Clinical Study of Guided Bone Regeneration and/or Bone Grafts in the Treatment of Ligature-induced Peri-implantitis Defects in Dogs
|
|
|
- Abner Payne
- 6 years ago
- Views:
Transcription
1 Braz Dent J (2001) 12(2): Treatment of peri-implantitis in dogs ISSN Clinical Study of Guided Bone Regeneration and/or Bone Grafts in the Treatment of Ligature-induced Peri-implantitis Defects in Dogs Francisco H. NOCITI Jr. 1 Raul G. CAFFESSE 2 Enilson A. SALLUM 1 Maria Ângela N. MACHADO 1 Cristine M. STEFANI 1 Antonio Wilson SALLUM 1 1 Department of Prosthodontics and Periodontics, Division of Periodontics, School of Dentistry at Piracicaba, UNICAMP, Piracicaba, SP, Brazil 2 Department of Stomatology, Division of Periodontics, Univeristy of Texas-Dental Branch, Houston, TX, USA This study evaluated, by clinical analysis, the hard tissue response following treatment of ligature-induced peri-implantitis defects in 5 dogs. The mandibular premolars were removed from both sides of the jaw. After 3 months of healing, two titanium implants were placed on each side of the mandible. Following abutment connection, 3 months later, experimental peri-implantitis was induced by the placement of cotton ligatures in a submarginal position. Ligatures and abutments were removed after one month and the bony defects were randomly assigned to one of the following treatments: debridement (DE), debridement plus guided bone regeneration (GBR), debridement plus mineralized bone graft (BG) and debridement plus guided bone regeneration associated with mineralized bone graft (GBR+BG). The peri-implant bone defects were clinically measured before and 5 months post-treatment. Results showed a higher percentage of vertical bone fill for GBR+BG (27.77 ± 14.07) followed by GBR (21.78 ± 16.19), BG (21.26 ± 6.87), DE (14.03 ± 5.6). However, there were no statistically significant differences between any of the treatments proposed (one way repeated measures analysis of variance, P=0.265). Key Words: peri-implantitis, bioabsorbable membrane, bone graft. INTRODUCTION The long-term predictability of osseointegrated implants has been documented (1). Nevertheless, a significant number of early and late complications have also been reported (2). Current hypothesis associates bacterial infection and/or biomechanical overload as etiologic factors of late implant failure (3). Progressive bone loss around functioning dental implants is of special concern, because it may jeopardize the longterm prosthetic prognosis. The peri-implant bone destruction observed during the implant maintenance phase (peri-implantitis) has symptomatology similar to that of periodontitis, i.e., redness, increased probing depth, suppuration, radiographic bone loss. Several procedures have been described for the treatment of the inflammatory component and the resulting bony defect associated with infection of the peri-implant mucosa, including antimicrobial therapy, resective or regenerative procedures (4-7). Optimal treatment of peri-implantitis must include regeneration of lost bone in direct contact with the implant surface previously exposed to bacterial products. Clinical studies using guided bone regeneration for the treatment of periimplantitis defects present inconclusive results (4,5,8-10). Therefore, the purpose of the present study was to clinically evaluate the hard tissue healing in terms of defect fill following treatment of experimentally ligature-induced peri-implantitis defects using a bioabsorbable membrane (Bio-Guide, Osteohealth Co., Correspondence: Francisco H. Nociti Jr., Faculdade de Odontologia de Piracicaba, UNICAMP, Av. Limeira, 901 Bairro Areião, Piracicaba, SP, Brasil. Tel: Fax: nociti@fop.unicamp.br
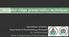
2 128 F.H. Nociti Jr. et al. New York, USA) and/or heterologous mineralized bone graft (Bio-Oss, Osteohealth Co.). MATERIAL AND METHODS Five 2-year-old mongrel dogs with good general health were used in this study (approximately 15 kg body weight). The animals received 1.5 ml/10 kg of acepromazine (Univet S.A., São Paulo, SP, Brazil) followed by intravenous injection of 25% sodium thiopental solution (0.5 ml/kg, Cristália Produtos Químicos e Farmacêuticos Ltda., Itapira, SP, Brazil) and local administration of 2% xylocaine (1:50,000 epinephrine, Merrel Lepetit Farmacêutica Ltda., Santo Amaro, SP, Brazil) in all surgical procedures (Figure 1). At the beginning of the experiment, all mandibular premolars were removed. After 3 months of healing, full-thickness flaps were elevated and two screw-shaped CP titanium implants with rough acid-etched surfaces (Napio System, Napio, Bauru, SP, Brazil) with a length of 8.5 mm, an outer diameter of 3.75 mm, and a pitch height of 0.6 mm, were placed bilaterally and the mucoperiosteal flaps sutured. Three months later, mucoperiosteal flaps were elevated and titanium abutments were connected. Two weeks after the abutment connection, alginate impressions were taken and occlusal acrylic stents were prepared for pre- and post-treatment measurements of bony defect depth. The stents were reduced and polished for better adaptation. Six points were marked on the surface of the stent around the implant: mesio-buccal, mid-buccal, disto-buccal, mesio-lingual, mid-lingual and disto-lingual. Cotton ligatures were placed in a submarginal position around the abutments and the dogs were fed with a soft diet to promote plaque accumulation and induce peri-implant inflammation with loss of bone. After 1 month of plaque accumula- Plaque control Plaque control weeks Extraction of mandibular premolars Placement of the implants Abutment Impression Treatment connection and ligatures Clinical measurements X X Figure 1. Study design. Figure 3. Radiographic appearance of the bone loss around the implants 1 month after placing the ligatures. Note that the morphology of the peri-implant bone defects was wide and circumferential. Figure 2. Clinical aspect of the peri-implant mucosa 1 month after ligature placement. Figure 4. Clinical appearance of the bony defects after debridement.
3 Treatment of peri-implantitis in dogs 129 tion, significant inflammation could be seen at the periimplant mucosa (Figure 2) and bone loss was radiographically detected (Figure 3). At this time, the ligatures were removed, and a plaque-control regime was initiated (hygienic phase) consisting of daily brushing and topical application of 0.12% chlorhexidine gluconate. In addition, metronidazole hydrochloride (250 mg/day, Flagyl, Rhodia Farma Ltda., São Paulo, SP, Brazil) was given systemically for 3 weeks. Two weeks after the beginning of the hygienic phase, full-thickness flaps were elevated. The abutments were removed and the granulation tissue around the implants was carefully removed using teflon hand curettes (Figure 4). The implant surface was treated with an air-powder abrasive instrument (Profi I, Dabi Atlante, Ribeirão Preto, SP, Brazil) for 30 s. The peri-implant bony defects were clinically evaluated and pretreatment depth of the defect, i.e., the distance from the top of the stent to the bottom of the peri-implant bone defect, was recorded using an orthodontic wire (0.8 mm) and an electronic digital caliper (accurate to 0.01 mm) for the six sites around each implant. All linear measurements throughout the study were performed by a calibrated examiner. The defects were randomly assigned to one of the following treatments: DE: debridement, GBR: debridement plus guided bone regeneration (Bio-Guide ), BG: debridement plus mineralized bone graft (Bio-Oss ), GBR+BG: debridement plus the association of guided bone regeneration and bone graft. The flaps were repositioned and sutured. Systemic metronidazole administration (250 mg/ day, Flagyl) was continued for the following week, and 0.12% chlorhexidine gluconate spray was topically Table 1. Percentage of vertical bone fill according to treatment. Treatment Vertical bone fill (%) DE ± 5.60 GBR ± BG ± 6.87 GBR + BG ± Means ± SD (ANOVA, P=0.265). DE: debridement; GBR: debridement plus guided bone regeneration; BG: debridement plus mineralized bone graft; GBR + BG: debridement plus guided bone regeneration/ mineralized bone graft. applied twice a day for the next 5 months. At that time, a mucoperiosteal flap was elevated and post-treatment measurements were obtained by the same method previously described. The experimental design used (complete randomized block design) provided a total of 20 peri-implant defects (five implants per treatment group) for statistical analysis. The six values obtained for each implant were averaged to obtain a mean value for the bony defect depth pre- and post-treatment. Mean hard tissue fill was obtained subtracting post-treatment mean value from pre-treatment mean value for each treatment. The data were statistically analyzed by one way repeated measures analysis of variance (ANOVA). RESULTS Clinical signs of peri-implant inflammation were reduced after 2 weeks of plaque control and systemic antimicrobial administration. In 2 sites, an exposure of the membrane occurred after 3 months of healing. The portion of collagen membrane that was exposed showed a progressive resorption and disappeared after 2 weeks of exposure. The peri-implant tissues around the exposed membranes did not have an inflammatory process. The other 18 sites remained covered by the soft tissues until the end of the experimental period. After 5 months of healing, newly formed hard tissue was observed filling the defects around the implants for all treatments (Table 1). GBR+BG had the best vertical bone fill followed by GBR, BG, and DE; however, the differences among treatments were not statistically significant. DISCUSSION The number of longitudinal studies evaluating different treatment options for peri-implantitis bony defects is limited, probably due to the fact that the frequency of late implant failures is relatively low. Many different approaches have been tested to reduce inflammation at the peri-implant mucosa including subgingival irrigation of the peri-implant area with antiseptic agents (11), systemic antimicrobial treatment (12) and controlled-delivery devices for local application of tetracycline (13). In the present study, as suggested by Hürzeler et al. (5), an association of local and systemic treatment was used resulting in a marked reduction in clinical
4 130 F.H. Nociti Jr. et al. signs of inflammation in the peri-implant mucosa. Once the inflammatory process is controlled, an attempt can be made to improve or re-establish osseointegration using regenerative procedures. An increasing number of reports have been trying to document the predictability of using regenerative procedures to treat bone defects around implants, however the results have been inconclusive. Grunder et al. (4) evaluated the treatment of ligature-induced periimplantitis defects using guided bone regeneration around submerged and nonsubmerged implants in dogs. They concluded that guided bone regeneration did not enhance clinical parameters or bone formation around diseased implants. These results were in disagreement with findings reported by Dahlin et al. (14), Becker et al. (15) and Zablotsky et al. (16), showing new bone formation around exposed implant surfaces after the procedure. Factors such as plaque-contaminated implants, premature membrane exposure and type of bone defect may help to explain the different results. Hürzeler et al. (5) evaluated the treatment of ligature-induced peri-implantitis defects clinically and histologically using guided bone regeneration and/or two types of bone grafts compared with an instrumented control. They observed different degrees of hard tissue fill. Guided bone regeneration and the association of membrane and bone grafts resulted in the greatest hard tissue fill of the defects. The present investigation can be considered the first clinical study, in an animal model, to evaluate the treatment of bone defects resulting from ligature-induced peri-implantitis using regenerative procedures with a bioabsorbable membrane (Bio-Guide ) and a heterologous mineralized bone graft (Bio-Oss ) separately or in combination. Pre- and post-treatment clinical evaluations showed a nonsignificant variable degree of hard tissue fill of the bone defects after all treatment procedures (P=0.265). The chronic circumferential bone defects observed around the implants in the present investigation, after 1 month of plaque accumulation, were similar to those reported by Hürzeler et al. (5), and different from those reported by Grunder et al. (4). Therefore, it would be reasonable to affirm that one of the most critical factors for predictable hard tissue fill around dental implants previously exposed to contaminants is the peri-implant bone defect morphology. Incomplete surface detoxification could be another negative factor for bone growth onto a previously exposed implant surface. In the present study, the observation of defect fill by a bone-like tissue indicated that the procedures used to eliminate contaminants from the implant surface might have been efficient. However, the bone-implant contact cannot be clinically determined. Although there have been many clinical reports (4,5,8-10) showing hard tissue fill of bone defects around implants, some questions still remain to be answered: How much newly formed bone is in contact with the previously exposed implant surface? How much bone to implant contact is necessary to improve the prognosis of the implant? Is it really necessary to use local and/or systemic antimicrobials to treat periimplant infections? Could any growth factor be used alone or in combination with other regenerative therapies to improve bone formation around the exposed implant surface? What is the impact of individual variability on the bone regeneration achieved around dental implants exposed to contaminants? Within the limits of the present investigation, it can be concluded that no difference could be detected between the treatments. Nevertheless, due to the small sample size used, the findings should be considered with caution. RESUMO Nociti Jr FH, Caffesse RG, Sallum EA, Machado MAN, Stefani CM, Sallum AW. Estudo clínico da utilização de regeneração óssea guiada e/ou enxerto ósseo no tratamento de defeitos ósseos resultantes da peri-implantite induzida em cães. Braz Dent J 2001;12(2): O presente estudo avaliou, clinicamente, a resposta do tecido ósseo após o tratamento de defeitos resultantes da peri-implantite induzida por ligaduras em cães. Cinco cães foram utilizados. Os pré molares inferiores foram extraídos de ambos os lados da mandíbula. Após três meses, os intermediários foram conectados aos implantes e a peri-implantite induzida através da colocação de ligaduras em posição submarginal. Um mês mais tarde, as ligaduras e os intermediários foram removidos e os defeitos ósseos resultantes foram aleatoriamente divididos entre os seguintes tratamentos: descontaminação (DE), descontaminação associada a regeneração óssea guiada (GBR), descontaminação associada ao enxerto ósseo (BG) e descontaminação associada a regeneração óssea guiada e ao enxerto ósseo (GBR+BG). Os defeitos ósseos peri-implantares foram clinicamente avaliados antes a após 5 meses do tratamento. Os resultados demonstraram uma maior porcentagem de preenchimento ósseo vertical para GBR+BG (27,77 ± 14,07) seguido por GBR (21,78 ± 16,19), BG
5 Treatment of peri-implantitis in dogs 131 (21,26 ± 6,87), DE (14,03 ± 5,6). Entretanto, a análise de variância não detectou diferenças estatísticas em qualquer um dos tratamentos propostos (P=0,265). Assim, dentro dos limites do presente trabalho, concluiu-se que não há diferença entre os tratamentos investigados. Unitermos: peri-implantite, membrana absorvível, enxerto ósseo. REFERENCES 1. Albrektsson T, Zarb G, Worthington RA, Eriksson RA. The longterm efficacy of currently used dental implants. A review and prognosis criteria for success. Int J Oral Maxillofac Implants 1986;1: Worthington P, Bolender Cl, Taylor TD. The Swedish system of osseointegrated implants: Problems and complications encountered during a 4-year trial period. Int J Oral Maxillofac Implants 1987;2: Mombelli A, von Oosten MAC, Schurch E, Lang NP. The microbiota associated with successful or failing osseointegrated titanium implants. Oral Microbiol Immunol 1987;2: Grunder U, Hürzeler MB Schüpbach P, Strub JR. Treatment of ligature-induced peri-implantitis using guided tissue regeneration: A clinical and histologic study in beagle dog. Int J Oral Maxillofac Implants 1993;8: Hürzeler MB, Quiñones CR, Morrison EC, Caffesse RG. Treatment of peri-implantitis using guided bone regeneration and bone grafts, alone or in combination, in beagle dogs. Part 1: Clinical findings and histologic observations. Int J Oral Maxillofac Implants 1995;10: Persson LG, Ericson I, Berglundh T, Lindhe J. Guided bone regeneration in the treatment of peri-implantitis. Clin Oral Implants Res 1996;7: Wetzel AC, Vlassis J, Caffesse RG, Hämmerle CHF, Lang NP. Attempts to obtain re-osseointegration following experimental peri-implantitis in dogs. Clin Oral Implants Res 1999;10: Zitzmann NU, Naef R, Schärer P. Resorbable versus nonresorbable membranes in combination with Bio-Oss for guided bone regeneration. Int J Oral Maxillofac Implants 1997;12: Lorenzoni M, Pertl C, Keil C, Wegscheider WA. Treatment of peri-implant defects with guided bone regeneration: A comparative clinical study with various membranes and bone grafts. Int J Oral Maxillofac Implants 1998;13: Kohal RJ, Trejo PM, Wirshing C, Hürzeler MB, Caffesse RG. Comparison of bioabsorbable and bioinert membranes for guided bone regeneration around non-submerged implants. An experimental study in mongrel dogs. Clin Oral Implants Res 1999;10: Lavigne SE, Krust-Bray KS, Williams KB, Killoy WJ, Theisen F. Effects of subgingival irrigation with chlorhexidine on the periodontal status of patients with HA-coated Integral dental implants. Int J Oral Maxillofac Implants 1994;9: Mombelli A, Lang NP. Antimicrobial treatment of peri-implant infections. Clin Oral Implants Res 1992;3: Flemmig TF. Infektionen bei osseointegrierten Implantaten Hintergründe und klinische Impliktionen. Implantologie 1994;1: Dahlin C, Sennerby L, Lekholm U, Linde A, Nyman S. Generation of new bone around titanium implants using a membrane technique: An experimental study in rabbits. Int J Oral Maxillofac Implants 1989;4: Becker W, Becker BE, Handelsman M, Ochsenbein C, Albrektsson T. Guided tissue regeneration for implants placed into extraction sockets. A study in dogs. J Periodontol 1991;62: Zablotsky MH, Meffert RM, Caudill R, Evans G. Histologic and clinical comparisons of guided tissue regeneration on dehisced hydroxylapatite-coated and titanium endosseous implant surface: A pilot study. Int J Oral Maxillofac Implants 1991;1: Accepted February 20, 2001
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Interest in and studies on osseointegration
 CASE REPORT A Two-Stage Surgical Approach to the Treatment of Severe Peri-Implant Defect: A 30-Month Clinical Follow- Up Report Jong-Eun Kim, DDS, MSD 1 Ha-Young Kim, DDS, MSD 1 Jung-Bo Huh, DDS, MSD,
CASE REPORT A Two-Stage Surgical Approach to the Treatment of Severe Peri-Implant Defect: A 30-Month Clinical Follow- Up Report Jong-Eun Kim, DDS, MSD 1 Ha-Young Kim, DDS, MSD 1 Jung-Bo Huh, DDS, MSD,
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Over the past few decades, an improved
 RESEARCH SANDBLASTED/ACID-ETCHED VS SMOOTH- SURFACE IMPLANTS: IMPLANT MOBILITY AND CLINICAL REACTION TO EXPERIMENTALLY INDUCED PERI-IMPLANTITIS IN BEAGLE DOGS Rodrigo Tadashi Martines, DDS; Wilson Roberto
RESEARCH SANDBLASTED/ACID-ETCHED VS SMOOTH- SURFACE IMPLANTS: IMPLANT MOBILITY AND CLINICAL REACTION TO EXPERIMENTALLY INDUCED PERI-IMPLANTITIS IN BEAGLE DOGS Rodrigo Tadashi Martines, DDS; Wilson Roberto
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys
 The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Case Presentation. Overall Health. Oral Hygiene. Chief Complaint. I hate my upper denture. I can t taste food. I want an implant solution
 Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
Asufficient quantity of bone is an essential prerequisite
 Clinical Evaluation of a Bilayered Collagen Membrane (Bio-Gide) Supported by Autografts in the Treatment of Bone Defects Around Implants Georges Tawil, DDS, DSc, OD 1 /Georgina El-Ghoule, DDS 2 /Muhieddine
Clinical Evaluation of a Bilayered Collagen Membrane (Bio-Gide) Supported by Autografts in the Treatment of Bone Defects Around Implants Georges Tawil, DDS, DSc, OD 1 /Georgina El-Ghoule, DDS 2 /Muhieddine
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
The Original remains unique.
 The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Long-term Results of Implants Treated with Guided Bone Regeneration: A 5-year Prospective Study
 Long-term Results of Implants Treated with Guided Bone Regeneration: A 5-year Prospective Study Nicola Ursula Zitzmann, Dr Med Dent 1 /Peter Schärer, Prof Dr Med Dent, MS 2 / Carlo Paolo Marinello, Prof
Long-term Results of Implants Treated with Guided Bone Regeneration: A 5-year Prospective Study Nicola Ursula Zitzmann, Dr Med Dent 1 /Peter Schärer, Prof Dr Med Dent, MS 2 / Carlo Paolo Marinello, Prof
Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region
 CLINICAL REPORT 269 George Nikou, Dimitris Nikolidakis, Peter Thoolen, Anton Sculean Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region KEY WORDS
CLINICAL REPORT 269 George Nikou, Dimitris Nikolidakis, Peter Thoolen, Anton Sculean Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region KEY WORDS
As an increasing number of
 LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
The effect of peri-implant bone exposure on soft tissue healing and bone loss in two adjacent implants
 Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH
 JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH How to cite this article: DESHPANDE S S, SARIN S P, PARKHEDKAR R D.PLATFORM SWITCHING OF DENTAL IMPLANTS: PANACEA FOR CRESTAL BONE LOSS?. Journal of Clinical
JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH How to cite this article: DESHPANDE S S, SARIN S P, PARKHEDKAR R D.PLATFORM SWITCHING OF DENTAL IMPLANTS: PANACEA FOR CRESTAL BONE LOSS?. Journal of Clinical
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis.
 Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
Failures in implant therapy. Biological and mechanical complications. Their prevention management. Dr. Katalin Csurgay Dr.
 Failures in implant therapy. Biological and mechanical complications. Their prevention management. Dr. Katalin Csurgay Dr. Tatiana Shkolnik Complications could be: Doctor related Patient related Early
Failures in implant therapy. Biological and mechanical complications. Their prevention management. Dr. Katalin Csurgay Dr. Tatiana Shkolnik Complications could be: Doctor related Patient related Early
Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study
 R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
Early implant placement: 3D radiographic study on the fate of buccal wall
 Early implant placement: 3D radiographic study on the fate of buccal wall A. Lanza 1-2, F. Scognamiglio 1, G. De Marco 1, F. Di Francesco 1, F. Femiano 1-3, M. Lanza 4, A. Itro 5 1 DD-Multidisciplinary
Early implant placement: 3D radiographic study on the fate of buccal wall A. Lanza 1-2, F. Scognamiglio 1, G. De Marco 1, F. Di Francesco 1, F. Femiano 1-3, M. Lanza 4, A. Itro 5 1 DD-Multidisciplinary
We Want to Keep You Smiling. Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide
 We Want to Keep You Smiling Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong Bone for a Healthier Smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
We Want to Keep You Smiling Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong Bone for a Healthier Smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
Posterior mandible and vertical augmentation
 CASE REPORT Bilateral Vertical Ridge Augmentation With Block Grafts and Guided Bone Regeneration in the Posterior Mandible: A Case Report Maria A. Peñarrocha* Jose A. Vina Laura Maestre David Peñarrocha-Oltra
CASE REPORT Bilateral Vertical Ridge Augmentation With Block Grafts and Guided Bone Regeneration in the Posterior Mandible: A Case Report Maria A. Peñarrocha* Jose A. Vina Laura Maestre David Peñarrocha-Oltra
Resorbable vs Non-resorbable Barriers with Immediate Implantation after Functional Loading under Overdenture
 Sahar Elkholy, Hussein Elcharkawi RESEARCH ARTICLE 10.5005/jp-journals-10029-1160 Resorbable vs Non-resorbable Barriers with Immediate Implantation after Functional Loading under Overdenture 1 Sahar Elkholy,
Sahar Elkholy, Hussein Elcharkawi RESEARCH ARTICLE 10.5005/jp-journals-10029-1160 Resorbable vs Non-resorbable Barriers with Immediate Implantation after Functional Loading under Overdenture 1 Sahar Elkholy,
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Please visit the C.E. Pavilion to validate your course attendance Or If There s a Line Go cdapresents.com
 UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
Straumann SmartOne. Stage 4 Af terc are and maintenance. Step 2 Maintenance visit
 Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Successful Bone Formation at Immediate Transmucosal Implants: A Clinical Report
 Successful Bone Formation at Immediate Transmucosal Implants: A Clinical Report Christoph H.F. Hämmerle, PD Dr med dent*/urs Brägger, Prof Dr med dent*/ Bruno Schmid, Dr med dent**/niklaus P. Lang, Prof
Successful Bone Formation at Immediate Transmucosal Implants: A Clinical Report Christoph H.F. Hämmerle, PD Dr med dent*/urs Brägger, Prof Dr med dent*/ Bruno Schmid, Dr med dent**/niklaus P. Lang, Prof
Augmentation of Peri-implant Bone Defects with Different Bone Grafts and Guided Bone Regeneration: A Pilot Experimental Study in the Dog
 Original J.Hard Tissue Biology.15(3): 82-88,2006 Journal of Hard Tissue Biology 15[3] (2006) p82-88 2006The Society for Regenerative Hard Tissue Biology Printed in Japan, All rights reserved. CODEN-JHTBFF,
Original J.Hard Tissue Biology.15(3): 82-88,2006 Journal of Hard Tissue Biology 15[3] (2006) p82-88 2006The Society for Regenerative Hard Tissue Biology Printed in Japan, All rights reserved. CODEN-JHTBFF,
Successful osseointegration of implants has been
 Therapeutic Management for Immediate Implant Placement in Sites with Periapical Deficiencies Where Coronal Bone Is Present: Technique and Case Report Cyril I. Evian, DMD 1 /Ahmed Al-Momani, BDS 2 /Edwin
Therapeutic Management for Immediate Implant Placement in Sites with Periapical Deficiencies Where Coronal Bone Is Present: Technique and Case Report Cyril I. Evian, DMD 1 /Ahmed Al-Momani, BDS 2 /Edwin
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
The use of dental implants to restore. Coated vs Uncoated Implants: Bone Defect Configurations After Progressive Peri-implantitis in Dogs RESEARCH
 RESEARCH Coated vs Uncoated Implants: Bone Defect Configurations After Progressive Peri-implantitis in Dogs Marwa Madi, MDS 1 * Osama Zakaria, MDS, PhD 2 Shohei Kasugai, DDS, PhD 2 In this study, hydroxyapatite
RESEARCH Coated vs Uncoated Implants: Bone Defect Configurations After Progressive Peri-implantitis in Dogs Marwa Madi, MDS 1 * Osama Zakaria, MDS, PhD 2 Shohei Kasugai, DDS, PhD 2 In this study, hydroxyapatite
Effect of thread size on the implant neck area: preliminary results at 1 year of function
 Young-Il Kang* Dong-Won Lee* Kwang-Ho Park Ik-Sang Moon Effect of thread size on the implant neck area: preliminary results at 1 year of function Authors affiliations: Young-Il Kang*, Dong-Won Lee*, Ik-Sang
Young-Il Kang* Dong-Won Lee* Kwang-Ho Park Ik-Sang Moon Effect of thread size on the implant neck area: preliminary results at 1 year of function Authors affiliations: Young-Il Kang*, Dong-Won Lee*, Ik-Sang
Periimplant Regeneration Fenestration
 Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
BOUCHLARIOTOU, Ioana, et al. Abstract
 Article Long-term stability of osseointegrated implants in bone regenerated with a collagen membrane in combination with a deproteinized bovine bone graft: 5- year follow-up of 20 implants BOUCHLARIOTOU,
Article Long-term stability of osseointegrated implants in bone regenerated with a collagen membrane in combination with a deproteinized bovine bone graft: 5- year follow-up of 20 implants BOUCHLARIOTOU,
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Many factors are known to influence the success of
 CLINICAL The Role of Two Different Collagen Membranes for Dehiscence Defect Around Implants in Humans Dong-Woon Lee, DDS, MSD 1,2 Kyeong-Taek Kim, DDS, MSD 1 Yon-Soo Joo, DDS 1 Mi-Kyung Yoo, DDS, MSD 1
CLINICAL The Role of Two Different Collagen Membranes for Dehiscence Defect Around Implants in Humans Dong-Woon Lee, DDS, MSD 1,2 Kyeong-Taek Kim, DDS, MSD 1 Yon-Soo Joo, DDS 1 Mi-Kyung Yoo, DDS, MSD 1
Failures in Endosseous Dental Implants A Literature review
 Eswaran Arumugam et al/ International Journal of Biomedical Research 2015; 6(10): 756-762. 756 International Journal of Biomedical Research ISSN: 0976-9633 (Online); 2455-0566 (Print) Journal DOI: 10.7439/ijbr
Eswaran Arumugam et al/ International Journal of Biomedical Research 2015; 6(10): 756-762. 756 International Journal of Biomedical Research ISSN: 0976-9633 (Online); 2455-0566 (Print) Journal DOI: 10.7439/ijbr
Periimplant Regeneration Fenestration
 Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
CASE REPORT MEGAGEN IMPLANT. AnyRidge. CLINICAL CASE REPORT Davide Farronato, DDs, PhD, PD, AP
 AnyRidge CLINICAL CASE REPORT Davide Farronato, DDs, PhD, PD, AP AnyRidge Clinical Case Ⅰ. Dr. Davide Farronato Baseline - fractured tooth Baseline - fractured tooth #25 Rx view Atraumatic avulsion technique
AnyRidge CLINICAL CASE REPORT Davide Farronato, DDs, PhD, PD, AP AnyRidge Clinical Case Ⅰ. Dr. Davide Farronato Baseline - fractured tooth Baseline - fractured tooth #25 Rx view Atraumatic avulsion technique
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps
 CLINICAL AND RESEARCH REPORTS Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps Jay R. Beagle Despite the continued debate regarding the need for
CLINICAL AND RESEARCH REPORTS Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps Jay R. Beagle Despite the continued debate regarding the need for
Antimicrobial Treatment of Peri-implant Diseases
 Antimicrobial Treatment of Peri-implant Diseases Lisa J. A. Heitz-Mayfield, BDS, MDSc, Odont Dr 1 /Niklaus P. Lang, DDS, MS, PhD 2 Purpose: To review the literature on the treatment of peri-implant diseases.
Antimicrobial Treatment of Peri-implant Diseases Lisa J. A. Heitz-Mayfield, BDS, MDSc, Odont Dr 1 /Niklaus P. Lang, DDS, MS, PhD 2 Purpose: To review the literature on the treatment of peri-implant diseases.
Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident
 Case Report 13 2011 Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident Dr Hitoshi Minagawa Tokyo, Japan Prosthetics Dr Hitoshi Minagawa successfully completed his studies
Case Report 13 2011 Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident Dr Hitoshi Minagawa Tokyo, Japan Prosthetics Dr Hitoshi Minagawa successfully completed his studies
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1.
 Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Immediate Implant Placement Along With Guided Bone Regeneration In Mandibular Anterior Region A Case Report.
 IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
RELIABLE WHEN IT COUNTS. The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4
 RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
Areview of recent studies concerning molar. Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report
 Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Improved osseiointegration techniques have led to
 Experimentally Induced Peri-implantitis: A Review of Different Treatment Methods Described in the Literature Monika Baron, MD 1 /Robert Haas, DMD, MD 2 / Orhun Dörtbudak, DMD, MD 3 /Georg Watzek, DMD,
Experimentally Induced Peri-implantitis: A Review of Different Treatment Methods Described in the Literature Monika Baron, MD 1 /Robert Haas, DMD, MD 2 / Orhun Dörtbudak, DMD, MD 3 /Georg Watzek, DMD,
Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans
 Research Article J Periodontal Implant Sci 2011;41:60-66 doi: 10.5051/jpis.2011.41.2.60 Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans Ji Young
Research Article J Periodontal Implant Sci 2011;41:60-66 doi: 10.5051/jpis.2011.41.2.60 Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans Ji Young
Alveolar ridge preservation techniques
 Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
The use of the LiteTouch Er:YAG laser in peri-implantitis treatment
 The use of the LiteTouch Er:YAG laser in peri-implantitis treatment Authors_Prof. Tzi Kang Peng, Taiwan & Prof. Georgi Tomov, Bulgaria _Introduction With oral implantology experience its Renaissance, the
The use of the LiteTouch Er:YAG laser in peri-implantitis treatment Authors_Prof. Tzi Kang Peng, Taiwan & Prof. Georgi Tomov, Bulgaria _Introduction With oral implantology experience its Renaissance, the
Alveolar Ridge Preservation:
 Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Influence of the position of. implants placed immediately into extraction sockets: An experimental study in dogs
 Influence of the position of implants placed immediately into extraction sockets: An experimental study in dogs Abstract Enzo De Santis, * Luiz A. Salata, Flávia Priscila Pereira, Sara Ferraris, Fabio
Influence of the position of implants placed immediately into extraction sockets: An experimental study in dogs Abstract Enzo De Santis, * Luiz A. Salata, Flávia Priscila Pereira, Sara Ferraris, Fabio
Implant Placement in Maxillary Anterior Region Along with Soft and Hard Tissue Grafting- A Case Report.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
CEMENT-RETAINED PROSTHESES INCREASE RISK OF PERI-IMPLANTITIS WHEN COMPARED TO SCREW- RETAINED PROSTHESES
 Braz J Periodontol - September 2014 - volume 24 - issue 03 CEMENT-RETAINED PROSTHESES INCREASE RISK OF PERI-IMPLANTITIS WHEN COMPARED TO SCREW- RETAINED PROSTHESES Rachel de Queiroz Ferreira Rodrigues
Braz J Periodontol - September 2014 - volume 24 - issue 03 CEMENT-RETAINED PROSTHESES INCREASE RISK OF PERI-IMPLANTITIS WHEN COMPARED TO SCREW- RETAINED PROSTHESES Rachel de Queiroz Ferreira Rodrigues
We want to keep you smiling. Bone regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide
 We want to keep you smiling Bone regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong bone for a healthier smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
We want to keep you smiling Bone regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong bone for a healthier smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
SPECIAL SUPPLEMENT. Inside this issue: 2014 No. 3. Peri-implant disease Implant surface: An evolution Summaries of select scientific publications
 www.jird.com SPECIAL SUPPLEMENT Inside this issue: Peri-implant disease Implant surface: An evolution Summaries of select scientific publications Official Publication of The Institute for Implant and Reconstructive
www.jird.com SPECIAL SUPPLEMENT Inside this issue: Peri-implant disease Implant surface: An evolution Summaries of select scientific publications Official Publication of The Institute for Implant and Reconstructive
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter
 THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
Effect of GBR in Combination with Deproteinized Bovine Bone Mineral on the Healing of Calvarial Defects in Rabbits
 Original Article Effect of GBR in Combination with Deproteinized Bovine Bone Mineral on the Healing of Calvarial Defects in Rabbits AA. Khoshkhoonejad 1, A. Miremadi 2, AR. Rokn 2,3, B. Eslami 4, M. Dehghan
Original Article Effect of GBR in Combination with Deproteinized Bovine Bone Mineral on the Healing of Calvarial Defects in Rabbits AA. Khoshkhoonejad 1, A. Miremadi 2, AR. Rokn 2,3, B. Eslami 4, M. Dehghan
Predictable Synthetic Bone Grafting Procedures for Implant Reconstruction: Part Two
 CLINICAL ARTICLE IJCID Predictable Synthetic Bone Grafting Procedures for Implant Reconstruction: Part Two Predictable Synthetic Bone Grafting Procedures for Implant Reconstruction: Part Two 1 Scott D
CLINICAL ARTICLE IJCID Predictable Synthetic Bone Grafting Procedures for Implant Reconstruction: Part Two Predictable Synthetic Bone Grafting Procedures for Implant Reconstruction: Part Two 1 Scott D
Endosseous cylindric implants are well accepted
 Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Treatment Concepts for PERI-IMPLANTITIS
 Treatment Concepts for PERI-IMPLANTITIS CONTENT Definition, diagnosis and prevalence 3 Risk factors and preventive measures 5 Latest evidence on the treatment of peri-implantitis 6 Clinical Cases Regenerative
Treatment Concepts for PERI-IMPLANTITIS CONTENT Definition, diagnosis and prevalence 3 Risk factors and preventive measures 5 Latest evidence on the treatment of peri-implantitis 6 Clinical Cases Regenerative
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
Bone Density Around Titanium Implants May Be Influenced by Intermittent Cigarette Smoke Inhalation: A Histometric Study in Rats
 Bone Density Around Titanium Implants May Be Influenced by Intermittent Cigarette Smoke Inhalation: A Histometric Study in Rats Francisco Humberto Nociti, Jr, DDS, MS, PhD 1 /João Batista César Neto, DDS
Bone Density Around Titanium Implants May Be Influenced by Intermittent Cigarette Smoke Inhalation: A Histometric Study in Rats Francisco Humberto Nociti, Jr, DDS, MS, PhD 1 /João Batista César Neto, DDS
Guided bone regeneration around 1-stage nonsubmerged dental implants with periimplant bone defects: A retrospective case series study
 Guided bone regeneration around 1-stage nonsubmerged dental implants with periimplant bone defects: A retrospective case series study Abstract Objective Amparo Aloy Prósper, a David Peñarrocha Oltra, a
Guided bone regeneration around 1-stage nonsubmerged dental implants with periimplant bone defects: A retrospective case series study Abstract Objective Amparo Aloy Prósper, a David Peñarrocha Oltra, a
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 67 Efficacy Evaluation of a New Buccal Bone Plate Preservation Technique: A Pilot Study Federico Brugnami, DDS* Alfonso Caiazzo, DDS**
The International Journal of Periodontics & Restorative Dentistry 67 Efficacy Evaluation of a New Buccal Bone Plate Preservation Technique: A Pilot Study Federico Brugnami, DDS* Alfonso Caiazzo, DDS**
A simple approach to preserve keratinized mucosa around implants using a pre-fabricated implantretained stent: a report of two cases
 Case Report J Periodontal Implant Sci 2010;40:194-200 doi: 10.5051/jpis.2010.40.4.194 A simple approach to preserve keratinized mucosa around implants using a pre-fabricated implantretained stent: a report
Case Report J Periodontal Implant Sci 2010;40:194-200 doi: 10.5051/jpis.2010.40.4.194 A simple approach to preserve keratinized mucosa around implants using a pre-fabricated implantretained stent: a report
The International Journal of Periodontics & Restorative Dentistry
 The nternational Journal of Periodontics & Restorative Dentistry 2009 BY QUNTESSENCE PUBLSHNG CO, NC. PRNTNG OF THS DOCUMENT S RESTRCTED TO PERSONAL USE ONLY. NO PART OF THS ARTCLE 549 Time Sequence of
The nternational Journal of Periodontics & Restorative Dentistry 2009 BY QUNTESSENCE PUBLSHNG CO, NC. PRNTNG OF THS DOCUMENT S RESTRCTED TO PERSONAL USE ONLY. NO PART OF THS ARTCLE 549 Time Sequence of
Key words: Peri- implant Mucositis, Peri- implantitis, Peri- implant Diseases, Treatment
 PERIODONTOLOGY 2000 Management of peri- implant mucositis and peri- implantitis Elena Figuero 1, Filippo Graziani 2, Ignacio Sanz 1, David Herrera 1,3, Mariano Sanz 1,3 1. Section of Graduate Periodontology,
PERIODONTOLOGY 2000 Management of peri- implant mucositis and peri- implantitis Elena Figuero 1, Filippo Graziani 2, Ignacio Sanz 1, David Herrera 1,3, Mariano Sanz 1,3 1. Section of Graduate Periodontology,
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
Porous titanium granules in the treatment of peri-implant osseous defects a 7-year follow-up study
 Andersen et al. International Journal of Implant Dentistry (2017) 3:50 DOI 10.1186/s40729-017-0106-2 International Journal of Implant Dentistry SHORT REPORT Open Access Porous titanium granules in the
Andersen et al. International Journal of Implant Dentistry (2017) 3:50 DOI 10.1186/s40729-017-0106-2 International Journal of Implant Dentistry SHORT REPORT Open Access Porous titanium granules in the
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report
 Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Esthetic management of multiple missing anterior teeth A Case report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
Root Surface Defect Produced by Hand Instruments and Ultrasonic Scaler with Different Power Settings: an In Vitro Study
 58 Braz Dent J (2009) 20(1): 58-63 R.C.V. Casarin et al. ISSN 0103-6440 Root Surface Defect Produced by Hand Instruments and Ultrasonic Scaler with Different Power Settings: an In Vitro Study Renato Corrêa
58 Braz Dent J (2009) 20(1): 58-63 R.C.V. Casarin et al. ISSN 0103-6440 Root Surface Defect Produced by Hand Instruments and Ultrasonic Scaler with Different Power Settings: an In Vitro Study Renato Corrêa
The healing of an extraction socket often produces
 Immediate One-Stage Postextraction Implant: A Human Clinical and Histologic Case Report Roberto Cornelini, MD, DDS 1 /Antonio Scarano, DDS 2 /Ugo Covani, MD, DDS 3 / Giovanna Petrone, DDS 2 /Adriano Piattelli,
Immediate One-Stage Postextraction Implant: A Human Clinical and Histologic Case Report Roberto Cornelini, MD, DDS 1 /Antonio Scarano, DDS 2 /Ugo Covani, MD, DDS 3 / Giovanna Petrone, DDS 2 /Adriano Piattelli,
Working together as a team, the periodontist
 The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants
 Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Many of the problems reported by conventional
 Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
Hiron Andreaza da Cunha, MS 1 /Carlos Eduardo Francischone, DMD 2 /Hugo Nary Filho, DDS 3 / Rubelisa Cândido Gomes de Oliveira, BDS 4
 A Comparison Between Cutting Torque and Resonance Frequency in the Assessment of Primary Stability and Final Torque Capacity of and TiUnite Single-Tooth Implants Under Immediate Loading Hiron Andreaza
A Comparison Between Cutting Torque and Resonance Frequency in the Assessment of Primary Stability and Final Torque Capacity of and TiUnite Single-Tooth Implants Under Immediate Loading Hiron Andreaza
Evidence-based decision making in periodontal tooth prognosis
 Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study
 Original Article Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study P. Singh, H. G. Garge*, V. S. Parmar, M. Viswambaran*, M. M. Goswami*
Original Article Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study P. Singh, H. G. Garge*, V. S. Parmar, M. Viswambaran*, M. M. Goswami*
Implant osseointegration and successful restoration
 Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Reclaiming the Lost Bastion for Successful Implant Therapy: A Case Series
 Rima Jaiswal et al Case Report 10.5005/jp-journals-10012-1146 Reclaiming the Lost Bastion for Successful Implant Therapy: A Case Series 1 Rima Jaiswal, 2 S Mahantesha, 3 S Ashwini ABSTRACT Introduction:
Rima Jaiswal et al Case Report 10.5005/jp-journals-10012-1146 Reclaiming the Lost Bastion for Successful Implant Therapy: A Case Series 1 Rima Jaiswal, 2 S Mahantesha, 3 S Ashwini ABSTRACT Introduction:
Peri-implant Augmentation
 Indication Sheet PIR3 Peri-implant Augmentation Early implantation with simultaneous GBR for contour augmentation using the technique by Prof. Daniel Buser and Prof. Urs Belser, University of Berne, Switzerland
Indication Sheet PIR3 Peri-implant Augmentation Early implantation with simultaneous GBR for contour augmentation using the technique by Prof. Daniel Buser and Prof. Urs Belser, University of Berne, Switzerland
01/05/2014. Background. Minimally invasive tooth extraction. Thomas Dietrich Professor of Oral Surgery University of Birmingham, School of Dentistry
 Background Remodelling of alveolar bone following extraction Minimally invasive tooth extraction Thomas Dietrich Professor of Oral Surgery University of Birmingham, School of Dentistry 2 weeks 4 weeks
Background Remodelling of alveolar bone following extraction Minimally invasive tooth extraction Thomas Dietrich Professor of Oral Surgery University of Birmingham, School of Dentistry 2 weeks 4 weeks
Vertical Augmentation
 Indication Sheet V Dr. Mauro Merli Vertical Augmentation Vertical alveolar ridge augmentation by means of the fence technique with Geistlich biomaterials > Original publication of the technique on PubMed;
Indication Sheet V Dr. Mauro Merli Vertical Augmentation Vertical alveolar ridge augmentation by means of the fence technique with Geistlich biomaterials > Original publication of the technique on PubMed;
Redefining Regeneration
 Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Cytoflex Barrier Membrane Clinical Evaluation
 Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
A Multicenter Report on 1,022 Consecutively Placed ITI Implants: A 7-Year Longitudinal Study
 A Multicenter Report on 1,022 Consecutively Placed ITI Implants: A 7-Year Longitudinal Study Daniel Brocard, DCD, DSO 1 /Pierre Barthet, DCD, DSO 2 /Eric Baysse, DCD 1 / Jean François Duffort, DCD, DSO
A Multicenter Report on 1,022 Consecutively Placed ITI Implants: A 7-Year Longitudinal Study Daniel Brocard, DCD, DSO 1 /Pierre Barthet, DCD, DSO 2 /Eric Baysse, DCD 1 / Jean François Duffort, DCD, DSO
Deploying Alpha-Bio Tec s NeO Selftapping Implant in an Atrophic Crest: Vestibular-Cortical Stabilization with Bone Graft
 The Atrophic crest Deploying Alpha-Bio Tec s NeO Selftapping Implant in an Atrophic Crest: Vestibular-Cortical Stabilization with Bone Graft Dr. Paolo Borelli DDS, Italy Dr. Massimiliano Favetti DDS, Italy
The Atrophic crest Deploying Alpha-Bio Tec s NeO Selftapping Implant in an Atrophic Crest: Vestibular-Cortical Stabilization with Bone Graft Dr. Paolo Borelli DDS, Italy Dr. Massimiliano Favetti DDS, Italy
