Giant keratocystic odontogenic tumor: a challenging diagnosis
|
|
|
- Myron Knight
- 5 years ago
- Views:
Transcription
1 Article / Clinical Case Report Rachna Kaushik a, Kumar Pushpanshu a, Silky Rajesh Punyani b, Vineet Raj c Kaushik R, Pushpanshu K, Punyani SR, Raj V.. Autopsy Case Rep [Internet]. 2016;6(3): ABSTRACT The keratocystic odontogenic tumor, although a benign lesion, is peculiarly aggressive with a high recurrence rate. Its involvement with the maxillary antrum is atypical. We report the unusual case of a 20-year-old male patient with an extensive antral tumor associated with an impacted third molar, which was initially misdiagnosed as a dentigerous cyst. Clinical, radiographic, and histopathologic aspects were analyzed to provide useful information for the correct diagnosis, treatment, and prognosis within a multidisciplinary approach. Keywords Carnoy s solution; Molar, Third; Maxillary Sinus; Odontogenic Tumors. INTRODUCTION The odontogenic keratocyst (OKC) was first described by Philipsen in 1956 as an odontogenic cyst with a keratinous epithelial lining and its distinctive histological features were elaborated by Pindborg and Hansen in However, in 1967, Toller suggested that the OKC should rather be regarded as a benign neoplasm and not as a typical cyst. 2 Ever since Mikulicz presented the first case of OKC, in 1876, as a dermoid cyst, this interesting lesion has been the subject of debate owing to its varied origin, debated development, peculiar behavior, unique tendency to recur, and disputed treatment modalities. 3 Keratocystic odontogenic tumors (KCOTs) are very aggressive with high mitotic counts and epithelial turnover rates, and a relatively high recurrence rate. 4 Additionally, the epithelial lining is not as inactive as that of other cysts and appears to have an innate growth potential, as observed with a benign tumor. 1 These are designated as a consistent finding in Gorlin syndrome. 5 Based on their biological behavior, neoplastic features, and recent research in genetics, the WHO in 2005 reclassified OKC as KCOT, which is now defined as a benign unicystic or multicystic, intraosseous tumor of odontogenic origin, with a characteristic lining of parakeratinized stratified squamous epithelium and potential for aggressive, infiltrative behavior. 6,7 KCOT is a benign developmental intraosseous neoplasm of the jaws arising from cell rests of the dental lamina (the oral epithelial lining of the developing tooth follicle) and an extension of basal cells of overlying oral epithelium. 1 KCOT is predominant in males; it occurs mainly in the second and third decade of life, and is most frequently found in the posterior body of the mandible and ascending ramus. 7 In the maxilla, the canine region is the most common location for KCOT, and it is quite a Department of Dentistry - SriKrishna Medical College & Hospital, Muzaffarpur India. b Department of Oral Medicine and Radiology - People s Dental Academy, Bhopal India. c Department of Oral Pathology - Chandra Dental College, Barabanki India. Autopsy and Case Reports. ISSN Copyright This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium provided the article is properly cited.
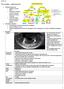
2 unusual for it to occur in the maxillary sinus. Less than 1% of KCOTs are involved with the maxillary sinus. 4,8 Clinically, KCOT is a fast-growing expansive lesion when it is involved near the maxillary sinus. It could easily expand to an enormous size occupying the entire maxilla. Maxillary sinus is a less dense structure, thus allowing the rapid growth of the lesion. 7 Such an extensive lesion involving an unusual site often presents with diagnostic and, therefore, therapeutic challenges. The purpose of this report is to present a rare case of KCOT in the maxillary sinus associated with an impacted tooth in a young Asian male. In addition, we discuss relevant issues about the diagnosis, management, and prognosis of these lesions, within a multidisciplinary approach. CASE REPORT A 20-year-old male patient reported for an evaluation of a right-side, unilateral, painless facial swelling of 6 months duration. The patient was apparently healthy with no significant medical, dental, or surgical history. On systematic clinical examination, a diffused swelling was evident, which extended from the right ala of the nose to the right outer canthus of the eye mediolaterally, and from the infra-orbital region to the level of right commissure, without the presence of lymphadenopathy (Figure 1). A thorough intraoral examination disclosed a diffuse soft swelling of 5 3 cm diameter along the right maxillary alveolus, which caused the obliteration of the buccal vestibule and extended from the maxillary right canine to the maxillary right second molar region. Upon digital compression, the swelling was soft and fluctuant in consistency, which indicated buccal cortical plate resorption. All teeth were negative to percussion and mobility tests. No visual disturbance or nasal obstruction were reported or observed. Routine laboratory parameters were normal. Radiological examination depicted a single unilocular radiolucency with smooth, corticated margins extending from the root apex of the right maxillary canine to the right maxillary tuberosity region. The radiolucency was associated with an impacted maxillary right third molar displacing it superiorly into the opacified right maxillary antrum. Destruction of the posterior wall of the sinus was also evident. The involved teeth showed no deviation; however, slightly resorbed roots were detected with right maxillary first and second premolars and right maxillary first molar. To visualize the lesion in more detail, computed tomography (CT) was performed, which revealed a large, well defined, non-enhancing, hypodense osteolytic lesion ( cm) with a well defined margin. The lesion involved the right maxillary bone and the maxillary sinus, and caused complete opacification of the right antrum and displacement of the right maxillary third molar to the anteromedial wall of the sinus (Figure 2). The expansile cystic lesion caused thinning of the antral walls and erosion of the buccal cortical bone of the right maxillary bone. Based on these observations, a tentative pre-operative diagnosis of dentigerous cyst associated with the right maxillary third molar was proposed. An incisional biopsy was performed and the histopathological examination of hematoxylin and eosin stained sections revealed a cystic mass lined by a parakeratinized stratified squamous epithelium of variable thickness (four to eight cell layers). The epithelium showed a lack of rete ridges, a distinctive basal layer with palisaded and hyperchromatic nuclei, surface corrugations, and detachment from the capsule in focal areas (Figure 3A). The connective tissue capsule Figure 1. Extraoral (frontal) view showing a swelling over the right maxillary region. 42
3 Kaushik R, Pushpanshu K, Punyani SR, Raj V Figure 2. Axial CT of the sinuses. A - Complete opacification of the right antrum; B - Thinning and irregular destruction of the antral walls is evident; C - Displacement of right maxillary third molar; D - Coronal view showing the extensive lesion involving the right antrum and infiltrating into the right nasal cavity. Figure 3. A - Photomicrograph of cyst wall showing parakeratinized lining epithelium with basal palisading and surface corrugations. Note the separation of epithelium from the underlying capsule (H&E, 200X); B - Photomicrograph of the lesion showing keratin-filled daughter cysts within the cystic capsule (H&E, 100X). 43
4 was loose to moderately dense, and was fibro cellular in nature showing spindle shaped fibroblasts and foci of chronic inflammatory infiltrate composed of lymphocytes, macrophages, and plasma cells. A few daughter cysts and odontogenic rests were also seen within the capsule (Figure 3B). The histopathological findings were suggestive of KCOT. After careful evaluation, the expansile maxillary tumor was enucleated as a whole using the Caldwell-Luc procedure. The associated impacted right maxillary third molar was simultaneously removed to avoid tumor fragmentation, and prophylactic chemical cauterization was done using Carnoy s solution. Betadine irrigation was performed and the borders of the wound were then sutured. The wound healed uneventfully, showing no recurrent sign during the follow-up period of more than 6 years. DISCUSSION KCOT, formerly believed to be a cyst, has certain uniquely distinguishable clinical and histologic features. 5 The term odontogenic keratocyst, as it was previously named, is nonspecific and only indicates keratin formation. The production of keratin is attributed to epithelial squamous metaplasia, which can lead to the keratinization of other odontogenic cysts (dentigerous, radicular, and residual cysts) as well. 9,10 The WHO s re-classification of this lesion from cyst to tumor underscores its potential aggressive nature, which indeed is the main difference between KCOT and other jaw cysts. It has an active epithelial component having an innate growth potential and a relatively high recurrence rate. The epithelial lining demonstrates a high mitotic activity and turnover rate. 1,4 The increased cell activity is confirmed by elevated levels of oxidative enzymes and acid phosphatase, which is indicative of high metabolic and lysosomal activities. The active epithelial lining may rarely develop into squamous cell carcinoma. 11 The epithelium of KCOT has decreased apoptotic activity, allowing the survival of genetically unstable cells. The higher epithelial proliferation rate, and the inhibition of apoptosis of the damaged cells, are important steps in tumor development. 7 KCOT exhibits unique growth and biological behavior compared to common cysts, wherein the growth is due to the active proliferation of the epithelial lining. Most of the commonly occurring cysts grow mainly because of the osmotic pressure of the cystic fluid. This pushing type of growth causes the buccal and lingual cortical plate expansion. KCOT, however, behaves like a benign tumor growing by extension rather than by expansion. Here, the osmotic pressure of the cystic fluid is quite low; thus, the extension is along the path of least resistance. The lesion mainly involves the cancellous bone and grows in the anteroposterior direction with little evidence of cortical expansion in the initial stages. They are poor bone resorbers that invade the compact bone much later. 1,8,10 Clinically, KCOTs are often asymptomatic; however, they occasionally may cause swelling, pain, discharge, teeth mobility, and invasion of adjacent structures. If secondarily infected, symptoms like pain, swelling, and discharge are not uncommon, wherein the lesion can be easily confused with inflammatory conditions like sinusitis. In this case, the patient had a localized asymptomatic swelling, which is the most commonly reported symptom. 4 The swelling was soft and fluctuant, indicating buccal cortical plate resorption, which is not uncommon with large KCOTs in the posterior maxilla. 12 The anatomical structure, loose maxillary bone density, and empty space of the maxillary antrum may be the contributing factors for the development of such an expansile tumor in the present case. KCOTs may cause the radicular displacement of adjacent teeth, but root resorption is rare. 5 Contrary to this, none of the teeth showed any deviation; however, rhizolysis was detected in three teeth of our patient. Radiographically, KCOT appears as well-defined radiolucency with an osteosclerotic rim, which may be unilocular or multilocular. 4 Multilocularity of these lesions is attributed to their tendency to expand through the marrow spaces owing to their active epithelium. 13 Scalloped margins are observed in the long standing lesions due to the regional resorption of the surrounding bone. 8 Even though KCOTs present a varied radiographic appearance, the lack of cortical expansion appears to be the only reliable radiographic parameter compared with odontogenic cysts or ameloblastomas. 6 KCOT can occur anywhere within the jaws and can resemble other lesions that present with similar radiological features. Therefore, many cystic and neoplastic lesions can be considered as the differential diagnosis. These include dentigerous cysts, lateral periodontal cysts, radicular cysts, ameloblastomas, 44
5 Kaushik R, Pushpanshu K, Punyani SR, Raj V adenomatoid odontogenic tumors, odontogenic myxomas, simple bone cysts, central giant cell granulomas, arteriovenous malformations, and a number of fibro-osseous lesions. It has been shown that an unerupted tooth is involved in the lesion in 25-40% of cases. Thus, clinically and radiologically, it mimics a dentigerous cyst, as was the scenario in the reported case. Therefore, a thorough preoperative differentiation between these lesions is of utmost importance as it leads to the choice of surgical method. 4,14 With KCOT involving the maxillary antrum being a rarity, its detection solely by plain radiography may result in misdiagnosis. 1 CT and/or magnetic resonance imaging (MRI) examinations can eliminate the superimposition of anatomical structures leading to the three-dimensional geometric accuracy. 14 Additionally, these examinations may help to assess the infiltration following cortical perforation and soft tissue involvement. 5 Therefore, CT/MRI can aid both diagnosis and preoperative preparation of these lesions involving a rare site, compared to the traditional two dimensional views. Even with highly suggestive clinical and radiographic features, KCOT can often be misdiagnosed and even more so when it involves the maxilla. Therefore, the best way to confirm its diagnosis is by recognizing its characteristic histopathologic features. 2 The histopathologic features of KCOT are confirmatory with distinctly different epithelial lining. However, these classic features may be altered by inflammation, which can lead to confusion. 6 Histologically, it has the characteristic lining of parakeratinized stratified squamous epithelium with an aggressive clinical presentation. 4 Previously considered a subtype, the orthokeratotic variety is currently considered as an innocent entity and is still believed to be a developmental odontogenic cyst. 14 Histopathologic diagnosis is particularly important for adequate treatment planning and, hence, for preventing recurrences. 1 KCOT has a high rate of recurrence (up to 60%), which is comparable only to ameloblastoma. 15 The involvement of a tooth the third molar in particular is considered to be an important risk factor for the development of recurrence. 6 In the present case, KCOT involved the right maxillary antrum along with the right maxillary impacted third molar. The likelihood of recurrences depends on numerous variables, which are yet to be clearly determined. There is no consensus regarding the best treatment option of KCOT, which must be managed in a case-by-case manner. The surgical treatment aims to control potential recurrence with the least possible morbidity. 5,6 Following careful assessment, we decided on an antral cystectomy using the Caldwell-Luc procedure, followed by treatment of the cavity with Carnoy s solution. The Caldwell-Luc procedure provides a direct view of the maxillary sinus, and Carnoy s solution kills the epithelial remnants or satellite cysts. 1 Carnoy s solution is a tissue fixative that kills epithelial remnants in the osseous margin because it can penetrate bone to a depth of 1.54 mm. 8 KCOTs involving the maxillary sinus invariably become large expanded lesions, which present challenges in achieving complete hemostasis in the anatomically delicate areas. 7 Such cases, therefore, require a multidisciplinary collaboration between different specializations with careful treatment planning for a favorable prognosis, including the absence of KCOT recurrence. Due to the frequent recurrence of KCOT, patients are recommended to be kept under long-term supervision as recurrences can occur up to 10 years after treatment. However, it is more common during the first 5-7 years. 6 Our patient was observed for 6 years after treatment with no evidence of recurrence. CONCLUSION The reclassification of KCOT from cyst to tumor underscores its aggressiveness, which should motivate the clinician to manage the disease aggressively. The lesion is unique in terms of its high recurrence rate, and it is a good mimic owing to its variety of clinical and radiographic appearances. Thus, only a cautious approach aided with wisely chosen diagnostic tests can help to make a preoperative diagnosis of this challenging tumor in an unusual site. REFERENCES 1. Kwon HI, Lim WB, Kim JS, et al. Odontogenic Keratocyst associated with an ectopic tooth in the Maxillary sinus: a report of two cases and a review of the literature. Korean J Pathol. 2011;45(Suppl 1):S org/ /koreanjpathol s1.s5. 2. Chaudhary S, Sinha A, Barua P, Mallikarjuna R. Keratocystic odontogenic tumour (KCOT) misdiagnosed 45
6 as a dentigerous cyst. BMJ Case Rep. 2013;2013 PMid: El-Hajj G, Anneroth G. Odontogenic keratocysts: a retrospective clinical and histologic study. Int J Oral Maxillofac Surg. 1996;25(2): org/ /s (96) PMid: Cakur B, Miloglu O, Yolcu U, Göregen M, Gürsan N. Keratocystic odontogenic tumor invading the right maxillary sinus: a case report. J Oral Sci. 2008;50(3): PMid: Grasmuck EA, Nelson BL. Keratocystic odontogenic tumor. Head Neck Pathol. 2010;4(1): org/ /s x. PMid: Sánchez-Burgos R, González-Martín Moro J, Pérez- Fernández E, Burgueño-García M. Clinical, radiological and therapeutic features of keratocystic odontogenic tumours: a study over a decade. J Clin Exp Dent. 2014;6(3):e jced PMid: Byun JH, Kang YH, Choi MJ, Park BW. Expansile keratocystic odontogenic tumor in the maxilla: immunohistochemical studies and review of literature. J Korean Assoc Oral Maxillofac Surg. 2013;39(4): org/ /jkaoms PMid: Gupta A, Rai B, Nair MA, Bhut MK. Keratocystic odontogenic tumor with impacted maxillary third molar involving the right maxillary antrum: an unusual case report. Indian J Dent Res. 2011;22(1): dx.doi.org/ / PMid: Regezi JA, Sdubba JJ. Oral pathology: clinical-pathologic correlations. 2nd ed. Philadelphia: W.B. Saunders Company; p R.A.Cawson, E.W.Odell. Cawson s essentials of oral pathology and oral medicine. 8th ed. Edinburgh: Churchill Livingstone; Scharffetter K, Balz-Herrmann C, Lagrange W, Koberg W, Mittermayer C. Proliferation kinetics-study of the growth of keratocysts: morpho-functional explanation for recurrences. J Craniomaxillofac Surg. 1989;17(5): PMid: Makowski GJ, McGuff S, Van Sickels JE. Squamous cell carcinoma in a maxillary odontogenic keratocyst. J Oral Maxillofac Surg. 2001;59(1): org/ /joms PMid: Haring JI, Van Dis ML. Odontogenic keratocysts: a clinical, radiographic, and histopathologic study. Oral Surg Oral Med Oral Pathol. 1988;66(1): org/ / (88) PMid: Koçak-Berberoğlu H, Çakarer S, Brkić A, Gürkan-Koseoglu B, Altuğ-Aydil B, Keskin C. Three-dımensıonal cone- beam computed tomography for dıagnosıs of keratocystıc odontogenıc tumours; evaluatıon of four cases. Med Oral Patol Oral Cir Bucal. 2012;17(6):e org/ /medoral PMid: DelBalso AM. An approach to the diagnostic imaging of jaw lesions, dental implants, and the temporomandibular joint. Radiol Clin North Am. 1998;36(5):855-90, vi. PMid: Conflict of interest: None Submitted on: March 9 th, 2016 Accepted on: June 21 st, 2016 Correspondence Kumar Pushpanshu Department of Dentistry - SriKrishna Medical College & Hospital Muzaffarpur, Bihar India Pin code: Phone: +91 (85) drpushpanshu@yahoo.co.in 46
Origin of Odontogenic Cysts & Tumors
 Origin of Odontogenic Cysts & Tumors Odontogenic Apparatus Origin of Odontogenic Cysts & Tumors Odontogenic Apparatus Remnants of dental lamina Reduced enamel epithelium Odontogenic rests Basal cell layer
Origin of Odontogenic Cysts & Tumors Odontogenic Apparatus Origin of Odontogenic Cysts & Tumors Odontogenic Apparatus Remnants of dental lamina Reduced enamel epithelium Odontogenic rests Basal cell layer
Management of Keratocystic Odontogenic Tumour With Marsupialisation, Enucleation and Carnoy s Solution Application: A Case Report
 Management of Keratocystic Odontogenic Tumour With Marsupialisation, Enucleation and Carnoy s Solution Application: A Case Report Aydin Ozkan 1, Gurkan Rasit Bayar 2, Hasan Ayberk Altug 2, Metin Sencimen
Management of Keratocystic Odontogenic Tumour With Marsupialisation, Enucleation and Carnoy s Solution Application: A Case Report Aydin Ozkan 1, Gurkan Rasit Bayar 2, Hasan Ayberk Altug 2, Metin Sencimen
An Expansile Large Odontogenic Keratocyst Maxilla: A Case Report.
 RESEARCH AND REVIEWS: JOURNAL OF DENTAL SCIENCES An Expansile Large Odontogenic Keratocyst Maxilla: A Case Report. Nasib Chand Khabra 1, Ish Pandhi 1 *, Kiran DN 2, Sunil Alipuria 1, Bhawna Gulati 1, and
RESEARCH AND REVIEWS: JOURNAL OF DENTAL SCIENCES An Expansile Large Odontogenic Keratocyst Maxilla: A Case Report. Nasib Chand Khabra 1, Ish Pandhi 1 *, Kiran DN 2, Sunil Alipuria 1, Bhawna Gulati 1, and
Orthokeratinized Odontogenic Cyst: A Rarity
 aijoc AIJOC Case Report 1 Heena Sonawane, 2 Freny R Karjodkar, 3 Kaustubh Sansare, 4 Nimish Prakash ABSTRACT Orthokeratinized odontogenic cyst (OOC) was first identified as the rare variant of keratocystic
aijoc AIJOC Case Report 1 Heena Sonawane, 2 Freny R Karjodkar, 3 Kaustubh Sansare, 4 Nimish Prakash ABSTRACT Orthokeratinized odontogenic cyst (OOC) was first identified as the rare variant of keratocystic
Squamous Cell Carcinoma Arising in a Residual Cyst: A Case Report
 Squamous Cell Carcinoma Arising in a Residual Cyst: A Case Report Abstract Aim: The purpose of this report is to present a case of squamous cell carcinoma (SCC) arising from a mandibular residual cyst.
Squamous Cell Carcinoma Arising in a Residual Cyst: A Case Report Abstract Aim: The purpose of this report is to present a case of squamous cell carcinoma (SCC) arising from a mandibular residual cyst.
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Orthokeratinized Odontogenic Cyst: A Case Report- A Milder Variant of OKC or an Independent Entity Mariyam
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Orthokeratinized Odontogenic Cyst: A Case Report- A Milder Variant of OKC or an Independent Entity Mariyam
Glandular Odontogenic Cyst Coexisting with a Dentigerous Cyst: Case Report
 SmyrnaMed Case 2018;2(1): 1-5 ISSN (Online): 2564-6869 www.smyrnamed.com Glandular Odontogenic Cyst Coexisting with a Dentigerous Cyst: Case Report Assist.Prof.Dr. Serap Keskin Tunç 1, Dt. Erkan Feslihan
SmyrnaMed Case 2018;2(1): 1-5 ISSN (Online): 2564-6869 www.smyrnamed.com Glandular Odontogenic Cyst Coexisting with a Dentigerous Cyst: Case Report Assist.Prof.Dr. Serap Keskin Tunç 1, Dt. Erkan Feslihan
Keratocystic Odontogenic Tumor : What radiologist needs to know?
 Keratocystic Odontogenic Tumor : What radiologist needs to know? Poster No.: C-0444 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit K. El Karzazi, J. M. Villanueva Rincón, R. Corrales,
Keratocystic Odontogenic Tumor : What radiologist needs to know? Poster No.: C-0444 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit K. El Karzazi, J. M. Villanueva Rincón, R. Corrales,
A CLINICOPATHOLOGIC STUDY OF ODONTOGENIC KERATOCYST (OKC) AND THE ROLE OF AgNORs IN CELL PROLIFERATION
 A CLINICOPATHOLOGIC STUDY OF ODONTOGENIC KERATOCYST (OKC) AND THE ROLE OF AgNORs IN CELL PROLIFERATION * Vindhya Savithri **Sudha S ***Shameena P.M ****Ipe Varghese Abstract : The histologic pattern of
A CLINICOPATHOLOGIC STUDY OF ODONTOGENIC KERATOCYST (OKC) AND THE ROLE OF AgNORs IN CELL PROLIFERATION * Vindhya Savithri **Sudha S ***Shameena P.M ****Ipe Varghese Abstract : The histologic pattern of
Keratocystic Odontogenic Tumor (KCOT) in Maxillary Sinus arising from an Infected Dentigerous Cyst
 Keratocystic Odontogenic Tumor (KCOT) in Maxillary Sinus arising from an Infected Dentigerous Cyst N R Chourasia, Abhishek Singh Payak, Preeti Bhadouria Department of Oral and Maxillofacial Surgery, Rishiraj
Keratocystic Odontogenic Tumor (KCOT) in Maxillary Sinus arising from an Infected Dentigerous Cyst N R Chourasia, Abhishek Singh Payak, Preeti Bhadouria Department of Oral and Maxillofacial Surgery, Rishiraj
Large Dentigerous Cyst
 Volume 16.2.1 Feb 2016 This Lecture Series qualifies for 0.5 Informal CPD Learning Hours Large Dentigerous Cyst By Dr Hassem Geha A 55 year-old male presented with a painless swelling in the right mandible.
Volume 16.2.1 Feb 2016 This Lecture Series qualifies for 0.5 Informal CPD Learning Hours Large Dentigerous Cyst By Dr Hassem Geha A 55 year-old male presented with a painless swelling in the right mandible.
Arun V Subramaniam et al. / International Journal of Biopharmaceutics. 2014; 5(3): International Journal of Biopharmaceutics
 225 e- ISSN 0976-1047 Print ISSN 2229-7499 International Journal of Biopharmaceutics Journal homepage: www.ijbonline.com IJB ODONTOGENIC KERATOCYSTS: VARIOUS RADIOGRAPHIC APPEARANCES Arun Subramaniam*
225 e- ISSN 0976-1047 Print ISSN 2229-7499 International Journal of Biopharmaceutics Journal homepage: www.ijbonline.com IJB ODONTOGENIC KERATOCYSTS: VARIOUS RADIOGRAPHIC APPEARANCES Arun Subramaniam*
Treatment Modalities of Odontogenic Keratocyst of Maxilla and Mandible: Our Experience
 wjd Parveen Akhter Lone et al Original Research 10.5005/jp-journals-10015-1344 Treatment Modalities of Odontogenic Keratocyst of Maxilla and Mandible: Our Experience 1 Parveen Akhter Lone, 2 Mohan Singh,
wjd Parveen Akhter Lone et al Original Research 10.5005/jp-journals-10015-1344 Treatment Modalities of Odontogenic Keratocyst of Maxilla and Mandible: Our Experience 1 Parveen Akhter Lone, 2 Mohan Singh,
Disclosure. Educational Objectives. Terminology. Odontogenic Cysts. Terminology
 Disclosure Lisa J. Koenig BChD, DDS, MS Professor & Program Director, Oral Medicine and Oral Radiology Marquette University School of Dentistry Consultant to Soredex for the Scanora 3D and 3Dx Author/Editor
Disclosure Lisa J. Koenig BChD, DDS, MS Professor & Program Director, Oral Medicine and Oral Radiology Marquette University School of Dentistry Consultant to Soredex for the Scanora 3D and 3Dx Author/Editor
Case Report Basal Cell Ameloblastoma of Mandible: A Rare Case Report with Review
 Case Reports in Dentistry Volume 2013, Article ID 187820, 4 pages http://dx.doi.org/10.1155/2013/187820 Case Report Basal Cell Ameloblastoma of Mandible: A Rare Case Report with Review Hemant Shakya, 1
Case Reports in Dentistry Volume 2013, Article ID 187820, 4 pages http://dx.doi.org/10.1155/2013/187820 Case Report Basal Cell Ameloblastoma of Mandible: A Rare Case Report with Review Hemant Shakya, 1
IN THE NAME OF GOD. Dr.kheirandish DDS,MSC Oral and maxillofacial pathology
 IN THE NAME OF GOD Dr.kheirandish DDS,MSC Oral and maxillofacial pathology ODONTOGENIC CYSTS AND TUMORS Chapter 15 I. DENTIGEROUS CYST II. III. IV. ERUPTION CYST ODONTOGENIC KERATOCYST Orthokeratinized
IN THE NAME OF GOD Dr.kheirandish DDS,MSC Oral and maxillofacial pathology ODONTOGENIC CYSTS AND TUMORS Chapter 15 I. DENTIGEROUS CYST II. III. IV. ERUPTION CYST ODONTOGENIC KERATOCYST Orthokeratinized
A Case Report on Surgical Management of Odontogenic Keratocyst
 World Journal of Medical Sciences 10 (2): 212-216, 2014 ISSN 1817-3055 IDOSI Publications, 2014 DOI: 10.5829/idosi.wjms.2014.10.2.82185 A Case Report on Surgical Management of Odontogenic Keratocyst 1
World Journal of Medical Sciences 10 (2): 212-216, 2014 ISSN 1817-3055 IDOSI Publications, 2014 DOI: 10.5829/idosi.wjms.2014.10.2.82185 A Case Report on Surgical Management of Odontogenic Keratocyst 1
Differential Diagnosis of Radiolucent Lesions of the Jaws
 Differential Diagnosis of Radiolucent Lesions of the Jaws Multilocular Multilocular Radiolucencies Odontogenic Keratocyst Botryoid Odontogenic Cyst Glandular odontogenic Cyst Invasive Ameloblastoma Central
Differential Diagnosis of Radiolucent Lesions of the Jaws Multilocular Multilocular Radiolucencies Odontogenic Keratocyst Botryoid Odontogenic Cyst Glandular odontogenic Cyst Invasive Ameloblastoma Central
Cone Beam Computed Tomography Findings in Calcifying Cystic Odontogenic Tumor Associated with Odontome: A Case Report
 Phulambrikar T., et al. Dent Shiraz Univ Med Sci., December 2015; 16(4): 374-379. Case Report Cone Beam Computed Tomography Findings in Calcifying Cystic Odontogenic Tumor Associated with Odontome: A Case
Phulambrikar T., et al. Dent Shiraz Univ Med Sci., December 2015; 16(4): 374-379. Case Report Cone Beam Computed Tomography Findings in Calcifying Cystic Odontogenic Tumor Associated with Odontome: A Case
Case Report An Unusual Case of Tooth in the Floor of the Orbit: The Libyan Experience
 Case Reports in Dentistry Volume 2012, Article ID 954789, 5 pages doi:10.1155/2012/954789 Case Report An Unusual Case of Tooth in the Floor of the Orbit: The Libyan Experience Y. Naresh Shetty, Irfan Adil
Case Reports in Dentistry Volume 2012, Article ID 954789, 5 pages doi:10.1155/2012/954789 Case Report An Unusual Case of Tooth in the Floor of the Orbit: The Libyan Experience Y. Naresh Shetty, Irfan Adil
高雄醫學大學 口腔醫學院 口腔病理影像科 牙科 X 光影像判讀 教學範例
 高雄醫學大學 口腔醫學院 口腔病理影像科 牙科 X 光影像判讀 教學範例 Content Image No. 001 Dentigerous cyst over left upper embedded canine--------------------- 頁 1 Image No. 002---------------------------------------------------------------
高雄醫學大學 口腔醫學院 口腔病理影像科 牙科 X 光影像判讀 教學範例 Content Image No. 001 Dentigerous cyst over left upper embedded canine--------------------- 頁 1 Image No. 002---------------------------------------------------------------
Problem diagnoses. Current issues in Anatomic pathology. Problem Diagnoses in Tumors of the Oral Cavity 5/29/2009
 Current issues in Anatomic pathology Problem Diagnoses in Tumors of the Oral Cavity Richard Jordan DDS PhD FRCPath Professor of Oral Pathology & Pathology Director, UCSF Oral Pathology Diagnostic Laboratory
Current issues in Anatomic pathology Problem Diagnoses in Tumors of the Oral Cavity Richard Jordan DDS PhD FRCPath Professor of Oral Pathology & Pathology Director, UCSF Oral Pathology Diagnostic Laboratory
The clinical appearance and diagnosis of odontogenic cysts. SE Arc-Állcsont-Szájsebészeti és Fogászati Klinika BUDAPEST
 The clinical appearance and diagnosis of odontogenic cysts SE Arc-Állcsont-Szájsebészeti és Fogászati Klinika BUDAPEST DEFINITION A cyst is a sac with walls of connective tissue, lined by epithelium, containing
The clinical appearance and diagnosis of odontogenic cysts SE Arc-Állcsont-Szájsebészeti és Fogászati Klinika BUDAPEST DEFINITION A cyst is a sac with walls of connective tissue, lined by epithelium, containing
MALIGNANT TUMOURS OF THE JAWS
 MALIGNANT TUMOURS OF THE JAWS MALIGNANT TUMOURS OF THE JAWS Squamous cell carcinoma Osteogenic sarcoma Chondrosarcoma Fibrosarcoma Malignant lymphomas (incl. Burkitt s) Multiple myeloma Ameloblastoma Secondary
MALIGNANT TUMOURS OF THE JAWS MALIGNANT TUMOURS OF THE JAWS Squamous cell carcinoma Osteogenic sarcoma Chondrosarcoma Fibrosarcoma Malignant lymphomas (incl. Burkitt s) Multiple myeloma Ameloblastoma Secondary
Ameloblastomatous Gorlin s cyst
 319 Journal of Oral Science, Vol. 49, No. 4, 319-323, 2007 Case Report Ameloblastomatous Gorlin s cyst Mala Kamboj 1) and Manish Juneja 2) 1) Department of Oral Pathology and Microbiology, U.P. King George
319 Journal of Oral Science, Vol. 49, No. 4, 319-323, 2007 Case Report Ameloblastomatous Gorlin s cyst Mala Kamboj 1) and Manish Juneja 2) 1) Department of Oral Pathology and Microbiology, U.P. King George
Key words: Third molar, Impacted tooth, Tooth Eruption, Molar, Mandible, Unerupted Tooth.
 JOURNAL OF CASE REPORTS 2014;4(2):286-290 OPG and CBCT Finding s of an Ectopic Third Molar in the Sub-condylar Region Tatu Joy E 1, Farakath Khan 1, Shameel Mohammed 2 From the Department of Oral Medicine
JOURNAL OF CASE REPORTS 2014;4(2):286-290 OPG and CBCT Finding s of an Ectopic Third Molar in the Sub-condylar Region Tatu Joy E 1, Farakath Khan 1, Shameel Mohammed 2 From the Department of Oral Medicine
A Case Report of Odontogenic Keratocyst in Anterior Mandibule Position
 A Case Report of Odontogenic Keratocyst in Anterior Mandibule Position Malihe Moeini 1, Seyed Ehsan Anvar 2, Rasool Barzegari Bafghi 3* 1.Resident of Oral and Maxillofacial Radiology, Faculty of Dentistry,
A Case Report of Odontogenic Keratocyst in Anterior Mandibule Position Malihe Moeini 1, Seyed Ehsan Anvar 2, Rasool Barzegari Bafghi 3* 1.Resident of Oral and Maxillofacial Radiology, Faculty of Dentistry,
An unusual site of Adenomatoid Odontogenic Tumor: A rare case report
 J. Int Oral Health 2010 Case Report All right reserved An unusual site of Adenomatoid Odontogenic Tumor: A rare case report Sapna Panjwani*, Anjana Bagewadi**, Vaishali Keluskar*** *Post Graduate Student
J. Int Oral Health 2010 Case Report All right reserved An unusual site of Adenomatoid Odontogenic Tumor: A rare case report Sapna Panjwani*, Anjana Bagewadi**, Vaishali Keluskar*** *Post Graduate Student
CENTRAL GIANT CELL GRANULOMA PRESENTING AS UNILOCULAR RADIOLUCENCY IN POSTERIOR MANDIBLE A CASE REPORT
 IJCRR Section: Healthcare Sci. Journal Impact Factor 4.016 Case Report CENTRAL GIANT CELL GRANULOMA PRESENTING AS UNILOCULAR RADIOLUCENCY IN POSTERIOR MANDIBLE A CASE REPORT S. Aruleena Shaminey 1, G.
IJCRR Section: Healthcare Sci. Journal Impact Factor 4.016 Case Report CENTRAL GIANT CELL GRANULOMA PRESENTING AS UNILOCULAR RADIOLUCENCY IN POSTERIOR MANDIBLE A CASE REPORT S. Aruleena Shaminey 1, G.
AMELOBLASTIC FIBROMA: A RARE CASE REPORT
 Case Report International Journal of Dental and Health Sciences Volume 04, Issue 03 AMELOBLASTIC FIBROMA: A RARE CASE REPORT Namratha Patil 1 1.Sr lecturer, dept of oral medicine and radiology, KAHES VK
Case Report International Journal of Dental and Health Sciences Volume 04, Issue 03 AMELOBLASTIC FIBROMA: A RARE CASE REPORT Namratha Patil 1 1.Sr lecturer, dept of oral medicine and radiology, KAHES VK
MULTILOCULAR AMELOBLASTOMA OF MANDIBLE-A CASE REPORT
 International Journal of Advancements in Research & Technology, Volume 2, Issue2, February-2013 1 MULTILOCULAR AMELOBLASTOMA OF MANDIBLE-A CASE REPORT DR SANTOSH KUMAR SUBUDHI*, DR SUMIT DASH**, DR.K..PREMANANDA***,
International Journal of Advancements in Research & Technology, Volume 2, Issue2, February-2013 1 MULTILOCULAR AMELOBLASTOMA OF MANDIBLE-A CASE REPORT DR SANTOSH KUMAR SUBUDHI*, DR SUMIT DASH**, DR.K..PREMANANDA***,
TRAUMATIC BONE CYST OF IDIOPATHIC ORIGIN? A REPORT OF TWO CASES
 Traumatic Bone Cyst Kumar S. et al 183 CASE REPORT TRAUMATIC BONE CYST OF IDIOPATHIC ORIGIN? A REPORT OF TWO CASES Kumar Satish 1, S. Padmashree 1, Jayalekshmy Rema 1 ABSTRACT BACKGROUND: Traumatic bone
Traumatic Bone Cyst Kumar S. et al 183 CASE REPORT TRAUMATIC BONE CYST OF IDIOPATHIC ORIGIN? A REPORT OF TWO CASES Kumar Satish 1, S. Padmashree 1, Jayalekshmy Rema 1 ABSTRACT BACKGROUND: Traumatic bone
INFLAMMATORY DENTIGEROUS CYST OR INFLAMMATORY CYSTIC LESIONS OF MIXED DENTITION?: A REPORT OF THREE CASES
 Case Report International Journal of Dental and Health Sciences Volume 03, Issue 03 INFLAMMATORY DENTIGEROUS CYST OR INFLAMMATORY CYSTIC LESIONS OF MIXED DENTITION?: A REPORT OF THREE CASES Pritam K Mankapure
Case Report International Journal of Dental and Health Sciences Volume 03, Issue 03 INFLAMMATORY DENTIGEROUS CYST OR INFLAMMATORY CYSTIC LESIONS OF MIXED DENTITION?: A REPORT OF THREE CASES Pritam K Mankapure
Case Report Unicystic Ameloblastoma with Mural Proliferation Managed by Conservative Treatment
 Case Reports in Pathology Volume 2016, Article ID 3089540, 4 pages http://dx.doi.org/10.1155/2016/3089540 Case Report Unicystic Ameloblastoma with Mural Proliferation Managed by Conservative Treatment
Case Reports in Pathology Volume 2016, Article ID 3089540, 4 pages http://dx.doi.org/10.1155/2016/3089540 Case Report Unicystic Ameloblastoma with Mural Proliferation Managed by Conservative Treatment
Maxilla and mandible benign lesions: Radiologic Findings and Differential Diagnosis in CT
 Maxilla and mandible benign lesions: Radiologic Findings and Differential Diagnosis in CT Poster No.: C-0964 Congress: ECR 2012 Type: Scientific Exhibit Authors: N. Lopez 1, E. Marcos Naranjo 2, M. D.
Maxilla and mandible benign lesions: Radiologic Findings and Differential Diagnosis in CT Poster No.: C-0964 Congress: ECR 2012 Type: Scientific Exhibit Authors: N. Lopez 1, E. Marcos Naranjo 2, M. D.
Dentigerous cyst associated with an impacted mesiodens: report of 2 cases
 Imaging Science in Dentistry 2012; 42 : 255-60 http://dx.doi.org/10.5624/isd.2012.42.4.255 Dentigerous cyst associated with an impacted mesiodens: report of 2 cases Neha Khambete, Rahul Kumar*, Mukund
Imaging Science in Dentistry 2012; 42 : 255-60 http://dx.doi.org/10.5624/isd.2012.42.4.255 Dentigerous cyst associated with an impacted mesiodens: report of 2 cases Neha Khambete, Rahul Kumar*, Mukund
Epithelial Sources. Rests of Serres Rests of Malassez Reduced Enamel Epithelium Surface Mucosa
 ODONTOGENIC CYSTS Epithelial Sources Rests of Serres Rests of Malassez Reduced Enamel Epithelium Surface Mucosa Epithelial Sources Surface Epithelium Rests of Serres Reduced Enamel Epithelium Rests of
ODONTOGENIC CYSTS Epithelial Sources Rests of Serres Rests of Malassez Reduced Enamel Epithelium Surface Mucosa Epithelial Sources Surface Epithelium Rests of Serres Reduced Enamel Epithelium Rests of
[ 06-10] Dr. B. Siva Reddy, Dr. B. Ajay Reginald, Dr. D. Sireesha, Dr. Meda Samatha India Abstract: Keywords ARTICLE 20/07/ /09/2018
![[ 06-10] Dr. B. Siva Reddy, Dr. B. Ajay Reginald, Dr. D. Sireesha, Dr. Meda Samatha India Abstract: Keywords ARTICLE 20/07/ /09/2018 [ 06-10] Dr. B. Siva Reddy, Dr. B. Ajay Reginald, Dr. D. Sireesha, Dr. Meda Samatha India Abstract: Keywords ARTICLE 20/07/ /09/2018](/thumbs/87/95905171.jpg) Dentigerous Cyst Associated with an Impacted Mesiodens: A Rare Case Report with Review of Literature [PP: 06-10] Dr. B. Siva Reddy, Dr. B. Ajay Reginald, Dr. D. Sireesha, Dr. Meda Samatha, Department of
Dentigerous Cyst Associated with an Impacted Mesiodens: A Rare Case Report with Review of Literature [PP: 06-10] Dr. B. Siva Reddy, Dr. B. Ajay Reginald, Dr. D. Sireesha, Dr. Meda Samatha, Department of
Glandular odontogenic cyst associated with ameloblastoma: Case report and review of the literature
 Journal section: Oral Medicine and Pathology Publication Types: Case Report doi:10.4317/jced.53775 http://dx.doi.org/10.4317/jced.53775 : Case report and review of the literature Timothée Cousin 1, Samuel
Journal section: Oral Medicine and Pathology Publication Types: Case Report doi:10.4317/jced.53775 http://dx.doi.org/10.4317/jced.53775 : Case report and review of the literature Timothée Cousin 1, Samuel
EXTENSIVE PERIAPICAL CYST IN THE MAXILLARY SINUS A CASE REPORT
 May, 2012 INTERNATIONAL DENTAL JOURNAL OF STUDENT S RESEARCH: CASE REPORT Article Code: IDJSR 0002 EXTENSIVE PERIAPICAL CYST IN THE MAXILLARY SINUS A CASE REPORT Authors Bouguezzi Adel, DDS, Resident 1
May, 2012 INTERNATIONAL DENTAL JOURNAL OF STUDENT S RESEARCH: CASE REPORT Article Code: IDJSR 0002 EXTENSIVE PERIAPICAL CYST IN THE MAXILLARY SINUS A CASE REPORT Authors Bouguezzi Adel, DDS, Resident 1
PACIFIC JOURNAL OF MEDICAL SCIENCES ISSN:
 PACIFIC JOURNAL OF MEDICAL SCIENCES {Formerly: Medical Sciences Bulletin} ISSN: 2072 1625 Pac. J. Med. Sci. (PJMS) www.pacjmedsci.com. Email: pacjmedsci@gmail.com. ADENOMATOID ODONTOGENIC TUMOR WITH RARE
PACIFIC JOURNAL OF MEDICAL SCIENCES {Formerly: Medical Sciences Bulletin} ISSN: 2072 1625 Pac. J. Med. Sci. (PJMS) www.pacjmedsci.com. Email: pacjmedsci@gmail.com. ADENOMATOID ODONTOGENIC TUMOR WITH RARE
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 3/ Issue 18/May 05, 2014 Page 4859
 CYSTIC DEGENERATION IN FOLLICULAR AMELOBLASTOMA: A CASE REPORT Neeraj Kumar 1, Niharika Rathore 2, Hemant Shakya 3, Anshuman Jamdade 4, Puneet Chitlangia 5 HOW TO CITE THIS ARTICLE: Neeraj Kumar, Niharika
CYSTIC DEGENERATION IN FOLLICULAR AMELOBLASTOMA: A CASE REPORT Neeraj Kumar 1, Niharika Rathore 2, Hemant Shakya 3, Anshuman Jamdade 4, Puneet Chitlangia 5 HOW TO CITE THIS ARTICLE: Neeraj Kumar, Niharika
Inter-radicular Radiolucencies
 Inter-radicular Radiolucencies Differential Diagnosis Laterally Displaced Radicular Cyst Accessory canals Root fracture Lateral Periodontal Cyst Botryoid variant Odontogenic Keratocyst Incisive Canal Cyst
Inter-radicular Radiolucencies Differential Diagnosis Laterally Displaced Radicular Cyst Accessory canals Root fracture Lateral Periodontal Cyst Botryoid variant Odontogenic Keratocyst Incisive Canal Cyst
Case Report Keratocystic Odontogenic Tumor with an Ectopic Tooth in Maxilla
 Case Reports in Dentistry Volume 2013, Article ID 232096, 4 pages http://dx.doi.org/10.1155/2013/232096 Case Report Keratocystic Odontogenic Tumor with an Ectopic Tooth in Maxilla Basavaraj T. Bhagawati,
Case Reports in Dentistry Volume 2013, Article ID 232096, 4 pages http://dx.doi.org/10.1155/2013/232096 Case Report Keratocystic Odontogenic Tumor with an Ectopic Tooth in Maxilla Basavaraj T. Bhagawati,
SQUAMOUS ODONTOGENIC TUMOUR: REPORT OF FIVE CASES FROM NIGERIA AND REVIEW OF LITERATURE
 African Journal of Oral Health Volume 3 Numbers 1&2, 2006:1-5 REFEREED ARTICLE SQUAMOUS ODONTOGENIC TUMOUR: REPORT OF FIVE CASES FROM NIGERIA AND REVIEW OF LITERATURE Adebiyi K.E., Odukoya O., Taiwo, E.O.
African Journal of Oral Health Volume 3 Numbers 1&2, 2006:1-5 REFEREED ARTICLE SQUAMOUS ODONTOGENIC TUMOUR: REPORT OF FIVE CASES FROM NIGERIA AND REVIEW OF LITERATURE Adebiyi K.E., Odukoya O., Taiwo, E.O.
Ameloblastic Carcinoma of the Mandible: a Rare Case Report
 IBIMA Publishing Journal of Research and Practice in Dentistry http://www.ibimapublishing.com/journals/dent/dent.html Vol. 2015 (2015), Article ID 672596, 6 pages DOI: 10.5171/2015.672596 Case Report Ameloblastic
IBIMA Publishing Journal of Research and Practice in Dentistry http://www.ibimapublishing.com/journals/dent/dent.html Vol. 2015 (2015), Article ID 672596, 6 pages DOI: 10.5171/2015.672596 Case Report Ameloblastic
Unicystic Ameloblastoma of mandible. Aggresive treatment A myth or a need. Case report and Extensive review of literature
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 12, Issue 2 (Nov.- Dec. 2013), PP 26-31 Unicystic Ameloblastoma of mandible. Aggresive treatment A myth
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 12, Issue 2 (Nov.- Dec. 2013), PP 26-31 Unicystic Ameloblastoma of mandible. Aggresive treatment A myth
Ortho keratinized Odontogenic Cyst of Mandible: A Rare Case Report
 Journal of Dental School 2015; 33(3): 233-237 Case Report Ortho keratinized Odontogenic Cyst of Mandible: A Rare Case Report 1 Soudabeh Sargolzaei 1 Fatemeh Mashhadi Abbas *2 Leila Hesami Moghadam 3 Sanaa
Journal of Dental School 2015; 33(3): 233-237 Case Report Ortho keratinized Odontogenic Cyst of Mandible: A Rare Case Report 1 Soudabeh Sargolzaei 1 Fatemeh Mashhadi Abbas *2 Leila Hesami Moghadam 3 Sanaa
Incidental finding of dentigerous cyst - a case report
 Case Report Incidental finding of dentigerous cyst - a case report Pulivarthi Sushma 1, Sowbhagya M.B 2, Balaji P 3, Mahesh Kumar T.S 4 1 Postgraduate, 2 Reader, 3 Professor and Head of department, 4 Senior
Case Report Incidental finding of dentigerous cyst - a case report Pulivarthi Sushma 1, Sowbhagya M.B 2, Balaji P 3, Mahesh Kumar T.S 4 1 Postgraduate, 2 Reader, 3 Professor and Head of department, 4 Senior
Pre-reading - radiolucencies
 Pre-reading - radiolucencies Multiple radiolucencies o Suggests a systemic cause o Most likely: cherubism or KCOT s of nevoid basal cell carcinoma syndrome o Sometimes: florid osseous dysplasia (if limited
Pre-reading - radiolucencies Multiple radiolucencies o Suggests a systemic cause o Most likely: cherubism or KCOT s of nevoid basal cell carcinoma syndrome o Sometimes: florid osseous dysplasia (if limited
Clinical details: Details of scan: CONE BEAM CT REPORT: Name: H. B. Gender: Reason for referral: Referred by:
 Name: H. B. Gender: Male DOB: 11/12/1950 Age: 64 Date taken: 16/11/2015 Date reported: 19/11/2015 Clinical details: Reason for referral: Referred by: Investigate symptoms related to left TMJ. Reconstructed
Name: H. B. Gender: Male DOB: 11/12/1950 Age: 64 Date taken: 16/11/2015 Date reported: 19/11/2015 Clinical details: Reason for referral: Referred by: Investigate symptoms related to left TMJ. Reconstructed
Autologous Bone Augmentation in Combination with an Ameloblastoma in the Maxillary Region- A Case Report?
 Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550023 Volume 2, Issue 2 Case Report Autologous Bone Augmentation in Combination with an Ameloblastoma in the Maxillary Region- A Case
Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550023 Volume 2, Issue 2 Case Report Autologous Bone Augmentation in Combination with an Ameloblastoma in the Maxillary Region- A Case
Odontogenic Keratocyst Masquerading as a Dentigerous Cyst in the Maxilla: A Case Report of an Unusual Presentation
 European Journal of Therapeutics DOI: 10.5152/EurJTher.2018.496 Case Report Odontogenic Keratocyst Masquerading as a Dentigerous Cyst in the Maxilla: A Case Report of an Unusual Presentation Arvind Karikal
European Journal of Therapeutics DOI: 10.5152/EurJTher.2018.496 Case Report Odontogenic Keratocyst Masquerading as a Dentigerous Cyst in the Maxilla: A Case Report of an Unusual Presentation Arvind Karikal
A case of orthokeratinized odontoge Title suspected to be a radicular cyst
 A case of orthokeratinized odontoge Title suspected to be a radicular cyst Onuki, M; Saito, A; Hosokawa, S; Oh Author(s) Hayakawa, H; Seta, S; Muramatsu, T; Journal Bulletin of Tokyo Dental College, 5
A case of orthokeratinized odontoge Title suspected to be a radicular cyst Onuki, M; Saito, A; Hosokawa, S; Oh Author(s) Hayakawa, H; Seta, S; Muramatsu, T; Journal Bulletin of Tokyo Dental College, 5
Odontomes and Odontogenic tumours
 Odontomes and Odontogenic tumours Odontomes Developmental hamartoma Hamartoma: normal tissue in abnormal location Any cells to be neoplastic it must be able to replicate, which is not seen in hamartoma
Odontomes and Odontogenic tumours Odontomes Developmental hamartoma Hamartoma: normal tissue in abnormal location Any cells to be neoplastic it must be able to replicate, which is not seen in hamartoma
Management of Plexiform Ameloblastoma in a 12 year old female: A Case Report
 Article ID: ISSN 2046-1690 Management of Plexiform Ameloblastoma in a 12 year old female: A Case Report Corresponding Author: Dr. Sheeraz Badal, Senior Lecturer, Dept of Oral & Maxillofacial Surgery, MIDSR,
Article ID: ISSN 2046-1690 Management of Plexiform Ameloblastoma in a 12 year old female: A Case Report Corresponding Author: Dr. Sheeraz Badal, Senior Lecturer, Dept of Oral & Maxillofacial Surgery, MIDSR,
INFECTED DENTIGEROUS CYST IN IMPACTED CANINE- A case report
 Case Report INFECTED DENTIGEROUS CYST IN IMPACTED CANINE- A case report Gazala Fatima Parveen, M.D. Akheel 1 Department of oral & maxillofacial surgery, MCDRC Lucknow, U.P.,India 1-Department of Oral &
Case Report INFECTED DENTIGEROUS CYST IN IMPACTED CANINE- A case report Gazala Fatima Parveen, M.D. Akheel 1 Department of oral & maxillofacial surgery, MCDRC Lucknow, U.P.,India 1-Department of Oral &
Squamous cell carcinoma of the maxillary sinus mimicking periodontitis
 Squamous cell carcinoma of the maxillary sinus mimicking periodontitis 저자저널명발행기관 NDSL URL Na, Ji Yeon ; Kang, Joo Hyun ; Choi, Seong-Ho ; Jeong, Ho-Gul ; Han, Sang-Sun 大韓齒科醫師協會誌 = The journal of the Korean
Squamous cell carcinoma of the maxillary sinus mimicking periodontitis 저자저널명발행기관 NDSL URL Na, Ji Yeon ; Kang, Joo Hyun ; Choi, Seong-Ho ; Jeong, Ho-Gul ; Han, Sang-Sun 大韓齒科醫師協會誌 = The journal of the Korean
IMAGING OF CYSTS OF THE JAWS July 2002 N. Serman
 IMAGING OF CYSTS OF THE JAWS July 2002 N. Serman This is an area where radiology plays an important role in assisting with the diagnosis, determining the size of the lesion and the relationship to adjacent
IMAGING OF CYSTS OF THE JAWS July 2002 N. Serman This is an area where radiology plays an important role in assisting with the diagnosis, determining the size of the lesion and the relationship to adjacent
JOURNAL TAOMFR Mandiblular Ameloblastic fibro-odontoma
 Ameloblastic Fibro-Odontoma of the Mandible with Emphasis on Evaluation Using Cone Beam Computed Tomography Jing-Yi Chen 1, Frank Lei 2, Yu-Fong Chen 3,4 * Divisions of 1 Oral Pathology, 2 Periodotology,
Ameloblastic Fibro-Odontoma of the Mandible with Emphasis on Evaluation Using Cone Beam Computed Tomography Jing-Yi Chen 1, Frank Lei 2, Yu-Fong Chen 3,4 * Divisions of 1 Oral Pathology, 2 Periodotology,
A Radiographic technique for differentiating enamel and dentin in odontogenic tumors
 ISPUB.COM The Internet Journal of Radiology Volume 12 Number 1 A Radiographic technique for differentiating enamel and dentin in odontogenic tumors D Shetty, A Urs, R Kaur Citation D Shetty, A Urs, R Kaur.
ISPUB.COM The Internet Journal of Radiology Volume 12 Number 1 A Radiographic technique for differentiating enamel and dentin in odontogenic tumors D Shetty, A Urs, R Kaur Citation D Shetty, A Urs, R Kaur.
Journal of Craniomaxillofacial Research. Odontogenic keratocyst of mandibular condylar region: A case report. Abbas Karimi 1,2, Reza Amirzargar 2*
 Journal of Craniomaxillofacial Research Vol. 5, No. 2 Spring 2018 Odontogenic keratocyst of mandibular condylar region: A case report Abbas Karimi 1,2, Reza Amirzargar 2* 1. Craniomaxillofacial Research
Journal of Craniomaxillofacial Research Vol. 5, No. 2 Spring 2018 Odontogenic keratocyst of mandibular condylar region: A case report Abbas Karimi 1,2, Reza Amirzargar 2* 1. Craniomaxillofacial Research
Peripheral Odontogenic Fibroma: A rare case report
 Annals of Dental Research (2013) Vol 3 (1): 10-14 HATAM Publishers: All Rights Reserved Annals of Dental Research www.hgpub.com www.adres.yolasite.com Case Report Peripheral Odontogenic Fibroma: A rare
Annals of Dental Research (2013) Vol 3 (1): 10-14 HATAM Publishers: All Rights Reserved Annals of Dental Research www.hgpub.com www.adres.yolasite.com Case Report Peripheral Odontogenic Fibroma: A rare
Case Report Intraosseous Follicular Adenomatoid Odontogenic Tumour A Case Report
 International Dentistry Volume 2009, Article ID 597483, 4 pages doi:10.1155/2009/597483 Case eport Intraosseous Follicular Adenomatoid Odontogenic Tumour A Case eport Farhan Durrani 1 and oyana Singh 2
International Dentistry Volume 2009, Article ID 597483, 4 pages doi:10.1155/2009/597483 Case eport Intraosseous Follicular Adenomatoid Odontogenic Tumour A Case eport Farhan Durrani 1 and oyana Singh 2
Case Report Cholesterol Granuloma in Odontogenic Cyst: An Enigmatic Lesion
 Volume 2016, Article ID 6105142, 5 pages http://dx.doi.org/10.1155/2016/6105142 Case Report Cholesterol Granuloma in Odontogenic Cyst: An Enigmatic Lesion Mala Kamboj, Anju Devi, and Shruti Gupta Department
Volume 2016, Article ID 6105142, 5 pages http://dx.doi.org/10.1155/2016/6105142 Case Report Cholesterol Granuloma in Odontogenic Cyst: An Enigmatic Lesion Mala Kamboj, Anju Devi, and Shruti Gupta Department
Conservative management of a dentigerous cyst associated with eruption of teeth in a 7-year-old girl: a case report
 SE REPORT https://doi.org/10.5125/jkaoms.2017.43.s1.s1 pissn 2234-7550 eissn 2234-5930 onservative management of a dentigerous cyst associated with eruption of teeth in a 7-year-old girl: a case report
SE REPORT https://doi.org/10.5125/jkaoms.2017.43.s1.s1 pissn 2234-7550 eissn 2234-5930 onservative management of a dentigerous cyst associated with eruption of teeth in a 7-year-old girl: a case report
Odontogenic Cysts - An Overview
 Namita V Nayyer Michaelina Macluskey and William Keys Odontogenic Cysts - An Overview Abstract: This article aims to discuss the clinical features, radiological assessment, histopathology and management
Namita V Nayyer Michaelina Macluskey and William Keys Odontogenic Cysts - An Overview Abstract: This article aims to discuss the clinical features, radiological assessment, histopathology and management
Case report: Central Giant Cell Granuloma of Mandible A Case Report
 Case report: Central Giant Cell Granuloma of Mandible A Case Report 1Dr Praveen Kumar, 2 Dr Balreddy P., 3 Dr Sridhar Reddy B., 4 Dr Sanjeev Naik, 5Dr. Sujitha Reddy Patil 1Post Graduate, Department of
Case report: Central Giant Cell Granuloma of Mandible A Case Report 1Dr Praveen Kumar, 2 Dr Balreddy P., 3 Dr Sridhar Reddy B., 4 Dr Sanjeev Naik, 5Dr. Sujitha Reddy Patil 1Post Graduate, Department of
Mucous and ciliated cell metaplasia in epithelial linings of odontogenic inflammatory and developmental cysts
 77 Journal of Oral Science, Vol. 47, No. 2, 77-81, 2005 Original Mucous and ciliated cell metaplasia in epithelial linings of odontogenic inflammatory and developmental cysts Yasunori Takeda, Yuko Oikawa,
77 Journal of Oral Science, Vol. 47, No. 2, 77-81, 2005 Original Mucous and ciliated cell metaplasia in epithelial linings of odontogenic inflammatory and developmental cysts Yasunori Takeda, Yuko Oikawa,
Surgical ciliated cyst of the maxilla: pathology of the maxillary sinus
 Archives of Orofacial Sciences The Journal of the School of Dental Sciences, USM Case Report Arch Orofac Sci (2017), 12(2): 105-109. Surgical ciliated cyst of the maxilla: pathology of the maxillary sinus
Archives of Orofacial Sciences The Journal of the School of Dental Sciences, USM Case Report Arch Orofac Sci (2017), 12(2): 105-109. Surgical ciliated cyst of the maxilla: pathology of the maxillary sinus
Common/Important Radiolucencies. B. Most Common Location Apex of permanent first molar, rare in primary teeth.
 Cincinnati Dental Association Breakfast at Tiffany s: The Jewels and Gems of Oral Pathology November 17, 2010 John A. Svirsky, DDS, MEd Virginia Commonwealth University 804-828-0547 FAX: 804-828-6234 EMAIL:
Cincinnati Dental Association Breakfast at Tiffany s: The Jewels and Gems of Oral Pathology November 17, 2010 John A. Svirsky, DDS, MEd Virginia Commonwealth University 804-828-0547 FAX: 804-828-6234 EMAIL:
Multiple Synchronous Central Giant Cell Granulomas of the Maxillofacial Region: A Case Report 1
 Multiple Synchronous Central Giant Cell Granulomas of the Maxillofacial Region: A Case Report 1 Min Seok Kang, M.D., Hak Jin Kim, M.D. Multifocal central giant cell granulomas (CGCG) in the maxillofacial
Multiple Synchronous Central Giant Cell Granulomas of the Maxillofacial Region: A Case Report 1 Min Seok Kang, M.D., Hak Jin Kim, M.D. Multifocal central giant cell granulomas (CGCG) in the maxillofacial
Case Report An Extrafollicular Adenomatoid Odontogenic Tumor Mimicking a Periapical Cyst
 Hindawi Case Reports in Radiology Volume 2018, Article ID 6987050, 5 pages https://doi.org/10.1155/2018/6987050 Case Report An Extrafollicular Adenomatoid Odontogenic Tumor Mimicking a Periapical Cyst
Hindawi Case Reports in Radiology Volume 2018, Article ID 6987050, 5 pages https://doi.org/10.1155/2018/6987050 Case Report An Extrafollicular Adenomatoid Odontogenic Tumor Mimicking a Periapical Cyst
Ossifying fibromas of the jaw bone: 20 cases
 (2010) 39, 57 63 2010 The British Institute of Radiology http://dmfr.birjournals.org CASE REPORT Ossifying fibromas of the jaw bone: 20 cases Y Liu 1, M You 1, H Wang*,1, Z Yang 1, J Miao 1, K Shimizutani
(2010) 39, 57 63 2010 The British Institute of Radiology http://dmfr.birjournals.org CASE REPORT Ossifying fibromas of the jaw bone: 20 cases Y Liu 1, M You 1, H Wang*,1, Z Yang 1, J Miao 1, K Shimizutani
A COMPARATIVE HISTOPATHOLOGICAL STUDY OF EPITHELIAL linings OF ODONTOGENIC CYSTS AND UNICYSTIC AMElOBlASTOMAS
 A COMPARATIVE HISTOPATHOLOGICAL STUDY OF EPITHELIAL linings OF ODONTOGENIC CYSTS AND UNICYSTIC AMElOBlASTOMAS J Sudiono, RB Zain. A Comparative Histopathological Study of Epithelial Linings of Odontogenic
A COMPARATIVE HISTOPATHOLOGICAL STUDY OF EPITHELIAL linings OF ODONTOGENIC CYSTS AND UNICYSTIC AMElOBlASTOMAS J Sudiono, RB Zain. A Comparative Histopathological Study of Epithelial Linings of Odontogenic
Management of a Dentigerous Cyst Associated with Inverted and Fused Mesiodens: A Rare Case Report
 Management of a Dentigerous Cyst Associated with Inverted and Fused Mesiodens: A Rare Case Report Kiran Patel 1, Nishtha Patel 2, Karthik Venkataraghavan 3 1 Sr. Lecturer, Department of Oral & Maxillofacial
Management of a Dentigerous Cyst Associated with Inverted and Fused Mesiodens: A Rare Case Report Kiran Patel 1, Nishtha Patel 2, Karthik Venkataraghavan 3 1 Sr. Lecturer, Department of Oral & Maxillofacial
Clinical, radiological and therapeutic features of keratocystic odontogenic tumours: a study over a decade
 Journal section: Oral Medicine and Pathology Publication Types: Research doi:10.4317/jced.51408 http://dx.doi.org/10.4317/jced.51408 Clinical, radiological and therapeutic features of keratocystic odontogenic
Journal section: Oral Medicine and Pathology Publication Types: Research doi:10.4317/jced.51408 http://dx.doi.org/10.4317/jced.51408 Clinical, radiological and therapeutic features of keratocystic odontogenic
Calcifying Odontogenic Cyst with Complex Odontoma: Histological and Immunohistochemical Features
 Case Report Calcifying Odontogenic Cyst with Complex Odontoma: Histological and Immunohistochemical Features Nooshin Mohtasham 1, Amin Rahpeyma 2, Saeedeh Khajeh Ahmadi 3, Mohsen Merati 4 1 Oral and Maxillofacial
Case Report Calcifying Odontogenic Cyst with Complex Odontoma: Histological and Immunohistochemical Features Nooshin Mohtasham 1, Amin Rahpeyma 2, Saeedeh Khajeh Ahmadi 3, Mohsen Merati 4 1 Oral and Maxillofacial
ISSN: Volume 4 Issue CHOLESTEROL GRANULOMA: AN UNCOMMON CLINICAL ENTITY OF THE MAXILLARY SINUS
 ISSN: 2250-0359 Volume 4 Issue 4 2014 CHOLESTEROL GRANULOMA: AN UNCOMMON CLINICAL ENTITY OF THE MAXILLARY SINUS Sunita Singh Sonia Chhabra Pansi Gupta Priya Malik Pt B.D. Sharma PGIMS, Rohtak, Haryana
ISSN: 2250-0359 Volume 4 Issue 4 2014 CHOLESTEROL GRANULOMA: AN UNCOMMON CLINICAL ENTITY OF THE MAXILLARY SINUS Sunita Singh Sonia Chhabra Pansi Gupta Priya Malik Pt B.D. Sharma PGIMS, Rohtak, Haryana
The concept of unicystic ameloblastoma (UA) was
 Publication Treatment of Giant Unicystic Ameloblastoma Suction Drainage and Secondary Curettage: a Case Report Bing LIU 1, Wen Feng ZHANG 1, Xin Ming CHEN 2, Zhi Jun SUN 3, Mohd Jamal Alsharif 1, Yi Fang
Publication Treatment of Giant Unicystic Ameloblastoma Suction Drainage and Secondary Curettage: a Case Report Bing LIU 1, Wen Feng ZHANG 1, Xin Ming CHEN 2, Zhi Jun SUN 3, Mohd Jamal Alsharif 1, Yi Fang
Acanthomatous Ameloblastoma- A Case Report
 Acanthomatous Ameloblastoma- A Case Report Geeta Singh 1, Rashmi Agarwal 2, Vimlesh Kumar 3, Deepak Passi 4 1 Assistant Professor, Department of Oral & Maxillofacial Surgery, King George Dental University,
Acanthomatous Ameloblastoma- A Case Report Geeta Singh 1, Rashmi Agarwal 2, Vimlesh Kumar 3, Deepak Passi 4 1 Assistant Professor, Department of Oral & Maxillofacial Surgery, King George Dental University,
Pericoronal radiolucency associated with incomplete crown
 Imaging Science in entistry 2013; 43: 295-301 http://dx.doi.org/10.5624/isd.2013.43.4.295 Pericoronal radiolucency associated with incomplete crown Kyung-Soo Nah 1, * 1 epartment of Oral and Maxillofacial
Imaging Science in entistry 2013; 43: 295-301 http://dx.doi.org/10.5624/isd.2013.43.4.295 Pericoronal radiolucency associated with incomplete crown Kyung-Soo Nah 1, * 1 epartment of Oral and Maxillofacial
Keratocystic odontogenic tumor: A biopsy service s experience with 104 solitary, multiple and recurrent lesions
 Journal section: Oral Medicine and Pathology Publication Types: Research doi:10.4317/medoral.21181 http://dx.doi.org/doi:10.4317/medoral.21181 Keratocystic odontogenic tumor: A biopsy service s experience
Journal section: Oral Medicine and Pathology Publication Types: Research doi:10.4317/medoral.21181 http://dx.doi.org/doi:10.4317/medoral.21181 Keratocystic odontogenic tumor: A biopsy service s experience
Successful Conservative Surgical Treatment of Ameloblastic Fibroma in the Posterior Maxilla : A Case Report
 http://dx.doi.org/10.5933/jkapd.2013.40.4.321 ISSN (print) 1226-8496 Successful Conservative Surgical Treatment of Ameloblastic Fibroma in the Posterior Maxilla : A Case Report Youngeun Lee 1, Hyojung
http://dx.doi.org/10.5933/jkapd.2013.40.4.321 ISSN (print) 1226-8496 Successful Conservative Surgical Treatment of Ameloblastic Fibroma in the Posterior Maxilla : A Case Report Youngeun Lee 1, Hyojung
International Journal of Current Medical and Pharmaceutical Research
 ISSN: 2395-6429 International Journal of Current Medical and Pharmaceutical Research Available Online at http://www.journalcmpr.com DOI: http://dx.doi.org/10.24327/23956429.ijcmpr20170169 RESEARCH ARTICLE
ISSN: 2395-6429 International Journal of Current Medical and Pharmaceutical Research Available Online at http://www.journalcmpr.com DOI: http://dx.doi.org/10.24327/23956429.ijcmpr20170169 RESEARCH ARTICLE
International Journal of Scientific Research and Innovative Technology ISSN: Vol. 4 No. 4; April 2017
 Frequency of Lesions Associated with Impacted Teeth in Patients Referring to the Department of Oral Pathology, Tabriz Faculty of Dentistry from 2004 to 2013 and Its Relationship with Age, Gender, Location
Frequency of Lesions Associated with Impacted Teeth in Patients Referring to the Department of Oral Pathology, Tabriz Faculty of Dentistry from 2004 to 2013 and Its Relationship with Age, Gender, Location
Glandular odontogenic cyst: A case report
 Imaging Science in Dentistry 2014; 44: 75-9 http://dx.doi.org/10.5624/isd.2014.44.1.75 Glandular odontogenic cyst: A case report Shahnaz S. Tambawala 1, *, Freny R. Karjodkar 1, Archana Yadav 2, Kaustubh
Imaging Science in Dentistry 2014; 44: 75-9 http://dx.doi.org/10.5624/isd.2014.44.1.75 Glandular odontogenic cyst: A case report Shahnaz S. Tambawala 1, *, Freny R. Karjodkar 1, Archana Yadav 2, Kaustubh
Unusual transmigration of canines report of two cases in a family
 ISSN: Electronic version: 1984-5685 RSBO. 2014 Jan-Mar;11(1):88-92 Case Report Article Unusual transmigration of canines report of two cases in a family Sulabha A. Narsapur 1 Sameer Choudhari 2 Shrishal
ISSN: Electronic version: 1984-5685 RSBO. 2014 Jan-Mar;11(1):88-92 Case Report Article Unusual transmigration of canines report of two cases in a family Sulabha A. Narsapur 1 Sameer Choudhari 2 Shrishal
Jaws: Cysts and Odontogenic Neoplasms
 Topic 10: Jaw Cysts General Features of Jaw Cysts Sources of Epithelium in Cysts Radiographic Features of Jaw Cysts Microscopic Features of Jaw Cysts Treatment and Prognosis of Jaw Cysts Classification
Topic 10: Jaw Cysts General Features of Jaw Cysts Sources of Epithelium in Cysts Radiographic Features of Jaw Cysts Microscopic Features of Jaw Cysts Treatment and Prognosis of Jaw Cysts Classification
Big Keratocystic Odontogenic Tumor of the Mandible: A Case Report
 Big Keratocytic Odontogenic Bruktawit K et al 491 CASE REPORT Big Keratocystic Odontogenic Tumor of the Mandible: A Case Report Bruktawit Kebede 1, Demerew Dejene 1, Abebe Teka 1, Biruk Girma 1, Evelyn
Big Keratocytic Odontogenic Bruktawit K et al 491 CASE REPORT Big Keratocystic Odontogenic Tumor of the Mandible: A Case Report Bruktawit Kebede 1, Demerew Dejene 1, Abebe Teka 1, Biruk Girma 1, Evelyn
Periapical central giant cell granuloma misdiagnosed as odontogenic cyst
 doi: 10.1111/j.1365-2591.2006.01107.x CLINICAL ARTICLE Periapical central giant cell granuloma misdiagnosed as odontogenic cyst T. Lombardi 1, M. Bischof 1,2, R. Nedir 1,2, D. Vergain 1, C. Galgano 3,
doi: 10.1111/j.1365-2591.2006.01107.x CLINICAL ARTICLE Periapical central giant cell granuloma misdiagnosed as odontogenic cyst T. Lombardi 1, M. Bischof 1,2, R. Nedir 1,2, D. Vergain 1, C. Galgano 3,
Ameloblastic Carcinoma-Secondary Type,A Rare Case Report and Distinction from Malignant Ameloblastoma
 Ameloblastic Carcinoma-Secondary Type,A Rare Case Report and Distinction from Malignant Ameloblastoma Rajesh B Dhirawani, Sumit Asrani, Anshalika Agrawal, Sauvik Singha* and Kshitij Aggarwal Department
Ameloblastic Carcinoma-Secondary Type,A Rare Case Report and Distinction from Malignant Ameloblastoma Rajesh B Dhirawani, Sumit Asrani, Anshalika Agrawal, Sauvik Singha* and Kshitij Aggarwal Department
Erupting Compound Odontome - A case report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 3 Ver. V. (Mar. 2014), PP 26-30 Erupting Compound Odontome - A case report Dr. Sahana Srinath
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 3 Ver. V. (Mar. 2014), PP 26-30 Erupting Compound Odontome - A case report Dr. Sahana Srinath
Proceedings of the 36th World Small Animal Veterinary Congress WSAVA
 www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: http://www.ivis.org October 14(Fri) ~ 17(Mon) 2011 ICC Jeju, Korea 2011 WSAVA
www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: http://www.ivis.org October 14(Fri) ~ 17(Mon) 2011 ICC Jeju, Korea 2011 WSAVA
RADIOGRAPHIC INTERPRETATION Differential Diagnosis
 RADIOGRAPHIC INTERPRETATION Differential Diagnosis MODULE 1: The Introduction. Chief complaint Demographics Age Sex Race Historical findings Physical findings Clinical Radiographic Location Maxilla/mandible
RADIOGRAPHIC INTERPRETATION Differential Diagnosis MODULE 1: The Introduction. Chief complaint Demographics Age Sex Race Historical findings Physical findings Clinical Radiographic Location Maxilla/mandible
Radiographic features of cysts and benign tumors of the jaws. Cyst. Effects on adjacent structures. Types. Odontogenic Cysts. Non-Odontogenic cysts
 Radiographic features of cysts and benign tumors of the jaws Cyst A Cyst is a benign pathologic cavity filled with fluid, lined by epithelium, and surrounded by a connective tissue wall Steven R. Singer,
Radiographic features of cysts and benign tumors of the jaws Cyst A Cyst is a benign pathologic cavity filled with fluid, lined by epithelium, and surrounded by a connective tissue wall Steven R. Singer,
Odontogenic Keratocyst: The Northwestern USA Experience
 Volume 1 Number 2 Winter Issue, 2000 Odontogenic Keratocyst: The Northwestern USA Experience Abstract Odontogenic keratocyst (OKC) is a cyst of tooth origin with an aggressive clinical behavior including
Volume 1 Number 2 Winter Issue, 2000 Odontogenic Keratocyst: The Northwestern USA Experience Abstract Odontogenic keratocyst (OKC) is a cyst of tooth origin with an aggressive clinical behavior including
Ameoblastic carcinoma of mandible - A rare case report with review of literature
 Journal section: Oral Medicine and Pathology Publication Types: Case report doi:10.4317/jced.2.e100 Ameoblastic carcinoma of mandible - A rare case report with review of literature K Mubeen 1, Hemant Kumar
Journal section: Oral Medicine and Pathology Publication Types: Case report doi:10.4317/jced.2.e100 Ameoblastic carcinoma of mandible - A rare case report with review of literature K Mubeen 1, Hemant Kumar
Maxillary Sinus Measurements in Different Age Groups of Human Cadavers
 Tikrit Journal for Dental Sciences 1(2013)107-112 Maxillary Sinus Measurements in Different Age Groups of Human Cadavers Mohammad A. Abd-alla BDS, MSc., Ph.D. (1) Abdul-Jabbar J. Mahdi BDS, MSc., Ph.D.
Tikrit Journal for Dental Sciences 1(2013)107-112 Maxillary Sinus Measurements in Different Age Groups of Human Cadavers Mohammad A. Abd-alla BDS, MSc., Ph.D. (1) Abdul-Jabbar J. Mahdi BDS, MSc., Ph.D.
Erupted odontomas: a report of two unusual cases
 ISSN: Printed version: 1806-7727 Electronic version: 1984-5685 RSBO. 2012 Apr-Jun;9(2):199-203 Case Report Article Erupted odontomas: a report of two unusual cases Santosh Patil¹ Farzan Rahman² Shoaib
ISSN: Printed version: 1806-7727 Electronic version: 1984-5685 RSBO. 2012 Apr-Jun;9(2):199-203 Case Report Article Erupted odontomas: a report of two unusual cases Santosh Patil¹ Farzan Rahman² Shoaib
