VIPergic Innervation in the Gastrointestinal Tract of Diabetic Rats*)
|
|
|
- Hope Richardson
- 5 years ago
- Views:
Transcription
1 Hiroshima Journal of Medical Sciences Vol. 32, No. 4, 469,...,478, December, 1983 HIJM VIPergic Innervation in the Gastrointestinal Tract of Diabetic Rats*) Shinya KISHIMOT0 1 l, Satoko KUNITA 1 l, Akihiko KAMBARAo, Kazuma OKAMOT0, Satoru SHIMIZU 1 l, Masahiro Y AMAMOTon, Ha ssei KQHll, Kohichi SANQ 1 l, Gora KAJIYAMA 0, Akima MIYO~HI2l and Noboru Y ANAIHARA3l 1) The First Department of internal Medicine, Hiroshima University School of Medicine, 1-2-3, Kasumi, Minami-ku, Hiroshima 734, Japan. 2) Shizuoka General Hospital, Shizuoka 420, Japan 3) Shizuoka College of Pharmacy, Bioorganic chemistry, Oshika, Shizuoka 420, Japan (Received September 10, 1983) Key words: Diabetes, Gastroenteropathy, VJP nerves ABSTRACT Diabetic gastroenteropathy develor:ed in about 70 % of the rats with diabetes induced by streptozotocin. These rats were associated with diarrhea, gastric paresis, and small intestinal stasis. About 30% of the rats with diabetic gastroer.teropathy had narrowed and contracted segments of the lower esophagus and 70% of the colon of the rats showed dilated and contracted segments. Changes in the distribution of VIP-like immunoreactivities in nerve r:lexuses of the gastrointestinal wall which were observed with destruction of the autonomic nerves (both submucosal and myenteric plexuses) could be one of the plausible causes of diabetic gastroenteropathy induced by streptozotocin, although the precise mechanism of the development of diabetic gastroenteropathy in rats remains obscure. INTRODUCTION Dysfunton of the gastrointestinal tract in diabetic gastroenteropathy is known to occur in patients with long standing diabetes mellitus 12 l. Diabetic gastroenteropathy has been associated with gastric paresis, small intestinal stasis, and colonic dysfunction, whose involved clinical symptoms are nausea, vomiting, diarrhea ar d constipation. The causes of diabetic gastroenteropathy have been searched in r:eripheral autonomic neuropathy 3 l. Recent reviews have shown that pei::tidergic nerves coexist in autonomic nearves in the gastrointestinal wall. It is therefore interesting and meaningful to ascertain the changes in the peptidergic nerves of the gut wall in diabetic gastroenteropathy. In the present study, immunocytochemical observations of the peptidergic nerves were made on the nerve plexuses of the gastrointestinal wall in rats with diabetes induced by streptozotocin. MATERIALS AND METHODS Experimental Animals and Diabetes Male wistar rats, weighing 180 grams, were used in this study. Diabetes were produced by injecting 50 mg per kg of strer;tozotocin into the tail vein. The injection was done as quickly as possible because of the instability of strer;tozotocin solution. Strer;tozotocin solution was dissolved in citric buffer at ph 4. 5 and 1 ml of the buffer cor:taining 50 mg per kg of streptozotcin. The rats treated in this manner were kept and fed in a conventional manner for 6 months ar:.d then were killed by decapitation. Before * 1 **a~. ~mfi~ ~m~~. ~*-m. m* fi. w*~~. A~.~~~-. wwmm.~~~~.~~ m~: ;fi)jj(~7-:; r O)yfjft~v:::.tovt0V I P('f11!b1$~
2 470 S, Kishimoto et al. killing the rats, urine of all rats were checked for glycosuria. Blood was drawn from each rat for evaluating insulin before and after glucose instillation into the stomach. Preparation for Morphology and Immur:ocytochemistry The abdomen of decapitated rats was opened and examined at the macroscopic level for abnormal changes in the gastroir.testinal tract from the lower esophagus to rectum. Twotissus sample (1 x 1 cm) was taken from the following parts of the gastrointestir.al tract and pancreas: lower portion of the esor hagus, body and artrum of the stomach, pyloric sphir:cter, duodenum, jejunum, ileum, colon (cor:tracted and dilated segments), ar.d rancreas. Conventional Histopathology Each tissue sample of one group was fixed in Bouin's solution for 4 hours and then three micrcn-wax tissue sectiors were prer:ared in the usual manner. The tissue sections were stair:ed with hematoxylin and eosin for historathology. Indirect Immur:of1uorescert method 4 l Each tissue sample of the other group was fixed in p-benzoquinone solution for 4 hours and then washed in 7 % of sucrose in phosphate buffered salir:e at ph Ten micror:-frozen tissue sections were prer:ared for immurostaining after fixatior;. The frozen tissue sectior:s were left to react with the primary antiserum of vasoactive intestinal per:tide (VIP) (dilution 1 : 100) for 18 hours at 4 C. The labeled secord layer was applied for 1 hour at room temperature. FITC cori jugated goat antirabbit globulin (MEL) was used at a solution of 1 : 100. Control for Immunocytochemistry In order to demm:strate that the immurocytochemical reactions were srecific, the following tests were r:erformed. (1) Prior to irnmunostatining, the diluted ar: tiserum was absc rbeci with synthetic VIP (10 ng). (2) Normal rabbit serum was used instead of the.rrimary ar.tiserum as the 1st layer. (3) The FITC secord layer was spr:lied alone. Evaluation of Glucose, Insulin, Par:creatic Glucagon, and Gastrin The levels of glucose in the blood at fasting and after glucose admir: istra ti on ir: to the sto m - ach were determir:ed by autoar alyzer. The levels of immunoreactive ir:sulin, r:ancreatic glucagon, and gastrin were determined by radioi:mrnunoassay. The amount of intubated glucose was 0. 4 g/2 ml. The rats were killed 10 and 30 minutes after glucose administration. The total number of rats used in this study was thirty. Control Rats were injected with citric buffer alone. RESULTS Morphology Macroscopically the pancreas appeared atrophied in rats treated with streptozotocin when compared to that in the controls. Microscopic examination of the pancreas in rats given streptozotocin showed a marked reduction in the number and size of islets. The islets were characterized by infrequent or diminished B cells and infiltration of inflammatory cells (Fig. 1.). Fibrotic charges were also found in both endocrine and exocrire pancreas. Endocrir:e Function of the Pancreas Blood sugar levels and immunoreactive insulin levels at fasting in rats with streptozotocin were ± mg/dl and 9. 3± U/ml, respectively, while the levels in control rats were 120.8±5.5mg/dl and 26.8±1.6(-LU/ml, respectively (Table 1). Thus, rats treated with strei:;tozotocin showed hyperglycemia and hypoijsulinemia. The rats had also gylcosuria. The levels of blood sugar and immunoreactive insulin of the rats given streptozotocin were ±65. 0 and ± mg/dl, and ±4. 8 and 10. 2±1. 111U/ml at 10 and 30 minutes after glucose administration, respectively. These morphological and endocrine data, thus, Fig. 1. Destroyed B cells and cell infiltration in islets of diabetic rats (HE: x 400).
3 VIPergic Innervation in the Gastrointestinal Tract 471 Table 1. Blood sugar (BS), immunoreactive insulin (IRI), immunoreactive glucagon (IRG) and immunoreactive gastrin (IRGa) in diabetic rats and control. BS (mg/dl) IRI (pu/ml) IRG (pg/ml IRGa (pg/ml) Control ± ± ±18. 0 c 80.1±4. 6 AGML (+) DM ± ± ± ± AGML (-) 105.1±13. 9 BS: Blood sugar, IRI: Immunoreactive insulin, IRG: Immunoreactive glucagon, IR Ga: Immunoreactive gastrin indicated that the rats treated with streptozotocin were diabetic. Morphology of the Gastrointestinal Tract Esophagus The lower portion of the esophagus in diabetic rats, being equivalent to the lower esophageal sphincter, was contracted and narrowed, while the proximal portion from the contracted portion was relaxed and loose. Histological examination showed that nerve plexuses were decreased and/or were not observed occasionally in tht contracted portion (Fig. 2). Being congruous with the changes of nerve plexuses, VIP immunoreactivities were reduced or dimin - ished at the immunocytochemical level (Fig. 3 A and B). Stomach Rich VIP immunoreactivities were observed in the nerve plexuses and nerve axons of the gastric body when compared to those in cor.trol rats (Fig. 4). Somewhat reduced VIP immu:r:oreactivities were seen in the nerve plexuses and nerve axons in pyloric sphincter muscle layer of diabetic rats, although the reactivities were not markedly different from those in the cor;trol rats (Fig. 5 A and B). Small Intestine Seventy percent of diabetic rats were associated with diarrhea. The small intestine of diabetic rats was, as a whole, dilated, which suggested stasis, and damaged (Fig. 6). Histological appearance, however, was almost normal. VIP immunoreactivities were rich in the r;roximal intestine in these rats (Fig. 7 A and B). Also relatively rich VIP immunoreactivities were observed in the distal small intestine and ileum which were also dilated (Fig. 8 A and B). Colon Contracted and dilated segments in the colon Fig. 2. A disappeared nerve plexus is noted in the contracted segment of esophagus in a diabetic rat (HE: x 400). of diabetic rats were observed at the macroscopic level (Fig. 6). Marked cellular infiltration and fibrotic changes were seen in colonic mucosa of diabetic rats by hematoxylin and eosin stain (Fig. 9). Furthermore, the regular architecture of the colonic mucosae of diabetic rats was scarcely observed. Neither nerve plexuses nor nerve axons were observed in the contracted segments, while a normal distribution of nerve plexuses was seen in the dilated segments of the colon (Fig. 10 A and B). VIP immuno
4 472 S. Kishimoto et al. Fig. 3. A: VIP-like immunoreactive nerves in the esophagus of a control rat. B: No VIP-like immunoreactive nerves are found in the contracted segment of esophagus in a diabetic rat (IF: x 200). Fig. 4. Relatively rich VIP-like immunoreactive nerve fibers and ganglia are found in the gastric; body of diabetic rats (IF: x 200),
5 VIPergic Innervation in the Gastrointestinal Tract 473 Fig. 5. A: Rich VIP-like immunoreactive nerve fibers and plexuses are found in the pylorus of a control rat. B: VIP-like immunoreactive nerve fibers and plexuses are also observed in the pylorus of a diabetic rat (IF: >< '.200). Fig. 6. A diabetic rat shows distended small intestine (small arrow) and large intestine (large arrow).
6 474 S. Kishimoto et al. Fig. 7. VIP-like immunoreactive nerve fibers and plexuses in the duodenum of the control (A) and diabetic rat (B). reactivities were completely destroyed in the contracted segments of the colon, which was well in accord with the destruction of nerve plexuses in the same area of the colon (Fig. 11 A and B). DISCUSSION Diabetic gastroe~teropathy is not well understood. It is said that diabetic gastroenteropathy develops as a result of dysfunction of the autonomic nerves, which inr.ervated gastrointestinal h~ct, as seen in diabetes of lor g duration. However, the pathophysiology of this impaired gastrointestinal function in diabetes remains undefined, althovgh several mechanisms have been imrlicated. These include autor:omic neuropathy, microangiorathy, changes in insulin and glucagon release, and metabolic disturbance. In recer.t years some brain-gut hormones or peptides including neuropeptides have been described to play some role in the pathophysiology of diabetic gastroenteropathy 23 >, although their physiological importance remains to be determined. It is a likely fact that the metabolic changes observed in diabetes will modify the release of thses hormones and peptides and alter their effects on gastrointestinal function. The purpose in the study was, therefore, to demonstrate on morphological and immunocytochemical bases the changes in nerve plexuses and distribution of vasoactive intestinal peptide (VIP), one of the brain-gut peptides (peptidergic nerves) which innervated gastrointestinal function, in rats with diabetic gastroenteropathy induced by streptozotocin. It is generally accepted that strei::tozotocin is diabetogenic in rats 6 9, io, 20 >. In the present study, hyperglycemia as well as hypoinsulinemia have been demonstrated in rats treated with streptozotocin. These rats, therefore, were difinitely diabetic. About 70 % of rats treated with streptozotocin were associated with diarrhea and malnutrition as well. When the abdomen of the rats was
7 VIPergic Innervation in the Gastrointestinal Tract 475 Fig. 8. Rich VIP-like immunoreactive nerve fibers and ganglionic cell bodies in the ileum of both a control (A) and a diabetic rat (B) (IF: A: x 200, B: x 400). Fig. 9. Marked cell-infiltration, fibrosis and nerve plexus (arrow) are observed in the dilated segment of the colon of a diabetic rat (HE: x 700 ). Fig. 1Q. One never plexus (A: HE: x 100) and VIP-like immunoreactive nerve (B: IF: x200) in the dilated segment of the colon in a diabetic rat.
8 476 S. Kishimoto et al. Fig. 11. Neither a nerve plexus (A: HE: x400) nor VIP-like immunoreative nerve (B: IF: x200) are found in the contracted segment of the colon in a diabeitc rat. Fig. 12. rat A marked dilated stomach in a diabetic opeaed, gastric paresis of varying degree (to gastric atony) (Fig. 12) and small intestinal dilatation and stasis were observed. These signs and morphological findings observed macroscopically were similar those observed in patients with diabetic gastroenteropathy. Furthermore, it was interesting that the dilated and constricted segments were found in the colon of the rats. These findi::igs suggest that rats associated with these signs and morphological fiindings similar t:::> diabetic gastroenteropathy observed in human cases have diabetic gastroenteropathy. The remaiol1g 30% of the rats did not show such signs and findings, although the rats were diabetic because the rats had glycosuria, hyi:erglycemia and hypoinsulinemia. The lower es'.)phagus of about 30 % of the rats with gastroenteropathy was contracted and r:arrowed, while the proximal esophagus from the contracted area was dilated. Nerve plexuses in the wall of the cor,tracted area of the esophagus were destroyed and VIP immunoreactivities were not observed concomittantly in the same area. Since the esophageal smooth muscle
9 VIPergic Innervation in the Gastrointestinal Tract 477 seemed to be normal at the microscopical level, these nerve changes may influence the pathogenesis of contraction of the lower esophagus. As the esophagus is largely innervated by the vagus nerve, esophageal motor disturbance is considered to be a dysfur:.ction of esophageal innervation 21 25l. In addition to this, the present study showed that destruction of VIPergic innervation may play a role in esophageal contraction. The mechanism may be similar to that observed in cases of Hirschspru~g's disease and Chagas disease 19 l. On the contrary, autonomic and VIPergic innervation of the esophageal wall was almost normal in a large number of rats with diabetic gastroer.teropathy without esophageal contraction. Contraction of the e sophagus was not observed in any of the diabetic rats without gastroenteropathy and in control rats as well. Gastric retention (paresis) as well as delayed gastric emi:tying have been considered to be late complications of diabetes l. The enlarged stomach with retention in rats with gastroenteropathy observed in the r-resent study was similar to those (gastric paresis) in human diabetic cases. Rich VIP-like immunoreactivities were found in the mucosa and muscle layers of glandular stomach in these rats, suggesting that VIP in the nerves may be one of the pathophysiological causes of gastric retention and delayed gastric emptying because one of physiological actions of VIP is relaxation of smooth muscles 22 i. Abnormality of nerve plexuses in the glandular stomach was not noted. VIP-like immunoreactivities were not different in pyloric sphincter from rats with gastroenteropathy and without gastroenteropathy as well as control rats. The etiology of gastric stasis observed in diabetes, however, remains unresolved. In view of the frequent association with peripheral autonomic neuropathy which is a similar condition found after vagotomy 27 l, it is likely that visceral neuropathy is important in the etiology. Actually, in the another study, immunocytochemical VIP immunoreactivities were normal or rich in the gastric body mucosa and muscle layers in truncal vagotomized rats with marked gastric stasis 14 l. This finding supports the role of VIP in gastric stasis. Hyperglydemia and glucagon have also been shown to play a role in delayed gastric emptying in non-diabetic human cases with duodenal ulceration 2 7 i. A high concen - tration of blood glucagon was not observed in rats with gastric stasis in the present study. Therefore, pancreatic glucagon does not seem to play any role in the mechanism of delayed gastric emptying in rats with gastric paresis in the present study. Hypergastrinemia has been observed in rats with gastroenteropathy. This many be due to ga3tric retention and atrophic gastritis 13 l. Small intestinal dilation and stasis were observed in rats with diabetic gastroenteropathy. However, no specific lesions except thin and fragile wall were observed in enteric ganglia, mucosa, muscle, and microvasculature at light microscopic level. These support that there is no evidence of histological abnormalities which affect the intestinal sympathetic or parasympathetic nerves and the submucosal or myenteric plexuses in human cases l. It is very interesting that there were rich VIP-like immunoreactivities in almost all mucosa, muscle, and ganglia of the small intestine in rats with gastroenteropathy in the present study. The evidence also suggests that VIP may participate in the pathogenesis of small intestinal stasis in rats with diabetic gastroenteropathy as in the case of gastric paresis. The mechanism why VIP immunoreactivities increased, however, remains uncertain. Constipation has been reported to be a common feature of diabetic neuropathy in human cases 17 21l. In the present study, however, 70% of the rats with diabetic gastroenteropathy had diarrhea. Macroscopic findings showed dilated and contracted (narrowing) segments in the colon of these rats. Microscopical evidence, however, was very interesting. Thickened muscle layer was found in the contracted segments of the colon where neither nerve myenteric plexuses nor VIP nerves existed, while flattened mucosa associated with fibrotic changes and cellular infiltration were observed in the dilated segments where myenteric plexuses and VIP nerves were found. These findings were very similar to those observed in the diseased segments of Hirschsprung's disease and Chagas disease 19 l as well. These suggest that VIP existing in the nerve neurones of the colon may play an important role in the pathognomonic changes in the colon of rats with diabetic gastroenteropathy. In the contrast with these
10 478 S, Kishimoto et al. observations, little changes were observed in rats without diabetic gastroenteropathy and no abnormal changes were observed in the colon of control animals. These suprort the rathognomonic role of VIP mentioned above in rats with diabetic gastroenteropathy. Finally, the mechar.ism of develormer.t of macroscopical and histological abnormalities including destroyed myer.i.teric plexuses observed in the gastrointestir al tracts remains obscure. The direct toxic action of strertozctocin on the autonomic nerves in the gastroir.testir:al tract 18 ' could be denied since 6 mor:ths had passed after the injection. The results observed in the present study were the chronic effects of strei::tozotocin-induced diabetes on the gastrointestinal tract in rats. The results suggest that one of the brain-gut hormones (peptides), VIP, in the gastrointinal tract of the present study modified the release and exerted its effect on the gastrointestiral tract. Furtheremore, metabolic disturbances 18 ' induced by diabetes after strei::tozotocin administration may be a more peausible cause of the developmer.t of diabetic gastroenteropathy. REFERENCES l, Berge, K. G., Sprague, R. G. and Bennet, W. A The intestinal tract in diabetic diarrhea. A pathologic study. Diabetes 5 : Bloom, S. R Gastrointestinal hormones. Int. Rev. Physiol. 12: T.i-l.03. 3; Clements, R. S. Jr Diabetic neuropathy New concepts of its etiology. Diabetes 28 : Coons, A.H., Leduc, E. H. and Connolly, J.M Studies on antibody production l : A method for the histochemical demonstration of specific antibody and its application to a study of the hyperimmune rabbit. J. Exp. Med. 102 : Drewes, V. M., and Olsen, S Histological changes in the small bowel in diabetes mellitus: A study of peroral biopsy specimens. Acta Path. Microb. Scand. 63 : Evans, J. S., Gerritsen, G. C., Mann, K. M. and Owen, S. P Antitumor and hyperglycemic activity of streptozotocin and its cofactor. Cancer Chemother. Rep. 48 : Hall, W. H. and Sanders, L. L Gastric emptying of hypertonic glucose in diabetes mellitus and duodenal ulcer. South. Med. J. 69 : Hodges, F. J., Rundles, R. W. and Hanelin, J Roentgenologic study of small intestine II. Dysfunction associated with neurologic disease. Radiology 49 : Junod, A., Lambert, A. E., Orci, L., Pictet, R., Gonet~ A. E. and Renold, A. E Studies of the diabetogenic action of streptozotocin. Proc. Soc. Exp. Biol. Med. 126 : Junod, A., Lambert, A. E., Stauffer, W. and Renold, A. E Diabetogenic action of streptozotocin: Relationship of dose to metabolic response. J. Clin. Invest. 48 : Kassander, P Asymptomatic gastric retention in diabetes (gastroparesis diabeticorum). Ann. Int. Med. 48 : Katz, L.A. and Spiro, H. W Gastrointestinal manifestations of diabetes. New Engl. J. Med. 275 : Kishimoto, S., Shimizu, S., Yamamoto, M. et al Gastric morphology, gastrin and samatostatin in experimental gastritis in mice. 32 : Kishimoto, S Unpablished data. 15. Malins, J.M. and French, J.M Diabetic diarrhea. Quart. J. Med. 26 : Marshak, R.H. and Maklansky, A Diabetic gastropathy. Am. J. Dig. Dis. 9 : Mayne, N. M Neuropathy in the diabetic and non-diabetic populations. Lancet2 : Monckton, G. and Pehowich, E Autonomic neuropathy in the streptozotocin diabetic rat. Le J. Cand. D. Sci. Neural. 7 : Polak, J.M. and Bloom, S. R Distribution of neuropeptides and their influence on disease, p Gut Peptides edited by A. Miyoshi. Kodansha. 20. Rakieten, N., Raldeten, M. L. and Nadkarni, M. V Studies on the diabetogenic action of streptozotocin. Cancer Chemother. Rep. 29 : Rundles, R. W. 1:145. Diabetic neuropathy. General review with report of 125 cases. 24 : Said, S. I VIP overiew p Gut Hormones edited by S. R. Bloom and J. M. Polak Churchill Livingston London. 23. Scarpello, J. H.B. and Sladen, G. E. l!j78. Diabetes and the gut. Gut 19 : Smith, B Neuropathy of the oesophagus in diabetes mellitus. J. Neural. Neurosurg. Psychiat 37 : Texter, E. C. Jr., Danovitch, S. H., Kuhl, W. J. et al Physiologic studies of autonomicnervous-system dysfunction accompanying diabetes mellitus. Am. J. Dig. Dis. 7 : Vinik, I.E., Kern, F., Jr. and Struthers, J. E. Lr Malabsorption and the diarrhea of diabetes mellitus.gastroent. 43: Wooten, R. ~.and Meriwether, T. W. III Diabetic gastric atony. Med. Assoc, 176 : Zitomer, B. R., Gramm, H.F. and Kozak, G. P Gastric neuropathy in diabetes mellitus: Clinical and radiologic observations. Metabolism 17 :
Overview of digestion or, gut reactions - to food
 Key concepts in Digestion. Indigestion module Overview of digestion or, gut reactions - to food Prof. Barry Campbell Gastroenterology Cellular & Molecular Physiology e-mail: bjcampbl@liv.ac.uk http://pcwww.liv.ac.uk/~bjcampbl
Key concepts in Digestion. Indigestion module Overview of digestion or, gut reactions - to food Prof. Barry Campbell Gastroenterology Cellular & Molecular Physiology e-mail: bjcampbl@liv.ac.uk http://pcwww.liv.ac.uk/~bjcampbl
INTRODUCTION TO GASTROINTESTINAL FUNCTIONS
 1 INTRODUCTION TO GASTROINTESTINAL FUNCTIONS 2 Learning outcomes List two main components that make up the digestive system Describe the 6 essential functions of the GIT List factors (neurological, hormonal
1 INTRODUCTION TO GASTROINTESTINAL FUNCTIONS 2 Learning outcomes List two main components that make up the digestive system Describe the 6 essential functions of the GIT List factors (neurological, hormonal
What part of the gastrointestinal (GI) tract is composed of striated muscle and smooth muscle?
 CASE 29 A 34-year-old man presents to his primary care physician with the complaint of increased difficulty swallowing both solid and liquid foods. He notices that he sometimes has more difficulty when
CASE 29 A 34-year-old man presents to his primary care physician with the complaint of increased difficulty swallowing both solid and liquid foods. He notices that he sometimes has more difficulty when
University of Buea. Faculty of Health Sciences. Programme in Medicine
 Faculty of Health Sciences University of Buea Wednesday, 28 th January 2009 Time: 8 00-10 00 Programme in Medicine MED 303 (Gastrointestinal Physiology) EXAMS (2008-2009) Identify the letter of the choice
Faculty of Health Sciences University of Buea Wednesday, 28 th January 2009 Time: 8 00-10 00 Programme in Medicine MED 303 (Gastrointestinal Physiology) EXAMS (2008-2009) Identify the letter of the choice
Overview of digestion or, gut reactions - to food
 1 Key concepts in Digestion. Indigestion module Overview of digestion or, gut reactions to food Prof. Barry Campbell Gastroenterology Cellular & Molecular Physiology email: bjcampbl@liv.ac.uk http://pcwww.liv.ac.uk/~bjcampbl
1 Key concepts in Digestion. Indigestion module Overview of digestion or, gut reactions to food Prof. Barry Campbell Gastroenterology Cellular & Molecular Physiology email: bjcampbl@liv.ac.uk http://pcwww.liv.ac.uk/~bjcampbl
Overview of digestion
 Key concepts in Digestion. Overview of digestion introduction to the GI system Prof. Barry Campbell Cellular & Molecular Physiology e-mail: bjcampbl@liv.ac.uk http://pcwww.liv.ac.uk/~bjcampbl DIGESTION
Key concepts in Digestion. Overview of digestion introduction to the GI system Prof. Barry Campbell Cellular & Molecular Physiology e-mail: bjcampbl@liv.ac.uk http://pcwww.liv.ac.uk/~bjcampbl DIGESTION
Physiological processes in the GI tract:
 Gastrointestinal physiology for medical students General principal of gastrointestinal function Motility, nervous control and blood circulation Physiological processes in the GI tract: Motility Secretion
Gastrointestinal physiology for medical students General principal of gastrointestinal function Motility, nervous control and blood circulation Physiological processes in the GI tract: Motility Secretion
For more information about how to cite these materials visit
 Author: John Williams, M.D., Ph.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Non-commercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author: John Williams, M.D., Ph.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Non-commercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Digestive system L 2. Lecturer Dr. Firdous M. Jaafar Department of Anatomy/Histology section
 Digestive system L 2 Lecturer Dr. Firdous M. Jaafar Department of Anatomy/Histology section objectives 1-Describe the general structure of digestive tract: a-mucosa. b-submucosa. c-muscularis externa d-adventitia
Digestive system L 2 Lecturer Dr. Firdous M. Jaafar Department of Anatomy/Histology section objectives 1-Describe the general structure of digestive tract: a-mucosa. b-submucosa. c-muscularis externa d-adventitia
Invited Revie W. Hirschsprung's disease - immunohistochemical findings. Histology and H istopathology
 Histol Histopath (1 994) 9: 615-629 Histology and H istopathology Invited Revie W Hirschsprung's disease - immunohistochemical findings L.T. Larsson Department of Pediatric Surgery, University of Lund,
Histol Histopath (1 994) 9: 615-629 Histology and H istopathology Invited Revie W Hirschsprung's disease - immunohistochemical findings L.T. Larsson Department of Pediatric Surgery, University of Lund,
Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, ,
 IDP Biological Systems Gastrointestinal System Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, 504-568-2669, jbresl@lsuhsc.edu Overall Learning Objectives 1. Characterize
IDP Biological Systems Gastrointestinal System Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, 504-568-2669, jbresl@lsuhsc.edu Overall Learning Objectives 1. Characterize
Overview of Gastroenterology
 Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Overview of Gastroenterology Gastroenterology Made Really Simple! Food Waste
Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Overview of Gastroenterology Gastroenterology Made Really Simple! Food Waste
Gastrointestinal Anatomy and Physiology. Bio 219 Napa Valley College Dr. Adam Ross
 Gastrointestinal Anatomy and Physiology Bio 219 Napa Valley College Dr. Adam Ross Functions of digestive system Digestion Breakdown of food (chemically) using enzymes, acid, and water Absorption Nutrients,
Gastrointestinal Anatomy and Physiology Bio 219 Napa Valley College Dr. Adam Ross Functions of digestive system Digestion Breakdown of food (chemically) using enzymes, acid, and water Absorption Nutrients,
2. A digestive organ that is not part of the alimentary canal is the: a. stomach b. liver c. small intestine d. large intestine e.
 Chapter 14 The Digestive System and Body Metabolism Review Questions Multiple Choice: 1. Which of the following terms are synonyms? a. Gastrointestinal tract b. Digestive system c. Digestive tract d. Alimentary
Chapter 14 The Digestive System and Body Metabolism Review Questions Multiple Choice: 1. Which of the following terms are synonyms? a. Gastrointestinal tract b. Digestive system c. Digestive tract d. Alimentary
(A) Diarrhea. (B) Stomach cramps. (C) Dehydration due to excess fluid loss. (D) A, B, and C are correct. (E) Only answer B is correct.
 Human Anatomy - Problem Drill 21: The Digestive System Question No. 1 of 10 1. A 26-year-old male is treated in the emergency department for severe gastrointestinal disturbance. Which of the following
Human Anatomy - Problem Drill 21: The Digestive System Question No. 1 of 10 1. A 26-year-old male is treated in the emergency department for severe gastrointestinal disturbance. Which of the following
Oesophageal motor changes in diabetes mellitus
 Thorax (1976), 31, 278. Oesophageal motor changes in diabetes mellitus I. M. STEWART, D. J. HOSKING, B. J. PRESTON, and M. ATKINSON General Hospital, Nottingham Stewart, I. M., Hosking, D. J., Preston,
Thorax (1976), 31, 278. Oesophageal motor changes in diabetes mellitus I. M. STEWART, D. J. HOSKING, B. J. PRESTON, and M. ATKINSON General Hospital, Nottingham Stewart, I. M., Hosking, D. J., Preston,
Soft palate elevates, closing off the nasopharynx. Hard palate Tongue Bolus Epiglottis. Glottis Larynx moves up and forward.
 The Cephalic Phase Chemical and mechanical digestion begins in the mouth Saliva is an exocrine secretion Salivary secretion is under autonomic control Softens and lubricates food Chemical digestion: salivary
The Cephalic Phase Chemical and mechanical digestion begins in the mouth Saliva is an exocrine secretion Salivary secretion is under autonomic control Softens and lubricates food Chemical digestion: salivary
Insulin and the brain. Mary ET Boyle, Ph. D. Department of Cognitive Science UCSD
 Insulin and the brain Mary ET Boyle, Ph. D. Department of Cognitive Science UCSD 1921 Banting & Macleod Nobel Prize 1923 White, M. F. (2003) Science Berg, J. M., Tymoczko, J. L. and Stryer, L. (2007) Biochemistry
Insulin and the brain Mary ET Boyle, Ph. D. Department of Cognitive Science UCSD 1921 Banting & Macleod Nobel Prize 1923 White, M. F. (2003) Science Berg, J. M., Tymoczko, J. L. and Stryer, L. (2007) Biochemistry
Table 1 Clinical findings of diabetics. hypoglycemic agent
 Table 1 Clinical findings of diabetics 1)oral hypoglycemic agent Fig. 3 The ratio of primary bile acid to total bile acid Fig. 1 Fecal wet weight Fig. 4 Fecal fatty acid Fig. 2 Fecal bile acid excretion
Table 1 Clinical findings of diabetics 1)oral hypoglycemic agent Fig. 3 The ratio of primary bile acid to total bile acid Fig. 1 Fecal wet weight Fig. 4 Fecal fatty acid Fig. 2 Fecal bile acid excretion
Asma Karameh. -Shatha Al-Jaberi محمد خطاطبة -
 -2 Asma Karameh -Shatha Al-Jaberi محمد خطاطبة - 1 P a g e Gastrointestinal motilities Chewing: once you introduce the first bolus to the mouth you started what we call chewing reflex appears by muscle
-2 Asma Karameh -Shatha Al-Jaberi محمد خطاطبة - 1 P a g e Gastrointestinal motilities Chewing: once you introduce the first bolus to the mouth you started what we call chewing reflex appears by muscle
The Nervous System. Autonomic Division. C h a p t e r. PowerPoint Lecture Slides prepared by Jason LaPres North Harris College Houston, Texas
 C h a p t e r 17 The Nervous System Autonomic Division PowerPoint Lecture Slides prepared by Jason LaPres North Harris College Houston, Texas Copyright 2009 Pearson Education, Inc., publishing as Pearson
C h a p t e r 17 The Nervous System Autonomic Division PowerPoint Lecture Slides prepared by Jason LaPres North Harris College Houston, Texas Copyright 2009 Pearson Education, Inc., publishing as Pearson
Introduction to Gastrointestinal Physiology and GI Hormones Jack Grider, Ph.D
 Introduction to Gastrointestinal Physiology and GI Hormones Jack Grider, Ph.D OBJECTIVES: 1. Describe the general organization of the gut. 2. Identify the levels of neural control and describe the interaction
Introduction to Gastrointestinal Physiology and GI Hormones Jack Grider, Ph.D OBJECTIVES: 1. Describe the general organization of the gut. 2. Identify the levels of neural control and describe the interaction
2.4 Autonomic Nervous System
 2.4 Autonomic Nervous System The ANS regulates visceral activities normally outside the realm of consciousness and voluntary control: Circulation. Digestion. Sweating. Pupillary size. The ANS consists
2.4 Autonomic Nervous System The ANS regulates visceral activities normally outside the realm of consciousness and voluntary control: Circulation. Digestion. Sweating. Pupillary size. The ANS consists
Propulsion and mixing of food in the alimentary tract Chapter 63
 Propulsion and mixing of food in the alimentary tract Chapter 63 Types of GI movements: Propulsive movement-peristalsis Propulsion: controlled movement of ingested foods, liquids, GI secretions, and sloughed
Propulsion and mixing of food in the alimentary tract Chapter 63 Types of GI movements: Propulsive movement-peristalsis Propulsion: controlled movement of ingested foods, liquids, GI secretions, and sloughed
20 2 Stomach Fig. 2.1 An illustration showing different patterns of the myenteric plexus peculiar to the regions in the guinea-pig stomach stained wit
 Stomach 2 The stomach is unique in that ICC have a different distribution in proximal and distal regions of the same organ. ICC-CM and ICC-LM are densely distributed throughout the thick circular and longitudinal
Stomach 2 The stomach is unique in that ICC have a different distribution in proximal and distal regions of the same organ. ICC-CM and ICC-LM are densely distributed throughout the thick circular and longitudinal
,. 1\)... ubj«pcl: Doclo1: M. Khatatbeh Handout # 1 8/4/ Gastreintestinal System. Lecture#: 1. Gastrointestinal Physiology
 Lecture#: 1 Mc:di
Lecture#: 1 Mc:di
Alimentary Canal (I)
 Alimentary Canal (I) Esophagus and Stomach (Objectives) By the end of this lecture, the student should be able to discuss the microscopic structure in correlation with the function of the following organs:
Alimentary Canal (I) Esophagus and Stomach (Objectives) By the end of this lecture, the student should be able to discuss the microscopic structure in correlation with the function of the following organs:
Human Anatomy and Physiology - Problem Drill 15: The Autonomic Nervous System
 Human Anatomy and Physiology - Problem Drill 15: The Autonomic Nervous System Question No. 1 of 10 Which of the following statements is correct about the component of the autonomic nervous system identified
Human Anatomy and Physiology - Problem Drill 15: The Autonomic Nervous System Question No. 1 of 10 Which of the following statements is correct about the component of the autonomic nervous system identified
Bio& 242 Unit 1 / Lecture 4
 Bio& 242 Unit 1 / Lecture 4 system: Gastric hormones GASTRIN: Secretion: By enteroendocrine (G) in gastric pits of the mucosa. Stimulus: Stomach distention and acid ph of chyme causes Gastrin. Action:
Bio& 242 Unit 1 / Lecture 4 system: Gastric hormones GASTRIN: Secretion: By enteroendocrine (G) in gastric pits of the mucosa. Stimulus: Stomach distention and acid ph of chyme causes Gastrin. Action:
Why would fatty foods aggravate the patient s RUQ pain? What effect does cholecystokinin (CCK) have on gastric emptying?
 CASE 28 A 43-year-old woman presents to the emergency department with the acute onset of abdominal pain. Her pain is located to the right upper quadrant (RUQ) and radiates to the right shoulder. She reports
CASE 28 A 43-year-old woman presents to the emergency department with the acute onset of abdominal pain. Her pain is located to the right upper quadrant (RUQ) and radiates to the right shoulder. She reports
Adrenergic fibres in the human intestine
 Gut, 1968, 9, 678-682 Adrenergic fibres in the human intestine L. CAPURSO,1 C. A. FRIEDMANN, AND A. G. PARKS From the Research Department, St Mark's Hospital, London, and the London Hospital, Whitechapel,
Gut, 1968, 9, 678-682 Adrenergic fibres in the human intestine L. CAPURSO,1 C. A. FRIEDMANN, AND A. G. PARKS From the Research Department, St Mark's Hospital, London, and the London Hospital, Whitechapel,
(b) Stomach s function 1. Dilution of food materials 2. Acidification of food (absorption of dietary Fe in small intestine) 3. Partial chemical digest
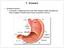 (1) General features a) Stomach is widened portion of gut-tube: between tubular and spherical; Note arranged of smooth muscle tissue in muscularis externa. 1 (b) Stomach s function 1. Dilution of food
(1) General features a) Stomach is widened portion of gut-tube: between tubular and spherical; Note arranged of smooth muscle tissue in muscularis externa. 1 (b) Stomach s function 1. Dilution of food
Daniel Hirsch, MD Director of Neonatology Somerset Medical Center Assistant Professor of Pediatrics UMDNJ RWJMS
 Daniel Hirsch, MD Director of Neonatology Somerset Medical Center Assistant Professor of Pediatrics UMDNJ RWJMS Daniel Hirsch, MD Director of Neonatology Somerset Medical Center Assistant Professor of
Daniel Hirsch, MD Director of Neonatology Somerset Medical Center Assistant Professor of Pediatrics UMDNJ RWJMS Daniel Hirsch, MD Director of Neonatology Somerset Medical Center Assistant Professor of
Ingestion Digestion- Absorption- Elimination
 DIGESTIVE SYSTEM 1 FUNCTIONS Organization GI tract==mouth anus Accessory organs Salivary glands, liver, pancreas, gallbladder Major Functions: Ingestion-mouth, teeth, tongue Digestion- chemical and mechanical
DIGESTIVE SYSTEM 1 FUNCTIONS Organization GI tract==mouth anus Accessory organs Salivary glands, liver, pancreas, gallbladder Major Functions: Ingestion-mouth, teeth, tongue Digestion- chemical and mechanical
Gastrointestinal Physiology
 Gastrointestinal Physiology Digestion and Absorption Definition Digestion: i Food dis dissolved d and broken down. Physical digestion: Propulsion and mixing of food by muscle in the alimentary tract. Chemical
Gastrointestinal Physiology Digestion and Absorption Definition Digestion: i Food dis dissolved d and broken down. Physical digestion: Propulsion and mixing of food by muscle in the alimentary tract. Chemical
GRANULOLYSIS IN A CELLS OF ENDOCRINE PANCREAS AND EXPERIMENTAL DIABETES IN ANIMALS
 Published Online: 1 August, 1968 Supp Info: http://doi.org/10.1083/jcb.38.2.462 Downloaded from jcb.rupress.org on December 25, 2018 GRANULOLYSIS IN A CELLS OF ENDOCRINE PANCREAS IN SPONTANEOUS AND EXPERIMENTAL
Published Online: 1 August, 1968 Supp Info: http://doi.org/10.1083/jcb.38.2.462 Downloaded from jcb.rupress.org on December 25, 2018 GRANULOLYSIS IN A CELLS OF ENDOCRINE PANCREAS IN SPONTANEOUS AND EXPERIMENTAL
Neuroendocrine Tumors
 Neuroendocrine Tumors Neuroendocrine tumors arise from cells that release a hormone in response to a signal from the nervous system. Neuro refers to the nervous system. Endocrine refers to the hormones.
Neuroendocrine Tumors Neuroendocrine tumors arise from cells that release a hormone in response to a signal from the nervous system. Neuro refers to the nervous system. Endocrine refers to the hormones.
1-It is to prevent back flow of fecal content from colon into small intestine.
 Function of the ileocecal valve: 1-It is to prevent back flow of fecal content from colon into small intestine. 2-The wall of the ileum for several centimeters preceding valve has a thickened muscular
Function of the ileocecal valve: 1-It is to prevent back flow of fecal content from colon into small intestine. 2-The wall of the ileum for several centimeters preceding valve has a thickened muscular
OPERATIVE TREATMENT OF ULCER DISEASE
 Página 1 de 8 Copyright 2001 Lippincott Williams & Wilkins Greenfield, Lazar J., Mulholland, Michael W., Oldham, Keith T., Zelenock, Gerald B., Lillemoe, Keith D. Surgery: Scientific Principles & Practice,
Página 1 de 8 Copyright 2001 Lippincott Williams & Wilkins Greenfield, Lazar J., Mulholland, Michael W., Oldham, Keith T., Zelenock, Gerald B., Lillemoe, Keith D. Surgery: Scientific Principles & Practice,
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 24 The Digestive System Introduction The purpose of this chapter is to Identify the anatomical components of the digestive system as well as their
Principles of Anatomy and Physiology 14 th Edition CHAPTER 24 The Digestive System Introduction The purpose of this chapter is to Identify the anatomical components of the digestive system as well as their
I. Neural Control of Involuntary Effectors. Chapter 9. Autonomic Motor Nerves. Autonomic Neurons. Autonomic Ganglia. Autonomic Neurons 9/19/11
 Chapter 9 I. Neural Control of Involuntary Effectors The Autonomic Nervous System Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Autonomic
Chapter 9 I. Neural Control of Involuntary Effectors The Autonomic Nervous System Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Autonomic
Autonomic Nervous System Dr. Ali Ebneshahidi
 Autonomic Nervous System Dr. Ali Ebneshahidi Nervous System Divisions of the nervous system The human nervous system consists of the central nervous System (CNS) and the Peripheral Nervous System (PNS).
Autonomic Nervous System Dr. Ali Ebneshahidi Nervous System Divisions of the nervous system The human nervous system consists of the central nervous System (CNS) and the Peripheral Nervous System (PNS).
Chapter 26 The Digestive System
 Chapter 26 The Digestive System Digestive System Gastroenterology is the study of the stomach and intestine. Digestion Catabolism Absorption Anabolism The actions of the digestive system are controlled
Chapter 26 The Digestive System Digestive System Gastroenterology is the study of the stomach and intestine. Digestion Catabolism Absorption Anabolism The actions of the digestive system are controlled
Composed by Natalia Leonidovna Svintsitskaya, Associate professor of the Chair of Human Anatomy, Candidate of Medicine
 Theoretical background to the study of the autonomic nervous system. Sympathetic and parasympathetic divisions of the autonomic nervous system. Features of the structure, function Composed by Natalia Leonidovna
Theoretical background to the study of the autonomic nervous system. Sympathetic and parasympathetic divisions of the autonomic nervous system. Features of the structure, function Composed by Natalia Leonidovna
The Autonomic Nervous
 Autonomic Nervous System The Autonomic Nervous Assess Prof. Fawzia Al-Rouq System Department of Physiology College of Medicine King Saud University LECTUR (1) Functional Anatomy & Physiology of Autonomic
Autonomic Nervous System The Autonomic Nervous Assess Prof. Fawzia Al-Rouq System Department of Physiology College of Medicine King Saud University LECTUR (1) Functional Anatomy & Physiology of Autonomic
DIGESTIVE TRACT ESOPHAGUS
 DIGESTIVE TRACT From the lower esophagus to the lower rectum four fundamental layers comprise the wall of the digestive tube: mucosa, submucosa, muscularis propria (externa), and adventitia or serosa (see
DIGESTIVE TRACT From the lower esophagus to the lower rectum four fundamental layers comprise the wall of the digestive tube: mucosa, submucosa, muscularis propria (externa), and adventitia or serosa (see
Chapter 15: The Autonomic Nervous System. Copyright 2009, John Wiley & Sons, Inc.
 Chapter 15: The Autonomic Nervous System Comparison of Somatic and Autonomic Nervous Systems Comparison of Somatic and Autonomic Nervous Systems Anatomy of Autonomic Motor Pathways Preganglionic neuron
Chapter 15: The Autonomic Nervous System Comparison of Somatic and Autonomic Nervous Systems Comparison of Somatic and Autonomic Nervous Systems Anatomy of Autonomic Motor Pathways Preganglionic neuron
- Digestion occurs during periods of low activity - Produces more energy than it uses. - Mucosa
 Introduction Digestive System Chapter 29 Provides processes to break down molecules into a state easily used by cells - A disassembly line: Starts at the mouth and ends at the anus Digestive functions
Introduction Digestive System Chapter 29 Provides processes to break down molecules into a state easily used by cells - A disassembly line: Starts at the mouth and ends at the anus Digestive functions
MCAT Biology Problem Drill 20: The Digestive System
 MCAT Biology Problem Drill 20: The Digestive System Question No. 1 of 10 Question 1. During the oral phase of swallowing,. Question #01 A. Initially, the food bolus is moved to the back of the tongue and
MCAT Biology Problem Drill 20: The Digestive System Question No. 1 of 10 Question 1. During the oral phase of swallowing,. Question #01 A. Initially, the food bolus is moved to the back of the tongue and
Chapter 14 The Autonomic Nervous System Chapter Outline
 Chapter 14 The Autonomic Nervous System Chapter Outline Module 14.1 Overview of the Autonomic Nervous System (Figures 14.1 14.3) A. The autonomic nervous system (ANS) is the involuntary arm of the peripheral
Chapter 14 The Autonomic Nervous System Chapter Outline Module 14.1 Overview of the Autonomic Nervous System (Figures 14.1 14.3) A. The autonomic nervous system (ANS) is the involuntary arm of the peripheral
ParasymPathetic Nervous system. Done by : Zaid Al-Ghnaneem
 ParasymPathetic Nervous system Done by : Zaid Al-Ghnaneem In this lecture we are going to discuss Parasympathetic, in the last lecture we took sympathetic and one of the objectives of last lecture was
ParasymPathetic Nervous system Done by : Zaid Al-Ghnaneem In this lecture we are going to discuss Parasympathetic, in the last lecture we took sympathetic and one of the objectives of last lecture was
Pancreas Fox Chapter 18 part 2 (also Chapter 19.3 & 19.4)
 Vert Phys PCB3743 Pancreas Fox Chapter 18 part 2 (also Chapter 19.3 & 19.4) T. Houpt, Ph.D. Anatomy of Digestive System Peristalsis Stomach and Acid Secretion Liver and Bile Secretion Pancreas and pancreatic
Vert Phys PCB3743 Pancreas Fox Chapter 18 part 2 (also Chapter 19.3 & 19.4) T. Houpt, Ph.D. Anatomy of Digestive System Peristalsis Stomach and Acid Secretion Liver and Bile Secretion Pancreas and pancreatic
AUTONOMIC NERVOUS SYSTEM PART I: SPINAL CORD
 AUTONOMIC NERVOUS SYSTEM PART I: SPINAL CORD How is the organization of the autonomic nervous system different from that of the somatic nervous system? Peripheral Nervous System Divisions Somatic Nervous
AUTONOMIC NERVOUS SYSTEM PART I: SPINAL CORD How is the organization of the autonomic nervous system different from that of the somatic nervous system? Peripheral Nervous System Divisions Somatic Nervous
Module 2 Heartburn Glossary
 Absorption Antacids Antibiotic Module 2 Heartburn Glossary Barrett s oesophagus Bloating Body mass index Burping Chief cells Colon Digestion Endoscopy Enteroendocrine cells Epiglottis Epithelium Absorption
Absorption Antacids Antibiotic Module 2 Heartburn Glossary Barrett s oesophagus Bloating Body mass index Burping Chief cells Colon Digestion Endoscopy Enteroendocrine cells Epiglottis Epithelium Absorption
The stomach is formed of three parts: -
 The stomach is formed of three parts: - (a) CARDIAC STOMACH: - It receives the oesophagus through Cardiac aperture guarded by a cardiac sphincter which prevents regurgitation of food. (b) FUNDIC PART:
The stomach is formed of three parts: - (a) CARDIAC STOMACH: - It receives the oesophagus through Cardiac aperture guarded by a cardiac sphincter which prevents regurgitation of food. (b) FUNDIC PART:
DIGESTIVE PHYSIOLOGY
 DIGESTIVE PHYSIOLOGY GASTROINTESTINAL PHYSIOLOGY Ingested foodstuff contributes to an increase in the overall weight of the animal, but does not become an integral part of the structure or metabolic activities
DIGESTIVE PHYSIOLOGY GASTROINTESTINAL PHYSIOLOGY Ingested foodstuff contributes to an increase in the overall weight of the animal, but does not become an integral part of the structure or metabolic activities
1. GASTROINTESTINAL PHYSIOLOGY
 1. GASTROINTESTINAL PHYSIOLOGY FOOD INGESTION Ingested foodstuff contributes to an increase in the overall weight of the animal, but does not become an integral part of the structure or metabolic activities
1. GASTROINTESTINAL PHYSIOLOGY FOOD INGESTION Ingested foodstuff contributes to an increase in the overall weight of the animal, but does not become an integral part of the structure or metabolic activities
Augmentation of Cysteamine and Mepirizole-Induced Lesions in the Rat Duodenum and Stomach by Histamine or Indomethacin
 Augmentation of Cysteamine and Mepirizole-Induced Lesions in the Rat Duodenum and Stomach by Histamine or Indomethacin Hironori TANAKA, Yoshimi KUWAHARA and Susumu OKABE Department of Applied Pharmacology,
Augmentation of Cysteamine and Mepirizole-Induced Lesions in the Rat Duodenum and Stomach by Histamine or Indomethacin Hironori TANAKA, Yoshimi KUWAHARA and Susumu OKABE Department of Applied Pharmacology,
GASTROINTESTINAL PHYSIOLOGY PHYSIOLOGY DEPARTMENT KAMPALA INTERNATIONAL UNIVERSITY DAR ES SALAAM TANZANIA
 GASTROINTESTINAL PHYSIOLOGY PHYSIOLOGY DEPARTMENT KAMPALA INTERNATIONAL UNIVERSITY DAR ES SALAAM TANZANIA Anatomy of the GI Tract The GI tract is essentially a hollow tube connecting the mouth to the anus.
GASTROINTESTINAL PHYSIOLOGY PHYSIOLOGY DEPARTMENT KAMPALA INTERNATIONAL UNIVERSITY DAR ES SALAAM TANZANIA Anatomy of the GI Tract The GI tract is essentially a hollow tube connecting the mouth to the anus.
It passes through the diaphragm at the level of the 10th thoracic vertebra to join the stomach
 The esophagus is a tubular structure (muscular, collapsible tube ) about 10 in. (25 cm) long that is continuous above with the laryngeal part of the pharynx opposite the sixth cervical vertebra The esophagus
The esophagus is a tubular structure (muscular, collapsible tube ) about 10 in. (25 cm) long that is continuous above with the laryngeal part of the pharynx opposite the sixth cervical vertebra The esophagus
- Digestion occurs during periods of low activity - Produces more energy than it uses. 3 Copyright 2016 by Elsevier Inc. All rights reserved.
 Introduction Digestive System Chapter 29 Provides processes to break down molecules into a state easily used by cells - A disassembly line: Starts at the mouth and ends at the anus Digestive functions
Introduction Digestive System Chapter 29 Provides processes to break down molecules into a state easily used by cells - A disassembly line: Starts at the mouth and ends at the anus Digestive functions
BIOCHEMISTRY ondmolecular BIOLOGY INTERNATIONAL Poges
 Vol. 40, No. 3, October 1996 BIOCHEMISTRY ondmolecular BIOLOGY INTERNATIONAL Poges 515-520 ATTENUATION BY NICOTINAMIDE OF THE STREPTOZOCIN INDUCED EARLY HYPERGLYCAEMIA IN FASTING RATS Kai K. Wong Department
Vol. 40, No. 3, October 1996 BIOCHEMISTRY ondmolecular BIOLOGY INTERNATIONAL Poges 515-520 ATTENUATION BY NICOTINAMIDE OF THE STREPTOZOCIN INDUCED EARLY HYPERGLYCAEMIA IN FASTING RATS Kai K. Wong Department
Digestive System Module 4: The Stomach *
 OpenStax-CNX module: m49286 1 Digestive System Module 4: The * Donna Browne Based on The by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0
OpenStax-CNX module: m49286 1 Digestive System Module 4: The * Donna Browne Based on The by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0
Evaluation of Serosal Nerves in Hirschsprung Disease
 Evaluation of Serosal Nerves in Hirschsprung Disease Mudassira and Anwar ul Haque Department of Pathology, Pakistan Institute of Medical Sciences, Islamabad. Introduction: For the diagnosis of Hirschsprung
Evaluation of Serosal Nerves in Hirschsprung Disease Mudassira and Anwar ul Haque Department of Pathology, Pakistan Institute of Medical Sciences, Islamabad. Introduction: For the diagnosis of Hirschsprung
Strain Differences in the Diabetogenic Activity of Streptozotocin in Mice
 1110 Biol. Pharm. Bull. 29(6) 1110 1119 (2006) Vol. 29, No. 6 Strain Differences in the Diabetogenic Activity of Streptozotocin in Mice Koji HAYASHI, Rhyoji KOJIMA, and Mikio ITO* Laboratory of Analytical
1110 Biol. Pharm. Bull. 29(6) 1110 1119 (2006) Vol. 29, No. 6 Strain Differences in the Diabetogenic Activity of Streptozotocin in Mice Koji HAYASHI, Rhyoji KOJIMA, and Mikio ITO* Laboratory of Analytical
Chapter 20 The Digestive System Exam Study Questions
 Chapter 20 The Digestive System Exam Study Questions 20.1 Overview of GI Processes 1. Describe the functions of digestive system. 2. List and define the four GI Processes: 20.2 Functional Anatomy of the
Chapter 20 The Digestive System Exam Study Questions 20.1 Overview of GI Processes 1. Describe the functions of digestive system. 2. List and define the four GI Processes: 20.2 Functional Anatomy of the
Eliades, Erlandson, Ruiz UW-L Journal of Undergraduate Research XVII (2014)
 Effects of Hibernation on the Enteric Nervous System of the Thirteenlined Ground Squirrels. Lauren Eliades, Martin Erlandson, Amelia Ruiz Faculty Sponsors: Dr. Sumei Liu and Dr. Scott Cooper, Department
Effects of Hibernation on the Enteric Nervous System of the Thirteenlined Ground Squirrels. Lauren Eliades, Martin Erlandson, Amelia Ruiz Faculty Sponsors: Dr. Sumei Liu and Dr. Scott Cooper, Department
Pathology of Intestinal Obstruction. Dr. M. Madhavan, MBBS., MD., MIAC, Professor of Pathology Saveetha Medical College
 Pathology of Intestinal Obstruction Dr. M. Madhavan, MBBS., MD., MIAC, Professor of Pathology Saveetha Medical College Pathology of Intestinal Obstruction Objectives list the causes of intestinal obstruction
Pathology of Intestinal Obstruction Dr. M. Madhavan, MBBS., MD., MIAC, Professor of Pathology Saveetha Medical College Pathology of Intestinal Obstruction Objectives list the causes of intestinal obstruction
The Anorectal Myenteric Plexus: Its Relation to Hypoganglionosis of the Colon
 The Anorectal Myenteric Plexus: Its Relation to Hypoganglionosis of the Colon ARTHUR G. WEINBERG, M.D. The Children's Hospital of Akron and Case-Western Reserve University School of Medicine, Akron, Ohio
The Anorectal Myenteric Plexus: Its Relation to Hypoganglionosis of the Colon ARTHUR G. WEINBERG, M.D. The Children's Hospital of Akron and Case-Western Reserve University School of Medicine, Akron, Ohio
Anatomy: Know Your Abdomen
 Anatomy: Know Your Abdomen Glossary Abdomen - part of the body below the thorax (chest cavity); separated by the diaphragm. Anterior - towards the front of the body. For example, the umbilicus is anterior
Anatomy: Know Your Abdomen Glossary Abdomen - part of the body below the thorax (chest cavity); separated by the diaphragm. Anterior - towards the front of the body. For example, the umbilicus is anterior
Gastrointestinal physiology II.
 Gastrointestinal physiology II. 62. Functions of the upper GI tract: chewing, salivation, swallowing. 63. Motor functions of the stomach. Vomiting (emesis). 1 Motor functions of the mouth and the oral
Gastrointestinal physiology II. 62. Functions of the upper GI tract: chewing, salivation, swallowing. 63. Motor functions of the stomach. Vomiting (emesis). 1 Motor functions of the mouth and the oral
Gastrointestinal Physiology Structure and Innervation of the Gastrointestinal Tract Gastrointestinal Smooth Muscle Functions as a Syncytium.
 Gastrointestinal Physiology Structure and Innervation of the Gastrointestinal Tract Structure of the gastrointestinal (GI) tract, Layers of the Gastrointestinal Tract 1. Mucosa: including A lining epithelium,
Gastrointestinal Physiology Structure and Innervation of the Gastrointestinal Tract Structure of the gastrointestinal (GI) tract, Layers of the Gastrointestinal Tract 1. Mucosa: including A lining epithelium,
Done by: Dina Sawadha & Mohammad Abukabeer
 Done by: Dina Sawadha & Mohammad Abukabeer The stomach *the stomach is a dilated part of the gastro intestinal tract, it's "J" shape. *the lower surface of the stomach ( the greater curvature ) reaches
Done by: Dina Sawadha & Mohammad Abukabeer The stomach *the stomach is a dilated part of the gastro intestinal tract, it's "J" shape. *the lower surface of the stomach ( the greater curvature ) reaches
Fig Glossopharyngeal nerve transmits signals to medulla oblongata. Integrating center. Receptor. Baroreceptors sense increased blood pressure
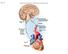 Fig. 5. Integrating center Glossopharyngeal nerve transmits signals to medulla oblongata Receptor 3 Vagus nerve transmits inhibitory signals to cardiac pacemaker Baroreceptors sense increased blood pressure
Fig. 5. Integrating center Glossopharyngeal nerve transmits signals to medulla oblongata Receptor 3 Vagus nerve transmits inhibitory signals to cardiac pacemaker Baroreceptors sense increased blood pressure
A. Incorrect! The esophagus connects the pharynx and the stomach.
 Human Physiology - Problem Drill 19: Digestive Physiology and Nutrition Question No. 1 of 10 Instructions: (1) Read the problem and answer choices carefully, (2) Work the problems on paper as 1. This organ
Human Physiology - Problem Drill 19: Digestive Physiology and Nutrition Question No. 1 of 10 Instructions: (1) Read the problem and answer choices carefully, (2) Work the problems on paper as 1. This organ
Two main groups Alimentary canal continuous coiled hollow tube Accessory digestive organs
 Digestion Breakdown of ingested food Absorption of nutrients into the blood Metabolism Production of cellular energy (ATP) Constructive and degradative cellular activities Two main groups Alimentary canal
Digestion Breakdown of ingested food Absorption of nutrients into the blood Metabolism Production of cellular energy (ATP) Constructive and degradative cellular activities Two main groups Alimentary canal
CHAPTER 15 LECTURE OUTLINE
 CHAPTER 15 LECTURE OUTLINE I. INTRODUCTION A. The autonomic nervous system (ANS) regulates the activity of smooth muscle, cardiac muscle, and certain glands. B. Operation of the ANS to maintain homeostasis,
CHAPTER 15 LECTURE OUTLINE I. INTRODUCTION A. The autonomic nervous system (ANS) regulates the activity of smooth muscle, cardiac muscle, and certain glands. B. Operation of the ANS to maintain homeostasis,
Small intestine. Small intestine
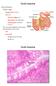 General features Tubular organ longest part; 5-6 m most of chemical digestion absorption of nutrients reabsorption of H2O occurs. Two structural features; maximize the lumenal surface area villi microvilli
General features Tubular organ longest part; 5-6 m most of chemical digestion absorption of nutrients reabsorption of H2O occurs. Two structural features; maximize the lumenal surface area villi microvilli
Digestive Lecture Test Questions Set 4
 Digestive Lecture Test Questions Set 4 1. Which of the following is not associated directly with the small intestine: a. villi b. circular folds c. microvilli d. haustrae e. secretin 2. The largest (longest)
Digestive Lecture Test Questions Set 4 1. Which of the following is not associated directly with the small intestine: a. villi b. circular folds c. microvilli d. haustrae e. secretin 2. The largest (longest)
Gastrointestinal Motility 2: Intestinal and Colonic Motility Jack Grider, Ph.D.
 Gastrointestinal Motility 2: Intestinal and Colonic Motility Jack Grider, Ph.D. OBJECTIVES: 1. Contrast the types of motility in the small intestine. 2. Describe the neural circuits that mediate peristalsis.
Gastrointestinal Motility 2: Intestinal and Colonic Motility Jack Grider, Ph.D. OBJECTIVES: 1. Contrast the types of motility in the small intestine. 2. Describe the neural circuits that mediate peristalsis.
Small Intestine, Large Intestine and anal cannel
 Small Intestine, Large Intestine and anal cannel 32409 Small intestine Large intestine Small intestine General Structure of the Digestive Tract rat 32409 Epithelium with goblet cells and absorptive cells
Small Intestine, Large Intestine and anal cannel 32409 Small intestine Large intestine Small intestine General Structure of the Digestive Tract rat 32409 Epithelium with goblet cells and absorptive cells
Energy, Chemical Reactions and Enzymes
 Phosphorylation Hydrolysis Energy, Chemical Reactions and Enzymes Chapter 2 (selections) What is Energy? Energy is the capacity to do work Potential Energy Kinetic Energy Chemical Bond Energy Like a rechargeable
Phosphorylation Hydrolysis Energy, Chemical Reactions and Enzymes Chapter 2 (selections) What is Energy? Energy is the capacity to do work Potential Energy Kinetic Energy Chemical Bond Energy Like a rechargeable
Pancreas & Biliary System. Dr. Vohra & Dr. Jamila
 Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Lab activity manual - Histology of the digestive system. Lab activity 1: esophagus stomach - small intestines
 Lab activity manual - Histology of the digestive system Jeanne Adiwinata Pawitan Prerequisite: Histology of the 4 basic tissues In this module we learn about the histology of the digestive system, from
Lab activity manual - Histology of the digestive system Jeanne Adiwinata Pawitan Prerequisite: Histology of the 4 basic tissues In this module we learn about the histology of the digestive system, from
Helicobacter and gastritis
 1 Helicobacter and gastritis Dr. Hala Al Daghistani Helicobacter pylori is a spiral-shaped gram-negative rod. H. pylori is associated with antral gastritis, duodenal (peptic) ulcer disease, gastric ulcers,
1 Helicobacter and gastritis Dr. Hala Al Daghistani Helicobacter pylori is a spiral-shaped gram-negative rod. H. pylori is associated with antral gastritis, duodenal (peptic) ulcer disease, gastric ulcers,
Abstract. Abnormal peristaltic waves like aperistalsis of the esophageal body, high amplitude and broader waves,
 Original Article Esophageal Motility Disorders in Diabetics Waquaruddin Ahmed, Ejaz Ahmed Vohra Department of Medicine, Dr. Ziauddin Medical University, Karachi. Abstract Objective: To see the presence
Original Article Esophageal Motility Disorders in Diabetics Waquaruddin Ahmed, Ejaz Ahmed Vohra Department of Medicine, Dr. Ziauddin Medical University, Karachi. Abstract Objective: To see the presence
The Autonomic Nervous System Outline of class lecture for Physiology
 The Autonomic Nervous System Outline of class lecture for Physiology 1 After studying the endocrine system you should be able to: 1. Describe the organization of the nervous system. 2. Compare and contrast
The Autonomic Nervous System Outline of class lecture for Physiology 1 After studying the endocrine system you should be able to: 1. Describe the organization of the nervous system. 2. Compare and contrast
Chp. 16: AUTONOMIC N.S. (In Review: Peripheral N. S.)
 Chp. 16: AUTONOMIC N.S. (In Review: Peripheral N. S.) Peripheral nerves contain both motor and sensory neurons Among the motor neurons, some of these are somatic and innervate skeletal muscles while some
Chp. 16: AUTONOMIC N.S. (In Review: Peripheral N. S.) Peripheral nerves contain both motor and sensory neurons Among the motor neurons, some of these are somatic and innervate skeletal muscles while some
Dr. Patsy Smyth, FNP-BC
 Dr. Patsy Smyth, FNP-BC Gastroparesis literally translated means stomach paralysis. Gastroparesis is a syndrome characterized by delayed gastric emptying in absence of mechanical obstruction of the stomach.
Dr. Patsy Smyth, FNP-BC Gastroparesis literally translated means stomach paralysis. Gastroparesis is a syndrome characterized by delayed gastric emptying in absence of mechanical obstruction of the stomach.
PHYSIOLOGY OF THE DIGESTIVE SYSTEM
 Student Name CHAPTER 26 PHYSIOLOGY OF THE DIGESTIVE SYSTEM D igestion is the process of breaking down complex nutrients into simpler units suitable for absorption. It involves two major processes: mechanical
Student Name CHAPTER 26 PHYSIOLOGY OF THE DIGESTIVE SYSTEM D igestion is the process of breaking down complex nutrients into simpler units suitable for absorption. It involves two major processes: mechanical
Includes mouth, pharynx, esophagus, stomach, small intestine, large intestine, rectum, anus. Salivary glands, liver, gallbladder, pancreas
 Chapter 14 The Digestive System and Nutrition Digestive System Brings Nutrients Into the Body The digestive system includes Gastrointestinal (GI) tract (hollow tube) Lumen: space within this tube Includes
Chapter 14 The Digestive System and Nutrition Digestive System Brings Nutrients Into the Body The digestive system includes Gastrointestinal (GI) tract (hollow tube) Lumen: space within this tube Includes
Sphincters heartburn diaphragm The Stomach gastric glands pepsin, chyme The Small Intestine 1-Digestion Is Completed in the Small Intestine duodenum
 Sphincters are muscles that encircle tubes and act as valves. The tubes close when the sphincters contract and they open when the sphincters relax. When food or saliva is swallowed, the sphincter relaxes
Sphincters are muscles that encircle tubes and act as valves. The tubes close when the sphincters contract and they open when the sphincters relax. When food or saliva is swallowed, the sphincter relaxes
The Digestive System. What is the advantage of a one-way gut? If you swallow something, is it really inside you?
 The Digestive System What is the advantage of a one-way gut?! If you swallow something, is it really inside you? Functions and Processes of the Digestive System: Move nutrients, water, electrolytes from
The Digestive System What is the advantage of a one-way gut?! If you swallow something, is it really inside you? Functions and Processes of the Digestive System: Move nutrients, water, electrolytes from
HISTOLOGY. GIT Block 432 Histology Team. Lecture 1: Alimentary Canal (1) (Esophagus & Stomach) Done by: Ethar Alqarni Reviewed by: Ibrahim Alfuraih
 HISTOLOGY Lecture 1: Alimentary Canal (1) (Esophagus & Stomach) Done by: Ethar Alqarni Reviewed by: Ibrahim Alfuraih Color Guide: Black: Slides. Red: Important. Green: Doctor s notes. Blue: Explanation.
HISTOLOGY Lecture 1: Alimentary Canal (1) (Esophagus & Stomach) Done by: Ethar Alqarni Reviewed by: Ibrahim Alfuraih Color Guide: Black: Slides. Red: Important. Green: Doctor s notes. Blue: Explanation.
VIPergic Innervation of the Gall Bladder 1n Health and Disease*)
 Hiroshima Journal of Medical Sciences Vol. 33, No. 2, 185~191, June, 1984 HIJM 33-26 185 VIPergic Innervation of the Gall Bladder 1n Health and Disease*) Shinya KISHIMOTO, Kazuma OKAMOTO, Satoru SHIMIZU,
Hiroshima Journal of Medical Sciences Vol. 33, No. 2, 185~191, June, 1984 HIJM 33-26 185 VIPergic Innervation of the Gall Bladder 1n Health and Disease*) Shinya KISHIMOTO, Kazuma OKAMOTO, Satoru SHIMIZU,
e. Undigested material is compacted and stored until the colon is full. When the colon is full, a signal to empty it is sent by sensors in the walls
 Digestive System 1. General a. Animals obtain energy by breaking food molecules into smaller pieces. b. The basic fuel molecules are amino acids, lipids and sugars c. Digestion is the chemical breakdown
Digestive System 1. General a. Animals obtain energy by breaking food molecules into smaller pieces. b. The basic fuel molecules are amino acids, lipids and sugars c. Digestion is the chemical breakdown
Causes of pancreatic insufficiency. Eugen Dumitru
 Causes of pancreatic insufficiency Eugen Dumitru Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes 3. The Consequences Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes
Causes of pancreatic insufficiency Eugen Dumitru Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes 3. The Consequences Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes
Physiology Unit 4 DIGESTIVE PHYSIOLOGY
 Physiology Unit 4 DIGESTIVE PHYSIOLOGY In Physiology Today Functions Motility Ingestion Mastication Deglutition Peristalsis Secretion 7 liters/day! Exocrine/endocrine Digestion Absorption Digestion of
Physiology Unit 4 DIGESTIVE PHYSIOLOGY In Physiology Today Functions Motility Ingestion Mastication Deglutition Peristalsis Secretion 7 liters/day! Exocrine/endocrine Digestion Absorption Digestion of
Autonomic Nervous System
 Autonomic Nervous System Keri Muma Bio 6 Organization of the Nervous System Efferent Division Somatic Nervous System Voluntary control Effector = skeletal muscles Muscles must be excited by a motor neuron
Autonomic Nervous System Keri Muma Bio 6 Organization of the Nervous System Efferent Division Somatic Nervous System Voluntary control Effector = skeletal muscles Muscles must be excited by a motor neuron
Chapter 16. APR Enhanced Lecture Slides
 Chapter 16 APR Enhanced Lecture Slides See separate PowerPoint slides for all figures and tables pre-inserted into PowerPoint without notes and animations. Copyright The McGraw-Hill Companies, Inc. Permission
Chapter 16 APR Enhanced Lecture Slides See separate PowerPoint slides for all figures and tables pre-inserted into PowerPoint without notes and animations. Copyright The McGraw-Hill Companies, Inc. Permission
