A novel graft option after pterygium excision: platelet-rich fibrin for conjunctivoplasty
|
|
|
- Gwenda Wheeler
- 5 years ago
- Views:
Transcription
1 (2017) 31, Macmillan Publishers Limited, part of Springer Nature. All rights reserved X/17 CLINICAL STUDY A novel graft option after pterygium excision: platelet-rich fibrin for conjunctivoplasty HB Cakmak 1, G Dereli Can 2,MECan 3 and N Cagil 2 1 Department of Ophthalmology, Hacettepe University Faculty of Medicine, Ankara, Turkey 2 Department of Ophthalmology, Yildirim Beyazit University Faculty of Medicine, Ankara Ataturk Training and Research Hospital, Ankara, Turkey 3 Department of Ophthalmology, Ankara Kecioren Training and Research Hospital, Ankara, Turkey Correspondence: G Dereli Can, Department of Ophthalmology, Yildirim Beyazit University Faculty of Medicine, Ankara Ataturk Training and Research Hospital, Yasamkent Mah Sk. Gulbeng Sitesi No: 1-49, Yenimahalle, Ankara 06380, Turkey Tel: ; Fax: dereli_gmz@ hotmail.com Received: 12 February 2016 Accepted in revised form: 27 April 2017 Published online: 16 June 2017 Abstract Purpose To compare the surgical results, complications, and recurrence rates of primary pterygium excision with conjunctival autografts (CA) vs platelet-rich fibrin (PRF) grafts. Patients and methods A total of 35 eyes of 35 patients with primary pterygium were included in the study. The patients underwent excision of pterygium followed by closure of the bare sclera by CA (group 1, n = 20) vs PRF grafts (group 2, n = 15). The PRF was generated from the patients own whole-blood sample by centrifugation and pressing. The surgery times, intra/ postoperative complications, recurrence rates of pterygium, and changes in visual acuity (VA) were evaluated and compared within groups. Results The mean follow-up period was 14.3 ± 6.5 months (6 24 months). The mean preoperative and postoperative VAs were same (20/25) (P = 0.204). The mean surgery time was shorter in group 2 (22.1 ± 1.9 min) compared to group 1 (33.8 ± 7.8 min) (P = 0.001). The recurrence was observed only in one (6.6%) case of group 2, while none of the cases showed recurrence in group 1. Graft loss was observed in 2 (10%) cases in group 1, and 1 (6.6%) case in group 2. No other intra/ postoperative complications such as tear in the graft, excessive bleeding, scleral necrosis, graft necrosis, pannus formation, or symblepharon occurred in both groups. Conclusions This preliminary study showed encouraging results of the application of PRF for conjuntivoplasty after pterygium excision. The use of PRF in pterygium surgery is a simple, easily applicable, and a promising method with low rates of recurrence and complications. (2017) 31, ; doi: /eye ; published online 16 June 2017 Introduction Pterygium is a common worldwide ocular surface disease, which is a result of abnormal fibrovascular tissue proliferation originates from the degenerative conjunctiva and the underlying tenon. 1,2 Pterygium is more common in sunny, hot, dry, windy, dusty climate conditions, smoky environments, and tropical regions. 3,4 Ultraviolet radiation is the major risk factor, which damages cell proliferation cycle and induces abnormal cell proliferation, squamous metaplasia, goblet cell hyperplasia, inflammation, fibrosis, angiogenesis, and extracellular matrix breakdown. 5 Although the pathogenesis of pterygium remains unclear, it is acceptable as a stem cell disorder, which allows extension of the wing-shaped fibrovascular proliferation onto the cornea, and as an epithelia mesenchymal transition. 6,7 Today, there are many approaches to its treatment including leaving bare sclera, primary conjunctival closure, conjunctival autografts (CA), conjunctival-limbal autografts, and amniotic membrane transplantation (AMT). 5,8,9 Recurrence rates, the major concern after pterygium surgery, within these methods vary widely, therefore, adjunct metabolites like 5-fluorouracil (5-FU), mitomycin-c (MMC), or thiotepa have been used to improve the results. 4,8,9 However, there exists no surgical technique accepted as the gold standard treatment that prevents recurrence. Platelet-rich fibrin (PRF), described by Choukroun et al, 10 is a second-generation platelet concentrate, consists of many growth factors, cytokines, and glycoproteins such as vascular endothelial growth factor, plateletderived growth factor (PDGF), transforming growth factor-β, fibronectin, and
2 A novel graft option after pterygium excision 1607 thrombospondin, which have key roles in hemostasis and wound healing. 11,12 Because of PRF s natural fibrin framework properties, growth factors can keep their activity for a relatively longer period and stimulate cell migration, wound healing, and tissue regeneration effectively. 12,13 Additionally, the PRF provides temporary scaffold function for growing cells to migrate easily on/ into this membrane. 14 Beside these features, PRF clots can easily be transformed in dense fibrin membranes or cylinders by using suitable tools. Although the PRF has been used in oral, ear nose throat, orthopedic, and plastic surgeries as a biomaterial, it has not been employed for pterygium surgery until now. 14 We advocated that PRF is a novel autologous biomaterial and a suturable membrane for ocular surface reconstruction after pterygium excision. The aim of this study was to evaluate the efficacy and safety of PRF grafting in primary pterygium surgery. Materials and methods Subjects This was a prospective, comparative, non-randomized clinical trial conducted at the Department of Ophthalmology, Yildirim Beyazit University, Ataturk Training and Research Hospital, Ankara, Turkey, according to the tenets of the declaration of Helsinki. Approval was obtained from the Institutional Review Board of Yildirim Beyazit University Hospital and written informed consent was obtained from all participants after the explanation of the research design. We prospectively and consecutively enrolled a total of 35 pterygium patients with unilateral nasal primary pterygium infiltrating cornea 2 5 mm in size, who underwent pterygium excision between June 2013 and September The indications for pterygium surgery were as follows: reported growth by patient, prominent vascularization, and intractable symptoms of irritation. Patients with pseudopterygium, infection of the ocular surface or eyelids, a history of prior ocular surgery for pterygium, or systemic diseases that might have an effect on the healing of the surgical site were excluded. After pterygium diagnosis, details of two surgical techniques were discussed with patients before the operation. Possible peroperative and postoperative risks were explained in detail. PRP is a new surgical method and the possible complications and safety concerns were discussed. Patients were assigned to treatment groups according to their preference after a thorough discussion of each surgical techniques, concerning possible implications and complications. The patients were allocated into two groups: group 1 consists of 20 patients who underwent primary pterygium excision followed by closure of the bare sclera with CA, group 2 consists of 15 patients who underwent primary pterygium excision followed by closure of the bare sclera with PRF graft. Preparation of the PRF Blood samples were taken with a 24-gauge butterfly needle from the patient s antecubital vein, immediately before surgery in the operating room. Samples were collected in 10 ml glass tubes without anticoagulant in the operating room just before the operation. Blood samples were immediately centrifuged at r.p.m. for 12 min using a table centrifuge system (Hettich EBA-20; Hettich Holding GmbH & Co. ohg, Kirchlengern, Germany). The fibrin clot that formed in the middle part of the tube was removed (Figure 1a), and remnants of red blood cells were scraped off with gauze (Figure 1b). The clot was transferred to a PRF box (Medisoft Medical, Ankara, Turkey) and compressed, and the PRF membranes were obtained (Figure 1c). As soon as PRF membrane was prepared, it was sutured, without any delay. Figure 1 The preparation protocol of the PRF membrane. (a) The fibrin clots were concentrated (arrow) between the red blood cell corpuscles at the bottom and the acellular plasma at the top of the tubes. (b) Separation of the PRF clot from red blood cell layer. (c) The suturable membrane formation prepared from the fibrin clot by pressing in the PRF box. Note the semitransparency and smooth surface of the membrane.
3 1608 A novel graft option after pterygium excision Surgical technique All surgical procedures were performed by one surgeon (GDC) under topical (0.5% propacaine HCl: Alcaine; Alcon Inc., Forth Worth, TX, USA) and subconjunctival (lidocaine 10 mg/ml+epinephrine mg/ml: Jetokain; Adeka, Samsun, Turkey) anesthesia. After a careful dissection, pterygium head and a small part of its body were excised with the underlying tenon tissue from the cornea and the sclera using scissors. Residual pterygium tissue on the cornea was stripped with crescent knife. In group 1, the bare sclera was measured with caliper, and a same sized CA was harvested from superotemporal bulbar conjunctiva without damaging the limbus, and was placed on the bare sclera. The CA was oriented over the scleral bed in the way that the limbal side in the graft remained limbal, and secured to the surrounding conjunctiva with 4 6 separated 7/0 vicryl sutures (DLZ , FSSB, Jestetten, Germany). In group 2 the PRF, prepared just before the pterygium excision,wastrimmedtofit the size of the defect, and placed on the bare sclera. After orientation, it was secured with 4 6 separated 7/0 vicryl sutures (DLZ , FSSB, Jestetten, Germany) to the surrounding conjunctiva. The surgery times of both procedures, and complications occurred during the surgery such as excessive bleeding, tears in the grafts, scleral damage, or graft loss were recorded for comparison. Postoperatively, all subjects received an antibiotic eye drop (0.3% Ofloxacin: Exocin; Allergan Inc.) four times daily for 1 week, and lubricant eye drop (Polyvinyl Alcohol and Povidone: Refresh single; Allergan Inc., Parsippany, NJ, USA) four times daily for 6 weeks. In addition, corticosteroid eye drop (0.1% Fluorometholone and 0.025% Tetrahydrozoline Hydrochloride: Efemoline; Novartis Ophthalmics AG Hettlingen, Forth Worth, TX, USA) was prescribed three times per day starting from third postoperative day up to 3 weeks. Follow-up examinations After descriptive evaluation of the subjects including age, gender, medical and ocular history, a comprehensive ophthalmic evaluation of all cases including best spectacle corrected visual acuity (BSCVA), refraction, tonometry, slit-lamp biomicroscopy, and dilated fundus examination was performed before and after surgery. In the postoperative period the patients were visited on days 1, 3, 5, and 1 week, 1 month, 6 months, 12 months, and 24 months after surgery. Preoperative and postoperative slit-lamp examinations in which the grafted area was observed for the presence of injection, pigmentation, granuloma, melting, or infection were documented photographically at each visit in the same room conditions, and the same device settings. Efron scale for conjunctival redness was used to scale degree of postoperative inflammation at the end of 1 month. In this scale conjunctival redness graded as normal, trace, mild, moderate, and severe. 15 Additionally, conjunctival epithelialization on surgical margins was closely monitored with fluorescein staining. Presence of reaction against sutures evidenced by mucous secretion and excessive hyperemia on conjunctiva was noted. Recurrence was defined as a fibrovascular growth over the nasal cornea with conjunctival drag extending beyond the surgical limbus. Statistical analysis Data were coded, entered, and analyzed with Statistical Package for the Social Sciences software version 18.0 (SPSS Inc., Chicago, IL, USA). Results were expressed as mean ± SD. A Mann Whitney U-test was performed to analyze the changes in continuous variables. Categorical variables were tested with Chi-square test. A P-value of less than 0.05 is considered statistically significant. Power analysis was performed by using GPower 3.1 software (Dusseldorf, Germany). Results Demographics There were 6 (30%) female and 14 (70%) male subjects in group 1, 8 (53.4%) female and 7 (46.6%) male subjects in group 2 (P = 0.148). The mean age of the patients in group 1 and 2 was 49.3 ± 12.4 (between 27 and 75) years and 55.2 ± 13.5 (between 30 and 70) years, respectively (P = 0.551). The mean duration of the pterygium was 5.1 ± 4.6 (between 1 and 20) years in group 1 and 5.2 ± 2.7 (between 1 and 10) years in group 2 (P = 0.216). The size and morphology of pterygium were similar in both groups. Visual acuity The mean BSCVA was 20/25 preoperatively in group 1 and group 2, and it was not changed 12 months after the surgery in both groups (P = 0.204). None of the cases showed decrease in BSCVA. Surgery time and follow-up examinations The average surgical time for group 2 was shorter (22.1 ± 1.9 min) when compared to group 1 (33.8 ± 7.8 min) (P = 0.001). No intraoperative complication was noted for both groups. The mean follow-up period was 14.3 ± 6.5 months (6 24 months) for
4 A novel graft option after pterygium excision 1609 Figure 2 Sequential anterior segment photographs of a case. (a) Primary nasal pterygium, swollen on the limbal site, infiltrates cornea 2 mm (arrow), and mild moderate nasal conjunctival hyperemia. (b) PRF secured with separate 7/0 absorbable suture material on the bare sclera. Note the smooth transition between host conjunctiva and the membrane (arrows). (c) Postoperative first week slit-lamp examination. PRF dissolves, conjunctival epithelialization was completed, and limbal site was clear (arrow). (d) Postoperative sixth month slit-lamp examination. There was no recurrence, hyperemia, roughness, or other complications. both groups (P = 0.5). In early postoperative period, slitlamp examination revealed shorter durations of epithelialization of the defective zone in group 1 (3.5 ± 1.3 days) than in group 2 (4.0 ± 3.1 days). The difference was not statistically significant (P = 0.681). Graft loss was observed in 2 (10%) cases in group 1 and 1 (6.6%) case in group 2 on day 5 postoperatively (P = 0.207). Delayed epithelialization was also observed in those cases. Suture reaction was observed in 3 (15%) cases of group 1. In one of those cases, pyogenic granuloma formation was developed at the first postoperative month. Likewise, postoperative inflammation graded as moderate was observed in 6 (30%) cases in group 1. No suture reaction was observed in group 2 and the difference between two groups was not statistically significant with regard to suture reactions (P = 0.117). On the contrary, postoperative inflammation scores were significantly lower in group 2 (P = 0.020). In addition biomicroscopic evaluation revealed excessive mucous secretion in 5 (25%) cases in the early postoperative period, which decreased up to first week in group 1. Whereas, this condition was not observed in any cases in group 2. No other postoperative complications such as scleral necrosis, graft necrosis, pannus formation, or symblepharon occurred in both groups. On the sixth month postoperative visit, the recurrence was observed only in one (6.6%) case in group 2. Although the perioperative and early postoperative period was free of complications and the healing process proceeded smoothly in that case, the complaints including mild irritation sensation and hyperemia were started 4 months after surgery. A lubricant eye drop (Polyvinyl Alcohol and Povidone: Refresh single; Allergan Inc.) and a corticosteroid eye drop (0.1% Fluorometholone and 0.025% Tetrahydrozoline Hydrochloride: Efemoline; Novartis Ophthalmics AG Hettlingen) were prescribed four times daily for 6 weeks. According to the quiescent results of the biomicroscopic evaluation performed 2 months after the medical treatment, no other procedure was applied to that patient. Figure 2 shows sequential anterior segment photographs of a case, taken preoperatively, intraoperatively, and on postoperative seventh day and sixth month. Discussion Traditionally, several treatment modalities such as leaving bare sclera, primary conjunctival closure,
5 1610 A novel graft option after pterygium excision conjunctival with/without limbal auto-grafting, and AMT have been used for ocular surface reconstruction after pterygium excision. 4,5,8,9 However, the most common challenging problem is recurrence rate after pterygium surgery. 16 The risk factors of pterygium recurrence are as follows: pterygium type and size, age of patient, environmental conditions, recurrent pterygium, and surgical technique. 17 Furthermore, surgical trauma, postoperative inflammation, fibroblast proliferation, and deposition of extracellular matrix protein have been related with the mechanism of pterygium recurrence. 18,19 Therefore, the main successful target of pterygium surgery is to prevent recurrence. To this end, adjunctive anti-mitotic agents such as β-irradiation, thiotepa, 5-FU, and MMC have been commonly tried with pterygium excision to reduce the rate of recurrence. 4,8,9,20 Pterygium excision followed by leaving bare sclera is out of favor due to its high recurrence rates. Therefore, CA technique has gradually become a popular treatment for pterygium in the 1980s. 21 This technique has been reported to have low recurrence rates. However it has some important disadvantages like requirement of longer operating times, postoperative ocular irritation, and disruption of normal anatomy and microenvironment of the conjunctival tissue. 22 PRF described by Choukroun et al, 10 is a secondgeneration platelet concentrate, consists of 3-D polymerized autologous fibrin matrix with the incorporation of platelets, growth factors, cytokines, circulating stem cells, and small amount of leukocytes, which have key roles in hemostasis and wound healing. The intrinsic incorporation of these factors within this scaffold allows for their progressive and controlled release, as the fibrin mesh degrades. PRF releases autologous growth factors gradually, resulting in a stronger and more durable effect on cell proliferation, differentiation, migration, and matrix synthesis by binding to specific cell-surface receptors. 10,23 Moreover, PRF provided mechanical support to the migrating conjunctival and endothelial cells as a scaffold. The combination of mechanical and chemotactic support of autologous PRF makes it suitable for reconstruction, improvement, and/or maintenance of the ocular surface, and might offer many potential clinical advantages for pterygium surgery when compared to other methods. To the best of our knowledge, this is the first study investigating and comparing the efficacy, safety, recurrence, and complication rates of the PRF grafting vs CA after pterygium excision. In this current study, surgeries with both techniques resulted similar recurrence rates and graft loss. Recurrence rate in the current study could be interpreted as equal as other studies, and better than some reports like Prabhasawat et al 24 who reported recurrence rate 10.9% with AMT and some other reports have presented recurrence rate 8 39% with CA for primary pterygium. 20,22,24 28 Another important finding is that the PRF grafting resulted in milder postoperative inflammation, tissue reaction, and granuloma formation. 16,19 PRF also contains a large quantity of platelet and small amount of leukocyte cytokines, which can play a significant role in the selfregulation of inflammatory and infectious phenomena. 29,30 For this reason, PRF usage might yield a less pronounced postoperative inflammation. If this is the case, it has other implications beside a more comfortable convalesence period. Marked postoperative inflammation might be a stealth generator of recurrence, inducing cellular activity. Following the same line, these findings provide some support for the conceptual premise that PRF usage might have a great impact on diminishing recurrence rates. Current study revealed that the mean surgery time was shorter in PRF group than CA group about 10 min. Harvesting CA requires additional surgical steps and needs extra time. Shorter surgery times not only decrease surgery costs but also it supports higher patient satisfaction. In prolonged surgeries, patients feel much more pain, causing their cooperation lost due to decrease in effect of anesthesics. In addition, increase in the amount of surgical manipulations and duration of surgery might provoke a more severe postoperative inflammation. Additionally, PRF grafting does not cause any additional conjunctival tissue damage and helps to preserve normal conjunctival anatomy maximally. Autologous biomaterials are more superior and preferable than homologous and synthetic materials for reconstruction of the damaged tissues. Although this study compared two autologous technic for conjunctivoplasty, the PRF has more advantages when compared to other technics such as AMT, an allograft, which has the least reaction potential. The preparation of AMT is complicated and rather expensive, which requires a strong tissue banking expertise to prevent inadvertent complications. Moreover, contagion risk of some serious pathogens like hepatitis B and human immune deficiency virus always exists and cannot be excluded even in the presence of very strict procedures and measures. Although, immune reactions against autologous PRF do not arise, stringent preparation measures are mandatory to ensure sterility and to minimize pre and post-surgical infection risks. Preparation of PRF is easy and can be carried out with few instruments in the operation theater. However, GMP clean room facilities are mandatory for PRF
6 A novel graft option after pterygium excision 1611 preparation in some countries, particularly in European countries. PRF membrane is a suitable medium for microbial growth.therefore,thereisalwaysariskofspreadof infection and to minimize that risk, freshly prepared membranes must be sutured promptly without any delay. Freshly prepared PRF, even though has some similarities to conjunctiva or amniotic membrane, behaves in a different way during handling and suturing. In the learning phase, inadequate membrane suturing may cause membrane loss. In this study, membrane loss occurred in 1 case (case 5) (6.6%), in which delayed epithelialization and healing were observed in contrast to other cases. This study is a preliminary experience with the use of an autologous PRF for conjunctivoplasty after pterygium excision. Although healing responses of cases were impressive and recurrence rate was very low, some important limitations of this study must be taken into account. First, this study is an initial study andonlyalimitednumberofcaseswereincluded.a limited statistical power because of the modest sample size in the present study (n = 35) has a limiting role in significance of the statistical comparisons. A post hoc power analysis, with an observed effect size (0.267), resulted that an n of ~ 180 would be needed to obtain statistical power at the recommended 0.80 level. Resultsofthisstudy,considering its insufficient sample size and inadequate power, must be interpreted with due skepticism. Future randomized studies, employing larger sample sizes, and powerful enough to reach a robust decision, will yield more steadfast conclusions. Second, in the current study PRF grafting compared with only one autologous method and differences between other alternative methods remains to be compared. Third, patients with primary pterygium were enrolled in this study and results cannot be generalized to the cases with recurrent pterygium. Finally, long-term results are important when making choices among different alternative therapies, and this study covers only a mean of 14 months follow-up period. As a result, this initial study showed encouraging results and gave a positive impression that PRF grafting in pterygium surgery was a novel, simple, easily applicable, and a promising method with low rates of recurrence and complication. Prospective long-term follow-up studies that additionally compare other techniques with the PRF in larger case groups are required to understand the advantages of PRF grafting in pterygium surgery. Summary What was known before K Conjunctival autografts, conjunctival-limbal autografts, and amniotic membrane are the most preferred graft materials after pterygium excision. K Platelet-rich fibrin (PRF) has been used in oral, ear nose throat, orthopedic, and plastic surgeries as a graft biomaterial, however, it has not been employed for pterygium surgery until now. What this study adds K PRF grafting after pterygium excision is a simple, easily applicable, and a promising method with low rates of recurrence and complications. K PRF is a novel autologous biomaterial and a suturable membrane for ocular surface reconstruction after pterygium excision. Conflict of interest The authors declare no conflict of interest. Acknowledgements We would like to thank Duygu Kiliç for her help and advice on statistical analysis. References 1 Di Girolamo N, Chui J, Coroneo MT, Wakefield D. Pathogenesis of pterygia: role of cytokines, growth factors, and matrix metalloproteinases. Prog Retin Res 2004; 23: Kim KW, Park SH, Kim JC. Fibroblast biology in pterygia. Exp Res 2016; 142: Li L, Zhong H, Tian E, Yu M, Yuan Y, Yang W et al. Five-year incidence and predictors for pterygium in a rural community in China: the Yunnan minority eye study. Cornea 2015; 34 (12): Serghiou S, Patel CJ, Tan YY, Koay P, Ioannidis JP. Fieldwide meta-analyses of observational associations can map selective availability of risk factors and the impact of model specifications. J Clin Epidemiol 2016; 71: Chui J, Di Girolamo N, Wakefield D, Coroneo MT. The pathogenesis of pterygium: current concepts and their therapeutic implications. Ocul Surf 2008; 6: Hirst LW, Axelsen Ra, Schwab I. Pterygium and associated ocular surface squamous neoplasia. Arch Ophthalmol 2009; 127: Ando R, Kase S, Ohashi T, Dong Z, Fukuhara J, Kanda A et al. Tissue factor expression in human pterygium. Mol Vis 2011; 17: Mahdy MES, Bhatia J. Treatment of primary pterygium: role of limbal stem cells and conjunctival autograft transplantation. Oman J Ophthalmol 2009; 2: Taylan Sekeroglu H, Erdem E, Dogan NC, Yagmur M, Ersoz R, Dogan A. Sutureless amniotic membrane transplantation
7 1612 A novel graft option after pterygium excision combined with narrow-strip conjunctival autograft for pterygium. Int Ophthalmol 2011; 31: Dohan DM, Choukroun J, Diss A, Dohan SL, Dohan AJ, Mouhyi J et al. Platelet-rich fibrin (PRF): a second-generation platelet concentrate. Part I: technological concepts and evolution. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2006; 101: e Prakash S, Thakur A. Platelet concentrates: past, present and future. J Maxillofac Oral Surg 2011; 10: Clark RA. Fibrin and wound healing. Ann NY Acad Sci 2001; 936: Öncü E, Alaaddinoğlu E. The effect of platelet-rich fibrin on implant stability. Int J Oral Maxillofac Implants 2015; 30: Dohan Ehrenfest DM, Doglioli P, de Peppo GM, Del Corso M, Charrier J-B. Choukroun s platelet-rich fibrin (PRF) stimulates in vitro proliferation and differentiation of human oral bone mesenchymal stem cell in a dose-dependent way. Arch Oral Biol 2010; 55: Efron N (eds). Contact Lens Practice, 2nd ed. Butterworth- Heinemann: Oxford, UK, Said DG, Faraj La, Elalfy MS, Yeung A, Miri A, Fares U et al. Intra-lesional 5 fluorouracil for the management of recurrent pterygium. (Lond) 2013; 27: Alpay A, Uğurbaş SH, Erdoğan B. Comparing techniques for pterygium surgery. Clin Ophthalmol 2009; 3: Kwon SH, Kim HK. Analysis of recurrence patterns following pterygium surgery with conjunctival autografts. Medicine (Baltimore) 2015; 94(4): e Ling S, Li Q, Lin H, Li W, Wang T, Ye H et al. Comparative evaluation of lymphatic vessels in primary versus recurrent pterygium. (Lond) 2012; 26(11): Tsim NC, Young AL, Jhanji V, Ho M, Cheng LL. Combined conjunctival rotational autograft with 0.02% mitomycin C in primary pterygium surgery: a long-term follow-up study. Br J Ophthalmol 2015; 99(10): Kenyon KR, Wagoner MD, Hettinger ME. Conjunctival autograft transplantation for advanced and recurrent pterygium. Ophthalmology 1985; 92: Hall RC, Logan AJ, Wells AP. Comparison of fibrin glue with sutures for pterygium excision surgery with conjunctival autografts. Clin Exp Ophthalmol 2009; 37: Lee HJ, Choi BH, Jung JH, Zhu SJ, Lee SH, Huh JY et al. Maxillary sinus floor augmentation using autogenous bone grafts and platelet-enriched fibrin glue with simultaneous implant placement. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2007; 103: Prabhasawat P, Barton K, Burkett G, Tseng SC. Comparison of conjunctival autografts, amniotic membrane grafts, and primary closure for pterygium excision. Ophthalmology 1997; 104: Kurna SA, Altun A, Aksu B, Kurna R, Sengor T. Comparing treatment options of pterygium: limbal sliding flap transplantation, primary closing, and amniotic membrane grafting. Eur J Ophthalmol 2013; 23: Kocamis O, Bilgec M. Evaluation of the recurrence rate for pterygium treated with conjunctival autograft. Graefes Arch Clin Exp Ophthalmol 2014; 252: Kaufman SC, Jacobs DS, Lee WB, Deng SX, Rosenblatt MI, Shtein RM. Options and adjuvants in surgery for pterygium: a report by the American Academy of Ophthalmology. Ophthalmology 2013; 120: Tsim NC, Young AL, Jhanji V, Ho M, Cheng LL. Combined conjunctival rotational autograft with 0.02% mitomycin C in primary pterygium surgery: a long-term follow-up study. Br J Ophthalmol 2015; 99: El-Sharkawy H, Kantarci A, Deady J, Hasturk H, Liu H, Alshahat M et al. Platelet-rich plasma: growth factors and pro- and anti-inflammatory properties. J Periodontol 2007; 78: Naik B, Karunakar P, Jayadev M, Marshal VR. Role of platelet rich fibrin in wound healing: a critical review. J Conserv Dent 2013; 16:
Original Research Article
 STUDY OF EPITHELIAL PHENOTYPE AFTER PTERYGIUM EXCISION BY USING CONJUNCTIVAL IMPRESSION CYTOLOGY. Dr. Sachin O. Agrawal*, Dr. Sudhir Pendke, Dr. Ravi Chauhan Department of Ophthalmology, Indira Gandhi
STUDY OF EPITHELIAL PHENOTYPE AFTER PTERYGIUM EXCISION BY USING CONJUNCTIVAL IMPRESSION CYTOLOGY. Dr. Sachin O. Agrawal*, Dr. Sudhir Pendke, Dr. Ravi Chauhan Department of Ophthalmology, Indira Gandhi
Clinical study of sutureless and glue free conjunctival autograft in pterygium surgery
 Original Article Clinical udy of sutureless and glue free conjunctival autograft in pterygium surgery Satish Desai 1*, Amol T Wanjari 2 1 Assiant Professor, PG. Student, Department of Ophthalmology, Government
Original Article Clinical udy of sutureless and glue free conjunctival autograft in pterygium surgery Satish Desai 1*, Amol T Wanjari 2 1 Assiant Professor, PG. Student, Department of Ophthalmology, Government
The recurrence of pterygium after different modalities of surgical treatment
 Saudi Journal of Ophthalmology (2011) 25, 411 415 King Saud University Saudi Journal of Ophthalmology www.saudiophthaljournal.com www.ksu.edu.sa www.sciencedirect.com ORIGINAL ARTICLE The recurrence of
Saudi Journal of Ophthalmology (2011) 25, 411 415 King Saud University Saudi Journal of Ophthalmology www.saudiophthaljournal.com www.ksu.edu.sa www.sciencedirect.com ORIGINAL ARTICLE The recurrence of
JMSCR Volume 03 Issue 01 Page January 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Pterygium Excision and Conjunctival Autograft A Study Authors Dr. M. Premanandam 1, Dr. A. Geetha 2, Dr. Himabindu 3 1 MS, Associate Professor,
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Pterygium Excision and Conjunctival Autograft A Study Authors Dr. M. Premanandam 1, Dr. A. Geetha 2, Dr. Himabindu 3 1 MS, Associate Professor,
Suture Less and Glue Free Limbal Conjunctival Autografting following Pterygium Excision
 ORIGINALARTICLE Suture Less and Glue Free Limbal Conjunctival Autografting following Pterygium Excision Ashok Sharma, Hans Raj, Amit Vikram Raina Abstract A prospective interventional self-control study
ORIGINALARTICLE Suture Less and Glue Free Limbal Conjunctival Autografting following Pterygium Excision Ashok Sharma, Hans Raj, Amit Vikram Raina Abstract A prospective interventional self-control study
Pterygium Excision and Conjunctival-Limbal Autograft Transplantation: A Simplified Technique
 Pterygium Excision and Conjunctival-Limbal Autograft Transplantation: A Simplified Technique Kirti Nath Jha Professor of Ophthalmology Mahatma Gandhi Medical College & Research Institute,Pondy-Cuddalore
Pterygium Excision and Conjunctival-Limbal Autograft Transplantation: A Simplified Technique Kirti Nath Jha Professor of Ophthalmology Mahatma Gandhi Medical College & Research Institute,Pondy-Cuddalore
Outcome of surgical management of pterygium in Brunei Darussalam
 Original Article Brunei Int Med J. 2011; 7 (1): 8-14 Outcome of surgical management of pterygium in Brunei Darussalam Mohan RAMALINGAM, Nayan JOSHI, Jayasree NAIR, Nadir Ali Mohamad ALI Department of Ophthalmology,
Original Article Brunei Int Med J. 2011; 7 (1): 8-14 Outcome of surgical management of pterygium in Brunei Darussalam Mohan RAMALINGAM, Nayan JOSHI, Jayasree NAIR, Nadir Ali Mohamad ALI Department of Ophthalmology,
Conventional and Autograft Surgery for Pterygium: A Prospective Comparative Study
 Original Research Article Conventional and Autograft Surgery for Pterygium: A Prospective Comparative Study Farhat Abrar Assistant Professor, Department of Ophthalmology, Teerthanker Mahaveer Medical College
Original Research Article Conventional and Autograft Surgery for Pterygium: A Prospective Comparative Study Farhat Abrar Assistant Professor, Department of Ophthalmology, Teerthanker Mahaveer Medical College
Leukocyte - Platelet Rich Fibrin
 INTRA-LOCK Leukocyte - Platelet Rich Fibrin L-PRF is a 3-D autogenous combination of Platelet Rich Fibrin derived from the patient s blood 1. A simplifi ed chairside procedure results in the production
INTRA-LOCK Leukocyte - Platelet Rich Fibrin L-PRF is a 3-D autogenous combination of Platelet Rich Fibrin derived from the patient s blood 1. A simplifi ed chairside procedure results in the production
Comparison of Two Methods for the Treatment of Primary Pterygium: Amniotic Membrane Transplantation plus Intraoperative Mitomycin C, versus
 Comparison of Two Methods for the Treatment of Primary Pterygium: Amniotic Membrane Transplantation plus Intraoperative Mitomycin C, versus Conjunctival Rotational Autograft plus Intraoperative Mitomycin
Comparison of Two Methods for the Treatment of Primary Pterygium: Amniotic Membrane Transplantation plus Intraoperative Mitomycin C, versus Conjunctival Rotational Autograft plus Intraoperative Mitomycin
Comparative Study on the Use of Conjunctival Autograft With or Without Mitomycin-C in Pterygium Surgery
 Original Article Philippine Journal of OPHTHALMOLOGY Comparative Study on the Use of Conjunctival Autograft With or Without Mitomycin-C in Pterygium Surgery Archimedes L.D. Agahan, MD, Pamela P. Astudillo,
Original Article Philippine Journal of OPHTHALMOLOGY Comparative Study on the Use of Conjunctival Autograft With or Without Mitomycin-C in Pterygium Surgery Archimedes L.D. Agahan, MD, Pamela P. Astudillo,
Outcome of conjunctival autograft sutured with polyamide black sutures in pterygium surgery
 Original article Outcome of conjunctival autograft sutured with polyamide black sutures in pterygium surgery Department of Ophthalmology, Hassan Institute of Medical Sciences Hassan, Karnataka, India Abstract
Original article Outcome of conjunctival autograft sutured with polyamide black sutures in pterygium surgery Department of Ophthalmology, Hassan Institute of Medical Sciences Hassan, Karnataka, India Abstract
Reducing Postoperative Pterygium Recurrence: Comparison of Free Conjunctival Auto-Graft and Conjunctival Rotation Flap Techniques
 ORIGINAL ARTICLE Reducing Postoperative Pterygium Recurrence: Comparison of Free Conjunctival Auto-Graft and Conjunctival Rotation Flap Techniques Waseem Akhter, Ali Tayyab, Ayisha Kausar and Amena Masrur
ORIGINAL ARTICLE Reducing Postoperative Pterygium Recurrence: Comparison of Free Conjunctival Auto-Graft and Conjunctival Rotation Flap Techniques Waseem Akhter, Ali Tayyab, Ayisha Kausar and Amena Masrur
CLOSURE OF OROANTRAL COMMUNICATION WITH PLATELET-RICH FIBRIN
 Original rticle International Journal of Dental and Health Sciences Volume 03,Issue 05 CLOSURE OF ORONTRL COMMUNICTION WITH PLTELET-RICH FIRIN Waseem itar 1, Mounzer ssad 2 1. MSc, Department of oral and
Original rticle International Journal of Dental and Health Sciences Volume 03,Issue 05 CLOSURE OF ORONTRL COMMUNICTION WITH PLTELET-RICH FIRIN Waseem itar 1, Mounzer ssad 2 1. MSc, Department of oral and
PRACTICE GUIDELINES AND STANDARDS OF CARE FOR PTERYGIUM
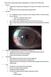 PRACTICE GUIDELINES AND STANDARDS OF CARE FOR PTERYGIUM I. II. Definition a. Triangular, fleshy, fibrovascular sheet originating from the conjunctiva and extending to corneal limbus and beyond. b. Typically
PRACTICE GUIDELINES AND STANDARDS OF CARE FOR PTERYGIUM I. II. Definition a. Triangular, fleshy, fibrovascular sheet originating from the conjunctiva and extending to corneal limbus and beyond. b. Typically
PRP Usage in Today's Implantology
 Volume 1, December 2004 www.implant.co.il PRP Usage in Today's Implantology by Dr. R. Shapira Introduction: Treating patients suffering from hematological disorders or using anticoagulant medications always
Volume 1, December 2004 www.implant.co.il PRP Usage in Today's Implantology by Dr. R. Shapira Introduction: Treating patients suffering from hematological disorders or using anticoagulant medications always
Amniotic membrane transplantation (AMT) without the use of sutures/fibrin glue
 Original article Amniotic membrane transplantation (AMT) without the use of sutures/fibrin glue Ajai Agrawal 1, VB Pratap 2 1 Department of Ophthalmology, Kalpana Chawla Government Medical College, Karnal,
Original article Amniotic membrane transplantation (AMT) without the use of sutures/fibrin glue Ajai Agrawal 1, VB Pratap 2 1 Department of Ophthalmology, Kalpana Chawla Government Medical College, Karnal,
Cut and Paste: No Suture, No Glue Conjunctival Autograft Technique for Pterygium Surgery - Our Experience
 Cut and Paste: No Suture, No Glue Conjunctival Autograft Technique for Pterygium Surgery - Our Experience Satish D Shet, Piyush Gupta, Yallappa B Bajantri, S Sahana ORIGINAL ARTICLE ABSTRACT Background:
Cut and Paste: No Suture, No Glue Conjunctival Autograft Technique for Pterygium Surgery - Our Experience Satish D Shet, Piyush Gupta, Yallappa B Bajantri, S Sahana ORIGINAL ARTICLE ABSTRACT Background:
Comparison of the surgical outcome between Wet Amniotic Membrane Graft (Wet AMG), Conjunctival Autograft (CAG) and Topical Mitomycin C (MMC)
 Original article Comparison of the surgical outcome between Wet Amniotic Membrane Graft (Wet AMG), Conjunctival Autograft (CAG) and Topical Mitomycin C (MMC) 1 Dr Pavitra Patel*, 2 Dr Sachin Daigavane,
Original article Comparison of the surgical outcome between Wet Amniotic Membrane Graft (Wet AMG), Conjunctival Autograft (CAG) and Topical Mitomycin C (MMC) 1 Dr Pavitra Patel*, 2 Dr Sachin Daigavane,
Pterygium is a degenerative disease of conjunctiva,
 Original Article A new technique of sutureless and glueless conjunctival autografting in pterygium surgery by thermocautery Arunava Kundu 1, Krishna Kanta Roy 1, Nazneen Nazm 1, Sampurna Mukherjee 1, Biplab
Original Article A new technique of sutureless and glueless conjunctival autografting in pterygium surgery by thermocautery Arunava Kundu 1, Krishna Kanta Roy 1, Nazneen Nazm 1, Sampurna Mukherjee 1, Biplab
Bone augmentation with maxgraft
 Patient information bone & tissue regeneration botiss biomaterials Bone augmentation with maxgraft established safe X100 natural Implantation stability is crucial for success Atrophy of the jaw bone loss
Patient information bone & tissue regeneration botiss biomaterials Bone augmentation with maxgraft established safe X100 natural Implantation stability is crucial for success Atrophy of the jaw bone loss
Surgical management of pterygium in a rural hospital using bare sclera versus conjunctival autograft technique
 International Journal of Research in Medical Sciences Dinesh P et al. Int J Res Med Sci. 2017May;5(5):2076-2080 www.msjonline.org pissn2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20171845
International Journal of Research in Medical Sciences Dinesh P et al. Int J Res Med Sci. 2017May;5(5):2076-2080 www.msjonline.org pissn2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20171845
Platelet-rich fibrin membrane in immediate dental implant loading
 original article Platelet-rich fibrin membrane in immediate dental implant loading Carlos Fernando de Almeida Barros MOURÃO 1, Natália Belmock Mascarenhas Freitas MOURÃO 2 104 Abstract / Introduction:
original article Platelet-rich fibrin membrane in immediate dental implant loading Carlos Fernando de Almeida Barros MOURÃO 1, Natália Belmock Mascarenhas Freitas MOURÃO 2 104 Abstract / Introduction:
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 3/ Issue 13/Mar 31, 2014 Page 3529
 CONJUNCTIVAL AUTOGRAFT FIXATION WITH PROTEIN COAGULATION AND BLOOD FIBRIN AS TISSUE ADHESIVE IN PTERYGIUM SURGERY Sooraj Singh Kubrey 1, Kavita Kumar 2, Shubhangi Kursange 3, Laxman Soni 4, Sanchit 5 HOW
CONJUNCTIVAL AUTOGRAFT FIXATION WITH PROTEIN COAGULATION AND BLOOD FIBRIN AS TISSUE ADHESIVE IN PTERYGIUM SURGERY Sooraj Singh Kubrey 1, Kavita Kumar 2, Shubhangi Kursange 3, Laxman Soni 4, Sanchit 5 HOW
Comparative Study of Amniotic Membrane Graft
 ORIGINAL RESEARCH Comparative Study of Giridhar Bellamkonda 1, Pragathi Kontham 2 ABSTRACT Introduction: Surgical excision remains principal mode of treatment for pterygium. Various techniques have been
ORIGINAL RESEARCH Comparative Study of Giridhar Bellamkonda 1, Pragathi Kontham 2 ABSTRACT Introduction: Surgical excision remains principal mode of treatment for pterygium. Various techniques have been
Comparison of prognostic value of Roper Hall and Dua classification systems in acute ocular burns
 1 Cornea and Refractive Surgery Services, Dr Rajendra Prasad Centre for Ophthalmic Sciences, All India Institute of Medical Sciences, New Delhi, India 2 Department of Biostatistics, All India Institute
1 Cornea and Refractive Surgery Services, Dr Rajendra Prasad Centre for Ophthalmic Sciences, All India Institute of Medical Sciences, New Delhi, India 2 Department of Biostatistics, All India Institute
Pattern of bone resorption after extraction
 Teeth loss Pattern of bone resorption after extraction 50% in 1st year 2/ 3 in first 3 months Reich KM, Huber CD, Lippnig WR, Um C, Watzek G, Tangl S. (2011, 17). Atrophy of Residual Alveolar Ridge following
Teeth loss Pattern of bone resorption after extraction 50% in 1st year 2/ 3 in first 3 months Reich KM, Huber CD, Lippnig WR, Um C, Watzek G, Tangl S. (2011, 17). Atrophy of Residual Alveolar Ridge following
Table 1. Characteristics of patients. Postoperative Comorbidity acuity band keratopathy. Visual Cause of. Case Age (Yr) Sex F/U (Month)
 착색양막을이용한띠각막병증의미용적치료 1459 Table 1. Characteristics of patients Case Age (Yr) Sex F/U (Month) Visual Cause of Postoperative Comorbidity acuity band keratopathy complications 1 19 M 13 NLP * PHPV Injection,
착색양막을이용한띠각막병증의미용적치료 1459 Table 1. Characteristics of patients Case Age (Yr) Sex F/U (Month) Visual Cause of Postoperative Comorbidity acuity band keratopathy complications 1 19 M 13 NLP * PHPV Injection,
Limbal-Conjunctival Autograft Transplantation for the Management of Primary Pterygium
 Limbal-Conjunctival Autograft Transplantation for the Management of Primary Pterygium Mahmoud Jabbarvand, MD, 1 Mohammad-Reza Khalili, MD 2 Mohammad-Taher Rajabi, MD 3 Abstract Purpose: To investigate
Limbal-Conjunctival Autograft Transplantation for the Management of Primary Pterygium Mahmoud Jabbarvand, MD, 1 Mohammad-Reza Khalili, MD 2 Mohammad-Taher Rajabi, MD 3 Abstract Purpose: To investigate
A Case Report of Recurrent Conjunctival Squamous Cell Carcinoma M Zhao 1, W Lin 2 *, Z Liu 2 ABSTRACT
 A Case Report of Recurrent Conjunctival Squamous Cell Carcinoma M Zhao 1, W Lin 2 *, Z Liu 2 ABSTRACT A case of recurrent squamous cell carcinoma of the conjunctiva is presented here. A 13-yearsold male
A Case Report of Recurrent Conjunctival Squamous Cell Carcinoma M Zhao 1, W Lin 2 *, Z Liu 2 ABSTRACT A case of recurrent squamous cell carcinoma of the conjunctiva is presented here. A 13-yearsold male
CHOUKROUN PRF SYSTEM
 CHOUKROUN PRF SYSTEM New DUO Centrifuge Customizable centrifuge! push button 4 colors panels are included with your DUO color code Bowl Mini tray Blood Collector Scissors THE CONCEPT The concept of CHOUKROUN
CHOUKROUN PRF SYSTEM New DUO Centrifuge Customizable centrifuge! push button 4 colors panels are included with your DUO color code Bowl Mini tray Blood Collector Scissors THE CONCEPT The concept of CHOUKROUN
STAB INCISION GLAUCOMA SURGERY (SIGS)
 STAB INCISION GLAUCOMA SURGERY (SIGS) Dr. Soosan Jacob, MS, FRCS, DNB Senior Consultant Ophthalmologist, Dr. Agarwal's Eye Hospital, Chennai, India dr_soosanj@hotmail.com Videos available in Youtube channel:
STAB INCISION GLAUCOMA SURGERY (SIGS) Dr. Soosan Jacob, MS, FRCS, DNB Senior Consultant Ophthalmologist, Dr. Agarwal's Eye Hospital, Chennai, India dr_soosanj@hotmail.com Videos available in Youtube channel:
CORNEAL CONDITIONS CORNEAL TRANSPLANTATION
 GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
Young patient s age determines pterygium recurrence after surgery.
 Young patient s age determines pterygium recurrence after surgery. Anguria P 1, Ntuli S 2, Carmichael T 1 1. Department of Neurosciences, Division of Ophthalmology, University of the Witwatersrand Johannesburg,
Young patient s age determines pterygium recurrence after surgery. Anguria P 1, Ntuli S 2, Carmichael T 1 1. Department of Neurosciences, Division of Ophthalmology, University of the Witwatersrand Johannesburg,
John Rawstron Christchurch 2015
 John Rawstron Christchurch 2015 John Rawstron Christchurch 2015 Nasal and temporal pterygiae (medial and lateral) pingueculum Body Neck Head Cap/hood Iles de Fuchs Stocker s line Pathogenesis UV light
John Rawstron Christchurch 2015 John Rawstron Christchurch 2015 Nasal and temporal pterygiae (medial and lateral) pingueculum Body Neck Head Cap/hood Iles de Fuchs Stocker s line Pathogenesis UV light
Pterygium Excision with Autologous Blood Autograft Fixation: Experience of a District Hospital of Bangladesh
 Original Article Pterygium Excision with Autologous Blood Autograft Fixation: Experience of a District Hospital of Bangladesh Huda MMU 1, Khaleque SA 2 Abstract A prospective interventional self-control
Original Article Pterygium Excision with Autologous Blood Autograft Fixation: Experience of a District Hospital of Bangladesh Huda MMU 1, Khaleque SA 2 Abstract A prospective interventional self-control
Post-operative outcomes of pterygium surgery using autologous blood and sutures: A comparative study
 Original Research Article Post-operative outcomes of pterygium surgery using autologous blood and sutures: A comparative study Pankaj Kumar 1,*, Shanti Pandey 2, GS Titiyal 3, Vivekanand Satyawali 4 1
Original Research Article Post-operative outcomes of pterygium surgery using autologous blood and sutures: A comparative study Pankaj Kumar 1,*, Shanti Pandey 2, GS Titiyal 3, Vivekanand Satyawali 4 1
L-PRF Leukocyte-Platelet Rich Fibrin
 Patient information bone & tissue regeneration botiss biomaterials L-PRF Leukocyte-Platelet Rich Fibrin innovative How to naturally support wound healing safe natural Wound healing What happens when a
Patient information bone & tissue regeneration botiss biomaterials L-PRF Leukocyte-Platelet Rich Fibrin innovative How to naturally support wound healing safe natural Wound healing What happens when a
Ocular Surface Reconstruction
 OCULAR SURFACE From Tissue Transplantation to Cell Therapy Abraham Solomon, MD Abstract: The most difficult part in ocular surface reconstruction for total limbal stem cell deficiency is restoring a healthy
OCULAR SURFACE From Tissue Transplantation to Cell Therapy Abraham Solomon, MD Abstract: The most difficult part in ocular surface reconstruction for total limbal stem cell deficiency is restoring a healthy
Subject Index. Atopic keratoconjunctivitis (AKC) management 16 overview 15
 Subject Index Acanthamoeba keratitis, see Infective keratitis Acute allergic conjunctivitis AKC, see Atopic keratoconjunctivitis Allergy acute allergic conjunctivitis 15 atopic keratoconjunctivitis 15
Subject Index Acanthamoeba keratitis, see Infective keratitis Acute allergic conjunctivitis AKC, see Atopic keratoconjunctivitis Allergy acute allergic conjunctivitis 15 atopic keratoconjunctivitis 15
Senile: flattening of vertical meridian, thinning of periphery, lack of luster
 Pterygia Etiology: triangular, fibrovascular, connective tissue overgrowths of bulbar conjunctiva onto cornea; distribution of ultraviolet energy- heat, wind, dust, dry atmosphere,higher prevalence nearer
Pterygia Etiology: triangular, fibrovascular, connective tissue overgrowths of bulbar conjunctiva onto cornea; distribution of ultraviolet energy- heat, wind, dust, dry atmosphere,higher prevalence nearer
Clinical and histologic evaluations of healing in an extraction socket filled with platelet-rich fibrin
 Journal of Dental Sciences (2011) 6, 116e122 available at www.sciencedirect.com journal homepage: www.e-jds.com Case Report Clinical and histologic evaluations of healing in an extraction socket filled
Journal of Dental Sciences (2011) 6, 116e122 available at www.sciencedirect.com journal homepage: www.e-jds.com Case Report Clinical and histologic evaluations of healing in an extraction socket filled
Prevalence of Pterygium and Outcome of Pterygium Surgery in Hilly Western Nepal: A Hospital based Study
 https://doi.org/10.22502/jlmc.v5i1.120 Original Research Article Prevalence of Pterygium and Outcome of Pterygium Surgery in Hilly Western Nepal: A Hospital based Study Laxmi Devi Manandhar, a Salma KC
https://doi.org/10.22502/jlmc.v5i1.120 Original Research Article Prevalence of Pterygium and Outcome of Pterygium Surgery in Hilly Western Nepal: A Hospital based Study Laxmi Devi Manandhar, a Salma KC
Fitting Keratoconus and Other Complicated Corneas
 Fitting Keratoconus and Other Complicated Corneas Christine W Sindt OD FAAO Professor, Clinical Ophthalmology Director, Contact Lens Service University of Iowa Disclosure Consultant: ALCON Vision Care
Fitting Keratoconus and Other Complicated Corneas Christine W Sindt OD FAAO Professor, Clinical Ophthalmology Director, Contact Lens Service University of Iowa Disclosure Consultant: ALCON Vision Care
Bone augmentation with biomaterials
 Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
Amniotic Membrane Transplantation In Ocular Surface Disorders
 Orginal Article Amniotic Membrane Transplantation In Ocular Surface Disorders Khalid Iqbal Talpur, Faiz Muhammad Halepota, Muhammad Pak J Ophthalmol 2005, Vol. 22 No. 3.................................................................................................
Orginal Article Amniotic Membrane Transplantation In Ocular Surface Disorders Khalid Iqbal Talpur, Faiz Muhammad Halepota, Muhammad Pak J Ophthalmol 2005, Vol. 22 No. 3.................................................................................................
PRE-DESCEMET S ENDOTHELIAL KERATOPLASTY (PDEK) DR ASHVIN AGARWAL
 PRE-DESCEMET S ENDOTHELIAL KERATOPLASTY (PDEK) DR ASHVIN AGARWAL Endothelial keratoplasty (EK) has evolved at a brisk pace and the volume of data accumulated over the past 10 years has demonstrated that
PRE-DESCEMET S ENDOTHELIAL KERATOPLASTY (PDEK) DR ASHVIN AGARWAL Endothelial keratoplasty (EK) has evolved at a brisk pace and the volume of data accumulated over the past 10 years has demonstrated that
Optometric Postoperative Cataract Surgery Management
 Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Topical anesthetic agent in primary pterygium surgery with autologous conjunctival graft
 ORIGINAL ARTICLE Proparacaine Hydrochloride 0.5 % as a sole topical anesthetic agent in primary pterygium surgery with autologous conjunctival graft: Our experience at tertiary care center,vadodara Aparna
ORIGINAL ARTICLE Proparacaine Hydrochloride 0.5 % as a sole topical anesthetic agent in primary pterygium surgery with autologous conjunctival graft: Our experience at tertiary care center,vadodara Aparna
The Clinical Application of Platelet-Rich Fibrin (Prf) and Allograft In Treatment Of Bony Defect - A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 12 Ver. IX (Dec. 2015), PP 16-20 www.iosrjournals.org The Clinical Application of Platelet-Rich
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 12 Ver. IX (Dec. 2015), PP 16-20 www.iosrjournals.org The Clinical Application of Platelet-Rich
ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT
 ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT * Mishal Piyush Shah 1 and Sheela Kumar Gujjari 2 1 Department of
ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT * Mishal Piyush Shah 1 and Sheela Kumar Gujjari 2 1 Department of
Tissue renewal and Repair. Nisamanee Charoenchon, PhD Department of Pathobiology, Faculty of Science
 Tissue renewal and Repair Nisamanee Charoenchon, PhD Email: nisamanee.cha@mahidol.ac.th Department of Pathobiology, Faculty of Science Topic Objectives 1. Describe processes of tissue repair, regeneration
Tissue renewal and Repair Nisamanee Charoenchon, PhD Email: nisamanee.cha@mahidol.ac.th Department of Pathobiology, Faculty of Science Topic Objectives 1. Describe processes of tissue repair, regeneration
CLINICAL INPUT RESPONSES
 CLINICAL INPUT RESPONSES Additional Comments With regard to the 9 indications listed above, there was lower range confidence that there is adequate evidence demonstrating that sutureless fixation human
CLINICAL INPUT RESPONSES Additional Comments With regard to the 9 indications listed above, there was lower range confidence that there is adequate evidence demonstrating that sutureless fixation human
Downloaded from Platelet-rich fibrin: A new paradigm in wound healing PLATELET-RICH FIBRIN: A NEW PARADIGM IN WOUND HEALING
 PLATELET-RICH FIBRIN: A NEW PARADIGM IN WOUND HEALING ISSN No. 2394-3971 Original Research Article Amol Manoj Karande 1, Rakshit Khandeparkar 2, Cherish Simon Vergeese 3, Hunny Jain 4. 1: Oral and Maxillofacial
PLATELET-RICH FIBRIN: A NEW PARADIGM IN WOUND HEALING ISSN No. 2394-3971 Original Research Article Amol Manoj Karande 1, Rakshit Khandeparkar 2, Cherish Simon Vergeese 3, Hunny Jain 4. 1: Oral and Maxillofacial
A study on changes in keratometry readings and astigmatism induced by pterygium before and after pterygium excision surgery
 Original Article A study on changes in keratometry readings and induced by pterygium before and after pterygium excision surgery Kshama B Popat*, Hetaj K. Sheth**, Vimal J. Vyas***, Matib M. Rangoonwala****,
Original Article A study on changes in keratometry readings and induced by pterygium before and after pterygium excision surgery Kshama B Popat*, Hetaj K. Sheth**, Vimal J. Vyas***, Matib M. Rangoonwala****,
The Original remains unique.
 The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
CLINICAL STUDY. AL Young 1,2, GYS Leung 1,2, LL Cheng 1,2, TTY Lau 1,2, PTH Lam 1,2 and DSC Lam 1,2,3
 (2009) 23, 1518 1523 & 2009 Macmillan Publishers Limited All rights reserved 0950-222X/09 $32.00 www.nature.com/eye CLINICAL STUDY Randomised controlled trial on the effectiveness of lidocaine gel vs tetracaine
(2009) 23, 1518 1523 & 2009 Macmillan Publishers Limited All rights reserved 0950-222X/09 $32.00 www.nature.com/eye CLINICAL STUDY Randomised controlled trial on the effectiveness of lidocaine gel vs tetracaine
Conjunctival displacement to the corneal side for oblique-parallel insertion in 25-gauge vitrectomy
 European Journal of Ophthalmology / Vol. 18 no. 5, 2008 / pp. 848-851 SHORT COMMUNICATIONS & CASE REPORTS Conjunctival displacement to the corneal side for oblique-parallel insertion in 25-gauge vitrectomy
European Journal of Ophthalmology / Vol. 18 no. 5, 2008 / pp. 848-851 SHORT COMMUNICATIONS & CASE REPORTS Conjunctival displacement to the corneal side for oblique-parallel insertion in 25-gauge vitrectomy
A Study to Compare Conjunctival Autografting with Sutures and Glue Free Sutureless Technique after Primary Pterygium Excision
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/573 A Study to Compare Conjunctival Autografting with Sutures and Glue Free Sutureless Technique after Primary Vasudha
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/573 A Study to Compare Conjunctival Autografting with Sutures and Glue Free Sutureless Technique after Primary Vasudha
INVELTYS (loteprednol etabonate ophthalmic suspension) 1%, for topical ophthalmic use Initial U.S. Approval: 1998
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use INVELTYS safely and effectively. See full prescribing information for INVELTYS. INVELTYS (loteprednol
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use INVELTYS safely and effectively. See full prescribing information for INVELTYS. INVELTYS (loteprednol
JMSCR Vol 05 Issue 06 Page June 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i6.141 Pterygium and Dry Eye- A Clinical Correlation
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i6.141 Pterygium and Dry Eye- A Clinical Correlation
Centre, Bhopal, India 3 Consultant at dental hospital Dubai, UAE
 DOI:10.21276/sjodr.2017.2.1.3 Saudi Journal of Oral and Dental Research Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-1300 (Print) ISSN 2518-1297
DOI:10.21276/sjodr.2017.2.1.3 Saudi Journal of Oral and Dental Research Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-1300 (Print) ISSN 2518-1297
Repeated bevacizumab injections versus mitomycin C in rotational conjunctival flap for prevention of pterygium recurrence
 AOP*** 1 Original Article Repeated bevacizumab injections versus mitomycin C in rotational conjunctival flap for prevention of pterygium recurrence Mustafa Ozsutcu, Emre Ayintap, Julide C U Akkan, Arif
AOP*** 1 Original Article Repeated bevacizumab injections versus mitomycin C in rotational conjunctival flap for prevention of pterygium recurrence Mustafa Ozsutcu, Emre Ayintap, Julide C U Akkan, Arif
Conjunctival Incisions for Strabismus Surgery: A Comparison of Techniques
 Techniques in Ophthalmology 5(3):125 129, 2007 P E D I A T R I C S U R G E R Y Conjunctival Incisions for Strabismus Surgery: A Comparison of Techniques David A. Sami, MD Pediatric Subspecialty Faculty
Techniques in Ophthalmology 5(3):125 129, 2007 P E D I A T R I C S U R G E R Y Conjunctival Incisions for Strabismus Surgery: A Comparison of Techniques David A. Sami, MD Pediatric Subspecialty Faculty
PRECISION PROGRAM. Injection Technique Quick-Reference Guide. Companion booklet for the Video Guide to Injection Technique
 Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Sutureless Intrascleral Pocket Technique of Transscleral Fixation of Intraocular Lens in Previous Vitrectomized Eyes
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(2):181-185 http://dx.doi.org/10.3341/kjo.2014.28.2.181 Case Report Sutureless Intrascleral Pocket Technique of Transscleral Fixation of Intraocular
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(2):181-185 http://dx.doi.org/10.3341/kjo.2014.28.2.181 Case Report Sutureless Intrascleral Pocket Technique of Transscleral Fixation of Intraocular
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome)
 Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Procedure Manual and Catalog
 Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
Comparative efficacy of β-irradiation and mitomycin-c in primary and recurrent pterygium
 European Journal of Ophthalmology / Vol. 11 n. 2, 2001 / pp. 126-132 Comparative efficacy of β-irradiation and mitomycin-c in primary and recurrent pterygium T. ŞIMŞEK, I. GÜNALP, H. ATILLA Department
European Journal of Ophthalmology / Vol. 11 n. 2, 2001 / pp. 126-132 Comparative efficacy of β-irradiation and mitomycin-c in primary and recurrent pterygium T. ŞIMŞEK, I. GÜNALP, H. ATILLA Department
Sclerokeratoplasty David S. Chu, M.D. Cases
 Sclerokeratoplasty David S. Chu, M.D. Cases Case 1 40 year-old female from Peru presented to our Service with inflamed OS for 2 months duration. Her symptoms began as red painful OS, which progressively
Sclerokeratoplasty David S. Chu, M.D. Cases Case 1 40 year-old female from Peru presented to our Service with inflamed OS for 2 months duration. Her symptoms began as red painful OS, which progressively
Clinical Review Criteria
 Clinical Review Criteria Autologous Platelet Derived Wound Healing Factors for Treatment of: Non Healing Cutaneous Wounds (Procuren) Non-Healing Fractures and the Associated GEM 21STM Device Platelet Rich
Clinical Review Criteria Autologous Platelet Derived Wound Healing Factors for Treatment of: Non Healing Cutaneous Wounds (Procuren) Non-Healing Fractures and the Associated GEM 21STM Device Platelet Rich
Cerasorb M DENTAL. O:\Zulassung\Cerasorb Dental Kanada 2013\Texte\Cerasorb M Dental final IFU docx
 Cerasorb M DENTAL Resorbable, pure-phase beta-tricalcium phosphate matrix with interconnecting porosity for bone regeneration for use in dental and maxillofacial surgery DESCRIPTION: Cerasorb M DENTAL
Cerasorb M DENTAL Resorbable, pure-phase beta-tricalcium phosphate matrix with interconnecting porosity for bone regeneration for use in dental and maxillofacial surgery DESCRIPTION: Cerasorb M DENTAL
Regenerative Tissue Matrix in Treatment of Wounds
 Regenerative Tissue Matrix in Treatment of Wounds Learning Objectives Differentiate between reparative and regenerative healing Review surgical techniques for applying a regenerative tissue scaffold to
Regenerative Tissue Matrix in Treatment of Wounds Learning Objectives Differentiate between reparative and regenerative healing Review surgical techniques for applying a regenerative tissue scaffold to
A Clinical Study of Conjunctival Autograft Using Fibrin Glue in Primary Pterygium Surgery
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 1 Ver. 17 January. (2018), PP 65-69 www.iosrjournals.org A Clinical Study of Conjunctival Autograft
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 1 Ver. 17 January. (2018), PP 65-69 www.iosrjournals.org A Clinical Study of Conjunctival Autograft
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS
 NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
WOUND CARE UPDATE. -Commonly Used Skin Substitute Products For Wound. -Total Contact Casting. Jack W. Hutter DPM, FACFAS, C. ped.
 WOUND CARE UPDATE -Commonly Used Skin Substitute Products For Wound Closure -Total Contact Casting Jack W. Hutter DPM, FACFAS, C. ped. Commonly Used Skin Substitute Products for Wound Closure why are they
WOUND CARE UPDATE -Commonly Used Skin Substitute Products For Wound Closure -Total Contact Casting Jack W. Hutter DPM, FACFAS, C. ped. Commonly Used Skin Substitute Products for Wound Closure why are they
History. Examination. Diagnosis/Course
 History A 51 year-old female with a history of chronic dry eyes and photosensitivity was referred for evaluation. She reported a five year history of symptoms of frequent irritation and photophobia in
History A 51 year-old female with a history of chronic dry eyes and photosensitivity was referred for evaluation. She reported a five year history of symptoms of frequent irritation and photophobia in
Comparison of Conjunctival Autograft and Intra-Operative Application of Mitomycin-C in Treatment of Primary Pterygium
 Original Article Comparison of Conjunctival Autograft and Intra-Operative Application of Mitomycin-C in Treatment of Primary Pterygium Zeeshan Kamil, Syeda Aisha Bokhari, Fawad Rizvi Pak J Ophthalmol 2011,
Original Article Comparison of Conjunctival Autograft and Intra-Operative Application of Mitomycin-C in Treatment of Primary Pterygium Zeeshan Kamil, Syeda Aisha Bokhari, Fawad Rizvi Pak J Ophthalmol 2011,
Long-term results of autologous cultivated oral mucosal epithelial transplantation in the scar phase of severe ocular surface disorders
 1 Department of Ophthalmology, Kyoto Prefectural University of Medicine, Graduate School of Medicine, Kyoto, Japan 2 Research Center for Inflammation and Regenerative Medicine, Doshisha University, Kyoto,
1 Department of Ophthalmology, Kyoto Prefectural University of Medicine, Graduate School of Medicine, Kyoto, Japan 2 Research Center for Inflammation and Regenerative Medicine, Doshisha University, Kyoto,
Clinical Usage Experience and Evaluation of Application of Platelet Rich Plasma Gel in Impacted Tooth Extraction: A Preliminary Study
 Fukui et al., Platelet-rich Plasma in Tooth Extraction ORIGINAL ARTICLE Clinical Usage Experience and Evaluation of Application of Platelet Rich Plasma Gel in Impacted Tooth Extraction: A Preliminary Study
Fukui et al., Platelet-rich Plasma in Tooth Extraction ORIGINAL ARTICLE Clinical Usage Experience and Evaluation of Application of Platelet Rich Plasma Gel in Impacted Tooth Extraction: A Preliminary Study
Case Report Managing Drawbacks in Unconventional Successful Glaucoma Surgery: A Case Report of Stent Exposure
 Case Reports in Ophthalmological Medicine Volume 2015, Article ID 847439, 4 pages http://dx.doi.org/10.1155/2015/847439 Case Report Managing Drawbacks in Unconventional Successful Glaucoma Surgery: A Case
Case Reports in Ophthalmological Medicine Volume 2015, Article ID 847439, 4 pages http://dx.doi.org/10.1155/2015/847439 Case Report Managing Drawbacks in Unconventional Successful Glaucoma Surgery: A Case
Case no.4. Subjective. Subjective (2) Caucasian female, 62 Y.O., consulting for a XXX opinion on her condition.
 Case no.4 Contact lenses: cause Subjective Caucasian female, 62 Y.O., consulting for a XXX opinion on her condition. Works as a lab technician for a veterenary surgeon No exposure to chemicals Had been
Case no.4 Contact lenses: cause Subjective Caucasian female, 62 Y.O., consulting for a XXX opinion on her condition. Works as a lab technician for a veterenary surgeon No exposure to chemicals Had been
EX-PRESS Glaucoma Filtration Device Surgical Procedure
 EX-PRESS Glaucoma Filtration Device Surgical Procedure Surgical Recommendations EX-PRESS Glaucoma Filtration Device preloaded device (plus 1 back-up) Sterile caliper Lid speculum Corneal forceps 0.12 forceps
EX-PRESS Glaucoma Filtration Device Surgical Procedure Surgical Recommendations EX-PRESS Glaucoma Filtration Device preloaded device (plus 1 back-up) Sterile caliper Lid speculum Corneal forceps 0.12 forceps
The Case FOR Oncoplastic Surgery in Small Breasts. Barbara L. Smith, MD, PhD Massachusetts General Hospital Harvard Medical School Boston, MA USA
 The Case FOR Oncoplastic Surgery in Small Breasts Barbara L. Smith, MD, PhD Massachusetts General Hospital Harvard Medical School Boston, MA USA Changing issues in breast cancer management Early detection
The Case FOR Oncoplastic Surgery in Small Breasts Barbara L. Smith, MD, PhD Massachusetts General Hospital Harvard Medical School Boston, MA USA Changing issues in breast cancer management Early detection
Pharmacologyonline 2: (2008) Young Researchers Gavasova and Budev EPULIS FISSURATUM CLINICAL APPEARANCE AND TREATMENT. Dr G.Gavasova, Dr I.
 EPULIS FISSURATUM CLINICAL APPEARANCE AND TREATMENT Dr G.Gavasova, Dr I.Budev Medical University, Faculty of Dental Medicine Oral Surgery Department Head: Prof. Dr D. Atanasov, Ph.D, MD. Summary Continuous
EPULIS FISSURATUM CLINICAL APPEARANCE AND TREATMENT Dr G.Gavasova, Dr I.Budev Medical University, Faculty of Dental Medicine Oral Surgery Department Head: Prof. Dr D. Atanasov, Ph.D, MD. Summary Continuous
Novel therapies for the treatment of persistent corneal epithelial defects
 Novel therapies for the treatment of persistent corneal epithelial defects Disclosures I have no financial interests in any of the techniques or products discussed. Bennie H. Jeng, M.D. Associate Professor
Novel therapies for the treatment of persistent corneal epithelial defects Disclosures I have no financial interests in any of the techniques or products discussed. Bennie H. Jeng, M.D. Associate Professor
BIOLOGICS STEM CELL AND PLATELET- RICH PLASMA FOR JOINT MANAGEMENT 1/10/ AAOS ANNUAL MEETING 2018 AAOS ANNUAL MEETING
 STEM CELL AND PLATELET- RICH PLASMA FOR JOINT MANAGEMENT BIOLOGICS o Injectable therapies that may suppress inflammation and promote regenerative pathways o Natural products that are harvested and are
STEM CELL AND PLATELET- RICH PLASMA FOR JOINT MANAGEMENT BIOLOGICS o Injectable therapies that may suppress inflammation and promote regenerative pathways o Natural products that are harvested and are
Injection Techniques Principles and Practice. Introduction. Learning Objectives 5/18/2015. Richard E. Castillo, OD, DO
 Injection Techniques Principles and Practice Richard E. Castillo, OD, DO Administering injections is considered a routine clinic activity Safety demands knowledge of: Anatomy & Physiology Pharmacology
Injection Techniques Principles and Practice Richard E. Castillo, OD, DO Administering injections is considered a routine clinic activity Safety demands knowledge of: Anatomy & Physiology Pharmacology
BEGO BIOMATERIALS When the result counts
 BEGO BIOMATERIALS When the result counts Partners in Progress INTRO Challenge what exists get the right answers We practise systematic thinking with a passion and we are never satisfied with the status
BEGO BIOMATERIALS When the result counts Partners in Progress INTRO Challenge what exists get the right answers We practise systematic thinking with a passion and we are never satisfied with the status
MULLERS MUSCLE-CONJUNCTIVAL RESECTION PTOSIS PROCEDURE
 Australian and New Zealand Journal of Ouhthalmology 1985; 13: 179-183 MULLERS MUSCLE-CONJUNCTIVAL RESECTION PTOSIS PROCEDURE ALLEN M. PUTTERMAN MD University Of lll~nois Eye and Ear Infirmary, Michael
Australian and New Zealand Journal of Ouhthalmology 1985; 13: 179-183 MULLERS MUSCLE-CONJUNCTIVAL RESECTION PTOSIS PROCEDURE ALLEN M. PUTTERMAN MD University Of lll~nois Eye and Ear Infirmary, Michael
ISSN: Volume 4 Issue Faciomaxillary prosthesis in rehabilitation. After maxillectomy. A clinical study
 ISSN: 2250-0359 Volume 4 Issue 4 2014 Faciomaxillary prosthesis in rehabilitation After maxillectomy A clinical study Prasad c Parimala V Vijjaykanth M Sivakumar P Department of Dental Surgery Govt. Stanley
ISSN: 2250-0359 Volume 4 Issue 4 2014 Faciomaxillary prosthesis in rehabilitation After maxillectomy A clinical study Prasad c Parimala V Vijjaykanth M Sivakumar P Department of Dental Surgery Govt. Stanley
CHOUKROUN PRF SYSTEM. WELCOME in the new concept of «SMART BLOOD GENERATION»
 CHOUKROUN PRF SYSTEM WELCOME in the new concept of «SMART BLOOD GENERATION» New centrifuge with switch button: 3 positions switch button Bowl Mini tray Blood Collector THE CONCEPT The concept of CHOUKROUN
CHOUKROUN PRF SYSTEM WELCOME in the new concept of «SMART BLOOD GENERATION» New centrifuge with switch button: 3 positions switch button Bowl Mini tray Blood Collector THE CONCEPT The concept of CHOUKROUN
SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM
 Page 1 of 5 SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM FML Liquifilm Sterile Eye Suspension COMPOSITION FML Liquifilm Sterile Eye Suspension contains: Fluorometholone 1,0 mg/ml Liquifilm
Page 1 of 5 SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM FML Liquifilm Sterile Eye Suspension COMPOSITION FML Liquifilm Sterile Eye Suspension contains: Fluorometholone 1,0 mg/ml Liquifilm
Astigmatic Outcomes of Temporal versus Nasal Clear Corneal Phacoemulsification
 Astigmatic Outcomes of Temporal versus Nasal Clear Corneal Phacoemulsification Mohammad Pakravan, MD; Homayoun Nikkhah, MD; Shahin Yazdani, MD Camelia Shahabi, MD; Massih Sedigh-Rahimabadi, MD Labbafinejad
Astigmatic Outcomes of Temporal versus Nasal Clear Corneal Phacoemulsification Mohammad Pakravan, MD; Homayoun Nikkhah, MD; Shahin Yazdani, MD Camelia Shahabi, MD; Massih Sedigh-Rahimabadi, MD Labbafinejad
A Guide to Administering
 A Guide to Administering INDICATIONS AND USAGE YUTIQ (fluocinolone acetonide intravitreal implant) 0.18 mg is indicated for the treatment of chronic non-infectious uveitis affecting the posterior segment
A Guide to Administering INDICATIONS AND USAGE YUTIQ (fluocinolone acetonide intravitreal implant) 0.18 mg is indicated for the treatment of chronic non-infectious uveitis affecting the posterior segment
REFERENCES for PLATELET RICH PLASMA (PRP)
 REFERENCES for PLATELET RICH PLASMA (PRP) Daif ET. Autologous blood injection as a new treatment modality for chronic recurrent temporomandibular joint dislocation. Oral Surg Oral Med Oral Pathol Oral
REFERENCES for PLATELET RICH PLASMA (PRP) Daif ET. Autologous blood injection as a new treatment modality for chronic recurrent temporomandibular joint dislocation. Oral Surg Oral Med Oral Pathol Oral
Tissue repair. (3&4 of 4)
 Tissue repair (3&4 of 4) What will we discuss today: Regeneration in tissue repair Scar formation Cutaneous wound healing Pathologic aspects of repair Regeneration in tissue repair Labile tissues rapid
Tissue repair (3&4 of 4) What will we discuss today: Regeneration in tissue repair Scar formation Cutaneous wound healing Pathologic aspects of repair Regeneration in tissue repair Labile tissues rapid
Comparison of management options for scleral buckle exposure
 Comparison of management options for scleral buckle exposure Abstract: Scleral buckling is a technique used for repair of rhegmatogenous retinal detachment in eyes with retinal breaks. This report demonstrates
Comparison of management options for scleral buckle exposure Abstract: Scleral buckling is a technique used for repair of rhegmatogenous retinal detachment in eyes with retinal breaks. This report demonstrates
Research Article Cytological Evaluation of Hyaluronic Acid on Wound Healing Following Extraction
 Cronicon OPEN ACCESS DENTAL SCIENCE Research Article Cytological Evaluation of Hyaluronic Acid on Wound Healing Following Extraction Gocmen Gokhan 1 *, Gonul O 1, Oktay NS 2, Pisiriciler R 2 and Goker
Cronicon OPEN ACCESS DENTAL SCIENCE Research Article Cytological Evaluation of Hyaluronic Acid on Wound Healing Following Extraction Gocmen Gokhan 1 *, Gonul O 1, Oktay NS 2, Pisiriciler R 2 and Goker
Role of ASOCT in Intracorneal Foreign Body
 Diagnostics Ocular Trauma Role of ASOCT in Intracorneal Foreign Body Tarun Arora MD, DNB, FICO Tarun Arora MD, DNB, FICO, Vijay Kumar Sharma MS, Rajesh Sinha MD, DNB, FRCS Cornea, Lens and Refractive Surgery
Diagnostics Ocular Trauma Role of ASOCT in Intracorneal Foreign Body Tarun Arora MD, DNB, FICO Tarun Arora MD, DNB, FICO, Vijay Kumar Sharma MS, Rajesh Sinha MD, DNB, FRCS Cornea, Lens and Refractive Surgery
