Dentoskeletal Stability in Conventional Orthognathic Surgery, Presurgical Orthodontic Treatment and Surgery-First Approach in Class-III Patients
|
|
|
- Jordan Dickerson
- 5 years ago
- Views:
Transcription
1 et al. 283 ReviewSeifi Article Dentoskeletal Stability in Conventional Orthognathic Surgery, Presurgical Orthodontic Treatment and Surgery-First Approach in Class-III Patients Massoud Seifi1, Negin-Sadat Matini2*, Amir-Reza Motabar3, Mahtab Motabar Department of Orthodontics, Dental School, Shahid Beheshti University of Medical Sciences, Tehran, Iran; Shahid Beheshti University of Medical Sciences, Tehran, Iran; Department of Plastic Surgery, BouAli Hospital, Azad Medical University, Tehran, Iran; Department of Periodontology, Dental School, Tehran University of Medical Sciences, Tehran, Iran *Corresponding Author: Negin-Sadat Matini, DDS; Shahid Beheshti University of Medical Sciences, Tehran, Iran. Tel: Received: January 22, 2018 Revised: July 26, 2018 Accepted: August 8, 2018 ABSTRACT For many years, the conventional approach to orthognathic surgery which was orthodontic treatment prior to orthognathic surgery has been the accepted method of treatment for skeletal class III malocclusion patients. This review compared the dentoskeletal stability of treatment results between conventional orthognathic surgery methods with presurgical orthodontic treatment and surgery-first approach in skeletal class III patients. The study protocol was based on Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA) statement for systematic review and meta-analysis. Electronic and manual searches for literature since 2011 were conducted. PubMed and Medline databases were accessed. Data extraction and analysis were performed by two independent individuals. Seven studies out of hundred-fourteen articles met the inclusion criteria and were selected for qualitative analysis. The included studies were 494 patients with skeletal class-iii malocclusion. Stability of treatment was compared between surgery-first approach and conventionally treated patients. The statistical analysis confirmed that surgeryfirst approach did not show more stability compared with presurgical orthodontics. The surgery-first approach shortened the overall treatment duration. However, more skeletal stability in conventional treatment was assessed. Both surgery-first approach and conventional treatment with presurgical orthodontics resulted in favorable skeletal changes in class-iii malocclusion patients. Moreover, these findings should be discussed further due to the variety of study designs, outcomes and biases. Current evidence in this field still needs to be expanded. The authors wish to see more well-designed randomized controlled trials with long-term follow ups to confirm the results. KEYWORDS Surgery-first; Orthodontics; Orthognathic surgery; Conventional approach Please cite this paper as: Seifi M, Matini NS, Motabar AR, Motabar M. Dentoskeletal Stability in Conventional Orthognathic Surgery, Presurgical Orthodontic Treatment and Surgery-First Approach in Class-III Patients. World J Plast Surg 2018;7(3): doi: /wjps
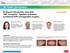
2 284 Maintaining dentoskeletal stability in patients INTRODUCTION For many years, the conventional approach to orthognathic surgery which include orthodontic treatment prior to orthognathic surgery has been the accepted method of treatment for skeletal class III malocclusion patients.1 However, there are some limitations such as long duration of the treatment and worsening of patients profile during pre-surgical orthodontics which decrease patient s compliance.2 The surgeryfirst approach have also been introduced as an alternative for the mentioned treatment plan. By the surgery-first approach, the need for any major orthodontic treatment preoperatively is diminished.3,4 In the conventional approach, dental decompensation is the result of presurgical orthodontics. In Class III malocclusion, the dental compensation usually evolves buccolabial flaring of the maxillary dentition and lingual tilt of mandibular dentition that will develop less class III appearance for patients and longer treatment time (for dental decompensation) with skeletal class III and mandibular prognathism.5 This probably is a disadvantage of the conventional approach due to less satisfaction of the patient.6 Through recent years, the surgery-first approach has become a popular treatment plan for patients regarding the factor that it may decrease the treatment duration by the reduction of preoperative orthodontics. This approach may lead to improved cooperation and has shown patients satisfaction with regards to immediate improvement of the facial profile or upper airway constriction.7-9 Also, increased tooth movement has been shown due to regional acceleratory phenomenon.10 It is reported that surgery-first approach can be performed in cases with mild crowding and proclined/retroclined anterior teeth, mild to moderate curve of Spee, mild vertical problem, and little or no transverse discrepancy.11 Although these advantages of surgeryfirst approach have led to acceptance of this treatment plan toward patients, it has not been fully investigated that this approach is more stable in post-operative occlusion compared with conventional approach.12 Proper dentoskeletal stability maintain more permanent results of the treatment. So it must be considered before a surgical method in order to ensure less relapse.13 Moreover, there is still no clear evidence regarding the stability of the results between surgery first and conventional approach under unstable postoperative dental and skeletal position.14 This study compared dentoskeletal stability between conventional orthognathic surgery, presurgical orthodontic treatment and surgery-first approach in skeletal class III patients. MATERIALS AND METHODS Search Strategy An Electronic search of PubMed was performed from 2011 to Based on the PICOS (participant, intervention, comparisons, outcome, and study designs), the inclusion criteria were non-syndromic adult patients with skeletal class III malocclusion who were treated with surgery-first approach or conventional approach. The outcome was to assess the postoperative stability between both approaches. Studies which had the least level of evidence, i.e. case reports were not included in the criteria. The search strategy was defined with the sequence as the following keywords: ( surgery first ) AND ( orthodontics ) OR ( orthognathic surgery ) AND ( orthodontics ) AND ( stability ). All publications were restricted for language and only English literatures were included. The exclusion criteria contained articles done on animals and in-vitro designs, case reports and reviews, studies referring to orthognathic surgery and orthodontics without determination of post-operative stability. The systematic review was also based on Preferred Reporting Items for systematic reviews and meta-analyses (PRISMA) diagram guidelines. A description of electronic search is provided on Figure 1. In details. Two independent authors performed eligibility assessment and the screening of title and abstracts. Any discussion regarding full-text selection was discussed with a third reviewer. Another different author checked the random selection of filtered articles. After the acceptance of each abstract articles the authors read the fulltext and included each full-text according to inclusion and exclusion criteria. Data Analysis Before carrying out the analysis and pooling the results, the heterogeneity hypothesis was tested using Chi-Square test. Then estimated effect size, the mean difference of change after
3 Seifi et al. 285 Fig. 1: PRISMA diagram for search strategy in systematic review. intervention between two treatments were pooled with adjustment for heterogeneity by using random effect model meta-analysis. The graphical display of these estimated results are shown in forest plot. RESULTS A total of 114 abstract were identified from the databases. However, only 7 articles matched the criteria. The PRISMA diagram gave a selection review of the search sequence. Table 1 summarized all included articles in the systematic review. Methodology quality could not be assessed with Cochrane Collaboration as none of the studies were clinical trials. The contents of the selected full-texts determined post-operative stability of the treatment by the comparison between lateral cephalometry analysis prior and after procedures. The excluded articles did not mention stability results of the treatment. A total of 311 patients with the mean age of 22.5 with the range of 18 to 37 were included. The sample size were not less than 37 and the maximum sample size was 61. Four studies reported Lefort I osteotomy with the addition of Bilateral Sagittal Split Osteotomy (BSSO), while 1 study only mentioned BSSO as surgical intervention. Occlusal stability was assessed by cephalometric analysis. Serial lateral cephalometric radiographs were obtained pre and post operatively. In order to compare dentoskeletal stability changes between selected articles, similar cephalometric parameters were identified. These 6 measurements included SellaNasion to A Point angle (SNA) which indicates the relative anterior-posterior position of the maxilla in relation to cranial base, Sella-Nasion to B Point angle (SNB) indicates the relative anterior-posterior position of the mandible in relation to cranial base, (B-point) the innermost point on the contour of the mandible between the incisor tooth and the bony chin, Overbite, Overjet and Angle between long axis of lower incisor and mandibular plane angle (IMPA). Overbite and overjet were commonly introduced as parameters for measuring occlusal stability. Hence, SNA, SNB, B-point and IMPA were included to demonstrate skeletal stability before and after the surgical procedure. Based on meta-analysis, there was no significant difference between occlusal stability of surgeryfirst approach compared with conventional treatment. These analyses were able to determine post-operative stability in both horizontal
4 Retrospective, cohort Identifying the parameters related to skeletal stability after orthognathic surgery in skeletal class III malocclusion using and to analyze the factors correlated with relapse Clarifying that OGS without presurgical orthodontics may be effective as the Conventional approach(ca) in correcting dentofacial deformities to compare the surgery first approach () with Conventional approach in terms of stability after mandibular setback in skeletal class III subjects Table 1: Summary of included articles in systematic review. Authors Origin Study type Sample Mean age Aim of study and year of size and at the time publication distribu- of surgery tion Taiwan N=45 ( male, 26 Ko et al., 2013 Prospective, case control Retrospective, N=61 (28 CA 21.6±3.5 cohort male, 33 23± CA, 23 Retrospective, N=12 (5 cohort male, 7 N=56 ( male, CA, 32 Bimaxillary surgery; 13.9 lefort I osteotomy, BSSO, and genioplasty (the latter only in 22 subjects) At 12 to 36 months follow-up relapse rate was not statistically significant between groups except for the lower anterior facial height ratio At debonding, 12.46% relapse. Mean B-point relapse, 1.44 Type of intervention Total Stability treatment time Bimaxillary surgery: 19.4 Lefort I osteotomy CA 22.3 with posterior impaction of the maxilla and BSSO or mandibular setback Mandibular surgery: BSSO SSRO 15.4 At debonding, mandible moved CA 22.5 anterioinferiorly. Average amounts of anterior relapse, 1.6 mm in the CA group and 2.4 mm in group. Vertical relapse pattern was similar, Relapse <1.5 mm more dominant in CA. significant association between degree of relapse and group difference ±2.37 The changes in arch width had no association with horizontal and vertical relapses of the mandible. Choi et al., 2015 Kim et al., 2014 Y k Kim et al., ±2.37 Evaluate the association between the transverse changes of arch dimension and postsurgical relapse of the mandible after mandibular setback with minimal orthodontic preparation without extraction 286 Maintaining dentoskeletal stability in patients
5 JY Kim et al., 2014 Park et al., 2016 Park et al., 2014 Retrospective, N=40 (25 case control male, CA, 20 Retrospective, N=37 (10 case series male, 17 Retrospective, N=60 (24 case control male, CA, 24 CA 25.25± ± ±4 CA 22.4± ±4.6 Comparison of postoperative stability following bimaxillary surgery performed either with or without preoperative orthodontic treatment Comparison of with CA in the amount and pattern of maxillary incisor inclination change in skeletal class III treated with extraction of the maxillary 1st pm and bimaxillary surgery Evaluation of postoperative stability of the treatment of mandibular prognathism treated with the (IVRO) Bimaxillary surgery: 14.7 Lefort 1 osteotomy + BSSO Bimaxillary surgery: 14±6 Lefort I osteotomy+ IVRO Bimaxillary surgery: NR Lefort 1 osteotomy + BSSO. Maxillary 1pms were extracted during surgery in the group No significant changes were observed in maxillary position after 1 year. The mandible had no significant relapse horizontally, but vertical relapse was significant at all time intervals, especially during the first 6 months postoperatively. Both anterior and posterior facial heights were decreased 1 year, and most changes occurred during the first 6 months postoperatively. No statistical differences were observed in the relapse rate between the two groups. NR Seifi et al. 287
6 288 Maintaining dentoskeletal stability in patients and vertical planes. The forest plot with mean difference of change after treatment and 95% CIs and the pooled estimates for mean difference of change of SNA were illustrated in Figure 2. As shown in this figure three studies assessed the SNA changes before and after the surgical procedure. However, neither showed significant difference between surgical-first and conventional approach with regards to SNA changes (overall: weighted mean difference (WMD)=0.66; 95%, CI=-0.42, 1.75). Figure 3 (overall: WMD=-0.07; 95%, CI=-0.40, 0.26) demonstrated four studies comparing SNB changes between two different treatment approaches, SNB had no significant difference in both mentioned treatments as the same result was shown for other parameters such as B point (overall: WMD=-0.53; 95%, CI=-1.21, 0.14), overbite (overall: WMD=-0.46; 95%, CI=-1.21, 0.28), overjet (overall: WMD=0.87; 95%, CI=0.28, 2.02), IMPA (overall: WMD=-3.91; 95%, CI=-12.63, 4.81) as are shown in Figure 4, 5, 6 and 7, respectively. Based on the meta-analysis, there was no significant difference in occlusal stability between surgery-first approach and the conventional approach based on the measured parameters. Fig. 2: Forest plot analysis for SNA. DISCUSSION This study included 3 retrospective cohort,12,15 1 prospective case control,16 2 retrospective case Fig. 3: Forest plot analysis for SNB. Fig. 4: Forest plot analysis for B-point.
7 Seifi et al. 289 Fig. 5: Forest plot analysis for overbite. Fig. 6: Forest plot analysis for overjet. Fig. 7: Forest plot analysis for IMPA. control,17,18 and 1 retrospective case series.19 Four studies reported Lefort I osteotomy with the addition of BSSO,12,16-18 while 1 study only mentioned BSSO as surgical intervention.15 In another study, patients underwent a Sagittal Split Ramus Osteotomy (SSRO)20 and the other study
8 290 Maintaining dentoskeletal stability in patients was a combination of Lefort 1 osteotomy and Intra Oral Vertical Ramus Osteotomy (IVRO).19 Ko et al. included genioplasty among other interventions.12 Ko et al. used monocortical plates and screws in each side of mandible and miniplates in each side of maxilla as postsurgical fixation.12 In Kim et al. s study, mandible was fixed with 4 miniplates in a monocortical fashion and intermaxillary elastics and also interocclusal splint were given to patients 4 to 6 weeks after the procedure.15 Two weeks of archwire and 8 mini implant were used as an intermaxillary fixation.20 Choi et al. also used mini plate as internal rigid fixation.16 However, in another study arch wires were used for 2-3 weeks as surgical fixation.19 Park et al. used metal plates and screws for fixation of mandible and a maxillomandibular fixation with surgical stent including ball clasps that were applied for 5 days in order to achieve retention.18 In the study by Ko et al., no presurgical orthodontics was performed in any patients. Kim et al. positioned inactive brackets for surgery-first group and had a presurgical orthodontic treatments included leveling, alignment and elimination of crowding for conventional approach group.15 In study by park et al., all patients in both surgery-first and conventional group received non-extraction orthodontic treatment for mandible and the maxillary premolar was extracted during the surgery for surgery-first group patients.17 Choi et al. positioned inactive braces 1 month prior to procedure due to intermaxillary fixation in conventional approach, also the presurgical orthodontics provided decompensation of teeth axes, and coordinating upper and lower arches.16 Two studies have assessed the stability after 6 months of follow up,18,20 however three studies have indicated a 12 months of post-operative examination12,16,19 and one study analyzed the patients after 22 months of follow up.15 Recently, surgery-first approach has been introduced in various surgical and also orthodontics publications. However, few studies have compared this approach with the conventional orthodontic-first approach in treatment of patients with skeletal class III malocclusion. Numbers of studies with clinical trial design for the mentioned subject is still rare.21 Despite the lack of relevant publication, surgery-first seems to have a shorter treatment time.7,19,22 The efficient orthodontic procedure in surgeryfirst approach is reported to be in relation with regional acceleratory phenomenon (RAP) which is the result of transient demineralization of the bones caused after surgical procedure Our aim in this systematic review was to compare the difference between surgery-first approach and the conventional approach in details. Dentoskeletal relapse is reported to have association with factors such as fixation method of bone plates, muscle contraction, maxillary constriction, curve of Spee, greater overbite and overjet. Better stability was exhibited in patients with flat curve of Spee and smaller overbite.12 Hence, some authors reported that its occurrence may be related to the surgical approach and the sequence of orthodontic treatment with surgery. Based on dentoskeletal stability, in surgeryfirst approach, better arch coordination can be resulted after the elimination of functional muscular forces in disproportional skeletal situation.26 After surgery, muscular loads will equilibrate and establish in proper position of teeth relative to apical base of the jaws and the jaws position will be more favored with less treatment duration. For instance, in class III mandibular prognathism, lower lip and mentalis muscle pressure against lower anterior teeth is a resisting functional load versus aligning orthodontic force. In disproportion skeletal situation, these contestant strains produce deleterious effects such as bone resorption, bone dehiscence, root resorption, and increased inflammation due to prolonged treatment time.26 When bringing jaws into appropriate position, a more balanced muscular force will be established. In the latter situation, orthodontic forces for alignment and leveling of teeth work optimal which means back-andforth and jiggling movements will be avoided. In transverse dimension, force of buccinators muscles, or so called the buccinator mechanism [upper and lower buccinator fibers, superior constrictor muscles (attached to pharyngeal tubercle), upper and lower orbicularis oris muscle fibers] is exerted to the maxillary and mandibular posterior teeth resulting linguoversion of them.26 This condition happens when perioral muscular force conquers the muscular force of the tongue. In rare cases, tongue force overcome the perioral muscular strain resulting outward positioning of the posterior teeth. These faciolingual positions that are described as torque
9 Seifi et al. 291 of teeth should be corrected in order to produce ideal interdigitation of dentition which is perquisite for occlusal stability. A moderate level of faciolingual discrepancies is consistent with Surgery-First Approach ()s. In Conventional Approach (CA), the mentioned discrepancies are never the less corrected by less limitations regarding complex skeletal problems. Again, in transverse dimension; contestant forces act as vying loads in contrast original situation versus corrected torque and adjusted posterior teeth relative to apical base.17,20 As in vertical dimension, surgery-first is able to position the tongue in a more proper relation with occlusal level, so less muscular resistance will be resulted for the later orthodontic treatment. According to the available data and authors studies, majority of skeletal and dental relapse takes place within short period after releasing inter maxillary fixation (IMF) postoperatively and initiation of the jaw function i.e. two to six months. The minimum follow-up period was 6 months in only two studies among all included studies in the present review. Based on the instability studies, it seems that dental and skeletal relapse are inevitable phenomena. Biologic boundaries are inherent limitation to the orthodontic tooth movement and skeletal repositioning.27 Apart from the mentioned general reason, surgery-first approach is a technique sensitive procedure. Even a highly experienced orthodontist/surgeon cannot clearly predict of the ideal post-treatment occlusal relationship. Improper fixation of the jaw pieces, malunion of healing osteotomized bone segments, loose IMFs (immediate or delayed loosening of the screws), incorrect position of the condyles relative to cranial base i.e. glenoid fossa, improper placement of the proximal/distal segments which leads to torqueing of the proximal parts, and inappropriate splint are among the factors that are noticeable in a technique sensitive orthognathic surgery.15 In addition to the consideration of the mentioned factors in skeletal stability, centric occlusion centric relation (CO-CR) discrepancies that are related to stability and function have a pivotal role in a sustained equilibrium of the functional matrix. Dental etiologic factors as a basis for relapse such as unstable position of the teeth regarding the biologic boundaries i.e. placement of the teeth outside of the jaw base functional matrix should not be taken for granted. Post-operative stability has not been fully investigated yet between these two approaches. Also, previous studies could not define precisely between different stabilities terminology. Authors of this review note that every skeletal instability leads to occlusal instability however, every occlusal instability is not equal to skeletal instability necessarily. Future caution must be taken to not confuse skeletal stability with occlusal stability and not to assess them with one another in upcoming clinical trials and case studies.15 Prior to the current study, it was unclear that which approach has gained more stability after the procedure. However, lack of patients and highlyqualified study designs are the limits in this systematic review. Another limit is related to population which all included studies were assessed. All included researches were applied in Asian population and were not performed on other populations such as Caucasians or Africans. So authors suggested alike studies on a diversion of population in order to investigate the stability outcomes of both approaches in patients. As it is explained in previous articles, the most definitive advantage of surgeryfirst approach is the shortening of treatment duration. However, by eliminating presurgical orthodontics, the surgeon may need to apply more invasive procedures. On the other hand, surgery-first approach may not be performed on patients with complex orthodontic deformities. Some articles reported the reliability of wearing splint in achieving a stable dentofacial position after surgery-first approach.15 Kim et al. reported the positioning of the maxilla as an important risk factor for mandibular relapse however the results showed same relapse in both explained surgical methods.15 Accelerating tooth movement is another aspect which may result rotational relapse.11 In addition to previous studies and the present systematic review, it was shown that long-term follow ups and a large homogenous samples are crucial in order to evaluate more exact arch dimensional changes. As the matter of dentoskeletal stability, no significant difference was shown between surgery-first approach and the conventional orthodontic-first approach for class III malocclusion patients. Practitioners
10 292 Maintaining dentoskeletal stability in patients are able to suggest both treatment plans as an appropriate method based on other occlusal and skeletal parameters. 9 ACKNOWLEDGMENT We would like to thank Sara Jambarsang (Biostatistician, Shahid Beheshti University of Medical Sciences, Tehran, Iran) for the statistical analysis. 10 CONFLICT OF INTEREST 11 The authors declare no conflict of interest. REFERENCES Worms FW, Isaacson RJ, Speidel TM. Surgical orthodontic treatment planning: profile analysis and mandibular surgery. Angle Orthod 1976;46:1-25. Nagasaka H, Sugawara J, Kawamura H, Nanda R. Surgery first skeletal Class III correction using the Skeletal Anchorage System. J Clin Orthod 2009;43: Huang CS, Hsu SS, Chen YR. Systematic review of the surgery-first approach in orthognathic surgery. Biomed J 2014;37: Yu HB, Mao LX, Wang XD, Fang B, Shen SG. The surgery-first approach in orthognathic surgery: a retrospective study of 50 cases. Int J Oral Maxillofac Surg 2015;44: Lee SJ, Kim TW, Nahm DS. Transverse implications of maxillary premolar extraction in Class III presurgical orthodontic treatment. Am J Orthod Dentofacial Orthop. 2006;129: Dowling PA, Espeland L, Krogstad O, Stenvik A, Kelly A. Duration of orthodontic treatment involving orthognathic surgery. Int J Adult Orthodon Orthognath Surg 1999;14: Choi JW, Lee JY, Yang SJ, Koh KS. The reliability of a surgery-first orthognathic approach without presurgical orthodontic treatment for skeletal class III dentofacial deformity. Ann Plast Surg 2015;74: Hernandez-Alfaro F, Guijarro-Martinez R, Peiro-Guijarro MA. Surgery first in orthognathic surgery: what have we learned? A comprehensive workflow based on 45 consecutive cases. J Oral Maxillofac Surg 2014;72: Leelasinjaroen P, Godfrey K, Manosudprasit M, Wangsrimongkol T, Surakunprapha P, Pisek P. Surgery first orthognathic approach for skeletal Class III malocclusion corrections-a literature review. J Med Assoc Thai 2012;95: Liou EJ, Chen PH, Wang YC, Yu CC, Huang CS, Chen YR. Surgery-first accelerated orthognathic surgery: postoperative rapid orthodontic tooth movement. J Oral Maxillofac Surg 2011;69: Baek SH, Ahn HW, Kwon YH, Choi JY. Surgery-first approach in skeletal class III malocclusion treated with 2-jaw surgery: evaluation of surgical movement and postoperative orthodontic treatment. J Craniofac Surg 2010;21: Ko EW, Lin SC, Chen YR, Huang CS. Skeletal and dental variables related to the stability of orthognathic surgery in skeletal Class III malocclusion with a surgery-first approach. J Oral Maxillofac Surg 2013;71: Choi SH, Yoo HJ, Lee JY, Jung YS, Choi JW, Lee KJ. Stability of pre-orthodontic orthognathic surgery depending on mandibular surgical techniques: SSRO vs IVRO. J Craniomaxillofac Surg 2016;44: Peiro-Guijarro MA, Guijarro-Martinez R, Hernandez-Alfaro F. Surgery first in orthognathic surgery: A systematic review of the literature. Am J Orthod Dentofacial Orthop 2016;149: Kim CS, Lee SC, Kyung HM, Park HS, Kwon TG. Stability of mandibular setback surgery with and without presurgical orthodontics. J Oral Maxillofac Surg 2014;72: Choi SH, Hwang CJ, Baik HS, Jung YS, Lee KJ. Stability of pre-orthodontic orthognathic surgery using intraoral vertical ramus osteotomy versus conventional treatment. J Oral Maxillofac Surg 2016;74: Park HM, Lee YK, Choi JY, Baek SH. Maxillary incisor inclination of skeletal Class III patients treated with extraction of the upper first premolars and two-jaw surgery: conventional orthognathic surgery vs surgeryfirst approach. Angle Orthod 2014;84: Park KH, Sandor GK, Kim YD. Skeletal stability of surgery-first bimaxillary orthognathic surgery for skeletal class III malocclusion, using standardized criteria. Int J Oral Maxillofac Surg 2016;45: Kim JY, Jung HD, Kim SY, Park HS, Jung
11 Seifi et al. 293 YS. Postoperative stability for surgery-first approach using intraoral vertical ramus osteotomy: 12 month follow-up. Br J Oral Maxillofac Surg 2014;52: Kim YK, Yun PY, Moon SW, Lee YS, Lee NK. Influence of the changes in arch width on postsurgical relapse after mandibular setback surgery with minimal orthodontics. J Oral Maxillofac Surg 2014;72: Min BK, Choi JY, Baek SH. Comparison of treatment duration between conventional three-stage method and surgery-first approach in patients with skeletal Class III malocclusion. J Craniofac Surg 2014;25: Liao YF, Chiu YT, Huang CS, Ko EW, Chen YR. Presurgical orthodontics versus no presurgical orthodontics: treatment outcome of surgical-orthodontic correction for skeletal class III open bite. Plast Reconstr Surg 2010;126: Sebaoun JD, Ferguson DJ, Wilcko MT, Wilcko WM. Alveolar osteotomy and rapid orthodontic treatments. Orthod Fr. 2007;78: Wilcko WM, Wilcko T, Bouquot JE, Ferguson DJ. Rapid orthodontics with alveolar reshaping: two case reports of decrowding. Int J Periodontics Restorative Dent 2001;21: Wilcko MT, Wilcko WM, Pulver JJ, Bissada NF, Bouquot JE. Accelerated osteogenic orthodontics technique: a 1-stage surgically facilitated rapid orthodontic technique with alveolar augmentation. J Oral Maxillofac Surg 2009;67: Berry DC. The buccinator mechanism. J Dent 1979;7: Posnick JC. Principles and Practice of Orthognathic Surgery: Elsevier Health Sciences; 2013.
Ortho-surgical Management of Severe Vertical Dysplasia: A Case Report
 Case Report Ortho-surgical Management of Severe Vertical Dysplasia: A Case Report 1 Vinni Arora, 2 Rekha Sharma, 3 Sachin Parashar 1 Senior Resident, 2 Professor and Head of Department, 3 Former Resident
Case Report Ortho-surgical Management of Severe Vertical Dysplasia: A Case Report 1 Vinni Arora, 2 Rekha Sharma, 3 Sachin Parashar 1 Senior Resident, 2 Professor and Head of Department, 3 Former Resident
Original Article. Han-Sol Song Sung-Hwan Choi Jung-Yul Cha Kee-Joon Lee Hyung-Seog Yu
 Original Article THE KOREAN JOURNAL of ORTHODONTICS pissn 2234-7518 eissn 2005-372X Comparison of changes in the transverse dental axis between patients with skeletal Class III malocclusion and facial
Original Article THE KOREAN JOURNAL of ORTHODONTICS pissn 2234-7518 eissn 2005-372X Comparison of changes in the transverse dental axis between patients with skeletal Class III malocclusion and facial
International Journal of Science & Technology ISSN (online): X Vol. 6 Issue 1, February 2016
 SURGERY FIRST ORTHOGNATHIC APPROACH: A REVIEW ARTICLE Dr. Kishore MSV, Professor and Head, Dr. Bachuwar Ankush, post graduate, Dr. Madhukar Reddy Rachala, Associate professor, Dr. Sattu Reddy Dharmender,
SURGERY FIRST ORTHOGNATHIC APPROACH: A REVIEW ARTICLE Dr. Kishore MSV, Professor and Head, Dr. Bachuwar Ankush, post graduate, Dr. Madhukar Reddy Rachala, Associate professor, Dr. Sattu Reddy Dharmender,
KJLO. A Sequential Approach for an Asymmetric Extraction Case in. Lingual Orthodontics. Case Report INTRODUCTION DIAGNOSIS
 KJLO Korean Journal of Lingual Orthodontics Case Report A Sequential Approach for an Asymmetric Extraction Case in Lingual Orthodontics Ji-Sung Jang 1, Kee-Joon Lee 2 1 Dream Orthodontic Clinic, Gimhae,
KJLO Korean Journal of Lingual Orthodontics Case Report A Sequential Approach for an Asymmetric Extraction Case in Lingual Orthodontics Ji-Sung Jang 1, Kee-Joon Lee 2 1 Dream Orthodontic Clinic, Gimhae,
Orthodontic and Orthognathic Surgical Correction of a Skeletal Class III Malocclusion
 Dental Medicine Research 30 2) 161 166, 2010 161 Case Report Orthodontic and Orthognathic Surgical Correction of a Skeletal Class III Malocclusion Tetsutaro Yamaguchi, Yoko Tomoyasu, Tatsuo Shirota*, Masashi
Dental Medicine Research 30 2) 161 166, 2010 161 Case Report Orthodontic and Orthognathic Surgical Correction of a Skeletal Class III Malocclusion Tetsutaro Yamaguchi, Yoko Tomoyasu, Tatsuo Shirota*, Masashi
Soft and Hard Tissue Changes after Bimaxillary Surgery in Chinese Class III Patients
 Original Article Soft and Hard Tissue Changes after Bimaxillary Surgery in Chinese Class III Patients Ming Tak Chew a Abstract: Cephalometric studies have shown that the Chinese race tends to have a greater
Original Article Soft and Hard Tissue Changes after Bimaxillary Surgery in Chinese Class III Patients Ming Tak Chew a Abstract: Cephalometric studies have shown that the Chinese race tends to have a greater
A Surgery-first Approach in Surgical-orthodontic Treatment of Mandibular Prognathism A Case Report
 Case Report 699 A Surgery-first Approach in Surgical-orthodontic Treatment of Mandibular Prognathism A Case Report Chung-Chih Yu, MD; Po-Hsun Chen 1, DDS, MS; Eric J.W. Liou 1, DDS, MS; Chiung-Shing Huang
Case Report 699 A Surgery-first Approach in Surgical-orthodontic Treatment of Mandibular Prognathism A Case Report Chung-Chih Yu, MD; Po-Hsun Chen 1, DDS, MS; Eric J.W. Liou 1, DDS, MS; Chiung-Shing Huang
Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization
 Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization Koroush Taheri Talesh, DDS, a Mohammad Hosein Kalantar Motamedi, DDS, b Mahdi Sazavar,
Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization Koroush Taheri Talesh, DDS, a Mohammad Hosein Kalantar Motamedi, DDS, b Mahdi Sazavar,
Professor, Department of Craniofacial Orthodontics, Chang Gung Memorial Hospital,
 Dr. Ellen Wen-Ching Ko, DDS, MS Professor, Department of Craniofacial Orthodontics, Chang Gung Memorial Hospital, Taipei, Taiwan Professor, Graduate Institute of Craniofacial and Dental Science, Chang
Dr. Ellen Wen-Ching Ko, DDS, MS Professor, Department of Craniofacial Orthodontics, Chang Gung Memorial Hospital, Taipei, Taiwan Professor, Graduate Institute of Craniofacial and Dental Science, Chang
Why Surgery-First? Surgery-First. How We Got Here. Point - The Case for Surgery-First Orthodontics. Conventional. What are the Problems?
 2014 Winter Conference February 7-9, 2014 Las Vegas, Nevada Point-Counterpoint: Surgery-First Point - The Case for Surgery-First Junji SUGAWARA Sendai, Japan Oral Maxillofac / Plastic Surgery Prosthodontics
2014 Winter Conference February 7-9, 2014 Las Vegas, Nevada Point-Counterpoint: Surgery-First Point - The Case for Surgery-First Junji SUGAWARA Sendai, Japan Oral Maxillofac / Plastic Surgery Prosthodontics
Correlation between Gonial Angle and Different Variables after Bilateral Sagittal Split Ramus Osteotomy
 Original Article Correlation between Gonial Angle and Different Variables after Bilateral Sagittal Split Ramus Osteotomy M. Bayat 1,2, M. Ja'farian 3, O. Ghassemi Habashi 4 1 Assistant Professor, Department
Original Article Correlation between Gonial Angle and Different Variables after Bilateral Sagittal Split Ramus Osteotomy M. Bayat 1,2, M. Ja'farian 3, O. Ghassemi Habashi 4 1 Assistant Professor, Department
Case Report: Long-Term Outcome of Class II Division 1 Malocclusion Treated with Rapid Palatal Expansion and Cervical Traction
 Case Report Case Report: Long-Term Outcome of Class II Division 1 Malocclusion Treated with Rapid Palatal Expansion and Cervical Traction Roberto M. A. Lima, DDS a ; Anna Leticia Lima, DDS b Abstract:
Case Report Case Report: Long-Term Outcome of Class II Division 1 Malocclusion Treated with Rapid Palatal Expansion and Cervical Traction Roberto M. A. Lima, DDS a ; Anna Leticia Lima, DDS b Abstract:
Skeletal Relapse after Correction of Mandibular Prognathism by Bilateral Sagittal Split Ramus Osteotomy
 Original Article Skeletal Relapse after Correction of Mandibular Prognathism by Bilateral Sagittal Split Ramus Osteotomy H. Mohajerani 1, M. Mehdizadeh 2, A. Khalighi Sigaroodi 3 1 Assistant Professor,
Original Article Skeletal Relapse after Correction of Mandibular Prognathism by Bilateral Sagittal Split Ramus Osteotomy H. Mohajerani 1, M. Mehdizadeh 2, A. Khalighi Sigaroodi 3 1 Assistant Professor,
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS CANDIDATE NUMBER:44 CASE NUMBER: 2 Year: 2010 ESLO 01 RÉSUMÉ OF CASE 5 CASE CATEGORY: CLASS II DIVISION 1 MALOCCLUSION A MALOCCLUSION WITH SIGNIFICANT MANDIBULAR
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS CANDIDATE NUMBER:44 CASE NUMBER: 2 Year: 2010 ESLO 01 RÉSUMÉ OF CASE 5 CASE CATEGORY: CLASS II DIVISION 1 MALOCCLUSION A MALOCCLUSION WITH SIGNIFICANT MANDIBULAR
SURGICAL - ORTHODONTIC TREATMENT OF CLASS II DIVISION 1 MALOCCLUSION IN AN ADULT PATIENT: A CASE REPORT
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 02 SURGICAL - ORTHODONTIC TREATMENT OF CLASS II DIVISION 1 MALOCCLUSION IN AN ADULT PATIENT: A CASE REPORT Amit Dahiya 1,Minakshi
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 02 SURGICAL - ORTHODONTIC TREATMENT OF CLASS II DIVISION 1 MALOCCLUSION IN AN ADULT PATIENT: A CASE REPORT Amit Dahiya 1,Minakshi
Mesial Step Class I or Class III Dependent upon extent of step seen clinically and patient s growth pattern Refer for early evaluation (by 8 years)
 Orthodontics and Dentofacial Development Overview Development of Dentition Treatment Retention and Relapse Growth of Naso-Maxillary Complex Develops postnatally entirely by intramenbranous ossification
Orthodontics and Dentofacial Development Overview Development of Dentition Treatment Retention and Relapse Growth of Naso-Maxillary Complex Develops postnatally entirely by intramenbranous ossification
Surgery-first approach using a three-dimensional virtual setup and surgical simulation for skeletal Class III correction
 Case Report THE KOREAN JOURNAL of ORTHODONTICS pissn 2234-7518 eissn 2005-372X Surgery-first approach using a three-dimensional virtual setup and surgical simulation for skeletal Class III correction Joon
Case Report THE KOREAN JOURNAL of ORTHODONTICS pissn 2234-7518 eissn 2005-372X Surgery-first approach using a three-dimensional virtual setup and surgical simulation for skeletal Class III correction Joon
Case Report. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System.
 Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
Severe Malocclusion: Appropriately Timed Treatment. This article discusses challenging issues clinicians face when treating
 Severe Malocclusion: The Importance of Appropriately Timed Treatment A Synchronized and Simultaneous Interdisciplinary Plan Using Cosmetic Dentistry Principles David M. Sarver, DMD, MS Abstract This article
Severe Malocclusion: The Importance of Appropriately Timed Treatment A Synchronized and Simultaneous Interdisciplinary Plan Using Cosmetic Dentistry Principles David M. Sarver, DMD, MS Abstract This article
Sample Case #1. Disclaimer
 ABO Sample Cases Disclaimer Sample Case #1 The following sample questions and answers were composed and vetted by a panel of experts in orthodontics and are intended to provide an example of the types
ABO Sample Cases Disclaimer Sample Case #1 The following sample questions and answers were composed and vetted by a panel of experts in orthodontics and are intended to provide an example of the types
Gentle-Jumper- Non-compliance Class II corrector
 15 CASE REPORT Gentle-Jumper- Non-compliance Class II corrector Amit Prakash 1,O.P.Mehta 2, Kshitij Gupta 3 Swapnil Pandey 4 Deep Kumar Suryawanshi 4 1 Senior lecturer Bhopal - INDIA 2 Professor Bhopal
15 CASE REPORT Gentle-Jumper- Non-compliance Class II corrector Amit Prakash 1,O.P.Mehta 2, Kshitij Gupta 3 Swapnil Pandey 4 Deep Kumar Suryawanshi 4 1 Senior lecturer Bhopal - INDIA 2 Professor Bhopal
Treatment duration and factors associated with the surgery-first approach: a twocenter
 Uribe et al. Progress in Orthodontics (2015) 16:29 DOI 10.1186/s40510-015-0101-1 RESEARCH Open Access Treatment duration and factors associated with the surgery-first approach: a twocenter study Flavio
Uribe et al. Progress in Orthodontics (2015) 16:29 DOI 10.1186/s40510-015-0101-1 RESEARCH Open Access Treatment duration and factors associated with the surgery-first approach: a twocenter study Flavio
ORTHODONTIC CORRECTION Of OCCLUSAL CANT USING MINI IMPLANTS:A CASE REPORT. Gupta J*, Makhija P.G.**, Jain V***
 ORTHODONTIC CORRECTION Of OCCLUSAL CANT USING MINI IMPLANTS:A CASE REPORT Gupta J*, Makhija P.G.**, Jain V*** Abstract: The inability of orthodontists to change the cant of the maxillary occlusal plane
ORTHODONTIC CORRECTION Of OCCLUSAL CANT USING MINI IMPLANTS:A CASE REPORT Gupta J*, Makhija P.G.**, Jain V*** Abstract: The inability of orthodontists to change the cant of the maxillary occlusal plane
Orthodontics-surgical combination therapy for Class III skeletal malocclusion
 [Downloaded free from http://www.contempclindent.org on Tuesday, July 16, 2013, IP: 164.100.31.82] Click here to download free Android application for this jou Orthodontics-surgical combination therapy
[Downloaded free from http://www.contempclindent.org on Tuesday, July 16, 2013, IP: 164.100.31.82] Click here to download free Android application for this jou Orthodontics-surgical combination therapy
Case Report. profile relaxed relaxed smiling. How would you treat this malocclusion?
 Pre-Treatment profile relaxed relaxed smiling How would you treat this malocclusion? Case R. C. 16 years, 9 months introduction This female adolescent with bilabial protrusion and flared upper anterior
Pre-Treatment profile relaxed relaxed smiling How would you treat this malocclusion? Case R. C. 16 years, 9 months introduction This female adolescent with bilabial protrusion and flared upper anterior
Crowded Class II Division 2 Malocclusion
 Class II Division 2 Malocclusion Crowded Class II Division 2 Malocclusion Clinicians: Drs. Chris Chang, Hsin-Yin Yeh, Sophia Pei-Wen Shu, W. Eugene Roberts Patient: Miss Jhan Pre-treatment Diagnosis An
Class II Division 2 Malocclusion Crowded Class II Division 2 Malocclusion Clinicians: Drs. Chris Chang, Hsin-Yin Yeh, Sophia Pei-Wen Shu, W. Eugene Roberts Patient: Miss Jhan Pre-treatment Diagnosis An
Post-operative stability of the maxilla treated with Le Fort I and horseshoe osteotomies in bimaxillary surgery
 European Journal of Orthodontics 24 (2002) 471 476 2002 European Orthodontic Society Post-operative stability of the maxilla treated with Le Fort I and horseshoe osteotomies in bimaxillary surgery Kiyoshi
European Journal of Orthodontics 24 (2002) 471 476 2002 European Orthodontic Society Post-operative stability of the maxilla treated with Le Fort I and horseshoe osteotomies in bimaxillary surgery Kiyoshi
OF LINGUAL ORTHODONTICS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: KDr. KP. kanarelis CASE NUMBER: 1 Year: 2010 WBLO 01 RESUME OF CASE 1 CASE CATEGORY: ADULT MALOCCLUSION NAME : IOANNIS.G BORN: 03.01.1989 SEX:
EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: KDr. KP. kanarelis CASE NUMBER: 1 Year: 2010 WBLO 01 RESUME OF CASE 1 CASE CATEGORY: ADULT MALOCCLUSION NAME : IOANNIS.G BORN: 03.01.1989 SEX:
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS CANDIDATE NUMBER: 44 CASE NUMBER: 1 Year: ESLO 01 RÉSUMÉ OF CASE 1 CASE CATEGORY: ADULT MALOCCLUSION NAME: K.N BORN: 03/03/1980 SEX: Male PRE-TREATMENT RECORDS:
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS CANDIDATE NUMBER: 44 CASE NUMBER: 1 Year: ESLO 01 RÉSUMÉ OF CASE 1 CASE CATEGORY: ADULT MALOCCLUSION NAME: K.N BORN: 03/03/1980 SEX: Male PRE-TREATMENT RECORDS:
Unilateral intraoral vertical ramus osteotomy based on preoperative three-dimensional simulation surgery in a patient with facial asymmetry
 CASE REPORT http://dx.doi.org/10.5125/jkaoms.2014.40.1.32 pissn 2234-7550 eissn 2234-5930 Unilateral intraoral vertical ramus osteotomy based on preoperative three-dimensional simulation surgery in a patient
CASE REPORT http://dx.doi.org/10.5125/jkaoms.2014.40.1.32 pissn 2234-7550 eissn 2234-5930 Unilateral intraoral vertical ramus osteotomy based on preoperative three-dimensional simulation surgery in a patient
Early Mixed Dentition Period
 REVIEW ARTIC CLE AODMR The Effects of a Prefabricated Functional Appliance in Early Mixed Dentition Period Toshio Iwata 1, Takashi Usui 2, Nobukazu Shirakawa 2, Toshitsugu Kawata 3 1 Doctor of Philosophy
REVIEW ARTIC CLE AODMR The Effects of a Prefabricated Functional Appliance in Early Mixed Dentition Period Toshio Iwata 1, Takashi Usui 2, Nobukazu Shirakawa 2, Toshitsugu Kawata 3 1 Doctor of Philosophy
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS CANDIDATE NUMBER : 13 Dr. Masatoshi Sana CASE NUMBER : Year : ESLO 01 RÉSUMÉ OF CASE 2 CASE CATEGORY: CLASS I MALOCCLUSION NAME: BORN: SEX: Yukari K. 08/03/1979
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS CANDIDATE NUMBER : 13 Dr. Masatoshi Sana CASE NUMBER : Year : ESLO 01 RÉSUMÉ OF CASE 2 CASE CATEGORY: CLASS I MALOCCLUSION NAME: BORN: SEX: Yukari K. 08/03/1979
ORTHOGNATHIC SURGERY
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Maxillary Expansion and Protraction in Correction of Midface Retrusion in a Complete Unilateral Cleft Lip and Palate Patient
 Case Report Maxillary Expansion and Protraction in Correction of Midface Retrusion in a Complete Unilateral Cleft Lip and Palate Patient Masayoshi Kawakami, DDS, PhD a ; Takakazu Yagi, DDS, PhD b ; Kenji
Case Report Maxillary Expansion and Protraction in Correction of Midface Retrusion in a Complete Unilateral Cleft Lip and Palate Patient Masayoshi Kawakami, DDS, PhD a ; Takakazu Yagi, DDS, PhD b ; Kenji
The ASE Example Case Report 2010
 The ASE Example Case Report 2010 The Requirements for Case Presentation in The Angle Society of Europe are specified in the Appendix I to the Bylaws. This example case report exemplifies how these requirements
The ASE Example Case Report 2010 The Requirements for Case Presentation in The Angle Society of Europe are specified in the Appendix I to the Bylaws. This example case report exemplifies how these requirements
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS Dr. Masatoshi Sana Year: ESLO 01 RÉSUMÉ OF CASE 8 CASE CATEGORY: TRANS / VERTICAL DISCREPANCY NAME: Akiko T. BORN : 15/03/1973 SEX: F PRE-TREATMENT RECORDS: AGE:
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS Dr. Masatoshi Sana Year: ESLO 01 RÉSUMÉ OF CASE 8 CASE CATEGORY: TRANS / VERTICAL DISCREPANCY NAME: Akiko T. BORN : 15/03/1973 SEX: F PRE-TREATMENT RECORDS: AGE:
Attachment G. Orthodontic Criteria Index Form Comprehensive D8080. ABBREVIATIONS CRITERIA for Permanent Dentition YES NO
 First Review IL HFS Dental Program Models Second Review Ortho cad Attachment G Orthodontic Criteria Index Form Comprehensive D8080 Ceph Film X-Rays Photos Narrative Patient Name: DOB: ABBREVIATIONS CRITERIA
First Review IL HFS Dental Program Models Second Review Ortho cad Attachment G Orthodontic Criteria Index Form Comprehensive D8080 Ceph Film X-Rays Photos Narrative Patient Name: DOB: ABBREVIATIONS CRITERIA
SURGICAL MODEL ACCURACY DEVICE. 25 years - manufacturing and distribution - around the globe research - design - manufacturing - distribution
 SURGICAL MODEL ACCURACY DEVICE 25 years - manufacturing and distribution - around the globe research - design - manufacturing - distribution 2 SMAD - SURGICAL MODEL ACCURACY DEVICE SMAD has be designed
SURGICAL MODEL ACCURACY DEVICE 25 years - manufacturing and distribution - around the globe research - design - manufacturing - distribution 2 SMAD - SURGICAL MODEL ACCURACY DEVICE SMAD has be designed
Cephalometric Analysis
 Cephalometric Analysis of Maxillary and Mandibular Growth and Dento-Alveolar Change Part III In two previous articles in the PCSO Bulletin s Faculty Files, we discussed the benefits and limitations of
Cephalometric Analysis of Maxillary and Mandibular Growth and Dento-Alveolar Change Part III In two previous articles in the PCSO Bulletin s Faculty Files, we discussed the benefits and limitations of
Case Report n 2. Patient. Age: ANB 8 OJ 4.5 OB 5.5
 Case Report n 2 Patient Age: 12.11 Diagnosis Angle cl.ii div.2 ANB 8 OJ 4.5 OB 5.5 Author: Dr. Case History The patient is a thirteen year old girl who exhibits delayed development, both physically and
Case Report n 2 Patient Age: 12.11 Diagnosis Angle cl.ii div.2 ANB 8 OJ 4.5 OB 5.5 Author: Dr. Case History The patient is a thirteen year old girl who exhibits delayed development, both physically and
Class II Correction with Invisalign Molar rotation.
 Tips from your peers to help you treat with confidence. Class II Correction with Invisalign Molar rotation. Dr. Mazyar Moshiri. Class II Correction with Invisalign Molar Rotation. Dr. Mazyar Moshiri. Orthodontic
Tips from your peers to help you treat with confidence. Class II Correction with Invisalign Molar rotation. Dr. Mazyar Moshiri. Class II Correction with Invisalign Molar Rotation. Dr. Mazyar Moshiri. Orthodontic
Research report for MSc Dent. University of Witwatersrand. Faculty of health science. Dr J Beukes. Student number: h
 Research report for MSc Dent University of Witwatersrand Faculty of health science Dr J Beukes Student number: 9507510h Supervisor: Prof JP Reyneke October 2011 1 1. Title 2. Aim 3. Introduction 4. Objectives
Research report for MSc Dent University of Witwatersrand Faculty of health science Dr J Beukes Student number: 9507510h Supervisor: Prof JP Reyneke October 2011 1 1. Title 2. Aim 3. Introduction 4. Objectives
Maxillary Growth Control with High Pull Headgear- A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 01 Ver. X January. (2018), PP 09-13 www.iosrjournals.org Maxillary Growth Control with High
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 01 Ver. X January. (2018), PP 09-13 www.iosrjournals.org Maxillary Growth Control with High
Treatment of Angle Class III. Department of Paedodontics and Orthodontics Dr. habil. Melinda Madléna associate professor
 Department of Paedodontics and Orthodontics Dr. habil. Melinda Madléna associate professor Disorders in Angle Class III The position of the lower jaw is foreward regarding to the upper jaw Mesialocclusion
Department of Paedodontics and Orthodontics Dr. habil. Melinda Madléna associate professor Disorders in Angle Class III The position of the lower jaw is foreward regarding to the upper jaw Mesialocclusion
The treatment options for nongrowing skeletal Class
 CASE REPORT Total distalization of the maxillary arch in a patient with skeletal Class II malocclusion Yoon Jeong Choi, a Jong-Suk Lee, b Jung-Yul Cha, c and Young-Chel Park d Seoul, Korea In nongrowing
CASE REPORT Total distalization of the maxillary arch in a patient with skeletal Class II malocclusion Yoon Jeong Choi, a Jong-Suk Lee, b Jung-Yul Cha, c and Young-Chel Park d Seoul, Korea In nongrowing
Angle Class II, division 2 malocclusion with deep overbite
 BBO Case Report Angle Class II, division 2 malocclusion with deep overbite Arno Locks 1 Angle Class II, division 2, malocclusion is characterized by a Class II molar relation associated with retroclined
BBO Case Report Angle Class II, division 2 malocclusion with deep overbite Arno Locks 1 Angle Class II, division 2, malocclusion is characterized by a Class II molar relation associated with retroclined
Treatment of Class II, Division 2 Malocclusion with Miniscrew Supported En-Masse Retraction: Is Deepbite Really an Obstacle for Extraction Treatment?
 TURKISH JOURNAL of DOI: 10.5152/TurkJOrthod.2017.17034 CASE REPORT Treatment of Class II, Division 2 Malocclusion with Miniscrew Supported En-Masse Retraction: Is Deepbite Really an Obstacle for Extraction
TURKISH JOURNAL of DOI: 10.5152/TurkJOrthod.2017.17034 CASE REPORT Treatment of Class II, Division 2 Malocclusion with Miniscrew Supported En-Masse Retraction: Is Deepbite Really an Obstacle for Extraction
MBT System as the 3rd Generation Programmed and Preadjusted Appliance System (PPAS) by Masatada Koga, D.D.S., Ph.D
 MBT System as the 3rd Generation Programmed and Preadjusted Appliance System (PPAS) by Masatada Koga, D.D.S., Ph.D Dr. Masatada Koga, D.D.S., Ph.D, is an assistant professor in the Department of Orthodontics
MBT System as the 3rd Generation Programmed and Preadjusted Appliance System (PPAS) by Masatada Koga, D.D.S., Ph.D Dr. Masatada Koga, D.D.S., Ph.D, is an assistant professor in the Department of Orthodontics
Midline Mandibular Osteotomy in an Asymmetric Patient
 Case Report Midline Mandibular Osteotomy in an Asymmetric Patient M. L. Anghinoni a ; A. S. Magri b ; A. Di Blasio c ; L. Toma d ; E. Sesenna e ABSTRACT This case report shows the possibility of the application
Case Report Midline Mandibular Osteotomy in an Asymmetric Patient M. L. Anghinoni a ; A. S. Magri b ; A. Di Blasio c ; L. Toma d ; E. Sesenna e ABSTRACT This case report shows the possibility of the application
A lingual orthodontic case with 3M Incognito Appliance System combined with orthognathic surgery.
 SM 3M Health Care Academy A lingual orthodontic case with 3M Incognito Appliance System combined with orthognathic surgery. Dr. B. Iglesias-Sánchez Dr. F. Hernandez-Alfaro Dr. J.C. Pérez-Varela DDS, MS.
SM 3M Health Care Academy A lingual orthodontic case with 3M Incognito Appliance System combined with orthognathic surgery. Dr. B. Iglesias-Sánchez Dr. F. Hernandez-Alfaro Dr. J.C. Pérez-Varela DDS, MS.
Nonsurgical Treatment of Adult Open Bite Using Edgewise Appliance Combined with High-Pull Headgear and Class III Elastics
 Case Report Nonsurgical Treatment of Adult Open Bite Using Edgewise Appliance Combined with High-Pull Headgear and Class III Elastics Isao Saito, DDS, PhD a ; Masaki Yamaki, DDS, PhD b ; Kooji Hanada,
Case Report Nonsurgical Treatment of Adult Open Bite Using Edgewise Appliance Combined with High-Pull Headgear and Class III Elastics Isao Saito, DDS, PhD a ; Masaki Yamaki, DDS, PhD b ; Kooji Hanada,
EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: Dr. Stefan Blasius Year: 2010 WBLO 01 EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: Dr. Stefan Blasius Year: 2010 WBLO 01 RÉSUMÉ
EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: Dr. Stefan Blasius Year: 2010 WBLO 01 EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: Dr. Stefan Blasius Year: 2010 WBLO 01 RÉSUMÉ
The Modified Twin Block Appliance in the Treatment of Class II Division 2 Malocclusions
 Journal of Orthodontics/Vol. 28/2001/271 280 The Modified Twin Block Appliance in the Treatment of Class II Division 2 Malocclusions F. M. V. DYER H. F. MCKEOWN P. J. SANDLER Department of Orthodontics,
Journal of Orthodontics/Vol. 28/2001/271 280 The Modified Twin Block Appliance in the Treatment of Class II Division 2 Malocclusions F. M. V. DYER H. F. MCKEOWN P. J. SANDLER Department of Orthodontics,
Postoperative mandibular stability after orthognathic surgery in patients with mandibular protrusion and mandibular deviation
 Wenli Lai, DDS, PhD Lecturer Department of Orthodontics West China College of Stomatology Sichuan University Chengdu, China Kazuhiro Yamada, DDS, PhD Lecturer Division of Orthodontics Department of Oral
Wenli Lai, DDS, PhD Lecturer Department of Orthodontics West China College of Stomatology Sichuan University Chengdu, China Kazuhiro Yamada, DDS, PhD Lecturer Division of Orthodontics Department of Oral
Class III malocclusion occurs in less than 5%
 CDABO CASE REPORT Orthodontic correction of a Class III malocclusion in an adolescent patient with a bonded RPE and protraction face mask Steven W. Smith, DDS, a and Jeryl D. English, DDS, MS b Dallas,
CDABO CASE REPORT Orthodontic correction of a Class III malocclusion in an adolescent patient with a bonded RPE and protraction face mask Steven W. Smith, DDS, a and Jeryl D. English, DDS, MS b Dallas,
Correction of a maxillary canine-first premolar transposition using mini-implant anchorage
 CASE REPORT Correction of a maxillary canine-first premolar transposition using mini-implant anchorage Mehmet Oguz Oztoprak, DDS, MSc, a Cigdem Demircan, DDS, b Tulin Arun, PhD, DDS, MSc c Transposition
CASE REPORT Correction of a maxillary canine-first premolar transposition using mini-implant anchorage Mehmet Oguz Oztoprak, DDS, MSc, a Cigdem Demircan, DDS, b Tulin Arun, PhD, DDS, MSc c Transposition
Non Extraction philosophy: Distalization using Jone s Jig appliance- a case report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 9 Ver. IV (Sep. 2014), PP 36-41 Non Extraction philosophy: Distalization using Jone s Jig appliance-
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 9 Ver. IV (Sep. 2014), PP 36-41 Non Extraction philosophy: Distalization using Jone s Jig appliance-
ISW for the treatment of adult anterior crossbite with severe crowding combined facial asymmetry case
 International Research Journal of Medicine and Biomedical Sciences Vol.3 (2),pp. 15-29, November 2018 Available online at http://www.journalissues.org/irjmbs/ https://doi.org/10.15739/irjmbs.18.004 Copyright
International Research Journal of Medicine and Biomedical Sciences Vol.3 (2),pp. 15-29, November 2018 Available online at http://www.journalissues.org/irjmbs/ https://doi.org/10.15739/irjmbs.18.004 Copyright
The America Association of Oral and Maxillofacial Surgeons classify occlusion/malocclusion in to the following three categories:
 Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
Correction of Class II Division 2 Malocclusion by Fixed Functional Class II Corrector Appliance: Case Report
 Case Report To cite: Kumar M, Sharma H, Bohara P. Correction of class II division 2 malocclusion by fixed functional class II corrector appliance: case report. Journal of contemporary orthodontics, February
Case Report To cite: Kumar M, Sharma H, Bohara P. Correction of class II division 2 malocclusion by fixed functional class II corrector appliance: case report. Journal of contemporary orthodontics, February
Angle Class II, division 2 malocclusion with severe overbite and pronounced discrepancy*
 O C a s e R e p o r t ngle Class II, division 2 malocclusion with severe overbite and pronounced discrepancy* Daniela Kimaid Schroeder** bstract This article reports the treatment of a young patient at
O C a s e R e p o r t ngle Class II, division 2 malocclusion with severe overbite and pronounced discrepancy* Daniela Kimaid Schroeder** bstract This article reports the treatment of a young patient at
Facial planning for orthodontists and oral surgeons
 ADVANCES IN ORTHODONTICS & DENTOFACIAL SURGERY Facial planning for orthodontists and oral surgeons G. William Arnett, DDS, FACD, a and Michael J. Gunson, DDS, MD b Santa Barbara, Calif The bite indicates
ADVANCES IN ORTHODONTICS & DENTOFACIAL SURGERY Facial planning for orthodontists and oral surgeons G. William Arnett, DDS, FACD, a and Michael J. Gunson, DDS, MD b Santa Barbara, Calif The bite indicates
Correction of Crowding using Conservative Treatment Approach
 Case Report Correction of Crowding using Conservative Treatment Approach Dr Tapan Shah, 1 Dr Tarulatha Shyagali, 2 Dr Kalyani Trivedi 3 1 Senior Lecturer, 2 Professor, Department of Orthodontics, Darshan
Case Report Correction of Crowding using Conservative Treatment Approach Dr Tapan Shah, 1 Dr Tarulatha Shyagali, 2 Dr Kalyani Trivedi 3 1 Senior Lecturer, 2 Professor, Department of Orthodontics, Darshan
The Long Term Outcome of Mandibular Orthognathic Surgery
 The Long Term Outcome of Mandibular Orthognathic Surgery Mohammed Ibrahim Al-Ajmi B.D.S (Ireland), MFDS RCPS (Glasgow) Thesis submitted for the degree of Doctorate of Clinical Dentistry (Oral and Maxillofacial
The Long Term Outcome of Mandibular Orthognathic Surgery Mohammed Ibrahim Al-Ajmi B.D.S (Ireland), MFDS RCPS (Glasgow) Thesis submitted for the degree of Doctorate of Clinical Dentistry (Oral and Maxillofacial
Orthognathic treatment of facial asymmetry due to temporomandibular joint ankylosis
 Orthognathic treatment of facial asymmetry due to temporomandibular joint ankylosis Ayse Gulsen 1, Serhat Sibar 2, Selahattin Ozmen 3 1 Department of Plastic, Reconstructive, and Aesthetic Surgery, Gazi
Orthognathic treatment of facial asymmetry due to temporomandibular joint ankylosis Ayse Gulsen 1, Serhat Sibar 2, Selahattin Ozmen 3 1 Department of Plastic, Reconstructive, and Aesthetic Surgery, Gazi
Treatment of a Patient with Class I Malocclusion and Severe Tooth Crowding Using Invisalign and Fixed Appliances
 36 Dental Medicine Research 34 1 36 40, 2014 Case Report Treatment of a Patient with Class I Malocclusion and Severe Tooth Crowding Using Invisalign and Fixed Appliances Yumiko OGURA, Wakana YANAGISAWA,
36 Dental Medicine Research 34 1 36 40, 2014 Case Report Treatment of a Patient with Class I Malocclusion and Severe Tooth Crowding Using Invisalign and Fixed Appliances Yumiko OGURA, Wakana YANAGISAWA,
Arch dimensional changes following orthodontic treatment with extraction of four first premolars
 Received: 14 June. 2015 Accepted: 7 Dec. 2015 Arch dimensional changes following orthodontic treatment with extraction of four first premolars Abstract Asghar Ebadifar DDS, MSc 1, Mohammad Hossien Shafazand
Received: 14 June. 2015 Accepted: 7 Dec. 2015 Arch dimensional changes following orthodontic treatment with extraction of four first premolars Abstract Asghar Ebadifar DDS, MSc 1, Mohammad Hossien Shafazand
Correction of Unilateral Scissor Bite using Periodontally Accelerated Osteogenic Orthodontics
 JIOS Case report Correction of Unilateral Scissor Bite using Periodontally 10.5005/jp-journals-10021-1272 Accelerated Osteogenic Orthodontics. Correction of Unilateral Scissor Bite using Periodontally
JIOS Case report Correction of Unilateral Scissor Bite using Periodontally 10.5005/jp-journals-10021-1272 Accelerated Osteogenic Orthodontics. Correction of Unilateral Scissor Bite using Periodontally
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 559 Failure of Orthodontic Mini-implants by Age, Sex, and Arch; Number of Primary Insertions; and Frequency of Reinsertions After Failure:
The International Journal of Periodontics & Restorative Dentistry 559 Failure of Orthodontic Mini-implants by Age, Sex, and Arch; Number of Primary Insertions; and Frequency of Reinsertions After Failure:
A Modified Three-piece Base Arch for en masse Retraction and Intrusion in a Class II Division 1 Subdivision Case
 Dhaval Ranjitbhai Lekhadia, Gautham Hegde RESEARCH ARTICLE 10.5005/jp-journals-10029-1149 A Modified Three-piece Base Arch for en masse Retraction and Intrusion in a Class II Division 1 Subdivision Case
Dhaval Ranjitbhai Lekhadia, Gautham Hegde RESEARCH ARTICLE 10.5005/jp-journals-10029-1149 A Modified Three-piece Base Arch for en masse Retraction and Intrusion in a Class II Division 1 Subdivision Case
Surgically assisted rapid palatal expansion (SARPE) prior to combined Le Fort I and sagittal osteotomies: A case report
 200 Carlos Alberto E. Tavares, DDS, MS, DOrth Professor Department of Orthodontics Associação Brasileira de Odontologia - RS Porto Alegre, Brazil Miguel Scheffer, DDS, MS Chairman Department of Oral and
200 Carlos Alberto E. Tavares, DDS, MS, DOrth Professor Department of Orthodontics Associação Brasileira de Odontologia - RS Porto Alegre, Brazil Miguel Scheffer, DDS, MS Chairman Department of Oral and
Post-graduate Student, Department of Oral and Maxillofacial Radiology, School of Dentistry, Isfahan University of Medical Sciences, Isfahan, Iran
 Journal section: Oral Surgery Publication Types: Research doi:10.4317/jced.53824 http://dx.doi.org/10.4317/jced.53824 Evaluation of orthognathic surgery on articular disc position and temporomandibular
Journal section: Oral Surgery Publication Types: Research doi:10.4317/jced.53824 http://dx.doi.org/10.4317/jced.53824 Evaluation of orthognathic surgery on articular disc position and temporomandibular
Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document.
 ORTHOGNATHIC SURGERY Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
ORTHOGNATHIC SURGERY Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
ISW for the treatment of moderate crowding dentition with unilateral second molar impaction
 International Research Journal of Public and Environmental Health Vol.5 (6),pp. 90-103, September 2018 Available online at https://www.journalissues.org/irjpeh/ https://doi.org/10.15739/irjpeh.18.013 Copyright
International Research Journal of Public and Environmental Health Vol.5 (6),pp. 90-103, September 2018 Available online at https://www.journalissues.org/irjpeh/ https://doi.org/10.15739/irjpeh.18.013 Copyright
Correction of Dentofacial Deformities (Orthognathic Surgery)
 Correction of Dentofacial Deformities (Orthognathic Surgery) BDS, MSc, German board of Oral and Maxillofacial Surgery ( Berlin-Germany), Doctoral degree by LBMS Definition Orthognathic surgery is a combination
Correction of Dentofacial Deformities (Orthognathic Surgery) BDS, MSc, German board of Oral and Maxillofacial Surgery ( Berlin-Germany), Doctoral degree by LBMS Definition Orthognathic surgery is a combination
Angle Class I malocclusion with anterior open bite treated with extraction of permanent teeth
 Angle Class I malocclusion with anterior open bite treated with extraction of permanent teeth Matheus Melo Pithon 1 This clinical case reports the orthodontic treatment of a Class I malocclusion with anterior
Angle Class I malocclusion with anterior open bite treated with extraction of permanent teeth Matheus Melo Pithon 1 This clinical case reports the orthodontic treatment of a Class I malocclusion with anterior
ORTHOGNATHIC SURGERY
 ORTHOGNATHIC SURGERY MEDICAL POLICY Effective Date: February 1, 2017 Review Dates: 1/93, 7/95, 10/97, 4/99, 10/00, 8/01, 12/01, 4/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11,
ORTHOGNATHIC SURGERY MEDICAL POLICY Effective Date: February 1, 2017 Review Dates: 1/93, 7/95, 10/97, 4/99, 10/00, 8/01, 12/01, 4/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11,
Sliding Mechanics with Microscrew Implant Anchorage
 Clinical Report Sliding Mechanics with Microscrew Implant Anchorage Hyo-Sang Park, DDS, MSD, PhD a ; Tae-Geon Kwon, DDS, MSD, PhD b Abstract: Three cases are illustrated. One was treated with maxillary
Clinical Report Sliding Mechanics with Microscrew Implant Anchorage Hyo-Sang Park, DDS, MSD, PhD a ; Tae-Geon Kwon, DDS, MSD, PhD b Abstract: Three cases are illustrated. One was treated with maxillary
Non-Surgical and Non-Extraction Treatment of a Severe Skeletal Class III Deep Bite Patient
 Case Report Non-Surgical and Non-Extraction Treatment of a Severe Skeletal Class III Deep Bite Patient Supachai Lertnimulchai 1 and Keith Godfrey 2 1 Private orthodontist, Amphoe Mueang, Nong Khai, Thailand
Case Report Non-Surgical and Non-Extraction Treatment of a Severe Skeletal Class III Deep Bite Patient Supachai Lertnimulchai 1 and Keith Godfrey 2 1 Private orthodontist, Amphoe Mueang, Nong Khai, Thailand
Skeletal class III maloeclusion treated using a non-surgieal approach supplemented with mini-implants: a case report
 Journal oforthodontîcz^ol 40, 2013, 256-263! CLINICAL SECTION Skeletal class III maloeclusion treated using a non-surgieal approach supplemented with mini-implants: a case report Marcel Marchiori Farret^
Journal oforthodontîcz^ol 40, 2013, 256-263! CLINICAL SECTION Skeletal class III maloeclusion treated using a non-surgieal approach supplemented with mini-implants: a case report Marcel Marchiori Farret^
An Adult Case of Skeletal Open Bite with a Severely Narrowed Maxillary Dental Arch
 Case Report An Adult Case of Skeletal Open Bite with a Severely Narrowed Maxillary Dental Arch Michiru Takeuchi, DDS a ; Eiji Tanaka, DDS, PhD b ; Daisuke Nonoyama, DDS c ; Junko Aoyama, DDS d ; Kazuo
Case Report An Adult Case of Skeletal Open Bite with a Severely Narrowed Maxillary Dental Arch Michiru Takeuchi, DDS a ; Eiji Tanaka, DDS, PhD b ; Daisuke Nonoyama, DDS c ; Junko Aoyama, DDS d ; Kazuo
TWO PHASE FOR A BETTER FACE!! TWIN BLOCK AND HEADGEAR FOLLOWED BY FIXED THERAPY FOR CLASS II CORRECTION
 Case Report NUJHS Vol. 5, No.2, June 2015, ISSN 2249-7110 TWO PHASE FOR A BETTER FACE!! TWIN BLOCK AND HEADGEAR FOLLOWED BY FIXED THERAPY FOR CLASS II CORRECTION 1 2 3 4 U S Krishna Nayak, Ashutosh Shetty,
Case Report NUJHS Vol. 5, No.2, June 2015, ISSN 2249-7110 TWO PHASE FOR A BETTER FACE!! TWIN BLOCK AND HEADGEAR FOLLOWED BY FIXED THERAPY FOR CLASS II CORRECTION 1 2 3 4 U S Krishna Nayak, Ashutosh Shetty,
Low-Force Mechanics Nonextraction. Estimated treatment time months (Actual 15 mos 1 week). Low-force mechanics.
 T.S. Age: 43 Years 1 Month Diagnosis: Class I Nonextraction Adult (severe crowding, very flat profile with tissue-grafting indications) Background: This case is very similar to the previous case of a 14-year-old.
T.S. Age: 43 Years 1 Month Diagnosis: Class I Nonextraction Adult (severe crowding, very flat profile with tissue-grafting indications) Background: This case is very similar to the previous case of a 14-year-old.
OF LINGUAL ORTHODONTICS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: KDr. KP. kanarelis CASE NUMBER: 2 Year: 2010 WBLO 01 RESUME OF CASE 2 CASE CATEGORY: ADULT MALOCCLUSION NAME : MARIA A. BORN: 18.04.1983 SEX:
EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: KDr. KP. kanarelis CASE NUMBER: 2 Year: 2010 WBLO 01 RESUME OF CASE 2 CASE CATEGORY: ADULT MALOCCLUSION NAME : MARIA A. BORN: 18.04.1983 SEX:
ISW for the Treatment of Bilateral Posterior Buccal Crossbite
 Journal of Dentistry and Oral Health Case report ISW for the Treatment of Bilateral Posterior Buccal Crossbite Chun-Shuo HUANG 1,2, Chien-Chih YU 3,*, Jian-Hong YU 1,2, and Yuan-Hou CHEN 1 1 Department
Journal of Dentistry and Oral Health Case report ISW for the Treatment of Bilateral Posterior Buccal Crossbite Chun-Shuo HUANG 1,2, Chien-Chih YU 3,*, Jian-Hong YU 1,2, and Yuan-Hou CHEN 1 1 Department
Nonextraction Treatment of Upper Canine Premolar Transposition in an Adult Patient
 Case Report Nonextraction Treatment of Upper Canine Premolar Transposition in an Adult Patient Shingo Kuroda a ; Yasuko Kuroda b Abstract: This article reports the successful treatment of a unilateral
Case Report Nonextraction Treatment of Upper Canine Premolar Transposition in an Adult Patient Shingo Kuroda a ; Yasuko Kuroda b Abstract: This article reports the successful treatment of a unilateral
Significant improvement with limited orthodontics anterior crossbite in an adult patient
 VARIA Significant improvement with limited orthodontics anterior crossbite in an adult patient Arzu Ari-Demirkaya Istanbul, Turkey Summary Objectives. Orthodontic treatment is known to last as long as
VARIA Significant improvement with limited orthodontics anterior crossbite in an adult patient Arzu Ari-Demirkaya Istanbul, Turkey Summary Objectives. Orthodontic treatment is known to last as long as
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Non-surgical management of skeletal malocclusions: An assessment of 100 cases
 Non-surgical management of skeletal malocclusions: An assessment of 100 cases In early 1970 s reduced risks associated with surgical procedures allowed the treatment planning process for skeletal malocclusions
Non-surgical management of skeletal malocclusions: An assessment of 100 cases In early 1970 s reduced risks associated with surgical procedures allowed the treatment planning process for skeletal malocclusions
For many years, patients with
 Dr. Robert Lowe is one of the great teachers in dentistry. Recently, he received the Gordon J. Christensen Award from the Chicago Dental Society in recognition of his excellence in teaching. Some of my
Dr. Robert Lowe is one of the great teachers in dentistry. Recently, he received the Gordon J. Christensen Award from the Chicago Dental Society in recognition of his excellence in teaching. Some of my
Removable appliances
 Removable appliances Melinda Madléna DMD, PhD associate professor Department of Pedodontics and Orthodontics Faculty of Dentistry Semmelweis University Budapest Classification of the orthodontic anomalies
Removable appliances Melinda Madléna DMD, PhD associate professor Department of Pedodontics and Orthodontics Faculty of Dentistry Semmelweis University Budapest Classification of the orthodontic anomalies
Research & Reviews: Journal of Dental Sciences
 Research & Reviews: Journal of Dental Sciences Orthodontic Camouflage of Skeletal Class I, Class II and Class III Malocclusion in Borderline Cases Report of Three Cases Dr. Seema Kapil Lahoti 1 *, Dr.
Research & Reviews: Journal of Dental Sciences Orthodontic Camouflage of Skeletal Class I, Class II and Class III Malocclusion in Borderline Cases Report of Three Cases Dr. Seema Kapil Lahoti 1 *, Dr.
ORTHO-SURGICAL MANAGEMENT OF SKELETAL CLASS III MALOCCLUSION WITH SEVERE TOOTH SIZE ARCH LENGTH DISCREPANCY
 Case Report ORTHO-SURGICAL MANAGEMENT OF SKELETAL CLASS III MALOCCLUSION WITH SEVERE TOOTH SIZE ARCH LENGTH DISCREPANCY SS Agarwal a, Karan Nehrab b, B Jayanc c, NK Sahoo d, ID Roy e, Mohit Sharma f 45
Case Report ORTHO-SURGICAL MANAGEMENT OF SKELETAL CLASS III MALOCCLUSION WITH SEVERE TOOTH SIZE ARCH LENGTH DISCREPANCY SS Agarwal a, Karan Nehrab b, B Jayanc c, NK Sahoo d, ID Roy e, Mohit Sharma f 45
S.H. Age: 15 Years 3 Months Diagnosis: Class I Nonextraction Severe crowding, very flat profile. Background:
 S.H. Age: 15 Years 3 Months Diagnosis: Class I Nonextraction Severe crowding, very flat profile Background: This case was selected to illustrate the long-term impact of treatment planning on the face and
S.H. Age: 15 Years 3 Months Diagnosis: Class I Nonextraction Severe crowding, very flat profile Background: This case was selected to illustrate the long-term impact of treatment planning on the face and
Fixed Twin Blocks. Guidelines for case selection are similar to those for removable Twin Block appliances.
 Fixed Twin Blocks Development of Fixed Twin Blocks Dr Clark has enjoyed the cooperation of Dynaflex in developing the Fixed Twin Block. Six years of clinical testing has confirmed that this technique produces
Fixed Twin Blocks Development of Fixed Twin Blocks Dr Clark has enjoyed the cooperation of Dynaflex in developing the Fixed Twin Block. Six years of clinical testing has confirmed that this technique produces
Class II Correction using Combined Twin Block and Fixed Orthodontic Appliances: A Case Report
 Case Report Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/506 Class II Correction using Combined Twin Block and Fixed Orthodontic Appliances: A Case Report Ahmed Alassiry Assistant
Case Report Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/506 Class II Correction using Combined Twin Block and Fixed Orthodontic Appliances: A Case Report Ahmed Alassiry Assistant
Virtual model surgery and wafer fabrication for orthognathic surgery
 Int. J. Oral Maxillofac. Surg. 2009; 38: 1306 1323 available online at http://www.sciencedirect.com Technical Note Orthognathic Surgery Virtual model surgery and wafer fabrication for orthognathic surgery
Int. J. Oral Maxillofac. Surg. 2009; 38: 1306 1323 available online at http://www.sciencedirect.com Technical Note Orthognathic Surgery Virtual model surgery and wafer fabrication for orthognathic surgery
Facial Soft Tissue Changes in Class III Patients Treated With Bimaxillary, Maxillary Advancement or Mandibular Set Back Orthognathic Surgery
 Facial Soft Tissue Changes in Class III Patients Treated With Bimaxillary, Maxillary Advancement or Mandibular Set Back Orthognathic Surgery Halise Aydemir 1, Ufuk Toygar-Memikoglu 2 1 Orthodontist, Turgut
Facial Soft Tissue Changes in Class III Patients Treated With Bimaxillary, Maxillary Advancement or Mandibular Set Back Orthognathic Surgery Halise Aydemir 1, Ufuk Toygar-Memikoglu 2 1 Orthodontist, Turgut
