Recognizing and Responding to Inadequately Treated Major Depressive Disorder (MDD)
|
|
|
- Catherine Charles
- 6 years ago
- Views:
Transcription
1 Objectives Recognizing and Responding to Inadequately Treated Major Depressive Disorder (MDD) Discuss the burden of MDD on the individual and society Explore the negative impact of residual symptoms Identify patient and treatment characteristics associated with a poor treatment response Discuss strategies to optimize pharmacotherapy Otsuka America Pharmaceutical, Inc., Rockville, MD 214 Otsuka America Pharmaceutical, Inc., Rockville, MD 3US14EBP436 July 214 advice or professional diagnosis. Users seeking medical advice should consult with their physician or other healthcare professional. Introduction 1. Burden of MDD 2. Residual symptoms in MDD 3. Response to Antidepressant Treatment in MDD 4. Evidence for the Treatment of Patients With MDD and Practical Guidelines 5. Summary Depression is the most common diagnosis among patients seen by psychiatrists in the US 1 MDD is a serious, chronic, disabling illness affecting more than 35 million people worldwide 2 MDD results in a substantial burden of disease to both the individual and society 3 Residual symptoms are common and cause significant psychosocial and occupational functional impairment 4,5 1. Duffy FF et al. Psychiatr Serv. 28;59(1): ; 2. World Health Organization. Fact Sheet on Depression. (212) 3. Kessler RC. Psychiatr Clin North Am. 212;35(1):1-14; 4. Romera I et al. Eur Psychiatry. 21;25(1):58-65; 5. Zimmerman M et al. Compr Psychiatry. 27;48(2): Lifetime Prevalence of MDD 25 Lifetime prevalence (%) BURDEN OF MDD Total Age (y) Overall lifetime prevalence of MDD across all ages is 16.6% 1. Kessler RC et al. Arch Gen Psychiatry. 25;62(6):
2 Link Between Depression and Other Illnesses High blood pressure Stroke Major 3% 24% Depression in the Past Year 7% 17% Asthma Heart 9% disease Diabetes When these rates were compared with subjects without reported mental illness in the past year, the differences in all chronic health conditions were statistically significantly different at the.5 level Accessed 29 April 214. Depression as a Risk Factor for Heart Disease: A Scientific Statement From the American Heart Association Based on a systematic literature review on depression and adverse medical outcomes after acute coronary syndrome (ACS) 53 studies and 4 meta-analyses met inclusion criteria The majority of relevant studies (21/32) suggest that depression is a risk factor for all-cause mortality after ACS. The majority of relevant studies (8/12) suggest that depression is a risk factor for cardiac mortality after ACS. The American Heart Association panel of authors suggests that depression should be elevated to the status of a risk factor for adverse medical outcomes in patients with ACS. 1. Lichtman JH et al. Circulation. 214;129. Epub ahead of print. Burden of Disease to the Individual Total Societal Costs (2) Physical MDD is a consistent predictor of the subsequent first onset of a variety of chronic physical disorders, including arthritis, asthma, cardiovascular disease, diabetes, chronic pain, and certain types of cancer Financial Incomes of people with MDD are substantially lower than those without depression Education MDD is associated with a 6% elevated risk of failure to complete secondary school than otherwise comparable youth 1. Kessler RC. Psychiatr Clin North Am. 212;35(1):1-14. Type of cost Dollars (in billions) Percentage of Total Cost/Case (in dollars) Total costs* ,118 Direct cost ,39 Inpatient ,127 Outpatient Pharmaceutical ,319 Suicide-related costs Workplace costs ,57 Absenteeism ,169 Presenteeism ,337 *Total costs = direct, suicide-related, and workplace costs. Note: Cost/case may not equal total cost divided by population estimates due to rounding. 1. reenberg PE et al. J Clin Psychiatry. 23;64(12): Outpatient Costs (1998/27) Lost Productive Time (hours per week) Dollars (in billions) Year Total outpatient treatment Mental health visits Psychotherapy Pharmaceutical Note: The 1998 expenditures have been inflated by the Consumer Price Index for medical care between 1998 and Marcus SC et al. Arch Gen Psychiatry. 21;67(12): Type of LPT MDD* Expected mean LPT in absence of depression Absenteeism 1.2 (.4).4 Presenteeism 7.2 (1.3) 1.1 Total LPT 8.4 (1.3) 1.5 Pain/weakness/fatigue 1. (1.2) 5.1 GI complaints 1.7 (1.5) 2. Panic/anxiety 9.3 (1.7) 4.1 Faintness/dizziness 8.9 (2.4) 4.5 Autonomic instability 9.5 (1.9) 6.5 Ears ringing/head or nose fullness 8.1 (1.2) 2.8 Sensory or nerve impairment 1. (1.4) 3.2 None 5.8 (3.7).8 GI, gastrointestinal; LPT, lost productive time. *Data reported as mean (standard error) hours per worker per week. 1. Stewart WF et al. JAMA. 23;289:
3 Suicide Risk Patients with MDD are roughly 2 times more likely to commit suicide than the general population Attempts at suicide among patients with MDD are highly associated with the occurrence and overall severity of MDD symptoms Increased time spent depressed is predictive of suicide attempts in this population 1. Sokero TP et al. Br J Psychiatry. 25;186: Suicidal Thoughts, Ideations, and Attempts Probability Ideation Attempts or completion Thoughts of death Day Note: Data based on 31 randomized controlled trials of fluoxetine and venlafaxine in patients with MDD. 1. Gibbons RD et al. Arch Gen Psychiatry. 212;69(6): Placebo Treated Incidence of Suicide Attempts Incidence (95% CI) of Suicide Attempts Major Depressive Episode Partial Remission Full Remission Over 5 years follow-up, risk of suicide attempts was 21-fold during a major depressive episode compared with full remission (N=332 vs 16 per 1, patient-years) Suicide Attempts in MDD: Depressionrelated Characteristics Characteristic Severity of depression at baseline, n (%) Mild Moderate Severe No suicide attempt (n=182) 11 (6) 99 (54) 72 (4) Suicide attempt (n=16) - 4 (25) 12 (75) P-value.2 Mean (SD) time to full remission, months 4. (4.7) 8.1 (7.5).2 Mean (SD) total time in depression, months 4.4 (4.7) 8.6 (7.1).2 Of the 41 discrete suicide attempts that occurred in the 16 patients over 18 months, 25 occurred during a major depressive episode, 12 during partial remission, and 4 during full remission The risk of a suicide attempt was almost 8-fold higher during a major depressive episode compared with a period of full remission (relative risk 7.54) Note: Data indicate the incidence rate per 1 patient-years based on Poisson distribution. 1. Holma KM et al. Am J Psychiatry. 21;167: SD, standard deviation. 1. Sokero TP et al. Br J Psychiatry. 25;186: Remission Is the Goal RESIDUAL SYMPTOMS IN MDD Remission Response Partial Response Nonresponse % Reduction in Score MADRS: total score 8 1 MADRS: 5% 1 HAM-D: 25% to 5% 2 HAM-D: < 25% 2 Remission also defined as attainment of a virtually asymptomatic status (17-item Hamilton Depression Rating Scale [HDRS] score 7) for at least 2 consecutive weeks Weisler R et al. CNS Spectrums. 29;14(6): ; 2. Nierenberg AA et al. J Clin Psychiatry. 21;62(suppl 16):5-9; 3. Frank E et al. Arch Gen Psychiatry. 1991;48: et al. 3
4 Prevalence and Types of Residual Symptoms Subjects (%) Distribution of Residual Symptoms in Full Responders N = 18 Common Unresolved or Residual MDD Symptoms Sleep disturbances (44%) Fatigue (38%) Diminished interest or pleasure (27%) Guilt ( 25%) Concentration difficulties ( 25%) Estimated frequencies 1 : Disturbances in mood ( 15%) Weight issues ( 15%) Disturbances in psychomotor activity ( 5%) Suicidal ideation ( 5%) Number of Residual Symptoms 1. Nierenberg AA et al. J Clin Psychiatry. 1999;6(4): Other residual/unresolved MDD symptoms include: core mood symptoms, 2 anxiety, 2,3 irritability and/or inner tension, 3 somatic symptoms (including pain), 2,4 sexual dysfunction, 3 and impairment of work and/or activities 2 1. Nierenberg AA et al. J Clin Psychiatry. 1999;6(4): Romera I et al. BMC Psychiatry. 213;13:51; 3. Trivedi MH et al. J Clin Psychiatry. 28;69(2): ; 4. Trivedi MH. J Clin Psychiatry. 24:6(Suppl 1) Residual Symptoms After Remission: STAR*D Symptom At least mild symptoms* (% of patients) At least moderate symptoms (% of patients) Weight increase Mid-nocturnal insomnia Increased appetite Sleep-onset insomnia Sad mood Hypersomnia Energy Concentration/decision making Weight decrease Early morning insomnia Restless Decreased appetite Involvement Outlook self Slowed down Suicidal ideation Defined as any 16-item Quick Inventory of Depressive Symptomatology, Self-Report (QIDS-SR16) item 1; Defined as any QIDS-SR16 item Nierenberg AA et al. Psychol Med. 21;4(1):41-5. Impact of Residual Symptoms on Patient Functioning and Outcomes Residual symptoms cause significant and often persistent psychosocial and occupational functional impairment 1,2,3 Patients being treated for MDD who have residual symptoms have an increased risk of depressive relapse 4,5 Author N Time Followed Relapsed Paykel months 76% of patients with residual symptoms 25% of patients with no residual symptoms Pintor years 91% of patients with partial remission 51% of patients with complete remission Patients with residual symptoms tend to have poor psychosocial functioning 6 1. Romera I et al. Eur Psychiatry. 21;25(1):58-65; 2. Zimmerman M et al. Compr Psychiatry. 27;48(2): ; 3. Fava M. J Psychopharm. 26;2(3):29-34; 4. Paykel ES et al. Psychol Med. 1995;25(6): ; 5. Pintor L et al. J Affect Disord. 24;82(2): ; 6. Romera I et al. BMC Psychiatry. 213;13:51. Predictors of Relapse and Recurrence in MDD Proportion Relapsing 1. Proportion of patients with ( ) and without ( ) residual symptoms relapsing after remission (log rank statistic = 17.43, df = 1, P <.1) Predictors of Relapse and Recurrence in MDD Survival Distribution Function A B C D Median Previous Weeks Recovery Episodes, n N Well, n Asymptomatic Asymptomatic Residual SSD Residual SSD Months to Relapse Weeks to First Prospective Relapse to Any Depressive Episode SSD, Subsyndromal Symptoms of Depression; Survival Distribution Function = Cumulative Proportion of Cases Surviving to Given Time Interval. 1. Paykel ES et al. Psychol Med. 1995;25: Judd LL et al. J Affect Discord. 1998;5:
5 Predictors of Relapse and Recurrence in MDD Predictors of Relapse and Recurrence in MDD Median Weeks to Relapse* Relapse in Patients With Partial and Complete Remission After 24 Months of Follow-up Type of Remission Relapse Yes No Partial Remission 48 (67.6%) 23 (32.4%) Complete Remission 17 (15.2%) 95 (84.8%) Improved Without Remission (n = 82) Remission (n = 155) *Relapse defined as onset of new major depressive episode. 1. Judd LL et al. J Affect Disord All proportions reflect percentage of relapse according to type of remission. 1. Pintor L et al. J Affect Disord. 23;73: Cumulative Proportion of Participants Without Relapse Comparison of STAR*D Participants Relapse During Follow-up Phase by Number of Acute Treatment Steps for STAR*D Participants Who Entered Follow-up Phase: In Remission Not In Remission 1. *Significant overall difference 1. *Significant overall difference among steps (x 2 = 23, df = 3, among steps (x 2 = 13, df = 3,.8 P <.1).8 P <.5) Step Step 2.4 Step 4 Step 3.4 Step Step 2 Step 4 Step Months of Follow-up 1. Rush AJ et al. Am J Psychiatry. 26;163: Impact of Residual Symptoms on Functioning Higher score indicates greater impairment 3. Score at Endpoint Nonresponse (n = 299) Remitted patients not significantly different from healthy controls on functioning levels at endpoint of 12-week treatment trial * Response (n = 122) Remission (n = 22) Healthy Controls (n = 482) SAS-SR Total SAS Work Composite Significant differences (P.5) for SAS work composite scores between response versus nonresponse (*), remission versus nonresponse ( ), remission versus response ( ). SAS-SR, Social Adjustment Scale-Self Report. 1. Miller IW et al. J Clin Psychiatry. 1998;59: Remission and Functioning Residual Symptoms and Functioning % of patients with normal functioning * 8 Normal functioning at endpoint (Month 6) was associated with a complete response at baseline (ie, after 3 months of acute antidepressant treatment). Note: Normal functioning defined as a Social and Occupational Functioning Assessment Scale score 8. *P < Romera I et al. Eur Psychiatry. 21;25: * 31 Baseline Month 3 Month 6 Complete remission Partial remission 77 * Residual Symptoms % of patients with residual symptoms Normal functioning at endpoint (Month 3) was associated with the absence of core mood symptoms (OR 8.7; 95% CI, ) and insomnia symptoms (OR 1.8; 95% CI, ) CI, confidence interval; OR, odds ratio. 1. Romera I et al. BMC Psychiatry. 213;13; 51. Remitters N=412 Non-remitters N=212 Core Insomnia Anxiety Somatic Moderate Pain 5
6 Remission as Goal of Treatment Significant Challenges Exist Surrounding the Treatment of MDD Only approximately 28% of patients treated for MDD achieve remission* following treatment with a single antidepressant 1 Partial response (indicated by a 25% to 49% reduction in depressive symptoms) is common 2 Patients not achieving a full remission typically suffer from troubling residual symptoms 2 Even patients considered to be fully remitted report experiencing at least one residual symptom 3,4 Ideally, the goal of treatment for MDD is for patients to achieve full remission 5 *Remission defined as a score of 5 on the Hamilton Depression Rating Scale. 1. Trivedi MH et al. Am J Psychiatry. 26;163:28-4; 2. Fava M. J Psychopharm. 26;2(3):29-34; 3. Paykel ES et al. Psychol Med. 1995;25(6): ; 4. Nierenberg AA et al. Psychol Med. 21;4(1):41-5; 5. Trivedi M. Psychiatry Weekly. May 21, 27. There is significant unmet need in the treatment of MDD: under-treatment due to misdiagnosis or underdiagnosis 1 low rates of adherence and persistence to therapy, 2 potentially influenced by: slow onset of action: antidepressants require 4 6 weeks to achieve full therapeutic effect 3 lack of efficacy: a significant proportion of patients fail to remit or only partially remit despite adequate therapy 4,5 poor tolerability: adverse events associated with pharmacologic agents may reduce adherence and persistence 3 low rates of guideline-concordant follow up 6 1. Nierenberg. Am J Manag Care. 21(suppl 11):353-66; 2. Cantrell, et al. Med Care. 26;44(4):3-33; 3. Gelenberg, et al. American Psychiatric Association. Practice guideline for the treatment of patients with major depressive disorder. 21; 4. Olchanski, et al. Clin Ther. 213;35(4):512-22; 5. Nierenberg, et al. Psychol Med. 21;4(1):41-5; 6. Chen, et al. Gen Hosp Psych. 21;32: Real-world Studies Show That <1/2 of Patients With MDD Receive an Adequate Course of Therapy Adherence to Therapy Is a Key Issue in Treating Patients With MDD A study of commercially insured people found that only 21.7% of those diagnosed with MDD received an adequate course of therapy 1 a : greater depressive symptom severity, functional impairment, duration of depression, and comorbidities were associated with higher probability of adequate treatment A national telephone survey found that only 25.3% of patients with a depressive disorder received an adequate course of therapy 2 b, c : patients with comorbid anxiety disorder were more likely to receive appropriate treatment a. Defined as: (1) 4 outpatient visits with a physician for pharmacotherapy, including either an antidepressant or mood stabilizer for 3 days; or (2) 8 outpatient visits for psychotherapy lasting 3 minutes each. b. Defined as receiving at least the minimum therapeutic dose of an antidepressant medication for 2months. c. Defined as 4 visits with a mental health specialist or PCP that included counseling for mental health problems. 1. Kessler, et al. JAMA. 23;289(23): ; 2. Young, et al. Arch Gen Psychiatry. 21;58(1): The association between prescriber specialty, follow-up visits, and proportion of patients to complete antidepressant regimen was estimated retrospectively using data from a large national health plan (N = 412) 1 : overall, less than half of patients completed the acute phase of therapy and approximately only 1/5 completed both the acute and continuation phase 1 These results suggest improved adherence to antidepressants is seen when proper provider support is in place and patients participate in frequent follow-up 47% Completed acute phase of therapy 1. Chen, et al. Gen Hosp Psych. 21;32: % Completed both acute and continuation phase of therapy The Majority of Patients Are Nonadherent Urgency to Treat Residual Symptoms APA Guidelines recommend that newly diagnosed patients remain on therapy for 6 9 months, yet over 4% of patients discontinue within 3 months 1 : studies show that 5% of MDD patients are adherent over the first 6 months of therapy, and 3% discontinue within the first month 2 premature discontinuation is associated with a 77% increase in the risk of a relapse 3 Physicians should check for nonadherence before assuming the drug is not effective Residual depressive symptoms are associated with an increased risk of relapse and poor psychosocial functioning 1,2 Adequate pharmacological intervention early in the disease is important to reduce the amount of the time in a depressed state, thereby decreasing the risk of suicide 1,2 1. Cantrell, et al. Med Care. 26;44(4):3-33; 2. Liu, et al. Clinicoecon Outcomes Res. 211;3:63-72; 3. Melfi, et al. Arch Gen Psychiatry. 1998;55(12): Fava M. J Psychopharmacology. 26;2(3): Sokero TP et al. Br J Psychiatry. 25;186:
7 Predicting Patient Response to Antidepressant Treatment Baseline Predictors RESPONSE TO ANTIDEPRESSANT TREATMENT IN MDD Sociodemographic Qualities Illness Characteristics Symptom Presentation Process Predictors Comorbid Conditions Change in Symptom Severity Treatmentrelated Side Effects Patient Adherence 1. Trivedi M. Psychiatry Weekly. May 21, 27. Baseline Characteristics Associated With a Poor Response to Antidepressant Treatment Baseline Characteristics Associated With a Better Response to Antidepressant Treatment Living alone Greater severity of depression Unemployed Lower income Higher neuroticism Anxious features Comorbid medical condition and/or personality disorder Longer duration of illness 1. Trivedi M. Psychiatry Weekly. May 21, 27. Married or cohabitating 1 Employment 2 Higher level of education 1 Negative family history of depression 1 Higher quality of life 1 Lower number of depressive episodes 1 Shorter illness histories 1 1. Trivedi M. Psychiatry Weekly. May 21, 27; 2. van der Lem R, et al. Soc Psychiatry Psychiatr Epidemiol. 213;48(6): The Delayed-onset Hypothesis of Antidepressant Treatment Initially believed that antidepressants take approximately 1 month for full antidepressant activity, with a delayed onset of action of at least 2 weeks 1 Methodological issues: Few prospective trials; majority of data based on post-hoc analyses, meta-analyses, and naturalistic studies 1 Randomized trials rely on significant drug/placebo differences in mean rating scale scores, which do not detect early significant symptom changes in individuals 1 Frequently used instruments such as the HAM-D are not very sensitive to treatment change 1 The weekly/bi-weekly measurements are too infrequent to detect early changes 1 The current cut-off point for a response of 5% improvement from baseline may be too strict to detect slight, but significant, early changes 1 A 2% cut-off may be more accurate, although somewhat arbitrarily determined 2 1. Möller HJ et al. Medicographia. 32;21: Ahn YM. Medicographia. 32;21:161. Early Improvement Is Common and Predicts Remission 1% 8% 6% 4% 2% Non-early improver (n = 212) % Early improvement Earlier onset of response before 2 weeks is common and highly predictive of later outcome 1-3 If no improvement is observed after 2 weeks, treatment should be adjusted or changed immediately 4 1. Henkel V et al. J Affect Disord. 28;115: ; 2. Nierenberg AA et al. Am J Psychiatry. 1995; 152:15-153; 3. Szegedi A et al. J Clin Psychiatry. 29;7: ; 4. Möller HJ et al. Medicographia. 32;21: Early improver (n = 493) Remitter (n = 347) Nonremitter (n = 358) Remission at discharge 7
8 Identifying the Inadequately Treated Patient Measurement tools for assessing severity of depression used during the first 2 4 weeks of antidepressant treatment can accurately predict the likelihood of a response or lack of response to treatment after a longer term (8 weeks) 1 Assessment tools to evaluate changes in symptom states during the first 4 weeks of treatment can also predict treatment response at 12 weeks 2 Dividing the HAM-D-17 into symptom clusters (mood, sleep/psychic anxiety, appetite, and somatic anxiety/weight) and evaluating change scores at 4 weeks correctly assigned up to 7% of patients as late responders or nonresponders at 12 weeks 1. Nirenberg AA et al. Am J Psychiatry. 2;157: ; 2. Trivedi MH et al. J Clin Psychiatry. 25;66(8): EVIDENCE FOR THE TREATMENT OF PATIENTS WITH MDD AND PRACTICAL GUIDELINES STAR*D Treatment Algorithm: Examining Different Treatment Strategies in a Real-world Setting Level 1 Initial treatment: SSRI STAR*D Results Symptom Remission a (% Patients) Level 1 1,2 SSRI (n = 3671) 28% Level 2 Switch to: SSRI, DNRI, SNRI, or cognitive therapy Augment with DNRI, 5-HT 1A partial agonist, or cognitive therapy Level SSRI (n = 238) DNRI (n = 239) SNRI (n = 25) Cognitive Therapy (n = 36) DNRI + SSRI (n = 279) 5HT-1A Partial Agonist + SSRI (n = 286) Cognitive Therapy + SSRI (n = 65) Level 3 Level 4 Level 2a Switch to: DNRI or SNRI* Switch to: NaSSA or TCA Augment with a mood stabilizer or thyroid hormone Switch to: MAOI or NaSSA combined with SNRI *Only for those who failed cognitive therapy; Only with DNRI, SSRI, or SNRI. DNRI, dopamine and norepinephrine reuptake inhibitor; MAOI, monoamine oxidase inhibitor; NaSSA, noradrenergic and specific serotonergic antidepressant; SNRI, serotonin norepinephrine reuptake inhibitor; SSRI, selective serotonin reuptake inhibitor; STAR*D, Sequenced Treatment Alternatives to Relieve Depression; TCA, tricyclic antidepressant. 1. Rush AJ et al. Am J Psychiatry. 23;16(2): % 21% 25% 25% 3% 3% 23% NaSSA TCA Mood Stabilizer Thyroid Hormone +ADT (n = 114) (n = 121) +ADT (n = 69) (n = 73) Level 3 6,7 12% 2% 16% 25% MAOI NaSSA + SNRI (n = 58) (n = 51) Level 4 8 7% 14% Note: Trial was not designed to directly compare switch or augmentation medication treatments. a Defined by exit score 7 on the HAM-D17. ADT, antidepressant therapy; HAM-D17, 17-item Hamilton Depression Rating Scale. 1. Rush AJ et al. Am J Psychiatry. 26;163: ; 5. Trivedi MH et al. N Engl J Med. 26;354(12): ; 2. Trivedi MH et al. Am J Psychiatry. 26;163(1):28-4; 6. Fava M et al. Am J Psychiatry. 26;163 (7): ; 7. Nierenberg AA et al. Am J Psychiatry. 26;163(9): ; 3. Rush AJ et al. N Engl J Med. 26;354(12): ; 8. McGrath PT et al. Am J Psychiatry. 26;163(9): Thase ME et al. Am J Psychiatry. 27;164(5): ; Combining Medications to Enhance Depression Outcomes (CO-MED) Study Design Randomly assigned (N=665) Acute Phase Combination SSRI + placebo (monotherapy) (n=224) DNRI + SSRI (n=221) SNRI + NaSSA (n=22) Continuation Phase Combination SSRI + placebo (monotherapy) (n=169) DNRI + SSRI (n=151) SNRI + NaSSA (n=159) CO-MED Results: Percentage of Patients Achieving Sustained Symptom Relief Patients Achieving Sustained Symptom Relief (%)* Monotherapy: SSRI + placebo (n=224) DNRI + SSRI (n=221) SNRI + NaSSA (n=22) Weeks (Acute Phase) 7 Months (Continuation Phase) DNRI, dopamine and norepinephrine reuptake inhibitor; NaSSA, noradrenergic and specific serotonergic antidepressant; SNRI, serotonin norepinephrine reuptake inhibitor; SSRI, selective serotonin reuptake inhibitor. 1. Rush AJ et al. Am J Psychiatry. 211;168(7): *Defined as scores of <8 and <6 on the 16-item Quick Inventory of Depressive Symptomatology Self-Report (QIDS-SR16) at the last two consecutive assessments. 1. Rush AJ et al. Am J Psychiatry. 211;168(7):
9 Revised APA Guidelines for the Acute-phase Treatment of MDD If no/partial response: Assess adherence and increase medication dosage or intensity of psychotherapy Start of medication trial and/or psychotherapy Initial weeks Full response: Continuation-phase treatment 4 8 weeks Reappraise treatment plan (Level I*) With medication: Optimize dose of current treatment (Level II*) Switch antidepressant (non-maoi: Level I; MAOI: Level II) Augment with a second agent (Level II/III) or psychotherapy (Level I) No / partial response ECT (Level I) With psychotherapy: Change intensity or type of psychotherapy (Level II) Combine psychotherapy with medication (Level II) *Level I = recommended with substantial clinical confidence; Level II = recommended with moderate clinical confidence; (Level III = may be recommended on the basis of individual circumstances). 1. Adapted from American Psychiatric Association. Practice Guideline for the Treatment of Patients With Major Depressive Disorder. 3rd ed. Arlington, VA: American Psychiatric Association; 21. Revised APA Guidelines: Augmentation Recommendations for No/Partial Response to Antidepressant Therapy Augmentation Options* Level of Clinical Confidence (I-III) Psychotherapy I Second Antidepressant Therapy Atypical Antipsychotic Thyroid Hormone Mood Stabilizer Anticonvulsant Psychostimulant Omega-3 Fatty Acid Folic Acid Anxiolytic or Sedative/Hypnotic *Classes of medication have been used in this table to replace some of the specific drug names. Includes non-maoi and MAOI antidepressants. Level I = recommended with substantial clinical confidence; Level II = recommended with moderate clinical confidence; (Level III = may be recommended on the basis of individual circumstances). 1. Adapted from American Psychiatric Association. Practice Guideline for the Treatment of Patients With Major Depressive Disorder. 3rd ed. Arlington, VA: American Psychiatric Association; 21. II III Treatment Guidelines: CANMAT CANMAT: Recommendations for Nonresponse or Incomplete Response to Initial ADT <2% improvement after 2 weeks of antidepressant treatment Change in treatment (eg, dose increase) 2% improvement after 4 6 weeks of antidepressant treatment Continue same treatment for 2 4 additional weeks before considering additional strategies First-line (Level 1 or Level 2 evidence, plus clinical support*) Switch to an agent with evidence for superiority SSRIs [Level 1] SNRIs [Level 1-2] Noradrenergic-serotonin modulator [Level 2] Add on another agent Mood stabilizer [Level 1] Atypical antipsychotics [Level 1-2] Second-line (Level 3 evidence or higher, plus clinical support*) Add on another agent DNRI [Level 2] Noradrenergic-serotonin modulator [Level 2] Atypical antipsychotic [Level 2] Thyroid hormone [Level 2] Switch to an agent with evidence for superiority, but with side effect limitations TCAs [Level 2] MAO inhibitors [Level 2] Third-line (Level 4 evidence or higher, plus clinical support*) Add on another agent Serotonin 5-HT 1A receptor partial agonist [Level 2] Psychostimulant [Level 2] Stimulants [Level 3] Atypical antipsychotic [Level 3] Level of Evidence Criteria 1=At least 2 RCTs with adequate sample sizes, preferably placebo controlled, and/or meta-analysis with narrow confidence intervals. 2=At least 1 RCT with adequate sample size and/or meta-analysis with wide confidence intervals. 3=Nonrandomized, controlled prospective studies or case series or high quality retrospective studies. 4=Expert opinion/consensus. 1. Lam RW et al. J Affect Disord. 29;117 (Suppl 1):S *Treatments with higher Levels of Evidence may be downgraded to lower Lines of Treatment due to clinical issues such as side effect or safety profile. Not all products in the therapeutic categories listed are indicated for adjunctive treatment in adult patients with MDD with an inadequate response to antidepressant therapy. Classes of medication have been used to replace some of the specific drug names. Levels of evidence and recommendations are represented for individual agents and should not be extrapolated to other agents in the same class. Please see the CANMAT Guidelines for further information on the specific drug recommendation options. 1. Lam RW et al. J Affective Disord. 29;117(suppl 1):S26-S43. International Consensus Statement on Optimizing Antidepressant Therapy Begin pharmacotherapy with an SSRI, SNRI, or DNRI After reaching a minimally effective dose, wait roughly 2 4 weeks to assess symptomatic improvement and tolerability before deciding how to optimize therapy: International Consensus Statement on Optimizing Antidepressant Therapy (cont) Assessment of symptomatic improvement and tolerability should occur every 2 weeks and at each assessment. Reasonable treatment options for partial or lack of efficacy include: Increase the Dose (for inadequate improvement but acceptable tolerability) Maintain the Current Dose (for adequate improvement and acceptable tolerability) Decrease the Dose (for adequate improvement but poor tolerability) Switch to a Different Agent (for inadequate improvement and poor tolerability) DNRI, dopamine and norepinephrine reuptake inhibitor; NaSSA, noradrenergic and specific serotonergic antidepressant; SNRI, serotonin norepinephrine reuptake inhibitor; SSRI, selective serotonin reuptake inhibitor. 1. Nutt DJ et al. J Clin Psychiatry. 21;71(suppl E1):e8. Modifying the antidepressant dose Switching to a different antidepressant DNRI, dopamine and norepinephrine reuptake inhibitor; NaSSA, noradrenergic and specific serotonergic antidepressant. 1. Nutt DJ et al. J Clin Psychiatry. 21;71(suppl E1):e8. Switching to augmentation/ combination strategies Augmentation/combination strategies include mood stabilizers, atypical antipsychotics, thyroid hormone, NaSSA, or DNRI 9
10 Nonpharmacologic Therapies for MD Categories of Care Care Strategies Psychotherapy Cognitive Behavioral Therapy (CBT) 1 Interpersonal Therapy 1 Group Therapy 1 Problem Solving Therapy 1 Future Directed Therapy (FDT) 2 Alternative Mind-Body Therapy Relaxation techniques (breathing exercises, meditation, etc.) 3 Yoga, tai chi, qigong 3 Family/Caregiver Involvement Family/caregiver involvement in the patient treatment plan facilitates day to day management of chronic difficulties of depression 4 Web-Based Intervention Deprexis (an interactive program that integrates multiple therapeutic approaches to depression) 5 1. American Psychiatric Association. Practice Guideline for the Treatment of Patients With Major Depressive Disorder. 3rd ed. Arlington, VA: American Psychiatric Association; 21; 2. Vilhauer JS et al. Innov Clin Neurosci. 213;1(3):12-2; 3. Bertisch SM et al. J Psychosom Res. 29;66(6): ; 4. Justin RG. Prim Care Companion. J Clin Psychiatry. 21;3(6):267; 5. Meyer B et al. J Med Internet Res. 29;11(2):e15. Challenges and Integrated Care Strategies for MDD Patient is feeling somewhat better following antidepressant treatment initiation but complains of lingering feelings of depressed mood Patient is feeling better with antidepressant therapy but complains of insomnia or aches and pains Patient is in obvious need of social support but is not interested in, or does not have access to, help (such as a support group) Patient complains that family members do not understand what they are going through and think family members are just angry and frustrated with them Patient is partially responding to antidepressant but expresses feelings of hopelessness and a general low satisfaction with life Measurement-based Care Summary Among practitioners, clinical treatment of depression is often associated with wide variations in dosage and duration of treatment 1 Measurement-based care was developed as a systematic approach to evaluate patient progress and eliminate variability in patient treatment among physicians In STAR*D, measurement-based care included the routine measurement of symptoms and side effects at each treatment visit; a treatment manual was used by treating physicians that detailed precisely when and how to modify medication regimens or doses based on results of assessments 2 A wide variety of physician-rated and patient-rated scales are currently available to evaluate patient symptoms, functioning ability, treatment progress, and side effects 3 For more information, please see: 1. Trivedi MH et al. Neuropsychopharmacology. 27;32(12): ; 2. Trivedi MH et al. Am J Psychiatry. 26;163(1):28-4; 3. Zimmerman M. Accessed October 1, 213. MDD is a serious, chronic, disabling illness affecting hundreds of millions of individuals worldwide Use of assessment tools and measurement-based care may facilitate patient-physician dialogue Residual symptoms are common and cause significant psychosocial and occupational functional impairment Over 9% of MDD patients experience residual symptoms during the course of treatment These patients are at increased risk for depressive relapse Patients with residual symptoms, relapse, and/or suicidality should receive increased vigilance and a more aggressive treatment approach (including combination therapy, psychotherapy, cognitive behavioral therapy, etc) 1
December 2014 MRC2.CORP.D.00011
 This program is paid for by Otsuka America Pharmaceutical, Inc. and Lundbeck, LLC. The speaker is a paid contractor of Otsuka America Pharmaceutical, Inc. advice or professional diagnosis. Users seeking
This program is paid for by Otsuka America Pharmaceutical, Inc. and Lundbeck, LLC. The speaker is a paid contractor of Otsuka America Pharmaceutical, Inc. advice or professional diagnosis. Users seeking
June 2015 MRC2.CORP.D.00030
 This program is paid for by Otsuka America Pharmaceutical, Inc. and Lundbeck, LLC. The speaker is a paid contractor of Otsuka America Pharmaceutical, Inc. June 2015 MRC2.CORP.D.00030 advice or professional
This program is paid for by Otsuka America Pharmaceutical, Inc. and Lundbeck, LLC. The speaker is a paid contractor of Otsuka America Pharmaceutical, Inc. June 2015 MRC2.CORP.D.00030 advice or professional
Measurement-based Scales in Major Depressive Disorder:
 This program is paid for by Otsuka Pharmaceutical Development & Commercialization, Inc. and Lundbeck, LLC. The speaker is a paid contractor of Otsuka Pharmaceutical Development and Commercialization, Inc.
This program is paid for by Otsuka Pharmaceutical Development & Commercialization, Inc. and Lundbeck, LLC. The speaker is a paid contractor of Otsuka Pharmaceutical Development and Commercialization, Inc.
Clinical Perspective on Conducting TRD Studies. Hans Eriksson, M.D., Ph.D., M.B.A. Chief Medical Specialist, H. Lundbeck A/S Valby, Denmark
 Clinical Perspective on Conducting TRD Studies Hans Eriksson, M.D., Ph.D., M.B.A. Chief Medical Specialist, H. Lundbeck A/S Valby, Denmark Overview of Presentation Treatment-Resistant Depression (TRD)
Clinical Perspective on Conducting TRD Studies Hans Eriksson, M.D., Ph.D., M.B.A. Chief Medical Specialist, H. Lundbeck A/S Valby, Denmark Overview of Presentation Treatment-Resistant Depression (TRD)
controls past MDD current MDD
 인제대학교서울백병원김원 * decreased appetite * decreased sleep * psychomotor agitaion * poor concentraion * psychomotor retardation * anhedonia depressed mood * low energy * guilt suicidal ideation * < 0.05 * total
인제대학교서울백병원김원 * decreased appetite * decreased sleep * psychomotor agitaion * poor concentraion * psychomotor retardation * anhedonia depressed mood * low energy * guilt suicidal ideation * < 0.05 * total
Guidelines MANAGEMENT OF MAJOR DEPRESSIVE DISORDER (MDD)
 MANAGEMENT OF MAJOR DEPRESSIVE DISORDER (MDD) Guidelines CH Lim, B Baizury, on behalf of Development Group Clinical Practice Guidelines Management of Major Depressive Disorder A. Introduction Major depressive
MANAGEMENT OF MAJOR DEPRESSIVE DISORDER (MDD) Guidelines CH Lim, B Baizury, on behalf of Development Group Clinical Practice Guidelines Management of Major Depressive Disorder A. Introduction Major depressive
KEY MESSAGES. It is often under-recognised and 30-50% of MDD cases in primary care and medical settings are not detected.
 KEY MESSAGES Major depressive disorder (MDD) is a significant mental health problem that disrupts a person s mood and affects his psychosocial and occupational functioning. It is often under-recognised
KEY MESSAGES Major depressive disorder (MDD) is a significant mental health problem that disrupts a person s mood and affects his psychosocial and occupational functioning. It is often under-recognised
Diagnosis & Management of Major Depression: A Review of What s Old and New. Cerrone Cohen, MD
 Diagnosis & Management of Major Depression: A Review of What s Old and New Cerrone Cohen, MD Why You re Treating So Much Mental Health 59% of Psychiatrists Are Over the Age of 55 AAMC 2014 Physician specialty
Diagnosis & Management of Major Depression: A Review of What s Old and New Cerrone Cohen, MD Why You re Treating So Much Mental Health 59% of Psychiatrists Are Over the Age of 55 AAMC 2014 Physician specialty
Augmentation and Combination Strategies in Antidepressants treatment of Depression
 Augmentation and Combination Strategies in Antidepressants treatment of Depression Byung-Joo Ham, M.D. Department of Psychiatry Korea University College of Medicine Background The response rates reported
Augmentation and Combination Strategies in Antidepressants treatment of Depression Byung-Joo Ham, M.D. Department of Psychiatry Korea University College of Medicine Background The response rates reported
Treating treatment resistant depression
 Treating treatment resistant depression These slides are the intellectual property of Ian Anderson and must not be reproduced Ian Anderson Neuroscience and Psychiatry Unit University of Manchester and
Treating treatment resistant depression These slides are the intellectual property of Ian Anderson and must not be reproduced Ian Anderson Neuroscience and Psychiatry Unit University of Manchester and
Suicide Risk and Melancholic Features of Major Depressive Disorder: A Diagnostic Imperative
 Suicide Risk and Melancholic Features of Major Depressive Disorder: A Diagnostic Imperative Robert I. Simon, M.D.* Suicide risk is increased in patients with Major Depressive Disorder with Melancholic
Suicide Risk and Melancholic Features of Major Depressive Disorder: A Diagnostic Imperative Robert I. Simon, M.D.* Suicide risk is increased in patients with Major Depressive Disorder with Melancholic
Adult Depression - Clinical Practice Guideline
 1 Adult Depression - Clinical Practice Guideline 05/2018 Diagnosis and Screening Diagnostic criteria o Please refer to Attachment A Screening o The United States Preventative Services Task Force (USPSTF)
1 Adult Depression - Clinical Practice Guideline 05/2018 Diagnosis and Screening Diagnostic criteria o Please refer to Attachment A Screening o The United States Preventative Services Task Force (USPSTF)
Depression and the Role of L-methylfolate
 Depression and the Role of L-methylfolate Depression is a chronic and recurrent disease affecting more than 18 million people in the United States, ranking it, along with heart disease, cancer and diabetes,
Depression and the Role of L-methylfolate Depression is a chronic and recurrent disease affecting more than 18 million people in the United States, ranking it, along with heart disease, cancer and diabetes,
Practice Matters: Screening and Referring Congregants with Major Depression
 International Journal of Faith Community Nursing Volume 1 Issue 3 Article 6 October 2015 Practice Matters: Screening and Referring Congregants with Major Depression Kim Link Western Kentucky University
International Journal of Faith Community Nursing Volume 1 Issue 3 Article 6 October 2015 Practice Matters: Screening and Referring Congregants with Major Depression Kim Link Western Kentucky University
Depression major depressive disorder. Some terms: Major Depressive Disorder: Major Depressive Disorder:
 Depression major depressive disorder Oldest recognized disorder: melancholia It is a positive and active anguish, a sort of psychical neuralgia wholly unknown to normal life. - William James "I am now
Depression major depressive disorder Oldest recognized disorder: melancholia It is a positive and active anguish, a sort of psychical neuralgia wholly unknown to normal life. - William James "I am now
Practice Guideline for the Treatment of Patients With Major Depressive Disorder: American Psychiatric Association
 Practice Guideline for the Treatment of Patients With Major Depressive Disorder: American Psychiatric Association Our clinical advisor adds updated advice on electroconvulsive therapy, transcranial magnetic
Practice Guideline for the Treatment of Patients With Major Depressive Disorder: American Psychiatric Association Our clinical advisor adds updated advice on electroconvulsive therapy, transcranial magnetic
Quality ID #411 (NQF 0711): Depression Remission at Six Months National Quality Strategy Domain: Effective Clinical Care
 Quality ID #411 (NQF 0711): Depression Remission at Six Months National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Outcome DESCRIPTION:
Quality ID #411 (NQF 0711): Depression Remission at Six Months National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Outcome DESCRIPTION:
Depression in the Medically Ill
 Mayo School of Continuous Professional Development Psychiatry in Medical Settings February 9 th, 2017 Depression in the Medically Ill David Katzelnick, M.D. Professor of Psychiatry, Mayo Clinic College
Mayo School of Continuous Professional Development Psychiatry in Medical Settings February 9 th, 2017 Depression in the Medically Ill David Katzelnick, M.D. Professor of Psychiatry, Mayo Clinic College
The Link Between Depression and Physical Symptoms
 The Link Between Depression and Physical Symptoms Madhukar H. Trivedi, M.D. Physical symptoms are common in depression, and, in fact, vague aches and pain are often the presenting symptoms of depression.
The Link Between Depression and Physical Symptoms Madhukar H. Trivedi, M.D. Physical symptoms are common in depression, and, in fact, vague aches and pain are often the presenting symptoms of depression.
Guilt Suicidality. Depression Co-Occurs with Medical Illness The rate of major depression among those with medical illness is significant.
 1-800-PSYCH If you are obsessive-compulsive, dial 1 repeatedly If you are paranoid-delusional, dial 2 and wait, your call is being traced If you are schizophrenic, a little voice will tell you what number
1-800-PSYCH If you are obsessive-compulsive, dial 1 repeatedly If you are paranoid-delusional, dial 2 and wait, your call is being traced If you are schizophrenic, a little voice will tell you what number
Graylands Hospital Drug Bulletin
 Graylands Hospital Drug Bulletin Antidepressant Combination and Augmentation Strategies North Metropolitan Area Mental Health Service October 2008 Vol 15 No.4 ISSN 1323-1251 Introduction Depression is
Graylands Hospital Drug Bulletin Antidepressant Combination and Augmentation Strategies North Metropolitan Area Mental Health Service October 2008 Vol 15 No.4 ISSN 1323-1251 Introduction Depression is
Adherence in A Schizophrenia:
 Understanding and Diagnosing Bipolar Disorder Treatment Promoting for Bipolar Treatment Disorder Adherence in A Schizophrenia: Resource for Providers Engagement Strategies for Health Care Providers, Case
Understanding and Diagnosing Bipolar Disorder Treatment Promoting for Bipolar Treatment Disorder Adherence in A Schizophrenia: Resource for Providers Engagement Strategies for Health Care Providers, Case
Supplementary Online Content
 Supplementary Online Content Lam RW, Levitt AJ, Levitan RD, et al. Efficacy of bright light treatment, fluoxetine, and the combination in patients with nonseasonal major depressive disorder: a randomized
Supplementary Online Content Lam RW, Levitt AJ, Levitan RD, et al. Efficacy of bright light treatment, fluoxetine, and the combination in patients with nonseasonal major depressive disorder: a randomized
2) Percentage of adult patients (aged 18 years or older) with a diagnosis of major depression or dysthymia and an
 Quality ID #370 (NQF 0710): Depression Remission at Twelve Months National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Prevention, Treatment, and Management of Mental Health
Quality ID #370 (NQF 0710): Depression Remission at Twelve Months National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Prevention, Treatment, and Management of Mental Health
How to treat depression with medication: Some rules of thumb
 How to treat depression with medication: Some rules of thumb R. Hamish McAllister-Williams, MD, PhD, FRCPsych Reader in Clinical Psychopharmacology Newcastle University Hon. Consultant Psychiatrist Regional
How to treat depression with medication: Some rules of thumb R. Hamish McAllister-Williams, MD, PhD, FRCPsych Reader in Clinical Psychopharmacology Newcastle University Hon. Consultant Psychiatrist Regional
Suitable dose and duration of fluvoxamine administration to treat depression
 PCN Psychiatric and Clinical Neurosciences 1323-13162003 Blackwell Science Pty Ltd 572April 2003 1098 Dose and duration of fluvoxamine S. Morishita and S. Arita 10.1046/j.1323-1316.2002.01098.x Original
PCN Psychiatric and Clinical Neurosciences 1323-13162003 Blackwell Science Pty Ltd 572April 2003 1098 Dose and duration of fluvoxamine S. Morishita and S. Arita 10.1046/j.1323-1316.2002.01098.x Original
Objectives. Objectives. A practice review. 02-Nov-16 MAJOR DEPRESSIVE DISORDER: NEW DEVELOPMENTS AND PRACTICAL IMPLICATIONS
 MAJOR DEPRESSIVE DISORDER: NEW DEVELOPMENTS AND PRACTICAL IMPLICATIONS Jon-Paul Khoo What is treatment resistance really? Database review 328 consecutive non-remitted MDD patients referred for private
MAJOR DEPRESSIVE DISORDER: NEW DEVELOPMENTS AND PRACTICAL IMPLICATIONS Jon-Paul Khoo What is treatment resistance really? Database review 328 consecutive non-remitted MDD patients referred for private
Clinical Significance of Anxiety in Depressed Patients Selecting an Antidepressant
 The Clinical Significance of Anxiety Disorders and the DSM-5 Anxious Distress Specifier in Depressed Patients Clinical Significance of Anxiety in Depressed Patients Selecting an Antidepressant Rhode Island
The Clinical Significance of Anxiety Disorders and the DSM-5 Anxious Distress Specifier in Depressed Patients Clinical Significance of Anxiety in Depressed Patients Selecting an Antidepressant Rhode Island
PRACTICAL MANAGEMENT OF DEPRESSION IN OLDER ADULTS. Lee A. Jennings, MD MSHS Assistant Professor Division of Geriatrics, UCLA
 CASE #1 PRACTICAL MANAGEMENT OF DEPRESSION IN OLDER ADULTS Lee A. Jennings, MD MSHS Assistant Professor Division of Geriatrics, UCLA OBJECTIVES Epidemiology Presentation in older adults Assessment Treatment
CASE #1 PRACTICAL MANAGEMENT OF DEPRESSION IN OLDER ADULTS Lee A. Jennings, MD MSHS Assistant Professor Division of Geriatrics, UCLA OBJECTIVES Epidemiology Presentation in older adults Assessment Treatment
Treatment strategies in major depression What to use when?
 Treatment strategies in major depression What to use when? Michael Bauer, MD, PhD Professor and Chair of Psychiatry University Hospital Carl Gustav Carus Technische Universität Dresden Germany First-line
Treatment strategies in major depression What to use when? Michael Bauer, MD, PhD Professor and Chair of Psychiatry University Hospital Carl Gustav Carus Technische Universität Dresden Germany First-line
Effective Date: 5/28/2014 Version: 2.0 (Revised: 10/12/2015) Approval By: CCC Clinical Delivery Steering Planned Review Date: (04/47/2017)
 Protocol Title: Depression & Generalized Anxiety Disorder Effective Date: 5/28/2014 Version: 2.0 (Revised: 10/12/2015) Approval By: CCC Clinical Delivery Steering Planned Review Date: (04/47/2017) Group
Protocol Title: Depression & Generalized Anxiety Disorder Effective Date: 5/28/2014 Version: 2.0 (Revised: 10/12/2015) Approval By: CCC Clinical Delivery Steering Planned Review Date: (04/47/2017) Group
Antidepressant Utilization in Bipolar Disorder: What Is the Evidence?
 Antidepressant Utilization in Bipolar Disorder: What Is the Evidence? 2018 Otsuka Pharmaceutical Development & Commercialization, Inc., Rockville, MD Lundbeck, LLC March 2018 MRC2.CORP.D.00336 Today s
Antidepressant Utilization in Bipolar Disorder: What Is the Evidence? 2018 Otsuka Pharmaceutical Development & Commercialization, Inc., Rockville, MD Lundbeck, LLC March 2018 MRC2.CORP.D.00336 Today s
Pharmacy Prior Authorization GMH/SA and Non-Title 19/21 SMI Non-Formulary and Prior Authorization Guidelines
 Non-Formulary Behavioral Health Medications ADHD medications for children under The patient must have a diagnosis for which the requested medication is: o Approved based on FDA indication and limits; OR
Non-Formulary Behavioral Health Medications ADHD medications for children under The patient must have a diagnosis for which the requested medication is: o Approved based on FDA indication and limits; OR
Some newer, investigational approaches to treating refractory major depression are being used.
 CREATED EXCLUSIVELY FOR FINANCIAL PROFESSIONALS Rx FOR SUCCESS Depression and Anxiety Disorders Mood and anxiety disorders are common, and the mortality risk is due primarily to suicide, cardiovascular
CREATED EXCLUSIVELY FOR FINANCIAL PROFESSIONALS Rx FOR SUCCESS Depression and Anxiety Disorders Mood and anxiety disorders are common, and the mortality risk is due primarily to suicide, cardiovascular
Multistate Outcome Analysis of Treatment MOAT
 Multistate Outcome Analysis of Treatment MOAT Charles L. Bowden, M.D. Presented with Fond Memories of an Outstanding Statistician and Investigative Scientist Andy Leon Design contributors to low generalizability
Multistate Outcome Analysis of Treatment MOAT Charles L. Bowden, M.D. Presented with Fond Memories of an Outstanding Statistician and Investigative Scientist Andy Leon Design contributors to low generalizability
Setting ambitious goals for patients with depression with a focus on functional recovery
 Setting ambitious goals for patients with depression with a focus on functional recovery The role of the overlooked cognitive symptoms in the treatment of depression Dr Andreas Papadopoulos Locum Consultant
Setting ambitious goals for patients with depression with a focus on functional recovery The role of the overlooked cognitive symptoms in the treatment of depression Dr Andreas Papadopoulos Locum Consultant
Primary Care: Referring to Psychiatry
 Primary Care: Referring to Psychiatry Carol Capitano, PhD, APRN-BC Assistant Professor, Clinical Educator University of New Mexico College of Nursing University of New Mexico Psychiatric Center Objectives
Primary Care: Referring to Psychiatry Carol Capitano, PhD, APRN-BC Assistant Professor, Clinical Educator University of New Mexico College of Nursing University of New Mexico Psychiatric Center Objectives
Clinical Use of Ketamine in Psychiatry
 Clinical Use of Ketamine in Psychiatry C. Sophia Albott, MD, MA Assistant Professor Department of Psychiatry and Behavioral Sciences University of Minnesota Medical School November 17, 2018 Disclosure
Clinical Use of Ketamine in Psychiatry C. Sophia Albott, MD, MA Assistant Professor Department of Psychiatry and Behavioral Sciences University of Minnesota Medical School November 17, 2018 Disclosure
Clinical Guideline for the Management of Bipolar Disorder in Adults
 Clinical Guideline for the Management of Bipolar Disorder in Adults Goal: To improve the quality of life of adults with bipolar disorder Identification and Treatment of Bipolar Disorder Criteria for Diagnosis:
Clinical Guideline for the Management of Bipolar Disorder in Adults Goal: To improve the quality of life of adults with bipolar disorder Identification and Treatment of Bipolar Disorder Criteria for Diagnosis:
Department of Psychiatry & Behavioral Sciences. University of Texas Medical Branch
 Depression in Childhood: Advances and Controversies in Treatment Karen Dineen Wagner, MD, PhD Marie B. Gale Centennial Professor & Vice Chair Department of Psychiatry & Behavioral Sciences Director, Division
Depression in Childhood: Advances and Controversies in Treatment Karen Dineen Wagner, MD, PhD Marie B. Gale Centennial Professor & Vice Chair Department of Psychiatry & Behavioral Sciences Director, Division
Is Depression management getting you down? G. Michael Allan Director Programs and Practice Support, CFPC Professor, Family Med, U of A
 Is Depression management getting you down? G. Michael Allan Director Programs and Practice Support, CFPC Professor, Family Med, U of A Faculty/Presenter Disclosures Faculty: Mike Allan Salary: College
Is Depression management getting you down? G. Michael Allan Director Programs and Practice Support, CFPC Professor, Family Med, U of A Faculty/Presenter Disclosures Faculty: Mike Allan Salary: College
Consultant Pharmacist Approach to Major Depressive Disorder
 Consultant Pharmacist Approach to Major Depressive Disorder ALAN OBRINGER RPH, CPH, CGP PRESIDENT/OWNER GUARDIAN PHARMACY OF ORLANDO Objectives What is Depression? Discuss the epidemiology of depression
Consultant Pharmacist Approach to Major Depressive Disorder ALAN OBRINGER RPH, CPH, CGP PRESIDENT/OWNER GUARDIAN PHARMACY OF ORLANDO Objectives What is Depression? Discuss the epidemiology of depression
Consultant Pharmacist Approach to Major Depressive Disorder ALAN OBRINGER RPH, CPH, CGP PRESIDENT/OWNER GUARDIAN PHARMACY OF ORLANDO
 Consultant Pharmacist Approach to Major Depressive Disorder ALAN OBRINGER RPH, CPH, CGP PRESIDENT/OWNER GUARDIAN PHARMACY OF ORLANDO Objectives What is Depression? Discuss the epidemiology of depression
Consultant Pharmacist Approach to Major Depressive Disorder ALAN OBRINGER RPH, CPH, CGP PRESIDENT/OWNER GUARDIAN PHARMACY OF ORLANDO Objectives What is Depression? Discuss the epidemiology of depression
Antidepressants. Dr Malek Zihlif
 Antidepressants The optimal use of antidepressant required a clear understanding of their mechanism of action, pharmacokinetics, potential drug interaction and the deferential diagnosis of psychiatric
Antidepressants The optimal use of antidepressant required a clear understanding of their mechanism of action, pharmacokinetics, potential drug interaction and the deferential diagnosis of psychiatric
8. DEPRESSION 1. Eve A. Kerr, M.D., M.P.H. and Kenneth A. Clark, M.D., M.P.H.
 8. DEPRESSION 1 Eve A. Kerr, M.D., M.P.H. and Kenneth A. Clark, M.D., M.P.H. We relied on the following sources to construct quality indicators for depression: the AHCPR Clinical Practice Guideline in
8. DEPRESSION 1 Eve A. Kerr, M.D., M.P.H. and Kenneth A. Clark, M.D., M.P.H. We relied on the following sources to construct quality indicators for depression: the AHCPR Clinical Practice Guideline in
DEPRESSION Eve A. Kerr, M.D., M.P.H.
 - 111-8. DEPRESSION Eve A. Kerr, M.D., M.P.H. We relied on the following sources to construct quality indicators for depression in adult women: the AHCPR Clinical Practice in Primary Care (Volumes 1 and
- 111-8. DEPRESSION Eve A. Kerr, M.D., M.P.H. We relied on the following sources to construct quality indicators for depression in adult women: the AHCPR Clinical Practice in Primary Care (Volumes 1 and
Depression. Content. Depression is common. Depression Facts. Depression kills. Depression attacks young people
 Content Depression Dr. Anna Lam Associate Consultant Department of Psychiatry, Queen Mary Hospital Honorary Clinical Assistant Professor Li Ka Shing Faculty of Medicine, The University of Hong Kong 1.
Content Depression Dr. Anna Lam Associate Consultant Department of Psychiatry, Queen Mary Hospital Honorary Clinical Assistant Professor Li Ka Shing Faculty of Medicine, The University of Hong Kong 1.
Is Depression management getting you down? G. Michael Allan Director Programs and Practice Support, CFPC Professor, Family Med, U of A
 Is Depression management getting you down? G. Michael Allan Director Programs and Practice Support, CFPC Professor, Family Med, U of A Faculty/Presenter Disclosures Faculty: Mike Allan Salary: College
Is Depression management getting you down? G. Michael Allan Director Programs and Practice Support, CFPC Professor, Family Med, U of A Faculty/Presenter Disclosures Faculty: Mike Allan Salary: College
1 1 Evidence-based pharmacotherapy of major depressive disorder. Michael J. Ostacher, Jeffrey Huffman, Roy Perlis, and Andrew A.
 1 1 Evidence-based pharmacotherapy of major depressive disorder Michael J. Ostacher, Jeffrey Huffman, Roy Perlis, and Andrew A. Nierenberg Massachusetts General Hospital and Harvard University, Boston,
1 1 Evidence-based pharmacotherapy of major depressive disorder Michael J. Ostacher, Jeffrey Huffman, Roy Perlis, and Andrew A. Nierenberg Massachusetts General Hospital and Harvard University, Boston,
Despite its prevalence in the managed. A Step Therapy Algorithm for the Treatment and Management of Chronic Depression REPORT
 REPORT A Step Therapy Algorithm for the Treatment and Management of Chronic Depression Jeffrey D. Dunn, PharmD, MBA; and John G. Tierney, MD Abstract Depression is a chronic and progressive condition that,
REPORT A Step Therapy Algorithm for the Treatment and Management of Chronic Depression Jeffrey D. Dunn, PharmD, MBA; and John G. Tierney, MD Abstract Depression is a chronic and progressive condition that,
ers_practice_parameter.pdf
 These Guidelines were based in part from on following: Treatment of Patients With Major Depressive Disorder from the American Psychiatric Association (APA) that was amended by the following Guideline Watch
These Guidelines were based in part from on following: Treatment of Patients With Major Depressive Disorder from the American Psychiatric Association (APA) that was amended by the following Guideline Watch
Clinical Perspective on Conducting Trials in Major Depressive Disorder. Justine M. Kent, M.D. Senior Director, Janssen R&D
 Clinical Perspective on Conducting Trials in Major Depressive Disorder Justine M. Kent, M.D. Senior Director, Janssen R&D Utility of the partial response construct In general, published clinical guidelines
Clinical Perspective on Conducting Trials in Major Depressive Disorder Justine M. Kent, M.D. Senior Director, Janssen R&D Utility of the partial response construct In general, published clinical guidelines
3. Depressione unipolare
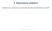 3. Depressione unipolare Depressione unipolare con mancata risposta al trattamento con SSRI Question: Should switching from SSRIs to another antidepressant class vs switching within class (SSRIs) be used
3. Depressione unipolare Depressione unipolare con mancata risposta al trattamento con SSRI Question: Should switching from SSRIs to another antidepressant class vs switching within class (SSRIs) be used
DEPRESSION 1 Eve Kerr, M.D., M.P.H.
 - 141-7. DEPRESSION 1 Eve Kerr, M.D., M.P.H. We relied on the following sources to construct quality indicators for depression in adult women: the AHCPR Clinical Practice in Primary Care (Volumes 1 and
- 141-7. DEPRESSION 1 Eve Kerr, M.D., M.P.H. We relied on the following sources to construct quality indicators for depression in adult women: the AHCPR Clinical Practice in Primary Care (Volumes 1 and
The Pharmacological Management of Bipolar Disorder: An Update
 Psychobiology Research Group The Pharmacological Management of Bipolar Disorder: An Update R. Hamish McAllister-Williams, MD, PhD, FRCPsych Reader in Clinical Psychopharmacology Newcastle University Hon.
Psychobiology Research Group The Pharmacological Management of Bipolar Disorder: An Update R. Hamish McAllister-Williams, MD, PhD, FRCPsych Reader in Clinical Psychopharmacology Newcastle University Hon.
Drug Surveillance 1.
 22 * * 3 1 2 3. 4 Drug Surveillance 1. 6-9 2 3 DSM-IV Anxious depression 4 Drug Surveillance GPRD A. (TCA) (SSRI) (SNRI) 20-77 - SSRI 1999 SNRI 2000 5 56 80 SSRI 1 1999 2005 2 2005 92.4, 2010 1999 3 1
22 * * 3 1 2 3. 4 Drug Surveillance 1. 6-9 2 3 DSM-IV Anxious depression 4 Drug Surveillance GPRD A. (TCA) (SSRI) (SNRI) 20-77 - SSRI 1999 SNRI 2000 5 56 80 SSRI 1 1999 2005 2 2005 92.4, 2010 1999 3 1
Depression in adults: treatment and management
 1 2 3 4 Depression in adults: treatment and management 5 6 7 8 Appendix V3: recommendations that have been deleted of changed from 2009 guideline Depression in adults: Appendix V3 1 of 22 1 Recommendations
1 2 3 4 Depression in adults: treatment and management 5 6 7 8 Appendix V3: recommendations that have been deleted of changed from 2009 guideline Depression in adults: Appendix V3 1 of 22 1 Recommendations
Effective Health Care
 Number 7 Effective Health Care Comparative Effectiveness of Second- Generation Antidepressants in the Pharmacologic Treatment of Adult Depression Executive Summary Background Depressive disorders such
Number 7 Effective Health Care Comparative Effectiveness of Second- Generation Antidepressants in the Pharmacologic Treatment of Adult Depression Executive Summary Background Depressive disorders such
Outline. Understanding Placebo Response in Psychiatry: The Good, The Bad, and The Ugly. Definitions
 Outline Understanding Placebo Response in Psychiatry: The Good, The Bad, and The Ugly Michael E. Thase, MD Professor of Psychiatry Perelman School of Medicine University of Pennsylvania and Philadelphia
Outline Understanding Placebo Response in Psychiatry: The Good, The Bad, and The Ugly Michael E. Thase, MD Professor of Psychiatry Perelman School of Medicine University of Pennsylvania and Philadelphia
Disclosure Information
 Disclosure Information I have no financial relationships to disclose. I will discuss the off label use of several depression and anxiety medications in pediatric population Pediatric Depression & Anxiety
Disclosure Information I have no financial relationships to disclose. I will discuss the off label use of several depression and anxiety medications in pediatric population Pediatric Depression & Anxiety
Depression in Late Life
 Depression in Late Life Robert Madan MD FRCPC Geriatric Psychiatrist Key Learnings Robert Madan MD FRCPC Key Learnings By the end of the session, participants will be able to List the symptoms of depression
Depression in Late Life Robert Madan MD FRCPC Geriatric Psychiatrist Key Learnings Robert Madan MD FRCPC Key Learnings By the end of the session, participants will be able to List the symptoms of depression
Depression & Anxiety in Adolescents
 Depression & Anxiety in Adolescents Objectives 1) Review diagnosis of anxiety and depression in adolescents 2) Provide overview of evidence-based treatment options 3) Increase provider comfort level with
Depression & Anxiety in Adolescents Objectives 1) Review diagnosis of anxiety and depression in adolescents 2) Provide overview of evidence-based treatment options 3) Increase provider comfort level with
The Role of the Family Physician in Managing Depression
 Middle East Journal of Family Medicine, 2004; Vol. 2 (2) The Role of the Family Physician in Managing Depression 1-Homoud F. Al-Zuabi, BSc.MBBCh.RCGP. Head of Ferdous Health Center Farwania Primary Health
Middle East Journal of Family Medicine, 2004; Vol. 2 (2) The Role of the Family Physician in Managing Depression 1-Homoud F. Al-Zuabi, BSc.MBBCh.RCGP. Head of Ferdous Health Center Farwania Primary Health
Taking Care: Child and Youth Mental Health TREATMENT OPTIONS
 Taking Care: Child and Youth Mental Health TREATMENT OPTIONS Open Learning Agency 2004 TREATMENT OPTIONS With appropriate treatment, more than 80% of people with depression get full relief from their symptoms
Taking Care: Child and Youth Mental Health TREATMENT OPTIONS Open Learning Agency 2004 TREATMENT OPTIONS With appropriate treatment, more than 80% of people with depression get full relief from their symptoms
Suboptimal Response in Psychotic & Mood Disorders: Causes, Consequences, and Management Strategies
 Suboptimal Response in Psychotic & Mood Disorders: Causes, Consequences, and Management Strategies Henry A. Nasrallah, MD Sydney W. Souers Professor and Chair, Department of Psychiatry, Saint Louis University,
Suboptimal Response in Psychotic & Mood Disorders: Causes, Consequences, and Management Strategies Henry A. Nasrallah, MD Sydney W. Souers Professor and Chair, Department of Psychiatry, Saint Louis University,
Start Low, Go Slow but Treat to Target
 Start Low, Go Slow but Treat to Target Pharmacotherapy for Depression, Anxiety and At-Risk Alcohol Use in Late Life September 29, 2014 Audio and Control Panel instruction On the phone? Raise your hand
Start Low, Go Slow but Treat to Target Pharmacotherapy for Depression, Anxiety and At-Risk Alcohol Use in Late Life September 29, 2014 Audio and Control Panel instruction On the phone? Raise your hand
Summary of guideline for the. treatment of depression RANZCP CLINICAL PRACTICE GUIDELINES ASSESSMENT
 RANZCP CLINICAL PRACTICE GUIDELINES Summary of guideline for the RANZCP CLINICAL PRACTICE GUIDELINES treatment of depression Pete M. Ellis, Ian B. Hickie and Don A. R. Smith for the RANZCP Clinical Practice
RANZCP CLINICAL PRACTICE GUIDELINES Summary of guideline for the RANZCP CLINICAL PRACTICE GUIDELINES treatment of depression Pete M. Ellis, Ian B. Hickie and Don A. R. Smith for the RANZCP Clinical Practice
Family Medicine Forum November 10, 2017 Montreal., Quebec. Jon Davine, CCFP, FRCP(C) Associate Professor, McMaster University
 APPROACH TO DEPRESSION IN PRIMARY CARE Family Medicine Forum November 10, 2017 Montreal., Quebec. Jon Davine, CCFP, FRCP(C) Associate Professor, McMaster University DISCLOSURE Speaker/Presenter Disclosure
APPROACH TO DEPRESSION IN PRIMARY CARE Family Medicine Forum November 10, 2017 Montreal., Quebec. Jon Davine, CCFP, FRCP(C) Associate Professor, McMaster University DISCLOSURE Speaker/Presenter Disclosure
Post-Stroke Depression Primary Care Stroke Update: What s New in Best Practice Prevention & Care
 Post-Stroke Depression Primary Care Stroke Update: What s New in Best Practice Prevention & Care Maria Hussain MD FRCPC Dallas Seitz MD PhD(c) FRCPC Division of Geriatric Psychiatry, Queen s University
Post-Stroke Depression Primary Care Stroke Update: What s New in Best Practice Prevention & Care Maria Hussain MD FRCPC Dallas Seitz MD PhD(c) FRCPC Division of Geriatric Psychiatry, Queen s University
TREATING MAJOR DEPRESSIVE DISORDER
 TREATING MAJOR DEPRESSIVE DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Major Depressive Disorder, Second Edition, originally published in April 2000.
TREATING MAJOR DEPRESSIVE DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Major Depressive Disorder, Second Edition, originally published in April 2000.
Patients in the MIDAS Project. Exclusion Due to Bipolarity or Psychosis. Results
 Things You Think You Know Things You Think You Know, That May Not Be True in the Diagnosis and Treatment of Depression Mark Zimmerman, MD Director of Outpatient Psychiatry Director of the Partial Hospital
Things You Think You Know Things You Think You Know, That May Not Be True in the Diagnosis and Treatment of Depression Mark Zimmerman, MD Director of Outpatient Psychiatry Director of the Partial Hospital
Mset, with some episodes clearly linked to environmental
 Prevention of Relapse and Recurrence in Depression: The Role of Long-Term Pharmacotherapy and Psychotherapy Andrew A. Nierenberg, M.D.; Timothy J. Petersen, Ph.D.; and Jonathan E. Alpert, M.D. Major depressive
Prevention of Relapse and Recurrence in Depression: The Role of Long-Term Pharmacotherapy and Psychotherapy Andrew A. Nierenberg, M.D.; Timothy J. Petersen, Ph.D.; and Jonathan E. Alpert, M.D. Major depressive
5 COMMON QUESTIONS WHEN TREATING DEPRESSION
 5 COMMON QUESTIONS WHEN TREATING DEPRESSION Do Antidepressants Increase the Possibility of Suicide? Will I Accidentally Induce Mania if I Prescribe an SSRI? Are Depression Medications Safe and Effective
5 COMMON QUESTIONS WHEN TREATING DEPRESSION Do Antidepressants Increase the Possibility of Suicide? Will I Accidentally Induce Mania if I Prescribe an SSRI? Are Depression Medications Safe and Effective
Session outline. Introduction to depression Assessment of depression Management of depression Follow-up Review
 Depression 1 Session outline Introduction to depression Assessment of depression Management of depression Follow-up Review 2 Activity 1: Person s story followed by group discussion Present the first person
Depression 1 Session outline Introduction to depression Assessment of depression Management of depression Follow-up Review 2 Activity 1: Person s story followed by group discussion Present the first person
Depressive and Bipolar Disorders
 Depressive and Bipolar Disorders Symptoms Associated with Depressive and Bipolar Disorders Characteristics of mood symptoms Affects a person s well being, school, work, or social functioning Continues
Depressive and Bipolar Disorders Symptoms Associated with Depressive and Bipolar Disorders Characteristics of mood symptoms Affects a person s well being, school, work, or social functioning Continues
Functional Assessment of Depression and Anxiety Disorders Relevant to Work Requirements
 Functional Assessment of Depression and Anxiety Disorders Relevant to Work Requirements Paul S. Appelbaum, MD Dollard Professor of Psychiatry, Medicine & Law Columbia University Overview Depression and
Functional Assessment of Depression and Anxiety Disorders Relevant to Work Requirements Paul S. Appelbaum, MD Dollard Professor of Psychiatry, Medicine & Law Columbia University Overview Depression and
Depression. Affects 6.7% of adult population Women affected twice as much as men Leading cause of disability from all medical illnesses
 Advances in Depression Research: A Report From NIMH Mayada Akil, M.D. Senior Advisor to the Director National Institute of Mental Health Depression Affects 6.7% of adult population Women affected twice
Advances in Depression Research: A Report From NIMH Mayada Akil, M.D. Senior Advisor to the Director National Institute of Mental Health Depression Affects 6.7% of adult population Women affected twice
Recommendation 1: Diagnosis of Generalized Anxiety Disorder (IΙΙ-2)
 Final GAD RECOMMENDATIONS & EVIDENCE Recommendation 1: Diagnosis of Generalized Anxiety Disorder (IΙΙ-2) It is recommended for general practitioners and other Primary Health Care doctors to consider the
Final GAD RECOMMENDATIONS & EVIDENCE Recommendation 1: Diagnosis of Generalized Anxiety Disorder (IΙΙ-2) It is recommended for general practitioners and other Primary Health Care doctors to consider the
BRAIN STIMULATION AN ALTERNATIVE TO DRUG THERAPY IN MATERNAL DEPRESSION?
 BRAIN STIMULATION AN ALTERNATIVE TO DRUG THERAPY IN MATERNAL DEPRESSION? Kira Stein, MD Medical Director West Coast Life Center Sherman Oaks, California CA Maternal Mental Health Initiative - 2013 2013
BRAIN STIMULATION AN ALTERNATIVE TO DRUG THERAPY IN MATERNAL DEPRESSION? Kira Stein, MD Medical Director West Coast Life Center Sherman Oaks, California CA Maternal Mental Health Initiative - 2013 2013
Long-term outcome of Treatment-Resistant Depression
 UNIVERSITÀ DI PISA FACOLTÀ DI MEDICINA E CHIRURGIA SCUOLA DI SPECIALIZZAZIONE DI PSICHIATRIA Direttore: Prof.ssa Liliana Dell Osso Tesi di specializzazione Long-term outcome of Treatment-Resistant Depression
UNIVERSITÀ DI PISA FACOLTÀ DI MEDICINA E CHIRURGIA SCUOLA DI SPECIALIZZAZIONE DI PSICHIATRIA Direttore: Prof.ssa Liliana Dell Osso Tesi di specializzazione Long-term outcome of Treatment-Resistant Depression
Presentation is Being Recorded
 Integrated Care for Depression & Anxiety Psychotropic Medication Management for Primary Care Providers Los Angeles County Department of Mental Health September 20, 2011 Presentation is Being Recorded Please
Integrated Care for Depression & Anxiety Psychotropic Medication Management for Primary Care Providers Los Angeles County Department of Mental Health September 20, 2011 Presentation is Being Recorded Please
Joel V. Oberstar, M.D. 1
 Diagnosis and Treatment of Depressive Disorders in Children and Adolescents Joel V. Oberstar, M.D. CEO & Chief Medical Officer Adjunct Assistant Professor of Psychiatry University of Minnesota Medical
Diagnosis and Treatment of Depressive Disorders in Children and Adolescents Joel V. Oberstar, M.D. CEO & Chief Medical Officer Adjunct Assistant Professor of Psychiatry University of Minnesota Medical
Managing Depression as a Chronic Condition. D. Green MD TOH/Bruyere Shared Care Program
 Managing Depression as a Chronic Condition D. Green MD TOH/Bruyere Shared Care Program None Financial disclosure Objectives To review key concepts relevant to understanding the course of depression To
Managing Depression as a Chronic Condition D. Green MD TOH/Bruyere Shared Care Program None Financial disclosure Objectives To review key concepts relevant to understanding the course of depression To
ANXIOUS DEPRESSION. Ned H. Kalin, MD University of Wisconsin Alan F. Schatzberg, MD Stanford University
 ANXIOUS DEPRESSION Ned H. Kalin, MD University of Wisconsin Alan F. Schatzberg, MD Stanford University NED H. KALIN, MD Disclosures!! Research/Grants: None!! Speakers Bureau: None!! Consultant: None!!
ANXIOUS DEPRESSION Ned H. Kalin, MD University of Wisconsin Alan F. Schatzberg, MD Stanford University NED H. KALIN, MD Disclosures!! Research/Grants: None!! Speakers Bureau: None!! Consultant: None!!
9/20/2011. Integrated Care for Depression & Anxiety: Psychotropic Medication Management for PCPs. Presentation is Being Recorded
 Integrated Care for Depression & Anxiety Psychotropic Medication Management for Primary Care Providers Los Angeles County Department of Mental Health September 20, 2011 Presentation is Being Recorded Please
Integrated Care for Depression & Anxiety Psychotropic Medication Management for Primary Care Providers Los Angeles County Department of Mental Health September 20, 2011 Presentation is Being Recorded Please
Depression in the Eldery Handout Package
 Depression in the Eldery Handout Package Depression in the Elderly 1 Learning Objectives Upon completion of this module, you should be able to: 1. State the prevalence and describe the consequences of
Depression in the Eldery Handout Package Depression in the Elderly 1 Learning Objectives Upon completion of this module, you should be able to: 1. State the prevalence and describe the consequences of
Depression Screening: An Effective Tool to Reduce Disability and Loss of Productivity
 Depression Screening: An Effective Tool to Reduce Disability and Loss of Productivity Kay n Campbell. EdD. RN-C. COHN-S, FAAOHN ICOH Cancun, Mexico March, 2012 What Is It? Common mental disorder Affects
Depression Screening: An Effective Tool to Reduce Disability and Loss of Productivity Kay n Campbell. EdD. RN-C. COHN-S, FAAOHN ICOH Cancun, Mexico March, 2012 What Is It? Common mental disorder Affects
Antidepressant Selection in Primary Care
 Antidepressant Selection in Primary Care R E B E C C A D. L E W I S, D O O O A S U M M E R C M E B R A N S O N, M O 1 5 A U G U S T 2 0 1 5 Objectives Understand the epidemiology of depression. Recognize
Antidepressant Selection in Primary Care R E B E C C A D. L E W I S, D O O O A S U M M E R C M E B R A N S O N, M O 1 5 A U G U S T 2 0 1 5 Objectives Understand the epidemiology of depression. Recognize
A Basic Approach to Mood and Anxiety Disorders in the Elderly
 A Basic Approach to Mood and Anxiety Disorders in the Elderly November 1 2013 Sarah Colman MD FRCPC Clinical Fellow, Geriatric Psychiatry Mount Sinai Hospital, University of Toronto Disclosure No conflict
A Basic Approach to Mood and Anxiety Disorders in the Elderly November 1 2013 Sarah Colman MD FRCPC Clinical Fellow, Geriatric Psychiatry Mount Sinai Hospital, University of Toronto Disclosure No conflict
The scope of the problem. Literature review
 Past Year: Novartis Ever: Alkermes, Amylin, Behringer- Ingelheim, Biovail, Bristol-Myers Squibb, Eli Lilly, Embryon, GlaxoSmithKline, Merck, Organon, Park-Davis, Pfizer, Sanolfi-Aventis, Smith-Kline Beacham,
Past Year: Novartis Ever: Alkermes, Amylin, Behringer- Ingelheim, Biovail, Bristol-Myers Squibb, Eli Lilly, Embryon, GlaxoSmithKline, Merck, Organon, Park-Davis, Pfizer, Sanolfi-Aventis, Smith-Kline Beacham,
Treatment of Bipolar disorder
 8/6/215 Treatment of Bipolar disorder Pichai Ittasakul, M.D. Department of Psychiatry, Ramathibodi Hospital, Mahidol University Bipolar disorder Manic-depressive Illness. is characterized by the occurrence
8/6/215 Treatment of Bipolar disorder Pichai Ittasakul, M.D. Department of Psychiatry, Ramathibodi Hospital, Mahidol University Bipolar disorder Manic-depressive Illness. is characterized by the occurrence
Psychiatry in Primary Care: What is the Role of Pharmacist?
 Psychiatry in Primary Care: What is the Role of Pharmacist? Benjamin Chavez, PharmD, BCPP, BCACP Clinical Associate Professor Director of Behavioral Health Pharmacy Services January 12, 2019 Disclosure
Psychiatry in Primary Care: What is the Role of Pharmacist? Benjamin Chavez, PharmD, BCPP, BCACP Clinical Associate Professor Director of Behavioral Health Pharmacy Services January 12, 2019 Disclosure
Depression: The Benefits of Early and Appropriate Treatment
 REPORTS Depression: The Benefits of Early and Appropriate Treatment Aron Halfin, MD Abstract Depression has a profound impact on patient health, individual and family quality of life, activities of daily
REPORTS Depression: The Benefits of Early and Appropriate Treatment Aron Halfin, MD Abstract Depression has a profound impact on patient health, individual and family quality of life, activities of daily
Bipolar Disorder 4/6/2014. Bipolar Disorder. Symptoms of Depression. Mania. Depression
 Bipolar Disorder J. H. Atkinson, M.D. Professor of Psychiatry HIV Neurobehavioral Research Programs University of California, San Diego KETHEA, Athens Slides courtesy of John Kelsoe, M.D. Bipolar Disorder
Bipolar Disorder J. H. Atkinson, M.D. Professor of Psychiatry HIV Neurobehavioral Research Programs University of California, San Diego KETHEA, Athens Slides courtesy of John Kelsoe, M.D. Bipolar Disorder
Depression After Traumatic Brain Injury (TBI)
 Depression After Traumatic Brain Injury (TBI) A resource for individuals with traumatic brain injury and their supporters This presentation is based on TBI Model Systems research and was developed with
Depression After Traumatic Brain Injury (TBI) A resource for individuals with traumatic brain injury and their supporters This presentation is based on TBI Model Systems research and was developed with
Application of Psychotropic Drugs in Primary Care
 Psychotropic Drugs Application of Psychotropic Drugs in Primary Care JMAJ 47(6): 253 258, 2004 Naoshi HORIKAWA Professor, Department of Psychiatry, Tokyo Women s Medical University Abstract: The incidence
Psychotropic Drugs Application of Psychotropic Drugs in Primary Care JMAJ 47(6): 253 258, 2004 Naoshi HORIKAWA Professor, Department of Psychiatry, Tokyo Women s Medical University Abstract: The incidence
Clinical guideline Published: 28 October 2009 nice.org.uk/guidance/cg90
 Depression in adults: recognition and management Clinical guideline Published: 28 October 2009 nice.org.uk/guidance/cg90 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Depression in adults: recognition and management Clinical guideline Published: 28 October 2009 nice.org.uk/guidance/cg90 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Challenges in identifying and treating bipolar depression: a guide
 Challenges in identifying and treating bipolar depression: a guide Dr. Paul Stokes Clinical Senior Lecturer, Centre for Affective Disorders, Department of Psychological Medicine Overview Challenges in
Challenges in identifying and treating bipolar depression: a guide Dr. Paul Stokes Clinical Senior Lecturer, Centre for Affective Disorders, Department of Psychological Medicine Overview Challenges in
Psychiatry Clinical Reviews Depression What Matters and Why?
 Mayo School of Continuous Professional Development Psychiatry Clinical Reviews Depression What Matters and Why? William V. Bobo, M.D., M.P.H. October 6-8, 2016 Intercontinental Chicago Magnificent Mile
Mayo School of Continuous Professional Development Psychiatry Clinical Reviews Depression What Matters and Why? William V. Bobo, M.D., M.P.H. October 6-8, 2016 Intercontinental Chicago Magnificent Mile
PSYCHOTROPIC MEDICATION AND THE WORKPLACE. Dr. Marty Ewer 295 Fullarton Road Parkside
 PSYCHOTROPIC MEDICATION AND THE WORKPLACE Dr. Marty Ewer 295 Fullarton Road Parkside 5063 82999281 Introduction Depression and anxiety commonly occur in people who work. The World Health Organization has
PSYCHOTROPIC MEDICATION AND THE WORKPLACE Dr. Marty Ewer 295 Fullarton Road Parkside 5063 82999281 Introduction Depression and anxiety commonly occur in people who work. The World Health Organization has
