Long-Term Effects From a Randomized Trial of Two Public Health Preventive Interventions for Parental Depression
|
|
|
- Garry Houston
- 5 years ago
- Views:
Transcription
1 Journal of Family Psychology Copyright 2007 by the American Psychological Association 2007, Vol. 21, No. 4, /07/$12.00 DOI: / Long-Term Effects From a Randomized Trial of Two Public Health Preventive Interventions for Parental Depression William R. Beardslee Judge Baker Children s Center and Children s Hospital Boston Tracy R. G. Gladstone Wellesley College, Judge Baker Children s Center, and Children s Hospital Boston Ellen J. Wright Brandeis University and Judge Baker Children s Center Peter Forbes Children s Hospital Boston This article presents long-term effects of a randomized trial evaluating 2 standardized, manual-based prevention strategies for families with parental mood disorder: informational lectures and a brief, clinician-based approach including child assessment and a family meeting. A sample of 105 families, in which at least 1 parent suffered from a mood disorder and at least 1 nondepressed child was within the 8- to 15-year age range, was recruited. Parents and children were assessed separately at baseline and every 9 to 12 months thereafter on behavioral functioning, psychopathology, and response to intervention. Both interventions produced sustained effects through the 6th assessment point, approximately 4.5 years after enrollment, with relatively small sample loss of families ( 14%). Clinician-based families had significantly more gains in parental child-related behaviors and attitudes and in childreported understanding of parental disorder. Child and parent family functioning increased for both groups and internalizing symptoms decreased for both groups, with no significant group differences. These findings demonstrate that brief, family-centered preventive interventions for parental depression may contribute to long-term, sustained improvements in family functioning. Keywords: parental depression, prevention, adolescents Supplemental materials: Adolescent depression is a public health problem of major proportions, with point prevalence rates ranging from 0.4% to 8.4% (Fleming & Offord, 1990). The lifetime prevalence of major depressive disorder in adolescents years of age is 14%. One of the most potent risk factors for adolescent depression is being the child of a depressed parent (Institute of Medicine, 1994); such a child William R. Beardslee, Judge Baker Children s Center and Department of Psychiatry, Children s Hospital Boston; Ellen J. Wright, Psychology Department, Brandeis University, and Judge Baker Children s Center; Tracy R. G. Gladstone, Wellesley Centers for Women, Wellesley College, Judge Baker Children s Center, and Department of Psychiatry, Children s Hospital Boston; Peter Forbes, Clinical Research Program, Children s Hospital Boston. This work was supported by NIMH Grant RO1 MH , the William T. Grant Foundation, the Overseas Shipholding Group, the Sidney A. Swensrud Foundation, and a William T. Grant Foundation Faculty Scholar Award (to William R. Beardslee). Correspondence concerning this article and requests for reprints should be addressed to William R. Beardslee, Department of Psychiatry, Children s Hospital Boston, 300 Longwood Avenue, Boston, MA william.beardslee@childrens.harvard.edu is about four times more likely to develop a mood disorder than is a child of a nondepressed parent (Beardslee, Versage, & Gladstone, 1998). In fact, by age 20, a child with an affectively ill parent has a 40% chance of having an episode of depression, and by age 25, this rate increases to 60% (Beardslee et al., 1993). Family factors may maintain depression in youth (Brent et al., 1997; Hammen, Rudolph, Weisz, Rao, & Burge, 1999) and are more salient than peer relationships are in predicting adolescent depressive symptoms (Sheeber, Hops, & Davis, 2001). Moreover, adverse family environments are among the most consistent risk factors for adolescent depression (Evans & Seligman, 2005). Yet, to date, intervention and prevention approaches to adolescent depression have focused on enhancing adolescent coping strategies with individual or group methods (e.g., Clarke et al., 2001; Jaycox, Reivich, Gilham, & Seligman, 1994), rather than with family-based approaches. Although several studies have incorporated traditional family therapy approaches to the treatment of child and adolescent depression, with some success (e.g., Diamond, Reis, Diamond, Siqueland, & Isaacs, 2002; Nelson, Barnard, & Cain, 2003), a recent meta-analysis (Horowitz & Garber, 2006) indicated that only three other family-based interventions had targeted 703
2 704 BEARDSLEE, WRIGHT, GLADSTONE, AND FORBES children and adolescents who were not yet clinically ill (Gillham & Reivich, 1999; Sandler et al., 1992; Shochet et al., 2001). None of these programs focused on children of depressed parents. Given the strong effects of parental depression on family functioning, the evidence that suggests family participation may enhance the benefits of treatment for depressed adolescents (Diamond et al., 2002), and the evidence of the benefits of family change in promoting resilience in teens (Asarnow, Scott, & Mintz, 2002; Diamond et al., 2002; Shochet et al., 2001), consideration of a family-based approach is warranted. Over the past 15 years, our group developed and tested two family-based preventive interventions for families with parental depression: informational lectures and a brief, clinician-based approach. We chose to focus on selective prevention (Institute of Medicine, 1994; i.e., interventions that targeted youth at elevated risk as a function of parental mood disorder; Beardslee, 1998). Our approaches targeted decreasing some risk factors inherent in the presence of parental mood disorder (e.g., family conflict and lack of parental focus; Beardslee, 2003) and targeted increasing factors that have been demonstrated to be protective when a parent suffers from mood disorders (e.g., increased involvement in outside activities, supportive adult and family relations, and increased family understanding; Beardslee & Podorefsky, 1988). Given the high rates of parental depression and the need for large-scale programs that could be disseminated widely, our approaches were designed for use by a range of practitioners from different disciplines and theoretical schools. Because parents with depression are likely to present in settings other than mental health clinics when seeking services for their children (U.S. Department of Health and Human Services, 2000), the interventions were designed for use by those who treat adults, children, and families in a wide variety of settings (e.g., pediatric clinics, primary care clinics, community settings). We targeted improved recognition and treatment of depression in youth as an intervention outcome, because most youths with depression are neither identified nor treated (U.S. Department of Health and Human Services, 2000), and we included education for parents about treatment for depression in adulthood. Rates of child difficulty are reduced more when parents with depression receive effective treatment than when they do not receive adequate treatment (Weissman et al., 2006). After standardizing the approaches, we conducted a pilot study in which the sample (N 36 families) was randomized on a 1/3:2/3 basis. The findings from this sample demonstrated the safety (Beardslee et al., 1997) and feasibility (Beardslee et al., 1993) of the approaches. Given that greater effects were observed in the clinician group and that both interventions were safe and useful, we undertook a randomized trial using a larger sample, with equal numbers of families assigned to each intervention condition. Again, relative to lecture group families, the clinician-facilitated group displayed greater parental change in variables that mediate both resilience in the offspring (e.g., improved child focus and communication) and greater understanding of parental mood disorder by the children at the 18-month (Beardslee et al., 1997) and the 30-month follow-up assessments (Beardslee, Gladstone, Wright, & Cooper, 2003). Both groups showed sustained gains, and a modest reduction in child internalizing symptoms was found for both groups (Beardslee et al., 2003) at the 30-month follow-up interval. Effective preventive interventions must show long-term effects (Institute of Medicine, 1994; National Advisory Mental Health Council Workgroup on Child and Adolescent Mental Health Intervention Development and Deployment, 2001). In this report, we address whether changes demonstrated at previous intervals (Beardslee et al., 1997, 2003) resulted in longer term effects for families by presenting analyses from the sixth assessment point, which occurred approximately 4.5 years after enrollment and randomization. We hypothesized that (a) parent-reported changes in family communication and understanding would be sustained over the longer follow-up interval and would be greater in the clinician group; (b) improvements in children s understanding of parents mood disorders would be sustained over the longer follow-up interval and would be greater in the clinician group; and (c) parental change in communication, functioning, and understanding would predict better understanding of parental mood disorder on the part of the offspring. On the basis of our previous analyses, we explored the following hypotheses: (a) Over the follow-up period, adolescents would show decreases in internalizing symptoms despite expected increases in this age group (e.g., Rao et al., 1995); (b) families that participated would be more likely to seek treatment for depressed children than would families in community samples; and (c) overall, family functioning would improve from baseline and would be sustained over time. Method Detailed descriptions of the sample, the measures, and the two interventions have been presented previously (Beardslee et al., 2003; Beardslee, Versage, Salt, & Wright, 1999). Participants and Procedures Dual- and single-parent families were eligible to participate if they had (a) at least one child 8 15 years of age and (b) at least one parent who had experienced an episode of mood disorder in the 18 months before contact. Parental exclusion criteria were serious current parental substance abuse or dependence, schizophrenia, current severe marital crisis, or other life crises (e.g., hospitalization) that would prevent the family s participation. Families also were excluded if parents were currently in marital therapy or family therapy more than twice monthly. Parents in psychotherapy for depression were not excluded. Youngsters were excluded if they had a current or a past history of major depression by parental report but were not excluded if they had experienced or been treated for other diagnoses (e.g., ADHD). We enrolled all eligible children in each family. All participants provided written informed consent, and the
3 LONG-TERM PREVENTION FOR PARENTAL DEPRESSION 705 children provided written assent at enrollment in accordance with human subjects standards. Any individual or family was free to discontinue participation at any point. The sample consisted of 105 families and included 21 families from the pilot sample and 84 families enrolled after the pilot period. 1 We recruited 53.6% of the sample from a large, prepaid HMO located in the Northeast. Mental health practitioners referred an additional 13.05%, 5.22% were recruited from support groups, and 9.57% responded to newspaper advertisements; 18.26% were recruited from a variety of other sources. Pilot families were randomized to treatment groups on a 2/3:1/3 basis (clinician facilitated: lecture). We used a balanced block randomization procedure for the other 84 families, with blocks of 4 stratified by family type (single parent or dual parent; Beardslee et al., 1999). Pilot measures, both pre- and post-intervention, were identical to those used after the pilot period, and there were no significant differences on study measures between the pilot and the nonpilot families. Assessments for all participants were conducted initially at Time 1 (T1), immediately after intervention at Time 2, and regularly for 9 12 months thereafter, at Time 3 through Time 6 (T3 T6). They were conducted by raters who were blind to assessment of other family members. Retention strategies included flexibility in location and timing of the assessment (within predefined limits) and small payments for each participant. It was impossible for individual assessors to be blind to group status, although child and parent assessors were kept blind to assessment information from each other. Intervention design. Both intervention strategies addressed poor communication, misunderstanding, feelings of guilt and blame, and lack of recognition of depression. To address putative protective factors, we designed both interventions to build support networks and outside activities for the children and to increase shared family understanding (Beardslee et al., 1999). Depression was presented as a family illness, and a cognitive framework was used (Beardslee et al., 1999). Parents were encouraged to get appropriate treatment for depression; if they were in treatment, we made contact with their clinicians before starting the preventive intervention to ensure coordination of their care. Both intervention groups were offered further sessions or telephone consultation at any point on request; the groups did not differ in their use of these extra sessions or referrals. Manuals specified the delivery of both interventions. Clinician-facilitated intervention. The clinician-facilitated intervention consisted of an average of seven sessions (M 6.7, SD 1.3; range 2 9) and included both separate meetings with parents and children and family meetings (Beardslee et al., 1999). Intervenors were licensed social workers or clinical psychologists who were rigorously trained in the intervention strategies. Training included case review; discussion of the manual; and, for many of the clinicians, role-playing with actors who played the parts of family members. Throughout the project, fidelity was ensured by ongoing supervision. Clinicians presented information about family experiences of mood disorder, obtained a history of parental mood disorder, assessed the functioning and concerns of the children, linked general information to each family s experience of depression, and helped parents prepare for and conduct a meeting in which the family discussed how it would deal with depression. Telephone contacts or refresher meetings occurred at 6- to 9-month intervals; they reviewed parental illness and addressed concerns that might have emerged during the interval. Using the manual and scripts, we developed a set of scales that assessed presence or absence of key intervention action during key sessions (i.e., sessions with the child, planning the family meeting, and the actual family meeting). The clinical interventions of 10 families were rated (37 sessions), and an overall score was obtained by summing the three ratings. Raters for fidelity were not project clinicians and had no knowledge of the families treatment. Overall, interrater reliability with the scales was excellent (intraclass correlations ranged from 0.89 to 0.99), and adherence to the protocol was similarly stellar (86.4% for the family meeting, 91.7% for the child session; Beardslee et al., 2003). Difference in adherence among the four clinicians was nonsignificant. Lecture intervention. The lecture intervention consisted of two meetings delivered in a group format, without children present, and of consultation as requested by families. The lecture was based on the same constructs as was the clinician-facilitated intervention, but we made no active attempt to link the psychoeducational material to each individual s life experiences. Lecture groups were formed as lecture families enrolled and contained an average of three families. William R. Beardslee delivered each lecture. We used a standardized scale that was based on content information from the lecture script to measure script adherence. A rater evaluated the videotapes for their adherence to the lecture script in regard to the presence or absence of 10 items from the first lecture and 27 from the second lecture. Ten videotapes (five of the first lectures and five of the second lectures, randomly selected) were rated, and the mean percent agreement was greater than 95% of the adherence to the protocol (Beardslee et al., 2003). Measures Demographic information. Family composition, socioeconomic status, and other demographic data obtained from heads of household at initial assessment were assessed with a measure developed by Larkin and Hirshfield (1997). Parental psychopathology. At T1, the Schedule for Affective Disorders and Schizophrenia Lifetime Version (Endicott & Spitzer, 1978), scored according to the 1 The pilot sample differed from the main sample in one respect. Originally, children were not interviewed directly at baseline in the pilot sample, although responses to the same self-reports were provided by the children. After the pilot study, 21 of the 36 pilot families consented to have their children interviewed. Thus, 1 year after enrollment, diagnostic data retrospective to time of enrollment were gathered for the children in these 21 pilot families. There were no significant differences on baseline measures for those who remained in the study and those who did not.
4 706 BEARDSLEE, WRIGHT, GLADSTONE, AND FORBES Research Diagnostic Criteria (Spitzer, Endicott, & Robins, 1978), was administered to the parent (or parents), consistent with our previous risk sample (Beardslee et al., 1996). It assesses affective illness (i.e., major depressive disorder, minor depression, intermittent depression, mania, hypomania, schizoaffective disorders), anxiety disorders, and substance abuse or dependence. Assessment of potential episodes in intervals after enrollment was done with the Streamlined Longitudinal Interval Continuation Evaluation. Psychometric properties for both versions have been well studied and are excellent (Keller et al., 1987). Child psychopathology. Each parent and child was interviewed with the Schedule for Affective Disorders and Schizophrenia for School-Age Children, Epidemiologic Version Revised, Lifetime Version (Puig-Antich, Orvaschel, Tabrizi, & Chambers, 1980) and was scored with the Diagnostic and Statistical Manual of Mental Disorders (3rd ed., rev.; American Psychiatric Association, 1987). 2 We combined information from both interviews using standard procedures described by Orvaschel, Puig-Antich, Chambers, Tabrizi, and Johnson (1982) to obtain a best estimate diagnosis. A shortened-interval version was used to cover the intervals (Keller, Shapiro, & Lavori, 1984). Reliability and validity properties have been well established (Ambrosini, 2000). Parental global functioning. For each parent, we used the Global Assessment Scale (GAS; Endicott, Spitzer, Fleiss, & Cohen, 1976) to obtain the individual s worst and current levels of functioning during each assessment interval and for the 18 months prior to enrollment. Extensive training was done with vignettes developed by the psychobiology of depression study of the National Institute of Mental Health, Clinical Research Branch. Child internalizing symptomatology. To assess degree of internalizing symptoms, we had children rate problem and adaptive behaviors on the Youth Self-Report (YSR) and the Young Adult Self-Report (YASR, used from age 18 forward; Achenbach & Edelbrock, 1987). The broadband internalizing t scores from both the YSR and the YASR were used for analyses. Internal consistency estimates were good ( s.84 and.80 for YSR internalizing and for YASR internalizing, respectively). Impact of the intervention parents. We administered the Semistructured Interview About the Intervention to each parent at baseline and at each follow-up assessment to assess parent-reported changes in eight behaviors (e.g., increased talking with children about depression) and nine attitudes (e.g., increased information about risk and resiliency in children) in regard to parenting, family communication, and understanding (Beardslee et al., 1999). We developed the interview to measure (a) the impact of parental affective disorders, (b) the impact of the interventions on family functioning, and (c) the degree to which the interventions addressed parents greatest concerns. Raters used information obtained from the Semistructured Interview About the Intervention to identify specific changes in illness-related behaviors and in attitudes attributed to project participation. To score positively, a parent must both report change and attribute it to the intervention. An interrater-reliability study, with raters blind to group membership, showed excellent intraclass correlations for total behaviors (r.94), total attitudes (r.92), and total changes (r.93; Beardslee et al., 1997). Internal consistency estimates were good (.78). Impact of the intervention children. The Semistructured Child Interview (Beardslee et al., 1999) provided information about children s perception of changes in the family, especially when describing their increased understanding. Independent raters, rating 20 transcribed and blinded interviews, generated excellent intraclass correlations (r.92; Beardslee et al., 1997). We generated change in understanding by combining the rater s score of improved understanding with the child s Likert rating of change (Beardslee et al., 2003). Internal consistency estimates were good (.84). Family functioning parents and children. To assess overall change in family functioning, we administered the Family Relationship Inventory (FRI; Holahan & Moos, 1983) at baseline and at each follow-up assessment to both parents and children. A 27-item measure, it consists of the three subscales (Cohesion, Expressiveness, and Conflict) of the relationship dimension of the Family Environment Scale (FES), a widely used, empirically derived measure of family functioning (Holahan & Moos, 1981). Estimates of internal consistency for this study were good (.83). Health care contacts. Treatment involvement at baseline and at follow-up intervals was elicited with a semistructured interview form, which allowed us to explore the impact of outside treatment on outcome variables. Information covered included whether participants had sought a variety of treatments for either medical or psychiatric difficulties (e.g., medication, mental health services, or lay services, such as talking to a religious leader) from baseline to the third assessment point and at each interval following. Interviewers elicited the information directly from individual parents, and child assessors interviewed the mothers about their children s participation until the adolescents became young adults. Young adults provided these data directly. Data Analytic Strategies In families in which there was only 1 parent with a mood disorder in the 18 months prior to enrollment, that parent was designated the identified patient (IP), and the non-ill parent was designated as a nonidentified patient (NIP). When both parents had experienced a mood disorder in the 18 months prior to baseline, the parent with the most severe or chronic mood disorder was designated as IP. Finally, at each assessment, a couple s GAS score was created. Used 2 We used diagnoses based on the Diagnostic and Statistical Manual to assess more typical childhood and adolescent disorders not covered by the Research Diagnostic Criteria (e.g., attentiondeficit/hyperactivity disorder, separation anxiety disorder) in addition to the affective disorders covered by the Schedule for Affective Disorders and Schizophrenia.
5 LONG-TERM PREVENTION FOR PARENTAL DEPRESSION 707 as a covariate, it reflected the lower of the two parents functioning scores. Because this study was concerned with developmental outcomes, we created a dichotomized developmental stage variable (younger than 14 years vs. 14 years and older). Calculated at each assessment, it allowed us to examine changes associated with early versus late adolescence. Because of time constraints and the assessment mode, not all outcome measures were obtained from all subjects at each assessment. In addition, a relatively small amount of nonresponse was due to dropout. To examine whether the dropouts and missing data affected the outcomes, we created a dichotomous completion status variable for each outcome for each subject. We considered all subjects who had data from all or all-but-one assessment (and who had completed the intervention) as completers and those with at least one point, but with two or more missing data points, as partial completers. We included this variable in all regressions to estimate differences in outcomes between those subjects with and without complete data and to adjust estimates of treatment group effects for nonresponse due to dropouts and missing data. We performed regression analyses with SAS Version 9.0 using generalized estimating equations, which provide unbiased estimates of treatment effects and tests of hypotheses when data are missing at random. Test statistics are chisquared and distributed under the null hypothesis. For parent outcomes, regressions adjusted for parent gender, IP status, the couple s worst GAS score, and completion status. For child outcomes, regressions adjusted for gender, developmental stage, and completion status. For outcomes measured at baseline and later assessments (parent FRI, child FRI, and child internalizing), we used two linear regression models. First, to test for postintervention differences in outcomes between treatment groups, we modeled the postintervention scores, adjusting the model for baseline score and covariates. Second, we tested for a sustained change from baseline by comparing the average baseline level with the average postintervention level. We also compared mean outcome levels within the postintervention assessments to examine the effect of time. Intervention Group Assessment Interaction Effects were tested for each outcome and were excluded when not significant. For outcomes without a baseline measure (child understanding and parent behavior and attitude changes), we tested for a treatment group difference by comparing the average outcome between groups across all assessments combined. We tested for a sustained change by comparing average postintervention levels for the groups combined. Effect sizes, which are included, clarify the magnitude of differences in outcomes between treatment groups and clarify the change in scores between the baseline and the follow-up assessments. The effect size is the observed difference expressed in standard deviation units and is calculated by taking the difference in the mean outcome divided by the pooled standard deviation. p values are two sided and are considered significant at the.05 level. Sample Composition Results At baseline, the sample consisted of 105 families. Of these, 97 completed the intervention, with gradual sample loss over the follow-up assessments (see Figure 1). Sample loss did not vary by intervention group. Because all children within the age range in each family were recruited, the number of children is larger than the number of families. Of the families, 12 (20%) in the clinician group and 8 (17%) in the lecture group were headed by single parents. Depending on assessment, parent behavior and attitudes scores were obtained for between 95% and 98% of participants, FRI scores were obtained for between 87% and 97% of parents and between 81% and 89% of children, child understanding scores were obtained for between 86% and 89% of the children, and internalizing outcomes were obtained for between 82% and 87% of the children. Of the families, 91 (87%) completed the T6 assessment point. The time from baseline to the sixth assessment averaged 53 months for both parents and children. It was longer in the clinician intervention for both parents and children: parents (M 50.0 months, SD 7.2 months, vs. M 56.1 months, SD 10.4 months), t(157) 4.11, p.001; children (M 49.8 months, SD 7.4 months vs. M 54.8 months, SD 9.9 months), t(112) 3.21, p.01. At baseline, 151 parents (79%; men 62%, women 93%) had ever had a mood disorder, with the most frequently diagnosed condition being major depression (men 39%, women 86%). In addition, 102 parents (54%) experienced nonaffective disorders, which included anxiety disorders and substance abuse. Of the parents, 110 had comorbid disorders (men 52%, women 76%; see Table 1). In the 18 months prior to baseline, both parents in 30 families (35% of two-parent families) had experienced a mood disorder. The average couple s worst GAS score was 50.4 (SD 11.8; range 25 70) in the same interval, which indicated significant family impairment. Similarly, in approximately 44% of couples, at least 1 parent met criteria for a nonaffective disorder in the past 18 months. The number of active illness episodes in the intervals declined slowly but remained high: The percentages of families that had at least one mood disorder were 90% from T1 to T3, 81% from T3 to T4, 72% from T4 to T5, and 66% from T5 to T6. Rates of nonaffective disorders showed corresponding decline from T1 to T3 (43%), from T3 to T4 (37%), from T4 to T5 (36%), and from T5 to T6 (31%). There were no significant differences in baseline demographics or in psychopathology between the intervention groups on parent or child variables. The mean age of the parents and of the children was 43 years and 12 years, respectively. The mean worst GAS score among the parents was 60. Of parents, 65% in the clinician group and 65% in the lecture group had major depression. The 8 families who dropped out between assessment and intervention were not different from the 97 families who completed the intervention on measures of global functioning or socioeconomic
6 708 BEARDSLEE, WRIGHT, GLADSTONE, AND FORBES Enrollment n = 105 families Randomized Clinician Lecture Allocated to intervention (n= 59 families) Received allocated intervention (n= 55 families) Discontinued or did not receive intervention (n= 4 families) Allocation Allocated to intervention (n=2 families) Received allocated intervention (n= 44 families) Discontinued or did not receive allocated intervention (n= 4 families) T3 Assessment Parents n = 97 Children n = 78 Follow-Up T3 Assessment Parents n = 76 Children n = 54 T4 Assessment Parents n = 98 Children n = 69 T4 Assessment Parents n=72 Children n=53 T5 Assessment Parents n=94 Children n=69 T5 Assessment Parents n=71 Children n=52 T6 Assessment Parents n=91 Children n=64 T6 Assessment Parents n=68 Children n=50 Figure 1. Study flow: intent to treat design. status. There were no significant differences between groups for completion status on any variable. Family Responses to Intervention Parents in the clinician group averaged 2.7 more childrelated behavior and attitude changes than lecture parents did: clinician and lecture (M 7.04, SD 3.0, vs. M 4.39, SD 2.7), effect size 0.84; 2 (1) 52.8, p The number of reported changes increased across the four follow-up assessments, 2 (3) 88.6, p.0001 (see Supplemental Figure 1). The IP reported 0.95 more changes than the NIP did, 2 (1) 4.53, p.05. Neither gender nor the couple s worst functioning predicted the parents response to intervention in this domain. The average number of changes made did not vary by completion status. Children s Change in Understanding of Parental Illness Children in the clinician group scored, on average, 0.7 points higher on improved understanding of parental mood disorder than those in the lecture group did across the four follow-up assessments: clinician and lecture (M 3.0, SD 2.1, vs. M 2.3, SD 2.1), effect size 0.33; 2 (1) 5.0, p.05 (see Supplemental Figure 2). Scores
7 LONG-TERM PREVENTION FOR PARENTAL DEPRESSION 709 Table 1 Individual Parental Psychopathology Lifetime diagnosis 18 mo. baseline T1 T3 T3 T4 T4 T5 T5 T6 Condition n % n % n % n % n % n % Any affective disorder Men Women Major depression Men Women Minor depression Men Women Intermittent depression Men Women Mania Men Women Hypomania Men Women Schizoaffective disorder Men Women Generalized anxiety disorder Men Women Phobic disorder Men Women Panic disorder Men Women Obsessive-compulsive disorder Men Women Alcohol abuse Men Women Drug abuse Men Women Comorbid disorders Men Women increased significantly over time, 2 (3) 9.0, p.05, but, with developmental stage in the model, this increase was not significant. On average, older children scored 0.6 points higher than younger children did, but the difference did not reach statistical significance. Completion status was a significant covariate, with completers scoring, on average, 0.95 points higher than partial completers did, 2 (1) 5.3, p.05. Connection Between Parent Change and Child Change in Understanding At each assessment, child understanding scores correlated significantly with concurrent couple-level parent changes in behavior and in attitudes (Spearman s r.26, p.01) and with parent changes at the previous assessment point (Spearman s r.28, p.01). Regression analysis indicated that concurrent parent changes significantly predicted child understanding, 2 (1) 14.1, p.001, as did previous parent changes, 2 (1) 18.3, p When we used both previous and concurrent parent changes to predict child understanding, parent changes from the previous assessment significantly predicted child understanding, 2 (1) 13.6, p.001, whereas concurrent changes were no longer significant. With previous parent changes in the model, neither completion status nor treatment group was a significant predictor of child understanding changes. Internalizing Symptomatology Overall, internalizing t scores decreased 3.2 points from baseline levels, 2 (1) 9.0, p.001; effect size 0.32.
8 710 BEARDSLEE, WRIGHT, GLADSTONE, AND FORBES Baseline levels significantly predicted later internalizing scores, 2 (1) 28.2, p With baseline scores in the model, there was no main effect for intervention group, but there was a main effect for gender, with girls scoring, on average, 3.7 points higher than boys did, 2 (1) 8.3, p.01; effect size In addition, completers scored, on average, 4.0 points lower than partial completers did, 2 (1) 4.1, p.05. Family Functioning Parent FRI scores increased, on average, 1.0 point from baseline, 2 (1) 11.2, p.001; effect size Controlling for baseline FRI, the intervention groups did not differ in postintervention FRI scores, 2 (1) 0.3, p.1. Baseline FRI values significantly predicted later FRI scores, 2 (1) 167.6, p.0001 (see Supplemental Figure 3). Controlling for baseline FRI, there was a main effect for IP status, with non-ill parents scoring 1.4 points higher on average, 2 (1) 7.99, p.01. A couple s worst GAS score predicted its FRI scores, 2 (1) 21.9, p.0001, with higher adaptive functioning levels predicting higher FRI scores. FRI scores averaged 2.2 points higher for participants with more complete data, 2 (1) 9.7, p.005. Child FRI scores increased, on average, 2.5 points from baseline, 2 (1) 19.3, p.0001; effect size Each postbaseline mean FRI level was significantly higher than baseline in pairwise post hoc comparisons, and means at the postbaseline assessments did not differ significantly. Adjusting for baseline FRI, the groups did not differ in postintervention FRI scores, 2 (1) 1.8, p.1; nor did FRI scores vary by completeness status, 2 (1) 0.74, p.1. Neither gender nor developmental stage predicted levels of family functioning (ps.1). A significant effect for baseline FRI was obtained, 2 (1) 5.40, p.05. Recognition and Treatment of Major Depression Children were excluded from the study when parents reported a history of major depression in the children by brief screening. However, data from the Schedule for Affective Disorders and Schizophrenia for School-Age Children revealed that 16 children had experienced an episode of major depression prior to baseline. Only 2 (13%) had been treated. Of the 16 children, 9 experienced an additional episode of major depression after baseline and 6 of these 9 (67%) received treatment. Of the 122 children with no baseline major depression, 17 (8 in the clinician group and 9 in the lecture group) developed at least one episode of major depression after intervention. By T6, 12 of the 17 (71%) had received treatment for at least one episode (6/8 in the clinician group and 6/9 in the lecture group). This finding suggests that recognition was much higher at postintervention assessments than at baseline: 12 of 17 (71%) versus 2 of 16 (13%), respectively; 2 (1) 11.4, p.001. Discussion This article presents one of the first reports of long-term, sustained, positive family change in response to familybased preventive intervention for parental mood disorders. As hypothesized, parents in the clinician group reported changes in illness-related behaviors and in attitudes that were sustained over time and were greater than those for the lecture group. IP parents reported more changes than NIP parents did, and group differences observed initially at T3 continued through T6. As hypothesized, children s understanding of parental mood disorder was sustained over time and was greater in the clinician group. Parental behavior and attitude changes and degree of child understanding of parental mood disorder were positively associated, which suggests that the interventions increased positive family interactions. Given the range of response within intervention groups, parent changes were more effective predictors of child change than group membership was. These findings are significant considering that children and parents were exposed to high levels of ongoing parental mood disorder, which would undermine interpersonal relationships. Adolescent internalizing symptoms diminished over time in both groups, although the youngsters were going through a period of increased risk (Rao et al., 1995) and would be expected to have increased depressive symptomatology (Lewinsohn, Rohde, & Seeley, 1998). This is an important prevention effect, as internalizing symptoms are predictors of and precursors to major depression. That girls fared worse than boys is consistent with the literature, which indicates that, at puberty, girls begin to display higher levels of depressive symptomatology (Angold, Costello, & Worthman, 1998). Unlike the low rates of recognition and treatment for youngsters with major depression prior to baseline, the rates of recognition and treatment of subsequent depression after intervention were much higher (including the rates for those not previously depressed). Approximately two thirds of these youngsters were recognized and were treated when depressed. We understand that this statement offers only a rough comparison, as, before intervention, the children were younger and were at an earlier developmental stage. As another comparison, with our own risk study of children who were drawn from the same HMO over a 4-year period, the majority of whose parents were depressed, only 30% of those with depression were recognized and were treated (Beardslee et al., 1996). Future studies with larger samples should examine what strategies are most effective in increasing recognition and treatment for depression in families at high risk for depression. As hypothesized, positive changes in family functioning were sustained over time. Increases in parent-reported changes in behaviors and attitudes and reports by parents and children of improved family functioning on the FRI provide multimodal support for this hypothesis. Group differences in family functioning were found on some, but not all, measures. In future analyses, we will explore withinand between-groups differences to determine which intervention strategy works best for which families.
9 LONG-TERM PREVENTION FOR PARENTAL DEPRESSION 711 Several characteristics of the intervention approaches may have contributed to their success. First, our approaches were strength based (Maton, Schellenbach, Leadbeater, & Solarz, 2004). Second, the clinician-facilitated program was flexible and was tailored to each family s needs. Third, these approaches focused on helping the family develop effective problem-solving strategies and coherent narratives about its experience with depression (Beardslee, 2003; Focht & Beardslee, 1996; Podorefsky, McDonald-Dowdell, & Beardslee, 2001). The value of family narratives in dealing with both physical and mental illness has come to be widely recognized (Pennebaker, 1997). Fourth, parents were assisted in obtaining treatment, and care was coordinated between our delivery of preventive intervention services and the clinician s provision of treatment for depression or for other illnesses. Finally, we believe that the continued support provided throughout the study for families in both groups influenced the sustained effects. This support included regularly scheduled assessments; consultation as requested; and, in the clinician group, regularly scheduled telephone meetings. The groups did not differ in terms of the use of consultation as requested. We believe that regularly scheduled assessments for both groups provided a reminder to participants of the goals presented in the intervention (Finn & Tonsager, 1997). We recommend regularly scheduled follow-ups and availability of consultation as requested by families as part of any long-term prevention strategy. Although findings from this study are promising, there are both strengths and limitations in our design that have important implications for future work in this area. First, we chose two forms of intervention that were compatible with public health approaches and did not elect to have a control group without intervention. We believed that not offering families some form of intervention would be unethical. Future studies should explore the effects of less intensive models of intervention than these two and thus should separate the effects of time and treatment in a clearer fashion. Given that these youngsters are passing through a crucial developmental epoch in adolescence (Conger & Ge, 1999; Ge & Conger, 1999), such designs would also allow exploration of normal developmental changes that these youngsters are undergoing versus changes related to their receiving preventive intervention. Second, the observed effects, although sustained, were small on some measures, as might be expected from a relatively brief intervention. For any individual measure, there was some sample loss. We have addressed the sample loss in two ways: (a) the general estimating equations take into account all available data and (b) completion status did not affect any group comparisons. The possibility of response bias on the respondents part should be considered, although this bias would operate equally for both interventions. The clinician intervention group was followed slightly longer than the lecture intervention group was, because it took longer to deliver and to schedule follow-up assessments, which could be done only after the clinician follow-up; however, given the lengthy follow-up period, this difference is unlikely to have affected the results. We also recognize that the assessors could not be blind to the intervention that the participants received, although we have demonstrated independent reliability for the ratings. Future studies with less intensive questionnaires can assess the outcomes while remaining blind to assessment conditions. Third, in addition to participating in these interventions, a large number of families received other treatment (e.g., medications for depression) over the follow-up period, and positive changes from this treatment may have contributed to the sustained effects that we report. In examining the effects of outside treatment, we found that participation in outside therapies did not affect the group differences in measures that were designed to detect changes in mediating variables (i.e., changes in parental behaviors and attitudes and children s improved understanding of parental mood disorder). However, families that sought and received outside therapy reported poorer functioning on the FRI and on the YSR/YASR. It is likely that the association between treatment seeking and either family functioning or youth internalizing symptomatology simply indicates that those who were more ill sought and received treatment. Our measure of outside treatment was a broad, nonspecific measure. Future studies should explore in greater detail the kind of treatment that parents receive and its impact on preventive interventions. Finally, the sample was largely white and middle class, and all of those sampled had health insurance. Similarly, rates of alcohol and substance abuse were low, which reflects the inclusion and exclusion criteria. Replication of these findings in other samples that represent different cultural and economic backgrounds and different levels of access to care is needed. Our initial, randomized replication with a sample of single-parent, urban women of color showed effects similar to those of our initial comparison trial (Podorefsky et al., 2001). The intervention has been used in the Netherlands, has been adapted for widespread use in Finland (Beardslee et al., in press), and has been successfully incorporated into a manual-based, cognitive behavioral, family-centered treatment for youngsters with depression and with inflammatory bowel disease (Szigethy et al., 2004). As we developed our preventive interventions, planning for dissemination was essential; thus, we chose strategies that could be used by a wide range of clinicians. In Finland, dissemination has occurred, as over 40 master trainers have been trained in the use of these and related methods; they, in turn, have trained over 500 clinicians (Toikka & Solantaus, 2006). Detailed manuals and training tapes are available from William R. Beardslee. Conducting this project made us aware of three larger problems with health care systems. First, in contrast to countries with national health insurance (Beardslee et al., in press), this country focuses far less on prevention than on treatment, despite evidence for the effectiveness of a wide array of prevention strategies (Institute of Medicine, 1994). Second, although completely compatible, prevention and clinical treatment require different orientations and approaches. Our prevention approach was timed for delivery when the family was not in crisis, and it focused on acquir-
10 712 BEARDSLEE, WRIGHT, GLADSTONE, AND FORBES ing new skills. It was based on the principle that parents could be effective parents despite their depression. It also addressed concerns that might arise several years from the point of intervention, as opposed to treatment whose maximal effect occurs during acute illness (Beardslee, 1998). Third, it remains difficult for us to combine child and parent care clinical approaches and/or reimbursement strategies in either prevention or treatment studies (Beardslee & Knitzer, 2003), both because health care systems are not integrated to encourage this and because clinicians often are trained to focus on either children or parents but not on both. Although the findings of this project are promising, there is still more to be learned about the effectiveness of these interventions. More methodologically rigorous work needs to be done, in part, before full-fledged dissemination is appropriate. Future research should also examine the relative cost-effectiveness of various prevention approaches. Given the chronic nature of depression and the evidence of sustained long-term effects from these relatively brief, standardized public health interventions, incorporation of family psychoeducational preventive approaches should be considered as part of clinical care for parents with depression. Future clinical and research programs should consider (a) involving the entire family, (b) teaching focused problem-solving strategies, (c) helping parents be effective in enhancing strengths in their youngsters, (d) including parental treatment referral as part of the intervention and the monitoring of effectiveness of parental treatment for depression, (e) providing support that helps staff learn and employ new methods, (f) developing shared understanding of the illness by families, and (g) providing long-term resources to families. References Achenbach, T. M., & Edelbrock, C. (1987). Manual for the Youth Self-Report and Profile. Burlington: University of Vermont. Ambrosini, P. J. (2000). Historical development and present status of the Schedule for Affective Disorders and Schizophrenia for School-Age Children (K SADS). Journal of the American Academy of Child and Adolescent Psychiatry, 39, American Psychiatric Association. (1987). Diagnostic and statistical manual of mental disorders (3rd ed., rev.). Washington, DC: Author. Angold, A., Costello, E. J., & Worthman, C. M. (1998). Puberty and depression: The roles of age, pubertal status and pubertal timing. Psychological Medicine, 28, Asarnow, J., Scott, C., & Mintz, J. (2002). A combined cognitive behavioral family education intervention for depressed children: A treatment development study. Cognitive Therapy and Research, 26, Beardslee, W. R. (1998). Prevention and the clinical encounter. American Journal of Orthopsychiatry, 68, Beardslee, W. R. (2003). When a parent is depressed: How to protect your children from the effects of depression in the family. New York: Little, Brown. (Originally published in 2002 as Out of the darkened room: When a parent is depressed: Protecting the children and strengthening the family.) Beardslee, W. R., Gladstone, T. R. G., Wright, E. J., & Cooper, A. B. (2003). A family-based approach to the prevention of depressive symptoms in children at risk: Evidence of parental and child change. Pediatrics, 112, e119 e131. Beardslee, W. R., Keller, M. B., Seifer, R., Lavori, P. W., Staley, J., Podorefsky, D., & Shera, D. (1996). Prediction of adolescent affective disorder: Effects of prior parental affective disorders and child psychopathology. Journal of the American Academy of Child and Adolescent Psychiatry, 35, Beardslee, W. R., & Knitzer, J. (2003). Strengths-based family mental health services: A family systems approach. In K. Maton, C. Schellenbach, B. Leadbeater, & A. Solarz (Eds.), Investing in children, youth, families, and communities: Strengths-based research and policy (pp ). Washington, DC: American Psychological Association. Beardslee, W. R., & Podorefsky, D. (1988). Resilient adolescents whose parents have serious affective and other psychiatric disorders: The importance of self-understanding and relationships. American Journal of Psychiatry, 149, Beardslee, W. R., Salt, P., Porterfield, K., Rothberg, P. C., van de Velde, P., Swatling, S., et al. (1993). Comparison of preventive interventions for families with parental affective disorder. Journal of the American Academy of Child and Adolescent Psychiatry, 32, Beardslee, W. R., Solantaus, T., van Doesum, K., & Hosman, C. (in press). Children of mentally ill parents: An opportunity for effective prevention all too often neglected. In C. Hosman, E. Jane-Llopis, & S. Saxena (Eds.), Prevention of mental disorders: Effective interventions and policy options. Oxford, England: Oxford University Press. Beardslee, W. R., Versage, E., & Gladstone, T. R. G. (1998). Children of affectively ill parents: A review of the past 10 years. Journal of the American Academy of Child and Adolescent Psychiatry, 37, Beardslee, W. R., Versage, E. M., Salt, P., & Wright, E. (1999). The development and evaluation of two preventive intervention strategies for children of depressed parents. In D. Cicchetti & S. L. Toth (Eds.), Rochester symposium on developmental psychopathology: Vol. IX. Developmental approaches to prevention and intervention (pp ). Rochester, NY: University of Rochester Press. Beardslee, W. R., Wright, E., Salt, P., Gladstone, T. R. G., Versage, E., & Rothberg, P. C. (1997). Examination of children s responses to two preventive intervention strategies over time. Journal of the American Academy of Child and Adolescent Psychiatry, 36, Brent, D., Holder, D., Kolko, D., Birmaher, B., Baugher, M., Roth, C., et al. (1997). A clinical psychotherapy trial for adolescent depression comparing cognitive, family, and supportive therapy. Archives of General Psychiatry, 54, Clarke, G. N., Hornbrook, M., Lynch, F., Polen, M., Gale, J., Beardslee, W. R., et al. (2001). A randomized trial of a group cognitive intervention for preventing depression in adolescent offspring of depressed parents. Archives of General Psychiatry, 58, Conger, R. D., & Ge, X. (1999). Conflict and cohesion in parent adolescent relations: Changes in emotional expression from early to midadolescence. In M. J. Cox & J. Brooks-Gunn (Eds.), Conflict and cohesion in families: Causes and consequences (pp ). Mahwah, NJ: Erlbaum. Diamond, G., Reis, B., Diamond, G., Siqueland, L., & Isaacs, L. (2002). Attachment-based family therapy for depressed adolescents: A treatment development study. Journal of the American Academy of Child and Adolescent Psychiatry, 41, Endicott, J., & Spitzer, R. L. (1978). A diagnostic interview: The schedule for affective disorders and schizophrenia. Archives of General Psychiatry, 35, Endicott, J., Spitzer, R. L., Fleiss, J. L., & Cohen, J. (1976). The
A Family-Based Approach to the Prevention of Depressive Symptoms in Children at Risk: Evidence of Parental and Child Change
 A Family-Based Approach to the Prevention of Depressive Symptoms in Children at Risk: Evidence of Parental and Child Change William R. Beardslee, MD* ; Tracy R. G. Gladstone, PhD* ; Ellen J. Wright, MA*;
A Family-Based Approach to the Prevention of Depressive Symptoms in Children at Risk: Evidence of Parental and Child Change William R. Beardslee, MD* ; Tracy R. G. Gladstone, PhD* ; Ellen J. Wright, MA*;
Research Article Increasing Understanding in Children of Depressed Parents: Predictors and Moderators of Intervention Response
 Hindawi Publishing Corporation Depression Research and Treatment Volume 2015, Article ID 347971, 9 pages http://dx.doi.org/10.1155/2015/347971 Research Article Increasing Understanding in Children of Depressed
Hindawi Publishing Corporation Depression Research and Treatment Volume 2015, Article ID 347971, 9 pages http://dx.doi.org/10.1155/2015/347971 Research Article Increasing Understanding in Children of Depressed
Adolescent Coping with Depression (CWD-A)
 This program description was created for SAMHSA s National Registry for Evidence-based Programs and Practices (NREPP). Please note that SAMHSA has discontinued the NREPP program and these program descriptions
This program description was created for SAMHSA s National Registry for Evidence-based Programs and Practices (NREPP). Please note that SAMHSA has discontinued the NREPP program and these program descriptions
The Prevention of Depression in Children and Adolescents: A Review
 In Review The Prevention of Depression in Children and Adolescents: A Review Tracy RG Gladstone, PhD 1 ; William R Beardslee, MD 2 Objective: To review the recent literature on the prevention of clinical
In Review The Prevention of Depression in Children and Adolescents: A Review Tracy RG Gladstone, PhD 1 ; William R Beardslee, MD 2 Objective: To review the recent literature on the prevention of clinical
Heidi Clayards Lynne Cox Marine McDonnell
 Heidi Clayards Lynne Cox Marine McDonnell Introduction to Interpersonal Psychotherapy (IPT) Adaptations from IPT to IPT-A Theoretical framework Description of treatment Review of the manual and demonstration
Heidi Clayards Lynne Cox Marine McDonnell Introduction to Interpersonal Psychotherapy (IPT) Adaptations from IPT to IPT-A Theoretical framework Description of treatment Review of the manual and demonstration
Review Article Pathways to Prevention for Children of Depressed Mothers: A Review of the Literature and Recommendations for Practice
 Depression Research and Treatment Volume 2012, Article ID 313689, 11 pages doi:10.1155/2012/313689 Review Article Pathways to Prevention for Children of Depressed Mothers: A Review of the Literature and
Depression Research and Treatment Volume 2012, Article ID 313689, 11 pages doi:10.1155/2012/313689 Review Article Pathways to Prevention for Children of Depressed Mothers: A Review of the Literature and
An Evaluation of the Brief Service Program at Children s Centre Thunder Bay. Children s Centre Thunder Bay. Conducted by. Suzanne Chomycz, M.A.
 An Evaluation of the Brief Service Program at Children s Centre Thunder Bay Children s Centre Thunder Bay Conducted by Suzanne Chomycz, M.A. Lakehead University 1 Acknowledgements Children s Centre Thunder
An Evaluation of the Brief Service Program at Children s Centre Thunder Bay Children s Centre Thunder Bay Conducted by Suzanne Chomycz, M.A. Lakehead University 1 Acknowledgements Children s Centre Thunder
The Relationship Between Clinical Diagnosis and Length of Treatment. Beth Simpson-Cullor. Senior Field Research Project. Social Work Department
 1 The Relationship Between Clinical Diagnosis and Length of Treatment Beth Simpson-Cullor Senior Field Research Project Social Work Department University of Tennessee at Chattanooga 2 Abstract Clinicians
1 The Relationship Between Clinical Diagnosis and Length of Treatment Beth Simpson-Cullor Senior Field Research Project Social Work Department University of Tennessee at Chattanooga 2 Abstract Clinicians
The comparison of behavioral and emotional problems in children with a bipolar parent and children with healthy parents in Zahedan, Iran, 2011
 The comparison of behavioral and emotional problems in children with a bipolar parent and children with healthy parents in Zahedan, Iran, 2011 Mahboubeh Firoozkouhi Moghaddam, Nour Mohammad Bakhshani,
The comparison of behavioral and emotional problems in children with a bipolar parent and children with healthy parents in Zahedan, Iran, 2011 Mahboubeh Firoozkouhi Moghaddam, Nour Mohammad Bakhshani,
Developing bipolar disorder. A study among children of patients with bipolar disorder Hillegers, Manon Hubertine Johanna
 University of Groningen Developing bipolar disorder. A study among children of patients with bipolar disorder Hillegers, Manon Hubertine Johanna IMPORTANT NOTE: You are advised to consult the publisher's
University of Groningen Developing bipolar disorder. A study among children of patients with bipolar disorder Hillegers, Manon Hubertine Johanna IMPORTANT NOTE: You are advised to consult the publisher's
Cognitive Behavioral Therapy Plus Motivational Interviewing Improves Outcome for Pediatric Obsessive Compulsive Disorder: A Preliminary Study
 Cognitive Behaviour Therapy Vol 39, No 1, pp. 24 27, 2010 Cognitive Behavioral Therapy Plus Motivational Interviewing Improves Outcome for Pediatric Obsessive Compulsive Disorder: A Preliminary Study Lisa
Cognitive Behaviour Therapy Vol 39, No 1, pp. 24 27, 2010 Cognitive Behavioral Therapy Plus Motivational Interviewing Improves Outcome for Pediatric Obsessive Compulsive Disorder: A Preliminary Study Lisa
APPENDIX 11: CASE IDENTIFICATION STUDY CHARACTERISTICS AND RISK OF BIAS TABLES
 APPENDIX 11: CASE IDENTIFICATION STUDY CHARACTERISTICS AND RISK OF BIAS TABLES 1 Study characteristics table... 3 2 Methodology checklist: the QUADAS-2 tool for studies of diagnostic test accuracy... 4
APPENDIX 11: CASE IDENTIFICATION STUDY CHARACTERISTICS AND RISK OF BIAS TABLES 1 Study characteristics table... 3 2 Methodology checklist: the QUADAS-2 tool for studies of diagnostic test accuracy... 4
Testing Mediators of Intervention Effects in Randomized Controlled Trials: An Evaluation of Three Depression Prevention Programs
 Journal of Consulting and Clinical Psychology 2010 American Psychological Association 2010, Vol. 78, No. 2, 273 280 0022-006X/10/$12.00 DOI: 10.1037/a0018396 Testing Mediators of Intervention Effects in
Journal of Consulting and Clinical Psychology 2010 American Psychological Association 2010, Vol. 78, No. 2, 273 280 0022-006X/10/$12.00 DOI: 10.1037/a0018396 Testing Mediators of Intervention Effects in
Patterns and Predictors of Subjective Units of Distress in Anxious Youth
 Behavioural and Cognitive Psychotherapy, 2010, 38, 497 504 First published online 28 May 2010 doi:10.1017/s1352465810000287 Patterns and Predictors of Subjective Units of Distress in Anxious Youth Courtney
Behavioural and Cognitive Psychotherapy, 2010, 38, 497 504 First published online 28 May 2010 doi:10.1017/s1352465810000287 Patterns and Predictors of Subjective Units of Distress in Anxious Youth Courtney
EDUCATIONAL PSYCHOLOGY (EPSY)
 Educational Psychology (EPSY) 1 EDUCATIONAL PSYCHOLOGY (EPSY) EPSY 1003 Learning to Learn Description: Learning effective strategies to succeed through online individualized assessment, positive attitude
Educational Psychology (EPSY) 1 EDUCATIONAL PSYCHOLOGY (EPSY) EPSY 1003 Learning to Learn Description: Learning effective strategies to succeed through online individualized assessment, positive attitude
TITLE: Practice parameters for the assessment and treatment of children and adolescents with posttraumatic stress disorder.
 Brief Summary TITLE: Practice parameters for the assessment and treatment of children and adolescents with posttraumatic stress disorder. SOURCE(S): Practice parameters for the assessment and treatment
Brief Summary TITLE: Practice parameters for the assessment and treatment of children and adolescents with posttraumatic stress disorder. SOURCE(S): Practice parameters for the assessment and treatment
PSYCHOPATHOLOGY AND DEVELOPMENT: TRAJECTORIES OF PSYCHOPATHOLOGY FROM EARLY ADOLESCENCE THROUGH YOUNG ADULTHOOD
 Psychopathology and Develoment, 1 PSYCHOPATHOLOGY AND DEVELOPMENT: TRAJECTORIES OF PSYCHOPATHOLOGY FROM EARLY ADOLESCENCE THROUGH YOUNG ADULTHOOD Marc S. Schulz*, Stuart T. Hauser**, Joseph P. Allen***,
Psychopathology and Develoment, 1 PSYCHOPATHOLOGY AND DEVELOPMENT: TRAJECTORIES OF PSYCHOPATHOLOGY FROM EARLY ADOLESCENCE THROUGH YOUNG ADULTHOOD Marc S. Schulz*, Stuart T. Hauser**, Joseph P. Allen***,
Correlates of Internalizing and Externalizing Behavior Problems: Perceived Competence, Causal Attributions, and Parental Symptoms
 Journal of Abnormal Child Psychology, Vol. 19, No. 2, 1991 Correlates of Internalizing and Externalizing Behavior Problems: Perceived Competence, Causal Attributions, and Parental Symptoms Bruce E. Compas,
Journal of Abnormal Child Psychology, Vol. 19, No. 2, 1991 Correlates of Internalizing and Externalizing Behavior Problems: Perceived Competence, Causal Attributions, and Parental Symptoms Bruce E. Compas,
Aggregation of psychopathology in a clinical sample of children and their parents
 Aggregation of psychopathology in a clinical sample of children and their parents PA R E N T S O F C H I LD R E N W I T H PSYC H O PAT H O LO G Y : PSYC H I AT R I C P R O B LEMS A N D T H E A S SO C I
Aggregation of psychopathology in a clinical sample of children and their parents PA R E N T S O F C H I LD R E N W I T H PSYC H O PAT H O LO G Y : PSYC H I AT R I C P R O B LEMS A N D T H E A S SO C I
An adult version of the Screen for Child Anxiety Related Emotional Disorders (SCARED-A)
 Netherlands Journal of Psychology / SCARED adult version 81 An adult version of the Screen for Child Anxiety Related Emotional Disorders (SCARED-A) Many questionnaires exist for measuring anxiety; however,
Netherlands Journal of Psychology / SCARED adult version 81 An adult version of the Screen for Child Anxiety Related Emotional Disorders (SCARED-A) Many questionnaires exist for measuring anxiety; however,
Co-Rumination Predicts the Onset of Depressive Disorders During Adolescence
 Journal of Abnormal Psychology 2011 American Psychological Association 2011, Vol. 120, No. 3, 752 757 0021-843X/11/$12.00 DOI: 10.1037/a0023384 BRIEF REPORT Co-Rumination Predicts the Onset of Depressive
Journal of Abnormal Psychology 2011 American Psychological Association 2011, Vol. 120, No. 3, 752 757 0021-843X/11/$12.00 DOI: 10.1037/a0023384 BRIEF REPORT Co-Rumination Predicts the Onset of Depressive
Cognitive Behavioral Therapy For Late Life Depression A Therapist Manual
 Cognitive Behavioral Therapy For Late Life Depression A Therapist Manual Anxiety likely contributes to poorer adaptive functioning, quality of life, and Using CBT to treat depression after stroke was first
Cognitive Behavioral Therapy For Late Life Depression A Therapist Manual Anxiety likely contributes to poorer adaptive functioning, quality of life, and Using CBT to treat depression after stroke was first
Hammen Publications since 2000
 Hammen, 1 Hammen Publications since 2000 Rao, U., Daley, S., & Hammen, C. (2000). Relationship between depression and substance use disorders in adolescent women during the transition to adulthood. Journal
Hammen, 1 Hammen Publications since 2000 Rao, U., Daley, S., & Hammen, C. (2000). Relationship between depression and substance use disorders in adolescent women during the transition to adulthood. Journal
S P O U S A L R ES E M B L A N C E I N PSYCHOPATHOLOGY: A C O M PA R I SO N O F PA R E N T S O F C H I LD R E N W I T H A N D WITHOUT PSYCHOPATHOLOGY
 Aggregation of psychopathology in a clinical sample of children and their parents S P O U S A L R ES E M B L A N C E I N PSYCHOPATHOLOGY: A C O M PA R I SO N O F PA R E N T S O F C H I LD R E N W I T H
Aggregation of psychopathology in a clinical sample of children and their parents S P O U S A L R ES E M B L A N C E I N PSYCHOPATHOLOGY: A C O M PA R I SO N O F PA R E N T S O F C H I LD R E N W I T H
SUMMARY AND DISCUSSION
 Risk factors for the development and outcome of childhood psychopathology SUMMARY AND DISCUSSION Chapter 147 In this chapter I present a summary of the results of the studies described in this thesis followed
Risk factors for the development and outcome of childhood psychopathology SUMMARY AND DISCUSSION Chapter 147 In this chapter I present a summary of the results of the studies described in this thesis followed
Problem Solved! with Arthur M. Nezu and Christine Maguth Nezu. How can one truly represent the problem-solving therapy (PST) approach in its
 Problem Solved! A review of the video Problem-Solving Therapy with Arthur M. Nezu and Christine Maguth Nezu Washington, DC: American Psychological Association, 2009. American Psychological Association
Problem Solved! A review of the video Problem-Solving Therapy with Arthur M. Nezu and Christine Maguth Nezu Washington, DC: American Psychological Association, 2009. American Psychological Association
The period from late adolescence to the mid-20s,
 Article Childhood and Adolescent Predictors of Major Depression in the Transition to Adulthood Helen Z. Reinherz, Sc.D. Angela D. Paradis, B.A. Rose M. Giaconia, Ph.D. Cecilia K. Stashwick, B.A. Garrett
Article Childhood and Adolescent Predictors of Major Depression in the Transition to Adulthood Helen Z. Reinherz, Sc.D. Angela D. Paradis, B.A. Rose M. Giaconia, Ph.D. Cecilia K. Stashwick, B.A. Garrett
Expressed Emotion-Criticism and Risk of Depression Onset in Children
 Journal of Clinical Child & Adolescent Psychology, 41(6), 771 777, 2012 Copyright # Taylor & Francis Group, LLC ISSN: 1537-4416 print=1537-4424 online DOI: 10.1080/15374416.2012.703122 Expressed Emotion-Criticism
Journal of Clinical Child & Adolescent Psychology, 41(6), 771 777, 2012 Copyright # Taylor & Francis Group, LLC ISSN: 1537-4416 print=1537-4424 online DOI: 10.1080/15374416.2012.703122 Expressed Emotion-Criticism
Focus of Today s Presentation. Partners in Healing Model. Partners in Healing: Background. Data Collection Tools. Research Design
 Exploring the Impact of Delivering Mental Health Services in NYC After-School Programs Gerald Landsberg, DSW, MPA Stephanie-Smith Waterman, MSW, MS Ana Maria Pinter, M.A. Focus of Today s Presentation
Exploring the Impact of Delivering Mental Health Services in NYC After-School Programs Gerald Landsberg, DSW, MPA Stephanie-Smith Waterman, MSW, MS Ana Maria Pinter, M.A. Focus of Today s Presentation
2010, Vol. 78, No. 2, X/10/$12.00 DOI: /a BRIEF REPORTS
 Journal of Consulting and Clinical Psychology 2010 American Psychological Association 2010, Vol. 78, No. 2, 260 267 0022-006X/10/$12.00 DOI: 10.1037/a0018935 The Impact of Perceived Interpersonal Functioning
Journal of Consulting and Clinical Psychology 2010 American Psychological Association 2010, Vol. 78, No. 2, 260 267 0022-006X/10/$12.00 DOI: 10.1037/a0018935 The Impact of Perceived Interpersonal Functioning
Child-Parent Psychotherapy Research Fact Sheet OVERVIEW
 Child-Parent Psychotherapy Research Fact Sheet OVERVIEW Child-Parent Psychotherapy (CPP) is an intervention model for children aged 0-5 who have experienced traumatic events and/or are experiencing mental
Child-Parent Psychotherapy Research Fact Sheet OVERVIEW Child-Parent Psychotherapy (CPP) is an intervention model for children aged 0-5 who have experienced traumatic events and/or are experiencing mental
Average length/number of sessions: 50
 Treatment Description Acronym (abbreviation) for intervention: CPP Average length/number of sessions: 50 Aspects of culture or group experiences that are addressed (e.g., faith/spiritual component, transportation
Treatment Description Acronym (abbreviation) for intervention: CPP Average length/number of sessions: 50 Aspects of culture or group experiences that are addressed (e.g., faith/spiritual component, transportation
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Drahota, A., Wood, J. J., Sze, K. M., & Van Dyke, M. (2011). Effects of cognitive behavioral therapy on daily living skills in children with high-functioning autism and
CRITICALLY APPRAISED PAPER (CAP) Drahota, A., Wood, J. J., Sze, K. M., & Van Dyke, M. (2011). Effects of cognitive behavioral therapy on daily living skills in children with high-functioning autism and
Pathways to Inflated Responsibility Beliefs in Adolescent Obsessive-Compulsive Disorder: A Preliminary Investigation
 Behavioural and Cognitive Psychotherapy, 2011, 39, 229 234 First published online 23 November 2010 doi:10.1017/s1352465810000810 Pathways to Inflated Responsibility Beliefs in Adolescent Obsessive-Compulsive
Behavioural and Cognitive Psychotherapy, 2011, 39, 229 234 First published online 23 November 2010 doi:10.1017/s1352465810000810 Pathways to Inflated Responsibility Beliefs in Adolescent Obsessive-Compulsive
Intergenerational Transmission of Depression : Test of an Interpersonal Stress Model in a Community Sample
 Intergenerational Transmission of Depression : Test of an Interpersonal Stress Model in a Community Sample Constance Hammen 1, Josephine H. Shih 1, Patricia A. Brennan 2 1 Department of Psychology, University
Intergenerational Transmission of Depression : Test of an Interpersonal Stress Model in a Community Sample Constance Hammen 1, Josephine H. Shih 1, Patricia A. Brennan 2 1 Department of Psychology, University
CHAPTER 2 CRITERION VALIDITY OF AN ATTENTION- DEFICIT/HYPERACTIVITY DISORDER (ADHD) SCREENING LIST FOR SCREENING ADHD IN OLDER ADULTS AGED YEARS
 CHAPTER 2 CRITERION VALIDITY OF AN ATTENTION- DEFICIT/HYPERACTIVITY DISORDER (ADHD) SCREENING LIST FOR SCREENING ADHD IN OLDER ADULTS AGED 60 94 YEARS AM. J. GERIATR. PSYCHIATRY. 2013;21(7):631 635 DOI:
CHAPTER 2 CRITERION VALIDITY OF AN ATTENTION- DEFICIT/HYPERACTIVITY DISORDER (ADHD) SCREENING LIST FOR SCREENING ADHD IN OLDER ADULTS AGED 60 94 YEARS AM. J. GERIATR. PSYCHIATRY. 2013;21(7):631 635 DOI:
Cognitive Therapy for Suicide Prevention
 This program description was created for SAMHSA s National Registry for Evidence-based Programs and Practices (NREPP). Please note that SAMHSA has discontinued the NREPP program and these program descriptions
This program description was created for SAMHSA s National Registry for Evidence-based Programs and Practices (NREPP). Please note that SAMHSA has discontinued the NREPP program and these program descriptions
Training school personnel to implement a universal school-based prevention of depression program under real-world conditions
 Journal of School Psychology 42 (2004) 343 357 Training school personnel to implement a universal school-based prevention of depression program under real-world conditions Paul H. Harnett a, *, Mark R.
Journal of School Psychology 42 (2004) 343 357 Training school personnel to implement a universal school-based prevention of depression program under real-world conditions Paul H. Harnett a, *, Mark R.
Mental Health is a Family Matter: Treating Depressed Mothers of Kids with Psychiatric Disorders
 Mental Health is a Family Matter: Treating Depressed Mothers of Kids with Psychiatric Disorders Holly A. Swartz, MD Associate Professor of Psychiatry Stacy Martin, MSEd, NCC, LPC Research Coordinator Western
Mental Health is a Family Matter: Treating Depressed Mothers of Kids with Psychiatric Disorders Holly A. Swartz, MD Associate Professor of Psychiatry Stacy Martin, MSEd, NCC, LPC Research Coordinator Western
Dealing with Feelings: The Effectiveness of Cognitive Behavioural Group Treatment for Women in Secure Settings
 Behavioural and Cognitive Psychotherapy, 2011, 39, 243 247 First published online 30 November 2010 doi:10.1017/s1352465810000573 Dealing with Feelings: The Effectiveness of Cognitive Behavioural Group
Behavioural and Cognitive Psychotherapy, 2011, 39, 243 247 First published online 30 November 2010 doi:10.1017/s1352465810000573 Dealing with Feelings: The Effectiveness of Cognitive Behavioural Group
Research in child anxiety disorders indicates
 A Longitudinal Study of Developmental Differences in Universal Preventive Intervention for Child Anxiety Sally Lock and Paula M. Barrett Griffith University, Australia The present paper presents the results
A Longitudinal Study of Developmental Differences in Universal Preventive Intervention for Child Anxiety Sally Lock and Paula M. Barrett Griffith University, Australia The present paper presents the results
CLINICAL BOTTOM LINE Early Intervention for Children With Autism Implications for Occupational Therapy
 Dawson, G., Rogers, S., Munson, J., Smith, M., Winter, J., Greenson, J.,... Varley, J. (2010). Randomized, controlled trial of an intervention for toddlers with autism: The Early Start Denver Model. Pediatrics,
Dawson, G., Rogers, S., Munson, J., Smith, M., Winter, J., Greenson, J.,... Varley, J. (2010). Randomized, controlled trial of an intervention for toddlers with autism: The Early Start Denver Model. Pediatrics,
Comorbidity With Substance Abuse P a g e 1
 Comorbidity With Substance Abuse P a g e 1 Comorbidity With Substance Abuse Introduction This interesting session provided an overview of recent findings in the diagnosis and treatment of several psychiatric
Comorbidity With Substance Abuse P a g e 1 Comorbidity With Substance Abuse Introduction This interesting session provided an overview of recent findings in the diagnosis and treatment of several psychiatric
When the Evidence Says, Yes, No, and Maybe So
 CURRENT DIRECTIONS IN PSYCHOLOGICAL SCIENCE When the Evidence Says, Yes, No, and Maybe So Attending to and Interpreting Inconsistent Findings Among Evidence-Based Interventions Yale University ABSTRACT
CURRENT DIRECTIONS IN PSYCHOLOGICAL SCIENCE When the Evidence Says, Yes, No, and Maybe So Attending to and Interpreting Inconsistent Findings Among Evidence-Based Interventions Yale University ABSTRACT
SECTION 1. Children and Adolescents with Depressive Disorder: Summary of Findings. from the Literature and Clinical Consultation in Ontario
 SECTION 1 Children and Adolescents with Depressive Disorder: Summary of Findings from the Literature and Clinical Consultation in Ontario Children's Mental Health Ontario Children and Adolescents with
SECTION 1 Children and Adolescents with Depressive Disorder: Summary of Findings from the Literature and Clinical Consultation in Ontario Children's Mental Health Ontario Children and Adolescents with
Development of a New Fear of Hypoglycemia Scale: Preliminary Results
 Development of a New Fear of Hypoglycemia Scale: Preliminary Results Jodi L. Kamps, 1 PHD, Michael C. Roberts, 2 PHD, ABPP, and R. Enrique Varela, 3 PHD 1 Children s Hospital of New Orleans, 2 University
Development of a New Fear of Hypoglycemia Scale: Preliminary Results Jodi L. Kamps, 1 PHD, Michael C. Roberts, 2 PHD, ABPP, and R. Enrique Varela, 3 PHD 1 Children s Hospital of New Orleans, 2 University
Youthdale Treatment Centres
 Youthdale Treatment Centres 227 Victoria Street, Toronto, ON M5B 1T8 PEG 205 Final Report August 1, 2007 Stephens R and Guerra R."Longitudinal functional and behavioural outcomes of youth with neuropsychiatric
Youthdale Treatment Centres 227 Victoria Street, Toronto, ON M5B 1T8 PEG 205 Final Report August 1, 2007 Stephens R and Guerra R."Longitudinal functional and behavioural outcomes of youth with neuropsychiatric
Substance Abuse Group Therapy
 Substance Abuse Group Therapy Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Chapter 1 This natural propensity in humans makes group therapy a powerful
Substance Abuse Group Therapy Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Chapter 1 This natural propensity in humans makes group therapy a powerful
Using a structured treatment, Friends for Life, in Norwegian outpatient clinics: results from a pilot study
 The Cognitive Behaviour Therapist: page 1 of 10 doi:10.1017/s1754470x08000160 ORIGINAL RESEARCH Using a structured treatment, Friends for Life, in Norwegian outpatient clinics: results from a pilot study
The Cognitive Behaviour Therapist: page 1 of 10 doi:10.1017/s1754470x08000160 ORIGINAL RESEARCH Using a structured treatment, Friends for Life, in Norwegian outpatient clinics: results from a pilot study
QUALITY ASSESSMENT (QA) MANUAL
 QUALITY ASSESSMENT (QA) MANUAL RFP-NIH-NIMH 98-DS-0008 Treatment for Adolescents with Depression Study (TADS) Principal Investigator: John S. March, MD, MPH. Duke University Medical Center with Duke Clinical
QUALITY ASSESSMENT (QA) MANUAL RFP-NIH-NIMH 98-DS-0008 Treatment for Adolescents with Depression Study (TADS) Principal Investigator: John S. March, MD, MPH. Duke University Medical Center with Duke Clinical
Study plan Department of Psychology B.A. in Psychology
 Plan Number: 6 08 2015 Study plan Department of Psychology B.A. in Psychology Plan Content The study plan for B.A. in Psychology includes (132) hours as follows: Number Type of the First University Requirements
Plan Number: 6 08 2015 Study plan Department of Psychology B.A. in Psychology Plan Content The study plan for B.A. in Psychology includes (132) hours as follows: Number Type of the First University Requirements
SUBSTANCE ABUSE A Quick Reference Handout by Lindsey Long
 Substance Abuse 1 SUBSTANCE ABUSE A Quick Reference Handout by Lindsey Long Diagnostic Criteria (APA, 2004) Within a 12 month period, a pattern of substance use leading to significant impairment or distress
Substance Abuse 1 SUBSTANCE ABUSE A Quick Reference Handout by Lindsey Long Diagnostic Criteria (APA, 2004) Within a 12 month period, a pattern of substance use leading to significant impairment or distress
Dr. Delphine Collin-Vézina, Ph.D.
 Interview Presentation Tier 2 Canada Research Chair Position School of Social Work McGill University Dr. Delphine Collin-Vézina, Ph.D. Career Path Academic Studies and Research Realizations Applied research
Interview Presentation Tier 2 Canada Research Chair Position School of Social Work McGill University Dr. Delphine Collin-Vézina, Ph.D. Career Path Academic Studies and Research Realizations Applied research
Disruptive Mood Dysregulation Disorder
 Walden University ScholarWorks School of Counseling Publications College of Social and Behavioral Sciences 2015 Disruptive Mood Dysregulation Disorder Brandy L. Gilea Walden University Rachel M. O Neill
Walden University ScholarWorks School of Counseling Publications College of Social and Behavioral Sciences 2015 Disruptive Mood Dysregulation Disorder Brandy L. Gilea Walden University Rachel M. O Neill
Dynamic Deconstructive Psychotherapy
 This program description was created for SAMHSA s National Registry for Evidence-based Programs and Practices (NREPP). Please note that SAMHSA has discontinued the NREPP program and these program descriptions
This program description was created for SAMHSA s National Registry for Evidence-based Programs and Practices (NREPP). Please note that SAMHSA has discontinued the NREPP program and these program descriptions
Counseling Clients With Late-Life Depression
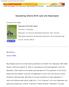 Counseling Clients With Late-Life Depression A review of the video Depression With Older Adults with Peter A. Lichtenberg Washington, DC: American Psychological Association, 2007. American Psychological
Counseling Clients With Late-Life Depression A review of the video Depression With Older Adults with Peter A. Lichtenberg Washington, DC: American Psychological Association, 2007. American Psychological
Critical Analysis of the Total Transformation Program (TTP) of Legacy Parenting for Helping Behavior Disordered Children and Teens
 Critical Analysis of the Total Transformation Program (TTP) of Legacy Parenting for Helping Behavior Disordered Children and Teens Patricia O. Quinn, MD, FAAP Director, National Center for Girls and Women
Critical Analysis of the Total Transformation Program (TTP) of Legacy Parenting for Helping Behavior Disordered Children and Teens Patricia O. Quinn, MD, FAAP Director, National Center for Girls and Women
Treating Depression in Disadvantaged Women: What is the evidence?
 Treating Depression in Disadvantaged Women: What is the evidence? Megan Dwight Johnson, MD MPH Associate Professor Medical Director, UWMC Inpatient Psychiatry Department of Psychiatry and Behavioral Sciences
Treating Depression in Disadvantaged Women: What is the evidence? Megan Dwight Johnson, MD MPH Associate Professor Medical Director, UWMC Inpatient Psychiatry Department of Psychiatry and Behavioral Sciences
Is Major Depressive Disorder or Dysthymia More Strongly Associated with Bulimia Nervosa?
 Is Major Depressive Disorder or Dysthymia More Strongly Associated with Bulimia Nervosa? Marisol Perez, 1 Thomas E. Joiner, Jr., 1 * and Peter M. Lewinsohn 2 1 Department of Psychology, Florida State University,
Is Major Depressive Disorder or Dysthymia More Strongly Associated with Bulimia Nervosa? Marisol Perez, 1 Thomas E. Joiner, Jr., 1 * and Peter M. Lewinsohn 2 1 Department of Psychology, Florida State University,
Pediatric Primary Care Mental Health Specialist Certification Exam. Detailed Content Outline
 Pediatric Primary Care Mental Health Specialist Certification Exam Detailed Content Outline Description of the Specialty The Pediatric Primary Care Mental Health Specialist (PMHS) builds upon the Advanced
Pediatric Primary Care Mental Health Specialist Certification Exam Detailed Content Outline Description of the Specialty The Pediatric Primary Care Mental Health Specialist (PMHS) builds upon the Advanced
Nova Scotia Board of Examiners in Psychology. Custody and Access Evaluation Guidelines
 Nova Scotia Board of Examiners in Psychology Custody and Access Evaluation Guidelines We are grateful to the Ontario Psychological Association and to the College of Alberta Psychologists for making their
Nova Scotia Board of Examiners in Psychology Custody and Access Evaluation Guidelines We are grateful to the Ontario Psychological Association and to the College of Alberta Psychologists for making their
A Pilot Study of Interpersonal Psychotherapy for Depressed Women with Breast Cancer
 A Pilot Study of Interpersonal Psychotherapy for Depressed Women with Breast Cancer CARLOS BLANCO, M.D., Ph.D.* JOHN C. MARKOWITZ, M.D.* DAWN L. HERSHMAN, M.D., M.S.# JON A. LEVENSON, M.D.* SHUAI WANG,
A Pilot Study of Interpersonal Psychotherapy for Depressed Women with Breast Cancer CARLOS BLANCO, M.D., Ph.D.* JOHN C. MARKOWITZ, M.D.* DAWN L. HERSHMAN, M.D., M.S.# JON A. LEVENSON, M.D.* SHUAI WANG,
Cognitive-Behavioral Assessment of Depression: Clinical Validation of the Automatic Thoughts Questionnaire
 Journal of Consulting and Clinical Psychology 1983, Vol. 51, No. 5, 721-725 Copyright 1983 by the American Psychological Association, Inc. Cognitive-Behavioral Assessment of Depression: Clinical Validation
Journal of Consulting and Clinical Psychology 1983, Vol. 51, No. 5, 721-725 Copyright 1983 by the American Psychological Association, Inc. Cognitive-Behavioral Assessment of Depression: Clinical Validation
PSYCHOLOGY (PSY) 440, 452, hours: elective courses based on the student s focus (applied or pre-doctoral)
 Psychology 115 (PSY) 435 DeGarmo Hall (309) 438-8651 Psychology.IllinoisState.edu Chairperson: J. Scott Jordan Programs Offered M.A./M.S. degrees in Clinical-Counseling Psychology; M.A./ M.S. degrees in
Psychology 115 (PSY) 435 DeGarmo Hall (309) 438-8651 Psychology.IllinoisState.edu Chairperson: J. Scott Jordan Programs Offered M.A./M.S. degrees in Clinical-Counseling Psychology; M.A./ M.S. degrees in
Students With Attention Deficit Hyperactivity Disorder
 On January 29, 2018 the Arizona State Board of Education approved a list of qualified professionals for identification of educational disabilities as developed by the Arizona Department of Education. Categories
On January 29, 2018 the Arizona State Board of Education approved a list of qualified professionals for identification of educational disabilities as developed by the Arizona Department of Education. Categories
CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION
 CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION What is the evidence that technology-based prevention interventions are an effective means of reducing substance use in adolescents? Fang, L., & Schinke,
CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION What is the evidence that technology-based prevention interventions are an effective means of reducing substance use in adolescents? Fang, L., & Schinke,
MARLYS STAUDT, MSW, Ph.D. EDUCATION
 MARLYS STAUDT, MSW, Ph.D. mstaudt@utk.edu (email) EDUCATION Ph.D, Washington University, George Warren Brown School of Social Work, St. Louis, Missouri. Dissertation: Use of Aftercare Services Following
MARLYS STAUDT, MSW, Ph.D. mstaudt@utk.edu (email) EDUCATION Ph.D, Washington University, George Warren Brown School of Social Work, St. Louis, Missouri. Dissertation: Use of Aftercare Services Following
Center for School Mental Health
 CSMH Updated 6.22.11 Summary of Free Assessment Measures Center for School Mental Health There are a number of assessment measures for clinicians that are available for free online. Below is a list of
CSMH Updated 6.22.11 Summary of Free Assessment Measures Center for School Mental Health There are a number of assessment measures for clinicians that are available for free online. Below is a list of
Introduction. PMDC Team
 Best Practices for Outpatient Program in Bipolar Disorder: Pediatric Mood Disorders Program at the University of Illinois at Chicago Julie A. Carbray PhD, PMHN-CNS Introduction five fold increase in diagnosis
Best Practices for Outpatient Program in Bipolar Disorder: Pediatric Mood Disorders Program at the University of Illinois at Chicago Julie A. Carbray PhD, PMHN-CNS Introduction five fold increase in diagnosis
Virginia Commonwealth University, b Harvard University and Judge Baker Children's Center, Online publication date: 23 April 2010
 This article was downloaded by: [Harvard Grad School of Education] On: 17 June 2010 Access details: Access Details: [subscription number 918775988] Publisher Routledge Informa Ltd Registered in England
This article was downloaded by: [Harvard Grad School of Education] On: 17 June 2010 Access details: Access Details: [subscription number 918775988] Publisher Routledge Informa Ltd Registered in England
Multi-Dimensional Family Therapy. Full Service Partnership Outcomes Report
 MHSA Multi-Dimensional Family Therapy Full Service Partnership Outcomes Report TABLE OF CONTENTS Enrollment 5 Discontinuance 5 Demographics 6-7 Length of Stay 8 Outcomes 9-11 Youth Outcome Questionnaire
MHSA Multi-Dimensional Family Therapy Full Service Partnership Outcomes Report TABLE OF CONTENTS Enrollment 5 Discontinuance 5 Demographics 6-7 Length of Stay 8 Outcomes 9-11 Youth Outcome Questionnaire
School-Based Prevention of Depressive Symptoms: A Randomized Controlled Study of the Effectiveness and Specificity of the Penn Resiliency Program
 Journal of Consulting and Clinical Psychology Copyright 2007 by the American Psychological Association 2007, Vol. 75, No. 1, 9 19 0022-006X/07/$12.00 DOI: 10.1037/0022-006X.75.1.9 School-Based Prevention
Journal of Consulting and Clinical Psychology Copyright 2007 by the American Psychological Association 2007, Vol. 75, No. 1, 9 19 0022-006X/07/$12.00 DOI: 10.1037/0022-006X.75.1.9 School-Based Prevention
Chapter 3. Psychometric Properties
 Chapter 3 Psychometric Properties Reliability The reliability of an assessment tool like the DECA-C is defined as, the consistency of scores obtained by the same person when reexamined with the same test
Chapter 3 Psychometric Properties Reliability The reliability of an assessment tool like the DECA-C is defined as, the consistency of scores obtained by the same person when reexamined with the same test
New Research in Depression and Anxiety
 New Research in Depression and Anxiety Robert Glassman Introduction Depression and anxiety are some of the most common disorders of childhood and adolescence. New research in these areas explores important
New Research in Depression and Anxiety Robert Glassman Introduction Depression and anxiety are some of the most common disorders of childhood and adolescence. New research in these areas explores important
Prospective Psychological Evaluation of Pediatric Heart and Heart Lung Recipients
 Prospective Psychological Evaluation of Pediatric Heart and Heart Lung Recipients Jo Wray, PHD, and Rosemary Radley-Smith, FRCP Department of Paediatrics, Harefield Hospital Objective To study psychological
Prospective Psychological Evaluation of Pediatric Heart and Heart Lung Recipients Jo Wray, PHD, and Rosemary Radley-Smith, FRCP Department of Paediatrics, Harefield Hospital Objective To study psychological
University of Groningen. Children of bipolar parents Wals, Marjolein
 University of Groningen Children of bipolar parents Wals, Marjolein IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Children of bipolar parents Wals, Marjolein IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
RESEARCH OBJECTIVE(S)
 Bearss, K., Johnson, C., Smith, T., Lecavalier, L., Swiezy, N., Aman, M.,... & Scahill, L. (2015). Effect of parent training vs parent education on behavioral problems in children with autism spectrum
Bearss, K., Johnson, C., Smith, T., Lecavalier, L., Swiezy, N., Aman, M.,... & Scahill, L. (2015). Effect of parent training vs parent education on behavioral problems in children with autism spectrum
FAMILY THERAPY OR FAMILY BASED INTERVENTION FOR CHILDREN AND ADOLESCENTS WHO SUFFER FROM PSYCHIATRIC DISORDERS
 Client HMSA: PQSR 2009 Measure Title FAMILY THERAPY OR FAMILY BASED INTERVENTION FOR CHILDREN AND ADOLESCENTS WHO SUFFER FROM PSYCHIATRIC DISORDERS Disease State Psychiatry Indicator Classification Disease
Client HMSA: PQSR 2009 Measure Title FAMILY THERAPY OR FAMILY BASED INTERVENTION FOR CHILDREN AND ADOLESCENTS WHO SUFFER FROM PSYCHIATRIC DISORDERS Disease State Psychiatry Indicator Classification Disease
Perinatal Depression: Current Management Issues
 Perinatal Depression: Current Management Issues Cindy-Lee Dennis, PhD Professor in Nursing and Psychiatry, University of Toronto Canada Research Chair in Perinatal Community Health Shirley Brown Chair
Perinatal Depression: Current Management Issues Cindy-Lee Dennis, PhD Professor in Nursing and Psychiatry, University of Toronto Canada Research Chair in Perinatal Community Health Shirley Brown Chair
The Anxiety Disorders Clinic for Children and Adolescents (TADCCA) at Aarhus University in Denmark ABSTRACT
 The Anxiety Disorder Clinic for Children and Adolescents (TADCCA) 115 The Anxiety Disorders Clinic for Children and Adolescents (TADCCA) at Aarhus University in Denmark MIKAEL THASTUM a,b a Department
The Anxiety Disorder Clinic for Children and Adolescents (TADCCA) 115 The Anxiety Disorders Clinic for Children and Adolescents (TADCCA) at Aarhus University in Denmark MIKAEL THASTUM a,b a Department
Sara Colalillo West Mall Vancouver, BC, V6T 1Z4 (604)
 Sara Colalillo 2136 West Mall Vancouver, BC, V6T 1Z4 (604) 360-2251 sara.colalillo@psych.ubc.ca EDUCATION Doctor of Philosophy, Clinical Psychology (2014 present), Vancouver, BC Dissertation: Associations
Sara Colalillo 2136 West Mall Vancouver, BC, V6T 1Z4 (604) 360-2251 sara.colalillo@psych.ubc.ca EDUCATION Doctor of Philosophy, Clinical Psychology (2014 present), Vancouver, BC Dissertation: Associations
Coping, Negative Cognitive Style and Depressive Symptoms in Children of Depressed Parents
 Cogn Ther Res (2013) 37:18 28 DOI 10.1007/s10608-012-9437-8 ORIGINAL ARTICLE Coping, Negative Cognitive Style and Depressive Symptoms in Children of Depressed Parents Jennifer P. Dunbar Laura McKee Aaron
Cogn Ther Res (2013) 37:18 28 DOI 10.1007/s10608-012-9437-8 ORIGINAL ARTICLE Coping, Negative Cognitive Style and Depressive Symptoms in Children of Depressed Parents Jennifer P. Dunbar Laura McKee Aaron
Life Events and Postpartum Depression in Tirana, Albania
 Life Events and Postpartum Depression in Tirana, Albania Daniela Meçe 1 Aleksander Moisiu University, Durres, Albania E-mail: danielamece@gmail.com Doi: 10.5901/mjss.2013.v4n4p311 Abstract The aim of this
Life Events and Postpartum Depression in Tirana, Albania Daniela Meçe 1 Aleksander Moisiu University, Durres, Albania E-mail: danielamece@gmail.com Doi: 10.5901/mjss.2013.v4n4p311 Abstract The aim of this
Family Group Cognitive Behavioral Preventive Intervention for Families of Depressed Parents: 18- and 24-Month Outcomes
 Journal of Consulting and Clinical Psychology 2011 American Psychological Association 2011, Vol. 79, No. 4, 488 499 0022-006X/11/$12.00 DOI: 10.1037/a0024254 Family Group Cognitive Behavioral Preventive
Journal of Consulting and Clinical Psychology 2011 American Psychological Association 2011, Vol. 79, No. 4, 488 499 0022-006X/11/$12.00 DOI: 10.1037/a0024254 Family Group Cognitive Behavioral Preventive
Examination of preventive interventions for families with depression: Evidence of change
 Development and Psychopathology, 9 (1997), 109 130 Copyright 1997 Cambridge University Press Printed in the United States of America Examination of preventive interventions for families with depression:
Development and Psychopathology, 9 (1997), 109 130 Copyright 1997 Cambridge University Press Printed in the United States of America Examination of preventive interventions for families with depression:
Avoidant Coping Moderates the Association between Anxiety and Physical Functioning in Patients with Chronic Heart Failure
 Avoidant Coping Moderates the Association between Anxiety and Physical Functioning in Patients with Chronic Heart Failure Eisenberg SA 1, Shen BJ 1, Singh K 1, Schwarz ER 2, Mallon SM 3 1 University of
Avoidant Coping Moderates the Association between Anxiety and Physical Functioning in Patients with Chronic Heart Failure Eisenberg SA 1, Shen BJ 1, Singh K 1, Schwarz ER 2, Mallon SM 3 1 University of
Diagnosis of Mental Disorders. Historical Background. Rise of the Nomenclatures. History and Clinical Assessment
 Diagnosis of Mental Disorders History and Clinical Assessment Historical Background For a long time confusion reigned. Every selfrespecting alienist, and certainly every professor, had his own classification.
Diagnosis of Mental Disorders History and Clinical Assessment Historical Background For a long time confusion reigned. Every selfrespecting alienist, and certainly every professor, had his own classification.
MHS PSYCHOPATHOLOGY IN COUNSELING
 MHS 6070 - PSYCHOPATHOLOGY IN COUNSELING This syllabus is a representative sample for this course. Specific information such as texts, assignments, and schedule may vary by semester. Catalog Description
MHS 6070 - PSYCHOPATHOLOGY IN COUNSELING This syllabus is a representative sample for this course. Specific information such as texts, assignments, and schedule may vary by semester. Catalog Description
Mental Health Rotation Educational Goals & Objectives
 Mental Health Rotation Educational Goals & Objectives Mental illness is prevalent in the general population and is commonly seen and treated in the office of the primary care provider. Educational experiences
Mental Health Rotation Educational Goals & Objectives Mental illness is prevalent in the general population and is commonly seen and treated in the office of the primary care provider. Educational experiences
Chronic and Episodic Stress in Children of Depressed Mothers
 Journal of Clinical Child & Adolescent Psychology, 45( 3), 270 278, 2016 Copyright # Taylor & Francis Group, LLC ISSN: 1537-4416 print=1537-4424 online DOI: 10.1080/15374416.2014.963859 Chronic and Episodic
Journal of Clinical Child & Adolescent Psychology, 45( 3), 270 278, 2016 Copyright # Taylor & Francis Group, LLC ISSN: 1537-4416 print=1537-4424 online DOI: 10.1080/15374416.2014.963859 Chronic and Episodic
New Jersey Department of Children and Families Policy Manual. Date: Chapter: A Health Services Subchapter: 1 Health Services
 New Jersey Department of Children and Families Policy Manual Manual: CP&P Child Protection and Permanency Effective Volume: V Health Date: Chapter: A Health Services 1-11-2017 Subchapter: 1 Health Services
New Jersey Department of Children and Families Policy Manual Manual: CP&P Child Protection and Permanency Effective Volume: V Health Date: Chapter: A Health Services 1-11-2017 Subchapter: 1 Health Services
Te Rau Hinengaro: The New Zealand Mental Health Survey
 Te Rau Hinengaro: The New Zealand Mental Health Survey Executive Summary Mark A Oakley Browne, J Elisabeth Wells, Kate M Scott Citation: Oakley Browne MA, Wells JE, Scott KM. 2006. Executive summary. In:
Te Rau Hinengaro: The New Zealand Mental Health Survey Executive Summary Mark A Oakley Browne, J Elisabeth Wells, Kate M Scott Citation: Oakley Browne MA, Wells JE, Scott KM. 2006. Executive summary. In:
Final Report of Activity February 21 st, 2006 to April 30 th, 2006 CHEO Grant 052
 Final Report of Activity February 21 st, 2006 to April 30 th, 2006 CHEO Grant 052 1- Title of Study: The prevalence of neuropsychiatric disorders in children and adolescents on an inpatient treatment unit:
Final Report of Activity February 21 st, 2006 to April 30 th, 2006 CHEO Grant 052 1- Title of Study: The prevalence of neuropsychiatric disorders in children and adolescents on an inpatient treatment unit:
JOHNNA L. KEEN, MSW, LCSW
 JOHNNA L. KEEN, MSW, LCSW EDUCATION Degree Concentration Year Institution M.S.W. Direct Practice 1994 Rutgers University B.A. Psychology 1988 Rowan University EXPERIENCE Year Position Location 2011-Present
JOHNNA L. KEEN, MSW, LCSW EDUCATION Degree Concentration Year Institution M.S.W. Direct Practice 1994 Rutgers University B.A. Psychology 1988 Rowan University EXPERIENCE Year Position Location 2011-Present
The DSM 5 and the Cultural Formulation Interview: What it is and how to implement it ANDRÉS HOYOS, MS, LCSW
 The DSM 5 and the Cultural Formulation Interview: What it is and how to implement it ANDRÉS HOYOS, MS, LCSW March 31, 2017 Objectives To understand the historical context and evolution of the cultural
The DSM 5 and the Cultural Formulation Interview: What it is and how to implement it ANDRÉS HOYOS, MS, LCSW March 31, 2017 Objectives To understand the historical context and evolution of the cultural
Incredible Years: Expected Effects and Recommendations for Monitoring Outcomes
 Incredible Years: Expected Effects and Recommendations for Monitoring Outcomes Submitted by Katie Rosanbalm, PhD Christina Christopoulos, PhD April, 2011 Bridging the gap between research and public policy
Incredible Years: Expected Effects and Recommendations for Monitoring Outcomes Submitted by Katie Rosanbalm, PhD Christina Christopoulos, PhD April, 2011 Bridging the gap between research and public policy
Hopelessness Predicts Suicide Ideation But Not Attempts: A 10-Year Longitudinal Study
 Suicide and Life-Threatening Behavior 1 2017 The American Association of Suicidology DOI: 10.1111/sltb.12328 Hopelessness Predicts Suicide Ideation But Not Attempts: A 10-Year Longitudinal Study TIANYOU
Suicide and Life-Threatening Behavior 1 2017 The American Association of Suicidology DOI: 10.1111/sltb.12328 Hopelessness Predicts Suicide Ideation But Not Attempts: A 10-Year Longitudinal Study TIANYOU
Parental Psychopathology & Childhood Treatment Response
 Parental Psychopathology & Childhood Treatment Response Mary A. Fristad, PhD, ABPP Professor, Psychiatry, Psychology & Human Nutrition The Ohio State University Division of Child & Adolescent Psychiatry
Parental Psychopathology & Childhood Treatment Response Mary A. Fristad, PhD, ABPP Professor, Psychiatry, Psychology & Human Nutrition The Ohio State University Division of Child & Adolescent Psychiatry
Accuracy of Interpersonal Stress Appraisals: Relationships between Mother and Adolescent. Daughter Depression. Cope Feurer
 Running Head: ACCURACY OF INTERPERSONAL APPRAISALS Accuracy of Interpersonal Stress Appraisals: Relationships between Mother and Adolescent Daughter Depression Cope Feurer University of North Carolina
Running Head: ACCURACY OF INTERPERSONAL APPRAISALS Accuracy of Interpersonal Stress Appraisals: Relationships between Mother and Adolescent Daughter Depression Cope Feurer University of North Carolina
DESIGN TYPE AND LEVEL OF EVIDENCE: Randomized controlled trial, Level I
 CRITICALLY APPRAISED PAPER (CAP) Hasan, A. A., Callaghan, P., & Lymn, J. S. (2015). Evaluation of the impact of a psychoeducational intervention for people diagnosed with schizophrenia and their primary
CRITICALLY APPRAISED PAPER (CAP) Hasan, A. A., Callaghan, P., & Lymn, J. S. (2015). Evaluation of the impact of a psychoeducational intervention for people diagnosed with schizophrenia and their primary
