Early Detection of Malignant Melanoma:The Roleof PhysicianExaminationand Self-Examinationof the Skin
|
|
|
- Jessie Collins
- 5 years ago
- Views:
Transcription
1 Early Detection of Malignant Melanoma:The Roleof PhysicianExaminationand Self-Examinationof the Skin Robert J. Friedman, M.D. Darrell S. Rigel, M.D. Alfred W. Kopf, M.D. Introduction Malignant melanoma is the leading cause of death from diseases of the skin. In 1985, about 22,000 people will develop newly recognized malignant melanomas; 5,500 people will die of the disease.' This ac counts for about 74 percent of all deaths from cutaneous cancers. The mortality rate from malignant melanoma is increasing faster than that of any other cancer except lung cancer.2 In the United States, about one in 150 people will develop a malignant melanoma during his or her lifetime, and this rate is esti mated to increase to one in 100 by the year Dr. Friedman is Clinical Instructor in the De partment of Dermatology of New York Univer sity School of Medicine, and Co-Director of the Pigmented Lesions Section, Oncology Section, of the Skin and Cancer Unit of New York Uni versity Medical Center, in New York, New York. Dr. Rigel is Clinical Instructor in the Department of Dermatology of New York University School of Medicine, and Co-Director of the Pigmented Lesions Section, Oncology Section, of the Skin and Cancer Unit of New York University Medi cal Center, in New York, New York. Dr. Kopf is Clinical Professor in the Department of Dermatology of New York University School of Medicine in New York, New York. This article was prepared in conjunction with the Task Force on Preventive Dermatology of the American Academy of Dermatology, and the American Cancer Society. There are two principal ways to reduce the morbidity and mortality from cuta neous malignant melanomas. The most di rect method would be to reduce the number of new tumors by identifying, eliminating, or counteracting the many factors that promote the development of malignant melanomasâ e.g., genetic influence, ex cessive exposure to ultraviolet light, im munologic defects, oncogenic viruses, and chemical carcinogens. Despite the many important research efforts designed to identify causal and promoting factors, however, this preventive strategy does not hold great promise for the short run. Thus, in 1985 and in the immediate future, the most important method of at tacking malignant melanoma is diagnosis at an early stage when the prognosis for cure by surgical removal is excellent. By performing careful, periodic, complete cu taneous examinations, by teaching patients the technique of routine self-examination of the skin, and by proper and timely use of diagnostic aids (particularly biopsy of the skin), physicians can improve the chances for early diagnosis and prompt eradication of malignant melanoma. Importance of Early Diagnosis The early diagnosis of malignant mela noma cannot be overemphasized.3-9 There is much evidence that thin malignant mel anomas have an excellent prognosis.3-'â 130 CA-A CANCERJOURNALFORCLINICIANS
2 C a U a Years Fig. 1. Ten-yearsurvival rate of patients with malignant melanoma (all stages), by lesion thick ness. Source: New York University Melanoma Cooperative Group, Breslow, in his fundamental study pub lished in 1970, showed that metastases did not develop in patients with malignant mel anomas less than 0.76 mm thick.â The excellent prognosis for patients who have such thin lesions excised has been repeat edly confirmed by others.'2â 9 Our experience with patients regis tered in the New York University Mela noma Cooperative Group2Â has been a 10-year survival rate of 99.5 percent for all stages of malignant melanoma less than 0.76 mm thick. In contrast, the rate was only 48 percent for those with malignant melanomas three mm and more in thick ness (Fig. I). There are, of course, rare exceptions, but the earlier the diagnosis â that is, the thinner the malignant melanomaâ and the earlier the surgical treatment, the greater the survival rate. Therefore, although we currently do not have the ability to prevent the development of malignant melanoma, we do have the ability to reduce the death rate from ma lignant melanoma to near zero through the recognition of such lesions when they are thin and virtually 100 percent curable by surgery. Patients can also participate in the identification of early malignant melano mas by using a thorough, easily taught method of cutaneous self-examination (de scribed on pages 141 and 146 to 150). Basic Factors in Early Diagnosis To make an early diagnosis, the physician must have a high index of suspicion for VOL.35,NO.3 MAY/JUNE
3 history of sunburns, and susceptible age. CommonBenignPigmentedLesions The most frequently encountered pig mented lesions are simple lentigines, â œ common molesâ (i.e., melanocytic nevi junctional, compound, intradermal), solar lentigines, and seborrheic keratoses. Fig. 2. Simple lentigo. Sharply defined, black reticulated, macular lesion with sharp jagged borders. â..â.. â œ 4 - lili@llflilfpfiirliif@ill@l1ltlijlfii1i.,,i1 SPECIMEN â _@_ DATE Fig. 3. Junction nevus. Sharply defined tan to brown macule. this tumor and thorough knowledge of: e The clinical characteristics of early ma lignant melanomas. â The clinical features of the common types of pigmented lesions that must be dif ferentiated from malignant melanomas. â The characteristics of precursor le sionsâ e.g., dysplastic nevi and certain congenital melanocytic nevi â thatmay give rise to malignant melanoma. â Other factors that increase the risk of developing a malignant melanoma e.g., familial history of malignant mel anoma, many melanocytic nevi, exces sive sun exposure, light complexion, Simple Lentigo (Fig. 2) A simple lentigo is a small (one to five mm), pigmented lesion. It is the initial stage of development of a common mole. The simple lentigo is a sharply defined, round, brown to black, macular lesion with smooth or jagged edges that may appear anywhere on the surface of the skin. The pigmen tation often has a reticulated (net-like) pat tern. Such a lesion generally arises in childhood but may appear later. Some sim ple lentigines are clinically indistinguish able from junctional nevi. Junctional Nevus (Fig. 3) A junctional nevus is generally a small (less than six mm, about 0.25 inch), macular, well-circumscribed, pigmented lesion with a smooth surface and relatively uniform pigmentation that ranges from light brown to very dark brown to black. It may appear at any site on the surface of the body, but occurs most often on areas exposed to the sun. A junctional nevus usually arises in childhood, but may lescence and young adulthood. It may per sist throughout adulthood in a junctional position or may develop into a compound or intradermal nevus as its cells proliferate and extend into the dermis (Fig. 4). Rarely do junctional nevi develop in people over the age of 40. The development of a mac ular, pigmented lesion in someone older than 40 years should alert the physician and patientâ to the possibility that it is an early malignant melanoma (Figs. 5a and Sb). Compound Nevus (Fig. 6) A compound nevus is generally a well 132 CA-ACANCERJOURNALFORCLINICIANS
4 Fig. 4. Progression of Melanocytic Nevi (a) Junctional: nevus cells present both singly and in uniform nests at the dermoepidermal junction. (b) Compound: nevus cells present both singly and in uniform nests at the dermoepidermal junction; and nests, cords, and strands of nevus cells in the dermis. (c) Intradermal: nests, cords, and strands of nevus cells in the Fig. 5. (a) Macular pigmented lesion on sole with some features of both an early malignant melanoma and an unusual junction nevus. (b) Progressionof the lesion two years later. Typical features of a thick malignant melanoma. VOL35,NO.3 MAY/JUNE
5 circumscribed, small (less than six mm), raised papule that is uniformly pigmented with a range of color from skin-colored to tan to shades of brown and a smooth or rough surface. It may have an excess of hair. It usually develops in late childhood, adolescence, or early adulthood. Fig. 6. Compound nevus. Small, well-circum scribed, uniformly pigmented, raised papule.,,.@.,; ii.*@, â œ â Iâ ; â..@ â œ â â â III.*@ Intradermal Nevus (Fig. 7) An intradermal nevus is generally a small (up to six mm) well-circumscribed papule that is usually uniform in pigmentation from skin-colored to tan or various shades of brown. The surface may be smooth or rough. Intradermal nevi may have an ex cess of hair. Solar Lentigo (Fig. 8) A solar lentigo is generally a uniform tan to brown macule, known to the lay pub lic as a â œ liver spot.â It is found on sun exposed skin in people with significantly sun-damaged skin. Common sites include the face, chest, and dorsa of the â P / â â â Fig. 7. Intradermal nevus. Small, well-circum scribed papule with minimal pigmentation. Seborrheic Keratosis (Fig. 9) A seborrheic keratosis is generally a ver rucous, round or ovoid, variably raised, light brown to black, sharply demarcated papule or plaque that ranges in diameter from a few millimeters to several centimeters. The sur face is generally â œ dullâ or â œ warty.â It often has a â œ stuck onâ appearance. Seborrheic keratoses are most commonly situated on the face, neck, and trunk. They are composed predominantly of proliferating keratino cytes (epidermal cells) and are not primarily of melanocytic origin. Fig.8. Solarlentigo.Tan,sharplydefined patch. Age as a Factor in the Onset and Diagnosis of Pigmented Lesions of the Skin The age of the patient is important to consider in making a differential diagno sis of pigmented lesions of the skin. Ma lignant melanomas rarely develop in childhood.2'-23 When they do occur in pre adolescents, they may develop de novo or 134 CA-ACANCERJOURNALFORCLINICIANS
6 Fig. 9. Seborrheic keratoses. Multiple, tan to darker brown, raised verrucous papules. Fig. 10. Asymmetry of early malignant mela noma. may originate in congenitally determined lesions like large congenital melanocytic nevi.212â 2'The most common benign pig mented lesions in children are ephelides (freckles), simple lentigines, and junc tional nevi. Compound nevi generally begin in childhood or adolescence; intra dermal nevi predominate in adulthood. The other common benign pigmented lesions (solar lentigines and seborrheic keratoses) usually begin later in adult life, generally from the 40s onward. The inci dence of malignant melanoma is very low in childhood and then increases with age.29'3â The mean age of presentation overall is approximately SO. However, any new pigmented lesion on the skin that de velops after age 403 and does not meet the criteria set forth for benign p'igmented lesions should be suspected of being a ma lignant melanoma or a precursor/marker lesion of a malignant melanoma (e.g., a dysplastic nevus). Clinical Characteristics ofearly MalignantMelanoma The clinically diagnostic features of early malignant melanoma (malignant mela noma in situ) are similar regardless of the anatomical site.4632 It is essential that physicians recognize these features. Un like benign pigmented lesions, which are generally round and symmetrical, early malignant melanomas are usually asym Fig. 11. Asymmetry of early malignant mela noma. metrical (Figs. 10 and 11). Unlike benign pigmented lesions, which generally have regular margins, the borders of early ma lignant melanomas are usually irregular (Figs. 12 and 13). Unlike benign pig mented lesions, which are generally uni form in color, macular malignant melanomas are variegated, ranging from various hues of tan and brown to black, and sometimes intermingled with red and white (Figs. 14â 17). Unlike most benign pigmented lesions, which generally have diameters less than six mm, the diameters of macular malignant melanomas when first identified are often more than six mm (Figs. 18â 20). These characteristic clinical features of early malignant melanoma can be easily VOL35.NO.3 MAY/JUNE
7 or the development of a new pigmented lesion, particularly after the age of 40, is of importance in alerting the physician to the possibility of a malignant melanoma. A malignant melanoma should be consid ered if any of the changes shown in Table 1 are Fig. 12. Border irregularity of early malignant melanoma. Fig. 13. Border irregularity of early malignant melanoma. remembered by thinking of ABCD: â A = Asymmetry. â B = Border irregularity. â C = Color variegation. â D = Diameter generally greater than six mm. Several clinical examples of the pro gression of malignant melanomas are il lustrated in Figures 21 to 24 for comparison with the early malignant melanomas de scribed above. The goal is to significantly reduce the number of these more advanced malignant melanomas, because they are associated with higher mortality rates. The diagnosis of malignant melanoma is based not only on clinical appearance, but also on history and symptomatology. Change in a preexisting melanocytic nevus PrecursorLesionsof Malignant Melanoma Recent evidence suggests that certain pig mented cutaneous lesions may give rise to malignant melanomas. These lesions in clude acquired abnormal melanocytic nevi known as dysplastic nevi, which are es pecially prevalent in certain melanoma prone families, but can also occur in the general population; and certain congenital melanocytic nevi. Dysplastic Nevus Dysplastic nevi are acquired pigmented le sions of the skin. Clinical and histological definitions of dysplastic nevi are evolv ing.@' In general, dysplastic nevi differ from common, acquired benign melanocytic nevi in several respects (Table 2). Some, how ever, cannot be distinguished clinically from malignant melanomas. Dysplastic nevi may occur in both familial and sporadic (non familial) settings. The clinical features of dysplastic nevi are similar, however, in both settings. Dysplastic nevi are typically larger than ordinary nevi, generally ranging from six to 12 mm or more in diameter (Fig. 25). They usually have both macular and ele vated (â œpebbly,â papular, nodular, or plaque) components (Fig. 26). The bor ders of dysplastic nevi, unlike those of common nevi, are often irregular and frequently so ill-defined that they fade imperceptibly into the surrounding skin (Fig. 27). Dysplastic nevi usually are variegated in color, ranging from tan to dark brown, at times with a prominent pink component (Fig. 28). These lesions may appear any where on the body, especially on the sun exposed areas of the trunk and extremities. However, they may also occur on sun-pro 136 CA-A CANCER JOURNAL FOR CLINICIANS
8 Fig. 14. Color variegation of early malignant melanoma. Note nuances of tans and browns. Fig. 15. Color variegation of early malignant melanoma. tected areas like the breasts, pubic area, buttocks, and scalp.35-4' Young adults generally have an aver age of 25 common melanocytic nevi, whereas individuals with dysplastic nevi may have more than 100 lesions. Common melanocytic nevi usually do not develop after the age of 40,31 whereas dysplastic nevi generally begin in adolescence and continue to appear throughout life.35-4' Dysplastic nevi may be familial or sporadic. Familial dysplastic nevi may be inherited as an autosomal dominant trait.35-4' The sporadic variant occurs in people who have no family history of either liiiiii.1iiiifitii I III It Fig. 16. Color variegation of malignant mela noma. Note the pink-red component at lower margin of lesion. The mortality rate from malignant melanoma is increasing at a rate faster than that from any other cancer except for lung cancer. dysplastic nevi or malignant melanomas. Overall, patients with dysplastic nevi have a reported lifetime risk for malignant mel anoma of approximately five to 10 percent, compared with the risk of about 0.7 percent for the general population.@â 4' The risk of developing malignant mel anoma is greater for those with one or more relatives with this tumor.4â The lifetime ;@i@i'i Fig. 17. Color variegation of early malignant melanoma. Irregularly marginated pigmented lesion and prominent central pinkish white components are indicative of spontaneous partial regression. VOL35,NO.3 MAY/JUNE
9 â I of malignant melanoma approaches a re ported 100 percent for those patients with dysplastic nevi who have both two or more first-degree relatives with cutaneous ma lignant melanomas and two or more with dysplastic Malignant melano mas in such individuals may arise either within the dysplastic nevi or apparently de novo in normal-appearing Fig. 18. Early malignant melanoma, approxi mately six mm in <â ;4i - FIg 19 Early malignant melanoma, approxi mately eight mm in diameter. Congenital Melanocytic Nevus By definition, a congenital melanocytic nevus is a lesion that contains nevus cells and is present at birth. Congenital melano cytic nevi can be categorized by size as follows:27@ â Smallâ less than 1.5 cm in diameter. â Mediumâ 1.5 to 19.9 cm in diameter. â Largeâ 20 cm or more in diameter. Congenital melanocytic nevi occur in about one percent of newborns;26 most of these nevi are small or medium-sized. The lifetime risk of malignant melanoma in pa tients with large congenital melanocytic nevi has been estimated to be about six percent,28 again, compared with a risk of 0.7 percent for the general population. The risk of a malignant melanoma developing in small and medium-sized congenital mel anocytic nevi has also been reported to be increased according to some investiga tors.42-40the magnitude of that risk, how ever, has not been established and is, therefore, still controversial. In sum, it has been found that malig nant melanomas may arise de novo as well as in association with preexisting melano cytic nevi. Dysplastic nevi may be both markers for malignant melanomas (i.e., identifying melanoma-prone individuals) or precursors of malignant melanomas (i.e., the dysplastic nevi themselves give rise to malignant melanomas). Again, large con genital melanocytic nevi (Fig. 29) also have a substantially greater risk of giving rise to malignant melanomas. Fig 20. Malignant melanoma in situ on sun damaged skin of cheek, approximately 18mm in largest diameter. Risk Factors for Development of Malignant Melanoma Epidemiologic data suggest that malignant melanomas may also be related to addi 138 CA-A CANCER JOURNAL FOR CLINICIANS
10 Fig. 21. Progression of malignant melanoma. plaque. 5_,JllIIJHhIJ IIlifi 111,11 1IIIUIIIIIIIIII I1J â PZCJME@ Fig. 22. Progression of malignant melanoma: plaque with nodule tional risk factors. Those at risk include: â People with light-colored eyes (blue, green, grey), light complexions, and light-colored hair, and those who are more easily sunburned.45 â Patients with xeroderma pigmentosum.40 â People who live near the equator.4' â People who have had severe sunburns, especially in childhood through their early teens to 20s.48 â People who work indoors and have pri marily outdoor recreational habits.49 â People with an increased number of mel anocytic nevi in childhood.5â Examination of the Skin: The First Step towards Diagnosis Unlike other cancers, which are generally hidden from view, malignant melanoma, as Dr. Neville Davis has said so inci sively,5' â œ writes its message in the skin with its own ink and it is there for all of us to see. Some see but do not compre hend.â It is our intent to make everyone see, understand, comprehend, and act. It has been demonstrated that there is a strong association between the length of survival of patients with malignant melanoma and the thickness of the lesion. Patients who have thin (less than 0.76 mm) malignant melanomas have a cure rate of close to 100 percent following surgical removal of the primary tumor. Fig. 23. Progression of malignant melanoma plaque with amelanotic nodule Ill.! I,I1@I'I@j1i1 CI@.4IN :,._..:..,_, :...) _â œ - -1)@II Fig 24. Progression of malignant melanoma with ulcerated nodule. VOL 35, NO. 3 MAY/JUNE
11 :cr.n Fig. 25. Dysplastic nevus measuring nine mm in diameter. Fig. 28. Dysplastic nevus with color variega tion from tan to IiIt,Ifl sf111.1 Fig. 26. Dysplastic nevus with features of a dark-target cm I@ I; 2j Fig. 27. Dysplastic nevus with papillated sur face and tan macular border fading into the surrounding skin (so-called â papillatedâ var iant). Early detection of breast cancer is fa cilitated by examinations by physicians and frequent self-examinations by women.52 Similarly, if malignant melanomas are to be identified when they are curable, complete and thorough examinations by physicians should be encouraged and taught, supplemented by frequent self examinations of the skin by patients. The following section describes a technique of systematic and thorough physician-examination of the skin and offers guidelines on teaching self examination of the skin. Examinationof the Skin by Physicians The equipment needed for complete ex amination of the skin is simple: examina tion table, source of bright light, and, occasionally, a magnifying lens (2 x â 4 x). The patient should lie on an exami nation table and the entire anterior surface of the body (including intertriginous areas) should be closely scrutinized for pig mented lesions. The next step is to look at the entire posterior aspect of the body (in cluding intertriginous areas). The scalp should also be thoroughly examined. An ordinary inexpensive blow dryer can be used, especially if hair is plentiful. All pigmented lesions should be care fully studied. Any lesion even remotely suggestive of a malignant melanoma should be given special attention.this includes 140 CA-A CANCER JOURNAL FOR CLINICIANS
12 obtaining an in-depth history and a biopsy. Remember the ABCDs (Asymmetry, Border irregularity, Color variegation, Di ameter â enlargement). A completeannualexaminationof the skin by a physician is recommended for everyone, supplemented by monthly self examinations by the patient. Patients with a personal or family history of malignant melanoma, as well as those with dysplastic nevi or any of the other risk factors, should have more frequent examinations by both their physicians and Self-Examination of the Skin Routine self-examination of the skin is in expensive, noninvasive, and free of danger. The patient takes part of the re sponsibility for identifying early malignant melanomas of the skin at a time when such lesions are curable. A thorough self-examination of the skin requires the patient to undress completely and have a full-length mirror, hand-held mirror, hand-held blow dryer, two chairs, and a well-lighted room. Right after bath ing is a good time for the examination. The first few times, the patient should spend a good deal of time inspecting the en â j Fig. 29. Giant congenital melanocytic nevus. By performing periodic complete cutaneous examinations, by teaching patients the technique of routine self-examination of the skin, and by proper use of diagnostic aids (particularly skin biopsy), physicians can improve the chances for early diagnosis and prompt eradication of malignant melanoma. tire surface of the skin. With experience, however, the self-examination should take only a few minutes. To look at parts of the skin surface that may be hard to seeâ for example, some areas of the back, scalp, and buttocksâ the patient may find it helpful to ask for the help of a spouse, relative, or friend. The self-examination should be carried out step by step as shown in the illustrations on pages 146 to 149. These pages can be photocopied and given to patients to en courage and facilitate their learning this critically important technique. Educational pamphlets for the public are also avail able through the American Academy of Dermatology or the American Cancer Society. It may be useful to measure unusual pigmented lesions and pinpoint their loca tions and sizes on body charts (Figs. 30 and 31). The blank body charts also may be photocopied and given to patients. The patient should see a physician if there are any newly discovered pigmented [Text continued on page 150/ VOL35,NO.3 MAY/JUNE
13 Fig. 30. Body chartsâ anteriorview and posterior view. 142 CA-A CANCER JOURNAL FOR CLINICIANS
14 â A Fig. 31. Photograph of patient with multiple dysplastic nevi. Body chart shows how these nevi are mapped. VOL 35, NO. 3 MAY/JUNE
15 144 CA-A CANCER JOURNAL FOR CLINICIANS
16 VOL 35,NO.3 MAY/JUNE
17 / Ij Step2 Hold your hands with the palms face up, as shown in the drawing. Look at your palms, fingers, spaces between the fingers and forearms. Then turn your hands over and ex amine the backs of your hands, fin gers, spaces between the fingers, fingernails, and forearms. Step 1 Make sure the room is well-lighted, and that you have nearby a full length mirror, a hand-held mirror, a hand-held blow dryer, and two chairs or stools. Undress com pletely. Step 3 Now position yourself in front of the full-length mirror. Hold up your arms, bent at the elbows, with your palms facing you. In the mirror, look at the backs of your forearms and elbows. Â 1985,AmericanCancer Society Inc., New York, N.Y. 146 CA-ACANCERJOURNALFORCLINICIANS
18 (Pt IF I Step Again using the full-length mirror, observe the entire front of your body. In turn, look at your face, neck, and arms. Turn your palms to face the mirror and look at your upper arms. Then look at your chest and abdomen; pubic area; thighs and lower legs. Step5 Still standing in front of the mirror, lift your arms over your head with the palms facing each other. Turn so that your right side is facing the mirror and look at the entire side of your bodyâ your hands and arms, underarms, sides of your trunk, thighs, and lower legs. Then turn, and repeat the process with your left side. VOL 35, NO. 3 MAY/JUNE
19 A. With your back toward the full length mirror, look at your buttocks and the backs of your thighs and lowerlegs. Step7 Now pick up the hand-held mirror. With your back still to the full-length mirror, examine the back of your neck, and your back and buttocks. Also examine the backs of your arms in this way. Some areas are hard to see, and you may find it helpful to ask your spouse or a friend to assist you. Â AmericanCancerSociety,Inc.,New York,N.Y. 148 CA-A CANCER JOURNAL FOR CLINICIANS
20 St 9 Sit down and prop up one leg on a chair or stool in front of you as shown. Using the hand-held mirror, examine the inside of the propped-up leg, beginning at the groin area and moving the mirror down the leg to your foot. Repeat the procedure for your other leg. Step 8 Use the hand-held mirror and the full-length mirror to look at your scalp. Because the scalp is diffi cult to examine, we suggest you also use a hand-held blow dryer turned to a cool setting, to lift the hair from the scalp. While some people find it easy to hold the mir ror in one hand and the dryer in the other, while looking in the full-length mirror, many do not. For the scalp examination in particular, then, you might ask your spouse or a friend to assist you. Ste 10Still sitting, cross one leg over the other. Use the hand-held mirror to examine the top of your foot, the toes, toenails, and spaces be tween the toes. Then look at the sole or bottom of your foot. Repeat the procedure for the other foot. VOL 35, NO. 3 MAY/JUNE
21 lesions or any significant changes in a preexisting pigmented lesion. Most early malignant melanomas are macular and grow in diameter for some time before they be come elevated. Flat lesions are almost al ways curable, whereas lesions that develop plaques, papules, or nodules have a greater risk for metastases.'6 The goal is to recog nize early malignant melanomas when they are flat and curable. In Summary The combination of routine physician examination of the skin coupled with self-examination provides a realistic op portunity for the identification of early malignant melanomas. Removal of such thin lesions can significantly reduce the mortal ity rate from this potentially serious form of cutaneous cancer. References 1. Silverberg E: Cancer statistics, CA 35:19â 35, KopfAW, Rigel DS, Friedman RJ: The rising incidence and mortality rate of malignant mela noma. J Dermatol SurgOncol 8:760â 761, Mihm MC Jr. Fitzpatrick TB, Brown MML, et al: Early detection of primary cutaneous ma lignant melanoma. A color atlas. N Engl J Med 289:989â 996, Ackerman AB: Clinical diagnosis of malig nant melanoma in situ, in Ackerman AB (ed): Pa thology of Malignant Melanoma. New York, Masson Publishing USA, Inc. 1981, pp 57â Sober AJ, Fitzpatrick TB, Mihm MC, et al: Early recognition of cutaneous melanoma. JAMA 242:2795â 2799, Ackerman AB: Malignant melanoma: A unifying concept. Hum Pathol 11:591â 595, Breslow A: Prognostic factors in the treat ment of cutaneous melanoma. J Cutan Pathol 6:208â 212, Fitzpatrick TB: Early recognition of primary cutaneous melanoma. Hosp Pract 17:67â 75, Clark WH Jr: Clinical diagnosis of cutaneous malignant melanoma (editorial). JAMA 236:484â 485, Clark WHir, From L, Bernardino EA, et al: The histogenesis and biologic behavior of pri mary human malignant melanomas of the skin. Cancer Res 29:705â 727, Breslow A: Thickness, cross-sectional areas, and depth of invasion in the prognosis of cuta neous melanoma. Ann Surg 172:902â 908, Balch CM, Murad TM, Soong SJ, et al: A multifactorial analysis of melanoma: Prognostic histopathological features comparing Clark's and Breslow's staging methods. Ann Surg 188:732â 742, McGovern Vi, Shaw HM, Milton GW, et al: Prognostic significance of the histological fea tures of malignant melanoma. Histopathology 3:385â 393, Day CL Jr. Mihm MC Jr, Lew RA, et al: Cu taneous malignant melanoma: Prognostic guide lines for physicians and patients. CA 32:113â 122, Breslow A, Cascinelli N, van der Esch EP, et al: Stage I melanoma of the limbs: Assess ment of prognosis by levels of invasion and maximum thickness. Tumori 64: , Funk W, Schmoeckel C, HÃ lzeld, et al: Prognostic classification of malignant melanoma by clinical criteria. BrJ Dermatol 111:129â 138, Wick MM, Sober AJ, Fitzpatrick Ti, et al: Clinical characteristics of early cutaneous mel anoma. Cancer 45:2684â 2686, Roses DF, Harris MN, Ackerman AB: Di agnosis and Management of Cutaneous Malig nant Melanoma. Philadelphia, WB Saunders Co. 1983, pp 126â BalchCM, MiltonGW, Shaw HM, etal: Cu taneous Melanoma: Clinical Management and Treatment Results Worldwide. Philadelphia, JB Lippincott Co, 1985, pp 63â NYU Melanoma Cooperative Group, un published observations, KopfAW, Ban RS, Rodrlguez-Sains RS, et al (eds): Malignant Melanoma. New York, Mas son Publishing USA, mc, 1979, pp 152â Lyall D: Malignant melanoma in infancy (letter). JAMA 202:1153, Trozak Di, Rowland WD, Hu F: Metastatic malignant melanoma in prepubertal children. Pediatrics 55:191â 204, Kaplan EN: The risk of malignancy in large congenital nevi. PlastReconstr Surg 53:42 lâ 428, Mark GJ, Mihm MC, Liteplo MG, et al: Congenital melanocytic nevi of the small and garment type. Clinical, histologic, and ultra 150 CA-A CANCER JOURNAL FOR CLINICIANS
22 structural studies. Hum Pathol 4:395â 418, Walton RG, Jacobs AH, Cox AJ: Pigmented lesions in newborn infants. Bri Dermatol95: , Kopf AW, Bart RS, Hennessey P: Congen ital nevocytic nevi and malignant melanomas. J AmAcadDermatol 1:123â 130, Rhodes AR, Wood WC, Sober AJ, et al: Nonepidermal origin of malignant melanoma associated with a giant congenital nevocellular nevus. Plant Reconstr Surg 67:782â 790, Kopf AW, Ban RS, Rodrlguez-Sains RS, et al (eds): Malignant Melanoma. New York, Masson Publishing USA, Inc, 1979, pp 1â CutlerSJ, Young ilir(eds): Third National Cancer Survey: Incidence Data. Nail Cancer Inst Monogr 41. DHEW Publication No. (NIH)75â 787. Bethesda, Md, National Cancer Institute, Jones RE ir, Cash ME, Ackerman AB: Ma lignant melanomas mistaken histologically for junctional nevi, in Ackerman AB (ed): Pathol ogy of Malignant Melanoma. New York, Man son Publishing USA, Inc. 1981, pp 93â Ackerman AB, Su WPD: The histology of cutaneous malignant melanoma, in Kopf AW, Ban RS, RodrIguez-Sains RS, et al (eds): Ma lignant Melanoma. New York, Masson Pub lishing USA, Inc, 1979, pp 25â Gumport SL, Harris MN, KopfAW: Diag nosis and management of common skin cancers. CA 31:79â 90, Rigel DS, Friedman Ri: Clinical manage ment of patients with dysplastic and congenital nevi. DermatolClin3:251â 255, Clark WH ir, Reimer RR, Greene M, et al: Origin of familial malignant melanomas from heritable melanocytic lesions. â œ The B-K Mole syndrome.â Arch Dermatol 114:732â 738, Elder DE, Greene MH, Bondi EE, etal: Ac quired melanocytic nevi and melanoma: The dysplastic nevus syndrome, in Ackerman AB(ed): Pathology of Malignant Melanoma. New York, Masson Publishing USA, Inc, 1981, pp 185â Greene MH, Fraumeni if: The hereditary variant of malignant melanoma, in Clark WH Jr, Goldman LI, Mastrangelo MJ (eds): Human Ma lignant Melanoma. New York, Grune & Strat ton, Inc. 1979, pp 139â Lynch HT, Fusaro RM, Danes BS, et al: A review of hereditary malignant melanoma in cluding biomarkers in familial atypical multiple mole melanoma syndrome. Cancer Genet Cy togenet 8:325â 358, Lynch HT, Fusaro RM, Pester J, et al: Familial, atypical multiple mole melanoma (FAMMM) syndrome: Genetic heterogeneity and malignantmelanoma.br i Cancer42:58â 70, Greene MH: The dysplastic nevus syn drome. New York, The Melanoma Letter of the Skin Cancer Foundation 1:2, Friedman Ri, Heilman ER, Rigel DS, et al: The dysplastic nevus: Clinical and patho logical features. DermatolClin 3:239â 249, Rhodes AR, Melski JW: Small congenital nevocellular nevi and the risk of cutaneous mel anoma. J Pediatr 100:219â 224, RhodesAR, SoberAJ,Day CL, etal:the malignant potential of small congenital nevocel lular nevi. An estimate of association based on a histologic study of 234 primary cutaneous mel anomas. J Am Acad Dermatol 6:230â 241, Arons MS. Hurwitz S: Congenital nevocel lular nevus: A review of the treatment contro versy and a report of 46 cases. PlantReconstr Surg 72:355â 365, GellenGA, KopfAW, Garfinkel L:Malig nant melanoma: A controlled study of possible associated factors. ArchDermatol99:43â 48, Kraemer KH: Xeroderma pigmentosum, in Demis Di, McGuire J (eds): Clinical Dermatol ogy, vol 4, unit 19â 7.Philadelphia, Harper & Row Publishers, Kopf AW, Knpke ML, Stern RS: Sun and malignant melanoma. J Am Acad Dermatol 11:674â 684, Lew RA, Sober AJ, Cook N, et al: Sun ex posure habits in patients with cutaneous mela noma: A cane control study. J Dermatol Surg Oncol9:981â 986, Rigel DS, Friedman RJ, KopfAW: Risk fac torsforthedevelopmentof malignantmela noma, in Proceedings of the National Clinical Dermatology Conference. Chicago, American AcademyofDermatology, Holman CDJ, Armstrong BK: Cutaneous malignant melanoma and indicators of total ac cumulated exposure to the sun: An analysis sep arating histogenetic types. I Nail Cancer Inst 73:75â 82, Davis N: Modern concepts of melanoma and its management. Ann Plant Surg 1:628â 629, Leis HP Jr: The diagnosis of breast cancer. CA 27:209â 231,1977. VOL35,NO.3 MAY/JUNE
Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc
 1 Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc Benign lesions Seborrheic Keratoses: Warty, stuck-on Genetics and birthdays Can start in late
1 Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc Benign lesions Seborrheic Keratoses: Warty, stuck-on Genetics and birthdays Can start in late
Dermatopathology: The tumor is composed of keratinocytes which show atypia, increase mitoses and abnormal mitoses.
 Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Clinical characteristics
 Skin Cancer Fernando Vega, MD Seattle Healing Arts Clinical characteristics Precancerous lesions Common skin cancers ACTINIC KERATOSIS Precancerous skin lesions Actinic keratoses Dysplastic melanocytic
Skin Cancer Fernando Vega, MD Seattle Healing Arts Clinical characteristics Precancerous lesions Common skin cancers ACTINIC KERATOSIS Precancerous skin lesions Actinic keratoses Dysplastic melanocytic
IT S FUNDAMENTAL MY DEAR WATSON! A SHERLOCKIAN APPROACH TO DERMATOLOGY
 IT S FUNDAMENTAL MY DEAR WATSON! A SHERLOCKIAN APPROACH TO DERMATOLOGY Skin, Bones, and other Private Parts Symposium Dermatology Lectures by Debra Shelby, PhD, DNP, FNP-BC, FADNP, FAANP Debra Shelby,
IT S FUNDAMENTAL MY DEAR WATSON! A SHERLOCKIAN APPROACH TO DERMATOLOGY Skin, Bones, and other Private Parts Symposium Dermatology Lectures by Debra Shelby, PhD, DNP, FNP-BC, FADNP, FAANP Debra Shelby,
Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more
 Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more common on the trunk; but extremities, head and neck are
Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more common on the trunk; but extremities, head and neck are
Morphologic characteristics of nevi associated with melanoma: a clinical, dermatoscopic and histopathologic analysis
 DERMATOLOGY PRACTICAL & CONCEPTUAL www.derm101.com Morphologic characteristics of nevi associated with melanoma: a clinical, dermatoscopic and histopathologic analysis Temeida Alendar 1, Harald Kittler
DERMATOLOGY PRACTICAL & CONCEPTUAL www.derm101.com Morphologic characteristics of nevi associated with melanoma: a clinical, dermatoscopic and histopathologic analysis Temeida Alendar 1, Harald Kittler
Dermatology for the PCP Deanna G. Brown, MD, FAAD Susong Dermatology Consulting Staff at CHI Memorial
 Dermatology for the PCP Deanna G. Brown, MD, FAAD Susong Dermatology Consulting Staff at CHI Memorial Cutaneous Oncology for the PCP Deanna G. Brown, MD, FAAD Susong Dermatology Consulting Staff at CHI
Dermatology for the PCP Deanna G. Brown, MD, FAAD Susong Dermatology Consulting Staff at CHI Memorial Cutaneous Oncology for the PCP Deanna G. Brown, MD, FAAD Susong Dermatology Consulting Staff at CHI
Photo Quiz Self-Test Your Diagnostic Acumen
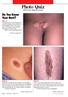 Do You Know Your Nevi? Case 1: The parents of a 3-year-old girl seek medical evaluation of the nodules on their daughter s back. The lesions have been present since birth and have grown with the child.
Do You Know Your Nevi? Case 1: The parents of a 3-year-old girl seek medical evaluation of the nodules on their daughter s back. The lesions have been present since birth and have grown with the child.
Malignant Melanoma Early Stage. A guide for patients
 This melanoma patient brochure is designed to help educate melanoma patients and their caregivers. It was developed under the guidance of Dr. Michael Smylie, Professor, Department of Oncology, University
This melanoma patient brochure is designed to help educate melanoma patients and their caregivers. It was developed under the guidance of Dr. Michael Smylie, Professor, Department of Oncology, University
Melanoma: The Basics. What is a melanocyte?
 Melanoma: The Basics What is a melanocyte? A melanocyte is a normal cell, found in the skin, which produces melanin. Melanin is a black or dark brown pigment that is seen in the skin, hair, and parts of
Melanoma: The Basics What is a melanocyte? A melanocyte is a normal cell, found in the skin, which produces melanin. Melanin is a black or dark brown pigment that is seen in the skin, hair, and parts of
Pathology of the skin. 2nd Department of Pathology, Semmelweis University
 Pathology of the skin 2nd Department of Pathology, Semmelweis University Histology of the skin Epidermis: Stratum corneum Stratum granulosum Stratum spinosum Stratum basale Dermis: papillary and reticular
Pathology of the skin 2nd Department of Pathology, Semmelweis University Histology of the skin Epidermis: Stratum corneum Stratum granulosum Stratum spinosum Stratum basale Dermis: papillary and reticular
Toby Maurer, MD University of California, San Francisco. Lifetime risk of an American developing melanoma
 Distinguishing Pigmented Skin Lesions and Melanoma Toby Maurer, MD University of California, San Francisco Epidemiology of Melanoma Lifetime risk of an American developing melanoma 1935: 1 in 1500 1980:
Distinguishing Pigmented Skin Lesions and Melanoma Toby Maurer, MD University of California, San Francisco Epidemiology of Melanoma Lifetime risk of an American developing melanoma 1935: 1 in 1500 1980:
Toby Maurer, MD University of California, San Francisco. Lifetime risk of an American developing melanoma
 Distinguishing Pigmented Skin Lesions and Melanoma Toby Maurer, MD University of California, San Francisco Epidemiology of Melanoma Lifetime risk of an American developing melanoma 1935: 1 in 1500 1980:
Distinguishing Pigmented Skin Lesions and Melanoma Toby Maurer, MD University of California, San Francisco Epidemiology of Melanoma Lifetime risk of an American developing melanoma 1935: 1 in 1500 1980:
المركب النموذج--- سبيتز وحمة = Type Spitz's Nevus, Compound SPITZ NEVUS 1 / 7
 SPITZ NEVUS 1 / 7 Epidemiology An annual incidence rate of 1.4 cases of Spitz nevus per 100,000 individuals has been estimated in Australia, compared with 25.4 per 100,000 individuals for cutaneous melanoma
SPITZ NEVUS 1 / 7 Epidemiology An annual incidence rate of 1.4 cases of Spitz nevus per 100,000 individuals has been estimated in Australia, compared with 25.4 per 100,000 individuals for cutaneous melanoma
VIP MedSpa Clinic News
 Maryam Hekmat, M.D. Inc. May 2017 VIP MedSpa Clinic News VIPMedSpaClinic.com 858-451-6500 11665 Avena Place, Suite 104 San Diego, CA 92128 Medical News Can B12 Shots Boost My Energy and Help Me Lose Weight?
Maryam Hekmat, M.D. Inc. May 2017 VIP MedSpa Clinic News VIPMedSpaClinic.com 858-451-6500 11665 Avena Place, Suite 104 San Diego, CA 92128 Medical News Can B12 Shots Boost My Energy and Help Me Lose Weight?
LENTIGO SIMPLEX. Epidemiology
 LENTIGO SIMPLEX Epidemiology The frequency of lentigo simplex in children and adults has not been determined. There does not appear to be a racial or gender predilection. Lentigo simplex is the most common
LENTIGO SIMPLEX Epidemiology The frequency of lentigo simplex in children and adults has not been determined. There does not appear to be a racial or gender predilection. Lentigo simplex is the most common
Living Beyond Cancer Skin Cancer Detection and Prevention
 Living Beyond Cancer Skin Cancer Detection and Prevention Cutaneous Skin Cancers Identification Diagnosis Treatment options Prevention What is the most common cancer in people? What is the most common
Living Beyond Cancer Skin Cancer Detection and Prevention Cutaneous Skin Cancers Identification Diagnosis Treatment options Prevention What is the most common cancer in people? What is the most common
SKIN CANCER. Most common cancer diagnosis 40% of all cancers
 SKIN CANCER Most common cancer diagnosis 40% of all cancers OBJECTIVES Review common and uncommon cancers of the skin. Special emphasis on melanoma and dysplastic nevus Review pathology/tnm/staging, which
SKIN CANCER Most common cancer diagnosis 40% of all cancers OBJECTIVES Review common and uncommon cancers of the skin. Special emphasis on melanoma and dysplastic nevus Review pathology/tnm/staging, which
Learning Objectives. Tanning. The Skin. Classic Features. Sun Reactive Skin Type Classification. Skin Cancers: Preventing, Screening and Treating
 Learning Objectives Skin Cancers: Preventing, Screening and Treating Robert A. Baldor, MD, FAAFP Professor, Family Medicine & Community Health University of Massachusetts Medical School Distinguish the
Learning Objectives Skin Cancers: Preventing, Screening and Treating Robert A. Baldor, MD, FAAFP Professor, Family Medicine & Community Health University of Massachusetts Medical School Distinguish the
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB. Friday, February 12, :30 am 11:00 am
 MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB Friday, February 12, 2012 9:30 am 11:00 am FACULTY COPY GOALS: Describe the basic clinical and morphologic features of various
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB Friday, February 12, 2012 9:30 am 11:00 am FACULTY COPY GOALS: Describe the basic clinical and morphologic features of various
Identifying Skin Cancer. Mary S. Stone MD Professor of Dermatology and Pathology University of Iowa Carver College of Medicine March, 2018
 Identifying Skin Cancer Mary S. Stone MD Professor of Dermatology and Pathology University of Iowa Carver College of Medicine March, 2018 American Cancer Society web site Skin Cancer Melanoma Non-Melanoma
Identifying Skin Cancer Mary S. Stone MD Professor of Dermatology and Pathology University of Iowa Carver College of Medicine March, 2018 American Cancer Society web site Skin Cancer Melanoma Non-Melanoma
Associated Detection Patterns, Lesion Characteristics, and Patient Characteristics
 1562 Thin Primary Cutaneous Melanomas Associated Detection Patterns, Lesion Characteristics, and Patient Characteristics Jennifer L. Schwartz, M.D. 1 Timothy S. Wang, M.D. 1 Ted A. Hamilton, M.S. 1 Lori
1562 Thin Primary Cutaneous Melanomas Associated Detection Patterns, Lesion Characteristics, and Patient Characteristics Jennifer L. Schwartz, M.D. 1 Timothy S. Wang, M.D. 1 Ted A. Hamilton, M.S. 1 Lori
VACAVILLE DERMATOLOGY
 Connecting the Dots on those Spots NANDAN V. KAMATH, M.D. VACAVILLE DERMATOLOGY Sources All of the photos were taken with permission from the Dermnet NZ website - Dermnet New Zealand after communicating
Connecting the Dots on those Spots NANDAN V. KAMATH, M.D. VACAVILLE DERMATOLOGY Sources All of the photos were taken with permission from the Dermnet NZ website - Dermnet New Zealand after communicating
Skin Cancer. 5 Warning Signs. American Osteopathic College of Occupational and Preventive Medicine OMED 2012, San Diego, Monday, October 8, 2012 C-1
 Skin Cancer AMERICAN OSTEOPATHIC COLLEGE OF OCCUPATIONAL & PREVENTIVE MEDICINE OMED 2012 October 8, 2012 E. Robert Wanat II, D.O., M.P.H. Learning Objectives: Identify the 3 Basic Types of Skin Cancer
Skin Cancer AMERICAN OSTEOPATHIC COLLEGE OF OCCUPATIONAL & PREVENTIVE MEDICINE OMED 2012 October 8, 2012 E. Robert Wanat II, D.O., M.P.H. Learning Objectives: Identify the 3 Basic Types of Skin Cancer
Multiple Primary Melanoma in a Thai Male: A Case Report
 Case Report Multiple Primary Melanoma in a Thai Male: A Case Report J Med Assoc Thai 2014; 97 (Suppl. 2): S234-S238 Full text. e-journal: http://www.jmatonline.com Kittisak Payapvipapong MD*, Pinyapat
Case Report Multiple Primary Melanoma in a Thai Male: A Case Report J Med Assoc Thai 2014; 97 (Suppl. 2): S234-S238 Full text. e-journal: http://www.jmatonline.com Kittisak Payapvipapong MD*, Pinyapat
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB. Friday, February 13, :30 am 11:00 am
 MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB Friday, February 13, 2009 9:30 am 11:00 am FACULTY COPY GOALS: Describe the basic clinical and morphologic features of various
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB Friday, February 13, 2009 9:30 am 11:00 am FACULTY COPY GOALS: Describe the basic clinical and morphologic features of various
Polypoid Melanoma, A Virulent Variant of the Nodular Growth Pattern
 Polypoid Melanoma, A Virulent Variant of the Nodular Growth Pattern ELIZABETH A. MANCI, M.D., CHARLES M. BALCH, M.D..TARIQ M. MURAD, M.D., PH.D., AND SENG/JAW SOONG, PH.D. Manci, Elizabeth A., Balch, Charles
Polypoid Melanoma, A Virulent Variant of the Nodular Growth Pattern ELIZABETH A. MANCI, M.D., CHARLES M. BALCH, M.D..TARIQ M. MURAD, M.D., PH.D., AND SENG/JAW SOONG, PH.D. Manci, Elizabeth A., Balch, Charles
An Overview of Melanoma. Harriet Kluger, M.D. Associate Professor Section of Medical Oncology Yale Cancer Center
 An Overview of Melanoma Harriet Kluger, M.D. Associate Professor Section of Medical Oncology Yale Cancer Center Melanoma Statistics Median age at presentation 45-55 55 years Incidence: 2003 54,200 cases
An Overview of Melanoma Harriet Kluger, M.D. Associate Professor Section of Medical Oncology Yale Cancer Center Melanoma Statistics Median age at presentation 45-55 55 years Incidence: 2003 54,200 cases
LUMPS AND BUMPS: AN ORGANIZED APPROACH TO DIAGNOSIS AND MANAGEMENT
 LUMPS AND BUMPS: AN ORGANIZED APPROACH TO DIAGNOSIS AND MANAGEMENT Tammy P. Than, M.S., O.D., F.A.A.O. The University of Alabama at Birmingham / School of Optometry 1716 University Blvd. Birmingham, AL
LUMPS AND BUMPS: AN ORGANIZED APPROACH TO DIAGNOSIS AND MANAGEMENT Tammy P. Than, M.S., O.D., F.A.A.O. The University of Alabama at Birmingham / School of Optometry 1716 University Blvd. Birmingham, AL
Wellness Along the Cancer Journey: Cancer Types Revised October 2015 Chapter 7: Skin Cancer
 Wellness Along the Cancer Journey: Cancer Types Revised October 2015 Chapter 7: Skin Cancer Cancer Types Rev. 10.20.15 Page 56 Skin Cancer Group Discussion True False Not Sure 1. People with darker skin
Wellness Along the Cancer Journey: Cancer Types Revised October 2015 Chapter 7: Skin Cancer Cancer Types Rev. 10.20.15 Page 56 Skin Cancer Group Discussion True False Not Sure 1. People with darker skin
MELANOMA. Some people are more likely to get a m Melanoma than others:
 MELANOMA This leaflet has been written to help you understand more about Melanoma. It tells you what is it, what causes it, what can be done about it, how it can be prevented, and where you can find out
MELANOMA This leaflet has been written to help you understand more about Melanoma. It tells you what is it, what causes it, what can be done about it, how it can be prevented, and where you can find out
Conflict of Interest 9/2/2014. Pathogenesis and Comparison of Atypical Spitz Nevi vs Benign Spitz, and Childhood Melanoma
 Pathogenesis and Comparison of Atypical Spitz Nevi vs Benign Spitz, and Childhood Melanoma Martin C. Mihm Jr., M.D., F.A.C.P. Harvard Medical School Brigham and Women s Hospital Dana Farber Cancer Center
Pathogenesis and Comparison of Atypical Spitz Nevi vs Benign Spitz, and Childhood Melanoma Martin C. Mihm Jr., M.D., F.A.C.P. Harvard Medical School Brigham and Women s Hospital Dana Farber Cancer Center
This is a repository copy of Easily missed? Amelanotic melanoma. White Rose Research Online URL for this paper:
 This is a repository copy of Easily missed? Amelanotic melanoma. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/127789/ Version: Accepted Version Article: Muinonen-Martin,
This is a repository copy of Easily missed? Amelanotic melanoma. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/127789/ Version: Accepted Version Article: Muinonen-Martin,
Lichenoid Tissue Reaction in Malignant Melanoma A Potential Diagnostic Pitfall
 natomic Pathology / LICHENOID TISSUE RECTION IN MLIGNNT MELNOM Lichenoid Tissue Reaction in Malignant Melanoma Potential Diagnostic Pitfall CPT Scott R. Dalton, MC, US, 1,3 Capt Matt. aptista, USF, MC,
natomic Pathology / LICHENOID TISSUE RECTION IN MLIGNNT MELNOM Lichenoid Tissue Reaction in Malignant Melanoma Potential Diagnostic Pitfall CPT Scott R. Dalton, MC, US, 1,3 Capt Matt. aptista, USF, MC,
Glenn D. Goldman, MD. Fletcher Allen Health Care. University of Vermont College of Medicine
 Glenn D. Goldman, MD Fletcher Allen Health Care University of Vermont College of Medicine Recognize and identify the main types of skin cancer Understand how and why Mohs surgery is utilized for the treatment
Glenn D. Goldman, MD Fletcher Allen Health Care University of Vermont College of Medicine Recognize and identify the main types of skin cancer Understand how and why Mohs surgery is utilized for the treatment
Glenn D. Goldman, MD. University of Vermont Medical Center. University of Vermont College of Medicine
 Glenn D. Goldman, MD University of Vermont Medical Center University of Vermont College of Medicine Recognize and identify the main types of skin cancer and their precursors Identify and understand new
Glenn D. Goldman, MD University of Vermont Medical Center University of Vermont College of Medicine Recognize and identify the main types of skin cancer and their precursors Identify and understand new
Melanoma. Kaushik Mukherjee MD A. Scott Pearson MD
 Melanoma Kaushik Mukherjee MD A. Scott Pearson MD Disclosures You still have to study Not all inclusive No Western blots Extensive use of Google Image Search and Sabiston Melanoma Basics 8 th most common
Melanoma Kaushik Mukherjee MD A. Scott Pearson MD Disclosures You still have to study Not all inclusive No Western blots Extensive use of Google Image Search and Sabiston Melanoma Basics 8 th most common
Abrupt Intralesional Color Change on Dermoscopy as a New Indicator of Early Superficial Spreading Melanoma in a Japanese Woman
 Published online: June 24, 2015 1662 6567/15/0072 0123$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Published online: June 24, 2015 1662 6567/15/0072 0123$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Cutaneous Melanoma: Epidemiology (USA) The Sentinel Node in Head and Neck Melanoma. Cutaneous Melanoma: Epidemiology (USA)
 The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
Melanoma and Dermoscopy. Disclosure Statement: ABCDE's of melanoma. Co-President, Usatine Media
 Melanoma and Dermoscopy Richard P. Usatine, MD, FAAFP Professor, Family and Community Medicine Professor, Dermatology and Cutaneous Surgery Medical Director, University Skin Clinic University of Texas
Melanoma and Dermoscopy Richard P. Usatine, MD, FAAFP Professor, Family and Community Medicine Professor, Dermatology and Cutaneous Surgery Medical Director, University Skin Clinic University of Texas
Dermoscopy: Recognizing Top Five Common In- Office Diagnoses
 Dermoscopy: Recognizing Top Five Common In- Office Diagnoses Vu A. Ngo, DO Department of Family Medicine and Dermatology Choctaw Nation Health Services Authority Learning Objectives Introduction to dermoscopy
Dermoscopy: Recognizing Top Five Common In- Office Diagnoses Vu A. Ngo, DO Department of Family Medicine and Dermatology Choctaw Nation Health Services Authority Learning Objectives Introduction to dermoscopy
with a sunscreen. He had red hair, blue eyes, and his on the skin of the back and abdomen (Fig. 2). The
 Journal ofmedical Genetics, 1978, 15, 352-356 Familial atypical multiple mole-melanoma syndrome HENRY T. LYNCH, BERT C. FRICHOT, III, AND JANE F. LYNCH From the Department ofpreventive Medicine/Public
Journal ofmedical Genetics, 1978, 15, 352-356 Familial atypical multiple mole-melanoma syndrome HENRY T. LYNCH, BERT C. FRICHOT, III, AND JANE F. LYNCH From the Department ofpreventive Medicine/Public
6/17/2018. Breaking Bad (Part 1) Dermoscopy of Brown(ish) Things. Bad?
 Breaking Bad (Part 1) Dermoscopy of Brown(ish) Things Jennie T. Clarke, MD ssociate Professor of Dermatology University of Utah School of Medicine Bad? 1 Brown(ish) Things Bad Melanoma Pigmented basal
Breaking Bad (Part 1) Dermoscopy of Brown(ish) Things Jennie T. Clarke, MD ssociate Professor of Dermatology University of Utah School of Medicine Bad? 1 Brown(ish) Things Bad Melanoma Pigmented basal
Frequency of moles in a defined population
 Journal of Epidemiology and Community Health, 1985, 39, 48-52 Frequency of moles in a defined population K R COOKE, G F S SPEARS, AND D C G SKEGG From the Department of Preventive and Social Medicine,
Journal of Epidemiology and Community Health, 1985, 39, 48-52 Frequency of moles in a defined population K R COOKE, G F S SPEARS, AND D C G SKEGG From the Department of Preventive and Social Medicine,
Mole mapping and monitoring. Dr Stephen Hayes. Associate Specialist in Dermatology, University Hospital Southampton
 Mole mapping and monitoring Dr Stephen Hayes Associate Specialist in Dermatology, University Hospital Southampton Outline of presentation The melanoma epidemic Benefits of early detection Risks of the
Mole mapping and monitoring Dr Stephen Hayes Associate Specialist in Dermatology, University Hospital Southampton Outline of presentation The melanoma epidemic Benefits of early detection Risks of the
Acral Melanoma in Japan
 Acral Melanoma in Japan MAKOTO SEUI, M.D., HIDEAKI TAKEMATSU, M.D., MICHIKO HOSOKAWA, M.D., MASAAKI OBATA, M.D., YASUSHI TOMITA, M.D., TAIZO KATO, M.D., MASAAKI TAKAHASHI, M.D., AND MARTIN C. MIHM, JR.,
Acral Melanoma in Japan MAKOTO SEUI, M.D., HIDEAKI TAKEMATSU, M.D., MICHIKO HOSOKAWA, M.D., MASAAKI OBATA, M.D., YASUSHI TOMITA, M.D., TAIZO KATO, M.D., MASAAKI TAKAHASHI, M.D., AND MARTIN C. MIHM, JR.,
Appendix : Dermoscopy
 Go Back to the Top To Order, Visit the Purchasing Page for Details APP Appendix : Dermoscopy Dermoscopy, also known as dermatoscopy, epiluminoscopy and epiluminescent microscopy, is an effective non-invasive
Go Back to the Top To Order, Visit the Purchasing Page for Details APP Appendix : Dermoscopy Dermoscopy, also known as dermatoscopy, epiluminoscopy and epiluminescent microscopy, is an effective non-invasive
MELANOMA. 4 Fitzroy Square, London W1T 5HQ Tel: Fax: Registered Charity No.
 MELANOMA This leaflet had been written to help you understand more about melanoma. It tells you what it is, what causes it, what can be done about it, how it can be prevented, and where you can find out
MELANOMA This leaflet had been written to help you understand more about melanoma. It tells you what it is, what causes it, what can be done about it, how it can be prevented, and where you can find out
Desmoplastic Melanoma R/O BCC. Clinical Information. 74 y.o. man with lesion on left side of neck r/o BCC
 R/O BCC Sabine Kohler, M.D. Professor of Pathology and Dermatology Dermatopathology Service Stanford University School of Medicine Clinical Information 74 y.o. man with lesion on left side of neck r/o
R/O BCC Sabine Kohler, M.D. Professor of Pathology and Dermatology Dermatopathology Service Stanford University School of Medicine Clinical Information 74 y.o. man with lesion on left side of neck r/o
Case Report Micromelanomas: A Review of Melanomas 2mmand a Case Report
 Case Reports in Oncological Medicine, Article ID 206260, 4 pages http://dx.doi.org/10.1155/2014/206260 Case Report Micromelanomas: A Review of Melanomas 2mmand a Case Report Sharad P. Paul 1,2,3 1 Skin
Case Reports in Oncological Medicine, Article ID 206260, 4 pages http://dx.doi.org/10.1155/2014/206260 Case Report Micromelanomas: A Review of Melanomas 2mmand a Case Report Sharad P. Paul 1,2,3 1 Skin
Finding Melanoma. Is not easy!
 Finding Melanoma Is not easy! Finding Melanoma Victoria mean depth at diagnosis is 1.5 mm. Melanoma 1.5mm Has Stage 1B Mortality 10% Melanoma Spotting a killer! Spotting a killer Visual Clues What are
Finding Melanoma Is not easy! Finding Melanoma Victoria mean depth at diagnosis is 1.5 mm. Melanoma 1.5mm Has Stage 1B Mortality 10% Melanoma Spotting a killer! Spotting a killer Visual Clues What are
p16 Genetic Test Reporting Counseling Protocol Flip Chart
 p16 Genetic Test Reporting Counseling Protocol Flip Chart Chromosomes, Gene, & Protein Cell Nucleus Chromosomes Gene Protein Adapted from Understanding Gene Testing,, NIH, 1995 Cancer Normal cell Disease
p16 Genetic Test Reporting Counseling Protocol Flip Chart Chromosomes, Gene, & Protein Cell Nucleus Chromosomes Gene Protein Adapted from Understanding Gene Testing,, NIH, 1995 Cancer Normal cell Disease
Springer Healthcare. Staging and Diagnosing Cutaneous Melanoma. Concise Reference. Dirk Schadendorf, Corinna Kochs, Elisabeth Livingstone
 Concise Reference Staging and Diagnosing Cutaneous Melanoma Dirk Schadendorf, Corinna Kochs, Elisabeth Livingstone Extracted from Handbook of Cutaneous Melanoma: A Guide to Diagnosis and Treatment Published
Concise Reference Staging and Diagnosing Cutaneous Melanoma Dirk Schadendorf, Corinna Kochs, Elisabeth Livingstone Extracted from Handbook of Cutaneous Melanoma: A Guide to Diagnosis and Treatment Published
Associate Clinical Professor of Dermatology MUSC
 Re-excision of Moderately Dysplastic Nevi: Should we or shouldn t we? John C. Maize, Jr, M.D. Dermatologist and Dermatopathologist Trident Dermatology, Charleston SC Associate Clinical Professor of Dermatology
Re-excision of Moderately Dysplastic Nevi: Should we or shouldn t we? John C. Maize, Jr, M.D. Dermatologist and Dermatopathologist Trident Dermatology, Charleston SC Associate Clinical Professor of Dermatology
Gross Appearance & Histology of Skin Cancer. Kyle Mannion M.D. January 21, 2005
 Gross Appearance & Histology of Skin Cancer Kyle Mannion M.D. January 21, 2005 Actinic Keratosis 5-20% will develop squamous/basal cell ca Almost solely from solar damage Usually develop during 4 th decade
Gross Appearance & Histology of Skin Cancer Kyle Mannion M.D. January 21, 2005 Actinic Keratosis 5-20% will develop squamous/basal cell ca Almost solely from solar damage Usually develop during 4 th decade
Associate Professor Amanda Oakley. Professor H. Peter Soyer. Academic Dermatologist The University of Queensland Brisbane. Dermatologist Hamilton
 Associate Professor Amanda Oakley Dermatologist Hamilton Professor H. Peter Soyer Academic Dermatologist The University of Queensland Brisbane 8:30-10:30 WS #3: Dermoscopy Workshop Part 1 11:00-13:00 WS
Associate Professor Amanda Oakley Dermatologist Hamilton Professor H. Peter Soyer Academic Dermatologist The University of Queensland Brisbane 8:30-10:30 WS #3: Dermoscopy Workshop Part 1 11:00-13:00 WS
Skin Cancer 101: Diagnosis and Management of the Most Common Cancer
 Skin Cancer 101: Diagnosis and Management of the Most Common Cancer Sarah Patton, PA-C, MSHS Skin Surgery Center www.skinsurgerycenter.com Seattle/Bellevue, WA Skin cancer Skin cancer is by far the most
Skin Cancer 101: Diagnosis and Management of the Most Common Cancer Sarah Patton, PA-C, MSHS Skin Surgery Center www.skinsurgerycenter.com Seattle/Bellevue, WA Skin cancer Skin cancer is by far the most
Total body photography in high risk patients
 Total body photography in high risk patients Doug Grossman, MD, PhD Department of Dermatology Huntsman Cancer Institute University of Utah Summer AAD F032 Practical Considerations for Patients with Melanoma
Total body photography in high risk patients Doug Grossman, MD, PhD Department of Dermatology Huntsman Cancer Institute University of Utah Summer AAD F032 Practical Considerations for Patients with Melanoma
BACK TO TABLE OF CONTENTS FOCUS ON MELANOMA Oncology Annual Report BAPTIST HEALTH LEXINGTON ONCOLOGY ANNUAL REPORT
 FOCUS ON MELANOMA 2014 Oncology Annual Report BAPTIST HEALTH LEXINGTON 1 2014 ONCOLOGY ANNUAL REPORT TABLE OF CONTENTS What is melanoma?...3 Who is at risk for melanoma?...3 What causes melanoma?...4 What
FOCUS ON MELANOMA 2014 Oncology Annual Report BAPTIST HEALTH LEXINGTON 1 2014 ONCOLOGY ANNUAL REPORT TABLE OF CONTENTS What is melanoma?...3 Who is at risk for melanoma?...3 What causes melanoma?...4 What
A PRACTICAL APPROACH TO ATYPICAL MELANOCYTIC LESIONS BIJAN HAGHIGHI M.D, DIRECTOR OF DERMATOPATHOLOGY, ST. JOSEPH HOSPITAL
 A PRACTICAL APPROACH TO ATYPICAL MELANOCYTIC LESIONS BIJAN HAGHIGHI M.D, DIRECTOR OF DERMATOPATHOLOGY, ST. JOSEPH HOSPITAL OBJECTIVES Discuss current trends and changing concepts in our understanding of
A PRACTICAL APPROACH TO ATYPICAL MELANOCYTIC LESIONS BIJAN HAGHIGHI M.D, DIRECTOR OF DERMATOPATHOLOGY, ST. JOSEPH HOSPITAL OBJECTIVES Discuss current trends and changing concepts in our understanding of
Dermatological Manifestations in the Elderly. Sanjay Siddha Staff Dermatologist UHN & MSH
 Dermatological Manifestations in the Elderly Sanjay Siddha Staff Dermatologist UHN & MSH Disclosure No actual or potential conflicts of interest or commercial relationships to declare Objectives Recognize
Dermatological Manifestations in the Elderly Sanjay Siddha Staff Dermatologist UHN & MSH Disclosure No actual or potential conflicts of interest or commercial relationships to declare Objectives Recognize
Basics in Dermoscopy
 Basics in Dermoscopy Manal Bosseila Professor of Dermatology, Cairo University Member of European Academy Dermatology & Venereology EADV Member of International Dermoscopy Society IDS Member of Aesthetic
Basics in Dermoscopy Manal Bosseila Professor of Dermatology, Cairo University Member of European Academy Dermatology & Venereology EADV Member of International Dermoscopy Society IDS Member of Aesthetic
Actinic keratosis (AK): Dr Sarma s simple guide
 Actinic keratosis (AK): Dr Sarma s simple guide Actinic keratosis is a very common lesion that you will see in your day-to-day practice. First, let me explain the name Actinic keratosis. It means keratosis
Actinic keratosis (AK): Dr Sarma s simple guide Actinic keratosis is a very common lesion that you will see in your day-to-day practice. First, let me explain the name Actinic keratosis. It means keratosis
Melanoma in the Older Person
 Review Article [1] August 01, 2004 Melanoma [2], Older Patients [3], Oncology Journal [4] By Susan M. Swetter, MD [5], Alan C. Geller, MPH, RN [6], and John M. Kirkwood, MD [7] Melanoma incidence and mortality
Review Article [1] August 01, 2004 Melanoma [2], Older Patients [3], Oncology Journal [4] By Susan M. Swetter, MD [5], Alan C. Geller, MPH, RN [6], and John M. Kirkwood, MD [7] Melanoma incidence and mortality
Skin Malignancies Non - Melanoma & Melanoma Marilyn Ng, MD Dept. of Surgery M&M Conference Downstate Medical Center July 19, 2012
 Skin Malignancies Non - Melanoma & Melanoma Marilyn Ng, MD Dept. of Surgery M&M Conference Downstate Medical Center July 19, 2012 Case Presentation 57 yo man with 3 month hx of a nonhealing < 1 cm right
Skin Malignancies Non - Melanoma & Melanoma Marilyn Ng, MD Dept. of Surgery M&M Conference Downstate Medical Center July 19, 2012 Case Presentation 57 yo man with 3 month hx of a nonhealing < 1 cm right
Oral and Maxillofacial Surgery Department
 Oral and Maxillofacial Surgery Department This leaflet explains: Lentigo Maligna What are the aims of this leaflet? This leaflet has been written to help you understand more about lentigo maligna and melanoma
Oral and Maxillofacial Surgery Department This leaflet explains: Lentigo Maligna What are the aims of this leaflet? This leaflet has been written to help you understand more about lentigo maligna and melanoma
SUBUNGUAL MALIGNANT MELANOMA ON THE RIGHT INDEX IN A DENTIST AFTER PROLONGED OCCUPATIONAL EXPOSURE TO X-RAYS
 SUBUNGUAL MALIGNANT MELANOMA ON THE RIGHT INDEX IN A DENTIST AFTER PROLONGED OCCUPATIONAL EXPOSURE TO X-RAYS J. HATZIS*, V. MAKROPOULOS**, N. AGNANTIS*** * Department of Skin and Venereal Diseases, University
SUBUNGUAL MALIGNANT MELANOMA ON THE RIGHT INDEX IN A DENTIST AFTER PROLONGED OCCUPATIONAL EXPOSURE TO X-RAYS J. HATZIS*, V. MAKROPOULOS**, N. AGNANTIS*** * Department of Skin and Venereal Diseases, University
You can also complete the survey over the phone with a trained interviewer by calling the study team toll free at
 Last modified: 0//08 0:0:5 AM Thank you very much for your participation in this important study. If you prefer, you can complete this survey online at www.stjude.org/ltfu-ask8. Your log-in ID is your
Last modified: 0//08 0:0:5 AM Thank you very much for your participation in this important study. If you prefer, you can complete this survey online at www.stjude.org/ltfu-ask8. Your log-in ID is your
Atypical Nevi When to Re-excise. Catherine Barry, DO Dermatopathologist
 Atypical Nevi When to Re-excise Catherine Barry, DO Dermatopathologist Why talk about skin cancer? Because it s the most common type of cancer! Non-melanoma Skin Cancers Basal Cell Carcinoma Squamous Cell
Atypical Nevi When to Re-excise Catherine Barry, DO Dermatopathologist Why talk about skin cancer? Because it s the most common type of cancer! Non-melanoma Skin Cancers Basal Cell Carcinoma Squamous Cell
Acquired melanocytic nevi in Egyptian patients: A clinicopathological study
 Acta Dermatovenerol APA Acta Dermatovenerologica Alpina, Pannonica et Adriatica ;:- doi:.8/v---8 Acquired melanocytic nevi in Egyptian patients: A clinicopathological study Mohamed A. El-Khalawany Abstract
Acta Dermatovenerol APA Acta Dermatovenerologica Alpina, Pannonica et Adriatica ;:- doi:.8/v---8 Acquired melanocytic nevi in Egyptian patients: A clinicopathological study Mohamed A. El-Khalawany Abstract
Regression 2/3/18. Histologically regression is characterized: melanosis fibrosis combination of both. Distribution: partial or focal!
 Regression Margaret Oliviero MSN, ARNP Harold S. Rabinovitz MD Histologically regression is characterized: melanosis fibrosis combination of both Distribution: partial or focal! Dermatoscopic terminology
Regression Margaret Oliviero MSN, ARNP Harold S. Rabinovitz MD Histologically regression is characterized: melanosis fibrosis combination of both Distribution: partial or focal! Dermatoscopic terminology
Melanocytic nevi, commonly referred to as
 Evaluation and Management of Melanocytic Nevi in Children Children with melanocytic nevi require proper counseling to discuss the risk for melanoma. Kara N. Shah, MD, PhD Melanocytic nevi, commonly referred
Evaluation and Management of Melanocytic Nevi in Children Children with melanocytic nevi require proper counseling to discuss the risk for melanoma. Kara N. Shah, MD, PhD Melanocytic nevi, commonly referred
Head and Neck Cancer How to recognize it in your office
 Head and Neck Cancer How to recognize it in your office Peter M Hunt, MD, FACS Associates in ENT/Head & Neck Surgery Director CHI Memorial Head & Neck and Melanoma Centers of Excellence September 8, 2018
Head and Neck Cancer How to recognize it in your office Peter M Hunt, MD, FACS Associates in ENT/Head & Neck Surgery Director CHI Memorial Head & Neck and Melanoma Centers of Excellence September 8, 2018
Histopathology of Melanoma
 THE YALE JOURNAL OF BIOLOGY AND MEDICINE 48, 409-416 (1975) Histopathology of Melanoma G. J. WALKER SMITH Department ofpathology, Yale University School ofmedicine, 333 Cedar Street, New Haven, Connecticut
THE YALE JOURNAL OF BIOLOGY AND MEDICINE 48, 409-416 (1975) Histopathology of Melanoma G. J. WALKER SMITH Department ofpathology, Yale University School ofmedicine, 333 Cedar Street, New Haven, Connecticut
Breslow Thickness and Clark Level Evaluation in Albanian Cutaneous Melanoma
 Research DOI: 10.6003/jtad.16104a2 Breslow Thickness and Clark Level Evaluation in Albanian Cutaneous Melanoma Daniela Xhemalaj, MD, Mehdi Alimehmeti, MD, Susan Oupadia, MD, Majlinda Ikonomi, MD, Leart
Research DOI: 10.6003/jtad.16104a2 Breslow Thickness and Clark Level Evaluation in Albanian Cutaneous Melanoma Daniela Xhemalaj, MD, Mehdi Alimehmeti, MD, Susan Oupadia, MD, Majlinda Ikonomi, MD, Leart
High Risk of Malignant Melanoma in Melanoma-Prone Families with Dysplastic Nevi
 High Risk of Malignant Melanoma in Melanoma-Prone Families with Dysplastic Nevi MARK H. GREENE, M.D.; WALLACE H. CLARK, Jr., M.D.; MARGARET A. TUCKER, M.D.; KENNETH H. KRAEMER, M.D.; DAVID E. ELDER, M.B.,
High Risk of Malignant Melanoma in Melanoma-Prone Families with Dysplastic Nevi MARK H. GREENE, M.D.; WALLACE H. CLARK, Jr., M.D.; MARGARET A. TUCKER, M.D.; KENNETH H. KRAEMER, M.D.; DAVID E. ELDER, M.B.,
Skin Tumors in Children
 AAD San Diego S021 2018 Skin Tumors in Children Jane M. Grant-Kels, MD,FAAD grant@uchc.edu Founding Chair Emeritus, Derm Dept, UCONN Vice Chair Dept of Dermatology Professor of Dermatology, Pathology and
AAD San Diego S021 2018 Skin Tumors in Children Jane M. Grant-Kels, MD,FAAD grant@uchc.edu Founding Chair Emeritus, Derm Dept, UCONN Vice Chair Dept of Dermatology Professor of Dermatology, Pathology and
Skin lesions The Good and the Bad. Dr Virginia Hubbard Ipswich Hospital NHS Trust Barts and the London School of Medicine and Dentistry
 Skin lesions The Good and the Bad Dr Virginia Hubbard Ipswich Hospital NHS Trust Barts and the London School of Medicine and Dentistry Case 1 32 year old woman Australian Lesion on back New hair growing
Skin lesions The Good and the Bad Dr Virginia Hubbard Ipswich Hospital NHS Trust Barts and the London School of Medicine and Dentistry Case 1 32 year old woman Australian Lesion on back New hair growing
They can develop anywhere on the skin and also inside the mouth. They can develop in normal skin or where there is an existing skin mole.
 What are malignant melanomas? Malignant melanomas are one type of skin cancer. They can develop anywhere on the skin and also inside the mouth. They can develop in normal skin or where there is an existing
What are malignant melanomas? Malignant melanomas are one type of skin cancer. They can develop anywhere on the skin and also inside the mouth. They can develop in normal skin or where there is an existing
Identifying Benign and Malignant Skin Lesions. No Disclosures. Common Benign Lesions. Benign Lesions 2/25/2018. Stucco Keratoses.
 Dermatology in Primary Care Identifying Benign and Malignant Skin Lesions Christy Quire Baker, APRN, FNP-BC, DCNP Dermatology Certified Nurse Practitioner No Disclosures Common Benign Lesions Seborrheic
Dermatology in Primary Care Identifying Benign and Malignant Skin Lesions Christy Quire Baker, APRN, FNP-BC, DCNP Dermatology Certified Nurse Practitioner No Disclosures Common Benign Lesions Seborrheic
 Page 1 of 15 Title Authored By Course No Contact Hours 2 Skin Cancer the Real Picture for Early Detection and Treatment Cheryl Sommer RN, MSN, ARNP SC120604 Purpose The purpose of this course is to provide
Page 1 of 15 Title Authored By Course No Contact Hours 2 Skin Cancer the Real Picture for Early Detection and Treatment Cheryl Sommer RN, MSN, ARNP SC120604 Purpose The purpose of this course is to provide
Katsuhiro Yamada, Natsuko Noguti, Masaaki Tsuda, Hazime Nagato, Naoko Hasunuma, Yoshihiro Umebayashi and Motomu Manabe
 Akita J Med 36 : 45-52, 2009 45 Katsuhiro Yamada, Natsuko Noguti, Masaaki Tsuda, Hazime Nagato, Naoko Hasunuma, Yoshihiro Umebayashi and Motomu Manabe (Received 22 December 2008, Accepted 15 January 2009)
Akita J Med 36 : 45-52, 2009 45 Katsuhiro Yamada, Natsuko Noguti, Masaaki Tsuda, Hazime Nagato, Naoko Hasunuma, Yoshihiro Umebayashi and Motomu Manabe (Received 22 December 2008, Accepted 15 January 2009)
Know who is at risk: LOOK! for ABCDs, rapidly changing lesions, do a biopsy when indicated
 Lindy P. Fox, MD Assistant Professor Director, Hospital Consultation Service Department of Dermatology University of California, San Francisco Applies to adults without history of malignancy or premalignant
Lindy P. Fox, MD Assistant Professor Director, Hospital Consultation Service Department of Dermatology University of California, San Francisco Applies to adults without history of malignancy or premalignant
Age and Gender Influences on Partner Assisted Skin Examination for Melanoma
 Age and Gender Influences on Partner Assisted Skin Examination for Melanoma Sara Ortiz, BA 1 ; Susan L Boone, MD 1 ; Jerod Stapleton, BS 2 ; Kimberly Mallet, PhD 2 : Rob Turrisi, PhD 2 ; June K. Robinson,
Age and Gender Influences on Partner Assisted Skin Examination for Melanoma Sara Ortiz, BA 1 ; Susan L Boone, MD 1 ; Jerod Stapleton, BS 2 ; Kimberly Mallet, PhD 2 : Rob Turrisi, PhD 2 ; June K. Robinson,
D thors have presented data on
 DEVELOPMENT AND ELIMINATION OF PIGMENTED MOLES, AND THE ANATOMICAL DISTRIBUTION OF PRIMARY MALIGNANT MELANOMA E. M. NICHOLLS, MD+ In Sydney, Australia, the number of pigmented moles per person increases
DEVELOPMENT AND ELIMINATION OF PIGMENTED MOLES, AND THE ANATOMICAL DISTRIBUTION OF PRIMARY MALIGNANT MELANOMA E. M. NICHOLLS, MD+ In Sydney, Australia, the number of pigmented moles per person increases
Dermoscopy. Sir William Osler. Dermoscopy. Dermoscopy. Melanoma USA Primary Care Update Faculty Disclosure Statement
 Diagnostic Ability: Pigmented Lesions Ted Rosen, MD Baylor College of Medicine Houston, Texas Enhanced 2010 Primary Care Update Faculty Disclosure Statement Ted Rosen, MD Speakers Bureau: Abbott, Amgen,
Diagnostic Ability: Pigmented Lesions Ted Rosen, MD Baylor College of Medicine Houston, Texas Enhanced 2010 Primary Care Update Faculty Disclosure Statement Ted Rosen, MD Speakers Bureau: Abbott, Amgen,
DERMATOLOGY PRACTICAL & CONCEPTUAL. Gabriel Salerni 1,2, Teresita Terán 3, Carlos Alonso 1,2, Ramón Fernández-Bussy 1 ABSTRACT
 DERMATOLOGY PRACTICAL & CONCEPTUAL www.derm101.com The role of dermoscopy and digital dermoscopy follow-up in the clinical diagnosis of melanoma: clinical and dermoscopic features of 99 consecutive primary
DERMATOLOGY PRACTICAL & CONCEPTUAL www.derm101.com The role of dermoscopy and digital dermoscopy follow-up in the clinical diagnosis of melanoma: clinical and dermoscopic features of 99 consecutive primary
Dermoscopy. Enhanced Diagnostic Ability: Pigmented Lesions. Ted Rosen, MD Baylor College of Medicine Houston, Texas
 Dermoscopy Enhanced Diagnostic Ability: Pigmented Lesions Ted Rosen, MD Baylor College of Medicine Houston, Texas Faculty Disclosure Statement No conflicts relevant to this workshop! Sir William Osler
Dermoscopy Enhanced Diagnostic Ability: Pigmented Lesions Ted Rosen, MD Baylor College of Medicine Houston, Texas Faculty Disclosure Statement No conflicts relevant to this workshop! Sir William Osler
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
ISPUB.COM. Seborrheic Keratosis: A Pictorial Review of the Histopathologic Variations. D Sarma, S Repertinger
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 2 Seborrheic Keratosis: A Pictorial Review of the Histopathologic Variations D Sarma, S Repertinger Citation D Sarma, S Repertinger.. The Internet
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 2 Seborrheic Keratosis: A Pictorial Review of the Histopathologic Variations D Sarma, S Repertinger Citation D Sarma, S Repertinger.. The Internet
Know who is at risk: LOOK! for ABCDs, rapidly changing lesions, do a biopsy when indicated
 Lindy P. Fox, MD Associate Professor Director, Hospital Consultation Service Department of Dermatology University of California, San Francisco Applies to adults without history of malignancy or premalignant
Lindy P. Fox, MD Associate Professor Director, Hospital Consultation Service Department of Dermatology University of California, San Francisco Applies to adults without history of malignancy or premalignant
Melanoma What It Is and How To Reduce Your Risk
 www.melanomafocus.com Melanoma What It Is and How To Reduce Your Risk 1 Melanoma What It Is And How To Reduce Your Risk What is melanoma? It is a potentially serious form of cancer, usually starting in
www.melanomafocus.com Melanoma What It Is and How To Reduce Your Risk 1 Melanoma What It Is And How To Reduce Your Risk What is melanoma? It is a potentially serious form of cancer, usually starting in
Skin Cancer. Dr Elizabeth Ogden Associate Specialist in Dermatology East and North Herts Dr Elizabeth Ogden
 Skin Cancer Dr Elizabeth Ogden Associate Specialist in Dermatology East and North Herts 13.10.16 Skin Cancer Melanoma mole cancer - is a true cancer which can metastasize and kill Non Melanoma skin cancer
Skin Cancer Dr Elizabeth Ogden Associate Specialist in Dermatology East and North Herts 13.10.16 Skin Cancer Melanoma mole cancer - is a true cancer which can metastasize and kill Non Melanoma skin cancer
Cutaneous Malignancies: A Primer COPYRIGHT. Marissa Heller, M.D.
 Cutaneous Malignancies: A Primer Marissa Heller, M.D. Associate Director of Dermatologic Surgery Department of Dermatology Beth Israel Deaconess Medical Center December 10, 2016 Skin Cancer Non-melanoma
Cutaneous Malignancies: A Primer Marissa Heller, M.D. Associate Director of Dermatologic Surgery Department of Dermatology Beth Israel Deaconess Medical Center December 10, 2016 Skin Cancer Non-melanoma
Clinical and Pathological Features of Cutaneous Malignant Melanoma: A Retrospective Analysis of 124 Japanese Patients
 Clinical and Pathological Features of Cutaneous Malignant Melanoma: A Retrospective Analysis of 24 Japanese Patients Yoshie Kuno, Kazuyuki Ishihara, Naoya Yamazaki and Kiyoshi Mukai 2 'Dermatology Division
Clinical and Pathological Features of Cutaneous Malignant Melanoma: A Retrospective Analysis of 24 Japanese Patients Yoshie Kuno, Kazuyuki Ishihara, Naoya Yamazaki and Kiyoshi Mukai 2 'Dermatology Division
What is melanoma? Melanoma dealing with the diagnosis. What is melanoma?
 Melanoma is a form of cancer which develops from that part of the skin which produces its colour. It grows from the cell which produces the brown pigment in our skin: the melanocyte. Often the melanoma
Melanoma is a form of cancer which develops from that part of the skin which produces its colour. It grows from the cell which produces the brown pigment in our skin: the melanocyte. Often the melanoma
STUDY. Analysis of the Melanoma Epidemic, Both Apparent and Real
 Analysis of the Melanoma Epidemic, Both Apparent and Real Data From the 1973 Through 1994 Surveillance, Epidemiology, and End Results Program Registry Leslie K. Dennis, PhD STUDY Background: The incidence
Analysis of the Melanoma Epidemic, Both Apparent and Real Data From the 1973 Through 1994 Surveillance, Epidemiology, and End Results Program Registry Leslie K. Dennis, PhD STUDY Background: The incidence
Skin Cancer - Non-Melanoma
 Skin Cancer - Non-Melanoma Introduction Each year, millions of people find out that they have skin cancer. Skin cancer is almost 100% curable if found early and treated right away. It is possible to prevent
Skin Cancer - Non-Melanoma Introduction Each year, millions of people find out that they have skin cancer. Skin cancer is almost 100% curable if found early and treated right away. It is possible to prevent
Atypical Histologic Features in Melanocytic Nevi
 The American Journal of Dermatopathology 22(5): 391 396, 2000 2000 Lippincott Williams & Wilkins, Inc., Philadelphia Atypical Histologic Features in Melanocytic Nevi Carmelo Urso, M.D. The atypical histologic
The American Journal of Dermatopathology 22(5): 391 396, 2000 2000 Lippincott Williams & Wilkins, Inc., Philadelphia Atypical Histologic Features in Melanocytic Nevi Carmelo Urso, M.D. The atypical histologic
