There is a paucity of postmortem histologic
|
|
|
- Kory Dennis
- 5 years ago
- Views:
Transcription
1 Postmortem Histologic Evaluation of Mandibular Titanium and Maxillary Hydroxyapatite-Coated Implants from 1 Patient Michael D. Rohrer, DDS, MS*/Randall R. Sobczak, DDS, FAGD**/ Hari S. Prasad, BS, MDT***/Harold F. Morris, DDS, MS**** Postmortem examination of human specimens is an extremely important aspect of evaluating the relative compatibility and long-term success of endosseous implant surfaces. The bone-implant interface of 5 commercially pure titanium screw-type mandibular implants after 85 months of service and 2 hydroxyapatite- (HA) coated maxillary implants after 38 months of service were examined. All implants were stable at the time of the patient s death. The mandibular implants had an average of 65% contact with bone and the maxillary implants had an average of 47% contact. The HA coating had separated from the maxillary implants in some areas and was free within surrounding connective tissue or surrounded by invaginating sulcular epithelium. The arrangement and pattern of bone contact appeared different between HA-coated and titanium implant surfaces. (INT J ORAL MAXILLOFAC IMPLANTS 1999;14: ) Key words: dental implant, Dental Implant Clinical Research Group, endosseous, histology, hydroxyapatite, osseointegration, postmortem, titanium There is a paucity of postmortem histologic information from long-term, prospective, controlled studies of dental implants. One of the most important questions to be answered is the relative compatibility and long-term success of the most common implant surfaces. The Dental Implant Clinical Research Group (DICRG) is one of the largest randomized scientific clinical studies of implants ever conducted in the United States and is ****Assistant Dean for Research, Professor of Oral and Maxillofacial Pathology, and Director, Hard Tissue Research Laboratory, College of Dentistry, University of Oklahoma Health Sciences Center, Oklahoma City, Oklahoma. ****Formerly Staff Dentist and Principal Investigator, Implant Programs, Department of Veterans Affairs, Puget Sound Health Care System, Seattle, Washington; Currently, Private Practice, Bothell, Washington. ****Research Assistant, Hard Tissue Research Laboratory, College of Dentistry, University of Oklahoma Health Sciences Center, Oklahoma City, Oklahoma. ****Director of Research, Department of Veterans Affairs Medical Center, Ann Arbor, Michigan. Reprint requests: Dr Michael D. Rohrer, College of Dentistry, University of Oklahoma Health Sciences Center, 1001 Stanton L. Young Blvd., Oklahoma City, OK Fax: the only study of endosseous dental implants conducted by an agency of the United States government. 1,2 Postmortem specimens from subjects in this study are becoming available for examination histologically and histomorphometrically. Since 1991, more than 3,000 implants have been placed and uncovered in more than 800 patients by more than 100 researchers of the DICRG. Because of the nature of the involvement of the subjects and their families in this highly controlled study, many are willing upon their deaths to submit postmortem specimens for examination. Specimens containing both titanium and hydroxyapatite- (HA) coated implants have been evaluated by undecalcified histologic techniques and histomorphometric analysis. 3 This particular study involves a patient who had received 5 screw-type titanium implants (Nobel Biocare, Göteborg, Sweden) in the anterior mandible prior to the initiation of the DICRG controlled study. Two maxillary HA-coated cylindric implants (Microvent, Core-Vent, Encino, CA) were placed as part of the study under a secondary protocol. At the time of the patient s death, the mandibular implants had been in place for 85 months and the maxillary implants had been in place for 38 months. The International Journal of Oral & Maxillofacial Implants 579
2 Patient Description Social History. The patient was a 77-year-old Caucasian male of Polish descent born in He used alcohol and tobacco prior to Medical History. The patient had suffered from beriberi as a prisoner of war, had bronchial asthma, and was allergic to sulfa. Dental History. The patient initially presented to the Seattle Veterans Affairs Dental Clinic in 1982 with only the mandibular left premolars remaining. The teeth had been restored with splinted crowns having extracoronal OSO attachments that retained a removable partial denture opposing a complete maxillary denture. The remaining teeth were extracted in February After 6 months of healing, 5 commercially pure (cp) 15-mm titanium screw-type implants were placed in the anterior mandible on July 31, Phase 2 uncovering was accomplished in November 1989, and the final fixed-detachable prosthesis was placed 1 year later, in November At the 1-month follow-up visit, it was noted that the patient complained of instability of his maxillary denture, which was now functioning against a very stable lower prosthesis. A 6-month implant prophylaxis was performed in May The prosthesis was removed, and excellent plaque control and gingival health were noted. The patient was unhappy with his maxillary denture and an occlusal equilibration was performed. One month later, it was noted that the patient s anterior maxillary ridge was becoming fibrous and mobile. His maxillary denture was relined in July 1991, and a new prosthesis fitted to the mouthpiece of his saxophone was placed 3 months later. The patient was stable for the next year and a half, until May 1993, when the maxillary denture was relined with tissue conditioner. One month later, 2 Microvent implants (3.25 mm 10 mm) were placed in the maxillary canine regions. The DICRG study protocol specified 5 implants for the completely edentulous maxilla. Only 2 were placed in this patient because of insufficient bone. Stage 2 surgery was performed on January 21, 1994, and 5- mm healing collars were placed. On February 8, it was noted that the healing was progressing slowly and that the healing collars were too short. Straight 4-mm abutments, 4-mm with ball attachments were placed on May 2, 1994, and the relined denture with ball/socket attachments was placed on May 18, Healing was reported as good at that visit. The patient next presented in late January of 1995 with the complaint of a loose denture in need of o-ring replacement. His gingival health was satisfactory, but the denture occlusal surfaces were very worn. Tissue conditioner was placed to correct for the anteroposterior rocking of the denture. It was also noted that the patient s health history had changed. He was then under treatment for hypertension and had had a stroke. His medications at this time included aspirin daily, nifedipine 3 times a day, Beconase nasal inhaler 3 puffs 3 times a day, albuterol 4 puffs twice a day, lasix and potassium every morning, ranitidine every morning for reflux, doxipine at bedtime, tipclopidine twice a day to inhibit platelet aggregation, and Fibercon. The mandibular implants were evaluated in June No suppuration was noted, and Periotest values were 6 to 5, indicating clinical integration. The fixed-detachable prosthesis was not mobile and was serviceable. The DICRG recall for the maxillary implants was performed in August The Gingival Index was graded at 2 for the mesial of the maxillary right canine implant and for the facial and distal of the maxillary left canine implant, with suppuration present. Periotest values were +2 and +4, respectively. Interprobe measurements were: right maxillary canine implant 3.5 mm mesial, 2.5 mm facial, 3.0 mm distal, 4.5 mm lingual; left maxillary canine implant 7.5 mm mesial, 3.5 mm facial, 7.0 mm distal, 5.0 mm lingual. Although Periotest values were in the positive range and pocket depths of over 3 mm were present, no mobility of the implants was noted. A culture was taken and the patient was started on tetracycline 250 mg 4 times daily for 14 days. A health history update was significant for recent episodes of pneumonia complicated by the patient s asthma. Culture results were negative, and the patient remained asymptomatic, with a marked decrease in suppuration on September 16. Later that month, the patient suffered another stroke with a residual left leg deficit and was unable to continue treatment. The patient returned in early December 1995 with an increase in the lingual pocket depth of the left maxillary canine implant to 11 mm, with a corresponding increase in suppuration. The maxillary implants remained non-mobile, and a repair procedure was scheduled for January At that appointment a decrease in suppuration was noted. The patient had been on antibiotics for his pneumonia. Probing depths had decreased slightly, to 3.5 mm buccal, 7.0 mm mesial, and 9.0 mm on the palatal and distal. A crestal incision revealed a 3-wall crater defect involving the palatal and extending toward the proximal of the maxil- 580 Volume 14, Number 4, 1999
3 Fig 1a Postmortem mandible with 5 cp titanium implants and the fixed-detachable prosthesis. Fig 1b Postmortem anterior maxilla with 2 HA-coated cylindric implants and ball attachments. lary left canine implant. The area was thoroughly curetted to remove granulation tissue, and the implant surface was smoothed using a white stone in a high-speed handpiece with copious irrigation. The implant was then detoxified for 3 minutes with a paste of tetracycline. OsteoGraf/N (CeraMed, Denver, CO) was placed in the defect and covered with a Gore-Tex barrier membrane (WL Gore, Flagstaff, AZ). Sutures were removed 5 days later and there was some swelling over the membrane. The patient was again seen on January 23 and showed normal healing. The patient was next seen on March 1, At that visit, the area of repair was intact, without erythema or purulence. The patient, however, had declined physically and was noticeably weak. His denture was relined with tissue conditioner so that he could resume wearing the prosthesis. At a 4-day follow-up visit, the gingival tissues appeared somewhat boggy in consistency and less firm than before, with the peri-implant gingiva at the facial aspect described as loose. The patient was instructed to minimize denture wear. During this time, the patient s health continued to decline, with several small strokes requiring his admission into a nursing care facility. He returned to the clinic on April 14, 1996, at which time it was noted that there was suppuration around the membrane; the membrane was diagnosed as infected. At membrane removal, the HA repair material was found to be encapsulated in fibrous connective tissue, which was left intact. The implant remained non-mobile. A postoperative prescription for tetracycline (250 mg for 7 days) was provided. One week later, healing was progressing in a slow but normal fashion, with some residual swelling and no purulence. On May 24, the repair side was well healed and alginate impressions were made of both arches in hopes of fabricating new prostheses. The patient was last seen 1 week later. His condition declined rapidly after that, and he died on August 30, Autopsy specimens were recovered on September 4. Specimen Preparation The anterior portions of the mandible and the maxilla were removed at autopsy (Fig 1), placed in 10% neutral buffered formalin and processed without decalcification. 4,5 The specimens were sectioned to a thickness of 5 mm through the center of the implants the maxillary specimens in a mesiodistal direction, and the mandibular specimens alternating mesiodistally and buccolingually. Following dehydration, infiltration and embedding were accomplished with a light-curing embedding resin (Technovit 7200 VLC, Kulzer-EXAKT, Norderstedt, Germany). The specimens were cut to a thickness of 150 µm on an EXAKT cutting/grinding system (EXAKT Apparatebau, Norderstedt, Germany), polished to a thickness of 40 µm using the EXAKT microgrinding system, stained with Stevenel s blue and Van Gieson s picro fuchsin, and viewed under conventional light and polarized light microscopy. Histomorphometric analyses of the light microscopic samples were made to determine the percentage of implant surface in contact with calcified bone, bone marrow, and gingival connective tissue. Photographs were taken with a medical macrolens system to produce 1.6 magnification of the implants in the bone. Transparencies were projected to a magnification of 75. A digital, programmable curvimeter (K&R Instruments, Orlando, FL) was used to measure the entire The International Journal of Oral & Maxillofacial Implants 581
4 Fig 2 (Left) Mesiodistal section of 2 mandibular cp titanium implants in situ for 85 months. Average bone contact = 68.5%; connective tissue = 14.5%; marrow = 17% (original magnification 1.6, Stevenel s blue and Van Gieson s picro fuchsin stain). Fig 3 (Right) Area at cervical of mandibular cp titanium implant in situ for 85 months. Bone contact occurs below level of crestal bone height between third and fourth thread. Epithelium (arrow) contacts implant down to level of bone attachment. Minimal inflammation is present (original magnification 10, Stevenel s blue and Van Gieson s picro fuchsin stain). perimeter of the implants. Linear measurements of the connective tissue, bone, and bone marrow contact were made for calculation of the percentage of contact with the implant. Connective tissue was defined as any fibrous tissue in contact with the implant coronal to the most coronal contact point of osseointegrated bone. This included any connective tissue lined by gingival epithelium. Bone contact was defined as intimate interface contact between the bone and the implant surface, with no soft tissue visible between the implant and the bone. Bone marrow was defined as interface contact between soft tissue and the implant surface apical to the most coronal contact point of osseointegrated bone. Results Light Microscopy. Low-power examination showed that the mandibular titanium implants were well integrated, with some crestal loss of bone, but with generally satisfactory height of bone on the implants. The buccolingual sections showed a relatively dense and continuous integration of bone to implant surface where the implants were close to the cortical bone of the buccal or lingual plates. The mesiodistal sections showed more bone marrow contact in the predominantly cancellous bone area (Fig 2). A higher-power view of the coronal area demonstrated some crestal bone loss in 3 of the implants; that is, bone contact with the implant more apical than the height of the crestal bone surrounding the implant. This generally was at the third thread. Sulcus epithelium was in contact with the implant to the point of bone contact (Fig 3). Very slight inflammation was present in the connective tissue. The bone bordering this ditch area exhibited a surface layer of osteoid tissue and osteoblasts, indicating active osteogenesis. The bone surrounding the apical portion of the implants was very dense. The bone in the apical vents was less dense but showed a high degree of bone contact. Polarization of the stained sections showed that the bone contacting the implants was mature and remodeled Haversian bone. Within the threads, the remodeled lamellar patterns consisted of much smaller osteons as opposed to the general, larger lamellar patterns of the bone farther from the implant (Fig 4a). The trabeculae in the cancellous bone area were generally oriented around the implant in a supporting, strut-like buttressing pattern (Fig 4b). Polarized light microscopy of the bone in this area also emphasized the remodeling pattern of the bone to conform to the architecture of the threads (Fig 4c). The amount of bone contact with the maxillary HA-coated implants was clearly less than with the mandibular implants; however, where there was contact it tended to be more continuous than in the titanium implants. Low-power mesiodistal views showed deep cratering of the bone around the implant from the maxillary right canine implant area and better bone contact with the implant in the maxillary left canine implant area. Particles of hydroxyapatite that were placed around the implant in an attempt at gaining greater bone support were also obvious. Higherpower views of the crestal area revealed that 582 Volume 14, Number 4, 1999
5 Fig 4a Polarized light view of area of bone within the threads of mandibular cp titanium implant in situ for 85 months. Polarization emphasizes the smaller osteons in the thread area compared to the generally larger lamellar patterns farther from the implant (original magnification 25, Stevenel s blue and Van Gieson s picro fuchsin stain). Fig 4b Polarized light view of cancellous bone surrounding mandibular cp titanium implant in situ for 85 months. Supporting trabeculae are arranged in a strut-like buttressing pattern (original magnification 6.25, Stevenel s blue and Van Gieson s picro fuchsin stain). Fig 4c Polarized light view of cancellous bone surrounding mandibular cp titanium implant in situ for 85 months. The polarization emphasizes the remodeling pattern of the bone to conform to the architecture of the threads (original magnification 25, Stevenel s blue and Van Gieson s picro fuchsin stain). epithelium from the gingiva followed the implant surface to well below the level of the crestal bone. Also, separation of the HA coating from the titanium surface in some areas was evident (Fig 5). Not all areas of the HA-coated implant not in intimate contact with the bone show the HA separation, but the epithelium had migrated along the entire HA surface to the point of first bone contact (Fig 6). Where bone was in tight apposition with the HA-coated implant, especially in the apical areas and within the apical vents, the bone was dense, solid, and mature. The character of this bone in contact with the HA was almost a continuous band of calcified bone, with 90% of the bone being calcified and 10% marrow (Fig 7). The bone had remodeled in the areas of implant contact to conform to the surface configuration of the implant (Fig 8). In some areas where new bone formed around the implant, loose pieces of HA coating were incorporated into the bone. Obviously the HA had separated from the implant in vivo, because the pieces of HA were surrounded by invaginating epithelium, and in some areas the epithelium was between the titanium surface and the separated HA coating (Fig 9). Histomorphometric Analysis. Histomorphometric analysis of the bone and soft tissue contact of the implants revealed 18% more contact with bone on the mandibular implants than the maxillary implants, with 47% of the maxillary implants with intimate bone contact and 65.4% of the mandibular implants with bone contact. Of the 2 maxillary HA-coated implants, there was much less bone contact on the right canine implant (38%) than on the left (56%). The bone contact on the mandibular implants was very uniform, ranging from a high of 72% to a low of 62%. A conspicuous difference between the HA-coated and cp titanium implants was seen in the amount of marrow contact. The maxillary HA-coated implants had an average of 5% marrow, and the mandibular cp titanium implants had an average of 19.4%. This is a measure of the continuity of the bone contact within the osseointegrated areas of the implants and indicates a more uninterrupted solid bone contact with the HA coating. The measurement for connective tissue contact is the measure of the amount of implant that is out of the bone and could actually represent gingival connective tissue, connective tissue lined by epithelium, or a portion of the implant totally exposed to The International Journal of Oral & Maxillofacial Implants 583
6 I Fig 5 Mesiodistal section of HA-coated maxillary right canine implant in situ for 38 months. Gingival epithelium (arrows) is in contact with the HA well apical to the level of bone. Separation of HA coating from the implant is seen (original magnification 6.25, Stevenel s blue and Van Gieson s picro fuchsin stain). Fig 6 Hydroxyapatite-coated maxillary right canine implant in situ for 38 months. The HA coating is tightly adherent to implant (I). Gingival epithelium has migrated all the way to the point of first bone contact (arrows). No inflammation is present in the connective tissue (original magnification 25, Stevenel s blue and Van Gieson s picro fuchsin stain). Fig 7 Apical area of HA-coated maxillary left canine implant in situ for 38 months. Tight contact of dense, solid, mature bone can be seen in almost continuous contact with the HA-coated implant (original magnification 6.25, Stevenel s blue and Van Gieson s picro fuchsin stain). I Fig 8 (Left) Polarized light view of apical vent area of HA-coated maxillary left canine implant in situ for 38 months. The polarization emphasizes the remodeling of the bone in contact with the implant to conform to the configuration of the implant surface. Note the difference in the lamellar pattern within the vent and the pattern of the bone surrounding the implant (original magnification 10, Stevenel s blue and Van Gieson s picro fuchsin stain). E Fig 9 (Right) Hydroxyapatite-coated maxillary right canine implant in situ for 38 months. Implant (I) and separated HA coating, which has been surrounded by invaginating sulcular epithelium (E), demonstrate that the HA coating had separated in situ (original magnification 25, Stevenel s blue and Van Gieson s picro fuchsin stain). 584 Volume 14, Number 4, 1999
7 Table 1 Bone and Soft Tissue Contact with Implants Amount of contact (%) Location/implant Bone Connective tissue Marrow Right maxilla/ha Left maxilla/ha Left mandible/titanium Left central mandible/titanium Central mandible/titanium Right central mandible/titanium Right mandible/titanium Average, maxilla Average, mandible the oral cavity. In regards to this parameter, the maxillary HA-coated implants were much less integrated, with an average of 48% not in bone, while the mandibular cp titanium implants showed an average of 15.2% coronal to the first bone contact. At least 2 sections of each implant were measured to arrive at the measurements for the bone and soft tissue contact. The measurements for all categories on all 7 implants can be seen in Table 1. Discussion This study of postmortem histologic features involving maxillary and mandibular implants with HA coatings and titanium surfaces is a valuable correlation between clinical parameters of implant success and actual implant osseointegration. Only a few studies of in situ implants in humans have been reported. 3,6 9 Although in this study the clinical parameters of peri-implant inflammation and pocket depth suggested that the maxillary HAcoated implants should have been less than satisfactory, they were acceptable to the patient. Regardless of the inflammation and loss of attachment, the stability and serviceability of the implants benefited the patient. The difference in the pattern of bone contact on the different types and locations of implants was interesting. Clinicians generally consider the bone of the mandible to be of higher quality than the maxilla and would assume that the quality and quantity of the osseointegration there would be greater. 10,11 Although the percentage of the bone contact was higher on the mandibular cp titanium implants, bone contact was more uniform and solid on the maxillary HA-coated implants. As can be seen in Figs 4b and 7, the bone contact patterns in the maxilla and mandible and therefore in HA-coated and titanium implants were very different. It is obvious that the bone was much higher coronally on the mandibular cp titanium implants than on the maxillary HA-coated implants. The average of 15.2% connective tissue contact on the mandibular cp titanium implants and 48% connective tissue contact on the maxillary HA-coated implants illustrates this. A major difference between the 2 areas and types of implant surfaces in this study is that in the area of bone contact, there is almost solid bone surrounding the maxillary HA-coated implants, with only 5% marrow contact. There is much more marrow in the mandibular cp titanium (19.4%), indicating more cancellous bone in tight contact with the implant. The surface of the maxillary HA-coated implants that was covered by connective tissue, which is coronal to any bone contact, showed a reasonably large amount of loss of HA from the surface of the implants. A feasible explanation for the presence of HA in the soft tissue adjacent to the maxillary left implant was the curettage and smoothing of the implant surface with a rotary white stone at the time of the surgical approach to the 3-wall defect. Separation of HA from the maxillary right implant can be seen in Fig 5, which is difficult to determine as pre- or postmortem. The use of polarized light in viewing the specimen sections emphasizes the remodeling pattern of the mature bone. As could be seen in Figs 4 and 8, the pattern of bone changed to accommodate the stresses placed upon it by the introduction of the implant. The functional forces transmitted through the implant to the bone seem to have influenced the remodeling pattern of the collagen structure of the bone. Bone in contact with the implant that is denser than the surrounding cancellous bone has been observed in other investigations. 3,12 The International Journal of Oral & Maxillofacial Implants 585
8 In this study, the surfaces of the implants, whether cp titanium or HA, were covered by gingival epithelium coronal to the area of first bone contact (Figs 3 and 5). This is similar to what was found in a postmortem study of 12 implants in 4 quadrants. 6 However, in another postmortem investigation involving a patient from the DICRG prospective study, the peri-implant mucosa showed clinical and histologic resemblance to the gingiva around natural teeth. In that study, a thin, nonkeratinized epithelium lacking rete ridges and looking like sulcular epithelium was present surrounding the necks of the implants. Coronal to the bone contact and between the bone and epithelium, connective tissue was tightly adherent to the implants, with bundles of collagen organized in the pattern of cervical gingival connective tissue. 3 Noticeable differences were seen in this study between the maxillary HA-coated implants and the mandibular cp titanium implants. However, because all of the implants were not placed according to the randomized protocol of the DICRG, it is difficult to discern differences that may be the result of location and function as opposed to surface coating. Additional postmortem examinations of patients who have been treated under prospective, controlled implant studies will help answer the question of the reaction of bone to the placement and long-term function of implants with various surfaces presented to the bone of the human jaws. Conclusion A postmortem histologic examination of the boneimplant interface of 5 cp titanium screw-type mandibular implants was carried out after 85 months of service and of 2 hydroxyapatite (HA) coated maxillary implants after 38 months of service. All implants were stable and satisfactory to the patient at the time of his death. The mandibular implants had an average of 65% contact with bone, and the maxillary implants had an average of 47% contact. The condition of the mandibular implants that had been in place for more than 7 years was excellent, with little inflammation around the implants and more than 80% of the length of the implants within bone. The maxillary HA-coated implants were stable, even though they had slightly less than 50% bone contact and had experienced peri-implantitis. They were considered stable by the clinicians and satisfactory by the patient. The HA coating appeared separated from the implants in some areas and in the area of the left maxillary implant it was both free within surrounding connective tissue and surrounded by invaginating sulcular epithelium. The presence of these HA fragments was most likely caused by instrumentation of the implant surface during surgical treatment of a bone defect in the area. The pattern and arrangement of bone contact was different between the maxillary HA-coated and the mandibular cp titanium implants. Acknowledgment The authors wish to thank Tom Sprowl, Hard Tissue Research Laboratory, University of Oklahoma College of Dentistry, for nondecalcified histology sections. References 1. Morris HF, Ochi S, Dental Implant Clinical Research Group (Planning Committee). The influence of implant design, application, and site on clinical performance and crestal bone: A multicenter, multidisciplinary clinical study. Implant Dent 1992;1: Morris HF, Ochi S. Clinical factors of importance to successful implant therapy. J Oral Maxillofac Surg 1997;55(suppl 5). 3. Dominici JT, Olson JW, Rohrer MD, Morris HF. Postmortem histologic evaluation of hydroxyapatite-coated cylinder and titanium alloy basket implants in situ for 37 months in the posterior mandible. Implant Dent 1997;6: Rohrer MD, Schubert CC. The cutting-grinding technique for histological preparation of undecalcified bone and boneanchored implants: Improvement in instrumentation and procedures. Oral Surg Oral Med Oral Pathol 1992;74: Donath K, Breuner G. A method for the study of undecalcified bones and teeth with the attached soft tissues: The Sage Schliff (sawing and grinding) technique. J Oral Pathol 1982;11: Rohrer MD, Bulard RA, Patterson MK. Maxillary and mandibular titanium implants 1 year after surgery: Histologic examination in a cadaver. Int J Oral Maxillofac Implants 1995;10: Nyström E, Kahnberg K, Albrektsson T. Treatment of the severely resorbed maxillae with bone graft and titanium implants: Histologic review of autopsy specimens. Int J Oral Maxillofac Implants 1993;8: GaRey DJ, Whittaker JM, James RA, Lozada JL. The histologic evaluation of the implant interface with heterograft and allograft materials An eight-month autopsy report, Part II. J Oral Implantol 1991;17: Wilson TG Jr, Schenk R, Buser D, Cochran D. Implants placed in immediate extraction sites: A report of histologic and histometric analyses of human biopsies. Int J Oral Maxillofac Implants 1998;13: Engquist B, Bergendal T, Kallus T, Linden U. A retrospective multicenter evaluation of osseointegrated implants supporting overdentures. Int J Oral Maxillofac Implants 1988;3: Jaffin RA, Berman CL. The excessive loss of Brånemark fixtures in type IV bone: A 5-year analysis. J Periodontol 1991;62: Misch CE. Density of bone: Effect on treatment plans, surgical approach, healing, and progressive bone loading. Int J Oral Implantol 1990;6: Volume 14, Number 4, 1999
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
STABILITY OF IMPLANTS AND NATURAL TEETH MONTHS OF FUNCTION AS DETERMINED BY THE PERIOTEST OVER 60 CLINICAL
 CLINICAL STABILITY OF IMPLANTS AND NATURAL TEETH AS DETERMINED BY THE PERIOTEST OVER 60 MONTHS OF FUNCTION Sheldon Winkler, DDS Harold F. Morris, DDS, MS J. Robert Spray, DDS KEY WORDS Implant Natural
CLINICAL STABILITY OF IMPLANTS AND NATURAL TEETH AS DETERMINED BY THE PERIOTEST OVER 60 MONTHS OF FUNCTION Sheldon Winkler, DDS Harold F. Morris, DDS, MS J. Robert Spray, DDS KEY WORDS Implant Natural
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note
 Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel
 PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
Pre op Failed endodontic treatment with sinus involvement.
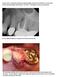 Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This
 1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Practical Advanced Periodontal Surgery
 Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Endosseous cylindric implants are well accepted
 Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
AO Certificate in Implant Dentistry Certificate
 AO Certificate in Implant Dentistry Certificate The AO Certificate in Implant Dentistry provides an opportunity for AO members to demonstrate that they have attained a level of education and experience
AO Certificate in Implant Dentistry Certificate The AO Certificate in Implant Dentistry provides an opportunity for AO members to demonstrate that they have attained a level of education and experience
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis.
 Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
Clinical Case Reports using Cytoplast GTR Barrier Membranes
 Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Advanced Probing Techniques
 Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
The restoration of partially and completely
 CLINICAL MANAGEMENT OF DENTAL IMPLANT FRACTURES. ACASE HISTORY Firas A. M. AL Quran, PhD, MSc Med; Bashar A. Rashan, MS; Ziad N. AL-Dwairi, PhD The widespread use of endosseous osseointegrated implants
CLINICAL MANAGEMENT OF DENTAL IMPLANT FRACTURES. ACASE HISTORY Firas A. M. AL Quran, PhD, MSc Med; Bashar A. Rashan, MS; Ziad N. AL-Dwairi, PhD The widespread use of endosseous osseointegrated implants
Implant Site Development Part I
 REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
Retreatment: Fractured Implants Due To Biomechanical Overload
 Glenn J. Wolfinger, DMD, FACP Retreatment: Fractured Implants Due To Biomechanical Overload Thomas J. Balshi, DDS, FACP he strength of osseointegration, T the biologic and biomechanical union of bone to
Glenn J. Wolfinger, DMD, FACP Retreatment: Fractured Implants Due To Biomechanical Overload Thomas J. Balshi, DDS, FACP he strength of osseointegration, T the biologic and biomechanical union of bone to
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
Long-term success of osseointegrated implants
 Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Evaluation of Titanium Implants Placed into Simulated Extraction Sockets: A Study in Dogs
 Evaluation of Titanium Implants Placed into Simulated Extraction Sockets: A Study in Dogs Ken Akimoto, DDS, MS*/William Becker, DDS, MS**/ Rutger Persson, DDS, Odont Dr***/David A. Baker, DDS, MS*/ Michael
Evaluation of Titanium Implants Placed into Simulated Extraction Sockets: A Study in Dogs Ken Akimoto, DDS, MS*/William Becker, DDS, MS**/ Rutger Persson, DDS, Odont Dr***/David A. Baker, DDS, MS*/ Michael
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1.
 Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
It has been proposed that partially edentulous maxillectomy
 CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study
 Original Article Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study P. Singh, H. G. Garge*, V. S. Parmar, M. Viswambaran*, M. M. Goswami*
Original Article Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study P. Singh, H. G. Garge*, V. S. Parmar, M. Viswambaran*, M. M. Goswami*
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Areview of recent studies concerning molar. Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report
 Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Clinical Perspectives
 Clinical Perspectives Inside This Issue: Revised Drilling Guidelines For Parallel Walled Implants Case Presentation By: Pär-Olov Östman, DDS, PhD, MD Volume 8, Issue 1 Recommended Drilling Guidelines For
Clinical Perspectives Inside This Issue: Revised Drilling Guidelines For Parallel Walled Implants Case Presentation By: Pär-Olov Östman, DDS, PhD, MD Volume 8, Issue 1 Recommended Drilling Guidelines For
In 1977, Lew1 developed a passive
 CLINICAL AN OVERVIEW OF THE LEW ATTACHMENT: CLINICAL REPORTS Jack Piermatti, DMD Sheldon Winkler, DDS KEY WORDS Lew attachment Atrophic mandible Subperiosteal implant Root form implant Although the Lew
CLINICAL AN OVERVIEW OF THE LEW ATTACHMENT: CLINICAL REPORTS Jack Piermatti, DMD Sheldon Winkler, DDS KEY WORDS Lew attachment Atrophic mandible Subperiosteal implant Root form implant Although the Lew
Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS
 Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
BASIC Level 1 Practitioner Certification
 Chapter 5 Place the Prosthesis Because dental implants are now an important and distinct part of prosthodontic dentistry, general dentists must be well versed in all aspects of the treatment option. The
Chapter 5 Place the Prosthesis Because dental implants are now an important and distinct part of prosthodontic dentistry, general dentists must be well versed in all aspects of the treatment option. The
Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report
 Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report 1 2 1 1 Mittal R, Saxena D, Rao S, Kumar M Abstract: Statement of Problem: Complete denture rehabilitation
Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report 1 2 1 1 Mittal R, Saxena D, Rao S, Kumar M Abstract: Statement of Problem: Complete denture rehabilitation
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental implants offer a predictable treatment
 Histologic evaluation of a 12-year-old threaded hydroxyapatite-coated implant placed in conjunction with subantral augmentation procedure: A clinical report Periklis Proussaefs, DDS, MS, a Henry-Savajol
Histologic evaluation of a 12-year-old threaded hydroxyapatite-coated implant placed in conjunction with subantral augmentation procedure: A clinical report Periklis Proussaefs, DDS, MS, a Henry-Savajol
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
SCD Case Study. The ability of the integrated implant to bear a load must be greater than the anticipated load during function.
 SCD Case Study Dental implants offer an effective and predictable way to replace teeth. Function, aesthetics and phonetics are regained. The long-term success clinically and aesthetically depends upon
SCD Case Study Dental implants offer an effective and predictable way to replace teeth. Function, aesthetics and phonetics are regained. The long-term success clinically and aesthetically depends upon
Implant osseointegration and successful restoration
 Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
This article is the third in a series for Oral Health
 VIEWPOINT Risk Factors in Implant Dentistry: Patient Local Related Risk Factors Murray Arlin, DDS, Dip. Perio Introduction This article is the third in a series for Oral Health magazine (August issues)
VIEWPOINT Risk Factors in Implant Dentistry: Patient Local Related Risk Factors Murray Arlin, DDS, Dip. Perio Introduction This article is the third in a series for Oral Health magazine (August issues)
Samantha W. Chou, D.M.D N. Southport Ave. Chicago, Illinois Phone: Fax:
 Samantha W. Chou, D.M.D. 2325 N. Southport Ave. Chicago, Illinois 60614 Phone: 312-608-6881 Fax: 773-296-0601 Samanthawchou@gmail.com What is our role as the dentist? "We live in a culture in which people
Samantha W. Chou, D.M.D. 2325 N. Southport Ave. Chicago, Illinois 60614 Phone: 312-608-6881 Fax: 773-296-0601 Samanthawchou@gmail.com What is our role as the dentist? "We live in a culture in which people
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Osseointegrated implant-supported
 CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Selection and arrangement of teeth in rpd
 Selection and arrangement of teeth in rpd upon completion of the articulator mounting and a thorough assessment of the occlusal requirements, the practitioner should be able to perform the proper arrangement
Selection and arrangement of teeth in rpd upon completion of the articulator mounting and a thorough assessment of the occlusal requirements, the practitioner should be able to perform the proper arrangement
During the last 30 years, endosseous oral
 Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Controlling Tissue Contours with a Prosthetically Driven Approach to Implant Dentistry
 Controlling Tissue Contours with a Prosthetically Driven Approach to Implant Dentistry Go online for in-depth content by Timothy F. Kosinski, DDS, MAGD With continual improvements in the design and production
Controlling Tissue Contours with a Prosthetically Driven Approach to Implant Dentistry Go online for in-depth content by Timothy F. Kosinski, DDS, MAGD With continual improvements in the design and production
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
Radiographic Stent for Simplified Placement of Implants in the Mandible
 10.5005/jp-journals-10026-1086 CASE REPORT Radiographic Stent for Simplified Placement of Implants in the Mandible ABSTRACT This article aims to present a modified yet simple technique for the placement
10.5005/jp-journals-10026-1086 CASE REPORT Radiographic Stent for Simplified Placement of Implants in the Mandible ABSTRACT This article aims to present a modified yet simple technique for the placement
Implants are a part of IMPLANT TREATMENT IN AN URBAN GENERAL DENTISTRY RESIDENCY PROGRAM: A7-YEAR RETROSPECTIVE STUDY CLINICAL
 CLINICAL IMPLANT TREATMENT IN AN URBAN GENERAL DENTISTRY RESIDENCY PROGRAM: A7-YEAR RETROSPECTIVE STUDY Clifford B. Starr, DMD Mohamed A. Maksoud, DMD KEY WORDS Dental implants General dentistry Resident
CLINICAL IMPLANT TREATMENT IN AN URBAN GENERAL DENTISTRY RESIDENCY PROGRAM: A7-YEAR RETROSPECTIVE STUDY Clifford B. Starr, DMD Mohamed A. Maksoud, DMD KEY WORDS Dental implants General dentistry Resident
An Introduction to Dental Implants
 An Introduction to Dental Implants Aims: This article provides an introduction to dental implants, outlining the categories of dental implants, the phases involved in implant dentistry and assessing a
An Introduction to Dental Implants Aims: This article provides an introduction to dental implants, outlining the categories of dental implants, the phases involved in implant dentistry and assessing a
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
The CMC approved a motion to accept all editorial action requests that remain on the consent calendar 21 Yea / 0 Nay / 0 Abstain
 PAGE 1 OF 14 Editorial Actions One or more member organizations requested that the following editorial action submissions be removed from the consent calendar and addressed individually: #s 4, 7, 8, 9,
PAGE 1 OF 14 Editorial Actions One or more member organizations requested that the following editorial action submissions be removed from the consent calendar and addressed individually: #s 4, 7, 8, 9,
Many of the problems reported by conventional
 Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
Many papers have reported on histologic
 Histologic Evaluation of Clinically Successful Osseointegrated Implants Retrieved from Irradiated Bone: A Report of 2 Patients Hidetaka Nakai, DDS*/Atsushi Niimi, DDS, DMSc**/Minoru Ueda, DDS, PhD*** The
Histologic Evaluation of Clinically Successful Osseointegrated Implants Retrieved from Irradiated Bone: A Report of 2 Patients Hidetaka Nakai, DDS*/Atsushi Niimi, DDS, DMSc**/Minoru Ueda, DDS, PhD*** The
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Patient's Guide to Dental Implants. an investment for a lifelong smile
 Patient's Guide to Dental Implants an investment for a lifelong smile Introduction Genicore is a specialized products and service provider to dental professionals in the United States. Genicore strategically
Patient's Guide to Dental Implants an investment for a lifelong smile Introduction Genicore is a specialized products and service provider to dental professionals in the United States. Genicore strategically
Benefits of CBCT in Implant Planning
 10.5005/jp-journals-10012-1032 CLINICAL SCIENCE 1 Gregori M Kurtzman, 2 Douglas F Dompkowski 1 Private General Practice in Silver Spring, Maryland, USA 2 Private Periodontal Practice in Bethesda, Maryland,
10.5005/jp-journals-10012-1032 CLINICAL SCIENCE 1 Gregori M Kurtzman, 2 Douglas F Dompkowski 1 Private General Practice in Silver Spring, Maryland, USA 2 Private Periodontal Practice in Bethesda, Maryland,
Prosthodonticstown. Immediate Implant Placement in Fresh Extraction Sites. clinical. Table I
 Prosthodonticstown clinical Immediate Implant Placement in Fresh Extraction Sites Charles A. Babbush, DDS, MScD Table I Benefits Of Immediate Implantation Improved prosthesis fabrication and/or design
Prosthodonticstown clinical Immediate Implant Placement in Fresh Extraction Sites Charles A. Babbush, DDS, MScD Table I Benefits Of Immediate Implantation Improved prosthesis fabrication and/or design
The influence of radiotherapy on osseointegration
 Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
US Implant System 2013 PROSTHETIC PROCEDURE
 US Implant System 2013 PROSTHETIC PROCEDURE Contents TS Implant System Cement retained restoration 06 Cement retained bridges with the Cement abutment system 18 Cement retained crown with the Angled abutment
US Implant System 2013 PROSTHETIC PROCEDURE Contents TS Implant System Cement retained restoration 06 Cement retained bridges with the Cement abutment system 18 Cement retained crown with the Angled abutment
S i m p l i c I t y, c o m f o r t, a e s t h e t i c s. axiom. The new dimension
 S i m p l i c I t y, c o m f o r t, a e s t h e t i c s axiom The new dimension 2 Implants by anthogyr axiom, t h e n e w g e n e r a t i o n i m p l a n t axiom characteristics represent the perfect synthesis
S i m p l i c I t y, c o m f o r t, a e s t h e t i c s axiom The new dimension 2 Implants by anthogyr axiom, t h e n e w g e n e r a t i o n i m p l a n t axiom characteristics represent the perfect synthesis
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants. by Timothy F. Kosinski, DDS, MAGD
 Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Lect. 14 Prosthodontics Dr. Osama
 Lect. 14 Prosthodontics Dr. Osama Principles of Removable Partial Denture Design Difference in Prosthesis Support and Influence on Design: For a tooth-supported prosthesis, the movement potential is less
Lect. 14 Prosthodontics Dr. Osama Principles of Removable Partial Denture Design Difference in Prosthesis Support and Influence on Design: For a tooth-supported prosthesis, the movement potential is less
In-Silico approach on Offset placement of implant-supported bridges placed in bone of different density in Orthodontics.
 In-Silico approach on Offset placement of implant-supported bridges placed in bone of different density in Orthodontics. Chandrasenan.P 1, Vishnu.G 2, Akshay K Nair 3 1M Tech student, Department of Mechanical
In-Silico approach on Offset placement of implant-supported bridges placed in bone of different density in Orthodontics. Chandrasenan.P 1, Vishnu.G 2, Akshay K Nair 3 1M Tech student, Department of Mechanical
Component parts of Chrome Cobalt Removable Partial Denture
 Lec. 5 د.بسام الطريحي Component parts of Chrome Cobalt Removable Partial Denture Major connectors: Are either bars or plates, the difference between them is in the amount of tissue covers. Plates are broad
Lec. 5 د.بسام الطريحي Component parts of Chrome Cobalt Removable Partial Denture Major connectors: Are either bars or plates, the difference between them is in the amount of tissue covers. Plates are broad
Then and Now. Implant Therapy:
 Implant Therapy: Then and Now by Timothy F. Kosinski, DDS, MAGD Implant dentistry has come a long way since blade and subperiostal implants were widely used. Improvements in implant design and site preparation
Implant Therapy: Then and Now by Timothy F. Kosinski, DDS, MAGD Implant dentistry has come a long way since blade and subperiostal implants were widely used. Improvements in implant design and site preparation
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior
 Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
UNDERSTANDING DENTAL IMPLANTS Comfort and Confidence Again
 502 Jefferson Highway N. Champlin, MN 55316 763 427-1311 www.moffittrestorativedentistry.com UNDERSTANDING DENTAL IMPLANTS Comfort and Confidence Again NEW TEETH FOR A NEW SMILE Do you avoid laughing aloud,
502 Jefferson Highway N. Champlin, MN 55316 763 427-1311 www.moffittrestorativedentistry.com UNDERSTANDING DENTAL IMPLANTS Comfort and Confidence Again NEW TEETH FOR A NEW SMILE Do you avoid laughing aloud,
Alveolar Ridge Preservation:
 Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Specialty Dentistry. Dentistry has nine specialty fields recognized by the American Dental Association
 Specialty Dentistry Dentistry has nine specialty fields recognized by the American Dental Association Dental Public Health Endodontics Oral and Maxillofacial Pathology Oral and Maxillofacial Radiology
Specialty Dentistry Dentistry has nine specialty fields recognized by the American Dental Association Dental Public Health Endodontics Oral and Maxillofacial Pathology Oral and Maxillofacial Radiology
Immediate Implant Placement:
 Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Dental Morphology and Vocabulary
 Dental Morphology and Vocabulary Palate Palate Palate 1 2 Hard Palate Rugae Hard Palate Palate Palate Soft Palate Palate Palate Soft Palate 4 Palate Hard Palate Soft Palate Maxillary Arch (Maxilla) (Uppers)
Dental Morphology and Vocabulary Palate Palate Palate 1 2 Hard Palate Rugae Hard Palate Palate Palate Soft Palate Palate Palate Soft Palate 4 Palate Hard Palate Soft Palate Maxillary Arch (Maxilla) (Uppers)
synocta Meso abutment for cement-retained restorations PROSTHETICS Step-by-step instructions
 synocta Meso abutment for cement-retained restorations PROSTHETICS Step-by-step instructions INTRODUCTION synocta Meso abutment for cement-retained restorations 1 The synocta Meso abutments, available
synocta Meso abutment for cement-retained restorations PROSTHETICS Step-by-step instructions INTRODUCTION synocta Meso abutment for cement-retained restorations 1 The synocta Meso abutments, available
From planning to surgery: a totally digital working flow for Leone implants placement
 Dr. Giancarlo Romagnuolo Roma, Italy From planning to surgery: a totally digital working flow for Leone implants placement Keywords guided surgery, 3D implant planning, single missing tooth, delayed immediate
Dr. Giancarlo Romagnuolo Roma, Italy From planning to surgery: a totally digital working flow for Leone implants placement Keywords guided surgery, 3D implant planning, single missing tooth, delayed immediate
The need for controlled clinical studies
 Factors Associated With Radiographic Vertical Bone Loss Around Implants Placed in a Clinical Study Michael C. Manz* * Previously, VA Medical Center, Ann Arbor, MI; currently, Department of Cariology, Restorative
Factors Associated With Radiographic Vertical Bone Loss Around Implants Placed in a Clinical Study Michael C. Manz* * Previously, VA Medical Center, Ann Arbor, MI; currently, Department of Cariology, Restorative
Young-Jin Park, DDS,* and Sung-Am Cho, DDS, MS, PhD
 J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants
 Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Immediate fixed teeth a treatment concept for edentulous patients
 52 Maxillary rehabilitation using the All-on-4 concept Immediate fixed teeth a treatment concept for edentulous patients DR DUSAN VASILJEVIC AND VLADAN VASILJEVIC, FRIEDEBURG, GERMANY The number of edentulous
52 Maxillary rehabilitation using the All-on-4 concept Immediate fixed teeth a treatment concept for edentulous patients DR DUSAN VASILJEVIC AND VLADAN VASILJEVIC, FRIEDEBURG, GERMANY The number of edentulous
Conus Concept: A Rewarding Complete Denture Treatment
 Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Frequency of the Various Classes of Removable Partial Dentures and Selection of Major Connectors and Direct/Indirect Retainers
 Turk J Med Sci 31 (2001) 445-449 TÜB TAK Filiz KEYF Frequency of the Various Classes of Removable Partial Dentures and Selection of Major Connectors and Direct/Indirect Retainers Received: November 30,
Turk J Med Sci 31 (2001) 445-449 TÜB TAK Filiz KEYF Frequency of the Various Classes of Removable Partial Dentures and Selection of Major Connectors and Direct/Indirect Retainers Received: November 30,
scientific compendium
 scientific compendium Zimmer Tapered Screw-Vent Implant Success Stories in Stability and Survival Rates Zimmer Tapered Screw-Vent Implant Scientific Compendium table of contents CLINICAL & PRE-CLINICAL
scientific compendium Zimmer Tapered Screw-Vent Implant Success Stories in Stability and Survival Rates Zimmer Tapered Screw-Vent Implant Scientific Compendium table of contents CLINICAL & PRE-CLINICAL
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Cytoflex Barrier Membrane Clinical Evaluation
 Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re. Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T
 Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/200
Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/200
A new approach with an in-situ self-hardening grafting material
 74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
