Polypoidal choroidal vasculopathy and photodynamic therapy with verteporfin
|
|
|
- Tiffany Posy Short
- 6 years ago
- Views:
Transcription
1 Graefe s Arch Clin Exp Ophthalmol (2005) 243: CLINICAL INVESTIGATION DOI /s Rufino M. Silva João Figueira M. Luz Cachulo Liliane Duarte José R. Faria de Abreu J. G. Cunha-Vaz Polypoidal choroidal vasculopathy and photodynamic therapy with verteporfin Received: 14 August 2004 Revised: 23 December 2004 Accepted: 5 January 2005 Published online: 28 April 2005 # Springer-Verlag 2005 R. M. Silva (*). J. Figueira. M. L. Cachulo. L. Duarte. J. R. Faria de Abreu. J. G. Cunha-Vaz Department of Ophthalmology, University Hospital of Coimbra, Praceta Mota Pinto, 3000 Coimbra, Portugal rufino.silva@oftalmologia.co.pt Tel.: Fax: R. M. Silva. J. Figueira. M. L. Cachulo. L. Duarte. J. R. Faria de Abreu. J. G. Cunha-Vaz AIBILI Association for Innovation and Biomedical Research on Light and Image, Coimbra, Portugal J. G. Cunha-Vaz Centre of Ophthalmology, Institute of Biomedical Research on Light and Image, Faculty of Medicine, University of Coimbra, Coimbra, Portugal Abstract Background: We evaluated, in a nonrandomised, institutional, prospective study, the efficacy of photodynamic therapy (PDT) with verteporfin in age-related macular degeneration (AMD) eyes with polypoidal choroidal vasculopathy (PCV) and subfoveal exudation. Methods: A prospective clinical and angiographic study was done in 40 consecutive eyes with PCV treated with PDT using masked best-corrected visual acuity (VA) and fluorescein and indocyanine green angiographic features at baseline and over 2 years. Results: Twenty-one eyes completed 1-year follow-up and showed, after a mean 2.9 PDT sessions, VA improvement in 12 eyes, no change in five eyes, and VA decrease in four eyes. Leakage was absent at the retinal and choroidal level in 14 eyes at 1 year. Recurrence occurred in one eye during the first year. Six eyes completed 2 years of follow-up and showed, after a mean 4 PDT sessions, VA improvement in five eyes and VA decrease in one eye. Leakage was absent at the retinal and choroidal level in five eyes. Recurrence occurred in four of these six eyes during the second year of follow-up. No serious adverse events were observed during the 2 years of follow-up. Conclusions: PDT with verteporfin was shown to be safe and effective for treating AMD eyes with PCV with subfoveal involvement. VA improvement and absence of leakage were achieved, respectively, in 57.1% and 66.6% of the eyes at 1 year. Recurrences were more frequent during the second year of follow-up. Keywords Polypoidal choroidal vasculopathy. PDT. Photodynamic therapy. Laser treatment. AMD Introduction Polypoidal choroidal vasculopathy (PCV) has been described for the last two decades [8, 13]. In 1985, Stern and colleagues [8] referred to it as multiple recurrent serosanguinous retinal pigment epithelial detachments in black women. In 1990, Yannuzzi et al. [13] further described orange subretinal lesions as polypoidal dilations arising from the choroidal vascular network and proposed the name idiopathic polypoidal choroidal vasculopathy. Indocyanine green angiography (ICG) was pointed out as superior to fluorescein angiography (FA) for detecting and characterizing these lesions [3, 7, 12]. Actually, atypical cases of age-related macular degeneration (AMD), when reexamined with ICG angiography, have been found to be present in about 8 13% of white patients with clinical appearance of exudative AMD [2, 12]. The natural course of the disease is associated with chronic, multiple, recurrent serosanguinous detachments of the retinal pigment epithelium (RPE) and neurosensory retina, and long-term preservation of good vision is possible [10]. Photodynamic therapy (PDT) using verteporfin has been shown to be
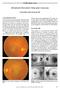
2 974 effective and safe in patients with subfoveal PCV [1, 6]. However, definitive clinical trials to establish the efficacy and safety of PDT in PCV are needed to confirm these observations. The purpose of this study was to evaluate, in a nonrandomised, institutional, prospective study, the efficacy and safety of PDT with Visudyne (verteporfin) in neovascular AMD eyes with PCV and subfoveal involvement. Materials and methods A prospective institutional study was performed in 40 consecutive eyes from 35 patients, 14 men and 21 women, with AMD and PCV who were treated with PDT with verteporfin between May 2000 and June Inclusion criteria included the following: (1) symptomatic macular PCV with subfoveal exudation on FA, (2) juxtafoveal, subfoveal, or extrafoveal active macular polypoidal lesions on ICG, (3) best-corrected initial visual acuity (VA) 20/40, (4) greatest linear dimension of active lesion 5,400 μm, (5) signs of AMD in the study eye. Exclusion criteria included the following: (1) previous treatment for PCV (such as laser photocoagulation), (2) other fundus diseases such as diabetic retinopathy, vasculitis, high myopia ( 6 diopters), vein or artery occlusion, epiretinal membrane, angioid streaks, juxtafoveal telangiectasias type 2, trauma, or intraocular infection or inflammation, (3) any systemic contraindication to verteporfin or angiographic dyes, (4) choroidal neovascularisation (CNV) secondary to other causes such as high myopia, pseudohistoplasmosis, or idiopathic, (5) RPE tear or ripping, (6) absence of signs of AMD in the study eye and fellow eye. The patients were observed at 3-month intervals. Clinical observation, fundoscopy, fundus photography, FA, ICG, and masked VA evaluation with Early Treatment Diabetic Retinopathy Study (ETDRS) charts were performed at each visit. PDT treatments or retreatments were applied in the presence of subfoveal juxta or extrafoveal active polypoidal lesions on ICG and subfoveal exudation on FA (Figs. 1, 2). Lesions were considered active in the presence of early and late hyperfluorescence on ICG and subfoveal leakage on FA. PDT treatments were performed within 3-month intervals using the standard protocols of the Treatment of Agerelated Macular Degeneration with Photodynamic Therapy (TAP) [9] and Verteporfin in Photodynamic Therapy (VIP) [11] trials, with a few modifications. The same light dose of 50 J/cm 2 and the same 3-month intervals between treatments were used. However, we chose to treat the lesion with the size visualised on ICG (largest diameter plus 1 mm). When more than one polypoidal vascular lesion was present and separated by more than 1 mm, two treatments with different spot sizes were used. Not all the haemorrhage area Fig. 1 Case 15. Color picture (a) and ICG (b) at baseline. Subfoveal polypoidal lesion on ICG and ring of lipid exudation on color picture. At 1 year and after one PDT treatment, almost complete reabsorption of lipid exudation is observed on color picture (c). FA shows late staining, and on ICG there is a complete regression of polyps (d and e). VA improved from 20/320 to 20/200.
3 975 Fig. 2 Case 4. Subfoveal polypoidal lesion with lipid exudation at baseline: a color picture, b early ICG, and c late ICG. One year later and after two PDT sessions, there was reabsorption of lipid exudation and complete regression of polypoidal subfoveal lesions (d color picture, e early ICG, f late ICG). VA improved from 20/400 to 20/250. was included in the area to be treated, unlike the standard protocols in TAP [9] and VIP [11]. In the presence of extensive haemorrhages, only 500 μm of the haemorrhage adjacent to the PCV visualised on ICG was included in the treatment spot. Retreatments were applied if ICG showed any juxtafoveal, extrafoveal, or subfoveal vascular polypoidal active lesion associated with subfoveal leakage on FA. We considered the recurrence of PCV to be present when an active ICG lesion and subfoveal FA leakage reappeared following at least two consecutive visits (3- month intervals) with no treatment (equaling a 9-month interval). All patients were older than 60 years of age at the time of diagnosis and presented with signs of AMD, including at least one intermediate drusen (between 63 and 125 μm) and focal areas of hyper- and/or hypopigmentation, and/or large drusens ( 125 μm). Only patients with 12 or more of follow-up were considered for the evaluation of results. The criteria for diagnosis of PCV are summarised in Table 1. The diagnosis was positive only in the presence of ICG features, and treatment was performed if an active lesion was evident and subfoveal leakage was observed on FA. In all cases, stereo color and red-free fundus photographs and stereo fluorescein and digital ICG angiograms were obtained with the Topcon ImageNet system. Images were reviewed by two independent reviewers (R.S., J.R.F. A.) at each 3-month interval and before any decision for treatment/no treatment/retreatment. Any disagreement was resolved by a third reviewer (J.G.C.V.). VA was tested by a masked observer using the ETDRS chart, and the best-corrected VA was obtained in all patients. The evolution of VA was classified into three groups: VA improvement (one or more lines), unchanged,
4 976 Table 1 Diagnosis criteria for PCV (RPE retinal pigment epithelium, CNV choroidal neovascularisation) Biomicroscopy and stereo red-free photography FA ICG Reddish-orange lesions Hypopigmentation of RPE Subretinal and sub-rpe haemorrhages Hard exudates Serosanguinous detachment of the RPE and neurosensory retina CNV Early and intermediate phases: dilated network of inner choroidal vessels with terminal hyperfluorescent aneurysm-like dilatations or polyps Late phases: two patterns (1) washout (nonleaking lesions), (2) hyperfluorescence (active lesions) and VA loss (less than three lines, with severe meaning loss of three or more lines). The study was approved by an internal review committee and conducted in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki. Each included patient signed an informed consent form after being instructed on the experimental character of the PDT treatment for PCV. Results Forty consecutive eyes of 35 patients, 21 women and 14 men, with an average age of 76.3±5 years (range 60 87) were enrolled in the study. These eyes represented 10% of all consecutive AMD eyes submitted to PDT between May 2000 and June Eighteen patients aged 75.6±7.6 years, nine men and nine women representing 21 eyes, completed 1 year of follow-up. PCV lesions were subfoveal in 20 eyes and juxtafoveal in one eye (case 8, Table 2). The mean number of PDT sessions was 2.9±0.9. VA improved in 12 eyes Table 2 Evolution of VA, number of PDT sessions, presence or absence of ICG active lesions and FA leakage (exudation), and recurrences at 12 and 24 (SD standard deviation) Initial VA 20/ VA 12 20/ No treat 12 Lines 12 VA 24 Lines 24 No treat 24 Clinical/ angiographic status 12 Clinical/ angiographic status at 24 Recurrences 1. AC No exudation 2. AC Exudation 3. AFS Exudation 4. ADS No exudation 5. CHC Exudation No exudation Recurrence 6. CHC Exudation No exudation Recurrence 7. EJ No exudation 8. ES No exudation No exudation Recurrence at 1 year 9. FPSD Exudation 10. FPSD No exudation 11. JSM No exudation 12. JNM No exudation 13. JP No exudation 14. JPF No exudation 15. MFN No exudation No exudation 16. MGB No exudation 17. MFB No exudation 18. MR Exudation 19. MIVC No exudation Exudation Recurrence 20. MJSF Exudation No exudation Recurrence 21. MRF No exudation Mean SD Range
5 977 (57.1%) and was unchanged in five eyes (23.8%). VA decreased in four eyes (19%) by less than three lines in one eye and by three lines in three eyes (Table 2). Mean initial VA acuity of these 21 eyes was 20/ (range 20/40 to 20/400), and mean final VA at 12 was 20/ (range 20/25 to 20/640). Leakage was absent at the retinal and choroidal level in 14 eyes (66.6%) at 1 year. Recurrence occurred in one eye during the first year (case 8, Table 2). The number of eyes with VA less than 20/200 decreased from six at time of enrollment to four at 1 year. The number of eyes with VA 20/50 increased from four to six during the same period. Six eyes completed 2 years of follow-up and showed, after 4±2.2 PDT sessions, VA improvement in five eyes (less than three lines) and VA decrease in one eye (one line). Mean initial VA acuity of these six eyes was 20/ (range 20/40 to 20/320), and mean VA at 24 was 20/63 2 (range 20/40 to 20/200). Recurrence occurred in four of these eyes during the second year of follow-up (Table 2). Leakage was absent at the retinal and choroidal level in five of these six eyes at 2 years. Severe subretinal and sub-rpe haemorrhage occurred in one eye (case 13) more than 1 month after the PDT session, causing significant VA loss and fibrosis. VA decrease occurred in three other eyes at 1 year (cases 7, 10, 17) and in another eye between the 18- and 24-month visits (case 6). Subfoveal fibrosis was responsible for VA decrease in cases 6 and 7, and subfoveal atrophy was related to VA decrease in cases 10 and 17. Baseline classification of the neovascular lesion of the study eye, using only FA, showed occult choroidal neovascularisation (OCNV) in all 21 eyes. ICG showed a dilated network of inner choroidal vessels with terminal hyperfluorescent aneurysm-like dilatations and/or polyps in all the cases. No significant side effects were observed during the study, including RPE ripping or tears, severe acute VA loss, development of secondary CNV, photosensitivity, low back pain, or catheter-induced complications. Discussion Our study evaluated the safety and efficacy of PDT with Visudyne in AMD eyes with juxtafoveal or subfoveal PCV on ICG and subfoveal exudation on FA. As far as we know, only a prospective study was published until now regarding PDT in PCV [1]. PCV is a relatively well-defined entity [2 4, 7, 8, 10, 12, 13]. In our study, all the eyes presented signs of AMD, and the diagnosis of PCV was based on clinical and angiographic features (Table 1). In the presence of recurrent serous-sanguineous subretinal and/or sub-rpe detachments, the diagnosis is evident. When only FA is performed, these exudative lesions are classified in most cases as occult without classic CNV. ICG shows a typical pattern of choroidal vessels with terminal hyperfluorescent aneurysm-like dilations or polyps in the early and/or intermediate phases. In late phases these lesions may become hypofluorescent due to a washout effect (inactive lesions), or they may remain hyperfluorescent-active lesions. All the cases we submitted to PDT with Visudyne presented juxtafoveal or subfoveal ICG-active lesions and exudation on FA, with VA loss due to these lesions. We found that PDT was effective and safe for treating PCV in AMD eyes in a series of 21 eyes at 1 year of follow-up. A total of 12 eyes (57.1%) showed some VA improvement at 1 year, with six eyes (28.5%) gaining three lines. The small group of six eyes with 2 years of follow-up showed VA improvement in 83.3% of cases (less than three lines) and VA loss in 16.6% of the eyes (one line). The higher final VA at 2 years when compared with the final VA at 12 is not a result of progressive VA improvement. In fact, these six eyes presented a higher initial VA, and three out of six had some VA decrease between 12 and 24. Recurrence of active lesions occurred in 4.7% of the eyes during the first year of follow-up and in 66.6% during the second year. The higher recurrence rate in eyes with longer follow-up was not followed by significant VA loss. In our series all patients were Caucasian. Females represented 50% of the patients with 1 year of follow-up and 60% of the 35 patients included in the study. This is in accordance with other series with predominantly white or black populations, in which 18 47% of the patients were male [5, 12]. Our study has one important limitation: It had no control group. If we consider FA classification, almost all of these eyes would have clinical indications for PDT (OCNV with small lesions and/or VA 20/50). A control group would not be ethically acceptable in these cases. The natural course of the disease is becoming progressively better understood. The disease has a remitting relapsing course and is associated clinically with chronic, multiple, recurrent serosanguinous detachments of the RPE and neurosensory retina. Long-term preservation of good vision can be obtained. Approximately half the patients with PCV lesions in the posterior pole may have a favourable course without treatment [10]. In the remaining half, the disorder may persist for a long time with occasional repeated bleeding and leakage, resulting in severe macular damage and VA loss. Eyes with a cluster of grapelike polypoidal dilations of the vessels may have a higher risk for severe visual loss [10]. Most of the series analysing the natural history of PCV describe lesions in the posterior pole, differentiating macular from extramacular and/or peripapillary polyps [1, 4, 5, 10, 12, 13]. Macular involvement ranged from 25% [12] to 94% [10]. The analysis of VA outcome must consider location of polyps. Kwok et al. [4] followed the natural history of nine eyes with macular involvement after a follow-up ranging from 5 to 60 and found VA improvement of two lines in
6 978 only one eye (11.1%), VA change of one line in one eye, and VA decrease of two lines in seven eyes (77.7%). Uyama et al. [10] followed 14 eyes with PCV (13 with macular involvement) for a mean period of 39.9 and described VA improvement of two lines in five eyes (35.7%) and VA decrease of two lines in four eyes (28.5%). In our series we only treated eyes with macular involvement and juxtafoveal or subfoveal lesions. Despite this, PDT treatment with Visudyne has shown better results at 1 year than natural history. VA stabilisation or improvement was achieved in 80.9% (gain of two lines in 47.6%), and VA loss of two lines was present in 19% of the eyes. Laser photocoagulation has been proposed for treating PCV lesions [4, 5, 10]. VA decrease of two lines has been shown to occur in 24 44% of the treated eyes with peripapillary and/or macular extrafoveal lesions [4, 5, 10]. Laser treatment of juxtafoveal or subfoveal lesions is not feasible and will promote immediate VA loss. PDT with Visudyne is an alternative. As far as we know, only a prospective study was published until now on PDT in PVC. Chan et al. [1] reported that from a group of 22 PCV eyes from 21 Asian patients (four extrafoveal, two juxtafoveal, and 16 subfoveal lesions) treated with a mean number of 1.6 PDT sessions, 21 (95%) had achieved a VA stabilisation or improvement at 1 year of follow-up. In 13 eyes (59%) there was a VA gain of two lines, and in 50% of the cases had a final VA of 20/50. Three of the four eyes with extrafoveal lesions showed an improvement of three lines, with a final VA of 20/50. Our results are not as impressive. However, there are some differences between the series regarding potential impact on VA prognosis. The presence of extrafoveal lesions is one of them and is responsible for 27% of the cases with a final VA of 20/50 and for 23% of the eyes with VA gain of two lines in the series of Chan etal. [1]. Other differences are related to race (all of our patients are Caucasian), AMD (all of them had signs of AMD in both eyes), and older age (mean of 75.6 years in our series vs. mean of 66.6 years in Chan et al. s series [1]). How these factors contribute is yet to be established. We have treated only AMD patients with juxtafoveal or subfoveal PCV active lesions. Only one eye presented a juxtafoveal lesion, and its behaviour was apparently similar to subfoveal lesions, with the exception of being the only one with a recurrence in the first year of follow-up. Most patients with evidence of PCV in one eye eventually develop similar lesions in the fellow eye [2]. We found bilateral PCV in 14.3% of the patients. However, 31.4% of the 35 patients presented disciform scar in the contralateral eye. The nature of the neovascular lesion originating the disciform scar was impossible to establish at that point. A PCV origin could not be ruled out in these cases. The selection of the spot size for PDT may be a controversial issue. The ICG hot spots would probably indicate the size of the lesions to be treated. As other authors have done [1], we chose to treat the lesion with the size visualised on ICG (largest diameter plus 1 mm). Leakage was absent at the retinal and choroidal level in 66.6% and 83.3% of the treated eyes at 12 and 24, respectively (Table 3). The number of treatments necessary to close the PCV lesion was widely variable (range of one to six over 24 ). The mean number of treatments was 1.9 and four at 12 and 24, respectively. These numbers are lower than the number of PDT sessions necessary to treat predominantly classic, OCNV, or minimally classic lesions [9, 11]. However, they are higher than those shown by Chan et al. [1]. One of the characteristics of PCV is the existence of recurrent subretinal and sub-rpe serosanguinous detachment. During follow-up, recurrence of exudation occurred in one eye up to 12 and in four of the six eyes during the second year of follow-up. The longer the follow-up, the higher the probability of recurrence. More cases with longer follow-up times are necessary to evaluate the recurrence rate in PCV eyes treated with PDT. How PDT affects recurrence rate is yet to be determined. VA decrease was not related to recurrence rate. In conclusion, PDT with verteporfin is effective and safe for treating active PCV lesions with subfoveal exudation. VA improvement and absence of leakage at 1 year occurred, respectively, in 57.1% and 66.6% of the eyes. The longer the follow-up, the greater the probability of recurrence. Table 3 VA change, absence of leakage, and number of treatments at 12 and 24 Followup (N=) 12 (N=21) 24 (N=6) VA improvement 12 eyes (57.1%) <3 lines: 6 eyes (28.5%) =3 lines: 6 eyes (28.5%) 5 eyes (83.3%) <3 lines: 83.3% VA no change VA decrease % Absence of leakage 5 eyes 23.8% 4 eyes 14 eyes (66.6%) 1 2 lines: 1 eye (4.7%) =3 lines: 3 eyes (14.2%) 0 1 eye 5 eyes (16.6%) (83.3%) <3 lines: 16.6% No treatments: SD (range) 2.9±0.9 (1 4) 4±2.2 (1 6)
7 979 References 1. Chan WM, Lam DSC, Lai TYY, Liu DTL, Li KKW, Yao Y, Wong TH (2004) Photodynamic therapy with verteprofin for symptomatic polypoidal choroidal vasculopathy. Ophthalmology 111: Ciardella AP, Donsoff IM, Huang SJ, Costa DL, Yannuzzi LA (2004) Polypoidal choroidal vasculopathy. Surv Ophthalmol 49: Guyer DR, Yannuzzi LA, Slakter JS, Sorenson JA, Hope-Ross M, Orlock DR (1994) Digital indocyanine-green video angiography of occult choroidal neovascularisation. Ophthalmology 101: Kwok AK, Lay TY, Chan CW, et al. (2002) Polypoidal choroidal vasculopathy in Chinese patients. Br J Ophthalmol 86: Lafaut BA, Leys AM, Snyers B, et al. (2000) Polypoidal choroidal vasculopathy in Caucasians. Graefes Arch Cin Exp Ophthalmol 238: Quaranta M, Maget-Faysse M, Coscas G (2002) Exudative idiopathic polypoidal choroidal vasculopathy and photodynamic therapy with verteporfin. Am J Ophthalmol 134: Spaide RF, Yannuzzi LA, Slakter JS, Sorenson J, Orlach DA (1995) Indocyanine green videoangiography of idiopathic polypoidal horoidal vasculopathy. Retina 15: Stern RM, Zakov N, Zegarra H, Gutman FA (1985) Multiple recurrent serosanguinous retinal pigment epithelial detachments in black women. Am J Ophthalmol 100: Bresller NM, Treatment of Age-related Macular Degeneration with Photodynamic Therapy (TAP) Study Group (2001) Photodynamic therapy of subfoveal choroidal neovascularisation in age-related macular degeneration with verteporfin. Two-year results of 2 randomized clinical trials TAP report 2. Arch Ophthalmol 119: Uyama M, Wada M, Nagai Y, Matsubara T, Matsunaga H, Fukushima I, Takahashi K, Matsumura M (2002) Polypoidal choroidal vasculopathy: natural history. Am J Ophthalmol 133: Verteporfin in Photodynamic Therapy Study Group (2001) Verteporfin therapy of subfoveal choroidal neovascularisation in age-related macular degeneration: two-year results of a randomized clinical trial including lesions with occult with no classic choroidal neovascularization Verteporfin in Photodynamic Therapy Report 2. Am J Ophthalmol 131: Yannuzzi LA, Ciardella A, Spaide RF, Rabb M, Freund KB, Orlock DA (1997) The expanding clinical spectrum of idiopathic polypoidal choroidal vasculopathy. Arch Ophthalmol 115: Yannuzzi LA, Sorenson J, Spaide RF, Lipson B (1990) Idiopathic polypoidal choroidal vasculopathy (IPCV). Retina 10:1 8
Stabilization of visual acuity with photodynamic therapy in eyes with chorioretinal anastomoses
 Graefe s Arch Clin Exp Ophthalmol (2004) 242:368 376 CLINICAL INVESTIGATION DOI 10.1007/s00417-003-0844-0 Rufino M. Silva José R. Faria de Abreu António Travassos José G. Cunha-Vaz Stabilization of visual
Graefe s Arch Clin Exp Ophthalmol (2004) 242:368 376 CLINICAL INVESTIGATION DOI 10.1007/s00417-003-0844-0 Rufino M. Silva José R. Faria de Abreu António Travassos José G. Cunha-Vaz Stabilization of visual
연령연관황반변성에서망막혈관종성증식과동반된망막색소상피박리의임상양상과일차적인광역학치료의결과
 연령연관황반변성에서망막혈관종성증식과동반된망막색소상피박리의임상양상과일차적인광역학치료의결과 40 Table. Clinical characteristics and results of patients undergoing photodynamic therapy for retinal angiomatous proliferation Patients No. Age/ sex Eye
연령연관황반변성에서망막혈관종성증식과동반된망막색소상피박리의임상양상과일차적인광역학치료의결과 40 Table. Clinical characteristics and results of patients undergoing photodynamic therapy for retinal angiomatous proliferation Patients No. Age/ sex Eye
Authors. Introduction. Introduction. Materials and Methods. Objective 10/27/2015
 Idiopathic Polypoidal Choroidal Vasculopathy (IPCV) in Thai Population Presenting with Choroidal Neovascularization (CNV) A multicenter study Authors Yonrawee Piyacomn 1, Chavakij Bhoomibunchoo 1, Yosanan
Idiopathic Polypoidal Choroidal Vasculopathy (IPCV) in Thai Population Presenting with Choroidal Neovascularization (CNV) A multicenter study Authors Yonrawee Piyacomn 1, Chavakij Bhoomibunchoo 1, Yosanan
CENTRAL SEROUS CHORIORETINOPATHY (CSC) IS
 Association Between the Efficacy of Half-Dose Photodynamic Therapy With Indocyanine Green Angiography and Optical Coherence Tomography Findings in the Treatment of Central Serous Chorioretinopathy MASSIMO
Association Between the Efficacy of Half-Dose Photodynamic Therapy With Indocyanine Green Angiography and Optical Coherence Tomography Findings in the Treatment of Central Serous Chorioretinopathy MASSIMO
The Natural History of Occult Choroidal Neovascularisation Associated With Age-related Macular Degeneration. A Systematic Review
 Review Article 145 The Natural History of Occult Choroidal Neovascularisation Associated With Age-related Macular Degeneration. A Systematic Review Antonio Polito, 1 MD, Miriam Isola, 2 MHS, Paolo Lanzetta,
Review Article 145 The Natural History of Occult Choroidal Neovascularisation Associated With Age-related Macular Degeneration. A Systematic Review Antonio Polito, 1 MD, Miriam Isola, 2 MHS, Paolo Lanzetta,
Fluorescein Angiography
 Last revision: October 2011 by Luis Arias Fluorescein Angiography Authors: Luis Arias, MD Hospital Universitari de Bellvitge - University of Barcelona. Spain Jordi Monés, MD Institut de la Màcula i de
Last revision: October 2011 by Luis Arias Fluorescein Angiography Authors: Luis Arias, MD Hospital Universitari de Bellvitge - University of Barcelona. Spain Jordi Monés, MD Institut de la Màcula i de
P olypoidal choroidal vasculopathy (PCV), first described
 602 EXTENDED REPORT The origins of polypoidal choroidal vasculopathy M Yuzawa, R Mori, A Kawamura... Br J Ophthalmol 2005;89:602 607. doi: 10.1136/bjo.2004.049296 See end of article for authors affiliations...
602 EXTENDED REPORT The origins of polypoidal choroidal vasculopathy M Yuzawa, R Mori, A Kawamura... Br J Ophthalmol 2005;89:602 607. doi: 10.1136/bjo.2004.049296 See end of article for authors affiliations...
Department of Ophthalmology, Kangnam Sacred Heart Hospital, College of Medicine, Hallym University, Seoul, Korea
 Department of Ophthalmology, Kangnam Sacred Heart Hospital, College of Medicine, Hallym University, Seoul, Korea Purpose: To investigate the factors that affect final vision following photodynamic therapy
Department of Ophthalmology, Kangnam Sacred Heart Hospital, College of Medicine, Hallym University, Seoul, Korea Purpose: To investigate the factors that affect final vision following photodynamic therapy
Current indications for photodynamic therapy in medical retina practice
 réalités Current indications for photodynamic therapy in medical retina practice No. 254 September 2018 OPHTALMOLOGIQUES SUMMARY: In medical retina practice, the use of photodynamic therapy (PDT) revolutionised
réalités Current indications for photodynamic therapy in medical retina practice No. 254 September 2018 OPHTALMOLOGIQUES SUMMARY: In medical retina practice, the use of photodynamic therapy (PDT) revolutionised
MONTHLY ADMINISTERED INTRAVITREOUS PHARmacotherapy
 Polypoidal Choroidal Vasculopathy Masquerading as Neovascular Age-Related Macular Degeneration Refractory to Ranibizumab ALEXANDROS N. STANGOS, JAGDEEP SINGH GANDHI, JAYASHREE NAIR-SAHNI, HEINRICH HEIMANN,
Polypoidal Choroidal Vasculopathy Masquerading as Neovascular Age-Related Macular Degeneration Refractory to Ranibizumab ALEXANDROS N. STANGOS, JAGDEEP SINGH GANDHI, JAYASHREE NAIR-SAHNI, HEINRICH HEIMANN,
Eye (2014) 28, & 2014 Macmillan Publishers Limited All rights reserved X/14 M Ho, ECF Lo, AL Young and DTL Liu
 (2014) 28, 1469 1476 & 2014 Macmillan Publishers Limited All rights reserved 0950-222X/14 www.nature.com/eye Outcome of polypoidal choroidal vasculopathy at 1 year by combined therapy of photodynamic therapy
(2014) 28, 1469 1476 & 2014 Macmillan Publishers Limited All rights reserved 0950-222X/14 www.nature.com/eye Outcome of polypoidal choroidal vasculopathy at 1 year by combined therapy of photodynamic therapy
Department of Ophthalmology, University Hospital of Santiago de Compostela, Ramon Baltar S/N, Santiago de Compostela, Spain 2
 Case Reports in Medicine Volume 2012, Article ID 897097, 10 pages doi:10.1155/2012/897097 Case Report Verteporfin Photodynamic Therapy Combined with Intravitreal Ranibizumab for Polypoidal Choroidal Vasculopathy
Case Reports in Medicine Volume 2012, Article ID 897097, 10 pages doi:10.1155/2012/897097 Case Report Verteporfin Photodynamic Therapy Combined with Intravitreal Ranibizumab for Polypoidal Choroidal Vasculopathy
Despite our growing knowledge of the
 OVERVIEW OF AVAILABLE TREATMENTS FOR NEOVASCULAR AGE-RELATED MACULAR DEGENERATION * Carl D. Regillo, MD ABSTRACT Although potential treatments for neovascular age-related macular degeneration represent
OVERVIEW OF AVAILABLE TREATMENTS FOR NEOVASCULAR AGE-RELATED MACULAR DEGENERATION * Carl D. Regillo, MD ABSTRACT Although potential treatments for neovascular age-related macular degeneration represent
Retina Conference. Janelle Fassbender, MD, PhD University of Louisville Department of Ophthalmology and Visual Sciences 09/04/2014
 Retina Conference Janelle Fassbender, MD, PhD University of Louisville Department of Ophthalmology and Visual Sciences 09/04/2014 Subjective CC/HPI: 64 year old Caucasian female referred by outside ophthalmologist
Retina Conference Janelle Fassbender, MD, PhD University of Louisville Department of Ophthalmology and Visual Sciences 09/04/2014 Subjective CC/HPI: 64 year old Caucasian female referred by outside ophthalmologist
Photodynamic therapy (PDT) for Central Serous Retinopathy (CSR)/ Polypoidal Choroidal Vasculopathy (PCV)
 Photodynamic therapy (PDT) for Central Serous Retinopathy (CSR)/ Polypoidal Choroidal Vasculopathy (PCV) About photodynamic therapy for Retinal Conditions The macula is the central part of the retina at
Photodynamic therapy (PDT) for Central Serous Retinopathy (CSR)/ Polypoidal Choroidal Vasculopathy (PCV) About photodynamic therapy for Retinal Conditions The macula is the central part of the retina at
VERTEPORFIN IN PHOTODYNAMIC THERAPY STUDY GROUP
 Verteporfin Therapy of Subfoveal Choroidal Neovascularization in Age-related Macular Degeneration: Two-year Results of a Randomized Clinical Trial Including Lesions With Occult With No Classic Choroidal
Verteporfin Therapy of Subfoveal Choroidal Neovascularization in Age-related Macular Degeneration: Two-year Results of a Randomized Clinical Trial Including Lesions With Occult With No Classic Choroidal
Evaluation of efficacy of eplerenone in the management of chronic central serous choroidoretinopathy
 Original article: Evaluation of efficacy of eplerenone in the management of chronic central serous choroidoretinopathy Dr. Sushant Madaan* Department of Ophthalmology, NIMS Medical College and Hopsital,Jaipur,
Original article: Evaluation of efficacy of eplerenone in the management of chronic central serous choroidoretinopathy Dr. Sushant Madaan* Department of Ophthalmology, NIMS Medical College and Hopsital,Jaipur,
Clinical Characteristics of Polypoidal Choroidal Vasculopathy Associated with Chronic Central Serous Chorioretionopathy
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(1):15-20 http://dx.doi.org/10.3341/kjo.2012.26.1.15 Original Article Clinical Characteristics of Polypoidal Choroidal Vasculopathy Associated
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(1):15-20 http://dx.doi.org/10.3341/kjo.2012.26.1.15 Original Article Clinical Characteristics of Polypoidal Choroidal Vasculopathy Associated
Principal Investigator: Mårten Brelen, Assistant Professor Department of Ophthalmology & Visual Sciences (DOVS), CUHK
 RESEARCH PROTOCOL Title: Subthreshold micropulse yellow (577 nm) laser versus half-dose photodynamic therapy for central serous chorioretinopathy : a randomized controlled pilot study Principal Investigator:
RESEARCH PROTOCOL Title: Subthreshold micropulse yellow (577 nm) laser versus half-dose photodynamic therapy for central serous chorioretinopathy : a randomized controlled pilot study Principal Investigator:
Key words: Choroidal neovascularisation, Laser coagulation, Retinal imaging
 420 Mini Review The Role of Optical Coherence Tomography (OCT) in the Diagnosis and Management of Retinal Angiomatous Proliferation (RAP) in Patients with Age-related Macular Degeneration Antonio Polito,
420 Mini Review The Role of Optical Coherence Tomography (OCT) in the Diagnosis and Management of Retinal Angiomatous Proliferation (RAP) in Patients with Age-related Macular Degeneration Antonio Polito,
Vitreous haemorrhage in massive hemorrhagic polypoidal choroidal vasculopathy: clinical characteristics and surgical outcomes
 DOI 10.1186/s40942-015-0025-4 International Journal of Retina and Vitreous ORIGINAL ARTICLE Open Access Vitreous haemorrhage in massive hemorrhagic polypoidal choroidal vasculopathy: clinical characteristics
DOI 10.1186/s40942-015-0025-4 International Journal of Retina and Vitreous ORIGINAL ARTICLE Open Access Vitreous haemorrhage in massive hemorrhagic polypoidal choroidal vasculopathy: clinical characteristics
CLINICAL SCIENCES. Verteporfin Therapy for Subfoveal Choroidal Neovascularization in Age-Related Macular Degeneration
 CLINICAL SCIENCES Verteporfin Therapy for Subfoveal Choroidal Neovascularization in Age-Related Macular Degeneration Three-Year Results of an Open-Label Extension of 2 Randomized Clinical Trials TAP Report
CLINICAL SCIENCES Verteporfin Therapy for Subfoveal Choroidal Neovascularization in Age-Related Macular Degeneration Three-Year Results of an Open-Label Extension of 2 Randomized Clinical Trials TAP Report
Photodynamic Therapy for Treatment of Subfoveal Choroidal Neovascularization in Exudative Age-Related Macular Degeneration
 Clinical Medicine Journal Vol. 4, No. 4, 2018, pp. 60-66 http://www.aiscience.org/journal/cmj ISSN: 2381-7631 (Print); ISSN: 2381-764X (Online) Photodynamic Therapy for Treatment of Subfoveal Choroidal
Clinical Medicine Journal Vol. 4, No. 4, 2018, pp. 60-66 http://www.aiscience.org/journal/cmj ISSN: 2381-7631 (Print); ISSN: 2381-764X (Online) Photodynamic Therapy for Treatment of Subfoveal Choroidal
Abstract Aims To analyse the histopathology of classic and occult choroidal neovascular membrane surgical specimens in age
 Br J Ophthalmol 2000;84:239 243 239 ORIGINAL ARTICLES Clinical science Clinicopathological correlation in exudative age related macular degeneration: histological diverentiation between classic and occult
Br J Ophthalmol 2000;84:239 243 239 ORIGINAL ARTICLES Clinical science Clinicopathological correlation in exudative age related macular degeneration: histological diverentiation between classic and occult
World Sight Day Case Studies. Mark Frost Screening Manager South East London DESP
 World Sight Day 2015 Case Studies Mark Frost Screening Manager South East London DESP Introduction All of the following cases have been identified in our screening programme over the last 3 years. The
World Sight Day 2015 Case Studies Mark Frost Screening Manager South East London DESP Introduction All of the following cases have been identified in our screening programme over the last 3 years. The
MEDICAL POLICY SUBJECT: PHOTODYNAMIC THERAPY FOR EFFECTIVE DATE: 07/20/00 SUBFOVEAL CHOROIDAL NEOVASCULARIZATION
 MEDICAL POLICY SUBJECT: PHOTODYNAMIC THERAPY FOR PAGE: 1 OF: 8 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: PHOTODYNAMIC THERAPY FOR PAGE: 1 OF: 8 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
Retinal pigment epithelial detachments in the elderly:
 British Journal of Ophthalmology, 1985, 69, 397-403 Retinal pigment epithelial detachments in the elderly: classification and outcome A G CASSWELL, D KOHEN, AND A C BIRD From Moorfields Eye Hospital, City
British Journal of Ophthalmology, 1985, 69, 397-403 Retinal pigment epithelial detachments in the elderly: classification and outcome A G CASSWELL, D KOHEN, AND A C BIRD From Moorfields Eye Hospital, City
POLYPOIDAL CHOROIDAL VASCULOPATHY, DIAGNOSIS AND MANAGEMENT
 GENERAL REVIEW POLYPOIDAL CHOROIDAL VASCULOPATHY, DIAGNOSIS AND MANAGEMENT COPPENS G., SPIELBERG L., LEYS A. ABSTRACT Polypoidal Choroidal Vasculopathy (PCV) was first identified in 1985. Initially considered
GENERAL REVIEW POLYPOIDAL CHOROIDAL VASCULOPATHY, DIAGNOSIS AND MANAGEMENT COPPENS G., SPIELBERG L., LEYS A. ABSTRACT Polypoidal Choroidal Vasculopathy (PCV) was first identified in 1985. Initially considered
Retinal Pigment Epithelial Tears (Rips) in the ERA of Anti Vegf - When and Why?
 Original Article Retinal Pigment Epithelial Tears (Rips) in the ERA of Anti Vegf - When and Why? Dr Sreelekha S. MS, DNB, DO, FRCS, Dr Manoj Soman DNB, FICO, FRCS, Dr. Unni Nair MS, FRCS, Dr. Ruminder
Original Article Retinal Pigment Epithelial Tears (Rips) in the ERA of Anti Vegf - When and Why? Dr Sreelekha S. MS, DNB, DO, FRCS, Dr Manoj Soman DNB, FICO, FRCS, Dr. Unni Nair MS, FRCS, Dr. Ruminder
Spontaneous Large Serous Retinal Pigment Epithelial Tear
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Clinical Trials Related to Age Related Macular Degeneration
 Clinical Trials Related to Age Related Macular Degeneration Kirti Singh MD, DNB, FRCS Kirti Singh MD, DNB, FRCS, Pooja Jain MBBS, Nitasha Ahir MBBS, Divya Jain MD, DNB Guru Nanak Eye Centre, Maulana Azad
Clinical Trials Related to Age Related Macular Degeneration Kirti Singh MD, DNB, FRCS Kirti Singh MD, DNB, FRCS, Pooja Jain MBBS, Nitasha Ahir MBBS, Divya Jain MD, DNB Guru Nanak Eye Centre, Maulana Azad
Bilateral Elevated Macular Lesions
 Challenging Case Bilateral Elevated Macular Lesions Section Editor: Alireza Ramezani, MD Case presentation A 65-year-old woman presented with decreased vision in both eyes of 2 months duration. She reported
Challenging Case Bilateral Elevated Macular Lesions Section Editor: Alireza Ramezani, MD Case presentation A 65-year-old woman presented with decreased vision in both eyes of 2 months duration. She reported
DOME SHAPED MACULOPATHY. Ιωάννης Ν. Βαγγελόπουλος Χειρ. Οφθαλμίατρος - Βόλος
 DOME SHAPED MACULOPATHY Ιωάννης Ν. Βαγγελόπουλος Χειρ. Οφθαλμίατρος - Βόλος DOME SHAPED MACULOPATHY-DEFINITIONS The entity Dome Shaped Macula ( DSM ) was first described by Gaucher and associates in 2008
DOME SHAPED MACULOPATHY Ιωάννης Ν. Βαγγελόπουλος Χειρ. Οφθαλμίατρος - Βόλος DOME SHAPED MACULOPATHY-DEFINITIONS The entity Dome Shaped Macula ( DSM ) was first described by Gaucher and associates in 2008
Ophthalmology Macular Pathways
 Ophthalmology Macular Pathways Age related Macular Degeneration Diabetic Macular Oedema Macular Oedema secondary to Central Retinal Macular Oedema secondary to Branch Retinal CNV associated with pathological
Ophthalmology Macular Pathways Age related Macular Degeneration Diabetic Macular Oedema Macular Oedema secondary to Central Retinal Macular Oedema secondary to Branch Retinal CNV associated with pathological
Fluorescein and Indocyanine Green Videoangiography of Choroidal Melanomas
 luorescein and Indocyanine Green Videoangiography of Choroidal Melanomas Leyla S. Atmaca, igen Batioğlu and Pelin Atmaca Eye Clinic, Ankara University Medical School, Ankara, Turkey Purpose: This study
luorescein and Indocyanine Green Videoangiography of Choroidal Melanomas Leyla S. Atmaca, igen Batioğlu and Pelin Atmaca Eye Clinic, Ankara University Medical School, Ankara, Turkey Purpose: This study
The limited number of currently approved
 CLINICAL TRIALS OF VERTEPORFIN AND PEGAPTANIB: WHAT ARE THE RESULTS? * William F. Mieler, MD ABSTRACT Currently available treatment options for the management of choroidal neovascularization (CNV) in age-related
CLINICAL TRIALS OF VERTEPORFIN AND PEGAPTANIB: WHAT ARE THE RESULTS? * William F. Mieler, MD ABSTRACT Currently available treatment options for the management of choroidal neovascularization (CNV) in age-related
Indocyanine Green Angiography Findings in Central Serous Chorioretinopathy
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. III (May. 2016), PP 11-21 www.iosrjournals.org Indocyanine Green Angiography Findings
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. III (May. 2016), PP 11-21 www.iosrjournals.org Indocyanine Green Angiography Findings
Long-term Management of AMD. Motasem Al-latayfeh, MD Assistant Prof. Ophthalmology Hashemite University Jordan
 Long-term Management of AMD Motasem Al-latayfeh, MD Assistant Prof. Ophthalmology Hashemite University Jordan DEFINITION 1 Age-related macular degeneration (AMD) is a disorder of the macula characterized
Long-term Management of AMD Motasem Al-latayfeh, MD Assistant Prof. Ophthalmology Hashemite University Jordan DEFINITION 1 Age-related macular degeneration (AMD) is a disorder of the macula characterized
AGE-RELATED MACULAR DEGENERATION IS THE LEADing
 Photodynamic Therapy for Age-related Macular Degeneration in a Clinical Setting: Visual Results and Angiographic Patterns RUTH AXER-SIEGEL, MD, RITA EHRLICH, MD, YUVAL YASSUR, MD, IRIT ROSENBLATT, MD,
Photodynamic Therapy for Age-related Macular Degeneration in a Clinical Setting: Visual Results and Angiographic Patterns RUTH AXER-SIEGEL, MD, RITA EHRLICH, MD, YUVAL YASSUR, MD, IRIT ROSENBLATT, MD,
ZEISS AngioPlex OCT Angiography. Clinical Case Reports
 Clinical Case Reports Proliferative Diabetic Retinopathy (PDR) Case Report 969 PROLIFERATIVE DIABETIC RETINOPATHY 1 1-year-old diabetic female presents for follow-up of proliferative diabetic retinopathy
Clinical Case Reports Proliferative Diabetic Retinopathy (PDR) Case Report 969 PROLIFERATIVE DIABETIC RETINOPATHY 1 1-year-old diabetic female presents for follow-up of proliferative diabetic retinopathy
IQ 532 Micropulse Green Laser treatment for Refractory Chronic Central Serous Retinopathy
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Report IQ 532 Micropulse Green Laser treatment for Refractory Chronic Central Serous Retinopathy Fawwaz Al Mamoori* Medical Retina Department, Eye Specialty Hospital,
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Report IQ 532 Micropulse Green Laser treatment for Refractory Chronic Central Serous Retinopathy Fawwaz Al Mamoori* Medical Retina Department, Eye Specialty Hospital,
Photodynamic Therapy for Choroidal Neovascularization
 Photodynamic Therapy for Choroidal Neovascularization Policy Number: 9.03.08 Last Review: 10/2014 Origination: 10/2000 Next Review: 10/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will
Photodynamic Therapy for Choroidal Neovascularization Policy Number: 9.03.08 Last Review: 10/2014 Origination: 10/2000 Next Review: 10/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will
SUMMARY. Heather Casparis, MD,* and Neil M. Bressler, MD MARINA AND ANCHOR
 The following are summaries of selected presentations and posters from the American Society of Retina Specialists and European VitreoRetinal Society Annual Meeting held September 9 13, 2006, in Cannes,
The following are summaries of selected presentations and posters from the American Society of Retina Specialists and European VitreoRetinal Society Annual Meeting held September 9 13, 2006, in Cannes,
Original Policy Date
 MP 9.03.08 Photocoagulation of Macular Drusen Medical Policy Section Miscellaneous Policies Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return
MP 9.03.08 Photocoagulation of Macular Drusen Medical Policy Section Miscellaneous Policies Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return
Age Related Macular Degeneration - An Overview Ajay Kapoor MS, Nishank Mittal MBBS, MS, Fel.(V.R.), Ankur Gupta MBBS, DNB,Fel.(V.R.
 MEDICAL OPHTHALMOLOGY Age Related Macular Degeneration - An Overview Ajay Kapoor MS, Nishank Mittal MBBS, MS, Fel.(V.R.), Ankur Gupta MBBS, DNB,Fel.(V.R.) Age related macular degeneration (AMD) is one
MEDICAL OPHTHALMOLOGY Age Related Macular Degeneration - An Overview Ajay Kapoor MS, Nishank Mittal MBBS, MS, Fel.(V.R.), Ankur Gupta MBBS, DNB,Fel.(V.R.) Age related macular degeneration (AMD) is one
! Honoraria. " Kemin " Nicox " Review of Optometry " Optometric Management " VSP. ! Scientific Advisory Boards
 Financial Disclosure: JP Choroid Chronicles Joseph J. Pizzimenti, OD, FAAO pizzimen@nova.edu! Honoraria " Kemin " Nicox " Review of Optometry " Optometric Management " VSP! Scientific Advisory Boards "
Financial Disclosure: JP Choroid Chronicles Joseph J. Pizzimenti, OD, FAAO pizzimen@nova.edu! Honoraria " Kemin " Nicox " Review of Optometry " Optometric Management " VSP! Scientific Advisory Boards "
FEP Medical Policy Manual
 FEP Medical Policy Manual Last Review: September 2016 Next Review: September 2017 Related Policies 9.03.20 Intraocular Radiation Therapy for Age-Related Macular Degeneration Photodynamic Therapy for Choroidal
FEP Medical Policy Manual Last Review: September 2016 Next Review: September 2017 Related Policies 9.03.20 Intraocular Radiation Therapy for Age-Related Macular Degeneration Photodynamic Therapy for Choroidal
I n the Western world, age related macular degeneration
 207 SCIENTIFIC REPORT Clinicopathological findings of choroidal neovascularisation following verteporfin photodynamic therapy F Gelisken, B A Lafaut, W Inhoffen, M Voelker, S Grisanti, K U Bartz-Schmidt...
207 SCIENTIFIC REPORT Clinicopathological findings of choroidal neovascularisation following verteporfin photodynamic therapy F Gelisken, B A Lafaut, W Inhoffen, M Voelker, S Grisanti, K U Bartz-Schmidt...
NATURAL COURSE OF PATIENTS DISCONTINUING TREATMENT FOR AGE-RELATED MACULAR DEGENERATION AND FACTORS ASSOCIATED WITH VISUAL PROGNOSIS
 NATURAL COURSE OF PATIENTS DISCONTINUING TREATMENT FOR AGE-RELATED MACULAR DEGENERATION AND FACTORS ASSOCIATED WITH VISUAL PROGNOSIS JAE HUI KIM, MD,* YOUNG SUK CHANG, MD, JONG WOO KIM, MD* Purpose: To
NATURAL COURSE OF PATIENTS DISCONTINUING TREATMENT FOR AGE-RELATED MACULAR DEGENERATION AND FACTORS ASSOCIATED WITH VISUAL PROGNOSIS JAE HUI KIM, MD,* YOUNG SUK CHANG, MD, JONG WOO KIM, MD* Purpose: To
I diopathic central serous (chorio)retinopathy (CSR) is a
 1483 EXTENDED REPORT Evaluation of central serous retinopathy with en face optical coherence tomography M E J van Velthoven, F D Verbraak, P M Garcia, R O Schlingemann, R B Rosen, M D de Smet... See end
1483 EXTENDED REPORT Evaluation of central serous retinopathy with en face optical coherence tomography M E J van Velthoven, F D Verbraak, P M Garcia, R O Schlingemann, R B Rosen, M D de Smet... See end
Description. Section: Other Effective Date: July 15, Subsection: Vision Original Policy Date: December 7, 2011 Subject: Page: 1 of 23
 Last Review Status/Date: June 2015 Page: 1 of 23 Description Photodynamic therapy (PDT) is a treatment modality designed to selectively occlude ocular choroidal neovascular tissue. The therapy is a 2-step
Last Review Status/Date: June 2015 Page: 1 of 23 Description Photodynamic therapy (PDT) is a treatment modality designed to selectively occlude ocular choroidal neovascular tissue. The therapy is a 2-step
Therapeutic Effect of Diode Laser Photodynamic Therapy with ICG Dye in ARMD: A Case Report
 Therapeutic Effect of Diode Laser Photodynamic Therapy with ICG Dye in ARMD: A Case Report Chang Kyoon Yoon, MD, Seung Eun Kyoung, MD, Moo Hwan Chang, MD Department of Ophthalmology, Dankook University
Therapeutic Effect of Diode Laser Photodynamic Therapy with ICG Dye in ARMD: A Case Report Chang Kyoon Yoon, MD, Seung Eun Kyoung, MD, Moo Hwan Chang, MD Department of Ophthalmology, Dankook University
CASE STUDIES CURRENT AND FUTURE TREATMENT OPTIONS FOR NEOVASCULAR AGE-RELATED MACULAR DEGENERATION * Discussion led by Neil M.
 CURRENT AND FUTURE TREATMENT OPTIONS FOR NEOVASCULAR AGE-RELATED MACULAR DEGENERATION * Discussion led by Neil M. Bressler, MD Dr Bressler: The overview articles in this monograph summarize safety, efficacy,
CURRENT AND FUTURE TREATMENT OPTIONS FOR NEOVASCULAR AGE-RELATED MACULAR DEGENERATION * Discussion led by Neil M. Bressler, MD Dr Bressler: The overview articles in this monograph summarize safety, efficacy,
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Multivariate Analysis of Intravitreal Injection of Anti-VEGF Bevacizumab in the Treatment
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Multivariate Analysis of Intravitreal Injection of Anti-VEGF Bevacizumab in the Treatment
Although photocoagulation and photodynamic PROCEEDINGS PEGAPTANIB SODIUM FOR THE TREATMENT OF AGE-RELATED MACULAR DEGENERATION *
 PEGAPTANIB SODIUM FOR THE TREATMENT OF AGE-RELATED MACULAR DEGENERATION Evangelos S. Gragoudas, MD ABSTRACT In December 24, the US Food and Drug Administration (FDA) approved pegaptanib sodium. Pegaptanib
PEGAPTANIB SODIUM FOR THE TREATMENT OF AGE-RELATED MACULAR DEGENERATION Evangelos S. Gragoudas, MD ABSTRACT In December 24, the US Food and Drug Administration (FDA) approved pegaptanib sodium. Pegaptanib
Polypoidal Choroidal Vasculopathy with Feeder Vessels: Characteristics, Fellow Eye Findings, and Long-term Treatment Outcomes
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(3):230-239 https://doi.org/10.3341/kjo.2016.0035 Original Article Polypoidal Choroidal Vasculopathy with Feeder Vessels: Characteristics, Fellow
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(3):230-239 https://doi.org/10.3341/kjo.2016.0035 Original Article Polypoidal Choroidal Vasculopathy with Feeder Vessels: Characteristics, Fellow
FEEDER VESSEL TREATMENT
 THERAPEUTIC OPTIONS FOR NEOVASCULAR AGE-RELATED MACULAR DEGENERATION * Discussion led by Donald J. D'Amico, MD Dr D Amico: The overview articles in this monograph highlight findings from clinical trials
THERAPEUTIC OPTIONS FOR NEOVASCULAR AGE-RELATED MACULAR DEGENERATION * Discussion led by Donald J. D'Amico, MD Dr D Amico: The overview articles in this monograph highlight findings from clinical trials
Transpupillary thermotherapy (TTT) for the treatment of choroidal neovascularisation
 Br J Ophthalmol 2001;85:173 178 173 King s College Hospital, Denmark Hill, London SE5 9RS, UK R S B Newsom J C McAlister M Saeed J D A McHugh Correspondence to: Mr R S B Newsom, Department of Vitreoretinal
Br J Ophthalmol 2001;85:173 178 173 King s College Hospital, Denmark Hill, London SE5 9RS, UK R S B Newsom J C McAlister M Saeed J D A McHugh Correspondence to: Mr R S B Newsom, Department of Vitreoretinal
High-dose antioxidants for central serous chorioretinopathy; The randomized placebo-controlled study
 Ratanasukon et al. BMC Ophthalmology 2012, 12:20 RESEARCH ARTICLE Open Access High-dose antioxidants for central serous chorioretinopathy; The randomized placebo-controlled study Mansing Ratanasukon *,
Ratanasukon et al. BMC Ophthalmology 2012, 12:20 RESEARCH ARTICLE Open Access High-dose antioxidants for central serous chorioretinopathy; The randomized placebo-controlled study Mansing Ratanasukon *,
CENTENE PHARMACY AND THERAPEUTICS NEW DRUG REVIEW 2Q17 April May
 BRAND NAME Lucentis GENERIC NAME ranibizumab MANUFACTURER Genentech, Inc. DATE OF APPROVAL June 30, 2006 PRODUCT LAUNCH DATE July 13, 2006 REVIEW TYPE Review type 1 (RT1): New Drug Review Full review of
BRAND NAME Lucentis GENERIC NAME ranibizumab MANUFACTURER Genentech, Inc. DATE OF APPROVAL June 30, 2006 PRODUCT LAUNCH DATE July 13, 2006 REVIEW TYPE Review type 1 (RT1): New Drug Review Full review of
Efficacy of Anti-VEGF Agents in the Treatment of Age-Related Macular Degeneration
 Efficacy of Anti-VEGF Agents in the Treatment of Age-Related Macular Degeneration Marilita M. Moschos Abstract- Purpose: To evaluate by OCT and mf-erg the macular function in eyes with CNV due to ARMD
Efficacy of Anti-VEGF Agents in the Treatment of Age-Related Macular Degeneration Marilita M. Moschos Abstract- Purpose: To evaluate by OCT and mf-erg the macular function in eyes with CNV due to ARMD
Ocular perfusion pressure and choroidal thickness in eyes with polypoidal choroidal vasculopathy, wet-age-related macular degeneration, and normals
 (2013) 27, 1038 1043 & 2013 Macmillan Publishers Limited All rights reserved 0950-222X/13 www.nature.com/eye CLINICAL STUDY Ocular perfusion pressure and choroidal thickness in eyes with polypoidal choroidal
(2013) 27, 1038 1043 & 2013 Macmillan Publishers Limited All rights reserved 0950-222X/13 www.nature.com/eye CLINICAL STUDY Ocular perfusion pressure and choroidal thickness in eyes with polypoidal choroidal
CLINICAL SCIENCES. Leopard-Spot Pattern of Yellowish Subretinal Deposits in Central Serous Chorioretinopathy
 CLINICAL SCIENCES Leopard-Spot Pattern of Yellowish Subretinal Deposits in Central Serous Chorioretinopathy Tomohiro Iida, MD; Richard F. Spaide, MD; Anton Haas, MD; Lawrence A. Yannuzzi, MD; Lee M. Jampol,
CLINICAL SCIENCES Leopard-Spot Pattern of Yellowish Subretinal Deposits in Central Serous Chorioretinopathy Tomohiro Iida, MD; Richard F. Spaide, MD; Anton Haas, MD; Lawrence A. Yannuzzi, MD; Lee M. Jampol,
Supplementary Online Content
 Supplementary Online Content Koh A, Lai TYY, Takahashi K, et al; the EVEREST II Study Group. Efficacy and safety of ranibizumab with or without verteporfin photodynamic therapy for polypoidal choroidal
Supplementary Online Content Koh A, Lai TYY, Takahashi K, et al; the EVEREST II Study Group. Efficacy and safety of ranibizumab with or without verteporfin photodynamic therapy for polypoidal choroidal
Clinical Policy Title: Ocular photodynamic therapy (OPDT) with Visudyne (verteporfin) for macular degeneration treatment
 Clinical Policy Title: Ocular photodynamic therapy (OPDT) with Visudyne (verteporfin) for macular degeneration treatment Clinical Policy Number: 10.02.04 Effective Date: January 1, 2016 Initial Review
Clinical Policy Title: Ocular photodynamic therapy (OPDT) with Visudyne (verteporfin) for macular degeneration treatment Clinical Policy Number: 10.02.04 Effective Date: January 1, 2016 Initial Review
Since /01/2014 Private practice Ophthalmology, Retinal Medical Specialty and AMD, private office
 Corinne GONZALEZ Ophthalmology (MD, Ph.D ) Retinal Medical Specialist SELARL CABINET DOCTEUR GONZALEZ 27, Boulevard des Minimes 31 200 Toulouse! 05 34 40 77 30 e-mail : cabinet.dr.gonzalez@wanadoo.fr Fax
Corinne GONZALEZ Ophthalmology (MD, Ph.D ) Retinal Medical Specialist SELARL CABINET DOCTEUR GONZALEZ 27, Boulevard des Minimes 31 200 Toulouse! 05 34 40 77 30 e-mail : cabinet.dr.gonzalez@wanadoo.fr Fax
Retinal Pigment Epithelial Detachment
 SURVEY OF OPHTHALMOLOGY VOLUME 52 NUMBER 3 MAY JUNE 2007 MAJOR REVIEW Retinal Pigment Epithelial Detachment Shiri Zayit-Soudry, MD, 1,3 Iris Moroz, MD, 2,3 and Anat Loewenstein, MD 1,3 1 Department of
SURVEY OF OPHTHALMOLOGY VOLUME 52 NUMBER 3 MAY JUNE 2007 MAJOR REVIEW Retinal Pigment Epithelial Detachment Shiri Zayit-Soudry, MD, 1,3 Iris Moroz, MD, 2,3 and Anat Loewenstein, MD 1,3 1 Department of
Characteristics and racial variations of polypoidal choroidal vasculopathy in tertiary centers in the United States and United Kingdom
 DOI 10.1186/s40942-017-0060-4 International Journal of Retina and Vitreous ORIGINAL ARTICLE Open Access Characteristics and racial variations of polypoidal choroidal vasculopathy in tertiary centers in
DOI 10.1186/s40942-017-0060-4 International Journal of Retina and Vitreous ORIGINAL ARTICLE Open Access Characteristics and racial variations of polypoidal choroidal vasculopathy in tertiary centers in
Comparative Study of Experimental Choroidal Neovascularization by Optical Coherence Tomography and Histopathology
 Comparative Study of Experimental Choroidal Neovascularization by Optical Coherence Tomography and Histopathology Toshio Fukuchi, Kanji Takahashi, Masanobu Uyama and Miyo Matsumura Department of Ophthalmology,
Comparative Study of Experimental Choroidal Neovascularization by Optical Coherence Tomography and Histopathology Toshio Fukuchi, Kanji Takahashi, Masanobu Uyama and Miyo Matsumura Department of Ophthalmology,
Fundus autofluorescence in exudative age-related macular degeneration
 Fundus autofluorescence in exudative age-related macular degeneration Q. Peng*, Y. Dong* and P.Q. Zhao Department of Ophthalmology, Xinhua Hospital Affiliated to Shanghai JiaoTong University School of
Fundus autofluorescence in exudative age-related macular degeneration Q. Peng*, Y. Dong* and P.Q. Zhao Department of Ophthalmology, Xinhua Hospital Affiliated to Shanghai JiaoTong University School of
Nonvisible subthreshold micropulse diode laser (810 nm) treatment of central serous chorioretinopathy: A pilot study
 European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 934-940 Nonvisible subthreshold micropulse diode laser (810 nm) treatment of central serous chorioretinopathy: A pilot study P. LANZETTA, F.
European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 934-940 Nonvisible subthreshold micropulse diode laser (810 nm) treatment of central serous chorioretinopathy: A pilot study P. LANZETTA, F.
Photodynamic Therapy (PDT) for agerelated
 Page 1 of 5 Photodynamic Therapy (PDT) for agerelated eye conditions Introduction This leaflet gives you information about Photodynamic Therapy (PDT) for the age--related eye conditions macular degeneration
Page 1 of 5 Photodynamic Therapy (PDT) for agerelated eye conditions Introduction This leaflet gives you information about Photodynamic Therapy (PDT) for the age--related eye conditions macular degeneration
Photodynamic therapy. in the treatment of subfoveal choroidal neovascu larisation
 Photodynamic therapy SIMON HARDING in the treatment of subfoveal choroidal neovascu larisation Abstract Sub foveal choroidal neovascularisation (CNV) is a major cause of visual disability, with agerelated
Photodynamic therapy SIMON HARDING in the treatment of subfoveal choroidal neovascu larisation Abstract Sub foveal choroidal neovascularisation (CNV) is a major cause of visual disability, with agerelated
CLINICAL SCIENCES. Treatment of Retinal Angiomatous Proliferation in Age-Related Macular Degeneration
 CLINICAL SCIENCES Treatment of Retinal Angiomatous Proliferation in Age-Related Macular Degeneration A Series of 104 Cases of Retinal Angiomatous Proliferation Ferdinando Bottoni, MD; Amedeo Massacesi,
CLINICAL SCIENCES Treatment of Retinal Angiomatous Proliferation in Age-Related Macular Degeneration A Series of 104 Cases of Retinal Angiomatous Proliferation Ferdinando Bottoni, MD; Amedeo Massacesi,
Transpupillary thermotherapy for central serous chorioretinopathy
 VOL. 32 NO. PHILIPPINE JOURNAL O Ophthalmology JANUARY CASE REPORT JUNE 2007 Harvey S. Uy, D, 2 arlah Angela. Salvosa, D 2 Pik Sha Chan, D Pearl T. Villalon, D 2 Asian Eye Institute akati, Philippines
VOL. 32 NO. PHILIPPINE JOURNAL O Ophthalmology JANUARY CASE REPORT JUNE 2007 Harvey S. Uy, D, 2 arlah Angela. Salvosa, D 2 Pik Sha Chan, D Pearl T. Villalon, D 2 Asian Eye Institute akati, Philippines
Corinne GONZALEZ Ophthalmology (MD, Ph.D ) Retinal Medical Specialist
 Corinne GONZALEZ Ophthalmology (MD, Ph.D ) Retinal Medical Specialist PRESENT PROFESSIONAL POSITION OPHTALMOLOGIST DOCTOR, Private practice Retinal medical Specialist, DMLA in particular Installation year
Corinne GONZALEZ Ophthalmology (MD, Ph.D ) Retinal Medical Specialist PRESENT PROFESSIONAL POSITION OPHTALMOLOGIST DOCTOR, Private practice Retinal medical Specialist, DMLA in particular Installation year
R&M Solutions
 Mohamed Hosny El-Bradey, MD., Assistant Professor of Ophthalmology, Tanta University. Wael El Haig, MD., Professor of Ophthalmology. Zagazeeg University. 1 Myopic CNV is considered the most common vision
Mohamed Hosny El-Bradey, MD., Assistant Professor of Ophthalmology, Tanta University. Wael El Haig, MD., Professor of Ophthalmology. Zagazeeg University. 1 Myopic CNV is considered the most common vision
Complete regression of branching vascular network in polypoidal choroidal vasculopathy by ranibizumab and photodynamic therapy, two case reports
 Iesato et al. BMC Ophthalmology (2018) 18:284 https://doi.org/10.1186/s12886-018-0952-6 CASE REPORT Open Access Complete regression of branching vascular network in polypoidal choroidal vasculopathy by
Iesato et al. BMC Ophthalmology (2018) 18:284 https://doi.org/10.1186/s12886-018-0952-6 CASE REPORT Open Access Complete regression of branching vascular network in polypoidal choroidal vasculopathy by
F luorescence angiography (FL-A) with fluorescein (FL)
 1609 EXTENDED REPORT Lower limits of fluorescein and indocyanine green dye for digital cslo fluorescence angiography A Bindewald, O Stuhrmann, F Roth, S Schmitz-Valckenberg, H-M Helb, A Wegener, N Eter,
1609 EXTENDED REPORT Lower limits of fluorescein and indocyanine green dye for digital cslo fluorescence angiography A Bindewald, O Stuhrmann, F Roth, S Schmitz-Valckenberg, H-M Helb, A Wegener, N Eter,
Thinking Beyond Wet Age-Related Macular Degeneration
 Ophthalmic Deliberations ISSN 0972-0200 Thinking Beyond Wet Age-Related Macular Degeneration Neha Goel, Atul Kumar, Mahesh P Shanmugam, Muna Bhende, Raja Narayanan, Hidetaka Matsumoto Atul Kumar MD, FAMS
Ophthalmic Deliberations ISSN 0972-0200 Thinking Beyond Wet Age-Related Macular Degeneration Neha Goel, Atul Kumar, Mahesh P Shanmugam, Muna Bhende, Raja Narayanan, Hidetaka Matsumoto Atul Kumar MD, FAMS
Optical Coherence Tomography in Diabetic Retinopathy. Mrs Samantha Mann Consultant Ophthalmologist Clinical Lead of SEL-DESP
 Optical Coherence Tomography in Diabetic Retinopathy Mrs Samantha Mann Consultant Ophthalmologist Clinical Lead of SEL-DESP Content OCT imaging Retinal layers OCT features in Diabetes Some NON DR features
Optical Coherence Tomography in Diabetic Retinopathy Mrs Samantha Mann Consultant Ophthalmologist Clinical Lead of SEL-DESP Content OCT imaging Retinal layers OCT features in Diabetes Some NON DR features
S ubfoveal fibrovascular membranes can lead to a loss of
 809 SCIENTIFIC REPORT Expression of pigment epithelium derived factor and vascular endothelial growth factor in choroidal neovascular membranes and polypoidal choroidal vasculopathy M Matsuoka, N Ogata,
809 SCIENTIFIC REPORT Expression of pigment epithelium derived factor and vascular endothelial growth factor in choroidal neovascular membranes and polypoidal choroidal vasculopathy M Matsuoka, N Ogata,
Retinal pigment epithelial atrophy over polypoidal choroidal vasculopathy lesions during ranibizumab monotherapy
 Hikichi et al. BMC Ophthalmology (2016) 16:55 DOI 10.1186/s12886-016-0237-x RESEARCH ARTICLE Retinal pigment epithelial atrophy over polypoidal choroidal vasculopathy lesions during ranibizumab monotherapy
Hikichi et al. BMC Ophthalmology (2016) 16:55 DOI 10.1186/s12886-016-0237-x RESEARCH ARTICLE Retinal pigment epithelial atrophy over polypoidal choroidal vasculopathy lesions during ranibizumab monotherapy
Disease-Specific Fluorescein Angiography
 Ruth E. Picchiottino, CRA Disease-Specific Fluorescein Angiography 15 Disease-Specific Fluorescein Angiography Recommendations for tailoring retinal fluorescein angiography to diabetic retinopathy, macular
Ruth E. Picchiottino, CRA Disease-Specific Fluorescein Angiography 15 Disease-Specific Fluorescein Angiography Recommendations for tailoring retinal fluorescein angiography to diabetic retinopathy, macular
for anti-vegf therapy
 Review Article Singapore Med J 2011, 52(4) 232 Eye and Retina Surgeons, Camden Medical Centre, 1 Orchard Boulevard, Singapore 248649 Koh A, MBBS, MMed, FAMS Ong SG, FRCSE, FRCOphth, FAMS Ophthalmic Surgeon,
Review Article Singapore Med J 2011, 52(4) 232 Eye and Retina Surgeons, Camden Medical Centre, 1 Orchard Boulevard, Singapore 248649 Koh A, MBBS, MMed, FAMS Ong SG, FRCSE, FRCOphth, FAMS Ophthalmic Surgeon,
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
Michael P. Blair, MD Retina Consultants, Ltd Libertyville/Des Plaines, Illinois Clinical Associate University of Chicago 17 October 2015
 Michael P. Blair, MD Retina Consultants, Ltd Libertyville/Des Plaines, Illinois Clinical Associate University of Chicago 17 October 2015 So What Parts of the Eye Retina are Affected by VHL Neural tissue
Michael P. Blair, MD Retina Consultants, Ltd Libertyville/Des Plaines, Illinois Clinical Associate University of Chicago 17 October 2015 So What Parts of the Eye Retina are Affected by VHL Neural tissue
Photocoagulation of disciform macular lesions
 British Journal of Ophthalmology, 1979, 63, 669-673 Photocoagulation of disciform macular lesions with krypton laser A. C. BIRD AND R. H. B. GREY From the Institute of Ophthalmology, Moorfields Eye Hospital,
British Journal of Ophthalmology, 1979, 63, 669-673 Photocoagulation of disciform macular lesions with krypton laser A. C. BIRD AND R. H. B. GREY From the Institute of Ophthalmology, Moorfields Eye Hospital,
Risk factors of a reduced response to ranibizumab treatment for neovascular age-related macular degeneration evaluation in a clinical setting
 Korb et al. BMC Ophthalmology 2013, 13:84 RESEARCH ARTICLE Open Access Risk factors of a reduced response to ranibizumab treatment for neovascular age-related macular degeneration evaluation in a clinical
Korb et al. BMC Ophthalmology 2013, 13:84 RESEARCH ARTICLE Open Access Risk factors of a reduced response to ranibizumab treatment for neovascular age-related macular degeneration evaluation in a clinical
Opinion 4 December 2013
 The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 4 December 2013 LUCENTIS 10 mg/ml, solution for injection Vial of 0.23 ml (CIP: 34009 378 101 5 9) Applicant: Novartis
The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 4 December 2013 LUCENTIS 10 mg/ml, solution for injection Vial of 0.23 ml (CIP: 34009 378 101 5 9) Applicant: Novartis
CLINICAL SCIENCES. Visual Outcomes Following Macular Translocation With 360 Peripheral Retinectomy
 CLINICAL SCIENCES Visual Outcomes Following Macular Translocation With 360 Peripheral Retinectomy James C. Lai, MD; Deborah J. Lapolice, MS; Sandra S. Stinnett, DrPH; Carsten H. Meyer, MD; Luz M. Arieu,
CLINICAL SCIENCES Visual Outcomes Following Macular Translocation With 360 Peripheral Retinectomy James C. Lai, MD; Deborah J. Lapolice, MS; Sandra S. Stinnett, DrPH; Carsten H. Meyer, MD; Luz M. Arieu,
The legally binding text is the original French version
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 12 September 2007 INFRACYANINE 25 mg/10 ml, powder and solvent for solution for injection 25 mg vial with one 10 ml
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 12 September 2007 INFRACYANINE 25 mg/10 ml, powder and solvent for solution for injection 25 mg vial with one 10 ml
Original Article Intravitreal injections of ranibizumab in treatment of idiopathic choroidal neovascularization
 Int J Clin Exp Med 2016;9(2):3780-3784 www.ijcem.com /ISSN:1940-5901/IJCEM0017597 Original Article Intravitreal injections of ranibizumab in treatment of idiopathic choroidal neovascularization Donghua
Int J Clin Exp Med 2016;9(2):3780-3784 www.ijcem.com /ISSN:1940-5901/IJCEM0017597 Original Article Intravitreal injections of ranibizumab in treatment of idiopathic choroidal neovascularization Donghua
Comparison of Indocyanine Green and Fluorescein Angiography of Choroidal Neovascularization
 ELSEVIER Comparison of Indocyanine Green and Fluorescein Angiography of Choroidal Neovascularization Ichiro Fukushima, Kanae Kusaka, Kanji Takahashi, Naoko Kishimoto, Tetsuya Nishimura, Hiroshi Ohkuma
ELSEVIER Comparison of Indocyanine Green and Fluorescein Angiography of Choroidal Neovascularization Ichiro Fukushima, Kanae Kusaka, Kanji Takahashi, Naoko Kishimoto, Tetsuya Nishimura, Hiroshi Ohkuma
Intraocular Radiation Therapy for Age-Related Macular Degeneration
 Medical Policy Manual Medicine, Policy No. 134 Intraocular Radiation Therapy for Age-Related Macular Degeneration Next Review: April 2019 Last Review: June 2018 Effective: August 1, 2018 IMPORTANT REMINDER
Medical Policy Manual Medicine, Policy No. 134 Intraocular Radiation Therapy for Age-Related Macular Degeneration Next Review: April 2019 Last Review: June 2018 Effective: August 1, 2018 IMPORTANT REMINDER
A Comparative Study of Age Related Macular Degeneration In Relation To SD-OCTand Fundus Photography.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 11 Ver. III (Nov. 2015), PP 33-37 www.iosrjournals.org A Comparative Study of Age Related Macular
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 11 Ver. III (Nov. 2015), PP 33-37 www.iosrjournals.org A Comparative Study of Age Related Macular
Indocyanine Green Angiographic Findings of Chorioretinal Folds
 Indocyanine Green Angiographic Findings of Chorioretinal Folds Miho Haruyama, Mitsuko Yuzawa, Akiyuki Kawamura, Chikayo Yamazaki and Youko Matsumoto Department of Ophthalmology, Nihon University School
Indocyanine Green Angiographic Findings of Chorioretinal Folds Miho Haruyama, Mitsuko Yuzawa, Akiyuki Kawamura, Chikayo Yamazaki and Youko Matsumoto Department of Ophthalmology, Nihon University School
Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
 Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
The College of Optometrists - Learning outcomes for the Professional Certificate in Medical Retina
 Learning outcomes for the Professional Certificate in Medical Retina, incorporating diabetic retinopathy screening and age related macular degeneration The professional certificate is a prerequisite to
Learning outcomes for the Professional Certificate in Medical Retina, incorporating diabetic retinopathy screening and age related macular degeneration The professional certificate is a prerequisite to
