A Functional Analysis of the Influence of b 3 -adrenoceptors on the Rat Micturition Cycle
|
|
|
- Lenard Walsh
- 5 years ago
- Views:
Transcription
1 /347/2/ $ THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS J Pharmacol Exp Ther 347: , November 2013 Copyright ª 2013 by The American Society for Pharmacology and Experimental Therapeutics A Functional Analysis of the Influence of b 3 -adrenoceptors on the Rat Micturition Cycle Prajni Sadananda, 1 Marcus J. Drake, Julian F. R. Paton, and Anthony E. Pickering School of Physiology & Pharmacology, Medical Sciences Building (P.S., J.F.R.P., A.E.P.), and School of Clinical Sciences (M.J.D.), University of Bristol, Bristol, United Kingdom Received June 18, 2013; accepted September 4, 2013 ABSTRACT Dysfunctions of the lower urinary tract, such as overactive bladder syndrome and incontinence, are the product of storage failure. Spontaneous regional bladder wall movements [nonmicturition contractions (NMCs)] are proposed to generate afferent activity that signals volume status to the central nervous system. The sympathetic nervous system, via activation of b-adrenoceptors (b-ars), causes bladder relaxation and promotes urine storage. We hypothesized that b-ar regulation of micturition is mediated by suppression of NMCs. We used an unanesthetized, decerebrate, artificially perfused rat preparation that allows simultaneous cystometry with external urethral sphincter and pelvic afferent nerve recordings. Systemic isoprenaline (10 nm to 1 mm) increased intervoid interval and bladder compliance accompanied by a decrease in NMC amplitude, voiding pressure, and voiding threshold. Isoprenaline also reduced arterial pressure and increased heart rate. The b 3 - AR agonist mirabegron ( nm) increased intervoid interval Introduction Dysfunctions of the lower urinary tract (LUT), such as overactive bladder (OAB), urgency, incontinence, and nocturia, signify failures of urine storage (Abrams et al., 2002). The mechanisms by which the bladder signals its volume status to the central nervous system are key to understanding such failures of storage. During the storage phase of micturition, a progressive increase in sympathetic activity releases noradrenaline that is believed to act on b-adrenoceptors (b-ars) on the bladder wall to produce smooth muscle relaxation. This increases bladder compliance and enables continued lowpressure filling of the bladder (reviewed in Fowler et al., 2008). When a storage threshold is reached (and the environmental context is permissive), parasympathetic muscarinic receptor activation evokes detrusor contraction and emptying of bladder contents. This work was supported by unrestricted funding from Astellas Pharma Inc. [Grant AG2009/00508]. A.E.P. is the recipient of a Wellcome Senior Clinical Research Fellowship [Grant ]. 1 Current affiliation: Department of Anatomy and Neuroscience, University of Melbourne, Parkville, Victoria, Australia. dx.doi.org/ /jpet and bladder compliance and reduced NMC amplitude, yet preserved active voiding function and had no effect on arterial pressure or heart rate. All of these effects of mirabegron were blocked by the selective b 3 -AR antagonist N-[[3-[(2S)- 2-hydroxy-3-[[2-[4-[(phenylsulfonyl)amino] phenyl]ethyl]amino]propoxy]phenyl]methyl]-acetamide (L748,337), which alone shortened intervoid interval and decreased bladder compliance suggesting the presence of a basal b 3 -AR mediated sympathetic tone. Similar effects of mirabegron were seen in an acetic acid sensitized bladder preparation and in preparations after loss of spinobulbar reflex bladder control. The b 3 -AR mediated increase in intervoid interval correlated with increased bladder compliance but not with the decrease in NMC amplitude. These findings indicate that b 3 -adrenoceptors have a selective effect that improves urine storage by increasing compliance without affecting the active components of voiding. The major roles of b-ar and muscarinic receptors in regulating bladder function in health and disease have made them attractive drug targets for treatment of bladder pathophysiology (Andersson and Wein, 2004; Hood and Andersson, 2013). It is worth noting that voiding dysfunctions, such as poor stream and incomplete bladder emptying, can arise in conjunction with storage problems. Thus, the development of therapies for storage dysfunction needs to consider the potential adverse effect of impaired voiding function. All of the known b-ar subtypes (1, 2, and 3) have been localized in human and rat bladders (Yamaguchi and Chapple, 2007), and detrusor relaxant actions have been described particularly for b 2 - and b 3 -AR, with some variation across species. Importantly, the relatively restricted distribution of the b 3 -AR subtype on the bladder has led to the development and recent licensing of selective agonists as treatments for OAB (Michel et al., 2011). However, it remains unclear how b 3 -AR activation functionally improves urine storage via direct relaxant effects on bladder smooth muscle (Takeda et al., 2000) or via changes in afferent transmission (Aizawa et al., 2012) with or without urothelial mediation. We have developed and characterized a novel model for integrated functional physiological and pharmacological studies ABBREVIATIONS: ANOVA, analysis of variance; b-ar, b-adrenoceptor; DAPR, decerebrate artificially perfused rat; EMG, electromyogram; EUS, external urinary sphincter; L748,337, N-[[3-[(2S)-2-hydroxy-3-[[2-[4-[(phenylsulfonyl)amino] phenyl]ethyl]amino]propoxy]phenyl]methyl]-acetamide; LUT, lower urinary tract; NMC, non-micturition contraction; ns, not significant; OAB, overactive bladder; PAN, pelvic afferent nerve. 506
2 of the complete rat micturition cycle in an unanesthetized preparation: the decerebrate artificially perfused rat (DAPR) (Pickering and Paton, 2006; Sadananda et al., 2011), a variant of the working heart brainstem preparation (Paton, 1996). This has intact LUT-spinal-brainstem reflex loops and demonstrates autonomic tone, the presence of which is crucial for normal bladder function. It also facilitates both nerve and sphincter recordings and enables the precise control of the composition of the perfusate for pharmacological investigations analogous to in vitro conditions. We previously observed that loss of autonomic tone in the DAPR (both pharmacological with hexamethonium ganglion blockade and pathological with loss of brainstem function) enhanced nonmicturition contraction (NMC) amplitude and reduced intervoid interval (Sadananda et al., 2011). This led us to hypothesize that the sympathetic drive acts to suppress NMCs which are proposed to be part of a volume assessment reflex mechanism (Drake et al., 2001), and hence facilitate urine storage. We aimed to test this proposal by investigating the role of b-ar agonists on the micturition cycle with a focus on the functional effect of b 3 -agonism, given the predominant role of the b3 subtype in mediating bladder relaxation (Igawa et al., 1999). We show that both nonselective b-ar and selective b 3 -AR agonism with mirabegron prolonged the intervoid interval and increased bladder compliance while suppressing NMC amplitude but not frequency. The b 3 -AR mediated effects promote storage without associated impairment of voiding function and are also seen in an acid-sensitized bladder pathological model. However, counter to our original hypothesis, we show that the increase in the intervoid interval correlates with the degree of increase in bladder compliance produced by b 3 -AR activation, but not with the reduction in NMC amplitude, nor with changed afferent sensitivity. Materials and Methods All experiments and procedures conformed to the UK Animals (Scientific Procedures) Act 1986 and were approved by our institutional ethics review committee. Preparation. The procedures for the DAPR preparation were as previously described (Pickering and Paton, 2006; Sadananda et al., 2011) and are outlined here in brief. Female Wistar rats (40 90 g, P20 P28) were deeply anesthetized with halothane until loss of paw withdrawal reflex. Following a midline laparotomy, the stomach, spleen, and free intestine were vascularly isolated with ligatures and removed. The animals were precollicularly decerebrated and the halothane anesthesia was withdrawn. The preparation was chilled in ice-cold Ringer s solution and a midline sternotomy was performed. The lungs were removed and both atria were incised to avoid venous congestion during subsequent arterial perfusion. An incision at the apex of the heart allowed insertion of the perfusion cannula (Ø 1.25 mm; DLR-4 Braintree Scientific, Braintree, MA) into the ascending aorta. The preparation was arterially perfused with carbogen-gassed Ringer s solution (composition described in Drugs and Solutions ), containing Ficoll-70 (1.25%; Sigma-Aldrich, St. Louis, MO), at 32 C at 30 ml/min. The arterial perfusion pressure was monitored via the second lumen of the cannula. Once perfusate flow was initiated, the heart resumed beating and rhythmic respiratory muscle contractions were seen within minutes, signaling the return of brainstem function (typically as arterial perfusion pressure reached mm Hg). Recordings. Simultaneous recordings of phrenic nerve, bladder pressure, electromyogram (EMG) of the external urinary sphincter (EUS), and pelvic afferent nerve (PAN) activity were recorded using Role of b 3 -adrenoceptors in Rat Micturition 507 custom built amplifiers (Electronic Workshop, School of Physiology & Pharmacology), digitized using a micro1401 (Cambridge Electronic Design, Cambridge, UK) and analyzed using Spike2 software (Cambridge Electronic Design). Rhythmic, ramping phrenic nerve activity gave a continuous physiological index of brainstem viability (Paton, 1996). The ECG was visible on the phrenic nerve recording, and heart rate was derived from the ECG. To allow EUS-EMG recording, the pubic symphysis was cut in the midline, and a glass suction electrode (tip diameter 200 mm) was placed slightly lateral to the midline directly below the bladder neck under visual control. The bladder afferent nerve was identified on the left and recorded proximal to the major pelvic ganglion, where it became the PAN. Both phrenic nerve and PAN were recorded with glass suction electrodes. A 30G needle was inserted into the bladder dome for pressure monitoring and fluid infusion. Cystometry Protocol. For cystometry, both ureters were cut and ligated to stop natural filling from the kidneys. The bladder was filled by constant infusion with an artificial urine saline solution (Sadananda et al., 2011) at a flow rate of 20 ml/min, which was chosen to produce relatively frequent (every 3 4 minutes) and stable voids. For all drugs, at least four stable control voiding contractions (typically over a period of 20 minutes) were elicited before systemic administration of the drug. The following micturition parameters were measured from a minimum of four cycles under each condition (see Fig. 1): 1. Baseline pressure: The lowest bladder pressure at the start of the filling phase. 2. Threshold pressure: The bladder pressure at the point where the EUS-EMG changes in activity from tonic to bursting, indicating the initiation of voiding (Maggi et al., 1986). 3. Voiding pressure: The peak bladder pressure achieved during the bursting phase of the EUS-EMG. 4. Voiding period: Determined from the duration of EUS-EMG bursting. 5. Intervoid interval: Time between voids. 6. Compliance: Obtained from the linear regression fit to the volume-infused versus bladder pressure relationship during the filling phase from the end of one void to the initiation of the next (at the threshold point). 7. NMCs: The peak to trough amplitude and inter-event interval of successive bladder pressure waves that were not associated with EUS-EMG bursting. The NMCs were identified (using a Spike2 function) by searching the intervoid regions for pressure waves of duration.5 seconds and amplitude.0.1 mm Hg and were manually verified. Acute, acetic acid bladder sensitization was performed by switching to continuous intravesical infusion of acid at a ph of 5.5 (Zhang et al., 2003; Yamaguchi and Chapple, 2007; Sadananda et al., 2009; Parsons and Drake, 2011). The change in micturition parameters was observed within minutes of starting the infusion, and the sensitization continued for the remaining duration of the experiment. Drugs and Solutions. The composition of the modified Ringer s solution used for arterial perfusion was as follows (in mm): NaCl (125), NaHCO 3 (24), KCl (3), CaCl 2 (2.5), MgSO 4 (1.25), KH 2 PO 4 (1.25), and dextrose (10); ph 7.3 after carbogenation (95% O 2 /5% CO 2 ). All drugs and salts were from Sigma-Aldrich unless otherwise stated. b-adrenergic agents were the nonselective agonist isoprenaline (1 nm to 1 mm), the b 1 receptor selective antagonist metoprolol (10 nm), the b 3 receptor selective agonist mirabegron (1 nm to 1 mm; Astellas Pharma), and b 3 -selective antagonist N-[[3-[(2S)-2-hydroxy-3-[[2-[4- [(phenylsulfonyl)amino] phenyl]ethyl]amino]propoxy]phenyl]methyl]- acetamide (L748,337, 3 mm; Tocris, Bristol, UK). Isoprenaline (100 mm stock) was dissolved with 1 mm ascorbic acid to prevent oxidation (final ph 7.25 when diluted to 1 mm in carbogenated modified Ringer s). Mirabegron (100 mm stock) was dissolved in 20% 2-hydroxypropylb -cyclodextrin solvent. L748,337 (30 mm stock) was dissolved in
3 508 Sadananda et al. Fig. 1. Micturition parameters recorded in DAPR preparation. (A) Cystometrogram showing two voiding contractions under control conditions (continuous infusion at 20 ml/min). The start of voiding is signaled by the onset of EUS bursting [seen in (B) on an expanded time base] from which the threshold pressure is derived. The intervoid interval is measured between the threshold points of successive voids. Voiding pressure is the maximal pressure during the EUS bursting phase. The baseline pressure is the trough pressure after a void once the bladder has relaxed, allowing filling to recommence. During the filling phase, the bladder pressure gradually ramps, with superimposed nonmicturition contractions whose peak-trough amplitude and period were quantified. The pelvic nerve recording showed characteristic responses during the filling and voiding phases, with bursts of activity corresponding to the NMCs, correlated with changes in bladder pressure and EUS activity. Note the preparation also showed increases in heart rate, arterial perfusion pressure, and phrenic nerve activity during each void, indicating global autonomic changes during micturition. (EUS, phrenic, and pelvic nerve recordings rectified and integrated with a time constant of 200 ms.) dimethylsulfoxide. For all other agents, aqueous stock solutions were prepared and diluted in Ringer s solution prior to administration. All drugs were added systemically to the perfusate at the final stated concentrations. Perfusion of Ringer s containing either 2-hydroxypropyl-b-cyclodextrin, dimethylsulfoxide, or ascorbic acid alone (0.2%, 0.03%, and 10 mm, respectively) was without effect on micturition parameters. Analysis. The effect of all of the agents was assayed against the micturition parameters (listed previously) as well as on integrated EUS-EMG, pelvic afferent nerve, and phrenic nerve activity alongside heart rate and arterial perfusion pressure (Fig. 1). Results are expressed as the mean 6 S.E., where normally distributed, or as the median [interquartile range]. Data were compared by paired t test or repeated-measures analysis of variance (ANOVA) with Dunnett s or
4 Bonferroni s post-hoc analysis and a significance threshold of P, The relationship between changes in NMC amplitude, compliance, and intervoid intervals was explored using linear regression. All data analyses were performed using Prism 5 (GraphPad software, La Jolla, CA). Results Cystometry in the DAPR under control conditions (with a continuous infusion of artificial urine at 20 ml/min) showed a baseline pressure of mm Hg with threshold and peak voiding pressures of and mm Hg, respectively (n 5 15). The intervoid interval was 181 seconds [ ] (n 5 18), and in time control experiments, these pressures and intervals remained stable for up to 3 hours (n 5 7). Actions of Systemic b-ar Agonists on the Micturition Cycle. Arterial infusion of isoprenaline (1 nm to 1 mm) caused a concentration-dependent decrease in threshold pressure and voiding pressure at all doses from 100 nm (Fig. 2, A C; n 5 4). At the highest concentration (1 mm; n 5 5), isoprenaline reduced threshold pressure by % (P, 0.02) and voiding pressure by % (P, 0.008). Isoprenaline increased both intervoid interval (by % of control) and bladder compliance ( % of control; P ) but did not significantly change baseline bladder pressure. The duration of the voiding phase was reduced by % (P ; n 5 6), but voiding remained complete. Notably, isoprenaline also caused a dose-dependent Role of b 3 -adrenoceptors in Rat Micturition 509 decrease in arterial perfusion pressure (Fig. 2D; from control of to mm Hg at 100 nm isoprenaline; P ) and an increase in heart rate (from to beats per minute; P ; n 5 6). In a further set of experiments, repetition of the same incrementing isoprenaline dose protocol in the presence of metoprolol (10 nm; b 1 -AR antagonist) produced a similar profile of effects on bladder/micturition parameters in all six preparations, including reducing threshold pressure by % (P, 0.04) and voiding pressure by % (P ; n 5 6) and increasing compliance ( % of control; P ) and intervoid interval (180% 6 42% of control; P, 0.05) in all preparations. Isoprenaline still decreased perfusion pressure in the presence of metoprolol but no longer caused a significant change in heart rate, providing evidence of its b 1 -AR antagonist activity. The metoprolol-resistant effects of isoprenaline on micturition suggested that they may be mediated by a b 2 - and/or b 3 - AR mechanism, so we tested the actions of incremental dosing with mirabegron, a b 3 -selective agonist (1 nm to 1 mm). Mirabegron (100 nm) increased the intervoid interval ( %; P ; n 5 7; Fig. 3, A and B), increased bladder compliance in all preparations ( %; P ; n 5 7; Fig. 3C), and produced a decrease in threshold pressure (Fig. 3D). However, at this concentration, there was no change in voiding pressure (Fig. 3E), baseline pressure, or duration of voiding phase, nor was there a change in arterial perfusion Fig. 2. Dose-response to systemic isoprenaline infusion. (A) Incremental dosing with isoprenaline (10 nm to 1 mm in the perfusate) prolonged the intervoid interval, reduced voiding pressure, and lowered arterial perfusion pressure. The pooled data showed significant reductions in voiding pressure (B) at isoprenaline $100 nm, threshold pressure (C) at isoprenaline $100 nm, and arterial perfusion pressure (D) at isoprenaline $10 nm. (Repeatedmeasures ANOVA with Dunnett s post-hoc tests: *P, 0.05; **P, 0.01; ***P, )
5 510 Sadananda et al. Fig. 3. Influence of b 3 -adrenoceptors on storage and voiding. (A) Incremental dosing with mirabegron in the perfusate (steps from 10 nm to 1 mm shown) increased the intervoid interval (100 nm; pooled data in red; n =7;P, 0.05) (B), bladder compliance (100 nm; pooled data in red; n = 7;P, 0.01) (C), and threshold pressure (D) without changing the voiding pressure (E). (F) Application of the b 3 -adrenoceptor antagonistl748,337 (3 mm) alone had the opposite effect shortening the intervoid interval suggesting the presence of a basal sympathetic tone to the bladder. (Repeated-measures ANOVA with Dunnett s post-hoc tests: *P, 0.05; **P, 0.01; P, ) pressure or heart rate. Only at the highest concentration (1 mm) did mirabegron reduce arterial perfusion pressure (from to mm Hg; P ; Fig. 3A), although heart rate was still unchanged. The actions of mirabegron (100 nm) to prolong the intervoid interval and increase compliance were blocked by the coapplication of the b 3 -AR antagonist L748,337 (3 mm, n 5 3; Table 1), and mirabegron now appeared to shorten the intervoid interval as well as increase voiding pressure. However, L748,337 alone was noted to reduce the intervoid interval (from to seconds; P, 0.05) and increase voiding pressure ( to mm Hg; P, 0.05) and baseline pressure ( to mm Hg; P, 0.05) (Fig. 3F). These findings indicate that there is ongoing sympathetic tone in the DAPR which acts via b 3 -ARs to promote urine storage. There was no significant additional effect of mirabegron (100 nm) upon these changes evoked by the b 3 -AR antagonist. Actions of Systemic b-ar Agonists on Nonmicturition Contractions. NMCs were readily apparent in most preparations with an amplitude of mm Hg and inter-nmc interval of seconds (n 5 17) in controls. Within preparations, NMC amplitude and frequency were maintained throughout the course of the experiment as long as brainstem control remained intact (as reflected by the eupnoeic pattern of phrenic nerve activity; Paton, 1996; Pickering and
6 TABLE 1 Effect of mirabegron in the presence of L748,337 Control Mirabegron + L748,337 IVI (n =3) * Voiding pressure (n =3) * Threshold pressure (n = 3) Baseline pressure (n = 3) Compliance (n = 3) IVI, intervoid interval. * P, 0.05, paired t test. Paton, 2006), but as we have noted previously (Sadananda et al., 2011), they showed a progressive increase in amplitude as bladder volume increased during the filling cycle (see Fig. 4A). The amplitude of NMCs was reduced by both isoprenaline ( %; P ; n 5 6; 1 mm; Fig. 4C) and mirabegron ( %; P, ; n 5 5; 100 nm; Fig. 4, A and D) in all preparations (Fig. 4A). NMC frequency was not significantly altered in the presence of mirabegron [inter-nmc interval for Role of b 3 -adrenoceptors in Rat Micturition 511 control vs. mirabegron: vs seconds, not significant (ns); Fig. 4D] or isoprenaline (Fig. 4E). The b 3 -AR antagonist, L748,337 increased NMC amplitude by % (P ; n 5 3) but had no effect on NMC frequency. The level of pelvic afferent nerve activity during NMCs and during voids was not altered by mirabegron (Fig. 4B) with maintained afferent sensitivity to bladder pressure [ control vs mv.s/mmhginthepresenceofmirabegron;n 5 3, ns). b 3 -AR Agonism in Pathological Models of Micturition. We have previously noted that NMCs are enhanced when spinal-brainstem autonomic control of the lower urinary tract is lost (Sadananda et al., 2011), which mimics the situation after spinal injury or autonomic neuropathy. Under these conditions, the NMCs changed in morphology with abnormally high amplitude ( mm Hg; n 5 6). In such preparations, mirabegron (100 nm) still reduced NMC amplitude by % (n 5 4; P ; see example in Fig. 5). The basal pelvic afferent nerve activity level diminished with the decrease in baseline bladder pressure on Fig. 4. Nonmicturition contractions are attenuated by b 3 -adrenoceptor agonists. (A) Application of mirabegron (100 nm) increased the intervoid interval and decreased the amplitude of NMCs. [Pelvic nerve activity was rectified and integrated time constant 200 ms (purple) and 2 seconds (black).] (B) Pelvic afferent nerve activity retained the same sensitivity to bladder pressure in the presence of mirabegron, still showing marked increases in activity during NMCs and during voids. (Correlation analysis using rectified and integrated pelvic nerve activity with time constant 500 ms.) Pooled data showed that both isoprenaline (1 mm; n =4;P, 0.01) (C) and mirabegron (100 nm; n =5;P, 0.01) (D) significantly reduced NMC amplitude (individual paired data in black and means inred)withoutanactiononthefrequencyof occurrence of the NMCs (E and F). (Paired t test: **P, 0.01.)
7 512 Sadananda et al. mirabegron administration, but the amplitude of the bursts of increased pelvic nerve activity associated with each NMC was preserved (n 5 4; see Fig. 5). Acute acetic acid sensitization (intravesical application at ph 5.5; n 5 7) produced the anticipated increase in voiding frequency ( to seconds; P ; see Fig. 6A) accompanied by a decrease in compliance ( to ml/mm Hg; P, 0.05). Acetic acid had no effect on NMC amplitude (control vs. acid: vs mm Hg) or frequency. Mirabegron (100 nm; n 5 5 preparations; Fig. 6, B and C) reversed the acid-induced shortening of the intervoid interval ( to seconds; P ) and the decreased bladder compliance ( to ml/mm Hg), but had no effect upon NMC amplitude (acid vs. acid1mirabegron mm Hg, ns). The restoration of the intervoid interval by mirabegron in the acid-sensitized preparation without an action on NMCs suggested that the b 3 receptor agonist might be exerting its main beneficial effect by increasing bladder compliance. Therefore, we performed correlation analysis on the data set from naive preparations to look at the relationships between mirabegron (100 nm)-induced changes in intervoid interval, NMC amplitude, and bladder compliance (Fig. 7). A positive correlation was found between the intervoid interval and compliance (linear regression; R ; P, 0.05), but there was no evident relationship to NMC amplitude. Furthermore, there appeared to be no significant relationship between compliance and NMC amplitude, suggesting that they may be independently regulated. Discussion We have undertaken a detailed examination of the mechanism of action of b-ar agonists on micturition in a functionally preserved, nonanesthetized rat preparation. We have shown that systemic administration of nonselective b-ar and b 3 - AR selective agents promotes storage by increasing bladder capacity and hence prolongation of the intervoid interval. This action was also seen following acute acetic acid bladder sensitization. These b-ar mediated effects are associated with increased bladder compliance and a decrease in the amplitude of non-micturition contractions. The selective b 3 -AR agonist mirabegron (Takasu et al., 2007) produced these effects on filling without changing active voiding parameters (unlike the nonselective b-ar agonist) or producing hemodynamic disturbances (see also Takeda et al., 2000). Selective b 3 -AR antagonism reduced bladder capacity and intervoid interval, indicating that there is a basal sympathetic tone acting via b 3 -AR to promote urine storage. These findings are consistent with an existing body of literature indicating that sympathoactivation via b-ar promotes urine storage both in rodents and in humans (reviews: Furuta et al., 2006; Yamaguchi and Chapple, 2007; Michel et al., 2011). These studies have shown roles for both b 2 - and b 3 -AR mediated effects on the detrusor (Longhurst and Levendusky, 1999; Morita et al., 2000; Michel and Vrydag, 2006), on signaling from the urothelium (Otsuka et al., 2008; Deba et al., 2009; Masunaga et al., 2010; Kullmann et al., 2011), and, latterly, afferent nerve signaling (Kanai et al., 2011; Aizawa et al., 2012). Much of these data have been gathered from in vitro studies or in vivo studies without intact micturition cycles, and as such, the importance of each mechanism in the regulation of the micturition cycle has been difficult to ascertain. We have taken advantage of the decerebrate, arterially perfused rat preparation (Pickering and Paton, 2006; Sadananda et al., 2011) which allows cystometry to assess both filling and voiding parameters while enabling in vitro like control over dosing of b-ar agonists and antagonists. In particular, we have been able to focus on the differential effects of these agents on bladder compliance, contractility, NMCs, and afferent signaling, and how these changes influence volume sensing and voiding frequency. As well as increasing intervoid interval, we observed that b-ar agonists consistently reduced NMC amplitude (but not frequency). Such spontaneous bladder motions may form part of a detection mechanism that signals bladder fullness to the central nervous system (Drake et al., 2001). Based on our previous observations that NMC amplitude was increased following loss of autonomic control (pharmacological or pathological; Sadananda et al., 2011), we hypothesized that Fig. 5. Pathologically augmented nonmicturition contractions are suppressed by b 3 -adrenoceptor agonist. After loss of brainstem-spinal control, micturition ceased, and the amplitude and morphology of NMCs and pelvic afferent activity were pathologically increased (shown on left, bladder at constant volume). Systemic infusion of mirabegron (100 nm) decreased both the amplitude of the NMCs and the pelvic afferent nerve activity (mirroring the reduction in bladder pressure) without a change in bladder volume. Note that the smaller NMCs in the presence of mirabegron still evoked similarsized bursts of afferent discharge. Pelvic nerve activity was rectified and integrated, shown here with two time constants: 200 ms (purple) and 2 seconds (black).
8 Role of b 3 -adrenoceptors in Rat Micturition 513 b-ar sympathomimetic agents would decrease NMC amplitude and thereby promote urine storage. We observed that b-ar agonists both reduced NMC amplitude and increased the intervoid interval. However, contrary to our original hypothesis, the increase in intervoid interval was not correlated with the degree of change in amplitude of NMCs, suggesting that these mechanisms are likely to be independent. The b-ar agonist evoked increase in intervoid interval was, instead, correlated with an increase in bladder compliance. In the case of b 3 -AR agonism, this increase in compliance was not accompanied by an alteration in the active voiding parameters, suggesting it did not produce a change in detrusor contractility (unlike the nonselective b-ar agonists). This result indicates that the effects of b 3 -AR agonism are not achieved by directly opposing parasympathetic actions. Thus, the mirabegron-induced change in compliance is mediated independent of an action on active contractility. An important caveat to these conclusions regarding the mechanism of action of b 3 -AR on urine storage should be noted: namely, that the intravesical pressure change of the NMCs may not be the physiologically relevant feature of the event. It may be that the movement-induced localized change in bladder wall stretch is the relevant signal to the bladder afferents (Drake et al., 2001) indeed, afferent nerve recordings in the presence of mirabegron suggested that this afferent signaling was preserved even though the amplitude of the NMCs was smaller. It is also worth noting that the threshold pressure for the initiation of voids was lowered by the b 3 -AR agonists, suggesting that there was no attenuation in the afferent signaling of bladder pressure. This was supported by our pelvic Fig. 6. Intravesical acetic acid sensitization of the lower urinary tract is reversed by b 3 -adrenoceptor agonist. (A) Intravesical infusion of acetic acid (ph 5.5) shortened the intervoid interval and decreased bladder compliance. Systemic infusion of mirabegron (10 and 100 nm), in the continued presence of intravesical acetic acid, prolonged the intervoid interval ($10 nm; P, 0.05; n = 7) (B) and increased bladder compliance (100 nm; P, 0.01; n = 7) (C) without significantly changing NMC amplitude. (Paired t test: *P, 0.05, and repeated-measures ANOVA with Dunnett s multiple comparison test versus acidsensitized condition: #P, 0.05; ##P, 0.01.) afferent nerve recordings that showed preserved afferent signaling in response to dynamic changes in bladder pressure (both NMCs and during voiding contractions) in the presence of b 3 -AR agonist. This appears to contrast with recent reports from in vitro (Kanai et al., 2011) and in vivo (Aizawa et al., 2012) studies showing a decrease in afferent nerve activities by b 3 -AR agonists. This disparity will require further investigation, but our findings may be explained by the presence of dynamic bladder motions seen in our preparation with intact micturition that may provide a more physiological afferent activation. The selective b 3 -AR agonist mirabegron improved urine storage and bladder compliance without attenuating voiding pressure, unlike the nonselective b agonist isoprenaline. Thus, it is plausible that the effect of isoprenaline on voiding pressure is mediated via b 1 /b 2 -AR receptors to oppose parasympathetic contractile responses. In addition to the reduced voiding pressure, we also noted that isoprenaline shortened the duration of the voiding phase (unlike mirabegron). Although we did not directly study urethral outflow function, this shortening of the voiding phase may be consistent with activation of b 2 -adrenoceptors that have a dilator function in the rat urethra (unlike b 3 ) (Michel and Vrydag, 2006) such dilation may allow more rapid evacuation of bladder contents. This lowered LUT outflow resistance could in itself account for the lowered voiding pressure in the presence of isoprenaline rather than a direct action on the detrusor, but this will require further experimental verification. Nonetheless, the features of selective b 3 -AR agonism are clinically relevant to OAB, as they suggest that storage function can be improved
9 514 Sadananda et al. Fig. 7. Mirabegron-induced increase in the intervoid interval is correlated with the degree of increase in compliance. (A) Linear regression analysis showed a positive correlation between the change in compliance and the degree of increase in the intervoid interval for each preparation (R 2 =0.45;P, 0.05; n = 7). (B) In contrast, there was no significant correlation between the change in NMC amplitude and the intervoid interval (n = 5). (C) The NMC amplitude change was also independent of the mirabegron-induced changes in bladder compliance (n = 5). Given this profile of action under physiological conditions, we next investigated the effect of b 3 -AR agonism in pathological models. First, mirabegron reversed the abnormally high amplitude of NMCs seen after loss of brainstem control in the DAPR preparation. Second, following acid sensitization to mimic acute bladder overactivity (Zhang et al., 2003), mirabegron increased the intervoid interval and compliance without an effect on NMC amplitude. This observation again implies that the effects of b 3 -AR agonism on storage are not mediated through a reduction in NMC amplitude. Although it has previously been noted in chronic models of lower urinary tract dysfunction such as bladder outlet obstruction (Hood and Andersson, 2013) that b 3 -AR agonism suppresses NMCs, it has not yet been demonstrated whether this action produces an improvement in urine storage in this pathological model. Technical Aspects of the Use of the DAPR. An advantage of the DAPR illustrated in this study is the ability to assay the systemic effects of pharmacological agents on multiple organ systems (relatively independent of preparation viability) and thus detect potential side effects. This was illustrated in the current investigation in which isoprenaline was shown to increase heart rate (via b 1 -AR) and reduce arterial perfusion pressure. These actions were not seen with mirabegron except at the highest dose, where it caused a mild hypotensive effect. The DAPR approach requires the use of young rats typically younger than 4 weeks of age. Although there is some debate over the age at which rat micturition is fully mature (Yamaguchi and Chapple, 2007; Kanai et al., 2011; Zvarova and Zvara, 2012), we found coordinated and complete bladder emptying in all our preparations as described previously (Sadananda et al., 2011). It should be noted that, for cystometry, we chose to use a bladder infusion rate (20 ml/ min) that produced a relatively short intervoid interval (typically less than 5 minutes) to allow drug responses to be assayed expeditiously, permitting repeated dosing studies with washouts. Conclusions Treatments for bladder storage dysfunctions such as OAB must possess a number of specific features: they must enhance bladder capacity and/or compliance while preserving the active voiding phase, and they should be well tolerated systemically. Previous therapies have focused on direct relaxation of the detrusor muscle, resulting in improved storage, but potentially adversely affecting voiding function, when contraction is required. In our current study, we found b 3 -AR agonism promoted urinary storage without impairing the voiding phase, and was relatively free of off-target cardiorespiratory side effects. Intriguingly, we also demonstrate a basal tone of sympathetically mediated b 3 activation that regulates lower urinary tract function and speculate that loss of such tone could play a role in the pathogenesis of conditions such as OAB. without affecting voiding characteristics. This is an important aspect, as storage disorders can coexist with impaired voiding function. Acknowledgments The authors are grateful to Dr. Cees Korstanje and Dr. Frank Perabo for their insights and productive discussions.
10 Authorship Contributions Participated in research design: Sadananda, Pickering, Paton, Drake. Conducted experiments: Sadananda. Performed data analysis: Sadananda, Pickering. Wrote or contributed to the writing of the manuscript: Sadananda, Pickering, Paton, Drake. References Abrams P, Cardozo L, Fall M, Griffiths D, Rosier P, Ulmsten U, van Kerrebroeck P, Victor A, and Wein A (2002) The standardisation of terminology of lower urinary tract function: report from the Standardisation Sub-committee of the International Continence Society. Am J Obstet Gynecol 187: Aizawa N, Homma Y, and Igawa Y (2012) Effects of mirabegron, a novel b3-adrenoceptor agonist, on primary bladder afferent activity and bladder microcontractions in rats compared with the effects of oxybutynin. Eur Urol 62: Andersson KE and Wein AJ (2004) Pharmacology of the lower urinary tract: basis for current and future treatments of urinary incontinence. Pharmacol Rev 56: Deba A, Palea S, Rouget C, Westfall TD, and Lluel P (2009) Involvement of beta(3)- adrenoceptors in mouse urinary bladder function: role in detrusor muscle relaxation and micturition reflex. Eur J Pharmacol 618: Drake MJ, Mills IW, and Gillespie JI (2001) Model of peripheral autonomous modules and a myovesical plexus in normal and overactive bladder function. Lancet 358: Fowler CJ, Griffiths D, and de Groat WC (2008) The neural control of micturition. Nat Rev Neurosci 9: Furuta A, Thomas CA, Higaki M, Chancellor MB, Yoshimura N, and Yamaguchi O (2006) The promise of beta3-adrenoceptor agonists to treat the overactive bladder. Urol Clin North Am 33: Hood B and Andersson KE (2013) Common theme for drugs effective in overactive bladder treatment: inhibition of afferent signaling from the bladder. Int J Urol 20: Igawa Y, Yamazaki Y, Takeda H, Hayakawa K, Akahane M, Ajisawa Y, Yoneyama T, Nishizawa O, and Andersson KE (1999) Functional and molecular biological evidence for a possible beta3-adrenoceptor in the human detrusor muscle. Br J Pharmacol 126: Kanai A, Wyndaele JJ, Andersson KE, Fry C, Ikeda Y, Zabbarova I, and De Wachter S (2011) Researching bladder afferents-determining the effects of b(3) -adrenergic receptor agonists and botulinum toxin type-a. Neurourol Urodyn 30: Kullmann FA, Downs TR, Artim DE, Limberg BJ, Shah M, Contract D, de Groat WC, and Rosenbaum JS (2011) Urothelial beta-3 adrenergic receptors in the rat bladder. Neurourol Urodyn 30: Longhurst PA and Levendusky M (1999) Pharmacological characterization of betaadrenoceptors mediating relaxation of the rat urinary bladder in vitro. Br J Pharmacol 127: Role of b 3 -adrenoceptors in Rat Micturition 515 Maggi CA, Giuliani S, Santicioli P, and Meli A (1986) Analysis of factors involved in determining urinary bladder voiding cycle in urethan-anesthetized rats. Am J Physiol 251:R250 R257. Masunaga K, Chapple CR, McKay NG, Yoshida M, and Sellers DJ (2010) The b3- adrenoceptor mediates the inhibitory effects of b-adrenoceptor agonists via the urothelium in pig bladder dome. Neurourol Urodyn 29: Michel MC, Ochodnicky P, Homma Y, and Igawa Y (2011) b-adrenoceptor agonist effects in experimental models of bladder dysfunction. Pharmacol Ther 131: Michel MC and Vrydag W (2006) Alpha1-, alpha2- and beta-adrenoceptors in the urinary bladder, urethra and prostate. Br J Pharmacol 147 (Suppl 2):S88 S119. Morita T, Iizuka H, Iwata T, and Kondo S (2000) Function and distribution of beta3- adrenoceptors in rat, rabbit and human urinary bladder and external urethral sphincter. J Smooth Muscle Res 36: Otsuka A, Shinbo H, Matsumoto R, Kurita Y, and Ozono S (2008) Expression and functional role of beta-adrenoceptors in the human urinary bladder urothelium. Naunyn Schmiedebergs Arch Pharmacol 377: Parsons BA and Drake MJ (2011) Animal models in overactive bladder research. Handb Exp Pharmacol (202): Paton JF (1996) A working heart-brainstem preparation of the mouse. J Neurosci Methods 65: Pickering AE and Paton JF (2006) A decerebrate, artificially-perfused in situ preparation of rat: utility for the study of autonomic and nociceptive processing. J Neurosci Methods 155: Sadananda P, Drake MJ, Paton JF, and Pickering AE (2011) An exploration of the control of micturition using a novel in situ arterially perfused rat preparation. Front Neurosci 5: Sadananda P, Shang F, Liu L, Mansfield KJ, and Burcher E (2009) Release of ATP from rat urinary bladder mucosa: role of acid, vanilloids and stretch. Br J Pharmacol 158: Takasu T, Ukai M, Sato S, Matsui T, Nagase I, Maruyama T, Sasamata M, Miyata K, Uchida H, and Yamaguchi O (2007) Effect of (R)-2-(2-aminothiazol-4-yl)-49-2-[(2- hydroxy-2-phenylethyl)amino]ethyl acetanilide (YM178), a novel selective beta3- adrenoceptor agonist, on bladder function. J Pharmacol Exp Ther 321: Takeda H, Yamazaki Y, Akahane M, Igawa Y, Ajisawa Y, and Nishizawa O (2000) Role of the beta(3)-adrenoceptor in urine storage in the rat: comparison between the selective beta(3)-adrenoceptor agonist, CL316, 243, and various smooth muscle relaxants. J Pharmacol Exp Ther 293: Yamaguchi O and Chapple CR (2007) Beta3-adrenoceptors in urinary bladder. Neurourol Urodyn 26: Zhang X, Igawa Y, Ishizuka O, Nishizawa O, and Andersson KE (2003) Effects of resiniferatoxin desensitization of capsaicin-sensitive afferents on detrusor overactivity induced by intravesical capsaicin, acetic acid or ATP in conscious rats. Naunyn Schmiedebergs Arch Pharmacol 367: Zvarova K and Zvara P (2012) Urinary bladder function in conscious rat pups: a developmental study. Am J Physiol Renal Physiol 302:F1563 F1568. Address correspondence to: Anthony E. Pickering, School of Physiology and Pharmacology, University of Bristol, University Walk, Bristol BS8 1TD, UK. Tony.Pickering@bristol.ac.uk
Overactive Bladder; OAB. Aδ silent C. Adenosine triphosphate; ATP SD g n Key words
 25-32 2009 SD 200-270g n 28 4 1 2 3 4 PE-50 4-5 0.25 60 C Key words acupuncture stimulation overactive bladder rat bladder irritation C C fiber Received November 17, 2008; Accepted January 9, 2009 I Overactive
25-32 2009 SD 200-270g n 28 4 1 2 3 4 PE-50 4-5 0.25 60 C Key words acupuncture stimulation overactive bladder rat bladder irritation C C fiber Received November 17, 2008; Accepted January 9, 2009 I Overactive
On the Site and Mechanism of Action of β3-adrenoceptor Agonists in the Bladder
 Official Journal of Korean Continence Society / Korean Society of Urological Research / The Korean Children s Continence and Enuresis Society / The Korean Association of Urogenital Tract Infection and
Official Journal of Korean Continence Society / Korean Society of Urological Research / The Korean Children s Continence and Enuresis Society / The Korean Association of Urogenital Tract Infection and
University of Bristol - Explore Bristol Research
 Ito, H., Drake, M. J., Fry, C. H., Kanai, A. J., & Pickering, A. E. (2018). Characterization of mouse neuro-urological dynamics in a novel decerebrate arterially perfused mouse (DAPM) preparation. Neurourology
Ito, H., Drake, M. J., Fry, C. H., Kanai, A. J., & Pickering, A. E. (2018). Characterization of mouse neuro-urological dynamics in a novel decerebrate arterially perfused mouse (DAPM) preparation. Neurourology
What is on the Horizon in Drug Therapy for OAB?
 What is on the Horizon in Drug Therapy for OAB? K-E Andersson, MD, PhD Wake Forest Institute for Regenerative Medicine Wake Forest University School of Medicine Winston Salem, North Carolina Disclosures
What is on the Horizon in Drug Therapy for OAB? K-E Andersson, MD, PhD Wake Forest Institute for Regenerative Medicine Wake Forest University School of Medicine Winston Salem, North Carolina Disclosures
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Original Article. Annals of Rehabilitation Medicine INTRODUCTION
 Original Article Ann Rehabil Med 2014;38(3):342-346 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.342 Annals of Rehabilitation Medicine Phasic Changes in Bladder Compliance
Original Article Ann Rehabil Med 2014;38(3):342-346 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.342 Annals of Rehabilitation Medicine Phasic Changes in Bladder Compliance
Beta3-Adrenoceptor Agonists: Possible Role in the Treatment of Overactive Bladder
 www.kjurology.org DOI:10.4111/kju.2010.51.12.811 Review Article Beta3-Adrenoceptor Agonists: Possible Role in the Treatment of Overactive Bladder Yasuhiko Igawa, Naoki Aizawa, Yukio Homma 1 Department
www.kjurology.org DOI:10.4111/kju.2010.51.12.811 Review Article Beta3-Adrenoceptor Agonists: Possible Role in the Treatment of Overactive Bladder Yasuhiko Igawa, Naoki Aizawa, Yukio Homma 1 Department
Physiologic Anatomy and Nervous Connections of the Bladder
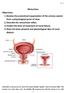 Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Alpha antagonists from initial concept to routine clinical practice
 european urology 50 (2006) 635 642 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Alpha antagonists from initial concept to routine clinical practice
european urology 50 (2006) 635 642 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Alpha antagonists from initial concept to routine clinical practice
Signal transduction underlying the control of urinary bladder smooth muscle tone Puspitoayu, E.
 UvA-DARE (Digital Academic Repository) Signal transduction underlying the control of urinary bladder smooth muscle tone Puspitoayu, E. Link to publication Citation for published version (APA): Puspitoayu,
UvA-DARE (Digital Academic Repository) Signal transduction underlying the control of urinary bladder smooth muscle tone Puspitoayu, E. Link to publication Citation for published version (APA): Puspitoayu,
Role of Animal Models
 Division of Urology, Department of Surgery, Duke University Medical Center Institute for Medical Research, Durham Veteran s Affairs Medical Center Role of Animal Models Matthew O. Fraser, PhD 9th Annual
Division of Urology, Department of Surgery, Duke University Medical Center Institute for Medical Research, Durham Veteran s Affairs Medical Center Role of Animal Models Matthew O. Fraser, PhD 9th Annual
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
The Inhibitory Role of Acetylcholine and Muscarinic Receptors in Bladder Afferent Activity
 EUROPEAN UROLOGY 58 (2010) 22 28 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Neuro-urology Editorial by Delphine Behr-Roussel and François A. Giuliano
EUROPEAN UROLOGY 58 (2010) 22 28 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Neuro-urology Editorial by Delphine Behr-Roussel and François A. Giuliano
This Special Report supplement
 ...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
The Evidence for Antimuscarinic Agents in Female Mixed Urinary Incontinence
 european urology supplements 5 (2006) 849 853 available at www.sciencedirect.com journal homepage: www.europeanurology.com The Evidence for Antimuscarinic Agents in Female Mixed Urinary Incontinence Stefano
european urology supplements 5 (2006) 849 853 available at www.sciencedirect.com journal homepage: www.europeanurology.com The Evidence for Antimuscarinic Agents in Female Mixed Urinary Incontinence Stefano
Neural Control of Lower Urinary Tract Function. William C. de Groat University of Pittsburgh Medical School
 Neural Control of Lower Urinary Tract Function William C. de Groat University of Pittsburgh Medical School Disclosures Current funding: NIH Grants, DK093424, DK-091253, DK-094905, DK-090006. Other financial
Neural Control of Lower Urinary Tract Function William C. de Groat University of Pittsburgh Medical School Disclosures Current funding: NIH Grants, DK093424, DK-091253, DK-094905, DK-090006. Other financial
Diagnosis and Mangement of Nocturia in Adults
 Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
Neural control of the lower urinary tract in health and disease
 Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
Normal micturition involves complex
 NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
Overactive bladder can result from one or more of the following causes:
 Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Anticholinergic medication use for female overactive bladder in the ambulatory setting in the United States.
 Página 1 de 6 PubMed darifenacin vs solifenacin Display Settings:, Sorted by Recently Added Results: 5 1. Int Urogynecol J. 2013 Oct 25. [Epub ahead of print] Anticholinergic medication use for female
Página 1 de 6 PubMed darifenacin vs solifenacin Display Settings:, Sorted by Recently Added Results: 5 1. Int Urogynecol J. 2013 Oct 25. [Epub ahead of print] Anticholinergic medication use for female
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests. Amelyn R.
 Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Non-adrenergic, non-cholinergic, non-purinergic contractions of the urothelium/lamina propria of the pig bladder
 Bond University epublications@bond Faculty of Health Sciences & Medicine Publications Faculty of Health Sciences & Medicine 10-1-2012 Non-adrenergic, non-cholinergic, non-purinergic contractions of the
Bond University epublications@bond Faculty of Health Sciences & Medicine Publications Faculty of Health Sciences & Medicine 10-1-2012 Non-adrenergic, non-cholinergic, non-purinergic contractions of the
A Multicenter, Double-blind, Randomized, Placebo-controlled Trial of the b3-adrenoceptor Agonist Solabegron for Overactive Bladder
 EUROPEAN UROLOGY 62 (2012) 834 840 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Voiding Dysfunction Editorial by Christopher R. Chapple on pp. 841 842
EUROPEAN UROLOGY 62 (2012) 834 840 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Voiding Dysfunction Editorial by Christopher R. Chapple on pp. 841 842
Japan. J. Pharmacol. 50, (1989) 327. Effects of Central Nervous System-Acting Drugs on Urinary Bladder Contraction in Unanesthetized Rats
 Japan. J. Pharmacol. 50, 327-332 (1989) 327 Effects of Central Nervous System-Acting Drugs on Urinary Bladder Contraction in Unanesthetized Rats Hitoshi KONTANI, Mikiko NAKAGAWA and Takeshi SAKAI Department
Japan. J. Pharmacol. 50, 327-332 (1989) 327 Effects of Central Nervous System-Acting Drugs on Urinary Bladder Contraction in Unanesthetized Rats Hitoshi KONTANI, Mikiko NAKAGAWA and Takeshi SAKAI Department
Naoki Wada, Seiji Matsumoto, Masafumi Kita, Kazumi Hashizume and Hidehiro Kakizaki
 bs_bs_banner International Journal of Urology (1) 1, 15 1 doi: 1.1111/iju.157 Original Article: Clinical Investigation Decreased urinary nerve growth factor reflects prostatic volume reduction and relief
bs_bs_banner International Journal of Urology (1) 1, 15 1 doi: 1.1111/iju.157 Original Article: Clinical Investigation Decreased urinary nerve growth factor reflects prostatic volume reduction and relief
THE ACONTRACTILE BLADDER - FACT OR FICTION?
 THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
Overactive Bladder Syndrome
 Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Objectives. Key Outlines:
 Objectives! Iden8fy and describe the Func8onal Anatomy of Urinary Bladder! Describe the mechanism of filling and emptying of the urinary bladder! Cystometrogram! Appreciate neurogenic control of the mechanism
Objectives! Iden8fy and describe the Func8onal Anatomy of Urinary Bladder! Describe the mechanism of filling and emptying of the urinary bladder! Cystometrogram! Appreciate neurogenic control of the mechanism
Chapter 23. Micturition and Renal Insufficiency
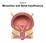 Chapter 23 Micturition and Renal Insufficiency Voiding Urine Between acts of urination, the bladder is filling. detrusor muscle relaxes urethral sphincters are tightly closed accomplished by sympathetic
Chapter 23 Micturition and Renal Insufficiency Voiding Urine Between acts of urination, the bladder is filling. detrusor muscle relaxes urethral sphincters are tightly closed accomplished by sympathetic
PREPARED FOR: U.S. Army Medical Research and Materiel Command Fort Detrick, Maryland
 Award Number: W81XWH-12-1-0445 TITLE: An investigation into the nature of non-voiding contractions resulting from detrusor hyperreflexia in neurogenic bladders following spinal cord injury PRINCIPAL INVESTIGATOR:
Award Number: W81XWH-12-1-0445 TITLE: An investigation into the nature of non-voiding contractions resulting from detrusor hyperreflexia in neurogenic bladders following spinal cord injury PRINCIPAL INVESTIGATOR:
The Time-Frequency Analysis of the Pudendo-to-Pudendal Nerve and Pelvic-to-Pudendal Nerve Reflexes in Anesthetized Intact Rats
 Journal of Medical and Biological Engineering, 24(1): 17-22 17 The Time-Frequency Analysis of the Pudendo-to-Pudendal Nerve and Pelvic-to-Pudendal Nerve Reflexes in Anesthetized Intact Rats Hui-Yi Chang
Journal of Medical and Biological Engineering, 24(1): 17-22 17 The Time-Frequency Analysis of the Pudendo-to-Pudendal Nerve and Pelvic-to-Pudendal Nerve Reflexes in Anesthetized Intact Rats Hui-Yi Chang
Male lower urinary tract symptoms and α 1D -adrenoceptors. and Karl-Erik Andersson 2. Winston Salem, NC, USA
 Male lower urinary tract symptoms and α 1D -adrenoceptors Osamu Ishizuka, 1 Tetsuya Imamura, 1 Yoshiki Kurizaki, 1 Osamu Nishizawa 1 and Karl-Erik Andersson 2 1 Department of Urology, Shinshu University
Male lower urinary tract symptoms and α 1D -adrenoceptors Osamu Ishizuka, 1 Tetsuya Imamura, 1 Yoshiki Kurizaki, 1 Osamu Nishizawa 1 and Karl-Erik Andersson 2 1 Department of Urology, Shinshu University
Neural control of the lower urinary tract
 Neural control of the lower urinary tract Jalesh N. Panicker Consultant Neurologist and Honorary Senior Lecturer The National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen
Neural control of the lower urinary tract Jalesh N. Panicker Consultant Neurologist and Honorary Senior Lecturer The National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen
Urinary System and Fluid Balance. Urine Production
 Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Characterization of bladder and external urethral activity in mice with or without spinal cord injury a comparison study with rats
 Am J Physiol Regul Integr Comp Physiol 31: R752 R758, 216. First published January 27, 216; doi:1.1152/ajpregu.45.215. Characterization of bladder and external urethral activity in mice with or without
Am J Physiol Regul Integr Comp Physiol 31: R752 R758, 216. First published January 27, 216; doi:1.1152/ajpregu.45.215. Characterization of bladder and external urethral activity in mice with or without
Characterization of bladder and external urethral activity in mice with or without spinal cord injury a comparison study with rats
 Am J Physiol Regul Integr Comp Physiol 31: R752 R758, 216. First published January 27, 216; doi:1.1152/ajpregu.45.215. Characterization of bladder and external urethral activity in mice with or without
Am J Physiol Regul Integr Comp Physiol 31: R752 R758, 216. First published January 27, 216; doi:1.1152/ajpregu.45.215. Characterization of bladder and external urethral activity in mice with or without
Department of Urology, Yantai Affiliated Hospital of Binzhou Medicine University, Yantai, China. 3
 Official Journal of Korean Continence Society / Korean Society of Urological Research / The Korean Children s Continence and Enuresis Society / The Korean Association of Urogenital Tract Infection and
Official Journal of Korean Continence Society / Korean Society of Urological Research / The Korean Children s Continence and Enuresis Society / The Korean Association of Urogenital Tract Infection and
TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury. Original Policy Date
 MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
INTRODUCTION. IN a previous paper(l) we have been able to show that adrenaline may
 REVERSAL OF THE ACTION OF ADRENALINE. BY B. A. McSWINEY AND G. L. BROWN. (From the Department of Physiology, University of Manchester.) INTRODUCTION. IN a previous paper(l) we have been able to show that
REVERSAL OF THE ACTION OF ADRENALINE. BY B. A. McSWINEY AND G. L. BROWN. (From the Department of Physiology, University of Manchester.) INTRODUCTION. IN a previous paper(l) we have been able to show that
Neuropathic Bladder. Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014
 Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
3/20/10. Prevalence of OAB Men: 16.0% Women: 16.9% Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Dry. Population (millions) Wet
 1 Prevalence of OAB Men: 16.0% Women: 16.9% Stewart WF, et al. World J Urol. 2003;20:327-336. Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Stewart WF, et al. World J Urol. 2003;20:327-336.
1 Prevalence of OAB Men: 16.0% Women: 16.9% Stewart WF, et al. World J Urol. 2003;20:327-336. Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Stewart WF, et al. World J Urol. 2003;20:327-336.
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Physiology & Neurophysiology of lower U.T.
 Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
CHAPTER 6. M.D. Eckhardt, G.E.P.M. van Venrooij, T.A. Boon. hoofdstuk :49 Pagina 89
 hoofdstuk 06 19-12-2001 09:49 Pagina 89 Urethral Resistance Factor (URA) Versus Schäfer s Obstruction Grade and Abrams-Griffiths (AG) Number in the Diagnosis of Obstructive Benign Prostatic Hyperplasia
hoofdstuk 06 19-12-2001 09:49 Pagina 89 Urethral Resistance Factor (URA) Versus Schäfer s Obstruction Grade and Abrams-Griffiths (AG) Number in the Diagnosis of Obstructive Benign Prostatic Hyperplasia
The effect of indomethacin on the muscarinic induced contractions in the isolated normal guinea pig urinary bladder
 Rahnama i et al. BMC Urology 2013, 13:8 RESEARCH ARTICLE Open Access The effect of indomethacin on the muscarinic induced contractions in the isolated normal guinea pig urinary bladder Mohammad S Rahnama
Rahnama i et al. BMC Urology 2013, 13:8 RESEARCH ARTICLE Open Access The effect of indomethacin on the muscarinic induced contractions in the isolated normal guinea pig urinary bladder Mohammad S Rahnama
Urethral pressure measurement in stress incontinence: does it help?
 Int Urol Nephrol (2009) 41:491 495 DOI 10.1007/s11255-008-9506-9 UROLOGY - ORIGINAL PAPER Urethral pressure measurement in stress incontinence: does it help? Bassem S. Wadie Æ Ahmed S. El-Hefnawy Received:
Int Urol Nephrol (2009) 41:491 495 DOI 10.1007/s11255-008-9506-9 UROLOGY - ORIGINAL PAPER Urethral pressure measurement in stress incontinence: does it help? Bassem S. Wadie Æ Ahmed S. El-Hefnawy Received:
Urinary Incontinence in Women: Never an Acceptable Consequence of Aging
 Urinary Incontinence in Women: Never an Acceptable Consequence of Aging Catherine A. Matthews, MD Associate Professor Chief, Urogynecology and Pelvic Reconstructive Surgery University of North Carolina,
Urinary Incontinence in Women: Never an Acceptable Consequence of Aging Catherine A. Matthews, MD Associate Professor Chief, Urogynecology and Pelvic Reconstructive Surgery University of North Carolina,
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN
 Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Efficacy and Safety of Propiverine and Solifenacin for the Treatment of Female Patients with Overactive Bladder: A Crossover Study
 LUTS () 3, 36 4 ORIGINAL ARTICLE Efficacy and Safety of Propiverine and Solifenacin for the Treatment of Female Patients with Overactive Bladder: A Crossover Study Naoki WADA, Masaki WATANABE, Masafumi
LUTS () 3, 36 4 ORIGINAL ARTICLE Efficacy and Safety of Propiverine and Solifenacin for the Treatment of Female Patients with Overactive Bladder: A Crossover Study Naoki WADA, Masaki WATANABE, Masafumi
Involuntary Detrusor Contractions: Correlation of Urodynamic Data to Clinical Categories
 Neurourology and Urodynamics 20:249±257 (2001) Involuntary Detrusor Contractions: Correlation of Urodynamic Data to Clinical Categories Lauri J. Romanzi, Asnat Groutz, Dianne M. Heritz, and Jerry G. Blaivas*
Neurourology and Urodynamics 20:249±257 (2001) Involuntary Detrusor Contractions: Correlation of Urodynamic Data to Clinical Categories Lauri J. Romanzi, Asnat Groutz, Dianne M. Heritz, and Jerry G. Blaivas*
Patient Information. Basic Information on Overactive Bladder Symptoms. pubic bone. urethra. scrotum. bladder. vaginal canal
 Patient Information English Basic Information on Overactive Bladder Symptoms The underlined terms are listed in the glossary. What is the bladder? pubic bone bladder seminal vesicles prostate rectum The
Patient Information English Basic Information on Overactive Bladder Symptoms The underlined terms are listed in the glossary. What is the bladder? pubic bone bladder seminal vesicles prostate rectum The
TREATMENT OF OVERACTIVE BLADDER IN ADULTS FUGA 2016 KGH
 TREATMENT OF OVERACTIVE BLADDER IN ADULTS FUGA 2016 KGH CONTENTS Overactive bladder (OAB) Treatment of OAB Beta-3 adrenoceptor agonist (Betmiga ) - Panacea? LASER treatment - a flash in the pan or the
TREATMENT OF OVERACTIVE BLADDER IN ADULTS FUGA 2016 KGH CONTENTS Overactive bladder (OAB) Treatment of OAB Beta-3 adrenoceptor agonist (Betmiga ) - Panacea? LASER treatment - a flash in the pan or the
Antimuscarinic drugs in detrusor overactivity and the overactive bladder syndrome: motor or sensory actions?
 Review Article SENSORY ACTIONS OF ANTIMUSCARINICS FINNEY et al. Antimuscarinic drugs in detrusor overactivity and the overactive bladder syndrome: motor or sensory actions? STEVEN M. FINNEY, KARL-ERIK
Review Article SENSORY ACTIONS OF ANTIMUSCARINICS FINNEY et al. Antimuscarinic drugs in detrusor overactivity and the overactive bladder syndrome: motor or sensory actions? STEVEN M. FINNEY, KARL-ERIK
A New Method for Urinary Bladder. Hyperactivity in Conscious Rats
 A New Method for Urinary Bladder Hyperactivity in Conscious Rats January 2010 Manabu MITOBE A New Method for Urinary Bladder Hyperactivity in Conscious Rats A Dissertation Submitted to the Graduate School
A New Method for Urinary Bladder Hyperactivity in Conscious Rats January 2010 Manabu MITOBE A New Method for Urinary Bladder Hyperactivity in Conscious Rats A Dissertation Submitted to the Graduate School
Neuromodulation and the pudendal nerve
 Neuromodulation and the pudendal nerve Stefan De Wachter, MD, PhD, FEBU Professor of Urology University of Antwerpen, Belgium Chairman dept of Urology, UZA Disclosures Consultant speaker: Astellas, Medtronic,
Neuromodulation and the pudendal nerve Stefan De Wachter, MD, PhD, FEBU Professor of Urology University of Antwerpen, Belgium Chairman dept of Urology, UZA Disclosures Consultant speaker: Astellas, Medtronic,
Efficacy and Adverse Effects of Solifenacin in the Treatment of Lower Urinary Tract Symptoms in Patients With Overactive Bladder
 Urol Sci 21;21(1):38 43 ORIGINAL ARTICLE Efficacy and Adverse Effects of Solifenacin in the Treatment of Lower Urinary Tract Symptoms in Patients With Overactive Bladder Yih-Chou Chen, Chia-Yen Chen, Hann-Chorng
Urol Sci 21;21(1):38 43 ORIGINAL ARTICLE Efficacy and Adverse Effects of Solifenacin in the Treatment of Lower Urinary Tract Symptoms in Patients With Overactive Bladder Yih-Chou Chen, Chia-Yen Chen, Hann-Chorng
The Urinary System 15PART B. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART B Ureters Slender tubes attaching the kidney to the bladder Continuous with
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART B Ureters Slender tubes attaching the kidney to the bladder Continuous with
Regulation of the Urinary Bladder Chapter 26
 Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Dr Jonathan Evans Paediatric Nephrologist
 How do I manage a patient with intractable daytime wetting: Dr Jonathan Evans Paediatric Nephrologist Of 107 children aged 11-12 with day-wetting 91 (85%) were dry at 15-16 yr Swithinbank et al BJU 1998
How do I manage a patient with intractable daytime wetting: Dr Jonathan Evans Paediatric Nephrologist Of 107 children aged 11-12 with day-wetting 91 (85%) were dry at 15-16 yr Swithinbank et al BJU 1998
김준철 가톨릭대학교의과대학비뇨기과학교실
 비뇨기계자율신경병증의치료 김준철 가톨릭대학교의과대학비뇨기과학교실 Introduction Urologic complications have increasingly become a concern in those affected by DM Genitourinary problems are included among these complications, related
비뇨기계자율신경병증의치료 김준철 가톨릭대학교의과대학비뇨기과학교실 Introduction Urologic complications have increasingly become a concern in those affected by DM Genitourinary problems are included among these complications, related
Development of mathematical model for lower urinary tract dysfunctions
 Development of mathematical model for lower urinary tract dysfunctions Mohanad A.Deaf 1, Mohamed A.A.Eldosoky 1, Ahmed M. El-Garhy 2, Hesham W.Gomma 2, Ahmed S.El-Azab 3 Dept. of Biomedical Engineering,
Development of mathematical model for lower urinary tract dysfunctions Mohanad A.Deaf 1, Mohamed A.A.Eldosoky 1, Ahmed M. El-Garhy 2, Hesham W.Gomma 2, Ahmed S.El-Azab 3 Dept. of Biomedical Engineering,
URINARY INCONTINENCE. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
Chapter 14 The Autonomic Nervous System Chapter Outline
 Chapter 14 The Autonomic Nervous System Chapter Outline Module 14.1 Overview of the Autonomic Nervous System (Figures 14.1 14.3) A. The autonomic nervous system (ANS) is the involuntary arm of the peripheral
Chapter 14 The Autonomic Nervous System Chapter Outline Module 14.1 Overview of the Autonomic Nervous System (Figures 14.1 14.3) A. The autonomic nervous system (ANS) is the involuntary arm of the peripheral
Contribution of the External Urethral Sphincter to Urinary Void Size in Unanesthetized Unrestrained Rats
 Neurourology and Urodynamics 35:696 702 (2016) Contribution of the External Urethral Sphincter to Urinary Void Size in Unanesthetized Unrestrained Rats Brandon K. LaPallo, 1 Jonathan R. Wolpaw, 1,2 * Xiang
Neurourology and Urodynamics 35:696 702 (2016) Contribution of the External Urethral Sphincter to Urinary Void Size in Unanesthetized Unrestrained Rats Brandon K. LaPallo, 1 Jonathan R. Wolpaw, 1,2 * Xiang
INTERNATIONAL SPINAL CORD INJURY DATA SETS URINARY TRACT IMAGING BASIC DATA SET - COMMENTS
 1 INTERNATIONAL SPINAL CORD INJURY DATA SETS URINARY TRACT IMAGING BASIC DATA SET - COMMENTS The working-group consists of: Fin Biering-Sørensen representing the Executive Committee of The International
1 INTERNATIONAL SPINAL CORD INJURY DATA SETS URINARY TRACT IMAGING BASIC DATA SET - COMMENTS The working-group consists of: Fin Biering-Sørensen representing the Executive Committee of The International
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
URINARY SYSTEM. Urinary System
 URINARY SYSTEM Urinary System Kidney Functions Excretion Regulation of blood volume and pressure Regulation of electrolyte and ph levels Kidney Structure Gross Anatomy Fibrous Capsule Renal Cortex Renal
URINARY SYSTEM Urinary System Kidney Functions Excretion Regulation of blood volume and pressure Regulation of electrolyte and ph levels Kidney Structure Gross Anatomy Fibrous Capsule Renal Cortex Renal
Original Article. J Fac Med Baghdad 119. Nibbras I. AL-Hamdani* Ali W. Zeki*** Introduction:
 Original Article The Efficacy of Solifenacin Added to Α-Adrenergic Antagonists in the Treatment of Lower Urinary Tract Symptoms in Males with Benign Prostate Hyperplasia (The Iraqi Experience) Nibbras
Original Article The Efficacy of Solifenacin Added to Α-Adrenergic Antagonists in the Treatment of Lower Urinary Tract Symptoms in Males with Benign Prostate Hyperplasia (The Iraqi Experience) Nibbras
The new International Continence Society
 ROLE OF CYSTOMETRY IN EVALUATING PATIENTS WITH OVERACTIVE BLADDER ADAM J. FLISSER AND JERRY G. BLAIVAS ABSTRACT Overactive bladder (OAB) can be caused by a variety of conditions. We believe that cystometrography
ROLE OF CYSTOMETRY IN EVALUATING PATIENTS WITH OVERACTIVE BLADDER ADAM J. FLISSER AND JERRY G. BLAIVAS ABSTRACT Overactive bladder (OAB) can be caused by a variety of conditions. We believe that cystometrography
Bristol Urological Institute, Bristol, UK. The Warrell Unit, St Mary s Hospital, Manchester. UK.
 Disclosures Basic Principles of Urodynamics Andrew Gammie Bristol Urological Institute, Bristol, UK Albyn, Andromeda, Laborie, Mediwatch, MMS Project sponsorship T-Doc LLC Trial sponsorship with grateful
Disclosures Basic Principles of Urodynamics Andrew Gammie Bristol Urological Institute, Bristol, UK Albyn, Andromeda, Laborie, Mediwatch, MMS Project sponsorship T-Doc LLC Trial sponsorship with grateful
Comparison of Symptom Severity and Treatment Response in Patients with Incontinent and Continent Overactive Bladder
 European Urology European Urology 48 (2005) 110 115 Female UrologyöIncontinence Comparison of Symptom Severity and Treatment Response in Patients with Incontinent and Continent Overactive Bladder Martin
European Urology European Urology 48 (2005) 110 115 Female UrologyöIncontinence Comparison of Symptom Severity and Treatment Response in Patients with Incontinent and Continent Overactive Bladder Martin
New Treatment Modalities for Benign Prostatic Hyperplasia. Seung-June Oh, MD Department of Urology, Seoul National University Hospital
 New Treatment Modalities for Benign Prostatic Hyperplasia Seung-June Oh, MD Department of Urology, Seoul National University Hospital Options for Treating BPH Pharmacotherapy blocker Agents for BPH + OAB
New Treatment Modalities for Benign Prostatic Hyperplasia Seung-June Oh, MD Department of Urology, Seoul National University Hospital Options for Treating BPH Pharmacotherapy blocker Agents for BPH + OAB
Urinary Incontinence for the Primary Care Provider
 Urinary Incontinence for the Primary Care Provider Diana J Scott FNP-BC https://youtu.be/gmzaue1ojn4 1 Assessment of Urinary Incontinence Urge Stress Mixed Other overflow, postural, continuous, insensible,
Urinary Incontinence for the Primary Care Provider Diana J Scott FNP-BC https://youtu.be/gmzaue1ojn4 1 Assessment of Urinary Incontinence Urge Stress Mixed Other overflow, postural, continuous, insensible,
2/9/2008. Men Women. Prevalence of OAB. Men: 16.0% Women: 16.9% Prevalence (%) < Age (years)
 Definition Botox for Overactive Bladder Donna Y. Deng Assistant Professor UCSF Department of Urology Urinary urgency With or without urge incontinence Usually with frequency & nocturia International Continence
Definition Botox for Overactive Bladder Donna Y. Deng Assistant Professor UCSF Department of Urology Urinary urgency With or without urge incontinence Usually with frequency & nocturia International Continence
Ganglionic Blockers. Ganglion- blocking agents competitively block the action of
 Ganglionic Blockers Ganglion- blocking agents competitively block the action of acetylcholine and similar agonists at nicotinic (Nn) receptors of both parasympathetic and sympathetic autonomic ganglia.
Ganglionic Blockers Ganglion- blocking agents competitively block the action of acetylcholine and similar agonists at nicotinic (Nn) receptors of both parasympathetic and sympathetic autonomic ganglia.
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Yuan et al., Afr J Tradit Complement Altern Med. (2014) 11(4):
 IZALPININ FROM FRUITS OF ALPINIA OXYPHYLLA WITH ANTAGONISTIC ACTIVITY AGAINST THE RAT BLADDER CONTRACTILITY 120 Yuan Yuan 1,5#, Yin-Feng Tan 2,3,4#, Peng Xu 2,3,4, Hailong Li 2,3,4, Yong-Hui Li 2,3,4,
IZALPININ FROM FRUITS OF ALPINIA OXYPHYLLA WITH ANTAGONISTIC ACTIVITY AGAINST THE RAT BLADDER CONTRACTILITY 120 Yuan Yuan 1,5#, Yin-Feng Tan 2,3,4#, Peng Xu 2,3,4, Hailong Li 2,3,4, Yong-Hui Li 2,3,4,
Efficacy of Silodosin for Relieving Benign Prostatic Obstruction: Prospective Pressure Flow Study
 Efficacy of Silodosin for Relieving Benign Prostatic Obstruction: Prospective Pressure Flow Study Yoshihisa Matsukawa,* Momokazu Gotoh, Tomonori Komatsu, Yasuhito Funahashi, Naoto Sassa and Ryohei Hattori
Efficacy of Silodosin for Relieving Benign Prostatic Obstruction: Prospective Pressure Flow Study Yoshihisa Matsukawa,* Momokazu Gotoh, Tomonori Komatsu, Yasuhito Funahashi, Naoto Sassa and Ryohei Hattori
Comparative Influence of Imidafenacin and Oxybutynin on Voiding Function in Rats with Functional Urethral Obstruction
 306 Original Article Comparative Influence of Imidafenacin and Oxybutynin on Voiding Function in Rats with Functional Urethral Obstruction Authors Affiliation A. Fukata, T. Yamazaki Watarase Research Center,
306 Original Article Comparative Influence of Imidafenacin and Oxybutynin on Voiding Function in Rats with Functional Urethral Obstruction Authors Affiliation A. Fukata, T. Yamazaki Watarase Research Center,
Botulinum Toxin: Applications in Urology
 Botulinum Toxin: Applications in Urology Dr. Lee Jonat, PGY-4 Department of Urologic Sciences University of British Columbia Outline Mechanism of Action Technical Considerations Adverse Events Neurogenic
Botulinum Toxin: Applications in Urology Dr. Lee Jonat, PGY-4 Department of Urologic Sciences University of British Columbia Outline Mechanism of Action Technical Considerations Adverse Events Neurogenic
Mechanisms of Disease: central nervous system involvement in overactive bladder syndrome
 Mechanisms of Disease: central nervous system involvement in overactive bladder syndrome Karl-Erik Andersson SUMMARY The pathophysiology of overactive bladder syndrome (OABS) and detrusor overactivity
Mechanisms of Disease: central nervous system involvement in overactive bladder syndrome Karl-Erik Andersson SUMMARY The pathophysiology of overactive bladder syndrome (OABS) and detrusor overactivity
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Dysfunctional voiding
 Dysfunctional voiding The importance of assessment, diagnosis and treatment of dysfunctional voiding and its role in recurrent UTI Dr Dean Wallace Consultant Paediatric Nephrologist RMCH Objectives Development
Dysfunctional voiding The importance of assessment, diagnosis and treatment of dysfunctional voiding and its role in recurrent UTI Dr Dean Wallace Consultant Paediatric Nephrologist RMCH Objectives Development
Management of OAB. Lynsey McHugh. Consultant Urological Surgeon. Lancashire Teaching Hospitals
 Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Journal of Pharmacological Sciences
 Journal of Pharmacological Sciences 128 (2015) 65e70 HOSTED BY Contents lists available at ScienceDirect Journal of Pharmacological Sciences journal homepage: www.elsevier.com/locate/jphs Full paper The
Journal of Pharmacological Sciences 128 (2015) 65e70 HOSTED BY Contents lists available at ScienceDirect Journal of Pharmacological Sciences journal homepage: www.elsevier.com/locate/jphs Full paper The
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH
 MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline
 Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Definitions of IC: U.S. perspective. Edward Stanford MD MS FACOG FACS Western Colorado
 Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Long-term persistence with mirabegron in a real-world clinical setting
 International Journal of Urology (2018) 25, 501--506 doi: 10.1111/iju.13558 Original Article: Clinical Investigation Long-term persistence with in a real-world clinical setting Naoki Wada, Masaki Watanabe,
International Journal of Urology (2018) 25, 501--506 doi: 10.1111/iju.13558 Original Article: Clinical Investigation Long-term persistence with in a real-world clinical setting Naoki Wada, Masaki Watanabe,
Autonomic Nervous System. Part of the nervous system that controls most of the visceral functions of the body ( Automatically?
 Autonomic Response? Autonomic Nervous System Part of the nervous system that controls most of the visceral functions of the body ------ ( Automatically?) Classification Of CNS Autonomic Nervous System
Autonomic Response? Autonomic Nervous System Part of the nervous system that controls most of the visceral functions of the body ------ ( Automatically?) Classification Of CNS Autonomic Nervous System
Video-urodynamics. P J R Shah Institute of Urology and UCH
 Video-urodynamics P J R Shah Institute of Urology and UCH Bladder Function Storage Capacity and Pressure Emptying Pressure/flow/emptying URODYNAMIC INVESTIGATIONS Free urine flow rate Urethral pressure
Video-urodynamics P J R Shah Institute of Urology and UCH Bladder Function Storage Capacity and Pressure Emptying Pressure/flow/emptying URODYNAMIC INVESTIGATIONS Free urine flow rate Urethral pressure
