Nice CKD Clinical Guidelines 2014 The challenges and benefits they may bring toprimary care
|
|
|
- Thomasina Chase
- 5 years ago
- Views:
Transcription
1 Nice CKD Clinical Guidelines 2014 The challenges and benefits they may bring toprimary care Paula D Souza Senior CKD Nurse Specialist Royal Devon and Exeter Healthcare Trust Introduction Background What are the main aims of the guideline Overview of the new recommendations incorporating some of the perceived challenges and benefits of implementation Amended guidelines and other recommendations Summary 1
2 Background Moderate to severe CKD is associated with an increased risk of other significant adverse outcomes such as: acute kidney injury, falls, frailty and mortality The risk of developing CKD increases with age There is evidence that treatment can prevent or delay the progression of CKD, reduce or prevent the development of complications, and reduce the risk of cardiovascular disease CKD can progress to established renal failure, in a small but significant percentage of people What is the aim of the guideline Update NICE clinical guideline CG73 in areas where new information has become available Provide new guidance in areas where previously no evidence existed Promote strategies aimed at earlier identification and prevention of progression 2
3 New Recommendations Identification and investigation of people who have or are at risk of developing CKD Classification of CKD and identification of people at risk of CKD complications and progression The definition of CKD progression Self-management of CKD The relationship between acute kidney injury and CKD Pharmacotherapy for CKD Identification and investigation of people who have or are at risk of developing CKD Clinical laboratories are recommended to: Use the Chronic Kidney Disease Epidemiology Collaboration (CKD-EPI) creatinine equation to estimate GFRcreatinine, using creatinine assays with calibration traceable to standardised reference material Use creatinine assays that are specific (for example, enzymatic assays) and zero-biased compared with isotope dilution mass spectrometry (IDMS) Participate in UK national quality assessment schemes for creatinine 3
4 Why change from MDRD to CKD-EPI? Modification of Diet in Renal Disease study equation or MDRD uses serum creatinine to estimate GFR (2006) Easy to use It does not require weight or height variables because the results are reported normalised to 1.73m2 body surface area which is an accepted average adult surface area. It provides an estimated GFR measurement but not an actual GFR measurement It uses four variables age, sex, race and serum creatinine Problems with MDRD Not validated: < 18years of age Individuals with serious co-morbid conditions and hospitalised patients especially with AKI where you get rapidly changing creatinine levels People with extremes of muscle mass Less accurate in people with near normal kidney function egfr 90ml/min/m2 It is also not validated in the older person MDRD equation was developed in a population with sub-optimal kidney function its accuracy in predicting GFR is best reflected in those with mild kidney impairment (category G2) group not routinely monitored in primary care In severe renal impairment egfr<15ml/min its less sensitive 4
5 CKD-EPI CKD-EPI equation (2009) like the MDRD was developed to estimate GFR from serum creatinine Difference: CKD-Epidemiology Collaboration group developed equation to match the accuracy of the MDRD but at lower GFR <60 ml/min/1.73m 2 (category G3) Uses the same variables as MDRD but different coefficients Limitations similar to the MDRD group (e.g. elderly and extremes of muscle mass) However: It is also considered a more accurate way of estimating GFR in those with higher level of GFR (>60ml/min ) than the MDRD minimizing the over-diagnosis of CKD seen with MDRD equation fewer classifications More accurate in young individuals, women and whites Predictor of mortality and ESKD in a broad range of populations What are the challenges for primary care in relation to the use of either MDRD or CKD-EPI No challenges but continued education is needed regarding the accuracy of theses equations in certain sub-groups Education should include messages such as: If egfr is greater than 90ml/min/1.73m2, use an increase in serum creatinine concentration of more than 20% to infer significant reduction in kidney function (new 2014) Interpret egfrvalues of 60ml/min/1.73m2 or more with caution, bearing in mind that estimates of GFR become less accurate as true GFR increases (new 2014) Encourage looking at trends of egfr / serum creatinine 5
6 New reporting criteria Clinical laboratories should report GFR either as a whole number if it is 90 ml/min/1.73 m2 or less If > 90 ml/min/1.73 m2 report as this The new boy on the block Cystatin C Low molecular weight (13.3 kilodaltons) protein freely filtered in the glomerulus Not secreted, fully reabsorbed and broken down in the renal tubules making it an excellent marker of GFR If kidney function and GFR rate decline the cystatinc levels will rise Compared to creatininethe production of CystatinC is less influenced by a persons age, gender and size its considered a better reflection of GFR than serum creatinine Alone it has not been shown to be superior to the formula-adjusted estimations of kidney function, but combined with egfrcreatinine studies have shown it improves the estimation accuracy of GFR 6
7 Challenges for Primary Care Clinical When to test: Suggest considerationshould be given to using egfrcystatincat initial diagnosis to confirm or refute CKD in people with: an egfrcreatinineof ml/min/1.73 m2, sustained for at least 90 days ANDno proteinuria (albumin:creatinine ratio) [ACR] <3 mg/mmol or any other marker of kidney damage (new 2014) Message: Do not diagnose CKD in people with: an egfrcreatinine of ml/min/1.73 m2 AND an egfrcystatincof more > 60 ml/min/1.73 m2 AND no other marker of kidney disease (new 2014) Interpret with caution CystatinC levels have been reported to alter in some people with cancer and thyroid dysfunction Cigarette smoking and CRP may also influence levels 7
8 Cost Locally available for clinicians to request but commissioning needs to be agreed Benefits Correct Classification both patient and financial Predictor of new onset and or developing CVD 8
9 Classification of CKD and identification of people at risk of CKD complications and progression Who should be tested: Diabetes Hypertension Cardiovascular disease Vascular disease or cerebral vascular disease Structural renal tract disease, recurrent renal calculi or prostatic hypertrophy Multisystem diseases with potential kidney involvement e.g. systemic lupus erythematosus Family history of end-stage kidney disease (GFR category G5) or hereditary kidney disease Opportunistic detection of hematuria Acute Kidney Injury ( new 2014) Classification of CKD using a combination of GFR and ACR 9
10 Key Message Increased ACR is associated with increased risk adverse outcomes Decreased GFR is associated with increased risk of adverse outcomes Increased ACR and decreased GFR in combination multiply the risk of adverse outcomes Challenges and Benefits of the new classification system Challenges: Primary care may see it as too complicated getting used to stages rather than categories Not all practitioners have the discussion about CKD Benefits: A visual tool (heat map) ACR measurements have changed 10
11 Working together Investigating the cause of CKD: After having an informed discussion with the person with CKD agree a plan to establish the cause, particularly if the cause is thought to be treatable (e.g. urinary tract obstruction, nephrotoxic drugs or glomerular disease) Use the person s GFR and ACR categories to indicatetheir risk of adverse outcomes (e.g. CKD progression, acute kidney injury, all-cause mortality and cardiovascular events) and discuss this with them Monitoring Agree the frequency of monitoring (egfrcreatinine and ACR) with the person, with or at risk of CKD Bear in mind that CKD is not progressive in many people 11
12 Guide to frequency of monitoring of GFR for people with, or at risk of CKD Tailor individual monitoring according to: The underlying cause of CKD Past patterns of egfrand ACR Comorbidities, especially heart failure Changes to their treatment (such as renin-angiotensin-aldosterone system [RAAS] antagonists, NSAIDs and diuretics) Inter-current illness Whether they have chosen conservative management of CKD (new 2014) 12
13 Challenges and benefits of the new monitoring criteria Challenges: Slightly different from monthly to times per year Benefits: Visual reminder The clinician and person with CKD decide on frequency according to clinical need Aim: identify progressive CKD Be aware that people with CKD are at increased risk of progression to end-stage renal disease if they have eitherof the following: a sustained decrease in GFR of 25% or more over 12 months or a sustained decrease in GFR of 15 ml/min/1.73 m2 or more over 12 months (new 2014) In people with an new finding of reduced GFR, repeat the GFR with 2 weeks to exclude causes of acute deterioration of GFR e.g. AKIor reninangiotensin system antagonist (RASA) therapy (amended 2014) Chronic Kidney Disease: NICE guideline CG amended CG
14 Risk factors associated with progression Cardiovascular disease Proteinuria Acute Kidney Injury Hypertension Diabetes Smoking African, African-Caribbean or Asian family origin Chronic use of NSAIDs Untreated urinary outflow tract obstruction Acute Kidney Injury and CKD Monitor people for the development or progression of CKD for at least 2-3 years after acute kidney injury, even if serum creatininehas returned to baseline (new 2014) Advise people who have had acute kidney injury that they are at increased risk of CKD developing or progressing (new 2014) 14
15 Challenges and Benefits Challenges: Getting used to the new criteria Not all AKI is documented or recognised Is it 2 or 3 years? Benefits: Realistic position kidney function does fluctuate and may not necessitate referral Following AKI closer monitoring Self management Ensure that systems are in place to: Enable people with CKD to share in decision-making about their care Support self-management (this includes providing information about blood pressure, exercise, diet and medicines) and enable people to make informed choices Give people access to their medical data (including diagnosis, comorbidities, test results, treatments and correspondence) through information systems such as Renal Patient View, to encourage and help them to self-manage their CKD 15
16 Challenges and Benefits Challenges: Having the discussion time and knowledge People having access to their medical data Benefits: Encourage practitioners to be up to date Prompt discussion about treatment plan +/- referral Ensure all information is correct classification Informed cohort improve concordance Proteinuria: amended guidelines To detect and identify proteinuria use a urine ACR in preference to protein:creatinine ratio (PCR) ACR has greater sensitivity at low levels of proteinuria For quantification and monitoring of high levels of proteinuria (ACR > 70mg/mmol) PCR can be used as an alternative ACR is recommended for people with diabetes People without diabetes with a GFR of <60ml.min/1.73m2 quantify urinary albumin or urinary protein loss For initial detection of proteinuria if ACR 3mg/mmol-70mg/mmol a subsequent early morning urine should completed for confirmation If initial ACR is 70mg/mmol a repeat sample is not required Regard a confirmed ACR of 3mg/mmol as clinically important proteinuria Chronic Kidney Disease: NICE guideline CG amended CG
17 Other Recommendations: Blood pressure No change to parameters Offer a low-costrenin-angiotensin system antagonist to people with CKD and: diabetes and an ACR of 3 mg/mmol or more hypertension and an ACR of 30 mg/mmol or more an ACR of 70 mg/mmol or more (irrespective of hypertension or cardiovascular disease)(new 2014) Do not offer a combination of renin-angiotensin system antagonists to people with CKD (new 2014) Do not routinely offer a RASA therapy to people with a pre-treatment potassium of >5.0mmol/litre(amended 2014) Follow the treatment recommendations in Hypertension (NICE clinical guideline 127) for people with CKD, hypertension and an ACR of <3 mg/mmol, if they do not have diabetes (new 2014) Vitamin D supplement in the management of CKD-MBD Do not routinely offer vitamin D supplementation to manage or prevent CKD-mineral and bone disorders (new 2014) Offer cholecalciferolor ergocalciferolto treat vitamin D deficiency in people with CKD and vitamin D deficiency (new 2014) If vitamin D deficiency has been corrected and symptoms of CKDmineral and bone disorders persist, offer alfacalcidol(1-alphahydroxycholecalciferol) or calcitriol(1-25-dihydroxycholecalciferol) to people with stage 4 or 5 CKD (new 2014) Monitor serum calcium and phosphate concentrations in people receiving alfacalcidol or calcitriol supplements (new 2014) 17
18 Statins and oral antiplatelet and anticoagulant therapy Follow the recommendations in lipid modification ( NICE CG 181) for the use of statins in CKD (new 2014) Offerantiplatelet drugs to people with CKD for the secondary prevention of cardiovascular disease, but be aware of the increased risk of bleeding (new 2014) Consider apixaban in preference to warfarin in people with confirmed egfrof 30-50ml/min/1.73m2 and non-valvular atrial fibrillation who have one or more of the following risk factors: Prior stroke or transient ischemic attack Age 75 years or older Hypertension Diabetes mellitus Symptomatic heart failure (new 2014) () Other recommendations Do not offer low-protein diets (dietary protein intake less than g/kg/day) to people with CKD (new 2014) Consider oral sodium bicarbonate supplementation for people with both: a GFR less than 30ml/min/1.73m2 AND a serum bicarbonate concentration of less than 20 mmol/litre(new 2014) ) 18
19 Referral Criteria GFR less than 30 ml/min/1.73 m2 (with or without diabetes) ACR 70 mg/mmolor more, unless known to be caused by diabetes and already appropriately treated ACR 30 mg/mmol or more, together with hematuria Sustained decrease in GFR of 25% or more and a change in GFR category or sustained decrease in GFR of 15 ml/min/1.73 m2 or more Hypertension that remains poorly controlled despite the use of at least 4 antihypertensive drugs at therapeutic doses Known or suspected rare or genetic causes of CKD Suspected renal artery stenosis Chronic Kidney Disease: NICE guideline CG amended CG Summary Use CKD-EPI in preference to MDRD Combining egfrusing the CKD EPI equation and CystatinC may classify less people with a CKD in a small but significant sub-group Commissioning of new tests will need to be agreed The new classification and monitoring grid should help practitioners with appropriate monitoring and assist them in identifying people who are increased risk of adverse outcome Practitioners are encouraged to discuss diagnosis and treatment plans with individuals Defining progression is more appropriate and may avoid inappropriate referrals Monitoring following AKI is recognised as important Access to medical data may create some challenges Gives practical advise on managing some of the complications associated with CKD 19
20 Thank You Any Questions? 20
Clinical guideline Published: 23 July 2014 nice.org.uk/guidance/cg182
 Chronic kidney disease in adults: assessment and management Clinical guideline Published: 23 July 2014 nice.org.uk/guidance/cg182 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Chronic kidney disease in adults: assessment and management Clinical guideline Published: 23 July 2014 nice.org.uk/guidance/cg182 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
The National Quality Standards for Chronic Kidney Disease
 The National Quality Standards for Chronic Kidney Disease Dr Robert Lewis Chief of Service, Wessex Kidney Centre, Portsmouth Specialist Committee Member Quality Standard for Chronic Kidney Disease, NICE
The National Quality Standards for Chronic Kidney Disease Dr Robert Lewis Chief of Service, Wessex Kidney Centre, Portsmouth Specialist Committee Member Quality Standard for Chronic Kidney Disease, NICE
QUICK REFERENCE FOR HEALTHCARE PROVIDERS
 KEY MESSAGES 1 SCREENING CRITERIA Screen: Patients with DM and/or hypertension at least yearly. Consider screening patients with: Age >65 years old Family history of stage 5 CKD or hereditary kidney disease
KEY MESSAGES 1 SCREENING CRITERIA Screen: Patients with DM and/or hypertension at least yearly. Consider screening patients with: Age >65 years old Family history of stage 5 CKD or hereditary kidney disease
Swindon Diabetes Guidelines: Management of Chronic Kidney Disease Associated with Diabetes Mellitus
 Swindon Diabetes Guidelines: Management of Chronic Kidney Disease Associated with Diabetes Mellitus 1 Contents Executive Summary... 3 How to Screen for Diabetic Nephropathy... 4 What to Measure... 4 Frequency
Swindon Diabetes Guidelines: Management of Chronic Kidney Disease Associated with Diabetes Mellitus 1 Contents Executive Summary... 3 How to Screen for Diabetic Nephropathy... 4 What to Measure... 4 Frequency
National Institute for Health and Care Excellence
 National Institute for Health and Care Excellence 4-year surveillance (2017) Chronic kidney disease in adults (2014) NICE guideline CG182 Appendix A2: Summary of new evidence from surveillance Investigations
National Institute for Health and Care Excellence 4-year surveillance (2017) Chronic kidney disease in adults (2014) NICE guideline CG182 Appendix A2: Summary of new evidence from surveillance Investigations
Primary Care Approach to Management of CKD
 Primary Care Approach to Management of CKD This PowerPoint was developed through a collaboration between the National Kidney Foundation and ASCP. Copyright 2018 National Kidney Foundation and ASCP Low
Primary Care Approach to Management of CKD This PowerPoint was developed through a collaboration between the National Kidney Foundation and ASCP. Copyright 2018 National Kidney Foundation and ASCP Low
Summary of Recommendation Statements Kidney International Supplements (2013) 3, 5 14; doi: /kisup
 http://www.kidney-international.org & 2013 DIGO Summary of Recommendation Statements idney International Supplements (2013) 3, 5 14; doi:10.1038/kisup.2012.77 Chapter 1: Definition and classification of
http://www.kidney-international.org & 2013 DIGO Summary of Recommendation Statements idney International Supplements (2013) 3, 5 14; doi:10.1038/kisup.2012.77 Chapter 1: Definition and classification of
CKD and risk management : NICE guideline
 CKD and risk management : NICE guideline 2008-2014 Shahed Ahmed Consultant Nephrologist shahed.ahmed@rlbuht.nhs.uk Key points : Changing parameters of CKD and NICE guidance CKD and age related change of
CKD and risk management : NICE guideline 2008-2014 Shahed Ahmed Consultant Nephrologist shahed.ahmed@rlbuht.nhs.uk Key points : Changing parameters of CKD and NICE guidance CKD and age related change of
Supplement: Summary of Recommendation Statements CHAPTER 1: DEFINITION AND CLASSIFICATION OF CKD
 Supplement: Summary of Recommendation Statements CHAPTER 1: DEFINITION AND CLASSIFICATION OF CKD 1.1 DEFINITION OF CKD 1.1.1: CKD is defined as abnormalities of kidney structure or function, present for
Supplement: Summary of Recommendation Statements CHAPTER 1: DEFINITION AND CLASSIFICATION OF CKD 1.1 DEFINITION OF CKD 1.1.1: CKD is defined as abnormalities of kidney structure or function, present for
Bulletin Independent prescribing information for NHS Wales
 Bulletin Independent prescribing information for NHS Wales October 2017 Chronic kidney disease Chronic kidney disease (CKD) is a long-term irreversible deterioration in the function of the kidneys, often
Bulletin Independent prescribing information for NHS Wales October 2017 Chronic kidney disease Chronic kidney disease (CKD) is a long-term irreversible deterioration in the function of the kidneys, often
SERVICE SPECIFICATION 6 Conservative Management & End of Life Care
 SERVICE SPECIFICATION 6 Conservative Management & End of Life Care Table of Contents Page 1 Key Messages 2 2 Introduction & Background 2 3 Relevant Guidelines & Standards 2 4 Scope of Service 3 5 Interdependencies
SERVICE SPECIFICATION 6 Conservative Management & End of Life Care Table of Contents Page 1 Key Messages 2 2 Introduction & Background 2 3 Relevant Guidelines & Standards 2 4 Scope of Service 3 5 Interdependencies
CKD FOR INTERNISTS. Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College
 CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
Chronic Kidney Disease
 Chronic Kidney Disease Presence of kidney damage or decreased kidney function for three or more months, - necessary to distinguish CKD from acute kidney disease. Ascertained either by kidney biopsy or
Chronic Kidney Disease Presence of kidney damage or decreased kidney function for three or more months, - necessary to distinguish CKD from acute kidney disease. Ascertained either by kidney biopsy or
Management of early chronic kidney disease
 Management of early chronic kidney disease GREENLANE SUMMER GP SYMPOSIUM 2018 Jonathan Hsiao Renal and General Physician Introduction A growing public health problem in NZ and throughout the world. Unknown
Management of early chronic kidney disease GREENLANE SUMMER GP SYMPOSIUM 2018 Jonathan Hsiao Renal and General Physician Introduction A growing public health problem in NZ and throughout the world. Unknown
Creatinine & egfr A Clinical Perspective. Suheir Assady MD, PhD Dept. of Nephrology & Hypertension RHCC
 Creatinine & egfr A Clinical Perspective Suheir Assady MD, PhD Dept. of Nephrology & Hypertension RHCC CLINICAL CONDITIONS WHERE ASSESSMENT OF GFR IS IMPORTANT Stevens et al. J Am Soc Nephrol 20: 2305
Creatinine & egfr A Clinical Perspective Suheir Assady MD, PhD Dept. of Nephrology & Hypertension RHCC CLINICAL CONDITIONS WHERE ASSESSMENT OF GFR IS IMPORTANT Stevens et al. J Am Soc Nephrol 20: 2305
Office Management of Reduced GFR Practical advice for the management of CKD
 Office Management of Reduced GFR Practical advice for the management of CKD CKD Online Education CME for Primary Care April 27, 2016 Monica Beaulieu, MD FRCPC MHA CHAIR PROVINCIAL KIDNEY CARE COMMITTEE
Office Management of Reduced GFR Practical advice for the management of CKD CKD Online Education CME for Primary Care April 27, 2016 Monica Beaulieu, MD FRCPC MHA CHAIR PROVINCIAL KIDNEY CARE COMMITTEE
CKDinform: A PCP s Guide to CKD Detection and Delaying Progression
 CKDinform: A PCP s Guide to CKD Detection and Delaying Progression Learning Objectives Describe suitable screening tools, such as GFR and ACR, for proper utilization in clinical practice related to the
CKDinform: A PCP s Guide to CKD Detection and Delaying Progression Learning Objectives Describe suitable screening tools, such as GFR and ACR, for proper utilization in clinical practice related to the
Professor Suetonia Palmer
 Professor Suetonia Palmer Department of Medicine Nephrologist Christchurch Hospital Christchurch 14:00-14:55 WS #108: The Kidney Test - When To Test and When to Refer ( and When Not To) 15:05-16:00 WS
Professor Suetonia Palmer Department of Medicine Nephrologist Christchurch Hospital Christchurch 14:00-14:55 WS #108: The Kidney Test - When To Test and When to Refer ( and When Not To) 15:05-16:00 WS
Elevation of Serum Creatinine: When to Screen, When to Refer. Bruce F. Culleton, MD, FRCPC; and Jolanta Karpinski, MD, FRCPC
 Elevation of Serum Creatinine: When to Screen, When to Refer Bruce F. Culleton, MD, FRCPC; and Jolanta Karpinski, MD, FRCPC Presented at the University of Calgary s CME and Professional Development 2006-2007
Elevation of Serum Creatinine: When to Screen, When to Refer Bruce F. Culleton, MD, FRCPC; and Jolanta Karpinski, MD, FRCPC Presented at the University of Calgary s CME and Professional Development 2006-2007
5/10/2014. Observation, control of blood pressure. Observation, control of blood pressure and risk factors.
 Overview The Kidneys Nicola Barlow Clinical Biochemistry Department City Hospital Renal physiology Renal pathophysiology Acute kidney injury Chronic kidney disease Assessing renal function GFR Proteinuria
Overview The Kidneys Nicola Barlow Clinical Biochemistry Department City Hospital Renal physiology Renal pathophysiology Acute kidney injury Chronic kidney disease Assessing renal function GFR Proteinuria
Outline. Outline CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW 7/23/2013. Question 1: Which of these patients has CKD?
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
Figure 1 LVH: Allowed Cost by Claim Volume (Data generated from a Populytics analysis).
 Chronic Kidney Disease (CKD): The New Silent Killer Nelson Kopyt D.O. Chief of Nephrology, LVH Valley Kidney Specialists For the past several decades, the health care needs of Americans have shifted from
Chronic Kidney Disease (CKD): The New Silent Killer Nelson Kopyt D.O. Chief of Nephrology, LVH Valley Kidney Specialists For the past several decades, the health care needs of Americans have shifted from
Section Questions Answers
 Section Questions Answers Guide to CKD Screening and Evaluation -Alec Otteman, MD Delaying Progression - Paul Drawz, MD, MHS, MS 1. Modifiable risk factors for CKD include: a. Diabetes b. Hypertension
Section Questions Answers Guide to CKD Screening and Evaluation -Alec Otteman, MD Delaying Progression - Paul Drawz, MD, MHS, MS 1. Modifiable risk factors for CKD include: a. Diabetes b. Hypertension
A New Approach for Evaluating Renal Function and Predicting Risk. William McClellan, MD, MPH Emory University Atlanta
 A New Approach for Evaluating Renal Function and Predicting Risk William McClellan, MD, MPH Emory University Atlanta Goals Understand the limitations and uses of creatinine based measures of kidney function
A New Approach for Evaluating Renal Function and Predicting Risk William McClellan, MD, MPH Emory University Atlanta Goals Understand the limitations and uses of creatinine based measures of kidney function
Outline. Outline CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW. Question 1: Which of these patients has CKD?
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
Chronic Kidney Disease (CKD) and egfr: Decision and Dilemma. Dr Bhavna K Pandya Consultant Nephrologist University Hospital Aintree
 Chronic Kidney Disease (CKD) and egfr: Decision and Dilemma Dr Bhavna K Pandya Consultant Nephrologist University Hospital Aintree Topics CKD background egfr background Patient with egfr Referral Guidelines
Chronic Kidney Disease (CKD) and egfr: Decision and Dilemma Dr Bhavna K Pandya Consultant Nephrologist University Hospital Aintree Topics CKD background egfr background Patient with egfr Referral Guidelines
CHRONIC RENAL FAILURE: WHAT THE PRIMARY CARE CAN OFFER. The annual conference of the Lebanese Society of Family Medicine October 2017 Dr Hiba AZAR
 CHRONIC RENAL FAILURE: WHAT THE PRIMARY CARE CAN OFFER The annual conference of the Lebanese Society of Family Medicine October 2017 Dr Hiba AZAR OUTLINE: A journey through CKD Screening for CKD: The why,
CHRONIC RENAL FAILURE: WHAT THE PRIMARY CARE CAN OFFER The annual conference of the Lebanese Society of Family Medicine October 2017 Dr Hiba AZAR OUTLINE: A journey through CKD Screening for CKD: The why,
Stages of Chronic Kidney Disease (CKD)
 Early Treatment is the Key Stages of Chronic Kidney Disease (CKD) Stage Description GFR (ml/min/1.73 m 2 ) >90 1 Kidney damage with normal or GFR 2 Mild decrease in GFR 60-89 3 Moderate decrease in GFR
Early Treatment is the Key Stages of Chronic Kidney Disease (CKD) Stage Description GFR (ml/min/1.73 m 2 ) >90 1 Kidney damage with normal or GFR 2 Mild decrease in GFR 60-89 3 Moderate decrease in GFR
Introduction to Clinical Diagnosis Nephrology
 Introduction to Clinical Diagnosis Nephrology I. David Weiner, M.D. C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University of Florida College
Introduction to Clinical Diagnosis Nephrology I. David Weiner, M.D. C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University of Florida College
The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009
 The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009 Teresa Northcutt, RN BSN Primaris Program Manager, Prevention - CKD MO-09-01-CKD This material was prepared by Primaris,
The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009 Teresa Northcutt, RN BSN Primaris Program Manager, Prevention - CKD MO-09-01-CKD This material was prepared by Primaris,
Cystatin C (serum, plasma, urine)
 Cystatin C (serum, plasma, urine) 1 Name and description of analyte 1.1 Name of analyte Cystatin C (serum, plasma and urine) 1.2 Alternative names Cystatin 3, post-gamma-globulin, neuroendocrine basic
Cystatin C (serum, plasma, urine) 1 Name and description of analyte 1.1 Name of analyte Cystatin C (serum, plasma and urine) 1.2 Alternative names Cystatin 3, post-gamma-globulin, neuroendocrine basic
CKD & HT. Anne-Marie Angus
 CKD & HT Anne-Marie Angus Hypertension definitions Persisting BP >140/90 and HBPM >135/85 Stage 1 >140/90 (HBPM >135/85) Stage 2 >160/100 (HBPM >150/90) Severe >180/100 White coat HT Why treat? A major
CKD & HT Anne-Marie Angus Hypertension definitions Persisting BP >140/90 and HBPM >135/85 Stage 1 >140/90 (HBPM >135/85) Stage 2 >160/100 (HBPM >150/90) Severe >180/100 White coat HT Why treat? A major
Online clinical pathway for chronic kidney disease (CKD) in primary care. February 27, 2015 Dr. Kerry McBrien University of Calgary
 Online clinical pathway for chronic kidney disease (CKD) in primary care February 27, 2015 Dr. Kerry McBrien University of Calgary FACULTY/PRESENTER DISCLOSURE Faculty: Kerry McBrien Relationships with
Online clinical pathway for chronic kidney disease (CKD) in primary care February 27, 2015 Dr. Kerry McBrien University of Calgary FACULTY/PRESENTER DISCLOSURE Faculty: Kerry McBrien Relationships with
Primary Care Physicians and Clinicians. XXX on behalf of the Upper Midwest Fistula First Coalition. Chronic Kidney Disease (CKD) Resources
 August 10, 2007 To: From: RE: Primary Care Physicians and Clinicians XXX on behalf of the Upper Midwest Fistula First Coalition Chronic Kidney Disease (CKD) Resources Caring for patients with chronic kidney
August 10, 2007 To: From: RE: Primary Care Physicians and Clinicians XXX on behalf of the Upper Midwest Fistula First Coalition Chronic Kidney Disease (CKD) Resources Caring for patients with chronic kidney
ALLHAT RENAL DISEASE OUTCOMES IN HYPERTENSIVE PATIENTS STRATIFIED INTO 4 GROUPS BY BASELINE GLOMERULAR FILTRATION RATE (GFR)
 1 RENAL DISEASE OUTCOMES IN HYPERTENSIVE PATIENTS STRATIFIED INTO 4 GROUPS BY BASELINE GLOMERULAR FILTRATION RATE (GFR) 6 / 5 / 1006-1 2 Introduction Hypertension is the second most common cause of end-stage
1 RENAL DISEASE OUTCOMES IN HYPERTENSIVE PATIENTS STRATIFIED INTO 4 GROUPS BY BASELINE GLOMERULAR FILTRATION RATE (GFR) 6 / 5 / 1006-1 2 Introduction Hypertension is the second most common cause of end-stage
Seung Hyeok Han, MD, PhD Department of Internal Medicine Yonsei University College of Medicine
 Seung Hyeok Han, MD, PhD Department of Internal Medicine Yonsei University College of Medicine Age and Kidney Weight renal weight and thickening of the vascular intima Platt et al. Gerentology 1999;45:243-253
Seung Hyeok Han, MD, PhD Department of Internal Medicine Yonsei University College of Medicine Age and Kidney Weight renal weight and thickening of the vascular intima Platt et al. Gerentology 1999;45:243-253
Concept and General Objectives of the Conference: Prognosis Matters. Andrew S. Levey, MD Tufts Medical Center Boston, MA
 Concept and General Objectives of the Conference: Prognosis Matters Andrew S. Levey, MD Tufts Medical Center Boston, MA General Objectives Topics to discuss What are the key outcomes of CKD? What progress
Concept and General Objectives of the Conference: Prognosis Matters Andrew S. Levey, MD Tufts Medical Center Boston, MA General Objectives Topics to discuss What are the key outcomes of CKD? What progress
New indicators to be added to the NICE menu for the QOF and amendments to existing indicators
 New indicators to be added to the for the QOF and amendments to existing indicators 1 st September 2015 Version 1.1 This document was originally published on 3 rd August 2015, it has since been updated.
New indicators to be added to the for the QOF and amendments to existing indicators 1 st September 2015 Version 1.1 This document was originally published on 3 rd August 2015, it has since been updated.
Faculty/Presenter Disclosure
 CSI for CKD Unravelling the myths surrounding chronic kidney disease Practical Evidence for Informed Practice Oct 21 2016 Dr. Scott Klarenbach University of Alberta Slide 1: Option B (Presenter with NO
CSI for CKD Unravelling the myths surrounding chronic kidney disease Practical Evidence for Informed Practice Oct 21 2016 Dr. Scott Klarenbach University of Alberta Slide 1: Option B (Presenter with NO
Younger adults with a family history of premature artherosclerotic disease should have their cardiovascular risk factors measured.
 Appendix 2A - Guidance on Management of Hypertension Measurement of blood pressure All adults from 40 years should have blood pressure measured as part of opportunistic cardiovascular risk assessment.
Appendix 2A - Guidance on Management of Hypertension Measurement of blood pressure All adults from 40 years should have blood pressure measured as part of opportunistic cardiovascular risk assessment.
Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012
 Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012 Susan McKenna Renal Clinical Nurse Specialist Cavan General Hospital Renal patient population ACUTE RENAL FAILURE
Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012 Susan McKenna Renal Clinical Nurse Specialist Cavan General Hospital Renal patient population ACUTE RENAL FAILURE
5.2 Key priorities for implementation
 5.2 Key priorities for implementation From the full set of recommendations, the GDG selected ten key priorities for implementation. The criteria used for selecting these recommendations are listed in detail
5.2 Key priorities for implementation From the full set of recommendations, the GDG selected ten key priorities for implementation. The criteria used for selecting these recommendations are listed in detail
Guideline scope Hypertension in adults (update)
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Hypertension in adults (update) This guideline will update the NICE guideline on hypertension in adults (CG127). The guideline will be
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Hypertension in adults (update) This guideline will update the NICE guideline on hypertension in adults (CG127). The guideline will be
Outline. Outline 10/14/2014 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW. Question 1: Which of these patients has CKD?
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
Chronic Kidney Disease: Optimal and Coordinated Management
 Chronic Kidney Disease: Optimal and Coordinated Management Michael Copland, MD, FRCPC Presented at University of British Columbia s 42nd Annual Post Graduate Review in Family Medicine Conference, Vancouver,
Chronic Kidney Disease: Optimal and Coordinated Management Michael Copland, MD, FRCPC Presented at University of British Columbia s 42nd Annual Post Graduate Review in Family Medicine Conference, Vancouver,
Angiotensin Converting Enzyme inhibitor (ACEi) / Angiotensin Receptor Blocker (ARB) To STOP OR Not in Advanced Renal Disease
 Angiotensin Converting Enzyme inhibitor (ACEi) / Angiotensin Receptor Blocker (ARB) To STOP OR Not in Advanced Renal Disease Investigator Meeting 12 th September 2017 - Sheffield Prof Sunil Bhandari Consultant
Angiotensin Converting Enzyme inhibitor (ACEi) / Angiotensin Receptor Blocker (ARB) To STOP OR Not in Advanced Renal Disease Investigator Meeting 12 th September 2017 - Sheffield Prof Sunil Bhandari Consultant
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Wanner C, Inzucchi SE, Lachin JM, et al. Empagliflozin and
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Wanner C, Inzucchi SE, Lachin JM, et al. Empagliflozin and
Applying clinical guidelines treating and managing CKD
 Applying clinical guidelines treating and managing CKD Develop patient treatment plan according to level of severity. Source: Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group. KDIGO 2012
Applying clinical guidelines treating and managing CKD Develop patient treatment plan according to level of severity. Source: Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group. KDIGO 2012
Chronic kidney disease screening and assessment
 Care map information Information resources for patients and carers Aboriginal and Torres Strait Islanders DEFINITION OF CKD egfr
Care map information Information resources for patients and carers Aboriginal and Torres Strait Islanders DEFINITION OF CKD egfr
Early identification and management of chronic kidney disease in adults: summary of updated NICE guidance
 GUIDELINES Early identification and management of chronic kidney disease in adults: summary of updated NICE guidance Serena Carville, 1 David Wonderling, 1 Paul Stevens, 2 on behalf of the Guideline Development
GUIDELINES Early identification and management of chronic kidney disease in adults: summary of updated NICE guidance Serena Carville, 1 David Wonderling, 1 Paul Stevens, 2 on behalf of the Guideline Development
CHRONIC KIDNEY DISEASE DIAGNOSIS
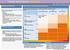 CHRONIC KIDNEY DISEASE DIAGSIS GFR categories, description and range WHO SHOULD BE TESTED FOR CKD CLASSIFICATION OF CKD USING egfr AND ACR CATEGORIES Offer testing for CKD using egfr, creatinine and ACR
CHRONIC KIDNEY DISEASE DIAGSIS GFR categories, description and range WHO SHOULD BE TESTED FOR CKD CLASSIFICATION OF CKD USING egfr AND ACR CATEGORIES Offer testing for CKD using egfr, creatinine and ACR
Management of New-Onset Proteinuria in the Ambulatory Care Setting. Akinlolu Ojo, MD, PhD, MBA
 Management of New-Onset Proteinuria in the Ambulatory Care Setting Akinlolu Ojo, MD, PhD, MBA Urine dipstick results Negative Trace between 15 and 30 mg/dl 1+ between 30 and 100 mg/dl 2+ between 100 and
Management of New-Onset Proteinuria in the Ambulatory Care Setting Akinlolu Ojo, MD, PhD, MBA Urine dipstick results Negative Trace between 15 and 30 mg/dl 1+ between 30 and 100 mg/dl 2+ between 100 and
Identifying and Managing Chronic Kidney Disease: A Practical Approach
 Identifying and Managing Chronic Kidney Disease: A Practical Approach S. Neil Finkle, MD, FRCPC Associate Professor Division of Nephrology, Department of Medicine, Dalhousie University Program Director,
Identifying and Managing Chronic Kidney Disease: A Practical Approach S. Neil Finkle, MD, FRCPC Associate Professor Division of Nephrology, Department of Medicine, Dalhousie University Program Director,
Chronic kidney disease (CKD) (Southampton pathway)
 Background information Patient information Key messages for this pathway Definitions and abbreviations used in this pathway Classification of CKD Diagnosis of CKD Summary of referral criteria Screening
Background information Patient information Key messages for this pathway Definitions and abbreviations used in this pathway Classification of CKD Diagnosis of CKD Summary of referral criteria Screening
Acute renal failure Definition and detection
 Acute renal failure Definition and detection Pierre Delanaye, MD, PhD Nephrology, Dialysis, Transplantation CHU Sart Tilman University of Liège BELGIUM Definition Acute Renal Failure Acute Kidney Injury
Acute renal failure Definition and detection Pierre Delanaye, MD, PhD Nephrology, Dialysis, Transplantation CHU Sart Tilman University of Liège BELGIUM Definition Acute Renal Failure Acute Kidney Injury
Evaluation of Chronic Kidney Disease KDIGO. Paul E de Jong University Medical Center Groningen The Netherlands
 Evaluation of Chronic Kidney Disease Paul E de Jong University Medical Center Groningen The Netherlands Evaluation and Management of CKD 1. Definition and classification of CKD 2. Definition and impact
Evaluation of Chronic Kidney Disease Paul E de Jong University Medical Center Groningen The Netherlands Evaluation and Management of CKD 1. Definition and classification of CKD 2. Definition and impact
Dr.Nahid Osman Ahmed 1
 1 ILOS By the end of the lecture you should be able to Identify : Functions of the kidney and nephrons Signs and symptoms of AKI Risk factors to AKI Treatment alternatives 2 Acute kidney injury (AKI),
1 ILOS By the end of the lecture you should be able to Identify : Functions of the kidney and nephrons Signs and symptoms of AKI Risk factors to AKI Treatment alternatives 2 Acute kidney injury (AKI),
ABCD and Renal Association Clinical Guidelines for Diabetic Nephropathy-CKD. Management of Dyslipidaemia and Hypertension in Adults Dr Peter Winocour
 ABCD and Renal Association Clinical Guidelines for Diabetic Nephropathy-CKD. Management of Dyslipidaemia and Hypertension in Adults Dr Peter Winocour Dr Indranil Dasgupta Rationale No national practical
ABCD and Renal Association Clinical Guidelines for Diabetic Nephropathy-CKD. Management of Dyslipidaemia and Hypertension in Adults Dr Peter Winocour Dr Indranil Dasgupta Rationale No national practical
CKD IN THE CLINIC. Session Content. Recommendations for commonly used medications in CKD. CKD screening and referral
 CKD IN THE CLINIC Family Physician Refresher Course Lisa M. Antes, MD April 19, 2017 No disclosures Session Content 1. 2. Recommendations for commonly used medications in CKD Basic principles /patient
CKD IN THE CLINIC Family Physician Refresher Course Lisa M. Antes, MD April 19, 2017 No disclosures Session Content 1. 2. Recommendations for commonly used medications in CKD Basic principles /patient
CKD at the primary and secondary care interface. Paul Cockwell Consultant Nephrologist Clinical Service Lead Renal Medicine, QEHB
 CKD at the primary and secondary care interface Paul Cockwell Consultant Nephrologist Clinical Service Lead Renal Medicine, QEHB The Health improvement Network (THIN): 6.7 million patients from 426 primary
CKD at the primary and secondary care interface Paul Cockwell Consultant Nephrologist Clinical Service Lead Renal Medicine, QEHB The Health improvement Network (THIN): 6.7 million patients from 426 primary
Case Studies: Renal and Urologic Impairments Workshop
 Case Studies: Renal and Urologic Impairments Workshop Justine Lee, MD, DBIM New York Life Insurance Co. Gina Guzman, MD, DBIM, FALU, ALMI Munich Re AAIM Triennial October, 2012 The Company You Keep 1 Case
Case Studies: Renal and Urologic Impairments Workshop Justine Lee, MD, DBIM New York Life Insurance Co. Gina Guzman, MD, DBIM, FALU, ALMI Munich Re AAIM Triennial October, 2012 The Company You Keep 1 Case
National Chronic Kidney Disease Audit
 National Chronic Kidney Disease Audit // National Report: Part 2 December 2017 Commissioned by: Delivered by: // Foreword by Fiona Loud And if, as part of good, patient-centred care, a record of your condition(s),
National Chronic Kidney Disease Audit // National Report: Part 2 December 2017 Commissioned by: Delivered by: // Foreword by Fiona Loud And if, as part of good, patient-centred care, a record of your condition(s),
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Solomon SD, Uno H, Lewis EF, et al. Erythropoietic response
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Solomon SD, Uno H, Lewis EF, et al. Erythropoietic response
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE General practice Indicators for the NICE menu
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE General practice Indicators for the NICE menu Indicator area: Pulse rhythm assessment for AF Indicator: NM146 Date: June 2017 Introduction There is evidence
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE General practice Indicators for the NICE menu Indicator area: Pulse rhythm assessment for AF Indicator: NM146 Date: June 2017 Introduction There is evidence
Diabetes and Kidney Disease. Kris Bentley Renal Nurse practitioner 2018
 Diabetes and Kidney Disease Kris Bentley Renal Nurse practitioner 2018 Aims Develop an understanding of Chronic Kidney Disease Understand how diabetes impacts on your kidneys Be able to recognise the risk
Diabetes and Kidney Disease Kris Bentley Renal Nurse practitioner 2018 Aims Develop an understanding of Chronic Kidney Disease Understand how diabetes impacts on your kidneys Be able to recognise the risk
מסקנות מיישום סטנדרטיזציה של בדיקת קראטינין : שימוש בנוסחאות לחישוב egfr
 מסקנות מיישום סטנדרטיזציה של בדיקת קראטינין : שימוש בנוסחאות לחישוב egfr תכנית המפגש: דרישות לסטנדרטיזציה של בדיקת קראטינין ד"ר מריאל קפלן, מנהלת אגף המעבדות, רמב"ם - הקריה הרפואית לבריאות האדם שימוש מושכל
מסקנות מיישום סטנדרטיזציה של בדיקת קראטינין : שימוש בנוסחאות לחישוב egfr תכנית המפגש: דרישות לסטנדרטיזציה של בדיקת קראטינין ד"ר מריאל קפלן, מנהלת אגף המעבדות, רמב"ם - הקריה הרפואית לבריאות האדם שימוש מושכל
Chronic Kidney Disease in Primary Care
 Clinical Stream Chronic Kidney Disease in Primary Care Dr Gerald Waters Dr Gerald Waters Renal Physician Chronic Kidney Disease Chronic Kidney Disease Normal functions of Kidneys Management of CKD Drugs
Clinical Stream Chronic Kidney Disease in Primary Care Dr Gerald Waters Dr Gerald Waters Renal Physician Chronic Kidney Disease Chronic Kidney Disease Normal functions of Kidneys Management of CKD Drugs
6/10/2014. Chronic Kidney Disease - General management and standard of care. Management of CKD according to stage (KDOQI 2002)
 Chronic Kidney Disease - General management and standard of care Dr Nathalie Demoulin, Prof Michel Jadoul Cliniques universitaires Saint-Luc Université Catholique de Louvain What should and can be done
Chronic Kidney Disease - General management and standard of care Dr Nathalie Demoulin, Prof Michel Jadoul Cliniques universitaires Saint-Luc Université Catholique de Louvain What should and can be done
VA/DoD Clinical Practice Guideline for the Management of Chronic Kidney Disease in Primary Care (2008) PROVIDER REFERENCE CARDS Chronic Kidney Disease
 VA/DoD Clinical Practice Guideline for the Management of Chronic Kidney Disease in Primary Care (2008) PROVIDER REFERECE CARDS Chronic Kidney Disease CKD VA/DoD Clinical Practice Guideline for the Management
VA/DoD Clinical Practice Guideline for the Management of Chronic Kidney Disease in Primary Care (2008) PROVIDER REFERECE CARDS Chronic Kidney Disease CKD VA/DoD Clinical Practice Guideline for the Management
NORTHERN IRELAND GUIDELINES FOR MANAGEMENT OF CHRONIC KIDNEY DISEASE
 NORTHERN IRELAND GUIDELINES FOR MANAGEMENT OF CHRONIC KIDNEY DISEASE Practical points for use of estimated GFR + quality outcome framework indicators Developed by GAIN and the Northern Ireland Nephrology
NORTHERN IRELAND GUIDELINES FOR MANAGEMENT OF CHRONIC KIDNEY DISEASE Practical points for use of estimated GFR + quality outcome framework indicators Developed by GAIN and the Northern Ireland Nephrology
Disclosures. Outline. Outline 5/23/17 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
Transforming Diabetes Care
 Transforming Diabetes Care Diabetic Kidney Disease: Prevention, Detection and Treatment Alexis Chettiar, ACNP-BC, PhD(c) 1 Polling Question - 1 What is your role as a healthcare provider? a) Dietitian
Transforming Diabetes Care Diabetic Kidney Disease: Prevention, Detection and Treatment Alexis Chettiar, ACNP-BC, PhD(c) 1 Polling Question - 1 What is your role as a healthcare provider? a) Dietitian
Renal function vs chemotherapy dosing
 Renal function vs chemotherapy dosing Jenny Casanova Senior Clinical Pharmacist Repatriation General Hospital Daw Park 1 Methods of estimating renal function Cockcroft-Gault (1976) C-G using ideal vs actual
Renal function vs chemotherapy dosing Jenny Casanova Senior Clinical Pharmacist Repatriation General Hospital Daw Park 1 Methods of estimating renal function Cockcroft-Gault (1976) C-G using ideal vs actual
Chronic Kidney Disease. Paul Cockwell Queen Elizabeth Hospital Birmingham
 Chronic Kidney Disease Paul Cockwell Queen Elizabeth Hospital Birmingham Paradigms for chronic disease 1. Acute and chronic disease is closely linked 2. Stratify risk and tailor interventions around failure
Chronic Kidney Disease Paul Cockwell Queen Elizabeth Hospital Birmingham Paradigms for chronic disease 1. Acute and chronic disease is closely linked 2. Stratify risk and tailor interventions around failure
Disclosures. Topics. Staging and GFR. K-DOQI Staging of Chronic Kidney Disease. Definition of Chronic Kidney Disease. Chronic Kidney Disease
 Disclosures Chronic Kidney Disease Consultant: Baxter Healthcare J. Kevin Tucker, M.D. Brigham and Women s Hospital Massachusetts General Hospital Topics Staging of chronic kidney disease (CKD) How to
Disclosures Chronic Kidney Disease Consultant: Baxter Healthcare J. Kevin Tucker, M.D. Brigham and Women s Hospital Massachusetts General Hospital Topics Staging of chronic kidney disease (CKD) How to
Objectives. Pre-dialysis CKD: The Problem. Pre-dialysis CKD: The Problem. Objectives
 The Role of the Primary Physician and the Nephrologist in the Management of Chronic Kidney Disease () By Brian Young, M.D. Assistant Clinical Professor of Medicine David Geffen School of Medicine at UCLA
The Role of the Primary Physician and the Nephrologist in the Management of Chronic Kidney Disease () By Brian Young, M.D. Assistant Clinical Professor of Medicine David Geffen School of Medicine at UCLA
Creatinine (serum, plasma)
 Creatinine (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Creatinine 1.2 Alternative names None 1.3 Description of analyte Creatinine is a heterocyclic nitrogenous compound (IUPAC
Creatinine (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Creatinine 1.2 Alternative names None 1.3 Description of analyte Creatinine is a heterocyclic nitrogenous compound (IUPAC
Assessing Renal Function: What you Didn t Know You Didn t Know
 Assessing Renal Function: What you Didn t Know You Didn t Know Presented By Tom Wadsworth PharmD, BCPS Associate Clinical Professor UAA/ISU Doctor of Pharmacy Program Idaho State University College of
Assessing Renal Function: What you Didn t Know You Didn t Know Presented By Tom Wadsworth PharmD, BCPS Associate Clinical Professor UAA/ISU Doctor of Pharmacy Program Idaho State University College of
Southern Derbyshire Shared Care Pathology Guidelines. AKI guidelines for primary care
 Southern Derbyshire Shared Care Pathology Guidelines AKI guidelines for primary care Contents: Flow Diagram: Recommended response time to AKI warning stage test results for adults in primary care 2 Table
Southern Derbyshire Shared Care Pathology Guidelines AKI guidelines for primary care Contents: Flow Diagram: Recommended response time to AKI warning stage test results for adults in primary care 2 Table
The evidence base for interventions to slow the progression of chronic kidney disease: Medical interventions. Jonathan Evans Paediatric Nephrologist
 The evidence base for interventions to slow the progression of chronic kidney disease: Medical interventions Jonathan Evans Paediatric Nephrologist CKD in adults Often unrecognised Preventable Major cardiovascular
The evidence base for interventions to slow the progression of chronic kidney disease: Medical interventions Jonathan Evans Paediatric Nephrologist CKD in adults Often unrecognised Preventable Major cardiovascular
Long-Term Care Updates
 Long-Term Care Updates January 2016 By Yunuo (Enora) Wu, PharmD Chronic kidney disease (CKD) is defined as kidney damage (including structural or functional abnormalities) or glomerular filtration rate
Long-Term Care Updates January 2016 By Yunuo (Enora) Wu, PharmD Chronic kidney disease (CKD) is defined as kidney damage (including structural or functional abnormalities) or glomerular filtration rate
Management of Hypertension. M Misra MD MRCP (UK) Division of Nephrology University of Missouri School of Medicine
 Management of Hypertension M Misra MD MRCP (UK) Division of Nephrology University of Missouri School of Medicine Disturbing Trends in Hypertension HTN awareness, treatment and control rates are decreasing
Management of Hypertension M Misra MD MRCP (UK) Division of Nephrology University of Missouri School of Medicine Disturbing Trends in Hypertension HTN awareness, treatment and control rates are decreasing
RENAL FUNCTION ASSESSMENT ASSESSMENT OF GLOMERULAR FUNCTION ASSESSMENT OF TUBULAR FUNCTION
 Measured GFR (mgfr mgfr) and Estimated t GFR (egfr egfr) R. Mohammadi Biochemist (Ph.D.) Faculty member of Medical Faculty RENAL FUNCTION ASSESSMENT ASSESSMENT OF GLOMERULAR FUNCTION ASSESSMENT OF TUBULAR
Measured GFR (mgfr mgfr) and Estimated t GFR (egfr egfr) R. Mohammadi Biochemist (Ph.D.) Faculty member of Medical Faculty RENAL FUNCTION ASSESSMENT ASSESSMENT OF GLOMERULAR FUNCTION ASSESSMENT OF TUBULAR
pat hways Key therapeutic topic Published: 26 February 2016 nice.org.uk/guidance/ktt16
 pat hways Anticoagulants, including non-vitamin K antagonist oral anticoagulants (NOACs) Key therapeutic topic Published: 26 February 2016 nice.org.uk/guidance/ktt16 Options for local implementation NICE
pat hways Anticoagulants, including non-vitamin K antagonist oral anticoagulants (NOACs) Key therapeutic topic Published: 26 February 2016 nice.org.uk/guidance/ktt16 Options for local implementation NICE
Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009
 www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers PROTEINURIA
www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers PROTEINURIA
HYPERTENSION IN CKD. LEENA ONGAJYOOTH, M.D., Dr.med RENAL UNIT SIRIRAJ HOSPITAL
 HYPERTENSION IN CKD LEENA ONGAJYOOTH, M.D., Dr.med RENAL UNIT SIRIRAJ HOSPITAL Stages in Progression of Chronic Kidney Disease and Therapeutic Strategies Complications Normal Increased risk Damage GFR
HYPERTENSION IN CKD LEENA ONGAJYOOTH, M.D., Dr.med RENAL UNIT SIRIRAJ HOSPITAL Stages in Progression of Chronic Kidney Disease and Therapeutic Strategies Complications Normal Increased risk Damage GFR
DISCLOSURES OUTLINE OUTLINE 9/29/2014 ANTI-HYPERTENSIVE MANAGEMENT OF CHRONIC KIDNEY DISEASE
 ANTI-HYPERTENSIVE MANAGEMENT OF CHRONIC KIDNEY DISEASE DISCLOSURES Editor-in-Chief- Nephrology- UpToDate- (Wolters Klewer) Richard J. Glassock, MD, MACP Geffen School of Medicine at UCLA 1 st Annual Internal
ANTI-HYPERTENSIVE MANAGEMENT OF CHRONIC KIDNEY DISEASE DISCLOSURES Editor-in-Chief- Nephrology- UpToDate- (Wolters Klewer) Richard J. Glassock, MD, MACP Geffen School of Medicine at UCLA 1 st Annual Internal
Disclosures. Outline. Outline 7/27/2017 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CKD: An update on recent developments. Robert Lewis Wessex Kidney Centre
 CKD: An update on recent developments Robert Lewis Wessex Kidney Centre Anatomy and functions of the kidney Calyces Key functions of the kidney Renal artery Renal vein Ureter Cortex Renal pelvis Medulla
CKD: An update on recent developments Robert Lewis Wessex Kidney Centre Anatomy and functions of the kidney Calyces Key functions of the kidney Renal artery Renal vein Ureter Cortex Renal pelvis Medulla
Identification, management and referral of adults with chronic kidney disease: concise guidelines
 Identification, management and referral of adults with chronic kidney disease: concise guidelines Abstract Chronic Kidney Disease (CKD) is often thought to be a relatively rare condition requiring specialist
Identification, management and referral of adults with chronic kidney disease: concise guidelines Abstract Chronic Kidney Disease (CKD) is often thought to be a relatively rare condition requiring specialist
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Chronic kidney disease: early identification and management of adults with chronic kidney disease in primary and secondary
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Chronic kidney disease: early identification and management of adults with chronic kidney disease in primary and secondary
2 Summary of NICE TA 249: Atrial fibrillation - Dabigatran Etexilate
 Service Notification in response to DHSSPS endorsed NICE Technology Appraisals NICE TA 249: Atrial fibrillation - Dabigatran Etexilate 1 Name of Commissioning Team Long Term Conditions Commissioning Team
Service Notification in response to DHSSPS endorsed NICE Technology Appraisals NICE TA 249: Atrial fibrillation - Dabigatran Etexilate 1 Name of Commissioning Team Long Term Conditions Commissioning Team
(KFTs) IACLD CME, Monday, February 20, Mohammad Reza Bakhtiari, DCLS, PhD
 Kidney Function Tests (KFTs) IACLD CME, Monday, February 20, 2012 Mohammad Reza Bakhtiari, DCLS, PhD Iranian Research Organization for Science & Technology (IROST) Tehran, Iran Composition and Properties
Kidney Function Tests (KFTs) IACLD CME, Monday, February 20, 2012 Mohammad Reza Bakhtiari, DCLS, PhD Iranian Research Organization for Science & Technology (IROST) Tehran, Iran Composition and Properties
Egyptian Hypertension Guidelines
 Egyptian Hypertension Guidelines 2014 Egyptian Hypertension Guidelines Dalia R. ElRemissy, MD Lecturer of Cardiovascular Medicine Cairo University Why Egyptian Guidelines? Guidelines developed for rich
Egyptian Hypertension Guidelines 2014 Egyptian Hypertension Guidelines Dalia R. ElRemissy, MD Lecturer of Cardiovascular Medicine Cairo University Why Egyptian Guidelines? Guidelines developed for rich
Outline. Outline. Introduction CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW 8/11/2011
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
Launch Meeting 3 rd April 2014, Lucas House, Birmingham
 Angiotensin Converting Enzyme inhibitor (ACEi) / Angiotensin Receptor Blocker (ARB) To STOP OR Not in Advanced Renal Disease Launch Meeting 3 rd April 2014, Lucas House, Birmingham Prof Sunil Bhandari
Angiotensin Converting Enzyme inhibitor (ACEi) / Angiotensin Receptor Blocker (ARB) To STOP OR Not in Advanced Renal Disease Launch Meeting 3 rd April 2014, Lucas House, Birmingham Prof Sunil Bhandari
Diabetes Mellitus. Eiman Ali Basheir. Mob: /1/2019
 Diabetes Mellitus Eiman Ali Basheir Mob: 091520385 27/1/2019 Learning Outcomes Discuss the WHO criteria for Diabetes Mellitus diagnosis Describe the steps taken to confirm diagnosis Interpret GTT. Discuss
Diabetes Mellitus Eiman Ali Basheir Mob: 091520385 27/1/2019 Learning Outcomes Discuss the WHO criteria for Diabetes Mellitus diagnosis Describe the steps taken to confirm diagnosis Interpret GTT. Discuss
Chapter 1: CKD in the General Population
 Chapter 1: CKD in the General Population Overall prevalence of CKD (Stages 1-5) in the U.S. adult general population was 14.8% in 2011-2014. CKD Stage 3 is the most prevalent (NHANES: Figure 1.2 and Table
Chapter 1: CKD in the General Population Overall prevalence of CKD (Stages 1-5) in the U.S. adult general population was 14.8% in 2011-2014. CKD Stage 3 is the most prevalent (NHANES: Figure 1.2 and Table
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest

 www.usrds.org www.usrds.org 1 1,749 + (2,032) 1,563 to
www.usrds.org www.usrds.org 1 1,749 + (2,032) 1,563 to