Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update
|
|
|
- Ambrose Jenkins
- 6 years ago
- Views:
Transcription
1 Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update Robert G. Micheletti, MD Assistant Professor of Dermatology and Medicine Director, Cutaneous Vasculitis Clinic, Penn Vasculitis Center Co-Director, Inpatient Consult Service University of Pennsylvania
2 Presentation Prodrome of fever, flu-like symptoms x 1-3 days Photophobia, conjunctival itching, dysphagia, skin tenderness Typically two or more mucous membranes Dusky atypical target lesions Denuded skin / epidermal detachment SJS < 10% BSA TEN > 30% BSA 1
3 Etiology and Pathogenesis Overall incidence of SJS/TEN 2-13 per million per year Risk factors include immune dysregulation: HIV infection 100-fold increase Autoimmune disease 50-fold increase in SLE patients Active malignancy (particularly hematologic) 30-to-60-fold increase J Invest Dermatol. 2016;136(7): Br J Dermatol Mar;166(3): Am J Clin Dermatol Feb;13(1):
4 Etiology and Pathogenesis Genetic factors HLA-B*15:02 (carbamazepine; OR 79.84, Asian)* HLA-A*31:01 (carbamazepine; all ethnic groups)* HLA-B*58:01 (allopurinol) *Pre-screening of HLA type recommended prior to starting carbamazepine Polymorphisms in Cyt P450 and other factors associated with decreased medication clearance N Engl J Med. 2011;364(12):1126. JAMA Dermatol. 2013;149(9):1025. J Dermatol Sci Feb;73(2):
5 Etiology and Pathogenesis Drug-specific CD8 T-cells and natural killer (NK) cells are the major inducers of keratinocyte apoptosis Drugs stimulate the immune system by binding to MHC-I and T- cell receptors, resulting in clonal expansion of cytotoxic T-cells These cells kill keratinocytes directly and indirectly via release of cytotoxic mediators: Soluble Fas ligand Perforin / granzyme Tumor necrosis factor Granulysin J Allergy Clin Immunol Dec;128(6):
6 Etiology and Pathogenesis Granulysin Produced and secreted by CD8 and NK cells Highly expressed in SJS/TEN Levels in blister fluid correlate with disease severity Reproducible cytotoxic effect on keratinocytes Thought responsible for apoptosis in SJS/TEN *Being studied as a diagnostic marker and treatment target for SJS/TEN Ann Intern Med. 2009;151(7):514. J Allergy Clin Immunol. 2008;122(5):992. Curr Opin Allergy Clin Immunol Aug;13(4): Curr Opin Allergy Clin Immunol Aug;15(4):
7 Etiology and Pathogenesis Medications are the most common cause of SJS/TEN Typically within 1-3 weeks (avg = 14 days) Unlikely after first 8 weeks of treatment Allopurinol* Anticonvulsants Sulfa antibiotics Nevirapine Oxicam NSAIDs *Most common in EuroSCAR (17.4%) J Am Acad Dermatol. 2008;58(1):25. 6
8 Etiology and Pathogenesis US Derm Hospitalist Study (377 adult patients) Most common cause of SJS/TEN, in 89.7%, was medication reaction, including common culprit drugs: Class of medications N=338 Antibiotics Trimethoprim/sulfamethoxazole β-lactam antibiotics Fluoroquinolones Antiepileptic/Mood stabilizers Lamotrigine Phenytoin Carbamazepine 165 (48.8%) 89 (26.3%) 42 (12.4%) 12 (3.6%) 83 (23.7%) 32 (9.5%) 30 (8.9%) 7 (2.1%) Allopurinol v 29 (8.6%) NSAIDs 18 (5.3%) v v v Micheletti et al, Society of Dermatology Hospitalists (submitted) 7
9 Etiology and Pathogenesis Derm Hospitalist Study: All patients with lamotrigine-induced SJS/TEN (n = 29) survived to discharge Exposure to phenytoin increased the risk of death (RR 3.82 ( )) High mortality among those receiving pip/tazo (Zosyn) (73%) drug or underlying disease state? For the most part, the specific drug trigger does not contribute significantly to mortality risk in SJS/TEN 8
10 Etiology and Pathogenesis Mycoplasma SJS trigger common in children Significant mucosal but minimal skin involvement Tend to have better outcomes Now recognized as a distinct entity, termed Mycoplasma-induced rash and mucositis (MIRM) Derm Hospitalist Study: 2% of cases attributed to Mycoplasma; mortality among infectious cases overall 8% J Am Acad Dermatol Feb;72(2): J Eur Acad Dermatol Venereol Mar;29(3):
11 Rapid Diagnosis a medical emergency When SJS/TEN is clinically obvious, institute therapy even if histologic confirmation is pending However, I do always perform a biopsy for completeness In one study, 1/3 of those biopsied received an alternate diagnosis based on histology Burns Feb 1. [Epub ahead of print]. 10
12 SJS Mimickers Transferred from an OSH, where he was diagnosed with SJS and treated in a burn unit Ultimate diagnosis = severe cutaneous lupus 11
13 SJS Mimickers Transferred from an OSH to our ICU for treatment of SJS/TEN; received IVIG Ultimate diagnosis = epidermolysis bullosa acquisita vs anti-epiligrin cicatricial pemphigoid 12
14 SJS Mimickers Patient with SLE on chronic immunosuppression Acute skin tenderness and widespread denuded skin concerning for SJS/TEN SSSS clinical pic Diagnosed with Staph scalded skin syndrome 13
15 SJS Mimickers Patient with acute leukemia 2-3 weeks s/p stem cell transplant Developed acute dusky erythema, erosions, mucositis, conjunctivitis SJS/TEN vs grade IV acute GVHD 14
16 SJS Mimickers Paraneoplastic pemphigus 15
17 Rapid Diagnosis a medical emergency When the diagnosis is in doubt, biopsy may be required to guide management Histologic appearance of SJS: Keratinocyte necrosis ranging from partial to full thickness (established lesions) Scant perivascular lymphohistiocytic inflammation 16
18 Rapid Diagnosis In our hospital, preliminary results of standard biopsy are available by the end of the following business day Alternative options: Frozen section biopsy Tzanck smear Jelly roll *Frozen section biopsy: Results typically available within minutes Take the time to discuss with pathology and determine the mechanism for this in your hospital 17
19 Rapid Diagnosis Jelly roll The blister roof can be submitted for frozen section Reveals full-thickness epidermal necrosis 18
20 Data-Driven Management Published overall mortality rate for SJS/TEN is 20-25% RegiSCAR cohort 6-week mortality: SJS = 12% SJS/TEN = 29% TEN = 46% Ther Adv Drug Saf. 2011;2(3):87. J Invest Dermatol May;133(5):
21 Data-Driven Management How do we give our patients the best chance for survival? What management is supported by the available evidence? 20
22 Data-Driven Management Stop the culprit drug Earlier withdrawal = better prognosis OR of death = 0.69 for each day sooner OR of death = 4.9 for drugs with long half lives Identification of the causative agent is a non-trivial exercise Causality assessment tools (e.g., ALDEN) may help but have problems with reliability and agreement No substitute for systematic approach by an expert (dermatologist) Arch Dermatol. 2000;136(3):323. Clin Pharmacol Ther. 2017;101:S5-S99. 21
23 Data-Driven Management Transfer the patient to an ICU or burn unit In one study, overall mortality = 32% Mortality of those transferred after > 1 week = 51% *Patients with mild SJS or SCORTEN of 0 or 1 should still be cared for in an ICU Mild SJS is a designation best made in retrospect; patients may progress rapidly from mild presentations Published guidelines suggest initial management of SJS/TEN patients in specialized centers due to risk of rapid progression regardless of initial % BSA involved Burns. 2016;42(4): J Burn Care Rehabil. 2002;23(2):87. 22
24 Data-Driven Management The level of care is a surrogate for supportive care: Fluids Electrolytes Temperature Nutrition Pain control Airway maintenance Wound care Infection surveillance Ophthalmology Gynecology Urology Hematology Role of dermatology Close diagnosis, identification of culprit drug Role Cleaning, Vaseline, Topical observation; Bacteremia of dermatology lubrication, steroids, non-stick in may as team steroid vaginal 27%: gauze require May Urethritis, develop 2/3-3/4 Parkland formula quarterback drops Enteral, profound urinary not parenteral retention neutropenia Staph, Amniotic Pseudomonas, Clean dilator, prolonged Critical membranes, / sterile Vaseline intubation role in patient Enterobacteriaceae technique scleral gauze advocacy spacers Medicine (Baltimore) Jan;89(1): J Am Acad Dermatol Aug;69(2):187.e1-187.e16. 23
25 Data-Driven Management Despite this, there is wide variability in supportive and systemic care: Survey of 102 burn centers showed variability in consultation of other services: Ophthalmology (66%) Dermatology (47%) Gynecology (13%) Burns Jun;42(4):
26 Data-Driven Management ICU versus Burn Center: Burn centers are highly skilled in wound care and fluid management, but do they have a dermatologist? Burn center may be less familiar with management of complex medical comorbidities Patients who are post-transplant, have autoimmune disease, etc. require specialized knowledge and care Dermatology hospitalists may be best positioned to provide the differential diagnosis, wound care, and advocacy patients need Both are better than non-specialized ward, but supportive care should be more homogeneous and studied prospectively J Am Acad Dermatol Jul;71(1):
27 Latest Evidence for Pharmacotherapies Besides supportive care, published literature has not consistently shown benefit from the use of any particular systemic therapy for SJS/TEN Case series and retrospective cohorts are limited by confounding factors, low numbers, and inherent biases that make drawing conclusions from existing data difficult 26
28 Latest Evidence for Pharmacotherapies Systemic Corticosteroids: Early observational studies indicated a higher complication and mortality rate EuroSCAR cohort suggested possible benefit to early steroids, though not statistically significant RegiSCAR cohort and systematic review: no mortality advantage over supportive care alone J Am Coll Surg. 1995;180(3):273 Ther Adv Drug Saf. 2011;2(3):87. J Am Acad Dermatol. 2008;58(1):33. J Invest Dermatol May;133(5):
29 Latest Evidence for Pharmacotherapies Systemic Corticosteroids: More recently, a meta-analysis of 96 studies in JAMA Dermatology, suggested there is a survival benefit While these results had limitations and were only marginally statistically significant, corticosteroids were felt to be promising On balance, despite concern for increased infection, early use of systemic steroids may be beneficial JAMA Dermatol. 2017;153(6):
30 Latest Evidence for Pharmacotherapies Intravenous Immunoglobulin: Data are limited and conflicting Thought to inhibit Fas FasL binding, but this is no longer considered the primary mediator of SJS Drugs. 2005;65(15):2085. Science. 1998;282(5388):490. Arch Dermatol. 2003;139(1):26. Arch Dermatol. 2003;139(1):39. Br J Dermatol Aug;167(2):
31 Latest Evidence for Pharmacotherapies Intravenous Immunoglobulin: Case series and a systematic review suggested highdose, early IVIG (>2g/kg total) improves survival However, a number of reviews, including the recent meta analysis from 2017, have shown no mortality benefit Drugs. 2005;65(15):2085. Science. 1998;282(5388):490. Arch Dermatol. 2003;139(1):26. Arch Dermatol. 2003;139(1):39. Br J Dermatol Aug;167(2):
32 Latest Evidence for Pharmacotherapies Intravenous Immunoglobulin: For these reasons, IVIG has fallen out of favor in Europe However, it continues to be an agent of choice for SJS/TEN among US dermatology hospitalists Br J Dermatol Nov;173(5):
33 Latest Evidence for Pharmacotherapies A survey of 131 US providers (academic dermatologists and burn centers) reported that: Majority do not use systemic steroids More likely to use IVIG if more severe disease majority use IVIG for SJS/TEN overlap and TEN Those who see SJS/TEN more frequently are more likely to use IVIG regardless of severity J Am Acad Dermatol Feb;74(2):
34 US Derm Hospitalist Study (377 adult patients) In our cohort managed by inpatient dermatologists, IVIG was used extensively, alone or in combination (55.6% of patients) Patients receiving IVIG had more severe disease at presentation: Higher median BSA involvement (30% vs 12%, p-value<0.01) Higher rate of TEN (28.0% vs 18.7%, p-value=0.01) Higher rates of severe ocular, oral, and genitourinary involvement (all p-values <0.05) compared to other treatment groups Micheletti et al, Society of Dermatology Hospitalists (submitted) 33
35 Latest Evidence for Pharmacotherapies Intravenous Immunoglobulin: In summary, no high quality evidence supports the use of IVIG in SJS/TEN However, those who receive it appear to be sicker to start with, and the effects of this and other confounders may not be completely accounted for by SCORTEN-predicted mortality Early in the disease course, a dose of 1g/kg/day x 3-4 days IVIG can be considered Potential side effects include clot / hyperviscosity Side effect profile more favorable than high-dose steroids Br J Dermatol Nov;173(5):
36 Latest Evidence for Pharmacotherapies Cyclosporine: Anti-apoptotic, inhibits T-cells, including CD8 T-cells Dose 3 to 5 mg/kg/day, tapered over one month Supported mostly by small, retrospective, and uncontrolled case series J Trauma. 2000;48(3):473. Cutis Jan;87(1):24-9. J Am Acad Dermatol 2012;67(4):
37 Latest Evidence for Pharmacotherapies Cyclosporine: Retrospective review of 64 patients Outcome of 15 who received cyclosporine (SMR = 0.43) better than 50 who received IVIG (SMR = 1.43) IVIG dose and timing varied widely Retrospective review of 44 patients Among 24 who received cyclosporine, SMR = 0.42 Open, Phase II trial of 29 patients: SCORTEN predicted mortality 2.75; actual = 0 Br J Dermatol. 2010;163(4):847. J Am Acad Dermatol. 2014;71(5):941. J Am Acad Dermatol. 2017;76(1):
38 Latest Evidence for Pharmacotherapies Cyclosporine: More recently, two 2017 studies suggested a mortality benefit of cyclosporine via meta-analysis and retrospective case series (49 patients) Increasing favor in Europe, but the actual number of treated patients remains small, and the drug has important side effects (renal, immunosuppression) JAMA Dermatol. 2017;153(6): J Invest Dermatol Oct;137(10):
39 Latest Evidence for Pharmacotherapies Cyclosporine: Letter-to-the-editor: Existing studies either exclude patients with renal insufficiency and other known SJS/TEN mortality risk factors altogether or do not report them In our cohort, renal failure was the greatest mortality RF Recent retrospective cohort study of 174 patients: No significant benefit from cyclosporine in 95 patients (versus 79 supportive care only) Acute renal failure more common in treatment group J Invest Dermatol Jan 21 [Epub ahead of print] 38
40 Latest Evidence for Pharmacotherapies Cyclosporine: In summary, cyclosporine is certainly deserving of further study, but there are reasons to temper enthusiasm Early use of cyclosporine in young, otherwise healthy patients at a dose of 3-5mg/kg/day is a reasonable treatment option, but we do not have enough data to recommend this in sicker patients JAMA Dermatol. 2017;153(6):
41 Latest Evidence for Pharmacotherapies Tumor Necrosis Factor (TNF) inhibitors: Thalidomide: Only double-blind, randomized, placebo-controlled TEN study Trial stopped early due to excess mortality (10/12 died, vs 3/10 in placebo) Suggested reason for caution with respect to TNF inhibitors for SJS/TEN Lancet. 1998;352(9140):
42 Latest Evidence for Pharmacotherapies Tumor Necrosis Factor (TNF) inhibitors: Etanercept: Case series in 8/2014 JAAD One 50mg injection 10 patients with good outcomes; no controls Infliximab: One 5mg/kg infusion Case reports only Pediatr Dermatol. 2014;31(4):532. J Am Acad Dermatol. 2014;71(2):
43 Latest Evidence for Pharmacotherapies Tumor Necrosis Factor (TNF) inhibitors: 96-patient randomized trial of etanercept versus corticosteroids SMR = 0.47 among those receiving etanercept (0.80 with corticosteroids) Decreased time to skin healing and lower rates of complications compared to corticosteroid group J Clin Invest Feb 5. [Epub ahead of print] 42
44 Latest Evidence for Pharmacotherapies Tumor Necrosis Factor (TNF) inhibitors: Recent experience with etanercept is promising 25mg or 50mg etanercept twice weekly until skin lesions healed J Clin Invest Feb 5. [Epub ahead of print] 43
45 US Derm Hospitalist Study (377 adult patients) Overall and subgroup mortality less than predicted by SCORTEN Predicted mortality for the overall cohort was 21.1%, vs 14.7% actual Adjusting for SCORTEN, mortality was lower in the steroid + IVIG group compared to IVIG or steroids alone and to supportive care only *Bias toward using IVIG to treat patients with more severe SJS/TEN *Only 5 patients treated with cyclosporine or etanercept In-hospital mortality SCORTEN predicted mortality, N (%) Overall N=368 IVIG only N=92 Steroid only N=116 IVIG + Steroid N=54 Supportive care N= (21.1) 21.6 (23.5) 20.8 (17.8) 11.6 (21.2) 22.7 (19.4) Observed mortality 54 (14.7) 17 (18.5) 15 (12.9) 6 (10.7) 16 (13.7) SMR (95%CI) 0.70 (0.58, 0.79) 0.79 (0.55, 0.92) 0.72 (0.48, 0.89) 0.52 (0.21, 0.79) 0.70 (0.47, 0.87) Micheletti et al, Society of Dermatology Hospitalists (submitted) 44
46 US Derm Hospitalist Study (377 adult patients) One of the largest existing SJS/TEN cohorts (largest in N America) Overall survival rate better than reported in the literature and better than predicted by SCORTEN: Published mortality rate 20-25% in our cohort, 14.7% Large systematic review reported SMR in our cohort, the SMR was 0.70 (0.58, 0.79) Ther Adv Drug Saf. 2011;2(3):87. Micheletti et al, Society of Dermatology Hospitalists (submitted). 45
47 US Derm Hospitalist Study (377 adult patients) Unclear if improved survival reflects excellent supportive care in tertiary centers, the presence of a consulting dermatologist, or inadequacy of SCORTEN as a predictive tool The optimal pharmacologic regimen remains uncertain Some small published series support steroids + IVIG Cyclosporine, etanercept, corticosteroids all reasonable Need better ways to account and adjust for prescriber practices, particularly with respect to IVIG severity bias Additional analysis of the cohort is ongoing J Burn Care Res Nov;33(6):e Indian J Dermatol Venereol Leprol. 2013;79(4):506. Micheletti et al, Society of Dermatology Hospitalists (submitted). 46
48 Latest Evidence for Pharmacotherapies At our institution, we favor: Admission of all SJS/TEN patients to the MICU At least 1:1 nursing care Daily dermatology and universal ophthalmology and gynecology consultation Early high-dose IVIG (1g/kg/day) x 3-4 days with a goal to try to stop progression (actively re-evaluating) Given as soon as the diagnosis is made (regardless of severity); early Rx may be the key with any treatment 47
49 Latest Evidence for Pharmacotherapies All retrospective studies and literature reviews are limited by heterogeneous populations, dosing, and confounding factors In general, a lack of consensus regarding the appropriate pharmacologic management of SJS/TEN persists, even among experienced providers 48
50 Next Steps Research priorities: Better understanding of the genetic and immunologic basis of disease with prospective sample collection Improved risk assessment so the reaction can be avoided Investigation of novel treatments to inhibit granulysin Br J Dermatol Nov;173(5):
51 Next Steps Research priorities: Systematic evaluation of SJS/TEN sequelae and quality of life Survey study Establish expert opinion standard for supportive care Delphi effort Br J Dermatol Aug;175(2): Br J Dermatol Nov;173(5):
52 Next Steps Research priorities: Revision of SCORTEN, which may overestimate mortality Improved prognostic model (SMR 0.99) Utilize existing networks to conduct a prospective SJS/TEN study and, ultimately, a randomized controlled trial J Invest Dermatol. 2017;137(5S):S37 51
53 Summary SJS/TEN is a severe cutaneous adverse drug reactions with published mortality of 20-25% Dermatologists play a critical role in diagnosing this disease, differentiating mimickers, identifying and stopping culprit drugs, and coordinating treatment efforts Much progress still to make with respect to pathogenesis, prevention, and management dermatologists can and should be at the forefront of these efforts 52
54 The Dermatology Foundation has supported & advanced my career.
55 Thank you University of Pennsylvania
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES. R e g i S C A R PATIENT'S DATA. Age country of birth
 REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
Bugs and Drugs: What s New in Hypersensitivity Reactions?
 Bugs and Drugs: What s New in Hypersensitivity Reactions? Erin Mathes, MD Associate Professor of Dermatology and Pediatrics University of California, San Francisco DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY
Bugs and Drugs: What s New in Hypersensitivity Reactions? Erin Mathes, MD Associate Professor of Dermatology and Pediatrics University of California, San Francisco DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY
Emergency Dermatology Dr Melissa Barkham
 Emergency Dermatology Dr Melissa Barkham Spotlight Seminar 30 th September 2010 Why is this important? Urgent recognition and treatment of dermatologic emergencies can be life saving and prevent long term
Emergency Dermatology Dr Melissa Barkham Spotlight Seminar 30 th September 2010 Why is this important? Urgent recognition and treatment of dermatologic emergencies can be life saving and prevent long term
Stevens Johnson Syndrome: How Diagnosis Impacts Disease Course
 Southern Adventist Univeristy KnowledgeExchange@Southern Graduate Research Projects Nursing 12-4-2015 Stevens Johnson Syndrome: How Diagnosis Impacts Disease Course Sharon K. Hart Southern Adventist University,
Southern Adventist Univeristy KnowledgeExchange@Southern Graduate Research Projects Nursing 12-4-2015 Stevens Johnson Syndrome: How Diagnosis Impacts Disease Course Sharon K. Hart Southern Adventist University,
To update the use of IVIG and CORTICOIDS IN management of SJS/ TEN To remind Doctors being careful when giving
 Present : Dr Pham Thi Minh Rang Internal Department No2-Hospital for children No2 AIMS To update the use of IVIG and CORTICOIDS IN management of SJS/ TEN To remind Doctors being careful when giving To
Present : Dr Pham Thi Minh Rang Internal Department No2-Hospital for children No2 AIMS To update the use of IVIG and CORTICOIDS IN management of SJS/ TEN To remind Doctors being careful when giving To
Future of Pediatrics: Blisters, Hives and Other Tales from the Emergency Room June 14 th, 2016
 A. Yasmine Kirkorian MD Assistant Professor of Dermatology & Pediatrics Children s National Health System George Washington University School of Medicine & Health Sciences Future of Pediatrics: Blisters,
A. Yasmine Kirkorian MD Assistant Professor of Dermatology & Pediatrics Children s National Health System George Washington University School of Medicine & Health Sciences Future of Pediatrics: Blisters,
Dilantin (phenytoin) ROBERT A. SCHWARTZ
 Dilantin (phenytoin) ROBERT A. SCHWARTZ Bailey & Galyen Attorney in Charge, Mass Tort Litigation Managing Attorney, Houston 18333 Egret Bay Blvd., Suite 120 Houston, Texas 77058 Toll Free: (866) 715-1529
Dilantin (phenytoin) ROBERT A. SCHWARTZ Bailey & Galyen Attorney in Charge, Mass Tort Litigation Managing Attorney, Houston 18333 Egret Bay Blvd., Suite 120 Houston, Texas 77058 Toll Free: (866) 715-1529
Correspondence should be addressed to Wanjarus Roongpisuthipong; rr
 Dermatology Research and Practice, Article ID 237821, 5 pages http://dx.doi.org/10.1155/2014/237821 Research Article Retrospective Analysis of Corticosteroid Treatment in Stevens-Johnson Syndrome and/or
Dermatology Research and Practice, Article ID 237821, 5 pages http://dx.doi.org/10.1155/2014/237821 Research Article Retrospective Analysis of Corticosteroid Treatment in Stevens-Johnson Syndrome and/or
Cutaneous Conditions Associated with Systemic Disease
 Cutaneous Conditions Associated with Systemic Disease Johnnie M Woodson, M.D., F.A.A.D. Assistant Professor of Dermatology University of Nevada School of Medicine Director of J. Woodson Dermatology & Associates,
Cutaneous Conditions Associated with Systemic Disease Johnnie M Woodson, M.D., F.A.A.D. Assistant Professor of Dermatology University of Nevada School of Medicine Director of J. Woodson Dermatology & Associates,
Five things not to miss in Dermatology. Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine
 Five things not to miss in Dermatology Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine Key Descriptives Fever, skin pain Purpura, necrosis Bullae, Mucosal, Skin sloughing
Five things not to miss in Dermatology Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine Key Descriptives Fever, skin pain Purpura, necrosis Bullae, Mucosal, Skin sloughing
Pediatric Dermatology
 Pediatric Dermatology --------- Emergencies & Urgencies Nicholas V. Nguyen, M.D. Director, Pediatric Dermatology Disclosures In the past 12 months, I have had the following financial relationships with
Pediatric Dermatology --------- Emergencies & Urgencies Nicholas V. Nguyen, M.D. Director, Pediatric Dermatology Disclosures In the past 12 months, I have had the following financial relationships with
Big rashes in little patients:
 ! Big rashes in little patients: Severe drug eruptions and cutaneous infections!! Marcia Hogeling, MD, FAAD Assistant Clinical Professor Director, Pediatric Dermatology Division of Dermatology David Geffen
! Big rashes in little patients: Severe drug eruptions and cutaneous infections!! Marcia Hogeling, MD, FAAD Assistant Clinical Professor Director, Pediatric Dermatology Division of Dermatology David Geffen
STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSIS IN CHILDREN: A LITERATURE REVIEW OF CURRENT TREATMENTS
 STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSIS IN CHILDREN: A LITERATURE REVIEW OF CURRENT TREATMENTS *Blanca R. Del Pozzo-Magaña, 1 Alejandro Lazo-Langner 2,3 1. Department of Pediatrics, University
STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSIS IN CHILDREN: A LITERATURE REVIEW OF CURRENT TREATMENTS *Blanca R. Del Pozzo-Magaña, 1 Alejandro Lazo-Langner 2,3 1. Department of Pediatrics, University
OXCARBAZEPINE-INDUCED STEVENS-JOHNSON SYNDROME: A CASE REPORT
 OXCARBAZEPINE-INDUCED STEVENS-JOHNSON SYNDROME: A CASE REPORT Lung-Chang Lin, 1,2 Ping-Chin Lai, 3 Sheau-Fang Yang, 4 and Rei-Cheng Yang 1,5 Departments of 1 Pediatrics and 4 Pathology, Kaohsiung Medical
OXCARBAZEPINE-INDUCED STEVENS-JOHNSON SYNDROME: A CASE REPORT Lung-Chang Lin, 1,2 Ping-Chin Lai, 3 Sheau-Fang Yang, 4 and Rei-Cheng Yang 1,5 Departments of 1 Pediatrics and 4 Pathology, Kaohsiung Medical
CARBAMAZEPINE INDUCED STEVENS JOHNSON SYNDROME- A CASE STUDY
 WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Ragesh SJIF Impact Factor 2.786 Volume 3, Issue 6, 1599-1604. Case Study ISSN 2278 4357 CARBAMAZEPINE INDUCED STEVENS JOHNSON SYNDROME- A CASE STUDY
WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Ragesh SJIF Impact Factor 2.786 Volume 3, Issue 6, 1599-1604. Case Study ISSN 2278 4357 CARBAMAZEPINE INDUCED STEVENS JOHNSON SYNDROME- A CASE STUDY
SKIN REACTIONS WITH PSYCHOTROPICS: A SYSTEMATIC REVIEW
 SKIN REACTIONS WITH PSYCHOTROPICS: A SYSTEMATIC REVIEW *Anderson Isaac, PharmD Candidate, 2019 Pooja Patel, PharmD Candidate, 2019 Katelyn Thomasson, PharmD Candidate, 2019 Erika Tillery, PharmD, BCPP,
SKIN REACTIONS WITH PSYCHOTROPICS: A SYSTEMATIC REVIEW *Anderson Isaac, PharmD Candidate, 2019 Pooja Patel, PharmD Candidate, 2019 Katelyn Thomasson, PharmD Candidate, 2019 Erika Tillery, PharmD, BCPP,
allergy Asia Pacific Stevens-Johnson syndrome and toxic epidermal necrolysis in Dr. Hasan Sadikin General Hospital Bandung, Indonesia from
 pissn -876 eissn -868 Original Article Asia Pac Allergy 6;6:-7 Stevens-Johnson syndrome and toxic epidermal necrolysis in Dr. Hasan Sadikin General Hospital Bandung, Indonesia from 9 Oki Suwarsa *, Wulan
pissn -876 eissn -868 Original Article Asia Pac Allergy 6;6:-7 Stevens-Johnson syndrome and toxic epidermal necrolysis in Dr. Hasan Sadikin General Hospital Bandung, Indonesia from 9 Oki Suwarsa *, Wulan
SJS/TEN spectrum. Stevens-Johnson syndrome (SJS) /Toxic Epidermal Necrolysis (TEN) 10/7/2016
 Jesse Keller MD Assistant Professor Oregon Health & Science University Stevens-Johnson syndrome (SJS) /Toxic Epidermal Necrolysis (TEN) Drug induced dermemergencies that exist on a spectrum Delayed reaction:
Jesse Keller MD Assistant Professor Oregon Health & Science University Stevens-Johnson syndrome (SJS) /Toxic Epidermal Necrolysis (TEN) Drug induced dermemergencies that exist on a spectrum Delayed reaction:
GOOD MORNING! AUGUST 5, 2014
 GOOD MORNING! AUGUST 5, 2014 PREP QUESTION During the health supervision visit of a term newborn boy, his mother relates that a cousins child died at age 4 months from sudden infant death syndrome. She
GOOD MORNING! AUGUST 5, 2014 PREP QUESTION During the health supervision visit of a term newborn boy, his mother relates that a cousins child died at age 4 months from sudden infant death syndrome. She
Skin Manifestations of Drug Reactions
 Skin Manifestations of Drug Reactions Dr Carol Hlela, Division of Dermatology Department of Medicine, University of Cape Town and Red Cross Children s Hospital What are the Skin Manifestations of Drug
Skin Manifestations of Drug Reactions Dr Carol Hlela, Division of Dermatology Department of Medicine, University of Cape Town and Red Cross Children s Hospital What are the Skin Manifestations of Drug
Introduction to Pemphigoid: Spectrum of Disease & Treatment
 Introduction to Pemphigoid: Spectrum of Disease & Treatment A Razzaque Ahmed, MD Center for Blistering Diseases Boston, MA A.Razzaque.Ahmed@tufts.edu centerforblisteringdiseases.com SPECTRUM OF PEMPHIGOID
Introduction to Pemphigoid: Spectrum of Disease & Treatment A Razzaque Ahmed, MD Center for Blistering Diseases Boston, MA A.Razzaque.Ahmed@tufts.edu centerforblisteringdiseases.com SPECTRUM OF PEMPHIGOID
A Case Report on Amoxicillin Induced Stevens- Johnson Syndrome
 Open Journal of Clinical & Medical Case Reports Volume 2 (2016) Issue 11 A Case Report on Amoxicillin Induced Stevens- Johnson Syndrome Rajendra Singh Airee*; Aastha Rawal; Binu Mathew; H. Doddayya Abstract
Open Journal of Clinical & Medical Case Reports Volume 2 (2016) Issue 11 A Case Report on Amoxicillin Induced Stevens- Johnson Syndrome Rajendra Singh Airee*; Aastha Rawal; Binu Mathew; H. Doddayya Abstract
Warfarin-induced toxic epidermal necrolysis in combination therapy of Henoch- Schönlein purpura nephritis: a case report
 Kasahara et al. BMC Nephrology (2017) 18:237 DOI 10.1186/s12882-017-0648-9 CASE REPORT Open Access Warfarin-induced toxic epidermal necrolysis in combination therapy of Henoch- Schönlein purpura nephritis:
Kasahara et al. BMC Nephrology (2017) 18:237 DOI 10.1186/s12882-017-0648-9 CASE REPORT Open Access Warfarin-induced toxic epidermal necrolysis in combination therapy of Henoch- Schönlein purpura nephritis:
Treatment with steroids and immunosuppressants
 Treatment with steroids and immunosuppressants Donna Culton, MD, PhD University of North Carolina IPPF 2017 Annual Patient Conference Newport Beach, CA September 16, 2017 Factors that will influence therapy
Treatment with steroids and immunosuppressants Donna Culton, MD, PhD University of North Carolina IPPF 2017 Annual Patient Conference Newport Beach, CA September 16, 2017 Factors that will influence therapy
Cutaneous Drug Reactions
 Cutaneous Drug Reactions Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada Copyright 2017 by Sea Courses
Cutaneous Drug Reactions Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada Copyright 2017 by Sea Courses
DERMATOLOGICAL EMERGENCIES. DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE
 DERMATOLOGICAL EMERGENCIES DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE Dermatological Emergencies INFECTIONS ERYTHRODERMA DRUG ERUPTIONS STEVENS-JOHNSON
DERMATOLOGICAL EMERGENCIES DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE Dermatological Emergencies INFECTIONS ERYTHRODERMA DRUG ERUPTIONS STEVENS-JOHNSON
EFAVIRENZ ASSOCIATED STEVENS-JOHNSON SYNDROME
 EFAVIRENZ ASSOCIATED STEVENS-JOHNSON SYNDROME To the Editor: Persons with human immunodeficiency virus (HIV) infection are highly susceptible to adverse dermatological reactions to specific medications
EFAVIRENZ ASSOCIATED STEVENS-JOHNSON SYNDROME To the Editor: Persons with human immunodeficiency virus (HIV) infection are highly susceptible to adverse dermatological reactions to specific medications
Drug Allergy A Guide to Diagnosis and Management
 Drug Allergy A Guide to Diagnosis and Management (Version 1 April 2015 updated April 2018) Author: Jed Hewitt Chief Pharmacist, Governance & Professional Practice Date of Preparation: April 2015 Updated:
Drug Allergy A Guide to Diagnosis and Management (Version 1 April 2015 updated April 2018) Author: Jed Hewitt Chief Pharmacist, Governance & Professional Practice Date of Preparation: April 2015 Updated:
Molecular Methods in the Diagnosis and Prognostication of Melanoma: Pros & Cons
 Molecular Methods in the Diagnosis and Prognostication of Melanoma: Pros & Cons Ben J. Friedman, MD Senior Staff Physician Department of Dermatology Department of Pathology and Laboratory Medicine Henry
Molecular Methods in the Diagnosis and Prognostication of Melanoma: Pros & Cons Ben J. Friedman, MD Senior Staff Physician Department of Dermatology Department of Pathology and Laboratory Medicine Henry
Positioning Biologics in Ulcerative Colitis
 Positioning Biologics in Ulcerative Colitis Bruce E. Sands, MD, MS Acting Chief, Gastrointestinal Unit Massachusetts General Hospital Associate Professor of Medicine Harvard Medical School Sequential Therapies
Positioning Biologics in Ulcerative Colitis Bruce E. Sands, MD, MS Acting Chief, Gastrointestinal Unit Massachusetts General Hospital Associate Professor of Medicine Harvard Medical School Sequential Therapies
Toxic Epidermal Necrolysis and SJS : Case Reports & Brief Review
 Case Report Toxic Epidermal Necrolysis and SJS : Case Reports & Brief Review Deepali P. Mohite*, Satyajitraje Tekade*, Amol Gadbail*, M. S. Chaudhary** Abstract : Toxic epidermal necrolysis (TEN) and Stevens
Case Report Toxic Epidermal Necrolysis and SJS : Case Reports & Brief Review Deepali P. Mohite*, Satyajitraje Tekade*, Amol Gadbail*, M. S. Chaudhary** Abstract : Toxic epidermal necrolysis (TEN) and Stevens
DERMATOLOGIC EMERGENCIES. Mary Evers D.O., F.A.O.C.D. Georgetown, Texas
 DERMATOLOGIC EMERGENCIES Mary Evers D.O., F.A.O.C.D. Georgetown, Texas SKIN EMERGENCIES??? Subclassifications: Autoimmune (Anaphylaxis, Vasculitis, Pemphigus) Erythroderma (AGEP, DRESS, SJS, TEN) Infectious
DERMATOLOGIC EMERGENCIES Mary Evers D.O., F.A.O.C.D. Georgetown, Texas SKIN EMERGENCIES??? Subclassifications: Autoimmune (Anaphylaxis, Vasculitis, Pemphigus) Erythroderma (AGEP, DRESS, SJS, TEN) Infectious
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Drug Allergy. These podcasts are designed to give medical students an overview of key topics in pediatrics. The audio
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Drug Allergy. These podcasts are designed to give medical students an overview of key topics in pediatrics. The audio
Cases of Non-Infectious Vulvovaginitis
 Cases of Non-Infectious Vulvovaginitis 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology
Cases of Non-Infectious Vulvovaginitis 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology
MEDICAL POLICY. Proprietary Information of YourCare Health Plan
 MEDICAL POLICY Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature generally recognized by the medical community.
MEDICAL POLICY Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature generally recognized by the medical community.
Stevens Johnson Syndrome and Toxic Epidermal Necrolysis Associated with Acetaminophen Use during Viral Infections
 BRIEF COMMUNICATION http://dx.doi.org/10.4110/in.2016.16.4.256 pissn 1598-2629 eissn 2092-6685 Stevens Johnson Syndrome and Toxic Epidermal Necrolysis Associated with Acetaminophen Use during Viral Infections
BRIEF COMMUNICATION http://dx.doi.org/10.4110/in.2016.16.4.256 pissn 1598-2629 eissn 2092-6685 Stevens Johnson Syndrome and Toxic Epidermal Necrolysis Associated with Acetaminophen Use during Viral Infections
Prevention of severe cutaneous adverse drug reactions: the emerging value of pharmacogenetic screening
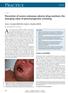 CMAJ Cases Prevention of severe cutaneous adverse drug reactions: the emerging value of pharmacogenetic screening Suran L. Fernando MB BS PhD, Andrew J. Broadfoot MB BS Previously published at www.cmaj.ca
CMAJ Cases Prevention of severe cutaneous adverse drug reactions: the emerging value of pharmacogenetic screening Suran L. Fernando MB BS PhD, Andrew J. Broadfoot MB BS Previously published at www.cmaj.ca
Update on systemic therapies and emerging treatments How do I choose a systemic agent?
 Update on systemic therapies and emerging treatments How do I choose a systemic agent? Amy S. Paller, M.D. Walter J. Hamlin Professor and Chair of Dermatology Professor of Pediatrics Northwestern University
Update on systemic therapies and emerging treatments How do I choose a systemic agent? Amy S. Paller, M.D. Walter J. Hamlin Professor and Chair of Dermatology Professor of Pediatrics Northwestern University
Mark A. Bechtel, MD Clinical Associate Professor Division Director, Dermatology Ohio State University Medical Center
 Dermatologic Emergencies Mark A. Bechtel, MD Clinical Associate Professor Division Director, Dermatology Ohio State University Medical Center Clinical Features of SJS/TEN Initial symptoms Fever, stinging
Dermatologic Emergencies Mark A. Bechtel, MD Clinical Associate Professor Division Director, Dermatology Ohio State University Medical Center Clinical Features of SJS/TEN Initial symptoms Fever, stinging
Kawasaki Disease Reconsidered New AHA Guidelines
 Kawasaki Disease Reconsidered New AHA Guidelines John Darby, MD Nisha Tamaskar, MD Stanford Shulman, MD Marietta DeGuzman, MD Kristin Sexson, MD, PhD Introductions John Darby, MD Texas Children s Hospital,
Kawasaki Disease Reconsidered New AHA Guidelines John Darby, MD Nisha Tamaskar, MD Stanford Shulman, MD Marietta DeGuzman, MD Kristin Sexson, MD, PhD Introductions John Darby, MD Texas Children s Hospital,
Paradoxial Safety Signals from Biologics
 Paradoxial Safety Signals from Biologics Christopher Ritchlin, MD, MPH Professor of Medicine Director, Translational Immunology Research Center University of Rochester Medical Center Rochester, NY Disclosures
Paradoxial Safety Signals from Biologics Christopher Ritchlin, MD, MPH Professor of Medicine Director, Translational Immunology Research Center University of Rochester Medical Center Rochester, NY Disclosures
Risk Factors and Management of Mood Stabilizer-associated Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis: A Mini-review
 140 Taiwanese Journal of Psychiatry (Taipei) Vol. 25 No. 3 2011 Overview Risk Factors and Management of Mood Stabilizer-associated Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis: A Mini-review Gen-Tang
140 Taiwanese Journal of Psychiatry (Taipei) Vol. 25 No. 3 2011 Overview Risk Factors and Management of Mood Stabilizer-associated Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis: A Mini-review Gen-Tang
Risk of Pneumocystosis among Patients Receiving Immunosuppressive Therapies: a population based analysis in the United States
 Risk of Pneumocystosis among Patients Receiving Immunosuppressive Therapies: a population based analysis in the United States Sergey Rekhtman MD, PharmD, MPH Amit Garg, MD Department of Dermatology Zucker
Risk of Pneumocystosis among Patients Receiving Immunosuppressive Therapies: a population based analysis in the United States Sergey Rekhtman MD, PharmD, MPH Amit Garg, MD Department of Dermatology Zucker
Coverage Criteria: Express Scripts, Inc. monograph dated 12/15/ months or as otherwise noted by indication
 BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Kineret (anakinra subcutaneous injection) Commercial HMO/PPO/CDHP
BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Kineret (anakinra subcutaneous injection) Commercial HMO/PPO/CDHP
Scratching the Surface: A Review of SJS/TEN
 Scratching the Surface: A Review of SJS/TEN Sarah Smith, PharmD Pharmacy Grand Rounds 2018 November 27, 2018 2018 MFMER slide 1 Toxic Epidermal Necrolysis Cutaneous Anthrax Stevens Johnson Syndrome Necrotizing
Scratching the Surface: A Review of SJS/TEN Sarah Smith, PharmD Pharmacy Grand Rounds 2018 November 27, 2018 2018 MFMER slide 1 Toxic Epidermal Necrolysis Cutaneous Anthrax Stevens Johnson Syndrome Necrotizing
Drug-induced stevens-johnson syndrome : Experience from a tertiary care hospital
 Original article: Drug-induced stevens-johnson syndrome : Experience from a tertiary care hospital *Arjun R 1,Mahalingeshwara Bhat K P 2, Sara C 1 1 PG student in General Medicine, KS Hegde Medical Acadamy,
Original article: Drug-induced stevens-johnson syndrome : Experience from a tertiary care hospital *Arjun R 1,Mahalingeshwara Bhat K P 2, Sara C 1 1 PG student in General Medicine, KS Hegde Medical Acadamy,
Dermatology Pearls for Inpatient Medicine. Dr Peter J Green MD FRCPC Professor, Division of Dermatology Dalhousie University
 Dermatology Pearls for Inpatient Medicine Dr Peter J Green MD FRCPC Professor, Division of Dermatology Dalhousie University Objectives 1. Review spectrum of cutaneous manifestations seen with inpatient
Dermatology Pearls for Inpatient Medicine Dr Peter J Green MD FRCPC Professor, Division of Dermatology Dalhousie University Objectives 1. Review spectrum of cutaneous manifestations seen with inpatient
Sidney Miller, MD, FACS Professor of Surgery Director of Research and Development Ohio State University Burn Center
 Management of the Burn Patient Sidney Miller, MD, FACS Professor of Surgery Director of Research and Development Ohio State University Burn Center American Burn Association Transfer Criteria Burn > 10%
Management of the Burn Patient Sidney Miller, MD, FACS Professor of Surgery Director of Research and Development Ohio State University Burn Center American Burn Association Transfer Criteria Burn > 10%
Department of Ophthalmology, Seoul National University College of Medicine, Seoul, Korea 2
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(5):331-340 http://dx.doi.org/10.3341/kjo.2013.27.5.331 Original Article Effect of Age and Early Intervention with a Systemic Steroid, Intravenous
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(5):331-340 http://dx.doi.org/10.3341/kjo.2013.27.5.331 Original Article Effect of Age and Early Intervention with a Systemic Steroid, Intravenous
Dr. Venkateswari. R. Dr. Janani Sankar s unit Kanchi Kamakoti CHILDS Trust Hospital
 Dr. Venkateswari. R. Dr. Janani Sankar s unit Kanchi Kamakoti CHILDS Trust Hospital Acknowledgements: KKCTH Dr. Ramkumar Consultant Dermatologist Dr. Ramprakash Consultant Ophthalmologist Dr. Prasad Manne
Dr. Venkateswari. R. Dr. Janani Sankar s unit Kanchi Kamakoti CHILDS Trust Hospital Acknowledgements: KKCTH Dr. Ramkumar Consultant Dermatologist Dr. Ramprakash Consultant Ophthalmologist Dr. Prasad Manne
Title: Cutaneous Adverse Drug Reactions in Indian population: A systematic review
 Title: Cutaneous Adverse Drug Reactions in Indian population: A systematic review Review question(s) To carry out a systematic review of the published evidence of the cutaneous adverse drug reactions in
Title: Cutaneous Adverse Drug Reactions in Indian population: A systematic review Review question(s) To carry out a systematic review of the published evidence of the cutaneous adverse drug reactions in
Stressed Out: Evaluating the Need for Stress Ulcer Prophylaxis in the ICU
 Stressed Out: Evaluating the Need for Stress Ulcer Prophylaxis in the ICU Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds November 8, 2016 2016 MFMER slide-1 Objectives Identify the significance
Stressed Out: Evaluating the Need for Stress Ulcer Prophylaxis in the ICU Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds November 8, 2016 2016 MFMER slide-1 Objectives Identify the significance
Interesting Case Series. Skin Grafting in Pyoderma Gangrenosum
 Interesting Case Series Skin Grafting in Pyoderma Gangrenosum Marco Romanelli, MD, PhD, Agata Janowska, MD, Teresa Oranges, MD, and Valentina Dini, MD, PhD Department of Dermatology, University of Pisa,
Interesting Case Series Skin Grafting in Pyoderma Gangrenosum Marco Romanelli, MD, PhD, Agata Janowska, MD, Teresa Oranges, MD, and Valentina Dini, MD, PhD Department of Dermatology, University of Pisa,
Rosacea Update: Rosacea pathogenesis. Rosacea genetics. Disclosures. Rosacea: Etiology? Th1/Th17 is activated in rosacea skin
 Winter Clinical Big Island 20 min Rosacea Update: 2017 Diane M. Thiboutot, M.D. Professor of Dermatology The Pennsylvania State University College of Medicine Hershey, PA Disclosures Investigator or consultant
Winter Clinical Big Island 20 min Rosacea Update: 2017 Diane M. Thiboutot, M.D. Professor of Dermatology The Pennsylvania State University College of Medicine Hershey, PA Disclosures Investigator or consultant
A Retrospective Study of Spectrum of Nevirapine Induced Cutaneous Drug Reactions in HIV Positive Patients
 Journal of US-China Medical Science 12 (2015) 85-89 doi: 10.17265/1548-6648/2015.02.008 D DAVID PUBLISHING A Retrospective Study of Spectrum of Nevirapine Induced Cutaneous Drug Reactions in HIV Positive
Journal of US-China Medical Science 12 (2015) 85-89 doi: 10.17265/1548-6648/2015.02.008 D DAVID PUBLISHING A Retrospective Study of Spectrum of Nevirapine Induced Cutaneous Drug Reactions in HIV Positive
Transplantation Immunology Booklet C
 Booklet C Pretest Correct Answers 3. (C) is correct. One of the major barriers to successful hematopoietic stem cell transplantation is the antigens coded for by the major histocompatibility gene complex.
Booklet C Pretest Correct Answers 3. (C) is correct. One of the major barriers to successful hematopoietic stem cell transplantation is the antigens coded for by the major histocompatibility gene complex.
Steroids for ARDS. Clinical Problem. Management
 Steroids for ARDS James Beck Clinical Problem A 60 year old lady re-presented to ICU with respiratory failure. She had previously been admitted for fluid management and electrolyte correction having presented
Steroids for ARDS James Beck Clinical Problem A 60 year old lady re-presented to ICU with respiratory failure. She had previously been admitted for fluid management and electrolyte correction having presented
Drug Class Prior Authorization Criteria Immune Globulins
 Drug Class Prior Authorization Criteria Immune Globulins Line of Business: Medicaid P & T Approval Date: August 16, 2017 Effective Date: August 16, 2017 This policy has been developed through review of
Drug Class Prior Authorization Criteria Immune Globulins Line of Business: Medicaid P & T Approval Date: August 16, 2017 Effective Date: August 16, 2017 This policy has been developed through review of
Psoriasis: Therapeutic goals
 Psoriasis: Therapeutic goals I want to die 50 45 impetiginization infliximab 600 40 35 30 400 25 20 15 200 10 5 0 22-ene 21-feb 23-mar 22-abr 22- may Efalizumab 6 doses: flare + REBOUND CSA 3 21-jun 21-jul
Psoriasis: Therapeutic goals I want to die 50 45 impetiginization infliximab 600 40 35 30 400 25 20 15 200 10 5 0 22-ene 21-feb 23-mar 22-abr 22- may Efalizumab 6 doses: flare + REBOUND CSA 3 21-jun 21-jul
September 12, 2015 Millie D. Long MD, MPH, FACG
 Update on Biologic Therapy in 2015 September 12, 2015 Millie D. Long MD, MPH, FACG Assistant Professor of Medicine Inflammatory Bowel Disease Center University of North Carolina-Chapel Hill Outline Crohn
Update on Biologic Therapy in 2015 September 12, 2015 Millie D. Long MD, MPH, FACG Assistant Professor of Medicine Inflammatory Bowel Disease Center University of North Carolina-Chapel Hill Outline Crohn
PEER REVIEW HISTORY ARTICLE DETAILS VERSION 1 - REVIEW
 PEER REVIEW HISTORY BMJ Paediatrics Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form and are provided with free text boxes to elaborate
PEER REVIEW HISTORY BMJ Paediatrics Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form and are provided with free text boxes to elaborate
Comprehensive survival analysis of a cohort of patients with Stevens-Johnson syndrome and toxic epidermal necrolysis.
 Comprehensive survival analysis of a cohort of patients with Stevens-Johnson syndrome and toxic epidermal necrolysis. Supplementary online-material Supplementary Table S1: Detailed descriptive analysis
Comprehensive survival analysis of a cohort of patients with Stevens-Johnson syndrome and toxic epidermal necrolysis. Supplementary online-material Supplementary Table S1: Detailed descriptive analysis
A Middle-Aged Man with Newly Diagnosed HIV Infection and Rash
 CLINICAL CASE OF THE MONTH A Middle-Aged Man with Newly Diagnosed HIV Infection and Rash Patrick Njoku, MD; Temeka Tate, MD; Sousan Zadeh, MD; Erin Hauck, MD; Anila Chaudhry, MD; Betty Lo-Blais, MD; Lee
CLINICAL CASE OF THE MONTH A Middle-Aged Man with Newly Diagnosed HIV Infection and Rash Patrick Njoku, MD; Temeka Tate, MD; Sousan Zadeh, MD; Erin Hauck, MD; Anila Chaudhry, MD; Betty Lo-Blais, MD; Lee
Case Report Cephazolin-Induced Toxic Epidermal Necrolysis Treated with Intravenous Immunoglobulin and N-Acetylcysteine
 Case Reports in Immunology Volume 2012, Article ID 931528, 4 pages doi:10.1155/2012/931528 Case Report Cephazolin-Induced Toxic Epidermal Necrolysis Treated with Intravenous Immunoglobulin and N-Acetylcysteine
Case Reports in Immunology Volume 2012, Article ID 931528, 4 pages doi:10.1155/2012/931528 Case Report Cephazolin-Induced Toxic Epidermal Necrolysis Treated with Intravenous Immunoglobulin and N-Acetylcysteine
Clinical profile of skin diseases in accident and emergency department attenders
 Hong Kong J. Dermatol. Venereol. (2007) 15, 4-9 Original Article Clinical profile of skin diseases in accident and emergency department attenders CY Chan, KL Kam, CA Graham, TH Rainer, NM Luk Skin problems
Hong Kong J. Dermatol. Venereol. (2007) 15, 4-9 Original Article Clinical profile of skin diseases in accident and emergency department attenders CY Chan, KL Kam, CA Graham, TH Rainer, NM Luk Skin problems
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: International Journal of Case Reports and Images (IJCRI) Type of Article: Case Report Title: A Case
: Online published version of an accepted article before publication in the final form. Journal Name: International Journal of Case Reports and Images (IJCRI) Type of Article: Case Report Title: A Case
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING
 AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
HIV-Associated Toxic Epidermal Necrolysis at San Francisco General Hospital: A 13-Year Retrospective Review
 HIV Clinical Management HIV-Associated Toxic Epidermal Necrolysis at San Francisco General Hospital: A 13-Year Retrospective Review Journal of the International Association of Providers of AIDS Care 2017,
HIV Clinical Management HIV-Associated Toxic Epidermal Necrolysis at San Francisco General Hospital: A 13-Year Retrospective Review Journal of the International Association of Providers of AIDS Care 2017,
CPC. Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand
 CPC Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand A 53 year-old woman with fever, facial swelling and rashes on face, trunk and upper extremities for 3
CPC Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand A 53 year-old woman with fever, facial swelling and rashes on face, trunk and upper extremities for 3
Michael P. Heffernan, M.D San Luis Dermatology & Laser Clinic Director, US Probity Medical Research
 Michael P. Heffernan, M.D San Luis Dermatology & Laser Clinic Director, US Probity Medical Research mpheffernanmd@gmail.com DISCLOSURES Consultant, Speaker, Investigator: Abbvie, Amgen, Brickell Biotech,
Michael P. Heffernan, M.D San Luis Dermatology & Laser Clinic Director, US Probity Medical Research mpheffernanmd@gmail.com DISCLOSURES Consultant, Speaker, Investigator: Abbvie, Amgen, Brickell Biotech,
Autoimmune Diseases with Oral Manifestations
 Autoimmune Diseases with Oral Manifestations Martin S. Greenberg DDS, FDS RCSEd Professor Emeritus Department of Oral Medicine University of Pennsylvania Disclosure Statement I have no actual or potential
Autoimmune Diseases with Oral Manifestations Martin S. Greenberg DDS, FDS RCSEd Professor Emeritus Department of Oral Medicine University of Pennsylvania Disclosure Statement I have no actual or potential
Cutaneous Adverse Drug Reactions in Domestic Animals. Katherine Doerr, DVM, Dip. ACVD. Veterinary Dermatology Center
 Cutaneous Adverse Drug Reactions in Domestic Animals Katherine Doerr, DVM, Dip. ACVD Veterinary Dermatology Center Maitland, Rockledge, Waterford Lakes, FL Not highly studied in veterinary medicine Unknown
Cutaneous Adverse Drug Reactions in Domestic Animals Katherine Doerr, DVM, Dip. ACVD Veterinary Dermatology Center Maitland, Rockledge, Waterford Lakes, FL Not highly studied in veterinary medicine Unknown
Summary of Risk Minimization Measures
 Table 6.1.4-1: Summary of Risk Minimization Measures Safety Concern Vaccination Hepatic and renal impairment Combination therapy Elderly Routine Risk Minimization Measures Specific subsection on vaccination
Table 6.1.4-1: Summary of Risk Minimization Measures Safety Concern Vaccination Hepatic and renal impairment Combination therapy Elderly Routine Risk Minimization Measures Specific subsection on vaccination
Prevalence and pattern of adverse cutaneous drug reactions presenting to a tertiary care hospital
 International Journal of Research in Dermatology Janardhan B et al. Int J Res Dermatol. 2017 Mar;3(1):74-78 http://www.ijord.com Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4529.intjresdermatol20164248
International Journal of Research in Dermatology Janardhan B et al. Int J Res Dermatol. 2017 Mar;3(1):74-78 http://www.ijord.com Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4529.intjresdermatol20164248
KEYTRUDA is also indicated in combination with pemetrexed and platinum chemotherapy for the
 FDA-Approved Indication for KEYTRUDA (pembrolizumab) in Combination With Carboplatin and Either Paclitaxel or Nab-paclitaxel for the Firstline Treatment of Patients With Metastatic Squamous Non Small Cell
FDA-Approved Indication for KEYTRUDA (pembrolizumab) in Combination With Carboplatin and Either Paclitaxel or Nab-paclitaxel for the Firstline Treatment of Patients With Metastatic Squamous Non Small Cell
Analysis of causation of Stevens Johnson Syndrome in a patient of rheumatoid arthritis with increased dose of methotrexate
 Original Research Article Analysis of causation of Stevens Johnson Syndrome in a patient of rheumatoid arthritis with increased dose of methotrexate Manab Nandy 1, Sangeeta De 2*, Mustafa Asad 2, Nirmal
Original Research Article Analysis of causation of Stevens Johnson Syndrome in a patient of rheumatoid arthritis with increased dose of methotrexate Manab Nandy 1, Sangeeta De 2*, Mustafa Asad 2, Nirmal
Key uncertainties around the evidence or technology are that the test has only been validated in biochemical studies.
 pat hways PredictSure-IBD for inflammatory bowel disease prognosis Medtech innovation briefing Published: 25 March 2019 nice.org.uk/guidance/mib178 Summary The technology described in this briefing is
pat hways PredictSure-IBD for inflammatory bowel disease prognosis Medtech innovation briefing Published: 25 March 2019 nice.org.uk/guidance/mib178 Summary The technology described in this briefing is
The Natural History of Psoriasis and Treatment Goals
 The Natural History of Psoriasis and Treatment Goals Psoriasis Epidemiology Prevalence Affects 2 3% of adult population (>7 million in US) Caucasians: 25% 2.5% African Americans: 1.3% (more likely to have
The Natural History of Psoriasis and Treatment Goals Psoriasis Epidemiology Prevalence Affects 2 3% of adult population (>7 million in US) Caucasians: 25% 2.5% African Americans: 1.3% (more likely to have
Comment on Association of bullous pemphigoid with malignancy: A systematic review and meta-analysis
 Accepted Manuscript Comment on Association of bullous pemphigoid with malignancy: A systematic review and meta-analysis Maglie Roberto, MD, Antiga Emiliano, MD, PhD, Caproni Marzia, MD, PhD PII: S0190-9622(17)32812-8
Accepted Manuscript Comment on Association of bullous pemphigoid with malignancy: A systematic review and meta-analysis Maglie Roberto, MD, Antiga Emiliano, MD, PhD, Caproni Marzia, MD, PhD PII: S0190-9622(17)32812-8
SKIN CANCER AFTER HSCT
 SKIN CANCER AFTER HSCT David Rice, PhD, MSN, RN, NP, NEA-BC Director, Education, Evidence-based Practice and Research City of Hope National Medical Center HOW THE EXPERTS TREAT HEMATOLOGIC MALIGNANCIES
SKIN CANCER AFTER HSCT David Rice, PhD, MSN, RN, NP, NEA-BC Director, Education, Evidence-based Practice and Research City of Hope National Medical Center HOW THE EXPERTS TREAT HEMATOLOGIC MALIGNANCIES
Difference of opinion? Michelle Moorhouse 24 Sep 2014
 Difference of opinion? Michelle Moorhouse 24 Sep 2014 Meet NN 52 years, female Nurse in pre-art clinic Referred Feb 2012 by dermatologist History of severe reactions to ART Erythema and bullous eruptions
Difference of opinion? Michelle Moorhouse 24 Sep 2014 Meet NN 52 years, female Nurse in pre-art clinic Referred Feb 2012 by dermatologist History of severe reactions to ART Erythema and bullous eruptions
Medical Therapy for Pediatric IBD: Efficacy and Safety
 Medical Therapy for Pediatric IBD: Efficacy and Safety Betsy Maxwell, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Pediatric IBD: Defining Remission
Medical Therapy for Pediatric IBD: Efficacy and Safety Betsy Maxwell, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Pediatric IBD: Defining Remission
Melanoma Immunotherapy. Nursing Perspective on Immune-Related Adverse Events: Patient education, Monitoring & Management
 Melanoma Immunotherapy Nursing Perspective on Immune-Related Adverse Events: Patient education, Monitoring & Management Mike Buljan, NP UCSF Medical Center Melanoma Oncology Disclosures None Only FDA-approved
Melanoma Immunotherapy Nursing Perspective on Immune-Related Adverse Events: Patient education, Monitoring & Management Mike Buljan, NP UCSF Medical Center Melanoma Oncology Disclosures None Only FDA-approved
Management of Chronic Idiopathic Urticaria
 9/3/216 Management of Chronic Idiopathic Urticaria Brian Berman, M.D., Ph.D. Professor Emeritus of Dermatology and Dermatologic Surgery, University of Miami Co-Director Center for Clinical and Cosmetic
9/3/216 Management of Chronic Idiopathic Urticaria Brian Berman, M.D., Ph.D. Professor Emeritus of Dermatology and Dermatologic Surgery, University of Miami Co-Director Center for Clinical and Cosmetic
Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino Jul-Aug; 21(4):423-7
 AMINOGLYCOSIDES Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino. 2007 Jul-Aug; 21(4):423-7 http://www.ncbi.nlm.nih.gov/pubmed/17882910 Evaluation of the in-vivo
AMINOGLYCOSIDES Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino. 2007 Jul-Aug; 21(4):423-7 http://www.ncbi.nlm.nih.gov/pubmed/17882910 Evaluation of the in-vivo
Tumor Necrosis Factor α Inhibitors in the Treatment of Toxic Epidermal Necrolysis
 ORIGINAL RESEARCH Tumor Necrosis Factor α Inhibitors in the Treatment of Toxic Epidermal Necrolysis Katelyn F. Woolridge, MD; Patrick L. Boler, MD, PharmD; Brian D. Lee, MD PRACTICE POINTS Controversy
ORIGINAL RESEARCH Tumor Necrosis Factor α Inhibitors in the Treatment of Toxic Epidermal Necrolysis Katelyn F. Woolridge, MD; Patrick L. Boler, MD, PharmD; Brian D. Lee, MD PRACTICE POINTS Controversy
Mechanisms of Drug Hypersensitivity Reactions
 18/5/213 Mechanisms of Drug Hypersensitivity Reactions Munir Pirmohamed NHS Chair of Pharmacogenetics Department of Molecular and Clinical Pharmacology Institute of Translational Medicine University of
18/5/213 Mechanisms of Drug Hypersensitivity Reactions Munir Pirmohamed NHS Chair of Pharmacogenetics Department of Molecular and Clinical Pharmacology Institute of Translational Medicine University of
Allergy, Atopy and Skin Cancer
 M. Shane Cahpman, MD, MBA: Dartmouth School of Medicine Boni E. Elewski, MD: University of Alabama Kenneth J. Tomecki, MD: Cleveland Clinic Ted Rosen, MD: Baylor College of Medicine Clinical and Therapeutic
M. Shane Cahpman, MD, MBA: Dartmouth School of Medicine Boni E. Elewski, MD: University of Alabama Kenneth J. Tomecki, MD: Cleveland Clinic Ted Rosen, MD: Baylor College of Medicine Clinical and Therapeutic
AOU Ospedali Riuniti - Ancona
 AOU Ospedali Riuniti - Ancona Ospedale Materno-Infantile di Alta Specializzazione G. Salesi UOC Pediatria Allergia a farmaci e infezioni: tra coesistenza e casualità fabrizio franceschini Drug Hypersensitivity
AOU Ospedali Riuniti - Ancona Ospedale Materno-Infantile di Alta Specializzazione G. Salesi UOC Pediatria Allergia a farmaci e infezioni: tra coesistenza e casualità fabrizio franceschini Drug Hypersensitivity
Azathioprine for Induction and Maintenance of Remission in Crohn s Disease
 Azathioprine for Induction and Maintenance of Remission in Crohn s Disease William J. Sandborn, MD Chief, Division of Gastroenterology Director, UCSD IBD Center Objectives Azathioprine as induction and
Azathioprine for Induction and Maintenance of Remission in Crohn s Disease William J. Sandborn, MD Chief, Division of Gastroenterology Director, UCSD IBD Center Objectives Azathioprine as induction and
7 Case reports Case series. 2 open label studies 131, Case reports
 TABLE e5. ALTERNATIVE TREATMENTS FOR ACTIVE THYROID EYE DISEASE (TED) Pharmacological Agent/Intervention Classification of Treatment/Mechanism of Action Study Design(s) Results of Randomized Study (if
TABLE e5. ALTERNATIVE TREATMENTS FOR ACTIVE THYROID EYE DISEASE (TED) Pharmacological Agent/Intervention Classification of Treatment/Mechanism of Action Study Design(s) Results of Randomized Study (if
Acute Graft-versus-Host Disease (agvhd) Udomsak Bunworasate Chulalongkorn University
 Acute Graft-versus-Host Disease (agvhd) Udomsak Bunworasate Chulalongkorn University Graft-versus-Host Disease (GVHD) Background GVHD is an immunologic reaction of the donor immune cells (Graft) against
Acute Graft-versus-Host Disease (agvhd) Udomsak Bunworasate Chulalongkorn University Graft-versus-Host Disease (GVHD) Background GVHD is an immunologic reaction of the donor immune cells (Graft) against
Field vs Lesional Therapies for AKs 3/2/2019, 9:00-12 AM
 Dilemmas and Challenges in Skin Cancer Therapies and Management Field vs Lesional Therapies for AKs 3/2/2019, 9:00-12 AM Roger I. Ceilley, M.D. Clinical Professor of Dermatology The University of Iowa
Dilemmas and Challenges in Skin Cancer Therapies and Management Field vs Lesional Therapies for AKs 3/2/2019, 9:00-12 AM Roger I. Ceilley, M.D. Clinical Professor of Dermatology The University of Iowa
건강한성인에서의오진하기쉬운포도구균성열상피부증후군의치험례. Staphylococcal Scalded Skin Syndrome in a Healthy Adult: Easy to Misdiagnose
 Archives of Hand and Microsurgery Arch Hand Microsurg 2018;23(4):271-276. https://doi.org/10.12790/ahm.2018.23.4.271 pissn 2586-3290 eissn 2586-3533 Case Report 건강한성인에서의오진하기쉬운포도구균성열상피부증후군의치험례 김홍일ㆍ곽찬이ㆍ박언주
Archives of Hand and Microsurgery Arch Hand Microsurg 2018;23(4):271-276. https://doi.org/10.12790/ahm.2018.23.4.271 pissn 2586-3290 eissn 2586-3533 Case Report 건강한성인에서의오진하기쉬운포도구균성열상피부증후군의치험례 김홍일ㆍ곽찬이ㆍ박언주
Dexamethasone Pulse Therapy for Stevens-Johnson Syndrome/ Toxic Epidermal Necrolysis
 Acta Derm Venereol 2007; 87: 144 148 CLINICAL REPORT Dexamethasone Pulse Therapy for Stevens-Johnson Syndrome/ Toxic Epidermal Necrolysis Sylvia H. Kardaun and Marcel F. Jonkman Center for Blistering Diseases,
Acta Derm Venereol 2007; 87: 144 148 CLINICAL REPORT Dexamethasone Pulse Therapy for Stevens-Johnson Syndrome/ Toxic Epidermal Necrolysis Sylvia H. Kardaun and Marcel F. Jonkman Center for Blistering Diseases,
DISCLOSURE. Relevant relationships with commercial entities none. Potential for conflicts of interest within this presentation none
 FEVER DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate potential bias N/A LEARNING OBJECTIVE
FEVER DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate potential bias N/A LEARNING OBJECTIVE
Scottish Medicines Consortium
 Scottish Medicines Consortium ustekinumab, 45mg solution for injection (Stelara ) No. (572/09) Janssen-Cilag Ltd 15 January 2010 The Scottish Medicines Consortium (SMC) has completed its assessment of
Scottish Medicines Consortium ustekinumab, 45mg solution for injection (Stelara ) No. (572/09) Janssen-Cilag Ltd 15 January 2010 The Scottish Medicines Consortium (SMC) has completed its assessment of
AIN. Decline in renal function characterized by an inflammatory infiltrate in the kidney interstitium
 AIN Decline in renal function characterized by an inflammatory infiltrate in the kidney interstitium Present in up to 27% of AKI biopsies 10% over 60yr olds Incidence increasing? Presentation Allergic
AIN Decline in renal function characterized by an inflammatory infiltrate in the kidney interstitium Present in up to 27% of AKI biopsies 10% over 60yr olds Incidence increasing? Presentation Allergic
Carbamazepine-Induced Incomplete Stevens-Johnson Syndrome: Report of a Case in Children without Mycoplasma pneumoniae Infection
 Case Report Carbamazepine-Induced Incomplete Stevens-Johnson Syndrome: Report of a Case in Children without Mycoplasma pneumoniae Infection J Med Assoc Thai 2015; 98 (Suppl. 7): S243-S247 Full text. e-journal:
Case Report Carbamazepine-Induced Incomplete Stevens-Johnson Syndrome: Report of a Case in Children without Mycoplasma pneumoniae Infection J Med Assoc Thai 2015; 98 (Suppl. 7): S243-S247 Full text. e-journal:
Primary Results Citation 2
 Table S1. Adalimumab clinical trials 1 ClinicalTrials.gov Rheumatoid Arthritis 3 NCT00195663 Breedveld FC, Weisman MH, Kavanaugh AF, et al. The PREMIER study. A multicenter, randomized, double-blind clinical
Table S1. Adalimumab clinical trials 1 ClinicalTrials.gov Rheumatoid Arthritis 3 NCT00195663 Breedveld FC, Weisman MH, Kavanaugh AF, et al. The PREMIER study. A multicenter, randomized, double-blind clinical
