The International Journal of Periodontics & Restorative Dentistry
|
|
|
- Lambert Walters
- 5 years ago
- Views:
Transcription
1 The International Journal of Periodontics & Restorative Dentistry
2 257 Minimally Invasive Surgical Technique and Enamel Matrix Derivative in Intrabony Defects: 2. Factors Associated with Healing Outcomes Pierpaolo Cortellini, MD, DDS* Giovanpaolo Pini-Prato, MD, DDS** Michele Nieri, MD, DDS** Maurizio S. Tonetti, DDS, MS*** This case cohort study was designed to evaluate the healing response of a minimally invasive surgical technique (MIST) in combination with enamel matrix derivative (EMD) in isolated deep intrabony defects. Forty deep intrabony defects were surgically accessed with the MIST. This technique was designed to limit the flap extent and reflection to reduce surgical trauma and increase flap stability. EMD was applied on the dried root surfaces. Surgery was performed with the aid of an operating microscope and microsurgical instruments. The 1-year clinical attachment level gain was 4.9 ± 1.7 mm. Seventy percent of defects gained 4 mm. Clinical attachment level gain was significantly associated with the depth of the three-wall component of the defect, with the intraoperative bleeding tendency of the defect, and with its interaction with the baseline amount of bone loss. Defect morphology and bleeding tendency seem to influence clinical outcomes from the use of MIST in combination with EMD. (Int J Periodontics Restorative Dent 2009;29: ) *Accademia Toscana di Ricerca Odontostomatologica (ATRO), Florence, Italy; European Research Group on Periodontology (ERGOPerio), Berne, Switzerland. **Professor, Department of Periodontology, Dental School, University of Florence, Italy. ***European Research Group on Periodontology (ERGOPerio), Berne, Switzerland. Correspondence to: Dr Pierpaolo Cortellini, Via Carlo Botta 16, Firenze, Italy; studiocortellini@cortellini.191.it. In the last 20 years, membranes, demineralized freeze-dried bone allograft, enamel matrix derivative (EMD), and combinations of membranes and fillers 1 6 have been successfully used in periodontal regenerative treatment of deep intrabony defects. A significant amount of variability in clinical results, however, has been consistently observed and explained in terms of differences in patient populations, defect morphology, surgical strategies, and operative protocols. Patient-associated factors, such as the level of self-performed oral hygiene, residual periodontal infections, and smoking habits, have been found to consistently influence the clinical outcomes of various regenerative strategies and materials. 4,7 12 Among defect-associated factors, the indicators of defect severity, including pocket depth, attachment loss, bone loss, and depth of the intrabony component of the defect, have been found to be consistently associated with the amounts of clinical attachment gained with all tested regenerative procedures. 4,7,9,10,13 15 Some morphologic characteristics of the defects, however, appear to be more approach-specific. Volume 29, Number 3, 2009
3 258 The defect angle (as assessed radiographically) has been found to affect clinical attachment level (CAL) gains when nonresorbable and resorbable barrier membranes 7,13,16 and EMD 11,17 are used, whereas defect angle did not show a significant impact on CAL gains when the defects were treated with titanium-reinforced expanded polytetrafluoroethylene membranes 9 or with resorbable membranes in combination with deproteinized bovine bone mineral. 18 Similarly, the number of residual bony walls did not seem to affect regeneration with barrier membranes alone 7,9,15 or in conjunction with deproteinized bovine bone mineral 4 but was significantly associated with outcomes following application of EMD in gel form. 11 Defect characteristics assessed during surgery, such as intraoperative bleeding tendency from the defect walls, have been found to negatively affect the final outcome of EMD-treated intrabony defects. 11 Observations from the cited studies have been used to develop clinical decision trees based on the morphology of the defect for the selection of the regenerative strategy, indicating the use of self-supporting (ie, titanium-reinforced) or supported membranes (ie, in combination with a filler material) in non space-maintaining defects, such as one-wall and/or wider defects, and the application of EMD or resorbable barrier membranes in the inherently more supportive twoto three-wall and/or narrower defects Surgical factors seem to greatly impact clinical outcomes as well. The different regenerative approaches are associated with clinical complications, the most frequent being flap dehiscence and exposure of the regenerative material, which is frequently observed with the use of barrier membranes and combined therapies. 4,10,13,15,23 26 The cited postsurgical complications were found to negatively influence the gain of clinical attachment. Reduced postoperative complications have been observed following the application of EMD. 11,27 In a controlled clinical trial, the absence of surgical complications was associated with improved outcomes. 27 The design of the surgical access and suturing technique in regenerative therapy has dramatically evolved in the last 20 years, from the use of conventional access flaps 13,23 sutured with external mattress sutures to the application of papilla preservation techniques associated with double-layer or single-layer internal mattress sutures to obtain a stable seal of the wound in the absence of tension The use of operating microscopes and microsurgical instruments has also been proposed to enhance the ability of the surgeon to properly handle the soft and hard tissues as well as the devices and materials involved in the regenerative treatment. 20,21 Recently, several authors have proposed the use of minimally invasive approaches in isolated or multiple defects. 35,36 Among these, a minimally invasive surgical technique (MIST) was proposed and tested in a preliminary case series. 34 Its main clinical objectives included a reduction of surgical trauma, an increase of flap/wound stability, stable primary closure of the wound, a reduction in surgical time, and minimal intraoperative and postoperative patient discomfort and morbidity. MIST was then tested in a case cohort; the clinical and patient outcomes of this case cohort study are reported elsewhere. 37 The specific aim of the present study was to identify defect factors associated with the 1-year changes in terms of CAL following application of the MIST in combination with EMD for the treatment of isolated deep intrabony defects. Method and materials Study population and experimental procedures The details of the patient population are described elsewhere. 37 All subjects had: (1) advanced periodontal disease but were in good general health; (2) at least one tooth with probing pocket depth and CAL loss of at least 5 mm associated with an intrabony defect of at least 2 mm; (3) fullmouth plaque scores (FMPS) 25%; (4) full-mouth bleeding scores (FMBS) 25%; (5) demonstrated a good level of compliance; and (6) teeth that were vital or had been properly treated with root canal therapy. Heavy smokers (> 10 cigarettes/day) were excluded. All subjects had received a cycle of cause-related therapy consisting of scaling and root planing, motivation, and oral hygiene instructions. Flap surgery for pocket elimination was performed, when indicated, in the remaining portions of the dentition of each patient before the regenerative treatment. All subjects gave informed written consent. Forty intrabony The International Journal of Periodontics & Restorative Dentistry
4 259 defects in 40 subjects that met the admission criteria were consecutively included in this cohort. Three months after completion of periodontal therapy, baseline clinical measurements were recorded, including FMPS, FMBS, probing depth (PD), and recession of the gingival margin (REC). The experimental sites were accessed with the MIST and carefully debrided. The procedure is described in detail elsewhere. 37 Measurements were made during surgery to characterize the defect anatomy, including the distance from the cementoenamel junction to the bottom of the defect (CEJ-BD), the total depth of the intrabony component of the defect (INFRA 38 ), and the bleeding tendency of the defect. When the defect showed bleeding tendency, bleeding was controlled by compacting wet, sterile gauze into the defect for 3 to 4 minutes. The root surface was cleansed with an ethylenediaminetetraacetic acid gel and EMD (Emdogain, Institut Straumann) was applied on the instrumented and dried root surfaces. Flaps were repositioned and sutured with modified internal mattress sutures. Patients were enrolled in a stringent postoperative supportive care program with weekly recalls for 6 weeks and then included in a 3-month periodontal supportive care program for 1 year. Outcome measures were obtained at 1 year. Periapical radiographs of the experimental sites were taken at baseline and at the 1-year follow-up. Data analysis Data were expressed as means ± standard deviations of 40 defects in 40 patients. No data points were missing. Comparisons between baseline and 1- year CAL, PD, and REC values were made using the paired Student t test ( =.05). Averages and 95% confidence intervals (CIs) were calculated for the differences between baseline and 1- year CAL, PD, and REC values. Percentage fill of the baseline intrabony component of the defect was calculated as ([CAL gain]/infra) 100. A multivariate linear regression analysis was carried out to predict changes in CAL (as a continuous variable) 1 year after the use of the MIST and application of EMD according to an a priori hypothesis; the selected variables were jointly entered in the model. The model included only variables related to defect morphology. As postulated in the a priori hypothesis, variables indicative of defect severity (CEJ-BD), the depth of the three-wall subcomponent, the radiographic defect angle as a descriptor of the defect morphology, and the bleeding tendency of the defect were entered into the model, along with the interaction between bleeding tendency of the defect and CEJ-BD. The variable CEJ-BD was selected as an indicator of disease severity 36 ; because it is highly correlated with CAL and INFRA, it can be used alone as a variable in a relatively small sample. The bleeding tendency of the defect was included following the observation that it was significantly greater in sites with greater baseline periodontal destruction (greater CEJ-BD or greater CAL). Patient-related variables were not considered, since those that could influence the outcomes had been controlled during cause-related therapy and heavy smokers and patients with poor oral hygiene or high levels of residual infection had been excluded. Results Clinical outcomes Details of the study population and clinical results were published previously. 37 In brief, 40 intrabony defects in 40 subjects (mean age 48.3 ± 9.8 years; range, 31 to 74 years; 14 men and 26 women; five smokers) were treated with the MIST + EMD. Average FMPS and FMBS were 13.1% ± 5.1% and 8.8% ± 3.3%, respectively. Defects presented with mean PD of 8.2 ± 1.9 mm, mean CAL of 10.0 ± 2.9 mm, and mean REC of 1.8 ± 1.6 mm. The mean intrabony component of the defects was 6.5 ± 2.3 mm. At 1 year, a CAL gain of 4.9 ± 1.7 mm (range, 3 to 9 mm; 95% CI, 4.3 to 5.4 mm) was associated with a residual PD of 3.0 ± 0.6 mm and a very limited increase of 0.4 ± 0.7 mm in REC (95% CI, 0.1 to 0.6 mm). Changes between baseline and 1 year in CAL and PD were clinically and statistically highly significant (mean PD change: 5.2 ± 1.7 mm, 95% CI, 4.7 to 5.8 mm; P <.0001). Changes in REC also reached statistical significance (P =.017). The data were stratified into four classes of CAL gain (Table 1). No sites lost attachment and no sites gained less than 3 mm of attachment, whereas 70% of sites gained 4 mm or more. The Volume 29, Number 3, 2009
5 260 Table 1 Baseline defect characteristics stratified by CAL gain as observed at 1 year after regenerative surgery CAL gain at 1 year Baseline characteristics < 3 mm 3 mm 4 5 mm 6 mm N (%) 0 12 (30.0%) 13 (32.5%) 15 (37.5%) PD 6.3 ± ± ± 1.2 CAL 7.8 ± ± ± 2.3 CEJ-BD 9.0 ± ± ± 2.6 INFRA 5.0 ± ± ± 2.3 Three-wall 1.9 ± ± ± 1.9 Two-wall 1.4 ± ± ± 1.8 One-wall 1.7 ± ± ± 1.2 Defect angle (deg) 31.9 ± ± ± 7.1 Intraoperative defect - 17% 31% 67% bleeding (prevalence) PD = probing depth; CAL = clinical attachment level; CEJ-BD = distance from cementoenamel junction to the bottom of the defect; INFRA = intrabony component of the defect. baseline characteristics of the defects clustered according to the different classes of CAL gain show that larger amounts of CAL gains were obtained in more severe defects, described in terms of PD, CAL, and bone loss, and intrabony component depth. The 1-year mean resolution of the defects was 77.6% ± 21.9% (range, 33.3% to 133.3%), and 12 sites (30%) reached 100% of the baseline intrabony component. Defect resolution ranging from 50% to 99% was observed in 26 sites (65%), while only two sites failed to reach 50% fill of the baseline intrabony component. Figure 1 depicts a patient treated with the MIST + EMD method. Multivariate analysis The multivariate analysis carried out to predict changes in CAL at 1 year after the application of MIST and EMD generated a highly statistically significant model (P <.0001) that explained 71% of the observed variability in CAL gains (Table 2). CAL gain was significantly associated with: (1) the bleeding tendency of the debrided defect during surgery, ie, bleeding defects resulted in greater amounts of CAL gain; (2) the interaction between the bleeding tendency of the defect and CEJ-BD, ie, deeper defects that bled showed the greatest amounts of CAL gain; and (3) the baseline depth of the three-wall intrabony subcomponent, ie, deeper three-wall components were associated with greater CAL gains. The baseline radiographic defect angle did not reach statistical significance. A subgroup analysis of 16 defects without a one-wall superficial component of the defect showed an overall tendency toward improved outcomes with respect to the total population in terms of CAL gain (5.1 ± 1.5 mm) and percent fill of the intrabony component of the defect (84.2% ± 27.1%). The International Journal of Periodontics & Restorative Dentistry
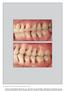
6 261 Fig 1a (left) Preoperative clinical view of the mandibular right second premolar. The tooth presents with a distal pocket that is 12 mm deep. Fig 1b (right) Baseline radiograph shows a deep and narrow intrabony defect reaching the apical third of the root. Fig 1c (left) Intraoperative view. The twoto three-wall intrabony defect is 12 mm deep. The total bone loss on the distal side amounts to 18 mm. An MIST approach was used to expose the residual bone contour and minimize flap reflection. Fig 1d (right) An internal modified mattress suture was applied to close the defectassociated interdental papillae. Fig 1e (left) A 3-mm probing depth was measured at 1 year. Fig 1f (right) The 1-year radiograph shows the resolution of the intrabony component of the defect. Table 2 Multivariate analysis Variable Estimate SE t ratio Prob > t Intercept CEJ-BD (mm) Bleeding tendency after debridement CEJ-BD bleeding tendency Depth three-wall component (mm) Radiographic angle (deg) The tested outcome was change in CAL (as a continuous variable) between baseline and 1 year. The model was highly significant (P <.001; R 2 = 0.71). Volume 29, Number 3, 2009
7 262 Discussion The treatment of 40 deep intrabony defects with the MIST in combination with EMD resulted in 1-year mean CAL gains of 4.9 ± 1.7 mm, associated with 3.0 ± 0.6 mm of residual PD and 0.4 ± 0.7 mm of increase in REC. 37 In this cohort, no sites lost attachment and no sites gained less than 3 mm of attachment. The majority of sites (70%) gained 4 mm or more of attachment at 1 year, and 37.5% of sites gained 6 mm or more. The reported outcomes were obtained in a patient population where the relevant patient-associated factors such as bacterial plaque, residual periodontal infection, and smoking habits were under optimal control. 4,7 12 Analysis of the baseline defect characteristics according to stratified classes of CAL gain (Table 1) and the results of the multivariate analysis (Table 2) allows for some interesting considerations. The largest amounts of CAL gain were obtained in sites that had been severely compromised by periodontal destruction. This observation is consistent with the data reported in many different regenerative studies. 4,7,9,10,13 15 The present study confirms the evidence that regenerative therapy is a treatment modality that can change the prognosis of severely compromised teeth, resulting in sizable amounts of CAL gain and PD reduction. Defect morphology, described in terms of residual bony walls, was also found to affect the final outcomes. Larger amounts of CAL gain were observed in sites with deeper threewall and two-wall subcomponents. In particular, the multivariate analysis (Table 2) showed a statistically significant correlation between the 1-year gain of CAL and the depth of the three-wall subcomponent. This confirms the observations of a previous EMD study 11 and other studies reporting on the application of nonresorbable and resorbable barrier membranes. 7,13,16 The more favorable outcomes in the three-wall intrabony subcomponents are generally explained in terms of greater support provided by the residual bony walls to the barriers and/or the repositioned gingival flaps. 7 The larger number of residual bony walls could also positively affect the blood clot stability, which is perceived as relevant for early healing events Another relevant finding of the present study is the evidence of improved outcomes in deep defects with an intraoperative bleeding tendency. In a previous EMD trial, 11 reduced CAL gains were observed at bleeding defects. This different response could be explained by the different intraoperative protocol for EMD application. In the present study, special care was taken to apply EMD on dried root and bone surfaces. When a defect showed a tendency to bleed, bleeding was controlled with compaction of wet, sterile gauze into the defect for a few minutes. After the gauze was removed, the area was carefully rinsed with saline and gently dried with air spray, and EMD was applied immediately. It may be that EMD is rapidly washed away in bleeding defects and thus fails to reach the root surfaces and the defect walls, thereby reducing the expression of its regenerative potential in bleeding defects. In contrast, when a dried root surface is The International Journal of Periodontics & Restorative Dentistry
8 263 present for EMD application, the potential for regeneration of bleeding defects seems to be greater than that seen at nonbleeding sites. These observations suggest the need to adopt a protocol for EMD delivery on dried root and bone surfaces. An interesting and novel observation was the interaction between the bleeding tendency of the defect and the severity of the bone destruction (CEJ-BD), which was highly significant. In this population, greater CAL gains were associated with increasing CEJ- BD depth in defects classified as bleeding. This was not seen in the nonbleeding defects. In other words, the bleeding tendency of the defects accounted for improved outcomes, and the improved outcomes, as expected, were correlated with the severity of the defects: the deeper defects gained more attachment. In fact, the observation of the lack of correlation between the severity of the defects and CAL gain in nonbleeding sites was unexpected. This might give rise to a series of hypotheses on the potential for regeneration expressed in bleeding or nonbleeding sites. Are bleeding defects better providers for regeneration? Do they support faster angiogenesis? Could this finding support a clinical effort to make nonbleeding sites bleed with additional bone instrumentation? The data from this paper do not allow definitive answers, but they raise questions regarding a potentially relevant issue. Further research is needed to explore this area. In conclusion, the application of the minimally invasive surgical technique in combination with enamel matrix derivative proved to be an efficacious surgical approach for the treatment of deep intrabony defects with a prevalent three-wall and two-wall morphology. The results were not significantly influenced by the radiographic defect angle and were more favorable in deep, bleeding defects, provided that bleeding was controlled during application of the enamel matrix derivative. Acknowledgments This study was partly supported by the Accademia Toscana di Ricerca Odontostomatologica (ATRO), Firenze, Italy, and by the European Research Group on Periodontology (ERGOPerio), Berne, Switzerland. Volume 29, Number 3, 2009
9 264 References 1. Reynolds MA, Aichelmann-Reidy ME, Branch-Mays GL, Gunsolley JC. The efficacy of bone replacement grafts in the treatment of periodontal osseous defects. A systematic review. Ann Periodontol 2003;8: Murphy KG, Gunsolley JC. Guided tissue regeneration for the treatment of periodontal intrabony and furcation defects. A systematic review. Ann Periodontol 2003;8: Trombelli L, Heitz-Mayfield LJ, Needleman I, Moles D, Scabbia A. A systematic review of graft materials and biological agents for periodontal intraosseous defects. J Clin Periodontol 2002;29(suppl 3): Tonetti MS, Cortellini P, Lang NP, et al. Clinical outcomes following treatment of human intrabony defects with GTR/bone replacement material or access flap alone. A multicenter randomized controlled clinical trial. J Clin Periodontol 2004;31: Esposito M, Grusovin MG, Coulthard P, Worthington HV. Enamel matrix derivative (Emdogain) for periodontal tissue regeneration in intrabony defects. Cochrane Database Syst Rev 2005 Oct 19;(4): CD Needleman IG, Worthington HV, Giedrys- Leeper E, Tucker RJ. Guided tissue regeneration for periodontal infra-bony defects. Cochrane Database Syst Rev 2006 Apr 19;(2):CD Tonetti MS, Pini Prato G, Cortellini P. Periodontal regeneration of human intrabony defects. IV. Determinants of healing response. J Periodontol 1993;64: Tonetti MS, Pini Prato G, Cortellini P. Effect of cigarette smoking on periodontal healing following GTR in infrabony defects. A preliminary retrospective study. J Clin Periodontol 1995;22: Tonetti MS, Pini-Prato G, Cortellini P. Factors affecting the healing response of intrabony defects following guided tissue regeneration and access flap surgery. J Clin Periodontol 1996;23: Cortellini P, Tonetti MS, Lang NP, et al. The simplified papilla preservation flap in the regenerative treatment of deep intrabony defects: Clinical outcomes and postoperative morbidity. J Periodontol 2001; 72: Tonetti MS, Lang NP, Cortellini P, et al. Enamel matrix proteins in the regenerative therapy of deep intrabony defects. J Clin Periodontol 2002;29: Heitz-Mayfield L, Tonetti MS, Cortellini P, Lang NP. Microbial colonization patterns predict the outcomes of surgical treatment of intrabony defects. J Clin Periodontol 2006;33: Falk H, Laurell L, Ravald N, Teiwik A, Persson R. Guided tissue regeneration therapy of 203 consecutively treated intrabony defects using a bioresorbable matrix barrier. Clinical and radiographic findings. J Periodontol 1997;68: Cortellini P, Carnevale G, Sanz M, Tonetti MS. Treatment of deep and shallow intrabony defects. A multicenter randomized controlled clinical trial. J Clin Periodontol 1998;25: Tonetti MS, Cortellini P, Suvan JE, et al. Generalizability of the added benefits of guided tissue regeneration in the treatment of deep intrabony defects. Evaluation in a multi-center randomized controlled clinical trial. J Periodontol 1998;69: Cortellini P, Tonetti MS. Radiographic defect angle influences the outcomes of GTR therapy in intrabony defects. 77th General Session of the IADR, Vancouver, Canada, March 10 13, Tsitoura E, Tucker R, Suvan J, Laurell L, Cortellini P, Tonetti M. Baseline radiographic defect angle of the intrabony defect as a prognostic indicator in regenerative periodontal surgery with enamel matrix derivative. J Clin Periodontol 2004;31: Liñares A, Cortellini P, Lang NP, Suvan J, Tonetti MS. Guided tissue regeneration/deproteinized bovine bone mineral or papilla preservation flaps alone for treatment of intrabony defects. II: Radiographic predictors and outcomes. J Clin Periodontol 2006;33: Cortellini P, Tonetti MS. Focus on intrabony defects: Guided tissue regeneration. Periodontol ;22: Cortellini P, Tonetti MS. Microsurgical approach to periodontal regeneration. Initial evaluation in a case cohort. J Periodontol 2001;72: Cortellini P, Tonetti MS. Clinical performance of a regenerative strategy for intrabony defects: Scientific evidence and clinical experience. J Periodontol 2005;76: Cortellini P. Reconstructive periodontal surgery: A challenge for modern periodontology. Int Dent J 2006;56(suppl 1): Cortellini P, Pini Prato G, Tonetti MS. Periodontal regeneration of human infrabony defects. I. Clinical measures. J Periodontol 1993;64: Nowzari H, Matian F, Slots J. Periodontal pathogens on polytetrafluorethylene membrane for guided tissue regeneration inhibit healing. J Clin Periodontol 1995; 22: Murphy KG. Postoperative healing complications associated with Gore-Tex Periodontal Material. Part II. Effect of complications on regeneration. Int J Periodontics Restorative Dent 1995;15: De Sanctis M, Zucchelli G, Clauser C. Bacterial colonization of barrier material and periodontal regeneration. J Clin Periodontol 1996;23: Sanz M, Tonetti MS, Zabalegui I, et al. Treatment of intrabony defects with enamel matrix proteins or barrier membranes: Results from a multicenter practice-based clinical trial. J Periodontol 2004;75: Cortellini P, Pini Prato G, Tonetti MS. The modified papilla preservation technique. A new surgical approach for interproximal regenerative procedures. J Periodontol 1995;66: Cortellini P, Pini Prato G, Tonetti MS. The simplified papilla preservation flap. A novel surgical approach for the management of soft tissues in regenerative procedures. Int J Periodontics Restorative Dent 1999;19: The International Journal of Periodontics & Restorative Dentistry
10 Murphy KG. Interproximal tissue maintenance in GTR procedures: Description of a surgical technique and 1-year reentry results. Int J Periodontics Restorative Dent 1996;16: Harrel SK, Rees TD. Granulation tissue removal in routine and minimally invasive procedures. Compend Contin Educ Dent 1995;16: Harrel SK, Nunn ME. Longitudinal comparison of the periodontal status of patients with moderate to severe periodontal disease receiving no treatment, non-surgical treatment, and surgical treatment utilizing individual sites for analysis. J Periodontol 2001;72: Wachtel H, Schenk G, Böhm S, Weng D, Zuhr O, Hürzeler MB. Microsurgical access flap and enamel matrix derivative for the treatment of periodontal intrabony defects: A controlled clinical study. J Clin Periodontol 2003;30: Cortellini P, Tonetti MS. A minimally invasive surgical technique with an enamel matrix derivative in the regenerative treatment of intrabony defects: A novel approach to limit morbidity. J Clin Periodontol 2007;34: Harrel SK, Wilson TG, Nunn ME. Prospective assessment of the use of enamel matrix proteins with minimally invasive surgery. J Periodontol 2005;76: Cortellini P, Nieri M, Pini Prato G, Tonetti MS. Single minimally invasive surgical technique with an enamel matrix derivative to treat multiple adjacent intra-bony defects: Clinical outcomes and patient morbidity. J Clin Periodontol 2008;35: Cortellini P, Tonetti MS. Minimally invasive surgical technique and enamel matrix derivative in intra-bony defects. I: Clinical outcomes and morbidity. J Clin Periodontol 2007;34: Cortellini P, Pini Prato G, Tonetti MS. Periodontal regeneration of human infrabony defects. II. Re-entry procedures and bone measures. J Periodontol 1993;64: Hiatt WH, Stallard RE, Butler ED, Badgett B. Repair following mucoperiosteal flap surgery with full gingival retention. J Periodontol 1968;39: Egelberg J. Regeneration and repair of periodontal tissues. J Periodontal Res 1987;22: Wikesjö UME, Nilvéus R. Periodontal repair in dogs: Effect of wound stabilization on healing. J Periodontol 1990;61: Haney JM, Nilvéus RE, McMillan PJ, Wikesjö UME. Periodontal repair in dogs: Expanded polytetrafluoroethylene barrier membrane supports wound stabilization and enhance bone regeneration. J Periodontol 1993;64: Volume 29, Number 3, 2009
Alarge number of sound clinical
 Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
The ultimate goal in periodontal
 Volume 71 Number 4 Interleukin-1 Gene Polymorphisms and Long-Term Stability Following Guided Tissue Regeneration Therapy* Massimo De Sanctis and Giovanni Zucchelli Background: Specific interleukin (IL)-1
Volume 71 Number 4 Interleukin-1 Gene Polymorphisms and Long-Term Stability Following Guided Tissue Regeneration Therapy* Massimo De Sanctis and Giovanni Zucchelli Background: Specific interleukin (IL)-1
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
Minimally invasive techniques for periodontal regeneration
 2016; 2(12): 230-234 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2016; 2(12): 230-234 www.allresearchjournal.com Received: 04-10-2016 Accepted: 05-11-2016 Dr. Rizwan M Sanadi Professor,
2016; 2(12): 230-234 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2016; 2(12): 230-234 www.allresearchjournal.com Received: 04-10-2016 Accepted: 05-11-2016 Dr. Rizwan M Sanadi Professor,
골내결손부에서의치주조직재생 : 증례보고
 ISSN 1229-5418 Implantology 2015; 19(4): 228~232 골내결손부에서의치주조직재생 : 증례보고 김설희, 김태일서울대학교치의학대학원치주과학교실 Periodontal Regeneration in Intrabony Defects: A Case Report Sul-hee Kim, Tae-il Kim Department of Periodontology,
ISSN 1229-5418 Implantology 2015; 19(4): 228~232 골내결손부에서의치주조직재생 : 증례보고 김설희, 김태일서울대학교치의학대학원치주과학교실 Periodontal Regeneration in Intrabony Defects: A Case Report Sul-hee Kim, Tae-il Kim Department of Periodontology,
SIdP Sessione Premio H.M. Goldman 2019 SIdP H.M. Goldman Award 2019 Session 19 th International Congress
 CLINICAL OUTCOMES OF THE ENTIRE PAPILLA PRESERVATION TECHNIQUE WITH AND WITHOUT BIOMATERIALS IN THE TREATMENT OF ISOLATED INTRABONY DEFECTS: A RANDOMISED- CONTROLLED CLINICAL TRIAL Serhat Aslan, 1 Nurcan
CLINICAL OUTCOMES OF THE ENTIRE PAPILLA PRESERVATION TECHNIQUE WITH AND WITHOUT BIOMATERIALS IN THE TREATMENT OF ISOLATED INTRABONY DEFECTS: A RANDOMISED- CONTROLLED CLINICAL TRIAL Serhat Aslan, 1 Nurcan
The Simplified Papilla Preservation Flap in the Regenerative Treatment of Deep Intrabony Defects: Clinical Outcomes and Postoperative Morbidity
 The Simplified Papilla Preservation Flap in the Regenerative Treatment of Deep Intrabony Defects: Clinical Outcomes and Postoperative Morbidity Pierpaolo Cortellini,* Maurizio S. Tonetti,* Niklaus P. Lang,
The Simplified Papilla Preservation Flap in the Regenerative Treatment of Deep Intrabony Defects: Clinical Outcomes and Postoperative Morbidity Pierpaolo Cortellini,* Maurizio S. Tonetti,* Niklaus P. Lang,
Which reconstructive procedures are effective for treating the periodontal intraosseous defect?
 Periodontology 2000, Vol. 37, 2005, 88 105 Printed in Denmark. All rights reserved Copyright Ó Blackwell Munksgaard 2005 PERIODONTOLOGY 2000 Which reconstructive procedures are effective for treating the
Periodontology 2000, Vol. 37, 2005, 88 105 Printed in Denmark. All rights reserved Copyright Ó Blackwell Munksgaard 2005 PERIODONTOLOGY 2000 Which reconstructive procedures are effective for treating the
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
A New Papilla Preservation Technique for Periodontal Regeneration of Severely Compromised Teeth. Jose A. Moreno Rodríguez and Raúl G.
 A New Papilla Preservation Technique for Periodontal Regeneration of Severely Compromised Teeth Jose A. Moreno Rodríguez and Raúl G. Caffesse Introduction: Periodontal regeneration of hopeless teeth represents
A New Papilla Preservation Technique for Periodontal Regeneration of Severely Compromised Teeth Jose A. Moreno Rodríguez and Raúl G. Caffesse Introduction: Periodontal regeneration of hopeless teeth represents
The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series
 CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
Straumann Emdogain May 25, 2011
 Straumann Emdogain May 25, 2011 Terms and Conditions of Institut Straumann AG regarding the use of the presentations contained in this Emdogain Scientific Evidence Presentation File Please note that this
Straumann Emdogain May 25, 2011 Terms and Conditions of Institut Straumann AG regarding the use of the presentations contained in this Emdogain Scientific Evidence Presentation File Please note that this
Dental Research Journal
 Dental Research Journal Case Report Treatment strategy for guided tissue regeneration in various class II furcation defect: Case series Pushpendra Kumar Verma 1, Ruchi Srivastava 1, K. K. Gupta 2, T. P.
Dental Research Journal Case Report Treatment strategy for guided tissue regeneration in various class II furcation defect: Case series Pushpendra Kumar Verma 1, Ruchi Srivastava 1, K. K. Gupta 2, T. P.
Evidence-based decision making in periodontal tooth prognosis
 Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Longitudinal Supportive Periodontal Therapy for Severe Chronic Periodontitis with Furcation Involvement: A 12-year Follow-up Report
 Bull Tokyo Dent Coll (2013) 54(4): 243 250 Case Report Longitudinal Supportive Periodontal Therapy for Severe Chronic Periodontitis with Furcation Involvement: A 12-year Follow-up Report Akiyo Komiya-Ito,
Bull Tokyo Dent Coll (2013) 54(4): 243 250 Case Report Longitudinal Supportive Periodontal Therapy for Severe Chronic Periodontitis with Furcation Involvement: A 12-year Follow-up Report Akiyo Komiya-Ito,
Optimization of the periodontal attachment before orthodontic treatment
 DOI: 10.1051/odfen/2017008 J Dentofacial Anom Orthod 2017;20:307 The authors Optimization of the periodontal attachment before orthodontic treatment S. Mouraret 1, J.-P. Forestier 2 1 Private practice
DOI: 10.1051/odfen/2017008 J Dentofacial Anom Orthod 2017;20:307 The authors Optimization of the periodontal attachment before orthodontic treatment S. Mouraret 1, J.-P. Forestier 2 1 Private practice
More than regeneration.
 Straumann Product Emdogain Information More than regeneration. Patient comfort. Straumann Emdogain More than regeneration. Peace of mind. Tooth Preservation with Straumann Emdogain Periodontitis is associated
Straumann Product Emdogain Information More than regeneration. Patient comfort. Straumann Emdogain More than regeneration. Peace of mind. Tooth Preservation with Straumann Emdogain Periodontitis is associated
Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report
 Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Clinical literature for therapeutic indications. Straumann Emdogain
 Clinical literature for therapeutic indications Straumann Emdogain Table of contents 1 Basic principles of periodontal regeneration with 2 Enamel Matrix Proteins 2 Straumann Emdogain in intrabony defects
Clinical literature for therapeutic indications Straumann Emdogain Table of contents 1 Basic principles of periodontal regeneration with 2 Enamel Matrix Proteins 2 Straumann Emdogain in intrabony defects
Contemporary Periodontal Surgery
 Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
Surgical Therapy. Tuesday, April 2, 13. Alessan"o Geminiani, DDS, MS
 Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic case report.
 European International Journal of Science and Technology Vol. 6 No. 5 July 2017 Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic
European International Journal of Science and Technology Vol. 6 No. 5 July 2017 Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic
Pierpaolo Cortellini 1,2, Gabrielle Stalpers 2, Aniello Mollo 3 and Maurizio S. Tonetti 2 1 Accademia Toscana di Ricerca
 J Clin Periodontol 2011; 38: 915 924 doi: 10.1111/j.1600-051X.2011.01768.x Periodontal regeneration versus extraction and prosthetic replacement of teeth severely compromised by attachment loss to the
J Clin Periodontol 2011; 38: 915 924 doi: 10.1111/j.1600-051X.2011.01768.x Periodontal regeneration versus extraction and prosthetic replacement of teeth severely compromised by attachment loss to the
Additional use of autogenous periosteal barrier membrane combined with regenerative therapy in the interproximal intrabony defects: case series
 https://doi.org/10.14368/jdras.2017.33.3.230 ISSN 2384-4353 eissn 2384-4272 Case Report Additional use of autogenous periosteal barrier membrane combined with regenerative therapy in the interproximal
https://doi.org/10.14368/jdras.2017.33.3.230 ISSN 2384-4353 eissn 2384-4272 Case Report Additional use of autogenous periosteal barrier membrane combined with regenerative therapy in the interproximal
Cytoflex Barrier Membrane Clinical Evaluation
 Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Periodontal Treatment Guide
 Periodontal Treatment Guide Teamwork for treating periodontal disease The treatment of patients with periodontal disease should involve the application of standard procedures based on commonly accepted
Periodontal Treatment Guide Teamwork for treating periodontal disease The treatment of patients with periodontal disease should involve the application of standard procedures based on commonly accepted
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
TOOTH PRESERVATION _Zahnerhalt.indd UG :49:51 Uhr
 TOOTH PRESERVATION WHY REPAIR WHEN YOU CAN REGENERATE? Regeneration is the more natural and reliable way of restoring the positive properties of body-inherent processes. The aim of regeneration is to
TOOTH PRESERVATION WHY REPAIR WHEN YOU CAN REGENERATE? Regeneration is the more natural and reliable way of restoring the positive properties of body-inherent processes. The aim of regeneration is to
Periodontal Regeneration
 Periodontal Regeneration Regeneration The most ideal treatment Attempts to recreate the tissues destroyed by periodontitis Cement, bone and ligament Reduces the risk for recession and sensitivity (could
Periodontal Regeneration Regeneration The most ideal treatment Attempts to recreate the tissues destroyed by periodontitis Cement, bone and ligament Reduces the risk for recession and sensitivity (could
Management of osseous defects in aggressive periodontitis: A report of four cases using different techniques
 www.edoriumjournals.com case series OPEN ACCESS Management of osseous defects in aggressive periodontitis: A report of four cases using different techniques Sangeeta Singh, Parul Sharma ABSTRACT Introduction:
www.edoriumjournals.com case series OPEN ACCESS Management of osseous defects in aggressive periodontitis: A report of four cases using different techniques Sangeeta Singh, Parul Sharma ABSTRACT Introduction:
Parthasaradhi T., et al. J Dent Shiraz Univ Med Sci., September 2015; 16(3):
 Case Report Management of a One-wall Intrabony Osseous Defect with Combination of Platelet Rich Plasma and Demineralized Bone Matrix- a Two-year Follow up Case Report Parthasaradhi Thakkalapati a, Chitraa.R.chandran
Case Report Management of a One-wall Intrabony Osseous Defect with Combination of Platelet Rich Plasma and Demineralized Bone Matrix- a Two-year Follow up Case Report Parthasaradhi Thakkalapati a, Chitraa.R.chandran
Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study
 R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
In infrabony defects (IBDs), regenerative
 Volume 88 Number 6 Long-Term Stability After Regenerative Treatment of Infrabony Defects: A Retrospective Case Series Katrin Nickles,* Bettina Dannewitz,* Kerstin Gallenbach,* Tatjana Ramich,* Susanne
Volume 88 Number 6 Long-Term Stability After Regenerative Treatment of Infrabony Defects: A Retrospective Case Series Katrin Nickles,* Bettina Dannewitz,* Kerstin Gallenbach,* Tatjana Ramich,* Susanne
Science Flash. Straumann Emdogain. Science Flash
 Science Flash Straumann Emdogain Science Flash TABLE OF CONTENTS -year success with Straumann Emdogain in intra-bony defects with enamel matrix proteins and guided tissue regeneration Comparison of recession
Science Flash Straumann Emdogain Science Flash TABLE OF CONTENTS -year success with Straumann Emdogain in intra-bony defects with enamel matrix proteins and guided tissue regeneration Comparison of recession
Gingival recession causes periodontal
 J Periodontol October 2005 Factors Affecting the Outcomes of Coronally Advanced Flap Root Coverage Procedure Lien-Hui Huang,* Rodrigo E.F. Neiva, and Hom-Lay Wang Background: The coronally advanced flap
J Periodontol October 2005 Factors Affecting the Outcomes of Coronally Advanced Flap Root Coverage Procedure Lien-Hui Huang,* Rodrigo E.F. Neiva, and Hom-Lay Wang Background: The coronally advanced flap
Surgical Procedure in Guided Tissue Regeneration with the. Inion GTR Biodegradable Membrane System
 Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
PERIODONTAL CASE PRESENTATION - 1
 PERIODONTAL CASE PRESENTATION - 1 Overview A 32 year-old patient presented with generalized aggressive periodontitis. Treatment included non-surgical therapy with adjunctive antibiotics and surgical treatment.
PERIODONTAL CASE PRESENTATION - 1 Overview A 32 year-old patient presented with generalized aggressive periodontitis. Treatment included non-surgical therapy with adjunctive antibiotics and surgical treatment.
Periodontal Disease. Radiology of Periodontal Disease. Periodontal Disease. The Role of Radiology in Assessment of Periodontal Disease
 Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Periodontal Regeneration a
 Pierpaolo Cortellini Advanced Training Workshop a Periodontal a Florence, Italy October 10 12, 2019 Periodontal October 10 12, 2019 The Advanced Training Workshop on Periodontal is an interactive course,
Pierpaolo Cortellini Advanced Training Workshop a Periodontal a Florence, Italy October 10 12, 2019 Periodontal October 10 12, 2019 The Advanced Training Workshop on Periodontal is an interactive course,
Many techniques have been proposed for root coverage:
 Case Series Localized Gingival Recessions Treated With the Original Envelope Technique: A Report of 50 Consecutive Patients Jaime A. Vergara* and Raul G. Caffesse Background: The surgical techniques used
Case Series Localized Gingival Recessions Treated With the Original Envelope Technique: A Report of 50 Consecutive Patients Jaime A. Vergara* and Raul G. Caffesse Background: The surgical techniques used
Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery
 CASE SERIES 1 OPEN ACCESS Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery Sangeeta ABSTRACT Introduction:
CASE SERIES 1 OPEN ACCESS Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery Sangeeta ABSTRACT Introduction:
Platelet-Rich Plasma and Bone Graft Combined with Partial Thickness Mucosal Flap Technique in the Treatment of Deep Intrabony Defects
 BALKAN JOURNAL OF STOMATOLOGY ISSN 1107-1141 TUPNBUPMPHJDBM!!TPDJFUZ Platelet-Rich Plasma and Bone Graft Combined with Partial Thickness Mucosal Flap Technique in the Treatment of Deep Intrabony Defects
BALKAN JOURNAL OF STOMATOLOGY ISSN 1107-1141 TUPNBUPMPHJDBM!!TPDJFUZ Platelet-Rich Plasma and Bone Graft Combined with Partial Thickness Mucosal Flap Technique in the Treatment of Deep Intrabony Defects
Long-term Clinical Outcome after Reconstruction of Periodontal Defects using a Bovine-Derived Xenograft: a Retrospective Cohort Study
 RESEARCH REPORTS Long-term Clinical Outcome after Reconstruction of Periodontal Defects using a Bovine-Derived Xenograft: a Retrospective Cohort Study Christina Tietmann, Frank Bröseler The present retrospective
RESEARCH REPORTS Long-term Clinical Outcome after Reconstruction of Periodontal Defects using a Bovine-Derived Xenograft: a Retrospective Cohort Study Christina Tietmann, Frank Bröseler The present retrospective
F.V. Ribeiro et al. Fernanda Vieira RIBEIRO Francisco Humberto Nociti JÚNIOR Enilson Antonio SALLUM Antonio Wilson SALLUM Márcio Zaffalon CASATI
 60 Braz Dent J (2010) 21(1): 60-67 F.V. Ribeiro et al. ISSN 0103-6440 Use of Enamel Matrix Protein Derivative with Minimally Invasive Surgical Approach in Intra-bony Periodontal Defects: Clinical and Patient-Centered
60 Braz Dent J (2010) 21(1): 60-67 F.V. Ribeiro et al. ISSN 0103-6440 Use of Enamel Matrix Protein Derivative with Minimally Invasive Surgical Approach in Intra-bony Periodontal Defects: Clinical and Patient-Centered
Osseous surgery in periodontal treatment
 SCIENTIFIC SESSION Osseous surgery in periodontal treatment Essayist: Roberto Pontoriero Introduction In periodontally involved patients, periodontal therapy usually results in various degrees of soft-tissue
SCIENTIFIC SESSION Osseous surgery in periodontal treatment Essayist: Roberto Pontoriero Introduction In periodontally involved patients, periodontal therapy usually results in various degrees of soft-tissue
Classifications for Gingival Recession: A Mini Review
 Galore International Journal of Health Sciences and Research Vol.3; Issue: 1; Jan.-March 2018 Website: www.gijhsr.com Review Article P-ISSN: 2456-9321 Classifications for Gingival Recession: A Mini Review
Galore International Journal of Health Sciences and Research Vol.3; Issue: 1; Jan.-March 2018 Website: www.gijhsr.com Review Article P-ISSN: 2456-9321 Classifications for Gingival Recession: A Mini Review
14/09/15. Assessment of Periodontal Disease. Outline. Why is Periodontal assessment needed? The Basics of Periodontal assessment
 Assessment of Periodontal Disease Dr Wendy Turner Outline Why is Periodontal assessment needed? The Basics of Periodontal assessment Probing: Basic Periodontal Examination for adults and children. Detailed
Assessment of Periodontal Disease Dr Wendy Turner Outline Why is Periodontal assessment needed? The Basics of Periodontal assessment Probing: Basic Periodontal Examination for adults and children. Detailed
Enamel matrix derivative (Emdogain ) for periodontal tissue regeneration in intrabony defects (Review)
 Enamel matrix derivative (Emdogain ) for periodontal tissue regeneration in intrabony defects (Review) Esposito M, Grusovin MG, Papanikolaou N, Coulthard P, Worthington HV This is a reprint of a Cochrane
Enamel matrix derivative (Emdogain ) for periodontal tissue regeneration in intrabony defects (Review) Esposito M, Grusovin MG, Papanikolaou N, Coulthard P, Worthington HV This is a reprint of a Cochrane
Delta Dental of Virginia Clinical Policy # 402
 Delta Dental of Virginia Clinical Policy # 402 Subject Mucogingival Surgery and Soft Tissue Grafting Originating Department Clinical Professional Services Signature Authority Dental Director Type: New
Delta Dental of Virginia Clinical Policy # 402 Subject Mucogingival Surgery and Soft Tissue Grafting Originating Department Clinical Professional Services Signature Authority Dental Director Type: New
Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition. By: Kimberly Hawrylyshyn
 Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition By: Kimberly Hawrylyshyn Background Periodontitis is a microbe induced inflammatory disease that
Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition By: Kimberly Hawrylyshyn Background Periodontitis is a microbe induced inflammatory disease that
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bridge Flap: A Sine Qua Non For Mucogingival Deformities Debajyoti Mondal, Anju L, Rajul Choradia, Somen
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bridge Flap: A Sine Qua Non For Mucogingival Deformities Debajyoti Mondal, Anju L, Rajul Choradia, Somen
AL-AZHAR. Dental Journal. Print ISSN Online ISSN ADJ-for Girls, Vol. 5, No. 1, January (2018) PP. 29:35
 AL-AZHAR Dental Journal F o r G i r l s The Official Publication of The Faculty of Dental Medicine For Girls, Al-Azhar University Cairo, Egypt. Print ISSN 2537-0308 Online ISSN 2537-0316 ADJ-for Girls,
AL-AZHAR Dental Journal F o r G i r l s The Official Publication of The Faculty of Dental Medicine For Girls, Al-Azhar University Cairo, Egypt. Print ISSN 2537-0308 Online ISSN 2537-0316 ADJ-for Girls,
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
68 r 2009 The Authors Journal compilation r 2009 John Wiley & Sons A/S
 J Clin Periodontol 2009; 36: 68 79 doi: 10.1111/j.1600-051X.2008.01346.x Does placement of a connective tissue graft improve the outcomes of coronally advanced flap for coverage of single gingival recessions
J Clin Periodontol 2009; 36: 68 79 doi: 10.1111/j.1600-051X.2008.01346.x Does placement of a connective tissue graft improve the outcomes of coronally advanced flap for coverage of single gingival recessions
Minimally invasive non-surgical approach for the treatment of periodontal intrabony defects: a retrospective analysis
 J Clin Periodontol 2015; doi: 10.1111/jcpe.12443 Minimally invasive non-surgical approach for the treatment of periodontal intrabony defects: a retrospective analysis Luigi Nibali 1,2, Daniela Pometti
J Clin Periodontol 2015; doi: 10.1111/jcpe.12443 Minimally invasive non-surgical approach for the treatment of periodontal intrabony defects: a retrospective analysis Luigi Nibali 1,2, Daniela Pometti
ELIMINATE POCKETS. Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease
 ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
Enamel matrix derivative (Emdogain ) for periodontal tissue regeneration in intrabony defects (Review)
 Enamel matrix derivative (Emdogain ) for periodontal tissue regeneration in intrabony defects (Review) Esposito M, Grusovin MG, Papanikolaou N, Coulthard P, Worthington HV This is a reprint of a Cochrane
Enamel matrix derivative (Emdogain ) for periodontal tissue regeneration in intrabony defects (Review) Esposito M, Grusovin MG, Papanikolaou N, Coulthard P, Worthington HV This is a reprint of a Cochrane
RESEARCH REVIEW. Gingival recession: a proposal for a new classification ISSN :
 RESEARCH REVIEW Gingival recession: a proposal for a new classification Shantipriya Reddy, Sanjay Kaul, Prasad M.G.S., Jaya Agnihotri, Amudha D., Soumya Kambali ABSTRACT An accurate diagnosis is often
RESEARCH REVIEW Gingival recession: a proposal for a new classification Shantipriya Reddy, Sanjay Kaul, Prasad M.G.S., Jaya Agnihotri, Amudha D., Soumya Kambali ABSTRACT An accurate diagnosis is often
Minimally invasive techniques for periodontal therapy
 Review Article DOI: 10.18231/2395-499X.2017.0003 Agraja Patil 1,*, Swapna Mahale 2, Chaitanya Joshi 3 1,3 PG Student, 2 Professor & HOD, Dept. of Periodontology, MGV KBH Dental College & Hospital, Nashik,
Review Article DOI: 10.18231/2395-499X.2017.0003 Agraja Patil 1,*, Swapna Mahale 2, Chaitanya Joshi 3 1,3 PG Student, 2 Professor & HOD, Dept. of Periodontology, MGV KBH Dental College & Hospital, Nashik,
Alveolar Ridge Preservation:
 Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Evaluation of Guided Tissue Regeneration Following Third Molar Extraction by Bone Scintigraphy Using Tc99m-MDP
 CASE REPORT Evaluation of Guided Tissue Regeneration Following Third Molar Extraction by Bone Scintigraphy Using Tc99m-MDP Orit Oettinger-Barak, Eli E. Machtei, Zohar Keidar, Dan Mahler, Imad Abu EL-Naaj,
CASE REPORT Evaluation of Guided Tissue Regeneration Following Third Molar Extraction by Bone Scintigraphy Using Tc99m-MDP Orit Oettinger-Barak, Eli E. Machtei, Zohar Keidar, Dan Mahler, Imad Abu EL-Naaj,
The Original remains unique.
 The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
TWO-STEP SURGICAL PROCEDURE FOR ROOT COVERAGE (FREE GINGIVAL GRAFT AND CORONALLY POSITIONED FLAP) - A CASE REPORT
 TWO-STEP SURGICAL PROCEDURE FOR ROOT COVERAGE (FREE GINGIVAL GRAFT AND CORONALLY POSITIONED FLAP) - A CASE REPORT Dr Prashant Bhusari*, Dr Apoorva Saxena**, Dr Jaya Jain***,Dr Rashmi Rathore***, Dr Aditi
TWO-STEP SURGICAL PROCEDURE FOR ROOT COVERAGE (FREE GINGIVAL GRAFT AND CORONALLY POSITIONED FLAP) - A CASE REPORT Dr Prashant Bhusari*, Dr Apoorva Saxena**, Dr Jaya Jain***,Dr Rashmi Rathore***, Dr Aditi
Please visit the C.E. Pavilion to validate your course attendance Or If There s a Line Go cdapresents.com
 UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
Treatment of Intrabony Periodontal Defects with Emdogain-TS - a Report of 26 Cases
 CLINICAL AND RESEARCH REPORTS Treatment of Intrabony Periodontal Defects with Emdogain-TS - a Report of 26 Cases Asta Miliauskaite, Matthias Hannig The aim of the present study was to present results after
CLINICAL AND RESEARCH REPORTS Treatment of Intrabony Periodontal Defects with Emdogain-TS - a Report of 26 Cases Asta Miliauskaite, Matthias Hannig The aim of the present study was to present results after
COMBINED PERIODONTAL-ENDODONTIC LESION. By Dr. P.K. Agrawal Sr. Prof and Head Dept. Of Periodontia Govt. Dental College, Jaipur
 COMBINED PERIODONTAL-ENDODONTIC LESION By Dr. P.K. Agrawal Sr. Prof and Head Dept. Of Periodontia Govt. Dental College, Jaipur Differential diagnosis For differential diagnostic purposed the endo-perio
COMBINED PERIODONTAL-ENDODONTIC LESION By Dr. P.K. Agrawal Sr. Prof and Head Dept. Of Periodontia Govt. Dental College, Jaipur Differential diagnosis For differential diagnostic purposed the endo-perio
Maryland AGD AE and Socket Grafting 2015
 The Goodacre Study 5 year retrospective study looked at Crown & Bridge Caries Single crowns 1% FPD abutments 17% Periodontal Involvement Single crowns
The Goodacre Study 5 year retrospective study looked at Crown & Bridge Caries Single crowns 1% FPD abutments 17% Periodontal Involvement Single crowns
MODIFIED SINGLE ROLL FLAP APPROACH FOR SIMULTANEOUS IMPLANT PLACEMENT AND GINGIVAL AUGMENTATION
 Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
Root Proximity Characteristics and Type of Alveolar Bone Loss: A Case-control Study
 Journal of the International Academy of Periodontology 011 13/3: 73-79 Root Proximity Characteristics and Type of Alveolar Bone Loss: A Case-control Study 1 1 1 Maria-Anna Loukideli, Alexandra Tsami, Eudoxie
Journal of the International Academy of Periodontology 011 13/3: 73-79 Root Proximity Characteristics and Type of Alveolar Bone Loss: A Case-control Study 1 1 1 Maria-Anna Loukideli, Alexandra Tsami, Eudoxie
GMJ, ASM 2013;2(S1):S120-S125 GULF MEDICAL JOURNAL
 Evaluate clinical effectiveness of autologous platelet rich plasma (PRP) using curasan technique in treating intrabony defects using regenerative material Bone graft / GTR membrane M Sesha Reddy College
Evaluate clinical effectiveness of autologous platelet rich plasma (PRP) using curasan technique in treating intrabony defects using regenerative material Bone graft / GTR membrane M Sesha Reddy College
Working together as a team, the periodontist
 The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
Regenerative Procedures and Orthodontics in the Treatment of Severe Intrabony Defects
 in the Treatment of Severe Intrabony Defects C. Tietmann, F. Bröseler, T. Axelrad, M. Franke, S. Jepsen Private Practice Periodontology, Aachen, Germany Department ofperiodontology, Operative andpreventivedentistry,
in the Treatment of Severe Intrabony Defects C. Tietmann, F. Bröseler, T. Axelrad, M. Franke, S. Jepsen Private Practice Periodontology, Aachen, Germany Department ofperiodontology, Operative andpreventivedentistry,
Efficacy of Lateral Pedicle Graft in the Treatment of Isolated Gingival Recession Defects
 International Journal of Pharmaceutical Science Invention ISSN (Online): 2319 6718, ISSN (Print): 2319 670X Volume 3 Issue 1 January 2014 PP.46-50 Efficacy of Lateral Pedicle Graft in the Treatment of
International Journal of Pharmaceutical Science Invention ISSN (Online): 2319 6718, ISSN (Print): 2319 670X Volume 3 Issue 1 January 2014 PP.46-50 Efficacy of Lateral Pedicle Graft in the Treatment of
Fundamental & Preventive Curvatures of Teeth and Tooth Development. Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L.
 Fundamental & Preventive Curvatures of Teeth and Tooth Development Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L. Dennis Proximal contact areas Contact areas are on the mesial and
Fundamental & Preventive Curvatures of Teeth and Tooth Development Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L. Dennis Proximal contact areas Contact areas are on the mesial and
Linking Research to Clinical Practice
 Is Non Surgical Periodontal Therapy Cost Effective? Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information
Is Non Surgical Periodontal Therapy Cost Effective? Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Chemicals in Surgical Periodontal Therapy
 Chemicals in Surgical Periodontal Therapy von Alexandrina L. Dumitrescu 1. Auflage Chemicals in Surgical Periodontal Therapy Dumitrescu schnell und portofrei erhältlich bei beck-shop.de DIE FACHBUCHHANDLUNG
Chemicals in Surgical Periodontal Therapy von Alexandrina L. Dumitrescu 1. Auflage Chemicals in Surgical Periodontal Therapy Dumitrescu schnell und portofrei erhältlich bei beck-shop.de DIE FACHBUCHHANDLUNG
A Promising Periodontal Procedure for the Treatment of Adjacent Gingival Recession Defects. Tolga Fikret Tözüm, DDS, PhD
 C L I N I C A L P R A C T I C E A Promising Periodontal Procedure for the Treatment of Adjacent Gingival Recession Defects Tolga Fikret Tözüm, DDS, PhD A b s t r a c t Various clinical reports on the reconstruction
C L I N I C A L P R A C T I C E A Promising Periodontal Procedure for the Treatment of Adjacent Gingival Recession Defects Tolga Fikret Tözüm, DDS, PhD A b s t r a c t Various clinical reports on the reconstruction
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
ORIGINAL ARTICLE. Introduction. Sujith Sukumar 1, Ivo Dřízhal 1, Josef Bukač 2, Vladimíra Paulusová 1, Shriharsha Pilathadka 1
 ORIGINAL ARTICLE SURGICAL TREATMENT OF PERIODONTAL INTRABONY DEFECTS WITH CALCIUM SULPHATE IN COMBINATION WITH BETA TRICALCIUM PHOSPHATE A 12-MONTH RETROSPECTIVE CLINICAL EVALUATION Sujith Sukumar 1, Ivo
ORIGINAL ARTICLE SURGICAL TREATMENT OF PERIODONTAL INTRABONY DEFECTS WITH CALCIUM SULPHATE IN COMBINATION WITH BETA TRICALCIUM PHOSPHATE A 12-MONTH RETROSPECTIVE CLINICAL EVALUATION Sujith Sukumar 1, Ivo
XIII CONGRESSO INTERNAZIONALE
 THE ASSOCIATION OF THE COMPOSITE IL-1 GENOTYPE WITH PERIODONTITIS PROGRESSION AND/OR TREATMENT OUTCOMES. A SYSTEMATIC REVIEW Associazione del genotipo IL-1 con la progressione della parodontite, e/o con
THE ASSOCIATION OF THE COMPOSITE IL-1 GENOTYPE WITH PERIODONTITIS PROGRESSION AND/OR TREATMENT OUTCOMES. A SYSTEMATIC REVIEW Associazione del genotipo IL-1 con la progressione della parodontite, e/o con
Bone Levels - From Hypothesis To Facts
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 6, Issue 5 (May.- Jun. 2013), PP 19-23 Bone Levels - From Hypothesis To Facts Savitha B 1, Priyanka
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 6, Issue 5 (May.- Jun. 2013), PP 19-23 Bone Levels - From Hypothesis To Facts Savitha B 1, Priyanka
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy
 Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS
 Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
WHAT IS THE PURPOSE OF WHAT WE DO? TEAM PERIODONTICS: WORKING TOGETHER TO IMPROVE PATIENT CARE YOU ARE THE PERIODONTISTS IN YOUR PRACTICE!
 Setter Periodontics 2075 SW 1 st Ave #2L Portland, OR 97201 503-222-9961 michael@setterperio.com WHAT IS THE PURPOSE OF WHAT WE DO? Gum Gardeners Study Club 2.27.17 TEAM PERIODONTICS: WORKING TOGETHER
Setter Periodontics 2075 SW 1 st Ave #2L Portland, OR 97201 503-222-9961 michael@setterperio.com WHAT IS THE PURPOSE OF WHAT WE DO? Gum Gardeners Study Club 2.27.17 TEAM PERIODONTICS: WORKING TOGETHER
Principles of Periodontal flap surgery. Dr.maryam khosravi
 Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
LANAP. Non-invasive laser gum therapy. LANAP Information Pack
 LANAP Non-invasive laser gum therapy LANAP Information Pack GumSurgeryConcord.com What is LANAP? LANAP vs Traditional Treatment Frequently Asked Questions Gum Tissue & Bone Regeneration Treatment Plan
LANAP Non-invasive laser gum therapy LANAP Information Pack GumSurgeryConcord.com What is LANAP? LANAP vs Traditional Treatment Frequently Asked Questions Gum Tissue & Bone Regeneration Treatment Plan
LANAP. The new solution to an old problem. LANAP Information Packet. What is LANAP? What is the Difference? Frequently Asked Questions
 LANAP The new solution to an old problem LANAP Information Packet What is LANAP? 2 What is the Difference? 5 Frequently Asked Questions 7 What is Biostimulation? 9 Treatment Plans 11 1 1 What are the Benefits?
LANAP The new solution to an old problem LANAP Information Packet What is LANAP? 2 What is the Difference? 5 Frequently Asked Questions 7 What is Biostimulation? 9 Treatment Plans 11 1 1 What are the Benefits?
Coverage of gingival recession defe Titletissue regeneration with and withou enamel matrix derivative in
 Coverage of gingival recession defe Titletissue regeneration with and withou enamel matrix derivative in a dog m Author(s) Fujita, T; Yamamoto, S; Ota, M; Shi Alternative Yamada, S International journal
Coverage of gingival recession defe Titletissue regeneration with and withou enamel matrix derivative in a dog m Author(s) Fujita, T; Yamamoto, S; Ota, M; Shi Alternative Yamada, S International journal
Educational Training Document
 Educational Training Document Table of Contents Part 1: Resource Document Disclaimer Page: 2 Part 2: Line Item Grade Sheets Page: 3 Release: 11/2016 Page 1 of 6 Part 1: Resource Document Disclaimer The
Educational Training Document Table of Contents Part 1: Resource Document Disclaimer Page: 2 Part 2: Line Item Grade Sheets Page: 3 Release: 11/2016 Page 1 of 6 Part 1: Resource Document Disclaimer The
Subject: Osseous Surgery Guideline #: Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017
 Clinical Guideline Subject: Osseous Surgery Guideline #: 04-205 Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017 Description This document addresses the procedure of osseous
Clinical Guideline Subject: Osseous Surgery Guideline #: 04-205 Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017 Description This document addresses the procedure of osseous
Michael K. McGuire,* E. Todd Scheyer,* and Martha Nunn
 J Periodontol November 2012 Evaluation of Human Recession Defects Treated With Coronally Advanced Flaps and Either Enamel Matrix Derivative or Connective Tissue: Comparison of Clinical Parameters at 10
J Periodontol November 2012 Evaluation of Human Recession Defects Treated With Coronally Advanced Flaps and Either Enamel Matrix Derivative or Connective Tissue: Comparison of Clinical Parameters at 10
12-Months Clinical Comparison between Osteoinductal and Emdogain for the Treatment of Intrabony Defects
 Seite 1 von 5 Int Poster J Dent Oral Med 2007, Vol 9 No 01, Poster 348 12-Months Clinical Comparison between and Emdogain for the Treatment of Intrabony Defects Language: English Authors: Assist. Prof.
Seite 1 von 5 Int Poster J Dent Oral Med 2007, Vol 9 No 01, Poster 348 12-Months Clinical Comparison between and Emdogain for the Treatment of Intrabony Defects Language: English Authors: Assist. Prof.
The partly epithelialized free gingival graft (pe-fgg) at lower incisors. A pilot study with implications for alignment of the mucogingival junction
 J Clin Periodontol 2012; 39: 674 680 doi: 10.1111/j.1600-051X.2012.01896.x The partly epithelialized free gingival graft (pe-fgg) at lower incisors. A pilot study with implications for alignment of the
J Clin Periodontol 2012; 39: 674 680 doi: 10.1111/j.1600-051X.2012.01896.x The partly epithelialized free gingival graft (pe-fgg) at lower incisors. A pilot study with implications for alignment of the
Clinical Comparison of Subepithelial Connective Tissue Grafts and Coronally Advanced Flaps with Emdogain in the Treatment of Gingival Recessions
 Original Article Clinical Comparison of Subepithelial Connective Tissue Grafts and Coronally Advanced Flaps with Emdogain in the Treatment of Gingival Recessions F. Haghighati 1,2, AA. Khoshkhoonejad 3,
Original Article Clinical Comparison of Subepithelial Connective Tissue Grafts and Coronally Advanced Flaps with Emdogain in the Treatment of Gingival Recessions F. Haghighati 1,2, AA. Khoshkhoonejad 3,
Surgical treatment of localized gingival recessions using coronally advanced flaps with or without subepithelial connective tissue graft
 Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.21043 http://dx.doi.org/doi:10.4317/medoral.21043 Surgical treatment of localized gingival recessions using coronally advanced
Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.21043 http://dx.doi.org/doi:10.4317/medoral.21043 Surgical treatment of localized gingival recessions using coronally advanced
Efficacy of Palatal Connective Tissue Graft as a Membrane in the Treatment of Intrabony Defects
 Journal of Periodontology & Implant Dentistry Research Article Efficacy of Palatal Connective Tissue Graft as a Membrane in the Treatment of Intrabony Defects Hamid Moghaddas 1 Leila Soltani 2 Omid Moghaddas
Journal of Periodontology & Implant Dentistry Research Article Efficacy of Palatal Connective Tissue Graft as a Membrane in the Treatment of Intrabony Defects Hamid Moghaddas 1 Leila Soltani 2 Omid Moghaddas
