The Identifiable Virtual Patient Model: Comparison of Simulation and Clinical Closed-Loop Study Results
|
|
|
- Hector Curtis
- 5 years ago
- Views:
Transcription
1 Journal of Diabetes Science and Technology Volume 6, Issue 2, March 202 Diabetes Technology Society ORIGINAL ARTICLE The Identifiable Virtual Patient Model: Comparison of Simulation and Clinical Closed-Loop Study Results Sami S., M.S., Stuart A. Weinzimer, M.D., 2 and Garry M. Steil, Ph.D. 3 Abstract Background: Optimizing a closed-loop insulin delivery algorithm for individuals with type diabetes can be potentially facilitated by a mathematical model of the patient. However, model simulation studies that evaluate changes to the control algorithm need to produce conclusions similar to those that would be obtained from a clinical study evaluating the same modification. We evaluated the ability of a low-order identifiable virtual patient (IVP) model to achieve this goal. Methods: Ten adult subjects (42.5 ±.5 years of age; 8.0 ± 3.5 years diabetes; 6.9 ± 0.8% hemoglobin Ac) previously characterized with the IVP model were studied following the procedures independently reported in a pediatric study assessing proportional integral derivative control with and without a 50% meal insulin bolus. Peak postprandial glucose levels with and without the meal bolus and use of supplemental carbohydrate to treat hypoglycemia were compared using two-way analysis of variance and chi-square tests, respectively. Results: The meal bolus decreased the peak postprandial glucose levels in both the adult-simulation and pediatricclinical study (23 ± 38 standard deviation to 205 ± 33 mg/dl and 226 ± 5 to 94 ± 47 mg/dl, respectively; p =.0472). No differences were observed between the peak postprandial levels obtained in the two studies (clinical and simulation study not different, p =.57; interaction p =.83) or in the use of supplemental carbohydrate (3 occurrences in 7 patient days of closed-loop control in the clinical-pediatric study; 7 occurrences over 20 patient days in the adult-simulation study, p =.29). Conclusions: Closed-loop simulations using an IVP model can predict clinical study outcomes in patients studied independently from those used to develop the model. J Diabetes Sci Technol 202;6(2): Author Affiliations: Independent Consultant, Germantown, Maryland; 2 Yale University, New Haven, Connecticut; and 3 Children s Hospital Boston & Harvard Medical School, Boston, Massachusetts Abbreviations: (ANOVA) analysis of variance, (CI) confidence interval, (CIR) carbohydrate-to-insulin ratio, (DIR) daily insulin requirement, (EGP) endogenous glucose production, (FCL) full closed loop, (FIR) finite impulse response, (GEZI) glucose effectiveness at zero insulin, (HbAc) hemoglobin Ac, (HCL) hybrid closed loop, (ISF) interstitial fluid, (IVP) identifiable virtual patient, (MARD) mean absolute relative difference, (NIH) National Institutes of Health, (PID) proportional integral derivative, (PD) pharmacodynamic, (PK) pharmacokinetic, (SC) subcutaneous, (SD) standard deviation, (SG) sensor glucose, (UVA) University of Virginia Keywords: algorithm, artificial pancreas, automated, closed loop, diabetes, insulin delivery, mathematical model Corresponding Author: Garry M. Steil, Ph.D., Children s Hospital Boston, 300 Longwood Avenue, Boston, MA 025; address garry.steil@childrens.harvard.edu 37
2 Introduction Metabolic modeling is widely believed to be essential to achieving a closed-loop insulin delivery system. As algorithms linking glucose-sensing and insulindelivery components become more complex, the ability to optimize design parameters and evaluate changes in system components using animal or clinical studies becomes increasingly impractical. Even the simplest of closed-loop algorithms may have multiple parameters that need to be adjusted. Improvements in the insulin formulation or the means of insulin delivery resulting in a more desirable pharmacokinetic/pharmacodynamic (PK/PD) response may require adjustments in closedloop parameters to capitalize on these developments. Glucose sensors have complex filtering/calibration routines that might also be optimized to effect an improvement in closed-loop performance. Closed-loop control parameters per se could potentially be optimized by empirical adjustments in much the same way as openloop control parameters e.g., glucose correction factors, carbohydrate-to-insulin ratios, basal rates, and insulinon-board are adjusted but changes in closed-loop parameters involve a putative higher risk. Animal studies can be conducted to mitigate some of this risk but animal models have limitations of their own. Insulin PK/ PD profiles, meal absorption profiles, and the diurnal variation in metabolic parameters in any given animal model may not accurately reflect those observed in humans. Generally, research groups seeking to develop closedloop algorithms have developed model simulators in parallel with their closed-loop algorithms, with the models being used to make key decisions in the design process. Examples include metabolic models developed in Karlsberg, Cambridge, 2 University of Virginia (UVA), 3 and Medtronic 4 6 that are paired with controllers developed at these same sites (Karlsburg, 7 Cambridge, 8,9 UVA, 0 and Medtronic 4 ). Of these, the Karlsburg model is now used primarily for optimizing open-loop insulin delivery; 5,6 however, the UVA simulator 3 is the only simulator accepted by the Food and Drug Administration as a replacement for animal studies. The model used to aid in developing the Medtronic proportional integral derivative (PID) algorithm is itself composed of a set of submodels: the identifiable twocompartment model of subcutaneous insulin absorption proposed by Sherwin and colleagues, 7 the so-called minimal model developed by Bergman and Cobelli, 8 2 and a two-compartment model of glucose appearance following meals developed by Hovorka and colleagues. 2 The combined model, termed identifiable virtual patient (IVP) model in this article, was shown to fit data obtained in the initial feasibility study of PID control with no significant residual error and with well-estimated parameters 6 (with initial closed-loop study reported ). Although the ability to fit data is a necessary component of model validation, more stringent criteria can be developed. 22,23 These include the ability of a model to reproduce results obtained in subjects that are independent from those used to develop the model. Ideally, the model should also be able to predict how a change in control parameters might impact an individual subject identified with the model and be able to predict regions of control stability (different combinations of control and patient parameters for which the closed-loop system provides acceptable control). In the present study, we evaluated the ability of the IVP model to satisfy the first of these additional criteria: the ability to reproduce closed-loop study results in subjects who are independent from those used to develop the model. Methods Ten virtual patients, 42.5 ±.5 years of age with diabetes for 8.0 ± 3.5 years, hemoglobin Ac (HbAc) of 6.9 ± 0.8%, and metabolic model parameters reported in the literature 6 were studied (i.e., simulated). Each subject was studied with the protocol and procedures reported in a clinical study of pediatric subjects assessing the impact of adding a meal insulin bolus to the Medtronic PID algorithm. 4 Briefly, in the clinical pediatric study, 2 closed-loop insulin delivery was started at 7 a.m. on day and continued through until 3 p.m. on day 2. Breakfast, lunch, and dinner were served at 8 a.m., 2 p.m., and 5 p.m. each day. Eight subjects were studied without meal boluses [full closed-loop (FCL); subject age: 6.8 ±.6 years, duration of diabetes: 6.9 ± 4.6 years, HbAc: 6.9 ± 0.8%]. Nine subjects were studied with a meal insulin bolus given 0 5 minutes in advance of the meal [hybrid closed-loop (HCL); subject age: 5. ±.0 years, duration of diabetes: 5.7 ± 2.9 years, HbAc: 7.3 ± 0.9%; meal bolus about one-half that which would normally be given to the subject based on their carbohydrate-to-insulin ratio (CIR)]. These procedures were repeated in the simulation study with the exception that each of the 0 adult virtual subjects was studied 372
3 once with FCL and once with HCL. For the simulation subjects, the CIR (g/unit) was obtained as 500/DIR (daily insulin requirement in Units). Meal size was not changed from that reported in the clinical study used to identify the virtual patients. The IVP model is composed of five equations characterizing the subcutaneous (SC) insulin concentration at the catheter site (I SC ), the concentration of insulin in plasma (I P ), insulin s effect (I EFF ) to lower plasma glucose (G), and the rate of appearance of glucose following meals (R A ): di SC (t) dt di P (t) dt di EFF (t) dt = = t I SC (t) + t 2 I P (t) + t ID(t) C I () t 2 I SC (t) (2) = p 2 I EFF (t) + p 2 S I I P (t) (3) dg(t) = (GEZI + I EFF ) G(t) + EGP + R A (t) (4) dt R A (t) = C H (t) V G t t e t t m (5) 2 m Model parameters τ and τ 2, (PK time constants, min); C I (insulin clearance, ml/min); p 2, (time constant for insulin action, min - ); S I (insulin sensitivity, ml/µu/min); GEZI (glucose effectiveness at zero insulin, min - ); EGP (endogenous glucose production, mg/dl/min); V G (glucose distribution volume, dl); and τ m (peak time of meal glucose appearance, one value for each meal) were identified during different time slots of varying length, with values in the first and third slots constrained to be identical (diurnal variation). Parameter values are reported in the original manuscript describing the identification procedure. 6 A glucose sensor was assumed to be placed in a SC interstitial fluid (ISF) fluid compartment described by dg ISF (t) = G ISF (t) + G P (t) (6) dt t SEN t SEN where, G P (t) is defined as the glucose concentration in plasma and G ISF (t) defined as the concentration of glucose in ISF. The ISF delay (τ SEN ) was fixed at 0 min. 24 Sensor glucose (SG) values were obtained each minute and processed in the identical manner to the clinical study. 2 SG was obtained by filtering the ISF signal with a seven-point, low-pass, finite impulse response (FIR) filter and the rate of change of SG (dsg / dt) estimated from an FIR filter, calculating the slope of SG versus time for the precious 5 min. 24 The PID algorithm was also configured identical to that reported for the clinical study, 2 with proportional (P), integral (I), and derivative (D) terms calculated at time points corresponding to minute-to-minute glucose values (time interval denoted as k): P(k) = K P [SG(k) G target ] (7) I(k) = I(k ) + K P T I [SG(k) G target ] (8) D(k) = K P T D dsg/dt(k) (9) PID(k) = P(k) + I(k) + D(k) (0) and integral term (basal) constrained by a wind-up protection routine defined by if SG > 80 mg/dl then I MAXA else if SG 60 mg/dl then I MAX = (G FIL 60) (I MAXA I MAXB ) I MAXB K P 20 else I MAXB () I MAXA was set to the maximum overnight basal rate plus 2.4 U/h, and I MAXB was set to K P (G target 60) to prevent the algorithm from delivering insulin with SG < 60 mg/dl and not increasing Gain K P was set in proportion to the subject s daily insulin requirement: K P =DIR/35000 where DIR is in U/day and the resulting K P is in (U/min)/(mg/dl). Derivative and integration times T D and T I were set to 90 and 450 min during the day (6 a.m. to 0 p.m.), and 60 and 50 min otherwise (night). Target glucose was 00 mg/dl during the day and 20 mg/dl during the night. The integrator initial condition [I(k )] was set to the subject s basal rate at the start of closed-loop control and thereafter constrained to be greater than 0. Although no changes were made in the virtual subject parameters or meal absorption parameters, the timing of each meal was modified to correspond to the timing 373
4 The Identifiable Virtual Patient Model: Comparison of Simulation and Clinical Closed-Loop Study Results in the clinical study. Breakfast, lunch, and dinner were moved from 8 a.m., p.m. and 6 p.m. to 8 a.m., 2 p.m., and 5 p.m. Supplemental carbohydrate (5 g with a peak appearance time τm = 5 min) was given in the event SG fell below 60 mg/dl. One subject was excluded from the simulation analysis for breakfast on day and dinner on day 2 as that subject, in the original closed-loop study, had requested to follow the Atkins diet routine during those meals (negligible carbohydrates with little or no meal response). Statistical Analysis as factors. Need for supplemental carbohydrate to treat hypoglycemia (SG < 60 mg/dl) was compared using a chi-square test. Results are reported as mean ± standard error of the mean unless otherwise noted. Simulations were performed using routines available in Matlab (Math Works, Natick, MA). Statistical analysis (two-way ANOVA, chi-square tests) was performed using GraphPad Prism version 5.04 for Windows (GraphPad Software, San Diego, CA). A posteriori power calculations were performed by Monte Carlo simulation using Mlab (Civilized Software, Silver Spring, MD). Results Presentation of the simulation study results follows that used by Weinzimer and colleagues2 in the report of the pediatric clinical study results, with Figures and 2 from that report reproduced here. Peak postprandial glucose level with and without meal bolus were compared using two-way analysis of variance (ANOVA) with study type (simulation vs clinical) and controller type (FCL vs HCL) Closed-loop control with meal bolus in the adult virtual patients (FCL; Figure A; Table ) resulted in similar peak postprandial glucose values to closed-loop control in the pediatric clinical subjects (Figure 2B; Table 2). This result was obtained despite differences in meal Figure. (A) Left panels show closed-loop simulation results in 0 adult virtual patients. (B) Right panels, adapted from Figure of Weinzimer and colleagues,2 show clinical data obtained in 8 pediatric subjects using the same protocol. Figure 2. (A) Left panel shows simulation of 24 h closed-loop control in 0 virtual adult subjects using FCL and the same algorithm modified by a meal bolus given by the subject 5 min in advance of a meal (HCL). Each subject was simulated twice with the same meal on both occasions. (B) Right panel shows results from a clinical study performed in pediatric subjects. Different patients (n = 8 and 9 for FCL and HCL, respectively) were studied with meals of their choosing (meal size shown in grams). 374
5 sizes [55 ± 27 standard deviations (SD), 88 ± 36, 69 ± 28 for adult virtual subjects vs 68 ± 24, 77 ± 26, and 99 ± 8 for the pediatric subjects; overall amount not different, p =.078 but with interaction, p =.023]. Time between peak insulin delivery and peak plasma insulin concentration during each meal was similar in the simulation and clinical studies but with the magnitude of insulin-delivery and concentrations being about two-thirds that observed in the pediatric clinical study (compare y-axis in lower panels for both). Table. Insulin Delivery and Glycemic Control Parameters in FCL versus HCL Virtual Simulation Study Table 2. Glycemic Control Parameters in FCL and HCL Subjects from Pediatric Clinical Study a a Reprinted with permission from Diabetes Care
6 Analyzed as independent studies, adding a meal bolus 5 min in advance of a meal lowered the peak postprandial glucose from 23 ± 38 to 205 ± 33 mg/dl in the adult simulation study (p =.008; Table ), and from 226 ± 5 to 94 ± 47 mg/dl in the clinical pediatric study (p =.04; Table 2 reproduced from original publication). Combining the simulation and clinical studies together and reanalyzing the data by two-way ANOVA showed the effect of the meal bolus to be significant with p =.047 and with no difference between the simulation and clinical studies (p =.57; interaction, p =.83). There were 3 occurrences of supplemental carbohydrate over 7 patient days in the clinical study versus 7 occurrences over 20 patient days in the simulation study (not different; p =.29, chi-square test). Sensor glucose was in the target range mg/dl 85% of the time in the clinical study versus 7% in the simulation. Mean absolute relative difference (MARD) introduced by the ISF delay and filter routine in the simulation study was 5.9%; MARD estimated from all sources of error was 3.9% in the pediatric clinical study. Discussion The present study showed that a low-order IVP simulator can reproduce clinical study results obtained in a population of subjects that are independent from those used to develop the model. Key observations made in the clinical study 2 used for comparison were that () 85% of all sensor glucose levels were between 70 and 80 mg/dl, (2) there was large intersubject variability in peak post-prandial glucose levels, (3) the closed-loop algorithm did not respond until 5 20 min into the meal, (4) peak insulin concentrations did not occur until 20 min after the meal started, and (5) plasma insulin concentration did not return to basal level until 8 0 h after dinner. These observations were all reproduced in the simulation study with only minor differences noted. Differences that were noted included a slightly lower percent of sensor glucose readings in target range (7 vs 85%, simulation vs clinical) and an increase in the use of supplemental carbohydrates (6 occurrences in 20 patient days vs 3 in 7). The difference in sensor values in the target range could potentially be attributed to the sensor underestimating glucose at high values in the clinical study. 2 Underestimation of sensor glucose can be due to nonlinearities in the sensor response, intrinsic offset in sensor current, or delays in glucose equilibration with ISF. 24 In our simulations, we included the delay in glucose equilibration with the SC ISF but did not simulate an offset in sensor current or nonlinearity in the sensor response. This resulted in a better MARD for the simulation than was reported in the pediatric study (5. vs 3.2%). Despite the better sensor, the virtual subjects still proved to be more difficult to control, with supplemental carbohydrate being used to correct hypoglycemia 7 times during 20 patient days of control in the simulation study and only 3 times in 7 patient days of real control. Although the difference was not statistically significant (p =.29), having a simulator that predicts the need for supplemental carbohydrate may be beneficial when testing algorithms for safety in advance of performing a clinical study. Minor differences were also observed in the relative magnitude of the breakfast versus lunch glucose excursions within each study. The two excursions were of similar magnitude in the simulation study, whereas the lunch excursion was smaller than the breakfast excursion in the clinical study. This may have been due to differences in the meal sizes consumed in each study. The meal sizes in the clinical study used to identify virtual patient subjects and the pediatric study used for comparison 2 were determined by the subjects, with the total amount of carbohydrate not different. However, while the total amount of carbohydrate consumed was not different, the distribution by meal was. Thus, to have the same ratio of breakfast to lunch carbohydrate in the two studies, the pediatric subjects would have had to consume 4% more carbohydrate at lunch in the FCL control subjects and 3% more in the HCL subjects. Still, despite the differences in patient population and relative carbohydrate consumed at each meal, the average closed-loop glucose profiles obtained in the simulation closely matched that of the clinical study despite insulin delivery rates that were approximately one-third less in the virtual subjects. Similar glucose profiles with different insulin delivery rates can be expected for a closed-loop system that adjusts insulin delivery rates to achieve the same target at the same rate. The inability to match all conditions in the simulation to those of the clinical study is nonetheless a limitation in the present study. The differences were, however, unavoidable, as IVP model parameters have not been published for pediatric subjects. Differences in the clinical versus simulation study design, population, and meals, may have masked our ability to detect differences between the simulation and clinical studies, or otherwise have affected the power of our statistical analysis. For example, in the simulation study, the difference in the peak postprandial glucose for breakfast on day 2 was significant [77 mg/dl with 95% confidence interval (CI) 376
7 (55.2 to 99.6); FCL vs HCL], whereas the same comparison in the clinical study was not [32.43 ± with 95% CI ( to 85.6)]. Effectively, the simulation study had more power to detect differences in peak postprandial glucose than the clinical study. However, rather than being an advantage, this suggests that there was an important component on variability that was not captured in the simulation. Conversely, the two-way ANOVA used to evaluate differences between the simulated and clinical results failed to detect differences in the peak postprandial glucose in the simulated and clinical data, raising the possibility that the comparison was underpowered. For the analysis performed, the peak postprandial values for breakfast, lunch, and dinner were combined leaving only study type (simulation vs clinical) and controller type (FCL vs HCL) as factors in the two-way ANOVA. However, combining breakfast, lunch, and dinner resulted in similar values [23 ± 35 (SD) vs 226 ± 5 for FCL, and 205 ± 38 vs 94 ± 47 for HCL]. As the difference was small, just 5 mg/dl for FCL, the power to detect significance was also low (3% estimated from Monte Carlo simulation). We estimate that to have detected a difference between simulated and clinical results, this difference would have needed to be at least 5% (~30 mg/dl) for both the FCL and HCL peak postprandial values (80% power). Given the limitations introduced by the nonmatched patient populations consuming different meals, further validation will be required to validate clinical closed-loop study results that can be reproduced with this simulator. The IVP model represents one of several models that could have been used for the simulations performed here. Other models include the KADIS simulator, the Cambridge simulator, 2 and the simulator developed at UVA. 3 It is not clear if the simulators yield significantly different results. Generally, equations for all the simulators are known but model parameters for individual subjects are often proprietary. The exceptions to this are the parameters for the 0 adult IVP subjects used here (reported in and colleagues) 6 and the 0 patients in each of the adult, pediatric, and child groups described in the UVA patent. 25 Equations for the different models differ primarily in number (model order) and the number of parameters. The trend has been to use high-order models for simulation, 26 although the parameters of such models are unidentifiable from data that is routinely collected in clinical studies (meal information, insulin delivery, and insulin and glucose concentrations). Lower order models are still well accepted for measuring metabolic parameters or as components of model predictive control algorithms. 26 However, low-order models do continue to be used as simulators. The KADIS model, for example, is identifiable from logbook or continuous glucose monitoring data. Once identified, the model is used to perform simulations to optimize open-loop therapy. 27 Although IVP model parameters are identifiable from the same routine data collection, the model is not suited for predicting a single future meal excursion as the model parameters are time-varying. Time-varying parameters were chosen as a basis for the model as it is well known that individuals with type diabetes can have high interand intraday variability in insulin requirements. As the IVP model is set up to capture this variability, it can only be used to predict average glucose responses that would be obtained by an individual on repeated days, or the average results obtained in a study involving multiple subjects. Results from the present study support its ability to predict results obtained across multiple subjects. The model has also been used as a guide in developing modifications to the PID controller, 4 which have been tested and shown to work well in subsequent clinical studies. 3 Nonetheless, given the limitations described earlier (nonmatched patient populations consuming different meals), further validation may still be required to assess its ability to reproduce other closed-loop clinical study results. Components of the IVP model specifically the twocompartment PK model described by Equations () and (2) have been used as components of different control algorithms. The PID closed-loop insulin delivery algorithm developed by Medtronic 3 and the MPC controller developed by Damiano and colleagues 28 both incorporated this characterization of the PK insulin response to predict plasma insulin concentrations during closed-loop insulin delivery. Noteworthy is that in both of these cases, 3,28 model parameters were preset to values obtained from the literature and no attempt was made to adjust or identify them in real time. In the study by Damiano and colleagues, 28 the insulin profiles were not well predicted in some individual cases, leading to poor control. However, when the parameters were retrospectively identified and the subjects studied on a subsequent occasion, both the real-time prediction and resulting control were substantially improved. Generally, closedloop controllers utilizing models as part of the control algorithm can be configured to identify the parameters of the model in real time; however, the ability of the real-time identification algorithms to track time-varying parameters needs to be carefully assessed. Subjects with parameters that differ substantially may need their parameters to be set off-line. 377
8 In summary, results presented in the original IVP model development and identification study 6 showed that the IVP model can be identified from routine insulin, glucose, and meal data. The present study showed that once a population of virtual patients is identified, that population can be used to perform closed-loop studies with the expected result not statistically different from that which would be obtained in a clinical study. Additional validation of the model, however, is required to confirm that the model can be used to optimize control in an individual subject or identify regions of control stability for the individual. Funding: This work was supported by National Institutes of Health (NIH) Grant #RO-DK6470 (Garry Steil). Stuart Weinzimer is supported by NIH Grant #R0 DK08568 and Juvenile Diabetes Research Fund Grant # Disclosures: Garry Steil and Sami were employed by Medtronic MiniMed during the performance of the clinical studies used to develop the IVP model and both have coauthored patents assigned to Medtronic. References:. Fischer U, Salzsieder E, Jutzi E, Albrecht G, Freyse EJ. Modelling the glucose-insulin system as a basis for the artificial beta cell. Biomed Biochim Acta. 984;43(5): Wilinska ME, Chassin LJ, Acerini CL, Allen JM, Dunger DB, Hovorka R. Simulation environment to evaluate closed-loop insulin delivery systems in type diabetes. J Diabetes Sci Technol. 200;4(): Kovatchev BP, Breton M, Dalla Man C, Cobelli C. In silico preclinical trials: a proof of concept in closed-loop control of type diabetes. J Diabetes Sci Technol. 2009;3(): Stocker D, S, Cortina GJ, Nitzan T, Plummer J, Steil GM, Mastrototaro J, inventors; Medtronic MiniMed, Inc., assignee. Virtual patient software system for educating and treating individuals with diabetes. United States patent application US 2006/ December Steil GM, Clark B, S, Rebrin K. Modeling insulin action for development of a closed-loop artificial pancreas. Diabetes Technol. Ther ;7(): S, Weinzimer S, Voskanyan G, Steil GM. Identification of intraday metabolic profiles during closed-loop glucose control in individuals with type diabetes. J Diabetes Sci Technol. 2009;3(5): Rebrin K, Fischer U, von Woedtke T, Abel P, Brunstein E. Automated feedback control of subcutaneous glucose concentration in diabetic dogs. Diabetologia. 989;32(8): Hovorka R, Allen JM, Elleri D, Chassin LJ, Harris J, Xing D, Kollman C, Hovorka T, Larsen AM, Nodale M, De Palma A, Wilinska ME, Acerini CL, Dunger DB. Manual closed-loop insulin delivery in children and adolescents with type diabetes: a phase 2 randomised crossover trial. Lancet. 200;375(976): Elleri D, Allen JM, Nodale M, Wilinska ME, Mangat JS, Larsen AM, Acerini CL, Dunger DB, Hovorka R. Automated overnight closedloop glucose control in young children with type diabetes. Diabetes Technol Ther. 20;3(4): Clarke WL, Anderson S, Breton M, Patek S, Kashmer L, Kovatchev B. Closed-loop artificial pancreas using subcutaneous glucose sensing and insulin delivery and a model predictive control algorithm: the Virginia experience. J Diabetes Sci Technol. 2009;3(5): Steil GM, Rebrin K, Darwin C, Hariri F, Saad MF. Feasibility of automating insulin delivery for the treatment of type diabetes. Diabetes. 2006;55(2): Weinzimer SA, Steil GM, Swan KL, Dziura J, Kurtz N, Tamborlane WV. Fully automated closed-loop insulin delivery versus semiautomated hybrid control in pediatric patients with type diabetes using an artificial pancreas. Diabetes Care. 2008;3(5): Steil GM, Palerm CC, Kurtz N, Voskanyan G, Roy A, Paz S, Kandeel FR. The effect of insulin feedback on closed loop glucose control. J Clin Endocrinol Metab. 20;96(5): S, Steil GM, inventors; Medtronic MiniMed, Inc., assignee. Apparatus and method for controlling insulin infusion with state variable feedback. United States patent US 7,806, Oct Augstein P, Vogt L, Kohnert KD, Heinke P, Salzsieder E. Translation of personalized decision support into routine diabetes care. J Diabetes Sci Technol. 200;4(6): Salzsieder E, Vogt L, Kohnert KD, Heinke P, Augstein P. Model-based decision support in diabetes care. Comput Methods Programs Biomed. 20;02(2): Insel PA, Kramer KJ, Sherwin RS, Liljenquist JE, Tobin JD, Andres R, Berman M. Modeling the insulin-glucose system in man. Fed Proc. 974;33(7):
9 8. Bergman RN, Ider YZ, Bowden CR, Cobelli C. Quantitative estimation of insulin sensitivity. Am J Physiol. 979;236(6):E Bergman RN, Phillips LS, Cobelli C. Physiologic evaluation of factors controlling glucose tolerance in man: measurement of insulin sensitivity and beta-cell glucose sensitivity from the response to intravenous glucose. J Clin Invest. 98;68(6): Bergman RN. Lilly lecture 989. Toward physiological understanding of glucose tolerance. Minimal- model approach. Diabetes. 989;38(2): Bergman RN. Minimal model: perspective from Horm Res. 2005;64(Suppl 3): Steil GM, Reifman J. Mathematical modeling research to support the development of automated insulin-delivery systems. J Diabetes Sci Technol. 2009;3(2): Steil GM, Hipszer B, Reifman J. Update on mathematical modeling research to support the development of automated insulin delivery systems. J Diabetes Sci Technol. 200;4(3): Rebrin K, Sheppard NF, Steil GM. Use of subcutaneous interstitial fluid glucose to estimate blood glucose: revisiting delay and sensor offset. J Diabetes Sci Technol. 200;4(5): Kovatchev BP, Breton MD, Cobelli C, Dalla Man C, inventors; University of Virginia Patent Foundation, assignee. Method, system and computer simulation environment for testing of monitoring and control strategies in diabetes. United States patent application US 200/ July Cobelli C, Dalla Man C, Sparacino G, Magni L, De Nicolao G, Kovatchev BP. Diabetes: models, signals, and control. IEEE Rev Biomed Eng. 2009;2: Salzsieder E, Vogt L, Kohnert KD, Heinke P, Augstein P. Modelbased decision support in diabetes care. Comput Methods Programs Biomed. 20;02(2): El-Khatib FH, Russell SJ, Nathan DM, Sutherlin RG, Damiano ER. A bihormonal closed-loop artificial pancreas for type diabetes. Sci Transl Med. 200;4;2(27):27ra
Effect of Insulin Feedback on Closed-Loop Glucose Control: A Crossover Study
 Journal of Diabetes Science and Technology Volume 6, Issue 5, September 2012 Diabetes Technology Society ORIGINAL ARTICLE Effect of Insulin Feedback on Closed-Loop Glucose Control: A Crossover Study Jessica
Journal of Diabetes Science and Technology Volume 6, Issue 5, September 2012 Diabetes Technology Society ORIGINAL ARTICLE Effect of Insulin Feedback on Closed-Loop Glucose Control: A Crossover Study Jessica
Closed-Loop Insulin Delivery Utilizing Pole Placement to Compensate for Delays in Subcutaneous Insulin Delivery
 Journal of Diabetes Science and Technology Volume 5, Issue 6, November 2011 Diabetes Technology Society SYMPOSIUM Closed-Loop Insulin Delivery Utilizing Pole Placement to Compensate for Delays in Subcutaneous
Journal of Diabetes Science and Technology Volume 5, Issue 6, November 2011 Diabetes Technology Society SYMPOSIUM Closed-Loop Insulin Delivery Utilizing Pole Placement to Compensate for Delays in Subcutaneous
Advancing closed-loop insulin delivery into a product. The Effect of Insulin Feedback on Closed Loop Glucose Control
 ORIGINAL Endocrine ARTICLE Research The Effect of Insulin Feedback on Closed Loop Glucose Control Garry M. Steil, Cesar C. Palerm, Natalie Kurtz, Gayane Voskanyan, Anirban Roy, Sachiko Paz, and Fouad R.
ORIGINAL Endocrine ARTICLE Research The Effect of Insulin Feedback on Closed Loop Glucose Control Garry M. Steil, Cesar C. Palerm, Natalie Kurtz, Gayane Voskanyan, Anirban Roy, Sachiko Paz, and Fouad R.
Abstract. Srinivas Laxminarayan, Ph.D., 1 Jaques Reifman, Ph.D., 1 and Garry M. Steil, Ph.D. 2 ORIGINAL ARTICLE. Background: Methods: Results:
 Journal of Diabetes Science and Technology Volume 6, Issue 6, November 2012 Diabetes Technology Society ORIGINAL ARTICLE Use of a Food and Drug Administration-Approved Type 1 Diabetes Mellitus Simulator
Journal of Diabetes Science and Technology Volume 6, Issue 6, November 2012 Diabetes Technology Society ORIGINAL ARTICLE Use of a Food and Drug Administration-Approved Type 1 Diabetes Mellitus Simulator
Continuous Glucose Monitoring Considerations for the Development of a Closed-Loop Artificial Pancreas System
 Journal of Diabetes Science and Technology Volume 5, Issue 6, November 2011 Diabetes Technology Society SYMPOSIUM Continuous Glucose Monitoring Considerations for the Development of a Closed-Loop Artificial
Journal of Diabetes Science and Technology Volume 5, Issue 6, November 2011 Diabetes Technology Society SYMPOSIUM Continuous Glucose Monitoring Considerations for the Development of a Closed-Loop Artificial
Fully Automated Closed-Loop Insulin Delivery vs. Semi-Automated Hybrid Control in Pediatric Patients with Type 1 Diabetes using an Artificial Pancreas
 Diabetes Care Publish Ahead of Print, published online February 5, 2008 Fully Automated Closed-Loop Insulin Delivery vs. Semi-Automated Hybrid Control in Pediatric Patients with Type 1 Diabetes using an
Diabetes Care Publish Ahead of Print, published online February 5, 2008 Fully Automated Closed-Loop Insulin Delivery vs. Semi-Automated Hybrid Control in Pediatric Patients with Type 1 Diabetes using an
A Closed-Loop Artificial Pancreas Using Model Predictive Control and a Sliding Meal Size Estimator. Abstract. Introduction
 Journal of Diabetes Science and Technology Volume 3, Issue 5, September 2009 Diabetes Technology Society SYMPOSIUM A Closed-Loop Artificial Pancreas Using Model Predictive Control and a Sliding Meal Size
Journal of Diabetes Science and Technology Volume 3, Issue 5, September 2009 Diabetes Technology Society SYMPOSIUM A Closed-Loop Artificial Pancreas Using Model Predictive Control and a Sliding Meal Size
Factors Influencing the Effectiveness of Glucagon for Preventing Hypoglycemia
 Journal of Diabetes Science and Technology Volume 4, Issue 6, November 2010 Diabetes Technology Society SYMPOSIUM Factors Influencing the Effectiveness of Glucagon for Preventing Hypoglycemia Jessica R.,
Journal of Diabetes Science and Technology Volume 4, Issue 6, November 2010 Diabetes Technology Society SYMPOSIUM Factors Influencing the Effectiveness of Glucagon for Preventing Hypoglycemia Jessica R.,
Bolus Estimation Rethinking the Effect of Meal Fat Content
 Bolus Estimation Rethinking the Effect of Meal Fat Content The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published
Bolus Estimation Rethinking the Effect of Meal Fat Content The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published
Diabetes Care 31: , 2008
 Emerging Treatments and Technologies O R I G I N A L A R T I C L E Fully Automated Closed-Loop Insulin Delivery Versus Semiautomated Hybrid Control in Pediatric Patients With Type 1 Diabetes Using an Artificial
Emerging Treatments and Technologies O R I G I N A L A R T I C L E Fully Automated Closed-Loop Insulin Delivery Versus Semiautomated Hybrid Control in Pediatric Patients With Type 1 Diabetes Using an Artificial
Diabetes Management: Current High Tech Innovations
 Diabetes Management: Current High Tech Innovations How Far We ve Come in the Last 40 Years William V. Tamborlane, MD Department of Pediatrics Yale School of Medicine Disclosures I am a consultant for:
Diabetes Management: Current High Tech Innovations How Far We ve Come in the Last 40 Years William V. Tamborlane, MD Department of Pediatrics Yale School of Medicine Disclosures I am a consultant for:
Mathematical Modeling Research to Support the Development of Automated Insulin-Delivery Systems
 Journal of Diabetes Science and Technology Volume 3, Issue 2, March 2009 Diabetes Technology Society MEETING PROCEEDINGS Mathematical Modeling Research to Support the Development of Automated Insulin-Delivery
Journal of Diabetes Science and Technology Volume 3, Issue 2, March 2009 Diabetes Technology Society MEETING PROCEEDINGS Mathematical Modeling Research to Support the Development of Automated Insulin-Delivery
Model-Based Sensor-Augmented Pump Therapy
 Journal of Diabetes Science and Technology Volume 7, Issue 2, March 2013 Diabetes Technology Society TECHNOLOGY REPORT Model-Based Sensor-Augmented Pump Therapy Benyamin, Ph.D., Gayane Voskanyan, Ph.D.,
Journal of Diabetes Science and Technology Volume 7, Issue 2, March 2013 Diabetes Technology Society TECHNOLOGY REPORT Model-Based Sensor-Augmented Pump Therapy Benyamin, Ph.D., Gayane Voskanyan, Ph.D.,
Research Proposal. 1. Background and Rationale
 1. Background and Rationale Insulin is secreted by the pancreatic beta cells and reduces blood glucose concentration (1). Glucagon is secreted by the pancreatic alpha cells and increases glucose concentration.
1. Background and Rationale Insulin is secreted by the pancreatic beta cells and reduces blood glucose concentration (1). Glucagon is secreted by the pancreatic alpha cells and increases glucose concentration.
Real-Time State Estimation and Long-Term Model Adaptation: A Two-Sided Approach toward Personalized Diagnosis of Glucose and Insulin Levels
 Journal of Diabetes Science and Technology Volume 6, Issue 5, September 202 Diabetes Technology Society ORIGINAL ARTICLE Real-Time State Estimation and Long-Term Model Adaptation: A Two-Sided Approach
Journal of Diabetes Science and Technology Volume 6, Issue 5, September 202 Diabetes Technology Society ORIGINAL ARTICLE Real-Time State Estimation and Long-Term Model Adaptation: A Two-Sided Approach
Carbohydrate Ratio Optimization and Adaptation Algorithm. Supplementary Figure 1. Schematic showing components of the closed-loop system.
 Basal Profile Adaptation Algorithm Carbohydrate Ratio Optimization and Adaptation Algorithm Supplementary Figure 1. Schematic showing components of the closed-loop system. The insulin pump and Dexcom G4
Basal Profile Adaptation Algorithm Carbohydrate Ratio Optimization and Adaptation Algorithm Supplementary Figure 1. Schematic showing components of the closed-loop system. The insulin pump and Dexcom G4
A Composite Model of Glucagon Glucose Dynamics for In Silico Testing of Bihormonal Glucose Controllers
 Journal of Diabetes Science and Technology Volume 7, Issue 4, July 2013 Diabetes Technology Society ORIGINAL ARTICLE A Composite Model of Glucagon Glucose Dynamics for In Silico Testing of Bihormonal Glucose
Journal of Diabetes Science and Technology Volume 7, Issue 4, July 2013 Diabetes Technology Society ORIGINAL ARTICLE A Composite Model of Glucagon Glucose Dynamics for In Silico Testing of Bihormonal Glucose
Insulin Administration for People with Type 1 diabetes
 Downloaded from orbit.dtu.dk on: Nov 17, 1 Insulin Administration for People with Type 1 diabetes Boiroux, Dimitri; Finan, Daniel Aaron; Poulsen, Niels Kjølstad; Madsen, Henrik; Jørgensen, John Bagterp
Downloaded from orbit.dtu.dk on: Nov 17, 1 Insulin Administration for People with Type 1 diabetes Boiroux, Dimitri; Finan, Daniel Aaron; Poulsen, Niels Kjølstad; Madsen, Henrik; Jørgensen, John Bagterp
NEW GENERATION CLOSED LOOP INSULIN DELIVERY SYSTEM
 NEW GENERATION CLOSED LOOP INSULIN DELIVERY SYSTEM Owais 1, Dawood A. Khan 2 1 Research Scholar, Department of Computer Science, University of Kashmir 2 Assistant Professor, Department of Computer Science,
NEW GENERATION CLOSED LOOP INSULIN DELIVERY SYSTEM Owais 1, Dawood A. Khan 2 1 Research Scholar, Department of Computer Science, University of Kashmir 2 Assistant Professor, Department of Computer Science,
Closing the loop, squaring the circle: Studies on insulin delivery, glucose monitoring and the artificial pancreas Luijf, Y.M.
 UvA-DARE (Digital Academic Repository) Closing the loop, squaring the circle: Studies on insulin delivery, glucose monitoring and the artificial pancreas Luijf, Y.M. Link to publication Citation for published
UvA-DARE (Digital Academic Repository) Closing the loop, squaring the circle: Studies on insulin delivery, glucose monitoring and the artificial pancreas Luijf, Y.M. Link to publication Citation for published
IDENTIFICATION OF LINEAR DYNAMIC MODELS FOR TYPE 1 DIABETES: A SIMULATION STUDY
 IDENTIFICATION OF LINEAR DYNAMIC MODELS FOR TYPE 1 DIABETES: A SIMULATION STUDY Daniel A. Finan Howard Zisser Lois Jovanovic Wendy C. Bevier Dale E. Seborg Department of Chemical Engineering University
IDENTIFICATION OF LINEAR DYNAMIC MODELS FOR TYPE 1 DIABETES: A SIMULATION STUDY Daniel A. Finan Howard Zisser Lois Jovanovic Wendy C. Bevier Dale E. Seborg Department of Chemical Engineering University
Reduced Hypoglycemia and Increased Time in Target Using Closed-Loop Insulin Delivery During Nights With or Without Antecedent Afternoon Exercise
 Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Reduced Hypoglycemia and Increased Time in Target Using Closed-Loop Insulin Delivery During Nights With or Without
Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Reduced Hypoglycemia and Increased Time in Target Using Closed-Loop Insulin Delivery During Nights With or Without
Model Identification Using Stochastic Differential Equation Grey-Box Models in Diabetes
 Journal of Diabetes Science and Technology Volume 7, Issue 2, March 2013 Diabetes Technology Society ORIGINAL ARTICLE Model Identification Using Stochastic Differential Equation Grey-Box Models in Diabetes
Journal of Diabetes Science and Technology Volume 7, Issue 2, March 2013 Diabetes Technology Society ORIGINAL ARTICLE Model Identification Using Stochastic Differential Equation Grey-Box Models in Diabetes
Preventing Hypoglycemia Using Predictive Alarm Algorithms and Insulin Pump Suspension
 DIABETES TECHNOLOGY & THERAPEUTICS Volume 11, Number 2, 29 Mary Ann Liebert, Inc. DOI: 1.189/dia.28.32 Preventing Hypoglycemia Using Predictive Alarm Algorithms and Insulin Pump Suspension Bruce Buckingham,
DIABETES TECHNOLOGY & THERAPEUTICS Volume 11, Number 2, 29 Mary Ann Liebert, Inc. DOI: 1.189/dia.28.32 Preventing Hypoglycemia Using Predictive Alarm Algorithms and Insulin Pump Suspension Bruce Buckingham,
IJESRT INTERNATIONAL JOURNAL OF ENGINEERING SCIENCES & RESEARCH TECHNOLOGY PID CONTROLLER FOR BLOOD GLUCOSE CONTROL Ajmal M M *, C R Srinivasan *
 [Ajmal* et al., 6(3): March, 217] Impact Factor: 4.116 IC Value: 3. IJESRT INTERNATIONAL JOURNAL OF ENGINEERING SCIENCES & RESEARCH TECHNOLOGY PID CONTROLLER FOR BLOOD GLUCOSE CONTROL Ajmal M M *, C R
[Ajmal* et al., 6(3): March, 217] Impact Factor: 4.116 IC Value: 3. IJESRT INTERNATIONAL JOURNAL OF ENGINEERING SCIENCES & RESEARCH TECHNOLOGY PID CONTROLLER FOR BLOOD GLUCOSE CONTROL Ajmal M M *, C R
VIRTUAL PATIENTS DERIVED FROM THE
 VIRTUAL PATIENTS DERIVED FROM THE CARELINK DATABASE Benyamin Grosman PhD Senior Principle Scientist Medtronic Diabetes WHY VIRTUAL PATIENT MODELING? Reduce the cost of clinical trials Use models in conjunction
VIRTUAL PATIENTS DERIVED FROM THE CARELINK DATABASE Benyamin Grosman PhD Senior Principle Scientist Medtronic Diabetes WHY VIRTUAL PATIENT MODELING? Reduce the cost of clinical trials Use models in conjunction
Artificial Pancreas Device Systems. Populations Interventions Comparators Outcomes. pump. pump
 Protocol Artificial Pancreas Device Systems (10130) Medical Benefit Effective Date: 04/01/18 Next Review Date: 01/19 Preauthorization Yes Review Dates: 03/15, 03/16, 03/17, 01/18 Preauthorization is required.
Protocol Artificial Pancreas Device Systems (10130) Medical Benefit Effective Date: 04/01/18 Next Review Date: 01/19 Preauthorization Yes Review Dates: 03/15, 03/16, 03/17, 01/18 Preauthorization is required.
Artificial Pancreas Systems: An Integrated Multivariable Adaptive Approach
 Preprints of the 19th World Congress The International Federation of Automatic Control Cape Town, South Africa August 24-29, 2014 Artificial Pancreas Systems: An Integrated Multivariable Adaptive Approach
Preprints of the 19th World Congress The International Federation of Automatic Control Cape Town, South Africa August 24-29, 2014 Artificial Pancreas Systems: An Integrated Multivariable Adaptive Approach
Reconstruction of Glucose in Plasma from Interstitial Fluid Continuous Glucose Monitoring Data: Role of Sensor Calibration
 Journal of Diabetes Science and Technology Volume 1, Issue 5, September 2007 Diabetes Technology Society SYMPOSIUM Reconstruction of Glucose in Plasma from Interstitial Fluid Continuous Glucose Monitoring
Journal of Diabetes Science and Technology Volume 1, Issue 5, September 2007 Diabetes Technology Society SYMPOSIUM Reconstruction of Glucose in Plasma from Interstitial Fluid Continuous Glucose Monitoring
In Silico Preclinical Trials: Methodology and Engineering Guide to Closed-Loop Control in Type 1 Diabetes Mellitus
 Journal of Diabetes Science and Technology Volume 3, Issue 2, March 2009 Diabetes Technology Society ORIGINAL ARTICLES In Silico Preclinical Trials: Methodology and Engineering Guide to Closed-Loop Control
Journal of Diabetes Science and Technology Volume 3, Issue 2, March 2009 Diabetes Technology Society ORIGINAL ARTICLES In Silico Preclinical Trials: Methodology and Engineering Guide to Closed-Loop Control
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Phillip M, Battelino T, Atlas E, et al. Nocturnal glucose control
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Phillip M, Battelino T, Atlas E, et al. Nocturnal glucose control
Simulation Environment to Evaluate Closed-Loop Insulin Delivery Systems in Type 1 Diabetes
 Journal of Diabetes Science and Technology Volume 4, Issue 1, January 2010 Diabetes Technology Society ORIGINAL ARTICLES Simulation Environment to Evaluate Closed-Loop Insulin Delivery Systems in Type
Journal of Diabetes Science and Technology Volume 4, Issue 1, January 2010 Diabetes Technology Society ORIGINAL ARTICLES Simulation Environment to Evaluate Closed-Loop Insulin Delivery Systems in Type
DESIGN AND CONTROL OF THE ARTIFICAL PANCREAS
 DESIGN AND CONTROL OF THE ARTIFICAL PANCREAS Eyal Dassau, Rebecca A. Harvey, Justin Lee, Howard Zisser and Francis J. Doyle III * Department of Chemical Engineering; University of California, Santa Barbara,
DESIGN AND CONTROL OF THE ARTIFICAL PANCREAS Eyal Dassau, Rebecca A. Harvey, Justin Lee, Howard Zisser and Francis J. Doyle III * Department of Chemical Engineering; University of California, Santa Barbara,
Proposed Clinical Application for Tuning Fuzzy Logic Controller of Artificial Pancreas utilizing a Personalization Factor
 Proposed Clinical Application for Tuning Fuzzy Logic Controller of Artificial Pancreas utilizing a Personalization Factor Richard Mauseth M.D 1,2, Youqing Wang 3,4,5, Eyal Dassau 3,4,5, Robert Kircher
Proposed Clinical Application for Tuning Fuzzy Logic Controller of Artificial Pancreas utilizing a Personalization Factor Richard Mauseth M.D 1,2, Youqing Wang 3,4,5, Eyal Dassau 3,4,5, Robert Kircher
Artificial Pancreas Device Systems. Populations Interventions Comparators Outcomes Individuals: With type 1 diabetes
 Protocol Artificial Pancreas Device Systems Medical Benefit Effective Date: 07/01/18 Next Review Date: 01/20 Preauthorization Yes Review Dates: 03/15, 03/16, 03/17, 01/18, 05/18, 01/19 Preauthorization
Protocol Artificial Pancreas Device Systems Medical Benefit Effective Date: 07/01/18 Next Review Date: 01/20 Preauthorization Yes Review Dates: 03/15, 03/16, 03/17, 01/18, 05/18, 01/19 Preauthorization
Diabetes Care Publish Ahead of Print, published online November 18, 2008
 Diabetes Care Publish Ahead of Print, published online November 18, 2008 Effect of Age of Infusion Site and Type of Rapid-Acting Analog on Pharmacodynamic Parameters of Insulin Boluses in Youth with TIDM
Diabetes Care Publish Ahead of Print, published online November 18, 2008 Effect of Age of Infusion Site and Type of Rapid-Acting Analog on Pharmacodynamic Parameters of Insulin Boluses in Youth with TIDM
The artificial pancreas: the next step in connectivity and digital treatment of type 1 diabetes
 The artificial pancreas: the next step in connectivity and digital treatment of type 1 diabetes Roman Hovorka PhD FMedSci University of Cambridge, UK Duality of interest declaration Advisory Panel: Research
The artificial pancreas: the next step in connectivity and digital treatment of type 1 diabetes Roman Hovorka PhD FMedSci University of Cambridge, UK Duality of interest declaration Advisory Panel: Research
The oral meal or oral glucose tolerance test. Original Article Two-Hour Seven-Sample Oral Glucose Tolerance Test and Meal Protocol
 Original Article Two-Hour Seven-Sample Oral Glucose Tolerance Test and Meal Protocol Minimal Model Assessment of -Cell Responsivity and Insulin Sensitivity in Nondiabetic Individuals Chiara Dalla Man,
Original Article Two-Hour Seven-Sample Oral Glucose Tolerance Test and Meal Protocol Minimal Model Assessment of -Cell Responsivity and Insulin Sensitivity in Nondiabetic Individuals Chiara Dalla Man,
Hypoglycemia Detection and Prediction Using Continuous Glucose Monitoring A Study on Hypoglycemic Clamp Data
 Journal of Diabetes Science and Technology Volume 1, Issue 5, September 2007 Diabetes Technology Society SYMPOSIUM Hypoglycemia Detection and Prediction Using Continuous Glucose Monitoring A Study on Hypoglycemic
Journal of Diabetes Science and Technology Volume 1, Issue 5, September 2007 Diabetes Technology Society SYMPOSIUM Hypoglycemia Detection and Prediction Using Continuous Glucose Monitoring A Study on Hypoglycemic
Optimal treatment of type 1 diabetes should. Original Article Feasibility of Automating Insulin Delivery for the Treatment of Type 1 Diabetes
 Original Article Feasibility of Automating Insulin Delivery for the Treatment of Type 1 Diabetes Garry M. Steil, 1 Kerstin Rebrin, 1 Christine Darwin, 2 Farzam Hariri, 2 and Mohammed F. Saad 3 An automated
Original Article Feasibility of Automating Insulin Delivery for the Treatment of Type 1 Diabetes Garry M. Steil, 1 Kerstin Rebrin, 1 Christine Darwin, 2 Farzam Hariri, 2 and Mohammed F. Saad 3 An automated
Agreement between Glucose Trends Derived from Three Simultaneously Worn Continuous Glucose Sensors
 Journal of Diabetes Science and Technology Volume 2, Issue 5, September 2008 Diabetes Technology Society ORIGINAL ARTICLES Agreement between Glucose Trends Derived from Three Simultaneously Worn Continuous
Journal of Diabetes Science and Technology Volume 2, Issue 5, September 2008 Diabetes Technology Society ORIGINAL ARTICLES Agreement between Glucose Trends Derived from Three Simultaneously Worn Continuous
JDRF Perspective on Closed Loop
 JDRF Perspective on Closed Loop Aaron J. Kowalski, Ph.D. Assistant Vice President Treatment Therapies Juvenile Diabetes Research Foundation International 1 Presenter Disclosure Aaron Kowalski Disclosed
JDRF Perspective on Closed Loop Aaron J. Kowalski, Ph.D. Assistant Vice President Treatment Therapies Juvenile Diabetes Research Foundation International 1 Presenter Disclosure Aaron Kowalski Disclosed
Active Insulin Infusion Using Fuzzy-Based Closed-loop Control
 Active Insulin Infusion Using Fuzzy-Based Closed-loop Control Sh. Yasini, M. B. Naghibi-Sistani, A. Karimpour Department of Electrical Engineering, Ferdowsi University of Mashhad, Mashhad, Iran E-mail:
Active Insulin Infusion Using Fuzzy-Based Closed-loop Control Sh. Yasini, M. B. Naghibi-Sistani, A. Karimpour Department of Electrical Engineering, Ferdowsi University of Mashhad, Mashhad, Iran E-mail:
Outpatient Glycemic Control with a Bionic Pancreas in Type 1 Diabetes
 original article Outpatient Glycemic with a Bionic Pancreas in Type 1 Diabetes Steven J. Russell, M.D., Ph.D., Firas H. El-Khatib, Ph.D., Manasi Sinha, M.D., M.P.H., Kendra L. Magyar, M.S.N., N.P., Katherine
original article Outpatient Glycemic with a Bionic Pancreas in Type 1 Diabetes Steven J. Russell, M.D., Ph.D., Firas H. El-Khatib, Ph.D., Manasi Sinha, M.D., M.P.H., Kendra L. Magyar, M.S.N., N.P., Katherine
Anomaly Detection in the Artificial Pancreas
 Anomaly Detection in the Artificial Pancreas Avila L., Martínez E. INGAR (CONICET-UTN) Abstract The integration of subcutaneous sensing and insulin delivery technologies with novel control strategies has
Anomaly Detection in the Artificial Pancreas Avila L., Martínez E. INGAR (CONICET-UTN) Abstract The integration of subcutaneous sensing and insulin delivery technologies with novel control strategies has
Novel Formulations to Modify Mealtime Insulin Kinetics
 Novel Formulations to Modify Mealtime Insulin Kinetics Alan Krasner, Roderike Pohl, Patrick Simms, Philip Pichotta, Robert Hauser, Errol De Souza Biodel, Inc. Danbury, CT Disclosure All authors are employees
Novel Formulations to Modify Mealtime Insulin Kinetics Alan Krasner, Roderike Pohl, Patrick Simms, Philip Pichotta, Robert Hauser, Errol De Souza Biodel, Inc. Danbury, CT Disclosure All authors are employees
Overnight Closed-Loop Insulin Delivery with Model Predictive Control: Assessment of Hypoglycemia and Hyperglycemia Risk Using Simulation Studies
 Journal of Diabetes Science and Technology Volume 3, Issue 5, September 2009 Diabetes Technology Society SYMPOSIUM Overnight Closed-Loop Insulin Delivery with Model Predictive Control: Assessment of Hypoglycemia
Journal of Diabetes Science and Technology Volume 3, Issue 5, September 2009 Diabetes Technology Society SYMPOSIUM Overnight Closed-Loop Insulin Delivery with Model Predictive Control: Assessment of Hypoglycemia
A Prospective Evaluation of Insulin Dosing Recommendations in Patients with Type 1 Diabetes at Near Normal Glucose Control: Bolus Dosing
 Journal of Diabetes Science and Technology Volume 1, Issue 1, January 2007 Diabetes Technology Society ORIGINAL ARTICLES A Prospective Evaluation of Insulin Dosing Recommendations in Patients with Type
Journal of Diabetes Science and Technology Volume 1, Issue 1, January 2007 Diabetes Technology Society ORIGINAL ARTICLES A Prospective Evaluation of Insulin Dosing Recommendations in Patients with Type
Achieving Open-loop Insulin Delivery using ITM Designed for T1DM Patients
 I. J. Computer Network and Information Security, 2012, 1, 52-58 Published Online February 2012 in MECS (http://www.mecs-press.org/) DOI: 10.5815/ijcnis.2012.01.07 Achieving Open-loop Insulin Delivery using
I. J. Computer Network and Information Security, 2012, 1, 52-58 Published Online February 2012 in MECS (http://www.mecs-press.org/) DOI: 10.5815/ijcnis.2012.01.07 Achieving Open-loop Insulin Delivery using
Inpatient Studies of a Kalman-Filter-Based Predictive Pump Shutoff Algorithm
 Journal of Diabetes Science and Technology Volume 6, Issue 5, September 2012 Diabetes Technology Society ORIGINAL ARTICLE Inpatient Studies of a Kalman-Filter-Based Predictive Pump Shutoff Algorithm Fraser,
Journal of Diabetes Science and Technology Volume 6, Issue 5, September 2012 Diabetes Technology Society ORIGINAL ARTICLE Inpatient Studies of a Kalman-Filter-Based Predictive Pump Shutoff Algorithm Fraser,
Diabetes Care 33: , 2010
 Emerging Treatment and Technology O R I G I N A L A R T I C L E MD-Logic Artificial Pancreas System A pilot study in adults with type 1 diabetes ERAN ATLAS, MSC 1 REVITAL NIMRI, MD 1 SHAHAR MILLER, BSC
Emerging Treatment and Technology O R I G I N A L A R T I C L E MD-Logic Artificial Pancreas System A pilot study in adults with type 1 diabetes ERAN ATLAS, MSC 1 REVITAL NIMRI, MD 1 SHAHAR MILLER, BSC
A Bihormonal Closed-Loop Artificial Pancreas for Type 1 Diabetes
 DIABETES A Bihormonal Closed-Loop Artificial Pancreas for Type 1 Diabetes Firas H. El-Khatib, 1 * Steven J. Russell, 2 * David M. Nathan, 2 Robert G. Sutherlin, 2 Edward R. Damiano 1 (Published 14 April
DIABETES A Bihormonal Closed-Loop Artificial Pancreas for Type 1 Diabetes Firas H. El-Khatib, 1 * Steven J. Russell, 2 * David M. Nathan, 2 Robert G. Sutherlin, 2 Edward R. Damiano 1 (Published 14 April
A Comparison of Time Delay in Three Continuous Glucose Monitors for Adolescents and Adults
 704443DSTXXX10.1177/1932296817704443Journal of Diabetes Science and TechnologySinha et al research-article2017 Original Article A Comparison of Time Delay in Three Continuous Glucose Monitors for Adolescents
704443DSTXXX10.1177/1932296817704443Journal of Diabetes Science and TechnologySinha et al research-article2017 Original Article A Comparison of Time Delay in Three Continuous Glucose Monitors for Adolescents
Algorithms for a Closed-Loop Artificial Pancreas: The Case for Model Predictive Control. B. Wayne Bequette, Ph.D.
 Journal of Diabetes Science and Technology Volume 7, Issue 6, November 2013 Diabetes Technology Society COMMENTARY Algorithms for a Closed-Loop Artificial Pancreas: The Case for Model Predictive Control
Journal of Diabetes Science and Technology Volume 7, Issue 6, November 2013 Diabetes Technology Society COMMENTARY Algorithms for a Closed-Loop Artificial Pancreas: The Case for Model Predictive Control
Diabetes Management Continuous Glucose Monitoring
 Progress with Closed-loop Systems in Type 1 Diabetes Lalantha Leelarathna 1 and Roman Hovorka 2 1. Clinical Research Associate; 2. Principal Research Associate, Institute of Metabolic Science, University
Progress with Closed-loop Systems in Type 1 Diabetes Lalantha Leelarathna 1 and Roman Hovorka 2 1. Clinical Research Associate; 2. Principal Research Associate, Institute of Metabolic Science, University
Bringing closed-loop home: recent advances in closed-loop insulin delivery
 REVIEW C URRENT OPINION Bringing closed-loop home: recent advances in closed-loop insulin delivery Hood Thabit and Roman Hovorka Purpose of review To highlight the recent advances in closed-loop research,
REVIEW C URRENT OPINION Bringing closed-loop home: recent advances in closed-loop insulin delivery Hood Thabit and Roman Hovorka Purpose of review To highlight the recent advances in closed-loop research,
Fayrouz Allam Tabbin Institute for Metallurgical Studies, Helwan, Egypt
 I.J. Intelligent Systems and Applications, 2012, 10, 58-71 Published Online September 2012 in MECS (http://www.mecs -press.org/) DOI: 10.5815/ijisa.2012.10.07 Evaluation of Using a Recurrent Neural Network
I.J. Intelligent Systems and Applications, 2012, 10, 58-71 Published Online September 2012 in MECS (http://www.mecs -press.org/) DOI: 10.5815/ijisa.2012.10.07 Evaluation of Using a Recurrent Neural Network
In Silico Evaluation of an Artificial Pancreas Combining Exogenous Ultrafast-Acting Technosphere Insulin with Zone Model Predictive Control
 Journal of Diabetes Science and Technology Volume 7, Issue 1, January 2013 Diabetes Technology Society ORIGINAL ARTICLE In Silico Evaluation of an Artificial Pancreas Combining Exogenous Ultrafast-Acting
Journal of Diabetes Science and Technology Volume 7, Issue 1, January 2013 Diabetes Technology Society ORIGINAL ARTICLE In Silico Evaluation of an Artificial Pancreas Combining Exogenous Ultrafast-Acting
Glucose Outcomes with the In-Home Use of a Hybrid Closed-Loop Insulin Delivery System in Adolescents and Adults with Type 1 Diabetes
 DIABETES TECHNOLOGY & THERAPEUTICS Volume 19, Number 3, 2017 Mary Ann Liebert, Inc. DOI: 10.1089/dia.2016.0421 ORIGINAL ARTICLE Glucose Outcomes with the In-Home Use of a Hybrid Closed-Loop Insulin Delivery
DIABETES TECHNOLOGY & THERAPEUTICS Volume 19, Number 3, 2017 Mary Ann Liebert, Inc. DOI: 10.1089/dia.2016.0421 ORIGINAL ARTICLE Glucose Outcomes with the In-Home Use of a Hybrid Closed-Loop Insulin Delivery
What is the role of insulin pumps in the modern day care of patients with Type 1 diabetes?
 What is the role of insulin pumps in the modern day care of patients with Type 1 diabetes? Dr. Fiona Wotherspoon Consultant in Diabetes and Endocrinology Dorset County Hospital Fiona.Wotherspoon@dchft.nhs.uk
What is the role of insulin pumps in the modern day care of patients with Type 1 diabetes? Dr. Fiona Wotherspoon Consultant in Diabetes and Endocrinology Dorset County Hospital Fiona.Wotherspoon@dchft.nhs.uk
Closing the loop, squaring the circle: Studies on insulin delivery, glucose monitoring and the artificial pancreas Luijf, Y.M.
 UvA-DARE (Digital Academic Repository) Closing the loop, squaring the circle: Studies on insulin delivery, glucose monitoring and the artificial pancreas Luijf, Y.M. Link to publication Citation for published
UvA-DARE (Digital Academic Repository) Closing the loop, squaring the circle: Studies on insulin delivery, glucose monitoring and the artificial pancreas Luijf, Y.M. Link to publication Citation for published
The Realities of Technology in Type 1 Diabetes
 The Realities of Technology in Type 1 Diabetes May 6, 2017 Rosanna Fiallo-scharer, MD Margaret Frederick, RN Disclosures I have no conflicts of interest to disclose I will discuss some unapproved treatments
The Realities of Technology in Type 1 Diabetes May 6, 2017 Rosanna Fiallo-scharer, MD Margaret Frederick, RN Disclosures I have no conflicts of interest to disclose I will discuss some unapproved treatments
Original Paper. In Silico Blood Glucose Control for Type 1 Diabetes with Meal Announcement Using Carbohydrate Intake and Glycemic Index
 Advanced Biomedical Engineering 5: 124 131, 2016. Original Paper DOI:10.14326/abe.5.124 In Silico Blood Glucose Control for Type 1 Diabetes with Meal Announcement Using Carbohydrate Intake and Glycemic
Advanced Biomedical Engineering 5: 124 131, 2016. Original Paper DOI:10.14326/abe.5.124 In Silico Blood Glucose Control for Type 1 Diabetes with Meal Announcement Using Carbohydrate Intake and Glycemic
Autonomous and Continuous Adaptation of a Bihormonal Bionic Pancreas in Adults and Adolescents With Type 1 Diabetes
 ORIGINAL Endocrine ARTICLE Research Autonomous and Continuous Adaptation of a Bihormonal Bionic Pancreas in Adults and Adolescents With Type 1 Diabetes Firas H. El-Khatib,* Steven J. Russell,* Kendra L.
ORIGINAL Endocrine ARTICLE Research Autonomous and Continuous Adaptation of a Bihormonal Bionic Pancreas in Adults and Adolescents With Type 1 Diabetes Firas H. El-Khatib,* Steven J. Russell,* Kendra L.
Multivariate Statistical Analysis to Detect Insulin Infusion Set Failure
 2011 American Control Conference on O'Farrell Street, San Francisco, CA, USA June 29 - July 01, 2011 Multivariate Statistical Analysis to Detect Insulin Infusion Set Failure Ruben Rojas, Winston Garcia-Gabin,
2011 American Control Conference on O'Farrell Street, San Francisco, CA, USA June 29 - July 01, 2011 Multivariate Statistical Analysis to Detect Insulin Infusion Set Failure Ruben Rojas, Winston Garcia-Gabin,
Future Direction of Artificial Pancreas. Roy W. Beck, MD, PhD. JAEB Center for Health Research Tampa, Florida
 Future Direction of Artificial Pancreas Roy W. Beck, MD, PhD JAEB Center for Health Research Tampa, Florida Financial Disclosures Dr. Beck does not have any personal conflicts of interest His employer,
Future Direction of Artificial Pancreas Roy W. Beck, MD, PhD JAEB Center for Health Research Tampa, Florida Financial Disclosures Dr. Beck does not have any personal conflicts of interest His employer,
A Bio-Inspired Glucose Controller Based on Pancreatic β-cell Physiology
 Journal of Diabetes Science and Technology Volume 6, Issue 3, May 2012 Diabetes Technology Society ORIGINAL ARTICLE A Bio-Inspired Glucose Controller Based on Pancreatic β-cell Physiology Pau, Ph.D., 1
Journal of Diabetes Science and Technology Volume 6, Issue 3, May 2012 Diabetes Technology Society ORIGINAL ARTICLE A Bio-Inspired Glucose Controller Based on Pancreatic β-cell Physiology Pau, Ph.D., 1
A Novel Index to Evaluate the Blood Glucose Controllability of Type I Diabetic Patients
 A Novel Index to Evaluate the Blood Glucose Controllability of Type I Diabetic Patients Germán Campetelli Estanislao Musulin, Marta S. Basualdo,, Alfredo Rigalli GIAIP-CIFASIS, CONICET-UNR-UPCAM III, Rosario,
A Novel Index to Evaluate the Blood Glucose Controllability of Type I Diabetic Patients Germán Campetelli Estanislao Musulin, Marta S. Basualdo,, Alfredo Rigalli GIAIP-CIFASIS, CONICET-UNR-UPCAM III, Rosario,
Effects of Measurement Frequency on Analytical Quality Required for Glucose Measurements in Intensive Care Units: Assessments by Simulation Models
 Clinical Chemistry 60:4 644 650 (2014) Endocrinology and Metabolism Effects of Measurement Frequency on Analytical Quality Required for Glucose Measurements in Intensive Care Units: Assessments by Simulation
Clinical Chemistry 60:4 644 650 (2014) Endocrinology and Metabolism Effects of Measurement Frequency on Analytical Quality Required for Glucose Measurements in Intensive Care Units: Assessments by Simulation
Research Article An Improved PID Algorithm Based on Insulin-on-Board Estimate for Blood Glucose Control with Type 1 Diabetes
 Computational and Mathematical Methods in Medicine Volume 215, Article ID 281589, 8 pages http://dx.doi.org/1.1155/215/281589 Research Article An Improved PID Algorithm Based on Insulin-on-Board Estimate
Computational and Mathematical Methods in Medicine Volume 215, Article ID 281589, 8 pages http://dx.doi.org/1.1155/215/281589 Research Article An Improved PID Algorithm Based on Insulin-on-Board Estimate
Model Identification using Continuous Glucose Monitoring Data for Type 1 Diabetes
 Downloaded from orbit.dtu.dk on: Mar 05, 018 Model Identification using Continuous Glucose Monitoring Data for Type 1 Diabetes Boiroux, Dimitri; Hagdrup, Morten; Mahmoudi, Zeinab; Poulsen, Niels Kjølstad;
Downloaded from orbit.dtu.dk on: Mar 05, 018 Model Identification using Continuous Glucose Monitoring Data for Type 1 Diabetes Boiroux, Dimitri; Hagdrup, Morten; Mahmoudi, Zeinab; Poulsen, Niels Kjølstad;
In Silico Preclinical Trials: A Proof of Concept in Closed-Loop Control of Type 1 Diabetes
 Journal of Diabetes Science and Technology Volume 3, Issue 1, January 2009 Diabetes Technology Society SYMPOSIUM In Silico Preclinical Trials: A Proof of Concept in Closed-Loop Control of Type 1 Diabetes
Journal of Diabetes Science and Technology Volume 3, Issue 1, January 2009 Diabetes Technology Society SYMPOSIUM In Silico Preclinical Trials: A Proof of Concept in Closed-Loop Control of Type 1 Diabetes
A switching based PID technique for blood glucose control.
 Biomedical Research 2017; 28 (19): 8477-8483 ISSN 0970-938X www.biomedres.info A switching based PID technique for blood glucose control. Muhammad Hamayun Qammar Kayani, Kainat Naeem Malik, Shaban Ahmad,
Biomedical Research 2017; 28 (19): 8477-8483 ISSN 0970-938X www.biomedres.info A switching based PID technique for blood glucose control. Muhammad Hamayun Qammar Kayani, Kainat Naeem Malik, Shaban Ahmad,
Artificial Pancreas Technologies: New Tools to Improve Diabetes Care Today and Tomorrow
 Artificial Pancreas Technologies: New Tools to Improve Diabetes Care Today and Tomorrow Mark D. DeBoer, MD, MSc., MCR University of Virginia Center for Diabetes Technologies October 2017 Learning Objectives
Artificial Pancreas Technologies: New Tools to Improve Diabetes Care Today and Tomorrow Mark D. DeBoer, MD, MSc., MCR University of Virginia Center for Diabetes Technologies October 2017 Learning Objectives
Continuous Glucose Monitoring: Changing Diabetes Behavior in Real Time and Retrospectively
 Journal of Diabetes Science and Technology Volume 2, Issue 3, May 2008 Diabetes Technology Society CONTROVERSIES in Continuous Glucose Monitoring Continuous Glucose Monitoring: Changing Diabetes Behavior
Journal of Diabetes Science and Technology Volume 2, Issue 3, May 2008 Diabetes Technology Society CONTROVERSIES in Continuous Glucose Monitoring Continuous Glucose Monitoring: Changing Diabetes Behavior
Automatic adaptation of basal therapy for Type 1 diabetic patients: a Run-to-Run approach
 Preprints of the 19th World Congress The International Federation of Automatic Control Automatic adaptation of basal therapy for Type 1 diabetic patients: a Run-to-Run approach Chiara Toffanin Alice Sandri
Preprints of the 19th World Congress The International Federation of Automatic Control Automatic adaptation of basal therapy for Type 1 diabetic patients: a Run-to-Run approach Chiara Toffanin Alice Sandri
A Novel Adaptive Basal Therapy Based on the Value and Rate of Change of Blood Glucose
 Journal of Diabetes Science and Technology Volume 3, Issue 5, September 29 Diabetes Technology Society SYMPOSIUM Novel daptive asal Therapy ased on the Value and Rate of Change of lood Glucose Youqing,
Journal of Diabetes Science and Technology Volume 3, Issue 5, September 29 Diabetes Technology Society SYMPOSIUM Novel daptive asal Therapy ased on the Value and Rate of Change of lood Glucose Youqing,
Alternative insulin delivery systems: how demanding should the patient be?
 Diabetologia (1997) 4: S97 S11 Springer-Verlag 1997 Alternative insulin delivery systems: how demanding should the patient be? K.S. Polonsky, M. M. Byrne, J. Sturis Department of Medicine, The University
Diabetologia (1997) 4: S97 S11 Springer-Verlag 1997 Alternative insulin delivery systems: how demanding should the patient be? K.S. Polonsky, M. M. Byrne, J. Sturis Department of Medicine, The University
Insulin Control System for Diabetic Patients by Using Adaptive Controller
 J. Basic. Appl. Sci. Res., 1(10)1884-1889, 2011 2011, TextRoad Publication ISSN 2090-4304 Journal of Basic and Applied Scientific Research www.textroad.com Insulin Control System for Diabetic Patients
J. Basic. Appl. Sci. Res., 1(10)1884-1889, 2011 2011, TextRoad Publication ISSN 2090-4304 Journal of Basic and Applied Scientific Research www.textroad.com Insulin Control System for Diabetic Patients
Diabetes II Insulin pumps; Continuous glucose monitoring system (CGMS) Ernest Asamoah, MD FACE FACP FRCP (Lond)
 Diabetes II Insulin pumps; Continuous glucose monitoring system (CGMS) Ernest Asamoah, MD FACE FACP FRCP (Lond) 9501366-011 20110401 Objectives Understand the need for insulin pumps and CGMS in managing
Diabetes II Insulin pumps; Continuous glucose monitoring system (CGMS) Ernest Asamoah, MD FACE FACP FRCP (Lond) 9501366-011 20110401 Objectives Understand the need for insulin pumps and CGMS in managing
AComparativeEffectivenessAnalysisof Three Continuous Glucose Monitors
 Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E AComparativeEffectivenessAnalysisof Three Continuous Glucose Monitors EDWARD R. DAMIANO, PHD 1 FIRAS H. EL-KHATIB,
Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E AComparativeEffectivenessAnalysisof Three Continuous Glucose Monitors EDWARD R. DAMIANO, PHD 1 FIRAS H. EL-KHATIB,
Simone Del Favero, PhD, Andrea Facchinetti, PhD, Giovanni Sparacino, PhD, and Claudio Cobelli, PhD
 DIA-2016-0413-ver9-Favero_3P.3d 03//17 12:40pm Page 1 DIABETES TECHNOLOGY & THERAPEUTICS Volume 19, Number 4, 2017 ª Mary Ann Liebert, Inc. DOI:.89/dia.2016.0413 ORIGINAL ARTICLE Retrofitting Real-Life
DIA-2016-0413-ver9-Favero_3P.3d 03//17 12:40pm Page 1 DIABETES TECHNOLOGY & THERAPEUTICS Volume 19, Number 4, 2017 ª Mary Ann Liebert, Inc. DOI:.89/dia.2016.0413 ORIGINAL ARTICLE Retrofitting Real-Life
The Artificial Pancreas
 SAGLB.DIA.15.2.87(2). Approved October 215 The Artificial Pancreas For scientific and medical purposes only The pancreas responds to changes in blood glucose by releasing insulin (β cells) to lower blood
SAGLB.DIA.15.2.87(2). Approved October 215 The Artificial Pancreas For scientific and medical purposes only The pancreas responds to changes in blood glucose by releasing insulin (β cells) to lower blood
Smith Predictor Sliding Mode Closed-loop Glucose Controller in Type 1 Diabetes
 Smith Predictor Sliding Mode Closed-loop Glucose Controller in Type 1 Diabetes Amjad Abu-Rmileh Winston Garcia-Gabin Research group on Statistics, Applied Economics and Health (GRECS), University of Girona,
Smith Predictor Sliding Mode Closed-loop Glucose Controller in Type 1 Diabetes Amjad Abu-Rmileh Winston Garcia-Gabin Research group on Statistics, Applied Economics and Health (GRECS), University of Girona,
Manual closed-loop insulin delivery in children and adolescents with type 1 diabetes: a phase 2 randomised crossover trial
 Manual closed-loop insulin delivery in children and adolescents with type 1 diabetes: a phase 2 randomised crossover trial Roman Hovorka, Janet M Allen, Daniela Elleri, Ludovic J Chassin, Julie Harris,
Manual closed-loop insulin delivery in children and adolescents with type 1 diabetes: a phase 2 randomised crossover trial Roman Hovorka, Janet M Allen, Daniela Elleri, Ludovic J Chassin, Julie Harris,
Probabilistic Evolving Meal Detection and Estimation of Meal Total Glucose Appearance
 Journal of Diabetes Science and Technology Volume 3, Issue 5, September 2009 Diabetes Technology Society SYMPOSIUM Probabilistic Evolving Meal Detection and Estimation of Meal Total Glucose Appearance
Journal of Diabetes Science and Technology Volume 3, Issue 5, September 2009 Diabetes Technology Society SYMPOSIUM Probabilistic Evolving Meal Detection and Estimation of Meal Total Glucose Appearance
Automated control of an adaptive bi-hormonal, dual-sensor artificial pancreas and evaluation during inpatient studies
 TBME-XXXX-XXXX (IN PRESS, 2014) 1 Automated control of an adaptive bi-hormonal, dual-sensor artificial pancreas and evaluation during inpatient studies Peter G. Jacobs, Member, IEEE, Joseph El Youssef,
TBME-XXXX-XXXX (IN PRESS, 2014) 1 Automated control of an adaptive bi-hormonal, dual-sensor artificial pancreas and evaluation during inpatient studies Peter G. Jacobs, Member, IEEE, Joseph El Youssef,
A Closed-Loop Artificial Pancreas Based on Risk Management
 Journal of Diabetes Science and Technology Volume 5, Issue 2, March 2011 Diabetes Technology Society ORIGINAL ARTICLES A Closed-Loop Artificial Pancreas Based on Risk Management Fraser, Ph.D., 1 B. Wayne
Journal of Diabetes Science and Technology Volume 5, Issue 2, March 2011 Diabetes Technology Society ORIGINAL ARTICLES A Closed-Loop Artificial Pancreas Based on Risk Management Fraser, Ph.D., 1 B. Wayne
The Role of Process Systems Engineering in the Quest for the Artificial Pancreas
 The Role of Process Systems Engineering in the Quest for the Artificial Pancreas Francis J. Doyle III Department of Chemical Engineering Biomolecular Science and Engineering Program Institute for Collaborative
The Role of Process Systems Engineering in the Quest for the Artificial Pancreas Francis J. Doyle III Department of Chemical Engineering Biomolecular Science and Engineering Program Institute for Collaborative
Glucose Clamp Algorithms and Insulin Time-Action Profiles. B. Wayne Bequette, Ph.D.
 Journal of Diabetes Science and Technology Volume 3, Issue 5, September 2009 Diabetes Technology Society SYMPOSIUM Glucose Clamp Algorithms and Insulin Time-Action Profiles B. Wayne, Ph.D. Abstract Motivation:
Journal of Diabetes Science and Technology Volume 3, Issue 5, September 2009 Diabetes Technology Society SYMPOSIUM Glucose Clamp Algorithms and Insulin Time-Action Profiles B. Wayne, Ph.D. Abstract Motivation:
Impact of sensing and infusion site dependent dynamics on insulin bolus based meal compensation
 Impact of sensing and infusion site dependent dynamics on insulin bolus based meal compensation Konstanze Kölle, Anders Fougner, Øyvind Stavdahl Department of Engineering Cybernetics, Norwegian University
Impact of sensing and infusion site dependent dynamics on insulin bolus based meal compensation Konstanze Kölle, Anders Fougner, Øyvind Stavdahl Department of Engineering Cybernetics, Norwegian University
Accuracy Requirements for a Hypoglycemia Detector: An Analytical Model to Evaluate the Effects of Bias, Precision, and Rate of Glucose Change
 Journal of Diabetes Science and Technology Volume 1, Issue 5, September 2007 Diabetes Technology Society SYMPOSIUM Accuracy Requirements for a Hypoglycemia Detector: An Analytical Model to Evaluate the
Journal of Diabetes Science and Technology Volume 1, Issue 5, September 2007 Diabetes Technology Society SYMPOSIUM Accuracy Requirements for a Hypoglycemia Detector: An Analytical Model to Evaluate the
CGM: Continuous Glucose Monitoring Making Sense of It All AW: ANCO/GEND/1016/0117
 CGM: Continuous Glucose Monitoring Making Sense of It All Objectives Review how to do a time effective interpretation of CGM and insulin pump download data Review how medications, lifestyle, and current
CGM: Continuous Glucose Monitoring Making Sense of It All Objectives Review how to do a time effective interpretation of CGM and insulin pump download data Review how medications, lifestyle, and current
More Than 1 Year of Hybrid Closed Loop in Pediatrics. Gregory P. Forlenza, MD Assistant Professor Barbara Davis Center
 More Than 1 Year of Hybrid Closed Loop in Pediatrics Gregory P. Forlenza, MD Assistant Professor Barbara Davis Center Disclosure Dr. Forlenza has served as a consultant for Abbott Diabetes Care and conducts
More Than 1 Year of Hybrid Closed Loop in Pediatrics Gregory P. Forlenza, MD Assistant Professor Barbara Davis Center Disclosure Dr. Forlenza has served as a consultant for Abbott Diabetes Care and conducts
SIMULATIONS OF A MODEL-BASED FUZZY CONTROL SYSTEM FOR GLYCEMIC CONTROL IN DIABETES
 Bulletin of the Transilvania University of Braşov Vol. 8 (57) No. 2-2015 Series I: Engineering Sciences SIMULATIONS OF A MODEL-BASED FUZZY CONTROL SYSTEM FOR GLYCEMIC CONTROL IN DIABETES C. BOLDIȘOR 1
Bulletin of the Transilvania University of Braşov Vol. 8 (57) No. 2-2015 Series I: Engineering Sciences SIMULATIONS OF A MODEL-BASED FUZZY CONTROL SYSTEM FOR GLYCEMIC CONTROL IN DIABETES C. BOLDIȘOR 1
The next five years in diabetes technology: closed-loop systems
 The next five years in diabetes technology: closed-loop systems J. H. (Hans) DeVries Academic Medical Center at the University of Amsterd, the Netherlands Keystone, CO, 19 July 2013 Disclosure AP@home,
The next five years in diabetes technology: closed-loop systems J. H. (Hans) DeVries Academic Medical Center at the University of Amsterd, the Netherlands Keystone, CO, 19 July 2013 Disclosure AP@home,
ARTIFICIAL ENDOCRINE PANCREAS: FROM BENCH TO BEDSIDE
 ARTIFICIAL ENDOCRINE PANCREAS: FROM BENCH TO BEDSIDE Ananda Basu MD, FRCP (UK) Professor of Medicine, Division of Endocrinology, Mayo Clinic, USA September 2015 COI/Funding/Support COI: None Funding: NIH:
ARTIFICIAL ENDOCRINE PANCREAS: FROM BENCH TO BEDSIDE Ananda Basu MD, FRCP (UK) Professor of Medicine, Division of Endocrinology, Mayo Clinic, USA September 2015 COI/Funding/Support COI: None Funding: NIH:
Artificial Pancreas: Model Predictive Control Design from Clinical Experience
 Journal of Diabetes Science and Technology Volume 7, Issue 6, November 2013 Diabetes Technology Society SYMPOSIUM Artificial Pancreas: Model Predictive Control Design from Clinical Experience Chiara, Ph.D.,
Journal of Diabetes Science and Technology Volume 7, Issue 6, November 2013 Diabetes Technology Society SYMPOSIUM Artificial Pancreas: Model Predictive Control Design from Clinical Experience Chiara, Ph.D.,
Design of the Health Monitoring System for the Artificial Pancreas: Low Glucose Prediction Module
 Journal of Diabetes Science and Technology Volume 6, Issue 6, November 2012 Diabetes Technology Society ORIGINAL ARTICLE Design of the Health Monitoring System for the Artificial Pancreas: Low Glucose
Journal of Diabetes Science and Technology Volume 6, Issue 6, November 2012 Diabetes Technology Society ORIGINAL ARTICLE Design of the Health Monitoring System for the Artificial Pancreas: Low Glucose
An event-based point of view on the control of insulin-dependent diabetes
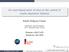 An event-based point of view on the control of insulin-dependent diabetes Brigitte Bidégaray-Fesquet Laboratoire Jean Kuntzmann Univ. Grenoble Alpes, France Réunion e-baccuss September 4th 20 Réunion e-baccuss,
An event-based point of view on the control of insulin-dependent diabetes Brigitte Bidégaray-Fesquet Laboratoire Jean Kuntzmann Univ. Grenoble Alpes, France Réunion e-baccuss September 4th 20 Réunion e-baccuss,
