Rethinking Recommendations for Use of Pneumococcal Vaccines in Adults
|
|
|
- Shawn Holt
- 6 years ago
- Views:
Transcription
1 VACCINES Bruce Gellin and John F. Modlin, Section Editors INVITED ARTICLE Rethinking Recommendations for Use of Pneumococcal Vaccines in Adults Cynthia G. Whitney, 1 William Schaffner, 2 and Jay C. Butler 3 1 Respiratory Diseases Branch, Division of Bacterial and Mycotic Diseases, National Center for Infectious Diseases, Centers for Disease Control and Prevention, Atlanta; 2 Department of Preventive Medicine, Vanderbilt University School of Medicine, Nashville, Tennessee; and 3 Arctic Investigations Program, National Center for Infectious Diseases, Centers for Disease Control and Prevention, Anchorage, Alaska Streptococcus pneumoniae remains a major cause of disease worldwide; the emergence of antibiotic-resistant strains emphasizes the importance of disease prevention by use of vaccines. Recent studies have provided information that is useful for the evaluation of current vaccine recommendations. Recommendations target most people who are at high risk for invasive pneumococcal disease. However, higher risk has also been identified for African Americans and smokers, but these groups are not specifically targeted by current recommendations. The vaccine is effective against invasive disease in immunocompetent people, although studies in immunocompromised subjects have found few subgroups in which the vaccine appears to be effective. Questions with regard to optimal timing and indications for revaccination remain a challenge, because the duration of protection and effectiveness of revaccination remain unknown. New pneumococcal vaccines appear promising but will need to be tested against the performance of the polysaccharide vaccine. Improving delivery of the currently available pneumococcal polysaccharide vaccine to adults who will benefit should be a high priority. Pneumococcus remains a major cause of morbidity and mortality worldwide in spite of the availability of vaccines. Although young children have the highest rates of pneumococcal disease, elderly persons and adults with certain chronic illnesses are also at high risk for invasive pneumococcal disease, and in industrialized countries, they are much more likely to die of pneumococcal disease than are children [1]. In spite of appropriate therapy, case-fatality rates for bacteremic pneumococcal pneumonia have a range of 7% 35% [2]. Pneumococci that are resistant to penicillin and to multiple agents are becoming increasingly common among patients in all age groups [3], which makes pneumococcal infections more difficult to treat. The emergence of antibiotic-resistant pneumococci has placed renewed emphasis on the importance of disease prevention. Pneumococcal vaccines were used as early as 1911 [4]. The first pneumococcal polysaccharide vaccines to be licensed in the United States, 2 different 6-valent formulations, were available shortly after World War II, but interest was very low in Received 28 December 2000; revised 9 March 2001; electronically published 30 July Reprints or correspondence: Dr. Cynthia G. Whitney, Centers for Disease Control and Prevention Mailstop C23, 1600 Clifton Rd. NE, Atlanta, GA (cgw3@cdc.gov). Clinical Infectious Diseases 2001; 33: by the Infectious Diseases Society of America. All rights reserved /2001/ $03.00 these vaccines and both were withdrawn from the market [5]. A 14-valent formulation was licensed in 1977, and in 1983, this vaccine was replaced by the 2 currently available 23-valent pneumococcal polysaccharide vaccines (Pneumovax 23, Merck; and Pnu-Immune 23, Wyeth-Ayerst Laboratories). Although pneumococcal polysaccharide vaccines are no longer new, new information has become available in the past few years regarding people who are at risk for pneumococcal infections and the performance of the polysaccharide vaccines in a variety of populations. Periodic review of new information is critical to ensure that vaccines are used in the best possible manner. We summarize the recent literature related to pneumococcal vaccines for adults and factors that should be considered for recommendations to prevent invasive pneumococcal disease and pneumococcal pneumonia in adults. CURRENT RECOMMENDATIONS FOR USE OF PNEUMOCOCCAL VACCINES IN ADULTS Pneumococcal polysaccharide vaccines are recommended for use in adults in many countries. In the United States, use of pneumococcal polysaccharide vaccines is recommended by several governmental and professional groups, including the Centers for Disease Control and Prevention s (CDC s) Advisory 662 CID 2001:33 (1 September) VACCINES
2 Committee on Immunization Practices (ACIP), the US Preventive Services Task Force, the American College of Physicians, the Infectious Diseases Society of America, the American College of Preventive Medicine, and the American Academy of Family Physicians [1, 6 11]. Although there are some minor differences in the recommendations, all these groups recommend vaccination for all adults aged 65 years and for selected people aged!65 years. According to the 1997 ACIP statement [1], people aged 2 64 years who have chronic illnesses that place them at moderate to high risk for pneumococcal disease or complications of pneumococcal disease should receive pneumococcal polysaccharide vaccine. These people include those with chronic cardiovascular disease (e.g., congestive heart failure or cardiomyopathies), chronic pulmonary disease (e.g., chronic obstructive pulmonary disease or emphysema, but not asthma), diabetes mellitus, alcoholism, chronic liver disease (e.g., cirrhosis), CSF leaks, or functional or anatomic asplenia. In addition, people who live in settings that may place them at higher risk for invasive pneumococcal disease or its complications (e.g., certain Alaska Native or American Indian populations or residents of long-term care facilities) should receive vaccine. The ACIP also recommends pneumococcal polysaccharide vaccine for immunocompromised people, which it defines as those with HIV infection or AIDS, hematologic or other generalized malignancy, chronic renal failure, and nephrotic syndrome, as well as those taking immunosuppressive therapy, including corticosteroids, and those who have undergone organ or bone marrow transplantation. The ACIP does not recommend routine revaccination. A second dose of vaccine is recommended 5 years after the first dose for persons with asplenia or for immunocompromised persons. In addition, persons 65 years who were vaccinated before age 65 years may be revaccinated a single time if at least 5 years have passed since their previous dose. The ACIP does not recommended multiple revaccinations because of insufficient data on the duration of protection and the safety of pneumococcal polysaccharide vaccines when administered 3 times. However, the committee states that the vaccine should be given to people with an indication who are unsure if they have previously received the vaccine. In their statement on the use of pneumococcal polysaccharide vaccine [1], the ACIP gave a value to the strength of their recommendations for various groups. The ACIP gave stronger recommendations for use of vaccine for elderly persons, persons with chronic conditions, and persons with asplenia, stating that there was moderate to strong epidemiologic evidence supporting the use of the vaccine in these groups at the time the recommendations were made. The ACIP s recommendations were less strong for vaccination of immunocompromised people, for persons involved in high-risk social situations, and for all revaccination recommendations, stating that there was limited or no evidence of vaccine effectiveness in these groups, but that the high risk of disease, potential benefits, and safety of the vaccine supported its use. Recommendations for pneumococcal polysaccharide vaccine issued in the 1996 report by the US Preventive Services Task Force [6] are similar to the ACIP statement with regard to both the groups for whom the vaccine is recommended and in the strength of the recommendations made. In contrast to the ACIP recommendations, the task force recommends vaccination of all institutionalized people aged 50 years. The task force, like the ACIP, does not recommend routine revaccination but rather states that revaccination may be appropriate for immunocompetent people at the highest risk for morbidity and mortality (e.g., people aged 75 years or with severe chronic disease) or for immunocompromised people. GROUPS AT RISK FOR PNEUMOCOCCAL DISEASE Young children and elderly persons. The risk of invasive pneumococcal disease is highest in young children, is low in older children and young adults who are immunocompetent, and increases with age (figure 1). According to provisional surveillance data from CDC s Active Bacterial Core surveillance [ABCs, 12], part of the Emerging Infections Program Network, annual incidence of invasive pneumococcal disease in 1999 was 7 cases per 100,000 population in adults aged years, 19 per 100,000 population in people aged years, 24 per 100,000 population in people aged years, and 61 per 100,000 population in people aged 65 years [12]. The measured incidence of invasive disease has varied markedly over time and between populations; a review of published studies performed among people aged 65 years found rates between Figure 1. Incidence of invasive pneumococcal disease in adults, by race and age group, From the Centers for Disease Control and Prevention s Active Bacterial Core Surveillance, unpublished data. VACCINES CID 2001:33 (1 September) 663
3 27 (Finland, ) and 83 (Ohio, ) per 100,000 population [13]. The likelihood of dying of an invasive pneumococcal disease also increases with age. Among adults with invasive pneumococcal disease, 7% of people aged years die of their illness, compared with 21% of those aged 65 years; people aged 65 years account for one-third of cases but over half of deaths from invasive pneumococcal disease [12]. Because the risk of disease and death increases with age, recommendations for vaccination should attempt to provide optimal protection for older adults. Certain ethnic groups. There are marked differences in risk for some racial/ethnic groups. The rate of invasive pneumococcal disease in African-American persons aged years exceeds that for white persons aged 65 years (figure 1), and African Americans at all ages have at least twice the risk of invasive pneumococcal disease as white persons in the United States [12, 14 17]. The higher disease incidence means that African-American adults are more likely to die of pneumococcal disease than whites, although case-fatality ratios for the 2 groups do not differ [17]. Rates of invasive pneumococcal infection are also higher among Alaska Natives [18] and certain other American Indian groups [19]. The reasons for these differences in risk of invasive disease are not well defined. Differences in the prevalence of chronic diseases, such as HIV infection, AIDS, or diabetes, may contribute to the differences in risk between racial and ethnic groups [18, 20]. However, studies that controlled for underlying diseases have still found higher risk of infection for African American persons than for persons of white race [20, 21]. Low socioeconomic status has also been suggested as an explanation for some of the racial and ethnic disparity, and recent studies have identified both poverty and African-American ethnicity as independent risk factors for invasive pneumococcal disease [14, 21, 22]. Although ACIP recommends that Alaska Natives and American Indians of all ages should receive pneumococcal polysaccharide vaccine because of high risk for invasive infection, current recommendations do not include African-American adults aged!65 years without underlying illnesses. The ACIP s new recommendations for use of pneumococcal conjugate vaccine in young children may be the first set of recommendations to suggest that clinicians should offer a vaccine to African Americans on the basis of the higher risk of disease in that race group [23]. Immunocompromised people and people with chronic illnesses. Immunocompromised people and people with certain chronic illness are at increased risk for invasive pneumococcal disease or for severe sequelae from their infections. People with chronic diseases that are ACIP indications for vaccine are twice as likely as others to die if they develop invasive pneumococcal disease [17]. The emergence of HIV and the subsequent development of highly active antiretroviral therapy (HAART) have had notable effects on the epidemiology of invasive pneumococcal disease in young adults. In a study from San Francisco that reviewed cases of invasive pneumococcal disease that occurred during , the rate of invasive pneumococcal disease in people with AIDS was 46 times higher than was the rate among people without known HIV infection [24]. In this population, a significant decrease in disease rates was noted among people with HIV or AIDS during this time period, possibly due to the increasing use of HAART. In some communities in the United States, HIV or AIDS is the most common underlying illness to be found in people who are years old and who have invasive pneumococcal disease [17, 20, 24]. Smokers. Smoking is not currently an indication for pneumococcal polysaccharide vaccine, but smoking has recently been identified as another major risk factor for invasive pneumococcal disease in adults. In population-based surveillance in Texas, smokers who were years old had 2.6 times the risk for invasive pneumococcal disease as nonsmokers who were the same age, and 31% of disease in the patients in this age group was attributable to smoking [14]. In a recent risk-factor study of immunocompetent adults aged years, 51% of disease in this population was attributed to smoking, and smoking conferred a greater risk of invasive pneumococcal disease than that of any other characteristic studied [21]. When researchers adjusted for other factors, people with invasive pneumococcal infection were 4.1 times more likely to be cigarette smokers than was the control group. The association increased with the number of cigarettes smoked and the number of years that the patient had smoked, indicating a dose-response relationship. Among current nonsmokers, case patients were more likely than were controls to be former smokers who had quit!10 years earlier or to be exposed to passive (secondhand) cigarette smoke. Residents of long-term care facilities. Pneumococcal disease is a major problem in long-term care facilities, and current vaccine recommendations suggest that institutionalized adults should receive polysaccharide vaccine. Not only are long-term care facility residents at high risk for sporadic pneumococcal disease as a result of their advanced age or the presence of chronic illnesses, but long-term care facilities also provide an optimal setting for pneumococcal outbreaks. Several outbreaks of infection have recently been reported, including one in which the outbreak strain was multidrug resistant [25 28]. Low vaccine coverage may facilitate institutional outbreaks of pneumococcal disease; at the time of these reported outbreaks,!10% of residents in the facilities had received pneumococcal polysaccharide vaccine. Outbreaks of pneumococcal disease are rare outside of institutional settings. The current ACIP recommendations account for most adults 664 CID 2001:33 (1 September) VACCINES
4 at high risk for invasive pneumococcal disease. According to CDC estimates, approximately one-third of all invasive pneumococcal cases occur in people aged 65 years and 38% occur in adults aged years (figure 2; ABCs, unpublished data). Among adults aged years, approximately two-thirds of cases occur in people who have a chronic medical condition that is an ACIP indication for pneumococcal polysaccharide vaccine [14, 20, 29]. Overall, 9000 cases (20%) of invasive pneumococcal disease in adults occur in people who do not currently have an indication for pneumococcal polysaccharide vaccine. Expanding the recommendations to include either all smokers, all African American persons, or all people aged 50 years may reduce the number of cases that occur in people without a vaccine indication to cases (table 1). VACCINATION WITH PNEUMOCOCCAL POLYSACCHARIDE VACCINE The currently available pneumococcal polysaccharide vaccines are designed to provide serotype-specific protection and include 25 mg of purified capsular polysaccharide antigens from each of 23 different serotypes. More than 90 pneumococcal serotypes and 140 serogroups, distinguishable by the structure of the polysaccharide capsule, have been identified as causing disease. A recent review of data from around the world found regional differences in distribution of serogroups, but 11 serogroups accounted for at least 75% of the isolates that caused invasive disease in adults in each geographic region [31]. In the United States, serotypes included in the 23-valent vaccine account for at least 85% 90% of strains that cause invasive disease in adults [1]. Vaccine antigens targeted against some serotypes may provide cross-protection against other serotypes in the same group [32]. Although recent studies that used molecular subtyping techniques have demonstrated that pneumococci have the ability to change their capsule type [33, 34], all capsular switching described to date has been between serotypes contained in the pneumococcal polysaccharide vaccine. Immunogenicity. Pneumococcal capsular polysaccharide vaccines provide protection by inducing serotype-specific antibodies that enhance opsonization, complement-dependent phagocytosis, and killing of pneumococci by leukocytes and other phagocytic cells. Concentrations of antibodies to pneumococcal polysaccharides increase within 1 week after vaccination and, for most vaccine antigens, remain greater than prevaccination levels for 15 years in healthy adults [35, 36]. In some people at increased risk of pneumococcal disease, such as elderly persons and those with certain underlying illnesses, immune responses to pneumococcal polysaccharides may be limited and antibody concentrations may decrease more rapidly after vaccination, compared with healthy adults [37 46]. However, the clinical relevance of antibody concentrations measured Figure 2. Projected number of invasive pneumococcal disease cases in the United States, by age group and vaccine indication, ACIP, Advisory Committee on Immunization Practices. From the Centers for Disease Control and Prevention s Active Bacterial Core Surveillance, unpublished data; Harrison et al. [20]; Bennett et al. [29]; and Pastor et al. [14]. after vaccination is difficult to determine because the quantity of antibodies that correlate with protection against pneumococcal disease has not been clearly defined. Measurements of antibody concentration do not take into consideration the functional activity of the antibody produced. Laboratory methods that assess the functional immune responses to vaccination, such as opsonophagocytic activity and antibody avidity for pneumococcal antigens, may prove to be a better way to predict protection and be more clinically relevant than are quantitative antibody measurements [47, 48]. Although substantial antibody responses may occur even among people aged 85 years, effectiveness may be reduced in very elderly persons because of functional differences in antibodies produced by people in this age group compared with younger vaccinees [49]. Immune responses are often not consistent among all 23 serotypes in the vaccine, and the magnitude of responses among vaccinees varies widely [50]. Genetic factors may play an important role in the response to polysaccharide antigens and could account for some of this variability [51]. Safety. On the basis of a quarter century of clinical experience, pneumococcal polysaccharide vaccines are considered safe [1]. Severe adverse effects (e.g., anaphylactic reactions) are rarely reported, and neurologic disorders (e.g., Guillain-Barré syndrome) have not been associated with administration of pneumococcal vaccine [52]. In a meta-analysis of 9 randomized controlled trials of pneumococcal vaccine efficacy, mild local reactions (e.g., pain at the injection site, erythema, and swelling) were observed among approximately one-third or fewer of patients who received the vaccine, and there were no reports of severe febrile or anaphylactic reactions [53]. In a prospective study of people aged years, large localized reaction (red- VACCINES CID 2001:33 (1 September) 665
5 Table 1. Number of cases of invasive pneumococcal disease (IPD) in the United States in persons with a vaccine indication, by various vaccination strategies. Age group, years Annual cases of IPD Based on current ACIP recommendations b No. of cases in persons with vaccine indication, by strategy a Current ACIP plus all smokers c Current ACIP plus all African Americans Current ACIP plus all people aged 50 years ,500 10,100 13,100 12,600 10, ,100 21,100 21,100 21,100 21,100 Total 45,800 37,200 42,000 40,600 40,400 NOTE. ACIP, Advisory Committee on Immunization Practices. a Estimates were made using 1998 postcensus population estimates and 1999 data from Active Bacterial Core Surveillance. b From [1]. The proportion of cases with an ACIP indication was assumed to be 100% for persons aged 65 years and 65% for persons aged years [14, 20, 29]. c Estimate based on smokers having 4.1 times the risk of invasive pneumococcal disease as nonsmokers [21] and a prevalence of smoking of 22.9% [30]. ness or swelling extending 4 inches [10.2 cm] around the injection site) were reported by 3% of vaccinees after the first dose of pneumococcal vaccine [54]. However, even these large localized reactions did not interfere with the activities of daily life and were self-limited. The mean interval from vaccination to complete resolution of symptoms was 3.6 days. Swelling, pain, and redness at the injection site have been associated with the higher prevaccination concentrations of anticapsular antibodies, indicating a localized Arthus-type reaction (type III hypersensitivity reaction) caused by formation of antibody-antigen complexes at the injection site [44, 54]. Intradermal administration may cause severe local reactions and is inappropriate [1]. Pneumococcal vaccine may cause transient increases in HIV replication [55, 56], but these studies were performed before the use of HAART became commonplace, so the clinical significance of this occurrence is unknown. This phenomenon has also been observed in HIV-infected people after they have been immunized with other vaccines [57] and during episodes of acute bacterial pneumonia [58]. One study, a randomized trial of 23-valent pneumococcal polysaccharide vaccine among HIVinfected adults in Uganda [59], found that the rates of all-cause pneumonia among people who were receiving pneumococcal vaccine were higher than they were among those who were given placebo. However, overall mortality during the followup period was the same (28%) in vaccine and placebo recipients. It is unclear whether these findings can be generalized outside of sub-saharan Africa. Studies evaluating safety and efficacy of pneumococcal vaccines in HIV-infected people in the United States who are being treated with HAART are in progress. Pneumococcal vaccines do not appear to alter the course of chronic, noninfectious diseases. Among 40 people with systemic lupus erythematosus randomized to receive pneumococcal polysaccharide vaccine or placebo, no changes in lupus activity were observed during follow-up [60]. The safety of pneumococcal polysaccharide vaccine during early pregnancy has not been evaluated in prospective studies, but no adverse consequences have been reported among newborns whose mothers were inadvertently vaccinated during pregnancy. Clinical impact. Prelicensure randomized, controlled trials of a single dose of pneumococcal polysaccharide vaccine were conducted in the 1970s among young, healthy South African gold miners, a group with high rates of pneumococcal pneumonia. Protective efficacy against pneumococcal pneumonia in these trials had a range of 76% 92% [61, 62]. In non-epidemic situations in industrialized countries, most pneumococcal disease in adults occurs in elderly persons or in people with chronic medical conditions. Pneumococcal polysaccharide vaccine efficacy has not consistently been proven in randomized, double-blind, controlled trials among elderly persons. Results of 1 randomized clinical trial suggested that the vaccine provided some protection against pneumococcal pneumonia among high-risk elderly people [63], whereas 2 other trials did not demonstrate efficacy against pneumonia or bronchitis in patients without bacteremia [64, 65]. The inability of these studies to document vaccine efficacy partly results from a lack of specific and sensitive diagnostic tests for nonbacteremic pneumococcal pneumonia. The diagnosis of pneumococcal pneumonia in the majority of patients in 2 of the trials [63, 65] was based on detection of rising antibodies to pneumolysin or pneumolysin immune complexes in patient serum. Subsequent work by Musher et al. [66] indicates that the latter assay, which was the basis for most of the diagnoses of pneumococcal pneumonia, is not specific. A nonspecific case definition of pneumococcal pneumonia would bias the findings of a trial to the null. In addition, these studies lacked statistical power to assess efficacy against bacteremia or meningitis. In the trial conducted by Örtqvist et al. [65] in Sweden, for example, the point estimate for vaccine efficacy against bacteremia was 79% ( P p.22; Fisher s exact test), but the power to detect a statistically significant difference in rates of invasive disease in vaccine and placebo recipients was only 5%. An additional trial among people aged 65 years in northern Finland who received influenza vaccination either alone or 666 CID 2001:33 (1 September) VACCINES
6 in combination with 23-valent pneumococcal polysaccharide vaccine showed that use of both vaccines had no advantage over use of influenza vaccine alone for prevention of pneumococcal pneumonia [67]. However, the diagnosis of pneumococcal pneumonia was also based primarily on pneumolysin serological testing in this study. Moreover, only 2 of the 7 cases of pneumococcal bacteremia occurred in people who received pneumococcal vaccine; therefore, the point estimate for protection against invasive disease was 60% (95% CI, 40 to 90) [67]. Two open trials have suggested protection against pneumococcal pneumonia among elderly residents of long-term care facilities [68, 69]. Although randomized, double-blind, controlled trials provide the greatest scientific rigor for evaluating pneumococcal vaccines, epidemiological studies, such as case-control and serotype distribution (indirect cohort) studies, offer a number of advantages. They permit rapid gathering of data with better statistical power to adequately evaluate vaccine effectiveness [70]. Moreover, ethical concerns about withholding a vaccine from control subjects make postlicensure randomized trials among people at highest risk of disease impractical. Finally, randomized trials evaluate vaccine performance under optimal conditions, whereas epidemiological studies provide a more pragmatic perspective by assessing the impact of a vaccine under ordinary conditions of clinical practice [71]. Postlicensure epidemiological studies have documented the effectiveness of pneumococcal polysaccharide vaccines for prevention of invasive infection (bacteremia and meningitis) among elderly persons and younger adults with certain chronic medical conditions [72 75]. Only 1 case-control study failed to demonstrate effectiveness against bacteremic disease [76] possibly because of study limitations, such as small sample size and incomplete ascertainment of vaccination status of patients. The overall rate of effectiveness against invasive pneumococcal disease among immunocompetent people aged 65 years is 75% [72]; however, efficacy may decrease with advancing age [74]. An indirect cohort analysis of CDC surveillance data indicates that polysaccharide vaccine is effective for the prevention of bacteremia and meningitis among people at increased risk for infection due to certain medical conditions, including diabetes mellitus, chronic heart and lung diseases, and anatomic asplenia (table 2) [72]. Although immunogenicity of polysaccharide vaccines is limited for persons with some immunocompromising conditions, it should be noted that the wide confidence intervals for many of the conditions for which effectiveness could not be confirmed may reflect small numbers of patient with nonvaccine serotype infections rather than reflecting a lack of benefit from the vaccine. A retrospective cohort study of all people aged 65 years who were enrolled in a managed care organization and who had chronic lung disease demonstrated significantly lower rates Table 2. Vaccine effectiveness among persons with chronic underlying medical conditions, based on indirect cohort analysis of Centers for Disease Control and Prevention surveillance data. Underlying conditions Effectiveness, % a 95% CI Effectiveness confirmed Anatomic asplenia COPD or asthma b Congestive heart failure Coronary vascular disease Diabetes mellitus Effectiveness not confirmed Alcoholism or cirrhosis! to 61 Chronic renal failure to 78 Hodgkin s disease to 89 Immunoglobulin deficiency to 95 Leukemia!0 634 to 72 Multiple myeloma!0 550 to 78 Non-Hodgkin s lymphoma to 92 Sickle cell disease to 88 NOTE. COPD, chronic obstructive pulmonary disease. a Vaccine effectiveness in indirect cohort analyses is calculated by comparing the proportion of invasive disease cases caused by serotypes included in the vaccine among vaccinated and unvaccinated people. No data are available for patients with HIV infection or who take immunosuppressive therapy. Adapted from [72]. b Asthma is no longer an Advisory Committee on Immunization Practices indication for pneumococcal polysaccharide vaccine. of all-cause pneumonia hospitalization and death among vaccinated persons, compared with unvaccinated people [77]. Rates of nonpneumonia hospitalization were similar in the 2 groups. In contrast to the findings of the trial in northern Finland [67], benefits of pneumococcal and influenza vaccinations were additive [77]. In a recent prospective study of residents in 5 nursing homes in Toronto, people developing any type of lower respiratory tract infections were less likely to have received pneumococcal vaccine than were those without these illnesses; however, the association was not statistically significant after controlling for other factors that influence the risk of lower respiratory infection, such as receipt of influenza vaccine [78]. The role of pneumococcal vaccine in people infected with HIV deserves special attention given the high rate of pneumococcal infection among people with HIV [24]. A nested casecontrol study from Baltimore in the early 1990s showed that people with pneumococcal disease and CD4 cell counts of 1200 cells/mm 3 were less likely to have received pneumococcal vaccine than were control subjects without pneumococcal disease [79]. In a case-control study conducted in Atlanta and San Francisco, 23-valent pneumococcal vaccine was 49% effective (95% CI, 12% 70%) for prevention of invasive pneumococcal disease in HIV-infected people aged years; however, in multivariable analysis, effectiveness was greater for white per- VACCINES CID 2001:33 (1 September) 667
7 sons (76%; 95% CI, 35% 91%) than it was for African-American persons (24%; 95% CI, 50% to 61%) [80]. Failure to demonstrate effectiveness among African-American persons may be due to limited power because of low vaccination rates for African-Americans, immunization at a more advanced stage of AIDS progression for African-American persons, or unmeasured factors. A randomized trial of 23-valent polysaccharide vaccine among HIV-infected people in Uganda showed no evidence of efficacy [59]. It should be noted that none of these studies was conducted among people who were receiving highly active antiretroviral agents, and no published study to date has evaluated the clinical impact of pneumococcal polysaccharide vaccine for persons receiving optimal antiretroviral therapy. Cost-effectiveness. On the basis of surveillance data collected in the late 1980s and early 1990s, and of vaccine effectiveness estimates from epidemiological studies, an analysis of cost-effectiveness of pneumococcal vaccination of all people aged 65 years for prevention of bacteremia and meningitis indicated that, from a social perspective, vaccination saved $8.27 per person vaccinated [81]. The cost savings associated with pneumococcal vaccination may be greater for elderly people who are at increased risk of serious pneumococcal disease due to certain chronic medical conditions. A review of pneumonia hospitalizations and deaths among elderly people with chronic lung disease in a managed care organization indicated that cost savings were between $115 and $512 over 2 years for each person vaccinated [77]. REVACCINATION Anecdotal reports suggest that the recommendations for revaccination with pneumococcal polysaccharide vaccine are a source of confusion for clinicians. (The term revaccination is used for second or third doses of pneumococcal polysaccharide vaccine and other vaccines that do not induce immune memory. The term booster dose should be reserved for subsequent doses of vaccines that induce immune memory). The ACIP recommends a one-time revaccination for people aged 65 years if the patient was first immunized before age 65 years and at least 5 years earlier [1]; this recommendation has been misinterpreted as suggesting revaccination every 5 years. Revaccination recommendations from the ACIP and US Preventive Services Task Force [6] differ, which may add to the confusion. Both groups agree that the evidence to support recommendations for revaccination is limited, and neither group strongly recommends revaccination for any population. Because the risk of developing invasive pneumococcal disease and of dying from it increase with age, the timing and frequency of revaccination to provide optimal protection are critical issues. There are limited data regarding how long protection provided by pneumococcal polysaccharide vaccines lasts, however. Concentrations of antibodies to pneumococcal polysaccharides remain greater than prevaccination levels for 15 years in healthy adults [35, 36] but decrease more rapidly in elderly persons and in those with certain underlying illnesses [37 46]. One epidemiologic study of polysaccharide vaccine effectiveness suggested lower effectiveness 5 years after vaccination in elderly persons [74]; another found no clear difference in effectiveness in people vaccinated at least 9 years earlier compared with people vaccinated more recently [72]. Revaccination with pneumococcal polysaccharide vaccine is associated with few systemic adverse events, although a recent large study found that local side effects are more common with revaccination than with initial vaccination [54]. This study compared the frequency of side effects in 901 patients who were aged years and who had never been immunized with those in 513 patients who were the same age and who had been immunized at least 5 years earlier. Local reactions of 4 inches (10.2 cm) were more common in revaccinated people (11%) than in people receiving their first dose (3%); healthy subjects had a 5-fold risk of a large local reaction after revaccination compared with initial vaccination. The likelihood of a large local reaction correlated with prevaccination antibody concentrations. Investigators found no difference in the frequency of systemic symptoms and no serious side effects in either group. Several studies have compared the immune response of revaccinees to first-time vaccine recipients [42, 54, 82 85]. In all studies but one [42], a study that mostly included Alaska Natives with chronic illnesses, peak antibody concentrations were lower after revaccination than they were after initial vaccination. Aging of the study subjects has been suggested as an explanation for the suboptimal immune response after revaccination, but the interval between immunizations was only 1 6 years [82 85]. A similar finding of hyporesponsiveness on revaccination has been well documented in children and young adults who had received a second dose of meningococcal serogroup C polysaccharide vaccine [86 89]; the reason for this finding is unknown. There are no studies that have measured the effectiveness of second or third doses of pneumococcal polysaccharide vaccine. Because the quantity of antibodies that correlate with protection against pneumococcal disease has not been clearly defined, it is unknown if the lower antibody levels seen on revaccination correlate with inferior protection. DELIVERING PNEUMOCOCCAL VACCINE Most patients who could benefit from pneumococcal polysaccharide vaccine have not yet received it. According to the 1997 Behavior Risk Factor Surveillance System, a phone survey of noninstitutionalized adults, only 46% of adults aged 65 years 668 CID 2001:33 (1 September) VACCINES
8 reported ever having received pneumococcal vaccine [90]. Coverage levels were significantly higher in 1997 than they were in 1995, when only 37% of respondents aged 65 years reported receiving vaccine [91]. Vaccine coverage levels differ by race and ethnic group, age, and health status; coverage is significantly lower among African-American persons (30% among African-Americans aged 65 years) and Hispanic persons (34%) than it is among non-hispanic white persons (47%) [91]. Only 17% of people years old with high-risk conditions reported previous receipt of pneumococcal vaccine in another national survey conducted in 1997 [92]. Use of vaccines in institutionalized adults also is suboptimal. Estimates from the 1997 National Nursing Home Survey indicate that only 28% of people in long-term care facilities had received pneumococcal vaccines [92]. The Healthy People 2010 objectives for pneumococcal immunization call for 90% of all people aged 65 years and 65% of high-risk adults years old to receive pneumococcal vaccine [93]. The reasons why pneumococcal vaccine has not been delivered more effectively to its targeted populations are numerous and varied. They relate to adult immunization issues generally and to pneumococcal vaccine specifically. Adults often do not visit physicians regularly, and when they do, many insurance plans do not cover provision of preventive services, including vaccines. Even in instances in which insurance plans include vaccine administration, payment to the physician usually is modest, providing little incentive to aggressively pursue immunization. Although many physicians wish to provide appropriate vaccine services to their patients, information about vaccine developments and recommendations may reach them only sporadically. Although pediatricians regularly receive updates regarding the childhood immunization schedule from public health agencies, professional societies, and vaccine manufacturers, these sources of continuing education are less likely to deliver vaccine information to physicians who care for adults. This type of information may be even less likely to reach medical subspecialists, such as rheumatologists, cardiologists, or nephrologists, who provide care for a substantial proportion of adults and who frequently are the sole source of medical care for their patients, many of whom have indications for immunization. Some features of the successful childhood immunization program in the United States are not applicable to adult immunization activities. The National Immunization Program provides funding and technical assistance to state and local health departments in providing immunization services to infants and children. Furthermore, in many states, school entry laws require nearly all children to be vaccinated with certain vaccines. Neither of these mechanisms is available to assist in the vaccination of adults; however, some states recently have instituted requirements that pneumococcal vaccine be offered to all patients admitted to long-term care facilities. Electronic immunization registries for tracking childhood immunizations are underway in some states; whether registries would be useful or feasible for improving adult immunization is unknown. Several factors specific to pneumococcal vaccine have impeded its more widespread use. Whereas an examination of national morbidity data clearly defines invasive pneumococcal disease as a substantial public health problem, clinicians may perceive the issue with less concern. Rates of invasive disease in the general population are sufficiently low such that even busy practitioners may go many years without encountering a case of pneumococcal bacteremia in their practice. Therefore, practitioners may not feel compelled to protect their patients against a risk that is perceived as remote. Although protection against pneumonia is considered important, the efficacy of the vaccine in preventing pneumonia continues to be treated with skepticism in the literature [65, 94]. Concern regarding side effects with revaccination may inhibit some clinicians from vaccinating patients, especially those patients with several doctors or whose vaccination records are missing or incomplete. Nevertheless, even many patients who feel negatively about vaccines would agree to receive pneumococcal vaccine if their health care provider offered it [95]. In addition, many options are available to improve vaccine delivery. Several studies have found that the use of standing orders orders that authorize nurses or pharmacists to administer vaccines according to a preapproved protocol and without direct physician involvement at the time of the interaction may be the best means of improving vaccine delivery to adults in hospitals, clinics, and long-term care facilities [96 98]. A recent review of interventions to improve rates of vaccination concluded that there was strong evidence that standing orders are effective in improving vaccination coverage in adults [99]. Standing orders for vaccine delivery are recommended by the Task Force on Community Preventive Services [100], the ACIP [92], and by the Canadian Community Health Practice Guidelines Working Group [101]. Other recommended methods of improving vaccine coverage among adults include the use of client and provider reminders, patient education, interventions that reduce client out-ofpocket costs, and assessment and feedback of provider vaccination rates; for populations that are difficult to reach, home visits or expanded access to health care settings may be needed [100]. Financial incentives, such as increasing reimbursement for vaccination, providing reimbursement for preventive health visits, or ensuring that insurers cover adult immunizations, could improve vaccine coverage. Changing pneumococcal vaccine recommendations to include all adults aged 50 years has been suggested as a means of simplifying the vaccine indications, harmonizing the indications with the expanded recommendations for influenza vac- VACCINES CID 2001:33 (1 September) 669
9 cine, and improving coverage among high-risk people aged!65 years. Research data are limited on whether such a strategy would raise coverage rates, although experience with other vaccines suggests that age-based recommendations might be effective. One study from Finland suggested that an age-based strategy was effective, but the age-based intervention that was used also included either mailed reminders or a mass media campaign [102]. Currently, at least 61 million adults in the United States have an indication for pneumococcal polysaccharide vaccine (table 3). If recommendations for pneumococcal polysaccharide vaccine were expanded to include all adults who are African American, who smoke, or who are aged 150 years, the number of adults with a vaccine indication would increase by million, depending on the strategy. Currently, only 2 manufacturers produce pneumococcal polysaccharide vaccine in the United States. In addition to concerns regarding the timing and effectiveness of revaccination, vaccine supply will need to be considered if health care providers were to begin immunizing new groups without causing relative shortages in vaccine availability for others at high risk. Adequacy of the vaccine supply has recently been a concern with influenza vaccine [103]. In 1994, orders for pneumococcal vaccine were delayed during a shortage that lasted a few months (R. Strikas, personal communication); the shortage was resolved after manufacturers increased capacity to keep up with increases in demand that had occurred from 1993 through NEW PNEUMOCOCCAL VACCINES Pneumococcal conjugate vaccines. A recent advancement in prevention of pneumococcal disease is the development of pneumococcal conjugate vaccines. A 7-valent pneumococcal conjugate vaccine was licensed in the United States for prevention of invasive pneumococcal disease in infants and young children in early 2000 [23] and is now licensed in several other countries. By conjugating polysaccharide antigens to a carrier protein, the immunologic responses elicited become T cell dependent. Memory B cells are produced and primed for booster responses rapid and dramatic increases in antibody concentrations to subsequent immunizations with pneumococcal polysaccharide [104]. Pneumococcal conjugate vaccines appear to be safe and to induce primary and booster antibody responses in infants and young children [104, 105]. A randomized trial of 7-valent pneumococcal conjugate vaccine among 37,000 infants enrolled in a large northern California health maintenance plan documented efficacy 190% for prevention of invasive pneumococcal disease caused by the 7 serotypes included in the vaccine [106]. Several other large randomized trials assessing the efficacy of conjugate vaccines to prevent invasive infection and acute otitis media in infants are ongoing. The role of conjugate vaccines among adults with underlying medical conditions and elderly persons remains to be determined. Preliminary data from studies of healthy people aged 50 years and of patients vaccinated after treatment for Hodgkin s disease indicate that antibody responses to pneumococcal conjugate vaccines have not been substantially better than responses to the polysaccharide vaccine [107, 108]. In one study, localized reactions (pain, stiffness, and induration at the injection site) were more common among people who received the conjugate vaccine, although these symptoms were generally mild [107]. In one family, administration of pneumococcal conjugate vaccine produced IgG responses in several people who lacked the capacity to respond to polysaccharide vaccine [109]. One approach to the use of conjugate vaccines in adults is to sequentially administer conjugate vaccine and 23-valent polysaccharide vaccine; giving conjugate vaccine first could prime the immune system, and the polysaccharide vaccine could then induce a booster response to the serotypes present in both vaccines as well as induce primary T cell independent responses to the serotypes in the 23-valent vaccine only [104, 110, 111]. A potential shortcoming of conjugate vaccines is that the number of serotypes that can be included may be limited [112], and people who are vaccinated would remain susceptible to most of the serotypes not included in the vaccine. Most con- Table 3. Number of adults in the United States with vaccine indications, according to various strategies. Age group, year(s) US population, millions According to current ACIP recommendations b No. of vaccine-eligible persons, in millions a Current ACIP plus all smokers Current ACIP plus all African Americans Current ACIP plus all persons aged 50 years Total NOTE. ACIP, Advisory Committee on Immunization Practices. a Estimates were made using 1998 postcensus population estimates and results from the 1997 National Health Interview Survey. Estimates of the number of vaccine-eligible people do not include people with immunocompromising conditions. b From [1]. 670 CID 2001:33 (1 September) VACCINES
10 jugate pneumococcal vaccines under evaluation contain capsular polysaccharides of 7 to 11 serotypes. Among preschoolaged children in the United States, the 7 most common serotypes (4, 14, 6B, 19F, 18C, 23F, and 9V) account for 80% of blood and CSF isolates in the United States, but only 50% of isolates among older children and adults [17, 23, 113]. Therefore, vaccine formulations that are based on the most prevalent serotypes among children may not provide optimal serotype coverage for prevention of pneumococcal infections in adults. However, immunogenicity and effectiveness are limited for polysaccharide vaccine for several pneumococcal serotypes that commonly cause serious infection in adults. If conjugate vaccines are more immunogenic against these serotypes in adults, overall effectiveness could theoretically be greater with conjugate vaccines, despite more limited serotype coverage [114]. Possible future pneumococcal vaccines. A promising approach for prevention of pneumococcal infections is to develop vaccines directed against noncapsular antigens common to all pneumococcal serotypes. Candidate antigens include a number of pneumococcal proteins: neuraminidase, autolysin, pneumolysin, pneumococcal surface proteins A and C (PspA and PspC), pneumococcal surface adhesin A (PsaA or 37-kDa protein), and putative proteinase maturation protein A (PpmA) [ ]. These proteins could not only provide protection against all pneumococcal serotypes, but they could also induce a T cell dependent response with immunologic memory. To date, only pneumolysin, PspA, and PsaA have been extensively examined for suitability as vaccine candidates, and only PspA has been tested in humans [120]. In this trial, vaccination with PspA led to an increase in circulating antibodies, and analysis of postvaccination serum samples showed increased binding to a variety of PspA and capsule types. Intranasal immunization of mice with PspA induced mucosal and systemic antibody responses, prevented pneumococcal colonization, and provided protection against systemic infection after intravenous, intratracheal, and intraperitoneal challenge [121]. A vaccine consisting of a live recombinant Salmonella typhimurium vaccine strain expressing pneumococcal PspA colonized gut-associated lymphoid tissues, spleens, and livers of orally immunized mice, induced serum and mucosal anti-pspa antibodies, and provided protection against challenge by a mouse-virulent Streptococcus pneumoniae [122]. An innovative approach to immunization involves introduction of a DNA plasmid carrying a protein-coding gene into the vaccine recipient s own cells, which leads to expression of an antigen that elicits an immune response (so-called DNA vaccines ). Such immunizing agents could be manufactured more easily and may be more stable during storage and distribution than vaccines composed of inactivated or attenuated microorganism, subcellular fractions, or recombinant proteins. Results of preliminary work on a pneumococcal DNA vaccine in laboratory animals are promising. Immunization of mice with a plasmid expressing PspA has been shown to induce a significant immune response and provided some protection against a challenge with intravenously administered serotype 3 S. pneumoniae [123]. However, a great deal of research remains to be done to clearly demonstrate safety, immunogenicity, and efficacy of DNA vaccines in humans. CONCLUSIONS Given the substantial morbidity and mortality caused by pneumococcal disease, periodic evaluations of the appropriateness of guidelines for use of pneumococcal vaccines are important. Several recent studies have provided information that is useful for the evaluation of current vaccine recommendations. The current recommendations for use of pneumococcal polysaccharide vaccines address most adults at high risk for invasive pneumococcal disease. African-American persons and smokers have recently been noted to have higher disease rates than do white persons and nonsmokers, and the increased risk in these groups is not specifically addressed by current recommendations. Discussions of changing vaccine recommendations should include whether the expected benefit from adding new groups to the recommendations outweighs the potential problems of cost and limited vaccine supply. Vaccine coverage is suboptimal, especially in minority groups and in high-risk people aged!65 years. Simplifying vaccine recommendations might improve coverage, as would promoting adoption of standing orders in nursing homes, hospitals, and clinics. Questions of when and how often to revaccinate also are important barriers to making rational decisions about who should receive pneumococcal vaccine before the age of 65 years. Little new evidence exists to clarify these questions. We have learned that revaccination results in more local side effects, but the frequency of side effects even with revaccination is relatively low, and side effects are self-limited. Immune responses appear to be less robust after revaccination than they are after an initial dose of polysaccharide vaccine. We do not know why this occurs, or in the absence of defined immunologic correlates of protection, if a lower immune response means that protection provided by the vaccine is reduced after revaccination. Because risk of disease and death from pneumococcal infection increase with age, the timing of initial and subsequent vaccine doses may be critical. If significant hyporesponsiveness occurs after revaccination, people who receive vaccine before the age of 65 years may respond less well when given the vaccine again later in life, when the risk of serious infection is greatest. In other words, if we only have 1 opportunity to provide an effective vaccine, when should that vaccine be given? What if we have 2 opportunities? Unfortunately, we do not know how many opportunities we have, and this uncertainty inhibits our VACCINES CID 2001:33 (1 September) 671
Streptococcus pneumoniae CDC
 Streptococcus pneumoniae CDC Pneumococcal Disease Infection caused by the bacteria, Streptococcus pneumoniae» otitis media 20 million office visits (28-55% Strep)» pneumonia 175,000 cases annually» meningitis
Streptococcus pneumoniae CDC Pneumococcal Disease Infection caused by the bacteria, Streptococcus pneumoniae» otitis media 20 million office visits (28-55% Strep)» pneumonia 175,000 cases annually» meningitis
Pneumococcal Disease and Pneumococcal Vaccines
 Pneumococcal Disease and Epidemiology and Prevention of - Preventable Diseases Note to presenters: Images of vaccine-preventable diseases are available from the Immunization Action Coalition website at
Pneumococcal Disease and Epidemiology and Prevention of - Preventable Diseases Note to presenters: Images of vaccine-preventable diseases are available from the Immunization Action Coalition website at
Haemophilus influenzae
 Haemophilus influenzae type b Severe bacterial infection, particularly among infants During late 19th century believed to cause influenza Immunology and microbiology clarified in 1930s Haemophilus influenzae
Haemophilus influenzae type b Severe bacterial infection, particularly among infants During late 19th century believed to cause influenza Immunology and microbiology clarified in 1930s Haemophilus influenzae
OREGON PUBLIC HEALTH, DHS IMMUNIZATION PROTOCOL FOR PHARMACISTS. PNEUMOCOCCAL POLYSACCHARIDE VACCINE 23-Valent Vaccine
 OREGON PUBLIC HEALTH, DHS IMMUNIZATION PROTOCOL FOR PHARMACISTS PNEUMOCOCCAL POLYSACCHARIDE VACCINE 23-Valent Vaccine Revisions as of 2/24/10 Pneumovax 23 should not be given concurrently with Zostavax
OREGON PUBLIC HEALTH, DHS IMMUNIZATION PROTOCOL FOR PHARMACISTS PNEUMOCOCCAL POLYSACCHARIDE VACCINE 23-Valent Vaccine Revisions as of 2/24/10 Pneumovax 23 should not be given concurrently with Zostavax
9/12/2018. Pneumococcal Disease and Pneumococcal Vaccines. Streptococcus pneumoniae. Pneumococcal Disease. Adult Track. Gram-positive bacteria
 Centers for Disease Control and Prevention National Center for Immunization and Respiratory Diseases Pneumococcal Disease and Pneumococcal Vaccines Adult Track Chapter 17 Photographs and images included
Centers for Disease Control and Prevention National Center for Immunization and Respiratory Diseases Pneumococcal Disease and Pneumococcal Vaccines Adult Track Chapter 17 Photographs and images included
Pneumococcal Vaccines. What s right for your clients?
 Pneumococcal Vaccines What s right for your clients? Vaccines Available - Pneumovax 23 A pneumococcal polysaccharide vaccine that includes 23 purified capsular polysaccharide antigens Vaccines Available
Pneumococcal Vaccines What s right for your clients? Vaccines Available - Pneumovax 23 A pneumococcal polysaccharide vaccine that includes 23 purified capsular polysaccharide antigens Vaccines Available
Alberta Health and Wellness Public Health Notifiable Disease Management Guidelines August Pneumococcal Disease, Invasive (IPD)
 August 2011 Pneumococcal Disease, Invasive (IPD) Revision Dates Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive) Case Definition August
August 2011 Pneumococcal Disease, Invasive (IPD) Revision Dates Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive) Case Definition August
Expanded Use of PCV13 & PPV23
 Expanded Use of PCV13 & PPV23 Dr. Jim Kellner Professor & Head Department of Pediatrics University of Calgary & Calgary Zone, Alberta Health Services Jim.Kellner@ahs.ca Objectives Explain the differences
Expanded Use of PCV13 & PPV23 Dr. Jim Kellner Professor & Head Department of Pediatrics University of Calgary & Calgary Zone, Alberta Health Services Jim.Kellner@ahs.ca Objectives Explain the differences
Recommendations for Using Pneumococcal Vaccines among Adults
 Recommendations for Using Pneumococcal Vaccines among Adults AI Collaborative Webinar February 2016 Tamara Pilishvili Respiratory Diseases Branch, CDC National Center for Immunization & Respiratory Diseases
Recommendations for Using Pneumococcal Vaccines among Adults AI Collaborative Webinar February 2016 Tamara Pilishvili Respiratory Diseases Branch, CDC National Center for Immunization & Respiratory Diseases
Recommendations for Using Pneumococcal Vaccines among Adults
 Recommendations for Using Pneumococcal Vaccines among Adults AI Collaborative Webinar July 2017 Tamara Pilishvili Respiratory Diseases Branch, CDC National Center for Immunization & Respiratory Diseases
Recommendations for Using Pneumococcal Vaccines among Adults AI Collaborative Webinar July 2017 Tamara Pilishvili Respiratory Diseases Branch, CDC National Center for Immunization & Respiratory Diseases
Series of 2 doses, 6-12 months apart. One dose is 720 Elu/0.5ml (GSK) or 25 u/0.5 ml (Merck)
 UTAH PREVENTIVE CARE RECOMMENDATIONS Adult - Ages 19 and Above IMMUNIZATIONS CONTENTS: General Instructions Hepatitis A Hepatitis B Human Papilloma Virus Influenza Meningococcal A, C, Y, W (MCV4) Meningococcal
UTAH PREVENTIVE CARE RECOMMENDATIONS Adult - Ages 19 and Above IMMUNIZATIONS CONTENTS: General Instructions Hepatitis A Hepatitis B Human Papilloma Virus Influenza Meningococcal A, C, Y, W (MCV4) Meningococcal
ACIP Recommendations for Pneumococcal 13-valent Conjugate and 23-valent Polysaccharide Vaccine Use among Adults
 ACIP Recommendations for Pneumococcal 13-valent Conjugate and 23-valent Polysaccharide Vaccine Use among Adults National Center for Immunization & Respiratory Diseases Respiratory Diseases Branch ACIP
ACIP Recommendations for Pneumococcal 13-valent Conjugate and 23-valent Polysaccharide Vaccine Use among Adults National Center for Immunization & Respiratory Diseases Respiratory Diseases Branch ACIP
Pneumococcal 13-valent Conjugate Vaccine Biological Page
 Pneumococcal 13-valent Conjugate Vaccine Biological Page Section 7: Biological Product Information Standard #: 07.291 Created by: Province-wide Immunization Program Standards and Quality Approved by: Province-wide
Pneumococcal 13-valent Conjugate Vaccine Biological Page Section 7: Biological Product Information Standard #: 07.291 Created by: Province-wide Immunization Program Standards and Quality Approved by: Province-wide
SUMMARY OF PRODUCT CHARACTERISTICS
 1. NAME OF THE MEDICINAL PRODUCT PNEUMOCOCCAL POLYSACCHARIDE VACCINE IP Solution for injection 0.5-mL single dose vials and prefilled syringes BRAND NAME: PNEUMOVAX 23 SUMMARY OF PRODUCT CHARACTERISTICS
1. NAME OF THE MEDICINAL PRODUCT PNEUMOCOCCAL POLYSACCHARIDE VACCINE IP Solution for injection 0.5-mL single dose vials and prefilled syringes BRAND NAME: PNEUMOVAX 23 SUMMARY OF PRODUCT CHARACTERISTICS
Vaccines for Primary Care Pneumococcal, Shingles, Pertussis
 Vaccines for Primary Care Pneumococcal, Shingles, Pertussis Devang Patel, M.D. Assistant Professor Chief of Service, MICU ID Service University of Maryland School of Medicine Pneumococcal Vaccine Pneumococcal
Vaccines for Primary Care Pneumococcal, Shingles, Pertussis Devang Patel, M.D. Assistant Professor Chief of Service, MICU ID Service University of Maryland School of Medicine Pneumococcal Vaccine Pneumococcal
Immunization Update: New CDC Recommendations. Blaise L. Congeni M.D. 2012
 Immunization Update: New CDC Recommendations Blaise L. Congeni M.D. 2012 Polysaccharide Vaccines Vaccine Hib capsule polysaccharide PRP (polyribose ribitol phosphate) Not protective in infants
Immunization Update: New CDC Recommendations Blaise L. Congeni M.D. 2012 Polysaccharide Vaccines Vaccine Hib capsule polysaccharide PRP (polyribose ribitol phosphate) Not protective in infants
Chapter 16 Pneumococcal Infection. Pneumococcal Infection. August 2015
 Chapter 16 16 PPV introduced for at risk 1996 PCV7 introduced for at risk 2002 and as routine 2008 PCV13 replaced PCV7 in 2010 NOTIFIABLE In some circumstances, advice in these guidelines may differ from
Chapter 16 16 PPV introduced for at risk 1996 PCV7 introduced for at risk 2002 and as routine 2008 PCV13 replaced PCV7 in 2010 NOTIFIABLE In some circumstances, advice in these guidelines may differ from
Table 1 23 Pneumococcal Capsular Types Included in PNEUMOVAX 23
 PRODUCT INFORMATION NAME OF THE MEDICINE: PNEUMOVAX 23 (pneumococcal vaccine, polyvalent, MSD) DESCRIPTION: PNEUMOVAX 23 (Pneumococcal Vaccine, Polyvalent, MSD), is a sterile, liquid vaccine for intramuscular
PRODUCT INFORMATION NAME OF THE MEDICINE: PNEUMOVAX 23 (pneumococcal vaccine, polyvalent, MSD) DESCRIPTION: PNEUMOVAX 23 (Pneumococcal Vaccine, Polyvalent, MSD), is a sterile, liquid vaccine for intramuscular
Vaccinations for Adults
 Case: Vaccinations for Adults Lisa Winston, MD University of California, San Francisco San Francisco General Hospital A 30-year old healthy woman comes for a routine visit. She is recently married and
Case: Vaccinations for Adults Lisa Winston, MD University of California, San Francisco San Francisco General Hospital A 30-year old healthy woman comes for a routine visit. She is recently married and
16 November 2017 National Immunisation Advisory Committee Recommendations for the 2017/2018 Influenza Vaccination Campaign
 16 November 2017 National Immunisation Advisory Committee Recommendations for the 2017/2018 Influenza Vaccination Campaign Please note the National Immunisation Advisory Committee (NIAC) has updated the
16 November 2017 National Immunisation Advisory Committee Recommendations for the 2017/2018 Influenza Vaccination Campaign Please note the National Immunisation Advisory Committee (NIAC) has updated the
41 Pneumococcal Disease
 41 Pneumococcal Disease Epidemiology and Prevention Abstract: Streptococcus pneumonie is a major cause of morbidity and mortality in very young, high-risk adults and elderly population. It kills almost
41 Pneumococcal Disease Epidemiology and Prevention Abstract: Streptococcus pneumonie is a major cause of morbidity and mortality in very young, high-risk adults and elderly population. It kills almost
Vaccines in Immunocompromised hosts
 Vaccines in Immunocompromised hosts Carlos del Rio, MD Emory Center for AIDS Research October 2013 Immunocompromised hosts Number has increased rapidly in the past decades Broad term that encompasses different
Vaccines in Immunocompromised hosts Carlos del Rio, MD Emory Center for AIDS Research October 2013 Immunocompromised hosts Number has increased rapidly in the past decades Broad term that encompasses different
Susan J. Rehm, MD, FACP, FIDSA Department of Infectious Disease Cleveland Clinic Cleveland, OH
 Improving Adult Vaccination Practices Preventing Pneumococcal Disease in Your High-Risk and Older Patients Susan J. Rehm, MD, FACP, FIDSA Department of Infectious Disease Cleveland Clinic Cleveland, OH
Improving Adult Vaccination Practices Preventing Pneumococcal Disease in Your High-Risk and Older Patients Susan J. Rehm, MD, FACP, FIDSA Department of Infectious Disease Cleveland Clinic Cleveland, OH
UPDATE ON IMMUNIZATION GUIDELINES AND PRACTICES
 DISCLOSURES UPDATE ON IMMUNIZATION GUIDELINES AND PRACTICES Nothing to disclose Kylie Mueller, Pharm.D., BCPS Clinical Specialist, Infectious Diseases Spartanburg Regional Medical Center LEARNING OBJECTIVES
DISCLOSURES UPDATE ON IMMUNIZATION GUIDELINES AND PRACTICES Nothing to disclose Kylie Mueller, Pharm.D., BCPS Clinical Specialist, Infectious Diseases Spartanburg Regional Medical Center LEARNING OBJECTIVES
Flu & Pneumonia Provider Toolkit
 Flu & Pneumonia Provider Toolkit 2018-2019 ILQI1809.1 Molina Healthcare and Providers Work Together to Protect Members from Flu & Pneumonia Molina Healthcare of Illinois (Molina) is continuing efforts
Flu & Pneumonia Provider Toolkit 2018-2019 ILQI1809.1 Molina Healthcare and Providers Work Together to Protect Members from Flu & Pneumonia Molina Healthcare of Illinois (Molina) is continuing efforts
BCG vaccine and tuberculosis
 PART 2: Vaccination for special risk groups 2.1 Vaccination for Aboriginal and Torres Strait Islander people Aboriginal and Torres Strait Islander people historically had a very high burden of infectious
PART 2: Vaccination for special risk groups 2.1 Vaccination for Aboriginal and Torres Strait Islander people Aboriginal and Torres Strait Islander people historically had a very high burden of infectious
Influenza. Influenza vaccines (WHO position paper) Weekly Epid. Record (2005, 80: ) 287
 Program Management 82_19 SAGE encouraged all countries to consider their preparedness for a potential influenza pandemic, recognizing that it would occur before strain-specific vaccine can be made in significant
Program Management 82_19 SAGE encouraged all countries to consider their preparedness for a potential influenza pandemic, recognizing that it would occur before strain-specific vaccine can be made in significant
Incidence per 100,000
 Streptococcus pneumoniae Surveillance Report 2005 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services Updated: March 2007 Background
Streptococcus pneumoniae Surveillance Report 2005 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services Updated: March 2007 Background
PNEUMOVAX 23 pneumococcal vaccine, polyvalent solution for injection
 PRODUCT INFORMATION PNEUMOVAX 23 pneumococcal vaccine, polyvalent solution for injection NAME OF THE MEDICINE PNEUMOVAX 23 (pneumococcal vaccine, polyvalent) DESCRIPTION PNEUMOVAX 23 (Pneumococcal Vaccine
PRODUCT INFORMATION PNEUMOVAX 23 pneumococcal vaccine, polyvalent solution for injection NAME OF THE MEDICINE PNEUMOVAX 23 (pneumococcal vaccine, polyvalent) DESCRIPTION PNEUMOVAX 23 (Pneumococcal Vaccine
3 rd dose. 3 rd or 4 th dose, see footnote 5. see footnote 13. for certain high-risk groups
 Figure 1. Recommended immunization schedule for persons aged 0 through 18 years 2013. (FOR THOSE WHO FALL BEHIND OR START LATE, SEE THE CATCH-UP SCHEDULE [FIGURE 2]). These recommendations must be read
Figure 1. Recommended immunization schedule for persons aged 0 through 18 years 2013. (FOR THOSE WHO FALL BEHIND OR START LATE, SEE THE CATCH-UP SCHEDULE [FIGURE 2]). These recommendations must be read
Update on Vaccine Recommendations. Objectives. Childhood Immunization Schedule At the Turn of the Century. New Horizons in Pediatrics April 30, 2017
 Centers for for Disease Disease Control Control and and Prevention Prevention National Center for Immunization and Respiratory Diseases Update on Vaccine Recommendations New Horizons in Pediatrics April
Centers for for Disease Disease Control Control and and Prevention Prevention National Center for Immunization and Respiratory Diseases Update on Vaccine Recommendations New Horizons in Pediatrics April
Jon Temte, MD/PhD Chair Wisconsin Council on Immunization Practices Professor of Family Medicine and Community Health
 Jon Temte, MD/PhD Chair Wisconsin Council on Immunization Practices Professor of Family Medicine and Community Health University of Wisconsin School of Medicine and Public Health Grand Rounds September
Jon Temte, MD/PhD Chair Wisconsin Council on Immunization Practices Professor of Family Medicine and Community Health University of Wisconsin School of Medicine and Public Health Grand Rounds September
Adult Immunization Rates
 Adult Immunization Rates California Immunization Coalition Summit May 5, 2014 Eileen Yamada, MD, MPH California Department of Public Health Immunization Branch Adult Immunization Rates California Data
Adult Immunization Rates California Immunization Coalition Summit May 5, 2014 Eileen Yamada, MD, MPH California Department of Public Health Immunization Branch Adult Immunization Rates California Data
Vaccine Preventable Diseases Among Adults
 Vaccine Preventable Diseases Among Adults Stephanie Borchardt, MPH, PhD Wisconsin Immunization Program Division of Public Health Wisconsin Department of Health Services November 17, 2016 At a Glance Burden
Vaccine Preventable Diseases Among Adults Stephanie Borchardt, MPH, PhD Wisconsin Immunization Program Division of Public Health Wisconsin Department of Health Services November 17, 2016 At a Glance Burden
Invasive Bacterial Disease
 Invasive Bacterial Disease All Streptococcus pneumoniae Electronic Disease Surveillance System Division of Surveillance and Disease Control Infectious Disease Epidemiology Program : 304-558-5358 or 800-423-1271
Invasive Bacterial Disease All Streptococcus pneumoniae Electronic Disease Surveillance System Division of Surveillance and Disease Control Infectious Disease Epidemiology Program : 304-558-5358 or 800-423-1271
RxVaccinate. Support. Objectives. Disclosures 7/8/2013. Pneumococcal Immunization Update
 RxVaccinate Pneumococcal Immunization Update Stephan L. Foster, Pharm.D., FAPhA, FNAP Professor and Vice-Chair College of Pharmacy University of Tennessee Health Science Center, Memphis, TN Liaison Member,
RxVaccinate Pneumococcal Immunization Update Stephan L. Foster, Pharm.D., FAPhA, FNAP Professor and Vice-Chair College of Pharmacy University of Tennessee Health Science Center, Memphis, TN Liaison Member,
2/16/2015 IMMUNIZATION UPDATE Kelly Ridgway, RPh February 21, Today s Overview NEW RECOMMENDATIONS
 IMMUNIZATION UPDATE 2015 Kelly Ridgway, RPh February 21, 2015 Today s Overview 1 2 3 4 5 6 Pneumococcal Vaccine Recommendations Meningococcal Vaccine Recommendations HPV Vaccine Recommendations Patient
IMMUNIZATION UPDATE 2015 Kelly Ridgway, RPh February 21, 2015 Today s Overview 1 2 3 4 5 6 Pneumococcal Vaccine Recommendations Meningococcal Vaccine Recommendations HPV Vaccine Recommendations Patient
Routine Adult Immunization: American College of Preventive Medicine Practice Policy Statement, updated 2002
 Routine Adult Immunization: American College of Preventive Medicine Practice Policy Statement, updated 2002 Ann R. Fingar, MD, MPH, and Byron J. Francis, MD, MPH Burden of suffering Vaccines are available
Routine Adult Immunization: American College of Preventive Medicine Practice Policy Statement, updated 2002 Ann R. Fingar, MD, MPH, and Byron J. Francis, MD, MPH Burden of suffering Vaccines are available
Pneumococcal vaccination in UK: an update. Dr Richard Pebody Immunisation Department Health Protection Agency Centre for Infections
 Pneumococcal vaccination in UK: an update Dr Richard Pebody Immunisation Department Health Protection Agency Centre for Infections Leading infectious causes of mortality, 2000 WHO estimates 3.5 Deaths
Pneumococcal vaccination in UK: an update Dr Richard Pebody Immunisation Department Health Protection Agency Centre for Infections Leading infectious causes of mortality, 2000 WHO estimates 3.5 Deaths
Update on Adult Immunization Strategies: Understanding the Current Recommendations
 Update on Adult Immunization Strategies: Understanding the Current Recommendations EDWARD A. DOMINGUEZ, MD, FACP, FIDSA Medical Director, Organ Transplant Infectious Diseases Methodist Dallas Medical Center,
Update on Adult Immunization Strategies: Understanding the Current Recommendations EDWARD A. DOMINGUEZ, MD, FACP, FIDSA Medical Director, Organ Transplant Infectious Diseases Methodist Dallas Medical Center,
Streptococcus Pneumoniae
 Streptococcus Pneumoniae (Invasive Pneumococcal Disease) DISEASE REPORTABLE WITHIN 24 HOURS OF DIAGNOSIS Per N.J.A.C. 8:57, healthcare providers and administrators shall report by mail or by electronic
Streptococcus Pneumoniae (Invasive Pneumococcal Disease) DISEASE REPORTABLE WITHIN 24 HOURS OF DIAGNOSIS Per N.J.A.C. 8:57, healthcare providers and administrators shall report by mail or by electronic
Use of 13-valent Pneumococcal Conjugate Vaccine and 23-valent Polysaccharide Vaccine in Adults with Immunocompromising Conditions
 Use of 13-valent Pneumococcal Conjugate Vaccine and 23-valent Polysaccharide Vaccine in Adults with Immunocompromising Conditions Tamara Pilishvili, MPH Respiratory Diseases Branch National Center for
Use of 13-valent Pneumococcal Conjugate Vaccine and 23-valent Polysaccharide Vaccine in Adults with Immunocompromising Conditions Tamara Pilishvili, MPH Respiratory Diseases Branch National Center for
Immunization of Adults in High Risk Populations. Carol A. Kurbis MD, CCFP, FRCPC WRHA Medical Officer of Health
 Immunization of Adults in High Risk Populations Carol A. Kurbis MD, CCFP, FRCPC WRHA Medical Officer of Health OBJECTIVES To review recommendations for immunization in adult populations, with a focus on
Immunization of Adults in High Risk Populations Carol A. Kurbis MD, CCFP, FRCPC WRHA Medical Officer of Health OBJECTIVES To review recommendations for immunization in adult populations, with a focus on
Pneumococcal Vaccination. Bottom Line. Gangrene from Pneumococcal Bacteremia
 Vaccination MSHO Performance Improvement Project Kristin L. Nichol, MD, MPH, MBA Professor of Medicine, University of Minnesota Chief of Medicine, Minneapolis VA Medical Cente Chair, MCAI Bottom Line disease
Vaccination MSHO Performance Improvement Project Kristin L. Nichol, MD, MPH, MBA Professor of Medicine, University of Minnesota Chief of Medicine, Minneapolis VA Medical Cente Chair, MCAI Bottom Line disease
2007 ACIP Recommendations for Influenza Vaccine. Anthony Fiore, MD, MPH Influenza Division, NCIRD, CDC
 2007 ACIP Recommendations for Influenza Vaccine Anthony Fiore, MD, MPH Influenza Division, NCIRD, CDC National Influenza Vaccine Summit April 19, 2007 Recommendation Changes for Influenza Vaccination:
2007 ACIP Recommendations for Influenza Vaccine Anthony Fiore, MD, MPH Influenza Division, NCIRD, CDC National Influenza Vaccine Summit April 19, 2007 Recommendation Changes for Influenza Vaccination:
Pneumococcal vaccines
 Pneumococcal vaccines Marco Aurélio Sáfadi, MD, PhD FCM da Santa Casa de São Paulo Challenges in establishing the baseline burden of disease, before implementing a vaccination program S. pneumoniae disease
Pneumococcal vaccines Marco Aurélio Sáfadi, MD, PhD FCM da Santa Casa de São Paulo Challenges in establishing the baseline burden of disease, before implementing a vaccination program S. pneumoniae disease
Deaths/yr Efficacy Use Prev Deaths/yr. Influenza 36,000 70% 60% 18,000. Pneumonia 40,000 60% 40% 20,000 HBV 6,000 90% 30% 4,000
 Tetanus, Diptheria, Pertussis,! Measles, Mumps, Rubella, Varicella, HPV, Polio Meningococcus, Pneumococcus,! Influenza, Hepatitis B, Hepatitis A,! H influenza, Rabies, Typhoid,! Yellow Fever, Japanese
Tetanus, Diptheria, Pertussis,! Measles, Mumps, Rubella, Varicella, HPV, Polio Meningococcus, Pneumococcus,! Influenza, Hepatitis B, Hepatitis A,! H influenza, Rabies, Typhoid,! Yellow Fever, Japanese
Policy and Procedure Manual
 Policy and Procedure Manual Medication Management MM.3-6 SUBJECT/TITLE: PURPOSE: DEFINITION: ADULT, INPATIENT PNEUMOCOCCAL AND SEASONAL INFLUENZA VACCINATION To ensure that adult inpatients who are candidates
Policy and Procedure Manual Medication Management MM.3-6 SUBJECT/TITLE: PURPOSE: DEFINITION: ADULT, INPATIENT PNEUMOCOCCAL AND SEASONAL INFLUENZA VACCINATION To ensure that adult inpatients who are candidates
Trends in Pneumonia and Influenza Morbidity and Mortality
 Trends in Pneumonia and Influenza Morbidity and Mortality American Lung Association Epidemiology and Statistics Unit Research and Health Education Division November 2015 Page intentionally left blank Introduction
Trends in Pneumonia and Influenza Morbidity and Mortality American Lung Association Epidemiology and Statistics Unit Research and Health Education Division November 2015 Page intentionally left blank Introduction
7/13/2016. Immunization Update Disclosures. Objectives. No financial disclosures to report
 Immunization Update 2016 Courtney A. Robertson, PharmD Clinical Assistant Professor University of Louisiana at Monroe School of Pharmacy Disclosures No financial disclosures to report Objectives Pharmacists
Immunization Update 2016 Courtney A. Robertson, PharmD Clinical Assistant Professor University of Louisiana at Monroe School of Pharmacy Disclosures No financial disclosures to report Objectives Pharmacists
Invasive Bacterial Disease
 Invasive Bacterial Disease Neisseria meningitidis, Haemophilus influenzae, and Group B Streptococcus (Streptococcus agalactiae) Case Report Form Electronic Disease Surveillance System Division of Surveillance
Invasive Bacterial Disease Neisseria meningitidis, Haemophilus influenzae, and Group B Streptococcus (Streptococcus agalactiae) Case Report Form Electronic Disease Surveillance System Division of Surveillance
Impact of Universal Infant Immunization with Pneumococcal (Streptococcus pneumonia) Conjugate Vaccines in Alaska
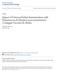 Pacific University CommonKnowledge School of Physician Assistant Studies Theses, Dissertations and Capstone Projects 8-2008 Impact of Universal Infant Immunization with Pneumococcal (Streptococcus pneumonia)
Pacific University CommonKnowledge School of Physician Assistant Studies Theses, Dissertations and Capstone Projects 8-2008 Impact of Universal Infant Immunization with Pneumococcal (Streptococcus pneumonia)
Getting national guidelines into practice: It takes more than education
 Getting national guidelines into practice: It takes more than education AI Collaborative Group 2 September 12, 2017 Lynette M. Wachholz, MN, ARNP, CPHQ Email: lwachholz@everettclinic.com The Everett Clinic
Getting national guidelines into practice: It takes more than education AI Collaborative Group 2 September 12, 2017 Lynette M. Wachholz, MN, ARNP, CPHQ Email: lwachholz@everettclinic.com The Everett Clinic
Bacterial diseases caused by Streptoccus pneumoniae in children
 Bacterial diseases caused by Streptoccus pneumoniae in children Bactermia 85% Bacterial pneumonia 66% Bacterial meningitis 50% Otitis media 40% Paranasal sinusitis 40% 0% 10% 20% 30% 40% 50% 60% 70% 80%
Bacterial diseases caused by Streptoccus pneumoniae in children Bactermia 85% Bacterial pneumonia 66% Bacterial meningitis 50% Otitis media 40% Paranasal sinusitis 40% 0% 10% 20% 30% 40% 50% 60% 70% 80%
Trends in Pneumonia and Influenza Morbidity and Mortality
 Trends in Pneumonia and Influenza Morbidity and Mortality American Lung Association Research and Program Services Epidemiology and Statistics Unit September 2008 Table of Contents Trends in Pneumonia and
Trends in Pneumonia and Influenza Morbidity and Mortality American Lung Association Research and Program Services Epidemiology and Statistics Unit September 2008 Table of Contents Trends in Pneumonia and
Andrew Kroger, MD, MPH National Center for Immunization and Respiratory Diseases MCH & Immunization Conference Anchorage, AK September 28, 2010
 2010 Immunization Update Andrew Kroger, MD, MPH National Center for Immunization and Respiratory Diseases MCH & Immunization Conference Anchorage, AK September 28, 2010 Disclosures No financial conflict
2010 Immunization Update Andrew Kroger, MD, MPH National Center for Immunization and Respiratory Diseases MCH & Immunization Conference Anchorage, AK September 28, 2010 Disclosures No financial conflict
PNEUMONIA : PROMISE FULFILLED? Regina Berba MD FPSMID
 PNEUMONIA : PROMISE FULFILLED? Regina Berba MD FPSMID Objectives of Lecture Know the quality of current evidence based guidelines on immunization Appreciate the performance of pneumonia vaccines in terns
PNEUMONIA : PROMISE FULFILLED? Regina Berba MD FPSMID Objectives of Lecture Know the quality of current evidence based guidelines on immunization Appreciate the performance of pneumonia vaccines in terns
Vaccine-Preventable Diseases in Colorado s Children 2009 Sean O Leary MD, Carl Armon PhD, Joni Reynolds, RNC, MSN, James Todd MD
 State of the Health of Colorado s Children Vaccine-Preventable Diseases in Colorado s Children 29 Sean O Leary MD, Carl Armon PhD, Joni Reynolds, RNC, MSN, James Todd MD Vaccines have been highly effective
State of the Health of Colorado s Children Vaccine-Preventable Diseases in Colorado s Children 29 Sean O Leary MD, Carl Armon PhD, Joni Reynolds, RNC, MSN, James Todd MD Vaccines have been highly effective
continuing education for pharmacists
 continuing education for pharmacists Pneumococcal Disease: Treatment and Prevention Volume XXXIV, No. 3 Donald L. Bennett, R.Ph., MBA, Clinical Assistant Professor, The Ohio State University College of
continuing education for pharmacists Pneumococcal Disease: Treatment and Prevention Volume XXXIV, No. 3 Donald L. Bennett, R.Ph., MBA, Clinical Assistant Professor, The Ohio State University College of
APEC Guidelines Immunizations
 Pregnancy provides an excellent opportunity to enhance a woman s protection against disease and to provide protection to the neonate during the first 3 to 6 months of life. Women of childbearing age should
Pregnancy provides an excellent opportunity to enhance a woman s protection against disease and to provide protection to the neonate during the first 3 to 6 months of life. Women of childbearing age should
11/17/2013 THE WHO, WHAT, WHEN, AND WHY OF ADULT VACCINATIONS. Pneumococcal Vaccines for Adults (PPV) Pneumococcal Vaccines
 THE WHO, WHAT, WHEN, AND WHY OF ADULT VACCINATIONS CAROL A. KAUFFMAN, MD VA ANN ARBOR HEALTHCARE SYSTEM UNIVERSITY OF MICHIGAN Will discuss: bacterial vaccines made of toxoids or polysaccharide capsular
THE WHO, WHAT, WHEN, AND WHY OF ADULT VACCINATIONS CAROL A. KAUFFMAN, MD VA ANN ARBOR HEALTHCARE SYSTEM UNIVERSITY OF MICHIGAN Will discuss: bacterial vaccines made of toxoids or polysaccharide capsular
To view past issues, go to: The New 13-Valent Pneumococcal Conjugate Vaccine (PCV13)
 From the Texas Department of State Health Services Immunization Branch The goal of the Vaccine Advisory is to disseminate, in a timely manner, practical information related to vaccines, vaccine-preventable
From the Texas Department of State Health Services Immunization Branch The goal of the Vaccine Advisory is to disseminate, in a timely manner, practical information related to vaccines, vaccine-preventable
The Role of the Pharmacist in Pneumococcal Vaccination
 The Role of the Pharmacist in Pneumococcal Vaccination The Role of the Pharmacist in Pneumococcal Vaccination Miranda Wilhelm, PharmD Clinical Associate Professor Department of Pharmacy Practice Southern
The Role of the Pharmacist in Pneumococcal Vaccination The Role of the Pharmacist in Pneumococcal Vaccination Miranda Wilhelm, PharmD Clinical Associate Professor Department of Pharmacy Practice Southern
Recommended Childhood Immunization Schedu...ates, January - December 2000, NP Central
 Recommended Childhood Immunization Schedule United States, January - December 2000 Vaccines 1 are listed under routinely recommended ages. Solid-colored bars indicate range of recommended ages for immunization.
Recommended Childhood Immunization Schedule United States, January - December 2000 Vaccines 1 are listed under routinely recommended ages. Solid-colored bars indicate range of recommended ages for immunization.
the benefits and potential side effects of pneumococcal immunization; and
 F883 483.80(d) Influenza and pneumococcal immunizations 483.80(d)(1) Influenza. The facility must develop policies and procedures to ensure that- (i) Before offering the influenza immunization, each resident
F883 483.80(d) Influenza and pneumococcal immunizations 483.80(d)(1) Influenza. The facility must develop policies and procedures to ensure that- (i) Before offering the influenza immunization, each resident
INFLUENZA VACCINATION AND MANAGEMENT SUMMARY
 INFLUENZA VACCINATION AND MANAGEMENT SUMMARY Morbidity and mortality related to influenza occur at a higher rate in people over 65 and those with underlying chronic medical conditions. Annual influenza
INFLUENZA VACCINATION AND MANAGEMENT SUMMARY Morbidity and mortality related to influenza occur at a higher rate in people over 65 and those with underlying chronic medical conditions. Annual influenza
2013 Adult Immunization Update. David H. Spach, MD Professor of Medicine Division of Infectious Diseases University of Washington, Seattle
 2013 Adult Immunization Update David H. Spach, MD Professor of Medicine Division of Infectious Diseases University of Washington, Seattle Adult Immunization Update Pertussis Vaccine Influenza Vaccine Zoster
2013 Adult Immunization Update David H. Spach, MD Professor of Medicine Division of Infectious Diseases University of Washington, Seattle Adult Immunization Update Pertussis Vaccine Influenza Vaccine Zoster
Update on Immunizations H. Keipp Talbot, M.D., M.P.H.
 Update on Immunizations H. Keipp Talbot, M.D., M.P.H. Vanderbilt University Medical Center 1 DISCLOSURES Financial Relationships with Relevant Commercial Interests Receive research funding from Sanofi
Update on Immunizations H. Keipp Talbot, M.D., M.P.H. Vanderbilt University Medical Center 1 DISCLOSURES Financial Relationships with Relevant Commercial Interests Receive research funding from Sanofi
EPIREVIEW INVASIVE PNEUMOCOCCAL DISEASE, NSW, 2002
 EPIREVIEW INVASIVE PNEUMOCOCCAL DISEASE, NSW, 2002 Robyn Gilmour Communicable Diseases Branch NSW Department of Health BACKGROUND Infection with the bacterium Streptococcus pneumoniae is a major cause
EPIREVIEW INVASIVE PNEUMOCOCCAL DISEASE, NSW, 2002 Robyn Gilmour Communicable Diseases Branch NSW Department of Health BACKGROUND Infection with the bacterium Streptococcus pneumoniae is a major cause
Superior Immune Response to Protein-conjugate vs. Free Pneumococcal. Polysaccharide Vaccine in COPD. for the COPD Clinical Research Network
 Page 32 of 37 Superior Immune Response to Protein-conjugate vs. Free Pneumococcal Polysaccharide Vaccine in COPD Mark T. Dransfield 1, Moon H. Nahm 1, MeiLan K. Han 2, Sarah Harnden 3, Gerard J. Criner
Page 32 of 37 Superior Immune Response to Protein-conjugate vs. Free Pneumococcal Polysaccharide Vaccine in COPD Mark T. Dransfield 1, Moon H. Nahm 1, MeiLan K. Han 2, Sarah Harnden 3, Gerard J. Criner
Impact of pneumococcal conjugate vaccine: US experience Stephanie Schrag Centers for Disease Control and Prevention Atlanta, GA
 Impact of pneumococcal conjugate vaccine: US experience Stephanie Schrag Centers for Disease Control and Prevention Atlanta, GA San Jose, Costa Rica, August 2007 Pneumococcal Conjugate Vaccine Introduction
Impact of pneumococcal conjugate vaccine: US experience Stephanie Schrag Centers for Disease Control and Prevention Atlanta, GA San Jose, Costa Rica, August 2007 Pneumococcal Conjugate Vaccine Introduction
Vaccines and Adults: Our Collective Challenge Webinar
 Vaccines and Adults: Our Collective Challenge Webinar Questions 1. What documentation would a pediatrician need to immunize adult parents to avoid some risk since they are non-patients of the practice
Vaccines and Adults: Our Collective Challenge Webinar Questions 1. What documentation would a pediatrician need to immunize adult parents to avoid some risk since they are non-patients of the practice
Journal Club 3/4/2011
 Journal Club 3/4/2011 Maternal HIV Infection and Antibody Responses Against Vaccine-Preventable Diseases in Uninfected Infants JAMA. 2011 Feb 9;305(6):576-84. Jones et al Dept of Pediatrics, Imperial College,
Journal Club 3/4/2011 Maternal HIV Infection and Antibody Responses Against Vaccine-Preventable Diseases in Uninfected Infants JAMA. 2011 Feb 9;305(6):576-84. Jones et al Dept of Pediatrics, Imperial College,
NOTE: The above recommendations must be read along with the footnotes of this schedule.
 Figure 1. Recommended immunization schedule for persons aged 0 through 18 years 2013. (FOR THOSE WHO FALL BEHIND OR START LATE, SEE THE CATCH-UP SCHEDULE [FIGURE 2]). These recommendations must be read
Figure 1. Recommended immunization schedule for persons aged 0 through 18 years 2013. (FOR THOSE WHO FALL BEHIND OR START LATE, SEE THE CATCH-UP SCHEDULE [FIGURE 2]). These recommendations must be read
These slides are the property of the presenter. Do not duplicate without express written consent.
 Cancer Survivorship Protecting Against Vaccine Preventable Diseases Heidi Loynes BSN, RN Immunization Nurse Educator Michigan Department of health and Human Services (MDHHS) loynesh@michigan.gov Are Vaccine-Preventable
Cancer Survivorship Protecting Against Vaccine Preventable Diseases Heidi Loynes BSN, RN Immunization Nurse Educator Michigan Department of health and Human Services (MDHHS) loynesh@michigan.gov Are Vaccine-Preventable
UNIVERSITY OF CALGARY. (IPD) in Adults with Underlying Comorbidities. Jason Lee Cabaj A THESIS SUBMITTED TO THE FACULTY OF GRADUATE STUDIES
 UNIVERSITY OF CALGARY The Influence of Childhood Conjugate Vaccine Introduction on Invasive Pneumococcal Disease (IPD) in Adults with Underlying Comorbidities by Jason Lee Cabaj A THESIS SUBMITTED TO THE
UNIVERSITY OF CALGARY The Influence of Childhood Conjugate Vaccine Introduction on Invasive Pneumococcal Disease (IPD) in Adults with Underlying Comorbidities by Jason Lee Cabaj A THESIS SUBMITTED TO THE
Platforms. Adolescent Immunization Update and the 16 Year Old Platform. Advisory Committee on Immunization Practices (ACIP)
 Adolescent Immunization Update and the 16 Year Old Platform William Atkinson, MD, MPH Associate Director for Immunization Education Immunization Action Coalition Advisory Committee on Immunization Practices
Adolescent Immunization Update and the 16 Year Old Platform William Atkinson, MD, MPH Associate Director for Immunization Education Immunization Action Coalition Advisory Committee on Immunization Practices
Immunizations to Reduce Disease H. Keipp Talbot, M.D., M.P.H.
 Immunizations to Reduce Disease H. Keipp Talbot, M.D., M.P.H. Vanderbilt University School of Medicine 1 DISCLOSURES Financial Relationships with Relevant Commercial Interests Receive research funding
Immunizations to Reduce Disease H. Keipp Talbot, M.D., M.P.H. Vanderbilt University School of Medicine 1 DISCLOSURES Financial Relationships with Relevant Commercial Interests Receive research funding
Impacto de la vacuna conjugada en EUA
 Impacto de la vacuna conjugada en EUA Richard Facklam, PhD, Distinguished Consultant, Retired, Centers for Disease Control and Prevention Atlanta, GA Bogotá, Colombia, February 2008 Pneumococcal Conjugate
Impacto de la vacuna conjugada en EUA Richard Facklam, PhD, Distinguished Consultant, Retired, Centers for Disease Control and Prevention Atlanta, GA Bogotá, Colombia, February 2008 Pneumococcal Conjugate
Pneumococcal Vaccine Introductions Dr. Carsten Mantel WHO/FCH/IVB/EPI
 Pneumococcal Vaccine Introductions 2012 Dr. Carsten Mantel WHO/FCH/IVB/EPI Pneumonia is leading cause of death in children < 5 yrs * Pneumococcus and Hib are the two leading causes of life-threatening
Pneumococcal Vaccine Introductions 2012 Dr. Carsten Mantel WHO/FCH/IVB/EPI Pneumonia is leading cause of death in children < 5 yrs * Pneumococcus and Hib are the two leading causes of life-threatening
Pneumococcal infection is one of. Epidemiology of Pneumococcal Disease ...PRESENTATIONS... Based on a presentation by Chris Van Beneden, MD, MPH
 ...PRESENTATIONS... Epidemiology of Pneumococcal Disease Based on a presentation by Chris Van Beneden, MD, MPH Presentation Summary Pneumococcus is a leading cause of pneumonia and meningitis in the United
...PRESENTATIONS... Epidemiology of Pneumococcal Disease Based on a presentation by Chris Van Beneden, MD, MPH Presentation Summary Pneumococcus is a leading cause of pneumonia and meningitis in the United
High Risk Conditions and Vaccination Gaps in Invasive Pneumococcal Disease Cases in Tennessee,
 High Risk Conditions and Vaccination Gaps in Invasive Pneumococcal Disease Cases in Tennessee, 2011-2016 Kinley Reed Candidate for Master of Public Health September 12, 2017 Outline Brief Introduction
High Risk Conditions and Vaccination Gaps in Invasive Pneumococcal Disease Cases in Tennessee, 2011-2016 Kinley Reed Candidate for Master of Public Health September 12, 2017 Outline Brief Introduction
Updated WHO position paper on pertussis vaccines. Geneva, Switzerland October 2010
 Updated WHO position paper on pertussis vaccines Geneva, Switzerland October 2010 Introduction Replaces the position paper on pertussis vaccines published in the Weekly Epidemiological Record in January
Updated WHO position paper on pertussis vaccines Geneva, Switzerland October 2010 Introduction Replaces the position paper on pertussis vaccines published in the Weekly Epidemiological Record in January
Adult Pneumococcal Disease
 Adult Pneumococcal Disease S. pneumoniae and pneumococcal disease The bacterium Streptococcus pneumoniae causes pneumococcal disease S. pneumoniae is commonly found in human nasopharynx (nose and throat)
Adult Pneumococcal Disease S. pneumoniae and pneumococcal disease The bacterium Streptococcus pneumoniae causes pneumococcal disease S. pneumoniae is commonly found in human nasopharynx (nose and throat)
HIV AND LUNG HEALTH. Stephen Aston Infectious Diseases SpR Royal Liverpool University Hospital
 HIV AND LUNG HEALTH Stephen Aston Infectious Diseases SpR Royal Liverpool University Hospital Introduction HIV infection exerts multiple effects on pulmonary immune responses: Generalised state of immune
HIV AND LUNG HEALTH Stephen Aston Infectious Diseases SpR Royal Liverpool University Hospital Introduction HIV infection exerts multiple effects on pulmonary immune responses: Generalised state of immune
Measure #111 (NQF 0043): Pneumococcal Vaccination Status for Older Adults National Quality Strategy Domain: Community/Population Health
 Measure #111 (NQF 0043): Pneumococcal Vaccination Status for Older Adults National Quality Strategy Domain: Community/Population Health 2017 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process
Measure #111 (NQF 0043): Pneumococcal Vaccination Status for Older Adults National Quality Strategy Domain: Community/Population Health 2017 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process
How to talk about typhoid: menu of messages
 How to talk about typhoid: menu of messages PATH/Rocky Prajapati The more we talk about typhoid, the better we ll be able to prioritize it. These messages were developed for use by anyone interested in
How to talk about typhoid: menu of messages PATH/Rocky Prajapati The more we talk about typhoid, the better we ll be able to prioritize it. These messages were developed for use by anyone interested in
Deployment of Combination Vaccines and STI vaccines
 Deployment of Combination Vaccines and STI vaccines Advancing Prevention Technologies for Sexual and Reproductive Health Symposium Berkeley, Ca March 24, 2009 Eileen Yamada, MD, MPH California Department
Deployment of Combination Vaccines and STI vaccines Advancing Prevention Technologies for Sexual and Reproductive Health Symposium Berkeley, Ca March 24, 2009 Eileen Yamada, MD, MPH California Department
Pneumococcal Vaccine Effectiveness. Steven Black, MD Center for Global Health Cincinnati Children s s Hospital Cincinnati, Ohio USA
 Pneumococcal Vaccine Effectiveness Steven Black, MD Center for Global Health Cincinnati Children s s Hospital Cincinnati, Ohio USA Overview Possible effectiveness outcomes for pneumococcal vaccines Pre-licensure
Pneumococcal Vaccine Effectiveness Steven Black, MD Center for Global Health Cincinnati Children s s Hospital Cincinnati, Ohio USA Overview Possible effectiveness outcomes for pneumococcal vaccines Pre-licensure
TDCJ OFFENDER IMMUNIZATION GUIDELINES
 TDCJ OFFENDER IMMUNIZATION GUIDELINES B-14.07 Immunizations Attachment A VACCINE WHO GETS IT * WHEN THEY GET IT DOSE/ROUTE HPV Vaccine Females age 9 to 26 years if not previously vaccinated. On Intake
TDCJ OFFENDER IMMUNIZATION GUIDELINES B-14.07 Immunizations Attachment A VACCINE WHO GETS IT * WHEN THEY GET IT DOSE/ROUTE HPV Vaccine Females age 9 to 26 years if not previously vaccinated. On Intake
Public Health Applications in Pharmacy
 1 Pharmacy 445 Public Health Applications in Pharmacy Jacqueline Gardner, Ph.D. Professor, Department of Pharmacy 2 Public or Community Health Distinct from clinical medicine, which focuses upon an individual
1 Pharmacy 445 Public Health Applications in Pharmacy Jacqueline Gardner, Ph.D. Professor, Department of Pharmacy 2 Public or Community Health Distinct from clinical medicine, which focuses upon an individual
September 14, All Medical Providers and Health Care Facilities. NYSDOH Bureau of Immunization
 September 14, 2009 TO: FROM: All Medical Providers and Health Care Facilities NYSDOH Bureau of Immunization HEALTH ADVISORY: Novel H1N1 Influenza Vaccine Information Please distribute to the Infection
September 14, 2009 TO: FROM: All Medical Providers and Health Care Facilities NYSDOH Bureau of Immunization HEALTH ADVISORY: Novel H1N1 Influenza Vaccine Information Please distribute to the Infection
B 型嗜血感冒桿菌感染及 其疫苗 衛生署疾病管制局 中區傳染病防治醫療網 王任賢指揮官
 B 型嗜血感冒桿菌感染及 其疫苗 衛生署疾病管制局 中區傳染病防治醫療網 王任賢指揮官 Haemophilus influenzae type b Severe bacterial infection, particularly among infants During late 19th century believed to cause influenza Immunology and microbiology
B 型嗜血感冒桿菌感染及 其疫苗 衛生署疾病管制局 中區傳染病防治醫療網 王任賢指揮官 Haemophilus influenzae type b Severe bacterial infection, particularly among infants During late 19th century believed to cause influenza Immunology and microbiology
Splenectomy Vaccine Protocol PIDPIC
 Splenectomy Vaccine Protocol PIDPIC 6.24.14 Rationale Spleen clears encapsulated bacteria and infected erythrocytes Serves as one of the largest lymphoid tissues where B cells are educated against encapsulated
Splenectomy Vaccine Protocol PIDPIC 6.24.14 Rationale Spleen clears encapsulated bacteria and infected erythrocytes Serves as one of the largest lymphoid tissues where B cells are educated against encapsulated
Title: Enhancing state-based surveillance for invasive pneumococcal disease
 09-ID-06 Committee: Infectious Diseases Title: Enhancing state-based surveillance for invasive pneumococcal disease I. tatement of the Problem: Cases of invasive pneumococcal disease among children less
09-ID-06 Committee: Infectious Diseases Title: Enhancing state-based surveillance for invasive pneumococcal disease I. tatement of the Problem: Cases of invasive pneumococcal disease among children less
HAEMOPHILUS INFLUENZAE INVASIVE DISEASE
 23 Annual Morbidity Report HAEMOPHILUS INFLUENZAE INVASIVE DISEASE CRUDE DATA 35 Annual Incidence a LA County.37 California b. United States c.2 Age at Diagnosis Mean 4. years Median 36. years Range Birth
23 Annual Morbidity Report HAEMOPHILUS INFLUENZAE INVASIVE DISEASE CRUDE DATA 35 Annual Incidence a LA County.37 California b. United States c.2 Age at Diagnosis Mean 4. years Median 36. years Range Birth
COUNTY OF MORRIS DEPARTMENT OF LAW & PUBLIC SAFETY OFFICE OF HEALTH MANAGEMENT
 1 COUNTY OF MORRIS DEPARTMENT OF LAW & PUBLIC SAFETY OFFICE OF HEALTH MANAGEMENT P.O. Box 900 Morristown, NJ 07963 (973) 631-5485 (973) 631-5490 Fax www.morrishealth.org 2012-2013 Influenza Season FREQUENTLY
1 COUNTY OF MORRIS DEPARTMENT OF LAW & PUBLIC SAFETY OFFICE OF HEALTH MANAGEMENT P.O. Box 900 Morristown, NJ 07963 (973) 631-5485 (973) 631-5490 Fax www.morrishealth.org 2012-2013 Influenza Season FREQUENTLY
Haemophilus influenzae Surveillance Report 2012 Oregon Active Bacterial Core Surveillance (ABCs) Center for Public Health Practice Updated: July 2014
 Haemophilus influenzae Surveillance Report 2012 Oregon Active Bacterial Core Surveillance (ABCs) Center for Public Health Practice Updated: July 2014 Background The Active Bacterial Core surveillance (ABCs)
Haemophilus influenzae Surveillance Report 2012 Oregon Active Bacterial Core Surveillance (ABCs) Center for Public Health Practice Updated: July 2014 Background The Active Bacterial Core surveillance (ABCs)
