Recognising, managing and preventing hypoglycaemia
|
|
|
- Corey Fowler
- 6 years ago
- Views:
Transcription
1 CPD Module Recognising, managing and preventing hypoglycaemia Debbie Hicks Since the discovery of insulin by Banting and Best in 1922, there have been a number of important developments in the treatment of diabetes. However, it is well known that a common side effect of blood-glucose-lowering treatments, such as insulin and sulphonylureas, is hypoglycaemia. Studies investigating the prevalence of hypoglycaemia have provided some alarming results. In particular, the Diabetes Control and Complications Trial (1993) reported a three-fold increase in severe hypoglycaemia and coma in intensively treated people with diabetes versus conventionally treated people. This CPD module discusses the potential causes of hypoglycaemia and circumstances in which hypoglycaemia risk is increased. The article also provides the signs and symptoms, as well as treatment and prevention. The global burden of diabetes is increasing. According to the latest figures by the International Diabetes Foundation (2012), more than 371 million people have diabetes worldwide and the prevalence of diabetes is increasing in every country. Furthermore, diabetes is predicted to become the seventh leading cause of death in the world by the year 2030 (World Health Organization, 2011) and it is the leading cause of blindness and kidney failure in developed countries. People with diabetes also have a greater risk of developing cardiovascular disease and this is a major cause of death in people with diabetes. The discovery of insulin by Banting and Best in 1922 was a major breakthrough in the treatment of type 1 diabetes and insulin use means that people with type 1 diabetes are no longer likely to die as a result of diagnosis. Further developments in the treatment of diabetes include the development of oral hypoglycaemic agents in the 1950s, including biguanides and sulphonylureas as treatment for type 2 diabetes. However, it is now widely accepted that hypoglycaemia is a side effect of both insulin and sulphonylureas rather than diabetes itself. This article is the first of two CPD modules on hypoglycaemia, which will explore many aspects of hypoglycaemia including recognition, treatment and prevention as well as the impact it has on the person with diabetes. The second article, which will be published in early 2014, will focus on the costs and complications of hypoglycaemia. Background Hypoglycaemia occurs when a person has a low level of blood glucose, usually <3.5 mmol/l. It can be termed as mild if it can be self-treated and severe if assistance is required from a third party (Diabetes Control and Complications Trial [DCCT], 1993). Hypoglycaemia is the most common side effect of insulin and sulphonylurea therapy. People with diabetes tend to under-report hypoglycaemia because they or their carers do not recognise what is happening. They may also be reluctant to talk about hypoglycaemia due to the risk of increased restrictions to their way Citation: Hicks D (2013) Recognising and managing hypoglycaemia. Journal of Diabetes Nursing 17: Article points 1. It is well known that blood glucose lowering therapies, such as insulin and sulphonylureas, can cause hypoglycaemia and studies have shown that prevalence of hypoglycaemia is high (Diabetes Control and Complications Trial, 1993). 2. Hypoglycaemia can be caused by: inappropriate insulin or sulphonylurea dosage; missing a meal; alcohol intake; taking part in physical activity without replacing lost glucose and increased sensitivity to insulin through weight loss or improved physical fitness. 3. It is crucial that people with diabetes who take either insulin or sulphonylureas receive the correct education to allow them to recognise and treat a hypoglycaemic episode and more importantly, prevent further hypoglycaemic episodes occurring. Key words - Hypoglycaemia - Insulin - Prevention - Sulphonylureas Author Debbie Hicks, Nurse Consultant in Diabetes, Enfield Community Services, Barnet, Enfield & Haringey Mental Health Trust, Enfield Journal of Diabetes Nursing Volume 17 No
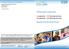
2 Page points 1. The Diabetes Control and Complications Trial (DCCT, 1993) reported a three-fold increase in severe hypoglycaemia and coma in intensively treated people with diabetes versus conventionally treated people. 2. In the 2012 National Diabetes Inpatient Audit of diabetes inpatients (Health and Social Care Information Centre, 2012), 20.4% had experienced mild hypoglycaemia (blood glucose of 3 4 mmol/l) and 10% had severe hypoglycaemia (blood glucose <3 mmol/l). 3. Hypoglycaemia can be caused by one factor or a combination of factors, such as inappropriate insulin or sulphonylurea dosage; missing a meal; alcohol intake; taking part in physical activity without replacing lost glucose and increased sensitivity to insulin through weight loss or improved physical fitness. Other factors are reduced renal function and lipohypertrophy. of life, such as loss of their driving licence or job. This under-reporting means that the actual number of people with diabetes who experience hypoglycaemia is unknown (Bailey and Day, 2010). Prevalence Studies investigating the prevalence of hypoglycaemia have provided some alarming results. The DCCT (1993) reported a three-fold increase in severe hypoglycaemia and coma in intensively treated people with diabetes versus conventionally treated people. An intensively treated individual with type 1 diabetes can experience up to 10 episodes of symptomatic hypoglycaemia per week and severe temporarily disabling hypoglycaemia at least once a year. An estimated 2 4% of deaths of people with type 1 diabetes have been attributed to hypoglycaemia (DCCT, 1993). Hypoglycaemia is also relatively common in type 2 diabetes, with prevalence rates of 70 80% in clinical trials using insulin to achieve good metabolic control (UK Hypoglycaemia Study, 2007). The UK Hypoglycaemia Study (2007) found that people with type 1 diabetes had an average of two self-treated episodes of hypoglycaemia per week while for those with type 2 diabetes, 39% on sulphonylureas had at least one episode each week. Furthermore, 51% of those who had been on insulin for less than 2 years had at least one episode each week and 60% of those taking insulin for more than 5 years had at least one episode each week. In the 2012 National Diabetes Inpatient Audit of diabetes inpatients (Health and Social Care Information Centre, 2012), 20.4% had experienced mild hypoglycaemia (blood glucose of 3 4 mmol/l) and 10% had severe hypoglycaemia (blood glucose <3 mmol/l). Figure 1 shows that just as many people taking sulphonylureas experienced severe hypoglycaemic episodes as those with type 2 diabetes taking insulin for less than two years (UK Hypoglycaemia Study, 2007). This study also showed that a person with type 2 diabetes who had been taking insulin for more than five years was just as likely to have a severe hypoglycaemic episode as someone with type 1 diabetes who had been on insulin for less than five years. Causes of hypoglycaemia Hypoglycaemia may be caused by a single factor or a combination of factors. The following list describes factors that can lead to a hypoglycaemic episode: l Insulin or sulphonylurea doses are inappropriate, for example, the dose does not match the lifestyle of the individual. If the person with diabetes is active at one part of the day when the insulin or sulphonylurea is peaking, this could precipitate a hypoglycaemic episode. l It is difficult to ensure the same amount of carbohydrate is taken at each meal every day. However, if the person with diabetes does not eat at a mealtime, either because they are distracted or during times of fasting, such as Ramadan, then the blood glucose levels will begin to fall and precipitate a hypoglycaemic episode. l When alcohol is drunk in certain quantities the glucose production from the liver is decreased. If insulin or sulphonylureas are taken they will continue to reduce the blood glucose level. Often alcohol is taken in the evening so it is crucial that people are educated to have a bedtime snack when drinking over the advised level of daily alcohol consumption (two units for women and three units for men) to prevent a hypoglycaemic episode occurring during the night. l When muscle is active it requires glucose for energy. If a person with diabetes is taking insulin or sulphonylureas they need to compensate for the activity by replacing the glucose, otherwise the glucose store will be depleted and hypoglycaemia will occur. Hypoglycaemia can occur during, 1 2 hours after, or up to 17 hours after exercise (Diedrich et al, 2002). l Sensitivity to insulin is increased following weight loss or improved physical fitness so it may be necessary to decrease the insulin or sulphonylurea dose to prevent hypoglycaemia occurring. It would not be appropriate to increase the glucose intake as this could cause weight gain. l As the renal function declines, the medication taken to control the blood glucose may need to be decreased to prevent hypoglycaemia. This is due to the delayed clearance of the medication which amplifies the glucose-lowering effect. l Lipohypertrophy, or fatty lumps at injection 256 Journal of Diabetes Nursing Volume 17 No
3 Figure 1. Results of the UK Hypoglycaemia Study (2007) showing occurrence of severe hypoglycaemia (reproduced with permission from Diabetalogica). SU= sulphonylurea. sites, caused mainly by poor site rotation and re-use of needles, can precipitate hypoglycaemia as the lipohypertrophic tissue does not allow the normal absorption of the insulin. If the insulin is absorbed too quickly then hypoglycaemia will follow. Hyperglycaemia is also possible if the insulin absorption is delayed (Vardar and Kizilci, 2007). Factors that increase risk of hypoglycaemia There are certain factors which may increase the risk of hypoglycaemia: l If a person with diabetes taking insulin or sulphonylureas has had a severe hypoglycaemic event, there is evidence to suggest that they are at an increased risk of having a further severe event within the next 24 hours (DCCT, 1993). l There is an increased risk of hypoglycaemia in a person who has had type 1 diabetes for a long time. This may be due to the recognition of the signs and symptoms diminishing over time. l Longer duration of use of insulin therapy in type 2 diabetes may also contribute to the increased risk of hypoglycaemia; again, this may be due to the recognition of the signs and symptoms diminishing over time. l Strict glycaemic control over a period of time, such as during pregnancy, may also increase the incidence of hypoglycaemia as the blood glucose level has to fall much less before it enters into the hypoglycaemia range. The person with diabetes may not sense the small decrease in the blood glucose level and it is not until the blood glucose level drops further that symptoms may be experienced. l Impaired awareness of hypoglycaemia develops when frequent episodes of hypoglycaemia lead to changes in how the body reacts to low blood glucose levels. The body stops releasing the hormone epinephrine and other stress hormones when blood glucose drops too low. The loss of the body s ability to release stress hormones after repeated episodes of hypoglycaemia is known as hypoglycaemia-associated autonomic failure. l The risk of severe or fatal hypoglycaemia associated with the use of oral hypoglycaemic agents and insulin increases exponentially with age. Furthermore, older adults with comorbidities, those using multiple medications and those who are frequently hospitalised are at greater risk from hypoglycaemia. As most people Page points 1. If a person with diabetes taking insulin or sulphonylureas has had a severe hypoglycaemic event, there is evidence to suggest that they are at an increased risk of having a further severe event within the next 24 hours (DCCT, 1993) 2. Strict glycaemic control over a period of time, such as during pregnancy, may also increase the incidence of hypoglycaemia as the blood glucose level has to fall much less before it enters the hypoglycaemia range. The person with diabetes may not sense the small decrease in the blood glucose level and it is not until the blood glucose level drops further that symptoms may be experienced. 3. Impaired awareness of hypoglycaemia develops when frequent episodes of hypoglycaemia lead to changes in how the body reacts to low blood glucose levels. The body stops releasing the hormone epinephrine and other stress hormones when blood glucose drops too low. Journal of Diabetes Nursing Volume 17 No
4 Page points 1. Once plasma glucose concentrations fall below 3.8 mmol/l, a sequence of responses is activated including: the release of neuroendocrine hormones; stimulation of the autonomic nervous system; and production of adrenergic and neuroglycopenic symptoms to protect the brain and limit systematic effects of hypoglycaemia. 2. A person with mild hypoglycaemia can be treated with g glucose. If the person does not feel better or if their blood glucose level is still less than 4 mmol/l after 5 10 minutes, treatment should be repeated. 3. In cases of severe hypoglycaemia the person affected will need someone else to treat them (DCCT, 1993), as they may not realise they are having a hypoglycaemic episode or may be unable to treat themselves. with type 2 diabetes are over 60 years of age, it is important to appreciate the idiosyncratic and age-specific manifestations of hypoglycemic symptoms, for example, confusion, dizziness, weakness, which could be confused with signs of dementia. l Nocturnal hypoglycaemia is not uncommon but can be missed as the individual is not woken by symptoms of low blood glucose, which can be due to the slow decrease in blood glucose. It is often the spouse or partner that is alerted to the hypoglycaemia due to the person with diabetes being restless or clammy (Allen and Frier, 2003). Signs and symptoms The brain depends on a continual supply of glucose and is vulnerable to any glucose deprivation. Unable to synthesise or store this primary source of energy, the brain is one of the first organs affected by lowered blood glucose levels. Once plasma glucose concentrations fall below the physiological range at a glycaemic threshold of <3.8 mmol/l, a sequence of responses is activated: the release of neuroendocrine hormones (also called counterregulatory or anti-insulin hormones); stimulation of the autonomic nervous system; and production of adrenergic and neuroglycopenic symptoms to protect the brain and limit systematic effects of hypoglycaemia. The normal physiological counterregulatory response to hypoglycaemia Box 1. Signs and symptoms of hypoglycaemia (Henderson et al, 2003). Adrenergic l Sweating l Light-headedness l Trembling/shaking l Hunger l Anxiety l Palpitations l Lip tingling l Irritability l Pallor Neuroglycopenic l Weak legs l Drowsiness l Poor concentration l Blurred vision l Headache l Confusion l Poor coordination l Slurred speech l Glazed eyes l Aggressive behaviour l Seizures l Loss of consciousness consists of suppression of insulin release and secretion of glucagon (Cryer et al, 2003). As the blood glucose begins to fall below normal levels, the adrenergic symptoms begin to be experienced (see Box 1). If treatment is not given, either because the person with diabetes is unaware of the falling blood glucose level or is unable to self-administer, then the symptoms will get worse and include further neuroglycopaenic symptoms as the brain struggles to function properly. These symptoms are shown in Box 1. Treatment of hypoglycaemia In cases of mild hypoglycaemia, g of glucose should be given; suitable treatments include: l 100 ml of Lucozade. l 150 ml of non-diet fizzy drink. l 200 ml of smooth orange juice. l Five or six dextrose tablets. l Four large jelly babies. l Seven large jelly beans. l Two tubes of glucose gel. If the person does not feel better or if their blood glucose level is still less than 4 mmol/l after 5 10 minutes, treatment should be repeated. When the person starts to feel better and if they are not due to eat a meal, they should eat some starchy food, such as a sandwich or a banana, and be monitored afterwards. In cases of severe hypoglycaemia the person affected will need someone else to treat them (DCCT, 1993), as they may not realise they are having a hypoglycaemic episode or may be unable to treat themselves. If the person is conscious and able to swallow safely, they should be given one of the suitable treatments listed above. Treatment should be repeated as required and the person should be accompanied until they have recovered. If the person is unconscious, they should be put in the recovery position (on their side with their head tilted back). Glucose treatment should not be put in their mouth. Glucagon can be injected if there is a trained person present. Otherwise, an ambulance should be called. The publication Recognition, treatment and prevention of hypoglycaemia in the community (TREND, 2011) provides a very helpful algorithm outlining the treatment pathway. 258 Journal of Diabetes Nursing Volume 17 No
5 The NICE Quality Standards for diabetes in adults (NICE, 2011) recommend that people with diabetes receive an ongoing review of treatment to minimise hypoglycaemia. If they have experienced a hypoglycaemic episode requiring medical attention they should be referred to a specialist diabetes team. Prevention It is crucial that people with diabetes who take either insulin or sulphonylureas receive the correct education to allow them to recognise and treat a hypoglycaemic episode and, more importantly, prevent further hypoglycaemic episodes occurring. Information should be provided to enable the person with diabetes to assess whether there is a potential risk of hypoglycaemia occurring and what steps are needed to prevent this. For example, if a person taking insulin decided they were going to take part in a prolonged period of exercise, such as a round of golf, they should be advised to check their blood glucose level prior to commencing the round but also to consume longacting carbohydrate, such as a muesli bar, before starting, or extra carbohydrate at the previous meal to prevent the blood glucose level dropping. If the activity involves short bursts of exercise, such as a game of football, then the carbohydrate would need to be much quicker in action, such as glucose tablets or a glucose drink. It is always advisable to check the blood glucose level after the extra activity and then 2 hours later as hypoglycaemia can often occur long after the activity has finished (Cryer, 2009). It is also important that anyone taking medication that can cause hypoglycaemia should carry an ID card that identifies the type of medication taken. All healthcare professionals working with people with diabetes should complete the NHS Diabetes (now part of NHS Improving Quality) e-learning module Safe management of hypoglycaemia. This module can be accessed at Other useful documents for healthcare professionals are The hospital management of hypoglycaemia in adults with diabetes mellitus (NHS Diabetes, 2010) and Recognition, treatment and prevention of hypoglycaemia in the community (TREND, 2011). Summary Hypoglycaemia is the cost associated with strict glycaemic control; it can cause significant morbidity and occasional mortality and can affect every aspect of daily living. Hypoglycaemia should be avoided at all costs in frail, elderly people, those people with established cardiovascular disease and people who are unable to recognise symptoms of hypoglycaemia. Every person with diabetes who takes either sulphonylureas or insulin therapy should be given the appropriate education to recognise, self treat and prevent hypoglycaemia. The second article will address the cost, complications and burden caused by hypoglycaemia. n Allen KV, Frier BM (2003) Nocturnal hypoglycemia: clinical manifestations and therapeutic strategies toward prevention. Endocr Pract 9: Bailey CJ, Day C (2010) Hypoglycaemia: a limiting factor. Br J Diabetes Vasc Dis 10: 2 4 Cryer PE, Davis SN, Shamoon H (2003) Hypoglycemia in diabetes. Diabetes Care 26: Cryer PE (2009) Hypoglycemia in diabetes: Pathophysiology, prevalence and prevention. American Diabetes Association, Alexandria, Virginia, USA Diabetes Control and Complications Trial Research Group (1993) The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med 329: Diedrich L, Sandoval D, Davis SN (2002) Hypoglycemia associated autonomic failure. Clin Auton Res 12: Health and Social Care Information Centre (2012) National Diabetes Inpatient Audit. Available at: diabetesinpatientaudit (accessed ) Henderson JN, Allen KV, Deary IJ, Frier BM (2003) Hypoglycaemia in insulin-treated type 2 diabetes: frequency, symptoms and impaired awareness. Diabet Med 20: International Diabetes Foundation (2012) IDF diabetes atlas update. Available at: (accessed ) NHS Diabetes (2010) The hospital management of hypoglycaemia in adults with diabetes mellitus. NHS Diabetes, Newcastle upon Tyne. Available at: (accessed ) NICE (2011) Diabetes in adults. QS6. NICE, London. Available at: (accessed ) TREND (2011) Recognition, treatment and prevention of hypoglycaemia in the community. SB Communications Group, London. Available at: (accessed ) UK Hypoglycaemia Study Group (2007) Risk of hypoglycaemia in types 1 and 2 diabetes: effects of treatment modalities and their duration. Diabetologia 50: Vardar B, Kizilci S (2007) Incidence of lipohypertrophy in diabetic people with diabetes and a study of influencing factors. Diabetes Res Clin Pract 77: World Health Organization (2011) Global status report on noncommunicable diseases WHO, Geneva. Available at: (accessed ) It is crucial that people with diabetes who take either insulin or sulphonylureas receive the correct education to allow them to recognise and treat a hypoglycaemic episode. Journal of Diabetes Nursing Volume 17 No
6 Online CPD activity Visit to record your answers and gain a certificate of participation Participants should read the preceding article before answering the multiple choice questions below. There is ONE correct answer to each question. After submitting your answers online, you will be immediately notified of your score. A pass mark of 70% is required to obtain a certificate of successful participation; however, it is possible to take the test a maximum of three times. A short explanation of the correct answer is provided. Before accessing your certificate, you will be given the opportunity to evaluate the activity and reflect on the module, stating how you will use what you have learnt in practice. The CPD centre keeps a record of your CPD activities and provides the option to add items to an action plan, which will help you to collate evidence for your annual appraisal. 1. During the Diabetes Control and Complications Trial how many episodes of hypoglycaemia were noted per week in the intensively treated group? A. 2 B. 4 C. 6 D What percentage of deaths in people with type 1 diabetes are attributed to hypoglycaemia? A. 1 2% B. 2 4% C. 5 7% D. 10% 3. Which of following can be causal factors of hypoglycaemia? A. Unplanned physical activity B. Excess alcohol C. Lipohypertrophy D. All of the above 4. Which of the following describes four adrenergic symptoms of hypoglycaemia? A. Pallor, palpitations, trembling and hunger B. Tingling of lips, confusion, pallor and anxiety C. Hunger, slurred speech, blurred vision and palpitations D. Sweating, trembling, drowsiness and pallor 5. Which of the following describes four neuroglycopaenic symptoms of hypoglycaemia? A. Confusion, hunger, slurred speech and drowsiness B. Coma, seizures, blurred vision and aggressiveness C. Anxiety, lack of concentration, pallor and poor coordination D. Drowsiness, confusion, palpitations and weak legs 6. What percentage of inpatients were recorded as having mild hypoglycaemia only in the 2012 National Diabetes Inpatient Audit report? A. 16% B. 18% C. 19% D. 20% 7. What is the appropriate amount of glucose to be given for a mild hypoglycaemic episode? A. 5 g B g C g D. 30 g 8. Which of the following contains the appropriate amount of glucose required to treat a hypoglycaemic episode? A. Four jelly beans B. One tube of glucose gel C. 100 ml of Lucozade D. 200 ml of diet lemonade 9. With regard to severe hypoglycaemia, which of the following statements is FALSE? A. A person will always be aware if they are experiencing severe hypoglycaemia B. A third party will be needed in order to treat severe hypoglycaemia C. If the person is unconscious, they should not be given glucose treatment orally D. Glucagon can be injected if there is a trained person present 10. With regard to prevention of hypoglycaemia during physical activity, which of the following is TRUE? A. Blood glucose should be checked before, immediately after and 2 hours after exercise B. For a prolonged period of physical activity, the person should eat long-acting carbohydrate C. For short bursts of activity, the person should consume fasteracting carbohydrates D. All of the above 260 Journal of Diabetes Nursing Volume 17 No
Hypoglyceamia and Exercise
 Hypoglyceamia and Exercise Noreen Barker Diabetes Specialist Nurse May 2016 Hypoglyceamia What is a hypo? Why are we concerned? Signs and symptoms Treatments Causes Hypo unawareness Managing diabetes and
Hypoglyceamia and Exercise Noreen Barker Diabetes Specialist Nurse May 2016 Hypoglyceamia What is a hypo? Why are we concerned? Signs and symptoms Treatments Causes Hypo unawareness Managing diabetes and
HYPOS. can strike twice
 HYPOS can strike twice A GUIDE FOR PEOPLE WITH DIABETES WHO HAVE HAD A HYPOGLYCAEMIC (low blood glucose) EVENT Section 1; The ambulance call out Section 2; Low blood glucose levels and how to manage them
HYPOS can strike twice A GUIDE FOR PEOPLE WITH DIABETES WHO HAVE HAD A HYPOGLYCAEMIC (low blood glucose) EVENT Section 1; The ambulance call out Section 2; Low blood glucose levels and how to manage them
Training booklet for understanding. Hypoglycaemia - LOW Blood glucose levels Hyperglycaemia - HIGH Blood glucose levels
 Integrated Community Diabetes Services The Poynt, Units 2-3 Poynters Road Luton, LU4 0LA Tel: 0333 405 3128 Training booklet for understanding Hypoglycaemia - LOW Blood glucose levels Hyperglycaemia -
Integrated Community Diabetes Services The Poynt, Units 2-3 Poynters Road Luton, LU4 0LA Tel: 0333 405 3128 Training booklet for understanding Hypoglycaemia - LOW Blood glucose levels Hyperglycaemia -
Help with hypos. Hypoglycaemia or a hypo is when your blood sugar level is less than 4.0mmol/L. Remember 4 is the floor!
 Other formats What is hypoglycaemia? Help with hypos If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign Language or translated
Other formats What is hypoglycaemia? Help with hypos If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign Language or translated
Essential advice for people with diabetes from Accu-Chek. Get the low-down on hypos
 Essential advice for people with diabetes from Accu-Chek Get the low-down on hypos The low-down on hypos If you have diabetes, a hypo is one of those things you have to deal with from time to time. FIRST
Essential advice for people with diabetes from Accu-Chek Get the low-down on hypos The low-down on hypos If you have diabetes, a hypo is one of those things you have to deal with from time to time. FIRST
Four is the Floor Symptoms can be felt at higher levels if control is poor Worth confirmation using BG meter if at all possible
 Sandra Coats Diabetes Specialist Nurse 1 Hypoglycaemia Hyperglycaemia Diabetes and Illness sick day Diabetic Ketoacidosis HONK/HHS 2 What is Hypoglycaemia BG levels below 4mmol/l. Four is the Floor Floor
Sandra Coats Diabetes Specialist Nurse 1 Hypoglycaemia Hyperglycaemia Diabetes and Illness sick day Diabetic Ketoacidosis HONK/HHS 2 What is Hypoglycaemia BG levels below 4mmol/l. Four is the Floor Floor
Soren Lilleore lives in Denmark and has Type 1 diabetes
 Soren Lilleore lives in Denmark and has Type 1 diabetes Novo Nordisk was one of the first companies to introduce insulin to the world more than 80 years ago. Since that time Novo Nordisk has been dedicated
Soren Lilleore lives in Denmark and has Type 1 diabetes Novo Nordisk was one of the first companies to introduce insulin to the world more than 80 years ago. Since that time Novo Nordisk has been dedicated
Get the low-down on hypos
 Are you prepared? Essential advice for people with diabetes from Accu-Chek 07299508001 Date of prep: May 2014 Having a hypo means your blood glucose is too low Test your blood glucose regularly and look
Are you prepared? Essential advice for people with diabetes from Accu-Chek 07299508001 Date of prep: May 2014 Having a hypo means your blood glucose is too low Test your blood glucose regularly and look
NDSS Helpline ndss.com.au
 Diabetes & Driving NDSS Helpline 1300 136 588 ndss.com.au The National Diabetes Services Scheme is an initiative of the Australian Government administered with Diabetes the assistance and driving of Diabetes
Diabetes & Driving NDSS Helpline 1300 136 588 ndss.com.au The National Diabetes Services Scheme is an initiative of the Australian Government administered with Diabetes the assistance and driving of Diabetes
Hypoglycaemia. Same as above, however Slightly more confused Dizziness Unable to treat self Too confused to eat/drink Slurred speech Unsteady on feet
 Looking after diabetes relies on balancing blood glucose increase from food with blood glucose fall from insulin s action. The body usually adjusts the insulin produced to match the blood glucose concentration,
Looking after diabetes relies on balancing blood glucose increase from food with blood glucose fall from insulin s action. The body usually adjusts the insulin produced to match the blood glucose concentration,
ANZCOR Guideline First aid Management of a Diabetic Emergency
 ANZCOR Guideline 9.2.9 First aid Management of a Diabetic Emergency Summary Who does this guideline apply to? This guideline applies to adult and child victims. Who is the audience for this guideline?
ANZCOR Guideline 9.2.9 First aid Management of a Diabetic Emergency Summary Who does this guideline apply to? This guideline applies to adult and child victims. Who is the audience for this guideline?
Hypoglycaemia. Information for patients Diabetes Service
 Hypoglycaemia Information for patients Diabetes Service What is hypoglycaemia? Hypoglycaemia or a hypo is the medical term for low blood glucose levels - that is a blood glucose level of less than 4 mmol/l.
Hypoglycaemia Information for patients Diabetes Service What is hypoglycaemia? Hypoglycaemia or a hypo is the medical term for low blood glucose levels - that is a blood glucose level of less than 4 mmol/l.
Do you have diabetes?
 Do you have diabetes? DAY AND NIGHT Are you being treated with insulin? Are you being treated with glucose lowering tablets called sulphonylureas? (ask your pharmacist) Have you experienced any of the
Do you have diabetes? DAY AND NIGHT Are you being treated with insulin? Are you being treated with glucose lowering tablets called sulphonylureas? (ask your pharmacist) Have you experienced any of the
Objectives. Why is blood glucose important? Hypoglycaemia. Hyperglycaemia. Acute Diabetes Emergencies (DKA,HONK)
 Acute Diabetes Emergencies Ross Buchan, DSN North Glasgow June 2017 Objectives Why is blood glucose important? Hypoglycaemia Hyperglycaemia Acute Diabetes Emergencies (DKA,HONK) Importance of Blood Glucose
Acute Diabetes Emergencies Ross Buchan, DSN North Glasgow June 2017 Objectives Why is blood glucose important? Hypoglycaemia Hyperglycaemia Acute Diabetes Emergencies (DKA,HONK) Importance of Blood Glucose
GUIDELINE FOR THE MANAGEMENT OF HYPOGLYCAEMIA IN ADULTS WITH DIABETES MELLITUS
 GUIDELINE FOR THE MANAGEMENT OF HYPOGLYCAEMIA IN ADULTS WITH DIABETES MELLITUS Guideline author Accountable Executive Lead Approving body Policy reference Diabetes Specialist Nurse Consultant Diabetologist
GUIDELINE FOR THE MANAGEMENT OF HYPOGLYCAEMIA IN ADULTS WITH DIABETES MELLITUS Guideline author Accountable Executive Lead Approving body Policy reference Diabetes Specialist Nurse Consultant Diabetologist
Hypoglycemia. When recognized early, hypoglycemia can be treated successfully.
 Hypoglycemia Introduction Hypoglycemia is a condition that causes blood sugar level to drop dangerously low. It mostly shows up in diabetic patients who take insulin. When recognized early, hypoglycemia
Hypoglycemia Introduction Hypoglycemia is a condition that causes blood sugar level to drop dangerously low. It mostly shows up in diabetic patients who take insulin. When recognized early, hypoglycemia
Objectives. Why is blood glucose important? Hypoglycaemia. Hyperglycaemia. Acute Diabetes Emergencies (DKA,HONK)
 Acute Diabetes Emergencies Ross Buchan, DSN North Glasgow September 2017 Objectives Why is blood glucose important? Hypoglycaemia Hyperglycaemia Acute Diabetes Emergencies (DKA,HONK) Importance of Blood
Acute Diabetes Emergencies Ross Buchan, DSN North Glasgow September 2017 Objectives Why is blood glucose important? Hypoglycaemia Hyperglycaemia Acute Diabetes Emergencies (DKA,HONK) Importance of Blood
THIS GUIDELINE REFERS TO ADULT PATIENTS WITH DIABETES
 Hypoglycaemia Aim(s) and objective(s) Hypoglycaemia (a hypo ) can occur as a consequence of diabetes treatment. It is a common problem among people with diabetes particularly those who are treated with
Hypoglycaemia Aim(s) and objective(s) Hypoglycaemia (a hypo ) can occur as a consequence of diabetes treatment. It is a common problem among people with diabetes particularly those who are treated with
TYPE 2 DIABETES AND STEROID TABLETS
 MEDICATION TYPE 2 DIABETES AND STEROID TABLETS WHY IS THIS LEAFLET FOR YOU? Taking steroid treatment when you have diabetes can make your blood glucose levels more difficult to control. This leaflet will
MEDICATION TYPE 2 DIABETES AND STEROID TABLETS WHY IS THIS LEAFLET FOR YOU? Taking steroid treatment when you have diabetes can make your blood glucose levels more difficult to control. This leaflet will
Hypoglycemia, Sick Days/DKA and Hospitalization
 Hypoglycemia, Sick Days/DKA and Hospitalization General survival skills for your client with diabetes at home and in Hospital Diabetes Canada guidelines for your client with diabetes while they are in
Hypoglycemia, Sick Days/DKA and Hospitalization General survival skills for your client with diabetes at home and in Hospital Diabetes Canada guidelines for your client with diabetes while they are in
DIABETES POLICY (Part of the Supporting Pupils with a Medical Condition Policy)
 DIABETES POLICY (Part of the Supporting Pupils with a Medical Condition Policy) Brockley Primary School It is important that children and young people with diabetes are properly supported in school. However,
DIABETES POLICY (Part of the Supporting Pupils with a Medical Condition Policy) Brockley Primary School It is important that children and young people with diabetes are properly supported in school. However,
the complete guide for controling hypoglycemia GLUCOSE
 the complete guide GLUCOSE for controling hypoglycemia Personal DATA Name Address Phone Diabetes Treatment Center: Name Address Phone In an urgent case contact with: Name Address Phone Presents other risk
the complete guide GLUCOSE for controling hypoglycemia Personal DATA Name Address Phone Diabetes Treatment Center: Name Address Phone In an urgent case contact with: Name Address Phone Presents other risk
Individual healthcare plan for Type 1 diabetes. for children/young people with diabetes in schools and Early Years settings
 Individual healthcare plan for Type 1 diabetes for children/young people with diabetes in schools and Early Years settings Individual healthcare plan for Type 1 diabetes for children/young people with
Individual healthcare plan for Type 1 diabetes for children/young people with diabetes in schools and Early Years settings Individual healthcare plan for Type 1 diabetes for children/young people with
TRUST CORE CLINICAL POLICY THE MANAGEMENT OF HYPOGLYCAEMIA IN ADULTS. Clinical Policies Group
 TRUST CORE CLINICAL POLICY THE MANAGEMENT OF HYPOGLYCAEMIA IN ADULTS APPROVAL Clinical Policies Group Date approved: 11 November 2013 EFFECTIVE FROM November 2013 DISTRIBUTION All clinical staff at Barts
TRUST CORE CLINICAL POLICY THE MANAGEMENT OF HYPOGLYCAEMIA IN ADULTS APPROVAL Clinical Policies Group Date approved: 11 November 2013 EFFECTIVE FROM November 2013 DISTRIBUTION All clinical staff at Barts
THE FACTS ABOUT FASTING DURING RAMADAN INFORMATION KIT FOR PEOPLE WITH TYPE 2 DIABETES
 THE FACTS ABOUT FASTING DURING RAMADAN INFORMATION KIT FOR PEOPLE WITH TYPE 2 DIABETES INTRODUCTION This information kit is designed to provide you with facts and practical advice about fasting during
THE FACTS ABOUT FASTING DURING RAMADAN INFORMATION KIT FOR PEOPLE WITH TYPE 2 DIABETES INTRODUCTION This information kit is designed to provide you with facts and practical advice about fasting during
Case study: Adult with uncontrolled type 2 diabetes of long duration and cardiovascular disease
 Case study: Adult with uncontrolled type 2 diabetes of long duration and cardiovascular disease Authored by Paul Zimmet and Richard Nesto on behalf of the Global Partnership for Effective Diabetes Management.
Case study: Adult with uncontrolled type 2 diabetes of long duration and cardiovascular disease Authored by Paul Zimmet and Richard Nesto on behalf of the Global Partnership for Effective Diabetes Management.
What is Diabetes? American Diabetes Association
 March 2015 What is Diabetes? Diabetes mellitus refers to a group of diseases that affect how your body uses blood sugar (glucose). Glucose is vital to your health because it's an important source of energy
March 2015 What is Diabetes? Diabetes mellitus refers to a group of diseases that affect how your body uses blood sugar (glucose). Glucose is vital to your health because it's an important source of energy
Do you have diabetes? Are you being treated with insulin or sulphonylureas?
 Do you have diabetes? Are you being treated with insulin or sulphonylureas? DAY AND NIGHT Have you experienced any of the following symptoms during the day or night? Hypo symptoms Unsettled / feeling 'off'
Do you have diabetes? Are you being treated with insulin or sulphonylureas? DAY AND NIGHT Have you experienced any of the following symptoms during the day or night? Hypo symptoms Unsettled / feeling 'off'
A GUIDE TO STARTING HUMALOG
 A GUIDE TO STARTING HUMALOG This booklet is intended only for those who have been prescribed Humalog. It is intended to be used in addition to the Patient Information Leaflet (PIL) which is included in
A GUIDE TO STARTING HUMALOG This booklet is intended only for those who have been prescribed Humalog. It is intended to be used in addition to the Patient Information Leaflet (PIL) which is included in
Hypoglycemia. Patient Education Diabetes Care Center. How to cope with low blood sugar. General Facts on Low Blood Sugar. Causes
 Patient Education How to cope with low blood sugar Recognizing the causes and symptoms of hypoglycemia can help you prepare for and respond to this condition when it arises. General Facts on Low Blood
Patient Education How to cope with low blood sugar Recognizing the causes and symptoms of hypoglycemia can help you prepare for and respond to this condition when it arises. General Facts on Low Blood
Dedicated To. Course Objectives. Diabetes What is it? 2/18/2014. Managing Diabetes in the Athletic Population. Aiden
 Managing Diabetes in the Athletic Population Dedicated To Aiden Michael Prybicien, LA, ATC, CSCS, CES, PES Athletic Trainer, Passaic High School Overlook Medical Center & Adjunct Faculty, William Paterson
Managing Diabetes in the Athletic Population Dedicated To Aiden Michael Prybicien, LA, ATC, CSCS, CES, PES Athletic Trainer, Passaic High School Overlook Medical Center & Adjunct Faculty, William Paterson
NDLS. Diabetes and Driving
 NDLS Diabetes and Driving This is an overview of driving with diabetes. The complete standards are published in Sláinte agus Tiomáint: Medical Fitness to Drive (MFTD) Guidelines. Be a responsible driver
NDLS Diabetes and Driving This is an overview of driving with diabetes. The complete standards are published in Sláinte agus Tiomáint: Medical Fitness to Drive (MFTD) Guidelines. Be a responsible driver
Type 1 Diabetes - Pediatrics
 Type 1 Diabetes - Pediatrics Introduction Type 1 diabetes prevents the body from removing sugar from the blood stream normally. Diabetes can lead to serious health problems if it is not treated. Currently
Type 1 Diabetes - Pediatrics Introduction Type 1 diabetes prevents the body from removing sugar from the blood stream normally. Diabetes can lead to serious health problems if it is not treated. Currently
 Diabetes Care Center Box 356176 1959 N.E. Pacific St. Seattle, WA 98195 206-598-4882 120457 University of Washington Medical Center Diabetes Care Center Arabic r02/2000 Patient Education Diabetes Care
Diabetes Care Center Box 356176 1959 N.E. Pacific St. Seattle, WA 98195 206-598-4882 120457 University of Washington Medical Center Diabetes Care Center Arabic r02/2000 Patient Education Diabetes Care
Pathway for Adult Patients with Diabetes attending the Emergency Department (ED) with Hypoglycaemia
 Leicestershirediabetes Guidelines Pathway for Adult Patients with Diabetes attending the Emergency Department (ED) with Hypoglycaemia Patient attends ED Support available from Diabetes Specialist Nurses
Leicestershirediabetes Guidelines Pathway for Adult Patients with Diabetes attending the Emergency Department (ED) with Hypoglycaemia Patient attends ED Support available from Diabetes Specialist Nurses
Hypoglycemia in congenital hyperinsulinism
 How a normal body works: Our body is constantly at work. Our cells need a source of energy, and this source of energy is called glucose. The process is quite simple; think of it like an assembly line.
How a normal body works: Our body is constantly at work. Our cells need a source of energy, and this source of energy is called glucose. The process is quite simple; think of it like an assembly line.
Managing diabetes can be difficult to balance with a busy lifestyle or partying.
 DRUGS AND DIABETES Managing diabetes can be difficult to balance with a busy lifestyle or partying. All drug use carries risk. We know that there are people who are diabetic who will choose to take drugs.
DRUGS AND DIABETES Managing diabetes can be difficult to balance with a busy lifestyle or partying. All drug use carries risk. We know that there are people who are diabetic who will choose to take drugs.
Type 1 Diabetes. Insulin
 Type 1 Diabetes Introduction Type 1 diabetes prevents the body from removing sugar from the blood stream normally. Diabetes can lead to serious health problems if it is not treated. Currently, there is
Type 1 Diabetes Introduction Type 1 diabetes prevents the body from removing sugar from the blood stream normally. Diabetes can lead to serious health problems if it is not treated. Currently, there is
!"#$%&'()*+,-./012&3!"#$%N!"#$%&'()OMMM QMMM!"#$%&'!"#()*+,-.!"#$%&'()*+,-./012priclJ kvirob^=e ÖäóÄìêáÇÉI=ÖäáéáòáÇÉF=!"
 !"#$!"#$%!"#$%&!"#$%&!"#$%&!"#$%&!"#$%&!"#$%&'()*+,-./012&3!"#$%N!"#$%&'()OMMM QMMM!"#$%&'!"#()*+,-.!"#$%&'()*+,-./012priclJ kvirob^=e ÖäóÄìêáÇÉI=ÖäáéáòáÇÉF=!"!"#$%&'()*+,-'()./012!"#$%&'%()*+,-./0$%1!"#$%&'()*+,-./0!"123
!"#$!"#$%!"#$%&!"#$%&!"#$%&!"#$%&!"#$%&!"#$%&'()*+,-./012&3!"#$%N!"#$%&'()OMMM QMMM!"#$%&'!"#()*+,-.!"#$%&'()*+,-./012priclJ kvirob^=e ÖäóÄìêáÇÉI=ÖäáéáòáÇÉF=!"!"#$%&'()*+,-'()./012!"#$%&'%()*+,-./0$%1!"#$%&'()*+,-./0!"123
Diabetes. For Employees of the Randolph County School System
 Diabetes For Employees of the Randolph County School System Diabetes Early detection and treatment of diabetes can decrease the risk of developing complications of diabetes Some symptoms of diabetes are
Diabetes For Employees of the Randolph County School System Diabetes Early detection and treatment of diabetes can decrease the risk of developing complications of diabetes Some symptoms of diabetes are
Teaching plan. Suggested group activities
 Teaching plan This lesson is designed to help workers learn about diabetes. To use this lesson for self-study, the learner should read the materials, do the case study activity, and take the test. For
Teaching plan This lesson is designed to help workers learn about diabetes. To use this lesson for self-study, the learner should read the materials, do the case study activity, and take the test. For
Diabetes Workbook Level 2
 Diabetes Workbook Level 2 Contents Diabetes Workbook 02 Pre Training Quiz 03 1. Introduction 04 2. Type 2 Diabetes 06 3. Nutrition 08 4. Exercise, Medication & Support 09 5. Hypoglycaemia 13 6. Hyperglycaemia
Diabetes Workbook Level 2 Contents Diabetes Workbook 02 Pre Training Quiz 03 1. Introduction 04 2. Type 2 Diabetes 06 3. Nutrition 08 4. Exercise, Medication & Support 09 5. Hypoglycaemia 13 6. Hyperglycaemia
MANAGING MEALTIME INSULIN
 MEDICATION MANAGING MEALTIME INSULIN kk WHY IS THIS LEAFLET FOR YOU? The blood glucose level in someone who does not have diabetes keeps remarkably steady despite variable meal sizes and amount of activity.
MEDICATION MANAGING MEALTIME INSULIN kk WHY IS THIS LEAFLET FOR YOU? The blood glucose level in someone who does not have diabetes keeps remarkably steady despite variable meal sizes and amount of activity.
Diabetic Emergencies. Chapter 15
 Diabetic Emergencies Chapter 15 Diabetes- is a disorder of glucose metabolism or difficulty metabolizing carbohydrates, fats and proteins Full name is diabetes mellitus which refers to the presence of
Diabetic Emergencies Chapter 15 Diabetes- is a disorder of glucose metabolism or difficulty metabolizing carbohydrates, fats and proteins Full name is diabetes mellitus which refers to the presence of
Certificate of Merit in Disorders of the Body Lesson 2: Epilepsy, Diabetes and Multiple Sclerosis
 Certificate of Merit in Disorders of the Body Lesson 2: Epilepsy, Diabetes and Multiple Sclerosis Epilepsy Epilepsy is a condition in which there is a sudden burst of electrical energy in the brain, which
Certificate of Merit in Disorders of the Body Lesson 2: Epilepsy, Diabetes and Multiple Sclerosis Epilepsy Epilepsy is a condition in which there is a sudden burst of electrical energy in the brain, which
Diet and reactive hypoglycaemia
 Diet and reactive hypoglycaemia Nutrition and Dietetics Patient Information Leaflet Introduction This leaflet is for people who have a condition called reactive hypoglycaemia. It gives information on what
Diet and reactive hypoglycaemia Nutrition and Dietetics Patient Information Leaflet Introduction This leaflet is for people who have a condition called reactive hypoglycaemia. It gives information on what
Diabetes Emergency Kit
 Diabetes Emergency Kit for: Last updated on / / Courtesy of www.laurenshope.com Diabetes General Information TREATMENT If the child is awake and can swallow, provide sugar immediately. Give 1/2 cup of
Diabetes Emergency Kit for: Last updated on / / Courtesy of www.laurenshope.com Diabetes General Information TREATMENT If the child is awake and can swallow, provide sugar immediately. Give 1/2 cup of
TO BE COMPLETED BY LICENSED HEALTH CARE PROFESSIONAL
 PART I OFFICE OF CATHOLIC SCHOOLS DIOCESE OF ARLINGTON DIABETES MEDICAL MANAGEMENT PLAN Page 1 of 5 TO BE COMPLETED BY PARENT OR GUARDIAN Student School Date of Birth Date of Diagnosis Grade/ Teacher Physical
PART I OFFICE OF CATHOLIC SCHOOLS DIOCESE OF ARLINGTON DIABETES MEDICAL MANAGEMENT PLAN Page 1 of 5 TO BE COMPLETED BY PARENT OR GUARDIAN Student School Date of Birth Date of Diagnosis Grade/ Teacher Physical
Type 2 Diabetes. What is diabetes? What is type 2 diabetes? What is type 1 diabetes? Understanding blood glucose and insulin
 Page 1 of 7 Type 2 Diabetes Type 2 diabetes occurs mainly in people aged over 40. The first-line treatment is diet, weight control and physical activity. If the blood sugar (glucose) level remains high
Page 1 of 7 Type 2 Diabetes Type 2 diabetes occurs mainly in people aged over 40. The first-line treatment is diet, weight control and physical activity. If the blood sugar (glucose) level remains high
In Hospital Management of Hypoglycaemia in Adults with Diabetes Mellitus
 In Hospital Management of Hypoglycaemia in Adults with Diabetes Mellitus This procedural document supersedes any previous guidelines in relation to this subject: PAT/T 49 v.2 In Hospital Management of
In Hospital Management of Hypoglycaemia in Adults with Diabetes Mellitus This procedural document supersedes any previous guidelines in relation to this subject: PAT/T 49 v.2 In Hospital Management of
How to manage Hypoglycaemia
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust How to manage Hypoglycaemia Nutrition & Dietetics Who is this leaflet for? The information in this leaflet tells you about:
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust How to manage Hypoglycaemia Nutrition & Dietetics Who is this leaflet for? The information in this leaflet tells you about:
Clinical Guidance. Management of hypoglycaemia in paediatric diabetes
 Clinical Guidance Management of hypoglycaemia in paediatric diabetes Summary This guidance is for the use of nurses and doctors management of children with diabetes suffering an episode of hypoglycaemia
Clinical Guidance Management of hypoglycaemia in paediatric diabetes Summary This guidance is for the use of nurses and doctors management of children with diabetes suffering an episode of hypoglycaemia
DIABETES AND ENTERAL FEEDING
 DIABETES AND ENTERAL FEEDING kk WHY IS THIS LEAFLET FOR YOU? This leaflet is for people with diabetes established on an enteral feeding regimen, and for the people who support them at home, in residential
DIABETES AND ENTERAL FEEDING kk WHY IS THIS LEAFLET FOR YOU? This leaflet is for people with diabetes established on an enteral feeding regimen, and for the people who support them at home, in residential
Diabetes. Introduction. Types of diabetes
 Diabetes Introduction Around 1.8 million people in the UK are diagnosed with diabetes each year. It is estimated that there are probably a further one million people who have diabetes without knowing it.
Diabetes Introduction Around 1.8 million people in the UK are diagnosed with diabetes each year. It is estimated that there are probably a further one million people who have diabetes without knowing it.
People with type 1 diabetes experience. Managing inpatient hypoglycaemia: The introduction of new national guidelines
 Managing inpatient hypoglycaemia: The introduction of new national guidelines Esther Walden, Debbie Stanisstreet Article points 1. The hospital environment presents major obstacles to good glycaemic control
Managing inpatient hypoglycaemia: The introduction of new national guidelines Esther Walden, Debbie Stanisstreet Article points 1. The hospital environment presents major obstacles to good glycaemic control
Policy for Supporting. Children and Young People with. Diabetes in Education
 Policy for Supporting Children and Young People with Diabetes in Education December 2011 POLICY FOR SUPPORTING CHILDREN AND YOUNG PEOPLE WITH DIABETES IN EDUCATION Contents 1. Introduction 2. Before a
Policy for Supporting Children and Young People with Diabetes in Education December 2011 POLICY FOR SUPPORTING CHILDREN AND YOUNG PEOPLE WITH DIABETES IN EDUCATION Contents 1. Introduction 2. Before a
Blood Glucose monitoring during extra-corporeal renal therapy and plasmapheresis.
 Blood Glucose monitoring during extra-corporeal renal therapy and plasmapheresis. Lead Clinician: Dr. R. Diwakar Implementation date: July 2013 Last updated: August 2017 Last review date: Planned review
Blood Glucose monitoring during extra-corporeal renal therapy and plasmapheresis. Lead Clinician: Dr. R. Diwakar Implementation date: July 2013 Last updated: August 2017 Last review date: Planned review
Hypoglycaemia. Parent Information Leaflet
 Hypoglycaemia Parent Information Leaflet July 2017 Definition Hypoglycaemia (hypo) in children with diabetes is a blood glucose of less than 4.0mmol/L. The first time your child has a hypo will be an anxious
Hypoglycaemia Parent Information Leaflet July 2017 Definition Hypoglycaemia (hypo) in children with diabetes is a blood glucose of less than 4.0mmol/L. The first time your child has a hypo will be an anxious
INFORMATION ON DRIVING AND DIABETES: GROUP 2 VEHICLES
 INFORMATION ON DRIVING AND DIABETES: GROUP 2 VEHICLES This information leaflet offers information on what is now required if you wish to hold a Group 2 Lorries, bus, taxi and HGV driving licence and to
INFORMATION ON DRIVING AND DIABETES: GROUP 2 VEHICLES This information leaflet offers information on what is now required if you wish to hold a Group 2 Lorries, bus, taxi and HGV driving licence and to
Placename CCG. Policies for the Commissioning of Healthcare
 Placename CCG Policies for the Commissioning of Healthcare Policy for the funding of insulin pumps and continuous glucose monitoring devices for patients with diabetes 1 Introduction 1.1 This document
Placename CCG Policies for the Commissioning of Healthcare Policy for the funding of insulin pumps and continuous glucose monitoring devices for patients with diabetes 1 Introduction 1.1 This document
Diabetes and pregnancy. diabetes. and. pregnancy
 Diabetes and pregnancy i diabetes and pregnancy www.glucomen.co.uk Diabetes and Pregnancy Diabetes is a medical condition where there is too much sugar (glucose) in the bloodstream. Glucose is the main
Diabetes and pregnancy i diabetes and pregnancy www.glucomen.co.uk Diabetes and Pregnancy Diabetes is a medical condition where there is too much sugar (glucose) in the bloodstream. Glucose is the main
Diabetes and Kidney Disease: Time to Act. Your Guide to Diabetes and Kidney Disease
 Diabetes and Kidney Disease: Time to Act Your Guide to Diabetes and Kidney Disease Diabetes is fast becoming a world epidemic Diabetes is reaching epidemic proportions worldwide. Every year more people
Diabetes and Kidney Disease: Time to Act Your Guide to Diabetes and Kidney Disease Diabetes is fast becoming a world epidemic Diabetes is reaching epidemic proportions worldwide. Every year more people
Hypoglycaemia (low blood sugar) & ketotic hypoglycaemia
 Information for parents and carers Hypoglycaemia (low blood sugar) & ketotic hypoglycaemia What is hypoglycaemia? Hypoglycemia is having a blood glucose (also known as blood sugar) level that is too low
Information for parents and carers Hypoglycaemia (low blood sugar) & ketotic hypoglycaemia What is hypoglycaemia? Hypoglycemia is having a blood glucose (also known as blood sugar) level that is too low
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Health Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Continuous subcutaneous insulin infusion for the treatment of diabetes (review) Final scope Appraisal objective To review
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Continuous subcutaneous insulin infusion for the treatment of diabetes (review) Final scope Appraisal objective To review
Essential advice for people with diabetes from Accu-Chek. The inside story on diabetes
 Essential advice for people with diabetes from Accu-Chek The inside story on diabetes What is diabetes? Glucose is a form of sugar that is found in food you eat. It is a vital energy source for your body
Essential advice for people with diabetes from Accu-Chek The inside story on diabetes What is diabetes? Glucose is a form of sugar that is found in food you eat. It is a vital energy source for your body
LOW BLOOD GLUCOSE (Hypoglycemia)
 Section Four DAILY CRISES In this section, you will learn about: Low blood glucose High blood glucose Diabetic Ketoacidosis Hyperosmolar Hyperglycemic Nonketotic Syndrome LOW BLOOD GLUCOSE (Hypoglycemia)
Section Four DAILY CRISES In this section, you will learn about: Low blood glucose High blood glucose Diabetic Ketoacidosis Hyperosmolar Hyperglycemic Nonketotic Syndrome LOW BLOOD GLUCOSE (Hypoglycemia)
7/28/17. Objectives: Hypoglycemia Unawareness in the Geriatric Patient: A Safety Concern. Disclaimer:
 Hypoglycemia Unawareness in the Geriatric Patient: A Safety Concern 29TH ANNUAL TNP CONFERENCE TRANSFORMING HEALTHCARE IN TEXAS SEPTEMBER 8, 2017 AUSTIN, TEXAS Kenneth Lowrance, DNP, APRN, CNS, FNP-BC,
Hypoglycemia Unawareness in the Geriatric Patient: A Safety Concern 29TH ANNUAL TNP CONFERENCE TRANSFORMING HEALTHCARE IN TEXAS SEPTEMBER 8, 2017 AUSTIN, TEXAS Kenneth Lowrance, DNP, APRN, CNS, FNP-BC,
Overview of Session 3 Taking Control of Your Diabetes (2)
 Overview of Session 3 Taking Control of Your Diabetes (2) Objectives of session 3 Objectives for this session are that participants will: Understand what a hypo & hyper are and how to treat these Know
Overview of Session 3 Taking Control of Your Diabetes (2) Objectives of session 3 Objectives for this session are that participants will: Understand what a hypo & hyper are and how to treat these Know
Placename CCG. Policies for the Commissioning of Healthcare
 Placename CCG Policies for the Commissioning of Healthcare Policy for the Provision of Continuous Glucose Monitoring and Flash Glucose Monitoring to patients with Diabetes Mellitus. This document is part
Placename CCG Policies for the Commissioning of Healthcare Policy for the Provision of Continuous Glucose Monitoring and Flash Glucose Monitoring to patients with Diabetes Mellitus. This document is part
Glycemic Management Hypoglycemic & Hyperglycemic Treatment Continuing Care
 Approved by: Glycemic Management Hypoglycemic & Hyperglycemic Continuing Care Senior Operating Officer, Addiction & Mental Health and Continuing Care, Edmonton Senior Operating Officer, Rural Services
Approved by: Glycemic Management Hypoglycemic & Hyperglycemic Continuing Care Senior Operating Officer, Addiction & Mental Health and Continuing Care, Edmonton Senior Operating Officer, Rural Services
Prepare for a healthy Ramadan What I should know about managing my type 2 diabetes during Ramadan
 Prepare for a healthy Ramadan What I should know about managing my type 2 diabetes during Ramadan www.diabetesalliance.co.uk This booklet is part of Dialogue, a patient support programme. It has been developed
Prepare for a healthy Ramadan What I should know about managing my type 2 diabetes during Ramadan www.diabetesalliance.co.uk This booklet is part of Dialogue, a patient support programme. It has been developed
The Signs, Symptoms, and Causes of Hypoglycemia
 The Signs, Symptoms, and Causes of Hypoglycemia Tam Doan PharmD, CDE, BC-ADM Clinical Pharmacist, Diabetes Care Manager Santa Clara Valley Medical Center Fruitdale, CA Agenda What is hypoglycemia? What
The Signs, Symptoms, and Causes of Hypoglycemia Tam Doan PharmD, CDE, BC-ADM Clinical Pharmacist, Diabetes Care Manager Santa Clara Valley Medical Center Fruitdale, CA Agenda What is hypoglycemia? What
AQA B3.3 Homeostasis LEVEL 3
 AQA B3.3 Homeostasis LEVEL 3 340 minutes 340 marks Page 1 of 49 Q1. To stay healthy, the amount of sodium in your body must not change very much. On average, a girl takes in 10 grams of sodium a day in
AQA B3.3 Homeostasis LEVEL 3 340 minutes 340 marks Page 1 of 49 Q1. To stay healthy, the amount of sodium in your body must not change very much. On average, a girl takes in 10 grams of sodium a day in
Standards of Care for Students with Type 1 Diabetes in School
 Standards of Care for Students with Type 1 Diabetes in School Purpose: To acknowledge and clarify the essential partnerships among parents or caregivers, students and school personnel in the care of students
Standards of Care for Students with Type 1 Diabetes in School Purpose: To acknowledge and clarify the essential partnerships among parents or caregivers, students and school personnel in the care of students
The National Diabetes Services Scheme (NDSS) is an initiative of the Australian Government administered by Diabetes Australia.
 ALCOHOL AND TYPE 1 DIABETES 1300 136 588 ndss.com.au The National Diabetes Services Scheme (NDSS) is an initiative of the Australian Government administered by Diabetes Australia. NDSS-003 RiskBehavRsc-Alcohol
ALCOHOL AND TYPE 1 DIABETES 1300 136 588 ndss.com.au The National Diabetes Services Scheme (NDSS) is an initiative of the Australian Government administered by Diabetes Australia. NDSS-003 RiskBehavRsc-Alcohol
Diabetes guidelines for schools, colleges & early year settings.
 Diabetes guidelines for schools, colleges & early year settings. Compiled by East of England Paediatric Diabetes Network Diabetes in Schools working group October 2012 2 Introduction Education is a cornerstone
Diabetes guidelines for schools, colleges & early year settings. Compiled by East of England Paediatric Diabetes Network Diabetes in Schools working group October 2012 2 Introduction Education is a cornerstone
Individual Health Care Plan-Diabetes
 Individual Health Care Plan-Diabetes Effective Date: School Year: 20 to 20 This plan should be completed by the student s diabetes care aide/health clerk and parents/guardians. It should be reviewed with
Individual Health Care Plan-Diabetes Effective Date: School Year: 20 to 20 This plan should be completed by the student s diabetes care aide/health clerk and parents/guardians. It should be reviewed with
Hypoglycaemia. Key messages All of us will remember a case of hypoglycaemia!!
 Hypoglycaemia Key messages All of us will remember a case of hypoglycaemia!! The frequency and severity of hypoglycaemia is commonly underes=mated and o>en mis- a@ributed to other condi=ons The symptoms
Hypoglycaemia Key messages All of us will remember a case of hypoglycaemia!! The frequency and severity of hypoglycaemia is commonly underes=mated and o>en mis- a@ributed to other condi=ons The symptoms
Managing your Diabetes during Ramadan
 Managing your Diabetes during Ramadan A Guide for Patients Introduction The holy month of Ramadan is a period of prayer, routine work, and charitable activities, with strict fasting where no food or drink
Managing your Diabetes during Ramadan A Guide for Patients Introduction The holy month of Ramadan is a period of prayer, routine work, and charitable activities, with strict fasting where no food or drink
2012 Edition. Part B: 3 3. DIABETES MELLITUS Effects of diabetes on driving Evidence of crash risk. 3.2.
 2012 Edition DIABETES MELLITUS 3. DIABETES MELLITUS Refer also to section 6 Neurological conditions, section 2 Cardiovascular conditions, section 8 Sleep disorders section 10 Vision eye disorders. 3.1
2012 Edition DIABETES MELLITUS 3. DIABETES MELLITUS Refer also to section 6 Neurological conditions, section 2 Cardiovascular conditions, section 8 Sleep disorders section 10 Vision eye disorders. 3.1
Executive Summary Management of Type 1 Diabetes Mellitus during illness in children and young people under 18 years (Sick Day Rules)
 Executive Summary Management of Type 1 Diabetes Mellitus during illness in children and young people under 18 years (Sick Day Rules) SETTING FOR STAFF PATIENTS Medical and nursing staff Children and young
Executive Summary Management of Type 1 Diabetes Mellitus during illness in children and young people under 18 years (Sick Day Rules) SETTING FOR STAFF PATIENTS Medical and nursing staff Children and young
Diabetes Medical Management Plan
 Diabetes Medical Management Plan 1 School District: School: School Year: Grade: Student Name: DOB: Provider Name: Phone #: Fax #: Blood Glucose Monitoring at School Blood Glucose Target Range: - mg/dl
Diabetes Medical Management Plan 1 School District: School: School Year: Grade: Student Name: DOB: Provider Name: Phone #: Fax #: Blood Glucose Monitoring at School Blood Glucose Target Range: - mg/dl
Study of hypoglycemia in elderly diabetes mellitus
 Original Research Article Study of hypoglycemia in elderly diabetes mellitus K. Babu Raj 1, R. Prabhakaran 2* 1 Reader, Department of Medicine, Rajah Muthiah Medical College, Annamalai University, Chidambaram,
Original Research Article Study of hypoglycemia in elderly diabetes mellitus K. Babu Raj 1, R. Prabhakaran 2* 1 Reader, Department of Medicine, Rajah Muthiah Medical College, Annamalai University, Chidambaram,
Policy for the Provision of Insulin Pumps for Patients with Diabetes Mellitus
 Policy for the Provision of Insulin Pumps for Patients with Diabetes Mellitus Version No. Changes Made Version of July 2018 V0.5 Changes made to the policy following patient engagement including: - the
Policy for the Provision of Insulin Pumps for Patients with Diabetes Mellitus Version No. Changes Made Version of July 2018 V0.5 Changes made to the policy following patient engagement including: - the
Pre-Dialysis Insulin Information for Patients with Type 2 Diabetes receiving haemodialysis
 Pre-Dialysis Insulin Information for Patients with Type 2 Diabetes receiving haemodialysis Exceptional healthcare, personally delivered 2 This leaflet is for patients with Type 2 diabetes who require insulin
Pre-Dialysis Insulin Information for Patients with Type 2 Diabetes receiving haemodialysis Exceptional healthcare, personally delivered 2 This leaflet is for patients with Type 2 diabetes who require insulin
Driving with Diabetes
 Driving with Diabetes Jan Broz Marketa Tolarova Jan Polak Brian Frier Assist. prof. Jan Broz, MD is an Assistant Professor of Internal Medicine at the Charles University 2nd Faculty of Medicine in Prague,
Driving with Diabetes Jan Broz Marketa Tolarova Jan Polak Brian Frier Assist. prof. Jan Broz, MD is an Assistant Professor of Internal Medicine at the Charles University 2nd Faculty of Medicine in Prague,
These results are supplied for informational purposes only.
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription Sponsor/company: sanofi-aventis ClinialTrials.gov
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription Sponsor/company: sanofi-aventis ClinialTrials.gov
Common Diabetes-related Terms
 Common Diabetes-related Terms A1C An A1C test measures a person's average blood glucose level over two to three months. Hemoglobin is the part of a red blood cell that carries oxygen to the cells and sometimes
Common Diabetes-related Terms A1C An A1C test measures a person's average blood glucose level over two to three months. Hemoglobin is the part of a red blood cell that carries oxygen to the cells and sometimes
What is Hypoglycemia?
 HYPOGLYCEMIA What is Hypoglycemia? Health Plan of Nevada Sierra Health and Life What is Hypoglycemia? Hypoglycemia, also known as low blood sugar, is usually defined as blood glucose below 70 mg/dl. However,
HYPOGLYCEMIA What is Hypoglycemia? Health Plan of Nevada Sierra Health and Life What is Hypoglycemia? Hypoglycemia, also known as low blood sugar, is usually defined as blood glucose below 70 mg/dl. However,
DIABETES MANAGEMENT POLICY
 DIABETES MANAGEMENT POLICY 1. PURPOSE St Hilda s is committed to providing a safe, healthy and supportive environment for all students. For students with diabetes, additional care must be taken to ensure
DIABETES MANAGEMENT POLICY 1. PURPOSE St Hilda s is committed to providing a safe, healthy and supportive environment for all students. For students with diabetes, additional care must be taken to ensure
DIABETES CARE TASKS AT SCHOOL: What Key Personnel Need to Know
 DIABETES CARE TASKS AT SCHOOL: What Key Personnel Need to Know HYPOGLYCEMIA Goal: Optimal Student Health and Learning Managing hypoglycemia is a vital piece of a comprehensive plan. 2 Learning Objectives
DIABETES CARE TASKS AT SCHOOL: What Key Personnel Need to Know HYPOGLYCEMIA Goal: Optimal Student Health and Learning Managing hypoglycemia is a vital piece of a comprehensive plan. 2 Learning Objectives
ZACHARY COMMUNITY SCHOOLS
 PARENTAL CONSENT/ RELEASE OF INFORMATION/ AND STUDENT WITH DIABETES CONTRACT Student s Name D.O.B. Parent/Guardian Home Phone # Work/Cell Phone # School Teacher Grade Physician Office # Fax # 1. I give
PARENTAL CONSENT/ RELEASE OF INFORMATION/ AND STUDENT WITH DIABETES CONTRACT Student s Name D.O.B. Parent/Guardian Home Phone # Work/Cell Phone # School Teacher Grade Physician Office # Fax # 1. I give
National Diabetes Inpatient Audit (NaDIA) 2016
 National Diabetes Inpatient Audit (NaDIA) 2016 DIABETES A summary report for people with diabetes and anyone interested in the quality of care for people with diabetes when they stay in hospital. Based
National Diabetes Inpatient Audit (NaDIA) 2016 DIABETES A summary report for people with diabetes and anyone interested in the quality of care for people with diabetes when they stay in hospital. Based
The most recent estimates suggest that. A study of inpatient diabetes care on medical wards. Saqib Javed, Yaser Javed, Kate Barnabas, Kalpana Kaushal
 A study of inpatient diabetes care on medical wards Saqib Javed, Yaser Javed, Kate Barnabas, Kalpana Kaushal Article points 1. It is well established that poor glycaemic control is associated with increased
A study of inpatient diabetes care on medical wards Saqib Javed, Yaser Javed, Kate Barnabas, Kalpana Kaushal Article points 1. It is well established that poor glycaemic control is associated with increased
special circumstances
 special circumstances circumstances circumstances circumstances circumstances Because so many factors affect your blood glucose, you need to be alert and flexible in how you take care of yourself. You
special circumstances circumstances circumstances circumstances circumstances Because so many factors affect your blood glucose, you need to be alert and flexible in how you take care of yourself. You
Hypoglycaemia in an inner-city accident
 Archives of Emergency Medicine, 1989, 6, 183-188 Hypoglycaemia in an inner-city accident and emergency department: a 12-month survey M. D. FEHER, P. GROUT, A. KENNEDY, R. S. ELKELES & R. TOUQUET Departments
Archives of Emergency Medicine, 1989, 6, 183-188 Hypoglycaemia in an inner-city accident and emergency department: a 12-month survey M. D. FEHER, P. GROUT, A. KENNEDY, R. S. ELKELES & R. TOUQUET Departments
DIABETES STRUCTURED EDUCATION IN WORCESTERSHIRE Information for Healthcare Professionals May 2011
 DIABETES STRUCTURED EDUCATION IN WORCESTERSHIRE Information for Healthcare Professionals May 2011 What is Structured Education? Diabetes Structured Education is referred to in the Diabetes NSF standards
DIABETES STRUCTURED EDUCATION IN WORCESTERSHIRE Information for Healthcare Professionals May 2011 What is Structured Education? Diabetes Structured Education is referred to in the Diabetes NSF standards
Elements for a Public Summary
 VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Schizophrenia Schizophrenia is a mental illness with a number of symptoms, including confused or unclear thinking and speech,
VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Schizophrenia Schizophrenia is a mental illness with a number of symptoms, including confused or unclear thinking and speech,
