Diabetes, Depression, and OASIS-C A GUIDE FOR HOME HEALTHCARE CLINICIANS
|
|
|
- Dinah May
- 5 years ago
- Views:
Transcription
1 Diabetes, Depression, and OASIS-C A GUIDE FOR HOME HEALTHCARE CLINICIANS Depression is significantly higher among elderly adults receiving home healthcare, particularly among adults with Type 2 diabetes. Depression leads to greater medical illness, functional impairment, and chronic pain. Opportunities are often missed to improve mental health and general medical outcomes when mental illness is underrecognized and undertreated. This article discusses the mandate by the Centers for Medicare & Medicaid Services (CMS), Outcome and Assessment Information Set C (OASIS-C) (2009) for the use of the Patient Health Questionnaire (PHQ-2) to screen for depression in home care patients, with special emphasis on the patient with diabetes. Depression is one of the most common mental health disorders and is predicted to be the second leading cause of disability worldwide by 2020 (Pignone et al., 2002). Among persons older than 65 years, one in six suffers from depression (Wang et al., 2005). According to Pickett et al. (2012), depression is significantly higher among elderly adults receiving home healthcare and leads to greater medical illness, functional impairment, and chronic pain. In 2003, Greenberg et al. described the economic burden of depression as substantial and the combined direct and indirect costs at $83.1 billion. Groups that have been identified to be at high risk for depression include minorities, women, patients with low socioeconomic status, and patients with physical disabilities or comorbid conditions (Acee, 2010). Opportunities are often missed to improve mental health and general medical outcomes when mental illness is underrecognized and undertreated (Brown et al., 2007). Beliefs that depression is normal with older age, as well as difficulties present in patients with cognitive deficits, make identification of depression in older adults challenging (Pignone et al., 2002). Depression is treatable, but first must be recognized, treated, and continuously monitored over time like any other chronic condition (Hall, 2012). Targeting depression in home care has been found to decrease hospitalization rates (Pickett et al., 2012). If left undetected or not fully treated, Anna M. Acee, EdD, ANP-BC, PMHNP-BC 362 Home Healthcare Nurse
2 2.1 HOURS Continuing Education The Centers for Medicare and Medicaid Services, Outcome and Assessment Information Set C has mandated the use of the Patient Health Questionnaire to screen for depression in homecare patients. vol. 32 no. 6 June 2014 Home Healthcare Nurse 363
3 depression is associated with higher costs, morbidity, risk of suicide, and mortality from other comorbid conditions (Beacham et al., 2008). Challenges in Managing Type 2 Diabetes and Depression A patient diagnosed with diabetes faces multiple self-management tasks each day to effectively manage this chronic illness. A daily regimen of monitoring blood glucose, meal planning, exercise, monitoring skin integrity, annual eye and dental exams, and frequent visits to the primary care provider (PCP) weigh heavily on these patients and serve as a constant reminder of the chronicity of their illness. The research has indicated that depressive disorders are higher among adults with diabetes than in the general population (Markowitz et al., 2011), with the incidence of major depression in patients with diabetes estimated to be 11% to 31% (Egede & Ellis, 2010). The research has indicated that patients with diabetes and depression have increased rates of mortality, cardiac events, hospitalizations, diabetes-related complications, functional impairment, healthcare costs, medical symptoms burden, and a decreased quality of life than patients with diabetes who are not depressed (Gonzalez et al., 2008). According to Katon (2011), comorbid depression is associated with poor adherence to self-care regimens, medical symptom burden, and functional impairment. People with Type 2 diabetes and major depression are at increased risk of microvascular and macrovascular complications (Lin et al., 2010) and up to 80% of patients with comorbid diabetes and depression will experience a relapse of depressive symptoms over a 5-year period (Ell et al., 2005). The risk of deterioration of depression symptoms over time emphasizes the need for ongoing screening for depression symptoms and treatment adherence (Hunt et al., 2012) and adjusting antidepressant therapy as needed over time (Culpepper, 2010). There is a positive relationship between poorer self-care and depressive symptoms (Markowitz et al., 2011) and inversely the higher the self-perception of health, the better the A1c levels (Acee & Fahs, 2012). Home healthcare nurses and other clinicians are well positioned to screen for depression and report the findings to the medical director or PCP. The barriers related to screening for depression include time constraints, difficulty assessing The Patient Health Questionnaire is a validated instrument that is widely used in primary care and is available in 48 languages. depressive symptoms with comorbid diabetes, clinician s lack of clinical expertise in assessing for mental health issues, patient s cultural taboos and fear of labeling, and cultural beliefs. Adding to this challenge, diagnosing depression in patients with diabetes is challenging due to the similarity of physical (e.g., weight loss and fatigue) or cognitive (e.g., trouble concentrating) symptoms. Assessing for Depression Centers for Medicare and Medicaid Services (CMS), Outcome and Assessment Information Set-C (OASIS-C) (2009) has mandated the use of the Patient Health Questionnaire (PHQ-2) to screen for depression in home care patients. The PHQ-2 assesses for two very significant signs of depression (including little interest or pleasure in doing things and experiencing a depressed mood) one of which is required to assess significant clinical depression. A score of 3 or higher is the recommended indicator for additional assessment. The PHQ-2 has been validated and showed wide variability in sensitivity (Gilbody et al., 2007). PHQ-9, the Next Step After a Positive PHQ-2 Any scores equal to or greater than 3 on the PHQ-2 should be referred to an advanced practice clinician (e.g., nurse practitioner, psychologist, physician) by the home healthcare team for diagnoses. CMS has recommended the use of the Patient Health Questionnaire-9 (PHQ-9) to further evaluate depressive symptoms during an initial visit and over time to monitor depressive symptoms and medication effectiveness in home care patients. The PHQ-9 is a nine-item screening 364 Home Healthcare Nurse
4 Table 1. Patient Health Questionnaire (PHQ-9) Over the last 2 weeks, how often have you been bothered by any of the following problems? (use ü to indicate your answer) Not at all Several Days More Than Half the Days Nearly Every Day 1. Little interest or pleasure in doing things Feeling down, depressed, or hopeless Trouble falling or staying asleep, or sleeping too much Feeling tired or having little energy Poor appetite or overeating Feeling bad about yourself or that you are a failure or have let yourself or your family down 7. Trouble concentrating on things, such as reading the newspaper or watching television watching television Moving or speaking so slowly that other people could have noticed. Or the opposite being so fidgety or restless that you have been moving around a lot more than usual Thoughts that you would be better off dead, or of hurting yourself in some way ADD COLUMNS TOTAL (Health care professional: For interpretation of TOTAL please refer to scoring card below.) 10. If you checked off any problems, how difficult have these Not difficult at all Somewhat difficult problems made it for you to do your work, take care of things at home, or get along with other people? Very difficult Extremely difficult PHQ-9 QUICK DEPRESSION ASSESSMENT For initial diagnosis: 1. Patient completes PHQ-9 Quick Depression Assessment. 2. Add score to determine severity. 3. Consider Major Depressive Disorder if there are at least 5./S in the shaded section (1 of which corresponds to Question #1 or #2). Consider Other Depressive Disorder if there are 2-4.Is in the shaded section (1 of which corresponds to Questions #1 or #2). Note. As the questionnaire relies on patient self-report, all responses should be verified by the clinician. A definitive diagnosis is made on clinical grounds, taking into account how well the patient understood the questionnaire and other relevant information from the patient. Diagnoses of major depressive disorder or other depressive disorder also require impairment of social, occupational, or other important areas of functioning (Question # 10) and ruling out normal bereavement, a history of a manic episode (bipolar disorder), and a physical disorder, medication, or other drug as the biological causes of the depressive symptoms. To monitor severity over time for newly diagnosed patients or patients in current treatment for depression: 1. Patients may complete questionnaires at baseline and at regular intervals [e.q., every 2 weeks) at home and bring them in at their next appointment for scoring, or they may complete the questionnaire during each scheduled appointment. 2. Add up.ü s by column. For every ü s: Several days = 1; More than half the days = 2; Nearly every day = Add together column scores to get a total score. 4. Refer to the PHQ-9 Scoring Card to interpret the total score. 5. Results may be included in patients files to assist you in setting up a treatment goal and determining degree of response, as well as guiding treatment intervention. PHQ-9 SCORING CARD FOR SEVERITY DETERMINATION for health professional use only Scoring - add up all checked boxes on PHQ-9 For every Not at all = 0; Several days = 1; More Than Half the Days = 2; Nearly Every Day = 3. Interpretation of Total Score Total Score Depression Severity 1 4 None 5 9 Mild depression Moderate depression Moderately severe depression Severe depression This PHQ-9 questionnaire is also available at Copyright Pfizer Inc. All rights reserved. Developed by On. Robert l. Spitzer, Janet B. Williams/ and Kurt Kroenke vol. 32 no. 6 June 2014 Home Healthcare Nurse 365
5 Table 2. Using Patient Health Questionnaire (PHQ-9) Diagnostic Assessment and Initiating Treatment PHQ-9 Symptoms and Impairment 1 to 4 symptoms, functional impairment PHQ-9 Severity Provisional Diagnosis < 10 Mild or minimal depressive symptoms Treatment Recommendations Reassurance and/or supportive counseling Patient self-management Recommend physical activity Educate patient to call if his or her condition deteriorates 2 to 4 symptoms, including Questions 1 and/or 2, plus functional impairment 5 symptoms, including Questions 1 and/or 2, plus functional impairment 5 symptoms, including Questions 1 and/or 2, plus functional impairment Moderate depressive symptoms (minor depression)** Moderately severe symptoms, major depression 20 Severe symptoms, major depression Watchful waiting Supportive counseling If no improvement after one or more months, use antidepressant or brief psychological counseling Patient preference for antidepressants and/or psychological counseling Antidepressants alone or in combination with psychological counseling Refer patient to psychiatrist or psychiatric nurse practitioner * Count the total number of symptoms in shaded sections of PHQ-9 from Table 2. **If symptoms present for > 2 years, chronic depression, or functional impairment is severe, remission with watchful waiting is unlikely, and immediate active treatment is indicated for moderate depressive symptoms (minor depression). Adapted with permission from Oxman, T. for 3CM, LLC, and the MacArthur Initiative on Depression and Primary Care, Source: Oxman T. Re-Engineering Systems for Primary Core Treatment of Depression: The Respect Depression Core Process. The Depression Initiative & Primary Care. Dartmouth Medical School. 2006: Version 9.11: 18. tool based on the diagnostic criteria for depression (Sheeran et al., 2010) (Table 1), with a scoring system based on duration/severity of particular symptoms (Kroenke et al., 2001). Depression is diagnosed when symptoms impact normal activities and persist for more than 2 weeks (Table 1). In 2002, the American Psychiatric Association outlined the diagnostic criteria for depression to include a positive response to at least one of the first two questions on the PHQ-9, indicating cardinal symptoms of persistent and pervasive low mood and loss of pleasure in usual activities. The PHQ-9 is a validated instrument that is widely used in primary care and is available in 48 languages (Multicultural Mental Health Resource Center, 2012). Patients with comorbidities (e.g., depression and diabetes) can be more thoroughly screened using the PHQ-9, because unlike the PHQ-2, it includes physical symptoms of depression. This tool is very user friendly, in that it can be administered and findings reviewed during the home visit. Home care staff may need to be trained to assess for any history or treatment of depression, or other mental health illness, substance abuse, or alcohol use. Evaluation of the findings from the PHQ-9 screen should then be interpreted by a physician, psychiatrist, psychologist, or advanced practice psychiatric nurse. The addition of this standardized tool will require agency approval and education for clinicians to assure reliability of results. Although the role of the home care nurse does not include diagnosis and treatment of depression, a review of the PHQ-9 is provided as a basic overview for better understanding of the signs and symptoms of depression. In order to make a diagnosis of major depression, a patient has had five or more depressive symptoms present for more than half the days over at least 2 weeks, with at least one of the symptoms being either depressed mood or inability to experience pleasure with activities that were at one time pleasurable (Kroenke et al., 2001). From the list of nine depressive symptoms, a patient indicates whether each symptom has bothered them during the last 2 weeks. The PHQ-9 can be used as both a diagnostic tool and a measurement of depression severity over time, to evaluate medication effectiveness and mental status (Spitzer et al., 1999). Based on a structured interview, the PHQ-9 has a high sensitivity (73%) and specificity (98%) (Kroenke et al., 2001). The PHQ-9 identifies clinical depression as a score of 10 or higher or a positive response to Item # 9: Thoughts of death or harming themselves (Bruce et al., 2011). A positive response to Item # 366 Home Healthcare Nurse
6 9 should be followed by questions to determine the level of risk and other influencing factors. When using the PHQ-9 for the first time to assess a patient s mood, the clinician must know that each item of the PHQ-9 ranges in severity from 0 to 3. The possible range of total scores is 0 to 27, with the higher score indicating more severe depression (Kroenke et al., 2001) (Table 2). The provider totals the checked boxes on the PHQ-9 based on the following: not at all = 0; several days = 1; more than half the days = 2; nearly every day = 3 (see Table 3 for the interpretation of total scores). The PHQ-9 assessment findings can help in determining first-line treatment options (e.g., watchful waiting, psychotherapy, or pharmacotherapy) (Table 3). Once diagnosed care will include ongoing monitoring, patient education, and selfmanagement support, which includes medication adherence, physical activity, and spending time in a nurturing environment (New York City Department of Health and Mental Hygiene, 2008). With mild depression (scores 5 9), the care provider can initiate supportive counseling and patient self-management, encourage physical activity, and educate the patient to report if his condition deteriorates (Table 3). With moderate depressive symptoms (scores 10 14), the patient will be monitored closely and provided with supportive counseling; if no improvement is observed in 1 month, an antidepressant may be indicated. For moderately severe depression (score 15 19), the care provider should determine the patient s preference for an antidepressant and/or psychotherapy. In the case of severe depression (major depression; score > 20), an antidepressant alone or in combination with psychotherapy is recommended; a referral to a psychiatric nurse practitioner or a psychiatrist is highly warranted (Spitzer et al., 1999). To determine the most appropriate treatment for a patient, the care provider should consider the severity of the patient s symptoms, psychosocial stressors, comorbid conditions, and patient s willingness to engage in increased physical activity. Additional factors that should be considered include the following: Table 3. Initial Response After 4 6 Weeks of an Adequate Dose of an Antidepressant PHQ-9 Treatment Response Treatment Plan Drop of 5 points from baseline Adequate No treatment change needed; follow-up in 4 weeks Drop in 2 4 points from baseline Possibly Inadequate May warrant an increase in antidepressant dose Drop of 1 point or no change or increase Inadequate Increase dose, augment, or switch; consider informal or formal psychiatric consultation, adding psychological counseling Initial Response to Psychological Counseling After 3 Sessions Over 4 6 Weeks PHQ-9 Treatment Response Treatment Plan Drop of > 5 points from baseline Adequate No treatment change needed; follow-up in 4 weeks Drop in 2 4 points from baseline Possibly Inadequate Probably no treatment change needed; share PHQ-9 score with psychotherapist Drop of 1 point or no change or increase Inadequate With depression-specific psychological counseling (CBT, PST, IPT*), discuss with therapist, consider adding antidepressant For patients satisfied in other type of psychological counseling, consider starting antidepressant For patients dissatisfied with psychological counseling, review treatment options and preferences The goal of acute phase treatment is remission of symptoms so that patients will have a reduction of the PHQ-9 to a score < 5. Patients who achieve this goal enter into the continuation phase in treatment. Patients who do not achieve this goal remain in acute phase treatment and require some alteration (dose increase, augmentation/switch/combination treatment). Patients who do not achieve remission after two adequate trials of antidepressant and/or psychological counseling by 20 to 30 weeks should have a psychiatric consultation for diagnostic and management suggestions. Note. CBT = Cognitive-Behavioral Therapy; IPT = Interpersonal Therapy; PHQ-9 = Patient Health Questionnaire; PST = Problem Solving Treatment. Adapted with permission from Oxman, T., for 3CM, LLC and the MacArthur Initiative on Depression and Primary Care, Source: Oxman T. Re-Engineering Systems for Primary Care Treatment of Depression: The Respect Depression Care Process. The Depression Initiative & Primary Care. Dartmouth Medical School. 2006: Version 9.11:48. vol. 32 no. 6 June 2014 Home Healthcare Nurse 367
7 Conduct assessment Using PHQ-2/M1730 PHQ-2 score: 0 2 PHQ-2 score: 3 or higher Repeat PHQ-2 weekly for fwo weeks; if 0 2 no further action; rescren for depression if symptoms arise during care or otherwise clincally indicated Conduct full PHQ-9 PHQ-9 score: <10 & no suicide ideation PHQ-9 score: 10 Suicidal ideation PHQ iteam 9 ( 1) Instruct patients with Depression Eduction Toolkit. Report PHQ-9 weekly for 2 wks; Follow Depression Care Management When PHQ-9 is positive ( 10) or if sucidal ideation emerges. Depression Care Management (DCM) Follow agency Suicide Risk Protocol when indicated Figure 1. Depression Screening Protocol. Reproduced from Bruce, M. L., Raue, P. J., Sheeran, T., Reilly, C., Pomerantz, J. C., Meyers, B. S.,..., Zukowski, D. (2011). Depression Care for Patients at Home (Depression CAREPATH): Home care depression care management protocol, part 2. Home Healthcare Nurse, 29(8), prior suicide attempt; significant comorbid anxiety, psychotic symptoms, or active substance abuse; access to firearms; living alone or with poor social supports; older adult male; recent loss or separation; hopelessness; preparatory acts (procuring means, putting affairs in order, warning statement, giving away personal belongings, suicidal notes); and family history of affective disorder, suicide, alcoholism (Intermountain Healthcare, 2008). If a patient expresses suicidal ideation or intent they should be immediately referred to their PCP for further evaluation. If the PCP is not available, the home care provider should consult with a psychiatrist or psychiatric nurse practitioner to determine which safety measures and treatment are needed (Intermountain Healthcare, 2008). If a patient requires ongoing mental evaluation and monitoring for depression, the patient should be referred to a home care mental health program where qualified mental health clinicians can oversee the patient s mental healthcare. It is important for the members of a home healthcare team to understand the role of the mental health team when managing a patient with comorbid depression. It has been recommended that the PHQ-9 be readministered 12 weeks after the beginning of treatment for depression (New York City Department of Health and Mental Hygiene, 2008). The patient s response to treatment (psychotherapy and/or medication) can be monitored primarily by the mental health home care provider (Table 3) in collaboration with the home healthcare team. Implications for Practice Depression is a very treatable condition, with research indicating that up to 70% to 80% of patients respond positively when adequate care is 368 Home Healthcare Nurse
8 provided (New York City Department of Health and Mental Hygiene, 2008). There is strong evidence that training a home care provider to detect depression symptoms will increase appropriate mental health referrals (Brown et al., 2007). Medicare s revised OASIS-C (2009) was implemented into practice in January 2010 and has streamlined many assessments and enhanced the section on depression. OASIS-C, recommends using the PHQ-2 assessment with all patients. Home healthcare providers need to be skilled at administering the PHQ-2 and referring patients who score positive on the PHQ-2 and would benefit from further evaluation using the PHQ-9 (Figure 1). For depression screening to be effective in patients with comorbidities, a collaborative framework needs to be in place between home care mental health services and home healthcare providers in order to satisfactorily diagnose, treat, and follow up home care patients. Anna M. Acee, EdD, ANP-BC, PMHNP-BC, is an Associate Professor, School of Nursing, Brooklyn Campus, Long Island University, Brooklyn, New York. The author and planners have disclosed no potential conflicts of interest, financial or otherwise. Address for correspondence: Anna M. Acee, EdD, ANP-BC, PMHNP-BC, 1 University Plaza, Brooklyn, NY (anna.acee@liu.edu). DOI: /NHH REFERENCES Acee, A. M. (2010). Detecting and managing depression in Type II diabetes: PHQ-9 is the answer! MEDSURG Nursing, 19(1), Acee, A. M., & Fahs, M. C. (2012). Can treating depression improve diabetic management? Nurse Practitioner, 37(1), American Psychiatric Association. (2002). Diagnostic and Statistical Manual IV-TR (pp ). Washington, DC: APA. Beacham, T., Williams, P. R., Askew, R., Walker, J., Schenk, L., & May, M. (2008). Insulin management: A guide for the home health nurse. Home Homecare Nurse, 26(7), Brown, E., Kaiser, R., & Gellis, Z. (2007). Screening and assessment of late-life depression in home healthcare: Issues and challenges. Annals of Long-term Care, 15(10), 2-7. Bruce, M. L., Raue, P. J., Sheeran, T., Reilly, C., Pomerantz, J. C., Meyers, B. S.,..., Zukowski, D. (2011). Depression Care for Patients at Home (Depression CAREPATH): Home care depression care management protocol, Part 2. Home Healthcare Nurse, 29(8), Centers for Medicare and Medicaid Services, (2009, September). OASIS-C Data Sets September 2009 for 1/1/2010 implementation. Retrieved from Initiatives-Patient-Assessment-Instruments/HomeHealth QualityInits/HHQIOASISDataSet.html Culpepper, L. (2010). Why do you need to move beyond first-line therapy for major depression? Journal of Clinical Psychiatry, 71(Suppl. 1), 4-9. Egede, L. E., & Ellis, C. (2010). Diabetes and depression: Global perspectives. Diabetes Research and Clinical Practice, 87(3), Ell, K., Unützer, J., Aranda, M., Sanchez, K., & Lee, P. J. (2005). Routine PHQ-9 depression screening in home health care: Depression, prevalence, clinical and treatment characteristics and screening implementation. Home Health Care Services Quarterly, 24(4), Gilbody, S., Richards, D., Brealey, S., & Hewitt, C. (2007). Screening for depression in medical settings with the Patient Health Questionnaire (PHQ): A diagnostic meta-analysis. Journal of General Internal Medicine, 22(11), Gonzalez, J. S., Safren, S. A., Delahanty, L. M., Cagliero, E., Wexler, D. J., Meigs, J. B., & Grant, R. W. (2008). Symptoms of depression prospectively predict poorer self-care in patients with Type 2 diabetes. Diabetes Medicine, 25(9), Greenberg, P. E., Kessler, R. C., Birnbaum, H. G., Leong, S. A., Lowe, S. W., Berglund, P. A., & Corey-Lisle, P. K. (2003). The economic burden of depression in the United States: How did it change between 1990 and 2000? Journal of Clinical Psychiatry, 64(12), Hall, M. (2012). Alcoholism & depression. Home Healthcare Nurse, 30(9), Hunt, C. W., Grant, J. S., & Pritchard, D. A. (2012). An empirical study of self-efficacy and social support in diabetes selfmanagement: Implications for home healthcare nurses. Home Healthcare Nurse, 30(4), Intermountain Healthcare. (2008). Care process model: Management of depression. December 2008 update. Retrieved from Katon, W. J. (2011). Epidemiology and treatment of depression in patients with chronic medical illness. Dialogues in Clinical Neuroscience, 13(1), Kroenke, K., Spitzer, R. L., & Williams, J. B. (2001). The PHQ-9: Validity of a brief depression severity measure. Journal of General Internal Medicine, 16(9), Lin, E. H., Rutter, C. M., Katon, W., Heckbert, S. R., Ciechanowski, P., Oliver, M. M.,..., Von Korff M. (2010). Depression and advanced complications of diabetes: A prospective cohort study. Diabetes Care, 33(2), Markowitz, S. M., Gonzalez, J. S., Wilkinson, J. L., & Safren, S. A. (2011). A review of treating depression in diabetes: Emerging findings. Psychosomatics, 52(1), Multicultural Mental Health Resource Center. (2012). PHQ in different languages. Retrieved from 9-multiple-languages New York City Department of Health and Mental Hygiene. (2008). City health information: Detecting and treating depression in adults. Retrieved from pdf/chi/chi26-9.pdf Pickett, Y., Raue, P. J., & Bruce, M. L. (2012). Late-life depression in home healthcare. Aging Health, 8(3), Pignone, M. P., Gaynes, B. N., Rushton, J. L., Burchell, C. M., Orleans, C. T., Mulrow, C. D., & Lohr, K. N. (2002). Screening for depression in adults: A summary of the evidence for the U.S. Preventive Services Task Force. Annals of Internal Medicine, 136(10), Retrieved from content/136/10/765.full.pdf-10/3/13 Sheeran, T., Reilly, C. F., Raue, P. J., Weinberger, M. I., Pomerantz, J., & Bruce, M. L. (2010). The PHQ-2 on OASIS-C: A new resource for identifying geriatric depression among home health patients. Home Healthcare Nurse, 28(2), Spitzer, R. L., Kroenke, K., & Williams, J. B. (1999). Validation and utility of a self-report version of PRIME-MD: The PHQ primary care study. Primary Care Evaluation of Mental Disorders. Patient Health Questionnaire. Journal of the American Medical Association, 282(18), Wang, P. S., Schneeweiss, S., Brookhart, M. A., Glynn, R. J., Mogun, H., Patrick, A. R., & Avorn, J. (2005). Suboptimal antidepressant use in the elderly. Journal of Clinical Psychopharmacology, 25(2), For 193 additional continuing nursing education activities related to home healthcare, go to nursingcenter.com/ce. vol. 32 no. 6 June 2014 Home Healthcare Nurse 369
PATIENT HEALTH QUESTIONNAIRE PHQ-9 FOR DEPRESSION
 PATIENT HEALTH QUESTIONNAIRE PHQ-9 FOR DEPRESSION USING PHQ-9 DIAGNOSIS AND SCORE FOR INITIAL TREATMENT SELECTION A depression diagnosis that warrants treatment or treatment change, needs at least one
PATIENT HEALTH QUESTIONNAIRE PHQ-9 FOR DEPRESSION USING PHQ-9 DIAGNOSIS AND SCORE FOR INITIAL TREATMENT SELECTION A depression diagnosis that warrants treatment or treatment change, needs at least one
Appendix B: Screening and Assessment Instruments
 Appendix B: Screening and Assessment Instruments Appendix B-1: Quick Guide to the Patient Health Questionnaire (PHQ) Purpose. The Patient Health Questionnaire (PHQ) is designed to facilitate the recognition
Appendix B: Screening and Assessment Instruments Appendix B-1: Quick Guide to the Patient Health Questionnaire (PHQ) Purpose. The Patient Health Questionnaire (PHQ) is designed to facilitate the recognition
LifeBridge Physician Network Care Path Depression, Substance Abuse June 26, 2015
 LifeBridge Physician Network Care Path Depression, Substance Abuse June 26, 2015 LBPN Care Path Aim: To develop and implement standard protocols, based on the best evidence, that provide a consistent clinical
LifeBridge Physician Network Care Path Depression, Substance Abuse June 26, 2015 LBPN Care Path Aim: To develop and implement standard protocols, based on the best evidence, that provide a consistent clinical
INSTRUCTION MANUAL Instructions for Patient Health Questionnaire (PHQ) and GAD-7 Measures
 PHQ and GAD-7 Instructions P. 1/9 INSTRUCTION MANUAL Instructions for Patient Health Questionnaire (PHQ) and GAD-7 Measures TOPIC PAGES Background 1 Coding and Scoring 2, 4, 5 Versions 3 Use as Severity
PHQ and GAD-7 Instructions P. 1/9 INSTRUCTION MANUAL Instructions for Patient Health Questionnaire (PHQ) and GAD-7 Measures TOPIC PAGES Background 1 Coding and Scoring 2, 4, 5 Versions 3 Use as Severity
RN Behavioral Health Care Manager in Primary Care Settings
 RN Behavioral Health Care Manager in Primary Care Settings Integrated Care and the Expanding Role of Nurses Seattle Airport Marriott, SeaTac, WA Tuesday, January 9, 2018 The Healthier Washington Practice
RN Behavioral Health Care Manager in Primary Care Settings Integrated Care and the Expanding Role of Nurses Seattle Airport Marriott, SeaTac, WA Tuesday, January 9, 2018 The Healthier Washington Practice
Chronic Condition Toolbook: Major Depressive Disorder. Focusing on Depression and Its Symptoms
 Chronic Condition Toolbook: Major Depressive Disorder Focusing on Depression and Its Symptoms Table of Contents Focusing on Major Depressive Disorder... 1 Major Depressive Disorder Algorithm... 2 The Importance
Chronic Condition Toolbook: Major Depressive Disorder Focusing on Depression and Its Symptoms Table of Contents Focusing on Major Depressive Disorder... 1 Major Depressive Disorder Algorithm... 2 The Importance
POST-STROKE DEPRESSION
 POST-STROKE DEPRESSION Stroke Annual Review March 7 th & 8 th, 2018 Justine Spencer, PhD, CPsych OVERVIEW What is Post-Stroke Depression (PSD)? Risk factors/predictors Impact of PSD Treatment and Management
POST-STROKE DEPRESSION Stroke Annual Review March 7 th & 8 th, 2018 Justine Spencer, PhD, CPsych OVERVIEW What is Post-Stroke Depression (PSD)? Risk factors/predictors Impact of PSD Treatment and Management
PHARMACY INFORMATION:
 Patient Name: Date of Birth: Referred by: Reason for Visit: Current psychiatric medications and doses: PHARMACY INFORMATION: Name of Pharmacy: Phone Number: Fax Number: Address: PRIMARY CARE PHYSICIAN
Patient Name: Date of Birth: Referred by: Reason for Visit: Current psychiatric medications and doses: PHARMACY INFORMATION: Name of Pharmacy: Phone Number: Fax Number: Address: PRIMARY CARE PHYSICIAN
Major Depressive Disorder Wellness Workbook
 Framing Major Depressive Disorder Major Depressive Disorder Wellness Workbook This Workbook belongs to you and you decide how to use it. You decide who to show it to and whether or not you want someone
Framing Major Depressive Disorder Major Depressive Disorder Wellness Workbook This Workbook belongs to you and you decide how to use it. You decide who to show it to and whether or not you want someone
Clinical Practice Guideline: Management of Major Depression in Primary Care
 Clinical Practice Guideline: Management of Major Depression in Primary Care Approved, CHP Quality Improvement Committee 3/27/01, 10/22/02, 10/28/03, 11/2/04, 11/1/05, 9/8/09, 5/10/11, 5/14/13, 5/12/15,
Clinical Practice Guideline: Management of Major Depression in Primary Care Approved, CHP Quality Improvement Committee 3/27/01, 10/22/02, 10/28/03, 11/2/04, 11/1/05, 9/8/09, 5/10/11, 5/14/13, 5/12/15,
Depression Assessment and Management. John Kern MD Clinical Professor University of Washington
 Depression Assessment and Management John Kern MD Clinical Professor University of Washington Handouts Antidepressant Treatment Flowchart Managing antidepressant nonresponse handouts 2 Diagnosis PHQ-9
Depression Assessment and Management John Kern MD Clinical Professor University of Washington Handouts Antidepressant Treatment Flowchart Managing antidepressant nonresponse handouts 2 Diagnosis PHQ-9
Objectives. Background and Significance. Background and Significance. Depression Screening: QIP in an Infectious Disease Primary Care Practice
 Depression Screening: QIP in an Infectious Disease Primary Care Practice Karen Holen Lyda MS NP Paul F. Cook PhD Steven C. Johnson MD Objectives Describe relevance of identifying depression in a clinic
Depression Screening: QIP in an Infectious Disease Primary Care Practice Karen Holen Lyda MS NP Paul F. Cook PhD Steven C. Johnson MD Objectives Describe relevance of identifying depression in a clinic
Treatment Algorithm Treatment Algorithm
 Treatment Algorithm Treatment Algorithm Primary Care Toolkit September 2015 Page 2 Adult (>18 years) Depression Flow Chart (Generic) Two Question Screen: PHQ-2 Annually, new adult patients, and when suspect
Treatment Algorithm Treatment Algorithm Primary Care Toolkit September 2015 Page 2 Adult (>18 years) Depression Flow Chart (Generic) Two Question Screen: PHQ-2 Annually, new adult patients, and when suspect
This product was developed by the RWJ Diabetes Self Management Program at Community Health Center, Inc. in Middleton, CT. Support for this product
 This product was developed by the RWJ Diabetes Self Management Program at Community Health Center, Inc. in Middleton, CT. Support for this product was provided by a grant from the Robert Wood Johnson Foundation
This product was developed by the RWJ Diabetes Self Management Program at Community Health Center, Inc. in Middleton, CT. Support for this product was provided by a grant from the Robert Wood Johnson Foundation
Brief Pain Inventory (Short Form)
 Brief Pain Inventory (Short Form) Study ID# Hospital# Do not write above this line Date: Time: Name: Last First Middle Initial 1) Throughout our lives, most of us have had pain from time to time (such
Brief Pain Inventory (Short Form) Study ID# Hospital# Do not write above this line Date: Time: Name: Last First Middle Initial 1) Throughout our lives, most of us have had pain from time to time (such
PATIENT NAME: DATE OF DISCHARGE: DISCHARGE SURVEY
 PATIENT NAME: DATE OF DISCHARGE: DISCHARGE SURVEY Please indicate whether you feel Living Hope Eating Disorder Treatment Center provided either Satisfactory or Unsatisfactory service for each number listed
PATIENT NAME: DATE OF DISCHARGE: DISCHARGE SURVEY Please indicate whether you feel Living Hope Eating Disorder Treatment Center provided either Satisfactory or Unsatisfactory service for each number listed
Care Team Training. Key Components of Collaborative Care. Collaborative Team Approach 4/21/2014 PCP. Core Program. New Roles. Psychiatric Consultant
 Team Training Key Components of Collaborative Collaborative Team Approach Patient PCP Manager New Roles Core Program Psychiatric Consultant Behavioral Health Clinicians Additional Clinic Resources Substance,
Team Training Key Components of Collaborative Collaborative Team Approach Patient PCP Manager New Roles Core Program Psychiatric Consultant Behavioral Health Clinicians Additional Clinic Resources Substance,
BEHAVIORAL HEALTH SCREENING TOOLS
 BEHAVIORAL HEALTH SCREENING TOOLS FOR THE CO-LOCATION OF BEHAVIORAL HEALTH SERVICES IN A PRIMARY CARESETTING Date: August 29, 2017 Introduction Today s Presenter Jacqueline Delmont, MD, MBA Delmont Healthcare
BEHAVIORAL HEALTH SCREENING TOOLS FOR THE CO-LOCATION OF BEHAVIORAL HEALTH SERVICES IN A PRIMARY CARESETTING Date: August 29, 2017 Introduction Today s Presenter Jacqueline Delmont, MD, MBA Delmont Healthcare
Making an IMPACT on late-life depression. Partnering with primary care providers can double the effect of treatment
 University of Massachusetts Boston From the SelectedWorks of Steven D Vannoy Fall September, 2006 Making an IMPACT on late-life depression. Partnering with primary care providers can double the effect
University of Massachusetts Boston From the SelectedWorks of Steven D Vannoy Fall September, 2006 Making an IMPACT on late-life depression. Partnering with primary care providers can double the effect
CBT Intake Form. Patient Name: Preferred Name: Last. First. Best contact phone number: address: Address:
 Patient Information CBT Intake Form Patient Name: Preferred Name: Last Date of Birth: _// Age: _ First MM DD YYYY Gender: Best contact phone number: Email address: _ Address: _ Primary Care Physician:
Patient Information CBT Intake Form Patient Name: Preferred Name: Last Date of Birth: _// Age: _ First MM DD YYYY Gender: Best contact phone number: Email address: _ Address: _ Primary Care Physician:
Measurement of Psychopathology in Populations. William W. Eaton, PhD Johns Hopkins University
 This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike License. Your use of this material constitutes acceptance of that license and the conditions of use of materials on this
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike License. Your use of this material constitutes acceptance of that license and the conditions of use of materials on this
INSOMNIA SEVERITY INDEX
 Name: Date: INSOMNIA SEVERITY INDEX For each of the items below, please circle the number that most closely corresponds to how you feel. 1. Please rate the CURRENT (i.e. last 2 weeks) severity of your
Name: Date: INSOMNIA SEVERITY INDEX For each of the items below, please circle the number that most closely corresponds to how you feel. 1. Please rate the CURRENT (i.e. last 2 weeks) severity of your
Bipolar Disorder Clinical Practice Guideline Summary for Primary Care
 Bipolar Disorder Clinical Practice Guideline Summary for Primary Care DIAGNOSIS AND CLINICAL ASSESSMENT Bipolar Disorder is categorized by extreme mood cycling; manifested by periods of euphoria, grandiosity,
Bipolar Disorder Clinical Practice Guideline Summary for Primary Care DIAGNOSIS AND CLINICAL ASSESSMENT Bipolar Disorder is categorized by extreme mood cycling; manifested by periods of euphoria, grandiosity,
Solution Title: Screening Can Improve Identification of Depression in Hospitalized Congestive Heart Failure Patients
 Solution Title: Screening Can Improve Identification of Depression in Hospitalized Congestive Heart Failure Patients Overview of Project Depression and heart disease affect millions of people worldwide.
Solution Title: Screening Can Improve Identification of Depression in Hospitalized Congestive Heart Failure Patients Overview of Project Depression and heart disease affect millions of people worldwide.
Mental Health measures workgroup Update. 14 th Washington Group meeting Buenos Aires 8-10 October 2014
 Mental Health measures workgroup Update 14 th Washington Group meeting Buenos Aires 8-10 October 2014 Overview Discussion document revised Key considerations Review of most commonly used instruments Proposal
Mental Health measures workgroup Update 14 th Washington Group meeting Buenos Aires 8-10 October 2014 Overview Discussion document revised Key considerations Review of most commonly used instruments Proposal
Implementing and Improving Depression Screenings in the Primary Care Setting. Janet Tennison, PhD, MSW, LCSW Behavioral Health Project Manager
 Implementing and Improving Depression Screenings in the Primary Care Setting Janet Tennison, PhD, MSW, LCSW Behavioral Health Project Manager Today s Objectives Participants will: Increase understanding
Implementing and Improving Depression Screenings in the Primary Care Setting Janet Tennison, PhD, MSW, LCSW Behavioral Health Project Manager Today s Objectives Participants will: Increase understanding
Penn State Altoona Integrated care model Health services Counseling Services Disability Services Health Promotion
 Penn State Altoona Integrated care model Health services Counseling Services Disability Services Health Promotion 4,000 undergraduates SAMHSA grant- 2009-2011 Topics Introduction Outcomes Statistics Screening
Penn State Altoona Integrated care model Health services Counseling Services Disability Services Health Promotion 4,000 undergraduates SAMHSA grant- 2009-2011 Topics Introduction Outcomes Statistics Screening
MATCP When the Severity of Symptoms Interferes with Progress
 MATCP 2017 When the Severity of Symptoms Interferes with Progress 1 Overview Stages of Change, or Readiness for Change Changing Behavior Medication Adherence Disruptive Behaviors Level of Care Tools including
MATCP 2017 When the Severity of Symptoms Interferes with Progress 1 Overview Stages of Change, or Readiness for Change Changing Behavior Medication Adherence Disruptive Behaviors Level of Care Tools including
Medicare Wellness Visit
 of Birth: Today s : Medicare Wellness Visit Dear Patient, Your Medicare benefits include an Annual Wellness Visit to assist in preventing illness or detect illness at an early stage. Your Annual Wellness
of Birth: Today s : Medicare Wellness Visit Dear Patient, Your Medicare benefits include an Annual Wellness Visit to assist in preventing illness or detect illness at an early stage. Your Annual Wellness
Jessica Gifford, LICSW Mental Health Educator Jessica Gifford, LICSW Mental Health Educator
 Alleviating Depression and Anxiety through Wellness Promotion Jessica Gifford, LICSW Mental Health Educator Jessica Gifford, LICSW Mental Health Educator Public Health Approach Mental Health is a public
Alleviating Depression and Anxiety through Wellness Promotion Jessica Gifford, LICSW Mental Health Educator Jessica Gifford, LICSW Mental Health Educator Public Health Approach Mental Health is a public
Welcome to NHS Highland Pain Management Service
 Welcome to NHS Highland Pain Management Service Information from this questionnaire helps us to understand your pain problem better. It is important that you read each question carefully and answer as
Welcome to NHS Highland Pain Management Service Information from this questionnaire helps us to understand your pain problem better. It is important that you read each question carefully and answer as
APPLYING THE INTEGRATED CARE APPROACH: PRACTICAL SKILLS FOR THE PSYCHIATRIC CONSULTANT WORKSHOP: ASSESSMENT AND TREATMENT IN COLLABORATIVE CARE
 APPLYING THE INTEGRATED CARE APPROACH: PRACTICAL SKILLS FOR THE PSYCHIATRIC CONSULTANT WORKSHOP: ASSESSMENT AND TREATMENT IN COLLABORATIVE CARE FUNDING ACKNOWLEDGEMENT Supported by Funding Opportunity
APPLYING THE INTEGRATED CARE APPROACH: PRACTICAL SKILLS FOR THE PSYCHIATRIC CONSULTANT WORKSHOP: ASSESSMENT AND TREATMENT IN COLLABORATIVE CARE FUNDING ACKNOWLEDGEMENT Supported by Funding Opportunity
These questionnaires are used by psychology services to help us understand how people feel. One questionnaire measures how sad people feel.
 ADAPTED PHQ-9 & GAD-7 QUESTIONNAIRES How to fill in these questionnaires: These questionnaires are used by psychology services to help us understand how people feel. One questionnaire measures how sad
ADAPTED PHQ-9 & GAD-7 QUESTIONNAIRES How to fill in these questionnaires: These questionnaires are used by psychology services to help us understand how people feel. One questionnaire measures how sad
Assessment in Integrated Care. J. Patrick Mooney, Ph.D.
 Assessment in Integrated Care J. Patrick Mooney, Ph.D. Purpose of assessment in integrated care: Assessment provides feedback to promote individual and group learning and change. Physicians Mental health
Assessment in Integrated Care J. Patrick Mooney, Ph.D. Purpose of assessment in integrated care: Assessment provides feedback to promote individual and group learning and change. Physicians Mental health
Treating Depression in Disadvantaged Women: What is the evidence?
 Treating Depression in Disadvantaged Women: What is the evidence? Megan Dwight Johnson, MD MPH Associate Professor Medical Director, UWMC Inpatient Psychiatry Department of Psychiatry and Behavioral Sciences
Treating Depression in Disadvantaged Women: What is the evidence? Megan Dwight Johnson, MD MPH Associate Professor Medical Director, UWMC Inpatient Psychiatry Department of Psychiatry and Behavioral Sciences
Screening for Depression and Suicide
 Screening for Depression and Suicide Christa Smith, PsyD Western Interstate Commission for Higher Education Boulder, Colorado 10/2/2008 Background My background A word about language Today stopics Why
Screening for Depression and Suicide Christa Smith, PsyD Western Interstate Commission for Higher Education Boulder, Colorado 10/2/2008 Background My background A word about language Today stopics Why
ADULT QUESTIONNAIRE. Date of Birth: Briefly describe the history and development of this issue from onset to present.
 ADULT QUESTIONNAIRE Name: Address: Preferred phone number to reach you: Is it okay to leave a message? Yes No (Please check one) Date of Birth: Reason(s) for seeking treatment at this time? Briefly describe
ADULT QUESTIONNAIRE Name: Address: Preferred phone number to reach you: Is it okay to leave a message? Yes No (Please check one) Date of Birth: Reason(s) for seeking treatment at this time? Briefly describe
Disorder. Objectives. Under Recognition/ Undertreatment. Making a Diagnosis
 Care Partners Primary Care Provider Lunch & Learn: Why PCPs Love Collaborative Care Presenter: Wayne Bentham, MD The advantage of the collaborative care model of depression management in primary care is
Care Partners Primary Care Provider Lunch & Learn: Why PCPs Love Collaborative Care Presenter: Wayne Bentham, MD The advantage of the collaborative care model of depression management in primary care is
Diabetes distress 7 A s model
 Diabetes and emotional health: A toolkit for health s supporting adults with type 1 or type 2 diabetes Diabetes distress 7 A s model AWARE Be AWARE that people with diabetes may experience diabetes distress
Diabetes and emotional health: A toolkit for health s supporting adults with type 1 or type 2 diabetes Diabetes distress 7 A s model AWARE Be AWARE that people with diabetes may experience diabetes distress
Integrated Care for Depression, Anxiety and PTSD. Introduction: Overview of Clinical Roles and Ideas
 Integrated Care for Depression, Anxiety and PTSD University of Washington An Evidence-based d Approach for Behavioral Health Professionals (LCSWs, MFTs, and RNs) Alameda Health Consortium November 15-16,
Integrated Care for Depression, Anxiety and PTSD University of Washington An Evidence-based d Approach for Behavioral Health Professionals (LCSWs, MFTs, and RNs) Alameda Health Consortium November 15-16,
Copyright 2011 Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited.
 416 Copyright 2011 Wolters Kluwer Health Lippincott Williams & Wilkins Illustrations by Denny Bond Depression Care for Patients at Home (Depression CAREPATH): INTERVENTION DEVELOPMENT AND IMPLEMENTATION,
416 Copyright 2011 Wolters Kluwer Health Lippincott Williams & Wilkins Illustrations by Denny Bond Depression Care for Patients at Home (Depression CAREPATH): INTERVENTION DEVELOPMENT AND IMPLEMENTATION,
Treating Patients with Depression Using Coordinated Medication Management. November 13, 2018
 Treating Patients with Depression Using Coordinated Medication Management November 13, 2018 Learning objectives Good Afternoon! Elisabeth Hager, MD, MMM Chief Medical Officer Southeast/Central Region 1)
Treating Patients with Depression Using Coordinated Medication Management November 13, 2018 Learning objectives Good Afternoon! Elisabeth Hager, MD, MMM Chief Medical Officer Southeast/Central Region 1)
Managing Depression as a Chronic Condition. D. Green MD TOH/Bruyere Shared Care Program
 Managing Depression as a Chronic Condition D. Green MD TOH/Bruyere Shared Care Program None Financial disclosure Objectives To review key concepts relevant to understanding the course of depression To
Managing Depression as a Chronic Condition D. Green MD TOH/Bruyere Shared Care Program None Financial disclosure Objectives To review key concepts relevant to understanding the course of depression To
Session outline. Introduction to depression Assessment of depression Management of depression Follow-up Review
 Depression 1 Session outline Introduction to depression Assessment of depression Management of depression Follow-up Review 2 Activity 1: Person s story followed by group discussion Present the first person
Depression 1 Session outline Introduction to depression Assessment of depression Management of depression Follow-up Review 2 Activity 1: Person s story followed by group discussion Present the first person
Christina Pucel Counseling 416 W. Main St Monongahela, PA /
 ADULT INTAKE Name: Gender: M F DOB: Address: City: State: Zip: Telephone: Home Mobile Highest Level Education: Occupation: Emergency Contact: Relationship: Phone: Referred by: Family Members: Name Gender
ADULT INTAKE Name: Gender: M F DOB: Address: City: State: Zip: Telephone: Home Mobile Highest Level Education: Occupation: Emergency Contact: Relationship: Phone: Referred by: Family Members: Name Gender
Postpartum Depression Screening
 Postpartum Depression Screening October 13, 2018 Deborah CowleyMD Psychiatrist Perinatal Consultant University of Washington Disclosures Perinatal Psychiatry Consultation Line/PAL for Moms UW Perinatal
Postpartum Depression Screening October 13, 2018 Deborah CowleyMD Psychiatrist Perinatal Consultant University of Washington Disclosures Perinatal Psychiatry Consultation Line/PAL for Moms UW Perinatal
Rasch-scaling of PHQ-9 and GAD-7 Consequences for repeated assessments. Jan R. Böhnke & Jaime Delgadillo
 Rasch-scaling of PHQ-9 and GAD-7 Consequences for repeated assessments Jan R. Böhnke & Jaime Delgadillo NHS::IAPT Improving Access to Psychological Therapies "Improving Access to Psychological Therapies
Rasch-scaling of PHQ-9 and GAD-7 Consequences for repeated assessments Jan R. Böhnke & Jaime Delgadillo NHS::IAPT Improving Access to Psychological Therapies "Improving Access to Psychological Therapies
Depression. Patients at Home
 Depression Patients at Home Illustration by Denny Bond High levels of depressive symptoms are common and contribute to poorer clinical outcomes even in geriatric patients who are already taking antidepressant
Depression Patients at Home Illustration by Denny Bond High levels of depressive symptoms are common and contribute to poorer clinical outcomes even in geriatric patients who are already taking antidepressant
Enhancing Treatment. Recognizing Depression and. Tools for successful patient management. Provider Communications. Health Net. Christian Aparicio,
 Provider Communications Recognizing Depression and Enhancing Treatment Tools for successful patient management Christian Aparicio, Health Net We offer tools and resources for improving member health. Contents
Provider Communications Recognizing Depression and Enhancing Treatment Tools for successful patient management Christian Aparicio, Health Net We offer tools and resources for improving member health. Contents
Quality ID #411 (NQF 0711): Depression Remission at Six Months National Quality Strategy Domain: Effective Clinical Care
 Quality ID #411 (NQF 0711): Depression Remission at Six Months National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Outcome DESCRIPTION:
Quality ID #411 (NQF 0711): Depression Remission at Six Months National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Outcome DESCRIPTION:
WELCOME TO AGEWELL MEDICAL ASSOCIATES
 WELCOME TO AGEWELL MEDICAL ASSOCIATES We offer the following checklist and suggestions to help make your first visit as easy and pleasant as possible. What to bring with you: [ ] All of your medications
WELCOME TO AGEWELL MEDICAL ASSOCIATES We offer the following checklist and suggestions to help make your first visit as easy and pleasant as possible. What to bring with you: [ ] All of your medications
2) Percentage of adult patients (aged 18 years or older) with a diagnosis of major depression or dysthymia and an
 Quality ID #370 (NQF 0710): Depression Remission at Twelve Months National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Prevention, Treatment, and Management of Mental Health
Quality ID #370 (NQF 0710): Depression Remission at Twelve Months National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Prevention, Treatment, and Management of Mental Health
Development, Implementation and Evaluation of a Psychiatric Home Care Evidence Based Practice. Rose Madden-Baer DNP MHSA BC-PHCNS CPHQ, CHCE, COS-C
 . Development, Implementation and Evaluation of a Psychiatric Home Care Evidence Based Practice Rose Madden-Baer DNP MHSA BC-PHCNS CPHQ, CHCE, COS-C Why develop a depression care model? Prevalence of depression
. Development, Implementation and Evaluation of a Psychiatric Home Care Evidence Based Practice Rose Madden-Baer DNP MHSA BC-PHCNS CPHQ, CHCE, COS-C Why develop a depression care model? Prevalence of depression
To: Our Medicare Patients. Subject: Your Welcome to Medicare Exam
 To: Our Medicare Patients Subject: Your Welcome to Medicare Exam Medicare covers a one-time Welcome to Medicare visit. The Welcome to Medicare visit must occur during your first twelve months as a Medicare
To: Our Medicare Patients Subject: Your Welcome to Medicare Exam Medicare covers a one-time Welcome to Medicare visit. The Welcome to Medicare visit must occur during your first twelve months as a Medicare
Help and Healing: Section 2: Treatment Planning. Treatment and Timelines. Depression Treatment Reference. Care Team Communication
 Help and Healing: Resources for Depression Care and Recovery Section 2: Treatment Planning Treatment and Timelines Depression Treatment Reference Care Team Communication Provider Education Tool - Questions
Help and Healing: Resources for Depression Care and Recovery Section 2: Treatment Planning Treatment and Timelines Depression Treatment Reference Care Team Communication Provider Education Tool - Questions
VA/DOD CLINICAL PRACTICE GUIDELINE
 VA/DOD CLIICAL PRACTICE GUIDELIE Management of Major Depressive Disorder (MDD) KE ELEMETS OF THE MDD GUIDELIE Screen annually for Depression (PHQ-2) Assess for Suicide Risk Obtain Standardized Symptom
VA/DOD CLIICAL PRACTICE GUIDELIE Management of Major Depressive Disorder (MDD) KE ELEMETS OF THE MDD GUIDELIE Screen annually for Depression (PHQ-2) Assess for Suicide Risk Obtain Standardized Symptom
Sleep Health Center. You have been scheduled for an Insomnia Treatment Program consultation to further discuss your
 Sleep Health Center You have been scheduled for an Insomnia Treatment Program consultation to further discuss your sleep. In the week preceding your appointment, please take the time to complete the enclosed
Sleep Health Center You have been scheduled for an Insomnia Treatment Program consultation to further discuss your sleep. In the week preceding your appointment, please take the time to complete the enclosed
Spring 2013 Geriatric Health Lecture Series on Alzheimer s Disease and Related Issues. Depression. Stephen Thielke, MD
 Spring 2013 Geriatric Health Lecture Series on Alzheimer s Disease and Related Issues Depression Stephen Thielke, MD Assistant Professor Department of Psychiatry and Behavioral Sciences University of Washington
Spring 2013 Geriatric Health Lecture Series on Alzheimer s Disease and Related Issues Depression Stephen Thielke, MD Assistant Professor Department of Psychiatry and Behavioral Sciences University of Washington
Depression: Assessment and Treatment For Older Adults
 Tool on Depression: Assessment and Treatment For Older Adults Based on: National Guidelines for Seniors Mental Health: the Assessment and Treatment of Depression Available on line: www.ccsmh.ca www.nicenet.ca
Tool on Depression: Assessment and Treatment For Older Adults Based on: National Guidelines for Seniors Mental Health: the Assessment and Treatment of Depression Available on line: www.ccsmh.ca www.nicenet.ca
Depression in Late Life Initiative
 Depression in Late Life Initiative made possible by the Archstone Foundation Depression in Late Life Request for Proposals (RFP) Care Partners: Bridging Families, Clinics, and Communities to Advance Late
Depression in Late Life Initiative made possible by the Archstone Foundation Depression in Late Life Request for Proposals (RFP) Care Partners: Bridging Families, Clinics, and Communities to Advance Late
A Guide to Behavioral Health Screenings: Utilizing Screening tools to Improve Identification of Depression and Alcohol Misuse in Primary Care
 A Guide to Behavioral Health Screenings: Utilizing Screening tools to Improve Identification of Depression and Alcohol Misuse in Primary Care HealthInsight New Mexico Team John Siebel, MD Medical Director
A Guide to Behavioral Health Screenings: Utilizing Screening tools to Improve Identification of Depression and Alcohol Misuse in Primary Care HealthInsight New Mexico Team John Siebel, MD Medical Director
PSYCHOLOGICAL CHALLENGES OF DIABETICS
 PSYCHOLOGICAL CHALLENGES OF DIABETICS Does Depression Correlate to Diabetic Foot Ulcer Outcomes? Garneisha Torrence, PGY-3 DVA Puget Sound Health Care System Disclosure No relevant financial or non-financial
PSYCHOLOGICAL CHALLENGES OF DIABETICS Does Depression Correlate to Diabetic Foot Ulcer Outcomes? Garneisha Torrence, PGY-3 DVA Puget Sound Health Care System Disclosure No relevant financial or non-financial
Primary Care: Referring to Psychiatry
 Primary Care: Referring to Psychiatry Carol Capitano, PhD, APRN-BC Assistant Professor, Clinical Educator University of New Mexico College of Nursing University of New Mexico Psychiatric Center Objectives
Primary Care: Referring to Psychiatry Carol Capitano, PhD, APRN-BC Assistant Professor, Clinical Educator University of New Mexico College of Nursing University of New Mexico Psychiatric Center Objectives
Practice Matters: Screening and Referring Congregants with Major Depression
 International Journal of Faith Community Nursing Volume 1 Issue 3 Article 6 October 2015 Practice Matters: Screening and Referring Congregants with Major Depression Kim Link Western Kentucky University
International Journal of Faith Community Nursing Volume 1 Issue 3 Article 6 October 2015 Practice Matters: Screening and Referring Congregants with Major Depression Kim Link Western Kentucky University
Depression. VNAA Best Practice for Home Health
 Depression VNAA Best Practice for Home Health Learning objectives The participant will be able to: Discuss two reasons why depression should be identified and treated Discuss two critical interventions
Depression VNAA Best Practice for Home Health Learning objectives The participant will be able to: Discuss two reasons why depression should be identified and treated Discuss two critical interventions
Adult Mental Health Services applicable to Members in the State of Connecticut subject to state law SB1160
 Adult Mental Health Services Comparison Create and maintain a document in an easily accessible location on such health carrier's Internet web site that (i) (ii) compares each aspect of such clinical review
Adult Mental Health Services Comparison Create and maintain a document in an easily accessible location on such health carrier's Internet web site that (i) (ii) compares each aspect of such clinical review
Annual Wellness Visit Form 2016
 Annual Wellness Visit Form 6 Initial G48/Subsequent G49 (circle one) Subjective: Past Medical History (mark X to confirm and note duration for chronic conditions only) Conditions Yrs Conditions Yrs Others:
Annual Wellness Visit Form 6 Initial G48/Subsequent G49 (circle one) Subjective: Past Medical History (mark X to confirm and note duration for chronic conditions only) Conditions Yrs Conditions Yrs Others:
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Major Depressive Disorder. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Major Depressive Disorder. These podcasts are designed to give medical students an overview of key topics in pediatrics.
Disclosure to Participants. Objectives. Origins of the ADA Position Statement
 Screening for Diabetes Distress and Depression: What Should the Diabetes Educator Do? Mary de Groot, Ph.D. Associate Professor, Indiana University School of Medicine Diabetes Translational Research Center
Screening for Diabetes Distress and Depression: What Should the Diabetes Educator Do? Mary de Groot, Ph.D. Associate Professor, Indiana University School of Medicine Diabetes Translational Research Center
PSYCHOTROPIC MEDICATION UTILIZATION PARAMETERS FOR CHILDREN AND YOUTH IN FOSTER CARE
 PSYCHOTROPIC MEDICATION UTILIZATION PARAMETERS FOR CHILDREN AND YOUTH IN FOSTER CARE Introduction and General Principles April 2017 Adapted for New Mexico from with permission from the Texas Department
PSYCHOTROPIC MEDICATION UTILIZATION PARAMETERS FOR CHILDREN AND YOUTH IN FOSTER CARE Introduction and General Principles April 2017 Adapted for New Mexico from with permission from the Texas Department
Integrating MH/SA Treatment in Primary Care Firm Clinics: The Behavioral Health Clinic
 Integrating MH/SA Treatment in Primary Care Firm Clinics: The Behavioral Health Clinic John D. Dingell VA Medical Center VISN 11 - Detroit, MI Objectives Upon completion of this session, participants will
Integrating MH/SA Treatment in Primary Care Firm Clinics: The Behavioral Health Clinic John D. Dingell VA Medical Center VISN 11 - Detroit, MI Objectives Upon completion of this session, participants will
Integrated Health and Well-Being
 Integrated Health and Well-Being CF Physical Health Health and Well-Being Mental Health 1 Depression A Continuum Normal Mood Lowering Abnormal Mood Lowering Abnormal Mood Lowering and Loss of Functioning
Integrated Health and Well-Being CF Physical Health Health and Well-Being Mental Health 1 Depression A Continuum Normal Mood Lowering Abnormal Mood Lowering Abnormal Mood Lowering and Loss of Functioning
SPIRIT CMTS Registry Example Patient for Care Manager Training
 SPIRIT CMTS Registry Example Patient for Care Manager Training Getting Started The following scenario is designed to help you learn how to use the Care Management Tracking System (CMTS) registry to facilitate
SPIRIT CMTS Registry Example Patient for Care Manager Training Getting Started The following scenario is designed to help you learn how to use the Care Management Tracking System (CMTS) registry to facilitate
Psychiatric Consultant Role in Collaborative Care Sept 12, 2013
 New York State Collaborative Care Initiative Psychiatric Consultant Role in Collaborative Care Sept 12, 2013 http://uwaims.org Presenter Building on 25 years of Research and Practice in Integrated Mental
New York State Collaborative Care Initiative Psychiatric Consultant Role in Collaborative Care Sept 12, 2013 http://uwaims.org Presenter Building on 25 years of Research and Practice in Integrated Mental
IMPACT Improving Mood Promoting Access to Collaborative Treatment
 IMPACT Improving Mood Promoting Access to Collaborative Treatment for Late-Life Depression Funded by John A. Hartford Foundation, California HealthCare Foundation, Robert Wood Johnson Foundation, Hogg
IMPACT Improving Mood Promoting Access to Collaborative Treatment for Late-Life Depression Funded by John A. Hartford Foundation, California HealthCare Foundation, Robert Wood Johnson Foundation, Hogg
Effective Treatment of Depression in Older African Americans: Overcoming Barriers
 Effective Treatment of Depression in Older African Americans: Overcoming Barriers R U T H S H I M, M D, M P H A S S I S T A N T P R O F E S S O R, D E P A R T M E N T O F P S Y C H I A T R Y A N D B E
Effective Treatment of Depression in Older African Americans: Overcoming Barriers R U T H S H I M, M D, M P H A S S I S T A N T P R O F E S S O R, D E P A R T M E N T O F P S Y C H I A T R Y A N D B E
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY
 Measure #134 (NQF 0418): Preventive Care and Screening: Screening for Clinical Depression and Follow-Up Plan National Quality Strategy Domain: Community/Population Health 2016 PQRS OPTIONS FOR INDIVIDUAL
Measure #134 (NQF 0418): Preventive Care and Screening: Screening for Clinical Depression and Follow-Up Plan National Quality Strategy Domain: Community/Population Health 2016 PQRS OPTIONS FOR INDIVIDUAL
Diabetes and Depression. Roshini Pinto-Powell, MD Stephen Noyes, LICSW, LADC William Gunn, PhD Beverly Bean, RN, C
 Diabetes and Depression Roshini Pinto-Powell, MD Stephen Noyes, LICSW, LADC William Gunn, PhD Beverly Bean, RN, C 2008 Learning Objectives State the risk factors for depression Identify the vulnerability
Diabetes and Depression Roshini Pinto-Powell, MD Stephen Noyes, LICSW, LADC William Gunn, PhD Beverly Bean, RN, C 2008 Learning Objectives State the risk factors for depression Identify the vulnerability
Lambeth Psychological Therapies
 Complaints procedure: If you are not happy about your experience with our service, you can speak to a member of staff directly; alternatively, you can contact the PALS Office. To make a formal complaint,
Complaints procedure: If you are not happy about your experience with our service, you can speak to a member of staff directly; alternatively, you can contact the PALS Office. To make a formal complaint,
Administering the PHQ-9 And Maximizing the Identification of Depression
 Administering the PHQ-9 And Maximizing the Identification of Depression Presented by: Dr. Robert Figlerski, Director of Behavioral Health Services Team Health, New York Region Office: 914-949-1199 email:
Administering the PHQ-9 And Maximizing the Identification of Depression Presented by: Dr. Robert Figlerski, Director of Behavioral Health Services Team Health, New York Region Office: 914-949-1199 email:
Depression among Older Adults. Prevalence & Intervention Strategies
 Depression among Older Adults Prevalence & Intervention Strategies Definition Depression is a complex syndrome complex characterized by mood disturbance plus variety of cognitive, psychological, and vegetative
Depression among Older Adults Prevalence & Intervention Strategies Definition Depression is a complex syndrome complex characterized by mood disturbance plus variety of cognitive, psychological, and vegetative
Relapse Prevention Webinar Agenda Relapse Prevention Planning
 Relapse Prevention Webinar Agenda Relapse Prevention Planning Rita Haverkamp, MSN, PMHCNS BC, CNS Expert Care Manager and AIMS Trainer By the end of the webinar you will be able to Describe what a RPP
Relapse Prevention Webinar Agenda Relapse Prevention Planning Rita Haverkamp, MSN, PMHCNS BC, CNS Expert Care Manager and AIMS Trainer By the end of the webinar you will be able to Describe what a RPP
Depression Care. Patient Education Script
 Everybody has the blues from time to time, or reacts to stressful life events with feelings of anxiety, sadness, or anger. Normally these feelings go away with time but when they persist, and are present
Everybody has the blues from time to time, or reacts to stressful life events with feelings of anxiety, sadness, or anger. Normally these feelings go away with time but when they persist, and are present
CONCORD INTERNAL MEDICINE MENTAL HEALTH PROTOCOL
 CONCORD INTERNAL MEDICINE MENTAL HEALTH PROTOCOL Douglas G. Kelling, Jr., MD Carla Gismondi-Eagan, MD, FACP George C. Monroe III, MD Revised April 8, 2012 The information contained in this protocol should
CONCORD INTERNAL MEDICINE MENTAL HEALTH PROTOCOL Douglas G. Kelling, Jr., MD Carla Gismondi-Eagan, MD, FACP George C. Monroe III, MD Revised April 8, 2012 The information contained in this protocol should
Mood Disorders for Care Coordinators
 Mood Disorders for Care Coordinators David A Harrison, MD, PhD Assistant Professor, Dept of Psychiatry & Behavioral Sciences University of Washington School of Medicine Introduction 1 of 3 Mood disorders
Mood Disorders for Care Coordinators David A Harrison, MD, PhD Assistant Professor, Dept of Psychiatry & Behavioral Sciences University of Washington School of Medicine Introduction 1 of 3 Mood disorders
AMPS : A Quick, Effective Approach To The Primary Care Psychiatric Interview
 AMPS : A Quick, Effective Approach To The Primary Care Psychiatric Interview February 7, 2012 Robert McCarron, D.O. Assosicate Clinical Professor Internal Medicine / Psychiatry / Pain Medicine UC Davis,
AMPS : A Quick, Effective Approach To The Primary Care Psychiatric Interview February 7, 2012 Robert McCarron, D.O. Assosicate Clinical Professor Internal Medicine / Psychiatry / Pain Medicine UC Davis,
Taking Care: Child and Youth Mental Health TREATMENT OPTIONS
 Taking Care: Child and Youth Mental Health TREATMENT OPTIONS Open Learning Agency 2004 TREATMENT OPTIONS With appropriate treatment, more than 80% of people with depression get full relief from their symptoms
Taking Care: Child and Youth Mental Health TREATMENT OPTIONS Open Learning Agency 2004 TREATMENT OPTIONS With appropriate treatment, more than 80% of people with depression get full relief from their symptoms
Supplementary Materials:
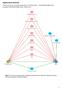 Supplementary Materials: Depression and risk of unintentional injury in rural communities a longitudinal analysis of the Australian Rural Mental Health Study (Inder at al.) Figure S1. Directed acyclic
Supplementary Materials: Depression and risk of unintentional injury in rural communities a longitudinal analysis of the Australian Rural Mental Health Study (Inder at al.) Figure S1. Directed acyclic
Oxleas CAMHS Dr Joanna Sales Clinical Director. Adolescent problems: Depression Deliberate Self Harm Early Intervention in Psychosis
 Oxleas CAMHS Dr Joanna Sales Clinical Director Adolescent problems: Depression Deliberate Self Harm Early Intervention in Psychosis PREVALENCE At any one time, the estimated number of children and young
Oxleas CAMHS Dr Joanna Sales Clinical Director Adolescent problems: Depression Deliberate Self Harm Early Intervention in Psychosis PREVALENCE At any one time, the estimated number of children and young
Denver Health s Roadmap to Reduce Racial Disparities: Telephonic Counseling for Depression and Anxiety
 Denver Health s Roadmap to Reduce Racial Disparities: Telephonic Counseling for Depression and Anxiety David Brody, MD Medical Director Denver Health Managed Care Plans Professor of Medicine University
Denver Health s Roadmap to Reduce Racial Disparities: Telephonic Counseling for Depression and Anxiety David Brody, MD Medical Director Denver Health Managed Care Plans Professor of Medicine University
Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents
 BadgerCare Plus Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice
BadgerCare Plus Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice
Summary of guideline for the. treatment of depression RANZCP CLINICAL PRACTICE GUIDELINES ASSESSMENT
 RANZCP CLINICAL PRACTICE GUIDELINES Summary of guideline for the RANZCP CLINICAL PRACTICE GUIDELINES treatment of depression Pete M. Ellis, Ian B. Hickie and Don A. R. Smith for the RANZCP Clinical Practice
RANZCP CLINICAL PRACTICE GUIDELINES Summary of guideline for the RANZCP CLINICAL PRACTICE GUIDELINES treatment of depression Pete M. Ellis, Ian B. Hickie and Don A. R. Smith for the RANZCP Clinical Practice
Help is at hand. Lambeth. Problems at work? Depressed? Stressed? Phobias? Anxious? Can t find work? Lambeth Psychological Therapies
 South London and Maudsley NHS Foundation Trust Problems at work? Lambeth Stressed? Depressed? Anxious? Phobias? Can t find work? Lambeth Psychological Therapies 020 3228 6747 Help is at hand Page 1 Are
South London and Maudsley NHS Foundation Trust Problems at work? Lambeth Stressed? Depressed? Anxious? Phobias? Can t find work? Lambeth Psychological Therapies 020 3228 6747 Help is at hand Page 1 Are
Obsessive-Compulsive Disorder Clinical Practice Guideline Summary for Primary Care
 Obsessive-Compulsive Disorder Clinical Practice Guideline Summary for Primary Care CLINICAL ASSESSMENT AND DIAGNOSIS (ADULTS) Obsessive-Compulsive Disorder (OCD) is categorized by recurrent obsessions,
Obsessive-Compulsive Disorder Clinical Practice Guideline Summary for Primary Care CLINICAL ASSESSMENT AND DIAGNOSIS (ADULTS) Obsessive-Compulsive Disorder (OCD) is categorized by recurrent obsessions,
Problem Summary. * 1. Name
 Problem Summary This questionnaire is an important part of providing you with the best health care possible. Your answers will help in understanding problems that you may have. Please answer every question
Problem Summary This questionnaire is an important part of providing you with the best health care possible. Your answers will help in understanding problems that you may have. Please answer every question
Depression intervention via referral, education, and collaborative treatment (Project DIRECT): a pilot study
 Executive summary of completed research Depression intervention via referral, education, and collaborative treatment (Project DIRECT): a pilot study Principal Investigator Jane McCusker, MD DrPH Co-investigators
Executive summary of completed research Depression intervention via referral, education, and collaborative treatment (Project DIRECT): a pilot study Principal Investigator Jane McCusker, MD DrPH Co-investigators
Psychiatry in a Collaborative System-Level and Practice-Level
 Psychiatry in a Collaborative System-Level and Practice-Level Robin M. Reed, MD, MPH Presentation for the North Carolina Psychiatric Association October 2 nd 2015 Disclosures I have no relevant financial
Psychiatry in a Collaborative System-Level and Practice-Level Robin M. Reed, MD, MPH Presentation for the North Carolina Psychiatric Association October 2 nd 2015 Disclosures I have no relevant financial
Please complete this form before your Doctor visit. We will review this together and make any changes needed.
 1 Medical History Please complete this form before your Doctor visit. We will review this together and make any changes needed. Name Date of Birth Date of visit What is your height? weight? Medical History,
1 Medical History Please complete this form before your Doctor visit. We will review this together and make any changes needed. Name Date of Birth Date of visit What is your height? weight? Medical History,
o Normal Balanced Diet for your Age o High in Carbohydrates o High in Fats o High in Protein o Other Diet
 HEALTH ASSESSMENT SCREENING FORM GO402 Welcome to G0438 First Annual G0439 Subsequent Other Code PATIENTS NAME: DATE OF BIRTH: DATE OF SERVICE: PLEASE LIST CURRENT MEDICATION, ALSO OVER THE COUNTER MEDICATIONS
HEALTH ASSESSMENT SCREENING FORM GO402 Welcome to G0438 First Annual G0439 Subsequent Other Code PATIENTS NAME: DATE OF BIRTH: DATE OF SERVICE: PLEASE LIST CURRENT MEDICATION, ALSO OVER THE COUNTER MEDICATIONS
