Pojednostavnjena protetička rehabilitacija pacijenta nakon uklanjanja oralnog karcinoma
|
|
|
- Tyler Daniels
- 5 years ago
- Views:
Transcription
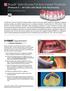
1 258 ACTA STOMATOLOGICA CROATICA Acta stomatol Croat. 2016;50(3): DOI: /asc50/3/9 PRIKAZ SLUČAJA CASE REPORT Josip Kranjčić 1, Nikola Džakula 2, Denis Vojvodić 1,3 Pojednostavnjena protetička rehabilitacija pacijenta nakon uklanjanja oralnog karcinoma Simplified Prosthetic Rehabilitation of a Patient after Oral Cancer Removal 1 Zavod za fiksnu protetiku Stomatološkog fakulteta Sveučilišta u Zagrebu, Zagreb, Hrvatska Department of Fixed Prosthodontics, School of Dental Medicine University of Zagreb, Zagreb, Croatia 2 Privatna stomatološka ordinacija, Zagreb, Hrvatska Private Dental Practice, Zagreb, Croatia 3 Klinički zavod za stomatološku protetiku Kliničke bolnice Dubrava, Zagreb, Hrvatska Clinical Department of Prosthodontics, Clinical Hospital Dubrava, Zagreb, Croatia Sažetak Terapija pacijenata s oralnim karcinomom složena je i zahtijeva multidisciplinaran pristup koji uključuje maksilofacijalnog i oralnog kirurga, onkologa i stomatološkog protetičara, a često je potrebna i psihološka pomoć. U ovom prikazu slučaja opisana je protetička rehabilitacija pacijentice nakon uklanjanja oralnoga karcinoma izradom resekcijske proteze. Resekcijska šupljina nalazi se na srednjem dijelu tvrdog nepca, a prema Aramanyju pripada trećem razredu maksilarnih defekata. Otisak ležišta proteze i resekcijske šupljine proveden je u dva koraka. Prvi je korak otisak ireverzibilnim hidrokoloidom za ležište proteze, a drugi, otisak resekcijske šupljine dobiven kondenzacijskim silikonskim materijalom s pomoću metalne baze resekcijske proteze. Resekcijskom protezom pacijentici su nadomješteni izgubljeni zubi te joj je, uz minimalne troškove, poboljšana oralna funkcija i estetika. Zaprimljen: 18. srpnja Prihvaćen: 1. rujna Adresa za dopisivanje Josip Kranjčić Stomatološki fakultet Sveučilišta u Zagrebu, Klinička bolnica Dubrava, Av. G. Šuška 6, Zagreb, Hrvatska tel: faks: kranjcic@sfzg.hr Ključne riječi novotvorine usta; nepčani obturator; stomatološka protetika; tehnike uzimanja otisaka Uvod Rak usne šupljine ubraja se u skupinu karcinoma glave i vrata te predstavlja bilo koje maligno tkivo u usnoj šupljini, bez obzira na to je li ono primarno oralna lezija, metastaza udaljenog tumora ili pak tumor koji se u usnu šupljinu proširio iz susjednog područja (1 3). Planocelularni karcinom razvija se u 90 posto slučajeva te čini do 3 posto svih karcinoma u Sjedinjenim Američkim Državama, u 9 posto slučajeva riječ je o karcinomu žlijezda slinovnica, sarkomu ili limfomu, a samo je u 1 posto slučajeva riječ o metastazama, najčešće iz pluća, dojke, prostate i bubrega (1 3). S obzirom na spol, češće obolijevaju muškarci (4). Čimbenici rizika od razvoja karcinoma usne šupljine su alkohol i duhan, ali i humani papiloma virus te ultraljubičasto zračenje (2 5). Terapija karcinoma usne šupljine agresivna je i obuhvaća kirurško uklanjanje te radioterapiju i kemoterapiju (6,7). Maksilektomija je naziv za odgovarajući kirurški zahvat kojim se uklanja dio, ili pak cijela gornja čeljust u postupku liječenja karcinoma (8). Introduction Oral cancer belongs to the group of head and neck cancers, and it represents any cancerous tissue in the oral cavity, regardless of being primarily oral lesion, tumor metastases or a distant tumor that has spread into the mouth from the adjacent area (1-3). Squamous cell carcinoma develops in 90% of cases and makes up 3% of all cancers in the United States. In 9% of cases, it is salivary glands cancer, or sarcoma, lymphoma, and metastases occur in only 1% of cases, usually from lung, breast, prostate and kidney (1-3). With regard to the gender, oral cancer is more common in men (4). Risk factors for oral cancer are alcohol, tobacco, or human papilloma virus, and ultraviolet radiation (2-5). Oral cancer therapy is usually aggressive and comprises surgical removal followed by radiotherapy and chemotherapy (6, 7). Maxillectomy is an appropriate surgical procedure which means that either a part or maxilla or the entire maxilla is removed in the process of surgical treatment of oral cancer (8). After surgical
2 Kranjčić et al. Rehabilitation with Obturator Prosthesis 259 Nakon kirurškog uklanjanja malignoga tkiva najčešće ostaje velik defekt tkiva uz oroantralnu komunikaciju, što pacijentu otežava funkciju žvakanja i gutanja hrane, govor, narušava estetiku te općenito umanjuje kvalitetu života povezanu s oralnim zdravljem. Zato je takvim pacijentima nužna odgovarajuća protetička terapija, što može biti dodatno otežano zbog posljedica provedene kirurške obrade, ali i radioterapije, poput trizmusa i ograničenog otvaranja usta (10 do 15 mm ili manje) (9). Trizmus se pojavljuje vrlo brzo nakon radioterapije i zato je potrebno odmah početi s vježbanjem žvačnih mišića s pomoću otvarača usta ili špatula za jezik. Ako se fizioterapija ne provodi, a trizmus postane kroničan, nastaju fibrozne promjene na žvačnim mišićima. Ograničeno otvaranje usta ne otežava samo žvačnu funkciju, nego i protetičku rehabilitaciju takvih pacijenata (9). Tradicionalno se u protetičkoj rehabilitaciji pacijenata nakon uklanjanja karcinoma izrađuju opturatori resekcijske proteze kako bi se zatvorila resekcijska šupljina primarno na tvrdom nepcu, ali i na zahvaćenom okolnom alveolarnom i mekom tkivu (8). Pojedini autori opisuju izradu resekcijske proteze retinirane na preostalim zubima, a drugi opisuju resekcijske proteze retinirane implantatima (6, 10 14). Predlaže se pričekati do šest mjeseci nakon kirurške terapije kako bi se tkiva resekcijske šupljine dimenzijski stabilizirala (najprije nastaje edem, a zatim njegova kontrakcija) i tek tada pristupiti izradi resekcijske proteze. U navedenom razdoblju može se izraditi privremena resekcijska proteza koja bi pacijentu omogućila bolju funkciju (9). Prema stajalištu Hauga (13), za izradu definitivne resekcijske proteze dovoljno je pričekati samo tri mjeseca nakon kirurškoga zahvata ili provedene radioterapije. Na oblik, a time i na stabilnost resekcijske proteze, utječu opseg kirurške resekcije te broj i raspored preostalih zuba. Uz retenciju proteze na preostalim zubima, važno je bazu proteze maksimalno proširiti na preostale strukture u usnoj šupljini. Naime, maksimalno proširena baza resekcijske proteze prenosi žvačne sile na preostali dio nepca i alveolarni greben te tako ublažava žvačni stres. Klasifikacija defekata gornje čeljusti prema Aramanyju u 6 klasa temelji se na međusobnom odnosu položaja resekcijske šupljine i preostalih retencijskih zuba te je dobrodošla pomoć pri planiranju metalnih baza resekcijskih proteza (15, 16). Prednost klasičnih resekcijskih proteza u odnosu na one retinirane implantatima jest relativno jednostavna i brža izrada, te lako održavanje oralne higijene, mogućnost kontrole tkiva resekcijske šupljine zbog mogućih tumorskih recidiva, ali i niža cijena, što je vrlo važno pacijentima lošijega imovnog stanja. Stoga je svrha ovoga rada bila prikazati izradu gornje resekcijske proteze nakon uklanjanja planocelularnog karcinoma gornje čeljusti, uz naglasak na jednostavnost i niže troškove ovog postupka. removal of cancerous tissue, a great tissue defect with oroantral communication remains, resulting in impaired function of chewing and swallowing, speech, esthetics, and generally impaired oral health related to quality of life. Therefore, in such patients it is necessary to perform appropriate prosthetic rehabilitation which can be additionally complicated by consequences of performed surgical, and radiation therapy such as trismus and limited mouth opening (10 to 15 mm or less) (9). Trismus begins shortly after radiotherapy, and therefore is necessary to start immediately with daily exercises of masticatory muscles using bite openers or a tongue blade. If physiotherapy is not carried out, trismus will become chronic with fibrosis of masticatory muscles. Limited mouth opening impairs masticatory function and prosthetic rehabilitation for such patients is a challenge for clinicians (9). Traditional approach in the prosthetic rehabilitation of patients after surgical removal of oral cancer is fabrication of obturator (resection) prosthesis in order to close acquired resection cavity primarily on the hard palate, but also on contiguous alveolar and soft tissue structures (8). Some authors described the fabrication of obturator prosthesis retained on the remaining teeth, while others described the obturator prosthesis retained by implants (6, 10-14). The period of 6 months after surgical treatment, when tissue of resection cavity becomes dimensionally stabilized (first tissue swelling, and then shrinkage), is usually sufficient for the beginning of the fabrication of the obturator prosthesis. During this period, temporary obturator prosthesis could be fabricated in order to enable better masticatory function (9). According to Haug (13), a sufficient period for the beginning of fabrication of definitive obturator prosthesis is up to 3 months after surgery, or 3 months after radiotherapy. The extension of surgical resection and the number and position of the remaining teeth affect the form as well as the stability of obturator prosthesis. Apart from the retention of prosthesis on the remaining teeth, it is important to expand the prosthesis base over the remaining oral structures. Maximal extension of obturator prosthesis base transmits masticatory forces to the remaining part of the palate and alveolar ridge, thus reducing masticatory stress. Aramany classification of maxillary defects in 6 classes is based on the relationship between the position of resection cavity and the remaining retention teeth, and is very helpful in the planning of the obturator prosthesis framework design (15, 16). The advantages of classic obturator prosthesis related to the obturator prosthesis retained on implants is relatively simple and faster fabrication, simple maintaining of oral hygiene, the ability to control possible tumor recurrence on resection cavity tissues, as well as lower price, which is very important among the patients of lower economic status. The aim of this paper was to present a fabrication of maxillary obturator prosthesis after surgical removal of maxillary squamous cell carcinoma with emphasis on simplicity and lower costs of this procedure. Prikaz slučaja Šest mjeseci nakon liječenja oralnog karcinoma 65-godišnja pacijentica dolazi u Klinički zavod za stomatološku protetiku Kliničke bolnice Dubrava radi protetičke rehabilitacije. Case report Six months after surgical treatment of oral cancer, a 65 year old patient visited Department of Prosthodontics at Clinical Hospital Dubrava seeking for prosthodontic reha-
3 260 Kranjčić i sur. Rehabilitacija resekcijskom protezom Slika 1. Intraoralni status pacijenta Figure 1 Patient s intraoral status. Slika 2. Metalna baza resekcijske proteze Figure 2 Cast framework of obturator prosthesis. Slika 3. Metalna baza resekcijske proteze s retencijskim elementima mrežica i retencijski kolčići ( ) te primarni sadreni radni model s prikazanim ulazom u resekcijsku šupljinu Figure 3 Cast framework of obturator prosthesis with retentive elements mesh and retentive dowels ( ), and primary working cast poured in dental stone with reproduced entrance of resection cavity. Slika 4. Otisak resekcijske šupljine kondenzacijskim silikonom na metalnoj bazi resekcijske proteze Figure 4 Condensation silicone impression of resection cavity on cast framework of obturator prosthesis. Slika 5. Primarni sadreni model s izrezanim dijelom ulaza u resekcijsku šupljinu (lijevo), te otisak resekcijske šupljine kondenzacijskim silikonom na metalnoj bazi resekcijske proteze (desno) Figure 5 Primary working cast with trimmed entrance to the resection cavity (left), and condensation silicone impression of resection cavity on cast framework of obturator prosthesis (right). Slika 6. Metalna baza resekcijske proteze s otiskom resekcijske šupljine postavljena na modificirani model pogled s bazalne strane modela Figure 6 Cast framework of obturator prosthesis with impression of resection cavity placed on modified model basal view. Slika 7. Izliven sekundarni dio modela u tvrdoj sadri (žuto) koji precizno prikazuje resekcijsku šupljinu, te postavljeni umjetni zubi na resekcijsku protezu Figure 7 Secondary part of working cast which precisely shows that resection cavity is poured in dental stone (yellow), and arranged artificial teeth in obturator prosthesis. Slika 8. Gotova resekcijska proteza Figure 8 Finished obturator prosthesis. Slika 9. Resekcijska proteza postavljena u usta pacijenta Figure 9 Obturator prosthesis inserted into the patient s mouth. Slika 10. Resekcijska proteza postavljena u usta pacijenta uz zatvaranje oroantralne komunikacije Figure 10 Obturator prosthesis inserted into the patient s mouth with closure of oro-antral communication.
4 Kranjčić et al. Rehabilitation with Obturator Prosthesis 261 Nakon kliničkoga pregleda zabilježena je Kennedyjeva klasa 4 gornjega zubnog luka s preostalim prvim i drugim molarom s desne strane te drugim molarom s lijeve strane. Resekcijski defekt nalazio se u središnjem dijelu tvrdoga nepca (klasa 3 prema Aramanyju) bez zahvaćanja alveolarnoga grebena i mekog nepca (slika 1.). Donja čeljust bila je djelomično ozubljena, ali bez defekta tkiva. Osmišljen je plan terapije prema kojem će se izraditi samo gornja resekcijska proteza s metalnom bazom (Co-Cr-Mo legura, Wironit, Bego, Bremen, Njemačka) retiniranom Bonwillovom kvačicom desno te obuhvatnom kvačicom s lijeve strane. Na donjoj čeljusti uopće nije bila planirana protetička terapija zbog lošijeg financijskog stanja pacijentice. Zbog djelomično izraženog trizmusa (udaljenost između gornjeg alveolarnog grebena u predjelu središnjih sjekutića i incizalnih bridova donjih središnjih sjekutića iznosila je oko 35 mm) koji se kod pacijentice pojavio kao posljedica radioterapije, nemoguće je bilo u jednom koraku precizno otisnuti usnu i resekcijsku šupljinu. Zato je to učinjeno u dva koraka. U prvom je uzet otisak od ireverzibilnog hidrokoloida alginata (Aroma Fine III; GC Corp, Tokio, Japan) kojim je precizno otisnut alveolarni greben s preostalim zubima, preostali dio tvrdog nepca te sam ulaz u resekcijsku šupljinu. Otisak je izliven u tvrdoj sadri (Moldano, Heraeus Kulzer, Hanau, Njemačka) te je uobičajenim postupkom izrađena metalna baza (Co-Cr-Mo legura, Wironit, Bego, Bremen, Njemačka) resekcijske proteze uz određene prilagodbe (slika 2.). Dio metalne baze resekcijske proteze koji prekriva resekcijsku šupljinu izrađen je poput mrežice s dva retencijska kolčića (slika 3.). Retentivni elementi metalne baze mrežica i kolčići prvotno služe kao nosači otisnog materijala u drugom koraku otiskivanja, a poslije kao retentivni elementi akrilatnog materijala opturatora. Metalna baza proteze retinirana je obuhvatnom kvačicom koja obuhvaća drugi molar s lijeve strane, te interdentalnom Bonwillovom kvačicom na prvom i drugom molaru s desne strane. Precizan otisak resekcijske šupljine (slika 4.) uzet je u drugom koraku kondenzacijskim silikonskim otisnim materijalom (Optosil/Xantopren L, Heraeus Kulzer, Hanau, Njemačka) te je s pomoću metalne baze resekcijske proteze, koja je poslužila kao žlica, unesen u usnu šupljinu. Unatoč trizmusu, a zbog odgovarajućeg oblika metalne baze, mogla se otisnuti cijela resekcijska šupljina te otisak izvaditi iz pacijentovih usta. Postojeći sadreni model smanjen je tako da je izrezan onaj dio koji je prikazivao ulaz u resekcijsku šupljinu. Metalna baza zajedno s otiskom resekcijske šupljine postavljena je na obrađeni model te je iz tvrde sadre (GC Fuji Rock, GC Europe, Leuven, Belgija) izliven otisak resekcijske šupljine i objedinjen s primarnim sadrenim modelom (slika 5. i 6.). U ustima pacijentice određeni su vertikalni i horizontalni međučeljusni odnosi, pri čemu je iznos slobodnoga interokluzijskoga prostora u položaju fiziološkog mirovanja iznosio 3 mm. Nakon što su postavljeni zubi (slika 7.), isprobani su u ustima pacijentice kako bi se provjerili okluzija i estetika. Slijedili su završni laboratorijski postupci pri izradi resekcijske proteze, a koristio se toplo polimerizirajući akrilat (Probase Hot; Ivoclar Vivadent, Schaan, Lihtenštajn), pri čemu je osim akrilatnih krila proteze napravljen i akrilatni optura- bilitation. During clinical examination, Kennedy Class 4 of maxillary dental arch was observed with remaining right first and second molars, and remaining left second molar. Resection cavity was located in the central part of the hard palate (class 3 according to Aramany classification), whereas the alveolar ridge and the soft palate were fully preserved (Figure 1). The mandible was partially edentulous but without abnormal tissue defects. Only the maxillary obturator prosthesis with metal framework (Co-Cr-Mo alloy, Wironit, Bego, Bremen, Germany) retained by Bonwill clasp on the right side, and by circumferential clasp on the left side was planned. Prosthetic treatment of the mandible was not planned due to the patient s low socio-economic status. Because of partially expressed trismus (the distance between the maxillary alveolar ridge in the central incisors area and incisal edges of mandibular central incisors was 35 mm), which occurred as a result of radiotherapy, it was impossible to make a precise one step impression of both, oral and resection cavity. Therefore, the two step impression technique was used. First step impression was made using irreversible hydrocolloid material (Aroma Fine III; GC Corp, Tokyo, Japan), and precisely captured alveolar ridge with remaining teeth, remaining part of the hard palate and only the entrance part of the resection cavity. The impression was poured in hard dental stone (Moldano, Heraeus Kulzer, Hanau, Germany), and the obturator prosthesis framework (Co-Cr-Mo alloy, Wironit, Bego, Bremen, Germany) was fabricated by standard procedure with certain modifications in design (Figure 2). Retentive mesh and dowels on obturator prosthesis framework (Figure 3) were added over the resection cavity to ensure retention for secondary impression material, as well as for the retention of a future acrylic resin bulb of the obturator. The obturator prosthesis framework engaged second left molar by circumferential clasp as well as first and second right molars by interdental Bonwill clasp. In the second impression step, a precise impression of the resection cavity (Figure 4) was made. Condensation silicone impression material (Optosil/Xantopren, Heraeus Kulzer, Hanau, Germany) was placed on the obturator prosthesis framework which served as a tray, and inserted into the oral cavity. Despite trismus, and because of the appropriate design of obturator prosthesis framework, it was possible to make impression of the entire resection cavity as well as to remove it from the patient s mouth. The stone cast was then modified; the part of the stone cast which corresponds to the entrance of resection cavity was cut out. Obturator prosthesis framework with silicon impression of the resection cavity was placed on the reduced stone cast. The adjacent impression was poured in dental stone (GC Fuji Rock, GC Europe, Leuven, Belgium) in order to produce definitive stone cast (Figures 5 and 6). In the patient s mouth, vertical and horizontal occlusal relationships were determined with interocclusal rest space of 3 mm at the physiologic rest position. After the artificial teeth were arranged (Figure 7), occlusion and esthetics were tested in the patient s mouth. The obturator prosthesis was finished by laboratory procedures using heat-curing acrylic resin (Probase Hot, Ivoclar
5 262 Kranjčić i sur. Rehabilitacija resekcijskom protezom tor (slika 8.) koji je obuhvatio retentivne elemente (mrežicu i kolčiće) na metalnoj bazi resekcijske proteze. Proteza je nakon toga završno obrađena i polirana. Pri predaji resekcijske proteze pacijentici (slike 9. i 10.) provjerena je točnost dosjeda proteze, osobito na rubovima resekcijske šupljine te su dodatno provjereni okluzijski kontakti artikulacijskim papirom (Arti-Fol; Dr Jean Bausch Gmbh & Co KG, Köln, Njemačka), a kvačice su aktivirane. Pacijentici su dane upute o higijeni resekcijske proteze, posebno opturatora koji ispunjava resekcijsku šupljinu kako bi se smanjila opasnost od infekcije zbog naseljavanja mikroorganizama na njegovoj površini. Preporučeni su i redoviti kontrolni pregledi svakih tri do šest mjeseci (ili prema potrebi), uz napomenu da će možda trebati podložiti resekcijsku protezu zbog promjena na koštanim i mekim tkivima njezina ležišta. Vivadent, Schaan, Liechtenstein), where both, acrylic base and acrylic bulb of the obturator (Figure 8), which covered retentive elements (mesh and dowels) on the obturator prosthesis framework, were fabricated. In the next step, the obturator prosthesis was finished and polished. At insertion of obturator prosthesis (Figures 9 and 10) the accuracy of obturator prosthesis fit was verified, especially on the edges of the resection cavity. The occlusion was tested by articulation paper (Arti-Fol, Dr. Jean Bausch GmbH & Co. KG, Cologne, Germany), and the clasps were activated. Hygiene instructions (especially for the obturator surgical site) were given to the patient in order to avoid possible infections due to microbial contamination of the obturator s surface. Regular follow-up every 3 to 6 months, or as needed was recommended to the patient, with a remark on possible need for obturator prosthesis relining procedure due to the occurring bone and mucosal tissue changes. Rasprava Terapija pacijenata s oralnim karcinomom zahtijeva multidisciplinaran pristup te uključuje maksilofacijalnog i oralnog kirurga, onkologa i stomatološkog protetičara, a često i psihološku pomoć (1, 17). Osnovna zadaća protetičke rehabilitacije u prikazanom kliničkom slučaju bila je izraditi odgovarajuću resekcijsku protezu kako bi se zatvorila komunikacija s nosnom šupljinom, nadomjestilo uklonjeno koštano tkivo i izgubljeni zubi te poboljšala oralna funkcija i estetika, a sve to uz što manje troškove za pacijenta. Protetička rehabilitacija pacijenata resekcijskim protezama svakako ima prednosti minimalan je dotok tekućine u nos i maksilarni sinus, omogućeno je žvakanje i gutanje te govor uz smanjenu ili uklonjenu hipernazalnost zbog razdvajanja usne od nosne šupljine (13, 18, 19). Izrada resekcijske proteze s opturatorom ne zahtijeva mnogo vremena, a resekcijska šupljina dostupna je pregledu kako bi se mogući recidiv tumora otkrio na vrijeme (13, 18). U slučaju djelomično ozubljenih pacijenata s dovoljno preostaloga alveolarnoga grebena i nepčane kosti, kirurško zatvaranje resekcijske šupljine nije prva opcija. Za takve pacijente, kao i u opisanom kliničkom slučaju, dobro je rješenje resekcijska proteza koja će funkcionirati kao klasična djelomična proteza. Uspjeh takve protetičke rehabilitacije ovisi o veličini i obliku zubnoga luka ostaloga nakon kirurškog uklanjanja karcinoma te o stanju mekih tkiva koja prekrivaju alveolarni greben i resekcijski defekt. U slučajevima s malo ili bez očuvane maksilarne kosti, izrada klasične resekcijske proteze otežana je i treba razmišljati o retenciji proteze implantatima (10, 12, 20). Aramanyjeva klasifikacija (15, 16) maksilarnih defekata pomaže u planiranju resekcijske proteze. U ovom kliničkom slučaju resekcijski defekt bio je u sredini tvrdog nepca, što je prema Aramanyju klasa 3, iako nisu bili očuvani svi zubi u zubnom luku. Resekcijska proteza retinirana je Bonwillovom i obuhvatnom kvačicom na molarima s retencijskim krakovima na bukalnim plohama te stabilizacijskim elementima na oralnim plohama zuba. Zbog lošijega financijskog stanja pacijentice, na preostalim molarima nisu Discussion An overall therapy of patients with oral cancer requires a multidisciplinary approach. It should include the maxillofacial surgeon, the oral surgeon, the oncologist, and the prosthodontist. Besides, the psychologist is often needed (1, 17). The aim of the prosthetic rehabilitation in the present case report was to fabricate appropriate obturator prosthesis in order to close communication with nasal cavity, replace lost bone tissue and teeth and improve oral function and esthetics. In addition, the aim was to accomplish this task at lowest cost. The prosthetic rehabilitation of patients with obturator prosthesis has the following advantages: fluid leakage into the nasal cavity and maxillary sinus is minimized; mastication, swallowing and speech with reduced or eliminated hipernasality are enabled due to separation between the oral and nasal cavity (13, 18, 19). The fabrication of the obturator prosthesis shortens the procedure time, and the resection cavity can be easily examined after removing the obturator prosthesis in order to detect tumor recurrence in time (13, 18). Surgical reconstruction of resection cavity should not be of primary consideration for partially dentate patients with remaining teeth and palatal bone after surgical resection. For such patients, as well as for the patient presented in this case report, the fabrication of obturator prosthesis which functions similarly to removable partial dental prosthesis would be a good solution. The success of prosthetic rehabilitation with obturator prosthesis depends on the size and shape of dental arch after surgical removal of cancer as well as on the quality of the soft tissue covering the alveolar ridge and resection cavity. In cases with little or no preserved maxillary bone, the fabrication of the classic obturator prosthesis is more difficult, and the retention of obturator prosthesis on implants may be a good solution (10, 12, 20). Aramany classification (15, 16) of maxillary defects is very helpful in planning of the obturator prosthesis. In this clinical case, Aramany class 3 defect was present. The resection cavity was located in central part of the hard palate; however, not all the teeth in dental arch were preserved. The obturator prosthesis was
6 Kranjčić et al. Rehabilitation with Obturator Prosthesis 263 izrađene modificirane krunice, no položaj i morfologija zuba bili su dovoljni za postizanje zadovoljavajuće retencije resekcijske proteze. Ozbiljan problem vezan za protetičku rehabilitaciju pacijenata nakon radioterapije jest trizmus, odnosno ograničeno otvaranje usta. Zato je klinička implikacija ovoga rada bila prikazati uzimanje otiska u dva koraka pri ograničenom otvaranju usta, uz naglasak na jednostavnost u postupku izrade i na finacijsku prihvatljivost kad je riječ o pacijentima lošijega financijskog statusa. Kao materijale izbora za izradu opturatora Depprich i suradnici (18) navode akrilate (polimetilmetakrilat), silikone i titanij. Nedostatak akrilata i silikona jest sklonost naseljavanju mikroorganizama zbog površinske poroznosti i hrapavosti, što može rezultirati prodorom mikroorganizama u unutrašnjost opturatora. Ovisno o općem zdravstvenom stanju pacijenta i patogenosti mikroorganizama može se pojaviti lokalna ili čak sistemska infekcija. U ovom je kliničkom slučaju opturator bio izrađen od toplinski polimerizirajućeg akrilata čija se površina može bolje ispolirati, što olakšava održavanje higijene i smanjuje nakupljanje mikroorganizama. Katkad, zbog osjetljivosti sluznice resekcijske šupljine, potrebno je opturator izraditi od mekog akrilata, iako će tada, zbog poroznosti materijala, održavanje higijene biti otežano. S druge strane, titanij ima dobra biomehanička svojstva, biokompatibilan je, male je težine i otporan na koroziju, ne izaziva alergije i može se izvrsno polirati. Nedostatak je to što ga je teško prilagođavati i podlagati, a i cijena takva protetičkog rada znatno je veća (18). Zaključak Protetska rehabilitacija nakon uklanjanja oralnog karcinoma složena je, te je izazov svakom protetičaru. Komplikacije nakon operacije i radioterapije, poput trizmusa, dodatno otežavaju protetičku rehabilitaciju. U dva koraka može se precizno otisnuti ležište buduće resekcijske proteze s resekcijskom šupljinom, osiguravajući dobar dosjed proteze i opturatora na ležištu, dobru retenciju i adekvatno zatvaranje resekcijske šupljine. U protetičkoj rehabilitaciji takvih pacijenata često je važno tražiti što jednostavnije rješenje koje omogućuje lagan pregled resekcijske šupljine, a uz to protetički rad učiniti što jeftinijim kako bi bio dostupan i pacijentima lošijega financijskog stanja. retained by Bonwill clasps and circumferential clasps on the molars with retention arms positioned on the buccal surfaces and stabilization elements on the oral surfaces of the teeth. Due to the patient s low socio-economic status, the remaining molars were not covered by crowns with rests. However, the locations and morphology of the teeth were satisfactory to establish retention of obturator prosthesis. A serious problem associated with the prosthetic rehabilitation of a patient after radiotherapy is trismus or limited mouth opening. In addition to the clinical implications discussed throughout this paper, the aim of this paper was to present a two-step impression technique with emphasis on the simplicity of obturator prosthesis fabrication as well as on economic acceptability for the patients of low socio-economic status. Depprich et al. (18) stated that acrylates (polymethyl methacrylate), silicone and titanium are commonly used materials for fabricating the obturator. Disadvantage of acrylates and silicones is in affinity to microorganisms contamination due to the surface porosity and roughness which can result in penetration of microorganisms into the interior of the obturator. Depending on the general health condition of the patient and pathogenicity of microorganisms, locally or even systemic infections can occur. In present clinical case obturator was made of heat-curing acrylic resin whose surface could be better polished thus facilitating hygiene and reduces the microorganisms accumulation. Sometimes, because of the vulnerability of resection cavity mucosa, it is necessary to use soft acrylates for obturator fabrication. In that case, obturator hygiene maintenance will be more difficult due to the surface porosity of the material. On the other hand, titanium has good biomechanical properties, it is biocompatible, low weight, corrosion resistant, nonallergic material, and its surface can be polished good. Disadvantage is that titanium is not easily to adjust or reline, and the price of such prosthetic appliance is higher (18). Conclusion Prosthetic rehabilitation after surgical removal of oral cancer is complex and challenging for prosthodontist. Trismus, as a complication after surgery and radiotherapy, complicates further prosthetic rehabilitation. Using the two-step impression technique it is possible to make an accurate impression of the denture-bearing area and the resection cavity, thus providing a good seating of obturator prosthesis, good retention, and adequate closure of the resection cavity. In prosthetic rehabilitation of such patients, it is important to search for simplified treatments which enable simple examination of resection cavity, and simultaneously, lower the costs in order to be acceptable to patients of low socio-economic status.
7 264 Kranjčić i sur. Rehabilitacija resekcijskom protezom Abstract The treatment of patients with oral cancer is complex: a multidisciplinary approach needs to be taken and maxillofacial and oral surgeons, an oncologist, a prosthodontist should be included, and a psychologist is often needed. This case report describes the prosthetic rehabilitation of a patient after surgical removal of oral cancer with obturator prosthesis. Resection cavity was located in central part of the hard palate and the condition belonged to Aramany class 3 maxillary defects. The two-step impression technique of denture bearing area and the resection cavity was performed. A primary impression-the impression of denture bearing area was made using irreversible hydrocolloid material, while the second impression the impression of resection cavity was made using condensation silicone material and obturator prosthesis framework. The obturator prosthesis replaced lost teeth, improved oral function and esthetics at minimal costs. Received: July 18, 2016 Accepted: September 1, 2016 Address for correspondence Josip Kranjčić University of Zagreb School of Dental Medicine Clinical Hospital Dubrava Av. G. Šuška 6, Zagreb, Croatia Phone: Fax: kranjcic@sfzg.hr Key words Mouth Neoplasms; Palatal Obturators; Prosthodontics; Dental Impression Technique References 1. Bilhan H, Geckili O, Bural C, Sonmez E, Guven E. Prosthetic rehabilitation of a patient after surgical reconstruction of the maxilla: a clinical report. J Prosthodont Jan;20(1): Srivastava R, Sharma R, Mishra S, Singh RB. Biochemical and molecular biological studies on oral cancer: an overview. Open Nutraceuticals J. 2011;4: Siegel MA, Kahn MA, Palazzolo MJ. Oral cancer: a prosthodontic diagnosis. J Prosthodont Jan;18(1): Rivera C. Essentials of oral cancer. Int J Clin Exp Pathol Sep 1;8(9): Macan D. O etiologiji karcinoma usne šupljine. Acta Stomatol Croat. 1996;30: Sullivan M, Gaebler C, Beukelman D, Mahanna G, Marshall J, Lydiatt D et al. Impact of palatal prosthodontic intervention on communication performance of patient s maxillectomy defects: a multilevel outcome study. Head Neck Jun;24(6): Ortegon SM, Martin JW, Lewin JS. A hollow delayed surgical obturator for a bilateral subtotal maxillectomy patient: a clinical report. J Prosthet Dent Jan;99(1): The glossary of prosthodontic terms. J Prosthet Dent Jul;94(1): Kramer, DC; Taylor, T-editors. Clinical maxillofacial prosthetics. 1 st ed. Carol Stream: Quintessence Publishing; Sharma AB, Beumer J. Reconstruction of maxillary defects: the case for prosthetic rehabilitation. J Oral Maxillofac Surg Dec;63(12): Al-Salehi SK, Calder ID, Lamb DJ. Magnetic retention for obturators. J Prosthodont May-Jun;16(3): Kim DD, Ghali GE. Dental implants in oral cancer reconstructions. Dent Clin North Am Oct;55(4): Haug SP. Maxillofacial prosthetic management of the maxillary resection patient. Atlas Oral Maxillofac Surg Clin North Am Mar;15(1): Cheng AC, Koticha TN, Tee-Khin N, Wee AG. Prosthodontic management of an irradiated maxillectomy patient with severe trismus using implant-supported prostheses: a clinical report. J Prosthet Dent May;99(5): Aramany MA. Basic principles of obturator design for partially edentulous patients. Part I: classification. J Prosthet Dent Dec;86(6): Aramany MA. Basic principles of obturator design for partially edentulous patients. Part II: design principles. J Prosthet Dent Dec;86(6): Bhasin AS, Singh V, Mantri SS. Rehabilitation of patient with acquired maxillary defect, using a closed hollow bulb obturator. Indian J Palliat Care Jan;17(1): Depprich R, Naujoks C, Lind D, Ommerborn M, Meyer U, Kubler NR et al. Evaluation of the quality of life of patients with maxillofacial defects after prosthodontic therapy with obturator prostheses. Int J Oral Maxillofac Surg Jan;40(1): Vojvodić D, Žabarović D. Retention of the lower complete dentures with the use of mini dental implants: case report. Acta Stomatol Croat. 2008;42: Parr GR, Tharp GE, Rahn A. Prosthodontic principles in the framework design of maxillary obturator prostheses. J Prosthet Dent May;93(5):
Prosthetic V. Removable dentures I.
 Prosthetic V. Removable dentures I. Removable dentures Partial Complete (full) lenka.roubalikova@tiscali.cz 2 Prosthetic dentistry replacement of Damaged teeth reconstruction of the crown (inlays, crowns)
Prosthetic V. Removable dentures I. Removable dentures Partial Complete (full) lenka.roubalikova@tiscali.cz 2 Prosthetic dentistry replacement of Damaged teeth reconstruction of the crown (inlays, crowns)
Frame designed partial prosthesis for the rehabilitation of a maxillectomy patient
 VARIA Frame designed partial prosthesis for the rehabilitation of a maxillectomy patient Sorin Popºor, Lia Maria Coman Târgu Mureº, Romania Summary This article is a case report and it describes a technique
VARIA Frame designed partial prosthesis for the rehabilitation of a maxillectomy patient Sorin Popºor, Lia Maria Coman Târgu Mureº, Romania Summary This article is a case report and it describes a technique
م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION
 Lec.1 م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION االسنان طب Prosthodontics is the branch of dentistry pertaining to the restoration and maintenance of oral function, comfort, appearance,
Lec.1 م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION االسنان طب Prosthodontics is the branch of dentistry pertaining to the restoration and maintenance of oral function, comfort, appearance,
Role of Maxillo-Facial Prosthodontist to Aid in Brachytherapy for Squamous Cell Carcinoma of Palate with Ancillary Prosthesis: A Case Report
 Journal of Dental & Oro-facial Research Vol. 14 Issue 01 Jan. 2018 Role of Maxillo-Facial Prosthodontist to Aid in Brachytherapy for Squamous Cell Carcinoma of Palate with Ancillary Prosthesis: A Case
Journal of Dental & Oro-facial Research Vol. 14 Issue 01 Jan. 2018 Role of Maxillo-Facial Prosthodontist to Aid in Brachytherapy for Squamous Cell Carcinoma of Palate with Ancillary Prosthesis: A Case
PROSTHETICREHABILITATION OFAHEMIMANDIBULECTOMY PATIENTWITHTWINOCCLUSION
 CASEREPORT PROSTHETICREHABILITATION OFAHEMIMANDIBULECTOMY PATIENTWITHTWINOCCLUSION Authors: Tejeswar Reddy B¹ Indira Padmaja B² Raja Reddy N³ 1 Post graduate, 2 Professor & HOD, 3 Reader, Address for correspondence:
CASEREPORT PROSTHETICREHABILITATION OFAHEMIMANDIBULECTOMY PATIENTWITHTWINOCCLUSION Authors: Tejeswar Reddy B¹ Indira Padmaja B² Raja Reddy N³ 1 Post graduate, 2 Professor & HOD, 3 Reader, Address for correspondence:
Three-dimensional finite element analysis of the application of attachment for obturator framework in unilateral maxillary defect
 Journal of Oral Rehabilitation 2007 Three-dimensional finite element analysis of the application of attachment for obturator framework in unilateral maxillary defect S. JIAN*, J. TING*, T. YING &W.DONG-MEI
Journal of Oral Rehabilitation 2007 Three-dimensional finite element analysis of the application of attachment for obturator framework in unilateral maxillary defect S. JIAN*, J. TING*, T. YING &W.DONG-MEI
Prosthodontic Rehabilitation of a Partially Edentulous Hemiglossectomy Patient: A Clinical Report
 case report 10.5005/jp-journals-10031-1067 Prosthodontic Rehabilitation of a Partially Edentulous Hemiglossectomy Patient: A Clinical Report 1 Ragini Sudhakar Sanaye, 2 Sabita M Ram, 3 Naisargi Shah, 4
case report 10.5005/jp-journals-10031-1067 Prosthodontic Rehabilitation of a Partially Edentulous Hemiglossectomy Patient: A Clinical Report 1 Ragini Sudhakar Sanaye, 2 Sabita M Ram, 3 Naisargi Shah, 4
An Alternative Prosthetic Approach for Rehabilitation of Two Edentulous Maxillectomy Patients: Clinical Report
 An Alternative Prosthetic Approach for Rehabilitation of Two Edentulous Maxillectomy Patients: Clinical Report Murat Yenisey, DDS, PhD, Şafak Külünk, DDS, PhD, & Necati Kaleli, DDS, PhD Department of Prosthodontics,
An Alternative Prosthetic Approach for Rehabilitation of Two Edentulous Maxillectomy Patients: Clinical Report Murat Yenisey, DDS, PhD, Şafak Külünk, DDS, PhD, & Necati Kaleli, DDS, PhD Department of Prosthodontics,
Cast Partial Denture Improving Emergence and Masticatory Function - A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 9 Ver. VI (Sep. 2015), PP 51-56 www.iosrjournals.org Cast Partial Denture Improving Emergence
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 9 Ver. VI (Sep. 2015), PP 51-56 www.iosrjournals.org Cast Partial Denture Improving Emergence
MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF PROSTHETIC DENTAL MEDICINE GOVERNMENT EXAMINATION SYLLABUS
 MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF PROSTHETIC DENTAL MEDICINE GOVERNMENT EXAMINATION SYLLABUS OF PROSTHETIC DENTAL MEDICINE ACADEMIC YEAR 2016/2017 1 1. Biomechanics of
MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF PROSTHETIC DENTAL MEDICINE GOVERNMENT EXAMINATION SYLLABUS OF PROSTHETIC DENTAL MEDICINE ACADEMIC YEAR 2016/2017 1 1. Biomechanics of
An Alternative Approach for Fabrication of a Hollow Maxillary Complete Denture: A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 4 Ver. IX (Apr. 2016), PP 68-72 www.iosrjournals.org An Alternative Approach for Fabrication
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 4 Ver. IX (Apr. 2016), PP 68-72 www.iosrjournals.org An Alternative Approach for Fabrication
ISSN: Volume 4 Issue Faciomaxillary prosthesis in rehabilitation. After maxillectomy. A clinical study
 ISSN: 2250-0359 Volume 4 Issue 4 2014 Faciomaxillary prosthesis in rehabilitation After maxillectomy A clinical study Prasad c Parimala V Vijjaykanth M Sivakumar P Department of Dental Surgery Govt. Stanley
ISSN: 2250-0359 Volume 4 Issue 4 2014 Faciomaxillary prosthesis in rehabilitation After maxillectomy A clinical study Prasad c Parimala V Vijjaykanth M Sivakumar P Department of Dental Surgery Govt. Stanley
A Comprehensive Prosthodontic Management of Subtotal Maxillectomy
 Manoj Kumar Sundar et al CASE REPORT 10.5005/jp-journals-10019-1118 A Comprehensive Prosthodontic Management of Subtotal Maxillectomy 1 Manoj Kumar Sundar, 2 GP Surendra Kumar, 3 Shruti Lakhanpal ABSTRACT
Manoj Kumar Sundar et al CASE REPORT 10.5005/jp-journals-10019-1118 A Comprehensive Prosthodontic Management of Subtotal Maxillectomy 1 Manoj Kumar Sundar, 2 GP Surendra Kumar, 3 Shruti Lakhanpal ABSTRACT
It has been proposed that partially edentulous maxillectomy
 CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
Removable partial dentures
 Removable partial dentures Feb, 4, 2015 McCracken's Removable Partial Prosthodontics, Twelfth Edition Carr, Alan B 1 Prosthesis that replaces the missing teeth and associated supporting structures in a
Removable partial dentures Feb, 4, 2015 McCracken's Removable Partial Prosthodontics, Twelfth Edition Carr, Alan B 1 Prosthesis that replaces the missing teeth and associated supporting structures in a
Lect. 14 Prosthodontics Dr. Osama
 Lect. 14 Prosthodontics Dr. Osama Principles of Removable Partial Denture Design Difference in Prosthesis Support and Influence on Design: For a tooth-supported prosthesis, the movement potential is less
Lect. 14 Prosthodontics Dr. Osama Principles of Removable Partial Denture Design Difference in Prosthesis Support and Influence on Design: For a tooth-supported prosthesis, the movement potential is less
Prosthodontic Management of Combination Syndrome Case with Metal Reinforced Maxillary Complete Denture and Mandibular Teeth supported Overdenture
 Case Report imedpub Journals www.imedpub.com Periodontics and Prosthodontics DOI: 10.21767/2471-3082.100041 Prosthodontic Management of Combination Syndrome Case with Metal Reinforced Maxillary Complete
Case Report imedpub Journals www.imedpub.com Periodontics and Prosthodontics DOI: 10.21767/2471-3082.100041 Prosthodontic Management of Combination Syndrome Case with Metal Reinforced Maxillary Complete
Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report
 Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report 1 2 1 1 Mittal R, Saxena D, Rao S, Kumar M Abstract: Statement of Problem: Complete denture rehabilitation
Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report 1 2 1 1 Mittal R, Saxena D, Rao S, Kumar M Abstract: Statement of Problem: Complete denture rehabilitation
Prosthetic Rehabilitation of Maxillectomy Defects- Clinical Outcomes
 Prosthetic Rehabilitation of Maxillectomy Defects- Clinical Outcomes Eleni D. Roumanas DDS Division of Advanced Prosthodontics and Weintraub Center for Reconstructive Biotechnology UCLA School of Dentistry
Prosthetic Rehabilitation of Maxillectomy Defects- Clinical Outcomes Eleni D. Roumanas DDS Division of Advanced Prosthodontics and Weintraub Center for Reconstructive Biotechnology UCLA School of Dentistry
PROSTHETIC REHABILITATION OF MAXILLARY DEFECTS: A REVIEW
 Review Article International Journal of Dental and Health Sciences Volume 01,Issue 04 PROSTHETIC REHABILITATION OF MAXILLARY DEFECTS: A REVIEW Sanjeeva Rao Olepu 1, Mithilesh Kumar 2,Ramu Rajesh Babu 3,Tanvi
Review Article International Journal of Dental and Health Sciences Volume 01,Issue 04 PROSTHETIC REHABILITATION OF MAXILLARY DEFECTS: A REVIEW Sanjeeva Rao Olepu 1, Mithilesh Kumar 2,Ramu Rajesh Babu 3,Tanvi
Removable Partial Dentures
 Removable Partial Dentures Replacement of missing teeth Fixed partial denture Removable partial denture Complete removable Transitional denture Partial removable Implant retained prosthodontics No prosthetic
Removable Partial Dentures Replacement of missing teeth Fixed partial denture Removable partial denture Complete removable Transitional denture Partial removable Implant retained prosthodontics No prosthetic
The CMC approved a motion to accept all editorial action requests that remain on the consent calendar 21 Yea / 0 Nay / 0 Abstain
 PAGE 1 OF 14 Editorial Actions One or more member organizations requested that the following editorial action submissions be removed from the consent calendar and addressed individually: #s 4, 7, 8, 9,
PAGE 1 OF 14 Editorial Actions One or more member organizations requested that the following editorial action submissions be removed from the consent calendar and addressed individually: #s 4, 7, 8, 9,
INCREASED RETENTION OF A PARTIAL DENTURE MAXILLARY OBTURATOR USING DENTAL IMPLANT
 INCREASED RETENTION OF A PARTIAL DENTURE MAXILLARY OBTURATOR USING DENTAL IMPLANT N. Yunus1, Z.A.A. Rahman 2. Increased retention of a partial denture maxillary obturator using dental implant. Annal Dent
INCREASED RETENTION OF A PARTIAL DENTURE MAXILLARY OBTURATOR USING DENTAL IMPLANT N. Yunus1, Z.A.A. Rahman 2. Increased retention of a partial denture maxillary obturator using dental implant. Annal Dent
Rehabilitation of Acquired Maxillary Defect with Precision Attachment Retained Hollow Bulb Obturator prosthesis: A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. X (July. 2017), PP 63-67 www.iosrjournals.org Rehabilitation of Acquired Maxillary Defect
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. X (July. 2017), PP 63-67 www.iosrjournals.org Rehabilitation of Acquired Maxillary Defect
"Artless solution to resolve the problem of retention in resorbed alveolar ridge cases"
 Article ID: ISSN 2046-1690 "Artless solution to resolve the problem of retention in resorbed alveolar ridge cases" Peer review status: No Corresponding Author: Dr. Khurshid Mattoo, Assistant Professor,
Article ID: ISSN 2046-1690 "Artless solution to resolve the problem of retention in resorbed alveolar ridge cases" Peer review status: No Corresponding Author: Dr. Khurshid Mattoo, Assistant Professor,
Maxillofacial prosthetics is a subspecialty of
 Invited Article Maxillofacial Prosthesis: A Review of Treatment Concepts for Better Prosthesis Prognosis Sanjay Prasad 1 ABSTRACT Maxillofacial prosthesis currently finds itself experiencing more change
Invited Article Maxillofacial Prosthesis: A Review of Treatment Concepts for Better Prosthesis Prognosis Sanjay Prasad 1 ABSTRACT Maxillofacial prosthesis currently finds itself experiencing more change
Immediate Complete Denture: A Case Report
 Human Journals Case Report July 2018 Vol.:10, Issue:1 All rights are reserved by Ruby et al. Immediate Complete Denture: A Case Report Keywords: immediate denture, dental prosthesis ABSTRACT Ruby*, Manish
Human Journals Case Report July 2018 Vol.:10, Issue:1 All rights are reserved by Ruby et al. Immediate Complete Denture: A Case Report Keywords: immediate denture, dental prosthesis ABSTRACT Ruby*, Manish
Denture relining as an indicator of residual ridge resorption
 ORIGINAL ARTICLE Denture relining as an indicator of residual ridge resorption Josip Kranjčić 1, Maja Kostelić Stunić 2, Asja Čelebić 3,4, Daniel Komar 1,4, Ketij Mehulić 1,4, Denis Vojvodić 1,5 1 Department
ORIGINAL ARTICLE Denture relining as an indicator of residual ridge resorption Josip Kranjčić 1, Maja Kostelić Stunić 2, Asja Čelebić 3,4, Daniel Komar 1,4, Ketij Mehulić 1,4, Denis Vojvodić 1,5 1 Department
Construction of Removable Partial Denture
 Construction of Removable Partial Denture Peter Hermann Department of Prosthodontics Semmelweis University Treatment options for edentulous spaces Fixed prosthodontics (crowns/bridges) Removable prosthodontics
Construction of Removable Partial Denture Peter Hermann Department of Prosthodontics Semmelweis University Treatment options for edentulous spaces Fixed prosthodontics (crowns/bridges) Removable prosthodontics
RELINING AND REBASING
 RELINING AND REBASING Relining: The process used to resurface the tissue side of a denture with new material layer, thus producing an accurate adaptation to the denture foundation area. Rebasing: The laboratory
RELINING AND REBASING Relining: The process used to resurface the tissue side of a denture with new material layer, thus producing an accurate adaptation to the denture foundation area. Rebasing: The laboratory
Relining and Rebasing of complete denture
 Relining and Rebasing of complete denture It is the procedures used to resurface the tissue-side of a denture with new material layer, thus producing an accurate adaptation to the denture foundation area.
Relining and Rebasing of complete denture It is the procedures used to resurface the tissue-side of a denture with new material layer, thus producing an accurate adaptation to the denture foundation area.
Case report: Lingualized occlusion -A better way for enhancing function & esthetic
 Case report: Lingualized occlusion -A better way for enhancing function & esthetic 1Dr. Vishrut Shah, 2 Dr. Sunil Dhaded, 3 Dr. Chandrashekar Sajjan 1Post graduate student, Department of Prosthodontics,
Case report: Lingualized occlusion -A better way for enhancing function & esthetic 1Dr. Vishrut Shah, 2 Dr. Sunil Dhaded, 3 Dr. Chandrashekar Sajjan 1Post graduate student, Department of Prosthodontics,
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note
 Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Evaluation of Speech in Patients with Partial Surgically Acquired Defects: Pre and Post Prosthetic Obturation
 Evaluation of Speech in Patients with Partial Surgically Acquired Defects: Pre and Post Prosthetic Obturation Abstract Aim: Maxillectomy often results in a high level of morbidity with significant psychological
Evaluation of Speech in Patients with Partial Surgically Acquired Defects: Pre and Post Prosthetic Obturation Abstract Aim: Maxillectomy often results in a high level of morbidity with significant psychological
Endocrinology Oral prosthetics in management of the head and neck cancer patient November 2003
 TITLE: Endocrinology Oral prosthetics in management of the head and neck cancer patient SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: November 12, 2003 RESIDENT PHYSICIAN: Jacques
TITLE: Endocrinology Oral prosthetics in management of the head and neck cancer patient SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: November 12, 2003 RESIDENT PHYSICIAN: Jacques
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
M.D.S. DEGREE EXAMINATION. (Revised Regulations) Branch VI PROSTHODONTICS. (For Candidates admitted from onwards)
 September 2008 [KT 389] Sub. Code: 2422. (Revised Regulations) Branch VI PROSTHODONTICS (For Candidates admitted from 2004-2005 onwards) Paper II REMOVABLE PROSTHODONTICS AND Time : Three hours Q.P. Code
September 2008 [KT 389] Sub. Code: 2422. (Revised Regulations) Branch VI PROSTHODONTICS (For Candidates admitted from 2004-2005 onwards) Paper II REMOVABLE PROSTHODONTICS AND Time : Three hours Q.P. Code
Overdenture: A Way of Preventive Prosthodontics
 CASE REPORT Overdenture: A Way of Preventive Prosthodontics Gorakhnath B Shinde 1 and Wadkar AP 2 Quick Response Code ABSTRACT: doi:... 1 Post Graduate Student 2 Professor and PG Guide Department of Prosthodontics
CASE REPORT Overdenture: A Way of Preventive Prosthodontics Gorakhnath B Shinde 1 and Wadkar AP 2 Quick Response Code ABSTRACT: doi:... 1 Post Graduate Student 2 Professor and PG Guide Department of Prosthodontics
Fixed Partial Dentures /FPDs/, Implant Supported. in implant prosthodontics
 Fixed Partial Dentures /FPDs/, Implant Supported Prosthesis/ISP/ in implant prosthodontics Prof.dr.Tamas Divinyi Semmelweis University, Faculty of Dentistry Department of Oral and Maxillofacial Surgery
Fixed Partial Dentures /FPDs/, Implant Supported Prosthesis/ISP/ in implant prosthodontics Prof.dr.Tamas Divinyi Semmelweis University, Faculty of Dentistry Department of Oral and Maxillofacial Surgery
INDIAN DENTAL JOURNAL
 REHABILITATION OF A COMPOSITE MAXILLA-MANDIBULAR RESECTION PATIENT BY GUIDE FLANGE AND OBTURATOR PROSTHESIS Dr. Shefali Goel 1 Dr. Neetu Singh 2 Dr. Balendra Pratap Singh 3 Dr. Pooran Chand 4 1, 2 Junior
REHABILITATION OF A COMPOSITE MAXILLA-MANDIBULAR RESECTION PATIENT BY GUIDE FLANGE AND OBTURATOR PROSTHESIS Dr. Shefali Goel 1 Dr. Neetu Singh 2 Dr. Balendra Pratap Singh 3 Dr. Pooran Chand 4 1, 2 Junior
The aim of this study was to evaluate the use of esthetic twin-flex clasp on remaining
 Cairo Dental Journal (24) Number (I), 163:169 January, 2008 Twin-Flex clasp as an esthetic approach for remaining central incisor abutment in unilateral maxillectomy cases Salah AF Hegazy 1 and Emiel AM
Cairo Dental Journal (24) Number (I), 163:169 January, 2008 Twin-Flex clasp as an esthetic approach for remaining central incisor abutment in unilateral maxillectomy cases Salah AF Hegazy 1 and Emiel AM
IMMEDIATE PARTIAL DENTURE PROSTHESIS - A CASE REPORT
 Case Report IMMEDIATE PARTIAL DENTURE PROSTHESIS - A CASE REPORT Abstract : 2 Vinaya Bhat & S. Sriram Balaji 2 Professor, P.G. Student, Department of Prosthodontics and Implantology, A.B. Shetty Memorial
Case Report IMMEDIATE PARTIAL DENTURE PROSTHESIS - A CASE REPORT Abstract : 2 Vinaya Bhat & S. Sriram Balaji 2 Professor, P.G. Student, Department of Prosthodontics and Implantology, A.B. Shetty Memorial
Chapter 12. Prosthodontics
 Chapter 12 Prosthodontics Golbarg Kolahi 1 Prosthesis [prahs-thee-sis] A replacement for a missing body part Golbarg Kolahi 2 Prosthesis In the dental field, it is a fixed or removable appliance replacing
Chapter 12 Prosthodontics Golbarg Kolahi 1 Prosthesis [prahs-thee-sis] A replacement for a missing body part Golbarg Kolahi 2 Prosthesis In the dental field, it is a fixed or removable appliance replacing
Original Research Article
 Medrech ISSN No. 2394-3971 Original Research Article CLINICAL VARIABLES ASSOCIATED WITH THE REHABILITATION OF A HEMIMANDIBULECTOMY PATIENT Manas Singh 1, Khurshid Mattoo 2, Lakshya Yadav 3 1 Department
Medrech ISSN No. 2394-3971 Original Research Article CLINICAL VARIABLES ASSOCIATED WITH THE REHABILITATION OF A HEMIMANDIBULECTOMY PATIENT Manas Singh 1, Khurshid Mattoo 2, Lakshya Yadav 3 1 Department
Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident
 Case Report 13 2011 Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident Dr Hitoshi Minagawa Tokyo, Japan Prosthetics Dr Hitoshi Minagawa successfully completed his studies
Case Report 13 2011 Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident Dr Hitoshi Minagawa Tokyo, Japan Prosthetics Dr Hitoshi Minagawa successfully completed his studies
Case Report Prosthetic Rehabilitation of Maxillary Defects Case Report
 Case Report Prosthetic Rehabilitation of Maxillary Defects Case Report Reena Luthra Department of Prosthodontics, Swami Devi Dyal Dental College &Hospital, Barwala, Haryana, India Corresponding Author:
Case Report Prosthetic Rehabilitation of Maxillary Defects Case Report Reena Luthra Department of Prosthodontics, Swami Devi Dyal Dental College &Hospital, Barwala, Haryana, India Corresponding Author:
TOOTH SUPPORTED MANDIBULAR OVERDENTURE: A FORGOTTEN CONCEPT
 TJPRC: International Journal of Prosthetic Dentistry & Research (TJPRC:IJPDR) Vol. 1, Issue 1, Jun 2017, 5-10 TJPRC Pvt. Ltd. TOOTH SUPPORTED MANDIBULAR OVERDENTURE: A FORGOTTEN CONCEPT ANSUIA GUPTA 1,
TJPRC: International Journal of Prosthetic Dentistry & Research (TJPRC:IJPDR) Vol. 1, Issue 1, Jun 2017, 5-10 TJPRC Pvt. Ltd. TOOTH SUPPORTED MANDIBULAR OVERDENTURE: A FORGOTTEN CONCEPT ANSUIA GUPTA 1,
METHODOLOGY OF PROSTHETIC TREATMENT IN PATIENTS WITH MAXILLECTOMY
 Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org Original article https://doi.org/10.5272/jimab.2018242.2043 Journal of IMAB - Annual Proceeding (Scientific Papers). 2018 Apr-Jun;24(2) METHODOLOGY
Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org Original article https://doi.org/10.5272/jimab.2018242.2043 Journal of IMAB - Annual Proceeding (Scientific Papers). 2018 Apr-Jun;24(2) METHODOLOGY
Making the Unstable Stable-A Case Series of Management of the Flabby Ridge
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 6 Ver. VIII (Jun. 2015), PP 67-71 www.iosrjournals.org Making the Unstable Stable-A Case Series
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 6 Ver. VIII (Jun. 2015), PP 67-71 www.iosrjournals.org Making the Unstable Stable-A Case Series
Saudi Journal of Oral and Dental Research. DOI: /sjodr. ISSN (Print) Dubai, United Arab Emirates Website:
 DOI:10.21276/sjodr Saudi Journal of Oral and Dental Research Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-1300 (Print) ISSN 2518-1297 (Online)
DOI:10.21276/sjodr Saudi Journal of Oral and Dental Research Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-1300 (Print) ISSN 2518-1297 (Online)
INDIAN JOURNAL OF DENTAL ADVANCEMENTS
 INDIAN JOURNAL OF DENTAL ADVANCEMENTS Journal homepage: www.nacd.in CASE REPORT Prosthetic Rehabilitation of A Unilateral Maxillary Defect with an Intermediate Obturator Mirna Garhnayak 1, Lokanath Garhnayak
INDIAN JOURNAL OF DENTAL ADVANCEMENTS Journal homepage: www.nacd.in CASE REPORT Prosthetic Rehabilitation of A Unilateral Maxillary Defect with an Intermediate Obturator Mirna Garhnayak 1, Lokanath Garhnayak
ISPUB.COM. Habitual Centric: A Case Report. Manisha, N Kathuria, A Gupta, N Gupta INTRODUCTION CASE REPORT
 ISPUB.COM The Internet Journal of Geriatrics and Gerontology Volume 6 Number 2 Habitual Centric: A Case Report Manisha, N Kathuria, A Gupta, N Gupta Citation Manisha, N Kathuria, A Gupta, N Gupta. Habitual
ISPUB.COM The Internet Journal of Geriatrics and Gerontology Volume 6 Number 2 Habitual Centric: A Case Report Manisha, N Kathuria, A Gupta, N Gupta Citation Manisha, N Kathuria, A Gupta, N Gupta. Habitual
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Prosthetic Rehabilitation of a Complete Bilateral Maxillectomy Patient: a Technical Report.
 Australian Journal of Basic and Applied Sciences, 3(2): 424-431, 2009 ISSN 1991-8178 Prosthetic Rehabilitation of a Complete Bilateral Maxillectomy Patient: a Technical Report. Namburi Suneel Kumar, Specialist
Australian Journal of Basic and Applied Sciences, 3(2): 424-431, 2009 ISSN 1991-8178 Prosthetic Rehabilitation of a Complete Bilateral Maxillectomy Patient: a Technical Report. Namburi Suneel Kumar, Specialist
Jordan University of Science and Technology Faculty of Applied Medical Sciences Department of Applied Dental Sciences Second Semester Course syllabus
 Jordan University of Science and Technology Faculty of Applied Medical Sciences Department of Applied Dental Sciences Second Semester Course syllabus Course Title Course Number Prerequisites Course Website
Jordan University of Science and Technology Faculty of Applied Medical Sciences Department of Applied Dental Sciences Second Semester Course syllabus Course Title Course Number Prerequisites Course Website
Frequency of the Various Classes of Removable Partial Dentures and Selection of Major Connectors and Direct/Indirect Retainers
 Turk J Med Sci 31 (2001) 445-449 TÜB TAK Filiz KEYF Frequency of the Various Classes of Removable Partial Dentures and Selection of Major Connectors and Direct/Indirect Retainers Received: November 30,
Turk J Med Sci 31 (2001) 445-449 TÜB TAK Filiz KEYF Frequency of the Various Classes of Removable Partial Dentures and Selection of Major Connectors and Direct/Indirect Retainers Received: November 30,
Cleft lip and palate; oronasal istula; prosthetic treatment; O ring attachment
 Open Journal of Clinical & Medical Case Reports Volume 4 (2018) Issue 6 ISSN 2379-1039 Prosthetic treatment of a unilateral left cleft lip and palate with anoronasal istula: A case report Yesiboli Yeerken,
Open Journal of Clinical & Medical Case Reports Volume 4 (2018) Issue 6 ISSN 2379-1039 Prosthetic treatment of a unilateral left cleft lip and palate with anoronasal istula: A case report Yesiboli Yeerken,
REMOVABLE PROSTHODONTICS
 REMOVABLE PROSTHODONTICS UnitedHealthcare Dental Coverage Guideline Guideline Number: DCG020.03 Effective Date: January 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...1 BENEFIT CONSIDERATIONS...1
REMOVABLE PROSTHODONTICS UnitedHealthcare Dental Coverage Guideline Guideline Number: DCG020.03 Effective Date: January 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...1 BENEFIT CONSIDERATIONS...1
Prosthodontic Treatment Of A Patient With Ectodermal Dysplasia: A Case Report
 ISPUB.COM The Internet Journal of Dental Science Volume 7 Number 2 Prosthodontic Treatment Of A Patient With Ectodermal Dysplasia: A Case Report I Sarikaya, A Güler Citation I Sarikaya, A Güler. Prosthodontic
ISPUB.COM The Internet Journal of Dental Science Volume 7 Number 2 Prosthodontic Treatment Of A Patient With Ectodermal Dysplasia: A Case Report I Sarikaya, A Güler Citation I Sarikaya, A Güler. Prosthodontic
Prosthetic Rehabilitation of a Velopharyngeal Defect: A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 4 Ver. X (Apr. 2015), PP 01-05 www.iosrjournals.org Prosthetic Rehabilitation of a Velopharyngeal
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 4 Ver. X (Apr. 2015), PP 01-05 www.iosrjournals.org Prosthetic Rehabilitation of a Velopharyngeal
MAURO FRADEANI, MD, DDS
 ESTHETIC REHABILITATION IN FIXED PROSTHODONTICS PROSTHETIC MAURO FRADEANI, MD, DDS Private Practice Pesaro and Milan, Italy TREATMENT A SYSTEMATIC APPROACH TO ESTHETIC, BIOLOGIC, AND FUNCTIONAL INTEGRATION
ESTHETIC REHABILITATION IN FIXED PROSTHODONTICS PROSTHETIC MAURO FRADEANI, MD, DDS Private Practice Pesaro and Milan, Italy TREATMENT A SYSTEMATIC APPROACH TO ESTHETIC, BIOLOGIC, AND FUNCTIONAL INTEGRATION
Stock Tray Modification for Two-Stage Impression Technique for Recording Flabby Ridges: Report of a Case Series
 I J Pre Clin Dent Res 2014;2(1):75-79 January-March All rights reserved International Journal of Preventive & Clinical Dental Research Stock Tray Modification for Two-Stage Impression Technique for Recording
I J Pre Clin Dent Res 2014;2(1):75-79 January-March All rights reserved International Journal of Preventive & Clinical Dental Research Stock Tray Modification for Two-Stage Impression Technique for Recording
SCD Case Study. Implant-supported overdentures
 SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
Double-casting method for fixed prosthodontics with functionally generated path
 Double-casting method for fixed prosthodontics with functionally generated path Shogo Minagi, DDS, PhD, a Toshiyuki Tanaka, DDS, b Takashi Sato, DDS, PhD, c and Tadashi Matsunaga, DDS, PhD d Department
Double-casting method for fixed prosthodontics with functionally generated path Shogo Minagi, DDS, PhD, a Toshiyuki Tanaka, DDS, b Takashi Sato, DDS, PhD, c and Tadashi Matsunaga, DDS, PhD d Department
Prosthodontic Rehabilitation with Overdenture Using Modified Impression Technique: A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 10 Ver.VII (Oct. 2015), PP 102-107 www.iosrjournals.org Prosthodontic Rehabilitation with Overdenture
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 10 Ver.VII (Oct. 2015), PP 102-107 www.iosrjournals.org Prosthodontic Rehabilitation with Overdenture
Ojaws is found to be a rare neoplasm of
 Abstract : A Combination Prosthesis -Magnet Retained Lip Plumper- A Case Report 1 2 3 4 Dhanpal S, Chitturi RK, Bhasmey SR, Mannava SP Acquired defects of the orofacial structures must be analysed as to
Abstract : A Combination Prosthesis -Magnet Retained Lip Plumper- A Case Report 1 2 3 4 Dhanpal S, Chitturi RK, Bhasmey SR, Mannava SP Acquired defects of the orofacial structures must be analysed as to
Samantha W. Chou, D.M.D N. Southport Ave. Chicago, Illinois Phone: Fax:
 Samantha W. Chou, D.M.D. 2325 N. Southport Ave. Chicago, Illinois 60614 Phone: 312-608-6881 Fax: 773-296-0601 Samanthawchou@gmail.com What is our role as the dentist? "We live in a culture in which people
Samantha W. Chou, D.M.D. 2325 N. Southport Ave. Chicago, Illinois 60614 Phone: 312-608-6881 Fax: 773-296-0601 Samanthawchou@gmail.com What is our role as the dentist? "We live in a culture in which people
INDIAN DENTAL JOURNAL
 ATTACHMENT RETAINED CAST PARTIAL DENTURE USING RHEIN 83 OT-CAP Dr. Charu Gupta 1 Dr. Harshul Sharma 2 Dr. Merrily Nongsiej 3 Dr. AbhinavShekhar 4 1 Senior Resident, Department of Prosthodontics, King George
ATTACHMENT RETAINED CAST PARTIAL DENTURE USING RHEIN 83 OT-CAP Dr. Charu Gupta 1 Dr. Harshul Sharma 2 Dr. Merrily Nongsiej 3 Dr. AbhinavShekhar 4 1 Senior Resident, Department of Prosthodontics, King George
Solid Zirconia Full-Arch Implant Prosthesis (Protocol C All-CAD with Multi-Unit Abutments) BruxZir. FIRST Appointment. The BruxZir
 (Protocol C All-CAD with Multi-Unit Abutments) Step-by-Step Restorative Protocol C The BruxZir Full-Arch Implant Prosthesis offers a fixed, all-zirconia implant solution for edentulous patients desiring
(Protocol C All-CAD with Multi-Unit Abutments) Step-by-Step Restorative Protocol C The BruxZir Full-Arch Implant Prosthesis offers a fixed, all-zirconia implant solution for edentulous patients desiring
Telescopic Retainers: An Old or New Solution? A Second Chance to Have Normal Dental Function
 Telescopic Retainers: An Old or New Solution? A Second Chance to Have Normal Dental Function Joseph B. Breitman, DMD, FACP, 1,2 Scott Nakamura, DMD, 3 Arnold L. Freedman, DDS, 4 & Irving L. Yalisove, DDS
Telescopic Retainers: An Old or New Solution? A Second Chance to Have Normal Dental Function Joseph B. Breitman, DMD, FACP, 1,2 Scott Nakamura, DMD, 3 Arnold L. Freedman, DDS, 4 & Irving L. Yalisove, DDS
A Study of Classification Systems for Maxillectomy Defects
 A Study of Classification Systems for Maxillectomy Defects Zubair Durrani FFDRCS, FRCS, FRCS (OMFS)* Syed Ghazanfar Hassan FFDRCS** Shomaila Ameer Alam BDS*** * Associate Professor & Consultant Oral and
A Study of Classification Systems for Maxillectomy Defects Zubair Durrani FFDRCS, FRCS, FRCS (OMFS)* Syed Ghazanfar Hassan FFDRCS** Shomaila Ameer Alam BDS*** * Associate Professor & Consultant Oral and
Long-term success of osseointegrated implants
 Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
An Obturator With A Soft Touch: A Case Report
 An Obturator With A Soft Touch: A Case Report Dr. Puneet Batra Abstract:- Factors that affect the management of maxillary defects are the presence of teeth, amount of remaining support area and defect
An Obturator With A Soft Touch: A Case Report Dr. Puneet Batra Abstract:- Factors that affect the management of maxillary defects are the presence of teeth, amount of remaining support area and defect
Case Report Total CAD/CAM Supported Method for Manufacturing Removable Complete Dentures
 Case Reports in Dentistry Volume 2016, Article ID 1259581, 5 pages http://dx.doi.org/10.1155/2016/1259581 Case Report Total CAD/CAM Supported Method for Manufacturing Removable Complete Dentures Arthur
Case Reports in Dentistry Volume 2016, Article ID 1259581, 5 pages http://dx.doi.org/10.1155/2016/1259581 Case Report Total CAD/CAM Supported Method for Manufacturing Removable Complete Dentures Arthur
Conus Concept: A Rewarding Complete Denture Treatment
 Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
Prosthodontic Management of Marginal. Hemimandibulectomy With Surgically Induced Lip Drop
 Prosthodontic Management of Marginal Hemimandibulectomy With Surgically Induced Lip Drop Dr. Krishna Prasad D. 1, Dr. Anupama Prasad D. 2, Dr. Anshul Bardia 3 Department of Prosthodontics and Crown & Bridge,
Prosthodontic Management of Marginal Hemimandibulectomy With Surgically Induced Lip Drop Dr. Krishna Prasad D. 1, Dr. Anupama Prasad D. 2, Dr. Anshul Bardia 3 Department of Prosthodontics and Crown & Bridge,
Selection and arrangement of teeth in rpd
 Selection and arrangement of teeth in rpd upon completion of the articulator mounting and a thorough assessment of the occlusal requirements, the practitioner should be able to perform the proper arrangement
Selection and arrangement of teeth in rpd upon completion of the articulator mounting and a thorough assessment of the occlusal requirements, the practitioner should be able to perform the proper arrangement
Module 2 Introduction to immediate full arch fixed implant treatment - surgical options
 Module 2 Introduction to immediate full arch fixed implant treatment - surgical options First Name Last Name Objectives Identify the need and opportunity to treat full arch patients with fixed detachable
Module 2 Introduction to immediate full arch fixed implant treatment - surgical options First Name Last Name Objectives Identify the need and opportunity to treat full arch patients with fixed detachable
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This
 1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
International Journal of Dentistry and Oral Science (IJDOS) ISSN:
 International Journal of Dentistry and Oral Science (IJDOS) ISSN: 2377-8075 A Novel Functional Impression Procedure for Distal-Extension Removable Partial Dentures Li QL *, Cao Y Case Report Department
International Journal of Dentistry and Oral Science (IJDOS) ISSN: 2377-8075 A Novel Functional Impression Procedure for Distal-Extension Removable Partial Dentures Li QL *, Cao Y Case Report Department
PROSTHETIC REHABILITATION OF MAXILLECTOMY PATIENT WITH TELESCOPIC DENTURES
 CASE REPORT PROSTHETIC REHABILITATION OF MAXILLECTOMY PATIENT WITH TELESCOPIC DENTURES ABSTRACT 1 C RAMU 2 T V PADMANABHAN 3 AHMED HASAN JIBRAN This article describes a technique of management of maxillectomy
CASE REPORT PROSTHETIC REHABILITATION OF MAXILLECTOMY PATIENT WITH TELESCOPIC DENTURES ABSTRACT 1 C RAMU 2 T V PADMANABHAN 3 AHMED HASAN JIBRAN This article describes a technique of management of maxillectomy
Articulation Performance of Patients Wearing Obturators with Different Buccal Extension Designs
 Articulation Performance of Patients Wearing Obturators with Different Buccal Extension Designs Suha Turkaslan a Timucin Baykul b M. Asim Aydin c M. Mustafa Ozarslan a Abstract Objectives: The primary
Articulation Performance of Patients Wearing Obturators with Different Buccal Extension Designs Suha Turkaslan a Timucin Baykul b M. Asim Aydin c M. Mustafa Ozarslan a Abstract Objectives: The primary
Jaw relation registration in RPD
 Jaw relation registration in RPD Why to Record the Jaw Relations? To establish and maintain a harmonious relationship with all oral structures and to provide a masticatory apparatus that is efficient and
Jaw relation registration in RPD Why to Record the Jaw Relations? To establish and maintain a harmonious relationship with all oral structures and to provide a masticatory apparatus that is efficient and
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
University of Groningen. Dental implants in maxillofacial prosthodontics Korfage, Anke
 University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Nagri D et al. Linear occlusion and Neutral Zone recording for severely resorbed ridges
 Doi:10.21276/ledent.2018.02.01.02 Case Report LINEAR OCCLUSION AND NEUTRAL ZONE RECORDING USING TISSUE CONDITIONER REPORT OF A SEVERELY RESORBED RIDGE Divya Nagri, 1Ashish Kakkar, 2Neeraj Mittal, 3Lovely
Doi:10.21276/ledent.2018.02.01.02 Case Report LINEAR OCCLUSION AND NEUTRAL ZONE RECORDING USING TISSUE CONDITIONER REPORT OF A SEVERELY RESORBED RIDGE Divya Nagri, 1Ashish Kakkar, 2Neeraj Mittal, 3Lovely
The Relining Method of Removable Denture with Magnetic Attachments
 The Relining Method of Removable Denture with Magnetic Attachments A. Hiraoka 1, T. Masuda 1, T. Tanaka 2, K. Hayashi 1, K. Shiraishi 1, R. Kanbara 1, Y. Nakamura 1, F. Ito 2, M. Okada 2 and Y. Tanaka
The Relining Method of Removable Denture with Magnetic Attachments A. Hiraoka 1, T. Masuda 1, T. Tanaka 2, K. Hayashi 1, K. Shiraishi 1, R. Kanbara 1, Y. Nakamura 1, F. Ito 2, M. Okada 2 and Y. Tanaka
Review article: Rehabilitation of glossectomy patient: Review
 Review article: Rehabilitation of glossectomy patient: Review Dr. Gunjan Gupta, Dr. Sunil Dhaded, Dr. Shalini B.N. A.M.E`S Dental College, Dept. of Prosthodontics, Raichur. India Corresponding author -
Review article: Rehabilitation of glossectomy patient: Review Dr. Gunjan Gupta, Dr. Sunil Dhaded, Dr. Shalini B.N. A.M.E`S Dental College, Dept. of Prosthodontics, Raichur. India Corresponding author -
Gingiva Solution SR Phonares II, IvoBase, SR Nexco
 Gingiva Solution SR Phonares II, IvoBase, SR Nexco Preface 5 Framework design 6 Framework preparation 8 Finishing of the denture base 10 Gingival modification 12 Mobile mucosa 14 Immobile mucosa 16 Lip
Gingiva Solution SR Phonares II, IvoBase, SR Nexco Preface 5 Framework design 6 Framework preparation 8 Finishing of the denture base 10 Gingival modification 12 Mobile mucosa 14 Immobile mucosa 16 Lip
Oral rehabilitation through preventive approach: Overdenture and fenestrated denture
 Case Report Oral rehabilitation through preventive approach: Overdenture and fenestrated denture Manu Rathee 1, Priyanka Boora 2, Poonam Malik 3* 1 Senior Professor and Head of Department, 2 PG Student,
Case Report Oral rehabilitation through preventive approach: Overdenture and fenestrated denture Manu Rathee 1, Priyanka Boora 2, Poonam Malik 3* 1 Senior Professor and Head of Department, 2 PG Student,
(Images are at the end of article)
 Long term provisionalization during periodontal surgery and extraction site tissue grafting: A Case Review Michael Tischler, DDS Diplomate American Board Of Oral Implantology/Implant Dentistry (Images
Long term provisionalization during periodontal surgery and extraction site tissue grafting: A Case Review Michael Tischler, DDS Diplomate American Board Of Oral Implantology/Implant Dentistry (Images
IMMEDIATEDENTURES: ACLINICALREVIEWANDCASEREPORT
 CASEREPORT IMMEDIATEDENTURES: ACLINICALREVIEWANDCASEREPORT Authors: 44 ABSTRACT Conventionally patients are advised to wait for a minimum period of 3 months, for fabrication of complete denture following
CASEREPORT IMMEDIATEDENTURES: ACLINICALREVIEWANDCASEREPORT Authors: 44 ABSTRACT Conventionally patients are advised to wait for a minimum period of 3 months, for fabrication of complete denture following
Locator retained mandibular complete prosthesis (isy Implant System)
 Locator retained mandibular complete prosthesis (isy Implant System) Mucosa-supported complete prostheses with poor fit greatly reduce people's quality of life. This is why the importance of implant-supported
Locator retained mandibular complete prosthesis (isy Implant System) Mucosa-supported complete prostheses with poor fit greatly reduce people's quality of life. This is why the importance of implant-supported
Occlusion and removable prosthodontics
 12 Occlusion and removable prosthodontics R. Jagger Synopsis Occlusal considerations for removable prostheses are essentially the same as for fixed restorations. The approach to establishing occlusion
12 Occlusion and removable prosthodontics R. Jagger Synopsis Occlusal considerations for removable prostheses are essentially the same as for fixed restorations. The approach to establishing occlusion
