Reduced mandibular range of motion in Duchenne Muscular Dystrophy: predictive factors
|
|
|
- Moses Cannon
- 5 years ago
- Views:
Transcription
1 J o u r n a l o f Oral Rehabilitation Journal of Oral Rehabilitation 2015 Reduced mandibular range of motion in Duchenne Muscular Dystrophy: predictive factors H. W. VAN BRUGGEN*, L. VAN DEN ENGEL-HOEK, M.H. STEENKS, E.M. BRONKHORST, N.H.J. CREUGERS*, I.J.M. DE GROOT & S.I. KALAYKOVA* *Department of Oral Function and Prosthetic Dentistry, College of Dental Science, Radboud University Nijmegen Medical Center, Nijmegen, Department of Oral-Maxillofacial Surgery, Prosthodontics and Special Dental Care, University Medical Center, Utrecht, Department of Rehabilitation, Radboud University Nijmegen Medical Center, Nijmegen, and Department of Preventive and Restorative Dentistry, College of Dental Science, Radboud University Nijmegen Medical Center, Nijmegen, The Netherlands SUMMARY Patients with Duchenne muscular dystrophy (DMD) experience negative effects upon feeding and oral health. We aimed to determine whether the mandibular range of motion in DMD is impaired and to explore predictive factors for the active maximum mouth opening (ammo). 23 patients with DMD (mean age years) and 23 controls were assessed using a questionnaire about mandibular function and impairments. All participants underwent a clinical examination of the masticatory system, including measurement of mandibular range of motion and variables related to mandibular movements. In all patients, quantitative ultrasound of the digastric muscle and the geniohyoid muscle and the motor function measure (MFM) scale were performed. The patients were divided into early and late ambulatory stage (AS), early non-ambulatory stage (ENAS) and late non-ambulatory stage (LNAS). All mandibular movements were reduced in the patient group (P < 0001) compared to the controls. Reduction in the ammo (<40 mm) was found in 26% of the total patient group. LNAS patients had significantly smaller mandibular movements compared to AS and ENAS (P < 005). Multiple linear regression analysis for ammo revealed a positive correlation with the body height and disease progression, with MFM total score as the strongest independent risk factor (R 2 = 071). Mandibular movements in DMD are significantly reduced and become more hampered with loss of motor function, including the sitting position, arm function, and neck and head control. We suggest that measurement of the ammo becomes a part of routine care of patients with DMD. KEYWORDS: Duchenne muscular dystrophy, masticatory system, mandibular range of motion, quantitative ultrasound, masticatory muscles, motor function measure Accepted for publication 22 December 2014 Introduction Duchenne muscular dystrophy (DMD) is, with an incidence of about 1: 4200 live male births, one of the most prevalent hereditary muscle diseases (1). It is caused by a defective gene for dystrophin, a protein that helps to keep muscle cells intact (2). DMD is characterised by progressive muscle weakness including the craniofacial muscles (3, 4). The weakness of the craniofacial muscles consequently affects the development and morphology of the craniofacial structures (5 8). Weakness of the jaw muscles, in combination with changes in the craniofacial morphology, may affect mandibular function, including mandibular range of motion (ROM) (4, 9). To our knowledge, predictive factors for a compromised mandibular ROM in patients with DMD have not been investigated yet. doi: /joor.12274
2 2 H. W. VAN BRUGGEN et al. The most important influencing factors upon the mandibular ROM in healthy subjects are the length of the mandible, functional capacity of the mandibular opening and closing muscles, morphology and status of the temporomandibular joint (TMJ), and pain conditions in the masticatory system (9, 10). Ultrasound measurements in patients with DMD of the masseter muscles and the suprahyoid muscles showed structural changes in these muscles indicating muscular dystrophy (4, 11). Hypothetically, the structural changes may lead to decreased strength of the muscles involved in mandibular movement and contribute to a limited mandibular ROM. Factors beyond the masticatory system may contribute to a reduction in the mandibular range of motion as well. Recent observations suggest a functional relationship between the cranio-cervical and the masticatory system (12, 13). As a consequence, gross motor function measurement, which includes assessment of posture, neck function and head control, might be predictive for the mandibular range of motion. The aim of our investigation was to determine whether the mandibular range of motion in DMD is impaired compared to that in healthy subjects and to explore predictive factors for the active maximum mouth opening (ammo) in DMD. Material and methods Participants Twenty-four patients with DMD aged from 6 to 38 years, participating in a swallowing study on DMD (11), and 24 age-matched healthy males were examined between May 2010 and February Patients were recruited by announcements of patient organisations. Only patients with an established diagnosis of DMD older than 5 years were eligible. Duchenne muscular dystrophy patients who were entirely dependent on tube feeding were excluded. The control group was recruited at a primary and a secondary school located in the western part of the Netherlands. Healthy students above 18 years were recruited at the College of Dental Sciences, Nijmegen, the Netherlands. Exclusion criteria for controls were the following: a history of neuromuscular disease, temporomandibular disorder, orthodontic treatment and morphologic dental malocclusion such as crossbite and a tendency to cross-bite. Protocol The participants in both the patient and the control group completed a questionnaire and underwent a clinical examination of the masticatory system including measurement of the mandibular range of motion. Additionally, the patients underwent quantitative muscle ultrasound imaging (QMUS) of the anterior belly of the digastric muscle and the geniohyoid muscle (14), and an assessment of their general physical abilities using the Motor Function Measure (MFM) (15). Questionnaire All subjects completed the questionnaire Screen, which was developed to assess pain in the head and neck region, mandibular function and related issues (16, 17). Clinical examination of the masticatory system All participants in this study were clinically examined following the validated procedure as described by Lobbezoo-Scholte et al. (18 21). This clinical examination included, among others, measurement of the mandibular range of motion, palpation of the masticatory muscles and the temporomandibular joints. All patients and controls were examined in the upright position with their heads supported in a neutral position. The following mandibular movements were assessed: active maximum mouth opening (ammo), passive maximum mouth opening (pmmo), protrusion, and left and right lateral range of motion. The overbite and overjet were also measured. The ammo was the distance measured between the incisal edges of the upper and lower central incisors plus the overbite. All measurements were recorded with a metal ruler (mm). We considered mandibular movements to be reduced: <40 mm for ammo, <8 mm for active lateral excursion and <5 mm for protrusion. The mobility of the temporomandibular joint was assessed by palpation of the lateral pole of the mandibular condyle during MMO with the index finger. Sliding of the mandibular condyle was assessed on a two-point scale: reduced meaning no or hardly any sliding of the lateral pole of the mandibular condyle and normal meaning sliding of the mandibular condyle to the
3 MUSCULAR DYSTROPHY AND MANDIBULAR MOVEMENT 3 crest of the articular eminence or beyond the crest of the articular eminence. The masseter and temporalis muscles were palpated to assess pain on palpation. The temporalis muscles were palpated bilaterally using the index and/or middle finger, applying firm pressure along the anterior, middle and posterior parts for 2 3 s. Then, the origin, the body and the insertion of the masseter are individually palpated for 2 3 s. Finally, the temporomandibular joints were palpated for 2 3 s. The left and right condyles were palpated in an open and closed mouth position. The lateral pole of each condyle was palpated anterior to the tragus of the ear and over the TMJ, and the posterior aspect of each condyle via the external acoustical meatus. Palpation pressure was firm (2 4 pounds) and was adjusted to the vulnerable patients, when appropriate (20, 22, 23). All pain reports of the participants during examination were recorded on a five-point Likert scale: 0 = no pain, 1 = mild, 2 = moderate, 3 = severe and 4 = very severe. Echo intensity imaging of the digastric and geniohyoid muscles In the patient group, QMUS was used to measure echo intensity of the digastric and geniohyoid muscles (11). These two muscles were selected because of their anatomical location. The diagnostic value of muscle ultrasound and the test retest reproducibility for the digastric muscle and the geniohyoid muscles was good (11). The region of interest was quantified by grey-scale analysis and calculation of z-scores (i.e. the amount of standard deviations below or above the mean of norm values), a reliable method with which changes in muscle architecture are assessed and compared with normal values (24, 25). The grey value of the mean of the left and right digastrics muscles and of the left and right geniohyoid muscle was expressed as z- scores. Z-score of < 2 and >2 is considered abnormal. Quantitative muscle ultrasound imaging of the digastric and geniohyoid muscles proved to be feasible in healthy children and young adults and is used for the detection of structural changes in these muscles (14). Medical information and general physical abilities In the patient group, information was gathered, among others, on body height, and baseline physical abilities were assessed by a physical therapist with expertise in paediatrics using a selection of MFM items. The MFM items have been previously been described (15). The items used in this study collect information about the sitting position, arm function, and neck and head control. The MFM items were scored on a four-point Likert scale and summed to comprise a total raw score (range 0 33), in which the maximum represents normal motor function. Based on the ambulatory function and the MFM, the patients were divided into early and late ambulatory stage (AS), early non-ambulatory stage (able to maintain posture) (ENAS) or late non-ambulatory stage (upper limb function and postural maintenance is increasingly limited) (LNAS) (26). Statistical analysis IBM SPSS version 20* was used to analyse the collected data. Mean and standard deviation were used to describe the average maximum mouth opening, the lateral excursions and the protrusion of the mandible in the patient and in control group. Paired Student s t-test was used to compare between-group continuous variable outcomes, and for dichotomous variables, the chi-square test was used. Patient data were further analysed using the three DMD stages. To compare test outcomes between the DMD stages, ANOVA was used for scale variables and chi-square test for dichotomous variables. Univariate and multivariate regression analyses were performed to determine which factors possibly affect the ammo within the patient group (dependent variable). The independent variables were age, body height, MFM total scores, MFM score item 13 14, ultrasound score of the digastric muscle and geniohyoid muscle. Results Participants Twenty-four patients with DMD were approached for inclusion in the study. One of the patients was excluded from the study because DMD was not genetically confirmed, and the signs and symptoms did not fit into the *IBM SPSS Statistics version 20, Inc., Chicago, IL, USA.
4 4 H. W. VAN BRUGGEN et al. Table 1. Group comparison and descriptive statistics of the mandibular range of motion during clinical examination in the patient group (n = 23) and in the control group (n = 23) Variables Mean age, years, month ammo (mm) (s.d.) range pmmo (mm) (s.d.) range Lateral ROM L/R (mm) Protrusion (mm) diagnosis of DMD. For analysis, the data of 23 patients and 23 age-matched males were used (Table 1). Patient characteristics of the total DMD sample as well as of the three stage groups are indicated in Table 2. Questionnaire Patient Control group group n = 23 n = 23 A limitation in the ability to open the mouth was noted in three patients (13%), and pain during opening the mouth was mentioned in four other patients (174%, Table 2). The maximum intensity of the recorded pain in these four patients was mild. Clinical examination of the masticatory system P-value 167 (77) 163 (67) (110) 546 (62) <00001* (111) 554(68) <00001* (30) 93 (17) <00001* (35) 93 (25) <00001* ammo: active maximum mouth opening, the maximum interincisal distance on opening as wide as possible plus the vertical overbite (limited MMO <40 mm). pmmo: passive maximum mouth opening, the maximum interincisal distance on active opening, with a slight overpressure on the edges of the upper and lower front teeth by the examiner plus the vertical overbite. Lateral ROM L/R: active mandibular lateral excursion, mean value between the left and right side. Protrusion: active forward movement of the mandible. Statistically significant differences (*) between the patient group and control group, tested with paired Student s t-tests. In six patients (261%), mild pain could be provoked during ammo, passive mouth opening, or palpation of the masseter muscle, temporalis muscle or the lateral pole of the TMJ. Four of these six patients belonged to the LNAS (Table 2). Active and passive maximum mouth opening, active mandibular lateral excursion and protrusion were significantly smaller in the patient group than in the control group (Table 1). In the patient group, 6 (26%) had a reduced ammo (<40 mm). The difference between the ammo and the pmmo in the patient and the control group was 1 mm. The LNAS had a statistically significant smaller ammo than the ENAS (Table 2). The active mandibular lateral excursion was reduced (<8 mm) in 16 patients (70%); all patients in the LNAS had a reduced lateral ROM. The LNAS had a statistically significant smaller lateral ROM than the ENAS (Table 2). The active mandibular protrusion was reduced (<5 mm) in seven patients (30%). The ENAS had a statistically significant smaller protrusion than the AS (Table 2). Clinical examination of the mobility of the temporomandibular joint revealed that 22 patients (960%) had a normal sliding of the mandibular condyle (Table 2). All controls had normal sliding of the mandibular condyle. Echo intensity imaging The echo intensity of the anterior belly of the digastric muscles, expressed as z-score, was found to be increased (z > 2) in 166% of the patients in the AS, 286% in ENAS and 500% in LNAS. The echo intensity of the geniohyoid muscles was increased in 500% of the patients in AS, 857% in ENAS and 900% in LNAS. There was a statistically significant difference between the AS and LNAS regarding the echo intensity of the geniohyoid muscles (Table 2). General physical abilities There was a significant difference in the MFM score between the ENAS and LNAS, and between AS and LNAS regarding the MFM total score (Table 2). There was a statistically significant difference between the ENAS and LNAS, and between AS and LNAS regarding the MFM items score. Predictive factors for the active maximum mouth opening Univariate linear regression analysis outcomes of potential predictors of ammo in patients with DMD are presented in Table 3. The univariate linear regres-
5 MUSCULAR DYSTROPHY AND MANDIBULAR MOVEMENT 5 Table 2. Characteristics of patients with Duchenne muscular dystrophy (n = 23) presented by stages. Mean and standard deviation of the measurements referred to as x (s.d.) or number of patient as n/% DMD stage P-value Variable Total (n = 23) AS (1) (n = 6) ENAS (2) (n = 7) LNAS (3) (n = 10) Age, years, month 167 (77) 84 (15) 150 (41) 228 (65) 0004* 0014* <0001* MFM, total raw score 201 (126) 325 (08) 269 (83) 79 (14) 0123 <0001* <0001* MFM item (25) 60 (0) 54 (10) 12 (14) 0172 <0001* <0001* ammo (mm) range 435 (110) 475 (79) 491 (92) 372 (111) * pmmo (mm) (s.d.) 443 (111) 483 (76) 501 (95) 378 (111) * 0060 range Lateral ROM L/R (mm) 64 (30) 73 (33) 82 (19) 47 (27) * Protrusion (mm) 47 (35) 70 (18) 49 (04) 32 (47) 0032* to6 EI digastric m., mean L/R 20 (31) 05 (14) 13 (25) 34 (38) (z-score) 13 to to EI geniohyoid (s.d.) 60 (52) 24 (30) 56 (52) 83 (53) * range m (z-score) Body height (cm) 1587 (219) 1308 (88) 1604 (160) 1743 (128) 0003* 0083 <0001* MMO reduced, subj 3/13% 1/17% 0/0% 2/20% 0585 Reduced TMJ sliding 1/4% 0/0% 0/0% 1/10% 1000 Pain provocation 6/26% 1/17% 1/14% 4/40% 0491 DMD, Duchenne muscular dystrophy; AS, Early and late ambulatory stage; ENAS, Early non-ambulatory stage; LNAS, Late nonambulatory stage. * Statistically significant difference between the DMD stages, tested with ANOVA for scale variables and with chi-square test for dichotomous outcome. The significance in the dichotomous outcomes relates to the variable being absent or present. MFM: Motor Function Measure, domain 2, items assessed axial en proximal motor capacities 12 items (total raw score 33 points); MFM score per item: 0 = does not initiate movement or starting position cannot be maintained; 1 = partially completes the exercise; 2 = completes the exercise with compensations; slowness or obvious clumsiness; and 3 = completes the exercise with a standard pattern. MFM items 13 14: item 13: seated on the chair without support of upper limbs or leaning against the back of the chair, maintains the sitting position, head and trunk in the axis; score 0 3; item14: seated on the chair or in their wheelchair. Head in flexion: from the fully flexed position, raises the head and maintains the raised position, head in the axis during the movement and when maintained; score 0 3. EI digastric L/R and geniohyoid muscles: echo intensity grey value (z-score) of the mean value of the left and right digastrics muscle and of the geniohyoid muscle; z-scores > 20; z-score < 2 and >2 is abnormal. MMO reduced, subjective: limitation in the ability to open the mouth noted by the patients in Screen or by anamnestic information. Sliding of the temporomandibular joint was assessed by palpation: reduced = no or hardly any sliding of the lateral pole of the mandibular condyle and normal = sliding to and beyond the crest of the articular eminence. Pain provocation during active mouth opening, passive mouth opening, or palpation of the masseter muscle, temporalis muscle or the lateral pole of the TMJ. sion analysis revealed negative correlations between the ammo and age, body height, ultrasound score of the digastric muscle and geniohyoid muscle, and positive correlations for the MFM variables. Because of the small number of patients, only two variables are used in our multiple linear regression analysis. Age and MFM variables are strongly correlated (Pearson correlation 0828; P =<0001) via disease progression, making age less informative. Therefore, we entered body height in the model, which in combination with MFM total raw score improved the model (R 2 = 071).
6 6 H. W. VAN BRUGGEN et al. Variable Effect 95% confidence interval for effect Lower bound Upper bound P-value R 2 Table 3. Univariate linear regression analysis of predictors of the impaired active maximal mouth opening (ammo) Age (in years) * 013 Body height (cm) MFM total raw score <0001* 057 MFM item * 037 EI digastric muscle (z-score) * 023 EI geniohyoid muscle (z-score) * 022 Discussion In this study, the impact of DMD on the mandibular movements was assessed by comparing the mandibular ROM of patients with those of a gender and agematched healthy control group. Also, mandibular ROM per ambulatory stage (AS, ENAS or LNAS) in the DMD group was examined. Predictive factors were established for reduced ammo in the patient group. This study shows that mandibular ROM was significantly lower in patients with DMD compared to controls. The decreased ammo in patients with DMD was primarily related to body height and higher disease severity, expressed by the motor function. Measurement of the mandibular movements is a standard procedure for evaluation of the musculoskeletal masticatory structures (18, 22). As an entity on itself, the active MMO is a parameter that can be established reliably, regardless of the severity of the limitation; the interobserver intra-class correlation coefficient (ICC) was 098, and the intra-observer ICC and inter-session ICC reliabilities both were 099 (27). In view of the wide range of variation of individual mandibular movements, it is difficult to set normal ranges and uniformity regarding the maximum movements. Suggested cut-off values for the ammo in healthy subjects vary between 40 and 44 mm for man; 38 and 42 mm for woman; and 35 and 40 for children (28 33). In accordance with the literature, we consider for our study <40 mm for ammo, <8 mm for active lateral excursion and <5 mm for protrusion as restricted. These values do not seem to be in conflict with other findings from the literature. In our study, we have incorporated the concept of the mandibular range of motion as an anatomical position (condyle in relation to the crest of the eminence next to the interincisal measurement of mandibular movements (34). Healthy individuals may perform normal opening with highly variable amounts of condylar translation, and variation in maximum incisor opening is largely explained by variation in the amount of mandibular rotation (35). It is mentioned in the literature that maximum incisor opening does not provide reliable information about condylar translation and its use as a diagnostic indicator of condylar movement is limited (35). A combination of the interincisal measurement of mandibular opening and assessment of the anatomical condylar position in relation to the crest of the eminence will improve establishing whether the impairment is intraarticular or not (34). Regarding ammo in patients with DMD compared to healthy controls, conflicting objective data can be found in the literature ranging from a reduced maximum mouth opening to a non-significant difference (3, 4). The mean reduction in the ammo of our patient group compared to the age and gender matched controls was 11 mm, which is a clinically relevant difference. In another study, MMOs of 391 mm (DMD patients, mean age 117 years) and 542 (healthy controls, mean age 119 years) were found (4). However, in a Japanese population, no significant difference between the DMD group and the control group was found, although the MMO of the patients tended to be less compared to controls (mean age 215 vs. 213, MMO 369 vs. 410 mm) (3). Despite the higher mean age in the latter study, the MMO was less than reported in the study of Botteron et al. (4) and our study. All studies included the vertical overbite in their measurements. Differences in ethnicity and instructions during the examination of the studied population in these studies may explain the variation of the ammo values.
7 MUSCULAR DYSTROPHY AND MANDIBULAR MOVEMENT 7 The mandibular ROM is influenced by many factors, that is age, gender, body height, ethnicity, status of the masticatory system, cervical column function, and head and neck posture (32, 36, 37). In patients with DMD, sonography indicated fatty infiltration related to the dystrophic changes of the masseter muscle and the suprahyoid muscles (4, 11). Muscle dystrophy may lead to muscle stiffness and consequently may hamper mouth opening and horizontal jaw movements. In our study, 5 of 6 patients with a limited MMO (<40 mm) had a normal sliding of the condyle, indicating that structural changes in the muscles may primarily be responsible for the reduced mandibular ROM in general and the ammo specifically. The differences between patients and controls regarding the mandibular ROM, and not only maximum mouth opening, indicates a more general muscle involvement than the muscles responsible for mouth opening and closing. The lateral pterygoid muscles play an important role in mouth opening but also in the control of horizontal mandibular movements such as protrusion and laterotrusion (38). In patients with spinal muscular atrophy, involvement of the lateral pterygoid muscle was found to play an important role in the impairment of the mandibular movement in this type of neuromuscular disorder (39). To our knowledge, the effect of DMD on the lateral pterygoid muscle is not investigated by MR imaging. In healthy individuals, the strength of the vertical component of the mouth opening muscle force (suprahyoid and indirectly the infra-hyoid muscles) is important in mouth opening (40). The structural changes found in the anterior belly of the digastric muscles and geniohyoid muscles in DMD may lead to a decreased strength and contribute to a limited maximum mouth opening. Our linear regression analysis confirms this hypothesis: the echo intensity of the digastrics and geniohyoid muscle correlated with the maximum mouth opening (Table 3). Moreover, the quantitative muscle ultrasound imaging in the patient group showed that the muscle echo intensity of the suprahyoid muscles increased gradually (z-sore > 2) with ambulatory loss (11). The influence of DMD on the suprahyoid (and probably the lateral pterygoid) muscles in our patients seems to follow a tendency like other physical characteristics that start to develop according to the stage of the disease. Table 4. Multiple linear regression analysis of predictors of the impaired active maximal mouth opening (ammo) Variable The study of L van de Engel-Hoek et al., 2012 showed the feasibility of quantitative muscle ultrasound of digastric muscles, the geniohyoid muscles in healthy subjects and patients with DMD (11). Quantitative muscle ultrasound imaging showed significant differences in echo intensity between healthy subjects and DMD patients, especially in the geniohyoid muscle. The anatomic location and structure of, for example, the mylohyoid muscle proved to be too thin to be measured and analysed. However, we do not expect that other oral muscles such as the mylohyoid muscles are spared from DMD. In this cohort of 23 boys and adults with DMD, the linear regression analysis revealed the severity of DMD, assessed by the MFM, and the height of the patient to be the strongest independent predictive factors for a restricted ammo (Table 4). Although age and height are generally related, in patients with DMD, due to the growth disturbances, height turned out to be a stronger independent factor for a restricted ammo than age (Table 4). A restricted mouth opening may hamper feeding, oral hygiene and dental care. Recognising this impairment and their predictive factors by medical staff, patients, parents and caretakers is a first step. Furthermore, in terms of management, it is important to take measures to slow down the development of the mouth opening reduction, possibly by developing a training programme. The programme has to be easy to implement in daily life and with low intensity aerobic exercises as suggested in other training programmes for patients with DMD (41, 42). Conclusion Effect 95% confidence interval for effect Lower bound Upper bound P-value (Constant) Body height (cm) * MFM total raw score <0001* R 2 = 071. Mandibular movements in DMD are significantly reduced compared to the healthy controls and become
8 8 H. W. VAN BRUGGEN et al. more hampered with loss of motor function, including the sitting position, arm function, and the neck and head control. We suggest that evaluation of the ammo as an expression of the reduced mandibular range of motion becomes a part of routine care of patients with DMD. Ethical approval The study was approved by the Committee on Research Involving Human Subjects of Arnhem and Nijmegen, the Netherlands (Registration Number 2009/331). Author contributions All authors contributed substantially to the design of the study, drafting the article and revising it and gave final approval of the version to be published. Declaration of conflicting interests The authors declared no potential conflicts of interest with respect to the authorship and/or publication of this article. Financial disclosure/funding This project was financially supported by the Duchenne Parent Project, the Netherlands. References 1. van Essen AJ, Busch HF, te Meerman GJ, ten Kate LP. Birth and population prevalence of Duchenne muscular dystrophy in The Netherlands. Hum Genet. 1992;88: Kanagawa M, Toda T. The genetic and molecular basis of muscular dystrophy: roles of cell matrix linkage in the pathogenesis. J Hum Genet. 2006;51: Ueki K, Nakagawa K, Yamamoto E. Bite force and maxillofacial morphology in patients with Duchenne-type muscular dystrophy. J Oral Maxillofac Surg. 2007;65: Botteron S, Verdebout CM, Jeannet PY, Kiliaridis S. Orofacial dysfunction in Duchenne muscular dystrophy. Arch Oral Biol. 2009;54: Kiliaridis S, Katsaros C. The effects of myotonic dystrophy and Duchenne muscular dystrophy on the orofacial muscles and dentofacial morphology. Acta Odontol Scand. 1998;56: Symons AL, Townsend GC, Hughes TE. Dental characteristics of patients with Duchenne muscular dystrophy. ASDC J Dent Child. 2002;69: Matsuyuki T, Kitahara T, Nakashima A. Developmental changes in craniofacial morphology in subjects with Duchenne muscular dystrophy. Eur J Orthod. 2006;28: Morel-Verdebout C, Botteron S, Kiliaridis S. Dentofacial characteristics of growing patients with Duchenne muscular dystrophy: a morphological study. Eur J Orthod. 2007;29: Dijkstra PU, Hof AL, Stegenga B, de Bont LG. Influence of mandibular height on mouth opening. J Oral Rehabil. 1999;26: van der Bilt A. Assessment of mastication with implications for oral rehabilitation: a review. J Oral Rehabil. 2011;38: van den Engel-Hoek L, Erasmus CE, Hendriks JC, Geurts AC, Klein WM, Pillen S et al. Oral muscles are progressively affected in Duchenne muscular dystrophy: implications for dysphagia treatment. J Neurol. 2013;260: Sonnesen L. Associations between the Cervical Vertebral Column and Craniofacial Morphology. Int J Dent. 2010;2010: Epub 2010 Jun La Touche R, Parıs-Alemany A, von Piekartz H, Mannheimer JS, Fernandez-Carnero J, Rocabado M. The influence of cranio-cervical posture on maximal mouth opening and pressure pain threshold in patients with myofascial temporomandibular pain disorders. Clin J Pain. 2011;27: Van Den Engel-Hoek L, Van Alfen N, De Swart BJ, De Groot IJ, Pillen S. Quantitative ultrasound of the tongue and submental muscles in children and young adults. Muscle Nerve. 2012;46: Berard C, Payan C, Hodgkinson I, Fermanian J, MFM Collaborative Study Group. A motor function measure for neuromuscular diseases. Construction and validation study. Neuromuscul Disord. 2005;15: De Leeuw JR, Steenks MH, Ros WJ, Lobbezoo-Scholte AM, Bosman F, Winnubst JA. Multidimensional evaluation of craniomandibular dysfunction. I: Symptoms and correlates. J Oral Rehabil. 1994;21: De Leeuw JR, Ros WJ, Steenks MH, Lobbezoo-Scholte AM, Bosman F, Winnubst JA. Multidimensional evaluation of craniomandibular dysfunction. II: pain assessment. J Oral Rehabil. 1994;21: Lobbezoo-Scholte AM, Steenks MH, Faber JA, Bosman F. Diagnostic value of orthopedic tests in patients with temporomandibular disorders. J Dent Res. 1993;72: Lobbezoo-Scholte AM, de Wijer A, Steenks MH, Bosman F. Interexaminer reliability of six orthopaedic tests in diagnostic subgroups of craniomandibular disorders. J Oral Rehabil. 1994;21: de Wijer A, Lobbezoo-Scholte AM, Steenks MH, Bosman F. Reliability of clinical findings in temporomandibular disorders. J Orofacial Pain. 1995;9: Steenks MH, de Wijer A, Bosman F. Orthopedic diagnostic tests for temporomandibular and cervical spine disorders. J Back Musculoskelet Rehabil. 1996;6: Schiffman E, Ohrbach R, Truelove E, Look J, Anderson G, Goulet JP et al. Diagnostic Criteria for Temporomandibular Disorders (DC/TMD) for Clinical and Research Applications:
9 MUSCULAR DYSTROPHY AND MANDIBULAR MOVEMENT 9 recommendations of the International RDC/TMD Consortium Network* and Orofacial Pain Special Interest Group. J Oral Facial Pain Headache. 2014;28: List T, John MT, Dworkin SF, Svensson P. Recalibration improves inter-examiner reliability of TMD examination. Acta Odontol Scand. 2006;64: Scholten RR, Pillen S, Verrips A, Zwarts MJ. Quantitative ultrasonography of skeletal muscles in children: normal values. Muscle Nerve. 2003;27: Pillen S, Verrips A, van Alfen N, Arts IM, Sie LT, Zwarts MJ. Quantitative skeletal muscle ultrasound: diagnostic value in childhood neuromuscular disease. Neuromuscul Disord. 2007;17: Bushby K, Finkel R, Birnkrant DJ, Case LE, Clemens PR, Cripe L et al., DMD Care Considerations Working Group Diagnosis and management of Duchenne muscular dystrophy, part 1: diagnosis, and pharmacological and psychosocial management. Lancet Neurol. 2010;9: Jager-Wittenaar H, Dijkstra PU, Vissink A, van Oort RP, Roodenburg JL. Variation in repeated mouth-opening measurements in head and neck cancer patients with and without trismus. Int J Oral Maxillofac Surg. 2009;38: Agerberg G. Maximal mandibular movements in young men and women. Sven Tandlak Tidskr. 1974;67: Helkimo M. Studies on function and dysfunction of the masticatory system. II. Index for anamnestic and clinical dysfunction and occlusal state. Swed Dent J. 1974;67: Landtwing K. Evaluation of the normal range of vertical mandibular opening in children and adolescents with special reference to age and stature. J Maxillofac Surg. 1978;6: Szentpetery A. Clinical utility of mandibular movement ranges. J Orofac Pain. 1993;7: Hirsh C, John MT, Lautenschl agher C, List T. Mandibular jaw movement capacity in year-old children and adolescents: normative values and the influence of gender, age and temporomandibular disorders. Eur J Oral Sci. 2006;114: M uller L, van Waes H, Langerweger C, Molinari L, Saurenmann RK. Maximal mouth opening capacity: percentiles for healthy children 4 17 years of age. Pediatr Rheumatol Online J. 2013;11: Heir GM. Assessment of the TMJ Patient. In: Fonseca RJ, Marciani RD, Turvey TA, eds. Oral and maxillofacial surgery, Vol. 2, 2nd edn. St Louis (MO): Elsevier; 2009: Travers KH, Buschang PH, Hayasaki H, Throckmorton GS. Associations between incisor and mandibular condylar movements during maximum mouth opening in humans. Arch Oral Biol. 2000;45: Kim DS, Choi SC, Lee SS, Heo MS, Huh KH, Hwang SJ et al. Correlation between 3-dimensional facial morphology and mandibular movement during maximum mouth opening and closing. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2010;110: Kuroda K, Saitoh I, Inada E, Takemoto Y, Iwasaki T, Iwase Y et al. Head motion may help mouth opening in children. Arch Oral Biol. 2011;56: Murray GM. The lateral Pterygoid muscle: function and dysfunction. Semin Orthod. 2012;18: Wadman GI, van Bruggen HW, Witkamp TD, Kalaykova SI, Stam M, van den Berg LH et al. Bulbar muscle MRI changes in patients with SMA with reduced mouth opening and dysphagia. Neurology. 2014;83: Koolstra JH. Dynamics of the human masticatory system. Crit Rev Oral Biol Med. 2002;13: Cup EH, Pieterse AJ, Ten Broek-Pastoor JM, Munneke M, van Engelen BG, Hendricks HT et al. Exercise therapy and other types of physical therapy for patients with neuromuscular diseases: a systematic review. Arch Phys Med Rehabil. 2007;88: Jansen M, de Groot IJ, van Alfen N, Geurts A. Physical training in boys with Duchenne Muscular Dystrophy: the protocol of the No Use is Disuse study. BMC Pediatr. 2010;10:55. Correspondence: Willemijn H. van Bruggen, Department of Oral Function and Prosthetic Dentistry, Radboud University Medical Center, PO Box 9101, 6500 HB Nijmegen, The Netherlands. Willemijn.vanBruggen@radboudumc.nl
An Index for the Measurement of Normal Maximum Mouth Opening
 A P P L I E D R E S E A R C H An Index for the Measurement of Normal Maximum Mouth Opening Khalid H. Zawawi, BDS Emad A. Al-Badawi, BDS, MS Silvia Lobo Lobo, DDS, MS Marcello Melis, DDS, RPharm Noshir
A P P L I E D R E S E A R C H An Index for the Measurement of Normal Maximum Mouth Opening Khalid H. Zawawi, BDS Emad A. Al-Badawi, BDS, MS Silvia Lobo Lobo, DDS, MS Marcello Melis, DDS, RPharm Noshir
4 Smallest detectable difference of maximal mouth opening in patients with painfully restricted temporomandibular joint function.
 4 Smallest detectable difference of maximal mouth opening in patients with painfully restricted temporomandibular joint function. Kropmans ThJB, Dijkstra PU, Stegenga B, Stewart R, de Bont LGM European
4 Smallest detectable difference of maximal mouth opening in patients with painfully restricted temporomandibular joint function. Kropmans ThJB, Dijkstra PU, Stegenga B, Stewart R, de Bont LGM European
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/141375
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/141375
Dental Issues in DMD. Elizabeth Vroom, DDS
 Dental Issues in DMD Elizabeth Vroom, DDS Changes in orofacial form and functions seen in DMD (most recommendations are expert opinions and not evidence based) Lack of dystrophin Muscle breakdown Fibrosis
Dental Issues in DMD Elizabeth Vroom, DDS Changes in orofacial form and functions seen in DMD (most recommendations are expert opinions and not evidence based) Lack of dystrophin Muscle breakdown Fibrosis
Introduction to Occlusion and Mechanics of Mandibular Movement
 Introduction to Occlusion and Mechanics of Mandibular Movement Dr. Pauline Hayes Garrett Department of Endodontics, Prosthodontics, and Operative Dentistry University of Maryland, Baltimore Assigned reading
Introduction to Occlusion and Mechanics of Mandibular Movement Dr. Pauline Hayes Garrett Department of Endodontics, Prosthodontics, and Operative Dentistry University of Maryland, Baltimore Assigned reading
AAO Foundation Award Final Report Drs. Peter H. Buschang and Gaylord S. Throckmorton
 Principal Investigator Co-Investigator AAO Foundation Award Final Report Drs. Peter H. Buschang and Gaylord S. Throckmorton Drs. J. English, M. Collins, and H. Hayasaki Secondary Investigators Award Type
Principal Investigator Co-Investigator AAO Foundation Award Final Report Drs. Peter H. Buschang and Gaylord S. Throckmorton Drs. J. English, M. Collins, and H. Hayasaki Secondary Investigators Award Type
Clinical measurement of maximum mouth opening in children and its relation with different facial types
 Research Article Clinical measurement of maximum mouth opening in children and its relation with different facial types M. Sridhar 1 *, Ganesh Jeevanandham 2 ABSTRACT Introduction: Maximal opening of the
Research Article Clinical measurement of maximum mouth opening in children and its relation with different facial types M. Sridhar 1 *, Ganesh Jeevanandham 2 ABSTRACT Introduction: Maximal opening of the
Evaluation of mandibular range of motion in Brazilian children and its correlation to age, height, weight, and gender
 Pediatric Dentistry Pediatric Dentistry Evaluation of mandibular range of motion in Brazilian children and its correlation to age, height, weight, and gender Letícia Mêlo de Sousa (a) Harumi Martins Nagamine
Pediatric Dentistry Pediatric Dentistry Evaluation of mandibular range of motion in Brazilian children and its correlation to age, height, weight, and gender Letícia Mêlo de Sousa (a) Harumi Martins Nagamine
Outline. Limiting your risk when treating patients with TMD. Temporomandibular Disorders 20/01/2014. TMD diagnosis. Condylar position and TMD risk
 Outline American Association of Orthodontists Limiting your risk when treating patients with TMD Ambra Michelotti michelot@unina.it TMD diagnosis Condylar position and TMD risk Occlusal interference and
Outline American Association of Orthodontists Limiting your risk when treating patients with TMD Ambra Michelotti michelot@unina.it TMD diagnosis Condylar position and TMD risk Occlusal interference and
CERVICAL SPINE SIGNS AND SYMPTOMS: PERPETUATING RATHER THAN PREDISPOSING FACTORS FOR TEMPOROMANDIBULAR DISORDERS IN WOMEN
 www.fob.usp.br/revista or www.scielo.br/jaos J Appl Oral Sci. 2007;15(4):259-64 CERVICAL SPINE SIGNS AND SYMPTOMS: PERPETUATING RATHER THAN PREDISPOSING FACTORS FOR TEMPOROMANDIBULAR DISORDERS IN WOMEN
www.fob.usp.br/revista or www.scielo.br/jaos J Appl Oral Sci. 2007;15(4):259-64 CERVICAL SPINE SIGNS AND SYMPTOMS: PERPETUATING RATHER THAN PREDISPOSING FACTORS FOR TEMPOROMANDIBULAR DISORDERS IN WOMEN
Anatomy and physiology of Temporomandibular Joint
 Anatomy and physiology of Temporomandibular Joint Temporomandibular joint (TMJ): It is the articulation of the condyle of the mandible, and the inter-articular disc; with the mandibular fossa (glenoid
Anatomy and physiology of Temporomandibular Joint Temporomandibular joint (TMJ): It is the articulation of the condyle of the mandible, and the inter-articular disc; with the mandibular fossa (glenoid
Muscles of mastication [part 1]
![Muscles of mastication [part 1] Muscles of mastication [part 1]](/thumbs/76/73586850.jpg) Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Citation for published version (APA): Koutris, M. (2013). Masticatory muscle pain: Causes, consequences, and diagnosis
 UvA-DARE (Digital Academic Repository) Masticatory muscle pain: Causes, consequences, and diagnosis Koutris, M. Link to publication Citation for published version (APA): Koutris, M. (2013). Masticatory
UvA-DARE (Digital Academic Repository) Masticatory muscle pain: Causes, consequences, and diagnosis Koutris, M. Link to publication Citation for published version (APA): Koutris, M. (2013). Masticatory
Fellowship. Digital Case Documentation Format for Fellowship Case Presentation. OCCLUSION CONNECTIONS Dot Dentistry
 Digital Case Documentation Format for Case Presentation TMD Candidate s Name: CLAYTON A. CHAN, D.D.S. Case No.: 1 Our Disciplines ORTHOPEDIC Patient s Initials: CL (EXAMPLE CASE) RESTORATIVE OCCLUSION
Digital Case Documentation Format for Case Presentation TMD Candidate s Name: CLAYTON A. CHAN, D.D.S. Case No.: 1 Our Disciplines ORTHOPEDIC Patient s Initials: CL (EXAMPLE CASE) RESTORATIVE OCCLUSION
Principle of Occlusion
 Principle of Occlusion Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Overview Principle of Occlusion Overview Principle of Occlusion Point centric Long centric Freedom
Principle of Occlusion Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Overview Principle of Occlusion Overview Principle of Occlusion Point centric Long centric Freedom
Concepts of occlusion Balanced occlusion. Monoplane occlusion. Lingualized occlusion. Figure (10-1)
 Any contact between teeth of opposing dental arches; usually, referring to contact between the occlusal surface. The static relationship between the incising or masticatory surfaces of the maxillary or
Any contact between teeth of opposing dental arches; usually, referring to contact between the occlusal surface. The static relationship between the incising or masticatory surfaces of the maxillary or
Evaluation of patients with temporomandibular disorders
 PEDODONTICS Clinical Measurement of Normal Maximum Mouth Opening in Children Youssef S. Abou-Atme, D.D.S., M.S.; Nada Chedid, D.D.S., M.S.; Marcello Melis, D.M.D., R.Pharm.; Khalid H. Zawawi, B.D.S., D.Sc.
PEDODONTICS Clinical Measurement of Normal Maximum Mouth Opening in Children Youssef S. Abou-Atme, D.D.S., M.S.; Nada Chedid, D.D.S., M.S.; Marcello Melis, D.M.D., R.Pharm.; Khalid H. Zawawi, B.D.S., D.Sc.
Case-control study of craniomandibular disorders in patients with fibromyalgia
 Journal section: Orofacial pain-tmjd Publication Types: Research doi:10.4317/jced.51816 http://dx.doi.org/10.4317/jced.51816 Case-control study of craniomandibular disorders in patients with fibromyalgia
Journal section: Orofacial pain-tmjd Publication Types: Research doi:10.4317/jced.51816 http://dx.doi.org/10.4317/jced.51816 Case-control study of craniomandibular disorders in patients with fibromyalgia
Temporomandibular disorders and the need for stomatognathic treatment in orthodontically treated and untreated girls
 European Journal of Orthodontics 22 (2000) 283 292 2000 European Orthodontic Society Temporomandibular disorders and the need for stomatognathic treatment in orthodontically treated and untreated girls
European Journal of Orthodontics 22 (2000) 283 292 2000 European Orthodontic Society Temporomandibular disorders and the need for stomatognathic treatment in orthodontically treated and untreated girls
Articulators. 5- Wax up and refining the occlusion for dental restorations.
 Articulators It is a mechanical device represents the TMJ, maxillary and mandibular arches. It can be used to hold the upper and lower casts according to their relationships to facilitate the purposes
Articulators It is a mechanical device represents the TMJ, maxillary and mandibular arches. It can be used to hold the upper and lower casts according to their relationships to facilitate the purposes
Up Date on TMD WHAT IS TMD? Temporomandibular Disorders (TMD)*: Donald Nixdorf DDS, MS
 Up Date on TMD Donald Nixdorf DDS, MS Associate Professor Division of TMD and Orofacial Pain WHAT IS TMD? Temporomandibular Disorders (TMD)*: MUSCLE and JOINT DISORDERS * Temporomandibular Muscle and Joint
Up Date on TMD Donald Nixdorf DDS, MS Associate Professor Division of TMD and Orofacial Pain WHAT IS TMD? Temporomandibular Disorders (TMD)*: MUSCLE and JOINT DISORDERS * Temporomandibular Muscle and Joint
Multi-site RDC/TMD Validation Study Specifications for TMD Examination Gold Standard Examiner. Version Date: Feb 10, 2005
 Multi-site RDC/TMD Validation Study Specifications for TMD Examination Gold Standard Examiner Version Date: Feb 10, 2005 Contents General Directions for Examination... 1 A. Expanded RDC Examination...
Multi-site RDC/TMD Validation Study Specifications for TMD Examination Gold Standard Examiner Version Date: Feb 10, 2005 Contents General Directions for Examination... 1 A. Expanded RDC Examination...
Different Non Surgical Treatment Modalities for Class III Malocclusion
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 9, Issue 6 (Sep.- Oct. 2013), PP 48-52 Different Non Surgical Treatment Modalities for Class III Malocclusion
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 9, Issue 6 (Sep.- Oct. 2013), PP 48-52 Different Non Surgical Treatment Modalities for Class III Malocclusion
The mandible moves, relative to the maxilla,
 2 PRACTICE The examination and recording of the : why and how S. J. Davies, 1 and R. M. J. Gray, 2 Before presenting how the examination and recording of the may be achieved, some attempt should be made
2 PRACTICE The examination and recording of the : why and how S. J. Davies, 1 and R. M. J. Gray, 2 Before presenting how the examination and recording of the may be achieved, some attempt should be made
Incidence of temporomandibular joint clicking in adolescents with and without unilateral posterior cross-bite: a 10-year follow-up study
 J o u r n a l o f Oral Rehabilitation Journal of Oral Rehabilitation 2016 43; 16 22 Incidence of temporomandibular joint clicking in adolescents with and without unilateral posterior cross-bite: a 10-year
J o u r n a l o f Oral Rehabilitation Journal of Oral Rehabilitation 2016 43; 16 22 Incidence of temporomandibular joint clicking in adolescents with and without unilateral posterior cross-bite: a 10-year
Y. H. SHEN*, Y. K. CHEN & S. Y. CHUANG Departments of *Oral and Maxillofacial Surgery, Oral Pathology. Introduction. Case report
 Journal of Oral Rehabilitation 2005 32; 332 336 Condylar resorption during active orthodontic treatment and subsequent therapy: report of a special case dealing with iatrogenic TMD possibly related to
Journal of Oral Rehabilitation 2005 32; 332 336 Condylar resorption during active orthodontic treatment and subsequent therapy: report of a special case dealing with iatrogenic TMD possibly related to
Arrangement of the artificial teeth:
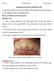 Lecture Prosthodontic Dr. Osama Arrangement of the artificial teeth: It s the placement of the teeth on a denture with definite objective in mind or it s the setting of teeth on temporary bases. Rules
Lecture Prosthodontic Dr. Osama Arrangement of the artificial teeth: It s the placement of the teeth on a denture with definite objective in mind or it s the setting of teeth on temporary bases. Rules
ChiroCredit.com Anatomy 226 INSTRUCTIONS/ASSIGNMENT FOR ANATOMICAL DISSECTION:
 ChiroCredit.com Anatomy 226 INSTRUCTIONS/ASSIGNMENT FOR ANATOMICAL DISSECTION: Once you click on the link to open the dissection module, the first thing you need to do is to be sure you can see all the
ChiroCredit.com Anatomy 226 INSTRUCTIONS/ASSIGNMENT FOR ANATOMICAL DISSECTION: Once you click on the link to open the dissection module, the first thing you need to do is to be sure you can see all the
Case Presentation #1 for the American Board of Craniofacial Pain July 2013
 Case Presentation #1 for the American Board of Craniofacial Pain July 2013 Case I Summary Presentation Pain in right temporomandibular joint with opening of mouth( 7 out of 10 ). Acute right non-reducing
Case Presentation #1 for the American Board of Craniofacial Pain July 2013 Case I Summary Presentation Pain in right temporomandibular joint with opening of mouth( 7 out of 10 ). Acute right non-reducing
JOHCD ABSTRACT INTRODUCTION MATERIALS AND METHODS /jp-journals
 Arun Kumar et al RESEARCH ARTICLE 10.5005/jp-journals-10062-0019 Measurement and Evaluation of the Normal Range of Maximal Mouth Opening and Its Correlation with Age, Body Height, Weight, and Gender in
Arun Kumar et al RESEARCH ARTICLE 10.5005/jp-journals-10062-0019 Measurement and Evaluation of the Normal Range of Maximal Mouth Opening and Its Correlation with Age, Body Height, Weight, and Gender in
OCCLUSION: PHYSIOLOGIC vs. NON-PHYSIOLOGIC
 Oral Anatomy and Occlusion Prosthodontic Component OCCLUSION: PHYSIOLOGIC vs. NON-PHYSIOLOGIC By: Dr. Babak Shokati, DDS, MSc. MSc. Prosthodontics Definition of Masticatory System by The Academy of Prosthodontics
Oral Anatomy and Occlusion Prosthodontic Component OCCLUSION: PHYSIOLOGIC vs. NON-PHYSIOLOGIC By: Dr. Babak Shokati, DDS, MSc. MSc. Prosthodontics Definition of Masticatory System by The Academy of Prosthodontics
Ascertaining of temporomandibular disorders (TMD) with clinical and instrumental methods in the group of young adults
 ORIGINAL PAPER Ascertaining of temporomandibular disorders (TMD) with clinical and instrumental methods in the group of young adults Anna Sójka 1, Juliusz Huber 2, Elżbieta Kaczmarek 3, Wiesław Hędzelek
ORIGINAL PAPER Ascertaining of temporomandibular disorders (TMD) with clinical and instrumental methods in the group of young adults Anna Sójka 1, Juliusz Huber 2, Elżbieta Kaczmarek 3, Wiesław Hędzelek
Definition and History of Orthodontics
 In the name of GOD Definition and History of Orthodontics Presented by: Dr Somayeh Heidari Orthodontist Reference: Contemporary Orthodontics Chapter 1 William R. Proffit, Henry W. Fields, David M.Sarver.
In the name of GOD Definition and History of Orthodontics Presented by: Dr Somayeh Heidari Orthodontist Reference: Contemporary Orthodontics Chapter 1 William R. Proffit, Henry W. Fields, David M.Sarver.
Upper Cross Syndrome: Assessment & Management in Family Practice HKDU Symposium Dec 2014
 Upper Cross Syndrome: Assessment & Management in Family Practice HKDU Symposium Dec 2014 Dr. Ngai Ho Yin Allen Family Medicine Specialist PGDipMusculoskeletal Medicine MBBS(HK), DCH(London), DFM(CUHK),
Upper Cross Syndrome: Assessment & Management in Family Practice HKDU Symposium Dec 2014 Dr. Ngai Ho Yin Allen Family Medicine Specialist PGDipMusculoskeletal Medicine MBBS(HK), DCH(London), DFM(CUHK),
The most common internal derangement within the human
 Two-year Natural Course of Anterior Disc Displacement with Reduction Stanimira Kalaykova, DDS PhD Student Amsterdam (ACTA) Research Institute MOVE University of Amsterdam and VU University Amsterdam Frank
Two-year Natural Course of Anterior Disc Displacement with Reduction Stanimira Kalaykova, DDS PhD Student Amsterdam (ACTA) Research Institute MOVE University of Amsterdam and VU University Amsterdam Frank
Sophie Kraaijenga 1, Lisette van der Molen 1, Harm van Tinteren 2, Frans Hilgers 1,3,4, Ludi Smeele 1,4,5,6
 Physical Therapy Treatment of myogenic temporomandibular disorder: a prospective randomized clinical trial, comparing a mechanical stretching device (TheraBiteH) with standard physical therapy exercise
Physical Therapy Treatment of myogenic temporomandibular disorder: a prospective randomized clinical trial, comparing a mechanical stretching device (TheraBiteH) with standard physical therapy exercise
Cervical Spine Exercise and Manual Therapy for the Autonomous Practitioner
 Cervical Spine Exercise and Manual Therapy for the Autonomous Practitioner Eric Chaconas PT, PhD, DPT, FAAOMPT Assistant Professor and Assistant Program Director Doctor of Physical Therapy Program Eric
Cervical Spine Exercise and Manual Therapy for the Autonomous Practitioner Eric Chaconas PT, PhD, DPT, FAAOMPT Assistant Professor and Assistant Program Director Doctor of Physical Therapy Program Eric
Diagnosis and Treatment of Temporomandibular Disorders (TMD) By: Aman Bhojani. Background & Etiology
 Diagnosis and Treatment of Temporomandibular Disorders (TMD) By: Aman Bhojani Background & Etiology TMD affects approximately 10-15% of the population, but only 5% seek treatment. Incidence peaks from
Diagnosis and Treatment of Temporomandibular Disorders (TMD) By: Aman Bhojani Background & Etiology TMD affects approximately 10-15% of the population, but only 5% seek treatment. Incidence peaks from
Attachment G. Orthodontic Criteria Index Form Comprehensive D8080. ABBREVIATIONS CRITERIA for Permanent Dentition YES NO
 First Review IL HFS Dental Program Models Second Review Ortho cad Attachment G Orthodontic Criteria Index Form Comprehensive D8080 Ceph Film X-Rays Photos Narrative Patient Name: DOB: ABBREVIATIONS CRITERIA
First Review IL HFS Dental Program Models Second Review Ortho cad Attachment G Orthodontic Criteria Index Form Comprehensive D8080 Ceph Film X-Rays Photos Narrative Patient Name: DOB: ABBREVIATIONS CRITERIA
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi. E. mail:
 The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
The Position of Anatomical Porion in Different Skeletal Relationships. Tarek. EL-Bialy* Ali. H. Hassan**
 The Position of Anatomical Porion in Different Skeletal Relationships Tarek. EL-Bialy* Ali. H. Hassan** Abstract Previous research has shown that the position of glenoid fossa differs in different skeletal
The Position of Anatomical Porion in Different Skeletal Relationships Tarek. EL-Bialy* Ali. H. Hassan** Abstract Previous research has shown that the position of glenoid fossa differs in different skeletal
Prosthetic Management of TMJ Disorders
 Prosthetic Management of TMJ Disorders Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Mohd@DrMohdAlfarsi.com @DrMohdAlfarsi DrMohdAlfarsi 056 224 2227 Overview Overview
Prosthetic Management of TMJ Disorders Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Mohd@DrMohdAlfarsi.com @DrMohdAlfarsi DrMohdAlfarsi 056 224 2227 Overview Overview
Temporomandibular Joint. Dr Noman ullah wazir
 Temporomandibular Joint Dr Noman ullah wazir Type of Joint TMJ is a Synovial joint between : The condylar head of the mandible. The mandibular fossa of squamous part of temporal bone. The joint cavity
Temporomandibular Joint Dr Noman ullah wazir Type of Joint TMJ is a Synovial joint between : The condylar head of the mandible. The mandibular fossa of squamous part of temporal bone. The joint cavity
The America Association of Oral and Maxillofacial Surgeons classify occlusion/malocclusion in to the following three categories:
 Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
Masseter muscle thickness and maxillary dental arch width
 European Journal of Orthodontics 25 (2003) 259 263 2003 European Orthodontic Society Masseter muscle thickness and maxillary dental arch width Stavros Kiliaridis*, Ioanna Georgiakaki* and Christos Katsaros**,
European Journal of Orthodontics 25 (2003) 259 263 2003 European Orthodontic Society Masseter muscle thickness and maxillary dental arch width Stavros Kiliaridis*, Ioanna Georgiakaki* and Christos Katsaros**,
Dr Mohammed Alfarsi Page 1 9 December Principles of Occlusion
 Dr Mohammed Alfarsi Page 1 9 December 2013 Principles of Occlusion Overview: The occlusion is a very large, yet easy to manage once properly understood, topic. Thus, no one handout is enough to fully understand
Dr Mohammed Alfarsi Page 1 9 December 2013 Principles of Occlusion Overview: The occlusion is a very large, yet easy to manage once properly understood, topic. Thus, no one handout is enough to fully understand
Intra-rater reliability of TMJ joint vibration a pilot study
 Intra-rater reliability of TMJ joint vibration a pilot study Magdalena Bakalczuk 1, Marcin Berger1, Michał Ginszt 2, Jacek Szkutnik 1, Sorochynska Solomiia 3, Piotr Majcher 2 1 Department of Functional
Intra-rater reliability of TMJ joint vibration a pilot study Magdalena Bakalczuk 1, Marcin Berger1, Michał Ginszt 2, Jacek Szkutnik 1, Sorochynska Solomiia 3, Piotr Majcher 2 1 Department of Functional
Temporomandibular Joint Clicking Noises Caused by a Multilocular Bone Cyst: A Case Report
 Temporomandibular Joint Clicking Noises Caused by a Multilocular Bone Cyst: A Case Report Abstract When diagnosing patients with temporomandibular disorder (TMD) symptoms, the possibility of unusual causes
Temporomandibular Joint Clicking Noises Caused by a Multilocular Bone Cyst: A Case Report Abstract When diagnosing patients with temporomandibular disorder (TMD) symptoms, the possibility of unusual causes
Assisted Bicycle Training Delays Functional Deterioration in Boys With Duchenne Muscular Dystrophy: The Randomized Controlled Trial No Use Is Disuse
 496326NNRXXX10.1177/1545968313496326Neurorehabilitation and Neural Repair XX(X)Jansen et al research-article2013 Clinical Research Article Assisted Bicycle Training Delays Functional Deterioration in Boys
496326NNRXXX10.1177/1545968313496326Neurorehabilitation and Neural Repair XX(X)Jansen et al research-article2013 Clinical Research Article Assisted Bicycle Training Delays Functional Deterioration in Boys
Screening orthodontic patients for temporomandibular disorders
 Clin Dent Rev (2017) 1:8 https://doi.org/10.1007/s41894-017-0007-z DIAGNOSIS Screening orthodontic patients for temporomandibular disorders Gary Klasser 1 Charles Greene 2 Received: 5 April 2017 / Accepted:
Clin Dent Rev (2017) 1:8 https://doi.org/10.1007/s41894-017-0007-z DIAGNOSIS Screening orthodontic patients for temporomandibular disorders Gary Klasser 1 Charles Greene 2 Received: 5 April 2017 / Accepted:
La Touche et al. The Journal of Headache and Pain (2015) 16:20 DOI /s
 La Touche et al. The Journal of Headache and Pain (2015) 16:20 DOI 10.1186/s10194-015-0500-1 RESEARCH ARTICLE Open Access Masticatory sensory-motor changes after an experimental chewing test influenced
La Touche et al. The Journal of Headache and Pain (2015) 16:20 DOI 10.1186/s10194-015-0500-1 RESEARCH ARTICLE Open Access Masticatory sensory-motor changes after an experimental chewing test influenced
Age peaks of different RDC/TMD diagnoses in a patient population
 journal of dentistry 38 (2010) 392 399 available at www.sciencedirect.com journal homepage: www.intl.elsevierhealth.com/journals/jden Age peaks of different RDC/TMD diagnoses in a patient population Daniele
journal of dentistry 38 (2010) 392 399 available at www.sciencedirect.com journal homepage: www.intl.elsevierhealth.com/journals/jden Age peaks of different RDC/TMD diagnoses in a patient population Daniele
Comparison between the external gonial angle in panoramic radiographs and lateral cephalograms of adult patients with Class I malocclusion
 425 Journal of Oral Science, Vol. 51, No. 3, 425-429, 2009 Original Comparison between the external gonial angle in panoramic radiographs and lateral cephalograms of adult patients with Class I malocclusion
425 Journal of Oral Science, Vol. 51, No. 3, 425-429, 2009 Original Comparison between the external gonial angle in panoramic radiographs and lateral cephalograms of adult patients with Class I malocclusion
Functional Outcomes of Temporomandibular Joint Ankylosis Treatments: A 10-year cohort study
 Regeneration, Reconstruction & Restoration Reconstruction Functional Outcomes of Temporomandibular Joint Ankylosis Treatments: A 10-year cohort study Mohammad Taghi Kiani a*, Mohammad Bayat b, Maryam Ajami
Regeneration, Reconstruction & Restoration Reconstruction Functional Outcomes of Temporomandibular Joint Ankylosis Treatments: A 10-year cohort study Mohammad Taghi Kiani a*, Mohammad Bayat b, Maryam Ajami
Response Type axium Adult Comprehensive Oral Examination (COE)
 Page 1 1. RADIOGRAPHIC EVALUATION 1001 Panoramic image (PAN) Maxillary sinuses Nasal cavity TMJ complex Mandibular canal visualization?bone anomalies (eg. radiopacity/radiolucency) Soft tissue abnormalities
Page 1 1. RADIOGRAPHIC EVALUATION 1001 Panoramic image (PAN) Maxillary sinuses Nasal cavity TMJ complex Mandibular canal visualization?bone anomalies (eg. radiopacity/radiolucency) Soft tissue abnormalities
APPENDIX A. MEDICAID ORTHODONTIC INITIAL ASSESSMENT FORM (IAF) You will need this scoresheet and a disposable ruler (or a Boley Gauge)
 APPENDIX A MEDICAID ORTHODONTIC INITIAL ASSESSMENT FORM (IAF) You will need this scoresheet and a disposable ruler (or a Boley Gauge) Name: _ I. D. Number: Conditions: 1. Cleft palate deformities 2. Deep
APPENDIX A MEDICAID ORTHODONTIC INITIAL ASSESSMENT FORM (IAF) You will need this scoresheet and a disposable ruler (or a Boley Gauge) Name: _ I. D. Number: Conditions: 1. Cleft palate deformities 2. Deep
TEMPORO-MANDIBULAR JOINT DISORDERS
 Disclaimer This movie is an educational resource only and should not be used to manage your dental health. All decisions about the management of TMJ Disorders must be made in conjunction with your Dental
Disclaimer This movie is an educational resource only and should not be used to manage your dental health. All decisions about the management of TMJ Disorders must be made in conjunction with your Dental
Characterization of Physiologic Occlusion
 Dental Journal Mahidol Dental Journal Original Article Nattaya Asawaworarit 1, Somsak Mitrirattanakul 2 1 B.Sc., D.D.S., Cert. in Clinical Science (Prosthodontics) Department of Masticatory Science Faculty
Dental Journal Mahidol Dental Journal Original Article Nattaya Asawaworarit 1, Somsak Mitrirattanakul 2 1 B.Sc., D.D.S., Cert. in Clinical Science (Prosthodontics) Department of Masticatory Science Faculty
assessed in 152 Brazilian children (78 boys and 74 girls), aged 8 to 12 (mean age 10.05
 www.scielo.br/jaos disorders Raquel Aparecida PIZOLATO 1, Frederico Silva de Freitas FERNANDES 2, Maria Beatriz Duarte GAVIÃO 3 1- Speech-Language Pathologist, MSc, Graduate student, Department of Community
www.scielo.br/jaos disorders Raquel Aparecida PIZOLATO 1, Frederico Silva de Freitas FERNANDES 2, Maria Beatriz Duarte GAVIÃO 3 1- Speech-Language Pathologist, MSc, Graduate student, Department of Community
Masticatory function after unilateral distal extension removable partial denture treatment: intra-individual comparison with opposite dentulous side
 J Med Dent Sci 2005; 52: 35 41 Original Article Masticatory function after unilateral distal extension removable partial denture treatment: intra-individual comparison with opposite dentulous side Wacharasak
J Med Dent Sci 2005; 52: 35 41 Original Article Masticatory function after unilateral distal extension removable partial denture treatment: intra-individual comparison with opposite dentulous side Wacharasak
Parotid Gland. Parotid Gland. Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible. Medial pterygoid.
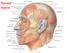 Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
Effect of Stomatognathic Alignment Exercise on Temporomandibular Joint Function and Swallowing Function of Stroke Patients with Limited Mouth Opening
 Effect of Stomatognathic Alignment Exercise on Temporomandibular Joint Function and Swallowing Function of Stroke Patients with Limited Mouth Opening J. Phys. Ther. Sci. 25: 1325 1329, 2013 Duck-Won Oh,
Effect of Stomatognathic Alignment Exercise on Temporomandibular Joint Function and Swallowing Function of Stroke Patients with Limited Mouth Opening J. Phys. Ther. Sci. 25: 1325 1329, 2013 Duck-Won Oh,
BUCCAL MUCOSA RIDGING AND TONGUE INDENTATION: INCIDENCE AND ASSOCIATED FACTORS
 Bull. Tokyo dent. Coll., Vol. 40, No. 2, pp. 71 78, May, 1999 71 Original Article BUCCAL MUCOSA RIDGING AND TONGUE INDENTATION: INCIDENCE AND ASSOCIATED FACTORS KATIUSKA PIQUERO, TOMOHIKO ANDO and KAORU
Bull. Tokyo dent. Coll., Vol. 40, No. 2, pp. 71 78, May, 1999 71 Original Article BUCCAL MUCOSA RIDGING AND TONGUE INDENTATION: INCIDENCE AND ASSOCIATED FACTORS KATIUSKA PIQUERO, TOMOHIKO ANDO and KAORU
JAMSS Speed-to-Treat Protocol For treatment of jaw joint and muscle sprain/strain injuries
 JAMSS Speed-to-Treat Protocol For treatment of jaw joint and muscle sprain/strain injuries INTRODUCTION What is Jaw Joint and Muscle Sprain/Strain (JAMSS)? Jaw Joint and Muscle Sprain/Strain (JAMSS) is
JAMSS Speed-to-Treat Protocol For treatment of jaw joint and muscle sprain/strain injuries INTRODUCTION What is Jaw Joint and Muscle Sprain/Strain (JAMSS)? Jaw Joint and Muscle Sprain/Strain (JAMSS) is
MEDICAL ASSISTANCE BULLETIN COMMONWEALTH OF PENNSYLVANIA DEPARTMENT OF PUBLIC WELFARE
 MEDICAL ASSISTANCE BULLETIN COMMONWEALTH OF PENNSYLVANIA DEPARTMENT OF PUBLIC WELFARE ISSUE DATE EFFECTIVE DATE NUMBER October 21,1996 October 28,1996 03-96-06 SUBJECT BY Information on New Procedures
MEDICAL ASSISTANCE BULLETIN COMMONWEALTH OF PENNSYLVANIA DEPARTMENT OF PUBLIC WELFARE ISSUE DATE EFFECTIVE DATE NUMBER October 21,1996 October 28,1996 03-96-06 SUBJECT BY Information on New Procedures
A jaw exerciser for fibrous ankylosis of the temporomandibular joint
 418 Australian Dental Journal, December, 1985 Volume 30, No. 6 A jaw exerciser for fibrous ankylosis of the temporomandibular joint M. Darveniza, M.D.Sc., F.R.A.C.D.S. Lecturer in Operative Dentistry,
418 Australian Dental Journal, December, 1985 Volume 30, No. 6 A jaw exerciser for fibrous ankylosis of the temporomandibular joint M. Darveniza, M.D.Sc., F.R.A.C.D.S. Lecturer in Operative Dentistry,
Prevalence of Temporomandibular Joint Dysfunction and Its Signs among the Partially Edentulous Patients in a Village of North Gujarat
 10.5005/jp-journals-10024-1466 Prevalence ORIGINAL of research Temporomandibular Joint Dysfunction and Its Signs among the Partially Edentulous Patients in a Village of North Gujarat Prevalence of Temporomandibular
10.5005/jp-journals-10024-1466 Prevalence ORIGINAL of research Temporomandibular Joint Dysfunction and Its Signs among the Partially Edentulous Patients in a Village of North Gujarat Prevalence of Temporomandibular
529-A Treatment and Management of the Edentulous Patient. Upon completion of this course the student should be able to:
 Course & Title: Session & Topic: 529-A Treatment and Management of the Edentulous Patient Jaw Relations General Goal: To understand the principles of orientational, horizontal and vertical jaw relations
Course & Title: Session & Topic: 529-A Treatment and Management of the Edentulous Patient Jaw Relations General Goal: To understand the principles of orientational, horizontal and vertical jaw relations
Joules, Genes, and Behaviors: Degeneration of The Human TMJ
 Joules, Genes, and Behaviors: Degeneration of The Human TMJ Jeffrey C. Nickel, DMD, MSc, PhD Associate Professor University of Missouri-Kansas City Department of Orthodontics and Dentofacial Orthopedics
Joules, Genes, and Behaviors: Degeneration of The Human TMJ Jeffrey C. Nickel, DMD, MSc, PhD Associate Professor University of Missouri-Kansas City Department of Orthodontics and Dentofacial Orthopedics
Okeson AAO May 3, 2016
 Orthodontic Therapy and : An Update Orthodontic Therapy and : An Update by Jeffrey P Okeson, DMD Professor and Chief, Division of Orofacial Pain Director, Orofacial Pain Program University of Kentucky
Orthodontic Therapy and : An Update Orthodontic Therapy and : An Update by Jeffrey P Okeson, DMD Professor and Chief, Division of Orofacial Pain Director, Orofacial Pain Program University of Kentucky
Case Report. A Novel Treatment of Recurrent Temporomandibular Joint Dislocation with Intermaxillary Fixation Using Microimplant: A Case Report
 JOMP Journal of Oral Medicine and Pain Case Report pissn 2288-9272 eissn 2383-8493 J Oral Med Pain 2014;39(4):156-162 http://dx.doi.org/10.14476/jomp.2014.39.4.156 A Novel Treatment of Recurrent Temporomandibular
JOMP Journal of Oral Medicine and Pain Case Report pissn 2288-9272 eissn 2383-8493 J Oral Med Pain 2014;39(4):156-162 http://dx.doi.org/10.14476/jomp.2014.39.4.156 A Novel Treatment of Recurrent Temporomandibular
Condylar Movement Assessment is Severe Attrition Patient Undergoing Orthodontic Treatment: Joint Vibrant Analysis Procedure
 Case Report imedpub Journals http://www.imedpub.com Journal of Dental and Craniofacial Research DOI: 10.21767/2576-392X.100004 Condylar Movement Assessment is Severe Attrition Patient Undergoing Orthodontic
Case Report imedpub Journals http://www.imedpub.com Journal of Dental and Craniofacial Research DOI: 10.21767/2576-392X.100004 Condylar Movement Assessment is Severe Attrition Patient Undergoing Orthodontic
Association of the Morphology of the Atlas Vertebra. with the Morphology of the Mandible
 MDJ Association of the Morphology of the Atlas Vertebra with the Morphology of the Mandible Dr. Hadeel Ali Hussein Al-Hashimi, B.D.S., M.Sc.* Dr. Zina Zuhair Al-Azawi, B.D.S., M.Sc.** Abstract Anatomy
MDJ Association of the Morphology of the Atlas Vertebra with the Morphology of the Mandible Dr. Hadeel Ali Hussein Al-Hashimi, B.D.S., M.Sc.* Dr. Zina Zuhair Al-Azawi, B.D.S., M.Sc.** Abstract Anatomy
Modelling of temporomandibular joint and FEM analysis
 Acta of Bioengineering and Biomechanics Vol. 8, No. 1, 2006 Modelling of temporomandibular joint and FEM analysis MARTINA FRIOVÁ, ZDENK HORÁK, SVATAVA KONVIKOVÁ Laboratory of Biomechanics, Department of
Acta of Bioengineering and Biomechanics Vol. 8, No. 1, 2006 Modelling of temporomandibular joint and FEM analysis MARTINA FRIOVÁ, ZDENK HORÁK, SVATAVA KONVIKOVÁ Laboratory of Biomechanics, Department of
KJLO. A Sequential Approach for an Asymmetric Extraction Case in. Lingual Orthodontics. Case Report INTRODUCTION DIAGNOSIS
 KJLO Korean Journal of Lingual Orthodontics Case Report A Sequential Approach for an Asymmetric Extraction Case in Lingual Orthodontics Ji-Sung Jang 1, Kee-Joon Lee 2 1 Dream Orthodontic Clinic, Gimhae,
KJLO Korean Journal of Lingual Orthodontics Case Report A Sequential Approach for an Asymmetric Extraction Case in Lingual Orthodontics Ji-Sung Jang 1, Kee-Joon Lee 2 1 Dream Orthodontic Clinic, Gimhae,
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Spinal muscular atrophy Report from observation charts
 Orofacial function of persons having Spinal muscular atrophy Report from observation charts The survey comprises 49 observation charts. Synonyms: SMA I (Werdnig-Hoffmann disease, SMA II, SMA III (Kugelberg-Welander
Orofacial function of persons having Spinal muscular atrophy Report from observation charts The survey comprises 49 observation charts. Synonyms: SMA I (Werdnig-Hoffmann disease, SMA II, SMA III (Kugelberg-Welander
Case Report. Hatice Gökalp, DDS, PhD a ; Hakan Türkkahraman, DDS b
 Case Report Changes in Position of the Temporomandibular Joint Disc and Condyle After Disc Repositioning Appliance Therapy: A Functional Examination and Magnetic Resonance Imaging Study Hatice Gökalp,
Case Report Changes in Position of the Temporomandibular Joint Disc and Condyle After Disc Repositioning Appliance Therapy: A Functional Examination and Magnetic Resonance Imaging Study Hatice Gökalp,
Dentofacial characteristics of women with oversized mandible and temporomandibular joint internal derangement
 Original Article Dentofacial characteristics of women with oversized mandible and temporomandibular joint internal derangement Beom-Seok Moon a ; Il-Hyung Yang b ; Sug-Joon Ahn c ABSTRACT Introduction:
Original Article Dentofacial characteristics of women with oversized mandible and temporomandibular joint internal derangement Beom-Seok Moon a ; Il-Hyung Yang b ; Sug-Joon Ahn c ABSTRACT Introduction:
Neuro-Occlusal Rehabilitation: Therapeutic by Direct and Indirect Tracks
 Cronicon OPEN ACCESS EC DENTAL SCIENCE Research Article Neuro-Occlusal Rehabilitation: Therapeutic by Direct and Indirect Tracks Amel Belkhiri* and Latifa Zenati SAAD Dahleb University, 12, rue AEK mechedel,
Cronicon OPEN ACCESS EC DENTAL SCIENCE Research Article Neuro-Occlusal Rehabilitation: Therapeutic by Direct and Indirect Tracks Amel Belkhiri* and Latifa Zenati SAAD Dahleb University, 12, rue AEK mechedel,
Horizontal Jaw Relation
 Horizontal Jaw Relation Horizontal Jaw Relation It is the relationship of the mandible to the maxilla in a horizontal plane. It can also be described as the relationship of the mandible to the maxilla
Horizontal Jaw Relation Horizontal Jaw Relation It is the relationship of the mandible to the maxilla in a horizontal plane. It can also be described as the relationship of the mandible to the maxilla
The Research Diagnostic Criteria for Temporomandibular Disorders. V: Methods Used to Establish and Validate Revised Axis I Diagnostic Algorithms
 The Research Diagnostic Criteria for Temporomandibular Disorders. V: Methods Used to Establish and Validate Revised Axis I Diagnostic Algorithms Eric L. Schiffman, DDS, MS Associate Professor Department
The Research Diagnostic Criteria for Temporomandibular Disorders. V: Methods Used to Establish and Validate Revised Axis I Diagnostic Algorithms Eric L. Schiffman, DDS, MS Associate Professor Department
Significant improvement with limited orthodontics anterior crossbite in an adult patient
 VARIA Significant improvement with limited orthodontics anterior crossbite in an adult patient Arzu Ari-Demirkaya Istanbul, Turkey Summary Objectives. Orthodontic treatment is known to last as long as
VARIA Significant improvement with limited orthodontics anterior crossbite in an adult patient Arzu Ari-Demirkaya Istanbul, Turkey Summary Objectives. Orthodontic treatment is known to last as long as
ORTHODONTIC INITIAL ASSESSMENT FORM (OIAF) w/ INSTRUCTIONS
 Use the accompanying Tip Sheet and How to Score the Orthodontic Initial Assessment Form for guidance in completion of the assessment form. You will need this score sheet and a disposable ruler (or a Boley
Use the accompanying Tip Sheet and How to Score the Orthodontic Initial Assessment Form for guidance in completion of the assessment form. You will need this score sheet and a disposable ruler (or a Boley
Jaw relation registration in RPD
 Jaw relation registration in RPD Why to Record the Jaw Relations? To establish and maintain a harmonious relationship with all oral structures and to provide a masticatory apparatus that is efficient and
Jaw relation registration in RPD Why to Record the Jaw Relations? To establish and maintain a harmonious relationship with all oral structures and to provide a masticatory apparatus that is efficient and
Exercise Therapy for Craniomandibular Disorders
 1137 Exercise Therapy for Craniomandibular Disorders Peter Nicolakis, MD, Burak Erdogmus, MD, Andreas Kopf, MD, Andreas Djaber-Ansari, MD, Eva Piehslinger, MD, PhD, Veronika Fialka-Moser, MD, PhD ABSTRACT.
1137 Exercise Therapy for Craniomandibular Disorders Peter Nicolakis, MD, Burak Erdogmus, MD, Andreas Kopf, MD, Andreas Djaber-Ansari, MD, Eva Piehslinger, MD, PhD, Veronika Fialka-Moser, MD, PhD ABSTRACT.
RESEARCH DIAGNOSTIC CRITERIA FOR TEMPOROMANDIBULAR DISORDERS
 DEPARTMENT OF ORAL MEDICINE OROFACIAL PAIN RESEARCH GROUP RESEARCH DIAGNOSTIC CRITERIA FOR TEMPOROMANDIBULAR DISORDERS AXIS I: CLINICAL PHYSICAL EXAMINATION FORMS AND SPECIFICATIONS INSTRUCTIONS FOR SCORING
DEPARTMENT OF ORAL MEDICINE OROFACIAL PAIN RESEARCH GROUP RESEARCH DIAGNOSTIC CRITERIA FOR TEMPOROMANDIBULAR DISORDERS AXIS I: CLINICAL PHYSICAL EXAMINATION FORMS AND SPECIFICATIONS INSTRUCTIONS FOR SCORING
Ultrasonographic Thickness of the Masseter Muscle in Growing Individuals with Unilateral Crossbite
 Original Article Ultrasonographic Thickness of the Masseter Muscle in Growing Individuals with Unilateral Crossbite Stavros Kiliaridis a ; Payam H. Mahboubi b ; Maarten C. Raadsheer c ; Christos Katsaros
Original Article Ultrasonographic Thickness of the Masseter Muscle in Growing Individuals with Unilateral Crossbite Stavros Kiliaridis a ; Payam H. Mahboubi b ; Maarten C. Raadsheer c ; Christos Katsaros
Temporomandibular joint internal derangements: Diagnosis, mechanisms and risk factors, and prognosis Kalaykova, S.I.
 UvA-DARE (Digital Academic Repository) Temporomandibular joint internal derangements: Diagnosis, mechanisms and risk factors, and prognosis Kalaykova, S.I. Link to publication Citation for published version
UvA-DARE (Digital Academic Repository) Temporomandibular joint internal derangements: Diagnosis, mechanisms and risk factors, and prognosis Kalaykova, S.I. Link to publication Citation for published version
Initial Doctor Questionnaire
 Initial Doctor Questionnaire DO NOT enter the patient in this study: if your patient does not have a TMD pain diagnosis if your patient does not need treatment at this time if you are not going to treat
Initial Doctor Questionnaire DO NOT enter the patient in this study: if your patient does not have a TMD pain diagnosis if your patient does not need treatment at this time if you are not going to treat
Prevalence of degree of saverity of temporomandibular join disorder based on sex and age group
 Prevalence of degree of saverity of temporomandibular join disorder based on sex and age group Luciana Dewanti Department of Prosthodontics Faculty of Dentistry Universitas Padjadjaran ABSTRACT Temporomandibular
Prevalence of degree of saverity of temporomandibular join disorder based on sex and age group Luciana Dewanti Department of Prosthodontics Faculty of Dentistry Universitas Padjadjaran ABSTRACT Temporomandibular
TitleTemporomandibular joint ankylosis: Mitarashi, S; Abe, S; Watanabe, H; Author(s) Hashimoto, M; Ide, Y
 TitleTemporomandibular joint ankylosis: Mitarashi, S; Abe, S; Watanabe, H; Author(s) Hashimoto, M; Ide, Y Cranio : the journal of craniomandi Journal 20(1): 67-71 URL http://hdl.handle.net/10130/1098 Right
TitleTemporomandibular joint ankylosis: Mitarashi, S; Abe, S; Watanabe, H; Author(s) Hashimoto, M; Ide, Y Cranio : the journal of craniomandi Journal 20(1): 67-71 URL http://hdl.handle.net/10130/1098 Right
Clinical evaluation of temporomandibular disorders in children and adolescents: a review of the literature
 TMJliterature 9-12-2009 16:53 Pagina 188 P. Toscano, P. Defabianis Department of Biomedical Sciences and Human Oncology Section of Paediatric Dentistry, Traumatology and orofacial malformations in the
TMJliterature 9-12-2009 16:53 Pagina 188 P. Toscano, P. Defabianis Department of Biomedical Sciences and Human Oncology Section of Paediatric Dentistry, Traumatology and orofacial malformations in the
Original Article. Articular disc displacement in mandibular asymmetry patients. Boonsiva Buranastidporn, Masataka Hisano and Kunimichi Soma
 J Med Dent Sci ; : 8 Original Article Articular disc displacement in mandibular asymmetry patients Boonsiva Buranastidporn, Masataka Hisano and Kunimichi Soma Orthodontic Science, Department of Orofacial
J Med Dent Sci ; : 8 Original Article Articular disc displacement in mandibular asymmetry patients Boonsiva Buranastidporn, Masataka Hisano and Kunimichi Soma Orthodontic Science, Department of Orofacial
Prevalence amongst adolescents in Bergen, Western Norway of temporomandibular disorders according to the DC/TMD criteria and examination protocol
 Prevalence amongst adolescents in Bergen, Western Norway of temporomandibular disorders according to the DC/TMD criteria and examination protocol Graue Anne Marit¹, Jokstad Asbjørn², Assmus Jörg³, Skeie
Prevalence amongst adolescents in Bergen, Western Norway of temporomandibular disorders according to the DC/TMD criteria and examination protocol Graue Anne Marit¹, Jokstad Asbjørn², Assmus Jörg³, Skeie
Removable appliances
 Removable appliances Melinda Madléna DMD, PhD associate professor Department of Pedodontics and Orthodontics Faculty of Dentistry Semmelweis University Budapest Classification of the orthodontic anomalies
Removable appliances Melinda Madléna DMD, PhD associate professor Department of Pedodontics and Orthodontics Faculty of Dentistry Semmelweis University Budapest Classification of the orthodontic anomalies
Horizontal jaw relations: The relationship of mandible to maxilla in a
 Horizontal relations Horizontal jaw relations: The relationship of mandible to maxilla in a horizontal plane (in anteroposterior and side to side direction). a- Protruded or forward relation. b-lateral
Horizontal relations Horizontal jaw relations: The relationship of mandible to maxilla in a horizontal plane (in anteroposterior and side to side direction). a- Protruded or forward relation. b-lateral
Dental Services Referral Form- Orthodontic Clinic
 Dental Services Referral Form- Orthodontic Clinic Date / / Title: Surname Given name Date of birth: Street address Suburb Postcode Name of Residential Facility (if applicable) Room: Phone - Home: Mobile:
Dental Services Referral Form- Orthodontic Clinic Date / / Title: Surname Given name Date of birth: Street address Suburb Postcode Name of Residential Facility (if applicable) Room: Phone - Home: Mobile:
Functional Unilateral Posterior Crossbite Effects on Mastication Movements Using Axiography
 Original Article Functional Unilateral Posterior Crossbite Effects on Mastication Movements Using Axiography Marco Antonio Canada Salioni a ; Silmara Elena Papa Pellizoni a ; Antonio Sérgio Guimarães b
Original Article Functional Unilateral Posterior Crossbite Effects on Mastication Movements Using Axiography Marco Antonio Canada Salioni a ; Silmara Elena Papa Pellizoni a ; Antonio Sérgio Guimarães b
