Risk factors of chronic periodontitis on healing response: a multilevel modelling analysis
|
|
|
- Alberta Webster
- 5 years ago
- Views:
Transcription
1 Song et al. BMC Medical Informatics and Decision Making (2017) 17:135 DOI /s RESEARCH ARTICLE Open Access Risk factors of chronic periodontitis on healing response: a multilevel modelling analysis J. Song, H. Zhao, C. Pan, C. Li, J. Liu and Y. Pan * Abstract Background: Chronic periodontitis is a multifactorial polygenetic disease with an increasing number of associated factors that have been identified over recent decades. Longitudinal epidemiologic studies have demonstrated that the risk factors were related to the progression of the disease. A traditional multivariate regression model was used to find risk factors associated with chronic periodontitis. However, the approach requirement of standard statistical procedures demands individual independence. Multilevel modelling (MLM) data analysis has widely been used in recent years, regarding thorough hierarchical structuring of the data, decomposing the error terms into different levels, and providing a new analytic method and framework for solving this problem. The purpose of our study is to investigate the relationship of clinical periodontal index and the risk factors in chronic periodontitis through MLM analysis and to identify high-risk individuals in the clinical setting. Methods: Fifty-four patients with moderate to severe periodontitis were included. They were treated by means of non-surgical periodontal therapy, and then made follow-up visits regularly at 3, 6, and 12 months after therapy. Each patient answered a questionnaire survey and underwent measurement of clinical periodontal parameters. Results: Compared with baseline, probing depth (PD) and clinical attachment loss (CAL) improved significantly after non-surgical periodontal therapy with regular follow-up visits at 3, 6, and 12 months after therapy. The null model and variance component models with no independent variables included were initially obtained to investigate the variance of the PD and CAL reductions across all three levels, and they showed a statistically significant difference (P < 0.001), thus establishing that MLM data analysis was necessary. Site-level had effects on PD and CAL reduction; those variables could explain 77 78% of PD reduction and 70 80% of CAL reduction at 3, 6, and 12 months. Other levels only explain 20 30% of PD and CAL reductions. Site-level had the greatest effect on PD and CAL reduction. Conclusions: Non-surgical periodontal therapy with regular follow-up visits had a remarkable curative effect. All three levels had a substantial influence on the reduction of PD and CAL. Site-level had the largest effect on PD and CAL reductions. Keywords: Chronic periodontitis, Risk factors, Prognosis, Multilevel modelling * Correspondence: yppan@cmu.edu.cn Department of Periodontics and Oral Biology, School of Stomatology, China Medical University, Shenyang , China The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Song et al. BMC Medical Informatics and Decision Making (2017) 17:135 Page 2 of 9 Background Chronic periodontitis is a multifactorial polygenetic disease with an increasing number of associated factors that have been identified over recent decades. Longitudinal epidemiologic studies have demonstrated that the risk factors were related to the progression of the disease [1, 2]. Plaque is an initial and necessary factor for the development of periodontal disease, but it alone does not necessitate periodontitis. The combined effects of different risk factors associated with periodontitis will eventually lead to periodontitis. Currently, some known risk factors associated with periodontitis include plaque, bleeding on probing (BOP), tooth position, age, gender, socio-economic position, smoking, stress-experience, obesity, systemic disease, and more [3 6].. In the past 30 years, one of the great advances in periodontology was the discovery of a huge difference in peoples susceptibility to periodontitis, which was mainly demonstrated in the occurrence, development, and response to treatment. Risk factor assessment and control have been paid increasing amounts of attention due to the belief that these are important parts of periodontal diagnosis and treatment [7]. Recently, researchers have proposed periodontal risk assessments (PRA) or periodontal risk calculators (PRC) [8, 9]. The basic idea is to put various periodontal risk factors together for analysis to help doctors more accurately analyse the progression and prognosis of diseases and then plan customized treatment for each individual. A traditional multivariate regression model was used to find risk factors associated with chronic periodontitis. However, the approach requirement of standard statistical procedures demands individual independence. If this is not done, the analysis will give incorrect or potentially misleading results. Another drawback is that in averaging lower level data to a higher level, the data is artificially simplified; consequently, the statistical power will appear biased. Multilevel modelling (MLM) data analysis has widely been used in recent years, regarding thorough hierarchical structuring of the data, decomposing the error terms into different levels, and providing a new analytic method and framework for solving this problem [10]. In much of periodontal research, statistical methods assume that the site observations are independent and use the mean values of sites to represent the full mouth. Periodontal data with an inherently hierarchical structure poses difficulties for analysis, as sites are clustered around a tooth, and teeth are clustered within the patient. The statistical approach of MLM may solve this problem. MLM has been widely used in education research, management, economics, sociology, psychology, and other fields but less for medical research [11]. In 1992, Albandar [12] stated that the application of multilevel modelling analysis on periodontal research may have important significance. Application of multilevel modelling analysis may provide a more accurate explanation of the natural hierarchical structure of the progression and healing responses after periodontal treatment [13]. MLM can provide a novel approach for periodontal disease research [14, 15]. The aim of the present study was to investigate, by means of multilevel analysis, risk factors that may affect moderate to severe periodontitis prognosis in Northern Chinese who have undergone non-surgical periodontal treatment. Methods Selection of patients The study sample comprised 54 patients who had been referred to the Department of Periodontics at the School of Stomatology, China Medical University, during the years 2012 through Based on sample size estimation of repeated measurement design, we calculated the statistical power using Stata Statistical power was close to 1 in our study. Our statistical power was high, therefore patient number was sufficient in our study. The patients had presented with moderate to severe periodontitis ((i) loss of at least 10 teeth, i.e., 18 existing teeth; or (ii) at least two interproximal sites (not on same tooth) with 6 mm clinical attachment loss and at least one interproximal site with 5 mm pocket depth; or (iii) at least two interproximal sites with 4 5 mm clinical attachment loss and no interproximal sites with clinical attachment loss of 6 mm, and the percentage of sites with pocket depth 4 mm in the upper tertile of the study population) [16]. All the patients received non-surgical periodontal treatments well as follow-up visits at 3, 6 and 12 months. Patients were included if they displayed the following features: 1. Were 35 to 60-years-old and from northeast China, with no prior periodontal or orthodontic treatment. 2. Had at least 16 standing teeth (excluding the third molars). 3. Had no serious mental illness or cognitive dysfunction. Patients were excluded if the patient interview revealed any of the following: 1. Known systemic diseases. 2. Patient did not consent to non-surgical periodontal therapy or regular follow-up visits. 3. A history of systemic antibiotic or periodontal treatment in the preceding 3 months. 4. Pregnant or lactating females. 5. Smoking cessation.
3 Song et al. BMC Medical Informatics and Decision Making (2017) 17:135 Page 3 of 9 Eligible patients who agreed to participate were asked to complete an in-person verbally administered survey. Written consent was obtained prior to the study participation. To ensure that each participant, regardless of his or her literacy level, understood and was willing to participate in the study, the consent form was read to all participants and they consented to the collection of data for the analysis of clinical research. Clinical measurements To obtain personal information, a questionnaire that included Gender(Male/Female), Age, Stress-experience(yes/ no), BMI, Education background(post graduation / graduate / senior school or below), Smokers, Socio-economic (More than USD = 1, USD =2, USD = 3, USD =4, less than USD = 5) was distributed among all the patients. Additional file 1. All patients received the same nonsurgical periodontal treatment, including oral hygiene instruction regarding brushing and inter-dental cleaning, and then regular follow-up visits at 3, 6, and 12 months after treatment. This was a 12-month prospective study. The data collection was conducted at baseline and 3, 6, and 12 months after completion of non-surgical periodontal treatment. The clinical examination and non-surgical periodontal treatment of all patients was performed by a calibrated examiner from the periodontic department. Four sites (mesio-buccal, mid-buccal, disto-buccal, and mid-lingual) per tooth were measured and recorded, excluding the third molars. PD, CAL, BOP, presence of plaque, mobility, and the number of missing teeth were probed with an automated controlled force periodontal probe (Florida Probe 32, Version 6, USA). Data analysis All data were entered in EpiData 3.1 and proofed for entry errors. SPSS12.0 and HLM6.0 statistical software were used to analyse the data. MLM data analysis was used to analyse PD and CAL reductions at the site level at 3, 6, and 12 months compared with baseline PD and CAL. The hierarchical analysis was constructed on three levels: the patient, the tooth, and the tooth site. The patient-level had 11 variables, including gender, age, smoker, BMI, stressexperience, socio-economic position, education level, the number of missing teeth, percentage sites with plaque at baseline, percentage sites with BOP at baseline, and percentage sites with PD 5 mm at baseline. The toothlevel had 2 variables, including tooth position and mobility. The site-level had 3 variables, including plaque at baseline, BOP at baseline, and surface of tooth. The total number of variables associated with all the three levels are shown in Table 1. Results In this study, 54 patients were investigated. A summary of each level and variable is described in Table 2. The mean age was 44.7 ± 1 years old, ranging from 35 to 59, and the sample was equally distributed in terms of gender (55.6% females). Fourteen patients were smokers among the males, and there were no female smokers. The mean BMI was 23.2 ± 0.5 kg/m 2. There were 5 patients who socioeconomic position in terms of income monthly was more than USD, 28 patients with USD, 13 patients with USD, 6 patients with , and 2 patients with less than USD. There were 5 patients with a post-graduate education level, 38 patients with a graduate level, and 11 patients with senior school or below. 57.4% (31/54) of the patients had stressexperience. The mean number of missing teeth was 1.5 ± 0.2. The sample included a total of 1431 teeth, included 641 anterior teeth, 413 premolars, and 377 M. There were 1131 teeth with mobility of 0, 202 teeth with mobility of 1, 80 teeth with mobility of 2, and 18 teeth with mobility of 3. The mean percentage sites with plaque at baseline were79.3% ± 1.6%. The mean percentage sites with BOP at baseline were 66.5% ± 2.0%. The mean percentage sites with PD 5 mm at baseline were 28.3% ± 1.8%. Sites with positive plaque index totaled 4547, while 3784 sites were positive in BOP index, making a total of 5724 sites at baseline. In response to non-surgical periodontal treatment, the full-mouth mean PD and CAL showed significant reductions at 3, 6, and 12 months compared with the baseline. The mean PD was 3.83 ± 0.17 mm at baseline, 2.04 ± 0.01 mm at 3 months, 2.01 ± 0.01 mm at 6 months, 1.19 ± 0.01 mm at 12 months. The mean CAL was 3.70 ± 0.03 mm at baseline, 3.04 ± 0.02 mm at 3 months, 2.98 ± 0.02 mm at 6 months, 2.89 ± 0.02 mm at 12 months. Multilevel statistical analysis Traditional statistical methods require individual independent variables, but the site-level observations in this study are not truly independent. Consequently, MLM analysis was used to investigate the possible factors in response to non-surgical periodontal treatment in terms of both PD and CAL reduction. Diversity of PD and CAL reductions between teeth The null model was the basis upon which to use MLM analysis. When different levels were determined to be correlated, MLM analysis was used; otherwise, a traditional statistical method was used. To investigate the reduction of PD and CAL across all three levels, the null model with the independent variables included were established (Table 3). Level 1 : Y ijk ¼ β ojk þ γ ijk
4 Song et al. BMC Medical Informatics and Decision Making (2017) 17:135 Page 4 of 9 Table 1 Variable assignment table Variables Assignment Patient -level Level 3 Age continuous variable Gender female =1, male =2 Smokers yes = 1, no = 0 BMI continuous variable Socio-economic More than USD = 1, USD =2, USD = 3, USD =4, less than USD = 5 Education background post graduation =1, graduate =2, senior school or below =3 Stress-experience yes = 1,no = 0 Number of missing teeth continuous variable % of sites with plaque at baseline continuous variable % of sites with BOP at baseline continuous variable % of sites with PD 5 mm at baseline continuous variable Tooth-level Level 2 Tooth position anterior = 1, premolar = 2, molar = 3 Mobility Do not have mobility = 0, mobility 1 mm = 1, 1 mm < mobility 2 mm = 2, mobility > 2 mm = 3 Site-level Level 1 Plaque at baseline presence = 1, absence = 0 BOP at baseline presence = 1, absence = 0 Surface of tooth 1 = buccal / lingual, 2 = mesiocclusion/distocclusion Level 2 : β ojk ¼ γ 00k þ μ ojk Level 3 : γ 00k ¼ π 000 þ e ook Y ijk, indicates the reduction in PD and CAL in patient Y, with i as the patient number, j as the tooth number, and k as the site number. Β ojk was the mean reduction of patient Y, γ 00k was the mean reduction of tooth β ojk, and π 000 was the mean reduction of site γ 00k. γ ijk represented the variation between the sites, which was the random component of Y ijk. μ ojk represented the variation between the teeth, which was the random component of β ojk.e ook represented the variation between the patients, which was the random component of γ 00k. The variance components showed that significant variations existed in all three levels (p < 0.001).Thus, it was necessary to use MLM analysis. The reduction of PD and CAL was significantly different among the teeth. Site-level significantly affected PD and CAL reductions: the variables could explain 77 78% of PD reduction and 70 80% of CAL reduction at 3, 6, and 12 months. As for the toothlevel, the variables could explain 11 12% of PD reduction and 10 11%of CAL reduction at 3,6,and 12 months.for patient-level effect on PD and CAL reductions, the variance explained 10 11% of PD reduction and 13 14% of CAL reduction at 3, 6, and 12 months. The influence of variables on PD and CAL reduction A total of 16 independent variables, with 11 on the patient level, 2 on the tooth level, and 3 on the site level, were included in the MLM analysis. Level-1: Y ijk ¼ β ojk þ β 1jk X 1ijk þ β 2jk X 2ijk þ β 3jk X 3ijk þ γ ijk Level-2: β ojk ¼ γ 00k þ γ 01k W 1jk þ γ 02k W 2jk þ μ ojk β 1jk ¼ γ 10k β 2jk ¼ γ 20k β 3jk ¼ γ 30k Level-3: γ 00k ¼ π 000 þ π 001 Z 00k þ π 002 Z 01k þ π 003 Z 03k þ π 004 Z 04k þ π 005 Z 05k þ π 006 Z 06k þ π 007 Z 07k þ π 008 Z 08k þ π009 Z 09k þ π 010 Z 10k þ π 011 Z 11k þ e ook γ 01k ¼ π 010 γ 02k ¼ π 020 The relationship of the risk factors and PD on healing response.
5 Song et al. BMC Medical Informatics and Decision Making (2017) 17:135 Page 5 of 9 Table 2 Baseline clinical and periodontal parameters by variables Variable Mean ± SD Patient -level (N = 54) Age (years) 44.7 ± 1 BMI(kg/ m 2 ) 23.2 ± 0.5 Number of missing teeth (N) 1.5 ± 0.2 % of sites with plaque at baseline 1.11 ± 0.15 a % of sites with BOP at baseline 0.97 ± 0.17 a % of sites with PD 5 mm at baseline 0.55 ± 0.15 a Variable N (%) Patient-level (N = 54) Gender Male 24(44.4%) Female 30(55.6%) Smokers Yes 14(25.9%) No 40(74.1%) Socio-economic More than USD 5 (9.3%) USD 28 (51.8%) USD 13 (24.1) USD 6 (11.1%) Less than USD = 5 2 (3.7%) Education background (N) post graduation 5 (9.3%) Graduate 38 (70.4%) senior school or below 11(20.3%) Stress-experience Yes 31(57.4%) No 23(42.6%) Tooth-level (N = 1431) Tooth position Anterior 641 (44.8%) Premolar 413 (28.9%) Molar 377 (26.3%) Mobility Do not have mobility 1131 (79.0%) mobility 1 mm 202 (14.1%) 1 mm < mobility 2 mm 80 (5.6%) mobility > 2 mm 18 (1.3%) Site-level (N = 5724) Plaque at baseline Presence 4547(79.4%) Absence 1177(20.6%) BOP at baseline Table 2 Baseline clinical and periodontal parameters by variables (Continued) Presence 3784(66.1%) Absence 1940(33.9%) Surface of tooth buccal / lingual 2862(50%) mesiocclusion/distocclusion 2862(50%) a: data after arcsine square root transformation A total of 5724 sites distributed on 1431 teeth in the 54 patients were included in this study. Compared with the baseline, the mean reduction in PD was 1.79 mm, 1.82 mm, 2.64 mm at 3, 6, and 12 months. At the site level, presence of BOP at baseline and the mesiocclusion/distocclusion surface of teeth showed a significantly greater reduction in PD at 3, 6, and 12 months (p < 0.05). The variables on the site level were reduced by 7%, 6%, 7% of PD reduction at 3, 6, and 12 months when compared with the corresponding Variance Component Models (Table 4). At the tooth level, more mobility showed significantly greater reduction in PD at 3, 6, and 12 months (p < 0.05). Table 3 Variance Components models for reduction in PD and CAL Variance SE Variance Components p The reduction in 3-month PD Patient (level-3) (10%) *** Tooth (level-2) (12%) *** Site (level-1) (78%) The reduction in 6-month PD Patient (level-3) (12%) *** Tooth (level-2) (11%) *** Site (level-1) (77%) The reduction in 12-month PD Patient (level-3) (11%) *** Tooth (level-2) (11%) *** Site (level-1) (78%) The reduction in 3-month CAL Patient (level-3) (16%) *** Tooth (level-2) (11%) *** Site (level-1) (73%) The reduction in 6-month CAL Patient (level-3) (14%) *** Tooth (level-2) (10%) *** Site (level-1) (76%) The reduction in 12-month CAL Patient (level-3) (13%) *** Tooth (level-2) (10%) *** Site (level-1) (77%) *** p<0.001
6 Song et al. BMC Medical Informatics and Decision Making (2017) 17:135 Page 6 of 9 Table 4 Random intercept models for reduction in PD and CAL Intercept Patient level PD 3-month Estimate 6-month Estimate 12-month Estimate CAL 3-month Estimate 6-month Estimate 12-month Estimate Gender 0.006(0.155) 0.068(0.131) 0.130(0.125) 0.869(0.267) 0.549(0.188) 0.517(0.265) Age 0.005(0.005) 0.006(0.005) 0.008(0.005) 0.011(0.011) 0.002(0.009) 0.009(0.009) BMI 0.010(0.016) 0.018(0.012) 0.000(0.015) 0.079(0.033) 0.012(0.020) 0.041(0.025) Smokers 0.088(0.150) 0.099(0.129) 0.068(0.135) 0.780(0.230) 0.866( (0.242 Socio-enconomic 0.043(0.054) 0.075(0.044) 0.045(0.061) 0.033(0.127) 0.039(0.092) 0.035(0.104) Education background 0.009(0.101) 0.041(0.079) 0.109(0.098) 0.013(0.210) 0.061(0.138) 0.091(0.175) Stress-experience 0.290(0.010) 0.268(0.076) 0.389(0.087) 0.190(0.183) 0.154(0.156) 0.093(0.168) Number of missing teeth 0.014(0.029) 0.004(0.024) 0.021(0.043) 0.015(0.070) 0.036(0.052) 0.033(0.819) % of sites with plaque at baseline 0.407(0.399) 0.240(0.308) 0.137(0.417) 1.326(0.962) 0.876(0.821) 1.302(0.642) % of sites with BOP at baseline 0.189(0.440) 0.005(0.238) 0.068(0429) 1.162(0.740) 0.907(0.615) 0.923(0.008) % of sites with PD 5mmat baseline Tooth-level 1.43(0.467) 2251(0.363) 1.468(0.495) 0.647(0.703) 1399(0.592) 1.032(0.743) Tooth position 0.062(0.035) 0.080(0.032) 0.047(0.039) 0.125(0.049) 0.136(0.039) 0.062(0.045) Mobility 0.211(0.057) 0.158(0.048) 0.190(0.054) 0.115(0.059) 0.057(0.070) 0.161(0.071) Site-level BOP at baseline 0.607(0.050) 0.563(0.051) 0.585(0.059) 0.542(0.073) 0.581(0.062) 0.691(0.065) Plaque at baseline 0.088(0.045) 0.056(0.048) 0.036(0.048) 0.009(0.067) 0.078(0.062) 0.064(0.063) Surface of tooth 0.254(0.030) 0.244(0.031) 0.202(0.031) 0.470(0.048) 0.547(0.045) 0.572(0.044) Variance Subject Tooth Site Total variance % reduction in variance Patient 50% 79% 65% 40% 48% 38% Tooth 25% 22% 20% 3% 7% 3% Site 7% 6% 6% 4% 8% 10% boldface representative P < 0.05 Anterior teeth showed a significantly greater reduction in PD only at 6 months (p < 0.05). The variables on the tooth level were reduced by 25%, 22%, and 20% of PD reduction at 3, 6, and 12 months when compared with the corresponding Variance Components Models (Table 4). At the patient level, no stress-experience and more percentage sites with PD 5 mm at baseline showed significant greater reductions in PD at 3, 6, and 12 months (p < 0.05). The variables on the patient level were reduced by 50%, 79%, and 65% of PD reduction at 3, 6, and 12 months when compared with the corresponding Variance Components Models (Table 4). The relationship of the risk factors and CAL on healing response A total of 5724 sites distributed on 1431 teeth in the 54 patients were included in this study. Compared with the baseline, the mean reduction in CAL was 0.66 mm, 0.72 mm, and 0.81 mm at 3, 6, and 12 months. At the site level, the presence of BOP at baseline and mesiocclusion/distocclusion surface of the tooth showed a significantly greater reduction in CAL at 3, 6, and 12 months (p < 0.05). The variables on the site level were reduced by 4%, 8%, and 10% of CAL reduction at 3, 6, and 12 months when compared with the corresponding Variance Components Models (Table 4). At the tooth level, the anterior teeth compared with the molars showed a significantly greater reduction in CAL at 3, 6, and 12 months (p < 0.05). More mobility showed a significantly greater reduction in CAL only at 12 months (p < 0.05). The variables for the tooth level were reduced by 3%, 7%, and 3% of CAL reduction at 3, 6, and 12 months when compared with the corresponding Variance Components Models (Table 4).
7 Song et al. BMC Medical Informatics and Decision Making (2017) 17:135 Page 7 of 9 At the patient level, females and non-smokers showed significantly greater reductions in CAL at 3, 6, and 12 months (p < 0.05). More percentage sites with PD 5 mm at baseline showed a significantly greater reduction in CAL only at 6 months (p < 0.05).The variables on the patient level were reduced by 40%, 48%, and 38% of CAL reduction at 3, 6, and 12 months when compared with the corresponding Variance Components Models (Table 4). Discussion The present study used variance component models to correctly specify the periodontal data structure and to compare the risk factors of moderate to severe periodontitis. The results of this study demonstrated that variances at each level were statistically significant, implying that ignoring any level may result in an erroneous finding. The variance components showed that the teeth variable was less similar than the subjects variable, and the sites variable was greater than both, implying that the reduction of PD and CAL is more substantial among different sites. Thus, the subject, tooth, and site levels should be considered when investigating the correlation structure of periodontal data. A previous study [17] used a periodontal pocket close situation as evaluation criteria for the efficacy of periodontal treatment. However, periodontal pocket close did not fully reflect the effects of basic treatment, especially for patients with moderate to severe periodontitis. Therefore, in this study we used not only PD reduction but also CAL reduction as indicators to evaluate the efficacy of non-surgical periodontal treatment for patients with severe chronic periodontitis. The results of the present study demonstrated that non-surgical periodontal treatment was significant for moderate to severe periodontitis. Site-level had the most effect on PD and CAL reductions. The result was the same as that in Tu YK s study [18]. Subject-level showed that males have a higher prevalence of clinical attachment loss. Studies by Hujoel et al. [19] have shown that male attachment loss is 3 mm, 4 mm, and 5 mm higher than 23%, 44%, and 55% that of females, respectively; that males consistently had more attachment loss than females at each age is not surprising due to males poor oral health awareness, self-care, and dental visiting practices, which may be related to hormones and oral hygiene habits [20]. Recent studies have shown that even after excluding smoking and oral hygiene, males still have higher morbidity, that relatively severe periodontitis may be related to differences in sex-specific immune function of the X chromosome differences, and that hormone secretion may lead to differences in the immune response of gender [21]. Male and female innate immunity and acquired immunity are quite different: the male body contains more IL-1β and TNF-α than the female body, but for these cytokines, infection and damage are closely linked. Smoking showed a negative impact on CAL reduction, which corroborates data reported in reviews on the effect of smoking on the outcome of periodontal treatment [22]. Smoking seriously affects periodontal health and inhibits osteoblast growth due to aggravated bone resorption. The random intercept models revealed an interaction between smoking and CAL reduction, yielding negative effect of smoking compared with non-smokers [23].Non-surgical periodontal therapy in patients with the poor treatment effect of smoking may inhibit fibroblast cell growth and attachment, affect the repair of periodontal tissue, affect periodontal tissue microcirculation, and impede periodontal tissue metabolism. Similar findings have previously been reported showing that smoking was a significant factor in determining the short-term clinical outcome of non-surgical periodontal treatment [24]. Stress-experience factors included stress, depression, anxiety, and tension. The higher the stress-experience, the higher the level of gingival sulcus fluid IL-6, which may affect immune function [25]. Pressure increases glucocorticoids to suppress the immune response of T cells, which makes it easy to accumulate plaque and affect the effectiveness of the treatment. The tooth-level covariates continued to show a linear relationship for the percentage of sites with PD 5mm at baseline and mobility. The main indicator of the degree of periodontal inflammation is PD. The more percentage of sites with PD 5 mm at baseline represents a more mobility-described infection and more severe inflammation, which means that then on-surgical periodontal treatment had room for improvement. During the period of observation, the premolars showed less overall change in CAL reduction than the anterior but more than the molars. Molars (M) are considered to have a more doubtful prognosis [26]. The presence of furcation defects, the divergence of roots, the dimensions of the furcation entrances, the concavities on the root surfaces, the cervical enamel projections, and even the more posterior position of the arches are considered factors that influence the establishment and progression of the periodontal destruction of molars. Due to the presence of molar root bifurcation, inflammation is not easy to control, and cleaning the rearward position is difficult. Because of the existence of premolar root surface concaves, infection is not easy to control. Among the site-level covariates, there were some new discoveries. BOP at baseline and surface of tooth showed positive predictions for PD reduction and CAL reduction with non-surgical periodontal treatment [27]. As we all know, plaque is the initial factor for periodontitis. However, the present study showed that the plaque at baseline and the percentage of sites with plaque at baseline had no significant effect on the prognosis of non-
8 Song et al. BMC Medical Informatics and Decision Making (2017) 17:135 Page 8 of 9 surgical periodontal treatment. Tomasi C et al. [17], in a multilevel approach of factors influencing the outcome of non-surgical periodontal treatment, showed that the aggregated variable of percentage of sites with plaque on the subject-level was not a significant factor, but the presence of plaque at site-level was identified as significant. The main difference is the reason for the research object selected: the Chinese people have relatively poor oral hygiene practices overall, with percentage of sites with plaque at baseline of more than 95%. Therefore, this study did not show an effect of the presence of plaque at the site-level. China is still a developing country; economic development is especially lacking in Northern China, where the socio-economic position and education level is low. The cost of treatment is expensive and not reimbursed, leading to poor awareness of dental initiative, poor oral hygiene, and poor attendance rates in accordance with the development of the treatment plan. Therefore, few patients meet the requirements of the treatment plan. Taken together, MLM was appropriately applied in the analysis of periodontal data. By means of the relevant data analysis, the risk factors that affected the prognosis of periodontitis could successfully be investigated. Accordingly, the effect of periodontal therapy could be enhanced along with proper control of the relevant risk factors. Although the one-factor evaluation was far from adequate for predicting disease prognosis, multi-factor analysis was overwhelmingly successful in evaluating the prognosis of individual periodontitis [24, 28]. For the reason that various risk factors showed different effects on disease and the same individual was affected by multiple risk factors at the same time, evaluation of the effect on disease prognosis from multiple risk factors on the same individual was particularly important in guiding our clinical work. Conclusions The study found that non-surgical periodontal treatment with regular follow-up visits had a remarkable curative effect for moderate to severe chronic periodontitis in terms of PD and CAL reductions. Periodontal data have been confirmed to have an inherently hierarchical structure. Use of MLM allowed determination of the impact of the patient, the tooth, and the tooth site factors on healing responses to non-surgical periodontal therapy in chronic periodontitis. Through MLM analysis found all three levels had a substantial influence on the reduction of PD and CAL. Site-level had the largest effect on PD and CAL reductions. Additional files Additional file 1: Periodontal risk factors. (DOC 30 kb) Abbreviations BOP: Bleeding on probing; CAL: Clinical attachment loss; MLM: Multilevel modelling; PD: Probing depth; PRA: Proposed periodontal risk assessments; PRC: Periodontal risk calculators Acknowledgements The study was funded through Liaoning Clinical Capability Construction Programs of Provincial Health and Family Planning Commission. The authors would like to thank Guoyuan Sui for help in the statistics. Funding This study was supported by a grant from the Liaoning Clinical Capability Construction Programs of Provincial Health and Family Planning Commission (No:LNCCC-C ). Availability of data and materials The data was presented in the article attachment named Data. Authors contributions Conceived and designed the experiments: YPP, JS. Performed the experiments: YPP, JS. Analyzed the data: JS. Contributed reagents/materials/ analysis tools: JS, HJZ, CLP, CL, JBL. Wrote the paper: JS. All the authors read and approved the final manuscript. Ethics approval and consent to participate All of Eligible patients who agreed to participate were asked to complete an in-person verbally administered survey. Written consent was obtained prior to the study participation. To ensure that each participant, regardless of his or her literacy level, understood and was willing to participate in the study, the consent form was read to all participants and they consented to the collection of data for the analysis of clinical research. And the research protocol was approved by the China Medical University ( ). Consent for publication Not applicable. Competing interests The authors declare that they have no competing interests. Publisher s Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. Received: 16 March 2017 Accepted: 4 September 2017 References 1. Heitz-Mayfield LJA. Disease progression: identification of high-risk groups and individuals for periodontitis. J Clin Periodontol. 2005;32(Suppl. 6): Borrell LN, Papapanou PN. Analytical epidemiology of periodontitis. J Clin Periodontol. 2005;32(Suppl. 6): Genco RJ, Borgnakke WS. Risk factors for periodontal disease. Periodontol. 2013;62(1): Ramseier CA. Potential impact of subject-based risk factor control on periodontitis. J Clin Periodontol. 2005;32(6): Bharti V, Khurana P. Metabolic syndrome and periodontal disease. J Indian Soc Periodontol. 2009;13(3): Otomo-Corgel J, Pucher JJ, Rethman MP, et al. State of the science: chronic periodontitis and systemic health. J Evid Based Dent Pract. 2012;12(3 Suppl): Pihlstrom BL. Periodontal risk assessment, diagnosis and treatment planning. Periodontol. 2001;25: Costa FO, Miranda LO, Pereira EJ, et al. Periodontal risk assessment (Pra) model in a sample of regular and irregular compliers under maintenance therapy: a 3-year prospective study. J Periodontol. 2012;83(3): Lindskog S, Blomlöf J, Persson I, et al. Validation of an algorithm for chronicperiodontitis risk assessment and prognostication: risk predictors, explanatory values, measures of quality, and clinical use. J Periodontol. 2010; 81(4): Peugh JL. A practical guide to multilevel modeling. J Sch Psychol. 2010; 48(1):
9 Song et al. BMC Medical Informatics and Decision Making (2017) 17:135 Page 9 of Kahn JH. Multilevel modeling: overview and applications to research incounseling psychology. J Couns Psychol. 2011;58(2): Albandar JM, Goldstein H. Multi-level statistical models in studies of periodontal diseases. J Periodontol. 1992;63(8): Chung H, Beretvas SN. The impact of ignoring multiple membership datastructures in multilevel models. Br J Math Stat Psychol. 2012;65(2): Burnside G, Pine CM, Williamson PR. Statistical power of multilevel Modelling in dental caries clinical trials: a simulation study. Caries Res. 2013;48(1): Axtelius B, Söderfeldt B, Attström R. A multilevel analysis of factors affecting pocket probing depth in patients responding differently to periodontal treatment. J Clin Periodontol. 1999;26(2): Wu X, Offenbacher S, Lopez NJ, et al. Association of interleukin-1 gene variations with moderate to severe chronic periodontitis in multiple ethnicities. J Periodontal Res. 2015;50: Tomasi C, Leyland AH, Wennström JL. Factors influencing the outcome ofnon-surgical periodontal treatment: a multilevel approach. J Clin Periodontol. 2007;34(8): Tu YK, Gilthorpe MS, Griffiths GS. The application of multilevel modeling in the analysis of longitudinal periodontal data part I: absolute levels of disease. J Periodontol. 2004;75(1): Hujoel PP, Loesche WJ, DeRouen TA. Assessment of relationships between site-specific variables. J Periodontol. 1990;61(6): Shiau HJ, Reynolds MA. Sex differences in destructive periodontal disease: exploring the biologic basis. J Periodontol. 2010;81(11): Tu YK, Gilthorpe MS, Griffiths GS, et al. The application of multilevel modeling in the analysis of longitudinal periodontal data part II: changes in disease levels over time. J Periodontol. 2004;75(1): Omasi C, Leyland AH, Wennström JL. Factors influencing the outcome of non-surgical periodontal treatment: a multilevel approach. J Clin Periodontol. 2007;34(8): Zeng J, Williams SM, Fletcher DJ, et al. Reexamining the association between smoking and periodontitis in the dunedin study with an enhanced analytical approach. J Periodontol. 2014;85(10): Wan CP, Leung WK, Wong MC, et al. Effects of smoking on healing response to non-surgical periodontal therapy: a multilevel modelling analysis. J Clin Periodontol. 2009;36(3): Saini R, Saini S, Saini SR. Periodontitis and psychological stress: a dental view. Ind Psychiatry J. 2010;19(1): Heitz-Mayfield L, Trombelli L, Heitz F, et al. A systematic review of the effect of surgical debridement vs. non-surgical debridement for the treatment of chronic periodontitis. J Clin Periodontol. 2002;29(Suppl3): Rahardjo A, Yoshihara A, Amarasena N, et al. Relationship between bleeding on probing and periodontal disease progression in community-dwelling older adults. J Clin Periodontol. 2005;32(11): Clarke P. When can group level clustering be ignored?multilevel models versus single-level models with sparse data. J Epidemiol Community Health. 2008;62(8): Submit your next manuscript to BioMed Central and we will help you at every step: We accept pre-submission inquiries Our selector tool helps you to find the most relevant journal We provide round the clock customer support Convenient online submission Thorough peer review Inclusion in PubMed and all major indexing services Maximum visibility for your research Submit your manuscript at
Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition. By: Kimberly Hawrylyshyn
 Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition By: Kimberly Hawrylyshyn Background Periodontitis is a microbe induced inflammatory disease that
Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition By: Kimberly Hawrylyshyn Background Periodontitis is a microbe induced inflammatory disease that
PERIODONTAL CASE PRESENTATION - 1
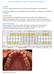 PERIODONTAL CASE PRESENTATION - 1 Overview A 32 year-old patient presented with generalized aggressive periodontitis. Treatment included non-surgical therapy with adjunctive antibiotics and surgical treatment.
PERIODONTAL CASE PRESENTATION - 1 Overview A 32 year-old patient presented with generalized aggressive periodontitis. Treatment included non-surgical therapy with adjunctive antibiotics and surgical treatment.
Mechanical Non Surgical Therapy: An Indispensable Tool
 IOSR Journal of Dental and Medical Sciences (JDMS) ISSN: 2279-0853, ISBN: 2279-0861. Volume 1, Issue 4 (Sep-Oct. 2012), PP 36-41 Mechanical Non Surgical Therapy: An Indispensable Tool 1 Ashu Bhardwaj,
IOSR Journal of Dental and Medical Sciences (JDMS) ISSN: 2279-0853, ISBN: 2279-0861. Volume 1, Issue 4 (Sep-Oct. 2012), PP 36-41 Mechanical Non Surgical Therapy: An Indispensable Tool 1 Ashu Bhardwaj,
Advanced Probing Techniques
 Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Alarge number of sound clinical
 Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report
 Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Linking Research to Clinical Practice
 Is Non Surgical Periodontal Therapy Cost Effective? Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information
Is Non Surgical Periodontal Therapy Cost Effective? Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information
Torsion bottle, a very simple, reliable, and cheap tool for a basic scoliosis screening
 Romano and Mastrantonio Scoliosis and Spinal Disorders (2018) 13:4 DOI 10.1186/s13013-018-0150-6 RESEARCH Open Access Torsion bottle, a very simple, reliable, and cheap tool for a basic scoliosis screening
Romano and Mastrantonio Scoliosis and Spinal Disorders (2018) 13:4 DOI 10.1186/s13013-018-0150-6 RESEARCH Open Access Torsion bottle, a very simple, reliable, and cheap tool for a basic scoliosis screening
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Dental Policy Subject: Teeth with a Poor or Guarded Prognosis Guideline #: Clinical Policy - 01 Publish Date: 03/15/2018 Status:
 Dental Policy Subject: Teeth with a Poor or Guarded Prognosis Guideline #: Clinical Policy - 01 Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/06/2018 Description This document addresses
Dental Policy Subject: Teeth with a Poor or Guarded Prognosis Guideline #: Clinical Policy - 01 Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/06/2018 Description This document addresses
Longitudinal Supportive Periodontal Therapy for Severe Chronic Periodontitis with Furcation Involvement: A 12-year Follow-up Report
 Bull Tokyo Dent Coll (2013) 54(4): 243 250 Case Report Longitudinal Supportive Periodontal Therapy for Severe Chronic Periodontitis with Furcation Involvement: A 12-year Follow-up Report Akiyo Komiya-Ito,
Bull Tokyo Dent Coll (2013) 54(4): 243 250 Case Report Longitudinal Supportive Periodontal Therapy for Severe Chronic Periodontitis with Furcation Involvement: A 12-year Follow-up Report Akiyo Komiya-Ito,
Evidence-based decision making in periodontal tooth prognosis
 Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Authors: Archita Kikani*, Mihir Shah**, Hiral Parikh***, Sandip Ladani****, Pratik Shah*****
 Original Research Kikani et al Socio-economic Position, Tobacco Habit, and Plaque: A Pathway To Severe Chronic Periodontitis Authors: Archita Kikani*, Mihir Shah**, Hiral Parikh***, Sandip Ladani****,
Original Research Kikani et al Socio-economic Position, Tobacco Habit, and Plaque: A Pathway To Severe Chronic Periodontitis Authors: Archita Kikani*, Mihir Shah**, Hiral Parikh***, Sandip Ladani****,
Clinical UM Guideline
 Clinical UM Guideline Subject: Teeth With A Poor or Guarded Prognosis Guideline #: Admin -01 Current Effective Date: 01/01/2016 Status: New Last Review Date: 02/08/2017 Description This document addresses
Clinical UM Guideline Subject: Teeth With A Poor or Guarded Prognosis Guideline #: Admin -01 Current Effective Date: 01/01/2016 Status: New Last Review Date: 02/08/2017 Description This document addresses
Effects of smoking on healing response to non-surgical periodontal therapy: A multilevel modelling analysis
 Title Effects of smoking on healing response to non-surgical periodontal therapy: A multilevel modelling analysis Author(s) Wan, CP; Leung, WK; Wong, MCM; Wong, RMS; Wan, P; Lo, ECM; Corbet, EF Citation
Title Effects of smoking on healing response to non-surgical periodontal therapy: A multilevel modelling analysis Author(s) Wan, CP; Leung, WK; Wong, MCM; Wong, RMS; Wan, P; Lo, ECM; Corbet, EF Citation
Periodontal Treatment Protocol Department of Orthodontics and Restorative Dentistry, Glenfield Hospital, Leicester
 Periodontal Treatment Protocol Department of Orthodontics and Restorative Dentistry, Glenfield Hospital, Leicester 1. Periodontal Assessment Signs of perio disease: - Gingivae become red/purple - Gingivae
Periodontal Treatment Protocol Department of Orthodontics and Restorative Dentistry, Glenfield Hospital, Leicester 1. Periodontal Assessment Signs of perio disease: - Gingivae become red/purple - Gingivae
Surgical Procedure in Guided Tissue Regeneration with the. Inion GTR Biodegradable Membrane System
 Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Disclaimer: The findings and conclusions in this presentation are those of the author and do not necessarily represent the official position of the
 Disclaimer: The findings and conclusions in this presentation are those of the author and do not necessarily represent the official position of the Centers for Disease Control and Prevention CDC-AAP Periodontal
Disclaimer: The findings and conclusions in this presentation are those of the author and do not necessarily represent the official position of the Centers for Disease Control and Prevention CDC-AAP Periodontal
Delta Dental of Virginia Clinical Policy # 402
 Delta Dental of Virginia Clinical Policy # 402 Subject Mucogingival Surgery and Soft Tissue Grafting Originating Department Clinical Professional Services Signature Authority Dental Director Type: New
Delta Dental of Virginia Clinical Policy # 402 Subject Mucogingival Surgery and Soft Tissue Grafting Originating Department Clinical Professional Services Signature Authority Dental Director Type: New
Takashi Yagisawa 1,2*, Makiko Mieno 1,3, Norio Yoshimura 1,4, Kenji Yuzawa 1,5 and Shiro Takahara 1,6
 Yagisawa et al. Renal Replacement Therapy (2016) 2:68 DOI 10.1186/s41100-016-0080-9 POSITION STATEMENT Current status of kidney transplantation in Japan in 2015: the data of the Kidney Transplant Registry
Yagisawa et al. Renal Replacement Therapy (2016) 2:68 DOI 10.1186/s41100-016-0080-9 POSITION STATEMENT Current status of kidney transplantation in Japan in 2015: the data of the Kidney Transplant Registry
The International Journal of Periodontics & Restorative Dentistry
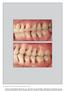 The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
Knowledge, Attitude and Practice about Oral Health among General Population of Peshawar
 SHORT COMMUNICATION Knowledge, Attitude and Practice about Oral Health among General Population of Peshawar Farzeen Khan, Aisha Ayub 3 and Zeeshan Kibria 1 ABSTRACT To determine the level of knowledge
SHORT COMMUNICATION Knowledge, Attitude and Practice about Oral Health among General Population of Peshawar Farzeen Khan, Aisha Ayub 3 and Zeeshan Kibria 1 ABSTRACT To determine the level of knowledge
Risk factors for chronic periodontitis in Sri Lankan adults: a population based case control study
 DOI 10.1186/s13104-017-2778-3 BMC Research Notes RESEARCH NOTE Risk factors for chronic periodontitis in Sri Lankan adults: a population based case control study Nimali Wellapuli 1 and Lilani Ekanayake
DOI 10.1186/s13104-017-2778-3 BMC Research Notes RESEARCH NOTE Risk factors for chronic periodontitis in Sri Lankan adults: a population based case control study Nimali Wellapuli 1 and Lilani Ekanayake
Objectives. Lecture 6 July 16, Operating premises of risk assessment. Page 1. Operating premises of risk assessment
 Page 1 Objectives Lecture 6 July 16, 2003 Linking populations, prevention, and risk assessment ohcd603 1 To understand the operating premises of risk assessment To be familiar with the different types
Page 1 Objectives Lecture 6 July 16, 2003 Linking populations, prevention, and risk assessment ohcd603 1 To understand the operating premises of risk assessment To be familiar with the different types
Periodontal Disease. Radiology of Periodontal Disease. Periodontal Disease. The Role of Radiology in Assessment of Periodontal Disease
 Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series
 CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
Dichotomizing partial compliance and increased participant burden in factorial designs: the performance of four noncompliance methods
 Merrill and McClure Trials (2015) 16:523 DOI 1186/s13063-015-1044-z TRIALS RESEARCH Open Access Dichotomizing partial compliance and increased participant burden in factorial designs: the performance of
Merrill and McClure Trials (2015) 16:523 DOI 1186/s13063-015-1044-z TRIALS RESEARCH Open Access Dichotomizing partial compliance and increased participant burden in factorial designs: the performance of
Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
 ull Tokyo Dent Coll (2017) 58(3): 177 186 Case Report doi:10.2209/tdcpublication.2016-0039 Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
ull Tokyo Dent Coll (2017) 58(3): 177 186 Case Report doi:10.2209/tdcpublication.2016-0039 Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
Prevalence of Periodontitis and its Association with Glycemic Control Among Patients with Type 2 Diabetes Mellitus Seen at St. Luke s Medical Center
 Philippine Journal of Internal Medicine Original Article Prevalence of Periodontitis and its Association with Glycemic Control Among Patients with Type 2 Diabetes Mellitus Seen at St. Luke s Medical Center
Philippine Journal of Internal Medicine Original Article Prevalence of Periodontitis and its Association with Glycemic Control Among Patients with Type 2 Diabetes Mellitus Seen at St. Luke s Medical Center
RESEARCH REVIEW. Gingival recession: a proposal for a new classification ISSN :
 RESEARCH REVIEW Gingival recession: a proposal for a new classification Shantipriya Reddy, Sanjay Kaul, Prasad M.G.S., Jaya Agnihotri, Amudha D., Soumya Kambali ABSTRACT An accurate diagnosis is often
RESEARCH REVIEW Gingival recession: a proposal for a new classification Shantipriya Reddy, Sanjay Kaul, Prasad M.G.S., Jaya Agnihotri, Amudha D., Soumya Kambali ABSTRACT An accurate diagnosis is often
Electronic Dental Records
 Electronic Dental Records Dr. Douglas K Benn, Professor of Maxillofacial Radiology & Director of Oral Diagnostic Systems, University of Florida and Health Conundrums LLC 8/2/2008 Dr Benn, University of
Electronic Dental Records Dr. Douglas K Benn, Professor of Maxillofacial Radiology & Director of Oral Diagnostic Systems, University of Florida and Health Conundrums LLC 8/2/2008 Dr Benn, University of
Response of molars and non-molars to a strict supragingival control in periodontal patients
 Periodontics Response of molars and non-molars to a strict supragingival control in periodontal patients Patrícia Daniela elchiors Angst (a) Flávia Benetti Piccinin (a) Rui Vicente Oppermann (a) Rosemary
Periodontics Response of molars and non-molars to a strict supragingival control in periodontal patients Patrícia Daniela elchiors Angst (a) Flávia Benetti Piccinin (a) Rui Vicente Oppermann (a) Rosemary
Assessment of periodontal status and oral hygiene habits in a group of adults with type I diabetes mellitus
 Assessment of periodontal status and oral hygiene habits in a group of adults with type I diabetes mellitus Doina Lucia Ghergic, Claudia Florina Andreescu, Catalina Grigore Constanta, Romania Summary Diabetes
Assessment of periodontal status and oral hygiene habits in a group of adults with type I diabetes mellitus Doina Lucia Ghergic, Claudia Florina Andreescu, Catalina Grigore Constanta, Romania Summary Diabetes
CT findings in patients with Cabazitaxel induced pelvic pain and haematuria: a case series
 Malalagama et al. Cancer Imaging (2017) 17:17 DOI 10.1186/s40644-017-0119-3 CASE SERIES CT findings in patients with Cabazitaxel induced pelvic pain and haematuria: a case series Geethal N. Malalagama
Malalagama et al. Cancer Imaging (2017) 17:17 DOI 10.1186/s40644-017-0119-3 CASE SERIES CT findings in patients with Cabazitaxel induced pelvic pain and haematuria: a case series Geethal N. Malalagama
An Overview of Gingival and Periodontal Diseases in 12 to 15 years using Gingivitis and Periodontitis Site Prevalence Index (WHO, 1978)
 10.5005/jp-journals-10015-1079 ORIGINL RESERCH WJD n Overview of Gingival and Periodontal Diseases in 12 to 15 years n Overview of Gingival and Periodontal Diseases in 12 to 15 years using Gingivitis and
10.5005/jp-journals-10015-1079 ORIGINL RESERCH WJD n Overview of Gingival and Periodontal Diseases in 12 to 15 years n Overview of Gingival and Periodontal Diseases in 12 to 15 years using Gingivitis and
The Importance of Implementing Oral Health Care Education in the Lehigh Valley
 The Importance of Implementing Oral Health Care Education in the Lehigh Valley Kayla Birde *1 and Christina Peters *1 Patricia Atno CDA, Charles Incalcaterra DMD 1 Lehigh Valley Health Network Dental Clinic-
The Importance of Implementing Oral Health Care Education in the Lehigh Valley Kayla Birde *1 and Christina Peters *1 Patricia Atno CDA, Charles Incalcaterra DMD 1 Lehigh Valley Health Network Dental Clinic-
THE MOUTH. The Missing Piece to Overall Wellness and Lower Medical Costs WHITE PAPER
 THE MOUTH The Missing Piece to Overall Wellness and Lower Medical Costs WHITE PAPER THE MOUTH The Missing Piece to Overall Wellness and Lower Medical Costs Executive Summary Chronic medical conditions
THE MOUTH The Missing Piece to Overall Wellness and Lower Medical Costs WHITE PAPER THE MOUTH The Missing Piece to Overall Wellness and Lower Medical Costs Executive Summary Chronic medical conditions
Patient had no significant findings in medical history. Her vital signs were 130/99, pulse 93.
 Julia Collins Den 1200 Journal #4 1. Demographics Patient is J.S. age 29, Heavy/II 2. Assessment Patient had no significant findings in medical history. Her vital signs were 130/99, pulse 93. Patient does
Julia Collins Den 1200 Journal #4 1. Demographics Patient is J.S. age 29, Heavy/II 2. Assessment Patient had no significant findings in medical history. Her vital signs were 130/99, pulse 93. Patient does
Periodontal Maintenance
 Periodontal Maintenance Friday, February 20, 2015 1:06 PM Periodontal disease control always begins with patient education - Plaque control, diet, smoking cessation, impact that systemic health has on
Periodontal Maintenance Friday, February 20, 2015 1:06 PM Periodontal disease control always begins with patient education - Plaque control, diet, smoking cessation, impact that systemic health has on
Optimization of the periodontal attachment before orthodontic treatment
 DOI: 10.1051/odfen/2017008 J Dentofacial Anom Orthod 2017;20:307 The authors Optimization of the periodontal attachment before orthodontic treatment S. Mouraret 1, J.-P. Forestier 2 1 Private practice
DOI: 10.1051/odfen/2017008 J Dentofacial Anom Orthod 2017;20:307 The authors Optimization of the periodontal attachment before orthodontic treatment S. Mouraret 1, J.-P. Forestier 2 1 Private practice
Does serum CA125 have clinical value for follow-up monitoring of postoperative patients with epithelial ovarian cancer? Results of a 12-year study
 Guo and Peng Journal of Ovarian Research (2017) 10:14 DOI 10.1186/s13048-017-0310-y RESEARCH Does serum CA125 have clinical value for follow-up monitoring of postoperative patients with epithelial ovarian
Guo and Peng Journal of Ovarian Research (2017) 10:14 DOI 10.1186/s13048-017-0310-y RESEARCH Does serum CA125 have clinical value for follow-up monitoring of postoperative patients with epithelial ovarian
Management of osseous defects in aggressive periodontitis: A report of four cases using different techniques
 www.edoriumjournals.com case series OPEN ACCESS Management of osseous defects in aggressive periodontitis: A report of four cases using different techniques Sangeeta Singh, Parul Sharma ABSTRACT Introduction:
www.edoriumjournals.com case series OPEN ACCESS Management of osseous defects in aggressive periodontitis: A report of four cases using different techniques Sangeeta Singh, Parul Sharma ABSTRACT Introduction:
DQA Measure Specifications: Administrative Claims-Based Measures Periodontal Evaluation in Adults with Periodontitis
 **Please read the DQA Measures User Guide prior to implementing this measure.** DQA Measure Specifications: Administrative Claims-Based Measures Periodontal Evaluation in Adults with Periodontitis Description:
**Please read the DQA Measures User Guide prior to implementing this measure.** DQA Measure Specifications: Administrative Claims-Based Measures Periodontal Evaluation in Adults with Periodontitis Description:
THE AMERICAN ACADEMY OF PERIODONTOLOGY
 THE AMERICAN ACADEMY OF PERIODONTOLOGY Suite 800 737 North Michigan Avenue Chicago, Illinois 60611-2690 www.perio.org 2005 The American Academy of Periodontology PDW PERIODONTAL DISEASES what you need
THE AMERICAN ACADEMY OF PERIODONTOLOGY Suite 800 737 North Michigan Avenue Chicago, Illinois 60611-2690 www.perio.org 2005 The American Academy of Periodontology PDW PERIODONTAL DISEASES what you need
EFFECT OF SMOKING ON BODY MASS INDEX: A COMMUNITY-BASED STUDY
 ORIGINAL ARTICLE. EFFECT OF SMOKING ON BODY MASS INDEX: A COMMUNITY-BASED STUDY Pragti Chhabra 1, Sunil K Chhabra 2 1 Professor, Department of Community Medicine, University College of Medical Sciences,
ORIGINAL ARTICLE. EFFECT OF SMOKING ON BODY MASS INDEX: A COMMUNITY-BASED STUDY Pragti Chhabra 1, Sunil K Chhabra 2 1 Professor, Department of Community Medicine, University College of Medical Sciences,
Delta Dental of Iowa Reference Code Listing
 4 Based on documentation received, this procedure does not meet the plan criteria to allow a benefit. 7 Service indicated is not a benefit. 12 Patient not eligible for service per contract limitation.
4 Based on documentation received, this procedure does not meet the plan criteria to allow a benefit. 7 Service indicated is not a benefit. 12 Patient not eligible for service per contract limitation.
Self-check with plaque disclosing solution improves oral hygiene in schoolchildren living in a children s home
 Nagashima et al. Archives of Public Health (2018) 76:50 https://doi.org/10.1186/s13690-018-0296-y RESEARCH Open Access Self-check with plaque disclosing solution improves oral hygiene in schoolchildren
Nagashima et al. Archives of Public Health (2018) 76:50 https://doi.org/10.1186/s13690-018-0296-y RESEARCH Open Access Self-check with plaque disclosing solution improves oral hygiene in schoolchildren
The ultimate goal in periodontal
 Volume 71 Number 4 Interleukin-1 Gene Polymorphisms and Long-Term Stability Following Guided Tissue Regeneration Therapy* Massimo De Sanctis and Giovanni Zucchelli Background: Specific interleukin (IL)-1
Volume 71 Number 4 Interleukin-1 Gene Polymorphisms and Long-Term Stability Following Guided Tissue Regeneration Therapy* Massimo De Sanctis and Giovanni Zucchelli Background: Specific interleukin (IL)-1
NATIONAL EXAMINING BOARD FOR DENTAL NURSES
 NATIONAL EXAMINING BOARD FOR DENTAL NURSES NATIONAL DIPLOMA EXAMINATION DENTAL CHARTING NEBDN is a limited company registered in England & Wales No. 5580200 Registered with the Charity Commisioners No.
NATIONAL EXAMINING BOARD FOR DENTAL NURSES NATIONAL DIPLOMA EXAMINATION DENTAL CHARTING NEBDN is a limited company registered in England & Wales No. 5580200 Registered with the Charity Commisioners No.
Periodontal Regeneration
 Periodontal Regeneration Regeneration The most ideal treatment Attempts to recreate the tissues destroyed by periodontitis Cement, bone and ligament Reduces the risk for recession and sensitivity (could
Periodontal Regeneration Regeneration The most ideal treatment Attempts to recreate the tissues destroyed by periodontitis Cement, bone and ligament Reduces the risk for recession and sensitivity (could
Examination and Treatment Protocols for Dental Caries and Inflammatory Periodontal Disease
 Examination and Treatment Protocols for Dental Caries and Inflammatory Periodontal Disease Dental Caries The current understanding of the caries process supports the shift in caries management from a restorative-only
Examination and Treatment Protocols for Dental Caries and Inflammatory Periodontal Disease Dental Caries The current understanding of the caries process supports the shift in caries management from a restorative-only
-70% Visible plaque index(vpi) -60% Bleeding on probing (BOP) -10% Probing depth (PD)
 Deep studies carried out by the Second University of Naples show the effectiveness of SoWash System and its accessories. After only 14 days use of SoWash System: -70% Visible plaque index(vpi) -60% Bleeding
Deep studies carried out by the Second University of Naples show the effectiveness of SoWash System and its accessories. After only 14 days use of SoWash System: -70% Visible plaque index(vpi) -60% Bleeding
Catherine A. Welch 1*, Séverine Sabia 1,2, Eric Brunner 1, Mika Kivimäki 1 and Martin J. Shipley 1
 Welch et al. BMC Medical Research Methodology (2018) 18:89 https://doi.org/10.1186/s12874-018-0548-0 RESEARCH ARTICLE Open Access Does pattern mixture modelling reduce bias due to informative attrition
Welch et al. BMC Medical Research Methodology (2018) 18:89 https://doi.org/10.1186/s12874-018-0548-0 RESEARCH ARTICLE Open Access Does pattern mixture modelling reduce bias due to informative attrition
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
The Clarion International Multidisciplinary Journal
 The Clarion Volume 3 Number 1 (2014) PP 8-12 The Clarion International Multidisciplinary Journal ISSN : 2277-1697 Periodontal treatment needs of a rural population of North East India Dilip Goswami Department
The Clarion Volume 3 Number 1 (2014) PP 8-12 The Clarion International Multidisciplinary Journal ISSN : 2277-1697 Periodontal treatment needs of a rural population of North East India Dilip Goswami Department
The dentogingival junction to the
 Volume 79 Number 10 RedefiningtheBiologicWidthinSevere, Generalized, Chronic Periodontitis: Implications for Therapy M. John Novak,* Huda M. Albather, and John M. Close Background: Previous studies demonstrated
Volume 79 Number 10 RedefiningtheBiologicWidthinSevere, Generalized, Chronic Periodontitis: Implications for Therapy M. John Novak,* Huda M. Albather, and John M. Close Background: Previous studies demonstrated
In-Network % of Negotiated Fee * % of Negotiated Fee * 100% 80% 50%
 Dental Metropolitan Life Insurance Company Network: PDP Plus Coverage Type Type A: Preventive (cleanings, exams, X-rays) Type B: Basic Restorative (fillings, extractions) Type C: Major Restorative (bridges,
Dental Metropolitan Life Insurance Company Network: PDP Plus Coverage Type Type A: Preventive (cleanings, exams, X-rays) Type B: Basic Restorative (fillings, extractions) Type C: Major Restorative (bridges,
History Why we need to classify?
 Aiming to Cover: MSc ADVANCED GENERAL DENTAL PRACTICE Classification & Recognition of Periodontal Disease Classification of periodontal disease Recognition of Disease DR MIKE MILWARD BDS (Birmingham),
Aiming to Cover: MSc ADVANCED GENERAL DENTAL PRACTICE Classification & Recognition of Periodontal Disease Classification of periodontal disease Recognition of Disease DR MIKE MILWARD BDS (Birmingham),
Maintenance in the Periodontally Compromised Patient. Dr. Van Vagianos January 22, 2009 Charlotte Dental Hygiene Study Club
 Maintenance in the Periodontally Compromised Patient Dr. Van Vagianos January 22, 2009 Charlotte Dental Hygiene Study Club Periodontal Maintenance for Natural Teeth and Implants What is Periodontal Maintenance?
Maintenance in the Periodontally Compromised Patient Dr. Van Vagianos January 22, 2009 Charlotte Dental Hygiene Study Club Periodontal Maintenance for Natural Teeth and Implants What is Periodontal Maintenance?
Periodontal disease is characterized by progressive periodontal pathogens. It is known that coronary heart disease is
 ISSN: 0975-766X CODEN: IJPTFI Available Online through Research Article www.ijptonline.com PREVALENCE OF PERIODONTAL DISEASES IN PATIENTS WITH CORONARY HEART DISEASE Niha Naveed* BDS student, Saveetha
ISSN: 0975-766X CODEN: IJPTFI Available Online through Research Article www.ijptonline.com PREVALENCE OF PERIODONTAL DISEASES IN PATIENTS WITH CORONARY HEART DISEASE Niha Naveed* BDS student, Saveetha
Sample Competency Forms
 Sample Competency Forms The competency and assessment forms and grading criteria included in this packet are suggestions only. Utilize and/or modify as it fits with your institution s practices. Procedures
Sample Competency Forms The competency and assessment forms and grading criteria included in this packet are suggestions only. Utilize and/or modify as it fits with your institution s practices. Procedures
CHAPTER 10. SUPPORTIVE PERIODONTAL THERAPY
 204 CHAPTER 10. SUPPORTIVE PERIODONTAL THERAPY Supportive Periodontal Therapy CHAPTER 10. SUPPORTIVE PERIODONTAL THERAPY DEFINITION Supportive Periodontal Treatment (Periodontal Maintenance, Preventive
204 CHAPTER 10. SUPPORTIVE PERIODONTAL THERAPY Supportive Periodontal Therapy CHAPTER 10. SUPPORTIVE PERIODONTAL THERAPY DEFINITION Supportive Periodontal Treatment (Periodontal Maintenance, Preventive
Natural History of Periodontitis
 Curr Oral Health Rep (2014) 1:286 294 DOI 10.1007/s40496-014-0034-7 EPIDEMIOLOGY (M LAINE, SECTION EDITOR) Natural History of Periodontitis Christoph A. Ramseier & Ho-Yan Duong & Eric Schmid Published
Curr Oral Health Rep (2014) 1:286 294 DOI 10.1007/s40496-014-0034-7 EPIDEMIOLOGY (M LAINE, SECTION EDITOR) Natural History of Periodontitis Christoph A. Ramseier & Ho-Yan Duong & Eric Schmid Published
Colorado Summit. Updates for Providers in the Colorado Medicaid Dental Program. This issue of the Colorado Summit will cover the following:
 Colorado Summit Updates for Providers in the Colorado Medicaid Dental Program Vol. 6 October 2015 This issue of the Colorado Summit will cover the following: Provider Revalidation Dental Hygiene Providers
Colorado Summit Updates for Providers in the Colorado Medicaid Dental Program Vol. 6 October 2015 This issue of the Colorado Summit will cover the following: Provider Revalidation Dental Hygiene Providers
SCIENTIFIC ARTICLES. 86 Stomatologija, Baltic Dental and Maxillofacial Journal, 2007, Vol. 9, No. 3 SUMMARY
 Stomatologija, Baltic Dental and Maxillofacial Journal, 9:86-9, 7 The relationship between the severity of malposition of the frontal teeth and periodontal health in age 5- and 5-44 Jolanta Pugaca, Ilga
Stomatologija, Baltic Dental and Maxillofacial Journal, 9:86-9, 7 The relationship between the severity of malposition of the frontal teeth and periodontal health in age 5- and 5-44 Jolanta Pugaca, Ilga
Prevalence of Gingival recession in Dental college students: A Clinical investigation
 American Journal of Advances in Medical Science www.arnaca.com eissn: 2347-2766 Original Research Article Prevalence of Gingival recession in Dental college students: A Clinical Ninad Moon 1, Prasant Pillai
American Journal of Advances in Medical Science www.arnaca.com eissn: 2347-2766 Original Research Article Prevalence of Gingival recession in Dental college students: A Clinical Ninad Moon 1, Prasant Pillai
Good news about dental benefits for employees of. LCMC Health
 Dental PPO Good news about dental benefits for employees of LCMC Health Why is dental health so important? Regular dental care does more than just improve smiles. Along with good oral hygiene, it can help
Dental PPO Good news about dental benefits for employees of LCMC Health Why is dental health so important? Regular dental care does more than just improve smiles. Along with good oral hygiene, it can help
Lars Jacobsson 1,2,3* and Jan Lexell 1,3,4
 Jacobsson and Lexell Health and Quality of Life Outcomes (2016) 14:10 DOI 10.1186/s12955-016-0405-y SHORT REPORT Open Access Life satisfaction after traumatic brain injury: comparison of ratings with the
Jacobsson and Lexell Health and Quality of Life Outcomes (2016) 14:10 DOI 10.1186/s12955-016-0405-y SHORT REPORT Open Access Life satisfaction after traumatic brain injury: comparison of ratings with the
MDJ Lower Arch Crowding In Relation To Periodontal Disease Vol.:5 No.:2 2008
 MDJ Lower Arch Crowding In Relation To Periodontal Disease Dr. Barzam Abdulwahab, B.D.S M.sc. (periodontics) Abstract A clinical examination was done to study the relationship between crowding and periodontal
MDJ Lower Arch Crowding In Relation To Periodontal Disease Dr. Barzam Abdulwahab, B.D.S M.sc. (periodontics) Abstract A clinical examination was done to study the relationship between crowding and periodontal
Comparison of Effectiveness of Two Designs of Interdental Toothbrushes in removing Dental Plaque
 RESEARCH ARTICLE Comparison of Effectiveness of Two Designs of Interdental Toothbrushes 10.5005/jp-journals-10029-1147 in removing Dental Plaque Comparison of Effectiveness of Two Designs of Interdental
RESEARCH ARTICLE Comparison of Effectiveness of Two Designs of Interdental Toothbrushes 10.5005/jp-journals-10029-1147 in removing Dental Plaque Comparison of Effectiveness of Two Designs of Interdental
effect of surgical debridement vs. non-surgical debridement for the treatment of chronic periodontitis.
 J Clin Periodontol 2002; 29(Suppl. 3): 92 102 Copyright # Blackwell Munksgaard 2002 Printed in Denmark. All rights reserved ISSN 1600-2865 Review article A systematic review of the effect of surgical debridement
J Clin Periodontol 2002; 29(Suppl. 3): 92 102 Copyright # Blackwell Munksgaard 2002 Printed in Denmark. All rights reserved ISSN 1600-2865 Review article A systematic review of the effect of surgical debridement
Effectiveness of the surgical torque limiter: a model comparing drill- and hand-based screw insertion into locking plates
 Ioannou et al. Journal of Orthopaedic Surgery and Research (2016) 11:118 DOI 10.1186/s13018-016-0458-y RESEARCH ARTICLE Effectiveness of the surgical torque limiter: a model comparing drill- and hand-based
Ioannou et al. Journal of Orthopaedic Surgery and Research (2016) 11:118 DOI 10.1186/s13018-016-0458-y RESEARCH ARTICLE Effectiveness of the surgical torque limiter: a model comparing drill- and hand-based
The Australian longitudinal study on male health sampling design and survey weighting: implications for analysis and interpretation of clustered data
 The Author(s) BMC Public Health 2016, 16(Suppl 3):1062 DOI 10.1186/s12889-016-3699-0 RESEARCH Open Access The Australian longitudinal study on male health sampling design and survey weighting: implications
The Author(s) BMC Public Health 2016, 16(Suppl 3):1062 DOI 10.1186/s12889-016-3699-0 RESEARCH Open Access The Australian longitudinal study on male health sampling design and survey weighting: implications
Multilevel analysis quantifies variation in the experimental effect while optimizing power and preventing false positives
 DOI 10.1186/s12868-015-0228-5 BMC Neuroscience RESEARCH ARTICLE Open Access Multilevel analysis quantifies variation in the experimental effect while optimizing power and preventing false positives Emmeke
DOI 10.1186/s12868-015-0228-5 BMC Neuroscience RESEARCH ARTICLE Open Access Multilevel analysis quantifies variation in the experimental effect while optimizing power and preventing false positives Emmeke
Interaction of lifestyle, behaviour or systemic diseases with dental caries and periodontal diseases
 Interaction of lifestyle, behaviour or systemic diseases with dental caries and periodontal diseases Andreas G. Schulte Prof. Dr. med. dent. Department of Special Care Dentistry University of Witten/Herdecke
Interaction of lifestyle, behaviour or systemic diseases with dental caries and periodontal diseases Andreas G. Schulte Prof. Dr. med. dent. Department of Special Care Dentistry University of Witten/Herdecke
Oral Health Matters from Head to Toe
 Oral Health Matters from Head to Toe Your Guide to Preventing and Treating Gum Disease for Overall Health Gums and Overall Health We all know that prevention is one of the keys to maintaining overall health.
Oral Health Matters from Head to Toe Your Guide to Preventing and Treating Gum Disease for Overall Health Gums and Overall Health We all know that prevention is one of the keys to maintaining overall health.
Studying the effectiveness of Farquhar's six-step method in motivating patients with chronic periodontitis about good oral hygiene
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. IV (July. 2017), PP 01-06 www.iosrjournals.org Studying the effectiveness of Farquhar's
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. IV (July. 2017), PP 01-06 www.iosrjournals.org Studying the effectiveness of Farquhar's
Subject: Osseous Surgery Guideline #: Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017
 Clinical Guideline Subject: Osseous Surgery Guideline #: 04-205 Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017 Description This document addresses the procedure of osseous
Clinical Guideline Subject: Osseous Surgery Guideline #: 04-205 Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017 Description This document addresses the procedure of osseous
Supplementary Online Content
 Supplementary Online Content Engebretson SP, Hyman LG, Michalowicz BS, et al. The effect of nonsurgical periodontal therapy on hemoglobin A1c levels among persons with type 2 diabetes and chronic periodontitis:
Supplementary Online Content Engebretson SP, Hyman LG, Michalowicz BS, et al. The effect of nonsurgical periodontal therapy on hemoglobin A1c levels among persons with type 2 diabetes and chronic periodontitis:
Comparison of Partial Recording Protocols in Disease Assessment among Periodontitis Patients in a Central Indian Population
 Journal section: Periodontology Publication Types: Research doi:10.4317/jced.3.e84 Comparison of Partial Recording Protocols in Disease Assessment among Periodontitis Patients in a Central Indian Population
Journal section: Periodontology Publication Types: Research doi:10.4317/jced.3.e84 Comparison of Partial Recording Protocols in Disease Assessment among Periodontitis Patients in a Central Indian Population
Adjusting the Oral Health Related Quality of Life Measure (Using Ohip-14) for Floor and Ceiling Effects
 Journal of Oral Health & Community Dentistry original article Adjusting the Oral Health Related Quality of Life Measure (Using Ohip-14) for Floor and Ceiling Effects Andiappan M 1, Hughes FJ 2, Dunne S
Journal of Oral Health & Community Dentistry original article Adjusting the Oral Health Related Quality of Life Measure (Using Ohip-14) for Floor and Ceiling Effects Andiappan M 1, Hughes FJ 2, Dunne S
Root Dentine Sensitivity
 Indian Medical Gazette JULY 2012 269 Original Study Root Dentine Sensitivity Jyoti Ajay Khade, Associate Professor, Dept. of Dentistry, Rajiv Gandhi Institute of Medical Sciences (RIMS) Adilabad, A.P.
Indian Medical Gazette JULY 2012 269 Original Study Root Dentine Sensitivity Jyoti Ajay Khade, Associate Professor, Dept. of Dentistry, Rajiv Gandhi Institute of Medical Sciences (RIMS) Adilabad, A.P.
A Pilot Study Comparing the Outcome of Scaling/Root Planing With and Without Perioscope Technology
 A Pilot Study Comparing the Outcome of Scaling/Root Planing With and Without Perioscope Technology Christine M. Blue, BSDH, MS; Patricia Lenton, RDH, MA; Scott Lunos, MS; Kjersta Poppe, RDH, MS; Joy Osborn,
A Pilot Study Comparing the Outcome of Scaling/Root Planing With and Without Perioscope Technology Christine M. Blue, BSDH, MS; Patricia Lenton, RDH, MA; Scott Lunos, MS; Kjersta Poppe, RDH, MS; Joy Osborn,
Dental Hygiene 10/16/2012 8/20/2012 8/29/2013 COURSE OUTLINE DHT 105 Dental Hygiene Clinic I - Preclinic 5 credit hours
 COURSE OUTLINE Dental Hygiene Clinic I - Preclinic 5 credit hours Course Description This course will introduce theories, rationales, and foundational knowledge for performing basic dental hygiene skills
COURSE OUTLINE Dental Hygiene Clinic I - Preclinic 5 credit hours Course Description This course will introduce theories, rationales, and foundational knowledge for performing basic dental hygiene skills
Screenings, Indices Their influence on the treatment plan (Berne concept)
 Screenings, Indices Their influence on the treatment plan (Berne concept) 1. 2. 3. 4. Garguilo AW, Wentz FM, Orban B. Dimensions and relations of thedentogingival junction in humans. J Periodontol 1961;
Screenings, Indices Their influence on the treatment plan (Berne concept) 1. 2. 3. 4. Garguilo AW, Wentz FM, Orban B. Dimensions and relations of thedentogingival junction in humans. J Periodontol 1961;
Analysis of TB prevalence surveys
 Workshop and training course on TB prevalence surveys with a focus on field operations Analysis of TB prevalence surveys Day 8 Thursday, 4 August 2011 Phnom Penh Babis Sismanidis with acknowledgements
Workshop and training course on TB prevalence surveys with a focus on field operations Analysis of TB prevalence surveys Day 8 Thursday, 4 August 2011 Phnom Penh Babis Sismanidis with acknowledgements
Unilateral lateral rectus muscle advancement surgery based on one-fourth of the angle of consecutive esotropia
 Kim and Lee BMC Ophthalmology (2017) 17:266 DOI 10.1186/s12886-017-0658-1 RESEARCH ARTICLE Open Access Unilateral lateral rectus muscle advancement surgery based on one-fourth of the angle of consecutive
Kim and Lee BMC Ophthalmology (2017) 17:266 DOI 10.1186/s12886-017-0658-1 RESEARCH ARTICLE Open Access Unilateral lateral rectus muscle advancement surgery based on one-fourth of the angle of consecutive
"Designing a fixed partial denture without a pontic"- Case report
 Article ID: ISSN 2046-1690 "Designing a fixed partial denture without a pontic"- Peer review status: No Corresponding Author: Dr. Khurshid Mattoo, Assistant Professor, Prosthodontics, College of Dental
Article ID: ISSN 2046-1690 "Designing a fixed partial denture without a pontic"- Peer review status: No Corresponding Author: Dr. Khurshid Mattoo, Assistant Professor, Prosthodontics, College of Dental
Referral of Patients. to the. Community Dental Referral Service. Hillingdon
 Referral of Patients to the Community Dental Referral Service In Hillingdon June 2012 1 Contents Page Background 3 Best use of Resources 3 Process for Referral 3-4 Acceptance Criteria for Specialist Treatment
Referral of Patients to the Community Dental Referral Service In Hillingdon June 2012 1 Contents Page Background 3 Best use of Resources 3 Process for Referral 3-4 Acceptance Criteria for Specialist Treatment
Data Analysis in Practice-Based Research. Stephen Zyzanski, PhD Department of Family Medicine Case Western Reserve University School of Medicine
 Data Analysis in Practice-Based Research Stephen Zyzanski, PhD Department of Family Medicine Case Western Reserve University School of Medicine Multilevel Data Statistical analyses that fail to recognize
Data Analysis in Practice-Based Research Stephen Zyzanski, PhD Department of Family Medicine Case Western Reserve University School of Medicine Multilevel Data Statistical analyses that fail to recognize
A Model for the Analysis of Caries Occurrence in Primary Molar Tooth Surfaces
 Original Paper DOI: 10.1159/000339390 Received: February 8, 2012 Accepted: April 17, 2012 Published online: $ $ $ A Model for the Analysis of Caries Occurrence in Primary Molar Tooth Surfaces J. Stephenson
Original Paper DOI: 10.1159/000339390 Received: February 8, 2012 Accepted: April 17, 2012 Published online: $ $ $ A Model for the Analysis of Caries Occurrence in Primary Molar Tooth Surfaces J. Stephenson
For all eligible employees of Louisiana Riverboat Gaming Partnership dba Diamond Jacks Casino - Bossier City, Policy # All Eligible Employees
 Dental insurance Benefit Highlights For all eligible employees of Louisiana Riverboat Gaming Partnership dba Diamond Jacks Casino - Bossier City, Policy # 902360 All Eligible Employees Effective date:
Dental insurance Benefit Highlights For all eligible employees of Louisiana Riverboat Gaming Partnership dba Diamond Jacks Casino - Bossier City, Policy # 902360 All Eligible Employees Effective date:
THE CALIFORNIA STATE UNIVERSITY DENTAL PROGRAM OVERVIEW
 THE CALIFORNIA STATE UNIVERSITY DENTAL PROGRAM OVERVIEW Plan Year: January 1, 2019 December 31, 2019 The California State University Dental Program consists of two types of plans: Delta Dental PPO and.
THE CALIFORNIA STATE UNIVERSITY DENTAL PROGRAM OVERVIEW Plan Year: January 1, 2019 December 31, 2019 The California State University Dental Program consists of two types of plans: Delta Dental PPO and.
Subdural hemorrhages in acute lymphoblastic leukemia: case report and literature review
 Yin et al. Chinese Neurosurgical Journal (2016) 2:25 DOI 10.1186/s41016-016-0045-4 CHINESE NEUROSURGICAL SOCIETY CASE REPORT CHINESE MEDICAL ASSOCIATION Subdural hemorrhages in acute lymphoblastic leukemia:
Yin et al. Chinese Neurosurgical Journal (2016) 2:25 DOI 10.1186/s41016-016-0045-4 CHINESE NEUROSURGICAL SOCIETY CASE REPORT CHINESE MEDICAL ASSOCIATION Subdural hemorrhages in acute lymphoblastic leukemia:
INTRODUCTION TO GUARDIAN CLINICAL POLICY
 DENTAL INSURANCE INTRODUCTION TO GUARDIAN CLINICAL POLICY April 26, 2018 Introduction and General Clinical Guidelines Prosthodontics Periodontics Oral Surgery General Anesthesia/IV Sedation Page 1 of 6
DENTAL INSURANCE INTRODUCTION TO GUARDIAN CLINICAL POLICY April 26, 2018 Introduction and General Clinical Guidelines Prosthodontics Periodontics Oral Surgery General Anesthesia/IV Sedation Page 1 of 6
Periodontal (Gum) Disease
 Periodontal (Gum) Disease If you have been told you have periodontal (gum) disease, you re not alone. An estimated 80 percent of American adults currently have some form of the disease. Periodontal diseases
Periodontal (Gum) Disease If you have been told you have periodontal (gum) disease, you re not alone. An estimated 80 percent of American adults currently have some form of the disease. Periodontal diseases
Seniors Oral Care
 For information about oral health care, please contact the Ontario Dental Association at 416-922-3900 or visit www.youroralhealth.ca The Ontario Dental Association gratefully acknowledges UBC ELDERS Education,
For information about oral health care, please contact the Ontario Dental Association at 416-922-3900 or visit www.youroralhealth.ca The Ontario Dental Association gratefully acknowledges UBC ELDERS Education,
Dental Policy. Subject: Prophylaxis Guideline #: Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/06/2018
 Dental Policy Subject: Prophylaxis Guideline #: 01-101 Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/06/2018 Description This document addresses the procedure of dental prophylaxis for
Dental Policy Subject: Prophylaxis Guideline #: 01-101 Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/06/2018 Description This document addresses the procedure of dental prophylaxis for
Periodontal Diagnosis Form
 Periodontal Diagnosis Form Notes on the use of the form 1. The form that follows is a comprehensive analysis of your patient, taking into account many factors that might contribute to oral conditions.
Periodontal Diagnosis Form Notes on the use of the form 1. The form that follows is a comprehensive analysis of your patient, taking into account many factors that might contribute to oral conditions.
