This study examined the potential financial
|
|
|
- Brook Jefferson
- 6 years ago
- Views:
Transcription
1 Impact of Dental Therapists on Productivity and Finances: II. Federally Qualified Health Centers Tryfon J. Beazoglou, Ph.D.; Howard L. Bailit, D.M.D., Ph.D.; Judy DeVitto, B.S.; Taegen McGowan, B.A., M.P.H.; Veronica Myne-Joslin, B.A. Abstract: This article estimates the impact of dental therapists treating children on Federally Qualified Health Center (FQHC) dental clinic finances and productivity. The analysis is based on twelve months of patient visit and financial data from large FQHC dental clinics (multiple delivery sites) in Connecticut and Wisconsin. Assuming dental therapists provide restorative, extraction, and pulpal services and dental hygienists continue to deliver all hygiene services, the maximum reduction in costs is about 6 percent. The limited impact of dental therapists on FQHC dental clinic finances is because 1) dental therapists only account for 17 percent of children services and 2) dentists are responsible for only 25 percent of clinic expenses and cost reductions are related to the difference between dental therapist and dentist wage rates. Dr. Beazoglou is Professor, Department of Craniofacial Sciences, School of Dental Medicine, University of Connecticut Health Center; Dr. Bailit is Professor Emeritus, Department of Community Medicine, School of Medicine, University of Connecticut Health Center; Ms. DeVitto is Administrative Manager, University of Connecticut Health Center Finance Corporation; Ms. McGowan is Research Assistant, Department of Community Medicine, School of Medicine, University of Connecticut Health Center; and Ms. Myne-Joslin is a data analyst, Cromwell, CT. Direct correspondence and requests for reprints to Dr. Tryfon Beazoglou, Department of Craniofacial Sciences, School of Dental Medicine, University of Connecticut Health Center, 263 Farmington Ave., Farmington, CT 06030; ; Beazoglou@nso1.uchc.edu. Keywords: access to care, federally qualified health centers, dental therapists, dentists, dental clinic finances, productivity Submitted for publication 10/12/11; accepted 5/2/12 This study examined the potential financial impact of dental therapists providing care to children within the four walls of Federally Qualified Health Center (FQHC) dental clinics. In some states, FQHCs can also deliver care to underserved patients in public settings such as schools and still receive their usual reimbursement rates. FQHC-operated, school-based dental programs are addressed in a separate article. 1 A detailed review of the dental therapy literature is available in the first article in this series. 2 FQHCs were established in the 1970s by the U.S. government (Health Resources and Services Administration, HRSA) to provide medical, dental, and behavioral health services to low-income and rural patients who do not have financial or physical access to the private delivery system. In part, FQHCs were established because in most states Medicaid fees are so low (for children and adults) that few dentists (or physicians) accept Medicaid-eligible patients. FQHCs are nonprofit organizations that receive prospective cost-based reimbursement (fee-per-visit) for the treatment of Medicaid patients. 3 For non- Medicaid, indigent dental patients (i.e., those unable to pay for all the care received), FQHCs charge a sliding scale fee-per-visit based on family income and size, following federal poverty guidelines. Part of the uncompensated care to indigent patients is covered by an annual 330 grant from the federal government. The contribution of the 330 grant funds to dental clinic revenues depends on the allocation of these funds among clinical divisions (e.g., medical, dental) within FQHCs. On average, the 330 grant pays for about 52 percent of all medical and dental services provided to indigent patients. The methods used to calculate the 330 grant awards are complex, and visit payment rates vary among FQHCs. Further, in some states the visit rate is dental-specific; others have one visit payment rate for all health services. Of the nation s 1,200 FQHCs, some 820 provide dental services (2009). These clinics employ 2,500 FTE (full-time equivalent) dentists and 1,120 FTE dental hygienists. 4 The literature on FQHC dental clinics is limited. All FQHCs are required to report to HRSA annually on their financial and clinical operations, but, for many important performance measures, medical and dental data are not presented separately. Some information is available from state studies of dental access disparities. The data suggest that most FQHC dental clinics have less than 1068 Journal of Dental Education Volume 76, Number 8
2 five operatories, two or fewer FTE dentists, and less than one FTE dental hygienist per dentist. 3,5-11 For FQHCs that provide dental care, dental patients account for about 10 percent of total FQHC revenues and expenses. In terms of dental clinic revenues, one study reported that 41.8 percent comes from grants, 6.5 percent from self-pay patients, 6.5 percent from private insurance, and 45.1 percent from public insurance (mainly Medicaid). 5 The dental safety net system (including FQHC dental clinics) has the capacity to treat about 8 to 9 million of the approximately 85 million people that have low incomes and limited financial access to dental services. 12 The safety net system consists of public and voluntary sector health facilities that care for the underserved. Besides FQHCs, the system includes local community dental clinics (non-fqhcs), dental schools, some hospitals, and public school clinics. Currently, FQHC dental clinics treat approximately 3.7 million people per year (2010). 4 Most patients (85 percent) have family incomes below 150 percent of the Federal Poverty Level (FPL), and about 50 percent of FQHC dental patients are children (eighteen years of age or younger). 5 Medicaid fee-for-service reimbursement rates are 30 to 70 percent below prevailing market fees in most states, and relatively few states provide more than emergency care for adults. As a result few private practitioners (i.e., <25 percent) accept Medicaid or indigent patients. 13 Nevertheless, private practices provide about two-thirds of the services to Medicaid patients (and substantial pro bono or reduced fee services for lower and middle-income patients). 14 Because of limited access to private offices and the limited size of the dental safety net, low-income patients have much lower utilization rates (approximately 30 percent of ever enrolled [one or more days] adults and children with annual visits) compared to those with private dental insurance or to people with family incomes 400 percent or above the FPL (approximately 60 percent). 10 Methods Economic Model FQHC dental clinics have excess demand for their services (represented by the horizontal lines in Figures 1 and 2). This is because of the large numbers of Medicaid and low-income patients (approximately 85 million), and because with low Medicaid fees, most private practices do not accept Medicaid patients. In addition, few Medicaid programs cover adults. In contrast, although limited in number and capacity (i.e., less than 4 million adult and child patients treated annually), FQHC dental clinics receive additional public funds to provide dental care to Medicaid and low-income patients of all ages. These are the primary reasons for excess patient demand. Figures 1 and 2 depict the supply and demand conditions in FQHC dental clinics where the prevailing price per unit of service is P 0 and the quantity demanded and supplied is Q 0. The introduction of a dental therapist entails the substitution of a higher price input (dentist time) by a lower price input (dental therapist time). This implies a shift of the supply function (S) to the right (S 1, Figure 2) along the demand function (D), other things being equal. The magnitude of the shift represents the cost difference between dental therapist time and dentist time used in the production of selected dental services. As the equilibrium shifts from point A to point B, the price per unit of dental services remains the same (P 0 ) and the quantity demanded and supplied increases to Q 1 (Figure 2). How much the utilization increases depend on the reduction in costs per unit of service (magnitude of shift of the supply) and the shape of the supply function. Level of training, scope of services, degree of supervision, and dental therapist wages determine changes in dental care costs. These interdependent dimensions are related to the productivity and efficiency of dental clinics employing dental therapists. In general, there is a positive relationship between the level of training (formal education or on-the-job), years of experience, and earnings. General dentists are trained for more years than dental therapists; dental hygienists are trained for more years than dental assistants; and it is assumed that dental therapists are trained for more years than dental hygienists. As a result, the wage rate of a dentist is expected to exceed that of a dental therapist and so on. For FQHC dental clinics to perform efficiently, each and all its resources (inputs) must be employed efficiently. This requires that, at the margin, the value generated by an input is equal to its remuneration (wage rate). Consider a dental service (e.g., a bitewing X-ray) that takes dentists, dental therapists, dental hygienists, or dental assistants the same time to perform. Efficient use of resources requires that the least costly input provides this service (i.e., dental assistants). Similarly, economic efficiency requires that dental hygienists rather than dental therapists or August 2012 Journal of Dental Education 1069
3 Price! S P0 A D 0 Q0 Quantity Demanded and Supplied Figure 1. FQHC dental clinic demand (D) and supply (S) without dental therapists Price S S1 P0 A C D P1 B 0 Q0 Q1 Quantity Demanded and Supplied Figure 2. FQHC dental clinic demand (D) and supply (S1) with dental therapists 1070 Journal of Dental Education Volume 76, Number 8
4 dentists provide prophylaxes and preventive services. Thus, it is economically irrational and inefficient to employ dental therapists to provide services now done by lesser trained personnel. In this analysis, dental therapist services do not include those performed by dental assistants and dental hygienists. Children s dental services provided by dentists that dental therapists can deliver are listed in Table 1. To estimate the cost reductions from having dental therapists perform these services, it is necessary to estimate the value of children services, the dentist share of service costs, and the wage differential between dentists and dental therapists. Equation 1 shows the potential cost reduction of employing a dental therapist, and equation 2 shows the percent cost reduction in total clinic revenues: (1) Potential Cost Reduction = X * s * (W D W DT )/W D. (2) Percent Cost Reduction = (X / Y) * s * (W D W DT )/W D. In these equations, X is the market value of a subset of dental services currently produced by dentists that dental therapists could produce; s is the dentist s percentage share in the cost of these services (dentist salary/total clinic expenses); W D is the wage rate of the dentist; W DT is the wage rate of the dental therapist; and Y is the market value (total revenues) of dental services produced by an FQHC dental clinic. Data Sources and Variables The collection of FQHC data was part of a separate study of FQHC dental clinic finances that preceded the current project. Working in cooperation with the National Network for Oral Health Access (NNOHA), FQHC dental clinics from around the country were asked to participate in the study if they had twelve months of electronic record data (patient visits) available. FQHCs were solicited from the NNOHA website, specific FQHCs recommended by NNOHA leaders, national NNOHA meetings, and an NNOHA-sponsored webinar. The information requested from the FQHCs included patient visits (date, clinic, provider, patient numbers, patient age, dental services [American Dental Association, ADA, codes], payer, and charge/s per visit or per service); description of clinic operations (provider and staff types, number and annual hours, number of operatories, and clinic square feet); and clinic finances (revenues from grants, patient care by payer, other sources, and expenses by expense category). Table 1. Dental therapist services ADA Code Procedure 2140 Amalgam, one-surface 2150 Amalgam, two-surfaces 2330 Composite, one-surface anterior 2331 Composite, two-surface anterior 2391 Composite, one-surface posterior 2392 Composite, two-surface posterior 2930 Stainless steel crown, primary 3110 Pulp cap, direct 3120 Pulp cap, indirect 3130 Pulpotomy 7140 Extraction, elevation/forceps removal These data were used to estimate the parameters in Equations 1 and 2. The variables used in the economic model are the following: Market value of dental services (Y). FQHC dental clinics have three primary payers: Medicaid, patient self-pay, and private insurance. Clinics charge a fee-per-visit for Medicaid and self-pay patients. The per-visit fee is a cost-based prospective reimbursement for Medicaid patients. The same fee-per-visit is applied to self-pay patients on a sliding scale, based on family size and income. As a result, the implicit price of specific dental procedures varies, depending on the payer and services provided to patients per visit. To have a standard way of comparing the value of services across patients, payers, and visits, the market value of dental services produced by clinics was calculated by applying the 2005 National Dental Advisory Service Comprehensive Fee Report for each service times its frequency. 15 Market value of dental therapist services (X). The market value of children services that dental therapists produce substituting for dentists (see Table 1) was estimated using the ADA average fee for each service. Dentist share of service costs. Based on the FQHC financial and service data, the dentist s share of service costs ranged between 17 percent and 32 percent with a mean value of 25 percent. As an initial conservative estimate, 30 percent was used in the calculations. Dentist s wage rate (W D ). An average compensation of $80 per hour (wages and fringe benefits) was based on discussions with FQHC dentists. Dental therapists wage rate (W DT ). The average compensation rate for dental hygienists, $40 per hour (wages and fringe benefits), was used as an initial conservative value. Actual dental therapist salaries are expected to be higher. August 2012 Journal of Dental Education 1071
5 Implicit Assumptions The assumptions underlying the analysis are the following: dental therapists are seamlessly integrated into FQHC dental clinics with no training costs; dental therapists are perfect substitutes for general dentists and provide all the services that they are legally able to provide; dental therapist cost reductions do not include costs associated with dentist supervision of dental therapists; dental therapists do not provide services currently performed by dental assistants and hygienists; and part-time dental therapist employment does not cause management inefficiencies related to patient scheduling, staff training, etc. These assumptions result in an upper boundary estimate (i.e., maximum impact possible) of the cost reduction for substituting dental therapists for dentists. Finally, sensitivity analyses were used to assess the relative impact of differences in dental therapist and dentist wage rates, dentist s share of total FQHC dental clinic expenses and share of children s services, and supply elasticity (the percent change in quantity supplied relative to the percent change in price). Results Cost Reduction and Utilization Increase The results are based on data from Connecticut and Wisconsin FQHCs. The Connecticut FQHC has seven dental clinic sites, and the Wisconsin FQHC has five large sites. These FQHCs were selected because of their size and data quality. Table 2 presents the annual number and market value of dental therapist-provided children services. All dental therapist services, mainly restorations and extractions, account for about 17 percent of children services, valued at 37 percent of total children services. Table 3 presents the potential upper boundary cost reductions from using dental therapists in FQHC dental clinics. Children services account for 26 to 37 percent of total FQHC dental revenues. The dentists contribution (i.e., wages) to the latter value is 30 percent. The absolute cost reduction from dental therapists under ideal conditions is up to $10,400 per dentist. As a percentage of child and total clinic service values, dental therapist cost reductions are about 5.6 percent and 1.6 percent, respectively. The expected increase in FQHC clinic dental services, given the estimated cost reduction from using dental therapists depends, on the elasticity of supply (percent change in utilization/percent change in costs). Since elasticity estimates are not available, a supply elasticity of 0.5 is assumed; this means that the percentage increase in utilization is equal to one-half the percentage reduction in costs. In this case, the increase in utilization is 1.9 percent to 2.8 percent. A less plausible supply elasticity is 1.0, which increases the estimated utilization increase by the same percentage reduction in costs. Sensitivity Analysis Based on Connecticut data, Table 4 shows the percentage and absolute dollar effects, respectively, of various dental therapist wage rates (ranging from $25 to $60 an hour) and dentist s share of FQHC dental clinic expenses (ranging from 20 to 40 per- Table 2. Mean number and value of annual dental therapist dental services provided to children (under age nineteen years) by FQHCs from Connecticut and Wisconsin Connecticut Wisconsin Value Value Services Number (000) Number (000) Restorations 5,427 $794 5,682 $1,103 Stainless steel crowns 121 $ $28 Pulp caps, pulpotomies 254 $ $23 Extractions 1,021 $ $84 Subtotal 6,823 $1,000 6,571 $1,138 Total children services 39,951 $2,660 55,259 $3,826 Total services, all patients 167,691 $9, ,091 $14, Journal of Dental Education Volume 76, Number 8
6 Table 3. Percentage and absolute annual cost reductions from substituting dental therapists for dentists treating children within the four walls of FQHCs from Connecticut and Wisconsin Connecticut Wisconsin Total value of all services (Y) $9,217,500 $14,562,737 Value of child services $2,660,020 $3,826,340 Value of child services provided by dentist (X) $999,604 $1,002,964 Dentist s share value of child services replaced by dental therapist (X*s) $299,881 $300,889 Number of FTE dentists Dental therapist absolute cost reduction (X*s*(WD-WDT)/WD) $149,941 $150,445 Dental therapist cost reduction per dentist $10,412 $7,918 Dental therapist percent cost reduction 5.6% 3.9% Dental therapist percent cost reduction for total services 1.6% 1.0% Note: The symbols for formulas 1 and 2 are in parentheses. Table 4. Effects of dental therapist wage differentials and dentist share of FQHC revenues on percent cost reductions Dentist Dental Therapist Dentist Dentist Dentist Dentist Dentist Wages Wages/Hr Share Share Share Share Share (W D ) (W DT ) (W D -W DT )/W D 20% 25% 30% 35% 40% $80 $ $80 $ $80 $ $80 $ $80 $ $80 $ $80 $ $80 $ cent). As the dental therapist wage rate increases, cost reductions per dentist are reduced from $9,432 (dentist s share 25 percent) to $3,430. When the dentist s share is 40 percent, the cost reductions per dentist decline from $18,865 to $6,860. As expected, cost reductions decline with increasing dental therapist wages and increase as the percentage of dentist share in the production of services increases. That is, the financial advantage of dental therapists decreases with increasing dental therapist incomes (relative to dentist incomes) and increases if dentists account for a larger share of total clinic production costs. The sensitivity analysis for the number of children per delivery site is shown in Table 5 (data from selected FQHC sites in Wisconsin and Connecticut). Actual data are presented for five FQHCs of different sizes (dentists, chairs, etc.) and numbers of children seen per year. For example, clinic A treats 359 children per year and clinic E treats 2,463 children per year. As the number of children increases, the absolute value of dental therapist cost reductions increases, but not the percent cost reductions. Also, the largest FQHC (E) does not have sufficient volume to employ a full-time dental therapist. That is, the range of dental therapist annual hours required in these clinics varies from 171 to 1,034. Since a full-time dental therapist is expected to work 2,000 hours per year (forty hours times fifty weeks), clinic E does not have sufficient volume of children services to employ a full-time dental therapist. Hence, to employ dental therapists full-time, they must work in multiple FQHC dental clinic sites. National Impact The estimated increase in utilization is 3 percent. This upper bound estimate is based on an expected maximum percent saving reduction of about 6 percent and an assumed supply elasticity of 0.5. In 2010, FQHC dental clinics treated 3.7 million patients, and 50 percent were children (1.85 million). Hence, the maximum estimated increase in utilization is 55,500 children (1.85 million times 3 percent). Based on 237 hours of dental therapist time per FTE dentist and 2,500 FTE dentists employed in FQHCs, August 2012 Journal of Dental Education 1073
7 Table 5. Dental therapist cost reductions in FQHC dental clinics of various sizez (A-E) Variables A B C D E Revenue/gross billing $816,890 $1,126,004 $1,885,304 $2,838,192 $4,059,469 Expenses $635,074 $1,048,240 $1,673,709 $3,203,895 $3,704,006 Chairs FTE dentists FTE dental hygienists FTE dental assistants Patients 1,503 3,593 4,872 4,793 7,315 Visits 5,321 7,814 12,597 11,505 17,596 Children (18 and under) 359 1,432 2,912 1,709 2,463 Visits for children 929 2,320 5,742 3,686 5,465 Value of children services $128,003 $263,086 $774,374 $688,658 $1,024,327 Value of dental therapist services $48,869 $57,376 $306,163 $163,080 $255,885 Dentist share value of child services $14,661 $17,213 $91,849 $48,226 $76,765 Dental therapist services ,067 1,139 1,668 Dental therapist hours per year , Dental therapist savings $7,330 $8,606 $45,924 $24,462 $38,383 % savings 5.73% 3.27% 5.93% 3.55% 3.75% 285 FTE dental therapists are needed to generate this increase in utilization. This estimate assumes that all FQHCs employ dental therapists; that dental therapists provide all restorative and other services legally allowed; that they average thirty-minute appointments; and that dentists do not spend any time supervising them. This estimate does not take into account broken appointments, sick leave, and related issues that reduce patient visits. Because some assumptions are problematic, the actual impact of dental therapists on access within the four walls of FQHCs is unknown but is likely to be substantially less. Discussion This study suggests that dental therapists providing care to children within the four walls of FQHCs will have a very modest impact on dental clinic finances and utilization. Specifically, dental therapists will generate a cost reduction of no more than 6 percent of total children costs. For the average FQHC, the absolute dollar cost reduction will be in the vicinity of $10,400 per dentist. The absolute cost reduction (but not the percentage) increases with more dentists. Extrapolating these data nationally, FQHCs have the capacity to employ about 285 dental therapists within their four walls. Under ideal conditions, these dental therapists have the potential to treat an additional 55,500 children. These are maximum estimates, and actual cost reductions and utilization are likely to be substantially lower. The primary reasons for the relatively limited impact of dental therapists on FQHC clinic productivity and finances are the following. First, the majority of children are reasonably healthy and do not require many dental therapist-level services. Based on Connecticut and Wisconsin data, about 70 percent of children services are diagnostic and preventive and only 17 percent restorative and extractions. Together, dental hygienists and dental therapists can provide about 95 percent of the care required by children treated in FQHCs. Second, most diagnostic and preventive services should be provided by dental hygienists, since they are trained to provide these services and presumably will have a lower wage rate than dental therapists. Third, dentists account for 25 percent or less of clinic operating costs. Seventy-five percent of expenses are related to other staff (e.g., dental hygienists, dental assistants, administrators), facilities, equipment, supplies, etc. These expenses continue whether dentists or dental therapists provide services. The cost reductions are mainly related to the difference in wage rates between dental therapists and dentists. These findings are in agreement with published reports from the United Kingdom that general dental practitioners who employ dental therapists do not generate an increase in net practice revenues and, in fact, may not cover dental therapist overhead costs. 16,17 The negative impact of dental therapists on 1074 Journal of Dental Education Volume 76, Number 8
8 net private practice revenues may explain the limited number of dental therapists in the United Kingdom and Australia. 18,19 Presumably, if they generated significant increases in net income, the demand for dental therapists would increase, and more would be educated. In developed countries, most dental therapists are employed in school-based clinics. There are several other barriers to the effective use of dental therapists in FQHCs. First, most FQHC dental clinics have five or fewer operatories and will find it difficult to employ dental therapists within their four walls. With two full-time dentists per clinic, for greater efficiency four chairs should be used by the dentists. In addition, most clinics employ about.5 dental hygienists per dentist (versus 1.5 per dentist in private general practices). FQHCs have a significant opportunity to see more patients and generate greater net revenues by employing more dental hygienists. This will require additional operatories and will further constrain the employment of dental therapists. Second, beyond facilities, dentists and other clinical and administrative personnel need formal training to work with dental therapists. These training programs do not exist (other than the one under development at the University of Minnesota), and currently, dental schools provide students and residents with minimal didactic and clinical experience working with dental hygienists and dental assistants. The exception is when students and residents rotate through community clinics and private practices. Third, based on the current structure of FQHC dental clinics, most will have to employ dental therapists on a part-time basis. Even the largest FQHC in this study with over four FTE dentists did not have enough child patients needing restorations and extractions to employ a full-time dental therapist. For FQHCs employing dental therapists part-time, they will have to schedule patients needing restorations and extractions on specific days and times. This will be a management challenge since clinics often have high broken appointment rates. Fourth, clinics have many other options to increase their capacity to see more patients and generate higher net revenues besides using dental therapists. As already noted, large increases in output can be expected from providing dentists more operatories, employing more dental hygienists and other staff, and, of course, improving basic management processes. Fifth, dental therapists are only legal in one state, and it may take ten to twenty years before the majority of states legalize this new occupation. Also, FQHCs have the capacity to employ relatively few dental therapists (285), so the value of starting new dental therapist training programs, regulatory mechanisms, etc. for this small number is questionable. There are situations in which dental therapists could be a significant advantage to community clinics. A good example is small frontier communities in Alaska, since it will always be difficult to recruit dentists, and especially culturally competent dentists, to these isolated tribal areas. Also, for clinics that have at least one full-time dentist and are unable to recruit additional dentists, dental therapists may offer an alternative. A 2006 study reported that 26 percent of rural clinics had open dentist positions. 20 A more recent investigation reported that 39 percent of surveyed clinic directors had open dentist positions. 21 However, these studies were completed before the current economic downturn, and now dental students are graduating with $200,000 or more debt. For both reasons, FQHCs offer new graduates the opportunity to significantly reduce their debt and at the same time make a reasonable salary. As such, FQHCs may have less difficulty recruiting and retaining dentists now than in the past. A related issue is the large increase in dental school graduates expected in the next ten years. Another possible opportunity is to have dental therapists provide care to adults. This issue needs further investigation, but at face value this option is unlikely to increase dental therapist cost reductions substantially. Adults have relatively less need for simple restorations and extractions than children. Also, most Medicaid programs do not cover adult dental care or adequately reimburse FQHCs for treating adults. The value of training dental therapists for more than 2.5 years is problematic. As seen in Table 4, this will lead to higher dental therapist salaries and decreased FQHC cost reductions. Also, since dental therapists and dental hygienists can provide 95 percent of children services, it is unlikely that more years of training and a wider scope of practice will have much impact. This may not be true with regard to treating adults, but it is unclear what percentage of adult services can be provided by dental hygienists and dental therapists. As part of this study, a model was developed that FQHCs can use to estimate the economic impact of employing dental therapists within their four walls. The data needed to make the estimates should be available to any FQHC that has an electronic dental record system. August 2012 Journal of Dental Education 1075
9 The major limitation of this study is that it is not based on empirical information from the actual operation of dental therapists working in FQHC clinics. Instead, using data from a small convenience sample of FQHC dental clinics, estimates are provided on the likely financial and utilization impact of dental therapists. Although basic information is available on the number and types of children services, there are many unknowns on how FQHCs will use dental therapists. Conclusions This study is an initial effort to examine the impact of dental therapists on FQHC productivity and finances treating children. The analysis suggests that dental therapists will have a modest effect on reducing costs and increasing utilization. Acknowledgments This study was supported by a grant from the Pew Center for the States. We want to thank the FQHCs that provided data for this study; the Board of the National Network for Oral Health Access, which was a strong supporter of this effort; and the many people who reviewed drafts of the project report and papers, including Drs. William Maas, Norman Tinanoff, Wayne Cottam, Gregory Nycz, Scott Wetterhall, Tim Brown, and Beth Mertz. We also recognize and appreciate the significant time and effort that the Pew staff, Ms. Shelly Gehshan and Mr. Andrew Snyder, put into all phases of this study. REFERENCES 1. Bailit HL, Beazoglou TJ, DeVitto J, McGowan T, Myne- Joslin V. Impact of dental therapists on productivity and finances: III. FQHC-run school-based dental care programs. J Dent Educ 2012;76(8): Bailit HL, Beazoglou TJ, DeVitto J, McGowan T, Myne-Joslin V. Impact of dental therapists on productivity and finances: I. Literature review. J Dent Educ 2012;76(8): Beazoglou T, Bailit H, Drozdowski M. Federally qualified health center dental program finances: a case study. Public Health Rep 2010;125: McFarland J. Presidential address at the annual National Network for Oral Health Access conference, Washington, DC, September 24, Ruddy G. Health center s role in addressing the oral health needs of the medically underserved. National Association of Community Health Centers, At: com/client/documents/issues-advocacy/policy-library/ research-data/research-reports/oral-health-report- FINAL.pdf. Accessed: November Beazoglou T, Heffley D, Lepowsky S, Douglass J, Lopez M, Bailit H. Dental safety net in Connecticut. J Am Dent Assoc 2005;136: Byck G, Cooksey J, Russinof H. Safety net dental clinics. J Am Dent Assoc 2005;136(7): Glassman P, Subar P. The California community clinic oral health capacity study: report to The California Endowment, At: sources/documents/pacific_communitycapacitysurvey- CAEndowmentReport pdf. Accessed: November Edelstein B. Update on disparities in oral health and access to dental care for America s children. Acad Pediatr 2009;9(6): Bailit H, D Adamo J. Improving access to oral health care for vulnerable and underserved populations. Unpublished paper prepared for Institute of Medicine consensus report: improving access to oral health care for vulnerable and underserved populations. 11. Institute of Medicine. Improving access to oral health care for vulnerable and underserved populations, At: to-oral-health-care-for-vulnerable-and-underserved- Populations.aspx. Accessed: September Bailit H, Beazoglou T, Demby N, McFarland J, Robinson P, Weaver R. Dental safety net: current capacity and potential for expansion. J Am Dent Assoc 2006;137(6): Borchgrevink A, Snyder A, Gehshan S. The effects of Medicaid reimbursement rates on access to dental care. Washington, DC: National Academy for State Health Policy, Beazoglou T, Bailit H, Myne V, Roth K. Supply and demand for dental services: Wisconsin Unpublished report to the Wisconsin Dental Association, national dental advisory service comprehensive fee report. 23 rd ed. Milwaukee: Yale Wasserman, D.M.D., Medical Publishers, Williams S, Bradley S, Godson J, Csikar J, Rowbotham J. Dental therapy in the United Kingdom: part 3. Financial aspects of current working practices. Br Dent J 2009;207: Harris R, Burnside G. The role of dental therapists working in four personal dental service pilots: type of patients seen, work undertaken, and cost-effectiveness within the context of dental practice. Br Dent J 2004;197: Nash DA, Friedman JW, Kardos TB, Kardos RL, Schwarz E, Satur J, et al. Dental therapists: a global perspective. Int Dent J 2008;58(2): Friedman J. The international dental therapist: history and current status. J Calif Dent Assoc 2011;36(1): Rosenblatt R, Andrilla H, Curtin T, Hart LG. Shortages of medical personnel at community health centers. JAMA 2006;295: Bolin KA. Survey of health center oral health providers. National Network for Oral Health Access. At: www. nnoha.org/goopages/pages_downloadgallery/download. php?filename=13902.pdf&orig_name=nnoha_salary_ survey_report_final_1210.pdf&cdpath=/nnoha_salary_ survey_report_final_1210.pdf. Accessed: December Journal of Dental Education Volume 76, Number 8
Dental access disparities are well documented. Dental Therapists in General Dental Practices: An Economic Evaluation
 Dental Therapists in General Dental Practices: An Economic Evaluation Tryfon J. Beazoglou, Ph.D.; Vickie F. Lazar, M.A., M.S.; Albert H. Guay, D.M.D.; Dennis R. Heffley, Ph.D.; Howard L. Bailit, D.M.D.,
Dental Therapists in General Dental Practices: An Economic Evaluation Tryfon J. Beazoglou, Ph.D.; Vickie F. Lazar, M.A., M.S.; Albert H. Guay, D.M.D.; Dennis R. Heffley, Ph.D.; Howard L. Bailit, D.M.D.,
Impact of Dental Therapists on Federally Qualified Health Center Finances
 Impact of Dental Therapists on Federally Qualified Health Center Finances HOWARD BAILIT, DMD, PHD TRYFON BEAZOGLOU, PHD SHELLY GEHSHAN, M PP Presentation to the National Network for Oral Health Access
Impact of Dental Therapists on Federally Qualified Health Center Finances HOWARD BAILIT, DMD, PHD TRYFON BEAZOGLOU, PHD SHELLY GEHSHAN, M PP Presentation to the National Network for Oral Health Access
An Analytical Review of the Pew Report Entitled, It Takes A Team and the Accompanying Productivity and Profit Calculator
 An Analytical Review of the Pew Report Entitled, It Takes A Team and the Accompanying Productivity and Profit Calculator The report, It Takes a Team, was released by the Pew Center on the States in December
An Analytical Review of the Pew Report Entitled, It Takes A Team and the Accompanying Productivity and Profit Calculator The report, It Takes a Team, was released by the Pew Center on the States in December
Access to dental care for low-income patients. Impact of Dental Therapists on Productivity and Finances: I. Literature Review
 Impact of Dental Therapists on Productivity and Finances: I. Literature Review Howard L. Bailit, D.M.D., Ph.D.; Tryfon J. Beazoglou, Ph.D.; Judy DeVitto, B.S.; Taegen McGowan, B.A., M.P.H.; Veronica Myne-Joslin,
Impact of Dental Therapists on Productivity and Finances: I. Literature Review Howard L. Bailit, D.M.D., Ph.D.; Tryfon J. Beazoglou, Ph.D.; Judy DeVitto, B.S.; Taegen McGowan, B.A., M.P.H.; Veronica Myne-Joslin,
Do Facts Matter? Shelly Gehshan Director, Pew Children s s Dental Campaign
 Agenda Pew Children s Dental Campaign Why dentists might oppose new workforce models Economics of new models in private practice Do Facts Matter? Shelly Gehshan Director, Pew Children s s Dental Campaign
Agenda Pew Children s Dental Campaign Why dentists might oppose new workforce models Economics of new models in private practice Do Facts Matter? Shelly Gehshan Director, Pew Children s s Dental Campaign
While the current crisis in state finances is
 Critical Issues in Dental Education State Financing of Dental Education: Impact on Supply of Dentists Howard L. Bailit, D.M.D., Ph.D.; Tryfon J. Beazoglou, Ph.D. Abstract: In 2000, the thirty-six states
Critical Issues in Dental Education State Financing of Dental Education: Impact on Supply of Dentists Howard L. Bailit, D.M.D., Ph.D.; Tryfon J. Beazoglou, Ph.D. Abstract: In 2000, the thirty-six states
The dental safety net system is made up of
 Are Dental Schools Part of the Safety Net? Howard L. Bailit, DMD, PhD Abstract: This article examines the current safety net activities of dental schools and reviews strategies by which schools could care
Are Dental Schools Part of the Safety Net? Howard L. Bailit, DMD, PhD Abstract: This article examines the current safety net activities of dental schools and reviews strategies by which schools could care
The supply of dental services is frequently associated
 Economic Impact of Dental Hygienists on Solo Dental Practices Vickie F. Lazar, M.A., M.S.; Albert H. Guay, D.M.D.; Tryfon J. Beazoglou, Ph.D. Abstract: The fact that a significant percentage of dentists
Economic Impact of Dental Hygienists on Solo Dental Practices Vickie F. Lazar, M.A., M.S.; Albert H. Guay, D.M.D.; Tryfon J. Beazoglou, Ph.D. Abstract: The fact that a significant percentage of dentists
Alternative Dental Workforce Models: Creating a Proposal and Developing a Consensus
 Alternative Dental Workforce Models: Creating a Proposal and Developing a Consensus Shelly Gehshan, MPP Director, Pew Children s Dental Campaign Pew Center on the States sgehshan@pewtrusts.org Why Do We
Alternative Dental Workforce Models: Creating a Proposal and Developing a Consensus Shelly Gehshan, MPP Director, Pew Children s Dental Campaign Pew Center on the States sgehshan@pewtrusts.org Why Do We
The Public and Private Dental Safety Net: Implementation of the ACA and their Roles in Access to Care for Medicaid and Expansion Populations
 Health Policy 12-1-2014 The Public and Private Dental Safety Net: Implementation of the ACA and their Roles in Access to Care for Medicaid and Expansion Populations Peter C. Damiano University of Iowa
Health Policy 12-1-2014 The Public and Private Dental Safety Net: Implementation of the ACA and their Roles in Access to Care for Medicaid and Expansion Populations Peter C. Damiano University of Iowa
Access to Dental Services in. Reimbursement Rates and Administrative Streamlining
 Access to Dental Services in Medicaid: The Effect of Reimbursement Rates and Administrative Streamlining Shelly Gehshan, M.P.P., and Andrew Snyder, M.P.A. National Academy for State Health Policy March
Access to Dental Services in Medicaid: The Effect of Reimbursement Rates and Administrative Streamlining Shelly Gehshan, M.P.P., and Andrew Snyder, M.P.A. National Academy for State Health Policy March
2015 Social Service Funding Application Non-Alcohol Funds
 2015 Social Service Funding Application Non-Alcohol Funds Applications for 2015 funding must be complete and submitted electronically to the City Manager s Office at ctoomay@lawrenceks.org by 5:00 pm on
2015 Social Service Funding Application Non-Alcohol Funds Applications for 2015 funding must be complete and submitted electronically to the City Manager s Office at ctoomay@lawrenceks.org by 5:00 pm on
2017 Social Service Funding Application Non-Alcohol Funds
 2017 Social Service Funding Application Non-Alcohol Funds Applications for 2017 funding must be complete and submitted electronically to the City Manager s Office at ctoomay@lawrenceks.org by 5:00 pm on
2017 Social Service Funding Application Non-Alcohol Funds Applications for 2017 funding must be complete and submitted electronically to the City Manager s Office at ctoomay@lawrenceks.org by 5:00 pm on
The National Perspective: States Working on New Providers
 The National Perspective: States Working on New Providers Shelly Gehshan, MPP Director, Pew Children s Dental Campaign Pew Center on the States sgehshan@pewtrusts.org What I ll Cover Cost of Delay report
The National Perspective: States Working on New Providers Shelly Gehshan, MPP Director, Pew Children s Dental Campaign Pew Center on the States sgehshan@pewtrusts.org What I ll Cover Cost of Delay report
CE Course Handout. Advancing Dental Education: Gies in the 21 st Century. Saturday, June 11, :00 p.m.-3:00 p.m.
 CE Course Handout Advancing Dental Education: Gies in the 21 st Century Saturday, June 11, 2016 2:00 p.m.-3:00 p.m. A Strategic Planning Project University of Connecticut Health Center Advancing Dental
CE Course Handout Advancing Dental Education: Gies in the 21 st Century Saturday, June 11, 2016 2:00 p.m.-3:00 p.m. A Strategic Planning Project University of Connecticut Health Center Advancing Dental
Scheduling by Design. NNOHA Orlando Dori Bingham
 Scheduling by Design NNOHA Orlando 2014 Dori Bingham What is Scheduling by Design? Use of the dental schedule to achieve three key strategic objectives: 1. Improved oral health status for patients 2. Maximum
Scheduling by Design NNOHA Orlando 2014 Dori Bingham What is Scheduling by Design? Use of the dental schedule to achieve three key strategic objectives: 1. Improved oral health status for patients 2. Maximum
Dental Therapy: A Workforce Option to Improve Access to Oral Health Care in Wisconsin
 Dental Therapy: A Workforce Option to Improve Access to Oral Health Care in Wisconsin Jane Koppelman, Research Director, Pew Dental Campaign Wisconsin Oral Health Conference September 26, 2018 Our Mission:
Dental Therapy: A Workforce Option to Improve Access to Oral Health Care in Wisconsin Jane Koppelman, Research Director, Pew Dental Campaign Wisconsin Oral Health Conference September 26, 2018 Our Mission:
Oral Health Care in California: State of the State. Dissemination Workshop August 4,2011
 Oral Health Care in California: State of the State Dissemination Workshop August 4,2011 Introduction 2011 IOM Reports on Oral Health Advancing Oral Health in America Improving Access to Oral Health Care
Oral Health Care in California: State of the State Dissemination Workshop August 4,2011 Introduction 2011 IOM Reports on Oral Health Advancing Oral Health in America Improving Access to Oral Health Care
Millions of Americans face significant barriers
 Dental School Applicants by State Compared to Population and Dentist Workforce Distribution Lauren E. Mentasti, B.S.; Edward A. Thibodeau, D.M.D., Ph.D. Abstract: Millions of Americans face significant
Dental School Applicants by State Compared to Population and Dentist Workforce Distribution Lauren E. Mentasti, B.S.; Edward A. Thibodeau, D.M.D., Ph.D. Abstract: Millions of Americans face significant
SNS Client Dashboard Data Survey Questions
 SNS Client Dashboard Data Survey Questions *This document lists the questions asked in the online SNS data survey; all responses should be submitted via the client portal Step 1 If your dental program
SNS Client Dashboard Data Survey Questions *This document lists the questions asked in the online SNS data survey; all responses should be submitted via the client portal Step 1 If your dental program
Seniors Plans to Teach at Some Point in Career, 2009
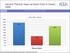 Seniors Plans to Teach at Some Point in Career, 2009 50% 45% 40% 35% 30% 25% 20% 15% 10% 5% 0% 44% Yes No Unsure 18% Plans to Teach 38% Source:, Senior Survey, 2009 Seniors Perceptions of Degree to Which
Seniors Plans to Teach at Some Point in Career, 2009 50% 45% 40% 35% 30% 25% 20% 15% 10% 5% 0% 44% Yes No Unsure 18% Plans to Teach 38% Source:, Senior Survey, 2009 Seniors Perceptions of Degree to Which
Dental Therapy Toolkit SUMMARY OF DENTAL THERAPY REGULATORY AND PAYMENT PROCESSES
 Dental Therapy Toolkit SUMMARY OF DENTAL THERAPY REGULATORY AND PAYMENT PROCESSES March, 2016 OFFICE OF RURAL HEALTH AND PRIMARY CARE EMERGING PROFESSIONS PROGRAM Acknowledgements This report was developed
Dental Therapy Toolkit SUMMARY OF DENTAL THERAPY REGULATORY AND PAYMENT PROCESSES March, 2016 OFFICE OF RURAL HEALTH AND PRIMARY CARE EMERGING PROFESSIONS PROGRAM Acknowledgements This report was developed
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Advanced Dental Health Practitioner (ADHP), 563, 564 Age, as barrier to oral health care, 525 Alcohol consumption, and tobacco use, oral
Index Note: Page numbers of article titles are in boldface type. A Advanced Dental Health Practitioner (ADHP), 563, 564 Age, as barrier to oral health care, 525 Alcohol consumption, and tobacco use, oral
Overview. An Advanced Dental Therapist in Rural Minnesota: Jodi Hager s Case Study Madelia Community Hospital and Clinics entrance
 An Advanced Dental Therapist in Rural Minnesota: Jodi Hager s Case Study Overview Rural communities face considerable challenges accessing oral health services. Compared to urban settings, fewer people
An Advanced Dental Therapist in Rural Minnesota: Jodi Hager s Case Study Overview Rural communities face considerable challenges accessing oral health services. Compared to urban settings, fewer people
Scheduling by Design. Dori Bingham Danielle Goldsmith. Strategies to Enhance Financial Sustainability, Access and the Completion of Phase 1 Treatments
 Scheduling by Design Strategies to Enhance Financial Sustainability, Access and the Completion of Phase 1 Treatments Dori Bingham Danielle Goldsmith Use of the dental schedule to achieve three key strategic
Scheduling by Design Strategies to Enhance Financial Sustainability, Access and the Completion of Phase 1 Treatments Dori Bingham Danielle Goldsmith Use of the dental schedule to achieve three key strategic
Christy Jo Fogarty, ADT, RDH, BSDH, MSOHP Advanced Dental Therapist Licensed Dental Hygienist
 Christy Jo Fogarty, ADT, RDH, BSDH, MSOHP Advanced Dental Therapist Licensed Dental Hygienist Neither I nor members of my immediate family have any financial interests to disclose relating to the content
Christy Jo Fogarty, ADT, RDH, BSDH, MSOHP Advanced Dental Therapist Licensed Dental Hygienist Neither I nor members of my immediate family have any financial interests to disclose relating to the content
The Health centers have become the largest primary care system in the United States. They provide timely treatment & preventive care There are more
 The Health centers have become the largest primary care system in the United States. They provide timely treatment & preventive care There are more than 700 new centers that have opened up as a result
The Health centers have become the largest primary care system in the United States. They provide timely treatment & preventive care There are more than 700 new centers that have opened up as a result
Lack of access to dental Medicaid services (Title
 ABSTRACT Dentists participation and children s use of services in the Indiana dental Medicaid program and SCHIP Assessing the impact of increased fees and administrative changes RYAN J. HUGHES, D.D.S.,
ABSTRACT Dentists participation and children s use of services in the Indiana dental Medicaid program and SCHIP Assessing the impact of increased fees and administrative changes RYAN J. HUGHES, D.D.S.,
STATE AND COMMUNITY MODELS FOR IMPROVING ACCESS TO DENTAL CARE FOR THE UNDERSERVED
 American Dental Association STATE AND COMMUNITY MODELS FOR IMPROVING ACCESS TO DENTAL CARE FOR THE UNDERSERVED October 2004 Executive Summary American Dental Association. State and Community Models for
American Dental Association STATE AND COMMUNITY MODELS FOR IMPROVING ACCESS TO DENTAL CARE FOR THE UNDERSERVED October 2004 Executive Summary American Dental Association. State and Community Models for
The Impact of Changing Workforce Models on Access to Oral Health Care Services
 The Impact of Changing Workforce Models on Access to Oral Health Care Services Presented by: Margaret Langelier, MSHSA Oral Health Workforce Research Center Center for Health Workforce Studies School of
The Impact of Changing Workforce Models on Access to Oral Health Care Services Presented by: Margaret Langelier, MSHSA Oral Health Workforce Research Center Center for Health Workforce Studies School of
Innovation in the Oral Health Service Delivery System
 Innovation in the Oral Health Service Delivery System Presented by: Simona Surdu, MD, PhD Oral Health Workforce Research Center Center for Health Workforce Studies School of Public Health, University at
Innovation in the Oral Health Service Delivery System Presented by: Simona Surdu, MD, PhD Oral Health Workforce Research Center Center for Health Workforce Studies School of Public Health, University at
Meeting the Oral Health Needs of Children
 Meeting the Oral Health Needs of Children Shelly Gehshan Director Advancing Children s Dental Health Initiative The Pew Center on the States 1 Why Does Oral Health Matter? Poor oral health can affect a
Meeting the Oral Health Needs of Children Shelly Gehshan Director Advancing Children s Dental Health Initiative The Pew Center on the States 1 Why Does Oral Health Matter? Poor oral health can affect a
Dental Therapy Toolkit LESSONS LEARNED
 Dental Therapy Toolkit LESSONS LEARNED March, 2016 Acknowledgements LESSONS LEARNED This report was developed through a partnership between the University of Minnesota, School of Dentistry, Metropolitan
Dental Therapy Toolkit LESSONS LEARNED March, 2016 Acknowledgements LESSONS LEARNED This report was developed through a partnership between the University of Minnesota, School of Dentistry, Metropolitan
Florida Department of Health: Oral Health Workforce
 Florida Department of Health: Oral Health Workforce Florida Board of Governors Meeting June 23, 2011 Tampa, Florida Amy Cober RD LD MPH Public Health Dental Program Florida Department of Health County
Florida Department of Health: Oral Health Workforce Florida Board of Governors Meeting June 23, 2011 Tampa, Florida Amy Cober RD LD MPH Public Health Dental Program Florida Department of Health County
Session 6: Dental Program Performance. Presenter: Danielle Apostolon, Senior Project Manager, Safety Net Solutions
 Session 6: Dental Program Performance Presenter: Danielle Apostolon, Senior Project Manager, Safety Net Solutions Key Objectives Overview of the important key data to track dental program performance Discuss
Session 6: Dental Program Performance Presenter: Danielle Apostolon, Senior Project Manager, Safety Net Solutions Key Objectives Overview of the important key data to track dental program performance Discuss
Sarah Wovcha, JD, MPH Executive Director Children s Dental Services
 Sarah Wovcha, JD, MPH Executive Director Children s Dental Services CDS Mission Statement: Since 1919 Children's Dental Services is dedicated to improving the oral health of children from families with
Sarah Wovcha, JD, MPH Executive Director Children s Dental Services CDS Mission Statement: Since 1919 Children's Dental Services is dedicated to improving the oral health of children from families with
Improving Access to Oral Health Care for Vulnerable and Underserved Populations
 Improving Access to Oral Health Care for Vulnerable and Underserved Populations Report of the Committee on Oral Health Access to Services Shelly Gehshan Director, Pew Children s Dental Campaign Committee
Improving Access to Oral Health Care for Vulnerable and Underserved Populations Report of the Committee on Oral Health Access to Services Shelly Gehshan Director, Pew Children s Dental Campaign Committee
State Case Study: Mid Level Providers in Connecticut
 State Case Study: Mid Level Providers in Connecticut Douglas B. Keck, DMD, MSHEd Carol J. Dingeldey, CAE Case Study: Mid Level Providers in Connecticut What we will cover: About Connecticut Setting the
State Case Study: Mid Level Providers in Connecticut Douglas B. Keck, DMD, MSHEd Carol J. Dingeldey, CAE Case Study: Mid Level Providers in Connecticut What we will cover: About Connecticut Setting the
Policy Benchmark 1: Having sealant programs in at least 25 percent of high-risk schools
 Policy Benchmark 1: Having sealant programs in at least 25 percent of high-risk schools Percentage of high-risk schools with sealant programs, 2010 75 100% 2 50 74% 7 25 49% 12 1 24% 23 None 7 Dental sealants
Policy Benchmark 1: Having sealant programs in at least 25 percent of high-risk schools Percentage of high-risk schools with sealant programs, 2010 75 100% 2 50 74% 7 25 49% 12 1 24% 23 None 7 Dental sealants
THE EARLY TREATMENT FOR HIV ACT: MEDICAID COVERAGE FOR PEOPLE LIVING WITH HIV
 THE EARLY TREATMENT FOR HIV ACT: MEDICAID COVERAGE FOR PEOPLE LIVING WITH HIV INTRODUCTION The Early Treatment for HIV Act (ETHA) would allow states to extend Medicaid coverage to uninsured, non-disabled
THE EARLY TREATMENT FOR HIV ACT: MEDICAID COVERAGE FOR PEOPLE LIVING WITH HIV INTRODUCTION The Early Treatment for HIV Act (ETHA) would allow states to extend Medicaid coverage to uninsured, non-disabled
Looking Back, Looking Forward
 Looking Back, Looking Forward An Empirical Look at Access to Dental Care in the United States Marko Vujicic, PhD Managing Vice President Health Policy Resources Center Agenda About Me Part 1 A Look Back
Looking Back, Looking Forward An Empirical Look at Access to Dental Care in the United States Marko Vujicic, PhD Managing Vice President Health Policy Resources Center Agenda About Me Part 1 A Look Back
The Oral Health Workforce & Access to Dental Care
 The Oral Health Workforce & Access to Dental Care Beth Mertz, PhD, MA National Health Policy Forum April 10, 2015 Objectives 1. Provide an overview of the current dental access and workforce landscape
The Oral Health Workforce & Access to Dental Care Beth Mertz, PhD, MA National Health Policy Forum April 10, 2015 Objectives 1. Provide an overview of the current dental access and workforce landscape
Highland Medical Center SLIDING FEE POLICY. HMC is here to serve the entire community, including people who may not have
 Highland Medical Center SLIDING FEE POLICY HMC is here to serve the entire community, including people who may not have regular access to health care because of distance and/or economics. In order to facilitate
Highland Medical Center SLIDING FEE POLICY HMC is here to serve the entire community, including people who may not have regular access to health care because of distance and/or economics. In order to facilitate
The Distribution and Composition of Arizona s Dental Workforce and Practice Patterns: Implications for Access to Care
 The Distribution and Composition of Arizona s Dental Workforce and Practice Patterns: Implications for Access to Care Center for California Health Workforce Studies July 2004 Elizabeth Mertz, MA Kevin
The Distribution and Composition of Arizona s Dental Workforce and Practice Patterns: Implications for Access to Care Center for California Health Workforce Studies July 2004 Elizabeth Mertz, MA Kevin
Salaries and Job Satisfaction of Health Center Dental Providers: 2013 Trends. Kenneth A Bolin, DDS, MPH
 Salaries and Job Satisfaction of Health Center Dental Providers: 2013 Trends Kenneth A Bolin, DDS, MPH NNOHA Webinar Series Archived presentations from the NNOHA webinar series are available online at
Salaries and Job Satisfaction of Health Center Dental Providers: 2013 Trends Kenneth A Bolin, DDS, MPH NNOHA Webinar Series Archived presentations from the NNOHA webinar series are available online at
Executive Summary. Burton Edelstein DDS MPH. Donald Schneider DDS MPH. R. Jeffrey Laughlin MPH
 SCHIP DENTAL PERFORMANCE OVER THE FIRST 10 YEARS: FINDINGS FROM THE LITERATURE AND A NEW ADA SURVEY Executive Summary Burton Edelstein DDS MPH Donald Schneider DDS MPH R. Jeffrey Laughlin MPH Prepared
SCHIP DENTAL PERFORMANCE OVER THE FIRST 10 YEARS: FINDINGS FROM THE LITERATURE AND A NEW ADA SURVEY Executive Summary Burton Edelstein DDS MPH Donald Schneider DDS MPH R. Jeffrey Laughlin MPH Prepared
Less than 40 percent of Medicaid-enrolled children in the study States received dental care during the study period.
 Children s Dental Care Access in Medicaid: The Role of Medical Care Use and Dentist Participation Tooth decay is one of the most preventable childhood diseases, yet dental care remains the most prevalent
Children s Dental Care Access in Medicaid: The Role of Medical Care Use and Dentist Participation Tooth decay is one of the most preventable childhood diseases, yet dental care remains the most prevalent
The Aging of the Population: Impacts on the Health Workforce
 The Aging of the Population: Impacts on the Health Workforce Presentation to the Advisory Committee on Interdisciplinary Community-Based Linkages Rockville, Maryland May 3, 2004 Jean Moore Director School
The Aging of the Population: Impacts on the Health Workforce Presentation to the Advisory Committee on Interdisciplinary Community-Based Linkages Rockville, Maryland May 3, 2004 Jean Moore Director School
Amendment 72 Increase Cigarette and Tobacco Taxes
 Amendment 72 Increase Cigarette and Tobacco Taxes ANALYSIS Amendment 72 proposes amending the Colorado Constitution to: increase the state tax on a pack of cigarettes from $0.84 to $2.59; increase the
Amendment 72 Increase Cigarette and Tobacco Taxes ANALYSIS Amendment 72 proposes amending the Colorado Constitution to: increase the state tax on a pack of cigarettes from $0.84 to $2.59; increase the
Access to Dental Care in the US
 Access to Dental Care in the US Time for Change?? Dr. Ana Karina Mascarenhas Immediate Past President, AAPHD Associate Dean of Research, Chief of Primary Care, Nova Southeastern University College of Dental
Access to Dental Care in the US Time for Change?? Dr. Ana Karina Mascarenhas Immediate Past President, AAPHD Associate Dean of Research, Chief of Primary Care, Nova Southeastern University College of Dental
MINNESOTA S ORAL HEALTH WORKFORCE October 2015
 MINNESOTA S ORAL HEALTH WORKFORCE 2012-2014 October 2015 2 Index Background Info 4-12 About this data Reference Maps 4-5 6-9 Additional Professional Information 10-12 All Oral Health Professions 12-30
MINNESOTA S ORAL HEALTH WORKFORCE 2012-2014 October 2015 2 Index Background Info 4-12 About this data Reference Maps 4-5 6-9 Additional Professional Information 10-12 All Oral Health Professions 12-30
Trends in the Provision of Oral Health Services by Federally Qualified Health Centers
 2018 Trends in the Provision of Oral Health Services by Federally Qualified Health Centers Center for Health Workforce Studies School of Public Health University at Albany, State University of New York
2018 Trends in the Provision of Oral Health Services by Federally Qualified Health Centers Center for Health Workforce Studies School of Public Health University at Albany, State University of New York
Meeting the Oral Health Care Needs of the Underserved
 Meeting the Oral Health Care Needs of the Underserved The rate and severity of oral disease is greater among people with special health care needs than in the general population due to difficulty in maintaining
Meeting the Oral Health Care Needs of the Underserved The rate and severity of oral disease is greater among people with special health care needs than in the general population due to difficulty in maintaining
Increasing Oral Health Access Through Clinic Expansion A NNOHA Promising Practice
 Increasing Oral Health Access Through Clinic Expansion A NNOHA Promising Practice By Ethan E. Kerns, DDS, Chief Dental Officer Salud Family Health Services Salud Family Health Salud Family Health Center,
Increasing Oral Health Access Through Clinic Expansion A NNOHA Promising Practice By Ethan E. Kerns, DDS, Chief Dental Officer Salud Family Health Services Salud Family Health Salud Family Health Center,
Pediatric Restorative Benefits: Potential for Fraud & Abuse
 1 Pediatric Restorative Benefits: Potential for Fraud & Abuse Part 2 The Medicaid-Commercial Spectrum, Media Reports of Abuse, U.S. Senate Study, Quest for the Facts and a Plan of Action Craig Kasten Wednesday
1 Pediatric Restorative Benefits: Potential for Fraud & Abuse Part 2 The Medicaid-Commercial Spectrum, Media Reports of Abuse, U.S. Senate Study, Quest for the Facts and a Plan of Action Craig Kasten Wednesday
National Dental Expenditure Flat Since 2008, Began to Slow in 2002
 National Dental Expenditure Flat Since 2008, Began to Slow in 2002 Author: Marko Vujicic, Ph.D. The Health Policy Institute (HPI) is a thought leader and trusted source for policy knowledge on critical
National Dental Expenditure Flat Since 2008, Began to Slow in 2002 Author: Marko Vujicic, Ph.D. The Health Policy Institute (HPI) is a thought leader and trusted source for policy knowledge on critical
The Oral Health Workforce in Maine
 The Oral Health Workforce in Maine December 2012 Prepared for: Maine Oral Health Funders Augusta, Maine Project Completed by: The Center for Health Workforce Studies School of Public Health, University
The Oral Health Workforce in Maine December 2012 Prepared for: Maine Oral Health Funders Augusta, Maine Project Completed by: The Center for Health Workforce Studies School of Public Health, University
Insurance Guide For Dental Healthcare Professionals
 Insurance Guide For Dental Healthcare Professionals Dental Benefits Basics What is dental insurance? Unlike traditional insurance, dental benefits are not meant to cover all oral healthcare needs. The
Insurance Guide For Dental Healthcare Professionals Dental Benefits Basics What is dental insurance? Unlike traditional insurance, dental benefits are not meant to cover all oral healthcare needs. The
Miami-Dade County Prepaid Dental Health Plan Demonstration: Less Value for State Dollars
 Miami-Dade County Prepaid Dental Health Plan Demonstration: Less Value for State Dollars Analysis commissioned by The Collins Center for Public Policy / Community Voices Miami AUGUST 2006 Author: Burton
Miami-Dade County Prepaid Dental Health Plan Demonstration: Less Value for State Dollars Analysis commissioned by The Collins Center for Public Policy / Community Voices Miami AUGUST 2006 Author: Burton
Biography for Brian J Quinlan DDS
 Biography for Brian J Quinlan DDS Northwestern University Dental School, Chicago, IL DDS 1986 Nothing Cum Laude Private practice, 3 locations: Chicago, Strum, WI & Twin Cities 1986-1991 Park Dental 1991-1996
Biography for Brian J Quinlan DDS Northwestern University Dental School, Chicago, IL DDS 1986 Nothing Cum Laude Private practice, 3 locations: Chicago, Strum, WI & Twin Cities 1986-1991 Park Dental 1991-1996
Contracting for Dental Services: Increase Access to Care
 Contracting for Dental Services: Increase Access to Care Irene V. Hilton, DDS, MPH Donald A. Simila, MSW, FACHE June 19, 2017 Objectives List scenarios in which health centers contract for dental services
Contracting for Dental Services: Increase Access to Care Irene V. Hilton, DDS, MPH Donald A. Simila, MSW, FACHE June 19, 2017 Objectives List scenarios in which health centers contract for dental services
Sarah Wovcha, J.D., M.P.H. Executive Director, In-House Counsel
 Sarah Wovcha, J.D., M.P.H. Executive Director, In-House Counsel Children s Dental Services (CDS) Portable Care Program Use of Advanced Dental Therapists in a portable care model and at CDS Need Definition
Sarah Wovcha, J.D., M.P.H. Executive Director, In-House Counsel Children s Dental Services (CDS) Portable Care Program Use of Advanced Dental Therapists in a portable care model and at CDS Need Definition
The Medicaid, Medicare, CHIP Services Dental Association is pleased to present Improving the Quality of Oral Healthcare through Case Management.
 The Medicaid, Medicare, CHIP Services Dental Association is pleased to present Improving the Quality of Oral Healthcare through Case Management. Improving the Quality of Oral Healthcare through Case Management
The Medicaid, Medicare, CHIP Services Dental Association is pleased to present Improving the Quality of Oral Healthcare through Case Management. Improving the Quality of Oral Healthcare through Case Management
Safety Net Solutions Benchmark Guide
 Safety Net Solutions Benchmark Guide How to use this guide: A benchmark is a point of reference from which measurements can be made. Benchmarks are for comparison only and are not precisely relative to
Safety Net Solutions Benchmark Guide How to use this guide: A benchmark is a point of reference from which measurements can be made. Benchmarks are for comparison only and are not precisely relative to
Article XIX DENTAL HYGIENIST COLLABORATIVE CARE PROGRAM
 Article XIX DENTAL HYGIENIST COLLABORATIVE CARE PROGRAM Pursuant to ACA 17-82-701-17-82-707 the Arkansas State Board of Dental Examiners herby promulgates these rules to implement the dental hygienist
Article XIX DENTAL HYGIENIST COLLABORATIVE CARE PROGRAM Pursuant to ACA 17-82-701-17-82-707 the Arkansas State Board of Dental Examiners herby promulgates these rules to implement the dental hygienist
CODA Guidelines for Dental Therapy Education: Implications for Expansion of Dental Therapy in the U.S.
 CODA Guidelines for Dental Therapy Education: Implications for Expansion of Dental Therapy in the U.S. Jane Koppelman, Research Director, Pew Dental Campaign Wisconsin Oral Health Conference September
CODA Guidelines for Dental Therapy Education: Implications for Expansion of Dental Therapy in the U.S. Jane Koppelman, Research Director, Pew Dental Campaign Wisconsin Oral Health Conference September
Redesign Dental for Maximum Efficiency. Mark Doherty DMD MPH Executive Director Safety Net Solutions
 Redesign Dental for Maximum Efficiency Mark Doherty DMD MPH Executive Director Safety Net Solutions Objectives Provide an overview of an effective, tried and true Redesign process Explain the 5 priority
Redesign Dental for Maximum Efficiency Mark Doherty DMD MPH Executive Director Safety Net Solutions Objectives Provide an overview of an effective, tried and true Redesign process Explain the 5 priority
HealthVoices. Health and Healthcare in Rural Georgia. The perspective of rural Georgians
 HealthVoices Health and Healthcare in Rural Georgia Issue 3, Publication #100, February 2017 Samantha Bourque Tucker, MPH; Hilton Mozee, BA; Gary Nelson, PhD The perspective of rural Georgians Rural Georgia
HealthVoices Health and Healthcare in Rural Georgia Issue 3, Publication #100, February 2017 Samantha Bourque Tucker, MPH; Hilton Mozee, BA; Gary Nelson, PhD The perspective of rural Georgians Rural Georgia
Dental Public Health Activity Descriptive Report
 Dental Public Health Activity Descriptive Report Practice Number: 04006 Submitted By: Office of Oral Health, Arizona Department of Health Services Submission Date: May 2002 Last Reviewed: September 2017
Dental Public Health Activity Descriptive Report Practice Number: 04006 Submitted By: Office of Oral Health, Arizona Department of Health Services Submission Date: May 2002 Last Reviewed: September 2017
Dental Therapists: Increasing Access to Dental Care. Kristen R. Boilini Pivotal Policy Consulting. Dental Care for AZ. Dental Care for AZ
 Dental Therapists: Increasing Access to Dental Care Kristen R. Boilini Pivotal Policy Consulting July 14, 2017 Why Dental Therapy? Vast rural areas and Tribal reservations 2.3 million Arizonans lack access
Dental Therapists: Increasing Access to Dental Care Kristen R. Boilini Pivotal Policy Consulting July 14, 2017 Why Dental Therapy? Vast rural areas and Tribal reservations 2.3 million Arizonans lack access
MEDICAID REIMBURSEMENT
 MEDICAID REIMBURSEMENT Medicaid for children under 20 Pays for exam, cleaning, and fluoride treatment every six months. $100 of x-rays per year. Pays for fillings, sealants, extractions, stainless steel
MEDICAID REIMBURSEMENT Medicaid for children under 20 Pays for exam, cleaning, and fluoride treatment every six months. $100 of x-rays per year. Pays for fillings, sealants, extractions, stainless steel
Dental PPO Plan. A plan to help you pay for the dental care you need. Accident & Health
 Dental PPO Plan A plan to help you pay for the dental care you need National General Accident and Health markets products underwritten by Time Insurance Company, National Health Insurance Company, Integon
Dental PPO Plan A plan to help you pay for the dental care you need National General Accident and Health markets products underwritten by Time Insurance Company, National Health Insurance Company, Integon
Access to Care: An International Perspective
 Access to Care: An International Perspective William R. Maas, DDS, MPH Director Division of Oral Health National Center for Chronic Disease Prevention and Health Promotion Centers for Disease Control and
Access to Care: An International Perspective William R. Maas, DDS, MPH Director Division of Oral Health National Center for Chronic Disease Prevention and Health Promotion Centers for Disease Control and
QUALITY, EFFECTIVENESS AND VALUE OF TELEHEALTH IN RURAL MINNESOTA SETTINGS. Sarah Wovcha, JD, MPH, Executive Director Minneapolis, MN
 QUALITY, EFFECTIVENESS AND VALUE OF TELEHEALTH IN RURAL MINNESOTA SETTINGS Sarah Wovcha, JD, MPH, Executive Director Minneapolis, MN Children s dental services Mission: Since 1919 Children's Dental Services
QUALITY, EFFECTIVENESS AND VALUE OF TELEHEALTH IN RURAL MINNESOTA SETTINGS Sarah Wovcha, JD, MPH, Executive Director Minneapolis, MN Children s dental services Mission: Since 1919 Children's Dental Services
Can dental therapists help the current, primarily of5ice-based, dental delivery system meet the needs of long-term care residents?
 An Advanced Dental Therapist in Long-Term Care: Heather Luebben s Case Study Overview The number of senior citizens (ages 65 and older) is expected to double to more than 98 million by 2060, when they
An Advanced Dental Therapist in Long-Term Care: Heather Luebben s Case Study Overview The number of senior citizens (ages 65 and older) is expected to double to more than 98 million by 2060, when they
Dental Care Remains the No. 1 Unmet Health Care Need for Children and Low-Income Adults
 Oral Health and Access to Dental Care for Ohioans, 2007 Dental Care Remains the No. 1 Unmet Health Care Need for Children and Low-Income Adults Oral Health and Access to Dental Care for Ohioans, 2007
Oral Health and Access to Dental Care for Ohioans, 2007 Dental Care Remains the No. 1 Unmet Health Care Need for Children and Low-Income Adults Oral Health and Access to Dental Care for Ohioans, 2007
Dental Public Health Activities & Practices
 Dental Public Health Activities & Practices Practice Number: 02001 Submitted By: Alaska Department of Health & Social Services, Division of Public Health Submission Date: February 2002 Last Updated: January
Dental Public Health Activities & Practices Practice Number: 02001 Submitted By: Alaska Department of Health & Social Services, Division of Public Health Submission Date: February 2002 Last Updated: January
Innovation in the Ranks; Expanding oral health care access in Arizona with advanced delivery and workforce models
 Innovation in the Ranks; Expanding oral health care access in Arizona with advanced delivery and workforce models Kavita Bernstein, Program Specialist Children s Health First Things First Megan Miks, Manager
Innovation in the Ranks; Expanding oral health care access in Arizona with advanced delivery and workforce models Kavita Bernstein, Program Specialist Children s Health First Things First Megan Miks, Manager
Background. North Dakota Oral Health Need
 Background In spring of 2014 the North Dakota Center for Rural Health was tasked with completing an objective assessment of oral health need and policy recommendations for North Dakota. This study was
Background In spring of 2014 the North Dakota Center for Rural Health was tasked with completing an objective assessment of oral health need and policy recommendations for North Dakota. This study was
Report on the Financial and Programmatic Feasibility of Establishing a Satellite Clinic of the VCU School of Dentistry in Wise County
 September 2007 Report on the Financial and Programmatic Feasibility of Establishing a Satellite Clinic of the VCU School of Dentistry in Wise County Advancing Virginia through Higher Education Report on
September 2007 Report on the Financial and Programmatic Feasibility of Establishing a Satellite Clinic of the VCU School of Dentistry in Wise County Advancing Virginia through Higher Education Report on
Phase I Planning Grant Application. Issued by: Caring for Colorado Foundation. Application Deadline: July 1, 2015, 5:00 PM
 Phase I Planning Grant Application Issued by: Caring for Colorado Foundation Application Deadline: July 1, 2015, 5:00 PM Executive Summary Caring for Colorado is currently accepting applications for SMILES
Phase I Planning Grant Application Issued by: Caring for Colorado Foundation Application Deadline: July 1, 2015, 5:00 PM Executive Summary Caring for Colorado is currently accepting applications for SMILES
Changes in Iowa Dentist Workforce Composition, : First in a Series of Issue Briefs
 Health Policy 5-1-2015 Changes in Iowa Dentist Workforce Composition, 1997-2013: First in a Series of Issue Briefs Julie Christine Reynolds University of Iowa Susan Christine McKernan University of Iowa
Health Policy 5-1-2015 Changes in Iowa Dentist Workforce Composition, 1997-2013: First in a Series of Issue Briefs Julie Christine Reynolds University of Iowa Susan Christine McKernan University of Iowa
Demonstrating Return on Investment for Community Health Worker Services Translating Science into Practice
 Demonstrating Return on Investment for Community Health Worker Services Translating Science into Practice May 11, 2017 The 8 th Annual Community Health Worker/Patient Navigator Conference Katharine London,
Demonstrating Return on Investment for Community Health Worker Services Translating Science into Practice May 11, 2017 The 8 th Annual Community Health Worker/Patient Navigator Conference Katharine London,
HRSA Oral Health Programs 2010 Dental Management Coalition June 27, 2010 Annapolis, MD
 HRSA Oral Health Programs 2010 Dental Management Coalition June 27, 2010 Annapolis, MD Jay R. Anderson, DMD, MHSA HRSA Chief Dental Officer US Department of Health and Human Services Health Resources and
HRSA Oral Health Programs 2010 Dental Management Coalition June 27, 2010 Annapolis, MD Jay R. Anderson, DMD, MHSA HRSA Chief Dental Officer US Department of Health and Human Services Health Resources and
Economic Impact of Regulating the Use of Amalgam Restorations
 Research Articles Economic Impact of Regulating the Use of Amalgam Restorations Tryfon Beazoglou, PhD a Stephen Eklund, DDS, DrPH b Dennis Heffley, PhD c Jonathan Meiers, DMD d L. Jackson Brown, DDS, PhD
Research Articles Economic Impact of Regulating the Use of Amalgam Restorations Tryfon Beazoglou, PhD a Stephen Eklund, DDS, DrPH b Dennis Heffley, PhD c Jonathan Meiers, DMD d L. Jackson Brown, DDS, PhD
Good news about dental benefits for employees of. LCMC Health
 Dental PPO Good news about dental benefits for employees of LCMC Health Why is dental health so important? Regular dental care does more than just improve smiles. Along with good oral hygiene, it can help
Dental PPO Good news about dental benefits for employees of LCMC Health Why is dental health so important? Regular dental care does more than just improve smiles. Along with good oral hygiene, it can help
Questions and Answers on 2009 H1N1 Vaccine Financing
 Questions and Answers on 2009 H1N1 Vaccine Financing General Financing Questions Considerations of financing distinguish between those related to the vaccine itself, the ancillary supplies needed to administer
Questions and Answers on 2009 H1N1 Vaccine Financing General Financing Questions Considerations of financing distinguish between those related to the vaccine itself, the ancillary supplies needed to administer
Oral Health Workforce: Options and Opportunities
 Oral Health Workforce: Options and Opportunities Burton L. Edelstein DDS MPH Senior Fellow in Public Policy, Children s Dental Health Project, Washington DC Professor of Dental Medicine and Health Policy
Oral Health Workforce: Options and Opportunities Burton L. Edelstein DDS MPH Senior Fellow in Public Policy, Children s Dental Health Project, Washington DC Professor of Dental Medicine and Health Policy
Water Fluoridation and Costs of Medicaid Treatment for Dental Decay -- Louisiana,
 MMWR September 03, 1999 / 48(34);753-757 Water Fluoridation and Costs of Medicaid Treatment for Dental Decay -- Louisiana, 1995-1996 Treatment costs for dental decay in young children can be substantial,
MMWR September 03, 1999 / 48(34);753-757 Water Fluoridation and Costs of Medicaid Treatment for Dental Decay -- Louisiana, 1995-1996 Treatment costs for dental decay in young children can be substantial,
Dental Public Health Activities & Practices
 Dental Public Health Activities & Practices Practice Number: 37002 Submitted By: North Dakota Department of Health, Family Health Division Submission Date: January 2010 Last Updated: January 2010 SECTION
Dental Public Health Activities & Practices Practice Number: 37002 Submitted By: North Dakota Department of Health, Family Health Division Submission Date: January 2010 Last Updated: January 2010 SECTION
Providing LARCs in a Federally Qualified Health Center Is it financially viable? A case study. Lisa Maldonado, MA, MPH Linda Prine, MD
 Providing LARCs in a Federally Qualified Health Center Is it financially viable? A case study Lisa Maldonado, MA, MPH Linda Prine, MD Mission The Reproductive Health Access Project trains and supports
Providing LARCs in a Federally Qualified Health Center Is it financially viable? A case study Lisa Maldonado, MA, MPH Linda Prine, MD Mission The Reproductive Health Access Project trains and supports
Paul Glassman DDS, MA, MBA Professor and Director of Community Oral Health University of the Pacific School of Dentistry San Francisco, CA
 Paul Glassman DDS, MA, MBA Professor and Director of Community Oral Health University of the Pacific School of Dentistry San Francisco, CA The US Health Care System is Undergoing Profound Change Drivers
Paul Glassman DDS, MA, MBA Professor and Director of Community Oral Health University of the Pacific School of Dentistry San Francisco, CA The US Health Care System is Undergoing Profound Change Drivers
STATES BEST PRACTICES IN IMPROVING STATE ORAL HEALTH PROGRAM WORKFORCE CAPACITY
 STATES BEST PRACTICES IN IMPROVING STATE ORAL HEALTH PROGRAM WORKFORCE CAPACITY UCSF DPH 175 Dental Public Health Lecture Series January 26, 2016 Dr. Harry Goodman Immediate Past-President, Association
STATES BEST PRACTICES IN IMPROVING STATE ORAL HEALTH PROGRAM WORKFORCE CAPACITY UCSF DPH 175 Dental Public Health Lecture Series January 26, 2016 Dr. Harry Goodman Immediate Past-President, Association
BARBARA AVED ASSOCIATES
 BARBARA AVED ASSOCIATES April 2018 Table of Contents INTRODUCTION... 2 METHODS... 3 FINDINGS... 4 I. Extent of Emergency Department Use for Preventable Dental Conditions... 4 II. Utilization of Dental
BARBARA AVED ASSOCIATES April 2018 Table of Contents INTRODUCTION... 2 METHODS... 3 FINDINGS... 4 I. Extent of Emergency Department Use for Preventable Dental Conditions... 4 II. Utilization of Dental
The Impact of Oral Disease on Colorado s Children
 The Impact of Oral Disease on Colorado s Children Colorado Health Institute 303 E. 17 th Avenue, Suite 930 Denver, Colorado 80203 www.coloradohealthinstitute.org June 2010 Table of Contents Introduction...
The Impact of Oral Disease on Colorado s Children Colorado Health Institute 303 E. 17 th Avenue, Suite 930 Denver, Colorado 80203 www.coloradohealthinstitute.org June 2010 Table of Contents Introduction...
COLUMBIA ST. MARY S MILWAUKEE FY15 COMMUNITY IMPACT REPORT CONTENTS
 HEALTH CONTENTS FY15 Community Impact Report Accomplishments Summary Page 2 Infant Mortality Pages 3-4 Children s Oral Health Access Page 5 Breast Cancer Screening Page 6 Access to Care Page 7-9 Financial
HEALTH CONTENTS FY15 Community Impact Report Accomplishments Summary Page 2 Infant Mortality Pages 3-4 Children s Oral Health Access Page 5 Breast Cancer Screening Page 6 Access to Care Page 7-9 Financial
I-Smile The Systematic Dental Home. Bob Russell, DDS, MPH Iowa Department of Public Health Cathy Coppes LBSW Iowa Department of Human Services
 I-Smile The Systematic Dental Home Bob Russell, DDS, MPH Iowa Department of Public Health Cathy Coppes LBSW Iowa Department of Human Services The Dental Home A Systematic Concept Dental decay is a multi-factorial,
I-Smile The Systematic Dental Home Bob Russell, DDS, MPH Iowa Department of Public Health Cathy Coppes LBSW Iowa Department of Human Services The Dental Home A Systematic Concept Dental decay is a multi-factorial,
Linking Research to Clinical Practice
 Is Non Surgical Periodontal Therapy Cost Effective? Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information
Is Non Surgical Periodontal Therapy Cost Effective? Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information
Access to Oral Health Care in Iowa
 Health Policy 2-1-2004 Access to Oral Health Care in Iowa Public Policy Center, The University of Iowa Copyright 2004 Public Policy Center, the University of Iowa Hosted by Iowa Research Online. For more
Health Policy 2-1-2004 Access to Oral Health Care in Iowa Public Policy Center, The University of Iowa Copyright 2004 Public Policy Center, the University of Iowa Hosted by Iowa Research Online. For more
Access to care and dental providers Minnesota Initiatives Leon Assael DMD CMM, Dean April
 Access to care and dental providers Minnesota Initiatives Leon Assael DMD CMM, Dean April 10. 2015 What is the status of oral health in America? David Satcher MD A silent epidemic of dental and oral diseases
Access to care and dental providers Minnesota Initiatives Leon Assael DMD CMM, Dean April 10. 2015 What is the status of oral health in America? David Satcher MD A silent epidemic of dental and oral diseases
