Duration of participation in continuous quality improvement: a key factor explaining improved delivery of Type 2 diabetes services
|
|
|
- Arnold Cunningham
- 6 years ago
- Views:
Transcription
1 Matthews et al. BMC Health Services Research 2014, 14:578 RESEARCH ARTICLE Open Access Duration of participation in continuous quality improvement: a key factor explaining improved delivery of Type 2 diabetes services Veronica Matthews 1*, Gill Schierhout 1, James McBroom 2, Christine Connors 3, Catherine Kennedy 4, Ru Kwedza 5, Sarah Larkins 6, Elizabeth Moore 7, Sandra Thompson 8, David Scrimgeour 9 and Ross Bailie 1 Abstract Background: It is generally recognised that continuous quality improvement (CQI) programs support development of high quality primary health care systems. However, there is limited evidence demonstrating their system-wide effectiveness. We examined variation in quality of Type 2 diabetes service delivery in over 100 Aboriginal and Torres Strait Islander primary health care centres participating in a wide-scale CQI project over the past decade, and determined the influence of health centre and patient level factors on quality of care, with specific attention to health centre duration of participation in a CQI program. Methods: We analysed over 10,000 clinical audit records to assess quality of Type 2 diabetes care of patients in 132 Aboriginal and Torres Strait Islander community health centres in five states/territories participating in the ABCD project for varying periods between 2005 and Process indicators of quality of care for each patient were calculated by determining the proportion of recommended guideline scheduled services that were documented as delivered. Multilevel regression models were used to quantify the amount of variation in Type 2 diabetes service delivery attributable to health centre or patient level factors and to identify those factors associated with greater adherence to best practice guidelines. Results: Health centre factors that were independently associated with adherence to best practice guidelines included longer participation in the CQI program, remoteness of health centres, and regularity of client attendance. Significantly associated patient level variables included greater age, and number of co-morbidities and disease complications. Health centre factors explained 37% of the differences in level of service delivery between jurisdictions with patient factors explaining only a further 1%. Conclusions: At the health centre level, Type 2 diabetes service delivery could be improved through long term commitment to CQI, encouraging regular attendance (for example, through patient reminder systems) and improved recording and coordination of patient care in the complex service provider environments that are characteristic of non-remote areas. Keywords: Quality improvement, Aboriginal & Torres Strait Islander populations, Type 2 diabetes mellitus, Primary health care, Variation in care * Correspondence: veronica.matthews@menzies.edu.au 1 Menzies School of Health Research, Brisbane, Queensland, Australia Full list of author information is available at the end of the article 2014 Matthews et al.; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly credited. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Matthews et al. BMC Health Services Research 2014, 14:578 Page 2 of 12 Background The international diabetes epidemic is expected to escalate over coming decades placing increasing economic and social pressures on health systems and communities [1-3]. In addition, socio-economic and ethnic inequities have been identified in provision of diabetes care [4]. Social determinants and lack of access to quality primary health care (PHC) services are important contributors to the inequity in health outcomes between Aboriginal and Torres Strait Islander communities and the Australian non-indigenous population. Over the past decade, there has been a significant increase in prevalence of diabetes in the Aboriginal and Torres Strait Islander population and they are now three times more likely to have diabetes compared to the non-indigenous Australian population [5]. Along with targeted prevention strategies, improvements in chronic disease care are necessary to reduce inequity, advance population health outcomes and lessen the burden on health care systems. Evidence indicates that improvements in quality of care and health outcomes can be achieved using integrated care frameworks and multifaceted improvement strategies targeting changes at all levels of the health system [6-9]. However, the effectiveness of local and large scale quality improvement approaches in health care remains uncertain with published studies showing considerable variation in levels of improvements achieved [10,11]. Australian Aboriginal and Torres Strait Islander primary health care setting There are a number of service sectors providing primary health care to Aboriginal and Torres Strait Islander communities. In recognition of the need for culturally appropriate care, Aboriginal and Torres Strait Islander community-controlled health services were developed over 40 years ago, employing a comprehensive care model with local Aboriginal and Torres Strait Islander participation and control in guiding, planning and delivery of services. The success of the community-controlled sector has led other health care providers to adopt community participatory processes in health service design, including a State and Territory government operated community health centre predominantly servicing an Indigenous community [12]. Both of these sectors are represented in metropolitan, remote and very remote locations across Australia. One21seventy/ABCD CQI program Over the past decade, a wide scale continuous quality improvement (CQI) program operating in both Aboriginal and Torres Strait Islander community controlled and government centres has included a focus on Type 2 diabetes. The Audit and Best Practice for Chronic Disease (ABCD) project employs a systems approach to improving PHC delivery utilising evidence-based clinical audit and system assessment tools to enable health centres to assess and reflect on system performance [13,14]. Typically, health centres conduct audits on an annual basis choosing from a suite of tools covering various aspects of PHC (including Type 2 diabetes, chronic kidney disease, coronary heart disease, maternal and child health, preventive health and mental health). A not-for-profit service agency, One21- seventy, develops and maintains evidence-based audit and systems assessment tools, provides online data services for automated reporting, benchmarking and interpretation, and training and site support for conducting audits according to standard protocols. Over 100 health centres using the One21seventy/ABCD tools have voluntarily provided their de-identified audit data to the ABCD National Research Partnership for analysis of variation in PHC service delivery. The aim of this study is to examine trends in the quality of Type 2 diabetes processes of care over time for participating health centres and identify the influence of regional, health centre, and individual patient level factors on delivery of services scheduled in current guidelines. Specifically, the analysis aimed to explore whether or not health centre duration of participation in the ABCD CQI program was associated with improvements in Type 2 diabetes service delivery. Methods Study context and design Table 1 shows completion rates of Type 2 diabetes audits by year of commencement in the project. Coinciding with stepped phases of research and geographical extensions of the project, a large number of health centres joined the program in 2006 (n = 41) and 2011 (n = 40). Participation in annual Type 2 diabetes audits is driven by health centre decision processes based on local priorities. As such, not all health centres completed Type 2 Table 1 Health centre participation in Type 2 diabetes audits by year of commencement First year of participation Completed baseline only Completed 1 2 cycles Completed 3 cycles Total n (%) n (%) n (%) (5) 11 (27) 28 (68) (20) 3 (30) 5 (50) (11) 3 (33) 5 (56) (0) 2 (22) 7 (78) (25) 9 (75) (33) 27 (68) (100) 11 Total 32 (24) 55 (42) 45 (34) 132
3 Matthews et al. BMC Health Services Research 2014, 14:578 Page 3 of 12 diabetes audits in consecutive years and CQI activity may have focussed on other clinical areas in-between diabetes audit cycles. This retrospective longitudinal study used Type 2 diabetes audit data to examine changes in quality of care over time and explore factors underlying variation in care delivery. Data collection Clinical audit records from 132 Aboriginal and Torres Strait Islander community health centres in five states/ territories participating in the ABCD project between 2005 and 2012 were analysed to assess quality of Type 2 diabetes care of patients. Clinical audits are generally completed by health centre staff trained in the use of One21seventy/ABCD tools and supported by quality improvement facilitators and/or One21seventy staff. The Type 2 diabetes audit tool was developed by an expert working group, with participation of chronic illness experts and health service staff from a number of jurisdictions across Australia. The tool is designed to enable services to assess their actual practice against best practice standards, and is accompanied by a protocol that includes reference to the guidelines that form the basis of the tool. Inter-rater validation tests were carried out as part of pilot testing. One21seventy/ABCD tools and protocols are regularly reviewed by expert reference groups to ensure continued alignment with best practice standards. Audit data are collected manually by health centres and directly entered into the One21seventy online database system. The criteria for inclusion in a Type 2 diabetes audit includes patients who: have a diagnosis of Type 2 diabetes; are aged 16 years or older; and have lived within community for six months or more in the last year. Where the eligible population is 30 or less, the audit protocol recommends that all eligible records at that health centre are audited. For 30 or more eligible clients, the protocol recommends and provides guidance for health centres to draw a sufficient number of records to achieve a precision of 90% or 95% confidence of the sample representing the population [15]. This sampling approach resulted in a total sample of 10,674 records available for analysis in this study. Ethics approval was obtained from research ethics committees in each jurisdiction (Human Research Ethics Committee of the Northern Territory Department of Health and Menzies School of Health Research (HREC- EC00153); Central Australian Human Research Ethics Committee (HREC-12-53); New South Wales Greater Western Area Health Service Human Research Committee (HREC/11/GWAHS/23); Queensland Human Research Ethics Committee Darling Downs Health Services District (HREC/11/QTDD/47); South Australian Aboriginal Health Research Ethics Committee ( ); Curtin University Human Research Ethics Committee (HR140/2008); Western Australian Country Health Services Research Ethics Committee (2011/27); Western Australia Aboriginal Health Information and Ethics Committee (111-8/05); University of Western Australia Human Research Ethics Committee (RA/4/1/5051)). Data analysis To assess Type 2 diabetes service delivery, the study measured 15 items from best practice guidelines used across the states and territories. The service items included laboratory investigations (albumin creatinine ratio, estimated glomerular filtration rate, full lipid profile and glycosylated haemoglobin), physical checks (weight, waist circumference, body mass index, blood pressure, visual acuity, dilated eye check, foot check) and counselling for certain risk factors (nutrition, physical activity, tobacco and alcohol use). Process of care performance for each patient was calculated by determining the proportion of services received out of the 15 scheduled services. A mean adherence to delivery of Type 2 diabetes services in a given health centre represented an overall performance score for the health centre in a given audit cycle. Each aggregate score was converted into a binary outcome variable that categorised higher performance as being within the top quartile of delivery across all health centres measured at baseline (greater than 76% service delivery). Health centre characteristics included length of participation in ABCD CQI, regularity of client attendance, size of service population, governance (community-controlled or government operated) and location based on the Australian Standard Geographical Classification (AGSC) system (very remote, remote or nonremote). For statistical analysis, rates of patient attendance were calculated based on the proportion of patients that did not attend in the previous six months prior to audit. A binary outcome variable was created that categorised a health centre as having lower regular attendance if more than 3% of patients did not attend within the previous six months. Patient level characteristics (sex, age, Indigenous status) were extracted from clinical records. Documented chronic health conditions (diabetes, hypertension, chronic heart disease and chronic kidney disease) were recorded as present or absent and co-morbidities were calculated by summing the recorded presence of each condition. Similarly, documented complications (retinopathy, neuropathy, foot ulcers and amputations) were recorded as present or absent and number of complications was calculated per individual. Multilevel mixed effects logistic regression models were used to quantify the variation in Type 2 diabetes service delivery attributable to health centre or patient level factors, allowing for the hierarchical structure of
4 Matthews et al. BMC Health Services Research 2014, 14:578 Page 4 of 12 the data (patients nested within health centres nested within jurisdictions). Crude odds ratios were calculated to measure the unadjusted association between the outcome and predictor variables. Non-significant variables were excluded from further analysis. Potential interactions were checked for significance. We adopted a stepwise modelling strategy starting with Model A that included the audit year variable only to test the influence of jurisdictions and health centres on Type 2 diabetes processes over time. Significant health centre (Model B) and then patient level variables (Model C) from the unadjusted analysis were introduced into the empty model. Predicted means and 95% confidence intervals were obtained from the regression analyses to rank jurisdictions and health centres according to their probability of providing a higher proportion of services compared to the overall mean probability (log odds scale). The reduction in variance due to the stepwise introduction of the different variables in the models was determined by the proportional change in variance (PCV) at different levels. The PCV provides an estimate of the extent to which health centre or patient level factors may explain individual differences in propensity for better health care delivery [16]. Median odds ratios (MORs) were calculated to help interpret variance in the odds ratio scale. The MOR is the increased (median) probability of receiving a high proportion of recommended care processes if a patient was to change health centre or jurisdiction [16,17]. If the MOR was equal to 1, there would be no difference between jurisdictions/health centres. If there were important differences between jurisdictions/ health centres, the MOR would be large. The accuracy of the variance estimates was evaluated by their standard error (SE). A p-value 0.05 was considered nonsignificant. Statistical analyses were conducted with STATA software, V.13. Results Of the 132 participating health centres, 79% were located in very remote or remote areas, 44% had a service population of 500 or fewer, and 73% were government operated (Table 2). In all jurisdictions, on average, approximately 90% of clients audited attended the health centre within the previous six months. By location, there Table 2 Characteristics of health centres and patients with Type 2 diabetes by jurisdiction (number & (%)) Far West New South Wales Northern Territory Queensland South Australia Western Australia Total number health centres Location Very remote 2 (33) 51 (82) 29 (66) 2 (33) 5 (36) 89 (67) Remote 1 (17) 9 (15) 4 (9) 0 2 (14) 16 (12) Non-remote 3 (50) 2 (3) 11 (25) 4 (67) 7 (50) 27 (20) Governance Government 0 44 (71) 44 (100) 3 (50) 6 (43) 97 (73) Community-controlled 6 (100) 18 (29) 0 3 (50) 8 (57) 35 (27) Service Population (33) 35 (56) 18 (41) 1 (17) 2 (14) 58 (44) (17) 12 (19) 11 (25) 2 (33) 0 26 (20) (50) 15 (24) 15 (34) 3 (50) 12 (86) 48 (36) Mean % (and range) clients that did not attend in last 6 months 21 (3 47) 4 (0 22) 12 (0 45) 25 (12 49) 17 (0 50) 10 (0 50) Duration of participation in ABCD CQI <1 year 0 14 (23) 12 (27) 2 (33) 4 (29) 32 (24) 1-2 years 0 26 (42) 19 (43) 4 (67) 6 (43) 55 (42) >3 years 6 (100) 22 (35) 13 (30) 0 4 (29) 45 (34) Number of patient records audited Age (years) mean & (range) 57 (19 94) 50 (15 91) 54 (15 97) 52 (16 86) 52 (17 88) 52 (15 97) Gender Male 441 (47) 1925 (40) 1587 (47) 136 (41) 472 (41) 4561 (43) Female 495 (53) 2924 (60) 1820 (53) 197 (59) 677 (59) 6113 (57) Indigenous status Indigenous 514 (55) 4684 (97) 2347 (69) 313 (94) 1071 (93) 8929 (84) Non-indigenous 384 (41) 127 (3) 591 (17) 20 (6) 56 (5) 1178 (11) Not recorded 38 (4) 38 (1) 469 (14) 0 22 (2) 567 (5) Two or more co-morbidities 770 (82) 3570 (74) 2326 (68) 210 (63) 677 (59) 7553 (71) Complications No complications 781 (83) 4185 (86) 2832 (83) 302 (91) 1000 (87) 9100 (85) 1-2 complications 148 (16) 613 (13) 510 (15) 27 (8) 134 (12) 1432 (13) >2 complications 7 (1) 51 (1) 65 (2) 4 (1) 15 (1) 142 (1) Total
5 Matthews et al. BMC Health Services Research 2014, 14:578 Page 5 of 12 Table 3 Percentage of clients that did not attend the health centre within the last six months by location Number of health centres Percent clients that did not attend in the last six months Location Mean SE Min Max Non-remote Remote Very Remote was a higher mean percentage of clients not attending within the previous six months in non-remote areas (25%) compared to remote (11%) and very remote areas (5%; Table 3). The mean age of patients was 52 years and 57% were female. Over 90% of records from the Northern Territory, Western Australia and South Australia were for Aboriginal or Torres Strait Islander people, compared to 69% in Queensland and 55% in Far West New South Wales health centres. Around 71% of patients had co-morbidities and 14% had one or more diabetes complications. These occurred more commonly in older patients (Table 4). Of all health services participating in the study around one third (34%) completed three or more cycles, 42% completed one to two cycles and 24% completed baseline audit only. This does not reflect attrition of health services, as some services commenced participation at differing time periods (Table 5). Of those health centres only completing baseline audits, 75% commenced ABCD CQI participation in 2011 or 2012 (Table 1). The distribution of remoteness of centres did not differ markedly by duration of participation in CQI, for example, 66%, 62% and 76% of health centres completing baseline, 1 2 audit cycles and 3 or more audit cycles respectively were from very remote areas. The distribution of health centres by governance showed that 47% of health centres that completed 3 or more cycles were community-controlled organisations and there was also an equal distribution of health centres by service population size that completed 3 or more cycles (Table 5). Wide variation in delivery of Type 2 diabetes services was evident across all health centres within an audit year and over time (Figure 1a). However, for those health centres that completed at least three audit cycles (n = 45) there was a trend of decreasing variation across successive cycles of CQI (Figure 1b). There were large improvements in service delivery in lower performing health centres from less than 20% in early cycles to 40-50% in later cycles (Figure 1b). In explaining this variation, the unadjusted logistic regression analysis showed that duration of participation in the ABCD CQI program, remoteness, regularity of patient attendance, patient age, level of co-morbidity and number of disease complications, were significantly associated with improved Type 2 diabetes service delivery (Table 6). Remoteness of health centres showed the strongest association with very remote and remote centres having 4.57 (95% CI ) and 2.55 (95% CI ) times the odds of being in the top quartile of Type 2 diabetes service delivery compared to non-remote centres. We tested the interaction between remoteness and duration of CQI participation and found significant improvement in service delivery with length of participation irrespective of health centre location. There was, however, a gradient of increasing odds of improvement from non-remote, to remote and very remote centres. The odds of receiving top quartile service delivery also increased with increasing age, co-morbidity and disease severity. Considering the likelihood of a correlation between patient age and disease status, we tested and found a significant interaction between these variables. All interaction terms were incorporated into the final adjusted model as shown in Table 7. There was a significant effect of time, with a steady increase in the odds of health centres being within the top quartile of Type 2 diabetes service delivery from baseline to Health centres had approximately three times greater odds of top quartile performance in 2012 compared to 2005/2006 (95% CI ) (Table 7, Model A). The effect of time diminished after adjusting for health centre and patient level factors (Table 7, Models B and C). The PCV in Model B (Table 7) shows that the addition of health centre factors explained 37% of the variation across jurisdictions and health centres. The longer the duration of participation in the ABCD CQI program, the Table 4 Clients with co-morbidities and disease complications by age group Number of chronic conditions documented Number of disease complications Age One condition 2 conditions None 1-2 >2 Total (years) n (%) n (%) n (%) n (%) n (%) 15 to < (65) 63 (35) 168 (94) 7 (4) 3 (2) to < (39) 1114 (61) 1693 (93) 110 (6) 27 (1) to < (29) 3035 (70) 3680 (85) 449 (10) 152 (4) 4281 >= (24) 3341 (76) 3559 (81) 602 (14) 224 (5) 4385 Total 3121 (29) 7553 (71) 9100 (85) 1168 (11) 406 (4) 10674
6 Matthews et al. BMC Health Services Research 2014, 14:578 Page 6 of 12 Table 5 Duration of CQI participation by health centre characteristic Completed Baseline only Completed 1 2 cycles Completed > =3 cycles Total n (%) n (%) n (%) n (%) Remoteness Non-Remote 6 (19) 16 (29) 5 (11) 27 (20) Remote 5 (16) 5 (9) 6 (13) 16 (12) Very Remote 21 (66) 34 (62) 34 (76) 89 (67) Total 32 (100) 55 (100) 45 (100) 132 (100) Governance Community-controlled 7 (22) 7 (13) 21 (47) 35 (27) Government 25 (78) 48 (87) 24 (53) 97 (73) Total 32 (100) 55 (100) 45 (100) 132 (100) Population <= (50) 28 (51) 14 (31) 58 (44) (6) 11 (20) 13 (29) 26 (20) > = (44) 16 (29) 18 (40) 48 (36) Total 32 (100) 55 (100) 45 (100) 132 (100) greater the odds of being within the top quartile of service delivery, particularly for health centres in remote and very remote locations (remote:1 2 cycles OR = 2.92, 95% CI ; 3 cycles OR = 3.14, 95% CI ; very remote: 1 2 cycles OR = 4.03, 95% CI ; 3 cycles OR = 4.72, 95% CI ). Health centres with a higher proportion of patients that attended within the previous six months also had better odds of being within the top quartile (OR = 1.40; 95% CI ). The addition of patient level factors in Model C had a modest effect, accounting for a further 1% of the variation in service delivery across health centres and jurisdictions. In most age groups, patients with co-morbidities and disease complications had greater odds of receiving higher level care than those without these conditions. The variation in the odds of top quartile delivery was reduced between jurisdictions and health centres after accounting for health centre and patient variables from MOR STATE-HC =4.68(ModelA;Table7)toMOR STATE-HC = 3.38 (Model C; Table 7). Changes in predicted odds for top quartile service delivery after adjusting for time and health centre and patient factors are shown in Figures 2 and 3 respectively. The highest performing outlier after adjusting for health centre and patient characteristics (Figure 3b) is a centre from a non-remote area that had completed one ABCD CQI Type 2 diabetes audit cycle since it joined in This health centre is renowned for its clinical leadership and model of care suited to the local Aboriginal and Torres Strait Islander population; factors which are not accounted for in this current analysis. Discussion There were improvements over time in the level of Type 2 diabetes care across the diverse range of Aboriginal and Figure 1 Type 2 diabetes service delivery over time. Mean percent Type 2 diabetes service delivery by a) all health centres over audit years (n = 132) and b) health centres that have participated in CQI for 3 or more years (n = 45) over successive audit cycles.
7 Matthews et al. BMC Health Services Research 2014, 14:578 Page 7 of 12 Table 6 Unadjusted multilevel regression analysis of health centre and patient level factors on delivery of guideline scheduled Type 2 diabetes services (n = clients; 132 health centres) Outcome is >76% service delivery Unadjusted Predictors OR 95% CI p-values Audit Year 2005/ (reference) ( ) < ( ) < ( ) < ( ) < ( ) < ( ) < Health Centre Characteristics Location Non-remote 1.00 (reference) Remote 2.55 ( ) Very Remote 4.57 ( ) < Governance Government operated 1.00 (reference) Community-controlled 1.09 ( ) 0.75 Service population (reference) >500- < ( ) ( ) 0.37 Patient attendance in last 6 months Lower attendance 1.00 (reference) Higher attendance 1.57 ( ) < Duration of CQI participation Baseline 1.00 (reference) 1-2 cycles 1.86 ( ) < cycles 2.33 ( ) < Patient Characteristics Sex Male 1.00 (reference) Female 1.06 ( ) 0.24 Age (years) 15- < (reference) 25- < ( ) < ( ) < ( ) < Indigenous status Non-Indigenous 1.00 (reference) Indigenous 1.03 ( ) 0.80 Comorbidity One condition 1.00 (reference) 2 conditions 1.54 ( ) < Complications None 1.00 (reference) 1-2 complications 1.44 ( ) < >2 complications 1.77 ( ) Torres Strait Islander primary health centres participating in a wide-scale CQI project. The main factors associated with improvement were duration of participation in CQI, the location of the health centre, regularity of patient attendance and patient age, co-morbidity and disease severity. A significant proportion of the variation across jurisdictions and centres was explained by health centre factors within the model (37%). There is an independent relationship between the duration of participation in ABCD CQI and improved documented adherence to best practice guidelines, with centres that participated for 3 or more cycles having between 1.5 to 5 times the odds of top quartile service delivery to patients depending on location (Model C; Table 7). This finding indicates that health centres in varying geographical contexts appear to obtain benefits from sustained CQI participation. Long
8 Matthews et al. BMC Health Services Research 2014, 14:578 Page 8 of 12 Table 7 Adjusted multilevel regression analysis of health centre and patient level factors on delivery of guideline scheduled Type 2 diabetes services (n = 10,674 clients; 132 health centres) Outcome is >76% service delivery Empty Model A Model B Model C Predictors Fixed effects OR 95% CI OR 95% CI OR 95% CI Audit Year 2005/ (reference) 1.00 (reference) 1.00 (reference) ( )*** 1.14 ( ) 1.20 ( ) ( )*** 1.21 ( ) 1.30 ( )* ( )*** 1.35 ( )* 1.40 ( )* ( )*** 1.16 ( ) 1.17 ( ) ( )*** 1.25 ( ) 1.24 ( ) ( )*** 1.18 ( ) 1.17 ( ) Health Centre Characteristics Location X duration of CQI participation Non-remote: Baseline 1.00 (reference) 1.00 (reference) 1-2 cycles 1.53 ( )* 1.47 ( )* 3 cycles 1.62 ( )* 1.55 ( ) Remote: Baseline 1.00 (reference) 1.00 (reference) 1-2 cycles 2.92 ( )** 2.91 ( )** 3 cycles 3.14 ( )** 3.29 ( )** Very Remote: Baseline 1.00 (reference) 1.00 (reference) 1-2 cycles 4.03 ( )*** 4.31 ( )*** 3 cycles 4.72 ( )*** 5.05 ( )*** Patient attendance in last 6 months Lower attendance 1.00 (reference) 1.00 (reference) Higher attendance 1.40 ( )*** 1.40 ( )*** Patient Characteristics (Age X disease status) 15- < 25 years: Comorbidity One condition 1.00 (reference) 2 or more conditions 1.83 ( ) 15- < 25 years: Complications None 1.00 (reference) 1-2 complications 0.87 ( ) >2 complications 5.82 ( ) 25- < 40 years: Comorbidity One condition 1.00 (reference) 2 or more conditions 1.38 ( )** 25- < 40 years: Complications None 1.00 (reference) 1-2 complications 2.40 ( )*** >2 complications 1.73 ( ) 40- < 55 years: Comorbidity One condition 1.00 (reference) 2 or more conditions 1.43 ( )*** 40- < 55 years: Complications None 1.00 (reference) 1-2 complications 1.32 ( )* >2 complications 1.17 ( ) 55 years: Comorbidity One condition 1.00 (reference) 2 or more conditions 1.26 ( )* 55 years: Complications None 1.00 (reference) 1-2 complications 1.29 ( )* >2 complications 1.45 ( )*
9 Matthews et al. BMC Health Services Research 2014, 14:578 Page 9 of 12 Table 7 Adjusted multilevel regression analysis of health centre and patient level factors on delivery of guideline scheduled Type 2 diabetes services (n = 10,674 clients; 132 health centres) (Continued) Random effects (intercepts) State (variance (SE)) 1.41 (0.99) 0.72 (0.53) 0.69 (0.51) MOR STATE PCV (% explained variance) 49% 51% Health Centre (variance (SE)) 1.21 (0.19) 0.93 (0.15) 0.94 (0.15) MOR HC PCV (% explained variance) 23% 23% State & Health Centre (variance) MOR STATE-HC PCV (% explained variance) 37% 38% Patient (variance (SE)) 0.13 (0.072) 0.07 (0.03) 0.02 (0.012) PCV (% explained variance) 44% 81% *p < 0.05; **p < 0.01; ***p < MOR (Median odds ratio): odds of receiving top quartile service delivery if a patient was to change health centre or jurisdiction [17]. PCV (Proportional change in variance): percent variation explained in odds for better health care delivery by introduction of health centre or patient level factors [16]. term commitment to CQI was also associated with improvements in health centres at the lower range of performance, with an increase in the lowest levels of adherence to best practice guidelines from less than 20% to approximately 40% over three audit cycles (Figure 1b). Health centres located in very remote (ASGC-RA 5) and remote areas (ASGC-RA 4) had increased odds of greater improvement in care processes over audit cycles compared to non-remote health centres. The ASGC-RA classification system is based on physical distance of the community to the nearest urban area and reflects access to goods and services [18]. The greater odds of a higher level of service delivery in these areas may reflect less complex service environments where the centre may be the single primary health care provider and some distance away from other providers. The availability of multiple service providers in non-remote locations provides a challenge for primary health care centres in coordinating and monitoring comprehensive delivery of care to patients with chronic disease. Yet, the quality of care shown by remote health centres has occurred in service environments characterised by high staff turnover, high use of locums and limited access to specialist services. Higher levels of service delivery in these areas may be due to the implementation of specific models of primary health care delivery (for example, hub and spoke and outreach services) designed to overcome barriers of remote geography, dispersed populations and to improve coordination of care [19]. CQI may have contributed in part to the development of these models of care as indicated in a recent evaluation of the CQI Strategy in the Northern Territory that suggested CQI processes led to Figure 2 Variation in adherence to guidelines on best practice Type 2 diabetes service delivery before adjustment. Ranking of a) jurisdictions and b) health centres according to their average delivery of Type 2 diabetes services relative to the overall average delivery as predicted from the regression Model A (adjusting for audit year only). Uncertainty around this estimate is illustrated by 95% confidence intervals.
10 Matthews et al. BMC Health Services Research 2014, 14:578 Page 10 of 12 Figure 3 Variation in adherence to guidelines on best practice Type 2 diabetes service delivery after adjustment. Ranking of a) jurisdictions and b) health centres according to their average delivery of Type 2 diabetes services relative to the overall average delivery as predicted from the regression Model C (adjusting for health centre and patient level factors). Uncertainty around this estimate is illustrated by 95% confidence intervals. positive changes in health centre practices and an increase in service delivery outputs [20]. Best practice Type 2 diabetes care dictates that patients receive certain services at regular intervals. It is unsurprising that health centres with a higher percentage of patients ( 3%) not attending in the previous six months had lower odds of providing best practice care. While non-remote health centres had on average 25% clients not attending in the previous six months compared to 11% and 5% of patients in remote and very remote areas respectively (Table 3), there was no significant statistical interaction between regularity of patient attendance and remoteness of health centres with respect to delivery of Type 2 diabetes care. The addition of patient-level characteristics into the model explained only a small component of the variation between health centres and jurisdictions (1%). There was an increasing trend of co-morbidity and disease severity with age (Table 4) and those patients who were older, had co-morbidities and/or complications were more likely to have greater odds of receiving top quartile service delivery. Within most age groups, patients with comorbidities and complications had greater odds of receiving more services compared to those without. This finding may reflect more opportunities for providing care or greater emphasis on managing high risk patients. Higher levels of care for high need patients along with general improvements in overall standards of care should contribute to a reduction in the Type 2 diabetes disease burden on health care systems and improved population health outcomes. There was a consistent trend of increasing odds of top quartile service delivery over audit years compared to the baseline year 2005/6 apart from a flattening out period in 2010 (Table 7, Model A). The period marked a new expansion phase for the ABCD project with new centres joining and the commencement of a nationwide CQI service support agency (One21seventy) designed to assist with implementation of the ABCD CQI tools and processes. Also in 2010, two jurisdictions implemented a network of regional CQI facilitators to support health centres with their CQI activities. The number of health centres participating and the number of audits undertaken, including Type 2 diabetes, increased substantially from 2011 once the new support infrastructure was in place. Jurisdictional differences in the odds of health centres being within the top quartile of service delivery may be attributed to the variable state-wide level support systems as well as the staggered commencement of participation in the ABCD project. Employment of regional positions that supported collaboration and information exchange across health centres was a key explanatory factor for improved performance at health centre level over time [21]. The top two ranked jurisdictions with respect to odds of top quartile delivery, before and after adjusting for health centre and patient factors (Figures 2a and 3a), are those that participated for more years in ABCD and/or have a regional CQI facilitator network. Similar factors have been attributed to the success of a long term diabetes quality of care project in a remote community of Western Australia [22]. Learnings from jurisdictions where there is well established macro-level CQI infrastructure can support the development of similar structures in other jurisdictions [23]. The investigation of patient, health centre and jurisdictional level factors that underlie variation in adherence to best practice Type 2 diabetes care has been made possible by the availability of the extensive CQI audit dataset from health centres participating in the ABCD
11 Matthews et al. BMC Health Services Research 2014, 14:578 Page 11 of 12 National Research Partnership. The voluntary nature of participation in this study by health centres, however, limits the generalisability of study findings. In addition, as data are collected from client records, service delivery may be underestimated due to poor documentation. Although a strength of this study design is the ability to correct for a range of known confounding factors, it is also recognised that the associations identified in this study, may be due, in part, to other unmeasured confounders. For example, there may be factors associated with longer term participation in CQI that may be responsible for the demonstrated improvements in adherence to best practice guidelines, such as well-functioning community health centres with good leadership and workforce stability that are both more likely to maintain CQI processes, and to achieve better results in diabetes management. The exemplary centre in Figure 3b is a case in point where their level of service delivery is amongst the best despite relatively limited participation in ABCD CQI to date. As mentioned, the health centre is renowned for its clinical leadership and model of care built around its own local CQI processes. To elucidate other potentially confounding factors enabling quality improvement, further quantitative and qualitative studies are planned to examine micro-, meso- and macro-level factors that have facilitated sustained improvement in high performing health centres [24]. It is important to note that it is through participation in the CQI initiative that data are available for the sort of analysis presented in this study. There are currently no other sources of comparable data in Australian primary care that would enable establishment of a comparison group not participating in the CQI program. Conclusions The findings of this study suggest that at the health centre level, the quality of Type 2 diabetes care for Aboriginal and Torres Strait Islander communities is associated with long term commitment to a CQI program. Sustained participation has particularly benefitted remote and very remote health centres and health centres performing at the lower range of service provision. Our findings suggest that improving regularity of patient attendance, better coordination and documentation of care within non-remote multiple service provider environments and sharing lessons from the successes of care coordination in remote areas has the potential to improve care delivery across the spectrum of health centres. Further understanding of system wide factors that underpin jurisdictional variation in delivery of care will assist health managers and policy makers to understand and develop macro-level strategies to improve quality of Type 2 diabetes care in Aboriginal and Torres Strait Islander communities. Abbreviations ABCD: Audit and Best Practice for Chronic Disease; ASGC: Australian Standard Geographical Classification; CQI: Continuous quality improvement; MOR: Median odds ratio; OR: Odds ratio; PCV: Proportional change in variance; PHC: Primary health care; SE: Standard error. Competing interests The authors declare that they have no competing interests. Authors contributions VM performed the statistical analysis and drafted the manuscript. GS conceived the study, participated in its design, assisted with statistical analysis and drafting of the manuscript. RB conceived the study and assisted with interpretation. JM assisted with statistical analysis. CC, CK, RK, SL, EM, ST and DS were instrumental with data acquisition and interpretation. All authors read and approved the final manuscript. Acknowledgements The development of this manuscript would not have been possible without the active support, enthusiasm and commitment of members of the ABCD National Research Partnership especially the participating primary health care centres that have provided de-identified audit data. The ABCD National Research Partnership Project is supported by funding from the National Health and Medical Research Council (#545267) and the Lowitja Institute, and by in-kind and financial support from a range of Community Controlled and Government agencies. RB s work is supported by an ARC Future Fellowship (#FT ). RK s current affiliation is the New South Wales Agency for Clinical Innovation, Sydney, Australia. Statistical advice from Mark Chatfield is gratefully acknowledged. Author details 1 Menzies School of Health Research, Brisbane, Queensland, Australia. 2 School of Environment, Griffith University, Brisbane, Queensland, Australia. 3 Department of Health, Darwin, Northern Territory, Australia. 4 Maari Ma Health Aboriginal Corporation, Broken Hill, Far West New South Wales, Australia. 5 Queensland Health, Cairns, Queensland, Australia. 6 School of Medicine & Dentistry, James Cook University, Townsville, Queensland, Australia. 7 Aboriginal Medical Services Alliance Northern Territory, Alice Springs, Northern Territory, Australia. 8 Western Australian Centre for Rural Health, University of Western Australia, Geraldton, Western Australia, Australia. 9 Aboriginal Health Council of South Australia, Adelaide, South Australia, Australia. Received: 29 March 2014 Accepted: 3 November 2014 References 1. Speight J, Browne J, Holmes-Truscott E, Hendrieckx C, Pouwer F, on behalf of the Diabetes MILES Australia reference group: Diabetes MILES Australia 2011 Survey Report. Melbourne: Diabetes Australia; Shaw JE, Sicree RA, Zimmet PZ: Global estimates of the prevalence of diabetes for 2010 and Diabetes Res Clin Pract 2010, 87: Zhang P, Zhang X, Brown J, Vistisen D, Sicree R, Shaw J, Nichols G: Global healthcare expenditure on diabetes for 2010 and Diabetes Res Clin Pract 2010, 87: Ricci-Cabello I, Ruiz-Pérez I, De Labry-Lima AO, Márquez-Calderón S: Do social inequalities exist in terms of the prevention, diagnosis, treatment, control and monitoring of diabetes? A systematic review. Health Soc Care Community 2010, 18: Australian Bureau of Statistics: Aboriginal and Torres Strait Islander Health Survey: First Results, Australia Canberra: ABS Cat No ; Ricci-Cabello I, Ruiz-Pérez I, Nevot-Cordero A, Rodríguez-Barranco M, Sordo L, Gonçalves DC: Health care interventions to improve the quality of diabetes care in African americans: a systematic review and metaanalysis. Diabetes Care 2013, 36: Tricco A, Ivers N, Grimshaw J, Moher D, Turner L, Galipeau J, Halperin I, Vachon B, Ramsay T, Manns B: Effectiveness of quality improvement strategies on the management of diabetes: a systematic review and meta-analysis. Lancet 2012, 379:
12 Matthews et al. BMC Health Services Research 2014, 14:578 Page 12 of Gardner K, Dowden M, Togni S, Bailie R: Understanding uptake of continuous quality improvement in Indigenous primary health care: lessons from a multi-site case study of the audit and best practice for chronic disease project. Implement Sci 2010, 5: Coleman K, Austin BT, Brach C, Wagner EH: Evidence on the chronic care model in the new millennium. Health Aff 2009, 28: Si D, Bailie R, Dowden M, Kennedy C, Cox R, O Donoghue L, Liddle H, Kwedza R, Connors C, Thompson S, Burke H, Brown A, Weeramanthri T: Assessing quality of diabetes care and its variation in Aboriginal community health centres in Australia. Diab Metabol Res Rev 2010, 26: Powell AE, Rushmer RK: A Systematic Narrative Review of Quality Improvement Models in Health Care. Dundee: Social Dimensions of Health Institute, University of Dundee & St Andrews; Hayman NE, White NE, Spurling GK: Improving Indigenous patients access to mainstream health services: the Inala experience. Med J Aust 2009, 190: Bailie R, Matthews V, Brands J, Schierhout G: A systems-based partnership learning model for strengthening primary healthcare. Implement Sci 2013, 8: Bailie RS, Si D, O Donoghue L, Dowden M: Indigenous health: effective and sustainable health services through continuous quality improvement. Med J Aust 2007, 186: One21seventy: Vascular and Metabolic Syndrome Management Clinical Audit Protocol. Brisbane: Menzies School of Health Research; Merlo J, Chaix B, Ohlsson H, Beckman A, Johnell K, Hjerpe LR, Larsen K: A brief conceptual tutorial of multilevel analysis in social epidemiology: using measures of clustering in multilevel logistic regression to investigate contextual phenomena. J Epidemiol Community Health 2006, 60: Larsen K, Merlo J: Appropriate assessment of neighbourhood effects on individual health: integrating random and fixed effects in multilevel logistic regression. Am J Epidemiol 2005, 161: Australian Bureau of Statistics: Statistical Geography Volume 1 - Australian Standard Geographical Classification. Canberra: ABS Cat No ; Wakerman J, Humphreys JS, Wells R, Kuipers P, Entwistle P, Jones J: Primary health care delivery models in rural and remote Australia: a systematic review. BMC Health Serv Res 2008, 8: Allen and Clarke: Evaluation of the Northern Territory Continuous Quality Improvement Investment Strategy: Final Report. Canberra: Department of Health; Schierhout G, Hains J, Si D, Kennedy C, Cox R, Kwedza R, O Donoghue L, Fittock M, Brands J, Lonergan K, Bailie R: Evaluating the effectiveness of a multifaceted, multilevel continuous quality improvement program in primary health care: developing a realist theory of change. Implement Sci 2013, 8: Marley JV, Nelson C, O Donnell V, Atkinson D: Quality indicators of diabetes care: an example of remote-area Aboriginal primary health care over 10 years. Med J Austr 2012, 197: Wise M, Angus S, Harris E, Parker S: National Appraisal of Continuous Quality Improvement Initiatives in Aboriginal and Torres Strait Islander Primary Health Care. Melbourne: The Lowitja Institute; Larkins S, Patrao T, Thompson S, Elston J, Connors C, Ward J, Matthews V, Kwedza R, Bailie R: Understanding quality improvement in Aboriginal and Torres Strait Islander primary health care: lessons from the best to better the rest [abstract]. In Sydney: PHCRIS conference: July 2013; [ 3&catid=1506&page=2&subcat=all&showHidden=1] Accessed: 03/03/2014. doi: /s Cite this article as: Matthews et al.: Duration of participation in continuous quality improvement: a key factor explaining improved delivery of Type 2 diabetes services. BMC Health Services Research :578. Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color figure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
Sarah Larkins, Annette Panzera, Michelle Redman MacLaren, + co authors
 Lessons from the best to better the rest: quality improvement in Indigenous primary health care National Rural Health Alliance Conference, Darwin, May 2015 Sarah Larkins, Annette Panzera, Michelle Redman
Lessons from the best to better the rest: quality improvement in Indigenous primary health care National Rural Health Alliance Conference, Darwin, May 2015 Sarah Larkins, Annette Panzera, Michelle Redman
Nattabi et al. BMC Infectious Diseases (2017) 17:148 DOI /s z
 Nattabi et al. BMC Infectious Diseases (2017) 17:148 DOI 10.1186/s12879-017-2241-z RESEARCH ARTICLE Open Access Wide variation in sexually transmitted infection testing and counselling at Aboriginal primary
Nattabi et al. BMC Infectious Diseases (2017) 17:148 DOI 10.1186/s12879-017-2241-z RESEARCH ARTICLE Open Access Wide variation in sexually transmitted infection testing and counselling at Aboriginal primary
Non-Government Organisations and a Collaborative Model for Rural, Remote and Indigenous Health
 Non-Government Organisations and a Collaborative Model for Rural, Remote and Indigenous Health Pat Field National Director, Rural Remote and Indigenous Programs, Heart Foundation of Australia 5th National
Non-Government Organisations and a Collaborative Model for Rural, Remote and Indigenous Health Pat Field National Director, Rural Remote and Indigenous Programs, Heart Foundation of Australia 5th National
Engaging stakeholders in prioritising and addressing evidence-practice gaps in maternal health care
 Engaging stakeholders in prioritising and addressing evidence-practice gaps in maternal health care Melanie Gibson-Helm 1, Jodie Bailie 2, Veronica Matthews 2, Alison Laycock 2, Jacqueline Boyle 1, Ross
Engaging stakeholders in prioritising and addressing evidence-practice gaps in maternal health care Melanie Gibson-Helm 1, Jodie Bailie 2, Veronica Matthews 2, Alison Laycock 2, Jacqueline Boyle 1, Ross
MAKING A DIFFERENCE CHRONIC CONDITIONS PREVENTION AND MANAGEMENT FOR ABORIGINAL CLIENTS IN THE NORTHERN TERRITORY
 MAKING A DIFFERENCE CHRONIC CONDITIONS PREVENTION AND MANAGEMENT FOR ABORIGINAL CLIENTS IN THE NORTHERN TERRITORY Dr Christine Connors and Liz Kasteel Chronic Conditions Strategy Unit NT Department of
MAKING A DIFFERENCE CHRONIC CONDITIONS PREVENTION AND MANAGEMENT FOR ABORIGINAL CLIENTS IN THE NORTHERN TERRITORY Dr Christine Connors and Liz Kasteel Chronic Conditions Strategy Unit NT Department of
Rural and remote health care research funding at NHMRC opportunities and barriers
 and remote health care research funding at NHMRC opportunities and barriers Dr Timothy Dyke Strategic Policy Group 2 September 2014 Presentation Outline NHMRC strategies NHMRC funding of rural and remote
and remote health care research funding at NHMRC opportunities and barriers Dr Timothy Dyke Strategic Policy Group 2 September 2014 Presentation Outline NHMRC strategies NHMRC funding of rural and remote
The Cancer Council NSW. Submission to the Legislative Assembly Public Accounts Committee. Inquiry into NSW State Plan Reporting
 The Cancer Council NSW Submission to the Legislative Assembly Public Accounts Committee Inquiry into NSW State Plan Reporting December 2007 2 Inquiry into NSW State Plan Reporting The Cancer Council NSW
The Cancer Council NSW Submission to the Legislative Assembly Public Accounts Committee Inquiry into NSW State Plan Reporting December 2007 2 Inquiry into NSW State Plan Reporting The Cancer Council NSW
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Murray PHN When submitting this Activity Work Plan 2016-2018 to the Department
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Murray PHN When submitting this Activity Work Plan 2016-2018 to the Department
School of Rural Health Strategic plan
 School of Rural Health Strategic plan 2017-22 Contents Strategic intent 4 Goals 5 Strategic goals 2017-22 6 The University of Sydney School of Rural Health 2017 22 Strategic Plan October 2017 The School
School of Rural Health Strategic plan 2017-22 Contents Strategic intent 4 Goals 5 Strategic goals 2017-22 6 The University of Sydney School of Rural Health 2017 22 Strategic Plan October 2017 The School
Burden of end-stage renal disease
 Summary of Indigenous health: End-stage renal disease Neil Thomson and Sasha Stumpers Australian Indigenous HealthInfoNet, Edith Cowan University www.healthinfonet.ecu.edu.au This summary of end-stage
Summary of Indigenous health: End-stage renal disease Neil Thomson and Sasha Stumpers Australian Indigenous HealthInfoNet, Edith Cowan University www.healthinfonet.ecu.edu.au This summary of end-stage
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Murray PHN When submitting this Activity Work Plan 2016-2018 to the Department
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Murray PHN When submitting this Activity Work Plan 2016-2018 to the Department
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Gippsland When submitting this Activity Work Plan 2016-2018 to the Department
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Gippsland When submitting this Activity Work Plan 2016-2018 to the Department
The Aboriginal Maternal and Infant Health Service: a decade of achievement in the health of women and babies in NSW
 The Aboriginal Maternal and Infant Health Service: a decade of achievement in the health of women and babies in NSW Elisabeth Murphy A,B and Elizabeth Best A A Maternity, Children and Young People s Health
The Aboriginal Maternal and Infant Health Service: a decade of achievement in the health of women and babies in NSW Elisabeth Murphy A,B and Elizabeth Best A A Maternity, Children and Young People s Health
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Hunter New England & Central Coast Please note: This Activity Work Plan was developed in response to the HNECC PHN
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Hunter New England & Central Coast Please note: This Activity Work Plan was developed in response to the HNECC PHN
Updated Activity Work Plan : Drug and Alcohol Treatment. Western NSW PHN
 Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment Western NSW PHN 1 Overview This Drug and Alcohol Treatment Activity Work Plan covers the period from 1 July 2016 to 30 June 2019 and is
Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment Western NSW PHN 1 Overview This Drug and Alcohol Treatment Activity Work Plan covers the period from 1 July 2016 to 30 June 2019 and is
The first step to Getting Australia s Health on Track
 2017 The first step to Getting Australia s Health on Track Heart Health is the sequential report to the policy roadmap Getting Australia s Health on Track and outlines a national implementation strategy
2017 The first step to Getting Australia s Health on Track Heart Health is the sequential report to the policy roadmap Getting Australia s Health on Track and outlines a national implementation strategy
Updated Activity Work Plan : Drug and Alcohol Treatment
 Web Version HPRM DOC/17/1043 Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment This Drug and Alcohol Treatment Activity Work Plan template has the following parts: 1. The updated strategic
Web Version HPRM DOC/17/1043 Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment This Drug and Alcohol Treatment Activity Work Plan template has the following parts: 1. The updated strategic
Monitoring and Evaluation Framework for the Tackling Indigenous Smoking Programme
 Monitoring and Evaluation Framework for the Tackling Indigenous Smoking Programme 30 June 2016 Introduction... 3 Context the TIS programme... 4 2.1 TIS programme objectives... 5 2.2 The delivery of the
Monitoring and Evaluation Framework for the Tackling Indigenous Smoking Programme 30 June 2016 Introduction... 3 Context the TIS programme... 4 2.1 TIS programme objectives... 5 2.2 The delivery of the
Clinical audit for occupational therapy intervention for children with autism spectrum disorder: sampling steps and sample size calculation
 DOI 10.1186/s13104-015-1247-0 CORRESPONDENCE Open Access Clinical audit for occupational therapy intervention for children with autism spectrum disorder: sampling steps and sample size calculation Scott
DOI 10.1186/s13104-015-1247-0 CORRESPONDENCE Open Access Clinical audit for occupational therapy intervention for children with autism spectrum disorder: sampling steps and sample size calculation Scott
INDIGENOUS MALE HEALTH
 INDIGENOUS MALE HEALTH A report for Indigenous males, their families and communities, and those committed to improving Indigenous male health Dr Mark Wenitong Executive Officer, Australian Indigenous Doctors
INDIGENOUS MALE HEALTH A report for Indigenous males, their families and communities, and those committed to improving Indigenous male health Dr Mark Wenitong Executive Officer, Australian Indigenous Doctors
BRIDGING THE GAP. Know your population How bad is it? Is it changing? Why the difference? The continuum of care
 Aboriginal & Torres Strait Islander diabetes and coronary heart disease BRIDGING THE GAP Graeme Maguire Cairns Base Hospital James Cook University Deaths per 1 population 1 1 8 6 4 8 6 4 1977 1981 Ischaemic
Aboriginal & Torres Strait Islander diabetes and coronary heart disease BRIDGING THE GAP Graeme Maguire Cairns Base Hospital James Cook University Deaths per 1 population 1 1 8 6 4 8 6 4 1977 1981 Ischaemic
A Framework for Optimal Cancer Care Pathways in Practice
 A to Guide Care Cancer Care A for Care in Practice SUPPORTING CONTINUOUS IMPROVEMENT IN CANCER CARE Developed by the National Cancer Expert Reference Group to support the early adoption of the A to Guide
A to Guide Care Cancer Care A for Care in Practice SUPPORTING CONTINUOUS IMPROVEMENT IN CANCER CARE Developed by the National Cancer Expert Reference Group to support the early adoption of the A to Guide
National Cross Cultural Dementia Network (NCCDN) A Knowledge Network of value
 National Cross Cultural Dementia Network (NCCDN) A Knowledge Network of value One in eight Australians with dementia do not speak English at home. Dementia does not discriminate; it affects all people
National Cross Cultural Dementia Network (NCCDN) A Knowledge Network of value One in eight Australians with dementia do not speak English at home. Dementia does not discriminate; it affects all people
Improving health service delivery through telehealth expansion in Queensland
 Improving health service delivery through telehealth expansion in Queensland Andrew Bryett, Acting Director, Statewide Telehealth Services, Queensland Health, Australia Queensland 22% of the land mass
Improving health service delivery through telehealth expansion in Queensland Andrew Bryett, Acting Director, Statewide Telehealth Services, Queensland Health, Australia Queensland 22% of the land mass
Primary Health Networks Drug and Alcohol Treatment Services Funding. Updated Activity Work Plan : Drug and Alcohol Treatment
 Primary Health Networks Drug and Alcohol Treatment Services Funding Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment Adelaide PHN This Activity Work Plan is an update to the 2016-18 Activity
Primary Health Networks Drug and Alcohol Treatment Services Funding Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment Adelaide PHN This Activity Work Plan is an update to the 2016-18 Activity
PCC4U. Uptake of the PCC4U Resources. Funded by the Australian Government through the National Palliative Care Program
 Issue No. 19 July 2010 The Australian Government has committed to improving the quality of care provided to Australians at end of life, by supporting the inclusion of palliative care education as an integral
Issue No. 19 July 2010 The Australian Government has committed to improving the quality of care provided to Australians at end of life, by supporting the inclusion of palliative care education as an integral
SUBMISSION. Inquiry into the Hearing Health and Wellbeing of Australia
 ROYAL AUSTRALASIAN COLLEGE OF SURGEONS AUSTRALIAN SOCIETY OF OTOLARYNGOLOGY HEAD AND NECK SURGERY SUBMISSION Inquiry into the Hearing Health and Wellbeing of Australia Date 23 December 2016 The Royal Australasian
ROYAL AUSTRALASIAN COLLEGE OF SURGEONS AUSTRALIAN SOCIETY OF OTOLARYNGOLOGY HEAD AND NECK SURGERY SUBMISSION Inquiry into the Hearing Health and Wellbeing of Australia Date 23 December 2016 The Royal Australasian
NATIONAL ORAL HEALTH PLAN MONITORING GROUP. KEY PROCESS AND OUTCOME PERFORMANCE INDICATORS Second follow-up report
 NATIONAL ORAL HEALTH PLAN MONITORING GROUP KEY PROCESS AND OUTCOME PERFORMANCE INDICATORS Second follow-up report 22-28 ARCPOH NOVEMBER 29 ACTION AREA ONE POPULATION ORAL HEALTH... 1 INDICATOR 1: NATIONAL
NATIONAL ORAL HEALTH PLAN MONITORING GROUP KEY PROCESS AND OUTCOME PERFORMANCE INDICATORS Second follow-up report 22-28 ARCPOH NOVEMBER 29 ACTION AREA ONE POPULATION ORAL HEALTH... 1 INDICATOR 1: NATIONAL
Sandra Meihubers AM. PO Box 495, Newport Beach, NSW Australia. ABN Phone:
 Sandra Meihubers AM CURRICULUM VITAE PO Box 495, Newport Beach, NSW 2106. Australia. ABN 91 152 056 619 Phone: 02 99731179 0418 405 757 E-Mail: sm495@ozemail.com.au Background Dr Sandra Meihubers is a
Sandra Meihubers AM CURRICULUM VITAE PO Box 495, Newport Beach, NSW 2106. Australia. ABN 91 152 056 619 Phone: 02 99731179 0418 405 757 E-Mail: sm495@ozemail.com.au Background Dr Sandra Meihubers is a
Policy Statement Delivery of Oral Health: Special groups: Aboriginal and Torres Strait Islander Australians
 Policy Statement 2.3.5 Delivery of Oral Health: Special groups: Aboriginal and Torres Strait Islander Australians Position Summary Research must be funded to better understand the dental needs and issues
Policy Statement 2.3.5 Delivery of Oral Health: Special groups: Aboriginal and Torres Strait Islander Australians Position Summary Research must be funded to better understand the dental needs and issues
Public Health Association of Australia: Policy-at-a-glance Domestic and Family Violence Policy
 Public Health Association of Australia: Policy-at-a-glance Domestic and Family Violence Policy Key message: PHAA will 1. Advocate for full implementation and resourcing of the National Plan to Reduce Violence
Public Health Association of Australia: Policy-at-a-glance Domestic and Family Violence Policy Key message: PHAA will 1. Advocate for full implementation and resourcing of the National Plan to Reduce Violence
Accessibility and quality of mental health services in rural and remote Australia. August Recommendations
 AMSANT submission to the Senate Community Affairs References Committee Inquiry: Accessibility and quality of mental health services in rural and remote Australia August 2018 Recommendations 1) Mental health
AMSANT submission to the Senate Community Affairs References Committee Inquiry: Accessibility and quality of mental health services in rural and remote Australia August 2018 Recommendations 1) Mental health
NPA LAS REVIEW ADVISORY GROUP WORKSHOP 19 OCTOBER 2018
 NPA LAS 2015-2020 REVIEW ADVISORY GROUP WORKSHOP 19 OCTOBER 2018 OBJECTIVES The review team wants to road test key findings, focusing on those which are contested Update the Advisory Group on progress
NPA LAS 2015-2020 REVIEW ADVISORY GROUP WORKSHOP 19 OCTOBER 2018 OBJECTIVES The review team wants to road test key findings, focusing on those which are contested Update the Advisory Group on progress
Women s Health Association of Victoria
 Women s Health Association of Victoria PO Box 1160, Melbourne Vic 3001 Submission to the Commonwealth Government on the New National Women s Health Policy 1 July, 2009. Contact person for this submission:
Women s Health Association of Victoria PO Box 1160, Melbourne Vic 3001 Submission to the Commonwealth Government on the New National Women s Health Policy 1 July, 2009. Contact person for this submission:
Don t Make Smokes Your Story Aboriginal and Torres Strait Islander anti-smoking campaign
 Don t Make Smokes Your Story Aboriginal and Torres Strait Islander anti-smoking campaign Jennifer Taylor 1, Kellie Mastersen 1 1 Australian Government Department of Health Introduction Don t Make Smokes
Don t Make Smokes Your Story Aboriginal and Torres Strait Islander anti-smoking campaign Jennifer Taylor 1, Kellie Mastersen 1 1 Australian Government Department of Health Introduction Don t Make Smokes
The elements of cancer and palliative care reform in Victoria
 The elements of cancer and palliative care reform in Victoria Dr Chris Brook Executive Director Rural and Regional Health and Aged Care Services Department of Human Services 1 Overview Rural and regional
The elements of cancer and palliative care reform in Victoria Dr Chris Brook Executive Director Rural and Regional Health and Aged Care Services Department of Human Services 1 Overview Rural and regional
The NGO has worked with the AMS and REHC to achieve the following:
 Providing eye care to remote Indigenous communities in the Northern Territory: a case study examining success factors and challenges from a collaborative approach between a NGO and AMS Tricia Keys 1, Maree
Providing eye care to remote Indigenous communities in the Northern Territory: a case study examining success factors and challenges from a collaborative approach between a NGO and AMS Tricia Keys 1, Maree
E. A Public Health Oriented Palliative Care System in Australia
 E. A Public Health Oriented Palliative Care System in Australia Overview Similar to other developed countries, Australia s population is ageing and there is increasing demand for equitable access to high
E. A Public Health Oriented Palliative Care System in Australia Overview Similar to other developed countries, Australia s population is ageing and there is increasing demand for equitable access to high
Our footprints: a traveller s guide to the COAG implementation process in Western Australia
 Our footprints: a traveller s guide to the COAG implementation process in Western Australia Beverley Stone 1, Kevin Cox 1, Rosalie Miles 1, Susan Powe 1, Vicki O Donnell, Linda Waters 1 WA Country Health
Our footprints: a traveller s guide to the COAG implementation process in Western Australia Beverley Stone 1, Kevin Cox 1, Rosalie Miles 1, Susan Powe 1, Vicki O Donnell, Linda Waters 1 WA Country Health
Primary Health Networks Greater Choice for At Home Palliative Care
 Primary Health Networks Greater Choice for At Home Palliative Care Brisbane South PHN When submitting the Greater Choice for At Home Palliative Care Activity Work Plan 2017-2018 to 2019-2020 to the Department
Primary Health Networks Greater Choice for At Home Palliative Care Brisbane South PHN When submitting the Greater Choice for At Home Palliative Care Activity Work Plan 2017-2018 to 2019-2020 to the Department
Cancer survival for Aboriginal and Torres Strait Islander Australians: a national study of survival rates and excess mortality
 Cancer survival for Aboriginal and Torres Strait Islander Australians: a national study of survival rates and excess mortality Author R. Condon, John, Zhang, Xiaohua, Baade, Peter, Griffiths, Kalinda,
Cancer survival for Aboriginal and Torres Strait Islander Australians: a national study of survival rates and excess mortality Author R. Condon, John, Zhang, Xiaohua, Baade, Peter, Griffiths, Kalinda,
Towards a Decadal Plan for Australian Nutrition Science September 2018
 Towards a Decadal Plan for Australian Nutrition Science September 2018 The Dietitians Association of Australia (DAA) is the national association of the dietetic profession with over 6,400 members, and
Towards a Decadal Plan for Australian Nutrition Science September 2018 The Dietitians Association of Australia (DAA) is the national association of the dietetic profession with over 6,400 members, and
Impact on children and youth mental health
 1% Impact on children and youth mental health Establishment of Australia s first intensive outpatient program for young people aged 14-24 with eating disorders Development and trial of a mobile phone-based
1% Impact on children and youth mental health Establishment of Australia s first intensive outpatient program for young people aged 14-24 with eating disorders Development and trial of a mobile phone-based
Guidelines for indigenous allied health, indigenous enrolled nurses, Aboriginal health workers and Aboriginal health practitioners applying for
 Guidelines for indigenous allied health, indigenous enrolled nurses, Aboriginal health workers and Aboriginal health practitioners applying for Credentialling as a Diabetes Educator Guidelines for indigenous
Guidelines for indigenous allied health, indigenous enrolled nurses, Aboriginal health workers and Aboriginal health practitioners applying for Credentialling as a Diabetes Educator Guidelines for indigenous
Cardiovascular Disease Risk Prediction in Indigenous Australians
 Cardiovascular Disease Risk Prediction in Indigenous Australians ELIZABETH LM BARR (MPH, PHD) NATIONAL HEART FOUNDATION POST-DOC FELLOW Cardiac Care in the NT Annual Workshop 2017 is proudly supported
Cardiovascular Disease Risk Prediction in Indigenous Australians ELIZABETH LM BARR (MPH, PHD) NATIONAL HEART FOUNDATION POST-DOC FELLOW Cardiac Care in the NT Annual Workshop 2017 is proudly supported
Evaluation of a multi-component community tobacco intervention in three remote Australian Aboriginal communities
 Evaluation of a multi-component community tobacco intervention in three remote Australian Aboriginal communities Abstract Objectives: To assess the effect of community tobacco interventions in Aboriginal
Evaluation of a multi-component community tobacco intervention in three remote Australian Aboriginal communities Abstract Objectives: To assess the effect of community tobacco interventions in Aboriginal
April 2019 NATIONAL POLICY PLATFORM
 April 2019 NATIONAL POLICY PLATFORM There are crisis services available 24/7 if you or someone you know is in distress Lifeline: 13 11 14 www.lifeline.org.au people took their own lives in 2017 1 Over
April 2019 NATIONAL POLICY PLATFORM There are crisis services available 24/7 if you or someone you know is in distress Lifeline: 13 11 14 www.lifeline.org.au people took their own lives in 2017 1 Over
strategic plan strong teeth strong body strong mind Developed in partnership with Rotary Clubs of Perth and Heirisson
 strategic plan 2012-2016 strong teeth strong body strong mind CONTENTS Introduction 2 Key Result Area 1 Dental Health Education 5 Key Result Area 2 Dental Treatment 7 Key Result Area 3 Advocacy 9 Key
strategic plan 2012-2016 strong teeth strong body strong mind CONTENTS Introduction 2 Key Result Area 1 Dental Health Education 5 Key Result Area 2 Dental Treatment 7 Key Result Area 3 Advocacy 9 Key
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 South Eastern Melbourne PHN When submitting this Activity Work Plan 2016-2018 to the Department of Health, the PHN
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 South Eastern Melbourne PHN When submitting this Activity Work Plan 2016-2018 to the Department of Health, the PHN
The updated incidences and mortalities of major cancers in China, 2011
 DOI 10.1186/s40880-015-0042-6 REVIEW Open Access The updated incidences and mortalities of major cancers in China, 2011 Wanqing Chen *, Rongshou Zheng, Hongmei Zeng and Siwei Zhang Abstract Introduction:
DOI 10.1186/s40880-015-0042-6 REVIEW Open Access The updated incidences and mortalities of major cancers in China, 2011 Wanqing Chen *, Rongshou Zheng, Hongmei Zeng and Siwei Zhang Abstract Introduction:
Needle and Syringe Programs - 17 October 2013
 Needle and Syringe Programs - 17 October 2013 ANCD Position Paper: Needle and Syringe Programs MEDIA RELEASE 17 October 2013 The Australian National Council on Drugs (ANCD) has today released a position
Needle and Syringe Programs - 17 October 2013 ANCD Position Paper: Needle and Syringe Programs MEDIA RELEASE 17 October 2013 The Australian National Council on Drugs (ANCD) has today released a position
NIDAC Online Consultation 1: Alcohol. Summary of Findings
 NIDAC Online Consultation 1: Alcohol Summary of Findings 1 BACKGROUND Between 28 March and 30 April 2011, NIDAC undertook an online consultation on alcohol using Survey Monkey, a specialised online survey
NIDAC Online Consultation 1: Alcohol Summary of Findings 1 BACKGROUND Between 28 March and 30 April 2011, NIDAC undertook an online consultation on alcohol using Survey Monkey, a specialised online survey
Executive Summary 10
 Executive Summary 10 In this section 12 Introduction 13 Radiation Oncology Services in Australia Key Issues 15 2012-2022 Strategic Directions and Objectives for the Radiation Oncology Sector 17 Policy
Executive Summary 10 In this section 12 Introduction 13 Radiation Oncology Services in Australia Key Issues 15 2012-2022 Strategic Directions and Objectives for the Radiation Oncology Sector 17 Policy
We are nearly there. Close the Gap for Vision
 We are nearly there Close the Gap for Vision Executive summary Australia is on the verge of closing the gap in Indigenous eye health Elimination of trachoma Sight restoration for ~4,000 Indigenous Australians
We are nearly there Close the Gap for Vision Executive summary Australia is on the verge of closing the gap in Indigenous eye health Elimination of trachoma Sight restoration for ~4,000 Indigenous Australians
Pre-budget Submission
 Health equality in the bush: realising physiotherapists potential to improve health outcomes and reduce preventable hospital admissions Letter from Melissa Locke APA President Physiotherapists are one
Health equality in the bush: realising physiotherapists potential to improve health outcomes and reduce preventable hospital admissions Letter from Melissa Locke APA President Physiotherapists are one
NATIONAL RURAL HEALTH ALLIANCE. Pre-Budget Submission
 NATIONAL RURAL HEALTH ALLIANCE Pre-Budget Submission 2018-19 Introduction The National Rural Health Alliance (the Alliance) is Australia s peak representative body for rural and remote health. We are committed
NATIONAL RURAL HEALTH ALLIANCE Pre-Budget Submission 2018-19 Introduction The National Rural Health Alliance (the Alliance) is Australia s peak representative body for rural and remote health. We are committed
The Cancer Council NSW
 The Cancer Council NSW Submission to the Legislative Assembly Social Issues Committee Inquiry into closing the gap: Overcoming Indigenous disadvantage January 2008 2 Inquiry into Closing the Gap Overcoming
The Cancer Council NSW Submission to the Legislative Assembly Social Issues Committee Inquiry into closing the gap: Overcoming Indigenous disadvantage January 2008 2 Inquiry into Closing the Gap Overcoming
Physical activity. Policy endorsed by the 50th RACGP Council 9 February 2008
 This paper provides a background to the Royal Australian College of General Practitioners (RACGP) current position on physical activity, as set out in the RACGP Guidelines for preventive activities in
This paper provides a background to the Royal Australian College of General Practitioners (RACGP) current position on physical activity, as set out in the RACGP Guidelines for preventive activities in
Palliative Care. Working towards the future of quality palliative care for all
 Palliative Care Working towards the future of quality palliative care for all FEBRUARY 2019 Recommended citation Palliative Care Australia 2018, Palliative Care 2030 working towards the future of quality
Palliative Care Working towards the future of quality palliative care for all FEBRUARY 2019 Recommended citation Palliative Care Australia 2018, Palliative Care 2030 working towards the future of quality
Bobby Goldsmith Foundation Strategic Plan
 Bobby Goldsmith Foundation Strategic Plan 2016 2020 OUR VISION... 3 OUR MISSION... 3 THE NEEDS OF PEOPLE WITH HIV TODAY... 3 OUR ROLE... 4 OUR APPROACH... 5 OUR OUTCOMES... 5 OUR GOALS... 5 OUR STRATEGIES...
Bobby Goldsmith Foundation Strategic Plan 2016 2020 OUR VISION... 3 OUR MISSION... 3 THE NEEDS OF PEOPLE WITH HIV TODAY... 3 OUR ROLE... 4 OUR APPROACH... 5 OUR OUTCOMES... 5 OUR GOALS... 5 OUR STRATEGIES...
Telecommunications Universal Service Obligation
 Mr Paul Lindwall Commissioner Productivity Commission Inquiry into Telecommunications Universal Service Obligation Dear Mr Lindwall Telecommunications Universal Service Obligation The National Rural Health
Mr Paul Lindwall Commissioner Productivity Commission Inquiry into Telecommunications Universal Service Obligation Dear Mr Lindwall Telecommunications Universal Service Obligation The National Rural Health
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Adelaide PHN This template was used to submit the Primary Health Network s (PHN s) Activity Work Plans to the Department
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Adelaide PHN This template was used to submit the Primary Health Network s (PHN s) Activity Work Plans to the Department
Overview. HIV and the First Peoples of Australia Our Story, Our Time, Our Journey. Social Determinants of Health. Our Story Education.
 HIV and the First Peoples of Australia Our Story, Our Time, Our Journey Friday 18th July, 2014 Sydney Associate Professor James Ward Baker IDI Deputy Program Head, Aboriginal and Torres Strait Islander
HIV and the First Peoples of Australia Our Story, Our Time, Our Journey Friday 18th July, 2014 Sydney Associate Professor James Ward Baker IDI Deputy Program Head, Aboriginal and Torres Strait Islander
Cancer in Australia: Actual incidence data from 1991 to 2009 and mortality data from 1991 to 2010 with projections to 2012
 bs_bs_banner Asia-Pacific Journal of Clinical Oncology 2013; 9: 199 213 doi: 10.1111/ajco.12127 ORIGINAL ARTICLE Cancer in Australia: Actual incidence data from 1991 to 2009 and mortality data from 1991
bs_bs_banner Asia-Pacific Journal of Clinical Oncology 2013; 9: 199 213 doi: 10.1111/ajco.12127 ORIGINAL ARTICLE Cancer in Australia: Actual incidence data from 1991 to 2009 and mortality data from 1991
DRUG AND ALCOHOL TREATMENT ACTIVITY WORK PLAN
 DRUG AND ALCOHOL TREATMENT ACTIVITY WORK PLAN 2016-2019 1 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-2019 Primary Health Tasmania t: 1300 653 169 e: info@primaryhealthtas.com.au
DRUG AND ALCOHOL TREATMENT ACTIVITY WORK PLAN 2016-2019 1 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-2019 Primary Health Tasmania t: 1300 653 169 e: info@primaryhealthtas.com.au
Volunteering in NHSScotland Developing and Sustaining Volunteering in NHSScotland
 NG11-07 ing in NHSScotland Developing and Sustaining ing in NHSScotland Outcomes The National Group for ing in NHS Scotland agreed the outcomes below which formed the basis of the programme to develop
NG11-07 ing in NHSScotland Developing and Sustaining ing in NHSScotland Outcomes The National Group for ing in NHS Scotland agreed the outcomes below which formed the basis of the programme to develop
Mental health and Aboriginal people and communities
 Mental health and Aboriginal people and communities 10-year mental health plan technical paper Contents Background...1 Aboriginal communities and the experience of poor mental health...2 Policy and program
Mental health and Aboriginal people and communities 10-year mental health plan technical paper Contents Background...1 Aboriginal communities and the experience of poor mental health...2 Policy and program
An epidemic of renal failure among Australian Aboriginals
 emja Australia The Medical Journal of Home Issues emja shop Classifieds Contact More... Topics Search Login Buy full access An epidemic of renal failure among Australian Aboriginals Janine L Spencer, Desiree
emja Australia The Medical Journal of Home Issues emja shop Classifieds Contact More... Topics Search Login Buy full access An epidemic of renal failure among Australian Aboriginals Janine L Spencer, Desiree
Available from Deakin Research Online:
 This is the published version: Stevens,M and Paradies,Y 2014, Changes in exposure to 'life stressors' in the Aboriginal and Torres Strait Islander population, 2002 to 2008., BMC Public Health, vol. 14,
This is the published version: Stevens,M and Paradies,Y 2014, Changes in exposure to 'life stressors' in the Aboriginal and Torres Strait Islander population, 2002 to 2008., BMC Public Health, vol. 14,
Preventing substance misuse among indigenous peoples: a comparative review
 Preventing substance misuse among indigenous peoples: a comparative review Dennis Gray, Drug Research Institute, Curtin University of Technology INTRODUCTION The aim of this presentation is to report on
Preventing substance misuse among indigenous peoples: a comparative review Dennis Gray, Drug Research Institute, Curtin University of Technology INTRODUCTION The aim of this presentation is to report on
Submission to the Commonwealth Government on the New National Women s Health Policy
 Submission to the Commonwealth Government on the New National Women s Health Policy 1 July, 2009. Authorised and written by: Patty Kinnersly, CEO, Women s Health Grampians Contact person for this submission:
Submission to the Commonwealth Government on the New National Women s Health Policy 1 July, 2009. Authorised and written by: Patty Kinnersly, CEO, Women s Health Grampians Contact person for this submission:
Consumer Consultant. PTBA (ichris) Community Mental Health. Owner Angela Micheletto
 Position Description Position Title Position Number Consumer Consultant PTBA (ichris) Position Status Part time, 0.6 0.8 EFT, until 30 September 2017 Program Area Award/Agreement/ Classification Reports
Position Description Position Title Position Number Consumer Consultant PTBA (ichris) Position Status Part time, 0.6 0.8 EFT, until 30 September 2017 Program Area Award/Agreement/ Classification Reports
4 th A-TRAC Symposium
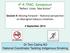 4 th A-TRAC Symposium Reflect. Unite. Take Action Session 4: Moving Forward National perspective on Aboriginal tobacco initiatives 4 September 2014 Dr Tom Calma AO National Coordinator Tackling Indigenous
4 th A-TRAC Symposium Reflect. Unite. Take Action Session 4: Moving Forward National perspective on Aboriginal tobacco initiatives 4 September 2014 Dr Tom Calma AO National Coordinator Tackling Indigenous
Heart health CHD management gaps in general practice
 professional practice Nancy Huang MBBS, DipRACOG, MPH, is National Manager Clinical Programs, Heart Foundation, Melbourne, Victoria. nancy.huang@heartfoundation.org.au Marcus Daddo BSc(Hons), is Manager
professional practice Nancy Huang MBBS, DipRACOG, MPH, is National Manager Clinical Programs, Heart Foundation, Melbourne, Victoria. nancy.huang@heartfoundation.org.au Marcus Daddo BSc(Hons), is Manager
Primary Health Networks
 Primary Health Networks Activity Work Plan 2016-17 to 2018-19 Budget Central and Eastern Sydney PHN When submitting this Activity Work Plan 2016-2018 to the Department of Health, the PHN must ensure that
Primary Health Networks Activity Work Plan 2016-17 to 2018-19 Budget Central and Eastern Sydney PHN When submitting this Activity Work Plan 2016-2018 to the Department of Health, the PHN must ensure that
Initiatives in Australia
 Initiatives in Australia closing disparities in cancer for Indigenous Australians Professor Gail Garvey gail.garvey@menzies.edu.au Apology Ten Year Anniversary 'Sorry' apology to Stolen Generations.
Initiatives in Australia closing disparities in cancer for Indigenous Australians Professor Gail Garvey gail.garvey@menzies.edu.au Apology Ten Year Anniversary 'Sorry' apology to Stolen Generations.
Eye Care in Action: Optometry in Aboriginal health services
 Eye Care in Action: Optometry in Aboriginal health services Anna Morse & Luke Arkapaw Public Health Division Brien Holden Vision Institute A multidisciplinary collaborative global research, development,
Eye Care in Action: Optometry in Aboriginal health services Anna Morse & Luke Arkapaw Public Health Division Brien Holden Vision Institute A multidisciplinary collaborative global research, development,
Participation in cervical screening by Indigenous women in the Northern Territory: a longitudinal study
 in cervical screening by Indigenous women in the Northern Territory: a longitudinal study Philippa L Binns and John R Condon The incidence of cervical cancer and mortality from the disease have been declining
in cervical screening by Indigenous women in the Northern Territory: a longitudinal study Philippa L Binns and John R Condon The incidence of cervical cancer and mortality from the disease have been declining
Dentist labour force projections,
 AIHW Dental Statistics and Research Unit Research Report No. 43 Dentist labour force projections, 200 2020 This report provides dentist labour force projections from 200 to the year 2020. In 2007 the establishment
AIHW Dental Statistics and Research Unit Research Report No. 43 Dentist labour force projections, 200 2020 This report provides dentist labour force projections from 200 to the year 2020. In 2007 the establishment
Rural and Remote Health James Cook University ISSN
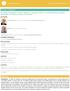 Rural and Remote Health James Cook University ISSN 1445-6354 ORIGINAL RESEARCH AUTHORS 1 John Humphreys PhD, Emeritus Professor, john.humphreys@monash.edu 2 David Lyle PhD, Head of Department * Veronica
Rural and Remote Health James Cook University ISSN 1445-6354 ORIGINAL RESEARCH AUTHORS 1 John Humphreys PhD, Emeritus Professor, john.humphreys@monash.edu 2 David Lyle PhD, Head of Department * Veronica
Aboriginal and Torres Strait Islander Services: 2016/17 in review
 Aboriginal and Torres Strait Islander Services: 216/17 in review Aboriginal and Torres Strait Islander adults and children access Australian Hearing s services in a wide range of locations: in Hearing
Aboriginal and Torres Strait Islander Services: 216/17 in review Aboriginal and Torres Strait Islander adults and children access Australian Hearing s services in a wide range of locations: in Hearing
Statement about the release of the National Ice Taskforce Report, release of two Review report and various announcements by the Australian Government
 Statement about the release of the National Ice Taskforce Report, release of two Review report and various announcements by the Australian Government 9 December 2015 The Network of Australian State and
Statement about the release of the National Ice Taskforce Report, release of two Review report and various announcements by the Australian Government 9 December 2015 The Network of Australian State and
City of Moonee Valley Draft MV 2040 Strategy
 + City of Moonee Valley Draft MV 2040 Strategy Your neighbourhood, your vision May 2018 Contact: Louise Sadler (Acting)Director of Strategy, Advocacy and Community Engagement Women s Health West 317-319
+ City of Moonee Valley Draft MV 2040 Strategy Your neighbourhood, your vision May 2018 Contact: Louise Sadler (Acting)Director of Strategy, Advocacy and Community Engagement Women s Health West 317-319
Stroke incidence and case-fatality among Indigenous and non-indigenous populations in the Northern Territory of Australia,
 Stroke incidence and case-fatality among Indigenous and non-indigenous populations in the Northern Territory of Australia, 1999 2011 Jiqiong You 1 *, John R. Condon 2, Yuejen Zhao 1, and Steven L. Guthridge
Stroke incidence and case-fatality among Indigenous and non-indigenous populations in the Northern Territory of Australia, 1999 2011 Jiqiong You 1 *, John R. Condon 2, Yuejen Zhao 1, and Steven L. Guthridge
SUMMARY OF RESULTS FROM INDIGENOUS SUICIDE PREVENTION PROGRAMS DELIVERED BY INDIGENOUS PSYCHOLOGICAL SERVICES Westerman, 2007
 SUMMARY OF RESULTS FROM INDIGENOUS SUICIDE PREVENTION PROGRAMS DELIVERED BY INDIGENOUS PSYCHOLOGICAL SERVICES Westerman, 2007 Studies continue to point to the escalating number of suicides amongst Aboriginal
SUMMARY OF RESULTS FROM INDIGENOUS SUICIDE PREVENTION PROGRAMS DELIVERED BY INDIGENOUS PSYCHOLOGICAL SERVICES Westerman, 2007 Studies continue to point to the escalating number of suicides amongst Aboriginal
The first year counts: cancer survival among Indigenous and non-indigenous Queenslanders
 The first year counts: cancer survival among Indigenous and non-indigenous Queenslanders 1997-2006 Author Cramb, Susanna M., Garvey, Gail, Valery, Patricia C., Williamson, John D., Baade, Peter D. Published
The first year counts: cancer survival among Indigenous and non-indigenous Queenslanders 1997-2006 Author Cramb, Susanna M., Garvey, Gail, Valery, Patricia C., Williamson, John D., Baade, Peter D. Published
SUBMISSION FROM THE NATIONAL AUTISTIC SOCIETY SCOTLAND
 SUBMISSION FROM THE NATIONAL AUTISTIC SOCIETY SCOTLAND 1. The National Autistic Society (Scotland) is part of the UK s leading charity for people affected by autism 1. Founded in 1962, by a group of parents
SUBMISSION FROM THE NATIONAL AUTISTIC SOCIETY SCOTLAND 1. The National Autistic Society (Scotland) is part of the UK s leading charity for people affected by autism 1. Founded in 1962, by a group of parents
Growing an optometry workforce for Aboriginal and Torres Strait Islander communities
 Growing an optometry workforce for Aboriginal and Torres Strait Islander communities Genevieve Napper 1, Luke Arkapaw 2, Mitchell Anjou 3, Anna Morse 2, Michelle Pollard 2 1 Australian College of Optometry;
Growing an optometry workforce for Aboriginal and Torres Strait Islander communities Genevieve Napper 1, Luke Arkapaw 2, Mitchell Anjou 3, Anna Morse 2, Michelle Pollard 2 1 Australian College of Optometry;
Q uitting smoking reduces the
 Smoking cessation advice and nonpharmacological support in a national sample of smokers and ex-smokers David P Thomas MB BS, PhD, FAFPHM 1 Pele T Bennet BHSc 2 Viki L Briggs BA, GDipIndigHlthProm, MPH
Smoking cessation advice and nonpharmacological support in a national sample of smokers and ex-smokers David P Thomas MB BS, PhD, FAFPHM 1 Pele T Bennet BHSc 2 Viki L Briggs BA, GDipIndigHlthProm, MPH
The barriers and facilitators of supporting self care in Mental Health NHS Trusts
 The barriers and facilitators of supporting self care in Mental Health NHS Trusts Executive Summary for the National Institute for Health Research Service Delivery and Organisation programme April 2010
The barriers and facilitators of supporting self care in Mental Health NHS Trusts Executive Summary for the National Institute for Health Research Service Delivery and Organisation programme April 2010
Oral health trends among adult public dental patients
 DENTAL STATISTICS & RESEARCH Oral health trends among adult public dental patients DS Brennan, AJ Spencer DENTAL STATISTICS AND RESEARCH SERIES Number 30 Oral health trends among adult public dental patients
DENTAL STATISTICS & RESEARCH Oral health trends among adult public dental patients DS Brennan, AJ Spencer DENTAL STATISTICS AND RESEARCH SERIES Number 30 Oral health trends among adult public dental patients
At the heart of health promotion: Health Promotion Policy & Advocacy. Rachelle Foreman
 . At the heart of health promotion: Australian About the Heart Maps Foundation & Health Promotion Policy & Advocacy Rachelle Foreman I would like to pay my respects to the Traditional Owners of the land
. At the heart of health promotion: Australian About the Heart Maps Foundation & Health Promotion Policy & Advocacy Rachelle Foreman I would like to pay my respects to the Traditional Owners of the land
bulletin criminal justice Police drug diversion in Australia Key Points Jennifer Ogilvie and Katie Willis
 criminal justice bulletin Police drug diversion in Australia Key Points Jennifer Ogilvie and Katie Willis Diversion involves the redirection of offenders away from conventional criminal justice processes.
criminal justice bulletin Police drug diversion in Australia Key Points Jennifer Ogilvie and Katie Willis Diversion involves the redirection of offenders away from conventional criminal justice processes.
NT Aboriginal Health KPIs: health, data and change Territory style. Pasqualina Coffey AMSANT
 NT Aboriginal Health KPIs: health, data and change Territory style Pasqualina Coffey AMSANT Overview NT Indigenous health care landscape Development of CQI and clinical indicators in the NT NT AHKPIs governance
NT Aboriginal Health KPIs: health, data and change Territory style Pasqualina Coffey AMSANT Overview NT Indigenous health care landscape Development of CQI and clinical indicators in the NT NT AHKPIs governance
Cancer screening: Breast
 Cancer control in NSW: 2016 Cancer screening: Breast Introduction In NSW, breast cancer accounted for 27.4 per cent of all new cancer cases in women, and 14.6 per cent of all cancer mortality in women
Cancer control in NSW: 2016 Cancer screening: Breast Introduction In NSW, breast cancer accounted for 27.4 per cent of all new cancer cases in women, and 14.6 per cent of all cancer mortality in women
ceptions of Perceptions of mental health service delivery among staff and Indigenous consumers: it's still about communication
 ceptions of Perceptions of mental health service delivery among staff and Indigenous consumers: it's still about communication Diann Eley, Louise Young, Keith Hunter, Peter Baker, Ernest Hunter and Dominique
ceptions of Perceptions of mental health service delivery among staff and Indigenous consumers: it's still about communication Diann Eley, Louise Young, Keith Hunter, Peter Baker, Ernest Hunter and Dominique
Caring for cancer patients with comorbidity
 Caring for cancer patients with comorbidity Comorbidity among Indigenous Australian cancer patients Chair: Diana Sarfati Speaker: Patricia Valery Session code: CTS.2.143-2 www.worldcancercongress.org Aboriginal
Caring for cancer patients with comorbidity Comorbidity among Indigenous Australian cancer patients Chair: Diana Sarfati Speaker: Patricia Valery Session code: CTS.2.143-2 www.worldcancercongress.org Aboriginal
Hepatitis C capacity strengthening program with Aboriginal Medical Services in regional Australia
 Hepatitis C capacity strengthening program with Aboriginal Medical Services in regional Australia Written and presented by: Beth Wilson ASHM is a signatory to the ACFID Code of Conduct and is committed
Hepatitis C capacity strengthening program with Aboriginal Medical Services in regional Australia Written and presented by: Beth Wilson ASHM is a signatory to the ACFID Code of Conduct and is committed
Gill Schierhout 1*, Tricia Nagel 1, Damin Si 3, Christine Connors 2, Alex Brown 4 and Ross Bailie 1
 Schierhout et al. International Journal of Mental Health Systems 2013, 7:16 RESEARCH Open Access Do competing demands of physical illness in type 2 diabetes influence depression screening, documentation
Schierhout et al. International Journal of Mental Health Systems 2013, 7:16 RESEARCH Open Access Do competing demands of physical illness in type 2 diabetes influence depression screening, documentation
KEY QUESTIONS What outcome do you want to achieve for mental health in Scotland? What specific steps can be taken to achieve change?
 SCOTTISH GOVERNMENT: NEXT MENTAL HEALTH STRATEGY Background The current Mental Health Strategy covers the period 2012 to 2015. We are working on the development of the next strategy for Mental Health.
SCOTTISH GOVERNMENT: NEXT MENTAL HEALTH STRATEGY Background The current Mental Health Strategy covers the period 2012 to 2015. We are working on the development of the next strategy for Mental Health.
