The only US Food and Drug Administration-approved
|
|
|
- Kory Wilkinson
- 5 years ago
- Views:
Transcription
1 Quantitative Assessment of Core/Penumbra Mismatch in Acute Stroke CT and MR Perfusion Imaging Are Strongly Correlated When Sufficient Brain Volume Is Imaged Pamela W. Schaefer, MD; Elizabeth R. Barak, MD; Shahmir Kamalian, MD; Leila Rezai Gharai, MD; Lee Schwamm, MD; Ramon Gilberto Gonzalez, MD, PhD; Michael H. Lev, MD Background and Purpose Our purpose was to determine (1) the correlation between quantitative CT and MR measurements of infarct core, penumbra, and mismatch; and (2) whether the difference between these measurements would alter patient selection for stroke clinical trials. Methods We studied 45 patients with acute middle cerebral artery stroke imaged a mean of 3.8 hours after onset (range,.48 to 8.35 hours) who underwent CT perfusion and MR diffusion (DWI)/perfusion imaging within 3 hours of each other. The DWI and MR-mean transit time (MTT) abnormalities were visually segmented using a semiautomated commercial analysis program. The CT-cerebral blood volume) and CT-MTT lesions were automatically segmented using a relative cerebral blood volume threshold of.56 and a relative MTT threshold of 1.5 on commercially available software. Percent mismatch was defined as [(MTT DWI)/DWI volume] 1. Pearson correlation coefficients were calculated. Results There were significant correlations for DWI versus CT-cerebral blood volume lesion volumes (r 2.88, P.1), for MR-MTT versus CT-MTT lesion volumes(r 2.86, P.1), and for MR-MTT/DWI versus CT-MTT/CT-cerebral blood volume mismatch lesion volumes(r 2.81, P.1). MR perfusion and CT perfusion agreed for determining: (1) infarct core versus 1 ml in 41 of 45 (91.1%); (2) MTT lesion size versus 2 cm diameter in 42 of 45 (93.3%); (3) mismatch versus 2% in 41 of 45 (91.1%); and (4) inclusion versus exclusion from trial enrollment in 38 of 45 (84.4%) patients. Six of 7 disagreements were due to inadequate CT coverage. Conclusion Advanced MR and CT perfusion imaging measurements of core/penumbra mismatch for patient selection in stroke trials are highly correlated when CT perfusion coverage is sufficient to include most of the ischemic region. Although MR is currently the preferred imaging method for determining core and penumbra, CT perfusion is comparable and potentially more available. (Stroke. 28;39: ) Key Words: acute ischemic acute stroke CT MRI penumbra perfusion CT imaging perfusion MR imaging The only US Food and Drug Administration-approved medical therapy for acute stroke to date is intravenous tissue plasminogen activator administered within 3 hours of symptom onset. However, there is increasing evidence that identification of potentially salvageable brain tissue with advanced MR and CT imaging may allow the selection of patients who can be effectively and safely treated with intravenous thrombolysis for up to 9 hours postictus. 1 5 Specifically, the mismatch between infarct core (brain likely to be irreversibly infarcted regardless of treatment) and ischemic penumbra (hypoperfused brain at risk for infarction in the absence of reperfusion) may identify patients with both a low hemorrhagic risk (small core) and a high likelihood of treatment benefit (large penumbra). In clinical practice, the core can be operationally defined using either MR diffusion-weighted imaging (DWI) or CT cerebral blood volume imaging (CT-CBV), and penumbra with either MR or CT perfusion-weighted imaging (MRP or CTP). However, the major completed clinical trials supporting the use of intravenous thrombolysis beyond 3 hours (Desmoteplase in Acute Ischemic Stroke [DIAS], Dose Escalation of Desmoteplase for Acute Ischemic Stroke [DEDAS], and Diffusion and Perfusion Imaging Evaluation for Understanding Stroke Evolution [DEFUSE]) and trials still in Received December 21, 27; final revision received March 17, 28; accepted March 31, 28. From the Departments of Radiology (P.W.S., E.R.B., S.K., L.R.G., R.G.G., M.H.L.) and Neurology (L.S.), Massachusetts General Hospital, Harvard Medical School, Boston, Mass. Correspondence to Pamela W. Schaefer, MD, Department of Radiology, Division of Neuroradiology, Gray 273A, Massachusetts General Hospital, 55 Fruit Street, Boston, MA pschaefer@partners.org 28 American Heart Association, Inc. Stroke is available at DOI: /STROKEAHA
2 Schaefer et al CT and MR Core/Penumbra Mismatch Correlate Strongly 2987 Table 1. Patient Demographics Mean* Range Age NIHSS* Time to first image 3:39 :29 8:21 Time CTP to MRI :42 :8 2:8 Sex 21 male 24 female Side 22 left 21 right *NIHSS is expressed as median rather than mean because it is not a normal distribution. progress (Echoplanar Imaging Thrombolysis Evaluation Trial [EPITHET], ReoPro Retavase Reperfusion of Stroke Safety Study Imaging Evaluation [ROSIE], and MR and Recanalization of Stroke Clots Using Embolectomy [MR RESCUE]) have all used DWI/MRP mismatch for patient selection. 1 3,6 CT scanners are much more widely available and accessible in emergency rooms than are MRI scanners and imaging patients with acute stroke as rapidly as possible is of paramount importance. Therefore, we sought to determine if CTP can be used in place of MRP for patient selection in clinical trials. Specifically, 3 inclusion criteria for major clinical trials aimed at extending the time window for intravenous thrombolysis beyond 3 hours are: (1) mean transit time (MTT) lesion diameter 2 cm; (2) core lesion size one third of the middle cerebral artery (MCA) territory (approximately 1 ml); and (3) core/penumbra mismatch 2%. We therefore sought to determine: (1) the correlation between quantitative CT and MR measurement of mismatch; and (2) whether the difference between these measurements, using current clinical protocols, would alter patient selection for stroke clinical trials. Methods Patient Selection This retrospective study was approved by our Institutional Review Board and was compliant with the Health Insurance Portability and Accountability Act. Review of our radiology database from June 24 to August 26 identified 47 consecutive patients with acute MCA and/or anterior cerebral artery stroke who had: (1) CTP within 9 hours of symptom onset; (2) MR diffusion and perfusion imaging within 3 hours subsequent to CTP; (3) unilateral stroke; (4) no evidence of old infarction; and (5) technically adequate images from both CTP and MRP. For our patients with acute stroke, we routinely obtain CTP and MRP. Initially, the patient receives a noncontrast CT and CT angiography to determine whether the patient is a candidate for recanalization therapy. We obtain a CTP because with only a few extra minutes of scanning and automated software, we can obtain quantitative core penumbra mismatch data very rapidly. We then transfer the patient to the MR scanner and obtain DWI and MRP because MRP has better coverage (whole brain) than CTP and unlike CTP has been widely accepted in clinical trials. Two of these cases were subsequently excluded after review of the imaging due to reperfusion between the CTP and MRP acquisitions. Ultimately, 45 patients were included; their demographic and clinical characteristics are shown in Table 1. Thirty-four patients had proximal vascular occlusions (internal carotid artery, M1 or M2), 2 had distal anterior cerebral artery occlusions, one had a distal MCA occlusion, and 8 had no visible occlusion on CT and/or MR angiogram. The National Institutes of Health Stroke Scale (NIHSS) score was performed by the admitting neurologist. In 4 patients, an admission NIHSS was not recorded and was recalculated from the well-documented admission neurological examination. 7 For one additional patient, an NIHSS score was not recorded and the admission note was insufficiently detailed to recalculate one. No patients were treated with intra-arterial recanalization procedures before CT or MR perfusion imaging. Six patients underwent intraarterial recanalization after both studies. Twenty patients received intravenous tissue plasminogen activator, 9 before imaging, 4 between CTP and MRP, and 7 after both studies. MRI Image Acquisition MR imaging was performed on a 1.5-Tesla Signa whole-body scanner (GE Medical Systems, Milwaukee, Wis) with echo planar capabilities. DWI images were obtained using single-shot, spin echo echoplanar imaging with sampling of the entire diffusion tensor. Six high b-value images corresponding to diffusion measurements in different gradient directions were acquired in addition to a single low b-value image. Double inversion pulses were used to help reduce eddy current effects. The high b value was 1 s/mm 2 and the low b value was s/mm 2. A TR of 5 ms was used. The TE for each scan was the minimum possible, typically between 9 and 1 ms. Other parameters are field of view of cm, image matrix of pixels, slice thickness of 5 mm with 1-mm gap, and 5 signal averages. As many axial slices as were needed to cover the entire brain were included, typically 22 to 25. Isotropic DWI images and apparent diffusion coefficient maps were reviewed. Perfusion-weighted imaging was performed using a dynamic susceptibility contrast technique. Serial echoplanar gradient echo images were acquired with TR/TE of 15/4 ms, field of view 22 cm, matrix , and slice thickness 5 mm with a 1-mm interslice gap. A complete volume of 16 slices was acquired every 1.5 seconds and 46 such volumes were acquired so that the total imaging time required by the sequence was 1 minute 9 seconds. Ten seconds after the beginning of image acquisition, 2 ml of gadopentetate dimeglumine.5 mmol/ml was administered through a peripheral intravenous catheter at a rate of 5 ml/s. This was followed immediately by the administration of 2 ml of normal saline at the same rate. MRI Image Processing Dynamic susceptibility contrast images were used to generate signal intensity-versus-time curves for each pixel in the imaged volume. These curves were integrated to yield maps of CBV for each pixel. Cerebral blood flow was calculated for each pixel by deconvolution using the singular value decomposition technique. 8,9 A global arterial input function was derived from the MCA ipsilateral to each patient s infarct. Vascular MTT was calculated by dividing CBV by cerebral blood flow. Postprocessing Image Analysis of MRI Visually detected DWI and MTT abnormalities were manually segmented by a research assistant using a semiautomated commercial analysis program (Analyze 7.; AnalyzeDirect). Final outlines were manually edited by a single experienced neuroradiologist. For each patient, volumes and percent mismatches were calculated using all DWI and MTT slices and using only those slices that covered regions that were also covered with CTP. Percent mismatch was defined as [(MTT DWI)/DWI] 1%. Cases were classified according to DWI lesion size (greater or less than 1 ml), mismatch (greater or less than 2%), and MTT lesion volume (greater or less than 4.19 ml the volume of a sphere with a diameter of 2 cm). CT Perfusion Image Acquisition CTP imaging was performed on a multidetector helical scanner (16- or 64-slice LightSpeed; GE Healthcare). Image acquisition was performed as a cine series (45 to 7 seconds at one image[s]) beginning 5 seconds after power injection (through a peripheral intravenous catheter, 18 to 2 gauge) of 35 to 4 ml of contrast
3 2988 Stroke November 28 A DWI vs CT-CBV lesion volume 1-2 mm slices 4-8 mm slices B DWI vs CT-CBV lesion volume with matched slices DWI lesion volume (ml) 2 1 y = 3.25x R 2 =.54 y = 1.49x R 2 =.94 DWI lesion volume (ml) 2 1 y = 1.8x R 2 =.88 MR-MTT lesion volume (ml) MR Mismatch Volume C E CT-CBV lesion volume (ml) MR-MTT vs CT-MTT lesion volume D 1-2 mm slices 4-8 mm slices y = 3.1x R 2 =.31 y = 1.39x R 2 = CT-MTT lesion volume (ml) MR vs CT Mismatch Volume 1-2 mm slices 4-8 mm slices y = 2.44x R 2 =.9 y = 1.2x R 2 = CT Mismatch volume MR-MTT lesion volume (ml) MR Mismatch Volume F CT-CBV lesion volume (ml) MR-MTT vs CT-MTT lesion volume with matched slices y = 1.3x R 2 = CT-MTT lesion volume (ml) MR vs CT Mismatch Volume with matched slices y =.94x R 2 = CT Mismatch Volume Figure 1. A F, Graphs of correlations between MRP and CTP core, penumbra, and mismatch volumes. Correlations of CT-CBV versus MR-DWI lesion volumes in 1 to 2 mm (R 2.54, slope 3.25) and 4 to 8 mm (R 2.94, slope 1.49) thick CTP slices. B, Correlation of CT-CBV versus MR-DWI lesion volumes in matched (R 2.88, slope 1.8) slices. C, Correlation of CT-MTT versus MR-MTT in 1 to 2 (R 2.31, slope 3.) and 4 to 8 mm (R 2.8, slope 1.39) thick CTP slices. D, Correlation of CT-MTT versus MR-MTT in matched slices (R 2.86, slope 1.3). E, Correlations of MR (MTT DWI) versus CT (MTT CBV) mismatch volumes in 1 to 2 (R 2.9, slope 2.44) and 4 to 8 mm (R 2.69, slope 1.2) thick CTP slices. F, Correlations of MR (MTT DWI) versus CT (MTT CBV) mismatch volumes in matched slices (R 2.81, slope.94). All correlation coefficients significantly improve with increasing slab thickness (P.5 for Group 2 versus Group 1). The higher correlation coefficient values for the CT-MTT versus MR-MTT lesion volumes and the CT versus MR mismatch volumes when the MRI volumes were calculated using only those slices that corresponded to the imaged CTP slabs, however, are not significantly different from the corresponding values in Group 2 (P.5). R 2 Pearson correlation coefficient; y slope. 1 to 2 mm Group 1, 4 to 8 mm Group 2. (Isovue 37; Bracco Diagnostics, Princeton, NJ) at 5 to 7 ml/s with a normal saline chaser bolus. Imaging parameters were 8 kvp, 2 ma, 1-second rotation time. Coverage consisted of slabs positioned parallel and superior to the orbital roof (to avoid radiation to the lens). On the 16-slice scanner, each slab consisted of one or 2 slices of 1-mm thickness or 4 slices of 5-mm thickness. On the 64-slice scanner, each bolus administration of contrast resulted in a 4-mm slab consisting of 8 slices of 5-mm thickness. Four patients received 2 such contrast bolus injections resulting in 2 4-mm slabs for a total of 8-mm coverage. CT Perfusion Image Processing and Analysis For CTP analysis, CBV and MTT maps were created from CTP data with commercially available semiautomated perfusion analysis software (Philips Brain Perfusion 24; Philips Medical System). The arterial input region of interest was selected from the MCA con-
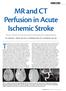
4 Schaefer et al CT and MR Core/Penumbra Mismatch Correlate Strongly 2989 Figure 2. MRP and CTP images. Good correlation between CTP and MRP lesion volumes and mismatch measurement. A 67-year-old man with NIHSS 18 and acute right MCA stroke; CTP performed 3:46 after symptom onset with 4 mm of coverage (CT-CBV [dark gray], 43.2 ml; CT-MTT (light gray), ml; mismatch volume, ml; mismatch percent 239.1), MRP performed :38 after CTP (DWI, 64.6 ml; MR-MTT, 21. ml; mismatch volume, ml; mismatch percent, 196.). tralateral to the infarct. The venous input region of interest was selected from the superior sagittal sinus. Infarct core was segmented based on a CBV threshold of 56% relative to the opposite side. The threshold chosen was based on the results of a pilot study, which compared DWI and CBV lesion volumes using thresholds of 46%, 56%, and 66% of the contralateral normal side as well as a 2 ml/1-g absolute threshold; the DWI CBV correlation was optimal using the 56% threshold. 1 Ischemic penumbra was segmented based on a MTT threshold of 15% relative to the contralateral side; this threshold was chosen based on a prior published report. 11 Using these thresholds, the software calculated the areas of the CBV and MTT lesions for each slice. These areas were multiplied by the slice thickness (5 mm or 1 mm) to determine the CBV and MTT lesion volumes. For patients with 2 CTP slabs, CBV and MTT volumes were calculated for each slab and summed for a total volume. Total CTP slab thickness was recorded as follows: 3 patients had 1 mm, 14 patients 2 mm, 24 patients 4 mm, and 4 patients 8 mm thickness. Percent volume mismatch was defined as [(MTT CBV)/ CBV] 1%. Cases were classified according to CBV lesion size (greater or less than 1 ml), CBV/MTT mismatch (greater or less than 2%), and MTT lesion volume (greater or less than 4.19 ml). Statistical Analysis Pearson correlations were used to compare CTP CBV versus MRI DWI lesion size, CTP MTT versus MRI MTT lesion size, and CT mismatch volume versus MR mismatch volume. Fisher s z transformation was used to determine whether Pearson correlation coefficients were statistically significantly different. Kappa statistics were calculated for agreement between CTP and MRP clinical trial selection criteria. Results Patient demographics are shown in Table 1. Mean DWI lesion volume was 48.6 ml ( to 247 ml) and mean CT-CBV lesion volume was 23. ml ( to 156 ml; r 2.74; P.1). Mean MR-MTT lesion volume was ml (.4 to 388 ml), and mean CT-MTT lesion volume was 78 ml (.2 to 36 ml; r 2.45; P.1). Mean MR-MTT/DWI difference was ml (.1 to 246.4) and mean CT-MTT/ CBV difference was ml (.7 to 247.4; r 2.34; P.1). The patients were divided into 2 groups according to the thickness of the CTP slab; Group 1 included 17 patients with 1- or 2-mm thickness and Group 2 included 28 patients with 4- or 8-mm thickness. For Group 1, there were statistically significant correlations between MR-DWI and CT-CBV lesion volumes (r 2.54, P.1) and between CT-MTT and MR-MTT lesion volumes (r 2.31, P.1), but not between CT and MR mismatch volumes. For Group 2, there were statistically significant correlations among all 3 comparison pairs, and all 3 correlation coefficients were significantly higher than the corresponding values for Group 1 with r 2.94 (P.1) for DWI versus CT-CBV, r 2.8 (P.1) for CT-MTT versus MR-MTT and r 2.69 (P.1) for CT-MTT/CBV mismatch volume versus MR-MTT/DWI mismatch volume. The correlation coefficients for CT versus MR-MTT (r 2.86, P.1) and CT versus MR mismatch volume (r 2.81, P.1) further improved when MRI volumes were calculated using only those slices that corresponded to the imaged CTP slabs, although they were not significantly different (P.5) from the corresponding values in Group 2 (Figures 1 and 2; Table 2). Patient selection with CTP versus MRP maps, using 3 different clinical trial inclusion and exclusion criteria, is summarized in Table 3. For determination of infarct core greater versus less than 1 ml, the CT-CBV lesion volume agreed with the MR-DWI lesion volume in 91% of cases (kappa.56). All 4 cases of disagreement (one with 1 mm, one with 2 mm, and 2 with 4-mm coverage) resulted from the CTP slab not covering the entire lesion. For determination of MTT lesion volume greater versus less than 4.19 ml, CT-MTT lesion volume agreed with MR-MTT lesion volume in 93% of cases (kappa.63). For the 2 cases (one with 2-mm and one with 4-mm CTP coverage) in which the CT-MTT lesion volume was less than and the MR-MTT volume was greater than 4.19 ml, the CTP slab placement did not cover the lesion. For the one case (with 4-mm coverage) in which the CT-MTT lesion volume was greater than and the MR-MTT lesion volume was less than 4.19 ml, the automated CTP software segmentation was incorrect (Supplemental Figure I, available online at stroke.ahajournals.org). For determination of whether mismatch was greater or less than 2%, the CT mismatch agreed
5 299 Stroke November 28 Table 2. Correlation of Advanced CT versus MR Lesion Volume Values All Patients 1 to 2 mm (Group 1) 4 to 8 mm (Group 2) Same Coverage for CTP and MRP (matched slices) r 2 P Value r 2 P Value r 2 P Value r 2 P Value CT-CBV versus MR-DWI lesion volumes *.1.94**.1.88***.1 CT-MTT versus MR-MTT lesion volumes CT-MTT minus CBV versus MR-MTT minus DWI lesion volumes For CT-CBV versus MR-DWI, the difference in r 2 between ** and *** is not significant at P.8. The difference between * and ** is significant at P.1 as well as between * and *** at.1. For CT versus MR-MTT, the difference in r 2 between and is not significant at P.18. The difference between and is significant at P.1 as well as between and at.1. For mismatch volumes, the difference in r 2 between and is not significant at P.13. The difference between and is significant at P.1 as well as between and at.1. with MR mismatch in 91% of cases (kappa.31). In 4 cases, the MRP mismatch was less than 2% and the CTP mismatch was greater than 2%. In 3 of these cases (2 with 2-mm and one with 4-mm coverage), the MTT lesion size was very small ( 4.19 ml), making percentage mismatch less reliable, whereas the fourth case (with 4-mm coverage) had the incorrect CTP segmentation previously described. Finally, we combined these criteria to determine the agreement between CTP and MRP for patient selection in clinical trial enrollment (Tables 3 and 4). For MR versus CT core volume less than 1 ml, penumbra volume 4.19 ml and mismatch 2%, we found an 84% agreement (kappa.54; Figure 1). Two patients (one with 2-mm and one with 4-mm CTP coverage) met selection criteria for clinical trial enrollment based on MRP but not CTP findings, because the CTP slab did not fully cover the ischemic lesion and so the CT-MTT volume was inaccurately determined to be less than 4.19 ml. Four patients (one with 1-mm, one with 2-mm, and 2 with 4-mm CTP coverage) met selection criteria for clinical trial enrollment based on CTP but not MRP findings, again due to inadequate CTP coverage, with underestimation of the CT-CBV volume at 1 ml. One patient (with 4-mm CTP coverage) met selection criteria for clinical trial enrollment based on CT but not MR findings, because the CTP segmentation overestimated MTT lesion size and mismatch. When we excluded cases of disagreement attributable to inadequate CTP coverage, overall agreement for patient selection in a clinical trial increased to 97.8% (kappa.91). Table 3. Discussion Advanced MR and CTP imaging measurements of core/ penumbra mismatch for patient selection in stroke clinical trials are strongly correlated when CTP coverage is sufficient to include most of the ischemic region using currently standard scanning protocols. Specifically, when using the combined criteria of ischemic core lesion (CT-CBV or MR-DWI) 1 ml, penumbra-core (CT-MTT/CBV and MR-MTT/DWI) mismatch of 2%, and penumbra (CT- MTT or MR-MTT) 2 cm diameter, we found an overall 84% agreement between CTP and MRP for enrollment selection. In addition, we found a greater than 9% agreement between CTP and MRP when each criterion was considered individually. Moreover, the majority of cases of disagreement could be attributed to inadequate CT coverage. When we exclude cases of disagreement due to inadequate CT coverage, overall agreement for patient selection increased to 97.8% (kappa.91). These results validate the use of advanced CT imaging for the selection of patients for acute stroke clinical trials. One reason that these results are important is that the success of an acute stroke clinical trial depends on assessing core and penumbra mismatch lesion size in a rapid and reproducible manner across multiple centers. We have demonstrated that commercially available CTP software allows clinically feasible, rapid automatic segmentation and volumetric measurement of CBV lesion size, MTT lesion size, and mismatch lesion size that correlates well with semiautomated volumet- Comparison of Clinical Trial Patient Selection Criteria Agreement for CTP versus MRP* Inclusion Criterion MRP and CTP Both Agreed MR and CTP Both Disagreed MR Disagreed CT Disagreed Percent Agreement 1 ml DWI/CT-CBV ml MTT % Mismatch Both Include Both Exclude MRP Exclude CTP Exclude Percent Agreement Clinical trial inclusion *Agreed: measurement satisfied inclusion criterion: core (MR-DWI, CT-CBV) 1 ml, penumbra (MR-MTT, CT-MTT) 4.19 ml, and mismatch (MR-MTT/DWI, CT-MTT/CBV 2%. Disagreed: measurement did not satisfy inclusion criterion: core (MR-DWI, CT-CBV) 1 ml, penumbra (MR-MTT, CT-MTT) 4.19 ml, and mismatch (MR-MTT/DWI, CT-MTT/CBV) 2%. Include: MRP or CTP satisfied all three criteria. Exclude: MRP or CTP did not meet at least one criterion.
6 Schaefer et al CT and MR Core/Penumbra Mismatch Correlate Strongly 2991 Table 4. Patients in Whom There Was a Discrepancy Between CTP and MRP for Clinical Trial Selection Criteria CT-CBV, ml MR-DWI, ml CT-MTT, ml MR-MTT, ml CT Mismatch, % MR Mismatch, % CTP Slab Thickness, mm Patient 1* Patient Patient Patient Patient Patient NC Patient *For patients 1 to 4, the CTP measurement of infarct core (CT-CBV) was less than, whereas the MR measurement of core (DWI) was 1 ml. For patients 5 and 6, the CT measurement of penumbra (CT-MTT) was less than, whereas the MR measurement of penumbra (MR-MTT) was 4.19 ml. For patient 7, the MR measurement of penumbra (MR-MTT) was less than, whereas the CT measurement of penumbra (CT-MTT) was 4.19 ml; and the MR measurement of mismatch (MTT-DWI) was less than, whereas the CT measurement of mismatch (MTT-CBV) was 2% percent. The CT segmented lesions were in different locations than those segmented on MRI. NC indicates not calculable because the denominator is. ric measurement of DWI lesion size, MR-MTT lesion size, and MR percent mismatch lesion size. Such software is currently commercially available from multiple vendors, including both Philips and GE Healthcare. Because semiautomated segmentation methods for calculating DWI and MTT are relatively time-consuming and impractical in the acute stroke setting, and there are no commercially available automatic segmentation tools for MRP, the selection criteria for most MR-based clinical trials have been based on subjective visual assessment of DWI lesion volume being less than one third of the MCA territory (or less than approximately 1 ml) and the DWI/transit time mismatch being greater than 2%. Compared with quantitative analyses, these subjective visual assessments have the potential to have poorer reliability. Our results are also noteworthy for other reasons. Imaging patients with acute stroke as rapidly as possible is of paramount importance. In general, CT scanners are more widely available and accessible in emergency rooms than are MRI scanners, and acute stroke CT (noncontrast CT, CT angiography, and CTP) scan time is generally less than that of acute stroke MR (DWI, MR angiography, and MRP) scan time. Furthermore, patients undergoing CT scanning do not require extensive screening to assure that they do not have metal in or on their bodies, and they do not require specialized (MR-compatible, nonferromagnetic) monitoring equipment. In addition, CT scanning costs less than MR scanning. We are aware of only one other study that compared CTP and MRP in selecting stroke patients for acute treatment. 12 In that study, the authors found 97.6% agreement between CTP and MRP for patient selection. The higher agreement between the 2 modalities in that study can be explained in part by the fact that CTP coverage was 4 cm in all cases, whereas some of our cases had only 1 or 2 cm of coverage. Indeed, in our study, when we exclude cases of disagreement due to inadequate CT coverage, overall agreement for patient selection increased to 97.8%. It is also noteworthy that their comparison was based on visual assessment, whereas ours was based on quantitative assessment. The major drawback of CTP for acute stroke imaging is limited coverage. Indeed, most of the discrepancies between CTP and MRP in our study could be attributed to the CTP slab not covering the entire lesion. This limitation will be minimized going forward as more centers purchase 64-slice scanners, which allow 4 cm of coverage per slab. However, there was disagreement between CTP and MRP for patient selection in 4 of our subjects, even with 4-mm coverage. Therefore, one should consider using 2 contrast boluses or shuttle mode scanning technique, both of which can double coverage. 13 When selecting the slab to be covered in a CTP acquisition, careful consideration of the clinical data, noncontrast CT, and CT angiography findings can also increase the likelihood of appropriate coverage of the ischemic lesion. The limitations of our study are as follows. Because CTP and MRP were performed up to 2 hours 8 minutes apart and stroke is a dynamic process, it is possible that in some patients, lesion core and ischemic penumbra volume changed between the CTP and MRP acquisitions. We excluded 2 clear cases of this phenomenon before enrollment but cannot be certain that more subtle cases were missed. Furthermore, we chose thresholds for CT-CBV and CT-MTT based on limited prior studies; it is possible that different thresholds are more appropriate and would provide a stronger correlation between CTP and MRP. In addition, we segmented MR-DWI and MTT abnormalities based on visual assessment. It is possible that choosing MR lesion volumes based on DWI and/or MTT thresholds could also improve the correlation between CT and MRI. We also chose clinical trial patient selection criteria (one third of the MCA territory for core and 2% mismatch for penumbra) based on the major large trials using mismatch surveyed in the introduction. A one third of MCA territory cutoff seems reasonable for core, because analysis of the ECASS 11 data determined that there was an increased risk of symptomatic intracranial hemorrhage in patients with hypoattenuation in greater than one third of the MCA territory on unenhanced CT. 14 However, it is possible that different selection criteria using different thresholds are more appropriate, especially for penumbra, and therefore would yield different results. Indeed, this has recently been suggested by a more detailed analysis of the DEFUSE data. 15 Moreover, although MTT or some measure of transit time has become the de facto penumbral measure of choice for major stroke trials, it remains unproven which perfusion imaging parameter provides the best differentiation between
7 2992 Stroke November 28 infarct core and penumbra in different clinical settings. It is possible that another parameter such as cerebral blood flow provides better differentiation between core and penumbra by excluding patients with benign oligemia and that we would not obtain the same results had we used other parameters In summary, validation and standardization of both the MR and CT definitions for core and penumbra are required. Conclusion Although MR is currently the preferred imaging method for measuring core, penumbra, and mismatch, CTP is quantitative and often more available. Criteria for patient selection for clinical trials are highly correlated for MR and CTP imaging when CTP coverage is sufficient to include the majority of the ischemic region. Acknowledgments We acknowledge Elkan Halpern, PhD, for assistance with our statistical analysis. Disclosures MHL: GE Healthcare (modest), Bracco (modest), and Vernalis (modest); LHS is on the medical advisory board of CoAxia, Inc; RGG received a National Institutes of Health Research Grant, Berlex Consultant (modest). References 1. Hacke W, Albers G, Al-Rawi Y, Bogousslavsky J, Davalos A, Eliasziw M, Fischer M, Furlan A, Kaste M, Lees KR, Soehngen M, Warach S. The Desmoteplase in Acute Ischemic Stroke Trial (DIAS): a phase II MRI-based 9-hour window acute stroke thrombolysis trial with intravenous desmoteplase. Stroke. 25;36: Furlan AJ, Eyding D, Albers GW, Al-Rawi Y, Lees KR, Rowley HA, Sachara C, Soehngen M, Warach S, Hacke W. Dose Escalation of Desmoteplase for Acute Ischemic Stroke (DEDAS): evidence of safety and efficacy 3 to 9 hours after stroke onset. Stroke. 26;37: Albers GW, Thijs VN, Wechsler L, Kemp S, Schlaug G, Skalabrin E, Bammer R, Kakuda W, Lansberg MG, Shuaib A, Coplin W, Hamilton S, Moseley M, Marks MP. Magnetic resonance imaging profiles predict clinical response to early reperfusion: the diffusion and perfusion imaging evaluation for understanding stroke evolution (DEFUSE) study. Ann Neurol. 26;6: Thomalla G, Schwark C, Sobesky J, Bluhmki E, Fiebach JB, Fiehler J, Zaro Weber O, Kucinski T, Juettler E, Ringleb PA, Zeumer H, Weiller C, Hacke W, Schellinger PD, Rother J. Outcome and symptomatic bleeding complications of intravenous thrombolysis within 6 hours in MRIselected stroke patients: comparison of a German multicenter study with the pooled data of ATLANTIS, ECASS, and NINDS tpa trials. Stroke. 26;37: Kohrmann M, Juttler E, Fiebach JB, Huttner HB, Siebert S, Schwark C, Ringleb PA, Schellinger PD, Hacke W. MRI versus CT-based thrombolysis treatment within and beyond the 3 h time window after stroke onset: a cohort study. Lancet Neurol. 26;5: Lev MH. CT/NIHSS mismatch for detection of salvageable brain in acute stroke triage beyond the 3-hour time window: overrated or undervalued? Stroke. 27;38: Kasner SE, Cucchiara BL, McGarvey ML, Luciano JM, Liebeskind DS, Chalela JA. Modified National Institutes of Health Stroke Scale can be estimated from medical records. Stroke. 23;34: Ostergaard L, Sorensen AG, Kwong KK, Weisskoff RM, Gyldensted C, Rosen BR. High resolution measurement of cerebral blood flow using intravascular tracer bolus passages. Part II: experimental comparison and preliminary results. Magn Reson Med. 1996;36: Ostergaard L, Weisskoff RM, Chesler DA, Gyldensted C, Rosen BR. High resolution measurement of cerebral blood flow using intravascular tracer bolus passages. Part I: mathematical approach and statistical analysis. Magn Reson Med. 1996;36: Kamalian S, Joshi M, Goldmakher GV, Gonzalez RG, Schaefer PW, Lev MH. CTP segmentation of infarct core: optimization of the CT-CBV/ MR-DWI correlation using relative: not absolute thresholds. Radiologic Society of North America 93rd Scientific Assembly and Annual Meeting. 27: Wintermark M, Flanders AE, Velthuis B, Meuli R, van Leeuwen M, Goldsher D, Pineda C, Serena J, van der Schaaf I, Waaijer A, Anderson J, Nesbit G, Gabriely I, Medina V, Quiles A, Pohlman S, Quist M, Schnyder P, Bogousslavsky J, Dillon WP, Pedraza S. Perfusion-CT assessment of infarct core and penumbra: receiver operating characteristic curve analysis in 13 patients suspected of acute hemispheric stroke. Stroke. 26;37: Wintermark M, Meuli R, Browaeys P, Reichhart M, Bogousslavsky J, Schnyder P, Michel P. Comparison of CT perfusion and angiography and MRI in selecting stroke patients for acute treatment. Neurology. 27; 68: Roberts HC, Roberts TP, Dillon WP. CT perfusion flow assessment: up and coming or off and running? AJNR Am J Neuroradiol. 21;22: Larrue V, von Kummer RR, Muller A, Bluhmki E. Risk factors for severe hemorrhagic transformation in ischemic stroke patients treated with recombinant tissue plasminogen activator: a secondary analysis of the European Australasian Acute Stroke Study (ECASS II). Stroke. 21;32: Kakuda W, Lansberg MG, Thijs VN, Kemp S, Bammer R, Wechsler L, Moseley M, Marks MP, Albers GW; DEFUSE Investigators. Optimal definition for PWI/DWI mismatch in acute ischemic stroke patients. J Cereb Blood Flow Metab. 28;28: Schaefer PW, Roccatagliata L, Ledezma C, Hoh B, Schwamm LH, Koroshetz W, Gonzalez RG, Lev MH. First-pass quantitative CT perfusion identifies thresholds for salvageable penumbra in acute stroke patients treated with intra-arterial therapy. AJNR Am J Neuroradiol. 26;27: Butcher KS, Parsons M, MacGregor L, Barber PA, Chalk J, Bladin C, Levi C, Kimber T, Schultz D, Fink J, Tress B, Donnan G, Davis S. Refining the perfusion diffusion mismatch hypothesis. Stroke. 25;36: Murphy BD, Fox AJ, Lee DH, Sahlas DJ, Black SE, Hogan MJ, Coutts SB, Demchuk AM, Goyal M, Aviv RI, Symons S, Gulka IB, Beletsky V, Pelz D, Hachinski V, Chan R, Lee TY. Identification of penumbra and infarct in acute ischemic stroke using computed tomography perfusionderived blood flow and blood volume measurements. Stroke. 26;37:
Optimal definition for PWI/DWI mismatch in acute ischemic stroke patients
 & 08 ISCBFM All rights reserved 0271-678X/08 $30.00 www.jcbfm.com Brief Communication Optimal definition for PWI/DWI mismatch in acute ischemic stroke patients Wataru Kakuda 1, Maarten G Lansberg 2, Vincent
& 08 ISCBFM All rights reserved 0271-678X/08 $30.00 www.jcbfm.com Brief Communication Optimal definition for PWI/DWI mismatch in acute ischemic stroke patients Wataru Kakuda 1, Maarten G Lansberg 2, Vincent
Rapid Assessment of Perfusion Diffusion Mismatch
 Rapid Assessment of Perfusion Diffusion Mismatch Ken Butcher, MD, PhD; Mark Parsons, PhD, FRACP; Louise Allport, FRACP; Sang Bong Lee, PhD; P. Alan Barber, PhD, ZRACP; Brian Tress, FRACR; Geoffrey A. Donnan,
Rapid Assessment of Perfusion Diffusion Mismatch Ken Butcher, MD, PhD; Mark Parsons, PhD, FRACP; Louise Allport, FRACP; Sang Bong Lee, PhD; P. Alan Barber, PhD, ZRACP; Brian Tress, FRACR; Geoffrey A. Donnan,
Comparison of Magnetic Resonance Imaging Mismatch Criteria to Select Patients for Endovascular Stroke Therapy
 Comparison of Magnetic Resonance Imaging Mismatch Criteria to Select Patients for Endovascular Stroke Therapy Nishant K. Mishra, MBBS, PhD, FESO; Gregory W. Albers, MD; Søren Christensen, PhD; Michael
Comparison of Magnetic Resonance Imaging Mismatch Criteria to Select Patients for Endovascular Stroke Therapy Nishant K. Mishra, MBBS, PhD, FESO; Gregory W. Albers, MD; Søren Christensen, PhD; Michael
Modifi ed CT perfusion contrast injection protocols for improved CBF quantifi cation with lower temporal sampling
 Investigations and research Modifi ed CT perfusion contrast injection protocols for improved CBF quantifi cation with lower temporal sampling J. Wang Z. Ying V. Yao L. Ciancibello S. Premraj S. Pohlman
Investigations and research Modifi ed CT perfusion contrast injection protocols for improved CBF quantifi cation with lower temporal sampling J. Wang Z. Ying V. Yao L. Ciancibello S. Premraj S. Pohlman
Subject: Anthem Policy Mechanical Embolectomy for Treatment of Acute Stroke
 John Whitney, MD Office of Medical Policy, Technology, Assessment and Credentialing WellPoint, Inc. 233 South Wacker Dr., Ste 3900 Chicago, IL 60606 (518) 367-5422 John.whitney@wellpoint.com Subject: Anthem
John Whitney, MD Office of Medical Policy, Technology, Assessment and Credentialing WellPoint, Inc. 233 South Wacker Dr., Ste 3900 Chicago, IL 60606 (518) 367-5422 John.whitney@wellpoint.com Subject: Anthem
Reperfusion therapy improves outcomes of patients with acute
 Published September 25, 2014 as 10.3174/ajnr.A4103 ORIGINAL RESEARCH BRAIN Combining MRI with NIHSS Thresholds to Predict Outcome in Acute Ischemic Stroke: Value for Patient Selection P.W. Schaefer, B.
Published September 25, 2014 as 10.3174/ajnr.A4103 ORIGINAL RESEARCH BRAIN Combining MRI with NIHSS Thresholds to Predict Outcome in Acute Ischemic Stroke: Value for Patient Selection P.W. Schaefer, B.
There is interest in studying core and penumbra to investigate
 CT Cerebral Blood Flow Maps Optimally Correlate With Admission Diffusion-Weighted Imaging in Acute Stroke but Thresholds Vary by Postprocessing Platform Shahmir Kamalian, MD; Shervin Kamalian, MD; Matthew
CT Cerebral Blood Flow Maps Optimally Correlate With Admission Diffusion-Weighted Imaging in Acute Stroke but Thresholds Vary by Postprocessing Platform Shahmir Kamalian, MD; Shervin Kamalian, MD; Matthew
Title: Stability of Large Diffusion/Perfusion Mismatch in Anterior Circulation Strokes for 4 or More Hours
 Author's response to reviews Title: Stability of Large Diffusion/Perfusion Mismatch in Anterior Circulation Strokes for 4 or More Hours Authors: Ramon G. Gonzalez (rggonzalez@partners.org) Reza Hakimelahi
Author's response to reviews Title: Stability of Large Diffusion/Perfusion Mismatch in Anterior Circulation Strokes for 4 or More Hours Authors: Ramon G. Gonzalez (rggonzalez@partners.org) Reza Hakimelahi
Reperfusion of the ischemic penumbra (ie, at-risk but
 Refinement of the Magnetic Resonance Diffusion-Perfusion Mismatch Concept for Thrombolytic Patient Selection Insights From the Desmoteplase in Acute Stroke Trials Steven Warach, MD, PhD; Yasir Al-Rawi,
Refinement of the Magnetic Resonance Diffusion-Perfusion Mismatch Concept for Thrombolytic Patient Selection Insights From the Desmoteplase in Acute Stroke Trials Steven Warach, MD, PhD; Yasir Al-Rawi,
CTP imaging has been used in the admission evaluation of
 Published January 12, 2012 as 10.3174/ajnr.A2809 ORIGINAL RESEARCH Shervin Kamalian Shahmir Kamalian A.A. Konstas M.B. Maas S. Payabvash S.R. Pomerantz P.W. Schaefer K.L. Furie R.G. González M.H. Lev CT
Published January 12, 2012 as 10.3174/ajnr.A2809 ORIGINAL RESEARCH Shervin Kamalian Shahmir Kamalian A.A. Konstas M.B. Maas S. Payabvash S.R. Pomerantz P.W. Schaefer K.L. Furie R.G. González M.H. Lev CT
Rapid identification of a major diffusion/perfusion mismatch in distal internal carotid artery or middle cerebral artery ischemic stroke
 Rapid identification of a major diffusion/perfusion mismatch in distal internal carotid artery or middle cerebral artery ischemic stroke The Harvard community has made this article openly available. Please
Rapid identification of a major diffusion/perfusion mismatch in distal internal carotid artery or middle cerebral artery ischemic stroke The Harvard community has made this article openly available. Please
The Declaration of Helsinki 1 stipulates that patients who
 Brain Lesion Volume and Capacity for Consent in Stroke Trials Potential Regulatory Barriers to the Use of Surrogate Markers Krishna A. Dani, MRCP; Michael T. McCormick, MRCP; Keith W. Muir, MD, FRCP Background
Brain Lesion Volume and Capacity for Consent in Stroke Trials Potential Regulatory Barriers to the Use of Surrogate Markers Krishna A. Dani, MRCP; Michael T. McCormick, MRCP; Keith W. Muir, MD, FRCP Background
Multidetector CT (MDCT) is widely used in the clinical field and becoming the new standard in radiological
 Focused Issue of This Month MDCT Application in Neuroimaging SeungKoo Lee, MD Department of Radiology, Yonsei University College of Medicine Email : slee@yumc.yonsei.ac.kr J Korean Med Assoc 2007; 50(1):
Focused Issue of This Month MDCT Application in Neuroimaging SeungKoo Lee, MD Department of Radiology, Yonsei University College of Medicine Email : slee@yumc.yonsei.ac.kr J Korean Med Assoc 2007; 50(1):
Can the Ischemic Penumbra Be Identified on Noncontrast CT of Acute Stroke?
 Can the Ischemic Penumbra Be Identified on Noncontrast CT of Acute Stroke? Keith W. Muir, MD, FRCP; Jonathan Baird-Gunning, BSc; Leighton Walker, FRCR; Tracey Baird, MRCP; Michael McCormick, MRCP; Shelagh
Can the Ischemic Penumbra Be Identified on Noncontrast CT of Acute Stroke? Keith W. Muir, MD, FRCP; Jonathan Baird-Gunning, BSc; Leighton Walker, FRCR; Tracey Baird, MRCP; Michael McCormick, MRCP; Shelagh
Neuroimaging for acute ischemic stroke: current challenges
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2014 Neuroimaging for acute ischemic stroke: current challenges Wegener, Susanne
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2014 Neuroimaging for acute ischemic stroke: current challenges Wegener, Susanne
Immediate Changes in Stroke Lesion Volumes Post Thrombolysis Predict Clinical Outcome
 Immediate Changes in Stroke Lesion Volumes Post Thrombolysis Predict Clinical Outcome Marie Luby, PhD; Steven J. Warach, MD, PhD; Zurab Nadareishvili, MD, PhD; José G. Merino, MD, MPhil Background and
Immediate Changes in Stroke Lesion Volumes Post Thrombolysis Predict Clinical Outcome Marie Luby, PhD; Steven J. Warach, MD, PhD; Zurab Nadareishvili, MD, PhD; José G. Merino, MD, MPhil Background and
Reliability of CT Perfusion in the Evaluation of the Ischaemic Penumbra
 Reliability of CT Perfusion in the Evaluation of the Ischaemic Penumbra JOSÉ EDUARDO ALVES, ÂNGELO CARNEIRO, JOÃO XAVIER Department of Neuroradiology, Centro Hospitalar do Porto; Porto, Portugal Key words:
Reliability of CT Perfusion in the Evaluation of the Ischaemic Penumbra JOSÉ EDUARDO ALVES, ÂNGELO CARNEIRO, JOÃO XAVIER Department of Neuroradiology, Centro Hospitalar do Porto; Porto, Portugal Key words:
occlusions. Cerebral perfusion is driven fundamentally by regional cerebral
 Appendix Figures Figure A1. Hemodynamic changes that may occur in major anterior circulation occlusions. Cerebral perfusion is driven fundamentally by regional cerebral perfusion pressure (CPP). In response
Appendix Figures Figure A1. Hemodynamic changes that may occur in major anterior circulation occlusions. Cerebral perfusion is driven fundamentally by regional cerebral perfusion pressure (CPP). In response
Stroke is the leading cause of serious, long-term disability
 Cost-Effectiveness of Patient Selection Using Penumbral-Based MRI for Intravenous Thrombolysis Stephanie R. Earnshaw, PhD; Dan Jackson, MSc; Ray Farkouh, PhD; Lee Schwamm, MD Background and Purpose Better
Cost-Effectiveness of Patient Selection Using Penumbral-Based MRI for Intravenous Thrombolysis Stephanie R. Earnshaw, PhD; Dan Jackson, MSc; Ray Farkouh, PhD; Lee Schwamm, MD Background and Purpose Better
Early identification of tissue at risk of infarction after
 Predicting Tissue Outcome From Acute Stroke Magnetic Resonance Imaging Improving Model Performance by Optimal Sampling of Training Data Kristjana Yr Jonsdottir, PhD, MSc; Leif Østergaard, DMSc, PhD, MD,
Predicting Tissue Outcome From Acute Stroke Magnetic Resonance Imaging Improving Model Performance by Optimal Sampling of Training Data Kristjana Yr Jonsdottir, PhD, MSc; Leif Østergaard, DMSc, PhD, MD,
Analysis of DWI ASPECTS and Recanalization Outcomes of Patients with Acute-phase Cerebral Infarction
 J Med Dent Sci 2012; 59: 57-63 Original Article Analysis of DWI ASPECTS and Recanalization Outcomes of Patients with Acute-phase Cerebral Infarction Keigo Shigeta 1,2), Kikuo Ohno 1), Yoshio Takasato 2),
J Med Dent Sci 2012; 59: 57-63 Original Article Analysis of DWI ASPECTS and Recanalization Outcomes of Patients with Acute-phase Cerebral Infarction Keigo Shigeta 1,2), Kikuo Ohno 1), Yoshio Takasato 2),
Treatment with intravenous tissue plasminogen activator
 RAPID Automated Patient Selection for Reperfusion Therapy A Pooled Analysis of the Echoplanar Imaging Thrombolytic Evaluation Trial (EPITHET) and the Diffusion and Perfusion Imaging Evaluation for Understanding
RAPID Automated Patient Selection for Reperfusion Therapy A Pooled Analysis of the Echoplanar Imaging Thrombolytic Evaluation Trial (EPITHET) and the Diffusion and Perfusion Imaging Evaluation for Understanding
Effect of Collateral Blood Flow on Patients Undergoing Endovascular Therapy for Acute Ischemic Stroke
 Effect of Collateral Blood Flow on Patients Undergoing Endovascular Therapy for Acute Ischemic Stroke Michael P. Marks, MD; Maarten G. Lansberg, MD; Michael Mlynash, MD; Jean-Marc Olivot, MD; Matus Straka,
Effect of Collateral Blood Flow on Patients Undergoing Endovascular Therapy for Acute Ischemic Stroke Michael P. Marks, MD; Maarten G. Lansberg, MD; Michael Mlynash, MD; Jean-Marc Olivot, MD; Matus Straka,
Hypoperfusion Intensity Ratio Predicts Infarct Progression and Functional Outcome in the DEFUSE 2 Cohort
 Hypoperfusion Intensity Ratio Predicts Infarct Progression and Functional Outcome in the DEFUSE 2 Cohort Jean Marc Olivot, MD, PhD; Michael Mlynash, MD, MS; Manabu Inoue, MD, PhD; Michael P. Marks, MD;
Hypoperfusion Intensity Ratio Predicts Infarct Progression and Functional Outcome in the DEFUSE 2 Cohort Jean Marc Olivot, MD, PhD; Michael Mlynash, MD, MS; Manabu Inoue, MD, PhD; Michael P. Marks, MD;
ACUTE STROKE IMAGING
 ACUTE STROKE IMAGING Mahesh V. Jayaraman M.D. Director, Inter ventional Neuroradiology Associate Professor Depar tments of Diagnostic Imaging and Neurosurger y Alper t Medical School at Brown University
ACUTE STROKE IMAGING Mahesh V. Jayaraman M.D. Director, Inter ventional Neuroradiology Associate Professor Depar tments of Diagnostic Imaging and Neurosurger y Alper t Medical School at Brown University
Whole brain CT perfusion maps with paradoxical low mean transit time to predict infarct core
 Whole brain CT perfusion maps with paradoxical low mean transit time to predict infarct core Poster No.: B-292 Congress: ECR 2011 Type: Scientific Paper Topic: Neuro Authors: S. Chakraborty, M. E. Ahmad,
Whole brain CT perfusion maps with paradoxical low mean transit time to predict infarct core Poster No.: B-292 Congress: ECR 2011 Type: Scientific Paper Topic: Neuro Authors: S. Chakraborty, M. E. Ahmad,
While MR imaging is superior in the diagnosis of acute
 ORIGINAL RESEARCH X.-C. Wang P.-Y. Gao J. Xue G.-R. Liu L. Ma Identification of Infarct Core and Penumbra in Acute Stroke Using CT Perfusion Source Images BACKGROUND AND PURPOSE: CT perfusion (CTP) mapping
ORIGINAL RESEARCH X.-C. Wang P.-Y. Gao J. Xue G.-R. Liu L. Ma Identification of Infarct Core and Penumbra in Acute Stroke Using CT Perfusion Source Images BACKGROUND AND PURPOSE: CT perfusion (CTP) mapping
Perfusion-weighted imaging (PWI) and diffusionweighted
 Apparent Diffusion Coefficient Thresholds Do Not Predict the Response to Acute Stroke Thrombolysis Poh-Sien Loh, FRACP; Ken S. Butcher, MD, PhD, FRCP(C), FRACP; Mark W. Parsons, PhD, FRACP; Lachlan MacGregor,
Apparent Diffusion Coefficient Thresholds Do Not Predict the Response to Acute Stroke Thrombolysis Poh-Sien Loh, FRACP; Ken S. Butcher, MD, PhD, FRCP(C), FRACP; Mark W. Parsons, PhD, FRACP; Lachlan MacGregor,
CT/MRI 第 42 回日本脳卒中学会講演シンポジウム 総説 はじめに. MRI magnetic resonance imaging DWI diffusion-weighted. DWI/CBF malignant profile
 第 42 回日本脳卒中学会講演シンポジウム 総説 CT/MRI 1 要旨 rt-pa MRI magnetic resonance imaging DWI diffusion-weighted image Tmax time-to-maximum DWI/PWI perfusion image mismatch CT computed tomography CBF cerebral blood flow
第 42 回日本脳卒中学会講演シンポジウム 総説 CT/MRI 1 要旨 rt-pa MRI magnetic resonance imaging DWI diffusion-weighted image Tmax time-to-maximum DWI/PWI perfusion image mismatch CT computed tomography CBF cerebral blood flow
The association between neurological deficit in acute ischemic stroke and mean transit time
 Neuroradiology (2006) 48: 69 77 DOI 10.1007/s00234-005-0012-9 DIAGNOSTIC NEURORADIOLOGY Peter D. Schellinger Lawrence L. Latour Chen-Sen Wu Julio A. Chalela Steven Warach The association between neurological
Neuroradiology (2006) 48: 69 77 DOI 10.1007/s00234-005-0012-9 DIAGNOSTIC NEURORADIOLOGY Peter D. Schellinger Lawrence L. Latour Chen-Sen Wu Julio A. Chalela Steven Warach The association between neurological
Characterization and Evolution of Diffusion MR Imaging Abnormalities in Stroke Patients Undergoing Intra-Arterial Thrombolysis
 AJNR Am J Neuroradiol 25:951 957, June/July 2004 Characterization and Evolution of Diffusion MR Imaging Abnormalities in Stroke Patients Undergoing Intra-Arterial Thrombolysis Pamela W. Schaefer, Alvand
AJNR Am J Neuroradiol 25:951 957, June/July 2004 Characterization and Evolution of Diffusion MR Imaging Abnormalities in Stroke Patients Undergoing Intra-Arterial Thrombolysis Pamela W. Schaefer, Alvand
Remission of diffusion lesions in acute stroke magnetic resonance imaging
 ORIGINAL RESEARCH Remission of diffusion lesions in acute stroke magnetic resonance imaging F. A. Fellner 1, M. R. Vosko 2, C. M. Fellner 1, D. Flöry 1 1. AKH Linz, Institute of Radiology, Austria. 2.
ORIGINAL RESEARCH Remission of diffusion lesions in acute stroke magnetic resonance imaging F. A. Fellner 1, M. R. Vosko 2, C. M. Fellner 1, D. Flöry 1 1. AKH Linz, Institute of Radiology, Austria. 2.
BY MARILYN M. RYMER, MD
 Lytics, Devices, and Advanced Imaging The evolving art and science of acute stroke intervention. BY MARILYN M. RYMER, MD In 1996, when the US Food and Drug Administration (FDA) approved the use of intravenous
Lytics, Devices, and Advanced Imaging The evolving art and science of acute stroke intervention. BY MARILYN M. RYMER, MD In 1996, when the US Food and Drug Administration (FDA) approved the use of intravenous
Downloaded from by on March 11, 2019
 Imaging-Based Endovascular Therapy for Acute Ischemic Stroke due to Proximal Intracranial Anterior Circulation Occlusion Treated Beyond 8 Hours From Time Last Seen Well Retrospective Multicenter Analysis
Imaging-Based Endovascular Therapy for Acute Ischemic Stroke due to Proximal Intracranial Anterior Circulation Occlusion Treated Beyond 8 Hours From Time Last Seen Well Retrospective Multicenter Analysis
Benign Oligemia Despite a Malignant MRI Profile in Acute Ischemic Stroke
 CASE REPORT J Clin Neurol 2010;6:41-45 Print ISSN 1738-6586 / On-line ISSN 2005-5013 10.3988/jcn.2010.6.1.41 Benign Oligemia Despite a Malignant MRI Profile in Acute Ischemic Stroke Oh Young Bang, MD a
CASE REPORT J Clin Neurol 2010;6:41-45 Print ISSN 1738-6586 / On-line ISSN 2005-5013 10.3988/jcn.2010.6.1.41 Benign Oligemia Despite a Malignant MRI Profile in Acute Ischemic Stroke Oh Young Bang, MD a
Prediction of Hemorrhage in Acute Ischemic Stroke Using Permeability MR Imaging
 AJNR Am J Neuroradiol 26:2213 2217, October 2005 Technical Note Prediction of Hemorrhage in Acute Ischemic Stroke Using Permeability MR Imaging Andrea Kassner, Timothy Roberts, Keri Taylor, Frank Silver,
AJNR Am J Neuroradiol 26:2213 2217, October 2005 Technical Note Prediction of Hemorrhage in Acute Ischemic Stroke Using Permeability MR Imaging Andrea Kassner, Timothy Roberts, Keri Taylor, Frank Silver,
Background. Recommendations for Imaging of Acute Ischemic Stroke: A Scientific Statement From the American Heart Association
 for Imaging of Acute Ischemic Stroke: A Scientific Statement From the American Heart Association An Scientific Statement from the Stroke Council, American Heart Association and American Stroke Association
for Imaging of Acute Ischemic Stroke: A Scientific Statement From the American Heart Association An Scientific Statement from the Stroke Council, American Heart Association and American Stroke Association
Biomedical Research 2017; 28 (17):
 Biomedical Research 2017; 28 (17): 7578-7582 ISSN 0970-938X www.biomedres.info Fusion images of perfusion- and diffusion-weighted MR imaging: A simple diagnostic approach of ischemic penumbra selection
Biomedical Research 2017; 28 (17): 7578-7582 ISSN 0970-938X www.biomedres.info Fusion images of perfusion- and diffusion-weighted MR imaging: A simple diagnostic approach of ischemic penumbra selection
Dynamic susceptibility contract-enhanced MRI is increasingly
 Influence of Arterial Input Function on Hypoperfusion Volumes Measured With Perfusion-Weighted Imaging Vincent N. Thijs, MD; Diederik M. Somford, MD; Roland Bammer, PhD; Wim Robberecht, MD, PhD; Michael
Influence of Arterial Input Function on Hypoperfusion Volumes Measured With Perfusion-Weighted Imaging Vincent N. Thijs, MD; Diederik M. Somford, MD; Roland Bammer, PhD; Wim Robberecht, MD, PhD; Michael
Predicting Cerebral Ischemic Infarct Volume with Diffusion and Perfusion MR Imaging
 AJNR Am J Neuroradiol 23:1785 1794, November/December 2002 Predicting Cerebral Ischemic Infarct Volume with Diffusion and Perfusion MR Imaging Pamela W. Schaefer, George J. Hunter, Julian He, Leena M.
AJNR Am J Neuroradiol 23:1785 1794, November/December 2002 Predicting Cerebral Ischemic Infarct Volume with Diffusion and Perfusion MR Imaging Pamela W. Schaefer, George J. Hunter, Julian He, Leena M.
Dong Gyu Na, Vincent N. Thijs, Gregory W. Albers, Michael E. Moseley, and Michael P. Marks. AJNR Am J Neuroradiol 25: , September 2004
 AJNR Am J Neuroradiol 25:1331 1336, September 2004 Diffusion-Weighted MR Imaging in Acute Ischemia: Value of Apparent Diffusion Coefficient and Signal Intensity Thresholds in Predicting Tissue at Risk
AJNR Am J Neuroradiol 25:1331 1336, September 2004 Diffusion-Weighted MR Imaging in Acute Ischemia: Value of Apparent Diffusion Coefficient and Signal Intensity Thresholds in Predicting Tissue at Risk
MR and CT Perfusion in Acute Ischemic Stroke The uses, methods, and risks associated with these alternative imaging modalities.
 MR and CT Perfusion in Acute Ischemic Stroke The uses, methods, and risks associated with these alternative imaging modalities. BY CATALINA C. IONITA, MD; EVE A. GUTERMAN; AND LEE R. GUTERMAN, PHD, MD
MR and CT Perfusion in Acute Ischemic Stroke The uses, methods, and risks associated with these alternative imaging modalities. BY CATALINA C. IONITA, MD; EVE A. GUTERMAN; AND LEE R. GUTERMAN, PHD, MD
IMAGING IN ACUTE ISCHEMIC STROKE
 IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
CT Perfusion Parameter Values in Regions of Diffusion Abnormalities
 AJNR Am J Neuroradiol 25:1205 1210, August 2004 CT Perfusion Parameter Values in Regions of Diffusion Abnormalities Marcello Galvez, Gerald E. York, II, and James D. Eastwood BACKGROUND AND PURPOSE: Dynamic
AJNR Am J Neuroradiol 25:1205 1210, August 2004 CT Perfusion Parameter Values in Regions of Diffusion Abnormalities Marcello Galvez, Gerald E. York, II, and James D. Eastwood BACKGROUND AND PURPOSE: Dynamic
MEDICAL POLICY EFFECTIVE DATE: 12/18/08 REVISED DATE: 12/17/09, 03/17/11, 05/19/11, 05/24/12, 05/23/13, 05/22/14
 MEDICAL POLICY SUBJECT: CT (COMPUTED TOMOGRAPHY) PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical
MEDICAL POLICY SUBJECT: CT (COMPUTED TOMOGRAPHY) PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical
Clinical-Diffusion Mismatch Predicts the Putative Penumbra With High Specificity
 Clinical-Diffusion Mismatch Predicts the Putative Penumbra With High Specificity Jane Prosser, FRACP; Ken Butcher, MD, PhD, FRCP(C); Louise Allport, FRACP; Mark Parsons, PhD, FRACP; Lachlan MacGregor,
Clinical-Diffusion Mismatch Predicts the Putative Penumbra With High Specificity Jane Prosser, FRACP; Ken Butcher, MD, PhD, FRCP(C); Louise Allport, FRACP; Mark Parsons, PhD, FRACP; Lachlan MacGregor,
Imaging for Acute Stroke
 Imaging for Acute Stroke Nine case studies detailing the impact of imaging on stroke therapy. BY ANSAAR T. RAI, MD Ischemic stroke is a dynamic process, and the term stroke in evolution precisely underscores
Imaging for Acute Stroke Nine case studies detailing the impact of imaging on stroke therapy. BY ANSAAR T. RAI, MD Ischemic stroke is a dynamic process, and the term stroke in evolution precisely underscores
Medical Policy. MP Computed Tomography Perfusion Imaging of the Brain
 Medical Policy MP 6.01.49 BCBSA Ref. Policy: 6.01.49 Last Review: 09/28/2017 Effective Date: 09/28/2017 Section: Radiology Related Policies 2.01.54 Endovascular Procedures for Intracranial Arterial Disease
Medical Policy MP 6.01.49 BCBSA Ref. Policy: 6.01.49 Last Review: 09/28/2017 Effective Date: 09/28/2017 Section: Radiology Related Policies 2.01.54 Endovascular Procedures for Intracranial Arterial Disease
ORIGINAL ARTICLE. Chang Y. Ho & Sajjad Hussain & Tariq Alam & Iftikhar Ahmad & Isaac C. Wu & Darren P. O Neill
 DOI 10.1007/s10140-012-1102-8 ORIGINAL ARTICLE Accuracy of CT cerebral perfusion in predicting infarct in the emergency department: lesion characterization on CT perfusion based on commercially available
DOI 10.1007/s10140-012-1102-8 ORIGINAL ARTICLE Accuracy of CT cerebral perfusion in predicting infarct in the emergency department: lesion characterization on CT perfusion based on commercially available
IST-3 Perfusion and angiography studies: Image acquisition and analysis protocol. Date: Authors: T Carpenter, JM Wardlaw Version: 5
 IST-3 Perfusion and angiography studies: Image acquisition and analysis protocol. Date: 20091024 Authors: T Carpenter, JM Wardlaw Version: 5 Methods: 1) Acquisition Due to the diverse range of scanners
IST-3 Perfusion and angiography studies: Image acquisition and analysis protocol. Date: 20091024 Authors: T Carpenter, JM Wardlaw Version: 5 Methods: 1) Acquisition Due to the diverse range of scanners
IMAGING IN ACUTE ISCHEMIC STROKE
 IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
Comparison of 10 Perfusion MRI Parameters in 97 Sub-6-Hour Stroke Patients Using Voxel-Based Receiver Operating Characteristics Analysis
 Comparison of 10 Perfusion MRI Parameters in 97 Sub-6-Hour Stroke Patients Using Voxel-Based Receiver Operating Characteristics Analysis Søren Christensen, MSc; Kim Mouridsen, PhD; Ona Wu, PhD; Niels Hjort,
Comparison of 10 Perfusion MRI Parameters in 97 Sub-6-Hour Stroke Patients Using Voxel-Based Receiver Operating Characteristics Analysis Søren Christensen, MSc; Kim Mouridsen, PhD; Ona Wu, PhD; Niels Hjort,
Experimental Assessment of Infarct Lesion Growth in Mice using Time-Resolved T2* MR Image Sequences
 Experimental Assessment of Infarct Lesion Growth in Mice using Time-Resolved T2* MR Image Sequences Nils Daniel Forkert 1, Dennis Säring 1, Andrea Eisenbeis 2, Frank Leypoldt 3, Jens Fiehler 2, Heinz Handels
Experimental Assessment of Infarct Lesion Growth in Mice using Time-Resolved T2* MR Image Sequences Nils Daniel Forkert 1, Dennis Säring 1, Andrea Eisenbeis 2, Frank Leypoldt 3, Jens Fiehler 2, Heinz Handels
The role of diffusion and perfusion MRI for the identification
 The Physiological Significance of the Time-to-Maximum (Tmax) Parameter in Perfusion MRI Fernando Calamante, PhD; Søren Christensen, PhD; Patricia M. Desmond, MD, FRANZCR; Leif Østergaard, MD, PhD; Stephen
The Physiological Significance of the Time-to-Maximum (Tmax) Parameter in Perfusion MRI Fernando Calamante, PhD; Søren Christensen, PhD; Patricia M. Desmond, MD, FRANZCR; Leif Østergaard, MD, PhD; Stephen
Advanced imaging of acute ischemic stroke has the. Cerebral Blood Flow Is the Optimal CT Perfusion Parameter for Assessing Infarct Core
 Cerebral Blood Flow Is the Optimal CT Perfusion Parameter for Assessing Infarct Core Bruce C.V. Campbell, MBBS, BMedSc, FRACP; Søren Christensen, PhD; Christopher R. Levi, MBBS, FRACP; Patricia M. Desmond,
Cerebral Blood Flow Is the Optimal CT Perfusion Parameter for Assessing Infarct Core Bruce C.V. Campbell, MBBS, BMedSc, FRACP; Søren Christensen, PhD; Christopher R. Levi, MBBS, FRACP; Patricia M. Desmond,
The role of CT perfusion in patients selection for acute treatment
 The role of CT perfusion in patients selection for acute treatment Enrico Fainardi Unità Operativa di Neuroradiologia, Dipartimento di Neuroscienze e Riabilitazione, Azienda Ospedaliero-Universitaria,
The role of CT perfusion in patients selection for acute treatment Enrico Fainardi Unità Operativa di Neuroradiologia, Dipartimento di Neuroscienze e Riabilitazione, Azienda Ospedaliero-Universitaria,
Tmax Determined Using a Bayesian Estimation Deconvolution Algorithm Applied to Bolus Tracking Perfusion Imaging: A Digital Phantom Validation Study
 Magn Reson Med Sci 2017; 16; 32 37 doi:10.2463/mrms.mp.2015-0167 Published Online: March 21, 2016 MAJOR PAPER Tmax Determined Using a Bayesian Estimation Deconvolution Algorithm Applied to Bolus Tracking
Magn Reson Med Sci 2017; 16; 32 37 doi:10.2463/mrms.mp.2015-0167 Published Online: March 21, 2016 MAJOR PAPER Tmax Determined Using a Bayesian Estimation Deconvolution Algorithm Applied to Bolus Tracking
This study is the culmination of work performed in response
 ORIGINAL RESEARCH J.M. Provenzale K. Shah U. Patel D.C. McCrory Systematic Review of CT and MR Perfusion Imaging for Assessment of Acute Cerebrovascular Disease BACKGROUND AND PURPOSE: Perfusion imaging
ORIGINAL RESEARCH J.M. Provenzale K. Shah U. Patel D.C. McCrory Systematic Review of CT and MR Perfusion Imaging for Assessment of Acute Cerebrovascular Disease BACKGROUND AND PURPOSE: Perfusion imaging
A Topographic Study of the Evolution of the MR DWI/PWI Mismatch Pattern and Its Clinical Impact A Study by the EPITHET and DEFUSE Investigators
 A Topographic Study of the Evolution of the MR DWI/PWI Mismatch Pattern and Its Clinical Impact A Study by the EPITHET and DEFUSE Investigators Toshiyasu Ogata, MD; Yoshinari Nagakane, MD; Soren Christensen,
A Topographic Study of the Evolution of the MR DWI/PWI Mismatch Pattern and Its Clinical Impact A Study by the EPITHET and DEFUSE Investigators Toshiyasu Ogata, MD; Yoshinari Nagakane, MD; Soren Christensen,
Wake-Up Stroke: Clinical and Neuroimaging Characteristics
 Original Paper DOI: 10.1159/000278929 Received: April 21, 2009 Accepted: November 4, 2009 Published online: January 30, 2010 Wake-Up Stroke: Clinical and Neuroimaging Characteristics Gisele S. Silva a,
Original Paper DOI: 10.1159/000278929 Received: April 21, 2009 Accepted: November 4, 2009 Published online: January 30, 2010 Wake-Up Stroke: Clinical and Neuroimaging Characteristics Gisele S. Silva a,
Rescuing the ischemic penumbra is the central premise of
 Perfusion-CT Assessment of Infarct Core and Penumbra Receiver Operating Characteristic Curve Analysis in 130 Patients Suspected of Acute Hemispheric Stroke Max Wintermark, MD; Adam E. Flanders, MD; Birgitta
Perfusion-CT Assessment of Infarct Core and Penumbra Receiver Operating Characteristic Curve Analysis in 130 Patients Suspected of Acute Hemispheric Stroke Max Wintermark, MD; Adam E. Flanders, MD; Birgitta
Thrombolysis is the only proven pharmacological treatment
 Perfusion Thresholds in Acute Stroke Thrombolysis K. Butcher, MD, PhD, FRCP(C); M. Parsons, PhD, FRACP; T. Baird, MBBS; A. Barber, PhD, FRANZ; G. Donnan, MD, FRACP; P. Desmond, FRACR; B. Tress, FRACR;
Perfusion Thresholds in Acute Stroke Thrombolysis K. Butcher, MD, PhD, FRCP(C); M. Parsons, PhD, FRACP; T. Baird, MBBS; A. Barber, PhD, FRANZ; G. Donnan, MD, FRACP; P. Desmond, FRACR; B. Tress, FRACR;
Imaging Stroke: Is There a Stroke Equivalent of the ECG? Albert J. Yoo, MD Director of Acute Stroke Intervention Massachusetts General Hospital
 Imaging Stroke: Is There a Stroke Equivalent of the ECG? Albert J. Yoo, MD Director of Acute Stroke Intervention Massachusetts General Hospital Disclosures Penumbra, Inc. research grant (significant) for
Imaging Stroke: Is There a Stroke Equivalent of the ECG? Albert J. Yoo, MD Director of Acute Stroke Intervention Massachusetts General Hospital Disclosures Penumbra, Inc. research grant (significant) for
Multiparametric MRI and CT Models of Infarct Core and Favorable Penumbral Imaging Patterns in Acute Ischemic Stroke
 Multiparametric MRI and CT Models of Infarct Core and Favorable Penumbral Imaging Patterns in Acute Ischemic Stroke Chelsea S. Kidwell, MD; Max Wintermark, MD; Deidre A. De Silva, MD; Timothy J. Schaewe,
Multiparametric MRI and CT Models of Infarct Core and Favorable Penumbral Imaging Patterns in Acute Ischemic Stroke Chelsea S. Kidwell, MD; Max Wintermark, MD; Deidre A. De Silva, MD; Timothy J. Schaewe,
Early and accurate detection of tissue at risk of infarction
 The Role of Bolus Delay and Dispersion in Predictor Models for Stroke Lisa Willats, PhD; Alan Connelly, PhD; Soren Christensen, PhD; Geoffrey A. Donnan, MD, FRACP; Stephen M. Davis, MD, FRACP; Fernando
The Role of Bolus Delay and Dispersion in Predictor Models for Stroke Lisa Willats, PhD; Alan Connelly, PhD; Soren Christensen, PhD; Geoffrey A. Donnan, MD, FRACP; Stephen M. Davis, MD, FRACP; Fernando
Perfusion Patterns of Ischemic Stroke on Computed Tomography Perfusion
 Journal of Stroke 2013;15(3):164-173 http://dx.doi.org/10.5853/jos.2013.15.3.164 Review Perfusion Patterns of Ischemic Stroke on Computed Tomography Perfusion Longting Lin, a Andrew Bivard, b Mark W. Parsons
Journal of Stroke 2013;15(3):164-173 http://dx.doi.org/10.5853/jos.2013.15.3.164 Review Perfusion Patterns of Ischemic Stroke on Computed Tomography Perfusion Longting Lin, a Andrew Bivard, b Mark W. Parsons
The Alberta Stroke Program Early CT Score (ASPECTS) is a
 ORIGINAL RESEARCH K. Lin O. Rapalino M. Law J.S. Babb K.A. Siller B.K. Pramanik Accuracy of the Alberta Stroke Program Early CT Score during the First 3 Hours of Middle Cerebral Artery Stroke: Comparison
ORIGINAL RESEARCH K. Lin O. Rapalino M. Law J.S. Babb K.A. Siller B.K. Pramanik Accuracy of the Alberta Stroke Program Early CT Score during the First 3 Hours of Middle Cerebral Artery Stroke: Comparison
Acute Ischemic Stroke Imaging. Ronald L. Wolf, MD, PhD Associate Professor of Radiology
 Acute Ischemic Stroke Imaging Ronald L. Wolf, MD, PhD Associate Professor of Radiology Title of First Slide of Substance An Illustrative Case 2 Disclosures No financial disclosures Off-label uses of some
Acute Ischemic Stroke Imaging Ronald L. Wolf, MD, PhD Associate Professor of Radiology Title of First Slide of Substance An Illustrative Case 2 Disclosures No financial disclosures Off-label uses of some
Clinical profile of patients with acute ischemic stroke receiving intravenous thrombolysis (rtpa-alteplase)
 International Journal of Advances in Medicine Jagini SP et al. Int J Adv Med. 2018 Feb;5(1):164-169 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20180078
International Journal of Advances in Medicine Jagini SP et al. Int J Adv Med. 2018 Feb;5(1):164-169 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20180078
Translent CT hyperattenuation after intraarterial thrombolysis in stroke. Contrast extravasation or hemorrhage
 Translent CT hyperattenuation after intraarterial thrombolysis in stroke. Contrast extravasation or hemorrhage Poster No.: C-0053 Congress: ECR 2013 Type: Scientific Exhibit Authors: A. Losa Palacios,
Translent CT hyperattenuation after intraarterial thrombolysis in stroke. Contrast extravasation or hemorrhage Poster No.: C-0053 Congress: ECR 2013 Type: Scientific Exhibit Authors: A. Losa Palacios,
Diagnostic improvement from average image in acute ischemic stroke
 Diagnostic improvement from average image in acute ischemic stroke N. Magne (1), E.Tollard (1), O. Ozkul- Wermester (2), V. Macaigne (1), J.-N. Dacher (1), E. Gerardin (1) (1) Department of Radiology,
Diagnostic improvement from average image in acute ischemic stroke N. Magne (1), E.Tollard (1), O. Ozkul- Wermester (2), V. Macaigne (1), J.-N. Dacher (1), E. Gerardin (1) (1) Department of Radiology,
OBJECTIVES: INTRODUCTION ADVANCES IN ACUTE STROKE CARE
 Brian A. Stettler, MD Assistant Professor, Department of Emergency Medicine, University of Cincinnati College of Medicine Member, Greater Cincinnati/Northern Kentucky Stroke Team Cincinnati, Ohio OBJECTIVES:
Brian A. Stettler, MD Assistant Professor, Department of Emergency Medicine, University of Cincinnati College of Medicine Member, Greater Cincinnati/Northern Kentucky Stroke Team Cincinnati, Ohio OBJECTIVES:
Diffusion-weighted Magnetic Resonance Imaging in the Emergency Department
 298 / = Abstract = Diffusion-weighted Magnetic Resonance Imaging in the Emergency Department Sung Pil Chung, M.D, Suk Woo Lee, M.D., Young Mo Yang, M.D., Young Rock Ha, M.D., Seung Whan Kim, M.D., and
298 / = Abstract = Diffusion-weighted Magnetic Resonance Imaging in the Emergency Department Sung Pil Chung, M.D, Suk Woo Lee, M.D., Young Mo Yang, M.D., Young Rock Ha, M.D., Seung Whan Kim, M.D., and
Update on Early Acute Ischemic Stroke Interventions
 Update on Early Acute Ischemic Stroke Interventions Diana Goodman MD Lead Neurohospitalist Maine Medical Center Assistant Professor of Neurology, Tufts University School of Medicine I have no disclosures
Update on Early Acute Ischemic Stroke Interventions Diana Goodman MD Lead Neurohospitalist Maine Medical Center Assistant Professor of Neurology, Tufts University School of Medicine I have no disclosures
Part 1 of this review established the clinical context of CT
 PHYSICS REVIEW A.A. Konstas G.V. Goldmakher T.-Y. Lee M.H. Lev Theoretic Basis and Technical Implementations of CT Perfusion in Acute Ischemic Stroke, Part 2: Technical Implementations SUMMARY: CT perfusion
PHYSICS REVIEW A.A. Konstas G.V. Goldmakher T.-Y. Lee M.H. Lev Theoretic Basis and Technical Implementations of CT Perfusion in Acute Ischemic Stroke, Part 2: Technical Implementations SUMMARY: CT perfusion
Thrombus hounsfield unit on CT predicts vascular recanalization in stroke patients
 Thrombus hounsfield unit on CT predicts vascular recanalization in stroke patients Poster No.: C-2616 Congress: ECR 2010 Type: Scientific Exhibit Topic: Neuro Authors: H. F.Termes, J. Puig, J. Daunis-i-Estadella,
Thrombus hounsfield unit on CT predicts vascular recanalization in stroke patients Poster No.: C-2616 Congress: ECR 2010 Type: Scientific Exhibit Topic: Neuro Authors: H. F.Termes, J. Puig, J. Daunis-i-Estadella,
Without reperfusion therapy, almost 80% of patients with
 ORIGINAL RESEARCH V. Puetz P.N. Sylaja M.D. Hill S.B. Coutts I. Dzialowski U. Becker G. Gahn R. von Kummer A.M. Demchuk CT Angiography Source Images Predict Final Infarct Extent in Patients with Basilar
ORIGINAL RESEARCH V. Puetz P.N. Sylaja M.D. Hill S.B. Coutts I. Dzialowski U. Becker G. Gahn R. von Kummer A.M. Demchuk CT Angiography Source Images Predict Final Infarct Extent in Patients with Basilar
The Value of Apparent Diffusion Coefficient Maps in Early Cerebral Ischemia
 AJNR Am J Neuroradiol 22:1260 1267, August 2001 The Value of Apparent Diffusion Coefficient Maps in Early Cerebral Ischemia Patricia M. Desmond, Amanda C. Lovell, Andrew A. Rawlinson, Mark W. Parsons,
AJNR Am J Neuroradiol 22:1260 1267, August 2001 The Value of Apparent Diffusion Coefficient Maps in Early Cerebral Ischemia Patricia M. Desmond, Amanda C. Lovell, Andrew A. Rawlinson, Mark W. Parsons,
Ischemic stroke is one of the most common causes of death
 Stroke Lesion Volumes and Outcome Are Not Different in Hemispheric Stroke Side Treated With Intravenous Thrombolysis Based on Magnetic Resonance Imaging Criteria Amir Golsari, MD; Bastian Cheng, MD; Jan
Stroke Lesion Volumes and Outcome Are Not Different in Hemispheric Stroke Side Treated With Intravenous Thrombolysis Based on Magnetic Resonance Imaging Criteria Amir Golsari, MD; Bastian Cheng, MD; Jan
Impact of Slow Blood Filling via Collaterals on Infarct Growth: Comparison of Mismatch and Collateral Status
 Journal of Stroke 2017;19(1):88-96 Original Article Impact of Slow Blood Filling via Collaterals on Infarct Growth: Comparison of Mismatch and Collateral Status Jeong Pyo Son, a,b Mi Ji Lee, c Suk Jae
Journal of Stroke 2017;19(1):88-96 Original Article Impact of Slow Blood Filling via Collaterals on Infarct Growth: Comparison of Mismatch and Collateral Status Jeong Pyo Son, a,b Mi Ji Lee, c Suk Jae
Assessing Tissue Viability with MR Diffusion and Perfusion Imaging
 AJNR Am J Neuroradiol 24:436 443, March 2003 Assessing Tissue Viability with MR Diffusion and Perfusion Imaging Pamela W. Schaefer, Yelda Ozsunar, Julian He, Leena M. Hamberg, George J. Hunter, A. Gregory
AJNR Am J Neuroradiol 24:436 443, March 2003 Assessing Tissue Viability with MR Diffusion and Perfusion Imaging Pamela W. Schaefer, Yelda Ozsunar, Julian He, Leena M. Hamberg, George J. Hunter, A. Gregory
EPITHET Positive Result After Reanalysis Using Baseline Diffusion-Weighted Imaging/Perfusion-Weighted Imaging Co-Registration
 EPITHET Positive Result After Reanalysis Using Baseline Diffusion-Weighted Imaging/Perfusion-Weighted Imaging Co-Registration Yoshinari Nagakane, MD, PhD; Soren Christensen, PhD; Caspar Brekenfeld, MD;
EPITHET Positive Result After Reanalysis Using Baseline Diffusion-Weighted Imaging/Perfusion-Weighted Imaging Co-Registration Yoshinari Nagakane, MD, PhD; Soren Christensen, PhD; Caspar Brekenfeld, MD;
Acute Stroke Treatment: Current Trends 2010
 Acute Stroke Treatment: Current Trends 2010 Helmi L. Lutsep, MD Oregon Stroke Center Oregon Health & Science University Overview Ischemic Stroke Neuroprotectant trials to watch for IV tpa longer treatment
Acute Stroke Treatment: Current Trends 2010 Helmi L. Lutsep, MD Oregon Stroke Center Oregon Health & Science University Overview Ischemic Stroke Neuroprotectant trials to watch for IV tpa longer treatment
Association of Early CT Abnormalities, Infarct Size, and Apparent Diffusion Coefficient Reduction in Acute Ischemic Stroke
 AJNR Am J Neuroradiol 25:933 938, June/July 2004 Association of Early CT Abnormalities, Infarct Size, and Apparent Diffusion Coefficient Reduction in Acute Ischemic Stroke Diederik M. Somford, Michael
AJNR Am J Neuroradiol 25:933 938, June/July 2004 Association of Early CT Abnormalities, Infarct Size, and Apparent Diffusion Coefficient Reduction in Acute Ischemic Stroke Diederik M. Somford, Michael
Reliable Perfusion Maps in Stroke MRI Using Arterial Input Functions Derived From Distal Middle Cerebral Artery Branches
 Reliable Perfusion Maps in Stroke MRI Using Arterial Input Functions Derived From Distal Middle Cerebral Artery Branches Martin Ebinger, MD; Peter Brunecker, MSc; Gerhard J. Jungehülsing, MD; Uwe Malzahn,
Reliable Perfusion Maps in Stroke MRI Using Arterial Input Functions Derived From Distal Middle Cerebral Artery Branches Martin Ebinger, MD; Peter Brunecker, MSc; Gerhard J. Jungehülsing, MD; Uwe Malzahn,
Stroke Treatment Beyond Traditional Time Windows. Rishi Gupta, MD, MBA
 Stroke Treatment Beyond Traditional Time Windows Rishi Gupta, MD, MBA Director, Stroke and Neurocritical Care Endovascular Neurosurgery Wellstar Health System THE PAST THE PRESENT 2015 American Heart Association/American
Stroke Treatment Beyond Traditional Time Windows Rishi Gupta, MD, MBA Director, Stroke and Neurocritical Care Endovascular Neurosurgery Wellstar Health System THE PAST THE PRESENT 2015 American Heart Association/American
Intravenous thrombolysis with recombinant tissue plasminogen
 ORIGINAL RESEARCH BRAIN Susceptibility-Diffusion Mismatch Predicts Thrombolytic Outcomes: A Retrospective Cohort Study M. Lou, Z. Chen, J. Wan, H. Hu, X. Cai, Z. Shi, and J. Sun ABSTRACT BACKGROUND AND
ORIGINAL RESEARCH BRAIN Susceptibility-Diffusion Mismatch Predicts Thrombolytic Outcomes: A Retrospective Cohort Study M. Lou, Z. Chen, J. Wan, H. Hu, X. Cai, Z. Shi, and J. Sun ABSTRACT BACKGROUND AND
There are many factors determining the fate of hypoperfused
 Regional Ischemic Vulnerability of the Brain to Hypoperfusion The Need for Location Specific Computed Tomography Perfusion Thresholds in Acute Stroke Patients Seyedmehdi Payabvash, MD; Leticia C.S. Souza,
Regional Ischemic Vulnerability of the Brain to Hypoperfusion The Need for Location Specific Computed Tomography Perfusion Thresholds in Acute Stroke Patients Seyedmehdi Payabvash, MD; Leticia C.S. Souza,
INTERVENTIONAL NEURORADIOLOGY
 Neuroradiology (2012) 54:579 588 DOI 10.1007/s00234-011-0944-1 INTERVENTIONAL NEURORADIOLOGY Perfusion-CT guided intravenous thrombolysis in patients with unknown-onset stroke: a randomized, double-blind,
Neuroradiology (2012) 54:579 588 DOI 10.1007/s00234-011-0944-1 INTERVENTIONAL NEURORADIOLOGY Perfusion-CT guided intravenous thrombolysis in patients with unknown-onset stroke: a randomized, double-blind,
Detecting and rescuing the ischemic penumbra is the main
 Influence of the Arterial Input Function on Absolute and Relative Perfusion-Weighted Imaging Penumbral Flow Detection A Validation With 15 O-Water Positron Emission Tomography Olivier Zaro-Weber, MD; Walter
Influence of the Arterial Input Function on Absolute and Relative Perfusion-Weighted Imaging Penumbral Flow Detection A Validation With 15 O-Water Positron Emission Tomography Olivier Zaro-Weber, MD; Walter
CT perfusion scans are widely applied to assess ischemia (low
 Published April 17, 2014 as 10.3174/ajnr.A3935 ORIGINAL RESEARCH BRAIN Early Basal Ganglia Hyperperfusion on CT Perfusion in Acute Ischemic Stroke: A Marker of Irreversible Damage? V. Shahi, J.E. Fugate,
Published April 17, 2014 as 10.3174/ajnr.A3935 ORIGINAL RESEARCH BRAIN Early Basal Ganglia Hyperperfusion on CT Perfusion in Acute Ischemic Stroke: A Marker of Irreversible Damage? V. Shahi, J.E. Fugate,
How to Interpret CT/CTA for Acute Stroke in the Age of Endovascular Clot Retrieval
 How to Interpret CT/CTA for Acute Stroke in the Age of Endovascular Clot Retrieval Peter Howard MD FRCPC Disclosures No conflicts to disclose How to Interpret CT/CTA for Acute Stroke in the Age of Endovascular
How to Interpret CT/CTA for Acute Stroke in the Age of Endovascular Clot Retrieval Peter Howard MD FRCPC Disclosures No conflicts to disclose How to Interpret CT/CTA for Acute Stroke in the Age of Endovascular
Endovascular Treatment Updates in Stroke Care
 Endovascular Treatment Updates in Stroke Care Autumn Graham, MD April 6-10, 2017 Phoenix, AZ Endovascular Treatment Updates in Stroke Care Autumn Graham, MD Associate Professor of Clinical Emergency Medicine
Endovascular Treatment Updates in Stroke Care Autumn Graham, MD April 6-10, 2017 Phoenix, AZ Endovascular Treatment Updates in Stroke Care Autumn Graham, MD Associate Professor of Clinical Emergency Medicine
EFFECTIVENESS OF CTA AND CTP IN GUIDING MANAGEMENT DECISIONS FOR ACUTE STROKE
 EFFECTIVENESS OF CTA AND CTP IN GUIDING MANAGEMENT DECISIONS FOR ACUTE STROKE Jon Benton MS-4, Chirag Dani MD, Vincent Persaud MD, Bilal A. Manzer, Macksood Aftab DO, MHA OBJECTIVES 1. Utility of advanced
EFFECTIVENESS OF CTA AND CTP IN GUIDING MANAGEMENT DECISIONS FOR ACUTE STROKE Jon Benton MS-4, Chirag Dani MD, Vincent Persaud MD, Bilal A. Manzer, Macksood Aftab DO, MHA OBJECTIVES 1. Utility of advanced
Broadening the Stroke Window in Light of the DAWN Trial
 Broadening the Stroke Window in Light of the DAWN Trial South Jersey Neurovascular and Stroke Symposium April 26, 2018 Rohan Chitale, MD Assistant Professor of Neurological Surgery Vanderbilt University
Broadening the Stroke Window in Light of the DAWN Trial South Jersey Neurovascular and Stroke Symposium April 26, 2018 Rohan Chitale, MD Assistant Professor of Neurological Surgery Vanderbilt University
Clinical Sciences. Arterial Spin Labeling Versus Bolus-Tracking Perfusion in Hyperacute Stroke
 Clinical Sciences Arterial Spin Labeling Versus Bolus-Tracking Perfusion in Hyperacute Stroke Andrew Bivard, PhD; Venkatesh Krishnamurthy, MRCP, FRACP; Peter Stanwell, PhD; Christopher Levi, MBBS, FRACP;
Clinical Sciences Arterial Spin Labeling Versus Bolus-Tracking Perfusion in Hyperacute Stroke Andrew Bivard, PhD; Venkatesh Krishnamurthy, MRCP, FRACP; Peter Stanwell, PhD; Christopher Levi, MBBS, FRACP;
New therapies directed at acute middle cerebral artery
 Regional Angiographic Grading System for Collateral Flow Correlation With Cerebral Infarction in Patients With Middle Cerebral Artery Occlusion Jane J. Kim, MD; Nancy J. Fischbein, MD; Ying Lu, PhD; Daniel
Regional Angiographic Grading System for Collateral Flow Correlation With Cerebral Infarction in Patients With Middle Cerebral Artery Occlusion Jane J. Kim, MD; Nancy J. Fischbein, MD; Ying Lu, PhD; Daniel
