Short implants versus longer implants in vertically augmented posterior mandibles: A randomised controlled trial with 5-year after loading follow-up
|
|
|
- Buck Tyler Boone
- 6 years ago
- Views:
Transcription
1 RANDOMISED CONTROLLED CLINICAL TRIAL 359 Pietro Felice, Gioacchino Cannizzaro, Carlo Barausse, Roberto Pistilli, Marco Esposito Short implants versus longer implants in vertically augmented posterior mandibles: A randomised controlled trial with 5-year after loading follow-up Key words bovine anorganic bone, inlay graft, short dental implants, sinus lift, vertical augmentation Objectives: To evaluate whether 6.6-mm long implants could be a suitable alternative to longer implants placed in vertically augmented atrophic posterior mandibles. Materials and methods: Sixty partially edentulous patients having 7 to 8 mm of residual crestal height and at least 5.5 mm thickness measured on CT scans above the mandibular canal were randomised according to a parallel group design. They were either to receive 1 to 3 submerged 6.6-mm long implants or 9.6 mm or longer implants (30 patients per group) placed in vertically augmented bone. Bone was augmented with interpositional anorganic bovine bone blocks covered by resorbable barriers. Grafts were left to heal for 5 months before implant placement. Four months after provisional acrylic prostheses were delivered, they were replaced, after 4 months, by definitive metal-ceramic prostheses. Outcome measures were: prosthesis and implant failures; complications; and radiographic peri-implant marginal bone level changes. All patients were followed up to 5 years after loading. Results: Five years after loading, 8 patients dropped out: 3 from the short implant group and 5 from the augmented group. The augmentation procedure failed in 2 patients and only 6.6-mm long implants could be inserted. There were no statistically significant differences for prosthesis and implant failures. Five prostheses failed in 4 patients of the short implant group versus 5 prostheses in 5 patients in the augmented group (Fishers exact test P = 1.0; difference in proportions = 0.07; 95% CI to 0.43). Five short implants failed in 3 patients versus 3 long implants in 3 patients (Fishers exact test P = 1.00 difference in proportions = 0.00; 95% CI to 0.43). There were statistically more complications in augmented patients (25 complications in 21 augmented patients versus 6 complications in 6 patients of the short implant group) (Fishers exact test P < ; difference in proportions = 0.60; 95% CI 0.38, 0.82). Both groups gradually lost peri-implant bone in a statistically significant way. Five years after loading, short implant group patients lost an average of 1.49 mm peri-implant bone compared with 2.34 mm in the augmented group. Short implants experienced statistically significantly less bone loss (0.82 mm, 95% CI 0.48; 1.16, P < ) than long implants. Conclusions: When residual bone height over the mandibular canal is between 7 to 8 mm, 6.6 mm short implants could be an interesting alternative to vertical augmentation in posterior atrophic mandibles since the treatment is faster, cheaper and associated with less morbidity. Longer follow-ups may still be needed to confirm these results, however the medium-term prognosis (5 years after loading) of short implants is at least as good as those of longer implants placed vertically in augmented mandibles. Pietro Felice, MD, DDS, PhD Researcher, Department of Periodontology and Implantology, University of Bologna, Bologna Italy Gioacchino Cannizzaro, MD, DDS Private practice, Pavia, Italy Carlo Barausse, DDS Resident, Department of Periodontology and Implantology, University of Bologna, Bologna, Italy Roberto Pistilli, MD Resident, Oral and Maxillofacial Unit, San Filippo Neri Hospital, Rome, Italy Marco Esposito, DDS, PhD Freelance researcher and Associate Professor, Department of Biomaterials, The Sahlgrenska Academy at Göteborg University, Sweden Correspondence to: Marco Esposito, Casella Postale 34, Arcore (MB), Italy espositomarco@ hotmail.com Conflict of interest statement: Biomet 3i, manufacturer of the implants used in this investigation, partially supported this trial. However data properties belonged to the authors and by no means did Biomet 3i interfere with the conduct of the trial or the publication of the results.
2 360 Felice et al Introduction Short implants could be an alternative to vertical augmentation procedures when the available bone height does not allow the placement of dental implants longer than 7 mm However, followups longer than 3 years are still lacking with the exception of a 10-year follow-up trial that considered 11-mm long implants as short implants 12. When the residual amount of mandibular bone height is less than 10 mm, implant supported prostheses are considered at a higher risk of failure 13, therefore more invasive procedures either to vertically augment the bone or to transpose the alveolar inferior nerve 18 are used to allow placement of longer implants. While it has been shown that it is possible to vertically augment bone with different procedures, these techniques are associated with significant postoperative morbidity and complications, can be expensive and technique sensitive, and require long treatment periods (up to 1 year) 1. On the contrary, the effectiveness of nerve transposition procedures has never been evaluated in proper comparative trials. Nerve transposition is technically demanding and can be associated with a substantial amount of permanent loss of nerve sensitivity, therefore nowadays is rarely used. Short implants could be a simpler, cheaper and faster alternative to vertical bone augmentation, if they will provide similar success rates. The definition of short implants is controversial since some authors consider short implants with a length of 7 mm to 10 mm 13, whereas other authors consider short implants with a designed intrabony length of 8 mm or less 19. Nevertheless, it is commonly perceived that implants 7 mm or shorter may not have as good a long-term prognosis as longer implants have. While it is common sense to use longer implants when bone heights allow it, it remains unclear how to proceed in the presence of residual mandibular bone height ranging from between 5 mm to 8 mm. Trials with follow-ups up to 1 year after loading suggest that short implants may be a good, if not a better alternative to longer implants placed in vertically augmented bone However, follow-ups to 3 years after loading are still too short for recommending the use of short implants, since their long-term prognosis is practically unknown. Therefore, longer follow-ups, ideally up to 10 years, are needed. The aim of this randomised controlled trial was to compare the outcome of partial fixed prostheses supported by 6.6-mm long implants (Nanotite, External Hex, Biomet 3i, Palm Beach, FL, USA) with prostheses supported by identical 9.6 mm or longer implants placed in posterior mandibles vertically augmented with an interpositional block of anorganic bovine bone (Bio-Oss; Geistlich Pharma, Wolhusen, Switzerland). The present investigation reports data to 5 years after loading. Previous publications reported data at 5 months 3, 1 year 5 and 3 years 10 after loading. In previous publications of this same study, different heights of short implant were reported: 7 mm 3,5 and 6.3 mm 10, respectively at 5 month, 1 and 3 years post-loading. This was due to the confusing information provided by the manufacturer: the actual height of the short implants from the apex to the collar to be potentially in contact with bone is 6.6 mm. This misunderstanding was due because the manufacturer, when describing the total length of its implants, also included in the measurement the height of the external hexagon. This should not be considered for calculating the exact total implant length since the external hexagon, needed to engage the abutment, does not go in contact with bone. The present article is reported according to the CONSORT statement for improving the quality of reports of parallel-group randomised trials ( Materials and methods Any patient with partial edentulism in the posterior mandible, having residual bone height of 7 mm to 8 mm and thickness of at least 5.5 mm above the inferior alveolar canal, requiring 2 to 3 adjacent implants, who was 18 or older and able to sign an informed consent form, was eligible for inclusion in this trial. Patient eligibility in terms of bone dimensions above the alveolar inferior canal was determined on computer tomography (CT) scans. Patients were not admitted in the study if any of the following exclusion criteria was present: (i) general contraindications to implant surgery; (ii) subjected to irradiation in the head and neck area less than 1 year before; (iii) under chemotherapy for malignant tumour; (iv) treated or under treatment with
3 Felice et al 361 intravenous amino-bisphosphonates; (v) affected by untreated periodontitis or having poor oral hygiene and motivation; (vi) uncontrolled diabetes; (vii) pregnant or lactating; (viii) substance abusers; (ix) psychiatric problems or unrealistic expectations; (x) lack of opposite occluding dentition in the area intended for implant placement; (xi) acute infection in the area intended for implant placement; (xii) patients participating in other trials, if the present protocol could not be followed; (xiii) referred only for implant placement; (xiv) extraction sites with less than 3 months of healing. Patients were divided into three groups according to what they declared: non-smokers; moderate smokers (up to 10 cigarettes per day); and heavy smokers (more than 10 cigarettes per day). Patients were recruited and treated in three different private practices by the same operators (Pietro Felice performed all the surgical and Paolo Censi all the prosthetic procedures), using similar and standardised procedures. The principles outlined in the Declaration of Helsinki on clinical research involving human subjects were followed. All patients received through explanations and signed a written informed consent form prior to being enrolled in the trial. After consent was given, eligible patients were randomised according to a parallel group design to receive either 6.6-mm long or an interpositional block of anorganic bovine bone (Bio-Oss) to allow placement of identical implants at least 9.6-mm long. Study models were used to plan the amount of vertical augmentation required by the patients. Within 10 days prior to bone augmentation and implant placement, patients underwent at least one a session of oral hygiene instructions and professionally delivered periodontal maintenance when required. Prior to augmentation, patients received 1 g of amoxicillin and clavulanic acid (or erythromycin 500 mg if allergic to penicillin) starting the night before the intervention, twice a day, for 7 days. All patients were treated under local anaesthesia using articain with adrenaline 1: No intravenous sedation was used. At the augmentation procedure, a surgical template was used to indicate the planned implant position. A paracrestal incision was made through the buccal area, respecting the emergence of the mental nerve, to expose the alveolar ridge. A mucoperiosteal flap was carefully retracted on the buccal side, trying to minimise tensions to the mental nerve. A horizontal osteotomy was made approximately 2 mm to 4 mm above the mandibular canal using a piezosurgery device (Mectron Piezosurgery Device; Mectron, Carasco Genoa, Italy), being very careful not to damage the lingual periosteum. Two oblique cuts were made, the mesial cut being at least 2 mm distal to the last tooth in the arch. The height of the osteotomised segment had to be of at least 3 mm to minimise the risk of its accidental fracture when inserting the stabilising screw. The segment was then raised in a coronal direction and a Bio-Oss block was trimmed to the desired height and shape, interposed between the raised fragment and the basal bone, and fixed with titanium miniplates and miniscrews (Gebrüder Martin, Tuttlingen, Germany) to both the basal and the crestal bone segment. Gaps were filled with particulated Bio-Oss from the block. The grafted area was covered with a resorbable barrier (Bio-Gide, Geistlich Pharma). Periosteal incisions were made to release the flaps as coronally as needed and the flaps were sutured with Vicryl 4.0 sutures (Ethicon FS-2, St-Stevens-Woluwe, Belgium), until the incisions were perfectly sealed. Ibuprofen 600 mg was prescribed to be taken 2 to 4 times a day during meals for as long as required. Patients were instructed to use corsodyl gel 1% twice a day for 2 weeks and then 0.2 chlorhexidine mouthwashes twice a day for up to the second month, to have a soft diet for 1 week, and to avoid brushing and trauma on the surgical sites. No removable prosthesis was allowed. Patients were seen after 3 days and sutures were removed after 10 days. All patients subjected to vertical augmentation were recalled for additional postoperative check-ups 1, 2, 3 and 4 months after the augmentation procedure. Five months after augmentation, a CT scan was taken to plan implant placement, miniplates were removed, knife edge ridges were flattened to reach a thickness of at least 5.5 mm when needed, and implants were inserted under local anaesthesia. Two g of amoxicillin (or erythromycin 500 mg) were administered 1 h prior to implant placement. Two to three 6.6-mm long (short implant group) or 9.6-mm long implants or longer (augmented group) were inserted under
4 362 Felice et al prosthetic guidance using a surgical template after crestal incision and flap elevation. Nanotite parallel walled Biomet 3i dental implants, of 4 mm diameter, with external connection, made of titanium alloy (Ti6Al4V) were used. The Nanotite implants are dual etched and then partially covered (about 50% of the surface) with nanoscale calcium phosphate crystals; this surface modification procedure is termed DCD (discrete crystalline deposition). The operator used 6.6-mm long implants for the test group, and the longer possible length (9.6 mm, 11.2 mm, 12.6 mm, and 14.6 mm) for the augmented group. The standard placement procedure as recommended by the manufacturer was used. Drills with increasing diameters (2 mm, 2.8 mm, and 3.5 mm)) were used to prepare the implant sites. Implant sites were slightly underprepared and the surgical unit was settled with a torque of 25 Ncm. In all cases, the head of the implants was placed supracrestally so that the neck of the implant (0.6 mm in height) was not embedded into bone. Resistance at implant insertion was recorded (<25 Ncm; <35 Ncm; <45 Ncm; >50 Ncm in this latter case the manual wrench was used to seat the implant). Cover screws were placed and implants were submerged. Flap closure was obtained with vicryl 4.0. Intraoral radiographs (baseline) were made with the paralleling technique. In the case that the bone levels around the study implants were hidden or difficult to be estimated, a second radiograph was made. Ibuprofen 600 mg was prescribed to be taken 2 to 4 times a day during meals, as long as required. Patients were instructed to use 0.2 chlorhexidine mouthwash for 1 min twice a day for 2 weeks, to have a soft diet for 1 week, and to avoid brushing and trauma on the surgical sites. No removable prosthesis was allowed. Sutures were removed after 10 days. After 4 months of submerged healing, implants were exposed, manually tested for stability and an impression with the pick-up impression copings was taken. Provisional screw-retained acrylic restorations rigidly joining the implants were delivered on prefabricated abutments (Biomet 3i). Occlusal surfaces were in slight contact with the opposite dentition. Intraoral radiographs of the study implants were taken. Four months after delivery of the provisional prostheses, implants were manually tested for stability. Then definitive screw-retained or provisionally cemented metal-ceramic restorations rigidly joining the implants with occlusal surfaces in ceramic were delivered on titanium-based UCLA abutments (Biomet 3i). Patients were enrolled in an oral hygiene program with recall visits every 4 months for the entire duration of the study. Follow-ups were conducted by different independent outcome assessors (Gerardo Pellegrino; Elisa Soardi; Carlo Barausse) together with the surgical operator. This study tested the null hypothesis that there were no differences in the clinical outcome between the two procedures against the alternative hypothesis of a difference. Outcome measures were: 1. Prosthesis failure: planned prosthesis which could not be placed due to implant failure(s), loss of the prosthesis secondary to implant failure(s) and remake of the prosthesis for any reasons. 2. Implant failure: implant mobility, removal of stable implants dictated by progressive marginal bone loss or infection and any mechanical complications rendering the implant not usable (e.g. implant facture). The stability of individual implants was measured at delivery of the provisional prostheses (4 months after implant placement), at delivery of the definitive prostheses (4 months after delivery of the provisional prostheses), at 1, 3 and 5 years after loading after prosthesis removal, by tightening abutment screws with a torque of 15 Ncm. 3. Any biological or prosthetic complications. 4. Time (days) needed to fully recover mental sensitivity after the augmentation procedure (augmented group) and implant placement (short implant group). This outcome was reported in a previous publication Peri-implant marginal bone level changes evaluated on intraoral radiographs taken with the paralleling technique at implant placement, 1, 3 and 5 years after loading. Radiographs were scanned and digitised into JPG files, converted to TIFF format with a 600 dpi resolution, then stored in a personal computer. Peri-implant marginal bone levels were measured using the UTHSCSA Image Tool 3.0 (The University of Texas Health Science Center, San Antonio, USA) software. The software
5 Felice et al 363 was calibrated for every single image using the known implant neck diameter. Measurements of the mesial and distal bone crest level adjacent to each implant were made to the nearest 0.01 mm and averaged at patient level and then at group level. The measurements were taken parallel to the implant axis. Reference points for the linear measurements were: the most coronal margin of the implant collar and the most coronal point of bone-to-implant contact. One dentist (Gerardo Pellegrino, subsequently replaced by Elisa Soardi and then by Carlo Barausse) not involved in the treatment of the patients performed all clinical and radiographic assessments without knowing group allocation, therefore the outcome assessors were blind. However the Bio- Oss augmented sites could be identified on radiographs because they appeared more radioopaque and implants were longer. The sample size was calculated for the primary outcome measures (implant failure): a two-group continuity corrected chi-square test with a two-sided significance level will have 80% power to detect the difference between a proportion of and a proportion of for patients experiencing at least one implant failure (odds ratio of 3.857) when the sample size in each group is 72. However, it was decided to recruit only 30 patients in each group, since that was the number of patients the sponsor was willing to sponsor in terms of free implants. A computer generated restricted randomisation list was created. Only one of the investigators (Marco Esposito), not involved in the selection and treatment of the patients, was aware of the random sequence and could have access to the random list stored in his password protected portable computer. The random codes were enclosed in sequentially numbered, identical, opaque, sealed envelopes. Envelopes were opened sequentially after eligible patients signed the informed consent form to be enrolled in the trial. Therefore, treatment allocation was concealed to the investigators in charge of enrolling and treating the patients. All data analysis was carried out according to a pre-established analysis plan. A biostatistician with expertise in dentistry analysed the data, without knowing the group codes. The patient was the statistical unit of the analyses. Differences in the proportion of patients with prosthesis failures, implant failures and complications (dichotomous outcomes) were compared between the groups using the Fisher s exact probability test. Differences of means at patient level for continuous outcomes (bone levels) between groups were compared by t tests. Comparisons between each of the time points and the baseline measurements were made by paired tests, to detect any changes in marginal peri-implant bone levels. An analysis of co-variance was used to compare the mean radiographic values at 1, 3 and 5 years, with the baseline value as a covariate. All statistical comparisons were conducted at the 0.05 level of significance. Results Sixty patients were considered eligible and were consecutively enrolled in the trial. For additional information about non-eligible patients, please look elsewhere 3. All patients were treated according to the allocated interventions. At the 5-year postloading endpoint, 8 patients dropped out, 5 from the augmented group and 3 from the short implant group. One patient from the short implant group decided for financial reasons to have the prosthesis made in Croatia, and then she refused to attend the follow-ups. Three patients did not come back at the 3-year evaluation, 1 patient from the short implant group due to having moved away and the remaining 2 patients, both from the augmented group, because they did not wish to attend the maintenance and follow-up controls. One patient of the short implant group disappeared after the 3-year follow-up and could not be contacted any longer. The remaining 3 patients dropped out after the 3-year follow-up from the augmented group: one moved abroad 3-and-a-half years after loading; another moved abroad 4 years after loading; and the last one was seen 3 years and 4 months after loading, but after that we did not manage keep in contact with her any further. The data of all remaining patients was evaluated in the statistical analyses. The following deviations from the protocol occurred:
6 364 Felice et al Fig 1 Sequence of periapical radiographs showing one of the patients treated with interpositional block xenograft and longer implants, which were positioned slightly supracrestally: (a) just after implant placement; (b) initial loading with a provisional prosthesis; (c) 1 year after loading follow-up; (d) 3 years after loading followup; (e) 5 years after loading follow-up. The peri-implant marginal bone levels remained substantially unaltered in this patient. a b c d e In one patient of the short implant group, the upper two implant threads remained exposed at implant placement. A titanium mesh was placed to regenerate bone and was stabilised with the cover screws. In one patient of the short implant group, the metal framework of the definitive prosthesis was not fitting perfectly; therefore it was sectioned and the patient rehabilitated with two single crowns instead of receiving a prosthesis splinting the two implants together. The great majority of the implants belonging to the short implant group and some belonging to the vertically augmented group, become exposed during healing because of their supracrestal position, so in only four patients of the short implant group, versus 24 patients of the augmented group, a surgical exposure of the implant was necessary. Patients were recruited and subjected to vertical bone augmentation from June 2007 to April The last final prosthesis was inserted in December The follow-up was to 5 years after implant loading (Figs 1a to 1e and Figs 2a to 2e). The main baseline patient characteristics are presented in Table 1. Sixty-one implants were placed in the augmented group and 60 in the short implant group. There were no apparent significant baseline imbalances between the two groups. The main results are summarised in Table 2. Five prostheses in the augmented group and 5 prostheses of four patients in the short implant group were considered as failures, the difference being not statistically significant (Fishers exact test P = 1.0; difference in proportions = 0.07; 95% CI to 0.43). In the augmented group three prostheses could not be placed at the planned time because of early implant failures. The remaining two prostheses were remade for aesthetic reasons after fracture of the ceramic lining at 19 months after loading, and at 4 and a half years. In the short implant group, one prosthesis could not be placed at the planned time because of an early implant failure. One patient come to the practice, 16 months after loading, with the prostheses in her hand and the failed implant attached to it asking whether it was possible to screw it back; the same patient came back 3 and a half years after loading with the new prosthesis fractured and with an implant attached to it. Another prosthesis was remade for aesthetic reasons after fracture of the ceramic lining 27 months after loading; finally another patient came back, 4 years after loading, with a prosthesis
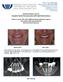
7 Felice et al 365 a b c Fig 2 Sequence of periapical radiographs showing one of the patients treated with 6.6- mm long implants, which were positioned slightly supracrestally: (a) just after implant placement; (b) initial loading with a provisional prosthesis; (c) 1 year after loading follow-up; (d) 3 years after loading follow-up; (e) 5 years after loading follow-up. Some peri-implant marginal bone loss occurred in this patient over the 5-year period, especially at the distal implant. d e Table 1 Patient and intervention characteristics. Long implants (n = 30) Short implants (n = 30) Females Mean age at implant insertion (range) 55 (43 67) 56 (40 83) Smokers 11 moderate 11 moderate + 1 heavy Total number of inserted implants Implants placed with <25 Ncm torque 12 (6 patients) 4 (2 patients) Mean length of placed implants 10.8 mm 6.6 mm Table 2 Summary of the main results up to 5 years after loading. Long implants (n = 25) Short implants (n = 27) P value Prosthesis failures (patients)* 5 (5) 5 (4) 1.00 Implant failures (patients) 3 (3) 5 (3) 1.00 Augmentation procedure failures 2 Not applicable Not applicable Complications (patients) 25 (21) 6 (6) < * Two patients in each group were not wearing their prosthesis at the moment of writing this article. in her hand and the two implants attached to it. At the end of the 5-year follow-up, two prostheses per group were not in function. Three implants failed in three patients of the augmented group prior to loading versus 5 implants in three patients of the short implant group: one patient lost an implant prior to loading; one patient lost 2 implants at 16 months and at 3 and a half years after loading; and the last patient lost both her implants 4 years after loading. Only the latter patient reported minor ailment at implants. The differences in proportions of implant failures were not statistically significant (Fishers exact test P = 1.00 difference in proportions = 0.00; 95% CI to 0.43).
8 366 Felice et al Table 3 Mean radiographic peri-implant marginal bone levels between groups and time periods. Short implants Long implants Implant placement Loading* 1 year after loading* 3 years after loading* 5 years after loading* N Mean (SD) 95% CI N Mean (SD) 95% CI N Mean (SD) 95% CI N Mean (SD) 95% CI N Mean (SD) 95% CI (0.41) 0.63, (0.53) 1.17, (0.54) 1.59, (0.46) 1.78, (0.47) 2.05, (0.28) 0.55, (0.42) 1.06, (0.42) 1.49, (0.75) 2.14, (0.74) 2.71, 3.32 * All changes from baseline statistically different (P <0.001). Twenty-five complications occurred in 21 patients of the augmented group versus 5 complications in 5 patients of the short implant group. The difference in proportions was statistically significant (Fishers exact test P < ; difference in proportions = 0.60; 95% CI 0.38, 0.82). No permanent paraesthesia of the alveolar inferior nerve occurred. In the augmented group, in three patients the Bio- Oss blocks fractured into many pieces at placement. In two of these patients, no clinically useful bone gain was obtained and only 6.6-mm long implants could be placed, instead of the 9.6 mm or longer implants as planned (the data of these two patients were analysed according to an intention-to-treat analysis). Sixteen patients had a transient postoperative paraesthesia of the mental nerve lasting 1 to 6 days and 4 patients had a soft tissue dehiscence at augmented sites 10 to 30 days after augmentation. One of the patients with dehiscence previously experienced a temporary paraesthesia. Twenty-five months after loading, the abutment screw become loose in one patient who already experienced a postoperative soft tissue dehiscence and the ceramic lining of another prostheses fractured 19 months post-loading. In the short implant groups, 2 patients had a transient post-implantation paraesthesia of the lower lip/chin lasting 2 days. Two patients experienced loosening of the abutment screws at 22 and 32 months post-loading, one patient had the ceramic lining of the prosthesis fractured 27 months after loading, and one patient had a fracture of the prosthesis 3-and-a-half years after loading. Both groups gradually lost a statistically significant amount of marginal peri-implant bone (P <0.001) at loading, 1, 3 and 5 years after loading (Table 3). At loading, patients with short implants lost an average of 0.58 mm peri-implant bone versus 0.56 mm for patients with long implants (Table 3). One year after loading, patients of both groups lost an average of 1 mm of peri-implant bone (Table 3). Three years after loading, patients with short implants lost 1.24 mm of peri-implant bone versus 1.76 mm of patients with longer implants (Table 3). Five years after loading, patients with short implants lost 1.49 mm of peri-implant bone versus 2.34 mm of patients with longer implants (Table 3). At 5 years after loading, there was a statistically significant difference between the two groups for peri-implant bone loss; when an analysis of covariance is applied (P <0.0001), short implants lost less bone (0.82 mm, 95% CI 0.48, 1.16; Table 4). Discussion This trial was designed to evaluate whether short implants could be used to support partial fixed prostheses in posterior mandibles having 7 mm to 8 mm of residual bone height above the mandibular canal. Implants 6.6-mm long were compared with implants at least 9.6-mm long placed in vertically augmented bone with interpositional blocks of anorganic bovine bone. Both techniques were able to achieve the planned goals and displayed similar clinical outcomes, but short implants did it with less morbidity, in a shorter time and at a lower cost. One additional surgical intervention with an additional healing time of 5 months was required to vertically augment bone. In addition, augmentation procedures are also more technically demanding than placing short implants. The main potential disadvantage with short implants is marginal bone loss. In fact, 5 years after loading, short implants are supported on average by only 4.4 mm of bone; the 2.2 mm remaining portion
9 Felice et al 367 Table 4 Comparison of mean changes in peri-implant marginal bone levels at different time periods between groups. Baseline loading Baseline 1 year after loading Baseline 3 years after loading Baseline 5 years after loading N Mean (SD) 95% CI N Mean (SD) 95% CI N Mean (SD) 95% CI N Mean (SD) 95% CI Short implants (0.30) -0.69, (0.36) -1.14, (0.36) -1.39, (0.40) -1.66, Long implants (0.29) -0.69, (0.31) -1.11, (0.72) -2.04, (0.75) -2.65, P value for groups 0.87* 0.90* 0.002* <0.0001* * Analysis of covariance at loading, 1, 3 and 5 years after loading with baseline as a covariate. of the implants is not supported because either the bone was gradually resorbed or because the implant was placed slightly supracrestally. If bone loss will progress, short implants may be at higher risk of premature failure. Therefore it is fundamental to wait for follow-ups up to 10 years, before being able to provided evidence-based recommendations on best therapeutic option. On the other hand, our results are encouraging since apparently short implants lost 0.8 mm less peri-implant marginal bone than longer implants. However, it is difficult to explain why short implants lost less bone than longer implants in augmented bone, but it may be that this phenomenon has to be put in correlation with the augmentation procedure. The present findings are in substantial agreement with other randomised controlled trials (RCTs) testing the same hypothesis under similar clinical conditions 4,6,8,9,11,20. These trials also suggested that short implants can also provide good clinical outcomes at least up to 1 year in function in maxillae, when compared to longer implants placed in lifted sinuses and augmented maxillas 4,6-9,11,20-22, even when immediately loaded if inserted with a torque superior to 40 Ncm 23, 24. All these trials suggest that short implants can be a reliable if not preferable solution to augmentation procedures for placing longer implants. The main question that remains to be answered is whether the long-term prognosis of short implants is comparable to that of longer implants in augmented bone. In fact, it may be possible that after several years of function, short implants might start to fail more often due to progressive marginal bone loss/ overload. Only longer follow-ups will provide a reliable answer to this question. Therefore we still need to be careful when suggesting any therapeutic options to our patients, since we actually do not know the long-term prognosis of short implants in patients with reduced bone heights. We used interpositional bone substitute block for vertical bone augmentation in the mandible simply because we felt that this technique was more reliable in our hands than other vertical augmentation procedures. However, the handling of block made of anorganic bovine sintered bone was unpractical because they easily fragmented during modelling, therefore we now prefer to use real blocks of animal origin 8,9,11,20. Several techniques are currently used to vertically augment the posterior mandible, and a few of them have been piloted in RCTs: various guided bone regeneration (GBR) procedures ; alveolar distraction osteogenesis 14,15 ; onlay bone grafting 15 ; and the use of interpositional bone grafts 4,25,26. Both autogenous bone and bone substitutes can be used, but a pilot study 26,27 suggested that bone substitute blocks might be a valid if not preferable option than autogenous bone harvested from the iliac crest for interpositional grafts, since patient discomfort is greatly reduced. The main limitation of the present trial is the small sample size, however it will be possible to combine the present findings with those of similar trials in a meta-analysis 1 to increase the sample size. Both techniques were tested in real clinical conditions and patient inclusion criteria were broad, therefore the results of the present investigation can be generalised to other settings treating patients with similar characteristics. However, the surgeon was experienced with both techniques and this factor might limit the extrapolations of the results. In addition, a 5-year follow-up may be still too short to make definitive statements on which could be the best treatment option. Longer follow-up periods and larger sample sizes are needed and these trials are currently ongoing.
10 368 Felice et al Conclusions When the residual bone height over the mandibular canal is between 7 mm to 8 mm, 6.6 mm short implants or longer implants placed in vertically augmented bone achieved good and similar results, however, short implants might preferable since the treatment is faster, cheaper and associated with less morbidity than vertical augmentation. These 5-year results must be confirmed by longer follow-ups. References 1. Esposito M, Grusovin MG, Felice P, Karatzopoulos G, Worthington HV, Coulthard P. Interventions for replacing missing teeth: horizontal and vertical bone augmentation techniques for dental implant treatment. Cochrane Database of Systematic Reviews: Chichester, UK: John Wiley & Sons, Esposito M, Felice P, Worthington HV. Interventions for replacing missing teeth: augmentation procedures of the maxillary sinus. Cochrane Database of Systematic Reviews: Chichester, UK: John Wiley & Sons, Felice P, Cannizzaro G, Checchi V, Pellegrino G, Censi P, Esposito M. Vertical bone augmentation versus 7-mm-long dental implants in posterior atrophic mandibles. Results of a randomised controlled clinical trial of up to 4 months after loading. Eur J Oral Implantol 2009;2: Felice P, Checchi V, Pistilli R, Scarano A, Pellegrino G, Esposito M. Bone augmentation versus 5 mm long dental implants in posterior atrophic jaws. Four-month post-loading results from a randomised controlled clinical trial. Eur J Oral Implantol 2009;2: Felice P, Pellegrino G, Checchi L, Pistilli R, Esposito M. Vertical augmentation with interpositional blocks of anorganic bovine bone vs. 7-mm-long implants in posterior mandibles: 1-year results of a randomized clinical trial. Clin Oral Implants Res 2010;21: Esposito M, Pellegrino G, Pistilli R, Felice P. Rehabilitation of posterior atrophic edentulous jaws: prostheses supported by 5 mm short implants or by longer implants in augmented bone? One-year results from a pilot randomised clinical trial. Eur J Oral Implantol 2011;4: Felice P, Soardi E, Pellegrino G, Pistilli R, Marchetti C, Gessaroli M, Esposito M. Treatment of the atrophic edentulous maxilla: short implants versus bone augmentation for placing longer implants. Five-month post-loading results of a pilot randomised controlled trial. Eur J Oral Implantol 2011;4: Pistilli R, Felice P, Cannizzaro G, Piatelli M, Corvino V, Barausse C, Buti J, Soardi E, Esposito M. Posterior atrophic jaws rehabilitated with prostheses supported by 6 mm long 4 mm wide implants or by longer implants in augmented bone. One-year post-loading results from a pilot randomised controlled trial. Eur J Oral Implantol 2013;6: Pistilli R, Felice P, Piattelli M, Gessaroli M, Soardi E, Barausse C, Buti J, Corvino V. Posterior atrophic jaws rehabilitated with prostheses supported by 5 x 5 mm implants with a novel nanostructured calcium-incorporated titanium surface or by longer implants in augmented bone. One-year results from a randomised controlled trial. Eur J Oral Implantol 2013;6: Esposito M, Cannizzaro G, Soardi E, Pellegrino G, Pistilli R, Felice P. A 3-year post-loading report of a randomised controlled trial on the rehabilitation of posterior atrophic mandibles: short implants or longer implants in vertically augmented bone? Eur J Oral Implantol 2011;4: Esposito M, Cannizzaro G, Soardi E, Pistilli R, Piattelli M, Corvino V, Felice P. Posterior atrophic jaws rehabilitated with prostheses supported by 6 mm short 4 mm wide implants or by longer implants in augmented bone. Preliminary results from a pilot randomised controlled trial. Eur J Oral Implantol 2012;5: Stellingsma K, Raghoebar GM, Visser A, Vissink A, Meijer HJ. The extremely resorbed mandible, 10-year results of a randomized controlled trial on 3 treatment strategies. Clin Oral Implants Res 2014;25: das Neves FD, Fones D, Bernardes SR, do Prado CJ, Neto AJ. Short implants - an analysis of longitudinal studies. Int J Oral Maxillofac Implants 2006;21: Chiapasco M, Romeo E, Casentini P, Rimondini L. Alveolar distraction osteogenesis vs. vertical guided bone regeneration for the correction of vertically deficient edentulous ridges: a 1-3-year prospective study on humans. Clin Oral Implants Res 2004;15: Chiapasco M, Zaniboni M, Rimondini L. Autogenous onlay bone grafts vs. alveolar distraction osteogenesis for the correction of vertically deficient edentulous ridges: a 2-4- year prospective study on humans. Clin Oral Implants Res 2007;18: Merli M, Migani M, Esposito M. Vertical ridge augmentation with autogenous bone grafts: resorbable barriers supported by ostheosynthesis plates versus titanium-reinforced barriers. A preliminary report of a blinded, randomized controlled clinical trial. Int J Oral Maxillofac Implants 2007;22: Fontana F, Santoro F, Maiorana C, Iezzi G, Piattelli A, Simion M. Clinical and histologic evaluation of allogenic bone matrix versus autogenous bone chips associated with titanium-reinforced e-ptfe membrane for vertical ridge augmentation: a prospective pilot study. Int J Oral Maxillofac Implants 2008;23: Rosenquist B. Implant placement in combination with nerve transpositioning: Experiences with the first 100 cases. Int J Oral Maxillofac Implants 1994;9: Renouard F, Nisand D. Impact of implant length and diameter on survival rates. Clin Oral Implants Res 2006;17(Suppl 2): Felice P, Pistilli R, Piattelli M, Soardi E, Corvino V, Esposito M. Posterior atrophic jaws rehabilitated with prostheses supported by 5 x 5 mm implants with a novel nanostructured calcium-incorporated titanium surface or by longer implants in augmented bone. Preliminary results from a randomised controlled trial. Eur J Oral Implantol 2012;5: Cannizzaro G, Felice P, Leone M, Viola P, Esposito M. Early loading of hydroxyapatite coated implants in the atrophic posterior maxilla: lateral sinus lift with autogenous bone and Bio-Oss versus crestal mini-sinus lift and 8 mm implants. A randomised controlled clinical trial. Eur J Oral Implantol 2009;2: Cannizzaro G, Felice P, Minciarelli AF, Leone M, Viola P, Esposito M. Early implant loading in the atrophic posterior maxilla: 1-stage lateral versus crestal sinus lift and 8 mm hydroxyapatite-coated implants. A 5-year randomised controlled trial. Eur J Oral Implantol 2013;6: Cannizzaro G, Leone M, Torchio C, Viola P, Esposito M. Immediate versus early loading of 7 mm long flapless-placed single implants: a split-mouth randomised controlled clinical trial. Eur J Oral Implantol 2008;1:
11 Felice et al 24. Cannizzaro G, Felice P, Leone M, Ferri V, Viola P, Esposito M. Immediate versus early loading of 6.5 mm-long flapless-placed single implants: a 4-year after loading report of a split-mouth randomised controlled trial. Eur J Oral Implantol 2012;5: Bianchi A, Felice P, Lizio G, Marchetti C. Alveolar distraction osteogenesis versus inlay bone grafting in posterior mandibular atrophy: a prospective study. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2008;105: Felice P, Marchetti C, Piattelli A, Pellegrino G, Checchi V, Worthington H, Esposito M. Vertical ridge augmentation of the atrophic posterior mandible with interpositional block grafts: bone from the iliac crest versus bovine anorganic bone. Results up to delivery of the final prostheses from a splitmouth, randomised controlled clinical trial. Eur J Oral Implantol 2008;1: Felice P, Marchetti C, Iezzi G, Piattelli A, Worthington H, Pellegrino G, Esposito M. Vertical augmentation of the posterior mandible with inlay grafts: bone from the iliac crest versus bovine bone. Clinical and histological results up to 1 year after loading from a randomized-controlled clinical trial. Clin Oral Implants Res 2009;20:
Pietro Felice, Gioacchino Cannizzaro, Vittorio Checchi, Claudio Marchetti, Gerardo Pellegrino, Paolo Censi, Marco Esposito
 RANDOMISED CONTROLLED CLINICAL TRIAL Publication 7 Pietro Felice, Gioacchino Cannizzaro, Vittorio Checchi, Claudio Marchetti, Gerardo Pellegrino, Paolo Censi, Marco Esposito Vertical bone augmentation
RANDOMISED CONTROLLED CLINICAL TRIAL Publication 7 Pietro Felice, Gioacchino Cannizzaro, Vittorio Checchi, Claudio Marchetti, Gerardo Pellegrino, Paolo Censi, Marco Esposito Vertical bone augmentation
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Vertical Augmentation
 Indication Sheet V Dr. Mauro Merli Vertical Augmentation Vertical alveolar ridge augmentation by means of the fence technique with Geistlich biomaterials > Original publication of the technique on PubMed;
Indication Sheet V Dr. Mauro Merli Vertical Augmentation Vertical alveolar ridge augmentation by means of the fence technique with Geistlich biomaterials > Original publication of the technique on PubMed;
Clinical Perspectives
 Clinical Perspectives Inside This Issue: Revised Drilling Guidelines For Parallel Walled Implants Case Presentation By: Pär-Olov Östman, DDS, PhD, MD Volume 8, Issue 1 Recommended Drilling Guidelines For
Clinical Perspectives Inside This Issue: Revised Drilling Guidelines For Parallel Walled Implants Case Presentation By: Pär-Olov Östman, DDS, PhD, MD Volume 8, Issue 1 Recommended Drilling Guidelines For
Vittorio Checchi, Pietro Felice, Giovanni Zucchelli, Carlo Barausse, Maurizio Piattelli, Roberto Pistilli, Giovanni Grandi, Marco Esposito
 RANDOMISED CONTROLLED CLINICAL TRIAL 263 Vittorio Checchi, Pietro Felice, Giovanni Zucchelli, Carlo Barausse, Maurizio Piattelli, Roberto Pistilli, Giovanni Grandi, Marco Esposito Wide diameter immediate
RANDOMISED CONTROLLED CLINICAL TRIAL 263 Vittorio Checchi, Pietro Felice, Giovanni Zucchelli, Carlo Barausse, Maurizio Piattelli, Roberto Pistilli, Giovanni Grandi, Marco Esposito Wide diameter immediate
Pietro Felice, Carlo Barausse, Rodolfo Blasone, Gianpaolo Favaretto, Claudio Stacchi, Matteo Calvo, Carlo Marin, Jacopo Buti, Marco Esposito
 RANDOMISED CONTROLLED CLINICAL TRIAL 397 Pietro Felice, Carlo Barausse, Rodolfo Blasone, Gianpaolo Favaretto, Claudio Stacchi, Matteo Calvo, Carlo Marin, Jacopo Buti, Marco Esposito A comparison of two
RANDOMISED CONTROLLED CLINICAL TRIAL 397 Pietro Felice, Carlo Barausse, Rodolfo Blasone, Gianpaolo Favaretto, Claudio Stacchi, Matteo Calvo, Carlo Marin, Jacopo Buti, Marco Esposito A comparison of two
Guided surgery as a way to simplify surgical implant treatment in complex cases
 52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
Narrow-diameter implants in premolar and molar areas
 2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
18: Felice P. In response. Implant Dent Jun;24(3): doi: /ID PubMed PMID:
 1: Felice P, Zucchelli G, Cannizzaro G, Barausse C, Diazzi M, Trullenque-Eriksson A, Esposito M. Immediate, immediate-delayed (6 weeks) and delayed (4 months) post-extractive single implants: 4-month post-loading
1: Felice P, Zucchelli G, Cannizzaro G, Barausse C, Diazzi M, Trullenque-Eriksson A, Esposito M. Immediate, immediate-delayed (6 weeks) and delayed (4 months) post-extractive single implants: 4-month post-loading
Nicola De Angelis, Pietro Felice, Gerardo Pellegrino, Andrea Camurati, Paolo Gambino,
 RANDOMISED CONTROLLED CLINICAL TRIAL 313 Nicola De Angelis, Pietro Felice, Gerardo Pellegrino, Andrea Camurati, Paolo Gambino, Marco Esposito Guided bone regeneration with and without a bone substitute
RANDOMISED CONTROLLED CLINICAL TRIAL 313 Nicola De Angelis, Pietro Felice, Gerardo Pellegrino, Andrea Camurati, Paolo Gambino, Marco Esposito Guided bone regeneration with and without a bone substitute
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space
 Case Report Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space Nidhi Bhatia 1, Shweta Bali 2, Meenu Taneja Bhasin 3, Priyanka Aggarwal 4, Vaibhav Joshi
Case Report Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space Nidhi Bhatia 1, Shweta Bali 2, Meenu Taneja Bhasin 3, Priyanka Aggarwal 4, Vaibhav Joshi
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Deploying Alpha-Bio Tec s NeO Selftapping Implant in an Atrophic Crest: Vestibular-Cortical Stabilization with Bone Graft
 The Atrophic crest Deploying Alpha-Bio Tec s NeO Selftapping Implant in an Atrophic Crest: Vestibular-Cortical Stabilization with Bone Graft Dr. Paolo Borelli DDS, Italy Dr. Massimiliano Favetti DDS, Italy
The Atrophic crest Deploying Alpha-Bio Tec s NeO Selftapping Implant in an Atrophic Crest: Vestibular-Cortical Stabilization with Bone Graft Dr. Paolo Borelli DDS, Italy Dr. Massimiliano Favetti DDS, Italy
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Keywords: Biomechanics, Biostatistics, Maxilla, Maxillary sinus, Sinus floor augmentation.
 Research Article Journal of Periodontal J Periodontal Implant Sci 2013;43:58-63 http://dx.doi.org/10.5051/jpis.2013.43.2.58 Peri-implant bone length changes and survival rates of implants penetrating the
Research Article Journal of Periodontal J Periodontal Implant Sci 2013;43:58-63 http://dx.doi.org/10.5051/jpis.2013.43.2.58 Peri-implant bone length changes and survival rates of implants penetrating the
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1.
 Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior
 Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Interventions for replacing missing teeth: augmentation procedures of the maxillary sinus.
 Interventions for replacing missing teeth: augmentation procedures of the maxillary sinus. Esposito M, Grusovin MG, Rees J, Karasoulos D, Felice P, Alissa R, Worthington HV, Coulthard P. Cochrane Database
Interventions for replacing missing teeth: augmentation procedures of the maxillary sinus. Esposito M, Grusovin MG, Rees J, Karasoulos D, Felice P, Alissa R, Worthington HV, Coulthard P. Cochrane Database
SCD Case Study. Implant-supported overdentures
 SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
From planning to surgery: a totally digital working flow for Leone implants placement
 Dr. Giancarlo Romagnuolo Roma, Italy From planning to surgery: a totally digital working flow for Leone implants placement Keywords guided surgery, 3D implant planning, single missing tooth, delayed immediate
Dr. Giancarlo Romagnuolo Roma, Italy From planning to surgery: a totally digital working flow for Leone implants placement Keywords guided surgery, 3D implant planning, single missing tooth, delayed immediate
It would be desirable to regenerate bone vertically
 Vertical Ridge Augmentation with Autogenous Bone Grafts: Resorbable Barriers Supported by Ostheosynthesis Plates Versus Titanium-Reinforced Barriers. A Preliminary Report of a Blinded, Randomized Controlled
Vertical Ridge Augmentation with Autogenous Bone Grafts: Resorbable Barriers Supported by Ostheosynthesis Plates Versus Titanium-Reinforced Barriers. A Preliminary Report of a Blinded, Randomized Controlled
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Basic information on the. Straumann Pro Arch TL. Straumann Pro Arch TL
 Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Conus Concept: A Rewarding Complete Denture Treatment
 Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Posterior mandible and vertical augmentation
 CASE REPORT Bilateral Vertical Ridge Augmentation With Block Grafts and Guided Bone Regeneration in the Posterior Mandible: A Case Report Maria A. Peñarrocha* Jose A. Vina Laura Maestre David Peñarrocha-Oltra
CASE REPORT Bilateral Vertical Ridge Augmentation With Block Grafts and Guided Bone Regeneration in the Posterior Mandible: A Case Report Maria A. Peñarrocha* Jose A. Vina Laura Maestre David Peñarrocha-Oltra
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
Interventions for replacing missing teeth: horizontal and vertical bone augmentation techniques for dental implant treatment (Review)
 Interventions for replacing missing teeth: horizontal and vertical bone augmentation techniques for dental implant treatment (Review) Esposito M, Grusovin MG, Felice P, Karatzopoulos G, Worthington HV,
Interventions for replacing missing teeth: horizontal and vertical bone augmentation techniques for dental implant treatment (Review) Esposito M, Grusovin MG, Felice P, Karatzopoulos G, Worthington HV,
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
Vertical Bone Augmentation for Implant Placement in the Mandible a Systematic. Review
 Vertical Bone Augmentation for Implant Placement in the Mandible a Systematic Review A dissertation submitted to the University of Manchester for the degree of Master of Science in Dentistry (Oral and
Vertical Bone Augmentation for Implant Placement in the Mandible a Systematic Review A dissertation submitted to the University of Manchester for the degree of Master of Science in Dentistry (Oral and
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
Featured Patient Case #1: Complete Mouth Reconstruction with Hybrid Restorations
 Philip L. Fava II, DMD, MDSc Robert A. Levine, DDS, FCPP, FISPPS 9880 Bustleton Ave, Suite 211 Philadelphia, PA 19115 PADentalImplants.com 215-677-8686 Featured Patient Case #1: Complete Mouth Reconstruction
Philip L. Fava II, DMD, MDSc Robert A. Levine, DDS, FCPP, FISPPS 9880 Bustleton Ave, Suite 211 Philadelphia, PA 19115 PADentalImplants.com 215-677-8686 Featured Patient Case #1: Complete Mouth Reconstruction
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
 Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
Immediate Implant Placement Along With Guided Bone Regeneration In Mandibular Anterior Region A Case Report.
 IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
Oral Health and Dentistry
 Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Table of Contents. 1 Immediate occlusal loading of NanoTite PREVAIL Implants: A prospective 1-year clinical and radiographic study
 Table of Contents 1 Immediate occlusal loading of NanoTite PREVAIL Implants: A prospective 1-year clinical and radiographic study 3 Immediate provisionalization of NanoTite Implants in support of single-tooth
Table of Contents 1 Immediate occlusal loading of NanoTite PREVAIL Implants: A prospective 1-year clinical and radiographic study 3 Immediate provisionalization of NanoTite Implants in support of single-tooth
Implant Placement in Maxillary Anterior Region Along with Soft and Hard Tissue Grafting- A Case Report.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants. by Timothy F. Kosinski, DDS, MAGD
 Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Localized Maxillary Ridge Augmentation Using Onlay Technique with a Xenograft Block for Dental Implant Placement A Case Series
 Localized Maxillary Ridge Augmentation Using Onlay Technique with a Xenograft Block for Dental Implant Placement A Case Series Hassan Maghaireh - BDS, MFDS RCSEd, MSc Implants Head of the International
Localized Maxillary Ridge Augmentation Using Onlay Technique with a Xenograft Block for Dental Implant Placement A Case Series Hassan Maghaireh - BDS, MFDS RCSEd, MSc Implants Head of the International
JMSCR Vol 06 Issue 07 Page July 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i7.101 Immediate Implant Following
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i7.101 Immediate Implant Following
It would be desirable to be able to regenerate bone
 Vertical one ugmentation with Dental Implant Placement: Efficacy and omplications ssociated with 2 Different Techniques. Retrospective ohort Study Mauro Merli, MD, DDS 1 /Massimo Migani, DDS 1 /Francesco
Vertical one ugmentation with Dental Implant Placement: Efficacy and omplications ssociated with 2 Different Techniques. Retrospective ohort Study Mauro Merli, MD, DDS 1 /Massimo Migani, DDS 1 /Francesco
Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident
 Case Report 13 2011 Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident Dr Hitoshi Minagawa Tokyo, Japan Prosthetics Dr Hitoshi Minagawa successfully completed his studies
Case Report 13 2011 Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident Dr Hitoshi Minagawa Tokyo, Japan Prosthetics Dr Hitoshi Minagawa successfully completed his studies
INTRODUCTION. General Information. Important Warning
 S u r g i c a l M a n u a l F o r M a g i x D e n t a l I m p l a n t INTRODUCTION General Information Read this manual carefully before starting treatment. This manual should be used as a reference guide
S u r g i c a l M a n u a l F o r M a g i x D e n t a l I m p l a n t INTRODUCTION General Information Read this manual carefully before starting treatment. This manual should be used as a reference guide
LIVE SURGERY SEMINAR VERTICAL AND HORIZONTAL BONE AUGMENTATION WITH XENOGENIC BLOCKS
 LIVE SURGERY SEMINAR VERTICAL AND HORIZONTAL BONE AUGMENTATION WITH XENOGENIC BLOCKS OsteoBiol Sp-Block OsteoBiol Dual-Block VENICE DENTAL CENTER 7 TH JULY 2012 VERTICAL AND HORIZONTAL BONE AUGMENTATION
LIVE SURGERY SEMINAR VERTICAL AND HORIZONTAL BONE AUGMENTATION WITH XENOGENIC BLOCKS OsteoBiol Sp-Block OsteoBiol Dual-Block VENICE DENTAL CENTER 7 TH JULY 2012 VERTICAL AND HORIZONTAL BONE AUGMENTATION
DIGITAL DIAGNOSIS AND TREATMENT PLANNING FOR PLACEMENT AND RESTORATION OF SINGLE IMPLANTS IN THE POSTERIOR MAXILLA By Timothy Kosinski, DDS
 DIGITAL DIAGNOSIS AND TREATMENT PLANNING FOR PLACEMENT AND RESTORATION OF SINGLE IMPLANTS IN THE POSTERIOR MAXILLA By Timothy Kosinski, DDS Dental implants have undergone many positive advances in recent
DIGITAL DIAGNOSIS AND TREATMENT PLANNING FOR PLACEMENT AND RESTORATION OF SINGLE IMPLANTS IN THE POSTERIOR MAXILLA By Timothy Kosinski, DDS Dental implants have undergone many positive advances in recent
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Hex-Lock Abutment System. Restorative Manual
 System Restorative Manual 32 Restorative options with s s are manufactured from titanium alloy and used as the support foundation for single- or multiple-unit cement-retained, partially edentulous fixed
System Restorative Manual 32 Restorative options with s s are manufactured from titanium alloy and used as the support foundation for single- or multiple-unit cement-retained, partially edentulous fixed
4766 Research Dr. San Antonio, TX insightdentalsystems.com
 OVERVIEW OF THE INSIGHT DENTAL IMPLANT DELIVERY SYSTEM The IDS system comes in a unit dose implant system where its advantage provides sterile instrumentation in one single-use kit. It is organized to
OVERVIEW OF THE INSIGHT DENTAL IMPLANT DELIVERY SYSTEM The IDS system comes in a unit dose implant system where its advantage provides sterile instrumentation in one single-use kit. It is organized to
GUIDED BONE & TISSUE REGENERATION 2-DAY MASTERCLASS (CHOOSE LONDON OR PARIS) DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND
 GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY MASTERCLASS (CHOOSE LONDON OR PARIS) This hands-on course will be delivered in small group workshops and will equip the
GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY MASTERCLASS (CHOOSE LONDON OR PARIS) This hands-on course will be delivered in small group workshops and will equip the
IOS & The Sirona Connect System Clinician Procedure
 Clinician Procedure Surgeon (Please ensure that these instructions are forwarded to the restorative clinician.) STEP 1: Select a BellaTek Encode Healing Abutment with the appropriate restorative platform
Clinician Procedure Surgeon (Please ensure that these instructions are forwarded to the restorative clinician.) STEP 1: Select a BellaTek Encode Healing Abutment with the appropriate restorative platform
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Contents Graduate Diploma of Dental Implantology
 Graduate Diploma of Dental Implantology Information Brochure Contents Graduate Diploma of Dental Implantology DOH 551 Introduction to Dental Implants and Basic Restorative Implantology Module 1 Fundamentals
Graduate Diploma of Dental Implantology Information Brochure Contents Graduate Diploma of Dental Implantology DOH 551 Introduction to Dental Implants and Basic Restorative Implantology Module 1 Fundamentals
Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants
 Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Long-term success of osseointegrated implants
 Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
Implant Restorations: A Step-By-Step Guide
 Implant Restorations: A Step-By-Step Guide Drago, Carl DDS, MS ISBN-13: 9780813828831 Table of Contents Contributors. Foreword. Acknowledgments. Chapter 1. Introduction To Implant Dentistry. 1. Introduction.
Implant Restorations: A Step-By-Step Guide Drago, Carl DDS, MS ISBN-13: 9780813828831 Table of Contents Contributors. Foreword. Acknowledgments. Chapter 1. Introduction To Implant Dentistry. 1. Introduction.
A new approach with an in-situ self-hardening grafting material
 74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
Case study 25. Implantology Solutions for Atrophic Maxilla Using Short Implants. Dr. Ariel Labanca Mitre
 Case study 25 Implantology Solutions for Atrophic Maxilla Using Short Implants Dr. Ariel Labanca Mitre Oral Implantology Specialist Prosthodontics Specialist Implantology Solutions for Atrophic Maxilla
Case study 25 Implantology Solutions for Atrophic Maxilla Using Short Implants Dr. Ariel Labanca Mitre Oral Implantology Specialist Prosthodontics Specialist Implantology Solutions for Atrophic Maxilla
CASE REPORT. CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration
 Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
A PERIO-PROSTHETIC. with the BIO-GLASS. DR. Mirko Paoli (DDS) DT. Roberto Fabris ABUTMENT SYSTEM
 A PERIO-PROSTHETIC with the TREATMENT use of ABUTMENT SYSTEM BIO-GLASS DR. Mirko Paoli (DDS) DT. Roberto Fabris 110 SUMMER 2015 The implant therapy in dentistry has allowed the modification of prosthetic
A PERIO-PROSTHETIC with the TREATMENT use of ABUTMENT SYSTEM BIO-GLASS DR. Mirko Paoli (DDS) DT. Roberto Fabris 110 SUMMER 2015 The implant therapy in dentistry has allowed the modification of prosthetic
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
Osseointegrated implant-supported
 CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
Osseointegrated dental implants have been used for
 Use of Distraction Osteogenesis for Repositioning of an Osseointegrated Implant: A Case Report Gustavo Mendonça, DDS, MS 1 /Daniela Baccelli Silveira Mendonça, DDS 2 / Alfredo Júlio Fernandes Neto, DDS,
Use of Distraction Osteogenesis for Repositioning of an Osseointegrated Implant: A Case Report Gustavo Mendonça, DDS, MS 1 /Daniela Baccelli Silveira Mendonça, DDS 2 / Alfredo Júlio Fernandes Neto, DDS,
4. What about age? There is no age limit. After puberty, anyone can get dental implants.
 Dental Implants 1. What are Osseointegrated implants? Osseointegrated implants are a new generation of dental implants in Rio de Janeiro, introduced in the 1960 s, they come in different shapes and sizes.
Dental Implants 1. What are Osseointegrated implants? Osseointegrated implants are a new generation of dental implants in Rio de Janeiro, introduced in the 1960 s, they come in different shapes and sizes.
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
Vertical and horizontal alveolar ridge augmentation
 CLINICAL SIMULTANEOUS VERTICAL GUIDED BONE REGENERATION AND GUIDED TISSUE REGENERATION IN THE POSTERIOR MAXILLA USING RECOMBINANT HUMAN PLATELET-DERIVED GROWTH FACTOR: A CASE REPORT Istvan Urban, DMD,
CLINICAL SIMULTANEOUS VERTICAL GUIDED BONE REGENERATION AND GUIDED TISSUE REGENERATION IN THE POSTERIOR MAXILLA USING RECOMBINANT HUMAN PLATELET-DERIVED GROWTH FACTOR: A CASE REPORT Istvan Urban, DMD,
GUIDED BONE & TISSUE REGENERATION 2-DAY LIVE COURSE DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND
 GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY LIVE COURSE Soft tissue management is the key to achieve aesthetic success. Periodontal and peri-implant soft tissue management
GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY LIVE COURSE Soft tissue management is the key to achieve aesthetic success. Periodontal and peri-implant soft tissue management
Ridge Split Procedure
 Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
Innovative Treatment Concepts IN ORAL AND MAXILLOFACIAL SURGERY
 Innovative Treatment Concepts IN ORAL AND MAXILLOFACIAL SURGERY LEADING REGENERATION CLINICAL CASES Dr. J. Aranda Onlay grafting for horizontal augmentation 8 Prof. Dr. D. Buser et al. Onlay grafting for
Innovative Treatment Concepts IN ORAL AND MAXILLOFACIAL SURGERY LEADING REGENERATION CLINICAL CASES Dr. J. Aranda Onlay grafting for horizontal augmentation 8 Prof. Dr. D. Buser et al. Onlay grafting for
Immediate Restorations on Implants in the Esthetic Area
 CLINICAL SCIENCE IJOICR Immediate Restorations on Implants in the Esthetic Area Immediate Restorations on Implants in the Esthetic Area 1 Pedro Peña Martinez, 2 Ramón Palomero Langner, 3 Ramón Palomero
CLINICAL SCIENCE IJOICR Immediate Restorations on Implants in the Esthetic Area Immediate Restorations on Implants in the Esthetic Area 1 Pedro Peña Martinez, 2 Ramón Palomero Langner, 3 Ramón Palomero
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel
 PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
The Use Of 6mm Long Implants In Cases With Limited Bone Height: A Preliminary 6-Month Clinical Study
 26 News No.26 January 2011 The Use Of 6mm Long Implants In Cases With Limited Bone Height: A Preliminary 6-Month Clinical Study Make it Simple 2 The Use Of 6mm Long Implants In Cases With Limited Bone
26 News No.26 January 2011 The Use Of 6mm Long Implants In Cases With Limited Bone Height: A Preliminary 6-Month Clinical Study Make it Simple 2 The Use Of 6mm Long Implants In Cases With Limited Bone
Exclusion Criteria. Subjects were excluded if they were smokers and if they had residual mandible height after
 Stability of Implants Placed in Augmented Posterior Mandible after Alveolar Osteotomy Using Resorbable Nonceramic Hydroxyapatite or Intraoral Autogenous Bone: 12-Month Follow-Up Alexandre M. Dottore, DDS;*
Stability of Implants Placed in Augmented Posterior Mandible after Alveolar Osteotomy Using Resorbable Nonceramic Hydroxyapatite or Intraoral Autogenous Bone: 12-Month Follow-Up Alexandre M. Dottore, DDS;*
soft-tissue regrowth. Pre-treatment. Implants placed with surgical guide for cemented crowns through the incisal edges.
 Extraction of #7 and 8 with Immediate Astra A discussion among dental professionals on the message boards of Dentaltown.com. A terrific case from Dr. Scott Erikson that takes you through the entire process
Extraction of #7 and 8 with Immediate Astra A discussion among dental professionals on the message boards of Dentaltown.com. A terrific case from Dr. Scott Erikson that takes you through the entire process
The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up
 643 The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up Marco Aurélio Bianchini, DDS, MSc, PhD 1 André R. Buttendorf,
643 The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up Marco Aurélio Bianchini, DDS, MSc, PhD 1 André R. Buttendorf,
It is well-known that osseointegrated implants do not
 Infraposition of Implant-Retained Maxillary Incisor Crown Placed in an Adult Patient: Case Report Roberto Cocchetto, MD, DDS 1 /Luigi Canullo, DDS 2 /Renato Celletti, MD, DDS 3 Several studies have clearly
Infraposition of Implant-Retained Maxillary Incisor Crown Placed in an Adult Patient: Case Report Roberto Cocchetto, MD, DDS 1 /Luigi Canullo, DDS 2 /Renato Celletti, MD, DDS 3 Several studies have clearly
EDI Journal. Techniques to control or avoid cement around implant-retained restorations. European Journal for Dental Implantologists TOPIC
 ISSN 1862-2879 Issue 4/2013 Vol. 9 EDI Journal European Journal for Dental Implantologists TOPIC Techniques to control or avoid cement around implant-retained restorations»edi News: Coming up: 9th BDIZ
ISSN 1862-2879 Issue 4/2013 Vol. 9 EDI Journal European Journal for Dental Implantologists TOPIC Techniques to control or avoid cement around implant-retained restorations»edi News: Coming up: 9th BDIZ
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
A novel technique for fabrication of immediate provisional restorations
 Clinical A novel technique for fabrication of immediate provisional restorations Pär-Olov Östman 1 Prosthetic rehabilitation of the edentulous patient with implant-supported restorations is a commonly
Clinical A novel technique for fabrication of immediate provisional restorations Pär-Olov Östman 1 Prosthetic rehabilitation of the edentulous patient with implant-supported restorations is a commonly
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note
 Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
S i m p l i c I t y, c o m f o r t, a e s t h e t i c s. axiom. The new dimension
 S i m p l i c I t y, c o m f o r t, a e s t h e t i c s axiom The new dimension 2 Implants by anthogyr axiom, t h e n e w g e n e r a t i o n i m p l a n t axiom characteristics represent the perfect synthesis
S i m p l i c I t y, c o m f o r t, a e s t h e t i c s axiom The new dimension 2 Implants by anthogyr axiom, t h e n e w g e n e r a t i o n i m p l a n t axiom characteristics represent the perfect synthesis
Surgical Manual. Step By Step Techniques
 Surgical Manual Step By Step Techniques Table of Contents Pre-Surgical 1 8 Measurement of Bone 2 Bone Classification 3 Implant Size Selection 4 5 Surgical Template Fabrication 6 8 Instrumentation 9 11
Surgical Manual Step By Step Techniques Table of Contents Pre-Surgical 1 8 Measurement of Bone 2 Bone Classification 3 Implant Size Selection 4 5 Surgical Template Fabrication 6 8 Instrumentation 9 11
AO Certificate in Implant Dentistry Certificate
 AO Certificate in Implant Dentistry Certificate The AO Certificate in Implant Dentistry provides an opportunity for AO members to demonstrate that they have attained a level of education and experience
AO Certificate in Implant Dentistry Certificate The AO Certificate in Implant Dentistry provides an opportunity for AO members to demonstrate that they have attained a level of education and experience
Case report: Replacement of failing 2 stage implants by basal implants and conventional bridgework
 Case report: Replacement of failing 2 stage implants by basal implants and conventional bridgework Authors Dr. Aleksandar Lazarov Solunska Str. 3 BG-1000 Sofia Bulgaria Email: alex.lazarov@yahoo.co.uk
Case report: Replacement of failing 2 stage implants by basal implants and conventional bridgework Authors Dr. Aleksandar Lazarov Solunska Str. 3 BG-1000 Sofia Bulgaria Email: alex.lazarov@yahoo.co.uk
SURGICAL MANUAL. Step By Step Techniques
 SURGICAL MANUAL Step By Step Techniques TABLE OF CONTENTS PRE-SURGICAL 1 8 MEASUREMENT OF BONE.......................... 2 BONE CLASSIFICATION........................... 3 IMPLANT SIZE SELECTION.........................
SURGICAL MANUAL Step By Step Techniques TABLE OF CONTENTS PRE-SURGICAL 1 8 MEASUREMENT OF BONE.......................... 2 BONE CLASSIFICATION........................... 3 IMPLANT SIZE SELECTION.........................
Devoted to the Advancement of Implant Dentistry
 Devoted to the Advancement of Implant Dentistry Devoted to the Advancement of Implant Dentistry Our ultimate goal is to provide you and your patients with the highest standards in implant case planning
Devoted to the Advancement of Implant Dentistry Devoted to the Advancement of Implant Dentistry Our ultimate goal is to provide you and your patients with the highest standards in implant case planning
International Journal of Applied Dental Sciences 2018; 4(1): Dr. Renu gupta, Dr. RP Luthra, Suhani Kukreja
 2018; 4(1): 213-218 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2018; 4(1): 213-218 2018 IJADS www.oraljournal.com Received: 06-11-2017 Accepted: 07-12-2017 Dr. Renu gupta Professor and head, Department
2018; 4(1): 213-218 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2018; 4(1): 213-218 2018 IJADS www.oraljournal.com Received: 06-11-2017 Accepted: 07-12-2017 Dr. Renu gupta Professor and head, Department
