NIH Public Access Author Manuscript Am J Geriatr Psychiatry. Author manuscript; available in PMC 2013 September 16.
|
|
|
- Heather Golden
- 5 years ago
- Views:
Transcription
1 NIH Public Access Author Manuscript Published in final edited form as: Am J Geriatr Psychiatry December ; 17(12): doi: /jgp.0b013e3181b972d1. Cost-related medication nonadherence among beneficiaries with depression following Medicare Part D Kara Zivin, PhD 1,2, Jeanne M. Madden, PhD 3,4, Amy J. Graves, MPH 3,4, Fang Zhang, PhD 3,4, and Stephen B. Soumerai, ScD 3,4 1 Department of Veterans Affairs, Health Services Research and Development (HSR&D) Center of Excellence, Serious Mental Illness Treatment Research and Evaluation Center (SMITREC), Ann Arbor, MI 2 Department of Psychiatry, University of Michigan Medical School, Ann Arbor, MI 3 Department of Ambulatory Care and Prevention, Harvard Medical School, Boston, MA 4 Harvard Pilgrim Health Care, Boston, MA Abstract Context Cost-related medication nonadherence (CRN) was problematic for Medicare beneficiaries with depressive symptoms prior to Medicare Part D. Objective To estimate changes in CRN and forgoing basic needs to pay for drugs among Medicare beneficiaries with and without depressive symptoms following Part D implementation. Design and Setting We compared changes in outcomes between 2005 and 2006 before and after Part D with changes between 2004 and 2005 using logistic regression to control for demographic characteristics, health status, and historical trends. Participants The community-dwelling sample of the Medicare Current Beneficiary Survey (n=24,234). Main Outcome Measures Self-reports of CRN (skipping or reducing doses, not obtaining prescriptions) and spending less on basic needs to afford medicines. Results The unadjusted annual prevalence of CRN among beneficiaries with depressive symptoms was 27% (2004), 27% (2005), and 24% (2006), compared to 13%, 12%, and 9% among beneficiaries without depressive symptoms. The annual prevalence of spending less on basic needs was 22% (2004), 23% (2005), and 19% (2006), compared to 8%, 9%, and 5% among beneficiaries without depressive symptoms. Controlling for historical changes and demographic characteristics, CRN did not decline among beneficiaries with depressive symptoms compared to beneficiaries without depressive symptoms (ratio of Part D changes 0.98; 95% CI, ). Respondents with depressive symptoms appeared less likely to spend less on basic needs compared to individuals without depressive symptoms (0.70; 95% CI, 0.49, 1.01), however this difference was not statistically significant. Conclusions Despite a Medicare Part D goal to improve medication adherence among mentally ill beneficiaries, the disparity in economic access to medications between beneficiaries with and without depressive symptoms did not improve after the start of Part D. Corresponding Author: Kara Zivin, PhD, University of Michigan Medical School, Department of Psychiatry, Rachel Upjohn Building, 4250 Plymouth Road, Box 5765, Ann Arbor, MI kzivin@umich.edu; Phone: x56009; fax
2 Zivin et al. Page 2 Keywords depression; Medicare Part D; cost-related nonadherence to medications Introduction Methods Sample and data source Measures The initiation of the Medicare Part D prescription drug benefit in 2006 was the largest change in coverage since Medicare's inception in 1965.(1) Prior to the availability of the prescription drug benefit, cost-related medication nonadherence (CRN) was a significant problem for many Medicare beneficiaries, particularly those who lacked prescription medication coverage.(2-6) Recent research has indicated that there have been improvements in CRN since the implementation of Medicare Part D in 2006; however, those with poor health or multiple somatic illnesses had higher rates of CRN before Part D implementation and experienced no declines in CRN associated with Part D drug coverage.(3) CRN was found to be particularly problematic prior to Part D among Medicare beneficiaries reporting depressive symptoms.(7-9) These beneficiaries were more likely to be women and to report lower incomes, lower functional status, more comorbidities, and fair or poor health status.(7) Given the importance of medication adherence for health outcomes and wellbeing,(10-13) there were concerns about how patients with mental illness would fare once Part D began.(14, 15) As a result, the Department of Health and Human Services exempted most medications for mental illness from formulary exclusions.(16) Using data from the Medicare Current Beneficiary Survey (MCBS),(17) two years before and one year after the initiation of Part D ( ), we sought to determine the annual prevalence and changes in CRN among Medicare beneficiaries with and without depressive symptoms after initiation of Medicare Part D). The MCBS is a nationally representative, longitudinal survey of disabled and elderly Medicare beneficiaries. Respondents are selected in rotating three-year panels, including four fall interviews, and participate based on Medicare enrollment files from the Centers for Medicare and Medicaid Services (CMS) using a stratified area-probability design.(18) Each fall, approximately 15,700 beneficiaries are surveyed. Additional details about MCBS sampling techniques and data collection are available elsewhere.(2, 3) CRN was our primary outcome measure of interest, and was based on responses to questions developed in our prior research and implemented in the MCBS since 2004.(2, 5, 6, 19) These measures have been shown to be valid and reliable measures of cost-related nonadherence to medications.(2, 3, 19) As in these previous studies, we constructed a summary indicator of CRN for analysis that took the value yes if a respondent indicated yes/ever during the current year on any of the following: skipped doses to make the medicine last longer ; taken smaller doses of a medicine to make the medicine last longer ; or any medicines prescribed for you that you did not get in combination with (a reason or the main reason) you did not obtain the medicine was you thought it would cost too much or decide not to fill or refill a prescription because it was too expensive. We also examined a separate question that asked beneficiaries if they spent less money on food, heat, or other basic needs so that [they] would have money for medicine. (2)
3 Zivin et al. Page 3 Statistical analysis Depressive symptoms, our key independent variable of interest, were measured using two questions in the MCBS that address specific DSM-IV criteria,(20) namely sadness and anhedonia, both known as strong indicators of depression.(21) The following two items formed the basis for our study's composite depressive symptom indicator: (1) In the past 12 months, how much of the time did you feel sad, blue, or depressed? and (2) In the past 12 months, have you had 2 weeks or more when you lost interest or pleasure in things that you usually cared about or enjoyed? Based on previously published methods,(7, 22) those responding all of the time or most of the time to the first item ( time depressed ) and/or responding affirmatively to the second item ( lost interest ) were classified as having depressive symptoms. We also examined demographic and clinical characteristics from the MCBS that could potentially influence medication adherence including: sex, age group (<55, 55-64, 65-74, 75-84, 85), income (<$25,000 and $25,000), race (black, white, or other), Hispanic ethnicity, educational attainment (above high school, high school diploma, no diploma), a count of self-reported comorbid medical conditions (0-1, 2-3, 4), a count of limitations in functional status or activities of daily living (ADL: 0, 1-2, 3), a measure of self-rated health (excellent, very good, or good versus fair or poor), and an indicator of prescription drug coverage. All measures were determined in each study year, thus a respondent's status on time varying characteristics could change during the study period. First, we estimated the rates of demographic and clinical characteristics among Medicare beneficiaries with and without depressive symptoms in 2004, 2005, and 2006, which were weighted to represent the entire non-institutionalized Medicare population using annual cross-sectional survey weights provided in the MCBS.(23) Next, we examined the relationship between depressive symptoms and the unadjusted annual prevalence of CRN and spending less on basic needs in 2004, 2005, and 2006 using Chi-square statistics. As in a previous study,(3) we used separate logistic regression models to predict the odds of CRN and spending less on basic needs respectively, by year. We stratified our analyses by the presence of depressive as defined above. The key covariates in these models were two indicators for response year (2006 and 2005, with 2004 as the reference year). Additional covariates controlled for sex, age group, income, race, number of morbidities, self-rated health, and number of years participation(3) in MCBS. We calculated a ratio of two odds ratios (namely 2006 versus 2005 relative to 2005 versus 2004) for beneficiaries with and without depressive symptoms, controlling for historical year-to-year changes in the absence of Part D.(3) Finally, we calculated a ratio of changes in outcomes following Part D among the beneficiaries with versus without depressive symptoms. All of the models used MCBS survey weights and controlled for clustering at the sampling unit, which is part of the MCBS study design,(18) and for repeated measures (e.g. non-independence of responses) over time. We chose to use a population-based approach to examine changes in CRN regardless of coverage status, which had the advantage of avoiding selection biases due to the likelihood that beneficiaries who enrolled in a prescription drug plan either before or after Part D were sicker.(24, 25) This approach also controlled for changes within specific types of drug coverage (e.g. HMO, employer) concurrent with and closely related to Part D implementation.(3) However, we examined (in data not shown) whether including an indicator of whether or not a beneficiary had any type of prescription drug coverage, or a specific type of drug coverage and found that this approach had little to no impact on estimates of changes in CRN and spending less on basic needs after Part D implementation.
4 Zivin et al. Page 4 Results In additional sensitivity analyses, we examined whether there was a differential impact of Part D on disabled (age <65) versus elderly ( 65) beneficiaries with and without depressive symptoms. Given that the disabled group with depressive symptoms was relatively small (less than 7% of our sample) we thought it would be unlikely that we would detect CRN differences and changes in spending less on basic needs in this population. However, the overall Part D effects were similar in both the disabled and elderly groups (with all results from the elderly population being almost identical to the overall population) so we chose to present the more parsimonious findings from the entire Medicare population as a whole, while using age groups in our adjusted analyses. All statistical analyses were conducted using Stata version 10 (StataCorp LP, College Station, Texas). This study was approved by the Human Subjects Committee of Harvard Pilgrim Health Care. Our sample included 14,500 Medicare beneficiaries who were interviewed as part of the MCBS in 2004, 14,701 in 2005, and 14,732 in Of these, 2,662, 2,611, and 2,662 (18% in all years) were classified as having depressive symptoms in 2004, 2005, and 2006 respectively. As shown in Table 1, people with depressive were more likely than those without depressive symptoms to be female, nonelderly disabled, poor, and sick (in terms of comorbid medical conditions, number of ADL limitations, and self-rated health). For example, in all years, more than 55% of beneficiaries with depressive symptoms reported their self-rated health as fair or poor, whereas only approximately 20% of beneficiaries without depressive symptoms reported fair or poor health. The unadjusted, weighted annual prevalence of CRN among beneficiaries with depressive symptoms was 27% in 2004, 27% in 2005, and 24% after Part D implementation in 2006, compared to 13%, 12%, and 9% among beneficiaries without depressive symptoms (Figure 1). The annual prevalence of spending less on basic needs was 22% in 2004, 23% in 2005, and 19% in 2006, compared to 8%, 9%, and 5% among beneficiaries without depressive symptoms. Thus, the disparity between CRN among beneficiaries with and without depressive symptoms, expressed as a simple ratio of rates, was 2.1 in 2004, 2.3 in 2005, and 2.7 in 2006, and the disparity for spending less on basic needs between beneficiaries with and without depressive symptoms was 2.6 in 2004 and 2005, and 3.7 in Table 2 shows the adjusted changes in CRN and spending less on basic needs after the implementation of Part D among beneficiaries with and without depressive symptoms. Controlling for historical changes (2005 versus 2004) and demographic characteristics, there were significant decreases in spending less among beneficiaries with depressive symptoms (ratio of ORs, 0.72; 95% CI, 0.52, 0.99, df=82, Wald t-test= 2.04), but there were no significant changes in CRN among beneficiaries with depressive symptoms (ratio of ORs, 0.85; 95% CI, , df=82, Wald t-test= 1.17). Among beneficiaries without depressive symptoms, there were greater decreases in spending less on basic needs (ratio of ORs, 0.50; 95% CI, 0.40, 0.63, df=82, Wald t-test= 5.95) and significant decreases in CRN (ratio of ORs 0.83; 95% CI, 0.70, 0.97, df=82, Wald t-test= 2.32). Comparing changes in outcomes before and after the drug benefit between respondents with and without depressive symptoms (which were non-significant for those with depressive symptoms and significant for those without depressive symptoms; see Table 2), there were no significant differences in rates of CRN among beneficiaries with versus without depressive symptoms (ratio of Part D changes 0.98; 95% CI, , df=82, Wald t-test= 0.13). Respondents with depressive symptoms appeared to experience smaller declines in
5 Zivin et al. Page 5 Comment spending less for basic needs after Part D than did those without depressive symptoms, though this difference was not statistically significant (ratio 0.70; 95% CI, 0.49, 1.01, df=82, Wald t-test= 1.94). Part D was hailed as(26) a contributor to increased access to prescription medications for Medicare beneficiaries. In 2004, 23% of elderly beneficiaries lacked prescription drug coverage, whereas in 2006, less than 10% lacked coverage. More than 6 million beneficiaries newly acquired coverage as a result of Part D.(24, 27, 28) However, despite increased coverage, previous research has indicated that overall rates of cost-related medication nonadherence and spending less on basic needs improved only somewhat after Part D began, and that there was no decline in CRN and spending less on basic needs among sicker beneficiaries.(3) In this study, we found that rates of CRN did not decrease significantly among beneficiaries with depressive symptoms, while they did among beneficiaries without depressive symptoms. Furthermore, while spending less on basic needs declined among beneficiaries with and without depressive symptoms after Part D, this decline was somewhat greater among beneficiaries without depressive symptoms. Beneficiaries with depressive symptoms experienced substantially higher overall rates of CRN and spending less on basic needs that persisted after the implementation of Part D, and the disparities between rates of CRN and spending less on basic needs among those with compared to those without depressive symptoms actually increased slightly between 2004 and There are a number of possible explanations for the different experiences of beneficiaries with and without depressive symptoms. Although our models controlled for poorer health at baseline among beneficiaries with depressive symptoms, there may be residual differences in health status that contribute to our findings. Specific coverage policies may also play a role. For example, beneficiaries who were dually eligible for Medicare and Medicaid were automatically switched from prior Medicaid drug coverage to a Part D plan, and Part D plans may have had less generous access to antidepressant medications than Medicaid plans. (29) While Part D excluded antidepressants from formulary restrictions, antidepressants were more often subject to prior authorization policies which are known to reduce access to these medications, which could have also led to an increase in CRN.(30, 31) Beneficiaries with depressive symptoms may have been more likely to have Medicaid coverage prior to Part D, as they had lower income levels. Furthermore, for beneficiaries who either switched from another drug coverage plan (e.g., Medicaid or employer-based) to Part D, or who had no prior drug coverage and did not enroll in Part D, rates of CRN and spending less on basic needs would not be expected to have declined substantially. Beneficiaries with depressive symptoms use more medications and therefore have higher drug costs given the substantial burden of cost-sharing in Part D plans. The standard plan requires 25% cost-sharing by the patient from the first dollar of benefits, though many actuarially equivalent plans have complex tier structures and overall patient cost-sharing greater than 25%. In addition, an unusual feature of Medicare Part D poses special cost burdens for sicker patients in the standard plan's prescription drug coverage gap known as the doughnut hole (100% cost sharing after first $2,250 in total drug costs).(28) The majority of Part D enrollees do not have coverage in the doughnut hole,(32) and many beneficiaries are not even aware of the coverage gap until they suddenly encounter it.(33, 34) Both the ordinary cost-sharing and the coverage gap weigh more heavily on depressed and ill patients, and could lead to CRN and spending less on basic needs. Conversely,
6 Zivin et al. Page 6 beneficiaries with depressive symptoms may have been less likely to have spending in the doughnut hole if they were eligible for low income subsidies. Conclusions These findings from Medicare beneficiaries with depressive symptoms raise questions about progress toward mental health parity in the era of Part D prescription medication coverage. Patient advocates argue that antidiscrimination measures are needed to achieve greater insurance equity across disease groups.(35) In fact, published rules governing access to medications in the Medicare drug benefit attempted to protect most psychotropic drug classes from formulary exclusions.(16) Yet mentally ill beneficiaries are more likely to have greater disease and disability burdens and needs for medication coverage at the same time that they have lower incomes and face higher out-of-pocket drug costs as well as greater challenges accessing medications,(7, 36, 37) such as prior authorization, and fail first policies for psychotropic medications.(38) It appears that the insurance expansion represented by Part D may have helped beneficiaries with depressive symptoms who may have greater medication needs less than beneficiaries without depressive symptoms.(39) It is important to look at not only the overall effect of Part D on CRN and spending less on basic needs but also at relative effects for vulnerable subpopulations to determine whether there are ways for policymakers to ensure reasonable equity in meeting coverage needs. While these are nationally representative, longitudinal data on CRN and spending less on basic needs among Medicare beneficiaries with depressive symptoms, there are several limitations to discuss. To date, Part D claims data are not available in the MCBS on prescription drug plans and formularies for individual Medicare beneficiaries,(27) so we cannot link individual CRN and spending less on basic needs to coverage of specific medications or classes of drugs including antidepressant medications or other psychotropic medications. Also, we have no information on actual medication utilization among patients with or without depression because the MCBS Cost and Use data files for 2006 are not available yet.(3) Although our reliable measures of CRN(19) and spending less on basic needs have been available in the MCBS since 2004, a longer pre-policy series would have permitted a stronger assessment of the impact of Part D implementation in 2006, yet this data was not available. Furthermore, this analysis included data from only the first year after Part D implementation. However, the 2006 round of MCBS interviews were conducted in the last three months of 2006, which was after the launch of Part D. These early findings should be followed up over time to determine the longer term implications of Part D coverage on beneficiaries with depressive symptoms. In conclusion, we found that Medicare beneficiaries with depressive symptoms, who are sicker and may have more intensive medication use than beneficiaries without depressive symptoms, were somewhat less likely to have improved economic access to medications after Part D than beneficiaries without depressive symptoms. Furthermore, the disparity in economic access between beneficiaries with and without depressive symptoms actually grew slightly wider after Part D. While more long-term data may help to shape future Medicare policy, a growing body of research suggests that eliminating the doughnut hole, reducing coinsurance, and automatically extending coverage to the near poor may be worth considering in better meeting the needs of vulnerable populations, such as those with mental illness.
7 Zivin et al. Page 7 Acknowledgments References This study was funded by grant #R01AG (Impact of Medicare Drug Benefit on Use and Cost-related Underuse of Medicines) from the National Institute on Aging (NIA) to Dr. Soumerai, and the Harvard Pilgrim Health Care Foundation. Drs. Zhang and Soumerai are investigators in the HMO Research Network Center for Education and Research in Therapeutics, supported by the U.S. Agency for Healthcare Research and Quality (Grant #2U18HS010391). Dr. Zivin was supported by a National Institute on Aging Pilot Faculty Grant to the Michigan Center on the Demography of Aging (MiCDA) (KZ), and the Rachel Upjohn Clinical Scholar Award (KZ). This work was conducted at the Department of Ambulatory Care and Prevention, Harvard Medical School and Harvard Pilgrim Health Care. 1. Greenwald LM. Medicare part D data: major changes on the horizon. Medical Care. 2007; 45:S9 12. [PubMed: ] 2. Soumerai SB, Pierre-Jacques M, Zhang F, et al. Cost-related medication nonadherence among elderly and disabled Medicare beneficiaries: a national survey 1 year before the Medicare drug benefit. Archives of Internal Medicine. 2006; 166: [PubMed: ] 3. Madden JM, Graves AJ, Zhang F, et al. Cost-related medication nonadherence and spending on basic needs following implementation of Medicare Part D. JAMA. 2008; 299: [PubMed: ] 4. Hanson, K.; Neuman, T.; Voris, M. Understanding the Health-Care Needs and Experiences of People with Disabilities. The Henry J. Kaiser Family Foundation; Menlo Park, CA: Safran DG, Neuman P, Schoen C, et al. Prescription Drug Coverage And Seniors: Findings From A 2003 National Survey. Health Affairs. 2005:W [PubMed: ] 6. Safran DG, Neuman P, Schoen C, et al. Prescription drug coverage and seniors: how well are states closing the gap? Health Affairs. 2002; (Suppl Web Exclusives):W [PubMed: ] 7. Bambauer KZ, Safran DG, Ross-Degnan D, et al. Depression and cost-related medication nonadherence in Medicare beneficiaries. Archives of General Psychiatry. 2007; 64: [PubMed: ] 8. Briesacher BA, Gurwitz JH. Soumerai SB: Patients at-risk for cost-related medication nonadherence: a review of the literature. Journal of General Internal Medicine. 2007; 22: [PubMed: ] 9. Piette JD, Heisler M, Wagner TH. Cost-related medication underuse among chronically III adults: the treatments people forgo, how often, and who is at risk. American Journal of Public Health. 2004; 94: [PubMed: ] 10. Melfi CA, Chawla AJ, Croghan TW, et al. The effects of adherence to antidepressant treatment guidelines on relapse and recurrence of depression. Archives of General Psychiatry. 1998; 55: [PubMed: ] 11. Maidment R, Livingston G, Katona C. Just keep taking the tablets: adherence to antidepressant treatment in older people in primary care. International Journal of Geriatric Psychiatry. 2002; 17: [PubMed: ] 12. Alexopoulos GS, Buckwalter K, Olin J, et al. Comorbidity of late life depression: an opportunity for research on mechanisms and treatment. Biological Psychiatry. 2002; 52: [PubMed: ] 13. Simon GE, Manning WG, Katzelnick DJ, et al. Cost-effectiveness of systematic depression treatment for high utilizers of general medical care. Archives of General Psychiatry. 2001; 58: [PubMed: ] 14. Simoni-Wastila L, Zuckerman IH, Shaffer T, et al. Drug use patterns in severely mentally ill medicare beneficiaries: impact of discontinuities in drug coverage. Health Services Research. 2008; 43: [PubMed: ] 15. Medicare Rights Center. Clearing Hurdles and Hitting Walls Restrictions Undermine Part D Coverage of Mental Health Drugs. Medicare Rights Center; New York, NA: Elliott RA, Majumdar SR, Gillick MR, et al. Benefits and consequences for the poor and the disabled. New England Journal of Medicine. 2005; 353: [PubMed: ]
8 Zivin et al. Page Adler GS. A profile of the Medicare Current Beneficiary Survey. Health Care Financing Review. 1994; 15: [PubMed: ] 18. Centers for Medicare and Medicaid Services (CMS) Technical Documentation for the Medicare Current Beneficiary Study Pierre-Jacques M, Safran DG, Zhang F, et al. Reliability of New Measures of Cost-Related Medication Nonadherence. Medical Care. 2008; 46: [PubMed: ] 20. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders DSM- IV. American Psychiatric Association; Washington, DC: Kroenke K, Spitzer RL, Williams JB. The Patient Health Questionnaire-2: validity of a two-item depression screener. Medical Care. 2003; 41: [PubMed: ] 22. Waldo DR. Symptoms of depression among aged Medicare enrollees Health Care Financing Review. 2004; 26: [PubMed: ] 23. Centers for Medicare and Medicaid Services (CMS). Technical Documentation for the Medicare Current Beneficiary Survey (MCBS), 2003 Access to Care, Section 5: Sample Design and Guidelines for Preparing Statistics (available on CD-ROM). Office of the Actuary; Levy, H.; Weir, DR. Take-Up of Medicare Part D and the SSA Subsidy Early Results from the Health and Retirement Study. University of Michigan; Ann Arbor, MI: Heiss F, McFadden D, Winter J. Who failed to enroll in Medicare Part D, and why? Early results. Health Affairs. 2006; 25:w [PubMed: ] 26. McClellan MB. Testimony of Mark McClellan, MD, PhD, Administrator CMS Before the Senate Special Committee on Aging. Hearing on Generic Drug Utilization in the Medicare Prescription Drug Benefit Stuart B. Where are the Medicare Part D claims data? Annals of Internal Medicine. 2008; 148: [PubMed: ] 28. Henry, J.; Kaiser Family Foundation. The Medicare Prescription Drug Benefit. Henry J. Kaiser Family Foundation; Bernasek, C.; Farkas, J.; Felman, H., et al. Case Study Michigan's Medicaid Prescription Drug Benefit. The Henry J. Kaiser Family Foundation; Washington, DC: Adams AS, Zhang F, LeCates RF, et al. Prior authorization for antidepressants in Medicaid: effects among disabled dual enrollees. Archives of Internal Medicine. 2009; 169: [PubMed: ] 31. Huskamp HA, Stevenson DG, Donohue JM, et al. Coverage and prior authorization of psychotropic drugs under Medicare Part D. Psychiatric Services. 2007; 58: [PubMed: ] 32. Henry, J.; Kaiser Family Foundation. Overview of Medicare Part D Organizations, Plans and Benefits By Enrollment in 2006 and Henry J. Kaiser Family Foundation; Menlo Park, CA: Hsu J, Fung V, Price M, et al. Medicare beneficiaries knowledge of Part D prescription drug program benefits and responses to drug costs. JAMA. 2008; 299: [PubMed: ] 34. Reed M, Brand R, Newhouse JP, et al. Coping with prescription drug cost sharing: knowledge, adherence, and financial burden. Health Services Research. 2008; 43: [PubMed: ] 35. Barry CL. The political evolution of mental health parity. Harvard Review of Psychiatry. 2006; 14: [PubMed: ] 36. Briesacher, B.; Stuart, B.; Doshi, J., et al. Medicare's Disabled Beneficiaries The Forgotten Population in the Debate Over Drug Benefits. The Commonwealth Fund (publication #573) and the Henry J. Kaiser Family Foundation (publication #6054); Hall JP, Kurth NK, Moore JM. Transition to Medicare Part D: an early snapshot of barriers experienced by younger dual eligibles with disabilities. The American journal of managed care. 2007; 13: [PubMed: ] 38. Donohue JM, Frank RG. Estimating Medicare Part D's impact on medication access among dually eligible beneficiaries with mental disorders. Psychiatric Services. 2007; 58: [PubMed: ]
9 Zivin et al. Page Richman BD. Insurance expansions: do they hurt those they are designed to help? Health Affairs. 2007; 26: [PubMed: ]
10 Zivin et al. Page 10 Figure. Rates of reported Cost-Related Nonadherence (CRN) and Spending Less on Basic Needs (Spent Less) According to Depressive Symptom Status
11 Zivin et al. Page 11 TABLE 1 Demographic and Health Characteristics of Community-Dwelling Medicare Beneficiaries by Self-Reported Depressive Symptom Status a, b 2004, N=14, , N=14, , N=14,732 Depressive Symptoms N=2,662 No Depressive Symptoms N=11,784 X 2 Depressive Symptoms N=2,611 No Depressive Symptoms N=12,019 X 2 Depressive Symptoms N=2,662 No Depressive Symptoms N=11,991 X 2 Characteristic % % p-value % % p-value % % p-value Female Sex g g Age, y c < g g g Income, US$ <$25, g g g Race Black g g White Other Hispanic Ethnicity g g Education >High school g g g High school diploma No high school diploma No. of physical morbidities d g g g
12 Zivin et al. Page , N=14, , N=14, , N=14,732 Depressive Symptoms N=2,662 No Depressive Symptoms N=11,784 X 2 Depressive Symptoms N=2,611 No Depressive Symptoms N=12,019 X 2 Depressive Symptoms N=2,662 No Depressive Symptoms N=11,991 X 2 Characteristic % % p-value % % p-value % % p-value No. of limitations in ADL e g g g Self-reported health status Excellent, very good, or good g g g Fair or poor Medication coverage None g g g Partial Employer Medicaid/Part D f a Depression symptoms defined as answering all or most of the time to In the past 12 months, how much of the time did you feel sad, blue, or depressed? or answering yes to In the past 12 months, have you had 2 weeks or more when you lost interest or pleasure in things that you usually cared about or enjoyed? b Percentage bases exclude those with missing values. Values were missing for no more than 2% of respondents per characteristic. Percentages calculated with national survey weights. Race and Hispanic ethnicity were defined by investigators. c Respondents younger than 65 years were defined as disabled. d Physical morbidities include cardiac disease, hypertension, cerebrovascular disease, lung disease, cancer, diabetes mellitus, arthritis, dementia, and other neurological conditions. Mental morbidities (psychiatric disorder and depression) are excluded. e ADL=activities of daily living. Limitations in ADL indicate reduced functional status. f Medicaid medication coverage in 2004 and 2005; Part D medication coverage in 2006 g X 2 significant at p<0.01
13 Zivin et al. Page 13 TABLE 2 Changes in Cost-Related Nonadherence and Spending Less on Basic Needs Following Part D Implementation Group Depressive Symptoms No Depressive Symptoms Depressive Symptoms / No Depressive Symptoms (Part D effect) Outcome measure Test 2005 vs vs vs vs vs vs vs Cost-related nonadherence OR (95% CI) 1.01 (0.84, 1.21) 0.86 (0.75, 0.98) 0.85 (0.65, 1.12) p= (0.82, 0.96) 0.74 (0.65, 0.84) 0.83 (0.71, 0.97) p= (0.73, 1.32) p=0.896 Wald t-test (df) 0.09 (99) 2.23 (99) 1.17 (82) 3.06 (99) 4.62 (99) 2.32 (82) 0.13 (82) Spent less on basic needs OR (95% CI) 1.08 (0.88, 1.32) 0.77 (0.65, 0.92) 0.72 (0.52, 0.99) 1.09 (0.95, 1.24) 0.55 (0.46, 0.65) 0.50 (0.40, 0.63) p=0.044 p< (0.49, 1.01) p=0.055 Wald t-test (df) 0.73 (99) 2.92 (99) 2.04 (82) 1.20 (99) 7.02 (99) 5.95 (82) 1.94 (82) * Models adjusted for sex, age group, income level, race, general health status, number of physical morbidities, and number of years participation in MCBS Significant at p<0.05 Ratios <1 suggest the decline in CRN among those with depressive symptoms is less than the decline among those without depressive symptoms
The High Cost-related Medication Non-adherence Rate among Medicare- Medicaid Dual-eligible Diabetes Patients
 Research Article imedpub Journals http://www.imedpub.com Journal of Health & Medical Economics ISSN 2471-9927 DOI: 10.21767/2471-9927.100019 The High Cost-related Medication Non-adherence Rate among Medicare-
Research Article imedpub Journals http://www.imedpub.com Journal of Health & Medical Economics ISSN 2471-9927 DOI: 10.21767/2471-9927.100019 The High Cost-related Medication Non-adherence Rate among Medicare-
Inhaler Costs and Medication Nonadherence Among Seniors With Chronic Pulmonary Disease
 CHEST Original Research Inhaler Costs and Medication Nonadherence Among Seniors With Chronic Pulmonary Disease Peter J. Castaldi, MD ; William H. Rogers, PhD ; Dana Gelb Safran, ScD ; and Ira B. Wilson,
CHEST Original Research Inhaler Costs and Medication Nonadherence Among Seniors With Chronic Pulmonary Disease Peter J. Castaldi, MD ; William H. Rogers, PhD ; Dana Gelb Safran, ScD ; and Ira B. Wilson,
Pharmacy Policies in Medicaid What You Need to Know to Improve Treatment Access
 Pharmacy Policies in Medicaid What You Need to Know to Improve Treatment Access Stephen B. Soumerai, ScD Professor of Ambulatory Care and Prevention Harvard Medical School and Harvard Pilgrim Health Care
Pharmacy Policies in Medicaid What You Need to Know to Improve Treatment Access Stephen B. Soumerai, ScD Professor of Ambulatory Care and Prevention Harvard Medical School and Harvard Pilgrim Health Care
Prevalence And Trends In Obesity Among Aged And Disabled U.S. Medicare Beneficiaries,
 Trends Prevalence And Trends In Obesity Among Aged And Disabled U.S. Medicare Beneficiaries, 1997 2002 The rise in obesity among beneficiaries, along with expansions in treatment coverage, could greatly
Trends Prevalence And Trends In Obesity Among Aged And Disabled U.S. Medicare Beneficiaries, 1997 2002 The rise in obesity among beneficiaries, along with expansions in treatment coverage, could greatly
medicaid and the The Role of Medicaid for People with Diabetes
 on medicaid and the uninsured The Role of for People with Diabetes November 2012 Introduction Diabetes is one of the most prevalent chronic conditions and a leading cause of death in the United States.
on medicaid and the uninsured The Role of for People with Diabetes November 2012 Introduction Diabetes is one of the most prevalent chronic conditions and a leading cause of death in the United States.
January 16, Dear Administrator Verma:
 Ms. Seema Verma Administrator Centers for Medicare and Medicaid Services Department of Health and Human Services Attention: CMMI New Direction P.O. Box 8011 Baltimore, MD 21244-1850 Re: (CMS-4182-P) Medicare
Ms. Seema Verma Administrator Centers for Medicare and Medicaid Services Department of Health and Human Services Attention: CMMI New Direction P.O. Box 8011 Baltimore, MD 21244-1850 Re: (CMS-4182-P) Medicare
METHODS RESULTS. Supported by funding from Ortho-McNeil Janssen Scientific Affairs, LLC
 PREDICTORS OF MEDICATION ADHERENCE AMONG PATIENTS WITH SCHIZOPHRENIC DISORDERS TREATED WITH TYPICAL AND ATYPICAL ANTIPSYCHOTICS IN A LARGE STATE MEDICAID PROGRAM S.P. Lee 1 ; K. Lang 2 ; J. Jackel 2 ;
PREDICTORS OF MEDICATION ADHERENCE AMONG PATIENTS WITH SCHIZOPHRENIC DISORDERS TREATED WITH TYPICAL AND ATYPICAL ANTIPSYCHOTICS IN A LARGE STATE MEDICAID PROGRAM S.P. Lee 1 ; K. Lang 2 ; J. Jackel 2 ;
INTRODUCTION TO HEALTH SERVICES RESEARCH POPULATION HEALTH 796. Spring 2014 WARF Room 758 Monday 9:00 AM- 11:30 AM.
 INTRODUCTION TO HEALTH SERVICES RESEARCH POPULATION HEALTH 796 Spring 2014 WARF Room 758 Monday 9:00 AM- 11:30 AM Health Services Research is a multidisciplinary field, both basic and applied, that examines
INTRODUCTION TO HEALTH SERVICES RESEARCH POPULATION HEALTH 796 Spring 2014 WARF Room 758 Monday 9:00 AM- 11:30 AM Health Services Research is a multidisciplinary field, both basic and applied, that examines
Alzheimer s disease affects patients and their caregivers. experience employment complications,
 Alzheimer s Disease and Dementia A growing challenge The majority of the elderly population with Alzheimer s disease and related dementia are in fair to poor physical health, and experience limitations
Alzheimer s Disease and Dementia A growing challenge The majority of the elderly population with Alzheimer s disease and related dementia are in fair to poor physical health, and experience limitations
The standard Medicare Part D drug coverage is divided into 3
 Assessment of Drug Consumption Patterns for Medicare Part D Patients Alex Pedan, PhD; Jingsong Lu, MS; and Laleh T. Varasteh, RPh, MSF The standard Medicare Part D drug coverage is divided into 3 consecutive
Assessment of Drug Consumption Patterns for Medicare Part D Patients Alex Pedan, PhD; Jingsong Lu, MS; and Laleh T. Varasteh, RPh, MSF The standard Medicare Part D drug coverage is divided into 3 consecutive
Estimating Medicaid Costs for Cardiovascular Disease: A Claims-based Approach
 Estimating Medicaid Costs for Cardiovascular Disease: A Claims-based Approach Presented by Susan G. Haber, Sc.D 1 ; Boyd H. Gilman, Ph.D. 1 1 RTI International Presented at The 133rd Annual Meeting of
Estimating Medicaid Costs for Cardiovascular Disease: A Claims-based Approach Presented by Susan G. Haber, Sc.D 1 ; Boyd H. Gilman, Ph.D. 1 1 RTI International Presented at The 133rd Annual Meeting of
Stephen B. Soumerai, ScD Professor of Ambulatory Care and Prevention Harvard Medical School and Harvard Pilgrim Health Care
 Effect of Drug Utilization Controls and Coverage on Quality, Cost and Outcomes among Patients with Mental Illness Stephen B. Soumerai, ScD Professor of Ambulatory Care and Prevention Harvard Medical School
Effect of Drug Utilization Controls and Coverage on Quality, Cost and Outcomes among Patients with Mental Illness Stephen B. Soumerai, ScD Professor of Ambulatory Care and Prevention Harvard Medical School
Use Of Atypical Antipsychotic Drugs For Schizophrenia In Maine Medicaid Following A Policy Change
 Use Of Atypical Antipsychotic Drugs For Schizophrenia In Maine Medicaid Following A Policy Change Discontinuities in use of these critical drugs became apparent after Maine Medicaid instituted prior authorization
Use Of Atypical Antipsychotic Drugs For Schizophrenia In Maine Medicaid Following A Policy Change Discontinuities in use of these critical drugs became apparent after Maine Medicaid instituted prior authorization
Facilitating Access to Mental Health Services: A Look at Medicaid, Private Insurance, and the Uninsured
 June 2017 Fact Sheet Facilitating Access to Mental Health Services: A Look at Medicaid, Private Insurance, and the Uninsured In 2015, over 43 million adults had a mental illness and nearly 10 million had
June 2017 Fact Sheet Facilitating Access to Mental Health Services: A Look at Medicaid, Private Insurance, and the Uninsured In 2015, over 43 million adults had a mental illness and nearly 10 million had
Cost-Related Medication Underuse: Prevalence Among Hospitalized Managed Care Patients
 ORIGINAL RESEARCH Cost-Related Medication Underuse: Prevalence Among Hospitalized Managed Care Patients Niteesh K. Choudhry, MD, PhD 1 *, Uzaib Y. Saya, BA 1, William H. Shrank, MD, MSHS 1, Jeffrey O.
ORIGINAL RESEARCH Cost-Related Medication Underuse: Prevalence Among Hospitalized Managed Care Patients Niteesh K. Choudhry, MD, PhD 1 *, Uzaib Y. Saya, BA 1, William H. Shrank, MD, MSHS 1, Jeffrey O.
MARGUERITE E. BURNS EDUCATION
 MARGUERITE E. BURNS Department of Room 501 WARF Building Madison, WI 53726 Ph. 608-265-5282 Email: meburns@wisc.edu EDUCATION 1989 B.A. Political Science and French, 1992 M.A. Political Science, 2008 Ph.D.
MARGUERITE E. BURNS Department of Room 501 WARF Building Madison, WI 53726 Ph. 608-265-5282 Email: meburns@wisc.edu EDUCATION 1989 B.A. Political Science and French, 1992 M.A. Political Science, 2008 Ph.D.
Chapter 6: Healthcare Expenditures for Persons with CKD
 Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
Failure of Internet-based audit and feedback to improve quality of care delivered by primary care residents
 International Journal for Quality in Health Care 2005; Volume 17, Number 5: pp. 427 431 Advance Access Publication: 14 April 2005 Failure of Internet-based audit and feedback to improve quality of care
International Journal for Quality in Health Care 2005; Volume 17, Number 5: pp. 427 431 Advance Access Publication: 14 April 2005 Failure of Internet-based audit and feedback to improve quality of care
Disparities in Transplantation Caution: Life is not fair.
 Disparities in Transplantation Caution: Life is not fair. Tuesday October 30 th 2018 Caroline Rochon, MD, FACS Surgical Director, Kidney Transplant Program Hartford Hospital, Connecticut Outline Differences
Disparities in Transplantation Caution: Life is not fair. Tuesday October 30 th 2018 Caroline Rochon, MD, FACS Surgical Director, Kidney Transplant Program Hartford Hospital, Connecticut Outline Differences
Changing Patterns in Medication Use with Increasing Probability of Death for Older Medicare Beneficiaries
 Changing Patterns in Medication Use with Increasing Probability of Death for Older Medicare Beneficiaries Thomas Shaffer, MHS; Linda Simoni-Wastila, PhD, Wendy Toler, PharmD, Bruce Stuart, PhD, and Jalpa
Changing Patterns in Medication Use with Increasing Probability of Death for Older Medicare Beneficiaries Thomas Shaffer, MHS; Linda Simoni-Wastila, PhD, Wendy Toler, PharmD, Bruce Stuart, PhD, and Jalpa
Access to medically necessary healthcare is critical for successful patient outcomes, yet access
 ISSUE BRIEF 7 July 2018 Out-of-Pocket Costs and Specialty Medications Access to medically necessary healthcare is critical for successful patient outcomes, yet access is often impeded or blocked entirely
ISSUE BRIEF 7 July 2018 Out-of-Pocket Costs and Specialty Medications Access to medically necessary healthcare is critical for successful patient outcomes, yet access is often impeded or blocked entirely
2015 Survey on Prescription Drugs
 2015 Survey on Prescription Drugs AARP Research January 26, 2016 (For media inquiries, contact Gregory Phillips at 202-434-2544 or gphillips@aarp.org) https://doi.org/10.26419/res.00122.001 Objectives
2015 Survey on Prescription Drugs AARP Research January 26, 2016 (For media inquiries, contact Gregory Phillips at 202-434-2544 or gphillips@aarp.org) https://doi.org/10.26419/res.00122.001 Objectives
The Impact of Tiered Co-Pays A Survey of Patients and Pharmacists
 The Impact of Tiered Co-Pays A Survey of Patients and Pharmacists Research Report Conducted by Harris Interactive September, 2003 This study was completed on behalf of and with support from the National
The Impact of Tiered Co-Pays A Survey of Patients and Pharmacists Research Report Conducted by Harris Interactive September, 2003 This study was completed on behalf of and with support from the National
Insurance Coverage Changes for People with HIV Under the ACA
 Insurance Coverage Changes for People with HIV Under the ACA Jennifer Kates, Lindsey Dawson Prior to the Affordable Care Act (ACA), people with HIV faced limited access to insurance coverage due to several
Insurance Coverage Changes for People with HIV Under the ACA Jennifer Kates, Lindsey Dawson Prior to the Affordable Care Act (ACA), people with HIV faced limited access to insurance coverage due to several
Disability, race/ethnicity, and medication adherence among Medicare myocardial infarction survivors
 Outcomes, Health Policy, and Managed Care Disability, race/ethnicity, and medication adherence among Medicare myocardial infarction survivors Yuting Zhang, PhD, a Seo Hyon Baik, PhD, a Chung-Chou H. Chang,
Outcomes, Health Policy, and Managed Care Disability, race/ethnicity, and medication adherence among Medicare myocardial infarction survivors Yuting Zhang, PhD, a Seo Hyon Baik, PhD, a Chung-Chou H. Chang,
Cost-related Non-adherence to Medications among Patients with Diabetes and Chronic Pain: Factors beyond Finances
 Diabetes Care Publish Ahead of Print, published online September 3, 2009 Cost-related Non-adherence to Medications among Patients with Diabetes and Chronic Pain: Factors beyond Finances Running title:
Diabetes Care Publish Ahead of Print, published online September 3, 2009 Cost-related Non-adherence to Medications among Patients with Diabetes and Chronic Pain: Factors beyond Finances Running title:
HEALTH CARE EXPENDITURES ASSOCIATED WITH PERSISTENT EMERGENCY DEPARTMENT USE: A MULTI-STATE ANALYSIS OF MEDICAID BENEFICIARIES
 HEALTH CARE EXPENDITURES ASSOCIATED WITH PERSISTENT EMERGENCY DEPARTMENT USE: A MULTI-STATE ANALYSIS OF MEDICAID BENEFICIARIES Presented by Parul Agarwal, PhD MPH 1,2 Thomas K Bias, PhD 3 Usha Sambamoorthi,
HEALTH CARE EXPENDITURES ASSOCIATED WITH PERSISTENT EMERGENCY DEPARTMENT USE: A MULTI-STATE ANALYSIS OF MEDICAID BENEFICIARIES Presented by Parul Agarwal, PhD MPH 1,2 Thomas K Bias, PhD 3 Usha Sambamoorthi,
Prescription Switching and Reduced LDL-C Goal Attainment
 Prescription Switching and Reduced LDL-C Goal Attainment JoAnne M. Foody, MD, FACC, FAHA Brigham and Women's Hospital, Boston, MA Disclosures Consultant for Merck and Pfizer Why Address Adherence? Increasing
Prescription Switching and Reduced LDL-C Goal Attainment JoAnne M. Foody, MD, FACC, FAHA Brigham and Women's Hospital, Boston, MA Disclosures Consultant for Merck and Pfizer Why Address Adherence? Increasing
As the US population ages, the prevalence of chronic disease
 ORIGINAL ARTICLE Hospitalizations and Deaths Among Adults With Cardiovascular Disease Who Underuse Medications Because of Cost A Longitudinal Analysis Michele Heisler, MD, MPA,* Hwajung Choi, PhD, Allison
ORIGINAL ARTICLE Hospitalizations and Deaths Among Adults With Cardiovascular Disease Who Underuse Medications Because of Cost A Longitudinal Analysis Michele Heisler, MD, MPA,* Hwajung Choi, PhD, Allison
CHRONIC DISEASE PREVALENCE AMONG ADULTS IN OHIO
 OHIO MEDICAID ASSESSMENT SURVEY 2012 Taking the pulse of health in Ohio CHRONIC DISEASE PREVALENCE AMONG ADULTS IN OHIO Amy Ferketich, PhD Ling Wang, MPH The Ohio State University College of Public Health
OHIO MEDICAID ASSESSMENT SURVEY 2012 Taking the pulse of health in Ohio CHRONIC DISEASE PREVALENCE AMONG ADULTS IN OHIO Amy Ferketich, PhD Ling Wang, MPH The Ohio State University College of Public Health
Medicaid Cost Containment and Potential Effects on Diabetic Beneficiaries
 Medicaid Cost Containment and Potential Effects on Diabetic Beneficiaries White Paper October 2003 2003 The Health Strategies Consultancy LLC and Duke University, The Fuqua School of Business For more
Medicaid Cost Containment and Potential Effects on Diabetic Beneficiaries White Paper October 2003 2003 The Health Strategies Consultancy LLC and Duke University, The Fuqua School of Business For more
Behavioral Health Hospital and Emergency Department Health Services Utilization
 Behavioral Health Hospital and Emergency Department Health Services Utilization Rhode Island Fee-For-Service Medicaid Recipients Calendar Year 2000 Prepared for: Prepared by: Medicaid Research and Evaluation
Behavioral Health Hospital and Emergency Department Health Services Utilization Rhode Island Fee-For-Service Medicaid Recipients Calendar Year 2000 Prepared for: Prepared by: Medicaid Research and Evaluation
Racial Variation In Quality Of Care Among Medicare+Choice Enrollees
 Racial Variation In Quality Of Care Among Medicare+Choice Enrollees Black/white patterns of racial disparities in health care do not necessarily apply to Asians, Hispanics, and Native Americans. by Beth
Racial Variation In Quality Of Care Among Medicare+Choice Enrollees Black/white patterns of racial disparities in health care do not necessarily apply to Asians, Hispanics, and Native Americans. by Beth
Predictors of Employment and Productivity Among Returning National Guard Members
 Predictors of Employment and Productivity Among Returning National Guard Members Kara Zivin, Ph.D. VA National Serious Mental Illness Treatment Resource & Evaluation Center VA Ann Arbor HSR&D Center of
Predictors of Employment and Productivity Among Returning National Guard Members Kara Zivin, Ph.D. VA National Serious Mental Illness Treatment Resource & Evaluation Center VA Ann Arbor HSR&D Center of
Does Variation in the Physical Characteristics of Generic Drugs Affect Patients Experiences?
 Does Variation in the Physical Characteristics of Generic Drugs Affect Patients Experiences? Results from a National Survey of Pharmacists and Patients Ameet Sarpatwari, J.D., Ph.D. Instructor in Medicine,
Does Variation in the Physical Characteristics of Generic Drugs Affect Patients Experiences? Results from a National Survey of Pharmacists and Patients Ameet Sarpatwari, J.D., Ph.D. Instructor in Medicine,
Cost-Related Nonadherence to Medications Among Patients With Diabetes and Chronic Pain 2,3,4
 Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Cost-Related Nonadherence to Medications Among Patients With Diabetes and Chronic Pain Factors beyond finances JACOB
Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Cost-Related Nonadherence to Medications Among Patients With Diabetes and Chronic Pain Factors beyond finances JACOB
Financial Hardship in Cancer Survivors
 Financial Hardship in Cancer Survivors Robin Yabroff Robin.yabroff@hhs.gov The views expressed are those of the speaker and do not necessarily represent the official position of Department of Health and
Financial Hardship in Cancer Survivors Robin Yabroff Robin.yabroff@hhs.gov The views expressed are those of the speaker and do not necessarily represent the official position of Department of Health and
Medicaid Expansion & Adult Dental Benefits: Access to Dental Care among Low-Income Adults
 Medicaid Expansion & Adult Dental Benefits: Access to Dental Care among Low-Income Adults Astha Singhal BDS, MPH, PhD Assistant Professor, Health Policy & Health Services Research Boston University Henry
Medicaid Expansion & Adult Dental Benefits: Access to Dental Care among Low-Income Adults Astha Singhal BDS, MPH, PhD Assistant Professor, Health Policy & Health Services Research Boston University Henry
TIMOTHY A. WAIDMANN Senior Research Associate Health Policy Center The Urban Institute
 TIMOTHY A. WAIDMANN Senior Research Associate Health Policy Center The Urban Institute Education 1991 Ph.D., Economics, University of Michigan 1989 M.A., Economics, University of Michigan 1986 A.B., Economics,
TIMOTHY A. WAIDMANN Senior Research Associate Health Policy Center The Urban Institute Education 1991 Ph.D., Economics, University of Michigan 1989 M.A., Economics, University of Michigan 1986 A.B., Economics,
Impact of Florida s Medicaid Reform on Recipients of Mental Health Services
 Impact of Florida s Medicaid Reform on Recipients of Mental Health Services Jeffrey Harman, PhD John Robst, PhD Lilliana Bell, MHA The Quality of Behavioral Healthcare : A Drive for Change Through Research
Impact of Florida s Medicaid Reform on Recipients of Mental Health Services Jeffrey Harman, PhD John Robst, PhD Lilliana Bell, MHA The Quality of Behavioral Healthcare : A Drive for Change Through Research
State Health System Performance: A Detailed Look at the Lone Star State
 State Health System Performance: A Detailed Look at the Lone Star State How does Texas fare in the Commonwealth Fund Scorecard on State Health System Performance? A DETAILED LOOK AT THE LONE STAR STATE
State Health System Performance: A Detailed Look at the Lone Star State How does Texas fare in the Commonwealth Fund Scorecard on State Health System Performance? A DETAILED LOOK AT THE LONE STAR STATE
HEALTH DISPARITIES AMONG ADULTS IN OHIO
 OHIO MEDICAID ASSESSMENT SURVEY 2012 Taking the pulse of health in Ohio HEALTH DISPARITIES AMONG ADULTS IN OHIO Amy K. Ferketich, PhD 1 Ling Wang, MPH 1 Timothy R. Sahr, MPH, MA 2 1The Ohio State University
OHIO MEDICAID ASSESSMENT SURVEY 2012 Taking the pulse of health in Ohio HEALTH DISPARITIES AMONG ADULTS IN OHIO Amy K. Ferketich, PhD 1 Ling Wang, MPH 1 Timothy R. Sahr, MPH, MA 2 1The Ohio State University
SPECIAL ISSUE. Medicaid Prescription Drug Access Restrictions: Exploring the Effect on Patient Persistence With Hypertension Medications
 Medicaid Prescription Drug Access Restrictions: Exploring the Effect on Patient Persistence With Hypertension Medications Jerome Wilson, PhD; Kirsten Axelsen, MS; and Simon Tang, MPH Objective: To compare
Medicaid Prescription Drug Access Restrictions: Exploring the Effect on Patient Persistence With Hypertension Medications Jerome Wilson, PhD; Kirsten Axelsen, MS; and Simon Tang, MPH Objective: To compare
The Public and Private Dental Safety Net: Implementation of the ACA and their Roles in Access to Care for Medicaid and Expansion Populations
 Health Policy 12-1-2014 The Public and Private Dental Safety Net: Implementation of the ACA and their Roles in Access to Care for Medicaid and Expansion Populations Peter C. Damiano University of Iowa
Health Policy 12-1-2014 The Public and Private Dental Safety Net: Implementation of the ACA and their Roles in Access to Care for Medicaid and Expansion Populations Peter C. Damiano University of Iowa
The clinical and economic benefits of better treatment of adult Medicaid beneficiaries with diabetes
 The clinical and economic benefits of better treatment of adult Medicaid beneficiaries with diabetes September, 2017 White paper Life Sciences IHS Markit Introduction Diabetes is one of the most prevalent
The clinical and economic benefits of better treatment of adult Medicaid beneficiaries with diabetes September, 2017 White paper Life Sciences IHS Markit Introduction Diabetes is one of the most prevalent
The 465 medicines in development include: 142 for diabetes, which affects 10.9 million Americans age 65 and older;
 Medicines in Development Older Americans The Medicare Population and Leading Chronic Diseases presented by america s biopharmaceutical research companies Overview 2013 REPORT Biopharmaceutical Research
Medicines in Development Older Americans The Medicare Population and Leading Chronic Diseases presented by america s biopharmaceutical research companies Overview 2013 REPORT Biopharmaceutical Research
Per Capita Health Care Spending on Diabetes:
 Issue Brief #10 May 2015 Per Capita Health Care Spending on Diabetes: 2009-2013 Diabetes is a costly chronic condition in the United States, medical costs and productivity loss attributable to diabetes
Issue Brief #10 May 2015 Per Capita Health Care Spending on Diabetes: 2009-2013 Diabetes is a costly chronic condition in the United States, medical costs and productivity loss attributable to diabetes
MARGUERITE E. BURNS EDUCATION
 MARGUERITE E. BURNS Department of Population Health Sciences Room 501 WARF Building Madison, WI 53726 Ph. 608-265-5282 Email: meburns@wisc.edu EDUCATION 1989 B.A. Political Science and French, 1992 M.A.
MARGUERITE E. BURNS Department of Population Health Sciences Room 501 WARF Building Madison, WI 53726 Ph. 608-265-5282 Email: meburns@wisc.edu EDUCATION 1989 B.A. Political Science and French, 1992 M.A.
THE AFFORDABLE CARE ACT, MEDICAID & RYAN WHITE: THE HIV VOTE. Daniel Tietz, RN, JD Executive Director
 THE AFFORDABLE CARE ACT, MEDICAID & RYAN WHITE: THE HIV VOTE Daniel Tietz, RN, JD Executive Director dtietz@acria.org Overview The Affordable Care Act and HIV Medicaid Expansion or not? Ryan White filling
THE AFFORDABLE CARE ACT, MEDICAID & RYAN WHITE: THE HIV VOTE Daniel Tietz, RN, JD Executive Director dtietz@acria.org Overview The Affordable Care Act and HIV Medicaid Expansion or not? Ryan White filling
President Clinton's proposal for health reform contains a plan for
 DataWatch Paying For Mental Health And Substance Abuse Care by Richard G. Frank, Thomas G. McGuire, Darrel A, Regier, Ronald Manderscheid, and Albert Woodward Abstract: Fifty-four billion dollars was spent
DataWatch Paying For Mental Health And Substance Abuse Care by Richard G. Frank, Thomas G. McGuire, Darrel A, Regier, Ronald Manderscheid, and Albert Woodward Abstract: Fifty-four billion dollars was spent
PQS Summary of Pharmacy/ Medication-Related Updates in the CY 2020 Final Call Letter
 Managing Performance Information in a Quality Driven World PQS Summary of Pharmacy/ Medication-Related Updates in the CY 2020 Final Call Letter REGULATORY UPDATE PQS Summary of Pharmacy/ Medication-Related
Managing Performance Information in a Quality Driven World PQS Summary of Pharmacy/ Medication-Related Updates in the CY 2020 Final Call Letter REGULATORY UPDATE PQS Summary of Pharmacy/ Medication-Related
Between 1985 and 1999, as managed
 National In Use Of Medications In Office- Based Practice, 1985 1999 Drugs were discussed 59 percent more often in office visits in 1999 than in 1985, rising to a rate of 146 prescriptions per 100 visits.
National In Use Of Medications In Office- Based Practice, 1985 1999 Drugs were discussed 59 percent more often in office visits in 1999 than in 1985, rising to a rate of 146 prescriptions per 100 visits.
POSITION STATEMENT ON HEALTH CARE REFORM NADP PRINCIPLES FOR EXPANDING ACCESS TO DENTAL HEALTH BENEFITS
 POSITION STATEMENT ON HEALTH CARE REFORM THE NATIONAL ASSOCIATION OF DENTAL PLANS (NADP) is the nation s largest association of companies providing dental benefits. NADP members cover 136 million Americans
POSITION STATEMENT ON HEALTH CARE REFORM THE NATIONAL ASSOCIATION OF DENTAL PLANS (NADP) is the nation s largest association of companies providing dental benefits. NADP members cover 136 million Americans
Trends in Ohioans Health Status and Income
 October 200 Trends in Ohioans Health Status and Income Since 2005, household incomes in Ohio have steadily declined. In 2005, 65% of Ohio adults were living in households with an annual income over 200%
October 200 Trends in Ohioans Health Status and Income Since 2005, household incomes in Ohio have steadily declined. In 2005, 65% of Ohio adults were living in households with an annual income over 200%
Oral Health in Children in Iowa
 December 2012 Oral Health in Children in Iowa An Overview From the 2010 Iowa Child and Family Household Health Survey Peter C. Damiano Director Jean C. Willard Senior Research Assistant Ki H. Park Graduate
December 2012 Oral Health in Children in Iowa An Overview From the 2010 Iowa Child and Family Household Health Survey Peter C. Damiano Director Jean C. Willard Senior Research Assistant Ki H. Park Graduate
PREPARED BY THE CENTER FOR MEDICARE ADVOCACY, INC.
 MEDICARE DRUG CARDS PROVE INCONSISTENT AND PROVIDE FEW DISCOUNTS FOR MEDICARE BENEFICIARIES TRYING TO REDUCE THE COST OF THE TEN MOST POPULAR BRAND-NAME DRUGS USED BY SENIORS PREPARED BY THE CENTER FOR
MEDICARE DRUG CARDS PROVE INCONSISTENT AND PROVIDE FEW DISCOUNTS FOR MEDICARE BENEFICIARIES TRYING TO REDUCE THE COST OF THE TEN MOST POPULAR BRAND-NAME DRUGS USED BY SENIORS PREPARED BY THE CENTER FOR
A COMPREHENSIVE REPORT ISSUED BY THE AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGISTS IN PARTNERSHIP WITH:
 A COMPREHENSIVE REPORT ISSUED BY THE AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGISTS IN PARTNERSHIP WITH: Amputee Coalition of America Mended Hearts National Federation of the Blind National Kidney Foundation
A COMPREHENSIVE REPORT ISSUED BY THE AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGISTS IN PARTNERSHIP WITH: Amputee Coalition of America Mended Hearts National Federation of the Blind National Kidney Foundation
Value of Hospice Benefit to Medicaid Programs
 One Pennsylvania Plaza, 38 th Floor New York, NY 10119 Tel 212-279-7166 Fax 212-629-5657 www.milliman.com Value of Hospice Benefit May 2, 2003 Milliman USA, Inc. New York, NY Kate Fitch, RN, MEd, MA Bruce
One Pennsylvania Plaza, 38 th Floor New York, NY 10119 Tel 212-279-7166 Fax 212-629-5657 www.milliman.com Value of Hospice Benefit May 2, 2003 Milliman USA, Inc. New York, NY Kate Fitch, RN, MEd, MA Bruce
Trends and Variation in Oral Anticoagulant Choice in Patients with Atrial Fibrillation,
 Trends and Variation in Oral Anticoagulant Choice in Patients with Atrial Fibrillation, 2010-2017 Junya Zhu, PhD Department of Health Policy and Management January 23, 2018 Acknowledgments Co-Authors G.
Trends and Variation in Oral Anticoagulant Choice in Patients with Atrial Fibrillation, 2010-2017 Junya Zhu, PhD Department of Health Policy and Management January 23, 2018 Acknowledgments Co-Authors G.
Dental Care Remains the No. 1 Unmet Health Care Need for Children and Low-Income Adults
 Oral Health and Access to Dental Care for Ohioans, 2007 Dental Care Remains the No. 1 Unmet Health Care Need for Children and Low-Income Adults Oral Health and Access to Dental Care for Ohioans, 2007
Oral Health and Access to Dental Care for Ohioans, 2007 Dental Care Remains the No. 1 Unmet Health Care Need for Children and Low-Income Adults Oral Health and Access to Dental Care for Ohioans, 2007
APPENDIX: Supplementary Materials for Advance Directives And Nursing. Home Stays Associated With Less Aggressive End-Of-Life Care For
 Nicholas LH, Bynum JPW, Iwashnya TJ, Weir DR, Langa KM. Advance directives and nursing home stays associated with less aggressive end-of-life care for patients with severe dementia. Health Aff (MIllwood).
Nicholas LH, Bynum JPW, Iwashnya TJ, Weir DR, Langa KM. Advance directives and nursing home stays associated with less aggressive end-of-life care for patients with severe dementia. Health Aff (MIllwood).
PRESCRIPTION DRUG COSTS
 ORIGINAL INVESTIGATION The Role of Patient-Physician Trust in Moderating Medication nadherence Due to Cost Pressures John D. Piette, PhD; Michele Heisler, MD, MPA; Sarah Krein, PhD, RN; Eve A. Kerr, MD,
ORIGINAL INVESTIGATION The Role of Patient-Physician Trust in Moderating Medication nadherence Due to Cost Pressures John D. Piette, PhD; Michele Heisler, MD, MPA; Sarah Krein, PhD, RN; Eve A. Kerr, MD,
Medicare prescription drug coverage: A very long wait for a very modest benefit
 The American Journal of Medicine (2005) 118, 325-329 EDITORIAL Medicare prescription drug coverage: A very long wait for a very modest benefit James E. Dalen, MD, MPH, Douglas J. Hartz, BS, BPA Arizona
The American Journal of Medicine (2005) 118, 325-329 EDITORIAL Medicare prescription drug coverage: A very long wait for a very modest benefit James E. Dalen, MD, MPH, Douglas J. Hartz, BS, BPA Arizona
Helpful Resources for people with Diabetes
 Helpful Resources for people with Diabetes Help with Diabetes tablets and insulin The goal of the program is to help eligible uninsured and underinsured patients of all ages receive needed prescription
Helpful Resources for people with Diabetes Help with Diabetes tablets and insulin The goal of the program is to help eligible uninsured and underinsured patients of all ages receive needed prescription
Evidence from a Pharmacy Access Program TERESA B. GIBSON, PHD SENIOR DIRECTOR, HEALTH OUTCOMES OCTOBER 27, 2011
 Evidence from a Pharmacy Access Program TERESA B. GIBSON, PHD SENIOR DIRECTOR, HEALTH OUTCOMES OCTOBER 27, 2011 OVERVIEW Gibson TB, Mahoney J, Ranghell K, Cherney BJ, McElwee N. Value-Based Insurance Plus
Evidence from a Pharmacy Access Program TERESA B. GIBSON, PHD SENIOR DIRECTOR, HEALTH OUTCOMES OCTOBER 27, 2011 OVERVIEW Gibson TB, Mahoney J, Ranghell K, Cherney BJ, McElwee N. Value-Based Insurance Plus
Follow this and additional works at:
 The University of Toledo The University of Toledo Digital Repository Theses and Dissertations 2013 Factors associated with primary medication nonadherence and its effect on health service utilization among
The University of Toledo The University of Toledo Digital Repository Theses and Dissertations 2013 Factors associated with primary medication nonadherence and its effect on health service utilization among
Webinar Series: Diabetes Epidemic & Action Report (DEAR) for Washington State - How We Are Doing and How We Can Improve.
 Webinar Series: Diabetes Epidemic & Action Report (DEAR) for Washington State - How We Are Doing and How We Can Improve April 22, 2015 Qualis Health A leading national population health management organization
Webinar Series: Diabetes Epidemic & Action Report (DEAR) for Washington State - How We Are Doing and How We Can Improve April 22, 2015 Qualis Health A leading national population health management organization
USRDS UNITED STATES RENAL DATA SYSTEM
 USRDS UNITED STATES RENAL DATA SYSTEM Chapter 6: Medicare Expenditures for Persons With CKD Medicare spending for patients with CKD aged 65 and older exceeded $50 billion in 2013, representing 20% of all
USRDS UNITED STATES RENAL DATA SYSTEM Chapter 6: Medicare Expenditures for Persons With CKD Medicare spending for patients with CKD aged 65 and older exceeded $50 billion in 2013, representing 20% of all
Unmanaged Behavioral Health Puts Your Company At Risk. Presented by: Dr. Sam Mayhugh Integrated Behavioral Health
 Unmanaged Behavioral Health Puts Your Company At Risk Presented by: Dr. Sam Mayhugh Integrated Behavioral Health Behavioral Health Management Webinar Overview History of BH management Prevalence of behavioral
Unmanaged Behavioral Health Puts Your Company At Risk Presented by: Dr. Sam Mayhugh Integrated Behavioral Health Behavioral Health Management Webinar Overview History of BH management Prevalence of behavioral
Identifying Adult Mental Disorders with Existing Data Sources
 Identifying Adult Mental Disorders with Existing Data Sources Mark Olfson, M.D., M.P.H. New York State Psychiatric Institute Columbia University New York, New York Everything that can be counted does not
Identifying Adult Mental Disorders with Existing Data Sources Mark Olfson, M.D., M.P.H. New York State Psychiatric Institute Columbia University New York, New York Everything that can be counted does not
Medicare Part D was implemented in 2006 to provide prescription
 Effects of Coverage Gap Reform on Adherence to Diabetes Medications Feng Zeng, PhD; Bimal V. Patel, PharmD, MS; and Louis Brunetti, MD Objectives: To investigate the impact of Part D coverage gap reform
Effects of Coverage Gap Reform on Adherence to Diabetes Medications Feng Zeng, PhD; Bimal V. Patel, PharmD, MS; and Louis Brunetti, MD Objectives: To investigate the impact of Part D coverage gap reform
Getting Hypertension Under Control
 Getting Hypertension Under Control Learning Objectives EXPLAIN the factors involved in patient medication non-adherence. OUTLINE the results of studies focusing on medication adherence issues in patients
Getting Hypertension Under Control Learning Objectives EXPLAIN the factors involved in patient medication non-adherence. OUTLINE the results of studies focusing on medication adherence issues in patients
Issue Brief. Women are living longer than ever. A woman who is 65
 September 2000 Issue Brief Living Longer, Staying Well: Promoting Good Health for Older Women Karen Scott Collins and Erin Strumpf The Commonwealth Fund is a private foundation established in 1918 by Anna
September 2000 Issue Brief Living Longer, Staying Well: Promoting Good Health for Older Women Karen Scott Collins and Erin Strumpf The Commonwealth Fund is a private foundation established in 1918 by Anna
Health Issues for Aging Populations
 This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike License. Your use of this material constitutes acceptance of that license and the conditions of use of materials on this
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike License. Your use of this material constitutes acceptance of that license and the conditions of use of materials on this
Mental health planners and policymakers routinely rely on utilization
 DataWatch Measuring Outpatient Mental Health Care In The United States by Mark Olfson and Harold Alan Pincus Abstract: A standard definition of outpatient mental health care does not now exist. Data from
DataWatch Measuring Outpatient Mental Health Care In The United States by Mark Olfson and Harold Alan Pincus Abstract: A standard definition of outpatient mental health care does not now exist. Data from
The University of Mississippi School of Pharmacy
 LONG TERM PERSISTENCE WITH ACEI/ARB THERAPY AFTER ACUTE MYOCARDIAL INFARCTION: AN ANALYSIS OF THE 2006-2007 MEDICARE 5% NATIONAL SAMPLE DATA Lokhandwala T. MS, Yang Y. PhD, Thumula V. MS, Bentley J.P.
LONG TERM PERSISTENCE WITH ACEI/ARB THERAPY AFTER ACUTE MYOCARDIAL INFARCTION: AN ANALYSIS OF THE 2006-2007 MEDICARE 5% NATIONAL SAMPLE DATA Lokhandwala T. MS, Yang Y. PhD, Thumula V. MS, Bentley J.P.
This slide set provides an overview of the impact of type 1 and type 2 diabetes mellitus in the United States, focusing on epidemiology, costs both
 This slide set provides an overview of the impact of type 1 and type 2 diabetes mellitus in the United States, focusing on epidemiology, costs both direct and indirect and the projected burden of diabetes,
This slide set provides an overview of the impact of type 1 and type 2 diabetes mellitus in the United States, focusing on epidemiology, costs both direct and indirect and the projected burden of diabetes,
Diversity and Dementia
 Diversity and Dementia Kala M. Mehta, DSc, MPH January 17, 2012 Overview Background Incidence and Prevalence of Dementia Why are these differences found? What s important for diverse dementia patients
Diversity and Dementia Kala M. Mehta, DSc, MPH January 17, 2012 Overview Background Incidence and Prevalence of Dementia Why are these differences found? What s important for diverse dementia patients
Overweight and Obesity Rates Among Upstate New York Adults
 T H E F A C T S A B O U T Overweight and Obesity Rates Among Upstate New York Adults Upstate New York Obesity Rate: 27.5% Overweight Rate: 35.5% Increase in the combined overweight/ obesity rate from 2003
T H E F A C T S A B O U T Overweight and Obesity Rates Among Upstate New York Adults Upstate New York Obesity Rate: 27.5% Overweight Rate: 35.5% Increase in the combined overweight/ obesity rate from 2003
Trends in Pneumonia and Influenza Morbidity and Mortality
 Trends in Pneumonia and Influenza Morbidity and Mortality American Lung Association Epidemiology and Statistics Unit Research and Health Education Division November 2015 Page intentionally left blank Introduction
Trends in Pneumonia and Influenza Morbidity and Mortality American Lung Association Epidemiology and Statistics Unit Research and Health Education Division November 2015 Page intentionally left blank Introduction
Health Care Reform Update and Advocacy Priorities
 Health Care Reform Update and Advocacy Priorities Robert Greenwald Clinical Professor of Law Director, Center for Health Law and Policy Innovation of Harvard Law School October 2012 PRESENTATION OUTLINE
Health Care Reform Update and Advocacy Priorities Robert Greenwald Clinical Professor of Law Director, Center for Health Law and Policy Innovation of Harvard Law School October 2012 PRESENTATION OUTLINE
HHS Public Access Author manuscript Ann Intern Med. Author manuscript; available in PMC 2016 May 17.
 The Burden of Health Care Costs in the Last 5 Years of Life Amy S. Kelley, MD, MSHS 1,2, Kathleen McGarry, PhD 3, Rebecca Gorges, MA 1, and Jonathan S. Skinner, PhD 4,5 1 Icahn School of Medicine at Mount
The Burden of Health Care Costs in the Last 5 Years of Life Amy S. Kelley, MD, MSHS 1,2, Kathleen McGarry, PhD 3, Rebecca Gorges, MA 1, and Jonathan S. Skinner, PhD 4,5 1 Icahn School of Medicine at Mount
Research Article Recognition of Depression and Anxiety among Elderly Colorectal Cancer Patients
 Nursing Research and Practice Volume 2010, Article ID 693961, 8 pages doi:10.1155/2010/693961 Research Article Recognition of Depression and Anxiety among Elderly Colorectal Cancer Patients Amy Y. Zhang
Nursing Research and Practice Volume 2010, Article ID 693961, 8 pages doi:10.1155/2010/693961 Research Article Recognition of Depression and Anxiety among Elderly Colorectal Cancer Patients Amy Y. Zhang
Medicare Severity-adjusted Diagnosis Related Groups (MS-DRGs) Coding Adjustment
 American Hospital association December 2012 TrendWatch Are Medicare Patients Getting Sicker? Today, Medicare covers more than 48 million people, and that number is growing rapidly baby boomers are reaching
American Hospital association December 2012 TrendWatch Are Medicare Patients Getting Sicker? Today, Medicare covers more than 48 million people, and that number is growing rapidly baby boomers are reaching
Employers, in their role as health care purchasers, are
 Article Health and Disability Costs of Depressive Illness in a Major U.S. Corporation Benjamin G. Druss, M.D., M.P.H. Robert A. Rosenheck, M.D. William H. Sledge, M.D. Objective: Employers are playing
Article Health and Disability Costs of Depressive Illness in a Major U.S. Corporation Benjamin G. Druss, M.D., M.P.H. Robert A. Rosenheck, M.D. William H. Sledge, M.D. Objective: Employers are playing
Relations between diabetes status, comorbid conditions, and current mental health in older adult females
 Ment Health Fam Med (2018) 13: 715-719 2018 Mental Health and Family Medicine Ltd Research Article Relations between diabetes status, comorbid conditions, and current mental health in older adult females
Ment Health Fam Med (2018) 13: 715-719 2018 Mental Health and Family Medicine Ltd Research Article Relations between diabetes status, comorbid conditions, and current mental health in older adult females
Medicare Risk Adjustment for the Frail Elderly
 Medicare Risk Adjustment for the Frail Elderly John Kautter, Ph.D., Melvin Ingber, Ph.D., and Gregory C. Pope, M.S. CMS has had a continuing interest in exploring ways to incorporate frailty adjustment
Medicare Risk Adjustment for the Frail Elderly John Kautter, Ph.D., Melvin Ingber, Ph.D., and Gregory C. Pope, M.S. CMS has had a continuing interest in exploring ways to incorporate frailty adjustment
Are Racial/Ethnic Disparities in Youth Psychotropic Medication Due to Overuse by Whites?
 Are Racial/Ethnic Disparities in Youth Psychotropic Medication Due to Overuse by Whites? Benjamin Cook, PhD MPH Director, Center for Multicultural Mental Health Research Assistant Professor, Department
Are Racial/Ethnic Disparities in Youth Psychotropic Medication Due to Overuse by Whites? Benjamin Cook, PhD MPH Director, Center for Multicultural Mental Health Research Assistant Professor, Department
had non-continuous enrolment in Medicare Part A or Part B during the year following initial admission;
 Effectiveness and cost-effectiveness of implantable cardioverter defibrillators in the treatment of ventricular arrhythmias among Medicare beneficiaries Weiss J P, Saynina O, McDonald K M, McClellan M
Effectiveness and cost-effectiveness of implantable cardioverter defibrillators in the treatment of ventricular arrhythmias among Medicare beneficiaries Weiss J P, Saynina O, McDonald K M, McClellan M
Financial Impact of Emergency Department Visits by Adults for Dental Conditions in Maryland
 Financial Impact of Emergency Department by Adults for Dental Conditions in Maryland Background Access to dental care remains challenging for many children and adults. Lack of preventive care services
Financial Impact of Emergency Department by Adults for Dental Conditions in Maryland Background Access to dental care remains challenging for many children and adults. Lack of preventive care services
RESEARCH. What is already known about this subject. What this study adds
 RESEARCH Adherence and Persistence to Prescribed Medication Therapy Among Medicare Part D Beneficiaries on Dialysis: Comparisons of Benefit Type and Benefit Phase Haesuk Park, PhD; Karen L. Rascati, PhD;
RESEARCH Adherence and Persistence to Prescribed Medication Therapy Among Medicare Part D Beneficiaries on Dialysis: Comparisons of Benefit Type and Benefit Phase Haesuk Park, PhD; Karen L. Rascati, PhD;
Schizophrenia, a devastating chronic. Treatment Adherence Associated With Conventional and Atypical Antipsychotics in a Large State Medicaid Program
 Treatment Adherence Associated With Conventional and Atypical Antipsychotics in a Large State Medicaid Program Joseph Menzin, Ph.D. Luke Boulanger, M.A. Mark Friedman, M.D. Joan Mackell, Ph.D. John R.
Treatment Adherence Associated With Conventional and Atypical Antipsychotics in a Large State Medicaid Program Joseph Menzin, Ph.D. Luke Boulanger, M.A. Mark Friedman, M.D. Joan Mackell, Ph.D. John R.
SURVEY ABOUT YOUR PRESCRIPTION CHOICES
 Editor s Note: This online data supplement contains supplemental material that was not included with the published article by William Shrank and colleagues, Patients' Perceptions of Generic Medications,
Editor s Note: This online data supplement contains supplemental material that was not included with the published article by William Shrank and colleagues, Patients' Perceptions of Generic Medications,
Costs and Use of Oral Anti-cancer Medications among Senior Medicare Part D Beneficiaries
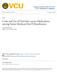 Virginia Commonwealth University VCU Scholars Compass Theses and Dissertations Graduate School 2012 Costs and Use of Oral Anti-cancer Medications among Senior Medicare Part D Beneficiaries Nantana Kaisaeng
Virginia Commonwealth University VCU Scholars Compass Theses and Dissertations Graduate School 2012 Costs and Use of Oral Anti-cancer Medications among Senior Medicare Part D Beneficiaries Nantana Kaisaeng
Apurba Chakraborty MBBS, MPH Dima M. Qato PharmD, MPH, PhD Professor Mark S. Dworkin MD, MPHTM The University of Illinois at Chicago
 Less is More: The Impact of Lower Pill Burden on Adherence to Antiretroviral Therapy among Treatment-Naive Patients with HIV Infection in the United States Apurba Chakraborty MBBS, MPH Dima M. Qato PharmD,
Less is More: The Impact of Lower Pill Burden on Adherence to Antiretroviral Therapy among Treatment-Naive Patients with HIV Infection in the United States Apurba Chakraborty MBBS, MPH Dima M. Qato PharmD,
OCTOBER 2011 MEDICAID AND HIV: A NATIONAL ANALYSIS
 OCTOBER 2011 MEDICAID AND HIV: A NATIONAL ANALYSIS MEDICAID AND HIV: A NATIONAL ANALYSIS OCTOBER 2011 Prepared by JEN KATES EXECUTIVE SUMMARY Medicaid, the nation s principal safety-net health insurance
OCTOBER 2011 MEDICAID AND HIV: A NATIONAL ANALYSIS MEDICAID AND HIV: A NATIONAL ANALYSIS OCTOBER 2011 Prepared by JEN KATES EXECUTIVE SUMMARY Medicaid, the nation s principal safety-net health insurance
CHCS. Multimorbidity Pattern Analyses and Clinical Opportunities: Dementia. Center for Health Care Strategies, Inc. FACES OF MEDICAID DATA SERIES
 CHCS Center for Health Care Strategies, Inc. FACES OF MEDICAID DATA SERIES Multimorbidity Pattern Analyses and Clinical Opportunities: Dementia December 2010 Cynthia Boyd, MD, MPH* Bruce Leff, MD* Carlos
CHCS Center for Health Care Strategies, Inc. FACES OF MEDICAID DATA SERIES Multimorbidity Pattern Analyses and Clinical Opportunities: Dementia December 2010 Cynthia Boyd, MD, MPH* Bruce Leff, MD* Carlos
Demand and Burden of Dental Care in Canadian Households. Mustafa Andkhoie, MPH PhD student, Epidemiology University of Saskatchewan May 27 th, 2015
 Demand and Burden of Dental Care in Canadian Households Mustafa Andkhoie, MPH PhD student, Epidemiology University of Saskatchewan May 27 th, 2015 Introduction Dental Health Expenditure In Canada second-largest
Demand and Burden of Dental Care in Canadian Households Mustafa Andkhoie, MPH PhD student, Epidemiology University of Saskatchewan May 27 th, 2015 Introduction Dental Health Expenditure In Canada second-largest
Brief Report Brief Report: Use of non-pharmacological strategies for pain relief in addiction treatment patients with chronic pain 1
 Brief Report Brief Report: Use of non-pharmacological strategies for pain relief in addiction treatment patients with chronic pain 1 Running head: Use of non-pharmacological treatments for pain Lewei (Allison)
Brief Report Brief Report: Use of non-pharmacological strategies for pain relief in addiction treatment patients with chronic pain 1 Running head: Use of non-pharmacological treatments for pain Lewei (Allison)
Medicaid s Role in Combating the Opioid Crisis
 1 Medicaid s Role in Combating the Opioid Crisis September 23, 2016 Deborah Bachrach Partner Manatt Health Assessing Innovations in Medicaid 1 Medicaid Started as Adjunct to Welfare Programs 2 Eligibility
1 Medicaid s Role in Combating the Opioid Crisis September 23, 2016 Deborah Bachrach Partner Manatt Health Assessing Innovations in Medicaid 1 Medicaid Started as Adjunct to Welfare Programs 2 Eligibility
