were included in the study. IOC findings included a single stone, multiple stones, nonpassage of contrast into the duodenum, dilated CBD, and poor visualization of the bile duct. Eighty-four percent of patients had ERCP only, 9% had EUS only, and 7% had EUS followed by ERCP. Sixty-five patients (57%) had CBD stones on ERCP or EUS. Older age, multiple stones, dilated CBD on IOC, and elevated postcholecystectomy bilirubin levels were the clinical variables with statistically significant differences on univariate analysis. On multivariable analysis, older age and elevated postcholecystectomy total bilirubin levels correlated with the presence of CBD stones on ERCP. Fifty-seven percent of patients referred for endoscopic evaluation after a positive IOC had CBD stones on ERCP. Patients with CBD stones after a positive IOC were more likely to be older with elevated postcholecystectomy total serum bilirubin levels. 240 Gastroenterology & Hepatology Volume 10, Issue 4 April 2014
2 PATIENTS MOST LIKELY TO HAVE A CBD STONE AFTER A POSITIVE IOC Laparoscopic cholecystectomy is regarded as the treatment of choice for cholecystitis and symptomatic cholelithiasis. 1,2 An intraoperative cholangiogram (IOC) is often performed during laparoscopic cholecystectomy to determine biliary patency, integrity, and anatomy. The incidence of common bile duct (CBD) stones found on IOC after cholecystectomy ranges from 8% to 15%. 1 Unfortunately, false-positive rates for IOCs are as high as 60% in some series. 3-5 It is unclear whether these rates are due to misinterpretation of the cholangiogram, passage of the stones prior to endoscopic intervention, or nonvisualization of stones at the time of their removal. After a positive IOC, a postoperative endoscopic retrograde cholangiopancreatography (ERCP) is indicated for stone removal. 6 ERCP is not an innocuous procedure. The complication rates for ERCP range from 2.5% to 11%. 7,8 The most common complications are post-ercp pancreatitis, infection, and bleeding. The identification of patients most likely to have a CBD stone at the time of the ERCP is important to limit patient exposure to potential complications. We describe a retrospective review of every ERCP and/or EUS related to a positive IOC performed at Wake Forest Baptist Medical Center in Winston-Salem, North Carolina between August 2003 and August The purpose of this study was to identify factors predictive of CBD stone(s) at the time of endoscopic evaluation after a positive IOC, thereby individualizing the intervention required for the patients to preemptively minimize or even eliminate the risks associated with postcholecystectomy ERCP. This study also describes the performance of endoscopic ultrasound (EUS) in detecting CBD stones in patients after a positive IOC. The study was approved by the Institutional Review Board of Wake Forest University Baptist Medical Center. Methods The following data were collected for all patients: patient demographics; indication for cholecystectomy; IOC findings; and blood tests before and after cholecystectomy, including liver function tests (LFTs; total bilirubin, direct bilirubin, transaminases, and alkaline phosphatase), peripheral white blood cell count, amylase, and lipase. The interval (in days) between the positive IOC and ERCP and/or EUS was documented. The indications for laparoscopic cholecystectomy were reviewed and divided into the following 5 categories: symptomatic cholelithiasis, cholecystitis, pancreatitis, gallbladder dyskinesia, and other causes. The positive findings on IOC that prompted referral for ERCP are divided into the following 6 categories: nonpassage of contrast into the duodenum, a single stone, multiple stones, dilated bile duct (>8 mm), poor visualization of the distal CBD, and palpable CBD stones at surgery. The findings on IOC were taken from the operative notes and from the record of the treating gastroenterologist. No IOC images were available to be reviewed independently. Patients with positive findings on IOC underwent ERCP and/or EUS for elevated liver enzymes pre- or postoperatively or for persistent abdominal pain, nausea, and/or vomiting. All ERCP and EUS procedures were performed by experienced gastroenterologists at Wake Forest Baptist Medical Center. The decision to perform EUS prior to ERCP was at the discretion of the endoscopist. Patients who did not proceed to ERCP after a negative EUS were called by the principal investigator and asked if they had ongoing biliary symptoms and whether they had undergone ERCP at a different facility. An ERCP was determined to be positive for stone(s) if the cholangiogram demonstrated filling defects consistent with stones or if stones were seen after a biliary sphincterotomy and CBD sweep. CBD stones seen on ERCP were removed using baskets or retrieval balloons. After stone removal, a cholangiogram was performed to ensure clearance of the bile duct. ERCP/EUS findings noted the presence of stone(s), whether there was a single stone or multiple stones, the size of the stone(s), and the diameter of the CBD. Statistical Analysis Univariate analysis was used to assess for statistically significant associations between potential clinical risk factors and whether or not a CBD stone was seen on ERCP. Continuous variables were reported as means and standard deviations if normally distributed and as medians and ranges if not normally distributed. Continuous variables were compared using t test or Wilcoxon rank sum test as appropriate. Categorical variables were compared using the chi-square test. Multivariable logistic regression analysis was also performed. The variables included in the model were all those significant on the univariate analysis. Statistical analysis was performed using Intercooled Stata 8.0 for Windows (Stata Corp). Results A total of 114 patients were included. None of the patients had any precholecystectomy evaluation of the bile ducts with either magnetic resonance cholangiopancreatography (MRCP) or EUS. The majority of cholecystectomies were performed at outside hospitals, and later patients were transferred to our medical center for ERCP/EUS. The indications for cholecystectomy include 49 (43%) patients with symptomatic cholelithiasis, 19 (17%) with Gastroenterology & Hepatology Volume 10, Issue 4 April
3 VADLAMUDI ET AL cholecystitis, 21 (18%) with pancreatitis, 7 (6%) with gallbladder dyskinesia (based on abnormal cholescintigraphy), 1 (1%) with acute cholangitis, and 17 (15%) with no record available in our database. Of the 19 patients who had cholecystitis, 13 (68%) had calculus type, and the remaining 6 (32%) had no record of the type. Operative notes were unavailable for review in 61 patients (54%), and, in 8 patients (7%), no indication for IOC was noted. The indication for performing an IOC was elevated liver enzymes in 20 patients, pancreatitis in 13 patients, CBD stone on preoperative abdominal ultrasound (US) in 4 patients, abnormal cystic duct anatomy in 2 patients, and CBD stone on computed tomography, CBD stone on magnetic resonance imaging, intraoperative cystic duct stone, CBD dilatation on preoperative abdominal US, gallbladder neck stone on preoperative abdominal US, and brisk outflow of bile from the cystic duct during the operation in 1 patient each. For patients who came to our institution with no operative notes, the findings noted on IOC were recorded by the gastroenterologist at the time of transfer as reported by the referring physician. All patients had successful ERCP and/or EUS. CBD stones were confirmed in 65 patients (57%), for a falsepositive IOC rate of 43%. The majority (84%) of patients underwent ERCP alone; however, a significant minority (16%) had EUS performed in addition to ERCP. The median time to ERCP and/or EUS after surgery was 4 days (range, 0-167). A single stone was identified on EUS and confirmed by ERCP in the patient who had the procedures 167 days after a positive IOC. Table 1 shows ERCP and EUS findings. Of the 10 patients who had no stone seen on EUS, 1 patient had an ERCP, which confirmed the presence of a stone. The ERCP was performed because there was some concern that the entirety of the bile duct was not visualized by EUS due to a periampullary diverticulum. All other patients were contacted by telephone. None had symptoms of biliary colic or required an ERCP after the EUS. Of the 8 patients with stones seen on EUS, 7 patients underwent subsequent ERCP at our center, and 1 patient was lost to follow-up. Six of the 7 patients investigated at our center had CBD stone(s) on ERCP; 1 patient had no stones at the time of the procedure. Being conservative and assuming that the 1 patient with a positive EUS for a CBD stone who was lost to follow-up was a false-positive, the sensitivity and specificity of EUS for detecting CBD stones in patients with a positive IOC in this study were 100% and 83%, respectively. A comparison of clinical factors in patients with or without confirmed CBD stones on ERCP or EUS is shown in Table 2. In our study, patients with confirmed CBD stones were more likely to be older, have multiple stones or a dilated duct on IOC, and have an elevated Table 1. ERCP and EUS Findings Procedure(s) ERCP only, n (%) 96 (84) EUS only, n (%) 10 (9) EUS followed by ERCP, n (%) 8 (7) ERCP Findings (n=104) No stones, n (%) 40 (38) Stone(s), n (%) 64 (62) Median CBD diameter on ERCP, mm (range) 10 (5-20) CBD dilated on ERCP, n (%) 45 (58) EUS Findings (n=18) No stones, n (%) 10 (56) Stone(s), n (%) 8 (44) Median CBD diameter on EUS, mm (range) 8 (4-18) CBD dilated on EUS, n (%) 7 (44) CBD, common bile duct; ERCP, endoscopic retrograde cholangiopancreatography; EUS, endoscopic ultrasound. total serum bilirubin postcholecystectomy. There was no significant difference in indication for cholecystectomy, precholecystectomy laboratory values, or days between positive IOC and ERCP and/or EUS in patients with or without confirmed CBD stones. Table 3 shows the results of the multivariable logistic analysis. Patients with a positive IOC who were older and had elevated postcholecystectomy serum bilirubin levels were more likely to have a stone seen on ERCP than those who were younger and had normal bilirubin levels. Discussion This is the largest study to date detailing ERCP findings after a positive IOC. In our study, 38% of patients (40 of 104 patients) who underwent postoperative ERCP for a positive IOC did not have CBD stones. A study by Frossard and colleagues indicated that spontaneous migration of CBD stones (especially those less than 8 mm in diameter) occurred in up to 21% of patients. 9 Spontaneous migration of stones into the duodenum and microlithiasis appeared to be the most likely explanations for negative ERCP results in our study. Overall, these data are consistent with prior reports indicating low rates of stone recovery on a postoperative ERCP. 3,10,11 Confirmation of microlithiasis would require crystal analysis of bile for calcium bilirubinate. This could not be accomplished in our study due to its retrospective design. IOC is mainly performed for 2 reasons: to detect choledocholithiasis and/or to confirm the integrity of the biliary system after the procedure. 12 Systematic reviews by Ford and colleagues and Sajid and colleagues indicate 242 Gastroenterology & Hepatology Volume 10, Issue 4 April 2014
4 PATIENTS MOST LIKELY TO HAVE A CBD STONE AFTER A POSITIVE IOC Table 2. Comparison of Patient Demographics, Indications for Cholecystectomy, IOC Findings, and Laboratory Values CBD Stones on ERCP or EUS No stones (n=49) Stones (n=65) P value Median Age, years (SD) 52 (13-93) 56 (14-92).03 Gender, n (%) Male 15 (32) 27 (42).27 Female 32 (68) 37 (58).34 IOC Findings, n (%) Nonpassage of contrast into the duodenum 7 (16) 7 (11).478 Single stone 19 (42) 26 (41).868 Multiple stones 12 (27) 30 (47).033 Dilated bile duct 0 (0) 5 (11).006 Poor visualization of the distal CBD 2 (4) 1 (2).365 Median Postcholecystectomy Laboratory Values AST, U/L ALT, U/L ALP, U/L Total bilirubin, mg/dl Direct bilirubin, mg/dl WBC count, Amylase, U/L Lipase, U/L Any Postoperative Liver Function Test Abnormality, n (%) 29 (88) 41 (82).47 ALP, alkaline phosphatase; ALT, alanine aminotransferase; AST, aspartate aminotransferase; CBD, common bile duct; ERCP, endoscopic retrograde cholangiopancreatography; EUS, endoscopic ultrasound; IOC, intraoperative cholangiogram; SD, standard deviation; WBC, white blood cell. no concrete evidence to support or reject the use of IOC during cholecystectomy. 12,13 As the interpretation of IOC depends on the reviewer, the accuracy of results can at times be in doubt. 14 In this context, biliary endoscopists are left to decide whether to proceed with ERCP and its inherent complications or pursue confirmatory imaging or clinical markers (eg, LFTs). In our study, none of the IOC findings accurately predicted the presence or absence of CBD stones, which is similar to findings in prior studies. 2 However, on multivariate analysis, patients who were older and had an elevated postcholecystectomy total serum bilirubin level were significantly more likely to have a CBD stone on ERCP. A study by Varadarajulu and colleagues identified abnormal LFTs as 1 of the variables that predicted the presence of CBD stones. 1 LFTs were shown to predict CBD stones in other studies, particularly in patients undergoing ERCP preoperatively Of all the LFTs analyzed in our data, only total serum bilirubin after the cholecystectomy predicted stones on ERCP (P value of.02 on univariate analysis). Ammori and colleagues advocate a wait-and-see policy for patients with small stones on IOC or follow-up with less invasive techniques, such as EUS or MRCP. 11 Those with definite CBD stones found on follow-up imaging would then undergo ERCP. The accuracy of both tests, particularly EUS, in the evaluation of CBD stones is greater than 95% Our results agreed with those of the study by Ammori and colleagues regarding follow-up of patients who had negative EUS findings. 11 EUS avoids the risk of pancreatitis seen with ERCP and can be very accurate in detecting CBD stones, even small ones in nondilated ducts. 22 EUS can be performed immediately before ERCP under the same sedation, avoiding the need for a second visit. In our study, we looked at the sensitivity and specificity of EUS for detecting CBD stones. The results showed that EUS had a high sensitivity (100%) and specificity (83%) for detecting a retained CBD stone, rendering it a useful screening study to perform before ERCP. There are several limitations of this study, including the study s retrospective design; the use of nonstandardized IOCs, with the subjects being referred from different hospitals with different imaging technologies; and the prolonged time period between positive IOC and endo- Gastroenterology & Hepatology Volume 10, Issue 4 April
5 VADLAMUDI ET AL Table 3. Estimated Odds Ratios Based on the Multivariable Logistic Regression Model* Variable Odds Ratio 95% CI Age Multiple stones seen on IOC Postcholecystectomy total bilirubin scopic imaging. As the patient numbers were small in our study, a larger study, performed prospectively, comparing EUS to ERCP for identifying CBD stones is the obvious next step. We have plans to initiate such a study at our institution in the near future. Summary In our 6-year retrospective analysis, 57% of the patients referred for ERCP after a positive IOC during laparoscopic cholecystectomy had confirmed CBD stone(s) on ERCP/EUS. Patients with CBD stones after a positive IOC were more likely to be older and have an elevated total serum bilirubin postcholecystectomy. We recommend using safer and less invasive imaging, such as EUS, in younger patients with normal LFTs and/or normal ducts and going straight to ERCP in elderly patients with abnormal LFTs and/or dilated ducts. The authors sincerely thank Dr Douglas Case of Wake Forest School of Medicine in Winston-Salem, North Carolina for his support with statistical analysis. The authors have no relevant conflicts of interest to disclose. References *Although significant in univariate analysis, the variable dilated bile duct on IOC was not included in this model because only 6 patients had this diagnosis. IOC, intraoperative cholangiogram. 1. Varadarajulu S, Eloubeidi MA, Wilcox CM, Hawes RH, Cotton PB. Do all patients with abnormal intraoperative cholangiogram merit endoscopic retrograde cholangiopancreatography? Surg Endosc. 2006;20(5): Spinn MP, Wolf DS, Verma D, Lukens FJ. Prediction of which patients with an abnormal intraoperative cholangiogram will have a confirmed stone at ERCP. Dig Dis Sci. 2010;55(5): Ryberg AA, Fitzgibbons RJ Jr, Tseng A, Maffi TR, Burr LJ, Doris PE. Abnormal cholangiograms during laparoscopic cholecystectomy. Is treatment always necessary? Surg Endosc. 1997;11(5): Korman J, Cosgrove J, Furman M, Nathan I, Cohen J. The role of endoscopic retrograde cholangiopancreatography and cholangiography in the laparoscopic era. Ann Surg. 1996;223(2): Levine SB, Lerner HJ, Leifer ED, Lindheim SR. Intraoperative cholangiography. A review of indications and analysis of age-sex groups. Ann Surg. 1983;198(6): Schmitt CM, Baillie J, Cotton PB. ERCP following laparoscopic cholecystectomy: a safe and effective way to manage CBD stones and complications. HPB Surg. 1995;8(3): Loperfido S, Angelini G, Benedetti G, et al. Major early complications from diagnostic and therapeutic ERCP: a prospective multicenter study. Gastrointest Endosc. 1998;48(1): Freeman ML. Adverse outcomes of ERCP. Gastrointest Endosc. 2002;56(6 suppl): S273-S Frossard JL, Hadengue A, Amouyal G, et al. Choledocholithiasis: a prospective study of spontaneous common bile duct stone migration. Gastrointest Endosc. 2000;51(2): Hainsworth PJ, Rhodes M, Gompertz RH, Armstrong CP, Lennard TW. Imaging of the common bile duct in patients undergoing laparoscopic cholecystectomy. Gut. 1994;35(7): Ammori BJ, Birbas K, Davides D, Vezakis A, Larvin M, McMahon MJ. Routine vs on demand postoperative ERCP for small bile duct calculi detected at intraoperative cholangiography. Clinical evaluation and cost analysis. Surg Endosc. 2000;14(12): Ford JA, Soop M, Du J, Loveday BP, Rodgers M. Systematic review of intraoperative cholangiography in cholecystectomy. Br J Surg. 2012;99(2): Sajid MS, Leaver C, Haider Z, Worthington T, Karanjia N, Singh KK. Routine on-table cholangiography during cholecystectomy: a systematic review. Ann R Coll Surg Engl. 2012;94(6): Sanjay P, Tagolao S, Dirkzwager I, Bartlett A. A survey of the accuracy of interpretation of intraoperative cholangiograms. HPB (Oxford). 2012;14(10): Katz D, Nikfarjam M, Sfakiotaki A, Christophi C. Selective endoscopic cholangiography for the detection of common bile duct stones in patients with cholelithiasis. Endoscopy. 2004;36(12): Bose SM, Mazumdar A, Prakash VS, Kocher R, Katariya S, Pathak CM. Evaluation of the predictors of choledocholithiasis: comparative analysis of clinical, biochemical, radiological, radionuclear, and intraoperative parameters. Surg Today. 2001;31(2): Onken JE, Brazer SR, Eisen GM, et al. Predicting the presence of choledocholithiasis in patients with symptomatic cholelithiasis. Am J Gastroenterol. 1996;91(4): Garrow D, Miller S, Sinha D, et al. Endoscopic ultrasound: a meta-analysis of test performance in suspected biliary obstruction. Clin Gastroenterol Hepatol. 2007;5(5): Fulcher AS, Turner MA, Capps GW, Zfass AM, Baker KM. Half-Fourier RARE MR cholangiopancreatography: experience in 300 subjects. Radiology. 1998;207(1): Palazzo L, Girollet PP, Salmeron M, et al. Value of endoscopic ultrasonography in the diagnosis of common bile duct stones: comparison with surgical exploration and ERCP. Gastrointest Endosc. 1995;42(3): Soto JA, Barish MA, Alvarez O, Medina S. Detection of choledocholithiasis with MR cholangiography: comparison of three-dimensional fast spin-echo and single- and multisection half-fourier rapid acquisition with relaxation enhancement sequences. Radiology. 2000;215(3): Sugiyama M, Atomi Y. Endoscopic ultrasonography for diagnosing choledocholithiasis: a prospective comparative study with ultrasonography and computed tomography. Gastrointest Endosc. 1997;45(2): Gastroenterology & Hepatology Volume 10, Issue 4 April 2014
Sex-related differences in predicting choledocholithiasis using current American Society of Gastrointestinal Endoscopy risk criteria
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Sex-related differences in predicting choledocholithiasis using current American Society of Gastrointestinal Endoscopy risk criteria Ankit Chhoda
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Sex-related differences in predicting choledocholithiasis using current American Society of Gastrointestinal Endoscopy risk criteria Ankit Chhoda
Presence of choledocholithiasis in patients undergoing cholecystectomy for mild biliary pancreatitis
 Original Article Presence of choledocholithiasis in patients undergoing cholecystectomy for mild biliary pancreatitis Pradhan S 1, Shah S 2, Maharjan S 2, Shah JN 3 1 2 2 3 Professor, Patan hospital Correspondence:
Original Article Presence of choledocholithiasis in patients undergoing cholecystectomy for mild biliary pancreatitis Pradhan S 1, Shah S 2, Maharjan S 2, Shah JN 3 1 2 2 3 Professor, Patan hospital Correspondence:
The authors have declared no conflicts of interest.
 Diagnostic Accuracy of Magnetic Resonance Cholangiopancreatography Versus Endoscopic Retrograde Cholangiopancreatography Findings in the Postorthotopic Liver Transplant Population Authors: *Ashok Shiani,
Diagnostic Accuracy of Magnetic Resonance Cholangiopancreatography Versus Endoscopic Retrograde Cholangiopancreatography Findings in the Postorthotopic Liver Transplant Population Authors: *Ashok Shiani,
Accuracy of ASGE criteria for the prediction of choledocholithiasis
 1130-0108/2016/108/6/309-314 Revista Española de Enfermedades Digestivas Copyright 2016 Arán Ediciones, S. L. Rev Esp Enferm Dig (Madrid) Vol. 108, N.º 6, pp. 309-314, 2016 ORIGINAL PAPERS Accuracy of
1130-0108/2016/108/6/309-314 Revista Española de Enfermedades Digestivas Copyright 2016 Arán Ediciones, S. L. Rev Esp Enferm Dig (Madrid) Vol. 108, N.º 6, pp. 309-314, 2016 ORIGINAL PAPERS Accuracy of
Magnetic Resonance Cholangiopancreatography (MRCP) in a District General Hospital
 Magnetic Resonance Cholangiopancreatography (MRCP) in a District General Hospital Poster No.: C-1790 Congress: ECR 2012 Type: Authors: Scientific Exhibit J. A. Maguire 1, H. Kasem 2, M. Akhtar 2, M. Strauss
Magnetic Resonance Cholangiopancreatography (MRCP) in a District General Hospital Poster No.: C-1790 Congress: ECR 2012 Type: Authors: Scientific Exhibit J. A. Maguire 1, H. Kasem 2, M. Akhtar 2, M. Strauss
ENDOSCOPIC TREATMENT OF A BILE DUCT
 HPB Surgery, 1990, Vol. 3, pp. 67-71 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
HPB Surgery, 1990, Vol. 3, pp. 67-71 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
Research Article The Diagnostic Accuracy of Linear Endoscopic Ultrasound for Evaluating Symptoms Suggestive of Common Bile Duct Stones
 Gastroenterology Research and Practice Volume 2016, Article ID 6957235, 5 pages http://dx.doi.org/10.1155/2016/6957235 Research Article The Diagnostic Accuracy of Linear Endoscopic Ultrasound for Evaluating
Gastroenterology Research and Practice Volume 2016, Article ID 6957235, 5 pages http://dx.doi.org/10.1155/2016/6957235 Research Article The Diagnostic Accuracy of Linear Endoscopic Ultrasound for Evaluating
ERCP and EUS: What s New and What Should We Do?
 ERCP and EUS: What s New and What Should We Do? Rajesh N. Keswani, MD Associate Professor of Medicine Division of Gastroenterology Northwestern University Feinberg School of Medicine EUS/ERCP in 2015 THE
ERCP and EUS: What s New and What Should We Do? Rajesh N. Keswani, MD Associate Professor of Medicine Division of Gastroenterology Northwestern University Feinberg School of Medicine EUS/ERCP in 2015 THE
The campaign on laboratory: focus on Gallstone Disease and ERCP
 The campaign on laboratory: focus on Gallstone Disease and ERCP Mauro Giuliani, MD, Specialist in Visceral Surgery, Vice Head Physician, Surgical Ward, Ospedale Regionale di Locarno Alberto Fasoli, MD,
The campaign on laboratory: focus on Gallstone Disease and ERCP Mauro Giuliani, MD, Specialist in Visceral Surgery, Vice Head Physician, Surgical Ward, Ospedale Regionale di Locarno Alberto Fasoli, MD,
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 96, No. 10, by Am. Coll. of Gastroenterology ISSN /01/$20.00
 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 96, No. 10, 2001 2001 by Am. Coll. of Gastroenterology ISSN 0002-9270/01/$20.00 Published by Elsevier Science Inc. PII S0002-9270(01)02807-6 Can Endoscopic
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 96, No. 10, 2001 2001 by Am. Coll. of Gastroenterology ISSN 0002-9270/01/$20.00 Published by Elsevier Science Inc. PII S0002-9270(01)02807-6 Can Endoscopic
Setting The study setting was hospital. The economic analysis was carried out in California, USA.
 Preoperative versus postoperative endoscopic retrograde cholangiopancreatography in mild to moderate gallstone pancreatitis: a prospective randomized trial Chang L, Lo S, Stabile B E, Lewis R J, Toosie
Preoperative versus postoperative endoscopic retrograde cholangiopancreatography in mild to moderate gallstone pancreatitis: a prospective randomized trial Chang L, Lo S, Stabile B E, Lewis R J, Toosie
Evidence-based guidelines for diagnosis of common bile duct stones Vanja Giljaca University Hospital Center Rijeka Department of Gastroenterology
 Evidencebased guidelines for diagnosis of common bile duct stones Vanja Giljaca University Hospital Center Rijeka Department of Gastroenterology Trusted evidence. Informed decisions. Better health. Outline
Evidencebased guidelines for diagnosis of common bile duct stones Vanja Giljaca University Hospital Center Rijeka Department of Gastroenterology Trusted evidence. Informed decisions. Better health. Outline
Predictors of abnormalities on magnetic resonance cholangiopancreatography: is there a role when the biliary tree is normal on previous imaging?
 ORIGINAL ARTICLE Annals of Gastroenterology (2019) 32, 1-6 Predictors of abnormalities on magnetic resonance cholangiopancreatography: is there a role when the biliary tree is normal on previous imaging?
ORIGINAL ARTICLE Annals of Gastroenterology (2019) 32, 1-6 Predictors of abnormalities on magnetic resonance cholangiopancreatography: is there a role when the biliary tree is normal on previous imaging?
Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study
 Study title Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study Primary Investigator: Kazuhide Matsushima, MD Co-Primary investigator: Zachary Warriner,
Study title Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study Primary Investigator: Kazuhide Matsushima, MD Co-Primary investigator: Zachary Warriner,
EAST MULTICENTER STUDY PROPOSAL
 EAST MULTICENTER STUDY PROPOSAL (Proposal forms must be completed in its entirety, incomplete forms will not be considered) GENERAL INFORMATION Study Title: Prospective Multi-Institutional Evaluation of
EAST MULTICENTER STUDY PROPOSAL (Proposal forms must be completed in its entirety, incomplete forms will not be considered) GENERAL INFORMATION Study Title: Prospective Multi-Institutional Evaluation of
Research Article Safety and Yield of Diagnostic ERCP in Liver Transplant Patients with Abnormal Liver Function Tests
 Diagnostic and erapeutic Endoscopy, Article ID 314927, 5 pages http://dx.doi.org/10.1155/2014/314927 Research Article Safety and Yield of Diagnostic ERCP in Liver Transplant Patients with Abnormal Liver
Diagnostic and erapeutic Endoscopy, Article ID 314927, 5 pages http://dx.doi.org/10.1155/2014/314927 Research Article Safety and Yield of Diagnostic ERCP in Liver Transplant Patients with Abnormal Liver
Appendix A: Summary of evidence from surveillance
 Appendix A: Summary of evidence from surveillance 2018 surveillance of Gallstone disease: diagnosis and management (2014) NICE guideline CG188 Summary of evidence from surveillance Studies identified in
Appendix A: Summary of evidence from surveillance 2018 surveillance of Gallstone disease: diagnosis and management (2014) NICE guideline CG188 Summary of evidence from surveillance Studies identified in
ERCP / PTC Surgical Laparoscopic vs open Timing and order of approach
 Choledocholithiasis Which Approach and When? Lygia Stewart, MD University of California, San Francisco 2010 Naffziger Post-Graduate Course Clinical Manifestations of Choledocholithiasis Asymptomatic (no
Choledocholithiasis Which Approach and When? Lygia Stewart, MD University of California, San Francisco 2010 Naffziger Post-Graduate Course Clinical Manifestations of Choledocholithiasis Asymptomatic (no
Department of General Surgery, Al Khor Hospital, Hamad Medical Corporation, Qatar 2
 International Scholarly Research Network ISRN Minimally Invasive Surgery Volume 2012, Article ID 469013, 5 pages doi:10.5402/2012/469013 Clinical Study Laparoscopic Intraoperative Cholangiography Interpretation
International Scholarly Research Network ISRN Minimally Invasive Surgery Volume 2012, Article ID 469013, 5 pages doi:10.5402/2012/469013 Clinical Study Laparoscopic Intraoperative Cholangiography Interpretation
Downloaded from jssu.ssu.ac.ir at 13:10 IRST on Saturday October 28th 2017
 Journal of Shahid Sadoughi University of Medical Sciences Vol. 21, No. 5, Nov-Dec 2013 Pages: 675-681 1392 5 21 675-681 : 3 2* 1 1392/8/ : -1-2 -3 1391/8/24 : (). :. 1390 200 :.. SPSS (%0/5) 200 (8%) (%9/5)19
Journal of Shahid Sadoughi University of Medical Sciences Vol. 21, No. 5, Nov-Dec 2013 Pages: 675-681 1392 5 21 675-681 : 3 2* 1 1392/8/ : -1-2 -3 1391/8/24 : (). :. 1390 200 :.. SPSS (%0/5) 200 (8%) (%9/5)19
Recurrent common bile duct stones as a late complication of endoscopic sphincterotomy
 Nzenza et al. BMC Gastroenterology (2018) 18:39 https://doi.org/10.1186/s12876-018-0765-3 RESEARCH ARTICLE Open Access Recurrent common bile duct stones as a late complication of endoscopic sphincterotomy
Nzenza et al. BMC Gastroenterology (2018) 18:39 https://doi.org/10.1186/s12876-018-0765-3 RESEARCH ARTICLE Open Access Recurrent common bile duct stones as a late complication of endoscopic sphincterotomy
CHOLANGIOGRAPHY IN PATIENTS WITH SUSPECTED DUCT STONES
 SAFETY AND OUTCOME OF SELECTIVE INTRA-OPERATIVE CHOLANGIOGRAPHY IN PATIENTS WITH SUSPECTED DUCT STONES Ihab Kadry, Mahmoud Reda, Hesham Ahmed and Mohamed ZaaZou. Department Of General Surgery Misr University
SAFETY AND OUTCOME OF SELECTIVE INTRA-OPERATIVE CHOLANGIOGRAPHY IN PATIENTS WITH SUSPECTED DUCT STONES Ihab Kadry, Mahmoud Reda, Hesham Ahmed and Mohamed ZaaZou. Department Of General Surgery Misr University
An angulated common bile duct predisposes to recurrent symptomatic bile duct stones after endoscopic stone extraction
 Surg Endosc (2006) 20: 1594 1599 DOI: 10.1007/s00464-005-0656-x Ó Springer Science+Business Media, Inc. 2006 An angulated common bile duct predisposes to recurrent symptomatic bile duct stones after endoscopic
Surg Endosc (2006) 20: 1594 1599 DOI: 10.1007/s00464-005-0656-x Ó Springer Science+Business Media, Inc. 2006 An angulated common bile duct predisposes to recurrent symptomatic bile duct stones after endoscopic
A scoring system for the prediction of choledocholithiasis: a prospective cohort study
 A scoring system for the prediction of choledocholithiasis: a prospective cohort study Bilal O. Al-Jiffry, a Samah Khayat, b Elfatih Abdeen, b Tasadooq Hussain, c Mohammed Yassin d From the a Department
A scoring system for the prediction of choledocholithiasis: a prospective cohort study Bilal O. Al-Jiffry, a Samah Khayat, b Elfatih Abdeen, b Tasadooq Hussain, c Mohammed Yassin d From the a Department
Role of hepatobiliary ultrasound in the diagnosis of choledocolitiasis
 Original articles Role of hepatobiliary ultrasound in the diagnosis of choledocolitiasis Andrea Piña, MD, 1 Martín Garzón, MD, 1 Jorge Iván Lizarazo, MD, 1 Juan Carlos Marulanda, MD, 1 Juan Carlos Molano,
Original articles Role of hepatobiliary ultrasound in the diagnosis of choledocolitiasis Andrea Piña, MD, 1 Martín Garzón, MD, 1 Jorge Iván Lizarazo, MD, 1 Juan Carlos Marulanda, MD, 1 Juan Carlos Molano,
Obstructive jaundice due to a blood clot after ERCP: a case report and review of the literature
 Zhu et al. BMC Gastroenterology (2018) 18:163 https://doi.org/10.1186/s12876-018-0898-4 CASE REPORT Open Access Obstructive jaundice due to a blood clot after ERCP: a case report and review of the literature
Zhu et al. BMC Gastroenterology (2018) 18:163 https://doi.org/10.1186/s12876-018-0898-4 CASE REPORT Open Access Obstructive jaundice due to a blood clot after ERCP: a case report and review of the literature
Duration of Pain Is Correlated With Elevation in Liver Function Tests in Patients With Symptomatic Choledocholithiasis
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:1077 1082 Duration of Pain Is Correlated With Elevation in Liver Function Tests in Patients With Symptomatic Choledocholithiasis ALA I. SHARARA, NABIL M.
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:1077 1082 Duration of Pain Is Correlated With Elevation in Liver Function Tests in Patients With Symptomatic Choledocholithiasis ALA I. SHARARA, NABIL M.
Making ERCP Easy: Tips From A Master
 Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Surveillance proposal consultation document
 Surveillance proposal consultation document 2018 surveillance of Gallstone disease: diagnosis and management (NICE guideline CG188) Proposed surveillance decision We propose to not update the NICE guideline
Surveillance proposal consultation document 2018 surveillance of Gallstone disease: diagnosis and management (NICE guideline CG188) Proposed surveillance decision We propose to not update the NICE guideline
Safety of endoscopic retrograde cholangiopancreatography in patients 80 years of age and older
 Original paper Safety of endoscopic retrograde cholangiopancreatography in patients 80 years of age and older Baydar Behlül 1, Serin Ayfer 2, Vatansever Sezgin 3, Kandemir Altay 3, Çelik Mustafa 3, Çekiç
Original paper Safety of endoscopic retrograde cholangiopancreatography in patients 80 years of age and older Baydar Behlül 1, Serin Ayfer 2, Vatansever Sezgin 3, Kandemir Altay 3, Çelik Mustafa 3, Çekiç
Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic Duct Obstruction: Is Endoscopic Sphincterotomy Needed?
 Gastroenterology Research and Practice Volume 2013, Article ID 375613, 6 pages http://dx.doi.org/10.1155/2013/375613 Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic
Gastroenterology Research and Practice Volume 2013, Article ID 375613, 6 pages http://dx.doi.org/10.1155/2013/375613 Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic
Routine Testing of Liver Function Before and After Elective Laparoscopic Cholecystectomy: Is It Necessary?
 Routine Testing of Liver Function Before and After Elective Laparoscopic Cholecystectomy: Is It Necessary? Nasir Zaheer Ahmad, FRCSI SCIENTIFIC PAPER ABSTRACT Background and Objectives: Liver function
Routine Testing of Liver Function Before and After Elective Laparoscopic Cholecystectomy: Is It Necessary? Nasir Zaheer Ahmad, FRCSI SCIENTIFIC PAPER ABSTRACT Background and Objectives: Liver function
Biliary tree dilation - and now what?
 Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
complication rates and/or incomplete clearance with need of intervention (ie, unfavorable outcomes).
 Research Original Investigation Natural Course vs Interventions to Clear Common Bile Duct Stones Data From the Swedish Registry for Gallstone Surgery and Endoscopic Retrograde Cholangiopancreatography
Research Original Investigation Natural Course vs Interventions to Clear Common Bile Duct Stones Data From the Swedish Registry for Gallstone Surgery and Endoscopic Retrograde Cholangiopancreatography
Endoscopic Ultrasonography Clinical Impact. Giancarlo Caletti. Gastroenterologia Università di Bologna. Caletti
 Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
In Woong Han 1, O Choel Kwon 1, Min Gu Oh 1, Yoo Shin Choi 2, and Seung Eun Lee 2. Departments of Surgery, Dongguk University College of Medicine 2
 Effect of Rowachol on Prevention of Postcholecystectomy Syndrome after Laparoscopic Cholecystectomy - Prospective multicenter Randomized controlled trial- In Woong Han 1, O Choel Kwon 1, Min Gu Oh 1, Yoo
Effect of Rowachol on Prevention of Postcholecystectomy Syndrome after Laparoscopic Cholecystectomy - Prospective multicenter Randomized controlled trial- In Woong Han 1, O Choel Kwon 1, Min Gu Oh 1, Yoo
Research Article Routine Cysticotomy and Flushing of the Cystic Duct in Patients with Low Risk of Common Duct Stones: Can It Be Beneficial?
 Hindawi Minimally Invasive Surgery Volume 2017, Article ID 9814389, 5 pages https://doi.org/10.1155/2017/9814389 Research Article Routine Cysticotomy and Flushing of the Cystic Duct in Patients with Low
Hindawi Minimally Invasive Surgery Volume 2017, Article ID 9814389, 5 pages https://doi.org/10.1155/2017/9814389 Research Article Routine Cysticotomy and Flushing of the Cystic Duct in Patients with Low
ORIGINAL ARTICLE. Endoscopic Retrograde Cholangiopancreatography Prior to Laparoscopic Cholecystectomy
 ORIGINAL ARTICLE Endoscopic Retrograde Cholangiopancreatography Prior to Laparoscopic Cholecystectomy A Common and Potentially Hazardous Technique That Can Be Avoided Bilal Alkhaffaf, MBChB, MRCS; Edward
ORIGINAL ARTICLE Endoscopic Retrograde Cholangiopancreatography Prior to Laparoscopic Cholecystectomy A Common and Potentially Hazardous Technique That Can Be Avoided Bilal Alkhaffaf, MBChB, MRCS; Edward
Pre-operative MRCP: is it necessary before routine laparoscopic cholecystectomy to exclude CBD stone-prospective study in tertiary care hospital
 International Surgery Journal Rao GB et al. Int Surg J. 2017 Nov;4(11):3633-3637 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20174636
International Surgery Journal Rao GB et al. Int Surg J. 2017 Nov;4(11):3633-3637 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20174636
REFERRAL GUIDELINES: GALLSTONES
 REFERRAL GUIDELINES: GALLSTONES Document Purpose To ensure patients with gallstones disease are managed appropriately in primary/ secondary care Oxford Radcliffe Hospital Surgical Department Surgical Registrar
REFERRAL GUIDELINES: GALLSTONES Document Purpose To ensure patients with gallstones disease are managed appropriately in primary/ secondary care Oxford Radcliffe Hospital Surgical Department Surgical Registrar
Endoscopic Papillary Balloon Dilation with Large Balloon after Limited Sphincterotomy for Retrieval of Choledocholithiasis
 Yonsei Medical Journal Vol. 47, No. 6, pp. 805-810, 2006 Endoscopic Papillary Balloon Dilation with Large Balloon after Limited Sphincterotomy for Retrieval of Choledocholithiasis Seungmin Bang, Myoung
Yonsei Medical Journal Vol. 47, No. 6, pp. 805-810, 2006 Endoscopic Papillary Balloon Dilation with Large Balloon after Limited Sphincterotomy for Retrieval of Choledocholithiasis Seungmin Bang, Myoung
SUNY Downstate Medical Center Kings County Hospital
 Management of Choledocholithiasis SUNY Downstate Medical Center Kings County Hospital Department of Surgery Grand Rounds Kiyanda Baldwin October 22, 2009 Case Presentation 43 y/o F c/o jaundice x 3 days
Management of Choledocholithiasis SUNY Downstate Medical Center Kings County Hospital Department of Surgery Grand Rounds Kiyanda Baldwin October 22, 2009 Case Presentation 43 y/o F c/o jaundice x 3 days
Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study
 Original article: Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study Kali CharanBansal Principal Specialist (General surgery)
Original article: Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study Kali CharanBansal Principal Specialist (General surgery)
Pre-operative prediction of difficult laparoscopic cholecystectomy
 International Surgery Journal http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151083 Pre-operative prediction of difficult laparoscopic
International Surgery Journal http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151083 Pre-operative prediction of difficult laparoscopic
Risk Factors for Conversion to Open Surgery in Patients With Acute Cholecystitis Undergoing Interval Laparoscopic Cholecystectomy
 Original Article 631 Risk Factors for Conversion to Open Surgery in Patients With Acute Cholecystitis Undergoing Interval Laparoscopic Cholecystectomy Kok-Ren Lim, 1 MRCS (Edin), Salleh Ibrahim, 1 FRCS
Original Article 631 Risk Factors for Conversion to Open Surgery in Patients With Acute Cholecystitis Undergoing Interval Laparoscopic Cholecystectomy Kok-Ren Lim, 1 MRCS (Edin), Salleh Ibrahim, 1 FRCS
ORIGINAL ARTICLE. Larissa University Hospital, Larissa, Greece
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Laparoendoscopic rendezvous may be an effective alternative to a failed preoperative endoscopic retrograde cholangiopancreatography in patients
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Laparoendoscopic rendezvous may be an effective alternative to a failed preoperative endoscopic retrograde cholangiopancreatography in patients
담낭절제술후발생한미리찌증후군의내시경적치료 1 예
 Case Report The Korean Journal of Pancreas and Biliary Tract 2014;19:199-203 http://dx.doi.org/10.15279/kpba.2014.19.4.199 pissn 1976-3573 eissn 2288-0941 담낭절제술후발생한미리찌증후군의내시경적치료 1 예 인하대학교의학전문대학원내과학교실 이정민
Case Report The Korean Journal of Pancreas and Biliary Tract 2014;19:199-203 http://dx.doi.org/10.15279/kpba.2014.19.4.199 pissn 1976-3573 eissn 2288-0941 담낭절제술후발생한미리찌증후군의내시경적치료 1 예 인하대학교의학전문대학원내과학교실 이정민
ISSN X (Print) Research Article. *Corresponding author Jitendra Singh Yadav
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(3B):966-970 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(3B):966-970 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Mirizzi syndrome with an unusual type of biliobiliary fistula a case report
 Kawaguchi et al. Surgical Case Reports (2015) 1:51 DOI 10.1186/s40792-015-0052-2 CASE REPORT Mirizzi syndrome with an unusual type of biliobiliary fistula a case report Tsutomu Kawaguchi 1,2*, Tadao Itoh
Kawaguchi et al. Surgical Case Reports (2015) 1:51 DOI 10.1186/s40792-015-0052-2 CASE REPORT Mirizzi syndrome with an unusual type of biliobiliary fistula a case report Tsutomu Kawaguchi 1,2*, Tadao Itoh
Arpit Amin, Yuriy Zhurov, George Ibrahim, Anthony Maffei, Jonathan Giannone, Thomas Cerabona, and Ashutosh Kaul
 Case Reports in Surgery Volume 2016, Article ID 1896368, 9 pages http://dx.doi.org/10.1155/2016/1896368 Case Report Combined Endoscopic and Management of Postcholecystectomy Mirizzi Syndrome from a Remnant
Case Reports in Surgery Volume 2016, Article ID 1896368, 9 pages http://dx.doi.org/10.1155/2016/1896368 Case Report Combined Endoscopic and Management of Postcholecystectomy Mirizzi Syndrome from a Remnant
Management of Gallbladder Disease
 Management of Gallbladder Disease Steven B. Johnson, MD, FACS, FCCM Professor and Chairman, Department of Surgery Program Director, Phoenix Integrated Surgical Residency University of Arizona College of
Management of Gallbladder Disease Steven B. Johnson, MD, FACS, FCCM Professor and Chairman, Department of Surgery Program Director, Phoenix Integrated Surgical Residency University of Arizona College of
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 8/27/2011 Radiology Quiz of the Week # 35 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 8/27/2011 Radiology Quiz of the Week # 35 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Enhanced recovery in the management of mild gallstone pancreatitis: a prospective cohort study
 Surg Today (2013) 43:643 647 DOI 10.1007/s00595-012-0364-9 ORIGINAL ARTICLE Enhanced recovery in the management of mild gallstone pancreatitis: a prospective cohort study Xin Zhao Da-Zhi Chen Ren Lang
Surg Today (2013) 43:643 647 DOI 10.1007/s00595-012-0364-9 ORIGINAL ARTICLE Enhanced recovery in the management of mild gallstone pancreatitis: a prospective cohort study Xin Zhao Da-Zhi Chen Ren Lang
Magnetic Resonance Cholangiography: Applications in Patients with Calculus Disease of the Biliary Tract
 Original Article Magnetic Resonance Cholangiography: Applications in Patients with Calculus Disease of the Biliary Tract Terrence H. Liu and Claude H. Organ, Jr., Department of Surgery, University of California
Original Article Magnetic Resonance Cholangiography: Applications in Patients with Calculus Disease of the Biliary Tract Terrence H. Liu and Claude H. Organ, Jr., Department of Surgery, University of California
Key Words: Choledocholithiasis; Endosonography; Cholangiopancreatography,
 Gut and Liver, Vol. 11, No. 2, March 2017, pp. 290-297 ORiginal Article Diagnostic Value of Endoscopic Ultrasonography in Symptomatic Patients with High and Intermediate Probabilities of Common Bile Duct
Gut and Liver, Vol. 11, No. 2, March 2017, pp. 290-297 ORiginal Article Diagnostic Value of Endoscopic Ultrasonography in Symptomatic Patients with High and Intermediate Probabilities of Common Bile Duct
Greater Manchester EUR Policy Statement on: Asymptomatic Gallstones GM Ref: GM061 Version: 0.2 (21 November 2018)
 Greater Manchester EUR Policy Statement on: Asymptomatic Gallstones GM Ref: GM061 Version: 0.2 (21 November 2018) Commissioning Statement Asymptomatic Gallstones Policy Exclusions (Alternative commissioning
Greater Manchester EUR Policy Statement on: Asymptomatic Gallstones GM Ref: GM061 Version: 0.2 (21 November 2018) Commissioning Statement Asymptomatic Gallstones Policy Exclusions (Alternative commissioning
CME Article Clinics in diagnostic imaging (115) Wai C T, Seto K Y, Sutedja D S
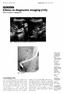 Medical Education Singapore Med.1 2007, 48 (4) : 361 CME Article Clinics in diagnostic imaging (115) Wai C T, Seto K Y, Sutedja D S fit. B CD - -0 o -5 r t -10 Fig. I US images of the upper right abdomen
Medical Education Singapore Med.1 2007, 48 (4) : 361 CME Article Clinics in diagnostic imaging (115) Wai C T, Seto K Y, Sutedja D S fit. B CD - -0 o -5 r t -10 Fig. I US images of the upper right abdomen
ACG Clinical Guideline: Management of Acute Pancreatitis
 ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
Title: Fasciola hepatica in the common bile duct: spyglass visualization and endoscopic extraction
 Title: Fasciola hepatica in the common bile duct: spyglass visualization and endoscopic extraction Authors: Edson Guzmán Calderón, Augusto Vera Calderón, Ramiro Díaz Ríos, Ronald Arcana López, Edgar Alva
Title: Fasciola hepatica in the common bile duct: spyglass visualization and endoscopic extraction Authors: Edson Guzmán Calderón, Augusto Vera Calderón, Ramiro Díaz Ríos, Ronald Arcana López, Edgar Alva
Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010
 Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010 Case Presentation 30 y.o. woman with 2 weeks of RUQ abdominal
Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010 Case Presentation 30 y.o. woman with 2 weeks of RUQ abdominal
Figure 2: Post-cholecystectomy biliary-like pain
 Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Magnetic resonance cholangiography compared with endoscopic retrograde cholangiography in the diagnosis of primary sclerosing cholangitis
 Original Article Magnetic resonance cholangiography compared with endoscopic retrograde cholangiography in the diagnosis of primary sclerosing cholangitis Hossein Ahrar, Mohamad Saleh Jafarpishe, Ali Hekmatnia,
Original Article Magnetic resonance cholangiography compared with endoscopic retrograde cholangiography in the diagnosis of primary sclerosing cholangitis Hossein Ahrar, Mohamad Saleh Jafarpishe, Ali Hekmatnia,
Single-stage management with combined tri-endoscopic approach. approach for concomitant cholecystolithiasis and choledocholithiasis
 Surg Endosc (2016) 30:5615 5620 DOI 10.1007/s00464-016-4918-6 and Other Interventional Techniques ENDOLUMINAL SURGERY Single-stage management with combined tri-endoscopic approach for concomitant cholecystolithiasis
Surg Endosc (2016) 30:5615 5620 DOI 10.1007/s00464-016-4918-6 and Other Interventional Techniques ENDOLUMINAL SURGERY Single-stage management with combined tri-endoscopic approach for concomitant cholecystolithiasis
Endoscopic Management of the Iatrogenic CBD Injury
 The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
Effects of age and cholecystectomy on common bile duct diameter as measured by endoscopic ultrasonography
 Surg Endosc (2013) 27:303 307 DOI 10.1007/s00464-012-2445-7 and Other Interventional Techniques Effects of age and cholecystectomy on common bile duct diameter as measured by endoscopic ultrasonography
Surg Endosc (2013) 27:303 307 DOI 10.1007/s00464-012-2445-7 and Other Interventional Techniques Effects of age and cholecystectomy on common bile duct diameter as measured by endoscopic ultrasonography
Cholecystectomy rate following endoscopic biliary interventions
 Original Article Brunei Int Med J. 2012; 8 (4): 166-172 Cholecystectomy rate following endoscopic biliary interventions Sky Lim 1, Lin Naing 1, Vui Heng Chong 2 1 Pengiran Anak Puteri Rashidah Sa adatul
Original Article Brunei Int Med J. 2012; 8 (4): 166-172 Cholecystectomy rate following endoscopic biliary interventions Sky Lim 1, Lin Naing 1, Vui Heng Chong 2 1 Pengiran Anak Puteri Rashidah Sa adatul
Endoscopic retrograde cholangiopancreatography versus intraoperative cholangiography for diagnosis of common bile duct stones (Review)
 Endoscopic retrograde cholangiopancreatography versus intraoperative cholangiography for diagnosis of common bile duct stones Gurusamy KS, Giljaca V, Takwoingi Y, Higgie D, Poropat G, Štimac D, Davidson
Endoscopic retrograde cholangiopancreatography versus intraoperative cholangiography for diagnosis of common bile duct stones Gurusamy KS, Giljaca V, Takwoingi Y, Higgie D, Poropat G, Štimac D, Davidson
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 Appendix B: Scope NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE Post publication note: The title of this guideline changed during development. This scope was published before the guideline
Appendix B: Scope NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE Post publication note: The title of this guideline changed during development. This scope was published before the guideline
Background. RUQ Ultrasound Normal, Recommend Clinical Correlation. Sohail R. Shah, MD, MSHA, FACS, FAAP Texas Children s Hosptial
 RUQ Ultrasound Normal, Recommend Clinical Correlation Sohail R. Shah, MD, MSHA, FACS, FAAP Texas Children s Hosptial Background Incidence of pediatric gallbladder disease continues to rise U.S. Pediatric
RUQ Ultrasound Normal, Recommend Clinical Correlation Sohail R. Shah, MD, MSHA, FACS, FAAP Texas Children s Hosptial Background Incidence of pediatric gallbladder disease continues to rise U.S. Pediatric
Cholecystectomy for acute gallstone pancreatitis: early vs delayed approach
 Scandinavian Journal of Surgery 99: 81 85, 2010 Cholecystectomy for acute gallstone pancreatitis: early vs delayed approach C. T. Wilson, M. A. de Moya Department of Trauma, Emergency Surgery, and Critical
Scandinavian Journal of Surgery 99: 81 85, 2010 Cholecystectomy for acute gallstone pancreatitis: early vs delayed approach C. T. Wilson, M. A. de Moya Department of Trauma, Emergency Surgery, and Critical
Management of Gallstone Pancreatitis: Effects of Deviation from Clinical Guidelines
 Management of Gallstone Pancreatitis: Effects of Deviation from Clinical Guidelines Kevin Sargen, Andrew N Kingsnorth Department of Surgery, Plymouth Postgraduate Medical School, Derriford Hospital. Plymouth.
Management of Gallstone Pancreatitis: Effects of Deviation from Clinical Guidelines Kevin Sargen, Andrew N Kingsnorth Department of Surgery, Plymouth Postgraduate Medical School, Derriford Hospital. Plymouth.
Title: The best approach to treat concomitant gallstones and. Authors: Jesús García-Cano, Francisco Domper
 Title: The best approach to treat concomitant gallstones and common bile duct stones. Is ERCP still needed? Authors: Jesús García-Cano, Francisco Domper DOI: 10.17235/reed.2019.6226/2019 Link: PubMed (Epub
Title: The best approach to treat concomitant gallstones and common bile duct stones. Is ERCP still needed? Authors: Jesús García-Cano, Francisco Domper DOI: 10.17235/reed.2019.6226/2019 Link: PubMed (Epub
Original Policy Date 12:2013
 MP 6.01.30 Magnetic Resonance Cholangiopancreatography Medical Policy Section Radiology Is12:2013sue 3:2005 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index Disclaimer
MP 6.01.30 Magnetic Resonance Cholangiopancreatography Medical Policy Section Radiology Is12:2013sue 3:2005 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index Disclaimer
What Should Be Done with Idiopathic Recurrent Pancreatitis That Remains Idiopathic after Standard Investigation?
 What Should Be Done with Idiopathic Recurrent Pancreatitis That Remains Idiopathic after Standard Investigation? John Baillie Division of Gastroenterology, Duke University Medical Center. Durham, NC, USA
What Should Be Done with Idiopathic Recurrent Pancreatitis That Remains Idiopathic after Standard Investigation? John Baillie Division of Gastroenterology, Duke University Medical Center. Durham, NC, USA
Case Report Uncommon Mixed Type I and II Choledochal Cyst: An Indonesian Experience
 Case Reports in Surgery Volume 2013, Article ID 821032, 4 pages http://dx.doi.org/10.1155/2013/821032 Case Report Uncommon Mixed Type I and II Choledochal Cyst: An Indonesian Experience Fransisca J. Siahaya,
Case Reports in Surgery Volume 2013, Article ID 821032, 4 pages http://dx.doi.org/10.1155/2013/821032 Case Report Uncommon Mixed Type I and II Choledochal Cyst: An Indonesian Experience Fransisca J. Siahaya,
Increased risk and severity of ERCP-related complications associated with asymptomatic common bile duct stones
 Increased risk and severity of ERCP-related complications associated with asymptomatic common bile duct stones Authors Hirokazu Saito 1, 2, Tatsuyuki Kakuma 3, Yoshihiro Kadono 4,AtsushiUrata 4,KentaroKamikawa
Increased risk and severity of ERCP-related complications associated with asymptomatic common bile duct stones Authors Hirokazu Saito 1, 2, Tatsuyuki Kakuma 3, Yoshihiro Kadono 4,AtsushiUrata 4,KentaroKamikawa
CHOLEDOCHOLITHIASIS IN PATIENTS WITH ACUTE GALLSTONE-RELATED DISEASE: RISK FACTORS, IMPACT OF ADMISSION DAY AND TREATMENT STRATEGY
 ARISTOTLE UNIVERSITY OF THESSALONIKI SCHOOL OF HEALTH SCIENCES FACULTY OF MEDICINE CHOLEDOCHOLITHIASIS IN PATIENTS WITH ACUTE GALLSTONE-RELATED DISEASE: RISK FACTORS, IMPACT OF ADMISSION DAY AND TREATMENT
ARISTOTLE UNIVERSITY OF THESSALONIKI SCHOOL OF HEALTH SCIENCES FACULTY OF MEDICINE CHOLEDOCHOLITHIASIS IN PATIENTS WITH ACUTE GALLSTONE-RELATED DISEASE: RISK FACTORS, IMPACT OF ADMISSION DAY AND TREATMENT
T-TUBE DRAINAGE VERSUS PRIMARY COMMON BILE DUCT CLOSURE AFTER OPEN CHOLEDOCHOTOMY
 T-TUBE DRAINAGE VERSUS PRIMARY COMMON BILE DUCT CLOSURE AFTER OPEN CHOLEDOCHOTOMY Khaled Ahmed El- Dabee, Abd Al-Lateif Ahmed, Mohamed Abdel Aziz Abdel Jawad, Taha Bahgat Salam, Ahmed Eisa Ahmed* and Saed
T-TUBE DRAINAGE VERSUS PRIMARY COMMON BILE DUCT CLOSURE AFTER OPEN CHOLEDOCHOTOMY Khaled Ahmed El- Dabee, Abd Al-Lateif Ahmed, Mohamed Abdel Aziz Abdel Jawad, Taha Bahgat Salam, Ahmed Eisa Ahmed* and Saed
Introduction of GB polyp
 Management of Gallbladder Polyp as Physician's View Sang Hyub Lee, MD, PhD Seoul National University College of Medicine Seoul National University Bundang Hospital Department of Internal Medicine Division
Management of Gallbladder Polyp as Physician's View Sang Hyub Lee, MD, PhD Seoul National University College of Medicine Seoul National University Bundang Hospital Department of Internal Medicine Division
Appendix I: GRADE profiles
 Appendix I: GRADE profiles GRADE and Modified GRADE approaches used in this guideline Standard GRADE approach Modified GRADE approach Criteria Effectiveness evidence (Developed by GRADE working group)
Appendix I: GRADE profiles GRADE and Modified GRADE approaches used in this guideline Standard GRADE approach Modified GRADE approach Criteria Effectiveness evidence (Developed by GRADE working group)
Sphincter of Oddi Dysfunction: What s the Verdict in 2014?
 SGNA March 2014 Sphincter of Oddi Dysfunction: What s the Verdict in 2014? Evan L. Fogel, M.D. Professor of Clinical Medicine ERCP Fellowship Director Division of Gastroenterology/Hepatology Indiana University
SGNA March 2014 Sphincter of Oddi Dysfunction: What s the Verdict in 2014? Evan L. Fogel, M.D. Professor of Clinical Medicine ERCP Fellowship Director Division of Gastroenterology/Hepatology Indiana University
Diagnosis of tumor extension in biliary carcinoma has. Differential Diagnosis and Treatment of Biliary Strictures
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
Primary Closure Versus T-tube Drainage After Open Choledochotomy
 Original Article Primary Closure Versus T-tube Drainage After Open Choledochotomy M. Ambreen, A.R. Shaikh, A. Jamal, J.N. Qureshi, A.G. Dalwani and M.M. Memon, Department of Surgery, Liaquat University
Original Article Primary Closure Versus T-tube Drainage After Open Choledochotomy M. Ambreen, A.R. Shaikh, A. Jamal, J.N. Qureshi, A.G. Dalwani and M.M. Memon, Department of Surgery, Liaquat University
Controversies in the management of acute pancreatitis
 Kathmandu University Medical Journal (3) Vol., No. 3, Issue 7, 3-7 Controversies in the management of acute pancreatitis Singh DR 1, Mehta A, Dangol UMS 3 1 Lecturer, Medical Officer, 3 Lecturer, Dept.
Kathmandu University Medical Journal (3) Vol., No. 3, Issue 7, 3-7 Controversies in the management of acute pancreatitis Singh DR 1, Mehta A, Dangol UMS 3 1 Lecturer, Medical Officer, 3 Lecturer, Dept.
Gallstones. Classification
 Gallstones Nariman Karanjia Tahir Ali Abstract Gallstones are extremely common in the UK and have a major effect on healthcare resources. Presentation depends on whether the stones occlude the cystic duct
Gallstones Nariman Karanjia Tahir Ali Abstract Gallstones are extremely common in the UK and have a major effect on healthcare resources. Presentation depends on whether the stones occlude the cystic duct
Naoyuki Toyota, Tadahiro Takada, Hodaka Amano, Masahiro Yoshida, Fumihiko Miura, and Keita Wada
 J Hepatobiliary Pancreat Surg (2006) 13:80 85 DOI 10.1007/s00534-005-1062-4 Endoscopic naso-gallbladder drainage in the treatment of acute cholecystitis: alleviates inflammation and fixes operator s aim
J Hepatobiliary Pancreat Surg (2006) 13:80 85 DOI 10.1007/s00534-005-1062-4 Endoscopic naso-gallbladder drainage in the treatment of acute cholecystitis: alleviates inflammation and fixes operator s aim
Primary Sclerosing Cholangitis and Cholestatic liver diseases. Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants
 Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Magnetic resonance cholangiopancreatography (MRCP) is an imaging. technique that is able to non-invasively assess bile and pancreatic ducts,
 SECRETIN AUGMENTED MRCP Riccardo MANFREDI, MD, MBA, FESGAR Magnetic resonance cholangiopancreatography (MRCP) is an imaging technique that is able to non-invasively assess bile and pancreatic ducts, in
SECRETIN AUGMENTED MRCP Riccardo MANFREDI, MD, MBA, FESGAR Magnetic resonance cholangiopancreatography (MRCP) is an imaging technique that is able to non-invasively assess bile and pancreatic ducts, in
ERCP complications and challenges in their diagnosis and management.
 ERCP complications and challenges in their diagnosis and management. Sandie R Thomson Chair of the Division of Gastroenterology, University of Cape Town ERCP Do I have a good Indication? . Algorithm for
ERCP complications and challenges in their diagnosis and management. Sandie R Thomson Chair of the Division of Gastroenterology, University of Cape Town ERCP Do I have a good Indication? . Algorithm for
MANAGEMENT OF COMPLICATED GALLSTONE DISEASE
 gastrointestinal tract and abdomen MANAGEMENT OF COMPLICATED GALLSTONE DISEASE Carmen L. Mueller, BSc(H), MD, FRCSC, Amy A. Neville, MD, FRCSC, MSc, and Gerald M. Fried, MD, FRCSC, FACS, FCAHS Gallstones
gastrointestinal tract and abdomen MANAGEMENT OF COMPLICATED GALLSTONE DISEASE Carmen L. Mueller, BSc(H), MD, FRCSC, Amy A. Neville, MD, FRCSC, MSc, and Gerald M. Fried, MD, FRCSC, FACS, FCAHS Gallstones
Aseries of credentialing guidelines for gastrointestinal endoscopic
 CURRENT ENDOSCOPIC PRACTICES THE EXPERTS SPEAK Canadian credentialing guidelines for endoscopic retrograde cholangiopancreatography Jonathon Springer MD FRCPC 1, Robert Enns MD FRCPC 2, Joseph Romagnuolo
CURRENT ENDOSCOPIC PRACTICES THE EXPERTS SPEAK Canadian credentialing guidelines for endoscopic retrograde cholangiopancreatography Jonathon Springer MD FRCPC 1, Robert Enns MD FRCPC 2, Joseph Romagnuolo
Bilirubin levels predict malignancy in patients with obstructive jaundice
 DOI:1.1111/j.1477-2574.211.312.x HPB ORIGINAL ARTICLE Bilirubin levels predict malignancy in patients with obstructive jaundice Giuseppe Garcea, Wee Ngu, Christopher P. Neal, Ashley R. Dennison & David
DOI:1.1111/j.1477-2574.211.312.x HPB ORIGINAL ARTICLE Bilirubin levels predict malignancy in patients with obstructive jaundice Giuseppe Garcea, Wee Ngu, Christopher P. Neal, Ashley R. Dennison & David
Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico
 Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques Associate Professor
Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques Associate Professor
Comparison between primary closure and T-tube drainage after open choledocotomy
 ISSN: 2203-1413 Vol.03 No.04 Comparison between primary closure and T-tube drainage after open choledocotomy Alireza Barband 1, Farzad Kakaei 1, Morteza Ghojazadeh 2, Abdolhamid Chavoshi Khamneh 1*, Morteza
ISSN: 2203-1413 Vol.03 No.04 Comparison between primary closure and T-tube drainage after open choledocotomy Alireza Barband 1, Farzad Kakaei 1, Morteza Ghojazadeh 2, Abdolhamid Chavoshi Khamneh 1*, Morteza
Natural history of Asymptomatic Bile Duct stones at time
 Ulster Med J2005; 74 (2) 108-112 Natural history of Asymptomatic Bile Duct stones at time of cholecystectomy Caddy GR, Kirby J, Kirk SJ, Allen MJ, Moorehead RJ, Tham TC Accepted 29 June 2005 STRUCTURED
Ulster Med J2005; 74 (2) 108-112 Natural history of Asymptomatic Bile Duct stones at time of cholecystectomy Caddy GR, Kirby J, Kirk SJ, Allen MJ, Moorehead RJ, Tham TC Accepted 29 June 2005 STRUCTURED
Endoscopic Management of Biliary Strictures. Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center
 Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
ORIGINAL ARTICLE. Prospective Randomized Trial of LC LCBDE vs ERCP/S LC for Common Bile Duct Stone Disease
 ORIGINAL ARTICLE Prospective Randomized Trial of LC LCBDE vs ERCP/S LC for Common Bile Duct Stone Disease Stanley J. Rogers, MD; John P. Cello, MD; Jan K. Horn, MD; Allan E. Siperstein, MD; William P.
ORIGINAL ARTICLE Prospective Randomized Trial of LC LCBDE vs ERCP/S LC for Common Bile Duct Stone Disease Stanley J. Rogers, MD; John P. Cello, MD; Jan K. Horn, MD; Allan E. Siperstein, MD; William P.
What Are Gallstones? GALLSTONES. Gallstones are pieces of hard, solid matter that form over time in. the gallbladder of some people.
 What Are Gallstones? Gallstones are pieces of hard, solid matter that form over time in the gallbladder of some people. The gallbladder sits under the liver and stores bile (a key digestive juice ). Gallstones
What Are Gallstones? Gallstones are pieces of hard, solid matter that form over time in the gallbladder of some people. The gallbladder sits under the liver and stores bile (a key digestive juice ). Gallstones
Endoscopic management of postoperative bile duct injuries: a single center experience.
 1- Endoscopic management of postoperative bile duct injuries: a single center experience. BACKGROUND/AIM: Biliary endoscopic procedures may be less invasive than surgery for management of postoperative
1- Endoscopic management of postoperative bile duct injuries: a single center experience. BACKGROUND/AIM: Biliary endoscopic procedures may be less invasive than surgery for management of postoperative
THE INTERVENTIONAL RADIOLOGIST CHRISTIAAN VAN DER LEIJ, MD. EBIR. INTERVENTIONAL RADIOLOGY MAASTRICHT UMC+
 THE INTERVENTIONAL RADIOLOGIST CHRISTIAAN, MD. EBIR. INTERVENTIONAL RADIOLOGY MAASTRICHT UMC+ DISCLOSURES None 78 Y/O FEMALE Painful RUQ Fever Lab: Raised Leukocytes/CRP CHOLECYSTITIS 3-9% patients ER
THE INTERVENTIONAL RADIOLOGIST CHRISTIAAN, MD. EBIR. INTERVENTIONAL RADIOLOGY MAASTRICHT UMC+ DISCLOSURES None 78 Y/O FEMALE Painful RUQ Fever Lab: Raised Leukocytes/CRP CHOLECYSTITIS 3-9% patients ER
