Thick vs. Thin Gingival Biotypes: A Key Determinant in Treatment Planning for Dental Implants
|
|
|
- Ernest Watts
- 6 years ago
- Views:
Transcription
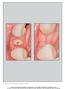
1 r s Thick vs. Thin Gingival Biotypes: A Key Determinant in Treatment Planning for Dental Implants richard t. kao, dds, phd; mark c. fagan, ms, dds; and gregory j. conte, ms, dmd abstract During the treatment planning process, it is important to recognize differences in gingival tissue can affect treatment outcomes. The concept that thick and thin gingival biotypes have different responses to inflammation and trauma was previously introduced. In this paper, this concept is expanded in that gingival biotypes dictate different procedures for implant site preparation. With appreciation of these differences, preparatory steps can be taken to create a more ideal implant placement site. authors Richard T. Kao, DDS, PhD, is in private practice in Cupertino, Calif., associate clinical professor, University of California, San Francisco, and associate adjunct professor, University of the Pacific Arthur A. Dugoni School of Dentistry, San Francisco. Mark C. Fagan, MS, DDS, is in private practice in San Jose, Calif., assistant clinical professor, University of California, San Francisco. Gregory J. Conte, MS, DMD, is in private practice in San Francisco. acknowledgment This paper is dedicated to Drs. Ivan Ancell and Joseph Zingale who helped guide the authors during our periodontal training in the development and thought process behind this paper. Previously, the importance of taking into consideration the differences in gingival tissue during treatment planning has been emphasized. Specifically, it was pointed out how thick and thin gingival biotypes respond differently to inflammation, restorative trauma, and parafunctional habits. 1,2 These traumatic events result in various types of periodontal defects, which respond to different treatments. The authors also pointed out how periodontal surgery techniques have made it possible to change a thin gingival biotype into a thick gingival form. This provides a more favorable restorative environment and increases the predictability of treatment outcomes. In this paper, the authors extend their earlier observations of thick vs. thin gingival tissues and describe why it is important to appreciate tissue biotypes during implant treatment planning. Thick and Thin Gingival Biotypes Historically, Ochsenbein and Miller have discussed the importance of thick vs. thin gingiva in restorative treatment planning. 1 In a population study, thick periodontal biotypes (85 percent) were found to be more prevalent than thin scalloped forms (15 percent). 3 Subsequently, the authors published a paper that further analyzed thick and thin tissue biotypes in terms of their gingival and osseous architecture. 2 Thick gingival tissue is probably the image most associated with periodontal health (figure 1a, table 1). The tissue is dense in appearance with a fairly large zone of attachment. The gingival topography is relatively flat with the suggestion of a thick underlying bony architecture. Surgical evaluation of these areas often reveals relatively thick underlying osseous forms (figure 1b). march
2 table 1 Characteristics of Thick Gingiva n Relatively flat soft tissue and bony architecture n Dense fibrotic soft tissue n Relatively large amount of attached gingiva n Thick underlying osseous form n Relatively resistant to acute trauma n Reacts to disease with pocket formation and infrabony defect formation 1a. figures 1a-b. The clinical presentation of thick gingiva and the type of osseous architecture associated with this gingival tissue type. 1b. table 2 Characteristics of Thin Gingiva n Highly scalloped soft tissue and bony architecture n Delicate friable soft tissue n Minimal amount of attached gingiva n Thin underlying bone characterized by bony dehiscence and fenestration n Reacts to insults and disease with gingival recession 2a. 2b. figures 2a-b. Clinical presentation of thin gingiva is characterized by thin friable tissue. It is associated with clefts, perforation, and gingival recession. table 3 Comparison of Tissue Response to Inflammation, Surgery and Tooth Extraction Inflammation Surgery Thick Gingival Biotype Soft tissue: Marginal inflammation; cyanosis; bleeding on probing; edema/ fibrotic changes Hard tissue: bone loss with pocket formation/infrabony defects Predicable soft and hard tissue contour after healing. Thin Gingival Biotype Soft tissue: Thin marginal redness and gingival recession Hard tissue: Rapid bone loss associated with soft tissue recession Difficult to predict where tissue will heal and stabilize Tooth Extraction Minimal ridge atrophy Ridge resorption in the apical and lingual direction Thin gingival tissue tends to be delicate and almost translucent in appearance (figures 2a-b, table 2). The tissue appears friable with a minimal zone of attached gingiva. The soft tissue is highly accentuated and often suggestive of thin or minimal bone over the labial roots. Surgical evaluation often reveals thin labial bone with the possible presence of fenesfigure 2c. The osseous architecture associated with this gingival tissue type is characterized by fenestration and dehiscence. tration and dehiscence (figure 2c). In the authors previous paper, it was suggested that since these two tissue biotypes have different gingival and osseous architectures, they exhibit different pathological responses when subjected to inflammatory, traumatic, or surgical insults 2 (table 3). These different responses dictate different treatment modalities. It also was noted that current periodontal surgical techniques have the potential to improve tissue quality, thereby enhancing the restorative environment. The paradigm shift proposed was that by taking into consideration the gingival tissue biotype during treatment planning, more appropriate strategies for periodontal management may be developed, resulting in more predictable treatment outcomes. 194 march 2008
3 Tissue Biotype in Implant Treatment Planning If osseous and gingival tissues are different for thick and thin tissue biotypes, it seems logical that these distinctions would significantly influence implant site preparation and treatment planning. This is consistent with previous observations that the stability of the osseous crest and soft tissue is directly proportional to the thickness of the bone and gingival tissue. 4,5 Thick bony plates associated with thick biotypes and thin plates with potential fenestrations and dehiscence associated with thin biotypes respond differently to extraction and have a different pattern of osseous remodeling following this procedure. The trauma induced by the extraction procedure is more likely to result in fracture of the labial plate in the thin biotype than in the thick one. Also, the remodeling process that follows over the next few months will result in more dramatic alveolar resorption in the apical and lingual direction for the ridge associated with thin biotypes. Even after initial alveolar ridge remodeling, the gingival tissue and bone are more likely to continue to recede, especially if the implant is labially inclined. This underscores the importance of appreciating gingival tissue biotypes during implant treatment planning. Furthermore, when these tissue biotypes are carefully considered, various periodontal and surgical strategies can be employed to improve the treatment outcome either by minimizing alveolar resorption or by providing a better tissue environment for implant placement. Extraction of Teeth in Thick vs. Thin Biotypes Though extractions should always be atraumatic, teeth with thin gingival biotypes merit more attention due to their association with thin figure 3a. Tooth No. 9 has a fractured root. figure 3c. The anchor post is placed through a perforation in an impression tray containing bite registration material. Using the tray as a base, the anchor post is ratcheted such that the root is elevated. alveolar plates. Possible strategies that should be considered include: n Minimizing leveraging forces toward the thin labial plate. Most of the manipulation should be focused on the interproximal area. n Sectioning the root(s) from the tooth, when possible, to improve the likelihood for elevation. n Using periotomes to expand and elevate the tooth with controlled force focused on the periodontal ligament space. The placement and elevation force should be focused on the interproximal space so leverage force is exerted on either the buccal or lingual plate. n Using a ratchet extraction device to apply reciprocating force on adjacent teeth while extruding the amputated root tip out the socket (figure 3). This may be the most effective and atraumatic approach for the broken tooth. The tooth is amputated to the level of the cementoenamel junction. After preparation of a post space, an anchoring device is used to engage the root. This device is passed through a quadrant tray with figure 3b. The crown is removed and the anchor post is placed into the root tip figure 3d. The extracted root. This technique is advantageous since there is no force placed on the socket and surrounding bone contact bite registration and impression material for the adjacent teeth. After the impression material has set, the anchoring device is ratcheted against the top of the quadrant tray. This strategy is atraumatic and applies no forces on the surrounding alveolar bone. Atraumatic extraction and preservation of the alveolar plate are essential if the site is to be used for implant placement. Excessive force is likely to fracture the alveolar plate and result in bone resorption and unpredictable bone healing. This is more pronounced with the thin alveolar plate associated with thin gingival biotypes. When compromise of the alveolar plate is suspected, it is essential to utilize ridge preservation or augmentation protocols. Ridge Preservation in Thick vs. Thin Biotypes Prevention of postextraction alveolar bone loss is critical in assuring implant success. Given the thin alveolar plate associated with thin periodontal biotypes, it is not unusual to see more extensive ridge march
4 figure 4a. Lower left lateral incisor No. 23 was extracted and extensive bone loss was present. A 12-mm tenting bone screw was placed to support the graft material and prevent collapse of the membrane. remodeling when compared to the thicker alveolar plate associated with thick biotypes. Not only is atraumatic extraction critical to minimize this postextraction remodeling, it is important to consider strategies to preserve the alveolar bone, such as socket preservation or ridge preservation procedures. A number of studies have shown that without intervention, significant alterations in most extraction ridge dimensions will occur. 6-9 This loss can be 1.5 to 2.0 mm over the first 12 months with most loss occurring during the initial three months. 9 A variety of approaches can be employed to address this problem, but most involve grafting the extraction socket and using membranes to support missing/perforated bony walls. Ridge preservation should be considered for most thin biotype cases and in thick biotype cases where excessive trauma or a previous history of endodontic surgery/fistula tracts may have compromised the alveolar plate. Classically, socket or ridge preservation involves the use of a graft material placed in the socket followed by a variety of other substances such as demineralized freeze-dried bone allograft, mineralized freeze-dried bone allograft, xenograft (mostly of bovine source), and alloplastic materials (b-tricalcium phosphate, durapatite, hydroxyapatite). Since the site will be used for implant placement approximately three months to four months after grafting, it is important to select a graft material that resorbs quickly since only newly formed bone will contribute figure 4b. Bone graft material and a resorbable membrane were placed, (Biomend Extend. Zimmer Dental. Carlsbad, Calif.) to the osseointegration of the dental implants. For that reason, slow resorption graft materials such as xenografts and nonresorbable alloplastic materials (durapatite, hydroxyapatite) should be avoided. When there is excessive volume of nonresorbable graft materials, there is inadequate room for bone ingrowth to provide implant osteointegration. Additionally, the ridge preservation strategy is only successful if the graft material is retained in the extraction socket. A variety of approaches can be utilized to achieve socket closure. These include the use of barrier membranes, tenting pins, collagen plugs, connective tissue grafts, free gingival grafts, acellular dermal grafts, and advancement of the buccal flap. An advanced case of socket preservation with regeneration of the labial plate and vertical dimension is seen in figure 4. Whereas simple cases with intact buccal and lingual plates can be easily managed with grafting and socket coverage, advanced cases may require space-maintaining devices such as tenting pins and membranes. All of these options work to a certain extent and the selection should be based on individual cases/requirements. When excessive bone is lost to resorption, leaving a narrow ridge with a large buccal deficiency or decreased vertical height, a block graft is generally the technique that yields predictable results The block graft material can be of autologous or allograft origin. Autologous graft material is commonly harvested from either the mandibular figure 4c. Re-entry at five months, which illustrates bone regeneration up to the top of the bone screw. ramus or mandibular symphysis. Allograft block grafts can be obtained from several commercial providers. The advantage of this technique is that the graft is placed as a block instead of in particulate form, providing increased structural support. A case of block grafting is presented where there is a narrowed anterior maxillary ridge defect (figure 5a). These situations generally require two-stage surgical procedures that included a bone graft surgery followed by implant placement after graft healing. In this situation, it is critical that soft tissue incisions be carefully planned to allow for flap relaxation over the increased volume gained by the graft and to ensure tensionless primary closure. Once adequate access was gained, the graft and recipient bed were prepared to obtain intimate, broad contact between the surfaces. The recipient bed was perforated to enhance revascularization and the graft was stabilized using fixation screws to maintain close bone contact and prevent graft rotation (figure 5b). Adequate primary fixation is essential for graft survival. Particulate bone can be packed around the block and a resorbable collagen membrane can be placed over the entire graft. The soft tissue flap is then advanced and sutured for primary closure. After a healing period of five to six months, the site can be re-entered and integration of the graft to the recipient bone confirmed. Using an appropriate surgical stent, implants can then be properly placed into the widened ridge (figure 5c). 196 march 2008
5 figure 5a. Extensive defect noted upon flap elevation. figure 6a. The initial defect after tooth extraction. The defect is mainly a three-wall defect with almost complete loss of facial bone. figure 6c. A pediculated connective tissue graft was used to cover the grafted defect, maintaining soft tissue height and width. In this second case of deficient alveolar ridge, it is essential to rebuild both the hard and soft tissue components in a single procedure to improve the esthetics and to minimize surgical visits (figure 6a). This case illustrates a three-wall defect, which has better regenerative potential than the one-wall type discussed previously. For this defect, particulate bone can be used as long as two critical components of regeneration are included: space maintenance and adequate soft tissue closure. In order to maintain the defect figure 5b. The area was prepared and a block allograft was trimmed and fixated with two bone screws (J Block Cortico-Cancellous Bone Allograft, Zimmer Dental). figure 6b. The defect was filled with FDBA and a tenting pin was placed for space maintenance. figure 6d. On re-entry, there is both adequate volume of hard, as well as soft, tissue for implant placement. Immediate Implants in Thick vs. Thin Biotypes Whether a practitioner chooses to place an implant as a delayed or immediate treatment will depend on the conditions of each case. A delayed implant approach might be taken when there is not enough thickness in periodontal tissues to predictably minimize alveolar resorption secondary to healing, or a lack of anchoring bone to ensure stabilization. The decision is also dependent on the practitioner s comfort level in available reconstructive techniques. For a thin biotype case, practitioners must be aware of the possibility of significant resorption, which may have an impact on esthetics. Furthermore, the loss of peri-implant structures may result in thin, transspace, a tenting pin was placed in the socket in an orientation to help support both the facial and vertical dimensions. Particulate freeze-dried bone allograft material was packed into the socket around the tenting pin, slightly overfilling the defect (figure 6b), and a resorbable collagen membrane was trimmed and placed over the graft material. Soft tissue closure over the membrane and graft is critical for proper healing. If the facial flap is advanced over the defect, the vestibular tissue will be figure 5c. Re-entry at six months. Note the excellent ridge width obtained and the ideal implant placement in the augmented site. pulled coronally, possibly resulting in a lack of adequate attached tissue, and thereby creating a thin case that will compromise future implant placement. A technique for covering the socket after tooth extraction using a pediculated connective tissue graft was described by Mathews. 12 Utilizing this closure technique over the grafted socket permitted complete soft tissue coverage. Additionally, it maintained both vertical and horizontal soft tissue components, and increased the thickness of facial attached tissue (figure 6c). After healing for five to six months, the site was re-entered and an implant was placed (figure 6d). This case illustrates the transformation of a severely thin defect into a more advantageous thick periodontium. march
6 figure 7a. Initial presentation of maxillary left central with fractured root. Relatively minor facial inflammation and recession are present. figure 7c. Radiograph of implant prior to implant exposure. figure 7b. Incisal view of immediate implant placement after tooth extraction. figure 7d. Final crown restoration. lucent tissue over the implant, which appears grayish, especially if the facial plate is lost and implant threads are exposed. In these cases, further bone and soft tissue grafting procedures may be necessary. However, once an implant is in place, it may be difficult to regain pre-extraction tissue contours. In a thick biotype environment, immediate placement of an implant can be completed with predictable results. 13 There also is evidence that placement of an immediate implant can help preserve the osseous structures. 14 Even in cases where there is relatively thick tissue present, simultaneous soft and hard tissue preservation/augmentation techniques along with immediate implant placement may be necessary to achieve the best esthetic outcome. Proper treatment planning between the implant surgeon and restorative dentist is essential when optimal esthetic results are desired. An illustrative case is a patient presented with a fracture in the root of the maxillary left central incisor (figure 7a). After appropriately evaluating periodontal tissue characteristics and other necessary surgical and restorative information, a treatment plan was developed that called for extraction of the tooth and immediate implant placement (figure 7b). After hard tissue grafting to fill the facial gap of the socket, closure of the implant-socket was completed with a pediculated connective tissue graft. 12 A radiograph (figure 7c) was taken prior to exposure of the implant. The implant was then exposed and the patient was referred back to his restorative dentist for placement of the final crown (figure 7d). Summary In this paper, the authors continue to develop the thesis that evaluation of gingival tissue biotypes is important in treatment planning. Since thick and thin gingival biotypes are associated with thick and thin osseous patterns, the two tissue types will respond differently to the trauma of extraction and have different patterns of osseous remodeling following the procedure. By understanding the nature of the tissue biotype, the practitioner can employ appropriate periodontal and surgical procedures to minimize alveolar resorption and provide a more favorable tissue environment for implant placement. This is especially important in thin periodontal biotypes where the thin alveolar plate is highly susceptible to remodeling. Additionally, these techniques when appropriately applied can save on treatment time and cost for patients. references 1. Ochsenbein C, Ross S, A re-evaluation of osseous surgery. Dent Clin North Am 13(1):87-102, January Kao RT, Pasquinelli K, Thick vs. thin gingival tissue: a key determinant in tissue response to disease and restorative treatment. J Calif Dent Assoc 30(7):521-6, July Olsson M, Lindhe J, Periodontal characteristics in individuals with varying forms of the upper central incisors. J Clin Periodontol 18:78-82, Tarnow DP, Magner AW, Fletcher P, The effect of the distance from the contact point to the crest of bone on the presence or absence of the interproximal dental papilla. J Periodontol 62: , Maynard JG Jr, Wilson RD, Physiologic dimensions of the periodontium significant to the restorative dentist. J Periodontol 50:170-4, Atwood DA, Postextraction changes in the adult mandible as illustrated by microradiographs and mid-sagittal section and serial cephalometric roentgenographs. J Prosthet Dent 13:810-6, Lekovic V, Kenny EB, et al, A bone regenerative approach to alveolar ridge maintenance following tooth extraction. J Periodontol 68:563-70, Pietrokovski J, Massler M, Alveolar ridge resorption following tooth extraction. J Prosthet Dent 17:21-7, Schropp L, Wenzel A, et al, Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12-month prospective study. Int J Periodontics Restorative Dent 23:313-23, Levin L, Nitzan D, Schwarz-Arad D, Success of dental implants placed in intraoral block bone grafts. J Periodontol 78(1):18-21, McCarthy C, Patel RR, et al, Dental implants and onlay grafts in the anterior maxilla: Analysis of clinical outcome. Int J Oral Maxillofac Implants 18(2):238-41, Mathews D, The pediculated connective tissue graft: a technique for improving unaesthetic implant restorations. Pract Proced Aesthet Dent 14(9):719-24, Sammartino G, Marenzi G, et al, Aesthetics in oral implantology: biological, clinical, surgical, and prosthetic aspects. Implant Dent Mar 16(1):24-65, Dennison HW, Kalk W, et al, Anatomic considerations for preventive implantation. Int J Oral Maxillofac Implants 8:191-6, to request a printed copy of this article, please contact/ Richard T. Kao, DDS, PhD, S. DeAnza Blvd., Suite D1, Cupertino, Calif., march 2008
Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants
 Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Limited bone availability makes implant placement challenging
 Bone Grafting: Essential Indications and Techniques in Implant Dentistry Limited bone availability makes implant placement challenging and sometimes unpredictable. Candidates for implant therapy must have
Bone Grafting: Essential Indications and Techniques in Implant Dentistry Limited bone availability makes implant placement challenging and sometimes unpredictable. Candidates for implant therapy must have
Immediate Implant Placement:
 Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
(Images are at the end of article)
 Long term provisionalization during periodontal surgery and extraction site tissue grafting: A Case Review Michael Tischler, DDS Diplomate American Board Of Oral Implantology/Implant Dentistry (Images
Long term provisionalization during periodontal surgery and extraction site tissue grafting: A Case Review Michael Tischler, DDS Diplomate American Board Of Oral Implantology/Implant Dentistry (Images
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
Working together as a team, the periodontist
 The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
All Dentistry is Cosmetic Betsy Bakeman, DDS Arkansas State Dental Association
 All Dentistry is Cosmetic Betsy Bakeman, DDS Arkansas State Dental Association Patients have traditionally sought treatment when concerned with the way their teeth look, function or feel. Over the past
All Dentistry is Cosmetic Betsy Bakeman, DDS Arkansas State Dental Association Patients have traditionally sought treatment when concerned with the way their teeth look, function or feel. Over the past
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Surgical reconstruction of lost papilla around implant with a modified technique: A case report
 Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
Socket Treatment. Procedure Guide
 Socket Treatment Procedure Guide www.implantdirect.com 888.649.6425 Extraction Healing and Ridge Resorption The Why Working with patients to educate them on the benefits of bone maintenance post extraction
Socket Treatment Procedure Guide www.implantdirect.com 888.649.6425 Extraction Healing and Ridge Resorption The Why Working with patients to educate them on the benefits of bone maintenance post extraction
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior
 Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
MODIFIED SINGLE ROLL FLAP APPROACH FOR SIMULTANEOUS IMPLANT PLACEMENT AND GINGIVAL AUGMENTATION
 Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation. Sanju P. Jose
 Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Patients esthetic demands and
 Predictable Periimplant Gingival Esthetics: Use of the Natural Tooth as a Provisional following Implant Placement ROBERT C. MARGEAS, DDS* ABSTRACT Maintaining the interdental papilla and bone height following
Predictable Periimplant Gingival Esthetics: Use of the Natural Tooth as a Provisional following Implant Placement ROBERT C. MARGEAS, DDS* ABSTRACT Maintaining the interdental papilla and bone height following
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques
 I J Pre Clin Dent Res 2014;1(2):49-53 April-June All rights reserved International Journal of Preventive & Clinical Dental Research Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and
I J Pre Clin Dent Res 2014;1(2):49-53 April-June All rights reserved International Journal of Preventive & Clinical Dental Research Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and
Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS
 Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Alveolar ridge preservation techniques
 Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
Then and Now. Implant Therapy:
 Implant Therapy: Then and Now by Timothy F. Kosinski, DDS, MAGD Implant dentistry has come a long way since blade and subperiostal implants were widely used. Improvements in implant design and site preparation
Implant Therapy: Then and Now by Timothy F. Kosinski, DDS, MAGD Implant dentistry has come a long way since blade and subperiostal implants were widely used. Improvements in implant design and site preparation
Implant Placement in Maxillary Anterior Region Along with Soft and Hard Tissue Grafting- A Case Report.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT
 MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
Clinical Case Reports using Cytoplast GTR Barrier Membranes
 Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Dental Implant Placement in the Maxillary Anterior Region: Guidelines for Aesthetic Success Michael Tischler, DDS
 Page 1 of 10 Issue Date: March 2005, Posted On: 5/2/2005 Dental Implant Placement in the Maxillary Anterior Region: Guidelines for Aesthetic Success Michael Tischler, DDS Figure 1. A 43-year-old female
Page 1 of 10 Issue Date: March 2005, Posted On: 5/2/2005 Dental Implant Placement in the Maxillary Anterior Region: Guidelines for Aesthetic Success Michael Tischler, DDS Figure 1. A 43-year-old female
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
Bone Grafting and Immediate Implant Placement in the Anterior
 Bone Grafting and Immediate Implant Placement in the Anterior by Timothy F. Kosinski, DDS, MAGD Whether a consequence of periodontal disease, caries or trauma to the root, losing an anterior tooth is psychologically
Bone Grafting and Immediate Implant Placement in the Anterior by Timothy F. Kosinski, DDS, MAGD Whether a consequence of periodontal disease, caries or trauma to the root, losing an anterior tooth is psychologically
Periimplant Regeneration Fenestration
 Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Principles of Periodontal flap surgery. Dr.maryam khosravi
 Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
Controlling Tissue Contours with a Prosthetically Driven Approach to Implant Dentistry
 Controlling Tissue Contours with a Prosthetically Driven Approach to Implant Dentistry Go online for in-depth content by Timothy F. Kosinski, DDS, MAGD With continual improvements in the design and production
Controlling Tissue Contours with a Prosthetically Driven Approach to Implant Dentistry Go online for in-depth content by Timothy F. Kosinski, DDS, MAGD With continual improvements in the design and production
Cytoflex Barrier Membrane Clinical Evaluation
 Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Extraction Defect: Assessment, Classification and Management
 International Extraction Journal Defect: of Clinical Assessment, Implant Dentistry, Classification January-April and Management 2009;1(1):1-11 Extraction Defect: Assessment, Classification and Management
International Extraction Journal Defect: of Clinical Assessment, Implant Dentistry, Classification January-April and Management 2009;1(1):1-11 Extraction Defect: Assessment, Classification and Management
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
REGENERATIONTIME. A Case Report by. Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option
 A Case Report by Dr. Daniel Gober Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option The Situation A 35 year old male presented in my practice with a
A Case Report by Dr. Daniel Gober Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option The Situation A 35 year old male presented in my practice with a
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS
 The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS LOCALIZED RECESSION ON TOOTH #25 DUE TO BONE RECESSION (PRE OP) Introduction Tissue grafting
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS LOCALIZED RECESSION ON TOOTH #25 DUE TO BONE RECESSION (PRE OP) Introduction Tissue grafting
Periimplant Regeneration Fenestration
 Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Periodontal Surgery
 Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
botiss dental bone & tissue regeneration biomaterials mucoderm 3D-Regenerative Tissue Graft strictly biologic
 dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
The patient gave a history of hypertension and gastritis for which was taking Lacidipine 4mg, Omeprazole 20mg and Simvastatin 40mg.
 A.S. was referred by her general dental practitioner for assessment for possible implant placement to restore the space where her bridge replacing her maxillary central incisors had recently failed. Fig
A.S. was referred by her general dental practitioner for assessment for possible implant placement to restore the space where her bridge replacing her maxillary central incisors had recently failed. Fig
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1.
 Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
RELIABLE WHEN IT COUNTS. The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4
 RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
A new approach with an in-situ self-hardening grafting material
 74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
Nicholas Caplanis DMD MS 6/13/2012
 Considerations In The Esthetic Zone Nick Caplanis DMD MS Private Practice Periodontics and Implant Surgery Mission Viejo, California Nick@drcaplanis.com Assistant Professor Loma Linda University Anatomic
Considerations In The Esthetic Zone Nick Caplanis DMD MS Private Practice Periodontics and Implant Surgery Mission Viejo, California Nick@drcaplanis.com Assistant Professor Loma Linda University Anatomic
( ) 2009;28(2):89-94
 ( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
Prosthodonticstown. Immediate Implant Placement in Fresh Extraction Sites. clinical. Table I
 Prosthodonticstown clinical Immediate Implant Placement in Fresh Extraction Sites Charles A. Babbush, DDS, MScD Table I Benefits Of Immediate Implantation Improved prosthesis fabrication and/or design
Prosthodonticstown clinical Immediate Implant Placement in Fresh Extraction Sites Charles A. Babbush, DDS, MScD Table I Benefits Of Immediate Implantation Improved prosthesis fabrication and/or design
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 67 Efficacy Evaluation of a New Buccal Bone Plate Preservation Technique: A Pilot Study Federico Brugnami, DDS* Alfonso Caiazzo, DDS**
The International Journal of Periodontics & Restorative Dentistry 67 Efficacy Evaluation of a New Buccal Bone Plate Preservation Technique: A Pilot Study Federico Brugnami, DDS* Alfonso Caiazzo, DDS**
Periodontal Disease. Radiology of Periodontal Disease. Periodontal Disease. The Role of Radiology in Assessment of Periodontal Disease
 Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Clinical cases by Dr. Fernando Rojas-Vizcaya. botiss. dental bone & tissue regeneration. biomaterials. strictly biologic
 Clinical cases by Dr. Fernando Rojas-Vizcaya dental bone & tissue regeneration botiss biomaterials strictly biologic botiss BTR system: BONE biologic potential bovine block & granules: pure bone mineral
Clinical cases by Dr. Fernando Rojas-Vizcaya dental bone & tissue regeneration botiss biomaterials strictly biologic botiss BTR system: BONE biologic potential bovine block & granules: pure bone mineral
The following resources related to this article are available online at jada.ada.org ( this information is current as of July 11, 2011):
 Implants or Pontics: Decision Making for Anterior Tooth Replacement Frank Spear J Am Dent Assoc 2009;140;1160-1166 The following resources related to this article are available online at jada.ada.org (
Implants or Pontics: Decision Making for Anterior Tooth Replacement Frank Spear J Am Dent Assoc 2009;140;1160-1166 The following resources related to this article are available online at jada.ada.org (
Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla
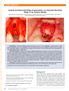 CASE REPORT Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla Alberto Monje,* Florencio Monje, Fernando Suarez,* Raúl González-García, Laura Villanueva-Alcojol,
CASE REPORT Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla Alberto Monje,* Florencio Monje, Fernando Suarez,* Raúl González-García, Laura Villanueva-Alcojol,
Dental Implant Treatment Planning and Restorative Considerations
 Dental Implant Treatment Planning and Restorative Considerations Aldo Leopardi, BDS, DDS, MS Practice Limited to Implant, Fixed and Removable Prosthodontics Greenwood Village, Colorado www.knowledgefactoryco.com
Dental Implant Treatment Planning and Restorative Considerations Aldo Leopardi, BDS, DDS, MS Practice Limited to Implant, Fixed and Removable Prosthodontics Greenwood Village, Colorado www.knowledgefactoryco.com
Implant Site Development Part I
 REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans
 Research Article J Periodontal Implant Sci 2011;41:60-66 doi: 10.5051/jpis.2011.41.2.60 Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans Ji Young
Research Article J Periodontal Implant Sci 2011;41:60-66 doi: 10.5051/jpis.2011.41.2.60 Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans Ji Young
Townie Guest Editorial. Gingival Attachment Loss: Evaluation and Surgical Options. Daniel J. Melker, DDS. fig. 1
 Gingival Attachment Loss: Evaluation and Surgical Options Daniel J. Melker, DDS Attached connective tissue (a.k.a. attached tissue) in the simplest terms is the body s only barrier between the underlying
Gingival Attachment Loss: Evaluation and Surgical Options Daniel J. Melker, DDS Attached connective tissue (a.k.a. attached tissue) in the simplest terms is the body s only barrier between the underlying
Evidence-based decision making in periodontal tooth prognosis
 Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Ridge Split Procedure
 Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery
 CASE SERIES 1 OPEN ACCESS Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery Sangeeta ABSTRACT Introduction:
CASE SERIES 1 OPEN ACCESS Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery Sangeeta ABSTRACT Introduction:
Pre op Failed endodontic treatment with sinus involvement.
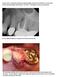 Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
Several extraction socket classifications have been
 Case Report Type 3 ReceSSion DefeCTS Clinical Management of Type 3 Recession Defects With Immediate Implant and Provisional Restoration Therapy: A Case Report Dennis P. Tarnow, DDS; and Stephen J. Chu,
Case Report Type 3 ReceSSion DefeCTS Clinical Management of Type 3 Recession Defects With Immediate Implant and Provisional Restoration Therapy: A Case Report Dennis P. Tarnow, DDS; and Stephen J. Chu,
Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques
 Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques Mohammad Assaf Assistant Professor, Faculty of Dentistry, Al-Quds University, Jerusalem, Palestine. ABSTRACT Correspondence
Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques Mohammad Assaf Assistant Professor, Faculty of Dentistry, Al-Quds University, Jerusalem, Palestine. ABSTRACT Correspondence
Dental implants certainly have
 CLINICAL Facial Wall Defect Grafting Techniques in Preparation for a Dental Implant by Timothy Kosinski, DDS, MAGD Dental implants certainly have become a popular method of restoring missing teeth. The
CLINICAL Facial Wall Defect Grafting Techniques in Preparation for a Dental Implant by Timothy Kosinski, DDS, MAGD Dental implants certainly have become a popular method of restoring missing teeth. The
Conventional immediate implant placement and immediate placement with socket-shield technique Which is better
 International Journal of Clinical Medicine Research 2014; 1(5): 176-180 Published online December 30, 2014 (http://www.aascit.org/journal/ijcmr) ISSN: 2375-3838 Conventional immediate implant placement
International Journal of Clinical Medicine Research 2014; 1(5): 176-180 Published online December 30, 2014 (http://www.aascit.org/journal/ijcmr) ISSN: 2375-3838 Conventional immediate implant placement
Inclusive Tooth Replacement System
 Optimizing Anterior Esthetics with the Inclusive Tooth Replacement System by Timothy F. Kosinski, DDS, MAGD Implant treatment has changed so much over the years. In the past it was acceptable to place
Optimizing Anterior Esthetics with the Inclusive Tooth Replacement System by Timothy F. Kosinski, DDS, MAGD Implant treatment has changed so much over the years. In the past it was acceptable to place
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Revisions for CDT 2016
 Revisions for CDT 2016 This document was developed from preliminary actions of the Code Maintenance Committee (CMC). This document has been compared to the CMC meeting notes and the ASCII file. This document
Revisions for CDT 2016 This document was developed from preliminary actions of the Code Maintenance Committee (CMC). This document has been compared to the CMC meeting notes and the ASCII file. This document
HDS PROCEDURE CODE GUIDELINES
 D4000 - D4999 Local anesthesia is usually considered to be part of Periodontal procedures. General Guidelines 1. Periodontal services are only benefited when performed on natural teeth for treatment of
D4000 - D4999 Local anesthesia is usually considered to be part of Periodontal procedures. General Guidelines 1. Periodontal services are only benefited when performed on natural teeth for treatment of
GBR membrane for ideal regeneration
 GBR membrane for ideal regeneration 1) i-gen Lingual Extension should be considered for a large defect. Need to have at least 1mm of space above the platform of a fixture: Make this space with a pre-existing
GBR membrane for ideal regeneration 1) i-gen Lingual Extension should be considered for a large defect. Need to have at least 1mm of space above the platform of a fixture: Make this space with a pre-existing
Alveolar Ridge Preservation:
 Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
GBR membrane for ideal regeneration. i-gen TM. 2mm. >2.5mm. Lingual Extension. >100 blunt angle
 REGENERATION 02/03 Design Concept GBR membrane for ideal regeneration i-gen TM Description Single A type Small IG1W4509 Single A type Regular IG1W5510 Single A type Wide IG1W6511 Single B type Small IG2W0918
REGENERATION 02/03 Design Concept GBR membrane for ideal regeneration i-gen TM Description Single A type Small IG1W4509 Single A type Regular IG1W5510 Single A type Wide IG1W6511 Single B type Small IG2W0918
Vertical and/or horizontal alveolar
 CLINICAL Vascularized Connective Tissue Flap for Bone Graft Coverage Alan S. Herford, DDS, MD 1 * Todd C. Cooper, DDS 1 Carlo Maiorana, DDS, MD 2 Marco Cicciù, DDS, PhD 2 Alveolar defects are characterized
CLINICAL Vascularized Connective Tissue Flap for Bone Graft Coverage Alan S. Herford, DDS, MD 1 * Todd C. Cooper, DDS 1 Carlo Maiorana, DDS, MD 2 Marco Cicciù, DDS, PhD 2 Alveolar defects are characterized
Osseous surgery in periodontal treatment
 SCIENTIFIC SESSION Osseous surgery in periodontal treatment Essayist: Roberto Pontoriero Introduction In periodontally involved patients, periodontal therapy usually results in various degrees of soft-tissue
SCIENTIFIC SESSION Osseous surgery in periodontal treatment Essayist: Roberto Pontoriero Introduction In periodontally involved patients, periodontal therapy usually results in various degrees of soft-tissue
Hyun-Jae Cho, Kun-Soo Jang, Ki-Hyun Jeong, Jae-Yun Jeon, Kyung-Gyun Hwang, Chang-Joo Park
 Vol. 33 No. 1, March 2014 Peri-implant gingival tissue changes following immediate placement of maxillary anterior single implant with a collagen-coated xenograft: A 1-year follow-up result Hyun-Jae Cho,
Vol. 33 No. 1, March 2014 Peri-implant gingival tissue changes following immediate placement of maxillary anterior single implant with a collagen-coated xenograft: A 1-year follow-up result Hyun-Jae Cho,
Practical Advanced Periodontal Surgery
 Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Educational Training Document
 Educational Training Document Table of Contents Part 1: Resource Document Disclaimer Page: 2 Part 2: Line Item Grade Sheets Page: 3 Release: 11/2016 Page 1 of 6 Part 1: Resource Document Disclaimer The
Educational Training Document Table of Contents Part 1: Resource Document Disclaimer Page: 2 Part 2: Line Item Grade Sheets Page: 3 Release: 11/2016 Page 1 of 6 Part 1: Resource Document Disclaimer The
Natural preservation of the emergence profile
 case report Natural preservation of the emergence profile Authors: Dr Umut Baysal & Dr Arzu Tuna, Germany Supplying single-tooth gaps with implants in the aesthetic zone is subject to strict evaluation.
case report Natural preservation of the emergence profile Authors: Dr Umut Baysal & Dr Arzu Tuna, Germany Supplying single-tooth gaps with implants in the aesthetic zone is subject to strict evaluation.
Esthetic management of multiple missing anterior teeth A Case report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
Over the years, mucogingival surgery
 The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation and Root Coverage: A Case Series Saroff Stephen Andrew Saroff, DDS, MSD 1 Abstract Over the years, mucogingival surgery has developed
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation and Root Coverage: A Case Series Saroff Stephen Andrew Saroff, DDS, MSD 1 Abstract Over the years, mucogingival surgery has developed
Uprighting Movement Relative to Defects Forced Eruption Alteration of the Gingival Embrasure Interactions with Implants
 Frank Celenza DDS Periodontist and Orthodontist Past President, Northeastern Society of Periodontists Associate Clinical Professor, New York University Member, ITI (International Team of Implantologists)
Frank Celenza DDS Periodontist and Orthodontist Past President, Northeastern Society of Periodontists Associate Clinical Professor, New York University Member, ITI (International Team of Implantologists)
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
Immediate implant placement in a single staged
 Bone and Crescent Shaped Free Gingival Grafting for Anterior Immediate Implant Placement: Technique and Case Report Han et al Thomas Han, DDS, MS 1 2 Abstract Immediate implant placement in a single staged
Bone and Crescent Shaped Free Gingival Grafting for Anterior Immediate Implant Placement: Technique and Case Report Han et al Thomas Han, DDS, MS 1 2 Abstract Immediate implant placement in a single staged
Bringing you Geistlich biocompatibility with improved application and handling benefits. Your combination for success
 Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
Horizontal bone augmentation by means of guided bone regeneration
 Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report
 Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
The Internatonal Journal of Periodontics & Restoraive Dentistry
 The Internatonal Journal of Periodontics & Restoraive Dentistry 3 Incisive Vessel Based Palatal Flap for the Reconstruction of Anterior Maxillary Soft Tissues [Au: Text has been edited heavily. Please
The Internatonal Journal of Periodontics & Restoraive Dentistry 3 Incisive Vessel Based Palatal Flap for the Reconstruction of Anterior Maxillary Soft Tissues [Au: Text has been edited heavily. Please
Course Objectives. HDA 2018 Dental Implant Complications. What are some common failures / problems we all encounter?
 HDA 2018 Dental Implant Complications 1 Course Objectives - Understand protocols for diagnosing and treatment planning to minimize complications - Recognize and manage intraoperative complications during
HDA 2018 Dental Implant Complications 1 Course Objectives - Understand protocols for diagnosing and treatment planning to minimize complications - Recognize and manage intraoperative complications during
Immediate Restorations on Implants in the Esthetic Area
 CLINICAL SCIENCE IJOICR Immediate Restorations on Implants in the Esthetic Area Immediate Restorations on Implants in the Esthetic Area 1 Pedro Peña Martinez, 2 Ramón Palomero Langner, 3 Ramón Palomero
CLINICAL SCIENCE IJOICR Immediate Restorations on Implants in the Esthetic Area Immediate Restorations on Implants in the Esthetic Area 1 Pedro Peña Martinez, 2 Ramón Palomero Langner, 3 Ramón Palomero
MUCOGINGIVAL THERAPY PERIODONTAL PLASTIC SURGERY
 MUCOGINGIVAL THERAPY PERIODONTAL PLASTIC SURGERY DR.H.Gharati Periodontist & Dental Implant Specialist Assistant Professor, School Of Dentistry Friedman(1957): DEFINITION Mucogingival surgery, Surgical
MUCOGINGIVAL THERAPY PERIODONTAL PLASTIC SURGERY DR.H.Gharati Periodontist & Dental Implant Specialist Assistant Professor, School Of Dentistry Friedman(1957): DEFINITION Mucogingival surgery, Surgical
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants. by Timothy F. Kosinski, DDS, MAGD
 Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A Case Series
 Journal of the International Academy of Periodontology 2012 14/3:62-68 One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A
Journal of the International Academy of Periodontology 2012 14/3:62-68 One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A
MASTERS SERIES 2010 ACCELERATED IMPLANT DENTISTRY EDUCATION. San Francisco April-September Miami March-August CREDIT HOURS
 MASTERS SERIES 2010 Level II Implant Continuum Advanced Continuum Miami March-August 2010 San Francisco April-September 2010 ACCELERATED IMPLANT DENTISTRY EDUCATION 120 CREDIT HOURS Arun K. Garg, D.M.D.
MASTERS SERIES 2010 Level II Implant Continuum Advanced Continuum Miami March-August 2010 San Francisco April-September 2010 ACCELERATED IMPLANT DENTISTRY EDUCATION 120 CREDIT HOURS Arun K. Garg, D.M.D.
